Endotracheal intubation is
|
|
|
- Brittany Rodgers
- 6 years ago
- Views:
Transcription
1 ClinicalArticle Unplanned Extubation in Adult Critical Care Quality Improvement and Education Payoff Amy L. Richmond, RN, CCRN Dena L. Jarog, RN, MSN, CCNS Vicki M. Hanson, RRT Endotracheal intubation is done many times a day in hospitals for patients who have or may have a problem with their airway. Once a patient is intubated, maintenance of the endotracheal tube is essential. In critical care units, the task of maintaining tube patency and placement is the responsibility of nursing and respiratory care professionals. For as long as patients have been intubated, the potential for unplanned removal of the endotracheal tube has been a source of concern. This concern has led nurses and other medical professionals to search for ways to decrease the occurrence of unplanned extubation. Unplanned extubation is defined as any accidental or purposeful removal of the endotracheal tube by a patient. 1-3 Because of a high rate of unplanned extubations 2.14% in the medical intensive care unit (MICU)/coronary care unit (CCU) and 2.32% in the surgical ICU (SICU) at a tertiary care hospital in north central Wisconsin, a quality control committee was formed to address methods for decreasing the unplanned extubation rate and increasing awareness of the rate of unplanned extubations. The committee consisted of staff from respiratory therapy, clinical nursing, and nursing Authors Amy L. Richmond is a critical care nurse in the surgical intensive care unit at St. Joseph s Hospital in Marshfield, Wis. She chairs the Endotracheal Tube Committee and has been instrumental in practice changes in critical care at St. Joseph s Hospital. Dena Jarog is the pediatric critical care clinical nurse specialist in the pediatric intensive care unit at St. Joseph s Hospital in Marshfield, Wis. Vicki Hanson is a respiratory therapist in the surgical and pediatric intensive care units at St. Joseph s Hospital in Marshfield, Wis. To purchase reprints, contact The InnoVision Group, 101 Columbia, Aliso Viejo, CA Phone, (800) or (949) (ext 532); fax, (949) ; , reprints@aacn.org. administration and a physician champion. As information and data were evaluated, the committee determined that although sedation and restraint were intermittently contributing factors to unplanned extubation, the techniques used for securing endotracheal tubes were the one factor that was consistently a problem. Staff members were using several different techniques to secure patients endotracheal tubes. Some patients had tube holders from other facilities that were unfamiliar to the staff; other patients had different methods of taping and products used. Some patients had their tube secured around their head; others had tape adhered to their bare skin. Because of the identified inconsistencies, the committee developed a plan to educate the nursing and respiratory care staff. The education consisted of training in new securing techniques, heightening awareness of patients activity levels, and improving knowledge about patients readiness for extubation. In this article, 32 CRITICALCARENURSE Vol 24, No. 1, FEBRUARY 2004
2 we address issues associated with unplanned extubations and how to decrease the occurrence of unplanned extubation by using a consistent securing technique. Literature Review A review of the literature revealed many studies 1,3-9 that expanded on old knowledge of unplanned extubation. Several studies 1,10-12 addressed factors that contributed to unplanned extubation and complications associated with those factors. Published reports 5,8-14 indicated that the frequency of unplanned extubation ranged from a low of 0.7% to a high of 25%. Quality improvement and education both played an important role in significantly decreasing rates of unplanned extubation. 11,12 Although some authors discussed new methods of securing endotracheal tubes, none provided information about the processes used to instruct staff in using the new methods properly. Whether securing techniques actually decrease the frequency of unplanned extubation in critical care populations also was not discussed. Methods St. Joseph s Hospital is a 500- bed, rural, tertiary care center. The subjects for this project were a convenience sample of all patients who had an unplanned extubation in the SICU and the CCU/MICU in a 2- year period. An intensivist, the respiratory care staff, and the nursing staff all perceived a high frequency of unplanned extubations in the adult critical care units during a 6-month period. The policy for securing endotracheal tubes was due for an update. Additionally, the products and techniques used to secure endotracheal tubes had changed, and those changes had not been incorporated into the policy and procedure. Therefore, staff members did not know how to use and secure endotracheal tubes properly. The committee thought that extubations could have been avoided if different techniques and possibly different products had been used to secure endotracheal tubes. To test this theory, the quality control committee developed a tool to track factors related to unplanned extubations (Figure 1). For each unplanned extubation, nurses in the critical care units were asked to enter information on the form. They were also required to complete an incident report, which was submitted to the quality control group and the risk management department at the hospital. Using incident reports, the tool developed by the committee, and the number of days that patients received mechanical ventilation, the committee was able to determine the frequency of unplanned extubations. Each quarter, the group met to discuss the unplanned extubations and determine a course of action to decrease the frequency of unplanned extubations in adult patients. Upon reviewing the data, the committee deemed the frequency of unplanned extubations to be too high, 2.32% in the SICU and 2.14% in the CCU/MICU. A review of the literature did not reveal any nationally accepted standard. Therefore, a goal was set to reduce the frequency of unplanned extubations to less than 0.8%; the committee thought that doing so would indicate a higher quality of care. To meet this goal, the quality control group investigated different tube holders in an effort to improve the security of the endotracheal tube. Evaluation of the tube holders required staff to receive instruction to ensure proper use of each holder. When this investigation was done, several manufacturers were producing endotracheal tube holders. The committee examined each of the holders available, looking at design, securability, ease of application, and durability once in place. They also wanted a device that allowed easy movement of the tube from side to side in order to maintain the integrity of the oral mucosa. Another feature important to the committee was that the holder maintain skin integrity beneath the area of application. This evaluation helped the committee narrow the field of prospective devices to 2, 1 (Hollister oral endotracheal attachment device) manufactured by Hollister, Inc (Libertyville, Ill) and 1 (Comfit) manufactured by Ackrad Laboratories, a CooperSurgical Company (Cranford, NJ). These 2 types of holders were tried by the staff of each unit. After determining which devices were to be evaluated, the committee created a teaching plan to prepare the nursing and respiratory staff to use the new devices. A new policy that included instruction in using each device was created and put into use. The existing policy and procedure for taping were updated to provide an alternative choice for securing endotracheal tubes. Handson instruction about each holder and the taping technique was provided to all staff members along CRITICALCARENURSE Vol 24, No. 1, FEBRUARY
3 with written information and posters demonstrating proper use of the tube holders. Instruction was offered for 2 weeks, with times dispersed over all shifts to facilitate staff compliance. During the in-service training sessions, the nursing and respiratory care staff were taught the manufacturers recommended application technique for the 2 tube holders. The staff were also taught a method of taping, using cloth tape circling behind the head and secured directly to the tube. A piece of tape was torn to a length that extends around the back of the patient s head, with adhesive ends long enough to wrap around the endotracheal tube and make the tube secure. An adhesive skin preparation was applied to the cheek area and the endotracheal tube to give a sticky base to which the tape could adhere. The upper loose ends were then wrapped around the endotracheal tube with the lower loose ends being brought up, over, and across the patient s upper lip to the opposite cheek. The current policy and procedure for using tape as a securing device was updated, and a new policy was created to describe the use of the new tube holder in order to maintain consistency among staff members when choosing and using securing devices. Once the training was complete, each device was evaluated for separate 3-month periods to allow for an application learning curve to level out. With each evaluation, the education provided for that securing device was reinforced. Results The focus of this project was education and process change. In order to show the change as effective, data were collected by using a tool developed by the quality improvement committee (Figure 1), assessing the factors thought to contribute most to unplanned extubation. The factors most cited in the literature were physical restraint, level of sedation, and activity and mental status of the patient at the time of unplanned extubation. 1,5,10,15 In the initial evaluation, the factor most commonly associated with unplanned extubation in the SICU and CCU at St. Joseph s was the technique used to secure the endotracheal tube. The tool used during data collection addressed the other common factors described in published reports and securing technique. When the data were analyzed, no pattern indicated that any of the other factors was a significant contributor to unplanned extubation. We decided to begin the education program with a single focus on securing the endotracheal tube and then branch out to educate staff members about the other factors once the staff had mastered securing. With this arrangement, we could be more certain that the extubations that were occurring were due to the level of sedation or restraint and not to use of poor technique to secure the tube. During this project, the unplanned extubation rates for 2 6-month periods were compared to determine whether the frequency of unplanned extubations decreased after extensive changes in the process of securing endotracheal tubes were coupled with intensive education about the changes. When the first 6 months preceding staff education was compared with the 6 months after staff education, an improvement in the rate of unplanned extubation was apparent among all patients studied (Figure 2). During the first 6 months before the education, for the 2 units (SICU and CCU/MICU) combined, a total of 495 patients were intubated for 1154 days. The next year, during a comparable 6-month period after the education, 523 patients in the 2 units were intubated for 1689 days. Pearson chi-square analysis indicated a significant decrease in the rate of unplanned extubation after extensive education. In the CCU/ MICU, the unplanned extubation rate decreased from 2.14% (9 extubations in 421 days) before to 0.87% (6 extubations in 689 days) after the education. In the SICU, the unplanned extubation rate decreased from 2.32% (17 extubations in 733 ventilator days) before to 1.0% (10 extubations in 1000 days) after the education (Figure 2). Pearson chi-square analysis of the number of extubations before and after the education program indicated a significance of.03 for the CCU/MICU and.002 for the ICU (P <.05). At the same time that the frequency of unplanned extubations decreased, the number of ventilator days increased (Figure 3). Discussion Unplanned extubation has been a problem for many institutions. 1,2,7,8,10,12,13,15 It has been several years since anyone has reported new information about rates of unplanned extubation and the impact of quality improvement. In an attempt to increase the quality of care for our patients, a new method of securing endotracheal tubes was taught and implemented. Before the in-service training sessions, rates of unplanned 34 CRITICALCARENURSE Vol 24, No. 1, FEBRUARY 2004
4 Date: Time: Unit: Pt Diagnosis/Injury/Surgery: Restraint type: Position of patient at time of extubation: Position of patient at time of extubation: Type of ETT holder: Where was the RN? Halter posy Bilateral wrist restraints Left wrist restraint only Right wrist restraint only Chair Bed: R, L, Supine, Prone Walking Chair Bed: R, L, Supine, Prone Walking Comfit Holister Tape: PICU P&P, OR, ED, Outlying facility or transport service In the room Out of the room How many patients did you have? Do you feel your assignment for your shift in any way contributed to the patient s unplanned extubation? Yes No Explain: Where was the RT? On the unit Off the unit Do you feel your assignment for your shift in any way contributed to the patient s unplanned extubation? Yes No Explain: What was the sedation level of the patient at the time of unplanned extubation? a) Adequately sedated b) Suddenly awake c) Inadequately sedated Please explain: Type of sedation: Type of paralytic: Versed: prn Norcuron: prn Ativan: prn Pavulon: prn Pain medications: MSO 4 : prn Other: Dilaudid: prn Figure 1 Unplanned extubation report form. This form is not part of the patient s permanent medical record. Abbreviations: ED, emergency department; ETT, endotracheal tube;, infusion; L, left; MSO 4, morphine sulfate; OR, operating room; PICU P&P, pediatric intensive care unit policy and procedure; prn, as needed; Pt, patient; R, right; RN, registered nurse; RT, respiratory therapist. Reprinted with permission of St. Joseph s Hospital, Marshfield, Wis. CRITICALCARENURSE Vol 24, No. 1, FEBRUARY
5 Percentage Intensive care unit 17 incidents 733 ventilator days Figure 2 Unplanned extubation rates for 6 months before and after education program on securing endotracheal tubes. extubation for the 2 units combined were as high as 2.34%. After staff education, unplanned extubation rates plummeted to 0.95% for the 2 units combined, indicating that education and attention to detail and quality can improve care of intubated patients. While the rate of unplanned extubations was decreasing, the facility instituted a new trauma service, which significantly increased the number of ventilator days in the critical care units. Although the number of ventilator days increased, the number of extubations decreased significantly (Figure 3). Limitations of the Study One limitation of this study is the method used to complete the data collection sheet. Although 1 person was responsible for collating collected data, all nursing and respiratory therapy staff were required to 10 incidents 1000 ventilator days Before education 9 incidents 421 ventilator days 6 incidents 689 ventilator days Coronary care unit understand the use of the tool and use it appropriately. Each time an unplanned extubation occurred, the staff person involved was required to No. of extubations After education SICU Before education CCU/MICU Number of extubations complete an incident report and a collection tool. At times the tool was not completed but an incident report was generated. Inconsistent data collection required the review of charts to fill in missing data. If documentation was not complete, it was difficult for the collator to go to the chart and fill in retrospective data. Another limitation of this study is that the committee did not use a formal database to collate information but rather tallied all results by hand. Because of this practice, only patients who had an unplanned extubation were followed up; therefore, patients having planned extubations could not be compared with patients who had an unplanned extubation. If a formal database had been used, all intubated patients might have been included in order to compare some of the interventions that were used successfully for patients who stayed intubated versus patients who had unplanned extubations. Sedation and/or use of SICU After education CCU/MICU Number of ventilator days Figure 3 Rates of unplanned extubation in the surgical intensive care unit (SICU) and the coronary care unit/medical intensive care unit (CCU/MICU) before and after the education program No. of ventilator days 36 CRITICALCARENURSE Vol 24, No. 1, FEBRUARY 2004
6 restraints, oral versus nasal intubation, and the need for reintubation after unplanned extubation also could have been compared in patients who remained intubated versus patients with unplanned extubations. Use of a formal database would have kept information together, with better accessibility for future comparisons and research. Conclusion For as long as patients have been intubated, the potential for unplanned removal has been a source of concern. This concern has led nurses and other medical professionals to search for ways to decrease the occurrence of unplanned extubation. In this project, a perceived problem was assessed, and a tool for data collection was created. The tool was used to collect data on unplanned extubation and was then used to clarify perceptions and assumptions, steps that led to a change in practice. This change was of great benefit to the patients and the staff, because it provided consistency for a method of securing endotracheal tubes, which led to better quality of care for the patients. The tool has been used consistently for some time. We plan to try to build a database in which information can be stored and collated to allow comparison of methods and types of sedation and to develop protocols for fast-track weaning parameters and alternatives for restraint; our hope is to further decrease the number of unplanned extubations. Acknowledgments We acknowledge the assistance and efforts of the following staff members at St. Joseph s Hospital and the Marshfield Clinic system in Marshfield, Wis: the nurses in the intensive care unit; the respiratory care practitioners; the nurses in the medical critical care unit; Rachel Boehning-Anderson, director of the respiratory care department; Donald Reinhardt and Jeff Thoma, hospital information systems; and Richard Berg, biostatistician. References 1. Grap MJ, Glass C, Lindamood MO. Factors related to unplanned extubation of endotracheal tubes. Crit Care Nurse. April 1995; 15: Atkins PM, Mion LC, Mendelson W, Palmer RM, Slomka J, Franko T. Characteristics and outcomes of patients who self-extubate from ventilatory support. Chest. 1997;112: Mion LC. Establishing alternatives to physical restraints in the acute care setting: a conceptual framework to assist nurses decision making. AACN Clin Issues. 1996;7: Happ MB. Treatment interference in acutely and critically ill adults. Am J Crit Care. 1998; 7: Sessler CN. Unplanned extubations: making progress using CQI. Intensive Care Med. 1997;23: Brown K, Thompson DG, Brooks L. Lowering the rate of unscheduled extubations. MCN Am J Matern Child Nurs. 1996;21: Crimlisk JT, Bernardo J, Blansfield JS, et al. Endotracheal reintubation: a closer look at a preventative condition. Clin Nurse Spec. 1996;11: Kapadia FN, Bajan KB, Raje KV. Airway accidents in intubated intensive care unit patients: an epidemiological study. Crit Care Med. 2000;28: Christie JM, Dethlefson M, Cane RD. Unplanned endotracheal extubation in the intensive care unit. J Clin Anesth. 1996;8: Chevron V, Menard JF, Richard JC, Girault C, Leroy J, Bonmarchand G. Unplanned extubation: risk factors of development and predictive criteria for reintubation. Crit Care Med. 1998;26: Maguire GP, DeLorenzo LJ, Moggio RA. Unplanned extubation in the intensive care unit: a quality of care concern. Crit Care Nurs Q. November 1994;17: Chiang AA, Lee KC, Lee JC, Wei CH. Effectiveness of a continuous quality improvement program aiming to reduce unplanned extubation: a prospective study. Intensive Care Med. 1996;22: Tominaga GT, Rudzwich H, Scannell G, Waxman K. Decreasing unplanned extubations in the surgical intensive care unit. Am J Surg. 1995;170: Carrion MI, Ayuso D, Marcos M, et al. Accidental removal of endotracheal and nasogastric tubes and intravascular catheters. Crit Care Med. 2000;28: Betbese AJ, Perez M, Bak E, Rialp G, Mancebo J. A prospective study of planned endotracheal extubation in intensive care unit patients. Crit Care Med. 1998;26:
Unplanned Extubation: A Local Experience
 O r i g i n a l A r t i c l e Singapore Med J 2002 Vol 43(10) : 504-508 Unplanned Extubation: A Local Experience L L Phoa, W Y Pek, W S Yap, A Johan Department of Respiratory Medicine Tan Tock Seng Hospital
O r i g i n a l A r t i c l e Singapore Med J 2002 Vol 43(10) : 504-508 Unplanned Extubation: A Local Experience L L Phoa, W Y Pek, W S Yap, A Johan Department of Respiratory Medicine Tan Tock Seng Hospital
[Downloaded free from on Wednesday, September 28, 2016, IP: ]
![[Downloaded free from on Wednesday, September 28, 2016, IP: ] [Downloaded free from on Wednesday, September 28, 2016, IP: ]](/thumbs/74/70428039.jpg) Original Article Unplanned extubation in the ICU: Impact on outcome and nursing workload Ayman Krayem, Ron Butler*, Claudio Martin* King Khalid National Guard Hospital, King Abdulaziz, Medical City - Jeddah,
Original Article Unplanned extubation in the ICU: Impact on outcome and nursing workload Ayman Krayem, Ron Butler*, Claudio Martin* King Khalid National Guard Hospital, King Abdulaziz, Medical City - Jeddah,
INFLUENCE OF PHYSICAL
 Critical Care Techniques INFLUENCE OF PHYSICAL RESTRAINT ON UNPLANNED EXTUBATION OF ADULT INTENSIVE CARE PATIENTS: A CASE-CONTROL STUDY By Li-Yin Chang, RN, MSN, Kai-Wei Katherine Wang, RN, PhD, and Yann-Fen
Critical Care Techniques INFLUENCE OF PHYSICAL RESTRAINT ON UNPLANNED EXTUBATION OF ADULT INTENSIVE CARE PATIENTS: A CASE-CONTROL STUDY By Li-Yin Chang, RN, MSN, Kai-Wei Katherine Wang, RN, PhD, and Yann-Fen
Factors Affecting Invasive Management after Unplanned Extubation in an Intensive Care Unit
 Korean J Crit Care Med 2015 August 30(3):164-170 / ISSN 2383-4870 (Print) ㆍ ISSN 2383-4889 (Online) Original Article Factors Affecting Invasive Management after Unplanned Extubation in an Intensive Care
Korean J Crit Care Med 2015 August 30(3):164-170 / ISSN 2383-4870 (Print) ㆍ ISSN 2383-4889 (Online) Original Article Factors Affecting Invasive Management after Unplanned Extubation in an Intensive Care
Self-Extubation in the Surgical Intensive Care Unit and Restraint Policy Change: A Retrospective Study
 Send Orders for Reprints to reprints@benthamscience.net 10 Open Medicine Journal, 2014, 1, 10-14 Open Access Self-Extubation in the Surgical Intensive Care Unit and Restraint Policy Change: A Retrospective
Send Orders for Reprints to reprints@benthamscience.net 10 Open Medicine Journal, 2014, 1, 10-14 Open Access Self-Extubation in the Surgical Intensive Care Unit and Restraint Policy Change: A Retrospective
Interfacility Protocol Protocol Title:
 Interfacility Protocol Protocol Title: Mechanical Ventilator Monitoring & Management Original Adoption Date: 05/2009 Past Protocol Updates 05/2009, 12/2013 Date of Most Recent Update: March 23, 2015 Medical
Interfacility Protocol Protocol Title: Mechanical Ventilator Monitoring & Management Original Adoption Date: 05/2009 Past Protocol Updates 05/2009, 12/2013 Date of Most Recent Update: March 23, 2015 Medical
WEANING READINESS & SPONTANEOUS BREATHING TRIAL MONITORING
 CLINICAL EVIDENCE GUIDE WEANING READINESS & SPONTANEOUS BREATHING TRIAL MONITORING Weaning readiness and spontaneous breathing trial monitoring protocols can help you make the right weaning decisions at
CLINICAL EVIDENCE GUIDE WEANING READINESS & SPONTANEOUS BREATHING TRIAL MONITORING Weaning readiness and spontaneous breathing trial monitoring protocols can help you make the right weaning decisions at
Optimize vent weaning and SBT outcomes. Identify underlying causes for SBT failures. Role SBT and weaning protocol have in respiratory care
 Optimize vent weaning and SBT outcomes Identify underlying causes for SBT failures Role SBT and weaning protocol have in respiratory care Lower risk of developing complications Lower risk of VAP, other
Optimize vent weaning and SBT outcomes Identify underlying causes for SBT failures Role SBT and weaning protocol have in respiratory care Lower risk of developing complications Lower risk of VAP, other
INTUBATION/RSI. PURPOSE: A. To facilitate secure, definitive control of the airway by endotracheal intubation in an expeditious and safe manner
 Manual: LifeLine Patient Care Protocols Section: Adult/Pediatrics Protocol #: AP1-009 Approval Date: 03/01/2018 Effective Date: 03/05/2018 Revision Due Date: 12/01/2018 INTUBATION/RSI PURPOSE: A. To facilitate
Manual: LifeLine Patient Care Protocols Section: Adult/Pediatrics Protocol #: AP1-009 Approval Date: 03/01/2018 Effective Date: 03/05/2018 Revision Due Date: 12/01/2018 INTUBATION/RSI PURPOSE: A. To facilitate
ARTICLE IN PRESS. doi: /j.jemermed TRAUMA PATIENTS CAN SAFELY BE EXTUBATED IN THE EMERGENCY DEPARTMENT
 doi:10.1016/j.jemermed.2009.05.033 The Journal of Emergency Medicine, Vol. xx, No. x, pp. xxx, 2009 Copyright 2009 Elsevier Inc. Printed in the USA. All rights reserved 0736-4679/09 $ see front matter
doi:10.1016/j.jemermed.2009.05.033 The Journal of Emergency Medicine, Vol. xx, No. x, pp. xxx, 2009 Copyright 2009 Elsevier Inc. Printed in the USA. All rights reserved 0736-4679/09 $ see front matter
A prolonged observational study of tracheal tube displacements: Benchmarking an incidence <0.5-1% in a medical-surgical adult intensive care unit
 Research Article A prolonged observational study of tracheal tube displacements: Benchmarking an incidence
Research Article A prolonged observational study of tracheal tube displacements: Benchmarking an incidence
Difficult weaning from mechanical ventilation
 Difficult weaning from mechanical ventilation Paolo Biban, MD Director, Neonatal and Paediatric Intensive Care Unit Division of Paediatrics, Major City Hospital Azienda Ospedaliera Universitaria Integrata
Difficult weaning from mechanical ventilation Paolo Biban, MD Director, Neonatal and Paediatric Intensive Care Unit Division of Paediatrics, Major City Hospital Azienda Ospedaliera Universitaria Integrata
REHABILITATION OF PATIENTS MANAGED IN ICU
 REHABILITATION OF PATIENTS MANAGED IN ICU RECOMMENDATIONS Safety to mobilize / exercise: on the website Recommendation 1 All critically ill patients nursed in ICU should be screened closely before active
REHABILITATION OF PATIENTS MANAGED IN ICU RECOMMENDATIONS Safety to mobilize / exercise: on the website Recommendation 1 All critically ill patients nursed in ICU should be screened closely before active
KICU Spontaneous Awakening Trial (SAT) Questionnaire
 KICU Spontaneous Awakening Trial (SAT) Questionnaire Please select your best answer(s): 1. What is your professional role? 1 Staff Nurse 2 Nurse Manager 3 Nurse Educator 4 Physician 5 Medical Director
KICU Spontaneous Awakening Trial (SAT) Questionnaire Please select your best answer(s): 1. What is your professional role? 1 Staff Nurse 2 Nurse Manager 3 Nurse Educator 4 Physician 5 Medical Director
Liberation from Mechanical Ventilation in Critically Ill Adults
 Liberation from Mechanical Ventilation in Critically Ill Adults 2017 ACCP/ATS Clinical Practice Guidelines Timothy D. Girard, MD, MSCI Clinical Research, Investigation, and Systems Modeling of Acute Illness
Liberation from Mechanical Ventilation in Critically Ill Adults 2017 ACCP/ATS Clinical Practice Guidelines Timothy D. Girard, MD, MSCI Clinical Research, Investigation, and Systems Modeling of Acute Illness
AGITATION ONSET, FREQUENCY, AND ASSOCIATED TEMPORAL FACTORS IN CRITICALLY ILL ADULTS. Patient Safety Issues
 Patient Safety Issues AGITATION ONSET, FREQUENCY, AND ASSOCIATED TEMPORAL FACTORS IN CRITICALLY ILL ADULTS By Ruth S. Burk, RN, PhD, ANP-BC, Mary Jo Grap, RN, PhD, Cindy L. Munro, RN, PhD, ANP-C, Christine
Patient Safety Issues AGITATION ONSET, FREQUENCY, AND ASSOCIATED TEMPORAL FACTORS IN CRITICALLY ILL ADULTS By Ruth S. Burk, RN, PhD, ANP-BC, Mary Jo Grap, RN, PhD, Cindy L. Munro, RN, PhD, ANP-C, Christine
PICU Sedation Holidays. Jorge G. Sainz MD FAAP Medical Director PICU Medical Director Transport
 Jorge G. Sainz MD FAAP Medical Director PICU Medical Director Transport jsainz@elpasochildrens.org 1. Define sedation holiday. Objectives 2. Review differences between adult and pediatric sedation in ICU
Jorge G. Sainz MD FAAP Medical Director PICU Medical Director Transport jsainz@elpasochildrens.org 1. Define sedation holiday. Objectives 2. Review differences between adult and pediatric sedation in ICU
CASE PRIMERS. Pediatric Anesthesia Fellowship Program. Laryngotracheal Reconstruction (LTR) Tufts Medical Center
 CASE PRIMERS Pediatric Anesthesia Fellowship Program Tufts Medical Center Department of Anesthesiology and Perioperative Medicine Division of Pediatric Anesthesia 800 Washington Street, Box 298 Boston,
CASE PRIMERS Pediatric Anesthesia Fellowship Program Tufts Medical Center Department of Anesthesiology and Perioperative Medicine Division of Pediatric Anesthesia 800 Washington Street, Box 298 Boston,
Policies and Procedures. I.D. Number: 1154
 Policies and Procedures Title: TRACHEOSTOMY TUBE CHANGE - PEDIATRIC I.D. Number: 1154 Authorization: [X ] SHR Nursing Practice Committee Source: Nursing Date Effective: October 2008 Date Revised: March
Policies and Procedures Title: TRACHEOSTOMY TUBE CHANGE - PEDIATRIC I.D. Number: 1154 Authorization: [X ] SHR Nursing Practice Committee Source: Nursing Date Effective: October 2008 Date Revised: March
VAP Prevention bundles
 VAP Prevention bundles Dr. Shafiq A.Alimad MD Head of medical department at USTH YICID workshop, 15-12-2014 Care Bundles What are they & why use them? What are Care Bundles? Types of Care Bundles available
VAP Prevention bundles Dr. Shafiq A.Alimad MD Head of medical department at USTH YICID workshop, 15-12-2014 Care Bundles What are they & why use them? What are Care Bundles? Types of Care Bundles available
ENDOTRACHEAL INTUBATION POLICY
 POLICY Indications: Ineffective ventilation with mask and t-piece, or mask and bag technique Inability to maintain a patent airway Need or anticipation of need for prolonged ventilation Need for endotracheal
POLICY Indications: Ineffective ventilation with mask and t-piece, or mask and bag technique Inability to maintain a patent airway Need or anticipation of need for prolonged ventilation Need for endotracheal
This interdisciplinary clinical support document provides guidelines for the safe establishment of an artificial airway.
 PURPOSE This interdisciplinary clinical support document provides guidelines for the safe establishment of an artificial airway. POLICY STATEMENTS Endotracheal intubation will be performed by the Most
PURPOSE This interdisciplinary clinical support document provides guidelines for the safe establishment of an artificial airway. POLICY STATEMENTS Endotracheal intubation will be performed by the Most
Collaborative Regional Benchmarking Group (North of England, North Yorkshire & Humber and West Yorkshire)
 Collaborative Regional Benchmarking Group (North of England, North Yorkshire & Humber and West Yorkshire) Best Practice Guidance Endo Tracheal Tube Care These recommendations are based on the current evidence
Collaborative Regional Benchmarking Group (North of England, North Yorkshire & Humber and West Yorkshire) Best Practice Guidance Endo Tracheal Tube Care These recommendations are based on the current evidence
(31189) Hypothermia Initiation Phase One
 Hypothermia Initiation Phase One Diagnosis Allergies For hypothermia tracking purposes only. Please do not uncheck.- Required Cardiac Emergency Tracking For hypothermia tracking purposes only. Consults
Hypothermia Initiation Phase One Diagnosis Allergies For hypothermia tracking purposes only. Please do not uncheck.- Required Cardiac Emergency Tracking For hypothermia tracking purposes only. Consults
The Impact of a Unique Airway Clearance System on Airway Mechanics in Ventilated Patients
 The Impact of a Unique Airway Clearance System on Airway Mechanics in Ventilated Patients Schofield, L. 1, Shorr, A.F. 2, Washington, J. 1, Carlson, M. 1, Wagner, W. 1.1 McLaren Northern Michigan Hospital,
The Impact of a Unique Airway Clearance System on Airway Mechanics in Ventilated Patients Schofield, L. 1, Shorr, A.F. 2, Washington, J. 1, Carlson, M. 1, Wagner, W. 1.1 McLaren Northern Michigan Hospital,
Aim: Reduction in the rate of CLD in ELBW infants (<1000 grams) by 30% from its baseline of 72 % by January 2016.
 LIVE (Less Invasive Ventilation of ELBW infants) HEALTHY WVU Children s Hospital, Morgantown, WV, USA Rebecca Tilley, RN; Jamie Karr, RT; Tiffany Blosser, RN; Christy Dixon, RT; Melinda Connolly, ANP;
LIVE (Less Invasive Ventilation of ELBW infants) HEALTHY WVU Children s Hospital, Morgantown, WV, USA Rebecca Tilley, RN; Jamie Karr, RT; Tiffany Blosser, RN; Christy Dixon, RT; Melinda Connolly, ANP;
Primary Screening and Ongoing Assessment, Diagnosis and Interventions
 Primary Screening and Ongoing Assessment, Diagnosis and Interventions Vicky Scott, RN, PhD Clinical Professor, School of Population and Public Health Faculty of Medicine, University of British Columbia
Primary Screening and Ongoing Assessment, Diagnosis and Interventions Vicky Scott, RN, PhD Clinical Professor, School of Population and Public Health Faculty of Medicine, University of British Columbia
PHYSICIAN'S ORDERS Mark in for desired orders. If is blank, order is inactive. VENTILATOR SEDATION / ANALGESIC / DELIRIUM ORDER
 Nursing Daily awakenings PHYSICIAN'S ORDERS Mark in for desired orders. If is blank, order is inactive. VENTILATOR SEDATION / ANALGESIC / DELIRIUM ORDER Do not perform daily awakenings: Rationale: Daily
Nursing Daily awakenings PHYSICIAN'S ORDERS Mark in for desired orders. If is blank, order is inactive. VENTILATOR SEDATION / ANALGESIC / DELIRIUM ORDER Do not perform daily awakenings: Rationale: Daily
What s New About Proning?
 1 What s New About Proning? J. Brady Scott, MSc, RRT-ACCS, AE-C, FAARC Director of Clinical Education and Assistant Professor Department of Cardiopulmonary Sciences Division of Respiratory Care Rush University
1 What s New About Proning? J. Brady Scott, MSc, RRT-ACCS, AE-C, FAARC Director of Clinical Education and Assistant Professor Department of Cardiopulmonary Sciences Division of Respiratory Care Rush University
Goal Directed Protocols
 James R Dexter MD FACP FCCP Goal Directed Protocols Complete a Task or Achieve a Goal? James R Dexter MD FACP FCCP jamesrdexter@gmail.com Medical Director Respiratory Care, Redlands Community Hospital
James R Dexter MD FACP FCCP Goal Directed Protocols Complete a Task or Achieve a Goal? James R Dexter MD FACP FCCP jamesrdexter@gmail.com Medical Director Respiratory Care, Redlands Community Hospital
Sedation Hold/Interruption and Weaning Protocol ( Wake-up and Breathe )
 PROTOCOL Sedation Hold/Interruption and Weaning Protocol ( Wake-up and Breathe ) Page 1 of 6 Scope: Population: Outcome: Critical care clinicians and providers. All ICU patients intubated or mechanically
PROTOCOL Sedation Hold/Interruption and Weaning Protocol ( Wake-up and Breathe ) Page 1 of 6 Scope: Population: Outcome: Critical care clinicians and providers. All ICU patients intubated or mechanically
The Art and Science of Weaning from Mechanical Ventilation
 The Art and Science of Weaning from Mechanical Ventilation Shekhar T. Venkataraman M.D. Professor Departments of Critical Care Medicine and Pediatrics University of Pittsburgh School of Medicine Some definitions
The Art and Science of Weaning from Mechanical Ventilation Shekhar T. Venkataraman M.D. Professor Departments of Critical Care Medicine and Pediatrics University of Pittsburgh School of Medicine Some definitions
Surgical intervention for a variety
 Volume 7, No.4 Recovery Strat eg i e s from the OR to Home I n T h i s I s s u e The increasing population of older adults will result in an increased amount of surgical procedures being performed on geriatric
Volume 7, No.4 Recovery Strat eg i e s from the OR to Home I n T h i s I s s u e The increasing population of older adults will result in an increased amount of surgical procedures being performed on geriatric
Spontaneous Breathing Trial and Mechanical Ventilation Weaning Process
 Page 1 of 5 ASSESSMENT INTERVENTION Patient receiving mechanical ventilation Baseline ventilatory mode/ settings RT and RN to assess criteria 1 for SBT Does patient meet criteria? RT to initiate SBT Does
Page 1 of 5 ASSESSMENT INTERVENTION Patient receiving mechanical ventilation Baseline ventilatory mode/ settings RT and RN to assess criteria 1 for SBT Does patient meet criteria? RT to initiate SBT Does
Extubation Failure & Delay in Brain-Injured Patients
 Extubation Failure & Delay in Brain-Injured Patients Niall D. Ferguson, MD, FRCPC, MSc Director, Critical Care Medicine University Health Network & Mount Sinai Hospital Associate Professor of Medicine
Extubation Failure & Delay in Brain-Injured Patients Niall D. Ferguson, MD, FRCPC, MSc Director, Critical Care Medicine University Health Network & Mount Sinai Hospital Associate Professor of Medicine
Cost Containment in the Intensive Care Unit: Chest Roentgenograms
 ISPUB.COM The Internet Journal of Pulmonary Medicine Volume 5 Number 2 Cost Containment in the Intensive Care Unit: Chest Roentgenograms G Diaz-Fuentes, R Rosen, L Menon Citation G Diaz-Fuentes, R Rosen,
ISPUB.COM The Internet Journal of Pulmonary Medicine Volume 5 Number 2 Cost Containment in the Intensive Care Unit: Chest Roentgenograms G Diaz-Fuentes, R Rosen, L Menon Citation G Diaz-Fuentes, R Rosen,
DELIRIUM MONITORING CARE UNIT AND PATIENT OUTCOMES IN A GENERAL INTENSIVE. Delirium Assessment
 Delirium Assessment DELIRIUM MONITORING AND PATIENT OUTCOMES IN A GENERAL INTENSIVE CARE UNIT By Lois Andrews, RN-BC, DNP, CCRN, ACNS-BC, Susan G. Silva, PhD, Susan Kaplan, RN, PhD, and Kathie Zimbro,
Delirium Assessment DELIRIUM MONITORING AND PATIENT OUTCOMES IN A GENERAL INTENSIVE CARE UNIT By Lois Andrews, RN-BC, DNP, CCRN, ACNS-BC, Susan G. Silva, PhD, Susan Kaplan, RN, PhD, and Kathie Zimbro,
Neonatal and Pediatric Securement From Salter
 Neonatal and Pediatric Securement From Salter The touch that says so much Striving to be #1 IN PATIENT SATISFACTION Now with options for ncpap,, and low flow therapy. Collaborative Innovation Today, Salter
Neonatal and Pediatric Securement From Salter The touch that says so much Striving to be #1 IN PATIENT SATISFACTION Now with options for ncpap,, and low flow therapy. Collaborative Innovation Today, Salter
CLINICAL CONSIDERATIONS FOR THE BUNNELL LIFE PULSE HIGH-FREQUENCY JET VENTILATOR
 CLINICAL CONSIDERATIONS FOR THE BUNNELL LIFE PULSE HIGH-FREQUENCY JET VENTILATOR 801-467-0800 Phone 800-800-HFJV (4358) Hotline TABLE OF CONTENTS Respiratory Care Considerations..3 Physician Considerations
CLINICAL CONSIDERATIONS FOR THE BUNNELL LIFE PULSE HIGH-FREQUENCY JET VENTILATOR 801-467-0800 Phone 800-800-HFJV (4358) Hotline TABLE OF CONTENTS Respiratory Care Considerations..3 Physician Considerations
Standardize comprehensive care of the patient with severe traumatic brain injury
 Trauma Center Practice Management Guideline Iowa Methodist Medical Center Des Moines Management of Patients with Severe Traumatic Brain Injury (GCS < 9) ADULT Practice Management Guideline Contact: Trauma
Trauma Center Practice Management Guideline Iowa Methodist Medical Center Des Moines Management of Patients with Severe Traumatic Brain Injury (GCS < 9) ADULT Practice Management Guideline Contact: Trauma
ECMO Extracorporeal Membrane Oxygenation
 ECMO Extracorporeal Membrane Oxygenation patienteducation.osumc.edu ECMO Table of Contents ECMO: Extracorporeal Membrane Oxygenation... 3 ECMO Treatment... 5 Care Team... 7 Discontinuing ECMO... 8 Notes,
ECMO Extracorporeal Membrane Oxygenation patienteducation.osumc.edu ECMO Table of Contents ECMO: Extracorporeal Membrane Oxygenation... 3 ECMO Treatment... 5 Care Team... 7 Discontinuing ECMO... 8 Notes,
The Ohio State University and The Bellevue Hospital Smoking Cessation Initiative - 1. Are you finally ready to stop smoking?
 The Ohio State University and The Bellevue Hospital Smoking Cessation Initiative - 1 Are you finally ready to stop smoking? If you are ready to stop smoking, you may be interested in a collaborative research
The Ohio State University and The Bellevue Hospital Smoking Cessation Initiative - 1 Are you finally ready to stop smoking? If you are ready to stop smoking, you may be interested in a collaborative research
GE Healthcare. Non Invasive Ventilation (NIV) For the Engström Ventilator. Relief, Relax, Recovery
 GE Healthcare Non Invasive Ventilation (NIV) For the Engström Ventilator Relief, Relax, Recovery COPD is currently the fourth leading cause of death in the world, and further increases in the prevalence
GE Healthcare Non Invasive Ventilation (NIV) For the Engström Ventilator Relief, Relax, Recovery COPD is currently the fourth leading cause of death in the world, and further increases in the prevalence
Tracheostomy. Hope Building Neurosurgery
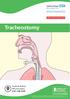 Tracheostomy Hope Building Neurosurgery 0161 206 5055 All Rights Reserved 2017. Document for issue as handout. Unique Identifier: CS36(17). Review date: November 2019 What is a tracheostomy? A tracheostomy
Tracheostomy Hope Building Neurosurgery 0161 206 5055 All Rights Reserved 2017. Document for issue as handout. Unique Identifier: CS36(17). Review date: November 2019 What is a tracheostomy? A tracheostomy
SARASOTA MEMORIAL HOSPITAL NURSING DEPARTMENT POLICY
 PS1070 SARASOTA MEMORIAL HOSPITAL NURSING DEPARTMENT POLICY TITLE: ADMISSION/DISCHARGE CRITERIA: CARDIOVASCULAR INTENSIVE Job Title of Reviewer: Director, CVICU EFFECTIVE DATE: REVIEWED/REVISED DATE: POLICY
PS1070 SARASOTA MEMORIAL HOSPITAL NURSING DEPARTMENT POLICY TITLE: ADMISSION/DISCHARGE CRITERIA: CARDIOVASCULAR INTENSIVE Job Title of Reviewer: Director, CVICU EFFECTIVE DATE: REVIEWED/REVISED DATE: POLICY
Tracheostomy. Information for patients and relatives
 Tracheostomy Information for patients and relatives page 2 What is a tracheostomy? A tracheostomy is a small hole (stoma) made at the front of the neck, which goes into the trachea (windpipe). A tube called
Tracheostomy Information for patients and relatives page 2 What is a tracheostomy? A tracheostomy is a small hole (stoma) made at the front of the neck, which goes into the trachea (windpipe). A tube called
IICU Staff Meeting Minutes May 15 and 16, 2013 IICU Conference Room
 IICU Staff Meeting Minutes May 15 and 16, 2013 IICU Conference Room 1) Decreasing Telemetry Alarms Janice Marlett, BSN, RN, Nursing Staff Educator To decrease tele alarms: Properly prep the skin Shave
IICU Staff Meeting Minutes May 15 and 16, 2013 IICU Conference Room 1) Decreasing Telemetry Alarms Janice Marlett, BSN, RN, Nursing Staff Educator To decrease tele alarms: Properly prep the skin Shave
Proprietary Acute Care Indicators
 Proprietary Acute Care Indicators Indicator 1a: Device-Associated Infections in the Intensive Care Unit Central Line-Associated Bloodstream Infections in the APICU, CCU, MICU, M/S ICU, & SICU Ventilator-Associated
Proprietary Acute Care Indicators Indicator 1a: Device-Associated Infections in the Intensive Care Unit Central Line-Associated Bloodstream Infections in the APICU, CCU, MICU, M/S ICU, & SICU Ventilator-Associated
Unplanned Extubation in Patients with Mechanical Ventilation: Experience in the Medical Intensive Care Unit of a Single Tertiary Hospital
 ORIGINAL ARTICLE http://dx.doi.org/10.4046/trd.2015.78.4.336 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2015;78:336-340 Unplanned Extubation in Patients with Mechanical Ventilation: Experience
ORIGINAL ARTICLE http://dx.doi.org/10.4046/trd.2015.78.4.336 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2015;78:336-340 Unplanned Extubation in Patients with Mechanical Ventilation: Experience
ADVANCED AIRWAY MANAGEMENT
 The Advanced Airway Management protocol should be used on all patients requiring advanced airway management procedures. This protocol is divided into three sections the Crash Airway Algorithm, the Rapid
The Advanced Airway Management protocol should be used on all patients requiring advanced airway management procedures. This protocol is divided into three sections the Crash Airway Algorithm, the Rapid
Scenario title. We re Coming Down Intrahospital Transfer post MET. Designed for (specific group) ICU MET team. Scenario Design team.
 Scenario title We re Coming Down Intrahospital Transfer post MET Designed for (specific group) ICU MET team Scenario Design team Name Maurice Le Guen Cameron Knott Organisation Austin Hospital Date of
Scenario title We re Coming Down Intrahospital Transfer post MET Designed for (specific group) ICU MET team Scenario Design team Name Maurice Le Guen Cameron Knott Organisation Austin Hospital Date of
ASPIRUS WAUSAU HOSPITAL, INC. Passion for excellence. Compassion for people. SUBJECT: END TIDAL CARBON DIOXIDE MONITORING (CAPNOGRAPHY)
 Passion for excellence. Compassion for people. P&P REF : NEW 7-2011 ONBASE POLICY ID: 13363 REPLACES: POLICY STATUS : FINAL DOCUMENT TYPE: Policy EFFECTIVE DATE: 4/15/2014 PROPOSED BY: Respiratory Therapy
Passion for excellence. Compassion for people. P&P REF : NEW 7-2011 ONBASE POLICY ID: 13363 REPLACES: POLICY STATUS : FINAL DOCUMENT TYPE: Policy EFFECTIVE DATE: 4/15/2014 PROPOSED BY: Respiratory Therapy
Cell Phones and Pagers
 FALLS Cell Phones and Pagers Please turn your cell phones off or turn the ringer down during the session. If you must answer a call, please be considerate of other attendees and leave the room before you
FALLS Cell Phones and Pagers Please turn your cell phones off or turn the ringer down during the session. If you must answer a call, please be considerate of other attendees and leave the room before you
Joint Theater Trauma System Clinical Practice Guideline
 Page 1 of 7 Joint Theater Trauma System Clinical Practice Guideline TRAUMA AIRWAY MANAGEMENT Original Release/Approval 18 Dec 2004 Note: This CPG requires an annual review. Reviewed: May 2012 Approved:
Page 1 of 7 Joint Theater Trauma System Clinical Practice Guideline TRAUMA AIRWAY MANAGEMENT Original Release/Approval 18 Dec 2004 Note: This CPG requires an annual review. Reviewed: May 2012 Approved:
Universal Screening for Palliative Needs
 P A L L I A T I V E C A R E NO PATIENT LEFT BEHIND Universal Screening for Palliative Needs BY MARY HICKS, RN, MSN, APRN AND ELIZABETH DISTEFANO, RN, BSN How can health care providers be confident their
P A L L I A T I V E C A R E NO PATIENT LEFT BEHIND Universal Screening for Palliative Needs BY MARY HICKS, RN, MSN, APRN AND ELIZABETH DISTEFANO, RN, BSN How can health care providers be confident their
All bedside percutaneously placed tracheostomies
 Page 1 of 5 Scope: All bedside percutaneously placed tracheostomies Population: All ICU personnel Outcomes: To standardize and outline the steps necessary to safely perform a percutaneous tracheostomy
Page 1 of 5 Scope: All bedside percutaneously placed tracheostomies Population: All ICU personnel Outcomes: To standardize and outline the steps necessary to safely perform a percutaneous tracheostomy
Exclusion Criteria 1. Operator or supervisor feels specific intra- procedural laryngoscopy device will be required.
 FELLOW Study Data Analysis Plan Direct Laryngoscopy vs Video Laryngoscopy Background Respiratory failure requiring endotracheal intubation occurs in as many as 40% of critically ill patients. Procedural
FELLOW Study Data Analysis Plan Direct Laryngoscopy vs Video Laryngoscopy Background Respiratory failure requiring endotracheal intubation occurs in as many as 40% of critically ill patients. Procedural
Early Mobility: The Experiences of Two ICUs
 Early Mobility: The Experiences of Two ICUs Sharon Dickinson MSN, RN, ANP, ACNS-BC, CCRN Clinical Nurse Specialist SICU/Rapid Response Sarah Taylor MSN, RN, ACNS-BC Clinical Nurse Specialist TBICU University
Early Mobility: The Experiences of Two ICUs Sharon Dickinson MSN, RN, ANP, ACNS-BC, CCRN Clinical Nurse Specialist SICU/Rapid Response Sarah Taylor MSN, RN, ACNS-BC Clinical Nurse Specialist TBICU University
sounds are distant with inspiratory crackles. He sits on the edge of his chair, leaning forward, with both hands on his
 I NTE R P R ETI N G A R T E R I A L B L O O D G A S E S : EASY AS A B C Take this step-by-step approach to demystify the parameters of oxygenation, ventilation, acid-base balance. BY WILLIAM C. PRUITT,
I NTE R P R ETI N G A R T E R I A L B L O O D G A S E S : EASY AS A B C Take this step-by-step approach to demystify the parameters of oxygenation, ventilation, acid-base balance. BY WILLIAM C. PRUITT,
Improved IPGM: Demonstrating the Value to both Patients and Hospitals
 Improved IPGM: Demonstrating the Value to both Patients and Hospitals Osama Hamdy, MD, PhD, FACE Medical Director, Inpatient Diabetes Program Joslin Diabetes Center Harvard Medical School, Boston, MA Cost
Improved IPGM: Demonstrating the Value to both Patients and Hospitals Osama Hamdy, MD, PhD, FACE Medical Director, Inpatient Diabetes Program Joslin Diabetes Center Harvard Medical School, Boston, MA Cost
Vents, LVADs, and Hospice Oh My!
 Vents, LVADs, and Hospice Oh My! Colleen Gilmore RN, MSN, ANP-BC Patrick White MD, HMDC, FACP, FAAHPM 1 Disclosure: White, Patrick, M.D. Patrick White M.D. has financial interests to disclose. Potential
Vents, LVADs, and Hospice Oh My! Colleen Gilmore RN, MSN, ANP-BC Patrick White MD, HMDC, FACP, FAAHPM 1 Disclosure: White, Patrick, M.D. Patrick White M.D. has financial interests to disclose. Potential
NRP Raising the Bar for Providers and Instructors
 NRP 2011 Raising the Bar for Providers and Instructors What is the same? 1. Minimum course requirement is Lessons 1 through 4 and Lesson 9. The NRP Provider Card requires renewal every 2 years. Your facility
NRP 2011 Raising the Bar for Providers and Instructors What is the same? 1. Minimum course requirement is Lessons 1 through 4 and Lesson 9. The NRP Provider Card requires renewal every 2 years. Your facility
POLICY. Number: Title: APPLICATION OF NON INVASIVE VENTILATION FOR ACUTE RESPIRATORY FAILURE. Authorization
 POLICY Number: 7311-60-024 Title: APPLICATION OF NON INVASIVE VENTILATION FOR ACUTE RESPIRATORY FAILURE Authorization [ ] President and CEO [ x ] Vice President, Finance and Corporate Services Source:
POLICY Number: 7311-60-024 Title: APPLICATION OF NON INVASIVE VENTILATION FOR ACUTE RESPIRATORY FAILURE Authorization [ ] President and CEO [ x ] Vice President, Finance and Corporate Services Source:
Reducing Unplanned Extubations in the NICU. abstract
 QUALITY REPORT Reducing Unplanned Extubations in the NICU AUTHORS: Lori Merkel, MS, BSN, CPHQ, RNC-NIC, Kimberly Beers, RRT-NPS, Mary M. Lewis, MSN, RNC-NIC, Joy Stauffer, BSN, RNC-NIC, Dennis J. Mujsce,
QUALITY REPORT Reducing Unplanned Extubations in the NICU AUTHORS: Lori Merkel, MS, BSN, CPHQ, RNC-NIC, Kimberly Beers, RRT-NPS, Mary M. Lewis, MSN, RNC-NIC, Joy Stauffer, BSN, RNC-NIC, Dennis J. Mujsce,
Rehabilitation and Restorative Care
 170 25 Rehabilitation and Restorative Care 1. Define important words in this chapter 2. Discuss rehabilitation and restorative care 3. Describe the importance of promoting independence 4. Explain the complications
170 25 Rehabilitation and Restorative Care 1. Define important words in this chapter 2. Discuss rehabilitation and restorative care 3. Describe the importance of promoting independence 4. Explain the complications
Simulation 3: Post-term Baby in Labor and Delivery
 Simulation 3: Post-term Baby in Labor and Delivery Opening Scenario (Links to Section 1) You are an evening-shift respiratory therapist in a large hospital with a level III neonatal unit. You are paged
Simulation 3: Post-term Baby in Labor and Delivery Opening Scenario (Links to Section 1) You are an evening-shift respiratory therapist in a large hospital with a level III neonatal unit. You are paged
St. Jude Children's Research Hospital. September 9, 2014 Final Report
 The Impact of a Play-Based Procedural Preparation and Support Intervention for Children Undergoing Cranial Radiation for Treatment of a Central Nervous System Tumor St. Jude Children s Research Hospital
The Impact of a Play-Based Procedural Preparation and Support Intervention for Children Undergoing Cranial Radiation for Treatment of a Central Nervous System Tumor St. Jude Children s Research Hospital
The use of proning in the management of Acute Respiratory Distress Syndrome
 Case 3 The use of proning in the management of Acute Respiratory Distress Syndrome Clinical Problem This expanded case summary has been chosen to explore the rationale and evidence behind the use of proning
Case 3 The use of proning in the management of Acute Respiratory Distress Syndrome Clinical Problem This expanded case summary has been chosen to explore the rationale and evidence behind the use of proning
Elsevier Mechanical Ventilation Test Bank Questions
 Elsevier Test Bank Questions Free PDF ebook Download: Elsevier Test Bank Questions Download or Read Online ebook elsevier mechanical ventilation test bank questions in PDF Format From The Best User Guide
Elsevier Test Bank Questions Free PDF ebook Download: Elsevier Test Bank Questions Download or Read Online ebook elsevier mechanical ventilation test bank questions in PDF Format From The Best User Guide
Capnography: Creating a Culture of Safety! An Interview With Peggy Lange, RT!
 Capnography: Creating a Culture of Safety An Interview With Peggy Lange, RT Pat Iyer Hi, this is a podcast from the Physician-Patient Alliance for Health & Safety. The podcast that we're presenting today
Capnography: Creating a Culture of Safety An Interview With Peggy Lange, RT Pat Iyer Hi, this is a podcast from the Physician-Patient Alliance for Health & Safety. The podcast that we're presenting today
Tube Fasteners. Tube. Fasteners
 Tube Fasteners Tube Fasteners Confidence is in the air. Provide an extra measure of protection with confidence. The AnchorFast Guard oral endotracheal tube fastener features an integrated tube protection
Tube Fasteners Tube Fasteners Confidence is in the air. Provide an extra measure of protection with confidence. The AnchorFast Guard oral endotracheal tube fastener features an integrated tube protection
A NEW direction for subglottic secretion management
 A NEW direction for subglottic secretion management The SIMEX Subglottic Aspiration System, cuff M and cuff S are the most advanced solution for the aspiration of subglottic secretion, featuring all new
A NEW direction for subglottic secretion management The SIMEX Subglottic Aspiration System, cuff M and cuff S are the most advanced solution for the aspiration of subglottic secretion, featuring all new
Respiratory Care Services
 Respiratory Care Services Who we are 45 Licensed Respiratory Care Practitioners & 3 per diem Hospital assistants Out patient services Limited to Asthma Clinic Pilot In-patient services Primarily intensive
Respiratory Care Services Who we are 45 Licensed Respiratory Care Practitioners & 3 per diem Hospital assistants Out patient services Limited to Asthma Clinic Pilot In-patient services Primarily intensive
Ventilator Associated
 Ventilator Associated Pneumonia: Key and Controversial Issues Christopher P. Michetti, MD, FACS Inova Fairfax Hospital, Falls Church, VA Forrest Dell Moore, MD, FACS Banner Healthcare System, Phoenix,
Ventilator Associated Pneumonia: Key and Controversial Issues Christopher P. Michetti, MD, FACS Inova Fairfax Hospital, Falls Church, VA Forrest Dell Moore, MD, FACS Banner Healthcare System, Phoenix,
SARASOTA MEMORIAL HOSPITAL NURSING DEPARTMENT POLICY
 PS1006 SARASOTA MEMORIAL HOSPITAL NURSING DEPARTMENT TITLE: PROPOFOL SEDATION PROTOCOL Job Title of Reviewer: Director, ICU :#: EFFECTIVE DATE: REVISED DATE: TYPE: 1/95 8/06, 5/09 DEPARTMENTAL INTERDEPARTMENTAL
PS1006 SARASOTA MEMORIAL HOSPITAL NURSING DEPARTMENT TITLE: PROPOFOL SEDATION PROTOCOL Job Title of Reviewer: Director, ICU :#: EFFECTIVE DATE: REVISED DATE: TYPE: 1/95 8/06, 5/09 DEPARTMENTAL INTERDEPARTMENTAL
X-ray (Radiography) - Chest
 Scan for mobile link. X-ray (Radiography) - Chest Chest x-ray uses a very small dose of ionizing radiation to produce pictures of the inside of the chest. It is used to evaluate the lungs, heart and chest
Scan for mobile link. X-ray (Radiography) - Chest Chest x-ray uses a very small dose of ionizing radiation to produce pictures of the inside of the chest. It is used to evaluate the lungs, heart and chest
Facilitating EndotracheaL Intubation by Laryngoscopy technique and Apneic Oxygenation Within the Intensive Care Unit (FELLOW)
 Facilitating EndotracheaL Intubation by Laryngoscopy technique and Apneic Oxygenation Within the Intensive Data Analysis Plan: Apneic Oxygenation vs. No Apneic Oxygenation Background Critically ill patients
Facilitating EndotracheaL Intubation by Laryngoscopy technique and Apneic Oxygenation Within the Intensive Data Analysis Plan: Apneic Oxygenation vs. No Apneic Oxygenation Background Critically ill patients
MASTER SYLLABUS
 MASTER SYLLABUS 2018-2019 A. Academic Division: Health Science B. Discipline: Respiratory Care C. Course Number and Title: RESP 2490 Practicum IV D. Course Coordinator: Tricia Winters, BBA, RRT, RCP Assistant
MASTER SYLLABUS 2018-2019 A. Academic Division: Health Science B. Discipline: Respiratory Care C. Course Number and Title: RESP 2490 Practicum IV D. Course Coordinator: Tricia Winters, BBA, RRT, RCP Assistant
Ventilator-Associated Event Prevention: Innovations
 Ventilator-Associated Event Prevention: Innovations Michael J. Apostolakos, MD Professor of Medicine Director, Adult Critical Care University of Rochester Mobility/Sedation in the ICU Old teaching: Keep
Ventilator-Associated Event Prevention: Innovations Michael J. Apostolakos, MD Professor of Medicine Director, Adult Critical Care University of Rochester Mobility/Sedation in the ICU Old teaching: Keep
SARASOTA MEMORIAL HOSPITAL NURSING DEPARTMENT POLICY
 PS1006 SARASOTA MEMORIAL HOSPITAL NURSING DEPARTMENT POLICY TITLE: MONITORING NEUROMUSCULAR BLOCKADE IN THE CRITICAL CARE Job Title of Reviewer: Director, ICU EFFECTIVE DATE: REVISED DATE: POLICY TYPE:
PS1006 SARASOTA MEMORIAL HOSPITAL NURSING DEPARTMENT POLICY TITLE: MONITORING NEUROMUSCULAR BLOCKADE IN THE CRITICAL CARE Job Title of Reviewer: Director, ICU EFFECTIVE DATE: REVISED DATE: POLICY TYPE:
Pain & Sedation Management in PICU. Marut Chantra, M.D.
 Pain & Sedation Management in PICU Marut Chantra, M.D. Pain Diseases Trauma Procedures Rogers Textbook of Pediatric Intensive Care, 5 th ed, 2015 Emotional Distress Separation from parents Unfamiliar
Pain & Sedation Management in PICU Marut Chantra, M.D. Pain Diseases Trauma Procedures Rogers Textbook of Pediatric Intensive Care, 5 th ed, 2015 Emotional Distress Separation from parents Unfamiliar
Interaction between Sedation and Weaning: How to Balance Them? Guillermo Castorena MD Fundacion Clinica Medica Sur Mexico
 Interaction between Sedation and Weaning: How to Balance Them? Guillermo Castorena MD Fundacion Clinica Medica Sur Mexico Balance is not that easy! Weaning Weaning is the liberation of a patient from
Interaction between Sedation and Weaning: How to Balance Them? Guillermo Castorena MD Fundacion Clinica Medica Sur Mexico Balance is not that easy! Weaning Weaning is the liberation of a patient from
NON INVASIVE LIFE SAVERS. Non Invasive Ventilation (NIV)
 Table 1. NIV: Mechanisms Of Action Decreases work of breathing Increases functional residual capacity Recruits collapsed alveoli Improves respiratory gas exchange Reverses hypoventilation Maintains upper
Table 1. NIV: Mechanisms Of Action Decreases work of breathing Increases functional residual capacity Recruits collapsed alveoli Improves respiratory gas exchange Reverses hypoventilation Maintains upper
IFT1 Interfacility Transfer of STEMI Patients. IFT2 Interfacility Transfer of Intubated Patients. IFT3 Interfacility Transfer of Stroke Patients
 IFT1 Interfacility Transfer of STEMI Patients IFT2 Interfacility Transfer of Intubated Patients IFT3 Interfacility Transfer of Stroke Patients Interfacility Transfer Guidelines IFT 1 TRANSFER INTERFACILITY
IFT1 Interfacility Transfer of STEMI Patients IFT2 Interfacility Transfer of Intubated Patients IFT3 Interfacility Transfer of Stroke Patients Interfacility Transfer Guidelines IFT 1 TRANSFER INTERFACILITY
Nasopharyngeal airways for craniofacial conditions
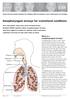 Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Nasopharyngeal airways for craniofacial conditions This information sheet from Great Ormond Street Hospital (GOSH)
Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Nasopharyngeal airways for craniofacial conditions This information sheet from Great Ormond Street Hospital (GOSH)
Sedation and Anesthesia Visiting Provider Inspection Review Form
 6 Crescent Road, Toronto, O Canada M4W 1T1 T: 416.961.6555 F: 416.961.5814 Toll Free: 1.800.565.4591 www.rcdso.org Sedation and Anesthesia Visiting Provider Inspection Review Form GEERAL IFORMATIO Inspection
6 Crescent Road, Toronto, O Canada M4W 1T1 T: 416.961.6555 F: 416.961.5814 Toll Free: 1.800.565.4591 www.rcdso.org Sedation and Anesthesia Visiting Provider Inspection Review Form GEERAL IFORMATIO Inspection
FAILURE OF NONINVASIVE VENTILATION FOR DE NOVO ACUTE HYPOXEMIC RESPIRATORY FAILURE: ROLE OF TIDAL VOLUME
 FAILURE OF NONINVASIVE VENTILATION FOR DE NOVO ACUTE HYPOXEMIC RESPIRATORY FAILURE: ROLE OF TIDAL VOLUME Guillaume CARTEAUX, Teresa MILLÁN-GUILARTE, Nicolas DE PROST, Keyvan RAZAZI, Shariq ABID, Arnaud
FAILURE OF NONINVASIVE VENTILATION FOR DE NOVO ACUTE HYPOXEMIC RESPIRATORY FAILURE: ROLE OF TIDAL VOLUME Guillaume CARTEAUX, Teresa MILLÁN-GUILARTE, Nicolas DE PROST, Keyvan RAZAZI, Shariq ABID, Arnaud
MT Custom Weaning Protocol for your Ventilator Patients SMARTCARE /PS
 MT-0913-2008 Custom Weaning Protocol for your Ventilator Patients SMARTCARE /PS 02 SmartCare /PS automates weaning The problem however is that no matter how good the written protocol is, physicians and
MT-0913-2008 Custom Weaning Protocol for your Ventilator Patients SMARTCARE /PS 02 SmartCare /PS automates weaning The problem however is that no matter how good the written protocol is, physicians and
Analysis of Causalities and Outcomes in Trauma Patients Who Self-Extubate
 Analysis of Causalities and Outcomes in Trauma Patients Who Self-Extubate Ana Negrete, PharmD, BCPS 1 Stephanie N Thompson, PhD 2 Julton Tomanguillo Chumbe, MD 3 Damayanti Samanta, MS 4 Audis Bethea, PharmD,
Analysis of Causalities and Outcomes in Trauma Patients Who Self-Extubate Ana Negrete, PharmD, BCPS 1 Stephanie N Thompson, PhD 2 Julton Tomanguillo Chumbe, MD 3 Damayanti Samanta, MS 4 Audis Bethea, PharmD,
Transcatheter Aortic Valve Replacement (TAVR)
 UW MEDICINE PATIENT EDUCATION Transcatheter Aortic Valve Replacement (TAVR) Treatment for aortic stenosis This handout explains when your doctor may advise TAVR to treat aortic stenosis. It includes the
UW MEDICINE PATIENT EDUCATION Transcatheter Aortic Valve Replacement (TAVR) Treatment for aortic stenosis This handout explains when your doctor may advise TAVR to treat aortic stenosis. It includes the
PEDIATRIC ASTHMA INPATIENT CARE MAP
 DATE PATIENT PEDIATRIC ASTHMA INPATIENT CARE MAP DOB HSC NO. PHIN Approved by the Winnipeg Regional Health Authority This Care Map is to be used as a guideline and in no way replaces sound clinical judgment
DATE PATIENT PEDIATRIC ASTHMA INPATIENT CARE MAP DOB HSC NO. PHIN Approved by the Winnipeg Regional Health Authority This Care Map is to be used as a guideline and in no way replaces sound clinical judgment
Outline. Local case study. Standardizing pediatric disaster response in King County
 Standardizing pediatric disaster response in King County Mary A. King, MD, MPH WAMI 2010 June 1, 2010 Outline Local case study Background on pediatric MCI King County barriers to pediatric disaster care
Standardizing pediatric disaster response in King County Mary A. King, MD, MPH WAMI 2010 June 1, 2010 Outline Local case study Background on pediatric MCI King County barriers to pediatric disaster care
Physiotherapy on the Intensive Care Unit. Information for patients, their family and carers
 Physiotherapy on the Intensive Care Unit Information for patients, their family and carers A team of Specialist Physiotherapists works in the Intensive Care Units within the Oxford University Hospitals
Physiotherapy on the Intensive Care Unit Information for patients, their family and carers A team of Specialist Physiotherapists works in the Intensive Care Units within the Oxford University Hospitals
Other methods for maintaining the airway (not definitive airway as still unprotected):
 Page 56 Where anaesthetic skills and drugs are available, endotracheal intubation is the preferred method of securing a definitive airway. This technique comprises: rapid sequence induction of anaesthesia
Page 56 Where anaesthetic skills and drugs are available, endotracheal intubation is the preferred method of securing a definitive airway. This technique comprises: rapid sequence induction of anaesthesia
Ventilating the paediatric patient. Lizzie Barrett Nurse Educator November 2016
 Ventilating the paediatric patient Lizzie Barrett Nurse Educator November 2016 Acknowledgements Kate Leutert NE PICU Children's Hospital Westmead Dr. Chloe Tetlow VMO Anaesthetist and Careflight Overview
Ventilating the paediatric patient Lizzie Barrett Nurse Educator November 2016 Acknowledgements Kate Leutert NE PICU Children's Hospital Westmead Dr. Chloe Tetlow VMO Anaesthetist and Careflight Overview
MASTER SYLLABUS
 A. Academic Division: Health Sciences B. Discipline: Respiratory Care MASTER SYLLABUS 2018-2019 C. Course Number and Title: RESP 2330 Advanced Life Support Procedures D. Course Coordinator: Tricia Winters,
A. Academic Division: Health Sciences B. Discipline: Respiratory Care MASTER SYLLABUS 2018-2019 C. Course Number and Title: RESP 2330 Advanced Life Support Procedures D. Course Coordinator: Tricia Winters,
The Dedicated Trauma Surgeon: A Retrospective Review on Patient Outcomes
 The Dedicated Trauma Surgeon: A Retrospective Review on Patient Outcomes Truong D. Ma, MD, MS;Tiffany D. Marchand, MD; M. D. Gothard, MS; Karen M. Gil, PhD; Richard L. George, MD, MSPH We have no disclosures
The Dedicated Trauma Surgeon: A Retrospective Review on Patient Outcomes Truong D. Ma, MD, MS;Tiffany D. Marchand, MD; M. D. Gothard, MS; Karen M. Gil, PhD; Richard L. George, MD, MSPH We have no disclosures
What is the next best step?
 Noninvasive Ventilation William Janssen, M.D. Assistant Professor of Medicine National Jewish Health University of Colorado Denver Health Sciences Center What is the next best step? 65 year old female
Noninvasive Ventilation William Janssen, M.D. Assistant Professor of Medicine National Jewish Health University of Colorado Denver Health Sciences Center What is the next best step? 65 year old female
Policies & Procedures. RNSP - RN Procedure. I.D. Number: 1097
 Policies & Procedures Title: ESOPHAGEAL TAMPONADE TUBE (MINNESOTA Tube) ASSISTING WITH INSERTION, CARE OF A PATIENT, ASSISTING WITH REMOVAL RNSP - RN Procedure I.D. Number: 1097 Authorization [x] Nursing
Policies & Procedures Title: ESOPHAGEAL TAMPONADE TUBE (MINNESOTA Tube) ASSISTING WITH INSERTION, CARE OF A PATIENT, ASSISTING WITH REMOVAL RNSP - RN Procedure I.D. Number: 1097 Authorization [x] Nursing
The Power of Purple* Polyurethane PICC. Patient Guide. Access Systems
 The Power of Purple* Polyurethane PICC Patient Guide Access Systems Preamble Your doctor is giving you a PowerPICC* catheter so that you can easily get the intravenous (IV) medicines you need. This catheter
The Power of Purple* Polyurethane PICC Patient Guide Access Systems Preamble Your doctor is giving you a PowerPICC* catheter so that you can easily get the intravenous (IV) medicines you need. This catheter
