New insights into the organophosphate-induced intermediate syndrome
|
|
|
- Patience Greene
- 5 years ago
- Views:
Transcription
1 191 Case report Haliga RE, et al. New insights into the organophosphate-induced intermediate syndrome DOI: /aiht New insights into the organophosphate-induced intermediate syndrome Raluca Ecaterina Haliga 1, Bianca Codrina Morarasu 2, Manuela Ursaru 3, Viorica Irimioaia 4, and Laurentiu Sorodoc 1 Department of Internal Medicine and Toxicology 1, Department of Internal Medicine 2, Department of Radiology and Imaging 3, Department of Neurology 4, Sf. Spiridon Clinical Emergency Hospital, University of Medicine and Pharmacy Gr. T. Popa Iasi, Romania [Received in March 2018; Similarity Check in March 2018; Accepted in May 2018] Acute organophosphate (OP) poisoning can be deadlier than any other type of chemical poisoning. So far, only a few cases have been described that include extensive neurological complications. We present an outstanding case of severe oral OP poisoning with intermediate syndrome developed on the fourth day after hospital admission. The clinical picture involved weakness of the proximal upper and lower limb muscles and several muscles supplied by motor cranial nerves, but, what is peculiar, the distal upper and lower limb muscles were also affected (forearms, hands, legs, and feet). To our knowledge, this is a unique presentation, as lower limb muscle weakness was reported only in the context of delayed polyneuropathy. Another remarkable feature was the involvement of six of the twelve cranial nerves, which makes this case of intermediate syndrome the first with such a spread of muscle weakness and provides new insights into the polymorphic clinical manifestations of acute OP poisoning. KEY WORDS: cholinesterase; lower limb muscle weakness; motor cranial nerves; myasthenia; poisoning Since Clermont developed the first synthetic organic phosphorus anticholinesterase compound in 1854, more than 50,000 organophosphate substances (OPs) have been discovered. Acute OP poisoning is frequent in developing countries with easy access to anticholinesterase insecticides. The World Health Organization estimates that it causes more than 250,000 deaths every year (1). In Romania we deal with severe poisoning, prolonged hospitalisation and high cost for this category of patients. Of particular interest are the neurological complications that can occur. There are three phases of neurological manifestation: acute cholinergic crisis (ACC), intermediate syndrome (IMS), and organophosphate-induced delayed polyneuropathy (OPIDP), first reported by Wadia (2). ACC develops in the first minutes to hours of OP poisoning. Due to the anticholinergic action, it affects muscarinic and nicotinic peripheral receptors and the central nervous system. The clinical picture is shaped by muscarinic and nicotinic symptoms (3). It involves the respiratory and cardiovascular system with rhinorrhoea, bronchospasm, bronchorrhoea, cough or severe respiratory distress, bradycardia and hypotension, gastrointestinal symptoms with nausea, vomiting, diarrhoea, and abdominal cramps, or neurological signs with fasciculation, muscle paralysis, dizziness, confusion, and seizures (4). These may be Correspondence to: Bianca Codrina Morarasu, Department of Internal Medicine, Sf. Spiridon Clinical Emergency Hospital, 1 Independentei St., Iasi, Romania, morarasu.bianca.codrina@gmail.com considered typical manifestations of ACC. More serious complications that can lead to death include coma and acute respiratory failure requiring mechanical intubation and ventilation (5). OPIDP emerges within two to four weeks after exposure to OP insecticides and is characterised by lower limb muscle weakness, followed by progress toward upper limb muscles. After affecting the pyramidal tract, it leads to extrapyramidal symptoms characterised by spasticity or abnormal reflexes. Recovery can be complete in young patients, but neurological impairment may persist in certain cases (6). IMS following acute OP poisoning is a complication with an incidence between 7.7 % and 84 % (7). This variability seems to be due to the great differences in defining IMS among studies. Generally, it appears two to four days after the cholinergic crisis in patients with severe and prolonged acetylcholinesterase (AChE) inhibition. The classic symptom defining IMS is weakness affecting the respiratory and limb girdle muscles, as well as muscles supplied by motor cranial nerves. (8) Uncommon presentations of IMS include extrapyramidal symptoms, bilateral vocal cord paralysis, or even all the three neurological phases in the same patient (9-10). All of these seem to reflect a pathophysiological dysfunction of the neuromuscular junction due to the accumulation of acetylcholine in the synaptic cleft. Other mechanisms include muscle necrosis, oxidative stress-related myopathy,
2 192 or persistent AChE inhibition (7). However, the pathophysiology underlying IMS is still not clear. Here we present a case of severe IMS with weakness involving proximal and distal limb muscles and several muscles supplied by motor cranial nerves following acute ingestion of diazinon in a suicidal attempt of a 49-year-old woman. To our knowledge, this is the first report of IMS with such particular clinical presentation. CASE REPORT A 49-year-old woman ingested about 200 ml of diazinon in a suicide attempt. She had no prior medical history of suicidal thoughts or attempts. After approximately one hour from the ingestion, her family found her unconscious on the farm field. She had pulse but was unresponsive and sweating profusely, so the family took her to the local hospital. About one hour later, she received gastric lavage and activated charcoal and was then referred to our emergency department where she arrived two hours later with drowsiness, temporal and spatial disorientation, slur, generalised tremor, diaphoresis, cough, epigastric pain, nausea, and vomiting of white foam. Physical examination revealed hypotension (blood pressure 85/60 mmhg), bradycardia (heart rate bpm), hypoxia (oxygen saturation was % even on oxygen therapy delivering O 2 at 4 L min -1 ), midsized pupils, diaphoresis, hypersalivation, rhonchi in the inferior lung fields, and epigastric tenderness. The baseline measurement of serum butyrylcholinesterase (BuChE) was 281 U L -1 (normal values U L -1 ). The chest X-ray (Figure 1) revealed a consolidation occupying the right inferior lung parenchyma. Antidote treatment was started while the patient was in the emergency department, with two vials of 250 mg obidoxime and nine vials of 1 mg atropine with titration, both given intravenously (IV). About two hours later, the patient was admitted to our toxicology department. On arrival, her blood pressure was 110/70 mmhg and heart rate 114 bpm. She presented with dry skin, midsize pupils, persistent epigastric pain, nausea, and insecticide breath. Electrocardiogram (ECG) showed sinus tachycardia, and the full laboratory profile revealed leukocytosis, neutrophilia, increased C-reactive protein (CRP), fibrinogen, and abnormal urine findings due to the urinary tract infection with E. coli. We continued antidote treatment with atropine and adjusted the doses to the signs of atropinisation; we started with one vial every 2 h for one day, then changed to every 4 h for the next three days, and finally to every 6 h for the next five days, after which atropine treatment was stopped. IV obidoxime was also continued for 72 h from admission to the toxicology department, and two units of fresh frozen plasma (FFP) were administered in the first two days. Serum BuChE was monitored regularly (Figure 2). The patient s general status improved with antidote treatment. Her haemodynamics was stable, oxygen saturation normal (no artificial ventilation was needed), pupils midsize, skin dry, and she was conscious and oriented. The cholinergic and digestive symptoms gradually receded and only a mild cough persisted. In spite of the atropine treatment, however, on the fourth day of admission to our toxicology department, the patient developed myoclonic twitches of the jaw and tremor of the head and arms. She complained of a generalised weakness and difficulty moving the limbs, standing, staying seated, and breathing due to respiratory muscle weakness. Neurological examination revealed myasthenia gravis due to OP poisoning. Her sensation was unaltered but with diminished tendon reflexes. Head computed tomography with contrast showed diffuse cerebral oedema (Figure 3). Lumbar puncture was normal. The treatment of the cerebral oedema started with a loop diuretic, but the patient s neurological status continued to decline. The next day she had the Glasgow Coma Score of 11, bilateral ptosis, and difficulty opening and closing her mouth. She could not chew, raise eyebrows, or smile. Clinical signs and symptoms of bulbar palsy were also present, along with dysphagia, hoarse voice, and inability to shrug or turn the head. Secretions from the respiratory tract were removed with bronchial endoscopy. Arterial blood gases were within the normal range. Electromyography was not performed. All these clinical, neurological, and radiological findings pointed to the diagnosis of an atypical Figure 1 X-ray of the patient poisoned with diazinon on admission
3 193 Haliga RE, et al. New insights into the organophosphate-induced intermediate syndrome Figure 2 Serum cholinesterase levels in the patient poisoned with diazinon over the 14 days of hospitalisation IMS due to severe OP poisoning. We introduced treatment with mannitol, group B vitamins, and haemoglobin glutamer (Actovegin) and kept the patient under close observation. To address respiratory and urinary tract infection we also introduced antibiotic treatment according to her antibiogram. The patient s neurological status improved in the days that followed. She fully recovered from muscle weakness, but the signs of facial nerve palsy remained. She was discharged after 14 days in hospital and had been followed up periodically for the next year. Discussion The clinical features and prognosis in OP poisoning depend on the type of pesticide, dose, route of administration, and the moment when treatment is initiated. With our patient, the culprit pesticide was a diethyl compound diazinon, the most common category of pesticide nowadays (11). A recent study by Peter et al. (12) showed that the diethyl group was associated with later onset and less severe symptoms than the dimethyl group of OPs. Also, the incidence of the IMS and the need for tracheostomy or intubation were significantly lower with the diethyl compounds. The diethyl group contains fat-soluble organophosphates that remain in the circulation in low levels and may persist for a longer period of time. After ingestion, diazinon causes a rise in acetylcholine concentration with subsequent stimulation of the muscarinic and nicotinic receptors shaping the acute cholinergic syndrome (11). On admission, our patient had the classic hallmarks of this syndrome with hypotension, bradycardia, cough, nausea, vomiting, and abdominal pain due to muscarinic effects, accompanied by nicotinic manifestations. Further confirmation of the diagnosis came with low serum BuChE, which is a common finding among patients poisoned with OPs (13). Several studies found that the severity of poisoning and the need for intubation rose with lower plasma or serum levels (14-15). However, whether the level of serum cholinesterase correlates with the severity of poisoning is still a matter of debate. In our case, serum BuChE was severely depressed, with only slight fluctuations throughout hospitalisation, despite optimal atropine and oxime therapy and the administration of two units of FFP over the first two days of admission to our toxicology department. This finding is consistent with the report by Pazooki et al. (16). In contrast, a prospective study (17) with 33 cases of OP poisoning, reported that nine patients treated only with atropine + pralidoxime developed IMS, while no IMS was observed in those who received atropine + pralidoxime + FFP. BuChE plasma levels were similar between the two groups on admission to the hospital, but in the FFP-treated group they increased by 461 U L -1 with every two bags of plasma given. BuChE provided with plasma might play a role in sequestrating OPs in the circulation and stop further AChE inhibition. This may become extremely important when AChE activity is extremely low. In addition, FFP provides other important molecules, such as esterases and proteases, which may counteract the OP effects. How successfully will depend on the type of OP pesticides (18). Further research is therefore needed to better understand the effects of BuChE on the central nervous system (17). IMS appears within the first 24 to 96 h of OP ingestion and can last up to six days. Recent studies, however, have shown that IMS may also occur outside this time frame, even after acute cholinergic crisis seems to have been resolved. Our patient s symptoms are the case in point: they
4 194 Figure 3 CT scan shows a discrete supra-tentorial loss of grey-white matter differentiation, with the effacement of the cerebral sulci and obliteration of supraselar and ambiens cisterns. There are no signs of uncal herniation seemed to have improved, but 72 h after admission, she developed a weakness in several muscle groups. Our findings correspond to the clinical features of IMS first described in 1987 (19) as weakness of the neck flexors, respiratory, proximal limb muscles, and certain muscles supplied by motor cranial nerves. One of the most important complications, however, is the respiratory failure requiring intubation and mechanical ventilation (20). It can appear in % of patients and directly correlates with the severity of poisoning. Other risk factors for intubation/ventilation include pneumonia, acute pulmonary oedema, or cardiovascular collapse (21). Our patient remained stable (under constant monitoring), even though she was severely poisoned and developed pneumonia. To the best of our knowledge, this is the first case reporting a distal limb muscle weakness. Our patient was unable to extend, flex or lift up her forearms, hands, legs, and feet. She was incapable to stand, sit, or walk. Her tendon reflexes were slower but the sensation was preserved. The weakness of the distal limbs was reported earlier only in the context of OPIDP, which develops two to three weeks after OPs poisoning. The clinical picture of OPIDP includes weakness and numbness in the lower limbs, followed by progression toward the upper limbs (6). Symptoms may last for up to two years, but recovery can be complete, especially in young patients. In our case, the symptoms regressed to full resolution until discharge from the hospital. Weakness in the muscle groups supplied by the 3 rd (bilateral ptosis), 5 th (inability to close the mouth or to chew), and 7 th (inability to smile and raise eyebrows) motor cranial nerve as well as the bulbar syndrome in our patient clearly point to multiple cranial nerve involvement. Literature does report that IMS may affect motor cranial nerves but not to such an extent (19, 22). In a study which evaluated IMS in 21 patients (23), 17 had weakness in the muscles supplied by motor cranial nerves and three had atypical manifestations with a relapse of acute cholinergic symptoms at the beginning of IMS. In our case, we noticed concomitant development of fasciculation in the jaw muscles and symptoms of IMS. This situation has already been reported in literature; De Bleecker et al. (14) observed that out of eight patients with IMS, six developed cholinergic symptoms, such as fasciculation, bradycardia, diarrhoea, sweating, lacrimation, and increased salivary and bronchial secretion. Conclusion Early recognition of muscle weakness before major complications appear can save lives. Our case stands out with an atypical IMS. First, it is quite uncommon (although not unheard of) that acute cholinergic symptoms such as muscle fasciculation should appear at this stage. Second, muscle weakness spread to the distal limbs, which has only been encountered in delayed polyneuropathy, bearing the risk of becoming a chronic condition. Fortunately, this symptom regressed within several days with the accompanying clinical manifestations. Third, six of the twelve cranial nerves were involved, which makes this case of IMS the first with such an large extent of muscle weakness. All these new findings in our case witness to the complex clinical picture of IMS that needs further research. Conflicts of interest None to declare. Acknowledgements We would like to thank our patient for consenting to the publication of this case report.
5 195 REFERENCES 1. World Health Organization. The Impact of Pesticides on Health: Preventing Intentional and Unintentional Deaths from Pesticide Poisoning, 2004 [displayed 7 May 2018]. Available at PesticidesHealth2.pdf 2. Wadia RS, Chitra S, Armin RB, Kiwallkar RS, Sardesai HV. Electrophysiological studies in acute organophosphate poisoning. J Neurol Neurosurg Psychiatry 1987;50: PMCID: PMC Singh G, Khurana D. Neurology of acute organophosphate poisoning. Neurol India 2009;57: doi: / Peter JV, Cherian AM. Organic insecticides. Anaesth Intensive Care 2000;28: PMID: Namba T. Cholinesterase inhibition by organophosphorus compounds and its clinical effects. B World Health Organ 1971;44: PMCID: PMC Lotti M, Moretto A. Organophosphate-induced delayed polyneuropathy. Toxicol Rev 2005;24: PMID: Yang CC, Deng JF. Intermediate syndrome following organophosphate insecticide poisoning. J Chin Med Assoc 2007;70: doi: /S (08) Karalliedde L, Baker D, Marrs TC. Organophosphateinduced intermediate syndrome: aetiology and relationships with myopathy. Toxicol Rev 2006;25:1-14. PMID: Sarkar S, Nandi M, Mondal R, Mandal SK. Organophosphorusinduced extrapyramidal intermediate syndrome in an adolescent suicide attempt survivor. J Neurosci Rural Pract 2014;5: doi: / Azazh A. Severe organophosphate poisoning with delayed cholinergic crisis, intermediate syndrome and organophosphate induced delayed polyneuropathy on succession. Ethiop J Health Sci 2011;21: PMCID: PMC Gallo MA, Lawryk NJ. Organic phosphorus pesticides. In: Hayes WJ, Laws ER, editors. Handbook of Pesticide Toxicology. San Diego (CA): Academic Press; p Peter JV, Jerobin J, Nair A, Bennett A, Samuel P, Chrispal A, Abraham OC, Mathews KP, Fleming JJ, Oommen A. Clinical profile and outcome of patients hospitalized with dimethyl and diethyl organophosphate poisoning. Clin Toxicol 2010;48: doi: / Chaudhary SC, Singh K, Sawlani KK, Jain N, Vaish AK, Atam V, Lal Patel M, Agarwal A. Prognostic significance of estimation of pseudocholinesterase activity and role of pralidoxime therapy in organophosphorous poisoning. Toxicol Int 2013;20: doi: / De Bleecker J, Van den Neucker K, Colardyn F. Intermediate syndrome in organophosphorus poisoning: a prospective study. Crit Care Med 1993;21: PMID: Areekul S, Srichairat S, Kirdudom P. Serum and red cell cholinesterase activity in people exposed to organophosphate insecticides. Southeast Asian J Trop Med Public Health 1981;12:94-8. PMID: Pazooki S, Solhi H, Vishteh HR, Shadnia S, Beigi MJ. Effectiveness of fresh frozen plasma as supplementary treatment in organophosphate poisoning. Med J Malaysia 2011;66: PMID: Güven M, Sungur M, Eser B, Sari I, Altuntaş F. The Effects of fresh frozen plasma on cholinesterase levels and outcomes in patients with organophosphate poisoning. J Toxicol Clin Toxicol 2004;42: doi: /CLT von der Wellen J, Bierwisch A, Worek F, Thiermann H, Wille T. Kinetics of pesticide degradation by human fresh frozen plasma (FFP) in vitro. Toxicol Lett 2016;244: doi: /j.toxlet Senanayake N, Karalliedde L. Neurotoxic effects of organophosphorus insecticides. An intermediate syndrome. N Engl J Med 1987;316: doi: / NEJM Eddleston M, Mohamed F, Davies JO, Eyer P, Worek F, Sheriff MH, Buckley NA. Respiratory failure in acute organophosphorus pesticide self-poisoning. QJM 2006;99: doi: /qjmed/hcl Peter JV, Sudarsan TI, Moran JL. Clinical features of organophosphate poisoning: A review of different classification systems and approaches. Indian J Crit Care Med 2014;18: doi: / De Bleecker J, Vogelaers D, Ceuterick C, Van Den Neucker K, Willems J, De Reuck J. Intermediate syndrome due to prolonged parathion poisoning. Acta Neurol Scand 1992;86: doi: /j tb05110.x 23. He F, Xu H, Qin F, Xu L, Huang J, He X. Intermediate myasthenia syndrome following acute organophosphates poisoning - an analysis of 21 cases. Hum Exp Toxicol 1998;17: doi: / Novi uvidi u intermedijarni sindrom uzrokovan trovanjem organofosfatnim pesticidom Akutno trovanje organofosfatima (OP) može biti smrtonosnije od bilo koje druge vrste trovanja kemikalijama. Dosada je opisano tek nekoliko slučajeva s neurološkim komplikacijama širokih razmjera. Ovdje donosimo prikaz jednog iznimnno teškog slučaja trovanja pacijentice diazinonom, u koje se intermedijarni sindrom javio četvrtoga dana hospitalizacije. Njezina klinička slika obuhvaćala je slabost u pojedinim mišićima proksimalnih dijelova gornjih udova povezanih s motornim kranijalnim živcima, ali ono što je neobično bila je slabost mišića u distalnim dijelovima donjih udova. Koliko znamo, to je jedinstven takav slučaj, s obzirom na to da je slabost u mišićima donjih udova opisana samo u kontekstu kasne polineuropatije. Uz to, ovaj se slučaj intermedijarnog sindroma ističe i dosad nezabilježenom zahvaćenošću šest od dvanaest kranijalnih živaca. Time je dobiven novi uvid u polimorfnu narav kliničkih manifestacija akutnog trovanja organofosfatima. KLJUČNE RIJEČI: kolinesteraze; mijastenija; motorni kranijalni živci; slabost mišića donjih udova
Int. J. Pharm. Sci. Rev. Res., 28(1), September October 2014; Article No. 12, Pages: 61-66
 Research Article Nashwa M. Radwan 1, Naglaa A. El-Nabarawy 2 1,2 Consultant of clinical toxicology, National Egyptian Center of Clinical & Environmental, Toxicological Research (NECTR) - Cairo University.
Research Article Nashwa M. Radwan 1, Naglaa A. El-Nabarawy 2 1,2 Consultant of clinical toxicology, National Egyptian Center of Clinical & Environmental, Toxicological Research (NECTR) - Cairo University.
Atropine therapy in acute anticholinesterase (Organophosphorus / carbamate) poisoning; adherence to current guidelines
 Atropine therapy in acute anticholinesterase (Organophosphorus / carbamate) poisoning; adherence to current guidelines 1,,3 1 3 Jayasinghe SS, Fernando A, Pathirana KD, K Kishanthi Gunasinghe 1 Department
Atropine therapy in acute anticholinesterase (Organophosphorus / carbamate) poisoning; adherence to current guidelines 1,,3 1 3 Jayasinghe SS, Fernando A, Pathirana KD, K Kishanthi Gunasinghe 1 Department
Adherence to the National Guidelines on the Management of Organophosphorus Poisoning
 Adherence to the National Guidelines on the Management of Organophosphorus Poisoning 1 1 Jayasinghe SS, FernandoA 1 Department of Pharmacology, Faculty of Medicine, University of Ruhuna, Galle, Sri Lanka
Adherence to the National Guidelines on the Management of Organophosphorus Poisoning 1 1 Jayasinghe SS, FernandoA 1 Department of Pharmacology, Faculty of Medicine, University of Ruhuna, Galle, Sri Lanka
Outcome of patients with OPC poisoning who require mechanical ventilation: a statistical analysis
 International Journal of Advances in Medicine Madala P et al. Int J Adv Med. 17 Apr;4(2):37-361 http://www.ijmedicine.com pissn 2349-39 eissn 2349-3933 Original Research Article DOI: http://dx.doi.org/.183/2349-3933.ijam17913
International Journal of Advances in Medicine Madala P et al. Int J Adv Med. 17 Apr;4(2):37-361 http://www.ijmedicine.com pissn 2349-39 eissn 2349-3933 Original Research Article DOI: http://dx.doi.org/.183/2349-3933.ijam17913
Clinical profile and outcome of intermediate syndrome in acute organophosphate poisoning
 International Journal of Advances in Medicine Velayudham R et al. Int J Adv Med. 2018 Feb;5(1):62-67 http://www.ijmedicine.com pissn 2349-3925 eissn 2349-3933 Original Research Article DOI: http://dx.doi.org/10.18203/2349-3933.ijam20175561
International Journal of Advances in Medicine Velayudham R et al. Int J Adv Med. 2018 Feb;5(1):62-67 http://www.ijmedicine.com pissn 2349-3925 eissn 2349-3933 Original Research Article DOI: http://dx.doi.org/10.18203/2349-3933.ijam20175561
Intermediate Syndrome After Organophosphate Ingestion
 TZU CHI MED J September 2007 Vol 19 No 3 available at http://health.elsevier.com/tcmj Tzu Chi Medical Journal Case Report Intermediate Syndrome After Organophosphate Ingestion Yen-Ta Huang 1,2,4 *, Pei-Chun
TZU CHI MED J September 2007 Vol 19 No 3 available at http://health.elsevier.com/tcmj Tzu Chi Medical Journal Case Report Intermediate Syndrome After Organophosphate Ingestion Yen-Ta Huang 1,2,4 *, Pei-Chun
By Dr. Magdy M. Awny. (nerve agent)
 By Dr. Magdy M. Awny (nerve agent) Pesticides Is any chemical substance or mixture of substances intended for preventing, destroying, repelling, or mitigating any pest are a group of insecticides or Organophosphorous
By Dr. Magdy M. Awny (nerve agent) Pesticides Is any chemical substance or mixture of substances intended for preventing, destroying, repelling, or mitigating any pest are a group of insecticides or Organophosphorous
Cholinergic receptors( cholinoceptors ) are two families muscarinic and nicotinic depending on their affinities to cholinomimetic agents(agents that
 Cholinergic drugs Cholinergic drugs Are drugs act on receptors that are activated by acetylcholine(ach) which is the neurotransmitter of the parasympathetic nervous system. ACH is synthesized in the cholinergic
Cholinergic drugs Cholinergic drugs Are drugs act on receptors that are activated by acetylcholine(ach) which is the neurotransmitter of the parasympathetic nervous system. ACH is synthesized in the cholinergic
Predicting the need for ventilatory support in organophosphorous compound poisoning
 International Journal of Research in Medical Sciences Philip SM. Int J Res Med Sci. 2018 Dec;6(12):4015-4021 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Original Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20184900
International Journal of Research in Medical Sciences Philip SM. Int J Res Med Sci. 2018 Dec;6(12):4015-4021 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Original Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20184900
Has little therapeutic value. Has multiple actions. Has short t ½ Activates muscarinic & nicotinic receptors. 10/17/2017 2
 Has little therapeutic value. Has multiple actions. Has short t ½ Activates muscarinic & nicotinic receptors. 10/17/2017 2 Muscarinic stimulation: On the CVS: -ve chronotropic & inotropic effects. Decrease
Has little therapeutic value. Has multiple actions. Has short t ½ Activates muscarinic & nicotinic receptors. 10/17/2017 2 Muscarinic stimulation: On the CVS: -ve chronotropic & inotropic effects. Decrease
Organophosphate Poisoning Aklilu A 203
 Organophosphate Poisoning Aklilu A 203 CASE REPORT SEVERE ORGANOPHOSPHATE POISONING WITH DELAYED CHOLINERGIC CRISIS, INTERMEDIATE SYNDROME AND ORGANOPHOSPHATE INDUCED DELAYED POLYNEUROPATHY ON SUCCESSION
Organophosphate Poisoning Aklilu A 203 CASE REPORT SEVERE ORGANOPHOSPHATE POISONING WITH DELAYED CHOLINERGIC CRISIS, INTERMEDIATE SYNDROME AND ORGANOPHOSPHATE INDUCED DELAYED POLYNEUROPATHY ON SUCCESSION
Human Physiology Lab (Biol 236L) Fall, 2015
 1 Human Physiology Lab (Biol 236L) Fall, 2015 Name: Nursing Case Study: Muscle Weakness Chief Complaint: A 26-year-old woman with muscle weakness in the face. Patient Presentation: A 26-year-old woman
1 Human Physiology Lab (Biol 236L) Fall, 2015 Name: Nursing Case Study: Muscle Weakness Chief Complaint: A 26-year-old woman with muscle weakness in the face. Patient Presentation: A 26-year-old woman
Autonomic Pharmacology: Cholinergic agonists
 Autonomic Pharmacology: Cholinergic agonists Öner Süzer www.onersuzer.com osuzer@istanbul.edu.tr Last update: 23.01.2013 1 Acetylcholine Acetylcholine (ACh), the naturally occurring neurotransmitter for
Autonomic Pharmacology: Cholinergic agonists Öner Süzer www.onersuzer.com osuzer@istanbul.edu.tr Last update: 23.01.2013 1 Acetylcholine Acetylcholine (ACh), the naturally occurring neurotransmitter for
Clinical Problems in Organophosphate Insecticide Poisoning: The Use of a Computerized Information System
 FUNDAMENTAL AND APPUED TOXICOLOGY 4, S2O9-S214 (1984) Clinical Problems in Organophosphate Insecticide Poisoning: The Use of a Computerized Information System ASHER HlRSHBERG AND YEHUDA LERMAN Research
FUNDAMENTAL AND APPUED TOXICOLOGY 4, S2O9-S214 (1984) Clinical Problems in Organophosphate Insecticide Poisoning: The Use of a Computerized Information System ASHER HlRSHBERG AND YEHUDA LERMAN Research
Cholinesterase-inhibiting Chemicals C 1
 BASF Chemical Emergency Medical Guidelines Cholinesterase-inhibiting Chemicals C 1 Information and recommendations for doctors at hospitals/emergency departments Patients whose vomitus, skin or clothing
BASF Chemical Emergency Medical Guidelines Cholinesterase-inhibiting Chemicals C 1 Information and recommendations for doctors at hospitals/emergency departments Patients whose vomitus, skin or clothing
BUTYRYLCHOLINESTERASE ACTIVITY BIOMARKER FOR PREDICTING THE OUTCOME IN ACUTE CHOLINESTERASE INHIBITOR POISONING A 30-YEAR RETROSPECTIVE ANALYSIS
 Rev. Med. Chir. Soc. Med. Nat., Iaşi 2014 vol. 118, no. 4 INTERNAL MEDICINE - PEDIATRICS ORIGINAL PAPERS BUTYRYLCHOLINESTERASE ACTIVITY BIOMARKER FOR PREDICTING THE OUTCOME IN ACUTE CHOLINESTERASE INHIBITOR
Rev. Med. Chir. Soc. Med. Nat., Iaşi 2014 vol. 118, no. 4 INTERNAL MEDICINE - PEDIATRICS ORIGINAL PAPERS BUTYRYLCHOLINESTERASE ACTIVITY BIOMARKER FOR PREDICTING THE OUTCOME IN ACUTE CHOLINESTERASE INHIBITOR
INTRODUTION. from atropos, one of the three fates, who according to Greek mythology,
 Introduction INTRODUTION Atropine, a naturally occurring tertiary amine, derives its name from atropos, one of the three fates, who according to Greek mythology, chose how a person die. The atropine, a
Introduction INTRODUTION Atropine, a naturally occurring tertiary amine, derives its name from atropos, one of the three fates, who according to Greek mythology, chose how a person die. The atropine, a
A Primer on Chemical Nerve Agents. Information for Public Health and EMS Workers
 A Primer on Chemical Nerve Agents Information for Public Health and EMS Workers This information was adapted and developed from a presentation by: Area Health Education Center of Southern Nevada 2 Chemical
A Primer on Chemical Nerve Agents Information for Public Health and EMS Workers This information was adapted and developed from a presentation by: Area Health Education Center of Southern Nevada 2 Chemical
BRAIN STEM CASE HISTORIES CASE HISTORY VII
 463 Brain stem Case history BRAIN STEM CASE HISTORIES CASE HISTORY VII A 60 year old man with hypertension wakes one morning with trouble walking. He is feeling dizzy and is sick to his stomach. His wife
463 Brain stem Case history BRAIN STEM CASE HISTORIES CASE HISTORY VII A 60 year old man with hypertension wakes one morning with trouble walking. He is feeling dizzy and is sick to his stomach. His wife
IJBCP International Journal of Basic & Clinical Pharmacology
 Print ISSN 2319-2003 Online ISSN 2279-0780 IJBCP International Journal of Basic & Clinical Pharmacology doi: 10.5455/2319-2003.ijbcp20140622 Research Article The utility of serial serum cholinesterase
Print ISSN 2319-2003 Online ISSN 2279-0780 IJBCP International Journal of Basic & Clinical Pharmacology doi: 10.5455/2319-2003.ijbcp20140622 Research Article The utility of serial serum cholinesterase
ORGANOPHOSPHORUS INSECTICIDE POISONING
 Abstract ORGANOPHOSPHORUS INSECTICIDE POISONING Pages with reference to book, From 27 To 31 Hamida Jamil ( Department of Medicine Unit II, Jinnah Postgraduate Medical Centre, Karachi. ) A review of 755
Abstract ORGANOPHOSPHORUS INSECTICIDE POISONING Pages with reference to book, From 27 To 31 Hamida Jamil ( Department of Medicine Unit II, Jinnah Postgraduate Medical Centre, Karachi. ) A review of 755
Drugs Affecting the Autonomic Nervous System-2 Cholinergic agents
 Drugs Affecting the Autonomic Nervous System-2 Cholinergic agents Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Cholinergic agents, Cholinomimetic drugs,
Drugs Affecting the Autonomic Nervous System-2 Cholinergic agents Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Cholinergic agents, Cholinomimetic drugs,
Pharmacology Autonomic Nervous System Lecture10
 Pharmacology Autonomic Nervous System Lecture10 Note : Most of the time in this lecture, the doctor was only reading from the slides, so I m going to write only the extra information he mentioned So Please
Pharmacology Autonomic Nervous System Lecture10 Note : Most of the time in this lecture, the doctor was only reading from the slides, so I m going to write only the extra information he mentioned So Please
Organophosphorous Compound Poisoning in Western Odisha: A Five Year Retrospective Study
 Original article Indian Journal of Forensic Medicine and Pathology 121 Organophosphorous Compound Poisoning in Western Odisha: A Five Year Retrospective Study Manoj Kumar Jena Abstract Background: Organophosphorous
Original article Indian Journal of Forensic Medicine and Pathology 121 Organophosphorous Compound Poisoning in Western Odisha: A Five Year Retrospective Study Manoj Kumar Jena Abstract Background: Organophosphorous
Cholinergic antagonists
 Cholinergic antagonists Cholinergic antagonists: They are also called anticholinergic drugs or cholinergic blockers, this group include: 1.Antimuscarinic agents ( atropine, ipratropium, scopolamine) 2.
Cholinergic antagonists Cholinergic antagonists: They are also called anticholinergic drugs or cholinergic blockers, this group include: 1.Antimuscarinic agents ( atropine, ipratropium, scopolamine) 2.
chlorpyriphos group when compared to other OP compounds. Keywords: organophosphate * Address for Correspondence:
 Research Article Clinical profile and outcome of organophosphate poisoning cases in a tertiary care hospital in central Kerala Edwin J George 1*, Jayaraj K 2, John J Manjaly 3, Raghunath M 4 1,2,3,4 Assistant
Research Article Clinical profile and outcome of organophosphate poisoning cases in a tertiary care hospital in central Kerala Edwin J George 1*, Jayaraj K 2, John J Manjaly 3, Raghunath M 4 1,2,3,4 Assistant
Parasympathetic Nervous System Part I
 Parasympathetic Nervous System Part I Edward JN Ishac, Ph.D. Professor Smith Building, Room 742 eishac@vcu.edu 828 2127 Department of Pharmacology and Toxicology Medical College of Virginia Campus of Virginia
Parasympathetic Nervous System Part I Edward JN Ishac, Ph.D. Professor Smith Building, Room 742 eishac@vcu.edu 828 2127 Department of Pharmacology and Toxicology Medical College of Virginia Campus of Virginia
A study of serum amylase levels in acute organophosphorous poisoning at Government Dharmapuri Medical College Hospital, Dharmapuri
 Original Research Article A study of serum amylase levels in acute organophosphorous poisoning at Government Dharmapuri Medical College Hospital, Dharmapuri P. Elango 1, G. Indumathi 2* 1 Assistant Professor,
Original Research Article A study of serum amylase levels in acute organophosphorous poisoning at Government Dharmapuri Medical College Hospital, Dharmapuri P. Elango 1, G. Indumathi 2* 1 Assistant Professor,
5.1 Alex.
 5.1 Alex http://tinyurl.com/neuromakessense Alex is a 20-year-old full-time national serviceman. His only past medical history is asthma, presents to A&E with a 4-day history of bilateral finger weakness
5.1 Alex http://tinyurl.com/neuromakessense Alex is a 20-year-old full-time national serviceman. His only past medical history is asthma, presents to A&E with a 4-day history of bilateral finger weakness
JMSCR Vol 06 Issue 12 Page December 2018
 JMSCR Vol 6 Issue 12 Page 28-39 December 218 www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 79.54 ISSN (e)-2347-176x ISSN (p) 2455-45 DOI: https://dx.doi.org/1.18535/jmscr/v6i12.6
JMSCR Vol 6 Issue 12 Page 28-39 December 218 www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 79.54 ISSN (e)-2347-176x ISSN (p) 2455-45 DOI: https://dx.doi.org/1.18535/jmscr/v6i12.6
Study of prognostic value of serum and RBC acetyle cholinesterase level in organophosphorus poisoning and its correlation with the outcome
 Original Research Article Study of prognostic value of serum and RBC acetyle cholinesterase level in organophosphorus poisoning and its correlation with the outcome Prakash Patel 1, Viralben P. Patel 2*,
Original Research Article Study of prognostic value of serum and RBC acetyle cholinesterase level in organophosphorus poisoning and its correlation with the outcome Prakash Patel 1, Viralben P. Patel 2*,
LOSS OF CONSCIOUSNESS & ASSESSMENT. Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT
 LOSS OF CONSCIOUSNESS & ASSESSMENT Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT OUTLINE Causes Head Injury Clinical Features Complications Rapid Assessment Glasgow Coma Scale Classification
LOSS OF CONSCIOUSNESS & ASSESSMENT Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT OUTLINE Causes Head Injury Clinical Features Complications Rapid Assessment Glasgow Coma Scale Classification
NEUROMUSCULAR BLOCKING AGENTS
 NEUROMUSCULAR BLOCKING AGENTS Edward JN Ishac, Ph.D. Associate Professor, Pharmacology and Toxicology Smith 742, 828-2127, Email: eishac@vcu.edu Learning Objectives: 1. Understand the physiology of the
NEUROMUSCULAR BLOCKING AGENTS Edward JN Ishac, Ph.D. Associate Professor, Pharmacology and Toxicology Smith 742, 828-2127, Email: eishac@vcu.edu Learning Objectives: 1. Understand the physiology of the
Expanded Case Summary 4: Botulism.
 Expanded Case Summary 4: Botulism. This case details the presentation and management of a patient admitted to the intensive care unit following a respiratory arrest with potential hypoxic brain injury.
Expanded Case Summary 4: Botulism. This case details the presentation and management of a patient admitted to the intensive care unit following a respiratory arrest with potential hypoxic brain injury.
CALL US...TM. Anticholinesterase (Organic Phosphorus and Carbamate) Pesticide Poisoning
 CALL US...TM The Official Newsletter of the California Poison Control System Volume 6, Number 2 Summer 2008 Anticholinesterase (Organic Phosphorus and Carbamate) Pesticide Poisoning Introduction Organic
CALL US...TM The Official Newsletter of the California Poison Control System Volume 6, Number 2 Summer 2008 Anticholinesterase (Organic Phosphorus and Carbamate) Pesticide Poisoning Introduction Organic
A study on glasgow coma scale score and QTC interval in predicting prognosis and outcome of organophosphate and carbamate poisoning
 Original Research Article A study on glasgow coma scale score and QTC interval in predicting prognosis and outcome of organophosphate and carbamate poisoning Raman Prabhakaran 1*, Marannan Navinkumar 2,
Original Research Article A study on glasgow coma scale score and QTC interval in predicting prognosis and outcome of organophosphate and carbamate poisoning Raman Prabhakaran 1*, Marannan Navinkumar 2,
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Study of Hyperglycemia and Its Association with Pseudocholinesterase Levels and Severity of
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Study of Hyperglycemia and Its Association with Pseudocholinesterase Levels and Severity of
ORGANOPHOSPHATE POISONING: 10 YEARS OF EXPERIENCE IN SOUTHERN TAIWAN
 ORGAOPHOSPHATE POISOIG: 10 YEARS OF EXPERIECE I SOUTHER TAIWA Jong-Rung Tsai, 1 Chau-Chyun Sheu, 1 Meng-Hsuan Cheng, 1 Jen-Yu Hung, 1 Chuan-Sheng Wang, 2 Inn-Wen Chong, 1,3 Ming-Shyang Huang, 1,3 and Jhi-Jhu
ORGAOPHOSPHATE POISOIG: 10 YEARS OF EXPERIECE I SOUTHER TAIWA Jong-Rung Tsai, 1 Chau-Chyun Sheu, 1 Meng-Hsuan Cheng, 1 Jen-Yu Hung, 1 Chuan-Sheng Wang, 2 Inn-Wen Chong, 1,3 Ming-Shyang Huang, 1,3 and Jhi-Jhu
Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials
 Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials 1 1. A high-risk bodily fluid for spreading infection is blood. 2. Items that can reduce the spread of infection include masks, gloves, and
Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials 1 1. A high-risk bodily fluid for spreading infection is blood. 2. Items that can reduce the spread of infection include masks, gloves, and
The role of plasmapheresis in organophosphate poisoning: Case reports of three pediatric patients
 The Turkish Journal of Pediatrics 2017; 59: 491-496 DOI: 10.24953/turkjped.2017.04.020 Case Report The role of plasmapheresis in organophosphate poisoning: Case reports of three pediatric patients Ufuk
The Turkish Journal of Pediatrics 2017; 59: 491-496 DOI: 10.24953/turkjped.2017.04.020 Case Report The role of plasmapheresis in organophosphate poisoning: Case reports of three pediatric patients Ufuk
CLINICAL REVIEW. Managing acute organophosphorus pesticide poisoning. Darren M Roberts, 1 Cynthia K Aaron 2
 For the full versions of these articles see bmj.com CLINICAL REVIEW Managing acute organophosphorus pesticide poisoning Darren M Roberts, 1 Cynthia K Aaron 2 1 South Asian Clinical Toxicology Research
For the full versions of these articles see bmj.com CLINICAL REVIEW Managing acute organophosphorus pesticide poisoning Darren M Roberts, 1 Cynthia K Aaron 2 1 South Asian Clinical Toxicology Research
Myasthenia Gravis. Mike Gilchrist 10/30/06
 Myasthenia Gravis Mike Gilchrist 10/30/06 Overview Background Pathogenesis Clinical Manifestations Diagnosis Treatment Associated Conditions Background Severe muscle disease Most common disorder of neuromuscular
Myasthenia Gravis Mike Gilchrist 10/30/06 Overview Background Pathogenesis Clinical Manifestations Diagnosis Treatment Associated Conditions Background Severe muscle disease Most common disorder of neuromuscular
Clinical profile of organophosphorus poisoning in a tertiary care hospital
 Original article Clinical profile of organophosphorus poisoning in a tertiary care hospital Dayanand Raddi, Anikethana G V Karnataka Institute of Medical Sciences, Hubli, Karnataka Corresponding author:
Original article Clinical profile of organophosphorus poisoning in a tertiary care hospital Dayanand Raddi, Anikethana G V Karnataka Institute of Medical Sciences, Hubli, Karnataka Corresponding author:
RMP section VI.2 Elements for Public Summary
 RMP section VI.2 Elements for Public Summary Product: Atropin Stragen, 0,1 mg/ml solution for injection in pre-filled syringe Atropin Stragen, 0,2 mg/ml solution for injection in pre-filled syringe RMP:
RMP section VI.2 Elements for Public Summary Product: Atropin Stragen, 0,1 mg/ml solution for injection in pre-filled syringe Atropin Stragen, 0,2 mg/ml solution for injection in pre-filled syringe RMP:
MYASTHENIA GRAVIS. Mr. D.Raju, M.pharm, Lecturer
 MYASTHENIA GRAVIS Mr. D.Raju, M.pharm, Lecturer OUTLINE Background Anatomy Pathophysiology Clinical Presentation Treatment BACKGROUND Acquired autoimmune disorder Clinically characterized by: Weakness
MYASTHENIA GRAVIS Mr. D.Raju, M.pharm, Lecturer OUTLINE Background Anatomy Pathophysiology Clinical Presentation Treatment BACKGROUND Acquired autoimmune disorder Clinically characterized by: Weakness
A Hypothesis Driven Approach to the Neurological Exam
 A Hypothesis Driven Approach to the Neurological Exam Vanja Douglas, MD Assistant Clinical Professor UCSF Department of Neurology Disclosures None 1 Purpose of Neuro Exam Screen asymptomatic patients Screen
A Hypothesis Driven Approach to the Neurological Exam Vanja Douglas, MD Assistant Clinical Professor UCSF Department of Neurology Disclosures None 1 Purpose of Neuro Exam Screen asymptomatic patients Screen
NEW ZEALAND DATA SHEET. Injection solution 2.5 mg/ml: a clear, colourless, particle-free solution containing 2.5 mg/ml Neostigmine methylsulphate.
 NEW ZEALAND DATA SHEET NAME OF MEDICINE NEOSTIGMINE METHYLSULPHATE INJECTION B.P. Solution for injection 2.5 mg/ml. PRESENTATIONS Injection solution 2.5 mg/ml: a clear, colourless, particle-free solution
NEW ZEALAND DATA SHEET NAME OF MEDICINE NEOSTIGMINE METHYLSULPHATE INJECTION B.P. Solution for injection 2.5 mg/ml. PRESENTATIONS Injection solution 2.5 mg/ml: a clear, colourless, particle-free solution
Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra hospital, Isfahan university of medical sciences
 Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra hospital, Isfahan university of medical sciences ٢ Level of consciousness is depressed Stuporous patients respond only to repeated
Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra hospital, Isfahan university of medical sciences ٢ Level of consciousness is depressed Stuporous patients respond only to repeated
Movement Disorders. Psychology 372 Physiological Psychology. Background. Myasthenia Gravis. Many Types
 Background Movement Disorders Psychology 372 Physiological Psychology Steven E. Meier, Ph.D. Listen to the audio lecture while viewing these slides Early Studies Found some patients with progressive weakness
Background Movement Disorders Psychology 372 Physiological Psychology Steven E. Meier, Ph.D. Listen to the audio lecture while viewing these slides Early Studies Found some patients with progressive weakness
Chapter 13. Learning Objectives. Learning Objectives 9/11/2012. Poisonings, Overdoses, and Intoxications
 Chapter 13 Poisonings, Overdoses, and Intoxications Learning Objectives Discuss use of activated charcoal in treatment of poisonings List treatment options for acetaminophen overdose List clinical manifestations
Chapter 13 Poisonings, Overdoses, and Intoxications Learning Objectives Discuss use of activated charcoal in treatment of poisonings List treatment options for acetaminophen overdose List clinical manifestations
The Spectrum of Intermediate Syndrome Following Acute Organophosphate Poisoning: A Prospective Cohort Study from Sri Lanka
 PLoS MEDICINE The Spectrum of Intermediate Syndrome Following Acute Organophosphate Poisoning: A Prospective Cohort Study from Sri Lanka Pradeepa Jayawardane 1,2*, Andrew H. Dawson 1,3, Vajira Weerasinghe
PLoS MEDICINE The Spectrum of Intermediate Syndrome Following Acute Organophosphate Poisoning: A Prospective Cohort Study from Sri Lanka Pradeepa Jayawardane 1,2*, Andrew H. Dawson 1,3, Vajira Weerasinghe
The Latest Approaches to Reversal of Neuromuscular Blocking Agents
 The Latest Approaches to Reversal of Neuromuscular Blocking Agents Janay Bailey, Pharm.D. Anesthesiology 2017; 126:173-90 Objectives Pharmacists Determine optimal paralytic choices in knowing if reversal
The Latest Approaches to Reversal of Neuromuscular Blocking Agents Janay Bailey, Pharm.D. Anesthesiology 2017; 126:173-90 Objectives Pharmacists Determine optimal paralytic choices in knowing if reversal
Neuromuscular Blockers
 Neuromuscular Blockers Joanne Leung joanneleung22@hotmail.com Oct 14, 2014 Objectives After this lecture, you should be able to: Describe the physiology of the neuromuscular junction Differentiate the
Neuromuscular Blockers Joanne Leung joanneleung22@hotmail.com Oct 14, 2014 Objectives After this lecture, you should be able to: Describe the physiology of the neuromuscular junction Differentiate the
Serial serum cholinesterase activities as a prognostic factor in organophosphate poisoned patients
 Hong Kong Journal of Emergency Medicine Serial serum cholinesterase activities as a prognostic factor in organophosphate poisoned patients HW Yun, DH Lee, JH Lee, YJ Cheon, YH Choi Objective: Organophosphate
Hong Kong Journal of Emergency Medicine Serial serum cholinesterase activities as a prognostic factor in organophosphate poisoned patients HW Yun, DH Lee, JH Lee, YJ Cheon, YH Choi Objective: Organophosphate
#10 part 1+ mind maps. cholinomimetics. made by lama shatat corrected by laith sorour date 25/10
 #10 part 1+ mind maps cholinomimetics made by lama shatat corrected by laith sorour date 25/10 Cholinergic Cholinergic agonists Direct (activates directly Cholinergic Receptor) ANS drugs Antagonists Adrenergic
#10 part 1+ mind maps cholinomimetics made by lama shatat corrected by laith sorour date 25/10 Cholinergic Cholinergic agonists Direct (activates directly Cholinergic Receptor) ANS drugs Antagonists Adrenergic
Poison (Toxicant): any substance or agent capable of producing a deleterious response in a biological system or living organism.
 Poison (Toxicant): any substance or agent capable of producing a deleterious response in a biological system or living organism. Poisoning= overdose toxicity intoxication= toxicity due to foreign substance
Poison (Toxicant): any substance or agent capable of producing a deleterious response in a biological system or living organism. Poisoning= overdose toxicity intoxication= toxicity due to foreign substance
DUODOTE AUTO-INJECTOR
 Hazardous Material (WMD) use only Indications The DuoDote may be administered by the EMT or Paramedic who have had adequate training in the on-site recognition and treatment of nerve agent exposure. Chemical
Hazardous Material (WMD) use only Indications The DuoDote may be administered by the EMT or Paramedic who have had adequate training in the on-site recognition and treatment of nerve agent exposure. Chemical
 Page 1 of 6 Title Authored By Course No Contact Hour 1 An Overview of Myasthenia Gravis Ray Lengel RN, FNP, MS MG2061208 Purpose The goal of this course is to provide an understanding about myasthenia
Page 1 of 6 Title Authored By Course No Contact Hour 1 An Overview of Myasthenia Gravis Ray Lengel RN, FNP, MS MG2061208 Purpose The goal of this course is to provide an understanding about myasthenia
Case 1. What does the CXR show? How would you manage this patient? Discussion overleaf.
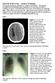 Tutorial of the week cerebral challenge. This has previously been published in Update in anaesthesia. Examples of investigations demonstrating typical appearances of commonly encountered conditions are
Tutorial of the week cerebral challenge. This has previously been published in Update in anaesthesia. Examples of investigations demonstrating typical appearances of commonly encountered conditions are
Mahmoud K. Elguindi et al.
 Mahmoud K. Elguindi et al. Electroneurophysiological Monitoring as an Early Severity Predictor in Acute Anticholinesterase Poisoned Patient and the Effect of Oxime Therapy Manipulation Mahmoud K. Elguindi
Mahmoud K. Elguindi et al. Electroneurophysiological Monitoring as an Early Severity Predictor in Acute Anticholinesterase Poisoned Patient and the Effect of Oxime Therapy Manipulation Mahmoud K. Elguindi
2:39 2: Dizziness and nausea Cerebral. 2:57 1: Vomiting Gastro-intestinal
 Supplemental: Table B: Detailed description of adverse events by time, treatment group and procedure T-spinal to incident T-spinal to PACU discharge Group THA/TKA Adverse event description Adverse event
Supplemental: Table B: Detailed description of adverse events by time, treatment group and procedure T-spinal to incident T-spinal to PACU discharge Group THA/TKA Adverse event description Adverse event
NATO UNCLASSIFIED NATO UNCLASSIFIED 2-1 ORIGINAL CHAPTER 2 NERVE AGENTS SECTION I - GENERAL
 NATO UNCLASSIFIED AMedP-6(B), Part III CHAPTER 2 NERVE AGENTS SECTION I - GENERAL 201. Introduction. The nerve agents (NA) are a group of particularly toxic chemical warfare agents. They were developed
NATO UNCLASSIFIED AMedP-6(B), Part III CHAPTER 2 NERVE AGENTS SECTION I - GENERAL 201. Introduction. The nerve agents (NA) are a group of particularly toxic chemical warfare agents. They were developed
Chapter 18 Neuromuscular Blocking Agents Study Guide and Application Exercise
 Chapter 18 Neuromuscular Blocking Agents Study Guide and Application Exercise 1. Read chapter 2. Review objectives (p.305) 3. Review key terms and definitions (p.305) Add: Cholinesterase inhibitor Vagal
Chapter 18 Neuromuscular Blocking Agents Study Guide and Application Exercise 1. Read chapter 2. Review objectives (p.305) 3. Review key terms and definitions (p.305) Add: Cholinesterase inhibitor Vagal
The Neurologic Examination. John W. Engstrom, M.D. University of California San Francisco School of Medicine
 The Neurologic Examination John W. Engstrom, M.D. University of California San Francisco School of Medicine Overview The Neurologic Examination Mental status demonstration/questions Cranial nerves demonstration/questions
The Neurologic Examination John W. Engstrom, M.D. University of California San Francisco School of Medicine Overview The Neurologic Examination Mental status demonstration/questions Cranial nerves demonstration/questions
An infected insect bite? Dr Estée Török Honorary Consultant in Infectious Diseases & Microbiology Addenbrooke s Hospital, Cambridge
 An infected insect bite? Dr Estée Török Honorary Consultant in Infectious Diseases & Microbiology Addenbrooke s Hospital, Cambridge Case history 48 year old man Presented to A&E with 48 hour history double
An infected insect bite? Dr Estée Török Honorary Consultant in Infectious Diseases & Microbiology Addenbrooke s Hospital, Cambridge Case history 48 year old man Presented to A&E with 48 hour history double
Anesthesia and Neuromuscular Blockade: A Guide for Hospital Pharmacists. Upon completion of this activity, participants will be better able to:
 Anesthesia and Neuromuscular Blockade: A Guide for Hospital Pharmacists EDUCATIONAL OBJECTIVES Upon completion of this activity, participants will be better able to: 1. Understand the use of neuromuscular
Anesthesia and Neuromuscular Blockade: A Guide for Hospital Pharmacists EDUCATIONAL OBJECTIVES Upon completion of this activity, participants will be better able to: 1. Understand the use of neuromuscular
Faculty of Clinical Forensic Medicine Committee 1/2018
 Guideline Subject: Clinical Forensic Assessment and Management of Non-Fatal Strangulation Approval Date: January 2018 Review Date: January 2021 Review By: Number: Faculty of Clinical Forensic Medicine
Guideline Subject: Clinical Forensic Assessment and Management of Non-Fatal Strangulation Approval Date: January 2018 Review Date: January 2021 Review By: Number: Faculty of Clinical Forensic Medicine
Identification number: TÁMOP /1/A
 Manifestation of Novel Social Challenges of the European Union in the Teaching Material of Medical Biotechnology Master s Programmes at the University of Pécs and at the University of Debrecen Identification
Manifestation of Novel Social Challenges of the European Union in the Teaching Material of Medical Biotechnology Master s Programmes at the University of Pécs and at the University of Debrecen Identification
PRODUCT INFORMATION. (RS)-N,N-Dimethyl-2-[(2-methylphenyl)phenylmethoxy]ethanamine dihydrogen 2-hydroxypropane-1,2,3-tricarboxylate
![PRODUCT INFORMATION. (RS)-N,N-Dimethyl-2-[(2-methylphenyl)phenylmethoxy]ethanamine dihydrogen 2-hydroxypropane-1,2,3-tricarboxylate PRODUCT INFORMATION. (RS)-N,N-Dimethyl-2-[(2-methylphenyl)phenylmethoxy]ethanamine dihydrogen 2-hydroxypropane-1,2,3-tricarboxylate](/thumbs/81/82665370.jpg) NORGESIC Orphenadrine citrate and paracetamol PRODUCT INFORMATION NAME OF THE MEDICINE Active ingredient: Chemical name: CAS number: 4682-36-4 Chemical structure: Orphenadrine citrate (RS)-N,N-Dimethyl-2-[(2-methylphenyl)phenylmethoxy]ethanamine
NORGESIC Orphenadrine citrate and paracetamol PRODUCT INFORMATION NAME OF THE MEDICINE Active ingredient: Chemical name: CAS number: 4682-36-4 Chemical structure: Orphenadrine citrate (RS)-N,N-Dimethyl-2-[(2-methylphenyl)phenylmethoxy]ethanamine
STUDY OF LEVELS OF SERUM CREATINE PHOSPHOKINASE AND LIVER ENZYMES AS A PROGNOSTIC INDICATORS IN ACUTE ORGANOPHOSPHORUS POISONING
 Original Article STUDY OF LEVELS OF SERUM CREATINE PHOSPHOKINASE AND LIVER ENZYMES AS A PROGNOSTIC INDICATORS IN ACUTE ORGANOPHOSPHORUS POISONING Banashankari S Kollur1, Mallanna S Mulimani2 Post graduate
Original Article STUDY OF LEVELS OF SERUM CREATINE PHOSPHOKINASE AND LIVER ENZYMES AS A PROGNOSTIC INDICATORS IN ACUTE ORGANOPHOSPHORUS POISONING Banashankari S Kollur1, Mallanna S Mulimani2 Post graduate
Respiratory failure in acute organophosphorus pesticide self-poisoning
 Q J Med 2006; 99:513 522 doi:10.1093/qjmed/hcl065 Respiratory failure in acute organophosphorus pesticide self-poisoning M. EDDLESTON 1,2,3, F. MOHAMED 2,3, J.O.J. DAVIES 2,4, P. EYER 2,5, F. WOREK 2,6,
Q J Med 2006; 99:513 522 doi:10.1093/qjmed/hcl065 Respiratory failure in acute organophosphorus pesticide self-poisoning M. EDDLESTON 1,2,3, F. MOHAMED 2,3, J.O.J. DAVIES 2,4, P. EYER 2,5, F. WOREK 2,6,
AUTOIMMUNE DISORDERS IN THE ACUTE SETTING
 AUTOIMMUNE DISORDERS IN THE ACUTE SETTING Diagnosis and Treatment Goals Aimee Borazanci, MD BNI Neuroimmunology Objectives Give an update on the causes for admission, clinical features, and outcomes of
AUTOIMMUNE DISORDERS IN THE ACUTE SETTING Diagnosis and Treatment Goals Aimee Borazanci, MD BNI Neuroimmunology Objectives Give an update on the causes for admission, clinical features, and outcomes of
NERVOUS SYSTEM NERVOUS SYSTEM. Somatic nervous system. Brain Spinal Cord Autonomic nervous system. Sympathetic nervous system
 SYNAPTIC NERVOUS SYSTEM NERVOUS SYSTEM CENTRAL NERVOUS SYSTEM PERIPHERAL NERVOUS SYSTEM Brain Spinal Cord Autonomic nervous system Somatic nervous system Sympathetic nervous system Parasympathetic nervous
SYNAPTIC NERVOUS SYSTEM NERVOUS SYSTEM CENTRAL NERVOUS SYSTEM PERIPHERAL NERVOUS SYSTEM Brain Spinal Cord Autonomic nervous system Somatic nervous system Sympathetic nervous system Parasympathetic nervous
Sample Case Study. The patient was a 77-year-old female who arrived to the emergency room on
 Sample Case Study The patient was a 77-year-old female who arrived to the emergency room on February 25 th with a chief complaint of shortness of breath and a deteriorating pulmonary status along with
Sample Case Study The patient was a 77-year-old female who arrived to the emergency room on February 25 th with a chief complaint of shortness of breath and a deteriorating pulmonary status along with
CENTRAL CARE POLICY SYMPTOMS OF ILLNESS. Policy: Consumers will be observed for symptoms of physical problems, distress, pain, or unusual behaviors.
 Page 1 of 5 CENTRAL CARE POLICY SYMPTOMS OF ILLNESS SUBJECT: SYMPTOMS OF ILLNESS ANNUAL REVIEW MONTH: June RESPONSIBLE FOR REVIEW: Director of Central Care LAST REVISION DATE: June 2009 Policy: Consumers
Page 1 of 5 CENTRAL CARE POLICY SYMPTOMS OF ILLNESS SUBJECT: SYMPTOMS OF ILLNESS ANNUAL REVIEW MONTH: June RESPONSIBLE FOR REVIEW: Director of Central Care LAST REVISION DATE: June 2009 Policy: Consumers
Post-Anesthesia Care In the ICU
 Post-Anesthesia Care In the ICU The following is based on current research and regional standards of care. At completion you will be able to identify Basic equipment needed at the bedside. Aldrete scoring
Post-Anesthesia Care In the ICU The following is based on current research and regional standards of care. At completion you will be able to identify Basic equipment needed at the bedside. Aldrete scoring
Organophosphate Induced Neuropathy - An Epidemic Case Report at Civil Hospital, Ahmedabad
 * Corresponding Author: Mrs. Yagna U. Shukla. Email: yagnshukla@yahoo.com BJKines-NJBAS Volume-7(2), December 2015 2015 Organophosphate Induced Neuropathy - An Epidemic Case Report at Civil Hospital, Ahmedabad
* Corresponding Author: Mrs. Yagna U. Shukla. Email: yagnshukla@yahoo.com BJKines-NJBAS Volume-7(2), December 2015 2015 Organophosphate Induced Neuropathy - An Epidemic Case Report at Civil Hospital, Ahmedabad
Principles of Drug Action
 Principles of Drug Action How Do Drugs Work? Drugs (usually small molecules) bind to proteins (large molecules) or nucleic acids (only a few) Drug target = binding site of drug (RICE) o Receptors o Ion
Principles of Drug Action How Do Drugs Work? Drugs (usually small molecules) bind to proteins (large molecules) or nucleic acids (only a few) Drug target = binding site of drug (RICE) o Receptors o Ion
Nervous System. Peripheral Nervous System ( PNS ) Central Nervous System ( CNS ) Somatic. Autonomic ( ANS ) Enteric.
 NERVOUS SYSTEM Nervous System Peripheral Nervous System ( PNS ) Central Nervous System ( CNS ) Efferent (Motor) Afferent (Sensor) Autonomic ( ANS ) Somatic Parasympathetic Sympathetic Enteric Autonomic
NERVOUS SYSTEM Nervous System Peripheral Nervous System ( PNS ) Central Nervous System ( CNS ) Efferent (Motor) Afferent (Sensor) Autonomic ( ANS ) Somatic Parasympathetic Sympathetic Enteric Autonomic
Unexplained Illness Patient Scenario
 Diagnosis and Management of Foodborne Illnesses A Primer for Physicians and Other Health Care Professionals Unexplained Illness Patient Scenario Unexplained Illness Patient Scenario American Medical Association
Diagnosis and Management of Foodborne Illnesses A Primer for Physicians and Other Health Care Professionals Unexplained Illness Patient Scenario Unexplained Illness Patient Scenario American Medical Association
Anterior Cervical Discectomy and Fusion for Cervical Radiculopathy or Cervical Myelopathy (ACDF)
 Anterior Cervical Discectomy and Fusion for Cervical Radiculopathy or Cervical Myelopathy (ACDF) About your condition The pressure from your bulging disc(s) might be causing your pain, numbness or weakness.
Anterior Cervical Discectomy and Fusion for Cervical Radiculopathy or Cervical Myelopathy (ACDF) About your condition The pressure from your bulging disc(s) might be causing your pain, numbness or weakness.
VACCINE-RELATED ALLERGIC REACTIONS
 VACCINE-RELATED ALLERGIC REACTIONS Management of Anaphylaxis IERHA Immunization Program September 2016 VACCINE-RELATED ADVERSE EVENTS Local reactions pain, edema, erythema Systemic reactions fever, lymphadenopathy
VACCINE-RELATED ALLERGIC REACTIONS Management of Anaphylaxis IERHA Immunization Program September 2016 VACCINE-RELATED ADVERSE EVENTS Local reactions pain, edema, erythema Systemic reactions fever, lymphadenopathy
MUSCLE RELAXANTS. Mr. D.Raju, M.pharm, Lecturer
 MUSCLE RELAXANTS Mr. D.Raju, M.pharm, Lecturer Muscle Relaxants are classified as: I)Peripherally acting A.Neuromuscular blocking agents:- 1) Depolarizing muscle relaxants. 2) Non-depolarizing muscle relaxants
MUSCLE RELAXANTS Mr. D.Raju, M.pharm, Lecturer Muscle Relaxants are classified as: I)Peripherally acting A.Neuromuscular blocking agents:- 1) Depolarizing muscle relaxants. 2) Non-depolarizing muscle relaxants
Nerve Agent/Organophosphate Pesticide Exposure Treatment
 Nerve Agent/Organophosphate Pesticide Exposure Treatment Purpose: This Protocol is intended for EMS personnel at all levels to assess and treat patients exposed to nerve agents and organophosphate pesticides.
Nerve Agent/Organophosphate Pesticide Exposure Treatment Purpose: This Protocol is intended for EMS personnel at all levels to assess and treat patients exposed to nerve agents and organophosphate pesticides.
CASO CLINICO: DELIRIUM O ENCEFALOPATIA ACUTA?
 15 Congresso Nazionale Associazione Nazionale Psicogeriatria FIRENZE PALAZZO DEI CONGRESSI 16/18 APRILE 2015 CASO CLINICO: DELIRIUM O ENCEFALOPATIA ACUTA? N. Latronico Università degli Studi di Brescia
15 Congresso Nazionale Associazione Nazionale Psicogeriatria FIRENZE PALAZZO DEI CONGRESSI 16/18 APRILE 2015 CASO CLINICO: DELIRIUM O ENCEFALOPATIA ACUTA? N. Latronico Università degli Studi di Brescia
Pharmacotherapy to protect the neuromuscular junction after acute organophosphorus pesticide poisoning
 Ann. N.Y. Acad. Sci. ISSN 0077-8923 ANNALS OF THE NEW YORK ACADEMY OF SCIENCES Issue: Countermeasures Against Chemical Threats Pharmacotherapy to protect the neuromuscular junction after acute organophosphorus
Ann. N.Y. Acad. Sci. ISSN 0077-8923 ANNALS OF THE NEW YORK ACADEMY OF SCIENCES Issue: Countermeasures Against Chemical Threats Pharmacotherapy to protect the neuromuscular junction after acute organophosphorus
High Yield Neurological Examination
 High Yield Neurological Examination Vanja Douglas, MD Sara & Evan Williams Foundation Endowed Neurohospitalist Chair Director, Neurohospitalist Division Associate Professor of Clinical Neurology UCSF Department
High Yield Neurological Examination Vanja Douglas, MD Sara & Evan Williams Foundation Endowed Neurohospitalist Chair Director, Neurohospitalist Division Associate Professor of Clinical Neurology UCSF Department
Weapons of Mass Destruction. Lesson Goal. Lesson Objectives 9/10/2012
 Weapons of Mass Destruction Lesson Goal To become familiarize with the concept of weapons of mass destruction (WMD), how these weapons might be used, and the type of treatment that would be appropriate
Weapons of Mass Destruction Lesson Goal To become familiarize with the concept of weapons of mass destruction (WMD), how these weapons might be used, and the type of treatment that would be appropriate
Competency Title: Continuous Positive Airway Pressure
 Competency Title: Continuous Positive Airway Pressure Trainee Name: ------------------------------------------------------------- Title: ---------------------------------------------------------------
Competency Title: Continuous Positive Airway Pressure Trainee Name: ------------------------------------------------------------- Title: ---------------------------------------------------------------
DYSPORT (Clostridium botulinum type A toxin-haemagglutinin complex)
 DYSPORT (Clostridium botulinum type A toxin-haemagglutinin complex) CONSUMER MEDICINE INFORMATION What is in this leaflet This leaflet answers some common questions about Dysport. It does not contain all
DYSPORT (Clostridium botulinum type A toxin-haemagglutinin complex) CONSUMER MEDICINE INFORMATION What is in this leaflet This leaflet answers some common questions about Dysport. It does not contain all
Organophosphate Poisoning Predicting the Need for Mechanical Ventilator Support
 Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2016/509 Organophosphate Poisoning Predicting the Need for Mechanical Ventilator Support Pavan Soni 1, M G Solu 2, V Garg
Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2016/509 Organophosphate Poisoning Predicting the Need for Mechanical Ventilator Support Pavan Soni 1, M G Solu 2, V Garg
PRACTICE GUIDELINE. DEFINITIONS: Mild head injury: Glasgow Coma Scale* (GCS) score Moderate head injury: GCS 9-12 Severe head injury: GCS 3-8
 PRACTICE GUIDELINE Effective Date: 9-1-2012 Manual Reference: Deaconess Trauma Services TITLE: TRAUMATIC BRAIN INJURY GUIDELINE OBJECTIVE: To provide practice management guidelines for traumatic brain
PRACTICE GUIDELINE Effective Date: 9-1-2012 Manual Reference: Deaconess Trauma Services TITLE: TRAUMATIC BRAIN INJURY GUIDELINE OBJECTIVE: To provide practice management guidelines for traumatic brain
QUESTION EXAMPLES ECG
 ACEM Fellowship VAQ Examination QUESTION EXAMPLES ECG ECG 1: A 16 year old boy with a congenital heart problem presents to your ED with syncopal episodes. An ECG is taken. Describe and interpret his ECG
ACEM Fellowship VAQ Examination QUESTION EXAMPLES ECG ECG 1: A 16 year old boy with a congenital heart problem presents to your ED with syncopal episodes. An ECG is taken. Describe and interpret his ECG
PROSTIGMIN (neostigmine bromide)
 PROSTIGMIN (neostigmine bromide) TABLETS DESCRIPTION: Prostigmin (neostigmine bromide), an anticholinesterase agent, is available for oral administration in 15 mg tablets. Each tablet also contains gelatin,
PROSTIGMIN (neostigmine bromide) TABLETS DESCRIPTION: Prostigmin (neostigmine bromide), an anticholinesterase agent, is available for oral administration in 15 mg tablets. Each tablet also contains gelatin,
Original Article. Section: Medicine INTRODUCTION MATERIALS AND METHODS
 DOI: 10.21276/aimdr.2018.4.3.ME6 Original Article ISSN (O):2395-2822; ISSN (P):2395-2814 Comparative Study of Current Dosing Practice of Atropine in Organophosphorus Poisoning at BLDE University Shri B
DOI: 10.21276/aimdr.2018.4.3.ME6 Original Article ISSN (O):2395-2822; ISSN (P):2395-2814 Comparative Study of Current Dosing Practice of Atropine in Organophosphorus Poisoning at BLDE University Shri B
Management of Severe Traumatic Brain Injury
 Guideline for North Bristol Trust Management of Severe Traumatic Brain Injury This guideline describes the following: Initial assessment and management of the patient with head injury Indications for CT
Guideline for North Bristol Trust Management of Severe Traumatic Brain Injury This guideline describes the following: Initial assessment and management of the patient with head injury Indications for CT
Med 536 Communicating About Prognosis Workshop. Case 2
 Med 536 Communicating About Prognosis Workshop Case 2 ID / CC: 33 year-old man with intracranial hemorrhage History of the Presenting Illness 33 year-old man with a prior history of melanoma of the neck
Med 536 Communicating About Prognosis Workshop Case 2 ID / CC: 33 year-old man with intracranial hemorrhage History of the Presenting Illness 33 year-old man with a prior history of melanoma of the neck
PHARMACOLOGICAL PROBLEMS
 PHARMACOLOGICAL PROBLEMS 1. A 69 year old woman suffering from CHF has been treated with.25 mg Digoxin tablet daily for last 3 months. But the heart failure is not controlled adequately. What will be the
PHARMACOLOGICAL PROBLEMS 1. A 69 year old woman suffering from CHF has been treated with.25 mg Digoxin tablet daily for last 3 months. But the heart failure is not controlled adequately. What will be the
Patho-physiology of nervous System Talk 2 Syndromes in neurosciences. Petr Maršálek Dept pathological physiology 1.Med. F. CUNI
 Patho-physiology of nervous System Talk 2 Syndromes in neurosciences Petr Maršálek Dept pathological physiology 1.Med. F. CUNI Talks on NS Talk 1 - Pain and Motor disorders Talk 2 - This - Syndromes in
Patho-physiology of nervous System Talk 2 Syndromes in neurosciences Petr Maršálek Dept pathological physiology 1.Med. F. CUNI Talks on NS Talk 1 - Pain and Motor disorders Talk 2 - This - Syndromes in
