May the longtime sun shine upon you, All love surround you, And the pure light within you Guide you on your way.
|
|
|
- Darcy Griffin
- 6 years ago
- Views:
Transcription
1
2
3 May the longtime sun shine upon you, All love surround you, And the pure light within you Guide you on your way.
4 Introduction Dying is a natural part of life, but many people do not have experience caring for someone during the dying process and find themselves navigating through new and unfamiliar territory. It is not uncommon to experience a wide range of emotions and a sense of uncertainty. At times you may feel that you are on a roller coaster, not knowing what to expect next. This booklet is designed to help you feel more confident in knowing what to expect and what you can do to care for someone in the final weeks and hours of life. Family members, friends, and caregivers can play an important role in providing comfort and support to someone entering this final phase of life. Sometimes it is not so much what you say or do, but just being present with another, that can provide a sense of reassurance and comfort. Each person s dying experience is unique, and no one can fully predict what it will be like or when it will occur. However, we hope the information contained in this booklet will provide some landmarks to help guide the way. Please contact hospice at any time for further information and support. It is our goal to respect the dignity of each person by providing quality comfort care. 1
5 Table of Contents Introduction...1 Developmental Milestones and Tasks...3 Withdrawal...4 Changes in Appetite...5 Changes in Elimination...6 Changes in Breathing...7 Changes in Body Temperature...8 Confusion and Disorientation...9 Restlessness and Agitation...11 Surge of Energy...13 Saying Goodbye...14 Review of Possible Signs and Symptoms...15 Moment of Death...17 Care for the Caregiver
6 End-of-Life Developmental Milestones and Tasks Source: Dr. Ira Byock Dr. Ira Byock is a leader and educator in promoting quality care at the end of life. Below is a framework he developed that outlines some of the issues many people may be contemplating as they approach death. His findings are included here as part of a holistic understanding of the dying process. Although the journey toward death may not be easy, it can often be a time of new insights, personal growth, and inner healing. Sense of completion with worldly affairs Sense of completion in relationships with community Sense of meaning about one s individual life Experiencing love of self Experiencing love of others Sense of completion in relationships with family and friends Acceptance of the finality of life of one s existence as an individual Sense of a new self (personhood) beyond personal loss Sense of meaning about life in general Surrendering to the transcendent, to the unknown letting go 3
7 Withdrawal It is common for people to begin to withdraw from friends, family, and the world around them as a normal part of the dying process. This process may begin as early as weeks before the death. The dying person may stay in bed all day and spend more time asleep than awake. With the withdrawal comes less of a need to communicate with others; touch and silence take on more meaning. People at this point may seem unresponsive and difficult to arouse or may appear to be in a coma-like state. This detaching from surroundings and relationships may be preparation for release and letting go. What you can do: Plan activities and visits for times of day when the person seems most alert. Because hearing remains intact to the end, speak to the person in your normal tone of voice. Identify yourself by name when you speak. Tell the person what you are going to do before you do it. For example: Bob, this is Karen. I m going to clean your mouth now. Remember not to say anything in front of the person that you wouldn t say if he or she were awake. 4
8 Changes in Appetite Near the end of life, it is natural for a person to no longer be interested in food or to be unable to eat or drink. Often nothing tastes good, and cravings come and go. This is often one of the hardest concepts for caregivers to accept because food is the way we nourish the body and share family time together. As the body naturally begins to slow down, it is no longer able to digest and assimilate food in the same way. Weight loss is expected and does not mean that the person is hungry or being starved by the absence of food. What you can do: Let the person be the guide; he or she will let you know if food or fluids are needed or wanted. Liquids are preferred to solids. Some people find thickened liquids easier to swallow. Small chips of ice or frozen juice may be refreshing in the mouth. If the person is able to swallow, fluids may be given in small amounts by syringe (without a needle) or dropper (ask the hospice nurse for guidance). There may be times when the taste or smell of familiar foods in small amounts is comforting. People who can t speak will sometimes cough, bite the spoon, clamp their teeth closed, turn their heads, or spit food out to let you know they don t want to eat. Respect the person s wishes by trying not to force food or drink. Often a person near death may appear thirsty but won t be able to drink water. Frequent mouth care may provide comfort; use swabs to keep the mouth and lips moist. 5
9 Changes in Elimination Incontinence is the loss of control of the bladder and bowels that can sometimes occur as the muscles in the lower body begin to relax. As people decline, the urine output usually diminishes, and the color is usually darker than normal. It may also be cloudy or have a strong odor. This is the normal response to the decreased fluid intake as well as decreased circulation through the kidneys. Unfortunately, incontinence can be a source of shame and embarrassment for many people. Keeping the person clean, dry, and comfortable, as well as preserving dignity, is the overall goal. What you can do: Adult disposable briefs and underpads on the bed may solve the problem. The nurse or home health aide can show you how to change these for someone in bed. In some situations it may be appropriate for the nurse to suggest placing a catheter (a tube) into the bladder to keep the person s skin from being constantly wet. There may be a few seconds of discomfort as the catheter is inserted, but then there is generally no awareness of it at all. The nurse may suggest that certain lotions or creams be applied to the skin periodically. To help maintain dignity, provide privacy when changing pads or providing personal care. Check the person frequently to ensure that he or she is kept dry and comfortable. 6
10 Changes in Breathing Breathing patterns often begin to change for those nearing the end of life. Breathing may slow down, or there may be rapid, shallow breaths followed by periods of no breathing. These periods can last 5 to 30 seconds, or even up to a full minute. This kind of breathing is not uncomfortable for the person but is a response to the body s weakening condition. Your hospice nurse, along with your physician, will assess and determine if oxygen would be a comfort measure at this time. Sometimes when individuals are so weak that they can t swallow, saliva gathers in the back of the throat and makes a rattling sound. Suctioning usually only increases the secretions and causes discomfort. This sound may be distressing to hear, but it does not indicate that the person is suffering. What you can do: Gently turning the person on his or her side may assist gravity to drain the secretions. Raising the head of the bed may also help. Your nurse may educate you about prescribed medications that will dry excess secretions. At this point the person is usually breathing with his or her mouth open. This will make the mouth very dry, so frequent mouth care is important. If breathing seems labored, your doctor may prescribe morphine or a similar medication to ease the breathing and provide comfort. 7
11 Changes in Body Temperature Fever As the body becomes weaker, so does the temperature control mechanism in the brain. This can cause the person to have a fever or cause the body to become cool. Sometimes a person may become sweaty and clammy with or without a fever. What you can do: If a fever develops, let your hospice nurse know. Often placing a cool wash cloth on the forehead and removing blankets may be all that is needed. However, your hospice nurse may suggest an over-the-counter pain reliever (such as acetaminophen) if the fever is high. As the fever lowers, the person may perspire, requiring a change of gown, pajamas, and sheets to provide more comfort. Consider using a fan or opening a window. If the person throws the covers off, it is important to remember that he or she may be warm even when you feel cool. Coolness As your loved one becomes weaker, his or her circulation decreases. You may notice that extremities feel cool to the touch and skin color may change. The hands and feet may become purplish, and the knees, ankles, and elbows may look blotchy. The person may appear pale and have a bluish cast around the lips and under the fingernails. This state doesn t cause any discomfort for the person and is a natural part of the dying process. What you can do: Use a warm blanket, but not an electric blanket. Continue to gently reposition the person, or provide gentle massage. 8
12 Confusion and Disorientation At times, people nearing the end of their life may have confusion about the time, their surroundings, and the identity of those around them. They may report seeing people or things that are not visible to others, and they may engage in conversation with others who are not visibly present or who have already died. People near the end of life will sometimes talk about travel, as though they are planning a journey. They may say things such as: I want to go home, I want to get my keys, I need to find my suitcase, or Where is the train/bus? This type of conversation is referred to as symbolic language, and may be one of the ways people let us know that they are preparing for death or are trying to tell us goodbye. When these symptoms are present, we may wonder if the person is taking too much medicine or not enough. Most often, these symptoms are a normal part of the dying process. The hospice nurse will assess the prescribed medication at each visit and determine along with the physician if it is the correct medicine at the correct dosage. What you can do: Report these symptoms to the hospice nurse or other hospice team members; they will assess and provide information on ways you can provide care and support at this time. If appropriate, gently try to reorient the person. Remind them of who you are and what you are going to be doing, and point out familiar landmarks in their surroundings. Provide reassurance by reminding them of your presence and support, and that you will take care of them and keep them safe. Sometimes limiting visitors can decrease the level of confusion or disorientation. 9
13 Allow and acknowledge whatever experience the person may be having, without trying to contradict or argue it away. This experience is real to them, even though it may not seem real to you. Listen carefully; there may be meaningful messages being shared in symbolic language. You may want to keep a journal to record some of the meaningful things that are shared. This may be a source of inspiration and comfort to share with other family members. You don t have to do or say anything to make things better. Just be there as fully as you can. Sogyal Rinpoche 10
14 Restlessness and Agitation At times, the person you are caring for may appear restless or unable to be still, and may pick at bed clothes or perform repetitive movements. This is not uncommon and may be due to a variety of physical or emotional reasons. Restlessness may be caused in part by a slowing down of circulation, causing less oxygen to flow to the brain. Sometimes restlessness or agitation can be a symptom of physical discomfort or pain. Emotional or spiritual concerns, such as an unresolved issue or unfinished task, can be worrisome and also cause feelings of uneasiness or restlessness. What you can do: Let the hospice nurse know if the person is agitated or restless. The nurse will assess for any underlying pain or discomfort. Continue with the medication regimen prescribed by the doctor. Utilize the hospice social worker and/or chaplain to address underlying concerns and provide emotional or spiritual support. Provide a reassuring presence by speaking slowly, calmly, and in a soothing way. If appropriate, help the person resolve issues and complete tasks. Sometimes offering to take over a task or suggesting it be delegated to another trusted person can provide relief. Try reading something inspirational or playing soft music. Holding hands or a light touch may be reassuring. 11
15 Use bed rails or have someone sit with the person to keep him or her safe. Consider use of a baby monitor while out of the room. Restraints may cause further agitation and are not encouraged. It may be useful to limit visitors at this time and to minimize outside distractions (loud noises, radio or TV, ringing phones). Some people find comfort in sharing memories about special occasions or holidays, family experiences, or the memory of a favorite place. Among the best things we can give each other are good memories. Henry Nouwen 12
16 Surge of Energy Dying loved ones may exhibit sudden unexplained surges of energy, which are usually short-lived. They may become unexpectedly alert and clear, ask to eat when they haven t had food for days, or they may want to get up to visit when they haven t been out of bed for weeks. This doesn t always happen in such dramatic ways but can be more subtle, such as being awake more when they have been sleeping most of the time. It is easy to see how this could be misunderstood and can give false hope that the individuals are getting better. It may be that they are marshalling all their physical strength for their last full-body experience in this life. What you can do: Enjoy this time for what it is. Use the time to reminisce and say goodbye. Be together holding hands. The things that matter most in our lives are not fantastic or grand. They are the moments when we touch one another, when we are there in the most attentive or caring way. Jack Kornfield 13
17 Saying Goodbye Many people have questions about saying goodbye and wonder whether it is appropriate to do so. Some are concerned that it will hasten death or communicate something unintended. Others may want to say goodbye but may not know what to say. In addition, some families have questions about whether they should give permission to let go. When and how to say goodbye is a personal decision, and there is no right or wrong way to do it. Some families have difficulty starting the conversation but find that once begun, it can be a gift. This time with your loved one is precious. What you can do: Take this opportunity while the person is alert to say or do what you need to. Listen to the wisdom of your heart, and follow its guidance. Some families begin these conversations with: What I love most about you... What I will always remember... What I will miss most about you... What I learned from you... What I will cherish... Some people may choose this time to say, I am sorry, share forgiveness, or let go of past conflicts. Some people may choose this time to share expressions of gratitude. It may be helpful to lie in bed with your loved one and hold them, or take their hand and say everything you need to say. Tears are a normal and natural part of saying goodbye, and could be a healthy expression of your love. 14
18 Review of Possible Signs and Symptoms of Approaching Death Because each person s dying process is unique to him or her, the outline below is only a general guide. People may exhibit some or all of these signs and symptoms at varying times. ONE TO THREE MONTHS Withdrawal from people and activities Communicating less Eating and drinking less Sleeping more ONE TO TWO WEEKS Disorientation and confusion Use of symbolic language ( I want to go home ) Talking to others not present in the room Physical changes: Increase or decrease in pulse Decrease in blood pressure Changes in skin color Irregularities in breathing Changes in body temperature, hot/cold Not eating, taking little or no fluids 15
19 DAYS TO HOURS Sleeping most of the time Surge of energy Restlessness Difficulty swallowing Further discoloration of skin Ongoing changes in breathing (long pauses between breaths) Rattling breath sounds Weak pulse Further decrease in blood pressure Decreased urine output or no urine Eyelids no longer able to close completely MINUTES Shallow breaths with longer pauses Mouth open Unresponsive In this life we cannot do great things. We can only do small things with great love. Mother Teresa 16
20 Moment of Death It is important to discuss with family members, caregivers, and friends what to do if they are present at the time of death. No one can accurately predict when death may occur. Some people die when others are present. Some take their last breaths when they are alone. When the person has died, there will be no breathing or heartbeat. There will be no response to your voice or touch. The eyes may be partly open, and the pupils will be unresponsive. The jaw will relax, and the mouth will open. Sometimes there will be loss of bowel and bladder control. No matter how well prepared you are, death can still feel like a shock. At the time of death, nothing needs to be done immediately other than calling hospice. There is no need to call 911 or notify the police. You may want to call a trusted friend or a family member to be with you at this time. What you can do: Please contact hospice. A nurse will visit. Please note that other team members may provide assistance as needed. When a nurse or other team members visit, some of the things they may do are: Confirm the death Remove any tubes that are present Offer to bathe and prepare the body Dispose of medications Call the funeral home, if you wish Provide support Notify the physician and your hospice team, and arrange for medical equipment to be removed 17
21 People honor the passing of their loved ones in a variety of ways. Some choose to have the funeral home come right away, while other families may choose to wait for a period of time before calling. Some of the ways in which you can honor your loved one are: bathing and dressing the body in special clothes, telling stories, lighting a candle, sharing a ritual from his or her spiritual tradition, placing flowers in the room, or playing special music. Let the funeral home staff know when you are ready for them to arrive. When they do come, you can decide whether you want to be present when they remove the body or wait in another part of the house. The funeral home will let you know about making arrangements for services. Our life is a faint tracing on the surface of mystery. Annie Dillard 18
22 Care for the Caregiver Caring for someone who is in the final weeks and days of life can be physically and emotionally demanding. It may feel overwhelming at times and leave you weary in body, mind, and spirit. In addition, some caregivers are often juggling other responsibilities such as work, household duties, caring for other family members, or addressing their own health concerns. Trying to balance another s care with your own needs for rest and nourishment is challenging, but important for your own wellbeing. What you can do: Take a deep breath several times a day. Deep breathing brings more oxygen to every cell and can refresh both body and mind. Go outside for a few minutes; smell and feel the fresh air. Take a walk or sit in your garden. If you have an exercise routine, try to adhere to it, as this can help decrease stress and boost energy. Lie down for 20 minutes or sit in a recliner with your feet up. Drink plenty of liquids, especially water. Follow a well-balanced diet, eating at regular intervals. Your health and nutrition are just as important as that of the person for which you are caring. Determine if calls or visits are helpful or would cause more stress. Limit these as a way of honoring your own needs and private time. Ask for help. Often family and friends want to help but do not know how. Keep a list of tasks to be done, such as shopping, going to the post office, walking the dog, or going to the pharmacy. Utilize a hospice volunteer visitor for respite or for help with errands. Share your concerns or feelings with a trusted friend, your spiritual counselor, or someone from your hospice team. 19
23 2008 by Hospice of Santa Cruz County. This booklet (published as When Death is Near and When the Time Comes) was created by Hospice of Santa Cruz County, a community-based, not-for-profit organization in Scotts Valley, California, that serves Santa Cruz and North Monterey counties. Through a generous grant from The California Endowment, Hospice of Santa Cruz County has moved forward in its ultimate goal of improving the delivery of end-of-life education, hospice, Transitions, and grief support services within the Latino community. All rights reserved. No part of this booklet may be reproduced without prior permission of the publisher. Printed in the United States of America. Published by Quality of Life Publishing Co. Naples, Florida Quality of Life Publishing Co. is an independent, mission-driven firm specializing in branded publications that help ease the way for those with life-limiting illnesses and their families. Visit HOW TO ORDER BRANDED COPIES: Call Quality of Life Publishing Co. during regular business hours (Eastern Time) toll free at or info@qolpublishing.com.
24
S A M P L E. Is Near. When Death. Logo A CAREGIVER S GUIDE
 When Death Is Near A CAREGIVER S GUIDE Logo Updated 2019. 2008 by Hospice of Santa Cruz County. This booklet (published as When Death is Near and When the Time Comes) was created by Hospice of Santa Cruz
When Death Is Near A CAREGIVER S GUIDE Logo Updated 2019. 2008 by Hospice of Santa Cruz County. This booklet (published as When Death is Near and When the Time Comes) was created by Hospice of Santa Cruz
ALONG THE FINAL JOURNEY
 ALONG THE FINAL JOURNEY A Guide for families and caregivers TABLE OF CONTENTS STARTING THE JOURNEY...2 ALONG THE JOURNEY... 3 Physical/Emotional Symptoms and Appropriate Comfort Measures Diminishing Appetite...
ALONG THE FINAL JOURNEY A Guide for families and caregivers TABLE OF CONTENTS STARTING THE JOURNEY...2 ALONG THE JOURNEY... 3 Physical/Emotional Symptoms and Appropriate Comfort Measures Diminishing Appetite...
Physical/Emotional Symptoms and Appropriate Comfort Measures
 Physical/Emotional Symptoms and Appropriate Comfort Measures A. Diminishing Appetite Page 2 B. Decreased Socialization Page 2 C. Sleeping Page 2 E. Changes in Pain Level Page 3 D. Incontinence Page 3 F.
Physical/Emotional Symptoms and Appropriate Comfort Measures A. Diminishing Appetite Page 2 B. Decreased Socialization Page 2 C. Sleeping Page 2 E. Changes in Pain Level Page 3 D. Incontinence Page 3 F.
Preparing for Approaching Death
 Preparing for Approaching Death Old Colony Hospice created this guide for our hospice family and caregivers by revising and adapting the following journal article: Hospice Techniques: Preparing for the
Preparing for Approaching Death Old Colony Hospice created this guide for our hospice family and caregivers by revising and adapting the following journal article: Hospice Techniques: Preparing for the
Palliative Care Victoria The Process of Dying Page 1. The Process of Dying. What to expect and how to help
 Palliative Care Victoria The Process of Dying Page 1 The Process of Dying What to expect and how to help Palliative Care Victoria The Process of Dying Page 2 About dying Dying is a natural part of life.
Palliative Care Victoria The Process of Dying Page 1 The Process of Dying What to expect and how to help Palliative Care Victoria The Process of Dying Page 2 About dying Dying is a natural part of life.
Preparing for Approaching Death By North Central Florida Hospice, Inc.
 Preparing for Approaching Death By North Central Florida Hospice, Inc. When a person enters the final stage of the dying process, two different dynamics are at work which are closely interrelated and interdependent.
Preparing for Approaching Death By North Central Florida Hospice, Inc. When a person enters the final stage of the dying process, two different dynamics are at work which are closely interrelated and interdependent.
Preparing for the Death of a Loved One. Information for Patients & Visitors
 Preparing for the Death of a Loved One Information for Patients & Visitors This booklet is provided to help you know what to expect when your loved one is dying. It may help you to respond in ways that
Preparing for the Death of a Loved One Information for Patients & Visitors This booklet is provided to help you know what to expect when your loved one is dying. It may help you to respond in ways that
What to expect in the last days and hours of life in the Intensive Care Unit (ICU)
 What to expect in the last days and hours of life in the Intensive Care Unit (ICU) Information for patients and caregivers Please visit the UHN Patient Education website for more health information: www.uhnpatienteducation.ca
What to expect in the last days and hours of life in the Intensive Care Unit (ICU) Information for patients and caregivers Please visit the UHN Patient Education website for more health information: www.uhnpatienteducation.ca
Precious Moments. Giving comfort and support when someone you love is dying.
 Precious Moments Giving comfort and support when someone you love is dying www.stjoes.ca When someone you love is dying When someone you love is dying, you may want to know how you can provide comfort
Precious Moments Giving comfort and support when someone you love is dying www.stjoes.ca When someone you love is dying When someone you love is dying, you may want to know how you can provide comfort
What to expect in the last few days of life
 What to expect in the last few days of life Contents Introduction... 3 What are the signs that someone is close to death?... 4 How long does death take?... 7 What can I do to help?... 7 Can friends and
What to expect in the last few days of life Contents Introduction... 3 What are the signs that someone is close to death?... 4 How long does death take?... 7 What can I do to help?... 7 Can friends and
Coping with dying. Information for families and carers
 Coping with dying Information for families and carers This leaflet describes some of the physical changes that happen to people as they start to die. It also covers what will happen immediately following
Coping with dying Information for families and carers This leaflet describes some of the physical changes that happen to people as they start to die. It also covers what will happen immediately following
Journey s End: What to Expect and What to Do When Giving Care at the End of Life
 Journey s End: What to Expect and What to Do When Giving Care at the End of Life 2009 Pathways Home Health & Hospice. All rights reserved. Journey s End: What to Expect and What to Do Just as our lives
Journey s End: What to Expect and What to Do When Giving Care at the End of Life 2009 Pathways Home Health & Hospice. All rights reserved. Journey s End: What to Expect and What to Do Just as our lives
What to expect in the last few days of life
 What to expect in the last few days of life Contents Introduction... 3 What are the signs that someone is close to death?... 4 How long does death take?... 6 What can I do to help?... 7 Can friends and
What to expect in the last few days of life Contents Introduction... 3 What are the signs that someone is close to death?... 4 How long does death take?... 6 What can I do to help?... 7 Can friends and
Journey towards new life...
 Journey towards new life... Dear Family, The staff of Maxville Manor accompanies you on this difficult journey. Our Residents are like family to us. In an effort to provide the support you need, we offer
Journey towards new life... Dear Family, The staff of Maxville Manor accompanies you on this difficult journey. Our Residents are like family to us. In an effort to provide the support you need, we offer
When Someone Close To You Is Dying
 Remember that preparing for a death can be difficult. We hope the information provided in this booklet may reduce the amount of stress you feel by giving you some information about what to expect. While
Remember that preparing for a death can be difficult. We hope the information provided in this booklet may reduce the amount of stress you feel by giving you some information about what to expect. While
When Someone Close To You Is Dying
 Remember that preparing for a death can be difficult We hope the information provided in this booklet may reduce the amount of stress you feel by giving you some information about what to expect While
Remember that preparing for a death can be difficult We hope the information provided in this booklet may reduce the amount of stress you feel by giving you some information about what to expect While
Preventing delirium while in hospital Tips for family, whānau, and friends who are supporting an older person
 Preventing delirium while in hospital Tips for family, whānau, and friends who are supporting an older person This brochure shares some simple ways you can help our care staff to prevent delirium, recognize
Preventing delirium while in hospital Tips for family, whānau, and friends who are supporting an older person This brochure shares some simple ways you can help our care staff to prevent delirium, recognize
Understanding late stage dementia Understanding dementia
 Understanding late stage dementia About this factsheet This factsheet is for relatives of people diagnosed with dementia. It provides information about what to expect as dementia progresses to late stage.
Understanding late stage dementia About this factsheet This factsheet is for relatives of people diagnosed with dementia. It provides information about what to expect as dementia progresses to late stage.
Managing Other Medical Conditions
 Managing Other Medical Conditions When Dementia is Part of the Picture Terms You Will NEED to Know - Advanced directives - Living Will - DNR orders - Durable HC-POA - Palliative care - Hospice care - Comfort
Managing Other Medical Conditions When Dementia is Part of the Picture Terms You Will NEED to Know - Advanced directives - Living Will - DNR orders - Durable HC-POA - Palliative care - Hospice care - Comfort
There For You. Your Compassionate Guide. World-Class Hospice Care Since 1979
 There For You Your Compassionate Guide World-Class Hospice Care Since 1979 What Is Hospice? Hospice is a type of care designed to provide support during an advanced illness. Hospice care focuses on comfort
There For You Your Compassionate Guide World-Class Hospice Care Since 1979 What Is Hospice? Hospice is a type of care designed to provide support during an advanced illness. Hospice care focuses on comfort
Palliative Care Asking the questions that matter to me
 Palliative Care Asking the questions that matter to me THE PALLIATIVE HUB Adult This booklet has been developed by the Palliative Care Senior Nurses Network and adapted with permission from Palliative
Palliative Care Asking the questions that matter to me THE PALLIATIVE HUB Adult This booklet has been developed by the Palliative Care Senior Nurses Network and adapted with permission from Palliative
Palliative Care and End of Life Care
 Palliative Care and End of Life Care 8/2012 Palliative Care Palliative care is specialized medical care for people with serious illness. This type of care is focused on providing patients with relief from
Palliative Care and End of Life Care 8/2012 Palliative Care Palliative care is specialized medical care for people with serious illness. This type of care is focused on providing patients with relief from
Session 15: Mindful Eating, Mindful Movement
 Session 15: Mindful Eating, Mindful Movement Are there times when you realize that you are still eating and simply haven t noticed that you are not even hungry anymore? Do you ever get to the end of a
Session 15: Mindful Eating, Mindful Movement Are there times when you realize that you are still eating and simply haven t noticed that you are not even hungry anymore? Do you ever get to the end of a
End of Life with Dementia Sue Quist RN, CHPN
 End of Life with Dementia Sue Quist RN, CHPN Objectives: Describe the Medicare hospice benefit and services. Discuss the Medicare admission criteria for hospice patients with dementia due to Alzheimer
End of Life with Dementia Sue Quist RN, CHPN Objectives: Describe the Medicare hospice benefit and services. Discuss the Medicare admission criteria for hospice patients with dementia due to Alzheimer
GASTRECTOMY. Date of Surgery. Please bring this booklet the day of your surgery. QHC#34
 GASTRECTOMY Date of Surgery Please bring this booklet the day of your surgery. QHC#34 What is a Gastrectomy? A Gastrectomy is the surgical removal of all or part of the stomach. The stomach is the digestion
GASTRECTOMY Date of Surgery Please bring this booklet the day of your surgery. QHC#34 What is a Gastrectomy? A Gastrectomy is the surgical removal of all or part of the stomach. The stomach is the digestion
Be Fit for Life Series. Key Number Five Increase Metabolism
 Key #5 Increase Metabolism Page 1 of 9 Be Fit for Life Series Key Number Five Increase Metabolism Sit or lie in a safe and comfortable position I want you to close your eyes keep them closed until I ask
Key #5 Increase Metabolism Page 1 of 9 Be Fit for Life Series Key Number Five Increase Metabolism Sit or lie in a safe and comfortable position I want you to close your eyes keep them closed until I ask
RELAXATION EXERCISES
 RELAXATION EXERCISES Relaxation technique 1: Breathing meditation for stress relief With its focus on full, cleansing breaths, deep breathing is a simple, yet powerful, relaxation technique. It s easy
RELAXATION EXERCISES Relaxation technique 1: Breathing meditation for stress relief With its focus on full, cleansing breaths, deep breathing is a simple, yet powerful, relaxation technique. It s easy
Ileal Conduit Diversion Surgery
 Here are some words and pictures to help you understand this surgery: Bladder: the bladder stores urine that is made by the kidneys Bowels: the bowels are the parts of the body that digest food and fluids.
Here are some words and pictures to help you understand this surgery: Bladder: the bladder stores urine that is made by the kidneys Bowels: the bowels are the parts of the body that digest food and fluids.
4/3/2014. Dame Cicely Sanders : Born in England Nursing Degree Social Work Degree Doctor Opened 1 st Stand Alone Hospice 1967
 Catherine Hausenfluke Independent Consultant 512-966-4955 Know More about Dying and Grief Come to Terms with Your Own Morality Understand Grief and What are the Rules Understand the Dying Process Relating
Catherine Hausenfluke Independent Consultant 512-966-4955 Know More about Dying and Grief Come to Terms with Your Own Morality Understand Grief and What are the Rules Understand the Dying Process Relating
for the grieving process How to cope as your loved one nears the end stages of IPF
 Preparing yourself for the grieving process How to cope as your loved one nears the end stages of IPF 3 As your loved one nears the end stages of IPF, it s important that you be there for him or her as
Preparing yourself for the grieving process How to cope as your loved one nears the end stages of IPF 3 As your loved one nears the end stages of IPF, it s important that you be there for him or her as
Preparing for Death. A guide for families and caregivers as death approaches PALLIATIVE & END OF LIFE
 PALLIATIVE & END OF LIFE Preparing for Death A guide for families and caregivers as death approaches In this booklet you will learn about: Things to consider when a loved one is seriously ill Checklist
PALLIATIVE & END OF LIFE Preparing for Death A guide for families and caregivers as death approaches In this booklet you will learn about: Things to consider when a loved one is seriously ill Checklist
Hospice Journey. A guide of signs, symptoms and caregiving
 Hospice Journey A guide of signs, symptoms and caregiving 1 This book is a guide to help you through the dying journey a natural part of life. A variety of changes can be seen as a body prepares for death.
Hospice Journey A guide of signs, symptoms and caregiving 1 This book is a guide to help you through the dying journey a natural part of life. A variety of changes can be seen as a body prepares for death.
Delirium A guide for caregivers
 Delirium A guide for caregivers Disclaimer This is general information developed by The Ottawa Hospital. It is not intended to replace the advice of a qualified health-care provider. Please consult your
Delirium A guide for caregivers Disclaimer This is general information developed by The Ottawa Hospital. It is not intended to replace the advice of a qualified health-care provider. Please consult your
Welcome to Greenfield Community Acupuncture!
 Welcome to Greenfield Community Acupuncture! Since our office runs differently than many acupuncture offices, please take the time to read this introduction to our clinic and to our community. If you still
Welcome to Greenfield Community Acupuncture! Since our office runs differently than many acupuncture offices, please take the time to read this introduction to our clinic and to our community. If you still
University Counselling Service
 Bereavement The death of someone close can be devastating. There are no right or wrong reactions to death, the way you grieve will be unique to you. How you grieve will depend on many factors including
Bereavement The death of someone close can be devastating. There are no right or wrong reactions to death, the way you grieve will be unique to you. How you grieve will depend on many factors including
COMMUNICATION ISSUES IN PALLIATIVE CARE
 COMMUNICATION ISSUES IN PALLIATIVE CARE Palliative Care: Communication, Communication, Communication! Key Features of Communication in Appropriate setting Permission Palliative Care Be clear about topic
COMMUNICATION ISSUES IN PALLIATIVE CARE Palliative Care: Communication, Communication, Communication! Key Features of Communication in Appropriate setting Permission Palliative Care Be clear about topic
Seniors Helping Seniors September 7 & 12, 2016 Amy Abrams, MSW/MPH Education & Outreach Manager Alzheimer s San Diego
 Dementia Skills for In-Home Care Providers Seniors Helping Seniors September 7 & 12, 2016 Amy Abrams, MSW/MPH Education & Outreach Manager Alzheimer s San Diego Objectives Familiarity with the most common
Dementia Skills for In-Home Care Providers Seniors Helping Seniors September 7 & 12, 2016 Amy Abrams, MSW/MPH Education & Outreach Manager Alzheimer s San Diego Objectives Familiarity with the most common
Approaching End of Life Some Thoughts... Information for Patients and Families
 Approaching End of Life Some Thoughts... Information for Patients and Families This pamphlet has been produced by the Cancer Care Program of North York General Hospital www.nygh.on.ca 4001 Leslie Street,
Approaching End of Life Some Thoughts... Information for Patients and Families This pamphlet has been produced by the Cancer Care Program of North York General Hospital www.nygh.on.ca 4001 Leslie Street,
ALZHEIMER S DISEASE, DEMENTIA & DEPRESSION
 ALZHEIMER S DISEASE, DEMENTIA & DEPRESSION Daily Activities/Tasks As Alzheimer's disease and dementia progresses, activities like dressing, bathing, eating, and toileting may become harder to manage. Each
ALZHEIMER S DISEASE, DEMENTIA & DEPRESSION Daily Activities/Tasks As Alzheimer's disease and dementia progresses, activities like dressing, bathing, eating, and toileting may become harder to manage. Each
ANESTHESIA. Planning Your Childbirth: Pain Relief During Labor and Delivery EACH WOMAN S LABOR IS
 ANESTHESIA & YOU Planning Your Childbirth: Pain Relief During Labor and Delivery EACH WOMAN S LABOR IS UNIQUE T he amount of pain a woman feels during labor may differ from that felt by another woman.
ANESTHESIA & YOU Planning Your Childbirth: Pain Relief During Labor and Delivery EACH WOMAN S LABOR IS UNIQUE T he amount of pain a woman feels during labor may differ from that felt by another woman.
CARING FOR PATIENTS WITH DEMENTIA:
 CARING FOR PATIENTS WITH DEMENTIA: LESSON PLAN Lesson overview Time: One hour This lesson teaches useful ways to work with patients who suffer from dementia. Learning goals At the end of this session,
CARING FOR PATIENTS WITH DEMENTIA: LESSON PLAN Lesson overview Time: One hour This lesson teaches useful ways to work with patients who suffer from dementia. Learning goals At the end of this session,
wrha.mb.ca a conversation about tube feeding a guide for clients, families and friends healthcare professional guide Healthcare Professional Guide
 a conversation about tube feeding a guide for clients, families and friends healthcare professional guide Health Care Professional Guide Pamphlet Information Healthcare Professional Guide If you are reading
a conversation about tube feeding a guide for clients, families and friends healthcare professional guide Health Care Professional Guide Pamphlet Information Healthcare Professional Guide If you are reading
Coach on Call. Letting Go of Stress. A healthier life is on the line for you! How Does Stress Affect Me?
 Coach on Call How Does Stress Affect Me? Over time, stress can affect the way you feel, think, and act. You need some time when you are free of stress. You need ways to get relief from stress. Without
Coach on Call How Does Stress Affect Me? Over time, stress can affect the way you feel, think, and act. You need some time when you are free of stress. You need ways to get relief from stress. Without
Controlling Worries and Habits
 THINK GOOD FEEL GOOD Controlling Worries and Habits We often have obsessional thoughts that go round and round in our heads. Sometimes these thoughts keep happening and are about worrying things like germs,
THINK GOOD FEEL GOOD Controlling Worries and Habits We often have obsessional thoughts that go round and round in our heads. Sometimes these thoughts keep happening and are about worrying things like germs,
Keeping Home Safe WHAT CAN YOU DO?
 Keeping Home Safe or dementia may have trouble knowing what is dangerous or making safe decisions. By helping him or her feel more relaxed and less confused at home, you can help stop accidents. trip because
Keeping Home Safe or dementia may have trouble knowing what is dangerous or making safe decisions. By helping him or her feel more relaxed and less confused at home, you can help stop accidents. trip because
TAKING CARE OF YOUR FEELINGS
 TAKING CARE OF YOUR FEELINGS A burn injury causes changes in your life. Even though the event or accident that caused the burn may be over, you may still experience strong emotional or physical reactions.
TAKING CARE OF YOUR FEELINGS A burn injury causes changes in your life. Even though the event or accident that caused the burn may be over, you may still experience strong emotional or physical reactions.
INFORMATION FOR PATIENTS, CARERS AND FAMILIES. Coping with dying
 INFORMATION FOR PATIENTS, CARERS AND FAMILIES Coping with dying This leaflet describes some of the physical changes that happen to people as they start to die. It anticipates some of the questions you
INFORMATION FOR PATIENTS, CARERS AND FAMILIES Coping with dying This leaflet describes some of the physical changes that happen to people as they start to die. It anticipates some of the questions you
Preparing for Death: Guidelines for Your Family, Loved Ones or Caregivers
 Preparing for Death: Guidelines for Your Family, Loved Ones or Caregivers Once your loved one has chosen to take this step, and make use of the aid-in-dying drug, you may be the one or one of several who
Preparing for Death: Guidelines for Your Family, Loved Ones or Caregivers Once your loved one has chosen to take this step, and make use of the aid-in-dying drug, you may be the one or one of several who
Understanding Your Own Grief Journey. Information for Teens
 Understanding Your Own Grief Journey Information for Teens Grief is a natural response to love and loss. People who are grieving experience a variety of feelings, sometimes in succession, sometimes at
Understanding Your Own Grief Journey Information for Teens Grief is a natural response to love and loss. People who are grieving experience a variety of feelings, sometimes in succession, sometimes at
A Caregiver s Guide: Congestive Heart Failure
 A Caregiver s Guide: Congestive Heart Failure This is a guide for family members, friends and other caregivers who are supporting someone who has congestive heart failure (CHF). This is a guide for family
A Caregiver s Guide: Congestive Heart Failure This is a guide for family members, friends and other caregivers who are supporting someone who has congestive heart failure (CHF). This is a guide for family
and breathing Relaxation techniques East and North Hertfordshire NHS Trust Patient Information Series PI 83 a patient s guide
 Relaxation and breathing techniques Patient Information Series PI 83 East and North Hertfordshire NHS Trust 2 a patient s guide Relaxation and breathing techniques Contents Introduction 4 When and where
Relaxation and breathing techniques Patient Information Series PI 83 East and North Hertfordshire NHS Trust 2 a patient s guide Relaxation and breathing techniques Contents Introduction 4 When and where
Session 16: Manage Your Stress
 Session 16: Manage Your Stress Stress is part of life. However, you can learn better ways to take care of yourself when faced with stress. Stress is not always bad. Some stress can make life interesting
Session 16: Manage Your Stress Stress is part of life. However, you can learn better ways to take care of yourself when faced with stress. Stress is not always bad. Some stress can make life interesting
keep track of other information like warning discuss with your doctor, and numbers of signs for relapse, things you want to
 Helping you set your brain free from psychosis. www.heretohelp.bc.ca This book was written by Sophia Kelly and the BC Schizophrenia Society, for the BC Partners for Mental Health and Addictions Information.
Helping you set your brain free from psychosis. www.heretohelp.bc.ca This book was written by Sophia Kelly and the BC Schizophrenia Society, for the BC Partners for Mental Health and Addictions Information.
UW MEDICINE PATIENT EDUCATION. Baby Blues and More DRAFT. Knowing About This in Advance Can Help
 UW MEDICINE PATIENT EDUCATION Baby Blues and More Recognizing and coping with postpartum mood disorders Some women have baby blues or more serious postpartum mood disorders. It helps to know about these
UW MEDICINE PATIENT EDUCATION Baby Blues and More Recognizing and coping with postpartum mood disorders Some women have baby blues or more serious postpartum mood disorders. It helps to know about these
CARING FOR YOUR CATHETER AT HOME
 CARING FOR YOUR CATHETER AT HOME After surgery (radical prostatectomy) for prostate cancer you will have a urinary catheter for a short period of time and will need to go home with the catheter still in
CARING FOR YOUR CATHETER AT HOME After surgery (radical prostatectomy) for prostate cancer you will have a urinary catheter for a short period of time and will need to go home with the catheter still in
PERINATAL PALLIATIVE CARE SUPPORTING FAMILIES AS THEY PREPARE TO WELCOME THEIR BABY AND TO SAY GOOD-BYE
 PERINATAL PALLIATIVE CARE SUPPORTING FAMILIES AS THEY PREPARE TO WELCOME THEIR BABY AND TO SAY GOOD-BYE Kathy Cromwell CT, MSW, LCSW Director, Hinds Hospice Angel Babies HINDS HOSPICE ANGEL BABIES Our
PERINATAL PALLIATIVE CARE SUPPORTING FAMILIES AS THEY PREPARE TO WELCOME THEIR BABY AND TO SAY GOOD-BYE Kathy Cromwell CT, MSW, LCSW Director, Hinds Hospice Angel Babies HINDS HOSPICE ANGEL BABIES Our
After Soft Tissue Sarcoma Treatment
 After Soft Tissue Sarcoma Treatment Living as a Cancer Survivor For many people, cancer treatment often raises questions about next steps as a survivor. What Happens After Treatment for Soft Tissue Sarcomas?
After Soft Tissue Sarcoma Treatment Living as a Cancer Survivor For many people, cancer treatment often raises questions about next steps as a survivor. What Happens After Treatment for Soft Tissue Sarcomas?
Understanding THE SYMPTOMS YOU SEE
 Understanding THE SYMPTOMS YOU SEE Z Human existence is rich with experiences that weave a completed quilt called life. As the quilt nears completion, there is no set calendar as to its final, beautiful
Understanding THE SYMPTOMS YOU SEE Z Human existence is rich with experiences that weave a completed quilt called life. As the quilt nears completion, there is no set calendar as to its final, beautiful
Understanding and preventing delirium in older people
 Understanding and preventing delirium in older people Tips for family, whānau, and friends As people get older, especially if they are unwell or living with a dementia, they have greater risk of developing
Understanding and preventing delirium in older people Tips for family, whānau, and friends As people get older, especially if they are unwell or living with a dementia, they have greater risk of developing
S A M P L E. Your Pain. Managing. Logo A GUIDE TO PAIN MEDICATION USE
 Managing Your Pain A GUIDE TO PAIN MEDICATION USE Logo Revised 2019. 2015 by Quality of Life Publishing Co. All rights reserved. No part of this booklet may be reproduced without prior permission of the
Managing Your Pain A GUIDE TO PAIN MEDICATION USE Logo Revised 2019. 2015 by Quality of Life Publishing Co. All rights reserved. No part of this booklet may be reproduced without prior permission of the
Participant s Guide Care at the End-of-Life
 Participant s Guide Care at the End-of-Life Module One Managing Resident Care Module Two Preparing the Family Module Three: After Death Credits Project Lead Paula McMenamin, MSW Content Experts Connie
Participant s Guide Care at the End-of-Life Module One Managing Resident Care Module Two Preparing the Family Module Three: After Death Credits Project Lead Paula McMenamin, MSW Content Experts Connie
After Adrenal Cancer Treatment
 After Adrenal Cancer Treatment Living as a Cancer Survivor For many people, cancer treatment often raises questions about next steps as a survivor. Lifestyle Changes After Treatment for Adrenal Cancer
After Adrenal Cancer Treatment Living as a Cancer Survivor For many people, cancer treatment often raises questions about next steps as a survivor. Lifestyle Changes After Treatment for Adrenal Cancer
Lesson 9 Anxiety and Relaxation Techniques
 The following presentation was originally developed for individuals and families by Achieva (a Western PA service provider). Now offered as a webcast production, ODP is providing this valuable resource
The following presentation was originally developed for individuals and families by Achieva (a Western PA service provider). Now offered as a webcast production, ODP is providing this valuable resource
Enhanced Recovery Programme Liver surgery
 Enhanced Recovery Programme Liver surgery General Surgery Patient information leaflet Introduction When you are admitted to hospital for your surgery you will be taking part in an enhanced recovery programme.
Enhanced Recovery Programme Liver surgery General Surgery Patient information leaflet Introduction When you are admitted to hospital for your surgery you will be taking part in an enhanced recovery programme.
Delirium: Information for Patients and Families
 health information Delirium: Information for Patients and Families 605837 Alberta Health Services, (2016/11) Resources Delirium in the Older Person Family Guide: search delirium at viha.ca Go to myhealth.alberta.ca
health information Delirium: Information for Patients and Families 605837 Alberta Health Services, (2016/11) Resources Delirium in the Older Person Family Guide: search delirium at viha.ca Go to myhealth.alberta.ca
What to Expect in the Last Days of Life: A Guide for Caregivers
 Inside this guide: Physical changes and needs Eating and drinking 2 Pain 3 Restlessness, agitation and disorientation Mouth, nose and eye care Weakness and sleepiness Changes in breathing Looking after
Inside this guide: Physical changes and needs Eating and drinking 2 Pain 3 Restlessness, agitation and disorientation Mouth, nose and eye care Weakness and sleepiness Changes in breathing Looking after
Lose Weight. without dieting.
 Lose Weight without dieting www.bronwendeklerk.com The Secret to Losing Weight Today I want to share a little secret with you. If you re reading this you have probably become despondent with dieting. Maybe
Lose Weight without dieting www.bronwendeklerk.com The Secret to Losing Weight Today I want to share a little secret with you. If you re reading this you have probably become despondent with dieting. Maybe
- copyright
 Relaxation Exercises Let s start with breathing! Your breathing is often the first thing to be affected by stress. When we are anxious we tend to hunch up the shoulders and breathe in a more rapid and
Relaxation Exercises Let s start with breathing! Your breathing is often the first thing to be affected by stress. When we are anxious we tend to hunch up the shoulders and breathe in a more rapid and
Tips on How to Better Serve Customers with Various Disabilities
 FREDERICTON AGE-FRIENDLY COMMUNITY ADVISORY COMMITTEE Tips on How to Better Serve Customers with Various Disabilities Fredericton - A Community for All Ages How To Welcome Customers With Disabilities People
FREDERICTON AGE-FRIENDLY COMMUNITY ADVISORY COMMITTEE Tips on How to Better Serve Customers with Various Disabilities Fredericton - A Community for All Ages How To Welcome Customers With Disabilities People
Tips on How to Manage Stress and Sleep
 Tips on How to Manage Stress and Sleep Insomnia Everyone has had those times of watching the clock, noting with misery how slowly the night is passing. Insomnia is repeated difficulty in falling asleep,
Tips on How to Manage Stress and Sleep Insomnia Everyone has had those times of watching the clock, noting with misery how slowly the night is passing. Insomnia is repeated difficulty in falling asleep,
A Guide to Help New Mothers Stay Smoke-Free
 A Guide to Help New Mothers Stay Smoke-Free 1 Welcome to motherhood! You have just been through a life-changing experience pregnancy and child birth. Having a plan to stay smoke-free is an important step.
A Guide to Help New Mothers Stay Smoke-Free 1 Welcome to motherhood! You have just been through a life-changing experience pregnancy and child birth. Having a plan to stay smoke-free is an important step.
CARING FOR THOSE YOU LOVE
 CARING FOR THOSE YOU LOVE PRESENTED BY: BILL CRAWFORD, Jr. Dementia Care Specialist COMFORT KEEPERS 8205 CAMP BOWIE WEST SUITE 216 FORT WORTH, TEXAS 76116 P: 817-560-8085 Bill Crawford, Jr., DCS, Director
CARING FOR THOSE YOU LOVE PRESENTED BY: BILL CRAWFORD, Jr. Dementia Care Specialist COMFORT KEEPERS 8205 CAMP BOWIE WEST SUITE 216 FORT WORTH, TEXAS 76116 P: 817-560-8085 Bill Crawford, Jr., DCS, Director
Relaxation Techniques
 Relaxation is needed for good health. It gives your body and mind a chance to rest and recover from high-stress situations. Your heart rate slows down, blood pressure decreases and muscles relax. Relaxation
Relaxation is needed for good health. It gives your body and mind a chance to rest and recover from high-stress situations. Your heart rate slows down, blood pressure decreases and muscles relax. Relaxation
Progression LATE STAGE. What is Alzheimer s disease? The late stage - what to expect
 Progression LATE STAGE This document is one in a five-part series on the stages of Alzheimer s disease and is written for the person with the disease, their family 1 and caregivers. The late stage of the
Progression LATE STAGE This document is one in a five-part series on the stages of Alzheimer s disease and is written for the person with the disease, their family 1 and caregivers. The late stage of the
CARING FOR SICK PEOPLE AT HOME
 PANDEMIC INFLUENZA CARING FOR SICK PEOPLE AT HOME What is pandemic flu? Pandemic flu means that a new strain of influenza has spread all over the world and is affecting a large number of people. During
PANDEMIC INFLUENZA CARING FOR SICK PEOPLE AT HOME What is pandemic flu? Pandemic flu means that a new strain of influenza has spread all over the world and is affecting a large number of people. During
Pain Relief During Labor and Delivery
 Pain Relief During Labor and Delivery Each woman's labor is unique. The amount of pain a woman feels during labor may differ from that felt by another woman. Pain depends on many factors, such as the size
Pain Relief During Labor and Delivery Each woman's labor is unique. The amount of pain a woman feels during labor may differ from that felt by another woman. Pain depends on many factors, such as the size
Grief and Loss. What is grief like?
 Grief and Loss What is grief like? Grief is our response to loss. It is the normal, natural and inevitable response to loss, and it can affect every part of our life, but it is varied and different for
Grief and Loss What is grief like? Grief is our response to loss. It is the normal, natural and inevitable response to loss, and it can affect every part of our life, but it is varied and different for
Teaching Family and Friends in Your Community
 2 CHAPTER Teaching Family and Friends in Your Community 9 Old people can remember when there were fewer problems with teeth and gums. Children s teeth were stronger and adults kept their teeth longer.
2 CHAPTER Teaching Family and Friends in Your Community 9 Old people can remember when there were fewer problems with teeth and gums. Children s teeth were stronger and adults kept their teeth longer.
Hospice Education Network - ELNEC: Geriatrics - Communication Module 6. two-wayway
 E L N E C End-of-Life Nursing Education Consortium Geriatric Curriculum Module 6: Communication at the End of Life Part I: Basic Communication Objectives: Describe basic principles of communication Explore
E L N E C End-of-Life Nursing Education Consortium Geriatric Curriculum Module 6: Communication at the End of Life Part I: Basic Communication Objectives: Describe basic principles of communication Explore
Thoughts on Living with Cancer. Healing and Dying. by Caren S. Fried, Ph.D.
 Thoughts on Living with Cancer Healing and Dying by Caren S. Fried, Ph.D. My Personal Experience In 1994, I was told those fateful words: You have cancer. At that time, I was 35 years old, a biologist,
Thoughts on Living with Cancer Healing and Dying by Caren S. Fried, Ph.D. My Personal Experience In 1994, I was told those fateful words: You have cancer. At that time, I was 35 years old, a biologist,
Introduction. Today we hope to provide tips and resources to help balance the challenges of caregiving and ensure that everyone is being cared for.
 Caregiver Wellness Introduction Being a caregiver can be both rewarding and challenging. It s easy to forget to tend to your own needs while caring for your loved one, but it is incredibly important. Today
Caregiver Wellness Introduction Being a caregiver can be both rewarding and challenging. It s easy to forget to tend to your own needs while caring for your loved one, but it is incredibly important. Today
Living well with and beyond cancer Information, support and practical advice to help you through treatment and beyond
 Living well with and beyond cancer Information, support and practical advice to help you through treatment and beyond Exceptional healthcare, personally delivered Introduction to this booklet Receiving
Living well with and beyond cancer Information, support and practical advice to help you through treatment and beyond Exceptional healthcare, personally delivered Introduction to this booklet Receiving
Validation Techniques in a Real World By Alisa Tagg, BA ACC/EDU AC-BC CADDCT CDP CDCS NAAP President
 What is Validation? This therapy was developed to attempt understanding what emotions patients with Alzheimer s disease are expressing and respond in a way that allows patients to express their emotions
What is Validation? This therapy was developed to attempt understanding what emotions patients with Alzheimer s disease are expressing and respond in a way that allows patients to express their emotions
In most cases, behavioural and psychological symptoms can be successfully managed without medication.
 MEDICATION People with dementia often develop changes as their condition progresses. These include changes in their behaviour and feelings, the things they think and how they perceive the world. Collectively,
MEDICATION People with dementia often develop changes as their condition progresses. These include changes in their behaviour and feelings, the things they think and how they perceive the world. Collectively,
MINTO PREVENTION & REHABILITATION CENTRE CENTRE DE PREVENTION ET DE READAPTATION MINTO. Preparing to Quit. About This Kit
 MINTO PREVENTION & REHABILITATION CENTRE CENTRE DE PREVENTION ET DE READAPTATION MINTO Preparing to Quit About This Kit There is no one best way to quit smoking. Your Heart Institute Prevention and Rehabilitation
MINTO PREVENTION & REHABILITATION CENTRE CENTRE DE PREVENTION ET DE READAPTATION MINTO Preparing to Quit About This Kit There is no one best way to quit smoking. Your Heart Institute Prevention and Rehabilitation
End-of-Life Care. Annual Education End-of-Life Care Mission Health System, Inc.
 Annual Education 2014 2013 Mission Health System, Inc. Why Cover This Subject? Patients who are near the end of their lives need to receive care that addresses their psychosocial, emotional, and spiritual
Annual Education 2014 2013 Mission Health System, Inc. Why Cover This Subject? Patients who are near the end of their lives need to receive care that addresses their psychosocial, emotional, and spiritual
Delirium Information for relatives, carers and patients
 Delirium Information for relatives, carers and patients Contents Part A Introduction What is delirium? Quotes from relatives or carers showing what might happen to a patient suffering from delirium How
Delirium Information for relatives, carers and patients Contents Part A Introduction What is delirium? Quotes from relatives or carers showing what might happen to a patient suffering from delirium How
STAY NOURISHED. Be happy and healthy as you age
 STAY NOURISHED Be happy and healthy as you age As we age physical changes to our bodies occur which can affect the way we think and feel about food. These changes can prevent us from having access to a
STAY NOURISHED Be happy and healthy as you age As we age physical changes to our bodies occur which can affect the way we think and feel about food. These changes can prevent us from having access to a
UW MEDICINE PATIENT EDUCATION. Baby Blues and More. Postpartum mood disorders DRAFT. Emotional Changes After Giving Birth
 UW MEDICINE PATIENT EDUCATION Baby Blues and More Postpartum mood disorders Some new mothers have baby blues or more serious postpartum mood disorders. This chapter gives ideas for things you can do to
UW MEDICINE PATIENT EDUCATION Baby Blues and More Postpartum mood disorders Some new mothers have baby blues or more serious postpartum mood disorders. This chapter gives ideas for things you can do to
Having suicidal thoughts?
 Having suicidal thoughts? Information for you, and for family, whänau, friends and support network Prepared by skylight for the New Zealand Guidelines Group CONTENTS Having Suicidal Thoughts? 1 Asking
Having suicidal thoughts? Information for you, and for family, whänau, friends and support network Prepared by skylight for the New Zealand Guidelines Group CONTENTS Having Suicidal Thoughts? 1 Asking
Accessibility. Serving Clients with Disabilities
 Accessibility Serving Clients with Disabilities Did you know that just over 15.5% of Ontarians have a disability? That s 1 in every 7 Ontarians and as the population ages that number will grow. People
Accessibility Serving Clients with Disabilities Did you know that just over 15.5% of Ontarians have a disability? That s 1 in every 7 Ontarians and as the population ages that number will grow. People
CHEMOTHERAPY. What should I expect?
 CHEMOTHERAPY What should I expect? WHAT IS CHEMOTHERAPY? Chemotherapy is treatment that uses drugs to stop the growth of cancer cells, either by killing the cells or by stopping them from dividing. Chemotherapy
CHEMOTHERAPY What should I expect? WHAT IS CHEMOTHERAPY? Chemotherapy is treatment that uses drugs to stop the growth of cancer cells, either by killing the cells or by stopping them from dividing. Chemotherapy
Feeling depressed? Feeling anxious? What may help. What may help
 2. EMOTIONAL NEEDS A long and serious illness takes its toll as much on the mind as it does on the body. Distress or emotional upset can arise at any time and can last for days, weeks, or even months.
2. EMOTIONAL NEEDS A long and serious illness takes its toll as much on the mind as it does on the body. Distress or emotional upset can arise at any time and can last for days, weeks, or even months.
The 5 Emotional First Aid Skills
 The 5 Emotional First Aid Skills Reach Out Provide a caring presence. Don t try to fix the survivor or help him look at the bright side. Get by the survivor s side at his level, listen, lightly touch,
The 5 Emotional First Aid Skills Reach Out Provide a caring presence. Don t try to fix the survivor or help him look at the bright side. Get by the survivor s side at his level, listen, lightly touch,
AFSP SURVIVOR OUTREACH PROGRAM VOLUNTEER TRAINING HANDOUT
 AFSP SURVIVOR OUTREACH PROGRAM VOLUNTEER TRAINING HANDOUT Goals of the AFSP Survivor Outreach Program Suggested Answers To Frequently Asked Questions on Visits Roadblocks to Communication During Visits
AFSP SURVIVOR OUTREACH PROGRAM VOLUNTEER TRAINING HANDOUT Goals of the AFSP Survivor Outreach Program Suggested Answers To Frequently Asked Questions on Visits Roadblocks to Communication During Visits
Esophagectomy Surgery
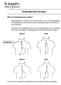 Esophagectomy Surgery What is esophagectomy surgery? Esophagectomy surgery is the removal part, or all, of the esophagus. The esophagus is the tube that your food goes down on the way to your stomach.
Esophagectomy Surgery What is esophagectomy surgery? Esophagectomy surgery is the removal part, or all, of the esophagus. The esophagus is the tube that your food goes down on the way to your stomach.
Mindfulness: Practice and Movement
 Mindfulness: Practice and Movement Being mindful can apply to the way our bodies move and feel. In between movement, the body gains benefits by focusing on the pauses or rest. What You Need Electronic
Mindfulness: Practice and Movement Being mindful can apply to the way our bodies move and feel. In between movement, the body gains benefits by focusing on the pauses or rest. What You Need Electronic
FAMILY AND FRIENDS. are an important part of every woman s journey with ovarian cancer
 FAMILY AND FRIENDS are an important part of every woman s journey with ovarian cancer Going for a walk with me, taking me out of the house, just distracting me from my problems were good and talking about
FAMILY AND FRIENDS are an important part of every woman s journey with ovarian cancer Going for a walk with me, taking me out of the house, just distracting me from my problems were good and talking about
Restlessness Emotional support Self care
 Comfort Airway Restlessness Emotional support Self care MED 12412 9/12 City of Hope Department of Supportive Care Medicine 1500 Duarte Road Duarte, CA 91010 August 2012 The following are recommendations
Comfort Airway Restlessness Emotional support Self care MED 12412 9/12 City of Hope Department of Supportive Care Medicine 1500 Duarte Road Duarte, CA 91010 August 2012 The following are recommendations
YOGA FOR ANXIETY SINEAD MC KIERNAN LOVE YOGA. Facebook Love Yoga.
 YOGA FOR ANXIETY SINEAD MC KIERNAN LOVE YOGA loveyogaclasses@gmail.com Tweet @sineadloveyoga Facebook Love Yoga ANXIETY; a feeling of worry, nervousness, or unease about something with an uncertain outcome.
YOGA FOR ANXIETY SINEAD MC KIERNAN LOVE YOGA loveyogaclasses@gmail.com Tweet @sineadloveyoga Facebook Love Yoga ANXIETY; a feeling of worry, nervousness, or unease about something with an uncertain outcome.
