Scope This guideline is aimed at all healthcare professionals involved in the care of infants within the neonatal service.
|
|
|
- Augustus Henry
- 5 years ago
- Views:
Transcription
1 UHL Neonatal Guideline: CPAP Nursing Care University Hospitals of Leicester NHS NHS Trust Nov 2018 Nov 2021 Scope This guideline is aimed at all healthcare professionals involved in the care of infants within the neonatal service. Aim To ensure that all infants receiving CPAP are optimally cared for and to reduce the incidence of nasal trauma. Key Points Traumatic injuries to the nose are a common complication of CPAP in neonates. The incidence of nasal trauma can be minimized by good fixation methods and nursing techniques. Hourly visual checks and two-hourly physical checks are required (listed in section 2.7) and are regularly audited. Some of the most important points are illustrated in Appendix Background Continuous Positive Airway Pressure (CPAP) is the application of positive pressure to the airway of a spontaneously breathing infant throughout the respiratory cycle. CPAP predominantly works by preventing collapse of the alveoli with marginal stability. The recruitment of more alveoli helps to increase the Functional Residual Capacity (FRC) thus improving oxygenation and decreasing intrapulmonary shunting. Endogenous surfactant is conserved; the breathing pattern regulates with stabilization of the rib cage, which reduces recession and increases efficiency of the diaphragm. Listed uses for CPAP on the Neonatal unit include; Respiratory Distress Syndrome (RDS) Apnoea of prematurity Prevention of extubation failure Transient Tachypnoea of the Newborn (TTN) Infants with Chronic Lung Disease (CLD) In practice CPAP consists of a controlled flow of gas administered to the baby using a flow driver to circulate humidified gas through a CPAP circuit to the larynx or nose. The level of care administered is measured by a pressure reading in cm H 2 O. In order to raise or lower the pressures given to the baby the flow of gas in L/m can be increased or decreased. UHL Neonatal Guideline: CPAP Nursing Care Page 1 of 10
2 The evidence, clinical studies and controversies regarding CPAP have been extensively reviewed elsewhere and are not discussed here. The guidelines focus mainly on the practical aspects of CPAP administration in neonates. 2. Practice Guidelines 2.1 PRIOR TO COMMENCING CPAP Infants should be nursed in a safe environment with access to suction, oxygen and resuscitation equipment at each cot side. CPAP drivers should be well maintained and cleaned. The flow should be set, initially at 8L/m and the oxygen at the infant s individual requirements. Initial PEEP (Positive End Expiratory Pressure) is set at 5cmH 2 O to 8cm H 2 O, however this is dependent on infant s current condition. Alarms on the CPAP driver should be set according to the manufacturer s guidance. 2.2 HUMIDIFICATION CPAP circuits used on the unit should be humidified at all times. Ensure that the humidifier is on and warmed prior to connecting to the infant. Sterile water for irrigation is used to fill the chamber. Don t over-fill the chambers or let them dry out Humidification is delivered to the infant at 37 C. Humidification and warming of the inspiratory gases is a very important aspect on CPAP. In normally breathing infants the flows are very low compared to the gas flows that occur when administering CPAP. High flow gases dry the mucosa, decrease the muco-ciliary function and increase the airway resistance. It is ideal to deliver gases at a chamber temperature of 37 C with humidity. UHL Neonatal Guideline: CPAP Nursing Care Page 2 of 10
3 2.3 CPAP HATS Ensure the correct size hat is used, as there are a variety of sizes available. Use the tape measure provided to guide you on the correct size. Measurements should be taken from the base of the neck to the middle of the forehead and back to the base (NOT the head circumference). Be aware that it may be necessary to go up or down a size to ensure the best fit. The hat should be put on the infant s head prior to connecting the generator. Ensuring that the ears are in a normal position and flat against the head, and fit from the brow to the nape of the neck. The open end of the hat should be tied off (not too tight) to ensure a snug and secure fit. Eyes should be clearly visible. The hat size should be regularly reviewed for correct sizing and changed when elasticity is lost or is dirty. 2.4 NASAL PRONGS/MASKS Use the sizing guide provided by the manufacturer to correctly gauge the size of the prongs/mask needed. Attach the prongs/mask to the generator prior to attaching to the infant. Bring the generator towards the nose and gently insert the prongs into position whilst supporting the weight of the equipment. Prongs should be positioned correctly so that they are square onto the nose and not tipped at an angle. They should NOT be pressed hard against the nasal septum (this is to prevent damage to the lateral walls of the nostrils and the nasal septum) Masks should be place evenly on the nose to create a seal and minimize gas leak especially to the eyes. The eyes should be clearly visible without any of the mask touching them. Prongs/mask should be kept clean, patent and free from obstruction. Alternate between prong and mask when the infant tolerates this. The prongs/mask are secured using the straps from the generator horizontally across the infant s cheeks. Do NOT over tighten. The exhaust tubing should be free so that pressure is not applied to the nose. Correct fitting of the prongs/mask, careful observation of the nose and immediate response to any indicators of nasal damage should be employed by carers. If skin protection (e.g. Duoderm) is needed, ensure that it is secure and cannot migrate over the nostrils blocking the airway. UHL Neonatal Guideline: CPAP Nursing Care Page 3 of 10
4 2.5 PRESSURES AND FLOW Initial PEEP is usually between 4-6cm H 2 O but greatly varies depending on the infant s condition. The flow is initially set at 8L/m. Pressure is achieved by altering the flow. Decisions on pressure should be made between the medical and nursing team and documented in the care plan and notes. Indications for adjusting the pressure are: o Degree of RDS o Effort of breathing o Blood gas o Chest X ray o Oxygen requirements o Apnoeas, bradycardias and desaturations The use of a dummy can help to settle a baby and create a better seal, which will help to maintain better pressures. If pressure needs to be significantly increased this could be an indication of a more serious problem such as a pneumothorax or need for intubation and ventilation. Medical review is required immediately. 2.6 GENERAL CARE Suction may be required, but this is individualized to the infant s needs. Monitoring of the infant s vital signs, heart rate, respiratory rate and oxygen saturations should be in place. Ensure that the infants face is kept clean from secretions. Clean behind the infant s ears during cares (as preterm infants may be nursed with CPAP for many weeks). An oro-gastric tube (OGT) is used in preference to a naso-gastric tube (NGT), to prevent distortion to the nostrils and ensure a good seal with the prongs or mask. The OGT should be aspirated prior to every feed to reduce gas and help prevent abdominal distention CPAP belly. If the infant is not having any feeds the OGT can be kept open on free drainage. Continue to aspirate the OGT every 4-6 hours. Mouth care will be needed due to the high flow gases causing the mouth to become very dry. Consideration must be given to the developmental needs of the baby and each should have individualized care to achieve this. The use of positioning aids should be used to maintain comfort and correct positioning. Time and care should be taken to ensure that the CPAP is secure, well fitted and safe. UHL Neonatal Guideline: CPAP Nursing Care Page 4 of 10
5 2.7 CARE OF THE NOSE AND FACE FOR INFANTS RECEIVING CPAP Traumatic injuries to the nose are the most common complication of CPAP in neonates. Nasal prongs may rub and damage the internal aspects of the nasal septum, whereas masks are found to cause trauma to the nasal septum and nasal philtrum or the bridge of the nose. Both problems can be minimized by good fixation methods and nursing techniques. Every hour check visually: The generator is positioned correctly The nose should not be pushed upwards or squashed The exhaust tubing should be free so that pressure is not applied to the nose. The eyes should be clearly visible Tapes should not be too tight or cause indentation Check humidification chamber for water level (Do not over-fill or allow to dry out!) 2-4 hourly physical checks Prongs/mask should be removed and pressure relieved from the nose and face. The nose should be inspected for signs of redness, indentation, bruising or bleeding. If skin protection (i.e. Duoderm) is needed ensure that it is secure and cannot migrate over the nostrils causing the airway to block. The ears should be inspected to ensure that they are not creased or folded. Remember to clean behind the ears. If there are any changes or concerns re-check in 1 hour and ask for a review. Document care on an ITU chart and record any findings in the notes. Prongs/mask should be checked to ensure that they are clean and patent prior to being place back on the infant s nose. 2.8 MONITORING INFANTS WITH CPAP Hourly observations should be recorded for each infant including: Heart Rate Respiratory rate Oxygen saturations PEEP Flow of gas FiO2 Humidity temperature Position of infant UHL Neonatal Guideline: CPAP Nursing Care Page 5 of 10
6 2.9 PARENTS Keep parents informed of progress on CPAP If baby is settled encourage parents to have a cuddle or Kangaroo care. References Cahill, S. Continuous Positive Airway Pressure (CPAP) Nursing Guidelines. NHS Forth Valley 2012 Alsop E.A, Cooke J, Gupta S, Sinha S.K. Nasal Trauma in preterm Infants receiving Continuous positive airway pressure. Arch Dis Child 2008; 93: n23 Chen SJ. Boo NY. Yong SC. Incidence of nasal trauma associated with nasal prong versus nasal mask during continuous positive airway pressure treatment in very low birth weight infants: a random control study Arch Dis Child Fetal Neonatal Ed 2005: 90 F480 doi: 1136/acd Fischer C, Bertelle V, Hohlfeld J., Forcada-Guex M, Stadelmann-Diaw C, Tolsa J. Nasal trauma due to continuous positive airway pressure in neonates. Arch Dis Child Fetal Neonatal Ed 2010; 95 F447-F451 doi:1136/acd Ho JJ, Subramaniam P, Henderson-Smart DJ, Davis PG. Continuous distending pressure for respiratory distress in preterm infants. Cochrane Databas of Systematic Reviews 2002, Issue 2. Art no CD McCoskey L. Nursing care guidelines for the prevention of nasal breakdown in neonates receiving nasal CPAP. Advances in neonatal care 2008; 8 (2), Shanmugananda K, Rawal J. Nasal trauma due to continuous positive airway pressure in Newborns. Arch Dis Child Fetal Neonatal Ed 2007; 92 F18doi: /adc Squires AJ, Hyndman M. Prevention of nasal injuries secondary to NCPAP application in the ELBW infant. Neonatal Network 2009; 28 (1) UHL Neonatal Guideline: CPAP Nursing Care Page 6 of 10
7 Audit Criteria Documentation of hourly and 2 to 4 hourly physical checks in all infants receiving CPAP (100%). Guideline Development August 2013 Sept 2015 Oct 2015 Nov 2018 Neonatal Guidelines Meeting text approved subject to amendments Amendments, appendices added (REM guidelines lead), Circulation to senior nurses. Neonatal Governance Meeting Guideline review and Neonatal Governance Meeting UHL Neonatal Guideline: CPAP Nursing Care Page 7 of 10
8 Appendix 1: Visible Eyes Ensure that the hat fits from the brow to the nape of the neck with the eyes clearly visible Fitting the Hat Use the tape measure provided to select the correct size of hat. Maintain Good Pressure The use of a dummy helps to create a better seal which helps to maintain good pressures. UHL Neonatal Guideline: CPAP Nursing Care Page 8 of 10
9 Avoid pressure to the nose Leave the exhaust tubing free so that pressure is not applied to the nose. Duoderm (or other hydrocolloid dressing) is not to be used as a pressure-relieving device. It is only to be used if the skin is red, non-blanching, bruised or broken. Duoderm should be changed every 24 hours or sooner if it becomes displaces. Document the use of duoderm and the reasons for its use in the notes. Regular inspection Every 1-2 hours, relieve the pressure from the nasal area by lifting the prongs/mask away from the infants face, allowing inspection of the area. If baby is pressure-dependent, consider 3-4 hourly pressure relief. Document in notes if baby is unable to tolerate more frequent pressure relief. Inspiration & Pressure lines Secure the tubes coming from the generator with the central Velcro strip. Split the inspiration and pressure lines and secure with the secondary Velcro strip. UHL Neonatal Guideline: CPAP Nursing Care Page 9 of 10
10 Appendix 2: STOP Poster (prevention of device-related pressure ulcers) UHL Neonatal Guideline: CPAP Nursing Care Page 10 of 10
Introducing Infant Flow Advance SIPAP. By Joanne Cookson March 2008
 Introducing Infant Flow Advance SIPAP By Joanne Cookson March 2008 Aim To introduce clinical practioners to the new SiPAP machine Objectives To define what is SiPAP To look at different modes able to be
Introducing Infant Flow Advance SIPAP By Joanne Cookson March 2008 Aim To introduce clinical practioners to the new SiPAP machine Objectives To define what is SiPAP To look at different modes able to be
South Central Neonatal Network Quality Care Group Working to provide a unified approach to excellence
 South Central Neonatal Network Quality Care Group Working to provide a unified approach to excellence Guideline framework for CPAP Approved by & date Date of publication Neonatal Network Board December
South Central Neonatal Network Quality Care Group Working to provide a unified approach to excellence Guideline framework for CPAP Approved by & date Date of publication Neonatal Network Board December
CONTINUOUS POSITIVE AIRWAY PRESSURE (CPAP) DEFINITION
 CONTINUOUS POSITIVE AIRWAY PRESSURE (CPAP) DEFINITION Method of maintaining low pressure distension of lungs during inspiration and expiration when infant breathing spontaneously Benefits Improves oxygenation
CONTINUOUS POSITIVE AIRWAY PRESSURE (CPAP) DEFINITION Method of maintaining low pressure distension of lungs during inspiration and expiration when infant breathing spontaneously Benefits Improves oxygenation
Practical Application of CPAP
 CHAPTER 3 Practical Application of CPAP Dr. Srinivas Murki Neonatologist Fernadez Hospital, Hyderabad. A.P. Practical Application of CPAP Continuous positive airway pressure (CPAP) applied to premature
CHAPTER 3 Practical Application of CPAP Dr. Srinivas Murki Neonatologist Fernadez Hospital, Hyderabad. A.P. Practical Application of CPAP Continuous positive airway pressure (CPAP) applied to premature
Clinical Guideline: Management of a baby on CPAP
 Clinical Guideline: Management of a baby on CPAP Authors: EOE Neonatal Benchmarking Group For use in: EoE Neonatal Units Guidance specific to the care of neonatal patients. Used by: For use in neonatal
Clinical Guideline: Management of a baby on CPAP Authors: EOE Neonatal Benchmarking Group For use in: EoE Neonatal Units Guidance specific to the care of neonatal patients. Used by: For use in neonatal
PUMANI bcpap GUIDELINES FOR CLINICIANS. An Overview of the Pumani bcpap, Indications for bcpap, and Instructions for Use
 An Overview of the Pumani bcpap, Indications for bcpap, and Instructions for Use What is bcpap? bcpap stands for bubble Continuous Positive Airway Pressure. Sometimes called Continuous Distending Pressure,
An Overview of the Pumani bcpap, Indications for bcpap, and Instructions for Use What is bcpap? bcpap stands for bubble Continuous Positive Airway Pressure. Sometimes called Continuous Distending Pressure,
SARASOTA MEMORIAL HOSPITAL DEPARTMENT POLICY
 PS1006 SARASOTA MEMORIAL HOSPITAL DEPARTMENT POLICY TITLE: NON-INVASIVE VENTILATION FOR THE Job Title of Reviewer: EFFECTIVE DATE: REVISED DATE: Director, Respiratory Care Services 126.685 (neo) 3/26/15
PS1006 SARASOTA MEMORIAL HOSPITAL DEPARTMENT POLICY TITLE: NON-INVASIVE VENTILATION FOR THE Job Title of Reviewer: EFFECTIVE DATE: REVISED DATE: Director, Respiratory Care Services 126.685 (neo) 3/26/15
Part I: How to Assemble the Pumani CPAP Part II: How to Prepare the Baby for CPAP Part III: How to Attach the Baby to the Pumani CPAP
 Pumani CPAP User Manual Table of Contents Part I: How to Assemble the Pumani CPAP 3 Pumani CPAP Components 4 Assembly Instructions 5-15 Part II: How to Prepare the Baby for CPAP 16-18 Part III: How to
Pumani CPAP User Manual Table of Contents Part I: How to Assemble the Pumani CPAP 3 Pumani CPAP Components 4 Assembly Instructions 5-15 Part II: How to Prepare the Baby for CPAP 16-18 Part III: How to
Acute Paediatric Respiratory Pathway
 Guideline for the use of high Flow Nasal Cannula Oxygen Therapy (Optiflow or Airvo) in Children with Bronchiolitis or an acute respiratory illness Introduction: High flow nasal cannula (HFNC) oxygen enables
Guideline for the use of high Flow Nasal Cannula Oxygen Therapy (Optiflow or Airvo) in Children with Bronchiolitis or an acute respiratory illness Introduction: High flow nasal cannula (HFNC) oxygen enables
NON INVASIVE LIFE SAVERS. Non Invasive Ventilation (NIV)
 Table 1. NIV: Mechanisms Of Action Decreases work of breathing Increases functional residual capacity Recruits collapsed alveoli Improves respiratory gas exchange Reverses hypoventilation Maintains upper
Table 1. NIV: Mechanisms Of Action Decreases work of breathing Increases functional residual capacity Recruits collapsed alveoli Improves respiratory gas exchange Reverses hypoventilation Maintains upper
I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device
 I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device II. Policy: Continuous Positive Airway Pressure CPAP by the Down's system will be instituted by Respiratory Therapy personnel
I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device II. Policy: Continuous Positive Airway Pressure CPAP by the Down's system will be instituted by Respiratory Therapy personnel
Title Neonatal and Paediatric High-Flow Nasal Cannula Oxygen Therapy Guideline. Department Paediatrics / Neonates Date Issued
 Document Control Title Author Neonatal and Paediatric High-Flow Nasal Cannula Oxygen Therapy Guideline Author s job title Directorate Medical Version Department Paediatrics / Neonates Date Issued Status
Document Control Title Author Neonatal and Paediatric High-Flow Nasal Cannula Oxygen Therapy Guideline Author s job title Directorate Medical Version Department Paediatrics / Neonates Date Issued Status
Advantages and disadvantages of different nasal CPAP systems in newborns
 Intensive Care Med (2004) 30:926 930 DOI 10.1007/s00134-004-2267-8 N E O N A T A L A N D P A E D I A T R I C I N T E N S I V E C A R E V. Buettiker M. I. Hug O. Baenziger C. Meyer B. Frey Advantages and
Intensive Care Med (2004) 30:926 930 DOI 10.1007/s00134-004-2267-8 N E O N A T A L A N D P A E D I A T R I C I N T E N S I V E C A R E V. Buettiker M. I. Hug O. Baenziger C. Meyer B. Frey Advantages and
Neonatal and Pediatric Securement From Salter
 Neonatal and Pediatric Securement From Salter The touch that says so much Striving to be #1 IN PATIENT SATISFACTION Now with options for ncpap,, and low flow therapy. Collaborative Innovation Today, Salter
Neonatal and Pediatric Securement From Salter The touch that says so much Striving to be #1 IN PATIENT SATISFACTION Now with options for ncpap,, and low flow therapy. Collaborative Innovation Today, Salter
Competency Title: Continuous Positive Airway Pressure
 Competency Title: Continuous Positive Airway Pressure Trainee Name: ------------------------------------------------------------- Title: ---------------------------------------------------------------
Competency Title: Continuous Positive Airway Pressure Trainee Name: ------------------------------------------------------------- Title: ---------------------------------------------------------------
I. Subject: Pressure Support Ventilation (PSV) with BiPAP Device/Nasal CPAP
 I. Subject: Pressure Support Ventilation (PSV) with BiPAP Device/Nasal CPAP II. Policy: PSV with BiPAP device/nasal CPAP will be initiated upon a physician's order by Respiratory Therapy personnel trained
I. Subject: Pressure Support Ventilation (PSV) with BiPAP Device/Nasal CPAP II. Policy: PSV with BiPAP device/nasal CPAP will be initiated upon a physician's order by Respiratory Therapy personnel trained
Surfactant Administration
 Approved by: Surfactant Administration Gail Cameron Senior Director Operations, Maternal, Neonatal & Child Health Programs Dr. Paul Byrne Medical Director, Neonatology Neonatal Policy & Procedures Manual
Approved by: Surfactant Administration Gail Cameron Senior Director Operations, Maternal, Neonatal & Child Health Programs Dr. Paul Byrne Medical Director, Neonatology Neonatal Policy & Procedures Manual
This is a pre-copyedited, author-produced PDF of an article accepted for publication in Journal of Neonatal Nursing following peer review.
 This is a pre-copyedited, author-produced PDF of an article accepted for publication in Journal of Neonatal Nursing following peer review. The version of record [Journal of Neonatal Nursing (February 2013)
This is a pre-copyedited, author-produced PDF of an article accepted for publication in Journal of Neonatal Nursing following peer review. The version of record [Journal of Neonatal Nursing (February 2013)
CHEST PHYSIOTHERAPY IN NICU PURPOSE POLICY STATEMENTS SITE APPLICABILITY PRACTICE LEVEL/COMPETENCIES. The role of chest physiotherapy in the NICU
 PURPOSE The role of chest physiotherapy in the NICU POLICY STATEMENTS In principle chest physiotherapy should be limited to those infants considered most likely to benefit with significant respiratory
PURPOSE The role of chest physiotherapy in the NICU POLICY STATEMENTS In principle chest physiotherapy should be limited to those infants considered most likely to benefit with significant respiratory
1.1.2 CPAP therapy is used for patients who are suffering from an acute type 1 respiratory failure (Pa02 <8kPa with a normal or low Pac02).
 Guidelines for initiating and managing CPAP (Continuous Positive Airway Pressure) on a general ward. B25/2006 1.Introduction and Who Guideline applies to 1.1.1 This document provides guidance for Healthcare
Guidelines for initiating and managing CPAP (Continuous Positive Airway Pressure) on a general ward. B25/2006 1.Introduction and Who Guideline applies to 1.1.1 This document provides guidance for Healthcare
5 Million neonatal deaths each year worldwide. 20% caused by neonatal asphyxia. Improvement of the outcome of 1 million newborns every year
 1 5 Million neonatal deaths each year worldwide 20% caused by neonatal asphyxia Improvement of the outcome of 1 million newborns every year International Liaison Committee on Resuscitation (ILCOR) American
1 5 Million neonatal deaths each year worldwide 20% caused by neonatal asphyxia Improvement of the outcome of 1 million newborns every year International Liaison Committee on Resuscitation (ILCOR) American
AEROSURF Phase 2 Program Update Investor Conference Call
 AEROSURF Phase 2 Program Update Investor Conference Call November 12, 2015 Forward Looking Statement To the extent that statements in this presentation are not strictly historical, including statements
AEROSURF Phase 2 Program Update Investor Conference Call November 12, 2015 Forward Looking Statement To the extent that statements in this presentation are not strictly historical, including statements
HeartCode PALS. PALS Actions Overview > Legend. Contents
 HeartCode PALS PALS Actions Overview > Legend Action buttons (round buttons) Clicking a round button initiates an action. Clicking this button, for example, checks the child s carotid pulse. Menu buttons
HeartCode PALS PALS Actions Overview > Legend Action buttons (round buttons) Clicking a round button initiates an action. Clicking this button, for example, checks the child s carotid pulse. Menu buttons
WILAflow Elite Neonatal Ventilator. Non-invasive treatment for the most delicate patients.
 EN WILAflow Elite Neonatal Ventilator Non-invasive treatment for the most delicate patients. 0197 Infant Ventilation redefined A new generation in Infant Ventilation WILAflow Elite is a microprocessor
EN WILAflow Elite Neonatal Ventilator Non-invasive treatment for the most delicate patients. 0197 Infant Ventilation redefined A new generation in Infant Ventilation WILAflow Elite is a microprocessor
Respiratory Physio Protocol for Paediatric Patients on BIPAP via a tracheotomy (uncuffed tube)
 This is an official Northern Trust policy and should not be edited in any way Respiratory Physio Protocol for Paediatric Patients on BIPAP via a tracheotomy (uncuffed tube) Reference Number: NHSCT/12/547
This is an official Northern Trust policy and should not be edited in any way Respiratory Physio Protocol for Paediatric Patients on BIPAP via a tracheotomy (uncuffed tube) Reference Number: NHSCT/12/547
INTRODUCTION The effect of CPAP works on lung mechanics to improve oxygenation (PaO 2
 2 Effects of CPAP INTRODUCTION The effect of CPAP works on lung mechanics to improve oxygenation (PaO 2 ). The effect on CO 2 is only secondary to the primary process of improvement in lung volume and
2 Effects of CPAP INTRODUCTION The effect of CPAP works on lung mechanics to improve oxygenation (PaO 2 ). The effect on CO 2 is only secondary to the primary process of improvement in lung volume and
Bilevel positive airway pressure (BPAP) non-invasive ventilation
 Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Bilevel positive airway pressure (BPAP) non-invasive ventilation This information sheet from Great Ormond Street
Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Bilevel positive airway pressure (BPAP) non-invasive ventilation This information sheet from Great Ormond Street
CHANHASSEN FIRE DEPARTMENT MEDICAL / RESCUE SKILLS
 CHANHASSEN FIRE DEPARTMENT MEDICAL / RESCUE SKILLS PRACTICAL STATIONS CHANHASSEN FIRE DEPARTMENT MEDICAL / RESCUE SKILLS 1. CARDIAC ARREST MANAGEMENT 2. AIRWAY & RESPIRATORY MANAGEMENT 3. SPINAL IMMOBILIZATION
CHANHASSEN FIRE DEPARTMENT MEDICAL / RESCUE SKILLS PRACTICAL STATIONS CHANHASSEN FIRE DEPARTMENT MEDICAL / RESCUE SKILLS 1. CARDIAC ARREST MANAGEMENT 2. AIRWAY & RESPIRATORY MANAGEMENT 3. SPINAL IMMOBILIZATION
Complex Care Hub Manual: Continuous Positive Airway Pressure (CPAP) Ventilation
 Complex Care Hub Manual: Continuous Positive Airway Pressure (CPAP) Ventilation Table of Contents 1. What is Continuous Positive Airway Pressure (CPAP)?... 2 2. Important information for support worker...
Complex Care Hub Manual: Continuous Positive Airway Pressure (CPAP) Ventilation Table of Contents 1. What is Continuous Positive Airway Pressure (CPAP)?... 2 2. Important information for support worker...
WILAflow Elite Neonatal Ventilator. Non-invasive treatment for the most delicate patients.
 EN WILAflow Elite Neonatal Ventilator Non-invasive treatment for the most delicate patients. 0197 Infant Ventilation redefined A new generation in Infant Ventilation WILAflow Elite is a microprocessor
EN WILAflow Elite Neonatal Ventilator Non-invasive treatment for the most delicate patients. 0197 Infant Ventilation redefined A new generation in Infant Ventilation WILAflow Elite is a microprocessor
Neonatal Respiratory Physiotherapy. Nicky Hawkes Advanced Respiratory Physiotherapist Oct 2011
 Neonatal Respiratory Physiotherapy Nicky Hawkes Advanced Respiratory Physiotherapist Oct 2011 Respiratory Physiotherapy?..Not just percussion! Assessment of baby s respiratory status and deciding what
Neonatal Respiratory Physiotherapy Nicky Hawkes Advanced Respiratory Physiotherapist Oct 2011 Respiratory Physiotherapy?..Not just percussion! Assessment of baby s respiratory status and deciding what
Yorkshire & Humber Neonatal ODN (South) Clinical Guideline
 Yorkshire & Humber Neonatal ODN (South) Clinical Guideline Title: Ventilation Author: Dr Cath Smith updated September 2017, written by Dr Elizabeth Pilling May 2011 Date written: May 2011 Review date:
Yorkshire & Humber Neonatal ODN (South) Clinical Guideline Title: Ventilation Author: Dr Cath Smith updated September 2017, written by Dr Elizabeth Pilling May 2011 Date written: May 2011 Review date:
10/17/2016 OXYGEN DELIVERY: INDICATIONS AND USE OF EQUIPMENT COURSE OBJECTIVES COMMON CAUSES OF RESPIRATORY FAILURE
 OXYGEN DELIVERY: INDICATIONS AND USE OF EQUIPMENT J U L I E Z I M M E R M A N, R N, M S N C L I N I C A L N U R S E S P E C I A L I S T E L O I S A C U T L E R, R R T, B S R C C L I N I C A L / E D U C
OXYGEN DELIVERY: INDICATIONS AND USE OF EQUIPMENT J U L I E Z I M M E R M A N, R N, M S N C L I N I C A L N U R S E S P E C I A L I S T E L O I S A C U T L E R, R R T, B S R C C L I N I C A L / E D U C
2007 Recertification Session. Airway review
 2007 Recertification Session Airway review Level of awareness: This is similar to the AVPU, the GCS is performed later Verbal, loud verbal, or pain stimulus. If pain stimulus, consider a trapezeus squeeze
2007 Recertification Session Airway review Level of awareness: This is similar to the AVPU, the GCS is performed later Verbal, loud verbal, or pain stimulus. If pain stimulus, consider a trapezeus squeeze
Tracheostomy and Ventilator Education Program Module 2: Respiratory Anatomy
 Tracheostomy and Ventilator Education Program Module 2: Respiratory Anatomy Disclaimer This material is intended for use by trained family members and caregivers of children with tracheostomies who are
Tracheostomy and Ventilator Education Program Module 2: Respiratory Anatomy Disclaimer This material is intended for use by trained family members and caregivers of children with tracheostomies who are
CLINICAL CONSIDERATIONS FOR THE BUNNELL LIFE PULSE HIGH-FREQUENCY JET VENTILATOR
 CLINICAL CONSIDERATIONS FOR THE BUNNELL LIFE PULSE HIGH-FREQUENCY JET VENTILATOR 801-467-0800 Phone 800-800-HFJV (4358) Hotline TABLE OF CONTENTS Respiratory Care Considerations..3 Physician Considerations
CLINICAL CONSIDERATIONS FOR THE BUNNELL LIFE PULSE HIGH-FREQUENCY JET VENTILATOR 801-467-0800 Phone 800-800-HFJV (4358) Hotline TABLE OF CONTENTS Respiratory Care Considerations..3 Physician Considerations
Simulation 3: Post-term Baby in Labor and Delivery
 Simulation 3: Post-term Baby in Labor and Delivery Opening Scenario (Links to Section 1) You are an evening-shift respiratory therapist in a large hospital with a level III neonatal unit. You are paged
Simulation 3: Post-term Baby in Labor and Delivery Opening Scenario (Links to Section 1) You are an evening-shift respiratory therapist in a large hospital with a level III neonatal unit. You are paged
Kugelman A, Riskin A, Said W, Shoris I, Mor F, Bader D.
 Heated, Humidified High-Flow Nasal Cannula (HHHFNC) vs. Nasal Intermittent Positive Pressure Ventilation (NIPPV) for the Primary Treatment of RDS, A Randomized, Controlled, Prospective, Pilot Study Kugelman
Heated, Humidified High-Flow Nasal Cannula (HHHFNC) vs. Nasal Intermittent Positive Pressure Ventilation (NIPPV) for the Primary Treatment of RDS, A Randomized, Controlled, Prospective, Pilot Study Kugelman
User Manual & Repair Manual
 User Manual & Repair Manual 0120 Introduction Complications due to premature birth, including respiratory distress, are the leading cause of child mortality worldwide. Bubble continuous positive airway
User Manual & Repair Manual 0120 Introduction Complications due to premature birth, including respiratory distress, are the leading cause of child mortality worldwide. Bubble continuous positive airway
Prepared by : Bayan Kaddourah RN,MHM. GICU Clinical Instructor
 Mechanical Ventilation Prepared by : Bayan Kaddourah RN,MHM. GICU Clinical Instructor 1 Definition Is a supportive therapy to facilitate gas exchange. Most ventilatory support requires an artificial airway.
Mechanical Ventilation Prepared by : Bayan Kaddourah RN,MHM. GICU Clinical Instructor 1 Definition Is a supportive therapy to facilitate gas exchange. Most ventilatory support requires an artificial airway.
Objectives. Apnea Definition and Pitfalls. Pathophysiology of Apnea. Apnea of Prematurity and hypoxemia episodes 5/18/2015
 Apnea of Prematurity and hypoxemia episodes Deepak Jain MD Care of Sick Newborn Conference May 2015 Objectives Differentiating between apnea and hypoxemia episodes. Pathophysiology Diagnosis of apnea and
Apnea of Prematurity and hypoxemia episodes Deepak Jain MD Care of Sick Newborn Conference May 2015 Objectives Differentiating between apnea and hypoxemia episodes. Pathophysiology Diagnosis of apnea and
Non Invasive Ventilation In Preterm Infants. Manuel Sanchez Luna Hospital General Universitario Gregorio Marañón Complutense University Madrid
 Non Invasive Ventilation In Preterm Infants Manuel Sanchez Luna Hospital General Universitario Gregorio Marañón Complutense University Madrid Summary Noninvasive ventilation begings in the delivery room
Non Invasive Ventilation In Preterm Infants Manuel Sanchez Luna Hospital General Universitario Gregorio Marañón Complutense University Madrid Summary Noninvasive ventilation begings in the delivery room
Heated Humidified High Flow Nasal Cannula Treatment (HHHFNC)
 Heated Humidified High Flow Nasal Cannula Treatment (HHHFNC) 1. Introduction and Who Guideline applies to Heated humidified high flow nasal cannula treatment (HHHFNC), otherwise called as High flow oxygen
Heated Humidified High Flow Nasal Cannula Treatment (HHHFNC) 1. Introduction and Who Guideline applies to Heated humidified high flow nasal cannula treatment (HHHFNC), otherwise called as High flow oxygen
IICU Staff Meeting Minutes May 15 and 16, 2013 IICU Conference Room
 IICU Staff Meeting Minutes May 15 and 16, 2013 IICU Conference Room 1) Decreasing Telemetry Alarms Janice Marlett, BSN, RN, Nursing Staff Educator To decrease tele alarms: Properly prep the skin Shave
IICU Staff Meeting Minutes May 15 and 16, 2013 IICU Conference Room 1) Decreasing Telemetry Alarms Janice Marlett, BSN, RN, Nursing Staff Educator To decrease tele alarms: Properly prep the skin Shave
Tracheostomy. Hope Building Neurosurgery
 Tracheostomy Hope Building Neurosurgery 0161 206 5055 All Rights Reserved 2017. Document for issue as handout. Unique Identifier: CS36(17). Review date: November 2019 What is a tracheostomy? A tracheostomy
Tracheostomy Hope Building Neurosurgery 0161 206 5055 All Rights Reserved 2017. Document for issue as handout. Unique Identifier: CS36(17). Review date: November 2019 What is a tracheostomy? A tracheostomy
LRI Children s Hospital
 LRI Children s Hospital Humidified High Flow Nasal Cannula (HHFNC) Oxygen Therapy Staff relevant to: Medical and Nursing staff Team approval date: 5.01.18 Version: 1 Revision due: January 2020 Written
LRI Children s Hospital Humidified High Flow Nasal Cannula (HHFNC) Oxygen Therapy Staff relevant to: Medical and Nursing staff Team approval date: 5.01.18 Version: 1 Revision due: January 2020 Written
Pediatric Patients. BCFPD Paramedic Education Program. EMS Education Paramedic Level
 Pediatric Patients BCFPD Program Basic Considerations Much of the initial patient assessment can be done during visual examination of the scene. Involve the caregiver or parent as much as possible. Allow
Pediatric Patients BCFPD Program Basic Considerations Much of the initial patient assessment can be done during visual examination of the scene. Involve the caregiver or parent as much as possible. Allow
Presented By : Kamlah Olaimat
 Presented By : Kamlah Olaimat 18\7\2010 Transient Tachpnea of the Definition:- newborn (TTN) TTN is a benign disease of near term or term infant who display respiratory distress shortly after delivery.
Presented By : Kamlah Olaimat 18\7\2010 Transient Tachpnea of the Definition:- newborn (TTN) TTN is a benign disease of near term or term infant who display respiratory distress shortly after delivery.
Noninvasive Mechanical Ventilation in Children ศ.พญ.อร ณวรรณ พฤทธ พ นธ หน วยโรคระบบหายใจเด ก ภาคว ชาก มารเวชศาสตร คณะแพทยศาสตร โรงพยาบาลรามาธ บด
 Noninvasive Mechanical Ventilation in Children ศ.พญ.อร ณวรรณ พฤทธ พ นธ หน วยโรคระบบหายใจเด ก ภาคว ชาก มารเวชศาสตร คณะแพทยศาสตร โรงพยาบาลรามาธ บด Noninvasive Mechanical Ventilation Provide support without
Noninvasive Mechanical Ventilation in Children ศ.พญ.อร ณวรรณ พฤทธ พ นธ หน วยโรคระบบหายใจเด ก ภาคว ชาก มารเวชศาสตร คณะแพทยศาสตร โรงพยาบาลรามาธ บด Noninvasive Mechanical Ventilation Provide support without
Ventilating the paediatric patient. Lizzie Barrett Nurse Educator November 2016
 Ventilating the paediatric patient Lizzie Barrett Nurse Educator November 2016 Acknowledgements Kate Leutert NE PICU Children's Hospital Westmead Dr. Chloe Tetlow VMO Anaesthetist and Careflight Overview
Ventilating the paediatric patient Lizzie Barrett Nurse Educator November 2016 Acknowledgements Kate Leutert NE PICU Children's Hospital Westmead Dr. Chloe Tetlow VMO Anaesthetist and Careflight Overview
Newborn Life Support. NLS guidance.
 Kelly Harvey, ANNP NWNODN, previously Wythenshawe Hospital has shared this presentation with the understanding that it is for personal use following your attendance at the 8th Annual Senior Neonatal Nursing
Kelly Harvey, ANNP NWNODN, previously Wythenshawe Hospital has shared this presentation with the understanding that it is for personal use following your attendance at the 8th Annual Senior Neonatal Nursing
October Paediatric Respiratory Workbook APCP RESPIRATORY COMMITTEE
 October 2017 Paediatric Respiratory Workbook APCP RESPIRATORY COMMITTEE This workbook is designed to introduce to you the difference between paediatric and adult anatomy and physiology. It will also give
October 2017 Paediatric Respiratory Workbook APCP RESPIRATORY COMMITTEE This workbook is designed to introduce to you the difference between paediatric and adult anatomy and physiology. It will also give
Interfacility Protocol Protocol Title:
 Interfacility Protocol Protocol Title: Mechanical Ventilator Monitoring & Management Original Adoption Date: 05/2009 Past Protocol Updates 05/2009, 12/2013 Date of Most Recent Update: March 23, 2015 Medical
Interfacility Protocol Protocol Title: Mechanical Ventilator Monitoring & Management Original Adoption Date: 05/2009 Past Protocol Updates 05/2009, 12/2013 Date of Most Recent Update: March 23, 2015 Medical
NON-INVASIVE VENTILATION. Lijun Ding 23 Jan 2018
 NON-INVASIVE VENTILATION Lijun Ding 23 Jan 2018 Learning objectives What is NIV The difference between CPAP and BiPAP The indication of the use of NIV Complication of NIV application Patient monitoring
NON-INVASIVE VENTILATION Lijun Ding 23 Jan 2018 Learning objectives What is NIV The difference between CPAP and BiPAP The indication of the use of NIV Complication of NIV application Patient monitoring
Critical Care Services: Equipment and Procedures Information for Patients, Relatives and Carers
 Critical Care Services: Equipment and Procedures Information for Patients, Relatives and Carers The Critical Care unit can be a frightening place for patients and visitors. Seeing a loved one attached
Critical Care Services: Equipment and Procedures Information for Patients, Relatives and Carers The Critical Care unit can be a frightening place for patients and visitors. Seeing a loved one attached
Minimizing Lung Damage During Respiratory Support
 Minimizing Lung Damage During Respiratory Support University of Miami Jackson Memorial Medical Center Care of the Sick Newborn 15 Eduardo Bancalari MD University of Miami Miller School of Medicine Jackson
Minimizing Lung Damage During Respiratory Support University of Miami Jackson Memorial Medical Center Care of the Sick Newborn 15 Eduardo Bancalari MD University of Miami Miller School of Medicine Jackson
CURRENT TRENDS IN NON-INVASIVE VENTILATION. Disclosures. Why not invasive ventilation? Objectives. Currently available modes
 CURRENT TRENDS IN NON-INVASIVE VENTILATION ----------------------------------------------------------- Karen Drinkard, RRT-NPS Neonatal Respiratory Clinical Specialist University of Washington Medical
CURRENT TRENDS IN NON-INVASIVE VENTILATION ----------------------------------------------------------- Karen Drinkard, RRT-NPS Neonatal Respiratory Clinical Specialist University of Washington Medical
Charisma High-flow CPAP solution
 Charisma High-flow CPAP solution Homecare PNEUMOLOGY Neonatology Anaesthesia INTENSIVE CARE VENTILATION Sleep Diagnostics Service Patient Support charisma High-flow CPAP solution Evidence CPAP therapy
Charisma High-flow CPAP solution Homecare PNEUMOLOGY Neonatology Anaesthesia INTENSIVE CARE VENTILATION Sleep Diagnostics Service Patient Support charisma High-flow CPAP solution Evidence CPAP therapy
Module 2: Facilitator instructions for Airway & Breathing Skills Station
 Module 2: Facilitator instructions for Airway & Breathing Skills Station 1. Preparation a. Assemble equipment beforehand. b. Make sure that you have what you need and that it is functioning properly. 2.
Module 2: Facilitator instructions for Airway & Breathing Skills Station 1. Preparation a. Assemble equipment beforehand. b. Make sure that you have what you need and that it is functioning properly. 2.
Equipment: NRP algorithm, MRSOPA table, medication chart, SpO 2 table Warm
 NRP Skills Stations Performance Skills Station OR Integrated Skills Station STATION: Assisting with and insertion of endotracheal tube (ETT) Equipment: NRP algorithm, MRSOPA table, medication chart, SpO
NRP Skills Stations Performance Skills Station OR Integrated Skills Station STATION: Assisting with and insertion of endotracheal tube (ETT) Equipment: NRP algorithm, MRSOPA table, medication chart, SpO
BiLevel Pressure Device
 PROCEDURE - Page 1 of 7 Purpose Scope Classes/ Goals Define indications and care settings for acute and chronic initiation of Noninvasive Positive Pressure Ventilation. Identify the role of Respiratory
PROCEDURE - Page 1 of 7 Purpose Scope Classes/ Goals Define indications and care settings for acute and chronic initiation of Noninvasive Positive Pressure Ventilation. Identify the role of Respiratory
NIV - BI-LEVEL POSITIVE AIRWAY PRESSURE (BIPAP)
 Introduction NIV - BI-LEVEL POSITIVE AIRWAY PRESSURE (BIPAP) Noninvasive ventilation (NIV) is a method of delivering oxygen by positive pressure mask that allows for the prevention or postponement of invasive
Introduction NIV - BI-LEVEL POSITIVE AIRWAY PRESSURE (BIPAP) Noninvasive ventilation (NIV) is a method of delivering oxygen by positive pressure mask that allows for the prevention or postponement of invasive
Positive Pressure Therapy
 Positive Pressure Therapy Positive Pressure Therapy...2 What is Sleep Apnea?....2 Positive Pressure Machines..................................................... 4 Types..................................................................................
Positive Pressure Therapy Positive Pressure Therapy...2 What is Sleep Apnea?....2 Positive Pressure Machines..................................................... 4 Types..................................................................................
Transnasal Humidified Rapid Insufflation Ventilatory Exchange (THRIVE): An Optimal Method of Preoxygenation for General Anaesthesia in Obstetrics
 Transnasal Humidified Rapid Insufflation Ventilatory Exchange (THRIVE): An Optimal Method of Preoxygenation for General Anaesthesia in Obstetrics Dr E McMaster, Dr E Gent, Dr T Mahendrayogam, Dr A Surendran
Transnasal Humidified Rapid Insufflation Ventilatory Exchange (THRIVE): An Optimal Method of Preoxygenation for General Anaesthesia in Obstetrics Dr E McMaster, Dr E Gent, Dr T Mahendrayogam, Dr A Surendran
Clinical Guideline: Heated Humidified High Flow Nasal Cannula (HHHFNC) Guideline
 EOE Neonatal ODN Clinical Guideline: Heated Humidified High Flow Nasal Cannula (HHHFNC) Guideline Authors: Dr Eliana Panayiotou and Dr Bharat Vakharia For use in: EoE Neonatal Units Guidance specific to
EOE Neonatal ODN Clinical Guideline: Heated Humidified High Flow Nasal Cannula (HHHFNC) Guideline Authors: Dr Eliana Panayiotou and Dr Bharat Vakharia For use in: EoE Neonatal Units Guidance specific to
Skill Evaluation Sheets
 Skill Evaluation Sheets Skill Drill 2-: How to Remove Gloves Skill Drill 4-: Primary Check: RAP-CAB Skill Drill 4-2: Perform a Secondary Check Skill Drill 5-: Adult CPR Skill Drill 5-2: Child CPR Skill
Skill Evaluation Sheets Skill Drill 2-: How to Remove Gloves Skill Drill 4-: Primary Check: RAP-CAB Skill Drill 4-2: Perform a Secondary Check Skill Drill 5-: Adult CPR Skill Drill 5-2: Child CPR Skill
The essential principles of tracheostomy care
 The essential principles of tracheostomy care Deborah Dawson Consultant Nurse Critical Care Excellence in specialist and community healthcare Key publications https://www.stgeorges.nhs.uk/gps-andclinicians/clinical-resources/tracheostomyguidelines/
The essential principles of tracheostomy care Deborah Dawson Consultant Nurse Critical Care Excellence in specialist and community healthcare Key publications https://www.stgeorges.nhs.uk/gps-andclinicians/clinical-resources/tracheostomyguidelines/
Carole Wegner RN, MSN And Lori Leiser CRT
 Airway Clearance Carole Wegner RN, MSN And Lori Leiser CRT Topics Suctioning and suctioning equipment Medications to facilitate t airway clearance Bronchial hygiene modalities Preparing for suctioning
Airway Clearance Carole Wegner RN, MSN And Lori Leiser CRT Topics Suctioning and suctioning equipment Medications to facilitate t airway clearance Bronchial hygiene modalities Preparing for suctioning
Non-invasive Ventilation protocol For COPD
 NHS LANARKSHIRE MONKLANDS HOSPITAL Non-invasive Ventilation protocol For COPD April 2017 S Baird Review Date: Oct 2019 Approved by Medical Directorate Indications for Non-Invasive Ventilation (NIV) NIV
NHS LANARKSHIRE MONKLANDS HOSPITAL Non-invasive Ventilation protocol For COPD April 2017 S Baird Review Date: Oct 2019 Approved by Medical Directorate Indications for Non-Invasive Ventilation (NIV) NIV
Day-to-day management of Tracheostomies & Laryngectomies
 Humidification It is mandatory that a method of artificial humidification is utilised when a tracheostomy tube is in situ, for people requiring oxygen therapy dry oxygen should never be given to someone
Humidification It is mandatory that a method of artificial humidification is utilised when a tracheostomy tube is in situ, for people requiring oxygen therapy dry oxygen should never be given to someone
Adult Patients Going Home with a Tracheostomy
 Physiotherapy Department Adult Patients Going Home with a Tracheostomy Darent Valley Hospital Darenth Wood Road Dartford Kent DA2 8DA www.dvh.nhs.uk In case of emergencies you will need to dial 999 If
Physiotherapy Department Adult Patients Going Home with a Tracheostomy Darent Valley Hospital Darenth Wood Road Dartford Kent DA2 8DA www.dvh.nhs.uk In case of emergencies you will need to dial 999 If
Intensive Care Diary. information. Radnor Ward. Salisbury NHS Foundation Trust
 information Intensive Care Diary Radnor Ward Salisbury NHS Foundation Trust Contents The purpose of your diary Intensive Care Diary Admission Day - What happened? Why am I here? Visitor s Blog / World
information Intensive Care Diary Radnor Ward Salisbury NHS Foundation Trust Contents The purpose of your diary Intensive Care Diary Admission Day - What happened? Why am I here? Visitor s Blog / World
COBIS Management of airway burns and inhalation injury PAEDIATRIC
 COBIS Management of airway burns and inhalation injury PAEDIATRIC 1 A multidisciplinary team should provide the management of the child with inhalation injury. Childhood inhalation injury mandates transfer
COBIS Management of airway burns and inhalation injury PAEDIATRIC 1 A multidisciplinary team should provide the management of the child with inhalation injury. Childhood inhalation injury mandates transfer
GE Healthcare. Non Invasive Ventilation (NIV) For the Engström Ventilator. Relief, Relax, Recovery
 GE Healthcare Non Invasive Ventilation (NIV) For the Engström Ventilator Relief, Relax, Recovery COPD is currently the fourth leading cause of death in the world, and further increases in the prevalence
GE Healthcare Non Invasive Ventilation (NIV) For the Engström Ventilator Relief, Relax, Recovery COPD is currently the fourth leading cause of death in the world, and further increases in the prevalence
Chapter 10 The Respiratory System
 Chapter 10 The Respiratory System Biology 2201 Why do we breathe? Cells carry out the reactions of cellular respiration in order to produce ATP. ATP is used by the cells for energy. All organisms need
Chapter 10 The Respiratory System Biology 2201 Why do we breathe? Cells carry out the reactions of cellular respiration in order to produce ATP. ATP is used by the cells for energy. All organisms need
** SURFACTANT THERAPY**
 ** SURFACTANT THERAPY** Full Title of Guideline: Surfactant Therapy Author (include email and role): Stephen Wardle (V4) Reviewed by Dushyant Batra Consultant Neonatologist Division & Speciality: Division:
** SURFACTANT THERAPY** Full Title of Guideline: Surfactant Therapy Author (include email and role): Stephen Wardle (V4) Reviewed by Dushyant Batra Consultant Neonatologist Division & Speciality: Division:
1. Can you convince me that one should use CPAP and avoid mechanical ventilation?
 CHAPTER 12 FAQ's Dr Rhishikesh Thakre Neonatologist Aurangabad, Mahrashtra Following are bedside tips one learns with experience. So as to guide the newcomer who should not repeat the same mistakes, the
CHAPTER 12 FAQ's Dr Rhishikesh Thakre Neonatologist Aurangabad, Mahrashtra Following are bedside tips one learns with experience. So as to guide the newcomer who should not repeat the same mistakes, the
F: Respiratory Care. College of Licensed Practical Nurses of Alberta, Competency Profile for LPNs, 3rd Ed. 59
 F: Respiratory Care College of Licensed Practical Nurses of Alberta, Competency Profile for LPNs, 3rd Ed. 59 Competency: F-1 Airway Management F-1-1 F-1-2 F-1-3 F-1-4 F-1-5 Demonstrate knowledge and ability
F: Respiratory Care College of Licensed Practical Nurses of Alberta, Competency Profile for LPNs, 3rd Ed. 59 Competency: F-1 Airway Management F-1-1 F-1-2 F-1-3 F-1-4 F-1-5 Demonstrate knowledge and ability
MODULE VII. Delivery and Immediate Neonatal Care
 MODULE VII Delivery and Immediate Neonatal Care NEONATAL ASPHYXIA About one million deaths per year In Latin America 12% of newborns suffer some degree of asphyxia Main cause of perinatal and neonatal
MODULE VII Delivery and Immediate Neonatal Care NEONATAL ASPHYXIA About one million deaths per year In Latin America 12% of newborns suffer some degree of asphyxia Main cause of perinatal and neonatal
Patent Ductus Arteriosus (PDA)
 Patent Ductus Arteriosus (PDA) A Parent Information Leaflet What is the Ductus Arteriosus? What is the Ductus Arteriosus? The Ductus Arteriosus is a small muscular blood vessel that joins the pulmonary
Patent Ductus Arteriosus (PDA) A Parent Information Leaflet What is the Ductus Arteriosus? What is the Ductus Arteriosus? The Ductus Arteriosus is a small muscular blood vessel that joins the pulmonary
ENDOTRACHEAL INTUBATION POLICY
 POLICY Indications: Ineffective ventilation with mask and t-piece, or mask and bag technique Inability to maintain a patent airway Need or anticipation of need for prolonged ventilation Need for endotracheal
POLICY Indications: Ineffective ventilation with mask and t-piece, or mask and bag technique Inability to maintain a patent airway Need or anticipation of need for prolonged ventilation Need for endotracheal
This interdisciplinary clinical support document provides guidelines for the safe establishment of an artificial airway.
 PURPOSE This interdisciplinary clinical support document provides guidelines for the safe establishment of an artificial airway. POLICY STATEMENTS Endotracheal intubation will be performed by the Most
PURPOSE This interdisciplinary clinical support document provides guidelines for the safe establishment of an artificial airway. POLICY STATEMENTS Endotracheal intubation will be performed by the Most
Airway Management From Brady s First Responder (8th Edition) 82 Questions
 Airway Management From Brady s First Responder (8th Edition) 82 Questions 1. What color will cyanotic skin be? p. 119 *A.) Blue B.) Red C.) Yellow D.) Green 2. Which is the primary path for air to enter
Airway Management From Brady s First Responder (8th Edition) 82 Questions 1. What color will cyanotic skin be? p. 119 *A.) Blue B.) Red C.) Yellow D.) Green 2. Which is the primary path for air to enter
Children & Young People s Directorate Paediatric-Neonatal Guidelines Checklist & Version Control Sheet
 Children & Young People s Directorate Paediatric-Neonatal Guidelines Checklist & Version Control Sheet 1. Name of Guideline / Policy/ Procedure 2. Purpose of Procedure/ Guidelines/ Protocol Guideline for
Children & Young People s Directorate Paediatric-Neonatal Guidelines Checklist & Version Control Sheet 1. Name of Guideline / Policy/ Procedure 2. Purpose of Procedure/ Guidelines/ Protocol Guideline for
H: Respiratory Care. Saskatchewan Association of Licensed Practical Nurses, Competency Profile for LPNs, 3rd Ed. 79
 H: Respiratory Care Saskatchewan Association of Licensed Practical Nurses, Competency Profile for LPNs, 3rd Ed. 79 Competency: H-1 Airway Management H-1-1 H-1-2 H-1-3 H-1-4 H-1-5 Demonstrate knowledge
H: Respiratory Care Saskatchewan Association of Licensed Practical Nurses, Competency Profile for LPNs, 3rd Ed. 79 Competency: H-1 Airway Management H-1-1 H-1-2 H-1-3 H-1-4 H-1-5 Demonstrate knowledge
Name and title of the investigators responsible for conducting the research: Dr Anna Lavizzari, Dr Mariarosa Colnaghi
 Protocol title: Heated, Humidified High-Flow Nasal Cannula vs Nasal CPAP for Respiratory Distress Syndrome of Prematurity. Protocol identifying number: Clinical Trials.gov NCT02570217 Name and title of
Protocol title: Heated, Humidified High-Flow Nasal Cannula vs Nasal CPAP for Respiratory Distress Syndrome of Prematurity. Protocol identifying number: Clinical Trials.gov NCT02570217 Name and title of
Advanced Airway Management. University of Colorado Medical School Rural Track
 Advanced Airway Management University of Colorado Medical School Rural Track Advanced Airway Management Basic Airway Management Airway Suctioning Oxygen Delivery Methods Laryngeal Mask Airway ET Intubation
Advanced Airway Management University of Colorado Medical School Rural Track Advanced Airway Management Basic Airway Management Airway Suctioning Oxygen Delivery Methods Laryngeal Mask Airway ET Intubation
Airway and Breathing
 Airway and Breathing ETAT Module 2 Adapted from Emergency Triage Assessment and Treatment (ETAT): Manual for Participants, World Health Organization, 2005 Learning Objectives Accurately determine whether
Airway and Breathing ETAT Module 2 Adapted from Emergency Triage Assessment and Treatment (ETAT): Manual for Participants, World Health Organization, 2005 Learning Objectives Accurately determine whether
CHILDREN S SERVICES. Patient information Leaflet BRONCHIOLITIS
 CHILDREN S SERVICES Patient information Leaflet BRONCHIOLITIS Sept 2014 INTRODUCTION This leaflet aims to help you understand bronchiolitis, how to make your child comfortable and when to contact for emergency
CHILDREN S SERVICES Patient information Leaflet BRONCHIOLITIS Sept 2014 INTRODUCTION This leaflet aims to help you understand bronchiolitis, how to make your child comfortable and when to contact for emergency
Guidelines and Best Practices for Vapotherm High Velocity Nasal Insufflation (Hi-VNI ) NICU POCKET GUIDE
 Guidelines and Best Practices for Vapotherm High Velocity Nasal Insufflation (Hi-VNI ) TM NICU POCKET GUIDE Patient Selection Diagnoses Patient presents with one or more of the following symptoms: These
Guidelines and Best Practices for Vapotherm High Velocity Nasal Insufflation (Hi-VNI ) TM NICU POCKET GUIDE Patient Selection Diagnoses Patient presents with one or more of the following symptoms: These
Von Reuss and CPAP, Disclosures CPAP. Noninvasive respiratory therapieswhy bother? Noninvasive respiratory therapies- types
 Noninvasive respiratory therapiesby a nose? NEO- The Conference for Neonatology February 21, 2014 Disclosures I have no relevant financial relationships to disclose or conflicts of interest to release.
Noninvasive respiratory therapiesby a nose? NEO- The Conference for Neonatology February 21, 2014 Disclosures I have no relevant financial relationships to disclose or conflicts of interest to release.
1.40 Prevention of Nosocomial Pneumonia
 1.40 Prevention of Nosocomial Pneumonia Purpose Audience Policy Statement: The guideline is designed to reduce the incidence of pneumonia and other acute lower respiratory tract infections. All UTMB healthcare
1.40 Prevention of Nosocomial Pneumonia Purpose Audience Policy Statement: The guideline is designed to reduce the incidence of pneumonia and other acute lower respiratory tract infections. All UTMB healthcare
Nasopharyngeal airways for craniofacial conditions
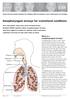 Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Nasopharyngeal airways for craniofacial conditions This information sheet from Great Ormond Street Hospital (GOSH)
Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Nasopharyngeal airways for craniofacial conditions This information sheet from Great Ormond Street Hospital (GOSH)
Care and Use of Nebulisers
 For further information visit: www.nhsdirect.nhs.uk www.lhch.nhs.uk www.dipex.org If you require a copy of this leaflet in any other format or language please contact us quoting the leaflet code and the
For further information visit: www.nhsdirect.nhs.uk www.lhch.nhs.uk www.dipex.org If you require a copy of this leaflet in any other format or language please contact us quoting the leaflet code and the
Oxygen & High flow nasal Oxygen therapy. Learning points. Why? 18/07/
 Oxygen & High flow nasal Oxygen therapy 13.07.2017 Learning points Update on BTS guidance May 2017 Help you understand the mechanism of action of high flow nasal oxygen therapy Help you think about the
Oxygen & High flow nasal Oxygen therapy 13.07.2017 Learning points Update on BTS guidance May 2017 Help you understand the mechanism of action of high flow nasal oxygen therapy Help you think about the
Provide guidelines for the management of mechanical ventilation in infants <34 weeks gestation.
 Page 1 of 5 PURPOSE: Provide guidelines for the management of mechanical ventilation in infants
Page 1 of 5 PURPOSE: Provide guidelines for the management of mechanical ventilation in infants
The Respiratory System
 13 PART A The Respiratory System PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB Organs of the Respiratory
13 PART A The Respiratory System PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB Organs of the Respiratory
