cardiac surgery: a review of 64 cases
|
|
|
- Cuthbert Weaver
- 5 years ago
- Views:
Transcription
1 Thorax (1968), 23, 652. The use of tracheostomy following major open cardiac surgery: a review of 64 cases JOHN C. NICHOLLS1 From the Brompton Hospital, London, S.W.3 Sixty-four tracheostomies performed in the period September 1965 to August 1966 in patients unfdergoing major open-heart surgery are reviewed. The indications and complications are classified, and the high incidence of secondary infection is discussed briefly. Tracheal stenosis or dilatation occurred in six patients (9 4%) and the contributory factors are discussed in greater detail. Tracheostomy is one of the oldest established procedures in surgical practice, but the indications for its use have undergone considerable changes, particularly in the last 25 years (Borman and Davidson, 1963). Its use is again under review (Lancet, 1967) and, as a result of the associated complications, many centres are using alternative methods, such as oro-tracheal and naso-tracheal intubation, even though they may have their own drawbacks (Tonkin and Harrison, 1966). It is therefore pertinent to review the use of tracheostomy in relation to one of the more recent indications-that is, after major open cardiac surgery. MATERIAL AND METHODS All patients admitted to the intensive care unit at the Brompton Hospital from 1 September 1965 to 31 August 1966 were assessed. The minimum period of follow-up was four months to allow for the development of late complications. Of 179 patients submitted to cardiopulmonary bypass surgery 68 required a tracheostomy for intermittent positive pressure respiration. The case records of 64 of these patients were examined; four were untraced. They consisted of a mixed population whose ages ranged from 6 to 63 years (average 34 years). Two patients had a second tracheostomy, and these are included as separate entities, as they were separated by a sufficient period of time and were, in any case, performed for different indications. There were 41 survivors (65%). TECHNIQUE AND MANAGEMENT All tracheostomies in this series were performed by a member of the sur- 1 Present address: West Herts Hospital, Hemel Hempstead, Herts 652 gical team, and all followed a common technique. Under general anaesthesia the method of Bjork (1960), using a transverse skin incision and constructing an anterior tracheal wall flap stitched to the subcutaneous tissues, was used. A plastic (Portex) cuffed tracheostomy tube, of the standard pattern and appropriate size, was inserted and the cuff was inflated just sufficiently to make an airtight seal. A dry dressing only, or skin sutures, were used, and the tracheostomy tube was then connected to a sterile respirator of the intermittent positive pressure type. During the period under review the nursing staff observed the following instructions for the management of the tracheostomy: The cuff was not released for the first 12 hours, and was then released for one minute every four hours following pharyngeal suction. It was then inflated again with just sufficient air to make an airtight seal. Tracheal suction was applied hourly, or more frequently if necessary, via a sterile rubber catheter held by sterile forceps. A 'no-touch' technique was desirable but was not always possible. The wound was cleaned with chlorhexidine (1: 1,000) and sprayed with Polybactrin four-hourly and a dry dressing was applied. (This might have been done more frequently if the dressing became moist.) A wound swab was taken and a trapped specimen of sputum was sent for culture the day following tracheostomy. These investigations were repeated every week unless more frequent results were required. When pathogenic organisms were cultured the patients were isolated or, as circumstances demanded, were moved into a different ward in the company of other patients with similar infecting organisms. Treatment with the appropriate systemic antibiotics was begun. The rooms were fumigated by a Hycolin spray for 24 hours before being brought back into use Ṫhe tracheostomy tube was only changed for specific indications.
2 The use of tracheostomy following major open cardiac surgery: a review of 64 cases RESULTS Tracheostomies were performed in 38 % of all patients who underwent cardiopulmonary bypass. Forty-seven (75%) were performed in the operating theatre, and the other 17 were performed in the intensive care unit. INDICATIONS All tracheostomies except one were performed as elective procedures and these are divided into three groups (Table I). The only TABLE I Group Indication NCosf I Pre-operative decision Operative decision Post-operative complications emergency tracheostomy was necessary for a patient in whom the endotracheal tube suddenly became blocked after 42 hours. The indications in group 1 were all multiple valve replacements, total correction of Fallot's tetralogy, clinical evidence of pulmonary oedema, or a raised pulmonary vascular resistance. One patient in this group had sustained a cardiac arrest seven days pre-operatively and a tracheostomy was performed at that time. In group 2 the following indications were used: a perfusion time longer than three hours, impaired cardiac function after total bypass, and suspected cerebral damage during operation due to anoxia or embolism. In one patient the sternum had to be left unsutured due to continued bleeding controllable only by packing. In both these groups the tracheostomy was performed at the end of the operation before the patient left the theatre. The post-operative complications (group 3) consisted of respiratory insufficiency after removal of the endotracheal tube, development of pulmonary oedema, development of a low output state, cerebral damage (unforeseen), and pulmonary em.boli. Tracheostomy was performed if any of the above was expected to last for a time exceeding 48 hours after the beginning of the operation, this being accepted at that time as the maximum for which an endotracheal tube would be left safely in situ. DURATION The mean period of intubation via the tracheostomy was 12-1 days (1-80 days), and for the survivors it was 14-7 days (2-80 days). Sixty-one patients were artificially ventilated for the whole of these periods (except for the 24-hour trial period before the tube was removed). In the remaining three patients weaning off artificial ventilation was prolonged, and these patients had a tracheostomy with intermittent ventilator support lasting 18 out of 26, 37 out of 63, and 3 out of 5 days. ENDOTRACHEAL INTUBATION This was performed in all patients, and the duration includes the time of operation. Forty-four patients had endotracheal intubation for 12 hours or less and one for 15 hours, being mainly those patients in groups 1 and 2. In 14 patients the endotracheal tube was in place for between 24 and 48 hours. The remaining five patients had endotracheal intubation exceeding 48 hours, the longest being 73 hours' continuous intubation followed by re-intubation 9 hours later for a further 6 hours before tracheostomy was performed. USE OF CURARE All patients were curarized for the period of operation, and its use was continued post-operatively for a period determined in consultation with the anaesthetist. Sedation was substituted as soon as the patients were able to tolerate the ventilator satisfactorily. In 20 patients no curare was required post-operatively. In the remaining 44, curare was necessary for an average period of 32 hours (2-120 hours). COMPLICATIONS 653 Infection In one patient infection was present before the tracheostomy was done and nine did not survive long enough for infection to become established. The patients fell into two groupsthose in whom the tracheostomy was performed in the theatre (38) and those in whom it was performed in the intensive care unit (16). In each case local, i.e., wound (if grown from the wound swab), and general (usually chest) infections were considered separately. Infection was determined by a positive culture and was thus not necessarily of clinical significance. Of the intensive care unit patients local infection occurred in 14 (87%) and general infection in all (100%). Six (16%) of the theatre patients showed no evidence of either local or general infection, 32 (82%) had a local infection, and 29 (74%) had a general infection. The incidence of infection did not show any direct relationship to the duration of tracheostomy or previous endotracheal intubation.
3 654 Pseudomonas pyocyanea, Escherichia coli, and Candida albicans were the commonest invading organisms. Stenosis This occurred in three patients (4-7%). In the first, the earliest evidence appeared 18 days after tracheostomy and was treated initially by repeated dilatations and eventually resection after 67 days. Death occurred at 94 days from a pyocyaneus septicaemia. The second patient developed a stricture 48 days post-operatively, which only required a single dilatation. Stenosis occurred in the third patient three months postoperatively and requires intermittent dilatation one year later. John C. Nicholls Dilatation Tracheal dilatation also occurred in three patients three, four, and six weeks postoperatively, and in all insertion of a large orotracheal tube was required for a time to maintain ventilation until a larger tracheostomy tube was inserted. Anoxic cardiac arrest, with eventual recovery, occurred in one patient when a large enough tube was not immediately available, and it was thus impossible to maintain satisfactory ventilation. Haemorrhage In two patients this was severe enough to require surgical intervention; in one bronchoscopy was necessary. Both episodes occurred on the seventh day and both patients were on anticoagulants. In three other patients there was some local bleeding which was controlled by conservative measures. Miscellaneous The following complications also occurred (in some cases in association with those previously mentioned). Food and fluids leaked temporarily around the tracheostomy tube above the balloon in two patients. In fourother patients, the tube was coughed up by one, blockage occurred at two days and required the tube to be changed in another, and a stitch abscess formed, resulting in a keloid scar, in the other two. Thus 17 complications other than infection occurred in 12 patients (19%). The complication was of a serious nature (stenosis, dilatation, and haemorrhage) in eight (12-5%). It is impossible to attribute any deaths solely to the tracheostomy in such a group of seriously ill patients. CLOSURE In only 16 of the 41 survivors was the time of closure of the wound recorded (closure implying disappearance of the air leak). This averaged 15-7 days (range 5-32), although in a further patient the wound was not fully healed two months later (following an 80-day tracheostomy). DISCUSSION This series forms a useful group of patients who have had tracheostomies performed and who were managed in a constant manner for a short period of time. They form their own control series for any one case, and the resulting complications can be considered by comparison with the uncomplicated cases. Two other similar series have been reported in recent years (Robertson, 1964; Trimble and Yao, 1966), but the series of McClelland (1965) and pf Neville, Spinazzola, Scicchitano, and Langston (1964) dealt with a wider selection of patients. Robertson, in his series in 1963, gave an overall incidence for tracheostomy of 32-4% in 389 patients undergoing open-heart surgery, which compares with the 38% in the present series. Only half of his patients were artificially ventilated, the main indication for tracheostomy being to allow efficient ventilation to continue. The other 50% were not ventilated artificially, but in a series of 50 patients reported by Trimble and Yao (1966) only one patient who had a tracheostomy was not artificially ventilated. This latter group is similar to the present series, and it may be that the prophylactic tracheostomies performed by Robertson would not now be done. In the present series, three cases were found in retrospect in which a tracheostomy may not have been necessary, because the patients recovered quickly, although this point is difficult to establish with any certainty; in the rest it would seem to have been essential. The indications for tracheostomy after open-heart surgery are continually changing and, as each new procedure becomes more firmly established, the necessity for a preoperative decision to perform a tracheostomy becomes less certain. Also, in the post-operative period attempts are being made to avoid tracheostomy by prolonged endotracheal intubation (Pracy, 1966; Lancet, 1967), although as recently as 1959 it was thought to be impossible to continue intermittent positive pressure respiration via an endotracheal tube for more than 24 hours (Cawthorne, Hewlett, and Ranger, 1959). The incidence of complications in the present series is higher than that previously reported, especially compared with Neville's series of mixed post-surgical cases (Neville et al., 1964), but it is lower than in the random series of McClelland
4 The use of tracheostomy following major open cardiac surgery: a review of 64 cases (1965). The reasons for this are not clear but may be related to the longer mean duration of tracheostomy of 14-7 days, compared with 6 5 days (Robertson, 1964) and 6 days (Trimble and Yao, 1966). The only complications reported in the latter series were infection (not detailed) in seven patients; in the former series complications consisted of an obstructed airway in several patients, haemorrhage in two, and anoxia during suction in one. The high incidence of infection in the present series is due to the inclusion of clinically nonsignificant infections, and possibly to the frequency with which specimens were taken. The only salient feature that emerged from the results was the markedly lower incidence of general infections resulting in the group submitted to tracheostomy in the theatre. The frequency was high despite all the precautions taken and, as in the patients described by Gotsman and Whitby (1964), was probably related to the hospital environment rather than to any other specific cause. Spalding (1966) was able to reduce lung infection by spraying the wound with Polybactrin every hour and using nystatin eight-hourly, and by the use of disposable polythene gloves when sucking out or touching the tracheostomy. Of the other complications, haemorrhage in a certain number of patients appears to be unavoidable, but stenosis and dilatation deserve special attention. The three patients who developed stenosis in this series showed no special common features (Table II) when compared with the series as a whole. TABLE II TABLE III The incidence of stenosis (4 7%) was slightly lower than in Gibson's (1967) series. The three factors which he included in the possible aetiology, namely overinflation of the cuff leading to pressure necrosis, a piston-like action from the ventilator leading to shearing forces, and secondary infection, were not all present in our three cases. Four of his patients required surgical treatment, whereas surgery was necessary in only one of the above patients. Tracheal dilatation has previously been reported in long-term cases (Lloyd and McClelland, 1964; Ringrose, 1965) and in our three patients certain common factors emerged. In two, leaking of food and fluids from the wound occurred after 9 and 18 days respectively; and both these eventually succumbed. The average age of the three patients (54 years) was higher than that of the whole series (34 years), as was the duration of the tracheostomy (55-5 days: 12-1 days), and all were massively infected at some stage. Two of the patients had endotracheal intubation for more than 24 hours, but the third was intubated only during operation. Two patients had prolonged periods of curarization, but the third required none (Table III). One patient was intolerant of the respirator for the first two weeks and there may have been considerable movement of the tracheostomy tube within the trachea. The numbers are too small for statistical analysis, but the above factors may be worthy of note. Tracheal lesions are common after tracheostomy (Stiles, 1965), but their incidence may be lessened by the use of non-irritant plastic tubes instead of the red rubber tubes that were used formerly. This Endo- Indication Age Duration Place Curare tracheal (years) (days) Performed (hours) Intubation InetoOucm Infection Outcome (hours) Pre-operative Theatre 48 9 Multiple Survived Pre-operative arrest Theatre 0 35 Multiple Died Emergency I.C.U Pre-tracheostomy Died 655
5 656 does not seem to have been the case when this series is compared with others. A prospective study of the histological changes found in tracheal mucosa following the use of these new tubes would be valuable. I should like to thank the following: Mr. W. Williams, who originally suggested the subject for this re iew; Mr. M. Paneth. for his help and encouragement; Mr. W. P. Cleland and Mr. P. Gadhiali. for advice; and Lord Brock and Mr. 0. S. Tubbs, for permission to study the patients under their care. REFERENCES Bjork V. 0. (1960). Partial resection of the only remaining lung with the aid of respirator treatment. J. thorac. cardiovasc. Surg., 39, 179. Borman, J., and Davidson, J. T. (1963). A history of tracheostomy: si spiritum ducit vivit (Cicero). Brit. J. Anaesth., 35, 388. Cawthome, T., Hewlett, A. B., and Ranger, D. (1959). Discussion: tracheostomy today. Proc. roy. Soc. Med., 52, 403. Gibson, P. (1967). Aetiology and repair of tracheal stenosis following tracheostomy and intermittent positive pressure respiration. Thorax, 22, 1. Gotsman, M. S., and Whitby, J. L. (1964). Respiratory infection following tracheostomy. Ibid., 19, 89. Leading article (1967). Endotracheal intubation or tracheostomy. Lancet, 1, 258. Lloyd, J. W., and McClelland, R. M. A. (1964). Tracheal dilatation. An unusual complication of tracheostomy. Ibid., 1, 83. John C. Nicholls McClelland, R. M. A. (1965). Complications of tracheostomy. Brit. med. J., 2, 567. Neville, W. E., Spinazzola, A., Scicchitano, L. P., and Langston, H. D. (1964). Tracheostomy and assisted ventilation. Use in respiratory insufficiency in the postsurgical patient. Arch. Surg., 89, 149. Pracy, R. (1966). Respiratory units: intermittent positive respiration: tracheostomy. Proc. roy. Soc. Med., 59, 35. Ringrose, E. W. (1965). Tracheal dilatation following prolonged use of a cuffed endotracheal tube. Med. J. Aust., 1, 591. Robertson, D. S. (1964). Tracheostomy and open heart surgery. Proc. roy. Soc. Med., 57, 855. Spalding, J. M. K. (1966). Respiratory units: intermittent positive pressure respiration: tracheostomy. Ibid., 59, 29. Stiles, P. J. (1965). Tracheal lesions after tracheostomy. Thorax, 20, 517. Tonkin, J. P., and Harrison, G. A. (1966). The effect on the larynx of prolonged endotracheal intubation. Med. J. Aust., 2, 581. Trimble, A. S., and Yao, J. (1966). Tracheostomy: surgical technique and sequelae in fifty cardiovascular patients. J. thorac. cardioi'asc. Surg., 51, 569. ADDENDUM Since the period of review management of the tracheostomy has been modified in respect of releasing the cuff; this is now deflated for one minute in every hour. Also several patients have been ventilated via the endotracheal tube for periods longer than 48 hours without apparent added complications, although analysis has not yet been undertaken. Thorax: first published as /thx on 1 November Downloaded from on 17 March 2019 by guest. Protected by copyright.
tracheostomies following open-heart surgery
 Thorax (1969), 24, 78. A review of the management of 14 elective tracheostomies following open-heart surgery R. D. MARSHALL From St. Bartholomew's Hospital, London' A retrospective survey of 14 cases of
Thorax (1969), 24, 78. A review of the management of 14 elective tracheostomies following open-heart surgery R. D. MARSHALL From St. Bartholomew's Hospital, London' A retrospective survey of 14 cases of
Tracheal Stenosis Following Cuffed Tube Tracheostomy
 Tracheal Stenosis Following Cuffed Tube Tracheostomy Anatomical Variation and Selected Treatment Armand A. Lefemine, M.D., Kenneth MacDonnell, M.D., and Hyung S. Moon, M.D. ABSTRACT Tracheal stenosis resulting
Tracheal Stenosis Following Cuffed Tube Tracheostomy Anatomical Variation and Selected Treatment Armand A. Lefemine, M.D., Kenneth MacDonnell, M.D., and Hyung S. Moon, M.D. ABSTRACT Tracheal stenosis resulting
Competency 1: General principles and equipment required to safely manage a patient with a tracheostomy tube.
 Competency 1: General principles and equipment required to safely manage a patient with a tracheostomy tube. Trainee Name: ------------------------------------------------------------- Title: ---------------------------------------------------------------
Competency 1: General principles and equipment required to safely manage a patient with a tracheostomy tube. Trainee Name: ------------------------------------------------------------- Title: ---------------------------------------------------------------
Tracheostomy. Information for patients and relatives
 Tracheostomy Information for patients and relatives page 2 What is a tracheostomy? A tracheostomy is a small hole (stoma) made at the front of the neck, which goes into the trachea (windpipe). A tube called
Tracheostomy Information for patients and relatives page 2 What is a tracheostomy? A tracheostomy is a small hole (stoma) made at the front of the neck, which goes into the trachea (windpipe). A tube called
All bedside percutaneously placed tracheostomies
 Page 1 of 5 Scope: All bedside percutaneously placed tracheostomies Population: All ICU personnel Outcomes: To standardize and outline the steps necessary to safely perform a percutaneous tracheostomy
Page 1 of 5 Scope: All bedside percutaneously placed tracheostomies Population: All ICU personnel Outcomes: To standardize and outline the steps necessary to safely perform a percutaneous tracheostomy
Emergency)tracheostomy)management)/)Patent)upper)airway)
 Emergency)tracheostomy)management)/)Patent)upper)airway) Call,for,airway,expert,help,,Look,,listen,&,feel,at,the,mouth,and,tracheostomy) A)Mapleson)C)system)(e.g.) Waters)circuit ))may)help)assessment)if)available)
Emergency)tracheostomy)management)/)Patent)upper)airway) Call,for,airway,expert,help,,Look,,listen,&,feel,at,the,mouth,and,tracheostomy) A)Mapleson)C)system)(e.g.) Waters)circuit ))may)help)assessment)if)available)
The essential principles of tracheostomy care
 The essential principles of tracheostomy care Deborah Dawson Consultant Nurse Critical Care Excellence in specialist and community healthcare Key publications https://www.stgeorges.nhs.uk/gps-andclinicians/clinical-resources/tracheostomyguidelines/
The essential principles of tracheostomy care Deborah Dawson Consultant Nurse Critical Care Excellence in specialist and community healthcare Key publications https://www.stgeorges.nhs.uk/gps-andclinicians/clinical-resources/tracheostomyguidelines/
Foundations of Critical Care Nursing Course. Tracheostomy Workbook
 Foundations of Critical Care Nursing Course Tracheostomy Workbook 1 Key Reference: Dawson D (2014) Essential principles:trachepstomy care in the adult patient, Nursing in Critical Care, Vol 19, 2 p.63-72.
Foundations of Critical Care Nursing Course Tracheostomy Workbook 1 Key Reference: Dawson D (2014) Essential principles:trachepstomy care in the adult patient, Nursing in Critical Care, Vol 19, 2 p.63-72.
RCH Trauma Guideline. Management of Traumatic Pneumothorax & Haemothorax. Trauma Service, Division of Surgery
 RCH Trauma Guideline Management of Traumatic Pneumothorax & Haemothorax Trauma Service, Division of Surgery Aim To describe safe and competent management of traumatic pneumothorax and haemothorax at RCH.
RCH Trauma Guideline Management of Traumatic Pneumothorax & Haemothorax Trauma Service, Division of Surgery Aim To describe safe and competent management of traumatic pneumothorax and haemothorax at RCH.
Use of the Silicone T-tube to Treat Tracheal Stenosis or Tracheal Injury
 Use of the Silicone T-tube to Treat Stenosis or Injury Chang-Jer Huang MD Backgound: stenosis or tracheal is a troublesome disease. Traditional temporary tracheostomy and reconstruction can resolve some
Use of the Silicone T-tube to Treat Stenosis or Injury Chang-Jer Huang MD Backgound: stenosis or tracheal is a troublesome disease. Traditional temporary tracheostomy and reconstruction can resolve some
TRACHEOSTOMY CARE. Tracheostomy- Surgically created hole that extends from the neck skin into the windpipe or trachea.
 1 TRACHEOSTOMY CARE Definitions: Trachea-Windpipe Tracheostomy- Surgically created hole that extends from the neck skin into the windpipe or trachea. Outer Cannula- The outer part of a trach tube. Usually
1 TRACHEOSTOMY CARE Definitions: Trachea-Windpipe Tracheostomy- Surgically created hole that extends from the neck skin into the windpipe or trachea. Outer Cannula- The outer part of a trach tube. Usually
Rota-Trach Double Lumen Tracheostomy Tube VITALTEC
 Rota-Trach Double Lumen Tracheostomy Tube VITALTEC Contents INTRODUCTION HISTORY REVIEW ANATOMY & PHYSIOLOGY OPERATIVE PROCEDURE THE RANGE OF TRACHEOSTOMY TUBES ROTA-TRACH TRACHEOSTOMY TUBE INTRODUCTION
Rota-Trach Double Lumen Tracheostomy Tube VITALTEC Contents INTRODUCTION HISTORY REVIEW ANATOMY & PHYSIOLOGY OPERATIVE PROCEDURE THE RANGE OF TRACHEOSTOMY TUBES ROTA-TRACH TRACHEOSTOMY TUBE INTRODUCTION
Cuff Diameter: A Quantitative
 Enlarging Intratracheal Tube Cuff Diameter: A Quantitative Roentgenographic Study of Its Value in the Early Prediction of Serious Tracheal Damage Faroque Khan, M.B., and Narayan C. Reddy, M.D. ABSTRACT
Enlarging Intratracheal Tube Cuff Diameter: A Quantitative Roentgenographic Study of Its Value in the Early Prediction of Serious Tracheal Damage Faroque Khan, M.B., and Narayan C. Reddy, M.D. ABSTRACT
Collaborative Regional Benchmarking Group (North of England, North Yorkshire & Humber and West Yorkshire)
 Collaborative Regional Benchmarking Group (North of England, North Yorkshire & Humber and West Yorkshire) Best Practice Guidance Endo Tracheal Tube Care These recommendations are based on the current evidence
Collaborative Regional Benchmarking Group (North of England, North Yorkshire & Humber and West Yorkshire) Best Practice Guidance Endo Tracheal Tube Care These recommendations are based on the current evidence
TRACHEOSTOMY. Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion
 TRACHEOSTOMY Definition Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion Indications for tracheostomy 1-upper airway obstruction with stridor, air hunger,
TRACHEOSTOMY Definition Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion Indications for tracheostomy 1-upper airway obstruction with stridor, air hunger,
Disclosures. Learning Objectives. Coeditor/author. Associate Science Editor, American Heart Association
 Tracheotomy Challenges for airway specialists Elizabeth H. Sinz, MD Professor of Anesthesiology & Neurosurgery Associate Dean for Clinical Simulation Disclosures Coeditor/author Associate Science Editor,
Tracheotomy Challenges for airway specialists Elizabeth H. Sinz, MD Professor of Anesthesiology & Neurosurgery Associate Dean for Clinical Simulation Disclosures Coeditor/author Associate Science Editor,
TRACHEOSTOMY 186 INTENSIVE CARE
 186 INTENSIVE CARE Table 7.4 Indications for tracheostomy Upper-airway obstruction Prolonged mechanical ventilation To facilitate bronchopulmonary toilet To maintain and protect the airway use of oral
186 INTENSIVE CARE Table 7.4 Indications for tracheostomy Upper-airway obstruction Prolonged mechanical ventilation To facilitate bronchopulmonary toilet To maintain and protect the airway use of oral
CARING FOR THE TRACHEOSTOMISED PATIENT: WHAT TO LOOK OUT FOR
 CARING FOR THE TRACHEOSTOMISED PATIENT: WHAT TO LOOK OUT FOR DR MOHD NAZRI ALI Anaesthesiologist & Intensivist HRPZ II, Kota Bharu, Kelantan Tracheostomy The Enabling Disability Tracheostomy Are becoming
CARING FOR THE TRACHEOSTOMISED PATIENT: WHAT TO LOOK OUT FOR DR MOHD NAZRI ALI Anaesthesiologist & Intensivist HRPZ II, Kota Bharu, Kelantan Tracheostomy The Enabling Disability Tracheostomy Are becoming
Kapitex Healthcare. making things clearer for tracheostomy patients
 Kapitex Healthcare making things clearer for tracheostomy patients preface In publishing this booklet, Kapitex Healthcare Ltd hopes to provide information and understanding for both the patient and carer
Kapitex Healthcare making things clearer for tracheostomy patients preface In publishing this booklet, Kapitex Healthcare Ltd hopes to provide information and understanding for both the patient and carer
ANWICU knowledge
 ANWICU knowledge www.anwicu.org.uk This presenta=on is provided by ANWICU We are a collabora=ve associa=on of ICUs in the North West of England. Permission to provide this presenta=on has been granted
ANWICU knowledge www.anwicu.org.uk This presenta=on is provided by ANWICU We are a collabora=ve associa=on of ICUs in the North West of England. Permission to provide this presenta=on has been granted
Review July Page 1 of 36. Title of Guideline. Contact Names and Job Title (authors) Directorate & Speciality
 Title of Guideline Contact Names and Job Title (authors) Directorate & Speciality Date of submission 06/07/2017 Date on which guideline must be reviewed Explicit definition of patient group to which it
Title of Guideline Contact Names and Job Title (authors) Directorate & Speciality Date of submission 06/07/2017 Date on which guideline must be reviewed Explicit definition of patient group to which it
Tracheostomy Sim Course
 Patients Name: Robert Smith Patients Age / DOB: 45 year old gentleman on medical ward Major Medical Problem Displaced tracheostomy tube Learning Goal Medical Early recognition of displaced tracheostomy
Patients Name: Robert Smith Patients Age / DOB: 45 year old gentleman on medical ward Major Medical Problem Displaced tracheostomy tube Learning Goal Medical Early recognition of displaced tracheostomy
Perforated duodenal ulcer in Reading from 1950 to 1959
 Gut, 1969, 1, 454-459 Perforated duodenal ulcer in Reading from 195 to 1959 PAUL CASSELL From the Royal Berkshire Hospital, Reading During the last 15 years there has been an evolution in the management
Gut, 1969, 1, 454-459 Perforated duodenal ulcer in Reading from 195 to 1959 PAUL CASSELL From the Royal Berkshire Hospital, Reading During the last 15 years there has been an evolution in the management
Clearing the air.. How to assist and rescue neck breathing patients. Presented by: Don Hall MCD, CCC/SLP Sarah Markel RRT, MHA
 Clearing the air.. How to assist and rescue neck breathing patients Presented by: Don Hall MCD, CCC/SLP Sarah Markel RRT, MHA Learning Objectives Define common terms identified with total (laryngectomy)
Clearing the air.. How to assist and rescue neck breathing patients Presented by: Don Hall MCD, CCC/SLP Sarah Markel RRT, MHA Learning Objectives Define common terms identified with total (laryngectomy)
CHEST DRAIN PROTOCOL
 CHEST DRAIN PROTOCOL Rationale The pleural membranes have an important role in effective lung expansion. The visceral pleura is a thin, smooth, serous membrane covering the surface of the lungs and is
CHEST DRAIN PROTOCOL Rationale The pleural membranes have an important role in effective lung expansion. The visceral pleura is a thin, smooth, serous membrane covering the surface of the lungs and is
Tracheostomy and laryngectomy airway emergencies: an overview for medical and nursing staff
 2013 Medical Journal Tracheostomy and laryngectomy airway emergencies: an overview for medical and nursing staff Steven Lobaz 1 and Paul Bush 2 1 ST6 and 2 Consultant Department of Anaesthesia and Intensive
2013 Medical Journal Tracheostomy and laryngectomy airway emergencies: an overview for medical and nursing staff Steven Lobaz 1 and Paul Bush 2 1 ST6 and 2 Consultant Department of Anaesthesia and Intensive
Tracheo-innominate artery fistula (TIF) is an uncommon
 Technique for Managing Tracheo-Innominate Artery Fistula Gorav Ailawadi, MD Tracheo-innominate artery fistula (TIF) is an uncommon complication (0.1-1%) following both open and percutaneous tracheostomy.
Technique for Managing Tracheo-Innominate Artery Fistula Gorav Ailawadi, MD Tracheo-innominate artery fistula (TIF) is an uncommon complication (0.1-1%) following both open and percutaneous tracheostomy.
I. Subject: Therapeutic Bronchoscopy and Bronchoscope Assisted Intubation
 I. Subject: Therapeutic Bronchoscopy and Bronchoscope Assisted Intubation II. Policy: Therapeutic flexible fiberoptic bronchoscopy procedures and bronchoscope assisted intubations will be performed by
I. Subject: Therapeutic Bronchoscopy and Bronchoscope Assisted Intubation II. Policy: Therapeutic flexible fiberoptic bronchoscopy procedures and bronchoscope assisted intubations will be performed by
Airway Management in the ICU
 Airway Management in the ICU New developments in management of epistaxis. April 28, 2008 Methods of airway control Non surgical BIPAP CPAP Mask ventilation Laryngeal Mask Intubation Surgical Cricothyrotomy
Airway Management in the ICU New developments in management of epistaxis. April 28, 2008 Methods of airway control Non surgical BIPAP CPAP Mask ventilation Laryngeal Mask Intubation Surgical Cricothyrotomy
PERFORATION OF THE TRACHEA AND BRONCHUS BY THE BRONCHOSCOPE
 Thlorax (1950), 5, 369. PERFORATION OF THE TRACHEA AND BRONCHUS BY THE BRONCHOSCOPE BY Fronm the Regional Thoracic Surgery Centre, Shotley Bridge Hospital, Newcastle-upon-Tyne (RECEIVED FOR PUBLICATION
Thlorax (1950), 5, 369. PERFORATION OF THE TRACHEA AND BRONCHUS BY THE BRONCHOSCOPE BY Fronm the Regional Thoracic Surgery Centre, Shotley Bridge Hospital, Newcastle-upon-Tyne (RECEIVED FOR PUBLICATION
Airway Management in a Patient with Klippel-Feil Syndrome Using Extracorporeal Membrane Oxygenator
 Airway Management in a Patient with Klippel-Feil Syndrome Using Extracorporeal Membrane Oxygenator Beckerman Z*, Cohen O, Adler Z, Segal D, Mishali D and Bolotin G Department of Cardiac Surgery, Rambam
Airway Management in a Patient with Klippel-Feil Syndrome Using Extracorporeal Membrane Oxygenator Beckerman Z*, Cohen O, Adler Z, Segal D, Mishali D and Bolotin G Department of Cardiac Surgery, Rambam
POLICY FOR THE PREVENTION AND CONTROL OF TUBERCULOSIS
 POLICY FOR THE PREVENTION AND CONTROL OF TUBERCULOSIS Policy No: 7.20 Approval Date: Review Date: Lead Director: Under Review Under Review Under Review Page 1 of 7 Polic y_for_the_prevention_and_control_of_tuberculosis
POLICY FOR THE PREVENTION AND CONTROL OF TUBERCULOSIS Policy No: 7.20 Approval Date: Review Date: Lead Director: Under Review Under Review Under Review Page 1 of 7 Polic y_for_the_prevention_and_control_of_tuberculosis
Results of Mitral Valve Replacement, with Special Reference to the Functional Tricuspid Insufficiency
 Results of Mitral Valve Replacement, with Special Reference to the Functional Tricuspid Insufficiency Ken-ichi ASANO, M.D., Masahiko WASHIO, M.D., and Shoji EGUCHI, M.D. SUMMARY (1) Surgical results of
Results of Mitral Valve Replacement, with Special Reference to the Functional Tricuspid Insufficiency Ken-ichi ASANO, M.D., Masahiko WASHIO, M.D., and Shoji EGUCHI, M.D. SUMMARY (1) Surgical results of
Waitin In The Wings. Esophageal/Tracheal Double Lumen Airway (Combitube ) Indications and Use for the Pre-Hospital Provider
 Waitin In The Wings Esophageal/Tracheal Double Lumen Airway (Combitube ) Indications and Use for the Pre-Hospital Provider 1 CombiTube Kit General Description The CombiTube is A double-lumen tube with
Waitin In The Wings Esophageal/Tracheal Double Lumen Airway (Combitube ) Indications and Use for the Pre-Hospital Provider 1 CombiTube Kit General Description The CombiTube is A double-lumen tube with
RSPT Tracheal Aspiration. Tracheal Aspiration. RSPT 1410 Tracheal Aspiration
 1 RSPT 1410 2 is the use of to facilitate the removal of secretions from the respiratory tract. Under normal circumstances, patients with normal coughing do not have difficulty in removing secretions.
1 RSPT 1410 2 is the use of to facilitate the removal of secretions from the respiratory tract. Under normal circumstances, patients with normal coughing do not have difficulty in removing secretions.
Extracorporeal Life Support Organization (ELSO) Guidelines for Pediatric Respiratory Failure
 Extracorporeal Life Support Organization (ELSO) Guidelines for Pediatric Respiratory Failure Introduction This pediatric respiratory failure guideline is a supplement to ELSO s General Guidelines for all
Extracorporeal Life Support Organization (ELSO) Guidelines for Pediatric Respiratory Failure Introduction This pediatric respiratory failure guideline is a supplement to ELSO s General Guidelines for all
Safer Tracheostomy Care Course
 Patients Name: Samira Patel Patients Age / DOB: 65 year old female on a general ward Major Medical Problem Blocked tracheostomy tube Learning Goal Medical Early recognition of respiratory distress Understanding
Patients Name: Samira Patel Patients Age / DOB: 65 year old female on a general ward Major Medical Problem Blocked tracheostomy tube Learning Goal Medical Early recognition of respiratory distress Understanding
Tracheostomy. Hope Building Neurosurgery
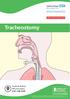 Tracheostomy Hope Building Neurosurgery 0161 206 5055 All Rights Reserved 2017. Document for issue as handout. Unique Identifier: CS36(17). Review date: November 2019 What is a tracheostomy? A tracheostomy
Tracheostomy Hope Building Neurosurgery 0161 206 5055 All Rights Reserved 2017. Document for issue as handout. Unique Identifier: CS36(17). Review date: November 2019 What is a tracheostomy? A tracheostomy
Options for Airway Management During Complex Resection and Reconstruction
 Options for Airway Management During Complex Resection and Reconstruction Brian E. Louie MD, FACS, FRCSC, MHA, MPH Director, Thoracic Research and Education Co-Director, Minimally Invasive Thoracic Surgery
Options for Airway Management During Complex Resection and Reconstruction Brian E. Louie MD, FACS, FRCSC, MHA, MPH Director, Thoracic Research and Education Co-Director, Minimally Invasive Thoracic Surgery
Discussing feline tracheal disease
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk Discussing feline tracheal disease Author : ANDREW SPARKES Categories : Vets Date : March 24, 2008 ANDREW SPARKES aims to
Vet Times The website for the veterinary profession https://www.vettimes.co.uk Discussing feline tracheal disease Author : ANDREW SPARKES Categories : Vets Date : March 24, 2008 ANDREW SPARKES aims to
Translaryngeal tracheostomy
 Translaryngeal tracheostomy Issued: August 2013 NICE interventional procedure guidance 462 guidance.nice.org.uk/ipg462 NICE has accredited the process used by the NICE Interventional Procedures Programme
Translaryngeal tracheostomy Issued: August 2013 NICE interventional procedure guidance 462 guidance.nice.org.uk/ipg462 NICE has accredited the process used by the NICE Interventional Procedures Programme
squamous-cell carcinoma1
 Thorax (1975), 30, 152. Local ablative procedures designed to destroy squamous-cell carcinoma1 J. M. LEE, FREDERICK P. STITIK, DARRYL CARTER, and R. ROBINSON BAKER Departments of Surgery, Pathology, and
Thorax (1975), 30, 152. Local ablative procedures designed to destroy squamous-cell carcinoma1 J. M. LEE, FREDERICK P. STITIK, DARRYL CARTER, and R. ROBINSON BAKER Departments of Surgery, Pathology, and
PYELOPLASTY (LAPAROSCOPIC AND OPEN PROCEDURE)
 PYELOPLASTY (LAPAROSCOPIC AND OPEN PROCEDURE) AN INFORMATION LEAFLET Written by: Department of Urology May 2011 Stockport: 0161 419 5698 Website: w w w. s t o c k p o r t. n h s. u k Tameside: 0161 922
PYELOPLASTY (LAPAROSCOPIC AND OPEN PROCEDURE) AN INFORMATION LEAFLET Written by: Department of Urology May 2011 Stockport: 0161 419 5698 Website: w w w. s t o c k p o r t. n h s. u k Tameside: 0161 922
Changing tracheostomy tubes
 Changing tracheostomy tubes Changing the tracheostomy tube should be a multidisciplinary decision. The first change should always be performed or supervised by a suitably trained member of the medical
Changing tracheostomy tubes Changing the tracheostomy tube should be a multidisciplinary decision. The first change should always be performed or supervised by a suitably trained member of the medical
Other methods for maintaining the airway (not definitive airway as still unprotected):
 Page 56 Where anaesthetic skills and drugs are available, endotracheal intubation is the preferred method of securing a definitive airway. This technique comprises: rapid sequence induction of anaesthesia
Page 56 Where anaesthetic skills and drugs are available, endotracheal intubation is the preferred method of securing a definitive airway. This technique comprises: rapid sequence induction of anaesthesia
Introducing the Fastrach-LMA. Prepared by Jim Medeiros, NREMT-P Regional Field Coordinator Lord Fairfax EMS Council
 Introducing the Fastrach-LMA Prepared by Jim Medeiros, NREMT-P Regional Field Coordinator Lord Fairfax EMS Council Objectives Review Anatomy of the Upper Airway Review LFEMSC LMA Protocol Discuss Indications
Introducing the Fastrach-LMA Prepared by Jim Medeiros, NREMT-P Regional Field Coordinator Lord Fairfax EMS Council Objectives Review Anatomy of the Upper Airway Review LFEMSC LMA Protocol Discuss Indications
Bergen Community College Division of Health Professions Department of Respiratory Care Fundamentals of Respiratory Critical Care
 Bergen Community College Division of Health Professions Department of Respiratory Care Fundamentals of Respiratory Critical Care Date Revised: January 2015 Course Description Student Learning Objectives:
Bergen Community College Division of Health Professions Department of Respiratory Care Fundamentals of Respiratory Critical Care Date Revised: January 2015 Course Description Student Learning Objectives:
Policies and Procedures. I.D. Number: 1154
 Policies and Procedures Title: TRACHEOSTOMY TUBE CHANGE - PEDIATRIC I.D. Number: 1154 Authorization: [X ] SHR Nursing Practice Committee Source: Nursing Date Effective: October 2008 Date Revised: March
Policies and Procedures Title: TRACHEOSTOMY TUBE CHANGE - PEDIATRIC I.D. Number: 1154 Authorization: [X ] SHR Nursing Practice Committee Source: Nursing Date Effective: October 2008 Date Revised: March
4/24/2017. Tracheal Stenosis. Tracheal Stenosis. Tracheal Stenosis. Tracheal Stenosis. Tracheal Stenosis Endoscopic & Surgical Management
 Endoscopic & Surgical Management Pressure ulceration Healing: granulation cicatrization contraction Ann Surg 1969;169:334-348 Gary Schwartz, MD Department of Thoracic Surgery and Lung Transplantation Baylor
Endoscopic & Surgical Management Pressure ulceration Healing: granulation cicatrization contraction Ann Surg 1969;169:334-348 Gary Schwartz, MD Department of Thoracic Surgery and Lung Transplantation Baylor
Policy x.xxx. Issued: Artificial Airways and Airway Care. ABC Home Medical Company Policy & Procedure Manual. A. Tracheostomy Tubes ( trach tubes)
 A. Tracheostomy Tubes ( trach tubes) A tracheotomy is a surgical procedure whereby an opening is cut into the trachea of the patient for the purpose of inserting a tube (trach tube). The trach tube allows
A. Tracheostomy Tubes ( trach tubes) A tracheotomy is a surgical procedure whereby an opening is cut into the trachea of the patient for the purpose of inserting a tube (trach tube). The trach tube allows
MRSA pneumonia mucus plug burden and the difficult airway
 Case report Crit Care Shock (2016) 19:54-58 MRSA pneumonia mucus plug burden and the difficult airway Ann Tsung, Brian T. Wessman An 80-year-old female with a past medical history of chronic obstructive
Case report Crit Care Shock (2016) 19:54-58 MRSA pneumonia mucus plug burden and the difficult airway Ann Tsung, Brian T. Wessman An 80-year-old female with a past medical history of chronic obstructive
Inhaled Foreign Bodies in Children
 Arch. Dis. Childh., 1966, 41, 402. Inhaled Foreign Bodies in Children An analysis of 40 cases CONSTANCE M. DAVIS From the Royal Liverpool Children's Hospital and Alder Hey Children's Hospital, Liverpool
Arch. Dis. Childh., 1966, 41, 402. Inhaled Foreign Bodies in Children An analysis of 40 cases CONSTANCE M. DAVIS From the Royal Liverpool Children's Hospital and Alder Hey Children's Hospital, Liverpool
Critical Care Monitoring. Indications. Pleural Space. Chest Drainage. Chest Drainage. Potential space. Contains fluid lubricant
 Critical Care Monitoring Indications 1-2- 2 Pleural Space Potential space Contains fluid lubricant Can fill with air, blood, plasma, serum, lymph, pus 3 1 Pleural Space Problems when contain abnormal substances:
Critical Care Monitoring Indications 1-2- 2 Pleural Space Potential space Contains fluid lubricant Can fill with air, blood, plasma, serum, lymph, pus 3 1 Pleural Space Problems when contain abnormal substances:
UMC HEALTH SYSTEM Lubbock, Texas :
 Consent for Commonly Performed Procedures in the Adult Critical Care Units I, the undersigned, understand that the adult intensive and intermediate care units ( critical care units ) are places where seriously
Consent for Commonly Performed Procedures in the Adult Critical Care Units I, the undersigned, understand that the adult intensive and intermediate care units ( critical care units ) are places where seriously
Nasopharyngeal airways for craniofacial conditions
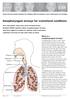 Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Nasopharyngeal airways for craniofacial conditions This information sheet from Great Ormond Street Hospital (GOSH)
Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Nasopharyngeal airways for craniofacial conditions This information sheet from Great Ormond Street Hospital (GOSH)
Steroid Therapy for Tracheal Stenosis in Children
 Steroid Therapy for Tracheal Stenosis in Children Clinical Experience in 4 Children with Severe Strictures H. Biemann Othersen, Jr., M.D. ABSTRACT Recently a refinement in the treatment of tracheal stenosis
Steroid Therapy for Tracheal Stenosis in Children Clinical Experience in 4 Children with Severe Strictures H. Biemann Othersen, Jr., M.D. ABSTRACT Recently a refinement in the treatment of tracheal stenosis
OSAMA A. ABDULMAJID, ABDELMOMEN M. EBEID, MOHAMED M. MOTAWEH, and IBRAHIM S. KLEIBO
 Aspirated foreign bodies in the tracheobronchial tree: report of 250 cases Thorax (1976), 31, 635. OSAMA A. ABDULMAJID, ABDELMOMEN M. EBEID, MOHAMED M. MOTAWEH, and IBRAHIM S. KLEIBO Thoracic Surgical
Aspirated foreign bodies in the tracheobronchial tree: report of 250 cases Thorax (1976), 31, 635. OSAMA A. ABDULMAJID, ABDELMOMEN M. EBEID, MOHAMED M. MOTAWEH, and IBRAHIM S. KLEIBO Thoracic Surgical
SORE THROAT AFTER ANAESTHESIA
 Brit. J. Anaesth. (1960), 32, 219 SORE THROAT AFTER ANAESTHESIA BY C. M. CONWAY, J. S. MILLER AND F. L. H. SUGDEN Department of Anaesthesia, Charing Cross Hospital Medical School, London, W.C.2 A sore
Brit. J. Anaesth. (1960), 32, 219 SORE THROAT AFTER ANAESTHESIA BY C. M. CONWAY, J. S. MILLER AND F. L. H. SUGDEN Department of Anaesthesia, Charing Cross Hospital Medical School, London, W.C.2 A sore
H: Respiratory Care. Saskatchewan Association of Licensed Practical Nurses, Competency Profile for LPNs, 3rd Ed. 79
 H: Respiratory Care Saskatchewan Association of Licensed Practical Nurses, Competency Profile for LPNs, 3rd Ed. 79 Competency: H-1 Airway Management H-1-1 H-1-2 H-1-3 H-1-4 H-1-5 Demonstrate knowledge
H: Respiratory Care Saskatchewan Association of Licensed Practical Nurses, Competency Profile for LPNs, 3rd Ed. 79 Competency: H-1 Airway Management H-1-1 H-1-2 H-1-3 H-1-4 H-1-5 Demonstrate knowledge
Chapter 40 Advanced Airway Management
 1 2 3 4 5 Chapter 40 Advanced Airway Management Advanced Airway Management The advanced airway management techniques discussed in this chapter are to introduce the EMT-B student to these procedures only.
1 2 3 4 5 Chapter 40 Advanced Airway Management Advanced Airway Management The advanced airway management techniques discussed in this chapter are to introduce the EMT-B student to these procedures only.
Tracheal Stenosis as a Complication of Tracheos tomy
 Tracheal Stenosis as a Complication of Tracheos tomy D. A. Murphy, M.D., L. D. MacLean, M.D., and A. R. C. Dobell, M.D. T racheal stenosis is a rare complication of tracheostomy. As Colles [5] wrote in
Tracheal Stenosis as a Complication of Tracheos tomy D. A. Murphy, M.D., L. D. MacLean, M.D., and A. R. C. Dobell, M.D. T racheal stenosis is a rare complication of tracheostomy. As Colles [5] wrote in
POSTGRADUATE INSTITUTE OF MEDICINE UNIVERSITY OF COLOMBO. MD (ANAESTHESIOLOGY) FINAL EXAMINATION AUGUST 2011 Time : 1.00 p.m p.m.
 POSTGRADUATE INSTITUTE OF MEDICINE UNIVERSITY OF COLOMBO MD (ANAESTHESIOLOGY) FINAL EXAMINATION AUGUST 2011 Date : 5 th August 2011 Time : 1.00 p.m. 4.00 p.m. Answer any three questions. Answer each question
POSTGRADUATE INSTITUTE OF MEDICINE UNIVERSITY OF COLOMBO MD (ANAESTHESIOLOGY) FINAL EXAMINATION AUGUST 2011 Date : 5 th August 2011 Time : 1.00 p.m. 4.00 p.m. Answer any three questions. Answer each question
Endoscopy. Pulmonary Endoscopy
 Pulmonary 1 Direct visualization of TB tree Developed in 1890 s to remove foreign bodies - rigid metal tube Advances added light system, Sx Flexible fiberoptic scopes introduced in early 1960 s 2 Used
Pulmonary 1 Direct visualization of TB tree Developed in 1890 s to remove foreign bodies - rigid metal tube Advances added light system, Sx Flexible fiberoptic scopes introduced in early 1960 s 2 Used
Kingdom; 2 University of Cambridge, Cambridge, United Kingdom
 P-111 TIMING OF TRACHEOSTOMY AND ASSOCIATED COMPLICATIONS IN CARDIOTHORACIC INTENSIVE CARE PATIENTS Zochios, Vasileios 1 ; Casey, Jessica 2 ; Vuylsteke, Alain 1 1 Cardiac Critical Care Unit, Papworth Hospital
P-111 TIMING OF TRACHEOSTOMY AND ASSOCIATED COMPLICATIONS IN CARDIOTHORACIC INTENSIVE CARE PATIENTS Zochios, Vasileios 1 ; Casey, Jessica 2 ; Vuylsteke, Alain 1 1 Cardiac Critical Care Unit, Papworth Hospital
What you need to know about having a vasectomy
 University Teaching Trust What you need to know about having a vasectomy Urology Hope Building 0161 206 5380 All Rights Reserved 2017. Document for issue as handout. What is a vasectomy? A vasectomy is
University Teaching Trust What you need to know about having a vasectomy Urology Hope Building 0161 206 5380 All Rights Reserved 2017. Document for issue as handout. What is a vasectomy? A vasectomy is
Tracheal stenosis in infants and children is typically characterized
 Slide Tracheoplasty for Congenital Tracheal Stenosis Peter B. Manning, MD Tracheal stenosis in infants and children is typically characterized by the presence of complete cartilaginous tracheal rings and
Slide Tracheoplasty for Congenital Tracheal Stenosis Peter B. Manning, MD Tracheal stenosis in infants and children is typically characterized by the presence of complete cartilaginous tracheal rings and
Indications for the Brock operation in current
 Thorax (1973), 28, 1. Indications for the Brock operation in current treatment of tetralogy of Fallot H. R. MATTHEWS and R. H. R. BELSEY Department of Thoracic Surgery, Frenchay Hospital, Bristol It is
Thorax (1973), 28, 1. Indications for the Brock operation in current treatment of tetralogy of Fallot H. R. MATTHEWS and R. H. R. BELSEY Department of Thoracic Surgery, Frenchay Hospital, Bristol It is
Adult Patients Going Home with a Tracheostomy
 Physiotherapy Department Adult Patients Going Home with a Tracheostomy Darent Valley Hospital Darenth Wood Road Dartford Kent DA2 8DA www.dvh.nhs.uk In case of emergencies you will need to dial 999 If
Physiotherapy Department Adult Patients Going Home with a Tracheostomy Darent Valley Hospital Darenth Wood Road Dartford Kent DA2 8DA www.dvh.nhs.uk In case of emergencies you will need to dial 999 If
Oral care & swallowing
 Oral care & swallowing Oral care is important as it has a role to play in preventing healthcare associated infections. Dental plaque and the oropharynx can become colonized by bacteria and a biofilm can
Oral care & swallowing Oral care is important as it has a role to play in preventing healthcare associated infections. Dental plaque and the oropharynx can become colonized by bacteria and a biofilm can
Heart Valve Replacement
 Heart Valve Replacement Introduction Sometimes people have serious problems with the valves in their hearts. A heart valve repair or replacement surgery restores or replaces a defective heart valve. If
Heart Valve Replacement Introduction Sometimes people have serious problems with the valves in their hearts. A heart valve repair or replacement surgery restores or replaces a defective heart valve. If
Airway complications on the general medical unit after prolonged ICU admission
 Airway complications on the general medical unit after prolonged ICU admission Palash Kar Discipline of Acute Care Medicine, University of Adelaide Intensive Care Unit, Royal Adelaide Hospital, Adelaide,
Airway complications on the general medical unit after prolonged ICU admission Palash Kar Discipline of Acute Care Medicine, University of Adelaide Intensive Care Unit, Royal Adelaide Hospital, Adelaide,
Tracheostomy discharge information. Information for community nurses, patients and carers
 Tracheostomy discharge information Information for community nurses, patients and carers What is a tracheostomy? A tracheostomy is a surgical incision (cut) through the neck tissues into the trachea leaving
Tracheostomy discharge information Information for community nurses, patients and carers What is a tracheostomy? A tracheostomy is a surgical incision (cut) through the neck tissues into the trachea leaving
Case Report. Management of recurrent distal tracheal stenosis using an endoprosthesis: a case report* Abstract. Introduction.
 121 Case Report Management of recurrent distal tracheal stenosis using an endoprosthesis: a case report* André Germano Leite 1, Douglas Kussler 2 Abstract The authors report the case of a patient with
121 Case Report Management of recurrent distal tracheal stenosis using an endoprosthesis: a case report* André Germano Leite 1, Douglas Kussler 2 Abstract The authors report the case of a patient with
Trans-catheter aortic valve implantation (TAVI) work up
 Trans-catheter aortic valve implantation (TAVI) work up You have been referred for an assessment known as a TAVI work up because you have been diagnosed with aortic stenosis. This factsheet explains the
Trans-catheter aortic valve implantation (TAVI) work up You have been referred for an assessment known as a TAVI work up because you have been diagnosed with aortic stenosis. This factsheet explains the
Insertion of a totally implantable vascular access device (TIVAD)
 Insertion of a totally implantable vascular access device (TIVAD) What is a TIVAD? A TIVAD is a long hollow tube that is inserted into one of the large veins in your body. One end of the tube sits in a
Insertion of a totally implantable vascular access device (TIVAD) What is a TIVAD? A TIVAD is a long hollow tube that is inserted into one of the large veins in your body. One end of the tube sits in a
Tracheostomy management Kate Regan MRCP FRCA Katharine Hunt FRCA
 Kate Regan MRCP FRCA Katharine Hunt FRCA The use of tracheostomy has increased over recent years. Traditionally, it was confined to the emergency management of upper airway obstruction; more recently,
Kate Regan MRCP FRCA Katharine Hunt FRCA The use of tracheostomy has increased over recent years. Traditionally, it was confined to the emergency management of upper airway obstruction; more recently,
1.40 Prevention of Nosocomial Pneumonia
 1.40 Prevention of Nosocomial Pneumonia Purpose Audience Policy Statement: The guideline is designed to reduce the incidence of pneumonia and other acute lower respiratory tract infections. All UTMB healthcare
1.40 Prevention of Nosocomial Pneumonia Purpose Audience Policy Statement: The guideline is designed to reduce the incidence of pneumonia and other acute lower respiratory tract infections. All UTMB healthcare
Right-Sided Bacterial Endocarditis
 New Concepts in the Treatment of the Uncontrollable Infection Agustin Arbulu, M.D., Ali Kafi, M.D., Norman W. Thorns, M.D., and Robert F. Wilson, M.D. ABSTRACT Our experience with 25 patients with right-sided
New Concepts in the Treatment of the Uncontrollable Infection Agustin Arbulu, M.D., Ali Kafi, M.D., Norman W. Thorns, M.D., and Robert F. Wilson, M.D. ABSTRACT Our experience with 25 patients with right-sided
1 Chapter 40 Advanced Airway Management 2 Advanced Airway Management The advanced airway management techniques discussed in this chapter are to
 1 Chapter 40 Advanced Airway Management 2 Advanced Airway Management The advanced airway management techniques discussed in this chapter are to introduce the EMT-B student to these procedures only. In
1 Chapter 40 Advanced Airway Management 2 Advanced Airway Management The advanced airway management techniques discussed in this chapter are to introduce the EMT-B student to these procedures only. In
Lobectomy with sleeve resection in the
 Thorax (970), 25, 60. Lobectomy with sleeve resection in the treatment of bronchial tumours G. M. REES and M. PANETH Brompton Hospital, London, S.W3 Fortysix patients with malignant tumours involving the
Thorax (970), 25, 60. Lobectomy with sleeve resection in the treatment of bronchial tumours G. M. REES and M. PANETH Brompton Hospital, London, S.W3 Fortysix patients with malignant tumours involving the
F: Respiratory Care. College of Licensed Practical Nurses of Alberta, Competency Profile for LPNs, 3rd Ed. 59
 F: Respiratory Care College of Licensed Practical Nurses of Alberta, Competency Profile for LPNs, 3rd Ed. 59 Competency: F-1 Airway Management F-1-1 F-1-2 F-1-3 F-1-4 F-1-5 Demonstrate knowledge and ability
F: Respiratory Care College of Licensed Practical Nurses of Alberta, Competency Profile for LPNs, 3rd Ed. 59 Competency: F-1 Airway Management F-1-1 F-1-2 F-1-3 F-1-4 F-1-5 Demonstrate knowledge and ability
COBIS Management of airway burns and inhalation injury PAEDIATRIC
 COBIS Management of airway burns and inhalation injury PAEDIATRIC 1 A multidisciplinary team should provide the management of the child with inhalation injury. Childhood inhalation injury mandates transfer
COBIS Management of airway burns and inhalation injury PAEDIATRIC 1 A multidisciplinary team should provide the management of the child with inhalation injury. Childhood inhalation injury mandates transfer
Autologous Pulmonary Valve Replacement of the Diseased Aortic Valve
 Autologous Pulmonary Valve Replacement of the Diseased Aortic Valve By L. GONZALEZ-LAvIN, M.D., M. GEENS. M.D., J. SOMERVILLE, M.D., M.R.C.P., ANm D. N. Ross, M.B., CH.B., F.R.C.S. SUMMARY Living tissue
Autologous Pulmonary Valve Replacement of the Diseased Aortic Valve By L. GONZALEZ-LAvIN, M.D., M. GEENS. M.D., J. SOMERVILLE, M.D., M.R.C.P., ANm D. N. Ross, M.B., CH.B., F.R.C.S. SUMMARY Living tissue
Cuffed Tracheal Tubes in Children - Myths and Facts. PD Dr. Markus Weiss Department of Anaesthesia University Children s Hospital Zurich Switzerland
 Cuffed Tracheal Tubes in Children - Myths and Department of Anaesthesia University Children s Hospital Zurich Switzerland PRO Reduced gas leak, low fresh gas flow Decreased atmospheric pollution Constant
Cuffed Tracheal Tubes in Children - Myths and Department of Anaesthesia University Children s Hospital Zurich Switzerland PRO Reduced gas leak, low fresh gas flow Decreased atmospheric pollution Constant
Surgical Management of Subglottic Stenosis
 Surgical Management of Subglottic Stenosis Cameron D. Wright, MD ubglottic stenosis is usually due to either endotracheal S tube ischemic necrosis or idiopathic larygotracheal stenosis. The ischemic area
Surgical Management of Subglottic Stenosis Cameron D. Wright, MD ubglottic stenosis is usually due to either endotracheal S tube ischemic necrosis or idiopathic larygotracheal stenosis. The ischemic area
Tracheostomy and Ventilator Education Program Module 2: Respiratory Anatomy
 Tracheostomy and Ventilator Education Program Module 2: Respiratory Anatomy Disclaimer This material is intended for use by trained family members and caregivers of children with tracheostomies who are
Tracheostomy and Ventilator Education Program Module 2: Respiratory Anatomy Disclaimer This material is intended for use by trained family members and caregivers of children with tracheostomies who are
Kevin K. Nunnink Extracorporeal Membrane Oxygenation Program
 PATIE NT I N FO R M ATI O N Kevin K. Nunnink Extracorporeal Membrane Oxygenation Program A family s guide to understanding this specialized treatment for cardiac and pulmonary complications Saint Luke
PATIE NT I N FO R M ATI O N Kevin K. Nunnink Extracorporeal Membrane Oxygenation Program A family s guide to understanding this specialized treatment for cardiac and pulmonary complications Saint Luke
TRACHEOBRONCHIAL FOREIGN BODY REMOVAL ADVICE IN DOGS AND CATS
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk TRACHEOBRONCHIAL FOREIGN BODY REMOVAL ADVICE IN DOGS AND CATS Author : MIKE STAFFORD-JOHNSON, MIKE MARTIN Categories : Vets
Vet Times The website for the veterinary profession https://www.vettimes.co.uk TRACHEOBRONCHIAL FOREIGN BODY REMOVAL ADVICE IN DOGS AND CATS Author : MIKE STAFFORD-JOHNSON, MIKE MARTIN Categories : Vets
Retroperineal Lymph Node Dissection (RPLND)
 Acute Services Division Information for patients about Retroperineal Lymph Node Dissection (RPLND) Introduction This booklet gives you information about surgery to remove the residual lymph nodes at the
Acute Services Division Information for patients about Retroperineal Lymph Node Dissection (RPLND) Introduction This booklet gives you information about surgery to remove the residual lymph nodes at the
Airway management problem during anaesthesia. Airway management problem in ICU / HDU. Airway management problem occurring in the Emergency Department
 4th National Audit Project of the Royal College of Anaesthetists: Major Complications of Airway Management in the UK Please select one form from the list below Airway management problem during anaesthesia
4th National Audit Project of the Royal College of Anaesthetists: Major Complications of Airway Management in the UK Please select one form from the list below Airway management problem during anaesthesia
Tracheostomy. Intensive Care Unit Patient Information Leaflet
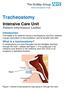 Tracheostomy Intensive Care Unit Patient Information Leaflet Introduction This leaflet is for patients having a tracheostomy and their relatives. It gives information on the procedure, and its benefits
Tracheostomy Intensive Care Unit Patient Information Leaflet Introduction This leaflet is for patients having a tracheostomy and their relatives. It gives information on the procedure, and its benefits
Ostium primum defects with cleft mitral valve
 Thorax (1965), 20, 405. VIKING OLOV BJORK From the Department of Thoracic Surgery, University Hospital, Uppsala, Sweden Ostium primum defects are common; by 1955, 37 operated cases had been reported by
Thorax (1965), 20, 405. VIKING OLOV BJORK From the Department of Thoracic Surgery, University Hospital, Uppsala, Sweden Ostium primum defects are common; by 1955, 37 operated cases had been reported by
Esophageal Perforation
 Esophageal Perforation Dr. Carmine Simone Thoracic Surgeon, Division of General Surgery Head, Division of Critical Care May 15, 2006 Overview Case presentation Radiology Pre-operative management Operative
Esophageal Perforation Dr. Carmine Simone Thoracic Surgeon, Division of General Surgery Head, Division of Critical Care May 15, 2006 Overview Case presentation Radiology Pre-operative management Operative
Trust Guidelines. Title: Guidelines for chest drain insertion
 Trust Guidelines Title: Guidelines for chest drain insertion Authors: Dr JCT Pepperell; Dr J Tipping; J Hansford Ratified by: Planned Care and Emergency & Urgent Care Divisional Governance Committees Active
Trust Guidelines Title: Guidelines for chest drain insertion Authors: Dr JCT Pepperell; Dr J Tipping; J Hansford Ratified by: Planned Care and Emergency & Urgent Care Divisional Governance Committees Active
Neuromuscular diseases (NMDs) include both hereditary and acquired diseases of the peripheral neuromuscular system. They are diseases of the
 Neuromuscular diseases (NMDs) include both hereditary and acquired diseases of the peripheral neuromuscular system. They are diseases of the peripheral nerves (neuropathies and anterior horn cell diseases),
Neuromuscular diseases (NMDs) include both hereditary and acquired diseases of the peripheral neuromuscular system. They are diseases of the peripheral nerves (neuropathies and anterior horn cell diseases),
pulmonary and critical care pearls
 pulmonary and critical care pearls A 63-Year-Old Woman With Subcutaneous Emphysema Following Endotracheal Intubation* Bassam Hashem, MD; James K. Smith, MD, FCCP; and W. Bruce Davis, MD, FCCP (CHEST 2005;
pulmonary and critical care pearls A 63-Year-Old Woman With Subcutaneous Emphysema Following Endotracheal Intubation* Bassam Hashem, MD; James K. Smith, MD, FCCP; and W. Bruce Davis, MD, FCCP (CHEST 2005;
Kelly procedure. How does the urinary system work? What is a Kelly procedure and why does my child need one?
 Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Kelly procedure This information sheet from Great Ormond Street Hospital (GOSH) explains the Kelly procedure used
Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Kelly procedure This information sheet from Great Ormond Street Hospital (GOSH) explains the Kelly procedure used
Inserting a percutaneous biliary drain and biliary stent (a tube to drain bile)
 Patient information - Radiology Unit Tel 0118 322 7991 Inserting a percutaneous biliary drain and biliary stent (a tube to drain bile) Introduction This leaflet tells you about the procedures known as
Patient information - Radiology Unit Tel 0118 322 7991 Inserting a percutaneous biliary drain and biliary stent (a tube to drain bile) Introduction This leaflet tells you about the procedures known as
Subglottic stenosis, with involvement of the lower larynx
 Laryngotracheal Resection and Reconstruction John D. Mitchell, MD n, Subglottic stenosis is being recognized with increasing frequency in adults, and may be the most frequent indication for airway intervention
Laryngotracheal Resection and Reconstruction John D. Mitchell, MD n, Subglottic stenosis is being recognized with increasing frequency in adults, and may be the most frequent indication for airway intervention
CHAPTER 7 Procedures on Respiratory System
 CHAPTER 7 Propunere noua clasificare proceduri folosind codificarea ICD-10-AM versiunea 3, 30 martie 2004 Procedures on Respiratory System BLOCK 520 Examination procedures on larynx 41764-03 Fibreoptic
CHAPTER 7 Propunere noua clasificare proceduri folosind codificarea ICD-10-AM versiunea 3, 30 martie 2004 Procedures on Respiratory System BLOCK 520 Examination procedures on larynx 41764-03 Fibreoptic
