Reliability of the Spinal Instability Neoplastic Scale
|
|
|
- Shonda Marshall
- 6 years ago
- Views:
Transcription
1 Musculoskeletal Imaging Original Research Fisher et al. Reliability of the Spinal Instability Neoplastic Scale Musculoskeletal Imaging Original Research Charles G. Fisher 1,2 Anne L. Versteeg 3 Rowan Schouten 4 Stefano Boriani 5 Peter P. Varga 6 Laurence D. Rhines 7 Manraj K. S. Heran 8,9 Norio Kawahara 10 Daryl Fourney 11 Jeremy J. Reynolds 12 Michael G. Fehlings 13,14 Ziya L. Gokaslan 15 Fisher CG, Versteeg AL, Schouten R, et al. Keywords: metastasis, neoplasm, radiologist reliability, spinal instability, spinal instability neoplastic scale (SINS), spine, validity DOI: /AJR Received November 13, 2013; accepted after revision February 19, L. D. Rhines received grant support for another work from Stryker. J. J. Reynolds received grant support for other works from Globus, DePuy Synthes, and Medtronic. Z. L. Gokaslan received grant support for other works from AOSpine, NREF, DePuy, US Spine and Spinal Kinetics, and the AO Foundation. This study received financial support from AOSpine International through the AOSpine Knowledge Forum Tumor. AOSpine is a clinical division of the AO Foundation, which is an independent medically guided not-for-profit organization. AJR 2014; 203: X/14/ American Roentgen Ray Society Reliability of the Spinal Instability Neoplastic Scale Among Radiologists: An Assessment of Instability Secondary to Spinal Metastases OBJECTIVE. The spinal instability neoplastic scale (SINS) is a new classification system for tumor-related spinal instability. The SINS may prove to be a valuable tool for radiologists to communicate with oncologists and surgeons in a standardized evidence-based manner. The objective of this study was to determine the inter- and intraobserver reliability and validity of the SINS among radiologists. MATERIALS AND METHODS. Thirty-seven radiologists from 10 international sites used the SINS to categorize the degree of spinal instability in 30 patients with spinal tumors. To assess validity, we compared the SINS scores assigned by the radiologists with the SINS scores of 11 spine oncology surgeons (reference standard). Each total SINS score (range, 0 18 points) was converted into one of the following three clinical categories: 0 6 points, stable; 7 12 points, potentially unstable; and points, unstable. In addition, each total SINS score was converted into a binary scale: 0 6 points was defined as stable, and 7 18 points was considered a current or possible instability for which surgical consultation is recommended. RESULTS. Radiologists using the SINS binary scale showed excellent (κ = 0.88) validity, substantial (κ = 0.76) interobserver agreement, and excellent (κ = 0.82) intraobserver reproducibility. Radiologists rated all unstable cases and 621 of 629 (98.7%) potentially unstable cases with a SINS score of 7 or more points, thus appropriately initiating a referral for surgical assessment. CONCLUSION. SINS is a reliable tool for radiologists rating tumor-related spinal instability. It accurately discriminates between stable and potentially unstable or unstable lesions and, therefore, can guide the need for surgical consultation. R ecent advances in systemic treatments have improved the survival rates of cancer patients, which has resulted in an increased incidence of spine metastatic disease [1 4]. Spinal metastases can create spinal column insta- bility and neural compression that can potentially result in significant pain, devastating neurologic consequences, or both. Early diagnosis and appropriate management are therefore crucial. The typical goals of spinal metastasis treatments are pain relief, the res- 1 Department of Orthopaedics, Division of Spine, University of British Columbia and Vancouver General Hospital, Vancouver, BC, Canada. 2 Blusson Spinal Cord Centre, 818 W 10th Ave, 6th Fl, Vancouver, BC V5Z 1M9, Canada. Address correspondence to C. G. Fisher (charles.fisher@vch.ca). 3 Department of Orthopaedics, University Medical Center Utrecht, Utrecht, The Netherlands. 4 Department of Orthopaedic Surgery and Musculoskeletal Medicine, Christchurch Hospital, Christchurch, New Zealand. 5 Department of Degenerative and Oncological Spine Surgery, Rizzoli Institute, Bologna, Italy. 6 National Center for Spinal Disorders and Buda Health Center, Budapest, Hungary. 7 Department of Neurosurgery, The University of Texas M. D. Anderson Cancer Center, Houston, TX. 8 Department of Radiology, University of British Columbia, Vancouver, BC, Canada. 9 Department of Diagnostic & Therapeutic Neuroradiology, Vancouver General Hospital, Vancouver, BC, Canada. 10 Department of Orthopedic Surgery, Kanazawa Medical University, Kahoku-gun, Japan. 11 Department of Surgery, Division of Neurosurgery, University of Saskatchewan, Royal University Hospital, Saskatoon, SK, Canada. 12 Spinal Division, Oxford University Hospital, NHS Trust, Oxford, UK. 13 Department of Neurosurgery, University of Toronto, Toronto, ON, Canada. 14 Krembil Neuroscience Centre, Toronto Western Hospital, University Health Network, Toronto, ON, Canada. 15 Department of Neurosurgery, The Johns Hopkins University School of Medicine, Baltimore, MD. AJR:203, October
2 Fisher et al. toration or preservation of neurologic function, and establishment of spinal stability. The latter is often the primary intention of the treatment. A range of therapeutic options provided by various subspecialists including medical and radiation oncologists, radiologists, and surgeons exists. Therefore, it is critical that the terminology used for the diagnosis and treatment of spinal instability due to metastases is standardized and evidence based so that the subspecialists can work together to facilitate optimal patient care. High-grade neurologic compression and mechanical instability are considered absolute indications for surgery [5, 6]. Although neurologic issues are relatively straightforward from a diagnostic perspective, spinal instability related to metastases is not, as evidenced by the facts that there is no established reference standard and that there are inconsistencies among spine oncology surgeons, the specialty most familiar with the anatomy and treatment of spine instability [7]. The diagnosis of spinal oncologic instability is even more difficult for the nonsurgical members of the multidisciplinary care team, possibly resulting in the underrecognition and underreferral of patients who may benefit from surgical stabilization [8, 9]. Diagnosing spinal stability is made difficult by the lack of consensus guidelines rating the relevance and validity of specific clinical and imaging findings. In response, the Spine Oncology Study Group (SOSG), an international cohort of spine oncology experts including oncology spine surgeons and oncologists, developed a tool to assess and grade spinal stability to assist in making treatment decisions and identifying patients requiring surgical assessment. SOSG defined spinal instability caused by metastatic disease as follows [7]: [the] loss of spinal integrity as a result of a neoplastic process that is associated with movement-related pain, symptomatic or progressive deformity, and/or neural compromise under physiologic loads. SOSG then integrated the best available literature and expert opinions to develop the spinal instability neoplastic scale (SINS) [7]. The SINS classifies spinal stability by adding together six radiographic and clinical components to create a total SINS score ranging from 0 to 18 (Table 1). The total SINS score is further divided into the following three clinical categories of stability: 0 6 points denotes the spine as stable; 7 12 points, as potentially unstable (Fig. 1); and points, as unstable TABLE 1: The Spinal Instability Neoplastic Scale (SINS) Classification According to Fisher et al. [7] Parameters Score (Points) Location Junctional (occiput C2, C7 T2, T11 L1, L5 S1) 3 Mobile spine (C3 C6, L2 L4) 2 Semirigid (T3 T10) 1 Rigid (S2 S5) 0 Pain a Yes 3 Occasional pain but not mechanical 1 Pain-free lesion 0 Bone lesion Lytic 2 Mixed (lytic/blastic) 1 Blastic 0 Radiographic spinal alignment Subluxation/translation present 4 De novo deformity (kyphosis/scoliosis) 2 Normal alignment 0 Vertebral body collapse > 50% collapse 3 < 50% collapse 2 No collapse with > 50% body involved 1 None of the above 0 Posterolateral involvement of spinal elements b Bilateral 3 Unilateral 1 None of the above 0 Note The scores for the six radiographic and clinical components were added together to yield a total SINS score ranging from 0 to 18. Reprinted with permission from [7]: Fisher CG, DiPaola CP, Ryken TC, et al. A novel classification system for spinal instability in neoplastic disease: an evidence-based approach and expert consensus from the Spine Oncology Study Group. Spine (Phila Pa 1976) 2010; 35:E1221 E1229. a Pain improvement with recumbency, pain with movement or loading of spine, or both. b Facet, pedicle, or costovertebral joint fracture or replacement with tumor. (Fig. 2). Based on a recommended threshold for surgical consultation, a binary scale was also created: stable (0 6 points) or a current or possible instability for which assessment by a spine surgeon is recommended (7 18 points). SOSG members using SINS showed 95.7% and 79.5% sensitivity and specificity, respectively, for the detection of potentially unstable or unstable spinal metastases [10]. Near-perfect interobserver reliability and intraobserver reliability were noted for distinctions among the three clinical categories of stability [10]. Although the SINS has not yet undergone prospective clinical validation, it represents the only classification system to date for diagnosing neoplastic spinal instability derived from evidence-based medicine. It is therefore critical that key physicians who will use it and advise on it specifically, radiologists assess the tool from a fundamental diagnostic test perspective before prospective clinical evaluation. The aim of this study was to assess the interand intraobserver reliability of the SINS score among radiologists who play a pivotal role in the evaluation of patients with spine metastases. Materials and Methods Patients This study received institutional review board approval before its commencement. The records for 30 cases of metastatic spine disease with patient-identifying information removed were reviewed at 10 international sites. The patients in the study group were 13 women (mean age, 60 years; 870 AJR:203, October 2014
3 Reliability of the Spinal Instability Neoplastic Scale age range, years) and 17 men (mean age, 64 years; age range, years). Lung (n = 6, 20%), prostate (n = 6, 20%), breast (n = 5, 17%), and myeloma (n = 4, 13%) were the most common primary malignancies, with 12 different tumor types represented overall. Lesions were spread across the cervical (C0 C7) spine (n = 6, 20%), thoracic (T1 T10) spine (n = 11, 37%), thoracolumbar (T11 L2) junction (n = 8, 27%), and low lumbar (L3 L5) regions (n = 5, 17%). For each case, demographic data, histopathologic diagnosis, and a pain description with A D B E Fig year-old man with multiple myeloma who presented with mild low back pain that is not aggravated by activities or movement. A E, Selected CT images of L5 lesion are provided: left parasagittal (A), midline sagittal (B), right parasagittal (C), coronal (D), and axial cut (E). Total spinal instability neoplastic scale (SINS) score was calculated as follows: junctional location, 3 points; pain but not mechanical, 1 point; lytic, 2 points; spinal alignment preserved, 0 points; less than 50% vertebral body collapse, 2 points; unilateral replacement of right pedicle with tumor, 1 point. Thus, total SINS score is 9 points ( = 9), which indicates potential instability for which surgical referral is recommended. an emphasis on movement-related pain were provided to simulate information typically provided to the radiologist. Representative preoperative radiographs, CT scans, and MR images followed. CT scans were provided for each assessment. After reviewing an instructional booklet and case examples on the application of the SINS, 37 radiologists from North America, Europe, and Asia independently assigned a SINS score to each case. From 6 to 8 weeks later, after the order of the cases was changed to minimize recall bias, the same radiologists scored the same cases a second time. All radiologists were working at academic centers and had been in practice for an average of 15 years (SD = 12 years) at the time of the study, and 36% had completed subspecialty training in neuroradiology. Although a true reference standard has not yet been determined, the best possible validity reference or reference standard was established by 11 experienced spine oncology surgeons, all of whom are familiar with the SINS classification and are members of the SOSG. They reviewed and rated each case C AJR:203, October
4 Fisher et al. once. For each case, the most frequent SINS score (i.e., the score assigned by most surgeons) became the reference standard score. In cases in which ties occurred, the two most frequent scores were averaged. For each case, the total SINS score, the three clinical categories (stability, potential instability, and instability), and the binary scale were analyzed. The mean number of years in practice for the spine surgeons was 13 years (SD, 12 years). A D Statistical Analysis Interobserver agreement (Fleiss kappa) for the radiologists and surgeons and intraobserver reproducibility (Cohen s kappa) among the radiologists were calculated for the total SINS score, the three clinical categories, and the binary scale [11, 12]. Validity was defined as the average kappa (Cohen s kappa) for agreement between the radiologists and the reference standard. The kappa coefficients were interpreted and translated into levels of agreement using the Landis and Koch [13] grading system (Table 2), where a kappa value of 1.0 implies perfect agreement. To produce CIs for the kappa estimates, we used a sampling distribution for the kappa statistic by means of bootstrapping, simulating 1000 B E Fig year-old woman with known metastatic sarcoma who presented with neck pain that was exacerbated by any movement but that improved with application of cervical collar. A E, Selected CT images of C4 lesion are provided: left parasagittal (A), midline sagittal (B), right parasagittal (C), coronal (D), and axial cut (E). Total spinal instability neoplastic scale (SINS) score was calculated as follows: mobile spine location, 2 points; mechanical pain, 3 points; lytic lesion, 2 points; kyphotic deformity, 2 points; more than 50% collapse, 3 points; bilateral posterolateral involvement, 3 points. Total SINS score is 15 points ( ), which indicates potential instability for which surgical referral is recommended. kappa estimates, and using the 2.5 and 97.5 percentiles for the CIs. All statistical analyses were performed using Stata software (version 12.0, StataCorp) for Microsoft Windows. Results Interobserver Agreement Interobserver agreement was substantial (κ = 0.76) and moderate (κ = 0.53) among radiologists for the binary scale and three clinical categories, respectively (Table 3). An analysis of the separate SINS components showed excellent agreement for location (κ = 0.94); sub- C 872 AJR:203, October 2014
5 Reliability of the Spinal Instability Neoplastic Scale stantial agreement for pain (κ = 0.73), bone lesion quality (κ = 0.65), and vertebral body collapse (κ = 0.61); and moderate agreement for spinal alignment (κ = 0.49) and posterolateral involvement of the spinal elements (κ = 0.55). The interobserver agreement among surgeons was excellent (κ = 0.83) and substantial (κ = 0.65) for the binary scale and three clinical categories, respectively. Intraobserver Reproducibility For the radiologists, intraobserver reproducibility was excellent (κ = 0.82) and substantial (κ = 0.69) for the binary scale and three clinical categories, respectively (Table 3). An analysis of the separate SINS components showed that intraobserver reproducibility was excellent for location (κ = 0.96) and pain (κ = 0.85) and was substantial for bone lesion quality (κ = 0.75), spinal alignment (κ = 0.69), vertebral body collapse (κ = 0.71), and posterolateral involvement of the spinal elements (κ = 0.68). Validity The level of agreement between radiologists and reference standard was excellent (κ = 0.88) for the binary scale and substantial (κ = 0.71) for the three clinical categories. Table 4 outlines the three clinical categories (0 6 points, stable; 7 12 points, potentially unstable; points, unstable) scored by the spine surgeons cross-tabulated with the scores by the radiologists. The radiologists recorded SINS scores of 7 points or greater for all the unstable cases and for 621 of the 629 (98.7%) potentially unstable cases. In other words, all unstable and 98.7% of potentially unstable patients would have been appropriately identified as requiring surgical assessment. Twenty percent of the cases that the surgeons identified as stable were considered potentially unstable by the radiologists. Discussion Given the multidisciplinary approach toward the treatment of patients with metastatic spine disease, it is important to establish a clear framework for proper referral among health care professionals to ensure the best supportive care is provided. Before the SINS, reliable and validated guidelines to assess tumor-related spinal instability did not exist, and this lack of a standard created variability in interpretations, referral patterns, and consequently patient management. Radiologists and the advanced imaging modalities (e.g., CT and MRI) they interpret have a critical role in the evaluation of spinal metastases and the treatment decisions for these TABLE 2: Levels of Agreement for Kappa Values Kappa Value Level of Agreement Slight Fair Moderate Substantial > 0.80 Excellent Note Adapted with permission from [13] (Landis JR, Koch GG. The measurement of observer agreement for categorical data. Biometrics 1977; 33: ). patients. It is therefore essential that radiologists have a reliable and valid tool on which to evaluate neoplastic instability something that they currently do not have. Although SINS has not undergone prospective clinical evaluation, it was derived using evidence-based medicine and is the closest thing to a reference standard that we have. This study has shown that, among radiologists, the SINS binary scale provides a reliable tool for rating tumor-related spinal instability with excellent validity, substantial interobserver agreement, and excellent intraobserver reproducibility. These results indicate that SINS is a tool that can accurately discriminate between stable and potentially unstable lesions, an important decision when considering the need for surgical consultation. Using radiographic features to help clinicians select the most appropriate treatment of metastatic spinal disease has been previously reported. Snyder et al. [14] used a CT-based structural rigidity analysis, which they referred to as CTRA, as a noninvasive method to predict vertebral fracture risk in breast cancer patients with spinal metastases and suggested that surgical stabilization be considered for patients identified with a high fracture risk. CTRA, however, requires additional software and is time-consuming, with an analysis time of 2 4 hours per patient, thereby currently limiting its use. Furthermore, unlike fractures in the appendicular skeleton, not all fractures in the spine are unstable; therefore, a more comprehensive approach to the assessment of spinal stability is necessary. In contrast, the SINS framework for assessing spinal instability is based on six common radiographic and clinical parameters and does not rely on sophisticated analysis methods. One study assessed the interrater reliability of a range of imaging features of spinal metastases and noted moderate or poor agreement for most criteria between musculoskeletal radiologists and orthopedic surgeons [15]. The set of radiologic components included in the SINS were selected by the SOSG by combining the best available literature and consensus expert opinion [7], an evidence-based medicine process. Using the surgeons consensus assessment as the reference for validity or reference standard is a limitation because SINS must be prospectively evaluated; however, in the early phases of the development of a classification system, these assumptions are necessary to ensure SINS is TABLE 3: Reliability Analysis of the Spinal Instability Neoplastic Scale (SINS) Among Radiologists and Surgeons (Reference Standard) Observers TABLE 4: Cross Tabulation of Clinical Categories Based on Spinal Instability Neoplastic Scale (SINS) Scores for 30 Cases Determined by Surgeons (Reference Standard) and 37 Radiologists Clinical Category Assigned by Radiologists a Interobserver Agreement (κ) Three Clinical Categories (95% CI) Clinical Category Assigned by Surgeons (No. of Interpretations) Stable Binary Scale (95% CI) Potentially Unstable Unstable Total Stable Potentially unstable Unstable Total a The radiologists first assessments were used for this analysis. Intraobserver Reproducibility (κ) Three Clinical Categories (95% CI) Binary Scale (95% CI) Radiologists 0.53 ( ) 0.76 ( ) 0.69 ( ) 0.82 ( ) Surgeons 0.65 ( ) 0.83 ( ) NA NA Note NA = not applicable. AJR:203, October
6 optimized before expensive and time-consuming prospective evaluation. Obtaining opinions from radiologists across seven international sites has enhanced the generalizability of this study s findings. In addition, an a priori power analysis ensured that a sufficient number of cases (n = 30) were included [16], and rearranging the case order before the second review minimized recall bias. Despite these strategies, some results of this study may have been skewed because the mock cases may not fully reflect real-life clinical settings. Radiologists depend on the referring clinician to describe the patient s pain characteristics and, in particular, its relationship to movement. For the radiologist-assigned SINS score to be accurate, this detail needs to be routinely provided as part of the radiology consultation. We are hopeful that as oncologists more commonly use SINS, this important characteristic will be provided. Furthermore, with the involvement of an integrated multidisciplinary team of specialists (oncologists, radiologists, pathologists, surgeons) becoming more prevalent in the care of oncology patients, the provision of the pain component of SINS to radiologists should be improved. The limited selection of images available for each case scenario may have negatively impacted on the reliability of measures such as discriminating between lytic and blastic lesions. The availability of complete sets of reconstructed CT and MR images and ability to scroll through these images may translate into better SINS reliability in the true clinical setting. The lack of images is a limitation of this study, but one that probably biases toward the null hypothesis. The statistical method for testing reliability also has limitations. The kappa statistic used in this study is influenced by different factors, such as the rater s prevalence, weighting, and bias. A low kappa value might reflect the inability of the tested classification or the raters to distinguish between two different categories that are closely related [17, 18]. Although a kappa value of between 0.81 and 1.0 arbitrarily translates into excellent agreement according to the widely accepted Landis and Koch [13] scale, this level of agreement may reflect an unacceptable difference in agreement in the clinical setting. Depending on the purpose of the score and the influence of the result, the margin of error that will be allowed must be determined [17, 18]. The reliability of SINS has been previously established among surgeons, and with this study, radiologists who play a pivotal role in advising oncologists about potentially serious problems related to neurologic compression and spinal instability. Although the current iteration of SINS has sound diagnostic Fisher et al. test parameters, it requires prospective clinical validation and may indeed undergo modification based on the results of these studies. For now, physicians involved in the evaluation and care of these complex patients have a reliable and provisionally valid tool to evaluate spinal instability secondary to metastatic disease something we have desperately needed for some time. Acknowledgments We are grateful to the radiologists who contributed to and participated in this study: Nafi Aygun, Sachin Gujar, Izlem Izbudak, Haris Sair, Ugo Albisinni, Eugenio Rimondi, Daniel Vanel, Alberto Zerbi, Mitesh Ganhdi, Greg Cowderoy, John McGuire, Jennifer Sommerville, Maria Gergely, Maria Puhl, Judit Sandor, Ildiko Takasc, Vince Kumar, Norman Leeds, Matthew Debnam, Komal Shah, Ramy Mansour, Eugene McNally, Simon Ostlere, James Teh, Tasha Ellchuk, Derek Fladeland, Haron Obaid, Sheldon Wiebe, Jason Chew, Jason Shewchuk, Talia Vertinsky, Mariko Doai, Toshifumi Gabata, Masataka Kitadate, Julia Fairbairn, Khalid Latief, and Rachel Musson. We thank our fellow spine surgeons who assisted in establishing the reference standard: Nicolas Dea, Adrienne Kelly, and Dennis Hartig. We also thank the following participating spine centers and their clinical personnel: University of British Columbia, BC Cancer Agency, and Vancouver Coastal Health, Vancouver, BC, Canada; University of Saskatchewan, Royal University Hospital, Saskatoon, SK, Canada; University of Toronto and Toronto Western Hospital Krembil Neuroscience Centre, Toronto, ON, Canada; The Johns Hopkins University School of Medicine, Baltimore, MD; The University of Texas M. D. Anderson Cancer Center, Houston, TX; Rizzoli Institute, Bologna, Italy; Oxford University Hospital NHS Trust, Oxford, UK; National Center for Spinal Disorders and Buda Health Center, Budapest, Hungary; Princess Alexandra Hospital, Brisbane Spine Reference Center, Brisbane, Australia; Kanazawa Medical University, Kahoku-gun, Japan; and Nottingham University Hospital NHS Trust Queen s Medical Centre, Nottingham, UK. We also thank AO Clinical Investigation and Documentation, especially Monica Daigl for performing the statistical analysis, and the AOSpine Knowledge Forum Tumor Steering Committee for managing and supporting this study. References 1. Hayat MJ, Howlader N, Reichman ME, Edwards BK. Cancer statistics, trends, and multiple primary cancer analyses from the Surveillance, Epidemiology, and End Results (SEER) program. Oncologist 2007; 12: Harel R, Angelov L. Spine metastases: current treatments and future directions. Eur J Cancer 2010; 46: Ortiz Gómez JA. The incidence of vertebral body metastases. Int Orthop 1995; 19: Falicov A, Fisher CG, Sparkes J, Boyd MC, Wing PC, Dvorak MF. Impact of surgical intervention on quality of life in patients with spinal metastases. Spine 2006; 31: Bilsky M, Smith M. Surgical approach to epidural spinal cord compression. Hematol Oncol Clin North Am 2006; 20: Bilsky MH, Azeem S. The NOMS framework for decision making in metastatic cervical spine tumors. Curr Opin Orthop 2007; 18: Fisher CG, DiPaola CP, Ryken TC, et al. A novel classification system for spinal instability in neoplastic disease: an evidence-based approach and expert consensus from the Spine Oncology Study Group. Spine (Phila Pa 1976) 2010; 35:E1221 E Eastley N, Newey M, Ashford RU. Skeletal metastases: the role of the orthopaedic and spinal surgeon. Surg Oncol 2012; 21: Galasko CS, Norris HE, Crank S. Spinal instability secondary to metastatic cancer. J Bone Joint Surg Am 2000; 82: Fourney DR, Frangou EM, Ryken TC, et al. Spinal instability neoplastic score: an analysis of reliability and validity from the Spine Oncology Study Group. J Clin Oncol 2011; 29: Cohen J. A coefficient of agreement for nominal scales. Educ Psychol Meas 1960; 20: Fleiss JL. Measuring nominal scale agreement among many raters. Psychol Bull 1971; 76: Landis JR, Koch GG. The measurement of observer agreement for categorical data. Biometrics 1977; 33: Snyder BD, Cordio MA, Nazarian A, et al. Noninvasive prediction of fracture risk in patients with metastatic cancer to the spine. Clin Cancer Res 2009; 15: Khan L, Mitera G, Probyn L, et al. Inter-rater reliability between musculoskeletal radiologists and orthopedic surgeons on computed tomography imaging features of spinal metastases. Curr Oncol 2011; 18:e282 e Scheffe H. The analysis of variance. New York, NY: Wiley, Kottner J, Audigé L, Brorson S, et al. Guidelines for reporting reliability and agreement studies (GRRAS) were proposed. J Clin Epidemiol 2011; 64: Sim J, Wright CC. The kappa statistic in reliability studies: use, interpretation, and sample size requirement. Phys Ther 2005; 85: AJR:203, October 2014
Reliability of the Spinal Instability Neoplastic Score (SINS) among radiation oncologists: an assessment of instability secondary to spinal metastases
 Fisher et al. Radiation Oncology 2014, 9:69 RESEARCH Open Access Reliability of the Spinal Instability Neoplastic Score (SINS) among radiation oncologists: an assessment of instability secondary to spinal
Fisher et al. Radiation Oncology 2014, 9:69 RESEARCH Open Access Reliability of the Spinal Instability Neoplastic Score (SINS) among radiation oncologists: an assessment of instability secondary to spinal
Interobserver agreement for the spine instability neoplastic score varies according to the experience of the evaluator
 CLINICAL SCIENCE Interobserver agreement for the spine instability neoplastic score varies according to the experience of the evaluator William Gemio Jacobsen Teixeira, I Pedro Ricardo de Mesquita Coutinho,
CLINICAL SCIENCE Interobserver agreement for the spine instability neoplastic score varies according to the experience of the evaluator William Gemio Jacobsen Teixeira, I Pedro Ricardo de Mesquita Coutinho,
Metastatic Spinal Disease
 Metastatic Spinal Disease Mr Neil Chiverton Consultant Spinal Surgeon, Sheffield Objectives The scale and nature of the problem NICE recommendations Surgical decision making Case illustrations Incidence
Metastatic Spinal Disease Mr Neil Chiverton Consultant Spinal Surgeon, Sheffield Objectives The scale and nature of the problem NICE recommendations Surgical decision making Case illustrations Incidence
agreed MSCC pathways and guidelines).
 Referral of Patients with Spinal Metastatic Disease and Suspected Metastatic Spinal Cord Compression (to be used in association with locally West Midlands Clinical Networks and Clinical Senate Coversheet
Referral of Patients with Spinal Metastatic Disease and Suspected Metastatic Spinal Cord Compression (to be used in association with locally West Midlands Clinical Networks and Clinical Senate Coversheet
Kim, Hyoungmin 1 ; Lee, Choon-Ki 1 ; Yeom, Jin S. 1 ; Lee, Jae Hyup 1 ; Lee, Suk- Joong 2 ; Chang, Bong-Soon 1
 The Predictive Value of the Spinal Instability Neoplastic Score (SINS) System for Adverse Events of Pathologic Fracture and Spinal Cord Compression in Patients with Single Spinal Metas tasis. Kim, Hyoungmin
The Predictive Value of the Spinal Instability Neoplastic Score (SINS) System for Adverse Events of Pathologic Fracture and Spinal Cord Compression in Patients with Single Spinal Metas tasis. Kim, Hyoungmin
A Novel Classification System for Spinal Instability in Neoplastic Disease
 A Novel Classification System for Spinal Instability in Neoplastic Disease An Evidence-Based Approach and Expert Consensus From the Spine Oncology Study Group Charles G. Fisher, MD, MHSc, FRCSC,* Christian
A Novel Classification System for Spinal Instability in Neoplastic Disease An Evidence-Based Approach and Expert Consensus From the Spine Oncology Study Group Charles G. Fisher, MD, MHSc, FRCSC,* Christian
Separation Surgery for Spinal Metastases: A Review on Surgical Treatment Goals
 WScJ : 5-9, 6 Separation Surgery for Spinal Metastases: A Review on Surgical Treatment Goals Gabriel A. Smith, Arunit J. Chugh, Michael Steinmetz Department of Neurosurgery, Case Western Reserve University
WScJ : 5-9, 6 Separation Surgery for Spinal Metastases: A Review on Surgical Treatment Goals Gabriel A. Smith, Arunit J. Chugh, Michael Steinmetz Department of Neurosurgery, Case Western Reserve University
Reliability of the AOSpine thoracolumbar spine injury classification system and thoracolumbar injury classification and severity score (TLICS)
 Editorial Page 1 of 5 Reliability of the AOSpine thoracolumbar spine injury classification system and thoracolumbar injury classification and severity score (TLICS) Jetan H. Badhiwala, Michael G. Fehlings
Editorial Page 1 of 5 Reliability of the AOSpine thoracolumbar spine injury classification system and thoracolumbar injury classification and severity score (TLICS) Jetan H. Badhiwala, Michael G. Fehlings
Surgical management of spinal osteoblastomas
 CLINICAL ARTICLE J Neurosurg Spine 27:321 327, 2017 Surgical management of spinal osteoblastomas Anne L. Versteeg, MD, 1 Nicolas Dea, MD, MSc, FRCSC, 2 Stefano Boriani, MD, 3 Peter P. Varga, MD, 4 Alessandro
CLINICAL ARTICLE J Neurosurg Spine 27:321 327, 2017 Surgical management of spinal osteoblastomas Anne L. Versteeg, MD, 1 Nicolas Dea, MD, MSc, FRCSC, 2 Stefano Boriani, MD, 3 Peter P. Varga, MD, 4 Alessandro
9:00-9:10 am Metastatic Epidural Cervical Spinal Cord Compression CSRS San Diego, 2015 Michael G. Fehlings, MD
 9:00-9:10 am Metastatic Epidural Cervical Spinal Cord Compression CSRS San Diego, 2015 Michael G. Fehlings, MD 1 BACKGROUND After the lungs and the liver, metastases most frequently arise in osseous tissues;
9:00-9:10 am Metastatic Epidural Cervical Spinal Cord Compression CSRS San Diego, 2015 Michael G. Fehlings, MD 1 BACKGROUND After the lungs and the liver, metastases most frequently arise in osseous tissues;
Imaging of bone metastases
 Imaging of bone metastases Antoine Feydy Service de Radiologie B Hôpital Cochin APHP Université Paris Descartes antoine.feydy@aphp.fr MEXICO 2016 INTRODUCTION Diagnostic Imaging Imaging Modalities Strengths,
Imaging of bone metastases Antoine Feydy Service de Radiologie B Hôpital Cochin APHP Université Paris Descartes antoine.feydy@aphp.fr MEXICO 2016 INTRODUCTION Diagnostic Imaging Imaging Modalities Strengths,
Surgical Treatment of Spine Surgery Experience Primary Spinal Neoplasms ( ) Ziya L. Gokaslan, MD, FACS Approximately 3500 spine tumor
 Surgical Treatment of Primary Spinal Neoplasms Ziya L. Gokaslan, MD, FACS Donlin M. Long Professor Professor of Neurosurgery, Oncology & Orthopaedic Surgery Vice Chairman Director of Spine Program Department
Surgical Treatment of Primary Spinal Neoplasms Ziya L. Gokaslan, MD, FACS Donlin M. Long Professor Professor of Neurosurgery, Oncology & Orthopaedic Surgery Vice Chairman Director of Spine Program Department
Magnetic Resonance Imaging Interpretation in Patients With Symptomatic Lumbar Spine Disc Herniations
 Magnetic Resonance Imaging Interpretation in Patients With Symptomatic Lumbar Spine Disc Herniations Comparison of Clinician and Radiologist Readings Jon D. Lurie, MD, MS,* David M. Doman, MD, Kevin F.
Magnetic Resonance Imaging Interpretation in Patients With Symptomatic Lumbar Spine Disc Herniations Comparison of Clinician and Radiologist Readings Jon D. Lurie, MD, MS,* David M. Doman, MD, Kevin F.
Recommendations for cross-sectional imaging in cancer management, Second edition
 www.rcr.ac.uk Recommendations for cross-sectional imaging in cancer management, Second edition Tumours of the spinal cord Faculty of Clinical Radiology www.rcr.ac.uk Contents Primary spinal cord tumours
www.rcr.ac.uk Recommendations for cross-sectional imaging in cancer management, Second edition Tumours of the spinal cord Faculty of Clinical Radiology www.rcr.ac.uk Contents Primary spinal cord tumours
SPINE. Oncology Symposium. Multidisciplinary JUNE 3-4, Conference Location:
 Multidisciplinary SPINE Oncology Symposium JUNE 3-4, 2016 Conference Location: Memorial Sloan Kettering Cancer Center Zuckerman Research Center 417 East 68th Street, New York, NY 10065 Course Overview
Multidisciplinary SPINE Oncology Symposium JUNE 3-4, 2016 Conference Location: Memorial Sloan Kettering Cancer Center Zuckerman Research Center 417 East 68th Street, New York, NY 10065 Course Overview
Observer variation for radiography, computed tomography, and magnetic resonance imaging of occult hip fractures
 Observer variation for radiography, computed tomography, and magnetic resonance imaging of occult hip fractures Collin, David; Dunker, Dennis; Gothlin, Jan H.; Geijer, Mats Published in: Acta Radiologica
Observer variation for radiography, computed tomography, and magnetic resonance imaging of occult hip fractures Collin, David; Dunker, Dennis; Gothlin, Jan H.; Geijer, Mats Published in: Acta Radiologica
J Korean Soc Spine Surg 2018 Jun;25(2): Originally published online June 30, 2018;
 Journal of Korean Society of Spine Surgery The Spinal Instability Neoplastic Score (SINS) as a Surgical Decision-Making Tool for the Treatment of Spine Metastasis Sang-Min Park, M.D., Hyoungmin Kim, M.D.,
Journal of Korean Society of Spine Surgery The Spinal Instability Neoplastic Score (SINS) as a Surgical Decision-Making Tool for the Treatment of Spine Metastasis Sang-Min Park, M.D., Hyoungmin Kim, M.D.,
Evaluation of prognostic scoring systems for bone metastases using single center data
 MOLECULAR AND CLINICAL ONCOLOGY 3: 1361-1370, 2015 Evaluation of prognostic scoring systems for bone metastases using single center data HIROFUMI SHIMADA 1, TAKAO SETOGUCHI 2, SHUNSUKE NAKAMURA 1, MASAHIRO
MOLECULAR AND CLINICAL ONCOLOGY 3: 1361-1370, 2015 Evaluation of prognostic scoring systems for bone metastases using single center data HIROFUMI SHIMADA 1, TAKAO SETOGUCHI 2, SHUNSUKE NAKAMURA 1, MASAHIRO
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/35777 holds various files of this Leiden University dissertation. Author: Wijffels, Mathieu Mathilde Eugene Title: The clinical and non-clinical aspects
Cover Page The handle http://hdl.handle.net/1887/35777 holds various files of this Leiden University dissertation. Author: Wijffels, Mathieu Mathilde Eugene Title: The clinical and non-clinical aspects
Decision Making Flowchart for Metastatic Spinal Cord Compression and Pathological Spinal Fractures
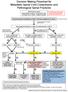 Decision Making Flowchart for Metastatic Spinal Cord Compression and Pathological Spinal Fractures All Referrals (see notes): Spinal Surgeons Locally or Trauma SpR at UHW Oncology SpR at Velindre / Singleton
Decision Making Flowchart for Metastatic Spinal Cord Compression and Pathological Spinal Fractures All Referrals (see notes): Spinal Surgeons Locally or Trauma SpR at UHW Oncology SpR at Velindre / Singleton
The use of surgery in the elderly. for management of metastatic epidural spinal cord compression
 The use of surgery in the elderly Bone Tumor Simulators for management of metastatic epidural spinal cord compression Justin E. Bird, M.D. Assistant Professor Orthopaedic Oncology and Spine Surgery Epidemiology
The use of surgery in the elderly Bone Tumor Simulators for management of metastatic epidural spinal cord compression Justin E. Bird, M.D. Assistant Professor Orthopaedic Oncology and Spine Surgery Epidemiology
8/3/2017. Spine SBRT: A Clinician's Update On Techniques and Outcomes. Disclosures. Outline
 Spine SBRT: A Clinician's Update On Techniques and Outcomes Chia-Lin (Eric) Tseng, MD FRCPC Radiation Oncologist Sunnybrook Health Sciences Centre University of Toronto August 3, 2017 Disclosures I have
Spine SBRT: A Clinician's Update On Techniques and Outcomes Chia-Lin (Eric) Tseng, MD FRCPC Radiation Oncologist Sunnybrook Health Sciences Centre University of Toronto August 3, 2017 Disclosures I have
Radiotherapy symptoms control in bone mets. Francesco Cellini GemelliART. Ernesto Maranzano,MD. Session 5: Symptoms management
 Session 5: Symptoms management Radiotherapy symptoms control in bone mets Francesco Cellini GemelliART Ernesto Maranzano,MD Director of Oncology Department Chief of Radiation Oncology Centre S. Maria Hospital
Session 5: Symptoms management Radiotherapy symptoms control in bone mets Francesco Cellini GemelliART Ernesto Maranzano,MD Director of Oncology Department Chief of Radiation Oncology Centre S. Maria Hospital
Disclosures. Disclosures 27/01/2019. Modern approach and pitfalls in metastatic spine surgery. None.. Jeremy Reynolds
 Modern approach and pitfalls in metastatic spine surgery Jeremy Reynolds Spine Lead Oxford Bone and Soft Tissue Sarcoma Service MSCC Lead Thames Valley Cancer Network Clinical Lead Oxford Spine 1 Disclosures
Modern approach and pitfalls in metastatic spine surgery Jeremy Reynolds Spine Lead Oxford Bone and Soft Tissue Sarcoma Service MSCC Lead Thames Valley Cancer Network Clinical Lead Oxford Spine 1 Disclosures
A Validated Classification for External Immobilization of the Cervical Spine
 72 Original Research A Validated Classification for External Immobilization of the Cervical Spine Micha Holla 1 Joske M. R. Huisman 1 Allard J. F. Hosman 1 1 Department of Orthopaedics, Radboud University
72 Original Research A Validated Classification for External Immobilization of the Cervical Spine Micha Holla 1 Joske M. R. Huisman 1 Allard J. F. Hosman 1 1 Department of Orthopaedics, Radboud University
Statistical Validation of the Grand Rapids Arch Collapse Classification
 Statistical Validation of the Grand Rapids Arch Collapse Classification David Burkard, BS Michelle Padley, CRTM John Anderson, MD Donald Bohay, MD John Maskill, MD Daniel Patton, MD Orthopaedic Associates
Statistical Validation of the Grand Rapids Arch Collapse Classification David Burkard, BS Michelle Padley, CRTM John Anderson, MD Donald Bohay, MD John Maskill, MD Daniel Patton, MD Orthopaedic Associates
SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT
 SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT 1 Anatomy 3 columns- Anterior, middle and Posterior Anterior- ALL, Anterior 2/3 rd body & disc. Middle- Posterior 1/3 rd of body & disc, PLL Posterior-
SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT 1 Anatomy 3 columns- Anterior, middle and Posterior Anterior- ALL, Anterior 2/3 rd body & disc. Middle- Posterior 1/3 rd of body & disc, PLL Posterior-
factor for identifying unstable thoracolumbar fractures. There are clinical and radiological criteria
 NMJ-Vol :2/ Issue:1/ Jan June 2013 Case Report Medical Sciences Progressive subluxation of thoracic wedge compression fracture with unidentified PLC injury Dr.Thalluri.Gopala krishnaiah* Dr.Voleti.Surya
NMJ-Vol :2/ Issue:1/ Jan June 2013 Case Report Medical Sciences Progressive subluxation of thoracic wedge compression fracture with unidentified PLC injury Dr.Thalluri.Gopala krishnaiah* Dr.Voleti.Surya
Classification of Thoracolumbar Spine Injuries
 Classification of Thoracolumbar Spine Injuries Guillem Saló Bru 1 IMAS. Hospitals del Mar i de l Esperança. ICATME. Institut Universitari Dexeus USP. UNIVERSITAT AUTÒNOMA DE BARCELONA Objectives of classification
Classification of Thoracolumbar Spine Injuries Guillem Saló Bru 1 IMAS. Hospitals del Mar i de l Esperança. ICATME. Institut Universitari Dexeus USP. UNIVERSITAT AUTÒNOMA DE BARCELONA Objectives of classification
Review Article Chondrosarcoma of the Mobile Spine and Sacrum
 Sarcoma Volume 2011, Article ID 274281, 4 pages doi:10.1155/2011/274281 Review Article Chondrosarcoma of the Mobile Spine and Sacrum Ryan M. Stuckey and Rex A. W. Marco Department of Orthopaedics, University
Sarcoma Volume 2011, Article ID 274281, 4 pages doi:10.1155/2011/274281 Review Article Chondrosarcoma of the Mobile Spine and Sacrum Ryan M. Stuckey and Rex A. W. Marco Department of Orthopaedics, University
The vertebral column is the primary osseous target of
 spine clinical article J Neurosurg Spine 23:228 232, 2015 Predictors of delayed failure of structural kyphoplasty for pathological compression fractures in cancer patients Gary Rajah, MD, 1 David Altshuler,
spine clinical article J Neurosurg Spine 23:228 232, 2015 Predictors of delayed failure of structural kyphoplasty for pathological compression fractures in cancer patients Gary Rajah, MD, 1 David Altshuler,
Page 1 of 6 PATIENT PRESENTATION
 PATIENT PRESENTATION Suspected spinal cord compression (severe pain or abnormal neurology, or incidental finding on MRI- not intended for traumatic injuries. If in emergency center, triage patient as emergent.)
PATIENT PRESENTATION Suspected spinal cord compression (severe pain or abnormal neurology, or incidental finding on MRI- not intended for traumatic injuries. If in emergency center, triage patient as emergent.)
Clinical Appropriateness Guidelines: Advanced Imaging
 Clinical Appropriateness Guidelines: Advanced Imaging Appropriate Use Criteria: Imaging of Bone Marrow Blood Supply Effective Date: September 5, 2017 Proprietary Date of Origin: 05/21/2007 Last revised:
Clinical Appropriateness Guidelines: Advanced Imaging Appropriate Use Criteria: Imaging of Bone Marrow Blood Supply Effective Date: September 5, 2017 Proprietary Date of Origin: 05/21/2007 Last revised:
Relationship Between Intraclass Correlation and Percent Rater Agreement
 Relationship Between Intraclass Correlation and Percent Rater Agreement When raters are involved in scoring procedures, inter-rater reliability (IRR) measures are used to establish the reliability of measures.
Relationship Between Intraclass Correlation and Percent Rater Agreement When raters are involved in scoring procedures, inter-rater reliability (IRR) measures are used to establish the reliability of measures.
The value of multidisciplinary tumor boards in cancer care
 The value of multidisciplinary tumor boards in cancer care Executive summary Tumor boards provide a collaborative, multidisciplinary approach to cancer care, bringing together oncology, radiology and pathology
The value of multidisciplinary tumor boards in cancer care Executive summary Tumor boards provide a collaborative, multidisciplinary approach to cancer care, bringing together oncology, radiology and pathology
The effect of early versus delayed radiation therapy on length of hospital stay in the palliative setting
 Original Article on Palliative Radiotherapy The effect of early versus delayed radiation therapy on length of hospital stay in the palliative setting Taylor R. Cushman 1, Shervin Shirvani 2, Mohamed Khan
Original Article on Palliative Radiotherapy The effect of early versus delayed radiation therapy on length of hospital stay in the palliative setting Taylor R. Cushman 1, Shervin Shirvani 2, Mohamed Khan
Upper Cervical Spine - Occult Injury and Trigger for CT Exam
 Upper Cervical Spine - Occult Injury and Trigger for CT Exam Main Menu Introduction Clinical clearance of C-SpineC Radiographic evaluation Norms for C-spineC Triggers for CT exam: Odontoid Lateral view
Upper Cervical Spine - Occult Injury and Trigger for CT Exam Main Menu Introduction Clinical clearance of C-SpineC Radiographic evaluation Norms for C-spineC Triggers for CT exam: Odontoid Lateral view
CP80 Version: V01. Acute Oncology Management Service Date approved: 8 th May 2015 Date ratified: 1 st June 2015 Review date: 1 st June 2017
 STANDARD OPERATING PROCEDURE (SOP) AND PATHWAY FOR THE MANAGEMENT OF PATIENTS WITH METASTATIC SPINAL CORD COMPRESSION (MSCC) WITHIN THE CHRISTIE (Refer to the Manchester Cancer Network MSCC Pathway flowchart)
STANDARD OPERATING PROCEDURE (SOP) AND PATHWAY FOR THE MANAGEMENT OF PATIENTS WITH METASTATIC SPINAL CORD COMPRESSION (MSCC) WITHIN THE CHRISTIE (Refer to the Manchester Cancer Network MSCC Pathway flowchart)
Case Conference: SBRT for spinal metastases D A N I E L S I M P S O N M D 3 / 2 7 / 1 2
 Case Conference: SBRT for spinal metastases D A N I E L S I M P S O N M D 3 / 2 7 / 1 2 Case 79 yo M with hx of T3N0 colon cancer diagnosed in 2008 metastatic liver disease s/p liver segmentectomy 2009
Case Conference: SBRT for spinal metastases D A N I E L S I M P S O N M D 3 / 2 7 / 1 2 Case 79 yo M with hx of T3N0 colon cancer diagnosed in 2008 metastatic liver disease s/p liver segmentectomy 2009
En bloc spondylectomy for spinal metastases: a review of techniques
 Neurosurg Focus 15 (5):Article 6, 2003, Click here to return to Table of Contents En bloc spondylectomy for spinal metastases: a review of techniques KEVIN C. YAO, M.D., STEFANO BORIANI, M.D., ZIYA L.
Neurosurg Focus 15 (5):Article 6, 2003, Click here to return to Table of Contents En bloc spondylectomy for spinal metastases: a review of techniques KEVIN C. YAO, M.D., STEFANO BORIANI, M.D., ZIYA L.
Malignant metastatic tumors of the upper cervical
 J Neurosurg Spine 21:886 891, 2014 AANS, 2014 Treatment of C-2 metastatic tumors with intraoperative transoral or transpedicular vertebroplasty and occipitocervical posterior fixation Clinical article
J Neurosurg Spine 21:886 891, 2014 AANS, 2014 Treatment of C-2 metastatic tumors with intraoperative transoral or transpedicular vertebroplasty and occipitocervical posterior fixation Clinical article
Hybrid bone scintigraphy in gastrointestinal malignancies Institutional Experience
 Hybrid bone scintigraphy in gastrointestinal malignancies Institutional Experience Nazia Rashid 1, Saima Riaz 1, Humayun Bashir 1, Shafqat Mehmood 2 1 Nuclear Medicine Department ad 2 Internal Medicine
Hybrid bone scintigraphy in gastrointestinal malignancies Institutional Experience Nazia Rashid 1, Saima Riaz 1, Humayun Bashir 1, Shafqat Mehmood 2 1 Nuclear Medicine Department ad 2 Internal Medicine
The surgical treatment of metastatic disease of the spine
 The surgical treatment of metastatic disease of the spine Péter Banczerowski National Institute of Neurosurgery, Budapest Spine tumours 15% of the primary tumours of the CNS affect the spine The spine
The surgical treatment of metastatic disease of the spine Péter Banczerowski National Institute of Neurosurgery, Budapest Spine tumours 15% of the primary tumours of the CNS affect the spine The spine
ASJ. Magnification Error in Digital Radiographs of the Cervical Spine Against Magnetic Resonance Imaging Measurements. Asian Spine Journal
 Asian Spine Journal Asian Spine Clinical Journal Study Asian Spine J 2013;7(4):267-272 Magnification http://dx.doi.org/10.4184/asj.2013.7.4.267 error in cervical spine 267 Magnification Error in Digital
Asian Spine Journal Asian Spine Clinical Journal Study Asian Spine J 2013;7(4):267-272 Magnification http://dx.doi.org/10.4184/asj.2013.7.4.267 error in cervical spine 267 Magnification Error in Digital
Spinal cord compression as a first presentation of cancer: A case report
 J Pain Manage 2013;6(4):319-322 ISSN: 1939-5914 Nova Science Publishers, Inc. Spinal cord compression as a first presentation of cancer: A case report Nicholas Lao, BMSc(C), Michael Poon, MD(C), Marko
J Pain Manage 2013;6(4):319-322 ISSN: 1939-5914 Nova Science Publishers, Inc. Spinal cord compression as a first presentation of cancer: A case report Nicholas Lao, BMSc(C), Michael Poon, MD(C), Marko
Metastatic Spinal Cord Compression (MSCC) Clinical guidelines and pathway
 Metastatic Spinal Cord Compression (MSCC) Clinical guidelines and pathway Version 2: May 2012 To be read in conjunction with NICE CG75 Developed by consensus by: Dr Peter Robson, Consultant Oncologist,
Metastatic Spinal Cord Compression (MSCC) Clinical guidelines and pathway Version 2: May 2012 To be read in conjunction with NICE CG75 Developed by consensus by: Dr Peter Robson, Consultant Oncologist,
Suspecting Tumors, or Could it be cancer?
 Suspecting Tumors, or Could it be cancer? Donna E. Reece, M.D. Princess Margaret Cancer Centre University Health Network Toronto, ON CANADA 07 February 2018 Background Low back pain is common However,
Suspecting Tumors, or Could it be cancer? Donna E. Reece, M.D. Princess Margaret Cancer Centre University Health Network Toronto, ON CANADA 07 February 2018 Background Low back pain is common However,
HIGH LEVEL - Science
 Learning Outcomes HIGH LEVEL - Science Describe the structure and function of the back and spine (8a) Outline the functional anatomy and physiology of the spinal cord and peripheral nerves (8a) Describe
Learning Outcomes HIGH LEVEL - Science Describe the structure and function of the back and spine (8a) Outline the functional anatomy and physiology of the spinal cord and peripheral nerves (8a) Describe
MODULE 1 BASIC COMPREHENSIVE COURSE 19 June 2017 PRELIMINARY PROGRAMME
 MODULE 1 BASIC COMPREHENSIVE COURSE 19 June 2017 PRELIMINARY PROGRAMME QUICK FACTS WHEN: WHERE: MAXIMUM ATTENDEES: REGISTRATION FEE: CME CREDITS: LANGUAGE: DRESS: IMPORTANT NOTE: 19 June 2017 Strasbourg,
MODULE 1 BASIC COMPREHENSIVE COURSE 19 June 2017 PRELIMINARY PROGRAMME QUICK FACTS WHEN: WHERE: MAXIMUM ATTENDEES: REGISTRATION FEE: CME CREDITS: LANGUAGE: DRESS: IMPORTANT NOTE: 19 June 2017 Strasbourg,
of the lumbar facet joints there
 Skeletal Radiol (1999) 28:215±219 International Skeletal Society 1999 A R T I C L E Dominik Weishaupt Marco Zanetti Norbert Boos Juerg Hodler MR imaging and CT in osteoarthritis of the lumbar facet joints
Skeletal Radiol (1999) 28:215±219 International Skeletal Society 1999 A R T I C L E Dominik Weishaupt Marco Zanetti Norbert Boos Juerg Hodler MR imaging and CT in osteoarthritis of the lumbar facet joints
Delayed surgery in neurologically intact patients affected by thoraco-lumbar junction burst fractures: to reduce pain and improve quality of life
 Original Study Delayed surgery in neurologically intact patients affected by thoraco-lumbar junction burst fractures: to reduce pain and improve quality of life Lorenzo Nigro 1, Roberto Tarantino 1, Pasquale
Original Study Delayed surgery in neurologically intact patients affected by thoraco-lumbar junction burst fractures: to reduce pain and improve quality of life Lorenzo Nigro 1, Roberto Tarantino 1, Pasquale
AO CLASSIFICATIONS THORACO-LUMBAR SPINAL INJURIES
 AO CLASSIFICATIONS THORACO-LUMBAR SPINAL INJURIES T H E A O / A S I F ( A R B E I T S G E M E I N S C H A F T F Ü R O S T E O S Y N T H E S E F R A G E N / A S S O C I A T I O N F O R T H E S T U D Y O
AO CLASSIFICATIONS THORACO-LUMBAR SPINAL INJURIES T H E A O / A S I F ( A R B E I T S G E M E I N S C H A F T F Ü R O S T E O S Y N T H E S E F R A G E N / A S S O C I A T I O N F O R T H E S T U D Y O
COMMITMENT &SOLUTIONS UNPARALLELED. Assessing Human Visual Inspection for Acceptance Testing: An Attribute Agreement Analysis Case Study
 DATAWorks 2018 - March 21, 2018 Assessing Human Visual Inspection for Acceptance Testing: An Attribute Agreement Analysis Case Study Christopher Drake Lead Statistician, Small Caliber Munitions QE&SA Statistical
DATAWorks 2018 - March 21, 2018 Assessing Human Visual Inspection for Acceptance Testing: An Attribute Agreement Analysis Case Study Christopher Drake Lead Statistician, Small Caliber Munitions QE&SA Statistical
Induction and Maintenance of Lordosis in MultiLevel ACDF Using Allograft. Saad Khairi, MD Jennifer Murphy Robert S. Pashman, MD
 Induction and Maintenance of Lordosis in MultiLevel ACDF Using Allograft Saad Khairi, MD Jennifer Murphy Robert S. Pashman, MD Purpose Is lordosis induced by multilevel cortical allograft ACDF placed on
Induction and Maintenance of Lordosis in MultiLevel ACDF Using Allograft Saad Khairi, MD Jennifer Murphy Robert S. Pashman, MD Purpose Is lordosis induced by multilevel cortical allograft ACDF placed on
Subaxial Cervical Spine Trauma
 Subaxial Cervical Spine Trauma Pooria Salari, MD Assistant Professor Of Orthopaedics Department of Orthopaedic Surgery St. Louis University School of Medicine St. Louis, Missouri, USA Initial Evaluation
Subaxial Cervical Spine Trauma Pooria Salari, MD Assistant Professor Of Orthopaedics Department of Orthopaedic Surgery St. Louis University School of Medicine St. Louis, Missouri, USA Initial Evaluation
Multidisciplinary Spine Oncology Symposium
 Multidisciplinary Spine Oncology Symposium Friday-Saturday, April 7-8, 2017 Memorial Sloan Kettering Cancer Center Zuckerman Research Center 417 East 68th Street New York, NY 10065 Multidisciplinary Spine
Multidisciplinary Spine Oncology Symposium Friday-Saturday, April 7-8, 2017 Memorial Sloan Kettering Cancer Center Zuckerman Research Center 417 East 68th Street New York, NY 10065 Multidisciplinary Spine
2 nd Annual Spine Trauma Summit May 20-21, 2016 at the Seattle Science Foundation AGENDA. Friday, May 20, 2016
 2 nd Annual Spine Trauma Summit May 20-21, 2016 at the Seattle Science Foundation AGENDA Friday, May 20, 2016 6:00pm 6:30pm 9:00pm Buffet Dinner Served (not accredited) Case Reviews and Discussions All
2 nd Annual Spine Trauma Summit May 20-21, 2016 at the Seattle Science Foundation AGENDA Friday, May 20, 2016 6:00pm 6:30pm 9:00pm Buffet Dinner Served (not accredited) Case Reviews and Discussions All
Bone Metastases. Sukanda Denjanta, M.Sc., BCOP Pharmacy Department, Chiangrai Prachanukroh Hospital
 Bone Metastases Sukanda Denjanta, M.Sc., BCOP Pharmacy Department, Chiangrai Prachanukroh Hospital 1 Outline Pathophysiology Signs & Symptoms Diagnosis Treatment Spinal Cord Compression 2 General Information
Bone Metastases Sukanda Denjanta, M.Sc., BCOP Pharmacy Department, Chiangrai Prachanukroh Hospital 1 Outline Pathophysiology Signs & Symptoms Diagnosis Treatment Spinal Cord Compression 2 General Information
A Worldwide Analysis of the Reliability and Perceived Importance of an Injury to the Posterior Ligamentous Complex in AO Type A Fractures
 378 Original Article GLOBAL SPINE JOURNAL THIEME A Worldwide Analysis of the Reliability and Perceived Importance of an Injury to the Posterior Ligamentous Complex in AO Type A Fractures Gregory D. Schroeder
378 Original Article GLOBAL SPINE JOURNAL THIEME A Worldwide Analysis of the Reliability and Perceived Importance of an Injury to the Posterior Ligamentous Complex in AO Type A Fractures Gregory D. Schroeder
A rare case of spinal injury: bilateral facet dislocation without fracture at the lumbosacral joint
 J Orthop Sci (2012) 17:189 193 DOI 10.1007/s00776-011-0082-y CASE REPORT A rare case of spinal injury: bilateral facet dislocation without fracture at the lumbosacral joint Kei Shinohara Shigeru Soshi
J Orthop Sci (2012) 17:189 193 DOI 10.1007/s00776-011-0082-y CASE REPORT A rare case of spinal injury: bilateral facet dislocation without fracture at the lumbosacral joint Kei Shinohara Shigeru Soshi
Neurosurgery (Orthopaedic PGY-1) Goals. Objectives
 Neurosurgery (Orthopaedic PGY-1) Length: 1 month of PGY-1 (Orthopaedic Designated Residents) or 1 month of PGY-2, -3, or -4 year Location: The Queen's Medical Center Primary Supervisor: William Obana,
Neurosurgery (Orthopaedic PGY-1) Length: 1 month of PGY-1 (Orthopaedic Designated Residents) or 1 month of PGY-2, -3, or -4 year Location: The Queen's Medical Center Primary Supervisor: William Obana,
Pott s kyphosis. University Affiliated Sixth People s Hospital, 600 Yishan Road, Shanghai , P.
 QJM Advance Access published November 17, 2014 Pott s kyphosis Author Names: Yi Zhang, Yong-Sheng Yu, Zheng-Hao Tang and Guo-Qing Zang Author Affiliations: Department of Infectious Diseases, Shanghai Jiao
QJM Advance Access published November 17, 2014 Pott s kyphosis Author Names: Yi Zhang, Yong-Sheng Yu, Zheng-Hao Tang and Guo-Qing Zang Author Affiliations: Department of Infectious Diseases, Shanghai Jiao
The Challenges of Managing Spine and Spinal Cord Injuries
 The Challenges of Managing Spine and Spinal Cord Injuries An Evolving Consensus and Opportunities for Change Michael G. Fehlings, MD, PhD, FRCS(C), FACS,* Jefferson R. Wilson, MD,* Marcel F. Dvorak, MD,
The Challenges of Managing Spine and Spinal Cord Injuries An Evolving Consensus and Opportunities for Change Michael G. Fehlings, MD, PhD, FRCS(C), FACS,* Jefferson R. Wilson, MD,* Marcel F. Dvorak, MD,
Signal intensity changes of the posterior elements of the lumbar spine in symptomatic adults
 ORIGINAL ARTICLE SPINE SURGERY AND RELATED RESEARCH Signal intensity changes of the posterior elements of the lumbar spine in symptomatic adults Kosuke Sugiura, Toshinori Sakai, Fumitake Tezuka, Kazuta
ORIGINAL ARTICLE SPINE SURGERY AND RELATED RESEARCH Signal intensity changes of the posterior elements of the lumbar spine in symptomatic adults Kosuke Sugiura, Toshinori Sakai, Fumitake Tezuka, Kazuta
Primary Bone Tumors: Spine Surgery Live -Video Techniques Mobile Spine
 Primary Bone Tumors: Spine Surgery Live -Video Techniques Mobile Spine Christopher Ames MD Professor of Neurosurgery and Orthopedic Surgery Director of Spine Tumor And Deformity Surgery UCSF Department
Primary Bone Tumors: Spine Surgery Live -Video Techniques Mobile Spine Christopher Ames MD Professor of Neurosurgery and Orthopedic Surgery Director of Spine Tumor And Deformity Surgery UCSF Department
APPROPRIATE USE GUIDELINES
 APPROPRIATE USE GUIDELINES Appropriateness of Advanced Imaging Procedures (MRI, CT, Bone Scan/PET) in Patients with Neck Pain CDI QUALITY INSTITUTE: PROVIDER LED ENTITY (PLE) Updated June, 2017 Contents
APPROPRIATE USE GUIDELINES Appropriateness of Advanced Imaging Procedures (MRI, CT, Bone Scan/PET) in Patients with Neck Pain CDI QUALITY INSTITUTE: PROVIDER LED ENTITY (PLE) Updated June, 2017 Contents
Case Report Traumatic Death due to Simultaneous Double Spine Fractures in Patient with Ankylosing Spondylitis
 Case Reports in Orthopedics Volume 2015, Article ID 590935, 4 pages http://dx.doi.org/10.1155/2015/590935 Case Report Traumatic Death due to Simultaneous Double Spine Fractures in Patient with Ankylosing
Case Reports in Orthopedics Volume 2015, Article ID 590935, 4 pages http://dx.doi.org/10.1155/2015/590935 Case Report Traumatic Death due to Simultaneous Double Spine Fractures in Patient with Ankylosing
Demonstration of active Side Shift Type1(Mirror Image ) in Right (Major) Thoracic curve.
 Side Shift The Development of a Classification System for the Use of The (modified) Side-Shift Approach to The Conservative Management of Scoliosis Tony Betts Royal National Orthopaedic Hospital Background
Side Shift The Development of a Classification System for the Use of The (modified) Side-Shift Approach to The Conservative Management of Scoliosis Tony Betts Royal National Orthopaedic Hospital Background
Workshop. Eric M. Massicotte, MD, MSc, MBA, FRCSC Associate Professor University of Toronto
 Workshop Eric M. Massicotte, MD, MSc, MBA, FRCSC Associate Professor University of Toronto Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored,
Workshop Eric M. Massicotte, MD, MSc, MBA, FRCSC Associate Professor University of Toronto Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored,
Am I eligible for the TOPS study? Possibly, if you suffer from one or more of the following conditions:
 Am I eligible for the TOPS study? Possibly, if you suffer from one or more of the following conditions: Radiating leg pain Greater leg / buttock pain than back pain Severe pain sets in when walking as
Am I eligible for the TOPS study? Possibly, if you suffer from one or more of the following conditions: Radiating leg pain Greater leg / buttock pain than back pain Severe pain sets in when walking as
Primary care referral criteria for musculoskeletal MRI scans
 Appendix 1 Primary care referral criteria for musculoskeletal MRI scans Accepted Criteria for Direct Access MRI Body Part Symptoms Imaging indicated Lumbar Spine Low Back Pain with adverse symptoms or
Appendix 1 Primary care referral criteria for musculoskeletal MRI scans Accepted Criteria for Direct Access MRI Body Part Symptoms Imaging indicated Lumbar Spine Low Back Pain with adverse symptoms or
BRIEFING PAPER THE USE OF RED FLAGS TO IDENTIFY SERIOUS SPINAL PATHOLOGY THE CHRISTIE, GREATER MANCHESTER & CHESHIRE. Version:
 BRIEFING PAPER THE USE OF RED FLAGS TO IDENTIFY SERIOUS SPINAL PATHOLOGY THE CHRISTIE, GREATER MANCHESTER & CHESHIRE Procedure Reference: Document Owner: Jackie Turnpenney Version: Accountable Committee:
BRIEFING PAPER THE USE OF RED FLAGS TO IDENTIFY SERIOUS SPINAL PATHOLOGY THE CHRISTIE, GREATER MANCHESTER & CHESHIRE Procedure Reference: Document Owner: Jackie Turnpenney Version: Accountable Committee:
A practical tool for locomotion scoring in sheep: Reliability when used by veterinary surgeons and sheep farmers
 See discussions, stats, and author profiles for this publication at: https://www.researchgate.net/publication/272945558 A practical tool for locomotion scoring in sheep: Reliability when used by veterinary
See discussions, stats, and author profiles for this publication at: https://www.researchgate.net/publication/272945558 A practical tool for locomotion scoring in sheep: Reliability when used by veterinary
Cement augmentation in spinal tumors: a systematic review comparing vertebroplasty and kyphoplasty
 35 35 43 Cement augmentation in spinal tumors: a systematic review comparing vertebroplasty and kyphoplasty Authors Josh E Schroeder¹, Erika Ecker², Andrea C Skelly², Leon Kaplan¹ Institutions ¹ Orthopedic
35 35 43 Cement augmentation in spinal tumors: a systematic review comparing vertebroplasty and kyphoplasty Authors Josh E Schroeder¹, Erika Ecker², Andrea C Skelly², Leon Kaplan¹ Institutions ¹ Orthopedic
Metastatic disease of the Spine
 Metastatic disease of the Spine Jwalant S. Mehta MS (Orth); MCh (Orth); D Orth; FRCS (Tr & Orth) Consultant Spine Surgeon The Royal Orthopaedic Hospital Birmingham Children s Hospital MSCC Metastatic Spinal
Metastatic disease of the Spine Jwalant S. Mehta MS (Orth); MCh (Orth); D Orth; FRCS (Tr & Orth) Consultant Spine Surgeon The Royal Orthopaedic Hospital Birmingham Children s Hospital MSCC Metastatic Spinal
Clinical Correlation of a New Practical MRI Method for Assessing Cervical Spinal Canal Compression
 Musculoskeletal Imaging Original Research Park et al. MRI Assessment of Cervical Spinal Canal Compression Musculoskeletal Imaging Original Research Hee-Jin Park 1,2 Sam Soo Kim 2 Eun-Chul Chung 1 So-Yeon
Musculoskeletal Imaging Original Research Park et al. MRI Assessment of Cervical Spinal Canal Compression Musculoskeletal Imaging Original Research Hee-Jin Park 1,2 Sam Soo Kim 2 Eun-Chul Chung 1 So-Yeon
National Imaging Associates, Inc. Clinical guidelines
 National Imaging Associates, Inc. Clinical guidelines Original Date: September 1997 THORACIC SPINE CT Page 1 of 5 CPT Codes: 72128, 72129, 72130 Last Review Date: May 2013 Guideline Number: NIA_CG_043
National Imaging Associates, Inc. Clinical guidelines Original Date: September 1997 THORACIC SPINE CT Page 1 of 5 CPT Codes: 72128, 72129, 72130 Last Review Date: May 2013 Guideline Number: NIA_CG_043
Heidi Lako-Adamson, MD, NRP, FAEMS FM Ambulance and Sanford EMS Education Medical Director
 Heidi Lako-Adamson, MD, NRP, FAEMS FM Ambulance and Sanford EMS Education Medical Director Spinal cord injury statistics. Definition of spinal motion restriction. Difference between spinal motion restriction
Heidi Lako-Adamson, MD, NRP, FAEMS FM Ambulance and Sanford EMS Education Medical Director Spinal cord injury statistics. Definition of spinal motion restriction. Difference between spinal motion restriction
Diffusion-weighted MR Imaging Offers No Advantage over Routine Noncontrast MR Imaging in the Detection of Vertebral Metastases
 AJNR Am J Neuroradiol 1:948 953, May Diffusion-weighted MR Imaging Offers No Advantage over Routine Noncontrast MR Imaging in the Detection of Vertebral Metastases Mauricio Castillo, Andres Arbelaez, J.
AJNR Am J Neuroradiol 1:948 953, May Diffusion-weighted MR Imaging Offers No Advantage over Routine Noncontrast MR Imaging in the Detection of Vertebral Metastases Mauricio Castillo, Andres Arbelaez, J.
Systematic review Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review (...)
 Systematic review Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review (...) 59 59 66 Cervical artificial disc replacement versus fusion in the cervical spine:
Systematic review Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review (...) 59 59 66 Cervical artificial disc replacement versus fusion in the cervical spine:
Revised Dec Spine MR Protocols
 Spine MR Protocols Sp 1: Cervical spine MRI without contrast Sp 2: Pre- and post-contrast cervical spine MRI Sp 3: Pre- and post-contrast cervical spine MRI (multiple sclerosis protocol) Sp 4: Thoracic
Spine MR Protocols Sp 1: Cervical spine MRI without contrast Sp 2: Pre- and post-contrast cervical spine MRI Sp 3: Pre- and post-contrast cervical spine MRI (multiple sclerosis protocol) Sp 4: Thoracic
OPTICAL TOPOGRAPHIC IMAGING FOR SPINAL INTRAOPERATIVE 3D NAVIGATION IN MINIMALLY INVASIVE APPROACHES: INITIAL PRECLINICAL EXPERIENCE
 OPTICAL TOPOGRAPHIC IMAGING FOR SPINAL INTRAOPERATIVE 3D NAVIGATION IN MINIMALLY INVASIVE APPROACHES: INITIAL PRECLINICAL EXPERIENCE Authors: Daipayan Guha 1, Raphael J akubovic 2, Shaurya Gupta 1, Albert
OPTICAL TOPOGRAPHIC IMAGING FOR SPINAL INTRAOPERATIVE 3D NAVIGATION IN MINIMALLY INVASIVE APPROACHES: INITIAL PRECLINICAL EXPERIENCE Authors: Daipayan Guha 1, Raphael J akubovic 2, Shaurya Gupta 1, Albert
Departement of Neurosurgery A.O.R.N A. Cardarelli- Naples.
 Percutaneous posterior pedicle screw fixation in the treatment of thoracic, lumbar and thoraco-lumbar junction (T12-L1) traumatic and pathological spine fractures. Report of 45 cases. G. Vitale, A. Punzo,
Percutaneous posterior pedicle screw fixation in the treatment of thoracic, lumbar and thoraco-lumbar junction (T12-L1) traumatic and pathological spine fractures. Report of 45 cases. G. Vitale, A. Punzo,
Introductory Lecture. Significance of results in cancer imaging
 Cancer Imaging (2001) 2, 1 5 Introductory Lecture Monday 15 October 2001, 09.10 09.50 Significance of results in cancer imaging Rodney H Reznek Professor of Diagnostic Imaging, St Bartholomew s Hospital,
Cancer Imaging (2001) 2, 1 5 Introductory Lecture Monday 15 October 2001, 09.10 09.50 Significance of results in cancer imaging Rodney H Reznek Professor of Diagnostic Imaging, St Bartholomew s Hospital,
Original Date: October 2015 LUMBAR SPINAL FUSION FOR
 National Imaging Associates, Inc. Clinical guidelines Original Date: October 2015 LUMBAR SPINAL FUSION FOR Page 1 of 9 INSTABILITY AND DEGENERATIVE DISC CONDITIONS FOR CMS (MEDICARE) MEMBERS ONLY CPT4
National Imaging Associates, Inc. Clinical guidelines Original Date: October 2015 LUMBAR SPINAL FUSION FOR Page 1 of 9 INSTABILITY AND DEGENERATIVE DISC CONDITIONS FOR CMS (MEDICARE) MEMBERS ONLY CPT4
COMPUTING READER AGREEMENT FOR THE GRE
 RM-00-8 R E S E A R C H M E M O R A N D U M COMPUTING READER AGREEMENT FOR THE GRE WRITING ASSESSMENT Donald E. Powers Princeton, New Jersey 08541 October 2000 Computing Reader Agreement for the GRE Writing
RM-00-8 R E S E A R C H M E M O R A N D U M COMPUTING READER AGREEMENT FOR THE GRE WRITING ASSESSMENT Donald E. Powers Princeton, New Jersey 08541 October 2000 Computing Reader Agreement for the GRE Writing
Thoracolumbar Spine Fractures
 Thoracolumbar Spine Fractures C. Craig Blackmore, MD, MPH Professor of Radiology Adjunct Professor of Health Services Harborview Injury Prevention and Research Center University of Washington Outline Who
Thoracolumbar Spine Fractures C. Craig Blackmore, MD, MPH Professor of Radiology Adjunct Professor of Health Services Harborview Injury Prevention and Research Center University of Washington Outline Who
ASJ. Detecting Facet Joint and Lateral Mass Injuries of the Subaxial Cervical Spine in Major Trauma Patients. Asian Spine Journal
 Asian Spine Journal Asian Spine Clinical Journal Study Asian Spine J 2015;9(3):327-337 http://dx.doi.org/10.4184/asj.2015.9.3.327 Facet joint injuries 327 Detecting Facet Joint and Lateral Mass Injuries
Asian Spine Journal Asian Spine Clinical Journal Study Asian Spine J 2015;9(3):327-337 http://dx.doi.org/10.4184/asj.2015.9.3.327 Facet joint injuries 327 Detecting Facet Joint and Lateral Mass Injuries
Cervical corpectomy for sub-axial retro-vertebral body lesions
 Eshra Egyptian Journal of Neurosurgery (2019) 33:2 https://doi.org/10.1186/s41984-018-0004-9 Egyptian Journal of Neurosurgery RESEARCH Open Access Cervical corpectomy for sub-axial retro-vertebral body
Eshra Egyptian Journal of Neurosurgery (2019) 33:2 https://doi.org/10.1186/s41984-018-0004-9 Egyptian Journal of Neurosurgery RESEARCH Open Access Cervical corpectomy for sub-axial retro-vertebral body
Original Article Clinics in Orthopedic Surgery 2015;7:
 Original Article Clinics in Orthopedic Surgery 2015;7:344-350 http://dx.doi.org/10.4055/cios.2015.7.3.344 Factors Affecting Survival in Patients Undergoing Palliative Spine Surgery for Metastatic Lung
Original Article Clinics in Orthopedic Surgery 2015;7:344-350 http://dx.doi.org/10.4055/cios.2015.7.3.344 Factors Affecting Survival in Patients Undergoing Palliative Spine Surgery for Metastatic Lung
Update on Management of Malignant Spinal Cord Compression. Heino Hugel Consultant in Palliative Medicine University Hospital Aintree
 Update on Management of Malignant Spinal Cord Compression Heino Hugel Consultant in Palliative Medicine University Hospital Aintree Current Guidelines The symptoms of MSCC may be subtle and therefore careful
Update on Management of Malignant Spinal Cord Compression Heino Hugel Consultant in Palliative Medicine University Hospital Aintree Current Guidelines The symptoms of MSCC may be subtle and therefore careful
Malignant Spinal Cord Compression (MSCC) Clinical Advisor Coordinator
 Malignant Spinal Cord Compression (MSCC) Clinical Advisor Coordinator Induction Training 2016 Version Control This is a controlled document please destroy all previous versions on receipt of a new version.
Malignant Spinal Cord Compression (MSCC) Clinical Advisor Coordinator Induction Training 2016 Version Control This is a controlled document please destroy all previous versions on receipt of a new version.
Reliability of Lichtman s classification for Kienböck s disease in 99 subjects
 Reliability of Lichtman s classification for Kienböck s disease in subjects Masaki Shin, M.D., Masahiro Tatebe, M.D., Hitoshi Hirata, M.D., Shukuki Koh, M.D., Takaaki Shinohara, M.D. Department of Hand
Reliability of Lichtman s classification for Kienböck s disease in subjects Masaki Shin, M.D., Masahiro Tatebe, M.D., Hitoshi Hirata, M.D., Shukuki Koh, M.D., Takaaki Shinohara, M.D. Department of Hand
Edward K. Nomoto, M.D.
 Page 1 of 5 Appointments CURRICULUM VITAE Edward K. Nomoto, M.D. 444 S. San Vicente Blvd, Suite 800 Los Angeles, CA 90048 (310) 423-9780 (work) Cedars-Sinai Medical Center, Spine Center Faculty, Orthopaedic
Page 1 of 5 Appointments CURRICULUM VITAE Edward K. Nomoto, M.D. 444 S. San Vicente Blvd, Suite 800 Los Angeles, CA 90048 (310) 423-9780 (work) Cedars-Sinai Medical Center, Spine Center Faculty, Orthopaedic
New Magnetic Resonance Imaging Grading System for Lumbar Neural Foramina Stenosis
 Original Article New Magnetic Resonance Imaging Grading System for Lumbar Neural Foramina Stenosis DOI: 10.7860/IJARS/2018/30862:2366 Radiology Section BINOJ VARGHESE v, ARUN C BABU ABSTRACT Introduction:
Original Article New Magnetic Resonance Imaging Grading System for Lumbar Neural Foramina Stenosis DOI: 10.7860/IJARS/2018/30862:2366 Radiology Section BINOJ VARGHESE v, ARUN C BABU ABSTRACT Introduction:
Does the Spine Surgeon s Experience Affect Fracture Classification, Assessment of Stability, and Treatment Plan in Thoracolumbar Injuries?
 Thomas Jefferson University Jefferson Digital Commons Rothman Institute Rothman Institute 6-1-2017 Does the Spine Surgeon s Experience Affect Fracture Classification, Assessment of Stability, and Treatment
Thomas Jefferson University Jefferson Digital Commons Rothman Institute Rothman Institute 6-1-2017 Does the Spine Surgeon s Experience Affect Fracture Classification, Assessment of Stability, and Treatment
Audit Report. National Audit of Paediatric Radiology Services in Hospitals
 Audit Report National Audit of Paediatric Radiology Services in Hospitals www.rcr.ac.uk 2 Contents Introduction 3 Standards 4 Material and methods 5 Results 6 Discussion 8 References 10 www.rcr.ac.uk 3
Audit Report National Audit of Paediatric Radiology Services in Hospitals www.rcr.ac.uk 2 Contents Introduction 3 Standards 4 Material and methods 5 Results 6 Discussion 8 References 10 www.rcr.ac.uk 3
CASE REPORT TOTAL EN BLOC SPONDYLECTOMY FOR L2 CHORDOMA: A CASE REPORT
 Nagoya J. Med. Sci. 73. 197 ~ 203, 2011 CASE REPORT TOTAL EN BLOC SPONDYLECTOMY FOR L2 CHORDOMA: A CASE REPORT NORIMITSU WAKAO 1, SHIRO IMAGAMA 1, ZENYA ITO 1, KEI ANDO 1, KENICHI HIRANO 1, RYOJI TAUCHI
Nagoya J. Med. Sci. 73. 197 ~ 203, 2011 CASE REPORT TOTAL EN BLOC SPONDYLECTOMY FOR L2 CHORDOMA: A CASE REPORT NORIMITSU WAKAO 1, SHIRO IMAGAMA 1, ZENYA ITO 1, KEI ANDO 1, KENICHI HIRANO 1, RYOJI TAUCHI
Original Policy Date
 MP 6.01.39 Positional Magnetic Resonance Imaging Medical Policy Section Radiology Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature search/12:2013 Return to Medical
MP 6.01.39 Positional Magnetic Resonance Imaging Medical Policy Section Radiology Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature search/12:2013 Return to Medical
