Diagnostic coding accuracy for traumatic spinal cord injuries
|
|
|
- Chad Short
- 5 years ago
- Views:
Transcription
1 (2009) 47, & 2009 International Society All rights reserved /09 $ ORIGINAL ARTICLE Diagnostic coding accuracy for traumatic spinal cord injuries EM Hagen 1,2, T Rekand 1, NE Gilhus 1,2 and M Gronning 1,2 1 Department of Neurology, Haukeland University Hospital, Bergen, Norway and 2 Department of Clinical Medicine, Section of Neurology, University of Bergen, Bergen, Norway Study design: Retrospective register study enhanced and verified by medical records. Objectives: To study whether electronic searches of discharge diagnosis are valid for epidemiological research of traumatic spinal cord injury (SCI), using the International Classification of Diseases (ICD). Settings: Haukeland University Hospital, Bergen, Norway Methods: We identified all hospital admissions with discharge codes suggesting a traumatic SCI from ICD-8 to ICD-10 in the electronic database at Haukeland University Hospital, and ascertained the cases by reviewing all hospital records. Results: 1080 patients had an ICD diagnostic code suggesting a traumatic SCI. Only 260 were verified when reviewing the hospital records. The ICD-10 codes had superior positive predictive values (PPV) and likelihood ratios (LR þ ) compared with the codes from ICD-8 and ICD-9. Combining seven codes from ICD-10 (S14.0, S14.1, S24.0, S24.1, S34.1, S34.3, T91.3) gave the highest sensitivity (0.83), specificity (0.97), PPV (0.88) and LR þ (30.23). Conclusion: Obtaining hospital discharge diagnoses solely from electronic databases overestimates the incidence of traumatic SCI. Identification of patients using ICD-10 codes is more complicated because acute traumatic SCI and traumatic SCI sequelae are listed with several codes. The latest ICD version proved to be most reliable when identifying patients with traumatic SCI. However, ICD data cannot be trusted without extensive validity checks for either research or for health planning and administration. (2009) 47, ; doi: /sc ; published online 7 October 2008 Keywords: traumatic spinal cord injury; ICD-8; ICD-9; ICD-10; discharge diagnoses; validation Introduction The incidence of traumatic spinal cord injuries (SCI) vary from 9.2 to 57.8 per million. 1 This variation is partly because of differences in definition, classification and procedures of patient identification. The International Classification of Diseases (ICD) has become the standard diagnostic classification for epidemiological and health management purposes, and has been subjected to continuous update and revision. The current version, ICD-10, was introduced in and has been used for somatic diseases at our hospital since Traumatic SCI based on ICD-8 3,4 and ICD-9 5,6 have been evaluated, but less so for ICD Although patient records should be the gold standard for accurate clinical information, administrative databases are widely searched, quickly and inexpensively, to obtain information for research as well as daily practice. 7 The reliability of information from such administrative databases Correspondence: Dr EM Hagen, Department of Neurology, Haukeland University Hospital, 5021 Bergen, Norway. ellen.merete.hagen@helse-bergen.no Received 15 May 2008; revised 21 August 2008; accepted 24 August 2008; published online 7 October 2008 can be questioned because of the inaccurate coding of the disease. Validity of the data is crucial for epidemiological research. In epidemiology comparison between time periods is of interest to identify the factors that determine the outcome and this paper illustrates how the changing diagnostic coding system influences the results using ICD 8, 9 and 10 to identify traumatic SCI. Such a diagnostic validity test may have direct implications for the planning of future research and for the clinical and administrative use of data from electronic databases. Materials and methods Definition of spinal cord injury Traumatic SCI was defined in accordance with Kraus et al. 8 as an acute, traumatic lesion of the spinal cord with varying degrees of motor and/or sensory deficit or paralysis. Although injuries of cauda equina were included, the definition excluded isolated injuries of other nerve roots. 9 Transient paresis or impermanent deficits lasting less than 1 week were not included.
2 368 Diagnostic coding accuracy for traumatic SCI Inclusion criteria Search codes describing traumatic spinal cord injury, both acute and sequelae, from ICD-8 and ICD-9 were included. 3 6,8,10 The codes from ICD-10 included codes that indicate a fracture or dislocation of the spinal column, concussion and edema of the spinal cord, trauma with SCI, other unspecified injuries of the spinal cord, injury of the cauda equina nerves and spinal cord, and sequelae of such injuries. Thus, we included 22 codes from ICD-10 to minimize possible under-reporting. All codes are listed in Table 1. Haukeland University Hospital serves three counties with a population of approximately 1 million. Most of the patients were admitted immediately after injury, but some were initially treated in local hospitals. Persons with minimal neurologic impairment on admission were included if their length of stay was greater than 1 week, 11,12 and 1 day for patients staying in the Department of Neurosurgery. There is only one Department of Neurosurgery in the region. Some Table 1 ICD codes used in the electronic case identification ICD x Fracture and fracture dislocation of vertebral column with spinal cord lesion 958.x Spinal cord lesion without evidence of spinal bone injury ICD Other paralytic syndromes Quadriplegia and quadriparesis Paraplegia 806.x Fracture of vertebral column with spinal cord lesion Late effect of spinal cord injury 952.x Spinal cord lesion without evidence of spinal bone injury ICD-10 G82 Paraplegia and tetraplegia S12.0 Fracture of first cervical vertebra S12.2 Fracture of other specified cervical vertebra S13.0 Traumatic rupture of cervical intervertebral disk S13.2 Dislocation of other and unspecified parts of neck S13.4 Sprain and strain of cervical spine S14.0 Concussion and edema of cervical spinal cord S14.1 Other and unspecified injuries of cervical spinal cord S22.0 Fracture of thoracic vertebra S23.1 Dislocation of thoracic vertebra S24.0 Concussion and edema of thoracic spinal cord S24.1 Other and unspecified injuries of thoracic spinal cord S32.0 Fracture of lumbar vertebra S33.1 Dislocation of lumbar vertebra S34.0 Concussion and edema of lumbar spinal cord S34.1 Other injury of lumbar spinal cord S34.3 Injury of cauda equina T06.0 Injuries of brain and cranial nerves with injuries of nerves and spinal cord at neck level T06.1 Injuries of nerves and spinal cord involving other multiple body regions T09.3 Injury of spinal cord, level unspecified T91.1 Sequelae of injuries, of poisoning and of other consequences of external causesfsequelae of injuries of neck and trunkfsequelae of fracture of spine T91.3 Sequelae of injuries, of poisoning and of other consequences of external causesfsequelae of injuries of neck and trunkfsequelae of injury of spinal cord An x indicates that all subcodes were included. The codes in bold are specific for traumatic SCI. patients were treated at other hospitals shortly after surgery. Both primary and later stays were included. Hospital discharge data The electronic discharge registry contained personal information about each patient, including an 11-digit national identification number, dates of admission and discharge, codes for one primary diagnosis and unlimited secondary diagnoses and codes for all surgical procedures performed. The clinical diagnoses and procedures with corresponding codes are made by the attending physician and written in the case summary prepared routinely at the end of the hospitalization. Local medical secretaries transfer this information to the electronic discharge registry. Data in the hospital discharge registry were reported using ICD-8 in the period , ICD-9 in the period and ICD-10 since August Case finding and ascertainment 1080 patients with a diagnostic code suggesting traumatic SCI were discharged from Haukeland University Hospital in the period , identified by computer search from the discharge registry using SQL-Database version 7.3, Microsoft Access Data were analyzed using SPSS release and STATA 9.0 (College Station, TX, USA). One author (EMH) reviewed all the complete patient records; and the other authors were consulted in all cases of doubt to reach a consensus. To detect any missing records, we compared the electronic searches with data from a local database at the Department of Neurology covering the period This database was extracted from a manual card-based system of discharge diagnoses at the Department. Most patients with persisting deficits would be transferred to the Department of Neurology, and the local database could act as a validation register. Statistical analysis Sensitivity was defined as the proportion of positives that were correctly identified, and specificity as the proportion of negatives that were correctly identified. The positive predictive value (PPV) is the proportion with a positive test result that was correctly diagnosed. The likelihood ratio (LR þ ) is the ratio of the probability of the specific test result in people who do have the disease compared to the probability in people who do not. The likelihood ratio of a positive test result (LR þ ) ¼ sensitivity/(1 specificity). We assessed the sensitivity, specificity, PPV and LR þ for each ICD code. Data were analyzed by using the statistical software STATA 9.0. The Western Norway Regional Committee for Medical Research Ethics, the Data Inspectorate and the Directorate for Health and Social Affairs approved the study. Results During the study period, 1080 patients were discharged from Haukeland University Hospital with one or more of the
3 Diagnostic coding accuracy for traumatic SCI 369 Table 2 Sensitivity, specificity, positive predictive value and likelihood ratio of search codes from ICD-8, ICD-9 and ICD-10 Code Sensitivity Specificity PPV LR+ ICD x x x+958.x ICD x x x+952.x ICD-10 G S S n/a S S S S n/a S T Combination Combination Abbreviations: LR+, likelihood ratio; PPV, positive predictive value. Combination 1: G82.4, S14.0, S14.1, S24.0, S24.1, S34.0, S34.1, S34.3, T91.3. Combination 2: S14.0, S14.1, S24.0, S24.1, S34.1, S34.3, T91.3. search codes (Table 1). Reviewing the complete patient records, only 260 of these patients (24.1%) were verified as having a traumatic SCI. The confirmed SCI patients had a total of 1107 hospital stays. 240 of these were primary admissions and 867 were follow-ups. The median number of stays was 2.5. Twenty-three patients with traumatic SCI included in the local database at the Department of Neurology, were not found in the electronic ICD-based search using multiple search codes. Of these, 22 did not have any relevant ICD search code, and one SCI patient was not at all registered in the hospital database. The proportion of patients verified with traumatic SCI were 77.5% during the period with ICD-8, 28.5% during the period with ICD-9 and 19.5% during the period with ICD-10, as shown in Table 2. Only one code was used at discharge in 99.6%, 92.4% and 76.5% of cases using ICD-8, ICD-9 and ICD-10, respectively, and two codes in 0.4%, 6.6% and 19.4%. Three codes were used only for a minority of stays in the last two revisions, for 1.0% and 4.1% of stays respectively. Table 2 shows the sensitivity, specificity, PPV and LR þ for each electronic search code for ICD-8, ICD-9 and ICD-10. The code 806.x (all subcodes included) from ICD-8 had the highest sensitivity and a high PPV. To achieve a higher sensitivity the number of search codes from each ICD version was reduced to the codes most specific for traumatic SCI. Using the codes 806.x, and 952.x from ICD-9, the proportion of verified patients increased to 34.7%. Using a combination of seven codes from ICD-10 the proportion of verified patients increased to 88% (Table 2). The code from ICD-9 had a low sensitivity, a high specificity, high PPV and high LR þ. The seven selected codes from ICD-10 had all a low sensitivity but a high specificity, high PPV and high LR þ. The LR þ for each single code varied from 0.39 to The highest ratio was for code from ICD-9. From ICD-10 the codes with highest LR þ were S14.0, S24.0, S24.1, S34.3 and T91.3 (Table 2). Combining two search codes in ICD-8 (806.x, 958.x) identified all patients with traumatic SCI. Combining the three ICD-9 codes 806.x, 907.2, 952.x did not identify 9.4% (14/149) of the patients with traumatic SCI. Using a combination of seven ICD-10 codes (S14.0, S14.1, S24.0, S24.1, S34.1, S34.3, T91.3) did not identify 16.2% (17/105) of the patients with traumatic SCI. Using the two codes from ICD-8, 20 of 89 possible patients (22.5%) did not have a traumatic SCI. Combining the three codes from ICD-9 and the seven codes from ICD-10, 65.3% and 12.0% of the included patients did not have a traumatic SCI, respectively. The most frequent diagnoses of the non-sci patients were nervous system injuries, cerebral palsy, whiplash associated disorders, traumatic brain injury and spine fractures without nervous system deficit. A combination of seven codes from ICD-10 (S14.0, S14.1, S24.0, S24.1, S34.1, S34.3 and T91.3) gave the optimal result regarding sensitivity, specificity, PPV and LR þ and better results than any ICD-8 and ICD-9 combinations. Discussion This study shows a low diagnostic accuracy for traumatic SCI using searches of discharge diagnoses in ICD-8, 9 and 10. Only 260 of 1080 potential traumatic SCI patients (24.1%) were confirmed as having a traumatic SCI after review of the patient records. The proportion of verified traumatic SCI was 77.5% for ICD-8, 28.5% for ICD-9 and 19.5% for ICD-10. Reducing the number of search codes from each ICD-version to the codes most specific for traumatic SCI increased the specificity as expected but decreased the sensitivity. There are substantial differences between ICD-8, 9 and ICD-10. However, all three versions were used during our study period. Therefore, the comparison of the ICD versions was made. A systematic review of 21 studies comparing the routine discharge diagnoses with the original medical record in Great Britain found the median coding accuracy declined from ICD-7 (96.5%) to ICD-8 (87%) and ICD-9 (77%). 14 Stroke coding accuracy was equally good with ICD-9 (90% correct) and ICD-10 (92% correct) in a study from Canada. 15 In the study from Great Britain the coding accuracy was higher for high-prevalence conditions (median 97%) than for low-prevalence conditions (median 91%). 14 Traumatic SCI is a low-prevalent condition. The code 806.x in ICD-8 had high sensitivity and PPV. Combining code 806.x and 958.x further increased the PPV. A study from USA 3 included four codes, 344, 805, 806 and 958. They found that the codes 806 and 958 had the highest validity. Combining the two codes 23.1% of SCI patients
4 370 Diagnostic coding accuracy for traumatic SCI were not identified. Because the codes 344 and 805 formed a large part of the data set, a later study restricted the search to the codes 806 and Only one of the 22 patients not found in the electronic search had been discharged with code 344 using only ICD-8. Adding this patient to the population 1 of 70 (1.4%) of the SCI patients were not identified using 806.x and 958.x. The PPV was very low (0.35) using a combination of three codes from ICD-9 (806.x, 952.x, 907.2) due to a higher number of patients with other diseases. A study from USA 5 found a higher overall PPV of 0.61 when using the two codes 806.x and 952.x. In our population, the code 806.x had the lowest specificity. PPV was lower for ICD-9 than for ICD-8. In UK hospital statistics diagnostic accuracy for SCI decreased from ICD-7 to ICD-8 and to ICD-9, probably because of more complex diagnostic classification. 14 In Finland more than half of the ICD-9 codes seemed to be misleading when comparing with the medical records. 6 When ICD-9 was used, some patients were coded with SCI, without any neurological deficits only fractures of the spine. They also found that after ICD-10 was introduced some cases with SCI were missed. Epidemiology relying only on ICD-9 codes will lead to significant overestimation. In our study, the overestimation using ICD-9 was mainly caused by incorrect use of code 806.x; that is, the code for fracture of vertebral column with spinal cord lesion given to patients with fractures with no spinal cord lesion. Such miscoding makes the data unreliable for epidemiological research and health care planning. We found that only 105 out of the 538 patients, who had one or more of the search codes from ICD-10, really had a traumatic SCI. Our selected ICD-10 discharge codes therefore grossly overestimate traumatic SCI as did the codes from ICD-8 and ICD-9. Most individual codes from ICD-10 had generally low sensitivity but high specificity, PPV and LR þ. ICD-10 differs substantially from previous ICD versions, and requires the use of multiple codes. These changes have influenced the proportion of patients verified. The codes indicate the anatomical location (cervical, thoracic and lumbar), and different codes for acute injury and sequelae are introduced. Our search covered many codes from ICD-10. The retrospective register-based epidemiological study from Finland 6 used 11 ICD-10 codes (S14.0, S14.1, S14.2, S24.0, S24.1, S24.2, S34.0, S34.1, S34.2, S34.3 and T91.3), and estimated the SCI prevalence rate to be 28 per The aim of the study was to identify all adult citizens (18 years or more) of Helsinki who had permanent sensory or motor deficits because of traumatic SCI. Cases were identified using the registers of the Kapyla Rehabilitation Centre, Helsinki University Central Hospital and the local organization for the disabled. They found that ICD-10 lacked sensitivity as 17 out of 152 patients were not identified. 6 In our study, we did not identify 16.2% of traumatic SCI patients using a combination of seven codes. An Australian study assessed the quality of ICD-10 coding in routinely collected hospital discharge data. Agreement of the principal diagnosis code was 85% at the 3-digit level in , improving to 87% in The code paraplegia had a sensitivity of 82% and a PPV of 85%. 16 However, the ICD diagnose G82 (paraplegia and tetraplegia) is a general diagnose describing a clinical picture and is not specific for traumatic SCI and not eligible for detecting patients. In our study, this code had low sensitivity and PPV. This clearly shows that the use of multiple codes is necessary to detect all patients. In our study, the codes S24.0 (Concussion and edema of thoracic spinal cord) and S24.1 (Other and unspecified injuries of thoracic spinal cord) had the highest LR þ, and 65.98, respectively. Injuries of the thoracic spinal cord are less frequent than injuries of the cervical and lumbar parts. These diagnoses have high specificity. When reducing the number of ICD-10 codes to seven by only selecting codes with high specificity, the proportion of patients with traumatic SCI verified increased to 88%, at the expense of losing 16.2% of the patients with traumatic SCI identified by the broad search. Thus a combination of seven codes from ICD-10 gave a higher specificity, PPV and LR þ compared to a combination of three codes from ICD-9. One of the major advantages of ICD-10 is that it is far more detailed than the previous ICD-versions. There are a total of codes in ICD-10 compared with 6969 in ICD-9. This permits more detailed clinical information. ICD-10 differs, however, substantially from the previous versions, and the possibilities for incorrect coding will affect the statistics. An international consortium presented in 2006 a list of highpriority methodological areas for researchers using health administrative data. The four most highly ranked priorities were the documentation of data fields in each country s hospital administrative data, the translation of patient safety indicators from ICD-9 to ICD-10, the development and validation of algorithms to verify the logic and internal consistency of coding in hospital abstract data, and interventional studies to enhance coding quality. 17 These measures may improve the quality of the databases in the future. The first diagnostic ICD-code should always describe the primary cause of the hospital stay. Incomplete coding of secondary diagnoses leads to under-reporting of all chronic disorders. 18 Many patients will have acute conditions or complications that take precedence in coding over chronic diseases. This may explain some missing patients also in our study. Causes of coding errors include lack of training and differences in coding tradition between departments. Other possibilities are ambiguity of terms, inaccurate or missing information in the patient record and variation and errors in clinical diagnoses. Local lists of limited code subsets may have been used, rather than the complete classification. The coding may also be biased by a tendency to repeat the codes used at previous stays because of convenience. Coding errors can occur during transcription by the physician or secretary. 19 Physicians in several specialties are involved in treating traumatic SCI. S-codes describe injuries related to a single body region, whereas T-codes include injuries to multiple or unspecified body regions. The latest ICD version proved to be most reliable when identifying patients with traumatic SCI. However, ICD data
5 Diagnostic coding accuracy for traumatic SCI 371 cannot be trusted without extensive validity checks for either research, health planning or administrative purposes. Acknowledgements We thank Alf M Aksland, Helse Vest IKT AS for retrieving the ICD-8 data. We are indebted to Harald Aurlien, Department of Clinical Medicine, Haukeland University Hospital for excellent technical assistance in developing the Microsoft Access database to retrieve ICD-9 and ICD-10 data, and to Jan Christian Broegger for assisting in analyzing the data in STATA 9.0. References 1 International Campaign for Cures of Injury Paralysis (ICCP). Table summarising published data on Injury. International Campaign for Cures of Injury Paralysis (ICCP), Available from: URL: iccp/index.php?option=com_content&task=view&id=13&itemid=28. 2 World Health Organization (WHO). ICD Implementation by countries. World Health Organization (WHO), Available from: URL: implementation/1.htm. 3 Webb Jr SB, Bracken MB, Wagner Jr FC. Retrospective versus prospective audit: a trial of two methods. Hosp Med Staff 1978; 7: Bracken MB, Freeman Jr DH, Hellenbrand K. Incidence of acute traumatic hospitalized spinal cord injury in the United States, Am J Epidemiol 1981; 113: Thurman DJ, Burnett CL, Jeppson L, Beaudoin DE, Sniezek JE. Surveillance of spinal cord injuries in Utah, USA. Paraplegia 1994; 32: Dahlberg A, Kotila M, Leppanen P, Kautiainen H, Alaranta H. Prevalence of spinal cord injury in Helsinki. 2005; 43: Humphries KH, Rankin JM, Carere RG, Buller CE, Kiely FM, Spinelli JJ. Co-morbidity data in outcomes research: are clinical data derived from administrative databases a reliable alternative to chart review? J Clin Epidemiol 2000; 53: Kraus JF, Franti CE, Riggins RS, Richards D, Borhani NO. Incidence of traumatic spinal cord lesions. J Chronic Dis 1975; 28: Maynard FM, Bracken MB, Creasey G, Ditunno JF, Donovan WH, Ducker TB et al. International standards for neurological and functional classification of spinal cord injury. 1997; 35: Thurman DJ, Sniezek J, Johnson D, Greenspan A, Smith SM. Guidelines for Surveillance of Central Nervous System. Atlanta, Georgia, US: US Department of Health and Human Services, Public Health Service, National Center for Injury Prevention and Control, Centers for Disease Control and Prevention, Atlanta, GA , USA. dxt9@cdc.gov, Marino RJ, Ditunno JF, Donovan WH, Maynard F. Neurologic recovery after traumatic spinal cord injury: data from the Model Injury Systems. Arch Phys Med Rehabil 1999; 80: Dryden DM, Saunders LD, Rowe BH, May LA, Yiannakoulias N, Svenson LW et al. The epidemiology of traumatic spinal cord injury in Alberta, Canada. Can J Neurol Sci 2003; 30: Hagen EM, Aarli JA, Gronning M. Patients with traumatic spinal cord injuries at the department of neurology, Haukeland Hospital Article in Norwegian. Tidsskr Nor Laegeforen 2001; 121: Campbell SE, Campbell MK, Grimshaw JM, Walker AE. A systematic review of discharge coding accuracy. J Public Health Med 2001; 23: Kokotailo RA, Hill MD. Coding of stroke and stroke risk factors using international classification of diseases, revisions 9 and 10. Stroke 2005; 36: Henderson T, Shepheard J, Sundararajan V. Quality of diagnosis and procedure coding in ICD-10 administrative data. Med Care 2006; 44: De Coster C, Quan H, Finlayson A, Gao M, Halfon P, Humphries KH et al. Identifying priorities in methodological research using ICD-9-CM and ICD-10 administrative data: report from an international consortium. BMC Health Serv Res 2006; 6: Iezzoni LI, Foley SM, Daley J, Hughes J, Fisher ES, Heeren T. Comorbidities, complications, and coding bias. Does the number of diagnosis codes matter in predicting in-hospital mortality? JAMA 1992; 267: Sorensen HT, Sabroe S, Olsen J. A framework for evaluation of secondary data sources for epidemiological research. Int J Epidemiol 1996; 25:
An introduction to the Barell body region by nature of injury diagnosis matrix
 91 SPECIAL FEATURE An introduction to the Barell body region by nature of injury diagnosis matrix V Barell*, L Aharonson-Daniel, L A Fingerhut, E J Mackenzie, A Ziv, V Boyko, A Abargel, M Avitzour, R Heruti...
91 SPECIAL FEATURE An introduction to the Barell body region by nature of injury diagnosis matrix V Barell*, L Aharonson-Daniel, L A Fingerhut, E J Mackenzie, A Ziv, V Boyko, A Abargel, M Avitzour, R Heruti...
Evaluating Sources of Traumatic Spinal Cord Injury Surveillance Data in Colorado
 American Journal of Epidemiology Copyright C 1997 by The Johns Hopkins University School of Hygiene and Public Health All rights reserved Vol. 148, No. 3 Printed In USA. Evaluating Sources of Traumatic
American Journal of Epidemiology Copyright C 1997 by The Johns Hopkins University School of Hygiene and Public Health All rights reserved Vol. 148, No. 3 Printed In USA. Evaluating Sources of Traumatic
Inter-rater reliability of the 1992 international standards for neurological and functional classi cation of incomplete spinal cord injury
 (2000) 38, 675 ± 679 ã 2000 International Medical Society of Paraplegia All rights reserved 1362 ± 4393/00 $15.00 www.nature.com/sc Inter-rater reliability of the 1992 international standards for neurological
(2000) 38, 675 ± 679 ã 2000 International Medical Society of Paraplegia All rights reserved 1362 ± 4393/00 $15.00 www.nature.com/sc Inter-rater reliability of the 1992 international standards for neurological
New Zealand Spinal Cord Injury Registry. First Annual Report August 2016 to July 2017
 New Zealand Spinal Cord Injury Registry First Annual Report August 216 to July 217 2 The New Zealand Spinal Cord Injury Registry (NZSCIR) would like to acknowledge the spinal service clinicians and coordinators
New Zealand Spinal Cord Injury Registry First Annual Report August 216 to July 217 2 The New Zealand Spinal Cord Injury Registry (NZSCIR) would like to acknowledge the spinal service clinicians and coordinators
Neurologic improvement after thoracic, thoracolumbar, and lumbar spinal cord (conus medullaris) injuries
 Thomas Jefferson University Jefferson Digital Commons Department of Orthopaedic Surgery Faculty Papers Department of Orthopaedic Surgery 1-2011 Neurologic improvement after thoracic, thoracolumbar, and
Thomas Jefferson University Jefferson Digital Commons Department of Orthopaedic Surgery Faculty Papers Department of Orthopaedic Surgery 1-2011 Neurologic improvement after thoracic, thoracolumbar, and
A Structural Service Plan: Towards Better and Safer Spine Surgeries. Department of Orthopaedics & Traumatology Tuen Mun Hospital
 A Structural Service Plan: Towards Better and Safer Spine Surgeries Department of Orthopaedics & Traumatology Tuen Mun Hospital Cheung KK Wong CY Chan Andrew Tse Alfred Chow YY Department of Orthopaedics
A Structural Service Plan: Towards Better and Safer Spine Surgeries Department of Orthopaedics & Traumatology Tuen Mun Hospital Cheung KK Wong CY Chan Andrew Tse Alfred Chow YY Department of Orthopaedics
Lumbosacral plexus lesion Lumbosacral plexus disorders G54.1 Neuralgic amyotrophy Neuralgic amyotrophy G
 ICD-9-CM and ICD-10-CM NEUROMUSCULAR DIAGNOSIS CODES Focal Neuropathy ICD-9-CM ICD-10-CM Mononeuropathy G56.00 Carpal tunnel syndrome 354.00 Other median nerve lesion 354.10 Lesion of ulnar nerve 354.20
ICD-9-CM and ICD-10-CM NEUROMUSCULAR DIAGNOSIS CODES Focal Neuropathy ICD-9-CM ICD-10-CM Mononeuropathy G56.00 Carpal tunnel syndrome 354.00 Other median nerve lesion 354.10 Lesion of ulnar nerve 354.20
Spinal injury. Structure of the spine
 Spinal injury Structure of the spine Some understanding of the structure of the spine (spinal column) and the spinal cord is important as it helps your Neurosurgeon explain about the part of the spine
Spinal injury Structure of the spine Some understanding of the structure of the spine (spinal column) and the spinal cord is important as it helps your Neurosurgeon explain about the part of the spine
Prediction of functional outcome after spinal cord injury: a task for the rehabilitation team and the patient
 () 8, 8 ± ã International Medical Society of Paraplegia All rights reserved ± / $. www.nature.com/sc Prediction of functional outcome after spinal cord injury: a task for the rehabilitation team and the
() 8, 8 ± ã International Medical Society of Paraplegia All rights reserved ± / $. www.nature.com/sc Prediction of functional outcome after spinal cord injury: a task for the rehabilitation team and the
Managetnent of Spinal Cord Injury a General Hospital in Rural India
 Parapicf{Ja 24 (1986) 110-33'5 1986 International Medical Society of Paraplegia Managetnent of Spinal Cord Injury a General Hospital in Rural India In V. Chacko, M.S. (Orth.),I B. Joseph, D.Orth., M.S.
Parapicf{Ja 24 (1986) 110-33'5 1986 International Medical Society of Paraplegia Managetnent of Spinal Cord Injury a General Hospital in Rural India In V. Chacko, M.S. (Orth.),I B. Joseph, D.Orth., M.S.
Functional outcome of patients with spinal cord injury: rehabilitation outcome study
 Clinical Rehabilitation 1999; 13: 457 463 Functional outcome of patients with spinal cord injury: rehabilitation outcome study MC Schönherr Rehabilitation Centre Beatrixoord, Haren and Department of Rehabilitation,
Clinical Rehabilitation 1999; 13: 457 463 Functional outcome of patients with spinal cord injury: rehabilitation outcome study MC Schönherr Rehabilitation Centre Beatrixoord, Haren and Department of Rehabilitation,
Demographic study of patients with vertebral column trauma in North-West of Iran trauma center
 ISSN: 2203-1413 Vol.05 No.01 Demographic study of patients with vertebral column trauma in North-West of Iran trauma center Samad Shams Vahdati 1, Ozgur tatli 2*, Seyedpooya Paknezhad 3, Neda Parnianfard
ISSN: 2203-1413 Vol.05 No.01 Demographic study of patients with vertebral column trauma in North-West of Iran trauma center Samad Shams Vahdati 1, Ozgur tatli 2*, Seyedpooya Paknezhad 3, Neda Parnianfard
AS THE NUMBER OF interventions proposed for study in
 ORIGINAL ARTICLE Upper- and Lower-Extremity Motor Recovery After Traumatic Cervical Spinal Cord Injury: An Update From the National Spinal Cord Injury Database Ralph J. Marino, MD, Stephen Burns, MD, Daniel
ORIGINAL ARTICLE Upper- and Lower-Extremity Motor Recovery After Traumatic Cervical Spinal Cord Injury: An Update From the National Spinal Cord Injury Database Ralph J. Marino, MD, Stephen Burns, MD, Daniel
OUTCOMES AND DATA 2016
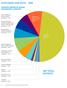 AND DATA 2016 SERVED BY REHAB IMPAIRMENT CATEGORY 20 patients 5.1% MAJOR MULTIPLE TRAUMA W/BRAIN OR SPINAL CORD INJURY 24 patients 6.2% TRAUMATIC 39 patients 10.0% AMPUTATION LOWER EXTREMITY 26 patients
AND DATA 2016 SERVED BY REHAB IMPAIRMENT CATEGORY 20 patients 5.1% MAJOR MULTIPLE TRAUMA W/BRAIN OR SPINAL CORD INJURY 24 patients 6.2% TRAUMATIC 39 patients 10.0% AMPUTATION LOWER EXTREMITY 26 patients
University of Groningen. Functional outcome after spinal cord injury Schonherr, Marleen C.
 University of Groningen Functional outcome after spinal cord injury Schonherr, Marleen C. IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it.
University of Groningen Functional outcome after spinal cord injury Schonherr, Marleen C. IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it.
SPINE EVALUATION AND CLEARANCE Basic Principles
 SPINE EVALUATION AND CLEARANCE Basic Principles General 1. Entire spine is immobilized during primary survey. 2. Radiographic clearance of the spine is not required before emergent surgical procedures.
SPINE EVALUATION AND CLEARANCE Basic Principles General 1. Entire spine is immobilized during primary survey. 2. Radiographic clearance of the spine is not required before emergent surgical procedures.
[FILE] SPINAL CORD INJURY TREATMENT GUIDELINES
![[FILE] SPINAL CORD INJURY TREATMENT GUIDELINES [FILE] SPINAL CORD INJURY TREATMENT GUIDELINES](/thumbs/77/76529822.jpg) 20 October, 2017 [FILE] SPINAL CORD INJURY TREATMENT GUIDELINES Document Filetype: PDF 428.48 KB 0 [FILE] SPINAL CORD INJURY TREATMENT GUIDELINES The time between the injury and treatment is a critical
20 October, 2017 [FILE] SPINAL CORD INJURY TREATMENT GUIDELINES Document Filetype: PDF 428.48 KB 0 [FILE] SPINAL CORD INJURY TREATMENT GUIDELINES The time between the injury and treatment is a critical
Spinal Cord Injury Transection Injury, Spinal Shock, and Hermiated Disc. Copyright 2014, 2011, 2006 by Saunders, an imprint of Elsevier, Inc.
 Spinal Cord Injury Transection Injury, Spinal Shock, and Hermiated Disc 1 Spinal Cord Injury Results from fracture and/or dislocation of vertebrae // Compresses, stretches, or tears spinal cord Cervical
Spinal Cord Injury Transection Injury, Spinal Shock, and Hermiated Disc 1 Spinal Cord Injury Results from fracture and/or dislocation of vertebrae // Compresses, stretches, or tears spinal cord Cervical
ACDF. Anterior Cervical Discectomy and Fusion. An introduction to
 An introduction to ACDF Anterior Cervical Discectomy and Fusion This booklet provides general information on ACDF. It is not meant to replace any personal conversations that you might wish to have with
An introduction to ACDF Anterior Cervical Discectomy and Fusion This booklet provides general information on ACDF. It is not meant to replace any personal conversations that you might wish to have with
SEVERAL STUDIES ON spinal cord injury (SCI) recovery. Early Versus Delayed Inpatient Spinal Cord Injury Rehabilitation: An Italian Study
 512 Early Versus Delayed Inpatient Spinal Cord Injury Rehabilitation: An Italian Study Giorgio Scivoletto, MD, Barbara Morganti, PT, Marco Molinari, MD, PhD ABSTRACT. Scivoletto G, Morganti B, Molinari
512 Early Versus Delayed Inpatient Spinal Cord Injury Rehabilitation: An Italian Study Giorgio Scivoletto, MD, Barbara Morganti, PT, Marco Molinari, MD, PhD ABSTRACT. Scivoletto G, Morganti B, Molinari
ORIGINAL ARTICLE Incidence of acute spinal cord injury in the Czech Republic: a prospective epidemiological study
 (217), 1 5 & 217 International Society All rights reserved 1362-4393/17 www.nature.com/sc ORIGINAL ARTICLE Incidence of acute spinal cord injury in the Czech Republic: a prospective epidemiological study
(217), 1 5 & 217 International Society All rights reserved 1362-4393/17 www.nature.com/sc ORIGINAL ARTICLE Incidence of acute spinal cord injury in the Czech Republic: a prospective epidemiological study
The Anatomy and Physiology of Spinal Cord Injury
 The Anatomy and Physiology of Spinal Cord Injury A Resource for Health Service Providers WA State Spinal Injury Unit Version 1 November 2013 Review Date November 2016 This document has been developed to
The Anatomy and Physiology of Spinal Cord Injury A Resource for Health Service Providers WA State Spinal Injury Unit Version 1 November 2013 Review Date November 2016 This document has been developed to
RADICULOPATHY AN INTRODUCTION TO
 AN INTRODUCTION TO RADICULOPATHY This booklet provides general information on radiculopathy. It is not meant to replace any personal conversations that you might wish to have with your physician or other
AN INTRODUCTION TO RADICULOPATHY This booklet provides general information on radiculopathy. It is not meant to replace any personal conversations that you might wish to have with your physician or other
102 Results RESULTS. Age Mean=S.D Range 42= years -84 years Number % <30 years years >50 years
 102 Results RESULTS A total of 50 cases were studied 39 males and 11females.Their age ranged between 16 years and 84 years (mean 42years). T1 and T2WI were acquired for all cases in sagittal and axial
102 Results RESULTS A total of 50 cases were studied 39 males and 11females.Their age ranged between 16 years and 84 years (mean 42years). T1 and T2WI were acquired for all cases in sagittal and axial
A test of the 1992 International Standards for Neurological and Functional Classi cation of Spinal Cord Injury
 Spinal Cord (1998) 36, 554 ± 560 1998 International Medical Society of Paraplegia All rights reserved 1362 ± 4393/98 $12.00 http://www.stockton-press.co.uk/sc A test of the 1992 International Standards
Spinal Cord (1998) 36, 554 ± 560 1998 International Medical Society of Paraplegia All rights reserved 1362 ± 4393/98 $12.00 http://www.stockton-press.co.uk/sc A test of the 1992 International Standards
Lecture 14: The Spinal Cord
 Lecture 14: The Spinal Cord M/O Chapters 16 69. Describe the relationship(s) between the following structures: root, nerve, ramus, plexus, tract, nucleus, and ganglion. 70. Trace the path of information
Lecture 14: The Spinal Cord M/O Chapters 16 69. Describe the relationship(s) between the following structures: root, nerve, ramus, plexus, tract, nucleus, and ganglion. 70. Trace the path of information
Central Cord Syndrome: Does early surgical intervention improve neurological outcome
 Central Cord Syndrome: Does early surgical intervention improve neurological outcome Ciara Stevenson, Jonathan Warnock, Suzanne Maguire, Niall Eames Department of Trauma and Orthopaedic Surgery, Royal
Central Cord Syndrome: Does early surgical intervention improve neurological outcome Ciara Stevenson, Jonathan Warnock, Suzanne Maguire, Niall Eames Department of Trauma and Orthopaedic Surgery, Royal
Specialised Services Commissioning Policy: CP141 Specialised Spinal Cord Injury Rehabilitation
 Specialised Services Commissioning Policy: CP141 Specialised Spinal Cord Injury Rehabilitation February 2018 Version 1.0 Document information Document purpose Document name Author Policy Specialised Spinal
Specialised Services Commissioning Policy: CP141 Specialised Spinal Cord Injury Rehabilitation February 2018 Version 1.0 Document information Document purpose Document name Author Policy Specialised Spinal
HERNIATED DISCS AN INTRODUCTION TO
 AN INTRODUCTION TO HERNIATED S This booklet provides general information on herniated discs. It is not meant to replace any personal conversations that you might wish to have with your physician or other
AN INTRODUCTION TO HERNIATED S This booklet provides general information on herniated discs. It is not meant to replace any personal conversations that you might wish to have with your physician or other
Nervous System: Spinal Cord and Spinal Nerves (Chapter 13)
 Nervous System: Spinal Cord and Spinal Nerves (Chapter 13) Lecture Materials for Amy Warenda Czura, Ph.D. Suffolk County Community College Eastern Campus Primary Sources for figures and content: Marieb,
Nervous System: Spinal Cord and Spinal Nerves (Chapter 13) Lecture Materials for Amy Warenda Czura, Ph.D. Suffolk County Community College Eastern Campus Primary Sources for figures and content: Marieb,
Cost of traumatic spinal cord injury in a population-based registry
 Spinal Cord (1996) 34, 470-480 1996 International Medical Society of Paraplegia All rights reserved 1362-4393/96 $12.00 Cost of traumatic spinal cord injury in a population-based registry Renee L Johnson
Spinal Cord (1996) 34, 470-480 1996 International Medical Society of Paraplegia All rights reserved 1362-4393/96 $12.00 Cost of traumatic spinal cord injury in a population-based registry Renee L Johnson
NEUROLOGICAL EXAMINATIONS: LOCALISATION AND GRADING
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk NEUROLOGICAL EXAMINATIONS: LOCALISATION AND GRADING Author : MARK LOWRIE Categories : Vets Date : June 16, 2014 MARK LOWRIE
Vet Times The website for the veterinary profession https://www.vettimes.co.uk NEUROLOGICAL EXAMINATIONS: LOCALISATION AND GRADING Author : MARK LOWRIE Categories : Vets Date : June 16, 2014 MARK LOWRIE
BACKGROUND ON INPATIENT REHAB FACILITIES (IRF)
 BACKGROUND ON INPATIENT REHAB FACILITIES (IRF) There are 1,140 IRFs in the US 1,000 rehab units within hospitals 217 freestanding rehabilitation hospitals 68% for-profit; 30% nonprofit. Most with designated
BACKGROUND ON INPATIENT REHAB FACILITIES (IRF) There are 1,140 IRFs in the US 1,000 rehab units within hospitals 217 freestanding rehabilitation hospitals 68% for-profit; 30% nonprofit. Most with designated
What to expect following spinal cord injury. Information for patients Therapy Services
 What to expect following spinal cord injury Information for patients Therapy Services Introduction This leaflet aims to explain what spinal cord injury is and what to expect over the next few months. What
What to expect following spinal cord injury Information for patients Therapy Services Introduction This leaflet aims to explain what spinal cord injury is and what to expect over the next few months. What
Tr a u m at i c injuries are major contributors to death
 J Neurosurg Spine 12:131 140, 2010 Epidemiological trends of spine and spinal cord injuries in the largest Canadian adult trauma center from 1986 to 2006 Clinical article Fa r h a d Pi r o u z m a n d,
J Neurosurg Spine 12:131 140, 2010 Epidemiological trends of spine and spinal cord injuries in the largest Canadian adult trauma center from 1986 to 2006 Clinical article Fa r h a d Pi r o u z m a n d,
Dynamic Spinal Visualization and Vertebral Motion Analysis
 Dynamic Spinal Visualization and Vertebral Motion Analysis Policy Number: 6.01.46 Last Review: 2/2019 Origination: 2/2006 Next Review: 2/2020 Policy Blue Cross and Blue Shield of Kansas City (Blue KC)
Dynamic Spinal Visualization and Vertebral Motion Analysis Policy Number: 6.01.46 Last Review: 2/2019 Origination: 2/2006 Next Review: 2/2020 Policy Blue Cross and Blue Shield of Kansas City (Blue KC)
PARAPLEGIA. B FIG. 6 A, B and C, Same patient three years after spinal grafting shows a most remarkable improvement of spinal deformity and posture.
 16 PARAPLEGIA A B FIG. 6 A, B and C, Same patient three years after spinal grafting shows a most remarkable improvement of spinal deformity and posture. a grotesque deformity of the spine and trunk with
16 PARAPLEGIA A B FIG. 6 A, B and C, Same patient three years after spinal grafting shows a most remarkable improvement of spinal deformity and posture. a grotesque deformity of the spine and trunk with
Acquired Brain Injury by Local Health Integration Network in Ontario
 Acquired Brain Injury by Local Health Integration Network in Research Team: Angela Colantonio, Principal Investigator Senior Research Scientist, Toronto Rehabilitation Institute UHN Professor of Occupational
Acquired Brain Injury by Local Health Integration Network in Research Team: Angela Colantonio, Principal Investigator Senior Research Scientist, Toronto Rehabilitation Institute UHN Professor of Occupational
Sir William Asher ANATOMY
 SPINAL CORD INJURY BASICS RELATED TO LIFE CARE PLANNING Lesson 1 Sir William Asher Picture the pathetic patient lying long abed, the urine leaking from his distended bladder, the lime draining from his
SPINAL CORD INJURY BASICS RELATED TO LIFE CARE PLANNING Lesson 1 Sir William Asher Picture the pathetic patient lying long abed, the urine leaking from his distended bladder, the lime draining from his
AROC Outcome Targets Report Inpatient Pathway 3
 AROC Outcome Targets Report Inpatient Pathway 3 Anywhere Hospital January 2013 December 2013 Australasian Faculty of Rehabilitation Medicine AROC impairment specific benchmarking process...3 Introducing
AROC Outcome Targets Report Inpatient Pathway 3 Anywhere Hospital January 2013 December 2013 Australasian Faculty of Rehabilitation Medicine AROC impairment specific benchmarking process...3 Introducing
Spinal Trauma. General Rehabilitation of Patient with Spinal Trauma. Common Spinal Injuries. Important Anatomical Structures at each Vertebral Level
 Asian Association for Dynamic Osteosynthesis Workshop on Management of Spinal Trauma 22 April 2007 (Sunday) Orthopaedic Learning Centre, PWH, Shatin, Hong Kong General Rehabilitation of Patient with Spinal
Asian Association for Dynamic Osteosynthesis Workshop on Management of Spinal Trauma 22 April 2007 (Sunday) Orthopaedic Learning Centre, PWH, Shatin, Hong Kong General Rehabilitation of Patient with Spinal
Mortality rates in geriatric patients with spinal cord injuries
 See the corresponding editorial and response in this issue, pp 275 276. J Neurosurg Spine 7:277 281, 2007 Mortality rates in geriatric patients with spinal cord injuries DANIEL R. FASSETT, M.D., 1 JAMES
See the corresponding editorial and response in this issue, pp 275 276. J Neurosurg Spine 7:277 281, 2007 Mortality rates in geriatric patients with spinal cord injuries DANIEL R. FASSETT, M.D., 1 JAMES
FUNCTIONAL OUTCOMES OF TRAUMATIC PARAPLEGIA PATIENTS: DOES SURGERY IMPROVE THE QUALITY OF LIFE?
 FUNCTIONAL OUTCOMES OF TRAUMATIC PARAPLEGIA PATIENTS: DOES SURGERY IMPROVE THE QUALITY OF LIFE? Original Article Orthopaedics R S Bajoria 1, Mahendra Panwar 2, Anand Rao 3, Sameer Gupta 4 1 - Associate
FUNCTIONAL OUTCOMES OF TRAUMATIC PARAPLEGIA PATIENTS: DOES SURGERY IMPROVE THE QUALITY OF LIFE? Original Article Orthopaedics R S Bajoria 1, Mahendra Panwar 2, Anand Rao 3, Sameer Gupta 4 1 - Associate
Latest Press Release. Mylan a1 blue pill real vs fake
 corp@stantec.com Latest Press Release Mylan a1 blue pill real vs fake S Approximate Synonyms. Cervical (neck) radiculitis; Cervical (neck) radiculopathy; Cervical radiculitis; Cervical radiculopathy; Ulnar
corp@stantec.com Latest Press Release Mylan a1 blue pill real vs fake S Approximate Synonyms. Cervical (neck) radiculitis; Cervical (neck) radiculopathy; Cervical radiculitis; Cervical radiculopathy; Ulnar
TRAUMATIC CAROTID &VERTEBRAL ARTERY INJURIES
 TRAUMATIC CAROTID &VERTEBRAL ARTERY INJURIES ALBERTO MAUD, MD ASSOCIATE PROFESSOR TEXAS TECH UNIVERSITY HEALTH SCIENCES CENTER EL PASO PAUL L. FOSTER SCHOOL OF MEDICINE 18TH ANNUAL RIO GRANDE TRAUMA 2017
TRAUMATIC CAROTID &VERTEBRAL ARTERY INJURIES ALBERTO MAUD, MD ASSOCIATE PROFESSOR TEXAS TECH UNIVERSITY HEALTH SCIENCES CENTER EL PASO PAUL L. FOSTER SCHOOL OF MEDICINE 18TH ANNUAL RIO GRANDE TRAUMA 2017
Title Protocol for the management of suspected cauda equine syndrome & decompensating spinal stenosis at NDDH
 Document Control Title Protocol for the management of suspected cauda equine syndrome & decompensating spinal stenosis at NDDH Author Author s job title Consultant T&O Directorate Scheduled Care Department
Document Control Title Protocol for the management of suspected cauda equine syndrome & decompensating spinal stenosis at NDDH Author Author s job title Consultant T&O Directorate Scheduled Care Department
Care Pathways for Enabling Recovery from Common Traffic Injuries: A Focus on the Injured Person
 Care Pathways for Enabling Recovery from Common Traffic Injuries: A Focus on the Injured Person Jessica J. Wong, DC, MPH, FCCSC Research Associate, UOIT-CMCC Centre for Disability Prevention and Rehabilitation
Care Pathways for Enabling Recovery from Common Traffic Injuries: A Focus on the Injured Person Jessica J. Wong, DC, MPH, FCCSC Research Associate, UOIT-CMCC Centre for Disability Prevention and Rehabilitation
Can. J. Neurol. Sci. 2003; 30:
 MOC Choice www.ccns.org ORIGINAL ARTICLE The Epidemiology of Traumatic Spinal Cord Injury in Alberta, Canada Donna M. Dryden, L. Duncan Saunders, Brian H. Rowe, Laura A. May, Niko Yiannakoulias, Lawrence
MOC Choice www.ccns.org ORIGINAL ARTICLE The Epidemiology of Traumatic Spinal Cord Injury in Alberta, Canada Donna M. Dryden, L. Duncan Saunders, Brian H. Rowe, Laura A. May, Niko Yiannakoulias, Lawrence
Trauma Registry Training. Exercises. Dee Vernberg Dan Robinson Digital Innovation (800) ex 4.
 Trauma Registry Training Exercises Dee Vernberg 785-296-0613 Dan Robinson 785-296-3180 Digital Innovation (800) 344-3668 ex 4 www.kstrauma.org For a copy of the Data Dictionary, please follow the below
Trauma Registry Training Exercises Dee Vernberg 785-296-0613 Dan Robinson 785-296-3180 Digital Innovation (800) 344-3668 ex 4 www.kstrauma.org For a copy of the Data Dictionary, please follow the below
The Nervous System PART C. PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College
 PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Nervous System 7 PART C Protection of the Central Nervous System Scalp and skin Skull and vertebral
PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Nervous System 7 PART C Protection of the Central Nervous System Scalp and skin Skull and vertebral
Selected Bibliography
 Selected Bibliography Journals Functional Anatomy of the Spinal Column Munro, D., 'Factors Governing the Stability of the Spine', Paraplegia, 3, 219 (1965) Romanes, G. T., 'The Arterial Supply of the Human
Selected Bibliography Journals Functional Anatomy of the Spinal Column Munro, D., 'Factors Governing the Stability of the Spine', Paraplegia, 3, 219 (1965) Romanes, G. T., 'The Arterial Supply of the Human
Comprehension of the common spine disorder.
 Objectives Comprehension of the common spine disorder. Disc degeneration/hernia. Spinal stenosis. Common spinal deformity (Spondylolisthesis, Scoliosis). Osteoporotic fracture. Anatomy Anatomy Anatomy
Objectives Comprehension of the common spine disorder. Disc degeneration/hernia. Spinal stenosis. Common spinal deformity (Spondylolisthesis, Scoliosis). Osteoporotic fracture. Anatomy Anatomy Anatomy
Correspondence to: Bharat Sutariya DOI: /ijmsph Received Date: Accepted Date:
 RESEARCH ARTICLE COMPARISON OF FUNCTIONAL AND NEUROLOGICAL OUTCOME OF CONSERVATIVE AND OPERATIVE MANAGEMENT IN PATIENTS WITH CERVICAL SPINE INJURY WITH COMPLETE QUADRIPLEGIA Amit Patel, Bharat Sutariya
RESEARCH ARTICLE COMPARISON OF FUNCTIONAL AND NEUROLOGICAL OUTCOME OF CONSERVATIVE AND OPERATIVE MANAGEMENT IN PATIENTS WITH CERVICAL SPINE INJURY WITH COMPLETE QUADRIPLEGIA Amit Patel, Bharat Sutariya
Ligamentous Integrity in Spinal Cord Injury without Radiographic Abnormality. Dr Anria Horn Dr Stewart Dix-Peek
 Ligamentous Integrity in Spinal Cord Injury without Radiographic Abnormality Dr Anria Horn Dr Stewart Dix-Peek Introduction Spinal Cord Injury Without Radiographic Abnormality SCIWORA Pang, Wilberger 1982
Ligamentous Integrity in Spinal Cord Injury without Radiographic Abnormality Dr Anria Horn Dr Stewart Dix-Peek Introduction Spinal Cord Injury Without Radiographic Abnormality SCIWORA Pang, Wilberger 1982
Hospital discharge data can be a potentially powerful data
 ORIGINAL ARTICLE Identification of Incident Injuries in Hospital Discharge Registers Rolf Gedeborg, a,b Henrik Engquist, a Lars Berglund, b and Karl Michaëlsson b,c Background: Hospital discharge data
ORIGINAL ARTICLE Identification of Incident Injuries in Hospital Discharge Registers Rolf Gedeborg, a,b Henrik Engquist, a Lars Berglund, b and Karl Michaëlsson b,c Background: Hospital discharge data
Icd 10 degenerative joint disease back
 Icd 10 degenerative joint disease back Search This article appeared in the January issue of the Radiology Coding & Compliance Expert. Many imaging studies are ordered because the patient is experiencing
Icd 10 degenerative joint disease back Search This article appeared in the January issue of the Radiology Coding & Compliance Expert. Many imaging studies are ordered because the patient is experiencing
MedStar Health considers Cough Assist Devices medically necessary for the following indications:
 MedStar Health, Inc. POLICY AND PROCEDURE MANUAL MP.047.MH Cough Assist Devices This policy applies to the following lines of business: MedStar Employee (Select) MedStar MA DSNP CSNP MedStar CareFirst
MedStar Health, Inc. POLICY AND PROCEDURE MANUAL MP.047.MH Cough Assist Devices This policy applies to the following lines of business: MedStar Employee (Select) MedStar MA DSNP CSNP MedStar CareFirst
TECHNICAL NOTES. for Spinal Fusion. June 2016
 TECHNICAL NOTES for Spinal Fusion June 2016 Pennsylvania Health Care Cost Containment Council Report Period: Calendar Year 2014 January 1, 2014 through December 31, 2014 Discharges 225 Market Street, Suite
TECHNICAL NOTES for Spinal Fusion June 2016 Pennsylvania Health Care Cost Containment Council Report Period: Calendar Year 2014 January 1, 2014 through December 31, 2014 Discharges 225 Market Street, Suite
Spontaneous Resolution of Spinal Canal Deformity After Burst Dispersion Fracture
 779 Spontaneous Resolution of Spinal Canal Deformity After Burst Dispersion Fracture T. M. H. Chakera 1 George Bedbrook C. M. Bradley3 We reviewed the records of 8 patients with 30 burst-dispersion spinal
779 Spontaneous Resolution of Spinal Canal Deformity After Burst Dispersion Fracture T. M. H. Chakera 1 George Bedbrook C. M. Bradley3 We reviewed the records of 8 patients with 30 burst-dispersion spinal
Accuracy of the Charlson Index Comorbidities Derived from a Hospital Electronic Database in a Teaching Hospital in Saudi Arabia
 Accuracy of the Charlson Index Comorbidities Derived from a Hospital Electronic Database in a Teaching Hospital in Saudi Arabia Accuracy of the Charlson Index Comorbidities Derived from a Hospital Electronic
Accuracy of the Charlson Index Comorbidities Derived from a Hospital Electronic Database in a Teaching Hospital in Saudi Arabia Accuracy of the Charlson Index Comorbidities Derived from a Hospital Electronic
River North Pain Management Consultants, S.C., Axel Vargas, M.D., Regional Anesthesiology and Interventional Pain Management.
 River North Pain Management Consultants, S.C., Axel Vargas, M.D., Regional Anesthesiology and Interventional Pain Management. Chicago, Illinois, 60611 Phone: (888) 951-6471 Fax: (888) 961-6471 Clinical
River North Pain Management Consultants, S.C., Axel Vargas, M.D., Regional Anesthesiology and Interventional Pain Management. Chicago, Illinois, 60611 Phone: (888) 951-6471 Fax: (888) 961-6471 Clinical
Rick Hansen Spinal Cord Injury Registry: special report
 Rick Hansen Spinal Cord Injury Registry: special report 11 13 acknowledgements Thank you to the dedicated clinicians, researchers and coordinators who collect, analyze and input data into the Rick Hansen
Rick Hansen Spinal Cord Injury Registry: special report 11 13 acknowledgements Thank you to the dedicated clinicians, researchers and coordinators who collect, analyze and input data into the Rick Hansen
One hospitalization with any of the defining diagnoses of spondylosis (see ICD9 and ICD10 code lists below) in any diagnostic position; or
 1 ORTHO 16 SPONDYLOSIS Includes spondylopathies due to asymptomatic and symptomatic degenerative changes of the bony spine (M47 and M48); Does not include ankylosing spondylitis (M45), other inflammatory
1 ORTHO 16 SPONDYLOSIS Includes spondylopathies due to asymptomatic and symptomatic degenerative changes of the bony spine (M47 and M48); Does not include ankylosing spondylitis (M45), other inflammatory
CERVICAL SPINE INJURIES IN THE ELDERLY
 CERVICAL SPINE INJURIES IN THE ELDERLY ISADOR H. LIEBERMAN, JOHN K. WEBB From University Hospital, Queen s Medical Centre, Nottingham, England We reviewed 41 patients over the age of 65 years (mean 76.5)
CERVICAL SPINE INJURIES IN THE ELDERLY ISADOR H. LIEBERMAN, JOHN K. WEBB From University Hospital, Queen s Medical Centre, Nottingham, England We reviewed 41 patients over the age of 65 years (mean 76.5)
Objectives. Comprehension of the common spine disorder
 Objectives Comprehension of the common spine disorder Disc degeneration/hernia Spinal stenosis Common spinal deformity (Spondylolisthesis, Scoliosis) Osteoporotic fracture Destructive spinal lesions Anatomy
Objectives Comprehension of the common spine disorder Disc degeneration/hernia Spinal stenosis Common spinal deformity (Spondylolisthesis, Scoliosis) Osteoporotic fracture Destructive spinal lesions Anatomy
SCIWORA Rozlyn McTeer BSN, RN, CEN Pediatric Trauma Coordinator Trauma Services OBJECTIVES DEFINITION 11/8/2017. Identify SCIWORA.
 SCIWORA Rozlyn McTeer BSN, RN, CEN Pediatric Trauma Coordinator Trauma Services Identify SCIWORA. OBJECTIVES Identify the population at risk. To identify anatomic and physiologic reasons for SCIWORA. To
SCIWORA Rozlyn McTeer BSN, RN, CEN Pediatric Trauma Coordinator Trauma Services Identify SCIWORA. OBJECTIVES Identify the population at risk. To identify anatomic and physiologic reasons for SCIWORA. To
Spine Pain Management Program
 Spine Pain Management Program Please complete the following information: Patient Name: Patient ID Number: Patient DOB: The procedure being requested is: Please check the indication (reason) for this procedure
Spine Pain Management Program Please complete the following information: Patient Name: Patient ID Number: Patient DOB: The procedure being requested is: Please check the indication (reason) for this procedure
NUMEROUS STUDIES HAVE addressed the incidence of
 332 ORIGINAL ARTICLE Trends in New Injuries, Prevalent Cases, and Aging With Spinal Cord Injury Michael J. DeVivo, DrPH, Yuying Chen, MD, PhD ABSTRACT. DeVivo MJ, Chen Y. Trends in new injuries, prevalent
332 ORIGINAL ARTICLE Trends in New Injuries, Prevalent Cases, and Aging With Spinal Cord Injury Michael J. DeVivo, DrPH, Yuying Chen, MD, PhD ABSTRACT. DeVivo MJ, Chen Y. Trends in new injuries, prevalent
Critical Review Form Diagnostic Test
 Critical Review Form Diagnostic Test The clinical presentation and impact of diagnostic delays on emergency department patients with spinal epidural abscess, J Emerg Med 2004; 26:285-291 Objectives: To
Critical Review Form Diagnostic Test The clinical presentation and impact of diagnostic delays on emergency department patients with spinal epidural abscess, J Emerg Med 2004; 26:285-291 Objectives: To
Case SCIWORA in patient with congenital block vertebra
 Case 15428 SCIWORA in patient with congenital block vertebra Lucas Walgrave 1, Charlotte Vanhoenacker 1-2, Thomas Golinvaux 3, Filip Vanhoenacker3-5 1: Leuven University Hospital, Department of Radiology,
Case 15428 SCIWORA in patient with congenital block vertebra Lucas Walgrave 1, Charlotte Vanhoenacker 1-2, Thomas Golinvaux 3, Filip Vanhoenacker3-5 1: Leuven University Hospital, Department of Radiology,
Neurological Conditions List by Practitioner Type MED-NEURODA~001
 Neurological Conditions List by Practitioner Type MED-NEURODA~001 Date: 26 May 2016 Foreword This guidance has been produced as part of a training programme for Healthcare Professionals approved by the
Neurological Conditions List by Practitioner Type MED-NEURODA~001 Date: 26 May 2016 Foreword This guidance has been produced as part of a training programme for Healthcare Professionals approved by the
Spinal injury is very common in Ireland: 19 per 100,000 (1). It poses a significant disease burden.
 MRI in traumatic spinal cord injury: a single national spinal centre experience and study of imaging features with clinical correlation with ASIA score and outcome Poster No.: C-1235 Congress: ECR 2011
MRI in traumatic spinal cord injury: a single national spinal centre experience and study of imaging features with clinical correlation with ASIA score and outcome Poster No.: C-1235 Congress: ECR 2011
Intrathecal Baclofen for CNS Spasticity
 Intrathecal Baclofen for CNS Spasticity Last Review Date: October 13, 2017 Number: MG.MM.ME.31bC7 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary
Intrathecal Baclofen for CNS Spasticity Last Review Date: October 13, 2017 Number: MG.MM.ME.31bC7 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary
Summary of Pediatric Trauma Patients
 Santa Rosa Memorial Hospital Trauma Services Summary of Pediatric Trauma Patients Reporting Dates Jan 1, 2004 May 31, 2006 The mission of the Santa Rosa Memorial Hospital Trauma Services is to provide
Santa Rosa Memorial Hospital Trauma Services Summary of Pediatric Trauma Patients Reporting Dates Jan 1, 2004 May 31, 2006 The mission of the Santa Rosa Memorial Hospital Trauma Services is to provide
What is a spinal cord injury?
 Spinal Cord Injury What is a spinal cord injury? A spinal cord injury (SCI) is when the spinal cord is damaged Such damage causes 2 things: - loss or change of movement (paralysis) - loss or change of
Spinal Cord Injury What is a spinal cord injury? A spinal cord injury (SCI) is when the spinal cord is damaged Such damage causes 2 things: - loss or change of movement (paralysis) - loss or change of
Risk Factors Predicting Mortality in Spinal Cord Injury in Nigeria
 Article ID: WMC00807 ISSN 2046690 Risk Factors Predicting Mortality in Spinal Cord Injury in Nigeria Corresponding Author: Dr. Ahidjo Kawu, Consultant Surgeon, Dept of Orthopaedics, UATH, Gwagwalada Abuja
Article ID: WMC00807 ISSN 2046690 Risk Factors Predicting Mortality in Spinal Cord Injury in Nigeria Corresponding Author: Dr. Ahidjo Kawu, Consultant Surgeon, Dept of Orthopaedics, UATH, Gwagwalada Abuja
RHABDOMYOLYSIS; EXERTIONAL
 1 MISC 20 RHABDOMYOLYSIS; EXERTIONAL Background This case definition was developed by the Armed Forces Health Surveillance Branch (AFHSB) for the purpose of epidemiological surveillance of exertional rhabdomyolysis.
1 MISC 20 RHABDOMYOLYSIS; EXERTIONAL Background This case definition was developed by the Armed Forces Health Surveillance Branch (AFHSB) for the purpose of epidemiological surveillance of exertional rhabdomyolysis.
AOSpine Severity. This. Disclaimer:
 AOSpine Classification and Injury Severity System for Traumatic Fractures of the Thoracolumbarr Spine This is the present form of the classification and injury severity system the AOSpine Knowledge Forum
AOSpine Classification and Injury Severity System for Traumatic Fractures of the Thoracolumbarr Spine This is the present form of the classification and injury severity system the AOSpine Knowledge Forum
SURGICAL SPINE INTERVENTION after traumatic spinal
 1818 Outcomes of Early Surgical Management Versus Late or No Surgical Intervention After Acute Spinal Cord Injury William McKinley, MD, Michelle A. Meade, PhD, Steven Kirshblum, MD, Barbara Barnard, DO
1818 Outcomes of Early Surgical Management Versus Late or No Surgical Intervention After Acute Spinal Cord Injury William McKinley, MD, Michelle A. Meade, PhD, Steven Kirshblum, MD, Barbara Barnard, DO
HIGH LEVEL - Science
 Learning Outcomes HIGH LEVEL - Science Describe the structure and function of the back and spine (8a) Outline the functional anatomy and physiology of the spinal cord and peripheral nerves (8a) Describe
Learning Outcomes HIGH LEVEL - Science Describe the structure and function of the back and spine (8a) Outline the functional anatomy and physiology of the spinal cord and peripheral nerves (8a) Describe
Introduction to Emergency Medical Care 1
 Introduction to Emergency Medical Care 1 OBJECTIVES 31.1 Define key terms introduced in this chapter. Slides 13 15, 17, 19, 28 31.2 Describe the components and function of the nervous system and the anatomy
Introduction to Emergency Medical Care 1 OBJECTIVES 31.1 Define key terms introduced in this chapter. Slides 13 15, 17, 19, 28 31.2 Describe the components and function of the nervous system and the anatomy
Head and Neck Cancers Data Quality Report Radiotherapy and Chemotherapy Data
 Head and Neck Cancers Data Quality Report Radiotherapy and Chemotherapy Data 1 This report has been compiled by Jinan Ridha, Analyst, Oxford Cancer Intelligence Unit (OCIU) With acknowledgements Mr Richard
Head and Neck Cancers Data Quality Report Radiotherapy and Chemotherapy Data 1 This report has been compiled by Jinan Ridha, Analyst, Oxford Cancer Intelligence Unit (OCIU) With acknowledgements Mr Richard
Incidental Durotomy/ Dural Tear.
 Incidental Durotomy/ Dural Tear www.fisiokinesiterapia.biz Objectives Define dural tear ( incidental durotomy ) Differentiate dural tears from other accidental punctures or lacerations I.D. Risk factors
Incidental Durotomy/ Dural Tear www.fisiokinesiterapia.biz Objectives Define dural tear ( incidental durotomy ) Differentiate dural tears from other accidental punctures or lacerations I.D. Risk factors
THE LUMBAR SPINE (BACK)
 THE LUMBAR SPINE (BACK) At a glance Chronic back pain, especially in the area of the lumbar spine (lower back), is a widespread condition. It can be assumed that 75 % of all people have it sometimes or
THE LUMBAR SPINE (BACK) At a glance Chronic back pain, especially in the area of the lumbar spine (lower back), is a widespread condition. It can be assumed that 75 % of all people have it sometimes or
Completing the Circle: Novel Methods for using PRO Scores in Shared Decision- Making and Patient Self-Management.
 Completing the Circle: Novel Methods for using PRO Scores in Shared Decision- Making and Patient Self-Management. Karon Cook, PhD, Northwestern University Chicago, IL Thursday, September 28, 2017 Relevant
Completing the Circle: Novel Methods for using PRO Scores in Shared Decision- Making and Patient Self-Management. Karon Cook, PhD, Northwestern University Chicago, IL Thursday, September 28, 2017 Relevant
NQF-ENDORSED VOLUNTARY CONSENSUS STANDARD FOR HOSPITAL CARE. Measure Information Form Collected For: CMS Outcome Measures (Claims Based)
 Last Updated: Version 4.3 NQF-ENDORSED VOLUNTARY CONSENSUS STANDARD FOR HOSPITAL CARE Measure Information Form Collected For: CMS Outcome Measures (Claims Based) Measure Set: CMS Readmission Measures Set
Last Updated: Version 4.3 NQF-ENDORSED VOLUNTARY CONSENSUS STANDARD FOR HOSPITAL CARE Measure Information Form Collected For: CMS Outcome Measures (Claims Based) Measure Set: CMS Readmission Measures Set
ICD-10-CM. International Classification of Diseases, 10th Revision, Clinical Modification
 ICD-10-CM International Classification of Diseases, 10th Revision, Clinical Modification ICD-10 stands for the International Statistical Classification of Diseases and Related Health Problems, 10 th revision
ICD-10-CM International Classification of Diseases, 10th Revision, Clinical Modification ICD-10 stands for the International Statistical Classification of Diseases and Related Health Problems, 10 th revision
UNIVERSITY OF CALGARY. Development and Validation of an ICD-10 Case Definition for Pediatric Traumatic Brain Injury
 UNIVERSITY OF CALGARY Development and Validation of an ICD-10 Case Definition for Pediatric Traumatic Brain Injury using Canadian Administrative Data by Jane Madison McChesney A THESIS SUBMITTED TO THE
UNIVERSITY OF CALGARY Development and Validation of an ICD-10 Case Definition for Pediatric Traumatic Brain Injury using Canadian Administrative Data by Jane Madison McChesney A THESIS SUBMITTED TO THE
Low back pain, radiculopathy left leg icd 10 code
 Home Search Low back pain, radiculopathy left leg icd 10 code 2018 ICD - 10 code for Radiculopathy is M54.1. Lookup the complete ICD 10 Code details for M54.1.. Low back pain ; M54.6 - Pain in thoracic
Home Search Low back pain, radiculopathy left leg icd 10 code 2018 ICD - 10 code for Radiculopathy is M54.1. Lookup the complete ICD 10 Code details for M54.1.. Low back pain ; M54.6 - Pain in thoracic
GMl GANGLIOSIDES IN THE TREATMENT OF SPINAL CORD INJURY: REPORT OF PRELIMINARY DATA ANALYSIS
 ACTA NEUROBIOL. EXP. 1990, 50: 515-521 Symposium "Recovery from brain damage: bel~avioral and neurochemical approaches" 4-7 July, 1989, Warsaw, Poland GMl GANGLIOSIDES IN THE TREATMENT OF SPINAL CORD INJURY:
ACTA NEUROBIOL. EXP. 1990, 50: 515-521 Symposium "Recovery from brain damage: bel~avioral and neurochemical approaches" 4-7 July, 1989, Warsaw, Poland GMl GANGLIOSIDES IN THE TREATMENT OF SPINAL CORD INJURY:
Stroke Special Project 640 and 740 Resource For Health Information Management Professionals
 Stroke Special Project 640 and 740 Resource For Health Information Management Professionals Linda Gould RPN Erin Kelleher, BA, CHIM Stefan Pagliuso PT, B.A. Kin(Hon.) Overview of this Resource Overview
Stroke Special Project 640 and 740 Resource For Health Information Management Professionals Linda Gould RPN Erin Kelleher, BA, CHIM Stefan Pagliuso PT, B.A. Kin(Hon.) Overview of this Resource Overview
S pinal injury in the paediatric trauma patient can have
 860 ORIGINAL ARTICLE Patterns and risks in spinal trauma B W Martin, E Dykes, F E Lecky... See end of article for authors affiliations... Correspondence to: Dr B W Martin, Hope Hospital, Stott Lane, Salford
860 ORIGINAL ARTICLE Patterns and risks in spinal trauma B W Martin, E Dykes, F E Lecky... See end of article for authors affiliations... Correspondence to: Dr B W Martin, Hope Hospital, Stott Lane, Salford
The New England Journal of Medicine A POPULATION-BASED STUDY OF SEIZURES AFTER TRAUMATIC BRAIN INJURIES
 A POPULATION-BASED STUDY OF SEIZURES AFTER TRAUMATIC BRAIN INJURIES JOHN F. ANNEGERS, PH.D., W. ALLEN HAUSER, M.D., SHARON P. COAN, M.S., AND WALTER A. ROCCA, M.D., M.P.H. ABSTRACT Background The risk
A POPULATION-BASED STUDY OF SEIZURES AFTER TRAUMATIC BRAIN INJURIES JOHN F. ANNEGERS, PH.D., W. ALLEN HAUSER, M.D., SHARON P. COAN, M.S., AND WALTER A. ROCCA, M.D., M.P.H. ABSTRACT Background The risk
ICD-10 FOR NEUROSURGERY NERVES- Part II
 ICD-10 FOR NEUROSURGERY NERVES- Part II J O H N F B I S H O P, P A - C, C P C, C P M A, C G S C, C P R C D I R E C T O R S U R G I C A L C O D I N G A N D A U D I T I N G S E R V I C E S S E N I O R M
ICD-10 FOR NEUROSURGERY NERVES- Part II J O H N F B I S H O P, P A - C, C P C, C P M A, C G S C, C P R C D I R E C T O R S U R G I C A L C O D I N G A N D A U D I T I N G S E R V I C E S S E N I O R M
Neck CTA: When? How? The Innsbruck Experience Marius C. Wick, M.D. Department of Radiology Karolinska University Hospital Solna Stockholm, Sweden
 Neck CTA: When? How? The Innsbruck Experience Marius C. Wick, M.D. Department of Radiology Karolinska University Hospital Solna Stockholm, Sweden No financial or non-financial competing interests to declare
Neck CTA: When? How? The Innsbruck Experience Marius C. Wick, M.D. Department of Radiology Karolinska University Hospital Solna Stockholm, Sweden No financial or non-financial competing interests to declare
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Achilles tendinopathy in dancers, 831 832 treatment of PRP in, 871 872 Achilles tendinopathy/tendonitis in ultramarathon athletes, 847
Index Note: Page numbers of article titles are in boldface type. A Achilles tendinopathy in dancers, 831 832 treatment of PRP in, 871 872 Achilles tendinopathy/tendonitis in ultramarathon athletes, 847
Objectives. Medicare Spending per Beneficiary: Analyzing MSPB Data to Identify Primary Drivers
 Medicare Spending per Beneficiary: Analyzing MSPB Data to Identify Primary Drivers August 22, 2017 Objectives Understand the basics of the hospital specific MSPB data files and reports Review the factors
Medicare Spending per Beneficiary: Analyzing MSPB Data to Identify Primary Drivers August 22, 2017 Objectives Understand the basics of the hospital specific MSPB data files and reports Review the factors
Neurovascular Observations Nursing Clinical Guideline
 Reference (include title, Patel, k., & McCann, P. A. (2012). The emergent assessment of supracondylar fractures of the paediatric humerus. Hand Surgery, 17(2), 161-165. From Medline Evidence level (I-)
Reference (include title, Patel, k., & McCann, P. A. (2012). The emergent assessment of supracondylar fractures of the paediatric humerus. Hand Surgery, 17(2), 161-165. From Medline Evidence level (I-)
Vertebral Axial Decompression
 Vertebral Axial Decompression Policy Number: 8.03.09 Last Review: 11/2018 Origination: 11/2005 Next Review: 11/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage
Vertebral Axial Decompression Policy Number: 8.03.09 Last Review: 11/2018 Origination: 11/2005 Next Review: 11/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage
Issues in Spinal Care Part I. The Program is Funded by: Laerdal Medical AS PO Box Stavanger Norway
 Issues in Spinal Care Part 1 Program Objectives By the end of this lecture, the participant should be able to... Understand the effect that improved equipment and training has had on Spinal Cord Injury
Issues in Spinal Care Part 1 Program Objectives By the end of this lecture, the participant should be able to... Understand the effect that improved equipment and training has had on Spinal Cord Injury
