Outline 11/13/2009. Yikes! This Kid has a Trach: Intervention. Community Settings
|
|
|
- Franklin Bruce
- 5 years ago
- Views:
Transcription
1 Yikes! This Kid has a Trach: Intervention In Community Settings Outline Pediatric Tracheostomy Anatomy and Physiology of Airway Timing and Indication Physiologic Complications Communication Options Low & High Tech Passy Muir Speaking Valve Evaluation Treatment Strategies Case Studies Identifying Resources Pediatric Airway Anatomy Softer, larger palate Lumen size is smaller Larynx is higher Close approximationof of larynx and tongue More cartilage (softer) 1
2 Timing of Pediatric Tracheostomy 85% are under 1 year of age (Albamonte et al. 1993) Average age 2 3 years old Critical time for development Practice and hear their own vocalizations Indications for Pediatric Tracheostomy Ventilation/pulmonary disorders Pulmonary toilet Neuromuscular disorders Airway obstruction Normal Trachea Image from Airway Atlas by John Sherry II, M.D. 2
3 Grade 3 Subglottic Stenosis Source: Laryngoscope 101: December 1991 Grade 4 complete obstruction Source: Laryngoscope 101: December 1991 Laryngomalacia Image from Airway Atlas by John Sherry II, M.D. 3
4 Tracheal Web Image from the Virtual Children s Hospital Vocal Cord Paralysis Source: American Academy of Otolaryngology Head and Neck Surgery Clinical Complications of Tracheostomy AIRFLOW 4
5 Effects of Tracheostomy on Communication Development Caregiver interaction(aradine, 1983) Voice quality Speech (Kaslon & Stein, 1989, Singer et al., 1989) 61% have articulation error Consonant and vowel errors Excessive use of phonological processes (stridency and liquid deviation, cluster reduction, fronting) Language Tracheostomy and Aspiration Laryngeal Tethering (Butcher 1982; Logeman, 1995) Decreased Sensation in the Oropharynx 2 (Feldman et al., 1966, Nash 1988) Reduced Airway Closure (Sasalo & Isaccson, 1988; Nash, 1988; Logeman, 1995) Reduced Subglottic Air Pressure (Sasaki & Isaacson, 1988, Gross et al, 1994 and 2004) Pediatric Studies Swallow Physiology 91% of 36 trach infants had swallowing disorders; 1/2 attributed to underlying neuro or anatomic deficits (Rosingh and Peek 1999) Higher incidence id of enteral lfeeding (Wilging 2000) Trach effect (Abraham 2000) Toddlers with trach Reduced laryngeal elevation Delayed swallow response penetration 5
6 Decreased Secretion Control and PEEP Removal of filtration & humidification Decreased cough Abraham (2009) All 50 children in study had secretion management issues 98% level of trachea 40% level of larynx 56% oral Communication Options Low Tech Thumbs up/down Eye blink system Squeeze Hand Kick or move leg/foot Any reliable body part movement Dry erase/magic slate Notepad/pen Sign Language Advantages: Readily available Inexpensive Easy to use/access Easy to use/access Disadvantages: limited Low Tech 6
7 Switches Communication Options High Tech Big Mac Switch/Voice Output Switches (toys, computer interface) Vi Voice output devices Computer based devices Dedicated Communication Devices Environmental Controls High Tech Advantages: Greater capability for higher and lower level patients Disadvantages: Expensive Reimbursement issues More complicated Requires greater skill of clinician Evaluation and attainment can be difficult and time consuming 7
8 Passy Muir Valve Restores Airflow to Upper Airway Clinical Benefits Improved swallow Improved voice Improved Secretion Management Abraham (2009) 24/49 children wearing PMV full time secretion management within normal limits in average of 2 weeks. 8
9 Cotreatment Expedites Decannulation and Weaning Restoration of normal physiology Utilization of expiratory muscles Accustomed to more normal breathing pattern Increased PEEP and oxygenation Able to communicate Less WOB, easier to tolerate Pediatric Studies PMV in children Cho Lieu study (1999) Retrospective evaluation 3 days 18 years old (50% under 1 year) Variety of airway pathologies and diverse medical problems 52 of 55 tolerated PMV Youngest children in study average 27 m. to decannulation Greatest period of speech development Every effort should be made to place a speaking valve when feasible 9
10 Passy Muir Valves Team Approach Multi disciplinary Patient Centered Policies and Procedures Psychological aspects General Differences Habilitation Behavioral considerations 10
11 Patient Selection Cognitive status Awake, responsive, attempting to communicate Medically stable Able to tolerate cuff deflation Able to manage secretions Factors Effecting Upper Airway Patency Size of Tracheostomy Tube Presence and Degree of Obstruction Edema Secretions To Assess for Upper Airway Patency Deflate cuff Finger occlude and voice or cough on exhalation Use mirrors, cotton, feathers, whistles or bubbles to assist with the oral exhalation process. 11
12 Placement Guidelines Patient education Patient position Suctioning Achieve complete cuff deflation Use the warning label provided with packaging Oxygenation Vital Signs Breath Sounds Color WOB Patient Responsiveness Baseline Measurements Distress Signs and Symptoms Increased RR, HR Anxiety and fear Restlessness Increased irritability Stridor Grunting (infants) Retractions Nasal flaring Head bobbing Sniffing position Decreased BS during auscultation Decreased chest movement Decreased LOC Decreased PaO2 (SaO2) Increased PaCo2 Paleness or cyanosis Decreased perfusion/mottling Bradycardia/hypotension (this is a late sign) 12
13 Guidelines Approach to Education Higher incidence of airway obstruction Normal baselines Reaction time Transitions may be gradual Children 0 6 months old Evaluation: Infant communication developmental scale Oral motor function and feeding skills Treatment: Parent education Early developmental milestones Non nutritive oral stimulation/ sucking Bottle feeding Double-click to edit Double-click to edit Double-click to edit 13
14 Children 6 24 months old Evaluation: Receptive and expressive language Play and cognition Oral feeding Skills Treatment: Parent education Facilitate oral exhalation Facilitate vocalization Augment with alternative communication systems as necessary Oral feeding PLAY,, PLAYP LAY,, PLAY! Goal 1# Increase Oral Exhalation Techniques Imitation Blowing Bubbles Whistles Horns, Kazoos Pinwheels Straws Cotton balls 14
15 Goal #2 Increase Voicing Activities Planes, trains and automobiles Play dough Rice and beans Animals Books Songs Toby Tracheasuarus Case Study: Rudy History: 28 week preemie H i li d6 h Hospitalized 6 months Rehospitalized 2 3x first year: Pneumonia/trached Tracheomalacia/subglottic stenosis D/C home 12 mo. with PMV and home nursing Referred for speech eval 15
16 Case Study: Rudy Evaluation: Babbling intermittently Does not tolerate PMV Developmental delay LT Goals: Utilize PMV waking hours Age appropriate speech skills Age appropriate language skills Caregiver education for feeding and s/l development Case Study: Rudy ST Goals: Utilize PMV 1 minute during play or eating 4/5 trials Produce /p,b,m/ in syllables during play or babbling 5x session Attempt animal/vehicle sounds 3 5x session Imitate oral movements/mouth play 5 x session Wave or vocalize to greet with 80% freq with min cues Laugh 2 x session Caregiver will verbalize understanding of PMV use Apply PMV before all meds and meals Demonstrate proper care and cleaning Mom s Perspective When he first got the trach, my aunt who is an RN, commented that he would be severely speech delayed once it came out. I was determined that such would not be the case, so we required him to wear a PMV as soon as we got it. He didn't like it, he would fuss when we put it on. But the doctors had said we could use it, and that he could work up to it. So we would put it on for so many minutes at a time & distract the heck out of him while he fussed. I held him at the window, would swing him, etc. It wasn't too long before he wore it all day. He had a home nurse until he was in his 3rd year, but attended church, took family trips out of state, and had a normal life except for water restrictions. His trach came out when he was 4. He wore a bandana for about 6 months while the hole closed, but we still let him play outside and do everything he could. 16
17 Rudy: A Great Outcome! Case Study: Deke History 2 years old 3p deletion syndrome Craniofacial deformities Trach: alternate airway/pulmonary toilet Chronic/long term Severe developmental delay Severe motor impairment G tube Respiratory treatments PM Ventilator Life expectancy: 5 7 years Case Study: Deke Evaluation: Severe/profound motor, cognitive, speech, language impairment Dysphagiadue to severely impaired oral motor skills Non Verbal Tracheostomized/does not tolerate PMV Ventilated at night 17
18 Case Study: Deke Long Term Goals: Tolerate PMV waking hours Oral motor skills adequate for words Use words or augmentative communication devices to express basic wants, needs, feelings and/or ideas Demonstrate understanding of cause/effect to control/interact with environment and play Case Study: Deke Short Term Goals: Utilize PMV for 30 seconds during play 3x per session (increase incrementally as possible) Participate in intensive oral motor program for increased strength, range of motion, and function of lips, cheeks, tongue and jaw 2 3x daily Vocalize while wearing PMV 3x per session Demonstrate reliable body movement to activate switch or AC device 3/5 trials Use AC device or toy to demonstrate cause/effect 5x per session (fan, talking picture frame, Big Mack, etc) Produce /p, b, m/in isolation/syllables during play 5x per session Case Study: Deke Outcome: Move mouth for kisses Laugh/giggle at fan, bubbles, grandma singing on Big Mack or in person Wears PMV waking hours Reduced need for suction/clearer upper airway Vocalizes with PMV: ma for mom and cooing and some babbling during play Activating switches with fist and foot Participating in some outdoor activities (swing, trick or treat in wagon with device) 18
19 Care, Cleaning Passy Muir Valves Allow to air dry Double-click to edit Double-click to edit 19
20 Children 3 years old School Age Evaluation: Receptive and expressive language Oral feeding Skills Treatment: Parent education Coordinate services with school, IEP Elimination of negative behaviors Intensive voice and speech therapy Additional Voice and Speech Goals Improve voice quality Weak Harsh, hyperfunctional Pitch Improve coordination of respiration and speech Improve articulation and phonology Swallowing and Feeding Goals PMV for assessment (clinical & instrumental) PMV for oral feeding Decrease sensitivity (facial/oral stimulation) Tastes Textures Feeding Equipment Positioning 20
21 Double-click to edit Resources Agencies/Individuals: Physician Hospital Based SLP, Nurse, Education Program DME, Home Care Agency Resources Web based Position Statements html html nts/pages/respiratory disease pediatric/childtrach1 12.html 21
22 Resources Web based Tracheostomy/Respiratory General Speaking Valve muir.com/ Trach Care %20Feb% pdf Resources Web based: Children s Hospital of Los Angeles 8D8F/Ventilation_Videos English.htm Cleveland Clinic Children s Hospital tion_guidelines.aspx /tracheostomy_care.aspx Phoenix Children s Hospital center/child healthtopics/tracheostomy.html Cincinnati Children s Hospital cpr.htm Resources Books: Kertoy, M. (2002). Children with Tracheostomies Resource Guide. Ontario, Canada: Singular Publishing Group, Inc. Bleile, K. editor(1993). The Care of Children with Long Term Tracheostomies. San Diego, CA: Singular Publishing Group, Inc. Bissel, C. (2000). Pediatric Tracheostomy Home Care Guide. Grafton, MA: Twin Enterprises, Inc. Dikeman, K.J., and Kazandjian, M. Communication and Swallowing Management of Tracheostomized and Ventilator Dependent Adults. Singular Publishing Group. 22
23 Educational Opportunities WEBINARS or SELF STUDY COURSES Basic Application Ventilator Application Advanced Pediatric Application Swallow and PMV Building a Trach Team Ventilator Basics for the Non RT Pediatric Ventilator Application muir.com ASHA, AARC and California Board of Nursing Credit References: Respiratory Care, April 2005, Vol 50, No 4 Respiratory Care, Sept 2006, Vol 51, No 9 Carron, J. et al. Pediatric tracheostomies: changing indications and outcomes. The Laryngoscope. 2000; 110(7): Lewis, C et al. Tracheostomy in pediatric patients. Archives of Otolaryngoloy yhead and Neck Surgery. 2003; 129: Care of the Child with a Chronic Tracheostomy; The official statement of the American Thoracic Society adopted July Can be located on website. Simon, B. et al. Communication development in young children with long term tracheostomies: preliminary report. International Journal of Pediatric Otorhinolaryngology. 1984; 6: Kertoy, M. et al. Speech and phonological characteristics of individual children with history of tracheostomy. Journal of Speech, Language, and Hearing Research. 1999; 42:
24 References: Abraham, S & Wolf, E. Swallowing physiology of toddlers with longterm tracheostomies: a preliminary study. Dysphagia. 2000; 15: Cho Lieu, J. et al. Passy Muir valve in children with tracheotomy. International Journal of Pediatric Otorhinolaryngology. 1999; 50: Abraham, S. Babies Bbi with ihtracheostomies: The challenge hll of providing specialized clinical care. The ASHA Leader Online. Waldowski, K. Baby Trachs. Advance for SLPs. Volume 12, Issue 26, page 6. Cordle, K. Speaking Valves for Infants. Advance for SLPs... Volume 16, Issue 11, page 9. Hofmann, L. et al. Passy Muir Speaking Valve use in a children hospital: An interdisciplinary approach. Perspectives on Voice and Voice Disorders. 2008; 18: References: Abraham, S. Clinical and Fluoroscopic Issues in the Management of Swallowing Disorders in Infants and Young Children with Tracheostomies. In Dysphagia in the Trach/Vent Population. ASHA Professional Development and Special Interest Division Harvey, G. Treatment of voice disorders in medically complex children. Language, Speech, and Hearing Services in Schools. 1996; 27: Woodnorth, G. Assessing and Managing Medically Fragile Children: Tracheostomy and Ventilatory Support. Language, Speech, and Hearing Services in Schools. 2004; 35: Kaslon WK, Stein RE: Chronic pediatric tracheostomy: Assessment and implications for habilitation of voice, speech and language on young children. Int J Pediatr Otorhinolaryngol 9: , 1985 Hill BP, Singer LT: Speech and language development after infant tracheostomy. J Speech Hearing Dis 55:15 20,
What are the Challenges? Spreading the Word in NICU. Need for NICU Care: Impact. Baby Trachs: Use of the Passy Muir Valve in the NICU to
 What are the Challenges? Baby Trachs: Use of the Passy Muir Valve in the NICU to Optimize Swallowing and Feeding Catherine S Shaker, MS/CCC SLP, BRS S and Cari Mutnick, MS/CCC SLP Florida Hospital for
What are the Challenges? Baby Trachs: Use of the Passy Muir Valve in the NICU to Optimize Swallowing and Feeding Catherine S Shaker, MS/CCC SLP, BRS S and Cari Mutnick, MS/CCC SLP Florida Hospital for
The Role of the Speech Language Pathologist & Spinal Cord Injury
 The Role of the Speech Language Pathologist & Spinal Cord Injury Facts According to the National Spinal Cord Injury Statistical Center (NSCISC) there are approxiamtely 12,000 new spinal cord injuries (SCI)
The Role of the Speech Language Pathologist & Spinal Cord Injury Facts According to the National Spinal Cord Injury Statistical Center (NSCISC) there are approxiamtely 12,000 new spinal cord injuries (SCI)
COMMUNICATION. Communication and Swallowing post Tracheostomy. Role of SLT. Impact of Tracheostomy. Normal Speech. Facilitating Communication
 Communication and Swallowing post Tracheostomy. Role of SLT 1. 2. 3. Management of communication needs. Management of swallowing issues. Working with the multidisciplinary team to facilitate weaning. Impact
Communication and Swallowing post Tracheostomy. Role of SLT 1. 2. 3. Management of communication needs. Management of swallowing issues. Working with the multidisciplinary team to facilitate weaning. Impact
Swallow Function: Passy-Muir Valve Use for Evaluation & Rehabilitation David A. Muir Course Outline Physiology of Swallow
 Swallow Function: Passy-Muir Valve Use for Evaluation & Rehabilitation Mary Spremulli, MA, CCC-SLP Passy-Muir Clinical Consultant spre713@hotmail.com (949) 833-8255 David A. Muir 23 year-old ventilator
Swallow Function: Passy-Muir Valve Use for Evaluation & Rehabilitation Mary Spremulli, MA, CCC-SLP Passy-Muir Clinical Consultant spre713@hotmail.com (949) 833-8255 David A. Muir 23 year-old ventilator
PMV ON OR OFF WITH SWALLOWING DOES IT MAKE A DIFFERENCE?
 PMV ON OR OFF WITH SWALLOWING DOES IT MAKE A DIFFERENCE? 1 Tedd Masiongale, MA, CCC-SLP Lorry Lewis, MS, CCC-SLP REASON FOR STUDY After several years of working with trach and ventilator dependent patients,
PMV ON OR OFF WITH SWALLOWING DOES IT MAKE A DIFFERENCE? 1 Tedd Masiongale, MA, CCC-SLP Lorry Lewis, MS, CCC-SLP REASON FOR STUDY After several years of working with trach and ventilator dependent patients,
Tracheostomy: Procedures, Timing and Tubes
 TRACHEOSTOMY: PROCEDURES, TIMING AND TUBES Gail M. Sudderth RRT Clinical Specialist Passy-Muir Inc. gsudderth@passy-muir.com (949) 833-8255 Objectives Explain how the timing of the tracheotomy and tube
TRACHEOSTOMY: PROCEDURES, TIMING AND TUBES Gail M. Sudderth RRT Clinical Specialist Passy-Muir Inc. gsudderth@passy-muir.com (949) 833-8255 Objectives Explain how the timing of the tracheotomy and tube
Where do we come from?
 Interdisciplinary Decision-Making with Patients Requiring Tracheostomy and Carrie Windhorst MS CCC-SLP Cheryl Wagoner MS CCC-SLP Ricque Harth MEd CCC-SLP Where do we come from? Welcome to Madonna Rehabilitation
Interdisciplinary Decision-Making with Patients Requiring Tracheostomy and Carrie Windhorst MS CCC-SLP Cheryl Wagoner MS CCC-SLP Ricque Harth MEd CCC-SLP Where do we come from? Welcome to Madonna Rehabilitation
PMV 2020 (CLEAR) INSTRUCTION BOOKLET. Touching Lives and Advancing Patient Care Through Education. David A. Muir Inventor of the PMV
 PASSY-MUIR LOW PROFILE TRACHEOSTOMY SWALLOWING AND SPEAKING VALVE PMV 2020 (CLEAR) INSTRUCTION BOOKLET David A. Muir Inventor of the PMV PASSY-MUIR LOW PROFILE TRACHEOSTOMY SWALLOWING AND SPEAKING VALVE
PASSY-MUIR LOW PROFILE TRACHEOSTOMY SWALLOWING AND SPEAKING VALVE PMV 2020 (CLEAR) INSTRUCTION BOOKLET David A. Muir Inventor of the PMV PASSY-MUIR LOW PROFILE TRACHEOSTOMY SWALLOWING AND SPEAKING VALVE
Developing a Speaking Valve Protocol in the NICU 5/17/2012
 Disclosures Developing a Speaking Valve Protocol in the NICU Melanie Stevens, MS-CCC/SLP Jen Finch, MA-CCC/SLP Leslie Justice, RN, MS, CPNP Erin Wishloff, BS/RRT-NPS Melanie Stevens, MS-CCC/SLP Disclosure:
Disclosures Developing a Speaking Valve Protocol in the NICU Melanie Stevens, MS-CCC/SLP Jen Finch, MA-CCC/SLP Leslie Justice, RN, MS, CPNP Erin Wishloff, BS/RRT-NPS Melanie Stevens, MS-CCC/SLP Disclosure:
Tracheostomy and Ventilator Education Program Module 10: Communication Supplies
 Tracheostomy and Ventilator Education Program Module 10: Communication Supplies Disclaimer This material is intended for use by trained family members and caregivers of children with tracheostomies who
Tracheostomy and Ventilator Education Program Module 10: Communication Supplies Disclaimer This material is intended for use by trained family members and caregivers of children with tracheostomies who
Respiratory Compromise and Swallowing
 Speech Pathology and Respiratory Care April 11, 2013 By Angela Parcaro-Tucker, MA, CCC-SLP, LSVT How can Speech Therapy help? 1 Respiratory Compromise and Swallowing Swallowing is a complex sequence of
Speech Pathology and Respiratory Care April 11, 2013 By Angela Parcaro-Tucker, MA, CCC-SLP, LSVT How can Speech Therapy help? 1 Respiratory Compromise and Swallowing Swallowing is a complex sequence of
TRACHEOSTOMY CARE. Tracheostomy- Surgically created hole that extends from the neck skin into the windpipe or trachea.
 1 TRACHEOSTOMY CARE Definitions: Trachea-Windpipe Tracheostomy- Surgically created hole that extends from the neck skin into the windpipe or trachea. Outer Cannula- The outer part of a trach tube. Usually
1 TRACHEOSTOMY CARE Definitions: Trachea-Windpipe Tracheostomy- Surgically created hole that extends from the neck skin into the windpipe or trachea. Outer Cannula- The outer part of a trach tube. Usually
Oral care & swallowing
 Oral care & swallowing Oral care is important as it has a role to play in preventing healthcare associated infections. Dental plaque and the oropharynx can become colonized by bacteria and a biofilm can
Oral care & swallowing Oral care is important as it has a role to play in preventing healthcare associated infections. Dental plaque and the oropharynx can become colonized by bacteria and a biofilm can
1/22/2014. Disclosure. Course Outline. Course Objectives EARLY INTERVENTION IN PERSONS WITH MINIMALLY CONSCIOUS STATE & TRACHEOSTOMY
 Welcome to Passy-Muir s Event Webinar: Pediatric Candidacy for Speaking Valve Use: Journeys to Success If you have not registered for this event, go to the Education Portal to complete your registration.
Welcome to Passy-Muir s Event Webinar: Pediatric Candidacy for Speaking Valve Use: Journeys to Success If you have not registered for this event, go to the Education Portal to complete your registration.
Airway and Ventilation. Emergency Medical Response
 Airway and Ventilation Lesson 14: Airway and Ventilation You Are the Emergency Medical Responder Your medical emergency response team has been called to the fitness center by building security on a report
Airway and Ventilation Lesson 14: Airway and Ventilation You Are the Emergency Medical Responder Your medical emergency response team has been called to the fitness center by building security on a report
Communication & The Mechanically Ventilated Patient. Megan Urban, MA, CCC-SLP Clinical Coordinator, Speech Pathology September 26, 2013
 Communication & The Mechanically Ventilated Patient Megan Urban, MA, CCC-SLP Clinical Coordinator, Speech Pathology September 26, 2013 Why is communication important? We had a young adult patient who sustained
Communication & The Mechanically Ventilated Patient Megan Urban, MA, CCC-SLP Clinical Coordinator, Speech Pathology September 26, 2013 Why is communication important? We had a young adult patient who sustained
Foundations of Critical Care Nursing Course. Tracheostomy Workbook
 Foundations of Critical Care Nursing Course Tracheostomy Workbook 1 Key Reference: Dawson D (2014) Essential principles:trachepstomy care in the adult patient, Nursing in Critical Care, Vol 19, 2 p.63-72.
Foundations of Critical Care Nursing Course Tracheostomy Workbook 1 Key Reference: Dawson D (2014) Essential principles:trachepstomy care in the adult patient, Nursing in Critical Care, Vol 19, 2 p.63-72.
SWALLOW PHYSIOLOGY IN PATIENTS WITH TRACH CUFF INFLATED OR DEFLATED: A RETROSPECTIVE STUDY
 SWALLOW PHYSIOLOGY IN PATIENTS WITH TRACH CUFF INFLATED OR DEFLATED: A RETROSPECTIVE STUDY Ruiying Ding, PhD, 1 Jeri A. Logemann, PhD 2 1 University of Wisconsin-Whitewater, Department of Communicative
SWALLOW PHYSIOLOGY IN PATIENTS WITH TRACH CUFF INFLATED OR DEFLATED: A RETROSPECTIVE STUDY Ruiying Ding, PhD, 1 Jeri A. Logemann, PhD 2 1 University of Wisconsin-Whitewater, Department of Communicative
Passy-MuirInc. Passy-Muir Tracheostomy and. Ventilator Speaking Valve. Resource Guide. Passy-Muir Tracheostomy and Ventilator Speaking Valves
 Passy-Muir Tracheostomy and Ventilator Speaking Valve Resource Guide Touching Lives and Advancing Patient Care Through Education Passy-MuirInc. Passy-Muir Tracheostomy and Ventilator Speaking Valves TABLE
Passy-Muir Tracheostomy and Ventilator Speaking Valve Resource Guide Touching Lives and Advancing Patient Care Through Education Passy-MuirInc. Passy-Muir Tracheostomy and Ventilator Speaking Valves TABLE
Tracheostomy in pediatric. Tran Quoc Huy, MD ENT department
 Tracheostomy in pediatric Tran Quoc Huy, MD ENT department 1. History 2. Indication 3. Tracheostomy vs Tracheal intubation 4. A systematic review 5. Decannulation 6. Swallowing 7. Communication concerns
Tracheostomy in pediatric Tran Quoc Huy, MD ENT department 1. History 2. Indication 3. Tracheostomy vs Tracheal intubation 4. A systematic review 5. Decannulation 6. Swallowing 7. Communication concerns
*gurgle* *snore* *slaver* Tracheostomy Emergencies with Trachy Tracey Helen Lyall ACCP LUHT 03/06/2016
 *gurgle* *snore* *slaver* Tracheostomy Emergencies with Trachy Tracey Helen Lyall ACCP LUHT 03/06/2016 Learning objectives Describe the difference in anatomy between a tracheotomy and a laryngectomy Understand
*gurgle* *snore* *slaver* Tracheostomy Emergencies with Trachy Tracey Helen Lyall ACCP LUHT 03/06/2016 Learning objectives Describe the difference in anatomy between a tracheotomy and a laryngectomy Understand
Pediatric Issue. Official Publication of Passy Muir
 Passy-Muir, Inc. FALL 2017 Volume 1, Issue 1 Pediatric Issue Official Publication of Passy Muir Welcome to Aerodigestive Health: Addressing Use of the Passy Muir Tracheostomy and Ventilator Swallowing
Passy-Muir, Inc. FALL 2017 Volume 1, Issue 1 Pediatric Issue Official Publication of Passy Muir Welcome to Aerodigestive Health: Addressing Use of the Passy Muir Tracheostomy and Ventilator Swallowing
Welcome to the Specialized Medical Services respiratory training webinar series!
 Welcome to the Specialized Medical Services respiratory training webinar series! SMS is your LTC facility single source for oxygen, medical equipment, respiratory care services and supplies nationwide.
Welcome to the Specialized Medical Services respiratory training webinar series! SMS is your LTC facility single source for oxygen, medical equipment, respiratory care services and supplies nationwide.
Tracheostomy and Ventilator Education Program Module 2: Respiratory Anatomy
 Tracheostomy and Ventilator Education Program Module 2: Respiratory Anatomy Disclaimer This material is intended for use by trained family members and caregivers of children with tracheostomies who are
Tracheostomy and Ventilator Education Program Module 2: Respiratory Anatomy Disclaimer This material is intended for use by trained family members and caregivers of children with tracheostomies who are
Upper Airway Obstruction
 Upper Airway Obstruction Adriaan Pentz Division of Otorhinolaryngology University of Stellenbosch and Tygerberg Hospital Stridor/Stertor Auditory manifestations of disordered respiratory function ie noisy
Upper Airway Obstruction Adriaan Pentz Division of Otorhinolaryngology University of Stellenbosch and Tygerberg Hospital Stridor/Stertor Auditory manifestations of disordered respiratory function ie noisy
October Paediatric Respiratory Workbook APCP RESPIRATORY COMMITTEE
 October 2017 Paediatric Respiratory Workbook APCP RESPIRATORY COMMITTEE This workbook is designed to introduce to you the difference between paediatric and adult anatomy and physiology. It will also give
October 2017 Paediatric Respiratory Workbook APCP RESPIRATORY COMMITTEE This workbook is designed to introduce to you the difference between paediatric and adult anatomy and physiology. It will also give
10/4/2010. Case Presentations. Children s Hospital Los Angeles
 Swallowing Series Case Presentations Children s Hospital Los Angeles Los Angeles, CA 1 Patient History 3 years 8 months of age Severe pulmonary hypoplasia secondaryto congenital diaphragmatic hernia (CDH)
Swallowing Series Case Presentations Children s Hospital Los Angeles Los Angeles, CA 1 Patient History 3 years 8 months of age Severe pulmonary hypoplasia secondaryto congenital diaphragmatic hernia (CDH)
Competency 1: General principles and equipment required to safely manage a patient with a tracheostomy tube.
 Competency 1: General principles and equipment required to safely manage a patient with a tracheostomy tube. Trainee Name: ------------------------------------------------------------- Title: ---------------------------------------------------------------
Competency 1: General principles and equipment required to safely manage a patient with a tracheostomy tube. Trainee Name: ------------------------------------------------------------- Title: ---------------------------------------------------------------
Tracheostomy. Hope Building Neurosurgery
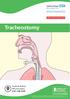 Tracheostomy Hope Building Neurosurgery 0161 206 5055 All Rights Reserved 2017. Document for issue as handout. Unique Identifier: CS36(17). Review date: November 2019 What is a tracheostomy? A tracheostomy
Tracheostomy Hope Building Neurosurgery 0161 206 5055 All Rights Reserved 2017. Document for issue as handout. Unique Identifier: CS36(17). Review date: November 2019 What is a tracheostomy? A tracheostomy
Respiratory Management of Facioscapulohumeral Muscular Dystrophy. Nicholas S. Hill, MD Tufts Medical Center Boston, MA
 Respiratory Management of Facioscapulohumeral Muscular Dystrophy Nicholas S. Hill, MD Tufts Medical Center Boston, MA Respiratory Involvement in FSHD Very variable time of onset rate of progression Muscles
Respiratory Management of Facioscapulohumeral Muscular Dystrophy Nicholas S. Hill, MD Tufts Medical Center Boston, MA Respiratory Involvement in FSHD Very variable time of onset rate of progression Muscles
McHenry Western Lake County EMS System Optional CE for Paramedics, EMT-B and PHRN s Croup vs. Epiglottitis. Optional #2 2017
 McHenry Western Lake County EMS System Optional CE for Paramedics, EMT-B and PHRN s Croup vs. Epiglottitis Optional #2 2017 The tones go out at 3 am for a child with difficulty breathing. As it is a kid
McHenry Western Lake County EMS System Optional CE for Paramedics, EMT-B and PHRN s Croup vs. Epiglottitis Optional #2 2017 The tones go out at 3 am for a child with difficulty breathing. As it is a kid
Other methods for maintaining the airway (not definitive airway as still unprotected):
 Page 56 Where anaesthetic skills and drugs are available, endotracheal intubation is the preferred method of securing a definitive airway. This technique comprises: rapid sequence induction of anaesthesia
Page 56 Where anaesthetic skills and drugs are available, endotracheal intubation is the preferred method of securing a definitive airway. This technique comprises: rapid sequence induction of anaesthesia
Neonatal Airway Disorders, Treatments, and Outcomes. Steven Goudy, MD Pediatric Otolaryngology Emory University Medical Center
 Neonatal Airway Disorders, Treatments, and Outcomes Steven Goudy, MD Pediatric Otolaryngology Emory University Medical Center Disclosure I have nothing to disclose Neonatal and Pediatric Tracheostomy Tracheostomy
Neonatal Airway Disorders, Treatments, and Outcomes Steven Goudy, MD Pediatric Otolaryngology Emory University Medical Center Disclosure I have nothing to disclose Neonatal and Pediatric Tracheostomy Tracheostomy
The Clinical Swallow Evaluation: What it can and cannot tell us. Introduction
 The Clinical Swallow Evaluation: What it can and cannot tell us Debra M. Suiter, Ph.D., CCC-SLP, BCS-S Director, Voice & Swallow Clinic Associate Professor, Division of Communication Sciences & Disorders
The Clinical Swallow Evaluation: What it can and cannot tell us Debra M. Suiter, Ph.D., CCC-SLP, BCS-S Director, Voice & Swallow Clinic Associate Professor, Division of Communication Sciences & Disorders
Stridor, Stertor, and Snoring: Pediatric Upper Airway Obstruction. Nathan Page, MD Pediatrics in the Red Rocks June?
 Stridor, Stertor, and Snoring: Pediatric Upper Airway Obstruction Nathan Page, MD Pediatrics in the Red Rocks June? I have no disclosures I do not plan to discuss unapproved or off label use of products
Stridor, Stertor, and Snoring: Pediatric Upper Airway Obstruction Nathan Page, MD Pediatrics in the Red Rocks June? I have no disclosures I do not plan to discuss unapproved or off label use of products
STRIDOR. Respiratory system. Lecture
 STRIDOR Stridor is a continuous inspiratory harsh sound produced by partial obstruction in the region of the larynx or trachea. Total obstruction cyanosis & death. Etiology Acute stridor Infectious croup
STRIDOR Stridor is a continuous inspiratory harsh sound produced by partial obstruction in the region of the larynx or trachea. Total obstruction cyanosis & death. Etiology Acute stridor Infectious croup
Analysis of Trans-Tracheal Measurements in Children Wearing Speaking Valves during Sleep
 ISSN: 2250-0359 Research Article Volume 8 Issue : 66 208 Analysis of Trans-Tracheal Measurements in Children Wearing Speaking Valves during Sleep Melodi Pirzada *, John Bishara, Jessica Shaw 2, Joy Eribo
ISSN: 2250-0359 Research Article Volume 8 Issue : 66 208 Analysis of Trans-Tracheal Measurements in Children Wearing Speaking Valves during Sleep Melodi Pirzada *, John Bishara, Jessica Shaw 2, Joy Eribo
Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing
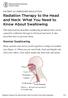 PATIENT & CAREGIVER EDUCATION Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing This information describes swallowing problems that can be caused by radiation therapy to the
PATIENT & CAREGIVER EDUCATION Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing This information describes swallowing problems that can be caused by radiation therapy to the
Tracheostomy. Information for patients and relatives
 Tracheostomy Information for patients and relatives page 2 What is a tracheostomy? A tracheostomy is a small hole (stoma) made at the front of the neck, which goes into the trachea (windpipe). A tube called
Tracheostomy Information for patients and relatives page 2 What is a tracheostomy? A tracheostomy is a small hole (stoma) made at the front of the neck, which goes into the trachea (windpipe). A tube called
Speech and Language Therapy. Kerrie McCarthy Senior Speech and Language Therapist
 Speech and Language Therapy Kerrie McCarthy Senior Speech and Language Therapist Contents 1. Voice disorders 2. Swallow disorders 3. Videofluroscopy 4. Adult Acquired Communication Disorders 5. How to
Speech and Language Therapy Kerrie McCarthy Senior Speech and Language Therapist Contents 1. Voice disorders 2. Swallow disorders 3. Videofluroscopy 4. Adult Acquired Communication Disorders 5. How to
8/8/2013. Disclaimer. Tracheostomy Care in the Home. Polling Question 1. Upper Airway and Respiratory System
 Disclaimer Appendix 3 Declaration of Vested Interest Form Name of presenter: Heather Murgatroyd RRT RPSGT Name of employer: DeVilbiss Healthcare Tracheostomy Care in the Home Heather Murgatroyd, RRT, RPSGT
Disclaimer Appendix 3 Declaration of Vested Interest Form Name of presenter: Heather Murgatroyd RRT RPSGT Name of employer: DeVilbiss Healthcare Tracheostomy Care in the Home Heather Murgatroyd, RRT, RPSGT
Tracheostomy management
 BJA Education, 15 (3): 149 153 (2015) doi: 10.1093/bjaceaccp/mku008 Advance Access Publication Date: 25 April 2014 Matrix reference 1C02, 2A01, 3A01 Tracheostomy management Katharine Hunt MBBS FRCA 1,
BJA Education, 15 (3): 149 153 (2015) doi: 10.1093/bjaceaccp/mku008 Advance Access Publication Date: 25 April 2014 Matrix reference 1C02, 2A01, 3A01 Tracheostomy management Katharine Hunt MBBS FRCA 1,
Anal Atresia FACTS: There is no known cause for anal atresia. Children with anal atresia can lead very happy lives post surgery!
 Anal Atresia FACTS: Anal atresia affects 1 in 5,000 births and is slightly more common in boys. There is no known cause for this condition. With anal atresia, any of the following can occur: The anal passage
Anal Atresia FACTS: Anal atresia affects 1 in 5,000 births and is slightly more common in boys. There is no known cause for this condition. With anal atresia, any of the following can occur: The anal passage
PEPP Course: PEPP BLS Pretest
 PEPP Course: PEPP BLS Pretest 1. What is the best way to administer oxygen to a child in moderate respiratory distress? Nasal cannula Simple mask Nonrebreathing mask Bag-valve-mask device 2. A 2-year-old
PEPP Course: PEPP BLS Pretest 1. What is the best way to administer oxygen to a child in moderate respiratory distress? Nasal cannula Simple mask Nonrebreathing mask Bag-valve-mask device 2. A 2-year-old
Airway Anatomy. Soft palate. Hard palate. Nasopharynx. Tongue. Oropharynx. Hypopharynx. Thyroid cartilage
 Airway Anatomy Hard palate Soft palate Tongue Nasopharynx Oropharynx Hypopharynx Thyroid cartilage Airway Anatomy Hyoid bone Thyroid cartilage Cricoid cartilage Trachea Cricothyroid membrane Airway Anatomy
Airway Anatomy Hard palate Soft palate Tongue Nasopharynx Oropharynx Hypopharynx Thyroid cartilage Airway Anatomy Hyoid bone Thyroid cartilage Cricoid cartilage Trachea Cricothyroid membrane Airway Anatomy
Slide 1. Slide 2. Slide 3. Introduction to the Electrolarynx. I have nothing to disclose and I have no proprietary interest in any product discussed.
 Slide 1 Introduction to the Electrolarynx CANDY MOLTZ, MS, CCC -SLP TLA SAN ANTONIO 2019 Slide 2 I have nothing to disclose and I have no proprietary interest in any product discussed. Slide 3 Electrolarynxes
Slide 1 Introduction to the Electrolarynx CANDY MOLTZ, MS, CCC -SLP TLA SAN ANTONIO 2019 Slide 2 I have nothing to disclose and I have no proprietary interest in any product discussed. Slide 3 Electrolarynxes
Pediatric Ingestion Injuries: Assessment & Treatment
 Pediatric Ingestion Injuries: Assessment & Treatment Benjamin L. Eithun, MSN, CRNP, RN, CPNP-AC, CCRN, TCRN Andrea L. Williams, PhD, RN UW Health & AFCH Case #1 Presentation Dispatched to Sandstone Ridge
Pediatric Ingestion Injuries: Assessment & Treatment Benjamin L. Eithun, MSN, CRNP, RN, CPNP-AC, CCRN, TCRN Andrea L. Williams, PhD, RN UW Health & AFCH Case #1 Presentation Dispatched to Sandstone Ridge
Policy x.xxx. Issued: Artificial Airways and Airway Care. ABC Home Medical Company Policy & Procedure Manual. A. Tracheostomy Tubes ( trach tubes)
 A. Tracheostomy Tubes ( trach tubes) A tracheotomy is a surgical procedure whereby an opening is cut into the trachea of the patient for the purpose of inserting a tube (trach tube). The trach tube allows
A. Tracheostomy Tubes ( trach tubes) A tracheotomy is a surgical procedure whereby an opening is cut into the trachea of the patient for the purpose of inserting a tube (trach tube). The trach tube allows
CARING FOR THE TRACHEOSTOMISED PATIENT: WHAT TO LOOK OUT FOR
 CARING FOR THE TRACHEOSTOMISED PATIENT: WHAT TO LOOK OUT FOR DR MOHD NAZRI ALI Anaesthesiologist & Intensivist HRPZ II, Kota Bharu, Kelantan Tracheostomy The Enabling Disability Tracheostomy Are becoming
CARING FOR THE TRACHEOSTOMISED PATIENT: WHAT TO LOOK OUT FOR DR MOHD NAZRI ALI Anaesthesiologist & Intensivist HRPZ II, Kota Bharu, Kelantan Tracheostomy The Enabling Disability Tracheostomy Are becoming
Prepared by : Bayan Kaddourah RN,MHM. GICU Clinical Instructor
 Mechanical Ventilation Prepared by : Bayan Kaddourah RN,MHM. GICU Clinical Instructor 1 Definition Is a supportive therapy to facilitate gas exchange. Most ventilatory support requires an artificial airway.
Mechanical Ventilation Prepared by : Bayan Kaddourah RN,MHM. GICU Clinical Instructor 1 Definition Is a supportive therapy to facilitate gas exchange. Most ventilatory support requires an artificial airway.
Bayfield-Ashland Counties EMS Council Pediatric Protocol PP-001 PREHOSPITAL CARE GUIDELINE
 INTRODUCTION: Pediatric emergencies may present a daunting challenge to prehospital care providers for a variety of reasons including: 1. The historical scarceness of primary training materials about the
INTRODUCTION: Pediatric emergencies may present a daunting challenge to prehospital care providers for a variety of reasons including: 1. The historical scarceness of primary training materials about the
Why Can t I breathe? Asthma vs. Vocal Cord Dysfunction (VCD) Lindsey Frohn, M.S., CCC-SLP Madonna Rehabilitation Hospital (Lincoln, NE)
 Why Can t I breathe? Asthma vs. Vocal Cord Dysfunction (VCD) Lindsey Frohn, M.S., CCC-SLP Madonna Rehabilitation Hospital (Lincoln, NE) Objectives Examine Vocal Cord Dysfunction Examine Exercise Induced
Why Can t I breathe? Asthma vs. Vocal Cord Dysfunction (VCD) Lindsey Frohn, M.S., CCC-SLP Madonna Rehabilitation Hospital (Lincoln, NE) Objectives Examine Vocal Cord Dysfunction Examine Exercise Induced
OVERCOMINGBARRIERS TO SPEAKING VALVE USE Success Through Teamwork 12/12/13. Passy Muir Inc. Clinical Consultant 1
 If you have not registered for this event, go to the Education Portal to complete your registration. ep.passy-muir.com o You will also have an opportunity to do this after the meeting ends. This is an
If you have not registered for this event, go to the Education Portal to complete your registration. ep.passy-muir.com o You will also have an opportunity to do this after the meeting ends. This is an
Respiratory Management in Pediatrics
 Respiratory Management in Pediatrics Children s Hospital Omaha Critical Care Transport Sue Holmer RN, C-NPT Objectives Examine the differences between the pediatric and adults airways. Recognize respiratory
Respiratory Management in Pediatrics Children s Hospital Omaha Critical Care Transport Sue Holmer RN, C-NPT Objectives Examine the differences between the pediatric and adults airways. Recognize respiratory
Evidence-Based Swallowing Related Issues in Patients with Tracheotomy Tubes
 Evidence-Based Swallowing Related Issues in Patients with Tracheotomy Tubes Steven B. Leder, Ph.D. Yale University School of Medicine Debra M. Suiter,, Ph.D. University of Memphis Impetus Swallowing Rx
Evidence-Based Swallowing Related Issues in Patients with Tracheotomy Tubes Steven B. Leder, Ph.D. Yale University School of Medicine Debra M. Suiter,, Ph.D. University of Memphis Impetus Swallowing Rx
The Pediatric Patient. Morgen Bernius, MD NCEMS Conference February 24, 2007
 The Pediatric Patient Morgen Bernius, MD NCEMS Conference February 24, 2007 Rule #1: Everyone Loves the Pediatric Patient Pediatrics in EMS Approximately 10% of all EMS treatment is for children younger
The Pediatric Patient Morgen Bernius, MD NCEMS Conference February 24, 2007 Rule #1: Everyone Loves the Pediatric Patient Pediatrics in EMS Approximately 10% of all EMS treatment is for children younger
PEDIATRIC EMERGENCIES Sandra Horning, MD Sacred Heart Medical Center Emergency Department
 PEDIATRIC EMERGENCIES Sandra Horning, MD Sacred Heart Medical Center Emergency Department Overview Roles of the EMS in Pediatric Care Growth and Development Assessment Airway Adjuncts and Intravenous Access
PEDIATRIC EMERGENCIES Sandra Horning, MD Sacred Heart Medical Center Emergency Department Overview Roles of the EMS in Pediatric Care Growth and Development Assessment Airway Adjuncts and Intravenous Access
Caring for Your TRACHEOSTOMY. Getting On with Your Life
 Caring for Your TRACHEOSTOMY Getting On with Your Life A New Pathway for Air Have you had a tracheostomy? Or, are you about to have one? If so, you may be wondering what the future holds for you. It s
Caring for Your TRACHEOSTOMY Getting On with Your Life A New Pathway for Air Have you had a tracheostomy? Or, are you about to have one? If so, you may be wondering what the future holds for you. It s
Reluctance or refusal to feed or eat. Understanding Feeding Aversion in a City Full of Foodies. Presentation Outline. Learning Objectives
 Understanding Feeding Aversion in a City Full of Foodies Amy Houtrow, MD, MPH Pediatric Physical Medicine & Rehabilitation UCSF Department of Pediatrics June 2, 2007 Learning Objectives Learners will be
Understanding Feeding Aversion in a City Full of Foodies Amy Houtrow, MD, MPH Pediatric Physical Medicine & Rehabilitation UCSF Department of Pediatrics June 2, 2007 Learning Objectives Learners will be
Communication and Swallowing with PSP/CBD. Megan DePuy, MBA, MS, CCC-SLP Private Speech Pathologist
 Communication and Swallowing with PSP/CBD Megan DePuy, MBA, MS, CCC-SLP Private Speech Pathologist A Speech Therapist? Why? Swallowing (Dysphagia) Speech (Dysarthria, Dysphonia) Language (Aphasia) An Experienced
Communication and Swallowing with PSP/CBD Megan DePuy, MBA, MS, CCC-SLP Private Speech Pathologist A Speech Therapist? Why? Swallowing (Dysphagia) Speech (Dysarthria, Dysphonia) Language (Aphasia) An Experienced
Anatomy Review. Anatomy Review. Respiratory Emergencies CHAPTER 16
 CHAPTER 16 Respiratory Emergencies Anatomy Review Anatomy Review 1 Pediatric Anatomy Airway structure differences Proportionally larger tongue Smaller, more flexible trachea Abdominal breathers Reasons
CHAPTER 16 Respiratory Emergencies Anatomy Review Anatomy Review 1 Pediatric Anatomy Airway structure differences Proportionally larger tongue Smaller, more flexible trachea Abdominal breathers Reasons
Respiratory Emergencies
 CHAPTER 16 Respiratory Emergencies Anatomy Review Anatomy Review Pediatric Anatomy Airway structure differences Proportionally larger tongue Smaller, more flexible trachea Abdominal breathers Reasons for
CHAPTER 16 Respiratory Emergencies Anatomy Review Anatomy Review Pediatric Anatomy Airway structure differences Proportionally larger tongue Smaller, more flexible trachea Abdominal breathers Reasons for
Pediatric Modified Barium Swallow Studies. Presented by Jody Bousquet, MA, CCC- SLP Susan Shonbrun, MS, CCC- SLP November 7, 2015
 Pediatric Modified Barium Swallow Studies Presented by Jody Bousquet, MA, CCC- SLP Susan Shonbrun, MS, CCC- SLP November 7, 2015 Definition * Modified Barium Swallow Study * Assesses swallow functions
Pediatric Modified Barium Swallow Studies Presented by Jody Bousquet, MA, CCC- SLP Susan Shonbrun, MS, CCC- SLP November 7, 2015 Definition * Modified Barium Swallow Study * Assesses swallow functions
Management of Pediatric Tracheostomy
 Management of Pediatric Tracheostomy Deepak Mehta Associate Professor Of Otolaryngology Director Pediatric Aerodigestive Center Definitions Tracheotomy: The making of an incision in the trachea The name
Management of Pediatric Tracheostomy Deepak Mehta Associate Professor Of Otolaryngology Director Pediatric Aerodigestive Center Definitions Tracheotomy: The making of an incision in the trachea The name
Small Volume Nebulizer Treatment (Hand-Held)
 Small Volume Aerosol Treatment Page 1 of 6 Purpose Policy Physician's Order Small Volume Nebulizer Treatment To standardize the delivery of inhalation aerosol drug therapy via small volume (hand-held)
Small Volume Aerosol Treatment Page 1 of 6 Purpose Policy Physician's Order Small Volume Nebulizer Treatment To standardize the delivery of inhalation aerosol drug therapy via small volume (hand-held)
REGION 1 EMERGENCY MEDICAL SERVICES STANDING MEDICAL ORDERS EMT Basic, EMT Intermediate, EMT Paramedic. SMO: Pediatric Assessment Guidelines
 REGION 1 EMERGENCY MEDICAL SERVICES STANDING MEDICAL ORDERS EMT Basic, EMT Intermediate, EMT Paramedic SMO: Pediatric Assessment Guidelines Overview: Pediatric patients account for about 10% or less of
REGION 1 EMERGENCY MEDICAL SERVICES STANDING MEDICAL ORDERS EMT Basic, EMT Intermediate, EMT Paramedic SMO: Pediatric Assessment Guidelines Overview: Pediatric patients account for about 10% or less of
Laryngoscopy Examinations
 Laryngoscopy Examinations Laryngoscopy is a visual examination of the back of the throat where the voice box (larynx) and vocal cords are located. The procedure is done by using hand mirrors and a light
Laryngoscopy Examinations Laryngoscopy is a visual examination of the back of the throat where the voice box (larynx) and vocal cords are located. The procedure is done by using hand mirrors and a light
Sun City Texas Computer Club. October 12, 2017
 Sun City Texas Computer Club October 12, 2017 Enhance Weak Speech To Better Communicate with Hearing Loss Dr. Natasha Dewald, AuD Hears To You Natasha@HearsToYouTx.com Dr. Natasha Dewald Education Undergraduate
Sun City Texas Computer Club October 12, 2017 Enhance Weak Speech To Better Communicate with Hearing Loss Dr. Natasha Dewald, AuD Hears To You Natasha@HearsToYouTx.com Dr. Natasha Dewald Education Undergraduate
Section 5: Communication. Part 1: Early Warning Signs. Theresa Golem. December 5, 2012
 Section 5: Communication Part 1: Early Warning Signs Theresa Golem December 5, 2012 Deficits in the area of communication are one of the key characteristics of autism spectrum disorders (ASD). Early warning
Section 5: Communication Part 1: Early Warning Signs Theresa Golem December 5, 2012 Deficits in the area of communication are one of the key characteristics of autism spectrum disorders (ASD). Early warning
Cough assist T70 for the Tracheostomy Child
 Patient and Family Education Cough assist 70 for the racheostomy Child with or without a ventilator What is a Cough assist device? he Cough assist 70 device removes mucus (secretions) from your child s
Patient and Family Education Cough assist 70 for the racheostomy Child with or without a ventilator What is a Cough assist device? he Cough assist 70 device removes mucus (secretions) from your child s
This interdisciplinary clinical support document provides guidelines for the safe establishment of an artificial airway.
 PURPOSE This interdisciplinary clinical support document provides guidelines for the safe establishment of an artificial airway. POLICY STATEMENTS Endotracheal intubation will be performed by the Most
PURPOSE This interdisciplinary clinical support document provides guidelines for the safe establishment of an artificial airway. POLICY STATEMENTS Endotracheal intubation will be performed by the Most
Clearing the air.. How to assist and rescue neck breathing patients. Presented by: Don Hall MCD, CCC/SLP Sarah Markel RRT, MHA
 Clearing the air.. How to assist and rescue neck breathing patients Presented by: Don Hall MCD, CCC/SLP Sarah Markel RRT, MHA Learning Objectives Define common terms identified with total (laryngectomy)
Clearing the air.. How to assist and rescue neck breathing patients Presented by: Don Hall MCD, CCC/SLP Sarah Markel RRT, MHA Learning Objectives Define common terms identified with total (laryngectomy)
TRACHEOSTOMY. Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion
 TRACHEOSTOMY Definition Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion Indications for tracheostomy 1-upper airway obstruction with stridor, air hunger,
TRACHEOSTOMY Definition Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion Indications for tracheostomy 1-upper airway obstruction with stridor, air hunger,
Respiratory Physio Protocol for Paediatric Patients on BIPAP via a tracheotomy (uncuffed tube)
 This is an official Northern Trust policy and should not be edited in any way Respiratory Physio Protocol for Paediatric Patients on BIPAP via a tracheotomy (uncuffed tube) Reference Number: NHSCT/12/547
This is an official Northern Trust policy and should not be edited in any way Respiratory Physio Protocol for Paediatric Patients on BIPAP via a tracheotomy (uncuffed tube) Reference Number: NHSCT/12/547
HEARING SCREENING Your baby passed the hearing screening. Universal Newborn
 Parents are important partners. They have the greatest impact upon their young child and their active participation is crucial. Mark Ross (1975) Universal Newborn HEARING SCREENING Your baby passed the
Parents are important partners. They have the greatest impact upon their young child and their active participation is crucial. Mark Ross (1975) Universal Newborn HEARING SCREENING Your baby passed the
The Respiratory System
 130 20 The Respiratory System 1. Define important words in this chapter 2. Explain the structure and function of the respiratory system 3. Discuss changes in the respiratory system due to aging 4. Discuss
130 20 The Respiratory System 1. Define important words in this chapter 2. Explain the structure and function of the respiratory system 3. Discuss changes in the respiratory system due to aging 4. Discuss
Passy-MuirInc. Clinical Inservice Outline. Touching Lives and Enhancing Patient Care Through Education
 Passy-MuirInc. Clinical Inservice Outline Touching Lives and Enhancing Patient Care Through Education Passy-Muir Tracheostomy & Ventilator Speaking Valves Clinical Inservice Outline I. Inventor, David
Passy-MuirInc. Clinical Inservice Outline Touching Lives and Enhancing Patient Care Through Education Passy-Muir Tracheostomy & Ventilator Speaking Valves Clinical Inservice Outline I. Inventor, David
Universal Newborn. Your baby has referred for another Hearing Screening or Diagnostic Hearing Test
 Parents are important partners. They have the greatest impact upon their young child and their active participation is crucial. Mark Ross (1975) Universal Newborn HEARING SCREENING Your baby has referred
Parents are important partners. They have the greatest impact upon their young child and their active participation is crucial. Mark Ross (1975) Universal Newborn HEARING SCREENING Your baby has referred
F: Respiratory Care. College of Licensed Practical Nurses of Alberta, Competency Profile for LPNs, 3rd Ed. 59
 F: Respiratory Care College of Licensed Practical Nurses of Alberta, Competency Profile for LPNs, 3rd Ed. 59 Competency: F-1 Airway Management F-1-1 F-1-2 F-1-3 F-1-4 F-1-5 Demonstrate knowledge and ability
F: Respiratory Care College of Licensed Practical Nurses of Alberta, Competency Profile for LPNs, 3rd Ed. 59 Competency: F-1 Airway Management F-1-1 F-1-2 F-1-3 F-1-4 F-1-5 Demonstrate knowledge and ability
Weaning from Mechanical Ventilation. Dr Azmin Huda Abdul Rahim
 Weaning from Mechanical Ventilation Dr Azmin Huda Abdul Rahim Content Definition Classification Weaning criteria Weaning methods Criteria for extubation Introduction Weaning comprises 40% of the duration
Weaning from Mechanical Ventilation Dr Azmin Huda Abdul Rahim Content Definition Classification Weaning criteria Weaning methods Criteria for extubation Introduction Weaning comprises 40% of the duration
Voice Disorders in Medically Complex Children
 Voice Disorders in Medically Complex Children Roger C. Nuss, MD, FACS Geralyn Harvey Woodnorth, M.A., CCC-SLP Department of Otolaryngology and Communication Enhancement Children s Hospital Boston Harvard
Voice Disorders in Medically Complex Children Roger C. Nuss, MD, FACS Geralyn Harvey Woodnorth, M.A., CCC-SLP Department of Otolaryngology and Communication Enhancement Children s Hospital Boston Harvard
Airway and Breathing
 Airway and Breathing ETAT Module 2 Adapted from Emergency Triage Assessment and Treatment (ETAT): Manual for Participants, World Health Organization, 2005 Learning Objectives Accurately determine whether
Airway and Breathing ETAT Module 2 Adapted from Emergency Triage Assessment and Treatment (ETAT): Manual for Participants, World Health Organization, 2005 Learning Objectives Accurately determine whether
Kapitex Healthcare. making things clearer for tracheostomy patients
 Kapitex Healthcare making things clearer for tracheostomy patients preface In publishing this booklet, Kapitex Healthcare Ltd hopes to provide information and understanding for both the patient and carer
Kapitex Healthcare making things clearer for tracheostomy patients preface In publishing this booklet, Kapitex Healthcare Ltd hopes to provide information and understanding for both the patient and carer
IAEM Clinical Guideline 9 Laryngomalacia. Version 1 September, Author: Dr Farah Mustafa
 IAEM Clinical Guideline 9 Laryngomalacia Version 1 September, 2016 Author: Dr Farah Mustafa Guideline lead: Dr Áine Mitchell, in collaboration with IAEM Clinical Guideline committee and Our Lady s Children
IAEM Clinical Guideline 9 Laryngomalacia Version 1 September, 2016 Author: Dr Farah Mustafa Guideline lead: Dr Áine Mitchell, in collaboration with IAEM Clinical Guideline committee and Our Lady s Children
H: Respiratory Care. Saskatchewan Association of Licensed Practical Nurses, Competency Profile for LPNs, 3rd Ed. 79
 H: Respiratory Care Saskatchewan Association of Licensed Practical Nurses, Competency Profile for LPNs, 3rd Ed. 79 Competency: H-1 Airway Management H-1-1 H-1-2 H-1-3 H-1-4 H-1-5 Demonstrate knowledge
H: Respiratory Care Saskatchewan Association of Licensed Practical Nurses, Competency Profile for LPNs, 3rd Ed. 79 Competency: H-1 Airway Management H-1-1 H-1-2 H-1-3 H-1-4 H-1-5 Demonstrate knowledge
Disclosures. Learning Objectives. Coeditor/author. Associate Science Editor, American Heart Association
 Tracheotomy Challenges for airway specialists Elizabeth H. Sinz, MD Professor of Anesthesiology & Neurosurgery Associate Dean for Clinical Simulation Disclosures Coeditor/author Associate Science Editor,
Tracheotomy Challenges for airway specialists Elizabeth H. Sinz, MD Professor of Anesthesiology & Neurosurgery Associate Dean for Clinical Simulation Disclosures Coeditor/author Associate Science Editor,
Role of the SLP: Pre-Surgical Assessment & Counseling
 Jenna MacKenzie, M.S., CCC-SLP & Nicole Palmer, M.S., CCC-SLP Texas Laryngectomy Association 2019 Conference Disclosures Neither presenters have any financial disclosures to report. Both presenters are
Jenna MacKenzie, M.S., CCC-SLP & Nicole Palmer, M.S., CCC-SLP Texas Laryngectomy Association 2019 Conference Disclosures Neither presenters have any financial disclosures to report. Both presenters are
Equipment: NRP algorithm, MRSOPA table, medication chart, SpO 2 table Warm
 NRP Skills Stations Performance Skills Station OR Integrated Skills Station STATION: Assisting with and insertion of endotracheal tube (ETT) Equipment: NRP algorithm, MRSOPA table, medication chart, SpO
NRP Skills Stations Performance Skills Station OR Integrated Skills Station STATION: Assisting with and insertion of endotracheal tube (ETT) Equipment: NRP algorithm, MRSOPA table, medication chart, SpO
What is the next best step?
 Noninvasive Ventilation William Janssen, M.D. Assistant Professor of Medicine National Jewish Health University of Colorado Denver Health Sciences Center What is the next best step? 65 year old female
Noninvasive Ventilation William Janssen, M.D. Assistant Professor of Medicine National Jewish Health University of Colorado Denver Health Sciences Center What is the next best step? 65 year old female
RSPT Tracheal Aspiration. Tracheal Aspiration. RSPT 1410 Tracheal Aspiration
 1 RSPT 1410 2 is the use of to facilitate the removal of secretions from the respiratory tract. Under normal circumstances, patients with normal coughing do not have difficulty in removing secretions.
1 RSPT 1410 2 is the use of to facilitate the removal of secretions from the respiratory tract. Under normal circumstances, patients with normal coughing do not have difficulty in removing secretions.
Compliance Department ELEMENTS OF EAR, NOSE AND THROAT EXAMINATION 11/2010
 Compliance Department ELEMENTS OF EAR, NOSE AND THROAT EXAMINATION 11/2010 System/ Body Area Constitutional Measurement of any three of the following seven vital signs: 1) sitting or standing blood pressure,
Compliance Department ELEMENTS OF EAR, NOSE AND THROAT EXAMINATION 11/2010 System/ Body Area Constitutional Measurement of any three of the following seven vital signs: 1) sitting or standing blood pressure,
The Effect of a Speaking Valve on Laryngeal Aspiration and Penetration in Children With Tracheotomies
 The Laryngoscope VC 2013 The American Laryngological, Rhinological and Otological Society, Inc. The Effect of a Speaking Valve on Laryngeal Aspiration and Penetration in Children With Tracheotomies Julina
The Laryngoscope VC 2013 The American Laryngological, Rhinological and Otological Society, Inc. The Effect of a Speaking Valve on Laryngeal Aspiration and Penetration in Children With Tracheotomies Julina
Feeding and Swallowing Problems in the Child with Special Needs
 Feeding and Swallowing Problems in the Child with Special Needs Joan Surfus, OTR/L, SWC Amy Lynch, MS, OTR/L Misericordia University This presentation is made possible, in part, by the support of the American
Feeding and Swallowing Problems in the Child with Special Needs Joan Surfus, OTR/L, SWC Amy Lynch, MS, OTR/L Misericordia University This presentation is made possible, in part, by the support of the American
Objectives. Case Presentation. Respiratory Emergencies
 Respiratory Emergencies Objectives Describe how to assess airway and breathing, including interpreting information from the PAT and ABCDEs. Differentiate between respiratory distress, respiratory failure,
Respiratory Emergencies Objectives Describe how to assess airway and breathing, including interpreting information from the PAT and ABCDEs. Differentiate between respiratory distress, respiratory failure,
10/17/2016 OXYGEN DELIVERY: INDICATIONS AND USE OF EQUIPMENT COURSE OBJECTIVES COMMON CAUSES OF RESPIRATORY FAILURE
 OXYGEN DELIVERY: INDICATIONS AND USE OF EQUIPMENT J U L I E Z I M M E R M A N, R N, M S N C L I N I C A L N U R S E S P E C I A L I S T E L O I S A C U T L E R, R R T, B S R C C L I N I C A L / E D U C
OXYGEN DELIVERY: INDICATIONS AND USE OF EQUIPMENT J U L I E Z I M M E R M A N, R N, M S N C L I N I C A L N U R S E S P E C I A L I S T E L O I S A C U T L E R, R R T, B S R C C L I N I C A L / E D U C
DIFFICULT ASTHMA. Dr. Prathyusha Dr. S.Balasubramanian KKCTH
 DIFFICULT ASTHMA Dr. Prathyusha Dr. S.Balasubramanian KKCTH CASE SUMMARY 11 yr old girl, Neyveli Treated as moderate persistent asthma x 5 years On Seroflo [ LABA + steroid ] 250 2 puffs BD and intermittent
DIFFICULT ASTHMA Dr. Prathyusha Dr. S.Balasubramanian KKCTH CASE SUMMARY 11 yr old girl, Neyveli Treated as moderate persistent asthma x 5 years On Seroflo [ LABA + steroid ] 250 2 puffs BD and intermittent
Respiration & Trunk control The Great Connection. Brief Review of Normal Development of the Rib Cage
 Respiration & Trunk control The Great Connection. are part of a complex combination of interactive systems. Muscles of respiration are part of the musculature of dynamic postural control. First 3 Years
Respiration & Trunk control The Great Connection. are part of a complex combination of interactive systems. Muscles of respiration are part of the musculature of dynamic postural control. First 3 Years
Facing Surgery for Throat Cancer? Learn about minimally invasive da Vinci Surgery for early to moderate stage throat cancer.
 Facing Surgery for Throat Cancer? Learn about minimally invasive da Vinci Surgery for early to moderate stage throat cancer. Surgery Options If you have been diagnosed with throat cancer, your doctor will
Facing Surgery for Throat Cancer? Learn about minimally invasive da Vinci Surgery for early to moderate stage throat cancer. Surgery Options If you have been diagnosed with throat cancer, your doctor will
Changing Your Trach Tube
 Patient & Family Guide 2017 Changing Your Trach Tube www.nshealth.ca Changing Your Trach Tube Your entire trach tube should be changed about once a month, or sooner if you notice an odour (smell) or get
Patient & Family Guide 2017 Changing Your Trach Tube www.nshealth.ca Changing Your Trach Tube Your entire trach tube should be changed about once a month, or sooner if you notice an odour (smell) or get
RESPIRATORY FAILURE. Michael Kelly, MD Division of Pediatric Critical Care Dept. of Pediatrics
 RESPIRATORY FAILURE Michael Kelly, MD Division of Pediatric Critical Care Dept. of Pediatrics What talk is he giving? DO2= CO * CaO2 CO = HR * SV CaO2 = (Hgb* SaO2 * 1.34) + (PaO2 * 0.003) Sound familiar??
RESPIRATORY FAILURE Michael Kelly, MD Division of Pediatric Critical Care Dept. of Pediatrics What talk is he giving? DO2= CO * CaO2 CO = HR * SV CaO2 = (Hgb* SaO2 * 1.34) + (PaO2 * 0.003) Sound familiar??
