Radiofrequency ablation of hepatocellular carcinoma as a bridge to liver transplantation
|
|
|
- Alicia Baker
- 5 years ago
- Views:
Transcription
1 DOI: /j x HPB ORIGINAL ARTICLE Radiofrequency ablation of hepatocellular carcinoma as a bridge to liver transplantation DerekA.DuBay 1 *, Charbel Sandroussi 1 *, John R. Kachura 2, Chia Sing Ho 2, J. Robert Beecroft 2, Charles M. Vollmer 3, Anand Ghanekar 1, Markus Guba 1, Mark S. Cattral 1, Ian D. McGilvray 1, David R. Grant 1 & Paul D. Greig 1 1 Liver Transplant Unit, Multiorgan Transplant Programme, University of Toronto, 2 Division of Vascular and Interventional Radiology, Department of Medical Imaging, Toronto General Hospital and Mount Sinai Hospital, University of Toronto, Toronto, Ontario, Canada, and 3 Division of General Surgery, Beth Israel Deaconess Medical Center, Harvard School of Medicine, Boston, MA, USA Abstracthpb_ Background: Radiofrequency ablation () of hepatocellular carcinoma (HCC) is widely utilized as a bridge to liver transplant with limited evidence to support efficacy. The purpose of the present study was to measure the effect of on time to drop-off in HCC-listed patients. Methods: Patients with Milan criteria tumours listed between January 1999 and June 2007 were stratified into (n = 77) and No Treatment groups (n = 93). Results: The primary effectiveness of was 83% (complete radiographic response). was associated with a longer median wait time to transplant (9.5 vs. 5 months). Tumour-specific drop-off events were equivalent between (21%) and No Treatment (12%) groups (P = 0.11). Controlling for wait time, there was no difference in overall (P = 0.56) or tumour-specific drop-off (P = 0.94). Furthermore, there were no differences in 5-year overall or tumour-free survivals from list date or transplant. Using multivariate analysis, the likelihood of receiving a transplant and patient survivals were associated with tumour characteristics (AFP, tumour number and size) and not with bridge therapy or waiting time. Discussion: allows patients to be maintained longer on the waiting list without negative consequences on drop-off or survival compared with no treatment. Post-transplant outcomes are affected more by tumour characteristics than or wait time. Keywords radiofrequency ablation, hepatocellular carcinoma, waiting list drop-off, Milan criteria, surgical treatment Received 28 June 2010; accepted 24 July 2010 Correspondence Paul D. Greig, NCSB, Toronto General Hospital, 585 University Avenue, Toronto, Ontario M5G 2N2, Canada. Tel: ; Fax: ; paul.greig@uhn.on.ca Introduction Liver transplantation is the most effective treatment for patients with hepatocellular carcinoma (HCC) arising in the setting of cirrhosis. 1 Liver transplant for HCC is only effective if the majority of patients awaiting transplantation survive and remain eligible to receive this treatment. 2 4 The primary goal of bridging therapy is to prevent waiting list drop-off by reducing tumour progression while secondary goals include the prevention of HCC recurrence and improving survival after liver transplantation. 5 9 In 2006, more than 50% of all patients listed for liver transplant *Contributed equally to first authorship. in the United States with a diagnosis of HCC received bridging therapy. 6 Although widely offered and applied, recent reviews have uniformly concluded that there is no evidence in the literature proving the efficacy of bridging therapies in maintaining patients on the list or improving post transplant survival. 5,8 12 Tumour ablation is a process whereby known or suspected HCC tumour nodules are destroyed by thermal or chemical injury via either a percutaneous or a surgical approach. Tumour destruction is then monitored by radiological measures. There are a variety of ablation techniques although radiofrequency ablation () has become the most common technique used in North America. 6 has been shown to be safe; with minimal morbidity and mortality both in transplant and non-transplant
2 HPB 25 populations There are several single centre reports of using as a bridge to transplant, documenting the safety of this intervention Although conceptually attractive, there are no controlled studies to suggest that truly impacts relevant HCC transplant patient outcomes. The present study was undertaken to determine the efficacy of as a bridge to transplant in patients with Milan criteria HCC. The primary aim was to determine whether increased the time taken to drop-off the waiting list. The secondary aims were to determine whether improved the chances of being transplanted, overall and disease-free survival (DFS). We hypothesized that as a bridge to transplant would decrease waiting list drop-off in a time to event model. Methods Ethics approval for this study was obtained from the Research Ethics Board of University Health Network (Protocol no CE). Patients During the period between January 1999 and June 2007, all patients with the diagnosis of HCC who were placed on the liver transplant waiting list or listed patients who developed an HCC while waiting for liver transplant were evaluated for this study. Only patients whose HCC tumour pattern fulfilled the Milan criteria were included in this study. These patients were identified using the Organ Transplant Tracking Registry (OTTR, HKS Medical Information Systems, Omaha, NE), which is an internal web-based electronic medical record that encompasses all patients evaluated for a solid organ transplant at the University Health Network, University of Toronto. For the purpose of the present study, the diagnosis of HCC was verified by review of the pretransplant radiological imaging, pre-transplant tumour histology (when performed) and the liver explant pathology. A total of 343 patients were listed and/or transplanted with a diagnosis of HCC. The following patients were excluded from this study: 105 patients with a tumour pattern that exceeded the Milan criteria, 24 patients with incidental tumours identified by explant pathology that were not suspected or recognized before transplant, 4 patients who received their procedures at a different institution and 3 patients who received a liver transplant at a different institution. An additional 18 patients with a history of a partial hepatectomy for HCC were excluded as these patients already had recurrent HCC and likely exhibited more aggressive tumour biology. To specifically analyse the effect of as bridging therapy vs. no treatment, Milan criteria patients who received bridging therapies other than were also excluded: 14 patients that received a percutaneous ethanol injection (PEI), 3 patients who received transarterial chemoembolization (TACE) therapy and 2 patients who received external beam radiotherapy. There were a total of 170 patients with the diagnosis of HCC recognized prior to transplant with a tumour pattern that radiographically fulfilled the Milan criteria: 77 patients received as a sole bridging therapy and 93 patients received no bridging therapy. Bridging therapy interventions were offered to patients at the University of Toronto beginning in 1999 and became our institution s recommended treatment (over TACE or PEI) for patients with small ( 4 cm),few( 3 lesions) unresectable HCCs that were remote from major biliary structures. Given the equipoise between and TACE as effective bridge therapy, evolved as our institutional standard for reasons of local expertise, resource availability and overall lower morbidity in favour of. Bridging therapies were offered to patients after review at a multidisciplinary HCC Tumour Review Board. as bridging therapy was recommended to patients with ablatable lesions who were expected to have a transplant wait time more than 3 months. Wait time was estimated based upon the patient s position on the transplant waiting list and availability of living liver donor. Specifically, if on the waiting list at the time of listing, the waiting time (current date minus list date) of the top tumour patient with the same ABO blood type was 3 months, or if the patent had a potential live donor volunteer to be assessed, then the patient was counselled by a Transplant Surgeon regarding the relative risks and benefits of bridge therapy, and no bridging therapy was recommended. Through surveillance with CT scans every 3 months, a Transplant Surgeon reassessed bridging recommendations if the live donor did not materialize, or if the waiting time was estimated to be an additional 2 3 months, the patient was counselled again, and bridge therapy was recommended. The use of as a bridging therapy over time has increased in frequency in parallel with the increased numbers of patients being listed for transplant and the prolongation of waiting times. Radiofrequency ablation therapy was delivered via a percutaneous approach in 97% of patients by one of three Interventional Radiologists. was provided to the remaining patients via open operations (3%) jointly by the interventional radiologist and transplant surgeon. Percutaneous procedures were performed on an outpatient basis with conscious sedation using titrated doses of intravenous midazolam and fentanyl, and utilizing ultrasound and/or CT guidance. A multi-tined LeVeen electrode (Boston Scientific Corporation, Natick, MA, USA) was used for most (79%) ablations. Technical details of the ablative therapies were prospectively entered into an Interventional Radiology database along with pre-intervention imaging characteristics and post-treatment radiological response. Pre-transplant clinical care Patients on the liver transplant waiting list with HCC were given a priority listing of 1T. The Canadian Liver Transplant allocation agreement assigns the following Medical Status to patients on the waiting list: (i) patients at home, (ii) patients hospitalized for a liver failure-related diagnosis, (iii) patients hospitalized with a
3 26 HPB creatinine >200 mm/l or grade 3 encephalopathy, or (iv) patients intubated in the intensive care unit. Organs are allocated according to the patient priority listing on a national and provincial level; the priority 1T lies between priorities 1 and As all tumour patients are eligible for a priority of at least 1T, waiting time is the dominant factor in the likelihood of being offered an organ. Patients were monitored by a transplant surgeon while on the liver transplant waiting list. Computed tomography (CT) or magnetic resonance imaging (MRI) was performed every 3 months. Indications for de-listing (i.e. drop-off or transplantation) were identified for all patients. Drop-off events were further classified into medical (cardiovascular, sepsis, upper gastrointestinal bleed and medically unfit) and tumour specific (lymph node metastases, peritoneal disease, tumour progression, pulmonary metastases, tumour rupture and vascular invasion). Study design This cohort study was a retrospective analysis. Patients were categorized into Radiofrequency Ablation or No Treatment groups. Primary outcomes were time to event analysis (listing to dropoff). Analyses were performed for both drop-off as a result of all causes (HCC-specific and medical aetiologies) as well as tumourspecific drop-off. Wait time was calculated from the date of listing until either transplant or delisting. For patients who developed HCC while on the list, wait time was adjusted to begin at the date of the diagnosis of HCC. Patients were censored at the time of transplant or at the time they refused transplant. Survival analysis was based upon the intention to treat. Statistical analysis Characteristics of the patients in each group were compared using t-tests and Mann Whitney U-tests for continuous outcomes and c 2 -tests of association for categorical outcomes. Survival analysis was performed by the University of Toronto Statistical Consulting Service using SAS statistical software (version 9.1, SAS Institute, Cary, NC, USA). The objective of the present study was to assess how various predictors could affect the risk of a patient dropping off the list while waiting for a transplant. As the probability of such an event (dropping off the list) must increase the longer a patient is on the list, we used survival analysis models which allowed us to test various predictors while controlling for differences between subjects due to differences in time on the list. Patient characteristics that we screened were: age at the time of listing, gender, blood type (O or not), treatment (yes or no), model for end-stage liver disease (MELD) score at the time of listing, AFP at the time of listing and aetiology. For categorical candidate predictor variables, we constructed Kaplan Meier survival curves of time to drop-off for each level of the predictor (SAS: Proc Lifetest) and used a log-rank test to test for differences in the survival function between the levels. We used Cox Regression (SAS : Proc Phreg) to assess the relationship between continuous predictors such as age and the survival function. The following predictors were not significant and were not used in subsequent models: aetiology (P = 0.37), MELD at list (P = 7) and gender (P = 0.59). Age was not significant (P = 9) but was retained in models because of its potential clinical importance. All other predictors were significant and were retained in the final models. We used Cox proportional hazard and logistic regression models to conduct a multivariate analysis of the candidate predictors, which allowed us to test for the significance of individual predictors while controlling for all other predictors in the model. Interactions were removed from the models if they were not significant and only final models are reported. After initial analysis of the whole cohort, further subgroup analysis was undertaken with 1:1 nearest neighbour propensity score matching. Waiting time, age, tumour number, tumour size, AFP and MELD score were incorporated into this analysis to ensure the relationship between predictor variables and outcome variables remained consistent across the vs. no treatment group. Results Patients and demographics Between January 1999 and June 2007, 170 patients who were listed for liver transplant with a diagnosis of HCC that fulfilled the Milan criteria by radiographic assessment either at the time of listing or while active on the waiting list were eligible for the primary analysis of this study. There were 77 patients that received as a sole bridging therapy and 93 patients that received no bridging therapy (Table 1). No patients were lost to follow-up. All patients have either received a liver transplant or have experienced a drop-off event. The only statistically significant difference in demographics (Table 1) between the groups was that fewer patients with a diagnosis of alcoholic liver disease received as a bridge to transplant (12% vs. 26% No Treatment, P = 2). Investigations could not identify any explanation for this observation. The mean listing medical MELD score at the time of listing was 14 in the group compared with 15 in the No Treatment group (Tables 1, P = 0.33). There was no difference in the type of transplant (live vs. deceased donor) between the and No Treatment group. The median waiting time to transplantation was significantly greater in the group compared with the No Treatment group (9.5 months vs. 5.0 months, P < 01). The differences in time on the list were most pronounced in the quartile of patients with the shortest waiting time (only 13% of the group was transplanted within 2.5 months of listing compared with 32% in the No Treatment group) and the longest waiting time quartile (35% of the group waited longer than 12.8 months compared with only 18% of the No Treatment group). Tumour characteristics The median alpha-fetoprotein levels at time of listing and the other tumour characteristics (including size and number) were similar between the and No Treatment groups (Table 1).
4 HPB 27 Table 1 Patient demographics at the time of listing No treatment Significance Total patients Age mean (range) Gender 5 Male 66 (86%) 75 (81%) Female 11 (14%) 18 (19%) Blood group 6 O 37 (48%) 41 (44%) A 31 (40%) 33 (35%) B 9 (12%) 15 (16%) AB 0 (0%) 4 (4%) Aetiology a Hepatitis B 17 (22%) 18 (19%) 6 Hepatitis C 49 (64%) 52 (56%) 0.31 Alcohol 9 (12%) 24 (26%) 2 NASH/ cryptogenic 3 (4%) 4 (4%) 9 Other 1 (1%) 5 (5%) 0.15 Tumour characteristics Mean number Mean maximal size 2.5 cm 2.4 cm Median AFP (Range) 28 0, , AFP > (21%) 21 (23%) 0.78 Mean MELD score (range) b Time on list (months) <01 < (13%) 30 (32%) (23%) 25 (27%) (29%) 21 (23%) > (35%) 17 (18%) Time on list median (range) 9.5 ( 51.1) 5.0 ( ) a Some patients had more than one aetiology of liver disease. b MELD scores reported are the medical MELD, without any exception points. MELD, model for end-stage liver disease; NASH, non-alcoholic steato-hepatitis. Table 2 Technical details and complications of the procedures Ablation access Percutaneous 75 (97%) Open surgical 2 (3%) Imaging guidance US 36 (47%) CT 8 (10%) CT & US 33 (43%) Total procedures 1 58 (75%) 2 12 (16%) 3 5 (6%) 4 2 (3%) Mean/ patient 1.4 (range 1 4) Number of tumours 1 tumour 70 (91%) ablated a 2 tumours 6 (8%) 3 tumors 0 (0%) 4 tumors 1 (1%) Mean number ablated 1.1 (range 1 4) Diameter of largest 2.6 cm (range 4.5 cm) tumour nodule a Ablation electrodes LeVeen 61 (79%) utilized Cool-tip 7 (9%) Berchtold 7 (9%) RITA StarBurst 2 (3%) Primary technique 83% (64/77) effectiveness ab Complications Major none Minor n = 2 Left portal vein thrombus Vasovagal reaction No deaths a Data presented for the first procedure only. b Defined as patients with a complete radiological response as measured on the first contrast enhanced imaging post-ablation. LeVeen electrode (Boston Scientific, Natick, MA); Cool-tip electrode (Covidien/Valleylab, Boulder, CO); Berchtold electrode (Integra Life- Sciences, Plainsboro, NJ); RITA StarBurst electrode (AngioDynamics, Queensbury, NY)., radiofrequency ablation; US, ultrasound; CT, computed tomography; cm, centimetres. Details of the procedures Details of the procedures are listed in Table 2. The procedures were performed by interventional radiologists on an outpatient basis using conscious sedation and percutaneous electrode insertion in 97% of the patients. The ablation electrodes were inserted into the HCC tumours using ultrasound (US) (47%), CT (10%) or a combination of US and CT localization (43%). The mean number of separate procedures was 1.4 per patient (range 1 4). The mean number of tumours treated per procedure was 1.1 and the mean largest tumour diameter was 2.6 cm. The primary technique effectiveness was 83% (64/77) as measured by a complete radiological (ablative) response on the first postprocedure contrast-enhanced imaging study. There were two minor complications of the interventions including asymptomatic left portal vein thrombosis and a vasovagal reaction that occurred immediately after application. Liver transplants have been performed in both of these patients with minor complications. There was one delayed tumour rupture three and a half months after ablation that was not attributed as a direct complication of the ablation. This patient did not receive a liver transplant. Patient drop-off from the waiting list analysis At the time of analysis, all patients in both groups had received a transplant, refused transplantation and were delisted, or dropped
5 28 HPB Table 3 Aetiology of patient drop-off from the liver transplant waiting list No treatment Significance Total patients Aetiology of drop-off Refused transplant* 7 (9%) 1 (1%) 1 Medical (total) 3 (4%) 5 (7%) 5 Cardiovascular 0 1 UGIB 1 0 Unfit 2 4 Tumor specific (total) 16 (21%) 11 (12%) 0.11 LN metastases 0 1 Peritoneal disease 1 0 Progression 0 2 Pulmonary metastases 5 0 Rupture 1 0 Vascular invasion 9 8 Transplant Deceased donor organ 45 (58%) 65 (69%) Live donor right lobe 6 (8%) 11 (12%) Transplant + Refused transplant 58 (75%) 77 (83%) 0.31 *6/7 patients who refused a transplant were interpreted to have a complete radiological response to tumour ablation. UGIB, upper gastro-intestinal bleed; LN, lymph node; HCC, hepatocellular carcinoma; MELD, model for end-stage liver disease. (a) Active on the list (%) No Treatment (b) Active on the list (%) No treatment P = No treatment P = off the waiting list for medical or tumour-specific reasons (Table 3). More patients in the group requested delisting from the waiting list (9% vs. 1% No Treatment, P = 1). Notably, six out of the seven requested delisting in the group because they had a sustained radiographical response. Of these six patients, four remain free of disease, one patient developed an additional HCC that was completely ablated and one patient developed a peri-ablation recurrence that was resected. There were similar percentages of patients who dropped-off for medical reasons (4% vs. 7% No Treatment, P = 5). For tumour-specific reasons, there was a trend towards a higher drop-off in the group (21% vs. 12% No Treatment, P = 0.11). The major differences in tumour events for the group were the development of pulmonary metastases in five, peritoneal disease in one and tumour rupture in one, compared with the No-treatment group who dropped-off for local progression in two and lymph node metastases in one. The development of vascular invasion was equivalent between groups (12% vs. 9% No Treatment, P = 3). Although there were numerically more drop-offs events in the group, the corresponding waiting time was also longer in the group, which would increase the probability of experiencing a drop-off event. Waiting time was controlled for using survival No Treatment Figure 1 (a) Overall drop-off from the waiting list. (b) Tumour-specific drop-off from the waiting list analysis modelling. There was no significant difference in the time to drop-off between the and No Treatment groups for all causes (medical + tumour; Fig. 1a) or for tumour-specific aetiology (Fig. 1b). The overall drop-off rate during the first 12 months after listing was approximately 2% per month for each group, and the rate of delisting for tumour specific drop-off events was approximately 1.7% per month. Transplantation Transplantation was achieved in 75% of those patients treated with as a bridge and 83% of those without treatment (P = 0.141). Tumour characteristics were most strongly associated with a reduction in the odds of achieving a transplant (Table 4). Patients with an AFP > 200 (OR 05, P < 01), greater number of tumours (OR 0.532, P = 37), bilobar disease (OR 0.344,
6 HPB 29 Table 4 Explant tumour characteristics No treatment Total patients Milan stage Within Milan 44 (76%) 61 (80%) 0.54 Outside Milan 14 (24%) 15 (20%) Microvascular invasion 11 (22%) 15 (19.7%) 0.76 Macrovascular invasion 2 (4%) 4 (5%) 0.75 Number of tumours (median) Size of largest tumour (median) Bilobar disease 18 (36%) 22 (29%) 05 Pathological grade Well differentiated 1 (2%) 8 (12%) 0.11 Moderately differentiated 39 (89%) 48 (74%) Poorly differentiated 9 (4%) 14 (8%) Significance P = 25), larger tumours (OR 65, P = 40) and a higher stage at listing (OR 0.155, P = 13) had a lower chance of being transplanted. This association was maintained on multivariate analysis for AFP > 200 (P < 01), higher tumour number (P = 13) and larger tumours (P = 14). The patients receiving did not have a lower odds of undergoing transplant despite a lower overall percentage of patients transplanted. After propensity matching of covariates the effect of on drop-off and achieveing transplantation was reanalysed. Good matching of covariates was achieved, with no statistically significant differences for the included covariates. With matching there was no difference in the treatment effect of on drop-off (t-statistic -2.26, P = 0.79) or achieving transplant (t-statistic -2.41, P = 0.79). Non-transplanted patients (waiting list drop-off events) The 1-, 3- and 5-year survival for those patients who were delisted was 87%, 76% and 55% for group, which was significantly higher than the No treatment group where the survival was 71%, 39%, 30% (P = 09). On univariate analysis, the risk of death was lower in females (HR 0.307, P = 41), and those receiving (HR 99, P = 14). On Multivariate analysis only was associated with a lower risk of dying. Tumour characteristics did not influence risk of death in those patients delisted. Explant pathology Details of the explant pathology are listed in Table 4. There were no statistically significant differences in explant pathology between those patients who received vs. No Treatment. Survivals There was no difference in the overall median follow-up time between the and No Treatment groups (41 vs. 46 months, (a) Overall Survival (%) 77 No Treatment 93 (b) Disease-free Survival (%) 77 No Treatment 93 No treatment P = No treatment P = Figure 2 (a) Overall survival in all hepatocellular carcinoma (HCC) patients. Time is calculated from the date of listing. (b) Tumour-free survival in all HCC patients. Time is calculated from the date of listing P = 4). After transplantation there was also no difference observed in the median follow-up time between the and No Treatment groups (30 vs. 41 months, P = 75). There was no significant difference in the overall survival (OS) (P = 0.75) or DFS (P = 4) as calculated from the time of listing (intent to treat analysis) between the and No Treatment groups. (Fig. 2a b) After liver transplant, there were nine deaths (four HCC/ five non-hcc related) and one HCC recurrence out of 51 patients transplanted (20% event rate). In comparison, there were 19 deaths (8 HCC/ 11 non-hcc) and 2 HCC recurrences in the 76 No Treatment group patients transplanted (25% event rate). The corresponding post-liver transplant OS (P = 0.76) and DFS (P = 6) curves did not demonstrate a statistical difference. (Fig. 3a b).
7 30 HPB (a) Overall Survival (%) 51 No Treatment 76 (b) Disease-free Survival (%) 51 No Treatment 76 Details of the predictors of survival are listed in Table 5. Based upon the intention to treat on both univariate and multivariate analysis, survival was lower in those patients with an AFP > 200 (P = 1) and a higher stage at listing (P = 08). Other tumour characteristics and treatment with were not significantly associated with OS. Discussion P = P = Figure 3 (a) Overall survival in hepatocellular carcinoma (HCC) patients that received a liver transplant. Time is calculated from the date of transplantation. (b) Tumour-free survival in HCC patients that received a liver transplant. Time is calculated from the date of transplantation The benefits of locoregional treatment for HCC patients prior to liver transplantation are unclear. 5,8 12 In a situation where the waiting time for liver transplantation is long, there is a perception by both the physicians and patients that not treating patients with HCC is unacceptable, despite the absence of evidence supporting short- or long-term benefit. The present study has demonstrated that can be safely performed for patients with tumours within the Milan Criteria. also appeared to allow patients to be maintained for a longer period of time on the transplant waiting list without any adverse effect on drop off, achieving transplant or post-transplant survival, a significant benefit when waiting times are prolonged. was safely performed percutaneously 97% of the time, with a high primary technique effectiveness of 83% and a very low complication rate. Six of the 77 patients treated with (intended as a bridge to transplant) had a sustained radiographical response such that these patients elected not to proceed with liver transplant. In the group of patients who were delisted, the survival in the group was superior compared with the No treatment group (55% vs. 30%), and was equivalent to other treatments with curative intent such as surgery thus became an effective destination therapy for a small portion of patients and avoided the need for liver transplant aclinically significant advantage to the use of. In the setting of a long waiting time for transplant, the durability of the response can be assessed and the need for transplantation for HCC be reconsidered. There was no significant difference in tumour-specific drop-off, although the incidence of drop-off events tended to be higher in the group. was not observed to halt the development of vascular invasion while on the transplant waiting list (12% vs. 9% No Treatment, P = NS). Moreover, the overall and tumourfree drop-off rates were equivalent when controlling for the longer waiting time in the group. As the majority of the patients were transplanted within 12 months, there were too few patients remaining in the survival analysis after 12 months to determine the efficacy of bridging therapy for those patients with a longer waiting time to transplantation, where the benefits of treatment may be most pronounced. Previous studies 18,25 have suggested that can reduce drop off on the waiting list compared with historical controls, however, these patients had longer waiting times than that those in our study and the cohorts used for comparison were not matched. Perhaps the most clinically important impact of for HCC patients that are typically transplanted within 1 year of listing is the ability of to maintain patient eligibility on the transplant list. This is important because, while a clinician may estimate a short waiting time, this study demonstrates that the waiting time may be unpredictably prolonged, as 41% of the no- group waited more than 5 months. The median time on the waiting list was significantly longer in the group (9.5 vs. 5 months) and despite this, the rate of transplantation and drop offs in the group were equivalent to those with much shorter waiting list times. Furthermore, the explant pathology was equivalent between these two groups suggesting that may halt the progression of tumour growth. The importance of being able to keep patients tumour burden within the Milan criteria without
8 HPB 31 Table 5 Logistic regression model for factors predicting achieving transplantation Variable Odds 95% confidence Significance Ratio Interval Univariate Multivariate Gender ns Age ns AFP > <01 <01 Waiting time ns ns Tumour number a Bilobar disease a ns Size of largest tumour a UNOS stage a ns a Data from time of listing. AFP, alpha fetoprotein;, radiofrequency ablation. increasing the rate of drop off or being detrimental to survival has implications for the priority given to these patients on the transplant waiting list. Although the time-to-drop-off was similar between the and No Treatment groups, there were some differences. The group experienced a greater incidence of drop-off for tumour events, notably pulmonary metastases (n = 5), peritoneal metastases (n = 1) and tumour rupture (n = 1). These unexpected events may be a reflection of the tumour biology but given that none of these were seen in the No Treatment group, they may also have occurred as a consequence of treatment. Peritoneal metastases and tumour rupture are a known, albeit very rare, direct complication of the ablation technique. Although the lung is a common destination for HCC metastases in advanced disease, pulmonary metastases should be a relatively uncommon event in patients with a HCC tumour pattern that fulfils the Milan criteria. During the ablation process, it is common to see micro-air bubbles escaping the ablation zone via the hepatic veins to the systemic circulation. If these contents contain viable tumour emboli, the lung would be the first microcirculation filter. This proposed mechanism, however, is purely speculative. The overall procedure-related local complication rates were similar to those published in the literature. In the present study, tumour characteristics were the best predictors of a failure to achieve transplantation and are probably reflective of the tumour biological behaviour. The main determinant of survival for non-resectable HCC within the Milan criteria is whether or not the patient is transplanted. Patients treated with achieved the same overall and tumour-free survival, despite significantly longer waiting times. Given the excellent post-transplant survival for HCC this finding is not unexpected, and is consistent with several recently published studies that posttransplant survival is equivalent for patients treated with. 5,8 12 It is also notable that the UNOS liver transplant review has suggested that patients who received bridging therapy on the waiting list had a slightly higher survival at 3 years (76% vs. 71%, P = 3). 6 There are also single centre reports suggesting that multimodal bridging therapies may increase post-transplant survival TACE is the predominant bridging therapy in the United States (60 70%) 6 and thus it is possible that TACE provides an additional survival benefit above that of. This study has limitations inherent to all retrospective analyses. Probably the most important one is whether or not this is an appropriate comparison between and No Treatment groups specifically whether the groups were at the same risk of dropoff or survival? For uniformity and generalizability, only patients with a HCC that fulfilled the Milan criteria were considered and the demographics and tumour characteristics were similar. To reduce confounding variables, patients treated with other bridging therapies (TACE, ethanol ablation, radiation) or previous hepatectomy were excluded. The major systemic bias in this study is the criteria used to select patients for : their tumours must have been safely ablatable and their wait time was predicted to exceed 3 months based upon their position on the blood-type specific waiting list and availability of a living liver donor. Thus, the patients may have been at a higher risk for drop-off as they were predictably on the wait list longer. The waitlist drop-off analysis, however, accounts for the difference in waiting times and demonstrated that the time to drop-off was similar between the groups for both tumour-specific and overall (medical and tumor-specific) indications. Furthermore, the nearest neighbour propensity score matching analysis demonstrated equivalent results between the and No Treatment groups. On the other hand, many in the No-treatment group may have been at higher risk for drop-off or recurrence if their tumours were not-ablatable for high-risk factors such as size, very exophytic nature or proximity to major biliary and vascular structures that might indicate having a worse or risky biology. These differences could only be normalized with a randomized prospective clinical trial. The present study analyses the largest reported single centre cohort of patients treated with as a bridge to liver transplant
9 32 HPB compared with a No-Treatment group treated during the same period. This study should be generalizable as it mirrors current clinical practice in many transplant centres with similar waiting times. Although no significant advantage of in waitlist dropoff or HCC recurrence was identified, the patients may have been at higher risk for these events because of the centre s criteria for selecting HCC patients for bridging and despite this, the patients were maintained for longer on the waiting list without any negative consequences with respect to drop-off or survival. Conflicts of interest None declared. References 1. Mazzaferro V, Regalia E, Doci R, Andreola S, Pulvirenti A, Bozzetti F et al. (1996) Liver transplantation for the treatment of small hepatocellular carcinomas in patients with cirrhosis. N Engl J Med 334: Llovet JM, Fuster J, Bruix J. (1999) Intention-to-treat analysis of surgical treatment for early hepatocellular carcinoma: resection versus transplantation. Hepatology 30: Shah SA, Cleary SP, Tan JC, Wei AC, Gallinger S, Grant DR et al. (2007) An analysis of resection vs transplantation for early hepatocellular carcinoma: defining the optimal therapy at a single institution. Ann Surg Oncol 14: Freeman RB, Edwards EB, Harper AM. (2006) Waiting list removal rates among patients with chronic and malignant liver diseases. Am J Transplant 6: Di Bisceglie AM. (2005) Pretransplant treatments for hepatocellular carcinoma: do they improve outcomes? Liver Transpl 11 (Suppl 2):S10 S Freeman RB, Jr, Steffick DE, Guidinger MK, Farmer DG, Berg CL, Merion RM. (2008) Liver and intestine transplantation in the United States, Am J Transplant 8(Pt 2): Greig PD. Treatment before liver transplant No treatment. Proceedings of the Fifth International Meeting, Hepatocellular Carcinoma: Eastern and Western Experiences Lubienski A. (2005) Hepatocellular carcinoma: interventional bridging to liver transplantation. Transplantation 80(Suppl):S113 S Schwartz M, Roayaie S, Uva P. (2007) Treatment of HCC in patients awaiting liver transplantation. Am J Transplant 7: Heckman JT, Devera MB, Marsh JW, Fontes P, Amesur NB, Holloway SE et al. (2008) Bridging locoregional therapy for hepatocellular carcinoma prior to liver transplantation. Ann Surg Oncol 15: Belghiti J, Carr BI, Greig PD, Lencioni R, Poon RT. (2008) Treatment before liver transplantation for HCC. Ann Surg Oncol 15: Lau WY, Lai EC. (2009) The current role of radiofrequency ablation in the management of hepatocellular carcinoma: a systematic review. Ann Surg 249: Curley SA, Izzo F, Ellis LM, Nicolas Vauthey J, Vallone P. (2000) Radiofrequency ablation of hepatocellular cancer in 110 patients with cirrhosis. Ann Surg 232: Lin SM, Lin CJ, Lin CC, Hsu CW, Chen YC. (2004) Radiofrequency ablation improves prognosis compared with ethanol injection for hepatocellular carcinoma < or =4 cm. Gastroenterology 127: Livraghi T, Meloni F, Di Stasi M, Rolle E, Solbiati L, Tinelli C et al. (2008) Sustained complete response and complications rates after radiofrequency ablation of very early hepatocellular carcinoma in cirrhosis: is resection still the treatment of choice? Hepatology 47: Shiina S, Teratani T, Obi S, Sato S, Tateishi R, Fujishima T et al. (2005) A randomized controlled trial of radiofrequency ablation with ethanol injection for small hepatocellular carcinoma. Gastroenterology 129: Fontana RJ, Hamidullah H, Nghiem H, Greenson JK, Hussain H, Marrero J et al. (2002) Percutaneous radiofrequency thermal ablation of hepatocellular carcinoma: a safe and effective bridge to liver transplantation. Liver Transpl 8: Lu DS, Yu NC, Raman SS, Lassman C, Tong MJ, Britten C et al. (2005) Percutaneous radiofrequency ablation of hepatocellular carcinoma as a bridge to liver transplantation. Hepatology 41: Mazzaferro V, Battiston C, Perrone S, Pulvirenti A, Regalia E, Romito R et al. (2004) Radiofrequency ablation of small hepatocellular carcinoma in cirrhotic patients awaiting liver transplantation: a prospective study. Ann Surg 240: Sala M, Llovet JM, Vilana R, Bianchi L, Sole M, Ayuso C et al. (2004) Initial response to percutaneous ablation predicts survival in patients with hepatocellular carcinoma. Hepatology 40: Bazarah SM, Peltekian KM, McAlister VC, Bitter-Suermann H, Mac- Donald AS. (2004) Utility of MELD and Child-Turcotte-Pugh scores and the Canadian waitlisting algorithm in predicting short-term survival after liver transplant. Clin Invest Med 27: Guglielmi A, Ruzzenente A, Valdegamberi A, Pachera S, Campagnaro T, D'Onofrio M et al. (2008) Radiofrequency ablation versus surgical resection for the treatment of hepatocellular carcinoma in cirrhosis. J Gastrointest Surg 12: Chen MS, Li JQ, Zheng Y, Guo RP, Liang HH, Zhang YQ et al. (2006) A prospective randomized trial comparing percutaneous local ablative therapy and partial hepatectomy for small hepatocellular carcinoma. Ann Surg 243: Lu MD, Kuang M, Liang LJ, Xie XY, Peng BG, Liu GJ et al. (2006) [Surgical resection versus percutaneous thermal ablation for early-stage hepatocellular carcinoma: a randomized clinical trial]. Zhonghua Yi Xue Za Zhi 86: Brillet PY, Paradis V, Brancatelli G, Rangheard AS, Consigny Y, Plessier A et al. (2006) Percutaneous radiofrequency ablation for hepatocellular carcinoma before liver transplantation: a prospective study with histopathologic comparison. AJR Am J Roentgenol 186(Suppl):S296 S Yao FY, Kinkhabwala M, LaBerge JM, Bass NM, Brown R, Jr, Kerlan R et al. (2005) The impact of pre-operative loco-regional therapy on outcome after liver transplantation for hepatocellular carcinoma. Am J Transplant 5(Pt 1): Fisher RA, Maluf D, Cotterell AH, Stravitz T, Wolfe L, Luketic V et al. (2004) Non-resective ablation therapy for hepatocellular carcinoma: effectiveness measured by intention-to-treat and dropout from liver transplant waiting list. Clin Transplant 18: Bharat A, Brown DB, Crippin JS, Gould JE, Lowell JA, Shenoy S et al. (2006) Pre-liver transplantation locoregional adjuvant therapy for hepatocellular carcinoma as a strategy to improve longterm survival. J Am Coll Surg 203:
Hepatocellular Carcinoma: Diagnosis and Management
 Hepatocellular Carcinoma: Diagnosis and Management Nizar A. Mukhtar, MD Co-director, SMC Liver Tumor Board April 30, 2016 1 Objectives Review screening/surveillance guidelines Discuss diagnostic algorithm
Hepatocellular Carcinoma: Diagnosis and Management Nizar A. Mukhtar, MD Co-director, SMC Liver Tumor Board April 30, 2016 1 Objectives Review screening/surveillance guidelines Discuss diagnostic algorithm
Living Donor Liver Transplantation for Hepatocellular Carcinoma: It Is All about Donors?
 Original Article Living Donor Liver Transplantation for Hepatocellular Carcinoma: It Is All about Donors? R. F. Saidi 1 *, Y. Li 2, S. A. Shah 2, N. Jabbour 2 1 Division of Organ Transplantation, Department
Original Article Living Donor Liver Transplantation for Hepatocellular Carcinoma: It Is All about Donors? R. F. Saidi 1 *, Y. Li 2, S. A. Shah 2, N. Jabbour 2 1 Division of Organ Transplantation, Department
Management of HepatoCellular Carcinoma
 9th Symposium GIC St Louis - 2010 Management of HepatoCellular Carcinoma Overview Pierre A. Clavien, MD, PhD Department of Surgery University Hospital Zurich Zurich, Switzerland Hepatocellular carcinoma
9th Symposium GIC St Louis - 2010 Management of HepatoCellular Carcinoma Overview Pierre A. Clavien, MD, PhD Department of Surgery University Hospital Zurich Zurich, Switzerland Hepatocellular carcinoma
Despite recent advances in the care of patients with
 Liver Transplantation for Hepatocellular Carcinoma: Lessons from the First Year Under the Model of End- Stage Liver Disease (MELD) Organ Allocation Policy Francis Y. Yao, 1,2 Nathan M. Bass, 1 Nancy L.
Liver Transplantation for Hepatocellular Carcinoma: Lessons from the First Year Under the Model of End- Stage Liver Disease (MELD) Organ Allocation Policy Francis Y. Yao, 1,2 Nathan M. Bass, 1 Nancy L.
PEER-REVIEW REPORT CLASSIFICATION LANGUAGE EVALUATION SCIENTIFIC MISCONDUCT CONCLUSION. [ Y] Accept [ ] Grade B: Very good
![PEER-REVIEW REPORT CLASSIFICATION LANGUAGE EVALUATION SCIENTIFIC MISCONDUCT CONCLUSION. [ Y] Accept [ ] Grade B: Very good PEER-REVIEW REPORT CLASSIFICATION LANGUAGE EVALUATION SCIENTIFIC MISCONDUCT CONCLUSION. [ Y] Accept [ ] Grade B: Very good](/thumbs/96/127805416.jpg) Reviewer s code: 03656588 Reviewer s country: China Date reviewed: 2017-06-08 [ ] Grade A: Excellent [ Y] Accept [ ] Grade B: Very good [ ] High priority for [ Y] Grade C: Good language [ ] Major revision
Reviewer s code: 03656588 Reviewer s country: China Date reviewed: 2017-06-08 [ ] Grade A: Excellent [ Y] Accept [ ] Grade B: Very good [ ] High priority for [ Y] Grade C: Good language [ ] Major revision
Living Donor Liver Transplantation Versus Deceased Donor Liver Transplantation for Hepatocellular Carcinoma: Comparable Survival and Recurrence
 LIVER TRANSPLANTATION 18:315-322, 2012 ORIGINAL ARTICLE Living Donor Liver Transplantation Versus Deceased Donor Liver Transplantation for Hepatocellular Carcinoma: Comparable Survival and Recurrence Lakhbir
LIVER TRANSPLANTATION 18:315-322, 2012 ORIGINAL ARTICLE Living Donor Liver Transplantation Versus Deceased Donor Liver Transplantation for Hepatocellular Carcinoma: Comparable Survival and Recurrence Lakhbir
HCC RADIOLOGIC DIAGNOSIS
 UCSF Transplant 2010 THE BEFORE AND AFTER HEPATOCELLULAR CARCINOMA MANAGEMENT Francis Yao, M.D. Professor of Clinical Medicine and Surgery Medical Director, Liver Transplantation University of California,
UCSF Transplant 2010 THE BEFORE AND AFTER HEPATOCELLULAR CARCINOMA MANAGEMENT Francis Yao, M.D. Professor of Clinical Medicine and Surgery Medical Director, Liver Transplantation University of California,
Liver transplantation: Hepatocellular carcinoma
 Liver transplantation: Hepatocellular carcinoma Alejandro Forner BCLC Group. Liver Unit. Hospital Clínic. University of Barcelona 18 de marzo 2015 3r Curso Práctico de Transplante de Órganos Sólidos Barcelona
Liver transplantation: Hepatocellular carcinoma Alejandro Forner BCLC Group. Liver Unit. Hospital Clínic. University of Barcelona 18 de marzo 2015 3r Curso Práctico de Transplante de Órganos Sólidos Barcelona
TREATMENT FOR HCC AND CHOLANGIOCARCINOMA. Shawn Pelletier, MD
 TREATMENT FOR HCC AND CHOLANGIOCARCINOMA Shawn Pelletier, MD Treatment for HCC Treatment strategies Curative first line therapy Thermal ablation vs Resection vs Transplant Other first line therapies TACE
TREATMENT FOR HCC AND CHOLANGIOCARCINOMA Shawn Pelletier, MD Treatment for HCC Treatment strategies Curative first line therapy Thermal ablation vs Resection vs Transplant Other first line therapies TACE
6/16/2016. Treating Hepatocellular Carcinoma: Deciphering the Clinical Data. Liver Regeneration. Liver Regeneration
 Treating : Deciphering the Clinical Data Derek DuBay, MD Associate Professor of Surgery Director of Liver Transplant Liver Transplant and Hepatobiliary Surgery UAB Department of Surgery Liver Regeneration
Treating : Deciphering the Clinical Data Derek DuBay, MD Associate Professor of Surgery Director of Liver Transplant Liver Transplant and Hepatobiliary Surgery UAB Department of Surgery Liver Regeneration
Hepatobiliary Malignancies Retrospective Study at Truman Medical Center
 Hepatobiliary Malignancies 206-207 Retrospective Study at Truman Medical Center Brandon Weckbaugh MD, Prarthana Patel & Sheshadri Madhusudhana MD Introduction: Hepatobiliary malignancies are cancers which
Hepatobiliary Malignancies 206-207 Retrospective Study at Truman Medical Center Brandon Weckbaugh MD, Prarthana Patel & Sheshadri Madhusudhana MD Introduction: Hepatobiliary malignancies are cancers which
Selection Criteria and Insertion of SIRT into HCC Treatment Guidelines
 Selection Criteria and Insertion of SIRT into HCC Treatment Guidelines 2 nd Asia Pacific Symposium on Liver- Directed Y-90 Microspheres Therapy 1st November 2014, Singapore Pierce Chow FRCSE PhD SIRT in
Selection Criteria and Insertion of SIRT into HCC Treatment Guidelines 2 nd Asia Pacific Symposium on Liver- Directed Y-90 Microspheres Therapy 1st November 2014, Singapore Pierce Chow FRCSE PhD SIRT in
Celsion Symposium New Paradigms in HCC Staging: HKLC vs. BCLC Staging
 Celsion Symposium New Paradigms in HCC Staging: HKLC vs. BCLC Staging Ronnie T.P. Poon, MBBS, MS, PhD Chair Professor of Hepatobiliary and Pancreatic Surgery Chief of Hepatobiliary and Pancreatic Surgery
Celsion Symposium New Paradigms in HCC Staging: HKLC vs. BCLC Staging Ronnie T.P. Poon, MBBS, MS, PhD Chair Professor of Hepatobiliary and Pancreatic Surgery Chief of Hepatobiliary and Pancreatic Surgery
Reconsidering Liver Transplantation for HCC in a Era of Organ shortage
 Reconsidering Liver Transplantation for HCC in a Era of Organ shortage Professor Didier Samuel Centre Hépatobiliaire Inserm-Paris Sud Research Unit 1193 Departement Hospitalo Universitaire Hepatinov Hôpital
Reconsidering Liver Transplantation for HCC in a Era of Organ shortage Professor Didier Samuel Centre Hépatobiliaire Inserm-Paris Sud Research Unit 1193 Departement Hospitalo Universitaire Hepatinov Hôpital
Surveillance for Hepatocellular Carcinoma
 Surveillance for Hepatocellular Carcinoma Marion G. Peters, MD John V. Carbone, MD, Endowed Chair Professor of Medicine Chief of Hepatology Research University of California San Francisco Recorded on April
Surveillance for Hepatocellular Carcinoma Marion G. Peters, MD John V. Carbone, MD, Endowed Chair Professor of Medicine Chief of Hepatology Research University of California San Francisco Recorded on April
Hepatocellular Carcinoma: Transplantation, Resection or Ablation?
 Hepatocellular Carcinoma: Transplantation, Resection or Ablation? Roberto Gedaly MD Chief, Abdominal Transplantation Transplant Service Line University of Kentucky Nothing to disclose Disclosure Objective
Hepatocellular Carcinoma: Transplantation, Resection or Ablation? Roberto Gedaly MD Chief, Abdominal Transplantation Transplant Service Line University of Kentucky Nothing to disclose Disclosure Objective
Liver Transplantation for Hepatocellular Carcinoma: Validation of the UCSF-Expanded Criteria Based on Preoperative Imaging
 American Journal of Transplantation 2007; 7: 2587 2596 Blackwell Munksgaard C 2007 The Authors Journal compilation C 2007 The American Society of Transplantation and the American Society of Transplant
American Journal of Transplantation 2007; 7: 2587 2596 Blackwell Munksgaard C 2007 The Authors Journal compilation C 2007 The American Society of Transplantation and the American Society of Transplant
9/10/2018. Liver Transplant for Hepatocellular Carcinoma (HCC): What is New? DISCLOSURES
 UCSF Transplant 2018: Pioneering Advances in Transplantation DISCLOSURES Liver Transplant for Hepatocellular Carcinoma (HCC): What is New? I have no relevant commercial interests or relationships to report
UCSF Transplant 2018: Pioneering Advances in Transplantation DISCLOSURES Liver Transplant for Hepatocellular Carcinoma (HCC): What is New? I have no relevant commercial interests or relationships to report
HPB ORIGINAL ARTICLE. Abstract. Keywords. Correspondence. Introduction
 DOI:1111/j.1477-2574.2009.00022.x HPB ORIGINAL ARTICLE Poorer survival in patients whose explanted hepatocellular carcinoma (HCC) exceeds Milan or UCSF Criteria. An analysis of liver transplantation in
DOI:1111/j.1477-2574.2009.00022.x HPB ORIGINAL ARTICLE Poorer survival in patients whose explanted hepatocellular carcinoma (HCC) exceeds Milan or UCSF Criteria. An analysis of liver transplantation in
INTRODUCTION. Journal of Surgical Oncology 2014;109:
 2014;109:533 541 Transplant Versus Resection for the Management of Hepatocellular Carcinoma Meeting Milan Criteria in the MELD Exception Era at a Single Institution in a UNOS Region with Short Wait Times
2014;109:533 541 Transplant Versus Resection for the Management of Hepatocellular Carcinoma Meeting Milan Criteria in the MELD Exception Era at a Single Institution in a UNOS Region with Short Wait Times
Hepatocellular Carcinoma. Markus Heim Basel
 Hepatocellular Carcinoma Markus Heim Basel Outline 1. Epidemiology 2. Surveillance 3. (Diagnosis) 4. Staging 5. Treatment Epidemiology of HCC Worldwide, liver cancer is the sixth most common cancer (749
Hepatocellular Carcinoma Markus Heim Basel Outline 1. Epidemiology 2. Surveillance 3. (Diagnosis) 4. Staging 5. Treatment Epidemiology of HCC Worldwide, liver cancer is the sixth most common cancer (749
Ontario s Adult Referral and Listing Criteria for Liver Transplantation
 Ontario s Adult Referral and Listing Criteria for Liver Transplantation Version 3.0 Trillium Gift of Life Network Ontario s Adult Referral & Listing Criteria for Liver Transplantation PATIENT REFERRAL
Ontario s Adult Referral and Listing Criteria for Liver Transplantation Version 3.0 Trillium Gift of Life Network Ontario s Adult Referral & Listing Criteria for Liver Transplantation PATIENT REFERRAL
Hepatocellular Carcinoma HCC Updated November 2015 by: Dr. Mohammed Alghamdi (Medical Oncology Fellow, University of Calgary)
 Hepatocellular Carcinoma HCC Updated November 2015 by: Dr. Mohammed Alghamdi (Medical Oncology Fellow, University of Calgary) Staff Reviewers: Dr. Yoo Joung Ko (Medical Oncologist, Sunnybrook Odette Cancer
Hepatocellular Carcinoma HCC Updated November 2015 by: Dr. Mohammed Alghamdi (Medical Oncology Fellow, University of Calgary) Staff Reviewers: Dr. Yoo Joung Ko (Medical Oncologist, Sunnybrook Odette Cancer
Treatment of Hepatocellular Carcinoma. Andrew J. Muir, MD MHS Division of Gastroenterology Duke University Medical Center
 Treatment of Hepatocellular Carcinoma Andrew J. Muir, MD MHS Division of Gastroenterology Duke University Medical Center Epidemiology of HCC: world The 5 th most common cancer worldwide > 500, 000 new
Treatment of Hepatocellular Carcinoma Andrew J. Muir, MD MHS Division of Gastroenterology Duke University Medical Center Epidemiology of HCC: world The 5 th most common cancer worldwide > 500, 000 new
Radiofrequency Ablation of Primary or Metastatic Liver Tumors
 Radiofrequency Ablation of Primary or Metastatic Liver Tumors Policy Number: 7.01.91 Last Review: 9/2018 Origination: 2/1996 Next Review: 9/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC)
Radiofrequency Ablation of Primary or Metastatic Liver Tumors Policy Number: 7.01.91 Last Review: 9/2018 Origination: 2/1996 Next Review: 9/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC)
NHS BLOOD AND TRANSPLANT ORGAN DONATION AND TRANSPLANTATION DIRECTORATE LIVER ADVISORY GROUP UPDATE ON THE HCC DOWN-STAGING SERVICE EVALUATION
 NHS BLOOD AND TRANSPLANT ORGAN DONATION AND TRANSPLANTATION DIRECTORATE LIVER ADVISORY GROUP UPDATE ON THE HCC DOWN-STAGING SERVICE EVALUATION 1. A service development evaluation to transplant down-staged
NHS BLOOD AND TRANSPLANT ORGAN DONATION AND TRANSPLANTATION DIRECTORATE LIVER ADVISORY GROUP UPDATE ON THE HCC DOWN-STAGING SERVICE EVALUATION 1. A service development evaluation to transplant down-staged
Hepatocellular Carcinoma (HCC): Who Should be Screened and How Do We Treat? Tom Vorpahl MSN, RN, ACNP-BC
 Hepatocellular Carcinoma (HCC): Who Should be Screened and How Do We Treat? Tom Vorpahl MSN, RN, ACNP-BC Objectives Identify patient risk factors for hepatocellular carcinoma (HCC) Describe strategies
Hepatocellular Carcinoma (HCC): Who Should be Screened and How Do We Treat? Tom Vorpahl MSN, RN, ACNP-BC Objectives Identify patient risk factors for hepatocellular carcinoma (HCC) Describe strategies
Multimodal therapy for hepatocellular carcinoma: A complementary approach to liver transplantation
 ORIGINAL ARTICLE Multimodal therapy for hepatocellular carcinoma: a complementary approach to liver transplantation., 2010; 9 (1): 23-32 January-March, Vol. 9 No.1, 2010: 23-32 23 ABSTRACT Multimodal therapy
ORIGINAL ARTICLE Multimodal therapy for hepatocellular carcinoma: a complementary approach to liver transplantation., 2010; 9 (1): 23-32 January-March, Vol. 9 No.1, 2010: 23-32 23 ABSTRACT Multimodal therapy
Department of Surgery, Samsung Medical Center, Sungkyunkwan University School of Medicine, Seoul, Korea
 ORIGINAL ARTICLE pissn -575 eissn -79 https://doi.org/1.17/astr.1.95..111 Annals of Surgical Treatment and Research Clinical usefulness of transarterial chemoembolization response prior to liver transplantation
ORIGINAL ARTICLE pissn -575 eissn -79 https://doi.org/1.17/astr.1.95..111 Annals of Surgical Treatment and Research Clinical usefulness of transarterial chemoembolization response prior to liver transplantation
Wait Time for Curative Intent Radio Frequency Ablation is Associated with Increased Mortality in Patients with Early Stage Hepatocellular Carcinoma
 ORIGINAL ARTICLE September-October, Vol. 16 No. 5, 2017: 765-771 765 The Official Journal of the Mexican Association of Hepatology, the Latin-American Association for Study of the Liver and the Canadian
ORIGINAL ARTICLE September-October, Vol. 16 No. 5, 2017: 765-771 765 The Official Journal of the Mexican Association of Hepatology, the Latin-American Association for Study of the Liver and the Canadian
Transcatheter Arterial Chemoembolization to Treat Primary or Metastatic Liver Malignancies
 Transcatheter Arterial Chemoembolization to Treat Primary or Metastatic Liver Malignancies Policy Number: 8.01.11 Last Review: 6/2018 Origination: 8/2005 Next Review: 6/2019 Policy Blue Cross and Blue
Transcatheter Arterial Chemoembolization to Treat Primary or Metastatic Liver Malignancies Policy Number: 8.01.11 Last Review: 6/2018 Origination: 8/2005 Next Review: 6/2019 Policy Blue Cross and Blue
Extending Indication: Role of Living Donor Liver Transplantation for Hepatocellular Carcinoma
 LIVER TRANSPLANTATION 13:S48-S54, 27 SUPPLEMENT Extending Indication: Role of Living Donor Liver Transplantation for Hepatocellular Carcinoma Satoru Todo, 1 Hiroyuki Furukawa, 2 Mitsuhiro Tada, 3 and the
LIVER TRANSPLANTATION 13:S48-S54, 27 SUPPLEMENT Extending Indication: Role of Living Donor Liver Transplantation for Hepatocellular Carcinoma Satoru Todo, 1 Hiroyuki Furukawa, 2 Mitsuhiro Tada, 3 and the
Paul Martin MD FACG. University of Miami
 Paul Martin MD FACG University of Miami 1 Liver cirrhosis of any cause Chronic C o c hepatitis epat t s B Risk increases with Male gender Age Diabetes Smoking ~5% increase in HCV-related HCC between 1991-28
Paul Martin MD FACG University of Miami 1 Liver cirrhosis of any cause Chronic C o c hepatitis epat t s B Risk increases with Male gender Age Diabetes Smoking ~5% increase in HCV-related HCC between 1991-28
Geographic Differences in Event Rates by Model for End-Stage Liver Disease Score
 American Journal of Transplantation 2006; 6: 2470 2475 Blackwell Munksgaard C 2006 The Authors Journal compilation C 2006 The American Society of Transplantation and the American Society of Transplant
American Journal of Transplantation 2006; 6: 2470 2475 Blackwell Munksgaard C 2006 The Authors Journal compilation C 2006 The American Society of Transplantation and the American Society of Transplant
Waitlist Priority for Hepatocellular Carcinoma Beyond Milan Criteria: A Potentially Appropriate Decision Without a Structured Approach
 American Journal of Transplantation 2014; 14: 79 87 Wiley Periodicals Inc. C Copyright 2013 The American Society of Transplantation and the American Society of Transplant Surgeons doi: 10.1111/ajt.12530
American Journal of Transplantation 2014; 14: 79 87 Wiley Periodicals Inc. C Copyright 2013 The American Society of Transplantation and the American Society of Transplant Surgeons doi: 10.1111/ajt.12530
Hepatocellular carcinoma (HCC) is the third
 Original Article / Transplantation Outcomes of loco-regional therapy for down-staging of hepatocellular carcinoma prior to liver transplantation Xian-Jie Shi, Xin Jin, Mao-Qiang Wang, Li-Xin Wei, Hui-Yi
Original Article / Transplantation Outcomes of loco-regional therapy for down-staging of hepatocellular carcinoma prior to liver transplantation Xian-Jie Shi, Xin Jin, Mao-Qiang Wang, Li-Xin Wei, Hui-Yi
RADIATION SEGMENTECTOMY. Robert J Lewandowski, MD
 RADIATION SEGMENTECTOMY Robert J Lewandowski, MD Robert Lewandowski, M.D. Consultant/Advisory Board: Cook Medical, LLC, Arsenal, BTG International, Boston Scientific Corp., ABK Reference Unlabeled/Unapproved
RADIATION SEGMENTECTOMY Robert J Lewandowski, MD Robert Lewandowski, M.D. Consultant/Advisory Board: Cook Medical, LLC, Arsenal, BTG International, Boston Scientific Corp., ABK Reference Unlabeled/Unapproved
Locoregional Treatments for HCC Applications in Transplant Candidates. Locoregional Treatments for HCC Applications in Transplant Candidates
 Locoregional Treatments for HCC Applications in Transplant Candidates Matthew Casey, MD March 31, 2016 Locoregional Treatments for HCC Applications in Transplant Candidates *No disclosures *Off-label uses
Locoregional Treatments for HCC Applications in Transplant Candidates Matthew Casey, MD March 31, 2016 Locoregional Treatments for HCC Applications in Transplant Candidates *No disclosures *Off-label uses
Surgical resection improves survival in pancreatic cancer patients without vascular invasion- a population based study
 Original article Annals of Gastroenterology (2013) 26, 346-352 Surgical resection improves survival in pancreatic cancer patients without vascular invasion- a population based study Subhankar Chakraborty
Original article Annals of Gastroenterology (2013) 26, 346-352 Surgical resection improves survival in pancreatic cancer patients without vascular invasion- a population based study Subhankar Chakraborty
PATIENTS AND METHODS. Data Source
 LIVER TRANSPLANTATION 20:1045 1056, 2014 ORIGINAL ARTICLE Waiting Time Predicts Survival After Liver Transplantation for Hepatocellular Carcinoma: A Cohort Study Using the United Network for Organ Sharing
LIVER TRANSPLANTATION 20:1045 1056, 2014 ORIGINAL ARTICLE Waiting Time Predicts Survival After Liver Transplantation for Hepatocellular Carcinoma: A Cohort Study Using the United Network for Organ Sharing
Liver resection for HCC
 8 th LIVER INTEREST GROUP Annual Meeting Cape Town 2017 Liver resection for HCC Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre The liver is almost unique in that treatment of the
8 th LIVER INTEREST GROUP Annual Meeting Cape Town 2017 Liver resection for HCC Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre The liver is almost unique in that treatment of the
Staging & Current treatment of HCC
 Staging & Current treatment of HCC Dr.: Adel El Badrawy Badrawy; ; M.D. Staging & Current ttt of HCC Early stage HCC is typically silent. HCC is often advanced at first manifestation. The selective ttt
Staging & Current treatment of HCC Dr.: Adel El Badrawy Badrawy; ; M.D. Staging & Current ttt of HCC Early stage HCC is typically silent. HCC is often advanced at first manifestation. The selective ttt
Guidelines for SIRT in HCC An Evolution
 Guidelines for SIRT in HCC An Evolution 2 nd Asia Pacific Symposium on Liver- Directed Y-90 Microspheres Therapy 1st November 2014, Singapore The challenge of HCC Surgery is potentially curative in early
Guidelines for SIRT in HCC An Evolution 2 nd Asia Pacific Symposium on Liver- Directed Y-90 Microspheres Therapy 1st November 2014, Singapore The challenge of HCC Surgery is potentially curative in early
HCC Imaging and Advances in Locoregional Therapy. David S. Kirsch MD Ochsner Clinic Foundation
 HCC Imaging and Advances in Locoregional Therapy David S. Kirsch MD Ochsner Clinic Foundation -Nothing to disclose Hepatic Imaging Primary imaging modalities include: US CT MR Angiography Nuclear medicine
HCC Imaging and Advances in Locoregional Therapy David S. Kirsch MD Ochsner Clinic Foundation -Nothing to disclose Hepatic Imaging Primary imaging modalities include: US CT MR Angiography Nuclear medicine
Combination transarterial chemoembolization and radiofrequency ablation therapy for early hepatocellular carcinoma
 ORIGINAL ARTICLE Korean J Intern Med 2016;31:242-252 Combination transarterial chemoembolization and radiofrequency ablation therapy for early hepatocellular carcinoma Myeong Jun Song 1, Si Hyun Bae 1,
ORIGINAL ARTICLE Korean J Intern Med 2016;31:242-252 Combination transarterial chemoembolization and radiofrequency ablation therapy for early hepatocellular carcinoma Myeong Jun Song 1, Si Hyun Bae 1,
RESEARCH ARTICLE. Validation of The Hong Kong Liver Cancer Staging System in Patients with Hepatocellular Carcinoma after Curative Intent Treatment
 DOI:10.22034/APJCP.2017.18.6.1697 RESEARCH ARTICLE Validation of The Hong Kong Liver Cancer Staging System in Patients with Hepatocellular Carcinoma after Curative Intent Treatment Alan Chuncharunee 1,
DOI:10.22034/APJCP.2017.18.6.1697 RESEARCH ARTICLE Validation of The Hong Kong Liver Cancer Staging System in Patients with Hepatocellular Carcinoma after Curative Intent Treatment Alan Chuncharunee 1,
hepatic artery chemoembolization (HACE) for hepatocellular Carcinoma in Patients Listed for Liver Transplantation
 American Journal of Transplantation 2004; 4: 782 787 Blackwell Munksgaard Copyright C Blackwell Munksgaard 2004 doi: 10.1111/j.1600-6143.2004.00413.x Hepatic Artery Chemoembolization for Hepatocellular
American Journal of Transplantation 2004; 4: 782 787 Blackwell Munksgaard Copyright C Blackwell Munksgaard 2004 doi: 10.1111/j.1600-6143.2004.00413.x Hepatic Artery Chemoembolization for Hepatocellular
Prediction of Progression-Free Survival in Patients Presenting with Hepatocellular Carcinoma Within the Milan Criteria
 LIVER TRANSPLANTATION 16:503-512, 2010 ORIGINAL ARTICLE Prediction of Progression-Free Survival in Patients Presenting with Hepatocellular Carcinoma Within the Milan Criteria Massimo De Giorgio, 1 * Stefano
LIVER TRANSPLANTATION 16:503-512, 2010 ORIGINAL ARTICLE Prediction of Progression-Free Survival in Patients Presenting with Hepatocellular Carcinoma Within the Milan Criteria Massimo De Giorgio, 1 * Stefano
Medical Policy. MP Radiofrequency Ablation of Primary or Metastatic Liver Tumors
 Medical Policy MP 7.01.91 BCBSA Ref. Policy: 7.01.91 Last Review: 08/20/2018 Effective Date: 08/20/2018 Section: Surgery Related Policies 7.01.75 Cryosurgical Ablation of Primary or Metastatic Liver Tumors
Medical Policy MP 7.01.91 BCBSA Ref. Policy: 7.01.91 Last Review: 08/20/2018 Effective Date: 08/20/2018 Section: Surgery Related Policies 7.01.75 Cryosurgical Ablation of Primary or Metastatic Liver Tumors
Inverse relationship between cirrhosis and massive tumours in hepatocellular carcinoma
 DOI:10.1111/j.1477-2574.2012.00507.x HPB ORIGINAL ARTICLE Inverse relationship between cirrhosis and massive tumours in hepatocellular carcinoma Umut Sarpel 1, Diego Ayo 2, Iryna Lobach 3, Ruliang Xu 4
DOI:10.1111/j.1477-2574.2012.00507.x HPB ORIGINAL ARTICLE Inverse relationship between cirrhosis and massive tumours in hepatocellular carcinoma Umut Sarpel 1, Diego Ayo 2, Iryna Lobach 3, Ruliang Xu 4
Bland Embolization Versus Chemoembolization of Hepatocellular Carcinoma Before Transplantation
 LIVER TRANSPLANTATION 20:536 543, 2014 ORIGINAL ARTICLE Bland Embolization Versus Chemoembolization of Hepatocellular Carcinoma Before Transplantation Michael D. Kluger, 1 Karim J. Halazun, 1 Ryan T. Barroso,
LIVER TRANSPLANTATION 20:536 543, 2014 ORIGINAL ARTICLE Bland Embolization Versus Chemoembolization of Hepatocellular Carcinoma Before Transplantation Michael D. Kluger, 1 Karim J. Halazun, 1 Ryan T. Barroso,
Liver Cancer: Diagnosis and Treatment Options
 Liver Cancer: Diagnosis and Treatment Options Fred Poordad, MD Chief, Hepatology University Transplant Center Professor of Medicine UT Health, San Antonio VP, Academic and Clinical Affairs, Texas Liver
Liver Cancer: Diagnosis and Treatment Options Fred Poordad, MD Chief, Hepatology University Transplant Center Professor of Medicine UT Health, San Antonio VP, Academic and Clinical Affairs, Texas Liver
Liver Transplantation for HCC Which Criteria?
 Liver Transplantation for HCC Which Criteria? Jacques Belghiti - François Durand Claire Francoz Hepato-Biliary-Pancreatic Liver Surgery and Liver Transplantation Unit Hôpital Beaujon (AP-HP), Clichy -
Liver Transplantation for HCC Which Criteria? Jacques Belghiti - François Durand Claire Francoz Hepato-Biliary-Pancreatic Liver Surgery and Liver Transplantation Unit Hôpital Beaujon (AP-HP), Clichy -
Percutaneous ablation: indications, techniques and results
 Percutaneous ablation: indications, techniques and results Giovan Giuseppe Di Costanzo Dipartimento dei Trapianti UOSC Epatologia AORN A Cardarelli - Napoli Treatment algorithm EASL, EORTC guidelines HCC
Percutaneous ablation: indications, techniques and results Giovan Giuseppe Di Costanzo Dipartimento dei Trapianti UOSC Epatologia AORN A Cardarelli - Napoli Treatment algorithm EASL, EORTC guidelines HCC
A) PUBLIC HEALTH B) PRESENTATION & DIAGNOSIS
 Hepatocellular Carcinoma HCC Updated November 2015 by: Dr. Mohammed Alghamdi (Medical Oncology Fellow, University of Calgary), April 2017 by Dr. Jenny Ko (Medical Oncologist, Abbotsford Centre, BC Cancer
Hepatocellular Carcinoma HCC Updated November 2015 by: Dr. Mohammed Alghamdi (Medical Oncology Fellow, University of Calgary), April 2017 by Dr. Jenny Ko (Medical Oncologist, Abbotsford Centre, BC Cancer
RETHINKING OUR APPROACH TO INTERMEDIATE-SIZE HCC
 SATELLITE SYMPOSIUM Emerging Horizons in HCC: From Palliation to Cure RETHINKING OUR APPROACH TO INTERMEDIATE-SIZE HCC Professor Riccardo Lencioni, MD, FSIR, EBIR University of Pisa School of Medicine,
SATELLITE SYMPOSIUM Emerging Horizons in HCC: From Palliation to Cure RETHINKING OUR APPROACH TO INTERMEDIATE-SIZE HCC Professor Riccardo Lencioni, MD, FSIR, EBIR University of Pisa School of Medicine,
Selection of patients of hepatocellular carcinoma beyond the Milan criteria for liver transplantation
 Title Selection of patients of hepatocellular carcinoma beyond the Milan criteria for liver transplantation Author(s) Chan, SC; Fan, ST Citation Hepatobiliary Surgery and Nutrition, 2013, v. 2 n. 2, p.
Title Selection of patients of hepatocellular carcinoma beyond the Milan criteria for liver transplantation Author(s) Chan, SC; Fan, ST Citation Hepatobiliary Surgery and Nutrition, 2013, v. 2 n. 2, p.
Surveillance for HCC Who, how Diagnosis of HCC Surveillance for HCC in Practice
 Surveillance for Hepatocellular Carcinoma Hashem B. El-Serag, MD, MPH Dan L. Duncan Professor of Medicine Chief, Gastroenterology and Hepatology Houston VA & Baylor College of Medicine Houston, TX Outline
Surveillance for Hepatocellular Carcinoma Hashem B. El-Serag, MD, MPH Dan L. Duncan Professor of Medicine Chief, Gastroenterology and Hepatology Houston VA & Baylor College of Medicine Houston, TX Outline
Hepatocellular Carcinoma in Qatar
 Hepatocellular Carcinoma in Qatar K. I. Rasul 1, S. H. Al-Azawi 1, P. Chandra 2 1 NCCCR, 2 Medical Research Centre, Hamad Medical Corporation, Doha, Qatar Abstract Objective The main aim of this study
Hepatocellular Carcinoma in Qatar K. I. Rasul 1, S. H. Al-Azawi 1, P. Chandra 2 1 NCCCR, 2 Medical Research Centre, Hamad Medical Corporation, Doha, Qatar Abstract Objective The main aim of this study
Total Tumor Volume and Alpha Fetoprotein for selection of transplant candidates. with hepatocellular carcinoma: a prospective validation
 Total Tumor Volume and Alpha Fetoprotein for selection of transplant candidates with hepatocellular carcinoma: a prospective validation Christian Toso 1, Glenda Meeberg 2, Roberto Hernandez-Alejandro 3,
Total Tumor Volume and Alpha Fetoprotein for selection of transplant candidates with hepatocellular carcinoma: a prospective validation Christian Toso 1, Glenda Meeberg 2, Roberto Hernandez-Alejandro 3,
Optimizing Patient Selection, Organ Allocation, and Outcomes in Liver Transplant (LT) Candidates with Hepatocellular Carcinoma (HCC)
 XXVI SETH Congress- 30 November 2017 Optimizing Patient Selection, Organ Allocation, and Outcomes in Liver Transplant (LT) Candidates with Hepatocellular Carcinoma (HCC) Neil Mehta, MD University of California,
XXVI SETH Congress- 30 November 2017 Optimizing Patient Selection, Organ Allocation, and Outcomes in Liver Transplant (LT) Candidates with Hepatocellular Carcinoma (HCC) Neil Mehta, MD University of California,
Percutaneous Ethanol Injection Therapy in the Treatment of Hepatocarcinoma Results Obtained from a Series of 88 Cases
 Percutaneous Ethanol Injection Therapy in the Treatment of Hepatocarcinoma Results Obtained from a Series of 88 Cases Mirela Danila, Ioan Sporea, Roxana Sirli, Alina Popescu Department of Gastroenterology
Percutaneous Ethanol Injection Therapy in the Treatment of Hepatocarcinoma Results Obtained from a Series of 88 Cases Mirela Danila, Ioan Sporea, Roxana Sirli, Alina Popescu Department of Gastroenterology
HCC: Is it an oncological disease? - No
 June 13-15, 2013 Berlin, Germany Prof. Oren Shibolet Head of the Liver Unit, Department of Gastroenterology Tel-Aviv Sourasky Medical Center and Tel-Aviv University HCC: Is it an oncological disease? -
June 13-15, 2013 Berlin, Germany Prof. Oren Shibolet Head of the Liver Unit, Department of Gastroenterology Tel-Aviv Sourasky Medical Center and Tel-Aviv University HCC: Is it an oncological disease? -
Liver Transplantation Evaluation: Objectives
 Liver Transplantation Evaluation: Essential Work-Up Curtis K. Argo, MD, MS VGS/ACG Regional Postgraduate Course Williamsburg, VA September 13, 2015 Objectives Discuss determining readiness for transplantation
Liver Transplantation Evaluation: Essential Work-Up Curtis K. Argo, MD, MS VGS/ACG Regional Postgraduate Course Williamsburg, VA September 13, 2015 Objectives Discuss determining readiness for transplantation
ORIGINAL ARTICLES LIVER, PANCREAS, AND BILIARY TRACT
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2011;9:989 994 ORIGINAL ARTICLES LIVER, PANCREAS, AND BILIARY TRACT Level of -Fetoprotein Predicts Mortality Among Patients With Hepatitis C Related Hepatocellular
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2011;9:989 994 ORIGINAL ARTICLES LIVER, PANCREAS, AND BILIARY TRACT Level of -Fetoprotein Predicts Mortality Among Patients With Hepatitis C Related Hepatocellular
Professor Norbert Bräu
 Sixth Annual BHIVA Conference for the Management of HIV/Hepatitis Co-Infection in collaboration with BASL and BVHG Professor Norbert Bräu James J Peters VA Medical Center, New York, USA COMPETING INTEREST
Sixth Annual BHIVA Conference for the Management of HIV/Hepatitis Co-Infection in collaboration with BASL and BVHG Professor Norbert Bräu James J Peters VA Medical Center, New York, USA COMPETING INTEREST
Hepatocellular Carcinoma in HIV-infected Patients A Growing Complication of Coinfection with HCV or HBV Mon, 31 May 2010
 Bronx VA Medical Center Mount Sinai School of Medicine Hepatocellular Carcinoma in HIV-infected Patients A Growing Complication of Coinfection with HCV or HBV Mon, 31 May 2010 Norbert Bräu, MD, MBA Associate
Bronx VA Medical Center Mount Sinai School of Medicine Hepatocellular Carcinoma in HIV-infected Patients A Growing Complication of Coinfection with HCV or HBV Mon, 31 May 2010 Norbert Bräu, MD, MBA Associate
Workup of a Solid Liver Lesion
 Workup of a Solid Liver Lesion Joseph B. Cofer MD FACS Chief Quality Officer Erlanger Health System Affiliate Professor of Surgery UTHSC-Chattanooga I have no financial or other relationships with any
Workup of a Solid Liver Lesion Joseph B. Cofer MD FACS Chief Quality Officer Erlanger Health System Affiliate Professor of Surgery UTHSC-Chattanooga I have no financial or other relationships with any
21/02/2014. Disclosures. HCC: predicting recurrence. Outline. Liver transplant: Beyond Milan?
 Disclosures HCC: predicting recurrence Peter Ghali, MD, FRCPC, MSc (epid) None relevant to this talk other than off-label use of sirolimus Toronto, February 2014 Outline Recurrence after what? Locoregional
Disclosures HCC: predicting recurrence Peter Ghali, MD, FRCPC, MSc (epid) None relevant to this talk other than off-label use of sirolimus Toronto, February 2014 Outline Recurrence after what? Locoregional
PAPER. Liver Transplantation for Hepatocellular Carcinoma
 PAPER Liver Transplantation for Hepatocellular Carcinoma Expanding Special Priority to Include III Disease Jeremy Goodman, MD; Sean C. Glasgow, MD; Mark Schnitzler, PhD; Jeffrey A. Lowell, MD; Surendra
PAPER Liver Transplantation for Hepatocellular Carcinoma Expanding Special Priority to Include III Disease Jeremy Goodman, MD; Sean C. Glasgow, MD; Mark Schnitzler, PhD; Jeffrey A. Lowell, MD; Surendra
The pediatric end-stage liver disease (PELD) score
 Selection of Pediatric Candidates Under the PELD System Sue V. McDiarmid, 1 Robert M. Merion, 2 Dawn M. Dykstra, 2 and Ann M. Harper 3 Key Points 1. The PELD score accurately predicts the 3 month probability
Selection of Pediatric Candidates Under the PELD System Sue V. McDiarmid, 1 Robert M. Merion, 2 Dawn M. Dykstra, 2 and Ann M. Harper 3 Key Points 1. The PELD score accurately predicts the 3 month probability
Hepatocellular Carcinoma Surveillance
 Amit G. Singal, MD, MS Hepatocellular Carcinoma Surveillance Postgraduate Course: Challenges in Management of Common Liver Diseases 308 1 Patient Case 69 year-old otherwise healthy male with compensated
Amit G. Singal, MD, MS Hepatocellular Carcinoma Surveillance Postgraduate Course: Challenges in Management of Common Liver Diseases 308 1 Patient Case 69 year-old otherwise healthy male with compensated
Surgical management of HCC. Evangelos Prassas Hepatobiliary and Pancreatic Surgery / Liver Transplantation Kings College Hospital / London
 Surgical management of HCC Evangelos Prassas Hepatobiliary and Pancreatic Surgery / Liver Transplantation Kings College Hospital / London Global distribution of HCC and staging systems WEST 1. Italy (Milan,
Surgical management of HCC Evangelos Prassas Hepatobiliary and Pancreatic Surgery / Liver Transplantation Kings College Hospital / London Global distribution of HCC and staging systems WEST 1. Italy (Milan,
Description. Section: Surgery Effective Date: October 15, 2014 Subsection: Surgery Original Policy Date: December 7, 2011 Subject:
 Last Review Status/Date: September 2014 Page: 1 of 20 Description In radiofrequency ablation (RFA), a probe is inserted into the center of a tumor and the noninsulated electrodes, which are shaped like
Last Review Status/Date: September 2014 Page: 1 of 20 Description In radiofrequency ablation (RFA), a probe is inserted into the center of a tumor and the noninsulated electrodes, which are shaped like
Advances in percutaneous ablation for hepatocellular carcinoma
 Advances in percutaneous ablation for hepatocellular carcinoma P. Nahon1,2,3 1 Hepatology, Jean Verdier Hospital, APHP, Bondy, France 2 Paris 13 university, Sorbonne Paris Cité, UFRSMBH, Bobigny, France
Advances in percutaneous ablation for hepatocellular carcinoma P. Nahon1,2,3 1 Hepatology, Jean Verdier Hospital, APHP, Bondy, France 2 Paris 13 university, Sorbonne Paris Cité, UFRSMBH, Bobigny, France
Chronic liver failure Assessment for liver transplantation
 Chronic liver failure Assessment for liver transplantation Liver Transplantation Dealing with the organ shortage Timing of listing must reflect length on waiting list Ethical issues Justice, equity, utility
Chronic liver failure Assessment for liver transplantation Liver Transplantation Dealing with the organ shortage Timing of listing must reflect length on waiting list Ethical issues Justice, equity, utility
Hepatocellular Carcinoma: A major global health problem. David L. Wood, MD Interventional Radiology Banner Good Samaritan Medical Center
 Hepatocellular Carcinoma: A major global health problem David L. Wood, MD Interventional Radiology Banner Good Samaritan Medical Center Hepatocellular Carcinoma WORLDWIDE The #2 Cancer Killer Overall cancer
Hepatocellular Carcinoma: A major global health problem David L. Wood, MD Interventional Radiology Banner Good Samaritan Medical Center Hepatocellular Carcinoma WORLDWIDE The #2 Cancer Killer Overall cancer
Management of Rare Liver Tumours
 Gian Luca Grazi Hepato-Biliary-Pancreatic Surgery National Cancer Institute Regina Elena Rome Fibrolamellar Carcinoma Mixed Hepato Cholangiocellular Carcinoma Hepatoblastoma Carcinosarcoma Primary Hepatic
Gian Luca Grazi Hepato-Biliary-Pancreatic Surgery National Cancer Institute Regina Elena Rome Fibrolamellar Carcinoma Mixed Hepato Cholangiocellular Carcinoma Hepatoblastoma Carcinosarcoma Primary Hepatic
WHAT IS THE BEST APPROACH FOR TRANS-ARTERIAL THERAPY IN HCC?
 WHAT IS THE BEST APPROACH FOR TRANS-ARTERIAL THERAPY IN HCC? Dr. Alexander Kim Chief, Vascular and Interventional Radiology, Medstar Georgetown University Hospital, USA DISCLAIMER Please note: The views
WHAT IS THE BEST APPROACH FOR TRANS-ARTERIAL THERAPY IN HCC? Dr. Alexander Kim Chief, Vascular and Interventional Radiology, Medstar Georgetown University Hospital, USA DISCLAIMER Please note: The views
HEPATOCELLULAR CARCINOMA: SCREENING, DIAGNOSIS, AND TREATMENT
 HEPATOCELLULAR CARCINOMA: SCREENING, DIAGNOSIS, AND TREATMENT INTRODUCTION: Hepatocellular carcinoma (HCC): Fifth most common cancer worldwide Third most common cause of cancer mortality In Egypt: 2.3%
HEPATOCELLULAR CARCINOMA: SCREENING, DIAGNOSIS, AND TREATMENT INTRODUCTION: Hepatocellular carcinoma (HCC): Fifth most common cancer worldwide Third most common cause of cancer mortality In Egypt: 2.3%
Organ allocation for liver transplantation: Is MELD the answer? North American experience
 Organ allocation for liver transplantation: Is MELD the answer? North American experience Douglas M. Heuman, MD Virginia Commonwealth University Richmond, VA, USA March 1998: US Department of Health and
Organ allocation for liver transplantation: Is MELD the answer? North American experience Douglas M. Heuman, MD Virginia Commonwealth University Richmond, VA, USA March 1998: US Department of Health and
Due to the disparity between organ availability and
 Use of Sorafenib in Patients With Hepatocellular Carcinoma Before Liver Transplantation: A Cost-Benefit Analysis While Awaiting Data on Sorafenib Safety Alessandro Vitale, 1 Michael L. Volk, 2 Davide Pastorelli,
Use of Sorafenib in Patients With Hepatocellular Carcinoma Before Liver Transplantation: A Cost-Benefit Analysis While Awaiting Data on Sorafenib Safety Alessandro Vitale, 1 Michael L. Volk, 2 Davide Pastorelli,
MP Transcatheter Arterial Chemoembolization to Treat Primary or Metastatic Liver Malignancies
 Medical Policy MP 8.01.11 BCBSA Ref. Policy: 8.01.11 Last Review: 07/25/2018 Effective Date: 07/25/2018 Section: Therapy Related Policies 7.01.75 Cryosurgical Ablation of Primary or Metastatic Liver Tumors
Medical Policy MP 8.01.11 BCBSA Ref. Policy: 8.01.11 Last Review: 07/25/2018 Effective Date: 07/25/2018 Section: Therapy Related Policies 7.01.75 Cryosurgical Ablation of Primary or Metastatic Liver Tumors
Learning Objectives. After attending this presentation, participants will be able to:
 Learning Objectives After attending this presentation, participants will be able to: Describe HCV in 2015 Describe how to diagnose advanced liver disease and cirrhosis Identify the clinical presentation
Learning Objectives After attending this presentation, participants will be able to: Describe HCV in 2015 Describe how to diagnose advanced liver disease and cirrhosis Identify the clinical presentation
UPDATE TO THE MANAGEMENT OF PATIENTS WITH HCC HCA
 UPDATE TO THE MANAGEMENT OF PATIENTS WITH HCC HUSSEIN K. MOHAMED MD, FACS. Transplant and Hepato-biliary Surgery Largo Medical Center HCA DISCLOSURE I have no financial relationship(s) relevant to the
UPDATE TO THE MANAGEMENT OF PATIENTS WITH HCC HUSSEIN K. MOHAMED MD, FACS. Transplant and Hepato-biliary Surgery Largo Medical Center HCA DISCLOSURE I have no financial relationship(s) relevant to the
Radiation Therapy for Liver Malignancies
 Outline Radiation Therapy for Liver Malignancies Albert J. Chang, M.D., Ph.D. Department of Radiation Oncology, UCSF March 23, 2014 Rationale for developing liver directed therapies Liver directed therapies
Outline Radiation Therapy for Liver Malignancies Albert J. Chang, M.D., Ph.D. Department of Radiation Oncology, UCSF March 23, 2014 Rationale for developing liver directed therapies Liver directed therapies
RFA for Liver Tumors: Does It Really Work? Heather Higgins, David L. Berger
 Hepatobiliary RFA for Liver Tumors: Does It Really Work? Heather Higgins, David L. Berger Department of Surgery, Massachusetts General Hospital, Boston, Massachusetts, USA Key Words. Radiofrequency ablation
Hepatobiliary RFA for Liver Tumors: Does It Really Work? Heather Higgins, David L. Berger Department of Surgery, Massachusetts General Hospital, Boston, Massachusetts, USA Key Words. Radiofrequency ablation
Tumor incidence varies significantly, depending on geographical location.
 Hepatocellular carcinoma is the 5 th most common malignancy worldwide with male-to-female ratio 5:1 in Asia 2:1 in the United States Tumor incidence varies significantly, depending on geographical location.
Hepatocellular carcinoma is the 5 th most common malignancy worldwide with male-to-female ratio 5:1 in Asia 2:1 in the United States Tumor incidence varies significantly, depending on geographical location.
Embolotherapy for Cholangiocarcinoma: 2016 Update
 Embolotherapy for Cholangiocarcinoma: 2016 Update Igor Lobko,MD Chief, Division Vascular and Interventional Radiology Long Island Jewish Medical Center GEST 2016 Igor Lobko, M.D. No relevant financial
Embolotherapy for Cholangiocarcinoma: 2016 Update Igor Lobko,MD Chief, Division Vascular and Interventional Radiology Long Island Jewish Medical Center GEST 2016 Igor Lobko, M.D. No relevant financial
Salvage Liver Transplantation for Recurrent Hepatocellular Carcinoma after Liver Resection: Retrospective Study of the Milan and Hangzhou Criteria
 Salvage Liver Transplantation for Recurrent Hepatocellular Carcinoma after Liver Resection: Retrospective Study of the Milan and Hangzhou Criteria Zhenhua Hu 1,2,3, Jie Zhou 1,2,3, Zhiwei Li 1,2,3, Jie
Salvage Liver Transplantation for Recurrent Hepatocellular Carcinoma after Liver Resection: Retrospective Study of the Milan and Hangzhou Criteria Zhenhua Hu 1,2,3, Jie Zhou 1,2,3, Zhiwei Li 1,2,3, Jie
Hepatocellular carcinoma in Sri Lanka - where do we stand?
 SCIENTIFIC ARTICLE Hepatocellular carcinoma in Sri Lanka - where do we stand? R.C. Siriwardana 1, C.A.H. Liyanage 1, M.B. Gunethileke 2 1. Specialist Gastrointestinal and Hepatobilliary Surgeon, Senior
SCIENTIFIC ARTICLE Hepatocellular carcinoma in Sri Lanka - where do we stand? R.C. Siriwardana 1, C.A.H. Liyanage 1, M.B. Gunethileke 2 1. Specialist Gastrointestinal and Hepatobilliary Surgeon, Senior
Indeterminate Pulmonary Nodules in Patients with Colorectal Cancer
 Indeterminate Pulmonary Nodules in Patients with Colorectal Cancer Jai Sule 1, Kah Wai Cheong 2, Stella Bee 2, Bettina Lieske 2,3 1 Dept of Cardiothoracic and Vascular Surgery, University Surgical Cluster,
Indeterminate Pulmonary Nodules in Patients with Colorectal Cancer Jai Sule 1, Kah Wai Cheong 2, Stella Bee 2, Bettina Lieske 2,3 1 Dept of Cardiothoracic and Vascular Surgery, University Surgical Cluster,
Disparities in Liver Transplant Allocation: An Update on MELD Allocation System
 Disparities in Liver Transplant Allocation: An Update on MELD Allocation System Naudia L. Jonassaint, MD MHS Assistant Professor of Medicine and Surgery University of Pittsburgh School of Medicine Historical
Disparities in Liver Transplant Allocation: An Update on MELD Allocation System Naudia L. Jonassaint, MD MHS Assistant Professor of Medicine and Surgery University of Pittsburgh School of Medicine Historical
Citation for published version (APA): Hompes, D. N. M. (2013). Advanced colorectal cancer: Exploring treatment boundaries.
 UvA-DARE (Digital Academic Repository) Advanced colorectal cancer: Exploring treatment boundaries Hompes, Daphne Link to publication Citation for published version (APA): Hompes, D. N. M. (2013). Advanced
UvA-DARE (Digital Academic Repository) Advanced colorectal cancer: Exploring treatment boundaries Hompes, Daphne Link to publication Citation for published version (APA): Hompes, D. N. M. (2013). Advanced
Natural History and Treatment Trends in Hepatocellular Carcinoma Subtypes: Insights From a National Cancer Registry
 2015;112:872 876 Natural History and Treatment Trends in Hepatocellular Carcinoma Subtypes: Insights From a National Cancer Registry PETER L. JERNIGAN, MD, KOFFI WIMA, MS, DENNIS J. HANSEMAN, PhD, RICHARD
2015;112:872 876 Natural History and Treatment Trends in Hepatocellular Carcinoma Subtypes: Insights From a National Cancer Registry PETER L. JERNIGAN, MD, KOFFI WIMA, MS, DENNIS J. HANSEMAN, PhD, RICHARD
Hepatocellular Carcinoma Recurrence After Liver Transplantation: an Analysis of Risk Factors and Incidence from Oregon Health & Science University
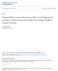 Portland State University PDXScholar University Honors Theses University Honors College 2016 Hepatocellular Carcinoma Recurrence After Liver Transplantation: an Analysis of Risk Factors and Incidence from
Portland State University PDXScholar University Honors Theses University Honors College 2016 Hepatocellular Carcinoma Recurrence After Liver Transplantation: an Analysis of Risk Factors and Incidence from
MANAGEMENT OF COLORECTAL METASTASES. Robert Warren, MD. The Postgraduate Course in General Surgery March 22, /22/2011
 MANAGEMENT OF COLORECTAL METASTASES Robert Warren, MD The Postgraduate Course in General Surgery March 22, 2011 Local Systemic LIVER TUMORS:THERAPEUTIC OPTIONS Hepatoma Cholangio. Neuroendo. Colorectal
MANAGEMENT OF COLORECTAL METASTASES Robert Warren, MD The Postgraduate Course in General Surgery March 22, 2011 Local Systemic LIVER TUMORS:THERAPEUTIC OPTIONS Hepatoma Cholangio. Neuroendo. Colorectal
OHSU Digital Commons. Oregon Health & Science University. Barry Schlansky. Scholar Archive. July 2013
 Oregon Health & Science University OHSU Digital Commons Scholar Archive July 2013 Waitlist time predicts survival after liver transplantation for hepatocellular carcinoma : a cohort study in the United
Oregon Health & Science University OHSU Digital Commons Scholar Archive July 2013 Waitlist time predicts survival after liver transplantation for hepatocellular carcinoma : a cohort study in the United
INTRODUCTION. Tae Yong Park, Young Chul Na, Won Hee Lee, Ji Hee Kim, Won Seok Chang, Hyun Ho Jung, Jong Hee Chang, Jin Woo Chang, Young Gou Park
 ORIGINAL ARTICLE Brain Tumor Res Treat 2013;1:78-84 / Print ISSN 2288-2405 / Online ISSN 2288-2413 online ML Comm Treatment Options of Metastatic Brain Tumors from Hepatocellular Carcinoma: Surgical Resection
ORIGINAL ARTICLE Brain Tumor Res Treat 2013;1:78-84 / Print ISSN 2288-2405 / Online ISSN 2288-2413 online ML Comm Treatment Options of Metastatic Brain Tumors from Hepatocellular Carcinoma: Surgical Resection
Jose Ramos. Role of Surgery in isolated hepatic metastasis from breast carcinoma, melanoma or sarcoma
 Role of Surgery in isolated hepatic metastasis from breast carcinoma, melanoma or sarcoma Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Evolution of liver resection Better understanding
Role of Surgery in isolated hepatic metastasis from breast carcinoma, melanoma or sarcoma Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Evolution of liver resection Better understanding
