Therapy Management of Burns
|
|
|
- Alaina Hodge
- 5 years ago
- Views:
Transcription
1 Care of Burns in Scotland Paediatric Guideline Therapy Management of Burns Reviewed by: Judith Montgomery (Specialist Physiotherapist, NHS Lothian) Caroline Grant (Paediatric MSK Physiotherapist, NHS Greater Glasgow and Clyde) Approved by the COBIS Steering Group Date reviewed: December 2018 Date of next review: December 2021 NOTE This guideline is not intended to be construed or to serve as a standard of care. Standards of care are determined on the basis of all clinical data available for an individual case and are subject to change as scientific knowledge and technology advance and patterns of care evolve. Adherence to guideline recommendations will not ensure a successful outcome in every case, nor should they be construed as including all proper methods of care or excluding other acceptable methods of care aimed at the same results. The ultimate judgement must be made by the appropriate healthcare professional(s) responsible for clinical decisions regarding a particular clinical procedure or treatment plan. This judgement should only be arrived at following discussion of the options with the patient, covering the diagnostic and treatment choices available. It is advised, however, that significant departures from the national guideline or any local guidelines derived from it should be fully documented in the patient s case notes at the time the relevant decision is taken. NSDxxxxxxV1
2 Contents 1) Aim ) Background ) Criteria for Therapy ) Recommended Therapy Intervention for the Acute Phase of Rehabilitation... 4 a) Respiratory... 4 b) Positioning... 5 c) Splinting... 6 d) Mobilisation ) Recommended Therapy Intervention for the Intermediate Phase of Rehabilitation... 7 a) Further Mobility... 7 b) Activities of Daily Living (ADL) and Occupational Performance Skills... 8 c) Scar Management... 8 d) Discharge planning ) Recommended Therapy Intervention for the Later Phase of Rehabilitation ) Discharge ) References Page 2 of 11
3 Aim This is a standard designed to assist and guide therapists in the management of a child following a burn in Scotland. This includes therapy management in Intensive Care, High Dependency, ward settings and as outpatients. Background A burn is a very common injury and can have a significant impact upon the individual s functional ability. Both Physiotherapy and Occupational Therapy therefore are vital in minimising/ preventing impairments to body functions and structures and restoring full independence (ANZBA, 2002 & Okhovatian & Zoubine, 2006). This guideline covers all aspects of burn therapy commencing with the acute phase which could be in Intensive Care, High Dependency and on the ward progressing through the intermediate phase of rehabilitation and on to later rehabilitation to restore them to their optimal functional level. Depending on the size, depth and location of the burn injury patients may not require all stages of therapy input (or any therapy input if they don t meet criteria below). To determine this all patients require an individual and continuously updated assessment (Burn Therapy Working Group, 2005 & Leveridge, 1991). The roles of the Physiotherapist and Occupational Therapist often overlap and differ between hospitals. For the purpose of this standard the Physiotherapist and Occupational Therapist will be referred to as the Burn Therapist. The most important point is that burn rehabilitation is multi- disciplinary, co-ordinated, individualised and holistic to optimise functional and cosmetic outcome (ANZBA, 2002 & Burn Therapy Working Group, 2005). It is also important that this standard is used in conjunction with the clinical reasoning skills of the Burn Therapist. Criteria for Therapy Patients following a burn may present with a wide range of signs and symptoms potentially affecting their respiratory, cardiovascular, neurological and orthopaedic systems. This is the recommended criteria that should be considered when making a referral to a Burn Therapist: Any patient who is/ has been intubated and ventilated Any patient who has a suspected/ known inhalation Any patient that has a pre-existing respiratory problem Any patient that has other respiratory problems as a result of the burn injury Any burn that is over a joint line or circumferential around a joint Any burn that will require pressure therapy e.g. following a skin graft Any patient developing or at risk of developing hypertrophic or keloid scarring Any patient with reduced mobility, range of movement and/ or muscle power since injury Any patient presenting with difficulties in Activities of Daily Living since injury Any patient following a burn that requires hand splinting Any patient that has hand function difficulties It is acknowledged that patients presenting with burn injuries that do not fit this criteria may require therapy assessment and management should be discussed with the Burn Therapist. Page 3 of 11
4 Therapists have a very important role to play in the burns team and where their input is required should be involved from day one of the child s admission or as early as the child is stable enough for therapy to commence. Recommended Therapy Intervention for the Acute Phase of Rehabilitation In the acute phase the burn injury will be in the early stages of wound healing undergoing frequent dressing changes and often requiring surgical intervention. The therapeutic management of the burn patient is determined by thorough assessment and formulation of a detailed list of problems and treatment goals and a detailed treatment/ management plan. This is in line with the documentation standard produced by the Chartered Society of Physiotherapy and local documentation policies (CSP, 2005). It is vital that the child and their family are educated regarding all aspects of the therapeutic treatment programme and are involved from the beginning in their child s treatment. Some parents/ families may find it distressing handling their child, especially if their injuries are extensive and/or disfiguring. Therefore it is important to involve them as much as possible in the rehabilitation process. For example involving parents and families with daily passive movements and assisting with functional skills when appropriate. This will help to improve compliance with home exercise programmes and scar management treatments. a) Respiratory Assessment of the child s respiratory status should be carried out and documented within 24 hours of admission, if required. This is in line with the standards produced by the Burn Therapy Standards Working Group and the Chartered Society of Physiotherapy (Burn Therapy Standards Working Group, 2005 & CSP, 2005). The Burn Therapist should clinically reason which physiotherapy chest treatment, if required is most appropriate depending on age, size and location of the burn. Ventilated patients Some children following a burn may require to be ventilated. This could be required if the child is suffering from stridor, facial burns, facial oedema and/ or smoke inhalation. The ventilated child may require chest physiotherapy. To clear secretions, manual chest physiotherapy techniques such as Autogenic Drainage (AD) along with manual hyperinflation may be considered. If the child has a chest burn use of any manual chest physiotherapy technique should be discussed with the relevant consultants. This is because manual techniques may cause further trauma to the burnt tissue which may result in superficial burns becoming deeper (Leveridge,1991 & Harden, 2002). Following a skin graft manual techniques are contraindicated due to the shearing forces which can cause a graft to fail. For additional information refer to the COBIS standard for Airway Burns and Inhalation Injury in Children Non- ventilated patients Prophylactic chest physiotherapy may be required for children that are at risk of developing chest symptoms (ANZBA, 2002). This is generally children that have prolonged reduced mobility, a pre-existing respiratory condition, chest wall burns and pain following surgical procedure. If the patient requires chest physiotherapy and is awake and compliant then Page 4 of 11
5 non manual Airway Clearance Techniques (ACT) such as incentive spirometry and Autogenic Drainage (AD) are advised. It is recommended that respiratory assessment and treatment continue until the child is symptom free and mobilising fully. b) Positioning Proper and early positioning is integral to the successful rehabilitation of a patient with a burn. The position of comfort after burn injury is typically the position that promotes deformity and therefore should be avoided. Therapeutic positioning is designed to reduce oedema by elevation of extremities and to preserve function by proper body alignment and the use of anti contracture positions. To ensure this, positioning should be assessed and managed within 24 hours of the child s admission (Whitehead & Serghiou, 2009). Every patient with a burn over a joint should have a positioning programme provided by the therapist and assessed regularly.it is essential that nursing staff should be shown how to carry this out, to ensure correct positioning at all times. A positioning chart could be utilised if appropriate. The optimum positioning for burn areas (anti-contracture positioning) is as follows: Head- elevated to reduce oedema Neck- maintained in midline and if burns are sustained to the anterior surface of the neck they should not have pillows behind their head. To position the neck in more extension a small towel/ roll can be placed behind their shoulders. There should be no rotation. A second mattress can also be used to gain an optimal position. Axilla- maintained at 90 abduction as a minimum or 110 if possible. Ensuring no pressure points exist, which may produce brachial plexus compression/ulnar nerve palsy at the elbow. There should be 10 of shoulder flexion to prevent brachial plexus injury. Positioning of the axilla can be difficult if the chest has also been grafted. An alternative can be to position the upper limb in a Bradford sling ensuring the elbow is mobilised regularly throughout the day. Shoulder and chest- if the patient is adopting a protracted/ flexed posture then if possible they should spend some time in prone lying. Maintenance of a semi-erect position will assist in movement of oedema away from the chest wall to more dependent tissues. Elbow- burns to the flexor aspect of the joint should be positioned in extension and supination on either pillows or in splints. The arms are elevated in the Bradford sling and should be removed for 10 minutes every hour and stretched into extension. Hand- all burns (unless superficial) should be elevated on pillows to help reduce oedema. The wrist should be maintained at 30 degrees extension and the MCPs at degrees flexion (to maintain collateral ligs on full stretch) and IPs in full extension (to prevent contracture of volar plate). Thumb in palmar abduction. Thermoplastic splints can be used to attain this position. Trunk- should be in midline. Hips- should be positioned in neutral and in 20 abduction. This can be done with pillows /towels/sandbags. Genital area- lower limbs should be positioned as for hip/ knee burns because patients will tend to adopt the foetal position with hips and knees flexed. Page 5 of 11
6 Knees- should be positioned in extension. There should not be a pillow underneath the knee joint. Ankles/ feet- plantar-grade. This is usually achieved by a pillow at the base of the foot holding the position or splints. The foot should be checked daily for pressure sores at the heels. Sheepskin or water filled surgical glove can be used as a protective cushioning. Toes (if clawing apparent)- neutral position with the foot in plantar flexion to gain a greater stretch along the plantar aspect of the foot. (Leveridge, 1991 & Vehmeyer-Heeman et al, 2005, Moore 2009). These positions may have to be adapted depending on the location of the burn and depending on if the young person has had skin grafts. c) Splinting Splinting is an extension of the therapeutic positioning programme and should be utilised when: A child is unable to voluntarily maintain proper positions Positioning is not effectively preventing contractures Immobilisation is required after skin grafting- this is particularly important at the axilla as contracture of the axilla following a skin graft is a common complication and a major concern for rehabilitation (Vehmeyer- Heeman et al, 2005) Full active range of movement is not being maintained with positioning and exercises The hands which are high risk for adopting poor postural positions (Leverige, 1991, ANZBA, 2002 & Whitehead & Serghiou, 2009) Burns to the neck are prone to contracting and splints such as soft and hard collars may be required if an optimal position cannot be maintained by pillows/ mattresses. These may have to be adapted if the child has a tracheostomy, central line or if the child has a splint for the axilla (Sharp et al, 2007). Splints may be made by the Burn Therapist, Medical Staff or Orthotic/ Orthopaedic Technicians and may require to be made in theatre. It is vital that splinting regimes are adhered to and there should be detailed instructions on how and when to apply the splint, how long it should be worn for and to observe for any signs of pressure areas. This information should be given to nursing staff that are caring for the patient, parents/ family and the child where appropriate. d) Mobilisation Range of movement (ROM) exercises should be commenced on the first day after admission and joint ranges of movement and muscle power must be documented on a chart on day one. These should be assessed and recorded on a daily basis until full active range of movement is achieved (Leveridge, 1991 & ANZBA, 2002). Where possible all joints including the affected and non- affected joints should be moved actively through their full range of motion. This should be done passively if the child cannot manage the full range of motion actively. This could take place in theatre or on the ward. In Page 6 of 11
7 some instances the range of movement exercises of the affected joints will occur only in theatre during dressing changes. The burn therapist may have to liaise with the pain team to ensure adequate analgesia prior to physiotherapy intervention (Stoddard et al, 2002). Individual exercise programmes should be issued as appropriate and family members should be educated in these to involve them in all aspects of the child s therapy. Particular attention should always be given to a burn injury of the hand. Assessment should include grip strength including gross grasp and pinch, functional grasps and bilateral use of hands. Mobilisation should commence once the child is medically stable and this can be when the child is in the Intensive Care and High Dependency settings. This should be discussed with the relevant consultants. In preparation the child should have spent some time upright in bed to reduce any vasovagal response to standing. If the child is too weak to commence mobilising then the use of hoists to transfer in to a chair and the use of tilt tables/ standing frames should be considered. If the child has had their burn grafted then mobilisation is contraindicated until the skin graft is stable. This normally takes 5-10 days to occur, but will differ between patients. During this time the grafted area is immobilised often in a splint. The wounds are normally inspected 3-5 days post-op and the consultant will document how well the graft has taken to the underlying tissue. Once the graft has taken 100% and/or the consultant has confirmed the graft is stable, range of movement exercises and mobilisation can occur. The Burn Therapist should ensure that the weight bearing status is discussed with the relevant consultant. Recommended Therapy Intervention for the Intermediate Phase of Rehabilitation This stage of rehabilitation predominantly occurs when the child has transferred from Intensive or High Dependency Care to a ward setting or occasionally home. Children will transition into this phase when they are medically stable and the amount of therapy that they require will vary depending on many factors such as burn location and size. Multi-disciplinary team working is vital at this point to ensure effective planning for discharge (Burn Therapy Standards Working Group, 2005). Interventions such as respiratory, positioning and splinting will still be required in this phase and will continue until the child has regained full active range of movement and full mobility. Therapy management in this stage will focus more on restoring function and commencing scar management. Clinical Psychology may be of benefit at this stage or in the later phase if the child or family require help coping/ adjusting with what has happened. Referral to relevant charity organisations may be considered at this stage e.g. Scottish Burned Children s Club (theburnsclub.org.uk) as they provide a network of support to burn survivor children and their families a) Further Mobility Where appropriate the therapy sessions will be based in the therapy department in the gym. Active and passive ranges of movements are vital in the acute phase of rehabilitation and may still be required in the intermediate phase. It is however recognised that these interventions have lowest compliance and activities of daily living are met with increased Page 7 of 11
8 compliance (Ekes & Marvin, 1985). Therefore at this stage in the rehabilitation it is important to consider incorporating sporting activities and the use of technology such as the Wii. Children at this stage of rehab who are still on the ward will require regular input and these treatment sessions could be in the therapy department. The amount of therapy input will be assessed on a daily basis and decreased as the child improves and progresses to discharge home. b) Activities of Daily Living (ADL) and Occupational Performance Skills At this stage the Burn Therapist should complete an assessment of the child s functional activities of daily living such as dressing, feeding and hygiene, if appropriate. Depending on the results input will be given to relearn/ adapt skills and/ or educate new strategies. Depending on the area which is burned some activities of daily living may become difficult without the aid of specialised equipment e.g. supported seating, adapted cutlery etc. Early assessment of the patient s functional ability will highlight any possible equipment that is required and allow time to ensure this is in place as and when required. The child s ability to participate in leisure activities should also be assessed and if required a developmental assessment of play skills completed. Liaison with the play therapist can be very beneficial. Returning to school should be considered at this stage and may require liaison between school and the Burn Therapist. Where appropriate an Additional Support for Learning (ASL) profile should be completed. c) Scar Management Once the burn has almost healed and resultant swelling has resolved the Burn Therapist will consider scar management treatments. These include pressure garments and silicone therapy. Both apply pressure and are thought to have an influence on the collagen remodelling phase of wound healing and therefore improve the appearance of the scar (Bloemen et al, 2008). Pressure garments and silicone therapy can be used in combination and this occurs when: The area has been grafted If hypertrophic scarring is evident over area of burn or donor area, once healed Pressure garments are custom made for each child. When the burn/ graft site has healed the child will be measured for a pressure garment. The burn may have to have cling film applied to cover it whilst the area is measured. Tubigrip or interim garments can be applied as a temporary measure if the burn has healed prior to the pressure garment being ready. Pressure garments must be worn for 23 hours daily until the scar is mature and may be worn for up to 18 months from injury or until scar is fully matured (Bloemen et al, 2008). It is vital that this is educated to parents and the child to increase compliance. The child should be reviewed approximately every three months to ensure that the garment is providing adequate pressure and continues to fit well as the child grows. It also gives the therapist an opportunity to review the scar. Silicone therapy on its own should be considered when: The surface area of the burn injury is small with minimal hypertrophy The location of the burn is an anatomical flexure or area of high movement The child may not be compliant with wearing a pressure garment Page 8 of 11
9 Silicone therapy comes in the form of sheets, gel and a spray. The format that should be prescribed depends on the age of the child, area and size of the burn. Parents should be educated to monitor for any signs of allergic reaction to the silicone and to discontinue use and contact their Burns Therapist should this occur. Massage and moisturising is an important part of scar management and parents should be educated to moisturise and massage the burn three- four times daily, once it has healed. They should use an emollient cream such as E45 or Diprobase and apply firm pressure. This is vital to break up the fibres in the scar tissue leaving it smoother and more supple (Leveridge, 1991). Silicone products can be used either in combination with pressure garments or as an isolated scar management treatment. d) Discharge planning The Burn Therapist along with the MDT is expected to ensure that transition from hospital to home is as seamless as possible and ensure continuing care is in place for discharge. The therapist must ensure that the following occur: Participation in medical case conferences/ ward rounds Refer to/ liaise with local Physiotherapists/ Occupational Therapists as required Ensure a follow-up therapy appointment has been given for continuing scar management e.g. silicone or pressure garment therapy if required Ensure the child has the appropriate equipment to enable mobility/ functional independence while at home/ school Ensure parents/ guardians have received all appropriate advice for home including provision and education of a home exercise programme where appropriate It is important to liaise closely with the parents/ carers as well as the child to ensure that all are fully involved and informed of plans for discharge. If appropriate this may require liaison with the discharge co-ordinator. Recommended Therapy Intervention for the Later Phase of Rehabilitation This is the phase of scar maturation and during this the Burn Therapist continues to assess, treat and provide support to both the child and family. If this phase of rehabilitation is being continued by another hospital a telephone referral and a detailed discharge summary should be sent. Both should be documented in the therapy notes. If the pressure garment process has been commenced then the pressure garments and the measurement sheets should be sent. If geographically possible the first garments should be fitted by the Burn Therapist that measured and then the child s care transferred. The child will return to the Burns Dressing Clinic (BDC) usually on a weekly (or more frequent basis) until their scar has healed. If the child still requires more therapy input to restore/ maximise functional ability they should be seen as an outpatient in the therapy department as well as at BDC. Page 9 of 11
10 Once discharged from BDC the child will be given a review appointment with the consultant. If continued physiotherapy is required the child will be seen at this review appointment. Once the child has regained maximal/ complete functional activity they will need to continue to see the Burn Therapist on a less regular basis for scar management only. At this stage parents should be encouraged to continue to keep their children active and advice on sporting activities given and/ or referral to local gym programmes can be made if appropriate. The child should now be established with wearing their pressure garment and/ or silicone therapy. The child should be reviewed every three months to monitor their scar and to reassess their therapy input. When the scar has fully matured or cosmetically has a good appearance (scar is flat, pale and soft) the child can stop pressure garment therapy. Parents should be educated to monitor for signs of the scar becoming hypertrophic and if observed should contact their Burn Therapist. All children should be reviewed by either the Burn Therapist after discontinuing pressure garment therapy or by medical staff. If the scar shows no signs of deterioration the child can be discharged from the Burn Therapist but may well have ongoing review by the Consultant especially if scar is over a joint. Discharge When the scar has fully matured and the child is ready to be discharged a copy of the discharge letter should be sent to the GP and to the relevant Consultant. Parents should always be advised that if they have any concerns with the appearance of the scar in the future they should contact their GP for re- referral to the Burns Clinic. Children may be re-referred to the Burns Therapist in the future if they have reconstructive surgery and require re- assessment and treatment. Page 10 of 11
11 References 1. Australian and New Zealand Burn Association (ANZBA) (2002) Occupational therapy and physiotherapy: principles and guidelines for burns patient management: Bloemen, M.C.T. et al (2008) Prevention and curative management of a hypertrophic scar formation; Burns 35: Burns Therapy Standards Working Group (2005) Standards of physiotherapy and occupational therapy practice in the management of burn injured adults and children; British Burn Association. 4. Chartered Society of Physiotherapy (2005) Core standards of physiotherapy practice; CSP. 5. Ekes, A. & Marvin, J. A. (1985) PT/OT forum, burn patient cooperation in physical and occupational therapy; Journal of Burn Care & Rehabilitation 6 (3): Fink, M.P. (1993) The efficacy of an oscillating bed in the prevention of lower respiratory tract Infection in critically ill victims of trauma; Chest 103: Harden, B. (2004) Emergency physiotherapy: Churchill Livingstone, Edinburgh. Jarrett, M.B. (2008) Physical outcomes of patients with burn injuries- a 12 month follow up; Journal of Burn Care & Research 29 (6): Leveridge, A (1991) Therapy for the burn patient: Chapman & Hall, London. Okhovatian, F. & Zoubine, N. (2006) A comparison between two burn rehabilitation protocols 33: Moore, M (Nov 2009) Hand Clinics, Rehabilitation of the Burnt Hand 9. Sharp, P.A. et al (2007) The effect of positioning devices and pressure therapy on outcome after full- thickness burns of the neck 28 (3): Stoddard, F.J. et al (2002) Treatment of pain in acutely burned children; Journal of Burn Care Rehabilitation 23: Whitehead, C. & Serghiou, M. (2009) A 12- Year Comparison of common therapeutic interventions in the burn unit; Journal of Burn Care Rehabilitation 30: Vehmeyer- Heeman, M. et al (2005) Axillary burns: extended grafting and early splinting prevents contractures 26 (6): Page 11 of 11
Erin P. Frazier, OTR/L Occupational Therapist Jessica Maher, PT, MSPT Physical Therapist
 Management of Burns for The Pediatric Patient Erin P. Frazier, OTR/L Occupational Therapist efrazier@mwph.org Jessica Maher, PT, MSPT Physical Therapist jmaher@mwph.org Mt. Washington Pediatric Hospital
Management of Burns for The Pediatric Patient Erin P. Frazier, OTR/L Occupational Therapist efrazier@mwph.org Jessica Maher, PT, MSPT Physical Therapist jmaher@mwph.org Mt. Washington Pediatric Hospital
A patient s guide to the. Excision of Soft Tissue Lesion from the Upper Limb
 A patient s guide to the Excision of Soft Tissue Lesion from the Upper Limb The Operation Before your operation one of the surgical team will discuss the surgical procedure with you and answer any questions
A patient s guide to the Excision of Soft Tissue Lesion from the Upper Limb The Operation Before your operation one of the surgical team will discuss the surgical procedure with you and answer any questions
Selective Dorsal Rhizotomy (SDR) Scotland Service Pathway
 Selective Dorsal Rhizotomy (SDR) Scotland Service Pathway This pathway should to be read in conjunction with the attached notes. The number in each text box refers to the note that relates to the specific
Selective Dorsal Rhizotomy (SDR) Scotland Service Pathway This pathway should to be read in conjunction with the attached notes. The number in each text box refers to the note that relates to the specific
PHYSIOTHERAPY PROTOCOLS FOR THE MANAGEMENT OF DIFFERENT TYPES OF BRACHIAL PLEXUS INJURIES
 PHYSIOTHERAPY PROTOCOLS FOR THE MANAGEMENT OF DIFFERENT TYPES OF BRACHIAL PLEXUS INJURIES Introduction As such, protocols in the management of brachial plexus injuries (BPI) are a bit of a misnomer. This
PHYSIOTHERAPY PROTOCOLS FOR THE MANAGEMENT OF DIFFERENT TYPES OF BRACHIAL PLEXUS INJURIES Introduction As such, protocols in the management of brachial plexus injuries (BPI) are a bit of a misnomer. This
Foot and ankle fractures
 Foot and ankle fractures Some fractures can be managed without surgery, but others require surgery to achieve the best possible outcome. Fractures and injuries to joints have a high risk of developing
Foot and ankle fractures Some fractures can be managed without surgery, but others require surgery to achieve the best possible outcome. Fractures and injuries to joints have a high risk of developing
Therapy following a neck of femur fracture
 INFORMATION FOR PATIENTS Therapy following a neck of femur fracture Name of patient: ffffffffffffffffffffffffffffffffffffffffffff Procedure: ffffffffffffffffffffffffffffffffffffffffffffffffffff Consultant:
INFORMATION FOR PATIENTS Therapy following a neck of femur fracture Name of patient: ffffffffffffffffffffffffffffffffffffffffffff Procedure: ffffffffffffffffffffffffffffffffffffffffffffffffffff Consultant:
This booklet has been developed to help guide you through your post-operative rehabilitation.
 Patient Information Physiotherapy following Breast Surgery Physiotherapy Directorate Keep this booklet as a reminder with your exercises long term. If you start to develop stiffness, pain, weakness, or
Patient Information Physiotherapy following Breast Surgery Physiotherapy Directorate Keep this booklet as a reminder with your exercises long term. If you start to develop stiffness, pain, weakness, or
American Burn Association Burn Rehabilitation Therapist Competency Tool Version 2
 This document is intended to establish a framework for basic practice standards related to burn rehabilitation and provide a common language for education programs to train burn rehabilitation therapists
This document is intended to establish a framework for basic practice standards related to burn rehabilitation and provide a common language for education programs to train burn rehabilitation therapists
Ratified by: Care and Clinical Policies Date: 17 th February 2016
 Clinical Guideline Reference Number: 0803 Version 5 Title: Physiotherapy guidelines for the Management of People with Multiple Sclerosis Document Author: Henrieke Dimmendaal / Laura Shenton Date February
Clinical Guideline Reference Number: 0803 Version 5 Title: Physiotherapy guidelines for the Management of People with Multiple Sclerosis Document Author: Henrieke Dimmendaal / Laura Shenton Date February
Essential intervention No.1 Health education and self-care KEY OBJECTIVES
 Essential intervention No.1 Health education and self-care Health education bridges the gap between health information and behaviour. The person affected by BU must have the knowledge, skills, resources,
Essential intervention No.1 Health education and self-care Health education bridges the gap between health information and behaviour. The person affected by BU must have the knowledge, skills, resources,
Physiotherapy Information following Anterior Cruciate Ligament (ACL) Reconstruction
 Physiotherapy Information following Anterior Cruciate Ligament (ACL) Reconstruction Name:... Surgery Date:... Graft:... Orthopaedic Outpatient Appointment Date: Time: Location: Contact Number: Contacting
Physiotherapy Information following Anterior Cruciate Ligament (ACL) Reconstruction Name:... Surgery Date:... Graft:... Orthopaedic Outpatient Appointment Date: Time: Location: Contact Number: Contacting
24 Hour Positioning, Passive Movements, Shoulder pain, Splinting, Use of Assistive Technology, Early Mobilisation, and the Home Environment.
 24 Hour Positioning, Passive Movements, Shoulder pain, Splinting, Use of Assistive Technology, Early Mobilisation, and the Home Environment. Christine Hogg Physiotherapy Team Leader and Vicky Thomas Senior
24 Hour Positioning, Passive Movements, Shoulder pain, Splinting, Use of Assistive Technology, Early Mobilisation, and the Home Environment. Christine Hogg Physiotherapy Team Leader and Vicky Thomas Senior
Bunion (hallux valgus deformity) surgery
 Bunion (hallux valgus deformity) surgery Bunion surgery is generally reserved for bunions that are severe and impacting on function. There most frequent surgical procedure used involves a medial incision
Bunion (hallux valgus deformity) surgery Bunion surgery is generally reserved for bunions that are severe and impacting on function. There most frequent surgical procedure used involves a medial incision
National Cancer Action Team. Rehabilitation Care Pathway Poor Mobility and Loss of Function
 National Cancer Action Team Rehabilitation Care Pathway Poor Mobility and Loss of Function Diagnosis & Care Planning Assess respiratory status especially in people with preexisting respiratory disease
National Cancer Action Team Rehabilitation Care Pathway Poor Mobility and Loss of Function Diagnosis & Care Planning Assess respiratory status especially in people with preexisting respiratory disease
Foot and ankle. Achilles tendon rupture repair. After surgery
 Foot and ankle Achilles tendon rupture repair There is no agreed single best treatment for Achilles tendon ruptures. Similar results can be achieved with non-surgical and surgical treatments. There is
Foot and ankle Achilles tendon rupture repair There is no agreed single best treatment for Achilles tendon ruptures. Similar results can be achieved with non-surgical and surgical treatments. There is
Range of motion and positioning
 Range of motion and positioning Learning guide Why is motion important? Most people take free, comfortable movement for granted. Motion is meant to be smooth and painless. The ligaments, tendons, muscles,
Range of motion and positioning Learning guide Why is motion important? Most people take free, comfortable movement for granted. Motion is meant to be smooth and painless. The ligaments, tendons, muscles,
Information and exercises following a proximal femoral replacement
 Physiotherapy Department Information and exercises following a proximal femoral replacement Introduction The hip joint is a type known as a ball and socket joint. The cup side of the joint is known as
Physiotherapy Department Information and exercises following a proximal femoral replacement Introduction The hip joint is a type known as a ball and socket joint. The cup side of the joint is known as
GG10Rehabilitation Programme for Arthroscopically Assisted Anterior Cruciate Ligament Reconstruction
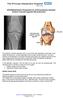 GG10Rehabilitation Programme for Arthroscopically Assisted Anterior Cruciate Ligament Reconstruction Femur ACL Graft Fibula Tibia The Anterior Cruciate Ligament (ACL) is one of the main ligaments in the
GG10Rehabilitation Programme for Arthroscopically Assisted Anterior Cruciate Ligament Reconstruction Femur ACL Graft Fibula Tibia The Anterior Cruciate Ligament (ACL) is one of the main ligaments in the
National Cancer Action Team. Rehabilitation Care Pathway Brain CNS
 National Cancer Action Team Rehabilitation Care Pathway Brain CNS Rehabilitation Care Pathway Brain CNS Diagnosis & Care Planning Drop Down Pathways Dysphagia Mobility/ loss of function Intervention D1
National Cancer Action Team Rehabilitation Care Pathway Brain CNS Rehabilitation Care Pathway Brain CNS Diagnosis & Care Planning Drop Down Pathways Dysphagia Mobility/ loss of function Intervention D1
Essential intervention No. 3 Oedema control KEY OBJECTIVES. Danger
 Essential intervention No. 3 Oedema control KEY OBJECTIVES To know what causes oedema. To know which kind of oedema needs to be referred for emergency surgery and why. To know the effects of oedema on
Essential intervention No. 3 Oedema control KEY OBJECTIVES To know what causes oedema. To know which kind of oedema needs to be referred for emergency surgery and why. To know the effects of oedema on
North of England Bone and Soft Tissue Tumour Service
 North of England Bone and Soft Tissue Tumour Service Guidelines for rehabilitation after replacement of the proximal femur Proximal femoral replacement surgery is usually carried out as part of treatment
North of England Bone and Soft Tissue Tumour Service Guidelines for rehabilitation after replacement of the proximal femur Proximal femoral replacement surgery is usually carried out as part of treatment
Exercises following Copeland Surface Replacement Arthroplasty (CSRA)
 Physiotherapy patient information Copeland Surface Replacement Arthroplasty Exercises following Copeland Surface Replacement Arthroplasty (CSRA) Introduction The Copeland Surface Replacement as it s name
Physiotherapy patient information Copeland Surface Replacement Arthroplasty Exercises following Copeland Surface Replacement Arthroplasty (CSRA) Introduction The Copeland Surface Replacement as it s name
Total Shoulder Arthroplasty / Hemi-arthroplasty (Elective)
 Total Shoulder Arthroplasty / Hemi-arthroplasty (Elective) Sling What can I do from day 1? Restrictions? Commence strengthening? Up to 3 weeks Active assisted/active supported within safe zone* Mobilise
Total Shoulder Arthroplasty / Hemi-arthroplasty (Elective) Sling What can I do from day 1? Restrictions? Commence strengthening? Up to 3 weeks Active assisted/active supported within safe zone* Mobilise
Ankle instability surgery
 Ankle instability surgery Ankle instability surgery is generally reserved for people with chronic ankle instability who have failed to respond to conservative treatment. The surgical technique used will
Ankle instability surgery Ankle instability surgery is generally reserved for people with chronic ankle instability who have failed to respond to conservative treatment. The surgical technique used will
Rehabilitation after shoulder dislocation
 Oxford University Hospitals NHS Trust Physiotherapy Department Rehabilitation after shoulder dislocation Information for patients This information leaflet gives you advice on rehabilitation after your
Oxford University Hospitals NHS Trust Physiotherapy Department Rehabilitation after shoulder dislocation Information for patients This information leaflet gives you advice on rehabilitation after your
ACL REHABILITATION. Key to Success
 ACL REHABILITATION The overall rehabilitation plan emphasises the importance of pre-operative exercises followed post operatively by early control of swelling and regaining full extension (straightening)
ACL REHABILITATION The overall rehabilitation plan emphasises the importance of pre-operative exercises followed post operatively by early control of swelling and regaining full extension (straightening)
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS
 Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
Your Orthotics service is changing
 Your Orthotics service is changing Important for referrers on changes effective from January 2015 Why is the service changing? As demand for the orthotics service increases and budgets remain relatively
Your Orthotics service is changing Important for referrers on changes effective from January 2015 Why is the service changing? As demand for the orthotics service increases and budgets remain relatively
Prevention and management of Pressure ulcers
 Prevention and management of Pressure ulcers A guide for patients, carers and relatives What is a pressure ulcer? Pressure ulcers are an injury to the skin and/or underlying tissues. They are also known
Prevention and management of Pressure ulcers A guide for patients, carers and relatives What is a pressure ulcer? Pressure ulcers are an injury to the skin and/or underlying tissues. They are also known
Shoulder Hemi-arthroplasty (Trauma)
 Shoulder Hemi-arthroplasty (Trauma) Sling What can I do from day 1? Restrictions? Commence strengthening? Trauma: Up to 6 Active assisted/active supported within safe zone* Mobilise unaffected joints e.g
Shoulder Hemi-arthroplasty (Trauma) Sling What can I do from day 1? Restrictions? Commence strengthening? Trauma: Up to 6 Active assisted/active supported within safe zone* Mobilise unaffected joints e.g
Total knee replacement
 Total knee replacement Inpatient and home exercises Information for patients MSK Orthopaedic Inpatients (Therapy) When you go home from hospital following your knee replacement, a referral will be made
Total knee replacement Inpatient and home exercises Information for patients MSK Orthopaedic Inpatients (Therapy) When you go home from hospital following your knee replacement, a referral will be made
Anterior Cruciate Ligament Reconstruction
 Anterior Cruciate Ligament Reconstruction Physiotherapy Department Patient information leaflet This patient information booklet is designed to provide you with information about the Anterior Cruciate Ligament
Anterior Cruciate Ligament Reconstruction Physiotherapy Department Patient information leaflet This patient information booklet is designed to provide you with information about the Anterior Cruciate Ligament
Exercises following arthroscopic (or open) anterior stabilisation
 Physiotherapy patient information Exercises following arthroscopic (or open) anterior stabilisation Introduction The shoulder joint is designed to give a large amount of movement, therefore support from
Physiotherapy patient information Exercises following arthroscopic (or open) anterior stabilisation Introduction The shoulder joint is designed to give a large amount of movement, therefore support from
Hip Arthroscopy Rehabilitation Protocol
 Hip Arthroscopy Rehabilitation Protocol 1. Concepts: a. Range of motion and weight bearing restrictions must be adhered to during the initial rehab process (4 total weeks of ROM and weight bearing restrictions)
Hip Arthroscopy Rehabilitation Protocol 1. Concepts: a. Range of motion and weight bearing restrictions must be adhered to during the initial rehab process (4 total weeks of ROM and weight bearing restrictions)
Current Concepts in Burn Rehabilitation
 Current Concepts in Burn Rehabilitation 7 th Congress of the Baltic Association of Rehabilitation Tallinn, Estonia September 2010 R. Scott Ward, PT, PhD Professor and Chair Department of Physical Therapy
Current Concepts in Burn Rehabilitation 7 th Congress of the Baltic Association of Rehabilitation Tallinn, Estonia September 2010 R. Scott Ward, PT, PhD Professor and Chair Department of Physical Therapy
1. Can self-propel, or use their foot to push (punt), a standard manual wheelchair 1 and be safe and able to do essential daily tasks.
 Disability Support Services Equipment and Modifications Competency Framework Wheeled Mobility and Postural Management Introduction The Wheeled Mobility and Postural Management Credential recognises that
Disability Support Services Equipment and Modifications Competency Framework Wheeled Mobility and Postural Management Introduction The Wheeled Mobility and Postural Management Credential recognises that
SPAH PHYSIOTHERAPY GUIDELINES FOR THE ACUTE MANAGEMENT OF ADULT AND PAEDIATRIC PATIENTS WITH SICKLE CELL DISEASE
 THIS DOCUMENT MUST NOT BE COPIED SPAH PHYSIOTHERAPY GUIDELINES FOR THE ACUTE MANAGEMENT OF ADULT AND PAEDIATRIC PATIENTS WITH SICKLE CELL DISEASE 1. Purpose of this document To provide guidelines for physiotherapy
THIS DOCUMENT MUST NOT BE COPIED SPAH PHYSIOTHERAPY GUIDELINES FOR THE ACUTE MANAGEMENT OF ADULT AND PAEDIATRIC PATIENTS WITH SICKLE CELL DISEASE 1. Purpose of this document To provide guidelines for physiotherapy
What to expect following spinal cord injury. Information for patients Therapy Services
 What to expect following spinal cord injury Information for patients Therapy Services Introduction This leaflet aims to explain what spinal cord injury is and what to expect over the next few months. What
What to expect following spinal cord injury Information for patients Therapy Services Introduction This leaflet aims to explain what spinal cord injury is and what to expect over the next few months. What
Humerus Fracture. Virtual Fracture Clinic Patient information
 Portsmouth Hospitals NHS Trust Virtual Fracture Clinic Patient information Humerus Fracture Specialist Support This leaflet can be made available in another language, large print or another format. Please
Portsmouth Hospitals NHS Trust Virtual Fracture Clinic Patient information Humerus Fracture Specialist Support This leaflet can be made available in another language, large print or another format. Please
TOTAL KNEE REPLACEMENT PATIENT INFORMATION LEAFLET
 TOTAL KNEE REPLACEMENT PATIENT INFORMATION LEAFLET This leaflet has been produced to help answer some questions you may have following your knee replacement. However if you still have any concerns or queries
TOTAL KNEE REPLACEMENT PATIENT INFORMATION LEAFLET This leaflet has been produced to help answer some questions you may have following your knee replacement. However if you still have any concerns or queries
Taking Action for Optimal Community and Long-Term stroke Care A Resource for Healthcare Providers
 Taking Action for Optimal Community and Long-Term stroke Care A Resource for Healthcare Providers Chapter 6: Activities and Participation Section 6.2: Positioning Copyright Information The Taking Action
Taking Action for Optimal Community and Long-Term stroke Care A Resource for Healthcare Providers Chapter 6: Activities and Participation Section 6.2: Positioning Copyright Information The Taking Action
Intermediate Postoperative Shoulder Stretching Exercises:
 Intermediate Postoperative Shoulder Stretching Exercises: - Videos are available on Dr. Witty s website. - These exercises can be started immediately after surgery to facilitate recovery and work together
Intermediate Postoperative Shoulder Stretching Exercises: - Videos are available on Dr. Witty s website. - These exercises can be started immediately after surgery to facilitate recovery and work together
Information and exercises following dynamic hip screw
 Physiotherapy Department Information and exercises following dynamic hip screw Introduction A dynamic hip screw is performed where the neck of femur has been fractured and where there is a good chance
Physiotherapy Department Information and exercises following dynamic hip screw Introduction A dynamic hip screw is performed where the neck of femur has been fractured and where there is a good chance
Stretching and Positioning Regime for Upper Limb
 Stretching and Positioning Regime for Upper Limb Physiotherapy Department Community & Therapy Services This leaflet has been designed to remind you of the exercises you have been taught, the correct techniques
Stretching and Positioning Regime for Upper Limb Physiotherapy Department Community & Therapy Services This leaflet has been designed to remind you of the exercises you have been taught, the correct techniques
Latissimus Dorsi Flap reconstruction Breast reconstruction
 Latissimus Dorsi Flap reconstruction Breast reconstruction 01935 384 352 yeovilhospital.nhs.uk Introduction Lots of women have surgery to reconstruct the breast after mastectomy. There are a variety of
Latissimus Dorsi Flap reconstruction Breast reconstruction 01935 384 352 yeovilhospital.nhs.uk Introduction Lots of women have surgery to reconstruct the breast after mastectomy. There are a variety of
Your Spasticity Management Service: Managing spasticity with Botulinum Toxin A in children with cerebral palsy
 Paediatric Unit information for parents and carers Your Spasticity Management Service: Managing spasticity with Botulinum Toxin A in children with cerebral palsy This leaflet is for children and young
Paediatric Unit information for parents and carers Your Spasticity Management Service: Managing spasticity with Botulinum Toxin A in children with cerebral palsy This leaflet is for children and young
Advice for patients following a Rotator Cuff Repair
 Contact Information Acute Musculoskeletal Therapy Team: 0151 676 5519 Advice for patients following a Rotator Cuff Repair Patient Advice and Liaison Service (PALS): 0151 430 1376 St Helens Hospital Marshall
Contact Information Acute Musculoskeletal Therapy Team: 0151 676 5519 Advice for patients following a Rotator Cuff Repair Patient Advice and Liaison Service (PALS): 0151 430 1376 St Helens Hospital Marshall
Charlotte Shoulder Institute
 Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Gill Orthopaedic Midtown Medical Plaza 1918 Randolph Rd., Suite 700 Charlotte, NC 28211 704-342-3544
Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Gill Orthopaedic Midtown Medical Plaza 1918 Randolph Rd., Suite 700 Charlotte, NC 28211 704-342-3544
Arthroscopic capsular release. Information for patients Orthopaedics - Upper Limb
 Arthroscopic capsular release Information for patients Orthopaedics - Upper Limb Introduction The Upper Limb Unit team would like you and your family to understand as much as possible about the operation
Arthroscopic capsular release Information for patients Orthopaedics - Upper Limb Introduction The Upper Limb Unit team would like you and your family to understand as much as possible about the operation
SCOTTISH MUSCLE NETWORK DUCHENNE MUSCULAR DYSTROPHY TRANSITION SOME USEFUL THINGS TO KNOW ABOUT HEALTH AROUND ADOLESCENCE
 SCOTTISH MUSCLE NETWORK DUCHENNE MUSCULAR DYSTROPHY TRANSITION SOME USEFUL THINGS TO KNOW ABOUT HEALTH AROUND ADOLESCENCE 02 Changes in our lives can be stressful and leaving school and moving into the
SCOTTISH MUSCLE NETWORK DUCHENNE MUSCULAR DYSTROPHY TRANSITION SOME USEFUL THINGS TO KNOW ABOUT HEALTH AROUND ADOLESCENCE 02 Changes in our lives can be stressful and leaving school and moving into the
WAHT-OCT-021 It is the responsibility of every individual to ensure this is the latest version as published on the Trust Intranet
 This guidance does not override the individual responsibility of health professionals to make appropriate decision according to the circumstances of the individual patient in consultation with the patient
This guidance does not override the individual responsibility of health professionals to make appropriate decision according to the circumstances of the individual patient in consultation with the patient
A Patient s Guide to Post-Operative Advice Following Pes Cavus
 A Patient s Guide to Post-Operative Advice Following Pes Cavus The Foot and Ankle unit at the Royal National Orthopaedic Hospital (RNOH) is a multi-disciplinary team. The team consists of three specialist
A Patient s Guide to Post-Operative Advice Following Pes Cavus The Foot and Ankle unit at the Royal National Orthopaedic Hospital (RNOH) is a multi-disciplinary team. The team consists of three specialist
Physiotherapy management
 Physiotherapy management Pre-operative Focus is on the objective assessment looking at ROM and muscle power. Using assessment findings, knowledge of prosthetic componentry and gait patterns, provide a
Physiotherapy management Pre-operative Focus is on the objective assessment looking at ROM and muscle power. Using assessment findings, knowledge of prosthetic componentry and gait patterns, provide a
Carpal Tunnel Syndrome
 Patient information Carpal Tunnel Syndrome i Important information for all patients having Carpal Tunnel surgery. Golden Jubilee National Hospital Agamemnon Street Clydebank, G81 4DY (: 0141 951 5000 www.nhsgoldenjubilee.co.uk
Patient information Carpal Tunnel Syndrome i Important information for all patients having Carpal Tunnel surgery. Golden Jubilee National Hospital Agamemnon Street Clydebank, G81 4DY (: 0141 951 5000 www.nhsgoldenjubilee.co.uk
Exercises and advice following your breast reconstruction surgery
 Exercises and advice following your breast reconstruction surgery This leaflet gives information to people who have had breast reconstructive surgery. It contains exercises that your physiotherapist would
Exercises and advice following your breast reconstruction surgery This leaflet gives information to people who have had breast reconstructive surgery. It contains exercises that your physiotherapist would
Your Orthotics service is changing
 Your Orthotics service is changing Important information for service users on changes effective from July 2015 Why is the service changing? As demand for the Orthotics service increases, Livewell Southwest
Your Orthotics service is changing Important information for service users on changes effective from July 2015 Why is the service changing? As demand for the Orthotics service increases, Livewell Southwest
Total Shoulder Rehab Protocol Dr. Payne
 Total Shoulder Rehab Protocol Dr. Payne Phase I Immediate Post Surgical Phase (0-4 weeks): Allow healing of soft tissue Maintain integrity of replaced joint Gradually increase passive range of motion (PROM)
Total Shoulder Rehab Protocol Dr. Payne Phase I Immediate Post Surgical Phase (0-4 weeks): Allow healing of soft tissue Maintain integrity of replaced joint Gradually increase passive range of motion (PROM)
A patient s guide to the. physiotherapy exercises and advice following excision of ilium with fibula strut
 A patient s guide to the physiotherapy exercises and advice following excision of ilium with fibula strut This booklet outlines the likely physiotherapy treatment you will receive while in hospital. Although
A patient s guide to the physiotherapy exercises and advice following excision of ilium with fibula strut This booklet outlines the likely physiotherapy treatment you will receive while in hospital. Although
Guidance for the Physiotherapy Management of Patients Undergoing Limb Reconstruction with a Circular Frame External Fixator.
 Guidance for the Physiotherapy Management of Patients Undergoing Limb Reconstruction with a Circular Frame External Fixator. Table of Contents INTRODUCTION... 2 TARGET AUDIENCE... 2 KEY CHANGES FROM PREVIOUS
Guidance for the Physiotherapy Management of Patients Undergoing Limb Reconstruction with a Circular Frame External Fixator. Table of Contents INTRODUCTION... 2 TARGET AUDIENCE... 2 KEY CHANGES FROM PREVIOUS
Above Knee Amputation: Post-op Information
 Above Knee Amputation: Post-op Information This package contains information to help as you begin the recovery process following your amputation. The topics included are: Emotions following an amputation.
Above Knee Amputation: Post-op Information This package contains information to help as you begin the recovery process following your amputation. The topics included are: Emotions following an amputation.
SHOULDER ARTHROSCOPY WITH ANTERIOR STABILIZATION / CAPSULORRHAPHY REHABILITATION PROTOCOL
 General Notes As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
General Notes As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
Exercises following rotator cuff repair (minor tear: less than 1cm)
 Physiotherapy patient information Rotator cuff repair (minor tear) Exercises following rotator cuff repair (minor tear: less than 1cm) Introduction The rotator cuff consists of four muscles and their tendons,
Physiotherapy patient information Rotator cuff repair (minor tear) Exercises following rotator cuff repair (minor tear: less than 1cm) Introduction The rotator cuff consists of four muscles and their tendons,
Greater Tuberosity Fracture Shoulder 6
 Greater Tuberosity Fracture Shoulder 6 Fracture Care Team: Shared Care Plan Eastbourne - 01323 414928 Conquest - 01424 757576 Email - esht.vfc@nhs.net This information leaflet follows up your recent telephone
Greater Tuberosity Fracture Shoulder 6 Fracture Care Team: Shared Care Plan Eastbourne - 01323 414928 Conquest - 01424 757576 Email - esht.vfc@nhs.net This information leaflet follows up your recent telephone
Elbow debridement (OK procedure)
 Elbow debridement (OK procedure) Information for patients The Nottingham Shoulder and Elbow Unit This document can be provided in different languages and formats. For more information please contact: Physiotherapy
Elbow debridement (OK procedure) Information for patients The Nottingham Shoulder and Elbow Unit This document can be provided in different languages and formats. For more information please contact: Physiotherapy
ACL RECONSTRUCTION PROTOCOL
 ACL RECONSTRUCTION PROTOCOL Name of Protocol/Regime ACL Reconstruction Consultant Updated On Updated By Review Date Mr Dawson 5/5/16 Barbara Pinguey/ Rachael Edgar 6/18 Please note that surgeons may have
ACL RECONSTRUCTION PROTOCOL Name of Protocol/Regime ACL Reconstruction Consultant Updated On Updated By Review Date Mr Dawson 5/5/16 Barbara Pinguey/ Rachael Edgar 6/18 Please note that surgeons may have
CANCER REHABILITATION PATHWAY - HAEMATOLOGY
 CANCER REHABILITATION PATHWAY - HAEMATOLOGY Statement: To be used in conjunction with Brain and CNS Rehabilitation Care Pathway as appropriate Diagnosis and Care Planning: The following symptom pathways
CANCER REHABILITATION PATHWAY - HAEMATOLOGY Statement: To be used in conjunction with Brain and CNS Rehabilitation Care Pathway as appropriate Diagnosis and Care Planning: The following symptom pathways
Total ankle replacement
 Total ankle replacement Initial rehabilitation phase 0-4 weeks To be safely and independently mobile with appropriate walking aid, adhering to weight bearing status To be independent with home exercise
Total ankle replacement Initial rehabilitation phase 0-4 weeks To be safely and independently mobile with appropriate walking aid, adhering to weight bearing status To be independent with home exercise
Elbow Replacement Guide
 Elbow Replacement Guide IM-CNOH-12 Rev. 1 Issue Date: March 2011 Review Date: March 2012 Founded 1908 C A P PA G H N AT I O N A L O RT H O PA E D I C H O S P I TA L FINGLAS, DUBLIN 11. TEL: 01 814 0429
Elbow Replacement Guide IM-CNOH-12 Rev. 1 Issue Date: March 2011 Review Date: March 2012 Founded 1908 C A P PA G H N AT I O N A L O RT H O PA E D I C H O S P I TA L FINGLAS, DUBLIN 11. TEL: 01 814 0429
Copyright Cardiff University
 This exercise programme has been developed by physiotherapists specifically for people with movement disorders. Exercise is not without its risks and this or any other exercise programme has potential
This exercise programme has been developed by physiotherapists specifically for people with movement disorders. Exercise is not without its risks and this or any other exercise programme has potential
Foot and Ankle Surgery
 Information about Foot and Ankle Surgery Statement of Use The information in this leaflet is intended solely for the person to whom it was given by the health care team and is provided as a general information
Information about Foot and Ankle Surgery Statement of Use The information in this leaflet is intended solely for the person to whom it was given by the health care team and is provided as a general information
Pressure Ulcers Patient Information Leaflet
 Pressure Ulcers Patient Information Leaflet Shining a light on the future Introduction This leaflet is about pressure ulcers and includes information about what they are what can cause them and how they
Pressure Ulcers Patient Information Leaflet Shining a light on the future Introduction This leaflet is about pressure ulcers and includes information about what they are what can cause them and how they
Pressure Ulcers Patient Information Leaflet
 Further information about the content, reference sources or production of this leaflet can be obtained from the Patient Information Centre. Pressure Ulcers Patient Information Leaflet This information
Further information about the content, reference sources or production of this leaflet can be obtained from the Patient Information Centre. Pressure Ulcers Patient Information Leaflet This information
Exercises following rotator cuff repair (major tear: 3-5cm and massive tear: more than 5cm)
 Physiotherapy patient information Rotator cuff repair (major/massive tear) Exercises following rotator cuff repair (major tear: 3-5cm and massive tear: more than 5cm) Introduction The rotator cuff consists
Physiotherapy patient information Rotator cuff repair (major/massive tear) Exercises following rotator cuff repair (major tear: 3-5cm and massive tear: more than 5cm) Introduction The rotator cuff consists
Advice for patients following a Slap Repair
 Contact Information Acute Musculoskeletal Therapy Team: 0151 676 5519 Patient Advice and Liaison Service (PALS): 0151 430 1376 Advice for patients following a Slap Repair St Helens Hospital Marshall Cross
Contact Information Acute Musculoskeletal Therapy Team: 0151 676 5519 Patient Advice and Liaison Service (PALS): 0151 430 1376 Advice for patients following a Slap Repair St Helens Hospital Marshall Cross
Total knee replacement: The enhanced recovery programme
 INFORMATION FOR PATIENTS Total knee replacement: The enhanced recovery programme This leaflet aims to explain the enhanced recovery programme after total knee replacement surgery, to outline certain common
INFORMATION FOR PATIENTS Total knee replacement: The enhanced recovery programme This leaflet aims to explain the enhanced recovery programme after total knee replacement surgery, to outline certain common
Protocol for the Management of Hip Arthroscopy Surgery
 Overall Aims of Surgery To decrease pain To increase range of motion (ROM) To increase hip/pelvis and lumbar stability To enable return to activities of daily living and sport Initial Post-operative Objectives
Overall Aims of Surgery To decrease pain To increase range of motion (ROM) To increase hip/pelvis and lumbar stability To enable return to activities of daily living and sport Initial Post-operative Objectives
Anterior Cruciate Ligament (ACL) Reconstruction. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Anterior Cruciate Ligament (ACL) Reconstruction An information guide Anterior Cruciate Ligament (ACL) Reconstruction Post-operative regime
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Anterior Cruciate Ligament (ACL) Reconstruction An information guide Anterior Cruciate Ligament (ACL) Reconstruction Post-operative regime
POST OP CLOSED BANKART PROCEDURE
 POST OP CLOSED BANKART PROCEDURE WEEKS 1-6 Do 1. Wear sling until advised otherwise 2. Keep dressing clean and dry 3. Do passive pendulum exercises to 90 degrees 4. Ice for 15 minutes after exercising
POST OP CLOSED BANKART PROCEDURE WEEKS 1-6 Do 1. Wear sling until advised otherwise 2. Keep dressing clean and dry 3. Do passive pendulum exercises to 90 degrees 4. Ice for 15 minutes after exercising
Charlotte Shoulder Institute
 Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
Proximal Humerus fracture Shoulder 7
 Proximal Humerus fracture Shoulder 7 Fracture Care Team: Shared Care Plan Eastbourne - 01323 414928 Conquest - 01424 757576 Email - esht.vfc@nhs.net This information leaflet follows up your recent telephone
Proximal Humerus fracture Shoulder 7 Fracture Care Team: Shared Care Plan Eastbourne - 01323 414928 Conquest - 01424 757576 Email - esht.vfc@nhs.net This information leaflet follows up your recent telephone
Reverse Total Shoulder Arthroplasty Protocol
 General Information: Reverse Total Shoulder Arthroplasty Protocol Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH) arthritis when it
General Information: Reverse Total Shoulder Arthroplasty Protocol Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH) arthritis when it
Lumbar decompression or discectomy
 Information and exercises Lumbar decompression or discectomy Introduction A lumbar decompression or discectomy is done to relieve pressure on the nerves in order to relieve pain and altered sensation.
Information and exercises Lumbar decompression or discectomy Introduction A lumbar decompression or discectomy is done to relieve pressure on the nerves in order to relieve pain and altered sensation.
INFORMATION FOR PATIENTS. Rotator cuff repair operation
 INFORMATION FOR PATIENTS Rotator cuff repair operation This booklet contains information about the shoulder surgery that you have been advised to have, and aims to answer some of the questions you may
INFORMATION FOR PATIENTS Rotator cuff repair operation This booklet contains information about the shoulder surgery that you have been advised to have, and aims to answer some of the questions you may
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R
 S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R H I P A R T H R O S C O P Y W I T H This protocol provides appropriate guidelines for the rehabilitation of patients following
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R H I P A R T H R O S C O P Y W I T H This protocol provides appropriate guidelines for the rehabilitation of patients following
Knee Replacement PROGRAM. Nightingale. Home Healthcare
 Knee Replacement PROGRAM TM Nightingale Home Healthcare With the help of Nightingale s experienced and professional rehabilitation team, you will be guided through a more complete and successful recovery
Knee Replacement PROGRAM TM Nightingale Home Healthcare With the help of Nightingale s experienced and professional rehabilitation team, you will be guided through a more complete and successful recovery
Preventing Pressure Ulcers
 Patient information Preventing Pressure Ulcers i Important information and care guide for patients at risk of pressure ulcers. Reproduced with kind permission from Healthcare Improvement Scotland Golden
Patient information Preventing Pressure Ulcers i Important information and care guide for patients at risk of pressure ulcers. Reproduced with kind permission from Healthcare Improvement Scotland Golden
Charlotte Shoulder Institute
 Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
FOOT AND ANKLE ARTHROSCOPY
 FOOT AND ANKLE ARTHROSCOPY Information for Patients WHAT IS FOOT AND ANKLE ARTHROSCOPY? The foot and the ankle are crucial for human movement. The balanced action of many bones, joints, muscles and tendons
FOOT AND ANKLE ARTHROSCOPY Information for Patients WHAT IS FOOT AND ANKLE ARTHROSCOPY? The foot and the ankle are crucial for human movement. The balanced action of many bones, joints, muscles and tendons
Exercises following stemmed hemiarthroplasty for trauma / fracture
 Physiotherapy patient information Stemmed hemiarthroplasty (Mr Malhas) Exercises following stemmed hemiarthroplasty for trauma / fracture Introduction A shoulder replacement is done following a fracture
Physiotherapy patient information Stemmed hemiarthroplasty (Mr Malhas) Exercises following stemmed hemiarthroplasty for trauma / fracture Introduction A shoulder replacement is done following a fracture
Preventing pressure ulcers
 Golden Jubilee National Hospital NHS National Waiting Times Centre Preventing pressure ulcers Patient information guide for adults at risk of pressure ulcers Agamemnon Street Clydebank, G81 4DY (: 0141
Golden Jubilee National Hospital NHS National Waiting Times Centre Preventing pressure ulcers Patient information guide for adults at risk of pressure ulcers Agamemnon Street Clydebank, G81 4DY (: 0141
HAND SURGERY- GUIDELINES for POST-OP TREATMENT and REFERRAL to HAND THERAPY
 HAND SURGERY- GUIDELINES for POST-OP TREATMENT and REFERRAL to HAND THERAPY Please use the specific hand therapy referral form. Always give at least one telephone number for the patient so that there is
HAND SURGERY- GUIDELINES for POST-OP TREATMENT and REFERRAL to HAND THERAPY Please use the specific hand therapy referral form. Always give at least one telephone number for the patient so that there is
Expert Transfers in Rehabilitation: A Safety and Utilisation Review
 Expert Transfers in Rehabilitation: A Safety and Utilisation Review Robert Mehan Meaghan Mackenzie Kim Brock Rehabilitation Care Centre NAHC 2007 - Hobart An important focus in stroke rehabilitation is
Expert Transfers in Rehabilitation: A Safety and Utilisation Review Robert Mehan Meaghan Mackenzie Kim Brock Rehabilitation Care Centre NAHC 2007 - Hobart An important focus in stroke rehabilitation is
Hand & Plastics Physiotherapy Department Extensor Tendon Repair Zone IV and above Information for patients
 Oxford University Hospitals NHS Trust Hand & Plastics Physiotherapy Department Extensor Tendon Repair Zone IV and above Information for patients Introduction You have had surgery to repair one or more
Oxford University Hospitals NHS Trust Hand & Plastics Physiotherapy Department Extensor Tendon Repair Zone IV and above Information for patients Introduction You have had surgery to repair one or more
PROM is not stretching!
 Dx: o Right o Left Shoulder Replacement/Hemiarthroplasty Rehab Date of Surgery: Patient Name: PT/OT: Please evaluate and treat. Follow attached protocol. 2-3 x per week x 6 weeks. Signature/Date: The intent
Dx: o Right o Left Shoulder Replacement/Hemiarthroplasty Rehab Date of Surgery: Patient Name: PT/OT: Please evaluate and treat. Follow attached protocol. 2-3 x per week x 6 weeks. Signature/Date: The intent
Weber B ankle fracture Information for patients Outpatient Fracture Care Team: Shared care plan
 Weber B ankle fracture Information for patients Outpatient Fracture Care Team: Shared care plan Orthopaedic Department Tunbridge Wells Hospital Tonbridge Road Pembury TN2 4QJ Telephone: 07734370108 Email:
Weber B ankle fracture Information for patients Outpatient Fracture Care Team: Shared care plan Orthopaedic Department Tunbridge Wells Hospital Tonbridge Road Pembury TN2 4QJ Telephone: 07734370108 Email:
NATIONAL REHABILITATION HOSPITAL SPINAL CORD SYSTEM OF CARE (SCSC) OUTPATIENT SCOPE OF SERVICE
 NATIONAL REHABILITATION HOSPITAL SPINAL CORD SYSTEM OF CARE (SCSC) OUTPATIENT SCOPE OF SERVICE Introduction: The Spinal Cord System of Care (SCSC) at the National Rehabilitation Hospital (NRH) provides
NATIONAL REHABILITATION HOSPITAL SPINAL CORD SYSTEM OF CARE (SCSC) OUTPATIENT SCOPE OF SERVICE Introduction: The Spinal Cord System of Care (SCSC) at the National Rehabilitation Hospital (NRH) provides
Clavicle (Collar bone) Fracture (undisplaced) Shoulder 4
 Clavicle (Collar bone) Fracture (undisplaced) Shoulder 4 Fracture Care Team: Shared Care Plan Eastbourne - 01323 414928 Conquest - 01424 757576 Email - esht.vfc@nhs.net This information leaflet follows
Clavicle (Collar bone) Fracture (undisplaced) Shoulder 4 Fracture Care Team: Shared Care Plan Eastbourne - 01323 414928 Conquest - 01424 757576 Email - esht.vfc@nhs.net This information leaflet follows
The Chailey Levels of Ability Assessment Charts
 The Chailey Levels of Ability Assessment Charts Assessment details NAME D.O.B. DIAGNOSIS DATE OF ASSESSMENT ASSESSMENT CENTRE NAME OF ASSESSOR Notes CHAILEY HERITAGE CLINICAL SERVICES Beggars Wood Road
The Chailey Levels of Ability Assessment Charts Assessment details NAME D.O.B. DIAGNOSIS DATE OF ASSESSMENT ASSESSMENT CENTRE NAME OF ASSESSOR Notes CHAILEY HERITAGE CLINICAL SERVICES Beggars Wood Road
Advice following Anterior Cruciate Ligament (ACL) reconstruction
 Advice following Anterior Cruciate Ligament (ACL) reconstruction Information for patients Mobilisation As soon as you feel well enough after the operation you will be able to get up and mobilise. You will
Advice following Anterior Cruciate Ligament (ACL) reconstruction Information for patients Mobilisation As soon as you feel well enough after the operation you will be able to get up and mobilise. You will
Routine For: OT - General Guidelines/Energy Conservation (Caregiver)
 GENERAL GUIDELINES - 9 Tips for Exercise: Body Mechanics for Helper - To protect back, stay as upright as possible and keep head in line with trunk. - Always position yourself as close as possible to the
GENERAL GUIDELINES - 9 Tips for Exercise: Body Mechanics for Helper - To protect back, stay as upright as possible and keep head in line with trunk. - Always position yourself as close as possible to the
