Robotic Surgery for Obstructive Sleep Apnea
|
|
|
- Easter Skinner
- 5 years ago
- Views:
Transcription
1 Curr Otorhinolaryngol Rep (2013) 1: DOI /s ROBOTIC SURGERY IN OTORHINOLARYNGOLOGY (MC SINGER & DJ TERRIS, SECTION EDITORS) Robotic Surgery for Obstructive Sleep Apnea Claudio Vicini Filippo Montevecchi J. Scott Magnuson Published online: 19 June 2013 Ó Springer Science+Business Media New York 2013 Abstract Nocturnal upper airway collapse often involves obstruction at the level of the tongue base. A number of surgical procedures have been developed in recent years to address this area in patients non-compliant with CPAP therapy. This paper outlines a novel way to treat obstructive sleep apnea related to lingual obstruction, utilizing the da Vinci Ò robotic surgical system. This technique offers significant potential advantages over other established approaches, and should be included in the surgical armamentarium of sleep surgeons. tongue. These include hyolingual advancement, tongue suture suspension, and various lingual resection techniques [1 6]. Typically, conventional tongue base resection is performed either via a transcervical approach or transorally with the aid of an endoscope for visualization [7 9]. These approaches each has significant potential limitations. The open techniques are technically difficult and morbid, and the transoral endoscopic approaches are hampered by relatively poor exposure and limited, non-articulated instrumentation. Keywords medicine TORS Apnea Tongue base Sleep Definitions Introduction Nocturnal upper airway collapse often involves obstruction at the level of the tongue base. In patients with obstructive sleep apnea (OSA) who are non-compliant with CPAP therapy a number of surgical procedures have been developed in recent years to address the area of the base of C. Vicini F. Montevecchi Otolaryngology-Head and Neck and Oral Surgery Unit, Special Surgery Department, Morgagni Pierantoni Hospital, University of Pavia in Forlì, Via Carlo Forlanini, 34, Forlì, Italy claudio@claudiovicini.com F. Montevecchi filo651@hotmail.com J. Scott Magnuson (&) Head and Neck Surgery, Center of Florida, Florida Hospital, Celebration Health, 410 Celebration Place, Suite 305, Celebration, FL 34747, USA scott.magnuson@flhosp.org Collectively, trans oral robotic surgery (TORS) procedures involve the precise excision of oral, pharyngeal and laryngeal tissue with a surgical robot. The robot facilitates these procedures with its articulated instruments and 3-dimension, high definition camera. TORS was pioneered by Weinstein and O Malley at the University of Pennsylvania as a minimally invasive technique for treatment of oropharyngeal cancers [10]. FDA approval for a number of adult head and neck indications was granted in December 2009 [11]. TORS has since become adopted worldwide and is considered by many practitioners to be the most effective and reproducible technique available for upper aerodigestive tract surgery. At face value, the outcomes of TORS appear equivalent to traditional transoral surgeries. However, numerous peer reviewed articles have shown that TORS allows the surgeon to perform procedures that otherwise could be done only through an open approach, but with less morbidity and improved quality of life (Fig. 1). Performing tongue base reduction (TBR) with the TORS approach allows for removal of a part of the base of the
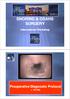
2 Curr Otorhinolaryngol Rep (2013) 1: Surgical procedures that have been performed concurrently with TORS TBR SGP include septal and turbinate surgery, as well as a number of variations of palate surgery, such as traditional uvulopalatopharyngoplasty, expansion sphincteroplasty, and Z-palatoplasty [15, 16]. Concurrent pharyngeal surgery may be carried out conventionally or robotically, according to the surgeon s preference and/or experience. Contraindications Fig. 1 Surgical field after tongue base reduction and before supraglottoplasty tongue from the foramen cecum to the vallecula. Note that in the context of sleep surgery, the term reduction is preferred to resection. TBR can include removal of lingual tonsillar tissue, tongue base musculature, or both. The amount of tissue resected can vary from several ml to more than 50 ml. This is determined by each individual patient s anatomy and degree of prolapse during sleep. Supraglottoplasty (SGP) refers to the adjunctive surgical management of collapsible epiglottic, arytenoid and/or aryepiglottic tissue. The suffix plasty includes a broad range of surgical maneuvers. Again, the specific manipulation utilized is tailored to the presenting pathology. Indications TORS TBR SGP can be used for appropriate cases of clinically significant OSA [12]. Most patients treated with this surgery have polysomnographic evidence of at least moderate to severe OSA (respiratory disturbance index C20) and excessive daytime somnolence (as documented by an Epworth Sleepiness Scale score [10). Ideal candidates for TORS intervention have significant obstruction at the tongue base (with a Cormack and Lehane grade of [2) and/or prolapse of adjacent supraglottic tissue. This is best determined by awake supine endoscopic exam or by druginduced sleep endoscopy (DISE). TORS tongue base surgery can be offered as a primary procedure to patients non-compliant with CPAP or as a secondary procedure after previous surgery failed to resolve the OSA. As per the surgeon s judgment associated nasal obstruction and excessive palate and tonsil tissue may be treated concurrent with TORS surgery. However, it has been reported that simultaneous multilevel surgery can increase the potential for postoperative morbidity [14]. There are several important contraindications to TORS TBR SGP. Surgery should not be offered to patients who are successfully treated with non-operative management. It is well accepted that OSA surgery should not be offered to patients who are tolerant of and compliant with CPAP therapy [13]. Other contraindications include comorbidities that result in an ASA score[2 or which would suggest that sleep surgery not be performed, such as significant or unstable cardiovascular disease, a history of a cerebrovascular accident, progressive neuromuscular disease, need for anticoagulation, or significant psychological instability. As with any surgery, adequate exposure is crucial. For TORS, surgeons must verify that a potential patient s anatomy will allow for sufficient exposure intraoperatively. Signs of potentially difficult exposure include significant retrognathia, an inability to hyperextend the neck, an interincisive distance \2.5 cm, and trismus. Significant micrognathia and macroglossia (with high modified Mallampati Friedman scores) can limit exposure for TORS, though we have operated on many such patients successfully. Preoperative Work-Up The preoperative workup is the same as what has been described for OSA surgery in general, including a polysomnographic evaluation, thorough sleep history, assessment of general medical health, and a comprehensive upper airway examination with awake fiberoptic endoscopy. In addition to the general ENT exam, this assessment should include notation of body mass index, neck circumference, tonsil size (grade 0 IV), modified Mallampati-Friedman Scoring (I IV), and Cormack and Lehane Scoring. Documentation of somnolence and sleep quality can include notation of the Epworth Sleepiness Scale score and results of any of the standardized subjective quality of life questionnaires (SF36, Stanford Sleepiness Scale, Beck Depression Index, etc.). Radiographic imaging is not essential, but when indicated can include panoramic radiography and lateral cephalometry, computerized tomography, and magnetic resonance imaging [17]. Though not
3 132 Curr Otorhinolaryngol Rep (2013) 1: routinely utilized by most surgeons before OSA surgery, neck CT or MRI can help in select cases to better define the pattern of soft tissue collapse and the relative mass of the obstructive lingual tissue. Imaging can also assist by demonstrating if tissue is primarily lymphatic (lingual tonsillar tissue), muscular, or both. In addition, druginduced fiberoptic sleep endoscopy (DISE) has been found to be a helpful determinant in site of obstruction determination [18, 19, 20, 21]. Though DISE is not yet a routine part of the preoperative evaluation of OSA patients in the US, there is a long track record of this procedure in Europe, and its adoption in the US appears to be growing. Anesthesia TORS TBR SGP is performed under general anesthesia [22]. The anesthesia and surgical team must be prepared for a difficult intubation, which could require the use of specialized instrumentation, such as a fiberoptic endoscope, GlideScope, or light wand. An extended anesthesia respiratory circuit is necessary, as the anesthesiologist is stationed at the foot of the bed. This allows for the surgical assistant to sit at the head of the bed without interference and allows for proper positioning of the robotic carts. They are placed along the sides of the patient s head as described for other TORS procedures. In Europe it is more customary to perform a tracheostomy immediately after intubation for lingual TORS surgery [23, 24]. This is not routinely advocated in the US and the surgery is done after either orotracheal or nasotracheal intubation with a small caliber endotracheal tube. Intravenous steroids are given to minimize lingual edema and for nausea prevention and intravenous broad-spectrum antibiotics are infused preoperatively per hospital protocol or surgeon preference. Instrumentation This surgery is performed with the da Vinci Ò Surgical System (Intuitive Surgical, Sunnyvale, CA). TORS requires either the S HD or the Si da Vinci Ò models; the Standard (or S) system is not sufficient for these procedures. This robotic equipment includes: High definition camera. A 0 and 30 camera is available with the robotic system. Both the 12 and the 8 mm diameter scope have excellent optics and allow for adequate working space in the mouth. They provide magnification up to 109, resulting in a clear 3D image, with easy identification of vessels and nerves. Two 5 mm articulated Endo Wrist Ò instrument arms, one placed on either side of the camera. A grasper is placed on one arm usually a 5 mm Maryland forceps is used and a spatula tip monopolar cautery in the other arm. A compatible laser fiber can be used in lieu of the cautery and is preferred by some surgeons. Though TORS surgery does not require much additional equipment beyond the robotic tools listed above, there are several other important instruments, which should be readily available on the operating room back table. It is best to have all of these instruments open and readily accessible. These include: Mouth gags: Two commonly used mouth gags include the Davis Meyer Ò gag (Karl Storz America) and the Feyh Kastenbauer Weinstein O Malley retractor (Gyrus ACMI, Germany). The Davis Meyer system includes multiple tongue blades of different lengths, each with integrated suction tubes for smoke evacuation, and is usually sufficient for the procedure. A small sized blade is usually best, especially in the initial TBR dissection. The FKWO gag has integrated adjustable cheek retractors but no suction ports on its various sized tongue blades; this retractor is sometimes superior to the Davis Meyer system for the SGP portion of the surgery. Headlight: A headlight is used when placing the mouth gag to assure adequate exposure. The robotic monopolar cautery is usually sufficient for hemostasis, although a vessel clip applier and an insulated bipolar forceps should be readily available. A tonsillectomy type suction cautery device is also sometimes needed. The bedside assistant may use a small diameter Yankauer suction device to suction blood and smoke from the surgical field. The suction device may also be used as a retractor. A few appropriate length forceps, hemostats, scissors, and other basic soft tissue instruments are occasionally needed. Surgical Team The bedside TORS team is composed of: The primary surgeon is seated at the robotic console. This console is situated in close proximity to the OR table, usually off to one side but within view of the operative site. The assistant (which may be a second surgeon) is seated at the head of the patient. The assistant retracts tissue, evacuates blood and smoke, adjusts the robotic arms
4 Curr Otorhinolaryngol Rep (2013) 1: and camera as needed to avoid robotic arm collisions, and assists with hemostasis via bipolar electrocoagulation or with use of vessel clips. An integrated microphone-loudspeaker system is built into the robotic system to improve communication between the primary surgeon and assistant. A surgical scrub technician, who aids in passing instruments and providing equipment is needed. of the tongue blade and amount of tongue retraction is adjusted so that the distal end of the blade ends just rostral to the superior limit of the planned resection in the midline (usually around the foramen cecum). It is not unusual at this point for the epiglottis to be obscured by the tongue base. If this is the case, it will come into view as the tongue reduction progresses. The robot is docked as per normal TORS protocol. Lingual Tonsillectomy Surgical Steps Tongue Base Reduction (TBR) TBR is based on the principles of TORS tongue base resection described in 2006 by O Malley et al. [25 ], and enlarges the anteroposterior airway dimension at the level of the tongue base. This reduction usually extends rostrally from the foramen cecum level to the vallecula; the SGP extension of the procedure can include vallecular mucosa and/or part of the epiglottis as necessary. The lateral oropharyngeal dimensions are not augmented with this surgery, and are better addressed by tonsillectomy with one of the variations of UPPP or lateral pharyngoplasty. As there can be considerable variation in anatomy between patients, the goal is not to remove a predetermined volume of tongue base but to improve the Cormack and Lehane grade from III or IV to at grade II or better [26]. Though it is safest to limit the tissue resection to the superficial layer of lingual lymphoid tissue, most cases require extension of the dissection into the lingual musculature. This deeper dissection can lead to exposure of the lingual artery and its dorsal branches, the hypoglossal nerve, and the lingual nerve. Though the volume of excised tissue is generally in the ml range, this can vary from as little as 7 ml to as much as 50 ml. The procedure is divided into several standardized steps, outlined below, and usually takes about 30 min to complete [27, 28, 29]. Exposure The intubated patient is placed supine, the neck is flexed, and the head is hyperextended and placed in the so-called sniffing position. If a planned tracheotomy is to be performed, it is done at this point. An upper dental arch tooth guard is placed to protect the area from trauma from the robotic camera and instrument arms. The tongue is pulled anteriorly with stay sutures and by using one of the two mouth gags. This maneuver can result in compression of the ventral tongue against the lower incisors. Consequently, consideration should also be given to use of a lower tooth guard to prevent any injury. The tongue base is then exposed with the appropriate mouth gag. The length (a) (b) (c) (d) (e) For the right side of the lingual tonsillectomy the Maryland forceps is placed in the left arm and the spatula tip cautery in the right arm. For the left side the instruments are switched. The 30 endoscope is positioned face up. The camera is set at relatively low magnification and wide-angle view to give a panoramic view of the tongue base at the beginning of the case. As the case progresses the magnification can be raised. The incision begins in the midline from the rostral end of the planned resection to the vallecula. The foramen cecum is a good landmark for the upper extent of this incision, as it is distal to the circumvallate papillae and is in the midline. This incision splits the lingual tonsillar tissue in the midline and extends down to the junction between lymphoid tissue and the underlying muscle. The borders of the right lingual tonsil are identified and marked with cautery to outline the resection margins. This extends superiorly from the sulcus terminalis, laterally from the amygalo-glossal sulcus, and inferiorly to the glosso-epiglottic sulcus. If the lingual tonsillar tissue is bulky enough that these landmarks are not visible, the central tongue base can first be debulked. The target tissue is then resected, with the deep plane at the lympho-muscular junction. This can usually be done in an en bloc fashion with minimal blood loss. The bedside assistant can facilitate this resection by using a suction or retracting device for counter traction of the tissue. The inferior limit of the surgical bed can be recognized by the bluish color of the vallecular mucosa. A number of small vessel branches from the lingual artery will be encountered and usually are taken care of easily with cautery. Larger vessels may be clipped as needed. Visualization of these vessels is improved by increasing the scope magnification. Additional tissue is removed as needed to assure a Cormack and Lehane grade of 2 or better. A minimal overall volume of 7 ml is recommended for alleviating obstruction. This may include muscle, with the following caveats, based on cadaveric dissections [29 31]:
5 134 Curr Otorhinolaryngol Rep (2013) 1: It is usually safe to remove a layer of muscle B10 mm within the entire tongue base. An additional 5 mm thick strip of muscle may generally be safely removed in the tongue base within 5 mm of the midline without encountering the hypoglossal nerves. This additional midline muscle resection should be done carefully and under sufficiently high magnification. It is of paramount importance to use the tongue base midline as the point of reference to minimize the risk to the hypoglossal nerve, lingual artery, and lingual neural branches. Because of inherent anatomic variability and tissue distortion from tongue retraction and mouth gag placement, precise localization of these structures is not possible. Supraglottoplasty (SGP) This optional step is performed at the same operative setting immediately after completion of the TBR. SGP is designed to ameliorate the inward inspiratory collapse of floppy and/or redundant epiglottic, aryepiglottic, and arytenoid mucosa [25, 27, 32]. This can include any or all of the following maneuvers and can usually be performed in 5 min or less: Resection of excessive tissue. Tissue removal to promote scarring and retraction. Use of sutures to increase tissue stability. Sectioning of tissue to release overly short ligaments. The two most common SGP techniques performed are the vertical midline suprahyoid epiglottic split and the horizontal epiglottic transection. Vertical Midline Supra-Hyoid Epiglottic Split The epiglottis is incised in the midline, following the medial glosso-epiglottic fold. This split begins at the epiglottic tip and extends caudally to a level C5 mm cephalad to the vallecula. A sufficient amount of epiglottic height should be left to minimize the chance for aspiration. Horizontal Epiglottic Transection The inferior extent of the midline epiglottic split is extended laterally on both sides. The plane of resection is cephalad to the pharyngo-epiglottic folds to minimize the chance for aspiration and to avoid bleeding from branches of the superior laryngeal vessels. In addition to stabilizing this supraglottic tissue, the secondary intention healing in the vallecula and adjacent areas from this procedure results in anterior advancement of the epiglottis. Caution has to be used to avoid overly aggressive resection of vallecular and epiglottic tissue as this can result in aspiration from fixation of the epiglottis to the tongue base. Case Conclusion and Postoperative Care The wound is inspected carefully to verify adequate hemostasis. Cautery or vessel clips are used as needed for persistent bleeding. A hemostatic agent can be applied to the exposed tissue in a thin layer. Some clinicians feel this may also help with postoperative discomfort. The tongue and airway are inspected for edema. If the patient has not undergone a tracheostomy the patient is assessed for extubation under observation in the OR. Overnight stay with continued intubation can be considered per surgeon s preference if necessary. Consideration should be given to placement of a nasogastric (NG) feeding tube, and some centers routinely use NG tubes for all TORS patients in the immediate postoperative period. This is per the surgeon s preference. Given the OSA, airway edema, and the potential for bleeding, it is advised that initial postoperative observation be undertaken in the appropriate monitored setting. In most institutions this would be the intensive care unit (or equivalent) rather than the typical postoperative hospital ward. Continuous pulse-oximetry is recommended. The patient should have suction available at all times at the bedside. The patient should be watched closely for bleeding, as there is a large area of exposed tissue at the surgical site which must undergo healing by secondary intention. As is the case with all such pharyngeal surgical defects, such as a simple tonsillectomy, the risk of postoperative bleeding has a bimodal distribution, with one peak within hours of surgery and the second approximately 7 10 days after surgery. Postoperative intravenous steroids can help with nausea, airway edema, and pain from the inflammatory response. It is advised to continue oral steroids post-discharge on a tapering dose, as some patients experience a significant crescendo of pain up to a week postoperatively. This is likely due to hyperinflammation or dissolution of the protective fibrinous exudative coating over the surgical site. In addition to steroid use, narcotics are used as needed, with close observation of respiratory rate and level of consciousness. The length of stay can vary considerably depending upon a number of variables and surgeon comfort level. Tracheostomy by itself necessitates a multi-day hospital stay. Other determinants include the presence or absence of other concurrent OSA procedures (UPPP, e.g.), general patient health, pain control, and swallowing ability.
6 Curr Otorhinolaryngol Rep (2013) 1: Table 1 Complications TORS for OSA (unpublished data from 75 consecutive patients) Operative complications Patients are followed closely after discharge. Diet is normalized as healing progresses, and formal therapist directed swallowing therapy is rarely needed (\10 % of cases). Postoperative polysomnography is performed once healing is complete, usually at least 3 6 months afterwards. Complications The largest series of patients to undergo TORS for OSA has been performed by Vicini et al. [28]. The most common operative complications include hypogeusia, transient pharyngeal edema and limited bleeding (Table 1). The pressure from the tongue blade attached to the mouth gag may cause temporary injury to the lingual nerve resulting in numbness that typically resolves in 1 4 weeks. Pharyngeal edema may also occur as a result of the pressure from the tongue blade and heat generated from the monopolar cautery. Both of these complications are directly related to the length of the operation and amount of time the patient is kept in suspension. Patients in suspension for less than 45 min are less likely to develop these complications. Late self limiting bleeding is uncommon and is reported to be 2.5 %. More severe complications (tooth injury, pharyngeal wall penetration, intraoperative bleeding requiring open control of vessels, and death) have not been reported. Results Percentage Transient hypogeusia Intra/post operative transient pharyngeal edema 3.16 Late self limiting bleeding 2.50 Teeth injury 0.0 Pharyngeal wall penetration 0.0 Intraoperative bleeding 0.0 Revision surgery 0.0 Death 0.0 Conversion to open 0.0 The series reported by Vicini et al. showed an improvement from a mean preoperative AHI 36.3 to a postoperative AHI Fifteen of the 20 patients in this series had a postoperative AHI less than 20 and only two patients had an AHI greater than 30. Improvements were also seen in Epworth Sleepiness Scale, lowest oxygen saturation and overall patient satisfaction. All improvements were found to be statistically significant. Conclusion TORS for OSA allows for tongue base resection with several advantages potential advantages over other tongue base resection procedures. This technique appears to be safe and effective. Additional studies, including comparison with other techniques are needed to assess the proper role of TORS in sleep surgery. Compliance with Ethics Guidelines This article does not contain any studies with human or animal subjects performed by any of the authors. Disclosure J. Scott Magnuson is a paid consultant, speaker, and instructor for Intuitive Surgical, Inc. Claudio Vicini and Filippo Montevecchi declare that they have no conflict of interest. References Papers of particular interest, published recently, have been highlighted as: Of importance Of major importance 1. Friedman M, Soans R, Gurpinar B, Lin HC, Joseph N. Evaluation of submucosal minimally invasive lingual excision technique for treatment of obstructive sleep apnea/hypopnea syndrome. Otolaryngol Head Neck Surg. 2008;139(3): Fujita S, Woodson BT, Clark JL, Wittig R. Laser midline glossectomy as a treatment for obstructive sleep apnea. Laryngoscope. 1991;101(8): Maturo SC, Mair EA. Coblation lingual tonsillectomy. Otolaryngol Head Neck Surg. 2006;135(3): Michelson SA. Radiofrequency tissue volume reduction of the tongue. In: Terris DJ, Goode RL, editors. Surgical management of sleep apnoea and snoring. New York: Taylor & Francis; Blumen MB, Coquille F, Rocchicioli C, Mellot F, Chabolle F. Radiofrequency tongue reduction through a cervical approach: a pilot study. Laryngoscope. 2006;116(10): Woodson BT. Innovative technique for lingual tonsillectomy and midline posterior glossectomy for obstructive sleep apnea. Oper Tech Otolaryngol Head Neck Surg. 2007;18: Chabolle F, Wagner I, Blumen MB, et al. Tongue base reduction with hyoepiglottoplasty: a treatment for severe obstructive sleep apnea. Laryngoscope. 1999;109(8): Sorrenti G, Piccin O, Mondini S, Ceroni AR. One-phase management of severe obstructive sleep apnea: tongue base reduction with hyoepiglottoplasty plus uvulopalatopharyngoplasty. Otolaryngol Head Neck Surg. 2006;135(6): Vicini C. Tongue-base reduction with hyoepiglottoplasty (TBRHE di chabolle). In: Vicini C, editor. Chirurgia della roncopatia. 1st ed. Lucca: Eureka; p O Malley BW Jr, Weinstein GS, Snyder W, Hockstein NG. Transoral robotic surgery (TORS) for base of tongue neoplasms. Laryngoscope. 2006;116(8): Weinstein GS, O Malley BW Jr, Magnuson JS, Carroll WR, Olsen KD, Daio L, Moore EJ, Holsinger FC. Transoral robotic surgery: a multicenter study to assess feasibility, safety, and surgical margins. Laryngoscope. 2012;122(8): doi: /lary
7 136 Curr Otorhinolaryngol Rep (2013) 1: Young T, Peppard PE, Gottlieb DJ. Epidemiology of obstructive sleep apnea: a population health perspective. Am J Respir Crit Care Med. 2002;165(9): Giles TL, Lasserson TJ, Smith BH, White J, Wright J, Cates CJ. Continuous positive airways pressure for obstructive sleep apnoea in adults. Cochrane Database Syst Rev. 2006;19(3):CD Sundaram S, Bridgman SA, Lim J, Lasserson TJ. Surgery for obstructive sleep apnoea. Cochrane Database Syst Rev. 2005;19(4):CD Cahali MB, Formigoni GG, Gebrim EM, Miziara ID. Lateral pharyngoplasty versus uvulopalatopharyngoplasty: a clinical, polysomnographic and computed tomography measurement comparison. Sleep. 2004;27(5): Pang KP, Woodson BT. Expansion sphincter pharyngoplasty: a new technique for the treatment of obstructive sleep apnea. Otolaryngol Head Neck Surg. 2007;137(1): Barkdull GC, Kohl CA, Patel M, Davidson TM. Computed tomography imaging of patients with obstructive sleep apnea. Laryngoscope. 2008;118(8): Abdullah VJ, Van Hasselt CA. Video sleep nasoendoscopy. In: Terris DJ, Goode RL, editors. Surgical management of sleep apnoea and snoring. 1st ed. New York: Taylor & Francis; Campanini A, Canzi P, De Vito A, Dallan I, Montevecchi F, Vicini C. Awake versus sleep endoscopy: personal experience in 250 OS- AHS patients. Acta Otorhinolaryngol Ital. 2010;30(2): patients underwent awake and sleep endoscopy. Sleep endoscopy was useful in determining the site of obstruction. 20. Pringle MB, Croft CB. A comparison of sleep nasoendopscopy and Muller manoeuvre. Clin Otolaryngol. 1991;16: Kezirian EJ. Nonresponders to pharyngeal surgery for obstructive sleep apnea: insights from drug-induced sleep endoscopy. Laryngoscope. 2011;121(6): doi: /lary Hillman DR, Loadsman JA, Platt PR, Eastwood PR. Obstructive sleep apnoea and anaesthesia. Sleep Med Rev. 2004;8(6): Campanini A, De Vito A, Frassineti S, Vicini C. Temporary tracheotomy in the surgical treatment of obstructive sleep apnea syndrome: personal experience. Acta Otorhinolaryngol Ital. 2003;23(6): Sun H, Lou W, Wang L, Wu Y. Clinical significance of preoperative tracheotomy in preventing perioperative OSAHS severe complications. Lin Chuang Er Bi Yan Hou Ke Za Zhi. 2005; 19(9): Vicini C, Montevecchi F, Tenti G, Canzi P, Dallan I, Tod H. Huntley. Transoral robotic surgery: tongue base reduction and supraglottoplasty for obstructive sleep apnea. Operative Technique in Otolaryngology. 2012;23(1): TORS (transoral robotic surgery) tongue base reduction technique described for patients with obstructive sleep apnea (OSA). 26. Cormack RS, Lehane J. Difficult tracheal intubation in obstetrics. Anaesthesia. 1984;39: Vicini C, Dallan I, Canzi P, Frassineti S, La Pietra MG, Montevecchi F. Transoral robotic tongue base resection in obstructive sleep apnoea-hypopnoea syndrome: a preliminary report.orl J Otorhinolaryngol Relat Spec. 2010;72(1):22 7. First paper to describe surgical outcomes for patients with OSA who underwent TORS with tongue base reduction. 28. Vicini C, Dallan I, Canzi P, Frassineti S, Nacci A, Seccia V, Panicucci E, Grazia La Pietra M, Montevecchi F, Tschabitscher M. Transoral robotic surgery of the tongue base in obstructive sleep apnea-hypopnea syndrome: anatomic considerations and clinical experience. Head Neck. 2012;34(1): doi: /hed This paper describes the pertinent anatomy of the tongue base from a transoral view for surgeons performing TORS. 29. Vicini C, Montevecchi F, Dallan I, Canzi P, Tenti G. Transoral robotic geniohyoidpexy as an additional step of transoral robotic tongue base reduction and supraglottoplasty: feasibility in a cadaver model. ORL J Otorhinolaryngol Relat Spec. 2011; 73(3): Sequert C, Lestang P, Baglin AC, Wagner I, Ferron JM, Chabolle F. Hypoglossal nerve in its intralingual trajectory: anatomy and clinical implications. Ann Otolaryngol Chir Cervicofac. 1999; 116(4): Lauretano AM, Li KK, Caradonna DS, Khosta RK, Fried MP. Anatomic location of the tongue base neurovascular bundle. Laryngoscope. 1997;107(8): Golz A, Goldenberg D, Westerman ST, Catalfumo FJ, Netzer A, Westerman LM, Joachims HZ. Laser partial epiglottidectomy as a treatment for obstructive sleep apnea and laryngomalacia. Ann Otol Rhinol Laryngol. 2000;109(12):
Trans Oral Robotic Surgery
 Trans Oral Robotic Surgery 1 by Leonardo da Vinci 2 Claudio Vicini, MD Filippo Montevecchi,MD Department of Special Surgery, Otolaryngology - Head & Neck Surgery Division, Oral Surgery Unit ( Head: Prof.
Trans Oral Robotic Surgery 1 by Leonardo da Vinci 2 Claudio Vicini, MD Filippo Montevecchi,MD Department of Special Surgery, Otolaryngology - Head & Neck Surgery Division, Oral Surgery Unit ( Head: Prof.
Otolaryngology -- Head and Neck Surgery
 Otolaryngology -- Head and Neck Surgery http://oto.sagepub.com/ Transoral Robotic Glossectomy for the Treatment of Obstructive Sleep Apnea-Hypopnea Syndrome Michael Friedman, Craig Hamilton, Christian
Otolaryngology -- Head and Neck Surgery http://oto.sagepub.com/ Transoral Robotic Glossectomy for the Treatment of Obstructive Sleep Apnea-Hypopnea Syndrome Michael Friedman, Craig Hamilton, Christian
Comparing Upper Airway Stimulation to Expansion Sphincter Pharyngoplasty: A Single University Experience
 771395AORXXX10.1177/0003489418771395Annals of Otology, Rhinology & LaryngologyHuntley et al research-article2018 Original Article Comparing Upper Airway Stimulation to Expansion Sphincter Pharyngoplasty:
771395AORXXX10.1177/0003489418771395Annals of Otology, Rhinology & LaryngologyHuntley et al research-article2018 Original Article Comparing Upper Airway Stimulation to Expansion Sphincter Pharyngoplasty:
Transoral Robotic Surgery for Treatment of Obstructive Sleep Apnea-Hypopnea Syndrome
 The Laryngoscope VC 2013 The American Laryngological, Rhinological and Otological Society, Inc. Transoral Robotic Surgery for Treatment of Obstructive Sleep Apnea-Hypopnea Syndrome Ho-Sheng Lin, MD; James
The Laryngoscope VC 2013 The American Laryngological, Rhinological and Otological Society, Inc. Transoral Robotic Surgery for Treatment of Obstructive Sleep Apnea-Hypopnea Syndrome Ho-Sheng Lin, MD; James
Hypertrophic lingual tonsils may obstruct the retrolingual
 Otolaryngology Head and Neck Surgery (2006) 134, 328-330 CLINICAL TECHNIQUES AND TECHNOLOGY Lingual Tonsillectomy Using Bipolar Radiofrequency Plasma Excision Sam Robinson, MB, BS, FRACS, Sandra L. Ettema,
Otolaryngology Head and Neck Surgery (2006) 134, 328-330 CLINICAL TECHNIQUES AND TECHNOLOGY Lingual Tonsillectomy Using Bipolar Radiofrequency Plasma Excision Sam Robinson, MB, BS, FRACS, Sandra L. Ettema,
Surgical Treatment of OSA. Han-Soo Bae, MD Monroe Ear Nose and Throat Associates May 5, 2017
 Surgical Treatment of OSA Han-Soo Bae, MD Monroe Ear Nose and Throat Associates May 5, 2017 Disclosure None Treatment of OSA PAP Oral appliance Surgery OSA and Mortality Surgical Treatment of OSA Surgery
Surgical Treatment of OSA Han-Soo Bae, MD Monroe Ear Nose and Throat Associates May 5, 2017 Disclosure None Treatment of OSA PAP Oral appliance Surgery OSA and Mortality Surgical Treatment of OSA Surgery
The surgical plane for lingual tonsillectomy: an anatomic study
 Son et al. Journal of Otolaryngology - Head and Neck Surgery (2016) 45:22 DOI 10.1186/s40463-016-0137-3 ORIGINAL RESEARCH ARTICLE Open Access The surgical plane for lingual tonsillectomy: an anatomic study
Son et al. Journal of Otolaryngology - Head and Neck Surgery (2016) 45:22 DOI 10.1186/s40463-016-0137-3 ORIGINAL RESEARCH ARTICLE Open Access The surgical plane for lingual tonsillectomy: an anatomic study
Robot-assisted, volumetric tongue base reduction and pharyngeal surgery for obstructive sleep apnea
 Operative Techniques in Otolaryngology (2012) 23, 48-55 Robot-assisted, volumetric tongue base reduction and pharyngeal surgery for obstructive sleep apnea Samuel Robinson, FRACS, a Suren Krishnan, OAM,
Operative Techniques in Otolaryngology (2012) 23, 48-55 Robot-assisted, volumetric tongue base reduction and pharyngeal surgery for obstructive sleep apnea Samuel Robinson, FRACS, a Suren Krishnan, OAM,
Does Drug-Induced Sleep Endoscopy Predict Surgical Success in Transoral Robotic Multilevel Surgery in Obstructive Sleep Apnea?
 The Laryngoscope VC 2016 The American Laryngological, Rhinological and Otological Society, Inc. Does Drug-Induced Sleep Endoscopy Predict Surgical Success in Transoral Robotic Multilevel Surgery in Obstructive
The Laryngoscope VC 2016 The American Laryngological, Rhinological and Otological Society, Inc. Does Drug-Induced Sleep Endoscopy Predict Surgical Success in Transoral Robotic Multilevel Surgery in Obstructive
TRANSORAL ROBOTIC SURGERY OF THE TONGUE BASE IN OBSTRUCTIVE SLEEP APNEA-HYPOPNEA SYNDROME: ANATOMIC CONSIDERATIONS AND CLINICAL EXPERIENCE
 ORIGINAL ARTICLE TRANSORAL ROBOTIC SURGERY OF THE TONGUE BASE IN OBSTRUCTIVE SLEEP APNEA-HYPOPNEA SYNDROME: ANATOMIC CONSIDERATIONS AND CLINICAL EXPERIENCE Claudio Vicini, MD, 1 Iacopo Dallan, MD, 2 Pietro
ORIGINAL ARTICLE TRANSORAL ROBOTIC SURGERY OF THE TONGUE BASE IN OBSTRUCTIVE SLEEP APNEA-HYPOPNEA SYNDROME: ANATOMIC CONSIDERATIONS AND CLINICAL EXPERIENCE Claudio Vicini, MD, 1 Iacopo Dallan, MD, 2 Pietro
Updated Friedman Staging System for Obstructive Sleep Apnea
 Updated Friedman Staging System for Obstructive Sleep Apnea Michael Friedman a, b Anna M. Salapatas b Lauren B. Bonzelaar c a Section of Sleep Surgery, Rush University Medical Center, and b Section of
Updated Friedman Staging System for Obstructive Sleep Apnea Michael Friedman a, b Anna M. Salapatas b Lauren B. Bonzelaar c a Section of Sleep Surgery, Rush University Medical Center, and b Section of
Surgical Options for the Successful Treatment of Obstructive Sleep Apnea
 Surgical Options for the Successful Treatment of Obstructive Sleep Apnea Benjamin J. Teitelbaum, MD, FACS Otolaryngology Head and Neck Surgery Saint Agnes Medical Center Fresno, California Terms Apnea
Surgical Options for the Successful Treatment of Obstructive Sleep Apnea Benjamin J. Teitelbaum, MD, FACS Otolaryngology Head and Neck Surgery Saint Agnes Medical Center Fresno, California Terms Apnea
Alexandria Workshop on
 Alexandria Workshop on 1 Snoring & OSA Surgery Course Director: Yassin Bahgat MD Claudio Vicini MD Course Board: Filippo Montevecchi MD Pietro Canzi MD Snoring & Obstructive ti Sleep Apnea The basic information
Alexandria Workshop on 1 Snoring & OSA Surgery Course Director: Yassin Bahgat MD Claudio Vicini MD Course Board: Filippo Montevecchi MD Pietro Canzi MD Snoring & Obstructive ti Sleep Apnea The basic information
Transoral robotic surgery for treatment of obstructive sleep apnea: factors predicting surgical response.
 Laryngoscope. 05 Apr;5(4):03-0. doi: 0.00/lary.4970. Epub 04 Oct 4. Transoral robotic surgery for treatment of obstructive sleep apnea: factors predicting surgical response. Lin HS, Rowley JA, Folbe AJ,
Laryngoscope. 05 Apr;5(4):03-0. doi: 0.00/lary.4970. Epub 04 Oct 4. Transoral robotic surgery for treatment of obstructive sleep apnea: factors predicting surgical response. Lin HS, Rowley JA, Folbe AJ,
Coblation-assisted Lewis and MacKay operation (CobLAMO): new technique for tongue reduction in sleep apnoea surgery
 University of Wollongong Research Online Faculty of Science, Medicine and Health - Papers Faculty of Science, Medicine and Health 2013 Coblation-assisted Lewis and MacKay operation (CobLAMO): new technique
University of Wollongong Research Online Faculty of Science, Medicine and Health - Papers Faculty of Science, Medicine and Health 2013 Coblation-assisted Lewis and MacKay operation (CobLAMO): new technique
Selecting Hypopharyngeal Surgery in OSA
 Selecting Hypopharyngeal Surgery in OSA Disclosures The following personal financial relationships with commercial interests relevant to this presentation: Eric J. Kezirian, MD, MPH Professor Eric.Kezirian@med.usc.edu
Selecting Hypopharyngeal Surgery in OSA Disclosures The following personal financial relationships with commercial interests relevant to this presentation: Eric J. Kezirian, MD, MPH Professor Eric.Kezirian@med.usc.edu
Surgery of the Hypopharynx So Many Choices. Overview 1/10/2018. Disclosures. Why Hypopharyngeal Surgery? AI RDI LSAT. Why hypopharyngeal surgery?
 Surgery of the Hypopharynx So Many Choices Eric J. Kezirian, MD, MPH Professor, Otolaryngology Head & Neck Surgery President, International Surgical Sleep Society Sleep-Doctor.com Eric.Kezirian@med.usc.edu
Surgery of the Hypopharynx So Many Choices Eric J. Kezirian, MD, MPH Professor, Otolaryngology Head & Neck Surgery President, International Surgical Sleep Society Sleep-Doctor.com Eric.Kezirian@med.usc.edu
Neuromuscular Stimulation for Sleep Apnea. Overview 1/24/2013. Disclosures. Midline Glossectomy. Palate + Hypopharyngeal Surgery: BMI
 Neuromuscular Stimulation for Sleep Apnea Disclosures The following personal financial relationships with commercial interests relevant to this presentation: Eric J. Kezirian, MD, MPH Director, Division
Neuromuscular Stimulation for Sleep Apnea Disclosures The following personal financial relationships with commercial interests relevant to this presentation: Eric J. Kezirian, MD, MPH Director, Division
SLEEP APNOEA DR TAN KAH LEONG ALVIN CO-DIRECTOR SLEEP LABORATORY SITE CHIEF SDDC (SLEEP) DEPARTMENT OF OTORHINOLARYNGOLOGY, HEAD & NECK SURGERY
 SLEEP APNOEA DR TAN KAH LEONG ALVIN CO-DIRECTOR SLEEP LABORATORY SITE CHIEF SDDC (SLEEP) DEPARTMENT OF OTORHINOLARYNGOLOGY, HEAD & NECK SURGERY
SLEEP APNOEA DR TAN KAH LEONG ALVIN CO-DIRECTOR SLEEP LABORATORY SITE CHIEF SDDC (SLEEP) DEPARTMENT OF OTORHINOLARYNGOLOGY, HEAD & NECK SURGERY
Soft tissue hypopharyngeal surgery for obstructive sleep apnea syndrome
 Oral Maxillofacial Surg Clin N Am 14 (2002) 371 376 Soft tissue hypopharyngeal surgery for obstructive sleep apnea syndrome B. Tucker Woodson, MD, FACS, ABSM Department of Otolaryngology and Human Communication,
Oral Maxillofacial Surg Clin N Am 14 (2002) 371 376 Soft tissue hypopharyngeal surgery for obstructive sleep apnea syndrome B. Tucker Woodson, MD, FACS, ABSM Department of Otolaryngology and Human Communication,
Goal of Evaluation. Overview. Characterize disorder to guide effective treatment 1/10/2018. Disclosures
 to Identify Sites of Obstruction in Patients with OSA Eric J. Kezirian, MD, MPH Professor, Otolaryngology Head & Neck Surgery President, International Surgical Sleep Society Sleep-Doctor.com Eric.Kezirian@med.usc.edu
to Identify Sites of Obstruction in Patients with OSA Eric J. Kezirian, MD, MPH Professor, Otolaryngology Head & Neck Surgery President, International Surgical Sleep Society Sleep-Doctor.com Eric.Kezirian@med.usc.edu
CHALLENGES IN PEDIATRIC OBSTRUCTIVE SLEEP APNEA. Amy S. Whigham, MD Assistant Professor
 CHALLENGES IN PEDIATRIC OBSTRUCTIVE SLEEP APNEA Amy S. Whigham, MD Assistant Professor Disclosures I have nothing to disclose. Outline Epidemiology Diagnosis Adenotonsillectomy Failure Treatment of Refractory
CHALLENGES IN PEDIATRIC OBSTRUCTIVE SLEEP APNEA Amy S. Whigham, MD Assistant Professor Disclosures I have nothing to disclose. Outline Epidemiology Diagnosis Adenotonsillectomy Failure Treatment of Refractory
11/19/2012 ก! " Varies 5-86% in men 2-57% in women. Thailand 26.4% (Neruntarut et al, Sleep Breath (2011) 15: )
 Snoring ก Respiratory sound generated in the upper airway during sleep that typically occurs during inspiration but may occur during expiration ICSD-2, 2005..... ก ก! Prevalence of snoring Varies 5-86%
Snoring ก Respiratory sound generated in the upper airway during sleep that typically occurs during inspiration but may occur during expiration ICSD-2, 2005..... ก ก! Prevalence of snoring Varies 5-86%
Snoring and Obstructive Sleep Apnea: Patient s Guide to Minimally Invasive Treatments Chapter 6
 Snoring and Obstructive Sleep Apnea: Patient s Guide to Minimally Invasive Treatments Chapter 6 MINIMALLY INVASIVE TREATMENTS OF SNORING AND SLEEP APNEA OVERVIEW The past decade has seen the rise of effective,
Snoring and Obstructive Sleep Apnea: Patient s Guide to Minimally Invasive Treatments Chapter 6 MINIMALLY INVASIVE TREATMENTS OF SNORING AND SLEEP APNEA OVERVIEW The past decade has seen the rise of effective,
Transoral robotic total laryngectomy: Report of 3 cases
 CASE REPORT Amy Chen, MD, Section Editor Transoral robotic total laryngectomy: Report of 3 cases Samuel Dowthwaite, MBBS, 1 Anthony C Nichols, MD, 1 John Yoo, MD, 1 Richard V. Smith, MD, 2 Sandeep Dhaliwal,
CASE REPORT Amy Chen, MD, Section Editor Transoral robotic total laryngectomy: Report of 3 cases Samuel Dowthwaite, MBBS, 1 Anthony C Nichols, MD, 1 John Yoo, MD, 1 Richard V. Smith, MD, 2 Sandeep Dhaliwal,
Obstructive Sleep Apnea- Hypopnea Syndrome and Snoring: Surgical Options
 Obstructive Sleep Apnea- Hypopnea Syndrome and Snoring: Surgical Options Joshua L. Kessler, MD, FACS Boston ENT Associates Clinical Instructor, Otology and Laryngology Harvard Medical School Why Consider
Obstructive Sleep Apnea- Hypopnea Syndrome and Snoring: Surgical Options Joshua L. Kessler, MD, FACS Boston ENT Associates Clinical Instructor, Otology and Laryngology Harvard Medical School Why Consider
OBSTRUCTIVE SLEEP APNEA and WORK Treatment Update
 OBSTRUCTIVE SLEEP APNEA and WORK Treatment Update David Claman, MD Professor of Medicine Director, UCSF Sleep Disorders Center 415-885-7886 Disclosures: None Chronic Sleep Deprivation (0 v 4 v 6 v 8 hrs)
OBSTRUCTIVE SLEEP APNEA and WORK Treatment Update David Claman, MD Professor of Medicine Director, UCSF Sleep Disorders Center 415-885-7886 Disclosures: None Chronic Sleep Deprivation (0 v 4 v 6 v 8 hrs)
Roles of Surgery in OSA MASM Annual Fall Conference 2017 October 14, 2017 Kathleen Yaremchuk, MD, MSA Chair, Department of Otolaryngology/Head and
 Roles of Surgery in OSA MASM Annual Fall Conference 2017 October 14, 2017 Kathleen Yaremchuk, MD, MSA Chair, Department of Otolaryngology/Head and Neck Surgery Senior Staff Sleep Medicine Henry Ford Hospital
Roles of Surgery in OSA MASM Annual Fall Conference 2017 October 14, 2017 Kathleen Yaremchuk, MD, MSA Chair, Department of Otolaryngology/Head and Neck Surgery Senior Staff Sleep Medicine Henry Ford Hospital
Pediatric Obstructive Sleep apnea An update What else is there to know?
 Pediatric Obstructive Sleep apnea An update What else is there to know? Garani S. Nadaraja, MD, FAAP Medical Director BCH-Oakland Clinical Assistant Professor Division of Pediatric Otolaryngology UCSF
Pediatric Obstructive Sleep apnea An update What else is there to know? Garani S. Nadaraja, MD, FAAP Medical Director BCH-Oakland Clinical Assistant Professor Division of Pediatric Otolaryngology UCSF
Transsubmental tongue-base suspension in treating patients with severe obstructive sleep apnoea after failed uvulopalatopharyngoplasty:
 CORRESPONDENCE: OUR EXPERIENCE Transsubmental tongue-base suspension in treating patients with severe obstructive sleep apnoea after failed uvulopalatopharyngoplasty: Our Experience Huang, T.-W.,* Su,
CORRESPONDENCE: OUR EXPERIENCE Transsubmental tongue-base suspension in treating patients with severe obstructive sleep apnoea after failed uvulopalatopharyngoplasty: Our Experience Huang, T.-W.,* Su,
Overview. Goal of Evaluation. DISE: Identifying the Sites of Obstruction in OSA. Characterize disorder to guide effective treatment.
 DISE: Identifying the Sites of Obstruction in OSA Eric J. Kezirian, MD, MPH Director, Division of Sleep Surgery Otolaryngology Head and Neck Surgery University of California, San Francisco ekezirian@ohns.ucsf.edu
DISE: Identifying the Sites of Obstruction in OSA Eric J. Kezirian, MD, MPH Director, Division of Sleep Surgery Otolaryngology Head and Neck Surgery University of California, San Francisco ekezirian@ohns.ucsf.edu
Obstructive sleep apnea (OSA) is a common disorder
 Original Research Sleep Medicine and Surgery Drug-Induced Sedation Endoscopy in the Evaluation of OSA Patients with Incomplete Oral Appliance Therapy Response Otolaryngology Head and Neck Surgery 2015,
Original Research Sleep Medicine and Surgery Drug-Induced Sedation Endoscopy in the Evaluation of OSA Patients with Incomplete Oral Appliance Therapy Response Otolaryngology Head and Neck Surgery 2015,
Corporate Medical Policy
 Corporate Medical Policy PALATOPHARYNGOPLASTY/UVULOPALATOPHARYGOPLASTY Description of Procedure or Service Palatopharyngoplasty refers to several surgical approaches for management of the upper airway,
Corporate Medical Policy PALATOPHARYNGOPLASTY/UVULOPALATOPHARYGOPLASTY Description of Procedure or Service Palatopharyngoplasty refers to several surgical approaches for management of the upper airway,
Hyoid Bone Suspension as a Part of Multilevel Surgery for Obstructive Sleep Apnea Syndrome
 266 Original Research THIEME Hyoid Bone Suspension as a Part of Multilevel Surgery for Obstructive Sleep Apnea Syndrome Abd Alzaher Tantawy 1 Sherif Mohammad Askar 1 Hazem Saeed Amer 1 Ali Awad 1 Mohammad
266 Original Research THIEME Hyoid Bone Suspension as a Part of Multilevel Surgery for Obstructive Sleep Apnea Syndrome Abd Alzaher Tantawy 1 Sherif Mohammad Askar 1 Hazem Saeed Amer 1 Ali Awad 1 Mohammad
Snoring: What Works?
 Snoring: What Works? Eric J. Kezirian, MD, MPH Director, Division of Sleep Surgery Otolaryngology Head and Neck Surgery University of California, San Francisco ekezirian@ohns.ucsf.edu Sleepsurgery.ucsf.edu
Snoring: What Works? Eric J. Kezirian, MD, MPH Director, Division of Sleep Surgery Otolaryngology Head and Neck Surgery University of California, San Francisco ekezirian@ohns.ucsf.edu Sleepsurgery.ucsf.edu
Contemporary Snoring Management
 Contemporary Snoring Management Eric J. Kezirian, MD, MPH Director, Division of Sleep Surgery Otolaryngology Head and Neck Surgery University of California, San Francisco ekezirian@ohns.ucsf.edu Sleepsurgery.ucsf.edu
Contemporary Snoring Management Eric J. Kezirian, MD, MPH Director, Division of Sleep Surgery Otolaryngology Head and Neck Surgery University of California, San Francisco ekezirian@ohns.ucsf.edu Sleepsurgery.ucsf.edu
Overview 1/20/2014. Disclosures. Update on Hypopharyngeal and Base of Tongue Management in OSA
 Update on Hypopharyngeal and Base of Management in OSA Disclosures The following personal financial relationships with commercial interests relevant to this presentation: Eric J. Kezirian, MD, MPH Professor
Update on Hypopharyngeal and Base of Management in OSA Disclosures The following personal financial relationships with commercial interests relevant to this presentation: Eric J. Kezirian, MD, MPH Professor
SURGERY FOR SNORING AND MILD OBSTRUCTIVE SLEEP APNOEA
 SURGERY FOR SNORING AND MILD OBSTRUCTIVE SLEEP APNOEA INTRODUCTION Snoring with or without excessive daytime somnolence, restless sleep and periods of apnoea are all manifestations of sleep disordered
SURGERY FOR SNORING AND MILD OBSTRUCTIVE SLEEP APNOEA INTRODUCTION Snoring with or without excessive daytime somnolence, restless sleep and periods of apnoea are all manifestations of sleep disordered
Tongue Coblation via the Ventral Approach for Obstructive Sleep Apnea Hypopnea Syndrome Surgery
 The Laryngoscope VC 2012 The American Laryngological, Rhinological and Otological Society, Inc. Tongue Coblation via the Ventral Approach for Obstructive Sleep Apnea Hypopnea Syndrome Surgery Tiening Hou,
The Laryngoscope VC 2012 The American Laryngological, Rhinological and Otological Society, Inc. Tongue Coblation via the Ventral Approach for Obstructive Sleep Apnea Hypopnea Syndrome Surgery Tiening Hou,
Temperature controlled radiofrequency ablation for OSA
 Temperature controlled radiofrequency ablation for OSA Ridhwan Y. Baba, M.B.B.S. *1, V.V.S. Ramesh Metta, M.B.B.S. 1, Arjun Mohan, M.B.B.S. 2, M. Jeffery Mador, M.D. 2 1 Department of Internal Medicine,
Temperature controlled radiofrequency ablation for OSA Ridhwan Y. Baba, M.B.B.S. *1, V.V.S. Ramesh Metta, M.B.B.S. 1, Arjun Mohan, M.B.B.S. 2, M. Jeffery Mador, M.D. 2 1 Department of Internal Medicine,
Unilateral Supraglottoplasty for Severe Laryngomalacia in Children. Nasser A Fageeh, MD, FRCSC, FACS*
 Bahrain Medical Bulletin, Vol. 37, No. 1, March 2015 Unilateral Supraglottoplasty for Severe Laryngomalacia in Children Nasser A Fageeh, MD, FRCSC, FACS* Objective: To study the efficacy of Unilateral
Bahrain Medical Bulletin, Vol. 37, No. 1, March 2015 Unilateral Supraglottoplasty for Severe Laryngomalacia in Children Nasser A Fageeh, MD, FRCSC, FACS* Objective: To study the efficacy of Unilateral
THE PATIENT STRONGLY MOTIVATED TOWARDS THE TREATMENT? & ENT
 SNORING & OSAHS SURGERY International Workshop Preoperative Diagnostic Protocol < 15 min Filippo Montevecchi M.D. Department of Special Surgery Head & Neck Surgery, Oral Surgery Unit (Head: C.Vicini) G.B.
SNORING & OSAHS SURGERY International Workshop Preoperative Diagnostic Protocol < 15 min Filippo Montevecchi M.D. Department of Special Surgery Head & Neck Surgery, Oral Surgery Unit (Head: C.Vicini) G.B.
11/7/2014. Disclosure Dr. Walvekar, I have the following relationship(s) with commercial interests.
 TORS & Supraglottic Laryngectomy Disclosure Dr. Walvekar, I have the following relationship(s) with commercial interests. Hood Laboratories Rec. Royalties Cook Industries Rec. Honoraria Medtronic Rec.
TORS & Supraglottic Laryngectomy Disclosure Dr. Walvekar, I have the following relationship(s) with commercial interests. Hood Laboratories Rec. Royalties Cook Industries Rec. Honoraria Medtronic Rec.
Modified Uvulopalatopharyngoplasty: The Extended Uvulopalatal Flap
 Modified Uvulopalatopharyngoplasty: The Extended Uvulopalatal Flap Hseuh-Yu Li, MD,* Kasey K. Li, MD, DDS, Ning-Hung Chen, MD, and Pa-Chun Wang, MD Objective: To investigate the surgical outcomes of a
Modified Uvulopalatopharyngoplasty: The Extended Uvulopalatal Flap Hseuh-Yu Li, MD,* Kasey K. Li, MD, DDS, Ning-Hung Chen, MD, and Pa-Chun Wang, MD Objective: To investigate the surgical outcomes of a
Copyright (c) 2012 Boston Children's Hospital 1
 SURGICAL MANAGEMENT OF PEDIATRIC OBSTRUCTIVE SLEEP RELATED BREATHING DISORDERS Gi Soo Lee, M.D. Ed.M. Department of Otolaryngology and Communication Enhancement Boston Children s Hospital REPORT OF FINANCIAL
SURGICAL MANAGEMENT OF PEDIATRIC OBSTRUCTIVE SLEEP RELATED BREATHING DISORDERS Gi Soo Lee, M.D. Ed.M. Department of Otolaryngology and Communication Enhancement Boston Children s Hospital REPORT OF FINANCIAL
Tolerance of Positive Airway Pressure following Site-Specific Surgery of Upper Airway
 34 The Open Sleep Journal, 2008, 1, 34-39 Open Access Tolerance of Positive Airway Pressure following Site-Specific Surgery of Upper Airway Ho-Sheng Lin *,#,1,2, Roger Toma #,2, Cara Glavin 2, Mark Toma
34 The Open Sleep Journal, 2008, 1, 34-39 Open Access Tolerance of Positive Airway Pressure following Site-Specific Surgery of Upper Airway Ho-Sheng Lin *,#,1,2, Roger Toma #,2, Cara Glavin 2, Mark Toma
Alexander C Vlantis. Total Laryngectomy 57
 07 Total Laryngectomy Alexander C Vlantis Total Laryngectomy 57 Total Laryngectomy STEP 1 INCISION AND POSITION OF STOMA A superiorly based apron flap incision is marked with the horizontal limb placed
07 Total Laryngectomy Alexander C Vlantis Total Laryngectomy 57 Total Laryngectomy STEP 1 INCISION AND POSITION OF STOMA A superiorly based apron flap incision is marked with the horizontal limb placed
Taste Disturbance Following Tongue Base Resection for OSA
 The Laryngoscope VC 2015 The American Laryngological, Rhinological and Otological Society, Inc. Taste Disturbance Following Tongue Base Resection for OSA Hsin-Ching Lin, MD, FACS; Michelle S. Hwang, BS;
The Laryngoscope VC 2015 The American Laryngological, Rhinological and Otological Society, Inc. Taste Disturbance Following Tongue Base Resection for OSA Hsin-Ching Lin, MD, FACS; Michelle S. Hwang, BS;
safety margin, To leave a functioning i larynx i.e. respiration, phonation & swallowing.
 The aim of the horizontal supra-glottic laryngectomy is: To remove the tumour with good safety margin, To leave a functioning i larynx i.e. respiration, phonation & swallowing. Disadvantages of classical
The aim of the horizontal supra-glottic laryngectomy is: To remove the tumour with good safety margin, To leave a functioning i larynx i.e. respiration, phonation & swallowing. Disadvantages of classical
Evaluation, Management and Long-Term Care of OSA in Adults
 Evaluation, Management and Long-Term Care of OSA in Adults AUGUST 2015 Providing diagnostic tools and therapies that are evidence-based is a key part of a successful sleep practice. This resource outlines
Evaluation, Management and Long-Term Care of OSA in Adults AUGUST 2015 Providing diagnostic tools and therapies that are evidence-based is a key part of a successful sleep practice. This resource outlines
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY
 OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY VERTICAL PARTIAL LARYNGECTOMY Management of small tumours involving the true vocal folds can be contentious. Tumour control is achieved
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY VERTICAL PARTIAL LARYNGECTOMY Management of small tumours involving the true vocal folds can be contentious. Tumour control is achieved
Perioperative Care in OSA Surgery
 Perioperative Care in OSA Surgery Overview Estimate of Major Peri-Op Complications Risk Factors for Airway Complications Peri-Operative Planning Avoidance of Complications Andrew N. Goldberg, MD, MSCE
Perioperative Care in OSA Surgery Overview Estimate of Major Peri-Op Complications Risk Factors for Airway Complications Peri-Operative Planning Avoidance of Complications Andrew N. Goldberg, MD, MSCE
Treating OSA? Don't Forget the Tongue
 From: ENT Today, January 2008 Treating OSA? Don't Forget the Tongue by Pippa Wysong Although otolaryngologic surgeons commonly focus on the palate when treating patients with obstructive sleep apnea (OSA),
From: ENT Today, January 2008 Treating OSA? Don't Forget the Tongue by Pippa Wysong Although otolaryngologic surgeons commonly focus on the palate when treating patients with obstructive sleep apnea (OSA),
RADICAL CYSTECTOMY. Solutions for minimally invasive urologic surgery
 RADICAL CYSTECTOMY Solutions for minimally invasive urologic surgery The da Vinci Surgical System High-definition 3D vision EndoWrist instrumentation Intuitive motion RADICAL CYSTECTOMY Maintains the oncologic
RADICAL CYSTECTOMY Solutions for minimally invasive urologic surgery The da Vinci Surgical System High-definition 3D vision EndoWrist instrumentation Intuitive motion RADICAL CYSTECTOMY Maintains the oncologic
Microsurgical Anatomy of the Terminal Hypoglossal Nerve Relevant for Neurostimulation in Obstructive Sleep Apnea.
 Neuromodulation. 05 Dec;8(8):7-8. doi: 0./ner.347. Epub 05 Sep 6. Microsurgical Anatomy of the Terminal Hypoglossal Nerve Relevant for Neurostimulation in Obstructive Sleep Apnea. Bassiri Gharb B, Tadisina
Neuromodulation. 05 Dec;8(8):7-8. doi: 0./ner.347. Epub 05 Sep 6. Microsurgical Anatomy of the Terminal Hypoglossal Nerve Relevant for Neurostimulation in Obstructive Sleep Apnea. Bassiri Gharb B, Tadisina
Uvulopalatopharyngoplasty with tonsillectomy in the treatment of severe OSAS
 B-ENT, 2009, 5, 245-250 Uvulopalatopharyngoplasty with tonsillectomy in the treatment of severe OSAS S. Gallina*, F. Dispenza**, G. Kulamarva***, A. Ballacchino**** and Riccardo Speciale**** *Dipartimento
B-ENT, 2009, 5, 245-250 Uvulopalatopharyngoplasty with tonsillectomy in the treatment of severe OSAS S. Gallina*, F. Dispenza**, G. Kulamarva***, A. Ballacchino**** and Riccardo Speciale**** *Dipartimento
Association of Palatine Tonsil Size and Obstructive Sleep Apnea in Adults
 The Laryngoscope VC 2017 The American Laryngological, Rhinological and Otological Society, Inc. Association of Palatine Tonsil Size and Obstructive Sleep Apnea in Adults Sebastian M. Jara, MD ; Edward
The Laryngoscope VC 2017 The American Laryngological, Rhinological and Otological Society, Inc. Association of Palatine Tonsil Size and Obstructive Sleep Apnea in Adults Sebastian M. Jara, MD ; Edward
EndoBlade Soft Tissue Release System
 Surgical Technique Endoscopic Gastroc Recession Endoscopic Plantar Fascia Release EndoBlade Soft Tissue Release System Endoscopic Gastroc Recession Arthrex has developed a comprehensive, completely disposable
Surgical Technique Endoscopic Gastroc Recession Endoscopic Plantar Fascia Release EndoBlade Soft Tissue Release System Endoscopic Gastroc Recession Arthrex has developed a comprehensive, completely disposable
Snoring. Forty-five percent of normal adults snore at least occasionally and 25
 Snoring Insight into sleeping disorders and sleep apnea Forty-five percent of normal adults snore at least occasionally and 25 percent are habitual snorers. Problem snoring is more frequent in males and
Snoring Insight into sleeping disorders and sleep apnea Forty-five percent of normal adults snore at least occasionally and 25 percent are habitual snorers. Problem snoring is more frequent in males and
LEVITAN S FIBREOPTIC STYLET: BEYOND BARRIERS. - Our Perspective.
 ISSN: 2250-0359 Volume 3 Issue 4 2013 LEVITAN S FIBREOPTIC STYLET: BEYOND BARRIERS - Our Perspective. Justin Ebenezer Sargunaraj * Dr.Balasubramaniam Thiagarajan * *Stanley Medical College ABSTRACT: This
ISSN: 2250-0359 Volume 3 Issue 4 2013 LEVITAN S FIBREOPTIC STYLET: BEYOND BARRIERS - Our Perspective. Justin Ebenezer Sargunaraj * Dr.Balasubramaniam Thiagarajan * *Stanley Medical College ABSTRACT: This
Airway/Breathing. Chapter 5
 Airway/Breathing Chapter 5 Airway/Breathing Introduction Skillful, rapid assessment and management of airway and ventilation are critical to preventing morbidity and mortality. Airway compromise can occur
Airway/Breathing Chapter 5 Airway/Breathing Introduction Skillful, rapid assessment and management of airway and ventilation are critical to preventing morbidity and mortality. Airway compromise can occur
EndoRelease ENDOSCOPIC CUBITAL TUNNEL RELEASE SYSTEM
 EndoRelease ENDOSCOPIC CUBITAL TUNNEL RELEASE SYSTEM SURGICAL TECHNIQUE Up p e r Ex t r e m i t y So l u t i o n s ENDOSCOPIC CUBITAL TUNNEL RELEASE SYSTEM Description: The EndoRelease Endoscopic Cubital
EndoRelease ENDOSCOPIC CUBITAL TUNNEL RELEASE SYSTEM SURGICAL TECHNIQUE Up p e r Ex t r e m i t y So l u t i o n s ENDOSCOPIC CUBITAL TUNNEL RELEASE SYSTEM Description: The EndoRelease Endoscopic Cubital
Research Article Drug-Induced Sleep Endoscopy Changes the Treatment Concept in Patients with Obstructive Sleep Apnoea
 BioMed Research International Volume 2016, Article ID 6583216, 5 pages http://dx.doi.org/10.1155/2016/6583216 Research Article Drug-Induced Sleep Endoscopy Changes the Treatment Concept in Patients with
BioMed Research International Volume 2016, Article ID 6583216, 5 pages http://dx.doi.org/10.1155/2016/6583216 Research Article Drug-Induced Sleep Endoscopy Changes the Treatment Concept in Patients with
Clinical Study Thirteen Years of Hyoid Suspension Experience in Multilevel OSAHS Surgery: The Short-Term Results of a Bicentric Study
 International Otolaryngology Volume 2013, Article ID 263043, 6 pages http://dx.doi.org/10.1155/2013/263043 Clinical Study Thirteen Years of Hyoid Suspension Experience in Multilevel OSAHS Surgery: The
International Otolaryngology Volume 2013, Article ID 263043, 6 pages http://dx.doi.org/10.1155/2013/263043 Clinical Study Thirteen Years of Hyoid Suspension Experience in Multilevel OSAHS Surgery: The
The Role of Modified Expansion Sphincter Pharyngoplasty in Multilevel Obstructive Sleep Apnea Syndrome Surgery
 432 Original Research THIEME The Role of Modified Expansion Sphincter Pharyngoplasty in Multilevel Obstructive Sleep Apnea Syndrome Surgery Francesco Lorusso 1 Francesco Dispenza 1 Domenico Michele Modica
432 Original Research THIEME The Role of Modified Expansion Sphincter Pharyngoplasty in Multilevel Obstructive Sleep Apnea Syndrome Surgery Francesco Lorusso 1 Francesco Dispenza 1 Domenico Michele Modica
Review Article Sleep Endoscopy in the Evaluation of Pediatric Obstructive Sleep Apnea
 Hindawi Publishing Corporation International Journal of Pediatrics Volume 2012, Article ID 576719, 6 pages doi:10.1155/2012/576719 Review Article Sleep Endoscopy in the Evaluation of Pediatric Obstructive
Hindawi Publishing Corporation International Journal of Pediatrics Volume 2012, Article ID 576719, 6 pages doi:10.1155/2012/576719 Review Article Sleep Endoscopy in the Evaluation of Pediatric Obstructive
Management of OSA. saurabh maji
 Management of OSA saurabh maji INTRODUCTION Obstructive sleep apnea is a major public health problem Prevalence of OSAS in INDIA is 2.4% to 4.96% in men and 1% to 2 % in women In the rest of the world
Management of OSA saurabh maji INTRODUCTION Obstructive sleep apnea is a major public health problem Prevalence of OSAS in INDIA is 2.4% to 4.96% in men and 1% to 2 % in women In the rest of the world
INGUINAL HERNIA REPAIR PROCEDURE GUIDE
 ROOM CONFIGURATION The following figure shows an overhead view of the recommended OR configuration for a da Vinci Inguinal Hernia Repair (Figure 1). NOTE: Configuration of the operating room suite is dependent
ROOM CONFIGURATION The following figure shows an overhead view of the recommended OR configuration for a da Vinci Inguinal Hernia Repair (Figure 1). NOTE: Configuration of the operating room suite is dependent
Pediatric partial cricotracheal resection: A new technique for the posterior cricoid anastomosis
 Otolaryngology Head and Neck Surgery (2006) 135, 318-322 ORIGINAL RESEARCH Pediatric partial cricotracheal resection: A new technique for the posterior cricoid anastomosis Mark E. Boseley, MD, and Christopher
Otolaryngology Head and Neck Surgery (2006) 135, 318-322 ORIGINAL RESEARCH Pediatric partial cricotracheal resection: A new technique for the posterior cricoid anastomosis Mark E. Boseley, MD, and Christopher
Microdebrider. Microdebrider. Mohamed Hesham,MD. The Management of Different Laryngeal Lesions. Dr. Ahmad Yassin 4/11/2013
 Microdebrider In The Management of Different Laryngeal Lesions Mohamed Hesham,MD Dr. Ahmad Yassin Otolaryngology Head&Neck Surgery Alexandria Faculty of Medicine Microdebrider The microdebrider is a powered
Microdebrider In The Management of Different Laryngeal Lesions Mohamed Hesham,MD Dr. Ahmad Yassin Otolaryngology Head&Neck Surgery Alexandria Faculty of Medicine Microdebrider The microdebrider is a powered
The incidence of early post-operative complications following uvulopalatopharyngoplasty: identification of predictive risk factors
 Kandasamy et al. Journal of Otolaryngology - Head and Neck Surgery 2013, 42:15 ORIGINAL RESEARCH ARTICLE Open Access The incidence of early post-operative complications following uvulopalatopharyngoplasty:
Kandasamy et al. Journal of Otolaryngology - Head and Neck Surgery 2013, 42:15 ORIGINAL RESEARCH ARTICLE Open Access The incidence of early post-operative complications following uvulopalatopharyngoplasty:
Effect of two types of mandibular advancement splints on snoring and obstructive sleep apnoea
 European Journal of Orthodontics 20 (1998) 293 297 1998 European Orthodontic Society Effect of two types of mandibular advancement splints on snoring and obstructive sleep apnoea J. Lamont*, D. R. Baldwin**,
European Journal of Orthodontics 20 (1998) 293 297 1998 European Orthodontic Society Effect of two types of mandibular advancement splints on snoring and obstructive sleep apnoea J. Lamont*, D. R. Baldwin**,
Multilevel airway obstruction including rare tongue base mass presenting as severe croup in an infant. Tara Brennan, MD 2,3
 Multilevel airway obstruction including rare tongue base mass presenting as severe croup in an infant Tara Brennan, MD 2,3 Jeffrey C. Rastatter, MD, FAAP 1,2 1 Department of Otolaryngology, Northwestern
Multilevel airway obstruction including rare tongue base mass presenting as severe croup in an infant Tara Brennan, MD 2,3 Jeffrey C. Rastatter, MD, FAAP 1,2 1 Department of Otolaryngology, Northwestern
Proposed GLOSSARY: Different sedative agents: Midazolam (M); Propofol (P) Different degrees of sedation (Minimal, Moderate, Deep) Proposal:
 SNORING & OSAHS SURGERY International Workshop Sleep Endoscopy > 15 min Filippo Montevecchi M.D. Department of Special Surgery Head & Neck Surgery, Oral Surgery Unit (Head: C.Vicini) G.B. Morgagni L.Pierantoni
SNORING & OSAHS SURGERY International Workshop Sleep Endoscopy > 15 min Filippo Montevecchi M.D. Department of Special Surgery Head & Neck Surgery, Oral Surgery Unit (Head: C.Vicini) G.B. Morgagni L.Pierantoni
Laser Cordectomy. Glottic Carcinoma
 Laser Cordectomy in Glottic Carcinoma Department of Otolaryngology gy Head & Neck Surgery Alexandria University Historical Review Endolaryngeal extirpation of vocal cord cancers is a controversial o issue
Laser Cordectomy in Glottic Carcinoma Department of Otolaryngology gy Head & Neck Surgery Alexandria University Historical Review Endolaryngeal extirpation of vocal cord cancers is a controversial o issue
ESP Step by Step:Tips & Trick Cartoon
 Step by Step:Tips & Trick Cartoon 02/05/2012 1 Evolution of Technique Pang & Tucker Woodson STUCK Sorrenti Vicini 02/05/2012 2 1 Tonsillectomy if TS in site, any size Otherwise TS fossa mucosectomy Maximum
Step by Step:Tips & Trick Cartoon 02/05/2012 1 Evolution of Technique Pang & Tucker Woodson STUCK Sorrenti Vicini 02/05/2012 2 1 Tonsillectomy if TS in site, any size Otherwise TS fossa mucosectomy Maximum
Surgical anatomy of the supraglottic larynx using the da Vinci robot
 ORIGINAL ARTICLE Surgical anatomy of the supraglottic larynx using the da Vinci robot Neerav Goyal, MD, MPH, Frederick Yoo, BA, Dhave Setabutr, MD, David Goldenberg, MD * Department of Surgery, Division
ORIGINAL ARTICLE Surgical anatomy of the supraglottic larynx using the da Vinci robot Neerav Goyal, MD, MPH, Frederick Yoo, BA, Dhave Setabutr, MD, David Goldenberg, MD * Department of Surgery, Division
Techniques of local anesthesia in the mandible
 Techniques of local anesthesia in the mandible The technique of choice for anesthesia of the mandible is the block injection and this is attributed to the absence of the advantages which are present in
Techniques of local anesthesia in the mandible The technique of choice for anesthesia of the mandible is the block injection and this is attributed to the absence of the advantages which are present in
Upper Airway Stimulation for Obstructive Sleep Apnea
 Upper Airway Stimulation for Obstructive Sleep Apnea Background, Mechanism and Clinical Data Overview Seth Hollen RPSGT 21 May 2016 1 Conflicts of Interest Therapy Support Specialist, Inspire Medical Systems
Upper Airway Stimulation for Obstructive Sleep Apnea Background, Mechanism and Clinical Data Overview Seth Hollen RPSGT 21 May 2016 1 Conflicts of Interest Therapy Support Specialist, Inspire Medical Systems
Biomedicine and Nursing 2017;3(1)
 Anesthetic concerns in transoral robotic surgery: initial experience of thirty-three cases. Ezgi ERKILIÇ, Elvin KESİMCİ, Halide CEYHAN, Mustafa AKSOY* Atatürk Training and Research Hospital, Anesthesiology
Anesthetic concerns in transoral robotic surgery: initial experience of thirty-three cases. Ezgi ERKILIÇ, Elvin KESİMCİ, Halide CEYHAN, Mustafa AKSOY* Atatürk Training and Research Hospital, Anesthesiology
Anatomy and Physiology. The airways can be divided in to parts namely: The upper airway. The lower airway.
 Airway management Anatomy and Physiology The airways can be divided in to parts namely: The upper airway. The lower airway. Non-instrumental airway management Head Tilt and Chin Lift Jaw Thrust Advanced
Airway management Anatomy and Physiology The airways can be divided in to parts namely: The upper airway. The lower airway. Non-instrumental airway management Head Tilt and Chin Lift Jaw Thrust Advanced
Anesthesia Considerations for Dynamic Upper Airway Evaluation
 Anesthesia Considerations for Dynamic Upper Airway Evaluation Mohamed Mahmoud MD Associate Professor of Anesthesia & Pediatrics Cincinnati Children s Hospital Medical Center Objectives Diagnosis of Sleep
Anesthesia Considerations for Dynamic Upper Airway Evaluation Mohamed Mahmoud MD Associate Professor of Anesthesia & Pediatrics Cincinnati Children s Hospital Medical Center Objectives Diagnosis of Sleep
Nicolette Mosinski MPAS, PA-C
 Nicolette Mosinski MPAS, PA-C 1. Impaired respiratory effort 2. Airway obstruction Observe patient for detection Rate Pattern Depth Accessory muscle use Evidence of injury Noises Silent manifestations
Nicolette Mosinski MPAS, PA-C 1. Impaired respiratory effort 2. Airway obstruction Observe patient for detection Rate Pattern Depth Accessory muscle use Evidence of injury Noises Silent manifestations
Tongue Base Reduction with Radiofrequency Tissue Ablation: Preliminary Results after Two Treatment Sessions
 SLEEP AND BREATHING VOL. 4, NO. 4, 2000 Tongue Base Reduction with Radiofrequency Tissue Ablation: Preliminary Results after Two Treatment Sessions BORIS A. STUCK, M.D., JOACHIM T. MAURER, M.D., and KARL
SLEEP AND BREATHING VOL. 4, NO. 4, 2000 Tongue Base Reduction with Radiofrequency Tissue Ablation: Preliminary Results after Two Treatment Sessions BORIS A. STUCK, M.D., JOACHIM T. MAURER, M.D., and KARL
ORIGINAL ARTICLE. First-Choice Treatment in Mild to Moderate Obstructive Sleep Apnea
 ORIGINAL ARTICLE First-Choice Treatment in Mild to Moderate Obstructive Sleep Apnea Single-Stage, Multilevel, Temperature-Controlled Radiofrequency Tissue Volume Reduction or Nasal Continuous Positive
ORIGINAL ARTICLE First-Choice Treatment in Mild to Moderate Obstructive Sleep Apnea Single-Stage, Multilevel, Temperature-Controlled Radiofrequency Tissue Volume Reduction or Nasal Continuous Positive
Difficult Airway. Department of Anesthesiology University of Colorado Health Sciences Center (prepared by Brenda A. Bucklin, M.D.)
 Difficult Airway Department of Anesthesiology University of Colorado Health Sciences Center (prepared by Brenda A. Bucklin, M.D.) Objectives Definition & incidence of the difficult airway Evaluation of
Difficult Airway Department of Anesthesiology University of Colorado Health Sciences Center (prepared by Brenda A. Bucklin, M.D.) Objectives Definition & incidence of the difficult airway Evaluation of
All bedside percutaneously placed tracheostomies
 Page 1 of 5 Scope: All bedside percutaneously placed tracheostomies Population: All ICU personnel Outcomes: To standardize and outline the steps necessary to safely perform a percutaneous tracheostomy
Page 1 of 5 Scope: All bedside percutaneously placed tracheostomies Population: All ICU personnel Outcomes: To standardize and outline the steps necessary to safely perform a percutaneous tracheostomy
Upper Airway Obstruction
 Upper Airway Obstruction Adriaan Pentz Division of Otorhinolaryngology University of Stellenbosch and Tygerberg Hospital Stridor/Stertor Auditory manifestations of disordered respiratory function ie noisy
Upper Airway Obstruction Adriaan Pentz Division of Otorhinolaryngology University of Stellenbosch and Tygerberg Hospital Stridor/Stertor Auditory manifestations of disordered respiratory function ie noisy
OSAS G. CAMMAROTO 1, F. MONTEVECCHI 2, G. D AGOSTINO 2, E. ZECCARDO 2, C. BELLINI 2, G. MECCARIELLO 2, C. VICINI 2
 ACTA OTORHINOLARYNGOLOGICA ITALICA Epub 207 May 22; doi: 0.4639/0392-00X-32 OSAS Palatal surgery in a transoral robotic setting (TORS): preliminary results of a retrospective comparison between uvulopalatopharyngoplasty
ACTA OTORHINOLARYNGOLOGICA ITALICA Epub 207 May 22; doi: 0.4639/0392-00X-32 OSAS Palatal surgery in a transoral robotic setting (TORS): preliminary results of a retrospective comparison between uvulopalatopharyngoplasty
This pamphlet has been designed as
 This pamphlet has been designed as an educational resource for patients with Obstructive Sleep Apnea (OSA). The successful use of CPAP requires no further intervention; however, not every patient is able,
This pamphlet has been designed as an educational resource for patients with Obstructive Sleep Apnea (OSA). The successful use of CPAP requires no further intervention; however, not every patient is able,
Transoral robotic surgery (TORS): a new tool for high risk tracheostomy decannulation
 ACTA OTORHINOLARYNGOLOGICA ITALICA 2017;37:46-50; doi: 10.14639/0392-100X-1134 Sleep apnoea Transoral robotic surgery (TORS): a new tool for high risk tracheostomy decannulation La chirurgia robotica transorale
ACTA OTORHINOLARYNGOLOGICA ITALICA 2017;37:46-50; doi: 10.14639/0392-100X-1134 Sleep apnoea Transoral robotic surgery (TORS): a new tool for high risk tracheostomy decannulation La chirurgia robotica transorale
(Surgically) Treating OSA in 2012 and Beyond
 (Surgically) Treating OSA in 2012 and Beyond Edward M. Weaver, MD, MPH Seattle VA Medical Center University of Washington Harborview Medical Center Acknowledgments This material is the result of work supported
(Surgically) Treating OSA in 2012 and Beyond Edward M. Weaver, MD, MPH Seattle VA Medical Center University of Washington Harborview Medical Center Acknowledgments This material is the result of work supported
Educational Session: Evaluation and Management of the Difficult Airway
 Educational Session: Evaluation and Management of the Difficult Airway Diane M. Birnbaumer, MD, FACEP 3/24/2010 7:30 AM - 8:30 AM The Difficult Airway What s Up YOUR Sleeve? Diane M. Birnbaumer, M.D.,
Educational Session: Evaluation and Management of the Difficult Airway Diane M. Birnbaumer, MD, FACEP 3/24/2010 7:30 AM - 8:30 AM The Difficult Airway What s Up YOUR Sleeve? Diane M. Birnbaumer, M.D.,
TRACHEOSTOMY. Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion
 TRACHEOSTOMY Definition Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion Indications for tracheostomy 1-upper airway obstruction with stridor, air hunger,
TRACHEOSTOMY Definition Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion Indications for tracheostomy 1-upper airway obstruction with stridor, air hunger,
Organ preservation in laryngeal cancer
 Organ preservation in laryngeal cancer Wojciech Golusiński Department of Head and Neck Surgery The Great Poland Cancer Centre, Poznan, Poland Poznan University of Medical Sciences, Poznan, Poland Silver
Organ preservation in laryngeal cancer Wojciech Golusiński Department of Head and Neck Surgery The Great Poland Cancer Centre, Poznan, Poland Poznan University of Medical Sciences, Poznan, Poland Silver
Outline. Major variables contributing to airway patency/collapse. OSA- Definition
 Outline Alicia Gruber Kalamas, MD Associate Clinical Professor of Anesthesia & Perioperative Care University of California, San Francisco September 2011 Definition Pathophysiology Patient Risk Factors
Outline Alicia Gruber Kalamas, MD Associate Clinical Professor of Anesthesia & Perioperative Care University of California, San Francisco September 2011 Definition Pathophysiology Patient Risk Factors
If you suspect airway problems, get a second opinion before you anaesthetise, not after!
 Assessing the airway It is more important to be aware of the various methods of dealing with difficult laryngoscopy than to expect to be able to accurately identify the rare difficult patients without
Assessing the airway It is more important to be aware of the various methods of dealing with difficult laryngoscopy than to expect to be able to accurately identify the rare difficult patients without
Pediatric obstructive sleep apnea Adenotonsillectomy and beyond (a surgeon s perspective)
 Pediatric obstructive sleep apnea Adenotonsillectomy and beyond (a surgeon s perspective) Tony Kille, MD Associate Professor Pediatric Otolaryngology American Family Children s Hospital Madison, WI Disclosures
Pediatric obstructive sleep apnea Adenotonsillectomy and beyond (a surgeon s perspective) Tony Kille, MD Associate Professor Pediatric Otolaryngology American Family Children s Hospital Madison, WI Disclosures
Oral cavity : consist of two parts: the oral vestibule and the oral cavity proper. Oral vestibule : is slit like space between.
 Oral cavity Oral cavity : consist of two parts: the oral vestibule and the oral cavity proper Oral vestibule : is slit like space between the teeth, buccal gingiva, lips, and cheeks 1 Oral cavity Oral
Oral cavity Oral cavity : consist of two parts: the oral vestibule and the oral cavity proper Oral vestibule : is slit like space between the teeth, buccal gingiva, lips, and cheeks 1 Oral cavity Oral
