Effectiveness of Mulligan s Technique and Spencer s Technique in Adjunct to Conventional Therapy in Frozen Shoulder: A Randomised Controlled Trial
|
|
|
- Michael Dean
- 6 years ago
- Views:
Transcription
1 (Volume 3, Issue 1) Available online at Effectiveness of Mulligan s Technique and Spencer s Technique in Adjunct to Conventional Therapy in Frozen Shoulder: A Randomised Controlled Trial Dr. B. Haveela 1, Dr. Praveen Dowle 2, Dr. P.Chandrashekar 3 1 Post Graduate Student, Nizam s Institute of Medical Sciences, Hyderabad 2 MPT (Musculoskeletal Sciences), Senior Physiotherapy Faculty, College of Physiotherapy, Nizam s Institute of Medical Sciences, Hyderabad 3 Head of Department, Department of Orthopaedics, Nizam s Institute of Medical Sciences, Hyderabad ABSTRACT Background: Frozen shoulder is a common condition with pain, stiffness and limited motion of the shoulder joint, resulting from the fibrosis and contracture of the glenohumeral joint capsule. Physical therapy treatment may include various manual mobilization techniques to regain extensibility of the shoulder capsule and in relieving pain and increase range of motion. Purpose: The purpose of the study was to compare and find out the effectiveness of Mulligan s technique and Spencer s technique individually when compared with conventional therapy in patients with frozen shoulder. Methods: 90 patients were selected randomly with frozen shoulder. The study included 3 groups, control group received Conventional therapy, mulligan s group received mulligan s technique MWM and conventional therapy, and spencer s group received Spencer s technique and conventional therapy. The period of intervention was 3 sessions per week for 6 weeks. The outcome measures included NPRS, goniometry and SPADI. ANOVA was done for inter group analysis, post hoc test was done for between group analysis and paired T- test was done for intra group analysis. Result: There was no significant difference in outcome measures of all the three groups at day 1. All the three groups showed significant difference (p- value <0.05) at 3 and 6 week in NPRS, shoulder ROM and SPADI. The mean difference and paired T-test values of mulligan s group was more when compared to control group and spencer s group at the end of 6 weeks Conclusion: In this study we found significant improvement statistically in all the outcome measures in control group, mulligan s group and spencer s group at 6 weeks of intervention. However the functional improvement in mulligan s group was better than control group and spencer group. Keywords: Frozen Shoulder, MWM, Mulligans Technique, and Spencer s Technique. 1. INTRODUCTION Frozen shoulder has been described as a painful condition associated with stiffness and difficulty in sleeping on the affected side. The condition can vary from mild to severe pain and from some to severe restriction in the movement; people with this condition struggle with basic activities of daily living such as difficulty in dressing, performing personal hygiene, overhead movements, and sleep disturbance. It is a condition of unknown etiology; it occurs in 2 5% of general adult population, 10 15% of the people with diabetes. It mainly affects the individuals of years of age with female predominance. 1, 4 it is said to be a self-limiting process. However in some patients, the disease can last much longer than 1 year. 7 Frozen shoulder can be defined as insidious and progressive loss of both active and passive shoulder mobility in the glenohumeral joint presumably due to capsular contracture. 1 recent studies showed inflammation and stiffness of the capsule surrounding the glenohumeral joint, greatly restricting motion and causing chronic pain 2. Much of the disease also involved structures outside the joint capsule. These structures can include coracohumeral ligament in the rotator interval, musculotendinous unit and the subacrominal bursa. 2,3 The onset of idiopathic frozen shoulder could be due to immunological, biochemical or hormonal imbalance, secondary risk factors include recent injury to the shoulder leading to lack of use due to pain or a recent shoulder surgery, 2018, All Rights Reserved Page 253
2 certain medical conditions such as diabetes mellitus, stroke, lung diseases, connective tissue diseases, thyroid, ischemic heart disease, inflammatory arthritis. 5,6 Physiotherapy methods such as active and active assisted exercises, pendular ex s, wand ex s, wall and ladder ex s, capsular stretching ex s and shoulder joint mobilization are often standard exercises in treating frozen shoulder. Electrotherapy modalities such as application of ultrasound, IFT, short-wave diathermy and LASER are used to relieve pain and promote hyperthermic effect to the tissues. Brain mulligan s technique known as mobilization with movement for peripheral joints combines sustained manual application of gliding" force to a joint by the therapist while the restricted upper limb movement is performed actively or passively by the patient to restore the reduced accessory glide and the result should be a pain free movement. 8 The spencer technique is a standardized series of shoulder treatments with broad application in diagnosis, treatment and prognosis. It is developed by Spencer, D.O. in this approach is a well-known osteopathic manipulative technique that focuses on mobilization of the glenohumeral and scapulothoracic joints. 10 It is an articulatory technique with seven different procedures, in this technique passive, smooth, rhythmic motion of the shoulder joint is done by the therapist to stretch contracted muscles, ligaments and capsule. Most of the force is applied at the end range of motion. 11 Very few studies have compared these two techniques, Mulligan s technique helps in repositioning the bone positional faults. 8 whereas Spencer s technique increases pain free range of motion through stretching the tissues; enhancing lymphatic flow and increase joint circulation. 11, As there are no studies in the literature which compared the effectiveness of these two techniques with the control group in frozen shoulder patients, hence the purpose of the present study was to compare and find out the effectiveness of mulligan s technique and spencer s technique individually when compared with conventional therapy on improvement of pain, functional disability and shoulder ROM in subjects with frozen shoulder. 2. MATERIALS AND METHODS We recruited 90 subjects from the outpatient Department of Physiotherapy, Nizam s Institute Of Medical Sciences, and Hyderabad. Subjects diagnosed as frozen shoulder by orthopedic department were included in the study. Institutional ethical committee approval was taken. Criteria for inclusion were age group of years of both genders, unilateral adhesive capsulitis, subjects who had restricted ROM (loss of 25% or greater relative to non-involved shoulder in one or multidirectional), Non diabetic subjects. Subjects were excluded if they had recent history of surgery on particular shoulder, Post traumatic and rotator cuff rupture, Neurological deficits affecting shoulder function, Pain or disorders of cervical spine, elbow, wrist or hand, tendon calcification, rheumatoid arthritis, osteoporosis, malignancies, pregnancy, open wounds or skin infections, a recent steroid injection and previous manipulation under anesthesia of effected shoulder. The subjects were randomly assigned into 3 groups by lottery method who met the inclusion criteria. Informed consent was taken from patient who met the criteria. Allocations were concealed. The outcome measures were blinded Pre-treatment evaluation was done on the first day as baseline measurement; the outcome measures numerical pain rating scale NPRS, shoulder pain and disability index SPADI and shoulder range of motion ROM were taken by the third person (physiotherapist) who was trained and the principal investigator was blinded. Group 1 received conventional therapy, Group 2 received mulligans technique MWM along with conventional therapy, and Group 3 received spencer s technique along with conventional therapy. At the end of session (day 1), the subjects were asked for any increase in pain. If no adverse response was reported, further sessions were carried out three sessions a week for six weeks. All the 3 groups were asked to continue conventional therapy exercises as home based program as the dosage mentioned below and within pain free limit. Follow up evaluation was done and documented at the end of 3 rd week, and 6 th week, all the final outcome measures were taken and data analysis between day1 to week 6 was done for the final result. There were 5 dropouts due to personal reasons. Conventional Therapy: Subjects received ultrasound therapy and exercise programme. The ultrasound treatment was given for sessions of 3MHz frequency with an intensity of 1.5 W / CM 2 for a period of 5 10 minutes duration. The exercise therapy programme includes active and active assisted range of motion exercises, isometric exercises, Codman s pendulum exercises, wand, pulley and finger ladder exercises, capsular stretching, pectoral stretch, scapular stabilization exercises, and warm water fermentation for (10 minutes). All were directed to do the same as Home Exercise Program (HEP) at least twice daily. Dosage: 3 sets for 10 repetitions with 2 minutes rest between sets for 6 weeks. Mulligan s group: Subjects received MWM and conventional therapy Mulligan s technique Mobilization with Movement The mulligan s technique was performed on the involved shoulder as described by mulligan 23. The treatment was administered by the physiotherapist who was trained in mulligan s technique. The therapist applied passive accessory glide as the patient moved the arm actively in the desired direction with in a pain free range. 2018, All Rights Reserved Page 254
3 To Increase Shoulder Flexion Patient positioned in relaxed supine position, the therapist stood laterally to the affected joint in stride stance and stabilize the scapula and clavicle with one hand and the distal end of humerus with the other. The belt is placed close to the shoulder joint line and is secured around the therapist s waist; the glide was given to distract the humerus laterally, while maintaining the glide patient was asked to perform slow active shoulder movement (flexion) and apply passive overpressure at the end of new available range. The therapist moved along the movement to sustain the glide along the treatment plane. Internal Rotation and External Rotation Patient positioned in supine, therapist stood lateral to the affected joint. The patients shoulder and elbow were placed in 90 of flexion, belt was placed close to the shoulder joint line and secured around the therapist s waist, and therapist pulled the belt laterally to distract the joint and stabilized the humerus by holding the distal end of humerus with both hands. Patient was then asked to perform the offending movement (internal and external rotation) actively, and give passive overpressure with the other hand at the end of new available range. Abduction Patient in a relaxed sitting position, belt was placed around the head of the humerus and postero-lateral and inferior glide was maintained. With one hand the therapist held the belt in place sustaining the glide. A counter pressure was also applied to the scapula with the therapist s other hand. The patient was asked to perform slow active shoulder movements to the end of pain free range (abduction). The glide was sustained during the movement and released after returning to the starting position. Patients were asked to continue conventional therapy as HEP Dosage: 3 sets for 10 repetitions with 1 minute rest between sets. 3 times a week for 6 weeks Spencer s Group Technique was performed on the involved shoulder as mentioned in the study conducted by Knebl et al., 10 DA Patriquin 9 and Nicholas NS 24 Spencer s Technique Patient positioned in side lying with the shoulder to be treated uppermost, the therapist stood in front of the patient stabilizing the superior aspect of the shoulder girdle, the fixed shoulder girdle provided a resistant structure against which to stretch the soft tissues around the glenohumeral articulation as the arm was used as a long lever. The therapist then supports the wrist and forearm of the patient and does passive, smooth, rhythmic back and forth motion of arm and is carried to the extreme limit permitted by the contracted muscles, ligaments and the capsule of the shoulder. Step 1 shoulder extension with elbow flexion: patients elbow was maintained in a flexed position and the arm was extended until the restricted barrier. Step 2 - shoulder flexion with elbow extension: patients flexed elbow was extended and moved anteriorly into shoulder flexion until the restricted barrier. Step 3 circumduction with compression: grasping the elbow of the patient with his shoulder in 90 abduction, moved the elbow in small clockwise and counter clockwise circles direction with compressive force. Step 4 circumduction with distraction: therapist maintained the traction of the patients shoulder joint in 90 of abduction and holding either elbow or wrist induced small clockwise and counter clockwise circles Step 5 shoulder abduction and internal rotation with elbow flexion: patient was asked to place his hand on therapists forearm for the support and then therapist performed abduction and internal rotation of patients arm Internal rotation (90 ) therapist placed the dorsum of the patient s hand behind his or her hip and moved the patients elbow anteriorly Step 6 - shoulder adduction and external rotation with elbow flexion: patient was asked to place his hand on therapists forearm for the support and then the therapist takes patients arm into adduction and external rotation. Step 7 - stretching tissue and pumping fluids with the arm extended: therapist interlocks his fingertips over the deltoid muscle, patient s hand was placed over the therapist shoulder, and the therapist slowly moved the arm away from the shoulder and released, repeated this 5 10 times if needed. Dosage: 3 sets for 10 repetitions with 1 minute rest between sets 3 times a week for 6 week 2018, All Rights Reserved Page 255
4 3. PROCEDURE 4. STATISTICAL ANALYSIS AND RESULT The study included 90 subjects out of which there were 5 drop out due to personal reasons.the findings of the present study indicate that out of 85 subjects in these sample 46 (54.1%) are females and 39 (45.9%) are males respectively. The present study shows the female predominance. 43 subjects left limb was affected and the percentage of (50.6%) and 42 subjects with right limb and percentage of (49.4%) and 37(43.5%) percent of care givers belong to age group of years, while 33 (38.3%) percent belong to age group of years, 9 (10.6%) percent belong to age group of >60 years and remaining 6 (7.1%) percent belong to age group of years. NPRS: There was no significant difference among control group, mulligan s group and spencer s group on day 1 since ANOVA f- value and P- value is more than A significant difference exists among Control Group, mulligan s and spencer s group at Week 3 and 6 since P-value is less than Results of multiple comparison showed no significant difference between control group and spencer s group in 3 rd week as the p value is greater than 0.05, and there was significant difference between control and mulligan s group, mulligan s and spencer s group. In 6 th week there was Significant difference (p<0.05) exists between all the three groups. GROUP TABLE 1: NPRS Paired t-test Paired Differences Mean T Df Sig. (2-tailed) Control DAY 1-WEEK Mulligan s DAY 1-WEEK Spencer s DAY 1-WEEK , All Rights Reserved Page 256
5 14.646, and respectively, as p value <0.05 hence there is significant difference when compared day1 to week RANGE OF MOTION There was no significant difference among control group, mulligan s group and spencer s group on day 1 flexion, abduction, internal rotation, external rotation and extension. Since p-value is greater than FLEXION: Week 3 flexion ANOVA f-value1.881 and P- value 0.159>0.05 hence there was no significant difference between groups, A significant difference was seen in week 6 since ANOVA f- value and p- value 0.001<0.05. Results of multiple comparison showed no significant difference between control and mulligan s group, control and spencer s group and mulligan s and spencer s group in 3 rd week as p-value 0.107, and >0.05. In 6 th week there was no significant difference between mulligan s and spencer s group as p- value >0.05, and there was significant difference between control and mulligan s group, control and spencer s group as (p<0.05). TABLE 2: ROM FLEXION Paired t-test GROUP Paired Differences Mean T Df Sig. (2-tailed) Control DAY 1-WEEK Mulligans DAY 1-WEEK Spencer s DAY 1-WEEK , and respectively, as p value <0.05 hence there is significant difference when compared day1 to week ABDUCTION: Week 3 abduction ANOVA f- value and p- value 0.000<0.05, week 6 ANOVA f- value and p- value 0.000<0.05.there was significant difference between groups. Results of multiple comparison showed no significant difference between control and spencer s group in 3 rd week as p-value 0.193>0.05, there was significant difference between control and mulligan s group, mulligan s and spencer s group as p<0.05. In 6 th week there was Significant difference (p<0.05) exists between all the three groups. GROUP TABLE 3: ROM ABDUCTION: Paired t-test Paired Differences T Df Sig. (2-tailed) Mean Control DAY 1-WEEK Mulligan s DAY 1-WEEK Spencer s DAY 1-WEEK , and respectively, as p value <0.05 hence there is significant difference when compared day1 to week INTERNAL ROTATION: Week 3 internal rotation ANOVA f- value and p- value 0.010<0.05, week 6 ANOVA f-value and p-value 0.001<0.05.there was significant difference between groups. Results of multiple comparison showed no significant difference between control and spencer, mulligan s and spencer s group in 3 rd week as p-value 0.164, >0.05, there was significant difference between control and mulligan s group as p<0.05. In 6 th week there was no significant difference between control and spencer s group as p-value >0.05, there was significant difference between control and mulligan s group, mulligan s and spencer s group as p<0.05. GROUP TABLE 4: ROM INTERNAL ROTATION: Paired t-test Paired Differences Mean T Df Sig. (2-tailed) Control DAY 1-WEEK Mulligan s DAY 1-WEEK Spencer s DAY 1-WEEK , and respectively, as p value <0.05 hence there is significant difference when compared day1 to week 2018, All Rights Reserved Page 257
6 EXTERNAL ROTAION: Week 3 external rotation ANOVA f- value and p value 0.050=0.05, week 6 ANOVA f-value and p-value 0.005<0.05. There was significant difference between groups. Results of multiple comparison showed no significant difference between control and mulligan s group, control and spencer s group in 3 rd week as p-value 0.070, >0.05, there was significant difference between mulligan s and spencer s group. In 6 th week there was no significant difference between control and spencer s group as p-value >0.05, there was significant difference between control and mulligan s group, mulligan s and spencer s group as p<0.05. TABLE 5: ROM EXTERNAL ROTATION: Paired t-test GROUP Paired Differences Mean T Df Sig. (2-tailed) Control DAY 1-WEEK Mulligan s DAY 1-WEEK Spencer s DAY 1-WEEK , and respectively, as p value <0.05 hence there is significant difference when compared day1 to week EXTENSION: Week 3 extension f- value and p- value 0.077>0.05, there was no significant difference between groups. Week 6 f-value and p- value 0.050=0.05, there was significant difference between groups. Results of multiple comparison showed no significant difference between control and spencer s group, mulligan s and spencer s group in 3 rd week as p-value 0.101, >0.05, there was significant difference between control and mulligan s group as p<0.05. in 6 th week there was no significant difference between control and spencer s group, mulligan s and spencer s group as p-value 0.495, >0.05, there was significant difference between control and mulligan s group as p<0.05. TABLE 6: ROM EXTENSION: Paired t-test GROUP Paired Differences Mean T df Sig. (2-tailed) Control DAY 1-WEEK Mulligan s DAY 1-WEEK Spencer s DAY 1-WEEK , and 1680 respectively, as p value <0.05 hence there is significant difference when compared day1 to week SHOULDER PAIN AND DISABILITY INDEX: There was no significant difference among control group, mulligan s group and spencer s group on day 1 since ANOVA f-value is and P- value >0.05. Week 3 ANOVA f-value and p-value 0.000<0.05, week 6 ANOVA f-value and p-value 0.000<0.05. Hence there was significant difference between groups. Results of multiple comparison showed no significant difference between mulligan s and spencer s group in 3 rd week as p-value 0.167>0.05, there was significant difference between control and mulligan s group, control and spencer s group as p<0.05. In 6 th week there was Significant difference (p<0.05) exists between all the three groups. TABLE 7: SPADI: Paired t-test GROUP Paired Differences Mean t Df Sig. (2-tailed) Control DAY 1-WEEK Mulligan s DAY 1-WEEK Spencer s DAY 1-WEEK , 2449 and respectively, as p value <0.05 hence there is significant difference when compared day1 to week 5. DISCUSSION This study was conducted to investigate the Effectiveness of mulligan s technique and spencer s technique in adjunct to conventional therapy in frozen shoulder PAIN: Decrease in pain score are probably because of mechanical and thermal effects in the tissues cause by the ultrasound, warm water fermentation, and joint mobilization. 2018, All Rights Reserved Page 258
7 Mulligan s technique is based on correction of positional faults and restoration of joint arthokinematics, which in turn permits pain free range of motion. It is also found to be effective by neurophysiological mechanism and production of initial hypoalgesia based on stimulation of peripheral mechanoreceptors and the inhibition of nociceptors and altering sympathetic nervous system. Spencer s technique is aimed to decrease pain by altering the circulatory pain biomarkers; it increases pain free range of motion by stretching the shoulder capsule and tight soft tissues, thus restoring specific joint motion. RANGE OF MOTION Shoulder ROM was measured with a standard Goniometer. The findings of the present investigation indicate that shoulder flexion, abduction, internal rotation, external rotation and extension have improved significantly in all the three groups evident by mean values Mulligan s mobilization with movement is a combination of active movement with simultaneous passive accessory mobilization. The active movement in this technique stimulates the proprioceptive tissues, such as the Golgi tendon organ by tendon stretch. MWM repositions the joint, causing it to track normally. MWM passively stretches the tightened soft tissues and shoulder capsule in frozen shoulder there by restores the normal extensibility of the shoulder capsule and tight soft tissues. Spencer s technique increases the pain free ROM by stretching the shoulder capsule and tight soft tissues, thus restoring specific joint motion. This technique when applied increases the lymphatic flow from the treatment area. With this technique the joint regains its normal ROM and resets neural reflexes. The passive repetitive translator movements, traction or gliding improves nutrition, circulation and lubrication in the joint structures. It reverses the negative changes in the joint, and normalizes arthokinematic gliding and rolling movement. The increased gliding will normalize the osteokinematic rotation and enable the restoration of shoulder mobility. Spadi Pain and Disability Index There is significant improvement in SPADI total score similarly improvement was noted when the total of shoulder pain and total of disability index scores were taken into consideration to assess all three groups for a period of six weeks The study suggests that control group receiving conventional therapy, mulligan s group receiving MWM along with conventional therapy and spencer s group receiving spencer s technique along with conventional therapy are equally effective in reducing pain and functional disability in patients suffering from frozen shoulder. However there is significant difference in mean scores of control group, mulligan s group and spencer s group when compared after six weeks of treatment, mulligan s group subjects showed greater percentage of improvement, it could be due to the added effect of gliding force to the joint. Hence this group is much better than control group and spencer s group and control group is least effective working group The results of this study are also in agreement with a study done by Shahbaz Nawaz Ansari et al., who stated that ultrasound therapy with end range mobilization produced better results than cryotherapy with stretching in reducing pain in frozen shoulder. The results of this study are also in agreement with a study conducted by Vinod Babu, P. Khyathi et al., who stated that MWM technique and Spencer s technique are clinically beneficial on improving pain, shoulder mobility and functional disability in the treatment of frozen shoulder. CONCLUSION All the three groups statistically showed improvement in pain, functional disability and shoulder ROM. However the functional improvement in mulligan s group was better than spencer s and control group. From the result obtained in the study we conclude that application of mulligan s MWM along with exercises and ultrasound therapy produces significant improvement in pain scores, shoulder range of motion and functional ability in frozen shoulder patients. 7. LIMITATIONS 1. Limited sample size 2. Results are applicable to subjects belonging to age group of years only 3. Short duration study(6 weeks) 4. Samples can be grouped according to severity of the condition and analyzed in future studies 8. SCOPE FOR FURTHER STUDY 1. Better results can be drawn if the study was conducted with large sample size for long duration. 2. Long term follow up of patients is recommended in further studies to long term effects of mulligan s and spencer s technique. 3. Sub grouping of age can be done and studied separately to draw significant results. 2018, All Rights Reserved Page 259
8 9. REFERENCES [1] Neviaser and Hannafin et al., 2010 Adhesive Capsulitis: A Review of Current Treatment. The American journal of sports medicine vol38 (11): [2] Hanuman Sigh, Mukesh Goyal, 2016 physiotherapeutic management of Adhesive Capsulitis: a review of literature. International journal of physiotherapy and research vol 4 (6): [3] PH Laubscher, Frozen shoulder: A review. S. A Orthopaedic journal Spring pg: [4] Wong P L K, Tan H C A, A review on frozen shoulder, Singapore Med vol51 (9): [5] Jason E et al., 2011 current review of adhesive capsulitis. Journal of shoulder and elbow surgery 20: [6] Ujwal L Yeole et al., 2017 effectiveness of movement with mobilization in adhesive capsulitis of shoulder: Randamised control trial. 4 (2). [7] Sedeeks S. Chey Andrew TH, Adhesive capsulitis: is arthroscopic capsular release necessary? Current review. OA Orthopedics pg: 1- [8] G. Doner et al., 2013 evaluation of mulligan s technique for adhesive capsulitis of the shoulder Journal of Rehabilitation Medicine 45: [9] Patriquin.D1992 The evolution of osteopathic manipulative treatment: The Spencer technique. Journal of American osteopathic association vol: 92 (9): [10] Knebl et al., 2002 improving functional ability in the elderly via the Spencer technique, an osteopathic manipulative treatment: A randomized controlled trial. Journal of American Osteopathic Association vol102 (7): [11] Eileen L. DiGiovanna, Stanley Schiowitz, Dennis J. Dowling. An Osteopathic Approach to Diagnosis and Treatment. 3rd ed. Lippincott Williams & Wilkins; [12] A. Giai Via et al Treatment of Adhesive capsulitis: a review. Muscles, Ligaments and Tendons journal 2012; 2 (2): [13] Shahbaz Nawaz Ansari et al., 2012 Effect of ultrasound therapy with end range mobilization over cryotherapy with capsular stretching on pain in frozen shoulder A comparative study International Journal of current research and review Vol:04 (24) : [14] Celik and Kaya Mutlu, 2015 Does adding mobilization to stretching improve outcomes for people with frozen shoulder? A randomized controlled clinical trial. Clinical Rehabilitation pg 1-9. [15] Wayne Hing 2008 Mulligan s mobilisation with movement: a review of the tenets and prescription of MWMs new Zealand Journal of Physiotherapy. Vol. 36 (3): [16] Veli Pekka Sipila The rationale for joint mobilization as a manual technique. Ortho sport Physical Therapy. [17] Linda Exelby 1996 Peripheral mobilizations with movement. Manual Therapy [18] Michner et al., Responsiveness of the numerical pain rating scale in patients with shoulder pain and the effect of surgical status. Journal of sports rehabilitation 11: [19] Joyce S. Sabari et al., Goniometric assessment of shoulder range of motion: Comparison of testing in supine and sitting position. Archieve of physical medicine and rehabilitation vol. 79: [20] SP. Rley et al., the shoulder pain and disability index: is it sensitive and responsive to immediate changes? Journal of manual therapy [21] P. Khyathi and Vinod Babu.k et al., Comparative effect of spencer s technique versus mulligan s technique for subjects with frozen shoulder a single blind study. International journal of physiotherapy. Vol; 2(2), [22] Yatheendra Kumar G, et al., Effect of high grade mobilization techniques and scapular stabilization exercises in frozen shoulder. International journal of physical education, sports and health; 2(1): [23] Mulligan B. Manual Therapy Nags, Snags, Mwm, etc. 5 th Ed; [24] Nicholas NS. Atlas of Osteopathic Techniques. 2nd ed. Philadelphia College of Osteopathic Medicine; , All Rights Reserved Page 260
Effectiveness of Gong s Mobilization on shoulder abduction in adhesive capsulitis: A Case Study
 Case Report: Effectiveness of Gong s Mobilization on shoulder abduction in adhesive capsulitis: A Case Study Sunil G. Harsulkar 1, Keerthi Rao 2, Chandra Iyer 3, Khatri S.M. 4 1Post-graduate student of
Case Report: Effectiveness of Gong s Mobilization on shoulder abduction in adhesive capsulitis: A Case Study Sunil G. Harsulkar 1, Keerthi Rao 2, Chandra Iyer 3, Khatri S.M. 4 1Post-graduate student of
Frozen Shoulder Syndrome Rehabilitation Using the Resistance Chair
 Frozen Shoulder Syndrome Rehabilitation Using the Resistance Chair General Information Frozen shoulder is a condition where the shoulder joint (glenohumeral joint) gradually becomes stiff, resulting in
Frozen Shoulder Syndrome Rehabilitation Using the Resistance Chair General Information Frozen shoulder is a condition where the shoulder joint (glenohumeral joint) gradually becomes stiff, resulting in
Nonoperative Treatment For Rotator Cuff Tendinitis/ Partial Thickness Tear Dr. Trueblood
 Nonoperative Treatment For Rotator Cuff Tendinitis/ Partial Thickness Tear Dr. Trueblood Relieving Pain Patients who present with SIS will have shoulder pain that is exacerbated with overhead activities.
Nonoperative Treatment For Rotator Cuff Tendinitis/ Partial Thickness Tear Dr. Trueblood Relieving Pain Patients who present with SIS will have shoulder pain that is exacerbated with overhead activities.
1-Apley scratch test.
 1-Apley scratch test. The patient attempts to touch the opposite scapula to test range of motion of the shoulder. 1-Testing abduction and external rotation( +ve sign touch the opposite scapula, -ve sign
1-Apley scratch test. The patient attempts to touch the opposite scapula to test range of motion of the shoulder. 1-Testing abduction and external rotation( +ve sign touch the opposite scapula, -ve sign
Arthroscopic SLAP Repair Protocol
 SPORTS & ORTHOPAEDIC SPECIALISTS Arthroscopic SLAP Repair Protocol 6-8 visits over 12 weeks Emphasis is on AAROM and a high repetition, low weight free weight program Address posterior capsular tightness
SPORTS & ORTHOPAEDIC SPECIALISTS Arthroscopic SLAP Repair Protocol 6-8 visits over 12 weeks Emphasis is on AAROM and a high repetition, low weight free weight program Address posterior capsular tightness
Conservative Massive Rotator Cuff Tear Protocol
 SPORTS & ORTHOPAEDIC SPECIALISTS Conservative Massive Rotator Cuff Tear Protocol 3-4 visits over 4-6 weeks Emphasis is on AAROM and a high repetition, low weight free weight program Emphasize improved
SPORTS & ORTHOPAEDIC SPECIALISTS Conservative Massive Rotator Cuff Tear Protocol 3-4 visits over 4-6 weeks Emphasis is on AAROM and a high repetition, low weight free weight program Emphasize improved
Shoulder Impingement Rehabilitation Recommendations
 Shoulder Impingement Rehabilitation Recommendations The following protocol can be utilized for conservative care of shoulder impingement as well as post- operative subacromial decompression (SAD) surgery.
Shoulder Impingement Rehabilitation Recommendations The following protocol can be utilized for conservative care of shoulder impingement as well as post- operative subacromial decompression (SAD) surgery.
Hemiplegic Shoulder Power Point for staff education sessions
 Appendix B Hemiplegic Shoulder Power Point for staff education sessions Jennifer Curry Physiotherapist, London Health Sciences Centre www.swostroke.ca Acknowledgements Maria Lung BSc (PT), MSc Train the
Appendix B Hemiplegic Shoulder Power Point for staff education sessions Jennifer Curry Physiotherapist, London Health Sciences Centre www.swostroke.ca Acknowledgements Maria Lung BSc (PT), MSc Train the
Distal Biceps Repair/Reconstruction Protocol
 SPORTS & ORTHOPAEDIC SPECIALISTS Distal Biceps Repair/Reconstruction Protocol 6-10 visits over 4-6 months Maintain shoulder ROM while immobilized during early phase of healing During recovery, pulling
SPORTS & ORTHOPAEDIC SPECIALISTS Distal Biceps Repair/Reconstruction Protocol 6-10 visits over 4-6 months Maintain shoulder ROM while immobilized during early phase of healing During recovery, pulling
Conservative Posterior Capsular Instability Protocol
 SPORTS & ORTHOPAEDIC SPECIALISTS Conservative Posterior Capsular Instability Protocol 4-6 visits over 6 weeks Primary instability often experiences secondary impingement. Therefore, to treat posterior
SPORTS & ORTHOPAEDIC SPECIALISTS Conservative Posterior Capsular Instability Protocol 4-6 visits over 6 weeks Primary instability often experiences secondary impingement. Therefore, to treat posterior
Bankart/ Anterior Capsulorrhaphy Repair Protocol
 SPORTS & ORTHOPAEDIC SPECIALISTS Bankart/ Anterior Capsulorrhaphy Repair Protocol 6-8 visits over 12 weeks Emphasis is on AAROM and a high repetition, low weight free weight program Address posterior capsular
SPORTS & ORTHOPAEDIC SPECIALISTS Bankart/ Anterior Capsulorrhaphy Repair Protocol 6-8 visits over 12 weeks Emphasis is on AAROM and a high repetition, low weight free weight program Address posterior capsular
Total Shoulder Rehab Protocol Dr. Payne
 Total Shoulder Rehab Protocol Dr. Payne Phase I Immediate Post Surgical Phase (0-4 weeks): Allow healing of soft tissue Maintain integrity of replaced joint Gradually increase passive range of motion (PROM)
Total Shoulder Rehab Protocol Dr. Payne Phase I Immediate Post Surgical Phase (0-4 weeks): Allow healing of soft tissue Maintain integrity of replaced joint Gradually increase passive range of motion (PROM)
Upper limb injuries II. Traumatology RHS 231 Dr. Einas Al-Eisa
 Upper limb injuries II Traumatology RHS 231 Dr. Einas Al-Eisa Capsulitis = inflammatory lesion of the glenohumeral joint capsule leading to: thickening and loss of joint volume painful stiffness of the
Upper limb injuries II Traumatology RHS 231 Dr. Einas Al-Eisa Capsulitis = inflammatory lesion of the glenohumeral joint capsule leading to: thickening and loss of joint volume painful stiffness of the
Rehabilitation Guidelines for Labral/Bankert Repair
 Rehabilitation Guidelines for Labral/Bankert Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Rehabilitation Guidelines for Labral/Bankert Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Int J Physiother. Vol 2(5), , October (2015) ISSN:
 Int J Physiother. Vol 2(5), 811-818, October (2015) ISSN: 2348-8336 ABSTRACT 1 Dr. Lipika Boruah P.T *2 Dr. Abhijit Dutta P.T 3 Dr. Pritam Deka P.T 4 Dr. Jeutishree Roy P.T Background: Joint mobilization
Int J Physiother. Vol 2(5), 811-818, October (2015) ISSN: 2348-8336 ABSTRACT 1 Dr. Lipika Boruah P.T *2 Dr. Abhijit Dutta P.T 3 Dr. Pritam Deka P.T 4 Dr. Jeutishree Roy P.T Background: Joint mobilization
The SUPPORT Trial: SUbacromial impingement syndrome and Pain: a randomised controlled trial Of exercise and injection
 The SUPPORT Trial: SUbacromial impingement syndrome and Pain: a randomised controlled trial Of exercise and injection SUPPORT Physiotherapy Intervention Training Manual Authors: Sue Jackson (SJ) Julie
The SUPPORT Trial: SUbacromial impingement syndrome and Pain: a randomised controlled trial Of exercise and injection SUPPORT Physiotherapy Intervention Training Manual Authors: Sue Jackson (SJ) Julie
Avon Office 2 Simsbury Rd. Avon, CT Office: (860) Fax: (860) REHABILITATION AFTER REVERSE SHOULDER ARTHROPLASTY
 Katherine J. Coyner, MD UCONN Musculoskeletal Institute Medical Arts & Research Building 263 Farmington Ave. Farmington, CT 06030 Office: (860) 679-6600 Fax: (860) 679-6649 www.drcoyner.com Avon Office
Katherine J. Coyner, MD UCONN Musculoskeletal Institute Medical Arts & Research Building 263 Farmington Ave. Farmington, CT 06030 Office: (860) 679-6600 Fax: (860) 679-6649 www.drcoyner.com Avon Office
Alternative Therapies for Adhesive Capsulitis: A Case Study LANIE ALPHIN
 Alternative Therapies for Adhesive Capsulitis: A Case Study LANIE ALPHIN Case Background 53 year old female Chief Complaint: Right shoulder pain for 6 months Diagnosis: Adhesive Capsulitis Imagining indicated
Alternative Therapies for Adhesive Capsulitis: A Case Study LANIE ALPHIN Case Background 53 year old female Chief Complaint: Right shoulder pain for 6 months Diagnosis: Adhesive Capsulitis Imagining indicated
Rehab protocol. Phase I: Immediate Post-Surgical Phase: Typically 0-4 weeks; 2 PT visits. Goals:
 Reverse Total shoulder arthroplasty Rehab protocol Phase I: Immediate Post-Surgical Phase: Typically 0-4 weeks; 2 PT visits Allow healing of soft tissue Maintain integrity of replaced joint Gradually increase
Reverse Total shoulder arthroplasty Rehab protocol Phase I: Immediate Post-Surgical Phase: Typically 0-4 weeks; 2 PT visits Allow healing of soft tissue Maintain integrity of replaced joint Gradually increase
Core deconditioning Smoking Outpatient Phase 1 ROM Other
 whereby the ball does not stay properly centered in the shoulder socket during shoulder movement. This condition may be associated with impingement of the rotator cuff on the acromion bone and coracoacromial
whereby the ball does not stay properly centered in the shoulder socket during shoulder movement. This condition may be associated with impingement of the rotator cuff on the acromion bone and coracoacromial
Reverse Bankart/Posterior Capsulorrhaphy Repair Protocol
 + SPORTS & ORTHOPAEDIC SPECIALISTS 8100 W. 78 th Street Edina, MN 55439 952-946-9777 www.womensorthocenter.com Reverse Bankart/Posterior Capsulorrhaphy Repair Protocol 6-10 visits over 16 weeks Emphasis
+ SPORTS & ORTHOPAEDIC SPECIALISTS 8100 W. 78 th Street Edina, MN 55439 952-946-9777 www.womensorthocenter.com Reverse Bankart/Posterior Capsulorrhaphy Repair Protocol 6-10 visits over 16 weeks Emphasis
Christopher K. Jones, MD Colorado Springs Orthopaedic Group
 Christopher K. Jones, MD Colorado Springs Orthopaedic Group 719-632-7669 Total Shoulder Replacement You have undergone a shoulder replacement procedure. The performance of the procedure is complete, but
Christopher K. Jones, MD Colorado Springs Orthopaedic Group 719-632-7669 Total Shoulder Replacement You have undergone a shoulder replacement procedure. The performance of the procedure is complete, but
2778 N. Webb Road Shoulder, Elbow, Wrist, Hand Wichita, KS and Arthroscopic Surgery Phone: Fax:
 Phase I: Protection Phase (Weeks 0-5) FOCUS: Passive range of motion (ROM). Minimize pain and inflammation. Maintain integrity of the repair. Regain full passive foward flexion of operated shoulder. Use
Phase I: Protection Phase (Weeks 0-5) FOCUS: Passive range of motion (ROM). Minimize pain and inflammation. Maintain integrity of the repair. Regain full passive foward flexion of operated shoulder. Use
Incorporating OMM to Enhance Your Clinical Practice Osteopathic diagnosis and approach to the upper extremity
 Incorporating OMM to Enhance Your Clinical Practice Osteopathic diagnosis and approach to the upper extremity Sheldon C. Yao, D.O. Acting Department Chair March 1, 2013 Clinical significance Upper extremity
Incorporating OMM to Enhance Your Clinical Practice Osteopathic diagnosis and approach to the upper extremity Sheldon C. Yao, D.O. Acting Department Chair March 1, 2013 Clinical significance Upper extremity
Biceps Tenodesis Protocol
 Biceps Tenodesis Protocol A biceps tenodesis procedure involves cutting of the long head of the biceps just prior to its insertion on the superior labrum and then anchoring the tendon along its anatomical
Biceps Tenodesis Protocol A biceps tenodesis procedure involves cutting of the long head of the biceps just prior to its insertion on the superior labrum and then anchoring the tendon along its anatomical
IJPHY ABSTRACT. Int J Physiother. Vol 3(5), , October (2016) ISSN: ORIGINAL ARTICLE
 Int J Physiother. Vol 3(5), 619-624, October (2016) ISSN: 2348-8336 ORIGINAL ARTICLE IJPHY ABSTRACT A COMPARATIVE STUDY ON THE EFFECTIVENESS OF MUSCLE ENERGY TECHNIQUES AND MOBILIZATION COUPLED WITH ULTRASOUND
Int J Physiother. Vol 3(5), 619-624, October (2016) ISSN: 2348-8336 ORIGINAL ARTICLE IJPHY ABSTRACT A COMPARATIVE STUDY ON THE EFFECTIVENESS OF MUSCLE ENERGY TECHNIQUES AND MOBILIZATION COUPLED WITH ULTRASOUND
TOTAL SHOULDER ARTHROPLASTY, HEMIARTHROPLASTY OR REVERSE ARTHROPLASTY
 TOTAL SHOULDER ARTHROPLASTY, HEMIARTHROPLASTY OR REVERSE ARTHROPLASTY Philosophy The following is an outline of the standard post-operative rehabilitation program following total shoulder arthroplasty.
TOTAL SHOULDER ARTHROPLASTY, HEMIARTHROPLASTY OR REVERSE ARTHROPLASTY Philosophy The following is an outline of the standard post-operative rehabilitation program following total shoulder arthroplasty.
This presentation is the intellectual property of the author. Contact them for permission to reprint and/or distribute.
 The Stiff Hand: Manual Therapy Sylvia Dávila, PT, CHT San Antonio, Texas Orthopedic Manual Therapy Common Applications Passive stretch Tensile force to tissue to increase extensibility of length & ROM
The Stiff Hand: Manual Therapy Sylvia Dávila, PT, CHT San Antonio, Texas Orthopedic Manual Therapy Common Applications Passive stretch Tensile force to tissue to increase extensibility of length & ROM
Limited Goals Program (Examples Include: Cuff Tear Arthropathy, Massive Irrepairable Rotator Cuff Tear, Selected Revision Surgeries)
 Limited Goals Program (Examples Include: Cuff Tear Arthropathy, Massive Irrepairable Rotator Cuff Tear, Selected Revision Surgeries) All information contained in this protocol is to be used as general
Limited Goals Program (Examples Include: Cuff Tear Arthropathy, Massive Irrepairable Rotator Cuff Tear, Selected Revision Surgeries) All information contained in this protocol is to be used as general
Rotator Cuff Repair Protocol for tear involving Subscapularis Tendon with or without Pectoralis Major Tendon Transfer
 Rotator Cuff Repair Protocol for tear involving Subscapularis Tendon with or without Pectoralis Major Tendon Transfer D. WATTS, MD Precautions: BASIS Tendon healing back to bone is a slow process that
Rotator Cuff Repair Protocol for tear involving Subscapularis Tendon with or without Pectoralis Major Tendon Transfer D. WATTS, MD Precautions: BASIS Tendon healing back to bone is a slow process that
Conservative Multi-Directional Capsular Instability Protocol
 SPORTS & ORTHOPAEDIC SPECIALISTS 8100 W. 78 th Street Edina, MN 55439 952-946-9777 www.womensorthocenter.com Conservative Multi-Directional Capsular Instability Protocol 4-6 visits over 6 weeks Primary
SPORTS & ORTHOPAEDIC SPECIALISTS 8100 W. 78 th Street Edina, MN 55439 952-946-9777 www.womensorthocenter.com Conservative Multi-Directional Capsular Instability Protocol 4-6 visits over 6 weeks Primary
ACTIVE AGING.
 Shoulder Pain Rehabilitation Protocol Rotator Cuff Syndrome Shoulder impingement The Resistance Chair Solution Shoulder Impingement a. Shoulder impingement is one of the most common causes of shoulder
Shoulder Pain Rehabilitation Protocol Rotator Cuff Syndrome Shoulder impingement The Resistance Chair Solution Shoulder Impingement a. Shoulder impingement is one of the most common causes of shoulder
Shoulder and Elbow ORTHOPAEDIC SYPMPOSIUM APRIL 8, 2017 DANIEL DOTY MD
 Shoulder and Elbow ORTHOPAEDIC SYPMPOSIUM APRIL 8, 2017 DANIEL DOTY MD Shoulder Articulations Glenohumeral Joint 2/3 total arc of motion Shallow Ball and Socket Joint Allows for excellent ROM Requires
Shoulder and Elbow ORTHOPAEDIC SYPMPOSIUM APRIL 8, 2017 DANIEL DOTY MD Shoulder Articulations Glenohumeral Joint 2/3 total arc of motion Shallow Ball and Socket Joint Allows for excellent ROM Requires
Bradley C. Carofino, M.D. Shoulder Specialist 230 Clearfield Avenue, Suite 124 Virginia Beach, Virginia Phone
 Subpectoral Bicep Tenodesis Protocol (Spreadsheet) Weeks 1-2 Modalities Treatment Restrictions Goals No active elbow flexion (6weeks) Full PROM shoulder and elbow PROM: Shoulder, elbow, forearm No active
Subpectoral Bicep Tenodesis Protocol (Spreadsheet) Weeks 1-2 Modalities Treatment Restrictions Goals No active elbow flexion (6weeks) Full PROM shoulder and elbow PROM: Shoulder, elbow, forearm No active
PROM is not stretching!
 Dx: o Right o Left Shoulder Replacement/Hemiarthroplasty Rehab Date of Surgery: Patient Name: PT/OT: Please evaluate and treat. Follow attached protocol. 2-3 x per week x 6 weeks. Signature/Date: The intent
Dx: o Right o Left Shoulder Replacement/Hemiarthroplasty Rehab Date of Surgery: Patient Name: PT/OT: Please evaluate and treat. Follow attached protocol. 2-3 x per week x 6 weeks. Signature/Date: The intent
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS
 Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
Rehabilitation Guidelines for Total Shoulder Arthroplasty and Hemi-arthroplasty
 Rehabilitation Guidelines for Total Shoulder Arthroplasty and Hemi-arthroplasty Josef K. Eichinger, MD General Information Total Recovery time is between 4-6 months depending on factors such as injury
Rehabilitation Guidelines for Total Shoulder Arthroplasty and Hemi-arthroplasty Josef K. Eichinger, MD General Information Total Recovery time is between 4-6 months depending on factors such as injury
Total Shoulder Arthroplasty / Hemiarthroplasty Protocol
 Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 Total Shoulder Arthroplasty / Hemiarthroplasty Protocol The intent of this protocol is to provide the
Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 Total Shoulder Arthroplasty / Hemiarthroplasty Protocol The intent of this protocol is to provide the
Charlotte Shoulder Institute
 Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
ADHESIVE CAPSULITIS (FROZEN SHOULDER)
 ADHESIVE CAPSULITIS (FROZEN SHOULDER) Frozen shoulder, or adhesive capsulitis is a condition that generally begins with the gradual onset of pain followed by a limitation of shoulder motion. The discomfort
ADHESIVE CAPSULITIS (FROZEN SHOULDER) Frozen shoulder, or adhesive capsulitis is a condition that generally begins with the gradual onset of pain followed by a limitation of shoulder motion. The discomfort
Shoulder Mobility Deficits. ICD-9-CM codes: Adhesive capsulitis of the shoulder
 Shoulder Mobility Deficits ICD-9-CM codes: 726.0 Adhesive capsulitis of the shoulder ICF codes: Activities and Participation Domain codes: d4452 Reaching (Using the hands and arms to extend outwards and
Shoulder Mobility Deficits ICD-9-CM codes: 726.0 Adhesive capsulitis of the shoulder ICF codes: Activities and Participation Domain codes: d4452 Reaching (Using the hands and arms to extend outwards and
REHABILITATION FOR SHOULDER FRACTURES & SURGERIES. Clavicle fractures Proximal head of humerus fractures
 REHABILITATION FOR SHOULDER FRACTURES & SURGERIES Clavicle fractures Proximal head of humerus fractures By Dr. Mohamed Behiry Lecturer Department of physical therapy for Orthopaedic and its surgery. Delta
REHABILITATION FOR SHOULDER FRACTURES & SURGERIES Clavicle fractures Proximal head of humerus fractures By Dr. Mohamed Behiry Lecturer Department of physical therapy for Orthopaedic and its surgery. Delta
Charlotte Shoulder Institute
 Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
Protocol S8 Physical Therapy Protocol for Arthroscopic Reverse Bankart Repair or Open Posterior Capsulorrhaphy
 Phase I: Protection Phase (0-5 weeks) Allow time for labral repair to heal. Gradually increase shoulder passive range of motion (ROM) Use pain medications as needed. Wear shoulder immobilizer for 5 weeks.
Phase I: Protection Phase (0-5 weeks) Allow time for labral repair to heal. Gradually increase shoulder passive range of motion (ROM) Use pain medications as needed. Wear shoulder immobilizer for 5 weeks.
Physical Examination of the Shoulder
 General setup Patient will be examined in both the seated and supine position so exam table needed 360 degree access to patient Expose neck and both shoulders (for comparison); female in gown or sports
General setup Patient will be examined in both the seated and supine position so exam table needed 360 degree access to patient Expose neck and both shoulders (for comparison); female in gown or sports
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS
 Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
Shoulder Joint Examination. Shoulder Joint Examination. Inspection. Inspection Palpation Movement. Look Feel Move
 Shoulder Joint Examination History Cuff Examination Instability Examination AC Joint Examination Biceps Tendon Examination Superior Labrum Examination Shoulder Joint Examination Inspection Palpation Movement
Shoulder Joint Examination History Cuff Examination Instability Examination AC Joint Examination Biceps Tendon Examination Superior Labrum Examination Shoulder Joint Examination Inspection Palpation Movement
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Effect of Muscle Energy Technique on Range Of Motion in Cases of Patients with Adhesive Capsulitis
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Effect of Muscle Energy Technique on Range Of Motion in Cases of Patients with Adhesive Capsulitis
ARTHROSCOPIC DECOMPRESSION PROTOCOL Dr. Steven Flores
 ARTHROSCOPIC DECOMPRESSION PROTOCOL Dr. Steven Flores This rehabilitation protocol has been developed for the patient following an arthroscopic decompression surgical procedure. The arthroscopic decompression
ARTHROSCOPIC DECOMPRESSION PROTOCOL Dr. Steven Flores This rehabilitation protocol has been developed for the patient following an arthroscopic decompression surgical procedure. The arthroscopic decompression
Jennifer L. Cook, MD Stephen A. Hanff, MD. Rotator Cuff Type I Repair (Small Large Tear)
 Jennifer L. Cook, MD Stephen A. Hanff, MD Florida Joint Care Institute 2165 Little Road, Trinity, Florida 34655 PH: (727) 372 6637 FAX: (727) 375 5044 Rotator Cuff Type I Repair (Small Large Tear) This
Jennifer L. Cook, MD Stephen A. Hanff, MD Florida Joint Care Institute 2165 Little Road, Trinity, Florida 34655 PH: (727) 372 6637 FAX: (727) 375 5044 Rotator Cuff Type I Repair (Small Large Tear) This
Arthroscopic Rotator Cuff Repair Protocol:
 Arthroscopic Rotator Cuff Repair Protocol: The intent of this protocol is to provide the therapist and patient with guidelines for the post-operative rehabilitation course after arthroscopic SLAP repair.
Arthroscopic Rotator Cuff Repair Protocol: The intent of this protocol is to provide the therapist and patient with guidelines for the post-operative rehabilitation course after arthroscopic SLAP repair.
SHOULDER ARTHROSCOPY WITH ANTERIOR STABILIZATION / CAPSULORRHAPHY REHABILITATION PROTOCOL
 General Notes As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
General Notes As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
IP: Sling for 6 weeks Week 0-6: Immobilisation + Pendulum exercise Week 6-4 Months: Active ROM 4 Months-on: Strengthening exercises
 Supplemental material 5 Table 1. Summary of rehabilitation programs postoperative. Author (year) Early Rehabilitation Conservative Rehabilitation Arndt et al., 2012 [35] First day postoperative-week 6:
Supplemental material 5 Table 1. Summary of rehabilitation programs postoperative. Author (year) Early Rehabilitation Conservative Rehabilitation Arndt et al., 2012 [35] First day postoperative-week 6:
ROTATOR CUFF TENDONITIS
 Daniel P. Duggan, D.O. The Sports Clinic 23961 Calle de la Magdalena, Suite 229 Laguna Hills, CA 92653 Phone: (949) 581-7001 Fax: (949) 581-8410 http://orthodoc.aaos.org/danielduggando The shoulder is
Daniel P. Duggan, D.O. The Sports Clinic 23961 Calle de la Magdalena, Suite 229 Laguna Hills, CA 92653 Phone: (949) 581-7001 Fax: (949) 581-8410 http://orthodoc.aaos.org/danielduggando The shoulder is
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article To Compare the Effectiveness of Maitland versus Mulligan Mobilisation in Idiopathic Adhesive
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article To Compare the Effectiveness of Maitland versus Mulligan Mobilisation in Idiopathic Adhesive
Superior Labrum Repair Protocol - SLAP
 Superior Labrum Repair Protocol - SLAP Stage I (0-4 weeks): Key Goals: Protect the newly repaired shoulder. Allow for decreased inflammation and healing. Maintain elbow, wrist and hand function. Maintain
Superior Labrum Repair Protocol - SLAP Stage I (0-4 weeks): Key Goals: Protect the newly repaired shoulder. Allow for decreased inflammation and healing. Maintain elbow, wrist and hand function. Maintain
Total Shoulder Arthroplasty / Hemiarthroplasty Therapy Protocol
 Total Shoulder Arthroplasty / Hemiarthroplasty Therapy Protocol The intent of this protocol is to provide the therapist with a guideline of the postoperative rehabilitation course of a patient that has
Total Shoulder Arthroplasty / Hemiarthroplasty Therapy Protocol The intent of this protocol is to provide the therapist with a guideline of the postoperative rehabilitation course of a patient that has
POST-SURGICAL POSTERIOR GLENOHUMERAL STABILIZATION REHABILITATION PROTOCOL (Capsulolabral Repair)
 Gregory N. Lervick, MD Andrew Anderson, PA-C 952-456-7111 POST-SURGICAL POSTERIOR GLENOHUMERAL STABILIZATION REHABILITATION PROTOCOL (Capsulolabral Repair) Open Arthroscopic Phase 1: Weeks 0-4 No shoulder
Gregory N. Lervick, MD Andrew Anderson, PA-C 952-456-7111 POST-SURGICAL POSTERIOR GLENOHUMERAL STABILIZATION REHABILITATION PROTOCOL (Capsulolabral Repair) Open Arthroscopic Phase 1: Weeks 0-4 No shoulder
Anterior Stabilization of the Shoulder: Distal Tibial Allograft
 Anterior Stabilization of the Shoulder: Distal Tibial Allograft Name: Diagnosis: Date: Date of Surgery: Phase I Immediate Post Surgical Phase (approximately Weeks 1-3) Minimize shoulder pain and inflammatory
Anterior Stabilization of the Shoulder: Distal Tibial Allograft Name: Diagnosis: Date: Date of Surgery: Phase I Immediate Post Surgical Phase (approximately Weeks 1-3) Minimize shoulder pain and inflammatory
Orthopedic Surgery and Sports Medicine FL License:
 Reverse Shoulder Arthroplasty Protocol: The intent of this protocol is to provide the therapist with a guideline for the post-operative rehabilitation course of a patient that has undergone a Reverse Shoulder
Reverse Shoulder Arthroplasty Protocol: The intent of this protocol is to provide the therapist with a guideline for the post-operative rehabilitation course of a patient that has undergone a Reverse Shoulder
It is most common in people between the age of 40 and 70 years and has been estimated to affect at least one person in 50 every year.
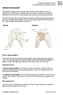 FROZEN SHOULDER The shoulder is designed to have a large amount of movement so that we can use our hands/arms in a wide variety of positions. Some movement occurs between the shoulder blade and chest wall.
FROZEN SHOULDER The shoulder is designed to have a large amount of movement so that we can use our hands/arms in a wide variety of positions. Some movement occurs between the shoulder blade and chest wall.
Anatomy. Introduction
 Anatomy Introduction Many adults (mostly women) between the ages of 40 and 60 years of age develop shoulder pain and stiffness called adhesive capsulitis. You may be more familiar with the term frozen
Anatomy Introduction Many adults (mostly women) between the ages of 40 and 60 years of age develop shoulder pain and stiffness called adhesive capsulitis. You may be more familiar with the term frozen
MOON SHOULDER GROUP NONOPERATIVE TREATMENT OF ROTATOR CUFF TENDONOPATHY PHYSICAL THERAPY GUIDELINES
 MOON SHOULDER GROUP NONOPERATIVE TREATMENT OF ROTATOR CUFF TENDONOPATHY PHYSICAL THERAPY GUIDELINES From: Kuhn JE. Exercise in the treatment of rotator cuff impingement. A systematic review and synthesized
MOON SHOULDER GROUP NONOPERATIVE TREATMENT OF ROTATOR CUFF TENDONOPATHY PHYSICAL THERAPY GUIDELINES From: Kuhn JE. Exercise in the treatment of rotator cuff impingement. A systematic review and synthesized
Frozen shoulder, also called adhesive capsulitis, causes pain and stiffness in the shoulder. Over time, the shoulder becomes very hard to move.
 1 Frozen Shoulder What is frozen shoulder? Frozen shoulder, also called adhesive capsulitis, causes pain and stiffness in the shoulder. Over time, the shoulder becomes very hard to move. Frozen shoulder
1 Frozen Shoulder What is frozen shoulder? Frozen shoulder, also called adhesive capsulitis, causes pain and stiffness in the shoulder. Over time, the shoulder becomes very hard to move. Frozen shoulder
Hemiplegic Shoulder. Incidence & Rationale. Shoulder Pain Assessment & Treatment
 Hemiplegic Shoulder Jeane Davis Fyfe OT, Senior Therapist Incidence & Rationale Up to 72% of stroke survivors will experience shoulder pain Shoulder pain may inhibit patient participation in rehabilitation
Hemiplegic Shoulder Jeane Davis Fyfe OT, Senior Therapist Incidence & Rationale Up to 72% of stroke survivors will experience shoulder pain Shoulder pain may inhibit patient participation in rehabilitation
TOTAL SHOULDER ARTHROPLASTY / HEMIARTHROPLASTY
 Teodoro P. Nissen, M.D., Q.M.E. Fellowship Trained Board Certified Joseph M. Centeno, M.D. Fellowship Trained Board Certified TOTAL SHOULDER ARTHROPLASTY / HEMIARTHROPLASTY Protocol: The intent of this
Teodoro P. Nissen, M.D., Q.M.E. Fellowship Trained Board Certified Joseph M. Centeno, M.D. Fellowship Trained Board Certified TOTAL SHOULDER ARTHROPLASTY / HEMIARTHROPLASTY Protocol: The intent of this
The Swimmer s Shoulder: An Osteopathic Approach
 The Swimmer s Shoulder: An Osteopathic Approach Mary Solomon, D.O. Rainbow Babies and Children s Hospital Cleveland, OH 440-914-7865 1 I have no relevant relationships/affiliations with any proprietary
The Swimmer s Shoulder: An Osteopathic Approach Mary Solomon, D.O. Rainbow Babies and Children s Hospital Cleveland, OH 440-914-7865 1 I have no relevant relationships/affiliations with any proprietary
Exploring the Rotator Cuff
 Exploring the Rotator Cuff Improving one s performance in sports and daily activity is a factor of neuromuscular efficiency and metabolic enhancements. To attain proficiency, reaction force must be effectively
Exploring the Rotator Cuff Improving one s performance in sports and daily activity is a factor of neuromuscular efficiency and metabolic enhancements. To attain proficiency, reaction force must be effectively
Phase I : Immediate Postoperative Phase- Protected Motion. (0-2 Weeks)
 Phase I : Immediate Postoperative Phase- Protected Motion (0-2 Weeks) Appointments Progression Criteria 2 weeks after surgery Rehabilitation appointments begin within 7-10 days of surgery, continue 1-2
Phase I : Immediate Postoperative Phase- Protected Motion (0-2 Weeks) Appointments Progression Criteria 2 weeks after surgery Rehabilitation appointments begin within 7-10 days of surgery, continue 1-2
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS
 Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
TALLGRASS ORTHOPEDIC & SPORTS MEDICINE. Phase I Immediate Post-Surgical Phase (Weeks 0-2) Date: Maintain/protect integrity of the repair
 TALLGRASS ORTHOPEDIC & SPORTS MEDICINE Name: Date of Surgery: Patient Flow Sheet Arthroscopic Rotator Cuff Repair Small to Medium Tears Benedict Figuerres, MD Phase I Immediate Post-Surgical Phase (Weeks
TALLGRASS ORTHOPEDIC & SPORTS MEDICINE Name: Date of Surgery: Patient Flow Sheet Arthroscopic Rotator Cuff Repair Small to Medium Tears Benedict Figuerres, MD Phase I Immediate Post-Surgical Phase (Weeks
Charlotte Shoulder Institute
 Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Gill Orthopaedic Midtown Medical Plaza 1918 Randolph Rd., Suite 700 Charlotte, NC 28211 704-342-3544
Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Gill Orthopaedic Midtown Medical Plaza 1918 Randolph Rd., Suite 700 Charlotte, NC 28211 704-342-3544
Biceps Tenotomy Protocol
 Biceps Tenotomy Protocol A biceps tenotomy procedure involves cutting of the long head of the biceps just prior to its insertion on the superior labrum. A biceps tenotomy is typically done when there is
Biceps Tenotomy Protocol A biceps tenotomy procedure involves cutting of the long head of the biceps just prior to its insertion on the superior labrum. A biceps tenotomy is typically done when there is
The Four Phases of Healing During Rehabilitation Following Rotator Cuff Surgery. Phase 1: Immediate postoperative period (weeks 0-6) Goals
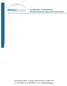 The Four Phases of Healing During Rehabilitation Following Rotator Cuff Surgery Phase 1: Immediate postoperative period (weeks 0-6) Maintain/protect integrity of repair Gradually increase PROM Diminish
The Four Phases of Healing During Rehabilitation Following Rotator Cuff Surgery Phase 1: Immediate postoperative period (weeks 0-6) Maintain/protect integrity of repair Gradually increase PROM Diminish
RN(EC) ENC(C) GNC(C) MN ACNP *** MECHANISM OF INJURY.. MOST IMPORTANT ***
 HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age - Certain conditions are more prevalent in particular age groups (i.e. Full rotator cuff tears are more common over the age of 45, traumatic injuries
HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age - Certain conditions are more prevalent in particular age groups (i.e. Full rotator cuff tears are more common over the age of 45, traumatic injuries
Anterior Labrum Repair Protocol
 Anterior Labrum Repair Protocol Stage I (0-4 weeks): Key Goals: Protect the newly repaired shoulder. Allow for decreased inflammation and healing. Maintain elbow, wrist and hand function. Maintain scapular
Anterior Labrum Repair Protocol Stage I (0-4 weeks): Key Goals: Protect the newly repaired shoulder. Allow for decreased inflammation and healing. Maintain elbow, wrist and hand function. Maintain scapular
Rehabilitation Guidelines for Large Rotator Cuff Repair
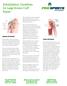 Rehabilitation Guidelines for Large Rotator Cuff Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the
Rehabilitation Guidelines for Large Rotator Cuff Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the
Rotator Cuff Repair Therapy Protocol
 Bart Eastwood D.O. 825 Davis st Blacksburg, VA 24060 540-951-6000 All information contained in this protocol is to be used as general guidelines only. Specific variations may be appropriate for each patient
Bart Eastwood D.O. 825 Davis st Blacksburg, VA 24060 540-951-6000 All information contained in this protocol is to be used as general guidelines only. Specific variations may be appropriate for each patient
Reverse Total Shoulder Arthroplasty Protocol
 General Information: Reverse Total Shoulder Arthroplasty Protocol Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH) arthritis when it
General Information: Reverse Total Shoulder Arthroplasty Protocol Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH) arthritis when it
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s R E V E R S E T O T A L S H O U L D E R A R T H R O P L A S T Y P R O T O C O L
 S p o r t s & O r t h o p a e d i c S p e c i a l i s t s R E V E R S E T O T A L S H O U L D E R A R T H R O P L A S T Y P R O T O C O L This protocol provides appropriate guidelines for the rehabilitation
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s R E V E R S E T O T A L S H O U L D E R A R T H R O P L A S T Y P R O T O C O L This protocol provides appropriate guidelines for the rehabilitation
30b Passive Stretches:! Technique Demo and Practice - Upper Body
 30b Passive Stretches:! Technique Demo and Practice - Upper Body 30b Passive Stretches:! Technique Demo and Practice - Upper Body! Class Outline" 5 minutes" "Attendance, Breath of Arrival, and Reminders
30b Passive Stretches:! Technique Demo and Practice - Upper Body 30b Passive Stretches:! Technique Demo and Practice - Upper Body! Class Outline" 5 minutes" "Attendance, Breath of Arrival, and Reminders
Work-related shoulder pain
 Work-related shoulder pain Stadler Kirsten M.B., Ch.B. (1987) (Pret), M. Med. (Orthop) (1998) (Stell.), Orthopaedic Surgeon, Room 333, Louis Leipoldt Medical Centre, Broadway Street, Bellville Cape Town
Work-related shoulder pain Stadler Kirsten M.B., Ch.B. (1987) (Pret), M. Med. (Orthop) (1998) (Stell.), Orthopaedic Surgeon, Room 333, Louis Leipoldt Medical Centre, Broadway Street, Bellville Cape Town
GUIDELINES FOR REHABILITATION Arthroscopic Rotator Cuff Repair
 Indications: Tearing of the rotator cuff tendon(s) insertion on the humerus. Procedure: Arthroscopic repair: Tear Size: supraspinatus, infraspinatus, subscapularis tendons. biceps tenodesis or tenotomy
Indications: Tearing of the rotator cuff tendon(s) insertion on the humerus. Procedure: Arthroscopic repair: Tear Size: supraspinatus, infraspinatus, subscapularis tendons. biceps tenodesis or tenotomy
Rotator Cuff Repair +/- Acromioplasty/Mumford. Phase I: 0 to 2 weeks after surgery
 Rotator Cuff Repair +/- Acromioplasty/Mumford 2. Ensure wound healing Phase I: 0 to 2 weeks after surgery 1. Sling: Use your sling all of the time. 2. Use of the affected arm: You may use your hand on
Rotator Cuff Repair +/- Acromioplasty/Mumford 2. Ensure wound healing Phase I: 0 to 2 weeks after surgery 1. Sling: Use your sling all of the time. 2. Use of the affected arm: You may use your hand on
Type Three Rotator Cuff Repair Arthroscopic Assisted with SAD Large to Massive Tears (Greater than 4 cm)
 Type Three Rotator Cuff Repair Arthroscopic Assisted with SAD Large to Massive Tears (Greater than 4 cm) Therapist Phone I. Phase I - Immediate Post-Surgical Phase (Day 1-10) Goals: Maintain Integrity
Type Three Rotator Cuff Repair Arthroscopic Assisted with SAD Large to Massive Tears (Greater than 4 cm) Therapist Phone I. Phase I - Immediate Post-Surgical Phase (Day 1-10) Goals: Maintain Integrity
Rehabilitation Guidelines for Shoulder Arthroscopy
 Rehabilitation Guidelines for Shoulder Arthroscopy The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Rehabilitation Guidelines for Shoulder Arthroscopy The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Rehabilitation Protocol: Massive Rotator Cuff Tear Repair
 Rehabilitation Protocol: Massive Rotator Cuff Tear Repair Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey
Rehabilitation Protocol: Massive Rotator Cuff Tear Repair Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey
Arthroscopic Bankart Repair Rehabilitation Protocol Dr. Mark Adickes
 Arthroscopic Bankart Repair Rehabilitation Protocol Dr. Mark Adickes Introduction: This rehabilitation protocol has been developed for the patient following an arthroscopic Bankart (anteroinferior labral
Arthroscopic Bankart Repair Rehabilitation Protocol Dr. Mark Adickes Introduction: This rehabilitation protocol has been developed for the patient following an arthroscopic Bankart (anteroinferior labral
Manual Therapy Techniques: Joint Mobilization and PNF Diagonal Patterns. Linda Gazzillo Diaz, Ed.D., ATC William Paterson University
 Manual Therapy Techniques: Joint Mobilization and PNF Diagonal Patterns Linda Gazzillo Diaz, Ed.D., ATC William Paterson University Assist in restoring joint motion by decreasing pain and stiffness Arthrokinematics
Manual Therapy Techniques: Joint Mobilization and PNF Diagonal Patterns Linda Gazzillo Diaz, Ed.D., ATC William Paterson University Assist in restoring joint motion by decreasing pain and stiffness Arthrokinematics
A Patient s Guide to Adhesive Capsulitis
 A Patient s Guide to Adhesive Capsulitis Orthopedic and Sports Medicine 825 South 8th Street, #550 Minneapolis, MN 55404 Phone: 612-333-5000 Fax: 612-333-6922 DISCLAIMER: The information in this booklet
A Patient s Guide to Adhesive Capsulitis Orthopedic and Sports Medicine 825 South 8th Street, #550 Minneapolis, MN 55404 Phone: 612-333-5000 Fax: 612-333-6922 DISCLAIMER: The information in this booklet
A discussion about Adhesive capsulitis 한상민
 A discussion about Adhesive capsulitis 한상민 Adhesive capsulitis Frozen shoulder Periarthritis Irritative capsulitis Scapulohumeral periarthritis Shoulder anatomy SC joint AC joint GH joint team ST joint
A discussion about Adhesive capsulitis 한상민 Adhesive capsulitis Frozen shoulder Periarthritis Irritative capsulitis Scapulohumeral periarthritis Shoulder anatomy SC joint AC joint GH joint team ST joint
Rotator Cuff Repair Protocol
 Rotator Cuff Repair Protocol Applicability: Physician Practices Date Effective: 11/2016 Department: Rehabilitation Services Supersedes: Rotator Cuff Repair (Beattie) Date Last Reviewed / or Date Last Revision:
Rotator Cuff Repair Protocol Applicability: Physician Practices Date Effective: 11/2016 Department: Rehabilitation Services Supersedes: Rotator Cuff Repair (Beattie) Date Last Reviewed / or Date Last Revision:
Biceps Tenodesis Protocol
 Robert K. Fullick, MD 6400 Fannin Street, Suite 1700 Houston, Texas 77030 Ph.: 713-486-7543 / Fx.: 713-486-5549 Biceps Tenodesis Protocol The intent of this protocol is to provide the clinician with a
Robert K. Fullick, MD 6400 Fannin Street, Suite 1700 Houston, Texas 77030 Ph.: 713-486-7543 / Fx.: 713-486-5549 Biceps Tenodesis Protocol The intent of this protocol is to provide the clinician with a
CENTER FOR ORTHOPAEDICS AND SPINE CARE PHYSICAL THERAPY PROTOCOL BENJAMIN J. DAVIS, MD Type Two Rotator Cuff Repair
 I. Phase I - Immediate Post-Surgical Phase (Day 1-10) Goals: Maintain Integrity of the Repair Gradually Increase Passive Range of Motion Diminish Pain and Inflammation Prevent Muscular Inhibition Passive
I. Phase I - Immediate Post-Surgical Phase (Day 1-10) Goals: Maintain Integrity of the Repair Gradually Increase Passive Range of Motion Diminish Pain and Inflammation Prevent Muscular Inhibition Passive
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s M A S S I V E R O T A T O R C U F F R E P A I R P R O T O C O L
 S p o r t s & O r t h o p a e d i c S p e c i a l i s t s M A S S I V E R O T A T O R C U F F R E P A I R P R O T O C O L This protocol provides appropriate guidelines for the rehabilitation of patients
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s M A S S I V E R O T A T O R C U F F R E P A I R P R O T O C O L This protocol provides appropriate guidelines for the rehabilitation of patients
Shoulder Arthroscopy with Rotator Cuff Repair Rehabilitation Protocol
 General Notes: As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
General Notes: As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
Anterior Stabilization of the Shoulder: Latarjet Protocol
 Robert K. Fullick, MD 6400 Fannin Street, Suite 1700 Houston, Texas 77030 Ph.: 713-486-7543 / Fx.: 713-486-5549 Anterior Stabilization of the Shoulder: Latarjet Protocol The intent of this protocol is
Robert K. Fullick, MD 6400 Fannin Street, Suite 1700 Houston, Texas 77030 Ph.: 713-486-7543 / Fx.: 713-486-5549 Anterior Stabilization of the Shoulder: Latarjet Protocol The intent of this protocol is
Charlotte Shoulder Institute
 Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
Post-Operative Instructions Glenoid Reconstruction using Fresh Distal Tibial Allograft
 Day of Surgery Post-Operative Instructions Glenoid Reconstruction using Fresh Distal Tibial Allograft A. Relax. Diet as tolerated. B. Icing is important for the first 5-7 days post-op. While the post-op
Day of Surgery Post-Operative Instructions Glenoid Reconstruction using Fresh Distal Tibial Allograft A. Relax. Diet as tolerated. B. Icing is important for the first 5-7 days post-op. While the post-op
