GUIDELINES FOR NASOPHARYNGEAL SUCTION OF A CHILD OR YOUNG ADULT
|
|
|
- Charleen Bell
- 5 years ago
- Views:
Transcription
1 ASSOCIATION OF PAEDIATRIC CHARTERED PHYSIOTHERAPISTS GUIDELINES FOR NASOPHARYNGEAL SUCTION OF A CHILD OR YOUNG ADULT APCP RESPIRATORY GROUP A Professional Network of The Chartered Society of Physiotherapy
2 Guideline for Nasopharyngeal Suction of a Child or Young Adult Introduction Throughout this guideline the term child / children can be taken to represent child / young person / young adult. This guideline has been produced to give those people undertaking nasopharyngeal suction in children an up-to-date evidence based guide, to ensure a safe and effective technique. Where evidence is lacking, consensus has been reached by specialist respiratory paediatric physiotherapists across the UK. It is intended that this is used as a template; additions may be needed to fit in with local policies. Background The aim of suctioning is to clear secretions, thus maintaining a patent airway, improving ventilation and oxygenation, and reducing the work of breathing. Suctioning is, however, an invasive procedure and adverse physiological effects can occur. These effects can be both 10, 17, 14, immediate and long term; a sound knowledge of the procedure is therefore required. 18 The procedure of suctioning is a common practice in the treatment of children with a variety of conditions. It is undertaken to remove excessive or retained secretions from a child s respiratory tract. This could be due to: Respiratory dysfunction/disease, causing an alteration in the type or quantity of secretions or disruption of the normal mucociliary clearance process Neurological disorders which inhibit or depress normal cough reflex An artificial airway in situ (suctioning via an artificial airway is not covered in this guideline, except a nasopharyngeal airway) The general principles of suctioning are the same, whether the child requires suction of the mouth, pharynx or via an artificial airway. 4, 5 Indications for Nasopharyngeal Suctioning Suctioning is a potentially hazardous procedure and should only be performed when there are clear indications that excessive pulmonary secretions are affecting the patency of the child s airway or the effective ventilation of the patient. 8 Suctioning should maximise removal of secretions with minimal tissue damage and hypoxia. It is an essential procedure that is determined by the child s clinical condition and not 1
3 predetermined intervals. The frequency of suctioning should be assessed for each child on an individual basis and should only be carried out when the child is unable to clear its own airway effectively. It should not be performed as a matter of routine. 12 An appropriate assessment must be undertaken to establish the need for suction. Evidence of retained secretions will be shown by one or more of the following: Visible, audible or palpable secretions Decreased oxygen saturation levels Increased oxygen requirements Coughing Poor cough / inability to generate effective spontaneous cough Reduced movement / breath sounds of the chest Signs of distress due to retained secretions i.e. increased work of breathing (nasal flaring / tracheal tug / costal recession), increased respiratory rate, tachycardia / 10, 14, 18 bradycardia, change of colour. Nasopharyngeal suction is indicated when there is evidence of retained secretions but the child is not able to clear the secretions independently and secretions are too low down in the airway for oral suction. Verbal Information Given to Child / Parent / Carer This must be obtained prior to this procedure being carried out. If the child is unable to give consent verbally, other ways of obtaining it must be explored, e.g. blinking, squeezing of the hand. If the child is unable to give any form of consent and not carrying out the procedure would be detrimental to their health, it is acceptable to proceed, providing the person performing the procedure is not aware of any documented evidence that the client has refused the procedure should the need arise. Guidance for patients who may not be competent to give informed consent, e.g. unconscious patients, some children, patients with severe mental health problems, confused patients and some patients with learning difficulties, consent is obtained whenever possible from parents, guardians, carers or others designated to act on the patients behalf. Verbal information given to children prior to consent to suctioning procedures 1. Reason for the selected suctioning procedure 2. Explanation of the equipment involved 3. Explanation of the practical procedure proposed 2
4 4. Explanation of any techniques used in conjunction with the suctioning procedure, e.g. postural drainage, vibrations, etc. 5. Discussion of relevant precautions / contraindications 6. Explanation of cleaning and equipment maintenance (may not need to be discussed before obtaining consent but will be covered by the end of the first treatment session, see individual procedures) 7. Informed consent will be obtained in initial assessment Important - The child should be made aware that they have a right to withdraw their consent at any point during the treatment. Contra-indications of Nasopharyngeal Suctioning 18, Unexplained haemoptysis (the coughing up of blood from the lungs or bronchi) or known clotting disorder Laryngospasm (stridor) Bronchospasm Basal skull fractures and other causes of cerebrospinal fluid leakage via the ear Pneumothorax Recent oesophageal or tracheal anastamoses (the joining of the branches of two blood vessels) and other forms of tracheobronchial trauma Occluded nasal passages Unexplained nasal bleeding Severe hypoxaemia / hypoxia Raised intracranial pressure Acute hypo or hypertension Suctioning should not be carried out if any of the above contra-indications are present unless assessed on an individual basis and with the agreement of the medical team. Equipment 1. An adequate supply of sterile suction catheters of the correct size and type: A diameter of less than half that of the diameter of the airway Multi-eyed catheters with 1 distal and 2 lateral ports with rounded ends and lateral ports that are smaller than the distal port It is preferable to use suction catheters with graduations and integrated valve for vacuum control 3
5 Selected suction catheter size should be documented in the child / young person s record 2. Suction unit with variable vacuum control: A vacuum pump with filter and clean tubing. Check the charge by switching it on and looking for charge levels. Look at machine to ensure all parts of the equipment are clean and intact. Check a charger is available. Check the pressure by switching it on; bend the tubing from the machine to the catheter to cut off air from the machine/ or place a finger over the end of the suction tubing -this will show the maximum pressure the machine can give. N.B. Maximum pressure is age appropriate and is essential to good care of the children. 3. Non-sterile gloves 4. Tap water for flushing. 5. Bag for waste. 6. Pulse Oximeter Pre-oxygenation / Post-oxygen Indications Suctioning removes oxygen from the airways and in some cases can cause hypoxia. Preoxygenation and/or post-oxygenation can minimise this risk but the need for this should be assessed on an individual basis in line with hospital / community policy, and documented 19, 20 within the child s health record. Children particularly at risk of hypoxia as a result of suctioning are: Those requiring oxygen therapy Those who have previously demonstrated desaturations during suctioning as confirmed by pulse oximetry Those with impaired respiratory or cardiac function NB. If, following clinical assessment, suction is indicated on an ongoing basis and oxygen is required, it will be necessary to liaise with the GP regarding oxygen provision if this isn t already available. 4
6 Nasopharyngeal Suction Pressure Guide Age mmhg Suction pressure Kpa Neonates years years years It is important that the lowest effective suction pressure is used, especially when secretions are loose. If secretions are not clearing with the above pressures, higher pressures can be used with caution up to a maximum of 150mmHg / 20Kpa. 18 Consideration should also be given to secretion mobilisation and other clearance techniques. These techniques must only be performed by those that have been taught by, and signed off as competent by, a respiratory physiotherapist. Procedure Rationale / Evidence 1) Assess the need for nasopharyngeal suction (see indications above): Whenever possible the child should be encouraged to clear their airway by coughing or other clearance techniques. If the child is able to clear their secretions independently, do not use suction. Suction should not be carried out as a matter of routine, only when there is evidence of retained secretions. Suction is an invasive and potentially dangerous procedure that may be traumatic to the child. It should therefore be used with care and thorough assessment, and when less invasive procedures are 16, 10, 17 in-effective. The major concerns are the possibility of: Respiratory distress Hypoxia Vomiting and risk of aspiration Tracheobronchial trauma and granulation or ulcer formation Pneumothorax in infants Raised intracranial pressure or arrhythmias if carina touched Intraventricular haemorrhages in premature infants Hypo or hypertension 17, 18, 5
7 2) Check all equipment is available and in working order. NB. Safety goggles are advised if there is a risk of contamination to the person who is undertaking the procedure. Suction equipment needs to be prepared and ready to use. To maintain safety of the person undertaking the procedure., 18 3) Explain and discuss the procedure with the child and family if possible. Gain consent (as above). To ensure understanding and consent is given. Encourage cooperation and reduce anxiety. 6, 10 4) Assessment observe the child s respiratory status and baseline values, e.g. heart rate, blood pressure, work of breathing and colour. Note the child s normal and accepted level of oxygen saturation level pre-suction. Maintain child s safety. To enable assessment of the effectiveness of treatment. 5) Prepare the child for the procedure. If able, position the child on their side, with their head turned to the side. Prevents the child s tongue from obstructing the airway. This is the preferred and safer position to reduce the risk of aspiration. 17, 18, 6) Wash hands using soap and water. Dry hands thoroughly. Reduces transmission of micro-organisms. 7 7) Choose an appropriate sized, graduated suction catheter, with side port suction control: Size of the suction catheter should be half the diameter of the smallest nostril. Depth of suction - with the child facing forward, measure from the nostril to the mid part of the ear lobe and down to the base of the neck. Record all details in the care plan. Suction can cause mucosal trauma and arrhythmias (abnormal heart rhythm). 18 Measured suction depth with multi eye catheters cause less trauma and arrhythmias. 18 The catheter tip will reach the naspharynx when measured as described. NB. If the child has a kyphoscoliosis measure both sides, add measurements together and divide by 2. A kyphoscoliosis is a abnormal curvature of the spine in which there is forward and sideways displacement. 6
8 8) Switch on the suction machine. With a gloved hand, test the suction equipment by placing the thumb over the end of the suction tubing for 5-10 seconds. Observe the pressure on the manometer of the suction machine and adjust as required. There is a risk of atelectasis (partial lung collapse) and hypoxia if the suction pressure 2, 4, 17 is too high. To minimise the risk of atelectasis and hypoxia. 12, 9) Attach a suction catheter to the suction tubing: peel back the catheter to expose the hard plastic connector leave the rest of the catheter in the protective cover To ensure sterility of the suction catheter. 10) Put a clean glove on the dominant hand. Do not touch anything EXCEPT the sterile part of the catheter. This gloved hand will be used to insert the sterile catheter into the nasopharyngeal airway. To maintain a clean technique., 21 11) Remove the suction catheter with gloved hand. To maintain a clean technique. 12) Hold the end of the suction catheter with gloved hand and the plastic connector with the ungloved hand. To maintain a clean technique. ) Check the child s observations and breathing pattern immediately prior to inserting the suction catheter To enable early recognition of any potential complications. To maintain the child s safety. 14) If identified on an individual basis, preoxygenate the child (if O 2 prescribed). To prevent hypoxia. 7
9 15) If required moisten the tip of the suction catheter in cooled, boiled water or apply a thin layer of sterile Aqua Gel to the tip of the suction catheter if required. Lubricate the tip of the suction catheter for easier insertion ) With no suction pressure applied insert the suction catheter diagonally into the nostril until the desired depth is reached. To avoid hitting the top of the nasal passage with the suction catheter and causing trauma. Nasopharynx Suction Catheter Oropharynx Oesophagus Larynx Trachea If resistance is felt DO NOT FORCE THE SUCTION CATHETER, pull back and gently reinsert the suction catheter. NB. The suction catheter must not be passed any further than the suprasternal notch, which is the dip at the front base of the neck. 17) At the desired depth apply constant suction for around 2 seconds (depending on the child), and then withdraw the suction catheter slowly. Suctioning should be quick and effective, i.e seconds for infants and 15 seconds for older children. The procedure should take no longer than seconds. The person suctioning must use their judgement to assess if a child can only tolerate shorter duration of suction based on their clinical symptoms Do not rotate, stir or trombone the catheter. To allow optimal secretion clearance and reduce the need for a second attempt. If the technique is too quick there is a risk that not all the secretions will be cleared. 8, 18 If it is too slow the child may become breathless and develop hypoxia. Prolonged suctioning or repeated insertion of the suction catheter may produce vagal stimulation, which can cause profound bradycardia. To prevent tissue damage and to enhance 11, 12 the child s comfort. 18 8
10 18) Monitor the child during and after the procedure using pre-suction baseline observations as a guideline. NB. If the child deteriorates during the procedure, stop suction immediately and reassess. Supply O 2 as indicated. 19) Assess the need for further suction. NB. Allow seconds before re-inserting a new suction catheter. To evaluate the effectiveness of suction and to determine if the procedure needs repeating. Allows for re-oxygenation ) Each suction catheter can be used more than once but for one episode of care only. There is no limitation on how many times the child is suctioned - it is decided on clinical need. To minimise the risk of infection to the child and person performing the procedure. Frequency of use of suction catheters, differ 4,, 15, 18 with local policy. Signs of successful suctioning: Child appears more comfortable Ensure the respiratory status is normal Ensure the observations have returned to the baseline values Removal of pulmonary secretions Improved oxygenation, saturations and/or colour Improved breath sounds and/or chest movement Auscultation may be used if trained in the skill Audible secretions have gone 21) Once the procedure is completed, discard the suction catheter by wrapping it around the gloved hand, disconnect from the suction tubing and pull the glove off, inside out. Safe disposal of equipment and prevention of cross infection. 9
11 22) Flush the suction tubing with water (from the container). NB. The container of water must be washed in hot soapy water, rinsed thoroughly, dried and re-filled with tap water. Secretions left in the suction tubing may decrease suction and provide an environment for growth of micro-organisms. To prevent growth of micro-organisms. 7, Turn off the suction machine. 23) Wean down the oxygen to the prescribed amount, to maintain oxygen saturations within normal limits for the child (if applicable). Normal oxygen delivery should resume after the procedure. 24) Ensure the suction machine is set up for the next episode of suction. To maintain the child s safety. To ensure sterility of the suction catheter. 3, 5, ) Wash hands using soap and water. Dry hands thoroughly. Reduces transmission of microorganisms. 7 26) Ensure the child has recovered from the procedure and he/she is left in a comfortable position. Promotes comfort and reduces anxiety. To influence future suction practice. 5 10
12 Modifications of Technique If retained secretions not being cleared consider: increasing pressure increasing size of catheter If getting trauma or if repeated suction needed: use aqua gel may need nasopharyngeal airway - discuss with medical team decrease size of catheter try other nostril use cool boiled water change type of catheter Difficult to get down airway: change nostril change position of child If nasogastric tube in place: recommend testing after suction to ensure it hasn't moved into the lungs to reduce the risk of aspiration use opposite nostril to the one with the nasogastric tube
13 References 1.Czarnik R.E.et al. Different effects of continuous versus intermittent suctioning on tracheal tissues. Heart and Lung. 1991;20(21): Carroll P. Safe Suctioning. Nursing. 1989; 19(9): Casteldine G. Nurse negligence in oral/nasal suctioning caused patients distress and put them at risk. British Journal of Nursing. 2006; 15(2): Glass A & Grap. Ten Tips for Safer Suctioning. American Journal of Nursing. 1995; 96(5): Great Ormond Street Hospital for Children s NHS Trust. Clinical Guideline: Airway Suction. Oct Available in: Clinical Standards Office at Hope House Children s Hospice. 6.Hope House Children s Hospices Consent Policy. Originated by: Kath Jones (Director of Care), Jon Mills (Social Work Team Manager). Approved by: Clinical Governance Committee. Issue date: May Review date: May Version 5. 7.Hope House Children s Hospices Infection Control Policy. Originated by: David Riffel (Hospice Coordinator) and James Lewis (Registered Nurse). Ratified by: Jenny Bate (Infection Control Nurse, Shropshire County NHS PCT). Issue date: January Review date: January Hough A. Physiotherapy in Respiratory Care: An Evidence Based Approach to Respiratory and Cardiac Management. 3 rd Edition. Nelson Thornes; , Mallet J & Dougherty L. Tracheostomy Care and Laryngectomy Voice Rehabilitation. The Royal Marsden NHS Trust. Manual of Clinical Nursing Procedures. 5 th ed. Oxford: Blackwell Science; Chapter Moore T. Suctioning Techniques for the removal of respiratory secretions. Nursing Standard. 2003; 18(9): NHS Warick & NHS Coventry. Coventry & Warwickshire Children & Young People s Interactive Competency Framework. 20 (accessed 7 Oct 20). Available from: Ritson P (Clinical Specialist Physiotherapist in Paediatric Intensive Care). Lecture Notes. Clinical Skills Workshop at Hope House Children s Hospice on Suction Techniques. Jan Available in: Clinical Standards Office at Hope House Children s Hospice., Royal Liverpool Children s NHS Trust. Competency Assessment Nasopharyngeal Suction. Oct Available in: Clinical Standards Office at Hope House Children s Hospice. 12
14 14, Royal Liverpool Children s NHS Trust. Competency Assessment Oral Suction. Oct Available in: Clinical Standards Office at Hope House Children s Hospice. 15, Scobie M, Copell B, Taylor A. et al. Effects of re-using suction catheters on occurance of pneumonia in children. Heart and Lung. 2001;30(3): , Thompson L. Suctioning adults with an artificial airway. Systemic review. No 9. The Joanna Briggs Institute for Evidence-Based Nursing and Midwifery 2000; cited in: Moore T. Suctioning techniques for the removal of respiratory secretions. Nursing Standard. 2003; 18(9): , Trigg E & Mohammed T. Practices in Children s Nursing. Guidelines for Hospital and Community. 3 rd ed. London: Churchill Livingstone; Birmingham Children s Hospital NHSFT. Guideline for Suction via a Tracheostomy in a child/young person at Birmingham Children s Hospital NHSFT and in the Community. July Knox AM (1993) Performing endotracheal suction on children: a literature review and implications for nursing practice. Intensive and critical care nursing 9: NHS Quality Improvement Scotland (2008). Caring for the child/ young person with a tracheostomy (online). Edinburgh: NHS Improvement Scotland. 21. Nursing and Midwifery Council. Code of Professional Conduct for the Nurse, Midwife and Health Visitor. 4 th ed. NMC London: 2002.
15 ASSOCIATION OF PAEDIATRIC CHARTERED PHYSIOTHERAPISTS GUIDANCE FOR PHYSIOTHERAPISTS: PAEDIATRIC MANUAL HANDLING ASSOCIATION OF PAEDIATRIC CHARTERED PHYSIOTHERAPISTS November 2015 A clinical interest group of the Chartered Society of Physiotherapy
RSPT Tracheal Aspiration. Tracheal Aspiration. RSPT 1410 Tracheal Aspiration
 1 RSPT 1410 2 is the use of to facilitate the removal of secretions from the respiratory tract. Under normal circumstances, patients with normal coughing do not have difficulty in removing secretions.
1 RSPT 1410 2 is the use of to facilitate the removal of secretions from the respiratory tract. Under normal circumstances, patients with normal coughing do not have difficulty in removing secretions.
LESSON ASSIGNMENT. Oral, Nasopharyngeal, and Nasotracheal Suctioning. After completing this lesson, you will be able to:
 LESSON ASSIGNMENT LESSON 4 Oral, Nasopharyngeal, and Nasotracheal Suctioning. LESSON ASSIGNMENT Paragraphs 4-1 through 4-4. LESSON OBJECTIVES After completing this lesson, you will be able to: 4-1. State/identify
LESSON ASSIGNMENT LESSON 4 Oral, Nasopharyngeal, and Nasotracheal Suctioning. LESSON ASSIGNMENT Paragraphs 4-1 through 4-4. LESSON OBJECTIVES After completing this lesson, you will be able to: 4-1. State/identify
TRACHEOSTOMY CARE. Tracheostomy- Surgically created hole that extends from the neck skin into the windpipe or trachea.
 1 TRACHEOSTOMY CARE Definitions: Trachea-Windpipe Tracheostomy- Surgically created hole that extends from the neck skin into the windpipe or trachea. Outer Cannula- The outer part of a trach tube. Usually
1 TRACHEOSTOMY CARE Definitions: Trachea-Windpipe Tracheostomy- Surgically created hole that extends from the neck skin into the windpipe or trachea. Outer Cannula- The outer part of a trach tube. Usually
Respiratory Physio Protocol for Paediatric Patients on BIPAP via a tracheotomy (uncuffed tube)
 This is an official Northern Trust policy and should not be edited in any way Respiratory Physio Protocol for Paediatric Patients on BIPAP via a tracheotomy (uncuffed tube) Reference Number: NHSCT/12/547
This is an official Northern Trust policy and should not be edited in any way Respiratory Physio Protocol for Paediatric Patients on BIPAP via a tracheotomy (uncuffed tube) Reference Number: NHSCT/12/547
Competency 1: General principles and equipment required to safely manage a patient with a tracheostomy tube.
 Competency 1: General principles and equipment required to safely manage a patient with a tracheostomy tube. Trainee Name: ------------------------------------------------------------- Title: ---------------------------------------------------------------
Competency 1: General principles and equipment required to safely manage a patient with a tracheostomy tube. Trainee Name: ------------------------------------------------------------- Title: ---------------------------------------------------------------
Carole Wegner RN, MSN And Lori Leiser CRT
 Airway Clearance Carole Wegner RN, MSN And Lori Leiser CRT Topics Suctioning and suctioning equipment Medications to facilitate t airway clearance Bronchial hygiene modalities Preparing for suctioning
Airway Clearance Carole Wegner RN, MSN And Lori Leiser CRT Topics Suctioning and suctioning equipment Medications to facilitate t airway clearance Bronchial hygiene modalities Preparing for suctioning
Introduction to Emergency Medical Care 1
 Introduction to Emergency Medical Care 1 OBJECTIVES 8.1 Define key terms introduced in this chapter. Slides 12 15, 21, 24, 31-34, 39, 40, 54 8.2 Describe the anatomy and physiology of the upper and lower
Introduction to Emergency Medical Care 1 OBJECTIVES 8.1 Define key terms introduced in this chapter. Slides 12 15, 21, 24, 31-34, 39, 40, 54 8.2 Describe the anatomy and physiology of the upper and lower
Protocol for performing chest clearance techniques by nursing staff
 Protocol for performing chest clearance techniques by nursing staff Rationale The main indications for performing chest clearance techniques (CCT) are to assist in the removal of thick, tenacious secretions
Protocol for performing chest clearance techniques by nursing staff Rationale The main indications for performing chest clearance techniques (CCT) are to assist in the removal of thick, tenacious secretions
1 SO7. Title of Guideline (must include the word Guideline (not. Oropharyngeal Suctioning Nursing Guideline. Contact Name and Job Title (author)
 Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Contact Name and Job Title (author) S07 Tracheal, Nasopharyngeal and Oropharyngeal Suctioning Nursing Guideline
Title of Guideline (must include the word Guideline (not protocol, policy, procedure etc) Contact Name and Job Title (author) S07 Tracheal, Nasopharyngeal and Oropharyngeal Suctioning Nursing Guideline
Adult Patients Going Home with a Tracheostomy
 Physiotherapy Department Adult Patients Going Home with a Tracheostomy Darent Valley Hospital Darenth Wood Road Dartford Kent DA2 8DA www.dvh.nhs.uk In case of emergencies you will need to dial 999 If
Physiotherapy Department Adult Patients Going Home with a Tracheostomy Darent Valley Hospital Darenth Wood Road Dartford Kent DA2 8DA www.dvh.nhs.uk In case of emergencies you will need to dial 999 If
Critical Care Services: Equipment and Procedures Information for Patients, Relatives and Carers
 Critical Care Services: Equipment and Procedures Information for Patients, Relatives and Carers The Critical Care unit can be a frightening place for patients and visitors. Seeing a loved one attached
Critical Care Services: Equipment and Procedures Information for Patients, Relatives and Carers The Critical Care unit can be a frightening place for patients and visitors. Seeing a loved one attached
Waitin In The Wings. Esophageal/Tracheal Double Lumen Airway (Combitube ) Indications and Use for the Pre-Hospital Provider
 Waitin In The Wings Esophageal/Tracheal Double Lumen Airway (Combitube ) Indications and Use for the Pre-Hospital Provider 1 CombiTube Kit General Description The CombiTube is A double-lumen tube with
Waitin In The Wings Esophageal/Tracheal Double Lumen Airway (Combitube ) Indications and Use for the Pre-Hospital Provider 1 CombiTube Kit General Description The CombiTube is A double-lumen tube with
Advanced Airway Management. University of Colorado Medical School Rural Track
 Advanced Airway Management University of Colorado Medical School Rural Track Advanced Airway Management Basic Airway Management Airway Suctioning Oxygen Delivery Methods Laryngeal Mask Airway ET Intubation
Advanced Airway Management University of Colorado Medical School Rural Track Advanced Airway Management Basic Airway Management Airway Suctioning Oxygen Delivery Methods Laryngeal Mask Airway ET Intubation
CHEST PHYSIOTHERAPY IN NICU PURPOSE POLICY STATEMENTS SITE APPLICABILITY PRACTICE LEVEL/COMPETENCIES. The role of chest physiotherapy in the NICU
 PURPOSE The role of chest physiotherapy in the NICU POLICY STATEMENTS In principle chest physiotherapy should be limited to those infants considered most likely to benefit with significant respiratory
PURPOSE The role of chest physiotherapy in the NICU POLICY STATEMENTS In principle chest physiotherapy should be limited to those infants considered most likely to benefit with significant respiratory
Nasopharyngeal airways for craniofacial conditions
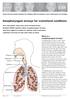 Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Nasopharyngeal airways for craniofacial conditions This information sheet from Great Ormond Street Hospital (GOSH)
Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Nasopharyngeal airways for craniofacial conditions This information sheet from Great Ormond Street Hospital (GOSH)
Administering Rescue Medication into Children for Prolonged Seizures
 Standard Operating Procedure 10 (SOP 10) Administering Rescue Medication into Children for Prolonged Seizures Why we have a procedure? Black Country Partnership NHS Trust (hereafter referred to as the
Standard Operating Procedure 10 (SOP 10) Administering Rescue Medication into Children for Prolonged Seizures Why we have a procedure? Black Country Partnership NHS Trust (hereafter referred to as the
Active Cycle of Breathing Technique
 Active Cycle of Breathing Technique Full Title of Guideline: Author (include email and role): Division & Speciality: Version: 3 Ratified by: Scope (Target audience, state if Trust wide): Review date (when
Active Cycle of Breathing Technique Full Title of Guideline: Author (include email and role): Division & Speciality: Version: 3 Ratified by: Scope (Target audience, state if Trust wide): Review date (when
Airway Management. DFMRT Casualty Care Examination Course. Revision notes for. January Les Gordon
 Airway Management Revision notes for DFMRT Casualty Care Examination Course January 2013 Les Gordon Indicating special information in Revision Notes presentations New information since Casualty Care in
Airway Management Revision notes for DFMRT Casualty Care Examination Course January 2013 Les Gordon Indicating special information in Revision Notes presentations New information since Casualty Care in
Basic Airway Management
 Basic Airway Management Dr. Madhurita Singh, Assoc. Professor, Dept. of Critical Care, CMC Vellore. This is the first module in a series on management of airway and ventilation in critically ill patients.
Basic Airway Management Dr. Madhurita Singh, Assoc. Professor, Dept. of Critical Care, CMC Vellore. This is the first module in a series on management of airway and ventilation in critically ill patients.
Other methods for maintaining the airway (not definitive airway as still unprotected):
 Page 56 Where anaesthetic skills and drugs are available, endotracheal intubation is the preferred method of securing a definitive airway. This technique comprises: rapid sequence induction of anaesthesia
Page 56 Where anaesthetic skills and drugs are available, endotracheal intubation is the preferred method of securing a definitive airway. This technique comprises: rapid sequence induction of anaesthesia
Clostridium difficile Specimen Collection
 Clostridium difficile Specimen Collection Collect stool specimens into a clean, airtight container with no preservative. All stool specimens should be tested as soon as possible. Ideally, stool specimens
Clostridium difficile Specimen Collection Collect stool specimens into a clean, airtight container with no preservative. All stool specimens should be tested as soon as possible. Ideally, stool specimens
2007 Recertification Session. Airway review
 2007 Recertification Session Airway review Level of awareness: This is similar to the AVPU, the GCS is performed later Verbal, loud verbal, or pain stimulus. If pain stimulus, consider a trapezeus squeeze
2007 Recertification Session Airway review Level of awareness: This is similar to the AVPU, the GCS is performed later Verbal, loud verbal, or pain stimulus. If pain stimulus, consider a trapezeus squeeze
Policy x.xxx. Issued: Artificial Airways and Airway Care. ABC Home Medical Company Policy & Procedure Manual. A. Tracheostomy Tubes ( trach tubes)
 A. Tracheostomy Tubes ( trach tubes) A tracheotomy is a surgical procedure whereby an opening is cut into the trachea of the patient for the purpose of inserting a tube (trach tube). The trach tube allows
A. Tracheostomy Tubes ( trach tubes) A tracheotomy is a surgical procedure whereby an opening is cut into the trachea of the patient for the purpose of inserting a tube (trach tube). The trach tube allows
Translaryngeal tracheostomy
 Translaryngeal tracheostomy Issued: August 2013 NICE interventional procedure guidance 462 guidance.nice.org.uk/ipg462 NICE has accredited the process used by the NICE Interventional Procedures Programme
Translaryngeal tracheostomy Issued: August 2013 NICE interventional procedure guidance 462 guidance.nice.org.uk/ipg462 NICE has accredited the process used by the NICE Interventional Procedures Programme
Neonatal Respiratory Physiotherapy. Nicky Hawkes Advanced Respiratory Physiotherapist Oct 2011
 Neonatal Respiratory Physiotherapy Nicky Hawkes Advanced Respiratory Physiotherapist Oct 2011 Respiratory Physiotherapy?..Not just percussion! Assessment of baby s respiratory status and deciding what
Neonatal Respiratory Physiotherapy Nicky Hawkes Advanced Respiratory Physiotherapist Oct 2011 Respiratory Physiotherapy?..Not just percussion! Assessment of baby s respiratory status and deciding what
I. Subject: Therapeutic Bronchoscopy and Bronchoscope Assisted Intubation
 I. Subject: Therapeutic Bronchoscopy and Bronchoscope Assisted Intubation II. Policy: Therapeutic flexible fiberoptic bronchoscopy procedures and bronchoscope assisted intubations will be performed by
I. Subject: Therapeutic Bronchoscopy and Bronchoscope Assisted Intubation II. Policy: Therapeutic flexible fiberoptic bronchoscopy procedures and bronchoscope assisted intubations will be performed by
Oral care & swallowing
 Oral care & swallowing Oral care is important as it has a role to play in preventing healthcare associated infections. Dental plaque and the oropharynx can become colonized by bacteria and a biofilm can
Oral care & swallowing Oral care is important as it has a role to play in preventing healthcare associated infections. Dental plaque and the oropharynx can become colonized by bacteria and a biofilm can
F: Respiratory Care. College of Licensed Practical Nurses of Alberta, Competency Profile for LPNs, 3rd Ed. 59
 F: Respiratory Care College of Licensed Practical Nurses of Alberta, Competency Profile for LPNs, 3rd Ed. 59 Competency: F-1 Airway Management F-1-1 F-1-2 F-1-3 F-1-4 F-1-5 Demonstrate knowledge and ability
F: Respiratory Care College of Licensed Practical Nurses of Alberta, Competency Profile for LPNs, 3rd Ed. 59 Competency: F-1 Airway Management F-1-1 F-1-2 F-1-3 F-1-4 F-1-5 Demonstrate knowledge and ability
Equipment: NRP algorithm, MRSOPA table, medication chart, SpO 2 table Warm
 NRP Skills Stations Performance Skills Station OR Integrated Skills Station STATION: Assisting with and insertion of endotracheal tube (ETT) Equipment: NRP algorithm, MRSOPA table, medication chart, SpO
NRP Skills Stations Performance Skills Station OR Integrated Skills Station STATION: Assisting with and insertion of endotracheal tube (ETT) Equipment: NRP algorithm, MRSOPA table, medication chart, SpO
10/17/2016 OXYGEN DELIVERY: INDICATIONS AND USE OF EQUIPMENT COURSE OBJECTIVES COMMON CAUSES OF RESPIRATORY FAILURE
 OXYGEN DELIVERY: INDICATIONS AND USE OF EQUIPMENT J U L I E Z I M M E R M A N, R N, M S N C L I N I C A L N U R S E S P E C I A L I S T E L O I S A C U T L E R, R R T, B S R C C L I N I C A L / E D U C
OXYGEN DELIVERY: INDICATIONS AND USE OF EQUIPMENT J U L I E Z I M M E R M A N, R N, M S N C L I N I C A L N U R S E S P E C I A L I S T E L O I S A C U T L E R, R R T, B S R C C L I N I C A L / E D U C
Vital Signs and Oxygen Administration
 Vital Signs and Oxygen Administration By Dr. Mohsen Dashti Patient Care and Management (202) May-9-2010 Vital Signs and Oxygen Administration What are the vital signs? Why do we need to know them? How
Vital Signs and Oxygen Administration By Dr. Mohsen Dashti Patient Care and Management (202) May-9-2010 Vital Signs and Oxygen Administration What are the vital signs? Why do we need to know them? How
H: Respiratory Care. Saskatchewan Association of Licensed Practical Nurses, Competency Profile for LPNs, 3rd Ed. 79
 H: Respiratory Care Saskatchewan Association of Licensed Practical Nurses, Competency Profile for LPNs, 3rd Ed. 79 Competency: H-1 Airway Management H-1-1 H-1-2 H-1-3 H-1-4 H-1-5 Demonstrate knowledge
H: Respiratory Care Saskatchewan Association of Licensed Practical Nurses, Competency Profile for LPNs, 3rd Ed. 79 Competency: H-1 Airway Management H-1-1 H-1-2 H-1-3 H-1-4 H-1-5 Demonstrate knowledge
The essential principles of tracheostomy care
 The essential principles of tracheostomy care Deborah Dawson Consultant Nurse Critical Care Excellence in specialist and community healthcare Key publications https://www.stgeorges.nhs.uk/gps-andclinicians/clinical-resources/tracheostomyguidelines/
The essential principles of tracheostomy care Deborah Dawson Consultant Nurse Critical Care Excellence in specialist and community healthcare Key publications https://www.stgeorges.nhs.uk/gps-andclinicians/clinical-resources/tracheostomyguidelines/
Positive Expiratory pressure (PEP), Acapella and Flutter
 Positive Expiratory pressure (PEP), Acapella and Flutter Full Title of Guideline: Author (include email and role): Division & Speciality: Version: 3 Ratified by: Scope (Target audience, state if Trust
Positive Expiratory pressure (PEP), Acapella and Flutter Full Title of Guideline: Author (include email and role): Division & Speciality: Version: 3 Ratified by: Scope (Target audience, state if Trust
Hypertonic Saline (7%) Administration Guideline (adults)
 Hypertonic Saline (7%) Administration Guideline (adults) Full Title of Guideline: Author (include email and role): Hypertonic Saline (7%) Administration Guideline for Practice (Adults) Clair Martin, Senior
Hypertonic Saline (7%) Administration Guideline (adults) Full Title of Guideline: Author (include email and role): Hypertonic Saline (7%) Administration Guideline for Practice (Adults) Clair Martin, Senior
Anatomy and Physiology. The airways can be divided in to parts namely: The upper airway. The lower airway.
 Airway management Anatomy and Physiology The airways can be divided in to parts namely: The upper airway. The lower airway. Non-instrumental airway management Head Tilt and Chin Lift Jaw Thrust Advanced
Airway management Anatomy and Physiology The airways can be divided in to parts namely: The upper airway. The lower airway. Non-instrumental airway management Head Tilt and Chin Lift Jaw Thrust Advanced
Airway and Ventilation. Emergency Medical Response
 Airway and Ventilation Lesson 14: Airway and Ventilation You Are the Emergency Medical Responder Your medical emergency response team has been called to the fitness center by building security on a report
Airway and Ventilation Lesson 14: Airway and Ventilation You Are the Emergency Medical Responder Your medical emergency response team has been called to the fitness center by building security on a report
Saline (0.9%) Nebuliser Guideline
 Saline (0.9%) Nebuliser Guideline Full Title of Guideline: Author (include email and role): Division & Speciality: Version: 3 Ratified by: Scope (Target audience, state if Trust wide): Review date (when
Saline (0.9%) Nebuliser Guideline Full Title of Guideline: Author (include email and role): Division & Speciality: Version: 3 Ratified by: Scope (Target audience, state if Trust wide): Review date (when
AIRWAY MANAGEMENT AND VENTILATION
 AIRWAY MANAGEMENT AND VENTILATION D1 AIRWAY MANAGEMENT AND VENTILATION Basic airway management and ventilation The laryngeal mask airway and Combitube Advanced techniques of airway management D2 Basic
AIRWAY MANAGEMENT AND VENTILATION D1 AIRWAY MANAGEMENT AND VENTILATION Basic airway management and ventilation The laryngeal mask airway and Combitube Advanced techniques of airway management D2 Basic
Pediatric Patients. BCFPD Paramedic Education Program. EMS Education Paramedic Level
 Pediatric Patients BCFPD Program Basic Considerations Much of the initial patient assessment can be done during visual examination of the scene. Involve the caregiver or parent as much as possible. Allow
Pediatric Patients BCFPD Program Basic Considerations Much of the initial patient assessment can be done during visual examination of the scene. Involve the caregiver or parent as much as possible. Allow
Tracheostomy discharge information. Information for community nurses, patients and carers
 Tracheostomy discharge information Information for community nurses, patients and carers What is a tracheostomy? A tracheostomy is a surgical incision (cut) through the neck tissues into the trachea leaving
Tracheostomy discharge information Information for community nurses, patients and carers What is a tracheostomy? A tracheostomy is a surgical incision (cut) through the neck tissues into the trachea leaving
Small Volume Nebulizer Treatment (Hand-Held)
 Small Volume Aerosol Treatment Page 1 of 6 Purpose Policy Physician's Order Small Volume Nebulizer Treatment To standardize the delivery of inhalation aerosol drug therapy via small volume (hand-held)
Small Volume Aerosol Treatment Page 1 of 6 Purpose Policy Physician's Order Small Volume Nebulizer Treatment To standardize the delivery of inhalation aerosol drug therapy via small volume (hand-held)
Bronchoscopy SICU Protocol
 Bronchoscopy SICU Protocol Updated January 2013 Outline Clinical indications Considerations Preparation Bronchoscopy technique Bronchoalveolar Lavage (BAL) Post-procedure Purpose Bronchoscopy is a procedure
Bronchoscopy SICU Protocol Updated January 2013 Outline Clinical indications Considerations Preparation Bronchoscopy technique Bronchoalveolar Lavage (BAL) Post-procedure Purpose Bronchoscopy is a procedure
TRANSFUSION OF BLOOD COMPONENTS ADMINISTRATION. All blood components are administered according to BOP DHB Policy and NZBS Guidelines.
 STANDARDS All blood components are administered according to BOP DHB Policy and NZBS Guidelines. EQUIPMENT IV administration set with 260 micron filter either integrated blood filter; or add on blood filter
STANDARDS All blood components are administered according to BOP DHB Policy and NZBS Guidelines. EQUIPMENT IV administration set with 260 micron filter either integrated blood filter; or add on blood filter
Your anaesthetic for heart surgery
 Your anaesthetic for heart surgery Information for patients and carers First Edition 2018 www.rcoa.ac.uk/patientinfo This leaflet gives you information about your anaesthetic for adult heart (cardiac)
Your anaesthetic for heart surgery Information for patients and carers First Edition 2018 www.rcoa.ac.uk/patientinfo This leaflet gives you information about your anaesthetic for adult heart (cardiac)
AIRWAY MANAGEMENT SUZANNE BROWN, CRNA
 AIRWAY MANAGEMENT SUZANNE BROWN, CRNA OBJECTIVE OF LECTURE Non Anesthesia Sedation Providers Review for CRNA s Informal Questions encouraged 2 AIRWAY MANAGEMENT AWARENESS BASICS OF ANATOMY EQUIPMENT 3
AIRWAY MANAGEMENT SUZANNE BROWN, CRNA OBJECTIVE OF LECTURE Non Anesthesia Sedation Providers Review for CRNA s Informal Questions encouraged 2 AIRWAY MANAGEMENT AWARENESS BASICS OF ANATOMY EQUIPMENT 3
1 Chapter 40 Advanced Airway Management 2 Advanced Airway Management The advanced airway management techniques discussed in this chapter are to
 1 Chapter 40 Advanced Airway Management 2 Advanced Airway Management The advanced airway management techniques discussed in this chapter are to introduce the EMT-B student to these procedures only. In
1 Chapter 40 Advanced Airway Management 2 Advanced Airway Management The advanced airway management techniques discussed in this chapter are to introduce the EMT-B student to these procedures only. In
1.40 Prevention of Nosocomial Pneumonia
 1.40 Prevention of Nosocomial Pneumonia Purpose Audience Policy Statement: The guideline is designed to reduce the incidence of pneumonia and other acute lower respiratory tract infections. All UTMB healthcare
1.40 Prevention of Nosocomial Pneumonia Purpose Audience Policy Statement: The guideline is designed to reduce the incidence of pneumonia and other acute lower respiratory tract infections. All UTMB healthcare
Tracheostomy. Information for patients and relatives
 Tracheostomy Information for patients and relatives page 2 What is a tracheostomy? A tracheostomy is a small hole (stoma) made at the front of the neck, which goes into the trachea (windpipe). A tube called
Tracheostomy Information for patients and relatives page 2 What is a tracheostomy? A tracheostomy is a small hole (stoma) made at the front of the neck, which goes into the trachea (windpipe). A tube called
Chapter 40 Advanced Airway Management
 1 2 3 4 5 Chapter 40 Advanced Airway Management Advanced Airway Management The advanced airway management techniques discussed in this chapter are to introduce the EMT-B student to these procedures only.
1 2 3 4 5 Chapter 40 Advanced Airway Management Advanced Airway Management The advanced airway management techniques discussed in this chapter are to introduce the EMT-B student to these procedures only.
Advanced Airway Management
 CHAPTER 37 Advanced Airway Management Airway Anatomy and Physiology Review Respiratory System: The Airway Respiratory System (Supine) Physiology: Factors of Adequate Breathing Functioning brainstem Open
CHAPTER 37 Advanced Airway Management Airway Anatomy and Physiology Review Respiratory System: The Airway Respiratory System (Supine) Physiology: Factors of Adequate Breathing Functioning brainstem Open
Interfacility Protocol Protocol Title:
 Interfacility Protocol Protocol Title: Mechanical Ventilator Monitoring & Management Original Adoption Date: 05/2009 Past Protocol Updates 05/2009, 12/2013 Date of Most Recent Update: March 23, 2015 Medical
Interfacility Protocol Protocol Title: Mechanical Ventilator Monitoring & Management Original Adoption Date: 05/2009 Past Protocol Updates 05/2009, 12/2013 Date of Most Recent Update: March 23, 2015 Medical
I. Subject: Medication Delivery by Metered Dose Inhaler (MDI)
 I. Subject: Medication Delivery by Metered Dose Inhaler (MDI) II. Policy: Aerosol medication administration by metered dose inhaler will be performed upon a physician's order by Respiratory Therapy personnel.
I. Subject: Medication Delivery by Metered Dose Inhaler (MDI) II. Policy: Aerosol medication administration by metered dose inhaler will be performed upon a physician's order by Respiratory Therapy personnel.
UMC HEALTH SYSTEM Lubbock, Texas :
 Consent for Commonly Performed Procedures in the Adult Critical Care Units I, the undersigned, understand that the adult intensive and intermediate care units ( critical care units ) are places where seriously
Consent for Commonly Performed Procedures in the Adult Critical Care Units I, the undersigned, understand that the adult intensive and intermediate care units ( critical care units ) are places where seriously
The Respiratory System
 130 20 The Respiratory System 1. Define important words in this chapter 2. Explain the structure and function of the respiratory system 3. Discuss changes in the respiratory system due to aging 4. Discuss
130 20 The Respiratory System 1. Define important words in this chapter 2. Explain the structure and function of the respiratory system 3. Discuss changes in the respiratory system due to aging 4. Discuss
Procedure for removal and reinsertion of an indwelling urethral catheter (female)
 Procedure for removal and reinsertion of an indwelling urethral catheter (female) Refer to National Infection Prevention and Control Manual for information on aseptic technique/cleaning equipment. Equipment
Procedure for removal and reinsertion of an indwelling urethral catheter (female) Refer to National Infection Prevention and Control Manual for information on aseptic technique/cleaning equipment. Equipment
Lesson 4-3: Cardiac Emergencies. CARDIAC EMERGENCIES Angina, AMI, CHF and AED
 Lesson 4-3: Cardiac Emergencies CARDIAC EMERGENCIES Angina, AMI, CHF and AED THREE FAMILIAR CARDIAC CONDITIONS Angina Pectoris Acute Myocardial Infarction Congestive Heart Failure ANGINA PECTORIS Chest
Lesson 4-3: Cardiac Emergencies CARDIAC EMERGENCIES Angina, AMI, CHF and AED THREE FAMILIAR CARDIAC CONDITIONS Angina Pectoris Acute Myocardial Infarction Congestive Heart Failure ANGINA PECTORIS Chest
This information will help you care for your tracheostomy while you re in the hospital and at home.
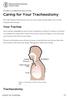 PATIENT & CAREGIVER EDUCATION Caring for Your Tracheostomy This information will help you care for your tracheostomy while you re in the hospital and at home. Your Trachea Your trachea (windpipe) is part
PATIENT & CAREGIVER EDUCATION Caring for Your Tracheostomy This information will help you care for your tracheostomy while you re in the hospital and at home. Your Trachea Your trachea (windpipe) is part
Tracheostomy. Hope Building Neurosurgery
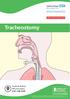 Tracheostomy Hope Building Neurosurgery 0161 206 5055 All Rights Reserved 2017. Document for issue as handout. Unique Identifier: CS36(17). Review date: November 2019 What is a tracheostomy? A tracheostomy
Tracheostomy Hope Building Neurosurgery 0161 206 5055 All Rights Reserved 2017. Document for issue as handout. Unique Identifier: CS36(17). Review date: November 2019 What is a tracheostomy? A tracheostomy
Tracheostomy and Ventilator Education Program Module 2: Respiratory Anatomy
 Tracheostomy and Ventilator Education Program Module 2: Respiratory Anatomy Disclaimer This material is intended for use by trained family members and caregivers of children with tracheostomies who are
Tracheostomy and Ventilator Education Program Module 2: Respiratory Anatomy Disclaimer This material is intended for use by trained family members and caregivers of children with tracheostomies who are
QOF indicator area: Chronic Obstructive Pulmonary disease (COPD)
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE QUALITY AND OUTCOMES FRAMEWORK (QOF) INDICATOR DEVELOPMENT PROGRAMME Cost impact statement: Chronic Obstructive Pulmonary Disease QOF indicator area:
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE QUALITY AND OUTCOMES FRAMEWORK (QOF) INDICATOR DEVELOPMENT PROGRAMME Cost impact statement: Chronic Obstructive Pulmonary Disease QOF indicator area:
CLINICAL CONSIDERATIONS FOR THE BUNNELL LIFE PULSE HIGH-FREQUENCY JET VENTILATOR
 CLINICAL CONSIDERATIONS FOR THE BUNNELL LIFE PULSE HIGH-FREQUENCY JET VENTILATOR 801-467-0800 Phone 800-800-HFJV (4358) Hotline TABLE OF CONTENTS Respiratory Care Considerations..3 Physician Considerations
CLINICAL CONSIDERATIONS FOR THE BUNNELL LIFE PULSE HIGH-FREQUENCY JET VENTILATOR 801-467-0800 Phone 800-800-HFJV (4358) Hotline TABLE OF CONTENTS Respiratory Care Considerations..3 Physician Considerations
Non-invasive Ventilation protocol For COPD
 NHS LANARKSHIRE MONKLANDS HOSPITAL Non-invasive Ventilation protocol For COPD April 2017 S Baird Review Date: Oct 2019 Approved by Medical Directorate Indications for Non-Invasive Ventilation (NIV) NIV
NHS LANARKSHIRE MONKLANDS HOSPITAL Non-invasive Ventilation protocol For COPD April 2017 S Baird Review Date: Oct 2019 Approved by Medical Directorate Indications for Non-Invasive Ventilation (NIV) NIV
I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device
 I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device II. Policy: Continuous Positive Airway Pressure CPAP by the Down's system will be instituted by Respiratory Therapy personnel
I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device II. Policy: Continuous Positive Airway Pressure CPAP by the Down's system will be instituted by Respiratory Therapy personnel
Clearing the air.. How to assist and rescue neck breathing patients. Presented by: Don Hall MCD, CCC/SLP Sarah Markel RRT, MHA
 Clearing the air.. How to assist and rescue neck breathing patients Presented by: Don Hall MCD, CCC/SLP Sarah Markel RRT, MHA Learning Objectives Define common terms identified with total (laryngectomy)
Clearing the air.. How to assist and rescue neck breathing patients Presented by: Don Hall MCD, CCC/SLP Sarah Markel RRT, MHA Learning Objectives Define common terms identified with total (laryngectomy)
Tracheostomy and laryngectomy airway emergencies: an overview for medical and nursing staff
 2013 Medical Journal Tracheostomy and laryngectomy airway emergencies: an overview for medical and nursing staff Steven Lobaz 1 and Paul Bush 2 1 ST6 and 2 Consultant Department of Anaesthesia and Intensive
2013 Medical Journal Tracheostomy and laryngectomy airway emergencies: an overview for medical and nursing staff Steven Lobaz 1 and Paul Bush 2 1 ST6 and 2 Consultant Department of Anaesthesia and Intensive
TRACHEOSTOMY. Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion
 TRACHEOSTOMY Definition Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion Indications for tracheostomy 1-upper airway obstruction with stridor, air hunger,
TRACHEOSTOMY Definition Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion Indications for tracheostomy 1-upper airway obstruction with stridor, air hunger,
CONTINUOUS POSITIVE AIRWAY PRESSURE (CPAP)
 CONTINUOUS POSITIVE AIRWAY PRESSURE (CPAP) Continuous Positive Airway Pressure (CPAP) may be used as an adjunctive therapy for the treatment of patients with suspected Acute Pulmonary Edema, Chronic Obstructive
CONTINUOUS POSITIVE AIRWAY PRESSURE (CPAP) Continuous Positive Airway Pressure (CPAP) may be used as an adjunctive therapy for the treatment of patients with suspected Acute Pulmonary Edema, Chronic Obstructive
Central venous access devices for children with lysosomal storage disorders
 Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Central venous access devices for children with lysosomal storage disorders This information explains about central
Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Central venous access devices for children with lysosomal storage disorders This information explains about central
NHS GREATER GLASGOW & CLYDE CONTROL OF INFECTION COMMITTEE STANDARD OPERATING PROCEDURE (SOP) INSERTION & MAINTENANCE OF INDWELLING
 Page Page 1 of 6 AIM STATEMENT REQUIREMENTS LOCATION TIMING PROCEDURE To minimise the risk of secondary infection as a result of urinary catheterisation. A urinary catheter bypasses the body s normal defence
Page Page 1 of 6 AIM STATEMENT REQUIREMENTS LOCATION TIMING PROCEDURE To minimise the risk of secondary infection as a result of urinary catheterisation. A urinary catheter bypasses the body s normal defence
PUMANI bcpap GUIDELINES FOR CLINICIANS. An Overview of the Pumani bcpap, Indications for bcpap, and Instructions for Use
 An Overview of the Pumani bcpap, Indications for bcpap, and Instructions for Use What is bcpap? bcpap stands for bubble Continuous Positive Airway Pressure. Sometimes called Continuous Distending Pressure,
An Overview of the Pumani bcpap, Indications for bcpap, and Instructions for Use What is bcpap? bcpap stands for bubble Continuous Positive Airway Pressure. Sometimes called Continuous Distending Pressure,
CCTC Minnesota Procedure: Minnesota Tube, Assisting with Insertion and Care of Patient
 CCTC Minnesota Procedure: Minnesota Tube, Assisting with Insertion and Care of Patient Purpose: To control bleeding from esophageal or gastric varices that have not responded to medical therapy (ie. Sclerotherapy,
CCTC Minnesota Procedure: Minnesota Tube, Assisting with Insertion and Care of Patient Purpose: To control bleeding from esophageal or gastric varices that have not responded to medical therapy (ie. Sclerotherapy,
CHANHASSEN FIRE DEPARTMENT MEDICAL / RESCUE SKILLS
 CHANHASSEN FIRE DEPARTMENT MEDICAL / RESCUE SKILLS PRACTICAL STATIONS CHANHASSEN FIRE DEPARTMENT MEDICAL / RESCUE SKILLS 1. CARDIAC ARREST MANAGEMENT 2. AIRWAY & RESPIRATORY MANAGEMENT 3. SPINAL IMMOBILIZATION
CHANHASSEN FIRE DEPARTMENT MEDICAL / RESCUE SKILLS PRACTICAL STATIONS CHANHASSEN FIRE DEPARTMENT MEDICAL / RESCUE SKILLS 1. CARDIAC ARREST MANAGEMENT 2. AIRWAY & RESPIRATORY MANAGEMENT 3. SPINAL IMMOBILIZATION
This information was created and reviewed through a partnership with the UAMS Patient and Family Advisory Councils.
 Tracheostomy Care You have a: Cuffed Tracheostomy Cuffless Tracheostomy What is a tracheostomy? A tracheostomy (sometimes called a trach rhymes with cake ) is a small opening, or stoma, in your throat.
Tracheostomy Care You have a: Cuffed Tracheostomy Cuffless Tracheostomy What is a tracheostomy? A tracheostomy (sometimes called a trach rhymes with cake ) is a small opening, or stoma, in your throat.
CONTROLLED DOCUMENT. Guidelines for the use of subcutaneous hydration in palliative care (hypodermoclysis) Controlled Document Number: CG259
 Guidelines for the use of subcutaneous hydration in palliative care (hypodermoclysis) CONTROLLED DOCUMENT CATEGORY: CLASSIFICATION: Controlled Document Number: Version Number: 1 Controlled Document Sponsor:
Guidelines for the use of subcutaneous hydration in palliative care (hypodermoclysis) CONTROLLED DOCUMENT CATEGORY: CLASSIFICATION: Controlled Document Number: Version Number: 1 Controlled Document Sponsor:
Upper Airway Obstruction
 Upper Airway Obstruction Adriaan Pentz Division of Otorhinolaryngology University of Stellenbosch and Tygerberg Hospital Stridor/Stertor Auditory manifestations of disordered respiratory function ie noisy
Upper Airway Obstruction Adriaan Pentz Division of Otorhinolaryngology University of Stellenbosch and Tygerberg Hospital Stridor/Stertor Auditory manifestations of disordered respiratory function ie noisy
B S D H UNLOCKING BARRIERS TO CARE
 B S D H UNLOCKING BARRIERS TO CARE Guidelines for the Development of Local Standards of Oral Health Care for Dependent, Dysphagic, Critically and Terminally Ill Patients Report of BSDH Working Group J.
B S D H UNLOCKING BARRIERS TO CARE Guidelines for the Development of Local Standards of Oral Health Care for Dependent, Dysphagic, Critically and Terminally Ill Patients Report of BSDH Working Group J.
Home Health Foundation, Inc. To create more permanent IV access for patients undergoing long term IV therapy.
 PROCEDURE ORIGINAL DATE: 06/99 Revised Date: 09/02 Home Health Foundation, Inc. SUBJECT: PURPOSE: MIDLINE CATHETER INSERTION To create more permanent IV access for patients undergoing long term IV therapy.
PROCEDURE ORIGINAL DATE: 06/99 Revised Date: 09/02 Home Health Foundation, Inc. SUBJECT: PURPOSE: MIDLINE CATHETER INSERTION To create more permanent IV access for patients undergoing long term IV therapy.
Face and Throat Injuries. Chapter 26
 Face and Throat Injuries Chapter 26 Anatomy of the Head Landmarks of the Neck Injuries to the Face Injuries around the face can lead to upper airway obstructions. Bleeding from the face can be profuse.
Face and Throat Injuries Chapter 26 Anatomy of the Head Landmarks of the Neck Injuries to the Face Injuries around the face can lead to upper airway obstructions. Bleeding from the face can be profuse.
POSTURAL DRAINAGE. To safely and effectively teach and supervise a service user undertaking Postural Drainage as a means of airways clearance.
 POSTURAL DRAINAGE AIM To safely and effectively teach and supervise a service user undertaking Postural Drainage as a means of airways clearance. To assess users ability to complete independent treatments
POSTURAL DRAINAGE AIM To safely and effectively teach and supervise a service user undertaking Postural Drainage as a means of airways clearance. To assess users ability to complete independent treatments
Intensive Care Diary. information. Radnor Ward. Salisbury NHS Foundation Trust
 information Intensive Care Diary Radnor Ward Salisbury NHS Foundation Trust Contents The purpose of your diary Intensive Care Diary Admission Day - What happened? Why am I here? Visitor s Blog / World
information Intensive Care Diary Radnor Ward Salisbury NHS Foundation Trust Contents The purpose of your diary Intensive Care Diary Admission Day - What happened? Why am I here? Visitor s Blog / World
COMMUNICATION. Communication and Swallowing post Tracheostomy. Role of SLT. Impact of Tracheostomy. Normal Speech. Facilitating Communication
 Communication and Swallowing post Tracheostomy. Role of SLT 1. 2. 3. Management of communication needs. Management of swallowing issues. Working with the multidisciplinary team to facilitate weaning. Impact
Communication and Swallowing post Tracheostomy. Role of SLT 1. 2. 3. Management of communication needs. Management of swallowing issues. Working with the multidisciplinary team to facilitate weaning. Impact
Procedure for removal and reinsertion of a supra pubic catheter
 Procedure for removal and reinsertion of a supra pubic catheter Equipment required collect prior to procedure Perform this procedure as an aseptic technique to minimise the risk of introducing Clean the
Procedure for removal and reinsertion of a supra pubic catheter Equipment required collect prior to procedure Perform this procedure as an aseptic technique to minimise the risk of introducing Clean the
Taking nose, throat and skin swabs. Clinical Skills
 Clinical Skills Taking nose, throat and skin swabs Carole Loveridge (Lecturer in Women s Health) Aims and Objectives Aims and Objectives The aim of this module is to facilitate learning regarding the purpose
Clinical Skills Taking nose, throat and skin swabs Carole Loveridge (Lecturer in Women s Health) Aims and Objectives Aims and Objectives The aim of this module is to facilitate learning regarding the purpose
BPG 03: Continuous Renal Replacement Therapy (CRRT)
 BPG 03: Continuous Renal Replacement Therapy (CRRT) Statement of Best Practice Patient s requiring Continuous Renal Replacement Therapy (CRRT) will receive appropriate therapy to meet their individual
BPG 03: Continuous Renal Replacement Therapy (CRRT) Statement of Best Practice Patient s requiring Continuous Renal Replacement Therapy (CRRT) will receive appropriate therapy to meet their individual
8/8/2013. Disclaimer. Tracheostomy Care in the Home. Polling Question 1. Upper Airway and Respiratory System
 Disclaimer Appendix 3 Declaration of Vested Interest Form Name of presenter: Heather Murgatroyd RRT RPSGT Name of employer: DeVilbiss Healthcare Tracheostomy Care in the Home Heather Murgatroyd, RRT, RPSGT
Disclaimer Appendix 3 Declaration of Vested Interest Form Name of presenter: Heather Murgatroyd RRT RPSGT Name of employer: DeVilbiss Healthcare Tracheostomy Care in the Home Heather Murgatroyd, RRT, RPSGT
Airway/Breathing. Chapter 5
 Airway/Breathing Chapter 5 Airway/Breathing Introduction Skillful, rapid assessment and management of airway and ventilation are critical to preventing morbidity and mortality. Airway compromise can occur
Airway/Breathing Chapter 5 Airway/Breathing Introduction Skillful, rapid assessment and management of airway and ventilation are critical to preventing morbidity and mortality. Airway compromise can occur
Effective Date: August 31, 2006 SUBJECT: CARE AND USE OF NEBULIZER AND INTERMITTENT POSITIVE PRESSURE BREATHING DEVICE
 COALINGA STATE HOSPITAL NURSING POLICY AND PROCEDURE MANUAL SECTION - Treatments POLICY NUMBER: 421 Effective Date: August 31, 2006 SUBJECT: CARE AND USE OF NEBULIZER AND INTERMITTENT POSITIVE PRESSURE
COALINGA STATE HOSPITAL NURSING POLICY AND PROCEDURE MANUAL SECTION - Treatments POLICY NUMBER: 421 Effective Date: August 31, 2006 SUBJECT: CARE AND USE OF NEBULIZER AND INTERMITTENT POSITIVE PRESSURE
Section 4.1 Paediatric Tracheostomy Introduction
 Bite- sized training from the GTC Section 4.1 Paediatric Tracheostomy Introduction This is one of a series of bite- sized chunks of educational material developed by the Global Tracheostomy Collaborative.
Bite- sized training from the GTC Section 4.1 Paediatric Tracheostomy Introduction This is one of a series of bite- sized chunks of educational material developed by the Global Tracheostomy Collaborative.
ADVANCED AIRWAY MANAGEMENT
 The Advanced Airway Management protocol should be used on all patients requiring advanced airway management procedures. This protocol is divided into three sections the Crash Airway Algorithm, the Rapid
The Advanced Airway Management protocol should be used on all patients requiring advanced airway management procedures. This protocol is divided into three sections the Crash Airway Algorithm, the Rapid
Effective Date: August 31, To provide guidelines for the proper administration of ear irrigation
 SUBJECT: EAR IRRIGATION 1. PURPOSE: COALINGA STATE HOSPITAL NURSING POLICY AND PROCEDURE MANUAL SECTION - Treatments POLICY NUMBER: 406 Effective Date: August 31, 2006 To provide guidelines for the proper
SUBJECT: EAR IRRIGATION 1. PURPOSE: COALINGA STATE HOSPITAL NURSING POLICY AND PROCEDURE MANUAL SECTION - Treatments POLICY NUMBER: 406 Effective Date: August 31, 2006 To provide guidelines for the proper
Critical Care of the Post-Surgical Patient
 Critical Care of the Post-Surgical Patient, Dr med vet, DEA, DECVIM-CA Many critically ill patients require surgical treatments. These patients often have multisystem abnormalities during the immediate
Critical Care of the Post-Surgical Patient, Dr med vet, DEA, DECVIM-CA Many critically ill patients require surgical treatments. These patients often have multisystem abnormalities during the immediate
RESPIRATORY REHABILITATION
 RESPIRATORY REHABILITATION By: Dr. Fatima Makee AL-Hakak University of kerbala College of nursing CHEST PHYSIOTHERAPY Chest physiotherapy (CPT) includes: 1.Postural drainage. 2.Chest percussion and vibration.
RESPIRATORY REHABILITATION By: Dr. Fatima Makee AL-Hakak University of kerbala College of nursing CHEST PHYSIOTHERAPY Chest physiotherapy (CPT) includes: 1.Postural drainage. 2.Chest percussion and vibration.
SOUTHERN HEALTH & SOCIAL CARE TRUST. Children & Young People s Directorate Procedure/Guidelines/Protocol Checklist & Version Control Sheet
 Children & Young People s Directorate Procedure/Guidelines/Protocol Checklist & Version Control Sheet 1 Name of Procedure/Guidelines/ Protocol: PROCEDURE FOR PERIPHERAL ARTERIAL CANNULATION 2 Purpose of
Children & Young People s Directorate Procedure/Guidelines/Protocol Checklist & Version Control Sheet 1 Name of Procedure/Guidelines/ Protocol: PROCEDURE FOR PERIPHERAL ARTERIAL CANNULATION 2 Purpose of
Urinary Catheter Passport SAMPLE COPY. A guide to looking after a urinary catheter. (for service users and healthcare workers) 2nd Edition
 Urinary Catheter Passport A guide to looking after a urinary catheter (for service users and healthcare workers) 2nd Edition Contact details Urinary Catheter Passport Service user Name Address Postcode
Urinary Catheter Passport A guide to looking after a urinary catheter (for service users and healthcare workers) 2nd Edition Contact details Urinary Catheter Passport Service user Name Address Postcode
Cough Assist. Information for patients, families and carers Therapy Services
 Cough Assist Information for patients, families and carers Therapy Services PROUD TO MAKE A DIFFERENCE SHEFFIELD TEACHING HOSPITALS NHS FOUNDATION TRUST page 2 of 16 Table of contents Why do I need a Cough
Cough Assist Information for patients, families and carers Therapy Services PROUD TO MAKE A DIFFERENCE SHEFFIELD TEACHING HOSPITALS NHS FOUNDATION TRUST page 2 of 16 Table of contents Why do I need a Cough
EMT. Chapter 8 Review
 EMT Chapter 8 Review 1. During the scene size-up, you should routinely determine all of the following, EXCEPT: A. the mechanism of injury or nature of illness. B. the ratio of pediatric patients to adult
EMT Chapter 8 Review 1. During the scene size-up, you should routinely determine all of the following, EXCEPT: A. the mechanism of injury or nature of illness. B. the ratio of pediatric patients to adult
Foundations of Critical Care Nursing Course. Tracheostomy Workbook
 Foundations of Critical Care Nursing Course Tracheostomy Workbook 1 Key Reference: Dawson D (2014) Essential principles:trachepstomy care in the adult patient, Nursing in Critical Care, Vol 19, 2 p.63-72.
Foundations of Critical Care Nursing Course Tracheostomy Workbook 1 Key Reference: Dawson D (2014) Essential principles:trachepstomy care in the adult patient, Nursing in Critical Care, Vol 19, 2 p.63-72.
Patient/Carer instructions for the administration of Subcutaneous Cytarabine
 Patient/Carer instructions for the administration of Subcutaneous Cytarabine This document covers the following information: What cytarabine is What subcutaneous means What happens if you decide to inject
Patient/Carer instructions for the administration of Subcutaneous Cytarabine This document covers the following information: What cytarabine is What subcutaneous means What happens if you decide to inject
Management of Upper Airway Obstruction in Pierre Robin Sequence
 Management of Upper Airway Obstruction in Pierre Robin Sequence South Wales Cleft Team Pierre Robin Sequence Triad of cleft palate, micrognathia and airway obstruction was described by St Hilaire in 1822,
Management of Upper Airway Obstruction in Pierre Robin Sequence South Wales Cleft Team Pierre Robin Sequence Triad of cleft palate, micrognathia and airway obstruction was described by St Hilaire in 1822,
