Liver transplantation for hepatocellular carcinoma: outcomes and treatment options for recurrence
|
|
|
- Hope Robinson
- 6 years ago
- Views:
Transcription
1 INVITED REVIEW Annals of Gastroenterology (2015) 28, 1-8 Liver transplantation for hepatocellular carcinoma: outcomes and treatment options for recurrence Robert S. Rahimi, James F. Trotter Baylor University Medical Center, Dallas, TX, USA Abstract Overall survival and recurrence rates after liver transplantation (LT) for hepatocellular carcinoma (HCC) vary, however observational data support the notion that patients with HCC have an overall worse long-term prognosis after LT compared to patients transplanted without HCC. Patient selection for LT in patients with HCC fluctuated as changes in the model for end-stage liver disease score was adjusted from 2002 to In the last decade, management of HCC patients on the waiting list has varied based on center experience. Since HCC patients have better access to the donor pool compared to non-hcc patients as evidenced by their lower dropout rate from the waiting list, living donation has been implemented in certain centers. Overall patient survival, recurrence free survival, and recurrence rates have been compared between living donor LT (LDLT) and deceased donor LT, with one meta-analysis reporting a lower disease free survival in LDLT, however overall patient survival and recurrence rates showed no at 1, 3 and 5 years. In patients exhibiting HCC recurrence, different modalities regarding immunosuppression and therapies have been evaluated. Currently there are no consensus treatment strategies regarding post-transplant HCC recurrence in patients not suitable for locoregional therapy, hence consideration of a mammalian target of rapamycin inhibitors with the addition of sorafenib might be a feasible option with close monitoring in clinical practice despite the notable toxicities. Keywords Cirrhosis, deceased-donor, liver cancer, living-donor, mtor, sirolimus, sorafenib Ann Gastroenterol 2015; 28 (4): 1-8 Introduction Hepatocellular carcinoma (HCC) is a major health concern worldwide, resulting from chronic liver injury and inflammation due to viral, non-viral and genetic etiologies. HCC has been found to be the second [1] or third [2] leading cause of cancer-related death worldwide, with the majority of cases occurring in the setting of cirrhosis [3]. As the epidemic of nonalcoholic fatty liver disease (NAFLD) and chronic hepatitis C virus continues to increase in the United States [2], HCC rates will rise accordingly. Prior to the model for endstage liver disease (MELD) and HCC exception allocation system, patients with HCC remained on the waiting list longer than candidates without HCC, resulting in fewer than 5% of liver transplantation (LT) being performed for HCC. However, once MELD and HCC exceptions were adopted at the national Annette C. and Harold C. Simmons Transplant Institute, Baylor University Medical Center, Dallas, TX, USA Conflict of Interest: ne Correspondence to: Robert S. Rahimi, MD, Baylor University Medical Center, 3410 Worth St Suite 860, Dallas, TX 75246, USA, Tel.: , Fax: , robert.rahimi@baylorhealth.edu Received 8 vember 2014; accepted 9 December 2014 level, the number of overall transplant recipients steadily increased from nearly 5,000 patients in 2002, to 6,069 patients in 2008, while HCC patients receiving LT steadily rose (from nearly 1,000 in 2002 to 1,656 in 2008), representing over 21% of liver transplants [4] (Fig. 1). In February 2002, patients with HCC were given transplant exception MELD scores at higher values for both T1 and T2 lesions, based on a 3-month mortality estimate in comparison to disease progression that would preclude LT [5]. Later, followup data indicated that these exception scores were too liberal for HCC, hence adjustments in the MELD exception prioritization scheme changed over time [6] (Table 1). In particular, half of the patients with T1 tumor criteria (one single lesion <2 cm) were discovered not to have HCC in the explanted liver [7]. As a result, HCC patients with T1 tumors do not receive MELD exception points for HCC. However, patients within T2 criteria (1 lesion 5 cm or two or three lesions 1 cm but 3 cm in size) received 22 MELD exception points. In addition, patients receive additional MELD exception points every 90 days representing a 10% increase in mortality [6]. To receive these exception points, patients must be restaged every 90 days with cross-sectional imaging of the abdomen and chest to ensure that these criteria continue to be met. Prior to 1996, restrictions on LT for HCC were more liberal, which resulted in 5-year overall survivals (OS) up to 50%. During that same year, Mazzaferro and colleagues introduced 2015 Hellenic Society of Gastroenterology
2 2 R. S. Rahimi and J. F. Trotter Table 1 Changes in the MELD prioritization exception scores for HCC over time using initial 3 month mortality risk estimates Original February 2003 April 2004 March 2005 Stage I 1 tumor<2 cm 15% risk=meld 24 8% risk=meld 20 0 risk=meld calculated 0 risk=meld calculated Stage II 1 tumor 2 5 cm or 2 3 tumors largest <3 cm MELD, model for end stage liver disease; HCC, hepatocellular carcinoma 30% risk=meld 29 15% risk=meld 24 15% risk=meld 24 15% risk=meld 22 # of Recipients Year of transplantation Source: SRTR Analysis. Data as of May 2009 Figure 1 The solid line represents the total amount of liver transplant recipients from (all etiologies except hepatocellular carcinoma [HCC]), in comparison to HCC liver recipients from the same era (dashed line) the Milan criteria (any solitary HCC 5 cm, or up to three lesions 3 cm each, without vascular invasion or metastasis) which resulted in 5-year transplant survival near 70%, with recurrence seen in less than 10% [8]. The importance of these independent prognostic factors matches post-transplant survival outcomes for most other liver transplant indications. Hence, a recent international consensus conference recommended using the Milan criteria as the benchmark for selecting HCC patients for LT, and when making comparisons to other suggested expansion criteria [9]. Patients that fall outside the Milan criteria have the potential to have ablative techniques to downsize large tumors in order to fall into the exception range for LT. This downstaging technique is an area of ongoing research, however, with the continued organ shortage, decisions regarding transplantation need to be considered with respect to the benefits regarding potential HCC patients, and balanced with the consequences for all potential liver recipients on the waiting list. This resulted in many attempts to expand the Milan criteria as it was considered too conservative, however, only the University of California San Francisco (UCSF) criteria (one tumor 6.5 cm, or three nodules with the largest 4.5 cm, and a total tumor diameter of 8 cm) have demonstrated comparable outcome data in its prospectively validated design [10,11]. As the donor pool has stayed relatively fixed in size over the years [12], increasing the MELD exception scores for HCC patients may deprive other candidates without HCC from a potential LT depending on regional variations. Although expansion of the Milan criteria has shown good outcomes in select individuals [10,13], it should be left up to the individual regions to come to an agreement regarding any proposal change on expanding the current Milan criteria. Caution should be taken when expanding tumor criteria as HCC recurrence post-lt is a continuum as described by the metro-ticket analogy [14]. The further distance you travel underground, you pay a higher ticket premium, which is analogous to the larger the HCC tumor, the higher price you pay for HCC recurrence post-lt. While the national MELD exception criteria are followed in most regions, some regions, namely region 4 and 5 have expanded their criteria slightly. Region 5 utilizes the UCSF criteria and region 4 uses locally derived staging criteria (one lesion 6 cm or up to three lesions [none larger than 5 cm] with a total tumor size of <9 cm) [13]. This review will discuss current concepts regarding LT in the HCC patient population. Management and outcomes of patients with HCC on the liver transplant waiting list Patients with a diagnosis of HCC that are within the Milan criteria, and are expected to be on the waiting list for more than a few months, are considered for locoregional treatments [radiofrequency ablation (RFA) and transarterial chemoembolization (TACE)] [15,16]. According to the most recent national dataset, locoregional therapies are being used more frequently in patients who received a LT (Fig. 2), albeit through a regional review board, since different regions vary widely on their acceptance of such patients for transplant, while the current system does not allow patients outside Milan criteria who undergo downstaging to receive HCC exception points. As of 2008, use of TACE therapies have seen a steady rise in that nearly 75% of patients underwent this type of treatment prior to receiving a LT, as compared to a slight decline to nearly one-third of individuals having RFA therapy prior to LT (Fig. 3). Depending on the transplant centers experience, size and location of the tumor(s), patients may benefit from locoregional procedures in the hopes of preventing progression beyond the Milan criteria, thereby maintaining their priority on the liver transplant waiting list [17,18]. Although the absolute benefit in preventing waitlist dropout rates with locoregional treatment is lacking, both patient survival (79% vs. 75%, P=0.03) and graft survival (76% vs. 71%, P=0.03) at 3 years after LT has shown more benefit for HCC patients receiving ablative therapy compared to those not receiving locoregional treatment [7]. However, the authors also demonstrated the adjusted patient survival at 1 year (85% vs.
3 Liver transplantation for HCC 3 70% 60% 50% 40% 30% 20% 10% 0% Year of transplantation Source: SRTR Analysis. Data as of May 2009 Figure 2 The proportion of hepatocellular carcinoma liver recipients that received any pre-transplant locoregional therapy by year of transplant from % 70% 60% 50% 40% 30% 20% 10% 0% TACE RFA Chemical Cryo Year of transplantation Source: SRTR Analysis. Data as of May 2009 Figure 3 The comparison of different non-surgical treatment modalities utilizing locoregional therapy from , prior to liver transplantation. The majority of treatment modalities remain steady over the years with the majority using transcatheter arterial chemoembolization (TACE) as a bridge to liver transplantation, followed by radiofrequency ablation (RFA) Cryo, cryotherapy 88%, P=0.003) and 3 years (74% vs. 81%, P<0.001) after LT were significantly worse in patients with HCC compared to those without HCC respectively. These therapies do not impact the actuarial wait time on the LT waiting list, however, it has been shown that patients with HCC tend to have shorter wait times with regards to non-hcc patients with comparison MELD scores of points at 1, 2, and 3 month intervals (Fig. 4). In turn, those with HCC have less dropout or death rates in comparison to patients without HCC that have MELD scores of 30 [7]. Furthermore, a detailed analysis demonstrated that once a patient is diagnosed with HCC, lower dropout rates are seen within the first year across all UNOS regions in these patients compared to non-hcc patients (Fig. 5) [19]. As HCC patients receive locoregional therapy in most cases, the potential to arrest tumor growth without impacting their position on the waiting list is seen as a major advantage. In fact, even if the HCC tumor is successfully ablated and the patient has no residual disease, patients are still eligible for Percent of Adult Candidates 80% 70% 60% 50% 40% 30% 20% 10% Transplanted With HCC Transplanted Without HCC 30 days 60 days 90 days 0% HCC >30 other Exc MELD Score Category Source: SRTR Analysis. Data as of May 2007 Figure 4 Waiting list candidates with or without hepatocellular carcinoma (HCC) who underwent liver transplantation within 1, 2 and 3 months are stratified by model for end stage liver disease (MELD) at a snapshot in time (January 1, 2006). A higher percentage of patients were transplanted with HCC within 3 months of listing compared to non-hcc patients even while exhibiting high MELD scores, or if the etiology of liver disease met other exception (EXc) criteria %Dropout US Region HCC n-hcc (Initial MELD < 21) = n-hcc (all) Figure 5 The percent dropout of eligible liver transplant recipients within 12 months of listing for hepatocellular carcinoma (HCC) and non-hcc patients according to region. Reprinted with permission from John Wiley and Sons MELD, model for end-stage liver disease tumor exception point upgrades every 3 months, resulting in an increase in LT priority compared to non-hcc patients. It has been suggested that an HCC priority score be implemented to allow for similar dropout and LT rates for both HCC and non-hcc patients, with the hopes of allowing equal access to LT and similar post-transplant outcomes [19]. The long waiting time (>2 years) for HCC in some regions in the US, namely region 5, has led to an instructive experiment of nature. As larger cohorts of patients with HCC have been followed after locoregional therapy for longer periods of time, there is a subset of patients who seem to progress very slowly with regard to HCC. Such patients are typically characterized by slow or no increase in tumor size for years after locoregional therapy. Since most of these patients have excellent hepatic function, their urgency for transplant is not apparent. As a result, there is a movement to allow such patients to continue to receive increased MELD score increments every 90 days, but to inactivate them when their MELD score is sufficiently high to actually receive a transplant. In doing so, patients with no or
4 4 R. S. Rahimi and J. F. Trotter slow tumor growth would be allowed to avoid liver transplant, thereby saving them the risk of the procedure and allowing sicker patients to have access to the limited donor pool. Living-donor LT (LDLT) versus deceased-donor LT (DDLT) As the need for donor livers exceeds organ availability in most countries, LDLT has been suggested as an alternative to alleviate the organ shortage and possibly allow recipient expansion criteria in patients with HCC in comparison to DDLT [20]. The purported advantage of LDLT in HCC patients is seemingly obvious. Patients with HCC have an urgent need for transplant and the availability of a living donor would likely shorten their time to surgery, thereby preventing disease progression which might occur while waiting for a deceased donor. Previous studies have shown conflicting results with respect to recurrence rates and OS [21-25], therefore, two recent meta-analyses were completed in order to evaluate overall outcomes in LDLT versus DDLT for patients with HCC [26,27]. In one meta-analysis [27], a total of 7 studies with 1310 subjects were used to compare patient survival, recurrence free survival (RFS) and recurrence rates in patients with HCC receiving a LDLT or a DDLT. In 5 studies comparing 792 patients, 1-year survival rates (OR 1.03, 95%CI , P=0.9) were similar in LDLT vs. DDLT recipients. Three-year patient survival was reported in 7 studies with 1283 patients (OR 1.07, 95%CI , P=0.69), while 4 studies with 740 patients reported 5-year survival (OR 0.64, 95%CI , P=0.18), all of which showed no s in overall patient survival for LDLT and DDLT recipients. In terms of RFS, the 1-year (3 studies with 796 patients; OR 0.86, 95% CI , P=0.54), 3-year (4 studies with 755 patients; OR 1.04, 95% CI , P=0.84) and 5-year (3 studies with 663 patients; OR 1.11, 95%CI , P=0.65) showed similar outcomes for LDLT and DDLT recipients. With regard to tumor recurrence rates, the 1- and 3-year recurrence rates were reported in 4 studies with 638 patients (1-year, OR 1.55, 95%CI , P=0.55; 3-year, OR 2.57, 95%CI , P=0.24), while 5-year recurrence rates were represented by 3 trials with 546 patients (OR 1.21, 95%CI , P=0.71). There were no significant s in recurrence rates between LDLT and DDLT recipients. In another meta-analysis [26], a total of 16 studies were used for comparison. The mean time from transplant to HCC recurrence ranged from 4.6 to 38 months, with the median time from recurrence to death ranging from 6 to 30.6 months. The disease free survival (DFS) was significantly shorter in patients receiving LDLT in 3 of 10 studies analyzed, with 3-year DFS ranging from % compared to % after DDLT. The overall hazard ratio (HR) was not significantly different when comparing cohort studies from eastern and western countries for DFS after LDLT vs. DDLT, however, the overall HR for DFS was 1.59 (95%CI , P=0.041) after LDLT when 8 cohort studies were combined. The HR for OS after LDLT compared with DDLT was 0.97 (95%CI , P=0.81). Therefore, this meta-analysis suggests that DFS is worse after LDLT compared to DDLT for HCC, however reports of underlying tumor biology are limited in those undergoing a shorter wait list time observed with LDLT (Table 2). Hence, more research is needed to determine if these observed s are truly due to underlying tumor biology or study bias. The finding that there is no apparent benefit in survival for HCC patients undergoing LDLT is somewhat surprising. The reasons for this are not entirely clear. However, one contributing factor may be that HCC patients selected for LDLT may have tumor characteristics associated with worse tumor biology than DDLT. The evidence supporting this claim is based on clinical experience as well as findings in the National Institutes of Health sponsored trial, the adult-to-adult living donor liver transplant study (A2ALL) [28]. In the report from this group, there was a trend toward LDLT recipients having worse tumor characteristics. The selection of such patients for LDLT could lead to worse outcomes. In addition, a study from the same group showed that recipients with HCC were more than twofold likely to have their donors approved for the operation. This might suggest that the transplant team may be more likely to approve donors for HCC patients based on the pressure to perform the surgery in desperate patients. Risk factors for HCC recurrence: mammalian targets of rapamycin (mtors) after LT HCC recurrence rates after LT are estimated to occur in up to 20% [9], and occur more frequently within the first 2 years [29,30], have limited treatment options, and result in an overall poor prognosis, with a median survival of less than 1 year [31]. These recurrence rates have been shown in post-lt patients predominantly to arise based on tumor biology including poorly differentiated tumors and macro/ microvascular invasion [14,32]. Some studies have suggested that immunosuppression (IS) with an mtor inhibitor may reduce the risk of HCC recurrence post-lt [33,34]. The use of mtor inhibitors is one such strategy used for both IS and Table 2 Summary of 1, 3, and 5 year outcomes based on meta analysis in patients with HCC receiving LDLT or DDLT and sirolimus based immunosuppression Patient (overall) survival Recurrence/ disease free survival Tumor recurrence rates LDLT DDLT SRL IS SRL free IS 3 year significantly decreased to no Increased Increased Decreased Decreased Decreased Increased LDLT, living-donor liver transplantation; DDLT, deceased-donor liver transplantation; SRL, sirolimus; IS, immunosuppression; HCC, hepatocellular carcinoma
5 Liver transplantation for HCC 5 anti-proliferative/anti-angiogenic properties that inhibits cell growth and survival [35-37]. The reluctance to use mtor in the early post-transplant setting could be due to poor wound healing and/or hepatic artery thrombosis [38]. In fact, sirolimus (SRL), the most widely prescribed mtor inhibitor in LT has received two black-box warnings against its use in liver transplant recipients based on an increased risk of hepatic artery thrombosis and death. Despite these warnings, up to 10% of liver recipients are administered this drug by one year after transplant. However, these mtor medications like SRL have been shown in multiple studies to reduce HCC recurrence rates when used as the main IS agent in patients receiving LT for HCC, even though higher rejection rates have been reported [39-41]. In 2011, a meta-analysis was conducted to determine if using SRL based regimens as IS after LT improves survival and recurrence of HCC in patients that had a diagnosis of HCC pre-transplant [33,34,39,40,42]. A total of 5 controlled studies from different countries (3 retrospective, 1 matched-cohort and a case-control study) included 2950 participants and found that SRL-based regimens improved overall 1-, 3-, and 5-year survival (OR 4.53, 95%CI ; OR 1.97, 95% CI ; OR 2.47, 95%CI ),respectively, compared to SRL-free regimens. One study compared the different mortality risks after LT using various IS protocols (Fig. 6) [33] and showed a significant in survival in patients using SRL-based IS. Furthermore, SRL-based regimens showed an overall decrease in tumor recurrence (OR 0.42, 95%CI ) compared to SRL-free regimens without any significant post-transplant complications observed between the two groups. An updated meta-analysis described outcomes in patients using SRL as the main IS agent who underwent LT for HCC [43]. Of these 5 studies [34,39,40,44,45], 474 total patients were Figure 6 The overall hazard ratios (±95% confidence interval) are represented on the x-axis of this horizontal box plot and compare the risk of mortality after liver transplantation using various immunosuppression regimens. Results were corrected for model for end-stage liver disease (MELD), year of transplant, primary liver disease (non-hepatocellular carcinoma [HCC]), age at transplant, and, when applicable, total tissue volume, α-fetoprotein, and pre-transplant HCC treatment. *Significant variables. Reprinted with permission from John Wiley and Sons MMF, mycophenolate mofetil included in the final analysis, of which 77% were male, with an average age around 56 years old, having a median follow up ranging from 18 to 49 months. The overall results suggest that the recurrence rate of HCC after LT was lower in the SRL group (5-13%) compared with patients using calcineurin inhibitors (CNIs) (17-39%) with an overall advantage in all categories for the SRL group: lower recurrence rate (OR 0.3, 95% CI , P<0.001), lower recurrence related mortality (OR 0.29, 95% CI , P=0.005), and lower overall mortality (OR=0.35, 95% CI , P<0.001) respectively. The overall 1-, 3-, and 5-year RFS was superior in the SRL group which ranged from 93-96%, 82-86% and 79-80%, while patients taking CNIs had worse overall RFS ranging from 70-78%, 64-65% and 54-60% during the same time frame respectively. The overall 1-, 3-, and 5-year OS was also much better in the SRL group (94-95%, 85%, and 80%) in comparison with the CNI group (79-83%, 66%, and 59-62%) respectively (Table 2). Similarly, overall mortality on pooled analysis was significantly lower in SRL-treated patients vs. the CNI group (OR=0.35, 95%CI , P<0.001). Although limitations exist in metaanalysis which include: non-randomized data, lack of subgroup analysis regarding patients exceeding the Milan criteria, and possible publication bias based on the different weighted studies, overall SRL seems to be safe, effective and potentially promising regarding the OS benefits for LT recipients having a pre-transplant diagnosis of HCC. However, more prospective studies are needed to determine if improvements in survival are due to SRL alone, or from reduction in CNIs. More recently, a systematic review compared everolimus (another mtor inhibitor) and SRL with CNI use on post-lt recurrence of HCC [46]. Of the 42 studies that included 3,666 HCC LT recipients analyzed, CNI use was associated with higher rates of HCC recurrence (448/3227 or 13.8%) compared to mtors (35/439 or 8%, P<0.001), although patients treated with CNIs had lower rates of microvascular invasion and higher proportion of HCC within Milan criteria. The rates of HCC recurrence did not differ if transplanted outside of Milan criteria when comparing CNI or mtor use, while locoregional therapy data was limited when analyzing the results. A subgroup analysis demonstrated that although patients taking everolimus had shorter follow-up data, overall HCC recurrence post-lt was less frequently observed compared to SRL use (8/196 or 4.1% vs. 23/218 or 10.5%, P=0.02). Furthermore, no data was available with respect to dosage and IS levels when mtors were used. Of note, one major between everolimus and SRL is that data using everolimus has led to FDA approval in LT recipients after 30 days without a black box warning [47]. Although the present analysis of multiple studies favors the use of mtor (everolimus >SRL) for LT in HCC patients compared to CNI use, these findings need longer patient follow up and comparable cohorts in order to make similar comparisons between everolimus and SRL use before final conclusions can be drawn. Furthermore, when comparing overall mtor and CNI use, the results were not significantly different when RCT studies were included, hence mtor superiority over CNI use for prevention of HCC recurrence post-lt remains controversial at this time.
6 6 R. S. Rahimi and J. F. Trotter To answer and address the issues above, a multicenter international randomized controlled trial is underway and is estimated to be completed in This study will analyze 5 year follow-up data to determine if the mtor inhibitor SRL can improve HCC RFS in LT recipients with a pre-transplant diagnosis of HCC compared to SRL-free regimens [48]. All eligible LT patients (deceased donor, split-liver, or living donors) with a histological diagnosis of HCC in the explanted liver, will be given 4-6 weeks of a CNI medication (mtor inhibitor-free), then randomized and separated into two groups: 1) mtor inhibitor-free IS; and 2) SRL containing IS±CNI 4-6 weeks later at a loading dose of 5 mg/day and 2 mg/day thereafter. Steroid reduction is encouraged by 3 months in both groups post-lt with a desired trough level for SRL of 4-10 ng/ml on routine lab analysis. Patients simultaneously using mycophenolic acid prodrugs and CNIs are expected to have these medications reduced by 50% with the ideal long-term goal of SRL monotherapy in arm two. Groups will be stratified into high (extending beyond Milan criteria, undergoing salvage transplantation or HCC in non-cirrhotic liver) or low risk (within Milan criteria). An estimated 255 patients per arm is expected, with the hypothesis of 5-year RFS of 60% in arm 1 and 72% in arm 2, which corresponds to a clinically relevant hazard ratio of If the hypothesis holds true, that mtor inhibition with SRL can improve RFS while providing adequate IS, then the standard of care regarding IS might change in the near future in patients with HCC post-lt. Sorafenib in combination with mtors for recurrent HCC after LT As sorafenib is a multikinase inhibitor of Raf, vascular endothelial- and platelet-derived growth factor receptors, it mediates cell proliferation and angiogenesis, resulting in an increase in OS and improvement in radiologic progression in patients with HCC [49]. However, there is limited data regarding the concomitant use of sorafenib and mtor inhibitors in patients post-lt with recurrent HCC [50-52]. It has been hypothesized that combination therapy could have synergistic effects [53,54]. A recent multicenter retrospective study evaluated patients with recurrent HCC after LT who were treated with mtor inhibitors and sorafenib during tumor relapse as patients were not candidates for locoregional therapy [55]. Two groups were assigned, with the first termed the safety population (n=31), who received sorafenib and an mtor inhibitor for either palliative or adjuvant treatment. This group consisted of 48% of the population diagnosed with chronic hepatitis C cirrhosis with HCC, while 52% had alcoholic cirrhosis of which only 7% were found to have incidental HCC. Most underwent DDLT (93%) and were within the Milan criteria. The second population was termed the efficacy group (n=26), who received the same two drug regimen, instead for systemic treatment for tumor relapse. There were no s in clinical parameters between the two groups. Once recurrence of HCC was confirmed, IS was switched in each patient to an mtor inhibitor (23 patients received everolimus, 8 received SRL). Then, after stable graft function, sorafenib was added at median times of 1.1 month after everolimus initiation and 1.4 months after SRL initiation. The starting dose was 400 mg/day in the majority of patients, as the toxicity or immunologic consequences were unknown with this combination. Sorafenib was later increased to a maximum tolerated dose of 800 mg/day, and maintained until toxicity, tumor progression, hepatic decompensation or death ensued. Radiologic follow up for treatment response was conducted every 12 weeks with assessments of tumor size as well as new lesions according to the Response Evaluation Criteria in Solid Tumors [56]. The overall results for dual administration of sorafenib and an mtor inhibitor in this study were described as follows. The median time from LT to recurrence was 22.6 months (range months), with nearly two-thirds (20/31) representing extrahepatic recurrence without liver involvement, about 19% having extrahepatic with hepatic recurrence, and nearly 16% having hepatic recurrence only. The antitumor efficacy had an overall clinical benefit rate of 53.8% (14/26 patients), with 3.8% (1/26) showing a partial response and the remaining 50% demonstrating disease stabilization. Patients with disease progression were seen in 38.5% (10/26), while 7.7% (2/26) could not be evaluated as sorafenib was given for <4 weeks and no imaging studies for tumor reassessment were obtained. The median OS after HCC relapse was about 40 months (95%CI months), while the median OS since the start of the treatment with sorafenib was 19.3 months (95%CI= months). After initiating sorafenib treatment, the median time to disease progression was 6.77 months (95%CI months). The most common toxicities experienced in this cohort of patients were: diarrhea (77.4%), asthenia (58.1%), and handfoot syndrome (54.8%); while serious adverse events leading to death was seen in 2 patients overall: the first patient experiencing uncontrolled gastric hemorrhage not related to portal hypertension or ulcer disease, and the other having a central nervous system hemorrhage 18 days after initiating therapy, in which treatment was stopped, however 4 weeks later the patient expired. The possible explanation resulting in the latter cause of bleeding was suspicion of, but unconfirmed leptomeningeal metastases. There were no recorded or suspected episodes of acute or chronic graft rejection related to mtor inhibitors and sorafenib. Concluding remarks Management of patients with HCC on the waiting list vary by different institutions, however, centers that have LDLT options should consider this as an alternative for patients with HCC as the donor pool is limited and the OS and tumor recurrence rates of HCC have similar outcomes compared to DDLT. Although DFS might be worse after LDLT, discussions should be undertaken with potential donors and recipients. Changes in IS with mtors have been
7 Liver transplantation for HCC 7 studied in recurrent HCC, and the addition of sorafenib to these regimens have shown promise in improving OS and delaying disease progression. Currently, a multicenter international randomized control trial is underway to address the issue of mtor IS ± sorafenib and recurrent HCC. References 1. Organization. WH. Mortality Database. WHO Statistical Information System El-Serag HB, Rudolph KL. Hepatocellular carcinoma: epidemiology and molecular carcinogenesis. Gastroenterology 2007;132: Colombo M, de Franchis R, Del Ninno E, et al. Hepatocellular carcinoma in Italian patients with cirrhosis. N Engl J Med 1991;325: Ioannou GN, Perkins JD, Carithers RL, Jr. Liver transplantation for hepatocellular carcinoma: impact of the MELD allocation system and predictors of survival. Gastroenterology 2008;134: Freeman RB, Jr., Wiesner RH, Harper A, et al. The new liver allocation system: moving toward evidence-based transplantation policy. Liver Transplant 2002;8: Washburn K. Model for end stage liver disease and hepatocellular carcinoma: a moving target. Transplant Rev (Orlando) 2010;24: Freeman RB, Jr., Steffick DE, Guidinger MK, et al. Liver and intestine transplantation in the United States, Am J Transplant 2008;8: Mazzaferro V, Regalia E, Doci R, et al. Liver transplantation for the treatment of small hepatocellular carcinomas in patients with cirrhosis. N Engl J Med 1996;334: Clavien PA, Lesurtel M, Bossuyt PM, et al. Recommendations for liver transplantation for hepatocellular carcinoma: an international consensus conference report. Lancet Oncol 2012;13:e11-e Yao FY, Ferrell L, Bass NM, et al. Liver transplantation for hepatocellular carcinoma: expansion of the tumor size limits does not adversely impact survival. Hepatology 2001;33: Yao FY, Xiao L, Bass NM, et al. Liver transplantation for hepatocellular carcinoma: validation of the UCSF-expanded criteria based on preoperative imaging. Am J Transplant 2007;7: Berg CL, Steffick DE, Edwards EB, et al. Liver and intestine transplantation in the United States Am J Transplant 2009;9: Onaca N, Davis GL, Goldstein RM, et al. Expanded criteria for liver transplantation in patients with hepatocellular carcinoma: a report from the International Registry of Hepatic Tumors in Liver Transplantation. Liver Transplant 2007;13: Mazzaferro V, Llovet JM, Miceli R, et al. Predicting survival after liver transplantation in patients with hepatocellular carcinoma beyond the Milan criteria: a retrospective, exploratory analysis. Lancet Oncol 2009;10: Millonig G, Graziadei IW, Freund MC, et al. Response to preoperative chemoembolization correlates with outcome after liver transplantation in patients with hepatocellular carcinoma. Liver Transplant 2007;13: Mazzaferro V, Battiston C, Perrone S, et al. Radiofrequency ablation of small hepatocellular carcinoma in cirrhotic patients awaiting liver transplantation: a prospective study. Ann Surg 2004;240: Maddala YK, Stadheim L, Andrews JC, et al. Drop-out rates of patients with hepatocellular cancer listed for liver transplantation: outcome with chemoembolization. Liver Transplant 2004;10: Yao FY, Bass NM, Nikolai B, et al. A follow-up analysis of the pattern and predictors of dropout from the waiting list for liver transplantation in patients with hepatocellular carcinoma: implications for the current organ allocation policy. Liver Transplant 2003;9: Washburn K, Edwards E, Harper A, et al. Hepatocellular carcinoma patients are advantaged in the current liver transplant allocation system. Am J Transplant 2010;10: Bhangui P, Vibert E, Majno P, et al. Intention-to-treat analysis of liver transplantation for hepatocellular carcinoma: living versus deceased donor transplantation. Hepatology 2011;53: Hwang S, Lee SG, Joh JW, et al. Liver transplantation for adult patients with hepatocellular carcinoma in Korea: comparison between cadaveric donor and living donor liver transplantations. Liver Transplant 2005;11: Fisher RA, Kulik LM, Freise CE, et al. Hepatocellular carcinoma recurrence and death following living and deceased donor liver transplantation. Am J Transplant 2007;7: Lo CM, Fan ST, Liu CL, et al. Living donor versus deceased donor liver transplantation for early irresectable hepatocellular carcinoma. Brit J Surg 2007;94: Vakili K, Pomposelli JJ, Cheah YL, et al. Living donor liver transplantation for hepatocellular carcinoma: Increased recurrence but improved survival. Liver Transplant 2009;15: Di Sandro S, Slim AO, Giacomoni A, et al. Living donor liver transplantation for hepatocellular carcinoma: long-term results compared with deceased donor liver transplantation. Transplant Proc 2009;41: Grant RC, Sandhu L, Dixon PR, et al. Living vs. deceased donor liver transplantation for hepatocellular carcinoma: a systematic review and meta-analysis. Clin Transplant 2013;27: Liang W, Wu L, Ling X, et al. Living donor liver transplantation versus deceased donor liver transplantation for hepatocellular carcinoma: a meta-analysis. Liver Transplant 2012;18: Kulik LM, Fisher RA, Rodrigo DR, et al. Outcomes of living and deceased donor liver transplant recipients with hepatocellular carcinoma: results of the A2ALL cohort. Am J Transplant 2012;12: Cescon M, Ravaioli M, Grazi GL, et al. Prognostic factors for tumor recurrence after a 12-year, single-center experience of liver transplantations in patients with hepatocellular carcinoma. J Transplant 2010; Kornberg A, Kupper B, Tannapfel A, et al. Long-term survival after recurrent hepatocellular carcinoma in liver transplant patients: clinical patterns and outcome variables. Eur J Surg Oncol 2010;36: Hollebecque A, Decaens T, Boleslawski E, et al. Natural history and therapeutic management of recurrent hepatocellular carcinoma after liver transplantation. Gastroenterol Clin Biol 2009;33: Herrero JI, Sangro B, Quiroga J, et al. Influence of tumor characteristics on the outcome of liver transplantation among patients with liver cirrhosis and hepatocellular carcinoma. Liver Transplant 2001;7: Toso C, Merani S, Bigam DL, et al. Sirolimus-based immunosuppression is associated with increased survival after liver transplantation for hepatocellular carcinoma. Hepatology 2010;51: Zimmerman MA, Trotter JF, Wachs M, et al. Sirolimusbased immunosuppression following liver transplantation for hepatocellular carcinoma. Liver Transplant 2008;14: Bjornsti MA, Houghton PJ. The TOR pathway: a target for cancer therapy. Nat Rev Cancer 2004;4: Price DJ, Grove JR, Calvo V, et al. Rapamycin-induced inhibition of the 70-kilodalton S6 protein kinase. Science 1992;257:
8 8 R. S. Rahimi and J. F. Trotter 37. Villanueva A, Chiang DY, Newell P, et al. Pivotal role of mtor signaling in hepatocellular carcinoma. Gastroenterology 2008;135: , 1983 e1-e Panaro F, Piardi T, Gheza F, et al. Causes of sirolimus discontinuation in 97 liver transplant recipients. Transplant Proc 2011;43: Vivarelli M, Dazzi A, Zanello M, et al. Effect of different immunosuppressive schedules on recurrence-free survival after liver transplantation for hepatocellular carcinoma. Transplantation 2010;89: Chinnakotla S, Davis GL, Vasani S, et al. Impact of sirolimus on the recurrence of hepatocellular carcinoma after liver transplantation. Liver Transplant 2009;15: Zimmerman MA, Trotter JF, Wachs M, et al. Predictors of longterm outcome following liver transplantation for hepatocellular carcinoma: a single-center experience. Transplant Int 2007;20: Zhou J, Wang Z, Wu ZQ, et al. Sirolimus-based immunosuppression therapy in liver transplantation for patients with hepatocellular carcinoma exceeding the Milan criteria. Transplant Proc 2008;40: Menon KV, Hakeem AR, Heaton ND. Meta-analysis: recurrence and survival following the use of sirolimus in liver transplantation for hepatocellular carcinoma. Aliment Pharmacol Ther 2013;37: cera A, Andorno E, Tagliamacco A, et al. Sirolimus therapy in liver transplant patients: an initial experience at a single center. Transplant Proc 2008;40: Toso C, Meeberg GA, Bigam DL, et al. De novo sirolimus-based immunosuppression after liver transplantation for hepatocellular carcinoma: long-term outcomes and side effects. Transplantation 2007;83: Cholongitas E, Mamou C, Rodriguez-Castro KI, et al. Mammalian target of rapamycin inhibitors are associated with lower rates of hepatocellular carcinoma recurrence after liver transplantation: a systematic review. Transplant Int 2014;27: Saliba F, De Simone P, Nevens F, et al. Renal function at two years in liver transplant patients receiving everolimus: results of a randomized, multicenter study. Am J Transplant 2013;13: Schnitzbauer AA, Zuelke C, Graeb C, et al. A prospective randomised, open-labeled, trial comparing sirolimus-containing versus mtor-inhibitor-free immunosuppression in patients undergoing liver transplantation for hepatocellular carcinoma. BMC Cancer 2010;10: Llovet JM, Ricci S, Mazzaferro V, et al. Sorafenib in advanced hepatocellular carcinoma. N Engl J Med 2008;359: Bhoori S, Toffanin S, Sposito C, et al. Personalized molecular targeted therapy in advanced, recurrent hepatocellular carcinoma after liver transplantation: a proof of principle. J Hepatol 2010;52: Kim R, El-Gazzaz G, Tan A, et al. Safety and feasibility of using sorafenib in recurrent hepatocellular carcinoma after orthotopic liver transplantation. Oncology 2010;79: Waidmann O, Hofmann WP, Zeuzem S, et al. mtor inhibitors and sorafenib for recurrent heptocellular carcinoma after orthotopic liver transplantation. J Hepatol 2011;54: Newell P, Toffanin S, Villanueva A, et al. Ras pathway activation in hepatocellular carcinoma and anti-tumoral effect of combined sorafenib and rapamycin in vivo. J Hepatol 2009;51: Wang Z, Zhou J, Fan J, et al. Effect of rapamycin alone and in combination with sorafenib in an orthotopic model of human hepatocellular carcinoma. Clin Cancer Res 2008;14: Gomez-Martin C, Bustamante J, Castroagudin JF, et al. Efficacy and safety of sorafenib in combination with mammalian target of rapamycin inhibitors for recurrent hepatocellular carcinoma after liver transplantation. Liver Transplant 2012;18: Therasse P, Arbuck SG, Eisenhauer EA, et al. New guidelines to evaluate the response to treatment in solid tumors. European Organization for Research and Treatment of Cancer, National Cancer Institute of the United States, National Cancer Institute of Canada. J Natl Cancer Inst 2000;92:
Living Donor Liver Transplantation for Hepatocellular Carcinoma: It Is All about Donors?
 Original Article Living Donor Liver Transplantation for Hepatocellular Carcinoma: It Is All about Donors? R. F. Saidi 1 *, Y. Li 2, S. A. Shah 2, N. Jabbour 2 1 Division of Organ Transplantation, Department
Original Article Living Donor Liver Transplantation for Hepatocellular Carcinoma: It Is All about Donors? R. F. Saidi 1 *, Y. Li 2, S. A. Shah 2, N. Jabbour 2 1 Division of Organ Transplantation, Department
Reconsidering Liver Transplantation for HCC in a Era of Organ shortage
 Reconsidering Liver Transplantation for HCC in a Era of Organ shortage Professor Didier Samuel Centre Hépatobiliaire Inserm-Paris Sud Research Unit 1193 Departement Hospitalo Universitaire Hepatinov Hôpital
Reconsidering Liver Transplantation for HCC in a Era of Organ shortage Professor Didier Samuel Centre Hépatobiliaire Inserm-Paris Sud Research Unit 1193 Departement Hospitalo Universitaire Hepatinov Hôpital
Management of HepatoCellular Carcinoma
 9th Symposium GIC St Louis - 2010 Management of HepatoCellular Carcinoma Overview Pierre A. Clavien, MD, PhD Department of Surgery University Hospital Zurich Zurich, Switzerland Hepatocellular carcinoma
9th Symposium GIC St Louis - 2010 Management of HepatoCellular Carcinoma Overview Pierre A. Clavien, MD, PhD Department of Surgery University Hospital Zurich Zurich, Switzerland Hepatocellular carcinoma
Optimizing Patient Selection, Organ Allocation, and Outcomes in Liver Transplant (LT) Candidates with Hepatocellular Carcinoma (HCC)
 XXVI SETH Congress- 30 November 2017 Optimizing Patient Selection, Organ Allocation, and Outcomes in Liver Transplant (LT) Candidates with Hepatocellular Carcinoma (HCC) Neil Mehta, MD University of California,
XXVI SETH Congress- 30 November 2017 Optimizing Patient Selection, Organ Allocation, and Outcomes in Liver Transplant (LT) Candidates with Hepatocellular Carcinoma (HCC) Neil Mehta, MD University of California,
Liver transplantation: Hepatocellular carcinoma
 Liver transplantation: Hepatocellular carcinoma Alejandro Forner BCLC Group. Liver Unit. Hospital Clínic. University of Barcelona 18 de marzo 2015 3r Curso Práctico de Transplante de Órganos Sólidos Barcelona
Liver transplantation: Hepatocellular carcinoma Alejandro Forner BCLC Group. Liver Unit. Hospital Clínic. University of Barcelona 18 de marzo 2015 3r Curso Práctico de Transplante de Órganos Sólidos Barcelona
Clinical Study Use of Adjuvant Sorafenib in Liver Transplant Recipients with High-Risk Hepatocellular Carcinoma
 Transplantation, Article ID 913634, 5 pages http://dx.doi.org/10.1155/2014/913634 Clinical Study Use of Adjuvant Sorafenib in Liver Transplant Recipients with High-Risk Hepatocellular Carcinoma Kirti Shetty,
Transplantation, Article ID 913634, 5 pages http://dx.doi.org/10.1155/2014/913634 Clinical Study Use of Adjuvant Sorafenib in Liver Transplant Recipients with High-Risk Hepatocellular Carcinoma Kirti Shetty,
Hepatocellular Carcinoma. Markus Heim Basel
 Hepatocellular Carcinoma Markus Heim Basel Outline 1. Epidemiology 2. Surveillance 3. (Diagnosis) 4. Staging 5. Treatment Epidemiology of HCC Worldwide, liver cancer is the sixth most common cancer (749
Hepatocellular Carcinoma Markus Heim Basel Outline 1. Epidemiology 2. Surveillance 3. (Diagnosis) 4. Staging 5. Treatment Epidemiology of HCC Worldwide, liver cancer is the sixth most common cancer (749
Extending Indication: Role of Living Donor Liver Transplantation for Hepatocellular Carcinoma
 LIVER TRANSPLANTATION 13:S48-S54, 27 SUPPLEMENT Extending Indication: Role of Living Donor Liver Transplantation for Hepatocellular Carcinoma Satoru Todo, 1 Hiroyuki Furukawa, 2 Mitsuhiro Tada, 3 and the
LIVER TRANSPLANTATION 13:S48-S54, 27 SUPPLEMENT Extending Indication: Role of Living Donor Liver Transplantation for Hepatocellular Carcinoma Satoru Todo, 1 Hiroyuki Furukawa, 2 Mitsuhiro Tada, 3 and the
Hepatocellular Carcinoma: Diagnosis and Management
 Hepatocellular Carcinoma: Diagnosis and Management Nizar A. Mukhtar, MD Co-director, SMC Liver Tumor Board April 30, 2016 1 Objectives Review screening/surveillance guidelines Discuss diagnostic algorithm
Hepatocellular Carcinoma: Diagnosis and Management Nizar A. Mukhtar, MD Co-director, SMC Liver Tumor Board April 30, 2016 1 Objectives Review screening/surveillance guidelines Discuss diagnostic algorithm
Transcatheter Arterial Chemoembolization to Treat Primary or Metastatic Liver Malignancies
 Transcatheter Arterial Chemoembolization to Treat Primary or Metastatic Liver Malignancies Policy Number: 8.01.11 Last Review: 6/2018 Origination: 8/2005 Next Review: 6/2019 Policy Blue Cross and Blue
Transcatheter Arterial Chemoembolization to Treat Primary or Metastatic Liver Malignancies Policy Number: 8.01.11 Last Review: 6/2018 Origination: 8/2005 Next Review: 6/2019 Policy Blue Cross and Blue
9/10/2018. Liver Transplant for Hepatocellular Carcinoma (HCC): What is New? DISCLOSURES
 UCSF Transplant 2018: Pioneering Advances in Transplantation DISCLOSURES Liver Transplant for Hepatocellular Carcinoma (HCC): What is New? I have no relevant commercial interests or relationships to report
UCSF Transplant 2018: Pioneering Advances in Transplantation DISCLOSURES Liver Transplant for Hepatocellular Carcinoma (HCC): What is New? I have no relevant commercial interests or relationships to report
Living donor liver transplantation for hepatocellular carcinoma in Seoul National University
 Original Article on Liver Transplantation for Hepatocellular Carcinoma Living donor liver transplantation for hepatocellular carcinoma in Seoul National University Suk Kyun Hong, Kwang-Woong Lee, Hyo-Sin
Original Article on Liver Transplantation for Hepatocellular Carcinoma Living donor liver transplantation for hepatocellular carcinoma in Seoul National University Suk Kyun Hong, Kwang-Woong Lee, Hyo-Sin
Liver Transplantation for HCC Which Criteria?
 Liver Transplantation for HCC Which Criteria? Jacques Belghiti - François Durand Claire Francoz Hepato-Biliary-Pancreatic Liver Surgery and Liver Transplantation Unit Hôpital Beaujon (AP-HP), Clichy -
Liver Transplantation for HCC Which Criteria? Jacques Belghiti - François Durand Claire Francoz Hepato-Biliary-Pancreatic Liver Surgery and Liver Transplantation Unit Hôpital Beaujon (AP-HP), Clichy -
Radiofrequency Ablation of Primary or Metastatic Liver Tumors
 Radiofrequency Ablation of Primary or Metastatic Liver Tumors Policy Number: 7.01.91 Last Review: 9/2018 Origination: 2/1996 Next Review: 9/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC)
Radiofrequency Ablation of Primary or Metastatic Liver Tumors Policy Number: 7.01.91 Last Review: 9/2018 Origination: 2/1996 Next Review: 9/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC)
Waitlist Priority for Hepatocellular Carcinoma Beyond Milan Criteria: A Potentially Appropriate Decision Without a Structured Approach
 American Journal of Transplantation 2014; 14: 79 87 Wiley Periodicals Inc. C Copyright 2013 The American Society of Transplantation and the American Society of Transplant Surgeons doi: 10.1111/ajt.12530
American Journal of Transplantation 2014; 14: 79 87 Wiley Periodicals Inc. C Copyright 2013 The American Society of Transplantation and the American Society of Transplant Surgeons doi: 10.1111/ajt.12530
Hepatocellular Carcinoma: Transplantation, Resection or Ablation?
 Hepatocellular Carcinoma: Transplantation, Resection or Ablation? Roberto Gedaly MD Chief, Abdominal Transplantation Transplant Service Line University of Kentucky Nothing to disclose Disclosure Objective
Hepatocellular Carcinoma: Transplantation, Resection or Ablation? Roberto Gedaly MD Chief, Abdominal Transplantation Transplant Service Line University of Kentucky Nothing to disclose Disclosure Objective
Despite recent advances in the care of patients with
 Liver Transplantation for Hepatocellular Carcinoma: Lessons from the First Year Under the Model of End- Stage Liver Disease (MELD) Organ Allocation Policy Francis Y. Yao, 1,2 Nathan M. Bass, 1 Nancy L.
Liver Transplantation for Hepatocellular Carcinoma: Lessons from the First Year Under the Model of End- Stage Liver Disease (MELD) Organ Allocation Policy Francis Y. Yao, 1,2 Nathan M. Bass, 1 Nancy L.
Liver transplantation for hepatocellular carcinoma: pre-transplant considerations and post-transplant management
 Review Article Page 1 of 9 Liver transplantation for hepatocellular carcinoma: pre-transplant considerations and post-transplant management Vladimir Marquez Division of Gastroenterology, University of
Review Article Page 1 of 9 Liver transplantation for hepatocellular carcinoma: pre-transplant considerations and post-transplant management Vladimir Marquez Division of Gastroenterology, University of
Living vs. deceased-donor liver transplantation for patients with hepatocellular carcinoma
 Review Article Living vs. deceased-donor liver transplantation for patients with hepatocellular carcinoma Kohei Ogawa, Yasutsugu Takada Department of HB and Breast Surgery, Ehime University, Ehime, Japan
Review Article Living vs. deceased-donor liver transplantation for patients with hepatocellular carcinoma Kohei Ogawa, Yasutsugu Takada Department of HB and Breast Surgery, Ehime University, Ehime, Japan
21/02/2014. Disclosures. HCC: predicting recurrence. Outline. Liver transplant: Beyond Milan?
 Disclosures HCC: predicting recurrence Peter Ghali, MD, FRCPC, MSc (epid) None relevant to this talk other than off-label use of sirolimus Toronto, February 2014 Outline Recurrence after what? Locoregional
Disclosures HCC: predicting recurrence Peter Ghali, MD, FRCPC, MSc (epid) None relevant to this talk other than off-label use of sirolimus Toronto, February 2014 Outline Recurrence after what? Locoregional
Selection Criteria and Insertion of SIRT into HCC Treatment Guidelines
 Selection Criteria and Insertion of SIRT into HCC Treatment Guidelines 2 nd Asia Pacific Symposium on Liver- Directed Y-90 Microspheres Therapy 1st November 2014, Singapore Pierce Chow FRCSE PhD SIRT in
Selection Criteria and Insertion of SIRT into HCC Treatment Guidelines 2 nd Asia Pacific Symposium on Liver- Directed Y-90 Microspheres Therapy 1st November 2014, Singapore Pierce Chow FRCSE PhD SIRT in
Factors predicting survival after post-transplant hepatocellular carcinoma recurrence
 J Hepatobiliary Pancreat Sci (2013) 20:342 347 DOI 10.1007/s00534-012-0528-4 ORIGINAL ARTICLE Factors predicting survival after post-transplant hepatocellular carcinoma recurrence Christian Toso Sonia
J Hepatobiliary Pancreat Sci (2013) 20:342 347 DOI 10.1007/s00534-012-0528-4 ORIGINAL ARTICLE Factors predicting survival after post-transplant hepatocellular carcinoma recurrence Christian Toso Sonia
Liver Transplantation for Hepatocellular Carcinoma: Validation of the UCSF-Expanded Criteria Based on Preoperative Imaging
 American Journal of Transplantation 2007; 7: 2587 2596 Blackwell Munksgaard C 2007 The Authors Journal compilation C 2007 The American Society of Transplantation and the American Society of Transplant
American Journal of Transplantation 2007; 7: 2587 2596 Blackwell Munksgaard C 2007 The Authors Journal compilation C 2007 The American Society of Transplantation and the American Society of Transplant
Hepatocellular Carcinoma (HCC): Who Should be Screened and How Do We Treat? Tom Vorpahl MSN, RN, ACNP-BC
 Hepatocellular Carcinoma (HCC): Who Should be Screened and How Do We Treat? Tom Vorpahl MSN, RN, ACNP-BC Objectives Identify patient risk factors for hepatocellular carcinoma (HCC) Describe strategies
Hepatocellular Carcinoma (HCC): Who Should be Screened and How Do We Treat? Tom Vorpahl MSN, RN, ACNP-BC Objectives Identify patient risk factors for hepatocellular carcinoma (HCC) Describe strategies
TREATMENT FOR HCC AND CHOLANGIOCARCINOMA. Shawn Pelletier, MD
 TREATMENT FOR HCC AND CHOLANGIOCARCINOMA Shawn Pelletier, MD Treatment for HCC Treatment strategies Curative first line therapy Thermal ablation vs Resection vs Transplant Other first line therapies TACE
TREATMENT FOR HCC AND CHOLANGIOCARCINOMA Shawn Pelletier, MD Treatment for HCC Treatment strategies Curative first line therapy Thermal ablation vs Resection vs Transplant Other first line therapies TACE
Liver Transplantation for Hepatocellular Carcinoma: An Appraisal of Current Controversies
 2235-1795/0014-0183$38.00/0 183 Review Liver Transplantation for Hepatocellular Carcinoma: An Appraisal of Current Controversies Yee Lee Cheah a Pierce K.H. Chow b,c,d a Hepatobiliary and Pancreatic Surgery,
2235-1795/0014-0183$38.00/0 183 Review Liver Transplantation for Hepatocellular Carcinoma: An Appraisal of Current Controversies Yee Lee Cheah a Pierce K.H. Chow b,c,d a Hepatobiliary and Pancreatic Surgery,
Department of Surgery, Samsung Medical Center, Sungkyunkwan University School of Medicine, Seoul, Korea
 ORIGINAL ARTICLE pissn -575 eissn -79 https://doi.org/1.17/astr.1.95..111 Annals of Surgical Treatment and Research Clinical usefulness of transarterial chemoembolization response prior to liver transplantation
ORIGINAL ARTICLE pissn -575 eissn -79 https://doi.org/1.17/astr.1.95..111 Annals of Surgical Treatment and Research Clinical usefulness of transarterial chemoembolization response prior to liver transplantation
6/16/2016. Treating Hepatocellular Carcinoma: Deciphering the Clinical Data. Liver Regeneration. Liver Regeneration
 Treating : Deciphering the Clinical Data Derek DuBay, MD Associate Professor of Surgery Director of Liver Transplant Liver Transplant and Hepatobiliary Surgery UAB Department of Surgery Liver Regeneration
Treating : Deciphering the Clinical Data Derek DuBay, MD Associate Professor of Surgery Director of Liver Transplant Liver Transplant and Hepatobiliary Surgery UAB Department of Surgery Liver Regeneration
NHS BLOOD AND TRANSPLANT ORGAN DONATION AND TRANSPLANTATION DIRECTORATE LIVER ADVISORY GROUP UPDATE ON THE HCC DOWN-STAGING SERVICE EVALUATION
 NHS BLOOD AND TRANSPLANT ORGAN DONATION AND TRANSPLANTATION DIRECTORATE LIVER ADVISORY GROUP UPDATE ON THE HCC DOWN-STAGING SERVICE EVALUATION 1. A service development evaluation to transplant down-staged
NHS BLOOD AND TRANSPLANT ORGAN DONATION AND TRANSPLANTATION DIRECTORATE LIVER ADVISORY GROUP UPDATE ON THE HCC DOWN-STAGING SERVICE EVALUATION 1. A service development evaluation to transplant down-staged
Living Donor Liver Transplantation Versus Deceased Donor Liver Transplantation for Hepatocellular Carcinoma: Comparable Survival and Recurrence
 LIVER TRANSPLANTATION 18:315-322, 2012 ORIGINAL ARTICLE Living Donor Liver Transplantation Versus Deceased Donor Liver Transplantation for Hepatocellular Carcinoma: Comparable Survival and Recurrence Lakhbir
LIVER TRANSPLANTATION 18:315-322, 2012 ORIGINAL ARTICLE Living Donor Liver Transplantation Versus Deceased Donor Liver Transplantation for Hepatocellular Carcinoma: Comparable Survival and Recurrence Lakhbir
WHAT IS THE BEST APPROACH FOR TRANS-ARTERIAL THERAPY IN HCC?
 WHAT IS THE BEST APPROACH FOR TRANS-ARTERIAL THERAPY IN HCC? Dr. Alexander Kim Chief, Vascular and Interventional Radiology, Medstar Georgetown University Hospital, USA DISCLAIMER Please note: The views
WHAT IS THE BEST APPROACH FOR TRANS-ARTERIAL THERAPY IN HCC? Dr. Alexander Kim Chief, Vascular and Interventional Radiology, Medstar Georgetown University Hospital, USA DISCLAIMER Please note: The views
HCC RADIOLOGIC DIAGNOSIS
 UCSF Transplant 2010 THE BEFORE AND AFTER HEPATOCELLULAR CARCINOMA MANAGEMENT Francis Yao, M.D. Professor of Clinical Medicine and Surgery Medical Director, Liver Transplantation University of California,
UCSF Transplant 2010 THE BEFORE AND AFTER HEPATOCELLULAR CARCINOMA MANAGEMENT Francis Yao, M.D. Professor of Clinical Medicine and Surgery Medical Director, Liver Transplantation University of California,
Celsion Symposium New Paradigms in HCC Staging: HKLC vs. BCLC Staging
 Celsion Symposium New Paradigms in HCC Staging: HKLC vs. BCLC Staging Ronnie T.P. Poon, MBBS, MS, PhD Chair Professor of Hepatobiliary and Pancreatic Surgery Chief of Hepatobiliary and Pancreatic Surgery
Celsion Symposium New Paradigms in HCC Staging: HKLC vs. BCLC Staging Ronnie T.P. Poon, MBBS, MS, PhD Chair Professor of Hepatobiliary and Pancreatic Surgery Chief of Hepatobiliary and Pancreatic Surgery
Surgical management of HCC. Evangelos Prassas Hepatobiliary and Pancreatic Surgery / Liver Transplantation Kings College Hospital / London
 Surgical management of HCC Evangelos Prassas Hepatobiliary and Pancreatic Surgery / Liver Transplantation Kings College Hospital / London Global distribution of HCC and staging systems WEST 1. Italy (Milan,
Surgical management of HCC Evangelos Prassas Hepatobiliary and Pancreatic Surgery / Liver Transplantation Kings College Hospital / London Global distribution of HCC and staging systems WEST 1. Italy (Milan,
OHSU Digital Commons. Oregon Health & Science University. Barry Schlansky. Scholar Archive. July 2013
 Oregon Health & Science University OHSU Digital Commons Scholar Archive July 2013 Waitlist time predicts survival after liver transplantation for hepatocellular carcinoma : a cohort study in the United
Oregon Health & Science University OHSU Digital Commons Scholar Archive July 2013 Waitlist time predicts survival after liver transplantation for hepatocellular carcinoma : a cohort study in the United
Surveillance for Hepatocellular Carcinoma
 Surveillance for Hepatocellular Carcinoma Marion G. Peters, MD John V. Carbone, MD, Endowed Chair Professor of Medicine Chief of Hepatology Research University of California San Francisco Recorded on April
Surveillance for Hepatocellular Carcinoma Marion G. Peters, MD John V. Carbone, MD, Endowed Chair Professor of Medicine Chief of Hepatology Research University of California San Francisco Recorded on April
Salvage Liver Transplantation for Recurrent Hepatocellular Carcinoma after Liver Resection: Retrospective Study of the Milan and Hangzhou Criteria
 Salvage Liver Transplantation for Recurrent Hepatocellular Carcinoma after Liver Resection: Retrospective Study of the Milan and Hangzhou Criteria Zhenhua Hu 1,2,3, Jie Zhou 1,2,3, Zhiwei Li 1,2,3, Jie
Salvage Liver Transplantation for Recurrent Hepatocellular Carcinoma after Liver Resection: Retrospective Study of the Milan and Hangzhou Criteria Zhenhua Hu 1,2,3, Jie Zhou 1,2,3, Zhiwei Li 1,2,3, Jie
Guidelines for SIRT in HCC An Evolution
 Guidelines for SIRT in HCC An Evolution 2 nd Asia Pacific Symposium on Liver- Directed Y-90 Microspheres Therapy 1st November 2014, Singapore The challenge of HCC Surgery is potentially curative in early
Guidelines for SIRT in HCC An Evolution 2 nd Asia Pacific Symposium on Liver- Directed Y-90 Microspheres Therapy 1st November 2014, Singapore The challenge of HCC Surgery is potentially curative in early
Living donor liver transplantation for hepatocellular carcinoma achieves better outcomes
 Review Article on Liver Transplantation for Hepatocellular Carcinoma Living donor liver transplantation for hepatocellular carcinoma achieves better outcomes Chih-Che Lin, Chao-Long Chen Liver Transplantation
Review Article on Liver Transplantation for Hepatocellular Carcinoma Living donor liver transplantation for hepatocellular carcinoma achieves better outcomes Chih-Che Lin, Chao-Long Chen Liver Transplantation
Treatment of Hepatocellular Carcinoma. Andrew J. Muir, MD MHS Division of Gastroenterology Duke University Medical Center
 Treatment of Hepatocellular Carcinoma Andrew J. Muir, MD MHS Division of Gastroenterology Duke University Medical Center Epidemiology of HCC: world The 5 th most common cancer worldwide > 500, 000 new
Treatment of Hepatocellular Carcinoma Andrew J. Muir, MD MHS Division of Gastroenterology Duke University Medical Center Epidemiology of HCC: world The 5 th most common cancer worldwide > 500, 000 new
INTRODUCTION. Journal of Surgical Oncology 2014;109:
 2014;109:533 541 Transplant Versus Resection for the Management of Hepatocellular Carcinoma Meeting Milan Criteria in the MELD Exception Era at a Single Institution in a UNOS Region with Short Wait Times
2014;109:533 541 Transplant Versus Resection for the Management of Hepatocellular Carcinoma Meeting Milan Criteria in the MELD Exception Era at a Single Institution in a UNOS Region with Short Wait Times
Optimization of immunosuppressive medication upon liver transplantation against HCC recurrence
 Review Article Optimization of immunosuppressive medication upon liver transplantation against HCC recurrence Shirin Elizabeth Khorsandi, Nigel Heaton Institute of Liver Studies, King s Healthcare Partners
Review Article Optimization of immunosuppressive medication upon liver transplantation against HCC recurrence Shirin Elizabeth Khorsandi, Nigel Heaton Institute of Liver Studies, King s Healthcare Partners
Hepatocellular Carcinoma: A major global health problem. David L. Wood, MD Interventional Radiology Banner Good Samaritan Medical Center
 Hepatocellular Carcinoma: A major global health problem David L. Wood, MD Interventional Radiology Banner Good Samaritan Medical Center Hepatocellular Carcinoma WORLDWIDE The #2 Cancer Killer Overall cancer
Hepatocellular Carcinoma: A major global health problem David L. Wood, MD Interventional Radiology Banner Good Samaritan Medical Center Hepatocellular Carcinoma WORLDWIDE The #2 Cancer Killer Overall cancer
Effects of Maintenance Immunosuppression With Sirolimus After Liver Transplant for Hepatocellular Carcinoma
 ORIGINAL ARTICLE YANIK ET AL. Effects of Maintenance Immunosuppression With Sirolimus After Liver Transplant for Hepatocellular Carcinoma Elizabeth L. Yanik, 1 Srinath Chinnakotla, 2 Sally K. Gustafson,
ORIGINAL ARTICLE YANIK ET AL. Effects of Maintenance Immunosuppression With Sirolimus After Liver Transplant for Hepatocellular Carcinoma Elizabeth L. Yanik, 1 Srinath Chinnakotla, 2 Sally K. Gustafson,
Total Tumor Volume and Alpha Fetoprotein for selection of transplant candidates. with hepatocellular carcinoma: a prospective validation
 Total Tumor Volume and Alpha Fetoprotein for selection of transplant candidates with hepatocellular carcinoma: a prospective validation Christian Toso 1, Glenda Meeberg 2, Roberto Hernandez-Alejandro 3,
Total Tumor Volume and Alpha Fetoprotein for selection of transplant candidates with hepatocellular carcinoma: a prospective validation Christian Toso 1, Glenda Meeberg 2, Roberto Hernandez-Alejandro 3,
Geographic Differences in Event Rates by Model for End-Stage Liver Disease Score
 American Journal of Transplantation 2006; 6: 2470 2475 Blackwell Munksgaard C 2006 The Authors Journal compilation C 2006 The American Society of Transplantation and the American Society of Transplant
American Journal of Transplantation 2006; 6: 2470 2475 Blackwell Munksgaard C 2006 The Authors Journal compilation C 2006 The American Society of Transplantation and the American Society of Transplant
Research Article A Decade of Experience Using mtor Inhibitors in Liver Transplantation
 Transplantation Volume 2011, Article ID 913094, 7 pages doi:10.1155/2011/913094 Research Article A Decade of Experience Using mtor Inhibitors in Liver Transplantation Jeffrey Campsen, 1, 2 Michael A. Zimmerman,
Transplantation Volume 2011, Article ID 913094, 7 pages doi:10.1155/2011/913094 Research Article A Decade of Experience Using mtor Inhibitors in Liver Transplantation Jeffrey Campsen, 1, 2 Michael A. Zimmerman,
Selection of patients of hepatocellular carcinoma beyond the Milan criteria for liver transplantation
 Title Selection of patients of hepatocellular carcinoma beyond the Milan criteria for liver transplantation Author(s) Chan, SC; Fan, ST Citation Hepatobiliary Surgery and Nutrition, 2013, v. 2 n. 2, p.
Title Selection of patients of hepatocellular carcinoma beyond the Milan criteria for liver transplantation Author(s) Chan, SC; Fan, ST Citation Hepatobiliary Surgery and Nutrition, 2013, v. 2 n. 2, p.
Following the introduction of adult-to-adult living
 LIVER FAILURE/CIRRHOSIS/PORTAL HYPERTENSION Liver Transplant Recipient Survival Benefit with Living Donation in the Model for Endstage Liver Disease Allocation Era Carl L. Berg, 1 Robert M. Merion, 2 Tempie
LIVER FAILURE/CIRRHOSIS/PORTAL HYPERTENSION Liver Transplant Recipient Survival Benefit with Living Donation in the Model for Endstage Liver Disease Allocation Era Carl L. Berg, 1 Robert M. Merion, 2 Tempie
Hepatocellular carcinoma
 Hepatocellular carcinoma Mary Ann Y. Huang, M.D., M.S., FAASLD Transplant hepatologist Peak Gastroenterology Associates Porter Adventist Hospital Denver, Colorado Background - Worldwide Hepatocellular
Hepatocellular carcinoma Mary Ann Y. Huang, M.D., M.S., FAASLD Transplant hepatologist Peak Gastroenterology Associates Porter Adventist Hospital Denver, Colorado Background - Worldwide Hepatocellular
EASL-EORTC Guidelines
 Pamplona, junio de 2008 CLINICAL PRACTICE GUIDELINES: PARADIGMS IN MANAGEMENT OF HCC EASL-EORTC Guidelines Bruno Sangro Clínica Universidad de Navarra. CIBERehd. Pamplona, Spain Levels of Evidence according
Pamplona, junio de 2008 CLINICAL PRACTICE GUIDELINES: PARADIGMS IN MANAGEMENT OF HCC EASL-EORTC Guidelines Bruno Sangro Clínica Universidad de Navarra. CIBERehd. Pamplona, Spain Levels of Evidence according
HEPATOCELLULAR CARCINOMA: SCREENING, DIAGNOSIS, AND TREATMENT
 HEPATOCELLULAR CARCINOMA: SCREENING, DIAGNOSIS, AND TREATMENT INTRODUCTION: Hepatocellular carcinoma (HCC): Fifth most common cancer worldwide Third most common cause of cancer mortality In Egypt: 2.3%
HEPATOCELLULAR CARCINOMA: SCREENING, DIAGNOSIS, AND TREATMENT INTRODUCTION: Hepatocellular carcinoma (HCC): Fifth most common cancer worldwide Third most common cause of cancer mortality In Egypt: 2.3%
Medical Policy. MP Radiofrequency Ablation of Primary or Metastatic Liver Tumors
 Medical Policy MP 7.01.91 BCBSA Ref. Policy: 7.01.91 Last Review: 08/20/2018 Effective Date: 08/20/2018 Section: Surgery Related Policies 7.01.75 Cryosurgical Ablation of Primary or Metastatic Liver Tumors
Medical Policy MP 7.01.91 BCBSA Ref. Policy: 7.01.91 Last Review: 08/20/2018 Effective Date: 08/20/2018 Section: Surgery Related Policies 7.01.75 Cryosurgical Ablation of Primary or Metastatic Liver Tumors
Hepatocellular Carcinoma HCC Updated November 2015 by: Dr. Mohammed Alghamdi (Medical Oncology Fellow, University of Calgary)
 Hepatocellular Carcinoma HCC Updated November 2015 by: Dr. Mohammed Alghamdi (Medical Oncology Fellow, University of Calgary) Staff Reviewers: Dr. Yoo Joung Ko (Medical Oncologist, Sunnybrook Odette Cancer
Hepatocellular Carcinoma HCC Updated November 2015 by: Dr. Mohammed Alghamdi (Medical Oncology Fellow, University of Calgary) Staff Reviewers: Dr. Yoo Joung Ko (Medical Oncologist, Sunnybrook Odette Cancer
Review Article Liver Transplantation for Hepatocellular Carcinoma beyond Milan Criteria: Multidisciplinary Approach to Improve Outcome
 ISRN Hepatology, Article ID 706945, 25 pages http://dx.doi.org/10.1155/2014/706945 Review Article Liver Transplantation for Hepatocellular Carcinoma beyond Milan Criteria: Multidisciplinary Approach to
ISRN Hepatology, Article ID 706945, 25 pages http://dx.doi.org/10.1155/2014/706945 Review Article Liver Transplantation for Hepatocellular Carcinoma beyond Milan Criteria: Multidisciplinary Approach to
HCC: Is it an oncological disease? - No
 June 13-15, 2013 Berlin, Germany Prof. Oren Shibolet Head of the Liver Unit, Department of Gastroenterology Tel-Aviv Sourasky Medical Center and Tel-Aviv University HCC: Is it an oncological disease? -
June 13-15, 2013 Berlin, Germany Prof. Oren Shibolet Head of the Liver Unit, Department of Gastroenterology Tel-Aviv Sourasky Medical Center and Tel-Aviv University HCC: Is it an oncological disease? -
Liver transplantation for hepatocellular carcinoma with live donors or extended criteria donors: a propensity score-matched comparison
 ORIGINAL ARTICLE Annals of Gastroenterology (2018) 31, 722-727 Liver transplantation for hepatocellular carcinoma with live donors or extended criteria donors: a propensity score-matched comparison Georgios
ORIGINAL ARTICLE Annals of Gastroenterology (2018) 31, 722-727 Liver transplantation for hepatocellular carcinoma with live donors or extended criteria donors: a propensity score-matched comparison Georgios
RESEARCH ARTICLE. Validation of The Hong Kong Liver Cancer Staging System in Patients with Hepatocellular Carcinoma after Curative Intent Treatment
 DOI:10.22034/APJCP.2017.18.6.1697 RESEARCH ARTICLE Validation of The Hong Kong Liver Cancer Staging System in Patients with Hepatocellular Carcinoma after Curative Intent Treatment Alan Chuncharunee 1,
DOI:10.22034/APJCP.2017.18.6.1697 RESEARCH ARTICLE Validation of The Hong Kong Liver Cancer Staging System in Patients with Hepatocellular Carcinoma after Curative Intent Treatment Alan Chuncharunee 1,
What Is the Real Gain After Liver Transplantation?
 LIVER TRANSPLANTATION 15:S1-S5, 9 AASLD/ILTS SYLLABUS What Is the Real Gain After Liver Transplantation? James Neuberger Organ Donation and Transplantation, NHS Blood and Transplant, Bristol, United Kingdom;
LIVER TRANSPLANTATION 15:S1-S5, 9 AASLD/ILTS SYLLABUS What Is the Real Gain After Liver Transplantation? James Neuberger Organ Donation and Transplantation, NHS Blood and Transplant, Bristol, United Kingdom;
The pediatric end-stage liver disease (PELD) score
 Selection of Pediatric Candidates Under the PELD System Sue V. McDiarmid, 1 Robert M. Merion, 2 Dawn M. Dykstra, 2 and Ann M. Harper 3 Key Points 1. The PELD score accurately predicts the 3 month probability
Selection of Pediatric Candidates Under the PELD System Sue V. McDiarmid, 1 Robert M. Merion, 2 Dawn M. Dykstra, 2 and Ann M. Harper 3 Key Points 1. The PELD score accurately predicts the 3 month probability
Chapter 6: Transplantation
 Chapter 6: Transplantation Introduction During calendar year 2012, 17,305 kidney transplants, including kidney-alone and kidney plus at least one additional organ, were performed in the United States.
Chapter 6: Transplantation Introduction During calendar year 2012, 17,305 kidney transplants, including kidney-alone and kidney plus at least one additional organ, were performed in the United States.
MP Transcatheter Arterial Chemoembolization to Treat Primary or Metastatic Liver Malignancies
 Medical Policy MP 8.01.11 BCBSA Ref. Policy: 8.01.11 Last Review: 07/25/2018 Effective Date: 07/25/2018 Section: Therapy Related Policies 7.01.75 Cryosurgical Ablation of Primary or Metastatic Liver Tumors
Medical Policy MP 8.01.11 BCBSA Ref. Policy: 8.01.11 Last Review: 07/25/2018 Effective Date: 07/25/2018 Section: Therapy Related Policies 7.01.75 Cryosurgical Ablation of Primary or Metastatic Liver Tumors
IS THERE A DIFFERENCE IN LIVER CANCER RATES IN PATIENTS WHO RECEIVE TREATMENT FOR HEPATITIS?
 IS THERE A DIFFERENCE IN LIVER CANCER RATES IN PATIENTS WHO RECEIVE TREATMENT FOR HEPATITIS? Dr. Sammy Saab David Geffen School of Medicine, Los Angeles, USA April 2018 DISCLAIMER Please note: The views
IS THERE A DIFFERENCE IN LIVER CANCER RATES IN PATIENTS WHO RECEIVE TREATMENT FOR HEPATITIS? Dr. Sammy Saab David Geffen School of Medicine, Los Angeles, USA April 2018 DISCLAIMER Please note: The views
Liver Cancer: Diagnosis and Treatment Options
 Liver Cancer: Diagnosis and Treatment Options Fred Poordad, MD Chief, Hepatology University Transplant Center Professor of Medicine UT Health, San Antonio VP, Academic and Clinical Affairs, Texas Liver
Liver Cancer: Diagnosis and Treatment Options Fred Poordad, MD Chief, Hepatology University Transplant Center Professor of Medicine UT Health, San Antonio VP, Academic and Clinical Affairs, Texas Liver
ORIGINAL ARTICLE. Received June 6, 2011; accepted September 8, 2011.
 LIVER TRANSPLANTATION 18:45-52, 2012 ORIGINAL ARTICLE Efficacy and Safety of Sorafenib in Combination With Mammalian Target of Rapamycin Inhibitors for Recurrent Hepatocellular Carcinoma After Liver Transplantation
LIVER TRANSPLANTATION 18:45-52, 2012 ORIGINAL ARTICLE Efficacy and Safety of Sorafenib in Combination With Mammalian Target of Rapamycin Inhibitors for Recurrent Hepatocellular Carcinoma After Liver Transplantation
Liver resection for HCC
 8 th LIVER INTEREST GROUP Annual Meeting Cape Town 2017 Liver resection for HCC Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre The liver is almost unique in that treatment of the
8 th LIVER INTEREST GROUP Annual Meeting Cape Town 2017 Liver resection for HCC Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre The liver is almost unique in that treatment of the
AASLD Washington DC, USA Dr. Alexander Kim Chief Vascular and Interventional Radiology, Medstar Georgetown University Hospital
 AASLD 2017 - Washington DC, USA Dr. Alexander Kim Chief Vascular and Interventional Radiology, Medstar Georgetown University Hospital THE CHANGING LANDSCAPE IN THE TREATMENT OF HCC DISCLAIMER Please note:
AASLD 2017 - Washington DC, USA Dr. Alexander Kim Chief Vascular and Interventional Radiology, Medstar Georgetown University Hospital THE CHANGING LANDSCAPE IN THE TREATMENT OF HCC DISCLAIMER Please note:
Bridging and downstaging treatments for hepatocellular carcinoma in patients on the waiting list for liver transplantation
 Online Submissions: http://www.wjgnet.com/esps/ bpgoffice@wjgnet.com doi:10.3748/wjg.v19.i43.7515 World J Gastroenterol 2013 November 21; 19(43): 7515-7530 ISSN 1007-9327 (print) ISSN 2219-2840 (online)
Online Submissions: http://www.wjgnet.com/esps/ bpgoffice@wjgnet.com doi:10.3748/wjg.v19.i43.7515 World J Gastroenterol 2013 November 21; 19(43): 7515-7530 ISSN 1007-9327 (print) ISSN 2219-2840 (online)
Therapeutic options for hepatocellular carcinoma
 GASTROENTEROLOGY 2005;128:1752 1764 Liver Transplantation for Hepatocellular Carcinoma ALEX S. BEFELER, PAUL H. HAYASHI, and ADRIAN M. DI BISCEGLIE Saint Louis University Liver Center, Saint Louis University,
GASTROENTEROLOGY 2005;128:1752 1764 Liver Transplantation for Hepatocellular Carcinoma ALEX S. BEFELER, PAUL H. HAYASHI, and ADRIAN M. DI BISCEGLIE Saint Louis University Liver Center, Saint Louis University,
Description. Section: Surgery Effective Date: October 15, 2014 Subsection: Surgery Original Policy Date: December 7, 2011 Subject:
 Last Review Status/Date: September 2014 Page: 1 of 20 Description In radiofrequency ablation (RFA), a probe is inserted into the center of a tumor and the noninsulated electrodes, which are shaped like
Last Review Status/Date: September 2014 Page: 1 of 20 Description In radiofrequency ablation (RFA), a probe is inserted into the center of a tumor and the noninsulated electrodes, which are shaped like
Transcatheter hepatic arterial chemoembolization may be considered medically necessary to
 Original Issue Date (Created): July 1, 2002 Most Recent Review Date (Revised): September 24, 2013 Effective Date: November 1, 2013 I. POLICY Hepatocellular carcinoma Transcatheter hepatic arterial chemoembolization
Original Issue Date (Created): July 1, 2002 Most Recent Review Date (Revised): September 24, 2013 Effective Date: November 1, 2013 I. POLICY Hepatocellular carcinoma Transcatheter hepatic arterial chemoembolization
Review on liver transplant for hepatocellular carcinoma
 Review Article Review on liver transplant for hepatocellular carcinoma Hellen Chiao, Chao-Hsiung Edward Yang, Catherine T. Frenette Department of Organ and Cell Transplantation, Scripps Green Hospital,
Review Article Review on liver transplant for hepatocellular carcinoma Hellen Chiao, Chao-Hsiung Edward Yang, Catherine T. Frenette Department of Organ and Cell Transplantation, Scripps Green Hospital,
Should the Liver Transplant Criteria for Hepatocellular Carcinoma Be Different for Deceased Donation and Living Donation?
 LIVER TRANSPLANTATION 17:S133-S138, 2011 SUPPLEMENT Should the Liver Transplant Criteria for Hepatocellular Carcinoma Be Different for Deceased Donation and Living Donation? David Grant, 1,2,5 Robert A.
LIVER TRANSPLANTATION 17:S133-S138, 2011 SUPPLEMENT Should the Liver Transplant Criteria for Hepatocellular Carcinoma Be Different for Deceased Donation and Living Donation? David Grant, 1,2,5 Robert A.
Current Concepts in Hepatocellular Carcinoma and Liver Transplantation: A Review and 2014 Update
 REVIEW ARTICLE Current Concepts in Hepatocellular Carcinoma and Liver Transplantation: 10.5005/jp-journals-10018-1123 A Review and 2014 Update Current Concepts in Hepatocellular Carcinoma and Liver Transplantation:
REVIEW ARTICLE Current Concepts in Hepatocellular Carcinoma and Liver Transplantation: 10.5005/jp-journals-10018-1123 A Review and 2014 Update Current Concepts in Hepatocellular Carcinoma and Liver Transplantation:
Hepatocellular carcinoma (HCC) is the third
 Intention-to-Treat Analysis of Liver Transplantation for Hepatocellular Carcinoma: Living Versus Deceased Donor Transplantation Prashant Bhangui, 1 Eric Vibert, 1,2,4 Pietro Majno, 5 Chady Salloum, 1 Paola
Intention-to-Treat Analysis of Liver Transplantation for Hepatocellular Carcinoma: Living Versus Deceased Donor Transplantation Prashant Bhangui, 1 Eric Vibert, 1,2,4 Pietro Majno, 5 Chady Salloum, 1 Paola
Increased hepatocellular carcinoma recurrence in women compared to men with high alpha fetoprotein at liver transplant
 ORIGINAL ARTICLE July-August, Vol. 15 No. 4, 2016: 545-549 545 The Official Journal of the Mexican Association of Hepatology, the Latin-American Association for Study of the Liver and the Canadian Association
ORIGINAL ARTICLE July-August, Vol. 15 No. 4, 2016: 545-549 545 The Official Journal of the Mexican Association of Hepatology, the Latin-American Association for Study of the Liver and the Canadian Association
MANAGEMENT OF COLORECTAL METASTASES. Robert Warren, MD. The Postgraduate Course in General Surgery March 22, /22/2011
 MANAGEMENT OF COLORECTAL METASTASES Robert Warren, MD The Postgraduate Course in General Surgery March 22, 2011 Local Systemic LIVER TUMORS:THERAPEUTIC OPTIONS Hepatoma Cholangio. Neuroendo. Colorectal
MANAGEMENT OF COLORECTAL METASTASES Robert Warren, MD The Postgraduate Course in General Surgery March 22, 2011 Local Systemic LIVER TUMORS:THERAPEUTIC OPTIONS Hepatoma Cholangio. Neuroendo. Colorectal
Supplementary webappendix
 Supplementary webappendix This webappendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Clavien P-A, Lesurtel M, Bossuyt PMM,
Supplementary webappendix This webappendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Clavien P-A, Lesurtel M, Bossuyt PMM,
PATIENTS AND METHODS. Data Source
 LIVER TRANSPLANTATION 20:1045 1056, 2014 ORIGINAL ARTICLE Waiting Time Predicts Survival After Liver Transplantation for Hepatocellular Carcinoma: A Cohort Study Using the United Network for Organ Sharing
LIVER TRANSPLANTATION 20:1045 1056, 2014 ORIGINAL ARTICLE Waiting Time Predicts Survival After Liver Transplantation for Hepatocellular Carcinoma: A Cohort Study Using the United Network for Organ Sharing
Transcatheter Arterial Chemoembolization (TACE) to Treat Primary or Metastatic Liver Malignancies
 Transcatheter Arterial Chemoembolization (TACE) to Treat Primary or Metastatic Liver Malignancies Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its
Transcatheter Arterial Chemoembolization (TACE) to Treat Primary or Metastatic Liver Malignancies Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its
ORIGINAL ARTICLE Gastroenterology & Hepatology INTRODUCTION
 ORIGINAL ARTICLE Gastroenterology & Hepatology http://dx.doi.org/10.3346/jkms.2013.28.8.1207 J Korean Med Sci 2013; 28: 1207-1212 The Model for End-Stage Liver Disease Score-Based System Predicts Short
ORIGINAL ARTICLE Gastroenterology & Hepatology http://dx.doi.org/10.3346/jkms.2013.28.8.1207 J Korean Med Sci 2013; 28: 1207-1212 The Model for End-Stage Liver Disease Score-Based System Predicts Short
9th Paris Hepatitis Conference
 9th Paris Hepatitis Conference Paris, 12 January 2016 Treatment of hepatocellular carcinoma: beyond international guidelines Massimo Colombo Chairman Department of Liver, Kidney, Lung and Bone Marrow Units
9th Paris Hepatitis Conference Paris, 12 January 2016 Treatment of hepatocellular carcinoma: beyond international guidelines Massimo Colombo Chairman Department of Liver, Kidney, Lung and Bone Marrow Units
Literature Review: Transplantation July 2010-June 2011
 Literature Review: Transplantation July 2010-June 2011 James Cooper, MD Assistant Professor, Kidney and Pancreas Transplant Program, Renal Division, UC Denver Kidney Transplant Top 10 List: July Kidney
Literature Review: Transplantation July 2010-June 2011 James Cooper, MD Assistant Professor, Kidney and Pancreas Transplant Program, Renal Division, UC Denver Kidney Transplant Top 10 List: July Kidney
Liver transplantation for hepatocellular carcinoma - non-cancer factors and implications for improving outcome beyond standard tumor criteria
 Kornberg et al. Hepatoma Res 2018;4:60 DOI: 10.20517/2394-5079.2018.86 Hepatoma Research Review Open Access Liver transplantation for hepatocellular carcinoma - non-cancer factors and implications for
Kornberg et al. Hepatoma Res 2018;4:60 DOI: 10.20517/2394-5079.2018.86 Hepatoma Research Review Open Access Liver transplantation for hepatocellular carcinoma - non-cancer factors and implications for
Hepatocellular Carcinoma Recurrence After Liver Transplantation: an Analysis of Risk Factors and Incidence from Oregon Health & Science University
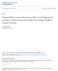 Portland State University PDXScholar University Honors Theses University Honors College 2016 Hepatocellular Carcinoma Recurrence After Liver Transplantation: an Analysis of Risk Factors and Incidence from
Portland State University PDXScholar University Honors Theses University Honors College 2016 Hepatocellular Carcinoma Recurrence After Liver Transplantation: an Analysis of Risk Factors and Incidence from
Liver Transplantation
 Liver Transplantation Dr Mathew Jacob - MRCS FRCS CCT (UK) Lead Consultant HPB/Transplant Surgeon Aster Integrated Liver Care Program AsterMedcity, kochi, kerala, India mathew@transplantationliver.com
Liver Transplantation Dr Mathew Jacob - MRCS FRCS CCT (UK) Lead Consultant HPB/Transplant Surgeon Aster Integrated Liver Care Program AsterMedcity, kochi, kerala, India mathew@transplantationliver.com
Disparities in Liver Transplant Allocation: An Update on MELD Allocation System
 Disparities in Liver Transplant Allocation: An Update on MELD Allocation System Naudia L. Jonassaint, MD MHS Assistant Professor of Medicine and Surgery University of Pittsburgh School of Medicine Historical
Disparities in Liver Transplant Allocation: An Update on MELD Allocation System Naudia L. Jonassaint, MD MHS Assistant Professor of Medicine and Surgery University of Pittsburgh School of Medicine Historical
NIH Public Access Author Manuscript J Surg Res. Author manuscript; available in PMC 2011 May 18.
 NIH Public Access Author Manuscript Published in final edited form as: J Surg Res. 2011 April ; 166(2): 189 193. doi:10.1016/j.jss.2010.04.036. Hepatocellular Carcinoma Survival in Uninsured and Underinsured
NIH Public Access Author Manuscript Published in final edited form as: J Surg Res. 2011 April ; 166(2): 189 193. doi:10.1016/j.jss.2010.04.036. Hepatocellular Carcinoma Survival in Uninsured and Underinsured
Hepatocellular Carcinoma Recurrence and Death Following Living and Deceased Donor Liver Transplantation
 American Journal of Transplantation 2007; 7: 1601 1608 Blackwell Munksgaard C 2007 The Authors Journal compilation C 2007 The American Society of Transplantation and the American Society of Transplant
American Journal of Transplantation 2007; 7: 1601 1608 Blackwell Munksgaard C 2007 The Authors Journal compilation C 2007 The American Society of Transplantation and the American Society of Transplant
Locoregional Treatments for HCC Applications in Transplant Candidates. Locoregional Treatments for HCC Applications in Transplant Candidates
 Locoregional Treatments for HCC Applications in Transplant Candidates Matthew Casey, MD March 31, 2016 Locoregional Treatments for HCC Applications in Transplant Candidates *No disclosures *Off-label uses
Locoregional Treatments for HCC Applications in Transplant Candidates Matthew Casey, MD March 31, 2016 Locoregional Treatments for HCC Applications in Transplant Candidates *No disclosures *Off-label uses
Hepatobiliary Malignancies Retrospective Study at Truman Medical Center
 Hepatobiliary Malignancies 206-207 Retrospective Study at Truman Medical Center Brandon Weckbaugh MD, Prarthana Patel & Sheshadri Madhusudhana MD Introduction: Hepatobiliary malignancies are cancers which
Hepatobiliary Malignancies 206-207 Retrospective Study at Truman Medical Center Brandon Weckbaugh MD, Prarthana Patel & Sheshadri Madhusudhana MD Introduction: Hepatobiliary malignancies are cancers which
Adult-to-adult living donor liver transplantation Triumphs and challenges
 Falk Symposium No. 163 on Chronic Inflammation of Liver and Gut Adult-to-adult living donor liver transplantation Triumphs and challenges ST Fan, MS, MD, PhD, DSc Professor Sun CY Chair of Hepatobiliary
Falk Symposium No. 163 on Chronic Inflammation of Liver and Gut Adult-to-adult living donor liver transplantation Triumphs and challenges ST Fan, MS, MD, PhD, DSc Professor Sun CY Chair of Hepatobiliary
Role of positron emission tomography/computed tomography in living donor liver transplantation for hepatocellular carcinoma
 Review Article on Liver Transplantation for Hepatocellular Carcinoma Role of positron emission tomography/computed tomography in living donor liver transplantation for hepatocellular carcinoma Seung Duk
Review Article on Liver Transplantation for Hepatocellular Carcinoma Role of positron emission tomography/computed tomography in living donor liver transplantation for hepatocellular carcinoma Seung Duk
Key Words: Everolimus; Living donor liver transplantation; Hepatocellular carcinoma; Hepatic artery thrombosis
 Ann Hepatobiliary Pancreat Surg 2017;21:205-211 https://doi.org/10.14701/ahbps.2017.21.4.205 Original Article Assessing the role of everolimus in reducing hepatocellular carcinoma recurrence after living
Ann Hepatobiliary Pancreat Surg 2017;21:205-211 https://doi.org/10.14701/ahbps.2017.21.4.205 Original Article Assessing the role of everolimus in reducing hepatocellular carcinoma recurrence after living
Review Article The Role of mtor Inhibitors in Liver Transplantation: Reviewing the Evidence
 Hindawi Publishing Corporation Journal of Transplantation Volume 2014, Article ID 845438, 45 pages http://dx.doi.org/10.1155/2014/845438 Review Article The Role of mtor Inhibitors in Liver Transplantation:
Hindawi Publishing Corporation Journal of Transplantation Volume 2014, Article ID 845438, 45 pages http://dx.doi.org/10.1155/2014/845438 Review Article The Role of mtor Inhibitors in Liver Transplantation:
Nexavar in advanced HCC: a paradigm shift in clinical practice
 Nexavar in advanced HCC: a paradigm shift in clinical practice Tim Greten Hanover Medical School, Germany Histopathological progression and molecular features of HCC Chronic liver disease Liver cirrhosis
Nexavar in advanced HCC: a paradigm shift in clinical practice Tim Greten Hanover Medical School, Germany Histopathological progression and molecular features of HCC Chronic liver disease Liver cirrhosis
HCC surgical approach: resection and transplantation indications and outcome
 SAMO, Friday 15th April 2011 Workshop on Primary liver tumors HCC surgical approach: resection and transplantation indications and outcome Gilles Mentha University Hospital of Geneva Hepatocellular Carcinoma
SAMO, Friday 15th April 2011 Workshop on Primary liver tumors HCC surgical approach: resection and transplantation indications and outcome Gilles Mentha University Hospital of Geneva Hepatocellular Carcinoma
Paul Martin MD FACG. University of Miami
 Paul Martin MD FACG University of Miami 1 Liver cirrhosis of any cause Chronic C o c hepatitis epat t s B Risk increases with Male gender Age Diabetes Smoking ~5% increase in HCV-related HCC between 1991-28
Paul Martin MD FACG University of Miami 1 Liver cirrhosis of any cause Chronic C o c hepatitis epat t s B Risk increases with Male gender Age Diabetes Smoking ~5% increase in HCV-related HCC between 1991-28
Worldwide Causes of HCC
 Approach to HCV Treatment in Patients with HCC JORGE L. HERRERA, MD, MACG UNIVERSITY OF SOUTH ALABAMA COLLEGE OF MEDICINE Worldwide Causes of HCC 60% 50% 40% 54% 30% 20% 10% 31% 15% 0% Hepatitis B Hepatitis
Approach to HCV Treatment in Patients with HCC JORGE L. HERRERA, MD, MACG UNIVERSITY OF SOUTH ALABAMA COLLEGE OF MEDICINE Worldwide Causes of HCC 60% 50% 40% 54% 30% 20% 10% 31% 15% 0% Hepatitis B Hepatitis
Study Objective and Design
 Randomized, Open Label, Multicenter, Phase II Trial of Transcatheter Arterial Chemoembolization (TACE) Therapy in Combination with Sorafenib as Compared With TACE Alone in Patients with Hepatocellular
Randomized, Open Label, Multicenter, Phase II Trial of Transcatheter Arterial Chemoembolization (TACE) Therapy in Combination with Sorafenib as Compared With TACE Alone in Patients with Hepatocellular
