Aspiration Pneumonia is Well Understood
|
|
|
- Stanley Mathews
- 5 years ago
- Views:
Transcription
1 Myths part 2
2 Aspiration Pneumonia is Well Understood
3 Aspiration Always Leads to Pneumonia Aspiration Pneumonia Research VF and FEES did not significantly predict aspiration pneumonia. Specifically, Documented aspiration of food or liquid on an instrumental swallow study were not predictors of pneumonia. Only 38% of those who aspirated developed pneumonia. Therefore, dysphagia by itself does not appear to cause aspiration pneumonia. Dysphagia and aspiration are necessary but not sufficient conditions for development of pneumonia. Langmore 1998
4 Aspiration Always Leads to Pneumonia Study of 515 patients with dementia and/or Parkinson s Disease 11% (52) of patients developed pneumonia in 3 months 9.8% using compensatory chin tuck (chin down) 8.4% with nectar thick liquids 15.0% with honey thick liquids Robbins 2008
5 PRANDIAL ASPIRATION AND PNEUMONIA IN AN ELDERLY POPULATION FOLLOWED OVER 3 YEARS FEINBERG 1996 Study followed 152 patients for 3 years 50 non aspirators, 51 minor aspirators, 51 major aspirators 21 PEGS 6 NGT Our results indicate that there is not a simple and obvious relation between prandial liquid aspiration and pneumonia. Artificial feeding does not seem to be a satisfactory solution for preventing pneumonia in elderly aspirators.
6 PRANDIAL ASPIRATION AND PNEUMONIA IN AN ELDERLY POPULATION FOLLOWED OVER 3 YEARS FEINBERG 1996 Status Months Pneumonia Episodes Frequency No Aspiration % Minor Aspiration % Major Aspiration/Oral feeding % Major Aspiration/Artificial Feeding % Total %
7 PRANDIAL ASPIRATION AND PNEUMONIA IN AN ELDERLY POPULATION FOLLOWED OVER 3 YEARS FEINBERG 1996 Mortality Rates Final Status Deaths PNA in pts who expired PNA considered cause of death Non aspirators 7 (19%) 5 (71%) 2 (43%) (NS) Minor aspirators 9 (24%) 7 (78%) 3 (33%) (NS) Major aspirators Oral feeding Major aspirators Artificial feeding 21 (45%) 10 (48%) 7 (33%) (NS) 26 (87%) 15 (58%) 14 (54%) Total 63 (41%) 37 (59%) 27 (43%)
8 PRANDIAL ASPIRATION AND PNEUMONIA IN AN ELDERLY POPULATION FOLLOWED OVER 3 YEARS FEINBERG1996 Conclusion: Results indicate that there is not a simple and obvious relation between aspiration and pneumonia. Artificial feeding does not seem to be a satisfactory solution for preventing pneumonia in elderly aspirators.
9 THE NATURAL HISTORY OF PATIENTS WHO ASPIRATE BOCK 2018 Dysphagia etiology was highly associated with increased development of pulmonary events for some patients, especially those with generalized nonspecific dysphagia due to deconditioning or frailty and esophageal dysphagia. Dietary modification recommendations at the time of VFSS (prohibition of oral intake or modification of food consistency) had no significant impact on time to first pulmonary event or survival Severity of aspiration as defined by PAS was not associated with altered overall survival
10 THE NATURAL HISTORY OF PATIENTS WHO ASPIRATE BOCK 2018 Recommendations for dietary modification to a nothing by mouth status or modified food consistency had no statistically significant association with development of pulmonary events or survival in patients with detectable or unsensed penetration or aspiration on VFSS compared to full-diet recommendation.
11 ASPIRATION AS A FUNCTION OF AGE, SEX, LIQUID TYPE, BOLUS VOLUME, AND BOLUS DELIVERY ACROSS THE HEALTHY ADULT LIFE SPAN BUTLER healthy adults across the life span produced 6404 test swallows. 50% of the participants penetrated on 1 or more swallows 18% of the participants aspirated on 1 or more swallows Adults in the 8 th and 9th decades demonstrated a greater difference in PAS scores with increasing liquid viscosity Females demonstrated consistent PAS scores across liquid volumes Males PAS scores increased with the 15 to 20 ml volumes The likelihood of aspiration and penetration increased significantly with increasing liquid fat content as well as age Increased volume also increased aspiration odds
12 BUT The Patient Has A Diagnosis of Aspiration Pneumonia
13 Aspiration Pneumonia: A Review of Modern Trends DiBardino, 2015 A host of literature, mostly in the elderly, stroke victims, and nursing home population, associates documented dysphagia and presence of dysphagia risk factors with pneumonia. The patient population itself confounds analysis, as a number of studies associate age itself to aspiration pneumonia. These data are generated from patients diagnosed with pneumonia with no discrimination between aspiration pneumonitis, as we have defined it, and traditional community acquired pneumonia (CAP).
14 Aspiration Pneumonia: A Review of Modern Trends DiBardino, 2015 Dysphagia literature examining pneumonia risk factors classifies all pneumonia with the term aspiration pneumonia and combines all patients with pneumonia to generate end points. Aspiration pneumonia represents 5% to 15% of pneumonias in the hospitalized population. The ICD-9 code based reviews suggest an increasing incidence, making it the second most common diagnosis in Medicare patients who are hospitalized [2,44]. However, higher reimbursement rates for this ICD-9 code than for CAP ICD-9 codes may falsely increase the frequency in this population.
15 Aspiration: /aspə rāsh(ə)n/: Noun: An Ambiguous Term Used for a Diagnosis of Uncertainty Ferguson 2018 The commonly used term, aspiration pneumonia, is misleading to clinicians and should be abandoned This terminology may be considered lazy or dangerous and are often used when the diagnosis is uncertain, leading to a false sense of security by clinicians. Often in the face of clinical uncertainty, the term aspiration event is utilized. There is no uniform definition for the term aspiration pneumonia, no gold standard test to diagnose aspiration
16 Aspiration: /aspə rāsh(ə)n/: Noun: An Ambiguous Term Used for a Diagnosis of Uncertainty Ferguson 2018 The nasopharynx, oropharynx, lung, and esophagus share the same microbiome because of chronic microaspiration that occurs naturally, which varies by diet, age, and geographic location
17 Aspiration: /aspə rāsh(ə)n/: Noun: An Ambiguous Term Used for a Diagnosis of Uncertainty Ferguson 2018 An attempt to delineate whether it is a regular pneumonia or an aspiration pneumonia on the basis of a speech therapy evaluation is needless and inaccurate as dysphagia and chronic silent aspiration are often not witnessed, and unlikely to reduce recurrent pneumonia. A patient with a history of head and neck cancer, previous stroke, or neurological disorder is commonly reflexively diagnosed with aspiration pneumonia despite a lack of findings of dysphagia. Good oral care for all patients, however, especially after stoke, may prevent recurrent pneumonia episodes as poor dentition, care, and changes in salivary flow are more likely to lead to [bacterial]colonization
18 Pillars of Aspiration Pneumonia Ashford 2016 ASPIRATION PNEUMONIA Poor Oral Health High Number of Aspiration Swallows Severely Impaired Health
19 Myth: SLPs understand how to prescribe diets
20 WHAT INFORMATION DO CLINICIANS USE IN RECOMENDING ORAL VERSES NONORAL FEEDING IN OPROPHARYNGEAL DYSPHAGIC PATIENTS LOGEMANN 2008 There is little evidence regarding types(s) of information clinicians use to make the recommendation for oral or non-oral feeding in patients with oropharyngeal dysphagia. Part 1: Several small groups of clinicians were surveyed to obtain the variables used to make oral verses non oral recommendation 46 variables were identified The list of 46 variables was given to clinicians to rank the top 10 variables that were important 13 variables were identified
21 WHAT INFORMATION DO CLINICIANS USE IN RECOMENDING ORAL VERSES NONORAL FEEDING IN OPROPHARYNGEAL DYSPHAGIC PATIENTS LOGEMANN 2008 Part 2: 20 MBSS videos were sent to 23 clinicians Decisions: Oral Partially oral with nonoral feeding Nonoral Include which of the 13 variables influenced their decision
22 Frequency Rank Criterion Frequency % Kappa 1 Amt of aspiration 79.6% Frequency of aspiration 70.4% Diagnosis 44.6% History of pneumonia 40.4% Ability to complete postures 35.4% Cough ability 35% Severity of medical condition 32.0% Recovery prognosis 26.7% Respiratory status 22.6% Silent aspiration 22.4% Patient wishes 21.5% Alertness 21.3% Secretion management 11.7%
23 The Influence Of Food Texture And Liquid Consistency Modification On Swallowing Physiology And Function Steele 2015 This systematic review identified major gaps in the understanding of the impact of liquid consistency and food texture on swallowing physiology, both in healthy and disordered populations. With respect to objective measures that might be used to guide the classification of thickened liquids and texture modified foods, the review identified an absence of convention, particularly in terms of the shear rates that are used for reporting apparent viscosity. Exceptionally limited information is available for objective measurement of texture-modified foods.
24 Changing Diet Texture Study evaluated dietary intake over the course of a day in hospitalized patients older than 60 years comparing intake in patients consuming a regular diet to those consuming a texture modified diet Patients on the modified diet had a significantly lower nutritional intake in terms of energy and protein. 54% of patients on a texture modified diet were recommended a nutritional supplement, compared with 24% of patients on a regular diet. Wright 2005
25 Changing Diet Texture Compared with the normal diet the puréed and liquid diets were the ones with the most reduced: energy (31.4% and 39.9%, respectively), protein (45.4% and 79.8%, respectively) lipid (41.0% and 76.0%, respectively) contents. Viganó 2011
26 Thickened Liquids Despite the lack of evidence to support first-line use of thickened liquids, many clinicians continue to believe they are an effective intervention. (Wang 2016) In a 2005 survey of speech-language pathologists, respondents prescribed thickened liquids to 25% to 75% of patients with dysphagia. (Garcia 2005)
27 Thickened Liquids The Influence of Food Texture and Liquid Consistency Modification on Swallowing Physiology and Function: A Systematic Review (Steele 2015) Qualitative synthesis revealed two key trends with respect to the impact of thickening liquids on swallowing: Thicker liquids reduce the risk of penetration aspiration, but also increase the risk of post-swallow residue in the pharynx.
28 Thickened Liquids No strong evidence is available supporting the use of thickened liquids as an intervention for patients with dysphagia. Sura et al Dehydration occurred to a significant degree in the presence of thickened liquids. Logemann 2003 Dehydration in the elderly can lead to: Hypotension Falls Constipation UTI Confusion Delirium Poor recovery from illness
29 Thickened Liquids Complications that may arise from thickeners: Slow gastric emptying Increase risk of reflux Reduce appetite
30 Thickening agents used for dysphagia management: effect on bioavailability of water, medication and feelings of satiety Cichero 2013 Dehydration may be due to physiological expectations that thick fluids will make them feel full Flavor suppression associated with increasing thickness provides little motivation to drink. The mucoadhesive qualities of thickeners leave the mouth feeling sticky after a drink rather than wet, resulting in continuing unresolved feelings of thirst Administration of medication with thickened liquids needs careful consideration and consultation with a pharmacist as effects of delayed dissolution and disintegration have been demonstrated
31 Thickening Agents Used For Dysphagia Management: Effect On Bioavailability Of Water, Medication And Feelings Of Satiety Cichero 2013 This literature review suggests that individuals prescribed very thick liquids (e.g. pudding-thick) will struggle to meet hydration needs orally. Individuals receiving moderately thick (e.g. honey-thick or nectar thick ) will also perceive their drinks to be more filling and will consume less than those on unthickened beverages. Use of Thickened Liquids in Skilled Nursing Facilities Castellanos 2004 A mean of 8.3% (range 0% to 28%) of residents were receiving thickened liquids, with considerable variation regions. Of those receiving thickened liquids, on average 60% received nectar/syrup thick, 33% received honey thick, and 6% received pudding/spoon thick.
32 Defining Physical Properties Of Fluids For Dysphagia Evaluation And Treatment Robbins 2002 The generally accepted clinical notion that manipulation of thicker (more viscous) substances reduces occurrence of aspiration, or modifies other bolus flow characteristics in dysphagic persons that produce an improved swallow, has little support, other than anecdotal, in the literature. Despite the paucity of data, the manipulation of thickness in the diet has become a cornerstone of dysphagia management practice.
33 HOW THICK IS THICK? MULTICENTER STUDY OF THE RHEOLOGICAL AND MATERIAL PROPERTY CHARACTERISTICS OF MEALTIME FLUIDS AND VIDEOFLUOROSCOPY FLUIDS CICHERO 2000 There is poor correlation between the viscosity of thickened liquids used during videofluoroscopic tests and the viscosity of liquids prepared to the same target levels for patients during mealtime.
34 The Horrible Taste Of Nectar And Honey Inappropriate Use Of Thickened Liquids In Dementia Wang 2016 Use of thickened liquids reduces videofluoroscopic evidence of aspiration in older adults with dementia but does not reduce the 3-month risk of pneumonia in the same population.
35 Malnutrition 15% of community-dwelling and home-bound elderly, 23% to 62% of hospitalized patients and up to 85% of nursing home residents suffer from malnutrition. Ahmed 2010
36 Malnutrition The prevalence of malnutrition increases in the geriatric population and is associated with a decline in: functional status impaired muscle function decreased bone mass immune dysfunction anemia Ahmed 2010
37 Malnutrition Effects of Malnutrition: reduced cognitive function poor wound healing delayed recovery from surgery higher hospital readmission rates mortality Ahmed 2010
38 Malnutrition Effects of malnutrition Respiratory problems Cardiac problems Infections DVT Multi-organ failure Brownie 2005
39 Malnutrition Brownie 2005 states: Malnutrition exacerbates existing medical conditions, increases risk of complications, leads to a decline in functional status and is associated with increased demands on medical services, lengthier hospital stays, readmission, early institutionalization and decreased survival time.
40 Malnutrition Aging is associated with decreased intracellular fluid and lean body mass. This correlates with altered physiological responses: Reduced cellular capacity to store water A decline in strength, balance and muscle mass Increased truncal obesity These changes predispose older people to dehydration, reduced basal metabolism, falls, injury, and central weight gain Noticeable changes in body composition often go unnoticed because the proportion of fat generally increases causing the total body weight to remain relativity stable. Brownie 2005
41 Malnutrition Modifying the consistency of solid food and/or liquid is a mainstay of compensatory intervention for patients with dysphagia. (Sura 2012) A recent survey (n=357) indicated : 53% of SLPs report they have no training in nutrition 77% of SLPs consult a dietitian 50% or less of the time when recommending a diet change 20% of SLPs report 0 consultations with a dietitian when changing a diet in the past 12 months Bice 2018
42 Malnutrition The nutritional consequence of a reduced lean body mass results in a reduced metabolic rate, and a proportional decline in total energy (caloric) requirements. This has serious implications for the diet, specifically in the adequacy of protein and micronutrient intake. In light of a reduced energy requirement, the quality of food selected by older people becomes vitally important, and food choices are a crucial determinant of optimal health. High-quality, nutrient dense foods are needed to preserve muscle mass. Brownie 2005
43 Malnutrition Diet software analysis in a particular study revealed modified diets contain fewer calories than regular diets (analyzed for a 5 week menu cycle). On average pureed trays provided 1700 kcal/day Regular texture provided 2100 kcal/day Another study directly analyzed food from 3 consecutive days in ten facilities. Average energy provided per day: Regular diet 2413 with 13% protein Chopped 2055 with 12% protein Pureed 2174 with 11% protein Keller 2012
44 Malnutrition A different study used weighted food records. Those on an altered diet consumed a significantly lower amount of energy (923 verses 1456 kcal) and protein (40 verses 60 g). A study using a plate waste method with 215 residents from several facilities found those who consumed an altered diet consumed significantly less energy, protein, calcium and vitamin D. Keller 2012
45 Malnutrition Study evaluated dietary intake over the course of a day in hospitalized patients older than 60 years, comparing intake in patients consuming a regular diet to those consuming a texture modified diet. Patients on the modified diet had a significantly lower nutritional intake in terms of energy and protein. 54% of patients on a texture modified diet were recommended a nutritional supplement, compared with 24% of patients on a regular diet. Wright 2005
46 Malnutrition Compared with the normal diet, the puréed and liquid diets were the ones with the most reduced: energy (31.4% and 39.9%, respectively), protein (45.4% and 79.8%, respectively) lipid (41.0% and 76.0%, respectively) contents. Viganó 2011
47 Malnutrition Patients who consumed an altered diet had decreased skeletal muscle mass Decrease FIM scores were independently related to texture modified diets Over half the patients on altered diets were malnourished Energy and protein intake were significantly lower Shimizu 2017
48 Malnutrition Traditional dietary intervention methods intended to improve the nutritional status of long-term care residents without dysphagia are not necessarily evidenced-based. Dunne 2007
49 Malnutrition Standardized markers or characteristics to diagnosis malnutrition include identification of two of six characteristics: insufficient energy intake weight loss loss of muscle mass bioelectric impedance (BIA) dual energy X-ray absorptiometry (DXA), computed tomography (CT) magnetic resonance imaging (MRI) Kline 2014
50 Malnutrition loss of subcutaneous fat localized or generalized fluid accumulation that may sometimes mask weight loss diminished functional status as measured by hand grip strength Kline 2014
51 Dysphagia and Dietary Levels in Skilled Nursing Facilities Groher nursing home residents on mechanically altered diets Swallowing evaluation including: Medical history Physical examination FEES MBSS Detailed observation of 2 meals Sustained attention Posture Self feeding skills
52 Dysphagia and Dietary Levels in Skilled Nursing Facilities GROHER 1995 Appropriate diet levels were determined by: Integrity of physical examination Xerostomia Deglutitory muscle strength Secretion and food management Cognitive status Ability to feed self History of aspiration pneumonia General health status Overall abilities during mealtime Diet level was not considered to be changed unless the resident tolerated for 30 days without >2% weight loss and no pneumonia
53 Dysphagia and Dietary Levels In Skilled Nursing Facilities Groher % were able to eat diets above the prescribed diet level 4% were consuming diets above an appropriate level 5% were considered to be at the appropriate diet level
54 Feed Tubes Are Safe
55 Feeding Tubes Make Patients Safe No published randomized trials that compare tube feeding with oral feeding. There is no data to suggest that tube feeding improves any of these clinically important outcomes and some data suggests it does not: Reduce risk of aspiration pneumonia Prolong survival Reduce the risk of pressure sores Reduce risk of infections Improve function Provide palliation Finucane 1999
56 Feeding Tubes Make Patients Safe Over the last 2 decades, research has failed to demonstrate benefits of tube feeding in patients with advanced dementia. Expert opinion and position statements by national organizations increasingly advocate against this practice. Mitchell 2016
57 Feeding Tubes Make Patients Safe Aspiration pneumonia is among the most serious complication of gastrostomy tube feedings. However, few data are available from the nursing home setting where tube feedings are used for extended periods. Reviewed 109 nursing facility charts in order to determine the incidence of, and risk factors for, aspiration pneumonia: 22.9% of gastrostomy tube-fed patients aspirated. A history of recent previous pneumonia was found in 40.7% of those who subsequently developed aspiration pneumonia. Cogen 1989
58 Aspiration = Risk
59 Risk can be measured/we can make our patients safe List of valid tools that measure patient risk of aspiration: The risk of aspiration is an emotional response of the clinician not a pathophysiology in the patient. -Dr. Michael Crary
60 Possible risk? Predictors Dependent for feeding Number of decayed teeth Multiple medical diagnoses Current smoker Number of medications Dependent for oral care Tube fed Langmore 1998
61 Risk can be measured/we can make our patients safe Healthy normals aspirate so What is a safe swallow? Maintain nutrition? Maintain hydration? No pneumonia? No coughing/choking? Patient feels they have good quality of life?
62
63 Imaging Assessments Result in Objective Information
64 Subjective Assessment of Videofluoroscopic Swallow Studies LEE 2017 Seventy-six VFSS videos of patients with dysphagia were presented to blinded, experienced speechlanguage pathologists and laryngologists Evaluators rated each video as normal or abnormal for hyoid elevation pharyngeal area pharyngeal area constriction (PCR) Pharyngoesophageal segment opening A blinded investigator assessed evaluators inter- and intrarater agreement and compared their responses to objectively measured results for these parameters to examine accuracy.
65 Subjective Assessment of Videofluoroscopic Swallow Studies LEE 2017 Evaluators correctly classified only 61.5% of VFSS videos as normal or abnormal Agreement was highly variable Accuracy: PCR at 71.6% Hyo-laryngeal elevation was 61.3% PES opening was 59.2% Pharyngeal area was 45.3% Evaluators unanimously agreed on a correct interpretation of a VFSS only 28% of the time
66 Subjective Assessment of Videofluoroscopic Swallow Studies LEE 2017 Subjective assessment of VFSS parameters is inconsistently accurate when compared with objective measurements, with accuracy ratings ranging from 45.3% to 71.6% for specific parameters
67 Interjudge Agreement in Videofluoroscopic Studies of Swallowing Wilcox therapists were given 3 recorded studies along with patient history and the results of the clinical swallow evaluation Clinicians spent 30 to 60 minutes reviewing the tape More time than usual Typically did not view tapes out of the radiology suite Clinicians reported they typically were only concerned with the presence or absence of aspiration Poor agreement across all areas
68 ELUCIDATING INCONSISTENCIES IN DYSPHAGIA DIAGNOSTICS: REDEFINING NORMAL PLOWMAN 2018 Clip Rated normal swallow within normal limits Rated normal swallow as disordered Average
69 Survey of Clinician Decision Making When Identifying Swallowing and Determining Treatment Vose Swallows Easy: swallow delay Moderate: swallow delay, duration of LVC, duration and amount of UES opening Complex: LVC reaction time, duration of LVC, amount and duration of UES opening
70 Easy Swallow 88% identified the issue 77% identified 5-9 issues 27% identified 10+ issues
71 Moderate Swallow identified all four issues 59% amount of UES opening 49% duration of UES opening 46% delayed swallow initiation 39% duration of LVC
72 Complex Swallow 0% identified all 4 impairments 68% amount of UES opening 65% LVC reaction time 54% duration of UES opening 53% duration of LVC
73 Observer Agreement of Measurements in FEES Pilz 2015 Two evaluators scored 60 FEES Prior to data collection raters completed an intensive training program on the rating scales of four visuoperceptual ordinal variables Piecemeal deglutition Post-swallow vallecular pooling Post-swallow pyriform sinus pooling Laryngeal penetration/aspiration
74 Observers Agreement on Measurements in FEES Pilz 2016 Intra- and inter-rater agreement on FEES measurements ranged from 0.76 to 0.93 (rater 1)and from 0.61 to 0.88 (rater 2) Bolus consistency resulted in decreased inter-rater agreement for all measured FEES variables during thin liquid swallows When rating on consensus, the raters deviated considerably from the scores they had previously given on the independent rating task
75 Dysphagia Therapy is Practiced as a Precise Science
76 WHAT IS USUAL CARE IN DYSPHAGIA REHABILITATION: A SURVEY OF USA DYSPHAGIA PRACTICE PATTERNS CARNABY 2013 The scope of dysphagia rehabilitation methods has been changing. Research has moved away from the use of behavioral compensations and maneuvers toward a greater emphasis on exercised-based therapy that emphasizes consistent, active muscle movement. Examples include: Lingual resistance exercises (IOPI) Expiratory Muscle Strength Training (EMST) McNeill Dysphagia Therapy Program (MDTP)
77 WHAT IS USUAL CARE IN DYSPHAGIA REHABILITATION: A SURVEY OF USA DYSPHAGIA PRACTICE PATTERNS CARNABY 2013 Data from new therapies suggests a stronger emphasis on exercise yields positive results that are superior to older management techniques of compensations and maneuvers. Although there is evidence supporting these active exercise approaches, it is unclear how many practicing SLPs are utilizing these techniques. Given this recent change in treatment emphasis, it is important to determine if practicing SLPs are incorporating best practice into their treatment approaches.
78 WHAT IS USUAL CARE IN DYSPHAGIA REHABILITATION: A SURVEY OF USA DYSPHAGIA PRACTICE PATTERNS CARNABY 2013 This study used a web-based survey method to target SLPs who treat adults with dysphagia in a variety of clinical settings throughout the US The ASHA s Special Interest Group 13 was used as the sampling frame because it provided a representative study population of experienced dysphagia clinicians.
79 WHAT IS USUAL CARE IN DYSPHAGIA REHABILITATION: A SURVEY OF USA DYSPHAGIA PRACTICE PATTERNS CARNABY surveys were analyzed Assessment information: 55% SLPs reported using either self-developed assessment/outcome measures 44% used facility-developed measures 37 % reported using published peer reviewed tools 29 % reported that they used only published tools with statistically confirmed validity
80 WHAT IS USUAL CARE IN DYSPHAGIA REHABILITATION: A SURVEY OF USA DYSPHAGIA PRACTICE PATTERNS CARNABY 2013 Therapy techniques used were derived from: 92% postgraduate CEU courses 70% learned from colleagues 44 % self developed 20% from professional journal articles
81 WHAT IS USUAL CARE IN DYSPHAGIA REHABILITATION: A SURVEY OF USA DYSPHAGIA PRACTICE PATTERNS CARNABY different techniques were recommended 3.9% were based on physiologic abnormality identified from data provided 96 different combinations were recommended with no single combination exactly repeated 58% did not match the patient's specific dysphagic symptoms 13% of interventions were exercise based
82 WHAT IS USUAL CARE IN DYSPHAGIA REHABILITATION: A SURVEY OF USA DYSPHAGIA PRACTICE PATTERNS CARNABY % of SLPs believed the patient improved more than 50% of the time (improving diet) 19% of SLPs reported return to full oral diet without restrictions as a typical outcome of therapy Common causes for not regaining pre-injury diet: Progression of premorbid disease Cognition
83 WHY DO CLINICIANS CHOOSE THE THERAPIES AND TECHNIQUES THEY DO? MCCURTIN 2017 Item/Technique % always/freq. use % never/rarely use 1 Texture modification Thickening liquid Positioning changes Double swallow Adapted utensils Volume regulation Physical support Effortful swallow Shaker maneuver
84 WHY DO CLINICIANS CHOOSE THE THERAPIES AND TECHNIQUES THEY DO? MCCURTIN 2017 Reason for using It is suitable for my clients Based on my clinical experience It is more concrete than abstract It is theoretically sound Experts recommend it % of responses I learned it in school
85 An Exercise is an Exercise is an Exercise
86 Exercise Principles In the study of exercise science, there are several universally accepted scientific exercise training principles that must be followed in order to get the most from exercise programs These fundamental rules are the force behind the ability to change any system
87 Exercise Principles Individual differences Overload Specificity Progression Adaptation Use/Disuse Reversibility
88 Individual Differences Patient s impairments have a different etiology Stroke Parkinson s Disease Cancer Many others Patients have different pathophysiology Imaging is necessary Patients have different availability Adapt therapy to the patient, not the patient to the program
89 Overload Exercise efforts that do not force the neuromuscular system beyond the level of usual activity will not elicit adaptations. By challenging the system beyond typical use, adaptations occur to accommodate the increased demand. Engaging in exercise that is not intense enough to push the system beyond the level of activity to which it is accustomed will not result in adaptation. Burkhead 2007 Examples: Lip protrusion and retraction Effortful swallow
90 The concept of One Rep Max Maximum muscle force output during a single repetition is called One Repetition Maximum or One Rep Max The number of reps that one can perform before fatiguing varies according to the percentage of the 1 RM Performing an exercise where more than 30 reps can be completed does not efficiently increase muscle strength % 1 RM REPS 100% 1 80% 10 60% 15 50% 20 40% 25 30% 30 Inadequate intensity to generate strength increases
91 Strength Training Early changes in strength training are generally the result of modifications in how the nervous system activates the muscle rather than a structural alteration in the muscle itself Improved performance may be the result of an increased number of motor units recruited or improved speed and coordination of motor unit recruitment These early alterations in neural activation can improve force production, coordination, and precision of movement. As a training program progresses, strength gains appear to be more the result of morphologic changes within muscle tissue (6 8 weeks)
92 Strength in swallowing What tools do we have to objectively measure strength? For example: Current standard of care during a CSE is to have the patient push their tongue against a tongue depressor to determine strength. Well, how much should they push and how good are we at assessing this? Does experience make us better at figuring it out? Clark 2003: Over all a weak to moderate correlation exists between the therapist vs IOPI measurements. In the study those with minimal experience (students) were better than experienced raters (0.696 verses 0.395).
93 Strength in swallowing The second issue is, are me measuring the right thing? Bu Sha 2000: Using a tongue protrusion task, normal adults generated the greatest force on a transducer 2.5 cm behind the teeth. Pharyngeal residue Strength? Spasticity/Tone? ROM? Sequencing? TBR?
94 Fatigue Kays 2010 Studied 22 healthy adults Two age groups (young adults and older adults) Measured P max and Endurance (50% of Pmax) twice before the meal and once after? Why the difference? No explanation Provided a meal of a bagel with peanut butter, carrot sticks, and 8 oz of chocolate milk All subjects showed reduced strength and endurance post meal. Young adults showed greater decrease in anterior tongue Pmax than older adults
95 Fatigue Ravenhorst-Bell 2012 N=20 all older adults Served the regular lunch at an ALF Measured Pmax and Endurance (50% of Pmax) After the meal both Pmax and Endurance improved to the level of statistical significance. Solomon 2006: The dilemma remains to explain and document the persistent issue of fatigue in the dysphagia literature
96 Fatigue Wouldn t we need to answer a few questions before using the word to describe our patient? Was there sufficient force before the task began? Fatigue verses some other condition How much force is needed to perform the activity? How was it measured before the activity started? How was it measured before the f-word was documented? What impact does fatigue have on the system?
97 Specificity This principle simply states that exercising a certain body part or component of the body primarily develops that part Change in performance related to exercise involves a complex constellation of both central and peripheral adaptations. Adding specificity to any training regimen directs the focus toward a common goal.
98 Specificity Swallowing is the best exercise for swallowing. Practicing something incorrectly only reinforces the incorrect pattern. Perfect practice makes perfect. Having someone with dysphagia consume a meal during therapy and simply counting the coughs, throat clears, etc., yields nothing. The patient is simply practicing a dysphagic swallow while the therapist is present. Diet trials and observation of meal times day after day needs to be removed from the tool box
99 Specificity Most motor skills do not generalize across tasks. Research supports this concept in swallowing therapy. Several of studies have documented increased size of cortical representation of the tongue following completion of a tongue protrusion activity. However, it does the activity does not result in an increase was of representation of the cortical masticatory area/swallow cortex. This indicates task specificity of plasticity in the motor cortex. It is important that training involves exercise that replicates the desired task: swallowing.
100 Progression In order to continue to make gains the load must be systematically and progressively increased To maximize gains over time, the absolute value of load placed on the muscle must be progressively adjusted over the course of the exercise program. This practice, known as progressive resistance, is necessary to maintain the relative physiologic load as a proportion of the maximal forcegenerating capacity. Burkhead 2007 How can this be accomplished in dysphagia therapy?
101 Progression Bolus selection is determined based on the patient s swallowing dysfunction: Increasing viscosity places an increase demand on pressure and force (Miller 1996, Watts 2015, Nagy 2015) Possibly challenges strength/pressure required Increasing bolus size requires a faster swallow Challenges timing, triggering, sequencing (Chi-Fishman 2002, Barikroo 2015) Bolus taste and temperature impact the swallow as well (Pelletier 2006) If the patient s swallow behavior does not meet the desired target consider changing the bolus (size, viscosity, taste, temperature)
102 Adaptation The activity must be performed with adequate duration for the system to realize there is a need for change. Exercise task must exceed usual levels of activity and be performed for an adequate duration (within a session and over time) to trigger the need for changing the system s response. With that premise, intensity can be defined on three levels: the mechanical or resistive load placed on the system amount or repetition of practice during the training regimen, and duration of training over time. Each of these levels of intensity has proven critical in bringing about neuromuscular adaptations.
103 Adaptation The length of therapy sessions and the time focused on actual treatment within each session matters For every minute you spend chatting with your patient you are wasting a minute of therapy Payment continues to decrease our available time with patients Make the most of the time you have
104 Use it or lose it (Use/Disuse) Animal studies have shown again and again how plasticity can be induced in the brain through extended training Synaptogenesis in the contralateral side of the brain in the presence of unilateral damage has occurred and been found to be dependent on behavior after the injury. Think about constraint therapy. Of course, the issue is there must be intentional good use. If simply random swallowing improved swallowing the fact that we swallow saliva and eat would be the only therapy we would ever need.
105 Use it or lose it (Use/Disuse) Practicing something incorrectly may only reinforce the aberrant patterns of behavior We have to use a skill or movement with increased competence-which can be measured in various ways such as efficiency and accuracy. Robbin 2008: The immediate lesson for the swallowing clinician, however is that trainingeven the training of a patient who is aspirating and at high risk for pulmonary or other health consequences-appears preferable to merely observing and documenting.
106 Reversibility Effects of training are lost when training stops and can gain the effects Detraining occurs within a relatively short time period after training ceases Performance reductions may occur in as little as two weeks or sooner
107 An Exercise is An Exercise Is An Exercise PART 2
108 Neuroplasticity Factors supporting the rehabilitation potential of many patients with dysphagia: Dysphagia research and clinical evidence indicate that positive neuroplastic changes are possible even in the presence of chronic conditions, multi-system atrophy and advanced age. Neuroplastic improvements following disease can include: Reorganization of cortical representation Increased efficiency of residual pathways Greater use of alternative descending pathways
109 Neuroplastic Principles When developing a treatment plan it is necessary to consider neuroplastic principles to maximize treatment impact - Use it or lose it - Use it and improve it - Repetition matters - Intensity matters - Plasticity is experience specific - Salience - Difficulty - Transference Kleim & Jones, JSLHR, 2008 Robbins et al, JSLHR 2008
110 Use It Or Lose It Factors that must be considered: What is being trained? How is the system being challenged? Is the system being used and engaged to maximize functional outcomes? Plowman 2016
111 Use It And Improve It With increased biological activity future functioning is enhanced. The object is not to merely use a function but to use it with increasing competence (efficiency/accuracy) Simply swallowing does not improve the swallow Goals must be determined and performance evaluated Plowman 2016
112 Repetition Matters Neural Substrates may be modified by extensive and prolonged practice Considerations for therapy: - number of repetitions - number of treatment sessions - treatment duration - speed of presentation Plowman 2016
113 Repetitions in 60 minutes TRIALS Kleim et al Reconsidering Swallowing: What is Normal How perspective impacts behavior Why understanding normal is important Reviewing normal physiology
114 Intensity Matters No adaptions will occur if the muscle(s) is not forced beyond typical activity level Plowman 2016
115 Specificity (Experience Specific) Consider what is being repeated and work to enhance accuracy, quality, coordination and strength Changes only occur in the neural substrates engaged in the trained behavior The type of training will determine the functional outcome (skill versus strength versus endurance) Plowman 2016
116 Salience Only behaviorally relevant experiences cause neuroplastic changes Best induced with movement that is purposeful and related to the behavior being trained The patient needs to be attentive to task The patient needs proprioceptive awareness of trial accuracy (errors/ success) Plowman 2016
117 Difficulty Difficulty level must be achievable to the patient - If the goal is unattainable the patient may lose interest and lose motivation Difficulty level must challenge the patient - This ensures attention and interest There must be systematic progression in targets - Progressive strength/load requirement - Increase demands on timing and coordination - Move to more complex/challenging food stimuli Plowman 2016
118 Transference Will training other systems target your goal and lead to functional improvements in swallowing? Is the training provided transferring to the targeted swallowing task? Plowman 2016
119 Conclusion
120 DETERMINING CLINICAL APPROPRIATENESS OF INTERVENTION What are my patient s wishes? What physiological Deficits that need to be rehabilitated? What are the research based interventions? Do I have a strong rationale?
121 Suggestions for Critical Evaluation of an Approach Where did you hear about it? Most responsible researchers will willingly offer their work for peer review and critique as a necessary step in working toward acceptance. Thus, research that eventually makes it to press has a much higher chance of presenting unbiased and well-substantiated information. Critically evaluate even what you read in journals with a keen eye on methodology, underlying theoretical support, and evaluative measures. Search the literature for replications of the research that supports the technique. Consider the professional and personal implications of utilization of the technique as being equally important as the possible implications for patient care. Recall your responsibility to the ASHA Code of Ethics under which we all practice. Huckabee 1997
122 In order to effectively treat dysphagia we must rely on EBP
Daniels SK & Huckabee ML (2008). Dysphagia Following Stroke. Muscles of Deglutition. Lateral & Mesial Premotor Area 6. Primary Sensory
 An Overview of Dysphagia in the Stroke Population Stephanie K. Daniels, PhD Michael E. DeBakey VA Medical Center PM & R, Baylor College of Medicine Communication Sciences and Disorders, University of Houston
An Overview of Dysphagia in the Stroke Population Stephanie K. Daniels, PhD Michael E. DeBakey VA Medical Center PM & R, Baylor College of Medicine Communication Sciences and Disorders, University of Houston
SWALLOWING DIFFICULTIES IN HD
 Nutrition, eating and swallowing needs, challenges and solutions Workshop SWALLOWING DIFFICULTIES IN HD Angela Nuzzi Speech and Language Pathologist (SLP) EHDN Language Coordinator - Italy The role of
Nutrition, eating and swallowing needs, challenges and solutions Workshop SWALLOWING DIFFICULTIES IN HD Angela Nuzzi Speech and Language Pathologist (SLP) EHDN Language Coordinator - Italy The role of
5 Things I Want You to Know About Dysphagia. Prof Maggie-Lee Huckabee The University of Canterbury Rose Centre for Stroke Recovery and Research
 5 Things I Want You to Know About Dysphagia Prof Maggie-Lee Huckabee The University of Canterbury Rose Centre for Stroke Recovery and Research 5 things 1) Why we can t diagnose dysphagia at bedside. 2)
5 Things I Want You to Know About Dysphagia Prof Maggie-Lee Huckabee The University of Canterbury Rose Centre for Stroke Recovery and Research 5 things 1) Why we can t diagnose dysphagia at bedside. 2)
Evidenced Based Practice in Dysphagia. Houston We Have a Problem
 Evidenced Based Practice in Dysphagia Houston We Have a Problem HOUSTON, WE HAVE A PROBLEM THE ALARM WILL SOUND, EVENTUALLY Rosenbeck 1995 In 1969 an alarm sounded throughout the aphasiology community
Evidenced Based Practice in Dysphagia Houston We Have a Problem HOUSTON, WE HAVE A PROBLEM THE ALARM WILL SOUND, EVENTUALLY Rosenbeck 1995 In 1969 an alarm sounded throughout the aphasiology community
Swallowing Screen Why? How? and So What? พญ.พวงแก ว ธ ต สก ลช ย ภาคว ชาเวชศาสตร ฟ นฟ คณะแพทยศาสตร ศ ร ราชพยาบาล
 Swallowing Screen Why? How? and So What? พญ.พวงแก ว ธ ต สก ลช ย ภาคว ชาเวชศาสตร ฟ นฟ คณะแพทยศาสตร ศ ร ราชพยาบาล Dysphagia in Stroke The incidence of dysphagia after stroke ranging from 23-50% 1 Location
Swallowing Screen Why? How? and So What? พญ.พวงแก ว ธ ต สก ลช ย ภาคว ชาเวชศาสตร ฟ นฟ คณะแพทยศาสตร ศ ร ราชพยาบาล Dysphagia in Stroke The incidence of dysphagia after stroke ranging from 23-50% 1 Location
Factors Associated With Compliance With Viscosity-Modified Diet Among Dysphagic Patients Jae Seong Shim, MD, Byung-Mo Oh, MD, Tai Ryoon Han, MD
 Original Article Ann Rehabil Med 2013;37(5):628-632 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2013.37.5.628 Annals of Rehabilitation Medicine Factors Associated With Compliance With
Original Article Ann Rehabil Med 2013;37(5):628-632 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2013.37.5.628 Annals of Rehabilitation Medicine Factors Associated With Compliance With
Normal and Abnormal Oral and Pharyngeal Swallow. Complications.
 ESPEN Congress Gothenburg 2011 Assessment and treatment of dysphagia What is the evidence? Normal and Abnormal Oral and Pharyngeal Swallow. Complications. Pere Clavé Educational Session. Assessment and
ESPEN Congress Gothenburg 2011 Assessment and treatment of dysphagia What is the evidence? Normal and Abnormal Oral and Pharyngeal Swallow. Complications. Pere Clavé Educational Session. Assessment and
Review of dysphagia in poststroke
 Review of dysphagia in poststroke patients Danielle Thompson, Speech and Language Therapist Northwick Park Hospital With acknowledgement to Mary McFarlane, Principal Speech and Language Therapist, Acute
Review of dysphagia in poststroke patients Danielle Thompson, Speech and Language Therapist Northwick Park Hospital With acknowledgement to Mary McFarlane, Principal Speech and Language Therapist, Acute
Clinical Swallowing Exam
 Clinical Evaluation Template 1 Clinical Exam Name: ID/Medical record number: Date of exam: Referred by: Reason for referral: Medical diagnosis: Date of onset of diagnosis: Other relevant medical history/diagnoses/surgery
Clinical Evaluation Template 1 Clinical Exam Name: ID/Medical record number: Date of exam: Referred by: Reason for referral: Medical diagnosis: Date of onset of diagnosis: Other relevant medical history/diagnoses/surgery
ESSD. EUGMS-ESSD Working Group on Oropharyngeal Dysphagia. 9 th Congress of the European Union Geriatric Medicine Society (EUGMS)
 ESSD EUGMS-ESSD Working Group on Oropharyngeal Dysphagia 9 th Congress of the European Union Geriatric Medicine Society (EUGMS) ESSD European Society for Swallowing Disorders (ESSD). ESSD Mission. The
ESSD EUGMS-ESSD Working Group on Oropharyngeal Dysphagia 9 th Congress of the European Union Geriatric Medicine Society (EUGMS) ESSD European Society for Swallowing Disorders (ESSD). ESSD Mission. The
Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing
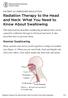 PATIENT & CAREGIVER EDUCATION Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing This information describes swallowing problems that can be caused by radiation therapy to the
PATIENT & CAREGIVER EDUCATION Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing This information describes swallowing problems that can be caused by radiation therapy to the
The Clinical Swallow Evaluation: What it can and cannot tell us. Introduction
 The Clinical Swallow Evaluation: What it can and cannot tell us Debra M. Suiter, Ph.D., CCC-SLP, BCS-S Director, Voice & Swallow Clinic Associate Professor, Division of Communication Sciences & Disorders
The Clinical Swallow Evaluation: What it can and cannot tell us Debra M. Suiter, Ph.D., CCC-SLP, BCS-S Director, Voice & Swallow Clinic Associate Professor, Division of Communication Sciences & Disorders
RECOMMENDATIONS & UPDATES IN THE MANAGEMENT OF POST- STROKE DYSPHAGIA
 RECOMMENDATIONS & UPDATES IN THE MANAGEMENT OF POST- STROKE DYSPHAGIA Feeding in the Acute Stroke Period: - Early initiation of feeding is beneficial w/c decreases the risk of infections, improve survival
RECOMMENDATIONS & UPDATES IN THE MANAGEMENT OF POST- STROKE DYSPHAGIA Feeding in the Acute Stroke Period: - Early initiation of feeding is beneficial w/c decreases the risk of infections, improve survival
Main Aspects of the Management of Neurogenic Dysphagia
 Main Aspects of the Management of Neurogenic Dysphagia Mario Prosiegel/München German Society of Neurology (DGN) prosiegel@t-online.de DYSPHAGIA October 8-10, 2015 Pavia, Italy Overview Diagnosis Causal
Main Aspects of the Management of Neurogenic Dysphagia Mario Prosiegel/München German Society of Neurology (DGN) prosiegel@t-online.de DYSPHAGIA October 8-10, 2015 Pavia, Italy Overview Diagnosis Causal
When Eating Becomes A Challenge Dysphagia
 When Eating Becomes A Challenge Dysphagia 1. DYSPHAGIA, WHAT IS IT? 2. IMPLICATIONS 3. ASSESSMENT 4. COMPENSATORY SWALLOWING AND EXERCISES 5. DIET TEXTURE ADJUSTMENTS Swallowing Dysfunction = Dysphagia
When Eating Becomes A Challenge Dysphagia 1. DYSPHAGIA, WHAT IS IT? 2. IMPLICATIONS 3. ASSESSMENT 4. COMPENSATORY SWALLOWING AND EXERCISES 5. DIET TEXTURE ADJUSTMENTS Swallowing Dysfunction = Dysphagia
Section K Swallowing/ Nutritional Status
 Instructor Guide Section K Swallowing/ Nutritional Status Objectives State the intent of Section K Swallowing and Nutritional Status. Describe how to conduct an assessment of a resident s nutritional status.
Instructor Guide Section K Swallowing/ Nutritional Status Objectives State the intent of Section K Swallowing and Nutritional Status. Describe how to conduct an assessment of a resident s nutritional status.
Filling the Nutritional Gap in Dysphagia
 Filling the Nutritional Gap in Dysphagia Krystel Ouaijan, RDN, MSc Nutrition Support Dietitian in Saint George Hospital UMC PhD in University of Geneva Krystel Ouaijan - Dubai -2018 1 Patient Profiles
Filling the Nutritional Gap in Dysphagia Krystel Ouaijan, RDN, MSc Nutrition Support Dietitian in Saint George Hospital UMC PhD in University of Geneva Krystel Ouaijan - Dubai -2018 1 Patient Profiles
Dysphagia as a Geriatric Syndrome Assessment and Treatment. Ashton Galyen M.A., CCC-SLP St. Vincent Indianapolis Acute Rehabilitation Unit
 Dysphagia as a Geriatric Syndrome Assessment and Treatment Ashton Galyen M.A., CCC-SLP St. Vincent Indianapolis Acute Rehabilitation Unit March 16, 2018 Ashton Galyen, M.A., CCC-SLP Master s degree in
Dysphagia as a Geriatric Syndrome Assessment and Treatment Ashton Galyen M.A., CCC-SLP St. Vincent Indianapolis Acute Rehabilitation Unit March 16, 2018 Ashton Galyen, M.A., CCC-SLP Master s degree in
Dysphagia and Swallowing. Jan Adams, DNP, MPA, RN and Karen Kern
 Dysphagia and Swallowing Jan Adams, DNP, MPA, RN and Karen Kern Scope of the Problem and Incidence 15 million people in the US have some form of Dysphagia. Every year, 1 million people are diagnosed with
Dysphagia and Swallowing Jan Adams, DNP, MPA, RN and Karen Kern Scope of the Problem and Incidence 15 million people in the US have some form of Dysphagia. Every year, 1 million people are diagnosed with
Dysphagia Treatment: What are We Doing, and Why?
 Dysphagia Treatment: What are We Doing, and Why? ASHA Convention, 2014; Orlando James L. Coyle, Ph.D., CCC SLP, BCS S University of Pittsburgh jcoyle@pitt.edu 1 Treatment 2 Aims, targets and ingredients
Dysphagia Treatment: What are We Doing, and Why? ASHA Convention, 2014; Orlando James L. Coyle, Ph.D., CCC SLP, BCS S University of Pittsburgh jcoyle@pitt.edu 1 Treatment 2 Aims, targets and ingredients
10/26/2017. Diagnostic Tests vs. Screening. Dysphagia Screening: What it is and what it is not
 Dysphagia Screening: What it is and what it is not Debra M. Suiter, Ph.D., CCC-SLP, BCS-S Director University of Kentucky Voice & Swallow Clinic Lexington, Kentucky ASHA's Preferred Practice Pattern on
Dysphagia Screening: What it is and what it is not Debra M. Suiter, Ph.D., CCC-SLP, BCS-S Director University of Kentucky Voice & Swallow Clinic Lexington, Kentucky ASHA's Preferred Practice Pattern on
Swallowing Disorders and Their Management in Patients with Multiple Sclerosis
 National Multiple Sclerosis Society 733 Third Avenue New York, NY 10017-3288 Clinical Bulletin Information for Health Professionals Swallowing Disorders and Their Management in Patients with Multiple Sclerosis
National Multiple Sclerosis Society 733 Third Avenue New York, NY 10017-3288 Clinical Bulletin Information for Health Professionals Swallowing Disorders and Their Management in Patients with Multiple Sclerosis
Speech and Language Therapy. Kerrie McCarthy Senior Speech and Language Therapist
 Speech and Language Therapy Kerrie McCarthy Senior Speech and Language Therapist Contents 1. Voice disorders 2. Swallow disorders 3. Videofluroscopy 4. Adult Acquired Communication Disorders 5. How to
Speech and Language Therapy Kerrie McCarthy Senior Speech and Language Therapist Contents 1. Voice disorders 2. Swallow disorders 3. Videofluroscopy 4. Adult Acquired Communication Disorders 5. How to
TREATMENT OF DYSPHAGIA IN PATIENTS AFTER STROKE IN ESTONIA
 TREATMENT OF DYSPHAGIA IN PATIENTS AFTER STROKE IN ESTONIA ANNE URIKO SPORTS MEDICINE AND REHABILITATION CLINIG OF TARTU UNIVERSITY HOSPITAL 17.09.2010 DYSPHAGIA DIFFICULTY MOVING FOOD FROM MOUTH TO STOMACH
TREATMENT OF DYSPHAGIA IN PATIENTS AFTER STROKE IN ESTONIA ANNE URIKO SPORTS MEDICINE AND REHABILITATION CLINIG OF TARTU UNIVERSITY HOSPITAL 17.09.2010 DYSPHAGIA DIFFICULTY MOVING FOOD FROM MOUTH TO STOMACH
DYSPHAGIA SCREENING and CLINICAL SWALLOW EVALUATIONS. Debra M. Suiter, Ph.D., CCC-SLP, BRS-S VA Medical Center-Memphis
 DYSPHAGIA SCREENING and CLINICAL SWALLOW EVALUATIONS Debra M. Suiter, Ph.D., CCC-SLP, BRS-S VA Medical Center-Memphis Suiter, ASHA, 2012 Diagnostic Tests vs. Screening Diagnostic tests are used when a
DYSPHAGIA SCREENING and CLINICAL SWALLOW EVALUATIONS Debra M. Suiter, Ph.D., CCC-SLP, BRS-S VA Medical Center-Memphis Suiter, ASHA, 2012 Diagnostic Tests vs. Screening Diagnostic tests are used when a
Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing
 PATIENT & CAREGIVER EDUCATION Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing This information describes swallowing problems that can be caused by radiation therapy to the
PATIENT & CAREGIVER EDUCATION Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing This information describes swallowing problems that can be caused by radiation therapy to the
Guideline of Videofluoroscopic Swallowing Study (VFSS) in Speech Therapy
 Page 1 of 9 Guideline of Videofluoroscopic Swallowing Study (VFSS) in Speech Therapy Version 1.0 Effective Date Document Number HKIST-C-VFG-v1 Author HKAST AR Sub-committee Custodian Chairperson of HKIST
Page 1 of 9 Guideline of Videofluoroscopic Swallowing Study (VFSS) in Speech Therapy Version 1.0 Effective Date Document Number HKIST-C-VFG-v1 Author HKAST AR Sub-committee Custodian Chairperson of HKIST
The Role of the Speech Language Pathologist & Spinal Cord Injury
 The Role of the Speech Language Pathologist & Spinal Cord Injury Facts According to the National Spinal Cord Injury Statistical Center (NSCISC) there are approxiamtely 12,000 new spinal cord injuries (SCI)
The Role of the Speech Language Pathologist & Spinal Cord Injury Facts According to the National Spinal Cord Injury Statistical Center (NSCISC) there are approxiamtely 12,000 new spinal cord injuries (SCI)
THE POTENTIAL IMPACT OF VITALSTIM THERAPY ON HEALTHCARE COSTS: A White PaperVitalStim Therapy has significant
 Dysphagia THE POTENTIAL IMPACT OF VITALSTIM THERAPY ON HEALTHCARE COSTS: A White PaperVitalStim Therapy has significant Contents potential to dramatically impact the health care costs arising from oropharyngeal
Dysphagia THE POTENTIAL IMPACT OF VITALSTIM THERAPY ON HEALTHCARE COSTS: A White PaperVitalStim Therapy has significant Contents potential to dramatically impact the health care costs arising from oropharyngeal
Chapter 19. Nutrition and Fluids. All items and derived items 2015, 2011 by Mosby, Inc., an imprint of Elsevier Inc. All rights reserved.
 Chapter 19 Nutrition and Fluids Nutrition Nutrition--processes involved in the ingestion, digestion, absorption & use of foods & fluids by the body. The person s diet affects physical & mental wellbeing
Chapter 19 Nutrition and Fluids Nutrition Nutrition--processes involved in the ingestion, digestion, absorption & use of foods & fluids by the body. The person s diet affects physical & mental wellbeing
Standardisation of Videofluoroscopy: Where is it taking us?
 Standardisation of Videofluoroscopy: Where is it taking us? Jodi Allen, Senior Speech and Language Therapist, The National Hospital for Neurology and Neurosurgery If somebody asked you. What do you start
Standardisation of Videofluoroscopy: Where is it taking us? Jodi Allen, Senior Speech and Language Therapist, The National Hospital for Neurology and Neurosurgery If somebody asked you. What do you start
OPTICS OPTimal nutrition by Informing and Capacitating family members of best nutrition practices OPTICS
 OPTICS OPTimal nutrition by Informing and Capacitating family members of best nutrition practices Educational Booklet for Families Version April 26 th 2016 Page 1 of 12 This information booklet was originally
OPTICS OPTimal nutrition by Informing and Capacitating family members of best nutrition practices Educational Booklet for Families Version April 26 th 2016 Page 1 of 12 This information booklet was originally
Palliative Care Swallowing Management HEATHER STORIE M.S.,CCC-SLP, BCS-S SPEECH LANGUAGE PATHOLOGY, BOARD CERTIFIED SWALLOWING SPECIALIST
 Palliative Care Swallowing Management HEATHER STORIE M.S.,CCC-SLP, BCS-S SPEECH LANGUAGE PATHOLOGY, BOARD CERTIFIED SWALLOWING SPECIALIST Objectives Gain a general understanding of normal swallowing Gain
Palliative Care Swallowing Management HEATHER STORIE M.S.,CCC-SLP, BCS-S SPEECH LANGUAGE PATHOLOGY, BOARD CERTIFIED SWALLOWING SPECIALIST Objectives Gain a general understanding of normal swallowing Gain
Nutrition at the Bedside
 Nutrition at the Bedside Linda Varnell, RD, LDN Clinical Dietitian February 26, 2010 Objectives Identify risk factors for malnutrition in the older adult Recognize physical signs of malnutrition Gain skills
Nutrition at the Bedside Linda Varnell, RD, LDN Clinical Dietitian February 26, 2010 Objectives Identify risk factors for malnutrition in the older adult Recognize physical signs of malnutrition Gain skills
Dysphagia after Stroke. Wendy Busby Stroke Service Dunedin Hospital
 Dysphagia after Stroke Wendy Busby Stroke Service Dunedin Hospital Incidence IN NEW ZEALAND 9,5000 new stroke per year Rate is decreasing More people surviving Major cause of disability in adults Prevalence
Dysphagia after Stroke Wendy Busby Stroke Service Dunedin Hospital Incidence IN NEW ZEALAND 9,5000 new stroke per year Rate is decreasing More people surviving Major cause of disability in adults Prevalence
2013 Charleston Swallowing Conference
 Providing Quality Affordable Continuing Education and Treatment Materials for over 30 years. 2013 Charleston Swallowing Conference Session 9 Bedside Assessment: What Does It Tell You? 10:00 11:30 am Saturday,
Providing Quality Affordable Continuing Education and Treatment Materials for over 30 years. 2013 Charleston Swallowing Conference Session 9 Bedside Assessment: What Does It Tell You? 10:00 11:30 am Saturday,
Stroke Management in the Long Term Care Setting - Clinical Practice Guideline. Continuing Professional Education Self-Study Course
 Stroke Management in the Long Term Care Setting - Clinical Practice Guideline Continuing Professional Education Self-Study Course Written by Liz Friedrich, MPH, RD, CSG, LDN, FAND Edited by Becky Dorner,
Stroke Management in the Long Term Care Setting - Clinical Practice Guideline Continuing Professional Education Self-Study Course Written by Liz Friedrich, MPH, RD, CSG, LDN, FAND Edited by Becky Dorner,
HOMES AND SENIORS SERVICES. APPROVAL DATE: August 1985 REVISION DATE: January 2015 REVIEW DATE: May 2018
 POLICY: Page 1 of 10 Residents who experience signs and symptoms associated with dysphagia will have their nutrition and hydration needs met in a safe, coordinated manner as managed by the interdisciplinary
POLICY: Page 1 of 10 Residents who experience signs and symptoms associated with dysphagia will have their nutrition and hydration needs met in a safe, coordinated manner as managed by the interdisciplinary
Critical Review: Is a chin-down posture more effective than thickened liquids in eliminating aspiration for patients with Parkinson s disease?
 Critical Review: Is a chin-down posture more effective than thickened liquids in eliminating aspiration for patients with Parkinson s disease? Nadia Torrieri, M.Cl.Sc. (SLP) Candidate The Unversity of
Critical Review: Is a chin-down posture more effective than thickened liquids in eliminating aspiration for patients with Parkinson s disease? Nadia Torrieri, M.Cl.Sc. (SLP) Candidate The Unversity of
Reluctance or refusal to feed or eat. Understanding Feeding Aversion in a City Full of Foodies. Presentation Outline. Learning Objectives
 Understanding Feeding Aversion in a City Full of Foodies Amy Houtrow, MD, MPH Pediatric Physical Medicine & Rehabilitation UCSF Department of Pediatrics June 2, 2007 Learning Objectives Learners will be
Understanding Feeding Aversion in a City Full of Foodies Amy Houtrow, MD, MPH Pediatric Physical Medicine & Rehabilitation UCSF Department of Pediatrics June 2, 2007 Learning Objectives Learners will be
PATIENT COMPLIANCE TIP SHEET Dietary Guidelines Following a Stroke
 PATIENT COMPLIANCE TIP SHEET Dietary Guidelines Following a Stroke A stroke may be very frightening to both the patient and family. It helps to remember that stroke survivors usually have at least some
PATIENT COMPLIANCE TIP SHEET Dietary Guidelines Following a Stroke A stroke may be very frightening to both the patient and family. It helps to remember that stroke survivors usually have at least some
Nutricia. Nutrition and Dysphagia
 Nutricia Nutrition and Dysphagia 1 Introduction What is Dysphagia? The inability to swallow normally or freely. Disorder in the swallowing process that does not allow safe passing of food from the mouth
Nutricia Nutrition and Dysphagia 1 Introduction What is Dysphagia? The inability to swallow normally or freely. Disorder in the swallowing process that does not allow safe passing of food from the mouth
Oral care & swallowing
 Oral care & swallowing Oral care is important as it has a role to play in preventing healthcare associated infections. Dental plaque and the oropharynx can become colonized by bacteria and a biofilm can
Oral care & swallowing Oral care is important as it has a role to play in preventing healthcare associated infections. Dental plaque and the oropharynx can become colonized by bacteria and a biofilm can
DYSPHAGIA MANAGEMENT IN ACUTE CARE AMANDA HEREFORD, MA, CCC- SLP
 DYSPHAGIA MANAGEMENT IN ACUTE CARE AMANDA HEREFORD, MA, CCC- SLP OVERVIEW Decision making re: swallowing in the medically compromised patient Swallow evaluation vs. Nursing Swallow Screening Instrumental
DYSPHAGIA MANAGEMENT IN ACUTE CARE AMANDA HEREFORD, MA, CCC- SLP OVERVIEW Decision making re: swallowing in the medically compromised patient Swallow evaluation vs. Nursing Swallow Screening Instrumental
Nutrition in children with special needs. Dr. Meenakshi J.
 Nutrition in children with special needs Dr. Meenakshi J. 1 Factors affecting growth and nutrition in children with special nutritional factors Inadequate intake primarily related to feeding dysfunction
Nutrition in children with special needs Dr. Meenakshi J. 1 Factors affecting growth and nutrition in children with special nutritional factors Inadequate intake primarily related to feeding dysfunction
Managing Nutrition and Unintended Weight Loss
 Managing Nutrition and Unintended Weight Loss Kathleen Niedert, PhD, RD, CSG, FADA, LNHA 2018 Spring Conference & Exhibitor Show May 2-3, 2018 OBJECTIVES Define the three main categories and three primary
Managing Nutrition and Unintended Weight Loss Kathleen Niedert, PhD, RD, CSG, FADA, LNHA 2018 Spring Conference & Exhibitor Show May 2-3, 2018 OBJECTIVES Define the three main categories and three primary
Karen Schoeneman Consul6ng 1
 + New Dining Standards of Practice How Do We Get There? Karen Schoeneman + How Did They Happen? 2 n CMS and Pioneer Network co-sponsored a symposium on the food and dining requirements, and culture change
+ New Dining Standards of Practice How Do We Get There? Karen Schoeneman + How Did They Happen? 2 n CMS and Pioneer Network co-sponsored a symposium on the food and dining requirements, and culture change
ROLE OF THE DIETITIAN. Aims of Dietetic Treatment NUTRITIONAL ISSUES WHY? MALNUTRITION NUTRITONAL MANAGEMENT OF MOTOR NEURONE DISEASE.
 NUTRITONAL MANAGEMENT OF MOTOR NEURONE DISEASE. ROLE OF THE DIETITIAN SALLY DARBY NEUROLOGY DIETITIAN Not just tube feeding Referral soon after diagnosis Advise on healthy eating for MND Monitor nutritional
NUTRITONAL MANAGEMENT OF MOTOR NEURONE DISEASE. ROLE OF THE DIETITIAN SALLY DARBY NEUROLOGY DIETITIAN Not just tube feeding Referral soon after diagnosis Advise on healthy eating for MND Monitor nutritional
15/11/2011. Swallowing
 Swallowing Swallowing starts from placement of the food in the mouth and continues until food enters the stomach. Dysphagia: any difficulty in moving food from mouth to stomach. Pharynx is shared for both
Swallowing Swallowing starts from placement of the food in the mouth and continues until food enters the stomach. Dysphagia: any difficulty in moving food from mouth to stomach. Pharynx is shared for both
Critical Review: Does treatment with levodopa improve swallowing function in patients with Parkinson s Disease?
 Copyright 2013 by Siwicky, M. Critical Review: Does treatment with levodopa improve swallowing function in patients with Parkinson s Disease? Siwicky, M. M.Cl.Sc SLP Candidate University of Western Ontario:
Copyright 2013 by Siwicky, M. Critical Review: Does treatment with levodopa improve swallowing function in patients with Parkinson s Disease? Siwicky, M. M.Cl.Sc SLP Candidate University of Western Ontario:
Dysphagia Identification and Management
 Dysphagia Identification and Management Presented By Speech-Language Pathologist Developmental Disabilities Administration DC Department on Disability Services Training Objectives After this training session
Dysphagia Identification and Management Presented By Speech-Language Pathologist Developmental Disabilities Administration DC Department on Disability Services Training Objectives After this training session
Information about Feeding Tubes
 Information about Feeding Tubes By Theresa Imperato, RN and Lorraine Danowski, RD What is a feeding tube? It is a small, flexible tube, about ¼ in diameter that is an alternative route for nourishment
Information about Feeding Tubes By Theresa Imperato, RN and Lorraine Danowski, RD What is a feeding tube? It is a small, flexible tube, about ¼ in diameter that is an alternative route for nourishment
Respiratory Swallow Coordination in Healthy Individuals
 Cloud Publications International Journal of Advanced Speech and Hearing Research 2012, Volume 1, Issue 1, pp. 1-9, Article ID Med-03 Research Article Open Access Respiratory Swallow Coordination in Healthy
Cloud Publications International Journal of Advanced Speech and Hearing Research 2012, Volume 1, Issue 1, pp. 1-9, Article ID Med-03 Research Article Open Access Respiratory Swallow Coordination in Healthy
Quick Death, Slow Death, Hopefully No Death
 Quick Death, Slow Death, Hopefully No Death Collaborative presentation on learning from choking and nutrition incidents in RWT. Introduction of IDDSI for food and fluids Why there is an NPSA Alert Safe
Quick Death, Slow Death, Hopefully No Death Collaborative presentation on learning from choking and nutrition incidents in RWT. Introduction of IDDSI for food and fluids Why there is an NPSA Alert Safe
Fact Sheet. VitalStim Therapy
 VitalStim Therapy Fact Sheet Dysphagia, or difficulty with swallowing, is a sorely neglected medical disorder that impacts as many as 15 million Americans, with approximately one million people annually
VitalStim Therapy Fact Sheet Dysphagia, or difficulty with swallowing, is a sorely neglected medical disorder that impacts as many as 15 million Americans, with approximately one million people annually
Dysphagia Management in TCP. Susan Smith and Vanessa Barkla Speech Pathologists, Ballarat Health Services May 2012
 Dysphagia Management in TCP Susan Smith and Vanessa Barkla Speech Pathologists, Ballarat Health Services May 2012 The role of the Speech Pathologist To assess swallowing status To provide management and
Dysphagia Management in TCP Susan Smith and Vanessa Barkla Speech Pathologists, Ballarat Health Services May 2012 The role of the Speech Pathologist To assess swallowing status To provide management and
VIDEOFLUOROSCOPIC SWALLOWING EXAM
 VIDEOFLUOROSCOPIC SWALLOWING EXAM INDENTIFYING INFORMATION May include the following: Name, ID/medical record number, date of birth, date of exam, referred by, reason for referral HISTORY/SUBJECTIVE INFORMATION
VIDEOFLUOROSCOPIC SWALLOWING EXAM INDENTIFYING INFORMATION May include the following: Name, ID/medical record number, date of birth, date of exam, referred by, reason for referral HISTORY/SUBJECTIVE INFORMATION
OPTICS OPTimal nutrition by Informing and Capacitating family members of best nutrition practices OPTICS
 OPTICS OPTimal nutrition by Informing and Capacitating family members of best nutrition practices Educational Booklet for Families Version June 16 2014 Page 1 of 11 This information booklet was originally
OPTICS OPTimal nutrition by Informing and Capacitating family members of best nutrition practices Educational Booklet for Families Version June 16 2014 Page 1 of 11 This information booklet was originally
SWALLOWING: HOW CAN WE HELP
 SWALLOWING: HOW CAN WE HELP Carol Romero-Clark, M.S., CCC-SLP University of New Mexico Hospital Speech Pathology Department November 10, 2017 What happens when you swallow? Mouth (Oral Phase) Your tongue
SWALLOWING: HOW CAN WE HELP Carol Romero-Clark, M.S., CCC-SLP University of New Mexico Hospital Speech Pathology Department November 10, 2017 What happens when you swallow? Mouth (Oral Phase) Your tongue
Pediatric Modified Barium Swallow Studies. Presented by Jody Bousquet, MA, CCC- SLP Susan Shonbrun, MS, CCC- SLP November 7, 2015
 Pediatric Modified Barium Swallow Studies Presented by Jody Bousquet, MA, CCC- SLP Susan Shonbrun, MS, CCC- SLP November 7, 2015 Definition * Modified Barium Swallow Study * Assesses swallow functions
Pediatric Modified Barium Swallow Studies Presented by Jody Bousquet, MA, CCC- SLP Susan Shonbrun, MS, CCC- SLP November 7, 2015 Definition * Modified Barium Swallow Study * Assesses swallow functions
PEG Tube use in the Elderly
 PEG Tube use in the Elderly Jeffrey Wallace MD, MPH Professor and Director of Clinical Geriatrics University of Colorado Denver October 5, 2009 A Common Dilemma 88 yo F w/alzheimers, CAD, HTN, OP, DVT
PEG Tube use in the Elderly Jeffrey Wallace MD, MPH Professor and Director of Clinical Geriatrics University of Colorado Denver October 5, 2009 A Common Dilemma 88 yo F w/alzheimers, CAD, HTN, OP, DVT
EATING SAFELY AND TALKING ABOUT IT KIERA N BERGGREN, MA/CCC-SLP, MS 2018 FSHD CONNECT CONFERENCE
 EATING SAFELY AND TALKING ABOUT IT KIERA N BERGGREN, MA/CCC-SLP, MS 2018 FSHD CONNECT CONFERENCE DISCLOSURES I have no personal financial relationships with commercial interests relevant to this presentation
EATING SAFELY AND TALKING ABOUT IT KIERA N BERGGREN, MA/CCC-SLP, MS 2018 FSHD CONNECT CONFERENCE DISCLOSURES I have no personal financial relationships with commercial interests relevant to this presentation
FLOOVIDEOFLUOROSCOPIC SWALLOW STUDIES: LOOKING BEYOND ASPIRATION. Brenda Sitzmann, MA, CCC-SLP (816)
 FLOOVIDEOFLUOROSCOPIC SWALLOW STUDIES: LOOKING BEYOND ASPIRATION Brenda Sitzmann, MA, CCC-SLP bksitzmann@cmh.edu (816) 302-8037 DISCLOSURES Ms. Sitzmann is speech-language pathologist at Children s Mercy
FLOOVIDEOFLUOROSCOPIC SWALLOW STUDIES: LOOKING BEYOND ASPIRATION Brenda Sitzmann, MA, CCC-SLP bksitzmann@cmh.edu (816) 302-8037 DISCLOSURES Ms. Sitzmann is speech-language pathologist at Children s Mercy
Screening and Clinical Assessment for Dysphagia: How to Decide.
 Screening and Clinical Assessment for Dysphagia: How to Decide. How to Decide. ASHA Convention 2014 James L. Coyle, Ph.D., CCC-SLP, BCS-S Associate Professor, Communication Science & Disorders, University
Screening and Clinical Assessment for Dysphagia: How to Decide. How to Decide. ASHA Convention 2014 James L. Coyle, Ph.D., CCC-SLP, BCS-S Associate Professor, Communication Science & Disorders, University
Session #: R10 CASE STUDIES IN DYSPHAGIA DIAGNOSIS, TREATMENT AND REDUCTION OF REHOSPITALIZATIONS
 Session #: R10 CASE STUDIES IN DYSPHAGIA DIAGNOSIS, TREATMENT AND REDUCTION OF REHOSPITALIZATIONS PRESENTERS Dr. ERIC BLICKER, CCC-SLP.D., BCS-S COMMUNITY CARE PARTNERS, INC. EMAIL: CEUCUSTOMERCARE@GMAIL.COM
Session #: R10 CASE STUDIES IN DYSPHAGIA DIAGNOSIS, TREATMENT AND REDUCTION OF REHOSPITALIZATIONS PRESENTERS Dr. ERIC BLICKER, CCC-SLP.D., BCS-S COMMUNITY CARE PARTNERS, INC. EMAIL: CEUCUSTOMERCARE@GMAIL.COM
Applied physiology. 7- Apr- 15 Swallowing Course/ Anatomy and Physiology
 Applied physiology Temporal measures: Oral Transit Time (OTT) Pharyngeal Delay Time (PDT) Pharyngeal Transit Time (PTT) Oropharyngeal Swallowing Efficiency Score (OPSE score) 7- Apr- 15 Swallowing Course/
Applied physiology Temporal measures: Oral Transit Time (OTT) Pharyngeal Delay Time (PDT) Pharyngeal Transit Time (PTT) Oropharyngeal Swallowing Efficiency Score (OPSE score) 7- Apr- 15 Swallowing Course/
Communication and Swallowing with PSP/CBD. Megan DePuy, MBA, MS, CCC-SLP Private Speech Pathologist
 Communication and Swallowing with PSP/CBD Megan DePuy, MBA, MS, CCC-SLP Private Speech Pathologist A Speech Therapist? Why? Swallowing (Dysphagia) Speech (Dysarthria, Dysphonia) Language (Aphasia) An Experienced
Communication and Swallowing with PSP/CBD Megan DePuy, MBA, MS, CCC-SLP Private Speech Pathologist A Speech Therapist? Why? Swallowing (Dysphagia) Speech (Dysarthria, Dysphonia) Language (Aphasia) An Experienced
Expiratory Muscle Strength Training. (EMST) and Dysphagia
 Expiratory Muscle Strength Training 2015 Adult Swallowing Group NSW Speech Pathology Evidence Based Practice Network Christian Wiley and Kylie Draper Hans Bogaardt - Academic Member (EMST) and Dysphagia
Expiratory Muscle Strength Training 2015 Adult Swallowing Group NSW Speech Pathology Evidence Based Practice Network Christian Wiley and Kylie Draper Hans Bogaardt - Academic Member (EMST) and Dysphagia
Neoplastic Disease KNH 406
 Neoplastic Disease KNH 406 Cancer Carcinogenesis - Etiology Genes may be affected by antioxidants, soy, protein, fat, kcal, alcohol Nutritional genomics study of genetic variations that cause different
Neoplastic Disease KNH 406 Cancer Carcinogenesis - Etiology Genes may be affected by antioxidants, soy, protein, fat, kcal, alcohol Nutritional genomics study of genetic variations that cause different
Chapter 20. Assisting With Nutrition and Fluids
 Chapter 20 Assisting With Nutrition and Fluids Food and water: Are physical needs Basics of Nutrition Are necessary for life A poor diet and poor eating habits: Increase the risk for diseases and infection
Chapter 20 Assisting With Nutrition and Fluids Food and water: Are physical needs Basics of Nutrition Are necessary for life A poor diet and poor eating habits: Increase the risk for diseases and infection
Feeding Assistant Training Session #2
 Feeding Assistant Training Session #2 Dr. Heidi J. Silver, PhD, RDN Mrs. Abbie Hudson, BS, RDN Vanderbilt Center for Quality Aging & Qsource Vanderbilt Center for Human Nutrition Why is Nutrition Important?
Feeding Assistant Training Session #2 Dr. Heidi J. Silver, PhD, RDN Mrs. Abbie Hudson, BS, RDN Vanderbilt Center for Quality Aging & Qsource Vanderbilt Center for Human Nutrition Why is Nutrition Important?
Assessing the Eating Needs of Personal Care Services (PCS) Beneficiaries Effective 12/1/2016
 Assessing the Eating Needs of Personal Care Services (PCS) Beneficiaries Effective 12/1/2016 The Freedom to Succeed November 22,2016 Content Introduction Signs and Symptoms Caring for Individuals with
Assessing the Eating Needs of Personal Care Services (PCS) Beneficiaries Effective 12/1/2016 The Freedom to Succeed November 22,2016 Content Introduction Signs and Symptoms Caring for Individuals with
ESPEN GUIDELINES. on clinical nutrition and hydration in geriatrics
 ESPEN GUIDELINES on clinical nutrition and hydration in geriatrics SUMMARY Malnutrition and dehydration are widespread in older people, and obesity is an increasing problem. A range of effective interventions
ESPEN GUIDELINES on clinical nutrition and hydration in geriatrics SUMMARY Malnutrition and dehydration are widespread in older people, and obesity is an increasing problem. A range of effective interventions
Guidance for Oral Nutritional Support in patients with disease related malnutrition
 Guidance for Oral Nutritional Support in patients with disease related malnutrition NICE (CG3, 6) define oral nutrition support (ONS) as the modification of food and fluid by: fortifying food with protein,
Guidance for Oral Nutritional Support in patients with disease related malnutrition NICE (CG3, 6) define oral nutrition support (ONS) as the modification of food and fluid by: fortifying food with protein,
Feeding and Swallowing Problems in the Child with Special Needs
 Feeding and Swallowing Problems in the Child with Special Needs Joan Surfus, OTR/L, SWC Amy Lynch, MS, OTR/L Misericordia University This presentation is made possible, in part, by the support of the American
Feeding and Swallowing Problems in the Child with Special Needs Joan Surfus, OTR/L, SWC Amy Lynch, MS, OTR/L Misericordia University This presentation is made possible, in part, by the support of the American
Swallowing problems. Patient information. Name: Date: Speech and Language Therapist: Reviewed: May 2016 Next review: June 2017 Version 1
 Patient information Swallowing problems Name: Date: Speech and Language Therapist: Golden Jubilee National Hospital Agamemnon Street Clydebank, G81 4DY (: 0141 951 5000 www.nhsgoldenjubilee.co.uk Reviewed:
Patient information Swallowing problems Name: Date: Speech and Language Therapist: Golden Jubilee National Hospital Agamemnon Street Clydebank, G81 4DY (: 0141 951 5000 www.nhsgoldenjubilee.co.uk Reviewed:
ROLE OF A DIETITIAN & KEEPING HYDRATED. Emily Capener Haematology Dietitian UHW
 ROLE OF A DIETITIAN & KEEPING HYDRATED Emily Capener Haematology Dietitian UHW We will cover: PART 1 What is a dietitian Where do dietitans work About an acute dietitians role - Screening - Food charts
ROLE OF A DIETITIAN & KEEPING HYDRATED Emily Capener Haematology Dietitian UHW We will cover: PART 1 What is a dietitian Where do dietitans work About an acute dietitians role - Screening - Food charts
NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE SCOPE. Nutrition support in adults: oral supplements, enteral and parenteral feeding.
 NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE 1 Guideline title SCOPE Nutrition support in adults: oral supplements, enteral and parenteral feeding. 1.1 Short title Nutrition support 2 Background a) The National
NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE 1 Guideline title SCOPE Nutrition support in adults: oral supplements, enteral and parenteral feeding. 1.1 Short title Nutrition support 2 Background a) The National
Dignity and Nutrition for Older People
 South Gloucestershire Community Health Services Dignity and Nutrition for Older People Lorraine Norris Nutrition and Dietetic Professional Lead South Gloucestershire Community Health November 9th 2011
South Gloucestershire Community Health Services Dignity and Nutrition for Older People Lorraine Norris Nutrition and Dietetic Professional Lead South Gloucestershire Community Health November 9th 2011
Managing the Patient with Dysphagia
 Managing the Patient with Dysphagia Patricia K. Lerner, MA, CCC, ASHA Fellow Board Certified Specialist in Swallowing & Swallowing Disorders Clinical Assistant Professor New York University School of Medicine
Managing the Patient with Dysphagia Patricia K. Lerner, MA, CCC, ASHA Fellow Board Certified Specialist in Swallowing & Swallowing Disorders Clinical Assistant Professor New York University School of Medicine
New Evidence-Based Support of a 3 Ounce Water Swallow Challenge Protocol
 New Evidence-Based Support of a 3 Ounce Water Swallow Challenge Protocol Steven B. Leder, Ph.D. Yale University School of Medicine New Haven, Connecticut Debra M. Suiter, Ph.D. VA Medical Center-Memphis
New Evidence-Based Support of a 3 Ounce Water Swallow Challenge Protocol Steven B. Leder, Ph.D. Yale University School of Medicine New Haven, Connecticut Debra M. Suiter, Ph.D. VA Medical Center-Memphis
Karen Schoeneman Consul6ng 1
 + The New Dining Practice Standards and CMS Feeding Tube Guidance Revisions Karen Schoeneman, Owner Karen Schoeneman Consulting + How Did The New Dining Standards Happen? 2 CMS and Pioneer Network co-sponsored
+ The New Dining Practice Standards and CMS Feeding Tube Guidance Revisions Karen Schoeneman, Owner Karen Schoeneman Consulting + How Did The New Dining Standards Happen? 2 CMS and Pioneer Network co-sponsored
MS Learn Online Feature Presentation Swallowing Difficulties in Multiple Sclerosis Featuring Patricia Bednarik, MS, CCC-SLP, MSCS
 Page 1 MS Learn Online Feature Presentation Swallowing Difficulties in Multiple Sclerosis Featuring, MS, CCC-SLP, MSCS >>Kate Milliken: Welcome to MS Learn Online. I am Kate Milliken. Swallowing is something
Page 1 MS Learn Online Feature Presentation Swallowing Difficulties in Multiple Sclerosis Featuring, MS, CCC-SLP, MSCS >>Kate Milliken: Welcome to MS Learn Online. I am Kate Milliken. Swallowing is something
Feeding and Oral Hygiene: How to Address the Challenges
 Feeding and Oral Hygiene: How to Address the Challenges Paige W. Roberts, OTR/L Occupational Therapist Pediatric Feeding Disorders Program Marcus Autism Center Disclaimer: This content is for personal
Feeding and Oral Hygiene: How to Address the Challenges Paige W. Roberts, OTR/L Occupational Therapist Pediatric Feeding Disorders Program Marcus Autism Center Disclaimer: This content is for personal
Role of Dining Services and Dietary Needs of the Resident, 2014
 Role of Dining Services and Dietary Needs of the Resident, 2014 It is the dining services role to provide quality meals and service to all residents that is as home-like as possible. This will be done
Role of Dining Services and Dietary Needs of the Resident, 2014 It is the dining services role to provide quality meals and service to all residents that is as home-like as possible. This will be done
Alexandra Butti M.Cl.Sc (SLP) Candidate Western University: School of Communication Sciences and Disorders
 Critical Review: Does ingesting water increase the risk for adverse health effects in adults with oropharyngeal dysphagia who have been determined to aspirate thin fluids?* Alexandra Butti M.Cl.Sc (SLP)
Critical Review: Does ingesting water increase the risk for adverse health effects in adults with oropharyngeal dysphagia who have been determined to aspirate thin fluids?* Alexandra Butti M.Cl.Sc (SLP)
Cover Page. The handle holds various files of this Leiden University dissertation
 Cover Page The handle http://hdl.handle.net/1887/32744 holds various files of this Leiden University dissertation Author: Heemskerk, Anne-Wil Title: Dysphagia in Huntington s disease Issue Date: 2015-04-15
Cover Page The handle http://hdl.handle.net/1887/32744 holds various files of this Leiden University dissertation Author: Heemskerk, Anne-Wil Title: Dysphagia in Huntington s disease Issue Date: 2015-04-15
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of transcutaneous neuromuscular electrical stimulation for oropharyngeal dysphagia
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of transcutaneous neuromuscular electrical stimulation for oropharyngeal dysphagia
financial costs social isolation medical risks
 Dysphagia, commonly known as swallowing problems, is quite common. A significant number of people in long-term elderly care suffer from some form of dysphagia. Treating the condition is a challenge for
Dysphagia, commonly known as swallowing problems, is quite common. A significant number of people in long-term elderly care suffer from some form of dysphagia. Treating the condition is a challenge for
Dysphagia (swallowing problems)
 Dysphagia (swallowing problems) Speech and Language Therapy Department Patient Information Leaflet Introduction This leaflet is for people who have dysphagia. It gives information on what this condition
Dysphagia (swallowing problems) Speech and Language Therapy Department Patient Information Leaflet Introduction This leaflet is for people who have dysphagia. It gives information on what this condition
B. Background Information B1. Summary Medical team (physicians, dentists, etc ): Ancillary care team (nursing, therapists, etc ):
 1 A. Preliminary Information Reason for referral: Chronological age (Adjusted age): Primary caregiver: Informant for evaluation: Primary language: Interpreter Family concerns Barriers to learning: B. Background
1 A. Preliminary Information Reason for referral: Chronological age (Adjusted age): Primary caregiver: Informant for evaluation: Primary language: Interpreter Family concerns Barriers to learning: B. Background
Meat. Chicken, steak, fish, beans, pork and veal products are members of the meat group.
 HOW NUTRITION AND FLUID NEEDS CHANGE WITH AGE Food and nutritional needs change as a person gets older and older. The need for a lot of calories decreases when a person gets older. These needs were highest
HOW NUTRITION AND FLUID NEEDS CHANGE WITH AGE Food and nutritional needs change as a person gets older and older. The need for a lot of calories decreases when a person gets older. These needs were highest
Management of oropharyngeal dysphagia
 Management of oropharyngeal dysphagia Course Objectives Know the normal anatomy of swallowing Know the normal physiology of swallowing Enumerate different etiologies of oropharyngeal dysphagia Be able
Management of oropharyngeal dysphagia Course Objectives Know the normal anatomy of swallowing Know the normal physiology of swallowing Enumerate different etiologies of oropharyngeal dysphagia Be able
Patient and Family Resource Guide to ALS. Section 6. Nutritional Support
 Patient and Family Resource Guide to ALS Section 6 Nutritional Support 6 5550 W. Touhy Avenue, Skokie IL, 60077 847 679 3311 lesturnerals.org info@lesturnerals.org Nutritional Support Many factors can
Patient and Family Resource Guide to ALS Section 6 Nutritional Support 6 5550 W. Touhy Avenue, Skokie IL, 60077 847 679 3311 lesturnerals.org info@lesturnerals.org Nutritional Support Many factors can
Critical Review: The effect of time and temperature on the viscosity of thickened liquids
 Critical Review: The effect of time and temperature on the viscosity of thickened liquids Buckland, S.A. M.Cl.Sc (S-LP) Candidate University of Western Ontario: School of Communication Sciences and Disorders
Critical Review: The effect of time and temperature on the viscosity of thickened liquids Buckland, S.A. M.Cl.Sc (S-LP) Candidate University of Western Ontario: School of Communication Sciences and Disorders
IVOR LEWIS Esophagogastrectomy
 IVOR LEWIS Esophagogastrectomy SPEECH-LANGUAGE PATHOLOGY S ROLE MAGGIE BOYD, MS, CCC/SLP Biography Maggie Boyd, MS, CCC-SLP is a dysphagia clinical specialist at UAB hospital. She has 14 years clinical
IVOR LEWIS Esophagogastrectomy SPEECH-LANGUAGE PATHOLOGY S ROLE MAGGIE BOYD, MS, CCC/SLP Biography Maggie Boyd, MS, CCC-SLP is a dysphagia clinical specialist at UAB hospital. She has 14 years clinical
Understanding your child s videofluoroscopic swallow study report
 Understanding your child s videofluoroscopic swallow study report This leaflet is given to you during your child s appointment in order to explain some of the words used by the speech and language therapist
Understanding your child s videofluoroscopic swallow study report This leaflet is given to you during your child s appointment in order to explain some of the words used by the speech and language therapist
Prescribing Guidelines for Oral Nutritional Supplements (ONS) for adults
 Worcestershire Area Prescribing Committee Prescribing Guidelines for Oral Nutritional Supplements (ONS) for adults September 2017 Review Date September 2020 Version 3.0 1 Version Control: Version Type
Worcestershire Area Prescribing Committee Prescribing Guidelines for Oral Nutritional Supplements (ONS) for adults September 2017 Review Date September 2020 Version 3.0 1 Version Control: Version Type
MDS 3.0. Acronyms. Terminology & Definitions 8/22/2016 CAA CAT ADL BMI BIMS PT/OT/ST QI QM MDS RAI OMRA (SOT) OBRA RUG CMS COT OMRA ARD
 MDS 3.0 Acronyms MDS RAI OMRA (SOT) OBRA RUG CMS COT OMRA ARD CAA CAT ADL BMI BIMS PT/OT/ST QI QM Terminology & Definitions Active Disease Diagnosis Acute Change in Mental Status Period Reference Date
MDS 3.0 Acronyms MDS RAI OMRA (SOT) OBRA RUG CMS COT OMRA ARD CAA CAT ADL BMI BIMS PT/OT/ST QI QM Terminology & Definitions Active Disease Diagnosis Acute Change in Mental Status Period Reference Date
Effects of Oral Health Screening on Aspiration Pneumonia Risk for Adults with Dementia in Residential Aged Care
 Wicking Dementia Research and Education Centre Effects of Oral Health Screening on Aspiration Pneumonia Risk for Adults with Dementia in Residential Aged Care L. Goldberg, J. Westbury, S. Langmore, L.
Wicking Dementia Research and Education Centre Effects of Oral Health Screening on Aspiration Pneumonia Risk for Adults with Dementia in Residential Aged Care L. Goldberg, J. Westbury, S. Langmore, L.
