Hospice Journey. A guide of signs, symptoms and caregiving
|
|
|
- Ira Skinner
- 6 years ago
- Views:
Transcription
1 Hospice Journey A guide of signs, symptoms and caregiving 1
2 This book is a guide to help you through the dying journey a natural part of life. A variety of changes can be seen as a body prepares for death. These changes usually begin in the final 1 to 3 months prior to death. None, one or all of the following signs may be present on your journey. You may see a slow or rapid progression of these signs as the body prepares for death. Just as we are all unique in how we live; we are also unique in how we die. 2
3 Hospice Journey A guide of signs, symptoms and caregiving Table of contents Pain... 4 Nutrition and dehydration... 6 Constipation... 8 Skin care... 9 Seizure precautions Physical changes Withdrawal Signs of death Preparing for when someone dies Notes
4 Pain control When people say they are having pain, it generally means they are hurting somewhere in their body. Pain can usually be controlled very well by medications. The person may have side effects such as drowsiness or nausea during the first few days of a new pain medication or an increased dose. But, most side effects usually pass in a few days. Constipation is common with the use of pain medication. See the constipation section of this book to help prevent this side effect. Medications can also be given to prevent nausea and vomiting. Non-verbal signs of pain 1. Moaning 2. Grimacing 3. Crying 4. Restlessness 5. Withdrawal 6. Weakness 7. Skin pale in color 8. Low or high blood pressure 9. Slow or fast heart rate 10. Problems breathing 11. Excessive sweating 12. Guarding, lack of mobility Verbal signs of pain Rank your pain on a scale of 0 10, with 0 being no pain and 10 being the worst pain you can imagine. 4
5 What you can do If there is pain most of the day, medication scheduled around the clock is more helpful than taking it only as needed. Try to stay on top of the pain. Don t wait until the pain gets really bad. Take your pain medicine when pain starts. Take your pain medication a half-hour before activities if activity makes pain worse. If you are having pain, relax and take deep breaths. When you are relaxed your muscles are not tense and pain medication will work better. Change your position, listen to relaxing music or dim the lights. Heat or cold may help. Only apply heat or cold for 20 minutes at a time. Allow at least 20 minutes between applications. Never apply ice or heat directly on the skin. Never fall asleep with a heating pad on. At times, the pain medication dose and/or frequency may need to be increased. If your pain medicine doesn t work as well as it used to talk to your nurse about what you can do for comfort. Use assistive devices as needed such as a walker, wheelchair, etc. 5
6 Nutrition and dehydration Nutrition is a big part of our lives. Our culture places a lot of importance on meals and the need for nutrition to heal and become stronger. Often feeding and preparing meals for a loved one are ways of showing love, concern and caring. One of the hardest things for the caregiver to accept is when the dying person no longer eats or drinks enough to stay alive. But, as the body changes, not wanting to eat or drink is a natural response. Food may not taste as good. Liquids may be preferred. It is common for hard to digest foods such as meats to be the first foods the person does not want. Next, the person may not want to eat vegetables. People who are terminally ill often are not hungry. Those who do become hungry usually only need small amounts of food or fluid to satisfy their hunger. Changes that happen with dehydration may produce a natural analgesic (pain relief) effect in the final days of life. Dehydration also causes: Less urine output or less need to use a bed pan, urinal or commode or fewer episodes of incontinence Fewer secretions in the lungs which may relieve coughing and congestion Less swelling which may decrease pressure symptoms The mouth to be dry this can be controlled with frequent oral care 6
7 What you can do Allow your loved one to direct their intake of food. Don t force food or fluid intake. It is a natural response to not want to eat or drink as the body prepares to die and weight loss can be expected. You may wish to try nutritional supplements. Offer 4 to 6 small meals or snacks throughout the day. More frequent, small meals may be more appealing than 3 large meals. Cool, bland or soft foods may be best. Change the times of meals to when the person is pain free and has the most energy. This is often the morning or mid-afternoon. Offer pain and/or nausea medicine one hour before mealtime. Cups with lids such as travel mugs or children s sippy cups allow the weak person to drink without worry of spilling. Provide frequent mouth cares. As the body becomes dehydrated, the mouth will get dry. Offer ice chips, use artificial saliva and moisturizer for the lips. Toothette swabs are also helpful in keeping the mouth moist. IV fluids are not routinely used by Hospice when a person begins to decline or is not drinking fluids. IV fluids can overload the body and cause more discomfort. Fever can occur as the body becomes dehydrated. First try removing extra blankets and use a lighter covering such as a sheet. Fever can be checked by placing a thermometer in the mouth or under the arm. A cool washcloth to the forehead or a sponge bath can offer comfort. If the fever still remains, medications may be given. 7
8 Constipation Constipation is common when a person is on pain medications. Usually the following interventions will be started at the same time as a pain medication. Besides pain medications, less activity or movement and less food and drink will also tend toward constipation. Nausea, vomiting and more pain may be felt when you are constipated. What you can do Try to increase fiber intake. Eat more fruits, vegetables and grains. Drink fluids as tolerated. Consider drinking a cup of a stimulant such as coffee or one-half to one cup of warm prune juice. Try taking a stool softener and/or stimulant. Be more active if you are able. 8
9 Skin care Good skin care can help make the dying person more comfortable. This becomes more important when your loved one has to stay in bed, eats and drinks less or is no longer able to control bladder or bowel function (incontinent). What you can do Daily personal care and hygiene. Encourage daily movement and activities as tolerated, even simple motion exercises to the arms and legs. Prevent rubbing and friction injuries. Use skin barrier creams or ointments. Apply liberally. There is no need to remove all the skin barrier cream or ointment every time. Use mineral oil to make removal of cream or ointment easier. Protective barrier creams or ointments may prevent fungal or yeast infections. Reposition the person every 2 hours for comfort. Encourage high protein, high calorie foods (as tolerated and desired). Pressure relief devices can be used for heels and elbows. Keep skin moisturized with a lotion of choice. Special padding or cushions can be used for the bed or chair. Tell your hospice nurse if any skin irritation or breakdown occurs. 9
10 Seizure precautions Take your medication to prevent or treat seizures as instructed by your doctor and hospice nurse. Seizures are rarely a severe threat but can be when a seizure is immediately followed by another and another. You may feel a warning sensation (aura) before a seizure. This will alert you that a seizure is about to happen. Confusion, disorientation and sleepiness often follow a seizure. When a person begins to have feelings of an aura or starts to seize, have the person lie down. Stay away from areas that would result in injury until the seizure stops. If they are in bed, pad side rails with a blanket to prevent injury. Do not try to restrain the person when a seizure happens. Position the person on their side to allow drainage of secretions and to keep the airway open. Do not put anything in the person s mouth. Call the hospice nurse for more instruction and help. 10
11 Physical changes The last 1 to 2 weeks of life During this time you will see many physical changes. You may see some or all of these changes: The heart rate may increase or decrease from the normal heart rate. This is the body s way of conserving energy. As the heart gets weaker, it won t pump as strongly as before. The blood pressure may drop. Body temperature may go back and forth between hot and cold. The skin may be clammy. The person may sweat more. The skin may turn a bluish or purple color (mottling). This may be seen first in the nailbeds, legs and arms. Breathing patterns may change as the body tries to conserve energy. The dying person may breathe faster or slower than usual. The depth of breaths may decrease and become more shallow. An irregular breathing pattern may be seen. Pauses in breathing (apnea) may occur. These pauses may last from a few seconds up to a minute. Congestion or a rattily sound may be heard when the dying person breaths. The cough is usually weak and does not always clear this congestion. Often congestion can be helped by turning the person on one side or the other. Little to no intake of food and fluids can be expected. Because the dying person is taking in fewer liquids there is less urine output. He or she may be incontinent of bladder or bowel. Confusion or disorientation may occur or be increased. They may see things and/or people that others do not see; and speak to people who are not there. The dying person may become unresponsive sometime before death. The person may have a glassy look in their eyes or they may shed tears. 11
12 What you can do Keep room quiet and peaceful. Put on and remove blankets as body temperature changes occur. Keep skin dry and clean. Accept help with bathing your loved one in bed. Moisten lips with lip balm. Talk to your loved one. Sit and hold their hand. Touch and hearing are the final senses to go. Consider getting a hospital bed so the head of the bed can be raised to ease breathing. Position your loved one so there is less congestion or rattily breathing. Medications may help with congestion. Continue to give medications as directed to help with pain, restlessness or shortness of breath. Use disposable diapers or disposable pads for incontinence to protect linen. Continue with oral cares. Swab mouth with a toothette moistened with water. Being there is one of the most comforting things you can do. 12
13 Withdrawal As a person accepts that they are dying, they may start to withdraw. They may lose interest in favorite activities, friends, and family. They may spend more time sleeping. While sleeping, a dying person is often reviewing their life. Caregivers and family may see a dying person working with their hands and arms in the air or picking at blankets while they are sleeping. At times, the dying person may also talk about leaving or going home. They may talk about deceased family members or friends. A dying person may become agitated and restless. What you can do Talk to the dying person. They may not be able to respond but they can hear you. Hold their hand, give a massage. Touch can be comforting. Keep the environment relaxed. Consider medications to help with anxiety or treat the underlying cause such as pain or shortness of breath. Encourage activities or offer distractions. Welcome visitors. But also be aware your loved one may not tolerate long visits or many visits in one day. Be honest with visitors. Ask them to limit visit time or tell them your loved one does not want visitors today. Help your loved one resolve any issues. Disorientation and confusion may occur before a person dies. 13
14 Signs of death may include Breathing cannot be seen or heard No heartbeat Loss of bladder or bowel control No response to your voice or touch Eyelids slightly open Eyes fixed on a certain spot Jaw relaxed and mouth slightly open What to do at the time of death Call Hospice. Do not call 911 or the ambulance. The hospice staff will help you confirm that the person has died. They will call the funeral home and the doctor. Although this may sound frightening, the hospice team s goal is to prepare you for what will happen. Your physical and emotional well-being is important to us. 14
15 Preparing for when someone dies This checklist will help you keep track of what needs to be done when someone dies. Not all of the items will be needed by everyone. It will be helpful to check off items as they are done. Look into items marked with an asterisk (*) before the death. Reminder: Most bank accounts and computers will be protected by passwords and pin numbers. Write this information down in advance. At the Time of Death Notify Hospice. They will contact the doctor and funeral home. Notify immediate family and close friends. Within Hours of Death Notify the Power of Attorney (POA). *Address organ, eye, or tissue donation as needed. *Find and review deceased s funeral and burial wishes. *Arrange care for children or other dependents. *Arrange care for pets. In the Next Few Days Notify family members and friends. *Make arrangements with funeral home (cremation, burial, funeral and/or memorial services) *Prepare and arrange for obituary. Have post office hold or forward mail. Cancel or rearrange home deliveries. Arrange for care or disposal of perishable property (food, plants, etc.) (Continued on next page) 15
16 Preparing for when someone dies (continued) After the Funeral Get death certificates (at least 6 copies for bank accounts and insurance policies). Keep records of all payments for funeral and other expenses. Tell Social Security and other agencies as needed. *Locate safe deposit box(es). Contact bank for safe deposit box procedures. *Locate important papers and documents. Some of the items you may need include: Birth and Marriage certificates Social Security Card for dependent children, spouse and deceased Recent federal tax returns Military records, discharge certificates Wills, codicils, and trusts Bank accounts, stocks, bonds, and real estate records Life insurance policies Investigate *Social Security Benefits (800) or *Life insurance *Veteran s burial allowance and benefits *Union or fraternal organization death benefits *Employee benefits including: vacation pay, death benefits, retirement plans, deferred compensation, final wages, and medical reimbursements *Refunds on insurance or canceled subscriptions *IRA accounts *Business, partnership and investment arrangements 16
17 As Needed Meet with attorney about estate. Meet with CPA for tax and accounting matters. Meet with life insurance agent to collect benefits or consider options. Deal with fire, theft, liability and auto insurance on deceased s property. Determine value of assets. Review credit cards and charge accounts, cancel if needed. Do not pay any of the deceased s debts until the attorney discusses this with the family. If there is a trust involved, arrange for any allocations and transfers. Arrange for final income tax return and estate tax return as needed. 17
18 18 Notes:
19 Notes: 19
20 Copyright 2017 Sanford. All rights reserved. The information provided is for educational purposes only, is not to be used as the basis for medical treatment, and is not a substitute for professional medical advice /17
Physical/Emotional Symptoms and Appropriate Comfort Measures
 Physical/Emotional Symptoms and Appropriate Comfort Measures A. Diminishing Appetite Page 2 B. Decreased Socialization Page 2 C. Sleeping Page 2 E. Changes in Pain Level Page 3 D. Incontinence Page 3 F.
Physical/Emotional Symptoms and Appropriate Comfort Measures A. Diminishing Appetite Page 2 B. Decreased Socialization Page 2 C. Sleeping Page 2 E. Changes in Pain Level Page 3 D. Incontinence Page 3 F.
Palliative Care Victoria The Process of Dying Page 1. The Process of Dying. What to expect and how to help
 Palliative Care Victoria The Process of Dying Page 1 The Process of Dying What to expect and how to help Palliative Care Victoria The Process of Dying Page 2 About dying Dying is a natural part of life.
Palliative Care Victoria The Process of Dying Page 1 The Process of Dying What to expect and how to help Palliative Care Victoria The Process of Dying Page 2 About dying Dying is a natural part of life.
ALONG THE FINAL JOURNEY
 ALONG THE FINAL JOURNEY A Guide for families and caregivers TABLE OF CONTENTS STARTING THE JOURNEY...2 ALONG THE JOURNEY... 3 Physical/Emotional Symptoms and Appropriate Comfort Measures Diminishing Appetite...
ALONG THE FINAL JOURNEY A Guide for families and caregivers TABLE OF CONTENTS STARTING THE JOURNEY...2 ALONG THE JOURNEY... 3 Physical/Emotional Symptoms and Appropriate Comfort Measures Diminishing Appetite...
Preparing for Approaching Death
 Preparing for Approaching Death Old Colony Hospice created this guide for our hospice family and caregivers by revising and adapting the following journal article: Hospice Techniques: Preparing for the
Preparing for Approaching Death Old Colony Hospice created this guide for our hospice family and caregivers by revising and adapting the following journal article: Hospice Techniques: Preparing for the
Preparing for the Death of a Loved One. Information for Patients & Visitors
 Preparing for the Death of a Loved One Information for Patients & Visitors This booklet is provided to help you know what to expect when your loved one is dying. It may help you to respond in ways that
Preparing for the Death of a Loved One Information for Patients & Visitors This booklet is provided to help you know what to expect when your loved one is dying. It may help you to respond in ways that
Precious Moments. Giving comfort and support when someone you love is dying.
 Precious Moments Giving comfort and support when someone you love is dying www.stjoes.ca When someone you love is dying When someone you love is dying, you may want to know how you can provide comfort
Precious Moments Giving comfort and support when someone you love is dying www.stjoes.ca When someone you love is dying When someone you love is dying, you may want to know how you can provide comfort
What to expect in the last days and hours of life in the Intensive Care Unit (ICU)
 What to expect in the last days and hours of life in the Intensive Care Unit (ICU) Information for patients and caregivers Please visit the UHN Patient Education website for more health information: www.uhnpatienteducation.ca
What to expect in the last days and hours of life in the Intensive Care Unit (ICU) Information for patients and caregivers Please visit the UHN Patient Education website for more health information: www.uhnpatienteducation.ca
Coping with dying. Information for families and carers
 Coping with dying Information for families and carers This leaflet describes some of the physical changes that happen to people as they start to die. It also covers what will happen immediately following
Coping with dying Information for families and carers This leaflet describes some of the physical changes that happen to people as they start to die. It also covers what will happen immediately following
What to expect in the last few days of life
 What to expect in the last few days of life Contents Introduction... 3 What are the signs that someone is close to death?... 4 How long does death take?... 6 What can I do to help?... 7 Can friends and
What to expect in the last few days of life Contents Introduction... 3 What are the signs that someone is close to death?... 4 How long does death take?... 6 What can I do to help?... 7 Can friends and
What to expect in the last few days of life
 What to expect in the last few days of life Contents Introduction... 3 What are the signs that someone is close to death?... 4 How long does death take?... 7 What can I do to help?... 7 Can friends and
What to expect in the last few days of life Contents Introduction... 3 What are the signs that someone is close to death?... 4 How long does death take?... 7 What can I do to help?... 7 Can friends and
Preparing for Approaching Death By North Central Florida Hospice, Inc.
 Preparing for Approaching Death By North Central Florida Hospice, Inc. When a person enters the final stage of the dying process, two different dynamics are at work which are closely interrelated and interdependent.
Preparing for Approaching Death By North Central Florida Hospice, Inc. When a person enters the final stage of the dying process, two different dynamics are at work which are closely interrelated and interdependent.
Tobacco Cessation Toolkit
 You notice physical s, like moments of dizziness, sweating, hands trembling or a mild headache. When using tobacco, nicotine increases your heart rate (by about 10 20 beats per minute) and blood pressure.
You notice physical s, like moments of dizziness, sweating, hands trembling or a mild headache. When using tobacco, nicotine increases your heart rate (by about 10 20 beats per minute) and blood pressure.
S A M P L E. Is Near. When Death. Logo A CAREGIVER S GUIDE
 When Death Is Near A CAREGIVER S GUIDE Logo Updated 2019. 2008 by Hospice of Santa Cruz County. This booklet (published as When Death is Near and When the Time Comes) was created by Hospice of Santa Cruz
When Death Is Near A CAREGIVER S GUIDE Logo Updated 2019. 2008 by Hospice of Santa Cruz County. This booklet (published as When Death is Near and When the Time Comes) was created by Hospice of Santa Cruz
Preparing for Death. A guide for families and caregivers as death approaches PALLIATIVE & END OF LIFE
 PALLIATIVE & END OF LIFE Preparing for Death A guide for families and caregivers as death approaches In this booklet you will learn about: Things to consider when a loved one is seriously ill Checklist
PALLIATIVE & END OF LIFE Preparing for Death A guide for families and caregivers as death approaches In this booklet you will learn about: Things to consider when a loved one is seriously ill Checklist
CHEMOTHERAPY. What should I expect?
 CHEMOTHERAPY What should I expect? WHAT IS CHEMOTHERAPY? Chemotherapy is treatment that uses drugs to stop the growth of cancer cells, either by killing the cells or by stopping them from dividing. Chemotherapy
CHEMOTHERAPY What should I expect? WHAT IS CHEMOTHERAPY? Chemotherapy is treatment that uses drugs to stop the growth of cancer cells, either by killing the cells or by stopping them from dividing. Chemotherapy
Delirium: Information for Patients and Families
 health information Delirium: Information for Patients and Families 605837 Alberta Health Services, (2016/11) Resources Delirium in the Older Person Family Guide: search delirium at viha.ca Go to myhealth.alberta.ca
health information Delirium: Information for Patients and Families 605837 Alberta Health Services, (2016/11) Resources Delirium in the Older Person Family Guide: search delirium at viha.ca Go to myhealth.alberta.ca
Ileal Conduit Diversion Surgery
 Here are some words and pictures to help you understand this surgery: Bladder: the bladder stores urine that is made by the kidneys Bowels: the bowels are the parts of the body that digest food and fluids.
Here are some words and pictures to help you understand this surgery: Bladder: the bladder stores urine that is made by the kidneys Bowels: the bowels are the parts of the body that digest food and fluids.
When Someone Close To You Is Dying
 Remember that preparing for a death can be difficult. We hope the information provided in this booklet may reduce the amount of stress you feel by giving you some information about what to expect. While
Remember that preparing for a death can be difficult. We hope the information provided in this booklet may reduce the amount of stress you feel by giving you some information about what to expect. While
When Someone Close To You Is Dying
 Remember that preparing for a death can be difficult We hope the information provided in this booklet may reduce the amount of stress you feel by giving you some information about what to expect While
Remember that preparing for a death can be difficult We hope the information provided in this booklet may reduce the amount of stress you feel by giving you some information about what to expect While
Lenvatinib (Lenvima ) ( len-va-ti-nib )
 Lenvatinib (Lenvima ) ( len-va-ti-nib ) How drug is given: By mouth Purpose: To treat thyroid cancer or other cancers How to take this drug This medicine can be taken with or without food. Take each dose
Lenvatinib (Lenvima ) ( len-va-ti-nib ) How drug is given: By mouth Purpose: To treat thyroid cancer or other cancers How to take this drug This medicine can be taken with or without food. Take each dose
H2O to Go! Hydration. It s easier than you think to get dehydrated. No water, no go...
 H2O to Go! Hydration You ve probably heard those narrators on the National Geographic specials say things like, Water gives life, or, Without water there could be no life. They may be overly dramatic,
H2O to Go! Hydration You ve probably heard those narrators on the National Geographic specials say things like, Water gives life, or, Without water there could be no life. They may be overly dramatic,
Managing Other Medical Conditions
 Managing Other Medical Conditions When Dementia is Part of the Picture Terms You Will NEED to Know - Advanced directives - Living Will - DNR orders - Durable HC-POA - Palliative care - Hospice care - Comfort
Managing Other Medical Conditions When Dementia is Part of the Picture Terms You Will NEED to Know - Advanced directives - Living Will - DNR orders - Durable HC-POA - Palliative care - Hospice care - Comfort
General Symptoms. Cold Weather Symptoms TG-272
 General Symptoms Cold Weather Symptoms Cold weather injuries can range from mild chapped skin to life-threatening hypothermia. To avoid cold weather injuries, you must be prepared. Being prepared means
General Symptoms Cold Weather Symptoms Cold weather injuries can range from mild chapped skin to life-threatening hypothermia. To avoid cold weather injuries, you must be prepared. Being prepared means
S A M P L E. Your Pain. Managing. Logo A GUIDE TO PAIN MEDICATION USE
 Managing Your Pain A GUIDE TO PAIN MEDICATION USE Logo Revised 2019. 2015 by Quality of Life Publishing Co. All rights reserved. No part of this booklet may be reproduced without prior permission of the
Managing Your Pain A GUIDE TO PAIN MEDICATION USE Logo Revised 2019. 2015 by Quality of Life Publishing Co. All rights reserved. No part of this booklet may be reproduced without prior permission of the
A Guide to Help You Reduce and Stop Using Tobacco
 Let s Talk Tobacco A Guide to Help You Reduce and Stop Using Tobacco Congratulations for taking this first step towards a healthier you! 1-866-710-QUIT (7848) albertaquits.ca It can be hard to stop using
Let s Talk Tobacco A Guide to Help You Reduce and Stop Using Tobacco Congratulations for taking this first step towards a healthier you! 1-866-710-QUIT (7848) albertaquits.ca It can be hard to stop using
POST-OP PAIN MANAGEMENT
 POST-OP PAIN MANAGEMENT You re Part of the Team Pain Management After Surgery Having a procedure or surgery to address a health issue can result in post-op (postoperative) pain. This pain can and should
POST-OP PAIN MANAGEMENT You re Part of the Team Pain Management After Surgery Having a procedure or surgery to address a health issue can result in post-op (postoperative) pain. This pain can and should
HOW TOBACCO AFFECTS ME
 HOW TOBACCO AFFECTS ME 1. 2. 3. 4. 5. 1. 2. 3. 4. 5 Ways I Notice How Tobacco Affects My Health or Body 1. 2. 3. 4. 5. 5 Reasons Why I use Tobacco 5. 5 Reasons Why I want to be Tobacco- Free WHY I WANT
HOW TOBACCO AFFECTS ME 1. 2. 3. 4. 5. 1. 2. 3. 4. 5 Ways I Notice How Tobacco Affects My Health or Body 1. 2. 3. 4. 5. 5 Reasons Why I use Tobacco 5. 5 Reasons Why I want to be Tobacco- Free WHY I WANT
A Caregiver s Guide: Congestive Heart Failure
 A Caregiver s Guide: Congestive Heart Failure This is a guide for family members, friends and other caregivers who are supporting someone who has congestive heart failure (CHF). This is a guide for family
A Caregiver s Guide: Congestive Heart Failure This is a guide for family members, friends and other caregivers who are supporting someone who has congestive heart failure (CHF). This is a guide for family
Preventing delirium while in hospital Tips for family, whānau, and friends who are supporting an older person
 Preventing delirium while in hospital Tips for family, whānau, and friends who are supporting an older person This brochure shares some simple ways you can help our care staff to prevent delirium, recognize
Preventing delirium while in hospital Tips for family, whānau, and friends who are supporting an older person This brochure shares some simple ways you can help our care staff to prevent delirium, recognize
SAFETYNET LEARNING TOOLS
 SAFETYNET LEARNING TOOLS Topic: Urinary Tract Infection Use the materials in this document to help others learn more about urinary tract infection. LEARNING TOOLS: 1. How to Say it Guide 2. Recognizing
SAFETYNET LEARNING TOOLS Topic: Urinary Tract Infection Use the materials in this document to help others learn more about urinary tract infection. LEARNING TOOLS: 1. How to Say it Guide 2. Recognizing
Pressure ulcers can develop in a relatively short time, therefore it is important to prevent them or notice and recognise early signs of damage.
 Preventing Pressure Damage A Guide for Patients and Carers What is pressure damage? A pressure ulcer, (previously often referred to as a bed sore or pressure sore ) is a localised area of damage to the
Preventing Pressure Damage A Guide for Patients and Carers What is pressure damage? A pressure ulcer, (previously often referred to as a bed sore or pressure sore ) is a localised area of damage to the
Your Grief and Loss. Support for Loved Ones
 Your Grief and Loss Support for Loved Ones Introduction A message from our caring staff The staff and Bereavement Care Team of Huntsville Hospital Health System extend our deepest sympathies to you and
Your Grief and Loss Support for Loved Ones Introduction A message from our caring staff The staff and Bereavement Care Team of Huntsville Hospital Health System extend our deepest sympathies to you and
INFORMATION FOR PATIENTS, CARERS AND FAMILIES. Coping with dying
 INFORMATION FOR PATIENTS, CARERS AND FAMILIES Coping with dying This leaflet describes some of the physical changes that happen to people as they start to die. It anticipates some of the questions you
INFORMATION FOR PATIENTS, CARERS AND FAMILIES Coping with dying This leaflet describes some of the physical changes that happen to people as they start to die. It anticipates some of the questions you
GASTRECTOMY. Date of Surgery. Please bring this booklet the day of your surgery. QHC#34
 GASTRECTOMY Date of Surgery Please bring this booklet the day of your surgery. QHC#34 What is a Gastrectomy? A Gastrectomy is the surgical removal of all or part of the stomach. The stomach is the digestion
GASTRECTOMY Date of Surgery Please bring this booklet the day of your surgery. QHC#34 What is a Gastrectomy? A Gastrectomy is the surgical removal of all or part of the stomach. The stomach is the digestion
Dr. Nuelle Knee Replacement: Discharge Care Instructions
 Dr. Nuelle Knee Replacement: Discharge Care Instructions Your Recovery Thank you for allowing us to help you with your knee replacement surgery. We hope that you had a good stay with us. These discharge
Dr. Nuelle Knee Replacement: Discharge Care Instructions Your Recovery Thank you for allowing us to help you with your knee replacement surgery. We hope that you had a good stay with us. These discharge
risk factors for falling
 Resource # 10 Page 1 of 8 1. Dizziness- What Can Cause Dizziness? Not eating regularly Change in body position (e.g. from sitting to standing) Low blood pressure High blood pressure Medication side effects
Resource # 10 Page 1 of 8 1. Dizziness- What Can Cause Dizziness? Not eating regularly Change in body position (e.g. from sitting to standing) Low blood pressure High blood pressure Medication side effects
Ibrutinib (Imbruvica )
 Ibrutinib (Imbruvica ) ( eye BROO ti nib ) How drug is given: by mouth Purpose: to stop the growth of cancer cells in lymphoma and other cancers How to take the drug Take each dose at the same time every
Ibrutinib (Imbruvica ) ( eye BROO ti nib ) How drug is given: by mouth Purpose: to stop the growth of cancer cells in lymphoma and other cancers How to take the drug Take each dose at the same time every
Trastuzumab (Herceptin )
 Trastuzumab (Herceptin ) About This Drug Trastuzumab is used to treat cancer. It is given in the vein (IV) Possible Side Effects Bone marrow depression. This is a decrease in the number of white blood
Trastuzumab (Herceptin ) About This Drug Trastuzumab is used to treat cancer. It is given in the vein (IV) Possible Side Effects Bone marrow depression. This is a decrease in the number of white blood
ANESTHESIA. Planning Your Childbirth: Pain Relief During Labor and Delivery EACH WOMAN S LABOR IS
 ANESTHESIA & YOU Planning Your Childbirth: Pain Relief During Labor and Delivery EACH WOMAN S LABOR IS UNIQUE T he amount of pain a woman feels during labor may differ from that felt by another woman.
ANESTHESIA & YOU Planning Your Childbirth: Pain Relief During Labor and Delivery EACH WOMAN S LABOR IS UNIQUE T he amount of pain a woman feels during labor may differ from that felt by another woman.
Preventing Pressure Ulcers
 Patient information Preventing Pressure Ulcers i Important information and care guide for patients at risk of pressure ulcers. Reproduced with kind permission from Healthcare Improvement Scotland Golden
Patient information Preventing Pressure Ulcers i Important information and care guide for patients at risk of pressure ulcers. Reproduced with kind permission from Healthcare Improvement Scotland Golden
Dexamethasone is used to treat cancer. This drug can be given in the vein (IV), by mouth, or as an eye drop.
 Dexamethasone Other Names: Decadron About This Drug Dexamethasone is used to treat cancer. This drug can be given in the vein (IV), by mouth, or as an eye drop. Possible Side Effects (More Common) Increased
Dexamethasone Other Names: Decadron About This Drug Dexamethasone is used to treat cancer. This drug can be given in the vein (IV), by mouth, or as an eye drop. Possible Side Effects (More Common) Increased
Smoking and Quitting Assessment
 Smoking and Quitting Assessment A. Which of the following describes you? q I m not interested in trying to quit smoking. q I know I need to quit smoking, but I m not quite ready yet. q I m ready to quit
Smoking and Quitting Assessment A. Which of the following describes you? q I m not interested in trying to quit smoking. q I know I need to quit smoking, but I m not quite ready yet. q I m ready to quit
MANAGING POST-OP PAIN AT HOME
 MANAGING POST-OP PAIN AT HOME Medicines and Self-Care After Surgery Managing Pain at Home Pain is expected after surgery. Know that you have a right to have this pain controlled. Managing pain helps you
MANAGING POST-OP PAIN AT HOME Medicines and Self-Care After Surgery Managing Pain at Home Pain is expected after surgery. Know that you have a right to have this pain controlled. Managing pain helps you
Improving Your Sleep During Your Hospital Stay
 PATIENT & CAREGIVER EDUCATION Improving Your Sleep During Your Hospital Stay This information will help you improve your sleep during your hospital stay. Sleeping well at night can make you feel better
PATIENT & CAREGIVER EDUCATION Improving Your Sleep During Your Hospital Stay This information will help you improve your sleep during your hospital stay. Sleeping well at night can make you feel better
Preventing pressure ulcers
 Golden Jubilee National Hospital NHS National Waiting Times Centre Preventing pressure ulcers Patient information guide for adults at risk of pressure ulcers Agamemnon Street Clydebank, G81 4DY (: 0141
Golden Jubilee National Hospital NHS National Waiting Times Centre Preventing pressure ulcers Patient information guide for adults at risk of pressure ulcers Agamemnon Street Clydebank, G81 4DY (: 0141
Coach on Call. Letting Go of Stress. A healthier life is on the line for you! How Does Stress Affect Me?
 Coach on Call How Does Stress Affect Me? Over time, stress can affect the way you feel, think, and act. You need some time when you are free of stress. You need ways to get relief from stress. Without
Coach on Call How Does Stress Affect Me? Over time, stress can affect the way you feel, think, and act. You need some time when you are free of stress. You need ways to get relief from stress. Without
Managing Your Pain with Oral Patient Controlled Analgesia (Oral PCA)
 Managing Your Pain with Oral Patient Controlled Analgesia (Oral PCA) UHN Information for patients and families Read this resource to learn: What it is Why it is important How it works Possible side effects
Managing Your Pain with Oral Patient Controlled Analgesia (Oral PCA) UHN Information for patients and families Read this resource to learn: What it is Why it is important How it works Possible side effects
May the longtime sun shine upon you, All love surround you, And the pure light within you Guide you on your way.
 May the longtime sun shine upon you, All love surround you, And the pure light within you Guide you on your way. Introduction Dying is a natural part of life, but many people do not have experience caring
May the longtime sun shine upon you, All love surround you, And the pure light within you Guide you on your way. Introduction Dying is a natural part of life, but many people do not have experience caring
21. Getting Tested for HIV
 21. Getting Tested for HIV Objectives By the end of this session, group members will be able to: Describe the process of HIV testing. List reasons for getting tested for HIV. Background notes It is not
21. Getting Tested for HIV Objectives By the end of this session, group members will be able to: Describe the process of HIV testing. List reasons for getting tested for HIV. Background notes It is not
Pressure Ulcers ecourse
 Pressure Ulcers ecourse Module 4.1: Prevention of Pressure Ulcers Handout College of Licensed Practical Nurses of Alberta (Canada) CLPNA.com and StudywithCLPNA.com CLPNA Pressure Ulcers ecourse Module
Pressure Ulcers ecourse Module 4.1: Prevention of Pressure Ulcers Handout College of Licensed Practical Nurses of Alberta (Canada) CLPNA.com and StudywithCLPNA.com CLPNA Pressure Ulcers ecourse Module
A Guide to Help New Mothers Stay Smoke-Free
 A Guide to Help New Mothers Stay Smoke-Free 1 Welcome to motherhood! You have just been through a life-changing experience pregnancy and child birth. Having a plan to stay smoke-free is an important step.
A Guide to Help New Mothers Stay Smoke-Free 1 Welcome to motherhood! You have just been through a life-changing experience pregnancy and child birth. Having a plan to stay smoke-free is an important step.
Wellness along the Cancer Journey: Palliative Care Revised October 2015
 Wellness along the Cancer Journey: Palliative Care Revised October 2015 Chapter 3: Addressing Cancer Pain as a part of Palliative Care Palliative Care Rev. 10.8.15 Page 360 Addressing Cancer Pain as Part
Wellness along the Cancer Journey: Palliative Care Revised October 2015 Chapter 3: Addressing Cancer Pain as a part of Palliative Care Palliative Care Rev. 10.8.15 Page 360 Addressing Cancer Pain as Part
In-Patient Radioactive Iodine ( 131 I) Treatment
 In-Patient Radioactive Iodine ( 131 I) Treatment Information for patients and families Princess Margaret Read this booklet to learn: what radioactive iodine treatment is what to expect instructions to
In-Patient Radioactive Iodine ( 131 I) Treatment Information for patients and families Princess Margaret Read this booklet to learn: what radioactive iodine treatment is what to expect instructions to
Bowel Resection Surgery (Open Method)
 Bowel Resection Surgery (Open Method) What is a bowel resection? A bowel resection is surgery to remove a part of the large or small intestine. These parts are shown on this diagram. small intestine large
Bowel Resection Surgery (Open Method) What is a bowel resection? A bowel resection is surgery to remove a part of the large or small intestine. These parts are shown on this diagram. small intestine large
Pain and Ways to Manage It
 Pain and Ways to Manage It FM.850.M311.PHC (R.Jul-15) 1 Contents This page intentionally left blank. What the words mean............................. 2 Why is it important to manage your pain?............
Pain and Ways to Manage It FM.850.M311.PHC (R.Jul-15) 1 Contents This page intentionally left blank. What the words mean............................. 2 Why is it important to manage your pain?............
Nivolumab. Other Names: Opdivo. About this Drug. Possible Side Effects (More Common) Warnings and Precautions
 Nivolumab Other Names: Opdivo About this Drug Nivolumab is used to treat cancer. It is given in the vein (IV). Possible Side Effects (More Common) Bone marrow depression. This is a decrease in the number
Nivolumab Other Names: Opdivo About this Drug Nivolumab is used to treat cancer. It is given in the vein (IV). Possible Side Effects (More Common) Bone marrow depression. This is a decrease in the number
CLINICAL GUIDELINES FOR END OF LIFE CARE MEDICATIONS IN LONG TERM CARE HOMES
 CLINICAL GUIDELINES F END OF LIFE CARE MEDICATIONS IN LONG TERM CARE HOMES OPENING STATEMENT: Insert Facility Name is committed to providing effective end-of-life symptom management to all residents. Symptom
CLINICAL GUIDELINES F END OF LIFE CARE MEDICATIONS IN LONG TERM CARE HOMES OPENING STATEMENT: Insert Facility Name is committed to providing effective end-of-life symptom management to all residents. Symptom
Palliative Care and End of Life Care
 Palliative Care and End of Life Care 8/2012 Palliative Care Palliative care is specialized medical care for people with serious illness. This type of care is focused on providing patients with relief from
Palliative Care and End of Life Care 8/2012 Palliative Care Palliative care is specialized medical care for people with serious illness. This type of care is focused on providing patients with relief from
Anxiety- Information and a self-help guide
 Anxiety- Information and a self-help guide Anxiety Anxiety can be a very normal and healthy response to stressful situations, such as paying bills or sitting an exam. However, it becomes a problem when
Anxiety- Information and a self-help guide Anxiety Anxiety can be a very normal and healthy response to stressful situations, such as paying bills or sitting an exam. However, it becomes a problem when
Colonic (Large Intestine) Manometry
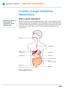 Patient and Family Education Colonic (Large Intestine) Manometry Manometry measures the pressure of contractions of the digestive tract. What is colonic manometry? The colon (also known as the large intestine)
Patient and Family Education Colonic (Large Intestine) Manometry Manometry measures the pressure of contractions of the digestive tract. What is colonic manometry? The colon (also known as the large intestine)
Preventing delirium while in the hospital
 Preventing delirium while in the hospital What is delirium? When an older person becomes ill and goes into the hospital, there is an increased risk of developing delirium and other problems. Delirium is
Preventing delirium while in the hospital What is delirium? When an older person becomes ill and goes into the hospital, there is an increased risk of developing delirium and other problems. Delirium is
Signs and Symptoms Of Common Health Concerns
 Signs and Symptoms Of Common Health Concerns New York Statewide School Health Services Center www.schoolhealthservicesny.com Phone: 585.617-2384 Fax: 585.352.9131 The pages in this chart list common symptoms
Signs and Symptoms Of Common Health Concerns New York Statewide School Health Services Center www.schoolhealthservicesny.com Phone: 585.617-2384 Fax: 585.352.9131 The pages in this chart list common symptoms
Patient & Family Guide. Nausea and Vomiting.
 Patient & Family Guide 2018 Nausea and Vomiting www.nscancercare.ca Efects of Cancer and Treatment: Nausea and Vomiting Dealing with the effects of cancer and treatment has improved over the years. As
Patient & Family Guide 2018 Nausea and Vomiting www.nscancercare.ca Efects of Cancer and Treatment: Nausea and Vomiting Dealing with the effects of cancer and treatment has improved over the years. As
Methotrexate. About This Drug. Possible Side Effects. Warnings and Precautions
 Methotrexate About This Drug Methotrexate is used to treat cancer. This drug is given in the vein (IV). Possible Side Effects Soreness of the mouth and throat. You may have red areas, white patches, or
Methotrexate About This Drug Methotrexate is used to treat cancer. This drug is given in the vein (IV). Possible Side Effects Soreness of the mouth and throat. You may have red areas, white patches, or
Oral Health Education
 e C ity Fre v a K I DS Oral Health Education for Pregnant Women, Children Birth through Age Five, and Their Families TM A Quick Reference for Home Visitors TM Cavity Free K I DS Cavity Free Kids Oral Health
e C ity Fre v a K I DS Oral Health Education for Pregnant Women, Children Birth through Age Five, and Their Families TM A Quick Reference for Home Visitors TM Cavity Free K I DS Cavity Free Kids Oral Health
- copyright
 Relaxation Exercises Let s start with breathing! Your breathing is often the first thing to be affected by stress. When we are anxious we tend to hunch up the shoulders and breathe in a more rapid and
Relaxation Exercises Let s start with breathing! Your breathing is often the first thing to be affected by stress. When we are anxious we tend to hunch up the shoulders and breathe in a more rapid and
At Home After Surgery
 Now that your surgery is done, your focus should be on healing. If you follow the recommendations listed in this section, you will help ensure that your new hip will last for the rest of your life. patients.d-h.org/ortho/hips
Now that your surgery is done, your focus should be on healing. If you follow the recommendations listed in this section, you will help ensure that your new hip will last for the rest of your life. patients.d-h.org/ortho/hips
keep track of other information like warning discuss with your doctor, and numbers of signs for relapse, things you want to
 Helping you set your brain free from psychosis. www.heretohelp.bc.ca This book was written by Sophia Kelly and the BC Schizophrenia Society, for the BC Partners for Mental Health and Addictions Information.
Helping you set your brain free from psychosis. www.heretohelp.bc.ca This book was written by Sophia Kelly and the BC Schizophrenia Society, for the BC Partners for Mental Health and Addictions Information.
Pain Relief During Labor and Delivery
 Pain Relief During Labor and Delivery Each woman's labor is unique. The amount of pain a woman feels during labor may differ from that felt by another woman. Pain depends on many factors, such as the size
Pain Relief During Labor and Delivery Each woman's labor is unique. The amount of pain a woman feels during labor may differ from that felt by another woman. Pain depends on many factors, such as the size
Chapter 20. Assisting With Nutrition and Fluids
 Chapter 20 Assisting With Nutrition and Fluids Food and water: Are physical needs Basics of Nutrition Are necessary for life A poor diet and poor eating habits: Increase the risk for diseases and infection
Chapter 20 Assisting With Nutrition and Fluids Food and water: Are physical needs Basics of Nutrition Are necessary for life A poor diet and poor eating habits: Increase the risk for diseases and infection
Midostaurin (Rydapt )
 Midostaurin (Rydapt ) ( mye doe STAW rin ) How drug is given: By mouth Purpose: To stop the growth of cancer cells in acute myeloid leukemia (AML) and other cancers. How to take this drug 1. Take this
Midostaurin (Rydapt ) ( mye doe STAW rin ) How drug is given: By mouth Purpose: To stop the growth of cancer cells in acute myeloid leukemia (AML) and other cancers. How to take this drug 1. Take this
Insomnia. F r e q u e n t l y A s k e d Q u e s t i o n s
 Insomnia Q: What is insomnia? A: Insomnia is a common sleep disorder. If you have insomnia, you may: Lie awake for a long time and have trouble falling asleep Wake up a lot and have trouble returning to
Insomnia Q: What is insomnia? A: Insomnia is a common sleep disorder. If you have insomnia, you may: Lie awake for a long time and have trouble falling asleep Wake up a lot and have trouble returning to
Preventing Pressure Ulcers
 Patient information Preventing Pressure Ulcers i Important information and care guide for patients at risk of pressure ulcers. Reproduced with kind permission from Healthcare Improvement Scotland Golden
Patient information Preventing Pressure Ulcers i Important information and care guide for patients at risk of pressure ulcers. Reproduced with kind permission from Healthcare Improvement Scotland Golden
Session 16: Manage Your Stress
 Session 16: Manage Your Stress Stress is part of life. However, you can learn better ways to take care of yourself when faced with stress. Stress is not always bad. Some stress can make life interesting
Session 16: Manage Your Stress Stress is part of life. However, you can learn better ways to take care of yourself when faced with stress. Stress is not always bad. Some stress can make life interesting
Pain Control After Surgery. Patient Information
 Pain Control After Surgery Patient Information What is Pain? Pain is an uncomfortable feeling that tells you something may be wrong in your body. Pain is your body s way of sending a warning to your brain.
Pain Control After Surgery Patient Information What is Pain? Pain is an uncomfortable feeling that tells you something may be wrong in your body. Pain is your body s way of sending a warning to your brain.
The 3 P s (Pain, Poop, Physical Therapy) for Post-Op Spinal Fusions
 The 3 P s (Pain, Poop, Physical Therapy) for Post-Op Spinal Fusions Pain control is a key part of your care after surgery. It can help speed recovery and improve the results of your surgery. This handout
The 3 P s (Pain, Poop, Physical Therapy) for Post-Op Spinal Fusions Pain control is a key part of your care after surgery. It can help speed recovery and improve the results of your surgery. This handout
for the grieving process How to cope as your loved one nears the end stages of IPF
 Preparing yourself for the grieving process How to cope as your loved one nears the end stages of IPF 3 As your loved one nears the end stages of IPF, it s important that you be there for him or her as
Preparing yourself for the grieving process How to cope as your loved one nears the end stages of IPF 3 As your loved one nears the end stages of IPF, it s important that you be there for him or her as
Palliative Care Asking the questions that matter to me
 Palliative Care Asking the questions that matter to me THE PALLIATIVE HUB Adult This booklet has been developed by the Palliative Care Senior Nurses Network and adapted with permission from Palliative
Palliative Care Asking the questions that matter to me THE PALLIATIVE HUB Adult This booklet has been developed by the Palliative Care Senior Nurses Network and adapted with permission from Palliative
In the Ageing Well Survey, 2007, skin care issues were among the top three health priorities identified by respondents.
 2 Caring For Your Skin Skin The Functions of the Skin Skin acts to protect internal organs from disease, excrete waste products, regulate body temperature and provide sensation through nerve endings. Skin
2 Caring For Your Skin Skin The Functions of the Skin Skin acts to protect internal organs from disease, excrete waste products, regulate body temperature and provide sensation through nerve endings. Skin
Is a LVAD the Right Treatment for Me? Decision Aid
 Is a LVAD the Right Treatment for Me? Decision Aid patienteducation.osumc.edu 2 Making an Informed Decision Review this book We give you this information to help you understand what the LVAD treatment
Is a LVAD the Right Treatment for Me? Decision Aid patienteducation.osumc.edu 2 Making an Informed Decision Review this book We give you this information to help you understand what the LVAD treatment
*521634* Sleep History Questionnaire. Name of primary care doctor:
 *521634* Today s Date: Sleep History Questionnaire Appointment Date: Please answer the following questions before coming to your appointment. Please arrive 15 minutes early with this packet filled out.
*521634* Today s Date: Sleep History Questionnaire Appointment Date: Please answer the following questions before coming to your appointment. Please arrive 15 minutes early with this packet filled out.
Open to the possibility of a multiple myeloma treatment that works in cells in your body at the DNA level
 If you have multiple myeloma and have already tried at least 2 other types of treatment Open to the possibility of a multiple myeloma treatment that works in cells in your body at the DNA level What is
If you have multiple myeloma and have already tried at least 2 other types of treatment Open to the possibility of a multiple myeloma treatment that works in cells in your body at the DNA level What is
Sunitinib. Other Names: Sutent. About This Drug. Possible Side Effects. Warnings and Precautions
 Sunitinib Other Names: Sutent About This Drug Sunitnib is used to treat cancer. It is given orally (by mouth). Possible Side Effects Headache Tiredness and weakness Soreness of the mouth and throat. You
Sunitinib Other Names: Sutent About This Drug Sunitnib is used to treat cancer. It is given orally (by mouth). Possible Side Effects Headache Tiredness and weakness Soreness of the mouth and throat. You
Delirium A guide for caregivers
 Delirium A guide for caregivers Disclaimer This is general information developed by The Ottawa Hospital. It is not intended to replace the advice of a qualified health-care provider. Please consult your
Delirium A guide for caregivers Disclaimer This is general information developed by The Ottawa Hospital. It is not intended to replace the advice of a qualified health-care provider. Please consult your
Taking Opioids Responsibly for Your Safety and the Safety of Others: Patient Information Guide on Long-term Opioid Therapy for Chronic Pain
 Taking Opioids Responsibly for Your Safety and the Safety of Others: Patient Information Guide on Long-term Opioid Therapy for Chronic Pain Department of Veterans Affairs (VA) and Department of Defense
Taking Opioids Responsibly for Your Safety and the Safety of Others: Patient Information Guide on Long-term Opioid Therapy for Chronic Pain Department of Veterans Affairs (VA) and Department of Defense
ten questions you might have about tapering (and room for your own) an informational booklet for opioid pain treatment
 ten questions you might have about tapering (and room for your own) an informational booklet for opioid pain treatment This booklet was created to help you learn about tapering. You probably have lots
ten questions you might have about tapering (and room for your own) an informational booklet for opioid pain treatment This booklet was created to help you learn about tapering. You probably have lots
Learn about Delirium. Information for patients and families
 Learn about Delirium Information for patients and families In this document you will find information about: What is delirium Signs Causes Treatment What you can do What is delirium? Delirium is sudden
Learn about Delirium Information for patients and families In this document you will find information about: What is delirium Signs Causes Treatment What you can do What is delirium? Delirium is sudden
Pharmacy Advisor Program. Specialized Health Support
 Pharmacy Advisor Program Specialized Health Support Contents Your Health and Your CVS Caremark Pharmacy Advisor Pharmacist...3 Keys to Your Health....4 Getting the Most from Your Medication...6 Feeling
Pharmacy Advisor Program Specialized Health Support Contents Your Health and Your CVS Caremark Pharmacy Advisor Pharmacist...3 Keys to Your Health....4 Getting the Most from Your Medication...6 Feeling
Dabrafenib (Tafinlar )
 Dabrafenib (Tafinlar ) ( da-braf-e-nib ) How drug is given: By mouth Purpose: To stop the growth of cancer cells in melanoma and other cancers. How to take this drug Take this medication on an empty stomach
Dabrafenib (Tafinlar ) ( da-braf-e-nib ) How drug is given: By mouth Purpose: To stop the growth of cancer cells in melanoma and other cancers. How to take this drug Take this medication on an empty stomach
Understanding Pain. Teaching Plan: Guidelines for Teaching this Lesson
 Understanding Pain Teaching Plan: Guidelines for Teaching this Lesson Lesson Overview This one-hour lesson plan is about pain and how your workers should respond to and care for residents with pain. You
Understanding Pain Teaching Plan: Guidelines for Teaching this Lesson Lesson Overview This one-hour lesson plan is about pain and how your workers should respond to and care for residents with pain. You
Imatinib (Gleevec ) ( eye-mat-eh-nib )
 Imatinib (Gleevec ) ( eye-mat-eh-nib ) How drug is given: by mouth Purpose: stops growth of cancer cells in leukemia, gastrointestinal stromal tumors (GIST), and other cancers How to take the drug by mouth
Imatinib (Gleevec ) ( eye-mat-eh-nib ) How drug is given: by mouth Purpose: stops growth of cancer cells in leukemia, gastrointestinal stromal tumors (GIST), and other cancers How to take the drug by mouth
Regorafenib (Stivarga )
 Page 1 of 5 Regorafenib (Stivarga ) About This Drug Regorafenib is used to treat cancer. It is given orally (by mouth). Possible Side Effects Bone marrow depression. This is a decrease in the number of
Page 1 of 5 Regorafenib (Stivarga ) About This Drug Regorafenib is used to treat cancer. It is given orally (by mouth). Possible Side Effects Bone marrow depression. This is a decrease in the number of
Dr. Nuelle Total/Partial Hip Replacement: Discharge Care Instructions
 Dr. Nuelle Total/Partial Hip Replacement: Discharge Care Instructions Your Recovery Thank you for allowing us to help you with your hip replacement surgery. We hope that you had a good stay with us. These
Dr. Nuelle Total/Partial Hip Replacement: Discharge Care Instructions Your Recovery Thank you for allowing us to help you with your hip replacement surgery. We hope that you had a good stay with us. These
Discharge Information following Bowel Surgery
 Discharge Information following Bowel Surgery Here is some information to help with your recovery at home and advice about returning to normal activities following bowel surgery. We hope this will be helpful
Discharge Information following Bowel Surgery Here is some information to help with your recovery at home and advice about returning to normal activities following bowel surgery. We hope this will be helpful
First Aid Preparedness Patsy Ramey, RN, BSN Clinical Resource Nurse Epilepsy Division
 First Aid Preparedness Patsy Ramey, RN, BSN Clinical Resource Nurse Epilepsy Division TRUST Time the seizure Remove glasses and anything tight around the neck Use something soft under their head STAY CALM
First Aid Preparedness Patsy Ramey, RN, BSN Clinical Resource Nurse Epilepsy Division TRUST Time the seizure Remove glasses and anything tight around the neck Use something soft under their head STAY CALM
Side Effects of Narcotic Pain Medication
 Side Effects of Narcotic Pain Medication Constipation is a treatable side effect (see constipation insert). It is advised to take some form of stool softener while taking narcotics. Ensure adequate fluids
Side Effects of Narcotic Pain Medication Constipation is a treatable side effect (see constipation insert). It is advised to take some form of stool softener while taking narcotics. Ensure adequate fluids
Concussion & You. A Handbook for Parents and Kids DEVELOPED BY CONCUSSION EXPERTS AT HOLLAND BLOORVIEW KIDS REHABILITATION HOSPITAL
 Concussion & You A Handbook for Parents and Kids DEVELOPED BY CONCUSSION EXPERTS AT HOLLAND BLOORVIEW KIDS REHABILITATION HOSPITAL Trusted experts in youth concussion www.hollandbloorview.ca/concussion
Concussion & You A Handbook for Parents and Kids DEVELOPED BY CONCUSSION EXPERTS AT HOLLAND BLOORVIEW KIDS REHABILITATION HOSPITAL Trusted experts in youth concussion www.hollandbloorview.ca/concussion
Radiation Therapy. This reference summary reviews what to expect during and after radiation therapy.
 Radiation Therapy Introduction Radiation therapy is a very common treatment for a variety of cancers. Radiation therapy, also called radiotherapy, is a cancer treatment that uses high doses of radiation
Radiation Therapy Introduction Radiation therapy is a very common treatment for a variety of cancers. Radiation therapy, also called radiotherapy, is a cancer treatment that uses high doses of radiation
information The Enhanced Recovery Programme for Total Hip Replacement (1 of 6) What will happen before I come into hospital?
 information If you need this information in another language or medium (audio, large print, etc) please contact the Customer Care Team on 0800 374 208 email: customercare@ salisbury.nhs.uk. You are entitled
information If you need this information in another language or medium (audio, large print, etc) please contact the Customer Care Team on 0800 374 208 email: customercare@ salisbury.nhs.uk. You are entitled
Living with Congestive Heart Failure
 Living with Congestive Heart Failure EPICORE CENTRE Division of Cardiology 213 Heritage Medical Research Centre University of Alberta Edmonton, AB T6G 2S2 Phone: (780) 492-8525 Fax: (780) 492-6059 Website:
Living with Congestive Heart Failure EPICORE CENTRE Division of Cardiology 213 Heritage Medical Research Centre University of Alberta Edmonton, AB T6G 2S2 Phone: (780) 492-8525 Fax: (780) 492-6059 Website:
