Guideline. Drugs & Therapeutics Committee
|
|
|
- Rose York
- 6 years ago
- Views:
Transcription
1 Physiotherapy Rehabilitation Guidelines for patients undergoing Lateral Ligament Reconstruction of the Ankle Document Type Date Approved Ratifying Body Related Documents Guideline 13/11/2017 Drugs & Therapeutics Committee Physiotherapy rehabilitation guidelines Pes Cavus Correction Physiotherapy rehabilitation guidelines Anterior ankle arthroscopy Physiotherapy rehabilitation guidelines Total Ankle Replacement Physiotherapy rehabilitation guidelines Subtalar and Hindfoot fusion Physiotherapy rehabilitation guidelines Hallux valgus deformity- Scarf Osteotomy Physiotherapy rehabilitation guidelines Tibialis Posterior Reconstruction Physiotherapy rehabilitation guidelines ACI of the ankle Author Owner (Executive Director) Directorate Superseded Documents Subject Review Date Joanna Benfield, Foot & Ankle Specialist Physiotherapist, RNOH Lucy Davies Operations Rehab Guidelines for Lateral Ligament Reconstruction of the Ankle (2008) Clinical, Clinical Units, Communication, Inpatient & Outpatient Services 13/11/2022 Ankle Page 1
2 Keywords and Phrases Consultation Group/Approving Bodies/Subject Matter Expert Rehabilitation, foot and ankle surgery, lateral ligament, anterior talofibular ligament, ATFL, calcaneofibular ligament, CFL, posterior talofibular ligament, PTFL, ankle sprain, instability, chronic ankle instability, CAI, mechanical instability, functional instability, Brostrum, Crisman-Snook, physiotherapy, complications, outcomes, milestones, function, treatment, exercise, pain relief, restrictions, limitations, sport, fitness, postural awareness, pain education, mobility, goals, precautions, compliance, ankle pain, leg pain, foot pain. Members of Foot and Ankle Unit Team (4 consultants, & Clinical Nurse Specialist) Members of Outpatient Musculoskeletal Physiotherapy Team (Band 5, 6, 7 and 8a staff members at Stanmore and Bolsover Street) Members of Inpatient Orthopaedic Physiotherapy Team (Band 7 and 8a staff members) Readership All staff (inc. Clinical) Ankle Page 2
3 Table of Contents 1. Equality Impact Assessment (EIA) Disclosure Statement Privacy Impact Assessment (PIA) Disclosure Statement Introduction and aims Definitions Duties and Responsibilities Body of Policy Monitoring and the effectiveness of this policy... 7 Appendix 1: Appendix 2: Appendix 3: Glossary of Terms Other linked trust policies and guidelines Extra sources of information and support Ankle Page 3
4 Equality Impact Assessment (EIA) Disclosure Statement Equality Impact Assessment (EIA) Disclosure Statement This policy was assessed on the 1st day of June 2017 for its impact on equality. The assessment determined that the policy will not have a significant negative impact on equality in relation to each of the protected staff/patient groups below: i.) Age; ii.) Sex (Male and Female); iii.) Disability (Learning Difficulties/Physical or Sensory Disability); iv.) Race or Ethnicity; v.) Religion and Belief; vi) Sexual Orientation (gay, lesbian or heterosexual); vii) Pregnancy and Maternity; vii) Gender Reassignment (The process of transitioning from one gender to another); viii) Marriage and Civil Partnership. Ankle Page 4
5 1. Privacy Impact Assessment (PIA) Disclosure Statement Privacy Impact Assessment (PIA) Disclosure Statement This policy was assessed on the 1 st day of June 2017 for its impact on privacy. The assessment determined that the policy will not have a significant negative impact on privacy of members of staff/patients. Ankle Page 5
6 2. Introduction and aims Please note that this is advisory information only. Individual / your experiences may differ from those described. All exercises must be demonstrated to a patient by a fully qualified physiotherapist. We cannot be held liable for the outcome of you undertaking any of the exercises / interventions shown here independently of direct supervision from the RNOH. As a specialist orthopaedic hospital we recognise that our broad and often complex patient group needs an individualised rehabilitation approach. Our emphasis is on patient-specific rehabilitation, which encourages recognition of those patients who may progress slower than others. These rehabilitation guidelines are therefore milestone driven and designed to provide an equitable rehabilitation service to all our patients. They will also limit unnecessary visits to the outpatient clinic at RNOHT by helping the patient and therapist to identify when specialist review is required. 3. Definitions See section Duties and Responsibilities Not applicable for this guideline. Ankle Page 6
7 5. Body of Policy Team Contact Details: Foot & Ankle Unit Consultants: Mr Singh, Mr Cullen, Mr Goldberg & Mr Welck Foot and Ankle Unit: Tel: (Please note that if ing from an address external to RNOH that this address is not secure so please do not include patient identifiable data) Physiotherapy Department: Tel: Ankle Page 7
8 Indications for surgery: Generally for Chronic Lateral Ankle Instability in patients who have failed to respond to conservative treatment. Possible complications: Infection Bleeding Nerve damage Deep Vein Thrombosis Pulmonary Embolism Scarring Persistent / Recurrent pain Recurrent instability Talo-crural and sub-talar joint stiffness Numbness/Pin s & Needles in the foot post-operatively Surgical techniques The technique(s) used will depend on the severity of the ankle instability and the quality of the lateral ligament complex. Surgery tends to include one of the following: Primary Anatomical (non-augmented) repair. Carried out by reattaching torn ligaments in order to regain lateral ankle stability. A Brostrom repair is the common technique used in an anatomical repair. Secondary Extrinsic (augmented) repair. The surgeon may use the peronei and re-route them, commonly through the lateral malleolus in order to gain greater stability. A Chrisman-Snook stabilisation is the commonly used technique at RNOH. Expected outcome: Improved function / mobility Improved pain relief, with decreased analgesic requirements Improved ankle-hindfoot complex stability Decreased requirement for orthotics Return to full sporting activity Full recovery may take up to twelve months Ankle Page 8
9 Pre-operatively The patient will be seen pre-operatively where able and with consent, the following will be assessed or discussed: Current functional levels General Health Social history and home set up Ability to mobilise, plus the provision of appropriate walking aids to be used post operatively Post-operative expectations Post-operative management explained, including the provision of bed exercises. Post-operatively Always check the operation notes, and the post-operative instructions. Discuss any deviation from routine guidelines with the team concerned. This is very important as the patient may have had a combination of techniques which may affect weightbearing status and progressions. Ankle Page 9
10 INITIAL REHABILITATION PHASE: 0-4 Weeks Goals: To be safely and independently mobile with appropriate walking aid, adhering to weight bearing status To be independent with home exercise programme as appropriate To understand self-management / monitoring, e.g. skin sensation, colour, swelling, temperature, circulation, elevation Restrictions: Ensure that weight bearing restrictions are adhered to: Primary Anatomical Repair and Secondary Anatomical Repair: o Back slab with foot in neutral dorsiflexion and maximum eversion for 2 weeks Non Weight Bearing (NWB). o Below Knee Plaster of Paris (BK POP) at 2 weeks. Full Weight Bearing (FWB). o POP removed at 4 weeks. Into ankle brace. FWB. No Range of Movement into Inversion for 6 weeks and care on Plantarflexion for 6 weeks to avoid stretching / stressing / damaging the repair site. Elevation If sedentary employment, may be able to return to work from 4 weeks postoperatively, as long as provisions to elevate leg, and no complications Treatment: Likely to be in Walker Boot or POP Pain-relief: Ensure adequate analgesia Elevation Exercises: teach circulatory exercises Education: teach how to monitor sensation, colour, circulation, temperature, swelling, and advise what to do if concerned Mobility: ensure patient independent with transfers and mobility, including stairs if necessary On discharge from ward: Independent and safe mobilising, including stairs if appropriate Independent with transfers Independent and safe with home exercise programme / monitoring Milestones to progress to next phase: Out of POP. Team to refer to physiotherapy at 4 weeks from clinic. Progression from NWB to FWB phase. Team to refer to physiotherapy if required to review safety of mobility / use of walking aids Adequate analgesia Ankle Page 10
11 RECOVERY REHABILITATION PHASE: 4 weeks- 12 weeks Goals: To be independently mobile unaided To achieve full range of movement Muscle strength: eversion grade 4 or 5 on Oxford scale Optimise normal movement Restrictions: No Range of Movement into Inversion until week 6, and care on Plantarflexion, to avoid stretching / stressing / damaging the repair site. Care on inversion and plantarflexion until week 12 Do not formally stretch ligament reconstruction into inversion or plantarflexion. It will naturally lengthen over a 6 month period Ensure adherence to weight bearing status To wear ankle brace until week 12, and longer if needed, until good stability and proprioceptive control No balance exercises until eversion grade 4 or 5 on Oxford scale achieved No impact exercise; i.e. jogging, aerobics Treatment: Pain relief Advice / Education Posture advice / education Mobility: ensure safely and independently mobile. Progress off walking aids once able. Gait Re-education Exercises: o Passive range of movement (PROM) / Active assisted range of movement (AAROM) / Active range of movement (AROM) (See restrictions above) o Strengthening exercises as appropriate o Core stability work o Balance / proprioception work once appropriate o Stretches of tight structures as appropriate (e.g. Achilles Tendon), not of ligament reconstruction o Review lower limb biomechanics and kinetic chain. Address issues as appropriate Swelling Management Manual Therapy: o Soft tissue techniques as appropriate o Joint mobilisations as appropriate Monitor sensation, swelling, colour, temperature, circulation Orthotics if required via surgical team Ankle Page 11
12 Hydrotherapy if appropriate Pacing advice as appropriate Milestones to progress to next phase: Muscle strength: eversion grade 4 or 5 on Oxford scale Full range of movement Neutral foot position when weight bearing / mobilising Failure to meet milestones: Refer back to team / Discuss with team Continue with outpatient physiotherapy if still progressing Ankle Page 12
13 INTERMEDIATE REHABILITATION PHASE: 12 weeks 6 months Goals: Independently mobile unaided out of brace Grade 4 or 5 muscle strength around ankle Optimise normal movement Return to low impact activity / sports Restrictions: Do not formally stretch ligament reconstruction into inversion or plantarflexion. It will naturally lengthen over a 6 month period To wear ankle brace until week 12, and longer if needed, until good stability and proprioceptive control No balance exercises until eversion grade 4 or 5 on Oxford scale achieved Treatment: Further progression of the above treatment: Pain relief Advice / Education Posture advice / education Mobility: Progression of mobility and function Wean from Brace: Once appropriate when has good stability and proprioceptive control Gait Re-education Exercises: o Range of movement o Progression of strengthening exercises as appropriate including of evertors. o Core stability work o Balance / proprioception work including progression to use of wobble boards, trampet, gym ball, dyna-cushion as appropriate o Stretches of tight structures as appropriate (e.g. Achilles Tendon), not of ligament reconstruction o Review lower limb biomechanics and kinetic chain. Address issues as appropriate. o Sports specific rehabilitation Swelling Management Manual Therapy: o Soft tissue techniques as appropriate o Joint mobilisations as appropriate ensuring awareness of those which may be fused and therefore not appropriate to mobilise Monitor sensation, swelling, colour, temperature, circulation Orthotics if required via surgical team Ankle Page 13
14 Hydrotherapy if appropriate Pacing advice as appropriate Milestones to progress to next phase: Independently mobile unaided out of brace Muscle strength: eversion grade 5 on Oxford scale Returned to low-impact activity / sports Failure to meet milestones: Refer back to team / Discuss with team Continue with outpatient physiotherapy if still progressing Ankle Page 14
15 FINAL REHABILITATION PHASE: 6 months 1 year Goals: Return to high impact sports if set as patient goal Normal evertor activity Single leg stand 10 seconds, eyes open and closed To be able to do multiple single leg heel raise Establish long term maintenance programme Treatment: Mobility / function: Progression of mobility and function, increasing dynamic control with specific training to functional goals Gait Re-education Exercises: o Progression of exercises including strengthening, balance and proprioception, core stability o Sports specific / functional exercises Swelling Management Manual therapy o Soft tissue techniques as appropriate o Joint mobilisations as appropriate ensuring awareness of those which may be fused and therefore not appropriate to mobilise Pacing advice Milestones for discharge: Independently mobile unaided Return to normal functional level Grade 5 eversion strength on Oxford scale Good proprioceptive control on single leg stand on operated limb Appropriate patient-specific functional goals achieved Return to sports if set as patient goal Ankle Page 15
16 FAILURE TO PROGRESS If a patient is failing to progress, then consider the following: POSSIBLE PROBLEM Swelling Pain Breakdown of wound e.g. inflammation, bleeding, infection Recurrent instability Numbness/altered sensation ACTION Ensure elevating leg regularly Use ice as appropriate if normal skin sensation and no contraindications Decrease amount of time on feet Pacing Use walking aids Circulatory exercises If decreases overnight, monitor closely If does not decrease overnight, refer back to surgical team or to GP Decrease activity Ensure adequate analgesia Elevate regularly Decrease weight bearing and use walking aids as appropriate Pacing Modify exercise programme as appropriate If persists, refer back to surgical team or to GP Refer to surgical team or to GP Refer back to surgical team Ensure exercises not too advanced for patient Address core stability Liaise with podiatrist/orthotics re: footwear Review immediate post-operative status if possible Ensure swelling under control If new onset or increasing refer back to surgical team or GP If static, monitor closely, but inform surgical team and refer back if deteriorates or if concerned 6. Monitoring and the effectiveness of this policy This guideline will be reviewed 5 yearly. Ankle Page 16
17 Ankle Page 17
18 Appendix 1: Glossary of Terms Not applicable. Ankle Page 18
19 Appendix 2: Other linked trust policies and guidelines Physiotherapy rehabilitation guidelines Pes cavus correction Physiotherapy rehabilitation guidelines Anterior ankle arthroscopy Physiotherapy rehabilitation guidelines Total Ankle Replacement Physiotherapy rehabilitation guidelines Subtalar and hindfoot fusion Physiotherapy rehabilitation guidelines Hallux valgus deformity- Scarf Osteotomy Physiotherapy rehabilitation guidelines Tibialis Posterior Reconstruction Physiotherapy rehabilitation guidelines ACI of the ankle All other RNOH Physiotherapy Rehabilitation Orthopaedic Post-operative Guidelines (Knee, Sarcoma Unit, Peripheral Nerve Injuries, Shoulder & Upper Limb, Spinal Surgery Unit) Ankle Page 19
20 Appendix 3: Extra sources of information and support Summary of evidence for physiotherapy guidelines A comprehensive literature search was carried out to identify research relating to rehabilitation for ankle instability and surgery for recurrent ankle instability and subsequent rehabilitation. After reviewing the articles and information, the physiotherapy guidelines were produced on the best available evidence. Baumhauer J, O Brien T (2002) Surgical Considerations in the Treatment of Ankle Instability. Journal of Athletic Training 37 (4) Burrus, M., Werner, B., Hadeed, M., Walker, J., Perumal, V. and Park, J. (2014). Predictors of Peroneal Pathology in Broström Gould Ankle Ligament Reconstruction for Lateral Ankle Instability. Foot & Ankle International, 36(3), pp Cheng M, Tho K (2002) Chrisman-Snook Ankle Ligament Reconstruction Outcomes A Local Experience. Singapore Med J 2002 Vol 43(12) : De Vries J, Krips R, Sierevelt I, Blankevoort L, Van Dijk C (2007) Interventions for treating chronic ankle stability. A Cochrane Review. Cochrane Database of Systematic Reviews. Issue 1 Fujii T, Kitaoka H, Watanabe K, Luo Z, An K (2006) Comparison of Modified Brostrom and Evans Procedure in Simulated Lateral Ankle Injury. Medicine & Science in Sports & Exercise 38 (6): Gribble et al (2016) Evidence review for the 2016 International Ankle Consortium consensus statement on the prevalence, impact and long-term consequences of lateral ankle sprains. British Journal of Sports Medicine (50) Hennrikus, W., Mapes, R., Lyons, P. and Lapoint, J. (1996). Outcomes of the Chrisman-Snook and Modified-Broström Procedures for Chronic Lateral Ankle Instability. The American Journal of Sports Medicine, 24(4), pp Hsu, A., Ardoin, G., Davis, W. and Anderson, R. (2015). Intermediate and Long-Term Outcomes of the Modified Brostrom-Evans Procedure for Lateral Ankle Ligament Reconstruction. Foot & Ankle Specialist, 9(2), pp Karlsson J, Lundin O, Lind K, Styf J (1999) Early mobilization vesus immobilization after ankle ligament stabilization. Scandinavian Journal of Medicine & Science in Sports 9: Karlsson J, Rudholm O, Bergsten T, Faxen E, Styf J (1995) Early range of motion training after ligament reconstruction of the ankle joint. Knee Surgery Sports Traumatology Arthroscopy 3: Kramer, D., Solomon, R., Curtis, C., Zurakowski, D. and Micheli, L. (2010). Clinical Results and Functional Evaluation of the Chrisman-Snook Procedure for Lateral Ankle Instability in Athletes. Foot & Ankle Specialist, 4(1), pp Ankle Page 20
21 Letts M, Davidson D, Mukhtar I (2003) Surgical Management of Chronic Lateral Ankle Instability in Adolescents. Journal of Pediatric Orthopaedics 23 (3) Li, H., Hua, Y., Li, H., Ma, K., Li, S. and Chen, S. (2017). Activity Level and Function 2 Years After Anterior Talofibular Ligament Repair: A Comparison Between Arthroscopic Repair and Open Repair Procedures. The American Journal of Sports Medicine, 45(9), pp Li, H., Zheng, J., Zhang, J., Hua, Y. and Chen, S. (2015). The Effect of Lateral Ankle Ligament Repair in Muscle Reaction Time in Patients with Mechanical Ankle Instability. International Journal of Sports Medicine, 36(12), pp Li, H., Zheng, J., Zhang, J., Cai, Y., Hua, Y. and Chen, S. (2015). The improvement of postural control in patients with mechanical ankle instability after lateral ankle ligaments reconstruction. Knee Surgery, Sports Traumatology, Arthroscopy, 24(4), pp Marsh J, Daigneault J, Polzhofer G (2006) Treatment of Ankle Instability in Children and Adolescents with a Modified Chrisman-Snook Repair: A Clinical and Patient-Based Outcome Study. Journal of Pediatric Orthopaedics 26 (1) Matheny, L., Johnson, N., Liechti, D. and Clanton, T. (2016). Activity Level and Function After Lateral Ankle Ligament Repair Versus Reconstruction. The American Journal of Sports Medicine, 44(5), pp Mattacola C & Dwyer M (2002) Rehabilitation of the Ankle after Acute Sprain or Chronic Instability. Journal of Athletic Training 37 (4) Miyamoto, W., Takao, M., Yamada, K. and Matsushita, T. (2014). Accelerated Versus Traditional Rehabilitation After Anterior Talofibular Ligament Reconstruction for Chronic Lateral Instability of the Ankle in Athletes. The American Journal of Sports Medicine, 42(6), pp Park, K., Lee, J., Suh, J., Shin, M. and Choi, W. (2016). Generalized Ligamentous Laxity Is an Independent Predictor of Poor Outcomes After the Modified Broström Procedure for Chronic Lateral Ankle Instability. The American Journal of Sports Medicine, 44(11), pp Pearce, C., Tourné, Y., Zellers, J., Terrier, R., Toschi, P. and Silbernagel, K. (2016). Rehabilitation after anatomical ankle ligament repair or reconstruction. Knee Surgery, Sports Traumatology, Arthroscopy, 24(4), pp Petrera, M., Dwyer, T., Theodoropoulos, J. and Ogilvie-Harris, D. (2014). Shortto Medium-term Outcomes After a Modified Broström Repair for Lateral Ankle Instability With Immediate Postoperative Weightbearing. The American Journal of Sports Medicine, 42(7), pp Russo, A. (2016). Treatment of chronic lateral ankle instability using the Brostrom-Gould procedure in athletes: long-term results. Joints. 4,(2), pp Sammarco, V. (2001). Complications of Lateral Ankle Ligament Reconstruction. Clinical Orthopaedics and Related Research, 391, pp Ankle Page 21
22 Shakked, R., Karnovsky, S. and Drakos, M. (2017). Operative treatment of lateral ligament instability. Current Reviews in Musculoskeletal Medicine, 10(1), pp Shibuya, N., Bazán, D., Evans, A., Agarwal, M. and Jupiter, D. (2016). Efficacy and Safety of Split Peroneal Tendon Lateral Ankle Stabilization. The Journal of Foot and Ankle Surgery, 55(4), pp So, E., Preston, N. and Holmes, T. (2017). Intermediate- to Long-Term Longevity and Incidence of Revision of the Modified Broström-Gould Procedure for Lateral Ankle Ligament Repair: A Systematic Review. The Journal of Foot and Ankle Surgery, 56(5), pp Tohyama, H., Beynnon, B., Pope, M., Haugh, L. and Renström, P. (1997). Laxity and flexibility of the ankle following reconstruction with the Chrisman- Snook procedure. Journal of Orthopaedic Research, 15(5), pp Tourné, Y. and Mabit, C. (2017). Lateral ligament reconstruction procedures for the ankle. Orthopaedics & Traumatology: Surgery & Research, 103(1), pp.s171-s181. White, W., McCollum, G. and Calder, J. (2015). Return to sport following acute lateral ligament repair of the ankle in professional athletes. Knee Surgery, Sports Traumatology, Arthroscopy, 24(4), pp Xu, H. and Lee, K. (2016). Modified Broström Procedure for Chronic Lateral Ankle Instability in Patients With Generalized Joint Laxity. The American Journal of Sports Medicine, 44(12), pp Xu, H., Choi, M., Kim, M., Park, K. and Lee, K. (2015). Gender Differences in Outcome After Modified Broström Procedure for Chronic Lateral Ankle Instability. Foot & Ankle International, 37(1), pp Yoo, J. and Yang, E. (2016). Clinical results of an arthroscopic modified Brostrom operation with and without an internal brace. Journal of Orthopaedics and Traumatology, 17(4), pp Ankle Page 22
23 This policy is available on request in large print and alternative languages. It is a manager s responsibility to ensure employees are aware of these options. * The following policies must be sent for review to the Local Counter Fraud Specialist: Fraud and Bribery Standard Financial Instructions Declaration of Interests Gifts and Hospitality Whistleblowing Disciplinary IT Anti-Money Laundering Managing Sickness Absence Secondary Employment Expenses Overpayment Financial Redress TOIL (Time off in Lieu) Code of Conduct/Standards of Business Conduct Data Protection Lone Worker Patient Transport Commercial Sponsorship Overseas Visitors Disclosure Ankle Page 23
Ankle instability surgery
 Ankle instability surgery Ankle instability surgery is generally reserved for people with chronic ankle instability who have failed to respond to conservative treatment. The surgical technique used will
Ankle instability surgery Ankle instability surgery is generally reserved for people with chronic ankle instability who have failed to respond to conservative treatment. The surgical technique used will
Total ankle replacement
 Total ankle replacement Initial rehabilitation phase 0-4 weeks To be safely and independently mobile with appropriate walking aid, adhering to weight bearing status To be independent with home exercise
Total ankle replacement Initial rehabilitation phase 0-4 weeks To be safely and independently mobile with appropriate walking aid, adhering to weight bearing status To be independent with home exercise
Bunion (hallux valgus deformity) surgery
 Bunion (hallux valgus deformity) surgery Bunion surgery is generally reserved for bunions that are severe and impacting on function. There most frequent surgical procedure used involves a medial incision
Bunion (hallux valgus deformity) surgery Bunion surgery is generally reserved for bunions that are severe and impacting on function. There most frequent surgical procedure used involves a medial incision
Foot and ankle fractures
 Foot and ankle fractures Some fractures can be managed without surgery, but others require surgery to achieve the best possible outcome. Fractures and injuries to joints have a high risk of developing
Foot and ankle fractures Some fractures can be managed without surgery, but others require surgery to achieve the best possible outcome. Fractures and injuries to joints have a high risk of developing
Foot and ankle. Achilles tendon rupture repair. After surgery
 Foot and ankle Achilles tendon rupture repair There is no agreed single best treatment for Achilles tendon ruptures. Similar results can be achieved with non-surgical and surgical treatments. There is
Foot and ankle Achilles tendon rupture repair There is no agreed single best treatment for Achilles tendon ruptures. Similar results can be achieved with non-surgical and surgical treatments. There is
Rehabilitation guidelines for patients undergoing Anterior Ankle Arthroscopy
 Rehabilitation guidelines for patients undergoing Anterior Ankle Arthroscopy At the RNOH, our emphasis is patient specific, which encourages recognition of those who may progress slower then others. We
Rehabilitation guidelines for patients undergoing Anterior Ankle Arthroscopy At the RNOH, our emphasis is patient specific, which encourages recognition of those who may progress slower then others. We
INITIAL REHABILITATION PHASE 0-4 weeks. Posterolateral Corner Injury
 Posterolateral Corner Injury Indications for Surgery The main indication of PLC reconstruction surgery is symptomatic instability following PLC injury. The aim of PLC reconstruction surgery is to restore
Posterolateral Corner Injury Indications for Surgery The main indication of PLC reconstruction surgery is symptomatic instability following PLC injury. The aim of PLC reconstruction surgery is to restore
Guideline. Drugs & Therapeutics Committee
 Physiotherapy Rehabilitation Guidelines for patients undergoing Total Ankle Replacement Document Type Date Approved Ratifying Body Related Documents Guideline 13/11/2017 Drugs & Therapeutics Committee
Physiotherapy Rehabilitation Guidelines for patients undergoing Total Ankle Replacement Document Type Date Approved Ratifying Body Related Documents Guideline 13/11/2017 Drugs & Therapeutics Committee
Overview. 20% of lateral ankle sprains can lead to chronic pain and instability (UW Sports Medicine, 2014)
 Overview Lateral ankle sprains are the most common sports injury (Godges & Klingman, 2014) Conservative treatment: o Aggressive rehabilitation, bracing, taping, and/or orthotics (UW Sports Medicine, 2014)
Overview Lateral ankle sprains are the most common sports injury (Godges & Klingman, 2014) Conservative treatment: o Aggressive rehabilitation, bracing, taping, and/or orthotics (UW Sports Medicine, 2014)
Dr. Huff Modified Brostrom Repair Rehabilitation Protocol:
 Dr. Huff Modified Brostrom Repair Rehabilitation Protocol: The intent of this protocol is to provide the clinician with a guideline of the post-operative rehabilitation course of a patient who has undergone
Dr. Huff Modified Brostrom Repair Rehabilitation Protocol: The intent of this protocol is to provide the clinician with a guideline of the post-operative rehabilitation course of a patient who has undergone
A Patient s Guide to Post-Operative Advice Following Pes Cavus
 A Patient s Guide to Post-Operative Advice Following Pes Cavus The Foot and Ankle unit at the Royal National Orthopaedic Hospital (RNOH) is a multi-disciplinary team. The team consists of three specialist
A Patient s Guide to Post-Operative Advice Following Pes Cavus The Foot and Ankle unit at the Royal National Orthopaedic Hospital (RNOH) is a multi-disciplinary team. The team consists of three specialist
POSTOP FOLLOW-UP & REHABILITATION FOLLOWING FOOT & ANKLE SURGERY
 1 POSTOP FOLLOW-UP & REHABILITATION FOLLOWING FOOT & ANKLE SURGERY The following instructions are general guidelines, but surgeon post-op instructions will dictate the individual patient's post-op management
1 POSTOP FOLLOW-UP & REHABILITATION FOLLOWING FOOT & ANKLE SURGERY The following instructions are general guidelines, but surgeon post-op instructions will dictate the individual patient's post-op management
V E R I TAS MGH 1811 MGH 1811 V E R I TAS. *Gerber JP. Persistent disability with ankle sprains. Foot Ankle Int 19: , 1998.
 MGH 1811 Management of Ankle Instability Richard J. de Asla, M.D. V E R I TAS MGH 1811 I have no potential conflicts with this presentation. V E R I TAS It s just a sprain Lateral Ankle Sprains Most common
MGH 1811 Management of Ankle Instability Richard J. de Asla, M.D. V E R I TAS MGH 1811 I have no potential conflicts with this presentation. V E R I TAS It s just a sprain Lateral Ankle Sprains Most common
A patient s guide to. Inferior Heel Pain
 A patient s guide to Inferior Heel Pain The Foot & Ankle Unit at the Royal National Orthopaedic Hospital is made up of a multi-disciplinary team. The team consists of four specialist orthopaedic foot and
A patient s guide to Inferior Heel Pain The Foot & Ankle Unit at the Royal National Orthopaedic Hospital is made up of a multi-disciplinary team. The team consists of four specialist orthopaedic foot and
Rehabilitation Guidelines for Patients Undergoing Precice Nail Lengthening. Joint Academic Committee. Holly Doyle. Aresh Nejad. Clinical 19/04/2021
 Rehabilitation Guidelines for Patients Undergoing Precice Nail Lengthening Date Approved 19/04/2018 Ratifying Body Related Documents Joint Academic Committee Physiotherapy rehabilitation guidelines Author
Rehabilitation Guidelines for Patients Undergoing Precice Nail Lengthening Date Approved 19/04/2018 Ratifying Body Related Documents Joint Academic Committee Physiotherapy rehabilitation guidelines Author
Sports Injuries of the Foot and Ankle Dominic Nielsen. Parkside Hospital Ashtead Hospital St George s
 Sports Injuries of the Foot and Ankle Dominic Nielsen Parkside Hospital Ashtead Hospital St George s Themes Ankle instability Ankle impingement Stress fractures 5 th MT fractures Peroneal subluxation Ankle
Sports Injuries of the Foot and Ankle Dominic Nielsen Parkside Hospital Ashtead Hospital St George s Themes Ankle instability Ankle impingement Stress fractures 5 th MT fractures Peroneal subluxation Ankle
Tibialis Posterior Tendon Dysfunction. Orthopaedic Department Patient Information Leaflet
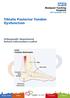 Tibialis Posterior Tendon Dysfunction Orthopaedic Department Patient Information Leaflet What is Tibialis Posterior Tendon Dysfunction? The Tibialis Posterior Tendon (see diagram) is an important structure
Tibialis Posterior Tendon Dysfunction Orthopaedic Department Patient Information Leaflet What is Tibialis Posterior Tendon Dysfunction? The Tibialis Posterior Tendon (see diagram) is an important structure
Protocol for the Management of Hip Arthroscopy Surgery
 Overall Aims of Surgery To decrease pain To increase range of motion (ROM) To increase hip/pelvis and lumbar stability To enable return to activities of daily living and sport Initial Post-operative Objectives
Overall Aims of Surgery To decrease pain To increase range of motion (ROM) To increase hip/pelvis and lumbar stability To enable return to activities of daily living and sport Initial Post-operative Objectives
A Patient s Guide to Adult-Acquired Flatfoot Deformity
 A Patient s Guide to Adult-Acquired Flatfoot Deformity Glendale Adventist Medical Center 1509 Wilson Terrace Glendale, CA 91206 Phone: (818) 409-8000 DISCLAIMER: The information in this booklet is compiled
A Patient s Guide to Adult-Acquired Flatfoot Deformity Glendale Adventist Medical Center 1509 Wilson Terrace Glendale, CA 91206 Phone: (818) 409-8000 DISCLAIMER: The information in this booklet is compiled
Anterior Cruciate Ligament Reconstruction
 Anterior Cruciate Ligament Reconstruction Physiotherapy Department Patient information leaflet This patient information booklet is designed to provide you with information about the Anterior Cruciate Ligament
Anterior Cruciate Ligament Reconstruction Physiotherapy Department Patient information leaflet This patient information booklet is designed to provide you with information about the Anterior Cruciate Ligament
WHAT IS THIS CONDITION? COMMON CAUSES:
 Mr Laurence James BSc MBBS MRCS(Eng) FRCS(Tr&Orth) Consultant Orthopaedic Surgeon Foot, Ankle and Sports Injuries WHAT IS THIS CONDITION? The posterior tibial tendon is an important structure that is normally
Mr Laurence James BSc MBBS MRCS(Eng) FRCS(Tr&Orth) Consultant Orthopaedic Surgeon Foot, Ankle and Sports Injuries WHAT IS THIS CONDITION? The posterior tibial tendon is an important structure that is normally
Christopher Kim, MD, Minh-Ha Hoang, DO, Scott G. Kaar, MD, William Mitchell, MD and Lauren Smith,PA-C
 Christopher Kim, MD, Minh-Ha Hoang, DO, Scott G. Kaar, MD, William Mitchell, MD and Lauren Smith,PA-C Department of Orthopaedic Surgery Sports Medicine and Shoulder Service Achilles Tendon Rupture Non-Operative
Christopher Kim, MD, Minh-Ha Hoang, DO, Scott G. Kaar, MD, William Mitchell, MD and Lauren Smith,PA-C Department of Orthopaedic Surgery Sports Medicine and Shoulder Service Achilles Tendon Rupture Non-Operative
Mr Keith Winters MBChB, FRACS (Orth) Specialist Orthopaedic Surgeon
 Mr Keith Winters MBChB, FRACS (Orth) Specialist Orthopaedic Surgeon Ph: (03) 9598 0691 Post op Instructions: Achilles Tendon Repair Recommended appliances for after your surgery: Crutches, walking frame
Mr Keith Winters MBChB, FRACS (Orth) Specialist Orthopaedic Surgeon Ph: (03) 9598 0691 Post op Instructions: Achilles Tendon Repair Recommended appliances for after your surgery: Crutches, walking frame
Index. Clin Sports Med 23 (2004) Note: Page numbers of article titles are in boldface type.
 Clin Sports Med 23 (2004) 169 173 Index Note: Page numbers of article titles are in boldface type. A Achilles enthesopathy, calcaneal spur with, 133 clinical presentation of, 135 136 definition of, 131
Clin Sports Med 23 (2004) 169 173 Index Note: Page numbers of article titles are in boldface type. A Achilles enthesopathy, calcaneal spur with, 133 clinical presentation of, 135 136 definition of, 131
Scar Engorged veins. Size of the foot [In clubfoot, small foot]
![Scar Engorged veins. Size of the foot [In clubfoot, small foot] Scar Engorged veins. Size of the foot [In clubfoot, small foot]](/thumbs/78/77722241.jpg) 6. FOOT HISTORY Pain: Walking, Running Foot wear problem Swelling; tingly feeling Deformity Stiffness Disability: At work; recreation; night; walk; ADL, Sports Previous Rx Comorbidities Smoke, Sugar, Steroid
6. FOOT HISTORY Pain: Walking, Running Foot wear problem Swelling; tingly feeling Deformity Stiffness Disability: At work; recreation; night; walk; ADL, Sports Previous Rx Comorbidities Smoke, Sugar, Steroid
North of England Bone and Soft Tissue Tumour Service
 North of England Bone and Soft Tissue Tumour Service Guidelines for rehabilitation after replacement of the proximal femur Proximal femoral replacement surgery is usually carried out as part of treatment
North of England Bone and Soft Tissue Tumour Service Guidelines for rehabilitation after replacement of the proximal femur Proximal femoral replacement surgery is usually carried out as part of treatment
Physiotherapy information for Achilles Tendinopathy
 Physiotherapy information for Achilles Tendinopathy What is Achilles Tendinopathy? Achilles Tendinopathy is a condition that can cause pain, swelling and weakness of the Achilles Tendon. This joins your
Physiotherapy information for Achilles Tendinopathy What is Achilles Tendinopathy? Achilles Tendinopathy is a condition that can cause pain, swelling and weakness of the Achilles Tendon. This joins your
Common Athletic Injuries of the Ankle
 Common Athletic Injuries of the Ankle Common Injuries of the Ankle in Athletes Ankle Sprains Chronic Lateral Ankle Instability Peroneal Tendon Injuries Achilles Tendon Tears Ankle Sprains What s an Ankle
Common Athletic Injuries of the Ankle Common Injuries of the Ankle in Athletes Ankle Sprains Chronic Lateral Ankle Instability Peroneal Tendon Injuries Achilles Tendon Tears Ankle Sprains What s an Ankle
Anterior Cruciate Ligament Reconstruction
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Anterior Cruciate Ligament Reconstruction Physiotherapy This patient information booklet is designed to provide you with information
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Anterior Cruciate Ligament Reconstruction Physiotherapy This patient information booklet is designed to provide you with information
Clin Podiatr Med Surg 19 (2002) Index
 Clin Podiatr Med Surg 19 (2002) 335 344 Index Note: Page numbers of article titles are in bold face type. A Accessory soleus muscle, magnetic resonance imaging of, 300 Achilles tendon injury of, magnetic
Clin Podiatr Med Surg 19 (2002) 335 344 Index Note: Page numbers of article titles are in bold face type. A Accessory soleus muscle, magnetic resonance imaging of, 300 Achilles tendon injury of, magnetic
Your Orthotics service is changing
 Your Orthotics service is changing Important for referrers on changes effective from January 2015 Why is the service changing? As demand for the orthotics service increases and budgets remain relatively
Your Orthotics service is changing Important for referrers on changes effective from January 2015 Why is the service changing? As demand for the orthotics service increases and budgets remain relatively
ACL Reconstruction Protocol (Allograft)
 ACL Reconstruction Protocol (Allograft) Week one Week two Initial Evaluation Range of motion Joint hemarthrosis Ability to contract quad/vmo Gait (generally WBAT in brace) Patella Mobility Inspect for
ACL Reconstruction Protocol (Allograft) Week one Week two Initial Evaluation Range of motion Joint hemarthrosis Ability to contract quad/vmo Gait (generally WBAT in brace) Patella Mobility Inspect for
FOOT AND ANKLE ARTHROSCOPY
 FOOT AND ANKLE ARTHROSCOPY Information for Patients WHAT IS FOOT AND ANKLE ARTHROSCOPY? The foot and the ankle are crucial for human movement. The balanced action of many bones, joints, muscles and tendons
FOOT AND ANKLE ARTHROSCOPY Information for Patients WHAT IS FOOT AND ANKLE ARTHROSCOPY? The foot and the ankle are crucial for human movement. The balanced action of many bones, joints, muscles and tendons
Your Orthotics service is changing
 Your Orthotics service is changing Important information for service users on changes effective from July 2015 Why is the service changing? As demand for the Orthotics service increases, Livewell Southwest
Your Orthotics service is changing Important information for service users on changes effective from July 2015 Why is the service changing? As demand for the Orthotics service increases, Livewell Southwest
Ankle Fracture Orthopaedic Department Patient Information Leaflet. Under review. Page 1
 Ankle Fracture Orthopaedic Department Patient Information Leaflet Page 1 Ankle Fracture Welcome to the Dudley Group NHS Foundation Trust. This leaflet will provide you with information regarding the diagnosis
Ankle Fracture Orthopaedic Department Patient Information Leaflet Page 1 Ankle Fracture Welcome to the Dudley Group NHS Foundation Trust. This leaflet will provide you with information regarding the diagnosis
Ankle Sprains and Their Imitators
 Ankle Sprains and Their Imitators Mark Halstead, MD Dr. Mark Halstead is the Associate Professor of the Departments of Orthopedics and Pediatrics at Washington University School of Medicine; Director of
Ankle Sprains and Their Imitators Mark Halstead, MD Dr. Mark Halstead is the Associate Professor of the Departments of Orthopedics and Pediatrics at Washington University School of Medicine; Director of
Anterior Cruciate Ligament (ACL) Reconstruction
 Further information Information on who to contact, i.e. web sites / telephone numbers of other departments / organisations which may be of help. How to contact us Watford General Hospital West Hertfordshire
Further information Information on who to contact, i.e. web sites / telephone numbers of other departments / organisations which may be of help. How to contact us Watford General Hospital West Hertfordshire
Ligament lesions of the ankle. Marc C. Attinger
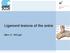 Ligament lesions of the ankle Marc C. Attinger Anatomy Mechanism of injury Each lig with its function during ROM in dorsiflexion/er ATFL slack, CFL tight in plantarflexion/ir CFL slack, ATFL tight Acute
Ligament lesions of the ankle Marc C. Attinger Anatomy Mechanism of injury Each lig with its function during ROM in dorsiflexion/er ATFL slack, CFL tight in plantarflexion/ir CFL slack, ATFL tight Acute
BUCKS MSK: FOOT AND ANKLE PATHWAY GP MANAGEMENT. Hallux Valgus. Assessment: Early Management. (must be attempted prior to any referral to imsk):
 Hallux Valgus Common condition: affecting around 28% of the adult population. Prevalence increases with age and in females. Observation: Lateral deviation of the great toe. May cause secondary irritation
Hallux Valgus Common condition: affecting around 28% of the adult population. Prevalence increases with age and in females. Observation: Lateral deviation of the great toe. May cause secondary irritation
Advice following Anterior Cruciate Ligament (ACL) reconstruction
 Advice following Anterior Cruciate Ligament (ACL) reconstruction Information for patients Mobilisation As soon as you feel well enough after the operation you will be able to get up and mobilise. You will
Advice following Anterior Cruciate Ligament (ACL) reconstruction Information for patients Mobilisation As soon as you feel well enough after the operation you will be able to get up and mobilise. You will
Comparison of outcomes in patients with generalized ligamentous laxity and without generalized laxity in the arthroscopic Modified Broströ m
 Comparison of outcomes in patients with generalized ligamentous laxity and without generalized laxity in the arthroscopic Modified Broströ m Operation for Chronic Lateral Ankle Instability NO CONFLICT
Comparison of outcomes in patients with generalized ligamentous laxity and without generalized laxity in the arthroscopic Modified Broströ m Operation for Chronic Lateral Ankle Instability NO CONFLICT
North of England Bone and Soft Tissue Tumour Service
 North of England Bone and Soft Tissue Tumour Service Guidelines for rehabilitation after proximal tibial replacement Proximal tibial replacement surgery is usually carried out as part of treatment for
North of England Bone and Soft Tissue Tumour Service Guidelines for rehabilitation after proximal tibial replacement Proximal tibial replacement surgery is usually carried out as part of treatment for
Ankle Arthritis PATIENT INFORMATION. The ankle joint. What is ankle arthritis?
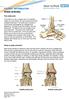 PATIENT INFORMATION Ankle Arthritis The ankle joint The ankle is a very complex joint. It is actually made up of two joints: the true ankle joint and the subtalar ankle joint. The ankle joint consists
PATIENT INFORMATION Ankle Arthritis The ankle joint The ankle is a very complex joint. It is actually made up of two joints: the true ankle joint and the subtalar ankle joint. The ankle joint consists
Post Operative Total Hip Replacement Protocol Brian J. White, MD
 Post Operative Total Hip Replacement Protocol Brian J. White, MD www.western-ortho.com The intent of this protocol is to provide guidelines for progression of rehabilitation. It is not intended to serve
Post Operative Total Hip Replacement Protocol Brian J. White, MD www.western-ortho.com The intent of this protocol is to provide guidelines for progression of rehabilitation. It is not intended to serve
3/6/2012 STATE OF THE ART: FOOT AND ANKLE GENERAL KNOWLEDGE 1. TRASP REHABILITATION CONTENTS. General knowledge Trasp Prevention
 STATE OF THE ART: FOOT AND ANKLE ILITATION Fabienne Van De Steene. CONTENTS General knowledge Trasp Prevention Rehab Ankle sprain CAI Achilles tendon Plantar fasciitis Take home message 2 1. TRASP Ankle
STATE OF THE ART: FOOT AND ANKLE ILITATION Fabienne Van De Steene. CONTENTS General knowledge Trasp Prevention Rehab Ankle sprain CAI Achilles tendon Plantar fasciitis Take home message 2 1. TRASP Ankle
Achilles Tendon Rupture
 43 Thames Street, St Albans, Christchurch 8013 Phone: (03) 356 1353 Website: philip-bayliss.com Achilles Tendon Rupture Summary Achilles tendon ruptures commonly occur in athletic individuals in their
43 Thames Street, St Albans, Christchurch 8013 Phone: (03) 356 1353 Website: philip-bayliss.com Achilles Tendon Rupture Summary Achilles tendon ruptures commonly occur in athletic individuals in their
Ankle Arthroscopy.
 Ankle Arthroscopy Key words: Ankle pain, ankle arthroscopy, ankle sprain, ankle stiffness, day case surgery, articular cartilage, chondral injury, chondral defect, anti-inflammatory medication Our understanding
Ankle Arthroscopy Key words: Ankle pain, ankle arthroscopy, ankle sprain, ankle stiffness, day case surgery, articular cartilage, chondral injury, chondral defect, anti-inflammatory medication Our understanding
ACHILLES TENDON REPAIR REHAB GUIDELINES
 ACHILLES TENDON REPAIR REHAB GUIDELINES Typically patients are discharged on the day of the operation or the next day. The leg is usually immobilized in a cast or hinged brace, ranging from 4-8 weeks.
ACHILLES TENDON REPAIR REHAB GUIDELINES Typically patients are discharged on the day of the operation or the next day. The leg is usually immobilized in a cast or hinged brace, ranging from 4-8 weeks.
Barriers Between Injury and Returnto-Work. Lower Extremity. Why the Extreme Variability
 Barriers Between Injury and Returnto-Work in the Lower Extremity Why the Extreme Variability Barriers to Diagnosis Failure or delay in reporting injury Employee expectations: Not really a serious injury
Barriers Between Injury and Returnto-Work in the Lower Extremity Why the Extreme Variability Barriers to Diagnosis Failure or delay in reporting injury Employee expectations: Not really a serious injury
Review relevant anatomy of the foot and ankle. Learn the approach to examining the foot and ankle
 Objectives Review relevant anatomy of the foot and ankle Learn the approach to examining the foot and ankle Learn the basics of diagnosis and treatment of ankle sprains Overview of other common causes
Objectives Review relevant anatomy of the foot and ankle Learn the approach to examining the foot and ankle Learn the basics of diagnosis and treatment of ankle sprains Overview of other common causes
Anterior Cruciate Ligament (ACL) Reconstruction. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Anterior Cruciate Ligament (ACL) Reconstruction An information guide Anterior Cruciate Ligament (ACL) Reconstruction Post-operative regime
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Anterior Cruciate Ligament (ACL) Reconstruction An information guide Anterior Cruciate Ligament (ACL) Reconstruction Post-operative regime
A Patient s Guide to Inter Digital Neuralgia (Morton s Neuroma)
 A Patient s Guide to Inter Digital Neuralgia (Morton s Neuroma) The foot and ankle unit at the Royal National Orthopaedic Hospital (RNOH) is a multi-disciplinary team. The team consists of two specialist
A Patient s Guide to Inter Digital Neuralgia (Morton s Neuroma) The foot and ankle unit at the Royal National Orthopaedic Hospital (RNOH) is a multi-disciplinary team. The team consists of two specialist
Sports Injuries of the Ankle and Ankle Arthritis. Mr Amit Amin Consultant Foot and Ankle Surgeon Parkside Hospital
 Sports Injuries of the Ankle and Ankle Arthritis Mr Amit Amin Consultant Foot and Ankle Surgeon Parkside Hospital Impingement Painful mechanical limitation of full ankle movement secondary to osseous
Sports Injuries of the Ankle and Ankle Arthritis Mr Amit Amin Consultant Foot and Ankle Surgeon Parkside Hospital Impingement Painful mechanical limitation of full ankle movement secondary to osseous
Dr Schock Achilles Tendon Repair Protocol
 Dr Schock Achilles Tendon Repair Protocol Phase 1- Maximum Protective Phase (2-4 post-op) Goals for Phase 1 Protect integrity of repair Minimize effusion ROM per guidelines listed Immobilization/Weight
Dr Schock Achilles Tendon Repair Protocol Phase 1- Maximum Protective Phase (2-4 post-op) Goals for Phase 1 Protect integrity of repair Minimize effusion ROM per guidelines listed Immobilization/Weight
LATERAL LIGAMENT SPRAIN OF THE ANKLE
 MUSCULOSKELETAL YOUR GUIDE TO LATERAL LIGAMENT SPRAIN OF THE ANKLE An IPRS Guide to provide you with exercises and advice to ease your condition Contents The ankle joint..................................................
MUSCULOSKELETAL YOUR GUIDE TO LATERAL LIGAMENT SPRAIN OF THE ANKLE An IPRS Guide to provide you with exercises and advice to ease your condition Contents The ankle joint..................................................
Rehabilitation Guidelines for Achilles Tendon Repair
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Achilles Tendon Repair The Achilles tendon is the strongest and thickest tendon in the body. It attaches the calf muscles (soleus and gastrocnemius)
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Achilles Tendon Repair The Achilles tendon is the strongest and thickest tendon in the body. It attaches the calf muscles (soleus and gastrocnemius)
Rehabilitation and Return to Play Following Achilles Tendon Repair
 Rehabilitation and Return to Play Following Achilles Tendon Repair Monte Wong PT, DPT, SCS, ATC, CSCS Assistant Athletic Trainer/Physical Therapist Philadelphia Eagles Mechanism of Injury 1.) forceful
Rehabilitation and Return to Play Following Achilles Tendon Repair Monte Wong PT, DPT, SCS, ATC, CSCS Assistant Athletic Trainer/Physical Therapist Philadelphia Eagles Mechanism of Injury 1.) forceful
Ankle Ligament Injury: Don t Worry- It s Only a Sprain Wes Jackson MD Orthopaedic Foot & Ankle
 Ankle Ligament Injury: Don t Worry- It s Only a Sprain Wes Jackson MD Orthopaedic Foot & Ankle Outline I. Epidemiology II. Classification and Types of Sprains III. Anatomy IV. Clinical Assessment and Imaging
Ankle Ligament Injury: Don t Worry- It s Only a Sprain Wes Jackson MD Orthopaedic Foot & Ankle Outline I. Epidemiology II. Classification and Types of Sprains III. Anatomy IV. Clinical Assessment and Imaging
NICHOLAS J. AVALLONE, M.D.
 NICHOLAS J. AVALLONE, M.D. www.dravallone.com ACHILLES TENDON REPAIR REHAB GUIDELINES DISCLAIMER: The intent of this protocol is to provide therapists with guidelines for rehabilitation based on a review
NICHOLAS J. AVALLONE, M.D. www.dravallone.com ACHILLES TENDON REPAIR REHAB GUIDELINES DISCLAIMER: The intent of this protocol is to provide therapists with guidelines for rehabilitation based on a review
A Patient s Guide to Ankle Sprain and Instability. Foot and Ankle Center of Massachusetts, P.C.
 A Patient s Guide to Ankle Sprain and Instability Welcome to Foot and Ankle Center of Massachusetts, where we believe in accelerating your learning curve with educational materials that are clearly written
A Patient s Guide to Ankle Sprain and Instability Welcome to Foot and Ankle Center of Massachusetts, where we believe in accelerating your learning curve with educational materials that are clearly written
ANTERIOR CRUCIATE LIGAMENT (ACL) INJURIES
 ANTERIOR CRUCIATE LIGAMENT (ACL) INJURIES WHAT IS THE ACL? The ACL is a very strong ligament on the inside of the knee. It runs from the femur (thigh bone) obliquely down to the Tibia (shin bone). The
ANTERIOR CRUCIATE LIGAMENT (ACL) INJURIES WHAT IS THE ACL? The ACL is a very strong ligament on the inside of the knee. It runs from the femur (thigh bone) obliquely down to the Tibia (shin bone). The
Physical Examination of the Foot & Ankle
 Inspection Standing, feet straight forward facing toward examiner Swelling Deformity Flatfoot (pes planus and hindfoot valgus) High arch (pes cavus and hindfoot varus) Peek-a-boo heel Varus Too many toes
Inspection Standing, feet straight forward facing toward examiner Swelling Deformity Flatfoot (pes planus and hindfoot valgus) High arch (pes cavus and hindfoot varus) Peek-a-boo heel Varus Too many toes
Ankle Arthroscopy. Day Surgery Unit Surgical Short Stay Physiotherapy Department. Royal Surrey County Hospital. Patient information leaflet
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Ankle Arthroscopy Day Surgery Unit Surgical Short Stay Physiotherapy Department Name of Patient: Date: Name of Physiotherapist:
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Ankle Arthroscopy Day Surgery Unit Surgical Short Stay Physiotherapy Department Name of Patient: Date: Name of Physiotherapist:
But it s only an ankle sprain. Ankle injuries are the most common injury to the lower limb as a result of sports.
 But it s only an ankle sprain Ankle injuries are the most common injury to the lower limb as a result of sports. Fortunately, most of them are minor and require little specific treatment, however, some
But it s only an ankle sprain Ankle injuries are the most common injury to the lower limb as a result of sports. Fortunately, most of them are minor and require little specific treatment, however, some
Ankle Pain After a Sprain.
 Ankle Pain After a Sprain www.fisiokinesiterapia.biz Anterior Drawer Stress Test Talar Tilt Talar Tilt (CFL) Difficult to isolate from subtalar ROM Slight plantar flexion (dorsi = relative subtalar isolation)
Ankle Pain After a Sprain www.fisiokinesiterapia.biz Anterior Drawer Stress Test Talar Tilt Talar Tilt (CFL) Difficult to isolate from subtalar ROM Slight plantar flexion (dorsi = relative subtalar isolation)
Jozef Murar, M.D. TCO Edina Crosstown 4010 W 65 th St, Edina, MN Tel: Fax:
 Jozef Murar, M.D. TCO Edina Crosstown 4010 W 65 th St, Edina, MN 55435 Tel: 952-456-7000 Fax: 952-832-0477 www.tcomn.com ACHILLES TENDON REHABILITATION PROTOCOL Pre-op: Gait training Post-op: Week 2 Post-op
Jozef Murar, M.D. TCO Edina Crosstown 4010 W 65 th St, Edina, MN 55435 Tel: 952-456-7000 Fax: 952-832-0477 www.tcomn.com ACHILLES TENDON REHABILITATION PROTOCOL Pre-op: Gait training Post-op: Week 2 Post-op
Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction
 Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These
Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These
Foot and ankle update
 Foot and ankle update Mr Ian Garnham Consultant Foot and Ankle Surgeon Whipps Cross University Hospital Hallux Rigidus Symptoms first ray and 1st MTP pain and swelling worse with push off or forced dorsiflexion
Foot and ankle update Mr Ian Garnham Consultant Foot and Ankle Surgeon Whipps Cross University Hospital Hallux Rigidus Symptoms first ray and 1st MTP pain and swelling worse with push off or forced dorsiflexion
Achilles Tendonitis and Tears
 Achilles Tendonitis and Tears The Achilles tendon is an important structure for normal ankle motion and normal function, even for daily activities such as walking. Achilles tendonitis can occur in patients
Achilles Tendonitis and Tears The Achilles tendon is an important structure for normal ankle motion and normal function, even for daily activities such as walking. Achilles tendonitis can occur in patients
Modified Brostrom-Evans-Gould technique for recurrent lateral ankle ligament instability
 Journal of Orthopaedic Surgery 2007;15(3):306-10 Modified Brostrom-Evans-Gould technique for recurrent lateral ankle ligament instability ZD Ng, S Das De Department of Orthopaedic Surgery, National University
Journal of Orthopaedic Surgery 2007;15(3):306-10 Modified Brostrom-Evans-Gould technique for recurrent lateral ankle ligament instability ZD Ng, S Das De Department of Orthopaedic Surgery, National University
.org. Posterior Tibial Tendon Dysfunction. Anatomy. Cause. Symptoms
 Posterior Tibial Tendon Dysfunction Page ( 1 ) Posterior tibial tendon dysfunction is one of the most common problems of the foot and ankle. It occurs when the posterior tibial tendon becomes inflamed
Posterior Tibial Tendon Dysfunction Page ( 1 ) Posterior tibial tendon dysfunction is one of the most common problems of the foot and ankle. It occurs when the posterior tibial tendon becomes inflamed
Guidance for the Physiotherapy Management of Patients Undergoing Limb Reconstruction with a Circular Frame External Fixator.
 Guidance for the Physiotherapy Management of Patients Undergoing Limb Reconstruction with a Circular Frame External Fixator. Table of Contents INTRODUCTION... 2 TARGET AUDIENCE... 2 KEY CHANGES FROM PREVIOUS
Guidance for the Physiotherapy Management of Patients Undergoing Limb Reconstruction with a Circular Frame External Fixator. Table of Contents INTRODUCTION... 2 TARGET AUDIENCE... 2 KEY CHANGES FROM PREVIOUS
A patient s guide to. ankle arthroscopy
 A patient s guide to ankle arthroscopy The foot and ankle unit at the Royal National Orthopaedic Hospital (RNOH) is a multi-disciplinary team. The team consists of three specialist orthopaedic foot and
A patient s guide to ankle arthroscopy The foot and ankle unit at the Royal National Orthopaedic Hospital (RNOH) is a multi-disciplinary team. The team consists of three specialist orthopaedic foot and
Anatomy and evaluation of the ankle.
 Anatomy and evaluation of the ankle www.fisiokinesiterapia.biz Ankle Anatomical Structures Tibia Fibular Talus Tibia This is the strongest largest bone of the lower leg. It bears weight and the bone creates
Anatomy and evaluation of the ankle www.fisiokinesiterapia.biz Ankle Anatomical Structures Tibia Fibular Talus Tibia This is the strongest largest bone of the lower leg. It bears weight and the bone creates
ACL Reconstruction Rehabilitation Allograft Kyle F. Chun, MD
 ACL Reconstruction Rehabilitation Allograft Kyle F. Chun, MD [ ] Meniscus Repair (If checked, WBAT in brace in full extension, ROM 0-90 x 6 wks; WBAT 0-90, ROM 0-120 weeks 7-12; WBAT/ROMAT 12+ weeks, no
ACL Reconstruction Rehabilitation Allograft Kyle F. Chun, MD [ ] Meniscus Repair (If checked, WBAT in brace in full extension, ROM 0-90 x 6 wks; WBAT 0-90, ROM 0-120 weeks 7-12; WBAT/ROMAT 12+ weeks, no
GG10Rehabilitation Programme for Arthroscopically Assisted Anterior Cruciate Ligament Reconstruction
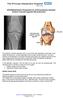 GG10Rehabilitation Programme for Arthroscopically Assisted Anterior Cruciate Ligament Reconstruction Femur ACL Graft Fibula Tibia The Anterior Cruciate Ligament (ACL) is one of the main ligaments in the
GG10Rehabilitation Programme for Arthroscopically Assisted Anterior Cruciate Ligament Reconstruction Femur ACL Graft Fibula Tibia The Anterior Cruciate Ligament (ACL) is one of the main ligaments in the
Investigation of the factors to affect the duration to return sports after the surgery of anterior talofibular ligament repair with arthroscopy
 Investigation of the factors to affect the duration to return sports after the surgery of anterior talofibular ligament repair with arthroscopy Hamamatsu University School of Medicine Mitsuru Hanada, Shoichi
Investigation of the factors to affect the duration to return sports after the surgery of anterior talofibular ligament repair with arthroscopy Hamamatsu University School of Medicine Mitsuru Hanada, Shoichi
A patient s guide to. preparing for foot and ankle surgery
 A patient s guide to preparing for foot and ankle surgery The foot and ankle unit at the Royal National Orthopaedic Hospital (RNOH) is a multi-disciplinary team. The team consists of three specialist orthopaedic
A patient s guide to preparing for foot and ankle surgery The foot and ankle unit at the Royal National Orthopaedic Hospital (RNOH) is a multi-disciplinary team. The team consists of three specialist orthopaedic
ACL Reconstruction Rehabilitation Bone Patellar Tendon Bone Graft Kyle F. Chun, MD
 ACL Reconstruction Rehabilitation Bone Patellar Tendon Bone Graft Kyle F. Chun, MD [ ] Meniscus Repair (If checked, WBAT in brace in full extension, ROM 0-90 x 6 wks; WBAT 0-90, ROM 0-120 weeks 7-12; WBAT/ROMAT
ACL Reconstruction Rehabilitation Bone Patellar Tendon Bone Graft Kyle F. Chun, MD [ ] Meniscus Repair (If checked, WBAT in brace in full extension, ROM 0-90 x 6 wks; WBAT 0-90, ROM 0-120 weeks 7-12; WBAT/ROMAT
Patient information. Total Ankle Replacement Trauma and Orthopaedic Directorate PIF 1335 V2
 Patient information Total Ankle Replacement Trauma and Orthopaedic Directorate PIF 1335 V2 Your Consultant has advised you that you are suitable to have a total ankle replacement. The aim of surgery is
Patient information Total Ankle Replacement Trauma and Orthopaedic Directorate PIF 1335 V2 Your Consultant has advised you that you are suitable to have a total ankle replacement. The aim of surgery is
Caring For Your Lateral Ankle Middlebury College
 Caring For Your Lateral Ankle Sprain @ Middlebury College ** severe sprains or medial (inner side of ankle) sprains may require a different program Anatomy, Pathology, and Classification of Ankle Sprains
Caring For Your Lateral Ankle Sprain @ Middlebury College ** severe sprains or medial (inner side of ankle) sprains may require a different program Anatomy, Pathology, and Classification of Ankle Sprains
Hindfoot / Midfoot Fusion (Arthrodesis) Orthopeadic Department Patient Information Leaflet
 Hindfoot / Midfoot Fusion (Arthrodesis) Orthopeadic Department Patient Information Leaflet There are often three reasons why this operation is performed: Pain - from osteoarthritis (OA) and rheumatoid
Hindfoot / Midfoot Fusion (Arthrodesis) Orthopeadic Department Patient Information Leaflet There are often three reasons why this operation is performed: Pain - from osteoarthritis (OA) and rheumatoid
KNEE REHABILITATION PROGRAMME. Patient Information & Exercise Folder
 KNEE REHABILITATION PROGRAMME Patient Information & Exercise Folder Mr D Raj FRCS (Tr & Orth) Consultant Lower Limb Orthopaedic Surgeon BOSTONIAN PRIVATE WING Pilgrim Hospital, Boston Lincolnshire PE21
KNEE REHABILITATION PROGRAMME Patient Information & Exercise Folder Mr D Raj FRCS (Tr & Orth) Consultant Lower Limb Orthopaedic Surgeon BOSTONIAN PRIVATE WING Pilgrim Hospital, Boston Lincolnshire PE21
Recognizing common injuries to the lower extremity
 Recognizing common injuries to the lower extremity Bones Femur Patella Tibia Tibial Tuberosity Medial Malleolus Fibula Lateral Malleolus Bones Tarsals Talus Calcaneus Metatarsals Phalanges Joints - Knee
Recognizing common injuries to the lower extremity Bones Femur Patella Tibia Tibial Tuberosity Medial Malleolus Fibula Lateral Malleolus Bones Tarsals Talus Calcaneus Metatarsals Phalanges Joints - Knee
King Khalid University Hospital
 King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: ACL RECONSTRUCTION +/- MENSICAL REPAIR 1. General Guidelines: Time lines in this rehabilitation protocol are
King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: ACL RECONSTRUCTION +/- MENSICAL REPAIR 1. General Guidelines: Time lines in this rehabilitation protocol are
Physical Therapy for the Lower Extremity: What You and Your Patient Should Expect from Rehab
 1 Physical Therapy for the Lower Extremity: What You and Your Patient Should Expect from Rehab Thomas Clennell, PT, DPT, SCS Physical Therapist UCSF Benioff Children s Hospital Oakland Sports Medicine
1 Physical Therapy for the Lower Extremity: What You and Your Patient Should Expect from Rehab Thomas Clennell, PT, DPT, SCS Physical Therapist UCSF Benioff Children s Hospital Oakland Sports Medicine
Achilles tendon rupture: management and rehabilitation
 Achilles tendon rupture: management and rehabilitation Introduction The Achilles tendon (or heel cord) is the largest tendon in the human body. It connects the calf muscles (gastrocnemius and soleus) to
Achilles tendon rupture: management and rehabilitation Introduction The Achilles tendon (or heel cord) is the largest tendon in the human body. It connects the calf muscles (gastrocnemius and soleus) to
Adam N. Whatley, M.D Main St., STE Zachary, LA Phone(225) Fax(225)
 Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 Total Knee Arthroplasty Protocol: The intent of this protocol is to provide the clinician with a guideline
Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 Total Knee Arthroplasty Protocol: The intent of this protocol is to provide the clinician with a guideline
WHAT DO HALLUX VALGUS AND BUNION MEAN?
 Mr Laurence James BSc MBBS MRCS(Eng) FRCS(Tr&Orth) Consultant Orthopaedic Surgeon Foot, Ankle and Sports Injuries WHAT DO HALLUX VALGUS AND BUNION MEAN? Hallux is Latin for great toe and Valgus is Latin
Mr Laurence James BSc MBBS MRCS(Eng) FRCS(Tr&Orth) Consultant Orthopaedic Surgeon Foot, Ankle and Sports Injuries WHAT DO HALLUX VALGUS AND BUNION MEAN? Hallux is Latin for great toe and Valgus is Latin
Lesser toe surgery. Exceptional healthcare, personally delivered
 Lesser toe surgery Exceptional healthcare, personally delivered Following your consultation with a member of the Foot and Ankle team you have been diagnosed as needing lesser toe surgery. This leaflet
Lesser toe surgery Exceptional healthcare, personally delivered Following your consultation with a member of the Foot and Ankle team you have been diagnosed as needing lesser toe surgery. This leaflet
Physiotherapy treatment
 Appendix A Physiotherapy treatment Principles [These principles are intended to provide the basis for and guide the individual physiotherapist s decisions for selecting treatment content, and deciding
Appendix A Physiotherapy treatment Principles [These principles are intended to provide the basis for and guide the individual physiotherapist s decisions for selecting treatment content, and deciding
Copyright 2004, Yoshiyuki Shiratori. All right reserved.
 Ankle and Leg Evaluation 1. History Chief Complaint: A. What happened? B. Is it a sharp or dull pain? C. How long have you had the pain? D. Can you pinpoint the pain? E. Do you have any numbness or tingling?
Ankle and Leg Evaluation 1. History Chief Complaint: A. What happened? B. Is it a sharp or dull pain? C. How long have you had the pain? D. Can you pinpoint the pain? E. Do you have any numbness or tingling?
Rehabilitation Protocol:
 Rehabilitation Protocol: Patellofemoral resurfacing: Osteochondral Autograft Transplantation (OATS), Autologous Chondrocyte Implantation (ACI) and Microfracture Department of Orthopaedic Surgery Lahey
Rehabilitation Protocol: Patellofemoral resurfacing: Osteochondral Autograft Transplantation (OATS), Autologous Chondrocyte Implantation (ACI) and Microfracture Department of Orthopaedic Surgery Lahey
Stabilisation of the shoulder joint
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Stabilisation of the shoulder joint Physiotherapy Department Information leaflet for Name of Patient: Date: Name of Physiotherapist:
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Stabilisation of the shoulder joint Physiotherapy Department Information leaflet for Name of Patient: Date: Name of Physiotherapist:
Proximal Medial Gastrocnemius Release (PMGR)
 Proximal Medial Gastrocnemius Release (PMGR) Physiotherapy and Orthopaedic Department Patient information leaflet Date: Name of Patient: Name of Physiotherapist: Telephone: 01483 464153 This leaflet has
Proximal Medial Gastrocnemius Release (PMGR) Physiotherapy and Orthopaedic Department Patient information leaflet Date: Name of Patient: Name of Physiotherapist: Telephone: 01483 464153 This leaflet has
Ankle, sub-talar or mid-foot joint fusion
 Ankle, sub-talar or mid-foot joint fusion This leaflet aims to answer your questions about having an ankle, sub-talar or mid-foot joint fusion. It explains the benefits, risks and alternatives, as well
Ankle, sub-talar or mid-foot joint fusion This leaflet aims to answer your questions about having an ankle, sub-talar or mid-foot joint fusion. It explains the benefits, risks and alternatives, as well
King Khalid University Hospital
 King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: PCL RECONSTRUCTION +/- ACL / MCL / LCL / POSTEROLATERAL CORNER 1. General Guidelines: Time lines in this rehabilitation
King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: PCL RECONSTRUCTION +/- ACL / MCL / LCL / POSTEROLATERAL CORNER 1. General Guidelines: Time lines in this rehabilitation
Patellar-quadriceps Tendon Repair Protocol
 Patellar-quadriceps Tendon Repair Protocol Applicability: Physician Practice Date Effective: 3/2017 Department: Rehabilitation Services Supersedes: none Date Last Reviewed / or Date Last Revision: 1/2018
Patellar-quadriceps Tendon Repair Protocol Applicability: Physician Practice Date Effective: 3/2017 Department: Rehabilitation Services Supersedes: none Date Last Reviewed / or Date Last Revision: 1/2018
Subtalar Fusion. Cornwall Foot and Ankle
 Subtalar Fusion Cornwall Foot and Ankle Tibia (shin bone) Talus (ankle bone) Calcaneum (heel bone) SUBTALAR JOINT SIDE VIEW OF ANKLE Patient Information on Subtalar Fusion (Arthrodesis) What is a subtalar
Subtalar Fusion Cornwall Foot and Ankle Tibia (shin bone) Talus (ankle bone) Calcaneum (heel bone) SUBTALAR JOINT SIDE VIEW OF ANKLE Patient Information on Subtalar Fusion (Arthrodesis) What is a subtalar
