New Discriminant Method for Identifying the Aggressive Disease Phenotype of Non-alcoholic Fatty Liver Disease
|
|
|
- Brent Wilkins
- 5 years ago
- Views:
Transcription
1 ORIGINAL ARTICLE New Discriminant Method for Identifying the Aggressive Disease Phenotype of Non-alcoholic Fatty Liver Disease Yusuke Kawamura 1,2, Kenji Ikeda 1,2, Yasuji Arase 1,2, Shunichiro Fujiyama 1,2, Tetsuya Hosaka 1,2, Masahiro Kobayashi 1,2, Satoshi Saitoh 1,2, Hitomi Sezaki 1,2, Norio Akuta 1,2, Fumitaka Suzuki 1,2, Yoshiyuki Suzuki 1,2 and Hiromitsu Kumada 1,2 Abstract Objective To detect the aggressive phenotype of non-alcoholic fatty liver disease (NAFLD) based on the initial laboratory data and clinical characteristics. Methods We enrolled 144 patients with histologically proven NAFLD. For the first analysis, 24 NAFLD patients underwent repeat biopsy to establish a discriminant formula for predicting the AP of NAFLD (D- APN). The AP was defined by NAFLD that had been maintained or progressed to a fibrotic stage beyond stage 2. In the second analysis, we analyzed the distribution of the AP in each stage of disease and the incidence of the PNPLA3 rs GG genotype in AP in 120 other patients. Results After the analysis, the following function was found to discriminate the disease phenotype: z=0.150 body mass index (kg/m 2 ) age (years) ln (AST) (IU/L) ln (m-ast) A positive result indicates the AP of NAFLD. The discriminant functions had a positive predictive value of 94% and a negative predictive value of 71%. The distribution of the AP and the incidence of the PNPLA3 GG genotype in the AP in each stage of the disease among the 120 patients were as follows: non-alcoholic fatty liver, 30%/33%; non-alcoholic steatohepatitis (NASH) stage 1, 53%/26%; stage 2, 71%/70%; stage 3, 92%/57%; and stage 4, 93%/64%; there was a significant increase in the incidence of the AP as the disease progressed (p<0.001). Conclusion The new discriminant formula was useful for predicting disease progression potential in NAFLD patients and the incidence of the PNPLA3 GG genotype was elevated according to the distribution of AP. Key words: non-alcoholic fatty liver disease, aggressive, phenotype, fibrosis, hepatocellular carcinoma () () Introduction Non-alcoholic fatty liver disease (NAFLD) is a common cause of chronic liver disease in Western countries (1-4) and - more recently - in many Asian nations (5, 6). In particular, patients with non-alcoholic steatohepatitis (NASH), a subcategory of NAFLD, are at increased risk of developing hepatocellular carcinoma (7). Similar to individuals with viral hepatitis, patients with NAFLD and advanced fibrosis have a higher risk of hepatocarcinogenesis (8-10). In addition, we often encounter patients who have the same fibrotic stage at diagnosis of NAFLD; however, during follow up, they present with different progression patterns (i.e., the progression of fibrosis will be extremely rapid in one patient and very slow in another - during the same follow-up period). Thus, there is a need to be able to identify the rapid progressive type, or the aggressive phenotype and the slow progressive type, or the indolent phenotype at an earlier fibrotic stage; this would enable the more intensive follow-up of patients with the aggressive phenotype. Department of Hepatology, Toranomon Hospital, Japan and Okinaka Memorial Institute for Medical Research, Toranomon Hospital, Japan Received for publication June 8, 2016; Accepted for publication October 12, 2016 Correspondence to Dr. Yusuke Kawamura, k-yusuke@toranomon.gr.jp 1459
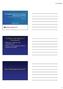
2 To date, several non-invasive scoring systems (NAFLD fibrosis score, BARD score, APRI and FIB-4 index) (11-14) have been constructed for the purpose of discriminating severe hepatic fibrosis from mild fibrosis; however, these scoring systems only estimate the current fibrotic stage, and cannot predict the speed of disease progression in the early stage of the disease. Thus, the first aim of the present retrospective study was to define the rapid progressive type, or aggressive phenotype of NAFLD using a non-invasive discriminant formula that does not depend on the various markers of fibrosis (i.e., hyaluronic acid, type-iv collagen 7S). Recently the impact of the PNPLA3 genotype on the pathogenesis and genetic risk of NAFLD appears to be straightforward (15-19), and Hotta et al. reported that the G- allele of rs was significantly associated with increases in the fibrotic stage in NAFLD patients, even after adjustment for age, gender, and BMI (17). Thus, another aim of the present study was to elucidate the relationship between the aggressive phenotype and the rs GG genotype. Study population Materials and Methods From January 1980 to July 2015, 220 patients were histopathologically diagnosed with NAFLD at Toranomon Hospital, Tokyo, Japan; 144 of these patients were enrolled in this retrospective study. The criteria for inclusion were as follows: (1) past daily alcohol intake of <20 g; (2) no underlying viral hepatitis, autoimmune hepatitis, drug-induced liver disease, or primary biliary cirrhosis; (3) no underlying systemic autoimmune diseases, such as systemic lupus erythematosus or rheumatoid arthritis; (4) no underlying metabolic diseases, such as hemochromatosis, alpha-1-antitrypsin deficiency, or Wilson disease; and (5) an analysis of the PNPLA3 rs genotype and m-ast (a marker of apoptosis) at the time of the initial biopsy. We divided these 144 patients into two groups. One group was the construct group, which included 24 patients who received repeat biopsy. In addition to the above-mentioned inclusion criteria, these patients also satisfied the following criteria: (1) all patients underwent examination for mitochondrial-ast (m-ast) (a marker of necroapoptosis) in several biopsies, (2) the fibrotic stage was maintained or progressed in comparison to the initial biopsy, and (3) the biopsies were performed over a period of more than one year. The other group was the validation group, which included 120 patients with histologically proven NAFLD. The study was approved by the Institutional Review Board of Toranomon Hospital. The definition of diabetes mellitus Diabetes mellitus was diagnosed based on the 2010 criteria of the American Diabetes Association (20). These criteria include: (1) casual plasma glucose 200 mg/dl; (2) fasting plasma glucose 126 mg/dl; and (3) 2-hour post-glucose (oral glucose tolerance test) 200 mg/dl. The determination of the PNPLA3 genotype PNPLA3 rs was genotyped with the TaqMan SNP genotyping assay (Applied Biosystems, Foster City, CA, USA). The histopathological examination of the liver Liver biopsy specimens were obtained using a 14-gauge modified Vim Silverman needle (Tohoku University style, Kakinuma Factory, Tokyo, Japan), a 16-gauge core tissue biopsy needle (Bard Peripheral Vascular, Tempe, AZ, USA) or surgical resection. Tissue was fixed in 10% formalin, and sections were stained with Hematoxylin and Eosin, Masson trichrome, silver impregnation, and periodic acid-schiff after diastase digestion. Fibrosis was scored using the five-grade scale proposed by Brunt et al. (21): stage 0, normal connective tissue; stage 1, pericellular or perivenular fibrosis in zone 3 (pericentral vein area); stage 2, zone 3 perisinusoidal/pericellular fibrosis with focal or extensive periportal fibrosis; stage 3, bridging or septal fibrosis; and stage 4, cirrhosis. NAFLD activity was scored using The NAFLD Activity Score (NAS), an eight-grade scale proposed by Kleiner et al. (22), which is determined based on the unweighted sum of the scores for steatosis (0-3), lobular inflammation (0-3), and ballooning degeneration (0-2). The definition of the disease phenotype of NAFLD (aggressive or indolent) In this study, we defined the aggressive phenotype as one that was maintained or progressed to a fibrotic stage of 2; in contrast, in patients with the indolent phenotype, the fibrotic stage was maintained at <2 after several biopsies (Fig. 1a). For example, a patient with stage 2 fibrosis at the first biopsy (Fig. 1b) and stage 3 fibrosis at the second biopsy (Fig. 1c), would be classified as having the aggressive phenotype. Statistical analysis Non-parametric procedures, including the chi-squared test and the Mann-Whitney U test, were employed for the analysis of background characteristics and laboratory data among the patients with each phenotype at the time of the first biopsy. The Cochran-Armitage trend test was used to investigate the significance of trends in the incidence of the aggressive phenotype and the rs GG genotype in patients with the aggressive phenotype based on pathological fibrotic stage. The Kolmogorov-Smirnov one-sample test was used to evaluate the normality of the distribution of the data. Because certain variables did not completely conform to a 1460
3 a Disease phenotype Histological staging First biopsy Repeated biopsy Number of patient Indolent phenotype of NAFLD NAFL 1 Maintained or progressed fibrotic stage under Aggressive phenotype of NAFLD Maintained or progressed fibrotic stage beyond Stage b c Figure 1. (a) The histological background and distribution of the aggressive and indolent phenotypes of NAFLD. (b) A 36-year-old man with stage 2 fibrosis at the time of the first biopsy (c); four years later he received a second biopsy that revealed stage 3 fibrosis, which is consistent with the aggressive phenotype. (Masson trichrome staining of liver tissue; Original magnification, 1 40) normal distribution, the bilirubin, AST, m-ast, ALT, GGT, triglyceride, and ferritin were subjected to natural logarithmic transformation. Following natural logarithmic transformation, each of the factors was normally or symmetrically distributed. After these procedures, the following discriminant analysis became rationally robust against deviations from normal distribution. All of the factors that were found to be at least marginally associated with the aggressive phenotype of NAFLD (p <0.05) in a univariate analysis were simultaneously entered into a multivariate discriminant analysis to predict the aggressive phenotype of NAFLD. The sensitivity, specificity, positive predictive value (PPV) and negative predictive value (NPV) for identifying the aggressive phenotype and the indolent phenotype were determined for this discriminant formula. Next, we validated the obtained predictive function using the data from the remaining 120 patients in the validation dataset. The data were analyzed using the SPSS software program (version 16.0 for Windows; SPSS, Chicago, IL, USA). Results The laboratory data for each phenotype (aggressive or indolent) in the construct group Table 1 summarizes the profiles and data of 24 NAFLD patients who received repeat biopsy, according to the disease phenotype (aggressive or indolent). Patients with the aggressive phenotype were significantly older and had significantly higher BMI, serum AST and m-ast values than those with the indolent phenotype. In addition, the serum ferritin level tended to be higher in patients with the aggressive phenotype. As for interval of the biopsy period, patients with the indolent phenotype presented with a significantly longer interval than those with the aggressive phenotype. The discriminant formula generated from the construct group After the analysis, we obtained the following formula: z= body mass index (kg/m 2 ) age (year) ln (AST) (IU/L) ln (m-ast) A positive result indicates the aggressive phenotype of liver disease, while a negative result indicates the indolent phenotype (discrimi- 1461
4 Table 1. Demographic Characteristics and Laboratory Data of the 24 Patients with Non-alcoholic Fatty Liver Disease according to Disease Phenotype in the Construct Group. Indolent phenotype (n=6) Aggressive phenotype (n=18) p value Gender, M:F, n 5:1 10: Age, years* 34 (26-44) 49.5 (33-65) Body mass index, kg/m 2 * 24.3 ( ) 27.9 ( ) Albumin, g/dl* 4.4 ( ) 4.3 ( ) Total bilirubin, mg/dl* 0.8 ( ) 0.9 ( ) AST, IU/L* 58.5 (29-72) 88.5 (36-150) ALT, IU/L* 95.5 (56-211) (41-281) γ-gtp, IU/L* 59 (17-178) 74.0 (26-505) Platelet count, 10 9 /L* 247 ( ) 200 ( ) Fasting blood sugar, mg/dl* 95.5 (92-112) 96.0 (65-273) Diabetes mellitus, yes/no 0/6 4/18 Total cholesterol, mg/dl* ( ) ( ) Triglycerides, mg/dl* (95-232) 129 (51-337) LDL-cholesterol, mg/dl* 133 ( ) 134 (99-205) HDL-cholesterol, mg/dl* 43 (35-54) 44 (31-84) Ferritin, ng/ml* 142 (16-536) 342 ( ) m-ast (IU/L)* 3.5 (2-5) 4.5 (2-17) NA score* 4 (1-6) 5 (2-7) Interval of biopsy, years* 10.1 ( ) 4.0 ( ) ALT: alanine aminotransferase, AST: aspartate aminotransferase, γ-gtp: gamma-glutamyl transpeptidase, HDL: high-density lipoprotein, LDH: lactate dehydrogenase, LDL: low-density lipoprotein, m-ast: mitochondrial-aspartate aminotransferase, NA score: NAFLD activity score *Expressed as median (range). Table 2. Distribution of Scores of the 120 Patients with Non-alcoholic Fatty Liver Disease in the Validation Group. NAFL (n=10) NASH Stage-1 (n=43) NASH Stage-2 (n=14) NASH Stage-3 (n=38) NASH Stage-4 (n=15) p value Age, years* 46.5 (24-78) 46.0 (23-73) 55.5 (35-70) 61.5 (29-83) 67 (36-85) <0.001 Body mass index, kg/m 2 * 24.3 ( ) 26.0 ( ) 25.8 ( ) 27.6 ( ) 26.2 ( ) AST, IU/L* 29.5 (14-55) 51.0 (23-164) 48.5 (25-139) 63 (17-198) 48 (26-152) m-ast (IU/L) * 4.5 ( 2-10) 4.0 ( 2-13) 4.0 ( 2-8) 5.0 ( 2-11) 4.0 ( 2-18) Score of discriminant formula* ( ) Number of aggressive phenotype (%) ( ) ( ) ( ) ( ) 3/10 (30%) 24/43 (53%) 10/14 (71%) 35/38 (92%) 14/15 (93%) <0.001 AST: aspartate aminotransferase, m-ast: mitochondrial-aspartate aminotransferase, NAFL: non-alcoholic fatty liver, NASH: non-alcoholic steatohepatitis *Expressed as median (range). Calculated with the following formula: z=0.150 body mass index (kg/m 2 ) age (years) ln (AST) (IU/L) ln (m-ast) nant formula for predicting the aggressive phenotype of NAFLD, named D-APN ). This discriminant formula has a sensitivity of 89%, a specificity of 83%, a PPV of 94%, and an NPV of 71%. The validation of the discriminant function The distribution of the scores of the 120 patients in the validation group is shown in Table 2. The discriminant formula scores were gradually elevated along with the stage of progression, and their distribution was significantly different among several stages of fibrosis. Fig. 2 shows the ratio of the aggressive phenotype and the PNPLA3 rs GG genotype in patients with the aggressive phenotype of NAFLD in each histological stage of NAFLD. The ratio of the aggressive phenotype of NAFLD was significantly elevated along with the stage of progression (p<0.001), and more than 70% of the patients with stage 2 fibrosis had the aggressive phenotype. Similarly, the incidence of the PNPLA3 rs GG genotype in patients with the aggressive phenotype was significantly elevated along with the stage of progression (p<0.001). 1462
5 Discriminant formula for predicted aggressive phenotype of NAFLD (D-APN) z=0.150 body mass index(kg/m 2 ) Age (year) ln (AST) (IU/L) ln (m-ast) (IU/L) (-) Indolent phenotype of NAFLD, (+) Aggressive phenotype of NAFLD Histological staging (Number) Disease phenotype (Number) The rate of AP The rate of PNPLA3 (rs738409) GG genotype in AP (% / number) NAFL (10) NASH stage 1 (43) (7) (3) (20) (23) 30 % (3/10) 53 % (23/43) *p< % (1/3) 26 % (6/23) *p<0.001 NASH stage 2 (14) (4) (10) (3) (35) (1) (14) 71 % (10/14) 70 % (7/10) NASH stage 3 (38) NASH stage 4 (15) 92 % (35/38) 93 % (14/15) 57 % (20/35) 64 % (9/14) *Cochran-Armitage trend analysis Figure 2. The distribution of the aggressive phenotype of NAFLD and the ratio of the PNPLA3 rs GG genotype in patients with the aggressive phenotype in the validation group of 120 NAFLD patients. Discussion In Japan, many patients with NAFLD are diagnosed by US alone, because liver biopsies are associated with the risk of major complications, including intraperitoneal bleeding. Although some non-invasive scoring systems (the NAFLD fibrosis score, the BARD score, and the APRI and FIB-4 indexes) have been used to predict fibrosis (11-14), these studies were principally aimed at differentiating the advanced stages of fibrosis (3 to 4) from mild stages of fibrosis (1 to 2). However, in daily clinical practice, we need to detect the rapidly progressive type at an earlier stage of disease, and we should follow these cases more intensively. In the present study, we created a discriminant formula to predict the aggressive phenotype of NAFLD that does not depend on the various markers of fibrosis. Similarly, some of the non-invasive scoring systems (the NAFLD fibrosis score, the BARD score, and the APRI and FIB-4 indexes) that are used for predicting fibrosis do not depend on the various fibrotic markers (11-14). There were two differences between our discriminant formula and the previously reported non-invasive scoring systems. First, our discriminant formula is can be used to predict the potential for disease progression in each NAFLD patient at the time of the first blood examination. Thus, in this study, we divided NAFLD patients into two disease phenotypes, the aggressive phenotype and the indolent phenotype, based on the disease stage in several biopsies. In patients with the aggressive phenotype, the stage of fibrosis was maintained at or progressed beyond 2. In patients with the indolent phenotype, the stage of fibrosis was maintained at <2. NASH stage 2 is defined by perisinusoidal and portal/periportal fibrosis, and fibrotic progression in this phase has very important clinical implications; the next stage of progression is fibrotic bridging. Recently, Vilar-Gomez et al. (23, 24) reported that weight loss (especially 10% weight loss) was highly associated with the level of improvement in the histological features and the resolution of NASH. However, in our study, in the cohort of the construct group, weight loss was observed between each liver biopsy in 3 of 6 patients (50%) [ 10% weight loss was observed in 1 of 6 patients (17%)] with the indolent phenotype. Similarly, weight loss was observed in 8 of 18 patients (44%) [ 10% weight loss was observed in 3 of 18 patients (17%)] with the aggressive phenotype. From this result, the use of the factor of weight loss alone may not be sufficient for predicting the resolution or progression of disease. Second, we used a marker of necroapoptosis, m-ast, to construct a new discriminant formula. CK-18(M30) is a prominent and specific marker of apoptosis in NAFLD that has been used in a clinical study in specialized tertiary care centers. Although several studies have reported the utility of CK-18(M30) as marker of apoptosis in NAFLD (25-29), it is not useful in daily clinical practice because it is not easy for all institutions (including primary and secondary care centers and general clinics) to obtain. Realistically, in daily clinical practice for NAFLD patients, a commerciallyavailable marker of necroapoptosis, such as m-ast, is more useful. In addition, our formula yielded very interesting results. 1463
6 Our estimation formula predicted the ratio of the aggressive phenotype in each fibrotic stage of NAFLD, the ratio was significantly elevated in accordance with the progression of fibrosis, and the incidence of the PNPLA3 GG genotype was significantly elevated in accordance with the distribution of the aggressive phenotype (Fig. 2). Recently, Singh et al. (30) reported that a low baseline AST:ALT ratio was a sensitive discriminant marker of the progression of fibrosis. In addition small proportion of these patients may rapidly progress to advanced fibrosis. Similarly, in our study population, five of the patients with the aggressive phenotype whose fibrotic stage was <2 at baseline presented a low baseline AST:ALT ratio (the median value was 0.47). However, the AST:ALT ratio changes along with the progression of the disease. Generally, the NASH patients with non-advanced fibrosis have a low AST:ALT ratio (<1.0), while those with advanced fibrosis have higher AST:ALT ratios. Progression is also associated with decreased fatty deposition. Stage 4 patients frequently present with ratios of 1.0. Similarly, in our study population, the median AST:ALT ratio in the validation group changed with each fibrotic stage as follows: stage 0, 0.67; stage 1, 0.55; stage 2, 0.57; stage 3, 0.77; and stage 4, Thus, 13 of the patients with the aggressive phenotype of NAFLD whose baseline stage of fibrosis was 2 presented higher baseline AST:ALT ratio values in comparison to the patients with the aggressive phenotype of NAFLD who had earlier stage of fibrosis at baseline (median AST:ALT ratio 0.75 vs. 0.47). Thus, the AST:ALT ratio is a useful marker for the early stages of NASH, but may not be sufficient for all stages of NASH. These results accurately reflect our impression of NAFLD in daily clinical medicine; the most important point was that almost 30% patients, even those with NAFL, who had the potential for rapidly progressive disease. However, the present study is associated with some limitations. First, the older age of the aggressive phenotype group influenced the definition of the aggressive phenotype, because older patients generally have advanced fibrosis. Second, we used 120 patients who did not receive a repeated biopsy for our validation group to predict the latent aggressive phenotype in this study; thus, we cannot be certain of the accuracy of these results in predicting the aggressive phenotype. Singh et al. (30) performed a systematic review and meta-analysis of paired-biopsy studies and reported that patients with NAFL progressed by 1 stage over 14.3 years, while those with NASH progressed by 1 stage over 7.1 years; however, the median follow-up period in our validation group was 4.4 years. Thus, the transaminase levels, platelet counts and body weight should be followed over a longer period to evaluate the utility of D-APN in a future study. Third, this was a retrospective single-center cohort study that evaluated a small number of patients. A further large-scale multicenter study is needed to evaluate this discriminant formula in a larger number of patients who receive repeat biopsy. However, we believe that this new discriminant formula will impact the routine clinical care of patients with NAFLD, especially those whose disease shows the potential for rapid progression. We also think that the progression of many high-risk patients to advanced liver disease, including decompensated liver cirrhosis and hepatocellular carcinoma, will be prevented by the early detection of disease progression using this discriminant formula. In conclusion, the new discriminant formula, named D- APN, was useful for predicting the NAFLD patients who had a high potential for disease progression, and the distribution of the aggressive phenotype was associated with the distribution of the PNPLA3 rs GG genotype. In addition, this formula is suitable for repeated use in daily clinical medicine. Its accuracy and reproducibility require further validation with larger numbers of patients in several countries besides Japan. The authors state that they have no Conflict of Interest (COI). Financial Support Okinaka Memorial Institute for Medical Research and Japanese Ministry of Health, Labour and Welfare. Acknowledgement This work was supported in part by grants from the Ministry of Health, Labour and Welfare in Japan and the Japan Agency for Medical Research and Development. References 1. Angulo P. Nonalcoholic fatty liver disease. N Engl J Med 346: , Williams R. Global challenges in liver disease. Hepatology 44: , Torres DM, Harrison SA. Diagnosis and therapy of nonalcoholic steatohepatitis. Gastroenterology 134: , Vuppalanchi R, Chalasani N. Nonalcoholic fatty liver disease and nonalcoholic steatohepatitis: selected practical issues in their evaluation and management. Hepatology 49: , Fan JG, Farrell GC. Epidemiology of non-alcoholic fatty liver disease in China. J Hepatol 50: , Watanabe S, Yaginuma R, Ikejima K, Miyazaki A. Liver diseases and metabolic syndrome. J Gastroenterol 43: , Adams LA, Lymp JF, St Sauver J, et al. The natural history of nonalcoholic fatty liver disease: a population-based cohort study. Gastroenterology 129: , Ratziu V, Bonyhay L, Di Martino V, et al. Survival, liver failure, and hepatocellular carcinoma in obesity-related cryptogenic cirrhosis. Hepatology 35: , Siegel AB, Zhu AX. Metabolic syndrome and hepatocellular carcinoma: two growing epidemics with a potential link. Cancer 115: , Kawamura Y, Arase Y, Ikeda K, et al. Large-scale long-term follow-up study of Japanese patients with non-alcoholic fatty liver disease for the onset of hepatocellular carcinoma. Am J Gastroenterol 107: , Angulo P, Hui JM, Marchesini G, et al. The NAFLD fibrosis score: a noninvasive system that identifies liver fibrosis in patients with NAFLD. Hepatology 45: , Harrison SA, Oliver D, Arnold HL, Gogia S, Neuschwander-Tetri BA. Development and validation of a simple NAFLD clinical scoring system for identifying patients without advanced disease. 1464
7 Gut 57: , Kruger FC, Daniels CR, Kidd M, et al. APRI: a simple bedside marker for advanced fibrosis that can avoid liver biopsy in patients with NAFLD/NASH. S Afr Med J 101: , Shah AG, Lydecker A, Murray K, et al. Comparison of noninvasive markers of fibrosis in patients with nonalcoholic fatty liver disease. Clin Gastroenterol Hepatol 7: , Romeo S, Kozlitina J, Xing C, et al. Genetic variation in PNPLA3 confers susceptibility to nonalcoholic fatty liver disease. Nat Genet 40: , Sookoian S, Castano GO, Burgueno AL, Gianotti TF, Rosselli MS, Pirola CJ. A nonsynonymous gene variant in the adiponutrin gene is associated with nonalcoholic fatty liver disease severity. J Lipid Res 50: , Hotta K, Yoneda M, Hyogo H, et al. Association of the rs polymorphism in PNPLA3 with liver damage and the development of nonalcoholic fatty liver disease. BMC Med Genet 11: 172, Kawaguchi T, Sumida Y, Umemura A, et al. Genetic polymorphisms of the human PNPLA3 gene are strongly associated with severity of non-alcoholic fatty liver disease in Japanese. PLoS One 7: e38322, Akuta N, Kawamura Y, Arase Y, et al. Relationships between genetic variations of PNPLA3, TM6SF2 and histological features of nonalcoholic fatty liver disease in Japan. Gut Liver 10: , American Diabetes Association. Diagnosis and classification of diabetes mellitus. Diabetes Care 33 Suppl 1: S62-S69, Brunt EM, Janney CG, Di Bisceglie AM, Neuschwander-Tetri BA, Bacon BR. Nonalcoholic steatohepatitis: a proposal for grading and staging the histological lesions. Am J Gastroenterol 94: , Kleiner DE, Brunt EM, Van Natta M, et al. Design and validation of a histological scoring system for nonalcoholic fatty liver disease. Hepatology 41: , Vilar-Gomez E, Martinez-Perez Y, Calzadilla-Bertot L, et al. Weight loss through lifestyle modification significantly reduces features of nonalcoholic steatohepatitis. Gastroenterology 149: e5; quiz e14-e15, Vilar-Gomez E, Yasells-Garcia A, Martinez-Perez Y, et al. Development and validation of a noninvasive prediction model for nonalcoholic steatohepatitis resolution after lifestyle intervention. Hepatology 63: , Alkhouri N, Carter-Kent C, Feldstein AE. Apoptosis in nonalcoholic fatty liver disease: diagnostic and therapeutic implications. Expert Rev Gastroenterol Hepatol 5: , Diab DL, Yerian L, Schauer P, et al. Cytokeratin 18 fragment levels as a noninvasive biomarker for nonalcoholic steatohepatitis in bariatric surgery patients. Clin Gastroenterol Hepatol 6: , Yilmaz Y, Dolar E, Ulukaya E, et al. Soluble forms of extracellular cytokeratin 18 may differentiate simple steatosis from nonalcoholic steatohepatitis. World J Gastroenterol 13: , Younossi ZM, Page S, Rafiq N, et al. A biomarker panel for nonalcoholic steatohepatitis (NASH) and NASH-related fibrosis. Obes Surg 21: , Feldstein AE, Wieckowska A, Lopez AR, Liu YC, Zein NN, McCullough AJ. Cytokeratin-18 fragment levels as noninvasive biomarkers for nonalcoholic steatohepatitis: a multicenter validation study. Hepatology 50: , Singh S, Allen AM, Wang Z, Prokop LJ, Murad MH, Loomba R. Fibrosis progression in nonalcoholic fatty liver vs nonalcoholic steatohepatitis: a systematic review and meta-analysis of pairedbiopsy studies. Clin Gastroenterol Hepatol 13: e1-e9; quiz e39-e40, The Internal Medicine is an Open Access article distributed under the Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License. To view the details of this license, please visit ( by-nc-nd/4.0/) The Japanese Society of Internal Medicine
New discriminant score to predict the fibrotic stage of non-alcoholic steatohepatitis in Japan
 Hepatol Int (215) 9:269 277 DOI 1.17/s1272-14-965-x ORIGINAL ARTICLE New discriminant score to predict the fibrotic stage of non-alcoholic steatohepatitis in Japan Yusuke Kawamura Kenji Ikeda Yasuji Arase
Hepatol Int (215) 9:269 277 DOI 1.17/s1272-14-965-x ORIGINAL ARTICLE New discriminant score to predict the fibrotic stage of non-alcoholic steatohepatitis in Japan Yusuke Kawamura Kenji Ikeda Yasuji Arase
Hepatocellular carcinoma is the most common liver-related complication in patients with histopathologically-confirmed NAFLD in Japan
 Akuta et al. BMC Gastroenterology (2018) 18:165 https://doi.org/10.1186/s12876-018-0900-1 RESEARCH ARTICLE Open Access Hepatocellular carcinoma is the most common liver-related complication in patients
Akuta et al. BMC Gastroenterology (2018) 18:165 https://doi.org/10.1186/s12876-018-0900-1 RESEARCH ARTICLE Open Access Hepatocellular carcinoma is the most common liver-related complication in patients
Background of the FIB-4 Index in Japanese Non-Alcoholic Fatty Liver Disease
 ORIGINAL ARTICLE Background of the FIB-4 Index in Japanese Non-Alcoholic Fatty Liver Disease Takashi Wada and Mikio Zeniya Abstract Objective We investigated the distribution and characteristics of the
ORIGINAL ARTICLE Background of the FIB-4 Index in Japanese Non-Alcoholic Fatty Liver Disease Takashi Wada and Mikio Zeniya Abstract Objective We investigated the distribution and characteristics of the
/ FIB4 Index , simple steatosis. FIB4 Index. FIB4 Index. FIB4 Index FIB4 Index. Sterling FIB4 Index. FIB4 Index AST AST ALT
 原 著 29 34-41, 2014 FIB4 Index 1 1 1 1 2 1 1 FIB4 Index FIB4 Index cut off 2.67 2.67 12,059 FIB4 IndexFIB4 Index 2.67 / FIB4 Index AST ALT FIB4 Index 2.67 161 1.3% FIB4 Index 5 FIB4 Index 1.1 5 1.6 FIB4
原 著 29 34-41, 2014 FIB4 Index 1 1 1 1 2 1 1 FIB4 Index FIB4 Index cut off 2.67 2.67 12,059 FIB4 IndexFIB4 Index 2.67 / FIB4 Index AST ALT FIB4 Index 2.67 161 1.3% FIB4 Index 5 FIB4 Index 1.1 5 1.6 FIB4
The classical metabolic work-up, approved by the Ethics Committee of the Antwerp
 SUPPLEMENTARY MATERIALS METHODS Metabolic work-up The classical metabolic work-up, approved by the Ethics Committee of the Antwerp University Hospital and requiring written informed consent, included a
SUPPLEMENTARY MATERIALS METHODS Metabolic work-up The classical metabolic work-up, approved by the Ethics Committee of the Antwerp University Hospital and requiring written informed consent, included a
CASE REPORT. Abstract. Introduction
 CASE REPORT A Customized Online Nutrition Guidance System Is Effective for Treating Patients with Nonalcoholic Fatty Liver Disease by Supporting Continuity of Diet Therapy at Home: A Pilot Study Tomonori
CASE REPORT A Customized Online Nutrition Guidance System Is Effective for Treating Patients with Nonalcoholic Fatty Liver Disease by Supporting Continuity of Diet Therapy at Home: A Pilot Study Tomonori
The role of non-invasivemethods in evaluating liver fibrosis of patients with non-alcoholic steatohepatitis
 The role of non-invasivemethods in evaluating liver fibrosis of patients with non-alcoholic steatohepatitis Objectives: Liver biopsy is the gold standard for diagnosing the extent of fibrosis in NAFLD/NASH;
The role of non-invasivemethods in evaluating liver fibrosis of patients with non-alcoholic steatohepatitis Objectives: Liver biopsy is the gold standard for diagnosing the extent of fibrosis in NAFLD/NASH;
Nonalcoholic Fatty Liver Disease: Definitions, Risk Factors, and Workup
 REVIEW REVIEW Nonalcoholic Fatty Liver Disease: Definitions, Risk Factors, and Workup Puneet Puri, M.B.B.S., M.D. and Arun J. Sanyal, M.B.B.S., M.D. Nonalcoholic fatty liver disease (NAFLD) is defined
REVIEW REVIEW Nonalcoholic Fatty Liver Disease: Definitions, Risk Factors, and Workup Puneet Puri, M.B.B.S., M.D. and Arun J. Sanyal, M.B.B.S., M.D. Nonalcoholic fatty liver disease (NAFLD) is defined
ALT and aspartate aminotransferase (AST) levels were measured using the α-ketoglutarate reaction (Roche,
 Supplemental Methods Analytical determinations ALT and aspartate aminotransferase (AST) levels were measured using the α-ketoglutarate reaction (Roche, Basel, Switzerland). Glucose, triglyceride, total
Supplemental Methods Analytical determinations ALT and aspartate aminotransferase (AST) levels were measured using the α-ketoglutarate reaction (Roche, Basel, Switzerland). Glucose, triglyceride, total
Challenges in the Diagnosis of Steatohepatitis
 The Bugaboos of Fatty Liver Disease: Ballooning and Fibrosis Hans Popper Hepatopathology Society Companion Meeting San Antonio, Tx March, 2017 David Kleiner, M.D., Ph.D. NCI/Laboratory of Pathology Challenges
The Bugaboos of Fatty Liver Disease: Ballooning and Fibrosis Hans Popper Hepatopathology Society Companion Meeting San Antonio, Tx March, 2017 David Kleiner, M.D., Ph.D. NCI/Laboratory of Pathology Challenges
In Search of New Biomarkers for Nonalcoholic Fatty Liver Disease
 REVIEW In Search of New Biomarkers for Nonalcoholic Fatty Liver Disease Ting-Ting Chan, M.R.C.P., and Vincent Wai-Sun Wong, M.D. Nonalcoholic fatty liver disease (NAFLD) affects 15% to 40% of the general
REVIEW In Search of New Biomarkers for Nonalcoholic Fatty Liver Disease Ting-Ting Chan, M.R.C.P., and Vincent Wai-Sun Wong, M.D. Nonalcoholic fatty liver disease (NAFLD) affects 15% to 40% of the general
Nonalcoholic fatty liver disease (NAFLD) is the most common
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2008;6:1249 1254 Cytokeratin 18 Fragment Levels as a Noninvasive Biomarker for Nonalcoholic Steatohepatitis in Bariatric Surgery Patients DIMA L. DIAB,* LISA YERIAN,
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2008;6:1249 1254 Cytokeratin 18 Fragment Levels as a Noninvasive Biomarker for Nonalcoholic Steatohepatitis in Bariatric Surgery Patients DIMA L. DIAB,* LISA YERIAN,
CDHNF & NASPGHAN A Partnership for Research and Education for Children s Digestive and Nutritional Health
 CDHNF & NASPGHAN A Partnership for Research and Education for Children s Digestive and Nutritional Health Obesity and NAFLD Definitions: Nonalcoholic steatohepatitis (NASH) and nonalcoholic fatty liver
CDHNF & NASPGHAN A Partnership for Research and Education for Children s Digestive and Nutritional Health Obesity and NAFLD Definitions: Nonalcoholic steatohepatitis (NASH) and nonalcoholic fatty liver
Update on Non-Alcoholic Fatty Liver Disease. Timothy R. Morgan, MD Chief, Hepatology, VA Long Beach Professor of Medicine, UCI
 Update on Non-Alcoholic Fatty Liver Disease Timothy R. Morgan, MD Chief, Hepatology, VA Long Beach Professor of Medicine, UCI February 3, 2018 Disclosure Clinical trials: Genfit Speaker s Bureau: none
Update on Non-Alcoholic Fatty Liver Disease Timothy R. Morgan, MD Chief, Hepatology, VA Long Beach Professor of Medicine, UCI February 3, 2018 Disclosure Clinical trials: Genfit Speaker s Bureau: none
Simple non-invasive fibrosis scoring systems can reliably exclude advanced fibrosis in patients with non-alcoholic fatty liver disease
 1 Liver Unit, Newcastle Upon Tyne Hospitals NHS Trust, Freeman Hospital, Newcastle upon Tyne, UK 2 Institute of Cellular Medicine, Faculty of Medical Sciences, Newcastle University, Newcastle Upon Tyne,
1 Liver Unit, Newcastle Upon Tyne Hospitals NHS Trust, Freeman Hospital, Newcastle upon Tyne, UK 2 Institute of Cellular Medicine, Faculty of Medical Sciences, Newcastle University, Newcastle Upon Tyne,
LIVER, PANCREAS, AND BILIARY TRACT
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:1028 1033 LIVER, PANCREAS, AND BILIARY TRACT Prevalence and Indicators of Portal Hypertension in Patients With Nonalcoholic Fatty Liver Disease FLAVIA D.
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:1028 1033 LIVER, PANCREAS, AND BILIARY TRACT Prevalence and Indicators of Portal Hypertension in Patients With Nonalcoholic Fatty Liver Disease FLAVIA D.
HEP DART 2017, Kona, Hawaii
 HEP DART 2017, Kona, Hawaii Rong Yu 1, Ke Xu 1, Jing Li 1, Tong Sun 1, Shengjiang Zhang 2, Jinhua Shao 2, Jin Sun 2, Qiong He 3, Jianwen Luo 3, Cheng Wang 4, Yudong Wang 4, Jing Chen 4, Vanessa Wu 4, George
HEP DART 2017, Kona, Hawaii Rong Yu 1, Ke Xu 1, Jing Li 1, Tong Sun 1, Shengjiang Zhang 2, Jinhua Shao 2, Jin Sun 2, Qiong He 3, Jianwen Luo 3, Cheng Wang 4, Yudong Wang 4, Jing Chen 4, Vanessa Wu 4, George
What is NAFLD?.NASH? Presenter Disclosure Information. Learning Objectives. Case 1: Rob. Questions Pertinent to Rob
 Presenter Disclosure Information 5 6pm Nonalcoholic Fatty Liver Disease (NAFLD): Another Obesity-Related Epidemic SPEAKER Elliot Tapper, MD The following relationships exist related to this presentation:
Presenter Disclosure Information 5 6pm Nonalcoholic Fatty Liver Disease (NAFLD): Another Obesity-Related Epidemic SPEAKER Elliot Tapper, MD The following relationships exist related to this presentation:
Akuta et al. BMC Gastroenterology (2016) 16:141 DOI /s
 Akuta et al. BMC Gastroenterology (2016) 16:141 DOI 10.1186/s12876-016-0557-6 RESEARCH ARTICLE Open Access Analysis of association between circulating mir-122 and histopathological features of nonalcoholic
Akuta et al. BMC Gastroenterology (2016) 16:141 DOI 10.1186/s12876-016-0557-6 RESEARCH ARTICLE Open Access Analysis of association between circulating mir-122 and histopathological features of nonalcoholic
AAIM: GI Workshop Follow Up to Case Studies. Non-alcoholic Fatty Liver Disease Ulcerative Colitis Crohn s Disease
 AAIM: GI Workshop Follow Up to Case Studies Non-alcoholic Fatty Liver Disease Ulcerative Colitis Crohn s Disease Daniel Zimmerman, MD VP and Medical Director, RGA Global October 2015 Non-alcoholic Fatty
AAIM: GI Workshop Follow Up to Case Studies Non-alcoholic Fatty Liver Disease Ulcerative Colitis Crohn s Disease Daniel Zimmerman, MD VP and Medical Director, RGA Global October 2015 Non-alcoholic Fatty
Nonalcoholic fatty liver disease (NAFLD) is
 HEPATOLOGY COMMUNICATIONS, VOL. 1, NO. 1, 2017 Effects of a Sodium-Glucose Cotransporter 2 Inhibitor in Nonalcoholic Fatty Liver Disease Complicated by Diabetes Mellitus: Preliminary Prospective Study
HEPATOLOGY COMMUNICATIONS, VOL. 1, NO. 1, 2017 Effects of a Sodium-Glucose Cotransporter 2 Inhibitor in Nonalcoholic Fatty Liver Disease Complicated by Diabetes Mellitus: Preliminary Prospective Study
CASE REPORT. Introduction. Case Report
 doi: 10.2169/internalmedicine.8754-16 Intern Med Advance Publication http://internmed.jp CASE REPORT The Improvement of the Hepatic Histological Findings in a Patient with Non-alcoholic Steatohepatitis
doi: 10.2169/internalmedicine.8754-16 Intern Med Advance Publication http://internmed.jp CASE REPORT The Improvement of the Hepatic Histological Findings in a Patient with Non-alcoholic Steatohepatitis
Fatty Liver Disease. Mark Thursz. Imperial College
 Fatty Liver Disease Mark Thursz Imperial College Non-Alcoholic Fatty Liver Disease UK adult obesity (BMI>30) 1980: 6% [M], 8% [F]. 1997: 17% [M], 20% [F]. By 2004, 23.6% of men and 23.8% of women were
Fatty Liver Disease Mark Thursz Imperial College Non-Alcoholic Fatty Liver Disease UK adult obesity (BMI>30) 1980: 6% [M], 8% [F]. 1997: 17% [M], 20% [F]. By 2004, 23.6% of men and 23.8% of women were
Liver Pathology in the 0bese
 Liver Pathology in the 0bese Rob Goldin Centre for Pathology, Imperial College r.goldin@imperial.ac.uk Ludwig et al. Non-alcoholic steatohepatitis: Mayo Clinic experiences with a hitherto unnamed disease.
Liver Pathology in the 0bese Rob Goldin Centre for Pathology, Imperial College r.goldin@imperial.ac.uk Ludwig et al. Non-alcoholic steatohepatitis: Mayo Clinic experiences with a hitherto unnamed disease.
Improving Access to Quality Medical Care Webinar Series
 Improving Access to Quality Medical Care Webinar Series Presented by The Arizona Telemedicine Program and the Southwest Telehealth Resource Center 2015 UA Board of Regents Welcome AZ, UT, CO, NM & NV FLEX
Improving Access to Quality Medical Care Webinar Series Presented by The Arizona Telemedicine Program and the Southwest Telehealth Resource Center 2015 UA Board of Regents Welcome AZ, UT, CO, NM & NV FLEX
Original Article. Significance of Hepatic Steatosis in Chronic Hepatitis B Infection INTRODUCTION
 Original Article Bhanthumkomol P, et al. THAI J GASTROENTEROL 2013 Vol. 14 No. 1 Jan. - Apr. 2013 29 Bhanthumkomol P 1 Charatcharoenwitthaya P 1 Pongpaiboon A 2 ABSTRACT Background: Significance of liver
Original Article Bhanthumkomol P, et al. THAI J GASTROENTEROL 2013 Vol. 14 No. 1 Jan. - Apr. 2013 29 Bhanthumkomol P 1 Charatcharoenwitthaya P 1 Pongpaiboon A 2 ABSTRACT Background: Significance of liver
Usefulness of Magnetic Resonance Imaging for the Diagnosis of Hemochromatosis with Severe Hepatic Steatosis in Nonalcoholic Fatty Liver Disease
 CASE REPORT Usefulness of Magnetic Resonance Imaging for the Diagnosis of Hemochromatosis with Severe Hepatic Steatosis in Nonalcoholic Fatty Liver Disease Yuichi Nozaki 1,NorikoSato 2, Tsuyoshi Tajima
CASE REPORT Usefulness of Magnetic Resonance Imaging for the Diagnosis of Hemochromatosis with Severe Hepatic Steatosis in Nonalcoholic Fatty Liver Disease Yuichi Nozaki 1,NorikoSato 2, Tsuyoshi Tajima
Aspartate aminotransferase-to-platelet ratio index in children with cholestatic liver diseases to assess liver fibrosis
 The Turkish Journal of Pediatrics 2015; 57: 492-497 Original Aspartate aminotransferase-to-platelet ratio index in children with cholestatic liver diseases to assess liver fibrosis Aysel Ünlüsoy-Aksu 1,
The Turkish Journal of Pediatrics 2015; 57: 492-497 Original Aspartate aminotransferase-to-platelet ratio index in children with cholestatic liver diseases to assess liver fibrosis Aysel Ünlüsoy-Aksu 1,
Pancreatic exocrine insufficiency: a rare cause of nonalcoholic steatohepatitis
 Pancreatic exocrine insufficiency: a rare cause of nonalcoholic steatohepatitis Naoki Tanaka 1, Akira Horiuchi 2, Takahide Yokoyama 3, Shigeyuki Kawa 1, and Kendo Kiyosawa 1 1 Department of Gastroenterology,
Pancreatic exocrine insufficiency: a rare cause of nonalcoholic steatohepatitis Naoki Tanaka 1, Akira Horiuchi 2, Takahide Yokoyama 3, Shigeyuki Kawa 1, and Kendo Kiyosawa 1 1 Department of Gastroenterology,
Nonalcoholic fatty liver disease (NAFLD) and nonalcoholic. Noninvasive Assessment of Nonalcoholic Fatty Liver Disease in Obese or Overweight Patients
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:1162 1168 Noninvasive Assessment of Nonalcoholic Fatty Liver Disease in Obese or Overweight Patients SVEN M. A. FRANCQUE,* AN VERRIJKEN, ILSE MERTENS, GUY
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:1162 1168 Noninvasive Assessment of Nonalcoholic Fatty Liver Disease in Obese or Overweight Patients SVEN M. A. FRANCQUE,* AN VERRIJKEN, ILSE MERTENS, GUY
NON-ALCOHOLIC FATTY LIVER DISEASE:
 NON-ALCOHOLIC FATTY LIVER DISEASE: ROLE OF THE PRIMARY PROVIDER Archita P. Desai, MD Assistant Professor of Medicine University of Arizona 25 th Annual Southwestern Conference on Medicine Outline Pathophysiology
NON-ALCOHOLIC FATTY LIVER DISEASE: ROLE OF THE PRIMARY PROVIDER Archita P. Desai, MD Assistant Professor of Medicine University of Arizona 25 th Annual Southwestern Conference on Medicine Outline Pathophysiology
Assessment of Liver Stiffness by Transient Elastography in Diabetics with Fatty Liver A Single Center Cross Sectional observational Study
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 6 Ver. IV (June. 2017), PP 49-53 www.iosrjournals.org Assessment of Liver Stiffness by Transient
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 6 Ver. IV (June. 2017), PP 49-53 www.iosrjournals.org Assessment of Liver Stiffness by Transient
NONALCOHOLIC FATTY LIVER DISEASE
 NONALCOHOLIC FATTY LIVER DISEASE Kiran Bambha, MD, MSc Hepatology and Liver Transplantation University of Colorado Denver April 13, 2012 Non-Alcoholic Fatty Liver Disease (NAFLD) Terminology Pathogenesis
NONALCOHOLIC FATTY LIVER DISEASE Kiran Bambha, MD, MSc Hepatology and Liver Transplantation University of Colorado Denver April 13, 2012 Non-Alcoholic Fatty Liver Disease (NAFLD) Terminology Pathogenesis
EVALUATION OF ABNORMAL LIVER TESTS
 EVALUATION OF ABNORMAL LIVER TESTS MIA MANABAT DO PGY6 MOA 119 TH ANNUAL SPRING SCIENTIFIC CONVENTION MAY 19, 2018 EVALUATION OF ABNORMAL LIVER TESTS Review of liver enzymes vs liver function tests Clinical
EVALUATION OF ABNORMAL LIVER TESTS MIA MANABAT DO PGY6 MOA 119 TH ANNUAL SPRING SCIENTIFIC CONVENTION MAY 19, 2018 EVALUATION OF ABNORMAL LIVER TESTS Review of liver enzymes vs liver function tests Clinical
Xiao-Ling Chi, Mei-Jie Shi, Huan-Ming Xiao, Yu-Bao Xie, and Gao-Shu Cai. Correspondence should be addressed to Xiao-Ling Chi;
 Evidence-Based Complementary and Alternative Medicine Volume 2016, Article ID 3743427, 6 pages http://dx.doi.org/10.1155/2016/3743427 Research Article The Score Model Containing Chinese Medicine Syndrome
Evidence-Based Complementary and Alternative Medicine Volume 2016, Article ID 3743427, 6 pages http://dx.doi.org/10.1155/2016/3743427 Research Article The Score Model Containing Chinese Medicine Syndrome
The role of ARFI and APRI in diagnosis of liver fibrosis on patients with common chronic liver diseases
 RESEARCH ARTICLE The role of ARFI and APRI in diagnosis of liver fibrosis on patients with common chronic liver diseases Objective: This study aimed to investigate the value of liver fibrosis assessment
RESEARCH ARTICLE The role of ARFI and APRI in diagnosis of liver fibrosis on patients with common chronic liver diseases Objective: This study aimed to investigate the value of liver fibrosis assessment
Steatotic liver disease
 Steatotic liver disease Fatty liver disease Prof. Dr. ANNE HOORENS Non-Neoplastic Liver Pathology December 8th 2018 Working Group of Digestive Pathology Belgian Society of Pathology OUTLINE NAFLD = Non-Alcoholic
Steatotic liver disease Fatty liver disease Prof. Dr. ANNE HOORENS Non-Neoplastic Liver Pathology December 8th 2018 Working Group of Digestive Pathology Belgian Society of Pathology OUTLINE NAFLD = Non-Alcoholic
NAFLD: evidence-based management. Curso de residentes AEEH Salvador Augustin, MD Liver Unit Vall d Hebron Hospital Barcelona, Spain
 NAFLD: evidence-based management Curso de residentes AEEH 2017 Salvador Augustin, MD Liver Unit Vall d Hebron Hospital Barcelona, Spain Clinical case - 55 yo female - Sent for incidental steatosis at abdominal
NAFLD: evidence-based management Curso de residentes AEEH 2017 Salvador Augustin, MD Liver Unit Vall d Hebron Hospital Barcelona, Spain Clinical case - 55 yo female - Sent for incidental steatosis at abdominal
Non-Alcoholic Fatty Liver Diseasean underestimated epidemic
 Non-Alcoholic Fatty Liver Diseasean underestimated epidemic Amir Shlomai MD,PhD Head, Department of Medicine D The Liver Institute Rabin Medical Center, Beilinson Hospital The IASLD semi-annual meeting-
Non-Alcoholic Fatty Liver Diseasean underestimated epidemic Amir Shlomai MD,PhD Head, Department of Medicine D The Liver Institute Rabin Medical Center, Beilinson Hospital The IASLD semi-annual meeting-
NASH PROGRESS IN THE LAST DECADE
 PROGRESS IN THE LAST DECADE Mitchell L. Shiffman, MD, FACG Director Health System Richmond and Newport News, VA Medical Group Good Help to Those in Need A GLOBAL HEALTH PROBLEM Nigeria Australia Spain
PROGRESS IN THE LAST DECADE Mitchell L. Shiffman, MD, FACG Director Health System Richmond and Newport News, VA Medical Group Good Help to Those in Need A GLOBAL HEALTH PROBLEM Nigeria Australia Spain
Nonalcoholic Fatty Liver Disease in Children: Typical and Atypical
 Nonalcoholic Fatty Liver Disease in Children: Typical and Atypical Disclosure Naim Alkhouri, MD discloses the following relationships with commercial companies: Membership in the Speakers Bureau for Alexion
Nonalcoholic Fatty Liver Disease in Children: Typical and Atypical Disclosure Naim Alkhouri, MD discloses the following relationships with commercial companies: Membership in the Speakers Bureau for Alexion
Obesity, metabolic syndrome (MetS), and type 2 diabetes
 Noninvasive Diagnosis of NASH and Liver Fibrosis Within the Spectrum of NAFLD Naim Alkhouri, MD, and Arthur J. McCullough, MD Dr. Alkhouri and Dr. McCullough are affiliated with the Department of Gastroenterology
Noninvasive Diagnosis of NASH and Liver Fibrosis Within the Spectrum of NAFLD Naim Alkhouri, MD, and Arthur J. McCullough, MD Dr. Alkhouri and Dr. McCullough are affiliated with the Department of Gastroenterology
NAFLD/NASH in Sub- Saharan Africa
 NAFLD/NASH in Sub- Saharan Africa Corné Kruger Gastroenterologist Durbanville Mediclinic Cape Town Liver Interest group meeting: Cape Town 2015 Introduction NAFLD is the most common liver disease disease
NAFLD/NASH in Sub- Saharan Africa Corné Kruger Gastroenterologist Durbanville Mediclinic Cape Town Liver Interest group meeting: Cape Town 2015 Introduction NAFLD is the most common liver disease disease
NON-ALCOHOLIC FATTY LIVER DISEASE (NAFLD) NON-ALCOHOLIC STEATOHEPATITIS (NASH) ADDRESSING A GROWING SILENT EPIDEMIC
 NON-ALCOHOLIC FATTY LIVER DISEASE () & NON-ALCOHOLIC STEATOHEPATITIS () ADDRESSING A GROWING SILENT EPIDEMIC PREVALENCE OF / USA Prevalence in Middle Age Patients San Antonio, Texas (Williams et al., Gastroenterology
NON-ALCOHOLIC FATTY LIVER DISEASE () & NON-ALCOHOLIC STEATOHEPATITIS () ADDRESSING A GROWING SILENT EPIDEMIC PREVALENCE OF / USA Prevalence in Middle Age Patients San Antonio, Texas (Williams et al., Gastroenterology
At Least 1 in 5 Patients in Your Practice Have Fatty Liver
 At Least 1 in 5 Patients in Your Practice Have Fatty Liver What Can You Tell Your Patients Magnus McLeod MD FRCPC Assistant Professor Dalhousie University 30-NOV-2017 NAFLD Non-Alcoholic Fatty Liver Disease
At Least 1 in 5 Patients in Your Practice Have Fatty Liver What Can You Tell Your Patients Magnus McLeod MD FRCPC Assistant Professor Dalhousie University 30-NOV-2017 NAFLD Non-Alcoholic Fatty Liver Disease
Prevalence of non-alcoholic fatty liver disease in type 2 diabetes mellitus patients in a tertiary care hospital of Bihar
 Original Research Article Prevalence of non-alcoholic fatty liver disease in type 2 diabetes mellitus patients in a tertiary care hospital of Bihar Naresh Kumar 1, Jyoti Kumar Dinkar 2*, Chandrakishore
Original Research Article Prevalence of non-alcoholic fatty liver disease in type 2 diabetes mellitus patients in a tertiary care hospital of Bihar Naresh Kumar 1, Jyoti Kumar Dinkar 2*, Chandrakishore
PEDIATRIC FOIE GRAS: NON-ALCOHOLIC FATTY LIVER DISEASE
 PEDIATRIC FOIE GRAS: NON-ALCOHOLIC FATTY LIVER DISEASE Updates on New insights into NAFLD and NASH pathophysiology New AASLD/AGA/ACG guidelines for NAFLD and NASH, as pertains to pediatrics Evidence-based
PEDIATRIC FOIE GRAS: NON-ALCOHOLIC FATTY LIVER DISEASE Updates on New insights into NAFLD and NASH pathophysiology New AASLD/AGA/ACG guidelines for NAFLD and NASH, as pertains to pediatrics Evidence-based
NON-ALCOHOLIC FATTY LIVER DISEASE (NAFLD) NON-ALCOHOLIC STEATOHEPATITIS (NASH) ADDRESSING A GROWING SILENT EPIDEMIC
 NON-ALCOHOLIC FATTY LIVER DISEASE () & NON-ALCOHOLIC STEATOHEPATITIS () ADDRESSING A GROWING SILENT EPIDEMIC PREVALENCE OF / USA Prevalence in Middle Age Patients San Antonio, Texas (Williams et al., Gastroenterology
NON-ALCOHOLIC FATTY LIVER DISEASE () & NON-ALCOHOLIC STEATOHEPATITIS () ADDRESSING A GROWING SILENT EPIDEMIC PREVALENCE OF / USA Prevalence in Middle Age Patients San Antonio, Texas (Williams et al., Gastroenterology
Linda Ferrell, MD Distinguished Professor Vice Chair Director of Surgical Pathology Dept of Pathology
 Linda Ferrell, MD Distinguished Professor Vice Chair Director of Surgical Pathology Dept of Pathology Nonalcoholic steatohepatitis and Fatty Liver Disease Liver manifestations of the obesity epidemic Changes
Linda Ferrell, MD Distinguished Professor Vice Chair Director of Surgical Pathology Dept of Pathology Nonalcoholic steatohepatitis and Fatty Liver Disease Liver manifestations of the obesity epidemic Changes
NAFLD and NASH: The Not-So-New Kids on the Block
 NAFLD and NASH: The Not-So-New Kids on the Block Mary E. Rinella, MD Associate Professor of Medicine Feinberg School of Medicine Northwestern University Chicago, Illinois This program is supported by an
NAFLD and NASH: The Not-So-New Kids on the Block Mary E. Rinella, MD Associate Professor of Medicine Feinberg School of Medicine Northwestern University Chicago, Illinois This program is supported by an
PROGRESSION TO FIBROSIS IN PATIENTS WITH NONALCOHOLIC FATTY LIVER DISEASE (NAFLD) THE VALUE OF NONINVASIVE MARKERS
 Supplement 1/2015, 4 th ISAA PROGRESSION TO FIBROSIS IN PATIENTS WITH NONALCOHOLIC FATTY LIVER DISEASE (NAFLD) THE VALUE OF NONINVASIVE MARKERS Denisa DOBRIN 1, Tiberiu Ioan NANEA 2, Cristian Mihai POMOHACI
Supplement 1/2015, 4 th ISAA PROGRESSION TO FIBROSIS IN PATIENTS WITH NONALCOHOLIC FATTY LIVER DISEASE (NAFLD) THE VALUE OF NONINVASIVE MARKERS Denisa DOBRIN 1, Tiberiu Ioan NANEA 2, Cristian Mihai POMOHACI
Fat, ballooning, plasma cells and a +ANA. Yikes! USCAP 2016 Evening Specialty Conference Cynthia Guy
 Fat, ballooning, plasma cells and a +ANA. Yikes! USCAP 2016 Evening Specialty Conference Cynthia Guy Goals Share an interesting case Important because it highlights a common problem that we re likely to
Fat, ballooning, plasma cells and a +ANA. Yikes! USCAP 2016 Evening Specialty Conference Cynthia Guy Goals Share an interesting case Important because it highlights a common problem that we re likely to
The Efficacy of Corticosteroid Therapy in a Patient with Nonalcoholic Steatohepatitis Overlapping Autoimmune Hepatitis: A Case Report
 doi: 10.2169/internalmedicine.8887-17 Intern Med Advance Publication http://internmed.jp CASE REPORT The Efficacy of Corticosteroid Therapy in a Patient with Nonalcoholic Steatohepatitis Overlapping Autoimmune
doi: 10.2169/internalmedicine.8887-17 Intern Med Advance Publication http://internmed.jp CASE REPORT The Efficacy of Corticosteroid Therapy in a Patient with Nonalcoholic Steatohepatitis Overlapping Autoimmune
Disclosure. Objectives. Smash the Nash: A practical approach to fatty liver disease
 Smash the Nash: A practical approach to fatty liver disease Bruce D. Askey, MS, ANP-BC Associate Lecturer North Andover, MA Adult Nurse Practitioner Dept. of Hepatology/Gastroenterology Guthrie Clinic
Smash the Nash: A practical approach to fatty liver disease Bruce D. Askey, MS, ANP-BC Associate Lecturer North Andover, MA Adult Nurse Practitioner Dept. of Hepatology/Gastroenterology Guthrie Clinic
Although nonalcoholic fatty liver disease (NAFLD) Decreased Survival of Subjects with Elevated Liver Function Tests During a 28-Year Follow-Up
 Decreased Survival of Subjects with Elevated Liver Function Tests During a 28-Year Follow-Up Cecilia Söderberg, 1 Per Stål, 2,3 Johan Askling, 1 Hans Glaumann, 3 Greger Lindberg, 3 Joel Marmur, 3 and Rolf
Decreased Survival of Subjects with Elevated Liver Function Tests During a 28-Year Follow-Up Cecilia Söderberg, 1 Per Stål, 2,3 Johan Askling, 1 Hans Glaumann, 3 Greger Lindberg, 3 Joel Marmur, 3 and Rolf
CASE REPORT. Introduction. Case Report
 doi: 10.2169/internalmedicine.8754-16 Intern Med 56: 2739-2744, 2017 http://internmed.jp CASE REPORT The Improvement of the Hepatic Histological Findings in a Patient with Non-alcoholic Steatohepatitis
doi: 10.2169/internalmedicine.8754-16 Intern Med 56: 2739-2744, 2017 http://internmed.jp CASE REPORT The Improvement of the Hepatic Histological Findings in a Patient with Non-alcoholic Steatohepatitis
Favorable efficacy of glecaprevir plus pibrentasvir as salvage therapy for HCV failures to prior direct acting antivirals regimens
 Received: 5 June 208 Accepted: 9 July 208 DOI: 0.002/jmv.25278 RESEARCH ARTICLE Favorable efficacy of glecaprevir plus pibrentasvir as salvage therapy for HCV failures to prior direct acting antivirals
Received: 5 June 208 Accepted: 9 July 208 DOI: 0.002/jmv.25278 RESEARCH ARTICLE Favorable efficacy of glecaprevir plus pibrentasvir as salvage therapy for HCV failures to prior direct acting antivirals
The effect of aerobic exercise on serum level of liver enzymes and liver echogenicity in patients with non-alcoholic fatty liver disease
 Gastroenterology and Hepatology From Bed to Bench. 2013 RIGLD, Research Institute for Gastroenterology and Liver Diseases ORIGINAL ARTICLE The effect of aerobic exercise on serum level of liver enzymes
Gastroenterology and Hepatology From Bed to Bench. 2013 RIGLD, Research Institute for Gastroenterology and Liver Diseases ORIGINAL ARTICLE The effect of aerobic exercise on serum level of liver enzymes
Serum Levels of CK18 M30 and Leptin Are Useful Predictors of Steatohepatitis and Fibrosis in Paediatric NAFLD
 ORIGINAL ARTICLE: HEPATOLOGY AND NUTRITION Serum Levels of CK18 M30 and Leptin Are Useful Predictors of Steatohepatitis and Fibrosis in Paediatric NAFLD Emer Fitzpatrick, y Ragai R. Mitry, y Alberto Quaglia,
ORIGINAL ARTICLE: HEPATOLOGY AND NUTRITION Serum Levels of CK18 M30 and Leptin Are Useful Predictors of Steatohepatitis and Fibrosis in Paediatric NAFLD Emer Fitzpatrick, y Ragai R. Mitry, y Alberto Quaglia,
ORIGINAL ARTICLE. Abstract. Introduction
 ORIGINAL ARTICLE Prognostic Factors for Regression from Impaired Glucose Tolerance to Normal Glucose Regulation in Japanese Patients with Nonalcoholic Fatty Liver Disease Chie Ogata, Yuki Ohmoto-Sekine,
ORIGINAL ARTICLE Prognostic Factors for Regression from Impaired Glucose Tolerance to Normal Glucose Regulation in Japanese Patients with Nonalcoholic Fatty Liver Disease Chie Ogata, Yuki Ohmoto-Sekine,
American Journal of Oral Medicine and Radiology
 American Journal of Oral Medicine and Radiology e - ISSN - XXXX-XXXX ISSN - 2394-7721 Journal homepage: www.mcmed.us/journal/ajomr PREVALENCE OF NONALCOHOLIC FATTY LIVER DISEASE AMONG TYPE 2 DIABETIC POPULATION
American Journal of Oral Medicine and Radiology e - ISSN - XXXX-XXXX ISSN - 2394-7721 Journal homepage: www.mcmed.us/journal/ajomr PREVALENCE OF NONALCOHOLIC FATTY LIVER DISEASE AMONG TYPE 2 DIABETIC POPULATION
HHS Public Access Author manuscript Clin Gastroenterol Hepatol. Author manuscript; available in PMC 2016 April 13.
 Relationship between changes in serum keratin 18 and changes in liver histology in children and adults with nonalcoholic fatty liver disease Raj Vuppalanchi 1, Ajay K. Jain 2, Ross Deppe 1, Katherine Yates
Relationship between changes in serum keratin 18 and changes in liver histology in children and adults with nonalcoholic fatty liver disease Raj Vuppalanchi 1, Ajay K. Jain 2, Ross Deppe 1, Katherine Yates
ABNORMAL LIVER FUNCTION TESTS. Dr Uthayanan Chelvaratnam Hepatology Consultant North Bristol NHS Trust
 ABNORMAL LIVER FUNCTION TESTS Dr Uthayanan Chelvaratnam Hepatology Consultant North Bristol NHS Trust INTRODUCTION Liver function tests Cases Non invasive fibrosis measurement Questions UK MORTALITY RATE
ABNORMAL LIVER FUNCTION TESTS Dr Uthayanan Chelvaratnam Hepatology Consultant North Bristol NHS Trust INTRODUCTION Liver function tests Cases Non invasive fibrosis measurement Questions UK MORTALITY RATE
NONALCOHOLIC FATTY LIVER DISEASE. Non-Alcoholic Fatty Liver Disease (NAFLD) Primary NAFLD. April 13, 2012
 NONALCOHOLIC FATTY LIVER DISEASE Kiran Bambha, MD University of Colorado Denver April 13, 2012 Non-Alcoholic Fatty Liver Disease (NAFLD) Primary NAFLD Simple Steatosis Fatty hepatocytes Intracellular fat
NONALCOHOLIC FATTY LIVER DISEASE Kiran Bambha, MD University of Colorado Denver April 13, 2012 Non-Alcoholic Fatty Liver Disease (NAFLD) Primary NAFLD Simple Steatosis Fatty hepatocytes Intracellular fat
Supplementary Table 1. The distribution of IFNL rs and rs and Hardy-Weinberg equilibrium Genotype Observed Expected X 2 P-value* CHC
 Supplementary Table 1. The distribution of IFNL rs12979860 and rs8099917 and Hardy-Weinberg equilibrium Genotype Observed Expected X 2 P-value* CHC rs12979860 (n=3129) CC 1127 1145.8 CT 1533 1495.3 TT
Supplementary Table 1. The distribution of IFNL rs12979860 and rs8099917 and Hardy-Weinberg equilibrium Genotype Observed Expected X 2 P-value* CHC rs12979860 (n=3129) CC 1127 1145.8 CT 1533 1495.3 TT
Early life determinants of Non-Alcoholic Fatty Liver Disease and NASH DR JULIANA MUIVA-GITOBU KENYA PAEDIATRIC ASSOCIATION CONFERENCE APRIL 2016.
 Early life determinants of Non-Alcoholic Fatty Liver Disease and NASH DR JULIANA MUIVA-GITOBU KENYA PAEDIATRIC ASSOCIATION CONFERENCE APRIL 2016. Outline Definition NAFLD and NASH Magnitude of the problem
Early life determinants of Non-Alcoholic Fatty Liver Disease and NASH DR JULIANA MUIVA-GITOBU KENYA PAEDIATRIC ASSOCIATION CONFERENCE APRIL 2016. Outline Definition NAFLD and NASH Magnitude of the problem
EFFECT OF ORAL SUPPLEMENTATION OF WHEY PROTEIN ISOLATE ON NON-ALCOHOLIC STEATOHEPATITIS PATIENTS
 42 EFFECT OF ORAL SUPPLEMENTATION OF WHEY PROTEIN ISOLATE ON NON-ALCOHOLIC STEATOHEPATITIS PATIENTS Prasong Tienboon MD, PhD. 1, Taned Chitapanarux MD. 2, Suwalee Pojchamarnwiputh MD. 3, Donrawee Leelarungrayub
42 EFFECT OF ORAL SUPPLEMENTATION OF WHEY PROTEIN ISOLATE ON NON-ALCOHOLIC STEATOHEPATITIS PATIENTS Prasong Tienboon MD, PhD. 1, Taned Chitapanarux MD. 2, Suwalee Pojchamarnwiputh MD. 3, Donrawee Leelarungrayub
Normal ALT for men 30 IU/L 36% US males abnormal. Abnl ALT. Assess alcohol use/meds. Recheck in 6-8 weeks. still pos
 Fatty liver disease Its not just for big boys anymore Ken Flora, MD, FAASLD, FACG, AGAF No disclosures Common situation Normal ALT for men 30 IU/L 36% US males abnormal Normal ALT for women 20 IU/L 28%
Fatty liver disease Its not just for big boys anymore Ken Flora, MD, FAASLD, FACG, AGAF No disclosures Common situation Normal ALT for men 30 IU/L 36% US males abnormal Normal ALT for women 20 IU/L 28%
Transient elastography in chronic liver diseases of other etiologies
 4 Post Meeting A.I.S.F. Unmet Clinical Needs in Hepatology: New and upcoming diagnostic tools" Transient elastography in chronic liver diseases of other etiologies Dr. Vincenza Calvaruso Gastroenterologia
4 Post Meeting A.I.S.F. Unmet Clinical Needs in Hepatology: New and upcoming diagnostic tools" Transient elastography in chronic liver diseases of other etiologies Dr. Vincenza Calvaruso Gastroenterologia
Non-Alcoholic Fatty Liver Disease
 Non-Alcoholic Fatty Liver Disease Varun Saxena, MD MAS Gastroenterology and Hepatology Kaiser Permanente South San Francisco Assistant Clinical Professor University of California San Francisco January
Non-Alcoholic Fatty Liver Disease Varun Saxena, MD MAS Gastroenterology and Hepatology Kaiser Permanente South San Francisco Assistant Clinical Professor University of California San Francisco January
広島大学学術情報リポジトリ Hiroshima University Institutional Repository
 広島大学学術情報リポジトリ Hiroshima University Institutional Repository Title Auther(s) Citation Issue Date DOI Atorvastatin improves disease activity of nonalcoholic steatohepatitis partly through its tumour necrosis
広島大学学術情報リポジトリ Hiroshima University Institutional Repository Title Auther(s) Citation Issue Date DOI Atorvastatin improves disease activity of nonalcoholic steatohepatitis partly through its tumour necrosis
M30 Apoptosense ELISA. A biomarker assay for detection and screening of NASH
 M30 Apoptosense ELISA A biomarker assay for detection and screening of NASH NASH A Global Disease In the Western countries, Non-Alcoholic Fatty Liver Disease (NAFLD) is the most common liver disease, strongly
M30 Apoptosense ELISA A biomarker assay for detection and screening of NASH NASH A Global Disease In the Western countries, Non-Alcoholic Fatty Liver Disease (NAFLD) is the most common liver disease, strongly
Significance of Hepatic Insulin Clearance in Patients with Chronic Hepatitis C and Non-alcoholic Fatty Liver Disease
 ORIGINAL ARTICLE Significance of Hepatic Insulin Clearance in Patients with Chronic Hepatitis C and Non-alcoholic Fatty Liver Disease Hisamitsu Miyaaki 1, Tatsuki Ichikawa 1,NaotaTaura 1, Satoshi Miuma
ORIGINAL ARTICLE Significance of Hepatic Insulin Clearance in Patients with Chronic Hepatitis C and Non-alcoholic Fatty Liver Disease Hisamitsu Miyaaki 1, Tatsuki Ichikawa 1,NaotaTaura 1, Satoshi Miuma
Non-Alcoholic Steatohepatitis (NASH): What the Gastroenterologist Should Know
 Non-Alcoholic Steatohepatitis (NASH): What the Gastroenterologist Should Know Naga P. Chalasani, MD, FACG Professor of Medicine and Cellular & Integrative Physiology Director, Division of GI and Hepatology
Non-Alcoholic Steatohepatitis (NASH): What the Gastroenterologist Should Know Naga P. Chalasani, MD, FACG Professor of Medicine and Cellular & Integrative Physiology Director, Division of GI and Hepatology
Update on Nonalcoholic Fatty Liver Disease. Kathleen E Corey, MD, MPH, MMSc Director, Mass General Fatty Liver Clinic
 Update on Nonalcoholic Fatty Liver Disease Kathleen E Corey, MD, MPH, MMSc Director, Mass General Fatty Liver Clinic Outline Defining the phenotypes of nonalcoholic fatty liver disease NAFLD Diagnostics
Update on Nonalcoholic Fatty Liver Disease Kathleen E Corey, MD, MPH, MMSc Director, Mass General Fatty Liver Clinic Outline Defining the phenotypes of nonalcoholic fatty liver disease NAFLD Diagnostics
Non alcoholic fatty liver and Non alcoholic Steatohepatitis. By Dr. Seham Seif
 Non alcoholic fatty liver and Non alcoholic Steatohepatitis By Dr. Seham Seif Definition NAFL describe a common clinicopathological conditions characterized by significant lipid deposition in the hepatocytes
Non alcoholic fatty liver and Non alcoholic Steatohepatitis By Dr. Seham Seif Definition NAFL describe a common clinicopathological conditions characterized by significant lipid deposition in the hepatocytes
Laboratory analysis of the obese child recommendations and discussion. MacKenzi Hillard May 4, 2011
 Laboratory analysis of the obese child recommendations and discussion MacKenzi Hillard May 4, 2011 aka: What to do with Fasting Labs The Obesity Epidemic The prevalence of obesity in adolescents has tripled
Laboratory analysis of the obese child recommendations and discussion MacKenzi Hillard May 4, 2011 aka: What to do with Fasting Labs The Obesity Epidemic The prevalence of obesity in adolescents has tripled
NON-ALCOHOLIC STEATOHEPATITIS AND NON-ALCOHOLIC FATTY LIVER DISEASES
 NON-ALCOHOLIC STEATOHEPATITIS AND NON-ALCOHOLIC FATTY LIVER DISEASES Preface Zobair M. Younossi xiii Epidemiology and Natural History of NAFLD and NASH 1 Janus P. Ong and Zobair M. Younossi Understanding
NON-ALCOHOLIC STEATOHEPATITIS AND NON-ALCOHOLIC FATTY LIVER DISEASES Preface Zobair M. Younossi xiii Epidemiology and Natural History of NAFLD and NASH 1 Janus P. Ong and Zobair M. Younossi Understanding
Liver biopsy as the gold standard for diagnosis. Pierre BEDOSSA
 Liver biopsy as the gold standard for diagnosis Pierre BEDOSSA 1 PATHOLOGY OF NAFLD CONFLICTS OF INTEREST Grants and funding from Genfit, Intercept, Allergan, Inventiva, OWL, Echosens CEO and funding of
Liver biopsy as the gold standard for diagnosis Pierre BEDOSSA 1 PATHOLOGY OF NAFLD CONFLICTS OF INTEREST Grants and funding from Genfit, Intercept, Allergan, Inventiva, OWL, Echosens CEO and funding of
NAFLD/NASH. Definitions. Pathology NASH. Vicki Shah PA-C, MMS Rush University Hepatology
 NAFLD/NASH Vicki Shah PA-C, MMS Rush University Hepatology Definitions NAFLD Evidence of hepatic steatosis by histology (5%) or imaging No causes for secondary fat accumulation EtOH, Drugs, hereditary
NAFLD/NASH Vicki Shah PA-C, MMS Rush University Hepatology Definitions NAFLD Evidence of hepatic steatosis by histology (5%) or imaging No causes for secondary fat accumulation EtOH, Drugs, hereditary
SAF score and mortality in NAFLD after up to 41 years of follow-up
 SAF score and mortality in NAFLD after up to 41 years of follow-up Hannes Hagström, Patrik Nasr, Mattias Ekstedt, Stergios Kechagias, Per Stal, Pierre Bedossa and Rolf Hultcrantz Journal Article N.B.:
SAF score and mortality in NAFLD after up to 41 years of follow-up Hannes Hagström, Patrik Nasr, Mattias Ekstedt, Stergios Kechagias, Per Stal, Pierre Bedossa and Rolf Hultcrantz Journal Article N.B.:
Clinical Model for NASH and Advanced Fibrosis in Adult Patients With Diabetes and NAFLD: Guidelines for Referral in NAFLD
 Diabetes Care 1 Clinical Model for NASH and Advanced Fibrosis in Adult Patients With Diabetes and NAFLD: Guidelines for Referral in NAFLD Jessica Bazick, 1 Michele Donithan, 2 Brent A. Neuschwander-Tetri,
Diabetes Care 1 Clinical Model for NASH and Advanced Fibrosis in Adult Patients With Diabetes and NAFLD: Guidelines for Referral in NAFLD Jessica Bazick, 1 Michele Donithan, 2 Brent A. Neuschwander-Tetri,
Serum fragmented cytokeratin 18 levels reflect the histological activity. score of nonalcoholic fatty liver disease more accurately than serum
 Serum fragmented cytokeratin 18 levels reflect the histological activity score of nonalcoholic fatty liver disease more accurately than serum alanine aminotransferase levels Masaru Tsutsui, BE, * Naoki
Serum fragmented cytokeratin 18 levels reflect the histological activity score of nonalcoholic fatty liver disease more accurately than serum alanine aminotransferase levels Masaru Tsutsui, BE, * Naoki
Case #1. Digital Slides 11/6/ year old woman presented with abnormal liver function tests. Liver Biopsy to r/o autoimmune hepatitis
 45 year old woman presented with abnormal liver function tests Liver Biopsy to r/o autoimmune hepatitis Further down. ANA 1: 160; ASMA 1:80 ANA 1: 160; ASMA 1:80 IgG = 14.5 g/l (upper normal range: 16)
45 year old woman presented with abnormal liver function tests Liver Biopsy to r/o autoimmune hepatitis Further down. ANA 1: 160; ASMA 1:80 ANA 1: 160; ASMA 1:80 IgG = 14.5 g/l (upper normal range: 16)
CIRROSI E IPERTENSIONE PORTALE NELLA DONNA
 Cagliari, 16 settembre 2017 CIRROSI E IPERTENSIONE PORTALE NELLA DONNA Vincenza Calvaruso, MD, PhD Ricercatore di Gastroenterologia Gastroenterologia & Epatologia, Di.Bi.M.I.S. Università degli Studi di
Cagliari, 16 settembre 2017 CIRROSI E IPERTENSIONE PORTALE NELLA DONNA Vincenza Calvaruso, MD, PhD Ricercatore di Gastroenterologia Gastroenterologia & Epatologia, Di.Bi.M.I.S. Università degli Studi di
NASH : Diagnosis and investigation. VII Workshop international, Curitiba, Brazil 29/08/2014
 NASH : Diagnosis and investigation VII Workshop international, Curitiba, Brazil 29/08/2014 Vlad Ratziu, Université Pierre et Marie Curie, Hôpital Pitié Salpêtrière, Paris, France Usual diagnostic circumstances
NASH : Diagnosis and investigation VII Workshop international, Curitiba, Brazil 29/08/2014 Vlad Ratziu, Université Pierre et Marie Curie, Hôpital Pitié Salpêtrière, Paris, France Usual diagnostic circumstances
PREVALENCE OF NAFLD & NASH
 - - PREVALENCE OF & USA Prevalence in Middle Age Patients San Antonio, Texas (Williams et al., Gastroenterology 2011; 140:124-31) Dallas Heart Study Prevalence Numbers (Browning et al., Hepatology 2004;40:1387-95)
- - PREVALENCE OF & USA Prevalence in Middle Age Patients San Antonio, Texas (Williams et al., Gastroenterology 2011; 140:124-31) Dallas Heart Study Prevalence Numbers (Browning et al., Hepatology 2004;40:1387-95)
2 nd International Workshop on NASH Biomarkers, Washington DC, May 5-6, 2017
 Hepatic Proton Density Fat Fraction Correlates With Histologic Measures of Steatosis and Is Responsive to Changes in Those Measures in a Multi-center Nonalcoholic Steatohepatitis Clinical Trial Michael
Hepatic Proton Density Fat Fraction Correlates With Histologic Measures of Steatosis and Is Responsive to Changes in Those Measures in a Multi-center Nonalcoholic Steatohepatitis Clinical Trial Michael
Internal Medicine Grand Rounds University of Texas Southwestern Medical Center October 5, 2018
 Internal Medicine Grand Rounds University of Texas Southwestern Medical Center October 5, 2018 Nonalcoholic Fatty Liver Disease (NAFLD) Turns 38-What Have We Learned? Jay D. Horton, M.D. This is to acknowledge
Internal Medicine Grand Rounds University of Texas Southwestern Medical Center October 5, 2018 Nonalcoholic Fatty Liver Disease (NAFLD) Turns 38-What Have We Learned? Jay D. Horton, M.D. This is to acknowledge
NAFLD & NASH. Naga Chalasani, MD, FACG Professor of Medicine and Cellular & Integrative Physiology Director, Division of GI and Hepatology
 NAFLD & NASH Naga Chalasani, MD, FACG Professor of Medicine and Cellular & Integrative Physiology Director, Division of GI and Hepatology Indiana University School of Medicine ACG Midwest Regional Course,
NAFLD & NASH Naga Chalasani, MD, FACG Professor of Medicine and Cellular & Integrative Physiology Director, Division of GI and Hepatology Indiana University School of Medicine ACG Midwest Regional Course,
Noninvasive Diagnosis and Staging of Liver Disease. Naveen Gara, MD
 Noninvasive Diagnosis and Staging of Liver Disease Naveen Gara, MD Outline Brief overview of the anatomy of liver Liver-related lab tests Chronic liver disease progression Estimation of liver fibrosis
Noninvasive Diagnosis and Staging of Liver Disease Naveen Gara, MD Outline Brief overview of the anatomy of liver Liver-related lab tests Chronic liver disease progression Estimation of liver fibrosis
Effect of lifetime alcohol consumption on the histological severity of non-alcoholic fatty liver disease
 Liver International ISSN 1478-3223 METABOLIC AND STEATOHEPATITIS Effect of lifetime alcohol consumption on the histological severity of non-alcoholic fatty liver disease Hellan K. Kwon 1, Joel K. Greenson
Liver International ISSN 1478-3223 METABOLIC AND STEATOHEPATITIS Effect of lifetime alcohol consumption on the histological severity of non-alcoholic fatty liver disease Hellan K. Kwon 1, Joel K. Greenson
Is increased red cell distribution width an indicating marker of nonalcoholic steatohepatitis and fibrotic stage?
 Online Submissions: http://www.wjgnet.com/esps/ bpgoffice@wjgnet.com doi:10.3748/wjg.v19.i42.7412 World J Gastroenterol 2013 November 14; 19(42): 7412-7418 ISSN 1007-9327 (print) ISSN 2219-2840 (online)
Online Submissions: http://www.wjgnet.com/esps/ bpgoffice@wjgnet.com doi:10.3748/wjg.v19.i42.7412 World J Gastroenterol 2013 November 14; 19(42): 7412-7418 ISSN 1007-9327 (print) ISSN 2219-2840 (online)
Development and validation of a simple index system to predict nonalcoholic fatty liver disease
 The Korean Journal of Hepatology 2011;17:19-26 DOI: 10.3350/kjhep.2011.17.1.19 Original Article Development and validation of a simple index system to predict nonalcoholic fatty liver disease Young Jin
The Korean Journal of Hepatology 2011;17:19-26 DOI: 10.3350/kjhep.2011.17.1.19 Original Article Development and validation of a simple index system to predict nonalcoholic fatty liver disease Young Jin
Serum YKL-40 as a marker of liver fibrosis in patients with non-alcoholic fatty
 Supplementary Information Serum YKL- as a marker of liver fibrosis in patients with non-alcoholic fatty liver disease Erina Kumagai 1,,#, Yohei Mano 1,#, Sachiyo Yoshio 1, Hirotaka Shoji 1, Masaya Sugiyama
Supplementary Information Serum YKL- as a marker of liver fibrosis in patients with non-alcoholic fatty liver disease Erina Kumagai 1,,#, Yohei Mano 1,#, Sachiyo Yoshio 1, Hirotaka Shoji 1, Masaya Sugiyama
Hepatology for the Nonhepatologist
 Hepatology for the Nonhepatologist Kenneth E. Sherman, MD, PhD Gould Professor of Medicine Director, Division of Digestive Diseases University of Cincinnati College of Medicine Cincinnati, Ohio Learning
Hepatology for the Nonhepatologist Kenneth E. Sherman, MD, PhD Gould Professor of Medicine Director, Division of Digestive Diseases University of Cincinnati College of Medicine Cincinnati, Ohio Learning
Managing abnormal LFTs in Primary care
 Managing abnormal LFTs in Primary care Summary guideline, April 2015 Sally Hull, Lucy Carter Managing abnormal LFTs in Primary care Draft guideline written by Dr Sally Hull and Dr Lucy Carter at CEG, with
Managing abnormal LFTs in Primary care Summary guideline, April 2015 Sally Hull, Lucy Carter Managing abnormal LFTs in Primary care Draft guideline written by Dr Sally Hull and Dr Lucy Carter at CEG, with
A Modification of the Brunt System for Scoring Liver Histology of Patients with Non-Alcoholic Fatty Liver Disease
 Arch Iran Med 2010; 13 (1): 38 44 Original Article A Modification of the Brunt System for Scoring Liver Histology of Patients with Non-Alcoholic Fatty Liver Disease Shahin Merat MD*, Farzaneh Khadem-Sameni
Arch Iran Med 2010; 13 (1): 38 44 Original Article A Modification of the Brunt System for Scoring Liver Histology of Patients with Non-Alcoholic Fatty Liver Disease Shahin Merat MD*, Farzaneh Khadem-Sameni
Evaluating Obese Persons With Abnormal Liver Chemistries
 Mary E. Rinella, MD, FAASLD Evaluating Obese Persons With Abnormal Liver Chemistries Postgraduate Course: Challenges in Management of Common Liver Diseases 275 1 25 year old obese Hispanic man with obesity,
Mary E. Rinella, MD, FAASLD Evaluating Obese Persons With Abnormal Liver Chemistries Postgraduate Course: Challenges in Management of Common Liver Diseases 275 1 25 year old obese Hispanic man with obesity,
Non-alcoholic fatty liver disease: time to take note and manage. Philip Newsome Professor of Hepatology & Director of Centre for Liver Research
 Non-alcoholic fatty liver disease: time to take note and manage Philip Newsome Professor of Hepatology & Director of Centre for Liver Research Disclosures Consultancy, Co-ordinating Investigator roles
Non-alcoholic fatty liver disease: time to take note and manage Philip Newsome Professor of Hepatology & Director of Centre for Liver Research Disclosures Consultancy, Co-ordinating Investigator roles
