Cross section of normal liver
|
|
|
- Florence Anderson
- 5 years ago
- Views:
Transcription
1 THE LIVER 1
2 Functions 1-processing of dietary amino acids, carbohydrates, lipids, and vitamins. 2-synthesis of serum proteins. 3-detoxification and excretion into bile of endogenous waste products and xenobiotics. 4- bile excresion 5- storage 2
3 Normal liver 3
4 Cross section of normal liver 4
5 Liver zones 5
6 -Surgical removal of 60% of the liver in a normal person is followed by minimal and transient hepatic impairment with restoration of most of its mass by regeneration within 4-6 weeks. -Perfect restoration may occur in persons who have sustained massive hepatic necrosis if the patient can survive the metabolic insult of liver failure. 6
7 % of hepatic function must be lost before hepatic failure ensues. - The balance may be moved toward decompensation by: A. systemic infections B. electrolyte disturbances C. major surgery D. heart failure E. GIT bleeding 7
8 CLINICAL SYNDROMES The major clinical syndromes of liver disease are: 1- hepatic failure 2- cirrhosis 3- portal hypertension 4- cholestasis. 8
9 Hepatic Failure -The most severe clinical consequence of liver disease. -It can occur due to: 1-insidious piecemeal destruction of hepatocytes. 2-repetitive symptomatic parenchymal damage. 3-sudden massive destruction. 9
10 Patterns of injury 1-Acute liver failure with massive hepatic necrosis. - Most often caused by drugs or viral hepatitis. - Clinical hepatic insufficiency progresses from onset of symptoms to hepatic encephalopathy within 2-3 weeks. - A course extending as long as 3 months is called subacute failure. - Massive hepatic necrosis. 10
11 2-Chronic liver disease. -The most common route to hepatic failure. - Mechanism: - A.hepatocytic (or parenchymal) damage - B.biliary disease - C.vascular disease - The end result is cirrhosis. 11
12 3-Hepatic dysfunction without overt necrosis. -Hepatocytes may be viable but unable to perform their normal metabolic function. -Causes: a. Mitochondrial injury in Reye syndrome b. Acute fatty liver of pregnancy c. Drug- or toxin-mediated injuries 12
13 Cirrhosis -Cirrhosis is among the top 10 causes of death in the Western world. -Its major causes include: 1- chronic viral infections 2- alcoholic or nonalcoholic steatohepatitis (NASH) 3- autoimmune diseases affecting hepatocytes and/or bile ducts 4- iron overload 13
14 5-Wilson disease 6-α-1- antitrypsin deficiency 7-Rare causes Galactosemia Tyrosinosis Glycogen storage disease III &IV Lipid storage disease Hereditary fructose intolerance Drug induced e.g methyldopa 14
15 -Cirrhosis is defined as a diffuse process characterized by fibrosis and the conversion of normal liver architecture into structurally abnormal nodules. -It is a diffuse process that includes: 1 Fibrous septa in the form of delicate bands or broad scars around multiple adjacent lobules. 2 Parenchymal nodules 15
16 -Nodules less than 3 mm in diameter=micronodules - Nodules larger than 3mm=macronodules - Hepatocytes in these nodules derive from two sources: (1) preexistent, long-lived hepatocytes that by the time cirrhosis is established display features of replicative senescence (2) newly formed hepatocytes capable of replication that are derived from stem/progenitor cells found adjacent to the canals of Hering and small bile ductules 16
17 Cirrhotic liver 17
18 Micronodular cirrhosis 18
19 Macronodular cirrhosis 19
20 20
21 Pathogenesis 1. Death of hepatocytes 2. Extracellular matrix deposition 3. Vascular reorganization 21
22 -In the normal liver ECM consists of collagen types I, III, V, and XI which is present only in the capsule, portal tracts, and around central veins. -Type IV collagen and other proteins present in the space between sinusoidal endothelial cells and hepatocytes (the space of Disse). -In cirrhosis, types I and III collagen and other ECM components are deposited in the space of Disse 22
23 - The major source of excess collagen in cirrhosis are the perisinusoidal stellate cells (Ito cells) which lie in the space of Disse. - Stellate cells normally function as storage cells for vitamin A. - Upon activation,stellate cells transform into myofibroblasts. 23
24 The stimuli for the activation of stellate cells and production of collagen are: 1.Reactive oxygen species 2.Growth factors 3.Cytokines such as TNF, IL-1, and lymphotoxins. 24
25 Activated stellate cells themselves produce growth factors, cytokines, and chemokines that cause their further proliferation and collagen synthesis in particular, transforming growth factor-β (TGF-β). 25
26 - Vascular injuries and changes also play significant roles in remodeling of the liver into a cirrhotic state. - Inflammation and thrombosis of portal veins, hepatic arteries, and/or central veins may lead to alternating zones of parenchymal hypoperfusion, with resulting parenchymal atrophy, and hyperperfusion, with overcompensating regeneration. 26
27 -The major vascular lesions that contribute to defects in liver function are: 1- Loss of sinusoidal endothelial cell fenestrations. 2- The development of portal vein hepatic vein and hepatic artery portal vein vascular shunts. 3- Loss of fenestrations and increased basement membrane thickness lead to increase in sinusoidal pressure and loss of solute exchange. (albumin, clotting factors, lipoproteins) 27
28 Clinical Features - Clinically silent. - Anorexia, weight loss, weakness, and, in advanced disease, frank debilitation. - Hepatic failure. 28
29 Complications 1 Progressive liver failure 2 Portal hypertension 3 The development of hepatocellular carcinoma 29
30 Portal Hypertension The intrahepatic causes are: 1- cirrhosis (most cases of portal hypertension). 2- schistosomiasis 3- massive fatty change 4- diffuse granulomatous diseases (e.g., sarcoidosis, miliary tuberculosis) 5-diseases affecting the portal microcirculation e.g nodular regenerative hyperplasia. 30
31 Mechanism of Portal hypertension in cirrhosis 1-Increased resistance to portal flow at the level of the sinusoids and compression of central veins by perivenular fibrosis and expanded parenchymal nodules. 2-Arterial and portal systems in the fibrous bands impose arterial pressure on the normally low-pressure portal venous system. 31
32 3-Increase in portal venous blood flow due to arterial vasodilation in the splanchnic circulation resulting from increased production of nitric oxide (NO) in the vascular bed. Reduced clearance of bacterial DNA absorbed from the gut that bypasses the Kupffer cells due to intrahepatic shunting of blood from portal to systemic circulation increases the production of NO. 32
33 Clinical consequences of portal hypertension 1. Ascites 2- Portosystemic Shunt 3- Hepatic encephalopathy 4- Splenomegaly 33
34 Ascites collection of excess fluid in the peritoneal cavity. clinically detectable when at least 500 ml have accumulated. 34
35 Ascites is a serous fluid containing as much as 3 g/dl of protein (largely albumin). The serum to ascites albumin gradient is 1.1 g/dl. The fluid may contain a scant number of mesothelial cells and mononuclear leukocytes. Influx of neutrophils suggests secondary Infection. The presence of red cells points to possible disseminated intraabdominal cancer. long-standing ascites may produce hydrothorax, more often on the right side. 35
36 Portosystemic Shunt Shunts develop wherever the systemic and portal circulations share capillary beds. Principal sites are: 1- veins around and within the rectum (hemorrhoids) 2- the cardioesophageal junction (esophagogastric varices). 3- the retroperitoneum. 4- the falciform ligament of the liver (involving periumbilical and abdominal wall collaterals). 36
37 Esophagogastric varices that appear in about 65% of persons with advanced cirrhosis of the liver causing massive hematemesis. Abdominal wall collaterals appear as dilated subcutaneous veins extending outward from the umbilicus (caput medusae). 37
38 Caput medusae-abdominal skin 38
39 Esophageal varicies 39
40 Hepatic Encephalopathy Hepatic encephalopathy may develop rapidly in acute liver failure or insidiously with gradually evolving chronic liver failure from cirrhosis. Hepatic encephalopathy show a spectrum of brain dysfunction ranging from subtle behavioral abnormalities to marked confusion and stupor to deep coma and death. 40
41 Associated neurologic signs include rigidity, hyperreflexia, nonspecific EEG changes, and, rarely, seizures. Characteristic is asterixis (also called flapping tremor) which is a pattern of nonrhythmic, rapid extension flexion movements of the head and extremities, best seen when the arms are held in extension with dorsiflexed wrists. 41
42 - In the brain there are only minor morphologic changes such as edema and an astrocytic reaction. - Two factors seem to be important in the genesis of this disorder: 1 Severe loss of hepatocellular function. 2 Shunting of blood from portal to systemic circulation around the chronically diseased liver. 42
43 - In the acute setting an elevation in blood ammonia which impairs neuronal function and promotes generalized brain edema. - In the chronic setting deranged neurotransmitter production. 43
44 Splenomegaly Long-standing congestion may cause congestive splenomegaly. Usually 1000 g or less (N<300gms). It is not necessarily correlated with other features of portal hypertension. Massive splenomegaly may secondarily induce a variety of hematologic abnormalities due to hypersplenism. 44
45 Hepatorenal Syndrome - Appears only with severe liver disease and is marked by the development of renal failure without primary abnormalities of the kidneys themselves. -Excluded by this definition are: 1 concomitant toxic damage to both the liver and the kidney as may occur in CCL4 & mushroom poisoning and the copper toxicity of Wilson disease. 2-circulatory collapse leads to acute tubular necrosis and renal failure. 45
46 -Kidney function promptly improves if hepatic failure is reversed. -The exact mechanism is unknown although splanchnic vasodilatation and systemic vasoconstriction leading to a severe reduction in renal blood flow particularly to the cortex. 46
47 DRUG- OR TOXIN-INDUCED LIVER DISEASE The liver is subject to injury from therapeutic and environmental chemicals. Injury may result from: 1- direct toxicity through hepatic conversion of a xenobiotic to an active toxin. 2- by immune mechanisms. 47
48 The injury may be immediate or take weeks to months to develop. drug-induced chronic hepatitis is clinically and histologically indistinguishable from chronic viral hepatitis or autoimmune hepatitis and hence serologic markers of viral infection are critical for making the distinction. 48
49 - Drug reactions are classified as: 1- predictable 2- unpredictable (idiosyncratic). 49
50 Predictable drug reactions may occur in anyone who accumulates a sufficient dose (dose-dependent). Unpredictable reactions depend on idiosyncrasies of the host: 1-the host's propensity to mount an immune response to drug related antigen. 2-the rate at which the host metabolizes the agent. 50
51 Predictable drugs: Acetaminophen Tetracycline Antineoplastic agents CCL4 Alcohol Unpredictable drugs Chlorpromazine Halothane Sulfonamides Methyldopa Allopurinol 51
52 -Patterns of injury 1-Hepatocellular necrosis 2-Cholestasis 3-Steatosis 4-Steatohepatitis 5-Fibrosis 6-Vascular lesions 7-Granuloma 8-Neoplasms benign & malignant 52
53 Pattern of Injury Morphology Examples Cholestatic Bland hepatocellular cholestasis, without inflammation Cholestatic hepatitis Cholestasis with lobular necroinflammatory activity Contraceptive Anabolic steroids Antibiotics; Phenothiazines Hepatocellular Spotty hepatocyte necrosis Methyldoya, Phenytoin necrosis Submassive necrosis, zone 3 Acetaminophen Halothane Massive necrosis Isoniazid, Phenytoin Steatosis Macrovesicular Ethanol, Methotrexate Corticosteroids Total parenteral nutrition 53
54 Steatohepatitis Microvesicular Mallory bodies Amiodarone, Ethanol Fibrosis and Periportal and Methotrexate, Isoniazid cirrhosis pericellular fibrosis Enalapril Granulomas non-caseating Sulfonamides Vascular lesions Sinusoidal obstruction High-dose chemotherapy syndrome (veno- Bush teas occlusivedisease) Budd-Chiari syndrome Sinusoidal dilatation Peliosis hepatis (blood-filled cavities) Oral contraceptives(ocp) Oral contraceptives (OCP) Anabolic steroids Tamoxifen 54
55 Neoplasms Hepatic adenoma HCC Cholangiocarcinoma Angiosarcoma OCP Anabolic steroids Thorotrast Thorotrast Thorotrast, Vinyl chloride 55
56 Drugs that may cause acute liver failure 1-Acetaminophen 2-Halothane 3-Antituberculosis drugs (rifampin, isoniazid) 4-Antidepressant monoamine oxidase inhibitors 5-Toxins as CCL 4 & mushroom poisoning 56
57 The most common cause (46% of cases of acute liver failure) is acetaminophen intoxication. 60% of these are a consequence of accidental overdosage. 57
58 Morphology: -Massive necrosis gm liver Submassive necrosis -Patchy necrosis 58
59 Hepatocellular necrosis caused by acetaminophen overdose. Confluent necrosis is seen in the perivenular region (large arrow) There is little inflammation. The residual normal tissue is indicated by the asterisk 59
60 Necrosis of hepatocytes 60
61 ACUTE AND CHRONIC HEPATITIS Acute and chronic forms of hepatitis are distinguished in part by duration and in part by the pattern of cell injury. Causative hepatotropic virus are hepatitis types A, B, C, D, and E. 61
62 The mononuclear inflammatory cell infiltrate predominates in all phases of hepatitic diseases because the inflammation is T cell mediated. 62
63 The distinction between acute and chronic hepatitis is based on: 1- the pattern of cell injury. 2- the severity of inflammation. 63
64 Morphologic features of acute hepatitis Enlarged, reddened liver; greenish if cholestatic Parenchymal Changes Swelling (ballooning degeneration) Cholestasis: canalicular bile plugs Mild fatty change of hepatocytes (HCV) Hepatocyte necrosis: isolated cells or clusters Cytolysis (rupture) Apoptosis (shrinkage) Bridging necrosis (portal-portal, central-central, portalcentral) 64
65 Lobular disarray: loss of normal architecture lobular hepatitis Regenerative changes: hepatocyte proliferation Sinusoidal cell reactive changes Accumulation of phagocytosed cellular debris in Kupffer cells. Influx of mononuclear cells into sinusoids. Portal tracts Inflammation: predominantly mononuclear. Inflammatory spillover into adjacent parenchyma with hepatocyte necrosis. 65
66 Morphologic features of chronic hepatitis Changes shared with acute hepatitis Hepatocyte injury, necrosis and apoptosis, and regeneration Sinusoidal cell reactive changes Portal tracts Inflammation Inerface hepatititis: spillover into adjacent parenchyma, with necrosis of hepatocytes. Bridging inflammation and necrosis Fibrosis: portal deposition, or portal and periportal deposition, or Formation of bridging fibrous septa. HBV: ground-glass hepatocytes (accumulation of HBsAg). HCV: bile duct epithelial cell proliferation, lymphoid aggregate formation. 66
67 Acute viral hepatitis showing disruption of lobular architecture, inflammatory cells in sinusoids, and apoptotic cells (arrow).
68 Ground-glass hepatocytes (arrow) in chronic hepatitis B, caused by accumulation of HBsAg in cytoplasm. 68
69 Fibrosis in chronic hepatitis 69
70 Autoimmune Hepatitis Chronic hepatitis with immunologic abnormalities -Histologic features are similar to chronic viral hepatitis -Indolent or severe course -Dramatic response to immunosuppressive therapy 70
71 Features: 1-Female predominance (70%) 2-Negative serelogy for viral Ags. 3- serum Ig (>2.5 g/dl) 4-High titers of autoantibodies (80% of cases) 5-The presence of other autoimmune diseases as RA, thyroiditis, sjogern syndrome, UC in 60% of the cases 71
72 The type of autoantibodies 1- Antinuclear antibodies 2- Antismooth muscle Abs anti actin anti troponin anti tropomyosin 3- liver/kidney microsomal Abs anti cytochrome P-450 components anti UDP-glucuronosyl transferases 3- Anti-soluble liver / pancreas antigen 72
73 Outcome Mild to severe chronic hepatitis Full remission is unusual Risk of cirrhosis is 5% which is the main cause of death 73
74 Alcoholic Liver Disease It accounts for 40-50% of deaths due to cirrhosis. More than 10 million Americans are alcoholics. Alcohol abuse is the fifth leading cause of death. 74
75 Alcohol-related fatty liver disease: (1) hepatic steatosis (90-100%) (2) alcoholic hepatitis (10-35%) (3) fibrosis and cirrhosis (8-20%) 75
76 Pathogenesis Short-term ingestion of as much as 80 g of ethanol per day generally produces mild, reversible hepatic changes (fatty liver). Chronic intake of g/day is considered a borderline risk factor for severe injury. 76
77 Women are more susceptible than men to hepatic injury due to decreased gastric metabolism of ethanol and differences in body composition. 77
78 Hepatocellular steatosis results from: (1) shunting of substrates away from catabolism and toward lipid biosynthesis. (2) impaired assembly and secretion of lipoproteins. (3) increased peripheral catabolism of fat. 78
79 Alcoholic hepatitis results from: Toxic by products of ethanol and its metabolites: 1- Acetaldehyde induces lipid peroxidation and acetaldehyde-protein adduct formation which may disrupt cytoskeleton and membrane function. 79
80 2- Direct Alcohol toxicity to cytoskeleton, mitochondrial function, and membrane fluidity. 3- Reactive oxygen species generated during oxidation of ethanol react with and damage membranes and proteins. 4-Reactive oxygen species also are produced by neutrophils, which infiltrate areas of hepatocyte necrosis. 80
81 5-Cytokine-mediated inflammation and cell injury. TNF is considered to be the main effector of injury; IL-1, IL-6, and IL-8 may also contribute. 81
82 The centrilobular region is most susceptible to toxic injury because the generation of acetaldehyde and free radicals is maximal in this region. Pericellular fibrosis and sinusoidal fibrosis develop in this area of the lobule. The prevalence of hepatitis C among persons with alcoholic disease is about 30% (and vice versa). 82
83 Cirrhosis develops in only a small fraction of chronic alcoholics. With complete abstinence some regression of scar can be seen in all cases. The micronodular liver transforms with regeneration into a macronodular cirrhotic organ. 83
84 Morphology Hepatocellular Steatosis Fatty liver with widespread steatosis is large (weighing 4-6 kg or more), soft, yellow, and greasy. It begins in centrilobular hepatocytes. The lipid droplets range from small (microvesicular) to large (macrovesicular). 84
85 Steatohepatitis. These changes typically are more pronounced with alcohol use than in NAFLD, but can be seen with variable degrees of prominence in fatty liver disease of any cause: 85
86 1 Hepatocyte ballooning. 2 Mallory-Denk bodies. These consist of tangled skeins of intermediate filaments (including ubiquitinated keratins 8 and 18) and are visible as eosinophilic cytoplasmic inclusions in degenerating hepatocytes. 3 Neutrophil infiltration. Predominantly neutrophilic infiltration may permeate the lobule and accumulate around degenerating hepatocytes, particularly those containing Mallory-Denk bodies. Lymphocytes and macrophages also may be seen in portal tracts or parenchyma 86
87 4 Steatohepatitis with fibrosis. 5 Micronodular or Laennec cirrhosis. 87
88 Alcoholic steatohepatitis 88
89 Cholestasis 89
90 Alcoholic steatohepatitis 90
91 Mallory-Denk bodies 91
92 Mallory-Denk bodies; clusters of inflammatory cells are also seen inset shows immunostaining for keratins 8 and 18 (brown) 92
93 Alcoholic Cirrhosis 93
94 Alcoholic Cirrhosis 94
95 Clinical Features Steatosis: Asymptomatic Hepatomegaly with mild elevations of serum bilirubin and alkaline phosphatase. 95
96 Alcoholic hepatitis: Can occur after just weeks or months of consistent use. The onset is typically acute and often follows a bout of particularly heavy drinking. Symptoms and laboratory abnormalities may range from minimal to severe. 96
97 malaise, anorexia, weight loss, upper abdominal discomfort, tender hepatomegaly, and fever. Hyperbilirubinemia, elevated alkaline phosphatase, and neutrophilic leukocytosis. Serum alanine aminotransferase and aspartate aminotransferase are elevated but usually remain below 500 U/ ml. 97
98 Each bout of hepatitis carries about a 10-20% risk of death. Cirrhosis appears in about one third of patients within a few years with repated bouts. 98
99 Cirrhosis: It is estimated that years of excessive drinking are necessary to develop alcoholic cirrhosis. The first signs of cirrhosis relate to complications of portal hypertension. Variceal hemorrhage or hepatic encephalopathy. Malaise, weakness, weight loss, and loss of appetite. 99
100 Cirrhosis may be clinically silent, discovered only at autopsy or when stress such as infection or trauma tips the balance toward hepatic insufficiency. Malnutrition and vitamin deficiencies (e.g., thiamine, vitamin B12). 100
101 The immediate causes of death are: 1 Hepatic failure 2 Massive gastrointestinal hemorrhage 3 Intercurrent infection 4 Hepatorenal syndrome 5 Hepatocellular carcinoma in 3-6% of cases 101
102 Nonalcoholic Fatty Liver Disease (NAFLD) It develops in persons who do not drink alcohol. The liver can show steatosis, steatohepatitis, and cirrhosis. 102
103 The term nonalcoholic steatohepatitis (NASH) is used to describe overt clinical features of liver injury similar to those induced by alcohol. 103
104 NAFLD is consistently associated with: 1 Type 2 diabetes (or family history of the condition) 2 Obesity, primarily central obesity (body mass index greater than 30 kg/m2 in whites and greater than 25 kg/m2 in Asians) 3 Dyslipidemia (hypertriglyceridemia, low HDL, highldl 4 Hypertension 104
105 Insulin resistance results in the accumulation of triglycerides in hepatocytes by: 1 Impaired oxidation of fatty acids 2 Increased synthesis and uptake of fatty acids 3 Decreased hepatic secretion of VLDL 105
106 Fat-laden hepatocytes are highly sensitive to lipid peroxidation products generated by oxidative stress, which can damage mitochondrial and plasma membranes, causing apoptosis. levels of TNF, IL-6, and of the MCP-1 chemokine increase, contributing to liver damage and inflammation. 106
107 NAFLD is the most common cause of incidental elevation of serum transaminases. Most persons with steatosis are asymptomatic. Patients with active steatohepatitis or fibrosis may also be asymptomatic, but some may have fatigue, malaise, right upper quadrant discomfort, or more severe symptoms of chronic liver disease. Liver biopsy is required for diagnosis. 107
108 The frequency of progression from steatosis to active steatohepatitis and then from active steatohepatitis to cirrhosis seems to be low. NAFLD is considered to be a significant contributor to the pathogenesis of cryptogenic cirrhosis. 108
109 Fatty change 109
110 fatty change 110
111 111
112 Primary Biliary Cirrhosis - Chronic progressive & often fatal cholestatic liver disease. -Non-suppurative granulomatous destruction of medium-sized intrahepatic bile ducts, portal inflammation & scarring. 112
113 Age 20-80yrs ( peak 40-50yrs) -F>M -Insidious onset -Pruritis, jaundice -Cirrhosis over 2 or more decades 113
114 PATHOGENESIS High titers of autoantibodies directed against several mitochondrial enzymes (>90%). Antimitochondrial pyruvate dehydrogenase autoantibodies. 114
115 Clinical Course The onset of PBC is insidious. Asymptomatic with elevated serum alkaline phosphatase. The diagnosis is usually made by demonstration of antimitochondrial antibodies and typical biopsy findings. 115
116 Patients often present with pruritus and usually prove to have advanced disease. Complications of cirrhosis over a period of 2 or more decades 116
117 MORPHOLOGY Interlobular bile ducts are actively destroyed by lymphocytic or plasmacytic inflammation with or without granulomas (the florid duct lesion). Portal tracts upstream from the damaged bile ducts show bile ductular proliferation and inflammation and necrosis of the adjacent periportal parenchyma. 117
118 Profound cholestasis in periportal/periseptal areas associated with feathery degeneration. Mallory-Denk bodies. 118
119 Primary biliary cirrhosis, end stage 119
120 Primary biliary cirrhosis 120
121 Ductular reaction in a fibrotic septum 121
122 Primary Sclerosing Cholangitis Chronic cholestatic disorder, characterized by progressive fibrosis and destruction of extrahepatic and intrahepatic bile ducts of all sizes. The changes in the ducts are patchy, cholangiography shows a characteristic beading in the affected segments of the biliary tree due to narrow strictures alternating with normal sized or dilated ducts. 122
123 -PSC and ulcerative colitis coexists in approximately 70% of affected patients. -The prevalence of PSC among persons with ulcerative colitis is about 4%. 123
124 The cause of PSC is unknown. There is association with ulcerative colitis linkage with certain HLA-DR alleles. Antinuclear cytoplasmic antibodies (ANCA) with a perinuclear localization present in 80% of cases. 124
125 Morphology The largest ducts have chronic inflammation with superimposed acute inflammation very similar to the mucosal lesions of ulcerative colitis. The smaller ducts often show mild inflammation but show a striking circumferential fibrosis often referred to as onion skinning around an increasingly atrophic duct lumen. 125
126 Duct loss leads to bile ductular proliferation, portal-portal septal fibrosis, and cirrhosis. The end-stage liver is therefore usually cirrhotic and green. 126
127 Primary sclerosing cholangitis. A bile duct undergoing degeneration is entrapped in a dense, onion-skin concentric scar. 127
128 Clinical Course M:F 2:1 3 rd -5 th decades of life Asymptomatic Persistently elevation of serum alkaline phosphatase. Acute cholangitis fever, right upper quadrant tenderness, and sometimes acute jaundice. At later stages may have progressive fatigue, pruritus, and chronic jaundice. Cholangiocarcinoma develops in 10-15% of patients with PSC, with a median time from diagnosis to malignant transformation of 5 years. 128
Liver Failure. The most severe clinical consequence of liver disease is liver failure:
 Liver diseases I The major primary diseases of the liver are: - Viral hepatitis, - Nonalcoholic fatty liver disease (NAFLD), - Alcoholic liver disease, - Hepatocellular carcinoma (HCC) Hepatic damage also
Liver diseases I The major primary diseases of the liver are: - Viral hepatitis, - Nonalcoholic fatty liver disease (NAFLD), - Alcoholic liver disease, - Hepatocellular carcinoma (HCC) Hepatic damage also
PITFALLS IN THE DIAGNOSIS OF MEDICAL LIVER DISEASE WITH TWO CONCURRENT ETIOLOGIES I HAVE NOTHING TO DISCLOSE CURRENT ISSUES IN ANATOMIC PATHOLOGY 2017
 CURRENT ISSUES IN ANATOMIC PATHOLOGY 2017 I HAVE NOTHING TO DISCLOSE Linda Ferrell PITFALLS IN THE DIAGNOSIS OF MEDICAL LIVER DISEASE WITH TWO CONCURRENT ETIOLOGIES Linda Ferrell, MD, UCSF THE PROBLEM
CURRENT ISSUES IN ANATOMIC PATHOLOGY 2017 I HAVE NOTHING TO DISCLOSE Linda Ferrell PITFALLS IN THE DIAGNOSIS OF MEDICAL LIVER DISEASE WITH TWO CONCURRENT ETIOLOGIES Linda Ferrell, MD, UCSF THE PROBLEM
Liver Diseases. Yasmine Lashine MD, PhD
 Liver Diseases Yasmine Lashine MD, PhD ILOs Recognize different causes of Live failure Recall and understand clinical picture and complication of Liver failure Discuss causes and clinical picture of hepatic
Liver Diseases Yasmine Lashine MD, PhD ILOs Recognize different causes of Live failure Recall and understand clinical picture and complication of Liver failure Discuss causes and clinical picture of hepatic
Basic patterns of liver damage what information can a liver biopsy provide and what clinical information does the pathologist need?
 Basic patterns of liver damage what information can a liver biopsy provide and what clinical information does the pathologist need? Rob Goldin r.goldin@imperial.ac.uk Fatty liver disease Is there fatty
Basic patterns of liver damage what information can a liver biopsy provide and what clinical information does the pathologist need? Rob Goldin r.goldin@imperial.ac.uk Fatty liver disease Is there fatty
Function: 1-Metabolic : Glucose. factors.. 3-Detoxification : Drugs, hormones, NH3. : Glycogen, TG, Fe, Cu, vit. 5-Excretory : Bile
 1 Liver Function: 1-Metabolic : Glucose 2-Synthetic : factors.. Albumin, clotting 3-Detoxification : Drugs, hormones, NH3 4-Storage vit : Glycogen, TG, Fe, Cu, 5-Excretory : Bile 2 - Net wt. 1400 1600gm
1 Liver Function: 1-Metabolic : Glucose 2-Synthetic : factors.. Albumin, clotting 3-Detoxification : Drugs, hormones, NH3 4-Storage vit : Glycogen, TG, Fe, Cu, 5-Excretory : Bile 2 - Net wt. 1400 1600gm
LIVER DISEASES. Pathology Department, Zhejiang University School of Medicine,
 LIVER DISEASES Pathology Department, Zhejiang University School of Medicine, 马丽琴,maliqin198@zju.edu.cn Viral Hepatitis Cirrhosis of liver Liver cancer Viral Hepatitis DEFINITION Primary hepatic infections
LIVER DISEASES Pathology Department, Zhejiang University School of Medicine, 马丽琴,maliqin198@zju.edu.cn Viral Hepatitis Cirrhosis of liver Liver cancer Viral Hepatitis DEFINITION Primary hepatic infections
Autoimmune Liver Diseases
 2nd Pannonia Congress of pathology Hepato-biliary pathology Autoimmune Liver Diseases Vera Ferlan Marolt Institute of pathology, Medical faculty, University of Ljubljana Slovenia Siofok, Hungary, May 2012
2nd Pannonia Congress of pathology Hepato-biliary pathology Autoimmune Liver Diseases Vera Ferlan Marolt Institute of pathology, Medical faculty, University of Ljubljana Slovenia Siofok, Hungary, May 2012
Liver, Pancreas and Gall Bladder Pathology
 Liver, Pancreas and Gall Bladder Pathology SCBM342 Systemic Pathology Witchuda Payuhakrit, Ph.D. (Pathobiology) Email: witchuda.pay@mahidol.ac.th Objectives 1. Understand etiology and pathogenesis of common
Liver, Pancreas and Gall Bladder Pathology SCBM342 Systemic Pathology Witchuda Payuhakrit, Ph.D. (Pathobiology) Email: witchuda.pay@mahidol.ac.th Objectives 1. Understand etiology and pathogenesis of common
Approach to the Patient with Liver Disease
 Approach to the Patient with Liver Disease Diagnosis of liver disease Careful history taking Physical examination Laboratory tests Radiologic examination and imaging studies Liver biopsy Liver diseases
Approach to the Patient with Liver Disease Diagnosis of liver disease Careful history taking Physical examination Laboratory tests Radiologic examination and imaging studies Liver biopsy Liver diseases
How to Approach a Medical Liver Biopsy. 9 th Bryan Warren School of Pathology Pancreatic and Liver Pathology. Sarajevo, 6 th -7 th November 2015
 1 A Brief Introduction to the Liver Sessions 9 th Bryan Warren School of Pathology Pancreatic and Liver Pathology Sarajevo, 6 th -7 th November 2015 Stefan Hübscher, Institute of Immunology & Immunotherapy,
1 A Brief Introduction to the Liver Sessions 9 th Bryan Warren School of Pathology Pancreatic and Liver Pathology Sarajevo, 6 th -7 th November 2015 Stefan Hübscher, Institute of Immunology & Immunotherapy,
Autoimmune Hepatobiliary Diseases PROF. DR. SABEHA ALBAYATI CABM,FRCP
 Autoimmune Hepatobiliary Diseases PROF. DR. SABEHA ALBAYATI CABM,FRCP Autoimmune hepatobiliary diseases The liver is an important target for immunemediated injury. Three disease phenotypes are recognized:
Autoimmune Hepatobiliary Diseases PROF. DR. SABEHA ALBAYATI CABM,FRCP Autoimmune hepatobiliary diseases The liver is an important target for immunemediated injury. Three disease phenotypes are recognized:
CHAPTER 1. Alcoholic Liver Disease
 CHAPTER 1 Alcoholic Liver Disease Major Lesions of Alcoholic Liver Disease Alcoholic fatty liver - >90% of binge and chronic drinkers Alcoholic hepatitis precursor of cirrhosis Alcoholic cirrhosis end
CHAPTER 1 Alcoholic Liver Disease Major Lesions of Alcoholic Liver Disease Alcoholic fatty liver - >90% of binge and chronic drinkers Alcoholic hepatitis precursor of cirrhosis Alcoholic cirrhosis end
Slide 7 demonstrates acute pericholangitisis with neutrophils around proliferating bile ducts.
 Many of the histologic images and the tables are from MacSween s Pathology of the Liver (5 th Edition). Other images were used from an online source called PathPedia.com. A few images from other sources
Many of the histologic images and the tables are from MacSween s Pathology of the Liver (5 th Edition). Other images were used from an online source called PathPedia.com. A few images from other sources
Extrahepatic Biliary Obstruction. Ductal Diseases: Stones Tumors. Acute Injury: Viral Hepatitis Toxin (APAP/Etoh) Reye s Shock.
 Extrahepatic Biliary Obstruction Stones Tumors Ductal Diseases: Ductal Diseases: Primary Biliary Primary Biliary Cirrhosis Cirrhosis Sclerosing Cholangitis Sclerosing Cholangitis Acute Injury: Viral Hepatitis
Extrahepatic Biliary Obstruction Stones Tumors Ductal Diseases: Ductal Diseases: Primary Biliary Primary Biliary Cirrhosis Cirrhosis Sclerosing Cholangitis Sclerosing Cholangitis Acute Injury: Viral Hepatitis
Nottingham Patterns of liver fibrosis and their clinical significance
 Nottingham 2006 Patterns of liver fibrosis and their clinical significance Alastair D Burt Professor of Pathology and Dean of Clinical Medicine University of Newcastle upon Tyne Collapse of reticulin
Nottingham 2006 Patterns of liver fibrosis and their clinical significance Alastair D Burt Professor of Pathology and Dean of Clinical Medicine University of Newcastle upon Tyne Collapse of reticulin
Linda Ferrell, MD Distinguished Professor Vice Chair Director of Surgical Pathology Dept of Pathology
 Linda Ferrell, MD Distinguished Professor Vice Chair Director of Surgical Pathology Dept of Pathology Nonalcoholic steatohepatitis and Fatty Liver Disease Liver manifestations of the obesity epidemic Changes
Linda Ferrell, MD Distinguished Professor Vice Chair Director of Surgical Pathology Dept of Pathology Nonalcoholic steatohepatitis and Fatty Liver Disease Liver manifestations of the obesity epidemic Changes
WEEK. MPharm Programme. Liver Biochemistry. Slide 1 of 49 MPHM14 Liver Biochemistry
 MPharm Programme Liver Biochemistry Slide 1 of 49 MPHM Liver Biochemistry Learning Outcomes Assess and evaluate the signs and symptoms of illness Assess and critically appraise a patients medication regimen,
MPharm Programme Liver Biochemistry Slide 1 of 49 MPHM Liver Biochemistry Learning Outcomes Assess and evaluate the signs and symptoms of illness Assess and critically appraise a patients medication regimen,
Histology. The pathology of the. bile ducts. pancreas. liver. The lecture in summary. Vt-2006
 Vt-2006 The pathology of the liver, bile ducts and pancreas Richard Palmqvist Docent, ST-läkare, Klin Pat Lab, Labcentrum The lecture in summary Introduction, histology & physiology in brief General phenomenon
Vt-2006 The pathology of the liver, bile ducts and pancreas Richard Palmqvist Docent, ST-läkare, Klin Pat Lab, Labcentrum The lecture in summary Introduction, histology & physiology in brief General phenomenon
DILI PATHOLOGY. PHILIP KAYE November 2017 BSG Pathology Winter Meeting
 DILI PATHOLOGY PHILIP KAYE November 2017 BSG Pathology Winter Meeting General Mechanisms Role of Liver Biopsy Outline Kleiner Categories Pathology! Differentials Severity Finally Drugs/Toxins may cause
DILI PATHOLOGY PHILIP KAYE November 2017 BSG Pathology Winter Meeting General Mechanisms Role of Liver Biopsy Outline Kleiner Categories Pathology! Differentials Severity Finally Drugs/Toxins may cause
Disorders of the Liver and Pancreas
 Disorders of the Liver and Pancreas Liver Lobule Hexagonal plates Sinusoids Triads Bile duct branch Arteriole Venuole Blood flows from periphery to Central vein Space of Dissé Lobular Microanatomy Hepatocytes
Disorders of the Liver and Pancreas Liver Lobule Hexagonal plates Sinusoids Triads Bile duct branch Arteriole Venuole Blood flows from periphery to Central vein Space of Dissé Lobular Microanatomy Hepatocytes
Basic patterns of liver damage what information can a liver biopsy provide and what clinical information does the pathologist need?
 Basic patterns of liver damage what information can a liver biopsy provide and what clinical information does the pathologist need? Rob Goldin r.goldin@imperial.ac.uk @robdgol FATTY LIVER DISEASE Brunt
Basic patterns of liver damage what information can a liver biopsy provide and what clinical information does the pathologist need? Rob Goldin r.goldin@imperial.ac.uk @robdgol FATTY LIVER DISEASE Brunt
Jaundice. Agnieszka Dobrowolska- Zachwieja, MD, PhD
 Jaundice Agnieszka Dobrowolska- Zachwieja, MD, PhD Jaundice definition Jaundice, as in the French jaune, refers to the yellow discoloration of the skin. It arises from the abnormal accumulation of bilirubin
Jaundice Agnieszka Dobrowolska- Zachwieja, MD, PhD Jaundice definition Jaundice, as in the French jaune, refers to the yellow discoloration of the skin. It arises from the abnormal accumulation of bilirubin
Cirrhosis and Portal Hypertension Gastroenterology Teaching Project American Gastroenterological Association
 CIRRHOSIS AND PORTAL HYPERTENSION Cirrhosis and Portal Hypertension Gastroenterology Teaching Project American Gastroenterological Association WHAT IS CIRRHOSIS? What is Cirrhosis? DEFINITION OF CIRRHOSIS
CIRRHOSIS AND PORTAL HYPERTENSION Cirrhosis and Portal Hypertension Gastroenterology Teaching Project American Gastroenterological Association WHAT IS CIRRHOSIS? What is Cirrhosis? DEFINITION OF CIRRHOSIS
Diseases of liver. Dr. Mohamed. A. Mahdi 4/2/2019. Mob:
 Diseases of liver Dr. Mohamed. A. Mahdi Mob: 0123002800 4/2/2019 Cirrhosis Cirrhosis is a complication of many liver disease. Permanent scarring of the liver. A late-stage liver disease. The inflammation
Diseases of liver Dr. Mohamed. A. Mahdi Mob: 0123002800 4/2/2019 Cirrhosis Cirrhosis is a complication of many liver disease. Permanent scarring of the liver. A late-stage liver disease. The inflammation
Supplemental Tables. Parasitic Schistosomiasis increase < 1. Genetic Hemochromatosis increase < 1. autoimmune Autoimmune hepatitis (AIH) increase < 1
 Supplemental Tables Supplemental Table 1 Various etiologies of liver cirrhosis and their association with liver stiffness and AST/ALT ratio Disease category Cause Example LS AST/ALT Inflammatory liver
Supplemental Tables Supplemental Table 1 Various etiologies of liver cirrhosis and their association with liver stiffness and AST/ALT ratio Disease category Cause Example LS AST/ALT Inflammatory liver
Steatotic liver disease
 Steatotic liver disease Fatty liver disease Prof. Dr. ANNE HOORENS Non-Neoplastic Liver Pathology December 8th 2018 Working Group of Digestive Pathology Belgian Society of Pathology OUTLINE NAFLD = Non-Alcoholic
Steatotic liver disease Fatty liver disease Prof. Dr. ANNE HOORENS Non-Neoplastic Liver Pathology December 8th 2018 Working Group of Digestive Pathology Belgian Society of Pathology OUTLINE NAFLD = Non-Alcoholic
Gastrointestinal System: Accessory Organ Disorders
 Gastrointestinal System: Accessory Organ Disorders Mary DeLetter, PhD, RN Associate Professor Dept. of Baccalaureate and Graduate Nursing Eastern Kentucky University Disorders of Accessory Organs Portal
Gastrointestinal System: Accessory Organ Disorders Mary DeLetter, PhD, RN Associate Professor Dept. of Baccalaureate and Graduate Nursing Eastern Kentucky University Disorders of Accessory Organs Portal
Liver failure &portal hypertension
 Liver failure &portal hypertension Objectives: by the end of this lecture each student should be able to : Diagnose liver failure (acute or chronic) List the causes of acute liver failure Diagnose and
Liver failure &portal hypertension Objectives: by the end of this lecture each student should be able to : Diagnose liver failure (acute or chronic) List the causes of acute liver failure Diagnose and
Digestive system L 4. Lecturer Dr. Firdous M. Jaafar Department of Anatomy/Histology section
 Digestive system L 4 Lecturer Dr. Firdous M. Jaafar Department of Anatomy/Histology section objectives 1-Describe the structure of liver. 2-Define liver lobule, and identify its zones. 3-Define portal
Digestive system L 4 Lecturer Dr. Firdous M. Jaafar Department of Anatomy/Histology section objectives 1-Describe the structure of liver. 2-Define liver lobule, and identify its zones. 3-Define portal
What Is Cirrhosis? CIRRHOSIS. Cirrhosis occurs when the liver is. by chronic conditions and diseases. permanently scarred or injured
 What Is Cirrhosis? Cirrhosis occurs when the liver is permanently scarred or injured by chronic conditions and diseases. Common causes of cirrhosis include: Long-term alcohol abuse. Chronic viral hepatitis
What Is Cirrhosis? Cirrhosis occurs when the liver is permanently scarred or injured by chronic conditions and diseases. Common causes of cirrhosis include: Long-term alcohol abuse. Chronic viral hepatitis
Steatosis/Steatohepatitis
 Prepared by Kurt Schaberg Introduction to Medical Liver Steatosis/Steatohepatitis Alcoholic Hepatitis Hepatocyte injury and inflammation resulting from chronic alcohol consumption AST/ALT ratio typically
Prepared by Kurt Schaberg Introduction to Medical Liver Steatosis/Steatohepatitis Alcoholic Hepatitis Hepatocyte injury and inflammation resulting from chronic alcohol consumption AST/ALT ratio typically
Biliary tract diseases of the liver
 Biliary tract diseases of the liver Digestive Diseases Course Bucharest 2016 Rob Goldin r.goldin@imperial.ac.uk How important are biliary tract diseases? Hepatology 2011 53(5):1608-17 Approximately 16%
Biliary tract diseases of the liver Digestive Diseases Course Bucharest 2016 Rob Goldin r.goldin@imperial.ac.uk How important are biliary tract diseases? Hepatology 2011 53(5):1608-17 Approximately 16%
Conflicts of Interest in the last 12 months
 STEATOHEPATITIS Richard K. Sterling, MD, MSc, FACP, FACG VCU Hepatology Professor of Medicine Chief, Section of Hepatology Virginia Commonwealth University Richmond, VA Conflicts of Interest in the last
STEATOHEPATITIS Richard K. Sterling, MD, MSc, FACP, FACG VCU Hepatology Professor of Medicine Chief, Section of Hepatology Virginia Commonwealth University Richmond, VA Conflicts of Interest in the last
Disorders of the Liver, Gallbladder and Pancreas
 Disorders of the Liver, Gallbladder and Pancreas Objectives: Disorders of the liver Disorders of the gall bladder Disorders of the pancreas Part 1: Disorders of the Liver 1 Jaundice: is a manifestation
Disorders of the Liver, Gallbladder and Pancreas Objectives: Disorders of the liver Disorders of the gall bladder Disorders of the pancreas Part 1: Disorders of the Liver 1 Jaundice: is a manifestation
Hepatitis. Causes: - infectious Hepatitis: viral, Bacterial, Parasitic, and Helminthic - Autoimmune Hepatitis - Drug- and Toxin (Alcohol) - Metabolic
 Liver diseases II Hepatitis Causes: - infectious Hepatitis: viral, Bacterial, Parasitic, and Helminthic - Autoimmune Hepatitis - Drug- and Toxin (Alcohol) - Metabolic infectious Hepatitis Several clinical
Liver diseases II Hepatitis Causes: - infectious Hepatitis: viral, Bacterial, Parasitic, and Helminthic - Autoimmune Hepatitis - Drug- and Toxin (Alcohol) - Metabolic infectious Hepatitis Several clinical
Interesting Cases from Liver Tumor Board. Jeffrey C. Weinreb, M.D.,FACR Yale University School of Medicine
 Interesting Cases from Liver Tumor Board Jeffrey C. Weinreb, M.D.,FACR Yale University School of Medicine jeffrey.weinreb@yale.edu Common Liver Diseases Hemangioma Cyst FNH Focal Fat/Sparing THID Non-Cirrhotic
Interesting Cases from Liver Tumor Board Jeffrey C. Weinreb, M.D.,FACR Yale University School of Medicine jeffrey.weinreb@yale.edu Common Liver Diseases Hemangioma Cyst FNH Focal Fat/Sparing THID Non-Cirrhotic
Non alcoholic fatty liver and Non alcoholic Steatohepatitis. By Dr. Seham Seif
 Non alcoholic fatty liver and Non alcoholic Steatohepatitis By Dr. Seham Seif Definition NAFL describe a common clinicopathological conditions characterized by significant lipid deposition in the hepatocytes
Non alcoholic fatty liver and Non alcoholic Steatohepatitis By Dr. Seham Seif Definition NAFL describe a common clinicopathological conditions characterized by significant lipid deposition in the hepatocytes
factors.. 3-Detoxification : Drugs, hormones, NH3 : Glycogen, TG, Fe, Cu,
 1 Liver Function: 1-Metabolic : Glucose 2-Synthetic : factors.. Albumin, clotting 3-Detoxification : Drugs, hormones, NH3 4-Storage vit : Glycogen, TG, Fe, Cu, 5-Excretory : Bile 2 - Net wt. 1400 1600gm
1 Liver Function: 1-Metabolic : Glucose 2-Synthetic : factors.. Albumin, clotting 3-Detoxification : Drugs, hormones, NH3 4-Storage vit : Glycogen, TG, Fe, Cu, 5-Excretory : Bile 2 - Net wt. 1400 1600gm
A Review of Liver Function Tests. James Gray Gastroenterology Vancouver
 A Review of Liver Function Tests James Gray Gastroenterology Vancouver Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored, or transmitted
A Review of Liver Function Tests James Gray Gastroenterology Vancouver Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored, or transmitted
LIVER SPECIALTY CONFERENCE USCAP Maha Guindi, M.D. Clinical Professor of Pathology Cedars-Sinai Medical Center Los Angeles, CA
 LIVER SPECIALTY CONFERENCE USCAP 2016 Maha Guindi, M.D. Clinical Professor of Pathology Cedars-Sinai Medical Center Los Angeles, CA Nothing to disclose Case History 47-year-old male, long standing ileal
LIVER SPECIALTY CONFERENCE USCAP 2016 Maha Guindi, M.D. Clinical Professor of Pathology Cedars-Sinai Medical Center Los Angeles, CA Nothing to disclose Case History 47-year-old male, long standing ileal
Disclosures Drug-induced Acute Liver Failure
 Disclosures Drug-induced Acute Liver Failure I have nothing to disclose. Raga Ramachandran, MD, PhD UCSF Pathology May 25, 2012 Acute liver failure (Fulminant hepatitis) Definition - onset of hepatic encephalopathy
Disclosures Drug-induced Acute Liver Failure I have nothing to disclose. Raga Ramachandran, MD, PhD UCSF Pathology May 25, 2012 Acute liver failure (Fulminant hepatitis) Definition - onset of hepatic encephalopathy
HEPETIC SYSTEMS BIOCHEMICAL HEPATOCYTIC SYSTEM HEPATOBILIARY SYSTEM RETICULOENDOTHELIAL SYSTEM
 EVALUATION OF LIVER FUNCTION R. Mohammadi Biochemist (Ph.D.) Faculty member of Medical Faculty HEPETIC SYSTEMS BIOCHEMICAL HEPATOCYTIC SYSTEM HEPATOBILIARY SYSTEM RETICULOENDOTHELIAL SYSTEM METABOLIC FUNCTION
EVALUATION OF LIVER FUNCTION R. Mohammadi Biochemist (Ph.D.) Faculty member of Medical Faculty HEPETIC SYSTEMS BIOCHEMICAL HEPATOCYTIC SYSTEM HEPATOBILIARY SYSTEM RETICULOENDOTHELIAL SYSTEM METABOLIC FUNCTION
Chapter 18 Liver and Gallbladder
 Chapter 18 Liver and Gallbladder 解剖學科徐淑媛 本堂重點 1. Liver : functions & histology 2. Gallbladder Physiology Liver Produce circulating plasma proteins Vitamin Iron Degradation Metabolism Bile manufacture (exocrine)
Chapter 18 Liver and Gallbladder 解剖學科徐淑媛 本堂重點 1. Liver : functions & histology 2. Gallbladder Physiology Liver Produce circulating plasma proteins Vitamin Iron Degradation Metabolism Bile manufacture (exocrine)
Primary Sclerosing Cholangitis and Cholestatic liver diseases. Ahsan M Bhatti MD, FACP Bhatti Gastroenterology Consultants
 Primary Sclerosing Cholangitis and Cholestatic liver diseases Ahsan M Bhatti MD, FACP Bhatti Gastroenterology Consultants I have nothing to disclose Educational Objectives What is PSC? Understand the cholestatic
Primary Sclerosing Cholangitis and Cholestatic liver diseases Ahsan M Bhatti MD, FACP Bhatti Gastroenterology Consultants I have nothing to disclose Educational Objectives What is PSC? Understand the cholestatic
-sheet 3. -Waseem Alhaj. Maha Shomaf
 -sheet 3 -Basheer egbaria -Waseem Alhaj Maha Shomaf 1 P a g e Viral hepatitis have many types each type is associated with different outcomes complication, some can result in acute one,others result in
-sheet 3 -Basheer egbaria -Waseem Alhaj Maha Shomaf 1 P a g e Viral hepatitis have many types each type is associated with different outcomes complication, some can result in acute one,others result in
Hepatitis. Dr. Mohamed. A. Mahdi 5/2/2019. Mob:
 Hepatitis Dr. Mohamed. A. Mahdi Mob: 0123002800 5/2/2019 Hepatitis Hepatitis means the inflammation of the liver. May cause by viruses or bacteria, parasites, radiation, drugs, chemical and toxins (alcohol).
Hepatitis Dr. Mohamed. A. Mahdi Mob: 0123002800 5/2/2019 Hepatitis Hepatitis means the inflammation of the liver. May cause by viruses or bacteria, parasites, radiation, drugs, chemical and toxins (alcohol).
Non-Cirrhotic Portal Hypertension and Incomplete Septal Cirrhosis. Stefan Hübscher, University of Birmingham, Birmingham B15 2TT, U.K.
 Non-Cirrhotic Portal Hypertension and Incomplete Septal Cirrhosis Stefan Hübscher, University of Birmingham, Birmingham B15 2TT, U.K. Non-Cirrhotic Portal Hypertension Problems with Liver Biopsy Diagnosis
Non-Cirrhotic Portal Hypertension and Incomplete Septal Cirrhosis Stefan Hübscher, University of Birmingham, Birmingham B15 2TT, U.K. Non-Cirrhotic Portal Hypertension Problems with Liver Biopsy Diagnosis
Viral Hepatitis (I) Luigi Terracciano Department of Pathology University Hospital Basel. Basel,
 Viral Hepatitis (I) Luigi Terracciano Department of Pathology University Hospital Basel Basel, 19. 04. 2016 Definition Hepatitis means inflammation of the liver characterized by a variable combination
Viral Hepatitis (I) Luigi Terracciano Department of Pathology University Hospital Basel Basel, 19. 04. 2016 Definition Hepatitis means inflammation of the liver characterized by a variable combination
Case n 1 ( B 92 / 4208 ) Case n 2 ( B 00 / 8249 ) Case n 3 ( B 98 / 8352 )
 Slide Seminar Case n 1 ( B 92 / 4208 ) 16 month-old girl. HBV serology +. Clinic in favour of chronic hepatitis. 4 portal triads! classification limited Viral B chronic hepatitis Mild activity (Fig. 1
Slide Seminar Case n 1 ( B 92 / 4208 ) 16 month-old girl. HBV serology +. Clinic in favour of chronic hepatitis. 4 portal triads! classification limited Viral B chronic hepatitis Mild activity (Fig. 1
Noncalculous Biliary Disease Dean Abramson, M.D. Gastroenterologists, P.C. Cedar Rapids. Cholestasis
 Noncalculous Biliary Disease Dean Abramson, M.D. Gastroenterologists, P.C. Cedar Rapids Cholestasis Biochemical hallmark Impaired bile flow from liver to small intestine Alkaline phosphatase is primary
Noncalculous Biliary Disease Dean Abramson, M.D. Gastroenterologists, P.C. Cedar Rapids Cholestasis Biochemical hallmark Impaired bile flow from liver to small intestine Alkaline phosphatase is primary
Key Points: Autoimmune Liver Disease: Update for Pathologists from the Hepatologist s Perspective. Jenny Heathcote, MD. University of Toronto
 Autoimmune Liver Disease: Update for Pathologists from the Hepatologist s Perspective Jenny Heathcote, MD University of Toronto Key Points: AILD comprise autoimmune hepatitis, primary biliary cirrhosis
Autoimmune Liver Disease: Update for Pathologists from the Hepatologist s Perspective Jenny Heathcote, MD University of Toronto Key Points: AILD comprise autoimmune hepatitis, primary biliary cirrhosis
)Liver diseases I and II)
 )Liver diseases I and II) The liver is vulnerable to a wide variety of metabolic, toxic, microbial, circulatory, and neoplastic insults. The major primary diseases of the liver are viral hepatitis, nonalcoholic
)Liver diseases I and II) The liver is vulnerable to a wide variety of metabolic, toxic, microbial, circulatory, and neoplastic insults. The major primary diseases of the liver are viral hepatitis, nonalcoholic
LIVER CIRRHOSIS. The liver extracts nutrients from the blood and processes them for later use.
 LIVER CIRRHOSIS William Sanchez, M.D. & Jayant A. Talwalkar, M.D., M.P.H. Advanced Liver Disease Study Group Miles and Shirley Fiterman Center for Digestive Diseases Mayo College of Medicine Rochester,
LIVER CIRRHOSIS William Sanchez, M.D. & Jayant A. Talwalkar, M.D., M.P.H. Advanced Liver Disease Study Group Miles and Shirley Fiterman Center for Digestive Diseases Mayo College of Medicine Rochester,
Gastroenterology. Certification Examination Blueprint. Purpose of the exam
 Gastroenterology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of the certified gastroenterologist
Gastroenterology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of the certified gastroenterologist
Interpreting Liver Function Tests
 PSH Clinical Guidelines Statement 2017 Interpreting Liver Function Tests Dr. Asad A Chaudhry Consultant Hepatologist, Chaudhry Hospital, Gujranwala, Pakistan. Liver function tests (LFTs) generally refer
PSH Clinical Guidelines Statement 2017 Interpreting Liver Function Tests Dr. Asad A Chaudhry Consultant Hepatologist, Chaudhry Hospital, Gujranwala, Pakistan. Liver function tests (LFTs) generally refer
Pancreatic exocrine insufficiency: a rare cause of nonalcoholic steatohepatitis
 Pancreatic exocrine insufficiency: a rare cause of nonalcoholic steatohepatitis Naoki Tanaka 1, Akira Horiuchi 2, Takahide Yokoyama 3, Shigeyuki Kawa 1, and Kendo Kiyosawa 1 1 Department of Gastroenterology,
Pancreatic exocrine insufficiency: a rare cause of nonalcoholic steatohepatitis Naoki Tanaka 1, Akira Horiuchi 2, Takahide Yokoyama 3, Shigeyuki Kawa 1, and Kendo Kiyosawa 1 1 Department of Gastroenterology,
Etiology of liver cirrhosis
 Liver cirrhosis 1 Liver cirrhosis Liver cirrhosis is the progressive replacement of normal hepatic cells by fibrous scar tissue, This scarring is accompanied by the loss of viable hepatocytes, which are
Liver cirrhosis 1 Liver cirrhosis Liver cirrhosis is the progressive replacement of normal hepatic cells by fibrous scar tissue, This scarring is accompanied by the loss of viable hepatocytes, which are
Cellular Injury. Intracellular degeneration. By Dr. Hemn Hassan Othman PhD, Pathology Fall /20/2018 1
 Cellular Injury Intracellular degeneration By Dr. Hemn Hassan Othman PhD, Pathology Fall 2018 10/20/2018 1 Types of cell injury Cell injury is divided into: 1. Reversible cell injury 2. Irreversible cell
Cellular Injury Intracellular degeneration By Dr. Hemn Hassan Othman PhD, Pathology Fall 2018 10/20/2018 1 Types of cell injury Cell injury is divided into: 1. Reversible cell injury 2. Irreversible cell
Chronic Biliary Disease. Dr Susan Davies & Dr Bill Griffiths
 Chronic Biliary Disease Dr Susan Davies & Dr Bill Griffiths Chronic Biliary Disease Terminology is confusing with pathologists and hepatologists using the same language BUT with different meanings. Chronic
Chronic Biliary Disease Dr Susan Davies & Dr Bill Griffiths Chronic Biliary Disease Terminology is confusing with pathologists and hepatologists using the same language BUT with different meanings. Chronic
New insights into fatty liver disease. Rob Goldin Centre for Pathology, Imperial College
 New insights into fatty liver disease Rob Goldin Centre for Pathology, Imperial College r.goldin@imperial.ac.uk Prevalence of NASH Global prevalence of NAFLD is 25% with highest prevalence in the Middle
New insights into fatty liver disease Rob Goldin Centre for Pathology, Imperial College r.goldin@imperial.ac.uk Prevalence of NASH Global prevalence of NAFLD is 25% with highest prevalence in the Middle
British Liver Transplant Group Pathology meeting September Leeds cases
 British Liver Transplant Group Pathology meeting September 2014 Leeds cases Leeds Case 1 Male 61 years Liver transplant for HCV cirrhosis with HCC in January 2014. Now raised ALT and bilirubin,? acute
British Liver Transplant Group Pathology meeting September 2014 Leeds cases Leeds Case 1 Male 61 years Liver transplant for HCV cirrhosis with HCC in January 2014. Now raised ALT and bilirubin,? acute
ACP-BSG meeting The liver in systemic inflammatory disorders. Dr Adrian C Bateman Southampton University Hospitals NHS Trust
 ACP-BSG meeting 10.12.09 The liver in systemic inflammatory disorders Dr Adrian C Bateman Southampton University Hospitals NHS Trust Wide range of diseases General inflammatory disorders Connective tissue
ACP-BSG meeting 10.12.09 The liver in systemic inflammatory disorders Dr Adrian C Bateman Southampton University Hospitals NHS Trust Wide range of diseases General inflammatory disorders Connective tissue
Evaluation of Liver Mass Lesions. American College of Gastroenterology 2013 Regional Postgraduate Course
 Evaluation of Liver Mass Lesions American College of Gastroenterology 2013 Regional Postgraduate Course Lewis R. Roberts, MB ChB, PhD Division of Gastroenterology and Hepatology Mayo Clinic College of
Evaluation of Liver Mass Lesions American College of Gastroenterology 2013 Regional Postgraduate Course Lewis R. Roberts, MB ChB, PhD Division of Gastroenterology and Hepatology Mayo Clinic College of
Liver Pathology: Cirrhosis, Hepatitis, and Primary Liver Tumors. Update and Diagnostic Problems
 SHORT COURSE Liver Pathology: Cirrhosis, Hepatitis, and Primary Liver Tumors. Update and Diagnostic Problems Linda Ferrell, M.D. Department of Anatomic Pathology, University of California San Francisco,
SHORT COURSE Liver Pathology: Cirrhosis, Hepatitis, and Primary Liver Tumors. Update and Diagnostic Problems Linda Ferrell, M.D. Department of Anatomic Pathology, University of California San Francisco,
Cirrhosis of the Liver
 235 60th Street, West New York, NJ 07093 T: (201) 854-4646 F: (201) 854-4647 810 Main Street, Hackensack, NJ 07601 T: (201) 488-0095 Cirrhosis of the Liver The liver, the largest organ in the body, is
235 60th Street, West New York, NJ 07093 T: (201) 854-4646 F: (201) 854-4647 810 Main Street, Hackensack, NJ 07601 T: (201) 488-0095 Cirrhosis of the Liver The liver, the largest organ in the body, is
Drug therapy in patient with hepatic impairment
 Drug therapy in patient with hepatic impairment Arzneimitteltherapie bei Leberinsuffizienz Dominik Wilke 03/04 Mai 2018 43. ADKA-Kongress, Stuttgart Functions of the Liver I Metabolism (Carbohydrates,
Drug therapy in patient with hepatic impairment Arzneimitteltherapie bei Leberinsuffizienz Dominik Wilke 03/04 Mai 2018 43. ADKA-Kongress, Stuttgart Functions of the Liver I Metabolism (Carbohydrates,
Patologia sistematica V Gastroenterologia Prof. Stefano Fiorucci Autoimmune liver diseases
 Patologia sistematica V Gastroenterologia Prof. Stefano Fiorucci Autoimmune liver diseases Harrison s Principles of Internal Medicine 18-19 Ed. 2012 e seguenti Chronic hepatitis classification by cause
Patologia sistematica V Gastroenterologia Prof. Stefano Fiorucci Autoimmune liver diseases Harrison s Principles of Internal Medicine 18-19 Ed. 2012 e seguenti Chronic hepatitis classification by cause
Function: 1-Metabolic : Glucose. factors.. 3-Detoxification : Drugs, hormones, NH3. : Glycogen, TG, Fe, Cu, vit. 5-Excretory : Bile
 1 Liver Function: 1-Metabolic : Glucose 2-Synthetic : factors.. Albumin, clotting 3-Detoxification : Drugs, hormones, NH3 4-Storage vit : Glycogen, TG, Fe, Cu, 5-Excretory : Bile 2 - Net wt. 1400 1600gm
1 Liver Function: 1-Metabolic : Glucose 2-Synthetic : factors.. Albumin, clotting 3-Detoxification : Drugs, hormones, NH3 4-Storage vit : Glycogen, TG, Fe, Cu, 5-Excretory : Bile 2 - Net wt. 1400 1600gm
Autoimmune Hepatitis: Histopathology
 REVIEW Autoimmune Hepatitis: Histopathology Stephen A. Geller M.D.*, Autoimmune hepatitis (AIH), a chronic hepatic necroinflammatory disorder, occurs mostly in women. AIH is characterized by prominent
REVIEW Autoimmune Hepatitis: Histopathology Stephen A. Geller M.D.*, Autoimmune hepatitis (AIH), a chronic hepatic necroinflammatory disorder, occurs mostly in women. AIH is characterized by prominent
Fat, ballooning, plasma cells and a +ANA. Yikes! USCAP 2016 Evening Specialty Conference Cynthia Guy
 Fat, ballooning, plasma cells and a +ANA. Yikes! USCAP 2016 Evening Specialty Conference Cynthia Guy Goals Share an interesting case Important because it highlights a common problem that we re likely to
Fat, ballooning, plasma cells and a +ANA. Yikes! USCAP 2016 Evening Specialty Conference Cynthia Guy Goals Share an interesting case Important because it highlights a common problem that we re likely to
MANAGEMENT OF LIVER CIRRHOSIS: PRACTICE ESSENTIALS AND PATIENT SELF-MANAGEMENT
 MANAGEMENT OF LIVER CIRRHOSIS: PRACTICE ESSENTIALS AND PATIENT SELF-MANAGEMENT Sherona Bau, ACNP The Pfleger Liver Institute 200 UCLA Medical Plaza, Suite 214 Los Angeles, CA 90095 September 30, 2017 I
MANAGEMENT OF LIVER CIRRHOSIS: PRACTICE ESSENTIALS AND PATIENT SELF-MANAGEMENT Sherona Bau, ACNP The Pfleger Liver Institute 200 UCLA Medical Plaza, Suite 214 Los Angeles, CA 90095 September 30, 2017 I
National Liver EQA Scheme. Open meeting, Glasgow March 24th 2004
 National Liver EQA Scheme Open meeting, Glasgow March 24th 2004 Participants meeting SOP8 Case discussion Are we quorate All please sign attendance sheet There were 20 EQA participants and 7 non-members
National Liver EQA Scheme Open meeting, Glasgow March 24th 2004 Participants meeting SOP8 Case discussion Are we quorate All please sign attendance sheet There were 20 EQA participants and 7 non-members
CrackCast Episode 28 Jaundice
 CrackCast Episode 28 Jaundice Episode overview: 1) Describe heme metabolism 2) List common pre-hepatic/hepatic/post-hepatic causes of jaundice Wisecracks: 1) What are clinical signs of liver disease? 2)
CrackCast Episode 28 Jaundice Episode overview: 1) Describe heme metabolism 2) List common pre-hepatic/hepatic/post-hepatic causes of jaundice Wisecracks: 1) What are clinical signs of liver disease? 2)
(C) Fig 5.1 Classical non alcoholic steatohepatitis (NASH). (A) Steatosis, hepatocyte ballooning, and inflammation (the trio of changes
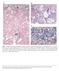 (A) (B) (C) Fig 5.1 Classical non alcoholic steatohepatitis (NASH). (A) Steatosis, hepatocyte ballooning, and inflammation (the trio of changes representing the minimal histological criteria of steatohepatitis)
(A) (B) (C) Fig 5.1 Classical non alcoholic steatohepatitis (NASH). (A) Steatosis, hepatocyte ballooning, and inflammation (the trio of changes representing the minimal histological criteria of steatohepatitis)
Liver Disease. By: Michael Martins
 Liver Disease By: Michael Martins Recently I have been getting a flurry of patients that have some serious liver complications. This week s literature review will be the dental management of the patients
Liver Disease By: Michael Martins Recently I have been getting a flurry of patients that have some serious liver complications. This week s literature review will be the dental management of the patients
EVALUATION OF ABNORMAL LIVER TESTS
 EVALUATION OF ABNORMAL LIVER TESTS MIA MANABAT DO PGY6 MOA 119 TH ANNUAL SPRING SCIENTIFIC CONVENTION MAY 19, 2018 EVALUATION OF ABNORMAL LIVER TESTS Review of liver enzymes vs liver function tests Clinical
EVALUATION OF ABNORMAL LIVER TESTS MIA MANABAT DO PGY6 MOA 119 TH ANNUAL SPRING SCIENTIFIC CONVENTION MAY 19, 2018 EVALUATION OF ABNORMAL LIVER TESTS Review of liver enzymes vs liver function tests Clinical
Morning Report Presentation. Sarah Hughes, MD January 11, 2005
 Morning Report Presentation Sarah Hughes, MD January 11, 2005 Primary Biliary Cirrhosis! PBC is a chronic, progressive, cholestatic liver disease of unknown cause that usually affects middle-aged women
Morning Report Presentation Sarah Hughes, MD January 11, 2005 Primary Biliary Cirrhosis! PBC is a chronic, progressive, cholestatic liver disease of unknown cause that usually affects middle-aged women
Anatomy of the biliary tract
 Harvard-MIT Division of Health Sciences and Technology HST.121: Gastroenterology, Fall 2005 Instructors: Dr. Jonathan Glickman Anatomy of the biliary tract Figure removed due to copyright reasons. Biliary
Harvard-MIT Division of Health Sciences and Technology HST.121: Gastroenterology, Fall 2005 Instructors: Dr. Jonathan Glickman Anatomy of the biliary tract Figure removed due to copyright reasons. Biliary
Hepatocytes produce. Proteins Clotting factors Hormones. Bile Flow
 R.J.Bailey MD Hepatocytes produce Proteins Clotting factors Hormones Bile Flow Trouble.. for the liver! Trouble for the Liver Liver Gall Bladder Common Alcohol Hep C Fatty Liver Cancer Drugs Viruses Uncommon
R.J.Bailey MD Hepatocytes produce Proteins Clotting factors Hormones Bile Flow Trouble.. for the liver! Trouble for the Liver Liver Gall Bladder Common Alcohol Hep C Fatty Liver Cancer Drugs Viruses Uncommon
PORTAL HYPERTENSION. Tianjin Medical University LIU JIAN
 PORTAL HYPERTENSION Tianjin Medical University LIU JIAN DEFINITION Portal hypertension is present if portal venous pressure exceeds 10mmHg (1.3kPa). Normal portal venous pressure is 5 10mmHg (0.7 1.3kPa),
PORTAL HYPERTENSION Tianjin Medical University LIU JIAN DEFINITION Portal hypertension is present if portal venous pressure exceeds 10mmHg (1.3kPa). Normal portal venous pressure is 5 10mmHg (0.7 1.3kPa),
Dhanpat Jain Yale University School of Medicine, New Haven, CT
 Dhanpat Jain Yale University School of Medicine, New Haven, CT Case history 15 years old female presented with fatigue. Found to have features suggestive of cirrhosis with esophageal varices, splenomegaly
Dhanpat Jain Yale University School of Medicine, New Haven, CT Case history 15 years old female presented with fatigue. Found to have features suggestive of cirrhosis with esophageal varices, splenomegaly
AMR in Liver Transplantation: Incidence
 AMR in Liver Transplantation: Incidence Primary AMR 1/3 to 1/2 of ABO-incompatible transplants Uncommon with ABO-compatible transplant Secondary AMR Unknown incidence: rarely tested Why is AMR uncommon
AMR in Liver Transplantation: Incidence Primary AMR 1/3 to 1/2 of ABO-incompatible transplants Uncommon with ABO-compatible transplant Secondary AMR Unknown incidence: rarely tested Why is AMR uncommon
Prognosis of untreated Primary Sclerosing Cholangitis (PSC) Erik Christensen Copenhagen, Denmark
 Prognosis of untreated Primary Sclerosing Cholangitis (PSC) Erik Christensen Copenhagen, Denmark Study of Prognosis of PSC Difficulties: Disease is rare The duration of the course of disease may be very
Prognosis of untreated Primary Sclerosing Cholangitis (PSC) Erik Christensen Copenhagen, Denmark Study of Prognosis of PSC Difficulties: Disease is rare The duration of the course of disease may be very
Improving Access to Quality Medical Care Webinar Series
 Improving Access to Quality Medical Care Webinar Series Presented by The Arizona Telemedicine Program and the Southwest Telehealth Resource Center 2015 UA Board of Regents Welcome AZ, UT, CO, NM & NV FLEX
Improving Access to Quality Medical Care Webinar Series Presented by The Arizona Telemedicine Program and the Southwest Telehealth Resource Center 2015 UA Board of Regents Welcome AZ, UT, CO, NM & NV FLEX
Dietary supplementation in treating non-alcoholic fatty liver disease Dr. Ahmad Saedi Associate Professor School of Nutritional Sciences and
 Dietary supplementation in treating non-alcoholic fatty liver disease Dr. Ahmad Saedi Associate Professor School of Nutritional Sciences and Dietetics Tehran University of Medical Sciences Honorary Academic
Dietary supplementation in treating non-alcoholic fatty liver disease Dr. Ahmad Saedi Associate Professor School of Nutritional Sciences and Dietetics Tehran University of Medical Sciences Honorary Academic
Hepatitis Panel/Acute Hepatitis Panel
 190.33 - Hepatitis Panel/Acute Hepatitis Panel This panel consists of the following tests: Hepatitis A antibody (HAAb), IgM antibody; Hepatitis B core antibody (HBcAb), IgM antibody; Hepatitis B surface
190.33 - Hepatitis Panel/Acute Hepatitis Panel This panel consists of the following tests: Hepatitis A antibody (HAAb), IgM antibody; Hepatitis B core antibody (HBcAb), IgM antibody; Hepatitis B surface
Pathology of the Liver and Biliary Tract 1 Normal Liver; Hepatic Injury, Response, and Failure
 Pathology of the Liver and Biliary Tract 1 Normal Liver; Hepatic Injury, Response, and Failure Shannon Martinson, August 2017 http://people.upei.ca/smartinson/ WELCOME! Dr Boute is the coordinator Course
Pathology of the Liver and Biliary Tract 1 Normal Liver; Hepatic Injury, Response, and Failure Shannon Martinson, August 2017 http://people.upei.ca/smartinson/ WELCOME! Dr Boute is the coordinator Course
End Stage Liver Disease & Disease Specific Indications for Liver Transplant. Susan Kang, RN, MSN, ANP-BC
 End Stage Liver Disease & Disease Specific Indications for Liver Transplant Susan Kang, RN, MSN, ANP-BC Introduction (https://www.srtr.org) What does the liver do? STORAGE METABOLIC DETOXIFICATION SYNTHETIC
End Stage Liver Disease & Disease Specific Indications for Liver Transplant Susan Kang, RN, MSN, ANP-BC Introduction (https://www.srtr.org) What does the liver do? STORAGE METABOLIC DETOXIFICATION SYNTHETIC
End Stage Liver Disease & Disease Specific Indications for Liver Transplant Susan Kang, RN, MSN, ANP BC
 End Stage Liver Disease & Disease Specific Indications for Liver Transplant Susan Kang, RN, MSN, ANP BC Introduction (https://www.srtr.org) 1 What does the liver do? STORAGE METABOLIC DETOXIFICATION SYNTHETIC
End Stage Liver Disease & Disease Specific Indications for Liver Transplant Susan Kang, RN, MSN, ANP BC Introduction (https://www.srtr.org) 1 What does the liver do? STORAGE METABOLIC DETOXIFICATION SYNTHETIC
Autoimmune hepatitis
 Autoimmune hepatitis: Autoimmune hepatitis a spectrum within a spectrum Alastair Burt Professor of Pathology and Dean of Clinical Medicine Newcastle University Spectrum of autoimmune liver disease Autoimmune
Autoimmune hepatitis: Autoimmune hepatitis a spectrum within a spectrum Alastair Burt Professor of Pathology and Dean of Clinical Medicine Newcastle University Spectrum of autoimmune liver disease Autoimmune
HOW TO DEAL WITH THOSE ABNORMAL LIVER ENZYMES David C. Twedt DVM, DACVIM Colorado State University Fort Collins, CO
 HOW TO DEAL WITH THOSE ABNORMAL LIVER ENZYMES David C. Twedt DVM, DACVIM Colorado State University Fort Collins, CO The identification of abnormal liver enzymes usually indicates liver damage but rarely
HOW TO DEAL WITH THOSE ABNORMAL LIVER ENZYMES David C. Twedt DVM, DACVIM Colorado State University Fort Collins, CO The identification of abnormal liver enzymes usually indicates liver damage but rarely
Drug Induced Liver Disease Role of the Pathologist. Disclosure. DILI can never be excluded. Romil Saxena, MD. Dr. Saxena has nothing to Disclose
 Drug Induced Liver Disease Role of the Pathologist Romil Saxena, MD Disclosure Dr. Saxena has nothing to Disclose DILI can never be excluded #1 DILI has no specific pattern of injury it can mimic any and
Drug Induced Liver Disease Role of the Pathologist Romil Saxena, MD Disclosure Dr. Saxena has nothing to Disclose DILI can never be excluded #1 DILI has no specific pattern of injury it can mimic any and
What is Liver Cancer? About the Liver
 Your liver is important and it has many functions. The top three are that it cleans your blood of toxins, gives you energy and produces bile for digestion. What is Liver Cancer? Cancer starts when cells
Your liver is important and it has many functions. The top three are that it cleans your blood of toxins, gives you energy and produces bile for digestion. What is Liver Cancer? Cancer starts when cells
Gastrointes*nal and Liver Pathology. Kris*ne Kra5s, M.D.
 Gastrointes*nal and Liver Pathology Kris*ne Kra5s, M.D. GI Pathology Outline Esophagus Stomach Intes*ne Liver Gallbladder Pancreas GI Pathology Outline Esophagus Stomach Intes*ne Liver Hepa**s Alcoholic
Gastrointes*nal and Liver Pathology Kris*ne Kra5s, M.D. GI Pathology Outline Esophagus Stomach Intes*ne Liver Gallbladder Pancreas GI Pathology Outline Esophagus Stomach Intes*ne Liver Hepa**s Alcoholic
Metabolic diseases of the liver
 Metabolic diseases of the liver Central role in metabolism Causes and mechanisms of dysfunction Clinical patterns of metabolic disease Clinical approach to problem-solving Specific disorders Liver s central
Metabolic diseases of the liver Central role in metabolism Causes and mechanisms of dysfunction Clinical patterns of metabolic disease Clinical approach to problem-solving Specific disorders Liver s central
Transplant Hepatology
 Transplant Hepatology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of the certified
Transplant Hepatology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of the certified
Overview of PSC Jayant A. Talwalkar, MD, MPH Associate Professor of Medicine Mayo Clinic Rochester, MN
 Overview of PSC Jayant A. Talwalkar, MD, MPH Associate Professor of Medicine Mayo Clinic Rochester, MN 2012 Annual Conference PSC Partners Seeking a Cure May 5, 2012 Primary Sclerosing Cholangitis Multifocal
Overview of PSC Jayant A. Talwalkar, MD, MPH Associate Professor of Medicine Mayo Clinic Rochester, MN 2012 Annual Conference PSC Partners Seeking a Cure May 5, 2012 Primary Sclerosing Cholangitis Multifocal
Pathology of The Liver - Practice. 2017/ semester
 Pathology of The Liver - Practice 2017/2018 2. semester Classification of Liver Diseases Non-neoplastic Metabolic diseases Congenital anomalies Circulatory disorders Hepatitis Infectious Toxic Autoimmune
Pathology of The Liver - Practice 2017/2018 2. semester Classification of Liver Diseases Non-neoplastic Metabolic diseases Congenital anomalies Circulatory disorders Hepatitis Infectious Toxic Autoimmune
UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES Discipline of Biochemistry and Molecular Biology
 UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES Discipline of Biochemistry and Molecular Biology 1 PBL SEMINAR ACUTE & CHRONIC ETHANOL EFFECTS An Overview Sites
UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES Discipline of Biochemistry and Molecular Biology 1 PBL SEMINAR ACUTE & CHRONIC ETHANOL EFFECTS An Overview Sites
Chapter 18 LIVER BILIARY TRACT
 Chapter 18 LIVER & BILIARY TRACT DUCT SYSTEM N O FIBROUS TISSUE PORTAL TRIAD CENTRAL VEIN PATTERNS OF HEPATIC INJURY Degeneration: Balooning, feathery degeneration, fat, pigment Inflammation:
Chapter 18 LIVER & BILIARY TRACT DUCT SYSTEM N O FIBROUS TISSUE PORTAL TRIAD CENTRAL VEIN PATTERNS OF HEPATIC INJURY Degeneration: Balooning, feathery degeneration, fat, pigment Inflammation:
