Obstructive Sleep Apnea: Effective Intervention & Care
|
|
|
- Shannon Simmons
- 6 years ago
- Views:
Transcription
1 Obstructive Sleep Apnea: Effective Intervention & Care Provider Training Modules Jonathan Freudman, MD 2016 Resonea Inc.
2 2016 Resonea Inc. Module III: Therapy for OSA
3 Module III: Therapy for OSA o Therapeutic goals o Interventions Patient education and support Lifestyle changes and behavioral modification CPAP Oral appliances Surgery o Interventions Overview for Mild, Moderate and Severe OSA o Follow-up 3
4 Module III: Therapeutic Goals for OSA o Improve the patient s quality of life Decrease daytime sleepiness Increase wellbeing, daytime performance Decrease other specific symptoms caused or aggravated by OSA o Decrease the patient s chances of OSA-associated complications Reduce the risk of hypertension, type II diabetes, cardiovascular disease, depression, stroke, erectile dysfunction, dementia or cognitive issues Reduce the risk of motor vehicle and other accidents o Improve the sleep environment for the bed partner 4
5 Module III: Patient Education & Support o Patient education and support are emphasized in chronic disease management o Especially important in OSA to help manage significant barriers Embarrassment regarding weight and/or snoring Fear regarding the disease (fear is not always a motivator can trigger denial) Fear and misconceptions pertaining to both PSG testing and CPAP treatment o Ten critically important OSA patient messaging points: 1) You will feel better if you are treated. 2) You will feel better if you are treated. 3) You will feel better if you are treated. 4) You will live healthier. 5) You will probably live longer. 6) Your bed partner will very likely be happier. 7) Your sex life will benefit from treatment. 8) Everyone else will be safer, because you will be less likely to cause an accident. 9) Most OSA treatments involve some effort, but are not painful and those who use them adjust well. 10) You will feel better if you are treated. 5
6 Module III: Primary Care Provider o Crucial role in patient education and support -- the art of medicine o Support Empathy Encouragement Empowerment o Educate to Motivate Emphasize the positive outcomes associated with OSA treatment Include a frank but compassionate discussion of the consequences and risks of not treating Not helpful to gloss over the importance of OSA, especially if non-treatment is being contemplated It is counterproductive to frighten the patient with a scenario that is grim and places blame some patients run away and don t come back Provide reassurance that people just like them do well with treatment. 6
7 Module III: Patient Education -- Be Specific o Emphasize the symptoms of OSA that are likely to improve with treatment: Daytime sleepiness and symptoms associated with daytime sleepiness Irritability, difficulty concentrating, memory problems, work performance, energy level, risk of accidents Snoring Other symptoms: headaches, GERD, sexual dysfunction, nocturia, o Reduction in risk of adverse health consequences associated with OSA: Hypertension Type II diabetes Depression Risk of stroke Risk of ASCVD Risk of heart failure Risk of erectile dysfunction Rate of motor vehicle accidents Risk of Alzheimer s disease or dementia Utilize Fight or Flight illustration to help patients understand the pathophysiology of OSA & why the consequences of untreated OSA are so profound. o OSA Treatment Options 7
8 Module III: Patient Education & Support Is An Ongoing Process o Crucial at time of diagnosis o Patients cannot always hear what is being said when first confronted with a diagnosis Denial common with all bad news These patients likely to be sleepy & may have a degree of cognitive impairment o Utilize Tools Written materials Graphics and videos English language proficiency may be a factor Literacy skills vary o Engage Others Spouse, friends and family Support groups/online communities o Repeat the messaging and provide ongoing support o Multidisciplinary chronic care management teams are an excellent vehicle for providing OSA patient education and support. 8
9 Module III: Lifestyle Changes & Behavior Modification Weight Reduction It is well known that weight reduction can reduce snoring Documented that patients with OSA who receive bariatric surgery have improvement in OSA Studies have also documented that obese patients with OSA achieve benefit (decreased AHI and decreased daytime sleepiness) with weight reduction programs ¹ As with any weight reduction program, maintenance of weight loss can be difficult, but some studies have shown persistence of OSA improvement even if some weight regained ² Exercise Often a component of weight loss programs Benefits of exercise for OSA have been demonstrated independent of weight loss 2014 meta-analysis that included 5 small randomized controlled trials showed that supervised exercise programs are associated with improved AHI, sleep efficiency, sleepiness, and cardiorespiratory fitness, even with minimal change in weight. ³ ¹ Kryger 2017 ² Kuna 2013, Johansson 2011, Tuomilehto 2010 ³ Iftikhar
10 Module III: Lifestyle & Behavior -- Alcohol & Other Sedatives Alcohol Consumption Promotes weight gain Depresses central nervous system Worsens snoring and exacerbates OSA events (apneas, hypopneas and oxygen desaturation) Can promote rebound insomnia Should be minimized in patients with OSA and avoided within 3 hours of bedtime. Other Sedatives can worsen OSA Benzodiazepines Barbiturates Antihistamines Opiates Sedating antidepressants Sedating anti-epileptics These should be avoided If absolutely necessary, regimens should be modified to reduce night-time sedative effects. 10
11 Module III: Lifestyle & Behavior -- Sleep Hygiene o People with OSA should avoid habits that disrupt their sleep patterns. o General practices of good sleep hygiene: Regular sleep schedule Use the bed for sleep and romance do not read, watch TV, etc. in bed Eliminate caffeinated beverages after mid-day No alcohol near bedtime Exercise regularly but not within 4 hours of bedtime Avoid use of computer/phone/tablet light-emitting screens before bedtime If you wake up, don t linger in bed worrying. Get up and read a book or magazine for a short time, before returning to bed. 11
12 Module III: Lifestyle & Behavior -- Sleep Position OSA in some people is associated with sleep position especially lying on the back. Changes in sleep position are not easy to accomplish. Various devices are available which restrict lying on back -- pillows, tennis ball contraptions, etc. It is difficult to track effectiveness and adherence to these maneuvers. Care providers should be skeptical of patient s claims that the problem has been solved with one of these devices. 12
13 Module III: Continuous Positive Airway Pressure (CPAP) o Mainstay of OSA treatment Safety and efficacy are well-documented in a large volume of high-quality clinical trials There is now a considerable body of experience treating OSA successfully with CPAP CPAP is safe and not painful Side effects if they occur ( e.g. bloating, irritation from mask) can be managed With proper instruction, patients adjust easily to the therapy o Pneumatic splint While the patient sleeps, pressurized air is pumped to a mask fitted to patient s nose and mouth (or nose only) Air passes through the nares into the patient s upper airway Pressure achieved is greater than the compressive pressure on the airway Pressurized air acts like a splint to prop the airway open o Since introduction into practice in the 1980 s, CPAP devices have improved: Now smaller, lighter, and quieter to operate More comfortable with advances in masks and nasal pillows Addition of heated humidifiers and heated hoses More form factors available for special uses, like travel 13
14 Module III: Benefits of CPAP Are Well-Established o Thirty five randomized controlled trials (RCTs) have demonstrated that CPAP ¹ Reduces AHI Lowers blood pressure Decreases day time sleepiness Improves quality of life across a range of disease severities, including cognitive function and depression o Observational studies in patients with moderate or severe OSA, who received CPAP vs. those who remained untreated, have demonstrated a decrease in cardiovascular mortality with CPAP treatment.² o A reduction in mortality with CPAP has not been demonstrated in RCTs: However, RCTs comparing CPAP with no treatment (or sham CPAP) have generally been of short duration. o RCTs and single arm studies (before and after CPAP) have demonstrated improvements in components of the metabolic syndrome, including glucose, lipids, and visceral fat, as well as blood pressure.³ ¹ Kryger 2017 ² Marti 2002, Campos-Rodriguez 2005, 2012 ³ Drager
15 Module III: Types of CPAP o Fixed-Dose CPAP Delivers positive airway pressure at a level that remains constant throughout the respiratory cycle The pressure setting is based on a titration study performed in the sleep lab While the patient sleeps and has OSA apneas and hypopneas, the technician starts CPAP at the lowest level and gradually increases the pressure until OSA events cease Ramp up pressures at the beginning of the night are sometimes used to improve comfort and tolerance of the device o Auto-Titrating CPAP or APAP Level of positive airway pressure varies in response to a change in air flow Throughout the night, as the physiology of sleep changes Over time - reflecting patient changes (e.g. weight or alcohol/sedative use) APAP can be used temporarily as a titration study to determine the pressure for fixed dose CPAP, or used for ongoing CPAP therapy. Studies, including RCTs, have documented equivalent outcomes with Fixed-Dose CPAP and APAP.¹ o Bi-level Positive Airway Pressure (BiPAP) is similar to CPAP Main difference is that BiPAP can be set to have a different pressure for inhalation and exhalation. BIPAP may be helpful in a subset of OSA patients who also have obesity/hypoventilation syndrome and central sleep apnea. ¹ Ayas
16 Module III: Limitations of CPAP o Must be used chronically - not a definitive treatment Use of CPAP for 6 hours or more per night is recommended and use for less than 4 hours per night has been proposed as a cut-off for non-adherence. Reported prevalence of noncompliance (use <4 hours/night) has varied from 29-83% ¹ Amongst OSA patients who were prescribed CPAP, compliance is realistically about 50%. Amongst compliant patients, the average duration of CPAP use is approximately five hours per night, across numerous studies.² o Factors associated with better CPAP compliance include: Severity of baseline OSA by AHI, and more importantly, degree of daytime sleepiness Patient s initial experience with CPAP - use during the first week of therapy Early experience with CPAP - especially mask fit and absence of mask leaks Psychosocial support, including frequent provider encounters, telehealth contacts and cognitive behavioral interventions ¹ Weaver 2016 ² Gay
17 Module III: Oral Appliances/Dental Devices o Oral appliances function to reposition the jaw, bringing the tongue and soft palate forward. Used during sleep Generally provided by a dentist, with medical assessment and follow-up also recommended The dentist providing oral appliances should have sufficient experience treating OSA and sufficient volume of fitting these appliances to be proficient. o Oral appliances help to reduce snoring. o Many studies, including dozens of RCTs, have documented that oral appliances are effective for treating OSA. o However, most studies that have compared oral appliances to CPAP have concluded that: CPAP is superior at improving AHI and oxyhemoglobin saturation (but not symptoms of daytime sleepiness).¹ Patients generally prefer oral appliances and demonstrate better adherence with these.¹ o Side effects are usually minor and may include jaw pain and changes to the bite with prolonged use. Oral appliances contraindicated in those with temperomandibular joint syndrome (TMJ). ¹ Cistulli
18 Module III: Surgery on Upper Airway o Surgery is generally a second line option in patients who have a surgically-correctable, upper airway obstructing lesion. o Usually reserved for patients who have failed CPAP and oral appliance therapy. o Sometimes employed in an adjunctive role to help patients who are struggling with CPAP or an oral appliance (e.g. relief of nasal obstruction). o Surgery can play a primary role in OSA management in patients with a surgically-correctable lesion that is causing apnea, such as severe tonsillar hypertrophy. o Surgical procedures utilized for OSA include: Nasal turbinate reduction Tonsillectomy/adenoidectomy Uvulopalatopharyngoplasty (UPPP) Maxillomandibular advancement (MMA) 18
19 Module III: Newer Approaches o Surgical implant of hypoglossal nerve stimulation device- one FDA approved product STAR trial¹ single arm (n=154); baseline AHI of 32 reduced to 15; baseline ESS of 11.6 reduced to 7.0; then responders were randomized to groups with stimulation turned on or group with sham treatment (stimulation off). In sham group, the AHI worsened, increasing toward baseline. Indicated for CPAP failures -- in moderate-to-severe OSA. Not in AASM guidelines and generally not covered by insurance. AAO-HNS (Head and Neck Surgeons) have issued a position statement on the therapy: American Academy of Otolaryngology-Head and Neck Surgery considers upper airway stimulation (UAS) via the hypoglossal nerve for the treatment of adult obstructive sleep apnea syndrome to be an effective, second-line treatment of moderate-to-severe obstructive sleep apnea in patients who are intolerant or unable to achieve benefit with positive pressure therapy (PAP). Not all adult patients are candidates for UAS therapy and appropriate polysomnographic, age, BMI and objective upper airway evaluation measures are required for proper patient selection. o Oral Pressure Therapy Mouthpiece attached to a suction unit One FDA approved device and generally not covered by insurance 63 patient single arm study; ² baseline AHI of 27.5 was reduced to 14.8 after 28 days of treatment Baseline ESS of 12.1 was reduced o 8.6 with treatment Also had single-night cross-over comparisons AHI was lower on treated nights. ¹ Strollo 2014 ² Colrain
20 Module III: Interventions Overview -- Patients With Mild OSA 1. Patient education and support: OSA pathophysiology, consequences and benefits of treatment 2. Behavioral modification: Weight loss and exercise Sedative medication avoidance Minimize alcohol. Sleep hygiene Sleeping in a non-supine position 3. Continuous Positive Airway Pressure (CPAP) therapy: Recommended for patients with mild OSA who have one or more clinical symptoms or physiologic sequelae attributable to OSA in particular, excessive daytime sleepiness. Medicare provides coverage for CPAP in patients with mild OSA (AHI 5-14), if associated with excessive daytime sleepiness, impaired neurocognitive function, mood disorders, insomnia, cardiovascular disease (eg, hypertension, ischemic heart disease), or a history of stroke. CPAP is recommended for patients with mild OSA even in the absence of symptoms, if they perform mission critical work (e.g. airline pilot, bus or truck drivers). 4. Oral appliances a viable alternative for those with mild OSA who decline or fail to adhere to CPAP. 20
21 Module III: Interventions Overview -- Patients With Moderate OSA 1. Patient education and support 2. Behavioral modification 3. Continuous Positive Airway Pressure (CPAP) therapy: Recommended as initial therapy for moderate OSA 4. Oral appliances are considered a reasonable alternative in patients with moderate OSA who decline or fail to adhere to CPAP. 5. Surgery can be considered an adjunct therapy for patients who are initially intolerant to CPAP, or if there is incomplete treatment of OSA with CPAP or oral appliances. 21
22 Module III: Interventions Overview -- Patients With Severe OSA 1. Patient education and support 2. Behavioral modification 3. Continuous Positive Airway Pressure (CPAP) therapy: Recommended as initial therapy for severe OSA 4. Oral appliances may be used with caution in patients with severe OSA, since variable efficacy of oral appliances has been reported in this patient population. 5. Surgery can be considered an adjunct therapy for patients who are initially intolerant to CPAP, or there is incomplete treatment of OSA with CPAP. 22
23 Module III: Interventions -- Follow-up All OSA patients require ongoing follow-up, for the purposes of: Further validation of the clinical diagnosis, Continued education and support, Determining adherence to lifestyle recommendations, Assessing adherence to therapy and response to CPAP or oral appliances, Considering the need for additional evaluations and interventions. DROWZLE App is a useful tool for patient follow-up: Allows frequent, systematic & objective monitoring of symptoms & personal risk factors Tracks change in daytime sleepiness scores with Epworth scale Overnight sound analysis can capture changes in sleep breathing, including apneas Can provide measurement of post-treatment improvement App provides links to educational information on OSA, plus patient resources available online Allows push-messaging to check patient progress or need for provider intervention Multi-disciplinary chronic care management teams are an excellent vehicle for providing ongoing follow-up care for patients with OSA. 23
24 Module III: References Ayas N, Patel S, Malhotra A, et al; Auto-titrating versus standard continuous positive airway pressure for the treatment of obstructive sleep apnea: results of a meta-analysis Sleep. 2004;27(2):249. Brown L, Lee W; Initiation of positive airway pressure therapy for obstructive sleep apnea in adults; UpToDate Oct 14, Campos-Rodriguez F, Martinez-Garcia MA, de la Cruz-Moron I, et al; Cardiovascular mortality in women with obstructive sleep apnea with or without continuous positive airway pressure treatment: a cohort study. Ann Intern Med 2012; 156:115. Campos-Rodriguez F, Peña-Griñan N, Reyes-Nuñez N, et al; Mortality in obstructive sleep apnea- hypopnea patients treated with positive airway pressure. Chest 2005; 128:624. Cistulli P, Collop N, Finlay G, editors); Oral appliances in the treatment of obstructive sleep apnea in adults; UpToDate January Colrain I, Black J, Siegel et al; A multicenter evaluation of oral pressure therapy for the treatment of obstructive sleep apnea Sleep Medicine September 2013 vol 14 issue Drager L, Togeiro S, Polotsky V et al; Obstructive Sleep Apnea: A Cardiometabolic Risk in Obesity and the Metabolic Syndrome J Am Coll Cardiol August 13; 62(7): Epstein L, Kristo D, Strollo P et al; Clinical guideline for evaluation and management of obstructive sleep apnea in adults; Adult Obstructive Sleep Apnea Task Force of the American Academy of Sleep Medicine J Clin Sleep Med 2009;5(3): Gay P, Weaver T, Loube D, et al; Evaluation of positive airway pressure treatment for sleep related breathing disorders in adults. Sleep 2006; 29:
25 Module III: References (continued) Iftikhar I, Kline C, Youngstedt S; Effects of exercise training on sleep apnea: a meta-analysis. Lung 2014; 192:175. Johansson K, Hemmingsson E, Harlid R, et al; Longer term effects of very low energy diet on obstructive sleep apnoea in cohort derived from randomised controlled trial: prospective observational follow-up study. BMJ 2011; 342:d3017. Kryger M, Collop N, Finlay G, editors); Management of obstructive sleep apnea in adults UpToDate February 3, 2016 Kuna T, Reboussin D, Borradaile K, et al; Long-term effect of weight loss on obstructive sleep apnea severity in obese patients with type 2 diabetes. Sleep 2013; 36:641. Marti S, Sampol G, Muñoz X, et al; Mortality in severe sleep apnoea/hypopnoea syndrome patients: impact of treatment. Eur Respir J 2002; 20:1511. Stollo P, Soose R, Maurer J, et al; Upper-Airway Stimulation for Obstructive Sleep Apnea NEJM 2014;370: Strohl K (Collop N, Finlay G, editors); Overview of obstructive sleep apnea in adults UpToDate June 24, 2016 Tuomilehto H, Gylling H, Peltonen M, et al; Sustained improvement in mild obstructive sleep apnea after a diet- and physical activity-based lifestyle intervention: postinterventional follow-up. Am J Clin Nutr 2010; 92:688. Weaver E and Kapur V [Collop, Eichler, editors]; Surgical treatment of obstructive sleep apnea in adults; UpToDate March 6, 2017 Weaver T (Collop N, Finlay G, editors); Adherence with continuous positive airway pressure (CPAP); UpToDate December 1,
A New, Clinically Proven Sleep Apnea Therapy for people unable to use CPAP.
 A New, Clinically Proven Sleep Apnea Therapy for people unable to use CPAP. Take Heart. If You Have OSA, You re Not Alone. Like you, more than 18 million Americans are estimated to have Obstructive Sleep
A New, Clinically Proven Sleep Apnea Therapy for people unable to use CPAP. Take Heart. If You Have OSA, You re Not Alone. Like you, more than 18 million Americans are estimated to have Obstructive Sleep
Inspire Therapy for Sleep Apnea
 Inspire Therapy for Sleep Apnea Patient Guide Giving You the FREEDOM TO SLEEP Like Everyone Else Take Comfort. Inspire therapy can help. Inspire therapy is a breakthrough implantable treatment option for
Inspire Therapy for Sleep Apnea Patient Guide Giving You the FREEDOM TO SLEEP Like Everyone Else Take Comfort. Inspire therapy can help. Inspire therapy is a breakthrough implantable treatment option for
Inspire Therapy for Sleep Apnea
 Inspire Therapy for Sleep Apnea Patient Guide Giving You the FREEDOM TO SLEEP Like Everyone Else Take Comfort. Inspire therapy can help. Inspire therapy is a breakthrough implantable treatment option for
Inspire Therapy for Sleep Apnea Patient Guide Giving You the FREEDOM TO SLEEP Like Everyone Else Take Comfort. Inspire therapy can help. Inspire therapy is a breakthrough implantable treatment option for
Evaluation, Management and Long-Term Care of OSA in Adults
 Evaluation, Management and Long-Term Care of OSA in Adults AUGUST 2015 Providing diagnostic tools and therapies that are evidence-based is a key part of a successful sleep practice. This resource outlines
Evaluation, Management and Long-Term Care of OSA in Adults AUGUST 2015 Providing diagnostic tools and therapies that are evidence-based is a key part of a successful sleep practice. This resource outlines
Inspire. therapy for sleep apnea. Giving you the freedom to sleep like everyone else
 Inspire therapy for sleep apnea Giving you the freedom to sleep like everyone else Take Comfort. Take Action. Inspire therapy can help. Here are some reasons people like you have chosen Inspire therapy
Inspire therapy for sleep apnea Giving you the freedom to sleep like everyone else Take Comfort. Take Action. Inspire therapy can help. Here are some reasons people like you have chosen Inspire therapy
OBSTRUCTIVE SLEEP APNEA and WORK Treatment Update
 OBSTRUCTIVE SLEEP APNEA and WORK Treatment Update David Claman, MD Professor of Medicine Director, UCSF Sleep Disorders Center 415-885-7886 Disclosures: None Chronic Sleep Deprivation (0 v 4 v 6 v 8 hrs)
OBSTRUCTIVE SLEEP APNEA and WORK Treatment Update David Claman, MD Professor of Medicine Director, UCSF Sleep Disorders Center 415-885-7886 Disclosures: None Chronic Sleep Deprivation (0 v 4 v 6 v 8 hrs)
Inspire Therapy for Sleep Apnea
 Inspire Therapy for Sleep Apnea Take Heart. If you have OSA, you re not alone. More than 18 million Americans are estimated to have Obstructive Sleep Apnea (OSA). OSA occurs when the tongue and other soft
Inspire Therapy for Sleep Apnea Take Heart. If you have OSA, you re not alone. More than 18 million Americans are estimated to have Obstructive Sleep Apnea (OSA). OSA occurs when the tongue and other soft
Obstructive Sleep Apnea Syndrome. Common sleep disorder causes high blood pressure and heart attacks
 Obstructive Sleep Apnea Syndrome Common sleep disorder causes high blood pressure and heart attacks Message: Sleep apnea is very common. It is estimated that 158 million people worldwide suffer from sleep
Obstructive Sleep Apnea Syndrome Common sleep disorder causes high blood pressure and heart attacks Message: Sleep apnea is very common. It is estimated that 158 million people worldwide suffer from sleep
Management of OSA. saurabh maji
 Management of OSA saurabh maji INTRODUCTION Obstructive sleep apnea is a major public health problem Prevalence of OSAS in INDIA is 2.4% to 4.96% in men and 1% to 2 % in women In the rest of the world
Management of OSA saurabh maji INTRODUCTION Obstructive sleep apnea is a major public health problem Prevalence of OSAS in INDIA is 2.4% to 4.96% in men and 1% to 2 % in women In the rest of the world
UPDATES IN SLEEP APNEA:
 UPDATES IN SLEEP APNEA: CPAP,CPAP COMPLIANCE, & ALTERNATIVES MICHELLE ZETOONY, DO, FCCP, FACOI BOARD CERTIFIED PULMONARY, CRITICAL CARE, SLEEP & INTERNAL MEDICINE CLEARWATER, FL DISCLOSURE I have no conflicts
UPDATES IN SLEEP APNEA: CPAP,CPAP COMPLIANCE, & ALTERNATIVES MICHELLE ZETOONY, DO, FCCP, FACOI BOARD CERTIFIED PULMONARY, CRITICAL CARE, SLEEP & INTERNAL MEDICINE CLEARWATER, FL DISCLOSURE I have no conflicts
in China Shanghai Office Beijing Office (+86) (+86)
 SLEEP Apnea in China Guide 2018-2019 Shanghai Office (+86) 21 2426 6400 Beijing Office (+86) 010 6464 0611 www.pacificprime.cn Follow us on WeChat t A comprehensive overview of sleep apnea Perhaps you
SLEEP Apnea in China Guide 2018-2019 Shanghai Office (+86) 21 2426 6400 Beijing Office (+86) 010 6464 0611 www.pacificprime.cn Follow us on WeChat t A comprehensive overview of sleep apnea Perhaps you
RESEARCH PACKET DENTAL SLEEP MEDICINE
 RESEARCH PACKET DENTAL SLEEP MEDICINE American Academy of Dental Sleep Medicine Dental Sleep Medicine Research Packet Page 1 Table of Contents Research: Oral Appliance Therapy vs. Continuous Positive Airway
RESEARCH PACKET DENTAL SLEEP MEDICINE American Academy of Dental Sleep Medicine Dental Sleep Medicine Research Packet Page 1 Table of Contents Research: Oral Appliance Therapy vs. Continuous Positive Airway
Helping You to Breathe Better, Sleep Easy & Live Well
 Helping You to Breathe Better, Sleep Easy & Live Well Your Guide to CPAP Therapy info@cansleep.ca Vancouver Island Lower Mainland Fraser Valley Sleep Apnea & Symptoms Obstructive Sleep Apnea (OSA) occurs
Helping You to Breathe Better, Sleep Easy & Live Well Your Guide to CPAP Therapy info@cansleep.ca Vancouver Island Lower Mainland Fraser Valley Sleep Apnea & Symptoms Obstructive Sleep Apnea (OSA) occurs
Inspire Therapy for Sleep Apnea
 Inspire Therapy for Sleep Apnea Patient Guide Giving You the FREEDOM TO SLEEP Like Everyone Else Take Comfort. Inspire therapy can help. Inspire therapy is a breakthrough implantable treatment option for
Inspire Therapy for Sleep Apnea Patient Guide Giving You the FREEDOM TO SLEEP Like Everyone Else Take Comfort. Inspire therapy can help. Inspire therapy is a breakthrough implantable treatment option for
WINDSOR DENTAL CARE 2224 WALKER ROAD SUITE 20 WINDSOR, ON N8W 5L7 PHONE FAX
 The quality of your sleep can impact you emotionally, physically and your overall general health. Poor sleep can cause chronic fatigue, daytime drowsiness, irritability and loss of focus. It affects your
The quality of your sleep can impact you emotionally, physically and your overall general health. Poor sleep can cause chronic fatigue, daytime drowsiness, irritability and loss of focus. It affects your
Sleep Medicine. Paul Fredrickson, MD Director. Mayo Sleep Center Jacksonville, Florida.
 Sleep Medicine Paul Fredrickson, MD Director Mayo Sleep Center Jacksonville, Florida Fredrickson.Paul@mayo.edu DISCLOSURES No relevant conflicts to report. Obstructive Sleep Apnea The most common sleep
Sleep Medicine Paul Fredrickson, MD Director Mayo Sleep Center Jacksonville, Florida Fredrickson.Paul@mayo.edu DISCLOSURES No relevant conflicts to report. Obstructive Sleep Apnea The most common sleep
11/13/2017. Jeremy Tabak MD, FAASM Medical Director Baptist Hospital Sleep Lab Medical Director Baptist Sleep Lab at Galloway
 Jeremy Tabak MD, FAASM Medical Director Baptist Hospital Sleep Lab Medical Director Baptist Sleep Lab at Galloway HypnoLaus study: OSA effect on mortality US Preventive Services Task Force recommendations
Jeremy Tabak MD, FAASM Medical Director Baptist Hospital Sleep Lab Medical Director Baptist Sleep Lab at Galloway HypnoLaus study: OSA effect on mortality US Preventive Services Task Force recommendations
SLEEP APNOEA DR TAN KAH LEONG ALVIN CO-DIRECTOR SLEEP LABORATORY SITE CHIEF SDDC (SLEEP) DEPARTMENT OF OTORHINOLARYNGOLOGY, HEAD & NECK SURGERY
 SLEEP APNOEA DR TAN KAH LEONG ALVIN CO-DIRECTOR SLEEP LABORATORY SITE CHIEF SDDC (SLEEP) DEPARTMENT OF OTORHINOLARYNGOLOGY, HEAD & NECK SURGERY
SLEEP APNOEA DR TAN KAH LEONG ALVIN CO-DIRECTOR SLEEP LABORATORY SITE CHIEF SDDC (SLEEP) DEPARTMENT OF OTORHINOLARYNGOLOGY, HEAD & NECK SURGERY
Positive Airway Pressure and Oral Devices for the Treatment of Obstructive Sleep Apnea
 Positive Airway Pressure and Oral Devices for the Treatment of Obstructive Sleep Apnea Policy Number: Original Effective Date: MM.01.009 11/01/2009 Line(s) of Business: Current Effective Date: HMO; PPO
Positive Airway Pressure and Oral Devices for the Treatment of Obstructive Sleep Apnea Policy Number: Original Effective Date: MM.01.009 11/01/2009 Line(s) of Business: Current Effective Date: HMO; PPO
Upper Airway Stimulation for Obstructive Sleep Apnea
 Upper Airway Stimulation for Obstructive Sleep Apnea Background, Mechanism and Clinical Data Overview Seth Hollen RPSGT 21 May 2016 1 Conflicts of Interest Therapy Support Specialist, Inspire Medical Systems
Upper Airway Stimulation for Obstructive Sleep Apnea Background, Mechanism and Clinical Data Overview Seth Hollen RPSGT 21 May 2016 1 Conflicts of Interest Therapy Support Specialist, Inspire Medical Systems
Obstructive Sleep Apnea: Effective Intervention & Care
 Obstructive Sleep Apnea: Effective Intervention & Care MeMD Telehealth Provider Training Modules Jonathan Freudman, MD 2016 Resonea Inc. 2016 Resonea Inc. Module IV: Best Practices To Improve CPAP Adherence
Obstructive Sleep Apnea: Effective Intervention & Care MeMD Telehealth Provider Training Modules Jonathan Freudman, MD 2016 Resonea Inc. 2016 Resonea Inc. Module IV: Best Practices To Improve CPAP Adherence
Helping You to Breathe Better, Sleep Easy & Live Well
 Helping You to Breathe Better, Sleep Easy & Live Well Your Guide to CPAP Therapy info@cansleep.ca Lower Mainland Vancouver Island Fraser Valley Sleep Apnea & Symptoms Obstructive Sleep Apnea (OSA) occurs
Helping You to Breathe Better, Sleep Easy & Live Well Your Guide to CPAP Therapy info@cansleep.ca Lower Mainland Vancouver Island Fraser Valley Sleep Apnea & Symptoms Obstructive Sleep Apnea (OSA) occurs
Treatment of Obstructive Sleep Apnea (OSA)
 MP9239 Covered Service: Prior Authorization Required: Additional Information: Yes when meets criteria below Yes as shown below None Prevea360 Health Plan Medical Policy: 1.0 A continuous positive airway
MP9239 Covered Service: Prior Authorization Required: Additional Information: Yes when meets criteria below Yes as shown below None Prevea360 Health Plan Medical Policy: 1.0 A continuous positive airway
Sleep Apnoea. Introduction Symptoms Causes Obtaining a Diagnosis Treatment Complications
 The most common forms of sleep apnoea are normally referred to as obstructive sleep apnoea (OSA) and relate to a condition which causes interruptions in breathing during sleep. People with obstructive
The most common forms of sleep apnoea are normally referred to as obstructive sleep apnoea (OSA) and relate to a condition which causes interruptions in breathing during sleep. People with obstructive
Positive Airway Pressure and Oral Devices for the Treatment of Obstructive Sleep Apnea
 Positive Airway Pressure and Oral Devices for the Treatment of Obstructive Sleep Apnea Policy Number: Original Effective Date: MM.01.009 11/01/2009 Line(s) of Business: Current Effective Date: HMO; PPO;
Positive Airway Pressure and Oral Devices for the Treatment of Obstructive Sleep Apnea Policy Number: Original Effective Date: MM.01.009 11/01/2009 Line(s) of Business: Current Effective Date: HMO; PPO;
Balboa Island Dentistry (949)
 Do You Snore? Are you always tired? Snoring is no laughing matter! It may be more than an annoying habit. It may be a sign of. How well do you sleep? Just about everyone snores occasionally. Even a baby
Do You Snore? Are you always tired? Snoring is no laughing matter! It may be more than an annoying habit. It may be a sign of. How well do you sleep? Just about everyone snores occasionally. Even a baby
Commissioning Policy Individual Funding Request
 Commissioning Policy Individual Funding Request Continuous Positive Airway Pressure (CPAP) Treatment of Obstructive Sleep Apnoea/Hypopnoea Syndrome (OSAHS) Criteria Based Access Policy Date Adopted: 13
Commissioning Policy Individual Funding Request Continuous Positive Airway Pressure (CPAP) Treatment of Obstructive Sleep Apnoea/Hypopnoea Syndrome (OSAHS) Criteria Based Access Policy Date Adopted: 13
Sleep Disordered Breathing
 Sleep Disordered Breathing SDB SDB Is an Umbrella Term for Many Disorders characterized by a lack of drive to breathe Results n repetitive pauses in breathing with no effort Occurs for a minimum of 10
Sleep Disordered Breathing SDB SDB Is an Umbrella Term for Many Disorders characterized by a lack of drive to breathe Results n repetitive pauses in breathing with no effort Occurs for a minimum of 10
Surgical Options for the Successful Treatment of Obstructive Sleep Apnea
 Surgical Options for the Successful Treatment of Obstructive Sleep Apnea Benjamin J. Teitelbaum, MD, FACS Otolaryngology Head and Neck Surgery Saint Agnes Medical Center Fresno, California Terms Apnea
Surgical Options for the Successful Treatment of Obstructive Sleep Apnea Benjamin J. Teitelbaum, MD, FACS Otolaryngology Head and Neck Surgery Saint Agnes Medical Center Fresno, California Terms Apnea
Snoring. Forty-five percent of normal adults snore at least occasionally and 25
 Snoring Insight into sleeping disorders and sleep apnea Forty-five percent of normal adults snore at least occasionally and 25 percent are habitual snorers. Problem snoring is more frequent in males and
Snoring Insight into sleeping disorders and sleep apnea Forty-five percent of normal adults snore at least occasionally and 25 percent are habitual snorers. Problem snoring is more frequent in males and
11/19/2012 ก! " Varies 5-86% in men 2-57% in women. Thailand 26.4% (Neruntarut et al, Sleep Breath (2011) 15: )
 Snoring ก Respiratory sound generated in the upper airway during sleep that typically occurs during inspiration but may occur during expiration ICSD-2, 2005..... ก ก! Prevalence of snoring Varies 5-86%
Snoring ก Respiratory sound generated in the upper airway during sleep that typically occurs during inspiration but may occur during expiration ICSD-2, 2005..... ก ก! Prevalence of snoring Varies 5-86%
Outcomes of Upper Airway Surgery in Obstructive Sleep Apnea
 Original Research Outcomes of Upper Airway Surgery in Obstructive Sleep Apnea Hadiseh Hosseiny 1, Nafiseh Naeimabadi 1, Arezu Najafi 1 *, Reihaneh Heidari 1, Khosro Sadeghniiat-Haghighi 1 1. Occupational
Original Research Outcomes of Upper Airway Surgery in Obstructive Sleep Apnea Hadiseh Hosseiny 1, Nafiseh Naeimabadi 1, Arezu Najafi 1 *, Reihaneh Heidari 1, Khosro Sadeghniiat-Haghighi 1 1. Occupational
Management of OSA in the Acute Care Environment. Robert S. Campbell, RRT FAARC HRC, Philips Healthcare May, 2018
 Management of OSA in the Acute Care Environment Robert S. Campbell, RRT FAARC HRC, Philips Healthcare May, 2018 1 Learning Objectives Upon completion, the participant should be able to: Understand pathology
Management of OSA in the Acute Care Environment Robert S. Campbell, RRT FAARC HRC, Philips Healthcare May, 2018 1 Learning Objectives Upon completion, the participant should be able to: Understand pathology
NON-INVASIVE VENTILATION MADE RIDICULOUSLY SIMPLE
 NON-INVASIVE VENTILATION MADE RIDICULOUSLY SIMPLE Jennifer Newitt, MD 3 rd year Pulmonary/Critical Care Fellow Mentor: Patrick Strollo Jr, MD Myth or Fact?!? Myth or Fact?!? Treatment for Obstructive
NON-INVASIVE VENTILATION MADE RIDICULOUSLY SIMPLE Jennifer Newitt, MD 3 rd year Pulmonary/Critical Care Fellow Mentor: Patrick Strollo Jr, MD Myth or Fact?!? Myth or Fact?!? Treatment for Obstructive
Update on Obstructive Sleep Apnea (OSA) With Oral Appliance Therapy (OAT) for the Health Care Professional
 Update on Obstructive Sleep Apnea (OSA) With Oral Appliance Therapy (OAT) for the Health Care Professional By Dr. Steven E. Todd, DMD, MaCSD, ABOI/ID Introduction and Objectives Discuss the impact of OSA
Update on Obstructive Sleep Apnea (OSA) With Oral Appliance Therapy (OAT) for the Health Care Professional By Dr. Steven E. Todd, DMD, MaCSD, ABOI/ID Introduction and Objectives Discuss the impact of OSA
The Agony or the Ecstasy. Familiar?
 The Agony or the Ecstasy Familiar? Snoring Related Complaints Drives wife from bedroom Girlfriend won t marry me Shakes entire house Ask me to leave movies and church Has had to leave boat so friends could
The Agony or the Ecstasy Familiar? Snoring Related Complaints Drives wife from bedroom Girlfriend won t marry me Shakes entire house Ask me to leave movies and church Has had to leave boat so friends could
Alaska Sleep Education Center
 Alaska Sleep Education Center The 3 Types of Sleep Apnea Explained: Obstructive, Central, & Mixed Posted by Kevin Phillips on Jan 28, 2015 6:53:00 PM Sleep apnea is a very common sleep disorder, affecting
Alaska Sleep Education Center The 3 Types of Sleep Apnea Explained: Obstructive, Central, & Mixed Posted by Kevin Phillips on Jan 28, 2015 6:53:00 PM Sleep apnea is a very common sleep disorder, affecting
What is Oral Appliance Therapy?
 You may have been diagnosed by your physician as required treatment for sleep-disordered breathing (snoring and/or obstructive sleep apnea). This condition may pose serious health risks since it disrupts
You may have been diagnosed by your physician as required treatment for sleep-disordered breathing (snoring and/or obstructive sleep apnea). This condition may pose serious health risks since it disrupts
Prefabricated Oral Appliances for Obstructive Sleep Apnea
 Medical Policy Manual Allied Health, Policy No. 36 Prefabricated Oral Appliances for Obstructive Sleep Apnea Next Review: May 2019 Last Review: April 2018 Effective: May 1, 2018 IMPORTANT REMINDER Medical
Medical Policy Manual Allied Health, Policy No. 36 Prefabricated Oral Appliances for Obstructive Sleep Apnea Next Review: May 2019 Last Review: April 2018 Effective: May 1, 2018 IMPORTANT REMINDER Medical
Obstructive Sleep Apnea
 Obstructive Sleep Apnea Introduction Obstructive sleep apnea is an interruption in breathing during sleep. It is caused by throat and tongue muscles collapsing and relaxing. This blocks, or obstructs,
Obstructive Sleep Apnea Introduction Obstructive sleep apnea is an interruption in breathing during sleep. It is caused by throat and tongue muscles collapsing and relaxing. This blocks, or obstructs,
Sleep and the Heart Reversing the Effects of Sleep Apnea to Better Manage Heart Disease
 1 Sleep and the Heart Reversing the Effects of Sleep Apnea to Better Manage Heart Disease Rami Khayat, MD Professor of Internal Medicine Director, OSU Sleep Heart Program Medical Director, Department of
1 Sleep and the Heart Reversing the Effects of Sleep Apnea to Better Manage Heart Disease Rami Khayat, MD Professor of Internal Medicine Director, OSU Sleep Heart Program Medical Director, Department of
THN. Sleep Therapy Study. ImThera. Information for Participants. Caution: Investigational device. Limited by United States law to investigational use.
 THN Sleep Therapy Study Information for Participants Caution: Investigational device. Limited by United States law to investigational use. ImThera Obstructive sleep apnea (OSA) is a very serious condition.
THN Sleep Therapy Study Information for Participants Caution: Investigational device. Limited by United States law to investigational use. ImThera Obstructive sleep apnea (OSA) is a very serious condition.
OBSTRUCTIVE SLEEP APNEA and WORK Treatment Update
 OBSTRUCTIVE SLEEP APNEA and WORK Treatment Update David Claman, MD Professor of Medicine Director, UCSF Sleep Disorders Center 415-885-7886 Disclosres: None Chronic Sleep Deprivation (0 v 4 v 6 v 8 hrs)
OBSTRUCTIVE SLEEP APNEA and WORK Treatment Update David Claman, MD Professor of Medicine Director, UCSF Sleep Disorders Center 415-885-7886 Disclosres: None Chronic Sleep Deprivation (0 v 4 v 6 v 8 hrs)
(HST) (95806, G0398, G0399)
 95800 Sleep study, unattended, simultaneous recording of, heart rate, oxygen saturation, respiratory analysis (e.g. by airflow or peripheral arterial tone), and sleep time 95801 Sleep study, unattended,
95800 Sleep study, unattended, simultaneous recording of, heart rate, oxygen saturation, respiratory analysis (e.g. by airflow or peripheral arterial tone), and sleep time 95801 Sleep study, unattended,
Learning Objectives. And it s getting worse. The Big Picture. Dr. Roger Roubal
 Learning Objectives How to screen for sleep apnea; questions to ask your patients Industry treatment guidelines; when to consider an oral appliance vs. a CPAP What goals/thresholds to set for successful
Learning Objectives How to screen for sleep apnea; questions to ask your patients Industry treatment guidelines; when to consider an oral appliance vs. a CPAP What goals/thresholds to set for successful
Index. sleep.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Accidents. See Motor vehicle accidents. Acetazolamide, in OSA therapy, 531 Acetylcholinesterase inhibitors, in OSA therapy, 532 533 Acromegaly,
Note: Page numbers of article titles are in boldface type. A Accidents. See Motor vehicle accidents. Acetazolamide, in OSA therapy, 531 Acetylcholinesterase inhibitors, in OSA therapy, 532 533 Acromegaly,
Sleep and the Heart. Physiologic Changes in Cardiovascular Parameters during Sleep
 Sleep and the Heart Rami N. Khayat, MD Professor of Internal Medicine Medical Director, Department of Respiratory Therapy Division of Pulmonary, Critical Care and Sleep Medicine The Ohio State University
Sleep and the Heart Rami N. Khayat, MD Professor of Internal Medicine Medical Director, Department of Respiratory Therapy Division of Pulmonary, Critical Care and Sleep Medicine The Ohio State University
Sleep and the Heart. Rami N. Khayat, MD
 Sleep and the Heart Rami N. Khayat, MD Professor of Internal Medicine Medical Director, Department of Respiratory Therapy Division of Pulmonary, Critical Care and Sleep Medicine The Ohio State University
Sleep and the Heart Rami N. Khayat, MD Professor of Internal Medicine Medical Director, Department of Respiratory Therapy Division of Pulmonary, Critical Care and Sleep Medicine The Ohio State University
Comparing Upper Airway Stimulation to Expansion Sphincter Pharyngoplasty: A Single University Experience
 771395AORXXX10.1177/0003489418771395Annals of Otology, Rhinology & LaryngologyHuntley et al research-article2018 Original Article Comparing Upper Airway Stimulation to Expansion Sphincter Pharyngoplasty:
771395AORXXX10.1177/0003489418771395Annals of Otology, Rhinology & LaryngologyHuntley et al research-article2018 Original Article Comparing Upper Airway Stimulation to Expansion Sphincter Pharyngoplasty:
Healthy Sleep. Frederick Tolle, M.D., dabsm Community Health Network
 Healthy Sleep Frederick Tolle, M.D., dabsm Community Health Network Adults should sleep 7 or more hours per night on a regular basis to promote optimal health. Getting less than 7 hours of sleep on average
Healthy Sleep Frederick Tolle, M.D., dabsm Community Health Network Adults should sleep 7 or more hours per night on a regular basis to promote optimal health. Getting less than 7 hours of sleep on average
Obstructive Sleep Apnea and COPD overlap syndrome. Financial Disclosures. Outline 11/1/2016
 Obstructive Sleep Apnea and COPD overlap syndrome Chitra Lal, MD, FCCP, FAASM Associate Professor of Medicine, Pulmonary, Critical Care, and Sleep, Medical University of South Carolina Financial Disclosures
Obstructive Sleep Apnea and COPD overlap syndrome Chitra Lal, MD, FCCP, FAASM Associate Professor of Medicine, Pulmonary, Critical Care, and Sleep, Medical University of South Carolina Financial Disclosures
Did you know more than a million Australians suffer from severe sleep apnoea?
 Did you know more than a million Australians suffer from severe sleep apnoea? Your comprehensive guide to curing sleep apnoea www.futuredental.com.au 1 Contents What is Obstructive Sleep Apnoea? 2 What
Did you know more than a million Australians suffer from severe sleep apnoea? Your comprehensive guide to curing sleep apnoea www.futuredental.com.au 1 Contents What is Obstructive Sleep Apnoea? 2 What
BTS sleep Course. Module 10 Therapies I: Mechanical Intervention Devices (Prepared by Debby Nicoll and Debbie Smith)
 BTS sleep Course Module 10 Therapies I: Mechanical Intervention Devices (Prepared by Debby Nicoll and Debbie Smith) S1: Overview of OSA Definition History Prevalence Pathophysiology Causes Consequences
BTS sleep Course Module 10 Therapies I: Mechanical Intervention Devices (Prepared by Debby Nicoll and Debbie Smith) S1: Overview of OSA Definition History Prevalence Pathophysiology Causes Consequences
Medicare C/D Medical Coverage Policy
 Medicare C/D Medical Coverage Policy Surgical Treatment of Obstructive Sleep Apnea Origination: June 26, 2000 Review Date: January 18, 2017 Next Review January, 2019 DESCRIPTION OF PROCEDURE OR SERVICE
Medicare C/D Medical Coverage Policy Surgical Treatment of Obstructive Sleep Apnea Origination: June 26, 2000 Review Date: January 18, 2017 Next Review January, 2019 DESCRIPTION OF PROCEDURE OR SERVICE
SNORING AND OBSTRUCTIVE SLEEP APNOEA WAYS TO DEAL WITH THESE PROBLEMS
 SNORING AND OBSTRUCTIVE SLEEP APNOEA WAYS TO DEAL WITH THESE PROBLEMS Laugh and the world laughs with you; snore and you sleep alone. These words by novelist Anthony Vergess ring true with all too many
SNORING AND OBSTRUCTIVE SLEEP APNOEA WAYS TO DEAL WITH THESE PROBLEMS Laugh and the world laughs with you; snore and you sleep alone. These words by novelist Anthony Vergess ring true with all too many
CPAP. The CPAP will be covered
 CPAP CPAP Did your patient have a face to face visit with the physician prior to having a sleep study that documented (1) Sleep History and symptoms and/or (2) Epworth Scale and/or (3) Physical Examination?
CPAP CPAP Did your patient have a face to face visit with the physician prior to having a sleep study that documented (1) Sleep History and symptoms and/or (2) Epworth Scale and/or (3) Physical Examination?
Data Management of the Sleep Disordered Breathing Patient
 Data Management of the Sleep Disordered Breathing Patient 1 AARC or AAST CEU credit As Allies in Better Sleep and Breathing, we make it our #1 priority to work in harmony with caregivers and patients to
Data Management of the Sleep Disordered Breathing Patient 1 AARC or AAST CEU credit As Allies in Better Sleep and Breathing, we make it our #1 priority to work in harmony with caregivers and patients to
Corporate Medical Policy
 Corporate Medical Policy PALATOPHARYNGOPLASTY/UVULOPALATOPHARYGOPLASTY Description of Procedure or Service Palatopharyngoplasty refers to several surgical approaches for management of the upper airway,
Corporate Medical Policy PALATOPHARYNGOPLASTY/UVULOPALATOPHARYGOPLASTY Description of Procedure or Service Palatopharyngoplasty refers to several surgical approaches for management of the upper airway,
ASK US. A Study for Obstructive Sleep Apnea Patients Using a New At-Home Sleep Test ARE YOU ABOUT THE STUDY #
 #15420040.0 A Study for Obstructive Sleep Apnea Patients Using a New At-Home Sleep Test STUDY DENTIST Dr. Michael Simmons DMD, MSc ARE YOU Struggling with or given up on CPAP and don t know what to do?
#15420040.0 A Study for Obstructive Sleep Apnea Patients Using a New At-Home Sleep Test STUDY DENTIST Dr. Michael Simmons DMD, MSc ARE YOU Struggling with or given up on CPAP and don t know what to do?
OSA - Obstructive sleep apnoea What you need to know if you think you might have OSA
 OSA - Obstructive sleep apnoea What you need to know if you think you might have OSA Obstructive sleep apnoea, or OSA, is a breathing problem that happens when you sleep. It can affect anyone men, women
OSA - Obstructive sleep apnoea What you need to know if you think you might have OSA Obstructive sleep apnoea, or OSA, is a breathing problem that happens when you sleep. It can affect anyone men, women
Dental Sleep Medicine Basics
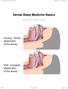 Dental Sleep Medicine Basics Written By: Patrick Tessier 2018 www.tap.wiki/ Page 1 of 8 INTRODUCTION Here are some basic aspect of Dental Sleep Medicine. This viewpoint is from an industry participant,
Dental Sleep Medicine Basics Written By: Patrick Tessier 2018 www.tap.wiki/ Page 1 of 8 INTRODUCTION Here are some basic aspect of Dental Sleep Medicine. This viewpoint is from an industry participant,
Sleep Apnea. Herbert A Berger, MD Pulmonary Division Department of Internal Medicine University of Iowa
 Sleep Apnea Herbert A Berger, MD Pulmonary Division Department of Internal Medicine University of Iowa Disclosures No Relevant Financial Interests to Report Objectives Learn the history and physical examination
Sleep Apnea Herbert A Berger, MD Pulmonary Division Department of Internal Medicine University of Iowa Disclosures No Relevant Financial Interests to Report Objectives Learn the history and physical examination
QUESTIONS FOR DELIBERATION
 New England Comparative Effectiveness Public Advisory Council Public Meeting Hartford, Connecticut Diagnosis and Treatment of Obstructive Sleep Apnea in Adults December 6, 2012 UPDATED: November 28, 2012
New England Comparative Effectiveness Public Advisory Council Public Meeting Hartford, Connecticut Diagnosis and Treatment of Obstructive Sleep Apnea in Adults December 6, 2012 UPDATED: November 28, 2012
Inspire Therapy for Obstructive Sleep Apnea. Clinical Data Update
 Inspire Therapy for Obstructive Sleep Apnea For OSA patients unable to tolerate or get consistent benefit from CPAP Clinical Data Update Summary of published long-term 3-year outcomes data Treatment Goals
Inspire Therapy for Obstructive Sleep Apnea For OSA patients unable to tolerate or get consistent benefit from CPAP Clinical Data Update Summary of published long-term 3-year outcomes data Treatment Goals
Frequently Asked Questions
 Q- What is Sleep Apnea? Frequently Asked Questions A- Sleep Apnea, sometimes known as the "silent killer" although there is usually nothing silent about it. It is associated with periodic loud snoring
Q- What is Sleep Apnea? Frequently Asked Questions A- Sleep Apnea, sometimes known as the "silent killer" although there is usually nothing silent about it. It is associated with periodic loud snoring
Positive Airway Pressure and Oral Devices for the Treatment of Obstructive Sleep Apnea
 Positive Airway Pressure and Oral Devices for the Treatment of Obstructive Sleep Apnea Policy Number: Original Effective Date: MM.01.009 11/01/2009 Line(s) of Business: Current Effective Date: HMO; PPO;
Positive Airway Pressure and Oral Devices for the Treatment of Obstructive Sleep Apnea Policy Number: Original Effective Date: MM.01.009 11/01/2009 Line(s) of Business: Current Effective Date: HMO; PPO;
Goals Session Putting it all Together
 Goals Session Putting it all Together Adherence to therapy Case presentations Treatment issues Charles Atwood, MD, FCCP, FAASM University of Pittsburgh Disclosures Advisory - Carecore National; Philips;
Goals Session Putting it all Together Adherence to therapy Case presentations Treatment issues Charles Atwood, MD, FCCP, FAASM University of Pittsburgh Disclosures Advisory - Carecore National; Philips;
What is SDB? Obstructive sleep apnea-hypopnea syndrome (OSAHS)
 Have a Good Sleep? Estimated 70 million Americans have clinically significant sleep problems Chronic insomnias report decreased quality of life, memory and attention problems, decreased physical health
Have a Good Sleep? Estimated 70 million Americans have clinically significant sleep problems Chronic insomnias report decreased quality of life, memory and attention problems, decreased physical health
Positive Pressure Therapy
 Positive Pressure Therapy Positive Pressure Therapy...2 What is Sleep Apnea?....2 Positive Pressure Machines..................................................... 4 Types..................................................................................
Positive Pressure Therapy Positive Pressure Therapy...2 What is Sleep Apnea?....2 Positive Pressure Machines..................................................... 4 Types..................................................................................
Emerging Nursing Roles in Collaborative Management of Sleep Disordered Breathing and Obstructive Sleep Apnoea
 Emerging Nursing Roles in Collaborative Management of Sleep Disordered Breathing and Obstructive Sleep Apnoea Sigma Theta Tau International 28th International Nursing Research Congress 27-31 July 2017
Emerging Nursing Roles in Collaborative Management of Sleep Disordered Breathing and Obstructive Sleep Apnoea Sigma Theta Tau International 28th International Nursing Research Congress 27-31 July 2017
Circadian Variations Influential in Circulatory & Vascular Phenomena
 SLEEP & STROKE 1 Circadian Variations Influential in Circulatory & Vascular Phenomena Endocrine secretions Thermo regulations Renal Functions Respiratory control Heart Rhythm Hematologic parameters Immune
SLEEP & STROKE 1 Circadian Variations Influential in Circulatory & Vascular Phenomena Endocrine secretions Thermo regulations Renal Functions Respiratory control Heart Rhythm Hematologic parameters Immune
Questions: What tests are available to diagnose sleep disordered breathing? How do you calculate overall AHI vs obstructive AHI?
 Pediatric Obstructive Sleep Apnea Case Study : Margaret-Ann Carno PhD, CPNP, D,ABSM for the Sleep Education for Pulmonary Fellows and Practitioners, SRN ATS Committee April 2014. Facilitator s guide Part
Pediatric Obstructive Sleep Apnea Case Study : Margaret-Ann Carno PhD, CPNP, D,ABSM for the Sleep Education for Pulmonary Fellows and Practitioners, SRN ATS Committee April 2014. Facilitator s guide Part
DOWNLOAD OR READ : TREATMENT FOR SNORING PROBLEMS PDF EBOOK EPUB MOBI
 DOWNLOAD OR READ : TREATMENT FOR SNORING PROBLEMS PDF EBOOK EPUB MOBI Page 1 Page 2 treatment for snoring problems treatment for snoring problems pdf treatment for snoring problems problem, presenting
DOWNLOAD OR READ : TREATMENT FOR SNORING PROBLEMS PDF EBOOK EPUB MOBI Page 1 Page 2 treatment for snoring problems treatment for snoring problems pdf treatment for snoring problems problem, presenting
CLINICAL MEDICAL POLICY
 Policy Name: Policy Number: Responsible Department(s): CLINICAL MEDICAL POLICY Hypoglossal Nerve Stimulation in the Treatment of Obstructive Sleep Apnea MP-079-MD-DE Medical Management Provider Notice
Policy Name: Policy Number: Responsible Department(s): CLINICAL MEDICAL POLICY Hypoglossal Nerve Stimulation in the Treatment of Obstructive Sleep Apnea MP-079-MD-DE Medical Management Provider Notice
ROBERT C. PRITCHARD DIRECTOR MICHAEL O. FOSTER ASSISTANT DIR. SLEEP APNEA
 ROBERT C. PRITCHARD DIRECTOR MICHAEL O. FOSTER ASSISTANT DIR. SLEEP APNEA A Person is physically qualified to drive a motor vehicle if that person; -(5) has no established medical history or clinical diagnosis
ROBERT C. PRITCHARD DIRECTOR MICHAEL O. FOSTER ASSISTANT DIR. SLEEP APNEA A Person is physically qualified to drive a motor vehicle if that person; -(5) has no established medical history or clinical diagnosis
The Clinician s Role in Educating Patients with Sleep Apnea
 The Clinician s Role in Educating Patients with Sleep Apnea Cindy Altman, RPSGT, R.EEG/EP T. Alegent Creighton Clinic/Omaha, NE Immediate Past President/BRPT The Early Years in Sleep 1929 1930 1950 s 1968
The Clinician s Role in Educating Patients with Sleep Apnea Cindy Altman, RPSGT, R.EEG/EP T. Alegent Creighton Clinic/Omaha, NE Immediate Past President/BRPT The Early Years in Sleep 1929 1930 1950 s 1968
GOT SLEEP? YOUR COMPLETE GUIDE TO UNDERSTANDING SLEEP APNEA
 Count me. I dare you. GOT SLEEP? YOUR COMPLETE GUIDE TO UNDERSTANDING SLEEP APNEA PRESENTED BY INTRODUCTION So what s the point of this ebook anyway? At The Maxillofacial Surgery Center, we want to inform
Count me. I dare you. GOT SLEEP? YOUR COMPLETE GUIDE TO UNDERSTANDING SLEEP APNEA PRESENTED BY INTRODUCTION So what s the point of this ebook anyway? At The Maxillofacial Surgery Center, we want to inform
Polysomnography (PSG) (Sleep Studies), Sleep Center
 Policy Number: 1036 Policy History Approve Date: 07/09/2015 Effective Date: 07/09/2015 Preauthorization All Plans Benefit plans vary in coverage and some plans may not provide coverage for certain service(s)
Policy Number: 1036 Policy History Approve Date: 07/09/2015 Effective Date: 07/09/2015 Preauthorization All Plans Benefit plans vary in coverage and some plans may not provide coverage for certain service(s)
Upper Airway Muscle Stimulation for Obstructive Sleep Apnea
 Upper Airway Muscle Stimulation for Obstructive Sleep Apnea M. Safwan Badr, MD, MBA Chair, Department of Medicine, Wayne State University School of Medicine. Staff Physician, John D. Dingell VA Medical
Upper Airway Muscle Stimulation for Obstructive Sleep Apnea M. Safwan Badr, MD, MBA Chair, Department of Medicine, Wayne State University School of Medicine. Staff Physician, John D. Dingell VA Medical
Positive Airway Pressure Systems for Sleep Disordered Breathing
 Positive Airway Pressure Systems for Sleep Disordered Breathing Lori Pickrell, RRT Account Manager Roberts Home Medical Lpickrell@robertshomemedical.com Objectives Upon completion of the session, attendees
Positive Airway Pressure Systems for Sleep Disordered Breathing Lori Pickrell, RRT Account Manager Roberts Home Medical Lpickrell@robertshomemedical.com Objectives Upon completion of the session, attendees
Obstructive Sleep Apnea: Effective Intervention & Care
 Obstructive Sleep Apnea: Effective Intervention & Care Provider Training Modules Jonathan Freudman, MD 2016 Resonea Inc. 2016 Resonea Inc. Module II: Confirming the Clinical Diagnosis of OSA Module II:
Obstructive Sleep Apnea: Effective Intervention & Care Provider Training Modules Jonathan Freudman, MD 2016 Resonea Inc. 2016 Resonea Inc. Module II: Confirming the Clinical Diagnosis of OSA Module II:
Obstructive Sleep Apnea in Truck Drivers
 Rocky Mountain Academy of Occupational and Environmental Medicine Denver, Colorado February 6, 2010 Obstructive Sleep Apnea in Truck Drivers Philip D. Parks, MD, MPH, MOccH Medical Director, Lifespan Health
Rocky Mountain Academy of Occupational and Environmental Medicine Denver, Colorado February 6, 2010 Obstructive Sleep Apnea in Truck Drivers Philip D. Parks, MD, MPH, MOccH Medical Director, Lifespan Health
Medical Affairs Policy
 Medical Affairs Policy Service: Sleep Disorder Treatment: Positive Airway Pressure Devices and Oral Appliances (CPAP, BPAP, BiPAP, BiPAP ST, BiPAP with backup, BiPAP -Auto SV, VPAP, VPAP Adapt, VPAP adapt
Medical Affairs Policy Service: Sleep Disorder Treatment: Positive Airway Pressure Devices and Oral Appliances (CPAP, BPAP, BiPAP, BiPAP ST, BiPAP with backup, BiPAP -Auto SV, VPAP, VPAP Adapt, VPAP adapt
Physician Dentist Collaboration
 Physician Dentist Collaboration Ronald S. Prehn, ThM, DDS Legal Perspective MD CAN LEGALLY MAKE PROPER DIAGNOSIS DDS CAN LEGALLY FABRICATE DENTAL SLEEP APPLIANCES Legal Perspective TWO PROFESSIONS WORK
Physician Dentist Collaboration Ronald S. Prehn, ThM, DDS Legal Perspective MD CAN LEGALLY MAKE PROPER DIAGNOSIS DDS CAN LEGALLY FABRICATE DENTAL SLEEP APPLIANCES Legal Perspective TWO PROFESSIONS WORK
Sleep Apnea: Diagnosis & Treatment
 Disclosure Sleep Apnea: Diagnosis & Treatment Lawrence J. Epstein, MD Sleep HealthCenters Harvard Medical School Chief Medical Officer for Sleep HealthCenters Sleep medicine specialty practice group Consultant
Disclosure Sleep Apnea: Diagnosis & Treatment Lawrence J. Epstein, MD Sleep HealthCenters Harvard Medical School Chief Medical Officer for Sleep HealthCenters Sleep medicine specialty practice group Consultant
Diabetes & Obstructive Sleep Apnoea risk. Jaynie Pateraki MSc RGN
 Diabetes & Obstructive Sleep Apnoea risk Jaynie Pateraki MSc RGN Non-REM - REM - Both - Unrelated - Common disorders of Sleep Sleep Walking Night terrors Periodic leg movements Sleep automatism Nightmares
Diabetes & Obstructive Sleep Apnoea risk Jaynie Pateraki MSc RGN Non-REM - REM - Both - Unrelated - Common disorders of Sleep Sleep Walking Night terrors Periodic leg movements Sleep automatism Nightmares
Sleep Apnea. What is sleep apnea? How does it occur? What are the symptoms?
 What is sleep apnea? Sleep Apnea Sleep apnea is a serious sleep problem. If you have it, you stop breathing for more than 10 seconds at a time many times while you sleep. Another term for this problem
What is sleep apnea? Sleep Apnea Sleep apnea is a serious sleep problem. If you have it, you stop breathing for more than 10 seconds at a time many times while you sleep. Another term for this problem
Sleep Diordered Breathing (Part 1)
 Sleep Diordered Breathing (Part 1) History (for more topics & presentations, visit ) Obstructive sleep apnea - first described by Charles Dickens in 1836 in Papers of the Pickwick Club, Dickens depicted
Sleep Diordered Breathing (Part 1) History (for more topics & presentations, visit ) Obstructive sleep apnea - first described by Charles Dickens in 1836 in Papers of the Pickwick Club, Dickens depicted
Update on Sleep Apnea Diagnosis and Treatment
 Update on Sleep Apnea Diagnosis and Treatment Damien Stevens MD Pulmonary/Critical Care/Sleep Medicine Medical Director KU Medical Center Sleep Laboratory Objectives Discuss physiology of sleep and obstructive
Update on Sleep Apnea Diagnosis and Treatment Damien Stevens MD Pulmonary/Critical Care/Sleep Medicine Medical Director KU Medical Center Sleep Laboratory Objectives Discuss physiology of sleep and obstructive
Continuous Positive Airway Pressure (CPAP)
 Patient Information Continuous Positive Airway Pressure (CPAP) Author: Pulmonary physiology, sleep and ventilation Produced and designed by the Communications Team Issue date July 2017 Expiry date July
Patient Information Continuous Positive Airway Pressure (CPAP) Author: Pulmonary physiology, sleep and ventilation Produced and designed by the Communications Team Issue date July 2017 Expiry date July
Rediscover the power of sleep
 Rediscover the power of sleep Patient Copy Apnea solutions for all ages Mobile Sleep Services Who We Are An experienced and well trained team of sleep care professionals consisting of Registered Sleep
Rediscover the power of sleep Patient Copy Apnea solutions for all ages Mobile Sleep Services Who We Are An experienced and well trained team of sleep care professionals consisting of Registered Sleep
Introducing the WatchPAT 200 # 1 Home Sleep Study Device
 Introducing the WatchPAT 200 # 1 Home Sleep Study Device Top 10 Medical Innovation for 2010 Cleveland Clinic Fidelis Diagnostics & Itamar Medical Fidelis Diagnostics founded in 2004, is a privately-held
Introducing the WatchPAT 200 # 1 Home Sleep Study Device Top 10 Medical Innovation for 2010 Cleveland Clinic Fidelis Diagnostics & Itamar Medical Fidelis Diagnostics founded in 2004, is a privately-held
OSA and COPD: What happens when the two OVERLAP?
 2011 ISRC Seminar 1 COPD OSA OSA and COPD: What happens when the two OVERLAP? Overlap Syndrome 1 OSA and COPD: What happens when the two OVERLAP? ResMed 10 JAN Global leaders in sleep and respiratory medicine
2011 ISRC Seminar 1 COPD OSA OSA and COPD: What happens when the two OVERLAP? Overlap Syndrome 1 OSA and COPD: What happens when the two OVERLAP? ResMed 10 JAN Global leaders in sleep and respiratory medicine
Combination Therapy. Albert Einstein 8/28/2018. Conflict of Interest Disclosure. Grant/Research Support
 Combination Therapy Conflict of Interest Disclosure 1. I do not have any potential conflicts of interest to disclose, OR 2. I wish to disclose the following potential conflicts of interest: Type of Potential
Combination Therapy Conflict of Interest Disclosure 1. I do not have any potential conflicts of interest to disclose, OR 2. I wish to disclose the following potential conflicts of interest: Type of Potential
Patient Adult Information History
 Patient Adult Information History Patient name: Age: Date: What is the main reason for today s evaluation? Infant History Birth delivery: Normal C-section Delayed Epidural Premature: No Yes If yes, how
Patient Adult Information History Patient name: Age: Date: What is the main reason for today s evaluation? Infant History Birth delivery: Normal C-section Delayed Epidural Premature: No Yes If yes, how
SLEEP SCREENING QUESTIONNAIRE
 SLEEP SCREENING QUESTIONNAIRE Please answer each question accurately and to the best of your knowledge, to help us obtain an accurate picture of your health and sleep issues, only this way will we be able
SLEEP SCREENING QUESTIONNAIRE Please answer each question accurately and to the best of your knowledge, to help us obtain an accurate picture of your health and sleep issues, only this way will we be able
2019 COLLECTION TYPE: MIPS CLINICAL QUALITY MEASURES (CQMS) MEASURE TYPE: Process
 Quality ID #277: Sleep Apnea: Severity Assessment at Initial Diagnosis National Quality Strategy Domain: Effective Clinical Care Meaningful Measure Area: Management of Chronic Conditions 2019 COLLECTION
Quality ID #277: Sleep Apnea: Severity Assessment at Initial Diagnosis National Quality Strategy Domain: Effective Clinical Care Meaningful Measure Area: Management of Chronic Conditions 2019 COLLECTION
WHAT YOU NEED TO KNOW ABOUT SLEEP APNEA
 WHAT YOU NEED TO KNOW ABOUT SLEEP APNEA Wayne Driscoll Clinical Education Specialist 2 SLEEP APNEA IN THE NEWS Carrie Fisher died from sleep apnea, other factors, coroner says USA Today NJ Transit engineer
WHAT YOU NEED TO KNOW ABOUT SLEEP APNEA Wayne Driscoll Clinical Education Specialist 2 SLEEP APNEA IN THE NEWS Carrie Fisher died from sleep apnea, other factors, coroner says USA Today NJ Transit engineer
Sleep Apnea Treatment Options, A Year After ASV
 Sleep Apnea Treatment Options, A Year After ASV Nancy Collop, MD, FAASM Emory University Associated Professional Sleep Societies, LLC 1 Conflict of Interest Disclosures for Speakers x 1. I do not have
Sleep Apnea Treatment Options, A Year After ASV Nancy Collop, MD, FAASM Emory University Associated Professional Sleep Societies, LLC 1 Conflict of Interest Disclosures for Speakers x 1. I do not have
