Strands & Standards INTRODUCTION TO PHYSICAL THERAPY
|
|
|
- Lindsay Fisher
- 5 years ago
- Views:
Transcription
1 Strands & Standards INTRODUCTION TO PHYSICAL THERAPY COURSE DESCRIPTION This course introduces students to the field of physical therapy through the history, medical terminology, documentation, therapy treatments, and pertinent legal and ethical considerations of the profession. Healthcare for a diverse population begins its thread in this course. Students will participate in clinical observations. License Type CTE or Secondary Education 6-12 Required Endorsement Exercise Science/Sports Medicine Intended Grade Level: Units of Credit: 1.0 Core Code: Prerequisite: None Skill Certification: 000 Test Weight: 1.0 Revised August 2016 Page 1 of 9
2 Strands & Standards <COURSE TITLE> Students will explore the fundamentals of rehabilitation medicine. Standard 1 Explore the rehabilitation therapy pathway. Define rehabilitation therapy Identify careers in the rehabilitation therapy pathway Explain the educational requirements for careers in the rehabilitation therapy pathway Compare and contrast job descriptions for careers in the rehabilitation therapy pathway Standard 2 Investigate the profession of physical therapy. Examine the roles and responsibilities of a physical therapist (hospital setting, long-term care facility, clinic, etc.) Identify the members and roles of the physical therapy team: (surgeon/physician/physician assistant, nurse, physical therapist, physical therapy assistant, physical therapy aide, athletic trainer, chiropractor, massage therapist, etc.) Standard 3 Explore the history of physical therapy. Create a historical timeline of the significant contributors, modalities, and treatments in physical therapy Compare and contrast current and historical modality treatment Standard 4 Explore the modern profession of physical therapy. Explore current trends in physical therapy Analyze current issues in physical therapy Identify innovative approaches in physical therapy Standard 5 Explain the role of the American Physical Therapy Association (APTA). Identify the functions of APTA Outline the Standards of Practice as defined by the APTA Describe the importance of involvement in APTA to further career development Standard 6 Create a career development plan within the physical therapy field. Explore educational offerings to enhance career development Compare and evaluate different types of educational opportunities Describe the benefits of mentoring as a career development tool (job shadows/internships) Describe the importance of involvement in organizations such as APTA to further career development Explore specialty areas within the field of physical therapy as described by the American Board of Physical Therapy Specialties (ABPTS) Medical, Legal, & Ethical-Students will identify the medical, legal, and ethical issues governing the clinical practice of physical therapy. Standard 1 Identify the rules and regulations of individually identifiable health information. Examine the Health Insurance Portability and Accountability Act (HIPAA) Identify consequences of violating Health Insurance Portability and Accountability Act (HIPAA) Explain personal responsibilities within the parameters of Health Insurance Portability and Accountability Act (HIPAA) Standard 2 Discuss desirable attitudes and behaviors when providing healthcare to diverse patients. Revised August 2016 Page 2 of 9
3 Describe cultural sensitivity in relation to healthcare Explore ways to treat the underserved and under-represented populations Identify ways that people from different cultures and backgrounds are stereotyped Describe the importance of treating patients as individuals Standard 3 Describe the required documentation related to physical therapy visits and treatment. Analyze medical records used in a physical therapy setting Create a SOAP note for each of the following conditions: musculoskeletal, neuromuscular, cardiovascular, and integumentary Standard 4 Discuss the Utah Physical Therapy Practice Act and how it relates to the roles and relationship between the physical therapy team. Identify the scope of practice of a physical therapist, physical therapist assistant, and a physical therapy aide Summarize the five parts of the Utah Physical Therapy Practice Act and identify the legal terms and discuss Standard 5 Investigate the various types of health insurance and the reimbursement process for physical therapy. Describe health insurance plans (premium, copay, deductible, etc.) Compare and contrast government funded plans and private insurance plans in regards to the number of reimbursed physical therapy visits Professionalism-Identify professional standards and characteristics of a physical therapy team. Standard 1 Describe the characteristics of an effective healthcare provider in personal and professional terms. Examine productivity and time management strategies Discuss implications of dress and other personal behaviors within the healthcare setting Identify best practices in respect to client relations Standard 2 Explain effective communication strategies of a physical therapist with patients and all members of the physical therapy team. Demonstrate appropriate verbal communication skills in a healthcare setting Demonstrate appropriate nonverbal communication skills in a healthcare setting Standard 3 Describe stressors that occur in personal and work life and how they might affect your ability to meet the needs of clients. Identify personal and workplace stressors that may have an effect on you behavior Describe stress management techniques that can be utilized in your personal life and in the workplace Terminology-Identify medical terminology related to the profession of physical therapy. Standard 1 Describe positional terminology in regards to the human body. Describe anatomical position Identify body planes and directional terms (sagittal, mid-sagittal, coronal/frontal, transverse/horizontal, superior, inferior, anterior, posterior, medial, lateral, proximal, distal, superficial, and deep) Standard 2 Compare and contrast body movements. Revised August 2016 Page 3 of 9
4 Flexion, extension, and hypertension Adduction and abduction Pronation and supination Retraction and protraction Elevation and depression Rotation and circumduction External rotation and internal rotation Lateral flexion (side-bending left and right) Inversion and eversion Dorsiflexion and plantar flexion Radial deviation and ulnar deviation Opposition Standard 3 Define terms associated to physical therapy Activities of daily living (ADLs) Ataxia Base of support Bilateral Calcaneal valgum Calcaneal varum Cervical Contracture Core Deformity Dissociation Distal Dynamic Extension External rotation Fine motor Flexion Genu valgum Genu varum Gross motor Hamstrings Hyperextension Hypermobility Hypertonic Hypotonic Internal rotation Instability Kinesthesia Kyphosis Long-sitting Lordosis Lumbar Manual therapy Midline Motor control Motor planning Obliquity Pes planus Prone Proprioception Proximal Quadriceps Revised August 2016 Page 4 of 9
5 Range of motion Recurvatum Reflex Ring sitting Sacral Side-sitting Spasticity Static Supine Symmetrical Tactile defensiveness Tailor-sitting Thoracic Tone (muscle) Unilateral Vestibular stimulation Weight shift Musculoskeletal-Students will examine physical therapy principles and methods of healing for musculoskeletal conditions. Standard 1 Identify conditions and injuries associated with the musculoskeletal systems. General conditions (osteoarthritis, osteoporosis, fibromyalgia, TMJ dysfunction) Shoulder injuries (rotator cuff tear, dislocation, frozen shoulder, tendinitis, fracture, shoulder impingement, thoracic outlet syndrome) Elbow injuries (golfer s elbow, tennis elbow, sprain, strain, fractures) Wrist injuries (carpal tunnel syndrome, sprain, strain, fractures) Neck and low back injuries (sprain, strain, disc herniation, stenosis, muscle spasm, posture, SI joint dysfunction, coccygodynia) Hip conditions (acetabular labral tears, bursitis, IT band tightness/syndrome, tendinitis, total knee replacement) Ankle injuries (Achilles tendinitis, peroneal tendinitis, sprain, strain, fractures) Foot and toe injuries (plantar fasciitis, tarsal tunnel syndrome, bunionectomies, sprain, strain, fractures) Standard 2 Identify how to assess musculoskeletal conditions. Current concerns General health Life style/adls/functional status (employment, activity level, recent or past injuries) Joint inspection/rom Muscle strength ADL/functional abilities Activity tolerance Standard 3 Explain the progress of a patient through the phases of physical therapy for musculoskeletal conditions. Identify short- and long-term goals Control inflammation and pain Increase range of motion Increase strength and function Return to normal function Standard 4 Model therapeutic exercises and modalities used to treat musculoskeletal conditions and injuries. Revised August 2016 Page 5 of 9
6 Manual therapy (mobilization, myofascial release, soft tissue mobilization) Strengthening (therapeutic exercises, stabilization) Range of motion (stretching) Modalities (traction, e-stimulation, ultrasound, heat/ice) Patient education Home exercise program (HEP) Standard 5 Compare and contrast assessment, therapeutic exercises, and modalities in an adult and a child patient. Modify the assessment for a pediatric patient Modify the therapeutic exercises and modalities for a pediatric patient Standard 6 Compare and contrast assessment, therapeutic exercises, and modalities in an adult and a geriatric patient. Modify the assessment for a geriatric patient Modify the therapeutic exercises and modalities for a geriatric patient Neuromuscular-Students will examine physical therapy principles and methods of healing for neuromuscular conditions. Standard 1 Identify conditions and injuries associated with the neuromuscular system. Parkinson s disease Guillian-Barre Syndrome Polio Multiple sclerosis (MS) Chronic inflammatory demyelinating neuropathy West Nile virus Cerebral palsy ALS Head injuries Spinal cord injuries Arthritis Inflammatory myopathies (polymyositis, dermatomyositis, inclusion body myositis) Multiple fractures and injuries Crush injuries Collagen vascular diseases Standard 2 Identify how to assess neuromuscular conditions. Impact on life expectancy Involvement of organ systems Family, social, community roles Impact of daily functioning (ambulation, ADLs, communication, nutritional status, community mobility, work performance) Muscle strength Joint contractures Pulmonary function Cardiomyopathy Intellectual capacity Standard 3 Explain the progress of a patient through the phases of physical therapy for neuromuscular conditions. Identify short- and long-term goals Control inflammation and pain Increase range of motion Increase strength and function Return to normal function Revised August 2016 Page 6 of 9
7 Standard 4 Model therapeutic exercises and modalities used to treat neuromuscular conditions and injuries. Manual therapy (mobilization, myofascial release, soft tissue mobilization) Strengthening (therapeutic exercises, stabilization) Range of motion (stretching) Modalities (traction, e-stimulation, ultrasound, heat/ice) Patient education Home exercise program (HEP) Assistive and adaptive devices (crutches, prostheses, wheelchairs) Standard 5 Compare and contrast assessment, therapeutic exercises, and modalities in an adult and child patient. Modify the assessment for a pediatric patient Modify the therapeutic exercises and modalities for a pediatric patient Standard 6 Compare and contrast assessment, therapeutic exercises, and modalities in an adult and a geriatric patient. Modify the assessment for a geriatric patient Modify the therapeutic exercises and modalities for a geriatric patient Cardiovascular-Students will examine physical therapy principles and methods of healing for cardiovascular conditions. Standard 1 Identify conditions and defects associated with the cardiovascular systems. Cardiomyopathy Heart failure Coronary artery disease Myocardial infarction Valvular disease Endocarditis Myocarditis Pericarditis Coronary artery-bypass graft (CABG) Valve replacement or repair Percutaneous transluminal coronary angioplasty Percutaneous coronary intervention Repair of atrial or ventricular septal defect Cox-Maxe procedure Trans myocardial laser revascularization Pericardiectomy Aortic aneurysm repair Radiofrequency ablation Pulmonary artery embolectomy Standard 2 Identify how to assess cardiovascular conditions. Onset and duration of symptoms Previous and ongoing medical and/or surgical treatment Lab results and diagnostic tests Social history Prior functional endurance level Home environment Family/caregiver support Family, professional, social, and community roles Patient s goals and expectations of returning to previous life roles Prior drug, tobacco, and alcohol use Current medications Revised August 2016 Page 7 of 9
8 Standard 3 Explain the progress of a patient through the phases of physical therapy for cardiovascular conditions. Exercises to improve mobility Determine cardiac responses to exercise and activity Increase flexibility Increase strength and function Increase aerobic exercise Independent exercise and conditioning Standard 4 Model therapeutic exercises and modalities used to treat cardiovascular conditions and defects. Standing and walking Low-impact aerobic exercises (treadmill, exercise bike, or rowing machine) Increase flexibility (ROM) Strength-training Standard 5 Compare and contrast assessment, therapeutic exercises, and modalities in an adult and a child patient. Modify the assessment for a pediatric patient Modify the therapeutic exercises and modalities for a pediatric patient Standard 6 Compare and contrast assessment, therapeutic exercises, and modalities in an adult and a geriatric patient. Modify the assessment for a geriatric patient Modify the therapeutic exercises and modalities for a geriatric patient Integumentary-Students will examine physical therapy principles and methods of healing for integumentary conditions. Standard 1 Identify conditions and injuries associated with the integumentary system. Burns Contusions Pressure ulcers Neuropathic ulcers Surgical wounds Vascular disease Abscess Traumatic injury Standard 2 Identify how to assess integumentary conditions. Patient history ADLs Ambulation (mobility) Strength Work/school activities Adequate mobility or dexterity to perform wound care Medical history Wound history System assessment Wound location and size Tunneling and undermining Wound characteristics (distinctness, thickness, attachment to the base of the wound, epithelialization/pigmentation) Standard 3 Explain the progress of a patient through the phases of physical therapy for integumentary conditions and injuries. Pain management Maximize movement and function (ROM and strengthening) Revised August 2016 Page 8 of 9
9 Facilitate wound healing (wound debridement and dressing application) Minimize scar/contracture development Standard 4 Model therapeutic exercises and modalities used to treat integumentary conditions and injuries. Hydrotherapy Thermotherapy Hyperbaric oxygen therapy Compression therapies (IPC, VAC) Electrotherapy Manual therapy (massage) ROM stretching Strengthening exercises Adaptive, protective, or assistive equipment Standard 5 Compare and contrast assessment, therapeutic exercises, and modalities in an adult and a child patient. Modify the assessment for a pediatric patient Modify the therapeutic exercises and modalities for a pediatric patient Standard 6 Compare and contrast assessment, therapeutic exercises, and modalities in an adult and a geriatric patient. Modify the assessment for a geriatric patient Modify the therapeutic exercises and modalities for a geriatric patient. Revised August 2016 Page 9 of 9
Introduction to Physical Therapy
 Introduction to Physical Therapy EXAM INFORMATION Items 53 Points 60 Prerequisites NONE Grade Level 11-12 Course Length ONE YEAR Career Cluster HEALTH CARE Performance Standards NOT INCLUDED Certificate
Introduction to Physical Therapy EXAM INFORMATION Items 53 Points 60 Prerequisites NONE Grade Level 11-12 Course Length ONE YEAR Career Cluster HEALTH CARE Performance Standards NOT INCLUDED Certificate
LABETTE COMMUNITY COLLEGE BRIEF SYLLABUS. Please check with the LCC bookstore for the required texts for this class.
 LABETTE COMMUNITY COLLEGE BRIEF SYLLABUS SPECIAL NOTE: This brief syllabus is not intended to be a legal contract. A full syllabus will be distributed to students at the first class session. TEXT AND SUPPLEMENTARY
LABETTE COMMUNITY COLLEGE BRIEF SYLLABUS SPECIAL NOTE: This brief syllabus is not intended to be a legal contract. A full syllabus will be distributed to students at the first class session. TEXT AND SUPPLEMENTARY
STUDY GUIDE a comprehensive review of the:
 STUDY GUIDE a comprehensive review of the: NFPT PERSONAL FITNESS TRAINERMANUAL Study & Reference: The Fundamentals for the CERTIFIED PERSONAL TRAINERR (CPT) Third Edition 2015 All Rights Reserved National
STUDY GUIDE a comprehensive review of the: NFPT PERSONAL FITNESS TRAINERMANUAL Study & Reference: The Fundamentals for the CERTIFIED PERSONAL TRAINERR (CPT) Third Edition 2015 All Rights Reserved National
Body Planes & Positions
 Learning Objectives Objective 1: Identify and utilize anatomical positions, planes, and directional terms. Demonstrate what anatomical position is and how it is used to reference the body. Distinguish
Learning Objectives Objective 1: Identify and utilize anatomical positions, planes, and directional terms. Demonstrate what anatomical position is and how it is used to reference the body. Distinguish
Contents. copyrighted material by PRO-ED, Inc. Chapter 1. Chapter 2. Chapter 3. Chapter 4. Chapter 5. Conditions in Athletic Injuries
 Acknowledgments xiii Introduction to the First Edition xv Introduction to the Second Edition xvii Chapter 1 Conditions in Athletic Injuries Anterior Cruciate Ligament (ACL) Tear 2 Biceps Tendon Strain
Acknowledgments xiii Introduction to the First Edition xv Introduction to the Second Edition xvii Chapter 1 Conditions in Athletic Injuries Anterior Cruciate Ligament (ACL) Tear 2 Biceps Tendon Strain
American Board of Physical Medicine & Rehabilitation. Part I Curriculum & Weights
 American Board of Physical Medicine & Rehabilitation Part I Curriculum & Weights Neurologic Disorders 30% Stroke Spinal Cord Injury Traumatic Brain Injury Neuropathies a) Mononeuropathies b) Polyneuropathies
American Board of Physical Medicine & Rehabilitation Part I Curriculum & Weights Neurologic Disorders 30% Stroke Spinal Cord Injury Traumatic Brain Injury Neuropathies a) Mononeuropathies b) Polyneuropathies
COURSE OUTLINE-IB 128: SPORTS MEDICINE INTRODUCTION
 COURSE OUTLINE-IB 128: SPORTS MEDICINE INTRODUCTION Definition of sports medicine Pre-participation physical exam Epidemiology of sports injuries injury rates for various sports sports risks relative to
COURSE OUTLINE-IB 128: SPORTS MEDICINE INTRODUCTION Definition of sports medicine Pre-participation physical exam Epidemiology of sports injuries injury rates for various sports sports risks relative to
0RTHOPEDIC MASSAGE. Orthopedic Massage Benefits. Orthopedic Massage Applications
 0RTHOPEDIC MASSAGE Orthopedic Massage involves therapeutic assessment, manipulation, and movement of locomotor soft tissues to eliminate pain and dysfunction throughout the body. It is more than a technique.
0RTHOPEDIC MASSAGE Orthopedic Massage involves therapeutic assessment, manipulation, and movement of locomotor soft tissues to eliminate pain and dysfunction throughout the body. It is more than a technique.
Table of Contents Treatment Guides Basic Activities of Daily Living Basic and Instrumental Activities of Daily Living 11 Bathing and Showering 13 Dres
 Treatment Guides Basic Activities of Daily Living Basic and Instrumental Activities of Daily Living 11 Bathing and Showering 13 Dressing 15 Feeding 18 Functional Communication 20 Functional Mobility 22
Treatment Guides Basic Activities of Daily Living Basic and Instrumental Activities of Daily Living 11 Bathing and Showering 13 Dressing 15 Feeding 18 Functional Communication 20 Functional Mobility 22
Medical Terminology. Anatomical Position, Directional Terms and Movements
 Medical Terminology Anatomical Position, Directional Terms and Movements What we will cover... Content Objectives Students will be able to gain a better understanding and application of medical terminology
Medical Terminology Anatomical Position, Directional Terms and Movements What we will cover... Content Objectives Students will be able to gain a better understanding and application of medical terminology
Post-op / Pre-op Page (ALREADY DONE)
 Post-op / Pre-op Page (ALREADY DONE) We offer individualized treatment plans based on your physician's recommendations, our evaluations, and your feedback. Most post-operative and preoperative rehabilitation
Post-op / Pre-op Page (ALREADY DONE) We offer individualized treatment plans based on your physician's recommendations, our evaluations, and your feedback. Most post-operative and preoperative rehabilitation
Health & Fitness. About Loudoun Sports Therapy
 Health & Fitness The Newsletter About Your Health And Caring For Your Body About Loudoun Sports Therapy The Physical Therapists at Loudoun Sports Therapy Center are medically trained, licensed professionals
Health & Fitness The Newsletter About Your Health And Caring For Your Body About Loudoun Sports Therapy The Physical Therapists at Loudoun Sports Therapy Center are medically trained, licensed professionals
What is Kinesiology? Basic Biomechanics. Mechanics
 What is Kinesiology? The study of movement, but this definition is too broad Brings together anatomy, physiology, physics, geometry and relates them to human movement Lippert pg 3 Basic Biomechanics the
What is Kinesiology? The study of movement, but this definition is too broad Brings together anatomy, physiology, physics, geometry and relates them to human movement Lippert pg 3 Basic Biomechanics the
Medical Terminology. Unit 2
 Medical Terminology Unit 2 Students will apply medical terminology. Objective 1: Identify and utilize anatomical positions, planes, and directional terms. Demonstrate what anatomical position is and how
Medical Terminology Unit 2 Students will apply medical terminology. Objective 1: Identify and utilize anatomical positions, planes, and directional terms. Demonstrate what anatomical position is and how
DART Diagnosis and Related Treatments
 DART Diagnosis and Related Treatments The DART Tool allows a user to obtain Treatment recommendations based on the disorder/condition. These recommendations are provided by ACOEM (American College of Occupational
DART Diagnosis and Related Treatments The DART Tool allows a user to obtain Treatment recommendations based on the disorder/condition. These recommendations are provided by ACOEM (American College of Occupational
SASTM.COM. Sound Assisted Soft Tissue Mobilization
 Sound Assisted Soft Tissue Mobilization SASTM is a form of instrument assisted soft tissue mobilization (IASTM). These instruments resonate better than any other products in the market! SASTM Seminar Overview
Sound Assisted Soft Tissue Mobilization SASTM is a form of instrument assisted soft tissue mobilization (IASTM). These instruments resonate better than any other products in the market! SASTM Seminar Overview
GLOSSARY. Active assisted movement: movement where the actions are assisted by an outside force.
 GLOSSARY The technical words used in this guide are listed here in alphabetic order. The first time one of these words is used in the guide, it is written in italics. Sometimes there is reference to a
GLOSSARY The technical words used in this guide are listed here in alphabetic order. The first time one of these words is used in the guide, it is written in italics. Sometimes there is reference to a
Medical Terminology. Anatomical Position, Directional Terms and Movements
 Medical Terminology Anatomical Position, Directional Terms and Movements What we will cover... Content Objectives Students will be able to gain a better understanding and application of medical terminology
Medical Terminology Anatomical Position, Directional Terms and Movements What we will cover... Content Objectives Students will be able to gain a better understanding and application of medical terminology
Clinical Information for Wheeled Mobility Page 1 of 6
 Clinical Information for Wheeled Mobility Page 1 of 6 PART A: PATIENT / PROVIDER INFORMATION - Please Print Name: Sponsor Soc. Sec. No: Address: City: St: Zip: Phone: ( ) Age: Sex: Height: Weight: Date
Clinical Information for Wheeled Mobility Page 1 of 6 PART A: PATIENT / PROVIDER INFORMATION - Please Print Name: Sponsor Soc. Sec. No: Address: City: St: Zip: Phone: ( ) Age: Sex: Height: Weight: Date
Phase II Health Sciences as Applied to Coaching.
 Phase II Health Sciences as Applied to Coaching www.topform.us Overview What is going to be covered today is.. Skeletal System Muscular System Most common injuries to know about in your sport Part One:
Phase II Health Sciences as Applied to Coaching www.topform.us Overview What is going to be covered today is.. Skeletal System Muscular System Most common injuries to know about in your sport Part One:
6.4 The Ankle. Body Divided into Planes. Health Services: Unit 6 Arms and Legs. Body Movement Vocabulary
 6.4 The Ankle Body Movement Vocabulary When fitness professionals refer to movement of the body, the pattern of movement is described from the anatomical position This position can best be described as
6.4 The Ankle Body Movement Vocabulary When fitness professionals refer to movement of the body, the pattern of movement is described from the anatomical position This position can best be described as
Chapter 8 8/23/2016. Body Mechanics and Patient Mobility. Introduction to Body Mechanics and Patient Mobility
 Chapter 8 Body Mechanics and Patient Mobility All items and derived items 2015, 2011, 2006 by Mosby, Inc., an imprint of Elsevier Inc. All rights reserved. Introduction to Body Mechanics and Patient Mobility
Chapter 8 Body Mechanics and Patient Mobility All items and derived items 2015, 2011, 2006 by Mosby, Inc., an imprint of Elsevier Inc. All rights reserved. Introduction to Body Mechanics and Patient Mobility
AMERICAN BOARD OF PHYSICAL THERAPY RESIDENCY AND FELLOWSHIP EDUCATION
 AMERICAN BOARD OF PHYSICAL THERAPY RESIDENCY AND FELLOWSHIP EDUCATION June 2017 American Physical Therapy Association 1111 North Fairfax Street Alexandria, VA 22314-1488 resfel@apta.org 703/706-3152 www.abptrfe.org
AMERICAN BOARD OF PHYSICAL THERAPY RESIDENCY AND FELLOWSHIP EDUCATION June 2017 American Physical Therapy Association 1111 North Fairfax Street Alexandria, VA 22314-1488 resfel@apta.org 703/706-3152 www.abptrfe.org
American Board of Physical Therapy Residency and Fellowship Education
 American Board of Physical Therapy Residency and Fellowship Education Description of Residency Practice Orthopaedics February 2017 American Physical Therapy Association 1111 North Fairfax Street Alexandria,
American Board of Physical Therapy Residency and Fellowship Education Description of Residency Practice Orthopaedics February 2017 American Physical Therapy Association 1111 North Fairfax Street Alexandria,
RN(EC) ENC(C) GNC(C) MN ACNP *** MECHANISM OF INJURY.. MOST IMPORTANT ***
 HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age of patient - Certain conditions are more prevalent in particular age groups (Hip pain in children may refer to the knee from Legg-Calve-Perthes
HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age of patient - Certain conditions are more prevalent in particular age groups (Hip pain in children may refer to the knee from Legg-Calve-Perthes
The Language of Anatomy. (Anatomical Terminology)
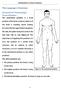 The Language of Anatomy (Anatomical Terminology) Terms of Position The anatomical position is a fixed position of the body (cadaver) taken as if the body is standing (erect) looking forward with the upper
The Language of Anatomy (Anatomical Terminology) Terms of Position The anatomical position is a fixed position of the body (cadaver) taken as if the body is standing (erect) looking forward with the upper
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Achilles tendonitis, criteria for full competition in, 164 165 description of, 164 patient education in, 165 prophylactic support in,
Index Note: Page numbers of article titles are in boldface type. A Achilles tendonitis, criteria for full competition in, 164 165 description of, 164 patient education in, 165 prophylactic support in,
bilateral, both before below elbow twice a day below knee bedrest
 Abbreviations Student Name: A approximately assessment assist active active assist abdominal aortic aneurysm active assistive range of motion abduction/adduction acromioclavicular joint anterior cruciate
Abbreviations Student Name: A approximately assessment assist active active assist abdominal aortic aneurysm active assistive range of motion abduction/adduction acromioclavicular joint anterior cruciate
Hip Arthroscopy Rehabilitation Protocol
 Hip Arthroscopy Rehabilitation Protocol 1. Concepts: a. Range of motion and weight bearing restrictions must be adhered to during the initial rehab process (4 total weeks of ROM and weight bearing restrictions)
Hip Arthroscopy Rehabilitation Protocol 1. Concepts: a. Range of motion and weight bearing restrictions must be adhered to during the initial rehab process (4 total weeks of ROM and weight bearing restrictions)
Unit 6 Orthopedic Physiotherapy
 Unit 6 Orthopedic Physiotherapy Task 1 Human Body Look at the diagram and study the main muscles of the body. Define which muscles have the following functions: Pectoral muscle lowers the arm. Intercostals
Unit 6 Orthopedic Physiotherapy Task 1 Human Body Look at the diagram and study the main muscles of the body. Define which muscles have the following functions: Pectoral muscle lowers the arm. Intercostals
Dorsal surface-the upper area or top of the foot. Terminology
 It is important to learn the terminology as it relates to feet to properly communicate with referring physicians when necessary and to identify the relationship between the anatomical structure of the
It is important to learn the terminology as it relates to feet to properly communicate with referring physicians when necessary and to identify the relationship between the anatomical structure of the
Post Operative Total Hip Replacement Protocol Brian J. White, MD
 Post Operative Total Hip Replacement Protocol Brian J. White, MD www.western-ortho.com The intent of this protocol is to provide guidelines for progression of rehabilitation. It is not intended to serve
Post Operative Total Hip Replacement Protocol Brian J. White, MD www.western-ortho.com The intent of this protocol is to provide guidelines for progression of rehabilitation. It is not intended to serve
Table of Contents 85 Treatment Guides 283 Handouts
 Table of Contents 85 Treatment Guides 283 Handouts ADLs and IADLs Activities of Daily Living Training Bathing and Showering Clothing Care Community Mobility Dressing Driving Feeding Functional Communication
Table of Contents 85 Treatment Guides 283 Handouts ADLs and IADLs Activities of Daily Living Training Bathing and Showering Clothing Care Community Mobility Dressing Driving Feeding Functional Communication
Contraindicated and High-Risk Exercises
 Contraindicated and High-Risk Exercises Young sub Kwon, Ph.D. ACSM RCEP, NSCA CSCS,*D Exercise Physiology Laboratory The University of New Mexico Albuquerque, NM, USA Introduction Any activity selected
Contraindicated and High-Risk Exercises Young sub Kwon, Ph.D. ACSM RCEP, NSCA CSCS,*D Exercise Physiology Laboratory The University of New Mexico Albuquerque, NM, USA Introduction Any activity selected
Mark Adickes, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas Phone: Fax:
 Mark Adickes, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas 77030 Phone: 713-986-6016 Fax: 713-986-5411 MENISCAL REPAIR PROTOCOL Longitudinal Meniscal Repair This rehabilitation
Mark Adickes, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas 77030 Phone: 713-986-6016 Fax: 713-986-5411 MENISCAL REPAIR PROTOCOL Longitudinal Meniscal Repair This rehabilitation
Physical Therapist. Lauren Sisco
 Physical Therapist Lauren Sisco What is a Physical Therapist? A physical therapist (PT) is a professional who examines an injured or ill patient and develops a care plan that encourages movement, reduces
Physical Therapist Lauren Sisco What is a Physical Therapist? A physical therapist (PT) is a professional who examines an injured or ill patient and develops a care plan that encourages movement, reduces
King Saud University College of Nursing Medical-surgical Nursing
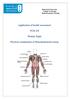 King Saud University College of Nursing Medical-surgical Nursing 1.Obtaining a health history: Ask about chief complain: History of presence of muscle pain (onset, location, Aggravating and alleviating
King Saud University College of Nursing Medical-surgical Nursing 1.Obtaining a health history: Ask about chief complain: History of presence of muscle pain (onset, location, Aggravating and alleviating
REMINDER. an exercise program. Senior Fitness Obtain medical clearance and physician s release prior to beginning
 Functional Forever: Exercise for Independent Living REMINDER Obtain medical clearance and physician s release prior to beginning an exercise program for clients with medical or orthopedic concerns. What
Functional Forever: Exercise for Independent Living REMINDER Obtain medical clearance and physician s release prior to beginning an exercise program for clients with medical or orthopedic concerns. What
Assessment Form Post Polio Syndrome and Late Effects of Polio
 FULL NAME: DATE OF BIRTH: PHONE NUMBER: CURRENT HOME ADDRESS: EMAIL ADDRESS: THERAPIST: REFERRAL SOURCE: CURRENT GP: NEXT OF KIN: ACC/NHI NUMBER: PATIENT GOALS OF TODAY S ASSESSMENT: MAIN PROBLEMS PATIENT
FULL NAME: DATE OF BIRTH: PHONE NUMBER: CURRENT HOME ADDRESS: EMAIL ADDRESS: THERAPIST: REFERRAL SOURCE: CURRENT GP: NEXT OF KIN: ACC/NHI NUMBER: PATIENT GOALS OF TODAY S ASSESSMENT: MAIN PROBLEMS PATIENT
Sensible Physical Limitations after Epidural Patching Procedures or Surgery. Laura Freed, MPT
 Sensible Physical Limitations after Epidural Patching Procedures or Surgery Laura Freed, MPT Introduction Spontaneous Intracranial Hypotension Patient Wife and Mother Physical Therapist (Belpre, OH) What
Sensible Physical Limitations after Epidural Patching Procedures or Surgery Laura Freed, MPT Introduction Spontaneous Intracranial Hypotension Patient Wife and Mother Physical Therapist (Belpre, OH) What
BIOMECHANICAL EXAMINATION OF THE PEDIATRIC LOWER EXTREMITY
 BIOMECHANICAL EXAMINATION OF THE PEDIATRIC LOWER EXTREMITY B.Resseque, D.P.M. ARCH HEIGHT OFF WEIGHTBEARING Evaluate arch height by placing a ruler from the heel to the first metatarsal head Compare arch
BIOMECHANICAL EXAMINATION OF THE PEDIATRIC LOWER EXTREMITY B.Resseque, D.P.M. ARCH HEIGHT OFF WEIGHTBEARING Evaluate arch height by placing a ruler from the heel to the first metatarsal head Compare arch
Hip Arthroscopy Rehabilitation Gluteus Medius Repair with or without Labral Debridement. Normalize gait pattern with brace (if indicated) and crutches
 General Guidelines: Hip Arthroscopy Rehabilitation Gluteus Medius Repair with or without Labral Debridement Normalize gait pattern with brace (if indicated) and crutches Weight-bearing: 20 lbs foot flat
General Guidelines: Hip Arthroscopy Rehabilitation Gluteus Medius Repair with or without Labral Debridement Normalize gait pattern with brace (if indicated) and crutches Weight-bearing: 20 lbs foot flat
LABETTE COMMUNITY COLLEGE BRIEF SYLLABUS. Please check with the LCC bookstore for the required texts for this class.
 LABETTE COMMUNITY COLLEGE BRIEF SYLLABUS SPECIAL NOTE: This brief syllabus is not intended to be a legal contract. A full syllabus will be distributed to students at the first class session. TEXT AND SUPPLEMENTARY
LABETTE COMMUNITY COLLEGE BRIEF SYLLABUS SPECIAL NOTE: This brief syllabus is not intended to be a legal contract. A full syllabus will be distributed to students at the first class session. TEXT AND SUPPLEMENTARY
Physical Therapy for Everyone
 Physical Therapy for Everyone Clarence Chan PT, DPT Assistant Professor C.Chan, 2007 Targeted Audience ALL OF US THAT ARE INTERESTED IN FEELING STRONGER AND HEALTHIER BY TAKING CARE OF OUR OWN BODY *NON
Physical Therapy for Everyone Clarence Chan PT, DPT Assistant Professor C.Chan, 2007 Targeted Audience ALL OF US THAT ARE INTERESTED IN FEELING STRONGER AND HEALTHIER BY TAKING CARE OF OUR OWN BODY *NON
MUSCULOSKELETAL DISORDERS: THE BIGGEST JOB SAFETY PROBLEM. What Are Musculoskeletal Disorders
 MUSCULOSKELETAL DISORDERS: THE BIGGEST JOB SAFETY PROBLEM What Are Musculoskeletal Disorders Every year more than 1.8 million workers in the United States suffer painful back and repetitive strain injuries,
MUSCULOSKELETAL DISORDERS: THE BIGGEST JOB SAFETY PROBLEM What Are Musculoskeletal Disorders Every year more than 1.8 million workers in the United States suffer painful back and repetitive strain injuries,
Yoga Anatomy & Physiology
 Yoga Anatomy & Physiology Anatomy & Physiology Anatomy- One of the basic essential sciences of medicine that studies the structure of an organism. Physiology- The biological study of the functions of living
Yoga Anatomy & Physiology Anatomy & Physiology Anatomy- One of the basic essential sciences of medicine that studies the structure of an organism. Physiology- The biological study of the functions of living
1-Apley scratch test.
 1-Apley scratch test. The patient attempts to touch the opposite scapula to test range of motion of the shoulder. 1-Testing abduction and external rotation( +ve sign touch the opposite scapula, -ve sign
1-Apley scratch test. The patient attempts to touch the opposite scapula to test range of motion of the shoulder. 1-Testing abduction and external rotation( +ve sign touch the opposite scapula, -ve sign
APPLICATION OF THE MOVEMENT SYSTEMS MODEL TO THE MANAGEMENT COMMON HIP PATHOLOGIES
 APPLICATION OF THE MOVEMENT SYSTEMS MODEL TO THE MANAGEMENT COMMON HIP PATHOLOGIES Tracy Porter, PT, DPT Des Moines University Department of Physical Therapy Objectives Review current literature related
APPLICATION OF THE MOVEMENT SYSTEMS MODEL TO THE MANAGEMENT COMMON HIP PATHOLOGIES Tracy Porter, PT, DPT Des Moines University Department of Physical Therapy Objectives Review current literature related
CLINICAL CONCEPTS FOR ORTHOPEDICS. CMS Clinical Concepts
 CLINICAL CONCEPTS FOR ORTHOPEDICS CMS Clinical Concepts ICD 10 LESSONS FROM OFFICE DOCUMENTATION Presented by Dr. Frankeny OUR CHALLENGE: CHANGING OUR DOCUMENTATION ICD 10 Learn the nomenclature Documenting
CLINICAL CONCEPTS FOR ORTHOPEDICS CMS Clinical Concepts ICD 10 LESSONS FROM OFFICE DOCUMENTATION Presented by Dr. Frankeny OUR CHALLENGE: CHANGING OUR DOCUMENTATION ICD 10 Learn the nomenclature Documenting
Physical Therapy DPT Curriculum Hunter College (Effective Spring 2016)
 Summer, Year # 1 (8 weeks) Physical Therapy DPT Curriculum Hunter College (Effective Spring 2016) (Includes new course numbering effective Spring 2016 and new course naming effective Spring 2018) Course
Summer, Year # 1 (8 weeks) Physical Therapy DPT Curriculum Hunter College (Effective Spring 2016) (Includes new course numbering effective Spring 2016 and new course naming effective Spring 2018) Course
Sports Medicine Unit 16 Elbow
 Sports Medicine Unit 16 Elbow I. Bones a. b. c. II. What movements does the elbow perform? a. Flexion b. c. Pronation d. III. Muscles in motion a. FLEXION (supinated) i Brachialis (pronated) ii (neutral)
Sports Medicine Unit 16 Elbow I. Bones a. b. c. II. What movements does the elbow perform? a. Flexion b. c. Pronation d. III. Muscles in motion a. FLEXION (supinated) i Brachialis (pronated) ii (neutral)
Terms of Movements by Prof. Dr. Muhammad Imran Qureshi
 Terms of Movements by Prof. Dr. Muhammad Imran Qureshi Three systems of the body work in coordination to perform various movements of the body. These are: A System of Bones (Osteology), A System of Muscles
Terms of Movements by Prof. Dr. Muhammad Imran Qureshi Three systems of the body work in coordination to perform various movements of the body. These are: A System of Bones (Osteology), A System of Muscles
Diagnosis: Gluteus Medius Tear, Labral Tear, CAM / Pincer
 Physical Therapy Prescription: Hip Arthroscopy Diagnosis: Gluteus Medius Tear, Labral Tear, CAM / Pincer Procedure: Gluteus Medius Repair, CAM / Pincer Decompression, Labral refixation / Capsular Shift
Physical Therapy Prescription: Hip Arthroscopy Diagnosis: Gluteus Medius Tear, Labral Tear, CAM / Pincer Procedure: Gluteus Medius Repair, CAM / Pincer Decompression, Labral refixation / Capsular Shift
Brennen Lucas, M.D. Advanced Orthopaedic Associates
 Brennen Lucas, M.D. Advanced Orthopaedic Associates 2778 N. Webb Rd. Wichita, KS 67226 316-631-1600 Fax: (316) 631-1674 1 (800) 362-0591 GUIDELINES FOR REHABILITATION FOLLOWING SURGICAL RECONSTRUCTION
Brennen Lucas, M.D. Advanced Orthopaedic Associates 2778 N. Webb Rd. Wichita, KS 67226 316-631-1600 Fax: (316) 631-1674 1 (800) 362-0591 GUIDELINES FOR REHABILITATION FOLLOWING SURGICAL RECONSTRUCTION
DIAGNOSTIC EVALUATION OF CERVICAL VS. SHOULDER PAIN: A PHYSIATRIST S PERSPECTIVE
 Russ Cantrell, M.D. Physical Medicine and Rehabilitation Orthopedic Sports Medicine and Spine Care Institute DIAGNOSTIC EVALUATION OF CERVICAL VS. SHOULDER PAIN: A PHYSIATRIST S PERSPECTIVE PHYSIATRIST
Russ Cantrell, M.D. Physical Medicine and Rehabilitation Orthopedic Sports Medicine and Spine Care Institute DIAGNOSTIC EVALUATION OF CERVICAL VS. SHOULDER PAIN: A PHYSIATRIST S PERSPECTIVE PHYSIATRIST
Functional Capacity Evaluation
 Functional Capacity Evaluation SAMPLE REPORT RETURN TO WORK Client Name: Frank T. Date of FCE: 1/05/2011 Therapist: Laurie T. Referrer: Dr. Smith Facility WorkWell Prevention & Care 11 East Superior Street,
Functional Capacity Evaluation SAMPLE REPORT RETURN TO WORK Client Name: Frank T. Date of FCE: 1/05/2011 Therapist: Laurie T. Referrer: Dr. Smith Facility WorkWell Prevention & Care 11 East Superior Street,
REACHING PEAK SPORTS PERFORMANCE AND PREVENTING INJURY
 The Athlete s Guide to REACHING PEAK SPORTS PERFORMANCE AND PREVENTING INJURY THE ATHLETE S GUIDE TO REACHING PEAK SPORTS PERFORMANCE AND PREVENTING INJURY Table of Contents Introduction...3 Common Sports
The Athlete s Guide to REACHING PEAK SPORTS PERFORMANCE AND PREVENTING INJURY THE ATHLETE S GUIDE TO REACHING PEAK SPORTS PERFORMANCE AND PREVENTING INJURY Table of Contents Introduction...3 Common Sports
Integrated Manual Therapy & Orthopedic Massage For Complicated Lower Extremity Conditions
 Integrated Manual Therapy & Orthopedic Massage For Complicated Lower Extremity Conditions Assessment Protocols Treatment Protocols Treatment Protocols Corrective Exercises Artwork and slides taken from
Integrated Manual Therapy & Orthopedic Massage For Complicated Lower Extremity Conditions Assessment Protocols Treatment Protocols Treatment Protocols Corrective Exercises Artwork and slides taken from
& & 392 & C1-C2
 Abbreviations...424 Abdominal Aortic Aneur... 302 Abdominal Rapid DDx...401 AC Sprain... 140 Acetabular Labral Tear... 222 Achilles Tendinopathy... 286 ACL Sprain/Tear... 236 Advanced Wobble Board... 395
Abbreviations...424 Abdominal Aortic Aneur... 302 Abdominal Rapid DDx...401 AC Sprain... 140 Acetabular Labral Tear... 222 Achilles Tendinopathy... 286 ACL Sprain/Tear... 236 Advanced Wobble Board... 395
THE SELECTIVE FUNCTIONAL MOVEMENT ASSESSMENT
 - 33 - THE SELECTIVE FUNCTIONAL MOVEMENT ASSESSMENT SFMA SCORING FP DP Active Cervical Flexion Active Cervical Extension Cervical Rotation Upper Extremity Pattern 1(MRE) Upper Extremity Pattern 2 (LRF)
- 33 - THE SELECTIVE FUNCTIONAL MOVEMENT ASSESSMENT SFMA SCORING FP DP Active Cervical Flexion Active Cervical Extension Cervical Rotation Upper Extremity Pattern 1(MRE) Upper Extremity Pattern 2 (LRF)
MT2 REMEDIAL MASSAGE GCMT 2007
 MT2 REMEDIAL MASSAGE GCMT 2007 DEFINITION Remedial Massage may be explained as the skilled, manual, therapeutic application of soft tissue remedial techniques which are selected and performed after careful
MT2 REMEDIAL MASSAGE GCMT 2007 DEFINITION Remedial Massage may be explained as the skilled, manual, therapeutic application of soft tissue remedial techniques which are selected and performed after careful
RECIPES FOR RATINGS !!! A. FIBROMYALGIA: 0% WPI P. 569 B. THORACIC OUTLET SYNDROME 0% WPI P. 569 C. MYOFASCIAL PAIN SYNDROME 0% WPI P.
 RECIPES FOR RATINGS 1. THE "0% WPI" RATINGS A. FIBROMYALGIA: 0% WPI P. 569 B. THORACIC OUTLET SYNDROME 0% WPI P. 569 C. MYOFASCIAL PAIN SYNDROME 0% WPI P. 569 D. TENDINITIS OF UPPER EXTREMITY 0% WPI P.
RECIPES FOR RATINGS 1. THE "0% WPI" RATINGS A. FIBROMYALGIA: 0% WPI P. 569 B. THORACIC OUTLET SYNDROME 0% WPI P. 569 C. MYOFASCIAL PAIN SYNDROME 0% WPI P. 569 D. TENDINITIS OF UPPER EXTREMITY 0% WPI P.
Travis G. - 1 Maak, - MD Sports Medicine University of Utah Orthopaedics 590 Wakara Way Salt Lake City, UT Tel: Fax:
 General Guidelines: Travis G. - 1 Maak, - MD Rehabilitation for Arthroscopic or Open Gluteus Medius Repair with or without Labral Debridement Normalize gait pattern with brace and crutches Weight-bearing:
General Guidelines: Travis G. - 1 Maak, - MD Rehabilitation for Arthroscopic or Open Gluteus Medius Repair with or without Labral Debridement Normalize gait pattern with brace and crutches Weight-bearing:
a. Demonstration & Practise of the Technique...4 b. Refining the Feel of the Technique...4 c. Practical Application to the Body Generally...
 Course Outline Course Overview Goltech Basic: Cross-Fibre Muscle Release...4 1. History & Development of Goltech...4 2. Musculo-Skeletal System as relevant to Goltech...4 3. Why Goltech cross-fibre muscle
Course Outline Course Overview Goltech Basic: Cross-Fibre Muscle Release...4 1. History & Development of Goltech...4 2. Musculo-Skeletal System as relevant to Goltech...4 3. Why Goltech cross-fibre muscle
COMMON CONDITIONS TREATED
 COMMON CONDITIONS TREATED Common Conditions Treated by Chiropractors, pages 2-9 Common Conditions Treated by Registered Massage Therapists, page 10 Common Conditions Treated with Medical Acupuncture, page
COMMON CONDITIONS TREATED Common Conditions Treated by Chiropractors, pages 2-9 Common Conditions Treated by Registered Massage Therapists, page 10 Common Conditions Treated with Medical Acupuncture, page
Prior authorization will not be required for outpatient speech therapy.*
 POLICY CHANGE: Authorization for All Outpatient Speech Therapy and Pediatric Outpatient Physical and Occupational Therapy NOT REQUIRED by Martin s Point Health Care Effective June 25, 2018 Thank you for
POLICY CHANGE: Authorization for All Outpatient Speech Therapy and Pediatric Outpatient Physical and Occupational Therapy NOT REQUIRED by Martin s Point Health Care Effective June 25, 2018 Thank you for
Hip Arthroscopy Labral Repair Protocol
 Hip Arthroscopy Labral Repair Protocol Applicability: Physician Practices Date Effective: 09/2013 Department: Rehabilitation Services Date Last Reviewed: 1/2018 Supersedes: n/a Administration Approval:
Hip Arthroscopy Labral Repair Protocol Applicability: Physician Practices Date Effective: 09/2013 Department: Rehabilitation Services Date Last Reviewed: 1/2018 Supersedes: n/a Administration Approval:
Page 1 of 6. Appendix 1
 Page 1 Appendix 1 Rotation Objectives and Schedule 1. Introductory Month 4 weeks 2. Total Joints 4 weeks a. Diagnosis and management of hip and knee arthritis b. Indications for surgery c. Implant selection;
Page 1 Appendix 1 Rotation Objectives and Schedule 1. Introductory Month 4 weeks 2. Total Joints 4 weeks a. Diagnosis and management of hip and knee arthritis b. Indications for surgery c. Implant selection;
Physical Exam. Jared Van Der Beek. Basics To Remember. Know the anatomy and how the muscles function.
 Physical Exam Jared Van Der Beek Jared@physio-puncture.com 1 Basics To Remember Know the anatomy and how the muscles function. Know what the special tests are looking for and understand why they are positive.
Physical Exam Jared Van Der Beek Jared@physio-puncture.com 1 Basics To Remember Know the anatomy and how the muscles function. Know what the special tests are looking for and understand why they are positive.
Body Organizations Flashcards
 1. What are the two main regions of the body? 2. What three structures are in the Axial Region? 1. Axial Region (Goes down midline of the body) 2. Appendicular Region (limbs) 3. Axial Region (Goes down
1. What are the two main regions of the body? 2. What three structures are in the Axial Region? 1. Axial Region (Goes down midline of the body) 2. Appendicular Region (limbs) 3. Axial Region (Goes down
After Arthroscopic Subacromial Decompression Intact Rotator Cuff (Distal Clavicle Resection)
 After Arthroscopic Subacromial Decompression Intact Rotator Cuff (Distal Clavicle Resection) Rehabilitation Protocol Phase 1: Weeks 0-4 Restrictions ROM 140 degrees of forward flexion 40 degrees of external
After Arthroscopic Subacromial Decompression Intact Rotator Cuff (Distal Clavicle Resection) Rehabilitation Protocol Phase 1: Weeks 0-4 Restrictions ROM 140 degrees of forward flexion 40 degrees of external
Year 2004 Paper one: Questions supplied by Megan
 QUESTION 47 A 58yo man is noted to have a right foot drop three days following a right total hip replacement. On examination there is weakness of right ankle dorsiflexion and toe extension (grade 4/5).
QUESTION 47 A 58yo man is noted to have a right foot drop three days following a right total hip replacement. On examination there is weakness of right ankle dorsiflexion and toe extension (grade 4/5).
Hip Arthroscopy Rehabilitation Protocol
 Hip Arthroscopy Rehabilitation Protocol This protocol is a generic outline of the postoperative management for patients undergoing hip arthroscopy. Depending on the exact diagnosis and the procedures performed,
Hip Arthroscopy Rehabilitation Protocol This protocol is a generic outline of the postoperative management for patients undergoing hip arthroscopy. Depending on the exact diagnosis and the procedures performed,
The causes of OA of the knee are multiple and include aging (wear and tear), obesity, and previous knee trauma or surgery. OA affects usually the
 The Arthritic Knee The causes of OA of the knee are multiple and include aging (wear and tear), obesity, and previous knee trauma or surgery. OA affects usually the medial compartment of the knee, and
The Arthritic Knee The causes of OA of the knee are multiple and include aging (wear and tear), obesity, and previous knee trauma or surgery. OA affects usually the medial compartment of the knee, and
intake form About You : General Health Information: Page 1`of 5 State/Province: Country: Zip/Postal Code: Address:
 intake form Page 1`of 5 About You : Name: Sex: Male Female Address: City: State/Province: Country: Zip/Postal Code: Home Phone Number: Mobile Phone Number: Email Address: Birthday: Marital Status: Married
intake form Page 1`of 5 About You : Name: Sex: Male Female Address: City: State/Province: Country: Zip/Postal Code: Home Phone Number: Mobile Phone Number: Email Address: Birthday: Marital Status: Married
SHOULDER ARTHROSCOPY WITH ANTERIOR STABILIZATION / CAPSULORRHAPHY REHABILITATION PROTOCOL
 General Notes As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
General Notes As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
Institute of Holistic Healthcare. Certificate in Orthopaedic Manipulative Therapy PROSPECTUS
 Institute of Holistic Healthcare Certificate in Orthopaedic Manipulative Therapy PROSPECTUS 2019 Contents Contents... 1 Aims:... 2 Objectives:... 2 Format of the Program:... 3 Program... 3 Continuing Professional
Institute of Holistic Healthcare Certificate in Orthopaedic Manipulative Therapy PROSPECTUS 2019 Contents Contents... 1 Aims:... 2 Objectives:... 2 Format of the Program:... 3 Program... 3 Continuing Professional
EASTERN ARIZONA COLLEGE Athletic Training Practicum I
 EASTERN ARIZONA COLLEGE Athletic Training Practicum I Course Design 2014-2015 Course Information Division Health & Physical Education Course Number HPE 292 Title Athletic Training Practicum I Credits 3
EASTERN ARIZONA COLLEGE Athletic Training Practicum I Course Design 2014-2015 Course Information Division Health & Physical Education Course Number HPE 292 Title Athletic Training Practicum I Credits 3
REHABILITATION PROTOCOL Criteria-Based Postoperative ACL Reconstruction Rehabilitation Protocol
 REHABILITATION PROTOCOL Criteria-Based Postoperative ACL Reconstruction Rehabilitation Protocol Phase I (Days 1 7) WEIGHTBEARING STATUS 1- Two crutches, weightbearing as tolerated. Exercises 1- Heel slides/wall
REHABILITATION PROTOCOL Criteria-Based Postoperative ACL Reconstruction Rehabilitation Protocol Phase I (Days 1 7) WEIGHTBEARING STATUS 1- Two crutches, weightbearing as tolerated. Exercises 1- Heel slides/wall
Top 100 Diagnosis Codes as Reported by HNS Physicians (Revised 08/30/16)
 Top 100 Diagnosis Codes as Reported by HNS Physicians (Revised 08/30/16) Disclaimer: The information in the HNS Code Translator is based on the General Equivalency Mapping (GEM) files published by CMS,
Top 100 Diagnosis Codes as Reported by HNS Physicians (Revised 08/30/16) Disclaimer: The information in the HNS Code Translator is based on the General Equivalency Mapping (GEM) files published by CMS,
WTC II Term 3 Notes & Assessments
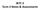 Term 3 Notes & Assessments Planes of Motion/Axes The body moves in a number of various ways and directions. In the past you have learned about the terminology for movements at specific joints, for example,
Term 3 Notes & Assessments Planes of Motion/Axes The body moves in a number of various ways and directions. In the past you have learned about the terminology for movements at specific joints, for example,
Musculoskeletal and Orthopaedic Conditions Treated
 General category Sub-categories Often used diagnosis/common terms Muscle and tendon pain and injuries Strains, tears/ruptures, contusions, lacerations, muscle pain, myofascial pain Tendinopathy, tendinitis,
General category Sub-categories Often used diagnosis/common terms Muscle and tendon pain and injuries Strains, tears/ruptures, contusions, lacerations, muscle pain, myofascial pain Tendinopathy, tendinitis,
Secrets and Staples of Training the Athletic Shoulder
 Secrets and Staples of Training the Athletic Shoulder Eric Beard Corrective Exercise Specialist Athletic Performance Enhancement Specialist EricBeard.com AthleticShoulder.com Presentation Overview Rationale
Secrets and Staples of Training the Athletic Shoulder Eric Beard Corrective Exercise Specialist Athletic Performance Enhancement Specialist EricBeard.com AthleticShoulder.com Presentation Overview Rationale
Toe walking gives rise to parental concern. Therefore, toe-walkers are often referred at the 3 years of age.
 IDIOPATHIC TOE WALKING Toe walking is a common feature in immature gait and is considered normal up to 3 years of age. As walking ability improves, initial contact is made with the heel. Toe walking gives
IDIOPATHIC TOE WALKING Toe walking is a common feature in immature gait and is considered normal up to 3 years of age. As walking ability improves, initial contact is made with the heel. Toe walking gives
Chapter 20: Muscular Fitness and Assessment
 Chapter 20: Muscular Fitness and Assessment American College of Sports Medicine. (2010). ACSM's resource manual for guidelines for exercise testing and prescription (6th ed.). New York: Lippincott, Williams
Chapter 20: Muscular Fitness and Assessment American College of Sports Medicine. (2010). ACSM's resource manual for guidelines for exercise testing and prescription (6th ed.). New York: Lippincott, Williams
Thoracolumbar Spine Conditions: Treatment and Return to Play
 Thoracolumbar Spine Conditions: Treatment and Return to Play C H R I S T O P H E R B U R K S, MD B I E N V I L L E O R T H O P A E D I C S P E C I A L I S T S O C E A N S P R I N G S, MS Thoracolumbar
Thoracolumbar Spine Conditions: Treatment and Return to Play C H R I S T O P H E R B U R K S, MD B I E N V I L L E O R T H O P A E D I C S P E C I A L I S T S O C E A N S P R I N G S, MS Thoracolumbar
Information contained in this curriculum guide is subject to change.
 Curriculum Overview The curriculum plan includes up to 55 required courses. During the first year students build on their prerequisite coursework through courses in the basic sciences and begin clinical
Curriculum Overview The curriculum plan includes up to 55 required courses. During the first year students build on their prerequisite coursework through courses in the basic sciences and begin clinical
Top 100 Diagnosis Codes as Reported by HNS Physicians
 Top 100 Diagnosis Codes as Reported by HNS Physicians Disclaimer: The information in the HNS Code Translator is based on the General Equivalency Mapping (GEM) files published by CMS, and are not intended
Top 100 Diagnosis Codes as Reported by HNS Physicians Disclaimer: The information in the HNS Code Translator is based on the General Equivalency Mapping (GEM) files published by CMS, and are not intended
Types of Body Movements
 Types of Body Movements Bởi: OpenStaxCollege Synovial joints allow the body a tremendous range of movements. Each movement at a synovial joint results from the contraction or relaxation of the muscles
Types of Body Movements Bởi: OpenStaxCollege Synovial joints allow the body a tremendous range of movements. Each movement at a synovial joint results from the contraction or relaxation of the muscles
REHABILITATION GUIDELINES FOR ARTHROSCOPIC CAPSULAR SHIFT
 REHABILITATION GUIDELINES FOR ARTHROSCOPIC CAPSULAR SHIFT The rehabilitation guidelines are presented in a criterion based progression. General time frames are given for reference to the average, but individual
REHABILITATION GUIDELINES FOR ARTHROSCOPIC CAPSULAR SHIFT The rehabilitation guidelines are presented in a criterion based progression. General time frames are given for reference to the average, but individual
Anatomy. Anatomy deals with the structure of the human body, and includes a precise language on body positions and relationships between body parts.
 Anatomy deals with the structure of the human body, and includes a precise language on body positions and relationships between body parts. Proper instruction on safe and efficient exercise technique requires
Anatomy deals with the structure of the human body, and includes a precise language on body positions and relationships between body parts. Proper instruction on safe and efficient exercise technique requires
Hip Arthroscopy Femoroacetabular Impingement (FAI) Ryan W. Hess, MD Tracey Pederson, PCC Office: (763) Fax: (763)
 Hip Arthroscopy Femoroacetabular Impingement (FAI) Ryan W. Hess, MD Tracey Pederson, PCC Office: (763) 302-2223 Fax: (763) 302-2401 GENERAL GUIDELINES: Despite the minimally invasive nature of hip arthroscopy,
Hip Arthroscopy Femoroacetabular Impingement (FAI) Ryan W. Hess, MD Tracey Pederson, PCC Office: (763) 302-2223 Fax: (763) 302-2401 GENERAL GUIDELINES: Despite the minimally invasive nature of hip arthroscopy,
EXERCISE PRESCRIPTION PART 1
 EXERCISE PRESCRIPTION PART 1 Michael McMurray, PT, DPT, OCS, FAAOMPT Orthopaedic Manual Physical Therapy Series Charlottesville 2017-2018 What is MET? An active rehabilitation system based in the biopsychosocial
EXERCISE PRESCRIPTION PART 1 Michael McMurray, PT, DPT, OCS, FAAOMPT Orthopaedic Manual Physical Therapy Series Charlottesville 2017-2018 What is MET? An active rehabilitation system based in the biopsychosocial
Adam N. Whatley, M.D Main St., STE Zachary, LA Phone(225) Fax(225)
 Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 Total Knee Arthroplasty Protocol: The intent of this protocol is to provide the clinician with a guideline
Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 Total Knee Arthroplasty Protocol: The intent of this protocol is to provide the clinician with a guideline
Reverse Total Shoulder Arthroplasty Protocol
 General Information: Reverse Total Shoulder Arthroplasty Protocol Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH) arthritis when it
General Information: Reverse Total Shoulder Arthroplasty Protocol Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH) arthritis when it
Session 4: Exercise Prescription for Musculoskeletal Disorders: Low Back Pain
 Session 4: Exercise Prescription for Musculoskeletal Disorders: Low Back Pain Course: Designing Exercise Prescriptions for Normal/Special Populations Presentation Created by Ken Baldwin, M.ED, ACSM-H/FI
Session 4: Exercise Prescription for Musculoskeletal Disorders: Low Back Pain Course: Designing Exercise Prescriptions for Normal/Special Populations Presentation Created by Ken Baldwin, M.ED, ACSM-H/FI
Course Information DPT 720 Professional Development (2 Credits) DPT 726 Evidenced-Based Practice in Physical Therapy I (1 Credit)
 Course Information DPT 720 Professional Development (2 Credits) This course introduces theories and experiences designed to develop professional socialization in students. Skills to accurately, sensitively
Course Information DPT 720 Professional Development (2 Credits) This course introduces theories and experiences designed to develop professional socialization in students. Skills to accurately, sensitively
Diagnostic Imaging Exams
 Guide for Chiropractors Diagnostic Imaging Exams CREATED FOR OUR CHIROPRACTIC PARTNERS This document has been prepared by the specialized, board-certified radiologists who interpret patient exams for Center
Guide for Chiropractors Diagnostic Imaging Exams CREATED FOR OUR CHIROPRACTIC PARTNERS This document has been prepared by the specialized, board-certified radiologists who interpret patient exams for Center
Module Eight. Application of Health Assessment NUR 225. Physical examination of Musculoskeletal System. King Saud University. Collage of Nursing
 King Saud University Collage of Nursing Medical Surgical Nursing depart Application of Health Assessment NUR 225 Module Eight Physical examination of Musculoskeletal System Obtaining a health history Ask
King Saud University Collage of Nursing Medical Surgical Nursing depart Application of Health Assessment NUR 225 Module Eight Physical examination of Musculoskeletal System Obtaining a health history Ask
