Guideline. Drugs & Therapeutics Committee
|
|
|
- Merilyn Park
- 5 years ago
- Views:
Transcription
1 Physiotherapy Rehabilitation Guidelines for patients undergoing Total Ankle Replacement Document Type Date Approved Ratifying Body Related Documents Guideline 13/11/2017 Drugs & Therapeutics Committee Physiotherapy rehabilitation guidelines Lateral ligament reconstruction of the ankle Physiotherapy rehabilitation guidelines Anterior ankle arthroscopy Physiotherapy rehabilitation guidelines Tibialis posterior reconstruction Physiotherapy rehabilitation guidelines Subtalar and hindfoot fusion Physiotherapy rehabilitation guidelines Hallux valgus deformity- Scarf Osteotomy Physiotherapy rehabilitation guidelines Pes Cavus correction Physiotherapy rehabilitation guidelines ACI of the ankle Author Owner (Executive Director) Directorate Superseded Documents Subject Joanna Benfield, Foot & Ankle Specialist Physiotherapist, RNOH Lucy Davies Operations Rehab Guidelines for Ankle Replacement (2014) Clinical, Clinical Units, Communication, Inpatient & Outpatient Services Review Date Keywords and Phrases 13/11/2022 Rehabilitation, ankle surgery, OA, osteoarthritis, total ankle replacement, physiotherapy, complications, outcomes, milestones, function, treatment, exercise, pain relief, restrictions, limitations, sport, fitness, postural awareness, pain education, mobility, goals, precautions, Physiotherapy Rehabilitation Guidelines for patients undergoing Total Ankle Replacement Page 1
2 compliance, knee pain, leg pain, foot pain Consultation Group/Approving Bodies/Subject Matter Expert Members of Foot and Ankle Unit Team (4 consultants, & Clinical Nurse Specialist) Members of Outpatient Musculoskeletal Physiotherapy Team (Band 5, 6, 7 and 8a staff members at Stanmore and Bolsover Street) Members of Inpatient Orthopaedic Physiotherapy Team (Band 7 and 8a staff members) Readership All staff (inc. Clinical) Physiotherapy Rehabilitation Guidelines for patients undergoing Total Ankle Replacement Page 2
3 Table of Contents 1. Equality Impact Assessment (EIA) Disclosure Statement Privacy Impact Assessment (PIA) Disclosure Statement Introduction and aims Definitions Duties and Responsibilities Body of Policy Monitoring and the effectiveness of this policy... 7 Appendix 1: Appendix 2: Appendix 3: Glossary of Terms Other linked trust policies and guidelines Extra sources of information and support Physiotherapy Rehabilitation Guidelines for patients undergoing Total Ankle Replacement Page 3
4 1. Equality Impact Assessment (EIA) Disclosure Statement Equality Impact Assessment (EIA) Disclosure Statement This policy was assessed on the 10th day of March 2017 for its impact on equality. The assessment determined that the policy will not have a significant negative impact on equality in relation to each of the protected staff/patient groups below: i.) Age; ii.) Sex (Male and Female); iii.) Disability (Learning Difficulties/Physical or Sensory Disability); iv.) Race or Ethnicity; v.) Religion and Belief; vi) Sexual Orientation (gay, lesbian or heterosexual); vii) Pregnancy and Maternity; vii) Gender Reassignment (The process of transitioning from one gender to another); viii) Marriage and Civil Partnership. Physiotherapy Rehabilitation Guidelines for patients undergoing Total Ankle Replacement Page 4
5 1. Privacy Impact Assessment (PIA) Disclosure Statement Privacy Impact Assessment (PIA) Disclosure Statement This policy was assessed on the 10th day of March 2017 for its impact on privacy. The assessment determined that the policy will not have a significant negative impact on privacy of members of staff/patients. Physiotherapy Rehabilitation Guidelines for patients undergoing Total Ankle Replacement Page 5
6 2. Introduction and aims Please note that this is advisory information only. Individual / your experiences may differ from those described. All exercises must be demonstrated to a patient by a fully qualified physiotherapist. We cannot be held liable for the outcome of you undertaking any of the exercises / interventions shown here independently of direct supervision from the RNOH. As a specialist orthopaedic hospital we recognise that our broad and often complex patient group needs an individualised rehabilitation approach. Our emphasis is on patient-specific rehabilitation, which encourages recognition of those patients who may progress slower than others. These rehabilitation guidelines are therefore milestone driven and designed to provide an equitable rehabilitation service to all our patients. They will also limit unnecessary visits to the outpatient clinic at RNOHT by helping the patient and therapist to identify when specialist review is required. 3. Definitions See section Duties and Responsibilities Not applicable for this guideline. 5. Body of Policy Physiotherapy Rehabilitation Guidelines for patients undergoing Total Ankle Replacement Page 6
7 Indications for Surgery Pain and decreased function not responsive to conservative treatment. Causes include post-traumatic osteoarthritis, primary osteoarthritis, Rheumatoid Arthritis, systemic joint disease, idiopathic arthritis. Possible Complications Infection Wound healing problems Persistent swelling Loosening / subsidence / migration of components Impingement Bleeding Nerve damage Deep Vein Thrombosis Pulmonary Embolism Non-union Persistent / recurrent pain Fracture of bone / components Tendon injuries Contractures Complex Regional Pain Syndrome If failure, may require subsequent revision ankle replacement or conversion to fusion or to below knee amputation Surgical Techniques The commonly used Total Ankle Replacement (TAR) prostheses at RNOH are the BOX Ankle Replacement (MatOrtho) or the Infinity Ankle System (Wright Medical Technology). The BOX is a three component, cementless, unconstrained, mobilebearing prosthesis. The Inifinity is a two component, cementless, semiconstrained prosthesis. The surgery may also include one or more of the following, depending on the clinical presentation of the patient: Tendo-Achilles lengthening Calcaneal osteotomy Tendon transfers Ligament reconstruction Other osteotomies or joint fusions Physiotherapy Rehabilitation Guidelines for patients undergoing Total Ankle Replacement Page 7
8 Clinical Trials A multi-centre randomised clinical trial is being led by the Royal National Orthopaedic Hospital comparing ankle replacement against ankle fusion (TARVA) further details can be found at Expected Outcome Improved function / mobility Improved pain relief Increased walking tolerance with decreased walking aid requirement Return to no-impact / low-impact sports may be possible but strenuous sport inadvisable Maintenance or improvement in range of movement (if the ankle was very stiff before surgery, range of motion may not be improved due to soft tissue constraints) Full recovery may take up to twelve months Pre-operatively The patient will be seen pre-operatively where able and with consent, the following will be assessed or discussed: Current functional levels General Health Social history and home set up Ability to mobilise, plus the provision of appropriate walking aids to be used post operatively Post-operative expectations Post-operative management explained, including the provision of bed exercises. Post-operatively Always check the operation notes, and the post-operative instructions. Discuss any deviation from routine guidelines with the team concerned. This is very important if the patient has had any other techniques as well as the Total Ankle Replacement as weight-bearing status and progressions may be different as well as other restrictions. Please ensure you follow the correct protocol from the relevant consultant the patient is under as there may be differences. Physiotherapy Rehabilitation Guidelines for patients undergoing Total Ankle Replacement Page 8
9 INITIAL REHABILITATION PHASE: 0-6 Weeks Goals: To be safely and independently mobile with appropriate walking aid, adhering to weight bearing status To be independent with home exercise programme as appropriate To understand self-management / monitoring, e.g. skin sensation, colour, swelling, temperature, circulation, elevation Exercises to strengthen core Restrictions: Ensure that weight bearing restrictions are adhered to: o Total Ankle Replacement (TAR) o Mr Singh / Mr Cullen / Mr Welck: Non weight bearing (NWB) for 2 weeks in Back Slab. Below Knee Plaster of Paris (BK POP) at 2 weeks. Progress to Full Weight Bearing (FWB) in POP. POP removed at 6 weeks. Into Aircast Boot. FWB. o Mr Goldberg: Non weight bearing (NWB) for 2 weeks in Back Slab or Aircast Boot. Below Knee Plaster of Paris (BK POP) at 2 weeks or continue with Aircast Boot. Progress to Full Weight Bearing (FWB) in POP / Aircast Boot. POP removed at 6 weeks and into Aircast Boot or continue with Aircast Boot. FWB. o If any other surgical technique used ensure you check any restrictions with team as these may differ from TAR alone Elevation If sedentary employment, may be able to return to work from 4 weeks postoperatively, as long as provisions to elevate leg, and no complications Treatment: Likely to be in Backslab / POP / Aircast Boot Pain-relief: Ensure adequate analgesia Elevation Exercises: teach circulatory exercises Education: teach how to monitor sensation, colour, circulation, temperature, swelling, and advise what to do if concerned Mobility: ensure patient independent with transfers and mobility, including stairs if necessary Physiotherapy Rehabilitation Guidelines for patients undergoing Total Ankle Replacement Page 9
10 On discharge from ward: Independent and safe mobilising, including stairs if appropriate Independent with transfers Independent and safe with home exercise programme / monitoring Milestones to progress to next phase: Out of POP. Team to refer to physiotherapy at 6 weeks from clinic. Progression from NWB to FWB phase. Team to refer to physiotherapy if required to review safety of mobility / use of walking aids Adequate analgesia Physiotherapy Rehabilitation Guidelines for patients undergoing Total Ankle Replacement Page 10
11 RECOVERY REHABILITATION PHASE: 6 weeks- 12 weeks Goals: Mr Singh / Mr Cullen / Mr Welck: Once advised by team bone healing is sufficient to come out of Aircast Boot: o To be independently mobile out of Aircast boot with walking aid as appropriate o To achieve optimal range of movement (as described in operation note) To address core stability and strength and control throughout kinetic chain within any restrictions Mr Goldberg: To remain independently and safely mobile in Aircast Boot with appropriate walking aid To address core stability and strength and control throughout kinetic chain within any restrictions Restrictions: Weight Bearing and POP / Aircast Boot progressions are dependent upon the bone healing of the individual patient. The surgical team will advise when to progress weight bearing and when to start to wean from / work out of Aircast Boot. Ensure that any weight bearing restrictions are adhered to Ensure that any post-operative instructions and advice from the team are adhered to as to when to progress from Aircast Boot and when it is ok to start work around the foot and ankle and out of the Aircast Boot. Mr Singh / Mr Cullen / Mr Welck: FWB in Aircast Boot from 6 weeks until advised by consultant can wean from this Mr Goldberg: FWB in Aircast Boot until 12 weeks or until advised by consultant. Into PUSH ankle brace at 12 weeks (FWB) or when advised by consultant Treatment: Pain relief Advice / Education Posture advice / education Mobility: ensure safely and independently mobile adhering to appropriate weight bearing restrictions. Progress off walking aids as appropriate once reaches FWB stage. Gait Re-education Wean out of Aircast boot once advised to do so and into normal footwear. Exercises: o Core stability work Physiotherapy Rehabilitation Guidelines for patients undergoing Total Ankle Replacement Page 11
12 o Review lower limb biomechanics and kinetic chain within any restrictions. Address issues as appropriate. o Range Of Movement (ROM) exercises of foot and ankle only when team advises can start these Passive (PROM) / Active assisted (AAROM) / Active ROM (AROM) o ROM exercises of other joints throughout kinetic chain as appropriate o Strengthening exercises of foot and ankle only when team advises can start these o Strengthening exercises of other muscles / muscle groups throughout kinetic chain as appropriate o Balance / proprioception work once appropriate o Stretches of tight structures as appropriate (e.g. Achilles Tendon) once team advises can start to work on these Swelling Management Manual Therapy: only when team advises can start to work out of boot / around foot and ankle: o Soft tissue techniques as appropriate o Joint mobilisations as appropriate Monitor sensation, swelling, colour, temperature, circulation Orthotics if required via surgical team Hydrotherapy if appropriate within restrictions once team advises can start this Pacing advice as appropriate Milestones to progress to next phase: Independently mobilising in Aircast boot +/- walking aid as appropriate Independent and safe with monitoring / self-management Adequate analgesia Failure to meet milestones: Refer back to team / Discuss with team Continue with outpatient physiotherapy if still progressing Physiotherapy Rehabilitation Guidelines for patients undergoing Total Ankle Replacement Page 12
13 INTERMEDIATE REHABILITATION PHASE: 12 weeks 6 months Goals: Once advised by team bone healing is sufficient to come out of Aircast Boot: o To be independently mobile out of Aircast boot with ankle brace / walking aid as appropriate o To achieve optimal range of movement (as described in operation note) o To optimise normal ankle and foot movement & restore gait o To be wearing normal footwear o Grade 4 or 5 muscle strength around ankle Optimise core stability and strength and control throughout kinetic chain within any restrictions Restrictions: Weight Bearing and POP / Aircast Boot progressions are dependent upon the bone healing of the individual patient. The surgical team will advise when to progress weight bearing and when to start to wean from / work out of Aircast Boot. Ensure that any weight bearing restrictions are adhered to Ensure that any post-operative instructions and advice from the team are adhered to as to when to progress from Aircast Boot and when it is ok to start work around the foot and ankle and out of the Aircast Boot. Mr Goldberg: Out of Aircast boot and into PUSH ankle brace FWB at 12 weeks, or when advised by consultant Mr Singh / Mr Cullen / Mr Welck: Team will advise when to wean from Aircast boot. No ankle brace Treatment: Further progression of the above treatment: Pain relief Advice / Education Posture advice / education Mobility: ensure safely and independently mobile adhering to restrictions. Progress off walking aids as appropriate. Gait Re-education Wean out of Aircast boot once advised to do so and into normal footwear. If patient unable to get into normal footwear advise to try Crocs or other wide fitting shoes. Exercises: o Core stability work o Review lower limb biomechanics and kinetic chain within any restrictions. Address issues as appropriate. Physiotherapy Rehabilitation Guidelines for patients undergoing Total Ankle Replacement Page 13
14 o Range Of Movement (ROM) exercises of foot and ankle only when team advises can start these PROM / AAROM / AROM o ROM exercises of other joints throughout kinetic chain as appropriate o Strengthening exercises of foot and ankle only when team advises can start these o Strengthening exercises of other muscles / muscle groups throughout kinetic chain as appropriate o Balance / proprioception work once appropriate o Stretches of tight structures as appropriate (e.g. Achilles Tendon) once team advises can start to work on these Swelling Management Manual Therapy: only when team advises can start to work out of boot / around foot and ankle: o Soft tissue techniques as appropriate o Joint mobilisations as appropriate Monitor sensation, swelling, colour, temperature, circulation Orthotics if required via surgical team Hydrotherapy if appropriate within restrictions once team advises can start this Pacing advice as appropriate Milestones to progress to next phase: Full range of movement Independently mobilising out of Aircast boot with ankle brace / walking aid as appropriate Wearing normal footwear Neutral foot position when weight bearing / mobilising Grade 4 or 5 muscle strength around ankle Failure to meet milestones: Refer back to team / Discuss with team Continue with outpatient physiotherapy if still progressing Physiotherapy Rehabilitation Guidelines for patients undergoing Total Ankle Replacement Page 14
15 FINAL REHABILITATION PHASE: 6 months 1 year Goals: Independently mobile unaided / with walking aid if required long term Return to gentle no-impact / low-impact sports Establish long term maintenance programme Grade 5 muscle strength around ankle Treatment: Mobility / function: Progression of mobility and function, increasing dynamic control with specific training to functional goals Gait Re-education Exercises: o Progression of exercises including range of movement, strengthening, transfer activation, balance and proprioception, core stability Swelling Management Manual Therapy: o Soft tissue techniques as appropriate o Joint mobilisations as appropriate Pacing advice Milestones for discharge: Independently mobile unaided / with walking aid if required long term Appropriate patient-specific functional goals achieved, eg. return to low/no impact sport Independent with long term maintenance programme Grade 5 muscle strength around ankle Physiotherapy Rehabilitation Guidelines for patients undergoing Total Ankle Replacement Page 15
16 FAILURE TO PROGRESS If a patient is failing to progress, then consider the following: POSSIBLE PROBLEM Swelling Pain Breakdown of Wound e.g inflammation, bleeding, infection Numbness / altered sensation ACTION Ensure elevating leg regularly Use ice as appropriate if normal skin sensation and no contraindications Decrease amount of time on feet Pacing Use walking aids Circulatory exercises If decreases overnight, monitor closely If does not decrease overnight, refer back to surgical team or to GP Decrease activity Ensure adequate analgesia Elevate regularly Decrease weight bearing and use walking aids as appropriate Pacing Modify exercise programme as appropriate If persists, refer back to surgical team or to GP Refer to surgical team or to GP Review immediate post-operative status if possible Ensure swelling under control If new onset or increasing refer back to surgical team or GP If static, monitor closely, but inform surgical team and refer back if deteriorates or if concerned Physiotherapy Rehabilitation Guidelines for patients undergoing Total Ankle Replacement Page 16
17 6. Monitoring and the effectiveness of this policy This guideline will be reviewed 5 yearly. Physiotherapy Rehabilitation Guidelines for patients undergoing Total Ankle Replacement Page 17
18 Appendix 1: Glossary of Terms Not applicable. Physiotherapy Rehabilitation Guidelines for patients undergoing Total Ankle Replacement Page 18
19 Appendix 2: Other linked trust policies and guidelines Physiotherapy rehabilitation guidelines Lateral ligament reconstruction of the ankle Physiotherapy rehabilitation guidelines Anterior ankle arthroscopy Physiotherapy rehabilitation guidelines Tibialis posterior reconstruction Physiotherapy rehabilitation guidelines Subtalar and hindfoot fusion Physiotherapy rehabilitation guidelines Hallux valgus deformity- Scarf Osteotomy Physiotherapy rehabilitation guidelines Pes Cavus correction Physiotherapy rehabilitation guidelines ACI of the ankle All other RNOH Physiotherapy Rehabilitation Orthopaedic Post-operative Guidelines (Knee, Sarcoma Unit, Peripheral Nerve Injuries, Shoulder & Upper Limb, Spinal Surgery Unit) Physiotherapy Rehabilitation Guidelines for patients undergoing Total Ankle Replacement Page 19
20 Appendix 3: Extra sources of information and support Summary of evidence for physiotherapy guidelines A comprehensive literature search was carried out to identify research relating to total ankle replacement and subsequent rehabilitation. After reviewing the articles and information, the physiotherapy guidelines were produced on the best available evidence. Assal, M., Ahmad, A., Lacraz, A., Courvoisier, D., Stern, R. and Crevoisier, X. (2011). Step activity monitoring to assess ambulation before and after total ankle arthroplasty. Foot and Ankle Surgery, 17(3), pp Bloch, B., Srinivasan, S. and Mangwani, J. (2015). Current Concepts in the Management of Ankle Osteoarthritis: A Systematic Review. The Journal of Foot and Ankle Surgery, 54(5), pp Brigido, S., Mulhern, J., Wobst, G. and Protzman, N. (2015). Preoperative and Postoperative Range of Motion: A Retrospective Comparison of Two Total Ankle Replacement Systems. The Journal of Foot and Ankle Surgery, 54(5), pp Buechel et al (2004) Twenty-year evaluation of cementless mobile-bearing Total Ankle Replacements. Clinical Orthopaedics and Related Research 424, Casartelli, N., Item-Glatthorn, J., Bizzini, M., Leunig, M. and Maffiuletti, N. (2013). Differences in gait characteristics between total hip, knee, and ankle arthroplasty patients: a six-month postoperative comparison. BMC Musculoskeletal Disorders, 14(1). Chopra, S., Rouhani, H., Assal, M., Aminian, K. and Crevoisier, X. (2013). Outcome of unilateral ankle arthrodesis and total ankle replacement in terms of bilateral gait mechanics. Journal of Orthopaedic Research, 32(3), pp Coetzee, J. and Castro, M. (2004). Accurate Measurement of Ankle Range of Motion after Total Ankle Arthroplasty. Clinical Orthopaedics and Related Research, 424, pp Coetzee, J., Petersen, D. and Stone, R. (2016). Comparison of Three Total Ankle Replacement Systems Done at a Single Facility. Foot & Ankle Specialist, 10(1), pp Conti S & Wong YS (2001) Complications of Total Ankle Replacement. Clinical Orthopaedics and Related Research 391, Conti, S., Dazen, D., Stewart, G., Green, A., Martin, R., Kuxhaus, L. and Miller, M. (2008). Proprioception after Total Ankle Arthroplasty. Foot & Ankle International, 29(11), pp Flavin, R., Coleman, S., Tenenbaum, S. and Brodsky, J. (2013). Comparison of Gait After Total Ankle Arthroplasty and Ankle Arthrodesis. Foot & Ankle International, 34(10), pp Physiotherapy Rehabilitation Guidelines for patients undergoing Total Ankle Replacement Page 20
21 Goldberg, A., Zaidi, R., Thomson, C., Doré, C., Skene, S., Cro, S., Round, J., Molloy, A., Davies, M., Karski, M., Kim, L. and Cooke, P. (2016). Total ankle replacement versus arthrodesis (TARVA): protocol for a multicentre randomised controlled trial: Table 1. BMJ Open, 6(9), p.e Goldberg A. (2016). Total ankle joint replacement. Drug and Therapeutics Bulletin, 54(2), pp Griesberg J & Hansen S (2003) Total Ankle Arthroplasty in the advanced flatfoot. Techniques in Foot and Ankle Surgery 2, (3): Gross, C., Hamid, K., Green, C., Easley, M., DeOrio, J. and Nunley, J. (2016). Operative Wound Complications Following Total Ankle Arthroplasty. Foot & Ankle International, 38(4), pp Gross, C., Lampley, A., Green, C., DeOrio, J., Easley, M., Adams, S. and Nunley, J. (2015). The Effect of Obesity on Functional Outcomes and Complications in Total Ankle Arthroplasty. Foot & Ankle International, 37(2), pp Hintermann, B., Knupp, M., Zwicky, L. and Barg, A. (2012). Total Ankle Replacement for Treatment of End-Stage Osteoarthritis in Elderly Patients. Journal of Aging Research, 2012, pp.1-8. Jones, C., Rush, S., Berlet, G., Regina, J., Penner, M., Brigido, S., Smith, W. and Brigido, S. (2015). Understanding the Postoperative Course and Rehabilitation Protocol for Total Ankle Arthroplasty. Foot & Ankle Specialist, 8(3), pp Kobayashi et al (2004) Ankle arthroplasties generate wear particles similar to knee arthroplasties. Clinical Orthopaedics and Related Research 424, Kotnis et al (2006) The management of failed ankle replacement. The Journal of Bone and Joint Surgery 88-B, (8): Lalonde K & Conti S (2006) Ankle arthritis: current status of ankle replacement versus fusion and other treatment modalities Current Opinion in Orthopaedics 17, (2): Lawton, C., Butler, B., Dekker, R., Prescott, A. and Kadakia, A. (2017). Total ankle arthroplasty versus ankle arthrodesis a comparison of outcomes over the last decade. Journal of Orthopaedic Surgery and Research, 12(1). Lee, K., Park, Y., Song, E., Yoon, T. and Jung, K. (2010). Static and Dynamic Postural Balance After Successful Mobile-Bearing Total Ankle Arthroplasty. Archives of Physical Medicine and Rehabilitation, 91(4), pp Macaulay, A., VanValkenburg, S. and DiGiovanni, C. (2015). Sport and activity restrictions following total ankle replacement: A survey of orthopaedic foot and ankle specialists. Foot and Ankle Surgery, 21(4), pp Martin, R., Stewart, G. and Conti, S. (2007). Posttraumatic Ankle Arthritis: An Update on Conservative and Surgical Management. Journal of Orthopaedic & Sports Physical Therapy, 37(5), pp Pagenstert, G., Horisberger, M., Leumann, A., Wiewiorski, M., Hintermann, B. and Valderrabano, V. (2011). Distinctive Pain Course during First Year after Physiotherapy Rehabilitation Guidelines for patients undergoing Total Ankle Replacement Page 21
22 Total Ankle Arthroplasty: A Prospective, Observational Study. Foot & Ankle International, 32(2), pp Prusinowska, A., Krogulec, Z., Turski, P., Przepiórski, E., Małdyk, P. and Księżopolska-Orłowska, K. (2015). Total ankle replacement surgical treatment and rehabilitation. Reumatologia/Rheumatology, 1, pp Rodrigues-Pinto, R., Muras, J., Martín Oliva, X. and Amado, P. (2013). Functional results and complication analysis after total ankle replacement. Foot and Ankle Surgery, 19(4), pp Roselló Añón, A., Martinez Garrido, I., Cervera Deval, J., Herrero Mediavilla, D., Sánchez González, M. and Vicent Carsí, V. (2014). Total ankle replacement in patients with end-stage ankle osteoarthritis: Clinical results and kinetic gait analysis. Foot and Ankle Surgery, 20(3), pp Schipper, O., Denduluri, S., Zhou, Y. and Haddad, S. (2015). Effect of Obesity on Total Ankle Arthroplasty Outcomes. Foot & Ankle International, 37(1), pp.1-7. Schuh, R., Hofstaetter, J., Krismer, M., Bevoni, R., Windhager, R. and Trnka, H. (2011). Total ankle arthroplasty versus ankle arthrodesis. Comparison of sports, recreational activities and functional outcome. International Orthopaedics, 36(6), pp Spirt et al (2004) Complications and failure after Total Ankle Arthroplasty. The Journal of Bone and Joint Surgery 86-A, (6): Stavrakis, A. and SooHoo, N. (2016). Trends in Complication Rates Following Ankle Arthrodesis and Total Ankle Replacement. The Journal of Bone and Joint Surgery, 98(17), pp Tenenbaum, S., Bariteau, J., Coleman, S. and Brodsky, J. (2017). Functional and clinical outcomes of total ankle arthroplasty in elderly compared to younger patients. Foot and Ankle Surgery, 23(2), pp Tochigi et al (2005) The effect of accuracy of implantation on range of movement of the Scandinavian Total Ankle Replacement. The Journal of Bone and Joint Surgery 87-B, (5): Valderrabano et al (2006) Sports and recreation activity of ankle arthritis patients before and after Total Ankle Replacement. The American Journal of Sports Medicine 34, (6): Valderrabano, V., Nigg, B., Tscharner, V., Frank, C. and Hintermann, B. (2007). J. Leonard Goldner Award 2006: Total Ankle Replacement in Ankle Osteoarthritis: An Analysis of Muscle Rehabilitation. Foot & Ankle International, 28(2), pp Valderrabano, V., Nigg, B., von Tscharner, V., Stefanyshyn, D., Goepfert, B. and Hintermann, B. (2007). Gait analysis in ankle osteoarthritis and total ankle replacement. Clinical Biomechanics, 22(8), pp Valderrabano, V., Tscharner, V., Nigg, B., Göpfert, B., Hintermann, B., Dick, W. and Frank, C. (2006). Muscle atrophy in ankle osteoarthritis and its rehabilitation with total ankle arthroplasty. Journal of Biomechanics, 39, p.s199. Physiotherapy Rehabilitation Guidelines for patients undergoing Total Ankle Replacement Page 22
23 Zaidi et al (2013). How do patients with end-stage ankle arthritis decide between two surgical treatments? A qualitative study. BMJ Open, 3 (7). Zaidi et al (2013). The outcome of total ankle replacement: a systematic review and meta-analysis. The Bone & Joint Journal, 95-B (11), Physiotherapy Rehabilitation Guidelines for patients undergoing Total Ankle Replacement Page 23
24 This policy is available on request in large print and alternative languages. It is a manager s responsibility to ensure employees are aware of these options. * The following policies must be sent for review to the Local Counter Fraud Specialist: Fraud and Bribery Standard Financial Instructions Declaration of Interests Gifts and Hospitality Whistleblowing Disciplinary IT Anti-Money Laundering Managing Sickness Absence Secondary Employment Expenses Overpayment Financial Redress TOIL (Time off in Lieu) Code of Conduct/Standards of Business Conduct Data Protection Lone Worker Patient Transport Commercial Sponsorship Overseas Visitors Disclosure Physiotherapy Rehabilitation Guidelines for patients undergoing Total Ankle Replacement Page 24
Total ankle replacement
 Total ankle replacement Initial rehabilitation phase 0-4 weeks To be safely and independently mobile with appropriate walking aid, adhering to weight bearing status To be independent with home exercise
Total ankle replacement Initial rehabilitation phase 0-4 weeks To be safely and independently mobile with appropriate walking aid, adhering to weight bearing status To be independent with home exercise
Bunion (hallux valgus deformity) surgery
 Bunion (hallux valgus deformity) surgery Bunion surgery is generally reserved for bunions that are severe and impacting on function. There most frequent surgical procedure used involves a medial incision
Bunion (hallux valgus deformity) surgery Bunion surgery is generally reserved for bunions that are severe and impacting on function. There most frequent surgical procedure used involves a medial incision
Ankle instability surgery
 Ankle instability surgery Ankle instability surgery is generally reserved for people with chronic ankle instability who have failed to respond to conservative treatment. The surgical technique used will
Ankle instability surgery Ankle instability surgery is generally reserved for people with chronic ankle instability who have failed to respond to conservative treatment. The surgical technique used will
Foot and ankle fractures
 Foot and ankle fractures Some fractures can be managed without surgery, but others require surgery to achieve the best possible outcome. Fractures and injuries to joints have a high risk of developing
Foot and ankle fractures Some fractures can be managed without surgery, but others require surgery to achieve the best possible outcome. Fractures and injuries to joints have a high risk of developing
Foot and ankle. Achilles tendon rupture repair. After surgery
 Foot and ankle Achilles tendon rupture repair There is no agreed single best treatment for Achilles tendon ruptures. Similar results can be achieved with non-surgical and surgical treatments. There is
Foot and ankle Achilles tendon rupture repair There is no agreed single best treatment for Achilles tendon ruptures. Similar results can be achieved with non-surgical and surgical treatments. There is
Rehabilitation guidelines for patients undergoing Anterior Ankle Arthroscopy
 Rehabilitation guidelines for patients undergoing Anterior Ankle Arthroscopy At the RNOH, our emphasis is patient specific, which encourages recognition of those who may progress slower then others. We
Rehabilitation guidelines for patients undergoing Anterior Ankle Arthroscopy At the RNOH, our emphasis is patient specific, which encourages recognition of those who may progress slower then others. We
Guideline. Drugs & Therapeutics Committee
 Physiotherapy Rehabilitation Guidelines for patients undergoing Lateral Ligament Reconstruction of the Ankle Document Type Date Approved Ratifying Body Related Documents Guideline 13/11/2017 Drugs & Therapeutics
Physiotherapy Rehabilitation Guidelines for patients undergoing Lateral Ligament Reconstruction of the Ankle Document Type Date Approved Ratifying Body Related Documents Guideline 13/11/2017 Drugs & Therapeutics
INITIAL REHABILITATION PHASE 0-4 weeks. Posterolateral Corner Injury
 Posterolateral Corner Injury Indications for Surgery The main indication of PLC reconstruction surgery is symptomatic instability following PLC injury. The aim of PLC reconstruction surgery is to restore
Posterolateral Corner Injury Indications for Surgery The main indication of PLC reconstruction surgery is symptomatic instability following PLC injury. The aim of PLC reconstruction surgery is to restore
POSTOP FOLLOW-UP & REHABILITATION FOLLOWING FOOT & ANKLE SURGERY
 1 POSTOP FOLLOW-UP & REHABILITATION FOLLOWING FOOT & ANKLE SURGERY The following instructions are general guidelines, but surgeon post-op instructions will dictate the individual patient's post-op management
1 POSTOP FOLLOW-UP & REHABILITATION FOLLOWING FOOT & ANKLE SURGERY The following instructions are general guidelines, but surgeon post-op instructions will dictate the individual patient's post-op management
A patient s guide to. Inferior Heel Pain
 A patient s guide to Inferior Heel Pain The Foot & Ankle Unit at the Royal National Orthopaedic Hospital is made up of a multi-disciplinary team. The team consists of four specialist orthopaedic foot and
A patient s guide to Inferior Heel Pain The Foot & Ankle Unit at the Royal National Orthopaedic Hospital is made up of a multi-disciplinary team. The team consists of four specialist orthopaedic foot and
A Patient s Guide to Post-Operative Advice Following Pes Cavus
 A Patient s Guide to Post-Operative Advice Following Pes Cavus The Foot and Ankle unit at the Royal National Orthopaedic Hospital (RNOH) is a multi-disciplinary team. The team consists of three specialist
A Patient s Guide to Post-Operative Advice Following Pes Cavus The Foot and Ankle unit at the Royal National Orthopaedic Hospital (RNOH) is a multi-disciplinary team. The team consists of three specialist
FOOT AND ANKLE ARTHROSCOPY
 FOOT AND ANKLE ARTHROSCOPY Information for Patients WHAT IS FOOT AND ANKLE ARTHROSCOPY? The foot and the ankle are crucial for human movement. The balanced action of many bones, joints, muscles and tendons
FOOT AND ANKLE ARTHROSCOPY Information for Patients WHAT IS FOOT AND ANKLE ARTHROSCOPY? The foot and the ankle are crucial for human movement. The balanced action of many bones, joints, muscles and tendons
Your Orthotics service is changing
 Your Orthotics service is changing Important for referrers on changes effective from January 2015 Why is the service changing? As demand for the orthotics service increases and budgets remain relatively
Your Orthotics service is changing Important for referrers on changes effective from January 2015 Why is the service changing? As demand for the orthotics service increases and budgets remain relatively
Hindfoot / Midfoot Fusion (Arthrodesis) Orthopeadic Department Patient Information Leaflet
 Hindfoot / Midfoot Fusion (Arthrodesis) Orthopeadic Department Patient Information Leaflet There are often three reasons why this operation is performed: Pain - from osteoarthritis (OA) and rheumatoid
Hindfoot / Midfoot Fusion (Arthrodesis) Orthopeadic Department Patient Information Leaflet There are often three reasons why this operation is performed: Pain - from osteoarthritis (OA) and rheumatoid
North of England Bone and Soft Tissue Tumour Service
 North of England Bone and Soft Tissue Tumour Service Guidelines for rehabilitation after replacement of the proximal femur Proximal femoral replacement surgery is usually carried out as part of treatment
North of England Bone and Soft Tissue Tumour Service Guidelines for rehabilitation after replacement of the proximal femur Proximal femoral replacement surgery is usually carried out as part of treatment
Rehabilitation Guidelines for Patients Undergoing Precice Nail Lengthening. Joint Academic Committee. Holly Doyle. Aresh Nejad. Clinical 19/04/2021
 Rehabilitation Guidelines for Patients Undergoing Precice Nail Lengthening Date Approved 19/04/2018 Ratifying Body Related Documents Joint Academic Committee Physiotherapy rehabilitation guidelines Author
Rehabilitation Guidelines for Patients Undergoing Precice Nail Lengthening Date Approved 19/04/2018 Ratifying Body Related Documents Joint Academic Committee Physiotherapy rehabilitation guidelines Author
Hindfoot/Midfoot Fusion (Arthrodesis)
 Hindfoot/Midfoot Fusion (Arthrodesis) There are often three reasons why this operation is performed: Pain - from osteoarthritis (OA) and rheumatoid arthritis (RA). Change of shape of foot or deformity.
Hindfoot/Midfoot Fusion (Arthrodesis) There are often three reasons why this operation is performed: Pain - from osteoarthritis (OA) and rheumatoid arthritis (RA). Change of shape of foot or deformity.
Your Orthotics service is changing
 Your Orthotics service is changing Important information for service users on changes effective from July 2015 Why is the service changing? As demand for the Orthotics service increases, Livewell Southwest
Your Orthotics service is changing Important information for service users on changes effective from July 2015 Why is the service changing? As demand for the Orthotics service increases, Livewell Southwest
Ankle Fracture Orthopaedic Department Patient Information Leaflet. Under review. Page 1
 Ankle Fracture Orthopaedic Department Patient Information Leaflet Page 1 Ankle Fracture Welcome to the Dudley Group NHS Foundation Trust. This leaflet will provide you with information regarding the diagnosis
Ankle Fracture Orthopaedic Department Patient Information Leaflet Page 1 Ankle Fracture Welcome to the Dudley Group NHS Foundation Trust. This leaflet will provide you with information regarding the diagnosis
Adam N. Whatley, M.D Main St., STE Zachary, LA Phone(225) Fax(225)
 Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 Total Knee Arthroplasty Protocol: The intent of this protocol is to provide the clinician with a guideline
Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 Total Knee Arthroplasty Protocol: The intent of this protocol is to provide the clinician with a guideline
Ankle Arthritis PATIENT INFORMATION. The ankle joint. What is ankle arthritis?
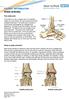 PATIENT INFORMATION Ankle Arthritis The ankle joint The ankle is a very complex joint. It is actually made up of two joints: the true ankle joint and the subtalar ankle joint. The ankle joint consists
PATIENT INFORMATION Ankle Arthritis The ankle joint The ankle is a very complex joint. It is actually made up of two joints: the true ankle joint and the subtalar ankle joint. The ankle joint consists
Tibialis Posterior Tendon Dysfunction. Orthopaedic Department Patient Information Leaflet
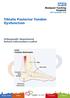 Tibialis Posterior Tendon Dysfunction Orthopaedic Department Patient Information Leaflet What is Tibialis Posterior Tendon Dysfunction? The Tibialis Posterior Tendon (see diagram) is an important structure
Tibialis Posterior Tendon Dysfunction Orthopaedic Department Patient Information Leaflet What is Tibialis Posterior Tendon Dysfunction? The Tibialis Posterior Tendon (see diagram) is an important structure
A Patient s Guide to Adult-Acquired Flatfoot Deformity
 A Patient s Guide to Adult-Acquired Flatfoot Deformity Glendale Adventist Medical Center 1509 Wilson Terrace Glendale, CA 91206 Phone: (818) 409-8000 DISCLAIMER: The information in this booklet is compiled
A Patient s Guide to Adult-Acquired Flatfoot Deformity Glendale Adventist Medical Center 1509 Wilson Terrace Glendale, CA 91206 Phone: (818) 409-8000 DISCLAIMER: The information in this booklet is compiled
WHAT IS THIS CONDITION? COMMON CAUSES:
 Mr Laurence James BSc MBBS MRCS(Eng) FRCS(Tr&Orth) Consultant Orthopaedic Surgeon Foot, Ankle and Sports Injuries WHAT IS THIS CONDITION? The posterior tibial tendon is an important structure that is normally
Mr Laurence James BSc MBBS MRCS(Eng) FRCS(Tr&Orth) Consultant Orthopaedic Surgeon Foot, Ankle and Sports Injuries WHAT IS THIS CONDITION? The posterior tibial tendon is an important structure that is normally
Protocol for the Management of Hip Arthroscopy Surgery
 Overall Aims of Surgery To decrease pain To increase range of motion (ROM) To increase hip/pelvis and lumbar stability To enable return to activities of daily living and sport Initial Post-operative Objectives
Overall Aims of Surgery To decrease pain To increase range of motion (ROM) To increase hip/pelvis and lumbar stability To enable return to activities of daily living and sport Initial Post-operative Objectives
Post Operative Total Hip Replacement Protocol Brian J. White, MD
 Post Operative Total Hip Replacement Protocol Brian J. White, MD www.western-ortho.com The intent of this protocol is to provide guidelines for progression of rehabilitation. It is not intended to serve
Post Operative Total Hip Replacement Protocol Brian J. White, MD www.western-ortho.com The intent of this protocol is to provide guidelines for progression of rehabilitation. It is not intended to serve
Ankle Arthritis and Ankle Replacement
 Ankle Arthritis and Ankle Replacement Ryan DeBlis, MD Disclosures I have no disclosures. 1 Diagnosis Ankle arthritis Majority (70%) of patients are post-traumatic (ie, after ankle fracture) Primary arthritis
Ankle Arthritis and Ankle Replacement Ryan DeBlis, MD Disclosures I have no disclosures. 1 Diagnosis Ankle arthritis Majority (70%) of patients are post-traumatic (ie, after ankle fracture) Primary arthritis
North of England Bone and Soft Tissue Tumour Service
 North of England Bone and Soft Tissue Tumour Service Guidelines for rehabilitation after proximal tibial replacement Proximal tibial replacement surgery is usually carried out as part of treatment for
North of England Bone and Soft Tissue Tumour Service Guidelines for rehabilitation after proximal tibial replacement Proximal tibial replacement surgery is usually carried out as part of treatment for
Anterior Cruciate Ligament (ACL) Reconstruction
 Further information Information on who to contact, i.e. web sites / telephone numbers of other departments / organisations which may be of help. How to contact us Watford General Hospital West Hertfordshire
Further information Information on who to contact, i.e. web sites / telephone numbers of other departments / organisations which may be of help. How to contact us Watford General Hospital West Hertfordshire
ACL Reconstruction Protocol (Allograft)
 ACL Reconstruction Protocol (Allograft) Week one Week two Initial Evaluation Range of motion Joint hemarthrosis Ability to contract quad/vmo Gait (generally WBAT in brace) Patella Mobility Inspect for
ACL Reconstruction Protocol (Allograft) Week one Week two Initial Evaluation Range of motion Joint hemarthrosis Ability to contract quad/vmo Gait (generally WBAT in brace) Patella Mobility Inspect for
Differences in Walking Mechanics Between Ankle Disarthrodesis and Primary Total Ankle Replacement
 Differences in Walking Mechanics Between Ankle Disarthrodesis and Primary Total Ankle Replacement Robin M. Queen, PhD Abigail L. Carpenter, MS Samuel B. Adams, Jr, MD Mark E. Easley, MD James A. Nunley,
Differences in Walking Mechanics Between Ankle Disarthrodesis and Primary Total Ankle Replacement Robin M. Queen, PhD Abigail L. Carpenter, MS Samuel B. Adams, Jr, MD Mark E. Easley, MD James A. Nunley,
A patient s guide to. ankle arthroscopy
 A patient s guide to ankle arthroscopy The foot and ankle unit at the Royal National Orthopaedic Hospital (RNOH) is a multi-disciplinary team. The team consists of three specialist orthopaedic foot and
A patient s guide to ankle arthroscopy The foot and ankle unit at the Royal National Orthopaedic Hospital (RNOH) is a multi-disciplinary team. The team consists of three specialist orthopaedic foot and
Mr Keith Winters MBChB, FRACS (Orth) Specialist Orthopaedic Surgeon
 Mr Keith Winters MBChB, FRACS (Orth) Specialist Orthopaedic Surgeon Ph: (03) 9598 0691 Post op Instructions: Achilles Tendon Repair Recommended appliances for after your surgery: Crutches, walking frame
Mr Keith Winters MBChB, FRACS (Orth) Specialist Orthopaedic Surgeon Ph: (03) 9598 0691 Post op Instructions: Achilles Tendon Repair Recommended appliances for after your surgery: Crutches, walking frame
ACL Reconstruction Rehabilitation Bone Patellar Tendon Bone Graft Kyle F. Chun, MD
 ACL Reconstruction Rehabilitation Bone Patellar Tendon Bone Graft Kyle F. Chun, MD [ ] Meniscus Repair (If checked, WBAT in brace in full extension, ROM 0-90 x 6 wks; WBAT 0-90, ROM 0-120 weeks 7-12; WBAT/ROMAT
ACL Reconstruction Rehabilitation Bone Patellar Tendon Bone Graft Kyle F. Chun, MD [ ] Meniscus Repair (If checked, WBAT in brace in full extension, ROM 0-90 x 6 wks; WBAT 0-90, ROM 0-120 weeks 7-12; WBAT/ROMAT
Ankle Replacement Surgery
 Ankle Replacement Surgery Ankle replacement surgery is performed to replace the damaged articular surfaces of the three bones of the ankle joint with artificial implants. This procedure is now being preferred
Ankle Replacement Surgery Ankle replacement surgery is performed to replace the damaged articular surfaces of the three bones of the ankle joint with artificial implants. This procedure is now being preferred
What variables influence final range of motion following Total Ankle Arthroplasty. Kevin T. Grosshans MD Mark S. Myerson MD
 What variables influence final range of motion following Total Ankle Arthroplasty Kevin T. Grosshans MD Mark S. Myerson MD Disclosures My disclosure is in the Final AOFAS Mobile App I have no potential
What variables influence final range of motion following Total Ankle Arthroplasty Kevin T. Grosshans MD Mark S. Myerson MD Disclosures My disclosure is in the Final AOFAS Mobile App I have no potential
Dr. Huff Modified Brostrom Repair Rehabilitation Protocol:
 Dr. Huff Modified Brostrom Repair Rehabilitation Protocol: The intent of this protocol is to provide the clinician with a guideline of the post-operative rehabilitation course of a patient who has undergone
Dr. Huff Modified Brostrom Repair Rehabilitation Protocol: The intent of this protocol is to provide the clinician with a guideline of the post-operative rehabilitation course of a patient who has undergone
.org. Posterior Tibial Tendon Dysfunction. Anatomy. Cause. Symptoms
 Posterior Tibial Tendon Dysfunction Page ( 1 ) Posterior tibial tendon dysfunction is one of the most common problems of the foot and ankle. It occurs when the posterior tibial tendon becomes inflamed
Posterior Tibial Tendon Dysfunction Page ( 1 ) Posterior tibial tendon dysfunction is one of the most common problems of the foot and ankle. It occurs when the posterior tibial tendon becomes inflamed
Rehabilitation after ankle injuries
 Rehabilitation after ankle injuries Ahmed Thabet, M.D. Assistant Professor Department of Orthopaedic Surgery & Rehabilitation Texas Tech University Health Sciences Center El Paso What are our objectives?
Rehabilitation after ankle injuries Ahmed Thabet, M.D. Assistant Professor Department of Orthopaedic Surgery & Rehabilitation Texas Tech University Health Sciences Center El Paso What are our objectives?
Patient information. Total Ankle Replacement Trauma and Orthopaedic Directorate PIF 1335 V2
 Patient information Total Ankle Replacement Trauma and Orthopaedic Directorate PIF 1335 V2 Your Consultant has advised you that you are suitable to have a total ankle replacement. The aim of surgery is
Patient information Total Ankle Replacement Trauma and Orthopaedic Directorate PIF 1335 V2 Your Consultant has advised you that you are suitable to have a total ankle replacement. The aim of surgery is
Midfoot Arthritis - Midfoot Fusion / Arthrodesis Surgery
 PATIENT INFORMATION Midfoot Arthritis - Midfoot Fusion / Arthrodesis Surgery The Midfoot The midfoot refers to the bones and joints that make up the arch and connect the forefoot to the hindfoot. Metatarsals
PATIENT INFORMATION Midfoot Arthritis - Midfoot Fusion / Arthrodesis Surgery The Midfoot The midfoot refers to the bones and joints that make up the arch and connect the forefoot to the hindfoot. Metatarsals
Anterior Cruciate Ligament Reconstruction
 Anterior Cruciate Ligament Reconstruction Physiotherapy Department Patient information leaflet This patient information booklet is designed to provide you with information about the Anterior Cruciate Ligament
Anterior Cruciate Ligament Reconstruction Physiotherapy Department Patient information leaflet This patient information booklet is designed to provide you with information about the Anterior Cruciate Ligament
A Patient s Guide to Inter Digital Neuralgia (Morton s Neuroma)
 A Patient s Guide to Inter Digital Neuralgia (Morton s Neuroma) The foot and ankle unit at the Royal National Orthopaedic Hospital (RNOH) is a multi-disciplinary team. The team consists of two specialist
A Patient s Guide to Inter Digital Neuralgia (Morton s Neuroma) The foot and ankle unit at the Royal National Orthopaedic Hospital (RNOH) is a multi-disciplinary team. The team consists of two specialist
ACL Reconstruction Rehabilitation Allograft Kyle F. Chun, MD
 ACL Reconstruction Rehabilitation Allograft Kyle F. Chun, MD [ ] Meniscus Repair (If checked, WBAT in brace in full extension, ROM 0-90 x 6 wks; WBAT 0-90, ROM 0-120 weeks 7-12; WBAT/ROMAT 12+ weeks, no
ACL Reconstruction Rehabilitation Allograft Kyle F. Chun, MD [ ] Meniscus Repair (If checked, WBAT in brace in full extension, ROM 0-90 x 6 wks; WBAT 0-90, ROM 0-120 weeks 7-12; WBAT/ROMAT 12+ weeks, no
Nursing Management: Musculoskeletal Trauma and Orthopedic Surgery. By: Aun Lauriz E. Macuja SAC_SN4
 Nursing Management: Musculoskeletal Trauma and Orthopedic Surgery By: Aun Lauriz E. Macuja SAC_SN4 The most common cause of musculoskeletal injuries is a traumatic event resulting in fracture, dislocation,
Nursing Management: Musculoskeletal Trauma and Orthopedic Surgery By: Aun Lauriz E. Macuja SAC_SN4 The most common cause of musculoskeletal injuries is a traumatic event resulting in fracture, dislocation,
A patient s guide to. preparing for foot and ankle surgery
 A patient s guide to preparing for foot and ankle surgery The foot and ankle unit at the Royal National Orthopaedic Hospital (RNOH) is a multi-disciplinary team. The team consists of three specialist orthopaedic
A patient s guide to preparing for foot and ankle surgery The foot and ankle unit at the Royal National Orthopaedic Hospital (RNOH) is a multi-disciplinary team. The team consists of three specialist orthopaedic
Guidance for the Physiotherapy Management of Patients Undergoing Limb Reconstruction with a Circular Frame External Fixator.
 Guidance for the Physiotherapy Management of Patients Undergoing Limb Reconstruction with a Circular Frame External Fixator. Table of Contents INTRODUCTION... 2 TARGET AUDIENCE... 2 KEY CHANGES FROM PREVIOUS
Guidance for the Physiotherapy Management of Patients Undergoing Limb Reconstruction with a Circular Frame External Fixator. Table of Contents INTRODUCTION... 2 TARGET AUDIENCE... 2 KEY CHANGES FROM PREVIOUS
Foot and ankle update
 Foot and ankle update Mr Ian Garnham Consultant Foot and Ankle Surgeon Whipps Cross University Hospital Hallux Rigidus Symptoms first ray and 1st MTP pain and swelling worse with push off or forced dorsiflexion
Foot and ankle update Mr Ian Garnham Consultant Foot and Ankle Surgeon Whipps Cross University Hospital Hallux Rigidus Symptoms first ray and 1st MTP pain and swelling worse with push off or forced dorsiflexion
Rehabilitation and Return to Play Following Achilles Tendon Repair
 Rehabilitation and Return to Play Following Achilles Tendon Repair Monte Wong PT, DPT, SCS, ATC, CSCS Assistant Athletic Trainer/Physical Therapist Philadelphia Eagles Mechanism of Injury 1.) forceful
Rehabilitation and Return to Play Following Achilles Tendon Repair Monte Wong PT, DPT, SCS, ATC, CSCS Assistant Athletic Trainer/Physical Therapist Philadelphia Eagles Mechanism of Injury 1.) forceful
Centre of musculoskeletal system
 Ortho cham zug Centre of excellence for the musculoskeletal system Your mobility, independence and quality of life are our aim. Because movement means life. Hirslanden A mediclinic international company
Ortho cham zug Centre of excellence for the musculoskeletal system Your mobility, independence and quality of life are our aim. Because movement means life. Hirslanden A mediclinic international company
Conversion of Pantalar fusion to total ankle replacement: A case Review. Key words: Pantalar fusion, non-union and total ankle replacement
 The Northern Ohio Foot and Ankle Journal Official Publication of the NOFA Foundation Conversion of Pantalar fusion to total ankle replacement: A case Review Author: Bryan Williams DPM 1 and Jonathan Sharpe
The Northern Ohio Foot and Ankle Journal Official Publication of the NOFA Foundation Conversion of Pantalar fusion to total ankle replacement: A case Review Author: Bryan Williams DPM 1 and Jonathan Sharpe
5 COMMON CONDITIONS IN THE FOOT & ANKLE
 5 COMMON CONDITIONS IN THE FOOT & ANKLE MICHAEL P. CLARE, MD FLORIDA ORTHOPAEDIC INSTITUTE TAMPA, FL USA IN A NUTSHELL ~ ALL ANATOMY & BIOMECHANICS >90% OF CONDITIONS IN FOOT & ANKLE DIAGNISED FROM GOOD
5 COMMON CONDITIONS IN THE FOOT & ANKLE MICHAEL P. CLARE, MD FLORIDA ORTHOPAEDIC INSTITUTE TAMPA, FL USA IN A NUTSHELL ~ ALL ANATOMY & BIOMECHANICS >90% OF CONDITIONS IN FOOT & ANKLE DIAGNISED FROM GOOD
Health-Related Quality of Life and Functional Outcomes in Ankle Arthritis Patients Based on Treating with and without Total Ankle Replacement Surgery
 Health-Related Quality of Life and Functional Outcomes in Ankle Arthritis Patients Based on Treating with and without Total Ankle Replacement Surgery Chayanin Angthong MD* * Division of Foot and Ankle
Health-Related Quality of Life and Functional Outcomes in Ankle Arthritis Patients Based on Treating with and without Total Ankle Replacement Surgery Chayanin Angthong MD* * Division of Foot and Ankle
The causes of OA of the knee are multiple and include aging (wear and tear), obesity, and previous knee trauma or surgery. OA affects usually the
 The Arthritic Knee The causes of OA of the knee are multiple and include aging (wear and tear), obesity, and previous knee trauma or surgery. OA affects usually the medial compartment of the knee, and
The Arthritic Knee The causes of OA of the knee are multiple and include aging (wear and tear), obesity, and previous knee trauma or surgery. OA affects usually the medial compartment of the knee, and
How is 1st MTP joint fusion carried out? Patient Information: Big Toe Fusion Metatarsophalangeal (MTP)
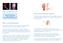 Patient Information: Big Toe Fusion Metatarsophalangeal (MTP) How is 1st MTP joint fusion carried out? You will be asked to wash your feet thoroughly on the day of operation and keep them clean, as this
Patient Information: Big Toe Fusion Metatarsophalangeal (MTP) How is 1st MTP joint fusion carried out? You will be asked to wash your feet thoroughly on the day of operation and keep them clean, as this
WHAT DO HALLUX VALGUS AND BUNION MEAN?
 Mr Laurence James BSc MBBS MRCS(Eng) FRCS(Tr&Orth) Consultant Orthopaedic Surgeon Foot, Ankle and Sports Injuries WHAT DO HALLUX VALGUS AND BUNION MEAN? Hallux is Latin for great toe and Valgus is Latin
Mr Laurence James BSc MBBS MRCS(Eng) FRCS(Tr&Orth) Consultant Orthopaedic Surgeon Foot, Ankle and Sports Injuries WHAT DO HALLUX VALGUS AND BUNION MEAN? Hallux is Latin for great toe and Valgus is Latin
TPO (Triple Pelvic Osteotomy) Information for young people
 Produced: Oct 2014 Ref: 201/02 Author: Clinical Support Review: May 2020 Royal Orthopaedic Hospital NHS Foundation Trust Patient Information Information for young people Welcome to the Royal Orthopaedic
Produced: Oct 2014 Ref: 201/02 Author: Clinical Support Review: May 2020 Royal Orthopaedic Hospital NHS Foundation Trust Patient Information Information for young people Welcome to the Royal Orthopaedic
YOUR TOTAL KNEE REPLACEMENT
 YOUR TOTAL KNEE REPLACEMENT Dr. M.S. Barrow Barrow Physiotherapy MBBch (Wits), FCS (SA) Orth. Waterfall City Hospital Orthopaedic Surgeon Tel: 011 304 7829 Suite 5, East Wing, Sunninghill Hospital www.barrowphysiotherapy.co.za
YOUR TOTAL KNEE REPLACEMENT Dr. M.S. Barrow Barrow Physiotherapy MBBch (Wits), FCS (SA) Orth. Waterfall City Hospital Orthopaedic Surgeon Tel: 011 304 7829 Suite 5, East Wing, Sunninghill Hospital www.barrowphysiotherapy.co.za
Common Foot and Ankle Conditions: How Can You Find Relief?
 Common Foot and Ankle Conditions: How Can You Find Relief? Your Feet and Ankles are Workhorses They bear a lot of weight They perform various movements Common Conditions That Cause Foot/Ankle Pain Plantar
Common Foot and Ankle Conditions: How Can You Find Relief? Your Feet and Ankles are Workhorses They bear a lot of weight They perform various movements Common Conditions That Cause Foot/Ankle Pain Plantar
Ankle, sub-talar or mid-foot joint fusion
 Ankle, sub-talar or mid-foot joint fusion This leaflet aims to answer your questions about having an ankle, sub-talar or mid-foot joint fusion. It explains the benefits, risks and alternatives, as well
Ankle, sub-talar or mid-foot joint fusion This leaflet aims to answer your questions about having an ankle, sub-talar or mid-foot joint fusion. It explains the benefits, risks and alternatives, as well
Periarticular knee osteotomy
 Periarticular knee osteotomy Turnberg Building Orthopaedics 0161 206 4803 All Rights Reserved 2018. Document for issue as handout. Knee joint The knee consists of two joints which allow flexion (bending)
Periarticular knee osteotomy Turnberg Building Orthopaedics 0161 206 4803 All Rights Reserved 2018. Document for issue as handout. Knee joint The knee consists of two joints which allow flexion (bending)
Foot and Ankle Surgery
 Information about Foot and Ankle Surgery Statement of Use The information in this leaflet is intended solely for the person to whom it was given by the health care team and is provided as a general information
Information about Foot and Ankle Surgery Statement of Use The information in this leaflet is intended solely for the person to whom it was given by the health care team and is provided as a general information
PATIENT INFORMATION THE DIFFERENCE IS MOVING.
 PATIENT INFORMATION THE DIFFERENCE IS MOVING. THIS BROCHURE IS WRITTEN TO HELP YOU MAKE AN INFORMED DECISION ABOUT YOUR SURGERY. Please read this entire brochure carefully. Keep this brochure. You may
PATIENT INFORMATION THE DIFFERENCE IS MOVING. THIS BROCHURE IS WRITTEN TO HELP YOU MAKE AN INFORMED DECISION ABOUT YOUR SURGERY. Please read this entire brochure carefully. Keep this brochure. You may
Total Hip Replacement Rehabilitation: Progression and Restrictions
 Total Hip Replacement Rehabilitation: Progression and Restrictions The success of total hip replacement (THR) is a result of predictable pain relief, improvements in quality of life, and restoration of
Total Hip Replacement Rehabilitation: Progression and Restrictions The success of total hip replacement (THR) is a result of predictable pain relief, improvements in quality of life, and restoration of
Knee arthroscopy. Physiotherapy Department. Patient information leaflet
 Knee arthroscopy Physiotherapy Department Patient information leaflet What is a knee arthroscopy? A knee arthroscopy is a type of keyhole surgery performed through small cuts in the skin. An instrument
Knee arthroscopy Physiotherapy Department Patient information leaflet What is a knee arthroscopy? A knee arthroscopy is a type of keyhole surgery performed through small cuts in the skin. An instrument
Patellar Tendon Repair Rehabilitation Guideline
 Patellar Tendon Repair Rehabilitation Guideline This rehabilitation program is designed to return the individual to their activities as quickly and safely as possible. It is designed for rehabilitation
Patellar Tendon Repair Rehabilitation Guideline This rehabilitation program is designed to return the individual to their activities as quickly and safely as possible. It is designed for rehabilitation
A patient s guide to. Radial Extracorporeal Shockwave Therapy (ESWT)
 A patient s guide to Radial Extracorporeal Shockwave Therapy (ESWT) The Foot & Ankle Unit at the Royal National Orthopaedic Hospital is made up of a multi-disciplinary team. The team consists of four specialist
A patient s guide to Radial Extracorporeal Shockwave Therapy (ESWT) The Foot & Ankle Unit at the Royal National Orthopaedic Hospital is made up of a multi-disciplinary team. The team consists of four specialist
Lumbar Decompression GUIDELINES FOR PATIENTS HAVING A. Lumbar Decompression
 ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 UPMC BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 GUIDELINES FOR PATIENTS HAVING A Lumbar Decompression Please stick addresograph
ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 UPMC BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 GUIDELINES FOR PATIENTS HAVING A Lumbar Decompression Please stick addresograph
ACL REHABILITATION. Key to Success
 ACL REHABILITATION The overall rehabilitation plan emphasises the importance of pre-operative exercises followed post operatively by early control of swelling and regaining full extension (straightening)
ACL REHABILITATION The overall rehabilitation plan emphasises the importance of pre-operative exercises followed post operatively by early control of swelling and regaining full extension (straightening)
Lesser toe deformities
 PATIENT INFORMATION Lesser toe deformities What are lesser toe deformities? Lesser toe deformities are caused by changes in normal anatomy that create an imbalance between the foot s muscle groups (intrinsic
PATIENT INFORMATION Lesser toe deformities What are lesser toe deformities? Lesser toe deformities are caused by changes in normal anatomy that create an imbalance between the foot s muscle groups (intrinsic
CEC ARTICLE: Special Medical Conditions Part 3: Hip and Knee Replacement C. Eggers
 CEC ARTICLE: Special Medical Conditions Part 3: Hip and Knee Replacement C. Eggers Joint replacement surgery removes a damaged joint and replaces it with a prosthesis or artificial joint. The purpose of
CEC ARTICLE: Special Medical Conditions Part 3: Hip and Knee Replacement C. Eggers Joint replacement surgery removes a damaged joint and replaces it with a prosthesis or artificial joint. The purpose of
Triple Pelvic Osteotomy(TPO)
 Produced: April 2015 Ref: 251/02 Author: Clinical Support Review: May 2020 Royal Orthopaedic Hospital NHS Foundation Trust Patient Information Osteotomy(TPO) Welcome to the Royal Orthopaedic Hospital (ROH).
Produced: April 2015 Ref: 251/02 Author: Clinical Support Review: May 2020 Royal Orthopaedic Hospital NHS Foundation Trust Patient Information Osteotomy(TPO) Welcome to the Royal Orthopaedic Hospital (ROH).
Barriers Between Injury and Returnto-Work. Lower Extremity. Why the Extreme Variability
 Barriers Between Injury and Returnto-Work in the Lower Extremity Why the Extreme Variability Barriers to Diagnosis Failure or delay in reporting injury Employee expectations: Not really a serious injury
Barriers Between Injury and Returnto-Work in the Lower Extremity Why the Extreme Variability Barriers to Diagnosis Failure or delay in reporting injury Employee expectations: Not really a serious injury
Subtalar Fusion. Cornwall Foot and Ankle
 Subtalar Fusion Cornwall Foot and Ankle Tibia (shin bone) Talus (ankle bone) Calcaneum (heel bone) SUBTALAR JOINT SIDE VIEW OF ANKLE Patient Information on Subtalar Fusion (Arthrodesis) What is a subtalar
Subtalar Fusion Cornwall Foot and Ankle Tibia (shin bone) Talus (ankle bone) Calcaneum (heel bone) SUBTALAR JOINT SIDE VIEW OF ANKLE Patient Information on Subtalar Fusion (Arthrodesis) What is a subtalar
THE TRUTH ABOUT OSTEOARTHRITIS. By GRAHAM NELSON RUSSELL VISSER
 THE TRUTH ABOUT OSTEOARTHRITIS By GRAHAM NELSON RUSSELL VISSER WWW.NWPG.COM.AU THE TRUTH ABOUT OSTEOARTHRITIS 2 ABOUT NORTHWEST PHYSIOTHERAPY GROUP Northwest Physiotherapy Group was first established as
THE TRUTH ABOUT OSTEOARTHRITIS By GRAHAM NELSON RUSSELL VISSER WWW.NWPG.COM.AU THE TRUTH ABOUT OSTEOARTHRITIS 2 ABOUT NORTHWEST PHYSIOTHERAPY GROUP Northwest Physiotherapy Group was first established as
Sports and Recreational Activities following Total Ankle Replacement
 12 Original Article THIEME Sports and Recreational Activities following Total Ankle Replacement Federico Giuseppe Usuelli 1 Andrea Pantalone 2 Camilla Maccario 1 Matteo Guelfi 2 Vincenzo Salini 2 1 Casco,
12 Original Article THIEME Sports and Recreational Activities following Total Ankle Replacement Federico Giuseppe Usuelli 1 Andrea Pantalone 2 Camilla Maccario 1 Matteo Guelfi 2 Vincenzo Salini 2 1 Casco,
NICHOLAS J. AVALLONE, M.D.
 NICHOLAS J. AVALLONE, M.D. www.dravallone.com ACHILLES TENDON REPAIR REHAB GUIDELINES DISCLAIMER: The intent of this protocol is to provide therapists with guidelines for rehabilitation based on a review
NICHOLAS J. AVALLONE, M.D. www.dravallone.com ACHILLES TENDON REPAIR REHAB GUIDELINES DISCLAIMER: The intent of this protocol is to provide therapists with guidelines for rehabilitation based on a review
Mr. Siva Chandrasekaran Orthopaedic Surgeon MBBS MSpMed MPhil (surg) FRACS
 Bunion Surgery Most people with bunions find pain relief with simple treatments to reduce pressure on the big toe, such as wearing wider shoes or using pads in their shoes. However, if these measures do
Bunion Surgery Most people with bunions find pain relief with simple treatments to reduce pressure on the big toe, such as wearing wider shoes or using pads in their shoes. However, if these measures do
Integra. Salto Talaris Total Ankle Prosthesis PATIENT INFORMATION
 Integra Salto Talaris Total Ankle Prosthesis PATIENT INFORMATION Fibula Articular Surface Lateral Malleolus Tibia Medial Malleolus Talus Anterior view of the right ankle region Talo-fibular Ligament Calcaneal
Integra Salto Talaris Total Ankle Prosthesis PATIENT INFORMATION Fibula Articular Surface Lateral Malleolus Tibia Medial Malleolus Talus Anterior view of the right ankle region Talo-fibular Ligament Calcaneal
ACHILLES TENDON REPAIR REHAB GUIDELINES
 ACHILLES TENDON REPAIR REHAB GUIDELINES Typically patients are discharged on the day of the operation or the next day. The leg is usually immobilized in a cast or hinged brace, ranging from 4-8 weeks.
ACHILLES TENDON REPAIR REHAB GUIDELINES Typically patients are discharged on the day of the operation or the next day. The leg is usually immobilized in a cast or hinged brace, ranging from 4-8 weeks.
Physical Therapy for the Lower Extremity: What You and Your Patient Should Expect from Rehab
 1 Physical Therapy for the Lower Extremity: What You and Your Patient Should Expect from Rehab Thomas Clennell, PT, DPT, SCS Physical Therapist UCSF Benioff Children s Hospital Oakland Sports Medicine
1 Physical Therapy for the Lower Extremity: What You and Your Patient Should Expect from Rehab Thomas Clennell, PT, DPT, SCS Physical Therapist UCSF Benioff Children s Hospital Oakland Sports Medicine
WHAT IS HIP ARTHROSCOPY?
 HIP ARTHROSCOPY Information for patients WHAT IS HIP ARTHROSCOPY? Hip arthroscopy is a minimally invasive procedure. An arthroscopic camera provides a magnified image of all parts of the joint. With the
HIP ARTHROSCOPY Information for patients WHAT IS HIP ARTHROSCOPY? Hip arthroscopy is a minimally invasive procedure. An arthroscopic camera provides a magnified image of all parts of the joint. With the
Advice following Anterior Cruciate Ligament (ACL) reconstruction
 Advice following Anterior Cruciate Ligament (ACL) reconstruction Information for patients Mobilisation As soon as you feel well enough after the operation you will be able to get up and mobilise. You will
Advice following Anterior Cruciate Ligament (ACL) reconstruction Information for patients Mobilisation As soon as you feel well enough after the operation you will be able to get up and mobilise. You will
Tendo Achilles rupture
 Tendo Achilles rupture Conservative and surgical management Therapy Department 01935 475 122 yeovilhospital.nhs.uk What is the Achilles tendon? The Achilles tendon is a large tendon at the back of the
Tendo Achilles rupture Conservative and surgical management Therapy Department 01935 475 122 yeovilhospital.nhs.uk What is the Achilles tendon? The Achilles tendon is a large tendon at the back of the
Physiotherapy information for Achilles Tendinopathy
 Physiotherapy information for Achilles Tendinopathy What is Achilles Tendinopathy? Achilles Tendinopathy is a condition that can cause pain, swelling and weakness of the Achilles Tendon. This joins your
Physiotherapy information for Achilles Tendinopathy What is Achilles Tendinopathy? Achilles Tendinopathy is a condition that can cause pain, swelling and weakness of the Achilles Tendon. This joins your
Calcaneus (Heel Bone) Fractures
 Page 1 of 8 Calcaneus (Heel Bone) Fractures A fracture of the calcaneus, or heel bone, can be a painful and disabling injury. This type of fracture commonly occurs during a high-energy event such as a
Page 1 of 8 Calcaneus (Heel Bone) Fractures A fracture of the calcaneus, or heel bone, can be a painful and disabling injury. This type of fracture commonly occurs during a high-energy event such as a
Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction
 Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These
Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These
Arthroscopy for Hip Osteoarthritis
 Appendix: Script #1: Health scenarios Arthroscopy for Hip Osteoarthritis Introduction Hip arthroscopy is a surgical procedure that gives doctors a clear view of the inside of the hip joint. This helps
Appendix: Script #1: Health scenarios Arthroscopy for Hip Osteoarthritis Introduction Hip arthroscopy is a surgical procedure that gives doctors a clear view of the inside of the hip joint. This helps
Physiotherapy following peri acetabular osteotomy (PAO) surgery
 Physiotherapy following peri acetabular osteotomy (PAO) surgery This leaflet explains more about returning to your everyday activities after your peri acetabular osteotomy (PAO). It explains the exercises
Physiotherapy following peri acetabular osteotomy (PAO) surgery This leaflet explains more about returning to your everyday activities after your peri acetabular osteotomy (PAO). It explains the exercises
WHAT IS ARTHRITIS OF THE BIG TOE (HALLUX RIGIDUS)?
 Mr Laurence James BSc MBBS MRCS(Eng) FRCS(Tr&Orth) Consultant Orthopaedic Surgeon Foot, Ankle and Sports Injuries WHAT IS ARTHRITIS OF THE BIG TOE (HALLUX RIGIDUS)? A common term for arthritis of the metatarsophalangeal
Mr Laurence James BSc MBBS MRCS(Eng) FRCS(Tr&Orth) Consultant Orthopaedic Surgeon Foot, Ankle and Sports Injuries WHAT IS ARTHRITIS OF THE BIG TOE (HALLUX RIGIDUS)? A common term for arthritis of the metatarsophalangeal
Total Ankle Arthroplasty for the Treatment of Symptomatic Nonunion following Tibiotalar Fusion
 Total Ankle Arthroplasty for the Treatment of Symptomatic Nonunion following Tibiotalar Fusion W I L L I A M P. H U N T I N G T O N, M. D. W. H O D G E S D A V I S, M. D. R O B E R T B. A N D E R S O N,
Total Ankle Arthroplasty for the Treatment of Symptomatic Nonunion following Tibiotalar Fusion W I L L I A M P. H U N T I N G T O N, M. D. W. H O D G E S D A V I S, M. D. R O B E R T B. A N D E R S O N,
Anterior Cruciate Ligament (ACL) Reconstruction Protocol
 Christopher M. Larson, MD Anterior Cruciate Ligament (ACL) Reconstruction Protocol **Please see the IMPORTANT NOTE for STRETCHING / KNEE EXTENSION on page 5** The intent of this protocol is to provide
Christopher M. Larson, MD Anterior Cruciate Ligament (ACL) Reconstruction Protocol **Please see the IMPORTANT NOTE for STRETCHING / KNEE EXTENSION on page 5** The intent of this protocol is to provide
Make sure you have properly fitting running shoes and break these in gradually. Never wear new running shoes for a race or a long run.
 Common Running Injuries We are delighted that you have decided to run in the next Bath Half Marathon and very much hope that you have good running shoes, undertake a regular training programme and don
Common Running Injuries We are delighted that you have decided to run in the next Bath Half Marathon and very much hope that you have good running shoes, undertake a regular training programme and don
Excision of Morton s Neuroma
 Excision of Morton s Neuroma Day Surgery Unit Patient information leaflet This leaflet outlines the risks, general advice and information about foot surgery called an excision of a Morton s Neuroma. If
Excision of Morton s Neuroma Day Surgery Unit Patient information leaflet This leaflet outlines the risks, general advice and information about foot surgery called an excision of a Morton s Neuroma. If
Achilles tendon rupture: management and rehabilitation
 Achilles tendon rupture: management and rehabilitation Introduction The Achilles tendon (or heel cord) is the largest tendon in the human body. It connects the calf muscles (gastrocnemius and soleus) to
Achilles tendon rupture: management and rehabilitation Introduction The Achilles tendon (or heel cord) is the largest tendon in the human body. It connects the calf muscles (gastrocnemius and soleus) to
Non weight bearing advice (post operative)
 Non weight bearing advice (post operative) Physiotherapy Department Patient information leaflet Who is this booklet for? This booklet is for post-operative patients who have been told that they will have
Non weight bearing advice (post operative) Physiotherapy Department Patient information leaflet Who is this booklet for? This booklet is for post-operative patients who have been told that they will have
Rehabilitation Protocol: Distal Femoral/Proximal Tibial Microfracture and Osteochondral Autograft Transplantation (OATS)
 Rehabilitation Protocol: Distal Femoral/Proximal Tibial Microfracture and Osteochondral Autograft Transplantation (OATS) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650
Rehabilitation Protocol: Distal Femoral/Proximal Tibial Microfracture and Osteochondral Autograft Transplantation (OATS) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650
Medial Patellofemoral Ligament Reconstruction Guidelines Brian Grawe Protocol
 Medial Patellofemoral Ligament Reconstruction Guidelines Brian Grawe Protocol Progression is based on healing constraints, functional progression specific to the patient. Phases and time frames are designed
Medial Patellofemoral Ligament Reconstruction Guidelines Brian Grawe Protocol Progression is based on healing constraints, functional progression specific to the patient. Phases and time frames are designed
Knee Replacement PROGRAM. Nightingale. Home Healthcare
 Knee Replacement PROGRAM TM Nightingale Home Healthcare With the help of Nightingale s experienced and professional rehabilitation team, you will be guided through a more complete and successful recovery
Knee Replacement PROGRAM TM Nightingale Home Healthcare With the help of Nightingale s experienced and professional rehabilitation team, you will be guided through a more complete and successful recovery
