Guillain-Barré Syndrome (GBS) Banu Anlar Hacettepe University, Ankara, Turkey
|
|
|
- Elaine Daniel
- 5 years ago
- Views:
Transcription
1 Guillain-Barré Syndrome (GBS) Banu Anlar Hacettepe University, Ankara, Turkey
2 Disorder of spinal roots and peripheral nerves Most common acquired polyneuropathy in children. 1-2/100,000 general population Lifetime likelihood for any individual: 1:1000. M/F: may differ between subtypes, 1.4 in our series
3 Average age 6.3 years old, youngest 3 mo. Rare neonatal form Post infectious. No history of infection in 30%. Common responsible agents: C.jejuni, EBV, CMV, HSV, m.pneumoniae*. Asymptomatic infection: C. jejuni 50% no GI Sx. Post-immunisation? Surgery, transplantation.
4 Clinically: Walking difficulty 2-3 weeks (mean 12 days) after infection. sensory symptoms 20-60% (pain, paresthesia, hypoesthesia), sometimes only Sx. Weakness typically ascendent and symmetrical, up to flaccid quadriplegia. Rarely: locked-in However: proximal predominance, non-ascending types too. Approx % become nonambulatory during the illness. Korinthenberg 2007
5 Criteria Progressive, relatively symmetrical weakness of two or more limbs because of neuropathy. Areflexia. Progression < 4 weeks. Exclusion of other causes. Supportive Relatively symmetric weakness accompanied by numbness and/or tingling. Mild sensory involvement. VII or other cranial nerve involvement. Absence of fever. Typical CSF findings Demyelination on ENMG.
6 autonomic dysfunction. urinary or bowel problems <24 hours. respiratory failure: 25%. bulbar palsy, arm weakness esp. in rapid progression
7 Neurological examination: symmetrical weakness. Persistent asymmetry is rare diminished or absent DTR 90% sensory deficit stocking- and-glove, cranial nerve involvement (VII, VIII,III, VI)
8 Autonomic disturbance: (sympathetic overactivity + parasympathetic underactivity*) Tachycardia, life-threatening arrhythmias, hypotension, hypertension Bladder function, esp. in nonambulatory severe cases. GI dysmotility*: abdominal distention, pain, cramps, constipation, ileus *due to autoimmune damage of vagal nerve (stomach, small intestine, and much of the colon) and sacral parasympathetics (distal colon).
9 Course Progression 1-4 weeks Plateau few weeks Improvement few mo-yrs In general benign, cure expected in 80%. Sequealae 10-20%, mortality 3-10%. Treatment-related clinical fluctuations: may occur within 8 weeks after starting immunotherapy: still considered monophasic. Slower progression (> 4 weeks): Subacute form Progression after 8 weeks from onset or marked deterioration despite appropriate immunotherapy: acute-onset CIDP rather than GBS.
10 (relatively) negative features for outcome: Time of onset to admission <7 days. Inability to cough. Inability to stand. Inability to lift the elbows. Inability to lift the head. Increases in liver enzyme. Forced vital capacity < ml/kg. Maximum inspiratory pressure <30 cm H 2 O. Maximum expiratory pressure <40 cm H 2 O. More than a 30% decrease in either forced vital capacity or maximum inspiratory pressure within 24 h
11 Clinical Variants
12 Miller-Fisher S Complaint: Diplopia. Ataxia. No weakness. Ptosis, pupillary reflex: III. Bickerstaff's brainstem encephalitis MRI in MFS: cranial n. enhancement in BBE: cranial n. enhancement and posterior fossa, white matter, thalamic lesions 30% Bickerstaff reported 8 patients: acute ophthalmoplegia, ataxia + drowsiness extensor plantar responses (40%), hyperreflexia, or hemisensory loss. 92% had an antecedent illness. Flaccid symmetrical tetraparesis 60% overlapping GBS facial diplegia (45%) bulbar palsy (34%) ENMG: motor axonal degeneration Serum anti-gq1b IgG antibody 66% BBE, MFS and GBS are within the same spectrum
13 Other variants of GBS Pharyngeal-cervical-brachial form Oropharyngeal form Isolated forms: Pure sensory * Pure autonomic Regional or asymmetric distribution DTR normal or brisk (10%) (antigm1 or antigd1a, AMAN) *Notturno 2008: pure acute sensory ataxic neuropathy with anti-gq1b and anti-gd1b 2/3:recent C. jejuni infection. Anti-GD1b, -GQ1b -GD1b,-GT1a. Motor nerve conduction: normal. Sensory nerves: reduced amplitude or absent action potentials. All recovered in 2 months and ENMG: in 3-5 months
14 MFS or acute ataxic neuropathy? Acute sensory ataxic neuropathy : profound sensory ataxia no ophthalmoplegia Romberg sign + ataxic GBS? acute sensory ataxic neuropathy ataxic GBS AntiGQ1b antibodies 18% 65% AntiGD1b IgG antibodies 35% 14% variants within a continuous spectrum
15 overlapping MFS (1/3 original patients drowsiness) Brainstem encephalitis who develop limb weakness can overlap with GBS. BBE can have absence of H reflex. Bickerstaff s patients: 50% hypo/areflexia GBS pharyngeal-cervical-brachial variant overlaps with BBE, MFS Overlap between: GBS-ADEM, GBS-myelitis
16 Electrophysiological-pathological-geographical subtypes: A. inflammatory demyelinating polyradiculoneuropathy (AIDP), A. motor and sensory axonal neuropathy (AMAN/AMSAN), AMSAN: adults<children, not geographic. Abrupt onset, rapid progression. Mechanical ventilation: freq. Outcome: usually residual disability Certain types are related to geography and season. In Western Europe, N.America, Australia, 80-90% of GBS in children: AIDP In Northern China, S.America and Japan, 50-70% of GBS in children: AMAN. In Turkey: 50% AIDP, 40% AMAN.
17 Axonal forms also associated with antiganglioside antibodies All GBS patients might show promptly reversible nerve conduction failure or axonal degeneration. This suggests a common pathogenetic mechanism of Abmediated dysfunction or disruption at the nodes of Ranvier, resulting in a continuum of nerve pathologies from transitory conduction failure to axonal degeneration.
18 In 40% of patients, nerve conduction studies within 1 st week may suggest neuropathy without showing criteria for electrophysiological subtype. ENMG results later change in 24 38% of patients: accurate classification depends on timing? Rather than broadly categorizing each subtype as an axonal or demyelinating neuropathy, we propose new diagnostic criteria based on an inclusive set of clinical features Wakerley, Uncini, Yuki for the GBS Classification Group Nat. Rev. Neurol. 10, (2014)
19 Differential diagnosis
20 Acute myelopathy: inflammation (myelitis), compression, ischemia. Brainstem encephalitis (Bickerstaff s) Acute anterior poliomyelitis: polio, also non-polio enterovirus Hyperreflexia, Babinski (corticospinal findings may be absent early). enterovirus 71: acute flaccid paraparesis. Australia,Cambodia. Prodromal diarrhoea, lethargy, irritability, nuchal rigidity. Then acute flaccid paraparesis up to 20%. West Nile virus (WNV): poliomyelitis syndrome, asymmetric paralysis: monoparesis-quadriparesis. Enterovi 68? Five cases.
21 Chronic inflam. demyelinating p.n.pathy (CIDP) may start acutely, progress rapidly (< 4 weeks). Clinical or ENG evidence of ongoing demyelination. Usually more proximal, usually no antecedent inf. CNS infection: GBS can present with meningismus and IICP Polymyositis: Bilateral proximal weakness over weeks-months. Patient ill, myalgia, fever, muscles tenderness. (GBS also: poorly localized pain on the back, buttocks, legs, muscle pain -irritability, and dysesthesia as many as 50% at presentation).
22 Neuromuscular transm. disorders: myasthenia (no sensory symptoms). Botulism (infantile) nausea, vomiting, constipation, ophthalmoplegia, ptosis, dilated pupils, blurred vision, dysphagia, dysarthria, urinary retention. No cranial involvement rules out botulism. Periodic paralyses with hypo K, hypo P Pseudoparalysis (trauma, JIA, ARF). Other polyneuropathies: CMV in immunosuppressed patients toxic (axonal). metabolic: Leigh S, vit B1/B12 def. critical illness, vasculitic, Lyme (endemic area, season; tick bite, CSF pleocytosis. Axonal) porphyria Usually more asymmetric. Axonal. In 50% weakness starts in the arms -- may be confused with pharyngeal-cervical-brachial GBS. Severe abdominal pain, psychiatric symptoms or seizures.
23 Diagnostic delays and errors in young children: Roodbol et al initially misdiagnosed delay until going to pediatrician Delay until GBS Dx Common Sx 23 preschool 68% 5 days 3 days refusal to walk leg pain 32 older 21% 5 days 0 days weakness, paresthesia myopathy, tonsillitis, meningitis, rheumatoid disorders, coxitis, discitis
24 Laboratory: may be normal in the first days. Diagnosis essentially clinical CSF protein Increased in 50% on day 1, in 90% day 15. pleocytosis: think infectious (HIV, CMV, Lyme), sarcoid, Leu/lymphoma ENMG abnormal after 2nd week: features of acquired demyelination. temporal dispersion, prolonged distal and F-wave latencies, non-uniform slowing conduction velocities, conduction block. In 1.week: 50-70% sural-sparing pattern in sensory n. normal in sural + abnormal in upper extremities (ulnar or median) Frequent, less specific: absent H-reflexes, low motor CMAP amplitudes on distal stimulation, prolonged F-wave responses. Related to prognosis: very low CMAPs on distal stimulation at initial testing: probability of poor outcome. Often non-diagnostic in the first week. Do not delay treatment, if GBS likely
25 Required for Diagnosis: Progressive weakness in two or more limbs. Areflexia (distal areflexia + proximal hyporeflexia enough if other features are consistent). Strongly Supportive of Diagnosis: Progression <4 weeks 50% by 2 wks, 80% by 3 wks, 90% by 4 wks. Relative symmetry, seldom absolute Mild sensory symptoms or signs. Cranial nerve VII 50 %, freq.bilateral. Autonomic dysfunction. Recovery begins 2-4 weeks after progression stops. Absence of fever at onset of neurologic symptoms.
26 THESE SUGGEST VARIANT CLINICAL FORMS: 1. Fever at onset of neuropathy 2. Severe sensory loss with pain 3. Progression >4 wks. 4. Cessation of progression- no recovery, or major residual deficit 5. Sphincter dysfunction (usually bladder only transiently) 6. CNS involvement (occasional patients: extensor plantar responses and ill-defined sensory levels) 7.Transient neck and back stiffness early in the course, resolution within days.
27 Cast doubt on the diagnosis Marked, persistent asymmetry Bladder or bowel dysfunction at onset. Persistent bladder or bowel dysfunction. Sharp sensory level. CSF: >50 mononuclear leukocytes or any polymorphonuclear leukocytes No CSF protein rise in 1-10 weeks after onset (rare).
28 Is autoimmune serology helpful in the diagnosis? 50-60% of acute-phase sera: Ab against at least one ganglioside Titers decrease with clinical improvement: cause, not a result, of nerve damage Anti-GQ1b and GT1a: Miller Fisher syndrome and GBS with ophthalmoplegia. Anti-GQ1b in ~95% of patients with acute MFS and approx. 2/3 of BBE. the anti-gq1b antibody syndrome. anti-gt1a: pharyngeal-cervical-brachial variant anti- GM1 and GM1b: AMAN BUT many centres test only for anti-gm1 and anti-gq1b and results are often delayed.
29 Gangliosides: Each ganglioside has particular distribution in the peripheral nervous system Biochemical analysis of extracts: GQ1b is present in cranial n. and spinal nerve roots (ventral and dorsal): III, IV, VI have higher content GQ1b interact with receptors or signal transducers; Abs may affect the function of the axon or Schwann cell impair nerve conduction Kusunoki 1999
30 GM1 on the surface of both axon (arrow) and dendrites of stage 3 neurons PATHOGENESIS Stage 5 neuron: dendrite (arrowheads) is devoid of GM1 staining. Ledesma et al 1999
31 Oculomotor nerve immunostained with anti-gq monoclonal Ab. unstained axoplasm surrounded by a stained portion. Chiba, Neurology 1993
32 Some Abs may be related to prognosis: Response to plasmapheresis may vary with the IgG subclass of the Ab Anti-ganglioside Abs are highly variable in specificity, avidity, titer and subclass. C. jejuni. GM1, GM1b, GD1a, GalNAc-GD1a and pure motor or axonal variants C. jejuni. also GQ1b and GT1a and oculomotor weakness GM1, GM1b, GD1a, GalNAc-GD1a : diarrhea. Patients with preceding diarrhea --poor recovery after IVIg. Preceding URTI and negative C. jejuni serology. IgG3 and IgG1-better recovery after IVIg. H. influenzae IOS:. GM1 CMV IgM against GM2, severe motor-sensory, frequent VII. nerve Yuki 2012
33 inf. agent Camp.jejuni Hem. infl. infection diarrhea URI molecular mimicry ganglioside ganglioside Ab to motor gangl. IgG1 (and IgA) IgG3 and IgG1 Neurological signs Pure motor Outcome after IVIg poor good
34 Polyclonal antibodies against GA1 GM1 GM1 GM1b GM2 GD1a GalNAc-GD1a GD1b GD2 GD3 GT1a GT1b GQ1b Neurological disease GBS, MMN,lower motor neuron dis., motor neuropathy, CIDP GBS, AMAN, MMN, lower motor neuron dis, ALS, motor neuropathy CIDP GBS GBS GBS, motor-sensory neuropathy AMAN, MMN, motor neuropathy GBS AMAN, motor neuropathy GBS ataxic GBS MMN CIDP, ataxic sensory neuropathy, Chr. ataxic sensory neuropathy w.ophthalmoplegia Chr. ataxic sensory neuropathy w.ophthalmoplegia Chr. ataxic sensory neuropathy w.ophthalmoplegia Oropharyngeal GBS, MFS, BBE, acute ophtalmoparesis Chr. ataxic sensory neuropathy w.ophthalmoplegia MFS, BBE,acute ophtalmoparesis, Chr. ataxic sensory neuropathy w.ophthalmoplegia
35 How Are Abs Synthesized? Both T-cell dependent and T-independent response against glycans Anti-GM1 antibodies in GBS: IgG1 or IgG3 subclass are T-cell-dependent T-cell-independent anti-gm1 IgM found at low level in normal individuals, but higher titers in neuropathy patients.
36 Immunogenicity of GM1 in humans: bovine brain gangliosides and purified GM1 were applied for treatment of various diseases a few patients developed GBS with antigm1 antibodies The New York Times 2008
37 Molecular mimicry or better fit hypothesis? B-lymphocytes undergo mutation of their V genes and modification of their binding sites. Some of these mutations produce a better fit in the IgM antibody/gm1 contact area, allowing new binding points (binding site expansion) that increase affinity for GM1. In most normal individuals, high-affinity B-lymphocytes are absent and there is no immune response to GM1. In GBS, the antibody response has class-switched from IgM to complement-fixing IgG1 and IgG3 isotypes. Control mechanism for drift: normal plasma contains Abs that block binding of pathogenic anti-gm1 antibodies IVIG may do the same
38 Effector mechanisms Nerve terminal damage after Ab and C binding: Demyelination earliest at proximal nerve roots and distal IM nerve twigs where the blood-nerve barriers are weak: the perisynaptic Schwann cell can be damaged by antiganglioside Ab. Activation of C pathway-- membrane attack complex --terminal axon cytoskeleton, mitochondria damage AIDP: demyelination, lymphocytic infiltration, macrophage-mediated clearance of myelin Axonal form: Target epitopes are likely the constituents of the axolemma of motor fibers. Macrophages attracted to Ranvier by C products dissect into the internodal periaxonal spaces, displace axons from inner Schwann cell plasmalemma, and cause axonal degeneration: more protracted course and incomplete recovery. Ab binding may alter Na+ channel function, causing conduction block: rapid improvement.
39 Genetic predisposition? A patient with severe tetraparesis, bulbar syndrome, and ophthalmoparesis. The nadir was reached within 1 day, requiring mechanical ventilation. Molecular analysis revealed a duplication at chromosome 17p , the genetic cause of Charcot-Marie-Tooth disease type 1A (CMT1A). (Munch et al 08)
40 Treatment: only supportive treatment reduces mortality. SPECIFIC Treatment: Admit to hospital Close follow-up during progressive phase (ventilation bag, tracheotomy set bedside). Intravenous immunoglobulin (IVIg) in the first 2-4 weeks of symptoms Plasmapheresis (PE) (1 plasma vol.50 ml/kg with 5% alb.) PE done after 7 days, IVIg given after 2 weeks benefit questionable.
41 Mild GBS: IVIg (2 PE for adults). Moderate/Severe GBS, bulbar GBS, BBE overlapping GBS: PE, IVIg (4 PE for adults). MFS:? Outcome good IVIG after PE: not significantly better than PE alone Pediatric trial comparing 2 g/kg IVIG over 2 days vs. 5 days: no difference in recovery. Two-day group: more early relapses. In children: moderate/severe GBS, IVIG the first-line drug protracted cases: IV steroids added to IVIG may hasten independent walking. If such therapy fails: PE Oral corticosteroids? combined with IVIg, may hasten recovery. Hughes et al Brain, 2007
42 Complications of IVIg: Certain do not respond, or even worsen after Expensive and not free of side effects Acute tubular necrosis: products with high sucrose. Anaphylactic reaction due to the IgA in patients with common variable immunodeficiency Immunoadsorption removes Ig from circulation, fewer side effects.
43 SYMPTOMATIC TREATMENT Monitoring and management for Respiratory and Airway Compromise Respiratory failure requiring mechanical ventilation: 20-30% of adults, 9% in our series Monitor signs of respiratory insufficiency: anxiety, pallor, restlesness, tachypnea, use of accessory muscles, asynchronous chest and abdomen movements, tachycardia At risk for mechanical ventilation: time from onset to admission <1 week, facial weakness, inability to cough, inability to lift head off pillow, atelectasis on chest X-ray demyelinating axonal? Sometimes mechanical ventilation is indicated because of severe bulbar dysfunction: secretions, risk of aspiration. (Burns, 2008)
44 Complications of mechanical ventilation: pneumonia, pulmonary embolus, bacteremia. Tracheostomy-when? 2 weeks following intubation, but if pulmonary function tests and strength are improving at 2 weeks, allow 1 more week Early tracheotomy improves patient comfort, airway safety, weaning. but complications: hemorrhage, infection, dislodgement of the tube
45 Autonomic Dysfunction: take care during patient care Severe dysautonomia most likely at clinical nadir (such as intensive care patient) but can also occur early in the disease Cardiac and hemodynamic disturbances: tachycardia, hypertension*, postural hypotension * --identify patients at risk for severe bradycardia, heart block, and asystole. Endotracheal suction and pharmacological agents may provoke bradycardia and asystole: hyperoxygenate before suction to minimize the effects of severe bradycardia. *labile; can be followed by hypotension. Do not leave patients at risk upright. Blood pressure and heart rate monitoring until clinical improvement *Disturbances of heart rate and blood pressure can also be due to: pulmonary embolus, sepsis, dehydration, pain, and electrolyte disturbance
46 Do: routine abdominal auscultation. Tx: Interrupt enteral feeding, nasogastric suctioning, and erythromycin. If possible, avoid narcotics Parenteral nutrition if > a few days.
47 Quadriplegic patients should not be left unattended in the sitting position without assessment of orthostatic hypotension. Intravascular volume should be maintained, particularly during positive-pressure ventilation. Drugs with hypotensive side effects should be avoided Arrhythmias frequently occur during suctioning. Succinylcholine should be avoided. Plasma exchange can cause hypotension and electrolyte disturbances.
48 Pain Management Back and extremity pain Not correlated with degree of disability. 1.try acetaminophen or nonsteroidal anti-inflammatory agents 2.as for neuropathic pain: GBP, CBZ, Amitriptylline
49 prevention of complications (bed sores, urinary infections, pulmonary complications or renal calculi due to immobilization) by: positioning, physical therapy and rehabilitation as soon as patient stable exercise regimen range-of-motion exercises to prevent shortening of weak muscles, joint contractures strength exercises, but avoid overworking muscles orthotics sensory reintegration techn., repetitive exercises for proprioceptive loss and ataxia Persistent fatigue is a common problem due to permanent axon loss
50 PROGNOSIS and OUTCOME Most of the recovery in first year, but even during 2-6 years Persistent disability in 20-30% of adults, much less in children more common with axonal, severe, mechanically ventilated patients rapid progression associated with long-term prognosis. In some studies, axonal involvement at initial ENMG also related to poorer outcome. GBS disability score at 2 weeks after admission, diarrhea age
51 Guillain-Barré Syndrome Disability Score 0 = healthy state 1 = minor symptoms and capable of running 2 = able to walk >10 m without assistance,unable to run 3 = able to walk 10 m across an open space with help 4 = bedridden or chairbound 5 = req.assisted ventilation for at least part of the day 6 = dead
52 Future Immunisations Withhold 1 year, then continue routine immunization Influenza, tetanus, and typhoid: associated with relapse Influenza vaccination: 1-2 additional GBS cases/10 6 doses. Weigh risk/benefit British GBS patients: 11/311 (3.5%) reported symptoms within 6 weeks of immunization No patient needed hospitalization or treatment.
53 Clinical Characteristics of Guillain-Barre Syndrome Çetin Okuyaz, Semra Kurul, and *the Turkish Guillain-Barre Study Group M:F 1.3 Age 6.7 ± 4.2 years (6.2) ENMG: 48% demyelinating, 38% axonal. Axonal-demyelinating: only difference in severity score: axonal worse at onset (p<0.022) CSF protein mg/dl, elevated in 82%. Clinical score (weakness) at onset and discharge: less in patients with increased CSF protein (demyelination rather than axonal, or timing of LP: milder cases admitted and investigated later, therefore protein higher ) Patients weaker at onset require ventilation, stay longer, and are weaker 6-12 months after discharge.
54 All Cases Electrophysiological subtypes p Demyelinating Axonal Age (y) 6.74 ± ± ± 4.34 y >0.05 Sex 130 M, 96 F 42 M, 38 F 49 M, 30 F >0.05 Duration (d) 7.93 ± ± ± 8.84 >0.05 weakness Duration (d) ± ± ± >0.05 hospitalization CSF protein mg/dl ± ± ± d >0.05 Distribution weakness % Parap. (53.4) Tetrap. (31.7) Tetrap.+ bulbar (14.9) Parap. (54.4) Tetrap. (34.2) Tetrap.+ bulbar (11.4) Parap. (43.0) Tetrap. (38.0) Tetrap.+ bulbar (19.0) >0.05 Sensory % >0.05 Sphincter % >0.05 Cranial n.% >0.05 Ventilation requirement % Treatment % None (24.8) IVIg (0.8) Plasmaph. (10.4) >0.05 None (28.3) IVIg (56.3) IVIg+Plasmaph.(15.0) None (26.6) IVIg (58.2) Plasmaph.(12.7) >0.05
55 9 year old girl admitted for progressive ascending weakness for 5 days. NE: can not stand up. DTR absent CSF cell count of /l and 89 mg/dl protein. NCV decreased. Case: IVIg 5 days no improvement. Headache, meningism on day 4 of IVIg CNS lesions can be silent
56 Alkan et al 2009
57 Case: 9 y.o. girl Lacroix et al 2010 fever for 10 days, productive cough, colicky abdominal pain, vomiting. Clarithromycin for interstitial pneumonia on chest X-ray. Also headache, diffuse leg pain, weakness PE: respiratory rate 30 breaths/min, pulse 100 /min. Retractions, nasal flaring, abdominal breathing. Oxygen saturation 88%. Hypoventilation of the right lung, wheezing, diffuse crackles. Blood pressure high (165/105 mm Hg). NE: Neck pain and stiffness on anterior flexion. DTR absent spinal cord CT normal Had to be intubated CSF normal A second lumbar puncture on day 6: marked increase of protein
58 Case 2-year-old girl transferred with lethargy, anorexia, and inability to walk for 1 day. Muscle tone decreased in all four extremities; able to sit briefly, unable to stand. CSF: Normal Worsens in 24 h: no movements in extremities 36 h: lethargic and difficult to arouse, unable to follow commands, no verbal output. small reactive pupils, eye movements intact. Motor examination, truncal hypotonia, poor head control, unable to sit w/o support. minimal spontaneous movements in extremities; briefly able to elevate upper and lower extremities against gravity. Feels noxious stimuli applied to all four extremities. DTR 2+ in biceps and triceps, absent in patella, and 1+ in Achilles. plantar responses flexor Neurological consultation. GBS?
59 Important part of PE Burke et al 2014
60 removal of the tick, lethargy significantly improved within hours Next day: strength near normal. (+) patellar reflex, but Achilles, biceps, and triceps reflexes absent able to walk and run without assistance 2 weeks: N the most frequent attachment site retroauricular skin. The pathophysiology of tick paralysis by ixobotoxin, the neurotoxin released by Dermacentor species, involves reduction of muscle action potential with sparing of neuromuscular transmission. nonspecific lethargy and weakness, acute ataxia, symmetric flaccid paralysis with areflexia.
61 Burke et al 2005
62
Supplementary Online Content
 Supplementary Online Content Stevens O, Claeys KG, Poesen K, Veroniek S, Van Damme P. Diagnostic challenges and clinical characteristics of hepatitis E virus associated Guillain- Barré syndrome. JAMA Neurol.
Supplementary Online Content Stevens O, Claeys KG, Poesen K, Veroniek S, Van Damme P. Diagnostic challenges and clinical characteristics of hepatitis E virus associated Guillain- Barré syndrome. JAMA Neurol.
Guillain-Barré Syndrome
 Guillain-Barré Syndrome Ouch! www.philippelefevre.com Guillain-Barré Syndrome Acute post-infective polyneuropathy Heterogeneous condition with several variant forms Lipid A Neuronal Ganglioside Pathogenesis
Guillain-Barré Syndrome Ouch! www.philippelefevre.com Guillain-Barré Syndrome Acute post-infective polyneuropathy Heterogeneous condition with several variant forms Lipid A Neuronal Ganglioside Pathogenesis
Guillain-Barré syndrome and related disorders
 Guillain-Barré syndrome and related disorders Dr Benjamin Wakerley Department of Neurology Gloucestershire Royal Hospital Disclosures Novartis - educational grant Guillain-Barré syndrome and related disorders
Guillain-Barré syndrome and related disorders Dr Benjamin Wakerley Department of Neurology Gloucestershire Royal Hospital Disclosures Novartis - educational grant Guillain-Barré syndrome and related disorders
Immune Mediated Neuropathies
 Immune Mediated Neuropathies Hernan Gatuslao, M.D. Assistant Professor Department of Neurology Virginia Commonwealth University School of Medicine AIDP and CIDP Acute inflammatory demyelinating polyneuropathy
Immune Mediated Neuropathies Hernan Gatuslao, M.D. Assistant Professor Department of Neurology Virginia Commonwealth University School of Medicine AIDP and CIDP Acute inflammatory demyelinating polyneuropathy
Miller Fisher Syndrome A variant of Guillan Barré Syndrome. Sarah I. Sheikh, BM BCh, MRCP
 Miller Fisher Syndrome A variant of Guillan Barré Syndrome Sarah I. Sheikh, BM BCh, MRCP History of GBS 1859 Jean Baptiste Octave Landry de Thézillat (1826-1865) published his observation on ascending
Miller Fisher Syndrome A variant of Guillan Barré Syndrome Sarah I. Sheikh, BM BCh, MRCP History of GBS 1859 Jean Baptiste Octave Landry de Thézillat (1826-1865) published his observation on ascending
Infection-Associated Neurological Syndromes
 Infection-Associated Neurological Syndromes Anand P, MD PhD Medical Director, BloodCenter of Wisconsin Assistant Professor, Medical College of Wisconsin ASFA Annual Meeting San Antonio, TX, May 8th, 2015
Infection-Associated Neurological Syndromes Anand P, MD PhD Medical Director, BloodCenter of Wisconsin Assistant Professor, Medical College of Wisconsin ASFA Annual Meeting San Antonio, TX, May 8th, 2015
Peripheral neuropathies, neuromuscular junction disorders, & CNS myelin diseases
 Peripheral neuropathies, neuromuscular junction disorders, & CNS myelin diseases Peripheral neuropathies according to which part affected Axonal Demyelinating with axonal sparing Many times: mixed features
Peripheral neuropathies, neuromuscular junction disorders, & CNS myelin diseases Peripheral neuropathies according to which part affected Axonal Demyelinating with axonal sparing Many times: mixed features
5.1 Alex.
 5.1 Alex http://tinyurl.com/neuromakessense Alex is a 20-year-old full-time national serviceman. His only past medical history is asthma, presents to A&E with a 4-day history of bilateral finger weakness
5.1 Alex http://tinyurl.com/neuromakessense Alex is a 20-year-old full-time national serviceman. His only past medical history is asthma, presents to A&E with a 4-day history of bilateral finger weakness
LE SYNDROME DE GUILLAIN-BARRE
 FORMATION UNIVERSITAIRE SPECIFIQUE (FUS) Enseignement interuniversitaire MASTER DE SPECIALISATION EN MEDECINE INTERNE Samedi 19 dećembre 2015 Institute of Neurosciences LE SYNDROME DE GUILLAIN-BARRE Peter
FORMATION UNIVERSITAIRE SPECIFIQUE (FUS) Enseignement interuniversitaire MASTER DE SPECIALISATION EN MEDECINE INTERNE Samedi 19 dećembre 2015 Institute of Neurosciences LE SYNDROME DE GUILLAIN-BARRE Peter
Immunopathology of Guillain- Barré syndrome. L. Magy Service de Neurologie Centre de Référence 'Neuropathies Périphériques Rares' CHU Limoges, France
 Immunopathology of Guillain- Barré syndrome L. Magy Service de Neurologie Centre de Référence 'Neuropathies Périphériques Rares' CHU Limoges, France What is Guillain-Barré syndrome? An immune-mediated
Immunopathology of Guillain- Barré syndrome L. Magy Service de Neurologie Centre de Référence 'Neuropathies Périphériques Rares' CHU Limoges, France What is Guillain-Barré syndrome? An immune-mediated
Case Report An Unusual Case of Recurrent Guillain-Barre Syndrome of a Different Subtype Five Years after Initial Diagnosis
 Case Reports in Neurological Medicine Volume 2013, Article ID 356157, 4 pages http://dx.doi.org/10.1155/2013/356157 Case Report An Unusual Case of Recurrent Guillain-Barre Syndrome of a Different Subtype
Case Reports in Neurological Medicine Volume 2013, Article ID 356157, 4 pages http://dx.doi.org/10.1155/2013/356157 Case Report An Unusual Case of Recurrent Guillain-Barre Syndrome of a Different Subtype
COPYRIGHT 2012 THE TRANSVERSE MYELITIS ASSOCIATION. ALL RIGHTS RESERVED
 The Transverse Myelitis Association...advocating for those with acute disseminated encephalomyelitis, neuromyelitis optica, optic neuritis and transverse myelitis ACUTE DISSEMINATED ENCEPHALOMYELITIS (ADEM)
The Transverse Myelitis Association...advocating for those with acute disseminated encephalomyelitis, neuromyelitis optica, optic neuritis and transverse myelitis ACUTE DISSEMINATED ENCEPHALOMYELITIS (ADEM)
Evaluation of Peripheral Neuropathy. Evaluation of Peripheral Neuropathy - Introduction
 Evaluation of Peripheral Neuropathy Chris Edwards, MD Ochsner Neurology, Main Campus Evaluation of Peripheral Neuropathy - Introduction A very common complaint in the clinic Presentation is variable Multiple
Evaluation of Peripheral Neuropathy Chris Edwards, MD Ochsner Neurology, Main Campus Evaluation of Peripheral Neuropathy - Introduction A very common complaint in the clinic Presentation is variable Multiple
ORIGINAL CONTRIBUTION. Continuous Spectrum of Pharyngeal-Cervical-Brachial Variant of Guillain-Barré Syndrome
 ORIGINAL CONTRIBUTION Continuous Spectrum of Pharyngeal-Cervical-Brachial Variant of Guillain-Barré Syndrome Takahide Nagashima, MD, PhD; Michiaki Koga, MD, PhD; Masaaki Odaka, MD, PhD; Koichi Hirata,
ORIGINAL CONTRIBUTION Continuous Spectrum of Pharyngeal-Cervical-Brachial Variant of Guillain-Barré Syndrome Takahide Nagashima, MD, PhD; Michiaki Koga, MD, PhD; Masaaki Odaka, MD, PhD; Koichi Hirata,
Seema Sikka, MD January 18, 2014 TRANSVERSE MYELITIS: A CLINICAL OVERVIEW
 Seema Sikka, MD January 18, 2014 TRANSVERSE MYELITIS: A CLINICAL OVERVIEW DISCLOSURES I have no industry relationships to disclose. I will not discuss off-label use. OBJECTIVES: TRANSVERSE MYELITIS Review
Seema Sikka, MD January 18, 2014 TRANSVERSE MYELITIS: A CLINICAL OVERVIEW DISCLOSURES I have no industry relationships to disclose. I will not discuss off-label use. OBJECTIVES: TRANSVERSE MYELITIS Review
The Neurologic Examination. John W. Engstrom, M.D. University of California San Francisco School of Medicine
 The Neurologic Examination John W. Engstrom, M.D. University of California San Francisco School of Medicine Overview The Neurologic Examination Mental status demonstration/questions Cranial nerves demonstration/questions
The Neurologic Examination John W. Engstrom, M.D. University of California San Francisco School of Medicine Overview The Neurologic Examination Mental status demonstration/questions Cranial nerves demonstration/questions
AUTOIMMUNE DISORDERS IN THE ACUTE SETTING
 AUTOIMMUNE DISORDERS IN THE ACUTE SETTING Diagnosis and Treatment Goals Aimee Borazanci, MD BNI Neuroimmunology Objectives Give an update on the causes for admission, clinical features, and outcomes of
AUTOIMMUNE DISORDERS IN THE ACUTE SETTING Diagnosis and Treatment Goals Aimee Borazanci, MD BNI Neuroimmunology Objectives Give an update on the causes for admission, clinical features, and outcomes of
Systematic Approach to Weakness Polat DURUKAN
 Systematic Approach to Weakness Polat DURUKAN Erciyes University Faculty of Medicine Department of EM, Kayseri, Turkey Subarachnoid hemorrhage? Hypoglycemia? Guillain-Barré syndrome? Sepsis? Dehydration
Systematic Approach to Weakness Polat DURUKAN Erciyes University Faculty of Medicine Department of EM, Kayseri, Turkey Subarachnoid hemorrhage? Hypoglycemia? Guillain-Barré syndrome? Sepsis? Dehydration
Risk Factors of Respiratory Failure in Children with Guillain-Barré Syndrome
 Pediatrics and Neonatology (2012) 53, 295e299 Available online at www.sciencedirect.com journal homepage: http://www.pediatr-neonatol.com ORIGINAL ARTICLE Risk Factors of Respiratory Failure in Children
Pediatrics and Neonatology (2012) 53, 295e299 Available online at www.sciencedirect.com journal homepage: http://www.pediatr-neonatol.com ORIGINAL ARTICLE Risk Factors of Respiratory Failure in Children
Guillain-Barré Syndrome in a Patient with Pneumococcal Meningitis
 Guillain-Barré Syndrome in a Patient with Pneumococcal Meningitis An Uncommon Complication of a Common Infection ACP Wisconsin, September 2017 Jesse Maupin, MD (PGY-2) University of Wisconsin Hospital
Guillain-Barré Syndrome in a Patient with Pneumococcal Meningitis An Uncommon Complication of a Common Infection ACP Wisconsin, September 2017 Jesse Maupin, MD (PGY-2) University of Wisconsin Hospital
A comparison of two patients with Guillain-Barre Syndrome J O H N C O R S I N O, S P T
 A comparison of two patients with Guillain-Barre Syndrome J O H N C O R S I N O, S P T Guillain-Barre Acute inflammatory demyelinating polyneuropathy Highly diverse presentation, course, outcome Miller-Fisher:
A comparison of two patients with Guillain-Barre Syndrome J O H N C O R S I N O, S P T Guillain-Barre Acute inflammatory demyelinating polyneuropathy Highly diverse presentation, course, outcome Miller-Fisher:
CIDP + MMN - how to diagnose and treat. Dr Hadi Manji
 CIDP + MMN - how to diagnose and treat Dr Hadi Manji Outline Introduction CIDP Diagnosis Clinical features MRI Nerve conduction tests Lumbar puncture Nerve biopsy Treatment IV Ig Steroids Plasma Exchnage
CIDP + MMN - how to diagnose and treat Dr Hadi Manji Outline Introduction CIDP Diagnosis Clinical features MRI Nerve conduction tests Lumbar puncture Nerve biopsy Treatment IV Ig Steroids Plasma Exchnage
SEMESTER Suriname study. The Suriname Meningo- encephalitis Study (SMS) Introduction. SMS- protocol version 3.4. Principal investigators:
 SEMESTER Suriname study The Suriname Meningo- encephalitis Study (SMS) Principal investigators: E.C.M. van Gorp 1,2 and S. Vreden 3 Participating investigators: H. Alberga 4, M. Baptista 5, R. Cruden 4,
SEMESTER Suriname study The Suriname Meningo- encephalitis Study (SMS) Principal investigators: E.C.M. van Gorp 1,2 and S. Vreden 3 Participating investigators: H. Alberga 4, M. Baptista 5, R. Cruden 4,
High Yield Neurological Examination
 High Yield Neurological Examination Vanja Douglas, MD Sara & Evan Williams Foundation Endowed Neurohospitalist Chair Director, Neurohospitalist Division Associate Professor of Clinical Neurology UCSF Department
High Yield Neurological Examination Vanja Douglas, MD Sara & Evan Williams Foundation Endowed Neurohospitalist Chair Director, Neurohospitalist Division Associate Professor of Clinical Neurology UCSF Department
Neurologic Examination
 John W. Engstrom, MD October 16, 2015 Neurologic Examination Overview The Neurologic Examination Neurologic Examination John W. Engstrom, M.D. Dept. of Neurology University of California, San Francisco
John W. Engstrom, MD October 16, 2015 Neurologic Examination Overview The Neurologic Examination Neurologic Examination John W. Engstrom, M.D. Dept. of Neurology University of California, San Francisco
Dysphagia as initial manifestation of Guillan-Barrè Syndrome in a child Elda Pitrolo, Simona Santucci, Chiara Cuzzupè, Filippo De Luca
 Clinical Case Seminar A7(1-5 ) Dysphagia as initial manifestation of Guillan-Barrè Syndrome in a child Elda Pitrolo, Simona Santucci, Chiara Cuzzupè, Filippo De Luca Department of Human Pathology of Adulthood
Clinical Case Seminar A7(1-5 ) Dysphagia as initial manifestation of Guillan-Barrè Syndrome in a child Elda Pitrolo, Simona Santucci, Chiara Cuzzupè, Filippo De Luca Department of Human Pathology of Adulthood
The Role of Cytomegalovirus, Haemophilus Influenzae and Epstein Barr Virus in Guillain Barre Syndrome
 ORIGINAL REPORT The Role of Cytomegalovirus, Haemophilus Influenzae and Epstein Barr Virus in Guillain Barre Syndrome Shahriar Nafissi 1, Zahra Vahabi 1, Maryam Sadeghi Ghahar 2, Ali Akbar Amirzargar 2,
ORIGINAL REPORT The Role of Cytomegalovirus, Haemophilus Influenzae and Epstein Barr Virus in Guillain Barre Syndrome Shahriar Nafissi 1, Zahra Vahabi 1, Maryam Sadeghi Ghahar 2, Ali Akbar Amirzargar 2,
S everal antibodies against gangliosides have been detected
 568 PAPER Central motor conduction in patients with anti-ganglioside antibody associated neuropathy syndromes and hyperreflexia Y Oshima, T Mitsui, H Yoshino, I Endo, M Kunishige, A Asano, T Matsumoto...
568 PAPER Central motor conduction in patients with anti-ganglioside antibody associated neuropathy syndromes and hyperreflexia Y Oshima, T Mitsui, H Yoshino, I Endo, M Kunishige, A Asano, T Matsumoto...
Central nervous system
 Central nervous system By Dr. Mohsen Dashti Clinical Medicine & Pathology 316 7 th Lecture Lecture outline Review of structure & function. Symptoms, signs & tests. Specific diseases. Review of structure
Central nervous system By Dr. Mohsen Dashti Clinical Medicine & Pathology 316 7 th Lecture Lecture outline Review of structure & function. Symptoms, signs & tests. Specific diseases. Review of structure
MOTOR NEURONE DISEASE
 MOTOR NEURONE DISEASE Dr Arun Aggarwal Department of Rehabilitation Medicine, RPAH Department of Neurology, Concord Hospital. Motor Neurone Disease Umbrella term in UK and Australia (ALS in USA) Neurodegenerative
MOTOR NEURONE DISEASE Dr Arun Aggarwal Department of Rehabilitation Medicine, RPAH Department of Neurology, Concord Hospital. Motor Neurone Disease Umbrella term in UK and Australia (ALS in USA) Neurodegenerative
Critical Illness Polyneuropathy CIP and Critical Illness Myopathy CIM. Andrzej Sladkowski
 Critical Illness Polyneuropathy CIP and Critical Illness Myopathy CIM Andrzej Sladkowski Potential causes of weakness in the ICU-1 Muscle disease Critical illness myopathy Inflammatory myopathy Hypokalemic
Critical Illness Polyneuropathy CIP and Critical Illness Myopathy CIM Andrzej Sladkowski Potential causes of weakness in the ICU-1 Muscle disease Critical illness myopathy Inflammatory myopathy Hypokalemic
Peripheral Neuropathies
 Peripheral Neuropathies ELBA Y. GERENA MALDONADO, MD ACTING ASSISTANT PROFESSOR UNIVERSITY OF WASHINGTON MEDICAL CENTER Objectives Definition Neurophysiology Evaluation of polyneuropathies Cases Summary
Peripheral Neuropathies ELBA Y. GERENA MALDONADO, MD ACTING ASSISTANT PROFESSOR UNIVERSITY OF WASHINGTON MEDICAL CENTER Objectives Definition Neurophysiology Evaluation of polyneuropathies Cases Summary
Appendix I (a) Human Surveillance Case Definition (Revised July 4, 2005)
 Section A: Case Definitions Appendix I (a) Human Surveillance Case Definition (Revised July 4, 2005) The current Case Definitions were drafted with available information at the time of writing. Case Definitions
Section A: Case Definitions Appendix I (a) Human Surveillance Case Definition (Revised July 4, 2005) The current Case Definitions were drafted with available information at the time of writing. Case Definitions
IVIG (intravenous immunoglobulin) Bivigam, Carimune NF, Flebogamma, Gammagard, Gammagard S/D, Gammaked, Gammaplex, Gamunex-C, Octagam, Privigen
 Pre - PA Allowance None Prior-Approval Requirements Diagnoses Patient must have ONE of the following documented indications: 1. Primary Immunodeficiency Disease (PID) with ONE of the a. Hypogammaglobulinemia,
Pre - PA Allowance None Prior-Approval Requirements Diagnoses Patient must have ONE of the following documented indications: 1. Primary Immunodeficiency Disease (PID) with ONE of the a. Hypogammaglobulinemia,
Case Classification West Nile Virus Neurological Syndrome (WNNS)
 WEST NILE VIRUS Case definition Case Classification West Nile Virus Neurological Syndrome (WNNS) CONFIRMED CASE West Nile Virus Neurological Syndrome (WNNS) Clinical criteria AND at least one of the confirmed
WEST NILE VIRUS Case definition Case Classification West Nile Virus Neurological Syndrome (WNNS) CONFIRMED CASE West Nile Virus Neurological Syndrome (WNNS) Clinical criteria AND at least one of the confirmed
A Hypothesis Driven Approach to the Neurological Exam
 A Hypothesis Driven Approach to the Neurological Exam Vanja Douglas, MD Assistant Clinical Professor UCSF Department of Neurology Disclosures None 1 Purpose of Neuro Exam Screen asymptomatic patients Screen
A Hypothesis Driven Approach to the Neurological Exam Vanja Douglas, MD Assistant Clinical Professor UCSF Department of Neurology Disclosures None 1 Purpose of Neuro Exam Screen asymptomatic patients Screen
GUILLAIN-BARRE SYNDROME
 GUILLAIN-BARRE SYNDROME tarek.sharshar@rpc.aphp.fr University of Versailles Saint-Quentin en Yvelines Raymond Poincaré Teaching Hospital Garches - France STATEMENTS 1. Guillain-Barré Syndrome (GBS) is
GUILLAIN-BARRE SYNDROME tarek.sharshar@rpc.aphp.fr University of Versailles Saint-Quentin en Yvelines Raymond Poincaré Teaching Hospital Garches - France STATEMENTS 1. Guillain-Barré Syndrome (GBS) is
Diagnosis and Management of Immune-mediated Neuropathies
 Continuing Medical Education 39 Diagnosis and Management of Immune-mediated Neuropathies Sung-Tsang Hsieh Abstract- Immune-mediate neuropathies, or inflammatory neuropathies are neuropathies due to the
Continuing Medical Education 39 Diagnosis and Management of Immune-mediated Neuropathies Sung-Tsang Hsieh Abstract- Immune-mediate neuropathies, or inflammatory neuropathies are neuropathies due to the
Il ruolo della diagnostica di laboratorio
 Cremona 9 giugno 2017 DIAGNOSI DIFFERENZIALE DELLE MALATTIE DEL SISTEMA NERVOSO PERIFERICO Il ruolo della diagnostica di laboratorio No conflicts of interest Wang Y et al. Mediators of Inflammatory 2015
Cremona 9 giugno 2017 DIAGNOSI DIFFERENZIALE DELLE MALATTIE DEL SISTEMA NERVOSO PERIFERICO Il ruolo della diagnostica di laboratorio No conflicts of interest Wang Y et al. Mediators of Inflammatory 2015
How to Think like a Neurologist Review of Exam Process and Assessment Findings
 Lehigh Valley Health Network LVHN Scholarly Works Neurology Update for the Non-Neurologist 2013 Neurology Update for the Non-Neurologist Feb 20th, 5:10 PM - 5:40 PM How to Think like a Neurologist Review
Lehigh Valley Health Network LVHN Scholarly Works Neurology Update for the Non-Neurologist 2013 Neurology Update for the Non-Neurologist Feb 20th, 5:10 PM - 5:40 PM How to Think like a Neurologist Review
TEXAS IMMUNIZATION CONFERENCE 2017 ACUTE FLACCID MYELITIS IN TEXAS
 TEXAS IMMUNIZATION CONFERENCE 2017 ACUTE FLACCID MYELITIS IN TEXAS Dr. Donald Murphey Dell Children s Medical Center, Dell Medical School, Austin, Texas Pediatric Infectious Diseases November 28, 2017
TEXAS IMMUNIZATION CONFERENCE 2017 ACUTE FLACCID MYELITIS IN TEXAS Dr. Donald Murphey Dell Children s Medical Center, Dell Medical School, Austin, Texas Pediatric Infectious Diseases November 28, 2017
Approach to a Neurologic Diagnosis
 Approach to a Neurologic Diagnosis Neurologic Diagnosis History Physical & Neurological Examination Ancillary Procedures 3 Questions Asked Focal neurologic deficits Increased intracranial pressure Signs
Approach to a Neurologic Diagnosis Neurologic Diagnosis History Physical & Neurological Examination Ancillary Procedures 3 Questions Asked Focal neurologic deficits Increased intracranial pressure Signs
Guillain-Barré Syndrome Beth A. Rosen. DOI: /pir
 Guillain-Barré Syndrome Beth A. Rosen Pediatrics in Review 2012;33;164 DOI: 10.1542/pir.33-4-164 The online version of this article, along with updated information and services, is located on the World
Guillain-Barré Syndrome Beth A. Rosen Pediatrics in Review 2012;33;164 DOI: 10.1542/pir.33-4-164 The online version of this article, along with updated information and services, is located on the World
A Case of Acute Sensory Neuropathy Associated with Contrast Enhancement of the Cauda Equina on Magnetic Resonance Imaging
 61 Case Report St. Marianna Med. J. Vol. 33, pp. 61 66, 2005 A Case of Acute Sensory Neuropathy Associated with Contrast Enhancement of the Cauda Equina on Magnetic Resonance Imaging Toshinari Kobayashi
61 Case Report St. Marianna Med. J. Vol. 33, pp. 61 66, 2005 A Case of Acute Sensory Neuropathy Associated with Contrast Enhancement of the Cauda Equina on Magnetic Resonance Imaging Toshinari Kobayashi
Dilemmas in the Management of Meningitis & Encephalitis HEADACHE AND FEVER. What is the best initial approach for fever, headache, meningisums?
 Dilemmas in the Management of Meningitis & Encephalitis Paul D. Holtom, MD Professor of Medicine and Orthopaedics USC Keck School of Medicine HEADACHE AND FEVER What is the best initial approach for fever,
Dilemmas in the Management of Meningitis & Encephalitis Paul D. Holtom, MD Professor of Medicine and Orthopaedics USC Keck School of Medicine HEADACHE AND FEVER What is the best initial approach for fever,
Paraparetic Guillain-Barré syndrome
 Paraparetic Guillain-Barré syndrome Bianca van den Berg, MD Christiaan Fokke, MD Judith Drenthen, MD Pieter A. van Doorn, MD, PhD Bart C. Jacobs, MD, PhD Correspondence to Dr. Jacobs: b.jacobs@erasmusmc.nl
Paraparetic Guillain-Barré syndrome Bianca van den Berg, MD Christiaan Fokke, MD Judith Drenthen, MD Pieter A. van Doorn, MD, PhD Bart C. Jacobs, MD, PhD Correspondence to Dr. Jacobs: b.jacobs@erasmusmc.nl
Appendix B: Provincial Case Definitions for Reportable Diseases
 Ministry of Health and Long-Term Care Infectious Diseases Protocol Appendix B: Provincial Case Definitions for Reportable Diseases Disease: West Nile Virus Illness Revised March 2017 West Nile Virus Illness
Ministry of Health and Long-Term Care Infectious Diseases Protocol Appendix B: Provincial Case Definitions for Reportable Diseases Disease: West Nile Virus Illness Revised March 2017 West Nile Virus Illness
Introduction and aims of the study
 Introduction and aims of the study 1 Chapter 1 Motor neuron diseases include the most incapacitating and life-threatening illnesses but also rather benign disorders with only mild symptoms and slow progression.
Introduction and aims of the study 1 Chapter 1 Motor neuron diseases include the most incapacitating and life-threatening illnesses but also rather benign disorders with only mild symptoms and slow progression.
Pediatric Patients. Neuromuscular Disease. Teera Kijmassuwan, MD Phetcharat Netmuy, B.N.S., MA Oranee Sanmaneechai, MD : Preceptor
 Patient Management Pediatric Patients with Neuromuscular Disease Teera Kijmassuwan, MD Phetcharat Netmuy, B.N.S., MA Oranee Sanmaneechai, MD : Preceptor Case Thai boy 1 year old Present with Respiratory
Patient Management Pediatric Patients with Neuromuscular Disease Teera Kijmassuwan, MD Phetcharat Netmuy, B.N.S., MA Oranee Sanmaneechai, MD : Preceptor Case Thai boy 1 year old Present with Respiratory
Post-Anesthesia Care In the ICU
 Post-Anesthesia Care In the ICU The following is based on current research and regional standards of care. At completion you will be able to identify Basic equipment needed at the bedside. Aldrete scoring
Post-Anesthesia Care In the ICU The following is based on current research and regional standards of care. At completion you will be able to identify Basic equipment needed at the bedside. Aldrete scoring
Patogenesi e terapia della Neuropatia Motoria Multifocale
 26 Settembre 2014 Patogenesi e terapia della Neuropatia Motoria Multifocale Francesca Gallia Neurologia 2, Ist. Clin. Humanitas Rozzano, Milano Multifocal Motor Neuropathy Rare disorder characterized by:
26 Settembre 2014 Patogenesi e terapia della Neuropatia Motoria Multifocale Francesca Gallia Neurologia 2, Ist. Clin. Humanitas Rozzano, Milano Multifocal Motor Neuropathy Rare disorder characterized by:
Brain and Central Nervous System Cancers
 Brain and Central Nervous System Cancers NICE guidance link: https://www.nice.org.uk/guidance/ta121 Clinical presentation of brain tumours History and Examination Consider immediate referral Management
Brain and Central Nervous System Cancers NICE guidance link: https://www.nice.org.uk/guidance/ta121 Clinical presentation of brain tumours History and Examination Consider immediate referral Management
A Practical Approach to Polyneuropathy SLOCUM DICKSON ANNUAL TEACHING DAY NOVEMBER 4, 2017
 A Practical Approach to Polyneuropathy SLOCUM DICKSON ANNUAL TEACHING DAY NOVEMBER 4, 2017 Disclosures Research support from Cytokinetics, Inc Catalyst, Inc Editorial fees from UptoDate. Objectives Describe
A Practical Approach to Polyneuropathy SLOCUM DICKSON ANNUAL TEACHING DAY NOVEMBER 4, 2017 Disclosures Research support from Cytokinetics, Inc Catalyst, Inc Editorial fees from UptoDate. Objectives Describe
Paraparesis. Differential Diagnosis. Ran brauner, Tel Aviv university
 Paraparesis Differential Diagnosis Ran brauner, Tel Aviv university Definition Loss of motor power to both legs Paraparesis (paraplegia) refers to partial (- paresis) or complete (-plegia) loss of voluntary
Paraparesis Differential Diagnosis Ran brauner, Tel Aviv university Definition Loss of motor power to both legs Paraparesis (paraplegia) refers to partial (- paresis) or complete (-plegia) loss of voluntary
Hyperreflexia in Guillain-Barré syndrome: relation with acute motor axonal neuropathy and anti-gm1 antibody
 18 Department of Neurology, Chiba University School of Medicine, Chiba, Japan S Kuwabara K Ogawara M Mori T Hattori Department of Neurology, Dokkyo University School of Medicine, Tochigi, Japan M Koga
18 Department of Neurology, Chiba University School of Medicine, Chiba, Japan S Kuwabara K Ogawara M Mori T Hattori Department of Neurology, Dokkyo University School of Medicine, Tochigi, Japan M Koga
Clinical and electrophysiologic features of childhood Guillain-Barré syndrome in Northeast China
 Journal of the Formosan Medical Association (2014) 113, 634e639 Available online at www.sciencedirect.com journal homepage: www.jfma-online.com ORIGINAL ARTICLE Clinical and electrophysiologic features
Journal of the Formosan Medical Association (2014) 113, 634e639 Available online at www.sciencedirect.com journal homepage: www.jfma-online.com ORIGINAL ARTICLE Clinical and electrophysiologic features
CNS third year med students Summary of midterm material H Awad
 CNS third year med students 2018 Summary of midterm material H Awad Dear All This presentation summaries the main important topics covered in the midterm material ( lectures 1-6) There will be two questions
CNS third year med students 2018 Summary of midterm material H Awad Dear All This presentation summaries the main important topics covered in the midterm material ( lectures 1-6) There will be two questions
Severe Chronic Inflammatory Demyelinating Polyneuropathy Ameliorated following High-dose (3 g/kg) Intravenous Immunoglobulin Therapy
 doi: 10.2169/internalmedicine.1723-18 http://internmed.jp CASE REPORT Severe Chronic Inflammatory Demyelinating Polyneuropathy Ameliorated following High-dose (3 g/kg) Intravenous Immunoglobulin Therapy
doi: 10.2169/internalmedicine.1723-18 http://internmed.jp CASE REPORT Severe Chronic Inflammatory Demyelinating Polyneuropathy Ameliorated following High-dose (3 g/kg) Intravenous Immunoglobulin Therapy
PRIMARY DISEASES OF MYELIN. By: Shifaa Al Qa qa
 PRIMARY DISEASES OF MYELIN By: Shifaa Al Qa qa Most diseases of myelin are primarily white matter disorders??? Myelinated axons most diseases of CNS myelin do not involve the peripheral nerves to any significant
PRIMARY DISEASES OF MYELIN By: Shifaa Al Qa qa Most diseases of myelin are primarily white matter disorders??? Myelinated axons most diseases of CNS myelin do not involve the peripheral nerves to any significant
Guide to the use of nerve conduction studies (NCS) & electromyography (EMG) for non-neurologists
 Guide to the use of nerve conduction studies (NCS) & electromyography (EMG) for non-neurologists What is NCS/EMG? NCS examines the conduction properties of sensory and motor peripheral nerves. For both
Guide to the use of nerve conduction studies (NCS) & electromyography (EMG) for non-neurologists What is NCS/EMG? NCS examines the conduction properties of sensory and motor peripheral nerves. For both
Guillain-Barré syndrome and related disorders
 Guillain-Barré syndrome and related disorders Artículo Amato AA RESUMEN En 1859, Landry describió una neuropatía caracterizada por parálisis severa ascendente. Posteriormente, Guillain, Barré y Strohl
Guillain-Barré syndrome and related disorders Artículo Amato AA RESUMEN En 1859, Landry describió una neuropatía caracterizada por parálisis severa ascendente. Posteriormente, Guillain, Barré y Strohl
Multifocal motor neuropathy: diagnostic criteria that predict the response to immunoglobulin treatment
 Multifocal motor neuropathy: diagnostic criteria that predict the response to immunoglobulin treatment 7 MMN RM Van den Berg-Vos, H Franssen, JHJ Wokke, HW Van Es, LH Van den Berg Annals of Neurology 2000;
Multifocal motor neuropathy: diagnostic criteria that predict the response to immunoglobulin treatment 7 MMN RM Van den Berg-Vos, H Franssen, JHJ Wokke, HW Van Es, LH Van den Berg Annals of Neurology 2000;
Anti-GQ1b IgG antibody syndrome: clinical and immunological range
 50 Department of Neurology, Dokkyo University School of Medicine, Kitakobayashi 880, Mibu, Shimotsuga, Tochigi 321 0293, Japan M Odaka N Yuki K Hirata Correspondence to: Dr Yuki yuki@dokkyomed.ac.jp Received
50 Department of Neurology, Dokkyo University School of Medicine, Kitakobayashi 880, Mibu, Shimotsuga, Tochigi 321 0293, Japan M Odaka N Yuki K Hirata Correspondence to: Dr Yuki yuki@dokkyomed.ac.jp Received
Acute Motor-dominant Polyneuropathy as Guillain-Barré Syndrome and Multiple Mononeuropathies in a Patient with Sjögren s Syndrome
 CASE REPORT Acute Motor-dominant Polyneuropathy as Guillain-Barré Syndrome and Multiple Mononeuropathies in a Patient with Sjögren s Syndrome Kenichiro Tanaka 1, Hiroyuki Nakayasu 1, Yutaka Suto 1, Shotaro
CASE REPORT Acute Motor-dominant Polyneuropathy as Guillain-Barré Syndrome and Multiple Mononeuropathies in a Patient with Sjögren s Syndrome Kenichiro Tanaka 1, Hiroyuki Nakayasu 1, Yutaka Suto 1, Shotaro
Comparison of electrophysiological findings in axonal and demyelinating Guillain-Barre syndrome
 Iranian Journal of Neurology Original Paper Iran J Neurol 2014; 13(3): 138-143 Comparison of electrophysiological findings in axonal and demyelinating Guillain-Barre syndrome Received: 9 Mar 2014 Accepted:
Iranian Journal of Neurology Original Paper Iran J Neurol 2014; 13(3): 138-143 Comparison of electrophysiological findings in axonal and demyelinating Guillain-Barre syndrome Received: 9 Mar 2014 Accepted:
THE ROLE OF THE ANTI GQ1B ANTIBODY IN DIFFERENTIAL. DIGNOSIS OF ACUTE OPTHALMOPARESIS
 THE ROLE OF THE ANTI GQ1B ANTIBODY IN DIFFERENTIAL. DIGNOSIS OF ACUTE OPTHALMOPARESIS Abstract Miller Fisher syndrome has a triad of total external ophthalmoplegia, ataxia and areflexia, Botulism is caused
THE ROLE OF THE ANTI GQ1B ANTIBODY IN DIFFERENTIAL. DIGNOSIS OF ACUTE OPTHALMOPARESIS Abstract Miller Fisher syndrome has a triad of total external ophthalmoplegia, ataxia and areflexia, Botulism is caused
Sample Case Study. The patient was a 77-year-old female who arrived to the emergency room on
 Sample Case Study The patient was a 77-year-old female who arrived to the emergency room on February 25 th with a chief complaint of shortness of breath and a deteriorating pulmonary status along with
Sample Case Study The patient was a 77-year-old female who arrived to the emergency room on February 25 th with a chief complaint of shortness of breath and a deteriorating pulmonary status along with
G uillain-barré syndrome (GBS) is a peripheral polyneuropathy
 767 PAPER Anti-GT1a IgG in Guillain-Barré syndrome M Koga, H Yoshino, M Morimatsu, N Yuki... See end of article for authors affiliations... Correspondence to: Dr M Koga, Department of Neurology, Dokkyo
767 PAPER Anti-GT1a IgG in Guillain-Barré syndrome M Koga, H Yoshino, M Morimatsu, N Yuki... See end of article for authors affiliations... Correspondence to: Dr M Koga, Department of Neurology, Dokkyo
Inflammatory neuropathies are uncommon but important to diagnose because they are treatable.
 MANAGEMENT OF INFLAMMATORY NEUROPATHIES See end of article for authors affiliations c GUILLAIN-BARRÉ Correspondence to: Dr Robert Hadden, West London Neurosciences Centre, Charing Cross Hospital, Fulham
MANAGEMENT OF INFLAMMATORY NEUROPATHIES See end of article for authors affiliations c GUILLAIN-BARRÉ Correspondence to: Dr Robert Hadden, West London Neurosciences Centre, Charing Cross Hospital, Fulham
AII-type: Select the most appropriate answer
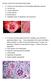 AII-type: Select the most appropriate answer ( )1. Choose one best answer for the following pathologic pictures. A. choroid cyst B. choroid papilloma C. pontine glioma D. ependymoma E. metastatic tumor
AII-type: Select the most appropriate answer ( )1. Choose one best answer for the following pathologic pictures. A. choroid cyst B. choroid papilloma C. pontine glioma D. ependymoma E. metastatic tumor
Pharyngeal-cervical-brachial variant of Guillain Barré syndrome
 Editor s choice Scan to access more free content Department of Medicine, National University Hospital, Singapore Correspondence to Professor Nobuhiro Yuki, Department of Medicine, National University of
Editor s choice Scan to access more free content Department of Medicine, National University Hospital, Singapore Correspondence to Professor Nobuhiro Yuki, Department of Medicine, National University of
42 y/o woman with unwitnessed episode of loss of consciousness and urinary incontinence
 Top Five Neurological Emergencies: When To Refer February 23, 2011 Jinny Tavee, MD Associate Professor Neurological Institute Cleveland Clinic Foundation 1 CASE 1 42 y/o woman with unwitnessed episode
Top Five Neurological Emergencies: When To Refer February 23, 2011 Jinny Tavee, MD Associate Professor Neurological Institute Cleveland Clinic Foundation 1 CASE 1 42 y/o woman with unwitnessed episode
American Board of Physical Medicine & Rehabilitation. Part I Curriculum & Weights
 American Board of Physical Medicine & Rehabilitation Part I Curriculum & Weights Neurologic Disorders 30% Stroke Spinal Cord Injury Traumatic Brain Injury Neuropathies a) Mononeuropathies b) Polyneuropathies
American Board of Physical Medicine & Rehabilitation Part I Curriculum & Weights Neurologic Disorders 30% Stroke Spinal Cord Injury Traumatic Brain Injury Neuropathies a) Mononeuropathies b) Polyneuropathies
SHASTA COUNTY Health and Human Services Agency
 FROM: 530 229 8447 TO: 15302293984 08/06/14 12:30 Pg 1 of 5 especially SHASTA COUNTY Health and Human Services Agency Public Health 2650RreslauerWay Redding, CA 96001-4297 (530) 229-8484 FAX (530) 225-3743
FROM: 530 229 8447 TO: 15302293984 08/06/14 12:30 Pg 1 of 5 especially SHASTA COUNTY Health and Human Services Agency Public Health 2650RreslauerWay Redding, CA 96001-4297 (530) 229-8484 FAX (530) 225-3743
MULTIPLE SCLEROSIS PROFILE
 MULTIPLE SCLEROSIS PROFILE What is Multiple Sclerosis? Multiple sclerosis (MS) is a chronic, inflammatory disease of unknown etiology that involves an immune-mediated attack on the central nervous system
MULTIPLE SCLEROSIS PROFILE What is Multiple Sclerosis? Multiple sclerosis (MS) is a chronic, inflammatory disease of unknown etiology that involves an immune-mediated attack on the central nervous system
Demyelinating Diseases of the Brain
 Department of Radiology University of California San Diego Demyelinating Diseases of the Brain John R. Hesselink, M.D. T1-Weighted Images Normal White Matter Contents Axons with envelope of myelin Neuroglia
Department of Radiology University of California San Diego Demyelinating Diseases of the Brain John R. Hesselink, M.D. T1-Weighted Images Normal White Matter Contents Axons with envelope of myelin Neuroglia
DISORDERS OF THE NERVOUS SYSTEM
 DISORDERS OF THE NERVOUS SYSTEM Bell Work What s your reaction time? Go to this website and check it out: https://www.justpark.com/creative/reaction-timetest/ Read the following brief article and summarize
DISORDERS OF THE NERVOUS SYSTEM Bell Work What s your reaction time? Go to this website and check it out: https://www.justpark.com/creative/reaction-timetest/ Read the following brief article and summarize
Electrodiagnostic studies comprising of electromyography (EMG) and nerve
 INTRODUCTION AND TERMINOLOGY Electrodiagnostic studies comprising of electromyography (EMG) and nerve conduction studies (NCS) are well-established objective methods for the diagnosis, quantification and
INTRODUCTION AND TERMINOLOGY Electrodiagnostic studies comprising of electromyography (EMG) and nerve conduction studies (NCS) are well-established objective methods for the diagnosis, quantification and
Case 1. Case Discussion. History. Present Illness. Impression. Physical Examination
 Case 1 Case Discussion R1 林吉倡 2013 / 01 / 02 13-yo Male BW: 45 kg DAY1 16:35 pm C/C: Epigastric pain since this morning TPR: 36.5/94/18 BP:133/83 SpO2: 100% GCS: 15 Triage: 2 Present Illness Sudden-onset
Case 1 Case Discussion R1 林吉倡 2013 / 01 / 02 13-yo Male BW: 45 kg DAY1 16:35 pm C/C: Epigastric pain since this morning TPR: 36.5/94/18 BP:133/83 SpO2: 100% GCS: 15 Triage: 2 Present Illness Sudden-onset
Guillain Barre Syndrome: A clinical observational study in Indian paediatric patients
 Guillain Barre Syndrome: A clinical observational study in Indian paediatric patients *Shikha Swaroop 1, Bakul B Javadekar 2 Sri Lanka Journal of Child Health, 2017; 46(3): 238-242 Abstract Background:
Guillain Barre Syndrome: A clinical observational study in Indian paediatric patients *Shikha Swaroop 1, Bakul B Javadekar 2 Sri Lanka Journal of Child Health, 2017; 46(3): 238-242 Abstract Background:
Mechanical Ventilation of the Patient with Neuromuscular Disease
 Mechanical Ventilation of the Patient with Neuromuscular Disease Dean Hess PhD RRT Associate Professor of Anesthesia, Harvard Medical School Assistant Director of Respiratory Care, Massachusetts General
Mechanical Ventilation of the Patient with Neuromuscular Disease Dean Hess PhD RRT Associate Professor of Anesthesia, Harvard Medical School Assistant Director of Respiratory Care, Massachusetts General
Electrophysiology in the Guillain-Barré Syndrome: Study of 30 Cases
 Journal of Bangladesh College of Physicians and Surgeons Vol. 24, No. 2, May 2006 Electrophysiology in the Guillain-Barré Syndrome: Study of 30 Cases NC KUNDU Summary: Thirty consecutive patients diagnosed
Journal of Bangladesh College of Physicians and Surgeons Vol. 24, No. 2, May 2006 Electrophysiology in the Guillain-Barré Syndrome: Study of 30 Cases NC KUNDU Summary: Thirty consecutive patients diagnosed
International Journal of Basic & Applied Physiology
 ELECTRODIAGNOSTIC FEATURES IN CLINICALLY SUSPECTED GUILLAIN BARRE SYNDROME Asha Shrivastava*, Rashmi Dave**, Sanjeev Shrivastava ***, Brajesh Sharma **** *Professor, ** JR III, *** Assistant Professor,
ELECTRODIAGNOSTIC FEATURES IN CLINICALLY SUSPECTED GUILLAIN BARRE SYNDROME Asha Shrivastava*, Rashmi Dave**, Sanjeev Shrivastava ***, Brajesh Sharma **** *Professor, ** JR III, *** Assistant Professor,
MYASTHENIA GRAVIS. Mr. D.Raju, M.pharm, Lecturer
 MYASTHENIA GRAVIS Mr. D.Raju, M.pharm, Lecturer OUTLINE Background Anatomy Pathophysiology Clinical Presentation Treatment BACKGROUND Acquired autoimmune disorder Clinically characterized by: Weakness
MYASTHENIA GRAVIS Mr. D.Raju, M.pharm, Lecturer OUTLINE Background Anatomy Pathophysiology Clinical Presentation Treatment BACKGROUND Acquired autoimmune disorder Clinically characterized by: Weakness
Role of MRI in acute disseminated encephalomyelitis
 Original Research Article Role of MRI in acute disseminated encephalomyelitis Shashvat Modiya 1*, Jayesh Shah 2, C. Raychaudhuri 3 1 1 st year resident, 2 Associate Professor, 3 HOD and Professor Department
Original Research Article Role of MRI in acute disseminated encephalomyelitis Shashvat Modiya 1*, Jayesh Shah 2, C. Raychaudhuri 3 1 1 st year resident, 2 Associate Professor, 3 HOD and Professor Department
ZKV and Guillain-Barré Syndrome. Silvia N. Tenembaum Pediatric Neurologist
 ZKV and Guillain-Barré Syndrome Silvia N. Tenembaum Pediatric Neurologist ZIKA VIRUS- BACKGROUND INFORMATION Arbovirus (Arthropod-borne virus) 1- Flaviviridae family: Dengue (DENV) West Nile (WNV) Yellow
ZKV and Guillain-Barré Syndrome Silvia N. Tenembaum Pediatric Neurologist ZIKA VIRUS- BACKGROUND INFORMATION Arbovirus (Arthropod-borne virus) 1- Flaviviridae family: Dengue (DENV) West Nile (WNV) Yellow
Encephalitis following Purified Chick-Embryo Cell Anti-Rabies Vaccination
 CASE REPORT JIACM 2003; 4(3): 251-9 Encephalitis following Purified Chick-Embryo Cell Anti-Rabies Vaccination NS Neki*, Ashok Khurana**, Ashok Duggal*** Abstract A case of encephalitis following purified
CASE REPORT JIACM 2003; 4(3): 251-9 Encephalitis following Purified Chick-Embryo Cell Anti-Rabies Vaccination NS Neki*, Ashok Khurana**, Ashok Duggal*** Abstract A case of encephalitis following purified
Clinical and Neurophysiological Pattern of Guillain-Barré Syndrome in Diabetic and Non Diabetic Patients
 Clinical and Neurophysiological Pattern of Guillain-Barré Syndrome in Diabetic and Non Diabetic Patients Shereen Zakarya Department of Neurology, Mansoura University ABSTRACT Objective: To study the clinical
Clinical and Neurophysiological Pattern of Guillain-Barré Syndrome in Diabetic and Non Diabetic Patients Shereen Zakarya Department of Neurology, Mansoura University ABSTRACT Objective: To study the clinical
Differential Diagnosis of Neuropathies and Compression. Dr Ashwin Pinto Consultant Neurologist Wessex Neurological Centre
 Differential Diagnosis of Neuropathies and Compression Dr Ashwin Pinto Consultant Neurologist Wessex Neurological Centre Outline of talk Mononeuropathies median and anterior interosseous nerve ulnar nerve
Differential Diagnosis of Neuropathies and Compression Dr Ashwin Pinto Consultant Neurologist Wessex Neurological Centre Outline of talk Mononeuropathies median and anterior interosseous nerve ulnar nerve
Adv Pathophysiology Unit 2: Neuro Page 1 of 8
 Adv Pathophysiology Unit 2: Neuro Page 1 of 8 Learning Objectives for this file: 1. Amaurosis fugax presentation & DDX 2. Clinical diagnostics 3. Case study & followup Adv Pathophysiology Unit 2: Neuro
Adv Pathophysiology Unit 2: Neuro Page 1 of 8 Learning Objectives for this file: 1. Amaurosis fugax presentation & DDX 2. Clinical diagnostics 3. Case study & followup Adv Pathophysiology Unit 2: Neuro
Myelitis= inflammation of the spinal cord
 Polio infection 1 Illustrate the epidemiology of the disease 2 Demonstrate the clinical features of polio infection 3 Enumerate the complications 4 Prevent and treat polio infection MUMPS 1 Identify the
Polio infection 1 Illustrate the epidemiology of the disease 2 Demonstrate the clinical features of polio infection 3 Enumerate the complications 4 Prevent and treat polio infection MUMPS 1 Identify the
Clinical Information on West Nile Virus (WNV) Infection
 Clinical Information on West Nile Virus (WNV) Infection Introduction In 1999, West Nile Virus (WNV), an Old World flavivirus, producing a spectrum of disease including severe meningoencephalitis, appeared
Clinical Information on West Nile Virus (WNV) Infection Introduction In 1999, West Nile Virus (WNV), an Old World flavivirus, producing a spectrum of disease including severe meningoencephalitis, appeared
Myasthenia gravis (MG) is an autoimmune disorder
 Brief Communication The clinical features of patients concurrent with Guillain-Barré syndrome and myasthenia gravis Junliang Yuan, MD, Juan Zhang, MD, ABSTRACT Bingwei Zhang, MD, Wenli Hu, MD. Objectives:
Brief Communication The clinical features of patients concurrent with Guillain-Barré syndrome and myasthenia gravis Junliang Yuan, MD, Juan Zhang, MD, ABSTRACT Bingwei Zhang, MD, Wenli Hu, MD. Objectives:
Vascular Disorders. Nervous System Disorders (Part B-1) Module 8 -Chapter 14. Cerebrovascular disease S/S 1/9/2013
 Nervous System Disorders (Part B-1) Module 8 -Chapter 14 Overview ACUTE NEUROLOGIC DISORDERS Vascular Disorders Infections/Inflammation/Toxins Metabolic, Endocrinologic, Nutritional, Toxic Neoplastic Traumatic
Nervous System Disorders (Part B-1) Module 8 -Chapter 14 Overview ACUTE NEUROLOGIC DISORDERS Vascular Disorders Infections/Inflammation/Toxins Metabolic, Endocrinologic, Nutritional, Toxic Neoplastic Traumatic
Making sense of Nerve conduction & EMG
 Making sense of Nerve conduction & EMG Drs R Arunachalam Consultant Clinical Neurophysiologist Wessex Neurological Centre Southampton University Hospital EMG/NCS EMG machine For the assessment of patients
Making sense of Nerve conduction & EMG Drs R Arunachalam Consultant Clinical Neurophysiologist Wessex Neurological Centre Southampton University Hospital EMG/NCS EMG machine For the assessment of patients
role of antiganglioside antibodies
 J Neurol Neurosurg Psychiatry 2000;68:191 195 191 Department of Neurology, Chiba University School of Medicine, 1 8 1 Inohana, Chuo-ku, Chiba 260 8670, Japan S Kuwabara K Ogawara K Mizobuchi M Mori T Hattori
J Neurol Neurosurg Psychiatry 2000;68:191 195 191 Department of Neurology, Chiba University School of Medicine, 1 8 1 Inohana, Chuo-ku, Chiba 260 8670, Japan S Kuwabara K Ogawara K Mizobuchi M Mori T Hattori
Pedro A. Mendez-Tellez, MD
 Critical Illness Polyneuropathy and Myopathy: Epidemiology and Risk Factors Pedro A. Mendez-Tellez, MD Johns Hopkins University Baltimore, Maryland, USA pmendez@jhmi.edu Conflict of Interest I have no
Critical Illness Polyneuropathy and Myopathy: Epidemiology and Risk Factors Pedro A. Mendez-Tellez, MD Johns Hopkins University Baltimore, Maryland, USA pmendez@jhmi.edu Conflict of Interest I have no
Case Number 1 Guillain-Barré Syndrome (GBS)
 Case Number 1 Guillain-Barré Syndrome (GBS) Maria Angela Grima Reviewed by: Dr. Nicola Aquilina Case summary: Demographic details: Mr. JS, male, Gudja Referred from: GP A 57-year-old Caucasian gentleman
Case Number 1 Guillain-Barré Syndrome (GBS) Maria Angela Grima Reviewed by: Dr. Nicola Aquilina Case summary: Demographic details: Mr. JS, male, Gudja Referred from: GP A 57-year-old Caucasian gentleman
Detection of Autoantibodies against Gangliosides in Guillain-Barré Syndrome
 ISSN 1735-1383 Iran. J. Immunol. September 2010, 7 (3), 198-201 Hong-Liang Zhang, Su-Jie Gao, Yi Yang, Jiang Wu Detection of Autoantibodies against Gangliosides in Guillain-Barré Syndrome Article Type:
ISSN 1735-1383 Iran. J. Immunol. September 2010, 7 (3), 198-201 Hong-Liang Zhang, Su-Jie Gao, Yi Yang, Jiang Wu Detection of Autoantibodies against Gangliosides in Guillain-Barré Syndrome Article Type:
