Huntington s disease. Eating and swallowing
|
|
|
- Nigel Dalton
- 5 years ago
- Views:
Transcription
1 Huntington s disease Eating and swallowing
2
3 People with Huntington s disease can experience difficulties with eating, drinking and swallowing. These can be among the most challenging aspects of this condition and can affect not only the person with Huntington s disease but also their family and carers. This fact sheet explains the signs of eating, drinking and swallowing difficulties, the reasons for these in Huntington s disease, key ways to manage them, and some handy hints for safer eating, drinking and swallowing. What are the signs of eating, drinking and swallowing problems? Common signs include: Physical difficulty self-feeding, i.e. using utensils to place food or drink in the mouth Difficulty controlling food or drink in the mouth Food or drink spilling forward out of the mouth Difficulty chewing food Difficulty actually swallowing Coughing or choking during or after swallowing the food or drink Bringing food or drink back up A wet, gurgle sounding voice
4 The sensation of food or drink catching in the throat; food sticking in the throat or a feeling that food or drink has gone down the wrong way Disinterest in eating and drinking Changes in appetite Heightened anxiety or fear of eating or drinking Enduring symptoms may include social isolation especially at meal-times, unexplained weight loss and/or frequent chest infections. It is important that where these symptoms are identified in the person with Huntington s disease, contact is made with their GP and/or medical team to request a referral to the local Speech & Language Therapy Service for specialist assessment and intervention. What are the effects of eating, drinking and swallowing problems? There are several reasons why eating, drinking and swallowing problems need to be managed properly: Aspiration is the technical term given when a foreign substance such as food, drink, saliva, refluxed acid and/or medication enters the airway to the lungs. Usually if this happens we describe it as something going down the wrong way and people will typically cough. If a person has eating, drinking and swallowing problems because of Huntington s disease they may
5 be at risk of aspiration. It is important to try and manage this risk of aspiration occurring because it can lead to chest infections and sometimes, aspiration pneumonia. Aspiration pneumonia is an infection of the lungs caused by accidental inhalation of a foreign substance into the lungs. It is a potentially serious, may be a fatal condition that requires attention from the medical team. Choking if a person has eating, drinking and swallowing problems because of Huntington s disease they may be at risk of choking and difficulty breathing because the airway to the lungs has been obstructed by for example food blocking the windpipe. Malnutrition is the condition that develops when the body does not get the right amount of nutrients (energy, protein, vitamins and minerals) that are necessary to maintain a healthy body. If a person has eating, drinking and swallowing problems because of Huntington s disease they may not be able to eat a balanced, high calorie diet that meets their individual needs for a healthy body and mind. Dehydration is the condition that develops when your body does not get enough fluids and salts, which may occur if the person with Huntington s disease because they have difficulty swallowing and drinking adequately.
6 Managing symptoms of Huntington s disease if the person with Huntington s disease has difficulty eating, drinking and swallowing other symptoms of their condition such as behaviour, concentration, memory, mood, choreiform movements and physical skills may be harder to control and manage. Quality of life eating and drinking is considered an essential part of daily living, which for most people is used to promote enjoyment, pleasure and socialisation. Where a person with Huntington s disease has eating, drinking and swallowing problems, they may feel that their own and their family/or carers quality of life is negatively affected. What are the reasons for eating, drinking and swallowing problems in people with Huntington s disease? Changes in the muscles used to eat, drink and swallow there are different muscle groups involved in the process of eating, drinking and swallowing. Upper limb muscles of the arm and hand are used to for example prepare meals and to place the food or drink in the mouth when eating and drinking. Muscles of the face and throat are used to for example chew food, control the food or drink in the mouth, pass it to the back of the mouth and down the throat, and to swallow.
7 Both these muscle groups can be affected by Huntington s disease, in particular muscle strength and range of muscle movement can change, which makes the action of eating, drinking and swallowing difficult. To add because of choreic movements, the control and co-ordination of these muscles groups can impact on the efficiency, effectiveness and time taking eating, drinking and swallowing. As a result of the physical changes in these muscles there can be specific problems across all phases of the actual swallow mechanism itself such as: Difficulty placing the food or fluid in the mouth; closing the lips together to keep the food or drink in the mouth; chewing the food or holding the drink in the mouth in preparation to transfer the food or drink to the back of the throat Co-ordination, timing and speed of transfer of the food or drink to the back of the throat; sometimes food or drink may transfer too quickly, too slowly and/or be uncoordinated Difficulty with food or drink being efficiently and effectively swallowed so as to enter the oesophagus (tube to the stomach) and not go down the wrong way into the airway to the lungs. Changes in appetite At different points during the condition, the person with Huntington s disease can
8 have changes in appetite. This can be for a variety of reasons such as changes in diet, actual difficulties eating, drinking and swallowing, fatigue and fear of spilling foods or choking, anxiety, frustration or an overall change in their mood such as depression. Any one or a combination of these factors can result in the person with Huntington s disease having a loss of appetite and although hungry, they may actually refuse to eat. Alternatively, people with Huntington s disease can have a voracious appetite. Even though they are eating frequently and often big meal portions, they always seem to be hungry. As a result of this they can have a tendency to take too big a mouthful of food and/or to cram as much food into their mouth. This can lead to spillage of food out of the mouth, storing of food in their cheeks and/or reduced control and coordination of the swallow mechanism and risk of aspiration or choking. Changes in cognition - as mentioned above, the person with Huntington s disease may experience anxiety and/or depression, which may manifest because of their difficulties with eating, drinking and swallowing. This may also arise because of changes in their cognition and mental health. Anxiety and stress often trigger visible chorea, which can then affect eating, drinking and swallowing. The actual fear of choking, drooling or the embarrassment
9 of making a mess while eating or drinking can actually increase the chance that it will happen. Where the person with Huntington s disease has a change in cognition, they may also have reduced insight, self-awareness and self-monitoring. As a result, some eating and drinking habits for example storing food in her their cheeks, taking too big a mouthful of food or drink, cramming food into their mouth may be difficult to self-manage. This is where the role of family and/or carer can aid the situation as they can act as a monitor and give advice when necessary. However, it is acknowledged that this may not be easy. Many people with Huntington s disease show great resistance to change in their life-style, which can make it difficult to introduce new habits and ideal food or drink textures to the daily routine. Weight loss in this condition has long been observed and is frequently attributed to involuntary choreic movements. Although many theories have been suggested, the cause of weight loss is still unclear. Most recent evidence proposes that the weight loss may be a manifestation of an underlying biochemical defect. Whatever the cause, the fact remains clear that a greater calorie intake is needed. Where weight loss is observed the person with Huntington s disease may not have sufficient energy;
10 making eating, drinking and swallowing an effortful, difficult and tiring activity. It is important where there are problems identified managing the weight of the person with Huntington s disease that contact is made with their GP and/or medical team to request a referral to the local Dietetic Service for specialist assessment and intervention. How are eating, drinking and swallowing problems assessed? Recognising the signs and symptoms of eating, drinking and swallowing difficulties is the first point from which assessment begins. The person with Huntington s disease, their family and/or carers are pivotal in identifying these difficulties and reporting any observations to their GP and/or specialist medical team involved. Once alerted that there are concerns about eating, drinking and swallowing, a referral should be made to the local Speech & Language Therapy Service. It is the role of a Speech & Language Therapist to assess eating, drinking and swallowing problems. Assessment may involve: Discussion with the person who has Huntington s disease, their family and/or carers.
11 Discussion with the medical team and other health and social care staff involved. Meal-time observation. Bedside swallow assessment, which is a noninvasive, non-instrumental clinical assessment of the person with Huntington s disease swallow function. In some cases, further tests such as a videofluoroscopy, which is a recorded dynamic continuous x-ray may be carried out to investigate in more detail the swallow function. This is typically carried out in a specialist x- ray clinic by a Radiologist and Speech and Language Therapist. How are eating, drinking and swallowing problems managed? From information obtained during assessment of eating, drinking and swallowing problems, the Speech & Language Therapist in collaboration with the person with Huntington s disease, their family, carers, medical team and other health and social care staff will develop a personalised care plan. This may involve: Food and fluid texture modification changes to the consistencies of food or fluid textures and advice on textures to avoid can be recommended by your local speech & language therapist so that that the person with Huntington s disease can easily and safely eat, drink and swallow.
12 Changes to meal times what time the person with Huntington s disease eat or drink throughout the day and evening, how often they eat and drink, and the portion size of their meal or drink may be reviewed to ensure it is the most suitable considering their daily presentation, mood, levels of fatigue, concentration and their medication regime to name a few factors. Changes to the meal-time environment it is important to set the scene ensuring the environment suits the person s individual needs, that can promote a pleasurable and safe place to eat and drink. For example, the dining area should have good lighting; it should be a calm and quiet area that is free from distractions such as lots of people present and/or television or music system being switched on. Advice on specialist eating and drinking equipment there are a variety of small aids from specialist crockery, cups, cutlery, place mats, tablecloths and straws that are available to help the person with Huntington s disease self-feed. Some of these items are readily obtained from shops, supermarkets or disability living centres and associated websites. However, it is important to seek specialist assessment and advice from a local occupational therapist before making any purchase. To access a local occupational therapist, contact your GP or medical team to request a referral to this service.
13 Advice on seating, posture and positioning at meal-times good body posture and head position are important for safe eating, drinking and swallowing. Ideally the person with Huntington s disease should be sitting upright in a chair, looking forward with their head held upright when eating and drinking. If they cannot sit in a chair then they should be sat comfortably as upright as possible in the bed or a wheelchair. In some cases, specifically designed seating aids, chairs and wheelchairs may be used to help promote optimal seating position especially where the person with Huntington s disease has body and/or head choreic movements. Where specialist seating and associated equipment is necessary it is important to access specific assessment and advice from your local physiotherapist and/or occupational therapist. They can be accessed by your GP or medical team making a referral to their Service. When considering optimal seating, posture and positioning it is vital to also consider access to and from the person with Huntington s disease especially in the case of emergency. Advice on assisted feeding dependent upon the individual skills of person with Huntington s disease, assisted feeding may take one or a combination of three forms.
14 Firstly, it may entail closely supervising the person with Huntington s disease self-feeding at meal-times. Secondly, it may be that someone supports the person with Huntington s disease self-feed by for example giving lots of physical and verbal prompts to help them self-feed and/or taking over feeding when they show signs of tiredness. Thirdly, as the condition progresses, the person with Huntington s disease may need to be fed their meal or given their drinks by family and/or carers. Dependent on the form of assisted feeding and support, advice can be given that is unique to the person with Huntington s disease, their family and/or carers individual needs. Alternative feeding method For some people with Huntington s disease eating, drinking and swallowing may become such a significant problem that a different method of feeding needs to be considered. Primarily this will include a gastrostomy, where a tube is inserted into the stomach via the abdomen. There are different forms in which a gastrostomy is offered, the difference being how the tube is inserted. The most common of these and that which most often is suggested for people with Huntington s disease is Percutaneous Endoscopic Gastrostomy (PEG).
15 There are advantages and disadvantages linked to this form of feeding and any decision made is unique to the individual with Huntington s disease, their circumstances and their specific needs. It is therefore crucial that in making a decision for alternative feeding, the person with Huntington s disease, their family, carers, medical team and health and social care staff carefully and thoroughly discuss the options available. Oral care Looking after your mouth, teeth and gums is a vital part of everyday living. It is particularly important when the person with Huntington s disease has eating, drinking or swallowing difficulties and maintaining a routine of oral care can be challenging. Regular visits to your local dentist are advisable. They can recommend the most appropriate oral care regime, most suitable toothbrush and toothpaste or mouthwash to use according to the person with Huntington s disease individual needs. Saliva management When the person with Huntington s disease has difficulty eating, drinking and swallowing, this may extend to difficulty managing their own saliva. This may present as problems with one or a combination of difficulties including:
16 Dry mouth Copious amounts of thin, watery saliva that the person with Huntington s disease may have difficulty controlling in their mouth and swallowing leading to for example drooling and/or a wet sounding voice A build-up of phlegm or thick, sticky tenacious mucous that may feel is sticking at the back of the throat and that looks stringy when the person with Huntington s disease cough to clear the product It is important to be aware of these difficulties and report this information to your local speech and language therapist for their assessment, practical advice and, liaison with the medical team and other health and social care team members to try and best manage the problem. Handy hints for safe eating, drinking and swallowing Every person with Huntington s disease problems eating, drinking and swallowing are unique to them and their situation. It is important for an individual care plan to be developed that considers their specific needs. However, here are some general helpful tips for safer eating, drinking and swallowing: Establish a routine at meal times; have meals and snacks at regular times across the day and evening.
17 Ensure the environment is calm, quiet and free from distractions e.g. turn off the TV or radio, and sit in a part of the room where there are fewer people. Try not to eat and drink alone. Allow yourself time to eat and drink. Take small mouthfuls of food or drink do not eat and drink at the same time. Make sure you have swallowed the first mouthful of food or drink before taking the next do not fill up your mouth with too much food or drink. Thoroughly chew your food; rest if you need to in between mouthfuls of food or drink. Ensure the food or drink is at the right temperature for you to eat, drink and swallow. Make food look attractive so you want to eat it. Ensure that you are alert, calm and sitting upright in a comfortable position when eating and drinking. Your head should be held upright in a mid-line position when swallowing food or drink. Concentrate on the task of eating and drinking talking in between courses of your meal or drink not during the activity itself. Rest before and after meals and drinks sit upright for at least 30 minutes after you have finished your meal or drink. Make sure family and carers are aware of your eating, drinking and swallowing problems and
18 where in place, are familiar with your individual care plan so they can support and encourage you. Speak with your speech and language therapist or medical team (GP, hospital doctor, nurse, dietician, occupational therapist or physiotherapist) if you need more help and information. A final point Throughout this fact sheet reference has been made to the role of health and social care staff to assess and offer intervention to meet the person with Huntington s disease individual needs. Where signs and symptoms of eating, drinking, swallowing and weight management are identified in the person with Huntington s disease, do not hesitate to consult your GP and/or medical team to request referral to the specialist clinical team: Speech and language therapy to assess and treat eating, drinking and swallowing difficulties Dietetics to assess and advise on nutrition, hydration needs, and weight management Physiotherapist to assess and advise on suitable body posture, head position and seating Occupational therapy to assess and advise on suitable seating and specialist feeding utensils Remember effective management of eating, drinking and swallowing problems should be a team approach
19 that includes the person with Huntington s disease, their family, carers, the medical team and health and social care professionals.
20 Further information Huntington s Disease Association Suite 24, Liverpool Science Park IC1, 131 Mount Pleasant, Liverpool, L3 5TF Phone Website: British Dietetic Association (BDA) 5th Floor, Charles House, 148/9 Great Charles Street Queensway, Birmingham, B3 3HT Phone: Website: British Association of Occupational Therapists and College of Occupational Therapists (BAOT/COT) Borough High Street, Southwark London, SE1 1LB Phone: Website: Disability Living Foundation (DLF) Harrow Road, London, W9 2HU Phone: Website: Dysphagia Online Website:
21 Chartered Society of Physiotherapy (CSP) 14 Bedford Row, London, WC1R 4ED Phone: Website: Royal College of Speech & Language Therapists (RCSLT) 2 White Hart Yard, London, SE1 1NX Phone: Website: Claire.Schofield@nchc.nhs.uk
22
23 Huntington s Eating and swallowing 03.18
24 Fact sheets available from the Huntington s Disease Association: General information about Huntington s disease and the Huntington s Disease Association Predictive testing for Huntington s disease Talking to children about Huntington s disease Information for teenagers A young adult's guide Eating and swallowing difficulties Huntington s disease and diet The importance of dental care Communication skills Behavioural problems Sexual problems Huntington s disease and the law Huntington s disease and driving Advice on life assurance, pensions, mortgages etc. Seating equipment and adaptations Checklist for choosing a care home Advance Decision to Refuse Treatment (ADRT) A carer's guide Challenging behaviour in Juvenile Huntington s disease A brief guide to Juvenile Huntington s disease for children s hospices and palliative care services A teacher s guide A young person with Juvenile Huntington s disease at school All fact sheets can be downloaded free of charge from our website or ordered by phone or info@hda.org.uk For a publication price list/order form, membership form, details of our Specialist Huntington s disease Advisers and local Branches and Support Groups, please phone or info@hda.org.uk Huntington s Disease Association Suite 24 Liverpool Science Park, IC1 131 Mount Pleasant, Liverpool L3 5TF phone info@hda.org.uk Registered charity no
Huntington s disease. The importance of dental care
 Huntington s disease The importance of dental care The Importance of dental care in Huntington s disease It should be stated from the outset that the teeth of people with Huntington s disease are no different
Huntington s disease The importance of dental care The Importance of dental care in Huntington s disease It should be stated from the outset that the teeth of people with Huntington s disease are no different
Huntington s disease General information about Huntington s and the Huntington's Disease Association
 Huntington s disease General information about Huntington s and the Huntington's Disease Association General information about Huntington s disease Huntington s disease (HD), is a hereditary disorder of
Huntington s disease General information about Huntington s and the Huntington's Disease Association General information about Huntington s disease Huntington s disease (HD), is a hereditary disorder of
Dysphagia Management in TCP. Susan Smith and Vanessa Barkla Speech Pathologists, Ballarat Health Services May 2012
 Dysphagia Management in TCP Susan Smith and Vanessa Barkla Speech Pathologists, Ballarat Health Services May 2012 The role of the Speech Pathologist To assess swallowing status To provide management and
Dysphagia Management in TCP Susan Smith and Vanessa Barkla Speech Pathologists, Ballarat Health Services May 2012 The role of the Speech Pathologist To assess swallowing status To provide management and
Swallowing problems. Patient information. Name: Date: Speech and Language Therapist: Reviewed: May 2016 Next review: June 2017 Version 1
 Patient information Swallowing problems Name: Date: Speech and Language Therapist: Golden Jubilee National Hospital Agamemnon Street Clydebank, G81 4DY (: 0141 951 5000 www.nhsgoldenjubilee.co.uk Reviewed:
Patient information Swallowing problems Name: Date: Speech and Language Therapist: Golden Jubilee National Hospital Agamemnon Street Clydebank, G81 4DY (: 0141 951 5000 www.nhsgoldenjubilee.co.uk Reviewed:
Eating and drinking in dementia
 Eating and drinking in dementia Patient infomation Nutrition and dietetics Clinical and diagnostic services centre This leaflet offers practical advice on how you can help someone with early stage dementia
Eating and drinking in dementia Patient infomation Nutrition and dietetics Clinical and diagnostic services centre This leaflet offers practical advice on how you can help someone with early stage dementia
Mouth care for people with dementia. Eating and Drinking. Staying well with dementia
 Mouth care for people with dementia Eating and Drinking Staying well with dementia 2 Dementia UK Eating and Drinking 3 Eating and drinking for a person with dementia People with dementia may experience
Mouth care for people with dementia Eating and Drinking Staying well with dementia 2 Dementia UK Eating and Drinking 3 Eating and drinking for a person with dementia People with dementia may experience
Understanding late stage dementia Understanding dementia
 Understanding late stage dementia About this factsheet This factsheet is for relatives of people diagnosed with dementia. It provides information about what to expect as dementia progresses to late stage.
Understanding late stage dementia About this factsheet This factsheet is for relatives of people diagnosed with dementia. It provides information about what to expect as dementia progresses to late stage.
What is Dysphagia? An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION What is Dysphagia? An information guide What is Dysphagia? If someone has dysphagia, this means they have difficulty in swallowing. Dysphagia
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION What is Dysphagia? An information guide What is Dysphagia? If someone has dysphagia, this means they have difficulty in swallowing. Dysphagia
Dysphagia (swallowing problems)
 Dysphagia (swallowing problems) Speech and Language Therapy Department Patient Information Leaflet Introduction This leaflet is for people who have dysphagia. It gives information on what this condition
Dysphagia (swallowing problems) Speech and Language Therapy Department Patient Information Leaflet Introduction This leaflet is for people who have dysphagia. It gives information on what this condition
Chef Rick Schmitt, CDM, CFPP Assistant Dining Director/Executive Chef Westminster Towers Rock Hill, SC
 Chef Rick Schmitt, CDM, CFPP Assistant Dining Director/Executive Chef Westminster Towers Rock Hill, SC Water/Hydration Food/Nutrition Shelter/Security Love/Acceptance/Belonging Definition A chronic or
Chef Rick Schmitt, CDM, CFPP Assistant Dining Director/Executive Chef Westminster Towers Rock Hill, SC Water/Hydration Food/Nutrition Shelter/Security Love/Acceptance/Belonging Definition A chronic or
Occupational therapy after stroke
 Call the Stroke Helpline: 0303 3033 100 or email: info@stroke.org.uk Occupational therapy after stroke This guide explains how occupational therapy can help your recovery and rehabilitation after a stroke.
Call the Stroke Helpline: 0303 3033 100 or email: info@stroke.org.uk Occupational therapy after stroke This guide explains how occupational therapy can help your recovery and rehabilitation after a stroke.
Mouth care for people with dementia. Eating and Drinking. Staying well with dementia
 Mouth care for people with dementia Eating and Drinking Staying well with dementia 2 Dementia UK Eating and drinking for a person with dementia People with dementia may experience problems with eating
Mouth care for people with dementia Eating and Drinking Staying well with dementia 2 Dementia UK Eating and drinking for a person with dementia People with dementia may experience problems with eating
ROLE OF THE DIETITIAN. Aims of Dietetic Treatment NUTRITIONAL ISSUES WHY? MALNUTRITION NUTRITONAL MANAGEMENT OF MOTOR NEURONE DISEASE.
 NUTRITONAL MANAGEMENT OF MOTOR NEURONE DISEASE. ROLE OF THE DIETITIAN SALLY DARBY NEUROLOGY DIETITIAN Not just tube feeding Referral soon after diagnosis Advise on healthy eating for MND Monitor nutritional
NUTRITONAL MANAGEMENT OF MOTOR NEURONE DISEASE. ROLE OF THE DIETITIAN SALLY DARBY NEUROLOGY DIETITIAN Not just tube feeding Referral soon after diagnosis Advise on healthy eating for MND Monitor nutritional
There are several reasons why a person with dementia may have a poor appetite and seem uninterested in eating.
 PBO 930022142 NPO 049-191 EATING If you are caring for someone with dementia you will want to ensure that they enjoy their food and that they eat a healthy, balanced diet. But for some people, as dementia
PBO 930022142 NPO 049-191 EATING If you are caring for someone with dementia you will want to ensure that they enjoy their food and that they eat a healthy, balanced diet. But for some people, as dementia
Assessing the Eating Needs of Personal Care Services (PCS) Beneficiaries Effective 12/1/2016
 Assessing the Eating Needs of Personal Care Services (PCS) Beneficiaries Effective 12/1/2016 The Freedom to Succeed November 22,2016 Content Introduction Signs and Symptoms Caring for Individuals with
Assessing the Eating Needs of Personal Care Services (PCS) Beneficiaries Effective 12/1/2016 The Freedom to Succeed November 22,2016 Content Introduction Signs and Symptoms Caring for Individuals with
Chapter 19. Nutrition and Fluids. All items and derived items 2015, 2011 by Mosby, Inc., an imprint of Elsevier Inc. All rights reserved.
 Chapter 19 Nutrition and Fluids Nutrition Nutrition--processes involved in the ingestion, digestion, absorption & use of foods & fluids by the body. The person s diet affects physical & mental wellbeing
Chapter 19 Nutrition and Fluids Nutrition Nutrition--processes involved in the ingestion, digestion, absorption & use of foods & fluids by the body. The person s diet affects physical & mental wellbeing
OPTICS OPTimal nutrition by Informing and Capacitating family members of best nutrition practices OPTICS
 OPTICS OPTimal nutrition by Informing and Capacitating family members of best nutrition practices Educational Booklet for Families Version June 16 2014 Page 1 of 11 This information booklet was originally
OPTICS OPTimal nutrition by Informing and Capacitating family members of best nutrition practices Educational Booklet for Families Version June 16 2014 Page 1 of 11 This information booklet was originally
2: Symptoms and management
 2: Symptoms and management This section will help you to find out about the likely symptoms of motor neurone disease (MND) and how these can be managed. The following information is an extracted section
2: Symptoms and management This section will help you to find out about the likely symptoms of motor neurone disease (MND) and how these can be managed. The following information is an extracted section
Chapter 23. Nutrition Needs. Copyright 2019 by Elsevier, Inc. All rights reserved.
 Chapter 23 Nutrition Needs Copyright 2019 by Elsevier, Inc. All rights reserved. Lesson 23.1 Define the key terms and key abbreviations in this chapter. Explain the purpose and use of the MyPlate symbol.
Chapter 23 Nutrition Needs Copyright 2019 by Elsevier, Inc. All rights reserved. Lesson 23.1 Define the key terms and key abbreviations in this chapter. Explain the purpose and use of the MyPlate symbol.
Oral care & swallowing
 Oral care & swallowing Oral care is important as it has a role to play in preventing healthcare associated infections. Dental plaque and the oropharynx can become colonized by bacteria and a biofilm can
Oral care & swallowing Oral care is important as it has a role to play in preventing healthcare associated infections. Dental plaque and the oropharynx can become colonized by bacteria and a biofilm can
DIET, NUTRITION AND HEAD AND NECK CANCER TREATMENT
 DIET, NUTRITION AND HEAD AND NECK CANCER TREATMENT DIET, NUTRITION AND HEAD AND NECK CANCER TREATMENT HOW HEAD AND NECK CANCER MAY AFFECT NUTRITION Head and neck cancer may make it hard to eat and drink.
DIET, NUTRITION AND HEAD AND NECK CANCER TREATMENT DIET, NUTRITION AND HEAD AND NECK CANCER TREATMENT HOW HEAD AND NECK CANCER MAY AFFECT NUTRITION Head and neck cancer may make it hard to eat and drink.
Nutrition and Feeding
 Nutrition and Feeding Introduction Within Neuromuscular conditions there can be a range of issues with feeding and nutrition. This may vary with different diagnoses. Normal, healthy growth is measured
Nutrition and Feeding Introduction Within Neuromuscular conditions there can be a range of issues with feeding and nutrition. This may vary with different diagnoses. Normal, healthy growth is measured
OPTICS OPTimal nutrition by Informing and Capacitating family members of best nutrition practices OPTICS
 OPTICS OPTimal nutrition by Informing and Capacitating family members of best nutrition practices Educational Booklet for Families Version April 26 th 2016 Page 1 of 12 This information booklet was originally
OPTICS OPTimal nutrition by Informing and Capacitating family members of best nutrition practices Educational Booklet for Families Version April 26 th 2016 Page 1 of 12 This information booklet was originally
SWALLOWING DIFFICULTIES IN HD
 Nutrition, eating and swallowing needs, challenges and solutions Workshop SWALLOWING DIFFICULTIES IN HD Angela Nuzzi Speech and Language Pathologist (SLP) EHDN Language Coordinator - Italy The role of
Nutrition, eating and swallowing needs, challenges and solutions Workshop SWALLOWING DIFFICULTIES IN HD Angela Nuzzi Speech and Language Pathologist (SLP) EHDN Language Coordinator - Italy The role of
Information leaflet for patients and families. Huntington Disease (HD)
 Information leaflet for patients and families Huntington Disease (HD) Introduction Huntington disease, or Huntington Chorea, (HD) is a slowly progressive disorder of the brain in adults. HD is an inherited
Information leaflet for patients and families Huntington Disease (HD) Introduction Huntington disease, or Huntington Chorea, (HD) is a slowly progressive disorder of the brain in adults. HD is an inherited
Occupational therapy after stroke
 Call the Stroke Helpline: 0303 3033 100 or email: info@stroke.org.uk Occupational therapy after stroke This guide explains how occupational therapy can help your recovery and rehabilitation after a stroke.
Call the Stroke Helpline: 0303 3033 100 or email: info@stroke.org.uk Occupational therapy after stroke This guide explains how occupational therapy can help your recovery and rehabilitation after a stroke.
Video Fluoroscopic Swallowing Exam (VFSE)
 Scan for mobile link. Video Fluoroscopic Swallowing Exam (VFSE) A video fluoroscopic swallowing exam (VFSE) uses a form of real-time x-ray called fluoroscopy to evaluate a patient s ability to swallow
Scan for mobile link. Video Fluoroscopic Swallowing Exam (VFSE) A video fluoroscopic swallowing exam (VFSE) uses a form of real-time x-ray called fluoroscopy to evaluate a patient s ability to swallow
4. Eating and drinking
 4. Eating and drinking This checklist can be downloaded from www.sunderlandactionforhealth.co.uk. It is free to use for personal use and with people you support. There are several important aspects of
4. Eating and drinking This checklist can be downloaded from www.sunderlandactionforhealth.co.uk. It is free to use for personal use and with people you support. There are several important aspects of
Meals make sense An audit checklist to consider how far a Care Home is implementing quality care re the mealtime experience.
 Meals make sense An audit checklist to consider how far a Care Home is implementing quality care re the mealtime experience. Place a tick in one of the 3 boxes Yes, No, Partly in relation to your Care
Meals make sense An audit checklist to consider how far a Care Home is implementing quality care re the mealtime experience. Place a tick in one of the 3 boxes Yes, No, Partly in relation to your Care
Swallowing Awareness Day
 awareness for youth and adults INSIDE: Facts about eating and drinking checklist General information 9, 2011 Facts for youth and adults on swallowing issues Dysphagia is the medical term for any difficulty
awareness for youth and adults INSIDE: Facts about eating and drinking checklist General information 9, 2011 Facts for youth and adults on swallowing issues Dysphagia is the medical term for any difficulty
Swallowing difficulties
 7A Swallowing difficulties Information for people with or affected by motor neurone disease With MND, you may experience changes to the way you swallow. You may also experience problems with managing your
7A Swallowing difficulties Information for people with or affected by motor neurone disease With MND, you may experience changes to the way you swallow. You may also experience problems with managing your
Chapter 20. Assisting With Nutrition and Fluids
 Chapter 20 Assisting With Nutrition and Fluids Food and water: Are physical needs Basics of Nutrition Are necessary for life A poor diet and poor eating habits: Increase the risk for diseases and infection
Chapter 20 Assisting With Nutrition and Fluids Food and water: Are physical needs Basics of Nutrition Are necessary for life A poor diet and poor eating habits: Increase the risk for diseases and infection
EATING WELL AND CANCER
 EATING WELL AND CANCER 2 Why is it important for people with cancer to eat well? If the person you care for has cancer, it is more important than ever that they eat well. Unfortunately, it is often at
EATING WELL AND CANCER 2 Why is it important for people with cancer to eat well? If the person you care for has cancer, it is more important than ever that they eat well. Unfortunately, it is often at
The road to recovery. The support available to help you with your recovery after stroke
 The road to recovery The road to recovery The support available to help you with your recovery after stroke We re for life after stroke Need to talk? Call our confidential Stroke Helpline on 0303 3033
The road to recovery The road to recovery The support available to help you with your recovery after stroke We re for life after stroke Need to talk? Call our confidential Stroke Helpline on 0303 3033
Tobacco Cessation Toolkit
 You notice physical s, like moments of dizziness, sweating, hands trembling or a mild headache. When using tobacco, nicotine increases your heart rate (by about 10 20 beats per minute) and blood pressure.
You notice physical s, like moments of dizziness, sweating, hands trembling or a mild headache. When using tobacco, nicotine increases your heart rate (by about 10 20 beats per minute) and blood pressure.
Living Life with Persistent Pain. A guide to improving your quality of life, in spite of pain
 Living Life with Persistent Pain A guide to improving your quality of life, in spite of pain Contents What is Persistent Pain? 1 The Science Bit 2 Pain & Stress 3 Coping with Stress 4 The importance of
Living Life with Persistent Pain A guide to improving your quality of life, in spite of pain Contents What is Persistent Pain? 1 The Science Bit 2 Pain & Stress 3 Coping with Stress 4 The importance of
Nasogastric Tube Patient Passport
 Nutrition and Dietetics Department Nasogastric Tube Patient Passport Please bring this booklet with you for all tube changes Patient Information If you need this information in another format or language
Nutrition and Dietetics Department Nasogastric Tube Patient Passport Please bring this booklet with you for all tube changes Patient Information If you need this information in another format or language
EATING SAFELY AND TALKING ABOUT IT KIERA N BERGGREN, MA/CCC-SLP, MS 2018 FSHD CONNECT CONFERENCE
 EATING SAFELY AND TALKING ABOUT IT KIERA N BERGGREN, MA/CCC-SLP, MS 2018 FSHD CONNECT CONFERENCE DISCLOSURES I have no personal financial relationships with commercial interests relevant to this presentation
EATING SAFELY AND TALKING ABOUT IT KIERA N BERGGREN, MA/CCC-SLP, MS 2018 FSHD CONNECT CONFERENCE DISCLOSURES I have no personal financial relationships with commercial interests relevant to this presentation
Chapter 27 & 28. Key Terms. Digestive System. Fig. 27-1, p. 443 Also known as the Gastrointestinal System (GI system)
 Chapter 27 & 28 Nutrition & Fluids Key Terms Aspiration Dehydration Edema Dysphagia Gastrostomy tube Intravenous therapy (IV) Digestive System Fig. 27-1, p. 443 Also known as the Gastrointestinal System
Chapter 27 & 28 Nutrition & Fluids Key Terms Aspiration Dehydration Edema Dysphagia Gastrostomy tube Intravenous therapy (IV) Digestive System Fig. 27-1, p. 443 Also known as the Gastrointestinal System
Dementia Care A Practical Guide to Swallowing Problems
 Nutrition and Dietetics Dementia Care A Practical Guide to Swallowing Problems People with dementia can experience difficulties with chewing and swallowing as their condition progresses. This may affect
Nutrition and Dietetics Dementia Care A Practical Guide to Swallowing Problems People with dementia can experience difficulties with chewing and swallowing as their condition progresses. This may affect
Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing
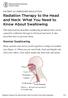 PATIENT & CAREGIVER EDUCATION Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing This information describes swallowing problems that can be caused by radiation therapy to the
PATIENT & CAREGIVER EDUCATION Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing This information describes swallowing problems that can be caused by radiation therapy to the
Patient and Family Resource Guide to ALS. Section 6. Nutritional Support
 Patient and Family Resource Guide to ALS Section 6 Nutritional Support 6 5550 W. Touhy Avenue, Skokie IL, 60077 847 679 3311 lesturnerals.org info@lesturnerals.org Nutritional Support Many factors can
Patient and Family Resource Guide to ALS Section 6 Nutritional Support 6 5550 W. Touhy Avenue, Skokie IL, 60077 847 679 3311 lesturnerals.org info@lesturnerals.org Nutritional Support Many factors can
E09 PEG. Expires end of March 2018 VITALITY.CO.UK
 VITALITY.CO.UK E09 PEG Expires end of March 2018 You can get more information and share your experiences at www.aboutmyhealth.org Tell us how useful you found this document at www.patientfeedback.org eidohealthcare.com
VITALITY.CO.UK E09 PEG Expires end of March 2018 You can get more information and share your experiences at www.aboutmyhealth.org Tell us how useful you found this document at www.patientfeedback.org eidohealthcare.com
Gastroscopy and dilatation/stent insertion
 Gastroscopy and dilatation/stent insertion GI Unit Patient Information Leaflet Introduction This leaflet is for patients who need dilatation of the oesophagus, which means stretching of the food pipe,
Gastroscopy and dilatation/stent insertion GI Unit Patient Information Leaflet Introduction This leaflet is for patients who need dilatation of the oesophagus, which means stretching of the food pipe,
Having a PEG tube inserted
 Having a PEG tube inserted This information leaflet is for patients who are having a PEG (Percutaneous Endoscopic Gastrostomy) tube inserted. It explains what is involved, what to expect and what significant
Having a PEG tube inserted This information leaflet is for patients who are having a PEG (Percutaneous Endoscopic Gastrostomy) tube inserted. It explains what is involved, what to expect and what significant
Advice for patients undergoing radiotherapy to the head and neck
 Advice for patients undergoing radiotherapy to the head and neck Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Advice for patients undergoing radiotherapy to the head and neck Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
NUTRITION CARE ALERTS
 APPENDIX 10 A NUTRITION CARE ALERTS and for Caregivers in Nursing Facilities or at Home Proper nutrition care is vital to the health and well-being of nursing facility residents and seniors living in their
APPENDIX 10 A NUTRITION CARE ALERTS and for Caregivers in Nursing Facilities or at Home Proper nutrition care is vital to the health and well-being of nursing facility residents and seniors living in their
Fatigue after stroke. What is post-stroke fatigue? Who is affected by post-stroke fatigue?
 Call the Stroke Helpline: 0303 3033 100 or email: info@stroke.org.uk Fatigue after stroke Fatigue affects half of all stroke survivors, but the signs of fatigue are not always obvious to other people and
Call the Stroke Helpline: 0303 3033 100 or email: info@stroke.org.uk Fatigue after stroke Fatigue affects half of all stroke survivors, but the signs of fatigue are not always obvious to other people and
whoah billy, that s no way to lift a heavy weight Stay healthy and happy at work with advice from the Chartered Society of Physiotherapy
 whoah billy, that s no way to lift a heavy weight yee-ow!! Stay healthy and happy at work with advice from the Chartered Society of Physiotherapy This leaflet has been compiled with the help of chartered
whoah billy, that s no way to lift a heavy weight yee-ow!! Stay healthy and happy at work with advice from the Chartered Society of Physiotherapy This leaflet has been compiled with the help of chartered
Role of Dining Services and Dietary Needs of the Resident, 2014
 Role of Dining Services and Dietary Needs of the Resident, 2014 It is the dining services role to provide quality meals and service to all residents that is as home-like as possible. This will be done
Role of Dining Services and Dietary Needs of the Resident, 2014 It is the dining services role to provide quality meals and service to all residents that is as home-like as possible. This will be done
SCOTTISH MUSCLE NETWORK DUCHENNE MUSCULAR DYSTROPHY TRANSITION SOME USEFUL THINGS TO KNOW ABOUT HEALTH AROUND ADOLESCENCE
 SCOTTISH MUSCLE NETWORK DUCHENNE MUSCULAR DYSTROPHY TRANSITION SOME USEFUL THINGS TO KNOW ABOUT HEALTH AROUND ADOLESCENCE 02 Changes in our lives can be stressful and leaving school and moving into the
SCOTTISH MUSCLE NETWORK DUCHENNE MUSCULAR DYSTROPHY TRANSITION SOME USEFUL THINGS TO KNOW ABOUT HEALTH AROUND ADOLESCENCE 02 Changes in our lives can be stressful and leaving school and moving into the
Dignity and Nutrition for Older People
 South Gloucestershire Community Health Services Dignity and Nutrition for Older People Lorraine Norris Nutrition and Dietetic Professional Lead South Gloucestershire Community Health November 9th 2011
South Gloucestershire Community Health Services Dignity and Nutrition for Older People Lorraine Norris Nutrition and Dietetic Professional Lead South Gloucestershire Community Health November 9th 2011
Radiotherapy to the face or neck (shell)
 Radiotherapy to the face or neck (shell) The name of your consultant is: The radiographer who explained the treatment to you is: You can contact us on: What is radiotherapy? Radiotherapy treats cancer
Radiotherapy to the face or neck (shell) The name of your consultant is: The radiographer who explained the treatment to you is: You can contact us on: What is radiotherapy? Radiotherapy treats cancer
Nutrition. A Guide. A guide to the nutrition of babies and children with liver disease
 A Guide A guide to the nutrition of babies and children with liver disease Why is nutrition so important?... 4 What is a nutritional assessment?... 5 Why do some children with liver disease have poor nutrition?...
A Guide A guide to the nutrition of babies and children with liver disease Why is nutrition so important?... 4 What is a nutritional assessment?... 5 Why do some children with liver disease have poor nutrition?...
Understanding your child s videofluoroscopic swallow study report
 Understanding your child s videofluoroscopic swallow study report This leaflet is given to you during your child s appointment in order to explain some of the words used by the speech and language therapist
Understanding your child s videofluoroscopic swallow study report This leaflet is given to you during your child s appointment in order to explain some of the words used by the speech and language therapist
Dysphagia Identification and Management
 Dysphagia Identification and Management Presented By Speech-Language Pathologist Developmental Disabilities Administration DC Department on Disability Services Training Objectives After this training session
Dysphagia Identification and Management Presented By Speech-Language Pathologist Developmental Disabilities Administration DC Department on Disability Services Training Objectives After this training session
Short-Term Side Effects from Head and Neck Radiation
 PATIENT EDUCATION patienteducation.osumc.edu Short-Term Side Effects from Head and Neck Radiation Side effects are problems caused by radiation therapy. These problems are different for each person and
PATIENT EDUCATION patienteducation.osumc.edu Short-Term Side Effects from Head and Neck Radiation Side effects are problems caused by radiation therapy. These problems are different for each person and
Information about Feeding Tubes
 Information about Feeding Tubes By Theresa Imperato, RN and Lorraine Danowski, RD What is a feeding tube? It is a small, flexible tube, about ¼ in diameter that is an alternative route for nourishment
Information about Feeding Tubes By Theresa Imperato, RN and Lorraine Danowski, RD What is a feeding tube? It is a small, flexible tube, about ¼ in diameter that is an alternative route for nourishment
Clinical Swallowing Exam
 Clinical Evaluation Template 1 Clinical Exam Name: ID/Medical record number: Date of exam: Referred by: Reason for referral: Medical diagnosis: Date of onset of diagnosis: Other relevant medical history/diagnoses/surgery
Clinical Evaluation Template 1 Clinical Exam Name: ID/Medical record number: Date of exam: Referred by: Reason for referral: Medical diagnosis: Date of onset of diagnosis: Other relevant medical history/diagnoses/surgery
RECOMMENDATIONS & UPDATES IN THE MANAGEMENT OF POST- STROKE DYSPHAGIA
 RECOMMENDATIONS & UPDATES IN THE MANAGEMENT OF POST- STROKE DYSPHAGIA Feeding in the Acute Stroke Period: - Early initiation of feeding is beneficial w/c decreases the risk of infections, improve survival
RECOMMENDATIONS & UPDATES IN THE MANAGEMENT OF POST- STROKE DYSPHAGIA Feeding in the Acute Stroke Period: - Early initiation of feeding is beneficial w/c decreases the risk of infections, improve survival
Eating and drinking with dementia
 Eating and drinking with dementia Information for patients, relatives and carers For more information, please contact: Department of Nutrition and Dietetics Scarborough Hospital Tel: 01723 342415 Woodlands
Eating and drinking with dementia Information for patients, relatives and carers For more information, please contact: Department of Nutrition and Dietetics Scarborough Hospital Tel: 01723 342415 Woodlands
Stay healthy and happy at work with advice from the Chartered Society of Physiotherapy
 Stay healthy and happy at work with advice from the Chartered Society of Physiotherapy Employment plays a big part in keeping you healthy just going out to work is good for you, both physically and mentally.
Stay healthy and happy at work with advice from the Chartered Society of Physiotherapy Employment plays a big part in keeping you healthy just going out to work is good for you, both physically and mentally.
Preventing Pressure Ulcers
 Patient information Preventing Pressure Ulcers i Important information and care guide for patients at risk of pressure ulcers. Reproduced with kind permission from Healthcare Improvement Scotland Golden
Patient information Preventing Pressure Ulcers i Important information and care guide for patients at risk of pressure ulcers. Reproduced with kind permission from Healthcare Improvement Scotland Golden
Dental Health E-presentation.
 Dental Health E-presentation www.healthycornwall.org.uk Learning Outcomes This short E-presentation has been developed to give you a basic understanding of the importance of good dental health and dental
Dental Health E-presentation www.healthycornwall.org.uk Learning Outcomes This short E-presentation has been developed to give you a basic understanding of the importance of good dental health and dental
Having a PEG tube inserted Information for patients and carers
 Sunderland Day Case Centre Endoscopy Having a PEG tube inserted Information for patients and carers www.medway.nhs.uk Checklist Things to remember before your procedure Read the booklet carefully. Fill
Sunderland Day Case Centre Endoscopy Having a PEG tube inserted Information for patients and carers www.medway.nhs.uk Checklist Things to remember before your procedure Read the booklet carefully. Fill
The first 6 weeks after gastric band/bypass surgery
 Patient information The first 6 weeks after gastric band/bypass surgery Eating and drinking In the first 4-6 weeks after the operation it is vital that you keep to the diet that we have advised in order
Patient information The first 6 weeks after gastric band/bypass surgery Eating and drinking In the first 4-6 weeks after the operation it is vital that you keep to the diet that we have advised in order
How Speech and Swallowing are Affected with ALS
 Patient Education How Speech and Swallowing are Affected with ALS This handout describes how ALS affects speech and swallowing. For speech issues it covers tips for listeners and speakers and what can
Patient Education How Speech and Swallowing are Affected with ALS This handout describes how ALS affects speech and swallowing. For speech issues it covers tips for listeners and speakers and what can
STAY NOURISHED. Be happy and healthy as you age
 STAY NOURISHED Be happy and healthy as you age As we age physical changes to our bodies occur which can affect the way we think and feel about food. These changes can prevent us from having access to a
STAY NOURISHED Be happy and healthy as you age As we age physical changes to our bodies occur which can affect the way we think and feel about food. These changes can prevent us from having access to a
Recovering at home. How will I feel when I get home? How should I look after my wound?
 How will I feel when I get home? Following your operation it is normal to have feelings of stress, anxiety or depression. Being affected emotionally is normal. It may help to talk about how you feel with
How will I feel when I get home? Following your operation it is normal to have feelings of stress, anxiety or depression. Being affected emotionally is normal. It may help to talk about how you feel with
The Children s Hospital, Oxford Sedation for clinical procedures Information for parents and carers
 The Children s Hospital, Oxford Sedation for clinical procedures Information for parents and carers What is sedation? Sedation can help your child by reducing anxiety before and during a clinical procedure,
The Children s Hospital, Oxford Sedation for clinical procedures Information for parents and carers What is sedation? Sedation can help your child by reducing anxiety before and during a clinical procedure,
INFORMATION FOR PATIENTS, CARERS AND FAMILIES. Coping with feelings of depression
 INFORMATION FOR PATIENTS, CARERS AND FAMILIES Coping with feelings of depression 1 Coping with feelings of depression There is no right or wrong way to feel when you or someone close to you has a terminal
INFORMATION FOR PATIENTS, CARERS AND FAMILIES Coping with feelings of depression 1 Coping with feelings of depression There is no right or wrong way to feel when you or someone close to you has a terminal
Speech and Language Therapy. Patient Information Leaflet Easy Read
 Speech and Language Therapy Patient Information Leaflet Easy Read This checklist can be downloaded from www.sunderlandactionforhealth.co.uk. It is free to use for personal use and with people you support.
Speech and Language Therapy Patient Information Leaflet Easy Read This checklist can be downloaded from www.sunderlandactionforhealth.co.uk. It is free to use for personal use and with people you support.
Nutrition Inspection Notebook (Updated April, 2011)
 Nutrition Inspection Notebook (Updated April, 2011) Publication code: HCR-0412-049 Name of Care Service: Address: Date of Inspection: Care Homes for Older People This Notebook is a tool to assist the Professional
Nutrition Inspection Notebook (Updated April, 2011) Publication code: HCR-0412-049 Name of Care Service: Address: Date of Inspection: Care Homes for Older People This Notebook is a tool to assist the Professional
Your anaesthetic for heart surgery
 Your anaesthetic for heart surgery Information for patients and carers First Edition 2018 www.rcoa.ac.uk/patientinfo This leaflet gives you information about your anaesthetic for adult heart (cardiac)
Your anaesthetic for heart surgery Information for patients and carers First Edition 2018 www.rcoa.ac.uk/patientinfo This leaflet gives you information about your anaesthetic for adult heart (cardiac)
How to look after your mouth. Cancer Services Information for patients
 How to look after your mouth Cancer Services Information for patients i Is my mouth at risk? There are many things that can affect your mouth. If you answer yes to any of the following, you may be at risk
How to look after your mouth Cancer Services Information for patients i Is my mouth at risk? There are many things that can affect your mouth. If you answer yes to any of the following, you may be at risk
Preventing delirium while in hospital Tips for family, whānau, and friends who are supporting an older person
 Preventing delirium while in hospital Tips for family, whānau, and friends who are supporting an older person This brochure shares some simple ways you can help our care staff to prevent delirium, recognize
Preventing delirium while in hospital Tips for family, whānau, and friends who are supporting an older person This brochure shares some simple ways you can help our care staff to prevent delirium, recognize
Tracheoesophageal Fistula and Esophageal Atresia
 Patient and Family Education Tracheoesophageal Fistula and Esophageal Atresia What is tracheoesophageal fistula? The word fistula means abnormal connection. Tracheoesophageal fistula (TEF) is a condition
Patient and Family Education Tracheoesophageal Fistula and Esophageal Atresia What is tracheoesophageal fistula? The word fistula means abnormal connection. Tracheoesophageal fistula (TEF) is a condition
Palliative Care Asking the questions that matter to me
 Palliative Care Asking the questions that matter to me THE PALLIATIVE HUB Adult This booklet has been developed by the Palliative Care Senior Nurses Network and adapted with permission from Palliative
Palliative Care Asking the questions that matter to me THE PALLIATIVE HUB Adult This booklet has been developed by the Palliative Care Senior Nurses Network and adapted with permission from Palliative
Bowel health and screening: carers guide. A booklet for carers of people who use easy read materials
 Bowel health and screening: carers guide A booklet for carers of people who use easy read materials Contents Page 3: About this booklet Page 4: What is the bowel? Page 5: Helping someone to have good bowel
Bowel health and screening: carers guide A booklet for carers of people who use easy read materials Contents Page 3: About this booklet Page 4: What is the bowel? Page 5: Helping someone to have good bowel
65+ YEARS OLD: KEEPING WELL WITH YOUR TYPE 2 DIABETES
 LIFESTYLE 65+ YEARS OLD: KEEPING WELL WITH YOUR TYPE 2 DIABETES WHY IS THIS LEAFLET FOR YOU? For many people, reaching the age of 65 and over can mean your life changes in many ways: You may have stoed
LIFESTYLE 65+ YEARS OLD: KEEPING WELL WITH YOUR TYPE 2 DIABETES WHY IS THIS LEAFLET FOR YOU? For many people, reaching the age of 65 and over can mean your life changes in many ways: You may have stoed
High dose (radical) radiotherapy to the lung or bronchus
 The Clatterbridge Cancer Centre NHS Foundation Trust High dose (radical) radiotherapy to the lung or bronchus Radiotherapy A guide for patients and carers Contents When radiotherapy is given... 1 Chemotherapy
The Clatterbridge Cancer Centre NHS Foundation Trust High dose (radical) radiotherapy to the lung or bronchus Radiotherapy A guide for patients and carers Contents When radiotherapy is given... 1 Chemotherapy
Enhanced Recovery Programme Liver surgery
 Enhanced Recovery Programme Liver surgery General Surgery Patient information leaflet Introduction When you are admitted to hospital for your surgery you will be taking part in an enhanced recovery programme.
Enhanced Recovery Programme Liver surgery General Surgery Patient information leaflet Introduction When you are admitted to hospital for your surgery you will be taking part in an enhanced recovery programme.
FACTSHEET F18 COPING WITH TIREDNESS
 COPING WITH TIREDNESS Many people with chest, heart and stroke conditions experience tiredness or fatigue. This factsheet explains some of the reasons why you might feel so tired. It also offers advice
COPING WITH TIREDNESS Many people with chest, heart and stroke conditions experience tiredness or fatigue. This factsheet explains some of the reasons why you might feel so tired. It also offers advice
Understanding Respiratory Illnesses
 Understanding Respiratory Illnesses Respiratory illnesses and the people you support Is a major cause of unplanned hospitalizations. Usually occur in fall and winter. It is important for you to Help people
Understanding Respiratory Illnesses Respiratory illnesses and the people you support Is a major cause of unplanned hospitalizations. Usually occur in fall and winter. It is important for you to Help people
Chapter 18 ECE 105 Feeding Toddlers and Young Children
 Chapter 18: Feeding Toddlers and Young Child ECE105 Profile of Toddlers and Preschoolers Toddlers (1-2 ½ year olds) are a challenge. They want to assert their independence but need and want limits. Toddlers
Chapter 18: Feeding Toddlers and Young Child ECE105 Profile of Toddlers and Preschoolers Toddlers (1-2 ½ year olds) are a challenge. They want to assert their independence but need and want limits. Toddlers
SAFETYNET LEARNING TOOLS
 SAFETYNET LEARNING TOOLS Topic: Respiratory Illness Use the materials in this document to help others learn more about respiratory illness. LEARNING TOOLS: 1. Understanding Respiratory Illness PowerPoint
SAFETYNET LEARNING TOOLS Topic: Respiratory Illness Use the materials in this document to help others learn more about respiratory illness. LEARNING TOOLS: 1. Understanding Respiratory Illness PowerPoint
Communication and Swallowing with PSP/CBD. Megan DePuy, MBA, MS, CCC-SLP Private Speech Pathologist
 Communication and Swallowing with PSP/CBD Megan DePuy, MBA, MS, CCC-SLP Private Speech Pathologist A Speech Therapist? Why? Swallowing (Dysphagia) Speech (Dysarthria, Dysphonia) Language (Aphasia) An Experienced
Communication and Swallowing with PSP/CBD Megan DePuy, MBA, MS, CCC-SLP Private Speech Pathologist A Speech Therapist? Why? Swallowing (Dysphagia) Speech (Dysarthria, Dysphonia) Language (Aphasia) An Experienced
Changes to your behaviour
 Life after stroke Changes to your behaviour Together we can conquer stroke Because there is so much to deal with after a stroke, it s normal for your behaviour to change in some way. In this booklet we
Life after stroke Changes to your behaviour Together we can conquer stroke Because there is so much to deal with after a stroke, it s normal for your behaviour to change in some way. In this booklet we
PEG Insertion. What is a PEG? What should I know before deciding? Consent form. On arrival to the Endoscopy Unit
 PEG Insertion What is a PEG? A PEG stands for Percutaneous Endoscopic Gastrostomy tube. It is a thin flexible feeding tube that passes through the skin of the abdomen and into the stomach. It allows liquid
PEG Insertion What is a PEG? A PEG stands for Percutaneous Endoscopic Gastrostomy tube. It is a thin flexible feeding tube that passes through the skin of the abdomen and into the stomach. It allows liquid
Tracheostomy. Hope Building Neurosurgery
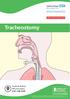 Tracheostomy Hope Building Neurosurgery 0161 206 5055 All Rights Reserved 2017. Document for issue as handout. Unique Identifier: CS36(17). Review date: November 2019 What is a tracheostomy? A tracheostomy
Tracheostomy Hope Building Neurosurgery 0161 206 5055 All Rights Reserved 2017. Document for issue as handout. Unique Identifier: CS36(17). Review date: November 2019 What is a tracheostomy? A tracheostomy
Cough Assist. Information for patients, families and carers Therapy Services
 Cough Assist Information for patients, families and carers Therapy Services PROUD TO MAKE A DIFFERENCE SHEFFIELD TEACHING HOSPITALS NHS FOUNDATION TRUST page 2 of 16 Table of contents Why do I need a Cough
Cough Assist Information for patients, families and carers Therapy Services PROUD TO MAKE A DIFFERENCE SHEFFIELD TEACHING HOSPITALS NHS FOUNDATION TRUST page 2 of 16 Table of contents Why do I need a Cough
Gastroscopy. GI Unit Patient Information Leaflet
 Gastroscopy GI Unit Patient Information Leaflet Introduction This leaflet is for people who are having a gastroscopy. It gives information on what a gastroscopy is, the benefits and risks of this and what
Gastroscopy GI Unit Patient Information Leaflet Introduction This leaflet is for people who are having a gastroscopy. It gives information on what a gastroscopy is, the benefits and risks of this and what
This section will help you to identify and manage some of the more difficult emotional responses you may feel after diagnosis.
 4: Emotional impact This section will help you to identify and manage some of the more difficult emotional responses you may feel after diagnosis. The following information is an extracted section from
4: Emotional impact This section will help you to identify and manage some of the more difficult emotional responses you may feel after diagnosis. The following information is an extracted section from
What to expect in the last few days of life
 What to expect in the last few days of life Contents Introduction... 3 What are the signs that someone is close to death?... 4 How long does death take?... 7 What can I do to help?... 7 Can friends and
What to expect in the last few days of life Contents Introduction... 3 What are the signs that someone is close to death?... 4 How long does death take?... 7 What can I do to help?... 7 Can friends and
Changing Patterns. healthyfutures.nhs.uk/llb
 Changing Patterns healthyfutures.nhs.uk/llb How do our eating habits develop? When we eat food that tastes good and gives us pleasure, endorphins (we like to think of them as happy chemicals) fill our
Changing Patterns healthyfutures.nhs.uk/llb How do our eating habits develop? When we eat food that tastes good and gives us pleasure, endorphins (we like to think of them as happy chemicals) fill our
Tracheostomy. Information for patients and relatives
 Tracheostomy Information for patients and relatives page 2 What is a tracheostomy? A tracheostomy is a small hole (stoma) made at the front of the neck, which goes into the trachea (windpipe). A tube called
Tracheostomy Information for patients and relatives page 2 What is a tracheostomy? A tracheostomy is a small hole (stoma) made at the front of the neck, which goes into the trachea (windpipe). A tube called
Session 15: Mindful Eating, Mindful Movement
 Session 15: Mindful Eating, Mindful Movement Are there times when you realize that you are still eating and simply haven t noticed that you are not even hungry anymore? Do you ever get to the end of a
Session 15: Mindful Eating, Mindful Movement Are there times when you realize that you are still eating and simply haven t noticed that you are not even hungry anymore? Do you ever get to the end of a
Eating, drinking and swallowing. A guide for carers of people living with a dementia
 Eating, drinking and swallowing A guide for carers of people living with a dementia When a person is living with a dementia they may experience difficulties with eating and drinking. As dementia progresses,
Eating, drinking and swallowing A guide for carers of people living with a dementia When a person is living with a dementia they may experience difficulties with eating and drinking. As dementia progresses,
Barium swallow for adults
 Barium swallow for adults Radiology Department Patient information leaflet This leaflet provides you with information about having a barium swallow. It explains what is involved and who you will meet.
Barium swallow for adults Radiology Department Patient information leaflet This leaflet provides you with information about having a barium swallow. It explains what is involved and who you will meet.
Radiotherapy to one side of the mouth and neck
 Clinical Oncology Radiotherapy to one side of the mouth and neck Consent information for patients Radiotherapy may be given on its own or with chemotherapy (separate information will be given about chemotherapy).
Clinical Oncology Radiotherapy to one side of the mouth and neck Consent information for patients Radiotherapy may be given on its own or with chemotherapy (separate information will be given about chemotherapy).
