Brachial Plexus Injury and Benign Paroxysmal Positional Vertigo Following a Fall: A Case Report
|
|
|
- David Charles
- 6 years ago
- Views:
Transcription
1 Governors State University OPUS Open Portal to University Scholarship All Capstone Projects Student Capstone Projects Spring 2015 Brachial Plexus Injury and Benign Paroxysmal Positional Vertigo Following a Fall: A Case Report Przemyslaw Ilczyk Governors State University Follow this and additional works at: Part of the Physical Therapy Commons Recommended Citation Ilczyk, Przemyslaw, "Brachial Plexus Injury and Benign Paroxysmal Positional Vertigo Following a Fall: A Case Report" (2015). All Capstone Projects For more information about the academic degree, extended learning, and certificate programs of Governors State University, go to Visit the Governors State Physical Therapy Department This Project Summary is brought to you for free and open access by the Student Capstone Projects at OPUS Open Portal to University Scholarship. It has been accepted for inclusion in All Capstone Projects by an authorized administrator of OPUS Open Portal to University Scholarship. For more information, please contact opus@govst.edu.
2 BRACHIAL PLEXUS INJURY AND BENIGN PAROXYSMAL POSITIONAL VERTIGO FOLLOWING A FALL. A CASE REPORT. By Przemyslaw Ilczyk M.A Academy of Physical Education, 2005 CAPSTONE PROJECT Submitted in partial fulfillment of the requirements For the Degree of Doctor of Physical Therapy Governors State University University Park, IL
3 ABSTRACT: Background: In the elderly population, research has shown that impairments of balance and strength are common reasons for falls. Falls constitute one of the main reasons for emergency department and hospital admissions, and are the second most common reason for brachial plexus injury. Another common symptom, after a fall and head trauma incident, is Benign Paroxysmal Positional Vertigo (BPPV). Approximately 50% of subjects with traumatic brain injury complain about positional vertigo. Research shows that traumatic BPPV is commonly misdiagnosed in clinical practice. Purpose: The purpose of this case report is to present interventions that were used to treat a patient with diagnoses of BPPV and brachial plexus injury following a fall. Case Description: The patient was a 67-year-old white male who presented to therapy with complaints of dizziness and shoulder weakness after a fall. He was referred to physical therapy by his physician with a diagnosis of brachial plexus injury and suspected BPPV. Outcomes: The dizziness symptoms associated with suspected BPPV were fully eliminated during the episode of care. The patient did not fully recover from the brachial plexus injury; however, he significantly improved his ability to perform activities of daily living. i
4 Discussion: Symptoms of BPPV sustained during a traumatic fall were effectively diagnosed by the Dix-Hallpike test and were successfully treated by the Epley canalith repositioning maneuver. Furthermore, the physical therapy treatment formed by neuromuscular re-education, strengthening and functional exercises, seemed to have a positive impact on patient s recovery process following traumatic brachial plexus injury. ii
5 INTRODUCTION: In older adults, falls are the leading cause of injury requiring admission to the emergency department or hospital and can sometimes be fatal. 1,2 Brachial plexus injury and dizziness associated with Benign Paroxysmal Positional Vertigo (BPPV) are common results of trauma related falls. 2,3 A significant amount of evidence describes treating patients with a single diagnosis of brachial plexus injury or BPPV; however, there is a gap in literature regarding the treatment strategy and progress of patients with multiple comorbidities. The purpose of this case report is to present the clinical reasoning and intervention strategy used by the physical therapy team during an eight-week treatment episode for a patient with comorbid BPPV and brachial plexus injury following a fall. The secondary purpose of this study is to report the patient s response to the implemented treatment. CASE DESCRIPTION: The patient was a 67-year-old white male who presented to therapy with complaints of dizziness after falling down the stairs at home and hitting his head about two weeks prior. He was admitted to the hospital one week after the incident. After hospitalization, he was referred to physical therapy by his physician with a diagnosis of brachial plexus injury and suspected Benign Paroxysmal Positional Vertigo (BPPV). The patient was a right hand 1
6 dominant barber who lived at home with his wife and was previously independent in work and all activities of daily living (ADLs). During the initial evaluation, the patient reported experiencing a spinning sensation when getting out of bed, looking up, or bending over. In the affected right arm, he denied paresthesia, but reported pain and weakness that limited raising his arm and impeded instrumental ADLs (IADLs) such as dressing and tooth brushing, and work activities such as cutting hair. Past medical history: The patient was previously diagnosed with prostate cancer, for which he was being treated for concurrently with physical therapy. Patient/family goals: The patient s goals for physical therapy included decreasing the dizziness episodes, improving active range of motion (AROM), and strengthening of his right shoulder in order to be independent in all activities he was able to perform prior to the accident. CLINICAL IMPRESSION: From the data collected during initial interview and from the review of clinical records, it was hypothesized that the dizziness symptoms were associated with BPPV and the impaired function of the right shoulder was due to brachial plexus injury, both resulted from the blunt trauma to the 2
7 head and shoulder during the fall. A study performed by Liu 3 suggests that BPPV is a common symptom after a head trauma. According to the author, approximately 50% of the subjects with traumatic brain injury complained about positional vertigo. 3 Research performed by Thatte et al. 4 reported that the most common cause of brachial plexus injury in adults is motor vehicles accidents, with falls as the second or third most common cause of the trauma to the brachial plexus. 2,4 EXAMINATION: To examine the patient s impairments and confirm the diagnosis of BPPV, the Dix-Hallpike test was used, as is supported in the research 1. The appropriateness of this test 1 and its excellent specificity of 100% 5 have been confirmed in the research. 5 If the test is positive, this population of patients with BPPV can be effectively treated by a special canalith repositioning maneuver. 3 To assess the limits of the patient s right shoulder AROM, the standard 12- inch goniometer and measurement procedure as explained by Mullaney et al. 6 were used. This study reported a high intra-tester, intra-class correlation coefficient (ICC) between goniometer and digital level, ranging from 0.91 to 0.99, which confirms that a goniometer is a reliable tool to measure patient s shoulder range of motion. 6 3
8 The manual muscle test (MMT) techniques, as explained in Hislop & Montgomery, 7 were used to evaluate the patient s bilateral upper extremity (UE) strength. The MMTs and AROM assessments were both performed with the patient in standing position. Before beginning the initial assessment, the patient completed the Disability of Arm, Shoulder and Hand (DASH) questionnaire. According to a study performed by Roy JS et al., the DASH reports an intraclass correlation coefficient (ICC) of , standard error of the measure (SEM) of , a minimal clinically important difference (MCID) of 10.2 and a minimal detectable change (MDC) of Assessment of the patient s posture alignment revealed a forward head posture in sitting and standing positions. A summary of the examination data is shown in Tables 1 and 2. Table #1: Initial neurological examination data. Dix-Hallpike test Right side Left side Results (+) Positive mild UBN (+) Positive severe UBN UBN: Upward Beating Nystagmu Table #2: Initial examination data. Tests DASH R shoulder AROM R shoulder MMT score Flex Abd IR ER Flex. Abd. ER Initial evaluation 50% HUB: R buttock Not tested 2/5 2/5 1/5 DASH The Disability of Arm Shoulder and Hand; AROM active range of motion; MMT manual muscle test; Flex Flexion; Abd Abduction; IR internal rotation; ER external rotation; HUB hand up back. 4
9 INTERVENTION: The patient attended minute physical therapy sessions 2-3 times a week for 8 weeks, equaling a total of 26 therapy sessions. During the first two sessions, the patient primarily received treatment for his BPPV symptoms. Each session, the Epley canalith repositioning maneuver was performed three times, exclusively for his left side due to fact that upward beating nystagmus (UBN) was most severe during left Dix-Hallpike test. It was suspected that, posterior semi-circular canal of patient s left inner ear was involved. 9 Before each intervention, the specific steps of the maneuver were explained and reviewed with the patient. After these sessions, the patient was instructed to stay in upright position and avoid bending forward or lying down on his left side for at least 24 hours, if possible. After the first therapy session, the patient reported that the dizziness symptoms significantly decreased. After the second physical therapy session, the symptoms were fully eliminated on both sides. However, the BPPV symptom resumed after 6 weeks, the Dix-Hallpike test was also performed at this time to confirm the diagnosis. At this point, the Epley maneuver was repeated 3 times on the left side for one session and 3 times on his right side during the following session. The patient was also given instructions on how to perform the Epley maneuver on his own if the symptoms returned. After those two sessions, the dizziness symptoms had stopped, and the patient remained clear of BPPV symptoms until discharge (Fig 1). 5
10 Figure 1: Progress of the BPPV symptoms. During the third session, the intervention for patient s right shoulder was implemented. Initially the shoulder intervention focused on active assisted range of motion (AAROM) exercises, specifically, pulleys and finger ladder min for each exercise (appendix A), active range of motion (AROM) exercises, specifically, wall washes and table washes, 7-15 minutes each exercise (appendix A), and upper body ergometer exercises, level 1 for 10 min. After the second week, more progressive resisted exercises concentrating on the eccentric work of the shoulder and parascapular muscles were implemented, specifically, wrist ripper with 2 lb. weight and Thera Bands (appendix A). All of the exercises were adjusted to the patient s progress by increasing resistance and number of repetitions 6
11 throughout the treatment. During week six, proprioceptive neuromuscular facilitation (PNF) strengthening exercises were added to the program (diagonal D1 flexion, extension, diagonal D2 flexion, extension). Initially, these exercises were performed without resistance, then progressed with yellow Thera bands. A research study performed by Sullivan et al. tested activity of the shoulder muscles during unilateral upper extremity PNF patterns using electromyography (EMG). The study confirmed that the intended shoulder muscles were active during these PNF patterns. 10 During the last phase of the plan of care, more functional activities were added. For example, patient performed activities such as placing and retrieving objects from a shelf at shoulder-height and above-shoulder. Due to specificity of the clinic specialized in mechanical diagnosis and therapy (McKenzie), retraction-extension exercise was used to improve patient s sitting and standing posture during each therapy session. The patient performed retraction-extension exercise for his cervical spine about 7-15 minutes each session. The patient was also instructed to perform his home exercise program (HEP) daily, three times per day. His HEP included 3 sets of 10 repetitions for each exercise: cervical retraction-extension, pulleys, wall washes, hand up back with belt, and table washes (appendix A). Later, the PNF strengthening exercises were also added. 10 All of the therapy interventions and the week they were performed are presented in Table 3 7
12 Table 3: Interventions. Intervention Week 1 Week 2 Week 3 Week 4 Week 5 Week 6 Week 7 1 X X X X X X X X 2 X X 3 X X X X X X X X 4 X X X X X X X X 5 X X X X X X X X 6 X X X X X X X 7 X X X X X X 8 X X X X X X 9 X X X 10 X X Week 8 1= patient education 6= neuromuscular re-education 2= Epley maneuver 7= active range of motion 3= range of motion exercise 8= progressive resistive exercise 4= active assisted range of motion 9= proprioceptive neuromuscular facilitation 5= upper body ergometer 10= functional training OUTCOMES: The subject of this case report can be considered a complex patient due to his vestibular, neuromuscular, and endocrine system diagnoses as well as other comorbidities. Recovery process for brachial plexus injury is often incomplete and expected to take 6 to 18 months. 11 During this episode of care, the patient showed progress in his shoulder ROM and strength with some deviations in his status. For example during week 5, the AROM of patient s involved shoulder decreased from 65 to 33 (Fig 2). The deviations were probably caused by return of his BPPV symptoms and clinical procedures associated with the patient s cancer diagnosis and 8
13 treatment. At the end of week 8 of physical therapy, patient s right shoulder ROM and strength were not within normal limits (WNL) yet, however, had significantly improved. In addition, his AROM improved from 15 to 74 of shoulder flexion, 10 to 64 of shoulder abduction, and in strength from 1/5 to 3/5 of shoulder external rotation since patient begun receiving physical therapy care (Fig 2 and Table 4). Overall, the patient presented with enhancement in his functional abilities. At the completion of the treatment, patient was able to perform ADLs and IADLs independently, such as washing his hair, brushing his teeth, donning and doffing a T-shirt, and placing and retrieving a 1 lb. dumbbell from an overhead shelf. Moreover, the dizziness symptoms associated with BPPV were fully eliminated by week 7 of treatment. At discharge, the patient reported that he was feeling at least 50% better since he started physical therapy treatment. However, the DASH score did not reflect this progress. At discharge, the DASH score was 10% worse than during the initial evaluation and changed from 50 to 55%. All the outcomes measures and data collected during this episode of care are provided in Table 4. DISCUSSION: The purpose of this case report is to present interventions that were used to treat a 67-year-old white male with diagnoses of BPPV and brachial 9
14 plexus injury following a fall. The patient attended 26 therapy sessions, Table 4: Outcomes Tests DASH R shoulder AROM R shoulder MMT Pain score Flex Abd IR ER Flex Abd ER IR on VAS Normal 0% /5 5/5 5/5 5/5 0/10 values Initial 50% HUB: R 2/5 2/5 1/5 3/10 evaluation buttock Week /5 3/5 2-/5 2-/5 Week HUB: R L4 Week /5 2+/5 3/5 2+/5 3/10 end range Week 8 55% /5 2+/5 3/5 3/5 DASH The Disability of Arm Shoulder and Hand; AROM active range of motion; MMT manual muscle test; Flex Flexion; Abd Abduction; IR internal rotation; ER external rotation; HUB hand up back. Figure 2: Progress of right shoulder AROM 10
15 Figure 3: Progress of right shoulder muscle strength Shoulder Strength MMT # out of Eval Week 3 Week 5 Week 6 D/C Flexion Abduction External Rotation Internal Rotation MMT: Manual muscle strength, #1.5=MMT 2-/5, #2=MMT 2/5, #2.5=MMT 2+/5, #3=MMT 3/3. which were concentrated mostly on the Epley canalith repositioning maneuver to decrease BPPV symptoms, neuromuscular re-education, therapeutic exercises and activities to improve AROM and muscle strength of his R shoulder. At discharge, patient presented with improved shoulder AROM an ability to perform ADLs. It is expected that the complexity of the subject associated with his comorbid diagnoses mentioned earlier had some impact on his recovery process. The cancer treatment, concurrent to physical therapy plan of care, seemed to have some impact on the patient s progress. During the fifth week of therapy, the patient underwent a lumbar procedure (spinal tap) as 11
16 part of his cancer treatment. The physician suggested the patient rest and lay down for an entire day after the procedure. Two days after this procedure, the patient presented to therapy with some decrease in right shoulder muscle strength and endurance from 3/5 to 2+/5, which also reflects as decreased shoulder flexion. Moreover, reappearance of the Benign Paroxysmal Positional Vertigo symptoms during the 6 th week of the therapy, also had impact on the patient s status. According to Mokri et al. 12 volume depletion of the cerebrospinal fluid (CSF) caused by CSF leak or by spinal tap diagnostic procedure, can cause descent of the brain, at the same time changing pressure in the perilymphatic fluid of the inner ear. In this situation altered hearing or vertigo symptoms can be present. 12 During episodes of vertigo and after the spinal tap procedure, the patient was unable to perform his home exercise program. Throughout these episodes, the patient spent most of the time in bed, which could be a reason why his progress in the therapy (AROM, strength and muscle endurance) fluctuated. However, at the end of the therapy care (26 visits), the patient reached all of his anticipated goals. He presented with significant improvements in AROM, strength, and muscle endurance, which reflected in his ability to perform all previous ADLs. Conversely, the meaningful improvement in the patient s ability to perform ADLs was not reflected in the patient s DASH score. It could not be explained why the initial evaluation score was better than discharge score. It 12
17 could only be hypothesized that the patient did not fully understand the instructions of the DASH questionnaire. Possibly he did not chose the most appropriate answers when completing the questionnaire, especially since, during the discharge assessment, he stated that his overall status and ability to perform ADLs had improved at least 50% since the beginning of the physical therapy. This case report supports the previous research evidence presented by Liu H. 3 that BPPV sustained during a traumatic fall can effectively be diagnosed by the Dix-Hallpike test and can successfully be treated by the Epley canalith repositioning maneuver. Moreover, this case report supports the clinical reasoning and appropriateness of the intervention used in this study to treat the patient with a post fall brachial plexus injury. Similar to the study published by Chambers et al., 11 this study confirmed that recovery of a brachial plexus injury is a lengthy process. The eight weeks of physical therapy was not sufficient to reach a full recovery; however, it represented satisfactory amount of time to improve patient s ability to perform ADLs. Furthermore, the length of treatment provided adequate time to educate the patient on how to advance his HEP in order to further improve his skills and progress toward full recovery after discharge. Limitations of the study: Due to the specificity of a case report, only a single subject s response to the interventions was presented. Therefore, these 13
18 findings cannot be generalized to other populations. More research is needed to confirm or refute these interventions as the best plan of care for BPPV, brachial plexus injury and symptom presentation. Conclusion: This case report presents one incidence of BPPV and brachial plexus injury as a result of fall. The physical therapy interventions presented in this study were effective for both BPPV and brachial plexus injury. Moreover, strategy used in this case report confirms that it is appropriate to resolve the BPPV first before addressing other issues such as brachial plexus injury. The current study presents the recovery process during 8 weeks episode of physical therapy. There is need for further study and follow-up, possibly after 6, 12 and 18 months, to monitor patient status in the process to recovery. 14
19 REFERENCES: 1. Shubert TE. Evidence-Based Exercise Prescription for Balance and Falls Prevention: A Current Review of the Literature... Exercise, Physical Activity and Aging (ExPAAC): Blending Research and Practice, July 29-31, Journal of Geriatric Physical Therapy. 2011;34(3): Chuang T-Y, Chiu F-Y, Tsai Y-A, Chiang S-C, Yen D-J, Cheng H. The comparison of electrophysiologic findings of traumatic brachial plexopathies in a tertiary care center. Injury. 2002;33(7): Liu H. Presentation and outcome of post-traumatic benign paroxysmal positional vertigo. Acta Oto-Laryngologica. 2012;132(8): Thatte MR, Babhulkar S, Hiremath A. Brachial plexus injury in adults: Diagnosis and surgical treatment strategies. Annals of Indian Academy of Neurology. 2013;16(1): Zainun Z, Zakaria MN, Sidek D, Ismail Z. Determination of Sensitivity & Specificity of Dix Hallpike Test (DHT) in Peripheral Vestibular Disordered Subjects. International Medical Journal. 2013;20(2): Mullaney MJ, McHugh MP, Johnson CP, Tyler TF. Reliability of shoulder range of motion comparing a goniometer to a digital level. Physiotherapy Theory & Practice. 2010;26(5): Hislop HJ, Avers D, Brown M. Daniels and Worthingham's Muscle Testing, Techniques of Manual Examination and Performance Testing. 8th ed. St. Louis, Missouri: Saunders; Roy JS, Macdermid JC, Woodhouse LJ. Measuring shoulder function: A systematic review of four questionnaires. Arthritis & Rheumatism: Arthritis Care & Research. 2009;61(5): Vannucchi P, Pecci R, Giannoni B. Posterior semicircular canal benign paroxysmal positional vertigo presenting with torsional downbeating nystagmus: an apogeotropic variant. Int J Otolaryngol. 2012;2012: Sullivan PE, Portney LG. Electromyographic activity of shoulder muscles during unilateral upper extremity proprioceptive neuromuscular facilitation patterns. Physical Therapy. 1980;60: Chambers JA, Hiles CL, Keene BP. Brachial plexus injury management in military casualties: who, what, when, why, and how. Military Medicine. 2014;179(6): Mokri B. Spontaneous intracranial hypotension. Curr Neurol Neurosci Rep. 2001;1(2): Physical Therapy: Weeks Charting my recovery from shoulder injury. Vol 2014: WordPress.com;
20 14. Healthy Mega Mall. 2011; Lifeline-Econo-Shoulder-Pulley_c11234_p htm. Accessed Dec. 1st Exercises After Breast Surgery. 2014; s-after-breast-surgery. Accessed Dec. 1st Thera-Band Exercises. Accessed Dec. 1st Wrist Ripper, Wrist Roller Training. 2014; ng_332_9425~product.html. Accessed Dec. 2nd
21 Appendix A: Therapeutic exercises. 1. Finger ladder Pulleys Wall washes 15 Thera band Wrist ripper: 17 17
Quick Guides Vestibular Diagnosis and Treatment:
 VNG - Balance Testing Quick Guides Vestibular Diagnosis and Treatment: A Physical Therapy Approach Dix-Hallpike Test for Diagnosis of BPPV Epley Canalith Repositioning Procedure (CRP) Semont Maneuver for
VNG - Balance Testing Quick Guides Vestibular Diagnosis and Treatment: A Physical Therapy Approach Dix-Hallpike Test for Diagnosis of BPPV Epley Canalith Repositioning Procedure (CRP) Semont Maneuver for
Rotator Cuff Repair Therapy Protocol
 Bart Eastwood D.O. 825 Davis st Blacksburg, VA 24060 540-951-6000 All information contained in this protocol is to be used as general guidelines only. Specific variations may be appropriate for each patient
Bart Eastwood D.O. 825 Davis st Blacksburg, VA 24060 540-951-6000 All information contained in this protocol is to be used as general guidelines only. Specific variations may be appropriate for each patient
Cross Country Education Leading the Way in Continuing Education and Professional Development.
 To comply with professional boards/associations standards: I declare that I or my family do not have any financial relationship in any amount, occurring in the last 12 months with a commercial interest
To comply with professional boards/associations standards: I declare that I or my family do not have any financial relationship in any amount, occurring in the last 12 months with a commercial interest
Shoulder Arthroscopy: Postop Instructions. Activites & Advice for in the Hospital and while at Home
 Dr. Mark Price MGH Sports Medicine Center 175 Cambridge Street, 4th floor Boston, MA 02114 www.massgeneral.org/ortho-sports-medicine/dr-price Shoulder Arthroscopy: Postop Instructions You will wake up
Dr. Mark Price MGH Sports Medicine Center 175 Cambridge Street, 4th floor Boston, MA 02114 www.massgeneral.org/ortho-sports-medicine/dr-price Shoulder Arthroscopy: Postop Instructions You will wake up
Because dizziness is an imprecise term, a major role of the clinician is to sort patients out into categories
 Dizziness and Imbalance Timothy C. Hain, MD Clinical Professor of Neurology, Otolaryngology, Physical Therapy Chicago Dizziness and Hearing 645 N. Michigan, Suite 410 312-274-0197 Lecture Goals 1. What
Dizziness and Imbalance Timothy C. Hain, MD Clinical Professor of Neurology, Otolaryngology, Physical Therapy Chicago Dizziness and Hearing 645 N. Michigan, Suite 410 312-274-0197 Lecture Goals 1. What
BENIGN PAROXYSMAL POSITIONAL VERTIGO (BPPV)
 5018 NE 15 TH AVE PORTLAND, OR 97211 FAX: (503) 229-8064 (800) 837-8428 INFO@VESTIBULAR.ORG VESTIBULAR.ORG BENIGN PAROXYSMAL POSITIONAL VERTIGO (BPPV) By Sheelah Woodhouse, BScPT WHAT IS BPPV? Benign Paroxysmal
5018 NE 15 TH AVE PORTLAND, OR 97211 FAX: (503) 229-8064 (800) 837-8428 INFO@VESTIBULAR.ORG VESTIBULAR.ORG BENIGN PAROXYSMAL POSITIONAL VERTIGO (BPPV) By Sheelah Woodhouse, BScPT WHAT IS BPPV? Benign Paroxysmal
MASSIVE ROTATOR CUFF REPAIR. REHABITATION PROTOCOL >3 cm
 MASSIVE ROTATOR CUFF REPAIR REHABITATION PROTOCOL >3 cm Phase I: (Protective Phase) Weeks 0 to 8 Goals: Minimize pain and inflammatory response Achieve ROM goals Establish stable scapula 1. Elbow, wrist
MASSIVE ROTATOR CUFF REPAIR REHABITATION PROTOCOL >3 cm Phase I: (Protective Phase) Weeks 0 to 8 Goals: Minimize pain and inflammatory response Achieve ROM goals Establish stable scapula 1. Elbow, wrist
Vestibular Evaluation
 Chris Carpino, MPT Vestibular Evaluation 1. History Most important aspect of evaluation (see DHI) 2. Vital Signs Check blood pressure in supine and sitting 3. Eye Exam 4. Positional Testing 5. Balance
Chris Carpino, MPT Vestibular Evaluation 1. History Most important aspect of evaluation (see DHI) 2. Vital Signs Check blood pressure in supine and sitting 3. Eye Exam 4. Positional Testing 5. Balance
REGENETEN Bioinductive Implant. Rehabilitation Protocol. for REGENETEN partial thickness tears without repair
 REGENETEN Bioinductive Implant Rehabilitation Protocol for REGENETEN partial thickness tears without repair Let s get you back to YOU. We must emphasize that this protocol is recommended ONLY for partial
REGENETEN Bioinductive Implant Rehabilitation Protocol for REGENETEN partial thickness tears without repair Let s get you back to YOU. We must emphasize that this protocol is recommended ONLY for partial
SMALL-MEDIUM ROTATOR CUFF REPAIR GUIDELINE
 SMALL-MEDIUM ROTATOR CUFF REPAIR GUIDELINE The rotator cuff is responsible for stabilization and active movement of the glenohumeral joint. An acute or overuse injury may cause the rotator cuff to be injured
SMALL-MEDIUM ROTATOR CUFF REPAIR GUIDELINE The rotator cuff is responsible for stabilization and active movement of the glenohumeral joint. An acute or overuse injury may cause the rotator cuff to be injured
Limited Goals Program (Examples Include: Cuff Tear Arthropathy, Massive Irrepairable Rotator Cuff Tear, Selected Revision Surgeries)
 Limited Goals Program (Examples Include: Cuff Tear Arthropathy, Massive Irrepairable Rotator Cuff Tear, Selected Revision Surgeries) All information contained in this protocol is to be used as general
Limited Goals Program (Examples Include: Cuff Tear Arthropathy, Massive Irrepairable Rotator Cuff Tear, Selected Revision Surgeries) All information contained in this protocol is to be used as general
Benign Paroxysmal Positional Vertigo
 Benign Paroxysmal Positional Vertigo Information for patients and families Read this booklet to learn about: What Benign Paroxysmal Positional Vertigo (BPPV) is Symptoms How your doctor will diagnose it
Benign Paroxysmal Positional Vertigo Information for patients and families Read this booklet to learn about: What Benign Paroxysmal Positional Vertigo (BPPV) is Symptoms How your doctor will diagnose it
International Journal of Medical and Exercise Science (Multidisciplinary, Peer Reviewed and Indexed Journal)
 ORIGINAL ARTICLE International Journal of Medical and Exercise Science (Multidisciplinary, Peer Reviewed and Indexed Journal) PHYSICAL THERAPY MANAGEMENT IN PATIENTS WITH CERVICOGENIC DIZZINESS-A CASE
ORIGINAL ARTICLE International Journal of Medical and Exercise Science (Multidisciplinary, Peer Reviewed and Indexed Journal) PHYSICAL THERAPY MANAGEMENT IN PATIENTS WITH CERVICOGENIC DIZZINESS-A CASE
Phase I : Immediate Postoperative Phase- Protected Motion. (0-2 Weeks)
 Phase I : Immediate Postoperative Phase- Protected Motion (0-2 Weeks) Appointments Progression Criteria 2 weeks after surgery Rehabilitation appointments begin within 7-10 days of surgery, continue 1-2
Phase I : Immediate Postoperative Phase- Protected Motion (0-2 Weeks) Appointments Progression Criteria 2 weeks after surgery Rehabilitation appointments begin within 7-10 days of surgery, continue 1-2
Latarjet Repair Rehabilitation Protocol
 General Notes: As tolerated should be understood to include with safety for the reconstruction/repair; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing
General Notes: As tolerated should be understood to include with safety for the reconstruction/repair; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing
Nonoperative Treatment For Rotator Cuff Tendinitis/ Partial Thickness Tear Dr. Trueblood
 Nonoperative Treatment For Rotator Cuff Tendinitis/ Partial Thickness Tear Dr. Trueblood Relieving Pain Patients who present with SIS will have shoulder pain that is exacerbated with overhead activities.
Nonoperative Treatment For Rotator Cuff Tendinitis/ Partial Thickness Tear Dr. Trueblood Relieving Pain Patients who present with SIS will have shoulder pain that is exacerbated with overhead activities.
CITY & HACKNEY PATHFINDER CLINICAL COMMISSIONING GROUP. Vertigo. (1) Vertigo. (4) Provisional Diagnosis. (5) Investigations. lasting days or weeks
 Authors: Dr Lucy O'Rouke and Mr N Eynon-Lewis Review date: January 2017 Vertigo (1) Vertigo (2) History (3) Examination (4) Provisional Diagnosis (5) Investigations (6) Medical Cause (7) Psychiatric Cause
Authors: Dr Lucy O'Rouke and Mr N Eynon-Lewis Review date: January 2017 Vertigo (1) Vertigo (2) History (3) Examination (4) Provisional Diagnosis (5) Investigations (6) Medical Cause (7) Psychiatric Cause
Monitoring of Caloric Response and Outcome in Patients With Benign Paroxysmal Positional Vertigo
 Otology & Neurotology 28:798Y800 Ó 2007, Otology & Neurotology, Inc. Monitoring of Caloric Response and Outcome in Patients With Benign Paroxysmal Positional Vertigo *Maria I. Molina, *Jose A. López-Escámez,
Otology & Neurotology 28:798Y800 Ó 2007, Otology & Neurotology, Inc. Monitoring of Caloric Response and Outcome in Patients With Benign Paroxysmal Positional Vertigo *Maria I. Molina, *Jose A. López-Escámez,
Home Exercise Program Progression and Components of the LTP Intervention. HEP Activities at Every Session Vital signs monitoring
 Home Exercise Program Progression and Components of the LTP Intervention HEP Activities at Every Session Vital signs monitoring Blood pressure, heart rate, Borg Rate of Perceived Exertion (RPE) and oxygen
Home Exercise Program Progression and Components of the LTP Intervention HEP Activities at Every Session Vital signs monitoring Blood pressure, heart rate, Borg Rate of Perceived Exertion (RPE) and oxygen
BPPV and Pitfalls in its Management. Reza Golrokhian Sani MD, Otolaryngologist- Head & Neck Surgeon Otologist & Neurotologist
 BPPV and Pitfalls in its Management Reza Golrokhian Sani MD, Otolaryngologist- Head & Neck Surgeon Otologist & Neurotologist Objectives 1-The best methods of diagnosis of BPV 2-How to differentiate between
BPPV and Pitfalls in its Management Reza Golrokhian Sani MD, Otolaryngologist- Head & Neck Surgeon Otologist & Neurotologist Objectives 1-The best methods of diagnosis of BPV 2-How to differentiate between
POST-SURGICAL POSTERIOR GLENOHUMERAL STABILIZATION REHABILITATION PROTOCOL (Capsulolabral Repair)
 Gregory N. Lervick, MD Andrew Anderson, PA-C 952-456-7111 POST-SURGICAL POSTERIOR GLENOHUMERAL STABILIZATION REHABILITATION PROTOCOL (Capsulolabral Repair) Open Arthroscopic Phase 1: Weeks 0-4 No shoulder
Gregory N. Lervick, MD Andrew Anderson, PA-C 952-456-7111 POST-SURGICAL POSTERIOR GLENOHUMERAL STABILIZATION REHABILITATION PROTOCOL (Capsulolabral Repair) Open Arthroscopic Phase 1: Weeks 0-4 No shoulder
Benign paroxysmal positional. Labyrinth. Canalolithiasis. Specialized dizzy clinic - most frequent diagnoses. Semicircular canals
 Specialized dizzy clinic - most frequent diagnoses Canalolithiasis Unclear vertigo/dizziness multisensory vertigo/dizziness Benign paroxysmal positional vertigo (BPPV) hands on unilateral vestibulopathy
Specialized dizzy clinic - most frequent diagnoses Canalolithiasis Unclear vertigo/dizziness multisensory vertigo/dizziness Benign paroxysmal positional vertigo (BPPV) hands on unilateral vestibulopathy
Dynamic Neuromobilization for the Treatment of Thoracic Outlet Syndrome Courtney Convey and Dr. Erickson
 Dynamic Neuromobilization for the Treatment of Thoracic Outlet Syndrome Courtney Convey and Dr. Erickson Abstract Title: Dynamic Neuromobilization for the Treatment of Thoracic Outlet Syndrome Background:
Dynamic Neuromobilization for the Treatment of Thoracic Outlet Syndrome Courtney Convey and Dr. Erickson Abstract Title: Dynamic Neuromobilization for the Treatment of Thoracic Outlet Syndrome Background:
Reverse Total Shoulder Arthroplasty Protocol
 General Information: Reverse Total Shoulder Arthroplasty Protocol Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH) arthritis when it
General Information: Reverse Total Shoulder Arthroplasty Protocol Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH) arthritis when it
Functional Limitation Reporting. Case Report on PQRS and G-Code reporting
 Functional Limitation Reporting Case Report on PQRS and G-Code reporting Patient Demographics! 66 year old male referred by Dr. Schriefer, a neurologist, for PT evaluation and treatment! Chief Complaint:
Functional Limitation Reporting Case Report on PQRS and G-Code reporting Patient Demographics! 66 year old male referred by Dr. Schriefer, a neurologist, for PT evaluation and treatment! Chief Complaint:
OBJECTIVES BALANCE EVALUATION COMMON CAUSES OF BALANCE DEFICITS POST TBI BRAIN INJURY BALANCE RELATIONSHIP
 OBJECTIVES Understand variables that contribute to balance deficits Understand the relationship between a brain injury and balance Become familiar with the components of a vestibular/balance assessment
OBJECTIVES Understand variables that contribute to balance deficits Understand the relationship between a brain injury and balance Become familiar with the components of a vestibular/balance assessment
Acute Vestibular Syndrome (AVS) 12/5/2017
 Sharon Hartman Polensek, MD, PhD Dept of Neurology, Emory University Atlanta VA Medical Center DIAGNOSTIC GROUPS FOR PATIENTS PRESENTING WITH DIZZINESS TO EMERGENCY DEPARTMENTS Infectious 2.9% Genitourinary
Sharon Hartman Polensek, MD, PhD Dept of Neurology, Emory University Atlanta VA Medical Center DIAGNOSTIC GROUPS FOR PATIENTS PRESENTING WITH DIZZINESS TO EMERGENCY DEPARTMENTS Infectious 2.9% Genitourinary
OrthoCarolina. Arthroscopic SLAP Lesion (Type II) Repair Protocol
 OrthoCarolina Arthroscopic SLAP Lesion (Type II) Repair Protocol Surgical Overview: SLAP, which stands for superior labrum anterior to posterior, lesions are labral detachments that originate posterior
OrthoCarolina Arthroscopic SLAP Lesion (Type II) Repair Protocol Surgical Overview: SLAP, which stands for superior labrum anterior to posterior, lesions are labral detachments that originate posterior
Functional Capacity Evaluation
 Functional Capacity Evaluation SAMPLE REPORT RETURN TO WORK Client Name: Frank T. Date of FCE: 1/05/2011 Therapist: Laurie T. Referrer: Dr. Smith Facility WorkWell Prevention & Care 11 East Superior Street,
Functional Capacity Evaluation SAMPLE REPORT RETURN TO WORK Client Name: Frank T. Date of FCE: 1/05/2011 Therapist: Laurie T. Referrer: Dr. Smith Facility WorkWell Prevention & Care 11 East Superior Street,
Benign Paroxysmal Positional Vertigo (a.k.a.) Diagnosis: Dix-Hallpike Maneuver. Case SH. BPPV nystagmus. Video Frenzel Goggles make it easier
 Canalith Repositioning for Benign Paroxysmal Positional Vertigo Benign Paroxysmal Positional Vertigo (a.k.a.) Timothy C. Hain, MD Departments of Neurology, Otolaryngology and Physical Therapy Northwestern
Canalith Repositioning for Benign Paroxysmal Positional Vertigo Benign Paroxysmal Positional Vertigo (a.k.a.) Timothy C. Hain, MD Departments of Neurology, Otolaryngology and Physical Therapy Northwestern
Avon Office 2 Simsbury Rd. Avon, CT Office: (860) Fax: (860) REHABILITATION AFTER REVERSE SHOULDER ARTHROPLASTY
 Katherine J. Coyner, MD UCONN Musculoskeletal Institute Medical Arts & Research Building 263 Farmington Ave. Farmington, CT 06030 Office: (860) 679-6600 Fax: (860) 679-6649 www.drcoyner.com Avon Office
Katherine J. Coyner, MD UCONN Musculoskeletal Institute Medical Arts & Research Building 263 Farmington Ave. Farmington, CT 06030 Office: (860) 679-6600 Fax: (860) 679-6649 www.drcoyner.com Avon Office
Particle Liberation Maneuvers for Benign Paroxysmal Positional Vertigo
 Particle Liberation Maneuvers for Benign Paroxysmal Positional Vertigo Ahmed A. El Degwi, MD* and Ayman E. El Sharabasy, MD** ENT Department * and Audiology Unit** Mansoura Faculty of Medicine Abstract
Particle Liberation Maneuvers for Benign Paroxysmal Positional Vertigo Ahmed A. El Degwi, MD* and Ayman E. El Sharabasy, MD** ENT Department * and Audiology Unit** Mansoura Faculty of Medicine Abstract
The Four Phases of Healing During Rehabilitation Following Rotator Cuff Surgery. Phase 1: Immediate postoperative period (weeks 0-6) Goals
 The Four Phases of Healing During Rehabilitation Following Rotator Cuff Surgery Phase 1: Immediate postoperative period (weeks 0-6) Maintain/protect integrity of repair Gradually increase PROM Diminish
The Four Phases of Healing During Rehabilitation Following Rotator Cuff Surgery Phase 1: Immediate postoperative period (weeks 0-6) Maintain/protect integrity of repair Gradually increase PROM Diminish
Deep Inferior Epigastric Perforator Breast Flap Reconstruction Protocol:
 Deep Inferior Epigastric Perforator Breast Flap Reconstruction Protocol: DAY 5-WEEK 2: Continue home exercise program per written patient handout. Continue appropriate incision care management per MD Maintain
Deep Inferior Epigastric Perforator Breast Flap Reconstruction Protocol: DAY 5-WEEK 2: Continue home exercise program per written patient handout. Continue appropriate incision care management per MD Maintain
Benign Paroxysmal Positional Vertigo (a.k.a.) Diagnosis: Dix-Hallpike Maneuver. Case SH. BPPV nystagmus. Video Frenzel Goggles make it easier
 Positional Vertigo Office Diagnosis and Treatment Timothy C. Hain, MD Departments of Neurology, Otolaryngology and Physical Therapy Northwestern University, Chicago, IL Janet O. Helminski, PhD Physical
Positional Vertigo Office Diagnosis and Treatment Timothy C. Hain, MD Departments of Neurology, Otolaryngology and Physical Therapy Northwestern University, Chicago, IL Janet O. Helminski, PhD Physical
ROTATOR CUFF REPAIR REHAB PROTOCOL
 Jayesh K. Patel, M.D. Trinity Clinic Orthopaedic and Sports Medicine 1327 Troup Hwy Tyler, TX 75701 (903) 510-8840 ROTATOR CUFF REPAIR REHAB PROTOCOL This rehabilitation protocol has been developed for
Jayesh K. Patel, M.D. Trinity Clinic Orthopaedic and Sports Medicine 1327 Troup Hwy Tyler, TX 75701 (903) 510-8840 ROTATOR CUFF REPAIR REHAB PROTOCOL This rehabilitation protocol has been developed for
Shoulder Arthroscopy with Posterior Labral Repair Rehabilitation Protocol
 General Notes: As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
General Notes: As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
ORTHOPEDIC AND SPORTS MEDICINE CENTER
 ORTHOPEDIC AND SPORTS MEDICINE CENTER SPORTS MEDICINE DIVISION COMBINED REHAB PROTOCOLS AAMC ORTHOPEDIC AND SPORTS MEDICINE SPECIALISTS Office: (410) 268-8862 Fax: (410) 268-0380 Rotator Cuff Repair Rehab
ORTHOPEDIC AND SPORTS MEDICINE CENTER SPORTS MEDICINE DIVISION COMBINED REHAB PROTOCOLS AAMC ORTHOPEDIC AND SPORTS MEDICINE SPECIALISTS Office: (410) 268-8862 Fax: (410) 268-0380 Rotator Cuff Repair Rehab
Subject: Vestibular Rehabilitation
 01-92502-14 Original Effective Date: 06/15/05 Reviewed: 09/27/18 Revised: 10/15/18 Subject: Vestibular Rehabilitation THIS MEDICAL COVERAGE GUIDELINE IS NOT AN AUTHORIZATION, CERTIFICATION, EXPLANATION
01-92502-14 Original Effective Date: 06/15/05 Reviewed: 09/27/18 Revised: 10/15/18 Subject: Vestibular Rehabilitation THIS MEDICAL COVERAGE GUIDELINE IS NOT AN AUTHORIZATION, CERTIFICATION, EXPLANATION
Charlotte Shoulder Institute
 Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
The Big 3 of Vertigo
 They feel it, you see it, few know it: Common vertigo conditions seen, but rarely diagnosed Peter Johns MD, FRCPC University of Ottawa pjohns@toh.ca Twitter @peterjohns84 The Big 3 of Vertigo BPPV Vestibular
They feel it, you see it, few know it: Common vertigo conditions seen, but rarely diagnosed Peter Johns MD, FRCPC University of Ottawa pjohns@toh.ca Twitter @peterjohns84 The Big 3 of Vertigo BPPV Vestibular
Total Shoulder Rehab Protocol Dr. Payne
 Total Shoulder Rehab Protocol Dr. Payne Phase I Immediate Post Surgical Phase (0-4 weeks): Allow healing of soft tissue Maintain integrity of replaced joint Gradually increase passive range of motion (PROM)
Total Shoulder Rehab Protocol Dr. Payne Phase I Immediate Post Surgical Phase (0-4 weeks): Allow healing of soft tissue Maintain integrity of replaced joint Gradually increase passive range of motion (PROM)
The SUPPORT Trial: SUbacromial impingement syndrome and Pain: a randomised controlled trial Of exercise and injection
 The SUPPORT Trial: SUbacromial impingement syndrome and Pain: a randomised controlled trial Of exercise and injection SUPPORT Physiotherapy Intervention Training Manual Authors: Sue Jackson (SJ) Julie
The SUPPORT Trial: SUbacromial impingement syndrome and Pain: a randomised controlled trial Of exercise and injection SUPPORT Physiotherapy Intervention Training Manual Authors: Sue Jackson (SJ) Julie
Throwers Ten Exercise Program
 The Thrower s Ten Program is designed to exercise the major muscles necessary for throwing. The Program s goal is to be an organized and concise exercise program. In addition, all exercises included are
The Thrower s Ten Program is designed to exercise the major muscles necessary for throwing. The Program s goal is to be an organized and concise exercise program. In addition, all exercises included are
Arthroscopic Rotator Cuff Repair Protocol:
 Arthroscopic Rotator Cuff Repair Protocol: The intent of this protocol is to provide the therapist and patient with guidelines for the post-operative rehabilitation course after arthroscopic SLAP repair.
Arthroscopic Rotator Cuff Repair Protocol: The intent of this protocol is to provide the therapist and patient with guidelines for the post-operative rehabilitation course after arthroscopic SLAP repair.
Arthroscopic Shoulder Surgery /Meniscectomy Recovery
 Arthroscopic Shoulder Surgery /Meniscectomy Recovery Arthroscopic Shoulder Surgery (Acromioplasty) Recovery Arthroscopic subacromial decompression (ASAD) is a surgical procedure with the goal of relieving
Arthroscopic Shoulder Surgery /Meniscectomy Recovery Arthroscopic Shoulder Surgery (Acromioplasty) Recovery Arthroscopic subacromial decompression (ASAD) is a surgical procedure with the goal of relieving
Electrical stimulation for reducing trapezius muscle dysfunction in cancer patients: traditional treatment protocols also work
 Electrical stimulation for reducing trapezius muscle dysfunction in cancer patients: traditional treatment protocols also work RE: Baldwin ERL, Baldwin TD, Lancaster JS, et al. Neuromuscular electrical
Electrical stimulation for reducing trapezius muscle dysfunction in cancer patients: traditional treatment protocols also work RE: Baldwin ERL, Baldwin TD, Lancaster JS, et al. Neuromuscular electrical
Adult Male Status Post Chronic Traumatic Brachial Plexus Injury: A Case Report
 Governors State University OPUS Open Portal to University Scholarship All Capstone Projects Student Capstone Projects Spring 2015 Adult Male Status Post Chronic Traumatic Brachial Plexus Injury: A Case
Governors State University OPUS Open Portal to University Scholarship All Capstone Projects Student Capstone Projects Spring 2015 Adult Male Status Post Chronic Traumatic Brachial Plexus Injury: A Case
Rehabilitation after Arthroscopic Posterior Bankart Repair
 Rehabilitation after Arthroscopic Posterior Bankart Repair Phase 1: 0 to 2 weeks after surgery POSTOPERATIVE INSTRUCTIONS You will wake up in the operating room. A sling and an ice pack will be in place.
Rehabilitation after Arthroscopic Posterior Bankart Repair Phase 1: 0 to 2 weeks after surgery POSTOPERATIVE INSTRUCTIONS You will wake up in the operating room. A sling and an ice pack will be in place.
Sensible Physical Limitations after Epidural Patching Procedures or Surgery. Laura Freed, MPT
 Sensible Physical Limitations after Epidural Patching Procedures or Surgery Laura Freed, MPT Introduction Spontaneous Intracranial Hypotension Patient Wife and Mother Physical Therapist (Belpre, OH) What
Sensible Physical Limitations after Epidural Patching Procedures or Surgery Laura Freed, MPT Introduction Spontaneous Intracranial Hypotension Patient Wife and Mother Physical Therapist (Belpre, OH) What
THROWER S TEN EXERCISE PROGRAM David Andrew Parker, MD
 THROWER S TEN EXERCISE PROGRAM David Andrew Parker, MD The thrower s ten exercise program has been designed to exercise the major muscles necessary to return to throwing. The program s goal is to be an
THROWER S TEN EXERCISE PROGRAM David Andrew Parker, MD The thrower s ten exercise program has been designed to exercise the major muscles necessary to return to throwing. The program s goal is to be an
Sterile gauze used at incision site. Check brace for rubbing or irritation. Compression garment at elbow to be used with physician s authorization
 ULNAR COLLATERAL LIGAMENT RECONSTRUCTION GUIDELINE Functional Outcome Measure KJOC (Appendix 1) should be completed at initial evaluation and at all identified times through guideline, Phase 1 Immediate
ULNAR COLLATERAL LIGAMENT RECONSTRUCTION GUIDELINE Functional Outcome Measure KJOC (Appendix 1) should be completed at initial evaluation and at all identified times through guideline, Phase 1 Immediate
Rotator Cuff Repair Protocol for tear involving Subscapularis Tendon with or without Pectoralis Major Tendon Transfer
 Rotator Cuff Repair Protocol for tear involving Subscapularis Tendon with or without Pectoralis Major Tendon Transfer D. WATTS, MD Precautions: BASIS Tendon healing back to bone is a slow process that
Rotator Cuff Repair Protocol for tear involving Subscapularis Tendon with or without Pectoralis Major Tendon Transfer D. WATTS, MD Precautions: BASIS Tendon healing back to bone is a slow process that
(PROTOCOL #18) REVERSE TOTAL SHOULDER ARTHROPLASTY PROTOCOL
 The following is a set of general guidelines. It is important to remember that each patient is different. The progression of the patient depends on many factors including age and medical health of the
The following is a set of general guidelines. It is important to remember that each patient is different. The progression of the patient depends on many factors including age and medical health of the
VESTIBULAR FUNCTION TESTING
 VESTIBULAR FUNCTION TESTING Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices
VESTIBULAR FUNCTION TESTING Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices
TALLGRASS ORTHOPEDIC & SPORTS MEDICINE THROWING ATHLETE EXERCISE PROGRAM TALLGRASSORTHOPEDICS.COM
 TALLGRASS ORTHOPEDIC & SPORTS MEDICINE THROWING ATHLETE EXERCISE PROGRAM TALLGRASSORTHOPEDICS.COM Patient Name: Date of Surgery: General Principles: The Throwing Athlete Exercise Program is designed to
TALLGRASS ORTHOPEDIC & SPORTS MEDICINE THROWING ATHLETE EXERCISE PROGRAM TALLGRASSORTHOPEDICS.COM Patient Name: Date of Surgery: General Principles: The Throwing Athlete Exercise Program is designed to
So Young Moon, M.D., Kwang-Dong Choi, M.D., Seong-Ho Park, M.D., Ji Soo Kim, M.D.
 So Young Moon, M.D., Kwang-Dong Choi, M.D., Seong-Ho Park, M.D., Ji Soo Kim, M.D. Background: Benign positional vertigo (BPV) is characterized by episodic vertigo and nystagmus provoked by head motion.
So Young Moon, M.D., Kwang-Dong Choi, M.D., Seong-Ho Park, M.D., Ji Soo Kim, M.D. Background: Benign positional vertigo (BPV) is characterized by episodic vertigo and nystagmus provoked by head motion.
Anterior Stabilization of the Shoulder: Distal Tibial Allograft
 Anterior Stabilization of the Shoulder: Distal Tibial Allograft Name: Diagnosis: Date: Date of Surgery: Phase I Immediate Post Surgical Phase (approximately Weeks 1-3) Minimize shoulder pain and inflammatory
Anterior Stabilization of the Shoulder: Distal Tibial Allograft Name: Diagnosis: Date: Date of Surgery: Phase I Immediate Post Surgical Phase (approximately Weeks 1-3) Minimize shoulder pain and inflammatory
Dizziness: Natural Treatment for Vertigo and BPPV
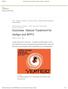 Wellness and WBV Studio Home» Bodywork» Massage» CranioSacral Therapy» Dizziness: Natural Treatment for Vertigo and BPPV CRANIOSACRAL THERAPY HOLISTIC HEALING Dizziness: Natural Treatment for Vertigo and
Wellness and WBV Studio Home» Bodywork» Massage» CranioSacral Therapy» Dizziness: Natural Treatment for Vertigo and BPPV CRANIOSACRAL THERAPY HOLISTIC HEALING Dizziness: Natural Treatment for Vertigo and
Benign paroxysmal positional vertigo: clinical characteristics of dizzy patients referred to a Falls and Syncope Unit
 Q J Med 2005; 98:357 364 Advance Access publication 8 April 2005 doi:10.1093/qjmed/hci057 Benign paroxysmal positional vertigo: clinical characteristics of dizzy patients referred to a Falls and Syncope
Q J Med 2005; 98:357 364 Advance Access publication 8 April 2005 doi:10.1093/qjmed/hci057 Benign paroxysmal positional vertigo: clinical characteristics of dizzy patients referred to a Falls and Syncope
Sasan Dabiri, MD, Assistant Professor
 Sasan Dabiri, MD, Assistant Professor Department of Otorhinolaryngology Head & Neck Surgery Amir A lam hospital Tehran University of Medical Sciences October 2015 Outlines Anatomy of Vestibular System
Sasan Dabiri, MD, Assistant Professor Department of Otorhinolaryngology Head & Neck Surgery Amir A lam hospital Tehran University of Medical Sciences October 2015 Outlines Anatomy of Vestibular System
Predictors of Protracted Recovery
 CONCUSSION MANAGEMENT SPECIALIST ON LINE CURRICULUM Protracted Recovery and Clinical Rehabilitation All rights reserved. Sports Medicine Concepts Concussion Management Specialist Program 1 Predictors of
CONCUSSION MANAGEMENT SPECIALIST ON LINE CURRICULUM Protracted Recovery and Clinical Rehabilitation All rights reserved. Sports Medicine Concepts Concussion Management Specialist Program 1 Predictors of
Reverse Total Shoulder Arthroplasty Protocol Shawn Hennigan, MD
 General Information: Reverse Total Shoulder Arthroplasty Protocol Shawn Hennigan, MD Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH)
General Information: Reverse Total Shoulder Arthroplasty Protocol Shawn Hennigan, MD Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH)
Neofitos Stefanides, M.D., P.C.
 Name: Date: Diagnosis: Date of Surgery: Rotator Cuff Physical Therapy Guidelines and Protocol General Guidelines: - Maintain surgical motion early, but don t push it. - Protect the repair (know what muscles
Name: Date: Diagnosis: Date of Surgery: Rotator Cuff Physical Therapy Guidelines and Protocol General Guidelines: - Maintain surgical motion early, but don t push it. - Protect the repair (know what muscles
 Appendix A: The American Society Of Shoulder And Elbow Therapists Arthroscopic Rotator Cuff Repair Rehabilitation Guide Phase 1 (POD 1 to ~ POW 6) GOALS: Maintain integrity of repair Minimize pain and
Appendix A: The American Society Of Shoulder And Elbow Therapists Arthroscopic Rotator Cuff Repair Rehabilitation Guide Phase 1 (POD 1 to ~ POW 6) GOALS: Maintain integrity of repair Minimize pain and
Dynamic Neural Mobilization as an Adjunct Intervention for a Patient with Cervical Radiculopathy: A Case Report.
 Dynamic Neural Mobilization as an Adjunct Intervention for a Patient with Cervical Radiculopathy: A. Kara Delie, SPT Kristine Erickson, PT, MS, NCS 1 Abstract: Title: Dynamic Neural Mobilization as an
Dynamic Neural Mobilization as an Adjunct Intervention for a Patient with Cervical Radiculopathy: A. Kara Delie, SPT Kristine Erickson, PT, MS, NCS 1 Abstract: Title: Dynamic Neural Mobilization as an
THROWERS TEN EXERCISE PROGRAM
 THROWERS TEN EXERCISE PROGRAM The Thrower s Ten Program is designed to exercise the major muscles necessary for throwing. The Program s goal is to be an organized and concise exercise program. In addition,
THROWERS TEN EXERCISE PROGRAM The Thrower s Ten Program is designed to exercise the major muscles necessary for throwing. The Program s goal is to be an organized and concise exercise program. In addition,
By: Sarah Van Winkle, SPT Dr. Jeff Sischo, PT, DPT, LAT, CSCS
 The Outcomes Following the Implementation of a Pelvic Floor Contraction with Lumbar Stabilization Exercises for a Patient with Low Back Pain: A Case Report By: Sarah Van Winkle, SPT Dr. Jeff Sischo, PT,
The Outcomes Following the Implementation of a Pelvic Floor Contraction with Lumbar Stabilization Exercises for a Patient with Low Back Pain: A Case Report By: Sarah Van Winkle, SPT Dr. Jeff Sischo, PT,
ANTERIOR SHOULDER STABILIZATION CLINICAL PRACTICE GUIDELINE
 ANTERIOR SHOULDER STABILIZATION CLINICAL PRACTICE GUIDELINE Background Ohio State s Anterior Shoulder Stabilization Rehabilitation Guideline is to be utilized following open or arthroscopic anterior shoulder
ANTERIOR SHOULDER STABILIZATION CLINICAL PRACTICE GUIDELINE Background Ohio State s Anterior Shoulder Stabilization Rehabilitation Guideline is to be utilized following open or arthroscopic anterior shoulder
Rotator Cuff Repair Protocol
 Protocol This rehabilitation protocol has been developed for the patient following a rotator cuff surgical procedure. This protocol will vary in length and aggressiveness depending on factors such as:
Protocol This rehabilitation protocol has been developed for the patient following a rotator cuff surgical procedure. This protocol will vary in length and aggressiveness depending on factors such as:
Anterior Stabilization of the Shoulder: Latarjet Protocol
 Robert K. Fullick, MD 6400 Fannin Street, Suite 1700 Houston, Texas 77030 Ph.: 713-486-7543 / Fx.: 713-486-5549 Anterior Stabilization of the Shoulder: Latarjet Protocol The intent of this protocol is
Robert K. Fullick, MD 6400 Fannin Street, Suite 1700 Houston, Texas 77030 Ph.: 713-486-7543 / Fx.: 713-486-5549 Anterior Stabilization of the Shoulder: Latarjet Protocol The intent of this protocol is
REHABILITATION GUIDELINES FOR ARTHROSCOPIC CAPSULAR SHIFT
 REHABILITATION GUIDELINES FOR ARTHROSCOPIC CAPSULAR SHIFT The rehabilitation guidelines are presented in a criterion based progression. General time frames are given for reference to the average, but individual
REHABILITATION GUIDELINES FOR ARTHROSCOPIC CAPSULAR SHIFT The rehabilitation guidelines are presented in a criterion based progression. General time frames are given for reference to the average, but individual
D: Doorway Stretch E: Towel Stretch for Pectoralis Minor Blackburn Exercises: 6 Positions A: Prone Horizontal Abduction (Neutral)
 D: Doorway Stretch Bring your shoulder into a horizontal position out to your side (abduction) and flex your elbow 90û Place your elbow against the edge of a doorway Lead forward and downwards with your
D: Doorway Stretch Bring your shoulder into a horizontal position out to your side (abduction) and flex your elbow 90û Place your elbow against the edge of a doorway Lead forward and downwards with your
PHASE I (Begin PT 3-5 days post-op) DOS:
 REHABILITATION GUIDELINES FOR POSTERIOR SHOULDER RECONSTRUCTION +/- LABRAL REPAIRS The rehabilitation guidelines are presented in a criterion based progression. General time frames are given for reference
REHABILITATION GUIDELINES FOR POSTERIOR SHOULDER RECONSTRUCTION +/- LABRAL REPAIRS The rehabilitation guidelines are presented in a criterion based progression. General time frames are given for reference
Journal of Sport Rehabilitation. The reliability of strength tests performed in elevated shoulder positions using a hand-held dynamometer
 The reliability of strength tests performed in elevated shoulder positions using a hand-held dynamometer Journal: Manuscript ID: JSR.2015-0034.R2 Manuscript Type: Technical Report Keywords: dynamometry,
The reliability of strength tests performed in elevated shoulder positions using a hand-held dynamometer Journal: Manuscript ID: JSR.2015-0034.R2 Manuscript Type: Technical Report Keywords: dynamometry,
ORIGINAL ARTICLE. A New Physical Maneuver for the Treatment of Benign Paroxysmal Positional Vertigo
 ORIGINAL ARTICLE Victor Vital, MD; Athanasia Printza, MD; Joseph Vital, MD; Stefanos Triaridis, MD; Miltiadis Tsalighopoulos, MD From the Department of Otolaryngology, Aristotle University of Thessaloniki,
ORIGINAL ARTICLE Victor Vital, MD; Athanasia Printza, MD; Joseph Vital, MD; Stefanos Triaridis, MD; Miltiadis Tsalighopoulos, MD From the Department of Otolaryngology, Aristotle University of Thessaloniki,
REVERSE TOTAL SHOULDER ARTHROPLASTY PROTOCOL
 Jennifer L. Cook, MD Stephen A. Hanff, MD Florida Joint Care Institute 2165 Little Road, Trinity, Florida 34655 PH: (727) 372 6637 FAX: (727) 375 5044 REVERSE TOTAL SHOULDER ARTHROPLASTY PROTOCOL Shoulder
Jennifer L. Cook, MD Stephen A. Hanff, MD Florida Joint Care Institute 2165 Little Road, Trinity, Florida 34655 PH: (727) 372 6637 FAX: (727) 375 5044 REVERSE TOTAL SHOULDER ARTHROPLASTY PROTOCOL Shoulder
Christopher K. Jones, MD Colorado Springs Orthopaedic Group
 Christopher K. Jones, MD Colorado Springs Orthopaedic Group 719-632-7669 Total Shoulder Replacement You have undergone a shoulder replacement procedure. The performance of the procedure is complete, but
Christopher K. Jones, MD Colorado Springs Orthopaedic Group 719-632-7669 Total Shoulder Replacement You have undergone a shoulder replacement procedure. The performance of the procedure is complete, but
Benign Paroxysmal Positional Vertigo. Jeff Walter PT, DPT, NCS
 Benign Paroxysmal Positional Vertigo Jeff Walter PT, DPT, NCS Benign Paroxysmal Positional Vertigo: (BPPV) Benign = not malignant Paroxysmal = recurrent, sudden intensification of symptoms Positional =
Benign Paroxysmal Positional Vertigo Jeff Walter PT, DPT, NCS Benign Paroxysmal Positional Vertigo: (BPPV) Benign = not malignant Paroxysmal = recurrent, sudden intensification of symptoms Positional =
Bradley C. Carofino, M.D. Shoulder Specialist 230 Clearfield Avenue, Suite 124 Virginia Beach, Virginia Phone
 Subpectoral Bicep Tenodesis Protocol (Spreadsheet) Weeks 1-2 Modalities Treatment Restrictions Goals No active elbow flexion (6weeks) Full PROM shoulder and elbow PROM: Shoulder, elbow, forearm No active
Subpectoral Bicep Tenodesis Protocol (Spreadsheet) Weeks 1-2 Modalities Treatment Restrictions Goals No active elbow flexion (6weeks) Full PROM shoulder and elbow PROM: Shoulder, elbow, forearm No active
AC reconstruction Protocol: Dr. Rolf
 AC reconstruction Protocol: Dr. Rolf The intent of this protocol is to provide the clinician with a guideline of the post-operative rehabilitation course of a patient that has undergone a AC reconstruction
AC reconstruction Protocol: Dr. Rolf The intent of this protocol is to provide the clinician with a guideline of the post-operative rehabilitation course of a patient that has undergone a AC reconstruction
Shoulder Exercises Phase 1 Phase 2
 Shoulder Exercises Phase 1 1. Pendulum exercise Bend over at the waist and let the arm hang down. Using your body to initiate movement, swing the arm gently forward and backward and in a circular motion.
Shoulder Exercises Phase 1 1. Pendulum exercise Bend over at the waist and let the arm hang down. Using your body to initiate movement, swing the arm gently forward and backward and in a circular motion.
Dizziness 101 E-Class TAKE HOME POINTS
 Dizziness 101 E-Class Dizziness is one of the most common reasons people seek medical care Important to consider the inner ear as a cause 5.5: Average number of providers seen if the inner ear wasn t considered
Dizziness 101 E-Class Dizziness is one of the most common reasons people seek medical care Important to consider the inner ear as a cause 5.5: Average number of providers seen if the inner ear wasn t considered
REHABILITATION GUIDELINES FOR ANTERIOR SHOULDER RECONSTRUCTION WITH BANKART REPAIR
 REHABILITATION GUIDELINES FOR ANTERIOR SHOULDER RECONSTRUCTION WITH BANKART REPAIR The rehabilitation guidelines are presented in a criterion based progression. General time frames are given for reference
REHABILITATION GUIDELINES FOR ANTERIOR SHOULDER RECONSTRUCTION WITH BANKART REPAIR The rehabilitation guidelines are presented in a criterion based progression. General time frames are given for reference
Rotator Cuff Repair Protocol
 Rotator Cuff Repair Protocol Applicability: Physician Practices Date Effective: 11/2016 Department: Rehabilitation Services Supersedes: Rotator Cuff Repair (Beattie) Date Last Reviewed / or Date Last Revision:
Rotator Cuff Repair Protocol Applicability: Physician Practices Date Effective: 11/2016 Department: Rehabilitation Services Supersedes: Rotator Cuff Repair (Beattie) Date Last Reviewed / or Date Last Revision:
Rehab protocol. Phase I: Immediate Post-Surgical Phase: Typically 0-4 weeks; 2 PT visits. Goals:
 Reverse Total shoulder arthroplasty Rehab protocol Phase I: Immediate Post-Surgical Phase: Typically 0-4 weeks; 2 PT visits Allow healing of soft tissue Maintain integrity of replaced joint Gradually increase
Reverse Total shoulder arthroplasty Rehab protocol Phase I: Immediate Post-Surgical Phase: Typically 0-4 weeks; 2 PT visits Allow healing of soft tissue Maintain integrity of replaced joint Gradually increase
VERTIGO. Tuesday 20 th February 2018 Dr Rukhsana Hussain. Disclaimers apply:
 VERTIGO Tuesday 20 th February 2018 Dr Rukhsana Hussain WHAT IS VERTIGO? 4 Vertigo is defined as an illusory sensation of motion of either the self or the surroundings in the absence of true motion. Explaining
VERTIGO Tuesday 20 th February 2018 Dr Rukhsana Hussain WHAT IS VERTIGO? 4 Vertigo is defined as an illusory sensation of motion of either the self or the surroundings in the absence of true motion. Explaining
Clinical Significance of Vestibular Evoked Myogenic Potentials in Benign Paroxysmal Positional Vertigo
 Otology & Neurotology 29:1162Y1166 Ó 2008, Otology & Neurotology, Inc. Clinical Significance of Vestibular Evoked Myogenic Potentials in Benign Paroxysmal Positional Vertigo *Won Sun Yang, Sung Huhn Kim,
Otology & Neurotology 29:1162Y1166 Ó 2008, Otology & Neurotology, Inc. Clinical Significance of Vestibular Evoked Myogenic Potentials in Benign Paroxysmal Positional Vertigo *Won Sun Yang, Sung Huhn Kim,
Top 35 Lower Body Exercises
 Top 35 Lower Body Exercises Calf Raise - Single Leg Stand on one leg, toes on edge of box Ankle hanging below toes Hold something for support Lift & lower body by extending the ankle of the stance leg
Top 35 Lower Body Exercises Calf Raise - Single Leg Stand on one leg, toes on edge of box Ankle hanging below toes Hold something for support Lift & lower body by extending the ankle of the stance leg
Vertigo. Definition. Causes. (Dizziness) Benign Paroxysmal Positional Vertigo (BPPV) Labyrinthitis. by Karen Schroeder, MS, RD
 Vertigo (Dizziness) by Karen Schroeder, MS, RD En Español (Spanish Version) Definition Vertigo is a feeling of spinning or whirling when you are not moving. It can also be an exaggerated feeling of motion
Vertigo (Dizziness) by Karen Schroeder, MS, RD En Español (Spanish Version) Definition Vertigo is a feeling of spinning or whirling when you are not moving. It can also be an exaggerated feeling of motion
Exercise 16: Theraband Series
 Exercise 16: Theraband Series Using the large rubber strip given to you by your therapist, tie the ends of the strip in a knot to form a large circular band. Then try the following exercises: A. Stand
Exercise 16: Theraband Series Using the large rubber strip given to you by your therapist, tie the ends of the strip in a knot to form a large circular band. Then try the following exercises: A. Stand
An Introduction to Dizziness and Vertigo
 An Introduction to Dizziness and Vertigo Tamara Mijovic MD CM FRCSC Clinical Assistant Professor Department of Otolaryngology Head and Neck Surgery Otology, Neurotology & Skull Base Surgery McGill University
An Introduction to Dizziness and Vertigo Tamara Mijovic MD CM FRCSC Clinical Assistant Professor Department of Otolaryngology Head and Neck Surgery Otology, Neurotology & Skull Base Surgery McGill University
Physical Therapy Intervention Strategies Post Ream and Run Hemiarthroplasty
 Physical Therapy Intervention Strategies Post Ream and Run Hemiarthroplasty Jessica Ottow, Student Physical Therapist Suzanne Ryer, MPT Faculty Mentor Abstract Background: Treatment of glenohumeral arthritis
Physical Therapy Intervention Strategies Post Ream and Run Hemiarthroplasty Jessica Ottow, Student Physical Therapist Suzanne Ryer, MPT Faculty Mentor Abstract Background: Treatment of glenohumeral arthritis
Rehabilitation Considerations for Post-Operative Rotator Cuff Repair. Adam Shutts, MSPT
 Rehabilitation Considerations for Post-Operative Rotator Cuff Repair Adam Shutts, MSPT Post-Operative Rotator Cuff Repair Delayed vs. early mobilization Differing rehabilitation strategies for different
Rehabilitation Considerations for Post-Operative Rotator Cuff Repair Adam Shutts, MSPT Post-Operative Rotator Cuff Repair Delayed vs. early mobilization Differing rehabilitation strategies for different
Arthroscopic SLAP Lesion Repair Rehabilitation Guideline
 Arthroscopic SLAP Lesion Repair Rehabilitation Guideline This rehabilitation program is designed to return the individual to their activities as quickly and safely as possible. It is designed for rehabilitation
Arthroscopic SLAP Lesion Repair Rehabilitation Guideline This rehabilitation program is designed to return the individual to their activities as quickly and safely as possible. It is designed for rehabilitation
POST OP CLOSED BANKART PROCEDURE
 POST OP CLOSED BANKART PROCEDURE WEEKS 1-6 Do 1. Wear sling until advised otherwise 2. Keep dressing clean and dry 3. Do passive pendulum exercises to 90 degrees 4. Ice for 15 minutes after exercising
POST OP CLOSED BANKART PROCEDURE WEEKS 1-6 Do 1. Wear sling until advised otherwise 2. Keep dressing clean and dry 3. Do passive pendulum exercises to 90 degrees 4. Ice for 15 minutes after exercising
REHABILITATION GUIDELINES FOR ROTATOR CUFF REPAIR FOR TYPE I TEARS (+/- SUBACROMINAL DECOMPRESSION)
 REHABILITATION GUIDELINES FOR ROTATOR CUFF REPAIR FOR TYPE I TEARS (+/- SUBACROMINAL DECOMPRESSION) The rehabilitation guidelines are presented in a criterion based progression. General time frames are
REHABILITATION GUIDELINES FOR ROTATOR CUFF REPAIR FOR TYPE I TEARS (+/- SUBACROMINAL DECOMPRESSION) The rehabilitation guidelines are presented in a criterion based progression. General time frames are
Shoulder Arthroscopy with Rotator Cuff Repair Rehabilitation Protocol
 General Notes: As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
General Notes: As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
After Arthroscopic Subacromial Decompression Intact Rotator Cuff (Distal Clavicle Resection)
 After Arthroscopic Subacromial Decompression Intact Rotator Cuff (Distal Clavicle Resection) Rehabilitation Protocol Phase 1: Weeks 0-4 Restrictions ROM 140 degrees of forward flexion 40 degrees of external
After Arthroscopic Subacromial Decompression Intact Rotator Cuff (Distal Clavicle Resection) Rehabilitation Protocol Phase 1: Weeks 0-4 Restrictions ROM 140 degrees of forward flexion 40 degrees of external
Latissimus dorsi tendon transfer protocol
 Department of Rehabilitation Services Physical Therapy The intent of this protocol is to provide the physical therapist with a guideline/treatment protocol for the postoperative rehabilitation management
Department of Rehabilitation Services Physical Therapy The intent of this protocol is to provide the physical therapist with a guideline/treatment protocol for the postoperative rehabilitation management
