(PROTOCOL #18) REVERSE TOTAL SHOULDER ARTHROPLASTY PROTOCOL
|
|
|
- Britton Briggs
- 5 years ago
- Views:
Transcription
1 The following is a set of general guidelines. It is important to remember that each patient is different. The progression of the patient depends on many factors including age and medical health of the patient and physician preferences. Any Bracing is discontinued ONLY UPON DIRECTION OF PHYSICIAN. General Information: Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH) arthritis when it is associated with irreparable rotator cuff damage, complex fractures as well as for a revision of a previously failed conventional Total Shoulder Arthroplasty (TSA) in which the rotator cuff tendons are deficient. It was initially designed and used in Europe in the late 1980 s by Grammont; and only received FDA approval for use in the United States in March of The rotator cuff is either absent or minimally involved with the rtsa; therefore, the rehabilitation for a patient following the rtsa is different than the rehabilitation following a traditional TSA. The surgeon, physical therapist and patient need to take this into consideration when establishing the postoperative treatment plan. SHOULDER DISLOCATION PERCAUTIONS: o No shoulder motion behind back. (NO combined shoulder adduction, internal rotation, and extension.) o No glenohumeral (GH) extension beyond neutral. **Precautions should be implemented for 12 weeks postoperatively unless surgeon specifically advises patient or therapist differently. Joint Protection: THERE IS A HIGHER RISK OF SHOULDER DISLOCATION FOLLOWING rtsa THAN A CONVENTIONAL TSA. o Avoidance of shoulder extension past neutral and the combination of shoulder adduction and internal rotation should be avoided for 12 weeks. o Patients with rtsa don t dislocate with the arm in abduction and external rotation. They typically dislocate with the arm in internal rotation and adduction in conjunction with extension. As such, Tucking in a shirt or performing bathroom / personal hygiene with the operative arm is a particularly dangerous activity particularly in the immediate peri-operative phase. Created on 07/01/2009 Page 1 of 8
2 Deltoid function: Stability and mobility of the shoulder joint is now dependent upon the deltoid and periscapular musculature. This concept becomes the foundation for the postoperative physical therapy management for a patient that has undergone rtsa. Typically patients achieve double the AROM from pre-op level. ROM: Expectation for range of motion gains should be set on a case-by-case basis depending upon underlying pathology. Normal/full active range of motion of the shoulder joint following rtsa is not expected. Reverse Total Shoulder Arthroplasty Biomechanics: The rtsa prosthesis reverses the orientation of the shoulder joint by replacing the glenoid fossa with a glenoid base plate and glenosphere and the humeral head with a shaft and concave cup. This prosthesis design alters the center of rotation of the shoulder joint by moving it medially and inferiorly. This subsequently increases the deltoid moment and deltoid tension, which enhances both the torque produced by the deltoid as well as the line of pull / action of the deltoid. This enhanced mechanical advantage of the deltoid compensates for the deficient RC as the deltoid becomes the primary elevator of the shoulder joint. This results in an improvement of shoulder elevation and often individuals are able to raise their upper extremity overhead. Phase I Precautions: o Sling is worn for 3-6weeks postoperatively. The use of a sling often may be extended for a total of 6 weeks, if the current rtsa procedure is a revision surgery or Tendon Transfer Procedure. o While lying supine, the distal humerus / elbow should be supported by a pillow or towel roll to avoid shoulder extension. Patients should be advised to always be able to visualize their elbow while lying supine. o No shoulder AROM. o No lifting of objects with operative extremity. o No supporting of body weight with involved extremity. o Keep incision clean and dry (no soaking/wetting for 2 weeks); No whirlpool, Jacuzzi, ocean/lake wading for 4 weeks. Created on 07/01/2009 Page 2 of 8
3 PHASE FUNCTIONAL PROGRESSION/ACTIVITIES GOALS/RESTRICTIONS Post op to 4 days OT elbow/hand ROM Putty and ADL modifications Begin PROM in supine after complete resolution of interscalene block. Forward flexion and elevation in the scapular plane in supine to 90 degrees. External rotation (ER) in scapular plane to available ROM as indicated by operative findings. Typically around degrees NO Internal Rotation Active/Active Assisted ROM (A/AAROM) of cervical spine, elbow, wrist and hand. Begin periscapular sub-maximal pain-free isometrics in the scapular plane. Frequent (4-5 times a day for about 20 minutes) cryotherapy. Continuous cryotherapy for the first 72 hours postoperatively, then frequent application (4-5 times a day for about 20 minutes). 4 days to 3 weeks Begin sub-maximal pain-free deltoid isometrics in scapular plane DASH baseline and every 4 weeks Insure patient is independent in bed mobility, transfers and ambulation. Insure proper sling fit/alignment/use. Instruct patient in proper positioning, posture, initial home exercise program. Provide patient/family with written home program including exercises and protocol information. Avoid shoulder extension when isolating posterior deltoid. Created on 07/01/2009 Page 3 of 8
4 PHASE FUNCTIONAL PROGRESSION/ACTIVITIES GOALS/RESTRICTIONS 3 weeks to 6 weeks Progress exercises listed above. Criteria for progression to the next phase (Phase II): Progress PROM: o Forward flexion and elevation in the scapular plane in supine to 120 degrees. o ER in scapular plane to tolerance, respecting soft tissue constraints. Tolerates shoulder PROM and isometrics; and, AROMminimally resistive program for elbow, wrist and hand. Patient demonstrates the ability to isometrically activate all components of the deltoid and periscapular musculature in the scapular plan. Gentle resisted exercise of elbow, wrist and hand. Continue frequent cryotherapy. 4 weeks Gradually restore AROM Begin shoulder AA/AROM as appropriate. o Forward flexion and elevation in scapular plane in supine with progression to sitting/standing. ER and IR in the scapular plane in supine with progression to sitting/standing. Control pain and inflammation. Allow continued healing of soft tissue / do not overstress healing tissue. Re-establish dynamic shoulder and scapular stability. Patient may begin to use hand of operative extremity for feeding and light activities of daily living including dressing, washing. Created on 07/01/2009 Page 4 of 8
5 Phase II Active Range of Motion / Early Strengthening Phase (Week 6 to 12): PHASE FUNCTIONAL PROGRESSION/ACTIVITIES GOALS/RESTRICTIONS 6 weeks to 8 weeks Continue progression of PROM (full PROM is not expected). Begin gentle glenohumeral IR behind back and ER sub-maximal pain free isometrics. Start PROM IR to tolerance (not to exceed 50 degrees) in the scapular plane. Initiate gentle scapulothoracic rhythmic stabilization and alternating isometrics in supine as appropriate. Begin gentle periscapular and deltoid sub-maximal pain free isotonic strengthening exercises, typically toward the end of the 8 th week. Progress strengthening of elbow, wrist and hand. Gentle glenohumeral and scapulothoracic joint mobilizations as indicated (Grade I and II). Continue use of cryotherapy as needed. BRACING DISCONTINUED UPON THE DIRECTION OF THE PHYSICIAN. Continue with PROM program. Precautions: Continue to avoid shoulder hyperextension. In the presence of poor shoulder mechanics avoid repetitive shoulder AROM exercises/activity. Restrict lifting of objects to no heavier than a coffee cup. No supporting of body weight by involved upper extremity. Created on 07/01/2009 Page 5 of 8
6 PHASE FUNCTIONAL PROGRESSION/ACTIVITIES GOALS/RESTRICTIONS 9 weeks to 12 weeks Continue with above exercises and functional activity progression. Begin AROM supine forward flexion and elevation in the plane of the scapula with light weights (1-3 lbs of kg) at varying degrees of trunk elevation as appropriate. (i.e. supine lawn chair progression with progression to sitting/standing). Progress to gentle glenohumeral IR and ER isotonic strengthening exercises in sidelying position with light weight (1-3 lbs or kg) and /or with light resistance resistive bands or sports cords. Criteria for progression to the next phase (Phase III): o Improving function of shoulder. o Patient demonstrates the ability to isotonically activate all components of the deltoid and periscapular musculature and is gaining strength. Created on 07/01/2009 Page 6 of 8
7 Phase III Moderate strengthening (Week 12+) PHASE FUNCTIONAL PROGRESSION/ACTIVITIES GOALS/RESTRICTIONS 12 weeks to 16 weeks Continue with the previous program as indicated. Progress to gentle resisted flexion, elevation in standing as appropriate. o Enhance functional use of operative extremity and advance functional activities. o Enhance shoulder mechanics, muscular strength and endurance. Precautions: o No lifting of objects heavier than 6 lbs with operative upper extremity o No sudden lifting or pushing activities. Activities: Gradually increase activity Golf: pitching wedge to start in approx 6 months Bowling: NOT RECOMMENDED Tennis: same start slow gradually increase activity Driving: able to drive, monitor meds, steer with other arm following post-op Shower: usually after first dressing with watertight dressing Throwing: 6 months Running: 3 months Refer to enclosed table for suggested exercises which optimize muscle function based on EMG activity. Created on 07/01/2009 Page 7 of 8
8 Phase IV continued Home Program (Typically 4 + months postop): Typically the patient is on a home exercise program at this stage to be performed 3-4 times per week with the focus on: o Continued strength gains o Continued progression toward a return to functional and recreational activities within limits as identified by progress made during rehabilitation and outlined by surgeon and physical therapist. Criteria for discharge from skilled therapy: o Patient is able to maintain pain free shoulder AROM demonstrating proper shoulder mechanics. (Typically degrees of elevation with functional ER of about 30 degrees.) o Typically able to complete light household and work activities. Approved By: Physician reserves the right to adjust these protocols for each patient. Signature: Date: Signature: Date: Balu Pisupati, PT Created on 07/01/2009 Page 8 of 8
Reverse Total Shoulder Arthroplasty Protocol
 General Information: Reverse Total Shoulder Arthroplasty Protocol Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH) arthritis when it
General Information: Reverse Total Shoulder Arthroplasty Protocol Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH) arthritis when it
Reverse Total Shoulder Arthroplasty Protocol Shawn Hennigan, MD
 General Information: Reverse Total Shoulder Arthroplasty Protocol Shawn Hennigan, MD Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH)
General Information: Reverse Total Shoulder Arthroplasty Protocol Shawn Hennigan, MD Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH)
Reverse Total Shoulder Protocol
 Marion Herring, M.D. OrthoVirginia PH: (804) 270-1305 FX: (804) 273-9294 www.orthovirginia.com Reverse Total Shoulder Protocol General Information: Reverse Total Shoulder Arthroplasty (rtsa) is designed
Marion Herring, M.D. OrthoVirginia PH: (804) 270-1305 FX: (804) 273-9294 www.orthovirginia.com Reverse Total Shoulder Protocol General Information: Reverse Total Shoulder Arthroplasty (rtsa) is designed
WILLIAM M. ISBELL, MD Jeremy R. Stinson PA-C
 WILLIAM M. ISBELL, MD Jeremy R. Stinson PA-C Post-Operative Rehabilitation Guidelines for Total Shoulder Arthroplasty (TSA) The intent of this protocol is to provide the physical therapist with a guideline/treatment
WILLIAM M. ISBELL, MD Jeremy R. Stinson PA-C Post-Operative Rehabilitation Guidelines for Total Shoulder Arthroplasty (TSA) The intent of this protocol is to provide the physical therapist with a guideline/treatment
Reverse Total Shoulder Arthroplasty with Latissimus dorsi tendon transfer Protocol:
 Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 Reverse Total Shoulder Arthroplasty with Latissimus dorsi tendon transfer Protocol: General Information:
Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 Reverse Total Shoulder Arthroplasty with Latissimus dorsi tendon transfer Protocol: General Information:
REVERSE TOTAL SHOULDER ARTHROPLASTY PROTOCOL
 Jennifer L. Cook, MD Stephen A. Hanff, MD Florida Joint Care Institute 2165 Little Road, Trinity, Florida 34655 PH: (727) 372 6637 FAX: (727) 375 5044 REVERSE TOTAL SHOULDER ARTHROPLASTY PROTOCOL Shoulder
Jennifer L. Cook, MD Stephen A. Hanff, MD Florida Joint Care Institute 2165 Little Road, Trinity, Florida 34655 PH: (727) 372 6637 FAX: (727) 375 5044 REVERSE TOTAL SHOULDER ARTHROPLASTY PROTOCOL Shoulder
Charlotte Shoulder Institute
 Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Gill Orthopaedic Midtown Medical Plaza 1918 Randolph Rd., Suite 700 Charlotte, NC 28211 704-342-3544
Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Gill Orthopaedic Midtown Medical Plaza 1918 Randolph Rd., Suite 700 Charlotte, NC 28211 704-342-3544
Reverse Total Shoulder
 Rehabilitation Protocol: Reverse Total Shoulder Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey Medical
Rehabilitation Protocol: Reverse Total Shoulder Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey Medical
Avon Office 2 Simsbury Rd. Avon, CT Office: (860) Fax: (860) REHABILITATION AFTER REVERSE SHOULDER ARTHROPLASTY
 Katherine J. Coyner, MD UCONN Musculoskeletal Institute Medical Arts & Research Building 263 Farmington Ave. Farmington, CT 06030 Office: (860) 679-6600 Fax: (860) 679-6649 www.drcoyner.com Avon Office
Katherine J. Coyner, MD UCONN Musculoskeletal Institute Medical Arts & Research Building 263 Farmington Ave. Farmington, CT 06030 Office: (860) 679-6600 Fax: (860) 679-6649 www.drcoyner.com Avon Office
TOTAL SHOULDER ARTHROPLASTY / HEMIARTHROPLASTY
 Teodoro P. Nissen, M.D., Q.M.E. Fellowship Trained Board Certified Joseph M. Centeno, M.D. Fellowship Trained Board Certified TOTAL SHOULDER ARTHROPLASTY / HEMIARTHROPLASTY Protocol: The intent of this
Teodoro P. Nissen, M.D., Q.M.E. Fellowship Trained Board Certified Joseph M. Centeno, M.D. Fellowship Trained Board Certified TOTAL SHOULDER ARTHROPLASTY / HEMIARTHROPLASTY Protocol: The intent of this
PROM is not stretching!
 Dx: o Right o Left Shoulder Replacement/Hemiarthroplasty Rehab Date of Surgery: Patient Name: PT/OT: Please evaluate and treat. Follow attached protocol. 2-3 x per week x 6 weeks. Signature/Date: The intent
Dx: o Right o Left Shoulder Replacement/Hemiarthroplasty Rehab Date of Surgery: Patient Name: PT/OT: Please evaluate and treat. Follow attached protocol. 2-3 x per week x 6 weeks. Signature/Date: The intent
Total Shoulder Rehab Protocol Dr. Payne
 Total Shoulder Rehab Protocol Dr. Payne Phase I Immediate Post Surgical Phase (0-4 weeks): Allow healing of soft tissue Maintain integrity of replaced joint Gradually increase passive range of motion (PROM)
Total Shoulder Rehab Protocol Dr. Payne Phase I Immediate Post Surgical Phase (0-4 weeks): Allow healing of soft tissue Maintain integrity of replaced joint Gradually increase passive range of motion (PROM)
Total Shoulder Arthroplasty / Hemiarthroplasty Protocol
 Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 Total Shoulder Arthroplasty / Hemiarthroplasty Protocol The intent of this protocol is to provide the
Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 Total Shoulder Arthroplasty / Hemiarthroplasty Protocol The intent of this protocol is to provide the
Orthopedic Surgery and Sports Medicine FL License:
 Reverse Shoulder Arthroplasty Protocol: The intent of this protocol is to provide the therapist with a guideline for the post-operative rehabilitation course of a patient that has undergone a Reverse Shoulder
Reverse Shoulder Arthroplasty Protocol: The intent of this protocol is to provide the therapist with a guideline for the post-operative rehabilitation course of a patient that has undergone a Reverse Shoulder
Rehabilitation Guidelines for Total Shoulder Arthroplasty and Hemi-arthroplasty
 Rehabilitation Guidelines for Total Shoulder Arthroplasty and Hemi-arthroplasty Josef K. Eichinger, MD General Information Total Recovery time is between 4-6 months depending on factors such as injury
Rehabilitation Guidelines for Total Shoulder Arthroplasty and Hemi-arthroplasty Josef K. Eichinger, MD General Information Total Recovery time is between 4-6 months depending on factors such as injury
Total Shoulder Arthroplasty / Hemiarthroplasty Therapy Protocol
 Total Shoulder Arthroplasty / Hemiarthroplasty Therapy Protocol The intent of this protocol is to provide the therapist with a guideline of the postoperative rehabilitation course of a patient that has
Total Shoulder Arthroplasty / Hemiarthroplasty Therapy Protocol The intent of this protocol is to provide the therapist with a guideline of the postoperative rehabilitation course of a patient that has
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS
 Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
Christopher K. Jones, MD Colorado Springs Orthopaedic Group
 Christopher K. Jones, MD Colorado Springs Orthopaedic Group 719-632-7669 Total Shoulder Replacement You have undergone a shoulder replacement procedure. The performance of the procedure is complete, but
Christopher K. Jones, MD Colorado Springs Orthopaedic Group 719-632-7669 Total Shoulder Replacement You have undergone a shoulder replacement procedure. The performance of the procedure is complete, but
Important rehabilitation management concepts to consider for a postoperative physical therapy RSA program are:
 : General Information: Reverse or Inverse Shoulder Arthroplasty (RSA) is designed specifically for the treatment of glenohumeral (GH) arthritis when it is associated with irreparable rotator cuff damage,
: General Information: Reverse or Inverse Shoulder Arthroplasty (RSA) is designed specifically for the treatment of glenohumeral (GH) arthritis when it is associated with irreparable rotator cuff damage,
TOTAL SHOULDER ARTHROPLASTY, HEMIARTHROPLASTY OR REVERSE ARTHROPLASTY
 TOTAL SHOULDER ARTHROPLASTY, HEMIARTHROPLASTY OR REVERSE ARTHROPLASTY Philosophy The following is an outline of the standard post-operative rehabilitation program following total shoulder arthroplasty.
TOTAL SHOULDER ARTHROPLASTY, HEMIARTHROPLASTY OR REVERSE ARTHROPLASTY Philosophy The following is an outline of the standard post-operative rehabilitation program following total shoulder arthroplasty.
Rehab protocol. Phase I: Immediate Post-Surgical Phase: Typically 0-4 weeks; 2 PT visits. Goals:
 Reverse Total shoulder arthroplasty Rehab protocol Phase I: Immediate Post-Surgical Phase: Typically 0-4 weeks; 2 PT visits Allow healing of soft tissue Maintain integrity of replaced joint Gradually increase
Reverse Total shoulder arthroplasty Rehab protocol Phase I: Immediate Post-Surgical Phase: Typically 0-4 weeks; 2 PT visits Allow healing of soft tissue Maintain integrity of replaced joint Gradually increase
Charlotte Shoulder Institute
 Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
Progression to the next phase based on clinical criteria and time frames as appropriate
 Indications Reverse total shoulder replacement is indicated for use in grossly rotator cuff deficient joints with severe arthropathy, or for use when a previous joint replacement has failed with a grossly
Indications Reverse total shoulder replacement is indicated for use in grossly rotator cuff deficient joints with severe arthropathy, or for use when a previous joint replacement has failed with a grossly
REVERSE SHOULDER ARTHROPLASTY
 William J. Robertson, MD TMI Sports Medicine 3533 Matlock Rd Arlington, TX 76015 Office: (817) 419-0303 Fax: (817) 468-5963 www.billrobertsonmd.com www.hipkneepreservation.com REVERSE SHOULDER ARTHROPLASTY
William J. Robertson, MD TMI Sports Medicine 3533 Matlock Rd Arlington, TX 76015 Office: (817) 419-0303 Fax: (817) 468-5963 www.billrobertsonmd.com www.hipkneepreservation.com REVERSE SHOULDER ARTHROPLASTY
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS
 Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
Arthroscopic Rotator Cuff Repair Protocol:
 Arthroscopic Rotator Cuff Repair Protocol: The intent of this protocol is to provide the therapist and patient with guidelines for the post-operative rehabilitation course after arthroscopic SLAP repair.
Arthroscopic Rotator Cuff Repair Protocol: The intent of this protocol is to provide the therapist and patient with guidelines for the post-operative rehabilitation course after arthroscopic SLAP repair.
Biceps Tenodesis Protocol
 Biceps Tenodesis Protocol A biceps tenodesis procedure involves cutting of the long head of the biceps just prior to its insertion on the superior labrum and then anchoring the tendon along its anatomical
Biceps Tenodesis Protocol A biceps tenodesis procedure involves cutting of the long head of the biceps just prior to its insertion on the superior labrum and then anchoring the tendon along its anatomical
Anterior Stabilization of the Shoulder: Distal Tibial Allograft
 Anterior Stabilization of the Shoulder: Distal Tibial Allograft Name: Diagnosis: Date: Date of Surgery: Phase I Immediate Post Surgical Phase (approximately Weeks 1-3) Minimize shoulder pain and inflammatory
Anterior Stabilization of the Shoulder: Distal Tibial Allograft Name: Diagnosis: Date: Date of Surgery: Phase I Immediate Post Surgical Phase (approximately Weeks 1-3) Minimize shoulder pain and inflammatory
Jennifer L. Cook, MD Stephen A. Hanff, MD. Rotator Cuff Type I Repair (Small Large Tear)
 Jennifer L. Cook, MD Stephen A. Hanff, MD Florida Joint Care Institute 2165 Little Road, Trinity, Florida 34655 PH: (727) 372 6637 FAX: (727) 375 5044 Rotator Cuff Type I Repair (Small Large Tear) This
Jennifer L. Cook, MD Stephen A. Hanff, MD Florida Joint Care Institute 2165 Little Road, Trinity, Florida 34655 PH: (727) 372 6637 FAX: (727) 375 5044 Rotator Cuff Type I Repair (Small Large Tear) This
The Four Phases of Healing During Rehabilitation Following Rotator Cuff Surgery. Phase 1: Immediate postoperative period (weeks 0-6) Goals
 The Four Phases of Healing During Rehabilitation Following Rotator Cuff Surgery Phase 1: Immediate postoperative period (weeks 0-6) Maintain/protect integrity of repair Gradually increase PROM Diminish
The Four Phases of Healing During Rehabilitation Following Rotator Cuff Surgery Phase 1: Immediate postoperative period (weeks 0-6) Maintain/protect integrity of repair Gradually increase PROM Diminish
Latissimus dorsi tendon transfer protocol
 Department of Rehabilitation Services Physical Therapy The intent of this protocol is to provide the physical therapist with a guideline/treatment protocol for the postoperative rehabilitation management
Department of Rehabilitation Services Physical Therapy The intent of this protocol is to provide the physical therapist with a guideline/treatment protocol for the postoperative rehabilitation management
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS
 Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
Post-Operative Instructions Glenoid Reconstruction using Fresh Distal Tibial Allograft
 Day of Surgery Post-Operative Instructions Glenoid Reconstruction using Fresh Distal Tibial Allograft A. Relax. Diet as tolerated. B. Icing is important for the first 5-7 days post-op. While the post-op
Day of Surgery Post-Operative Instructions Glenoid Reconstruction using Fresh Distal Tibial Allograft A. Relax. Diet as tolerated. B. Icing is important for the first 5-7 days post-op. While the post-op
Bradley C. Carofino, M.D. Shoulder Specialist 230 Clearfield Avenue, Suite 124 Virginia Beach, Virginia Phone
 Rehabilitation following Arthroscopic Rotator Cuff Repair: Medium Tears Phase I: Immediate Postsurgical Phase (Days 10-14) Precautions: No lifting of objects; No excessive arm motions; No excessive external
Rehabilitation following Arthroscopic Rotator Cuff Repair: Medium Tears Phase I: Immediate Postsurgical Phase (Days 10-14) Precautions: No lifting of objects; No excessive arm motions; No excessive external
Biceps Tenotomy Protocol
 Biceps Tenotomy Protocol A biceps tenotomy procedure involves cutting of the long head of the biceps just prior to its insertion on the superior labrum. A biceps tenotomy is typically done when there is
Biceps Tenotomy Protocol A biceps tenotomy procedure involves cutting of the long head of the biceps just prior to its insertion on the superior labrum. A biceps tenotomy is typically done when there is
AC reconstruction Protocol: Dr. Rolf
 AC reconstruction Protocol: Dr. Rolf The intent of this protocol is to provide the clinician with a guideline of the post-operative rehabilitation course of a patient that has undergone a AC reconstruction
AC reconstruction Protocol: Dr. Rolf The intent of this protocol is to provide the clinician with a guideline of the post-operative rehabilitation course of a patient that has undergone a AC reconstruction
Anterior Stabilization of the Shoulder: Latarjet Protocol
 Robert K. Fullick, MD 6400 Fannin Street, Suite 1700 Houston, Texas 77030 Ph.: 713-486-7543 / Fx.: 713-486-5549 Anterior Stabilization of the Shoulder: Latarjet Protocol The intent of this protocol is
Robert K. Fullick, MD 6400 Fannin Street, Suite 1700 Houston, Texas 77030 Ph.: 713-486-7543 / Fx.: 713-486-5549 Anterior Stabilization of the Shoulder: Latarjet Protocol The intent of this protocol is
Biceps Tenodesis Protocol
 Robert K. Fullick, MD 6400 Fannin Street, Suite 1700 Houston, Texas 77030 Ph.: 713-486-7543 / Fx.: 713-486-5549 Biceps Tenodesis Protocol The intent of this protocol is to provide the clinician with a
Robert K. Fullick, MD 6400 Fannin Street, Suite 1700 Houston, Texas 77030 Ph.: 713-486-7543 / Fx.: 713-486-5549 Biceps Tenodesis Protocol The intent of this protocol is to provide the clinician with a
Charlotte Shoulder Institute
 Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
Biceps Tenotomy Protocol
 Department of Rehabilitation Services Physical Therapy The intent of this protocol is to provide the clinician with a guideline of the postoperative rehabilitation course of a patient that has undergone
Department of Rehabilitation Services Physical Therapy The intent of this protocol is to provide the clinician with a guideline of the postoperative rehabilitation course of a patient that has undergone
UHealth Sports Medicine
 UHealth Sports Medicine Rehabilitation Guidelines for Arthroscopic Rotator Cuff Repair Type 1 Repairs (+/- subacromial decompression) The rehabilitation guidelines are presented in a criterion based progression.
UHealth Sports Medicine Rehabilitation Guidelines for Arthroscopic Rotator Cuff Repair Type 1 Repairs (+/- subacromial decompression) The rehabilitation guidelines are presented in a criterion based progression.
Type Three Rotator Cuff Repair Arthroscopic Assisted with SAD Large to Massive Tears (Greater than 4 cm)
 Type Three Rotator Cuff Repair Arthroscopic Assisted with SAD Large to Massive Tears (Greater than 4 cm) Therapist Phone I. Phase I - Immediate Post-Surgical Phase (Day 1-10) Goals: Maintain Integrity
Type Three Rotator Cuff Repair Arthroscopic Assisted with SAD Large to Massive Tears (Greater than 4 cm) Therapist Phone I. Phase I - Immediate Post-Surgical Phase (Day 1-10) Goals: Maintain Integrity
Shoulder Arthroscopy with Rotator Cuff Repair Rehabilitation Protocol
 General Notes: As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
General Notes: As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
Progression to the next phase based on Clinic Criteria and or Time Frames as Appropriate
 Bicep Tenodesis D. WATTS, M.D. Progression to the next phase based on Clinic Criteria and or Time Frames as Appropriate PHASE I PASSIVE RANG OF MOTION PHASE (STARTS APPROXIMATELY POST OP WEEKS 1-2) Minimize
Bicep Tenodesis D. WATTS, M.D. Progression to the next phase based on Clinic Criteria and or Time Frames as Appropriate PHASE I PASSIVE RANG OF MOTION PHASE (STARTS APPROXIMATELY POST OP WEEKS 1-2) Minimize
UHealth Sports Medicine
 UHealth Sports Medicine Rehabilitation Guidelines for Arthroscopic Rotator Cuff Repair Type 2 Repairs (+/- subacromial decompression) The rehabilitation guidelines are presented in a criterion based progression.
UHealth Sports Medicine Rehabilitation Guidelines for Arthroscopic Rotator Cuff Repair Type 2 Repairs (+/- subacromial decompression) The rehabilitation guidelines are presented in a criterion based progression.
Shoulder Arthroscopy with Posterior Labral Repair Rehabilitation Protocol
 General Notes: As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
General Notes: As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
Bradley C. Carofino, M.D. Shoulder Specialist 230 Clearfield Avenue, Suite 124 Virginia Beach, Virginia Phone
 Subpectoral Bicep Tenodesis Protocol (Spreadsheet) Weeks 1-2 Modalities Treatment Restrictions Goals No active elbow flexion (6weeks) Full PROM shoulder and elbow PROM: Shoulder, elbow, forearm No active
Subpectoral Bicep Tenodesis Protocol (Spreadsheet) Weeks 1-2 Modalities Treatment Restrictions Goals No active elbow flexion (6weeks) Full PROM shoulder and elbow PROM: Shoulder, elbow, forearm No active
SHOULDER ARTHROSCOPY WITH ANTERIOR STABILIZATION / CAPSULORRHAPHY REHABILITATION PROTOCOL
 General Notes As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
General Notes As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
CENTER FOR ORTHOPAEDICS AND SPINE CARE PHYSICAL THERAPY PROTOCOL BENJAMIN J. DAVIS, MD Type Two Rotator Cuff Repair
 I. Phase I - Immediate Post-Surgical Phase (Day 1-10) Goals: Maintain Integrity of the Repair Gradually Increase Passive Range of Motion Diminish Pain and Inflammation Prevent Muscular Inhibition Passive
I. Phase I - Immediate Post-Surgical Phase (Day 1-10) Goals: Maintain Integrity of the Repair Gradually Increase Passive Range of Motion Diminish Pain and Inflammation Prevent Muscular Inhibition Passive
Total Shoulder Arthroplasty
 1 Total Shoulder Arthroplasty Surgical indications and contraindications Anatomical Considerations: Total shoulder arthroplasty surgery involves the replacement of the humeral head and the glenoid articulating
1 Total Shoulder Arthroplasty Surgical indications and contraindications Anatomical Considerations: Total shoulder arthroplasty surgery involves the replacement of the humeral head and the glenoid articulating
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s R E V E R S E T O T A L S H O U L D E R A R T H R O P L A S T Y P R O T O C O L
 S p o r t s & O r t h o p a e d i c S p e c i a l i s t s R E V E R S E T O T A L S H O U L D E R A R T H R O P L A S T Y P R O T O C O L This protocol provides appropriate guidelines for the rehabilitation
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s R E V E R S E T O T A L S H O U L D E R A R T H R O P L A S T Y P R O T O C O L This protocol provides appropriate guidelines for the rehabilitation
Latarjet Repair Rehabilitation Protocol
 General Notes: As tolerated should be understood to include with safety for the reconstruction/repair; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing
General Notes: As tolerated should be understood to include with safety for the reconstruction/repair; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing
TALLGRASS ORTHOPEDIC & SPORTS MEDICINE. Phase I Immediate Post-Surgical Phase (Weeks 0-2) Date: Maintain/protect integrity of the repair
 TALLGRASS ORTHOPEDIC & SPORTS MEDICINE Name: Date of Surgery: Patient Flow Sheet Arthroscopic Rotator Cuff Repair Small to Medium Tears Benedict Figuerres, MD Phase I Immediate Post-Surgical Phase (Weeks
TALLGRASS ORTHOPEDIC & SPORTS MEDICINE Name: Date of Surgery: Patient Flow Sheet Arthroscopic Rotator Cuff Repair Small to Medium Tears Benedict Figuerres, MD Phase I Immediate Post-Surgical Phase (Weeks
Rotator Cuff Repair Protocol for tear involving Subscapularis Tendon with or without Pectoralis Major Tendon Transfer
 Rotator Cuff Repair Protocol for tear involving Subscapularis Tendon with or without Pectoralis Major Tendon Transfer D. WATTS, MD Precautions: BASIS Tendon healing back to bone is a slow process that
Rotator Cuff Repair Protocol for tear involving Subscapularis Tendon with or without Pectoralis Major Tendon Transfer D. WATTS, MD Precautions: BASIS Tendon healing back to bone is a slow process that
Type II SLAP lesions are created when the biceps anchor has pulled away from the glenoid attachment.
 Arthroscopic Superior Labral (SLAP) Repair Protocol-Type II, IV, and Complex Tears The intent of this protocol is to provide the clinician with a guideline of the post-operative rehabilitation course of
Arthroscopic Superior Labral (SLAP) Repair Protocol-Type II, IV, and Complex Tears The intent of this protocol is to provide the clinician with a guideline of the post-operative rehabilitation course of
Arthroscopic Labral Repair Protocol-Type II, IV, and Complex Tears:
 Arthroscopic Labral Repair Protocol-Type II, IV, and Complex Tears: The intent of this protocol is to provide the clinician with a guideline of the postoperative rehabilitation course of a patient that
Arthroscopic Labral Repair Protocol-Type II, IV, and Complex Tears: The intent of this protocol is to provide the clinician with a guideline of the postoperative rehabilitation course of a patient that
Rotator Cuff Repair Protocol
 Rotator Cuff Repair Protocol Applicability: Physician Practices Date Effective: 11/2016 Department: Rehabilitation Services Supersedes: Rotator Cuff Repair (Beattie) Date Last Reviewed / or Date Last Revision:
Rotator Cuff Repair Protocol Applicability: Physician Practices Date Effective: 11/2016 Department: Rehabilitation Services Supersedes: Rotator Cuff Repair (Beattie) Date Last Reviewed / or Date Last Revision:
Rotator Cuff Repair +/- Acromioplasty/Mumford. Phase I: 0 to 2 weeks after surgery
 Rotator Cuff Repair +/- Acromioplasty/Mumford 2. Ensure wound healing Phase I: 0 to 2 weeks after surgery 1. Sling: Use your sling all of the time. 2. Use of the affected arm: You may use your hand on
Rotator Cuff Repair +/- Acromioplasty/Mumford 2. Ensure wound healing Phase I: 0 to 2 weeks after surgery 1. Sling: Use your sling all of the time. 2. Use of the affected arm: You may use your hand on
Rotator Cuff Repair Protocol
 Rotator Cuff Repair Protocol Applicability: Physician Practices Date Effective: 11/2016 Department: Rehabilitation Services Supersedes: Rotator Cuff Repair (Beattie) Date Last Reviewed / or Date Last Revision:
Rotator Cuff Repair Protocol Applicability: Physician Practices Date Effective: 11/2016 Department: Rehabilitation Services Supersedes: Rotator Cuff Repair (Beattie) Date Last Reviewed / or Date Last Revision:
Mini Open Rotator Cuff Repair Small Tears < 1 cm
 Mini Open Rotator Cuff Repair Small Tears < 1 cm **It is the treating therapist s responsibility along with the referring physician s guidance to determine the actual progression of the patient within
Mini Open Rotator Cuff Repair Small Tears < 1 cm **It is the treating therapist s responsibility along with the referring physician s guidance to determine the actual progression of the patient within
No Financial Disclosures
 Rehabilitation Following Total and Reverse Shoulder Arthroplasty, PT, DPT, SCS, CSCS No Financial Disclosures Total Shoulder Arthroplasty Arthritic shoulder increasing in prevalence More active as we age
Rehabilitation Following Total and Reverse Shoulder Arthroplasty, PT, DPT, SCS, CSCS No Financial Disclosures Total Shoulder Arthroplasty Arthritic shoulder increasing in prevalence More active as we age
Rehabilitation Protocol: Arthroscopic Anterior Capsulolabral Repair of the Shoulder - Bankart Repair Rehabilitation Guidelines
 Rehabilitation Protocol: Arthroscopic Anterior Capsulolabral Repair of the Shoulder - Bankart Repair Rehabilitation Guidelines Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington
Rehabilitation Protocol: Arthroscopic Anterior Capsulolabral Repair of the Shoulder - Bankart Repair Rehabilitation Guidelines Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington
Anterior Labrum Repair Protocol
 Anterior Labrum Repair Protocol Stage I (0-4 weeks): Key Goals: Protect the newly repaired shoulder. Allow for decreased inflammation and healing. Maintain elbow, wrist and hand function. Maintain scapular
Anterior Labrum Repair Protocol Stage I (0-4 weeks): Key Goals: Protect the newly repaired shoulder. Allow for decreased inflammation and healing. Maintain elbow, wrist and hand function. Maintain scapular
Shawn Hennigan, MD Total Shoulder Arthroplasty Protocol. Phase 1 Maximum Protection (0-4 weeks)
 Shawn Hennigan, MD Total Shoulder Arthroplasty Protocol Goals for phase 1 Minimize Pain and inflammation Protect integrity of repair Initiate shoulder PROM Reduce muscular inhibition Maintain AROM of elbow,
Shawn Hennigan, MD Total Shoulder Arthroplasty Protocol Goals for phase 1 Minimize Pain and inflammation Protect integrity of repair Initiate shoulder PROM Reduce muscular inhibition Maintain AROM of elbow,
Mini Open Rotator Cuff Repair Large (3 5 cm)
 Mini Open Rotator Cuff Repair Large (3 5 cm) Size: small = < 1 cm, medium = 1 3 cm, large 3 5 cm, massive = > 5 cm **It is the treating therapist s responsibility along with the referring physician s guidance
Mini Open Rotator Cuff Repair Large (3 5 cm) Size: small = < 1 cm, medium = 1 3 cm, large 3 5 cm, massive = > 5 cm **It is the treating therapist s responsibility along with the referring physician s guidance
Rotator Cuff Repair Therapy Protocol
 Bart Eastwood D.O. 825 Davis st Blacksburg, VA 24060 540-951-6000 All information contained in this protocol is to be used as general guidelines only. Specific variations may be appropriate for each patient
Bart Eastwood D.O. 825 Davis st Blacksburg, VA 24060 540-951-6000 All information contained in this protocol is to be used as general guidelines only. Specific variations may be appropriate for each patient
Rehabilitation Protocol: Massive Rotator Cuff Tear Repair
 Rehabilitation Protocol: Massive Rotator Cuff Tear Repair Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey
Rehabilitation Protocol: Massive Rotator Cuff Tear Repair Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey
DISCHARGE INSTRUCTIONS & PHYSICAL THERAPY PROTOCOL: Biceps Tenodesis
 DISCHARGE INSTRUCTIONS & PHYSICAL THERAPY PROTOCOL: Biceps Tenodesis Initial recovery after shoulder surgery entails healing, controlling swelling and discomfort and regaining some shoulder motion. The
DISCHARGE INSTRUCTIONS & PHYSICAL THERAPY PROTOCOL: Biceps Tenodesis Initial recovery after shoulder surgery entails healing, controlling swelling and discomfort and regaining some shoulder motion. The
Arthroscopic Anterior Stabilization Rehab
 Arthroscopic Anterior Stabilization Rehab Phase I (0-3weeks) Sling immobilization-md directed Codmans/Pendulum exercises Wrist/Elbow ROM Gripping exercises FF-AAROM (supine)-limit to 90 o ER to 0 o Sub
Arthroscopic Anterior Stabilization Rehab Phase I (0-3weeks) Sling immobilization-md directed Codmans/Pendulum exercises Wrist/Elbow ROM Gripping exercises FF-AAROM (supine)-limit to 90 o ER to 0 o Sub
Superior Labrum Repair Protocol - SLAP
 Superior Labrum Repair Protocol - SLAP Stage I (0-4 weeks): Key Goals: Protect the newly repaired shoulder. Allow for decreased inflammation and healing. Maintain elbow, wrist and hand function. Maintain
Superior Labrum Repair Protocol - SLAP Stage I (0-4 weeks): Key Goals: Protect the newly repaired shoulder. Allow for decreased inflammation and healing. Maintain elbow, wrist and hand function. Maintain
Phase I: 0 to 3 weeks after surgery
 Dx: Right Left RTC (Massive) Repair Date of Surgery: Patient Name: PT/OT: Please evaluate and treat. Follow attached protocol. 2-3 x per week x 6 weeks. Signature/Date: 2. Ensure wound healing Phase I:
Dx: Right Left RTC (Massive) Repair Date of Surgery: Patient Name: PT/OT: Please evaluate and treat. Follow attached protocol. 2-3 x per week x 6 weeks. Signature/Date: 2. Ensure wound healing Phase I:
REHABILITATION GUIDELINES FOR ROTATOR CUFF REPAIR FOR TYPE II TEARS (MASSIVE)(+/- SUBACROMIAL DECOMPRESSION)
 REHABILITATION GUIDELINES FOR ROTATOR CUFF REPAIR FOR TYPE II TEARS (MASSIVE)(+/- SUBACROMIAL DECOMPRESSION) The rehabilitation guidelines are presented in a criterion based progression. General time frames
REHABILITATION GUIDELINES FOR ROTATOR CUFF REPAIR FOR TYPE II TEARS (MASSIVE)(+/- SUBACROMIAL DECOMPRESSION) The rehabilitation guidelines are presented in a criterion based progression. General time frames
Charlotte Shoulder Institute
 Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
Avon Office 2 Simsbury Rd. Avon, CT Office: (860) Fax: (860) Arthroscopic Posterior Labral Repair
 Katherine J. Coyner, MD UCONN Musculoskeletal Institute Medical Arts & Research Building 263 Farmington Ave. Farmington, CT 06030 Office: (860) 679-6600 Fax: (860) 679-6649 www.drcoyner.com Arthroscopic
Katherine J. Coyner, MD UCONN Musculoskeletal Institute Medical Arts & Research Building 263 Farmington Ave. Farmington, CT 06030 Office: (860) 679-6600 Fax: (860) 679-6649 www.drcoyner.com Arthroscopic
PHASE I (Begin PT 3-5 days post-op) DOS:
 REHABILITATION GUIDELINES FOR POSTERIOR SHOULDER RECONSTRUCTION +/- LABRAL REPAIRS The rehabilitation guidelines are presented in a criterion based progression. General time frames are given for reference
REHABILITATION GUIDELINES FOR POSTERIOR SHOULDER RECONSTRUCTION +/- LABRAL REPAIRS The rehabilitation guidelines are presented in a criterion based progression. General time frames are given for reference
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s T O T A L S H O U L D E R A R T H R O P L A S T Y P R O T O C O L
 S p o r t s & O r t h o p a e d i c S p e c i a l i s t s T O T A L S H O U L D E R A R T H R O P L A S T Y P R O T O C O L This protocol provides appropriate guidelines for the rehabilitation of patients
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s T O T A L S H O U L D E R A R T H R O P L A S T Y P R O T O C O L This protocol provides appropriate guidelines for the rehabilitation of patients
REHABILITATION FOLLOWING OPEN AND MINI-OPEN ROTATOR CUFF REPAIR
 REHABILITATION FOLLOWING OPEN AND MINI-OPEN ROTATOR CUFF REPAIR Post-Operative Physical Therapy Protocol Philip A. Davidson M.D. Phase I Immediate Post-Surgical Phase (Week 1-2) Maintain integrity of the
REHABILITATION FOLLOWING OPEN AND MINI-OPEN ROTATOR CUFF REPAIR Post-Operative Physical Therapy Protocol Philip A. Davidson M.D. Phase I Immediate Post-Surgical Phase (Week 1-2) Maintain integrity of the
 Appendix A: The American Society Of Shoulder And Elbow Therapists Arthroscopic Rotator Cuff Repair Rehabilitation Guide Phase 1 (POD 1 to ~ POW 6) GOALS: Maintain integrity of repair Minimize pain and
Appendix A: The American Society Of Shoulder And Elbow Therapists Arthroscopic Rotator Cuff Repair Rehabilitation Guide Phase 1 (POD 1 to ~ POW 6) GOALS: Maintain integrity of repair Minimize pain and
Rehabilitation Guidelines for Large Rotator Cuff Repair
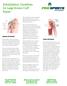 Rehabilitation Guidelines for Large Rotator Cuff Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the
Rehabilitation Guidelines for Large Rotator Cuff Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the
ULNAR COLLATERAL LIGAMENT (UCL) RECONSTRUCTION REHABILITATION PROTOCOL
 General Notes As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
General Notes As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
REHABILITATION PROTOCOL ARTHROSCOPIC ROTATOR CUFF REPAIR (1 and 2 tendon repairs <4cm²)
 Phil Davidson M.D. Eric Heiden M.D. Karen Heiden M.D. 2200 Park Ave, Bld. D, Ste. 100 Park City, Utah 84060 435.615.8822 435.615.8823 fax REHABILITATION PROTOCOL ARTHROSCOPIC ROTATOR CUFF REPAIR (1 and
Phil Davidson M.D. Eric Heiden M.D. Karen Heiden M.D. 2200 Park Ave, Bld. D, Ste. 100 Park City, Utah 84060 435.615.8822 435.615.8823 fax REHABILITATION PROTOCOL ARTHROSCOPIC ROTATOR CUFF REPAIR (1 and
Shoulder Hemi-arthroplasty (Trauma)
 Shoulder Hemi-arthroplasty (Trauma) Sling What can I do from day 1? Restrictions? Commence strengthening? Trauma: Up to 6 Active assisted/active supported within safe zone* Mobilise unaffected joints e.g
Shoulder Hemi-arthroplasty (Trauma) Sling What can I do from day 1? Restrictions? Commence strengthening? Trauma: Up to 6 Active assisted/active supported within safe zone* Mobilise unaffected joints e.g
MASSIVE ROTATOR CUFF REPAIR. REHABITATION PROTOCOL >3 cm
 MASSIVE ROTATOR CUFF REPAIR REHABITATION PROTOCOL >3 cm Phase I: (Protective Phase) Weeks 0 to 8 Goals: Minimize pain and inflammatory response Achieve ROM goals Establish stable scapula 1. Elbow, wrist
MASSIVE ROTATOR CUFF REPAIR REHABITATION PROTOCOL >3 cm Phase I: (Protective Phase) Weeks 0 to 8 Goals: Minimize pain and inflammatory response Achieve ROM goals Establish stable scapula 1. Elbow, wrist
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s M A S S I V E R O T A T O R C U F F R E P A I R P R O T O C O L
 S p o r t s & O r t h o p a e d i c S p e c i a l i s t s M A S S I V E R O T A T O R C U F F R E P A I R P R O T O C O L This protocol provides appropriate guidelines for the rehabilitation of patients
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s M A S S I V E R O T A T O R C U F F R E P A I R P R O T O C O L This protocol provides appropriate guidelines for the rehabilitation of patients
Phase I : Immediate Postoperative Phase- Protected Motion. (0-2 Weeks)
 Phase I : Immediate Postoperative Phase- Protected Motion (0-2 Weeks) Appointments Progression Criteria 2 weeks after surgery Rehabilitation appointments begin within 7-10 days of surgery, continue 1-2
Phase I : Immediate Postoperative Phase- Protected Motion (0-2 Weeks) Appointments Progression Criteria 2 weeks after surgery Rehabilitation appointments begin within 7-10 days of surgery, continue 1-2
Latissimus Dorsi Transfer
 Latissimus Dorsi Transfer 1. Defined a. Transfer of the latissimus dorsi from it insertion anteriorly on the proximal humeral shaft to a superior and posterior insertion on the humeral head in the subacromial
Latissimus Dorsi Transfer 1. Defined a. Transfer of the latissimus dorsi from it insertion anteriorly on the proximal humeral shaft to a superior and posterior insertion on the humeral head in the subacromial
Rehabilitation Guidelines for Labral/Bankert Repair
 Rehabilitation Guidelines for Labral/Bankert Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Rehabilitation Guidelines for Labral/Bankert Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Shoulder and Elbow ORTHOPAEDIC SYPMPOSIUM APRIL 8, 2017 DANIEL DOTY MD
 Shoulder and Elbow ORTHOPAEDIC SYPMPOSIUM APRIL 8, 2017 DANIEL DOTY MD Shoulder Articulations Glenohumeral Joint 2/3 total arc of motion Shallow Ball and Socket Joint Allows for excellent ROM Requires
Shoulder and Elbow ORTHOPAEDIC SYPMPOSIUM APRIL 8, 2017 DANIEL DOTY MD Shoulder Articulations Glenohumeral Joint 2/3 total arc of motion Shallow Ball and Socket Joint Allows for excellent ROM Requires
Arthroscopic SLAP Lesion Repair Rehabilitation Guideline
 Arthroscopic SLAP Lesion Repair Rehabilitation Guideline This rehabilitation program is designed to return the individual to their activities as quickly and safely as possible. It is designed for rehabilitation
Arthroscopic SLAP Lesion Repair Rehabilitation Guideline This rehabilitation program is designed to return the individual to their activities as quickly and safely as possible. It is designed for rehabilitation
REVERSE SHOULDER REPLACEMENT
 REVERSE SHOULDER REPLACEMENT The Reverse Shoulder Replacement is designed specifically for the use in shoulders with a deficient rotator cuff and arthritis, as well as other difficult shoulder reconstructive
REVERSE SHOULDER REPLACEMENT The Reverse Shoulder Replacement is designed specifically for the use in shoulders with a deficient rotator cuff and arthritis, as well as other difficult shoulder reconstructive
Total Shoulder Arthroplasty / Hemi-arthroplasty (Elective)
 Total Shoulder Arthroplasty / Hemi-arthroplasty (Elective) Sling What can I do from day 1? Restrictions? Commence strengthening? Up to 3 weeks Active assisted/active supported within safe zone* Mobilise
Total Shoulder Arthroplasty / Hemi-arthroplasty (Elective) Sling What can I do from day 1? Restrictions? Commence strengthening? Up to 3 weeks Active assisted/active supported within safe zone* Mobilise
Pectorlais Major Tendon Repair
 Dr. Mark Price MGH Sports Medicine Center 175 Cambridge Street, 4th floor Boston, MA 02114 www.massgeneral.org/ortho-sports-medicine/dr-price Pectorlais Major Tendon Repair The pectoralis major muscle
Dr. Mark Price MGH Sports Medicine Center 175 Cambridge Street, 4th floor Boston, MA 02114 www.massgeneral.org/ortho-sports-medicine/dr-price Pectorlais Major Tendon Repair The pectoralis major muscle
REHABILITATION GUIDELINES FOR ANTERIOR SHOULDER RECONSTRUCTION WITH BANKART REPAIR
 REHABILITATION GUIDELINES FOR ANTERIOR SHOULDER RECONSTRUCTION WITH BANKART REPAIR The rehabilitation guidelines are presented in a criterion based progression. General time frames are given for reference
REHABILITATION GUIDELINES FOR ANTERIOR SHOULDER RECONSTRUCTION WITH BANKART REPAIR The rehabilitation guidelines are presented in a criterion based progression. General time frames are given for reference
Anterior Stabilization of the Shoulder: Latarjet Protocol
 Anterior Stabilization of the Shoulder: Latarjet Protocol Dr. Abigail R. Hamilton, M.D. Shoulder instability may be caused from congenital deformity, recurrent overuse activity, and/or traumatic dislocation.
Anterior Stabilization of the Shoulder: Latarjet Protocol Dr. Abigail R. Hamilton, M.D. Shoulder instability may be caused from congenital deformity, recurrent overuse activity, and/or traumatic dislocation.
Charlotte Shoulder Institute
 Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
ROTATOR CUFF REPAIR REHAB PROTOCOL
 Jayesh K. Patel, M.D. Trinity Clinic Orthopaedic and Sports Medicine 1327 Troup Hwy Tyler, TX 75701 (903) 510-8840 ROTATOR CUFF REPAIR REHAB PROTOCOL This rehabilitation protocol has been developed for
Jayesh K. Patel, M.D. Trinity Clinic Orthopaedic and Sports Medicine 1327 Troup Hwy Tyler, TX 75701 (903) 510-8840 ROTATOR CUFF REPAIR REHAB PROTOCOL This rehabilitation protocol has been developed for
Shoulder Arthroscopy: Postop Instructions. Activites & Advice for in the Hospital and while at Home
 Dr. Mark Price MGH Sports Medicine Center 175 Cambridge Street, 4th floor Boston, MA 02114 www.massgeneral.org/ortho-sports-medicine/dr-price Shoulder Arthroscopy: Postop Instructions You will wake up
Dr. Mark Price MGH Sports Medicine Center 175 Cambridge Street, 4th floor Boston, MA 02114 www.massgeneral.org/ortho-sports-medicine/dr-price Shoulder Arthroscopy: Postop Instructions You will wake up
SHOULDER RESURFACING
 MGH Sports Medicine Center 175 Cambridge St., 4th floor Boston, MA 02114 http://orthodoc.aaos.org/mdprice SHOULDER RESURFACING The shoulder is a ball and socket joint that enables you to raise, twist,
MGH Sports Medicine Center 175 Cambridge St., 4th floor Boston, MA 02114 http://orthodoc.aaos.org/mdprice SHOULDER RESURFACING The shoulder is a ball and socket joint that enables you to raise, twist,
Diagnosis: s/p ( LEFT / RIGHT ) AC Joint Reconstruction -- Surgery Date:
 UCLA OUTPATIENT REHABILITATION SERVICES! SANTA MONICA! WESTWOOD 1000 Veteran Ave., A level Phone: (310) 794-1323 Fax: (310) 794-1457 1260 15 th St, Ste. 900 Phone: (310) 319-4646 Fax: (310) 319-2269 FOR
UCLA OUTPATIENT REHABILITATION SERVICES! SANTA MONICA! WESTWOOD 1000 Veteran Ave., A level Phone: (310) 794-1323 Fax: (310) 794-1457 1260 15 th St, Ste. 900 Phone: (310) 319-4646 Fax: (310) 319-2269 FOR
