Malignant Spinal Cord Compression (MSCC) Clinical Advisor Coordinator
|
|
|
- Cuthbert Maxwell
- 6 years ago
- Views:
Transcription
1 Malignant Spinal Cord Compression (MSCC) Clinical Advisor Coordinator Induction Training 2016
2 Version Control This is a controlled document please destroy all previous versions on receipt of a new version. Date Approved: March 2012 Review Date: March 2015 Version Date Issued Review Date Brief Summary of Change Owner s Name 1.0 March 2012 March a January 2014 March October 2016 October 2018 First Draft / NEYHCA branding and formatting Pathway revised and New referral form added Pathway revised and New referral form added MSCC Group / AOCEG MSCC Group / AOCEG For the latest version of these guidelines please see the NEYHCA (Cancer) website Please press control and click on the link below: Signature Sheet Agreement of the NEYHCA (Cancer) MSCC Clinical Advisor Induction Training 2012 These guidelines have been agreed by: Title Name Date Agreed Chair of the MSCC Group Dr Nabil El-Mahdawi Page 2 MSCC Clinical Advisor Induction Training Version 1.1 a January 2016
3 Chair of the MSCC Group Dr Nabil El-Mahdawi Chair of the Acute Oncology CEG Dr Lorcan O Toole Chair, NEYHCA Board / NEYHCA Cancer Management Group Mrs Allison Cooke The MSCC Group have agreed these guidelines Contents Version Control... 2 Signature Sheet... 2 Contents MSCC Induction Training... 4 Background... 4 The Need for an Educational Package... 4 Aetiology of MSCC... 4 Key Signs and Symptoms... 5 Referral pathways... 5 Management pathway... 6 MSCC Coordinator Pathway... 7 Specialist palliative care... 8 Rehabilitation and multi-professional referral... 8 Metastatic Spinal Cord Compression and timing of mobilisation Initial Presentation... 8 Audit... 9 MSCC Clinical Advisor Induction Training Version 1.1 Vs 1.1 January 2016 Page 3
4 Indicators of spinal instability... 9 Stable spine... 9 Discharge planning... 9 Competence of MSCC coordinators Presentations Appendix (i) MSCC Presentation Slides Appendix (ii) Article from Clinical Oncology (2002) Appendix (iii) MSCC Service Poster Appendix (iv) Pathway for Malignant / Metastatic Spinal Cord Compression (MSCC) Appendix (v) Metastatic / Malignant Spinal Cord Compression Referral Form MSCC Induction Training (This is also available as part of the MSCC Clinical Advisors Specification document) Background Malignant Spinal Cord Compression (MSCC) includes compression of the spinal cord. MSCC is a major cause of morbidity and is believed to occur in approximately 5% of all patients diagnosed with cancer. In approximately 85% of cases it results as a consequence of metastases from a primary tumour (3, 4) with cancers of the lung, prostate and breast accounting for around 50% of cases. Other cancers frequently associated with MSCC include lymphoma, renal, multiple myeloma, melanoma and sarcoma. The Need for an Educational Package Early diagnosis of MSCC whilst the patient is still ambulant is crucial in optimising patient outcomes. 9 Studies carried out in the United Kingdom (UK) over the last 10 years have identified several areas where increased awareness of this condition and specific aspects of treatment and rehabilitation could be improved. (10, 11, 12). The main issues identified were: Unacceptable delays in diagnosis and referral are common. Clinicians failed to consider a diagnosis of spinal cord compression resulting in delayed investigation and referral. There is a lack of formal referral procedures for patients with MSCC. Aetiology of MSCC The spinal column is the most common site of bony metastases with the thoracic spine being most frequently affected (70%), followed by lumbosacral (20%) and cervical (10%). Extradural compression of the spinal cord occurs due to tumour expansion into the epidural Page 4 MSCC Clinical Advisor Induction Training Version 1.1 a January 2016
5 space, usually from dissemination of malignant cells to the vertebral bodies or surrounding tissues via the vascular circulation. Direct extension from an intra-abdominal or intrathoracic primary adjacent to it or a primary malignancy arising in the vertebral body can also occur. Intradural spinal cord neoplasms (intramedullary and extramedullary) or metastases (intramedullary) can also present with symptoms of spinal cord compression. MSCC can be the presenting manifestation of a cancer or can be the sole site of recurrence. It is however, more common for it to occur where there is widely disseminated disease. Most patients will die as a result of their underlying cancer within a year of the diagnosis of spinal cord compression; however, patients with more favourable prognostic factors can survive beyond two years. Key Signs and Symptoms Remember: Taking to bed or needing a catheter, even in the absence of pain, should raise the possibility of MSCC. Pain Spinal pain must be treated as significant and should not be assumed to be degenerative disc disease. Radicular pain in a patient with cancer is a major cause of concern. Motor deficits Specific muscle weakness may emerge initially in the legs regardless of the level of compression. Compression of the lower cervical and upper thoracic nerve roots can present with upper limb weakness. The patient may complain of heavy or stiff limbs causing, for example, difficulty climbing stairs. Sensory deficits Paraesthesia and loss of sensation may develop progressing upwards from the toes in a stocking-like fashion eventually reaching the level of the lesion but is poorly localized to the site of the lesion. The patient may experience altered sensation to touch, pain and temperature. Autonomic dysfunction (usually late presenting symptoms) Sphincter disturbances can increase the tendency to constipation and/or urinary retention and this can progress to double incontinence. Referral pathways It has already been stated that patients with actual or potential MSCC may present in a variety of settings to any health care professional. The individual s presenting signs and symptoms and general physical condition will influence the likely referral and treatment pathway. Please see the flow chart pathway in regard to the MSCC coordinators. MSCC Clinical Advisor Induction Training Version 1.1 Vs 1.1 January 2016 Page 5
6 Management pathway Clinical assessment and examination of a patient with suspected spinal cord compression includes identification of risk factors, symptom evaluation of pain, sensory and motor function, and bowel and bladder function. To ensure patient on steroids (Dexamethasone 16 milligram/day (mg/d)). Suggest patient lies flat and advice on that they will require to maintain this position unless was advised by the spinal surgery team that the spine is stable. An emergency two-person ambulance with stretcher should be requested, to enable transfer of the patient from home to hospital. Admit direct to local hospital (avoiding Accident and Emergency, if possible). An urgent Magnetic Resonance Imaging (MRI) scan should be organised locally within 24hours. CT scan is an acceptable alternative if urgent MRI is not possible. If the individual is a hospice inpatient at the time of initial suspicion of MSCC, it would be preferable if an urgent local MRI could be arranged, rather than the patient having to be transferred as an in-patient to the local hospital. A Referral form must be completed and coordinator to facilitate telephone discussion with the on-call Oncologist and / or spinal surgery oncall is advised once clinical and radiological assessment has been performed. Ensure patient information has been handed to the patient and patient aware of the diagnosis and agreeing on the management plan before perusing into it. Page 6 MSCC Clinical Advisor Induction Training Version 1.1 a January 2016
7 MSCC Coordinator Pathway Suspected MSCC Outpatient, GP Coordinator Inpatient, including QCOH. Hospital team to arrange MRI Not known to oncology Known to oncology arrange bed in Queens Centre Acute admission: follow MSCC guidelines Inform oncologist Suspected MSCC Ward doctors to arrange urgent whole spine MRI MSCC confirmed, fill referral form and contact MSCC coordinator MSCC coordinator to contact oncologist and also neurosurgeon if needed Inoperable, Contact referring team & oncologist Operable, if patient wishes so advise contact to neurosurgery HRI Provide patient information on radiotherapy if patient suitable for treatment Best Supportive Care if not suitable for radiotherapy or not wish to have it Patient wishes to have radiotherapy Patient does not wish to have radiotherapy Arrange bed in Queens Centre and inform the team. Contact booking office. Team to complete management Form and submit to booking office MSCC Clinical Advisor Induction Training Version 1.1 Vs 1.1 January 2016 Page 7
8 Other points to consider pain and symptom management emotional/psychological support the need to consider spiritual needs and care family support rehabilitation/maximising potential discharge planning Assessment for hospice admission. Specialist palliative care Referral to the Specialist Palliative Care Service may be appropriate at any stage, from suspicion of MSCC, through diagnosis, treatment and rehabilitation to end of life care. It is particularly important when the issues are complex and are not able to be managed locally or when a multidisciplinary team approach to care has not been available but is required. Rehabilitation and multi-professional referral Rehabilitation should commence on diagnosis, encompassing the skills of various healthcare professions as appropriate. Referrals should be considered to the following multi-professional staff: Physiotherapist (within 24 hours of admission) Occupational Therapist (within 24 hours of admission) Social Worker (when needed) Other where relevant (Dietician, Speech and Language Therapist, Clinical Psychologist or Counsellor and Hospital Chaplain) Metastatic Spinal Cord Compression and timing of mobilisation Initial Presentation Assume spine unstable until MDT decision made regarding stability. Advise flat bed rest, one pillow with neutral spine alignment until confirmation of spinal stability. Stabilisation with a hard collar for patients with suspected cervical cord compression. (MSCC coordinators trained to fit collars). Spinal brace may be indicated for thoracic or lumbar lesions (liaise with consultant and neurosurgeons) Patient must be log rolled and use slipper pan and bottle/urinary catheter, cot sides in place Correct intervention for pressure relief Above knee TEDS to prevent thrombosis. Management pathway must be clearly documented and communicated to the team Page 8 MSCC Clinical Advisor Induction Training Version 1.1 a January 2016
9 Audit Retrospective audit of clinical practice shows wide variation in the timing of, and methods used to mobilise patients diagnosed with MSCC during treatment. In the past mobilisation has usually only been started only after radiotherapy or spinal stabilisation, or following an arbitrary period of bed rest. However there is no research evidence to support any of these approaches. NICE recommends that a decision about spinal stability has to be made by the MDT, ideally including surgeon, radiologist, oncologist and physiotherapist and documented in the medical record. Indicators of spinal instability Most reliable indicators of spinal instability are radiological findings (MRI) and clinical features such as mechanical pain and changing neurological features. Spinal instability, often with subluxation, can result in progressive kyphosis with extrusion of bone and disc into the spinal canal. It is characterised clinically by severe pain at the site of the lesion on attempted movement. Instability is likely to be present if any of the following are present: Severe pain at site of lesion, increasing on movement The tumour involves two or more adjacent vertebral bodies Both anterior and posterior elements at the same level are involved Involved vertebral bodies have collapsed to less than 50% of their original height The odontoid process has been destroyed leading to possible atlanto-axial subluxation (WOSCAN, West Of Scotland Cancer Network Guidelines for malignant spinal cord compression, 2007) Stable spine Once the spine is confirmed as stable, gentle mobilisation should be commenced as soon as possible, bearing in mind that this may be before, during or after definitive treatment. When pain is well controlled, gradual sitting should begin, from supine to 45 o initially and if tolerated, the patient should be encouraged to progress to 60 o and 90 o if able. Pain levels and neurological signs / symptoms must be monitored during this process. If there is a significant worsening of any of these, patients should be returned to a position where these changes reverse and the stability of the spine reassessed. (NICE, MSCC Guidelines, 2008) Discharge planning Discharge planning should commence as soon as possible following admission and certainly as soon as the diagnosis has been confirmed. The patient and their carers should be involved in all discussions to ensure their wishes are respected and that the goals of discharge planning are realistic and achievable. Where community staff has already been MSCC Clinical Advisor Induction Training Version 1.1 Vs 1.1 January 2016 Page 9
10 involved they should also be contacted for both a background report and to provide an update on the patient s status. A patient with MSCC may be discharged / transferred between various healthcare settings during their episode of care and therefore effective communication strategies must be ensured to facilitate a seamless process. Suspected MSCC Lie flat, neutral spine alignment and log roll Flow chart for decisions about timing and safety of mobilisation once MSCC suspected (NICE 2008) Conduct and review MRI Spine assessed as being unstable? (Bony or neurological instability) Yes Are surgery and / or radiotherapy appropriate? Yes Medical management, Dexamethasone, surgery and / or radiotherapy as appropriate No Graduated assessment of sitting once spinal shock settled or neurology stable (up to 60º over 4 hours) Fit brace or collar No Does spine remain stable? Significant increases in pain or neurological symptoms? Yes No Ongoing assessment and rehabilitation in unsupported sitting, standing, walking and ADLs Page 10 MSCC Clinical Advisor Induction Training Version 1.1 a January 2016 Discharge planning
11 Competence of MSCC coordinators A Registered nurse, at least band 6 Have read the educational package and attended the training and assessment sessions. Have high level of communication skills. Good experience with cancer patients. Familiar to the MSCC referral pathway and referral form. Attend educational sessions on MSCC. Aware of the MSCC and acute oncology guidelines In good contact with the MSCC coordinators representative at meetings. Have an access to the two yearly MSCC group meeting minutes. Happy to participate in ongoing MSCC audit. Presentations There is a presentation given with this training. The slides for the presentation have been added here as Appendix i. MSCC Clinical Advisor Induction Training Version 1.1 Vs 1.1 January 2016 Page 11
12 Appendix (i) MSCC Presentation Slides Page 12 MSCC Clinical Advisor Induction Training Version 1.1 a January 2016
13 MSCC Clinical Advisor Induction Training Version 1.1 Vs 1.1 January 2016 Page 13
14 Page 14 MSCC Clinical Advisor Induction Training Version 1.1 a January 2016
15 MSCC Clinical Advisor Induction Training Version 1.1 Vs 1.1 January 2016 Page 15
16 Page 16 MSCC Clinical Advisor Induction Training Version 1.1 a January 2016
17 MSCC Clinical Advisor Induction Training Version 1.1 Vs 1.1 January 2016 Page 17
18 Page 18 MSCC Clinical Advisor Induction Training Version 1.1 a January 2016
19 MSCC Clinical Advisor Induction Training Version 1.1 Vs 1.1 January 2016 Page 19
20 Page 20 MSCC Clinical Advisor Induction Training Version 1.1 a January 2016
21 MSCC Clinical Advisor Induction Training Version 1.1 Vs 1.1 January 2016 Page 21
22 Page 22 MSCC Clinical Advisor Induction Training Version 1.1 a January 2016
23 MSCC Clinical Advisor Induction Training Version 1.1 Vs 1.1 January 2016 Page 23
24 Page 24 MSCC Clinical Advisor Induction Training Version 1.1 a January 2016
25 MSCC Clinical Advisor Induction Training Version 1.1 Vs 1.1 January 2016 Page 25
26 Appendix (ii) Article from Clinical Oncology (2002) Page 26 MSCC Clinical Advisor Induction Training Version 1.1 a January 2016
27 MSCC Clinical Advisor Induction Training Version 1.1 Vs 1.1 January 2016 Page 27
28 Page 28 MSCC Clinical Advisor Induction Training Version 1.1 a January 2016
29 MSCC Clinical Advisor Induction Training Version 1.1 Vs 1.1 January 2016 Page 29
30 Page 30 MSCC Clinical Advisor Induction Training Version 1.1 a January 2016
31 MSCC Clinical Advisor Induction Training Version 1.1 Vs 1.1 January 2016 Page 31
32 Page 32 MSCC Clinical Advisor Induction Training Version 1.1 a January 2016
33 MSCC Clinical Advisor Induction Training Version 1.1 Vs 1.1 January 2016 Page 33
34 Page 34 MSCC Clinical Advisor Induction Training Version 1.1 a January 2016
35 Appendix (iii) MSCC Service Poster MSCC Clinical Advisor Induction Training Version 1.1 Vs 1.1 January 2016 Page 35
36 Page 36 MSCC Clinical Advisor Induction Training Version 1.1 a January 2016
37 Appendix (iv) Pathway for Malignant / Metastatic Spinal Cord Compression (MSCC) Hull and East Yorkshire Hospitals NHS Trust PATHWAY FOR MALIGNANT SPINAL CORD COMPRESSION (MSCC) (Adapted from NICE guidelines available at Patients with a known diagnosis of cancer The local MSCC coordinator should be contacted urgently (within 24 hours) to discuss the care of patients with known cancer and any symptoms suggestive of spinal metastases (see below) Patients without a known diagnosis of cancer Patients developing suspicious pain should be reviewed frequently and referred within 24 hours if they develop progressive pain or other symptoms suggestive of spinal metastases (see below) SYMPTOMS SUGGESTIVE OF SPINAL METASTASES Pain in the thoracic or cervical spine Progressive lumbar spinal pain Severe unremitting spinal pain Spinal pain aggravated by straining (for example, opening bowels, coughing or sneezing) Localised spinal tenderness Nocturnal spinal pain preventing sleep SYMPTOMS OR SIGNS SUGGESTIVE OF MSCC SHOULD BE VIEWED AS AN ONCOLOGICAL EMERGENCY The local MSCC coordinator should be contacted immediately to discuss the care of patients with or without known cancer with symptoms suggestive of spinal metastases who have any of the following neurological symptoms or who have neurological signs suggestive of MSCC or cauda equina compression Neurological symptoms include radicular pain, any limb weakness, difficulty in walking, sensory loss or bladder / bowel dysfunction MSCC Clinical Advisor Induction Training Version 1.1 Vs 1.1 January 2016 Page 37
38 Hull and East Yorkshire Hospitals NHS Trust FULL HISTORY AND CLINICAL ASSESSMENT MSCC suspected Nurse flat until stability of spine is known. Manage pain and other symptoms as required Start 16mgs of Dexamethasone immediately if no contraindications Continue dexamethasone 8mg bd with PPI until diagnosis confirmed DVT prophylaxis with LMWH if no contraindications MSCC not suspected Analgesia and investigation as required Refer as appropriate MRI arranged by referring team MRI result reported to referring team and MSCC coordinator MSCC confirmed on MRI scan MSCC Patients information Contact MSSC coordinator Tel: Tel: Or CHH Bleep 500 Complete referral form MSCC team decide on: Spinal stability and patient positioning Need for tissue diagnosis Preferred treatment Need for patient transfer MSCC excluded on MRI Treat as appropriate Treatment to start within 24 hours of diagnosis* Options include: Surgery (urgency depends on the neurological presentation) Radiotherapy Chemotherapy Best supportive care * For more information please refer to the local guideline. Rehabilitation should begin as soon as a diagnosis of MSCC is made Referral to: Physiotherapy within 24 hours Occupational therapy within 48 hours Social services Underlying malignant condition should be managed by appropriate team Plan for steroid reduction once definitive treatment complete Consider transfer to local hospital for continuing rehabilitation Page 38 MSCC Clinical Advisor Induction Training Version 1.1 a January 2016
39 Appendix (v) NEYHCA (Cancer) Metastatic / Malignant Spinal Cord Compression Referral Form Metastatic / Malignant Spinal Cord Compression (MSCC) Referral Form *Please fill all fields and do not use the return key during typing Please contact MSCC coordinator before sending on *(Failure to reach the MSCC coordinator please contact CHH bleep 500 or Registrar oncall) MSCC treatment referral: Date of referral : Time of referral: Date of admission: Referred by : Contact number: Extension: Bleep/Pager: Surname: Forename: DOB: Address: Telephone No. Patient Details and relevant information Previously known to Oncologist: Y / N Name: Oncologist aware of Referral: Y / N Prior MDT Discussion Y / N Hospital Date Outcome Primary: Background Tumour information Current Management: Chemo Radiotherapy Hormone Biological Best supportive care Previous MSCC: Y / N Date: Area affected: Treatment received: Radiotherapy Surgery Both Other: MSCC clinical information Time and Date of MSCC was first suspected: - Walking Status: Normal Unsteady: Y / N Since(date): Not Ambulant: Y Since (date): / N Spinal stable: Y / N / Not Known Recommandation: MRI Whole spine: Not Done (Reason: ) Done Location: Time - Date requested: - Time - Date done: - Outcome: Other relevant Information: Please complete this form as fully as possible MSCC Clinical Advisor Induction Training Version 1.1 Vs 1.1 January 2016 Page 39
CP80 Version: V01. Acute Oncology Management Service Date approved: 8 th May 2015 Date ratified: 1 st June 2015 Review date: 1 st June 2017
 STANDARD OPERATING PROCEDURE (SOP) AND PATHWAY FOR THE MANAGEMENT OF PATIENTS WITH METASTATIC SPINAL CORD COMPRESSION (MSCC) WITHIN THE CHRISTIE (Refer to the Manchester Cancer Network MSCC Pathway flowchart)
STANDARD OPERATING PROCEDURE (SOP) AND PATHWAY FOR THE MANAGEMENT OF PATIENTS WITH METASTATIC SPINAL CORD COMPRESSION (MSCC) WITHIN THE CHRISTIE (Refer to the Manchester Cancer Network MSCC Pathway flowchart)
Metastatic Spinal Cord Compression (MSCC) Clinical guidelines and pathway
 Metastatic Spinal Cord Compression (MSCC) Clinical guidelines and pathway Version 2: May 2012 To be read in conjunction with NICE CG75 Developed by consensus by: Dr Peter Robson, Consultant Oncologist,
Metastatic Spinal Cord Compression (MSCC) Clinical guidelines and pathway Version 2: May 2012 To be read in conjunction with NICE CG75 Developed by consensus by: Dr Peter Robson, Consultant Oncologist,
Update on Management of Malignant Spinal Cord Compression. Heino Hugel Consultant in Palliative Medicine University Hospital Aintree
 Update on Management of Malignant Spinal Cord Compression Heino Hugel Consultant in Palliative Medicine University Hospital Aintree Current Guidelines The symptoms of MSCC may be subtle and therefore careful
Update on Management of Malignant Spinal Cord Compression Heino Hugel Consultant in Palliative Medicine University Hospital Aintree Current Guidelines The symptoms of MSCC may be subtle and therefore careful
PATHWAY MANAGEMENT OF METASTATIC SPINAL CORD COMPRESSION (MSCC) THE CHRISTIE, GREATER MANCHESTER & CHESHIRE
 PATHWAY MANAGEMENT OF METASTATIC SPINAL CORD COMPRESSION (MSCC) THE CHRISTIE, GREATER MANCHESTER & CHESHIRE Procedure Reference: Document Owner: Dr V. Misra Version: Accountable Committee: V3 MSCC Network
PATHWAY MANAGEMENT OF METASTATIC SPINAL CORD COMPRESSION (MSCC) THE CHRISTIE, GREATER MANCHESTER & CHESHIRE Procedure Reference: Document Owner: Dr V. Misra Version: Accountable Committee: V3 MSCC Network
MANAGEMENT OF PATIENTS WITH METASTATIC SPINAL CORD COMPRESSION
 CLINICAL POLICY MANAGEMENT OF PATIENTS WITH METASTATIC SPINAL CORD COMPRESSION DOCUMENT REF: PCLASCORD (Version No. 1.4) Name and designation of policy author(s) Approved by (committee, group, manager)
CLINICAL POLICY MANAGEMENT OF PATIENTS WITH METASTATIC SPINAL CORD COMPRESSION DOCUMENT REF: PCLASCORD (Version No. 1.4) Name and designation of policy author(s) Approved by (committee, group, manager)
Guidelines for the Management. Malignant Spinal Cord Compression. Final Guideline
 Guidelines for the Management Of Malignant Spinal Cord Compression Final Guideline 1. Introduction 1.1 Aetiology of MSCC 1.2 Use of the guidelines 2. Summary of Pathway 2.1 Algorithms 2.2 Role of the MSCC
Guidelines for the Management Of Malignant Spinal Cord Compression Final Guideline 1. Introduction 1.1 Aetiology of MSCC 1.2 Use of the guidelines 2. Summary of Pathway 2.1 Algorithms 2.2 Role of the MSCC
Malignant Spinal cord Compression. Dr. Thiru Thirukkumaran Palliative Care Services - Northwest Tasmania
 Malignant Spinal cord Compression Dr. Thiru Thirukkumaran Palliative Care Services - Northwest Tasmania Background Statistics of SCC -1 Incidence of SCC Vertebral body metastases 85 % Para-vertebral (Lymphoma)
Malignant Spinal cord Compression Dr. Thiru Thirukkumaran Palliative Care Services - Northwest Tasmania Background Statistics of SCC -1 Incidence of SCC Vertebral body metastases 85 % Para-vertebral (Lymphoma)
Suspected spinal cord compression form
 Suspected spinal cord compression form Enter this form into the notes at the appropriate date in the Progress / Evaluation sheets. Please copy this form to Lisa Lewis, Medical PA (ext 4551), for audit
Suspected spinal cord compression form Enter this form into the notes at the appropriate date in the Progress / Evaluation sheets. Please copy this form to Lisa Lewis, Medical PA (ext 4551), for audit
Spinal cord compression: what it means and how it can be treated
 Spinal cord compression: what it means and how it can be treated Patient Information Oncology Department Author ID: Acute Oncology Nurse Specialist Leaflet Number: CC 036 Version: 2.1 Name of Leaflet:
Spinal cord compression: what it means and how it can be treated Patient Information Oncology Department Author ID: Acute Oncology Nurse Specialist Leaflet Number: CC 036 Version: 2.1 Name of Leaflet:
Palliative Care Emergencies
 Palliative Care Emergencies LAURA BARNFIELD What might constitute an emergency in Palliative Care? 1 Palliative Care Emergencies Major haemorrhage Metastatic Spinal Cord Compression (MSCC) Superior Vena
Palliative Care Emergencies LAURA BARNFIELD What might constitute an emergency in Palliative Care? 1 Palliative Care Emergencies Major haemorrhage Metastatic Spinal Cord Compression (MSCC) Superior Vena
MSCC CARE PATHWAYS & CASE STUDIES. By Michael Balloch Spine CNS
 MSCC CARE PATHWAYS & CASE STUDIES By Michael Balloch Spine CNS Aims To be familiar with the routes of MSCC prentaion How the guidelines work in practice Routes of presentation Generic intervention Managing
MSCC CARE PATHWAYS & CASE STUDIES By Michael Balloch Spine CNS Aims To be familiar with the routes of MSCC prentaion How the guidelines work in practice Routes of presentation Generic intervention Managing
Recognition & Treatment of Malignant Spinal Cord Compression Study Day
 Recognition & Treatment of Malignant Spinal Cord Compression Study Day 11 th May 2017 Dr Bernie Foran Consultant Clinical Oncologist & Honorary Senior Lecturer Weston Park Hospital Outline of Talk Clinical
Recognition & Treatment of Malignant Spinal Cord Compression Study Day 11 th May 2017 Dr Bernie Foran Consultant Clinical Oncologist & Honorary Senior Lecturer Weston Park Hospital Outline of Talk Clinical
Metastatic Spinal Disease
 Metastatic Spinal Disease Mr Neil Chiverton Consultant Spinal Surgeon, Sheffield Objectives The scale and nature of the problem NICE recommendations Surgical decision making Case illustrations Incidence
Metastatic Spinal Disease Mr Neil Chiverton Consultant Spinal Surgeon, Sheffield Objectives The scale and nature of the problem NICE recommendations Surgical decision making Case illustrations Incidence
agreed MSCC pathways and guidelines).
 Referral of Patients with Spinal Metastatic Disease and Suspected Metastatic Spinal Cord Compression (to be used in association with locally West Midlands Clinical Networks and Clinical Senate Coversheet
Referral of Patients with Spinal Metastatic Disease and Suspected Metastatic Spinal Cord Compression (to be used in association with locally West Midlands Clinical Networks and Clinical Senate Coversheet
Metastatic Spinal Cord Compression
 Metastatic Spinal Cord Compression Dr Zacharias Tasigiannopoulos Clinical Oncologist Colney centre Department of Oncology Norwich, UK Introduction 2-5% of cancer patients have an episode of MSCC Initial
Metastatic Spinal Cord Compression Dr Zacharias Tasigiannopoulos Clinical Oncologist Colney centre Department of Oncology Norwich, UK Introduction 2-5% of cancer patients have an episode of MSCC Initial
Recognition & Treatment of Malignant Spinal Cord Compression Study Day
 Recognition & Treatment of Malignant Spinal Cord Compression Study Day 16 th October 2014 Dr Bernie Foran Consultant Clinical Oncologist & Honorary Senior Lecturer Weston Park Hospital Outline of Talk
Recognition & Treatment of Malignant Spinal Cord Compression Study Day 16 th October 2014 Dr Bernie Foran Consultant Clinical Oncologist & Honorary Senior Lecturer Weston Park Hospital Outline of Talk
West Midlands Sarcoma Advisory Group
 West Midlands Sarcoma Advisory Group Guideline for the Initial Investigation and Referral to Specialist Sarcoma Multi Disciplinary Team for Suspected Bone Sarcoma Version History Version Date Brief Summary
West Midlands Sarcoma Advisory Group Guideline for the Initial Investigation and Referral to Specialist Sarcoma Multi Disciplinary Team for Suspected Bone Sarcoma Version History Version Date Brief Summary
Acute Oncology Services Clinical Forum: Metastatic Spinal Cord Compression. Tuesday 17 th September 2013
 Acute Oncology Services Clinical Forum: Metastatic Spinal Cord Compression Tuesday 17 th September 2013 Welcome, Introduction and Aims of the Event Dr Tom Newsom-Davis, LCA AOS Pathway Chair Why MSCC?
Acute Oncology Services Clinical Forum: Metastatic Spinal Cord Compression Tuesday 17 th September 2013 Welcome, Introduction and Aims of the Event Dr Tom Newsom-Davis, LCA AOS Pathway Chair Why MSCC?
GUIDELINES FOR RADIOTHERAPY IN SPINAL CORD COMPRESSION THE CHRISTIE, GREATER MANCHESTER & CHESHIRE. Version:
 GUIDELINES FOR RADIOTHERAPY IN SPINAL CORD COMPRESSION THE CHRISTIE, GREATER MANCHESTER & CHESHIRE Procedure Reference: Document Owner: Dr V. Misra Version: Accountable Committee: V4 Acute Oncology Group
GUIDELINES FOR RADIOTHERAPY IN SPINAL CORD COMPRESSION THE CHRISTIE, GREATER MANCHESTER & CHESHIRE Procedure Reference: Document Owner: Dr V. Misra Version: Accountable Committee: V4 Acute Oncology Group
Spinal cord compression
 Spinal cord compression Urology Department Patient Information Leaflet Introduction If you have been diagnosed with cancer, you need to know about spinal cord compression and the warning signs. This leaflet
Spinal cord compression Urology Department Patient Information Leaflet Introduction If you have been diagnosed with cancer, you need to know about spinal cord compression and the warning signs. This leaflet
GP Guidelines for the Management of Adult Patients with Gynaecological Cancers 2012
 GP Guidelines for the Management of Adult Patients with Gynaecological Cancers 2012 Version Control This is a controlled document please destroy all previous versions on receipt of a new version. Date
GP Guidelines for the Management of Adult Patients with Gynaecological Cancers 2012 Version Control This is a controlled document please destroy all previous versions on receipt of a new version. Date
North West London Trauma Network Spinal Pathway and Protocols
 North West London Trauma Network Spinal Pathway and Protocols 1. Spinal Clearance in the Trauma Patient Inclusions: All trauma patients who are not alert and orientated, unable to cooperate (including
North West London Trauma Network Spinal Pathway and Protocols 1. Spinal Clearance in the Trauma Patient Inclusions: All trauma patients who are not alert and orientated, unable to cooperate (including
The surgical treatment of metastatic disease of the spine
 The surgical treatment of metastatic disease of the spine Péter Banczerowski National Institute of Neurosurgery, Budapest Spine tumours 15% of the primary tumours of the CNS affect the spine The spine
The surgical treatment of metastatic disease of the spine Péter Banczerowski National Institute of Neurosurgery, Budapest Spine tumours 15% of the primary tumours of the CNS affect the spine The spine
What to expect following spinal cord injury. Information for patients Therapy Services
 What to expect following spinal cord injury Information for patients Therapy Services Introduction This leaflet aims to explain what spinal cord injury is and what to expect over the next few months. What
What to expect following spinal cord injury Information for patients Therapy Services Introduction This leaflet aims to explain what spinal cord injury is and what to expect over the next few months. What
Soft Tissue Tumour & Sarcoma Imaging Guidelines 2012
 Soft Tissue Tumour & Sarcoma Imaging Guidelines 2012 Version Control This is a controlled document please destroy all previous versions on receipt of a new version. Date Approved: March 2011 reissued April
Soft Tissue Tumour & Sarcoma Imaging Guidelines 2012 Version Control This is a controlled document please destroy all previous versions on receipt of a new version. Date Approved: March 2011 reissued April
Spinal Cord Compression Diagnosis and Management. Information for Shared Care Centres and Community Staff
 Reference: CG1412 Written by: Dr Daniel Yeomanson Peer reviewer Dr Jeanette Payne Approved: August 2016 Approved by D&TC: 10 th June 2016 Review Due: August 2019 Intended Audience This document contains
Reference: CG1412 Written by: Dr Daniel Yeomanson Peer reviewer Dr Jeanette Payne Approved: August 2016 Approved by D&TC: 10 th June 2016 Review Due: August 2019 Intended Audience This document contains
BRIEFING PAPER THE USE OF RED FLAGS TO IDENTIFY SERIOUS SPINAL PATHOLOGY THE CHRISTIE, GREATER MANCHESTER & CHESHIRE. Version:
 BRIEFING PAPER THE USE OF RED FLAGS TO IDENTIFY SERIOUS SPINAL PATHOLOGY THE CHRISTIE, GREATER MANCHESTER & CHESHIRE Procedure Reference: Document Owner: Jackie Turnpenney Version: Accountable Committee:
BRIEFING PAPER THE USE OF RED FLAGS TO IDENTIFY SERIOUS SPINAL PATHOLOGY THE CHRISTIE, GREATER MANCHESTER & CHESHIRE Procedure Reference: Document Owner: Jackie Turnpenney Version: Accountable Committee:
Humber NHS Foundation Trust. Joint Effort
 Joint Joint is a new community based musculoskeletal service that treats patients with complex problems of the spine, upper and lower limb. Joint s experienced Consultant Orthopaedic Surgeons and Extended
Joint Joint is a new community based musculoskeletal service that treats patients with complex problems of the spine, upper and lower limb. Joint s experienced Consultant Orthopaedic Surgeons and Extended
Management of Acute Oncological emergencies
 Management of Acute Oncological emergencies Malignant Spinal cord compression (MSCC) Neutropenic sepsis Superior vena caval obstruction Hypercalcemia Hyponatremia Bowel obstruction Brain Metastasis with
Management of Acute Oncological emergencies Malignant Spinal cord compression (MSCC) Neutropenic sepsis Superior vena caval obstruction Hypercalcemia Hyponatremia Bowel obstruction Brain Metastasis with
Title Protocol for the management of suspected cauda equine syndrome & decompensating spinal stenosis at NDDH
 Document Control Title Protocol for the management of suspected cauda equine syndrome & decompensating spinal stenosis at NDDH Author Author s job title Consultant T&O Directorate Scheduled Care Department
Document Control Title Protocol for the management of suspected cauda equine syndrome & decompensating spinal stenosis at NDDH Author Author s job title Consultant T&O Directorate Scheduled Care Department
NICE National Institute for Health and Clinical Excellence Metastic Spinal Cord Compression
 NICE - Metastic Spinal Cord Compression 26/11/2008 (Livello 2) NICE National Institute for Health and Clinical Excellence Metastic Spinal Cord Compression Documento Documento Documento Documento file:///c
NICE - Metastic Spinal Cord Compression 26/11/2008 (Livello 2) NICE National Institute for Health and Clinical Excellence Metastic Spinal Cord Compression Documento Documento Documento Documento file:///c
West Midlands Sarcoma Advisory Group
 West Midlands Sarcoma Advisory Group Guideline for the Initial Investigation and Referral to Sarcoma Specialist Multi Disciplinary Team for Suspected Sarcoma of Soft Tissue Extremities (limbs and trunk
West Midlands Sarcoma Advisory Group Guideline for the Initial Investigation and Referral to Sarcoma Specialist Multi Disciplinary Team for Suspected Sarcoma of Soft Tissue Extremities (limbs and trunk
Recognition & Treatment of Malignant Spinal Cord Compression
 Recognition & Treatment of Malignant Spinal Cord Compression Acute Oncology Study Day 15 th March 2018 Dr Bernie Foran Consultant Clinical Oncologist & Honorary Senior Lecturer Yorkshire & the Humber Weston
Recognition & Treatment of Malignant Spinal Cord Compression Acute Oncology Study Day 15 th March 2018 Dr Bernie Foran Consultant Clinical Oncologist & Honorary Senior Lecturer Yorkshire & the Humber Weston
Oncologic Emergencies: When to call the Radiation Oncologist
 Oncologic Emergencies: When to call the Radiation Oncologist Dr. Shrinivas Rathod Radiation Oncologist Radiation Oncology Program CancerCare Manitoba and University of Manitoba Disclosures Speaker s name:
Oncologic Emergencies: When to call the Radiation Oncologist Dr. Shrinivas Rathod Radiation Oncologist Radiation Oncology Program CancerCare Manitoba and University of Manitoba Disclosures Speaker s name:
Metastatic spinal cord compression (MSCC) What happens? MSCC. MSCC is a palliative care emergency. Signs/symptoms
 A patient with suspected metastatic spinal cord compression and the dilemma of non-resident status Sandra Notley CNS-Palliative Care 1 Metastatic spinal cord compression (MSCC) Is indentation, displacement
A patient with suspected metastatic spinal cord compression and the dilemma of non-resident status Sandra Notley CNS-Palliative Care 1 Metastatic spinal cord compression (MSCC) Is indentation, displacement
HIGH LEVEL - Science
 Learning Outcomes HIGH LEVEL - Science Describe the structure and function of the back and spine (8a) Outline the functional anatomy and physiology of the spinal cord and peripheral nerves (8a) Describe
Learning Outcomes HIGH LEVEL - Science Describe the structure and function of the back and spine (8a) Outline the functional anatomy and physiology of the spinal cord and peripheral nerves (8a) Describe
Primary care referral criteria for musculoskeletal MRI scans
 Appendix 1 Primary care referral criteria for musculoskeletal MRI scans Accepted Criteria for Direct Access MRI Body Part Symptoms Imaging indicated Lumbar Spine Low Back Pain with adverse symptoms or
Appendix 1 Primary care referral criteria for musculoskeletal MRI scans Accepted Criteria for Direct Access MRI Body Part Symptoms Imaging indicated Lumbar Spine Low Back Pain with adverse symptoms or
Decision Making Flowchart for Metastatic Spinal Cord Compression and Pathological Spinal Fractures
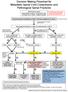 Decision Making Flowchart for Metastatic Spinal Cord Compression and Pathological Spinal Fractures All Referrals (see notes): Spinal Surgeons Locally or Trauma SpR at UHW Oncology SpR at Velindre / Singleton
Decision Making Flowchart for Metastatic Spinal Cord Compression and Pathological Spinal Fractures All Referrals (see notes): Spinal Surgeons Locally or Trauma SpR at UHW Oncology SpR at Velindre / Singleton
Physiotherapy Following Your Spinal Discectomy
 Physiotherapy Following Your Spinal Discectomy Patient information How to contact us Physiotherapy Department Watford General Hospital West Hertfordshire Hospitals NHS Trust Vicarage Road, Watford, Hertfordshire,
Physiotherapy Following Your Spinal Discectomy Patient information How to contact us Physiotherapy Department Watford General Hospital West Hertfordshire Hospitals NHS Trust Vicarage Road, Watford, Hertfordshire,
Gynae Cancer Multi Disciplinary Team Patient Information
 Gynae Cancer Multi Disciplinary Team Patient Information Introduction This booklet is for people who have been diagnosed with gynaecological cancers which include cancer of the cervix, ovary, vulva, vagina
Gynae Cancer Multi Disciplinary Team Patient Information Introduction This booklet is for people who have been diagnosed with gynaecological cancers which include cancer of the cervix, ovary, vulva, vagina
LOTHIAN LUMBAR SPINE PATHWAYS
 LOTHIAN LUMBAR SPINE PATHWAYS Patient Completes STarT Back form Assess patient and screen for Red Flags. If present refer to Appendix 1 Establish if Neurogenic. If so refer to Appendix 2 Children under
LOTHIAN LUMBAR SPINE PATHWAYS Patient Completes STarT Back form Assess patient and screen for Red Flags. If present refer to Appendix 1 Establish if Neurogenic. If so refer to Appendix 2 Children under
Referral guide for acute oncology emergencies
 Referral guide for acute oncology emergencies 1 st Edition v 1.0 London Cancer March 2013 To be used in conjunction with London Cancer clinical guidelines for acute oncology emergencies; A Guide to Acute
Referral guide for acute oncology emergencies 1 st Edition v 1.0 London Cancer March 2013 To be used in conjunction with London Cancer clinical guidelines for acute oncology emergencies; A Guide to Acute
Recommendations for cross-sectional imaging in cancer management, Second edition
 www.rcr.ac.uk Recommendations for cross-sectional imaging in cancer management, Second edition Tumours of the spinal cord Faculty of Clinical Radiology www.rcr.ac.uk Contents Primary spinal cord tumours
www.rcr.ac.uk Recommendations for cross-sectional imaging in cancer management, Second edition Tumours of the spinal cord Faculty of Clinical Radiology www.rcr.ac.uk Contents Primary spinal cord tumours
Posterior Lumbar Decompression for Spinal Stenosis
 Posterior Lumbar Decompression for Spinal Stenosis Issue 6: March 2016 Review date: February 2019 Following your recent MRI scan and consultation with your spinal surgeon you have been diagnosed with
Posterior Lumbar Decompression for Spinal Stenosis Issue 6: March 2016 Review date: February 2019 Following your recent MRI scan and consultation with your spinal surgeon you have been diagnosed with
Urology Multi Disciplinary Team Patient Information
 Urology Multi Disciplinary Team Patient Information Introduction This booklet is for people who have been diagnosed with urological cancers which include prostate, bladder, kidney, testicular and penile
Urology Multi Disciplinary Team Patient Information Introduction This booklet is for people who have been diagnosed with urological cancers which include prostate, bladder, kidney, testicular and penile
Ratified by: Care and Clinical Policies Date: 17 th February 2016
 Clinical Guideline Reference Number: 0803 Version 5 Title: Physiotherapy guidelines for the Management of People with Multiple Sclerosis Document Author: Henrieke Dimmendaal / Laura Shenton Date February
Clinical Guideline Reference Number: 0803 Version 5 Title: Physiotherapy guidelines for the Management of People with Multiple Sclerosis Document Author: Henrieke Dimmendaal / Laura Shenton Date February
A Best Practice Clinical Care Pathway for Major Amputation Surgery
 A Best Practice Clinical Care Pathway for Major Amputation Surgery April 2016 Introduction The perioperative mortality rate after major lower limb amputation in the UK is unacceptably high in modern medical
A Best Practice Clinical Care Pathway for Major Amputation Surgery April 2016 Introduction The perioperative mortality rate after major lower limb amputation in the UK is unacceptably high in modern medical
Salisbury Foundation Trust Radiology Department Referral Guidelines for Primary Care: Musculoskeletal Imaging
 Salisbury Foundation Trust Radiology Department Referral Guidelines for Primary Care: Musculoskeletal Imaging These guidelines have been issued in conjunction with the Royal College of Radiology referral
Salisbury Foundation Trust Radiology Department Referral Guidelines for Primary Care: Musculoskeletal Imaging These guidelines have been issued in conjunction with the Royal College of Radiology referral
Brain and Central Nervous System Cancers
 Brain and Central Nervous System Cancers NICE guidance link: https://www.nice.org.uk/guidance/ta121 Clinical presentation of brain tumours History and Examination Consider immediate referral Management
Brain and Central Nervous System Cancers NICE guidance link: https://www.nice.org.uk/guidance/ta121 Clinical presentation of brain tumours History and Examination Consider immediate referral Management
The use of surgery in the elderly. for management of metastatic epidural spinal cord compression
 The use of surgery in the elderly Bone Tumor Simulators for management of metastatic epidural spinal cord compression Justin E. Bird, M.D. Assistant Professor Orthopaedic Oncology and Spine Surgery Epidemiology
The use of surgery in the elderly Bone Tumor Simulators for management of metastatic epidural spinal cord compression Justin E. Bird, M.D. Assistant Professor Orthopaedic Oncology and Spine Surgery Epidemiology
NATIONAL REHABILITATION HOSPITAL SPINAL CORD SYSTEM OF CARE (SCSC) OUTPATIENT SCOPE OF SERVICE
 NATIONAL REHABILITATION HOSPITAL SPINAL CORD SYSTEM OF CARE (SCSC) OUTPATIENT SCOPE OF SERVICE Introduction: The Spinal Cord System of Care (SCSC) at the National Rehabilitation Hospital (NRH) provides
NATIONAL REHABILITATION HOSPITAL SPINAL CORD SYSTEM OF CARE (SCSC) OUTPATIENT SCOPE OF SERVICE Introduction: The Spinal Cord System of Care (SCSC) at the National Rehabilitation Hospital (NRH) provides
Review date: February Lumbar Discectomy
 Review date: February 2019 Lumbar Discectomy Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed as having a lumbar disc protrusion, resulting in nerve root
Review date: February 2019 Lumbar Discectomy Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed as having a lumbar disc protrusion, resulting in nerve root
The in-hospital management of COPD-exacerbation includes three core processes:
 Appendix 1A. Process flow for in-hospital management of COPDexacerbation The in-hospital management of COPD-exacerbation includes three core processes: 1. Diagnostic assessment 2. Pharmacological management
Appendix 1A. Process flow for in-hospital management of COPDexacerbation The in-hospital management of COPD-exacerbation includes three core processes: 1. Diagnostic assessment 2. Pharmacological management
Herniated Disk in the Lower Back
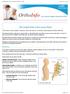 Herniated Disk in the Lower Back This article is also available in Spanish: Hernia de disco en la columna lumbar (topic.cfm?topic=a00730). Sometimes called a slipped or ruptured disk, a herniated disk
Herniated Disk in the Lower Back This article is also available in Spanish: Hernia de disco en la columna lumbar (topic.cfm?topic=a00730). Sometimes called a slipped or ruptured disk, a herniated disk
Cervical laminectomy for spinal cord compression. Information for patients Neurosurgery
 Cervical laminectomy for spinal cord compression Information for patients Neurosurgery What is a compression of the spinal cord and how has it been caused? The bones in our back are called vertebras and
Cervical laminectomy for spinal cord compression Information for patients Neurosurgery What is a compression of the spinal cord and how has it been caused? The bones in our back are called vertebras and
SELF ASSESSMENT REPORT (MULTI-DISCIPLINARY TEAM)
 SELF ASSESSMENT REPORT (MULTI-DISCIPLINARY TEAM) Network Trust MDT MDT Lead Clinician ASWCN TAUNTON AND SOMERSET Taunton Lung MDT (11-2C-1) - 2011/12 Dr Sarah Foster Compliance Self Assessment LUNG MDT
SELF ASSESSMENT REPORT (MULTI-DISCIPLINARY TEAM) Network Trust MDT MDT Lead Clinician ASWCN TAUNTON AND SOMERSET Taunton Lung MDT (11-2C-1) - 2011/12 Dr Sarah Foster Compliance Self Assessment LUNG MDT
Spinal injury. Structure of the spine
 Spinal injury Structure of the spine Some understanding of the structure of the spine (spinal column) and the spinal cord is important as it helps your Neurosurgeon explain about the part of the spine
Spinal injury Structure of the spine Some understanding of the structure of the spine (spinal column) and the spinal cord is important as it helps your Neurosurgeon explain about the part of the spine
Upper GI Malignancies Imaging Guidelines for the Management of Gastric, Oesophageal & Pancreatic Cancers 2012
 Upper GI Malignancies Imaging Guidelines for the Management of Gastric, Oesophageal & Pancreatic Cancers 2012 Version Control This is a controlled document please destroy all previous versions on receipt
Upper GI Malignancies Imaging Guidelines for the Management of Gastric, Oesophageal & Pancreatic Cancers 2012 Version Control This is a controlled document please destroy all previous versions on receipt
Guidelines for the Management of Bladder Cancer West Midlands Expert Advisory Group for Urological Cancer
 Guidelines for the Management of Bladder Cancer West Midlands Expert Advisory Group for Urological Cancer West Midlands Clinical Networks and Clinical Senate Coversheet for Network Expert Advisory Group
Guidelines for the Management of Bladder Cancer West Midlands Expert Advisory Group for Urological Cancer West Midlands Clinical Networks and Clinical Senate Coversheet for Network Expert Advisory Group
National Breast Cancer Audit next steps. Martin Lee
 National Breast Cancer Audit next steps Martin Lee National Cancer Audits Current Bowel Cancer Head & Neck Cancer Lung cancer Oesophagogastric cancer New Prostate Cancer - undergoing procurement Breast
National Breast Cancer Audit next steps Martin Lee National Cancer Audits Current Bowel Cancer Head & Neck Cancer Lung cancer Oesophagogastric cancer New Prostate Cancer - undergoing procurement Breast
2010 National Audit of Dementia (Care in General Hospitals)
 Royal College of Psychiatrists 2010 National Audit of Dementia (Care in General Hospitals) Organisational checklist results and commentary for: Barking, Havering and Redbridge Hospitals NHS Trust The 2010
Royal College of Psychiatrists 2010 National Audit of Dementia (Care in General Hospitals) Organisational checklist results and commentary for: Barking, Havering and Redbridge Hospitals NHS Trust The 2010
Acute Oncology. Protocols & Competencies Acute Oncology Introduction
 Acute Oncology Protocols & Competencies Acute Oncology Introduction Acute Oncology elearning Module Throughout the Acute Oncology FACTS elearning courses you will be able to access Network Protocols by
Acute Oncology Protocols & Competencies Acute Oncology Introduction Acute Oncology elearning Module Throughout the Acute Oncology FACTS elearning courses you will be able to access Network Protocols by
2010 National Audit of Dementia (Care in General Hospitals) North West London Hospitals NHS Trust
 Royal College of Psychiatrists 2010 National Audit of Dementia (Care in General Hospitals) Organisational checklist results and commentary for: rth West London Hospitals NHS Trust The 2010 national audit
Royal College of Psychiatrists 2010 National Audit of Dementia (Care in General Hospitals) Organisational checklist results and commentary for: rth West London Hospitals NHS Trust The 2010 national audit
Common Treatment Related Sideeffects. Radical Prostatectomy Urinary Effects. Survivorship what is the unmet need?
 Side Effects of Prostate Cancer Treatment Christian Smith Clinician Nurse, Velindre Cancer Centre Common Treatment Related Sideeffects Urinary RP, EBRT, Brachy Bowel EBRT & Brachy Sexual All treatment
Side Effects of Prostate Cancer Treatment Christian Smith Clinician Nurse, Velindre Cancer Centre Common Treatment Related Sideeffects Urinary RP, EBRT, Brachy Bowel EBRT & Brachy Sexual All treatment
Posterior Lumbar Spinal Fusion
 Posterior Lumbar Spinal Fusion Information to help patients prepare for a Posterior Lumbar Spinal Fusion Operation Directorates of Orthopaedic and Rheumatology, and Neurosciences Produced: February 2007
Posterior Lumbar Spinal Fusion Information to help patients prepare for a Posterior Lumbar Spinal Fusion Operation Directorates of Orthopaedic and Rheumatology, and Neurosciences Produced: February 2007
A Journey Down The Canal
 A Journey Down The Canal Radiological Assessment of Spinal Cord Masses John Berry-Candelario HMS III Gillian Lieberman, MD BIDMC Objectives Patient review Anatomy of the spine Imaging techniques Classification
A Journey Down The Canal Radiological Assessment of Spinal Cord Masses John Berry-Candelario HMS III Gillian Lieberman, MD BIDMC Objectives Patient review Anatomy of the spine Imaging techniques Classification
SPINAL CORD DISEASE IN DOGS PART TWO: MOST LIKELY CAUSES
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk SPINAL CORD DISEASE IN DOGS PART TWO: MOST LIKELY CAUSES Author : RITA GONÇALVES Categories : Vets Date : April 7, 2014 RITA
Vet Times The website for the veterinary profession https://www.vettimes.co.uk SPINAL CORD DISEASE IN DOGS PART TWO: MOST LIKELY CAUSES Author : RITA GONÇALVES Categories : Vets Date : April 7, 2014 RITA
Placename CCG. Policies for the Commissioning of Healthcare. Policy for Managing Back Pain- Spinal Injections
 Placename CCG Policies for the Commissioning of Healthcare Policy for Managing Back Pain- Spinal Injections 1 Introduction 1.1 This document is part of a suite of policies that the CCG uses to drive its
Placename CCG Policies for the Commissioning of Healthcare Policy for Managing Back Pain- Spinal Injections 1 Introduction 1.1 This document is part of a suite of policies that the CCG uses to drive its
2010 National Audit of Dementia (Care in General Hospitals) Chelsea and Westminster Hospital NHS Foundation Trust
 Royal College of Psychiatrists 2010 National Audit of Dementia (Care in General Hospitals) Organisational checklist results and commentary for: NHS Foundation Trust The 2010 national audit of dementia
Royal College of Psychiatrists 2010 National Audit of Dementia (Care in General Hospitals) Organisational checklist results and commentary for: NHS Foundation Trust The 2010 national audit of dementia
Developing spinal cord compression care guidelines at WPH
 Developing spinal cord compression care guidelines at WPH Spinal cord compression team: Sue Banks, Jean Buchanan, Dr Bernie Foran, Suzanne Hodson, Liz Kirkham, Rebecca Mills, Jan Siddall, Rebecca Walsh,
Developing spinal cord compression care guidelines at WPH Spinal cord compression team: Sue Banks, Jean Buchanan, Dr Bernie Foran, Suzanne Hodson, Liz Kirkham, Rebecca Mills, Jan Siddall, Rebecca Walsh,
Breast Cancer Multi Disciplinary Team Patient Information
 Breast Cancer Multi Disciplinary Team Patient Information Introduction This booklet is for people who have been diagnosed with breast cancer. It tells you about the breast multidisciplinary team and other
Breast Cancer Multi Disciplinary Team Patient Information Introduction This booklet is for people who have been diagnosed with breast cancer. It tells you about the breast multidisciplinary team and other
GUIDELINES FOR THE DIAGNOSIS AND MANAGEMENT OF ADULTS AT RISK OF AND WITH METASTATIC SPINAL CORD COMPRESSION
 GUIDELINES FOR THE DIAGNOSIS AND MANAGEMENT OF ADULTS AT RISK OF AND WITH METASTATIC SPINAL CORD COMPRESSION Policy author Accountable Executive Lead Approving body Policy reference Consultant Palliative
GUIDELINES FOR THE DIAGNOSIS AND MANAGEMENT OF ADULTS AT RISK OF AND WITH METASTATIC SPINAL CORD COMPRESSION Policy author Accountable Executive Lead Approving body Policy reference Consultant Palliative
How a fully integrated Acute Oncology Service can benefit the busy medical unit
 How a fully integrated Acute Oncology Service can benefit the busy medical unit Dr. Pauline Leonard MD FRCP Consultant Medical Oncologist Whittington Health Over the next 35 mins Briefly remind you of
How a fully integrated Acute Oncology Service can benefit the busy medical unit Dr. Pauline Leonard MD FRCP Consultant Medical Oncologist Whittington Health Over the next 35 mins Briefly remind you of
Cancer of Unknown Primary (CUP) Protocol
 1 Department of Oncology. Cancer of Unknown Primary (CUP) Protocol Version: Document type: Document sponsor Designation Document author [ s] Designation[s] Approving committee / Group Ratified by: Date
1 Department of Oncology. Cancer of Unknown Primary (CUP) Protocol Version: Document type: Document sponsor Designation Document author [ s] Designation[s] Approving committee / Group Ratified by: Date
Wound care Keep your wound clean and dry. You do not need to have a dressing over it unless you are told otherwise by your hospital staff.
 After thoracic or lumbar spinal surgery We ve given you this factsheet because you have recently had thoracic or lumbar spinal surgery at Wessex Spinal Unit. It contains useful information and advice that
After thoracic or lumbar spinal surgery We ve given you this factsheet because you have recently had thoracic or lumbar spinal surgery at Wessex Spinal Unit. It contains useful information and advice that
Chiropractic. Information for GPs and healthcare professionals
 Chiropractic Information for GPs and healthcare professionals What is chiropractic? Diagnosis, assessment and treatment Chiropractic is a primary healthcare profession that specialises in the diagnosis,
Chiropractic Information for GPs and healthcare professionals What is chiropractic? Diagnosis, assessment and treatment Chiropractic is a primary healthcare profession that specialises in the diagnosis,
Lumbar Nerve Root Decompression for Foraminal Stenosis
 Lumbar Nerve Root Decompression for Foraminal Stenosis Issue 5: March 2016 Review date: February 2019 Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed as
Lumbar Nerve Root Decompression for Foraminal Stenosis Issue 5: March 2016 Review date: February 2019 Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed as
2010 National Audit of Dementia (Care in General Hospitals) Guy's and St Thomas' NHS Foundation Trust
 Royal College of Psychiatrists 2010 National Audit of Dementia (Care in General Hospitals) Organisational checklist results and commentary for: Guy's and St Thomas' NHS Foundation Trust The 2010 national
Royal College of Psychiatrists 2010 National Audit of Dementia (Care in General Hospitals) Organisational checklist results and commentary for: Guy's and St Thomas' NHS Foundation Trust The 2010 national
National Hospital for Neurology and Neurosurgery. Muscle biopsy Centre for Neuromuscular Diseases
 National Hospital for Neurology and Neurosurgery Muscle biopsy Centre for Neuromuscular Diseases If you would like this document in another language or format or if you require the services of an interpreter
National Hospital for Neurology and Neurosurgery Muscle biopsy Centre for Neuromuscular Diseases If you would like this document in another language or format or if you require the services of an interpreter
What is Acute Oncology? Kay McCallum Acute Oncology Advanced Nurse Practitioner John Radcliffe Hospital Oxford September 2015
 What is Acute Oncology? Kay McCallum Acute Oncology Advanced Nurse Practitioner John Radcliffe Hospital Oxford September 2015 What is Acute Oncology? Outline of Talk Concept of Acute Oncology Service (AOS)
What is Acute Oncology? Kay McCallum Acute Oncology Advanced Nurse Practitioner John Radcliffe Hospital Oxford September 2015 What is Acute Oncology? Outline of Talk Concept of Acute Oncology Service (AOS)
Laparotomy for large retroperitoneal mass:
 Laparotomy for large retroperitoneal mass: procedure-specific information UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Laparotomy for large retroperitoneal mass: procedure-specific information UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Guidelines for the Management of Prostate Cancer West Midlands Expert Advisory Group for Urological Cancer
 Guidelines for the Management of Prostate Cancer West Midlands Expert Advisory Group for Urological Cancer West Midlands Clinical Networks and Clinical Senate Coversheet for Network Expert Advisory Group
Guidelines for the Management of Prostate Cancer West Midlands Expert Advisory Group for Urological Cancer West Midlands Clinical Networks and Clinical Senate Coversheet for Network Expert Advisory Group
Occupational Therapy and Physiotherapy in Stroke and Neurology Inpatient Services
 Occupational Therapy and Physiotherapy in Stroke and Neurology Inpatient Services Information for patients Welcome to the Stroke and Neurology inpatient therapy team. As part of your stay you may be assessed
Occupational Therapy and Physiotherapy in Stroke and Neurology Inpatient Services Information for patients Welcome to the Stroke and Neurology inpatient therapy team. As part of your stay you may be assessed
Radiotherapy symptoms control in bone mets. Francesco Cellini GemelliART. Ernesto Maranzano,MD. Session 5: Symptoms management
 Session 5: Symptoms management Radiotherapy symptoms control in bone mets Francesco Cellini GemelliART Ernesto Maranzano,MD Director of Oncology Department Chief of Radiation Oncology Centre S. Maria Hospital
Session 5: Symptoms management Radiotherapy symptoms control in bone mets Francesco Cellini GemelliART Ernesto Maranzano,MD Director of Oncology Department Chief of Radiation Oncology Centre S. Maria Hospital
Skull Base Tumour Service. The Multi-Disciplinary Team (MDT) Explained. Jan 2018 v1
 Skull Base Tumour Service The Multi-Disciplinary Team (MDT) Explained Jan 2018 v1 Skull base tumours grow in the bones of the skull that form the bottom of the head and the body ridge between the nose
Skull Base Tumour Service The Multi-Disciplinary Team (MDT) Explained Jan 2018 v1 Skull base tumours grow in the bones of the skull that form the bottom of the head and the body ridge between the nose
Suspecting Tumors, or Could it be cancer?
 Suspecting Tumors, or Could it be cancer? Donna E. Reece, M.D. Princess Margaret Cancer Centre University Health Network Toronto, ON CANADA 07 February 2018 Background Low back pain is common However,
Suspecting Tumors, or Could it be cancer? Donna E. Reece, M.D. Princess Margaret Cancer Centre University Health Network Toronto, ON CANADA 07 February 2018 Background Low back pain is common However,
Acute Oncology Induction Training Specification
 Acute Oncology Induction Training Specification Author: Acute Oncology/Cancer of Unknown Primary Clinical Network Group (AO/CUP CNG) V. 2.0 Agreed: 30.11.2012 Reviewed: May 2015 Review : May 2016 MCCN
Acute Oncology Induction Training Specification Author: Acute Oncology/Cancer of Unknown Primary Clinical Network Group (AO/CUP CNG) V. 2.0 Agreed: 30.11.2012 Reviewed: May 2015 Review : May 2016 MCCN
Blackburn with Darwen Clinical Commissioning Group and East Lancashire Clinical Commissioning Group. Policies for the Commissioning of Healthcare
 Blackburn with Darwen Clinical Commissioning Group and East Lancashire Clinical Commissioning Group Policies for the Commissioning of Healthcare Policy for Managing Back Pain Spinal /Facet Joint and Epidural
Blackburn with Darwen Clinical Commissioning Group and East Lancashire Clinical Commissioning Group Policies for the Commissioning of Healthcare Policy for Managing Back Pain Spinal /Facet Joint and Epidural
11. Spinal cord injury
 11. Spinal cord injury Introduction Always think spinal (vertebral) and/or spinal cord injury (SCI) in children with trauma. Remember SCIWORA cord injury may be present without abnormalities on routine
11. Spinal cord injury Introduction Always think spinal (vertebral) and/or spinal cord injury (SCI) in children with trauma. Remember SCIWORA cord injury may be present without abnormalities on routine
A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH)
 A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH) 6565 Fannin Street Houston, TX 77030 Phone: 713-790-3333 DISCLAIMER: The information in this booklet is compiled from a variety of sources.
A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH) 6565 Fannin Street Houston, TX 77030 Phone: 713-790-3333 DISCLAIMER: The information in this booklet is compiled from a variety of sources.
Faster Cancer Treatment Indicators: Use cases
 Faster Cancer Treatment Indicators: Use cases 2014 Date: October 2014 Version: Owner: Status: v01 Ministry of Health Cancer Services Final Citation: Ministry of Health. 2014. Faster Cancer Treatment Indicators:
Faster Cancer Treatment Indicators: Use cases 2014 Date: October 2014 Version: Owner: Status: v01 Ministry of Health Cancer Services Final Citation: Ministry of Health. 2014. Faster Cancer Treatment Indicators:
COLLEGE OF PHYSICIANS AND SURGEONS OF NOVA SCOTIA SUMMARY OF DECISION OF INVESTIGATION COMMITTEE C. Dr. John Kirkpatrick
 COLLEGE OF PHYSICIANS AND SURGEONS OF NOVA SCOTIA SUMMARY OF DECISION OF INVESTIGATION COMMITTEE C Dr. John Kirkpatrick Investigation Committee C of the College of Physicians and Surgeons of Nova Scotia
COLLEGE OF PHYSICIANS AND SURGEONS OF NOVA SCOTIA SUMMARY OF DECISION OF INVESTIGATION COMMITTEE C Dr. John Kirkpatrick Investigation Committee C of the College of Physicians and Surgeons of Nova Scotia
NATIONAL REHABILITATION HOSPITAL (NRH) THE SPINAL CORD SYSTEM OF CARE (SCSC) PROGRAMME INPATIENT SCOPE OF SERVICE
 NATIONAL REHABILITATION HOSPITAL (NRH) THE SPINAL CORD SYSTEM OF CARE (SCSC) PROGRAMME INPATIENT SCOPE OF SERVICE NATIONAL REHABILITATION HOSPITAL SCOPE OF SERVICE FOR THE SPINAL CORD SYSTEM OF CARE PROGRAMME
NATIONAL REHABILITATION HOSPITAL (NRH) THE SPINAL CORD SYSTEM OF CARE (SCSC) PROGRAMME INPATIENT SCOPE OF SERVICE NATIONAL REHABILITATION HOSPITAL SCOPE OF SERVICE FOR THE SPINAL CORD SYSTEM OF CARE PROGRAMME
South East Coast Operational Delivery Network. Critical Care Rehabilitation
 South East Coast Operational Delivery Networks Hosted by Medway Foundation Trust South East Coast Operational Delivery Network Background Critical Care Rehabilitation The optimisation of recovery from
South East Coast Operational Delivery Networks Hosted by Medway Foundation Trust South East Coast Operational Delivery Network Background Critical Care Rehabilitation The optimisation of recovery from
Simple removal of the kidney (simple nephrectomy): procedure-specific information
 PATIENT INFORMATION Simple removal of the kidney (simple nephrectomy): procedure-specific information What is the evidence base for this information? This leaflet includes advice from consensus panels,
PATIENT INFORMATION Simple removal of the kidney (simple nephrectomy): procedure-specific information What is the evidence base for this information? This leaflet includes advice from consensus panels,
Wendy Field Advanced Physiotherapy Practitioner June 2018
 Wendy Field Advanced Physiotherapy Practitioner June 2018 Radiculopathy???? Lumbar radicular pain is where the clinician suspects the pain is coming from a lumbar nerve root. Essentially we are looking
Wendy Field Advanced Physiotherapy Practitioner June 2018 Radiculopathy???? Lumbar radicular pain is where the clinician suspects the pain is coming from a lumbar nerve root. Essentially we are looking
Selective Dorsal Rhizotomy (SDR) Scotland Service Pathway
 Selective Dorsal Rhizotomy (SDR) Scotland Service Pathway This pathway should to be read in conjunction with the attached notes. The number in each text box refers to the note that relates to the specific
Selective Dorsal Rhizotomy (SDR) Scotland Service Pathway This pathway should to be read in conjunction with the attached notes. The number in each text box refers to the note that relates to the specific
Nepal Spinal Cord Injury Working Group
 Nepal Spinal Cord Injury Working Group 19 June 2015 Overview by Fiona Stephenson Rehabilitation Cluster Meeting Aim of the Nepal SCI Working Group Ascertain numbers of patients with SCI Find key actors
Nepal Spinal Cord Injury Working Group 19 June 2015 Overview by Fiona Stephenson Rehabilitation Cluster Meeting Aim of the Nepal SCI Working Group Ascertain numbers of patients with SCI Find key actors
LCA Lung Clinical Forum. 21 st October 2014
 LCA Lung Clinical Forum 21 st October 2014 Welcome Dr Liz Sawicka Chair - LCA Lung Pathway Group Succession planning Dr Kate Haire Consultant in Public Health Medicine, LCA Commissioning Intentions for
LCA Lung Clinical Forum 21 st October 2014 Welcome Dr Liz Sawicka Chair - LCA Lung Pathway Group Succession planning Dr Kate Haire Consultant in Public Health Medicine, LCA Commissioning Intentions for
