04/11/2014. Swallowing Disorders in Older Adults. Disclosures. Aging in America Administration on Aging. Outline. Changes with Aging
|
|
|
- Isabel Lindsey
- 5 years ago
- Views:
Transcription
1 Disclosures The author has no financial or nonfinancial relationships relevant to the content of this presentation Heather M Clark PhD CCC/SLP Minnesota Speech-Language-Hearing Association April 11, MFMER slide MFMER slide-2 Outline Age-related changes affecting swallowing function Assessment of dysphagia in older adults Management of dysphagia in older adults Aging in America Administration on Aging 41.4 million people over age 65 Over one in every eight, or 13.3%, of the population is an older American 79.7 million people over age 65 in million people over age 85 in 2040 Persons reaching age 65 have an average life expectancy of an additional 19.2 years MFMER slide MFMER slide-4 Changes with Aging Reduced sense of smell and taste Increased risk of xerostomia secondary to medications and illness Increased risk of tooth decay and gum disease Reduced esophageal motility Increased prevalence of GERD Slowed gastric emptying Heightened satiety schmoop.com Changes with Aging Decrease in neurons Reduced production of neurotransmitters Slowed neuronal conduction Slowed response times 2014 MFMER slide MFMER slide-6 1
2 Sarcopenia Reduction in muscle mass, strength, and endurance associated with aging Begins in 30 s, accelerates after age 75 (3-5% per decade) Causes Hormonal changes Changes in protein synthesis Nutrition Inactivity Changes in motor unit configurations iofbonehealth.org Sarcopenia in the Oropharyngeal Musculature Reduced lingual strength apparent by age 60 (Clark and Solomon, 2012; Youmans, Youmans, & Stierwalt 2009) Reduced lingual thickness is associated with poor nutritional status (Tamura et al 2012) Age-related changes in swallowing physiology (see Sarcopenia Resources) Increased oral and pharyngeal transit times More posterior/inferior bolus location at initiation of pharyngeal swallow More frequent pharyngeal residue More frequent laryngeal penetration See Sarcopenia Resources by Specialty Board on Swallowing & Swallowing Disorders 2014 MFMER slide MFMER slide-8 Respiratory Musculature Changes in respiratory system associated with aging (see Kim & Sapienza, 2005) Reduced lung elasticity, increased chest wall stiffness Reduced respiratory muscle strength Resistance exercise Inspiratory muscle training improves ventilatory capacity Expiratory muscle training improves nonventilatory functions (cough, swallow, speech) Laryngeal Musculature Intrinsic: Control vocal cord closure and tension Extrinsic: Contribute to hyolaryngeal elevation, epiglottic inversion, UES dilation Age-related changes Laryngeal cartilages ossify, making them less flexible Muscles atrophy, affecting strength as well as bulk for achieving vocal cord closure 2014 MFMER slide MFMER slide-10 Velopharyngeal Musculature Velar movements Contribute to posterior seal preventing premature spillage Prevent flow of bolus into nasopharynx Facilitate pharyngeal pressure generation to enhance bolus transit Pharyngeal constriction Pharyngeal pressures vary with swallowing condition Weakness presumed to contribute to residue 2014 MFMER slide-11 Lingual Musculature Evidence of lingual sarcopenia Animal models (e.g., Schaser et al 2011) Human studies (Beuhring et al, 2013; Clark and Solomon, 2012; Robbins et al, 1995; Tamura et al, 2012; Youmans, Youmans, & Stierwalt 2009) Contributes to multiple aspects of oropharyngeal swallow Oral containment Bolus manipulation Bolus transit (oral and pharyngeal) Oral phase dysphagia more common in patients with lingual weakness (Clark et al, 2003; Reddy et al, 1990; Robinovitch et al, 1991; Stierwalt & Youmans, 2007; Yoshida et al, 2006) 2014 MFMER slide-12 2
3 Orofacial Musculature Lip and Cheek Presumed association with anterior spillage and/or residue in lateral sulci (No studies were identified that specifically associated objectively measured labiobuccal weakness with oral dysphagia) Jaw Presumed to influence chewing effectiveness and efficiency Video of presbyphagia DVD # MFMER slide MFMER slide-14 Dysphagia-related Conditions in Aging Vascular (e.g., CVA) Neuromuscular (e.g., ALS) Movement (e.g., PD) Neurocognitive (e.g., AD, PPA) Respiratory (e.g., COPD) Gastrointestinal Neoplastic Infectious (community and hospital acquired) Assessment Considerations Older Adults 2014 MFMER slide MFMER slide-16 History Relevant co-morbidities Independence with food preparation Diet restrictions associated with co-morbidities or preference Prosthodontic fit Appetite Oral Structure and Function Dentition and prosthodontics Xerostomia Strength/functional reserve 2014 MFMER slide MFMER slide-18 3
4 Clinical and Instrumental Exam Observe clinical signs and evidence of physiologic impairment Consider variations associated with healthy aging Expands range of WNL/WFL Does not change severity ratings of identified dysphagia Management Considerations Older Adults 2014 MFMER slide MFMER slide-20 Candidacy for therapy Age should not be an independent indicator for candidacy Additional factors (examples) Resources (availability of SLP, transportation, funding, etc) Cognitive resources Physical limitations Sensori-perception Mobility or posture Self-feeding Treatment Targets 2014 MFMER slide MFMER slide-22 A Framework for Managing Dysphagia A Framework for Managing Dysphagia Structural and Functional Impairments Rehabilitative Clinical Signs Adaptive (Compensatory) Structural and Functional Impairments Structural impairments Clefts Resections Trauma Functional impairments Forces and pressures Speed and timing 2014 MFMER slide MFMER slide-24 4
5 A Framework for Managing Dysphagia Bolus containment Bolus manipulation Bolus transit Airway protection Clinical Signs Adaptive 2014 MFMER slide MFMER slide-26 Adaptive strategies Address clinical signs Manipulate the swallowing context to facilitate safety Do not induce permanent physiologic change Are effective only when in use Are effective immediately Effectiveness can be assessed during initial evaluation Adaptive strategies Postural changes Swallowing maneuvers Common sense behavioral modifications Somatosensory stimulation Diet modifications 2014 MFMER slide MFMER slide-28 Adaptive strategies Postural changes use gravity and/or pressure changes to contain or redirect the bolus Swallowing maneuvers alter the intensity or timing of swallowing behaviors augment swallow with volitional airway protection Adaptive strategies Common sense modifying bolus size serial swallows alternating solids and liquids moistening solids 2014 MFMER slide MFMER slide-30 5
6 Adaptive strategies Somatosensory stimulation Visual Taste Temperature Tactile Diet modifications manipulate Viscosity Elasticity Particulateness Adaptive Oral Containment 2014 MFMER slide MFMER slide-32 Oral Containment Adaptive : Oral Containment Lip, tongue, jaw and/or velar weakness or coordination Reduced sensitivity Xerostomia Anterior spillage Premature spillage Lateral sulci residue Anterior Spillage bolus placement on strong side head tilt to strong side Rehabilitative Adaptive (Compensatory) side lying posterior bolus placement assisted labial closure thickened liquids 2014 MFMER slide MFMER slide-34 Adaptive : Oral Containment Adaptive : Oral Containment Premature Posterior Spillage head tilt forward thickened liquids reduced particulateness of solids Lateral sulci residue Bolus placement on strong side Head tilt to strong side Sidelying heighten sensory awareness (temperature, taste) Reduce particulateness Finger sweep 2014 MFMER slide MFMER slide-36 6
7 Bolus preparation/manipulation Adaptive Bolus Preparation Lip, tongue, jaw and/or velar weakness or coordination Inadequate dentition Reduced sensitivity Xerostomia Rehabilitative Failure to respond to food stimuli Ineffective mastication Prolonged preparation Adaptive (Compensatory) 2014 MFMER slide MFMER slide-38 Adaptive : Bolus Preparation Adaptive : Bolus Preparation Agnosia Prolonged or incomplete mastication Modify elasticity of solids Targeted chewing rates Small bites Artificial saliva Additional sauces/gravies 2014 MFMER slide MFMER slide-40 Oral Transit Tongue weakness Reduced sensitivity Xerostomia Bradyphagia Oral residue Vallecular residue Adaptive Oral Transit Rehabilitative Adaptive (Compensatory) 2014 MFMER slide MFMER slide-42 7
8 Adaptive : Oral Transit Adaptive : Oral Transit Bradyphagia Oral residue Bolus placement on strong side Head tilt to strong side Reduce particulateness Thicken liquids Small bites Additional sauces/gravies Alternate solids and liquids Finger sweeps 2014 MFMER slide MFMER slide-44 Adaptive : Oral Transit Vallecular Residue Reduce particulateness Serial swallows Alternate solids and liquids Effortful swallow Head turn to weak* side Head tilt to strong* side Adaptive Bolus Transit 2014 MFMER slide MFMER slide-46 Pharyngeal Transit Adaptive : Bolus Transit Tongue weakness Pharyngeal weakness Impaired hyo-laryngeal excursion Impaired UES dilation Reduced sensitivity Xerostomia Nasopharyngeal Reflux Vallecular residue Pyriform residue Nasopharyngeal Reflux Upright posture Effortful swallow Thickened liquids Prosthetics Rehabilitative Adaptive (Compensatory) 2014 MFMER slide MFMER slide-48 8
9 Adaptive : Bolus Transit Effortful Swallow Vallecular Residue Reduce particulateness Serial swallows Alternate solids and liquids Effortful swallow Head turn to weak* side Head tilt to strong* side Linguapalatal pressure (Hind et al, 2001) Tongue base to pharyngeal wall pressure (Lazarus et al, 2002) Hyolaryngeal excursion (Hind et al, 2001) Pharyngeal pressure (peak & duration; earlier onsets) (Huckabee et al, 2005) Submental muscle activity (Huckabee et al, 2005) Duration of UES opening (Hind et al, 2001; Hiss et al 2005) Esophageal peristaltic amplitudes (Lever et al, 2007) Raises hyolaryngeal complex prior to the swallow (Bulow et al, 1999) Reduced penetration (Bulow et al 2001) 2014 MFMER slide MFMER slide-50 Adaptive : Bolus Transit Surface NMES to Neck Pyriform Residue for vallecular residue Mendelsohn VitalStim Condition Effects Normals: reduced laryngeal and hyoid elevation during stimulation (Humbert et al, 2006) Patients Stimulation on: hyoid lowers at rest, improved swallowing on some measures, not on others (Ludlow et al, 2007) Stimulation over time: greater improvement with VS compared to TDT; improved oral intake and swallowing physiology (not laryngeal elevation) (Shaw et al, 2007) 2014 MFMER slide MFMER slide-52 Airway Protection Adaptive Airway Protection Delayed pharyngeal response Reduced hyo-laryngeal excursion Reduced laryngeal closure Impaired sensitivity Impaired cough Rehabilitative P/A before the swallow P/A during the swallow P/A after the swallow Adaptive (Compensatory) 2014 MFMER slide MFMER slide-54 9
10 Adaptive : Airway Protection Adaptive : Airway Protection Penetration/Aspiration before the swallow Head down (chin tuck) posture Thermotactile stimulation Penetration/Aspiration during the swallow Super supraglottic swallow maneuver Supraglottic swallow maneuver Modified food textures 2014 MFMER slide MFMER slide-56 Adaptive : Airway Protection Penetration/Aspiration after the swallow Any strategies addressing residue Supraglottic swallow maneuver Position changes Semi-reclined Sidelying Evidence Supporting Use of Adaptive Techniques Thermal-tactile Stimulation TTS + oral stim + oral massage + digital manipulation improved swallowing physiology (but not occurrence of pneumonia or LOS) 4 studies with normal subjects during a single session 2 showed no effect 1 showed shorter latency with cold+tactile+sour, 1 showed brisk response 2 studies with patient groups during a single testing session Reduced stage transition time (stroke pts) No effect (neurologic pts with delayed swallow response) 2014 MFMER slide MFMER slide-58 Evidence Supporting Use of Adaptive Techniques Bolus Manipulations (taste, texture, temperature, volume, viscosity) Most studies examine single exposure effects There is a lack of evidence of the importance of texture modified foods and thickened fluids related to the amount of diet intake for adults with acute dysphagia There is some evidence of that thickened fluid cannot increase fluid intake for persons with acute and chronic dysphagia Evidence Supporting Use of Adaptive Techniques Bolus Manipulations (taste, texture, temperature, volume, viscosity) There is some evidence that special made and nutritional enriched texture modified food (pureed and minced) and thickened fluid (nectar, honey and pudding consistency) can increase the nutritional status of elderly persons with chronic dysphagia 2014 MFMER slide MFMER slide-60 10
11 Postural Changes Most studies examine single-exposure effects, but at least one reported positive rehabilitation outcomes Swallowing Maneuvers Most studies examine single exposure effects on swallowing physiology Chin tuck and supraglottic swallow Single session: inconsistent effects Long term: generally beneficial 2014 MFMER slide MFMER slide-62 Rehabilitative strategies Rehabilitative Target underlying physiologic impairment Intend to induce relatively permanent change in physiology Generally require time to become effective (dosage) Targets should reflect impairments identified during assessment should be consistent with current models of neuromuscular rehabilitation and motor learning 2014 MFMER slide MFMER slide-64 Rehabilitative strategies Strength Range Structure Neurophysiology Preventing/Slowing/Reversing Sarcopenia Resistance Exercise (see Vella & Kravitz, 2002; Liu & Latham, 2009) Strength gains with exercise similar to those shown in younger individuals Stimulates release of relevant hormones May enhance the benefit of nutritional and hormonal interventions General Principles (American College of Sports Medicine, do not address swallowing musculature) 2-4 days per week minutes 1-2 exercises per muscle group reps 65-75% of maximum 2014 MFMER slide MFMER slide-66 11
12 Rehabilitative Oral Containment Lip, tongue, jaw and/or velar weakness or coordination Reduced sensitivity Xerostomia Rehabilitative Anterior spillage Premature spillage Prolonged preparation Adaptive (Compensatory) 2014 MFMER slide MFMER slide-68 Rehabilitative : Bolus Containment Lip Screen Lip weakness Strengthening Facercise; mookychick.co.uk Facial-Flex; blaisemedical.com 2014 MFMER slide-69 Retrospective (uncontrolled study) of stroke pts showed improved strength and swallow function 2014 MFMER slide-70 Orofacial Strengthening Outcomes Improved oropharyngeal swallow efficiency following range of motion and/or coordination exercises (Logemann et al,1997) Greater weight gain with standard oral motor exercise plus dietary supplement than supplement alone in healthy elderly (Kikutani et al, 2006) Improved lip strength and swallowing capacity in stroke patients (Haag & Aniko, 2008) No change in lip or cheek strength following 4 weeks of training with high resistance straws (Clark & Shelton, 2011) Rehabilitative : Bolus Containment Reduced Tactile Sensation No evidence showing stimulation has direct effects on sensation 2014 MFMER slide MFMER slide-72 12
13 Rehabilitative : Bolus Containment Rehabilitative : Bolus Containment Reduced Taste or Olfactory Sensation?? Lingual weakness Strengthening 2014 MFMER slide MFMER slide-74 Lingual Strengthening Must involve resistance and overload (traditional OME likely insufficient) Specificity effects Observed for strength/endurance (Clark, 2012) Not observed for direction of movement in the context of maximum contraction (Clark et al., 2009) Observed for functional aspects of lingual movements (Clark & Shelton, 2011) Lingual muscle training can result in non-specific functional outcomes Training of anterior lingual elevation improves swallowing function (Robbins et al, 2005, 2007; Yeates et al, 2008) Lingual Strengthening: IOPI 2014 MFMER slide MFMER slide-76 Lingual Strengthening: IOPI Lingual Strengthening: Ora-Light 2014 MFMER slide MFMER slide-78 13
14 High Resistance Straws 2014 MFMER slide MFMER slide MFMER slide MFMER slide-82 Lingual Strengthening -- Outcomes Increased tongue strength (too many references to list) Increased lingual volume (Robbins et al, 2005) Improved swallowing pressures in healthy aging adults (Robbins et al, 2005) Increased swallowing pressures and reduced airway invasion (Robbins et al, 2007) Improved bolus control on videofluoroscopy (Yeates et al, 2008) Improved functional dietary intake by mouth (Yeates et al, 2008) Rehabilitative : Bolus Containment Buccal weakness Strengthening 2014 MFMER slide MFMER slide-84 14
15 Rehabilitative : Bolus Containment Rehabilitative : Bolus Containment Velar weakness? Exercise for velar depression? Hypophagia LSVT Sharkawi et al demonstrated improved swallowing (did not report effects on drooling) 2014 MFMER slide MFMER slide-86 Bolus preparation/manipulation Rehabilitative Bolus Preparation Lip, tongue, jaw and/or velar weakness or coordination Inadequate dentition Reduced sensitivity Xerostomia Rehabilitative Failure to respond to food stimuli Ineffective mastication Prolonged preparation Adaptive (Compensatory) 2014 MFMER slide MFMER slide-88 Rehabilitative : Bolus Preparation Rehabilitative : Bolus Preparation Lip, tongue, jaw and/or velar weakness or coordination Lip and tongue weakness addressed above Reduced jaw strength or ROM Strengthening Stretching Inadequate dentition Dental consult Reduced sensitivity Addressed above 2014 MFMER slide MFMER slide-90 15
16 Jaw Strengthening High resistance chewing gum Ingervall & Sitsanis (1987) Tzakis et al (1989) Chewy Tubes Jaw Stretching Active & Passive ROM mj-exerciser-and-jaw-exercise-for-tmj 2014 MFMER slide MFMER slide-92 Jaw Strengthening Outcomes Immediate decrease in chewing efficiency following exercise with high resistance chewing gum (Tzakis, M. G., et al. 1989) Rehabilitative : Bolus Preparation Xerostomia Modify medications Parasympathetic stimulating drugs Electrical stimulation 2014 MFMER slide MFMER slide-94 Oral Transit Tongue weakness Reduced sensitivity Xerostomia Oral residue Vallecular residue Oral Transit Rehabilitative Adaptive (Compensatory) 2014 MFMER slide MFMER slide-96 16
17 Rehabilitative : Oral Transit Tongue weakness Reduced sensitivity Xerostomia Addressed above Addressed above Addressed above Pharyngeal Phase 2014 MFMER slide MFMER slide-98 Rehabilitative Bolus Transit Pharyngeal Transit Tongue weakness Velar weakness Pharyngeal weakness Impaired hyo-laryngeal excursion Impaired UES dilation Reduced sensitivity Xerostomia Rehabilitative Nasopharyngeal reflux Vallecular residue Pyriform residue Adaptive (Compensatory) 2014 MFMER slide MFMER slide-100 Rehabilitative : Pharyngeal Transit Velar weakness Traditional OME (blowing, sucking exercises) CPAP Effortful swallow McNeil Dysphagia Therapy Program Masako CPAP Constant Positive Airway Pressure Shown to improve velopharyngeal valving during speech (Kuehn et al, 2002) Swallowing outcomes not yet studied 2014 MFMER slide MFMER slide
18 Rehabilitative : Pharyngeal Transit Pharyngeal weakness Masako Effortful swallow LSVT NMES McNeil Dysphagia Therapy Program Masako (Anterior Tongue Anchor) Original studies focused on pharyngeal effects, potentially affects lingual retraction as well Outcomes (condition effects) Bulging of posterior pharyngeal wall (Fujiu & Logemann, 1996) Increased (Lazarus et al 2002) or decreased (Umeki et al 2009; Doeltgen, 2009) tongue base to pharyngeal wall contact pressures Increased UES relaxation pressures in older adults (Doeltgen, 2011) Training effects unknown 2014 MFMER slide MFMER slide-104 Effortful Swallow Clark & Shelton (submitted) 40 healthy adult participants 35 females / 5 males Mean age 23.7 years (range 18 to 59) Assigned to one of three training conditions Tongue elevation + ES (N=15) Resistance straw training + ES (N=18) ES only (N=7) Daily exercise for 4 weeks 3 sets of 10 repetitions 2014 MFMER slide MFMER slide-106 Outcome Measures Lingual swallowing pressure Submental semg Negative pressure Obtained during Noneffortful dry swallow Effortful dry swallow Tongue strength Lingual Swallowing Pressure Tongue + ES Straw + ES ES Only Training x Effort F(1, 37) = 15.2 p =.000 Noneffortful Training Effects t (39) =.703 p =.486 Effortful Training Effects t (39) = 4.73 p =.000 PreTraining PostTraining PreTraining PostTraining Noneffortful Effortful Training F(1, 37) = 9.66 p =.004 Effort F(1, 37) = p =.000 Group F(2, 37) = 3.33 p = MFMER slide MFMER slide
19 Conclusions Training effortful swallow (in isolation or with preparatory contraction) improves only effortful swallows Training with high resistance straws improves only effortful sips. ES and/or tongue exercise did not improved sipping strength 2014 MFMER slide MFMER slide-110 Effortful Swallow Training Outcomes Increased oral pressures during effortful swallows (Clark & Shelton, 2011) Increased cutaneous neck pressure during effortful swallow (Felix et al, 2008) Increased hyoid elevation (paired with NMES) (Park et al, 2009) NMES Uses electricity to cause muscle contraction Electrode Sites Surface Percutaneous Intramuscular Current parameters Amplitude, duration, & frequency Intensity Waveform (pulsed most common) Bursts Has been applied to limb musculature to increase strength, but is most often used in conjunction with active exercise 2014 MFMER slide MFMER slide-112 Electrical Stimulation Surface NMES to Neck VitalStim No impact on pharyngeal physiology, diet advancement or return to oral feeding (Kiger et al 2006) Overall swallowing severity improved more with VS compared to TTS (Freed et al 2001) or traditional treatment (Blumenfeld et al 2006) 2014 MFMER slide MFMER slide
20 Surface NMES to Neck Rehabilitative : Bolus Transit Carnaby-Mann & Crary (2007) Meta-analysis 7 studies accepted for analysis 255 patients studied 2 controlled trials 5 used before/after (case series) design All studies used Transcutaneous stimulation applied to throat 20% improvement in swallowing function (collapsed across all studies) but actual outcome measures varied across studies Methodological flaws not addressed Reduced hyo-laryngeal excursion (weakness) Shaker head lift Mendelsohn Expiratory muscle strength training Falsetto 2014 MFMER slide MFMER slide-116 Extrinsic Laryngeal Muscle Strengthening Strength (ROM) contributes to Airway protection Epiglottic inversion UES dilation Shaker Head Lifts Head lifts Isometric Isotonic Outcomes Significant change in functional swallowing measure (Shaker et al, 2002 participants aged 62-89) Improved laryngeal elevation and UES dilation (Easterling et al, 2005; Logemann et al, 2009; Shaker et al, 1997) MFMER slide MFMER slide-118 ISO SwallowingExercises.com ISO Swallowing Exercise Device Baseline Medical Services, Inc MFMER slide MFMER slide
21 Mendelsohn Sustained laryngeal elevation during swallow Technically a ROM or endurance exercise (no added resistance) Outcomes Prolonged UES opening in normal participants (Ding et al, 2002) Improved timing of pharyngeal events in a single subject during VFSS (Logemann et al 1990) 87% (39/45) of all patients increased their functional oral intake of food/liquid (Neumann, 1993; Crary et al, 2004) Expiratory Muscle Strength Training (EMST) Pressure threshold trainer Resistance set at 75% maximum expiratory pressure 5-6 sets of 5 breaths 3 or 5 days per week (Anand et al 2012) 4-8 weeks 2014 MFMER slide MFMER slide-122 Expiratory Muscle Strength Training (EMST) Training Outcomes (see Sapienza et al 2011) Increased expiratory pressures Improved cough Increased submental muscle activity, influencing hyolaryngeal elevation Improvements in P-A scale Airway Protection 2014 MFMER slide MFMER slide-124 Airway Protection Delayed pharyngeal response Reduced hyo-laryngeal excursion Reduced laryngeal closure Impaired sensitivity Impaired cough Rehabilitative P/A before the swallow P/A during the swallow P/A after the swallow Adaptive (Compensatory) 2014 MFMER slide-125 Rehabilitative Airway Protection 2014 MFMER slide
22 Rehabilitative : Airway Protection Rehabilitative : Airway Protection Delayed pharyngeal response Impaired hyo-laryngeal elevation Addressed above 2014 MFMER slide MFMER slide-128 Rehabilitative : Airway Protection Reduced laryngeal closure Laryngeal adduction exercises Intrinsic Laryngeal Muscle Strengthening Bearing down (push-pull) Case study reported improved swallowing function pairing laryngeal adduction exercise with semg biofeedback (Crary et al, 2004) LSVT (also targets respiratory musculature) LSVT with 8 patients with Idiopathic Parkinson Disease. 51% decrease in swallowing motility disorders (El Sharkawi et al, 2002) 2014 MFMER slide MFMER slide-130 Rehabilitative : Airway Protection Rehabilitative : Airway Protection Reduced laryngeal sensitivity? PMV in the context of tracheostomy Impaired cough Expiratory muscle training 2014 MFMER slide MFMER slide
23 Exercise-based Dysphagia Intervention Outcomes for Older Adults Many studies examining benefits for individuals with dysphagia have not excluded young adults, but the populations of interest (e.g., stroke patients) tended to be older No studies have demonstrated poorer response to exercisebased treatments by older participants compared to younger participants Medicare Issues 2014 MFMER slide MFMER slide-134 Contract # /0003 DynCorp Therapy PSC Final Therapy Review Protocols 30 November 2001 Dysphagia Protocol Indications for Dysphagia Evaluation Documentation within the medical record must include at least one of the following conditions: History of aspiration or high risk for aspiration; Nasal regurgitation, choking, or frequent coughing during swallowing; Wet gurgling voice quality after swallowing, or delayed or slow swallow reflex; Presence of oral motor disorders such as drooling, oral food retention, or leakage of food or liquids placed into the mouth; Impaired salivary gland performance and/or presence of local structural lesions in the oral cavity or pharynx; Contract # /0003 DynCorp Therapy PSC Final Therapy Review Protocols 30 November 2001 Dysphagia Protocol Indications for Dysphagia Evaluation In-coordination, sensation loss, postural difficulties or other neuromotor disturbances affecting oropharyngeal abilities necessary to close the oral cavity and/or to bite, chew, suck, shape and/or squeeze the food bolus into the upper esophagus while protecting the airway; Post-surgical reaction affecting ability to adequately use oropharyngeal structures for swallowing; Documented weight loss and/or malnutrition of undetermined etiology that would require an evaluation to rule out dysphagia; 2014 MFMER slide MFMER slide-136 Contract # /0003 DynCorp Therapy PSC Final Therapy Review Protocols 30 November 2001 Dysphagia Protocol Indications for Dysphagia Evaluation The presence of a tracheostomy, NG- or G-tube; reduced or inadequate laryngeal elevation, labial closure, airway management problems, velopharyngeal closure, laryngeal closure, or pharyngeal peristalsis; or criocopharyngeal dysfunction. Existence of other conditions affecting the structural or functional integrity of the pharyngeal area. Examples of Information to be Included In Documentation of Skilled Services Use terminology that reflects the clinician's technical knowledge. Indicate the rationale (how the service relates to functional goal), type, and complexity of activity. Because patient has residue in the mouth with solids, putting him at risk to aspirate that material, he performed tongue sweeps of the buccal cavity with minimal cues on 80% of solid boluses MFMER slide Documentation-of-Skilled-and-Unskilled-Care-for-Medicare- Beneficiaries/ 2014 MFMER slide
24 Examples of Information to be Included In Documentation of Skilled Services Report objective data showing progress toward goal, such as accuracy of task performance speed of response/response latency frequency/number of responses or occurrences (e.g., patient swallowed 6/10 PO trials of ½ tsp boluses of puree textures with no delay in swallow initiation); number/type of cues level of independence in task completion (e.g., patient verbally described all compensatory strategies to maximize swallow safety independently, but required minimal verbal cues from SLP/caregiver to safely implement them at mealtimes) 2014 MFMER slide-139 Examples of Information to be Included In Documentation of Skilled Services Specify feedback provided to patient/caregiver about performance Explain decision making that result in modifications to treatment activities or the POC. Explain how modifications resulted in a functional change (e.g., patient's attention is enhanced by environmental cues and restructuring during mealtime, allowing her to consume at least 50% of meal without redirection). Explain advances based on functional change (e.g., coughing has decreased to less than 2x/6 oz. drink; liquids upgraded from nectar to thin). Documentation-of-Skilled-and-Unskilled-Care-for-Medicare- Beneficiaries/ 2014 MFMER slide-140 Examples of Information to be Included In Documentation of Skilled Services Explain decision making that result in modifications to treatment activities or the POC. Indicate additional goals or activities Indicate dropped or reduced activities (e.g., cuing hierarchy was modified to limit tactile cues to enable greater independence in patient's use of compensatory strategies at mealtimes). Elaborate on patient/caregiver education or training Evaluate patient s/caregiver s response to training Documentation Short-term goal Pt will safely consume mechanical soft diet with thin liquids x 3 meals per day with 1 overt s/s of aspiration to meet all nutrition/hydration needs. Documentation-of-Skilled-and-Unskilled-Care-for-Medicare- Beneficiaries/ 2014 MFMER slide Documentation-of-Skilled-and-Unskilled-Care-for-Medicare- Beneficiaries/ 2014 MFMER slide-142 Documentation Unskilled progress note Pt has been tolerating mechanical soft/thin liquid diet well. Comment: This progress note does not reflect change in status as a result of skilled intervention. Skilled progress note Pt has been seen for 8 treatment sessions during this period. Pt's diet was upgraded from puree/nectar thick liquids to mechanical soft/thin liquid diet. Pt safely consumed 3 trial meals at lunch with no overt signs and symptoms of aspiration. Pt requires mod verbal cues to safely implement compensatory strategies. The shortterm goal has been updated to include trials of regular texture foods. Plan of care includes caregiver education prior to discharge MFMER slide-143 Documentation Unskilled discharge note Pt has made progress during treatment. Pt and wife educated on use of swallow strategies for safety. Recommend discharge SLP services at this time. Comment: This note does not detail skilled intervention, patient's functional change in status, or skilled aspects of caregiver training. Documentation-of-Skilled-and-Unskilled-Care-for-Medicare- Beneficiaries/ 2014 MFMER slide
25 Documentation Skilled discharge note Skilled SLP services included caregiver education, dysphagia management, therapeutic diet upgrade trials, compensatory strategies (pacing, full oral clearance, cyclic ingestion, relaxation technique for controlled breathing) and discharge counseling. Pt currently has orders for mechanical soft with thin liquids x 2 meals (breakfast/lunch) but remains on puree at dinner. Significantly reduced swallow safety noted in evening due to increased cognitive-behavioral changes associated with sun-downing. Pt and his wife educated re: compensatory swallow strategies to improve safe and efficient swallowing with 100% return demonstration of strategies by his wife. SLP educated pt and family on the need to implement relaxation strategies while eating due to pt experiencing anxiety during meal times. Recommend pt returns home with home health SLP services to address swallow safety while maximizing efficient PO intake on mechanical soft diet with thin liquids. Concluding Remarks The knowledge and skills relevant for managing dysphagia in older adults have broader application Additional study is needed to demonstrate benefit of adaptive and rehabilitative strategies for older adults with dysphagia 2014 MFMER slide MFMER slide-146 References American College of Sports Medicine (no date) Resistance training and the older adult. Indianapolis IN: ACSM. Anand, S., El-Bashiti, N., & Sapienza, C. (2012). Effect of training frequency on maximum expiratory pressure. [Research Support, Non-U.S. Gov't]. American journal of speech-language pathology / American Speech- Language-Hearing Association, 21(4), doi: / (2012/ ) Questions & Discussion Ashford, J., McCabe, D., Wheeler-Hegland, K., Frymark, T., Mullen, R., Musson, N.,... Hammond, C. S. (2009). Evidence-based systematic review: Oropharyngeal dysphagia behavioral treatments. Part III--impact of dysphagia treatments on populations with neurological disorders. J Rehabil Res Dev, 46(2), Buehring, B., Hind, J., Fidler, E., Krueger, D., Binkley, N., & Robbins, J. (2013). Tongue Strength Is Associated with Jumping Mechanography Performance and Handgrip Strength but Not with Classic Functional Tests in Older Adults. Journal of the American Geriatrics Society. doi: /jgs Bulow, M., Olsson, R., & Ekberg, O. (2001). Videomanometric analysis of supraglottic swallow, effortful swallow, and chin tuck in patients with pharyngeal dysfunction. Dysphagia, 16(3), Bulow, M., Olsson, R., & Ekberg, O. (2002). Supraglottic swallow, effortful swallow, and chin tuck did not alter hypopharyngeal intrabolus pressure in patients with pharyngeal dysfunction. Dysphagia, 17(3), Burkhead, L. M., Sapienza, C. M., & Rosenbek, J. C. (2007). Strength-training exercise in dysphagia rehabilitation: principles, procedures, and directions for future research. Dysphagia, 22(3), doi: /s z Carnaby-Mann, G. D., & Crary, M. A. (2007). Examining the evidence on neuromuscular electrical stimulation for swallowing: a meta-analysis. Arch Otolaryngol Head Neck Surg, 133(6), MFMER slide MFMER slide-148 References Carnaby-Mann, G. D., & Crary, M. A. (2010). McNeill dysphagia therapy program: a case-control study. Arch Phys Med Rehabil, 91(5), doi: S (10)00081-X [pii] /j.apmr Clark, H., Lazarus, C., Arvedson, J., Schooling, T., & Frymark, T. (2009). Evidence-based systematic review: effects of neuromuscular electrical stimulation on swallowing and neural activation. [Research Support, Non-U.S. Gov't Review]. American journal of speech-language pathology / American Speech-Language-Hearing Association, 18(4), doi: / (2009/ ) Clark, H. M. (2012). Specificity of training in the lingual musculature. [Randomized Controlled Trial Research Support, Non-U.S. Gov't]. Journal of speech, language, and hearing research : JSLHR, 55(2), doi: / (2011/ ) Clark, H. M., Henson, P. A., Barber, W. D., Stierwalt, J. A., & Sherrill, M. (2003). Relationships among subjective and objective measures of tongue strength and oral phase swallowing impairments. [Research Support, Non- U.S. Gov't]. American journal of speech-language pathology / American Speech-Language-Hearing Association, 12(1), doi: / (2003/051) Clark, H. M., & Shelton, N. (2011). Augementing the effortful swallow: comparison of two training techniques. Paper presented at the Dysphagia Research Society, San Antonio, TX. Clark, H. M., & Solomon, N. P. (2012). Age and sex differences in orofacial strength. Dysphagia, 27(1), 2-9. doi: /s Connor, N. P., Russell, J. A., Wang, H., Jackson, M. A., Mann, L., & Kluender, K. (2009). Effect of tongue exercise on protrusive force and muscle fiber area in aging rats. [Research Support, N.I.H., Extramural]. Journal of speech, language, and hearing research : JSLHR, 52(3), doi: / (2008/ ) Crary, M. A., Carnaby Mann, G. D., Groher, M. E., & Helseth, E. (2004). Functional benefits of dysphagia therapy using adjunctive semg biofeedback. Dysphagia, 19(3), MFMER slide-149 References Ding, R., Larson, C. R., Logemann, J. A., & Rademaker, A. W. (2002). Surface electromyographic and electroglottographic studies in normal subjects under two swallow conditions: normal and during the Mendelsohn manuever. [Research Support, U.S. Gov't, P.H.S. Validation Studies]. Dysphagia, 17(1), Doeltgen, S. H., Macrae, P., & Huckabee, M. L. (2011). Pharyngeal pressure generation during tongue-hold swallows across age groups. [Comment]. American journal of speech-language pathology / American Speech- Language-Hearing Association, 20(2), doi: / (2011/ ) Doeltgen, S. H., Witte, U., Gumbley, F., & Huckabee, M. L. (2009). Evaluation of manometric measures during tongue-hold swallows. American journal of speech-language pathology / American Speech-Language-Hearing Association, 18(1), doi: / (2008/ ) Easterling, C., Grande, B., Kern, M., Sears, K., & Shaker, R. (2005). Attaining and maintaining isometric and isokinetic goals of the Shaker exercise. Dysphagia, 20(2), El Sharkawi, A., Ramig, L., Logemann, J. A., Pauloski, B. R., Rademaker, A. W., Smith, C. H.,... Werner, C. (2002). Swallowing and voice effects of Lee Silverman Voice Treatment (LSVT): a pilot study. J Neurol Neurosurg Psychiatry, 72(1), Fujui, M., & Logemann, J. A. (1996). Effect of a tongue-holding maneuver on posterior pharyngeal wall movement during deglutition. American Journal of Speech-Language Pathology, 5(1), Hagg, M., & Anniko, M. (2008). Lip muscle training in stroke patients with dysphagia. Acta Otolaryngol, 128(9), Hind, J. A., Nicosia, M. A., Roecker, E. B., Carnes, M. L., & Robbins, J. (2001). Comparison of effortful and noneffortful swallows in healthy middle-aged and older adults. Archives of Physical Medicine and Rehabilitation, 82, MFMER slide
26 References Johnson, A. M., & Connor, N. P. (2011). Effects of electrical stimulation on neuromuscular junction morphology in the aging rat tongue. [Research Support, N.I.H., Extramural]. Muscle Nerve, 43(2), doi: /mus Kim, J., Davenport, P., & Sapienza, C. (2009). Effect of expiratory muscle strength training on elderly cough function. [Research Support, Non-U.S. Gov't]. Archives of gerontology and geriatrics, 48(3), doi: /j.archger Kim, J., & Sapienza, C. M. (2005). Implications of expiratory muscle strength training for rehabilitation of the elderly: Tutorial. Journal of Rehabilitation Research and Development, 42(2), Kuehn, D. P., Imrey, P. B., Tomes, L., Jones, D. L., O'Gara, M. M., & Seaver, E. J., et al. (2002). Efficacy of continuous positive airway pressure for treatment of hypernasality. Cleft-Palate-Craniofacial Journal, 39, Latham, N. K., Bennett, D. A., Stretton, C. M., & Anderson, C. S. (2004). Systematic review of progressive resistance strength training in older adults. [Review]. The Journals of Gerontology. Series A, Biological Sciences and Medical Sciences, 59(1), Lazarus, C. L., Logemann, J. A., Song, C. W., Rademaker, A. W., & Kahrilas, P. J. (2002). Effects of voluntary maneuvers on tongue base function for swallowing. Folia Phoniatrica et Logopaedica, 54(4), Liu, C. J., & Latham, N. K. (2009). Progressive resistance strength training for improving physical function in older adults. [Meta-Analysis Review]. Cochrane database of systematic reviews(3), CD doi: / CD pub2 Logemann, J. A., & Kahrilas, P. J. (1990). Relearning to swallow after stroke--application of maneuvers and indirect biofeedback: a case study. Neurology, 40(7), Marcell, T. J. (2003). Sarcopenia: causes, consequences, and preventions. [Review]. The Journals of Gerontology. Series A, Biological Sciences and Medical Sciences, 58(10), M MFMER slide-151 References McCabe, D., Ashford, J., Wheeler-Hegland, K., Frymark, T., Mullen, R., Musson, N.,... Schooling, T. (2009). Evidence-based systematic review: Oropharyngeal dysphagia behavioral treatments. Part IV--impact of dysphagia treatment on individuals' postcancer treatments. J Rehabil Res Dev, 46(2), Neumann, S., Bartolome, G., Buchholz, D., & Proseigel, M. (1995). Swallowing therapy of neurologic patients: correlation of outcome with pretreatment variables and therapeutic methods. Dysphagia, 10, 1-5. Park, J. W., Oh, J. C., Lee, H. J., Park, S. J., Yoon, T. S., & Kwon, B. S. (2009). Effortful swallowing training coupled with electrical stimulation leads to an increase in hyoid elevation during swallowing. Dysphagia, 24(3), doi: /s Pitts, T., Bolser, D., Rosenbek, J., Troche, M., Okun, M. S., & Sapienza, C. (2009). Impact of expiratory muscle strength training on voluntary cough and swallow function in Parkinson disease. Chest, 135(5), Pitts, T., Bolser, D., Rosenbek, J., Troche, M., & Sapienza, C. (2008). Voluntary cough production and swallow dysfunction in Parkinson's disease. Dysphagia, 23(3), doi: /s x Reddy, N. P., Costarella, B. R., Grotz, R. C., & Canilang, E. P. (1990). Biomechanical measurements to characterize the oral phase of dysphagia. IEEE Trans Biomed Eng, 37(4), Robbins, J., Levine, R., Wood, J., Roecker, E. B., & Luschei, E. (1995). Age effects on lingual pressure generation as a risk factor for dysphagia. Journals of Gerontology Series A: Biological Sciences and Medical Sciences, 50(5), M Robinovitch, S. N., Herschler, C., & Romilly, D. P. (1991). A tongue force measurement system for the assessment of oral-phase swallowing disorders. Archives of Physical Medicine and Rehabilitation, 72, Schaser, A. J., Wang, H., Volz, L. M., & Connor, N. P. (2011). Biochemistry of the anterior, medial, and posterior genioglossus in the aged rat. [Research Support, N.I.H., Extramural]. Dysphagia, 26(3), doi: /s x 2014 MFMER slide-152 References Shaker, R., Easterling, C., Kern, M., Nitschke, T., Massey, B., Daniels, S.,... Dikeman, K. (2002). Rehabilitation of swallowing by exercise in tube-fed patients with pharyngeal dysphagia secondary to abnormal UES opening. Gastroenterology, 122(5), Shaker, R., Kern, M., Bardan, E., Taylor, A., Stewart, E. T., Hoffmann, R. G.,... Bonnevier, J. (1997). Augmentation of deglutitive upper esophageal sphincter opening in the elderly by exercise. Am J Physiol, 272(6 Pt 1), G Shaker, R., Li, Q., Ren, J., Townsend, W. F., Dodds, W. J., Martin, B. J.,... Rynders, A. (1992). Coordination of deglutition and phases of respiration: effect of aging, tachypnea, bolus volume, and chronic obstructive pulmonary disease. Am J Physiol, 263(5 Pt 1), G Shaker, R., Ren, J., Podvrsan, B., Dodds, W. J., Hogan, W. J., Kern, M.,... Hintz, J. (1993). Effect of aging and bolus variables on pharyngeal and upper esophageal sphincter motor function. Am J Physiol, 264(3 Pt 1), G Shaker, R., Ren, J., Zamir, Z., Sarna, A., Liu, J., & Sui, Z. (1994). Effect of aging, position, and temperature on the threshold volume triggering pharyngeal swallows. Gastroenterology, 107(2), Shelton, N. (2011). Resistance Straws and the Effortful Swallow Technique M.A., Appalachian State University, Boone, NC. Steele, C. M., & Huckabee, M. L. (2007). The influence of orolingual pressure on the timing of pharyngeal pressure events. Dysphagia, 22(1), doi: /s Tamura, F., Kikutani, T., Tohara, T., Yoshida, M., & Yaegaki, K. (2012). Tongue thickness relates to nutritional status in the elderly. [Research Support, Non-U.S. Gov't]. Dysphagia, 27(4), doi: /s z References Troche, M. S., Okun, M. S., Rosenbek, J. C., Musson, N., Fernandez, H. H., Rodriguez, R.,... Sapienza, C. M. (2010). Aspiration and swallowing in Parkinson disease and rehabilitation with EMST: a randomized trial. Neurology, 75(21), doi: 75/21/1912 [pii] /WNL.0b013e3181fef115 Tzakis, M. G., Kiliaridis, S., & Carlsson, G. E. (1989). Effect of chewing training on masticatory efficiency. Acta Odontol Scand, 47(6), Umeki, H., Takasaki, K., Enatsu, K., Tanaka, F., Kumagami, H., & Takahashi, H. (2009). Effects of a tongueholding maneuver during swallowing evaluated by high-resolution manometry. Otolaryngology--head and neck surgery : official journal of American Academy of Otolaryngology-Head and Neck Surgery, 141(1), doi: /j.otohns Wheeler-Hegland, K., Ashford, J., Frymark, T., McCabe, D., Mullen, R., Musson, N.,... Schooling, T. (2009). Evidence-based systematic review: Oropharyngeal dysphagia behavioral treatments. Part II--impact of dysphagia treatment on normal swallow function. J Rehabil Res Dev, 46(2), Yeates, E. M., Molfenter, S. M., & Steele, C. M. (2008). Improvements in tongue strength and pressuregeneration precision following a tongue-pressure training protocol in older individuals with dysphagia: three case reports. [Case Reports Research Support, Non-U.S. Gov't]. Clinical interventions in aging, 3(4), Yoshida, M., Kikutani, T., Tsuga, K., Utanohara, Y., Hayashi, R., & Akagawa, Y. (2006). Decreased tongue pressure reflects symptom of dysphagia. Dysphagia, 21(1), Youmans, S. R., Youmans, G. L., & Stierwalt, J. A. (2009). Differences in tongue strength across age and gender: is there a diminished strength reserve? Dysphagia, 24(1), MFMER slide MFMER slide
Daniels SK & Huckabee ML (2008). Dysphagia Following Stroke. Muscles of Deglutition. Lateral & Mesial Premotor Area 6. Primary Sensory
 An Overview of Dysphagia in the Stroke Population Stephanie K. Daniels, PhD Michael E. DeBakey VA Medical Center PM & R, Baylor College of Medicine Communication Sciences and Disorders, University of Houston
An Overview of Dysphagia in the Stroke Population Stephanie K. Daniels, PhD Michael E. DeBakey VA Medical Center PM & R, Baylor College of Medicine Communication Sciences and Disorders, University of Houston
Dysphagia as a Geriatric Syndrome Assessment and Treatment. Ashton Galyen M.A., CCC-SLP St. Vincent Indianapolis Acute Rehabilitation Unit
 Dysphagia as a Geriatric Syndrome Assessment and Treatment Ashton Galyen M.A., CCC-SLP St. Vincent Indianapolis Acute Rehabilitation Unit March 16, 2018 Ashton Galyen, M.A., CCC-SLP Master s degree in
Dysphagia as a Geriatric Syndrome Assessment and Treatment Ashton Galyen M.A., CCC-SLP St. Vincent Indianapolis Acute Rehabilitation Unit March 16, 2018 Ashton Galyen, M.A., CCC-SLP Master s degree in
Swallowing Screen Why? How? and So What? พญ.พวงแก ว ธ ต สก ลช ย ภาคว ชาเวชศาสตร ฟ นฟ คณะแพทยศาสตร ศ ร ราชพยาบาล
 Swallowing Screen Why? How? and So What? พญ.พวงแก ว ธ ต สก ลช ย ภาคว ชาเวชศาสตร ฟ นฟ คณะแพทยศาสตร ศ ร ราชพยาบาล Dysphagia in Stroke The incidence of dysphagia after stroke ranging from 23-50% 1 Location
Swallowing Screen Why? How? and So What? พญ.พวงแก ว ธ ต สก ลช ย ภาคว ชาเวชศาสตร ฟ นฟ คณะแพทยศาสตร ศ ร ราชพยาบาล Dysphagia in Stroke The incidence of dysphagia after stroke ranging from 23-50% 1 Location
Swallowing Strategies
 Department of Head and Neck Surgery Section of Speech Pathology & Audiology M.D. Anderson Cancer Center (713) 792-6525 Swallowing Strategies 1) POSTURAL CHANGES: a) Chin Tuck: (1) Delayed onset pharyngeal
Department of Head and Neck Surgery Section of Speech Pathology & Audiology M.D. Anderson Cancer Center (713) 792-6525 Swallowing Strategies 1) POSTURAL CHANGES: a) Chin Tuck: (1) Delayed onset pharyngeal
Clinical Swallowing Exam
 Clinical Evaluation Template 1 Clinical Exam Name: ID/Medical record number: Date of exam: Referred by: Reason for referral: Medical diagnosis: Date of onset of diagnosis: Other relevant medical history/diagnoses/surgery
Clinical Evaluation Template 1 Clinical Exam Name: ID/Medical record number: Date of exam: Referred by: Reason for referral: Medical diagnosis: Date of onset of diagnosis: Other relevant medical history/diagnoses/surgery
Exercise- Based Approaches to Dysphagia Rehabilitation
 Interventions Cichero J, Clavé P (eds): Stepping Stones to Living Well with Dysphagia. Nestlé Nutr Inst Workshop Ser, vol 72, pp 109 117, Nestec Ltd., Vevey/S. Karger AG., Basel, 2012 Exercise- Based Approaches
Interventions Cichero J, Clavé P (eds): Stepping Stones to Living Well with Dysphagia. Nestlé Nutr Inst Workshop Ser, vol 72, pp 109 117, Nestec Ltd., Vevey/S. Karger AG., Basel, 2012 Exercise- Based Approaches
SWALLOWING DIFFICULTIES IN HD
 Nutrition, eating and swallowing needs, challenges and solutions Workshop SWALLOWING DIFFICULTIES IN HD Angela Nuzzi Speech and Language Pathologist (SLP) EHDN Language Coordinator - Italy The role of
Nutrition, eating and swallowing needs, challenges and solutions Workshop SWALLOWING DIFFICULTIES IN HD Angela Nuzzi Speech and Language Pathologist (SLP) EHDN Language Coordinator - Italy The role of
Main Aspects of the Management of Neurogenic Dysphagia
 Main Aspects of the Management of Neurogenic Dysphagia Mario Prosiegel/München German Society of Neurology (DGN) prosiegel@t-online.de DYSPHAGIA October 8-10, 2015 Pavia, Italy Overview Diagnosis Causal
Main Aspects of the Management of Neurogenic Dysphagia Mario Prosiegel/München German Society of Neurology (DGN) prosiegel@t-online.de DYSPHAGIA October 8-10, 2015 Pavia, Italy Overview Diagnosis Causal
Rationale for strength and skill goals in tongue resistance training: A review
 Rationale for strength and skill goals in tongue resistance training: A review Catriona M. Steele, Gemma L. Bailey, Sonja M. Molfenter & Erin M. Yeates Authors: Catriona M. Steele, Ph.D., CCC-SLP, BRS-S
Rationale for strength and skill goals in tongue resistance training: A review Catriona M. Steele, Gemma L. Bailey, Sonja M. Molfenter & Erin M. Yeates Authors: Catriona M. Steele, Ph.D., CCC-SLP, BRS-S
Dysphagia Treatment: What are We Doing, and Why?
 Dysphagia Treatment: What are We Doing, and Why? ASHA Convention, 2014; Orlando James L. Coyle, Ph.D., CCC SLP, BCS S University of Pittsburgh jcoyle@pitt.edu 1 Treatment 2 Aims, targets and ingredients
Dysphagia Treatment: What are We Doing, and Why? ASHA Convention, 2014; Orlando James L. Coyle, Ph.D., CCC SLP, BCS S University of Pittsburgh jcoyle@pitt.edu 1 Treatment 2 Aims, targets and ingredients
15/11/2011. Swallowing
 Swallowing Swallowing starts from placement of the food in the mouth and continues until food enters the stomach. Dysphagia: any difficulty in moving food from mouth to stomach. Pharynx is shared for both
Swallowing Swallowing starts from placement of the food in the mouth and continues until food enters the stomach. Dysphagia: any difficulty in moving food from mouth to stomach. Pharynx is shared for both
Surgical Effects on Swallowing DYSPHAGIA AFTER TREATMENT FOR HNC: WHAT CAUSES IT? WHAT TREATMENT WORKS? Surgical Effects on Swallowing
 Susan Langmore, PhD, CCC-SLP, BRS-S Professor, BUMC, BU September 27, 2010 DYSPHAGIA AFTER TREATMENT FOR HNC: WHAT CAUSES IT? WHAT TREATMENT WORKS? Incidence of dysphagia after XRT VA study (Wolf; Terrell
Susan Langmore, PhD, CCC-SLP, BRS-S Professor, BUMC, BU September 27, 2010 DYSPHAGIA AFTER TREATMENT FOR HNC: WHAT CAUSES IT? WHAT TREATMENT WORKS? Incidence of dysphagia after XRT VA study (Wolf; Terrell
Dysphagia and Swallowing. Jan Adams, DNP, MPA, RN and Karen Kern
 Dysphagia and Swallowing Jan Adams, DNP, MPA, RN and Karen Kern Scope of the Problem and Incidence 15 million people in the US have some form of Dysphagia. Every year, 1 million people are diagnosed with
Dysphagia and Swallowing Jan Adams, DNP, MPA, RN and Karen Kern Scope of the Problem and Incidence 15 million people in the US have some form of Dysphagia. Every year, 1 million people are diagnosed with
The Clinical Swallow Evaluation: What it can and cannot tell us. Introduction
 The Clinical Swallow Evaluation: What it can and cannot tell us Debra M. Suiter, Ph.D., CCC-SLP, BCS-S Director, Voice & Swallow Clinic Associate Professor, Division of Communication Sciences & Disorders
The Clinical Swallow Evaluation: What it can and cannot tell us Debra M. Suiter, Ph.D., CCC-SLP, BCS-S Director, Voice & Swallow Clinic Associate Professor, Division of Communication Sciences & Disorders
Review of dysphagia in poststroke
 Review of dysphagia in poststroke patients Danielle Thompson, Speech and Language Therapist Northwick Park Hospital With acknowledgement to Mary McFarlane, Principal Speech and Language Therapist, Acute
Review of dysphagia in poststroke patients Danielle Thompson, Speech and Language Therapist Northwick Park Hospital With acknowledgement to Mary McFarlane, Principal Speech and Language Therapist, Acute
Feeding and Oral Hygiene: How to Address the Challenges
 Feeding and Oral Hygiene: How to Address the Challenges Paige W. Roberts, OTR/L Occupational Therapist Pediatric Feeding Disorders Program Marcus Autism Center Disclaimer: This content is for personal
Feeding and Oral Hygiene: How to Address the Challenges Paige W. Roberts, OTR/L Occupational Therapist Pediatric Feeding Disorders Program Marcus Autism Center Disclaimer: This content is for personal
Airway Protection: Clinical Management of Dysphagia and Dystussia in Neurodegenerative disease
 Airway Protection: Clinical Management of Dysphagia and Dystussia in Neurodegenerative disease Alexandra E. Brandimore, Ph.D. CCC/SLP MESPA Conference April 13, 2019 No conflicts of interest or disclosure
Airway Protection: Clinical Management of Dysphagia and Dystussia in Neurodegenerative disease Alexandra E. Brandimore, Ph.D. CCC/SLP MESPA Conference April 13, 2019 No conflicts of interest or disclosure
NIH T-32 Post-Doctoral Fellow, University of Florida, Departments of Neurology and Physiological Sciences (Fall 2008 Fall 2009)
 KAREN WHEELER HEGLAND, PH.D. WORK ADDRESS: University of Florida Department of Speech Language and Hearing Sciences Box 117420 Gainesville, FL 32611 EDUCATIONAL BACKGROUND: University of Florida, Undergraduate
KAREN WHEELER HEGLAND, PH.D. WORK ADDRESS: University of Florida Department of Speech Language and Hearing Sciences Box 117420 Gainesville, FL 32611 EDUCATIONAL BACKGROUND: University of Florida, Undergraduate
The Role of the Speech Language Pathologist & Spinal Cord Injury
 The Role of the Speech Language Pathologist & Spinal Cord Injury Facts According to the National Spinal Cord Injury Statistical Center (NSCISC) there are approxiamtely 12,000 new spinal cord injuries (SCI)
The Role of the Speech Language Pathologist & Spinal Cord Injury Facts According to the National Spinal Cord Injury Statistical Center (NSCISC) there are approxiamtely 12,000 new spinal cord injuries (SCI)
Effortful Pitch Glide: An Exercise for Potential Swallow Rehabilitation Evaluated by Dynamic MRI
 Effortful Pitch Glide: An Exercise for Potential Swallow Rehabilitation Evaluated by Dynamic MRI Keri Vasquez Miloro, MS, CCC-SLP, BRS-S William G. Pearson, Jr. PhD Susan Langmore, PhD, CCC-SLP, BRS-S
Effortful Pitch Glide: An Exercise for Potential Swallow Rehabilitation Evaluated by Dynamic MRI Keri Vasquez Miloro, MS, CCC-SLP, BRS-S William G. Pearson, Jr. PhD Susan Langmore, PhD, CCC-SLP, BRS-S
SUPER-SUPRAGLOTTIC SWALLOW IN IRRADIATED HEAD AND NECK CANCER PATIENTS
 SUPER-SUPRAGLOTTIC SWALLOW IN IRRADIATED HEAD AND NECK CANCER PATIENTS Jeri A. Logemann, PhD, 1 Barbara Roa Pauloski, PhD, 1 Alfred W. Rademaker, PhD, 2 Laura A. Colangelo, MS 2 1 Department of Communication
SUPER-SUPRAGLOTTIC SWALLOW IN IRRADIATED HEAD AND NECK CANCER PATIENTS Jeri A. Logemann, PhD, 1 Barbara Roa Pauloski, PhD, 1 Alfred W. Rademaker, PhD, 2 Laura A. Colangelo, MS 2 1 Department of Communication
Speech and Language Therapy. Kerrie McCarthy Senior Speech and Language Therapist
 Speech and Language Therapy Kerrie McCarthy Senior Speech and Language Therapist Contents 1. Voice disorders 2. Swallow disorders 3. Videofluroscopy 4. Adult Acquired Communication Disorders 5. How to
Speech and Language Therapy Kerrie McCarthy Senior Speech and Language Therapist Contents 1. Voice disorders 2. Swallow disorders 3. Videofluroscopy 4. Adult Acquired Communication Disorders 5. How to
TREATMENT OF DYSPHAGIA IN PATIENTS AFTER STROKE IN ESTONIA
 TREATMENT OF DYSPHAGIA IN PATIENTS AFTER STROKE IN ESTONIA ANNE URIKO SPORTS MEDICINE AND REHABILITATION CLINIG OF TARTU UNIVERSITY HOSPITAL 17.09.2010 DYSPHAGIA DIFFICULTY MOVING FOOD FROM MOUTH TO STOMACH
TREATMENT OF DYSPHAGIA IN PATIENTS AFTER STROKE IN ESTONIA ANNE URIKO SPORTS MEDICINE AND REHABILITATION CLINIG OF TARTU UNIVERSITY HOSPITAL 17.09.2010 DYSPHAGIA DIFFICULTY MOVING FOOD FROM MOUTH TO STOMACH
Temporal and Biomechanical Measurements of Upper Esophageal Sphincter (UES) Opening in Normal Swallowing
 Temporal and Biomechanical Measurements of Upper Esophageal Sphincter (UES) Opening in Normal Swallowing Youngsun Kim School of Hearing, Speech and Language Sciences, College of Health and Human Services,
Temporal and Biomechanical Measurements of Upper Esophageal Sphincter (UES) Opening in Normal Swallowing Youngsun Kim School of Hearing, Speech and Language Sciences, College of Health and Human Services,
Swallowing Disorders and Their Management in Patients with Multiple Sclerosis
 National Multiple Sclerosis Society 733 Third Avenue New York, NY 10017-3288 Clinical Bulletin Information for Health Professionals Swallowing Disorders and Their Management in Patients with Multiple Sclerosis
National Multiple Sclerosis Society 733 Third Avenue New York, NY 10017-3288 Clinical Bulletin Information for Health Professionals Swallowing Disorders and Their Management in Patients with Multiple Sclerosis
Dysphagia and the MBSS: Disclosures. Instrumental Assessment. The Disorder Guides the Treatment
 Dysphagia and the MBSS: The Disorder Guides the Treatment Jennifer Jones, PhD, CCC-SLP, BCS-S C/NDT Board Certified Specialist in Swallowing and Swallowing Disorders Certified in Neurodevelopmental Treatment
Dysphagia and the MBSS: The Disorder Guides the Treatment Jennifer Jones, PhD, CCC-SLP, BCS-S C/NDT Board Certified Specialist in Swallowing and Swallowing Disorders Certified in Neurodevelopmental Treatment
When Eating Becomes A Challenge Dysphagia
 When Eating Becomes A Challenge Dysphagia 1. DYSPHAGIA, WHAT IS IT? 2. IMPLICATIONS 3. ASSESSMENT 4. COMPENSATORY SWALLOWING AND EXERCISES 5. DIET TEXTURE ADJUSTMENTS Swallowing Dysfunction = Dysphagia
When Eating Becomes A Challenge Dysphagia 1. DYSPHAGIA, WHAT IS IT? 2. IMPLICATIONS 3. ASSESSMENT 4. COMPENSATORY SWALLOWING AND EXERCISES 5. DIET TEXTURE ADJUSTMENTS Swallowing Dysfunction = Dysphagia
Swallowing after a Total Laryngectomy
 Swallowing after a Total Laryngectomy Diane Longnecker, M.S.,CCC-SLP, BCS-S Baylor Institute for Rehabilitation at Baylor University Medical Center Dallas, TX Disclosure Statement No relevant financial
Swallowing after a Total Laryngectomy Diane Longnecker, M.S.,CCC-SLP, BCS-S Baylor Institute for Rehabilitation at Baylor University Medical Center Dallas, TX Disclosure Statement No relevant financial
2013 Charleston Swallowing Conference
 Providing Quality Affordable Continuing Education and Treatment Materials for over 30 years. 2013 Charleston Swallowing Conference Session 9 Bedside Assessment: What Does It Tell You? 10:00 11:30 am Saturday,
Providing Quality Affordable Continuing Education and Treatment Materials for over 30 years. 2013 Charleston Swallowing Conference Session 9 Bedside Assessment: What Does It Tell You? 10:00 11:30 am Saturday,
Reluctance or refusal to feed or eat. Understanding Feeding Aversion in a City Full of Foodies. Presentation Outline. Learning Objectives
 Understanding Feeding Aversion in a City Full of Foodies Amy Houtrow, MD, MPH Pediatric Physical Medicine & Rehabilitation UCSF Department of Pediatrics June 2, 2007 Learning Objectives Learners will be
Understanding Feeding Aversion in a City Full of Foodies Amy Houtrow, MD, MPH Pediatric Physical Medicine & Rehabilitation UCSF Department of Pediatrics June 2, 2007 Learning Objectives Learners will be
Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing
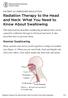 PATIENT & CAREGIVER EDUCATION Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing This information describes swallowing problems that can be caused by radiation therapy to the
PATIENT & CAREGIVER EDUCATION Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing This information describes swallowing problems that can be caused by radiation therapy to the
VIDEOFLUOROSCOPIC SWALLOWING EXAM
 VIDEOFLUOROSCOPIC SWALLOWING EXAM INDENTIFYING INFORMATION May include the following: Name, ID/medical record number, date of birth, date of exam, referred by, reason for referral HISTORY/SUBJECTIVE INFORMATION
VIDEOFLUOROSCOPIC SWALLOWING EXAM INDENTIFYING INFORMATION May include the following: Name, ID/medical record number, date of birth, date of exam, referred by, reason for referral HISTORY/SUBJECTIVE INFORMATION
Applied physiology. 7- Apr- 15 Swallowing Course/ Anatomy and Physiology
 Applied physiology Temporal measures: Oral Transit Time (OTT) Pharyngeal Delay Time (PDT) Pharyngeal Transit Time (PTT) Oropharyngeal Swallowing Efficiency Score (OPSE score) 7- Apr- 15 Swallowing Course/
Applied physiology Temporal measures: Oral Transit Time (OTT) Pharyngeal Delay Time (PDT) Pharyngeal Transit Time (PTT) Oropharyngeal Swallowing Efficiency Score (OPSE score) 7- Apr- 15 Swallowing Course/
Dysphagia Management in Stroke Rehabilitation
 Curr Phys Med Rehabil Rep (2014) 2:207 218 DOI 10.1007/s40141-014-0059-9 SWALLOWING DISORDERS (RE MARTIN, SECTION EDITOR) Dysphagia Management in Stroke Rehabilitation Danielle N. Johnson Hannah J. Herring
Curr Phys Med Rehabil Rep (2014) 2:207 218 DOI 10.1007/s40141-014-0059-9 SWALLOWING DISORDERS (RE MARTIN, SECTION EDITOR) Dysphagia Management in Stroke Rehabilitation Danielle N. Johnson Hannah J. Herring
RECOMMENDATIONS & UPDATES IN THE MANAGEMENT OF POST- STROKE DYSPHAGIA
 RECOMMENDATIONS & UPDATES IN THE MANAGEMENT OF POST- STROKE DYSPHAGIA Feeding in the Acute Stroke Period: - Early initiation of feeding is beneficial w/c decreases the risk of infections, improve survival
RECOMMENDATIONS & UPDATES IN THE MANAGEMENT OF POST- STROKE DYSPHAGIA Feeding in the Acute Stroke Period: - Early initiation of feeding is beneficial w/c decreases the risk of infections, improve survival
FLOOVIDEOFLUOROSCOPIC SWALLOW STUDIES: LOOKING BEYOND ASPIRATION. Brenda Sitzmann, MA, CCC-SLP (816)
 FLOOVIDEOFLUOROSCOPIC SWALLOW STUDIES: LOOKING BEYOND ASPIRATION Brenda Sitzmann, MA, CCC-SLP bksitzmann@cmh.edu (816) 302-8037 DISCLOSURES Ms. Sitzmann is speech-language pathologist at Children s Mercy
FLOOVIDEOFLUOROSCOPIC SWALLOW STUDIES: LOOKING BEYOND ASPIRATION Brenda Sitzmann, MA, CCC-SLP bksitzmann@cmh.edu (816) 302-8037 DISCLOSURES Ms. Sitzmann is speech-language pathologist at Children s Mercy
Management of oropharyngeal dysphagia
 Management of oropharyngeal dysphagia Course Objectives Know the normal anatomy of swallowing Know the normal physiology of swallowing Enumerate different etiologies of oropharyngeal dysphagia Be able
Management of oropharyngeal dysphagia Course Objectives Know the normal anatomy of swallowing Know the normal physiology of swallowing Enumerate different etiologies of oropharyngeal dysphagia Be able
2013, Bouchat-Laird, N.
 Critical Review: The Effect of Expiratory Muscle Strength Training (EMST) on Dysphagia in individuals with Idiopathic Parkinson s disease. Natasha Bouchat-Laird M.Cl.Sc (SLP) Candidate University of Western
Critical Review: The Effect of Expiratory Muscle Strength Training (EMST) on Dysphagia in individuals with Idiopathic Parkinson s disease. Natasha Bouchat-Laird M.Cl.Sc (SLP) Candidate University of Western
Safe swallowing strategies
 Learning Guide Safe swallowing strategies 27468 Apply safe swallowing strategies in a health or wellbeing setting Level 3 5 credits Name: Workplace: Issue 2.0 Copyright 2017 Careerforce All rights reserved.
Learning Guide Safe swallowing strategies 27468 Apply safe swallowing strategies in a health or wellbeing setting Level 3 5 credits Name: Workplace: Issue 2.0 Copyright 2017 Careerforce All rights reserved.
EATING SAFELY AND TALKING ABOUT IT KIERA N BERGGREN, MA/CCC-SLP, MS 2018 FSHD CONNECT CONFERENCE
 EATING SAFELY AND TALKING ABOUT IT KIERA N BERGGREN, MA/CCC-SLP, MS 2018 FSHD CONNECT CONFERENCE DISCLOSURES I have no personal financial relationships with commercial interests relevant to this presentation
EATING SAFELY AND TALKING ABOUT IT KIERA N BERGGREN, MA/CCC-SLP, MS 2018 FSHD CONNECT CONFERENCE DISCLOSURES I have no personal financial relationships with commercial interests relevant to this presentation
VitalStim in Swallowing Rehabilitation
 VitalStim in Swallowing Rehabilitation Meghan McAvoy, MS,CCC-SLP Mary Free Bed at Sparrow Hospital Disclosures No financial or non-financial disclosures Control of the swallow Both voluntary and involuntary
VitalStim in Swallowing Rehabilitation Meghan McAvoy, MS,CCC-SLP Mary Free Bed at Sparrow Hospital Disclosures No financial or non-financial disclosures Control of the swallow Both voluntary and involuntary
Swallowing disorder, aspiration: now what?
 Swallowing disorder, aspiration: now what? Poster No.: C-0691 Congress: ECR 2015 Type: Educational Exhibit Authors: A. Kavka, M. Kysilko, M. Rocek; Prague/CZ Keywords: Swallowing disorders, Dynamic swallowing
Swallowing disorder, aspiration: now what? Poster No.: C-0691 Congress: ECR 2015 Type: Educational Exhibit Authors: A. Kavka, M. Kysilko, M. Rocek; Prague/CZ Keywords: Swallowing disorders, Dynamic swallowing
Sapienza, C.M. (2008, invited). Respiratory muscle strength training. Current Opinion in Otolaryngology and Head and Neck Surgery, 16, 3,
 Pitts, T., Bolser, D., Rosenbek, J., Troche, M., & Sapienza, C. (2008). Voluntary cough production and swallow dysfunction in Parkinson's disease. Dysphagia, 23, 3, 297-301. Epub ahead of print. Cough
Pitts, T., Bolser, D., Rosenbek, J., Troche, M., & Sapienza, C. (2008). Voluntary cough production and swallow dysfunction in Parkinson's disease. Dysphagia, 23, 3, 297-301. Epub ahead of print. Cough
Oropharyngeal Dysphagia in Patients with COPD: A Systematic Review
 Oropharyngeal Dysphagia in Patients with COPD: A Systematic Review Lisa O Kane, B.A. Michael Groher, Ph.D. Boston University University of Redlands Boston, MA Redlands, CA ASHA Convention 2009 New Orleans
Oropharyngeal Dysphagia in Patients with COPD: A Systematic Review Lisa O Kane, B.A. Michael Groher, Ph.D. Boston University University of Redlands Boston, MA Redlands, CA ASHA Convention 2009 New Orleans
Palliative Care Swallowing Management HEATHER STORIE M.S.,CCC-SLP, BCS-S SPEECH LANGUAGE PATHOLOGY, BOARD CERTIFIED SWALLOWING SPECIALIST
 Palliative Care Swallowing Management HEATHER STORIE M.S.,CCC-SLP, BCS-S SPEECH LANGUAGE PATHOLOGY, BOARD CERTIFIED SWALLOWING SPECIALIST Objectives Gain a general understanding of normal swallowing Gain
Palliative Care Swallowing Management HEATHER STORIE M.S.,CCC-SLP, BCS-S SPEECH LANGUAGE PATHOLOGY, BOARD CERTIFIED SWALLOWING SPECIALIST Objectives Gain a general understanding of normal swallowing Gain
high-resolution manometry. Kumagami, Hidetaka; Takahashi, Haru Surgery Foundation Published by Mos
 NAOSITE: Nagasaki University's Ac Title Author(s) Citation Effects of a tongue-holding maneuve high-resolution manometry. Umeki, Hiroshi; Takasaki, Kenji; En Kumagami, Hidetaka; Takahashi, Haru Otolaryngology
NAOSITE: Nagasaki University's Ac Title Author(s) Citation Effects of a tongue-holding maneuve high-resolution manometry. Umeki, Hiroshi; Takasaki, Kenji; En Kumagami, Hidetaka; Takahashi, Haru Otolaryngology
Workbook. Apply safe swallowing strategies as a health assistant in an aged care, health or disability context. US Level 4 Credits 4. Name...
 Workbook Apply safe swallowing strategies as a health assistant in an aged care, health or disability context US 27468 Level 4 Credits 4 Name... US 27468 Level 4 Credits 4 All rights reserved. Careerforce
Workbook Apply safe swallowing strategies as a health assistant in an aged care, health or disability context US 27468 Level 4 Credits 4 Name... US 27468 Level 4 Credits 4 All rights reserved. Careerforce
Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing
 PATIENT & CAREGIVER EDUCATION Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing This information describes swallowing problems that can be caused by radiation therapy to the
PATIENT & CAREGIVER EDUCATION Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing This information describes swallowing problems that can be caused by radiation therapy to the
financial costs social isolation medical risks
 Dysphagia, commonly known as swallowing problems, is quite common. A significant number of people in long-term elderly care suffer from some form of dysphagia. Treating the condition is a challenge for
Dysphagia, commonly known as swallowing problems, is quite common. A significant number of people in long-term elderly care suffer from some form of dysphagia. Treating the condition is a challenge for
Respiratory Swallow Coordination in Healthy Individuals
 Cloud Publications International Journal of Advanced Speech and Hearing Research 2012, Volume 1, Issue 1, pp. 1-9, Article ID Med-03 Research Article Open Access Respiratory Swallow Coordination in Healthy
Cloud Publications International Journal of Advanced Speech and Hearing Research 2012, Volume 1, Issue 1, pp. 1-9, Article ID Med-03 Research Article Open Access Respiratory Swallow Coordination in Healthy
Feeding and Swallowing Problems in the Child with Special Needs
 Feeding and Swallowing Problems in the Child with Special Needs Joan Surfus, OTR/L, SWC Amy Lynch, MS, OTR/L Misericordia University This presentation is made possible, in part, by the support of the American
Feeding and Swallowing Problems in the Child with Special Needs Joan Surfus, OTR/L, SWC Amy Lynch, MS, OTR/L Misericordia University This presentation is made possible, in part, by the support of the American
Managing the Patient with Dysphagia
 Managing the Patient with Dysphagia Patricia K. Lerner, MA, CCC, ASHA Fellow Board Certified Specialist in Swallowing & Swallowing Disorders Clinical Assistant Professor New York University School of Medicine
Managing the Patient with Dysphagia Patricia K. Lerner, MA, CCC, ASHA Fellow Board Certified Specialist in Swallowing & Swallowing Disorders Clinical Assistant Professor New York University School of Medicine
HOMES AND SENIORS SERVICES. APPROVAL DATE: August 1985 REVISION DATE: January 2015 REVIEW DATE: May 2018
 POLICY: Page 1 of 10 Residents who experience signs and symptoms associated with dysphagia will have their nutrition and hydration needs met in a safe, coordinated manner as managed by the interdisciplinary
POLICY: Page 1 of 10 Residents who experience signs and symptoms associated with dysphagia will have their nutrition and hydration needs met in a safe, coordinated manner as managed by the interdisciplinary
Evidence-Based, Optimal Strength Exercise Parameters: Practice Considerations for Speech Therapists
 Evidence-Based, Optimal Strength Exercise Parameters: Practice Considerations for Speech Therapists Mark Richards, PT, MS, CEEAA Vice President of Clinical Services Accelerated Care Plus markprichards@comcast.net
Evidence-Based, Optimal Strength Exercise Parameters: Practice Considerations for Speech Therapists Mark Richards, PT, MS, CEEAA Vice President of Clinical Services Accelerated Care Plus markprichards@comcast.net
Pediatric Modified Barium Swallow Studies. Presented by Jody Bousquet, MA, CCC- SLP Susan Shonbrun, MS, CCC- SLP November 7, 2015
 Pediatric Modified Barium Swallow Studies Presented by Jody Bousquet, MA, CCC- SLP Susan Shonbrun, MS, CCC- SLP November 7, 2015 Definition * Modified Barium Swallow Study * Assesses swallow functions
Pediatric Modified Barium Swallow Studies Presented by Jody Bousquet, MA, CCC- SLP Susan Shonbrun, MS, CCC- SLP November 7, 2015 Definition * Modified Barium Swallow Study * Assesses swallow functions
Stage Transition And Laryngeal Closure In Poststroke Patients With Dysphagia
 Archived version from NCDOCKS Institutional Repository http://libres.uncg.edu/ir/asu/ Stage Transition And Laryngeal Closure In Poststroke Patients With Dysphagia By: Elizabeth Rachel Oommen Youngsun Kim
Archived version from NCDOCKS Institutional Repository http://libres.uncg.edu/ir/asu/ Stage Transition And Laryngeal Closure In Poststroke Patients With Dysphagia By: Elizabeth Rachel Oommen Youngsun Kim
Understanding your child s videofluoroscopic swallow study report
 Understanding your child s videofluoroscopic swallow study report This leaflet is given to you during your child s appointment in order to explain some of the words used by the speech and language therapist
Understanding your child s videofluoroscopic swallow study report This leaflet is given to you during your child s appointment in order to explain some of the words used by the speech and language therapist
Electrical Stimulation in the Treatment of Dysphagia Literature review. Baijens, 2008: Case report: Treatment of patient with opercular syndrome.
 Electrical Stimulation in the Treatment of Dysphagia Literature review Baijens, 2008: Case report: Treatment of patient with opercular syndrome. Design: Case study (Grade: D) Report on treatment outcomes
Electrical Stimulation in the Treatment of Dysphagia Literature review Baijens, 2008: Case report: Treatment of patient with opercular syndrome. Design: Case study (Grade: D) Report on treatment outcomes
Neuromuscular Electrical Stimulation in the Treatment of Dysphagia. A Summary of the Evidence. Empi St. Paul, MN
 Neuromuscular Electrical Stimulation in the Treatment of Dysphagia A Summary of the Evidence Empi St. Paul, MN Last updated February 4, 2010 Executive summary Neuromuscular electrical stimulation (NMES)
Neuromuscular Electrical Stimulation in the Treatment of Dysphagia A Summary of the Evidence Empi St. Paul, MN Last updated February 4, 2010 Executive summary Neuromuscular electrical stimulation (NMES)
Swallowing Course (RHS )
 Swallowing Course (RHS ) Dr/Mohamed Farahat Ibrahim, M.D., Ph.D. Professor, Consultant Phoniatrician (Communication and Swallowing Disorders) Chairman, Communication and Swallowing Disorders Unit (CSDU)
Swallowing Course (RHS ) Dr/Mohamed Farahat Ibrahim, M.D., Ph.D. Professor, Consultant Phoniatrician (Communication and Swallowing Disorders) Chairman, Communication and Swallowing Disorders Unit (CSDU)
Effect of posture on swallowing.
 Effect of posture on swallowing. Ahmad H. Alghadir, Hamayun Zafar, Einas S. Al-Eisa, Zaheen A. Iqbal Rehabilitation Research Chair, College of Applied Medical Sciences, King Saud University, Riyadh, KSA.
Effect of posture on swallowing. Ahmad H. Alghadir, Hamayun Zafar, Einas S. Al-Eisa, Zaheen A. Iqbal Rehabilitation Research Chair, College of Applied Medical Sciences, King Saud University, Riyadh, KSA.
SWALLOWING: HOW CAN WE HELP
 SWALLOWING: HOW CAN WE HELP Carol Romero-Clark, M.S., CCC-SLP University of New Mexico Hospital Speech Pathology Department November 10, 2017 What happens when you swallow? Mouth (Oral Phase) Your tongue
SWALLOWING: HOW CAN WE HELP Carol Romero-Clark, M.S., CCC-SLP University of New Mexico Hospital Speech Pathology Department November 10, 2017 What happens when you swallow? Mouth (Oral Phase) Your tongue
Why should we treat Dysphagia
 Why should we treat Dysphagia Dysphagia Market : Estimated 15 million adult patients in USA Frequently occurring condition in many disease states CVA is most frequent diagnosis 15% 10% 5% 5% 5% 60% CVA
Why should we treat Dysphagia Dysphagia Market : Estimated 15 million adult patients in USA Frequently occurring condition in many disease states CVA is most frequent diagnosis 15% 10% 5% 5% 5% 60% CVA
Cover Page. The handle holds various files of this Leiden University dissertation
 Cover Page The handle http://hdl.handle.net/1887/32744 holds various files of this Leiden University dissertation Author: Heemskerk, Anne-Wil Title: Dysphagia in Huntington s disease Issue Date: 2015-04-15
Cover Page The handle http://hdl.handle.net/1887/32744 holds various files of this Leiden University dissertation Author: Heemskerk, Anne-Wil Title: Dysphagia in Huntington s disease Issue Date: 2015-04-15
Expiratory Muscle Strength Training. (EMST) and Dysphagia
 Expiratory Muscle Strength Training 2015 Adult Swallowing Group NSW Speech Pathology Evidence Based Practice Network Christian Wiley and Kylie Draper Hans Bogaardt - Academic Member (EMST) and Dysphagia
Expiratory Muscle Strength Training 2015 Adult Swallowing Group NSW Speech Pathology Evidence Based Practice Network Christian Wiley and Kylie Draper Hans Bogaardt - Academic Member (EMST) and Dysphagia
«Einschluckstörungen»
 18. Fortbildungskurs der SGG Brunnen 20.04.2018 «Einschluckstörungen» Troubles de la déglutition Swallowing disorders Dr Valérie Schweizer Unité de Phoniatrie Service ORL et chirurgie cervicofaciale CHUV
18. Fortbildungskurs der SGG Brunnen 20.04.2018 «Einschluckstörungen» Troubles de la déglutition Swallowing disorders Dr Valérie Schweizer Unité de Phoniatrie Service ORL et chirurgie cervicofaciale CHUV
Correspondence should be addressed to Marziyeh Poorjavad;
 Stroke Research and Treatment, Article ID 918057, 7 pages http://dx.doi.org/10.1155/2014/918057 Review Article Surface Electrical Stimulation for Treating Swallowing Disorders after Stroke: A Review of
Stroke Research and Treatment, Article ID 918057, 7 pages http://dx.doi.org/10.1155/2014/918057 Review Article Surface Electrical Stimulation for Treating Swallowing Disorders after Stroke: A Review of
Communication and Swallowing with PSP/CBD. Megan DePuy, MBA, MS, CCC-SLP Private Speech Pathologist
 Communication and Swallowing with PSP/CBD Megan DePuy, MBA, MS, CCC-SLP Private Speech Pathologist A Speech Therapist? Why? Swallowing (Dysphagia) Speech (Dysarthria, Dysphonia) Language (Aphasia) An Experienced
Communication and Swallowing with PSP/CBD Megan DePuy, MBA, MS, CCC-SLP Private Speech Pathologist A Speech Therapist? Why? Swallowing (Dysphagia) Speech (Dysarthria, Dysphonia) Language (Aphasia) An Experienced
ALD 2015 KNOWLEDGE EXPERIENCE APPLICATION ALD 2015 KNOWLEDGE EXPERIENCE APPLICATION ALD 2015 KNOWLEDGE EXPERIENCE APPLICATION.
 ALD 2015 KNOWLEDGE EXPERIENCE APPLICATION Moving Tongues Beyond Frenectomy Grace Sun, DDS FAACD MALD MAGD MICOI Los Angeles ALD 2015 KNOWLEDGE EXPERIENCE APPLICATION Accredited Fellow, American Academy
ALD 2015 KNOWLEDGE EXPERIENCE APPLICATION Moving Tongues Beyond Frenectomy Grace Sun, DDS FAACD MALD MAGD MICOI Los Angeles ALD 2015 KNOWLEDGE EXPERIENCE APPLICATION Accredited Fellow, American Academy
DYSPHAGIA SCREENING and CLINICAL SWALLOW EVALUATIONS. Debra M. Suiter, Ph.D., CCC-SLP, BRS-S VA Medical Center-Memphis
 DYSPHAGIA SCREENING and CLINICAL SWALLOW EVALUATIONS Debra M. Suiter, Ph.D., CCC-SLP, BRS-S VA Medical Center-Memphis Suiter, ASHA, 2012 Diagnostic Tests vs. Screening Diagnostic tests are used when a
DYSPHAGIA SCREENING and CLINICAL SWALLOW EVALUATIONS Debra M. Suiter, Ph.D., CCC-SLP, BRS-S VA Medical Center-Memphis Suiter, ASHA, 2012 Diagnostic Tests vs. Screening Diagnostic tests are used when a
4/28/16. Today s Objectives. Evidence Based Decision Making in the Evaluation and Treatment of Dysphagia
 Evidence Based Decision Making in the Evaluation and Treatment of Dysphagia Megan Urban, MA, CCC-SLP, BCS-S Ashley Edds, MS, CCC-SLP April 29, 2016 Disclosures Financial Megan and Ashley are employed by
Evidence Based Decision Making in the Evaluation and Treatment of Dysphagia Megan Urban, MA, CCC-SLP, BCS-S Ashley Edds, MS, CCC-SLP April 29, 2016 Disclosures Financial Megan and Ashley are employed by
Effects of a Sour Bolus on Oropharyngeal Swallowing Measures in Patients With Neurogenic Dysphagia
 Journal of Speech and Hearing Research, Volume 38, 556-563, June 1995 Effects of a Sour Bolus on Oropharyngeal Swallowing Measures in Patients With Neurogenic Dysphagia Jeri A. Logemann Barbara Roa Pauloski
Journal of Speech and Hearing Research, Volume 38, 556-563, June 1995 Effects of a Sour Bolus on Oropharyngeal Swallowing Measures in Patients With Neurogenic Dysphagia Jeri A. Logemann Barbara Roa Pauloski
Medical Research Archives ORAL STRENGTH COMPARISONS ORAL STRENGTH COMPARISONS ACROSS AGE AND SEX IN HEALTHY VOLUNTEERS
 1 ACROSS AGE AND SEX IN HEALTHY VOLUNTEERS Scott R. Youmans Long Island University. Brooklyn Campus Email: scott.youmans@liu.edu Proper functioning of the oral musculature is crucial in the oral phases
1 ACROSS AGE AND SEX IN HEALTHY VOLUNTEERS Scott R. Youmans Long Island University. Brooklyn Campus Email: scott.youmans@liu.edu Proper functioning of the oral musculature is crucial in the oral phases
IVOR LEWIS Esophagogastrectomy
 IVOR LEWIS Esophagogastrectomy SPEECH-LANGUAGE PATHOLOGY S ROLE MAGGIE BOYD, MS, CCC/SLP Biography Maggie Boyd, MS, CCC-SLP is a dysphagia clinical specialist at UAB hospital. She has 14 years clinical
IVOR LEWIS Esophagogastrectomy SPEECH-LANGUAGE PATHOLOGY S ROLE MAGGIE BOYD, MS, CCC/SLP Biography Maggie Boyd, MS, CCC-SLP is a dysphagia clinical specialist at UAB hospital. She has 14 years clinical
Pharyngeal Effects of Bolus Volume, Viscosity, and Temperature in Patients With Dysphagia Resulting From Neurologic Impairment and in Normal Subjects
 Journal of Speech and Hearing Research, Volume 37, 1041-1049, October 1994 Pharyngeal Effects of Bolus Volume, Viscosity, and Temperature in Patients With Dysphagia Resulting From Neurologic Impairment
Journal of Speech and Hearing Research, Volume 37, 1041-1049, October 1994 Pharyngeal Effects of Bolus Volume, Viscosity, and Temperature in Patients With Dysphagia Resulting From Neurologic Impairment
COMMUNICATION AND SWALLOWING DISORDERS IN PARKINSON S DISEASE Challenges, Treatments, and Resources
 COMMUNICATION AND SWALLOWING DISORDERS IN PARKINSON S DISEASE Challenges, Treatments, and Resources Rosemary B. Loftin, M.S. CCC/SLP Supervisor of Speech Pathology Services Mayo Clinic Hospital Arizona
COMMUNICATION AND SWALLOWING DISORDERS IN PARKINSON S DISEASE Challenges, Treatments, and Resources Rosemary B. Loftin, M.S. CCC/SLP Supervisor of Speech Pathology Services Mayo Clinic Hospital Arizona
Critical Review: Is a chin-down posture more effective than thickened liquids in eliminating aspiration for patients with Parkinson s disease?
 Critical Review: Is a chin-down posture more effective than thickened liquids in eliminating aspiration for patients with Parkinson s disease? Nadia Torrieri, M.Cl.Sc. (SLP) Candidate The Unversity of
Critical Review: Is a chin-down posture more effective than thickened liquids in eliminating aspiration for patients with Parkinson s disease? Nadia Torrieri, M.Cl.Sc. (SLP) Candidate The Unversity of
Tongue strength: why? how?
 Tongue strength: why? how? Jan Vanderwegen Gwen Van Nuffelen University Hospital Saint-Pieter, Brussels University Hospital Antwerp, Antwerp University College Thomas More, Antwerp University of Ghent,
Tongue strength: why? how? Jan Vanderwegen Gwen Van Nuffelen University Hospital Saint-Pieter, Brussels University Hospital Antwerp, Antwerp University College Thomas More, Antwerp University of Ghent,
THE EFFECTS OF TWO REHABILITATION EXERCISES ON SUBMENTAL HYOLARYNGEAL MUSCULAR ACTIVITY. Teresa D. Hughes
 Running head: EFFECTS OF EXERCISES ON SUBMENTAL MUSCLE ACTIVITY THE EFFECTS OF TWO REHABILITATION EXERCISES ON SUBMENTAL HYOLARYNGEAL MUSCULAR ACTIVITY by Teresa D. Hughes Bachelor of Science, 2013 Texas
Running head: EFFECTS OF EXERCISES ON SUBMENTAL MUSCLE ACTIVITY THE EFFECTS OF TWO REHABILITATION EXERCISES ON SUBMENTAL HYOLARYNGEAL MUSCULAR ACTIVITY by Teresa D. Hughes Bachelor of Science, 2013 Texas
Dysphagia and Self Feeding in Acute Tetraplegia
 Dysphagia and Self Feeding in Acute Tetraplegia Danielle R. Karhut, OTR/L Robert Masterson, MS, CCC-SLP Spinal Cord Rehabilitation Unit UPMC Mercy Hospital/Centers for Rehab Services Pittsburgh, PA Tetraplegia
Dysphagia and Self Feeding in Acute Tetraplegia Danielle R. Karhut, OTR/L Robert Masterson, MS, CCC-SLP Spinal Cord Rehabilitation Unit UPMC Mercy Hospital/Centers for Rehab Services Pittsburgh, PA Tetraplegia
Assessing the Eating Needs of Personal Care Services (PCS) Beneficiaries Effective 12/1/2016
 Assessing the Eating Needs of Personal Care Services (PCS) Beneficiaries Effective 12/1/2016 The Freedom to Succeed November 22,2016 Content Introduction Signs and Symptoms Caring for Individuals with
Assessing the Eating Needs of Personal Care Services (PCS) Beneficiaries Effective 12/1/2016 The Freedom to Succeed November 22,2016 Content Introduction Signs and Symptoms Caring for Individuals with
Dysphagia Diagnostic Procedures
 The Role of Lingual Pressures In Dysphagia Screening Andrew Kaufman, BS Jackie Hind, MS Georgia Malandraki, PhD JoAnne Robbins, PhD American Speech Language Hearing Association Annual Meeting New Orleans,
The Role of Lingual Pressures In Dysphagia Screening Andrew Kaufman, BS Jackie Hind, MS Georgia Malandraki, PhD JoAnne Robbins, PhD American Speech Language Hearing Association Annual Meeting New Orleans,
Evidenced Based Practice in Dysphagia. Houston We Have a Problem
 Evidenced Based Practice in Dysphagia Houston We Have a Problem HOUSTON, WE HAVE A PROBLEM THE ALARM WILL SOUND, EVENTUALLY Rosenbeck 1995 In 1969 an alarm sounded throughout the aphasiology community
Evidenced Based Practice in Dysphagia Houston We Have a Problem HOUSTON, WE HAVE A PROBLEM THE ALARM WILL SOUND, EVENTUALLY Rosenbeck 1995 In 1969 an alarm sounded throughout the aphasiology community
DYSPHAGIA MANAGEMENT IN ACUTE CARE AMANDA HEREFORD, MA, CCC- SLP
 DYSPHAGIA MANAGEMENT IN ACUTE CARE AMANDA HEREFORD, MA, CCC- SLP OVERVIEW Decision making re: swallowing in the medically compromised patient Swallow evaluation vs. Nursing Swallow Screening Instrumental
DYSPHAGIA MANAGEMENT IN ACUTE CARE AMANDA HEREFORD, MA, CCC- SLP OVERVIEW Decision making re: swallowing in the medically compromised patient Swallow evaluation vs. Nursing Swallow Screening Instrumental
POST POLIO SYNDROME (PPS) AND ITS EFFECTS ON SWALLOWING BY: LINDSAY JORDAN
 POST POLIO SYNDROME (PPS) AND ITS EFFECTS ON SWALLOWING BY: LINDSAY JORDAN WHAT IS POST POLIO SYNDROME (PPS)? Post-polio syndrome (PPS) is a condition that affects polio survivors years after recovery
POST POLIO SYNDROME (PPS) AND ITS EFFECTS ON SWALLOWING BY: LINDSAY JORDAN WHAT IS POST POLIO SYNDROME (PPS)? Post-polio syndrome (PPS) is a condition that affects polio survivors years after recovery
When Swallowing Becomes Impossible
 University of Tennessee, Knoxville Trace: Tennessee Research and Creative Exchange University of Tennessee Honors Thesis Projects University of Tennessee Honors Program 5-2011 When Swallowing Becomes Impossible
University of Tennessee, Knoxville Trace: Tennessee Research and Creative Exchange University of Tennessee Honors Thesis Projects University of Tennessee Honors Program 5-2011 When Swallowing Becomes Impossible
Dysphagia Identification and Management
 Dysphagia Identification and Management Presented By Speech-Language Pathologist Developmental Disabilities Administration DC Department on Disability Services Training Objectives After this training session
Dysphagia Identification and Management Presented By Speech-Language Pathologist Developmental Disabilities Administration DC Department on Disability Services Training Objectives After this training session
Original Article. Annals of Rehabilitation Medicine INTRODUCTION
 Original Article Ann Rehabil Med 2012; 36: 512-520 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2012.36.4.512 Annals of Rehabilitation Medicine The Effect of Bedside Exercise Program
Original Article Ann Rehabil Med 2012; 36: 512-520 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2012.36.4.512 Annals of Rehabilitation Medicine The Effect of Bedside Exercise Program
Oro-pharyngeal and Esophageal Motility and Dysmotility John E. Pandolfino, MD, MSci
 Oro-pharyngeal and Esophageal Department of Medicine Feinberg School of Medicine Northwestern University 1 Oro-pharyngeal and Esophageal Motility Function: Oropharynx Transfer food Prevent aspiration Breathing
Oro-pharyngeal and Esophageal Department of Medicine Feinberg School of Medicine Northwestern University 1 Oro-pharyngeal and Esophageal Motility Function: Oropharynx Transfer food Prevent aspiration Breathing
Swallow Function: Passy-Muir Valve Use for Evaluation & Rehabilitation David A. Muir Course Outline Physiology of Swallow
 Swallow Function: Passy-Muir Valve Use for Evaluation & Rehabilitation Mary Spremulli, MA, CCC-SLP Passy-Muir Clinical Consultant spre713@hotmail.com (949) 833-8255 David A. Muir 23 year-old ventilator
Swallow Function: Passy-Muir Valve Use for Evaluation & Rehabilitation Mary Spremulli, MA, CCC-SLP Passy-Muir Clinical Consultant spre713@hotmail.com (949) 833-8255 David A. Muir 23 year-old ventilator
Deciphering Dysphagia with E-Stim 8 March 2015
 Deciphering Dysphagia with E-Stim 8 March 2015 Electrical Stimulation for Muscle Re-education in Swallowing Presented by: Russ Campbell, PT Sponsored by: HEMAX Health Products Company Limited New Options
Deciphering Dysphagia with E-Stim 8 March 2015 Electrical Stimulation for Muscle Re-education in Swallowing Presented by: Russ Campbell, PT Sponsored by: HEMAX Health Products Company Limited New Options
Videofluoroscopy quantification of laryngotracheal aspiration outcome in traumatic brain injury-related oropharyngeal dysphagia
 06. ORIGINAL ROSA TERRÉ 9/2/07 12:30 Página 7 1130-0108/2007/99/1/7-12 REVISTA ESPAÑOLA DE ENFERMEDADES DIGESTIVAS Copyright 2007 ARÁN EDICIONES, S. L. REV ESP ENFERM DIG (Madrid) Vol. 99. N. 1, pp. 7-12,
06. ORIGINAL ROSA TERRÉ 9/2/07 12:30 Página 7 1130-0108/2007/99/1/7-12 REVISTA ESPAÑOLA DE ENFERMEDADES DIGESTIVAS Copyright 2007 ARÁN EDICIONES, S. L. REV ESP ENFERM DIG (Madrid) Vol. 99. N. 1, pp. 7-12,
Swallow-respiratory coordination. Liza Bergström, Leg. logoped.
 Swallow-respiratory coordination Liza Bergström, Leg. logoped. Biological timeshare When we breathe, we don t swallow When we swallow, we don t breathe Body will always choose to breathe over anything
Swallow-respiratory coordination Liza Bergström, Leg. logoped. Biological timeshare When we breathe, we don t swallow When we swallow, we don t breathe Body will always choose to breathe over anything
Nutricia. Nutrition and Dysphagia
 Nutricia Nutrition and Dysphagia 1 Introduction What is Dysphagia? The inability to swallow normally or freely. Disorder in the swallowing process that does not allow safe passing of food from the mouth
Nutricia Nutrition and Dysphagia 1 Introduction What is Dysphagia? The inability to swallow normally or freely. Disorder in the swallowing process that does not allow safe passing of food from the mouth
Normal and Abnormal Oral and Pharyngeal Swallow. Complications.
 ESPEN Congress Gothenburg 2011 Assessment and treatment of dysphagia What is the evidence? Normal and Abnormal Oral and Pharyngeal Swallow. Complications. Pere Clavé Educational Session. Assessment and
ESPEN Congress Gothenburg 2011 Assessment and treatment of dysphagia What is the evidence? Normal and Abnormal Oral and Pharyngeal Swallow. Complications. Pere Clavé Educational Session. Assessment and
Effect of Palatal Surface Contouring Techniques on the Swallowing Function of Complete Denture Wearers.
 Effect of Palatal Surface Contouring Techniques on the Swallowing Function of Complete Denture Wearers. Tamer Abou-Elsaad 1, Ahmad Habib 2, Mohamed Elkhodary 2, and Abd-Allah Salem 2 1 Phoniatric Unit,
Effect of Palatal Surface Contouring Techniques on the Swallowing Function of Complete Denture Wearers. Tamer Abou-Elsaad 1, Ahmad Habib 2, Mohamed Elkhodary 2, and Abd-Allah Salem 2 1 Phoniatric Unit,
Neuromuscular Electrical Stimulation in the Early Intervention Population: A Series of Five Case Studies
 A Peer Reviewed Publication of the College of Health Care Sciences at Nova Southeastern University Dedicated to allied health professional practice and education http://ijahsp.nova.edu Vol. 10 No. 3 ISSN
A Peer Reviewed Publication of the College of Health Care Sciences at Nova Southeastern University Dedicated to allied health professional practice and education http://ijahsp.nova.edu Vol. 10 No. 3 ISSN
Speech and Swallowing in KD: Soup to Nuts. Neil C. Porter, M.D. Assistant Professor of Neurology University of Maryland
 Speech and Swallowing in KD: Soup to Nuts Neil C. Porter, M.D. Assistant Professor of Neurology University of Maryland Disclosures I will not be speaking on off-label use of medications I have no relevant
Speech and Swallowing in KD: Soup to Nuts Neil C. Porter, M.D. Assistant Professor of Neurology University of Maryland Disclosures I will not be speaking on off-label use of medications I have no relevant
Long Term Toxicities of Head & Neck Cancer Therapies. Faith Mutale Abramson Cancer Center University of Pennsylvania
 Long Term Toxicities of Head & Neck Cancer Therapies Faith Mutale Abramson Cancer Center University of Pennsylvania Head & Neck Cancer 2-3% of all cancers 1-2% of all cancer deaths Incidence includes:
Long Term Toxicities of Head & Neck Cancer Therapies Faith Mutale Abramson Cancer Center University of Pennsylvania Head & Neck Cancer 2-3% of all cancers 1-2% of all cancer deaths Incidence includes:
