Clinical, Electrophysiological and Histopathological Diagnosis of Chronic Polyradiculoneuropathy
|
|
|
- Denis Newman
- 5 years ago
- Views:
Transcription
1 Clinical, Electrophysiological and Histopathological Diagnosis of Chronic Polyradiculoneuropathy Hamdy N.A. El-Tallawy 1, Essam S. Darwish 1, Samyaa Ashour 2, Seyam S. Salem 3, Hesham S. Atta 4, Tarek A. Rageh 1 Departments of Neurology, Assiut University 1, Neurology, Ain Shams University 2, Clinical Neurophysiology, Cairo University 3, Pathology, Assiut University 4 ABSTRACT Peripheral neuropathies are among the most common neurological diseases. They are either inherited or acquired and are often associated with various disorders. This study was designed to 1- Evaluate the role of conventional and non-conventional neurophysiological studies in diagnosis of chronic polyneuropathy and 2- Evaluate the role of histopathologic study for diagnostic purposes.this study was carried out in the Neurology Department, Assiut University Hospital. The study was performed on 25 consecutive patients (20 males and 5 females) who were admitted to our department over the period of one year (May 1 st April 30 th, 2003). They were presented with manifestations of chronic polyneuropathy with duration of illness more than 6 months. Also, the study included age and sex matched 20 normal control individuals (14 males and 6 females).all patients and control were subjected to:a-complete history taking and clinical examination.b- Neurophysiological studies including (Distal latency, Nerve conduction, F response, H reflex, Conduction block study, and Quantitative electromyography)c- Sural nerve biopsy for patient group only. Patients were classified according to clinical and neurophysiological data in to 3 groups; Chronic inflammatory demyelinating polyneuropathy (CIDP), Hereditary polyneuropathy, and Polyneuropathy of undetermined aetiology. Comparison between three studied groups revealed; a statistical difference in the CMAP amplitude of ulnar nerve being more reduced in CIDP and those of undetermined aetiology compared to hereditary group. Conduction block were found mainly in CIDP group.sural nerve biopsy revealed segmental demyelination, axonal degeneration, active remyelination, axonal sprouting, and necrotizing vasculitis in different percentage among the three studied groups. (Egypt J. Neurol. Psychiat. Neurosurg., 2005, 42(2): ). INTRODUCTION The assessment and investigation of a possible neuropathy is one of the most common clinical problems facing the general neurologist. Studies of the prevalence of neuropathy in the community are rare but suggest a figure of between 2-8%, making peripheral neuropathy at least as common as stroke. Despite this high prevalence of neuropathy, it is only a small proportion of patients with neuropathies who are referred for detailed evaluation, principally those individuals with disabling disease, or with none of the obvious risk factors such as diabetes or alcoholism 1. The diagnosis of peripheral neuropathies can be frustrating, time consuming and costly. Careful clinical and electrodiagnostic assessment, with attention to the pattern of involvement and the type of nerve fibers mostly affected, narrows the different diagnosis and helps to focus the laboratory evaluation. A meticulous approach to 493
2 Egypt J. Neurol. Psychiat. Neurosurg. Vol. 42 (2) July 2005 the evaluation and differential diagnosis of a patient with peripheral neuropathy is essential, based on important elements of the clinical history and physical examination, the use of electromyography and nerve conduction studies, autonomic testing, cerebrospinal fluid analysis and nerve biopsy findings 2. Aim of the work is: 1. To evaluate the role of conventional and non conventional neuropsychological studies in diagnosis of chronic polyneuropathy (more than 6 months). 2. To evaluate the role of histopathologic study for diagnostic purposes. SUBJECTS AND METHODS The study includes all patients admitted to Neurology department, Assiut university hospital over the period of one year (From May1 st 2002 to April 30 th 2003), who presented with manifestations of chronic polyneuropathy with duration of illness more than 6 months. Twenty-five patients of chronic polyneuropathy (20 males and 5 females) were recruited along the period of the study whose age ranged from years with a mean age years. A group of 20 normal persons (14 males and 6 females) with a mean age years and age range years were chosen as a control group. Patients with polyneuropathy due to metabolic causes (Diabetes, renal diseases, liver diseases,.etc.) were excluded. All patients were subjected to: A) Complete history taking, clinical examination, both general and neurological; according to a standard neurological sheet, currently used in the Neurology department, Assiut University Hospital. B) Neurophysiological studies including: 1- Nerve conduction studies of the following nerves: median and ulnar nerves (Motor and sensory), common peroneal nerve (motor), and sural nerve (Sensory). 2- F response study of the following nerves: median, ulnar, and posterior tibial nerves. 3- H-reflex study of the posterior tibial nerve. 4- Conduction block study of the median and ulnar nerves. 5- Quantitative electromyography of the following muscles: abductor pollicis brevis, abductor digiti minimi, biceps, extensor digitorum brevis, and rectus femoris muscles. C) Nerve biopsy study: The nerve selected to be biopsed was the sural nerve. The sural nerve meets six criteria cited by Dyck and loufgren 3 for selection of a peripheral nerve for biopsy. The control group were subjected to complete clinical examination and the same neurophysiological studies. Patients were classified according to clinical and neurophysiological data into: Group 1: Twelve Patients (48%) diagnosed as Chronic Inflammatory Demyelinating Polyradiculoneuropathy (CIDP) who fulfilled criteria of Ad Hoc subcommittee for demyelinating neuropathy 4. Group 2: Nine Patients (36%) diagnosed as Hereditary Polyneuropathy. Group 3: Four Patients (16%) diagnosed as polyneuropathy of undermined aetiology. Consent: Written consents were taken from the patients after explaining to them the purpose of the study, steps of the work, benefits and risks. Agreement of the Ethical Committee of Faculty of Medicine Assiut University was taken. 494
3 RESULTS Quantitative EMG results: Statistical comparison was carried between the patients and control group using student s t test. 1- Amplitude: There was a statistically significant increase in the mean amplitude of Motor unit potentials of abductor pollicious brevis, Abductor digiti minimi and Extensor digitorum brevis muscles when compared with the control values. However, these finding were not detected from Biceps and Rectors femoris muscles. Eighty percent of cases had abnormal amplitude above the upper limit of normal range (mean for the control group + 2SD). 2- Duration: A statistically highly significant increase in the mean duration of MUPs of the all studied muscles was found when compared with the control group. Eighty four percent of cases had abnormal duration (above the upper limit of normal range). 3- Size index (area/ amplitude + log amplitude): There was a statistically highly significant increase in the mean size index of the studied muscles when compared with control group. Eighty four percent of cases had abnormal size index (above the upper limit of normal range). 4- Phase count: A statistically highly significant increase in the mean phase count of the studied muscles was found when compared to the control group. All cases were above upper limit of normal range. 5- Turn count: There was a statistically highly significant increase in the mean turn count of the studied muscles when compared to control group. All cases were above upper limit of normal range. 6- Polyphasic MUPs%: A statistically highly significant increase in the mean values of polyphasic MUPs% of the studied muscles was found when compared to the control group. All cases were above upper limit of normal range. There was a statistically highly significant positive correlation between the amplitude of MUPs and duration of illness (Fig. 1). No other statistically significant correlations were found between other parameters and duration of illness. There was a statistically significant negative correlation between size index and motor power (Fig. 2). Otherwise, no statistical significant correlations were found between other parameters and motor power. Neurophysiological data of the studied three groups: Comparison between the three above mentioned groups was done using ANOVA test. Table (1) shows a statistically significant difference in distal motor latencies of median and ulnar nerves, being prolonged in CIDP group compared to other groups. Also, a statistically significant reduction in the CMAP amplitude of ulnar nerve being more reduced in CIDP and those of undetermined aetiology compared to the hereditary group. Table (2) shows a statistically significant difference in distal sensory latencies of median and ulnar nerves, being more prolonged in CIDP group compared to the other two groups. Table (3) shows a statistically significant difference in F response latencies of median and ulnar nerves, being more prolonged in CIDP group compared to the other two groups. Comparison between the three groups for quantitative EMG parameters revealed no consistent statistically significant difference between the three groups apart from the following findings; A statistically significant difference in mean phase count of APB muscle was found between the three groups, being more in CIDP group compared to the other two groups. A statistically significant difference in mean amplitude of MUPs of EDB muscle was found, being higher in hereditary polyneuropathy group compared to the other two groups. Also a statistically significant difference in polyphasic MUPs % elicited from EDB muscle was found 495
4 Egypt J. Neurol. Psychiat. Neurosurg. Vol. 42 (2) July 2005 between different groups, being higher in CIDP group compared to the other two groups. Table (4) shows that, sural nerve biopsy from patients of CIDP revealed segmental demyelination in all patients (100%) with axonal degeneration in 5 patients (41.6%), 4 patients showed active remyelination (33.3%), and 6 patients showed axonal sprouting (50%). Sural nerve biopsy from patients of hereditary polyneuropathy demonstrated segmental demyelination in all patients (100%), with remyelination in 5 patients (55%) with no axonal degeneration could be detected. While biopsy of patients of polyneuropathy of undetermined etiology demonstrated axonal degeneration in 3 patients (75%), segmental demyelination in one patient (25%), and necrotizing vasculitis in 3 patients (75%). Fig. (1): Correlation between duration of illness and amplitude of MUPs. Fig. (2): Correlation between motor power and MUPs size index. 496
5 Table 1. Mean values±sd of motor conduction studies of the three studied groups. Parameter Group 1 Group 2 Group 3 Significance Distal latency 5.7± ± ± Median MCV 33.7± ± ± nerve Amplitude 2.8± ± ± Duration 18.0± ± ± Distal latency 4.5± ± ± Ulnar MCV 34.3± ± ± nerve Amplitude 2.4± ± ± Duration 18.4± ± ± Distal latency 7.3± ± ± Common MCV 26.9± ± ± peroneal Amplitude 0.6± ± ± nerve Duration 22.2± ± ± Significant: P< 0.05 * N.B.: Group 1: Chronic inflammatory demyelinating polyneuropathy (CIDP). Group 2: Hereditary polyneuropathy. Group 3: Polyneuropathy of undetermined etiology. Table 2. Mean values±sd of sensory conduction studies of the three studied groups. Parameter Group 1 Group 2 Group 3 Significance Median Distal latency 5.8± ± ± nerve SCV 30.6± ± ± Ulnar nerve Distal latency 5.5± ± ± SCV 31.2± ± ± Sural Distal latency ± ± ± nerve Distal latency ± ± ± SCV 22.9± ± ± Significant: P<0.05 Table 3. Mean values±sd of late response (F wave and H reflex) of the three studied groups. Parameter Group 1 Group 2 Group 3 Significance F response Median nerve 36.8± ± ± Ulnar nerve 38.8± ± ± Posterior tibial nerve 41.3± ± ± H reflex Posterior tibial nerve 38.7± ± ± Significant: P<0.05 Table 4. Pathological changes among the different studied groups. All patients Group (1) n=12 Group (2) n=9 Group (3) n=4 No. % No. % No. % No. % Segmental demyelination 22 88% % 9 100% 1 25% Active remyelination 9 36% % % 0 0% Onion bulb formation 9 36% % % 0 0% Schwann cell proferation 11 44% % % 1 25% Axonal degeneration 8 32% % 0 0% 3 75% Axonal sprouting 6 24% 6 50% 0 0% 0 0% Necrotizing vasculitis 3 12% 0 0% 0 0% 3 75% 497
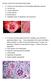
6 Egypt J. Neurol. Psychiat. Neurosurg. Vol. 42 (2) July 2005 Picture (1): Semithin transverse section of sural nerve biopsy (from a patient with CIDP) showing demyelination and presence of remyelination indicated by relatively thin myelinated axon in proportion to axon diameter (arrow). Picture (2): Semithin transverse section of sural nerve biopsy (from a case of hereditary polyneuropathy) showing segmental demyelination, schwann cell proliferation and onion bulb formation (arrow). Picture (3): Semithin transverse section of sural nerve biopsy (from a patient with polyneuropathy of undertermined aetiology) showing vasculitis of vasa nervosa appearing as fibrous scarring and thickening of vessel wall and endothelial proliferation with narrowing of vascular lumen (arrow). Picture (4): Semithin transverse section of sural nerve biopsy (from a case of CIDP) showing segmental demyelination, remyelination indicated by presence of relatively thin myelinated nerve fibers in proportion to their axon diameter, and axonal sprouting (arrow) appearing as four thin myelinated axons surrounded by one schwann cell (arrow). 498
7 Picture (5): Electron micrograph of ultrathin section of sural nerve biopsy (from a patient of hereditary polyneuropathy) shows decreased the numbers of myelinated nerve fibers with evidence of remyelination appearing as axons with relatively thin myelin sheath in proportion to their diameters. X Picture (6): Electron micrograph of ultrathin section of sural nerve biopsy (from a patient with polyneuropathy of undetermined aetiology) showing marked proliferation of endothelial lining of vasa nervosa with thickening of its wall (Vasculitis). X 2700 Picture (7): Electron micrograph of ultrathin section of sural nerve biopsy (from a patient with CIDP) showing decreased number of myelinated fibres with schwann cell proliferation. X
8 Egypt J. Neurol. Psychiat. Neurosurg. Vol. 42 (2) July 2005 DISCUSSION Clinicians use electrodiagnostic information to confirm clinical findings, localize specific subclinical abnormalities, and to identify the underlying pathophysiology. Although the primary role of clinical neurophysiology is diagnostic, test results may be sufficiently sensitive to identify sub-clinical findings and to monitor changes related to disease progression or treatment response 5. In this study, patients were considered to have peripheral neuropathy if confirmed by clinical examination as well as specific abnormal neurophysiological studies characteristic for polyneuropathy. Electromyography examination is an essential diagnostic tool in diagnosis of peripheral neuropathy and can be considered an extension of clinical examination. The wide spread use of computers in EMG machines led to the development of new testing procedures in the clinical EMG laboratory 6. In this study, we use Multi MUPs analysis method for quantitative EMG study in proximal and distal muscles of upper and lower limbs. There was statistically significant difference in the mean amplitude of MUAPs of the patients group compared to the control group. This was in agreement with Stalberg and Flack 7, who reported that the amplitude is a sensitive parameter in discriminating neurogenic from myogenic changes and stated that amplitude is typically increased in neuropathies, after collateral reinnervation and muscle fiber hypertrophy. The duration of MUAPs in our studied muscles showed a highly significant increase in patients compared to control group. These results agreed with Pfeiffer and Kunze 8, who also reported that the duration is a standard indicator for neuropathic changes. Also, positive correlation was found between the amplitude of MUAP and duration of illness in patients group. These results were in concordance with those of Terebuh and Johnson 9, who stated that with process of reinnervation, healthy motor axon give rise to extensive collaterals for dennervated muscle fibers (axonal sprouting), with a resultant increase in MUAP amplitude. As regard the size index (SI), there was a highly statistically significant increase in mean SI of patient group compared to control group. Also, there was a statistically significant negative correlation between SI and motor power of the studied muscles. These results agreed with Akaboshi 10, who stated that SI is an excellent parameter to distinguish neuropathic from normal MUAPs, and it is not affected by electrode position. The percentages of suggested subclassification of our patients are partially agreed with Barohn 11, who found, in his study on 402 consecutive patients referred to the University of Texas neuromuscular outpatients clinics, that hereditary neuropathy represent one third of the studied patients, acquired demyelinating polyneuropathy was found in 18%, and 23% of patients diagnosed as chronic sensory polyneuropathy with no identifiable cause, and the remaining patients had chronic polyneuropathy due to metabolic cause (renal, Hepatic, DM et) or toxin exposure. The slight difference between this study and our present study may be due to small number of our studied patients and exclusion of polyneuropathy of acute onset, and those due to metabolic causes. As regard clinical presentation of the studied groups in this study, a statistically significant more proximal motor weakness was observed among CIDP group compared to the other groups. A statistically significant radicular sensory impairment was observed among CIDP groups, and this can be explained by pathological involvement of proximal parts, of nerves and roots among these patients. This was further supported by the findings that measurement of late responses among the different groups in this study revealed prolonged F response latencies in CIDP group compared to the other groups which again confirms the involvement of proximal nerves and roots by the neuropathic process in CIDP patients. 500
9 These findings are consistent with Barohn and Saperstein 12, who stated that the finding of weakness in both proximal and distal muscle group in a symmetric fashion is the hallmark for acquired immune demyelinating polyneuropathies, both the acute form Guillian Barre syndrome and the chronic form CIDP. Neurophysiological assessment of the three groups shows statistically prolonged distal motor latencies and distal sensory latencies of median and ulnar nerves in CIDP group compared to the other groups. These results emphasize the value of distal latency as a sensitive parameter indicating demyelination process. These finding can be interpreted by the more severe and more rapid course of the neuropathic process in CIDP compared to hereditary polyneuropathy, in which the course of illness is more slower and show lesser degree of affection. Although in most cases, it is difficult to provide a clinical diagnosis based upon specific microscopic findings in the nerve biopsy, there are some conditions in which nerve biopsy can provide specific diagnostic information such as; vasculitis, amyloidosis, HNPP, leprosy, sarcoidosis and tumor infiltration 13. CIDP with purely demyelinating lesions was found in 7 patients (58.3%), and CIDP with mixed demyelinating and axonal lesions were found in 5 patients (41.7%). These finding are partially consistent with Villa 14 who found, on his study of 30 patients with CIDP, that all the studied sample showed demyelination, with 9 samples showed associative axonal degeneration. Also, Molenaar 15 found that 61% of patients with CIDP had sural nerve biopsy with predominantly demyelination. The relation of whether segmental demyelination and axonal degeneration are independent of each other, or whether there is interdependence between them, was the question of many previous studies. Said 16, through their work on patients with Guillian Barre syndrome, came to the conclusion that axonal degeneration developed independently of demyelination. Ashour 17 studied the histopathological changes in 36 cases of Guillian Barre syndrome. They demonstrated partial demyelination, remyelination with mild axonal degeneration in the studied biopsies. One patients in their studies showed marked axonal degeneration with no accompanying segmental demyelination. Axonal loss has more long-term prognostic impact than active demyelination, inflammatory infiltrates, or onion-bulb formations. Axonal degeneration occurs in varying degrees in lesions that are attributed primarily to demyelination. This phenomenon is evident in severe lesions of spinal roots and proximal nerve trunks in patients with Guillain-Barre syndrome 18. The axonal lesions occurring in the course of demyelinating neuropathy have been attributed to a bystander effect in inflammatory foci, to immune attack directed toward epitopes on the axon, or to increased endoneurial pressure 19. Therefore, in demyelinating disorders of the peripheral and central nervous systems, the longterm prognosis depends more on the amplitude of axonal loss, as recently emphasized in MS, than on demyelination 20. In group of patients with hereditary polyneuropathy, the following changes were observed in their sural nerve biopsies; segmental demyelination, remyelination, onion bulb formation and Schwann cell proliferation. These result correlate with the finding described by Dyck and Lambert 21, who stated that in cases of peroneal muscular atrophy (HSMN type one), the sural nerve biopsy showed reduced myelinated fiber density, hypertrophic onion bulb formation, and some axonal atrophy. In this group of common demyelinating Charcot-Marie-Tooth neuropathies (type 1A, 1B, 1C,) with autosomal dominant inheritance, no distinction between subtypes can be made based on morphology, and nerve biopsy does no more to establish prognosis than the combination of the clinical examination, electrophysiology and family history 22. In Dejerine-Sottas neuropathy, the nerve pathology demonstrates a spectrum of changes from congenital amyelination to hypomyelination and others show decreased numbers of nerve 501
10 Egypt J. Neurol. Psychiat. Neurosurg. Vol. 42 (2) July 2005 fibers, demyelination, remyelination, and onion bulb formation. Attempts have been made to classify these cases solely by morphology, but not all agree to this approach 23. Also in the type of Charcot-Marie-Tooth neuropathies (CMT2, CMT4 and CMTX), nerve biopsy has no specific picture enough to permit a definite diagnosis 24. In the third group of patients with undetermined polyneuropathy, the following changes in biopsies was observed; axonal degeneration in 3 patients, segmental demyelination in one patient, necrotizing vasculitis in endoneural vessels in 3 patients. Detection of vasculitis in sural nerve biopsy has special importance since this is a treatable condition. The advent of genetic tests for many neuropathies has reduced the need for biopsy, but it remains the primary method of establishing a diagnosis of vasculitic neuropathy when history is not available from elsewhere 25. These findings agreed with Molenaar 15, who stated that, although sural nerve biopsy may give much information about degree of demyelination, axonal injury and inflammatory cells infiltration, it is not confirmatory to diagnose CIDP. In addition, the pathologic changes of demyelination or remyelination are not unique to CIDP and can be demonstrated in other neuropathic disorders. It is important to emphasize that there is no diagnostic nerve biopsy findings for CIDP but only suggestive pathologic features 11. However, it is sometimes difficult to assess the activity of a chronic polyneuropathy. Nerve biopsy can be used to detect active nerve lesion and inflammatory cell infiltrate which reflect the stage of disease progression 26. Also, searching for axonal injury, manifestation of regeneration as; remyelination and axonal sprouting, may play an important role in detection of prognosis of these patients. In contrast, detection of blood vessels abnormalities such as necrotizing vasculitis in the studied nerve biopsy is a unique finding which is conclusive for the diagnosis of vasculitis and can t be diagnosed by any other mean of studies 22. Finally, on comparing the neurophysiological studies to the pathological finding in detecting the type of neuropathy, it was found that neurophysiological studies had a sensitivity of 87.5% in detecting of demyelinating form of polyneuropathy, 75% for axonal form of polyneuropathy, and only 40% for mixed form. These results magnify the role of neurophysiological studies in diagnosis of chronic polyneuropathies and detecting the underlying pathological mechanism. REFERENCES 1. Willison HJ and Winer JB. (2003): Clinical evaluation and investigation of neuropathy. J Neurol Neurosurg and psychiatry; 74:ii3. 2. Rosenberg NR, Portegies P, Visser M, Vermeulen M. (2001): Diagnostic investigation of patients with chronic polyneuropathy: evaluation of a clinical guideline J Neurol Neurosurg Psychiatry; 71: Dyck PJ, Loufgren RS. (1966): Methods of fascicular biopsy of human peripheral nerve for electrophysiogical and histological study. Mayo Clin Proc; 41: Research criteria for diagnosis of chronic inflammatory demyelinating polyneuropathy (CIDP). Report from an Ad Hoc Subcommittee of the American Academy of Neurology AIDS Task Force. Neurology 1991;41: Albers JW. (1993): Clinical neurophysiology of generalized polyneuopathy. J Clin Neurophsiol; 10: Stalberg E, Falck B, Sonoo M. (1995): Multi- MUP EMG analsis a two-year experience in daily clinical work. Electroenceph Clin Neurophysiol; 97: Stalberg E, Falck B. (1997): The role of electromyography in neurology. Electroencephalogr Clin Neurolphysiol; 103: Pfeiffer G, Kunze K. (1993): Frequency analysis and duration of motor unit potential: reliability and diagnostic usefulness. Electroencephal Clin Neurophysiol; 89: Terebuh BM, Johnson EW. (1997): Electrodiagnostic consultation including EMG examination. In Johnson EW andpease WS eds. Practical electromyography; 3 rd ed. Balltimore Wiliams and Wilkins. 502
11 10. Akaboshi K., Masakado Y., and Chino N. (2000): Quantitative EMG and motor unit recruitment threshold using a concentric needle with quadrifilar electrode. Muscle & Nerve; 23: Barohn RJ. (1998): Approach to pripheral neuropathy and neuronopathy. Semin Neurol; 18: Barohn RJ. Saperstien DS. (1998): Guillian-Barre syndrome and chronic inflammatory demyelinating polyneuropathy. Seminars in Neurology; 18: Mendell JR. (1998): Charcot-Tooth neuropathies and related disorders. Seminars in Neurology; 18: Villa Am, Molina H, Sanz OP, Sica RE. (1999): Chronic inflammatory demyelinating polyneuropathy. Findings in 30 patients. Medicina (B Aires); 59 (6): Molenaar DSM, Vermeulen M, de Haan R. (1998): Diagnostic value of sural nerve biopsy in chronic inflammatory demyelinating polyneuropathy. J Neurol Neurosurgy Psychiatry; 64: Said G, Saida K, Saida T, Asbury Ak. (1981): Axonal lesions in acute experimental demyelination: a sequential teased nerve fiber study. Neurology; 31 (4) : Ashour SM, Mostafa M, Gerard S, Mahran Z, Nawar N. (1987): Relationship between the clinical picture, pathological chamges and prognisi in Guillian Barre syndrome Sural nerve biopsy study MD thesis (faculty of Medicine, Ain Shams University). 18. Berciano J, Figols J, Garcia A, et al. (1997): Fulminant Guillain-Barre syndrome with universal inexcitability of peripheral nerves: a clinicopathological study. Muscle Nerve; 20: Griffin JW, LI CY, Ho TW, et al. (1996): Pathology of the motor-sensory axonal Guillain- Barre syndrome. Ann Neurol; 39: Trap BD, Peterson J, Ransohoff RM, Rudick R, Mork S, Bo L. (1998): Axonal transection in the lesions of multiple sclerosis. N Engl J Med; 338: Dyck PJ, Lambert EH. (1968a): Lower motor and primary sensory neuron diseases with peroneal muscular atrophy. Arch Neurol; 18: Dyck PJ, Giannini C, Lais A. (1993): Pathologic alterations of nerves. In: Dyck PJ,,et al, eds. Peripheral neuropathy. Philadelphia: WB Saunders,; Gabreels FA, Gabreels FF. (1993): Hereditary demyelinating motor and sensory neuropathy. Brain Pathol; 3: Sander S, Nicholson GA, Ouvrier RA et al. (1998): Charcot-Marie-Tooth disease: Histopathological features of the peripheral myelin protein (PMP22) duplication (CMTIA) and connexin 32 mutation (CMTX). Muscle Nerve; 21: Said G, Lacroix-Ciaudo C, Fujimura H, et al. (1988): The peripheral neuropathy of necrotizing arteritis: a clinicopathological study. Ann Neurol; 23: Bouchard C, Lacroix C, Plante V. et al. (1999): Clinicopathologic findings and prognosis of chronic inflammatory demelinating polyneuropathy. Neurology; 52 (3):
Diagnostic investigation of patients with chronic polyneuropathy: evaluation of a clinical guideline
 J Neurol Neurosurg Psychiatry 2001;71:205 209 205 Department of Neurology, Academic Medical Centre, University of Amsterdam, PO Box 22700, 1100 DE Amsterdam, The Netherlands N R Rosenberg P Portegies M
J Neurol Neurosurg Psychiatry 2001;71:205 209 205 Department of Neurology, Academic Medical Centre, University of Amsterdam, PO Box 22700, 1100 DE Amsterdam, The Netherlands N R Rosenberg P Portegies M
Guide to the use of nerve conduction studies (NCS) & electromyography (EMG) for non-neurologists
 Guide to the use of nerve conduction studies (NCS) & electromyography (EMG) for non-neurologists What is NCS/EMG? NCS examines the conduction properties of sensory and motor peripheral nerves. For both
Guide to the use of nerve conduction studies (NCS) & electromyography (EMG) for non-neurologists What is NCS/EMG? NCS examines the conduction properties of sensory and motor peripheral nerves. For both
Clinical and Neurophysiological Assessment of Cervical Radiculopathy
 Mohamed El-Khatib et al. Clinical and Neurophysiological Assessment of Cervical Radiculopathy Mohamed G. El-Khatib 1, Mohamed Saad 1, Seyam Saeed 2, Mohamed El-Sayed 1 Departments of Neurology, Mansoura
Mohamed El-Khatib et al. Clinical and Neurophysiological Assessment of Cervical Radiculopathy Mohamed G. El-Khatib 1, Mohamed Saad 1, Seyam Saeed 2, Mohamed El-Sayed 1 Departments of Neurology, Mansoura
Multifocal motor neuropathy: diagnostic criteria that predict the response to immunoglobulin treatment
 Multifocal motor neuropathy: diagnostic criteria that predict the response to immunoglobulin treatment 7 MMN RM Van den Berg-Vos, H Franssen, JHJ Wokke, HW Van Es, LH Van den Berg Annals of Neurology 2000;
Multifocal motor neuropathy: diagnostic criteria that predict the response to immunoglobulin treatment 7 MMN RM Van den Berg-Vos, H Franssen, JHJ Wokke, HW Van Es, LH Van den Berg Annals of Neurology 2000;
High resolution ultrasound in peripheral neuropathies
 3 rd Congress of the European Academy of Neurology Amsterdam, The Netherlands, June 24 27, 2017 Teaching Course 5 Advanced neurosonology - Level 3 High resolution ultrasound in peripheral neuropathies
3 rd Congress of the European Academy of Neurology Amsterdam, The Netherlands, June 24 27, 2017 Teaching Course 5 Advanced neurosonology - Level 3 High resolution ultrasound in peripheral neuropathies
COMPARISON OF ELECTRODIAGNOSTIC CRITERIA FOR PRIMARY DEMYELINATION IN CHRONIC POLYNEUROPATHY
 Three sets of electrodiagnostic criteria for establishing primary demyelination in chronic polyneuropathy are evaluated. Sensitivity is assessed in 7 patients with clinically established chronic inflammatory
Three sets of electrodiagnostic criteria for establishing primary demyelination in chronic polyneuropathy are evaluated. Sensitivity is assessed in 7 patients with clinically established chronic inflammatory
ELECTROPHYSIOLOGICAL FEATURES OF INHERITED DEMYELINATING NEUROPATHIES: A REAPPRAISAL IN THE ERA OF MOLECULAR DIAGNOSIS
 INVITED REVIEW ABSTRACT: The observation that inherited demyelinating neuropathies have uniform conduction slowing and that acquired disorders have nonuniform or multifocal slowing was made prior to the
INVITED REVIEW ABSTRACT: The observation that inherited demyelinating neuropathies have uniform conduction slowing and that acquired disorders have nonuniform or multifocal slowing was made prior to the
A/Professor Arun Aggarwal Balmain Hospital
 A/Professor Arun Aggarwal Balmain Hospital Nerve Conduction Studies Test to evaluate the function of motor / sensory nerves Evaluate Paraesthesia (numbness, tingling, burning) Weakness of arms and legs
A/Professor Arun Aggarwal Balmain Hospital Nerve Conduction Studies Test to evaluate the function of motor / sensory nerves Evaluate Paraesthesia (numbness, tingling, burning) Weakness of arms and legs
Critical Illness Polyneuropathy CIP and Critical Illness Myopathy CIM. Andrzej Sladkowski
 Critical Illness Polyneuropathy CIP and Critical Illness Myopathy CIM Andrzej Sladkowski Potential causes of weakness in the ICU-1 Muscle disease Critical illness myopathy Inflammatory myopathy Hypokalemic
Critical Illness Polyneuropathy CIP and Critical Illness Myopathy CIM Andrzej Sladkowski Potential causes of weakness in the ICU-1 Muscle disease Critical illness myopathy Inflammatory myopathy Hypokalemic
Making sense of Nerve conduction & EMG
 Making sense of Nerve conduction & EMG Drs R Arunachalam Consultant Clinical Neurophysiologist Wessex Neurological Centre Southampton University Hospital EMG/NCS EMG machine For the assessment of patients
Making sense of Nerve conduction & EMG Drs R Arunachalam Consultant Clinical Neurophysiologist Wessex Neurological Centre Southampton University Hospital EMG/NCS EMG machine For the assessment of patients
Peripheral Neuropathies
 Peripheral Neuropathies ELBA Y. GERENA MALDONADO, MD ACTING ASSISTANT PROFESSOR UNIVERSITY OF WASHINGTON MEDICAL CENTER Objectives Definition Neurophysiology Evaluation of polyneuropathies Cases Summary
Peripheral Neuropathies ELBA Y. GERENA MALDONADO, MD ACTING ASSISTANT PROFESSOR UNIVERSITY OF WASHINGTON MEDICAL CENTER Objectives Definition Neurophysiology Evaluation of polyneuropathies Cases Summary
Thank you to: L Magy, L Richard, N Couade, F Maquin
 «Crash course in the interpretation of peripheral nerve biopsies: which nerve to biopsy, tissue fixation: paraffin, semi thins, EM (common stains and immunos), identifying degenerating and regenerating
«Crash course in the interpretation of peripheral nerve biopsies: which nerve to biopsy, tissue fixation: paraffin, semi thins, EM (common stains and immunos), identifying degenerating and regenerating
Index. Note: Page numbers of article titles are in boldface type.
 Neurol Clin N Am 20 (2002) 605 617 Index Note: Page numbers of article titles are in boldface type. A ALS. See Amyotrophic lateral sclerosis (ALS) Amyotrophic lateral sclerosis (ALS) active denervation
Neurol Clin N Am 20 (2002) 605 617 Index Note: Page numbers of article titles are in boldface type. A ALS. See Amyotrophic lateral sclerosis (ALS) Amyotrophic lateral sclerosis (ALS) active denervation
Electrodiagnostic Measures
 Electrodiagnostic Measures E lectrodiagnostic assessments are sensitive, specific, and reproducible measures of the presence and severity of peripheral nerve involvement in patients with diabetes (1).
Electrodiagnostic Measures E lectrodiagnostic assessments are sensitive, specific, and reproducible measures of the presence and severity of peripheral nerve involvement in patients with diabetes (1).
Distal chronic spinal muscular atrophy involving the hands
 Journal ofneurology, Neurosurgery, and Psychiatry, 1978, 41, 653-658 Distal chronic spinal muscular atrophy involving the hands D. J. O'SULLIVAN AND J. G. McLEOD From St Vincent's Hospital, and Department
Journal ofneurology, Neurosurgery, and Psychiatry, 1978, 41, 653-658 Distal chronic spinal muscular atrophy involving the hands D. J. O'SULLIVAN AND J. G. McLEOD From St Vincent's Hospital, and Department
AII-type: Select the most appropriate answer
 AII-type: Select the most appropriate answer ( )1. Choose one best answer for the following pathologic pictures. A. choroid cyst B. choroid papilloma C. pontine glioma D. ependymoma E. metastatic tumor
AII-type: Select the most appropriate answer ( )1. Choose one best answer for the following pathologic pictures. A. choroid cyst B. choroid papilloma C. pontine glioma D. ependymoma E. metastatic tumor
Evaluation of Peripheral Neuropathy. Evaluation of Peripheral Neuropathy - Introduction
 Evaluation of Peripheral Neuropathy Chris Edwards, MD Ochsner Neurology, Main Campus Evaluation of Peripheral Neuropathy - Introduction A very common complaint in the clinic Presentation is variable Multiple
Evaluation of Peripheral Neuropathy Chris Edwards, MD Ochsner Neurology, Main Campus Evaluation of Peripheral Neuropathy - Introduction A very common complaint in the clinic Presentation is variable Multiple
Multifocal motor neuropathy: long-term clinical and electrophysiological assessment of intravenous immunoglobulin maintenance treatment
 Multifocal motor neuropathy: long-term clinical and electrophysiological assessment of intravenous immunoglobulin maintenance treatment 11 MMN RM Van den Berg-Vos, H Franssen, JHJ Wokke, LH Van den Berg
Multifocal motor neuropathy: long-term clinical and electrophysiological assessment of intravenous immunoglobulin maintenance treatment 11 MMN RM Van den Berg-Vos, H Franssen, JHJ Wokke, LH Van den Berg
CIDP + MMN - how to diagnose and treat. Dr Hadi Manji
 CIDP + MMN - how to diagnose and treat Dr Hadi Manji Outline Introduction CIDP Diagnosis Clinical features MRI Nerve conduction tests Lumbar puncture Nerve biopsy Treatment IV Ig Steroids Plasma Exchnage
CIDP + MMN - how to diagnose and treat Dr Hadi Manji Outline Introduction CIDP Diagnosis Clinical features MRI Nerve conduction tests Lumbar puncture Nerve biopsy Treatment IV Ig Steroids Plasma Exchnage
Motor and sensory nerve conduction studies
 3 rd Congress of the European Academy of Neurology Amsterdam, The Netherlands, June 24 27, 2017 Hands-on Course 2 Assessment of peripheral nerves function and structure in suspected peripheral neuropathies
3 rd Congress of the European Academy of Neurology Amsterdam, The Netherlands, June 24 27, 2017 Hands-on Course 2 Assessment of peripheral nerves function and structure in suspected peripheral neuropathies
Role of concentric needle Single Fiber Electromyography in detection of subclinical motor involvement in carpal tunnel syndrome
 Tawfeek et al. The Egyptian Journal of Neurology, Psychiatry and Neurosurgery (2018) 54:2 https://doi.org/10.1186/s41983-018-0004-4 The Egyptian Journal of Neurology, Psychiatry and Neurosurgery RESEARCH
Tawfeek et al. The Egyptian Journal of Neurology, Psychiatry and Neurosurgery (2018) 54:2 https://doi.org/10.1186/s41983-018-0004-4 The Egyptian Journal of Neurology, Psychiatry and Neurosurgery RESEARCH
Clinical and electrophysiologic features of childhood Guillain-Barré syndrome in Northeast China
 Journal of the Formosan Medical Association (2014) 113, 634e639 Available online at www.sciencedirect.com journal homepage: www.jfma-online.com ORIGINAL ARTICLE Clinical and electrophysiologic features
Journal of the Formosan Medical Association (2014) 113, 634e639 Available online at www.sciencedirect.com journal homepage: www.jfma-online.com ORIGINAL ARTICLE Clinical and electrophysiologic features
Yoshihisa Masakado, Michiyuki Kawakami, Kanjiro Suzuki, Leon Abe, Tetsuo Ota, and Akio Kimura
 REVIEW Clinical Neurophysiology in the Diagnosis of Peroneal Nerve Palsy Yoshihisa Masakado, Michiyuki Kawakami, Kanjiro Suzuki, Leon Abe, Tetsuo Ota, and Akio Kimura Keio University Tsukigase Rehabilitation
REVIEW Clinical Neurophysiology in the Diagnosis of Peroneal Nerve Palsy Yoshihisa Masakado, Michiyuki Kawakami, Kanjiro Suzuki, Leon Abe, Tetsuo Ota, and Akio Kimura Keio University Tsukigase Rehabilitation
Immune Mediated Neuropathies
 Immune Mediated Neuropathies Hernan Gatuslao, M.D. Assistant Professor Department of Neurology Virginia Commonwealth University School of Medicine AIDP and CIDP Acute inflammatory demyelinating polyneuropathy
Immune Mediated Neuropathies Hernan Gatuslao, M.D. Assistant Professor Department of Neurology Virginia Commonwealth University School of Medicine AIDP and CIDP Acute inflammatory demyelinating polyneuropathy
International Journal of Basic & Applied Physiology
 ELECTRODIAGNOSTIC FEATURES IN CLINICALLY SUSPECTED GUILLAIN BARRE SYNDROME Asha Shrivastava*, Rashmi Dave**, Sanjeev Shrivastava ***, Brajesh Sharma **** *Professor, ** JR III, *** Assistant Professor,
ELECTRODIAGNOSTIC FEATURES IN CLINICALLY SUSPECTED GUILLAIN BARRE SYNDROME Asha Shrivastava*, Rashmi Dave**, Sanjeev Shrivastava ***, Brajesh Sharma **** *Professor, ** JR III, *** Assistant Professor,
Compound Nerve Action Potential of Common Peroneal Nerve and Sural Nerve Action Potential in Common Peroneal Neuropathy
 J Korean Med Sci 2008; 23: 117-21 ISSN 1011-8934 DOI: 10.3346/jkms.2008.23.1.117 Copyright The Korean Academy of Medical Sciences Compound Nerve Action Potential of Common Peroneal Nerve and Sural Nerve
J Korean Med Sci 2008; 23: 117-21 ISSN 1011-8934 DOI: 10.3346/jkms.2008.23.1.117 Copyright The Korean Academy of Medical Sciences Compound Nerve Action Potential of Common Peroneal Nerve and Sural Nerve
Pediatric Aspects of EDX
 Pediatric Aspects of EDX Albert C. Clairmont, MD Associate Professor-Clinical The Ohio State University February 25, 2013 Objectives Overview of Pediatric Electrodiagnosis (EDX) Understand the different
Pediatric Aspects of EDX Albert C. Clairmont, MD Associate Professor-Clinical The Ohio State University February 25, 2013 Objectives Overview of Pediatric Electrodiagnosis (EDX) Understand the different
Nerve pathologic features differentiate POEMS syndrome from CIDP
 Piccione et al. Acta Neuropathologica Communications (2016) 4:116 DOI 10.1186/s40478-016-0389-1 RESEARCH Nerve pathologic features differentiate POEMS syndrome from CIDP Ezequiel A. Piccione 1, Janean
Piccione et al. Acta Neuropathologica Communications (2016) 4:116 DOI 10.1186/s40478-016-0389-1 RESEARCH Nerve pathologic features differentiate POEMS syndrome from CIDP Ezequiel A. Piccione 1, Janean
Clinical Aspects of Peripheral Nerve and Muscle Disease. Roy Weller Clinical Neurosciences University of Southampton School of Medicine
 Clinical Aspects of Peripheral Nerve and Muscle Disease Roy Weller Clinical Neurosciences University of Southampton School of Medicine Normal Nerves 1. Anterior Horn Cell 2. Dorsal root ganglion cell 3.
Clinical Aspects of Peripheral Nerve and Muscle Disease Roy Weller Clinical Neurosciences University of Southampton School of Medicine Normal Nerves 1. Anterior Horn Cell 2. Dorsal root ganglion cell 3.
Comparison of electrophysiological findings in axonal and demyelinating Guillain-Barre syndrome
 Iranian Journal of Neurology Original Paper Iran J Neurol 2014; 13(3): 138-143 Comparison of electrophysiological findings in axonal and demyelinating Guillain-Barre syndrome Received: 9 Mar 2014 Accepted:
Iranian Journal of Neurology Original Paper Iran J Neurol 2014; 13(3): 138-143 Comparison of electrophysiological findings in axonal and demyelinating Guillain-Barre syndrome Received: 9 Mar 2014 Accepted:
A Practical Approach to Polyneuropathy SLOCUM DICKSON ANNUAL TEACHING DAY NOVEMBER 4, 2017
 A Practical Approach to Polyneuropathy SLOCUM DICKSON ANNUAL TEACHING DAY NOVEMBER 4, 2017 Disclosures Research support from Cytokinetics, Inc Catalyst, Inc Editorial fees from UptoDate. Objectives Describe
A Practical Approach to Polyneuropathy SLOCUM DICKSON ANNUAL TEACHING DAY NOVEMBER 4, 2017 Disclosures Research support from Cytokinetics, Inc Catalyst, Inc Editorial fees from UptoDate. Objectives Describe
A family study of Charcot-Marie-Tooth disease
 Joturnal of Medical Genetics, 1982, 19, 88-93 A family study of Charcot-Marie-Tooth disease A P BROOKS* AND A E H EMERY From the University Department of Human Genetics, Western General Hospital, Edinburgh
Joturnal of Medical Genetics, 1982, 19, 88-93 A family study of Charcot-Marie-Tooth disease A P BROOKS* AND A E H EMERY From the University Department of Human Genetics, Western General Hospital, Edinburgh
For convenience values outside the normal range are bolded. Normal values for the specified patient are stated below the tables.
 Case tudy 8 or convenience values outside the normal range are bolded. Normal values for the specified patient are stated below the tables. History: 60 year-ol man with a history of left hand weakness
Case tudy 8 or convenience values outside the normal range are bolded. Normal values for the specified patient are stated below the tables. History: 60 year-ol man with a history of left hand weakness
Compound Action Potential, CAP
 Stimulus Strength UNIVERSITY OF JORDAN FACULTY OF MEDICINE DEPARTMENT OF PHYSIOLOGY & BIOCHEMISTRY INTRODUCTION TO NEUROPHYSIOLOGY Spring, 2013 Textbook of Medical Physiology by: Guyton & Hall, 12 th edition
Stimulus Strength UNIVERSITY OF JORDAN FACULTY OF MEDICINE DEPARTMENT OF PHYSIOLOGY & BIOCHEMISTRY INTRODUCTION TO NEUROPHYSIOLOGY Spring, 2013 Textbook of Medical Physiology by: Guyton & Hall, 12 th edition
Introduction and aims of the study
 Introduction and aims of the study 1 Chapter 1 Motor neuron diseases include the most incapacitating and life-threatening illnesses but also rather benign disorders with only mild symptoms and slow progression.
Introduction and aims of the study 1 Chapter 1 Motor neuron diseases include the most incapacitating and life-threatening illnesses but also rather benign disorders with only mild symptoms and slow progression.
PATTERNS OF NERVE CONDUCTION ABNORMALITIES IN POEMS SYNDROME
 ABSTRACT: Polyneuropathy, organomegaly, endocrinopathy, M protein, and skin changes (POEMS) syndrome is a rare cause of demyelinating and axonal neuropathy. POEMS syndrome and chronic inflammatory demyelinating
ABSTRACT: Polyneuropathy, organomegaly, endocrinopathy, M protein, and skin changes (POEMS) syndrome is a rare cause of demyelinating and axonal neuropathy. POEMS syndrome and chronic inflammatory demyelinating
A STUDY OF ASSESSMENT IN PERIPHERAL NEUROPATHY IN PATIENTS WITH NEWLY DETECTED THYROID DISORDERS IN A TERTIARY CARE TEACHING INSTITUTE
 A STUDY OF ASSESSMENT IN PERIPHERAL NEUROPATHY IN PATIENTS WITH NEWLY DETECTED THYROID DISORDERS IN A TERTIARY CARE TEACHING INSTITUTE Rajan Ganesan 1, Marimuthu Arumugam 2, Arungandhi Pachaiappan 3, Thilakavathi
A STUDY OF ASSESSMENT IN PERIPHERAL NEUROPATHY IN PATIENTS WITH NEWLY DETECTED THYROID DISORDERS IN A TERTIARY CARE TEACHING INSTITUTE Rajan Ganesan 1, Marimuthu Arumugam 2, Arungandhi Pachaiappan 3, Thilakavathi
Table 1: Nerve Conduction Studies (summarised)
 Table 1: Nerve Conduction Studies (summarised) Sensory nerve conduction 1 week* 3 months Superficial radial sensory Normal, symmetric SNAP and CV No change Median to digit II Normal, symmetric SNAP and
Table 1: Nerve Conduction Studies (summarised) Sensory nerve conduction 1 week* 3 months Superficial radial sensory Normal, symmetric SNAP and CV No change Median to digit II Normal, symmetric SNAP and
Case Report. Annals of Rehabilitation Medicine INTRODUCTION
 Case Report Ann Rehabil Med 2014;38(1):109-115 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2014.38.1.109 Annals of Rehabilitation Medicine Sonographic Evaluation of the Peripheral Nerves
Case Report Ann Rehabil Med 2014;38(1):109-115 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2014.38.1.109 Annals of Rehabilitation Medicine Sonographic Evaluation of the Peripheral Nerves
Comparison of diabetes patients with demyelinating diabetic sensorimotor polyneuropathy to those diagnosed with CIDP
 Comparison of diabetes patients with demyelinating diabetic sensorimotor polyneuropathy to those diagnosed with CIDP Samantha K. Dunnigan 1, Hamid Ebadi 1, Ari Breiner 1, Hans D. Katzberg 1, Leif E. Lovblom
Comparison of diabetes patients with demyelinating diabetic sensorimotor polyneuropathy to those diagnosed with CIDP Samantha K. Dunnigan 1, Hamid Ebadi 1, Ari Breiner 1, Hans D. Katzberg 1, Leif E. Lovblom
CLASSIFICATION OF PERIPHERAL NERVE DISEASES
 DIFFERENTIAL DIAGNOSIS OF NEUROGENIC DISORDERS & MYOPATHIES NEUROPATHY MYOPATHY Weakness distal proximal Sensory loss + 0 Loss of reflexes early late CSF protein elevated normal Electromyography neurogenic
DIFFERENTIAL DIAGNOSIS OF NEUROGENIC DISORDERS & MYOPATHIES NEUROPATHY MYOPATHY Weakness distal proximal Sensory loss + 0 Loss of reflexes early late CSF protein elevated normal Electromyography neurogenic
Imaging findings of Lower Extremity Peripheral Nerves in Charcot-Marie Tooth
 Original Research Imaging findings of Lower Extremity Peripheral Nerves in Charcot-Marie Tooth Jonelle M Petscavage-Thomas*, Sangeeta Chaudhary, Stephanie A Bernard, Eric A Walker and Gary A. Thomas Department
Original Research Imaging findings of Lower Extremity Peripheral Nerves in Charcot-Marie Tooth Jonelle M Petscavage-Thomas*, Sangeeta Chaudhary, Stephanie A Bernard, Eric A Walker and Gary A. Thomas Department
electrophysiological and nerve biopsy study
 Journal of Neurology, Neurosurgery, and Psychiatry 1984;47:543-548 Delayed neuropathy after organophosphorus insecticide (Dipterex) poisoning: a clinical, electrophysiological and nerve biopsy study C
Journal of Neurology, Neurosurgery, and Psychiatry 1984;47:543-548 Delayed neuropathy after organophosphorus insecticide (Dipterex) poisoning: a clinical, electrophysiological and nerve biopsy study C
A Comparison of Nerve Conduction Properties in Male and Female of 20 to 30 Years of Age Group
 A Comparison of Nerve Conduction Properties in Male and Female of 20 to 30 Years of Age Group Gakhar 1, M., Verma 2, S.K. and Lehri 3, A. 1 Research Scholar, Department of Sports Science, Punjabi University,
A Comparison of Nerve Conduction Properties in Male and Female of 20 to 30 Years of Age Group Gakhar 1, M., Verma 2, S.K. and Lehri 3, A. 1 Research Scholar, Department of Sports Science, Punjabi University,
International Journal of Ayurveda and Pharmaceutical Chemistry
 International Journal of Ayurveda and Pharmaceutical Chemistry Volume 7 Issue 2 2017 www.ijapc.com Managed by Green m RESEARCH ARTICLE www.ijapc.com e-issn 2350-0204 Role of an Advanced Diagnostic Technique
International Journal of Ayurveda and Pharmaceutical Chemistry Volume 7 Issue 2 2017 www.ijapc.com Managed by Green m RESEARCH ARTICLE www.ijapc.com e-issn 2350-0204 Role of an Advanced Diagnostic Technique
Nerve Conduction Study in Healthy Individuals: a Gender Based Study
 Original Article Nerve Conduction Study in Healthy Individuals: a Gender Based Study Dilip Thakur 1, BH Paudel 1, BK Bajaj 2, CB Jha 3 Department of Physiology 1 Internal Medicine 2 and Anatomy 3, BPKIHS
Original Article Nerve Conduction Study in Healthy Individuals: a Gender Based Study Dilip Thakur 1, BH Paudel 1, BK Bajaj 2, CB Jha 3 Department of Physiology 1 Internal Medicine 2 and Anatomy 3, BPKIHS
1/22/2019. Nerve conduction studies. Learning objectives: Jeffrey Allen MD University of Minnesota Minneapolis, MN
 Jeffrey Allen MD University of Minnesota Minneapolis, MN February 9, 2019 Learning objectives: Describe electrophysiologic features of peripheral nerve demyelination Identify electrophysiology findings
Jeffrey Allen MD University of Minnesota Minneapolis, MN February 9, 2019 Learning objectives: Describe electrophysiologic features of peripheral nerve demyelination Identify electrophysiology findings
Median-ulnar nerve communications and carpal tunnel syndrome
 Journal of Neurology, Neurosurgery, and Psychiatry, 1977, 40, 982-986 Median-ulnar nerve communications and carpal tunnel syndrome LUDWIG GUTMANN From the Department of Neurology, West Virginia University,
Journal of Neurology, Neurosurgery, and Psychiatry, 1977, 40, 982-986 Median-ulnar nerve communications and carpal tunnel syndrome LUDWIG GUTMANN From the Department of Neurology, West Virginia University,
EVALUATION OF HYPERPOLARIZATION POTENTIALS AND NERVE CONDUCTION PARAMETERS IN AXONAL NEUROPATHIC PATIENTS
 EVALUATION OF HYPERPOLARIZATION POTENTIALS AND NERVE CONDUCTION PARAMETERS IN AXONAL NEUROPATHIC PATIENTS Muhammad Abdul Azeem, Nabeeh Ibrahim Ali Rakkah, Muhammad Amir Mustufa, Anwar Ali *, Najamuddin
EVALUATION OF HYPERPOLARIZATION POTENTIALS AND NERVE CONDUCTION PARAMETERS IN AXONAL NEUROPATHIC PATIENTS Muhammad Abdul Azeem, Nabeeh Ibrahim Ali Rakkah, Muhammad Amir Mustufa, Anwar Ali *, Najamuddin
Ahmed Abbas, Mark Cook, Liong Hiew Fu, Alistair Lewthwaite, Colin Shirley, Yusuf A. Rajabally
 2016, Elsevier. Licensed under the Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International http://creativecommons.org/licenses/by-nc-nd/4.0/ Accepted Manuscript A case of POEMS mimicking
2016, Elsevier. Licensed under the Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International http://creativecommons.org/licenses/by-nc-nd/4.0/ Accepted Manuscript A case of POEMS mimicking
The near-nerve sensory nerve conduction in tarsal tunnel syndrome
 Journal of Neurology, Neurosurgery, and Psychiatry 1985;48: 999-1003 The near-nerve sensory nerve conduction in tarsal tunnel syndrome SHN J OH, HYUN S KM, BASHRUDDN K AHMAD From the Department ofneurology,
Journal of Neurology, Neurosurgery, and Psychiatry 1985;48: 999-1003 The near-nerve sensory nerve conduction in tarsal tunnel syndrome SHN J OH, HYUN S KM, BASHRUDDN K AHMAD From the Department ofneurology,
Clinical and Electrophysiological Abnormalities amongst the Patients of Diabetic Truncal Polyneuropathy
 Original Article GCSMC J Med Sci Vol (VI) No (II) July-December 2017 Clinical and Electrophysiological Abnormalities amongst the Patients of Diabetic Truncal Polyneuropathy Chilvana Patel*, Surya Murthy
Original Article GCSMC J Med Sci Vol (VI) No (II) July-December 2017 Clinical and Electrophysiological Abnormalities amongst the Patients of Diabetic Truncal Polyneuropathy Chilvana Patel*, Surya Murthy
Neuromuscular Respiratory Failure in Guillain-Barre Syndrome: Evaluation of Clinical and Electrodiagnostic Predictors
 Original Article Neuromuscular Respiratory Failure in Guillain-Barre Syndrome: Evaluation of Clinical and Electrodiagnostic Predictors Uma Sundar, Elizabeth Abraham, A Gharat, ME Yeolekar, Trupti Trivedi,
Original Article Neuromuscular Respiratory Failure in Guillain-Barre Syndrome: Evaluation of Clinical and Electrodiagnostic Predictors Uma Sundar, Elizabeth Abraham, A Gharat, ME Yeolekar, Trupti Trivedi,
Differential Diagnosis of Neuropathies and Compression. Dr Ashwin Pinto Consultant Neurologist Wessex Neurological Centre
 Differential Diagnosis of Neuropathies and Compression Dr Ashwin Pinto Consultant Neurologist Wessex Neurological Centre Outline of talk Mononeuropathies median and anterior interosseous nerve ulnar nerve
Differential Diagnosis of Neuropathies and Compression Dr Ashwin Pinto Consultant Neurologist Wessex Neurological Centre Outline of talk Mononeuropathies median and anterior interosseous nerve ulnar nerve
Charcot-Marie-Tooth disease (CMT) is the eponym
 ORIGINAL ARTICLE Charcot-Marie-Tooth Disease Subtypes and Genetic Testing Strategies Anita S.D. Saporta, MD, 1 Stephanie L. Sottile, BA, 1 Lindsey J. Miller, MS, 1 Shawna M.E. Feely, MS, 1 Carly E. Siskind,
ORIGINAL ARTICLE Charcot-Marie-Tooth Disease Subtypes and Genetic Testing Strategies Anita S.D. Saporta, MD, 1 Stephanie L. Sottile, BA, 1 Lindsey J. Miller, MS, 1 Shawna M.E. Feely, MS, 1 Carly E. Siskind,
DIFFERENTIAL DIAGNOSIS OF NEUROGENIC DISORDERS & MYOPATHIES
 DIFFERENTIAL DIAGNOSIS OF NEUROGENIC DISORDERS & MYOPATHIES NEUROPATHY MYOPATHY Weakness distal proximal Sensory dysfunction + 0 Loss of reflexes early late Serum enzymes +/- +++ CSF protein may be elevated
DIFFERENTIAL DIAGNOSIS OF NEUROGENIC DISORDERS & MYOPATHIES NEUROPATHY MYOPATHY Weakness distal proximal Sensory dysfunction + 0 Loss of reflexes early late Serum enzymes +/- +++ CSF protein may be elevated
Electrodiagnostic Variations in Guillain-Barré Syndrome - Retrospective Analysis of 95 Patients
 Original Article GCSMC J Med Sci Vol (VI) No (II) July-December 2017 Electrodiagnostic Variations in Guillain-Barré Syndrome - Retrospective Analysis of 95 Patients Chilvana Patel*, Surya Murthy Vishnubhakat**
Original Article GCSMC J Med Sci Vol (VI) No (II) July-December 2017 Electrodiagnostic Variations in Guillain-Barré Syndrome - Retrospective Analysis of 95 Patients Chilvana Patel*, Surya Murthy Vishnubhakat**
The clinical spectrum of Malaysian patients with. Chronic inflammatory demyelinating polyneuropathy
 Neurology Asia 2004; 9 : 39 45 The clinical spectrum of Malaysian patients with chronic inflammatory demyelinating polyneuropathy Khean Jin GOH, Wai Keong NG, Nee Kong CHEW, Chong Tin TAN Division of Neurology,
Neurology Asia 2004; 9 : 39 45 The clinical spectrum of Malaysian patients with chronic inflammatory demyelinating polyneuropathy Khean Jin GOH, Wai Keong NG, Nee Kong CHEW, Chong Tin TAN Division of Neurology,
Electrodiagnostics for Back & Neck Pain. Steven Andersen, MD Providence Physiatry Clinic
 Electrodiagnostics for Back & Neck Pain Steven Andersen, MD Providence Physiatry Clinic Electrodiagnostics Electromyography (EMG) Needle EMG exam (NEE) Nerve conduction studies (NCS) Motor Sensory Late
Electrodiagnostics for Back & Neck Pain Steven Andersen, MD Providence Physiatry Clinic Electrodiagnostics Electromyography (EMG) Needle EMG exam (NEE) Nerve conduction studies (NCS) Motor Sensory Late
Borderline Moderately out of normal range Severely out of normal range Technical
 Urgent Care Specialists 2200 Universal Drive, Boston, MA Phone: 761-621-5216 Fax: 761-564-0336 Report: EMG-1133-28616 Physician: Dr. John Smith Age Range: 40-59 Ref Phys: Dr. Joe Ranier Height Range cm:
Urgent Care Specialists 2200 Universal Drive, Boston, MA Phone: 761-621-5216 Fax: 761-564-0336 Report: EMG-1133-28616 Physician: Dr. John Smith Age Range: 40-59 Ref Phys: Dr. Joe Ranier Height Range cm:
ORIGINAL ARTICLE. Is Bell s palsy a component of polyneuropathy?
 ORIGINAL ARTICLE Is Bell s palsy a component of polyneuropathy? Tu ba Tunç MD, Erkan Tarhan MD,, Haldun O uz MD, Mustafa As m Þafak MD, Gülnihal Kutlu MD, Levent E. nan MD From Ministry of Health, Ankara
ORIGINAL ARTICLE Is Bell s palsy a component of polyneuropathy? Tu ba Tunç MD, Erkan Tarhan MD,, Haldun O uz MD, Mustafa As m Þafak MD, Gülnihal Kutlu MD, Levent E. nan MD From Ministry of Health, Ankara
ORIGINAL COMMUNICATION. IVIg dose increase
 J Neurol (2009) 256:608 614 DOI 10.1007/s00415-009-0130-0 ORIGINAL COMMUNICATION Andreas Baumann Christian W. Hess Matthias Sturzenegger IVIg dose increase in multifocal motor neuropathy A prospective
J Neurol (2009) 256:608 614 DOI 10.1007/s00415-009-0130-0 ORIGINAL COMMUNICATION Andreas Baumann Christian W. Hess Matthias Sturzenegger IVIg dose increase in multifocal motor neuropathy A prospective
Electrodiagnostic studies comprising of electromyography (EMG) and nerve
 INTRODUCTION AND TERMINOLOGY Electrodiagnostic studies comprising of electromyography (EMG) and nerve conduction studies (NCS) are well-established objective methods for the diagnosis, quantification and
INTRODUCTION AND TERMINOLOGY Electrodiagnostic studies comprising of electromyography (EMG) and nerve conduction studies (NCS) are well-established objective methods for the diagnosis, quantification and
PERIPHERAL NERVE CONDUCTION VELOCITIES AND HANDEDNESS IS THERE ANY CORELATION? (govt. Medical College surat.)(anirudha Apte-consultant Neurologist)
 6 PERIPHERAL NERVE CONDUCTION VELOCITIES AND HANDEDNESS IS THERE ANY CORELATION? ABSTRACT: SWAPNA APTE 1, ANIRUDHA APTE 2, HETAL THAKER 1 RAVI SAXENA 1 RINI TEKRIWAL 2, DHARITRI PARMAR 2. (govt. Medical
6 PERIPHERAL NERVE CONDUCTION VELOCITIES AND HANDEDNESS IS THERE ANY CORELATION? ABSTRACT: SWAPNA APTE 1, ANIRUDHA APTE 2, HETAL THAKER 1 RAVI SAXENA 1 RINI TEKRIWAL 2, DHARITRI PARMAR 2. (govt. Medical
Research Article Supramaximal Stimulus Intensity as a Diagnostic Tool in Chronic Demyelinating Neuropathy
 Neuroscience Journal Volume 2016, Article ID 6796270, 5 pages http://dx.doi.org/10.1155/2016/6796270 Research Article Supramaximal Stimulus Intensity as a Diagnostic Tool in Chronic Demyelinating Neuropathy
Neuroscience Journal Volume 2016, Article ID 6796270, 5 pages http://dx.doi.org/10.1155/2016/6796270 Research Article Supramaximal Stimulus Intensity as a Diagnostic Tool in Chronic Demyelinating Neuropathy
Index. Phys Med Rehabil Clin N Am 14 (2003) Note: Page numbers of article titles are in boldface type.
 Phys Med Rehabil Clin N Am 14 (2003) 445 453 Index Note: Page numbers of article titles are in boldface type. A Acid maltase deficiencies, electrodiagnosis of, 420, 422 Acquired peripheral neuropathy,
Phys Med Rehabil Clin N Am 14 (2003) 445 453 Index Note: Page numbers of article titles are in boldface type. A Acid maltase deficiencies, electrodiagnosis of, 420, 422 Acquired peripheral neuropathy,
Nerve Conduction Studies and EMG
 Nerve Conduction Studies and EMG Limitations of other methods of investigations of the neuromuscular system - Dr Rob Henderson, Neurologist Assessment of Weakness Thanks Peter Silburn PERIPHERAL NEUROPATHY
Nerve Conduction Studies and EMG Limitations of other methods of investigations of the neuromuscular system - Dr Rob Henderson, Neurologist Assessment of Weakness Thanks Peter Silburn PERIPHERAL NEUROPATHY
The second lumbrical-interossei latency difference in carpal tunnel syndrome: Is it a mandatory or a dispensable test?
 Alexandria Journal of Medicine (2013) 49, 199 205 Alexandria University Faculty of Medicine Alexandria Journal of Medicine www.sciencedirect.com ORIGINAL ARTICLE The second lumbrical-interossei latency
Alexandria Journal of Medicine (2013) 49, 199 205 Alexandria University Faculty of Medicine Alexandria Journal of Medicine www.sciencedirect.com ORIGINAL ARTICLE The second lumbrical-interossei latency
Case Report Central Nervous System Demyelination in a Charcot-Marie-Tooth Type 1A Patient
 Case Reports in Neurological Medicine Volume 2013, Article ID 243652, 4 pages http://dx.doi.org/10.1155/2013/243652 Case Report Central Nervous System Demyelination in a Charcot-Marie-Tooth Type 1A Patient
Case Reports in Neurological Medicine Volume 2013, Article ID 243652, 4 pages http://dx.doi.org/10.1155/2013/243652 Case Report Central Nervous System Demyelination in a Charcot-Marie-Tooth Type 1A Patient
NERVE CONDUCTION STUDY AMONG HEALTHY MALAYS. THE INFLUENCE OF AGE, HEIGHT AND BODY MASS INDEX ON MEDIAN, ULNAR, COMMON PERONEAL AND SURAL NERVES
 Malaysian Journal of Medical Sciences, Vol. 13, No. 2, July 2006 (19-23) ORIGINAL ARTICLE NERVE CONDUCTION STUDY AMONG HEALTHY MALAYS. THE INFLUENCE OF AGE, HEIGHT AND BODY MASS INDEX ON MEDIAN, ULNAR,
Malaysian Journal of Medical Sciences, Vol. 13, No. 2, July 2006 (19-23) ORIGINAL ARTICLE NERVE CONDUCTION STUDY AMONG HEALTHY MALAYS. THE INFLUENCE OF AGE, HEIGHT AND BODY MASS INDEX ON MEDIAN, ULNAR,
A Tale of Five Demyelinating Neuropathies
 Objectives A Tale of Five Demyelinating Neuropathies Tahseen Mozaffar, MD FAAN Professor and Vice Chair of Neurology Director, UC Irvine-MDA ALS and Neuromuscular Center Director, Neurology Residency Training
Objectives A Tale of Five Demyelinating Neuropathies Tahseen Mozaffar, MD FAAN Professor and Vice Chair of Neurology Director, UC Irvine-MDA ALS and Neuromuscular Center Director, Neurology Residency Training
3/17/2015. Amyotrophic lateral sclerosis Nerve conduction studies/electromyography Differential diagnosis Other motor neuron syndromes
 B. Jane Distad, MD Associate Professor Department of Neurology 2015 Amyotrophic lateral sclerosis Nerve conduction studies/electromyography Differential diagnosis Other motor neuron syndromes Spinal muscular
B. Jane Distad, MD Associate Professor Department of Neurology 2015 Amyotrophic lateral sclerosis Nerve conduction studies/electromyography Differential diagnosis Other motor neuron syndromes Spinal muscular
Traumatic Nerve Injuries. Nerve Injuries and Repair as Seen Through Electrodiagnostic Medicine
 Nerve Injuries and Repair as Seen Through Electrodiagnostic Medicine Ultra EMG February 2013 William S. Pease, M.D. Traumatic Nerve Injuries An orderly sequence of degeneration and regeneration follows
Nerve Injuries and Repair as Seen Through Electrodiagnostic Medicine Ultra EMG February 2013 William S. Pease, M.D. Traumatic Nerve Injuries An orderly sequence of degeneration and regeneration follows
Cervical radiculopathy: diagnostic aspects and non-surgical treatment Kuijper, B.
 UvA-DARE (Digital Academic Repository) Cervical radiculopathy: diagnostic aspects and non-surgical treatment Kuijper, B. Link to publication Citation for published version (APA): Kuijper, B. (2011). Cervical
UvA-DARE (Digital Academic Repository) Cervical radiculopathy: diagnostic aspects and non-surgical treatment Kuijper, B. Link to publication Citation for published version (APA): Kuijper, B. (2011). Cervical
Normative Data of Needle Electromyography, What Is Different in Iraqi Patients?
 NORMATIVE THE IRAQI POSTGRADUATE DATA OF MEDICAL NEEDLE JOURNAL ELECTROMYOGRAPHY Normative Data of Needle Electromyography, What Is Different in Iraqi Patients? Hasan Azeez Al-hamadani*,Zainulabdeen Abdulsamad
NORMATIVE THE IRAQI POSTGRADUATE DATA OF MEDICAL NEEDLE JOURNAL ELECTROMYOGRAPHY Normative Data of Needle Electromyography, What Is Different in Iraqi Patients? Hasan Azeez Al-hamadani*,Zainulabdeen Abdulsamad
LATE RESPONSES IN THE ELECTRODIAGNOSIS OF CERVICAL RADICULOPATHIES
 Neurology DOI: 10.15386/cjmed-382 LATE RESPONSES IN THE ELECTRODIAGNOSIS OF CERVICAL RADICULOPATHIES ANA MARIA GALAMB, IOAN DAN MINEA Department of Medical and Surgical Specialities, Faculty of Medicine,
Neurology DOI: 10.15386/cjmed-382 LATE RESPONSES IN THE ELECTRODIAGNOSIS OF CERVICAL RADICULOPATHIES ANA MARIA GALAMB, IOAN DAN MINEA Department of Medical and Surgical Specialities, Faculty of Medicine,
Conventional needle electromyography
 3 rd Congress of the European Academy of Neurology Amsterdam, The Netherlands, June 24 27, 2017 Hands-on Course 5 Electromyography: Surface, needle conventional and single fiber - Level 1-2 Conventional
3 rd Congress of the European Academy of Neurology Amsterdam, The Netherlands, June 24 27, 2017 Hands-on Course 5 Electromyography: Surface, needle conventional and single fiber - Level 1-2 Conventional
DSS-1. No financial disclosures
 DSS-1 No financial disclosures Clinical History 9 year old boy with past medical history significant for cerebral palsy, in-turning right foot, left clubfoot that was surgically corrected at 3 years of
DSS-1 No financial disclosures Clinical History 9 year old boy with past medical history significant for cerebral palsy, in-turning right foot, left clubfoot that was surgically corrected at 3 years of
Saeid Khosrawi, Farnaz Dehghan Department of Physical Medicine and Rehabilitation, Isfahan University of Medical Sciences, Isfahan, Iran
 Original Article Determination of the median nerve residual latency values in the diagnosis of carpal tunnel syndrome in comparison with other electrodiagnostic parameters Saeid Khosrawi, Farnaz Dehghan
Original Article Determination of the median nerve residual latency values in the diagnosis of carpal tunnel syndrome in comparison with other electrodiagnostic parameters Saeid Khosrawi, Farnaz Dehghan
THE ROLE OF NEURO-ELECTROPHYSIOLOGICAL DIAGNOSTIC TESTS IN CLINICAL MEDICINE S.O. MBUYA ABSTRACT
 52 EAST AFRICAN MEDICAL JOURNAL January 2006 East African Medical Journal Vol. 83 No. 1 January 2006 THE ROLE OF NEURO-ELECTROPHYSIOLOGICAL DIAGNOSTIC TESTS IN CLINICAL MEDICINE S.O. Mbuya, MBChB, MMed,
52 EAST AFRICAN MEDICAL JOURNAL January 2006 East African Medical Journal Vol. 83 No. 1 January 2006 THE ROLE OF NEURO-ELECTROPHYSIOLOGICAL DIAGNOSTIC TESTS IN CLINICAL MEDICINE S.O. Mbuya, MBChB, MMed,
Evaluation of nerve conduction abnormalities in type 2 diabetic patients
 Original article: Evaluation of nerve conduction abnormalities in type 2 diabetic patients 1Kannan K, 2 Sivaraj M 1Asst Professor, Dept of Physiology, kilpauk Medical College, Kilpauk, Chennai, Tamil Nadu,
Original article: Evaluation of nerve conduction abnormalities in type 2 diabetic patients 1Kannan K, 2 Sivaraj M 1Asst Professor, Dept of Physiology, kilpauk Medical College, Kilpauk, Chennai, Tamil Nadu,
Clinical and Neurophysiological Pattern of Guillain-Barré Syndrome in Diabetic and Non Diabetic Patients
 Clinical and Neurophysiological Pattern of Guillain-Barré Syndrome in Diabetic and Non Diabetic Patients Shereen Zakarya Department of Neurology, Mansoura University ABSTRACT Objective: To study the clinical
Clinical and Neurophysiological Pattern of Guillain-Barré Syndrome in Diabetic and Non Diabetic Patients Shereen Zakarya Department of Neurology, Mansoura University ABSTRACT Objective: To study the clinical
Abnormal EMG Patterns in Disease. Amanda C. Peltier, MD MS October 12, 2013
 Abnormal EMG Patterns in Disease Amanda C. Peltier, MD MS October 12, 2013 Disclosures I have no financial relationships to disclose that are relative to the content of my presentation. Basic Tenets of
Abnormal EMG Patterns in Disease Amanda C. Peltier, MD MS October 12, 2013 Disclosures I have no financial relationships to disclose that are relative to the content of my presentation. Basic Tenets of
A CASE OF GIANT AXONAL NEUROPATHY HEMANANTH T SECOND YEAR POST GRADUATE IN PAEDIATRICS INSTITUTE OF SOCIAL PAEDIATRICS GOVERNMENT STANLEY HOSPITAL
 A CASE OF GIANT AXONAL NEUROPATHY HEMANANTH T SECOND YEAR POST GRADUATE IN PAEDIATRICS INSTITUTE OF SOCIAL PAEDIATRICS GOVERNMENT STANLEY HOSPITAL CASE HISTORY Nine year old male child Second born Born
A CASE OF GIANT AXONAL NEUROPATHY HEMANANTH T SECOND YEAR POST GRADUATE IN PAEDIATRICS INSTITUTE OF SOCIAL PAEDIATRICS GOVERNMENT STANLEY HOSPITAL CASE HISTORY Nine year old male child Second born Born
Case Report An Unusual Case of Recurrent Guillain-Barre Syndrome of a Different Subtype Five Years after Initial Diagnosis
 Case Reports in Neurological Medicine Volume 2013, Article ID 356157, 4 pages http://dx.doi.org/10.1155/2013/356157 Case Report An Unusual Case of Recurrent Guillain-Barre Syndrome of a Different Subtype
Case Reports in Neurological Medicine Volume 2013, Article ID 356157, 4 pages http://dx.doi.org/10.1155/2013/356157 Case Report An Unusual Case of Recurrent Guillain-Barre Syndrome of a Different Subtype
MR Imaging of the Cauda Equina in Charcot-Marie-Tooth disease
 MR Imaging of the Cauda Equina in Charcot-Marie-Tooth disease Poster No.: C-0741 Congress: ECR 2015 Type: Scientific Exhibit Authors: Y. Tatewaki, S. Nishiyama, Y. Kato, T. Murata, S. Mugikura, L. Li,
MR Imaging of the Cauda Equina in Charcot-Marie-Tooth disease Poster No.: C-0741 Congress: ECR 2015 Type: Scientific Exhibit Authors: Y. Tatewaki, S. Nishiyama, Y. Kato, T. Murata, S. Mugikura, L. Li,
The Role of Hyperlipidemia on Nerve Conduction. Abdul Raheem H Dawoud, MB,ChB, Board* Shaymaa J Al Shareefi, MB,ChB, MSc* Hedef D El Yassin, PhD, **
 Bahrain Medical Bulletin, Vol. ٣٠, No. ٢, June ٢٠٠٨ The Role of Hyperlipidemia on Nerve Conduction Abdul Raheem H Dawoud, MB,ChB, Board* Shaymaa J Al Shareefi, MB,ChB, MSc* Hedef D El Yassin, PhD, ** Background:
Bahrain Medical Bulletin, Vol. ٣٠, No. ٢, June ٢٠٠٨ The Role of Hyperlipidemia on Nerve Conduction Abdul Raheem H Dawoud, MB,ChB, Board* Shaymaa J Al Shareefi, MB,ChB, MSc* Hedef D El Yassin, PhD, ** Background:
Muscle Weakness Or Paralysis With Compromise Of Peripheral Nerve
 Muscle Weakness Or Paralysis With Compromise Of Peripheral Nerve Muscle weakness or complete paralysis may be secondary to an interruption in the communication between the brain and nerve cells in the
Muscle Weakness Or Paralysis With Compromise Of Peripheral Nerve Muscle weakness or complete paralysis may be secondary to an interruption in the communication between the brain and nerve cells in the
Diabetic Neuropathy. Nicholas J. Silvestri, M.D.
 Diabetic Neuropathy Nicholas J. Silvestri, M.D. Types of Neuropathies Associated with Diabetes Mellitus p Chronic distal sensorimotor polyneuropathy p Focal compression neuropathies p Autonomic neuropathy
Diabetic Neuropathy Nicholas J. Silvestri, M.D. Types of Neuropathies Associated with Diabetes Mellitus p Chronic distal sensorimotor polyneuropathy p Focal compression neuropathies p Autonomic neuropathy
Sensory mononeuritis: differentiating pure neural leprosy from non-systemic vasculitic neuropathy
 Lepr Rev (2017) 88, 274 279 CASE REPORT Sensory mononeuritis: differentiating pure neural leprosy from non-systemic vasculitic neuropathy PINELOPI TSOUNI*, JOHANNES ALEXANDER LOBRINUS**, ANDREAS J. STECK*
Lepr Rev (2017) 88, 274 279 CASE REPORT Sensory mononeuritis: differentiating pure neural leprosy from non-systemic vasculitic neuropathy PINELOPI TSOUNI*, JOHANNES ALEXANDER LOBRINUS**, ANDREAS J. STECK*
Sciatic nerve motor conduction velocity studyt
 J. Neurol. Neurosurg. Psychiat., 1967, 30, 233 Sciatic nerve motor conduction velocity studyt C.-B. YAP AND T. HIROTA From the Department of Neurology and Psychiatry, Northwestern University Medical School,
J. Neurol. Neurosurg. Psychiat., 1967, 30, 233 Sciatic nerve motor conduction velocity studyt C.-B. YAP AND T. HIROTA From the Department of Neurology and Psychiatry, Northwestern University Medical School,
ORIGINAL CONTRIBUTION. Value of the Oral Glucose Tolerance Test in the Evaluation of Chronic Idiopathic Axonal Polyneuropathy
 ORIGINAL CONTRIBUTION Value of the Oral Glucose Tolerance Test in the Evaluation of Chronic Idiopathic Axonal Polyneuropathy Charlene Hoffman-Snyder, MSN, NP-BC; Benn E. Smith, MD; Mark A. Ross, MD; Jose
ORIGINAL CONTRIBUTION Value of the Oral Glucose Tolerance Test in the Evaluation of Chronic Idiopathic Axonal Polyneuropathy Charlene Hoffman-Snyder, MSN, NP-BC; Benn E. Smith, MD; Mark A. Ross, MD; Jose
F wave index: A diagnostic tool for peripheral neuropathy
 Indian J Med Res 145, March 2017, pp 353-357 DOI: 10.4103/ijmr.IJMR_1087_14 Quick Response Code: F wave index: A diagnostic tool for peripheral neuropathy G. R. Sathya 1, N. Krishnamurthy 1, Susheela Veliath
Indian J Med Res 145, March 2017, pp 353-357 DOI: 10.4103/ijmr.IJMR_1087_14 Quick Response Code: F wave index: A diagnostic tool for peripheral neuropathy G. R. Sathya 1, N. Krishnamurthy 1, Susheela Veliath
Hyperreflexia in Guillain-Barré syndrome: relation with acute motor axonal neuropathy and anti-gm1 antibody
 18 Department of Neurology, Chiba University School of Medicine, Chiba, Japan S Kuwabara K Ogawara M Mori T Hattori Department of Neurology, Dokkyo University School of Medicine, Tochigi, Japan M Koga
18 Department of Neurology, Chiba University School of Medicine, Chiba, Japan S Kuwabara K Ogawara M Mori T Hattori Department of Neurology, Dokkyo University School of Medicine, Tochigi, Japan M Koga
Hereditary distal spinal muscular atrophy
 Journal of Neurology, Neurosurgery, and Psychiatry, 1980, 43, 413-418 Hereditary distal spinal muscular atrophy with vocal cord paralysis I D YOUNG AND P S HARPER From the Section ofmedical Genetics, Department
Journal of Neurology, Neurosurgery, and Psychiatry, 1980, 43, 413-418 Hereditary distal spinal muscular atrophy with vocal cord paralysis I D YOUNG AND P S HARPER From the Section ofmedical Genetics, Department
Human nerve excitability
 Journal of Neurology, Neurosurgery, andpsychiatry, 1978, 41, 642-648 Human nerve excitability RICHARD E. MICHAEL P. POWERS", HERBERT M. SWICK, AND McQUILLEN From the Department of Neurology, University
Journal of Neurology, Neurosurgery, andpsychiatry, 1978, 41, 642-648 Human nerve excitability RICHARD E. MICHAEL P. POWERS", HERBERT M. SWICK, AND McQUILLEN From the Department of Neurology, University
Three patients in a Chinese family with hereditary sensory neuropathy mimicking leprosy
 Lepr Rev (2008) 79, 441 446 CASE REPORT Three patients in a Chinese family with hereditary sensory neuropathy mimicking leprosy JIANPING SHEN*, GUOCHENG ZHANG*, RONGDE YANG**, TINGYING HU** & MIN ZHOU*
Lepr Rev (2008) 79, 441 446 CASE REPORT Three patients in a Chinese family with hereditary sensory neuropathy mimicking leprosy JIANPING SHEN*, GUOCHENG ZHANG*, RONGDE YANG**, TINGYING HU** & MIN ZHOU*
NORMATIVE DATA OF UPPER LIMB NERVE CONDUCTION IN CENTRAL INDIA
 Indian J Physiol Pharmacol 2011; 55 (3) : 241 245 NORMATIVE DATA OF UPPER LIMB NERVE CONDUCTION IN CENTRAL INDIA SACHIN M. PAWAR, AVINASH B. TAKSANDE AND RAMJI SINGH* Department of Physiology, Mahatma
Indian J Physiol Pharmacol 2011; 55 (3) : 241 245 NORMATIVE DATA OF UPPER LIMB NERVE CONDUCTION IN CENTRAL INDIA SACHIN M. PAWAR, AVINASH B. TAKSANDE AND RAMJI SINGH* Department of Physiology, Mahatma
Neurophysiological Diagnosis of Birth Brachial Plexus Palsy. Dr Grace Ng Department of Paed PMH
 Neurophysiological Diagnosis of Birth Brachial Plexus Palsy Dr Grace Ng Department of Paed PMH Brachial Plexus Anatomy Brachial Plexus Cords Medial cord: motor and sensory conduction for median and ulnar
Neurophysiological Diagnosis of Birth Brachial Plexus Palsy Dr Grace Ng Department of Paed PMH Brachial Plexus Anatomy Brachial Plexus Cords Medial cord: motor and sensory conduction for median and ulnar
Charcot-Marie-Tooth Disease (CMT) Sometimes known as Hereditary Motor and Sensory neuropathy (HMSN) or Peroneal Muscular Atrophy (PMA)
 Version: 2 Published: January 2004 Updated: December 2009 Date of review: November 2011 Author: Dr.Hilton-Jones MD, FRCP, FRCPE Clinical Director, Oxford MDC Muscle and Nerve Centre, and revised by Dr.
Version: 2 Published: January 2004 Updated: December 2009 Date of review: November 2011 Author: Dr.Hilton-Jones MD, FRCP, FRCPE Clinical Director, Oxford MDC Muscle and Nerve Centre, and revised by Dr.
