Salbach et al. Implementation Science (2017) 12:100 DOI /s
|
|
|
- Beatrice Simon
- 6 years ago
- Views:
Transcription
1 Salbach et al. Implementation Science (2017) 12:100 DOI /s RESEARCH Open Access Facilitated interprofessional implementation of a physical rehabilitation guideline for stroke in inpatient settings: process evaluation of a cluster randomized trial Nancy M. Salbach 1,11*, Sharon Wood-Dauphinee 2, Johanne Desrosiers 3, Janice J. Eng 4, Ian D. Graham 5, Susan B. Jaglal 1, Nicol Korner-Bitensky 2, Marilyn MacKay-Lyons 6, Nancy E. Mayo 7, Carol L. Richards 8, Robert W. Teasell 9, Merrick Zwarenstein 10, Mark T. Bayley 11 and on behalf of the Stroke Canada Optimization of Rehabilitation By Evidence Implementation Trial (SCORE-IT) Team Abstract Background: The Stroke Canada Optimization of Rehabilitation by Evidence-Implementation Trial (SCORE-IT) showed that a facilitated knowledge translation (KT) approach to implementing a stroke rehabilitation guideline was more likely than passive strategies to improve functional walking capacity, but not gross manual dexterity, among patients in rehabilitation hospitals. This paper presents the results of a planned process evaluation designed to assess whether the type and number of recommended treatments implemented by stroke teams in each group would help to explain the results related to patient outcomes. Methods: As part of a cluster randomized trial, 20 rehabilitation units were stratified by language and allocated to a facilitated or passive KT intervention group. Sites in the facilitated group received the guideline with treatment protocols and funding for a part-time nurse and therapist facilitator who attended a 2-day training workshop and promoted guideline implementation for 16 months. Sites in the passive group received the guideline excluding treatment protocols. As part of a process evaluation, nurses, and occupational and physical therapists, blinded to study hypotheses, were asked to record their implementation of 18 recommended treatments targeting motor function, postural control and mobility using individualized patient checklists after treatment sessions for 2 weeks pre- and postintervention. The percentage of patients receiving each treatment pre- and post-intervention and between groups was compared after adjusting for clustering and covariates in a random-effects logistic regression analysis. (Continued on next page) * Correspondence: nancy.salbach@utoronto.ca 1 Department of Physical Therapy, University of Toronto, University Ave, Toronto, ON M5G 1V7, Canada 11 Toronto Rehabilitation Institute-University Health Network, 550 University Avenue, room (3-East) 3rd Floor University Wing, Toronto, ON M5G 2A2, Canada Full list of author information is available at the end of the article The Author(s) Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License ( which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver ( applies to the data made available in this article, unless otherwise stated.
2 Salbach et al. Implementation Science (2017) 12:100 Page 2 of 11 (Continued from previous page) Results: Data on treatment implementation from nine and eight sites in the facilitated and passive KT group, respectively, were available for analysis. The facilitated KT intervention was associated with improved implementation of sit-to-stand (p = 0.028) and walking (p = 0.043) training while the passive KT intervention was associated with improved implementation of standing balance training (p = 0.037), after adjusting for clustering at patient and provider levels and covariates. Conclusions: Despite multiple strategies and resources, the facilitated KT intervention was unsuccessful in improving integration of 18 treatments concurrently. The facilitated approach may not have adequately addressed barriers to integrating numerous treatments simultaneously and complex treatments that were unfamiliar to providers. Trial registration: Unique identifier-nct Keywords: Implementation, Facilitation, Interprofessional, Stroke, Rehabilitation, Guideline, Randomized controlled trial, Cluster randomization, Knowledge translation, Process evaluation Background Stroke is a chronic disabling condition [1] that is expected to affect an increasing number of individuals due to population growth and aging [2]. Clinical practice guidelines for inpatient stroke rehabilitation settings provide clear treatment recommendations aimed at improving motor function, postural control, and mobility [3 5]. Despite evidence that guideline adherence is associated with functional recovery [6] and patient satisfaction [7], studies conducted in Canada and in the UK reveal that guideline application is inconsistent [8 11]. To narrow these knowledge to practice gaps, the Knowledge to Action (KTA) Process [12] recommends an evaluation of barriers to knowledge use and tailoring of knowledge translation (KT) strategies to address those barriers. Research conducted by our team and others has shown that implementation of a stroke rehabilitation guideline in the inpatient hospital setting presents unique challenges [13, 14]. Owing to a broad research base [15, 16], stroke rehabilitation guidelines consist of an extensive number of treatment recommendations [3]. Although multiple efficacious treatments may be appropriate for a patient, there may be insufficient time to apply all of them thus requiring individual health professionals to prioritize and select [13]. This process is complicated by the recommendation to deliver stroke rehabilitation by a core interdisciplinary team consisting of physical and occupational therapists, nurses, and speech-language pathologists, physiatrists/physicians, social workers, and dietitians [3]. Team functioning and communication may affect how well members prioritize and coordinate implementation of treatment [13]. The complexity of efficacious treatments in terms of the number of steps and technical skill required also varies widely which has implications for education and training [13]. Finally, stroke can lead to heterogeneous profiles of sensorimotor, communication, and cognitive impairment that cause variable levels of disability. The type and magnitude of stroke-related deficits, the incidence of shoulder pain which occurs in almost 30% of patients [17], and patient preferences can further influence health providers decisions to apply a recommended treatment [13, 18]. A multi-component intervention is required to overcome the challenges to integrating stroke rehabilitation guidelines targeting improvement in motor function, postural control, and mobility. Facilitation, defined as the process of enabling (making easier) the implementation of evidence into practice (p. 579) [19, 20] is a recognized strategy and core component of the PARiHS (Promoting Action on Research Implementation in Health Services) framework [20 22] that could potentially enable collaboration within stroke teams to implement a comprehensive stroke rehabilitation guideline. Reviews of facilitation [19, 23] have characterized it as both an individual role incorporating project management and leadership and a process involving individuals and teams. Facilitators may use a range of strategies to assist individuals and teams to apply evidence in practice as facilitation should be tailored to the needs of the local context [19, 22, 23]. For example, a local facilitator may organize training sessions to address a need to build clinicians capacity to implement a specific treatment and check-in at regular intervals to help maintain motivation levels. Facilitators may also approach managers to enable the purchase of equipment or the re-organization of therapy space if these are the issues hindering practice change. In the context of inpatient stroke rehabilitation, employing multiple facilitators recruited from core health professional groups involved in interdisciplinary stroke rehabilitation teams was considered a novel and potentially effective strategy for enabling guideline implementation. In rehabilitation research, guideline provision combined with interactive educational sessions to review best practices has been associated with improved performance of recommended practices compared to mailing of the guideline among rehabilitation providers [24, 25]. Previous
3 Salbach et al. Implementation Science (2017) 12:100 Page 3 of 11 trials [24 26], however, have targeted adherence to 10 recommendations in one professional group and provided limited description of clustering effects and adjustment for covariates. No studies examined use of local facilitators from different professional groups to promote guideline implementation. The Stroke Canada Optimization of Rehabilitation by Evidence Implementation Trial (SCORE- IT) was a cluster randomized trial designed to evaluate the extent to which a multi-modal, facilitated KT approach to implementing a stroke rehabilitation guideline was more likely than passive strategies, such as mailing the guideline and educational materials, to improve patient function in the inpatient rehabilitation hospital setting (Bayley MT, Wood-Dauphinee S, Richards CL, Salbach NM, Desrosiers J, Eng JJ, et al.: Facilitated knowledge translation improves stroke rehabilitation outcomes: The SCORE-IT cluster randomized controlled trial, under review) [27]. Among patients with stroke treated at facilitated KT sites (n = 410), the odds of demonstrating a high level of functional walking capacity, measured using the 6-min walk test, were 1.63 times (95% CI: ) the odds observed among patients at passive KT sites (n =367)(Bayley MT, Wood-Dauphinee S, Richards CL, Salbach NM, Desrosiers J, Eng JJ, et al.: Facilitated knowledge translation improves stroke rehabilitation outcomes: The SCORE-IT cluster randomized controlled trial, under review). The facilitated KT intervention was not associated with gross manual dexterity (measured using the Box and Block Test) among patients with stroke (OR: 1.69, 95% CI: ). A mixed methods process evaluation was completed to help explain the results related to patient outcomes. In the qualitative process evaluation [27], focus groups were conducted with 33 nurses, therapists, and managers from 11 of the 20 study sites in the facilitated and passive KT groups to explore their experiences with SCORE-IT. The qualitative analysis yielded four themes describing factors that facilitated or hindered implementation of the KT interventions and clinical integration of the recommended treatments [27]. Themes included: presence/absence of facilitation, agreement that the intervention was practical, familiarity with the recommended treatments, and environmental factors (e.g., staff turnover, lack of space or equipment) [27]. Facilitating factors, such as the presence of an individual who provided stroke teams with support and motivation throughout the trial, and experience with using some of the treatment interventions, were described by participants in both study groups [27]. A fifth theme, namely improved team communication and interdisciplinary collaboration, was identified as an unexpected positive trial outcome that served to facilitate the clinical application of treatment interventions in both study groups [27]. While results from the qualitative process evaluation have increased our understanding of site, provider and treatment characteristics that may have influenced implementation of the study interventions and recommended treatments, the extent to which each recommended treatment was implemented has not been reported and may help to explain why the facilitated KT intervention was associated with improved functional walking capacity but not gross manual dexterity among patients. Thus, this paper presents the results of a quantitative process evaluation of SCORE-IT designed to evaluate the extent to which stroke teams implemented the recommended treatments targeting upper extremity (UE) and lower extremity (LE) motor function, postural control, and mobility in each intervention group. Methods A national, 2-parallel group cluster-randomized, pragmatic trial was conducted from 2007 to The effectiveness of a facilitated and passive KT intervention for implementing a stroke rehabilitation guideline was evaluated by comparing patient outcomes related to walking capacity and manual dexterity post-intervention. To understand how implementation of guideline recommendations may have influenced study outcomes related to patient function, stroke teams in each intervention group were asked to complete self-report checklists to record their implementation of 18 recommended treatments with each patient seen over a 2-week period pre- and post-intervention. The ethics board at each site and affiliated university approved the study protocol. Eligibility and recruitment Sites with designated rehabilitation beds, an interdisciplinary stroke team with at least one nurse, one physical therapist (PT) and one occupational therapist (OT), and regular inpatients post-stroke (i.e., 1 person post-stroke on the unit daily), were considered eligible. Sites with these characteristics were targeted as the treatment recommendations were developed for implementation primarily by nurses, PTs, and OTs in an inpatient rehabilitation setting [13]. Recruitment involved study leads sending letters of invitation to site managers/physiatrists and interviewing to screen for eligibility and obtain consent. All therapists and nurses working on the stroke rehabilitation unit were eligible to participate. A research assistant (RA) hired for each site obtained informed consent from rehabilitation providers. Details of patient eligibility and recruitment are described elsewhere (Bayley MT, Wood- Dauphinee S, Richards CL, Salbach NM, Desrosiers J, Eng JJ, et al.: Facilitated knowledge translation improves stroke rehabilitation outcomes: The SCORE-IT cluster randomized controlled trial, under review). Data collection Following recruitment, site representatives were asked to complete a site readiness checklist that required them to
4 Salbach et al. Implementation Science (2017) 12:100 Page 4 of 11 provide information on the language of documentation (English/French), university affiliation (full/partial or none), rehabilitation unit location (freestanding/integrated with a general hospital), and stroke patient volume (expected number of stroke patients/year). Site RAs abstracted patient sociodemographic and clinical data from health records. The outcome was change in the percentage of patients for which inpatient stroke teams implemented each recommended treatment pre- to post-intervention. All inpatients with stroke were expected to need the majority of treatments. For select treatments that are applied only when indicated (e.g., to reduce hand edema/shoulder pain), a similar proportion in each group was expected to require each treatment owing to randomization. A selfreport checklist was created for therapists to document name, profession, and which of the 18 recommended treatments was implemented for each patient. To mitigate social desirability bias [28], a section was added to the checklist where therapists could indicate that a treatment would have been implemented if time had permitted. A similar checklist was created for nurses to report on implementation of 7 treatments (sit-to-stand training, use of LE external support, walking practice, UE range of motion and/or stretching, interventions to prevent shoulder pain, task-specific training of the UE, and education of patients/caregivers on how to handle the affected UE). Site RAs oriented therapists and nurses, who were blinded to study hypotheses, to the checklists and asked them to complete a checklist at the end of every treatment session with patients post-stroke during a two-week period preand post-intervention. Randomization A biostatistician, not involved in study recruitment or data collection, used R statistical software to stratify hospitals by language of documentation (English/French) and randomly assign them to either the facilitated or passive KT group using a 1:1 allocation ratio. Site staff were informed of their group assignment following completion of pre-intervention data collection on treatment implementation. Interventions The SCORE-IT interventions are described in detail elsewhere (Bayley MT, Wood-Dauphinee S, Richards CL, Salbach NM, Desrosiers J, Eng JJ, et al.: Facilitated knowledge translation improves stroke rehabilitation outcomes: The SCORE-IT cluster randomized controlled trial, under review) [27]. Intervention development was guided by the KTA process and by the results of a qualitative study in which implementation of the stroke rehabilitation guideline was piloted at five inpatient rehabilitation hospitals in Canada [13]. Analysis of transcripts from focus groups involving 79 rehabilitation professionals (physical and occupational therapists, nurses, and directors/managers) identified lack of time, staffing issues, training/education, therapy selection and prioritization, equipment availability, and team functioning/communication as key barriers to guideline implementation. In alignment with the KTA process, the facilitated KT intervention was designed to address these barriers. The facilitated KT intervention included funding for two local facilitators, one nurse and one therapist, to provide 4 h per week of protected time to support guideline implementation over a 16-month period. Having a facilitator from both nursing and allied health was expected to facilitate interdisciplinary collaboration and address barriers related to team functioning and communication [13]. Facilitators attended a two-day workshop where they received media releases for promoting the guideline among clinicians, slide presentations of the treatment protocols, and training in how to apply treatments and run small group education/training sessions. This was designed to prepare facilitators to run local small group education/training sessions to address barriers related to inadequate education/training in how to apply the treatments in clinical practice for existing and new staff. Facilitators were also provided with an outline of strategies used to foster guideline implementation in the pilot study [13], a practice-change toolkit [29], and education in change management. They completed activities to compare current with recommended practice, identify barriers to practice change, and develop a plan that incorporated behavior change strategies to address local challenges to guideline implementation. This was expected to prepare facilitators to address other site-specific barriers related to, for example, insufficient equipment and motivation to change practice [13]. Stroke teams were provided with SCORE guideline booklets that included treatment recommendations and evidence-based treatment protocols and pocket reminder cards designed for therapists or nurses to enable quick and easy access to descriptions of protocols. These resources were expected to address barriers related to inadequate knowledge of and time to read recommendations [13]. Teleconferences and a web-based platform were provided for facilitators to communicate and share successful strategies. Sites in the passive group received SCORE guideline booklets that did not include treatment protocols, and a handbook [30] and educational video on the use of standardized assessment tools post-stroke. Clinicians were invited to join a list serve to ask questions and share their experiences with the trial. Sample size Post hoc power calculations were performed. Given 1381 observations available to analyze treatment implementation by nurses and therapists, accounting for clustering of
5 Salbach et al. Implementation Science (2017) 12:100 Page 5 of 11 observations within patients (mean patient-level intracluster correlation coefficient (ICC) across treatments of 0.12; mean cluster size of 8 observations per patient) yielded an effective sample size of 751 independent observations (375 per group) [31]. With 375 observations per group (2-sided alpha = 0.05) and a baseline implementation rate of 30%, there was 80% power to detect a between-group difference of 10% in the rate of treatment implementation. Given 547 observations available to analyze treatment implementation by therapists alone, accounting for clustering of observations within patients (mean patientlevel ICC across treatments of 0.09; mean cluster size of four observations per patient) yielded an effective sample size of 431 independent observations (215 per group). With 215 observations per group (2-sided alpha = 0.05) and a baseline implementation rate of 10%, there was 80% power to detect a between-group difference of 10% in the rate of treatment implementation. Analysis The unit of analysis was a binary variable that represented whether a patient received a recommended treatment or not during a treatment session. To account for potential clustering effects at the level of the hospital, provider, and patient, a random-effects logistic regression analysis was carried out in SAS v9.3. The analysis included the following steps. First, estimates of the unadjusted rate of treatment implementation within each group pre- and post-intervention, change pre- to post-intervention, and between-group comparison of change were obtained using proc. nlmixed. Next, tests for random variation at the site, provider and patient levels were performed. A significant test result (α = 0.05) in more than 33% of models was the criterion for including a clustering variable in all final models. A final model was constructed for each treatment with intervention group, evaluation time (pre or post), an interaction term of group by time, clustering variables and covariates entered as independent variables using proc. glimmix. Covariates included site location (freestanding/ integrated with a general hospital), and size of stroke service (expected #stroke patients/year), and patient motor function (Functional Independence Measure [32] (FIM) motor subscore) and comorbidity (Charlson score [33]) on admission. A significant interaction term (α = 0.05) was used to indicate whether change in the extent to which patients received a treatment was greater following the facilitated than following the passive KT intervention after adjusting for clustering and covariates. Results Figure 1 presents the CONSORT diagram describing the results of recruitment, randomization, and data collection. Of the 20 participating sites, 10 were randomized to the facilitated KT intervention and 10 were randomized to the passive KT intervention. Facilitators from all sites in the facilitated group attended the training workshop (Bayley MT, Wood-Dauphinee S, Richards CL, Salbach NM, Desrosiers J, Eng JJ, et al.: Facilitated knowledge translation improves stroke rehabilitation outcomes: The SCORE-IT cluster randomized controlled trial, under review). Three sites were removed from the Fig. 1 CONSORT flowchart
6 Salbach et al. Implementation Science (2017) 12:100 Page 6 of 11 Table 1 Site characteristics Characteristic Intervention group Facilitated (n = 9) Passive (n =8) English-language, n (%) 7 (78) 7 (88) Academic affiliation, n (%) None 5 (56) 4 (50) Partial 1 (11) 1 (13) Full 3 (33) 3 (38) Freestanding, n (%) 5 (56) 4 (50) Expected number of stroke patients/year, mean ± SD (Range) 95 ± 49 (22 160) 105 ± 72 (30 210) analysis because they had no data (n = 2) or only preintervention data (n = 1) due to technical issues with the database. Of the three sites removed, two were from the passive group and were non-academic, and located in a general hospital with 86 and 35 expected patients with stroke/year. The third site removed was from the facilitated group; it was a freestanding site, partiallyaffiliated with a university, with an expected volume of 90 patients with stroke/year. Thus, data from nine and eight sites in the facilitated and passive group, respectively, were analyzed. The CONSORT diagram indicates the number of unique providers and patients involved in this process evaluation, and the number of checklists submitted by providers pre- and post-intervention by study group. Table 1 describes characteristics of sites that provided process data. Just over half of the sites in the facilitated and passive groups had no academic affiliation and were freestanding rehabilitation hospitals. The expected number of patients with stroke admitted per year for sites in the facilitated and passive groups was, on average, 95 and 105, respectively. Table 2 describes characteristics of the patients for whom treatment implementation checklists were completed by intervention group and sampling time point. The median age of patients ranged from 62 to 73 years (depending on group, timepoint, and received treatments), with the majority being men (52 69%), ischemic stroke (64 76%), with some arm (CMSA median 2 3) and leg impairment (CMSA median 3). Charlson comorbidity score and the proportion of patients with ischemic stroke were significantly higher in the passive group pre-intervention and postintervention, respectively. Additional file 1: Table S1 describes checklist completion by provider group (see Additional file 1). Nurses contributed the greatest percentage of checklists in the Table 2 Patient characteristics on site admission by intervention group and sampling time point Characteristic 7 Treatments Implemented by RNs, OTs, and PTs 11 Treatments implemented by OTs, and PTs (score range/units) Facilitated group Passive group Facilitated group Passive group Pre * Post * Pre * Post * Pre * Post * Pre * Post * Patients, n Age in years 62 (57 77) 68 (60 78) 71 (62 79) 72 (65 79) 64 (57 77) 68 (60 78) 73 (62 79) 72 (64 79) Men, n (%) 34 (69) 26 (65) 16 (52) 25 (57) 27 (68) 26 (65) 15 (54) 22 (55) Type of stroke, n (%) Ischemic 37 (76) 25 (64) 20 (67) 30 (68) 30 (75) 25 (64) 19 (70) 26 (65) Hemorrhagic 8 (16) 12 (31) 6 (20) 5 (11) 6 (15) 12 (31) 6 (22) 5 (13) Unspecified 4 (8) 2 (5) 4 (13) 9 (20) 4 (10) 2 (5) 2 (7) 9 (23) Side of stroke, n (%) Right 25 (51) 25 (63) 14 (45) 20 (45) 20 (50) 25 (63) 13 (46) 18 (45) Left 22 (45) 14 (35) 15 (48) 23 (52) 19 (48) 14 (35) 13 (46) 21 (53) Brainstem 2 (4) 1 (3) 2 (6) 1 (2) 1 (3) 1 (3) 2 (7) 1 (3) Days post-stroke on admission 20 (13 28) 15 (9 26) 23 (11 41) 16 (10 34) 20 (13 28) 15 (9 26) 24 (11 44) 15 (10 29) Charlson Index (0 33) 2 (1 3) 2(1 3) 3 (2 4) 3(2 4) 2 (1 3) 2(1 3) 3 (2 4) 3(1 4) CMSA Arm (1 7) 2 (1 3) 3 (2 5) 2 (2 4) 2 (2 5) 2 (1 4) 3 (2 5) 2 (2 4) 2 (2 5) CMSA Leg (1 7) 3 (3 4) 3 (3 5) 3 (2 4) 3 (3 4) 3 (3 5) 3 (3 5) 3 (3 4) 3 (3 4) FIM motor (1 91) 33 (24 54) 46 (36 59) 35 (24 57) 48 (35 59) 32 (22 56) 46 (36 59) 41 (25 58) 49 (35 61) Abbreviations: CMSA Chedoke McMaster Stroke Assessment [30], FIM functional independence measure [32] * Values are median (P 25 -P 75 ) unless otherwise specified Data from 1 to 2 patients/analysis missing Between-group difference, p < Between-group difference, p < Data from 13 to 17 patients/analysis missing
7 Salbach et al. Implementation Science (2017) 12:100 Page 7 of 11 Table 3 Unadjusted intervention effect on change in implementation of 18 treatments Treatment Time Estimated % of times implemented (95% CI) Effect n Facilitated (F) group n Passive (P) group (Change F -Change P ) % (95% CI) 1. Sit-to-stand * Pre (17.3, 23.5) (29.5, 43.1) Post (33.4, 44.9) (27.9, 39.3) Change 18.7 (12.2, 25.3) 2.7 ( 11.5, 6.2) 21.4 (10.4, 32.4) 2. LE ROM and/or stretching (i.e. to Pre (10.1, 21.7) (3.4, 13.5) prevent spasticity and contractures) Post (5.5, 15.5) (11.3, 24.2) Change 5.4 ( 13.1, 2.3) 9.3 (1.1, 17.5) 14.7 ( 26.0, 3.5) 3. Use of LE external support (i.e. brace) Pre (5.3, 9.3) (10.0, 20.1) Post (5.4, 12.0) (12.8, 21.9) Change 1.4 ( 2.5, 5.3) 2.3 ( 4.5, 9.1) 0.9 ( 8.7, 6.9) 4. Task-specific training (i.e. stairs) * Pre (24.3, 39.2) (18.3, 34.2) Post (30.5, 46.5) (29.6, 46.0) Change 6.7 ( 4.3, 17.6) 11.5 (0.1, 22.9) 4.8 ( 20.6, 11.0) 5. Training for sitting balance * Pre (17.0, 30.7) (10.2, 23.7) Post (11.2, 23.7) (17.9, 32.5) Change 6.4 ( 15.6, 2.9) 8.2 ( 1.8, 18.2) 14.6 ( 28.2, 1.0) 6. Training for standing balance Pre (43.7, 59.6) (27.7, 45.1) Post (44.2, 60.7) (51.7, 68.3) Change 0.8 ( 10.7, 12.2) 23.6 (11.6, 35.6) 22.8 ( 39.4, 6.2) 7. FES for the LE Pre ( 0.6, 2.0) (0, 0) Post ( 0.7, 2.1) ( 0.7, 2.2) Change 0 ( 1.9, 1.9) 0.7 ( 0.7, 2.2) 0.7 ( 3.1, 1.7) 8. Walking practice Pre (13.1, 18.7) (25.0, 38.2) Post (33.4, 44.9) (27.2, 38.5) Change 23.2 (16.8, 29.6) 1.2 ( 7.4, 9.9) 22.0 (11.2, 32.8) 9. Treadmill walking practice Pre (0.1, 5.2) (2.2, 11.3) Post ( 0.5, 3.3) (1.4, 8.9) Change 1.3 ( 4.5, 2.0) 1.6 ( 7.5, 4.3) 0.3 ( ) 10. UE ROM and/or stretching (i.e. to Pre (10.1, 15.2) (15.9, 27.6) prevent spasticity and contractures) * Post (16.5, 26.2) (20.1, 30.5) Change 8.7 (3.2, 14.2) 3.5 ( 4.3, 11.4) 5.2 ( 4.4, 14.7) 11. Interventions to prevent shoulder Pre (21.7, 28.4) (19.2, 31.5) pain (i.e. sling) * Post (20.6, 30.9) (16.2, 26.1) Change 0.7 ( 5.5, 6.8) 4.3 ( 12.1, 3.6) 4.9 ( 5.1, 14.9) 12. Task-specific training (i.e. self-care Pre (25.4, 32.4) (30.5, 44.1) tasks) * Post (35.1, 46.8) (37.4, 49.4) Change 12.0 (5.3, 18.8) 6.1 ( 3.0, 15.2) 6.0 ( 5.4, 17.3) 13. Techniques to reduce hand edema * Pre (3.1, 11.4) (4.7, 15.6) Post (1.8, 9.4) (4.1, 13.7) Change 1.7 ( 7.3, 3.9) 1.3 ( 8.6, 6.0) 0 ( 9.6, 8.8) 14. Ice/heat or soft tissue massage Pre ( 0.5, 3.2) (3.4, 13.5) for shoulder Post (0.1, 5.5) (1.4, 8.9) Change 1.5 ( 1.8, 4.7) 3.3 ( 9.6, 3.0) 4.8 ( 2.3, 11.8)
8 Salbach et al. Implementation Science (2017) 12:100 Page 8 of 11 Table 3 Unadjusted intervention effect on change in implementation of 18 treatments (Continued) 15. FES for wrist/arm/shoulder * Pre ( 0.2, 4.2) ( 0.3, 5.4) Post ( 0.5, 3.3) ( 0.6, 3.5) Change 0.6 ( 3.5, 2.4) 1.1 ( 4.6, 2.4) 0.5 ( 4.1, 5.1) 16. Educate patient or caregiver on Pre (6.6, 11.0) (8.2, 17.7) how to handle arm or shoulder * Post (6.0, 12.9) (6.5, 13.8) Change 0.6 ( 3.5, 4.7) 2.8 ( 8.8, 3.2) 3.4 ( 3.9, 10.6) 17. UE constraint-induced therapy Pre (1.3, 8.0) (4.7, 15.6) Post ( 0.7, 2.1) (1.0, 7.9) Change 3.9 ( 7.6, 0.3) 5.7 ( 12.2, 0.8) 1.8 ( 5.6, 9.2) 18. Visual imagery to enhance Pre (0.1, 5.2) (1.1, 9.1) arm recovery Post (2.3, 10.3) (1.4, 8.9) Change 3.6 ( 1.1, 8.4) 0.1 ( 5.4, 5.6) 3.5 ( 3.7, 10.8) Abbreviations: n number of observations, CI confidence interval, LE lower extremity, ROM range of motion, FES functional electrical stimulation, UE upper extremity Italic text indicates statistically significant results * Demonstration and opportunity to practice during change management workshop Clinical protocol provided in SCORE guideline Clustering effect at provider level Clustering effect at patient level No longer significant after adjusting for clustering at the provider and patient level facilitated KT group (50 and 42%, pre- and post-intervention, respectively) and in the passive KT group (39 and 49%, pre- and post-intervention, respectively) for treatments that RNs, OTs, and PTs were asked to apply. Additional file 1: Table S2 provides the ICC value for the effect of clustering on treatment implementation at the site, provider and patient level for each of the 18 treatments. A significant effect of clustering on treatment implementation was observed at the site, provider and patient level in 0, 67, and 39% of models, respectively. The median ICC across treatments for sites, providers and patients was 0.06, 0.21, and 0.08, respectively. Additional file 1: Table S3 presents mean cluster sizes in terms of the number of providers per site, number of patients per provider, and number of checklist forms per patient pre- and post-intervention by study group (see Additional file 1). Cluster sizes at the site level indicated that the average number of providers contributing data to the analysis across groups and timepoints ranged from 10 to 15 for 7 treatments implemented by RNs, OTs, and PTs and from 5 to 7 for 11 treatments implemented by OTs and PTs. The average number of patients per provider contributing data to the analysis across groups, timepoints, and treatments ranged from 2 to 3. The average number of checklists completed per patient in the analysis across groups and timepoints ranged from 6 to 13 for 7 treatments implemented by RNs, OTs, and PTs and from 3 to 4 for 11 treatments implemented by OTs and PTs. Outcomes Table 3 presents unadjusted estimates of the percentage of patients receiving each treatment pre- and postintervention, the change in the percentage, and the between-group comparison. Seven of the 18 treatments, including training of sit-to-stand, sitting balance, and standing balance, task-specific training (i.e., stairs), walking practice, interventions to prevent shoulder pain, and task-specific training (i.e., self-care tasks), were being implemented at least 15% of the time in both groups at baseline. After adjusting for clustering at patient and provider levels and covariates, the facilitated KT intervention was associated with a significant improvement in the implementation of sit-to-stand training (p = 0.028) and walking practice (p = 0.043), and the passive KT intervention was associated with improved implementation of standing balance training (p = 0.037). Adjustment for the stratification variable did not change the interpretation of the results. Further analysis of which provider groups changed their practice (see Additional file 1: Table S4) revealed that the unadjusted percentage of patients receiving sit-tostand training was higher post- compared to preintervention for nurses (30 vs 10%), and PTs (67 vs 49%) in the facilitated group, and for PTs (58 vs 39%) in the passive group. The unadjusted percentage of patients receiving walking practice was higher post- compared to pre-intervention for nurses (14 vs 6%), OTs (37 vs 21%) and PTs (80 vs 70%) in the facilitated group, and for nurses (14 vs 11%), OTs (25 vs 14%) and PTs (76 vs 68%) in the passive group. The unadjusted percentage of patients receiving standing balance training was higher post- compared to pre-intervention for OTs (36 vs 34%) in the facilitated group, and OTs (38 vs 27%), and PTs (82 vs 45%) in the passive group.
9 Salbach et al. Implementation Science (2017) 12:100 Page 9 of 11 Discussion This is among the first process evaluations of a guideline implementation trial involving the use of interprofessional local facilitators in rehabilitation. Findings indicate that a facilitated KT intervention, with local nurse and therapist facilitators, tailoring of strategies to address local barriers, and a guideline with treatment protocols, was of limited effectiveness compared to passive guideline dissemination in improving short-term uptake of a comprehensive guideline by inpatient stroke rehabilitation teams. The process evaluation revealed that the facilitated KT intervention was associated with improved application of only two treatments (sit-to-stand training, walking practice), whereas the passive KT intervention was associated with improved application of one treatment (standing balance training). Results from this process evaluation suggest that superior functional walking capacity observed among patients post-stroke following the facilitated compared to the passive KT intervention (Bayley MT, Wood-Dauphinee S, Richards CL, Salbach NM, Desrosiers J, Eng JJ, et al.: Facilitated knowledge translation improves stroke rehabilitation outcomes: The SCORE-IT cluster randomized controlled trial, under review) resulted from an improved application of sit-to-stand and walking training by stroke teams. Process evaluation findings also indicate that the facilitated KT intervention was not associated with improved gross manual dexterity among patients because this intervention was not associated with improved uptake of treatments targeting UE function. Results from the current evaluation combined with findings from the qualitative process evaluation of SCORE-IT [27] may help to explain why sit-to-stand and walking practice were more likely than other treatments to be adopted in the facilitated KT group. Facilitation, specifically support and motivation that individuals provided to staff at sites in each group, was perceived to promote the implementation of the recommended treatments [27]. It is possible that facilitation of sit-to-stand and walking training was provided more consistently across sites in the facilitated KT group than in the passive KT group. Results of the qualitative analysis also showed that both familiarity and agreement with recommended treatments because they are clear and practical to follow [34, 35] likely helped to promote their uptake [27]. Sit-to-stand and walking training were implemented in at least 15% of patients in each group at baseline (unadjusted estimates) which suggests that some providers had the expertise to perform these treatments and considered them relevant. Sit-to-stand and walking training are also simple, taskoriented mobility treatments that are relevant to daily living. Complex treatments that either involve multiple steps (UE constraint-induced therapy) or technology (functional electrical stimulation, treadmill training) were rarely implemented at baseline and demonstrated either no change or reduced application post-intervention despite being supported by Level A evidence (i.e., evidence from at least one randomized controlled trial, meta-analysis, or systematic review). Based on the SCORE-IT qualitative findings, this was likely because health professionals found that these treatments were time-consuming, and required special training or equipment that was not consistently available across sites [27]. Finally, asking nurses to apply sit-to-stand and walking training, in addition to therapists, appeared an effective facilitated KT strategy as the percentage of patients receiving sit-to-stand and walking practice by nurses increased by 20% (vs a decrease of 11% in the control group) and 8% (vs 3% in the control group), respectively. Improved team communication and interprofessional collaboration were noted as an unintended outcome of SCORE-IT [27]. The improved practice of nurses, likely supported by the nurse facilitator in the facilitated KT group, was particularly influential in the current study as nurses provided a large proportion of the treatment data in the multivariable analysis. Standing balance training, which increased in the passive KT group, is also a simple task-oriented treatment. Because providers receiving facilitated KT were implementing standing balance training at a high rate at baseline (68% for PTs), they may have prioritized improving adoption of other treatments [13]. Results from the qualitative sub-study [27] indicate that a greater degree of facilitation of and/or agreement with the practicality of standing balance training in the passive compared to the facilitated group, may help to explain why this practice improved in the context of passive dissemination of the stroke rehabilitation guideline. Despite multiple strategies and resources, the facilitated KT intervention was unsuccessful in improving integration of 18 treatments concurrently. The facilitated approach may not have adequately addressed barriers to integrating numerous treatments simultaneously and complex treatments that were unfamiliar to providers. Targeting fewer treatments and providing individual hands-on training and access to an expert may be a more effective approach based on results from previous guideline implementation trials for low back pain [24] and whiplash [26] rehabilitation. Limitations The primary limitation of this process evaluation was the use of self-report measures of practice that cannot capture clinical judgment or patient preferences and are vulnerable to over-reporting. This limitation, however, would have affected both groups similarly. It could not be determined if treatments received were appropriate due to the unavailability of clinical data at the time implementation was evaluated. Results provide average rates of implementation after controlling for patient and hospital characteristics to optimize comparability between groups.
10 Salbach et al. Implementation Science (2017) 12:100 Page 10 of 11 Conclusions A facilitated KT intervention incorporating a guideline with treatment protocols and trained local nurse and therapist facilitators was of limited effectiveness compared to passive guideline dissemination in improving short-term uptake of a comprehensive guideline by inpatient stroke rehabilitation teams. Conducting this process evaluation as part of the trial was valuable as it revealed the nature of the practice change, in terms of the type of health providers involved and the type of and extent to which treatments were implemented, underpinning patient function outcomes observed in the main analysis. The combination of quantitative and qualitative process evaluation findings provided a basis for hypothesis generation related to designing KT interventions to overcome challenges to integrating treatments recommended in stroke rehabilitation guidelines in the context of interdisciplinary team care. Specifically, KT strategies that better address the need for staff training and team functioning to account for treatment complexity and prioritization post-stroke may be needed. Finally, the study design and analytical approach described in the current study, which involved consideration of multi-level clustering effects, and adjustment for site- and patient-level covariates, is innovative and will help to advance the field of implementation science in the context of rehabilitation guideline implementation. Additional file Additional file 1: Table S1. Checklist completion by provider group. Table S2. Intracluster correlation coefficients for the 18 recommended treatments. Table S3. Cluster sizes at the site, provider and patient level by study group and sampling time point. Table S4. Unadjusted rate of treatment implementation by healthcare professional and group pre- and post-intervention. (DOCX 21 kb) Abbreviations CI: Confidence Interval; CMSA: Chedoke McMaster Stroke Assessment; CONSORT: Consolidated Standards of Reporting Trials; FES: Functional Electrical Stimulation; FIM: Functional Independence Measure; ICC: Intracluster Correlation Coefficient; KT: Knowledge Translation; KTA: Knowledge to Action; LE: Lower Extremity; OR: Odds Ratio; OT: Occupational Therapist; PARiHS: Promoting Action on Research Implementation; PT: Physical Therapist; RA: Research Assistant; RN: Registered Nurse; ROM: Range of Motion; SCORE-IT: Stroke Canada Optimization of Rehabilitation by Evidence-Implementation Trial; UE: Upper Extremity Acknowledgements IDG is a recipient of a Canadian Institutes of Health Research Foundation Grant (FDN #143237). Funding A grant from the Canadian Stroke Network was used to fund the conduct of the study. The Toronto Rehabilitation Institute-University Health Network provided funding to support the analysis presented here. NMS was supported by Ontario Ministry of Research and Innovation Early Researcher and Canadian Institutes of Health Research New Investigator Awards to conduct this research. Availability of data and materials The datasets generated during and/or analyzed during the current study are not publicly available as participant consent and institutional approval for this activity were not obtained. Authors contributions MB, SWD, and IDG designed the study with input from the other co-authors. NMS planned the data analysis, and analyzed and interpreted the data regarding providers implementation of 18 treatments recommended in the stroke rehabilitation guideline and drafted the manuscript. All authors read and approved the final manuscript. Ethics approval and consent to participate The ethics board at each site and affiliated university approved the study protocol. Consent was obtained from site managers/physiatrists, and all therapists and nurses working on each stroke rehabilitation unit. Consent for publication Not applicable. Competing interests The authors declare that they have no competing interests. Publisher s Note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations. Author details 1 Department of Physical Therapy, University of Toronto, University Ave, Toronto, ON M5G 1V7, Canada. 2 School of Physical and Occupational Therapy, McGill University, 3630 Promenade Sir William Osler, Montreal, QC H3G 1Y5, Canada. 3 Faculty of Medicine and Health Sciences, Université de Sherbrooke, 3001, 12e avenue nord, Bureau FM-2208, Sherbrooke, QC J1H 5N4, Canada. 4 University of British Columbia, Wesbrook Mall, Vancouver, BC V6T 1Z3, Canada. 5 School of Epidemiology and Public Health, University of Ottawa, 600 Peter Morand Cres, Ottawa K1G 5Z3, Canada. 6 School of Physiotherapy, Dalhousie University, Office 405 Forrest Building, 5869 University Avenue, PO Box 15000, Halifax, NS B3H 4R2, Canada. 7 Division of Clinical Epidemiology, Division of Geriatrics, McGill University Health Center, Royal Victoria Hospital Site, Ross Pavilion R4.29, 687 Pine Ave W, Montreal, QC H3A 1A1, Canada. 8 Department of Rehabilitation, Faculty of Medicine, Université Laval and Centre de recherche en réadaptation et intégration sociale (CIRRIS), Institut de réadaptation en déficience physique de Québec (IRDPQ) Site Hamel, 525 Boul. Wilfrid-Hamel Est, Québec, QC G1M 2S8, Canada. 9 Parkwood Institute, 550 Wellington Road, London, ON N6C 0A7, Canada. 10 Schulich School of Medicine and Dentistry, Western University, Western Centre for Public Health and Family Medicine, 1151 Richmond St, London, ON N6A 3K7, Canada. 11 Toronto Rehabilitation Institute-University Health Network, 550 University Avenue, room (3-East) 3rd Floor University Wing, Toronto, ON M5G 2A2, Canada. Received: 31 October 2016 Accepted: 24 July 2017 References 1. Mayo NE, Wood-Dauphinee S, Cote R, Durcan L, Carlton J. Activity, participation, and quality of life 6 months poststroke. Arch Phys Med Rehabil. 2002;83: Krueger H, Koot J, Hall RE, O Callaghan C, Bayley M, Corbett D. Prevalence of individuals experiencing the effects of stroke in Canada: trends and projections. Stroke. 2015;46: Hebert D, Lindsay MP, McIntyre A, Kirton A, Rumney PG, Bagg S, et al. Canadian stroke best practice recommendations: stroke rehabilitation practice guidelines, update Int J Stroke. 2016;11: National Stroke Foundation. Clinical guidelines for stroke management Management Accessed 29 July Winstein CJ, Stein J, Arena R, Bates B, Cherney LR, Cramer SC, et al. Guidelines for adult stroke rehabilitation and recovery: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke. 2016;47(6):e98 e169.
11 Salbach et al. Implementation Science (2017) 12:100 Page 11 of Duncan PW, Horner RD, Reker DM, Samsa GP, Hoenig H, Hamilton B, et al. Adherence to postacute rehabilitation guidelines is associated with functional recovery in stroke. Stroke. 2002;33: Reker DM, Duncan PW, Horner BD, Hoenig H, Samsa GP, Hamilton BB, et al. Postacute stroke guideline compliance is associated with greater patient satisfaction. Arch Phys Med Rehabil. 2002;83: Menon-Nair A, Korner-Bitensky N, Ogourtsova T. Occupational therapists identification, assessment, and treatment of unilateral spatial neglect during stroke rehabilitation in Canada. Stroke. 2007;38: Salbach NM, Guilcher SJ, Jaglal SB. Physical therapists perceptions and use of standardized assessments of walking ability post-stroke. J Rehabil Med. 2011;43: Doyle L, MacKay-Lyons M. Utilization of aerobic exercise in adult neurological rehabilitation by physical therapists in Canada. J Neurol Phys Ther. 2013;37: Pollock A, Hazelton C, Brady M. Visual problems after stroke: a survey of current practice by occupational therapists working in UK stroke inpatient settings. Top Stroke Rehabil. 2011;18(Suppl 1): Graham ID, Logan J, Harrison MB, Straus SE, Tetroe J, Caswell W, et al. Lost in knowledge translation: time for a map? J Contin Educ Heal Prof. 2006;26: Bayley MT, Hurdowar A, Richards CL, Korner-Bitensky N, Wood-Dauphinee S, Eng JJ, et al. Barriers to implementation of stroke rehabilitation evidence: findings from a multi-site pilot project. Disabil Rehabil. 2012;34: Donnellan C, Sweetman S, Shelley E. Implementing clinical guidelines in stroke: a qualitative study of perceived facilitators and barriers. Health Policy. 2013;111: Evidence-Based Review of Stroke Rehabilitation. Heart & Stroke Foundation of Canada Accessed 29 July Stroke Engine. Heart & Stroke Foundation of Canada strokengine.ca/. Accessed 29 July Adey-Wakeling Z, Arima H, Crotty M, Leyden J, Kleinig T, Anderson CS, et al. Incidence and associations of hemiplegic shoulder pain poststroke: prospective population-based study. Arch Phys Med Rehabil. 2015;96: Pattison KM, Brooks D, Cameron JI, Salbach NM. Factors influencing physical therapists use of standardized measures of walking capacity poststroke across the care continuum. Phys Ther. 2015;95: Harvey G, Loftus-Hills A, Rycroft-Malone J, Titchen A, Kitson A, McCormack B, et al. Getting evidence into practice: the role and function of facilitation. J Adv Nurs. 2002;37: Kitson A, Harvey G, McCormack B. Enabling the implementation of evidence based practice: a conceptual framework. Qual Health Care. 1998;7: Rycroft-Malone J, Kitson A, Harvey G, McCormack B, Seers K, Titchen A, et al. Ingredients for change: revisiting a conceptual framework. Qual Saf Health Care. 2002;11: Kitson AL, Rycroft-Malone J, Harvey G, McCormack B, Seers K, Titchen A. Evaluating the successful implementation of evidence into practice using the PARiHS framework: theoretical and practical challenges. Implement Sci. 2008;3: Dogherty EJ, Harrison MB, Graham ID. Facilitation as a role and process in achieving evidence-based practice in nursing: a focused review of concept and meaning. Worldviews Evid-Based Nurs. 2010;7: Bekkering GE, Hendriks HJ, van Tulder MW, Knol DL, Hoeijenbos M, Oostendorp RA, et al. Effect on the process of care of an active strategy to implement clinical guidelines on physiotherapy for low back pain: a cluster randomised controlled trial. Qual Saf Health Care. 2005;14: Pennington L, Roddam H, Burton C, Russell I, Godfrey C, Russell D. Promoting research use in speech and language therapy: a cluster randomized controlled trial to compare the clinical effectiveness and costs of two training strategies. Clin Rehabil. 2005;19: Rebbeck T, Maher CG, Refshauge KM. Evaluating two implementation strategies for whiplash guidelines in physiotherapy: a cluster randomised trial. Aust J Physiother. 2006;52: Munce SEP, Graham ID, Salbach NM, Jaglal SB, Richards CL, Eng JJ, et al. Perspectives of health care professionals on the facilitators and barriers to the implementation of a stroke rehabilitation guidelines cluster randomized controlled trial. BMC Health Serv Res. 2017;17: Last JM. A dictionary of epidemiology. 3rd ed. New York: Oxford University Press; Registered Nurses' Association of Ontario: Toolkit: Implementation of best practice guidelines. 2nd ed ToolKit_2012_rev4_FA.pdf. Accessed 29 July Finch E, Brooks D, Stratford P, Mayo N. Physical rehabilitation outcome measures. Lippincott, Williams & Wilkins: Baltimore; Campbell MJ, Donner A, Klar N. Developments in cluster randomized trials and statistics in medicine. Statist Med. 2007;26: Granger CV, Hamilton BB, Linacre JM, Heinemann AW, Wright BD. Performance profiles of the functional independence measure. Am J Phys Med Rehabil. 1993;72: Tessier A, Finch L, Daskalopoulou SS, Mayo NE. Validation of the Charlson Comorbidity index for predicting functional outcome of stroke. Arch Phys Med Rehabil. 2008;89: Legare F, Ratte S, Gravel K, Graham ID. Barriers and facilitators to implementing shared decision-making in clinical practice: update of a systematic review of health professionals perceptions. Patient Educ Couns. 2008;73: Legare F, O Connor AM, Graham ID, Saucier D, Cote L, Blais J, et al. Primary health care professionals views on barriers and facilitators to the implementation of the Ottawa decision support framework in practice. Patient Educ Couns. 2006;63: Submit your next manuscript to BioMed Central and we will help you at every step: We accept pre-submission inquiries Our selector tool helps you to find the most relevant journal We provide round the clock customer support Convenient online submission Thorough peer review Inclusion in PubMed and all major indexing services Maximum visibility for your research Submit your manuscript at
Management of the Hemiplegic Arm: Implementing a Best Practice Protocol
 Background Information Appendix J Management of the Hemiplegic Arm: Implementing a Best Practice Protocol Dalia Abromaitis, OT Reg (Ont) Jennifer Curry, PT www.swostroke.ca Objectives Provide tools for
Background Information Appendix J Management of the Hemiplegic Arm: Implementing a Best Practice Protocol Dalia Abromaitis, OT Reg (Ont) Jennifer Curry, PT www.swostroke.ca Objectives Provide tools for
Champlain Assessment/Outcome Measures Forum February 22, 2010
 Champlain Assessment/Outcome Measures Forum February 22, 2010 Welcome Table Configurations Each table has a card with the name of the discipline(s) and the mix of professions Select the discipline of interest
Champlain Assessment/Outcome Measures Forum February 22, 2010 Welcome Table Configurations Each table has a card with the name of the discipline(s) and the mix of professions Select the discipline of interest
Downloaded from:
 Arnup, SJ; Forbes, AB; Kahan, BC; Morgan, KE; McKenzie, JE (2016) The quality of reporting in cluster randomised crossover trials: proposal for reporting items and an assessment of reporting quality. Trials,
Arnup, SJ; Forbes, AB; Kahan, BC; Morgan, KE; McKenzie, JE (2016) The quality of reporting in cluster randomised crossover trials: proposal for reporting items and an assessment of reporting quality. Trials,
Evaluation of a Knowledge Translation Strategy for Promoting Uptake of a Webbased Guide to HIV Rehabilitation
 International Forum on HIV and Rehabilitation Research Li Ka Shing Knowledge Institute, Toronto, Canada June 13-14, 2013 Evaluation of a Knowledge Translation Strategy for Promoting Uptake of a Webbased
International Forum on HIV and Rehabilitation Research Li Ka Shing Knowledge Institute, Toronto, Canada June 13-14, 2013 Evaluation of a Knowledge Translation Strategy for Promoting Uptake of a Webbased
From Good to Great OBJECTIVES. AOTA Centennial Vision Statement 10/14/2012
 From Good to Great Implementing evidence-based treatment and standardized outcome measures in in-patient rehabilitation LaMar Bolden, OTR, DPS Presented 10/28/2012 NJOTA conference OBJECTIVES Describe
From Good to Great Implementing evidence-based treatment and standardized outcome measures in in-patient rehabilitation LaMar Bolden, OTR, DPS Presented 10/28/2012 NJOTA conference OBJECTIVES Describe
10/12/2017. Disclaimers SELECTING STANDARDIZED OUTCOME MEASURES IN THE NEUROLOGICAL PATIENT POPULATION: PROCESS, BARRIERS AND APPLICATION
 SELECTING STANDARDIZED OUTCOME MEASURES IN THE NEUROLOGICAL PATIENT POPULATION: PROCESS, BARRIERS AND APPLICATION Stacia Britton, PT, DPT, NCS, CEEAA 2017 NCPTA Fall Conference Winston-Salem, North Carolina
SELECTING STANDARDIZED OUTCOME MEASURES IN THE NEUROLOGICAL PATIENT POPULATION: PROCESS, BARRIERS AND APPLICATION Stacia Britton, PT, DPT, NCS, CEEAA 2017 NCPTA Fall Conference Winston-Salem, North Carolina
USING WEB-BASED PRACTICE TO MAINTAIN DYSPHAGIA SCREENING SKILLS
 USING WEB-BASED PRACTICE TO MAINTAIN DYSPHAGIA SCREENING SKILLS TOR- BSST Rosemary Martino, PhD Associate Professor, Associate Chair Department of Speech-Language Pathology University of Toronto Lori Herlihy-O
USING WEB-BASED PRACTICE TO MAINTAIN DYSPHAGIA SCREENING SKILLS TOR- BSST Rosemary Martino, PhD Associate Professor, Associate Chair Department of Speech-Language Pathology University of Toronto Lori Herlihy-O
Anita Petzold, MSc 1,2, Nicol Korner-Bitensky, PhD 1,2, Nancy M. Salbach, PhD 3, Sara Ahmed, PhD 1,2, Anita Menon, MSc and Tatiana Ogourtsova, MSc 5
 J Rehabil Med 2012; 44: 118 124 ORIGINAL REPORT Increasing knowledge of best practices FOR occupational therapists treating post-stroke unilateral spatial neglect: results of a knowledge-translation intervention
J Rehabil Med 2012; 44: 118 124 ORIGINAL REPORT Increasing knowledge of best practices FOR occupational therapists treating post-stroke unilateral spatial neglect: results of a knowledge-translation intervention
Perception and use of gait measures among physical therapists in South Korea
 Original Article https://doi.org/10.14474/ptrs.2017.6.2.90 pissn 2287-7576 eissn 2287-7584 Phys Ther Rehabil Sci 2017, 6 (2), 90-95 www.jptrs.org Perception and use of gait measures among physical therapists
Original Article https://doi.org/10.14474/ptrs.2017.6.2.90 pissn 2287-7576 eissn 2287-7584 Phys Ther Rehabil Sci 2017, 6 (2), 90-95 www.jptrs.org Perception and use of gait measures among physical therapists
Measuring the Outcomes of Stroke Rehabilitation Results of a Canadian Stroke Strategy/Heart and Stroke Foundation National Consensus Panel
 Measuring the Outcomes of Stroke Rehabilitation Results of a Canadian Stroke Strategy/Heart and Stroke Foundation National Consensus Panel Objectives By the end of this presentation should be able to:
Measuring the Outcomes of Stroke Rehabilitation Results of a Canadian Stroke Strategy/Heart and Stroke Foundation National Consensus Panel Objectives By the end of this presentation should be able to:
Neurologic Upper Extremity: Function and Management
 Neurologic Upper Extremity: Function and Management A cademy Rehabilitation Institute of Chicago has been ranked Best Rehabilitation Hospital in America" every year since 1991 by U.S. News & World Report.
Neurologic Upper Extremity: Function and Management A cademy Rehabilitation Institute of Chicago has been ranked Best Rehabilitation Hospital in America" every year since 1991 by U.S. News & World Report.
Functional Independent Recovery among Stroke Patients at King Hussein Medical Center
 Functional Independent Recovery among Stroke Patients at King Hussein Medical Center Ali Al-Hadeed MD*, Amjad Banihani MD**, Tareq Al-Marabha MD* ABSTRACT Objective: To describe the functional independent
Functional Independent Recovery among Stroke Patients at King Hussein Medical Center Ali Al-Hadeed MD*, Amjad Banihani MD**, Tareq Al-Marabha MD* ABSTRACT Objective: To describe the functional independent
10/13/2017. The K2A Cycle. Focused Intensive Repetitive Step Training (FIRST)
 Walking the Walk: Translation of Scientific Findings into Clinical Practice September 14 and 15, 2017 State of the Science Chicago, IL T. George Hornby PT, PhD Jennifer Moore PT, DHSc, NCS The K2A Cycle
Walking the Walk: Translation of Scientific Findings into Clinical Practice September 14 and 15, 2017 State of the Science Chicago, IL T. George Hornby PT, PhD Jennifer Moore PT, DHSc, NCS The K2A Cycle
12/9/18. Implementing Meaningful Projects to Enhance EBP in your Clinic. Objectives. Overview
 Implementing Meaningful Projects to Enhance EBP in your Clinic Wendy Romney, PT, DPT, PhD, NCS Jenni Moore, PT, DHS, NCS Julie Tilson, PT, DPT, MS Susan Perry, PT, DPT Judith E Deutsch, PT, PhD, FAPTA
Implementing Meaningful Projects to Enhance EBP in your Clinic Wendy Romney, PT, DPT, PhD, NCS Jenni Moore, PT, DHS, NCS Julie Tilson, PT, DPT, MS Susan Perry, PT, DPT Judith E Deutsch, PT, PhD, FAPTA
CRITICALLY APPRAISED PAPER (CAP)
 CRITICALLY APPRAISED PAPER (CAP) FOCUSED QUESTION For patients with acute cerebral vascular accident, is virtual reality gaming more effective than standard recreational therapy for the improvement of
CRITICALLY APPRAISED PAPER (CAP) FOCUSED QUESTION For patients with acute cerebral vascular accident, is virtual reality gaming more effective than standard recreational therapy for the improvement of
Clinical audit for occupational therapy intervention for children with autism spectrum disorder: sampling steps and sample size calculation
 DOI 10.1186/s13104-015-1247-0 CORRESPONDENCE Open Access Clinical audit for occupational therapy intervention for children with autism spectrum disorder: sampling steps and sample size calculation Scott
DOI 10.1186/s13104-015-1247-0 CORRESPONDENCE Open Access Clinical audit for occupational therapy intervention for children with autism spectrum disorder: sampling steps and sample size calculation Scott
Physiotherapists in Canada, 2011 National and Jurisdictional Highlights
 pic pic pic Physiotherapists in Canada, 2011 National and Jurisdictional Highlights Spending and Health Workforce Our Vision Better data. Better decisions. Healthier Canadians. Our Mandate To lead the
pic pic pic Physiotherapists in Canada, 2011 National and Jurisdictional Highlights Spending and Health Workforce Our Vision Better data. Better decisions. Healthier Canadians. Our Mandate To lead the
A Clinician s Perspective of the ViaTherapy App for Upper Extremity Stroke Rehabilitation
 A Clinician s Perspective of the ViaTherapy App for Upper Extremity Stroke Rehabilitation Anik Laneville, OT Reg. (Ont.) Best Practice Occupational Therapist CRSN Dana Guest BSc. PT Best Practice Physiotherapist
A Clinician s Perspective of the ViaTherapy App for Upper Extremity Stroke Rehabilitation Anik Laneville, OT Reg. (Ont.) Best Practice Occupational Therapist CRSN Dana Guest BSc. PT Best Practice Physiotherapist
Whither knowledge translation: An international research agenda
 Whither knowledge translation 1 Whither knowledge translation: An international research agenda Ian D Graham a, Jacqueline Tetroe b a Vice President Knowledge Translation Canadian Institutes of Health
Whither knowledge translation 1 Whither knowledge translation: An international research agenda Ian D Graham a, Jacqueline Tetroe b a Vice President Knowledge Translation Canadian Institutes of Health
Stroke Rehab Definitions Framework Self-Assessment Tool Acute Integrated Stroke Unit
 rth & East GTA Stroke Network Stroke Rehab Definitions Framework Self-Assessment Tool Acute Integrated Stroke Unit Purpose of the Self-Assessment Tool: The GTA Rehab Network and the GTA regions of the
rth & East GTA Stroke Network Stroke Rehab Definitions Framework Self-Assessment Tool Acute Integrated Stroke Unit Purpose of the Self-Assessment Tool: The GTA Rehab Network and the GTA regions of the
SPINAL CORD INJURY Rehab Definitions Framework Self-Assessment Tool inpatient rehab Survey for Spinal Cord Injury (SCI)
 SPINAL CORD INJURY Rehab s Framework Self-Assessment Tool inpatient rehab Survey for Spinal Cord Injury (SCI) INTRODUCTION: In response to a changing rehab landscape in which rehabilitation is offered
SPINAL CORD INJURY Rehab s Framework Self-Assessment Tool inpatient rehab Survey for Spinal Cord Injury (SCI) INTRODUCTION: In response to a changing rehab landscape in which rehabilitation is offered
Original Article. Client-centred assessment and the identification of meaningful treatment goals for individuals with a spinal cord injury
 (2004) 42, 302 307 & 2004 International Society All rights reserved 1362-4393/04 $25.00 www.nature.com/sc Original Article Client-centred assessment and the identification of meaningful treatment goals
(2004) 42, 302 307 & 2004 International Society All rights reserved 1362-4393/04 $25.00 www.nature.com/sc Original Article Client-centred assessment and the identification of meaningful treatment goals
The Hand Hub. Mary P Galea Departments of Medicine and Rehabilitation Medicine (Royal Melbourne Hospital) The University of Melbourne
 The Hand Hub Mary P Galea Departments of Medicine and Rehabilitation Medicine (Royal Melbourne Hospital) The University of Melbourne What prompted this project? 30%-60% of stroke survivors fail to regain
The Hand Hub Mary P Galea Departments of Medicine and Rehabilitation Medicine (Royal Melbourne Hospital) The University of Melbourne What prompted this project? 30%-60% of stroke survivors fail to regain
Collaborative Research Grant Initiative: Mental Wellness in Seniors and Persons with Disabilities
 Predicting Potential for Positive Outcomes in a Slow-stream Rehabilitation Program Collaborative Research Grant Initiative: Mental Wellness in Seniors and Persons with Disabilities Ideas Fund Final Report
Predicting Potential for Positive Outcomes in a Slow-stream Rehabilitation Program Collaborative Research Grant Initiative: Mental Wellness in Seniors and Persons with Disabilities Ideas Fund Final Report
EVERY MINUTE COUNTS - Stroke Rehabilitation Intensity -
 EVERY MINUTE COUNTS - Stroke Rehabilitation Intensity - Presentation prepared by the Ontario Stroke Network Rehabilitation Intensity Working Group February 12, 2015 Objectives To provide context on why
EVERY MINUTE COUNTS - Stroke Rehabilitation Intensity - Presentation prepared by the Ontario Stroke Network Rehabilitation Intensity Working Group February 12, 2015 Objectives To provide context on why
Torsion bottle, a very simple, reliable, and cheap tool for a basic scoliosis screening
 Romano and Mastrantonio Scoliosis and Spinal Disorders (2018) 13:4 DOI 10.1186/s13013-018-0150-6 RESEARCH Open Access Torsion bottle, a very simple, reliable, and cheap tool for a basic scoliosis screening
Romano and Mastrantonio Scoliosis and Spinal Disorders (2018) 13:4 DOI 10.1186/s13013-018-0150-6 RESEARCH Open Access Torsion bottle, a very simple, reliable, and cheap tool for a basic scoliosis screening
Critically Appraised Paper for Efficacy of occupational therapy for patients with Parkinson's disease: A randomized controlled trial
 Dominican University of California Dominican Scholar Occupational Therapy Critically Appraised Papers Series Occupational Therapy 2017 Critically Appraised Paper for Efficacy of occupational therapy for
Dominican University of California Dominican Scholar Occupational Therapy Critically Appraised Papers Series Occupational Therapy 2017 Critically Appraised Paper for Efficacy of occupational therapy for
SENSe Implement: Changing clinical practice in sensory rehabilitation of the arm after stroke
 SENSe Implement: Changing clinical practice in sensory rehabilitation of the arm after stroke Leeanne Carey, Liana Cahill, Natasha Lannin and the SENSe Implement team. latrobe.edu.au CRICOS Provider 00115M
SENSe Implement: Changing clinical practice in sensory rehabilitation of the arm after stroke Leeanne Carey, Liana Cahill, Natasha Lannin and the SENSe Implement team. latrobe.edu.au CRICOS Provider 00115M
This Year in Review highlights some of the many initiatives undertaken within each strategic direction.
 This year s Annual Achievement Report provides a high level overview of the many successes in Toronto s stroke system. Through strategic leadership, the North & East GTA and the Toronto West Stroke Networks
This year s Annual Achievement Report provides a high level overview of the many successes in Toronto s stroke system. Through strategic leadership, the North & East GTA and the Toronto West Stroke Networks
2017 Report Card. 62 acute inpatient rehabilitation beds 13 DAYS
 Lovelace UNM Rehabilitation Hospital is dedicated helping each patient overcome the effects of illness and injury through our comprehensive inpatient and outpatient programs. Our highly specialized physicians
Lovelace UNM Rehabilitation Hospital is dedicated helping each patient overcome the effects of illness and injury through our comprehensive inpatient and outpatient programs. Our highly specialized physicians
Geriatric Certification
 Geriatric Certification Curriculum 2017 Geriatric Certification Program Program Director: Cody Thompson, PT, DPT, GCS, CSCS Program Description This program offers PTs and OTs the opportunity to develop
Geriatric Certification Curriculum 2017 Geriatric Certification Program Program Director: Cody Thompson, PT, DPT, GCS, CSCS Program Description This program offers PTs and OTs the opportunity to develop
CRITICALLY APPRAISED PAPER (CAP)
 CRITICALLY APPRAISED PAPER (CAP) Wu, C., Huang, P., Chen, Y., Lin, K., & Yang, H. (2013). Effects of mirror therapy on motor and sensory recovery in chronic stroke: A randomized controlled trial. Archives
CRITICALLY APPRAISED PAPER (CAP) Wu, C., Huang, P., Chen, Y., Lin, K., & Yang, H. (2013). Effects of mirror therapy on motor and sensory recovery in chronic stroke: A randomized controlled trial. Archives
Collected Scientific Research Relating to the Use of Osteopathy with Knee pain including iliotibial band (ITB) friction syndrome
 Collected Scientific Research Relating to the Use of Osteopathy with Knee pain including iliotibial band (ITB) friction syndrome Important: 1) Osteopathy involves helping people's own self-healing abilities
Collected Scientific Research Relating to the Use of Osteopathy with Knee pain including iliotibial band (ITB) friction syndrome Important: 1) Osteopathy involves helping people's own self-healing abilities
July 22, The Smoking Cessation Initiative Description- A Multi-Prong Approach: 1. RNAO Smoking Cessation (SC) Coordinators
 1 Registered Nurses Association of Ontario Smoking Cessation Nursing Best Practice Initiative Request for Proposal: Smoking Cessation Implementation Site 2013-2014 The Registered Nurses Association of
1 Registered Nurses Association of Ontario Smoking Cessation Nursing Best Practice Initiative Request for Proposal: Smoking Cessation Implementation Site 2013-2014 The Registered Nurses Association of
Course Descriptions for Courses in the Entry-Level Doctorate in Occupational Therapy Curriculum
 Course Descriptions for Courses in the Entry-Level Doctorate in Occupational Therapy Curriculum Course Name Therapeutic Interaction Skills Therapeutic Interaction Skills Lab Anatomy Surface Anatomy Introduction
Course Descriptions for Courses in the Entry-Level Doctorate in Occupational Therapy Curriculum Course Name Therapeutic Interaction Skills Therapeutic Interaction Skills Lab Anatomy Surface Anatomy Introduction
Education-only versus a multifaceted intervention for improving assessment of rehabilitation needs after stroke; a cluster randomised trial
 Lynch et al. Implementation Science (2016) 11:120 DOI 10.1186/s13012-016-0487-2 RESEARCH Open Access Education-only versus a multifaceted intervention for improving assessment of rehabilitation needs after
Lynch et al. Implementation Science (2016) 11:120 DOI 10.1186/s13012-016-0487-2 RESEARCH Open Access Education-only versus a multifaceted intervention for improving assessment of rehabilitation needs after
Rehab then what? Mandy Lau, OT Reg. (Ont.) Patient Flow Coordinator at Providence Healthcare
 Rehab then what? An integrated Rehab to Community Transition program Mandy Lau, OT Reg. (Ont.) Patient Flow Coordinator at Providence Healthcare Jessica Anderson Rehab to Community and Outreach coordinator
Rehab then what? An integrated Rehab to Community Transition program Mandy Lau, OT Reg. (Ont.) Patient Flow Coordinator at Providence Healthcare Jessica Anderson Rehab to Community and Outreach coordinator
2014 Report Card. 62 acute inpatient rehabilitation beds days
 Lovelace Rehabilitation Hospital is dedicated helping each patient overcome the effects of illness and injury through our comprehensive inpatient and outpatient programs. Our highly specialized physicians
Lovelace Rehabilitation Hospital is dedicated helping each patient overcome the effects of illness and injury through our comprehensive inpatient and outpatient programs. Our highly specialized physicians
Preparing Providers: Tools and Strategies to Enhance Health Services November 19, :50am
 Enhancing uptake of an online evidence-informed guide to HIV rehabilitation among occupational therapists, physiotherapists and speech-language pathologists Salbach N, Solomon P, O Brien K, Worthington
Enhancing uptake of an online evidence-informed guide to HIV rehabilitation among occupational therapists, physiotherapists and speech-language pathologists Salbach N, Solomon P, O Brien K, Worthington
Alcohol interventions in secondary and further education
 National Institute for Health and Care Excellence Guideline version (Draft for Consultation) Alcohol interventions in secondary and further education NICE guideline: methods NICE guideline Methods
National Institute for Health and Care Excellence Guideline version (Draft for Consultation) Alcohol interventions in secondary and further education NICE guideline: methods NICE guideline Methods
EDUCATION PROGRAMS. Educational Sessions for Long Term Care + Retirement
 EDUCATION PROGRAMS Educational Sessions for Long Term Care + Retirement GENERAL BACK CARE EDUCATION LIFT, TRANSFER AND REPOSITIONING TRAINING & Appropriate for any individual who is interested in learning
EDUCATION PROGRAMS Educational Sessions for Long Term Care + Retirement GENERAL BACK CARE EDUCATION LIFT, TRANSFER AND REPOSITIONING TRAINING & Appropriate for any individual who is interested in learning
Directors of Education Directors of Autism Intervention Program Directors of Community Agencies
 Ministry of Children and Youth Services Deputy Minister 14 th Floor 56 Wellesley St. W Toronto ON M5S 2S3 Tel: (416) 212-7432 Fax: (416) 325-5332 Ministry of Education Deputy Minister Mowat Block Queen
Ministry of Children and Youth Services Deputy Minister 14 th Floor 56 Wellesley St. W Toronto ON M5S 2S3 Tel: (416) 212-7432 Fax: (416) 325-5332 Ministry of Education Deputy Minister Mowat Block Queen
9/9/2016. By: Erica Ogilvie Rehab 540 Stroke Rehab University of Alberta Northwestern Ontario Regional Stroke Network
 By: Erica Ogilvie Rehab 540 Stroke Rehab University of Alberta Northwestern Ontario Regional Stroke Network Referred to as J.S. 60 year old Caucasian female 6 weeks post ischemic stroke Middle Cerebral
By: Erica Ogilvie Rehab 540 Stroke Rehab University of Alberta Northwestern Ontario Regional Stroke Network Referred to as J.S. 60 year old Caucasian female 6 weeks post ischemic stroke Middle Cerebral
Mark Jayes Highly Specialist Speech and Language Therapist HEE / NIHR Clinical Doctoral Research Fellow
 Mark Jayes Highly Specialist Speech and Language Therapist HEE / NIHR Clinical Doctoral Research Fellow 34% medical patients may lack capacity 1 Assessment is subjective, complex 2 Current practice is
Mark Jayes Highly Specialist Speech and Language Therapist HEE / NIHR Clinical Doctoral Research Fellow 34% medical patients may lack capacity 1 Assessment is subjective, complex 2 Current practice is
Review of Selected Physical Therapy Interventions for School Age Children with Disabilities
 Review of Selected Physical Therapy Interventions for School Age Children with Disabilities Prepared for the Center on Personnel Studies in Special Education EXECUTIVE SUMMARY by Susan K. Effgen University.
Review of Selected Physical Therapy Interventions for School Age Children with Disabilities Prepared for the Center on Personnel Studies in Special Education EXECUTIVE SUMMARY by Susan K. Effgen University.
OHTAC Recommendation
 OHTAC Recommendation Constraint-Induced Movement Therapy for Rehabilitation of Arm Dysfunction After Stroke in Adults. Presented to the Ontario Health Technology Advisory Committee in May 27, 2011 November
OHTAC Recommendation Constraint-Induced Movement Therapy for Rehabilitation of Arm Dysfunction After Stroke in Adults. Presented to the Ontario Health Technology Advisory Committee in May 27, 2011 November
FOCUSSED CLINICAL QUESTION:
 Treatment Critically Appraised Topic: Is daily passive muscle stretching effective at preventing losses of range of motion in adult spinal cord injured patients within a rehabilitation environment? Prepared
Treatment Critically Appraised Topic: Is daily passive muscle stretching effective at preventing losses of range of motion in adult spinal cord injured patients within a rehabilitation environment? Prepared
CRITICALLY APPRAISED PAPER (CAP)
 CRITICALLY APPRAISED PAPER (CAP) Dahl, A., Askim, T., Stock, R., Langørgen, E., Lydersen, S., & Indredavik, B. (2008). Short- and long-term outcome of constraint-induced movement therapy after stroke:
CRITICALLY APPRAISED PAPER (CAP) Dahl, A., Askim, T., Stock, R., Langørgen, E., Lydersen, S., & Indredavik, B. (2008). Short- and long-term outcome of constraint-induced movement therapy after stroke:
Dave Ure, OT Reg. (Ont.), CPA, CMA Coordinator
 Dave Ure, OT Reg. (Ont.), CPA, CMA Coordinator Development of the model In response to the request for proposal issued by the Ministry of Health and Long-Term Care in September 2001, the Southwestern Ontario
Dave Ure, OT Reg. (Ont.), CPA, CMA Coordinator Development of the model In response to the request for proposal issued by the Ministry of Health and Long-Term Care in September 2001, the Southwestern Ontario
NZ Organised Stroke Rehabilitation Service Specifications (in-patient and community)
 NZ Organised Stroke Rehabilitation Service Specifications (in-patient and community) Prepared by the National Stroke Network to outline minimum and strongly recommended standards for DHBs. Date: December
NZ Organised Stroke Rehabilitation Service Specifications (in-patient and community) Prepared by the National Stroke Network to outline minimum and strongly recommended standards for DHBs. Date: December
Standards of excellence
 The Accreditation Canada Stroke Distinction program was launched in March 2010 to offer a rigorous and highly specialized process above and beyond the requirements of Qmentum. The comprehensive Stroke
The Accreditation Canada Stroke Distinction program was launched in March 2010 to offer a rigorous and highly specialized process above and beyond the requirements of Qmentum. The comprehensive Stroke
Background. Ready 4 Rehabilitation in AHS
 Ready 4 Rehabilitation in AHS Ready 4 Rehabilitation in all Foundational Strategies: 1. Our Patients 2. Our People 3. Research & Innovation 4. Information Management & Technology Background Albertans want
Ready 4 Rehabilitation in AHS Ready 4 Rehabilitation in all Foundational Strategies: 1. Our Patients 2. Our People 3. Research & Innovation 4. Information Management & Technology Background Albertans want
Functional Electrical Stimulation-Assisted Walking: Enhancement of Voluntary Walking Function Among Persons with Severe Hemiplegia Post Stroke
 Functional Electrical Stimulation-Assisted Walking: Enhancement of Voluntary Walking Function Among Persons with Severe Hemiplegia Post Stroke Naaz Kapadia Date: May 10, 2010 Research Coordinator-Physiotherapist
Functional Electrical Stimulation-Assisted Walking: Enhancement of Voluntary Walking Function Among Persons with Severe Hemiplegia Post Stroke Naaz Kapadia Date: May 10, 2010 Research Coordinator-Physiotherapist
Mellen Center Approaches Exercise in MS
 Mellen Center Approaches Exercise in MS Framework: Physical exercise is generally recommended to promote fitness and wellness in individuals with or without chronic health conditions. Implementing and
Mellen Center Approaches Exercise in MS Framework: Physical exercise is generally recommended to promote fitness and wellness in individuals with or without chronic health conditions. Implementing and
Residential Care Fall and Fall Related Injury Prevention Toolkit. Introduction
 Residential Care Fall and Fall Related Injury Prevention Toolkit Introduction Residential Care Fall and Fall Related Injury Prevention Toolkit Executive Summary Residents of long term care (LTC) facilities
Residential Care Fall and Fall Related Injury Prevention Toolkit Introduction Residential Care Fall and Fall Related Injury Prevention Toolkit Executive Summary Residents of long term care (LTC) facilities
CJSP: On Reaffirming a Canadian School Psychology
 748212CJSXXX10.1177/0829573517748212Canadian Journal of School PsychologyEditorial editorial2017 Editorial CJSP: On Reaffirming a Canadian School Psychology Canadian Journal of School Psychology 1 5 The
748212CJSXXX10.1177/0829573517748212Canadian Journal of School PsychologyEditorial editorial2017 Editorial CJSP: On Reaffirming a Canadian School Psychology Canadian Journal of School Psychology 1 5 The
TOOLS TO IMPROVE CLINICAL REASONING FOR ASSESSMENT & TREATMENT Presented By: Michelle Green, PT, DPT, c/ndt, NCS
 TOOLS TO IMPROVE CLINICAL REASONING FOR ASSESSMENT & TREATMENT Presented By: Michelle Green, PT, DPT, c/ndt, NCS Carolina Clinical Education Consortium Spring Conference 2018 OBJECTIVES: Following completion
TOOLS TO IMPROVE CLINICAL REASONING FOR ASSESSMENT & TREATMENT Presented By: Michelle Green, PT, DPT, c/ndt, NCS Carolina Clinical Education Consortium Spring Conference 2018 OBJECTIVES: Following completion
Susan W. Muir PT PhD. Post-Doctoral Fellow Division of Geriatric Medicine Schulich School of Medicine & Dentistry University of Western Ontario
 Susan W. Muir PT PhD Post-Doctoral Fellow Division of Geriatric Medicine Schulich School of Medicine & Dentistry University of Western Ontario University of Toronto Rehabilitation Rounds June 14, 2012
Susan W. Muir PT PhD Post-Doctoral Fellow Division of Geriatric Medicine Schulich School of Medicine & Dentistry University of Western Ontario University of Toronto Rehabilitation Rounds June 14, 2012
Mental Health Peer Support in Primary Care
 Mental Health Peer Support in Primary Care Successful Implementations Mental Wellness Recovery 1 Faculty/Presenter Disclosure Faculty: Magda Czegledi Relationships that may introduce potential bias and/or
Mental Health Peer Support in Primary Care Successful Implementations Mental Wellness Recovery 1 Faculty/Presenter Disclosure Faculty: Magda Czegledi Relationships that may introduce potential bias and/or
Better Outcomes for Older People with Spinal Trouble (BOOST) Research Programme
 Better Outcomes for Older People with Spinal Trouble (BOOST) Research Programme Background Low back pain (LBP) is now recognised as the leading disabling condition in the world. LBP is a highly variable
Better Outcomes for Older People with Spinal Trouble (BOOST) Research Programme Background Low back pain (LBP) is now recognised as the leading disabling condition in the world. LBP is a highly variable
Physical Therapy. Program Information. Doctor of Physical Therapy (D.P.T.) Program Prerequisites UAB Equivalents
 The University of Alabama at Birmingham 1 Physical Therapy Degree Offered: Director (D.P.T.): D.P.T. Dr. David Morris Phone: (205) 934-3566 Website: Program Information www.uab.edu/pt The Doctor of Physical
The University of Alabama at Birmingham 1 Physical Therapy Degree Offered: Director (D.P.T.): D.P.T. Dr. David Morris Phone: (205) 934-3566 Website: Program Information www.uab.edu/pt The Doctor of Physical
Understanding test accuracy research: a test consequence graphic
 Whiting and Davenport Diagnostic and Prognostic Research (2018) 2:2 DOI 10.1186/s41512-017-0023-0 Diagnostic and Prognostic Research METHODOLOGY Understanding test accuracy research: a test consequence
Whiting and Davenport Diagnostic and Prognostic Research (2018) 2:2 DOI 10.1186/s41512-017-0023-0 Diagnostic and Prognostic Research METHODOLOGY Understanding test accuracy research: a test consequence
A snapshot of inpatient oncology rehabilitation: Patient profiles and rehab outcomes Rehabilitation Rounds, University of Toronto April 5, 2012
 A snapshot of inpatient oncology rehabilitation: Patient profiles and rehab outcomes Rehabilitation Rounds, University of Toronto April 5, 2012 Sara McEwen, PT, PhD Research Scientist, St. John s Rehab
A snapshot of inpatient oncology rehabilitation: Patient profiles and rehab outcomes Rehabilitation Rounds, University of Toronto April 5, 2012 Sara McEwen, PT, PhD Research Scientist, St. John s Rehab
Provincial Interprofessional Stroke Core Competency Framework with a TR Focus
 Provincial Interprofessional Stroke Core Competency Framework with a TR Focus Thursday June 1st, 2017 3:00 4:00 p.m. T14 Provincial TR Stroke Core Competencies Presenters Keli Cristofaro R/TRO Stroke Community
Provincial Interprofessional Stroke Core Competency Framework with a TR Focus Thursday June 1st, 2017 3:00 4:00 p.m. T14 Provincial TR Stroke Core Competencies Presenters Keli Cristofaro R/TRO Stroke Community
Occupational Therapy (OTHR)
 Occupational Therapy (OTHR) 1 Occupational Therapy (OTHR) Courses OTHR 5001. Developmental Perspectives in Occupational Therapy. 2 Credit Hours. This course explores human development and the relation
Occupational Therapy (OTHR) 1 Occupational Therapy (OTHR) Courses OTHR 5001. Developmental Perspectives in Occupational Therapy. 2 Credit Hours. This course explores human development and the relation
Needs Assessment and Plan for Integrated Stroke Rehabilitation in the GTA February, 2002
 Funding for this project has been provided by the Ministry of Health and Long-Term Care as part of the Ontario Integrated Stroke Strategy 2000. It should be noted that the opinions expressed are those
Funding for this project has been provided by the Ministry of Health and Long-Term Care as part of the Ontario Integrated Stroke Strategy 2000. It should be noted that the opinions expressed are those
Evaluation of the functional independence for stroke survivors in the community
 Asian J Gerontol Geriatr 2009; 4: 24 9 Evaluation of the functional independence for stroke survivors in the community ORIGINAL ARTICLE CKC Chan Bsc, DWC Chan Msc, SKM Wong MBA, MAIS, BA, PDOT ABSTRACT
Asian J Gerontol Geriatr 2009; 4: 24 9 Evaluation of the functional independence for stroke survivors in the community ORIGINAL ARTICLE CKC Chan Bsc, DWC Chan Msc, SKM Wong MBA, MAIS, BA, PDOT ABSTRACT
CRITICALLY APPRAISED PAPER (CAP)
 CRITICALLY APPRAISED PAPER (CAP) FOCUSED QUESTION Is the combination of occupational therapy (OT) and mental practice (MP), from either an internal or an external perspective, an effective intervention
CRITICALLY APPRAISED PAPER (CAP) FOCUSED QUESTION Is the combination of occupational therapy (OT) and mental practice (MP), from either an internal or an external perspective, an effective intervention
Are randomised controlled trials telling us what rehabilitation interventions work?
 Are randomised controlled trials telling us what rehabilitation interventions work? Focus on stroke Jane Burridge March 6 th 2014 Neurorehabilitation: facts, fears and the future Overview Stroke recovery
Are randomised controlled trials telling us what rehabilitation interventions work? Focus on stroke Jane Burridge March 6 th 2014 Neurorehabilitation: facts, fears and the future Overview Stroke recovery
Clinical utility of the Mellville-Nelson Self- Identified Goals Assessment
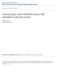 The University of Toledo The University of Toledo Digital Repository Master s and Doctoral Projects Clinical utility of the Mellville-Nelson Self- Identified Goals Assessment Ashley Obarski The University
The University of Toledo The University of Toledo Digital Repository Master s and Doctoral Projects Clinical utility of the Mellville-Nelson Self- Identified Goals Assessment Ashley Obarski The University
The Canadian contribution to the otolaryngology literature: a five year bibliometric analysis
 Gurberg et al. Journal of Otolaryngology - Head and Neck Surgery 2014, 43:47 ORIGINAL RESEARCH ARTICLE Open Access The Canadian contribution to the otolaryngology literature: a five year bibliometric analysis
Gurberg et al. Journal of Otolaryngology - Head and Neck Surgery 2014, 43:47 ORIGINAL RESEARCH ARTICLE Open Access The Canadian contribution to the otolaryngology literature: a five year bibliometric analysis
Low Tolerance Long Duration (LTLD) Stroke Demonstration Project
 Low Tolerance Long Duration (LTLD) Stroke Demonstration Project Interim Summary Report October 25 Table of Contents 1. INTRODUCTION 3 1.1 Background.. 3 2. APPROACH 4 2.1 LTLD Stroke Demonstration Project
Low Tolerance Long Duration (LTLD) Stroke Demonstration Project Interim Summary Report October 25 Table of Contents 1. INTRODUCTION 3 1.1 Background.. 3 2. APPROACH 4 2.1 LTLD Stroke Demonstration Project
Angela Colantonio, PhD 1, Gary Gerber, PhD 2, Mark Bayley, MD, FRCPC 1, Raisa Deber, PhD 3, Junlang Yin, MSc 1 and Hwan Kim, PhD candidate 1
 J Rehabil Med 2011; 43: 311 315 ORIGINAL REPORT Differential Profiles for Patients with Traumatic and Non- Traumatic Brain Injury Angela Colantonio, PhD 1, Gary Gerber, PhD 2, Mark Bayley, MD, FRCPC 1,
J Rehabil Med 2011; 43: 311 315 ORIGINAL REPORT Differential Profiles for Patients with Traumatic and Non- Traumatic Brain Injury Angela Colantonio, PhD 1, Gary Gerber, PhD 2, Mark Bayley, MD, FRCPC 1,
CRITICALLY APPRAISED PAPER (CAP)
 CRITICALLY APPRAISED PAPER (CAP) Kwon, J. Y., Chang, H. J., Yi, S. H., Lee, J. Y., Shin, H. Y., & Kim, Y. H. (2015). Effect of hippotherapy on gross motor function in children with cerebral palsy: A randomized
CRITICALLY APPRAISED PAPER (CAP) Kwon, J. Y., Chang, H. J., Yi, S. H., Lee, J. Y., Shin, H. Y., & Kim, Y. H. (2015). Effect of hippotherapy on gross motor function in children with cerebral palsy: A randomized
Lars Jacobsson 1,2,3* and Jan Lexell 1,3,4
 Jacobsson and Lexell Health and Quality of Life Outcomes (2016) 14:10 DOI 10.1186/s12955-016-0405-y SHORT REPORT Open Access Life satisfaction after traumatic brain injury: comparison of ratings with the
Jacobsson and Lexell Health and Quality of Life Outcomes (2016) 14:10 DOI 10.1186/s12955-016-0405-y SHORT REPORT Open Access Life satisfaction after traumatic brain injury: comparison of ratings with the
The Bobath concept today: What does the evidence really tell us?
 1 1 : What does the evidence really tell us? Central South Regional Stroke Network Hamilton, June 8, 2017 Julie Vaughan-Graham PT, PhD Post-Doctoral Fellow Department of Physical Therapy University of
1 1 : What does the evidence really tell us? Central South Regional Stroke Network Hamilton, June 8, 2017 Julie Vaughan-Graham PT, PhD Post-Doctoral Fellow Department of Physical Therapy University of
SPINAL CORD INJURY Rehab Definitions Framework Self-Assessment Tool Outpatient/ambulatory rehab Survey for Spinal Cord Injury (SCI)
 SPINAL CORD INJURY Rehab s Framework Self-Assessment Tool Outpatient/ambulatory rehab Survey for Spinal Cord Injury (SCI) INTRODUCTION: In response to a changing rehab landscape in which rehabilitation
SPINAL CORD INJURY Rehab s Framework Self-Assessment Tool Outpatient/ambulatory rehab Survey for Spinal Cord Injury (SCI) INTRODUCTION: In response to a changing rehab landscape in which rehabilitation
Takashi Yagisawa 1,2*, Makiko Mieno 1,3, Norio Yoshimura 1,4, Kenji Yuzawa 1,5 and Shiro Takahara 1,6
 Yagisawa et al. Renal Replacement Therapy (2016) 2:68 DOI 10.1186/s41100-016-0080-9 POSITION STATEMENT Current status of kidney transplantation in Japan in 2015: the data of the Kidney Transplant Registry
Yagisawa et al. Renal Replacement Therapy (2016) 2:68 DOI 10.1186/s41100-016-0080-9 POSITION STATEMENT Current status of kidney transplantation in Japan in 2015: the data of the Kidney Transplant Registry
How Many Years Clinical Practice is required to become an "Expert" Occupational Therapist?
 How Many Years Clinical Practice is required to become an "Expert" Occupational Therapist? Mehdi Rassafiani, BSc, MSc; Jenny Ziviani, PhD; Sylvia Rodger, PhD; Lenard Dalgleish, PhD (2005, June) Poster
How Many Years Clinical Practice is required to become an "Expert" Occupational Therapist? Mehdi Rassafiani, BSc, MSc; Jenny Ziviani, PhD; Sylvia Rodger, PhD; Lenard Dalgleish, PhD (2005, June) Poster
Technology to support a Community of Practice Promoting Healthy Built Environment Policies
 Technology to support a Community of Practice Promoting Healthy Built Environment Policies Kim Perrotta, HCBD Knowledge Translation & Communications Heart and Stroke Foundation Health Promotion Ontario
Technology to support a Community of Practice Promoting Healthy Built Environment Policies Kim Perrotta, HCBD Knowledge Translation & Communications Heart and Stroke Foundation Health Promotion Ontario
MSc Psychological Research Methods/ MPsych Advanced Psychology Module Catalogue / 2018
 MSc Psychological Research Methods/ MPsych Advanced Psychology Module Catalogue - 2017 / 2018 PSY555: Communication of Research for Psychology (Semester 2) 10 credits core PRM, option MPsych This module
MSc Psychological Research Methods/ MPsych Advanced Psychology Module Catalogue - 2017 / 2018 PSY555: Communication of Research for Psychology (Semester 2) 10 credits core PRM, option MPsych This module
PURPOSE OF THE SELF-ASSESSMENT TOOLS:
 Pulmonary Rehab s Framework Self-Assessment Tool Inpatient Rehab Survey for Pulmonary Rehab INTRODUCTION: In response to a changing rehab landscape in which rehabilitation is offered in many different
Pulmonary Rehab s Framework Self-Assessment Tool Inpatient Rehab Survey for Pulmonary Rehab INTRODUCTION: In response to a changing rehab landscape in which rehabilitation is offered in many different
Background: Traditional rehabilitation after total joint replacement aims to improve the muscle strength of lower limbs,
 REVIEWING THE EFFECTIVENESS OF BALANCE TRAINING BEFORE AND AFTER TOTAL KNEE AND TOTAL HIP REPLACEMENT: PROTOCOL FOR A SYSTEMATIC RE- VIEW AND META-ANALYSIS Background: Traditional rehabilitation after
REVIEWING THE EFFECTIVENESS OF BALANCE TRAINING BEFORE AND AFTER TOTAL KNEE AND TOTAL HIP REPLACEMENT: PROTOCOL FOR A SYSTEMATIC RE- VIEW AND META-ANALYSIS Background: Traditional rehabilitation after
COURSE ORIENTATION. Rehabilitation Health Science Department Master Program in Physical therapy Tests and Measurements (RHS-503)
 COURSE ORIENTATION Rehabilitation Health Science Department Master Program in Physical therapy Tests and Measurements (RHS-503) COURSE ORIENTATION Tests and Measurements (RHS-503) Mobile: +966542115404
COURSE ORIENTATION Rehabilitation Health Science Department Master Program in Physical therapy Tests and Measurements (RHS-503) COURSE ORIENTATION Tests and Measurements (RHS-503) Mobile: +966542115404
Older Adults Conference 2017 Saskatoon. Transforming the Care of Older Adults through Interprofessional Teams
 Older Adults Conference 2017 Saskatoon Transforming the Care of Older Adults through Interprofessional Teams The 2017 Older Adults Conference Transforming the Care of Older Adults through Interprofessional
Older Adults Conference 2017 Saskatoon Transforming the Care of Older Adults through Interprofessional Teams The 2017 Older Adults Conference Transforming the Care of Older Adults through Interprofessional
Can occupational therapy intervention focused on activities of daily living increase quality of life in people who have had a stroke?
 Pacific University CommonKnowledge Physical Function CATs OT Critically Appraised Topics 2008 Can occupational therapy intervention focused on activities of daily living increase quality of life in people
Pacific University CommonKnowledge Physical Function CATs OT Critically Appraised Topics 2008 Can occupational therapy intervention focused on activities of daily living increase quality of life in people
Measuring and Mapping the Rheumatology Workforce in Canada An update for: Royal College- National Speciality Societies Human Resource for Health
 Measuring and Mapping the Rheumatology Workforce in Canada An update for: Royal College- National Speciality Societies Human Resource for Health Dialogue June 2 nd 2017 Dr. Dianne Mosher The burden of
Measuring and Mapping the Rheumatology Workforce in Canada An update for: Royal College- National Speciality Societies Human Resource for Health Dialogue June 2 nd 2017 Dr. Dianne Mosher The burden of
Critical Review: Group Therapy for Post-Stroke Aphasia Rehabilitation
 Critical Review: Group Therapy for Post-Stroke Aphasia Rehabilitation Kristina Howatt Gerber M.Cl.Sc SLP Candidate University of Western Ontario: School of Communication Sciences and Disorders This critical
Critical Review: Group Therapy for Post-Stroke Aphasia Rehabilitation Kristina Howatt Gerber M.Cl.Sc SLP Candidate University of Western Ontario: School of Communication Sciences and Disorders This critical
CLINICAL OUTCOME VARIABLES SCALE: A RETROSPECTIVE
 J Rehabil Med 2010; 42: 609 613 ORIGINAL REPORT CLINICAL OUTCOME VARIABLES SCALE: A RETROSPECTIVE VALIDATION STUDY in patients after stroke Katherine Salter, BA 1, Jeffrey Jutai, PhD 1,2, Norine Foley,
J Rehabil Med 2010; 42: 609 613 ORIGINAL REPORT CLINICAL OUTCOME VARIABLES SCALE: A RETROSPECTIVE VALIDATION STUDY in patients after stroke Katherine Salter, BA 1, Jeffrey Jutai, PhD 1,2, Norine Foley,
Glen Sather Sports Medicine Clinic Research Strategy
 Glen Sather Sports Medicine Clinic Research Strategy 2015-2020 Vision: To be a centre of excellence in sport and exercise based musculoskeletal (MSK) and sports medicine care through innovative, clinically
Glen Sather Sports Medicine Clinic Research Strategy 2015-2020 Vision: To be a centre of excellence in sport and exercise based musculoskeletal (MSK) and sports medicine care through innovative, clinically
National Stroke Association s Guide to Choosing Stroke. Rehabilitation Services
 National Stroke Association s Guide to Choosing Stroke Rehabilitation Services Rehabilitation, often referred to as rehab, is an important part of stroke recovery. Through rehab, you: Re-learn basic skills
National Stroke Association s Guide to Choosing Stroke Rehabilitation Services Rehabilitation, often referred to as rehab, is an important part of stroke recovery. Through rehab, you: Re-learn basic skills
RxVACCINATE: A National Education and Practice Support Initiative to Increase Pharmacist Administered Pneumococcal Vaccinations.
 RxVACCINATE: A National Education and Practice Support Initiative to Increase Pharmacist Administered Pneumococcal Vaccinations. Pfizer Grant 45130: LOI Pneumococcal Disease Prevention Grant ID: 45130
RxVACCINATE: A National Education and Practice Support Initiative to Increase Pharmacist Administered Pneumococcal Vaccinations. Pfizer Grant 45130: LOI Pneumococcal Disease Prevention Grant ID: 45130
Systematic reviews and meta-analyses of observational studies (MOOSE): Checklist.
 Systematic reviews and meta-analyses of observational studies (MOOSE): Checklist. MOOSE Checklist Infliximab reduces hospitalizations and surgery interventions in patients with inflammatory bowel disease:
Systematic reviews and meta-analyses of observational studies (MOOSE): Checklist. MOOSE Checklist Infliximab reduces hospitalizations and surgery interventions in patients with inflammatory bowel disease:
THE APPLICATION OF COMMUNITY NEUROREHABILITATION USING A FAMILY-CENTRED APPROACH TO PERSONS WITH DISABILITY: A CASE STUDY IN STROKE SURVIVORS
 THE APPLICATION OF COMMUNITY NEUROREHABILITATION USING A FAMILY-CENTRED APPROACH TO PERSONS WITH DISABILITY: A CASE STUDY IN STROKE SURVIVORS Nomjit Nualnetr*, Waroonnapa Srisoparb**, Wichai Eungpinichpong***
THE APPLICATION OF COMMUNITY NEUROREHABILITATION USING A FAMILY-CENTRED APPROACH TO PERSONS WITH DISABILITY: A CASE STUDY IN STROKE SURVIVORS Nomjit Nualnetr*, Waroonnapa Srisoparb**, Wichai Eungpinichpong***
Table 2. Mapping graduate curriculum to Graduate Level Expectations (GDLEs) - MSc (RHBS) program
 Depth and breadth of knowledge demonstrate knowledge of the breadth of the field of Rehabilitation Science and within their discipline. demonstrate a sound understanding of the scope, perspectives, concepts,
Depth and breadth of knowledge demonstrate knowledge of the breadth of the field of Rehabilitation Science and within their discipline. demonstrate a sound understanding of the scope, perspectives, concepts,
Supporting Persons with Dementia Face the Decision and Effects of Hanging up the Keys
 TEAM TITLE List Team Members Supporting Persons with Dementia Face the Decision and Effects of Hanging up the Keys CCNA Team 16: Driving and Dementia Team Leaders: G. Naglie & M. Rapoport www.ccna-ccnv.ca
TEAM TITLE List Team Members Supporting Persons with Dementia Face the Decision and Effects of Hanging up the Keys CCNA Team 16: Driving and Dementia Team Leaders: G. Naglie & M. Rapoport www.ccna-ccnv.ca
CRITICALLY APPRAISED PAPER (CAP)
 CRITICALLY APPRAISED PAPER (CAP) Huseyinsinoglu, B. E., Ozdincler, A. R., & Krespi, Y. (2012). Bobath concept versus constraint-induced movement therapy to improve arm functional recovery in stroke patients:
CRITICALLY APPRAISED PAPER (CAP) Huseyinsinoglu, B. E., Ozdincler, A. R., & Krespi, Y. (2012). Bobath concept versus constraint-induced movement therapy to improve arm functional recovery in stroke patients:
PREVIOUS EMPLOYMENT. Associate OT : CJ Occupational Therapy * Assessment and treatment for adults with neurological conditions
 CURRICULUM VITAE Katie Hanagarth Green Owl Therapy Office 3, 36 Greenhill Street Stratford-upon-Avon CV37 6LE Tel: 01789 413960 / 07966 573317 Email: katie@greenowltherapy.co.uk - Web: www.greenowltherapy.co.uk
CURRICULUM VITAE Katie Hanagarth Green Owl Therapy Office 3, 36 Greenhill Street Stratford-upon-Avon CV37 6LE Tel: 01789 413960 / 07966 573317 Email: katie@greenowltherapy.co.uk - Web: www.greenowltherapy.co.uk
PROSPERO International prospective register of systematic reviews
 PROSPERO International prospective register of systematic reviews What is the application of ultrasound imaging in primary care for musculoskeletal disorders? Mark Karaczun, Toby Smith, Robert Fleetcroft,
PROSPERO International prospective register of systematic reviews What is the application of ultrasound imaging in primary care for musculoskeletal disorders? Mark Karaczun, Toby Smith, Robert Fleetcroft,
Making sense of Implementation
 Making sense of Implementation Dr Sharon Mickan Course Director MSc Evidence-Based Health Care Combine evidence to implement an effective clinical intervention using an effective Knowledge Translation
Making sense of Implementation Dr Sharon Mickan Course Director MSc Evidence-Based Health Care Combine evidence to implement an effective clinical intervention using an effective Knowledge Translation
