ORIGINAL PAPER. DDepartment of Neurosurgery, Nagoya University Graduate School of Medicine, Nagoya, Japan ABSTRACT
|
|
|
- Melinda Rose
- 6 years ago
- Views:
Transcription
1 Nagoya J. Med. Sci ~ 82, 2014 ORIGINAL PAPER A NOVEL METHOD FOR MANAGING WATER AND ELECTROLYTE BALANCE AFTER TRANSSPHENOIDAL SURGERY: PRELIMINARY STUDY OF MODERATE WATER INTAKE RESTRICTION KAZUHITO TAKEUCHI, MD; TETSUYA NAGATANI, MD, PhD; ERIKO OKUMURA, MD; and TOSHIHIKO WAKABAYASHI, MD, PhD DDepartment of Neurosurgery, Nagoya University Graduate School of Medicine, Nagoya, Japan ABSTRACT Hyponatremia is a common and potentially serious complication of transsphenoidal surgery (TSS). Since September 2009, we have implemented moderate water intake restriction (<2500 ml/day) after TSS in an attempt to prevent this complication. The aim of this study was to investigate the efficacy of a combination of moderate restriction of water intake plus antidiuretic hormone (arginine vasopressin [AVP]) replacement therapy in patients with diabetes insipidus (DI) for reducing the incidence of delayed hyponatremia after TSS. Patients treated from September 2005 to August 2009 were allowed to drink water freely after surgery (the control group), while patients treated from September 2009 to June 2012 were restricted to less than 2500 ml water per day (the water restriction group). To reduce the occurrence of hypernatremia, AVP replacement therapy was provided immediately after the development of DI. We retrospectively analyzed the incidence of hyponatremia, DI, and hypernatremia in patients following TSS. Hyponatremia incidence was significantly lower in the water restriction group (P = 0.017); however, there were no significant differences in DI incidence and hypernatremia incidence between the 2 groups. Under DI control with AVP replacement therapy, the water restriction group showed no significant difference in the daily self-rated thirst level for the patients with and without DI. Moderate water intake restriction in addition to AVP replacement therapy significantly decreases the incidence of hyponatremia without patient discomfort (extreme thirst) and other complications. However, further studies are required to determine the most effective amount of water and the optimal duration of postoperative water restriction. Key Words: Hyponatremia, Transsphenoidal Surgery, Pituitary Tumor, Syndrome of Inappropriate Secretion of Antidiuretic Hormone, Thirst INTRODUCTION Transsphenoidal surgery (TSS) is the first-line treatment for sellar and parasellar lesions, with the exception of some specific anatomical and histopathological conditions. Pituitary adenoma is the most common lesion treated using this approach. This surgery is less invasive and seldom results in serious complications; however, it can be the cause of disturbance in water and electro- Received: August 13, 2013; accepted: November 18, 2013 Corresponding author: Kazuhito Takeuchi, MD Department of Neurosurgery, Nagoya University, Graduate School of Medicine, 65 Tsurumai-cho, Showa-ku, Nagoya, Aichi , Japan Phone number: , Fax number: , mail@wajit.com 73
2 74 Kazuhito Takeuchi et al. lyte metabolism. Diabetes insipidus (DI) occurs in 10% to 50% of patients after TSS 4, 6, 11, 12, 14), while delayed hyponatremia is reported to occur in 1.8% to 35% of patients around postoperative day 7 9, 11, 13, 16, 19). Hyponatremia may become symptomatic, and prolonged hyponatremia may be life threatening 5, 9, 21). It is imperative to minimize risk factors for delayed hyponatremia after transsphenoidal tumor resection, because recent advances in neuroendoscopic techniques are less traumatic to the nasal apparatus, resulting in shorter hospital stays. Hyponatremia following TSS may arise because of deficiency in the supply of adrenocortical hormone, syndrome of inappropriate secretion of antidiuretic hormone (SIADH), and/or inappropriate fluid consumption 8, 13, 17). Although the causes of delayed hyponatremia following TSS are still unclear, some authors attribute this to SIADH and others suggest frequent coincidence with DI 8, 15, 20). We promote a novel method for managing water and electrolyte balance after TSS. We have previously managed water balance after TSS with free fluid intake and aggressive fluid replacement. In the present study, we adopted moderate restriction of postoperative water intake and reduced fluid replacement while carefully monitoring DI and body weight. We also monitored subjective sensation of thirst, as excessive thirst may hinder treatment compliance. To this end, we created a self-rated thirst level scale and assessed the relationship between thirst and DI in relation to delayed hyponatremia after TSS. The aim of the present study was to investigate the feasibility of moderate restriction of water intake to reduce the occurrence of delayed hyponatremia after TSS. PATIENTS AND METHODS Patient Population and Surgical Procedures In this retrospective study, we collected data from the charts of patients who had sellar and parasellar lesions and underwent purely endoscopic endonasal TSS from September 2005 to June A single surgeon (TN) performed all surgeries. Surgeries were performed under general anesthesia, with visualization provided by a 4-mm diameter rigid-lens endoscope. We operated through a unilateral nostril (usually on the right side), using a midline paraseptal approach to access the sphenoid sinus. This approach leaves the contralateral nostril intact and results in reduced postoperative nasal obstruction and less severe postoperative thirst due to oral breathing. The ipsilateral mucosa on the nasal septum was dissected to the level of the anterior wall of the sphenoid sinus. The bony septum was removed to expose the mucosa on the contralateral side. Routine wide-open sphenoidotomy was performed for all patients. Sellar and suprasellar procedures began with internal debulking of the tumor, followed by identification of the tumor capsule. In most cases, capsulectomy with an angled endoscope was possible. After tumor excision, we packed the tumor cavity with abdominal fat to prevent postoperative cerebrospinal fluid leakage. Nasal packing was removed immediately after extubation. Standard Protocol for Postoperative Management of Water and Electrolyte Balance In September 2009, we adopted a new protocol for managing water and electrolyte balance after TSS. The core concept of the present study is moderate restriction of water intake and adequate control of DI immediately after surgery. On the day of surgery and on postoperative day 1, the patients were intravenously administered 1000 ml sugar electrolyte maintenance transfusion solution containing 0.3% NaCl. On postoperative day 2, they were administered 500 ml sugar electrolyte maintenance transfusion solution. Postoperative patients were permitted to drink fluids 3 hours after returning to the ward. Patients without Cushing s disease were intravenously administered 100 mg hydrocortisone on the
3 FLUID MANAGEMENT AFTER PITUITARY SURGERY 75 Day 0 No Ordinary Unbearable Day 1 No Ordinary Unbearable Day 2 No Ordinary Unbearable Day 10 No Ordinary Unbearable Fig. 1. Thirst Questionnaire. Patients were required to circle a number depicting their own thirst level on this questionnaire each day, from the day of surgery to postoperative day 10. day of surgery and on postoperative day 1. An additional 100 mg was administered during the surgery. Fifty milligrams of hydrocortisone was administered on postoperative day 2, and 20 mg hydrocortisone was administered orally on postoperative days 3 and 4. For patients with Cushing s disease, cortisol replacement therapy was initiated upon confirmation of adrenal insufficiency. We prepared a printed form that the patients could use to record their thirst level. We represented thirst on a scale of 0 10, with 0 indicating no thirst and 10 indicating unbearable thirst. The midpoint of the scale (5) represented ordinary thirst (Fig. 1). The patients were instructed to keep the form at their bedside and were required to circle a number on 1 scale for each day. As a general rule, the patients were permitted to drink no more than 2500 ml water per day from postoperative day 1 to postoperative day 10. Blood tests for serum levels of electrolytes and endocrine function were performed 2 days before surgery and on postoperative days 1, 7, and 10. Hyponatremia was diagnosed if the serum sodium level was less than 135 meq/l. Hypernatremia was diagnosed if the serum sodium level was greater than 148 meq/l. Management of DI Urine volume was monitored every 2 hours on the day of surgery and on postoperative day 1, and every 8 hours from postoperative day 2 to postoperative day 10. We only observed balanced intake and fluid output on the day of the surgery and on postoperative day 1, because most patients were administered a relatively large volume of fluid during anesthesia. DI was diagnosed if urine volume reached 1000 ml/4 h and urine specific gravity fell below on or after postoperative day 2. From postoperative day 2, the patients received intravenous substitution
4 76 Kazuhito Takeuchi et al. therapy of vasopressin or were nasally administered deamino-8-d-arginine vasopressin (ddavp) if they were diagnosed with DI. The target volume of urine output for this treatment was defined as less than 1000 ml/4 h and less than 2500 ml/day. If body weight increased after surgery, administration of antidiuretic hormone (ADH) was discontinued. Study Design Patients in puerperium and those with a medical history of hyponatremia were excluded from the study. The remaining patients were categorized into the following 2 groups: control group, patients who were treated from September 2005 to August 2009 and were allowed to drink water freely after surgery; water restriction group, patients who were treated from September 2009 to June 2012 and were subjected to moderate water restriction. Demographics, tumor type and volume, incidence of hyponatremia, hypernatremia, and DI, operative time, intraoperative blood loss, intraoperative fluid balance, and average daily oral fluid intake between postoperative day 1 and postoperative day 7 or before the day of occurrence of hyponatremia were analyzed. Preoperative tumor volume was measured using a preoperative magnetic resonance imaging (MRI) scan and was calculated as follows: Volume (mm 3 ) = Width (mm) Height (mm) Depth (mm) 2 Statistical Analysis Statistical analyses were performed with the software package SPSS 19.0 J for Windows (SPSS Inc., IL, USA). Categorical variables were assessed with the Pearson chi-square test, and quantitative variables were compared with unpaired 2-tailed t tests. A P value 0.05 was considered statistically significant. Values are expressed as mean ± standard deviation. RESULTS A total of 191 patients with sellar lesions were treated using purely endoscopic endonasal TSS during this period. Two patients in puerperium and 4 patients with a medical history of hyponatremia were excluded. The remaining 185 patients were enrolled in the study. Clinical Characteristics Clinical characteristics (age, lesion type, and perioperative indices) for the 2 patient groups are summarized in Table 1. The water restriction group included 93 patients and the control group included 92 patients. The mean age was ± years in the water restriction group and ± years in the control group (P = 0.271). There were 52 women in the water restriction group and 44 women in the control group (P = 0.216). There were no statistically significant differences between these 2 groups with respect to clinical characteristics. Water and Electrolyte Disturbances Hyponatremia was observed in 5 patients in the water restriction group and 15 patients in the control group; this was a statistically significant difference (P = 0.017, Table 2). Among these patients, symptomatic hyponatremia was observed in only 1 patient in the water restriction group, as opposed to 6 patients in the control group, showing no significant difference (P = 0.052). There were 24 patients with DI and 3 patients with hypernatremia in the water restriction group and 27 patients with DI and 3 patients with hypernatremia in the control group; however,
5 FLUID MANAGEMENT AFTER PITUITARY SURGERY 77 Table 1 Characteristics of patients treated with endoscopic endonasal TSS. NF, non-functioning pituitary adenoma; GH, growth hormone secreting pituitary adenoma; PRL, prolactin secreting pituitary adenoma; ACTH, adrenocorticotropic hormone secreting pituitary adenoma Water Restriction Control P n Sex Female Male Age, y 48.99± ± Tumor type NF GH PRL 9 4 ACTH 4 6 Craniopharyngioma 3 1 Rathke s cleft cyst 2 1 meningioma 1 0 Tumor volume (mm 3 ) 5426± ± Table 2 Incidence of hyponatremia (with or without symptoms), diabetes insipidus (DI), and hypernatremia. Water Restriction Control P Hyponatremia 5 (5.4%) 15 (16.3%) Symptomatic 1 (1.1%) 6 (6.5%) Asymptomatic 4 (4.3%) 9 (9.8%) DI 21 (25.8%) 27 (29.3%) 0.48 Hypernatremia 3 (3.2%) 3 (3.3%) there was no statistically significant difference (P = and P = 0.989, respectively; Table 2). There were 24 patients with DI in the water restriction group and 27 patients in the control group, with no significant difference (P = 0.480). Three patients in the water restriction group had hypernatremia, with maximum serum sodium levels of 150 meq/l, 154 meq/l, and 148 meq/l respectively, and 3 patients in the control group had maximum serum sodium levels of 158 meq/l, 148 meq/l, and 151 meq/l, respectively. Isolated hyponatremia, combined DI and hyponatremia, and isolated DI were observed in 3, 2, and 22 patients, respectively, in the water restriction group, and 2, 13, and 14 patients, respectively, in the control group (Table 3). The incidence of both DI and hyponatremia in the same patient was significantly less in the water restriction group than in the control group (P = 0.003). Data on the average daily oral fluid intake of isolated hyponatremia patients, combined DI and hyponatremia patients, and isolated DI patients were available in 3 of 3, 2 of 2, and 19 of 22 patients in the water restriction group, respectively, and 2 of 2, 6 of 13, and 11 of 14
6 78 Kazuhito Takeuchi et al. Table 3 Intraoperative and postoperative measurements of water and electrolyte disturbances. *Average daily oral fluid intake during postoperative day 1 to day 7 or the day before incidence of hyponatremia. Isolated Hyponatremia Water Restriction Group Combined DI-Hyponatremia Isolated DI Isolated Hyponatremia Control Group DI-Hyponatremia Isolated DI n 3 (3.2%) 2 (2.2%) 22 (23.7%) 2 (2.2%) 13 (14.1%) 14 (15.2%) Sex Female Male Age, y 44.3 (26 70) 32.0 (28 36) (24 62) 53.5 (35 72) 54.3 (19 75) 48.1 (22 77) Intraoperative data Duration, min 208.6± ± ± ± ± ± 62.5 Blood loss, ml 30.0± ± ± ± ± ± 94.1 Fluid balance, ml 966.7± ± ± ± ± ± Post-operative data Oral fluid intake (ml)* ± ± ± ± ± ± patients in the control group, respectively. The average daily oral fluid intake was ± ml, ± ml, and ± ml in the water restriction group, respectively, and ± ml, ± ml, and ± ml in the control group, respectively (Table 3). Average daily oral fluid intake was greater than 2500 ml in 1 (50%) of 2 isolated hyponatremia patients, 5 (83.3%) of 6 combined DI and hyponatremia patients, and 6 (54.5%) of 11 isolated DI patients in the control group. There were no statistically significant differences between the 2 groups with respect to intraoperative data. Assessment of Thirst Level Only 37 of the 93 patients in the water restriction group evaluated their thirst level because the questionnaire was formulated after the treatment protocol had been initiated. These 37 patients included 9 patients with DI and 28 without DI (Fig. 2). There were no statistically significant differences in the thirst levels of patients with and without DI from the day of surgery to postoperative day 10. Illustrative Case in the Control Group A 47-year-old woman with a growth hormone-producing pituitary microadenoma detected on MRI underwent purely endoscopic endonasal TSS. Six hours after the surgery, she developed DI, and vasopressin was administered intravenously. On postoperative day 1, intravenous administration of vasopressin was switched to nasal administration of ddavp, which was continued until postoperative day 4. She was allowed to drink freely and exhibited polyuria and polydipsia. The maximum urine output (9693 ml/day) was observed on postoperative day 4. A subsequent decrease in urine output led to discontinuation of ddavp administration on postoperative day 5. Despite the alleviation of DI, the patient had been drinking ml/day from postoperative day 1 to postoperative day 7. She experienced headaches and nausea on postoperative day 8, and blood examination revealed hyponatremia (119 meq/l) on postoperative day 9. She was kept under water restriction after developing hyponatremia. Her symptoms and serum sodium level improved, and she was discharged from our department on postoperative day 18.
7 FLUID MANAGEMENT AFTER PITUITARY SURGERY 79 Fig. 2 Changes in the Thirst Level after Transsphenoidal Surgery. DISCUSSION Hyponatremia is a common electrolyte disturbance in the neurosurgical population. This 8, 15, complication is attributed to SIADH, cerebral salt wasting (CSW), and adrenal insufficiency 21). Hyponatremia following TSS has been reported by several authors. The reported incidence of this complication is approximately 30%, and it occurs about 7 days after surgery 3, 7, 11, 16). Approximately 20% of patients become symptomatic 21). The symptoms of hyponatremia are variable and include headache, nausea, vomiting, mental status disturbance, seizures, and coma 2, 5, 21). Therefore, if this complication occurs, patients may require additional treatment and longer hospital stay, even if there are no noticeable problems with the surgery itself. Insufficient or inappropriate treatment for this complication can induce other neurological disturbances, such as seizures, osmotic demyelination syndrome, coma, and even death 5, 15). The pathophysiology of delayed hyponatremia has been discussed extensively, and the main cause following TSS is believed to be the release of excessive antidiuretic hormone, presumably induced by surgical manipulation of the posterior pituitary gland and pituitary stalk 7, 18, 20). SIADH treatment is based on restriction of water intake. We evaluated this treatment by implementing moderate water restriction to prevent hyponatremia after TSS. To date, the method for preventing this complication has not been established. To the best of our knowledge, this is the first study to test a possible method for preventing hyponatremia following TSS. Occurrence of Hyponatremia We evaluated the usefulness of limiting oral fluid intake to 2500 ml/day from immediately
8 80 Kazuhito Takeuchi et al. after TSS to postoperative day 10. Previously identified risk factors for hyponatremia after TSS are older age, female sex, microadenomas, adrenocorticotropic hormone (ACTH)-producing tumors, and the presence of transient DI 7, 10, 13, 16, 17, 21). Although there were no significant differences in patient demographics or tumor-type distribution between the water restriction group and the control group, moderate water restriction significantly decreased the occurrence of this potentially life-threatening complication. Although there was no significant difference in the occurrence of symptomatic hyponatremia between the 2 groups, the occurrence of symptomatic hyponatremia tended to be quite low, because only 1 patient on water restriction developed symptomatic hyponatremia (1.1%) compared with 6 control patients (6.5%). The incidence of combined DI and hyponatremia was significantly lower in the water restriction group than in the control group. Olson et al. reported that two-thirds of normonatremic patients had dysfunctional arginine vasopressin (AVP) secretion under the water load test at 7 days after TSS, and that 9 of 23 patients actually developed hyponatremia after the water load test 13). Hence, even normonatremic patients can develop hyponatremia after this surgery 13). Thus, many patients may be susceptible to hyponatremia following TSS if exposed to excessive volitional fluid consumption. In this study, the average daily oral fluid intake was greater than 2500 ml in 83% of the combined DI and hyponatremia patients in the control group. On the other hand, patients restricted to 2500 ml/ day, especially those with DI, demonstrated a significantly reduced occurrence of hyponatremia. As revealed by the illustrative case discussed in the Results section, controlling water and osmotic balance is difficult when patients drink water freely. Patients occasionally drink water excessively after their urine output decreases, which can cause delayed hyponatremia after TSS in patients with DI. The reported incidence of combined DI and hyponatremia in this study is within the range of 4.5% 20% 1, 3, 7, 11, 13, 16, 21). We speculate that water restriction for patients with DI under antidiuretic hormone replacement therapy stabilizes net changes in body fluid content and facilitates the control of fluid and electrolyte balance. This moderate water restriction regimen has the potential to reduce the incidence of hyponatremia after surgery. Endoscopic TSS for Sellar Lesions Sigounas et al. reported that the incidence of DI can be reduced by treating patients with endoscopic surgery instead of microscopic surgery 18). Given that the main cause of both hyponatremia and DI is abnormal ADH secretion, endoscopic surgery may decrease the rate of postoperative hyponatremia. In this study, all patients underwent purely endoscopic endonasal TSS. The incidence of hyponatremia was 5.4% in the water restriction group and 16.3% in the control group. Recent large studies on delayed hyponatremia reported that hyponatremia occurs in 36.7% of patients treated with microscopic surgery 11). In comparison, the incidence of hyponatremia observed in the present study was relatively low, even in the control group. Transsphenoidal endoscopic surgery may reduce the incidence of postoperative hyponatremia. Complications of Moderate Water Restriction after TSS Dehydration is the most serious potential complication of water restriction, especially in patients with DI. There was no significant difference between the incidence of hypernatremia in the experimental and control groups. We implemented AVP replacement therapy to control the urine output immediately after approaching DI criteria to avoid dehydration. However, 3 patients in the experimental group developed DI. To reduce the incidence of hypernatremia among patients, water restriction therapy should be aborted until DI is brought under control. In our opinion, DI control is important for reducing not only the incidence of hypernatremia, but also the thirst level, which in turn reduces oral fluid intake. Some researchers have reported that ADH replacement therapy during the first 2 postoperative weeks can actually increase the risk for hyponatremia, and
9 FLUID MANAGEMENT AFTER PITUITARY SURGERY 81 thus, close monitoring of patient body weight and urine output is recommended, especially for patients undergoing ADH replacement therapy 7, 11, 12). ADH replacement therapy can be safe and can even decrease the incidence of hyponatremia if implemented together with water restriction therapy and can be withdrawn when the patient s body weight increases or when the patient s urine parameters no longer meet the criteria for DI. Alleviation of Thirst Our department has implemented various methods to reduce patient thirst. Nasal obstruction after TSS should be avoided, as this tends to increase patient thirst due to oral breathing. As a general rule, a hemilateral nasal approach via the right nostril was chosen to keep the left nostril intact. Nasal packing was not employed after surgery if cerebrospinal fluid leakage was not predicted in the intraoperative period. This provided patients a natural nasal airway via their intact left nostril. If nasal packing was necessary to prevent postoperative cerebrospinal fluid leakage, a breathable space was preserved in the nostril. The patients appeared to tolerate moderate water restriction if they frequently drank small amounts of water, rather than infrequent large amounts. There was no statistically significant difference in postoperative thirst level between water-restricted patients with DI and those without DI. Unfortunately, thirst level data were not available for all patients, but these findings suggest that thirst was not intolerable under moderate water restriction if the patients DI was sufficiently controlled. Limitations This study revealed that the incidence of hyponatremia in patients treated with water restriction after pituitary surgery was significantly lower than that in patients who drank water freely. While body weight, sex ratio, and tumor type distribution did not differ between groups, these factors were not considered when deciding on the maximum allowable volume; thus, all patients in the water restriction group were limited to 2500 ml/day immediately after surgery. Additional studies are also required to determine the optimal start and stop points for this regimen. This was a retrospective study, and we did not perform systematic daily endocrinological tests or water load tests. Therefore, uptake and excretion of electrolytes and daily changes in endocrine functions were not evaluated. Hence, a multicenter, prospective study including these tests is needed. CONCLUSION To our knowledge, this is the first study to test a potential method for preventing hyponatremia following TSS. Although there might be other causes of hyponatremia other than postoperative water excess, for example, adrenal insufficiency, moderate water restriction after pituitary surgery is a potentially effective and safe method to reduce hyponatremia. Indeed, hyponatremia after TSS is a largely preventable complication. Patients should not drink water freely after TSS, even if they are normonatremic and develop DI. The optimal amount and duration of water restriction are still unclear and require larger-scale multicenter trials. Funding: None Conflict of Interest: None
10 82 Kazuhito Takeuchi et al. REFERENCES 1) Adams JR, Blevins LS Jr., Allen GS, Verity DK, Devin JK: Disorders of water metabolism following transsphenoidal pituitary surgery: a single institution s experience. Pituitary 2006; 9: ) Adrogué HJ, Madias NE: Hyponatremia. N Engl J Med 2000; 342: ) Ausiello JC, Bruce JN, Freda PU: Postoperative assessment of the patient after transsphenoidal pituitary surgery. Pituitary 2008; 11: ) Ciric I, Ragin A, Baumgartner C, Pierce D: Complications of transsphenoidal surgery: results of a national survey, review of the literature, and personal experience. Neurosurgery 1997; 40: ) Gill G, Huda B, Boyd A, Skagen K, Wile D, Watson I, van Heyningen C: Characteristics and mortality of severe hyponatraemia a hospital-based study. Clin Endocrinol (Oxf) 2006; 65: ) Hans P, Stevenaert A, Albert A: Study of hypotonic polyuria after trans-sphenoidal pituitary adenomectomy. Intensive Care Med 1986; 12: ) Hensen J, Henig A, Fahlbusch R, Meyer M, Boehnert M, Buchfelder M: Prevalence, predictors and patterns of postoperative polyuria and hyponatraemia in the immediate course after transsphenoidal surgery for pituitary adenomas. Clin Endocrinol (Oxf) 1999; 50: ) Kamoi K, Tamura T, Tanaka K, Ishibashi M, Yamaji T: Hyponatremia and osmoregulation of thirst and vasopressin secretion in patients with adrenal insufficiency. J Clin Endocrinol Metab 1993; 77: ) Kelly DF, Laws ER Jr, Fossett D: Delayed hyponatremia after transsphenoidal surgery for pituitary adenoma: report of nine cases. J Neurosurg 1995; 83: ) Kinoshita Y, Tominaga A, Arita K, Sugiyama K, Hanaya R, Hama S, Sakoguchi T, Usui S, Kurisu K: Post-operative hyponatremia in patients with pituitary adenoma: post-operative management with a uniform treatment protocol. Endocr J 2011; 58: ) Kristof RA, Rother M, Neuloh G, Klingmueller D: Incidence, clinical manifestations, and course of water and electrolyte metabolism disturbances following transsphenoidal pituitary adenoma surgery: a prospective observational study. J Neurosurg 2009; 111: ) Nemergut EC, Zuo Z, Jane JA Jr, Laws ER Jr.: Predictors of diabetes insipidus after transsphenoidal surgery: a review of 881 patients. J Neurosurg 2005; 103: ) Olson BR, Gumowski J, Rubino D, Oldfield EH: Pathophysiology of hyponatremia after transsphenoidal pituitary surgery. J Neurosurg 1997; 87: ) Poon WS, Lolin YI, Yeung TF, Yip CP, Goh KY, Lam MK, Cockram C: Water and sodium disorders following surgical excision of pituitary region tumors. Acta Neurochir (Wien) 1996; 138: ) Rahman M, Friedman WA: Hyponatremia in neurosurgical patients: clinical guidelines development. Neurosurgery 2009; 65: ) Sane T, Rantakari K, Poranen A, Tähtelä R, Välimäki M, Pelkonen R: Hyponatremia after transsphenoidal surgery for pituitary tumors. J Clin Endocrinol Metab 1994; 79: ) Sata A, Hizuka N, Kawamata T, Hori T, Takano K: Hyponatremia after transsphenoidal surgery for hypothalamo-pituitary tumors. Neuroendocrinology 2006; 83: ) Sigounas DG, Sharpless JL, Cheng DM, Johnson TG, Senior BA, Ewend MG: Predictors and incidence of central diabetes insipidus after endoscopic pituitary surgery. Neurosurgery 2008; 62: ) Taylor SL, Tyrrell JB, Wilson CB: Delayed onset of hyponatremia after transsphenoidal surgery for pituitary adenomas. Neurosurgery 1995; 37: ) Ultmann MC, Hoffman GE, Nelson PB, Robinson AG: Transient hyponatremia after damage to the neurohypophyseal tracts. Neuroendocrinology 1992; 56: ) Zada G, Liu CY, Fishback D, Singer PA, Weiss MH: Recognition and management of delayed hyponatremia following transsphenoidal pituitary surgery. J Neurosurg 2007; 106:
Delayed Hyponatremia Following Transsphenoidal Surgery for Pituitary Adenoma
 Neurol Med Chir (Tokyo) 48, 489 494, 2008 Delayed Hyponatremia Following Transsphenoidal Surgery for Pituitary Adenoma Jae Il LEE, WonHoCHO*, ByungKwanCHOI, Seung Heon CHA, Geun Sung SONG, and Chang Hwa
Neurol Med Chir (Tokyo) 48, 489 494, 2008 Delayed Hyponatremia Following Transsphenoidal Surgery for Pituitary Adenoma Jae Il LEE, WonHoCHO*, ByungKwanCHOI, Seung Heon CHA, Geun Sung SONG, and Chang Hwa
cc/kg mmol/kg ADH i- Incidental ii- Hour glass iii- Diabetes Insipidus iv- Centeral diabetes insipidus v -Supra optic vi- Median emminance iii
 ( ) - ()... (DI) : DI. :. DI ( ) DI.... - DI. ( ) ( ) Immediate DI DI. Minirin DI DI DI (%) :. ( ) Delayed DI ( ) (%/) DI. Delayed DI (%) Immediate DI (%) DI.. (%/) (%/) (%/) Delayed DI. DI Minirin (%)
( ) - ()... (DI) : DI. :. DI ( ) DI.... - DI. ( ) ( ) Immediate DI DI. Minirin DI DI DI (%) :. ( ) Delayed DI ( ) (%/) DI. Delayed DI (%) Immediate DI (%) DI.. (%/) (%/) (%/) Delayed DI. DI Minirin (%)
Predictors of diabetes insipidus after transsphenoidal surgery: a review of 881 patients
 J Neurosurg 103:448 454, 2005 Predictors of diabetes insipidus after transsphenoidal surgery: a review of 881 patients EDWARD C. NEMERGUT, M.D., ZHIYI ZUO, M.D., PH.D., JOHN A. JANE JR., M.D., AND EDWARD
J Neurosurg 103:448 454, 2005 Predictors of diabetes insipidus after transsphenoidal surgery: a review of 881 patients EDWARD C. NEMERGUT, M.D., ZHIYI ZUO, M.D., PH.D., JOHN A. JANE JR., M.D., AND EDWARD
Peri-op Pituitary / Diabetes Insipidus/ Apoplexy Dr. Stan Van Uum, MD, PhD, FRCPC
 10 th Annual Canadian Endocrine Update 3 rd Canadian Endocrine Review Course Peri-op Pituitary / Diabetes Insipidus/ Apoplexy Dr. Stan Van Uum, MD, PhD, FRCPC 10 th Annual Canadian Endocrine Update Dr.
10 th Annual Canadian Endocrine Update 3 rd Canadian Endocrine Review Course Peri-op Pituitary / Diabetes Insipidus/ Apoplexy Dr. Stan Van Uum, MD, PhD, FRCPC 10 th Annual Canadian Endocrine Update Dr.
Delayed postoperative hyponatremia after transsphenoidal surgery: prevalence and associated factors
 J Neurosurg 119:1453 1460, 2013 AANS, 2013 Delayed postoperative hyponatremia after transsphenoidal surgery: prevalence and associated factors Clinical article Namath S. Hussain, M.D., M.B.A., 1 Mackenzie
J Neurosurg 119:1453 1460, 2013 AANS, 2013 Delayed postoperative hyponatremia after transsphenoidal surgery: prevalence and associated factors Clinical article Namath S. Hussain, M.D., M.B.A., 1 Mackenzie
Process / Evidence Class. Clinical Assessment / III
 Table 2: Endocrine Author Cozzi et al (2009) 1 Study Design: Prospectively followed case series. Fourteen patients had pre-op hypocortisolism. Patient Population: Seventy-two adult patients who underwent
Table 2: Endocrine Author Cozzi et al (2009) 1 Study Design: Prospectively followed case series. Fourteen patients had pre-op hypocortisolism. Patient Population: Seventy-two adult patients who underwent
Neuroendocrine challenges following hemispherectomy
 Neuroendocrine challenges following hemispherectomy Philip S. Zeitler MD. PhD Professor and Head Section of Endocrinology Children s Hospital Colorado University of Colorado Anschutz Medical Campus I am
Neuroendocrine challenges following hemispherectomy Philip S. Zeitler MD. PhD Professor and Head Section of Endocrinology Children s Hospital Colorado University of Colorado Anschutz Medical Campus I am
See the latest estimates for new cases of pituitary tumors in the US and what research is currently being done.
 About Pituitary Tumors Overview and Types If you have been diagnosed with a pituitary tumor or worried about it, you likely have a lot of questions. Learning some basics is a good place to start. What
About Pituitary Tumors Overview and Types If you have been diagnosed with a pituitary tumor or worried about it, you likely have a lot of questions. Learning some basics is a good place to start. What
Imaging pituitary gland tumors
 November 2005 Imaging pituitary gland tumors Neel Varshney,, Harvard Medical School Year IV Two categories of presenting signs of a pituitary mass Functional tumors present with symptoms due to excess
November 2005 Imaging pituitary gland tumors Neel Varshney,, Harvard Medical School Year IV Two categories of presenting signs of a pituitary mass Functional tumors present with symptoms due to excess
Urgent and Emergent Pituitary Conditions
 Urgent and Emergent Pituitary Conditions PANKAJ A. GORE, MD DIRECTOR, BRAIN AND SKULL BASE T UMOR SURGERY PROVIDENCE B R AIN AND S PINE I NSTITUTE Urgent and Emergent Pituitary Conditions Neurosurgical
Urgent and Emergent Pituitary Conditions PANKAJ A. GORE, MD DIRECTOR, BRAIN AND SKULL BASE T UMOR SURGERY PROVIDENCE B R AIN AND S PINE I NSTITUTE Urgent and Emergent Pituitary Conditions Neurosurgical
CSF Rhinorrhoea after Transsphenoidal Surgery
 ISPUB.COM The Internet Journal of Neurosurgery Volume 5 Number 1 CSF Rhinorrhoea after Transsphenoidal Surgery E Elgamal Citation E Elgamal. CSF Rhinorrhoea after Transsphenoidal Surgery. The Internet
ISPUB.COM The Internet Journal of Neurosurgery Volume 5 Number 1 CSF Rhinorrhoea after Transsphenoidal Surgery E Elgamal Citation E Elgamal. CSF Rhinorrhoea after Transsphenoidal Surgery. The Internet
Preliminary Experience with 3-Tesla MRI and Cushing s Disease
 TECHNICAL NOTE Preliminary Experience with 3-Tesla MRI and Cushing s Disease LouisJ.Kim,M.D., 1 Gregory P. Lekovic, M.D., Ph.D., J.D., 1 William L.White, M.D., 1 and John Karis, M.D. 2 ABSTRACT Because
TECHNICAL NOTE Preliminary Experience with 3-Tesla MRI and Cushing s Disease LouisJ.Kim,M.D., 1 Gregory P. Lekovic, M.D., Ph.D., J.D., 1 William L.White, M.D., 1 and John Karis, M.D. 2 ABSTRACT Because
Review Derleme. Mehtap Cakir. In tro duc ti on
 28 Review Derleme Water and Salt Metabolism Disorders Following Transsphenoidal Pituitary Surgery Transsfenoidal Hipofiz Cerrahisi Sonrası Görülen Sıvı Elektrolit Bozuklukları Selcuk University Meram School
28 Review Derleme Water and Salt Metabolism Disorders Following Transsphenoidal Pituitary Surgery Transsfenoidal Hipofiz Cerrahisi Sonrası Görülen Sıvı Elektrolit Bozuklukları Selcuk University Meram School
Lab bulletin. Copeptin
 b 24 w w w. b i o s c i e n t i a. c o m Lab bulletin Polyuria-polydipsia syndrome: improved differential diagnosis Pituitary surgery: easy monitoring for vasopressin deficiency Traumatic brain injury:
b 24 w w w. b i o s c i e n t i a. c o m Lab bulletin Polyuria-polydipsia syndrome: improved differential diagnosis Pituitary surgery: easy monitoring for vasopressin deficiency Traumatic brain injury:
DOWNLOAD OR READ : SYNDROME OF INAPPROPRIATE SECRETION OF ANTIDIURETIC HORMONE IN MALIGNANCY PDF EBOOK EPUB MOBI
 DOWNLOAD OR READ : SYNDROME OF INAPPROPRIATE SECRETION OF ANTIDIURETIC HORMONE IN MALIGNANCY PDF EBOOK EPUB MOBI Page 1 Page 2 syndrome of inappropriate secretion of antidiuretic hormone in malignancy
DOWNLOAD OR READ : SYNDROME OF INAPPROPRIATE SECRETION OF ANTIDIURETIC HORMONE IN MALIGNANCY PDF EBOOK EPUB MOBI Page 1 Page 2 syndrome of inappropriate secretion of antidiuretic hormone in malignancy
MANAGEMENT OF PATIENTS WITH PITUITARY DISORDERS ON THE NEUROSUGERY WARDS RESPONSIBILITIES OF THE METABOLIC REGISTRAR
 MANAGEMENT OF PATIENTS WITH PITUITARY DISORDERS ON THE NEUROSUGERY WARDS RESPONSIBILITIES OF THE METABOLIC REGISTRAR We have clear links with DCN and a responsibility for the management of patients with
MANAGEMENT OF PATIENTS WITH PITUITARY DISORDERS ON THE NEUROSUGERY WARDS RESPONSIBILITIES OF THE METABOLIC REGISTRAR We have clear links with DCN and a responsibility for the management of patients with
A Boy with Optic Glioma
 Clin Pediatr Endocrinol 1994;3(Suppl 4): 169-173 Copyright(C)1994 by The Japanese Society for Pediatric Endocrinology Taisuke Okada, Sumitaka Dohno, Yousei Shimasaki, Takashi Tomoda, Makiko Koga, Kumiko
Clin Pediatr Endocrinol 1994;3(Suppl 4): 169-173 Copyright(C)1994 by The Japanese Society for Pediatric Endocrinology Taisuke Okada, Sumitaka Dohno, Yousei Shimasaki, Takashi Tomoda, Makiko Koga, Kumiko
The efficacy and morbidity for transsphenoidal surgery. Morbidity of repeat transsphenoidal surgery assessed in more than 1000 operations
 J Neurosurg 121:67 74, 2014 AANS, 2014 Morbidity of repeat transsphenoidal surgery assessed in more than 1000 operations Clinical article Arman Jahangiri, B.S., Jeffrey Wagner, B.S., Sung Won Han, Corinna
J Neurosurg 121:67 74, 2014 AANS, 2014 Morbidity of repeat transsphenoidal surgery assessed in more than 1000 operations Clinical article Arman Jahangiri, B.S., Jeffrey Wagner, B.S., Sung Won Han, Corinna
Hypothalamus & Pituitary Gland
 Hypothalamus & Pituitary Gland Hypothalamus and Pituitary Gland The hypothalamus and pituitary gland form a unit that exerts control over the function of several endocrine glands (thyroid, adrenals, and
Hypothalamus & Pituitary Gland Hypothalamus and Pituitary Gland The hypothalamus and pituitary gland form a unit that exerts control over the function of several endocrine glands (thyroid, adrenals, and
Imaging The Turkish Saddle. Russell Goodman, HMS III Dr. Gillian Lieberman
 Imaging The Turkish Saddle Russell Goodman, HMS III Dr. Gillian Lieberman Learning Objectives Review the anatomy of the sellar region Discuss the differential diagnosis of sellar masses Discuss typical
Imaging The Turkish Saddle Russell Goodman, HMS III Dr. Gillian Lieberman Learning Objectives Review the anatomy of the sellar region Discuss the differential diagnosis of sellar masses Discuss typical
Iposodiemia: diagnosi e trattamento
 Iposodiemia: diagnosi e trattamento Enrico Fiaccadori Unita di Fisiopatologia dell Insufficienza Renale Acuta e Cronica Dipartimento di Medicina Clinica e Sperimentale Universita degli Studi di Parma Hyponatremia
Iposodiemia: diagnosi e trattamento Enrico Fiaccadori Unita di Fisiopatologia dell Insufficienza Renale Acuta e Cronica Dipartimento di Medicina Clinica e Sperimentale Universita degli Studi di Parma Hyponatremia
Neurohypophysis. AVP Receptors. Hyponatremia in Pituitary Disorders 9/29/2016. Lewis S. Blevins, Jr., M.D.
 in Pituitary Disorders Lewis S. Blevins, Jr., M.D. Neurohypophysis AVP secreting neurons in SON and PVN Osmo- and thirst receptors/centers in anterior hypothalamus Ascending pathways from ANS and brainstem
in Pituitary Disorders Lewis S. Blevins, Jr., M.D. Neurohypophysis AVP secreting neurons in SON and PVN Osmo- and thirst receptors/centers in anterior hypothalamus Ascending pathways from ANS and brainstem
Case Report A Case of Rathke s Cleft Cyst Associated with Transient Central Adrenal Insufficiency and Masked Diabetes Insipidus
 Hindawi Publishing Corporation Case Reports in Endocrinology Volume, Article ID 699, 6 pages http://dx.doi.org/.//699 Case Report A Case of Rathke s Cleft Cyst Associated with Transient Central Adrenal
Hindawi Publishing Corporation Case Reports in Endocrinology Volume, Article ID 699, 6 pages http://dx.doi.org/.//699 Case Report A Case of Rathke s Cleft Cyst Associated with Transient Central Adrenal
CCRN/PCCN Review Course May 30, 2013
 A & P Review CCRN/PCCN Review Course May 30, 2013 Endocrine Anterior pituitary Growth hormone: long bone growth Thyroid stimulating hormone: growth, thyroid secretion Adrenocorticotropic hormone: growth,
A & P Review CCRN/PCCN Review Course May 30, 2013 Endocrine Anterior pituitary Growth hormone: long bone growth Thyroid stimulating hormone: growth, thyroid secretion Adrenocorticotropic hormone: growth,
Endocrinological Outcome Among Treated Craniopharyngioma Patients
 Endocrinological Outcome Among Treated Craniopharyngioma Patients Afaf Al Sagheir, MD Head & Consultant, Section of Endocrinology/Diabetes Department of Pediatrics KFSH&RC Introduction Craniopharyngiomas
Endocrinological Outcome Among Treated Craniopharyngioma Patients Afaf Al Sagheir, MD Head & Consultant, Section of Endocrinology/Diabetes Department of Pediatrics KFSH&RC Introduction Craniopharyngiomas
Pathology of pituitary gland. By: Shifaa Qa qa
 Pathology of pituitary gland By: Shifaa Qa qa Sella turcica Adenohypophysis (80%): - epithelial cells - acidophil, basophil, chromophobe - Somatotrophs, Mammosomatotrophs, Corticotrophs, Thyrotrophs, Gonadotrophs
Pathology of pituitary gland By: Shifaa Qa qa Sella turcica Adenohypophysis (80%): - epithelial cells - acidophil, basophil, chromophobe - Somatotrophs, Mammosomatotrophs, Corticotrophs, Thyrotrophs, Gonadotrophs
Clinical significance of thickened sphenoid sinus mucosa in Rathke s cleft cyst
 SNI: General Neurosurgery OPEN ACCESS For entire Editorial Board visit : http://www.surgicalneurologyint.com Editor: C. David Hunt, M.D. Marquette General Neurosurgery, Brooklyn, NY, USA Original Article
SNI: General Neurosurgery OPEN ACCESS For entire Editorial Board visit : http://www.surgicalneurologyint.com Editor: C. David Hunt, M.D. Marquette General Neurosurgery, Brooklyn, NY, USA Original Article
Pituitary Tumors and Incidentalomas. Bijan Ahrari, MD, FACE, ECNU Palm Medical Group
 Pituitary Tumors and Incidentalomas Bijan Ahrari, MD, FACE, ECNU Palm Medical Group Background Pituitary incidentaloma: a previously unsuspected pituitary lesion that is discovered on an imaging study
Pituitary Tumors and Incidentalomas Bijan Ahrari, MD, FACE, ECNU Palm Medical Group Background Pituitary incidentaloma: a previously unsuspected pituitary lesion that is discovered on an imaging study
Immediate postoperative complications in transsphenoidal pituitary surgery: A prospective study
 ORIGINAL ARTICLE Page 335 Immediate postoperative complications in transsphenoidal pituitary surgery: A prospective study Tumul Chowdhury, Hemanshu Prabhakar 1, Parmod K. Bithal 1, Bernhard Schaller 2,
ORIGINAL ARTICLE Page 335 Immediate postoperative complications in transsphenoidal pituitary surgery: A prospective study Tumul Chowdhury, Hemanshu Prabhakar 1, Parmod K. Bithal 1, Bernhard Schaller 2,
JACK L. SNITZER, DO INTERNAL MEDICINE BOARD REVIEW COURSE 2018 PITUITARY
 JACK L. SNITZER, DO INTERNAL MEDICINE BOARD REVIEW COURSE 2018 PITUITARY JACK L. SNITZER, D.O. Peninsula Regional Endocrinology 1415 S. Division Street Salisbury, MD 21804 Phone:410-572-8848 Fax:410-572-6890
JACK L. SNITZER, DO INTERNAL MEDICINE BOARD REVIEW COURSE 2018 PITUITARY JACK L. SNITZER, D.O. Peninsula Regional Endocrinology 1415 S. Division Street Salisbury, MD 21804 Phone:410-572-8848 Fax:410-572-6890
Wales Critical Care & Trauma Network (North) Management of Hyponatraemia in Intensive Care Guidelines
 Wales Critical Care & Trauma Network (North) Management of Hyponatraemia in Intensive Care Guidelines Author: Richard Pugh June 2015 Guideline for management of hyponatraemia in intensive care Background
Wales Critical Care & Trauma Network (North) Management of Hyponatraemia in Intensive Care Guidelines Author: Richard Pugh June 2015 Guideline for management of hyponatraemia in intensive care Background
Pituitary adenoma is one of the common brain. Pituitary Adenoma Surgery: Retrospective Analysis of My Personal Experience
 Original Article Nepal Journal of Neuroscience 13:63-67, 2016 Prabin Shrestha, MD, PhD Anish M Singh, MS Address for correspondence: Prabin Shrestha, MD, PhD Email: prabinshrestha@hotmail.com Received,
Original Article Nepal Journal of Neuroscience 13:63-67, 2016 Prabin Shrestha, MD, PhD Anish M Singh, MS Address for correspondence: Prabin Shrestha, MD, PhD Email: prabinshrestha@hotmail.com Received,
Endoscopic Endonasal Surgery for Subdiaphragmatic Type Craniopharyngiomas
 Original Article doi: 10.2176/nmc.oa.2018-0028 Neurol Med Chir (Tokyo) 58, 260 265, 2018 Endoscopic Endonasal Surgery for Subdiaphragmatic Type Craniopharyngiomas Hiroshi NISHIOKA, 1,2 Yuichi NAGATA, 1
Original Article doi: 10.2176/nmc.oa.2018-0028 Neurol Med Chir (Tokyo) 58, 260 265, 2018 Endoscopic Endonasal Surgery for Subdiaphragmatic Type Craniopharyngiomas Hiroshi NISHIOKA, 1,2 Yuichi NAGATA, 1
Skullbase Lesions. Skullbase Surgery Open vs endoscopic. Choice Of Surgical Approaches 12/28/2015. Skullbase Surgery: Evolution
 Skullbase Lesions Skullbase Surgery Open vs endoscopic Prof Asim Mahmood,FRCS,FACS,FICS,FAANS, Professor of Neurosurgery Henry Ford Hospital Detroit, MI, USA Anterior Cranial Fossa Subfrontal meningioma
Skullbase Lesions Skullbase Surgery Open vs endoscopic Prof Asim Mahmood,FRCS,FACS,FICS,FAANS, Professor of Neurosurgery Henry Ford Hospital Detroit, MI, USA Anterior Cranial Fossa Subfrontal meningioma
Comparison of incidence of hyponatremia between intranasal and oral desmopressin in patients with central diabetes insipidus
 Endocrine Journal 2015, 62 (2), 195-200 Original Comparison of incidence of hyponatremia between intranasal and oral desmopressin in patients with central diabetes insipidus Yuko Kataoka 1), Sachi Nishida
Endocrine Journal 2015, 62 (2), 195-200 Original Comparison of incidence of hyponatremia between intranasal and oral desmopressin in patients with central diabetes insipidus Yuko Kataoka 1), Sachi Nishida
October 13, Surgical Nuances to Managing Cushing s Disease. Cortisol Regulation. Cushing s Syndrome Excess Cortisol. Sandeep Kunwar, M.D.
 Surgical Nuances to Managing Cushing s Disease Cortisol Regulation Sandeep Kunwar, M.D. Surgical Director, California Center for Pituitary Disorders Associate Clinical Professor, University of California,
Surgical Nuances to Managing Cushing s Disease Cortisol Regulation Sandeep Kunwar, M.D. Surgical Director, California Center for Pituitary Disorders Associate Clinical Professor, University of California,
Diseases of pituitary gland
 Diseases of pituitary gland A brief introduction Anterior lobe = adenohypophysis Posterior lobe = neurohypophysis The production of most pituitary hormones is controlled in large part by positively and
Diseases of pituitary gland A brief introduction Anterior lobe = adenohypophysis Posterior lobe = neurohypophysis The production of most pituitary hormones is controlled in large part by positively and
Pituitary Disorders. Eiman Ali Basheir Mob: /1/2019
 Pituitary Disorders Eiman Ali Basheir Mob: 0915020385 31/1/2019 Objectives By the end of this lecture the students will be able to: Understand basic Pituitary axis physiology State the common causes of
Pituitary Disorders Eiman Ali Basheir Mob: 0915020385 31/1/2019 Objectives By the end of this lecture the students will be able to: Understand basic Pituitary axis physiology State the common causes of
Long term outcome following repeat transsphenoidal surgery for recurrent endocrine-inactive pituitary adenomas
 Pituitary (2010) 13:223 229 DOI 10.1007/s11102-010-0221-z Long term outcome following repeat transsphenoidal surgery for recurrent endocrine-inactive pituitary adenomas Edward F. Chang Michael E. Sughrue
Pituitary (2010) 13:223 229 DOI 10.1007/s11102-010-0221-z Long term outcome following repeat transsphenoidal surgery for recurrent endocrine-inactive pituitary adenomas Edward F. Chang Michael E. Sughrue
Supplemental Information
 FROM THE AMERICAN ACADEMY OF PEDIATRICS Supplemental Information SUPPLEMENTAL FIGURE 2 Forest plot of all included RCTs using a random-effects model and M-H statistics with the outcome of hyponatremia
FROM THE AMERICAN ACADEMY OF PEDIATRICS Supplemental Information SUPPLEMENTAL FIGURE 2 Forest plot of all included RCTs using a random-effects model and M-H statistics with the outcome of hyponatremia
Disorders of water and sodium homeostasis. Prof A. Pomeranz 2017
 Disorders of water and sodium homeostasis Prof A. Pomeranz 2017 Pediatric (Nephrology) Tool Box Disorders of water and sodium homeostasis Pediatric Nephrology Tool Box Hyponatremiaand and Hypernatremia
Disorders of water and sodium homeostasis Prof A. Pomeranz 2017 Pediatric (Nephrology) Tool Box Disorders of water and sodium homeostasis Pediatric Nephrology Tool Box Hyponatremiaand and Hypernatremia
Hyponatraemia: confident diagnosis, effective treatment and avoiding disasters. Dr James Ahlquist Endocrinologist Southend Hospital
 Hyponatraemia: confident diagnosis, effective treatment and avoiding disasters Dr James Ahlquist Endocrinologist Southend Hospital Hyponatraemia: a common electrolyte disorder Electrolyte disorder Prevalence
Hyponatraemia: confident diagnosis, effective treatment and avoiding disasters Dr James Ahlquist Endocrinologist Southend Hospital Hyponatraemia: a common electrolyte disorder Electrolyte disorder Prevalence
ENDOCRINE OUTCOMES OF TRANS-SPHENOIDAL SURGERY FOR PITUITARY APOPLEXY VERSUS ELECTIVE SURGERY FOR PITUITARY ADENOMA
 ENDOCRINE PRACTICE Rapid Electronic Article in Press Rapid Electronic Articles in Press are preprinted manuscripts that have been reviewed and accepted for publication, but have yet to be edited, typeset
ENDOCRINE PRACTICE Rapid Electronic Article in Press Rapid Electronic Articles in Press are preprinted manuscripts that have been reviewed and accepted for publication, but have yet to be edited, typeset
Laurie A. Loevner, MD
 Laurie A. Loevner, MD Chief, Division of Neuroradiology UPHS Professor of Radiology, Otorhinolaryngology: Head & Neck Surgery, Neurosurgery, and Ophthalmology University of Pennsylvania Health System Disclosures
Laurie A. Loevner, MD Chief, Division of Neuroradiology UPHS Professor of Radiology, Otorhinolaryngology: Head & Neck Surgery, Neurosurgery, and Ophthalmology University of Pennsylvania Health System Disclosures
AACE/ACE Disease State Clinical Review
 AACE/ACE Disease State Clinical Review Whitney W. Woodmansee, MD 1 ; John Carmichael, MD 2 ; Daniel Kelly, MD 3 ; Laurence Katznelson, MD 4 ; on behalf of the AACE Neuroendocrine and Pituitary Scientific
AACE/ACE Disease State Clinical Review Whitney W. Woodmansee, MD 1 ; John Carmichael, MD 2 ; Daniel Kelly, MD 3 ; Laurence Katznelson, MD 4 ; on behalf of the AACE Neuroendocrine and Pituitary Scientific
Hyponatremia. Mis-named talk? Basic Pathophysiology
 Hyponatremia Great Lakes Hospital Medicine Symposium by Brian Wolfe, MD Assistant Professor of Internal Medicine University of Colorado Denver Mis-named talk? Why do we care about Hyponatremia? concentration
Hyponatremia Great Lakes Hospital Medicine Symposium by Brian Wolfe, MD Assistant Professor of Internal Medicine University of Colorado Denver Mis-named talk? Why do we care about Hyponatremia? concentration
Describe the epidemiology and clinical presentations of pituitary tumours:
 Pituitary Tumours: Describe the epidemiology and clinical presentations of pituitary tumours: 10-15% of all primary brain tumours More common in females Unselected autopsy studies 20-25% of population
Pituitary Tumours: Describe the epidemiology and clinical presentations of pituitary tumours: 10-15% of all primary brain tumours More common in females Unselected autopsy studies 20-25% of population
Syndrome of Inappropriate Secretion of Antidiuretic Hormone (SIADH) and Adrenal Insufficiency Induced by Rathke's Cleft Cyst: A Case Report
 Endocrine Journal 2000, 47 (4), 393-399 Syndrome of Inappropriate Secretion of Antidiuretic Hormone (SIADH) and Adrenal Insufficiency Induced by Rathke's Cleft Cyst: A Case Report HIROSHI IWAI, YASUHIRO
Endocrine Journal 2000, 47 (4), 393-399 Syndrome of Inappropriate Secretion of Antidiuretic Hormone (SIADH) and Adrenal Insufficiency Induced by Rathke's Cleft Cyst: A Case Report HIROSHI IWAI, YASUHIRO
Risk factors and rates of delayed symptomatic hyponatremia after transsphenoidal surgery: a systematic review
 Boston University OpenBU Theses & Dissertations http://open.bu.edu Boston University Theses & Dissertations 2016 Risk factors and rates of delayed symptomatic hyponatremia after transsphenoidal surgery:
Boston University OpenBU Theses & Dissertations http://open.bu.edu Boston University Theses & Dissertations 2016 Risk factors and rates of delayed symptomatic hyponatremia after transsphenoidal surgery:
ACROMEGALY OCCURRING IN A PATIENT WITH A PITUITARY ADENOMA, LYMPHOCYTIC HYPOPHYSITIS, AND A RATHKE CLEFT CYST
 Case Report ACROMEGALY OCCURRING IN A PATIENT WITH A PITUITARY ADENOMA, LYMPHOCYTIC HYPOPHYSITIS, AND A RATHKE CLEFT CYST Anupa Sharma, DO 1 ; Eric K.Richfield, MD, PhD 2 ; Sara E. Lubitz, MD 1 ABSTRACT
Case Report ACROMEGALY OCCURRING IN A PATIENT WITH A PITUITARY ADENOMA, LYMPHOCYTIC HYPOPHYSITIS, AND A RATHKE CLEFT CYST Anupa Sharma, DO 1 ; Eric K.Richfield, MD, PhD 2 ; Sara E. Lubitz, MD 1 ABSTRACT
BALANCE 13 DISORDERS OF WATER DISORDERS CHARACTERISED BY POLYDIPSIA AND POLYURIA. (vasopressin deficiency) 1 [primary] [secondary 6C] insipidus
![BALANCE 13 DISORDERS OF WATER DISORDERS CHARACTERISED BY POLYDIPSIA AND POLYURIA. (vasopressin deficiency) 1 [primary] [secondary 6C] insipidus BALANCE 13 DISORDERS OF WATER DISORDERS CHARACTERISED BY POLYDIPSIA AND POLYURIA. (vasopressin deficiency) 1 [primary] [secondary 6C] insipidus](/thumbs/80/80940031.jpg) Wit JM, Ranke MB, Kelnar CJH (eds): ESPE classification of paediatric endocrine diagnosis. 13. Disorders of water balance. Horm Res 2007;68(suppl 2):96 97 ESPE Code Diagnosis OMIM ICD10 13 DISORDERS OF
Wit JM, Ranke MB, Kelnar CJH (eds): ESPE classification of paediatric endocrine diagnosis. 13. Disorders of water balance. Horm Res 2007;68(suppl 2):96 97 ESPE Code Diagnosis OMIM ICD10 13 DISORDERS OF
A survey of pituitary incidentaloma in Japan
 European Journal of Endocrinology (2003) 149 123 127 ISSN 0804-4643 CLINICAL STUDY A survey of pituitary incidentaloma in Japan Naoko Sanno, Ken ichi Oyama, Shigeyuki Tahara, Akira Teramoto and Yuzuru
European Journal of Endocrinology (2003) 149 123 127 ISSN 0804-4643 CLINICAL STUDY A survey of pituitary incidentaloma in Japan Naoko Sanno, Ken ichi Oyama, Shigeyuki Tahara, Akira Teramoto and Yuzuru
Department of Neurosurgery and The California Center for Pituitary Disorders, University of California, San Francisco, California
 clinical article J Neurosurg 124:589 595, 2016 Improved versus worsened endocrine function after transsphenoidal surgery for nonfunctional pituitary adenomas: rate, time course, and radiological analysis
clinical article J Neurosurg 124:589 595, 2016 Improved versus worsened endocrine function after transsphenoidal surgery for nonfunctional pituitary adenomas: rate, time course, and radiological analysis
CENTENE PHARMACY AND THERAPEUTICS DRUG REVIEW 3Q17 July-August
 BRAND NAME Noctiva GENERIC NAME Desmopressin acetate nasal spray MANUFACTURER Serenity Pharmaceuticals DATE OF APPROVAL March 3, 2017 PRODUCT LAUNCH DATE TBD REVIEW TYPE Review type 1 (RT1): New Drug Review
BRAND NAME Noctiva GENERIC NAME Desmopressin acetate nasal spray MANUFACTURER Serenity Pharmaceuticals DATE OF APPROVAL March 3, 2017 PRODUCT LAUNCH DATE TBD REVIEW TYPE Review type 1 (RT1): New Drug Review
Original Article. Abstract. Introduction. Thinesh Kumran 1,2, Saffari Haspani 1,2, Jafri Malin Abdullah 1,4, Azmi Alias 1,2, Fan Rui Ven 3
 Original Article Factors Influencing Disconnection Hyperprolactinemia and Reversal of Serum Prolactin after Pituitary Surgery in a Non-Functioning Pituitary Macroadenoma Thinesh Kumran 1,2, Saffari Haspani
Original Article Factors Influencing Disconnection Hyperprolactinemia and Reversal of Serum Prolactin after Pituitary Surgery in a Non-Functioning Pituitary Macroadenoma Thinesh Kumran 1,2, Saffari Haspani
Metoclopramide Domperidone. HYPER- PROLACTINAEMIA: the true and the false problems
 Modern management of Hyperprolactinaemia Didier DEWAILLY, M.D. Department of Endocrine Gynaecology and Reproductive Medicine, Hôpital Jeanne de Flandre, C.H.R.U., 59037 Lille, France 1 Metoclopramide Domperidone
Modern management of Hyperprolactinaemia Didier DEWAILLY, M.D. Department of Endocrine Gynaecology and Reproductive Medicine, Hôpital Jeanne de Flandre, C.H.R.U., 59037 Lille, France 1 Metoclopramide Domperidone
Hyponatremia in Children with Acute Central Nervous System Diseases
 Bahrain Medical Bulletin, Volume 30, No 1, March 2008 Hyponatremia in Children with Acute Central Nervous System Diseases Lamia M Al Naama, PhD* Meaad Kadhum Hassan, CABP** Entisar A. Al Shawi, MSc***
Bahrain Medical Bulletin, Volume 30, No 1, March 2008 Hyponatremia in Children with Acute Central Nervous System Diseases Lamia M Al Naama, PhD* Meaad Kadhum Hassan, CABP** Entisar A. Al Shawi, MSc***
PITUITARY: JUST THE BASICS PART 2 THE PATIENT
 PITUITARY: JUST THE BASICS PART 2 THE PATIENT DISCLOSURE Relevant relationships with commercial entities none Potential for conflicts of interest within this presentation none Steps taken to review and
PITUITARY: JUST THE BASICS PART 2 THE PATIENT DISCLOSURE Relevant relationships with commercial entities none Potential for conflicts of interest within this presentation none Steps taken to review and
33 year old male with a history of resected craniopharyngioma (12 years ago) presents after a seizure. Jess Hwang 9/27/12
 33 year old male with a history of resected craniopharyngioma (12 years ago) presents after a seizure Jess Hwang 9/27/12 Craniopharyngioma history In 2000, at age 22, he presented with headache and blurry
33 year old male with a history of resected craniopharyngioma (12 years ago) presents after a seizure Jess Hwang 9/27/12 Craniopharyngioma history In 2000, at age 22, he presented with headache and blurry
Pituitary Tumors: adenoma, craniopharyngioma, rathke cyst
 Pituitary Tumors: adenoma, craniopharyngioma, rathke cyst Overview Tumors that grow from the pituitary gland can affect the whole body by interfering with normal hormone levels. They can also cause headaches
Pituitary Tumors: adenoma, craniopharyngioma, rathke cyst Overview Tumors that grow from the pituitary gland can affect the whole body by interfering with normal hormone levels. They can also cause headaches
Anesthetic Techniques in Endoscopic Sinus and Skull Base Surgery
 Anesthetic Techniques in Endoscopic Sinus and Skull Base Surgery Martha Cordoba Amorocho, MD Iuliu Fat, MD Supplement to Cordoba Amorocho M, Fat I. Anesthetic techniques in endoscopic sinus and skull base
Anesthetic Techniques in Endoscopic Sinus and Skull Base Surgery Martha Cordoba Amorocho, MD Iuliu Fat, MD Supplement to Cordoba Amorocho M, Fat I. Anesthetic techniques in endoscopic sinus and skull base
Pituitary adenomas in childhood and adolescence ISABELLE L. RICHMOND, M.D., PH.D., AND CHARLES B. WILSON, M.D.
 J Neurosurg 49:163-168, 1978 Pituitary adenomas in childhood and adolescence ISABELLE L. RICHMOND, M.D., PH.D., AND CHARLES B. WILSON, M.D. Department of Neurological Surgery, University of California
J Neurosurg 49:163-168, 1978 Pituitary adenomas in childhood and adolescence ISABELLE L. RICHMOND, M.D., PH.D., AND CHARLES B. WILSON, M.D. Department of Neurological Surgery, University of California
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Fenske W, Refardt J, Chifu I, et al. A copeptin-based approach
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Fenske W, Refardt J, Chifu I, et al. A copeptin-based approach
Pituitary Tumour Surgery. Remember to bring this handout to the hospital with you.
 Pituitary Tumour Surgery Remember to bring this handout to the hospital with you. 1 Pituitary Tumour Surgery Table of contents Page What is the pituitary gland?... 2 What is a pituitary tumour?... 3 Why
Pituitary Tumour Surgery Remember to bring this handout to the hospital with you. 1 Pituitary Tumour Surgery Table of contents Page What is the pituitary gland?... 2 What is a pituitary tumour?... 3 Why
The View through the Nose: ENT considerations for Pituitary/Skull Base Surgery
 The View through the Nose: ENT considerations for Pituitary/Skull Base Surgery Edsel Kim, M.D. Otolaryngology-Head and Neck Surgery The Oregon Clinic Providence Brain and Spine Institute Pituitary, Thyroid
The View through the Nose: ENT considerations for Pituitary/Skull Base Surgery Edsel Kim, M.D. Otolaryngology-Head and Neck Surgery The Oregon Clinic Providence Brain and Spine Institute Pituitary, Thyroid
Evaluation and Management of Pituitary Failure. Dr S. Ali Imran MBBS, FRCP (Edin), FRCPC Professor of Medicine Dalhousie University, Halifax, NS
 Evaluation and Management of Pituitary Failure Dr S. Ali Imran MBBS, FRCP (Edin), FRCPC Professor of Medicine Dalhousie University, Halifax, NS Conflict of Interest None Objectives Diagnostic approach
Evaluation and Management of Pituitary Failure Dr S. Ali Imran MBBS, FRCP (Edin), FRCPC Professor of Medicine Dalhousie University, Halifax, NS Conflict of Interest None Objectives Diagnostic approach
Pituitary, Parathyroid Pheochromocytomas & Paragangliomas: The 4 Ps of NETs
 Pituitary, Parathyroid Pheochromocytomas & Paragangliomas: The 4 Ps of NETs Shereen Ezzat, MD, FRCP(C), FACP Professor Of Medicine & Oncology Head, Endocrine Oncology Princess Margaret Hospital/University
Pituitary, Parathyroid Pheochromocytomas & Paragangliomas: The 4 Ps of NETs Shereen Ezzat, MD, FRCP(C), FACP Professor Of Medicine & Oncology Head, Endocrine Oncology Princess Margaret Hospital/University
Managing Acromegaly: Review of Two Cases
 Managing Acromegaly: Review of Two Cases INDICATION AND USAGE SIGNIFOR LAR (pasireotide) for injectable suspension is a somatostatin analog indicated for the treatment of patients with acromegaly who have
Managing Acromegaly: Review of Two Cases INDICATION AND USAGE SIGNIFOR LAR (pasireotide) for injectable suspension is a somatostatin analog indicated for the treatment of patients with acromegaly who have
182 Ligia Tataranu et al Endoscopic endonasal transsphenoidal approach
 182 Ligia Tataranu et al Endoscopic endonasal transsphenoidal approach Endoscopic endonasal transsphenoidal approach in the management of sellar and parasellar lesions: alternative surgical techniques,
182 Ligia Tataranu et al Endoscopic endonasal transsphenoidal approach Endoscopic endonasal transsphenoidal approach in the management of sellar and parasellar lesions: alternative surgical techniques,
Somatotroph Pituitary Adenomas (Acromegaly) The Diagnostic Pathway (11-2K-234)
 Somatotroph Pituitary Adenomas (Acromegaly) The Diagnostic Pathway (11-2K-234) Common presenting symptoms/clinical assessment: Pituitary adenomas are benign neoplasms of the pituitary gland. In patients
Somatotroph Pituitary Adenomas (Acromegaly) The Diagnostic Pathway (11-2K-234) Common presenting symptoms/clinical assessment: Pituitary adenomas are benign neoplasms of the pituitary gland. In patients
David Henley. Sir Charles Gairdner Hospital, Nedlands WA University of Western Australia. ESA Seminar Weekend, Melbourne Vic 27 th May 2017
 David Henley Sir Charles Gairdner Hospital, Nedlands WA University of Western Australia ESA Seminar Weekend, Melbourne Vic 27 th May 2017 Disclosures Received honoraria from Ipsen, Novartis, Servier, Bristol-Myers
David Henley Sir Charles Gairdner Hospital, Nedlands WA University of Western Australia ESA Seminar Weekend, Melbourne Vic 27 th May 2017 Disclosures Received honoraria from Ipsen, Novartis, Servier, Bristol-Myers
Intrasphenoidal Rathke's Cleft Cyst: Case presentation and review of the literature
 Romanian Neurosurgery Volume XXX Number 4 2016 October - December Article Intrasphenoidal Rathke's Cleft Cyst: Case presentation and review of the literature Umit Kocaman, Muhammet Bahadir Yilmaz, Hakan
Romanian Neurosurgery Volume XXX Number 4 2016 October - December Article Intrasphenoidal Rathke's Cleft Cyst: Case presentation and review of the literature Umit Kocaman, Muhammet Bahadir Yilmaz, Hakan
Trust Guideline for the Pituitary Tumour / other Pituitary Emergency
 A Clinical Guideline For Use in: By: For: Division responsible for document: AMU, Accident and emergency and all other clinical areas All Medical staff Management of patients with suspected pituitary tumours
A Clinical Guideline For Use in: By: For: Division responsible for document: AMU, Accident and emergency and all other clinical areas All Medical staff Management of patients with suspected pituitary tumours
Prolactin-Secreting Pituitary Adenomas (Prolactinomas) The Diagnostic Pathway (11-2K-234)
 Prolactin-Secreting Pituitary Adenomas (Prolactinomas) The Diagnostic Pathway (11-2K-234) Common presenting symptoms/clinical assessment: Pituitary adenomas are benign neoplasms of the pituitary gland.
Prolactin-Secreting Pituitary Adenomas (Prolactinomas) The Diagnostic Pathway (11-2K-234) Common presenting symptoms/clinical assessment: Pituitary adenomas are benign neoplasms of the pituitary gland.
Endoscopic Pituitary Surgery (transsphenoidal)
 Endoscopic Pituitary Surgery (transsphenoidal) Overview Endoscopic surgery is performed through the nose to remove tumors from the pituitary gland and skull base. In this minimally invasive surgery, the
Endoscopic Pituitary Surgery (transsphenoidal) Overview Endoscopic surgery is performed through the nose to remove tumors from the pituitary gland and skull base. In this minimally invasive surgery, the
Central Diabetes Insipidus
 Patient & Family Guide 2018 Central Diabetes Insipidus www.nshealth.ca Central Diabetes Insipidus What is central diabetes insipidus? Central diabetes insipidus (diabetes insipidus or DI) is a rare disorder
Patient & Family Guide 2018 Central Diabetes Insipidus www.nshealth.ca Central Diabetes Insipidus What is central diabetes insipidus? Central diabetes insipidus (diabetes insipidus or DI) is a rare disorder
NOCTIVA (desmopressin acetate) nasal spray
 NOCTIVA (desmopressin acetate) nasal spray Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Pharmacy
NOCTIVA (desmopressin acetate) nasal spray Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Pharmacy
15 month-old female with a cystic brain lesion. Magdalena Dumin, MD Pediatric Endocrinology Fellow University of Chicago December 4, 2014
 + 15 month-old female with a cystic brain lesion Magdalena Dumin, MD Pediatric Endocrinology Fellow University of Chicago December 4, 2014 + Chief Complaint 15 month-old female admitted to PICU for concern
+ 15 month-old female with a cystic brain lesion Magdalena Dumin, MD Pediatric Endocrinology Fellow University of Chicago December 4, 2014 + Chief Complaint 15 month-old female admitted to PICU for concern
Visual pathways in the chiasm
 Visual pathways in the chiasm Intracranial relationships of the optic nerve Fixation of the chiasm Chiasmatic pathologies The function of the optic chiasm may be altered by the presence of : 4) Artero
Visual pathways in the chiasm Intracranial relationships of the optic nerve Fixation of the chiasm Chiasmatic pathologies The function of the optic chiasm may be altered by the presence of : 4) Artero
Cerebral Salt Wasting
 Cerebral Salt Wasting Heather A Martin MSN, RN, CNRN, SCRN Swedish Medical Center 1 Disclosures none 2 2 The problem Hyponatremia is the most common disorder of electrolytes encountered in medical practice
Cerebral Salt Wasting Heather A Martin MSN, RN, CNRN, SCRN Swedish Medical Center 1 Disclosures none 2 2 The problem Hyponatremia is the most common disorder of electrolytes encountered in medical practice
Chapter 13 worksheet
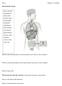 Name: Chapter 13 worksheet The Endocrine System Please label the: hypothalamus pineal gland pituitary gland thyroid gland parathyroid gland thymus heart stomach liver adrenal glands kidneys pancreas small
Name: Chapter 13 worksheet The Endocrine System Please label the: hypothalamus pineal gland pituitary gland thyroid gland parathyroid gland thymus heart stomach liver adrenal glands kidneys pancreas small
HYPONATRAEMIA: NUH GUIDELINE FOR INITIAL ASSESSMENT AND MANAGEMENT.
 HYPONATRAEMIA: NUH GUIDELINE FOR INITIAL ASSESSMENT AND MANAGEMENT. HYPONATRAEMIA: SODIUM < 130 MMOL/L SIGNIFICANT. Symptoms/signs usually only occur when sodium < 125 mmol/l. Acute hyponatraemia is less
HYPONATRAEMIA: NUH GUIDELINE FOR INITIAL ASSESSMENT AND MANAGEMENT. HYPONATRAEMIA: SODIUM < 130 MMOL/L SIGNIFICANT. Symptoms/signs usually only occur when sodium < 125 mmol/l. Acute hyponatraemia is less
TREATMENT OF CUSHING S DISEASE
 TREATMENT OF CUSHING S DISEASE Surgery, Radiation, Medication Peter J Snyder, MD Professor of Medicine Disclosures Novartis Research grant Pfizer Consultant Ipsen Research grant Cortendo Research grant
TREATMENT OF CUSHING S DISEASE Surgery, Radiation, Medication Peter J Snyder, MD Professor of Medicine Disclosures Novartis Research grant Pfizer Consultant Ipsen Research grant Cortendo Research grant
For more information about how to cite these materials visit
 Author(s): Roger Grekin, M.D., 2009 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Noncommercial Share Alike 3.0 License: http://creativecommons.org/licenses/by-nc-sa/3.0/
Author(s): Roger Grekin, M.D., 2009 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Noncommercial Share Alike 3.0 License: http://creativecommons.org/licenses/by-nc-sa/3.0/
Excretory System 1. a)label the parts indicated above and give one function for structures Y and Z
 Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- X- Y- Z- b) Which of the following is not a function of the organ shown? A. to produce
Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- X- Y- Z- b) Which of the following is not a function of the organ shown? A. to produce
Adrenal Ganglioneuroma Presenting With Adrenal Insufficiency After Unilateral Adrenalectomy
 ISPUB.COM The Internet Journal of Urology Volume 9 Number 1 Adrenal Ganglioneuroma Presenting With Adrenal Insufficiency After Unilateral Adrenalectomy S Bontha, N Sanalkumar, M Istarabadi, G Lepsien,
ISPUB.COM The Internet Journal of Urology Volume 9 Number 1 Adrenal Ganglioneuroma Presenting With Adrenal Insufficiency After Unilateral Adrenalectomy S Bontha, N Sanalkumar, M Istarabadi, G Lepsien,
Traumatic Brain Injury
 Traumatic Brain Injury Mark J. Harris M.D. Associate Professor University of Utah Salt Lake City USA Overview In US HI responsible for 33% trauma deaths. Closed HI 80% Missile / Penetrating HI 20% Glasgow
Traumatic Brain Injury Mark J. Harris M.D. Associate Professor University of Utah Salt Lake City USA Overview In US HI responsible for 33% trauma deaths. Closed HI 80% Missile / Penetrating HI 20% Glasgow
Repeat transsphenoidal surgery for Cushing's disease
 J Neurosurg 71:520-527, 1989 Repeat transsphenoidal surgery for Cushing's disease ROBERT B. FRIEDMAN, M.D., EDWARD H. OLDFIELD~ M.D., LYNNETTE K. NIEMAN, M.D., GEORGE P. CHROUSOS, M.D., JOHN L. DOPPMAN,
J Neurosurg 71:520-527, 1989 Repeat transsphenoidal surgery for Cushing's disease ROBERT B. FRIEDMAN, M.D., EDWARD H. OLDFIELD~ M.D., LYNNETTE K. NIEMAN, M.D., GEORGE P. CHROUSOS, M.D., JOHN L. DOPPMAN,
Dr. Dafalla Ahmed Babiker Jazan University
 Dr. Dafalla Ahmed Babiker Jazan University objectives Overview Definition of dehydration Causes of dehydration Types of dehydration Diagnosis, signs and symptoms Management of dehydration Complications
Dr. Dafalla Ahmed Babiker Jazan University objectives Overview Definition of dehydration Causes of dehydration Types of dehydration Diagnosis, signs and symptoms Management of dehydration Complications
After i.v injection 45% of the amount of desmopressin is found in the urine within 24 hours.
 MINIRIN Tablets 0.1 and 0.2 mg Declaration Tablets 0.1 mg. Each tablet contains desmopressin acetate 0.1 mg and excipients q.s Tablets 0.2 mg. Each tablet contains desmopressin acetate 0.2 mg and excipients
MINIRIN Tablets 0.1 and 0.2 mg Declaration Tablets 0.1 mg. Each tablet contains desmopressin acetate 0.1 mg and excipients q.s Tablets 0.2 mg. Each tablet contains desmopressin acetate 0.2 mg and excipients
Long-term results of gamma knife surgery for growth hormone producing pituitary adenoma: is the disease difficult to cure?
 J Neurosurg (Suppl) 102:119 123, 2005 Long-term results of gamma knife surgery for growth hormone producing pituitary adenoma: is the disease difficult to cure? TATSUYA KOBAYASHI, M.D., PH.D., YOSHIMASA
J Neurosurg (Suppl) 102:119 123, 2005 Long-term results of gamma knife surgery for growth hormone producing pituitary adenoma: is the disease difficult to cure? TATSUYA KOBAYASHI, M.D., PH.D., YOSHIMASA
Autoimmune hypophysitis may eventually become empty sella
 Neuroendocrinology Letters Volume 34 No. 2 2013 Autoimmune hypophysitis may eventually become empty sella Hua Gao*, You-you Gu*, Ming-cai Qiu Department of Endocrinology, Tianjin Medical University General
Neuroendocrinology Letters Volume 34 No. 2 2013 Autoimmune hypophysitis may eventually become empty sella Hua Gao*, You-you Gu*, Ming-cai Qiu Department of Endocrinology, Tianjin Medical University General
Abnormalities in serum sodium. David Metz Paediatric Nephrology
 Abnormalities in serum sodium David Metz Paediatric Nephrology Basics Total body sodium regulated by aldosterone and ANP Mediated by intravascular volume (not sodium) RAAS and intrarenal determines Na
Abnormalities in serum sodium David Metz Paediatric Nephrology Basics Total body sodium regulated by aldosterone and ANP Mediated by intravascular volume (not sodium) RAAS and intrarenal determines Na
The Endocrine System/Hormones
 The Endocrine System/Hormones Controls many body functions exerts control by releasing special chemical substances into the blood called hormones Hormones affect other endocrine glands or body systems
The Endocrine System/Hormones Controls many body functions exerts control by releasing special chemical substances into the blood called hormones Hormones affect other endocrine glands or body systems
Surgical therapeutic strategy for giant pituitary adenomas.
 Biomedical Research 2017; 28 (19): 8284-8288 ISSN 0970-938X www.biomedres.info Surgical therapeutic strategy for giant pituitary adenomas. Han-Shun Deng, Zhi-Quan Ding, Sheng-fan Zhang, Zhi-Qiang Fa, Qing-Hua
Biomedical Research 2017; 28 (19): 8284-8288 ISSN 0970-938X www.biomedres.info Surgical therapeutic strategy for giant pituitary adenomas. Han-Shun Deng, Zhi-Quan Ding, Sheng-fan Zhang, Zhi-Qiang Fa, Qing-Hua
CUSHING'S DISEASE. What is Cushing's Disease?
 CUSHING'S DISEASE What is Cushing's Disease? Cushing's Disease is a condition in which the adrenal glands overproduce certain hormones. The medical term for this disease is hyperadrenocorticism. The adrenal
CUSHING'S DISEASE What is Cushing's Disease? Cushing's Disease is a condition in which the adrenal glands overproduce certain hormones. The medical term for this disease is hyperadrenocorticism. The adrenal
Abstract. Introduction
 Clinical Features and Outcome of Surgery in 30 Patients with Acromegaly A. Chandna, N. Islam, A. Jabbar, L. Zuberi, N. Haque Endocrinology Section, Department of Medicine, Aga Khan University Hospital,
Clinical Features and Outcome of Surgery in 30 Patients with Acromegaly A. Chandna, N. Islam, A. Jabbar, L. Zuberi, N. Haque Endocrinology Section, Department of Medicine, Aga Khan University Hospital,
panhypopituitarism Pattawan Wongwijitsook Maharat Nakhon Ratchasima hospital 17 Nov 2013
 panhypopituitarism Pattawan Wongwijitsook Maharat Nakhon Ratchasima hospital 17 Nov 2013 PITUITARY GLAND (HYPOPHYSIS CEREBRI) The master of endocrine glands master of endocrine glands It is a small oval
panhypopituitarism Pattawan Wongwijitsook Maharat Nakhon Ratchasima hospital 17 Nov 2013 PITUITARY GLAND (HYPOPHYSIS CEREBRI) The master of endocrine glands master of endocrine glands It is a small oval
Pituitary Macroadenoma with Superior Orbital Fissure Syndrome
 1 CASE REPORT OPEN ACCESS Pituitary Macroadenoma with Superior Orbital Fissure Syndrome Tapan Nagpal, Ankit Singhania ABSTRACT Introduction: Pituitary adenomas are benign tumours which arise within the
1 CASE REPORT OPEN ACCESS Pituitary Macroadenoma with Superior Orbital Fissure Syndrome Tapan Nagpal, Ankit Singhania ABSTRACT Introduction: Pituitary adenomas are benign tumours which arise within the
