Keywords: malignant glaucoma; pars plana vitrectomy; risk factors; complications; intraocular pressure
|
|
|
- Rudolph Newton
- 5 years ago
- Views:
Transcription
1 Article Clinical Characteristics and Outcomes of Malignant Glaucoma after Different Procedures Treated with Pars Plana Vitrectomy: A 10-Year Retrospective Study Lina Krėpštė *, Reda Žemaitienė and Arūnas Miliauskas Department of Ophthalmology, Medical Academy, Lithuanian University of Health Sciences, Kaunas, Lithuania; reda.zemaitiene@kaunoklinikos.lt (R.Ž.); arunas.miliauskas@kaunoklinikos.lt (A.M.) * Correspondence: krepste@gmail.com; Tel.: Received: 27 July 2018; Accepted: 3 September 2018; Published: 5 September 2018 Abstract: Background and objectives: Despite established common risk factors, malignant glaucoma (MG) remains a rare condition with challenging management. We aimed to analyze differences in risk factors for MG after different surgeries and outcomes after pars plana vitrectomy (PPV). Materials and Methods: This retrospective study included cases of MG treated with PPV between January 2005 and December 2015 in the Department of Ophthalmology, Lithuanian University of Health Sciences, Kaunas, Lithuania. Results: A total of 39 cases were analyzed: 23 (59%) after cataract surgery, 13 (33.3%) after trabeculectomy, and 3 (7.7%) after other interventions. Characteristics among the groups did not differ. Intraocular lens refractive power was significantly higher in the cataract group, in which intraocular pressure (IOP) before MG was significantly greater in the affected eye. Normotension was achieved in 92.3%, and a normal anterior chamber in 75%. Additional measures included eye drops (n = 24), trabeculectomy (n = 5), bleb revision (n = 2), synechiotomy (n = 4), and cyclophotocoagulation (n = 1). The proportion of drop-free patients significantly increased after PPV compared with that before MG development (38.5% versus 15.4%). Complications were observed in 11 cases: choroidal detachments with spontaneous resolution (n = 2); retinal detachment (n = 1); constant mydriasis (n = 1), neovascular glaucoma (n = 1); obstruction of filtrating zone by iris (n = 1) and by blood clot (n = 1); posterior synechia formation causing IOP rise (n = 4 (all resolved after synechiotomy)). The cataract group experienced significantly fewer complications than the trabeculectomy group (17.4% vs. 53.8%, respectively). Conclusions: There were no differences in the risk of MG among the different surgeries. However, higher IOP in the predisposed eye (versus contra-lateral eye) could indicate additional risk of MG after cataract surgery. PPV afforded reliable treatment for MG and the possibility for glaucoma patients to discontinue topical treatment. Keywords: malignant glaucoma; pars plana vitrectomy; risk factors; complications; intraocular pressure 1. Introduction Malignant glaucoma (MG) is a condition involving acute shallowing of the anterior chamber (AC), usually accompanied by ocular hypertension, which is not resolved nor prevented by an iridotomy. The phrase malignant glaucoma was coined by von Graefe, who was the first to describe the condition [1]. Typically, MG occurs after eye surgery (spontaneous cases have also been reported) and may quickly alter the prognosis of otherwise uncomplicated surgery. Despite established common risk factors, MG remains a relatively rare condition. Although MG varies according to surgery type and study period, the most recent investigation reported an overall Medicina 2018, 54, 65; doi: /medicina
2 Medicina 2018, 54, 65 2 of 7 incidence of 2% over an 11-year period [2]. The exact pathogenesis of MG remains unclear, although several different mechanisms have been proposed, including entrapment of aqueous humor behind or within the vitreous, accumulation of fluid within the posterior chamber due to direct lens block, pressure difference(s) between the anterior and posterior compartments due to rotation of ciliary processes, or anterior hyaloid face obstruction [3]. Each of these mechanisms may play a role depending on the situation and, perhaps, on the surgery being performed. We aimed to analyze differences in risk factors among cases of MG after different surgeries, and outcomes after the MG was treated with pars plana vitrectomy (PPV). To our knowledge, this study involved the second largest sample of MGs treated with PPV [4] and the largest group of MGs treated after cataract surgery published to date [5,6]. 2. Materials and Methods The present study was performed at the Department of Ophthalmology, Lithuanian University of Health Sciences, a tertiary health care center, located in Kaunas, Lithuania. The study design was approved by Kaunas Regional Research Ethics Committee (P1-BE-2-26/2015). All cases of MG treated with PPV between January 2005 and December 2015 were retrospectively reviewed. Considering the retrospective nature of the study and the use of anonymized patient data, requirements for informed consent were waived. All cases were treated with complete PPV combined with moderate vitreous trimming, posterior capsulotomy, iridectomy, zonulohyaloidectomy, synechiotomy (if needed) and, in phakic patients, phacoemulsification with intraocular lens (IOL) implantation. Surgeries were performed by four vitreoretinal surgeons. Operations were started with dissection of the conjunctiva and pars plana incisions (three incisions in phakic eyes and two incisions in pseudophakic eyes). An infusion line was inserted via pars plana incision into the posterior chamber (in phakic eyes) or via a self-sealing clear corneal incision into the anterior chamber (in pseudophakic eyes). In phakic eyes, the infusion remained turned off and a limited core vitrectomy just to minimize intraocular pressure (IOP) and deepen the AC was performed. Then, standard cataract surgery and IOL implantation followed. After checking the successful penetration of the infusion line, the vitrectomy cutter and the lighter via pars plana incisions were introduced into the posterior chamber, the infusion was turned on, and the residual pars plana vitrectomy was started. A vitrectomy phacoemulsification vitrectomy approach in phakic MG cases has been described by Sharma et al. [7]. In pseudophakic eyes, the infusion line was turned on before inserting it into the anterior chamber. Then, the vitrectomy cutter and the lighter via pars plana incisions were introduced into the posterior chamber and the pars plana vitrectomy was started. First, posterior capsulotomy and peripheral iridotomy with zonulohyaloidectomy with the vitrectomy cutter were performed to create patent posterior anterior chambers communication, then the complete vitrectomy was performed. Pars plana incisions and conjunctiva were closed with 7/0 Vicryl sutures. Intracameral cefuroxime and subconjunctival antibiotic and steroid injections were given at the end of the surgery. An IOP-lowering and cyclopegic therapy was applied to all cases as adjunctive therapy while waiting for PPV. Cases were excluded from analysis if the diagnosis of MG, as the cause of ocular hypertension, was doubtful. If both eyes had MG and were treated with PPV, the second eye was included and previous MG status in the other eye was interpreted as a risk factor. Other risk factors or parameters considered were the female sex, age, hyperopia, diagnosis of angle closure glaucoma, axial length, AC depth before surgery, lens thickness, stage of cataract, IOL refractive power in diopters (D), IOP before, during and after MG, and time for MG to develop. PPV outcomes were evaluated according to effective IOP decrease (normotension was considered to be treatment success), deepening of the AC, the need for other measures, and complications.
3 Medicina 2018, 54, 65 3 of 7 Statistical analysis was performed using SPSS Version 20 (IBM Corporation, Armonk, NY, USA). The Shapiro-Wilk test was applied to determine how the variables are distributed. If the dataset followed a normal distribution, the mean with standard deviation was calculated, and means between groups were compared using Student s t-test. For non-normally distributed data, median and interquartile range (IQR) was calculated, and the non-parametric Mann Whitney U test was used. If data were non-normally distributed and related, the Wilcoxon signed-rank test was chosen. A receiver-operator characteristic curve (ROC) test for identification of cut-off value was used. Qualitative data were compared using the Pearson chi-squared test. The McNemar test was applied on non-normally distributed paired nominal data; p 0.05 was considered to be statistically significant. 3. Results Forty-three MG patients were treated with PPV during the study period, 39 of whom were ultimately included in the final analysis. Twenty-three (59%) cases developed MG after cataract surgery (group 1), 13 (33.3%) after trabeculectomy (group 2 (2 pseudophakic cases)), and 3 (7.7%) after other interventions (group 3). Patients in group 3 had different characteristics: MG development after peripheral iridotomy with neodymium-yttrium-aluminum garnet (Nd: YAG) laser in a 73-year-old woman, who underwent previous cataract surgery, followed by uveitis and trabeculectomy; MG after IOL exchange from the posterior to AC in a 67-year-old man, who underwent previous IOL repair after head trauma-caused IOL dislocation; and MG after covering of corneal transplant with amniotic membrane in a 65-year-old man. MG developed in 1, 20, and 6 days after intervention in these patients, respectively. Because group 3 consisted of three very different cases, this group was not included in the comparative analysis between the groups. The demographic characteristics and clinical parameters of the MG cases are summarized in Table 1; a comparison of data between groups 1 and 2 is also presented. IOL refractive power was significantly higher in cases after cataract surgery compared with cases after trabeculectomy, and a cut-off value of 25 D, with a sensitivity of 89% and specificity of 64%, was determined. Clinical Characteristics Table 1. Clinical characteristics of patients with malignant glaucoma (MG). Total (n = 39 Cases) Cases after Cataract Surgery (n = 23) Cases after Trabeculectomy (n = 13) Female sex (%) Age (years) 69.6 ± ± ± Glaucoma (%) Angle-closure glaucoma (%) MG in other eye (%) Hyperopia (%) Advanced cataract (%) Lens thickness (mm) 5.0 ( ) 5.1 ( ) 5.01 ( ) IOL refractive power (D) 24.5 ( ) 25.5 ( ) 24.0 ( ) D or higher IOL (%) AC depth (mm) 2.32 ( ) 2.34 ( ) 2.26 ( ) Axial length (mm) ± ± ± Corneal power (D) ( ) ( ) ( ) Astigmatism (D) 0.5 ( ) ( ) 0.5 ( ) Intraocular pressure (mmhg) during MG episode 40 ( ) 37 ( ) 41 ( ) in affected eye before MG 21 ( ) 19 ( ) 29 ( ) difference between the eyes 8 ( ) 5 ( ) 16 ( ) p 0.328
4 Medicina 2018, 54, 65 4 of 7 before MG Time to MG development (days) Median (interquartile range) 3.5 (1 11) 4.5 (1 11) 2 (1 6) longest time Normally distributed data were compared using t-test and presented as mean ± standard deviation. Non-normally distributed data were compared using nonparametric Mann-Whitney U test and presented as median with interquartile range. Anterior chamber; IOL, intraocular lens; D, diopters. IOP in the affected eye before intervention, which provoked MG, was significantly higher compared with IOP in the other eye: in the cataract group mmhg ( ) vs mmhg ( ) (p = 0.028), in the trabeculectomy group, 29 mmhg ( ) vs ( ) (p = 0.012). The median time from MG to PPV treatment was 8 days (IQR days), and did not differ between the groups. All cases, except for three, were treated within 55 days after development of MG. Exceptional cases were treated successfully after 198, 744, and 926 days, respectively, and only the last case needed IOP-lowering drops after PPV. The possible reason for the delay in the last case may have been moderate ocular hypertension (26.6 mmhg), which developed after cataract surgery. The other two cases were treated with other measures: the first was after cataract surgery followed by trabeculectomy; the second developed after trabeculectomy and was treated with oral acetazolamide, topical atropine and, later, anterior vitrectomy before undergoing PPV. The median follow-up time after PPV was 90 days ((IQR) days). The shortest follow-up time was 3 months. Normotension was achieved with PPV and additional measures, if needed, in 36 (92.3%) patients and was considered to be a successful treatment of MG. Additional measures included trabeculectomy in 5 cases, bleb revision in 2, synechiotomy in 4, trans-scleral cyclophotocoagulation in 1 case of neovascular glaucoma that involved retinal venous thrombosis before MG, and topical glaucoma treatment. IOP-lowering drops were needed in 24 (61.5%) cases; no difference between the groups was observed. The need for IOP-lowering drops before MG and after PPV decreased in the entire study group, and in all groups separately. The distribution of patients by the number of IOP-lowering medications used before MG and after MG was treated with PPV is shown in Table 2. A similar effect was observed within the groups. Successful cases were divided into groups according to the need for topical IOP-lowering treatment after PPV: drop-free group (15 cases [41.7%]) and drop-needed group (21 cases [58.3%]). The former group had significantly more drop-free patients before the development of MG compared with the drop-needed group: 5 cases (33.3%) and 1 case (4.8%), respectively (p = 0.023). No other parameter was statistically different between these groups. Table 2. Distribution of patients by the number of intraocular pressure-lowering medications used before development of malignant glaucoma (MG) and after it was treated with pars plana vitrectomy. Number of IOP Lowering Medications Before Surgery and Malignant Glaucoma, n (%) After Treatment of MG with Pars Plana Vitrectomy, n (%) 0 6 (15.4) 15 (38.5) (17.9) 4 (10.3) (38.5) 7 (17.9) (17.9) 8 (20.5) (10.3) 5 (12.8) IOP, intraocular pressure; NPar McNemar Test was applied. p Deepening of the AC was achieved in 90.3% of cases; restoration of normal or deep AC was achieved in 75% of cases after PPV. A significant difference was observed within the first two
5 Medicina 2018, 54, 65 5 of 7 groups: 80% of cataract and 33.3% of trabeculectomy cases exhibited normal or deep AC after treatment with PPV (p < 0.05). No association between AC status and IOP after PPV was observed. Three (7.7%) MG cases were considered to be unsuccessful due to failure to reach normal IOP with PPV and additional measures. One case was after a trabeculectomy, which was treated with atropine afterward for several years. Discontinuation of atropine drops always led to AC flattening and IOP elevation. After performing PPV, the AC remained flat, with IOP >30 mmhg. A trabeculectomy and later revisions of bleb were also unsuccessful. The other 2 unsuccessfully treated cases of MG developed 1 and 4 days after cataract surgeries with implantation of 35 D and 25 D IOLs, both underwent PPV 8 days after MG diagnoses, previously treated with 3 and 2 IOP-lowering medications, respectively, for angle-closure glaucoma and maximal IOP-lowering therapy during MG. Ocular hypertension (22.0 and 32.0 mmhg) persisted despite additional measures (AC restoration to normal depth, maximal topical treatment and, later, trabeculectomy, trans-scleral cyclophotocoagulation). Complications of varying severity after MG and PPV were observed in 11 cases: choroidal detachments with spontaneous resolution (n = 2); retinal detachment (n = 1); constant mydriasis (n = 1) in the cataract group and neovascular glaucoma (n = 1, which had experienced retinal venous thrombosis before the event); obstruction of filtrating zone by iris (n = 1) and by blood clot (n = 1); posterior synechia formation causing IOP rise (n =4 [all resolved after surgery]) in the trabeculectomy group. The cataract group experienced significantly fewer complications than the trabeculectomy group (17.4% vs. 53.8%, respectively). 4. Discussion We report 39 cases of MG, of which 23 developed after cataract surgery. According to our literature search, this is the largest number of MG cases after this type of surgery to be published to date [5,6]. All cases were treated with PPV. Although some centers follow stepwise treatment for MG [2,4,5], we use a more definitive approach. Because PPV addresses the main ocular structure involved in the pathogenesis of MG, we tend to perform PPV as first-line treatment by applying other measures (cycloplegics, topical and systemic IOP-lowering medications) as adjunctive therapy while waiting for surgery. While evaluating risk factors for MG, we observed a typical tendency in our study group. Our patients were mainly hyperopic females with short eyes and high refractive power corneas treated for glaucoma. Although differences in the prevalence of hyperopia and mean axial length between the cataract and trabeculectomy groups were not statistically significant, there was a tendency toward shorter eyes and more hyperopic patients in the MG group after cataract surgery. This observation was supported by the derivative parameter IOL refractive power. MG cases after cataract surgery had been implanted with IOLs of significantly higher diopters with a cut-off value of 25.0 D. This difference may reflect different pathological mechanisms involved in the development of MG after cataract surgery and trabeculectomy. An additional interesting and new detail is that MG that developed after cataract surgery was associated with IOP. Naturally, the trabeculectomy group had a higher IOP and a larger difference between the eyes before the surgery than did the cataract group. However, eyes before cataract surgery, which later provoked MG, also had a significantly higher IOP than their contralateral eyes. Therefore, we hypothesize that in addition to ocular hypertension (a known risk factor for MG [8]), a slightly higher IOP compared with the other eye could be a risk factor and should be considered while planning cataract surgery, especially in anatomically predisposed eyes. Whether preoperative lowering of IOP in such eyes could minimize the risk of MG, however, is unclear. Our study confirms the high effectiveness and acceptable safety profile of complete PPV with posterior capsulotomy, iridectomy and, in phakic cases, phacoemulsification with IOL implantation for treating MG. We observed only one vision-threatening complication (retinal detachment) that could be directly linked to PPV. Additionally, we observed no recurrence of MG. Except for some examples with obvious treatment failure before PPV (e.g., cycloplegics and anterior vitrectomy), our study was not designed to compare PPV with other treatment modalities.
6 Medicina 2018, 54, 65 6 of 7 According to the literature, the rate of immediate success with medical treatment is low and recurrence is high if cycloplegics are withdrawn [8]. It is difficult to discuss laser treatment modalities, such as laser capsulotomy, hyaloidotomy, and cyclophotocoagulation, confidently because the study groups were extremely small [8]. A study involving >10 cases reported an initial success rate of 67% after Nd:YAG laser hyaloidotomy, which diminished to 46.7% after 3 months [9]. Surgical options, described in the most recent review, are vitreous aspiration (we regard this to be a dangerous approach), anterior vitrectomy, and PPV with or without lensectomy. Although initial success is comparable between PPV and anterior vitrectomy, as well as between PPV with and without lensectomy, the recurrence rate always favors PPV with lensectomy [8]. The largest and the most recent study of MG cases treated with PPV reported a 100% success rate and 5.2% recurrence rate with PPV [4]. As the authors noted, most recurrences were caused by fibrin reaction that blocked iridectomy and, as such, we argue whether these cases could be considered as a recurrence of MG. In our study, we observed 4 cases of synechia formation and IOP elevation after PPV. We regard them as PPV complications because the conditions were resolved easily after synechiotomies. We did not observe associations between successful MG treatment and the status of AC after PPV. However, there was a significant difference between MG cases after cataract surgery and a trabeculectomy. Normal AC depth was achieved in most cataract cases (80%) and in only one-third of cases after a trabeculectomy. This could also reflect the different mechanism of MG. The retrospective nature of this study precluded us from evaluating other anterior chamber structural parameters, such as iris configuration or the position of the ciliary body, among others. Apart from successful treatment of MG, we demonstrate the possibility for glaucoma patients to reduce the need for IOP-lowering drops after PPV. Awareness of this should lower the threshold for performing simultaneous PPV, especially in the era of 23 G and higher PPV during other intraocular procedures in glaucomatous and anatomically predisposed eyes. Such a strategy would not only be effective in MG prevention, but also as a measure to withdraw or, at least, decrease topical treatment. 5. Conclusions MG after cataract surgery and trabeculectomy shared typical risk factors, including female sex, angle-closure glaucoma, and hyperopia. In addition, cases after cataract surgery tend to be implanted with IOLs of higher refractive power compared with trabeculectomy cases and to have a slightly higher IOP in the affected eye compared with the other eye, which could be also be regarded as indicating a higher risk of MG. Whether this risk could be minimized by preoperative IOP lowering remains unclear. PPV offers reliable and immediate treatment of MG with a low complication rate, as well as the possibility for glaucoma patients to reduce or discontinue IOP-lowering medications. Therefore, simultaneous PPV in anatomically predisposed eyes with glaucoma undergoing other intraocular surgery may be beneficial and less risky in the long-term. Author Contributions: Conceptualization, R.Ž.; Methodology, R.Ž.; Validation, L.K., R.Ž. and A.M.; Formal Analysis, L.K.; Investigation, L.K. and A.M.; Resources, A.M; Data Curation, L.K. and A.M.; Writing-Original Draft Preparation, L.K.; Writing-Review and Editing, L.K. and R.Ž.; Visualization, L.K.; Supervision, R.Ž.; Project Administration, R.Ž. Funding: This research received no external funding. Conflicts of Interest: The authors declare no conflict of interest. References 1. Graefe, A.V. Beitrag zur Pathologie und Therapie des Glaukoms. Arch. Ophthalmol. 1869, 15, Debrouwere, V.; Stalmans, P.; Van Calster, J.; Spileers, W.; Zeyen, T.; Stalmans, I. Outcomes of different management options for malignant glaucoma: A retrospective study. Graefe s Arch. Clin. Exp. Ophthalmol. 2012, 250, , doi: /s
7 Medicina 2018, 54, 65 7 of 7 3. Foreman-Larkin, J.; Netland, P.A.; Salim, S. Clinical Management of Malignant Glaucoma. J. Ophthalmol. 2015, 2015, , doi: /2015/ Balekudaru, S.; Choudhari, N.S.; Rewri, P.; George, R.; Bhende, P.S.; Bhende, M.; Lingam, V.; Lingam, G. Surgical management of malignant glaucoma: A retrospective analysis of fifty-eight eyes. Eye 2017, 31, 947, doi: /eye Varma, D.K.; Belovay, G.W.; Tam, D.Y.; Ahmed, I.I.K. Malignant glaucoma after cataract surgery. J. Cataract Refract. Surg. 2014, 40, , doi: /j.jcrs Zhou, C.; Qian, S.; Yao, J.; Tang, Y.; Qian, J.; Lu, Y.; Xu, G.; Sun, X. Clinical Analysis of 50 Chinese Patients with Aqueous Misdirection Syndrome: A Retrospective Hospital-based Study. J. Int. Med. Res. 2012, 40, , doi: / Sharma, A.; Sii, F.; Shah, P.; Kirkby, G.R. Vitrectomy Phacoemulsification Vitrectomy for the Management of Aqueous Misdirection Syndromes in Phakic Eyes. Ophthalmology 2006, 113, , doi: /j.ophtha Kaplowitz, K.; Yung, E.; Flynn, R.; Tsai, J.C. Current Concepts in the Treatment of Vitreous Block, Also Known as Aqueous Misdirection. Surv. Ophthalmol. 2015, doi: /j.survophthal Dave, P.; Senthil, S.; Rao, H.L.; Garudadri, C.S. Treatment outcomes in malignant glaucoma. Ophthalmology 2013, 120, , doi: /j.ophtha by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (
Objectives. Tubes, Ties and Videotape: Financial Disclosure. Five Year TVT Results IOP Similar
 Tubes, Ties and Videotape: Surgical Video of Glaucoma Implants and Financial Disclosure I have no financial interests or relationships to disclose. Herbert P. Fechter MD, PE Eye Physicians and Surgeons
Tubes, Ties and Videotape: Surgical Video of Glaucoma Implants and Financial Disclosure I have no financial interests or relationships to disclose. Herbert P. Fechter MD, PE Eye Physicians and Surgeons
Anterior segment imaging
 Article Date: 11/1/2016 Anterior segment imaging AS OCT vs. UBM vs. endoscope; case based approaches BY BENJAMIN BERT, MD, FACS AND BRIAN FRANCIS, MD, MS Currently, numerous imaging modalities are available
Article Date: 11/1/2016 Anterior segment imaging AS OCT vs. UBM vs. endoscope; case based approaches BY BENJAMIN BERT, MD, FACS AND BRIAN FRANCIS, MD, MS Currently, numerous imaging modalities are available
EXP11677SK. Financial Disclosure. None to be Declared EXP11677SK
 Financial Disclosure None to be Declared Presentation overview Glaucoma Surgical History Complications of trabeculectomy Express Device Specifications Surgical Steps Clinical advantages, indications and
Financial Disclosure None to be Declared Presentation overview Glaucoma Surgical History Complications of trabeculectomy Express Device Specifications Surgical Steps Clinical advantages, indications and
WGA. The Global Glaucoma Network
 The Global Glaucoma Network Fort Lauderdale April 30, 2005 Indications for Surgery 1. The decision for surgery should consider the risk/benefit ratio. Note: Although a lower IOP is generally considered
The Global Glaucoma Network Fort Lauderdale April 30, 2005 Indications for Surgery 1. The decision for surgery should consider the risk/benefit ratio. Note: Although a lower IOP is generally considered
Silicone oil pupillary block after laser retinopexy in aphakic eyes with presumed closed peripheral iridectomy: report of three cases
 Int Ophthalmol (2014) 34:913 917 DOI 10.1007/s10792-013-9862-z CASE REPORT Silicone oil pupillary block after laser retinopexy in aphakic eyes with presumed closed peripheral iridectomy: report of three
Int Ophthalmol (2014) 34:913 917 DOI 10.1007/s10792-013-9862-z CASE REPORT Silicone oil pupillary block after laser retinopexy in aphakic eyes with presumed closed peripheral iridectomy: report of three
Trabeculectomy combined with cataract extraction: a follow-up study
 British Journal of Ophthalmology, 1980, 64, 720-724 Trabeculectomy combined with cataract extraction: a follow-up study R. S. EDWARDS From the Birmingham and Midland Eye Hospital, Church Street, Birmingham
British Journal of Ophthalmology, 1980, 64, 720-724 Trabeculectomy combined with cataract extraction: a follow-up study R. S. EDWARDS From the Birmingham and Midland Eye Hospital, Church Street, Birmingham
Optometric Postoperative Cataract Surgery Management
 Financial Disclosures Optometric Postoperative Cataract Surgery Management David Dinh, OD Oak Cliff Eye Clinic Dallas Eye Consultants March 10, 2015 Comanagement Joint cooperation between two or more specialists
Financial Disclosures Optometric Postoperative Cataract Surgery Management David Dinh, OD Oak Cliff Eye Clinic Dallas Eye Consultants March 10, 2015 Comanagement Joint cooperation between two or more specialists
Program= Loma Linda University Program
 OPHTHALMOLOGY: PROGRAM REPORT (Main Table) Reporting Period: Total Experience of Residents Completing rams in 2008-2009 ram=2400521023 - Loma Linda University ram [PART 1 ] rams in the Nation: 115 Residents
OPHTHALMOLOGY: PROGRAM REPORT (Main Table) Reporting Period: Total Experience of Residents Completing rams in 2008-2009 ram=2400521023 - Loma Linda University ram [PART 1 ] rams in the Nation: 115 Residents
Marek Rwkas, 1 Karolina Krix-Jachym, 1 and Tomasz garnowski Introduction
 Ophthalmology Volume 2015, Article ID 873124, 6 pages http://dx.doi.org/10.1155/2015/873124 Clinical Study Evaluation of the Effectiveness of Surgical Treatment of Malignant Glaucoma in Pseudophakic Eyes
Ophthalmology Volume 2015, Article ID 873124, 6 pages http://dx.doi.org/10.1155/2015/873124 Clinical Study Evaluation of the Effectiveness of Surgical Treatment of Malignant Glaucoma in Pseudophakic Eyes
CLINICAL SCIENCES. Angle-closure Glaucoma Associated With Occult Annular Ciliary Body Detachment
 CLINICAL SCIENCES Angle-closure Glaucoma Associated With Occult Annular Ciliary Body Detachment Jeffrey M. Liebmann, MD; Robert N. Weinreb, MD; Robert Ritch, MD Objective: To evaluate the role of annular
CLINICAL SCIENCES Angle-closure Glaucoma Associated With Occult Annular Ciliary Body Detachment Jeffrey M. Liebmann, MD; Robert N. Weinreb, MD; Robert Ritch, MD Objective: To evaluate the role of annular
Management of Angle Closure Glaucoma Hospital Authority Convention 18 May 2015
 Management of Angle Closure Glaucoma Hospital Authority Convention 18 May 2015 Jimmy Lai Clinical Professor Department of Ophthalmology The University of Hong Kong 1 Primary Angle Closure Glaucoma PACG
Management of Angle Closure Glaucoma Hospital Authority Convention 18 May 2015 Jimmy Lai Clinical Professor Department of Ophthalmology The University of Hong Kong 1 Primary Angle Closure Glaucoma PACG
The Anterior Segment & Glaucoma Visual Recognition & Interpretation of Clinical Signs
 The Anterior Segment & Glaucoma Visual Recognition & Interpretation of Clinical Signs Quiz created by Jane Macnaughton MCOptom & Peter Chapman BSc MCOptom FBDO CET Accreditation C19095 2 CET Points (General)
The Anterior Segment & Glaucoma Visual Recognition & Interpretation of Clinical Signs Quiz created by Jane Macnaughton MCOptom & Peter Chapman BSc MCOptom FBDO CET Accreditation C19095 2 CET Points (General)
PRESENTED By DR. FAISAL ALMOBARAK, MD
 PRESENTED By DR. FAISAL ALMOBARAK, MD Early FAC associated with hypotony is an important complication after glaucoma filtering procedures, especially trabeculectomy. The reported incidence after trabeculectomy
PRESENTED By DR. FAISAL ALMOBARAK, MD Early FAC associated with hypotony is an important complication after glaucoma filtering procedures, especially trabeculectomy. The reported incidence after trabeculectomy
Transient Intraocular Pressure Elevation after Trabeculotomy and its Occurrence with Phacoemulsification and Intraocular Lens Implantation
 Transient Intraocular Pressure Elevation after Trabeculotomy and its Occurrence with Phacoemulsification and Intraocular Lens Implantation Masaru Inatani*, Hidenobu Tanihara, Takahito Muto*, Megumi Honjo*,
Transient Intraocular Pressure Elevation after Trabeculotomy and its Occurrence with Phacoemulsification and Intraocular Lens Implantation Masaru Inatani*, Hidenobu Tanihara, Takahito Muto*, Megumi Honjo*,
Citation BMC Ophthalmology, 2016, v. 16, article no. 64
 Title Recurrent acute angle-closure attack due to plateau iris syndrome after cataract extraction with or without argon laser peripheral iridoplasty: a case report Author(s) Choy, NKB; Chan, JCH; Chien,
Title Recurrent acute angle-closure attack due to plateau iris syndrome after cataract extraction with or without argon laser peripheral iridoplasty: a case report Author(s) Choy, NKB; Chan, JCH; Chien,
Review Article Clinical Management of Malignant Glaucoma
 Ophthalmology Volume 2015, Article ID 283707, 6 pages http://dx.doi.org/10.1155/2015/283707 Review Article Clinical Management of Malignant Glaucoma Julie Foreman-Larkin, 1 Peter A. Netland, 2 and Sarwat
Ophthalmology Volume 2015, Article ID 283707, 6 pages http://dx.doi.org/10.1155/2015/283707 Review Article Clinical Management of Malignant Glaucoma Julie Foreman-Larkin, 1 Peter A. Netland, 2 and Sarwat
Subject Index. Canaloplasty aqueous outflow system evaluation 110, 111 complications 118, 119 historical perspective 109, 110
 Subject Index Ab externo Schlemm canal surgery, see Canaloplasty, Viscocanalostomy Ab interno Schlemm canal surgery, see istent, Trabectome Adjustable sutures 14, 15 AGV glaucoma drainage implants 43,
Subject Index Ab externo Schlemm canal surgery, see Canaloplasty, Viscocanalostomy Ab interno Schlemm canal surgery, see istent, Trabectome Adjustable sutures 14, 15 AGV glaucoma drainage implants 43,
TRABECULECTOMY. Dr. Sandra M. Johnson, MD
 TRABECULECTOMY Dr. Sandra M. Johnson, MD FILTRATION OPTIONS Trabeculotomy, Schlemn s canal, internal Deep Non-penetrating Sclerectomy filtering to a scleral lake, or viscocanulostomy Trabeculectomy shunting
TRABECULECTOMY Dr. Sandra M. Johnson, MD FILTRATION OPTIONS Trabeculotomy, Schlemn s canal, internal Deep Non-penetrating Sclerectomy filtering to a scleral lake, or viscocanulostomy Trabeculectomy shunting
AC & ACG Instruction Course Surgical Treatments for PACG
 AC & ACG Instruction Course Surgical Treatments for PACG Presented by APGS Clement C.Y. THAM Professor, The Chinese University of Hong Kong Chief of Service, Hong Kong Eye Hospital Deputy Secretary-General,
AC & ACG Instruction Course Surgical Treatments for PACG Presented by APGS Clement C.Y. THAM Professor, The Chinese University of Hong Kong Chief of Service, Hong Kong Eye Hospital Deputy Secretary-General,
Choroidal detachment following retinal detachment surgery: An analysis and a new hypothesis to minimize its occurrence in high-risk cases
 European Journal of Ophthalmology / Vol. 14 no. 4, 2004 / pp. 325-329 Choroidal detachment following retinal detachment surgery: An analysis and a new hypothesis to minimize its occurrence in high-risk
European Journal of Ophthalmology / Vol. 14 no. 4, 2004 / pp. 325-329 Choroidal detachment following retinal detachment surgery: An analysis and a new hypothesis to minimize its occurrence in high-risk
SILICONE OIL INJECTION INDUCED GLAUCOMA: INCIDENCE AND MANAGEMENT
 SILICONE OIL INJECTION INDUCED GLAUCOMA: INCIDENCE AND MANAGEMENT Ahmad Elsayed Hudieb Department of Ophthalmology Faculty of Medicine, Al- Azhar University ABSTRACT Purpose: Intravitreal silicone oil
SILICONE OIL INJECTION INDUCED GLAUCOMA: INCIDENCE AND MANAGEMENT Ahmad Elsayed Hudieb Department of Ophthalmology Faculty of Medicine, Al- Azhar University ABSTRACT Purpose: Intravitreal silicone oil
Pediatric traumatic cataract Presentation and Management. Dr. Kavitha Kalaivani Pediatric ophthalmology Sankara Nethralaya Nov 7, 2017
 Pediatric traumatic cataract Presentation and Management Dr. Kavitha Kalaivani Pediatric ophthalmology Sankara Nethralaya Nov 7, 2017 Management of Traumatic Cataract Ocular trauma presents many problems
Pediatric traumatic cataract Presentation and Management Dr. Kavitha Kalaivani Pediatric ophthalmology Sankara Nethralaya Nov 7, 2017 Management of Traumatic Cataract Ocular trauma presents many problems
Chronicity. Narrow Minded. Course Outline. Acute angle closure. Subacute angle closure. Classification of Angle Closure 5/19/2014
 Chronicity Narrow Minded The management of narrow angles in the optometric practice Acute Subacute Chronic Aaron McNulty, OD, FAAO Course Outline Classification of Angle Closure Evaluation of narrow angles
Chronicity Narrow Minded The management of narrow angles in the optometric practice Acute Subacute Chronic Aaron McNulty, OD, FAAO Course Outline Classification of Angle Closure Evaluation of narrow angles
9/25/2017 CASE. 67 years old On 2 topical meds since 3 years. Rx: +3.0 RE LE
 CASE 67 years old On 2 topical meds since 3 years Rx: +3.0 /-0.5@65 RE +2.5/-0.5@115 LE IOP : 17 RE 19 LE CD: 0.5 RE 0.6 LE 1 67 years old On 2 topical meds since 3 years Rx: +3.0 /-0.5@65 RE +2.5/-0.5@115
CASE 67 years old On 2 topical meds since 3 years Rx: +3.0 /-0.5@65 RE +2.5/-0.5@115 LE IOP : 17 RE 19 LE CD: 0.5 RE 0.6 LE 1 67 years old On 2 topical meds since 3 years Rx: +3.0 /-0.5@65 RE +2.5/-0.5@115
NEW YORK UNIVERSITY SCHOOL OF MEDICINE DEPARTMENT OF OPHTHALMOLOGY EDUCATIONAL OBJECTIVES AND GOALS
 NEW YORK UNIVERSITY SCHOOL OF MEDICINE DEPARTMENT OF OPHTHALMOLOGY EDUCATIONAL OBJECTIVES AND GOALS Revision Date: 6/30/06 Distribution Date: 7/6/06 The Department of Ophthalmology at the NYU Medical Center
NEW YORK UNIVERSITY SCHOOL OF MEDICINE DEPARTMENT OF OPHTHALMOLOGY EDUCATIONAL OBJECTIVES AND GOALS Revision Date: 6/30/06 Distribution Date: 7/6/06 The Department of Ophthalmology at the NYU Medical Center
TRABECULECTOMY THE BEST AND WORST CANDIDATES
 TRABECULECTOMY THE BEST AND WORST CANDIDATES MICHAEL F. OATS, MD OPHTHALMIC CONSULTANTS OF BOSTON ASCRS 2014 FINANCIAL DISCLOSURES None TRABECULECTOMY Performed for over 100 years Most commonly performed
TRABECULECTOMY THE BEST AND WORST CANDIDATES MICHAEL F. OATS, MD OPHTHALMIC CONSULTANTS OF BOSTON ASCRS 2014 FINANCIAL DISCLOSURES None TRABECULECTOMY Performed for over 100 years Most commonly performed
LENS INDUCED GLAUCOMA
 LENS INDUCED GLAUCOMA PRESENTER P SHILPA RAVI 2 ND YEAR PG DEPT OF OPHTHALMOLOGY LENS INDUCED GLAUCOMA It is a form of secondary glaucoma where intraocular pressure is raised due to disorder in crystalline
LENS INDUCED GLAUCOMA PRESENTER P SHILPA RAVI 2 ND YEAR PG DEPT OF OPHTHALMOLOGY LENS INDUCED GLAUCOMA It is a form of secondary glaucoma where intraocular pressure is raised due to disorder in crystalline
Recurrent intraocular hemorrhage secondary to cataract wound neovascularization (Swan Syndrome)
 Recurrent intraocular hemorrhage secondary to cataract wound neovascularization (Swan Syndrome) John J. Chen MD, PhD; Young H. Kwon MD, PhD August 6, 2012 Chief complaint: Recurrent vitreous hemorrhage,
Recurrent intraocular hemorrhage secondary to cataract wound neovascularization (Swan Syndrome) John J. Chen MD, PhD; Young H. Kwon MD, PhD August 6, 2012 Chief complaint: Recurrent vitreous hemorrhage,
THE CURRENT TREATMENT OF GLAUCOMA IS DIrected
 Three-Year Follow-up of the Tube Versus Trabeculectomy Study STEVEN J. GEDDE, JOYCE C. SCHIFFMAN, WILLIAM J. FEUER, LEON W. HERNDON, JAMES D. BRANDT, AND DONALD L. BUDENZ, ON BEHALF OF THE TUBE VERSUS
Three-Year Follow-up of the Tube Versus Trabeculectomy Study STEVEN J. GEDDE, JOYCE C. SCHIFFMAN, WILLIAM J. FEUER, LEON W. HERNDON, JAMES D. BRANDT, AND DONALD L. BUDENZ, ON BEHALF OF THE TUBE VERSUS
Understanding Angle Closure
 Case Understanding Angle Closure Dominick L. Opitz, OD, FAAO Associate Professor Illinois College of Optometry 56 year old Caucasian Male Primary Eye Exam BCVA: 20/25 OD with+1.25 DS 20/25 OS with +1.75
Case Understanding Angle Closure Dominick L. Opitz, OD, FAAO Associate Professor Illinois College of Optometry 56 year old Caucasian Male Primary Eye Exam BCVA: 20/25 OD with+1.25 DS 20/25 OS with +1.75
EFFICACY AND SAFETY OF CANALOPLASTY IN SAUDI PATIENTS WITH UNCONTROLLED OPEN ANGLE GLAUCOMA
 EFFICACY AND SAFETY OF CANALOPLASTY IN SAUDI PATIENTS WITH UNCONTROLLED OPEN ANGLE GLAUCOMA DR.FAISAL ALMOBARAK ASSISTANT PROFESSOR AND CONSULTANT DEPARTMENT OF OPHTHALMOLOGY COLLEGE OF MEDICINE AND KING
EFFICACY AND SAFETY OF CANALOPLASTY IN SAUDI PATIENTS WITH UNCONTROLLED OPEN ANGLE GLAUCOMA DR.FAISAL ALMOBARAK ASSISTANT PROFESSOR AND CONSULTANT DEPARTMENT OF OPHTHALMOLOGY COLLEGE OF MEDICINE AND KING
Romanian Journal of Ophthalmology, Volume 59, Issue 4, October-December pp:
 Romanian Journal of Ophthalmology, Volume 59, Issue 4, October-December 2015. pp:243-247 GENERAL ARTICLE Intraoperative and postoperative complications in trabeculectomy, Clinical study Barac Ramona* **,
Romanian Journal of Ophthalmology, Volume 59, Issue 4, October-December 2015. pp:243-247 GENERAL ARTICLE Intraoperative and postoperative complications in trabeculectomy, Clinical study Barac Ramona* **,
Inaccuracy of Intraocular Lens Power Prediction for Cataract Surgery in Angle-Closure Glaucoma
 Original Article DOI 10.3349/ymj.2009.50.2.206 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 50(2):206-210, 2009 Inaccuracy of Intraocular Lens Power Prediction for Cataract Surgery in Angle-Closure
Original Article DOI 10.3349/ymj.2009.50.2.206 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 50(2):206-210, 2009 Inaccuracy of Intraocular Lens Power Prediction for Cataract Surgery in Angle-Closure
CONSENT FOR CATARACT SURGERY REQUEST FOR SURGICAL OPERATION / PROCEDURE AND ANAESTHETIC
 CONSENT FOR CATARACT SURGERY REQUEST FOR SURGICAL OPERATION / PROCEDURE AND ANAESTHETIC Your doctor has indicated that the condition of your eye appears stable and your cataract surgery and/or implantation
CONSENT FOR CATARACT SURGERY REQUEST FOR SURGICAL OPERATION / PROCEDURE AND ANAESTHETIC Your doctor has indicated that the condition of your eye appears stable and your cataract surgery and/or implantation
Anatomical results and complications after silicone oil removal
 Romanian Journal of Ophthalmology, Volume 61, Issue 4, October-December 2017. pp:261-266 GENERAL ARTICLE Anatomical results and complications after silicone oil removal Brănişteanu Daniel Constantin* **,
Romanian Journal of Ophthalmology, Volume 61, Issue 4, October-December 2017. pp:261-266 GENERAL ARTICLE Anatomical results and complications after silicone oil removal Brănişteanu Daniel Constantin* **,
Phacoemulsification versus Trabeculectomy in Medically Uncontrolled Chronic Angle- Closure Glaucoma without Cataract
 Phacoemulsification versus Trabeculectomy in Medically Uncontrolled Chronic Angle- Closure Glaucoma without Cataract Clement C. Y. Tham, FRCS, 1,2,3 Yolanda Y. Y. Kwong, FRCS, 1,2,3 Nafees Baig, FRCS,
Phacoemulsification versus Trabeculectomy in Medically Uncontrolled Chronic Angle- Closure Glaucoma without Cataract Clement C. Y. Tham, FRCS, 1,2,3 Yolanda Y. Y. Kwong, FRCS, 1,2,3 Nafees Baig, FRCS,
Surgical peripheral iridectomy via a clearcornea phacoemulsification incision for pupillary block following cataract surgery in acute angle closure
 Fang et al. BMC Ophthalmology (2018) 18:120 https://doi.org/10.1186/s12886-018-0786-2 TECHNICAL ADVANCE Open Access Surgical peripheral iridectomy via a clearcornea phacoemulsification incision for pupillary
Fang et al. BMC Ophthalmology (2018) 18:120 https://doi.org/10.1186/s12886-018-0786-2 TECHNICAL ADVANCE Open Access Surgical peripheral iridectomy via a clearcornea phacoemulsification incision for pupillary
MORE ON COMBINING OR NOT COMBINING...
 MORE ON COMBINING OR NOT COMBINING... A. GALAND* At the XVIII Congress of the European Society of Cataract and Refractive Surgeons (ESCRS) in Brussels, September 2 nd -6 th 2000, I was in charge of organizing
MORE ON COMBINING OR NOT COMBINING... A. GALAND* At the XVIII Congress of the European Society of Cataract and Refractive Surgeons (ESCRS) in Brussels, September 2 nd -6 th 2000, I was in charge of organizing
Measure #192: Cataracts: Complications within 30 Days Following Cataract Surgery Requiring Additional Surgical Procedures
 Measure #192: Cataracts: Complications within 30 Days Following Cataract Surgery Requiring Additional Surgical Procedures 2012 PHYSICIAN QUALITY REPORTING OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY
Measure #192: Cataracts: Complications within 30 Days Following Cataract Surgery Requiring Additional Surgical Procedures 2012 PHYSICIAN QUALITY REPORTING OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY
INTRODUCTION J. DAWCZYNSKI, E. KOENIGSDOERFFER, R. AUGSTEN, J. STROBEL. Department of Ophthalmology, University Hospital Jena, Jena - Germany
 European Journal of Ophthalmology / Vol. 17 no. 3, 2007 / pp. 363-367 Anterior segment optical coherence tomography for evaluation of changes in anterior chamber angle and depth after intraocular lens
European Journal of Ophthalmology / Vol. 17 no. 3, 2007 / pp. 363-367 Anterior segment optical coherence tomography for evaluation of changes in anterior chamber angle and depth after intraocular lens
Pseudophakic angle-closure from a Soemmering ring
 Suwan et al. BMC Ophthalmology (2016) 16:91 DOI 10.1186/s12886-016-0257-6 CASE REPORT Open Access Pseudophakic angle-closure from a Soemmering ring Yanin Suwan *, Bayasgalan Purevdorj, Chaiwat Teekhasaenee,
Suwan et al. BMC Ophthalmology (2016) 16:91 DOI 10.1186/s12886-016-0257-6 CASE REPORT Open Access Pseudophakic angle-closure from a Soemmering ring Yanin Suwan *, Bayasgalan Purevdorj, Chaiwat Teekhasaenee,
Trabeculectomy is the most commonly performed surgery
 ORIGINAL STUDY Standard Trabeculectomy and Ex-PRESS Miniature Glaucoma Shunt: A Comparative Study and Literature Review Elad Moisseiev, MD, Eran Zunz, MD, Rotem Tzur, MD, Shimon Kurtz, MD, and Gabi Shemesh,
ORIGINAL STUDY Standard Trabeculectomy and Ex-PRESS Miniature Glaucoma Shunt: A Comparative Study and Literature Review Elad Moisseiev, MD, Eran Zunz, MD, Rotem Tzur, MD, Shimon Kurtz, MD, and Gabi Shemesh,
KEY MESSAGES. Details of the evidence supporting these recommendations can be found in the above CPG, available on the following websites:
 QUICK REFERENCE FOR HEALTHCARE PROVIDERS KEY MESSAGES 1. Glaucoma is a chronic eye disease that damages the optic nerve, & can result in serious vision loss and irreversible blindness. 2. Glaucoma diagnosis
QUICK REFERENCE FOR HEALTHCARE PROVIDERS KEY MESSAGES 1. Glaucoma is a chronic eye disease that damages the optic nerve, & can result in serious vision loss and irreversible blindness. 2. Glaucoma diagnosis
Trabeculectomy A Review and 2 Year Follow Up
 ORIGINAL ARTICLE Trabeculectomy A Review and 2 Year Follow Up F Jaais, (MRCOphth) Department of Ophthalmology, University Malaya Medical Center, Faculty of Medicine, 50603 Kuala Lumpur Summary This study
ORIGINAL ARTICLE Trabeculectomy A Review and 2 Year Follow Up F Jaais, (MRCOphth) Department of Ophthalmology, University Malaya Medical Center, Faculty of Medicine, 50603 Kuala Lumpur Summary This study
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of microinvasive subconjunctival insertion of a trans-scleral gelatin stent for primary
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of microinvasive subconjunctival insertion of a trans-scleral gelatin stent for primary
Highlights On The Management Of Phacomorphic Glaucoma
 Highlights On The Management Of Phacomorphic Glaucoma Ahmed Aboueleinein What is phacomorphic glaucoma? It is a secondary angle closure glaucoma due to lens intumescence Advanced cataract or traumatic
Highlights On The Management Of Phacomorphic Glaucoma Ahmed Aboueleinein What is phacomorphic glaucoma? It is a secondary angle closure glaucoma due to lens intumescence Advanced cataract or traumatic
Choroidal Detachment after Filtering Surgery. Wan-Chen Ku, MD; Yin-Hsin Lin, MD; Lan-Hsin Chuang, MD; Ko-Jen Yang, MD
 Original Article 151 Choroidal Detachment after Filtering Surgery Wan-Chen Ku, MD; Yin-Hsin Lin, MD; Lan-Hsin Chuang, MD; Ko-Jen Yang, MD Results: Background: The purpose of this study is to report the
Original Article 151 Choroidal Detachment after Filtering Surgery Wan-Chen Ku, MD; Yin-Hsin Lin, MD; Lan-Hsin Chuang, MD; Ko-Jen Yang, MD Results: Background: The purpose of this study is to report the
ORIGINAL ARTICLE. SURGICAL RESULTS OF PARS PLANA VITRECTOMY COMBINED WITH SMALL INCISION CATARACT SURGERY V.D. Karthigeyan 1
 SURGICAL RESULTS OF PARS PLANA VITRECTOMY COMBINED WITH SMALL INCISION CATARACT SURGERY V.D. Karthigeyan 1 HOW TO CITE THIS ARTICLE: VD Karthigeyan. Surgical results of pars plana vitrectomy combined with
SURGICAL RESULTS OF PARS PLANA VITRECTOMY COMBINED WITH SMALL INCISION CATARACT SURGERY V.D. Karthigeyan 1 HOW TO CITE THIS ARTICLE: VD Karthigeyan. Surgical results of pars plana vitrectomy combined with
Aqueous Shunts and Stents for Glaucoma
 Protocol Aqueous Shunts and Stents for Glaucoma (90321) Medical Benefit Effective Date: 04/01/14 Next Review Date: 01/15 Preauthorization No Review Dates: 03/10, 03/11, 07/11, 01/12, 09/12, 01/13, 01/14
Protocol Aqueous Shunts and Stents for Glaucoma (90321) Medical Benefit Effective Date: 04/01/14 Next Review Date: 01/15 Preauthorization No Review Dates: 03/10, 03/11, 07/11, 01/12, 09/12, 01/13, 01/14
These devices, when FDA approved, are covered for patients with glaucoma that is not adequately controlled with medical therapy.
 Medical Policy Title: Aqueous Shunts and ARBenefits Approval: 10/26/2011 Devices for Glaucoma Effective Date: 01/01/2012 Document: ARB0168 Revision Date: Code(s): 66174, Transluminal dilation of aqueous
Medical Policy Title: Aqueous Shunts and ARBenefits Approval: 10/26/2011 Devices for Glaucoma Effective Date: 01/01/2012 Document: ARB0168 Revision Date: Code(s): 66174, Transluminal dilation of aqueous
Clinical study of traumatic cataract and its management
 Clinical study of traumatic cataract and its management Original article Manjula Mangane, M.R. Pujari, Chethan N. Murthy Department of Ophthalmology, Basaweshwar Teaching and General Hospital, Gulbarga,
Clinical study of traumatic cataract and its management Original article Manjula Mangane, M.R. Pujari, Chethan N. Murthy Department of Ophthalmology, Basaweshwar Teaching and General Hospital, Gulbarga,
Complication and Visual Outcome after Peadiatric Cataract Surgery with or Without Intra Ocular Lens Implantation
 Original Article Complication and Visual Outcome after Peadiatric with or Without Intra Ocular Lens Implantation Mazhar-ul-Hasan, Umair A. Qidwai, Aziz-ur-Rehman, Nasir Bhatti, Rashid H. Alvi Pak J Ophthalmol
Original Article Complication and Visual Outcome after Peadiatric with or Without Intra Ocular Lens Implantation Mazhar-ul-Hasan, Umair A. Qidwai, Aziz-ur-Rehman, Nasir Bhatti, Rashid H. Alvi Pak J Ophthalmol
ALTERNATIVES TO PHAKIC IMPLANT SURGERY
 Visian ICL Consent INTRODUCTION This information is being provided to you so that you can make an informed decision about having eye surgery to reduce or eliminate your nearsightedness. Only you and your
Visian ICL Consent INTRODUCTION This information is being provided to you so that you can make an informed decision about having eye surgery to reduce or eliminate your nearsightedness. Only you and your
Title. with prior vitrectomy. Author(s) Takashi. Issue Date Wichtig Editore.
 NAOSITE: Nagasaki University's Ac Title Author(s) Citation Spontaneous dislocation of in-the-b with prior vitrectomy Matsumoto, Makiko; Yamada, Koki; Ue Azusa; Tsuiki, Eiko; Kumagami, Take Takashi European
NAOSITE: Nagasaki University's Ac Title Author(s) Citation Spontaneous dislocation of in-the-b with prior vitrectomy Matsumoto, Makiko; Yamada, Koki; Ue Azusa; Tsuiki, Eiko; Kumagami, Take Takashi European
No-Touch Technique and a New Donor Adjuster for Descemet s Stripping Automated Endothelial Keratoplasty
 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
Surgical outcome of pars plana vitrectomy: a retrospective study in a peripheral tertiary eye care centre of Nepal
 Original article : a retrospective study in a peripheral tertiary eye care centre of Nepal Subedi S 1, Sharma MK 2, Sharma BR 2, Kansakar I 2, Dhakwa K 2, Adhikari RK 2 1.Nepal Eye Hospital, National Academy
Original article : a retrospective study in a peripheral tertiary eye care centre of Nepal Subedi S 1, Sharma MK 2, Sharma BR 2, Kansakar I 2, Dhakwa K 2, Adhikari RK 2 1.Nepal Eye Hospital, National Academy
Cataract. What is a Cataract?
 Cataract What is a Cataract? We all have a lens in our eye. This is positioned just behind the iris, which is the coloured ring in the eye that gives your eye its colour. The lens function is to focus
Cataract What is a Cataract? We all have a lens in our eye. This is positioned just behind the iris, which is the coloured ring in the eye that gives your eye its colour. The lens function is to focus
Intraoperative biometry for intraocular lens (IOL) power calculation at silicone oil removal
 European Journal of Ophthalmology / Vol. 13 no. 7, 2003 / pp. 622-626 Intraoperative biometry for intraocular lens (IOL) power calculation at silicone oil removal S.M. EL-BAHA, A. EI-SAMADONI, H.F. IDRIS,
European Journal of Ophthalmology / Vol. 13 no. 7, 2003 / pp. 622-626 Intraoperative biometry for intraocular lens (IOL) power calculation at silicone oil removal S.M. EL-BAHA, A. EI-SAMADONI, H.F. IDRIS,
Cataract. What is a Cataract?
 Cataract What is a Cataract? We all have a lens in our eye. This is positioned just behind the iris, which is the coloured ring in the eye that gives your eye its colour. The lens s function is to focus
Cataract What is a Cataract? We all have a lens in our eye. This is positioned just behind the iris, which is the coloured ring in the eye that gives your eye its colour. The lens s function is to focus
Pseudophakic pupillary-block glaucoma
 British Journal of Ophthalmology, 1977, 61, 329-333 DAVID WERNER AND MARTIN KABACK From the Department of Ophthalmology, Jewish General Hospital, Montreal, Canada SUMMARY Four cases of iris-supported pseudophakic
British Journal of Ophthalmology, 1977, 61, 329-333 DAVID WERNER AND MARTIN KABACK From the Department of Ophthalmology, Jewish General Hospital, Montreal, Canada SUMMARY Four cases of iris-supported pseudophakic
Ophthalmology. Juliette Stenz, MD
 Ophthalmology Juliette Stenz, MD Required Slide Disclosures NO SIGNIFICANT FINANCIAL, GENERAL, OR OBLIGATION INTERESTS TO REPORT Required Slide At the end of this session, students will be able to: 1.
Ophthalmology Juliette Stenz, MD Required Slide Disclosures NO SIGNIFICANT FINANCIAL, GENERAL, OR OBLIGATION INTERESTS TO REPORT Required Slide At the end of this session, students will be able to: 1.
SENARAI KADAR CAJ YANG TELAH MENDAPAT KELULUSAN ( JABATAN OFTALMOLOGI )
 SENARAI KADAR CAJ YANG TELAH MENDAPAT KELULUSAN ( JABATAN OFTALMOLOGI ) PTJ : JK.55 : JABATAN OFTALMOLOGI (JOFT) Sub PTJ : JK.55.01 : AM No Item Code / Name 1 1674 11674 - ANTERIOR CHAMBER WASHOUT 95.00
SENARAI KADAR CAJ YANG TELAH MENDAPAT KELULUSAN ( JABATAN OFTALMOLOGI ) PTJ : JK.55 : JABATAN OFTALMOLOGI (JOFT) Sub PTJ : JK.55.01 : AM No Item Code / Name 1 1674 11674 - ANTERIOR CHAMBER WASHOUT 95.00
Trabeculectomy is an effective method for lowering
 ORIGINAL STUDY Refractive Outcome of Cataract Surgery in Eyes With Prior Trabeculectomy: Risk Factors for Postoperative Myopia Oliver L. Yeh, MD, Karine D. Bojikian, MD, Mark A. Slabaugh, MD, and Philip
ORIGINAL STUDY Refractive Outcome of Cataract Surgery in Eyes With Prior Trabeculectomy: Risk Factors for Postoperative Myopia Oliver L. Yeh, MD, Karine D. Bojikian, MD, Mark A. Slabaugh, MD, and Philip
in Uveitis Euretina Hamburg 2013 Nicholas Jones Royal Eye Hospital Manchester, UK
 Cataract Surgery in Uveitis Euretina Hamburg 2013 Nicholas Jones Royal Eye Hospital Manchester, UK Cataract surgery in eyes with uveitis is not routine It requires much more pre-operative planning It may
Cataract Surgery in Uveitis Euretina Hamburg 2013 Nicholas Jones Royal Eye Hospital Manchester, UK Cataract surgery in eyes with uveitis is not routine It requires much more pre-operative planning It may
Review Article Malignant Glaucoma: A Review of the Modern Literature
 Ophthalmology Volume 2012, Article ID 852659, 6 pages doi:10.1155/2012/852659 Review Article Malignant Glaucoma: A Review of the Modern Literature H. Shahid and J. F. Salmon Oxford Eye Hospital, John Radcliffe
Ophthalmology Volume 2012, Article ID 852659, 6 pages doi:10.1155/2012/852659 Review Article Malignant Glaucoma: A Review of the Modern Literature H. Shahid and J. F. Salmon Oxford Eye Hospital, John Radcliffe
Aqueous Shunts and Stents for Glaucoma. (90321) (Formerly Aqueous Shunts for Glaucoma)
 Protocol Aqueous Shunts and Stents for Glaucoma (90321) (Formerly Aqueous Shunts for Glaucoma) Medical Benefit Effective Date: 01/01/13 Next Review Date: 01/14 Preauthorization* No Review Dates: 03/10,
Protocol Aqueous Shunts and Stents for Glaucoma (90321) (Formerly Aqueous Shunts for Glaucoma) Medical Benefit Effective Date: 01/01/13 Next Review Date: 01/14 Preauthorization* No Review Dates: 03/10,
Cataract surgery is the leading cause of malpractice claims (OMIC) Complicated CE/IOL: Choices the anterior segment surgeon can make
 Posterior Segment Complications and Management of Retained Lens Material Jay M. Stewart, MD Cataract surgery is the leading cause of malpractice claims (OMIC) Complicated CE/IOL: Choices the anterior segment
Posterior Segment Complications and Management of Retained Lens Material Jay M. Stewart, MD Cataract surgery is the leading cause of malpractice claims (OMIC) Complicated CE/IOL: Choices the anterior segment
MANAGEMENT OF NEOVASCULAR GLAUCOMA
 MSO EXPRESS: ISSUE 3 MANAGEMENT OF NEOVASCULAR GLAUCOMA Associate Professor Dr. Norlina Mohd Ramli, Dr. Ng Ker Hsin Associate Professor Dr. Norlina Mohd Ramli MBBS (UK) MRCOphth (UK) MS Ophthal (Mal) Fellowship
MSO EXPRESS: ISSUE 3 MANAGEMENT OF NEOVASCULAR GLAUCOMA Associate Professor Dr. Norlina Mohd Ramli, Dr. Ng Ker Hsin Associate Professor Dr. Norlina Mohd Ramli MBBS (UK) MRCOphth (UK) MS Ophthal (Mal) Fellowship
Role of Initial Preoperative Medical Management in Controlling Post-Operative Anterior Uveitis in Patients of Phacomorphic Glaucoma
 Original Article Role of Initial Preoperative Medical Management in Controlling Post-Operative Anterior Uveitis in Patients of Phacomorphic Glaucoma Irfan Qayyum Malik, M. Moin, A. Rehman, Mumtaz Hussain
Original Article Role of Initial Preoperative Medical Management in Controlling Post-Operative Anterior Uveitis in Patients of Phacomorphic Glaucoma Irfan Qayyum Malik, M. Moin, A. Rehman, Mumtaz Hussain
CHARTING THE NEW COURSE FOR MIGS
 CHARTING THE NEW COURSE FOR MIGS SEE WHAT S ON THE HORIZON CyPass Micro-Stent the next wave in micro-invasive glaucoma surgery. MICRO-INVASIVE GLAUCOMA SURGERY (MIGS) OFFERS A REVOLUTIONARY APPROACH TO
CHARTING THE NEW COURSE FOR MIGS SEE WHAT S ON THE HORIZON CyPass Micro-Stent the next wave in micro-invasive glaucoma surgery. MICRO-INVASIVE GLAUCOMA SURGERY (MIGS) OFFERS A REVOLUTIONARY APPROACH TO
Corporate Medical Policy
 Corporate Medical Policy Viscocanalostomy and Canaloplasty File Name: Origination: Last CAP Review: Next CAP Review: Last Review: viscocanalostomy_and_canaloplasty 11/2011 6/2017 6/2018 6/2017 Description
Corporate Medical Policy Viscocanalostomy and Canaloplasty File Name: Origination: Last CAP Review: Next CAP Review: Last Review: viscocanalostomy_and_canaloplasty 11/2011 6/2017 6/2018 6/2017 Description
Endocyclophotodestruction in Glaucoma Patients Undergoing Combined Surgery of Pars Plana Vitrectomy and Phacoemulsification
 e-issn 643-370 DOI: 0.269/MSM.89097 Received: 204.04.23 Accepted: 204.0.29 Published: 204.0. Endocyclophotodestruction in Glaucoma Patients Undergoing Combined Surgery of Pars Plana Vitrectomy and Phacoemulsification
e-issn 643-370 DOI: 0.269/MSM.89097 Received: 204.04.23 Accepted: 204.0.29 Published: 204.0. Endocyclophotodestruction in Glaucoma Patients Undergoing Combined Surgery of Pars Plana Vitrectomy and Phacoemulsification
STUDY OF EFFECTIVENESS OF LENS EXTRACTION AND PCIOL IMPLANTATION IN PRIMARY ANGLE CLOSURE GLAUCOMA Sudhakar Rao P 1, K. Revathy 2, T.
 STUDY OF EFFECTIVENESS OF LENS EXTRACTION AND PCIOL IMPLANTATION IN PRIMARY ANGLE CLOSURE GLAUCOMA Sudhakar Rao P 1, K. Revathy 2, T. Sreevathsala 3 HOW TO CITE THIS ARTICLE: Sudhakar Rao P, K. Revathy,
STUDY OF EFFECTIVENESS OF LENS EXTRACTION AND PCIOL IMPLANTATION IN PRIMARY ANGLE CLOSURE GLAUCOMA Sudhakar Rao P 1, K. Revathy 2, T. Sreevathsala 3 HOW TO CITE THIS ARTICLE: Sudhakar Rao P, K. Revathy,
Comparison Between 20- Gauge And 23-Gauge Vitrectomy In Diabetic Patients
 Asok Nataraj MS Abstract Aim: - Comparison Between 20- Gauge And 23-Gauge Vitrectomy In Diabetic Patients The purpose of this study was to directly compare the outcome, safety and efficacy of the 20G and
Asok Nataraj MS Abstract Aim: - Comparison Between 20- Gauge And 23-Gauge Vitrectomy In Diabetic Patients The purpose of this study was to directly compare the outcome, safety and efficacy of the 20G and
Sinus trabeculectomy. Preliminary results of IOO operations
 Brit. J. Ophthal. (I 972) 56, 833 Sinus trabeculectomy Preliminary results of IOO operations A. P. NESTEROV, N. V. FEDEROVA, AND Y. E. BATMANOV Department of Ophthalmology, Kazan Medical Institute, Kazan,
Brit. J. Ophthal. (I 972) 56, 833 Sinus trabeculectomy Preliminary results of IOO operations A. P. NESTEROV, N. V. FEDEROVA, AND Y. E. BATMANOV Department of Ophthalmology, Kazan Medical Institute, Kazan,
Primary Angle Closure Glaucoma
 www.eyesurgeonlondon.co.uk Primary Angle Closure Glaucoma What is Glaucoma? Glaucoma is a condition in which there is damage to the optic nerve. This nerve carries visual signals from the eye to the brain.
www.eyesurgeonlondon.co.uk Primary Angle Closure Glaucoma What is Glaucoma? Glaucoma is a condition in which there is damage to the optic nerve. This nerve carries visual signals from the eye to the brain.
Secondary management and outcome of massive suprachoroidal hemorrhage
 European Journal of Ophthalmology / Vol. 16 no. 6, 2006 / pp. 835-840 Secondary management and outcome of massive suprachoroidal hemorrhage E. FERETIS, S. MOURTZOUKOS, G. MANGOURITSAS, S.A. KABANAROU,
European Journal of Ophthalmology / Vol. 16 no. 6, 2006 / pp. 835-840 Secondary management and outcome of massive suprachoroidal hemorrhage E. FERETIS, S. MOURTZOUKOS, G. MANGOURITSAS, S.A. KABANAROU,
Myopic Shift After Intraocular Lens Implantation in Children Less Than Two Years of Age
 Original Article Myopic Shift After Intraocular Lens Implantation in Children Less Than Two Years of Age Suma Ganesh 1, Reena Gupta 2, Sumita Sethi 3, Chandra Gurung 4, Raman Mehta 5 1,5 Dr. Shroff s Charitable
Original Article Myopic Shift After Intraocular Lens Implantation in Children Less Than Two Years of Age Suma Ganesh 1, Reena Gupta 2, Sumita Sethi 3, Chandra Gurung 4, Raman Mehta 5 1,5 Dr. Shroff s Charitable
Department of Ophthalmology
 Department of Ophthalmology Period : 02/July/18 to 30/August/18 Semester : 7 th Semester Lecture Lesson Plan Sr. Date Topic Lesson plan Name of Faculty No. 1 02.07.18 Lens- Lens-Anatomy, Classification
Department of Ophthalmology Period : 02/July/18 to 30/August/18 Semester : 7 th Semester Lecture Lesson Plan Sr. Date Topic Lesson plan Name of Faculty No. 1 02.07.18 Lens- Lens-Anatomy, Classification
Primary angle closure (PAC) Pathogenesis: Pathogenesis 12/2/2016. Ying Han, MD, PhD Associate Professor of Ophthalmology Glaucoma Service, UCSF
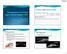 Primary angle closure (PAC) Ying Han, MD, PhD Associate Professor of Ophthalmology Glaucoma Service, UCSF Pathogenesis: Pupillary block and anterior lens movement Most common cause Normal pressure gradient
Primary angle closure (PAC) Ying Han, MD, PhD Associate Professor of Ophthalmology Glaucoma Service, UCSF Pathogenesis: Pupillary block and anterior lens movement Most common cause Normal pressure gradient
Corporate Medical Policy
 Corporate Medical Policy Aqueous Shunts and Devices for Glaucoma File Name: Origination: Last CAP Review: Next CAP Review: Last Review: aqueous_shunts_and_devices_for_glaucoma 3/2010 6/2017 6/2018 6/2017
Corporate Medical Policy Aqueous Shunts and Devices for Glaucoma File Name: Origination: Last CAP Review: Next CAP Review: Last Review: aqueous_shunts_and_devices_for_glaucoma 3/2010 6/2017 6/2018 6/2017
The Outcome Of 23 Gauge Pars Plana Vitrectomy Without Scleral Buckle For Management Of Rhegmatogenous Retinal Detachment. By:
 The Outcome Of 23 Gauge Pars Plana Vitrectomy Without Scleral Buckle For Management Of Rhegmatogenous Retinal Detachment. By: Mohamed El-Deeb, MD, M.Sc, ICO, FRCS. Vitreoretinal Consultant, Magrabi Eye
The Outcome Of 23 Gauge Pars Plana Vitrectomy Without Scleral Buckle For Management Of Rhegmatogenous Retinal Detachment. By: Mohamed El-Deeb, MD, M.Sc, ICO, FRCS. Vitreoretinal Consultant, Magrabi Eye
Advanced Eyecare of Orange County/ Kim T. Doan, M.D.
 Patient Information Sheet: Cataract Surgery And/Or Implantation of an Intraocular Lens This information is given to you so that you can prepare for the discussion with your eye surgeon. This document will
Patient Information Sheet: Cataract Surgery And/Or Implantation of an Intraocular Lens This information is given to you so that you can prepare for the discussion with your eye surgeon. This document will
Surgical Privileges Form: Ophthalmology
 Surgical Form: Ophthalmology Clinical Request Applicant s Name:. License No. (If Any):... Scope of Practice:. Facility:.. Date:... Category I: CORE PRIVILEGES 1. Admitting privileges 2. Admission history
Surgical Form: Ophthalmology Clinical Request Applicant s Name:. License No. (If Any):... Scope of Practice:. Facility:.. Date:... Category I: CORE PRIVILEGES 1. Admitting privileges 2. Admission history
84 Year Old with Rosacea
 84 Year Old with Rosacea S/p tap and injection of intravitreal vancomycin, ceftazidime, dexamethasone Post-injection day#1 Va HM IOP 14 mmhg Post-injection week#3 BCVA 20/20-3 (plano +0.50 x 180) IOP 23
84 Year Old with Rosacea S/p tap and injection of intravitreal vancomycin, ceftazidime, dexamethasone Post-injection day#1 Va HM IOP 14 mmhg Post-injection week#3 BCVA 20/20-3 (plano +0.50 x 180) IOP 23
Glaucoma is the second leading cause of blindness
 Int J Ophthalmol, Vol. 10, No. 1, Jan.18, 2017 www.ijo.cn Clinical Research Ex-PRESS implantation with phacoemulsification in POAG versus CPACG Jie Lan 1,2, Da-Peng Sun 2, Jie Wu 2, Ya-Ni Wang 2, Li-Xin
Int J Ophthalmol, Vol. 10, No. 1, Jan.18, 2017 www.ijo.cn Clinical Research Ex-PRESS implantation with phacoemulsification in POAG versus CPACG Jie Lan 1,2, Da-Peng Sun 2, Jie Wu 2, Ya-Ni Wang 2, Li-Xin
AB-INTERNO CANALOPLASTY THE MINIMALLY INVASIVE GLAUCOMA SURGERY THAT KEEPS ITS PROMISE
 WHITEPAPER AB-INTERNO CANALOPLASTY THE MINIMALLY INVASIVE GLAUCOMA SURGERY THAT KEEPS ITS PROMISE AB-INTERNO CANALOPLASTY: TREATMENT STEPS 12-MONTH CASE SERIES REVIEW ABiC Canaloplasty performed with an
WHITEPAPER AB-INTERNO CANALOPLASTY THE MINIMALLY INVASIVE GLAUCOMA SURGERY THAT KEEPS ITS PROMISE AB-INTERNO CANALOPLASTY: TREATMENT STEPS 12-MONTH CASE SERIES REVIEW ABiC Canaloplasty performed with an
Basic microsurgical suturing techniques for beginners
 ESCRS 2014 Basic microsurgical suturing techniques for beginners Trauma, sclera, trabeculectomy B.O. Bachmann Dept. of Ophthalmology, University of Cologne, Germany Financial interests: none Investigating
ESCRS 2014 Basic microsurgical suturing techniques for beginners Trauma, sclera, trabeculectomy B.O. Bachmann Dept. of Ophthalmology, University of Cologne, Germany Financial interests: none Investigating
Research Article Risk Factors of Malignant Glaucoma Occurrence after Glaucoma Surgery
 Hindawi Ophthalmology Volume 2017, Article ID 9616738, 6 pages https://doi.org/10.1155/2017/9616738 Research Article Risk Factors of Malignant Glaucoma Occurrence after Glaucoma Surgery Karolina Krix-Jachym,
Hindawi Ophthalmology Volume 2017, Article ID 9616738, 6 pages https://doi.org/10.1155/2017/9616738 Research Article Risk Factors of Malignant Glaucoma Occurrence after Glaucoma Surgery Karolina Krix-Jachym,
Nate Lighthizer, O.D., F.A.A.O. Assistant Professor, NSUOCO Assistant Dean, Clinical Care Services Director of CE Chief of Specialty Care Clinics
 Nate Lighthizer, O.D., F.A.A.O. Assistant Professor, NSUOCO Assistant Dean, Clinical Care Services Director of CE Chief of Specialty Care Clinics Chief of Electrodiagnostics Clinic lighthiz@nsuok.edu YAG
Nate Lighthizer, O.D., F.A.A.O. Assistant Professor, NSUOCO Assistant Dean, Clinical Care Services Director of CE Chief of Specialty Care Clinics Chief of Electrodiagnostics Clinic lighthiz@nsuok.edu YAG
Cornea/Anterior Segment OCT. User Experience
 Cornea/Anterior Segment OCT User Experience User Experience Case#1 Post Penetrating Keratoplasty Tokyo Medical University / Kohsei Chuo General Hospital Hideki Mori MD, PhD Almost eight years have passed
Cornea/Anterior Segment OCT User Experience User Experience Case#1 Post Penetrating Keratoplasty Tokyo Medical University / Kohsei Chuo General Hospital Hideki Mori MD, PhD Almost eight years have passed
Published in: British Journal of Ophthalmology. Document Version: Peer reviewed version
 Clear lens extraction for the management of primary angle closure glaucoma: surgical technique and refractive outcomes in the EAGLE cohort Day, A., Cooper, D., Burr, J. M., Foster, P., Friedman, D., Gazzard,
Clear lens extraction for the management of primary angle closure glaucoma: surgical technique and refractive outcomes in the EAGLE cohort Day, A., Cooper, D., Burr, J. M., Foster, P., Friedman, D., Gazzard,
CLINICAL SCIENCES. Postoperative Complications After Glaucoma Surgery for Primary Angle-Closure Glaucoma vs Primary Open-Angle Glaucoma
 ONLINE FIRST CLINICAL SCIENCES Postoperative Complications After Glaucoma Surgery for Primary Angle-Closure Glaucoma vs Primary Open-Angle Glaucoma Yar-Li Tan, MRCS; Pei-Fang Tsou, MBBS; Gavin S. Tan,
ONLINE FIRST CLINICAL SCIENCES Postoperative Complications After Glaucoma Surgery for Primary Angle-Closure Glaucoma vs Primary Open-Angle Glaucoma Yar-Li Tan, MRCS; Pei-Fang Tsou, MBBS; Gavin S. Tan,
Implantation of a corneal graft keratoprosthesis for severe corneal opacity in wet blinking eyes
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Implantation of a corneal graft keratoprosthesis for severe corneal opacity in wet blinking eyes The cornea
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Implantation of a corneal graft keratoprosthesis for severe corneal opacity in wet blinking eyes The cornea
TO DETERMINE THE LONG-TERM SAFETY AND EFFIcacy
 Five-year Follow-up of the Fluorouracil Filtering Surgery Study THE FLUOROURACIL FILTERING SURGERY STUDY GROUP* PURPOSE: To determine the efficacy and safety of subconjunctival 5-fluorouracil injections
Five-year Follow-up of the Fluorouracil Filtering Surgery Study THE FLUOROURACIL FILTERING SURGERY STUDY GROUP* PURPOSE: To determine the efficacy and safety of subconjunctival 5-fluorouracil injections
Cronicon EC OPHTHALMOLOGY. Research Article Trephine Assisted Trabeculectomy Technique. Idrees* Introduction
 Cronicon OPEN ACCESS EC OPHTHALMOLOGY Research Article Idrees* Al Dara Hospital and Medical Center at Riyadh, Saudi Arabia *Corresponding Author: Dr Idrees, Al Dara Hospital and Medical Center at Riyadh,
Cronicon OPEN ACCESS EC OPHTHALMOLOGY Research Article Idrees* Al Dara Hospital and Medical Center at Riyadh, Saudi Arabia *Corresponding Author: Dr Idrees, Al Dara Hospital and Medical Center at Riyadh,
Complete Visual Rehabilitation in a Patient with No Light Perception after Surgical Management of a Penetrating Open-Globe Injury: A Case Report
 Published online: June 23, 2015 1663 2699/15/0062 0204$39.50/0 This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial 3.0 Unported license (CC BY-NC)
Published online: June 23, 2015 1663 2699/15/0062 0204$39.50/0 This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial 3.0 Unported license (CC BY-NC)
Morning Report. copyright The University of Colorado. Ashley Laing 09/01/10 Preceptor- Dr. Pantcheva
 Morning Report Ashley Laing 09/01/10 Preceptor- Dr. Pantcheva Case Presentation CC: Right eye pain and headache HPI: 52 yo Caucasian male Presents to ED with OD pain/redness, decreased vision, headache
Morning Report Ashley Laing 09/01/10 Preceptor- Dr. Pantcheva Case Presentation CC: Right eye pain and headache HPI: 52 yo Caucasian male Presents to ED with OD pain/redness, decreased vision, headache
Secondary Glaucomas. Mr Nick Strouthidis MBBS MD PhD FRCS FRCOphth FRANZCO Consultant Ophthalmologist, Glaucoma Service, Moorfields Eye Hospital
 Secondary Glaucomas Mr Nick Strouthidis MBBS MD PhD FRCS FRCOphth FRANZCO Consultant Ophthalmologist, Glaucoma Service, Moorfields Eye Hospital Introduction: What is glaucoma? Glaucoma is the name given
Secondary Glaucomas Mr Nick Strouthidis MBBS MD PhD FRCS FRCOphth FRANZCO Consultant Ophthalmologist, Glaucoma Service, Moorfields Eye Hospital Introduction: What is glaucoma? Glaucoma is the name given
