Evaluation of thyroid dysfunction and postpartum depression in the postpartum female
|
|
|
- Jack Willis
- 6 years ago
- Views:
Transcription
1 The University of Toledo The University of Toledo Digital Repository Master s and Doctoral Projects Evaluation of thyroid dysfunction and postpartum depression in the postpartum female Catherine Gail Lindback The University of Toledo Follow this and additional works at: This Scholarly Project is brought to you for free and open access by The University of Toledo Digital Repository. It has been accepted for inclusion in Master s and Doctoral Projects by an authorized administrator of The University of Toledo Digital Repository. For more information, please see the repository's About page.
2 Evaluation of Thyroid Dysfunction and Postpartum Depression in the Postpartum Female Catherine Gail Lindback The University of Toledo 2012
3 ii Acknowledgments Thank you to my major advisor, Vivian Moynihan MD, MPH, for her constant support, guidance, and encouragement throughout this process. Also, thank you to her for her heartfelt dedication to physician assistant education.
4 iii Table of Contents I: Introduction...1 II: Methods...3 III: General Overview of Thyroid Function...4 IV: Hormonal Changes in Pregnancy and Postpartum Period...5 V: Endocrine Dysfunction in the Postpartum Female...8 VI: Postpartum Thyroid Dysfunction and Association with Postpartum Depression...10 VII: Current Screening Mechanisms for Postpartum Depression...13 VIII: Discussion...14 Conclusion...17 References...19 Abstract...22
5 1 Introduction The postnatal period is a time of great adjustment for new mothers. There is much joy and excitement associated with the long-awaited arrival of a new infant. Along with such joy and excitement comes a broad spectrum of alternate sensations including worry, fatigue, stress, and anxiety. Forty to eighty percent of postpartum women develop changes in mood, most often within two to three days of delivery, and experience symptoms ranging from great happiness to irritability, tearfulness, insomnia, and sadness (Pearlstein, Howard, Salisbury, & Zlotnick, 2009). These symptoms typically resolve within two weeks, but for some new mothers symptoms persist and worsen. Dramatic hormone changes during and after pregnancy play a significant role in the initiation of the above symptoms and associated disease states. Altered endocrine gland function with varying levels of estrogen and progesterone contribute to such symptoms. Postpartum depression arises in greater than 1 in 10 women up to a year after childbirth and requires appropriate medical attention in order to alleviate debilitating symptoms such as extreme fatigue, irritability, anxiety, depressed mood, and impaired concentration (Pearlstein et al., 2009). Postpartum thyroid dysfunction and postpartum thyroiditis are two associated medical conditions that share such symptoms. The prevalence of postpartum thyroid dysfunction is currently a topic of much debate and uncertainty in the medical community. Reported figures of the occurrence of this disease state vary significantly and universal screening standards do not exist at this time. Postpartum thyroid dysfunction, particularly postpartum thyroiditis, has been shown to be an overlooked condition with significant patient morbidity. Recurrent postpartum thyroiditis is observed in two thirds of all pregnancies with evidence of 20 to 60% of women developing permanent hypothyroidism
6 2 within 10 years of the initial event (Azizi, 2005). As a result, there is a need for heightened awareness of the symptoms associated with this disease both for afflicted patients and health care providers. In reviewing current research and clinical literature, there is a need to bring such evidence to the forefront and to devise an appropriate screening strategy with which to detect this underlying medical condition.
7 3 Methods Research was conducted using the following databases: CINAHL, Dissertation Abstracts, JAMA - Journal of American Medical Association, NIH - National Institutes of Health, ProQuest Nursing & Allied Health Source, PsycINFO, PsycLIT, and PubMed. Several search terms were used including: Endocrine disorders in the postpartum period, Endocrine dysfunction in the postpartum period, Evaluation of postpartum thyroid dysfunction, Postnatal period, Postpartum blues, Postpartum depression, Postpartum endocrine dysfunction, Postpartum hypothyroidism, Postpartum period, Postpartum thyroid dysfunction, Postpartum thyroid dysfunction and depression, Postpartum thyroid dysfunction and postpartum depression, Postpartum thyroid function screening, Postpartum thyroiditis, Postpartum thyroiditis and depression, Postpartum thyroiditis and postpartum depression, and Thyroid function screening in the postpartum period. All articles reviewed came from peer-reviewed journals and fell within a 12-year time frame. The research population lied within the United States and Europe and all articles were written in or translated into English. First tier studies consisted of original research articles evaluating large sample sizes of postpartum females. Second tier studies resembled first tier studies but consisted of smaller sample sizes from the population. Third tier studies consisted of general medical textbooks along with literature reviews of general articles containing relevant background information. Exclusion criteria included articles that were not associated with peer-reviewed journals, had serious identifiable methodological errors, and evidence of incorrect statistical analysis. I was wary of articles funded by particular corporations and associations and took the time to assess that the evidence presented was accurate and unbiased.
8 4 General Overview of Thyroid Function The thyroid gland is an endocrine gland consisting of clustered spheroid follicles lying in front and to the sides of the upper part of the trachea. The adult thyroid gland contains two lobes that wrap along the right and left aspects of the trachea. Each lobe is separated into three poles - upper, middle, and lower. Right and left thyroid lobes connect to form the thyroid isthmus at the anterior portion of the trachea just below the cricoid cartilage (Goldman & Ausiello, 2008). The clustered spheroid follicles contained in thyroid tissue contain thyrocytes that surround colloid. The main component of this colloid is thyroglobulin which is a thyrocyte-specific protein. Thyrocytes play an active role in the synthesis and secretion of thyroid hormone. Thyroid hormone increases oxygen consumption, thermogenesis, and expression of the low-density lipoprotein (LDL) receptor, resulting in accelerated LDL cholesterol degradation. Other physiologic effects of thyroid hormone include increased mental alertness, ventilatory drive, gastrointestinal motility, and bone turnover (Goldman & Ausiello, 2008). Overall, thyroid hormone helps regulate growth and development while controlling metabolism and body temperature and is therefore an essential factor in human life. Dietary iodine is an essential factor in thyroid hormone synthesis and secretion. Dietary iodine, mainly in the form of iodide (I - ), is absorbed from the gastrointestinal tract and distributed in extracellular fluid. From here, it is actively transported into thyrocytes where it is oxidized and later involved in the generation of thyroxine (T 4 ) and triiodothyronine (T 3 ), the thyroid hormones primarily responsible for regulation of metabolism (Goldman & Ausiello, 2008). As a result, dietary intake of iodine is of great significance in regulation of metabolism. The current recommended daily intake of iodine in the United States is 150 µg for optimal physiologic function and health (Zimmermann, 2009).
9 5 Hormonal Changes in Pregnancy and Postpartum Period Postpartum refers to the time period following delivery and extends to approximately six weeks after childbirth (Hacker, Gambone, & Hobel, 2010). Significant hormonal changes occur throughout pregnancy and their effects continue into the postpartum period. Placenta-derived human chorionic gonadotropin (hcg) has a thyroid-stimulating hormone (TSH) effect on the thyroid gland which can result in TSH suppression. Elevated estrogen levels lead to increased hepatic synthesis of thyroxine-binding globulin (TBG) and corticosteroid-binding globulin (CBG). TBG is the primary carrier protein for circulating thyroid hormone in the form of thyroxine (T 4 ). As a result, the body raises total circulating bound thyroid hormone. Adrenocorticotropic hormone (ACTH) and plasma cortisol levels increase late in the first trimester of pregnancy and remain elevated to the time of delivery with circulating cortisol primarily bound to CBG (Hacker et al., 2010). The pituitary gland is one of the most affected organs during this time, undergoing great anatomic and physiologic change. The pituitary gland is a pea-sized endocrine gland located at the base of the brain which helps control the release of hormones from other endocrine glands throughout the body and also releases hormones that directly affect body tissues. Pituitary gland volume is found to increase during pregnancy with the highest volume being observed during the first three postpartum days (Karaca, Tanriverdi, Unluhizarci, & Kelestimur, 2010). Pregnancy is associated with increased maternal hypothalamic-pituitary-adrenal (HPA) axis activity in which ACTH release from the anterior pituitary gland is increased in response to decreased free cortisol levels (Karaca et al., 2010). In addition, the thyroid-releasing hormone-thyroid-stimulating hormone (TRH-TSH) axis is altered throughout pregnancy due to the TSH effect of placental hcg on the thyroid gland. As
10 6 a result, maternal TSH levels decrease. TRH (thyroid-releasing hormone) is released from the hypothalamus and acts on the anterior lobe of the pituitary gland. TSH (thyrotropin or thyroidstimulating hormone) is a glycoprotein hormone produced by the anterior lobe of the pituitary gland that stimulates the growth and function of the thyroid gland. The changes in maternal thyroid function that occur throughout pregnancy usually plateau and resolve, but failure to adapt to these physiological changes can result in thyroid dysfunction (Mannisto et al., 2010). Significant changes in iodine metabolism occur during this time as well. After dietary consumption, iodine is absorbed by the stomach and duodenum and used in the production of thyroid hormone. Pregnancy increases demand on the maternal thyroid gland, with T 4 production increasing approximately 50% (Yarrington & Pearce, 2011). Increased iodine loss through excretion in urine also occurs and can potentially cause an increase in thyroid volume due to the resulting elevated levels of TSH (Lazarus, 2005). As a result of hormonal changes during pregnancy and throughout the postpartum period, changes in mood often occur. Dramatic changes in estrogen and progesterone levels occur during this time and are linked to such altered emotions (Steiner, Dunn, & Born, 2003). Postpartum blues refers to a period of great emotional change following childbirth. During this time, emotions of great joy and happiness may be present in the initial days after delivery followed by anxiety, irritability, confusion, and frequent crying episodes. Anywhere from 15 to 85% of women may experience symptoms of postpartum blues. Associated symptoms typically arise throughout the first five days after delivery. Symptoms typically resolve entirely after a short period and therefore do not require treatment. However in approximately 20% of cases, symptoms persist for more than three weeks and lead to a more serious disorder (Born, Zinga, & Steiner, 2004).
11 7 Postpartum depression is the new onset of depression during the postpartum period in which women experience disabling and persistent symptoms of depression, most frequently manifesting in the first 6 to 12 weeks after delivery, but onset of symptoms can occur even later following a period of initial stability. Symptoms include depressed mood, sleep disturbance, loss of appetite, lack of energy, anxiety, and suicidal thoughts. Overwhelming feelings of guilt or inadequacy in regards to the ability to care for the infant often arise. The new mother may also have an extreme preoccupation with the infant s safety and well-being. The prevalence of postpartum depression ranges between 10 to 15% in new mothers with reports of approximately 10% of women still experiencing symptoms one year after childbirth (Born et al., 2004).
12 8 Endocrine Dysfunction in the Postpartum Female Postpartum thyroid dysfunction is an immunological disorder occurring more frequently in women with particular human leukocyte antigen haplotypes. It is usually characterized by the presence of circulating thyroid peroxidase (TPO) antibodies in the bloodstream and is most often caused by postpartum thyroiditis (Lazarus, 2011). Postpartum thyroiditis is an autoimmune occurrence, in the postpartum period, of transient hyperthyroidism and/or transient hypothyroidism, with most women returning to the euthyroid state by one year postpartum. It is considered an exacerbation of an underlying autoimmune thyroiditis. Prevalence rates in the general population range from 0.9% to 11.7% (Nicholson, Robinson, Smallridge, Ladenson, & Powe, 2006). Autoimmune thyroiditis is often suppressed during pregnancy due to the physiologic suppression of immune activity during this time. It is subsequently potentiated in the postpartum period due to immunological rebound (Stagnaro-Green, 2002). Postpartum thyroiditis presents most commonly as hypothyroidism without preceding hyperthyroidism. In a study of 371 episodes of postpartum thyroiditis, hypothyroidism occurred in 43% of the cases without preceding hyperthyroidism. Hyperthyroidism alone occurred in 32% of the cases and hyperthyroidism followed by hypothyroidism occurred in 25% of reported cases (Stagnaro-Green, 2002). The hyperthyroid phase associated with postpartum thyroiditis occurs in the postpartum period between 2 and 10 months, most commonly presenting at three months. Symptoms include palpitations, nervousness, fatigue, and heat intolerance (Stagnaro-Green, 2002). The hypothyroid phase of postpartum thyroiditis occurs between 2 and 12 months into the postpartum period and is typically diagnosed around six months. Symptoms include decreased energy, depressed mood, impaired concentration, weight gain, dry skin, and cold
13 9 intolerance (Stagnaro-Green, 2002). Most women with postpartum thyroiditis are euthyroid at the completion of the first postpartum year, but permanent hypothyroidism is possible. Prospective studies have shown a prevalence rate of hypothyroidism of 23% and 29% at 3.5 to 8.7 years postpartum. Progression to permanent hypothyroidism was more common in women who presented with higher TSH levels and higher titers of thyroid peroxidase antibodies in the hypothyroid phase of postpartum thyroiditis (Stagnaro-Green, 2002).
14 10 Postpartum Thyroid Dysfunction and Association with Postpartum Depression Although a distinct relationship between postpartum thyroid dysfunction and postpartum depression is yet to be proven, an overlap of symptoms is evident. Common symptoms of postpartum depression include depressed mood, weight gain/loss, sleep disturbance, loss of appetite, lack of energy, and anxiety. These symptoms are also associated with postpartum thyroid dysfunction. There is a direct correlation between thyroid dysfunction and depression/anxiety in the generalized population. Abnormalities in thyroid function are associated with an increased frequency of psychiatric symptoms. Hyperthyroidism has been associated with anxiety, depression, and cognitive deficit while hypothyroidism has been associated with an increased incidence of depression (Lucas, Pizarro, Granada, Salinas, & Sanmarti (2001). The postpartum period is considered a time of heightened risk for developing psychiatric disorders. Women are particularly at risk of developing depression, having a 1 year prevalence, in general, of 8-12%, which rises to 15% during the postpartum period (Kuijpens, Vader, Drexhage, Wiersinga, van Son, & Pop, 2001). As a result, the possibility of postpartum thyroid dysfunction should be further investigated and screening considered. In a study conducted in June of 1997, 641 healthy Caucasian women were selected between their 36th week of pregnancy and fourth day postpartum for biological and clinical evaluation. Both clinical and laboratory follow-up continued throughout the postpartum period at one (n = 605), three (n = 552), six (n = 574), nine (n = 431), and twelve (n = 444) months (Lucas et al., 2001). Blood samples to determine free T 4 and TSH concentrations were drawn at each visit and subsequent thyroid antibodies were determined in patients with abnormal thyroid hormone concentrations. Reference ranges were 0.69 to 2.3 ng/dl for free T 4 and 0.4 to 4 miu/l for TSH. Reference ranges for thyroperoxidase and thyroglobulin antibodies were less than 66
15 11 IU/ml and less than 275 IU/ml. The Beck Depression Inventory (BDI) was administered at baseline and with each follow-up as a means of depression screening with total BDI scores of 21 and above being indicative of depression. Postpartum thyroid dysfunction was diagnosed in patients with the initial presentation of thyroid dysfunction in the postpartum period. Postpartum thyroiditis was considered to be present in women with overt or subclinical (only abnormalities in TSH concentrations, levels less than 0.1 miu/l) transient hyperthyroidism between 1 and 3 months postpartum and/or overt or subclinical hypothyroidism (only abnormalities in TSH concentrations, levels above 4 miu/l) between 3 and 6 months postpartum (Lucas et al., 2001). Throughout the study, 56 women developed postpartum thyroid dysfunction, corresponding to an incidence rate of 11%, with 45 women developing postpartum thyroiditis (incidence rate of 7.8%). Fifty women (incidence rate of 7.8%) scored greater than 21 on the BDI, but the diagnosis of postpartum depression was not confirmed. Out of these 50 women, five had a concurrent diagnosis of postpartum thyroid dysfunction. Eleven of the evaluated women (incidence rate of 1.8%) were diagnosed as having postpartum depression with a BDI score over 21 and required psychiatric treatment. Out of these 11 women, none had a concurrent diagnosis of postpartum thyroid dysfunction (Lucas et al., 2001). In a 2001 prospective observational study, 310 women were evaluated at 12 and 32 weeks gestation along with at 4, 12, 20, 28, and 36 weeks postpartum. TSH, free T 4, and TPO antibody testing was performed at each visit. Clinical thyroid dysfunction was defined as both abnormal TSH and free T 4 while subclinical thyroid dysfunction was defined as abnormal TSH in combination with normal free T 4. The TSH reference interval was defined as 0.15 to 2.0 mu/l while free T 4 was 8.7 to 19.6 pmol/l. In regards to TPO antibody testing, a concentration of
16 12 greater than 50 U/ml was considered positive. Depression was defined according to the Research Diagnostic Criteria in which one investigator established a syndromal diagnosis of depression during a semi-structured interview with the patient (Kuijpens et al., 2001). Results of this study showed that during pregnancy and in the early postpartum period, women with depression presented more often with elevated TPO antibody concentrations. In addition, both clinical and subclinical thyroid dysfunction in combination with depression were significantly more prevalent in TPO antibody positive women (Kuijpens et al., 2001). Overall, 41 women (14.1%) were found to be TPO antibody positive at some point in the postpartum period. Two hundred and thirty-two women (80%) remained euthyroid while seven women (2.4%) showed clinical thyroid dysfunction. One hundred and fifty-eight women (54.3%) presented with at least one episode of depression and 117 women (40.1%) had depression at one or more time(s) in the postpartum period. There is still no explanation for the relationship between particular forms of thyroid dysfunction and depression, but this study does suggest that TPO antibodies can be regarded as important markers for the future occurrence of depression in at-risk groups of patients (Kuijpens et al., 2001).
17 13 Current Screening Mechanisms for Postpartum Depression Postpartum depression, along with depression in general, is a major health problem that often goes undiagnosed. It is estimated that more than half of subjects do not seek professional care. Moreover, in subjects who visit their general practitioner, the diagnosis is missed in up to 50% of cases (Kuijpens et al., 2001). As a result, significant social, psychological, and financial burdens occur. Detection of postpartum depression at an early stage is crucial in alleviating such burdens and evaluation of potential causes is necessary. The Edinburgh Postnatal Depression Scale (EPDS) is currently the most common instrument utilized to screen for postpartum depression, having a sensitivity of 86% and specificity of 78% (Pedersen et al., 2007). The EPDS is a 10-item self-report questionnaire designed to identify symptoms of emotional distress in mothers during the postnatal period. A score above 10 requires repeat screening within 2 weeks and two scores above 12 require further assessment and treatment (Hanusa, Scholle, Haskett, Spadaro, & Wisner, 2008). Proper screening for postpartum depression is important because it is often the first step in the pathway to treatment. The EPDS should be utilized regularly at all postpartum examinations throughout the first postpartum year. Careful evaluation of results should be carried out and follow-up screenings administered as necessary. The EPDS was specifically developed for assessing postpartum depression and reduces the focus on specific somatic symptoms that are common to both women in the postpartum period and to women with depression (Hanusa et al., 2008). Routine use of the EPDS has consistently been shown to increase the detection of postpartum depression when compared to usual care and usage of other depression screening inventories (Sharp & Lipsky, 2002).
18 14 Discussion The incidence of postpartum thyroid dysfunction and its association with postpartum depression is an ongoing topic of much debate and uncertainty in the medical community. In reviewing current research and clinical literature, it is difficult to determine a direct correlation between postpartum thyroid dysfunction and postpartum depression. Specific studies exploring such a correlation are limited in number and provide inconclusive results. In the study of 641 healthy Caucasian women, postpartum thyroid dysfunction was diagnosed in only 56 women. In addition, subjects were evaluated between their 36th week of pregnancy and fourth day postpartum. This is a very limited time frame for diagnosis and evaluation of postpartum thyroid dysfunction and postpartum depression. A diagnosis of postpartum depression was derived using the Beck Depression Inventory, instead of the preferred Edinburgh Postnatal Depression Scale, with 50 women in the study scoring greater than 21 (incidence rate 7.8%; confidence interval 95%). Only five of these women had a simultaneous diagnosis of postpartum thyroid dysfunction. Eleven of the evaluated women were diagnosed as having postpartum depression and required psychiatric treatment (incidence rate 1.7%; confidence interval 95%). None of these women had a simultaneous diagnosis of postpartum thyroid dysfunction (Lucas et al., 2001). Despite the overlap of symptoms between postpartum thyroid dysfunction and postpartum depression, results of this study fail to show a correlation between the two. Instead, analysis of this study places focus on proper screening mechanisms for postpartum depression and the appropriate time frame in which to screen. Numerous studies have shown that the Edinburgh Postnatal Depression Scale accurately identifies women who are depressed or at risk of developing depression in the first six months postpartum and it is therefore the instrument of
19 15 choice in screening (Hanusa et al., 2008). The formal definition of the postpartum period extends to approximately six weeks after childbirth, but assessment of postpartum depression and potential postpartum thyroid dysfunction should not end here (Hacker et al., 2010). There are several reports of symptom onset after the six-week postnatal checkup. As a result, a longer period of clinical surveillance is warranted (Stowe, Hostetter, & Newport, 2004). In the 2001 prospective observational study, a much broader time frame existed in which to adequately diagnose and evaluate postpartum thyroid dysfunction and its potential correlation with postpartum depression. Both clinical and subclinical thyroid dysfunction were defined and appropriately measured in terms of TSH, free T 4, and TPO antibody testing at each visit. However, depression was defined according to the Research Diagnostic Criteria. As a result, a single investigator conducted a semi-structured interview with each subject in order to establish a diagnosis of depression. Such a method creates uncertainty regarding whether a standardized and accurate diagnosis of postpartum depression was made. Diagnoses of both clinical and subclinical thyroid dysfunction along with the diagnosis of depression were significantly more prevalent in TPO antibody positive subjects. As a result, a correlation between positive TPO antibody testing and postpartum depression is identified and further investigation is warranted (Kuijpens et al., 2001). Analysis of this study places emphasis on appropriate laboratory testing for diagnosis of postpartum thyroid dysfunction. Symptoms of postpartum thyroid dysfunction may be subtle and confused with postpartum depression, therefore complete testing is necessary (Swelam, Bakr, & Mansour, 2011). Laboratory testing includes thyroid function tests (serum TSH, T 3, and free T 4 ) along with TPO antibodies. Thyroid peroxidase (TPO) is an enzyme found on the surface of thyroid follicular cells and presence of serum TPO antibodies suggests an autoimmune
20 16 etiology of thyroid dysfunction. It is important to know that afflicted patients may become hypothyroid, hyperthyroid, or develop hyperthyroidism followed by hypothyroidism. As a result, complete laboratory testing is required for diagnosis and management (Swelam et al., 2011).
21 17 Conclusion At this time, a direct correlation between postpartum thyroid dysfunction and postpartum depression is yet to be proven, but a distinct overlap of symptoms between the two certainly exists. Such symptoms include depressed mood, weight gain/loss, sleep disturbance, loss of appetite, lack of energy, and anxiety. It is the presence of such symptoms in the postpartum female that warrants further investigation, evaluation, and treatment. Clinicians must be aware of such symptoms in their patients and utilize the appropriate screening instruments and testing mechanisms with which to arrive at the correct diagnosis. Clinicians must also obtain a greater understanding of postpartum thyroid dysfunction for it is a diagnosis that often goes unevaluated. A greater societal awareness of the potential onset of postpartum depression must exist as well, especially among pregnant and postpartum females. Postpartum depression is a common affliction in such a population that often goes unreported, undiagnosed, and ultimately untreated. Adverse and potentially severe consequences for mother, child, and immediate family result and persist without appropriate medical care. Clinicians must first and foremost listen to their patients with great attention and always take a detailed account of past medical history, family history, and social history. These are seemingly simple concepts, but can often be hastened or overlooked throughout the course of a busy day. In regards to pregnant and postpartum females, special focus must be placed on prior episodes of major depression, depression arising during previous pregnancies, personal or family history of thyroid dysfunction or autoimmune disorders, social support, and dietary intake. Although rare in the United States, iodine deficiency directly contributes to thyroid dysfunction. The current recommended daily intake of iodine in the United States must increase to 250 µg during pregnancy and postpartum due to maternal demands for increased T 4 production, iodine
22 18 transfer to the fetus, increase in renal iodine clearance, and excretion of iodine in breast milk. A urine iodine concentration of 100 µg/liter corresponds to an average daily intake of 150 µg (Zimmermann, 2009). Clinicians must know their practice demographics and be aware of areas throughout the United States where iodine deficiency is potentially prevalent, namely in the Midwest and Great Lakes regions of the country (Zimmermann, 2009). The Edinburgh Postnatal Depression Scale should be utilized at each postpartum visit throughout the first postpartum year. It is designed specifically for screening and early detection of postpartum depression. A score above 10 requires repeat screening within two weeks and two scores above 12 require further assessment and possible treatment for postpartum depression (Hanusa et al., 2008). A score of 10 or above should also create suspicion of underlying postpartum thyroid dysfunction. It is important to consider this diagnosis as a possible cause of postpartum depression symptoms and therefore order TSH, T 3, free T 4, and TPO antibody testing. A past medical history or family history positive for thyroid dysfunction or autoimmune disorders should initiate TSH, T 3, free T 4, and TPO antibody testing as well. Evaluation of thyroid dysfunction and depression in the postpartum female comprises an area of medicine that is still evolving. An overlap of symptoms between the two is evident, but a direct correlation remains unproven. The role of the clinician in proper diagnosis and subsequent treatment is essential. As a result, the clinician must keep these two related diagnoses in mind when caring for patients throughout the postpartum period.
23 19 References Azizi, F. (2005). The occurrence of permanent thyroid failure in patients with subclinical postpartum thyroiditis. European Journal of Endocrinology, 153 ( ). doi: /eje Born, L., Zinga, D., & Steiner, M. (2004). Challenges in identifying and diagnosing postpartum disorders. Primary Psychiatry, 11(3), Goldman, L., & Ausiello, D. (Eds.). (2008). Cecil medicine (23 rd ed.). Philadelphia, PA: Saunders. Hacker, N. F., Gambone, J. C., & Hobel, C. J. (Eds.). (2010). Hacker and Moore s essentials of obstetrics and gynecology (5 th ed.). Philadelphia, PA: Saunders. Hanusa, B. H., Scholle, S. H., Haskett, R. F., Spadaro, K., & Wisner, K. L. (2008). Screening for depression in the postpartum period: A comparison of three instruments. Journal of Women s Health, 17(4), doi: /jwh Karaca, Z., Tanriverdi, F., Unluhizarci, K., & Kelestimur, F. (2010). Pregnancy and pituitary disorders. European Journal of Endocrinology, 162, doi: /eje Kuijpens, J. L., Vader, H. L., Drexhage, H. A., Wiersinga, W. M., van Son, M. J., & Pop, V. J. (2001). Thyroid peroxidase antibodies during gestation are a marker for subsequent depression postpartum. European Journal of Endocrinology, 145, doi: /eje Lazarus, J. H. (2005). Thyroid disorders associated with pregnancy: Etiology, diagnosis, and management. Treatments in Endocrinology, 4(1), Lazarus, J. H. (2011). The continuing saga of postpartum thyroiditis. The Journal of Clinical Endocrinology & Metabolism, 96(3), doi: /jc
24 20 Lucas, A., Pizarro, E., Granada, M. L., Salinas, I., & Sanmarti, A. (2001). Postpartum thyroid dysfunction and postpartum depression: Are they two linked disorders? Clinical Endocrinology, 55(6), doi: /j x Mannisto, T., Vaarasmaki, M., Pouta, A., Hartikainen, A., Ruokonen, A., Surcel, H.,... Suvanto, E. (2010). Thyroid dysfunction and autoantibodies during pregnancy as predictive factors of pregnancy complications and maternal morbidity in later life. Journal of Clinical Endocrinology & Metabolism, 95(3), doi: /jc Nicholson, W. K., Robinson, K. A., Smallridge, R. C., Ladenson, P. W., & Powe, N. R. (2006). Prevalence of postpartum thyroid dysfunction: A quantitative review. Thyroid, 16(6), doi: /thy Pearlstein, T., Howard, M., Salisbury, A., & Zlotnick, C. (2009). Postpartum depression. American Journal of Obstetrics and Gynecology, 200(4), doi: /j.ajog Sharp, L. K., & Lipsky, M. S. (2002). Screening for depression across the lifespan: A review of measures for use in primary care settings. American Family Physician, 66(6), Stagnaro-Green, A. (2002). Postpartum thyroiditis. The Journal of Clinical Endocrinology & Metabolism, 87(9), doi: /jc Steiner, M., Dunn, E., & Born, L. (2003). Hormones and mood: From menarche to menopause and beyond. Journal of Affective Disorders, 74(1), doi: /s (02)
25 21 Stowe, Z. N., Hostetter, A. L., & Newport, D. J. (2005). The onset of postpartum depression: Implications for clinical screening in obstetrical and primary care. American Journal of Obstetrics and Gynecology, 192(2), doi: /j.ajog Swelam, E. S., Bakr, H. G., & Mansour, M. A. (2011). Postpartum thyroid dysfunction: A state of immunological dysregulation. Clinical Laboratory, 57(9-10), Yarrington, C., & Pearce, E. N. (2011). Iodine and pregnancy. Journal of Thyroid Research, 2011, 1-8. doi: /2011/ Zimmermann, M. B. (2009). Iodine deficiency. Endocrine Reviews, 30(4), doi: /er
26 22 Abstract Objective: To explore the potential correlation between postpartum thyroid dysfunction and postpartum depression and devise an appropriate strategy with which to detect and distinguish these conditions. Methods: Research was conducted using the following databases: CINAHL, Dissertation Abstracts, JAMA, NIH, ProQuest Nursing & Allied Health Source, PsycINFO, PsycLIT, and PubMed. Reviewed articles came from peer-reviewed journals and fell within a 12-year time frame. The research population lied within the United States and Europe and articles were written in or translated into English. Results: A direct correlation between postpartum thyroid dysfunction and postpartum depression is yet to be proven, but a distinct overlap of symptoms exists. Conclusion: The role of the clinician in proper diagnosis is essential. The clinician must keep these related diagnoses in mind when caring for patients throughout the postpartum period and utilize the Edinburgh Postnatal Depression Scale with TSH, T 3, free T 4, and TPO antibody testing when necessary.
Thyroid Function TSH Analyte Information
 Thyroid Function TSH Analyte Information 1 2013-05-01 Thyroid-stimulating hormone (TSH) Introduction Thyroid-stimulating hormone (thyrotropin, TSH) is a glycoprotein with molecular weight of approximately
Thyroid Function TSH Analyte Information 1 2013-05-01 Thyroid-stimulating hormone (TSH) Introduction Thyroid-stimulating hormone (thyrotropin, TSH) is a glycoprotein with molecular weight of approximately
Decoding Your Thyroid Tests and Results
 Decoding Your Thyroid Tests and Results Wondering about your thyroid test results? Learn about each test and what low, optimal, and high results may mean so you can work with your doctor to choose appropriate
Decoding Your Thyroid Tests and Results Wondering about your thyroid test results? Learn about each test and what low, optimal, and high results may mean so you can work with your doctor to choose appropriate
LABORATORY TESTS FOR EVALUATION OF THYROID DISORDERS
 LABORATORY TESTS FOR EVALUATION OF THYROID DISORDERS Maryam Tohidi Anatomical & clinical pathologist Research Institute for Endocrine Sciences THYROID GLAND (15-25 gr), (12-20 gr), 2 lobes connected by
LABORATORY TESTS FOR EVALUATION OF THYROID DISORDERS Maryam Tohidi Anatomical & clinical pathologist Research Institute for Endocrine Sciences THYROID GLAND (15-25 gr), (12-20 gr), 2 lobes connected by
Sample Type - Serum Result Reference Range Units. Central Thyroid Regulation Surrey & Activity KT3 4Q. Peripheral Thyroid D Function mark
 Thyroid Plus Sample Type - Serum Result Reference Range Units Central Thyroid Regulation Surrey & Activity KT3 4Q Total Thyroxine (T4)
Thyroid Plus Sample Type - Serum Result Reference Range Units Central Thyroid Regulation Surrey & Activity KT3 4Q Total Thyroxine (T4)
Women s Mental Health
 Women s Mental Health Linda S. Mullen, MD Director, Women s Mental Health Assistant Professor of Clinical Psychiatry in OB/GYN Columbia University & NewYork Presbyterian Hospital Departments of Psychiatry
Women s Mental Health Linda S. Mullen, MD Director, Women s Mental Health Assistant Professor of Clinical Psychiatry in OB/GYN Columbia University & NewYork Presbyterian Hospital Departments of Psychiatry
Balancing Hormone Function in Women By Meghna Thacker, NMD
 Balancing Hormone Function in Women By Meghna Thacker, NMD Hormone function is central to health and well being in both men as well as women. A problem encountered with any one endocrine gland can lead
Balancing Hormone Function in Women By Meghna Thacker, NMD Hormone function is central to health and well being in both men as well as women. A problem encountered with any one endocrine gland can lead
Thyroid Plus. Central Thyroid Regulation & Activity. Peripheral Thyroid Function. Thyroid Auto Immunity. Key Guide. Patient: DOB: Sex: F MRN:
 Thyroid Plus Patient: DOB: Sex: F MRN: Order Number: Completed: Received: Collected: Sample Type - Serum Result Reference Range Units Central Thyroid Regulation & Activity Total Thyroxine (T4) 127 127
Thyroid Plus Patient: DOB: Sex: F MRN: Order Number: Completed: Received: Collected: Sample Type - Serum Result Reference Range Units Central Thyroid Regulation & Activity Total Thyroxine (T4) 127 127
Thyroid Screen (Serum)
 Thyroid Screen (Serum) Patient: DOB: Sex: F MRN: Order Number: Completed: Received: Collected: Sample Type - Serum Result Reference Range Units Central Thyroid Regulation & Activity Total Thyroxine (T4)
Thyroid Screen (Serum) Patient: DOB: Sex: F MRN: Order Number: Completed: Received: Collected: Sample Type - Serum Result Reference Range Units Central Thyroid Regulation & Activity Total Thyroxine (T4)
Lecture title. Name Family name Country
 Lecture title Name Family name Country Nguyen Thy Khue, MD, PhD Department of Endocrinology HCMC University of Medicine and Pharmacy, MEDIC Clinic Hochiminh City, Viet Nam Provided no information regarding
Lecture title Name Family name Country Nguyen Thy Khue, MD, PhD Department of Endocrinology HCMC University of Medicine and Pharmacy, MEDIC Clinic Hochiminh City, Viet Nam Provided no information regarding
Approach to thyroid dysfunction
 Approach to thyroid dysfunction Alice Y.Y. Cheng, MD, FRCPC Twitter: @AliceYYCheng Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored, or
Approach to thyroid dysfunction Alice Y.Y. Cheng, MD, FRCPC Twitter: @AliceYYCheng Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored, or
Chapter I.A.1: Thyroid Evaluation Laboratory Testing
 Chapter I.A.1: Thyroid Evaluation Laboratory Testing Jennifer L. Poehls, MD and Rebecca S. Sippel, MD, FACS THYROID FUNCTION TESTS Overview Thyroid-stimulating hormone (TSH) is produced by the anterior
Chapter I.A.1: Thyroid Evaluation Laboratory Testing Jennifer L. Poehls, MD and Rebecca S. Sippel, MD, FACS THYROID FUNCTION TESTS Overview Thyroid-stimulating hormone (TSH) is produced by the anterior
Endocrine part two. Presented by Dr. Mohammad Saadeh The requirements for the Clinical Chemistry Philadelphia University Faculty of pharmacy
 Endocrine part two Presented by Dr. Mohammad Saadeh The requirements for the Clinical Chemistry Philadelphia University Faculty of pharmacy Cushing's disease: increased secretion of adrenocorticotropic
Endocrine part two Presented by Dr. Mohammad Saadeh The requirements for the Clinical Chemistry Philadelphia University Faculty of pharmacy Cushing's disease: increased secretion of adrenocorticotropic
THYROID HORMONES: An Overview
 1 SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY AND MOLECULAR BIOLOGY PBL SEMINAR MBBS III; BMLS & BDS Year 3 What are the Thyroid Hormones? THYROID
1 SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY AND MOLECULAR BIOLOGY PBL SEMINAR MBBS III; BMLS & BDS Year 3 What are the Thyroid Hormones? THYROID
BELIEVE MIDWIFERY SERVICES
 TITLE: THYROID DISEASE IN PREGNANCY EFFECTIVE DATE: July, 2013 POLICY STATEMENT: Pregnancy changes significantly the values influenced by the serum thyroid binding hormone level (i.e., total thyroxine,
TITLE: THYROID DISEASE IN PREGNANCY EFFECTIVE DATE: July, 2013 POLICY STATEMENT: Pregnancy changes significantly the values influenced by the serum thyroid binding hormone level (i.e., total thyroxine,
Understanding thyroid function tests. Dr. Colette George
 Understanding thyroid function tests Dr. Colette George Disclosures No financial disclosure I will present fictitious cases and thyroid function tests (TFTs) that are based on scenarios I commonly encounter.
Understanding thyroid function tests Dr. Colette George Disclosures No financial disclosure I will present fictitious cases and thyroid function tests (TFTs) that are based on scenarios I commonly encounter.
Hypothyroidism. Definition:
 Definition: Hypothyroidism Primary hypothyroidism is characterized biochemically by a high serum thyroidstimulating hormone (TSH) concentration and a low serum free thyroxine (T4) concentration. Subclinical
Definition: Hypothyroidism Primary hypothyroidism is characterized biochemically by a high serum thyroidstimulating hormone (TSH) concentration and a low serum free thyroxine (T4) concentration. Subclinical
HYPERTHYROIDISM. Hypothalamus. Thyrotropin-releasing hormone (TRH) Anterior pituitary gland. Thyroid-stimulating hormone (TSH) Thyroid gland T4, T3
 HYPERTHYROIDISM Hypothalamus Thyrotropin-releasing hormone (TRH) Anterior pituitary gland Thyroid-stimulating hormone (TSH) Thyroid gland T4, T3 In hyperthyroidism, there is an increased production of
HYPERTHYROIDISM Hypothalamus Thyrotropin-releasing hormone (TRH) Anterior pituitary gland Thyroid-stimulating hormone (TSH) Thyroid gland T4, T3 In hyperthyroidism, there is an increased production of
Thyroid Function. Thyroid Antibodies. Analyte Information
 Thyroid Function Thyroid Antibodies Analyte Information - 1-2013-04-30 Thyroid Antibodies Determination of thyroid autoantibodies are, besides TSH and FT4, one of the most important diagnostic parameters.
Thyroid Function Thyroid Antibodies Analyte Information - 1-2013-04-30 Thyroid Antibodies Determination of thyroid autoantibodies are, besides TSH and FT4, one of the most important diagnostic parameters.
Thyroid Gland 甲状腺. Huiping Wang ( 王会平 ), PhD Department of Physiology Rm C541, Block C, Research Building, School of Medicine Tel:
 Thyroid Gland 甲状腺 Huiping Wang ( 王会平 ), PhD Department of Physiology Rm C541, Block C, Research Building, School of Medicine Tel: 88208292 Outline Thyroid Hormones Types Biosynthesis Storage and Release
Thyroid Gland 甲状腺 Huiping Wang ( 王会平 ), PhD Department of Physiology Rm C541, Block C, Research Building, School of Medicine Tel: 88208292 Outline Thyroid Hormones Types Biosynthesis Storage and Release
Hypothyroidism in pregnancy. Nor Shaffinaz Yusoff Azmi Jabatan Perubatan Hospital Sultanah Bahiyah Kedah
 Hypothyroidism in pregnancy Nor Shaffinaz Yusoff Azmi Jabatan Perubatan Hospital Sultanah Bahiyah Kedah Agenda 1. Epidemiology and clinical characteristics of maternal hypothyroidism 2. Prevention and
Hypothyroidism in pregnancy Nor Shaffinaz Yusoff Azmi Jabatan Perubatan Hospital Sultanah Bahiyah Kedah Agenda 1. Epidemiology and clinical characteristics of maternal hypothyroidism 2. Prevention and
Thyroid and Antithyroid Drugs. Munir Gharaibeh, MD, PhD, MHPE Faculty of Medicine April 2014
 Thyroid and Antithyroid Drugs Munir Gharaibeh, MD, PhD, MHPE Faculty of Medicine April 2014 Anatomy and histology of the thyroid gland Located in neck adjacent to the 5 th cervical vertebra (C5). Composed
Thyroid and Antithyroid Drugs Munir Gharaibeh, MD, PhD, MHPE Faculty of Medicine April 2014 Anatomy and histology of the thyroid gland Located in neck adjacent to the 5 th cervical vertebra (C5). Composed
The Thyroid and Pregnancy OUTLINE OF DISCUSSION 3/19/10. Francis S. Greenspan March 19, Normal Physiology. 2.
 The Thyroid and Pregnancy Francis S. Greenspan March 19, 2010 OUTLINE OF DISCUSSION 1. Normal Physiology 2. Hypothyroidism 3. Hyperthyroidism 4. Thyroid Nodules and Cancer NORMAL PHYSIOLOGY Iodine Requirements:
The Thyroid and Pregnancy Francis S. Greenspan March 19, 2010 OUTLINE OF DISCUSSION 1. Normal Physiology 2. Hypothyroidism 3. Hyperthyroidism 4. Thyroid Nodules and Cancer NORMAL PHYSIOLOGY Iodine Requirements:
THE PHARMA INNOVATION - JOURNAL Assessment of Antithyroperoxidase Antibodies and Thyroid Hormones Among Sudanese Pregnant Women
 Received: 01-09-2013 Accepted: 30-09-2013 ISSN: 2277-7695 CODEN Code: PIHNBQ ZDB-Number: 2663038-2 IC Journal No: 7725 Vol. 2 No. 9 2013 Online Available at www.thepharmajournal.com THE PHARMA INNOVATION
Received: 01-09-2013 Accepted: 30-09-2013 ISSN: 2277-7695 CODEN Code: PIHNBQ ZDB-Number: 2663038-2 IC Journal No: 7725 Vol. 2 No. 9 2013 Online Available at www.thepharmajournal.com THE PHARMA INNOVATION
Thyroid hormones derived from two iodinated tyrosine molecules
 Thyroid Hormones OBJECTIVES Chemical nature of the thyroid hormones How different enzymes play a role in thyroid hormone formation? And what drugs affect them? Describe Function & Metabolism of thyroid
Thyroid Hormones OBJECTIVES Chemical nature of the thyroid hormones How different enzymes play a role in thyroid hormone formation? And what drugs affect them? Describe Function & Metabolism of thyroid
Unit Eleven - The Endocrine System
 Unit Eleven - The Endocrine System I. Introduction A. Overview: the endocrine system and nervous system work to control homeostasis within the body. The endocrine system operates at a much pace but the
Unit Eleven - The Endocrine System I. Introduction A. Overview: the endocrine system and nervous system work to control homeostasis within the body. The endocrine system operates at a much pace but the
Timothy Bilash MD MS OBG Northern Inyo Hospital, Bishop, CA October 20, :30 PM
 Thyroxine Deficiency in Pregnancy Timothy Bilash MD MS OBG Northern Inyo Hospital, Bishop, CA October 20, 2006 1:30 PM WHI Estrogen recap In http://courses.washington.edu/bonephys/opestrogen.html. from:
Thyroxine Deficiency in Pregnancy Timothy Bilash MD MS OBG Northern Inyo Hospital, Bishop, CA October 20, 2006 1:30 PM WHI Estrogen recap In http://courses.washington.edu/bonephys/opestrogen.html. from:
THYROID HORMONES & THYROID FUNCTION TESTS
 THYROID HORMONES & THYROID FUNCTION TESTS SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY AND MOLECULAR BIOLOGY CLINICAL BIOCHEMISTRY LECTURE BMLS III
THYROID HORMONES & THYROID FUNCTION TESTS SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY AND MOLECULAR BIOLOGY CLINICAL BIOCHEMISTRY LECTURE BMLS III
Common Issues in Management of Hypothyroidism
 Common Issues in Management of Hypothyroidism Family Medicine Refresher Course April 5, 2018 Janet A. Schlechte, M.D. Disclosure of Financial Relationships Janet A. Schlechte, M.D. has no relationships
Common Issues in Management of Hypothyroidism Family Medicine Refresher Course April 5, 2018 Janet A. Schlechte, M.D. Disclosure of Financial Relationships Janet A. Schlechte, M.D. has no relationships
Sanjay B. Dixit, M.D. BHS Endocrinology Associates November 11, 2017
 Sanjay B. Dixit, M.D. BHS Endocrinology Associates November 11, 2017 I will not be discussing this Outline of discussion Laboratory tests for thyroid function Diagnosis of hypothyroidism Treatment of
Sanjay B. Dixit, M.D. BHS Endocrinology Associates November 11, 2017 I will not be discussing this Outline of discussion Laboratory tests for thyroid function Diagnosis of hypothyroidism Treatment of
Postpartum Depression
 Clinical Medicine: Depression Postpartum Depression JMAJ 44(8): 354 358, 2001 Yoshiko MIYAOKA Department of Psychiatry, Tokyo Musashino Hospital Abstract: Both maternity blues and postpartum depression
Clinical Medicine: Depression Postpartum Depression JMAJ 44(8): 354 358, 2001 Yoshiko MIYAOKA Department of Psychiatry, Tokyo Musashino Hospital Abstract: Both maternity blues and postpartum depression
The Players. Liver Thyroid Adrenals Pancreas Reproductive System Pituitary Gut Bacteria
 The Players Part I Quick Review Understanding some of the key systems and their relationship to hormones is the best place to start It will help with some of the hormone interconnections Key to understanding
The Players Part I Quick Review Understanding some of the key systems and their relationship to hormones is the best place to start It will help with some of the hormone interconnections Key to understanding
Mastering the Thyroid
 + Mastering the Thyroid Physiology 2 A quick overview of how the thyroid is supposed to work Dysfunction 3 A quick overview of the ways in which thyroid dysfunction can occur Patterns 5 The 24 Patterns
+ Mastering the Thyroid Physiology 2 A quick overview of how the thyroid is supposed to work Dysfunction 3 A quick overview of the ways in which thyroid dysfunction can occur Patterns 5 The 24 Patterns
Hypothalamus & pituitary gland. Growth. Hormones Affecting Growth. Growth hormone (GH) GH actions. Suwattanee Kooptiwut, MD., MSc., Ph.D.
 Hypothalamus & pituitary gland Suwattanee Kooptiwut, MD., MSc., Ph.D. 1 2 Growth Hormones Affecting Growth Orderly sequences of maturation changes with increased weight and height Factors Genetic Nutrition
Hypothalamus & pituitary gland Suwattanee Kooptiwut, MD., MSc., Ph.D. 1 2 Growth Hormones Affecting Growth Orderly sequences of maturation changes with increased weight and height Factors Genetic Nutrition
Chapter 11 - Endocrine System
 Chapter 11 - Endocrine System 11.1 Introduction A. The endocrine system is made up of the cells, tissues, and organs that secrete hormones into body fluids. B. The body has two kinds of glands, exocrine
Chapter 11 - Endocrine System 11.1 Introduction A. The endocrine system is made up of the cells, tissues, and organs that secrete hormones into body fluids. B. The body has two kinds of glands, exocrine
The Endocrine System. I. Overview of the Endocrine System. II. Three Families of Hormones. III. Hormone Receptors. IV. Classes of Hormone Receptor
 The Endocrine System I. Overview of the Endocrine System A. Regulates long term metabolic processes B. Releases hormones from endocrine cells 1. Hormones are chemicals 2. Alter metabolism of cells 3. Release
The Endocrine System I. Overview of the Endocrine System A. Regulates long term metabolic processes B. Releases hormones from endocrine cells 1. Hormones are chemicals 2. Alter metabolism of cells 3. Release
Endocrine secretion cells secrete substances into the extracellular fluid
 Animal Hormones Concept 30.1 Hormones Are Chemical Messengers Endocrine secretion cells secrete substances into the extracellular fluid Exocrine secretion cells secrete substances into a duct or a body
Animal Hormones Concept 30.1 Hormones Are Chemical Messengers Endocrine secretion cells secrete substances into the extracellular fluid Exocrine secretion cells secrete substances into a duct or a body
Hypothyroidism. Causes. Diagnosis. Christopher Theberge
 Hypothyroidism Pronunciations: (Hypothyroidism) Hypothyroidism (under active thyroid) is a condition where the thyroid gland fails to secrete enough of the thyroid hormones thyroxine (T4) and triiodothyronine
Hypothyroidism Pronunciations: (Hypothyroidism) Hypothyroidism (under active thyroid) is a condition where the thyroid gland fails to secrete enough of the thyroid hormones thyroxine (T4) and triiodothyronine
Chapter 8.2 The Endocrine System
 Major Endocrine Organs Hypothalamus Pineal Gland Pituitary Gland Thyroid Gland Thymus Gland Adrenal Glands Pancreas Ovaries (Female) Testis (Male) Chapter 8.2 The Endocrine System The endocrine system
Major Endocrine Organs Hypothalamus Pineal Gland Pituitary Gland Thyroid Gland Thymus Gland Adrenal Glands Pancreas Ovaries (Female) Testis (Male) Chapter 8.2 The Endocrine System The endocrine system
Lothian Guidance for Diagnosis and Management of Thyroid Dysfunction in Pregnancy
 Lothian Guidance for Diagnosis and Management of Thyroid Dysfunction in Pregnancy Early diagnosis and good management of maternal thyroid dysfunction are essential to ensure minimal adverse effects on
Lothian Guidance for Diagnosis and Management of Thyroid Dysfunction in Pregnancy Early diagnosis and good management of maternal thyroid dysfunction are essential to ensure minimal adverse effects on
Iodine and Thyroid Hormones
 Iodine and Thyroid Hormones Iodine and Thyroid Hormones feed-back Iodine Deficiency Characteristics Iodine Deficiency None Mild Mode Severe Median urine iodine >100 50-99 20-49
Iodine and Thyroid Hormones Iodine and Thyroid Hormones feed-back Iodine Deficiency Characteristics Iodine Deficiency None Mild Mode Severe Median urine iodine >100 50-99 20-49
Endocrine part one. Presented by Dr. Mohammad Saadeh The requirements for the Clinical Chemistry Philadelphia University Faculty of pharmacy
 Endocrine part one Presented by Dr. Mohammad Saadeh The requirements for the Clinical Chemistry Philadelphia University Faculty of pharmacy HORMONES Hormones are chemicals released by a cell or a gland
Endocrine part one Presented by Dr. Mohammad Saadeh The requirements for the Clinical Chemistry Philadelphia University Faculty of pharmacy HORMONES Hormones are chemicals released by a cell or a gland
When the Bough Breaks
 Avoiding Crisis and the Loss of Life by Recognizing and Treating Angela Burling RN MSN Chris Raines MSN RN APRN-BC When the Bough Breaks Angela s Story Raines and Burling 1 A rare but devastatingcondition,
Avoiding Crisis and the Loss of Life by Recognizing and Treating Angela Burling RN MSN Chris Raines MSN RN APRN-BC When the Bough Breaks Angela s Story Raines and Burling 1 A rare but devastatingcondition,
Thyroid and Antithyroid Drugs. Dr. Alia Shatanawi Feb,
 Thyroid and Antithyroid Drugs Dr. Alia Shatanawi Feb, 24 2014 Anatomy and histology of the thyroid gland Located in neck adjacent to the 5 th cervical vertebra (C5). Composed of epithelial cells which
Thyroid and Antithyroid Drugs Dr. Alia Shatanawi Feb, 24 2014 Anatomy and histology of the thyroid gland Located in neck adjacent to the 5 th cervical vertebra (C5). Composed of epithelial cells which
Lothian Guidance for Diagnosis and Management of Thyroid Dysfunction in Pregnancy.
 Lothian Guidance for Diagnosis and Management of Thyroid Dysfunction in Pregnancy. Early diagnosis and good management of maternal thyroid dysfunction is essential to ensure minimal adverse effects on
Lothian Guidance for Diagnosis and Management of Thyroid Dysfunction in Pregnancy. Early diagnosis and good management of maternal thyroid dysfunction is essential to ensure minimal adverse effects on
HORMONES OF THE POSTERIOR PITUITARY
 HORMONES OF THE POSTERIOR PITUITARY HORMONES OF THE POSTERIOR PITUITARY In contrast to the hormones of the anterior lobe of the pituitary, those of the posterior lobe, vasopressin and oxytocin, are not
HORMONES OF THE POSTERIOR PITUITARY HORMONES OF THE POSTERIOR PITUITARY In contrast to the hormones of the anterior lobe of the pituitary, those of the posterior lobe, vasopressin and oxytocin, are not
Thyroid function testing in pregnancy: 2017 ATA guidelines update. Dr Simon Forehan
 Thyroid function testing in pregnancy: 2017 ATA guidelines update Dr Simon Forehan Several factors are known to tax gravid thyroid economy: Increased plasma volume TBG pool increased Renal clearance Feto-placental
Thyroid function testing in pregnancy: 2017 ATA guidelines update Dr Simon Forehan Several factors are known to tax gravid thyroid economy: Increased plasma volume TBG pool increased Renal clearance Feto-placental
Endocrine System. True or False
 True or False Endocrine System Some overweight people actually eat very little; their excess weight is caused by glands A woman who becomes anxious and depressed just before menstruating is suffering from
True or False Endocrine System Some overweight people actually eat very little; their excess weight is caused by glands A woman who becomes anxious and depressed just before menstruating is suffering from
The Endocrine System/Hormones
 The Endocrine System/Hormones Controls many body functions exerts control by releasing special chemical substances into the blood called hormones Hormones affect other endocrine glands or body systems
The Endocrine System/Hormones Controls many body functions exerts control by releasing special chemical substances into the blood called hormones Hormones affect other endocrine glands or body systems
university sciences of Isfahan university Com
 Introduce R. Gholamnezhad Lecturer of school of nursing & midwifery of Iran university Ph.D student tof Immunology, Sh School of medical sciences of Isfahan university E-Mail: Gholami278@gmail. Com Interpreting
Introduce R. Gholamnezhad Lecturer of school of nursing & midwifery of Iran university Ph.D student tof Immunology, Sh School of medical sciences of Isfahan university E-Mail: Gholami278@gmail. Com Interpreting
B-Resistance to the action of hormones, Hormone resistance characterized by receptor mediated, postreceptor.
 Disorders of the endocrine system 38 Disorders of endocrine system mainly are caused by: A-Deficiency or an excess of a single hormone or several hormones: - deficiency :can be congenital or acquired.
Disorders of the endocrine system 38 Disorders of endocrine system mainly are caused by: A-Deficiency or an excess of a single hormone or several hormones: - deficiency :can be congenital or acquired.
How to manage hypothyroid disease in pregnancy
 For mass reproduction, content licensing and permissions contact Dowden Health Media. FIRST OF 2 PARTS How to manage hypothyroid disease in pregnancy Pregnancy complicated by hypothyroidism puts mother
For mass reproduction, content licensing and permissions contact Dowden Health Media. FIRST OF 2 PARTS How to manage hypothyroid disease in pregnancy Pregnancy complicated by hypothyroidism puts mother
Slide notes: This presentation provides information on Graves disease, a systemic autoimmune disease. Epidemiology, pathology, complications,
 1 This presentation provides information on Graves disease, a systemic autoimmune disease. Epidemiology, pathology, complications, including ophthalmic complications, treatments (both permanent solutions
1 This presentation provides information on Graves disease, a systemic autoimmune disease. Epidemiology, pathology, complications, including ophthalmic complications, treatments (both permanent solutions
4) Thyroid Gland Defects - Dr. Tara
 4) Thyroid Gland Defects - Dr. Tara Thyroid Pituitary Axis TRH secreted in the hypothalamus stimulates production and Secretion of TSH TSH stimulates secretion of T3, T4 T4 has negative feedback on secretion
4) Thyroid Gland Defects - Dr. Tara Thyroid Pituitary Axis TRH secreted in the hypothalamus stimulates production and Secretion of TSH TSH stimulates secretion of T3, T4 T4 has negative feedback on secretion
Checking the Right Box at the Right Age: the Art of Pediatric Endocrine Testing
 Checking the Right Box at the Right Age: the Art of Pediatric Endocrine Testing Jean-Pierre Chanoine, MD Endocrinology and Diabetes Unit British Columbia s Children s Hospital Objectives 1. Interpret the
Checking the Right Box at the Right Age: the Art of Pediatric Endocrine Testing Jean-Pierre Chanoine, MD Endocrinology and Diabetes Unit British Columbia s Children s Hospital Objectives 1. Interpret the
Anatomy and Physiology. The Endocrine System
 Anatomy and Physiology The Endocrine System The endocrine system includes anything that secretes hormones directly into body fluids. Endocrine glands include: the thyroid, parathyroid, adrenal, kidney,
Anatomy and Physiology The Endocrine System The endocrine system includes anything that secretes hormones directly into body fluids. Endocrine glands include: the thyroid, parathyroid, adrenal, kidney,
Thyroid Disorders. January 2019
 Thyroid Disorders January 2019 What is the Thyroid? The thyroid is a small butterfly-shaped gland inside the neck, located in front of the trachea (windpipe) and below the larynx (voicebox). It produces
Thyroid Disorders January 2019 What is the Thyroid? The thyroid is a small butterfly-shaped gland inside the neck, located in front of the trachea (windpipe) and below the larynx (voicebox). It produces
Esther Briganti. Fetal And Maternal Health Beyond the Womb: hot topics in endocrinology and pregnancy. Endocrinologist and Clinician Researcher
 Fetal And Maternal Health Beyond the Womb: hot topics in endocrinology and pregnancy Esther Briganti Endocrinologist and Clinician Researcher Director, Melbourne Endocrine Associates Associate Professor,
Fetal And Maternal Health Beyond the Womb: hot topics in endocrinology and pregnancy Esther Briganti Endocrinologist and Clinician Researcher Director, Melbourne Endocrine Associates Associate Professor,
Limits of Liability/Disclaimer of Warranty
 Page 0 of 8 Limits of Liability/Disclaimer of Warranty The author, Brad Shook has made their best effort to produce a high quality and informative reference. The author makes no representation or warranties
Page 0 of 8 Limits of Liability/Disclaimer of Warranty The author, Brad Shook has made their best effort to produce a high quality and informative reference. The author makes no representation or warranties
the holtorf way proven path of evidence-based medicine and optimal wellness
 proven path of evidence-based medicine and optimal wellness 17 years ahead Get To Know The Facts: 17 Years Ahead There are hundreds of studies on the new way to approach thyroid treatment. But if your
proven path of evidence-based medicine and optimal wellness 17 years ahead Get To Know The Facts: 17 Years Ahead There are hundreds of studies on the new way to approach thyroid treatment. But if your
Thyroid gland defects. Dr. Tara Husain
 Thyroid gland defects Dr. Tara Husain Thyroid Pituitary Axis TRH secreted in the hypothalamus stimulates production and Secretion of TSH TSH stimulates secretion of T3,T4 T4 has negative feed back on secretion
Thyroid gland defects Dr. Tara Husain Thyroid Pituitary Axis TRH secreted in the hypothalamus stimulates production and Secretion of TSH TSH stimulates secretion of T3,T4 T4 has negative feed back on secretion
Can My Lab Work Tell Me I Am Depressed?
 1 Facebook: Brock Post Post 5 Can My Lab Work Tell Me I Am Depressed? Written by: Dr. Ryan Cedermark, DC, DACNB, RN, BSN, FNP Student (Chief Resident, CHC) Reviewed by: Dr. Brandon Brock, MSN, BSN, RN,
1 Facebook: Brock Post Post 5 Can My Lab Work Tell Me I Am Depressed? Written by: Dr. Ryan Cedermark, DC, DACNB, RN, BSN, FNP Student (Chief Resident, CHC) Reviewed by: Dr. Brandon Brock, MSN, BSN, RN,
BIOLOGY 2402 Anatomy and Physiology Lecture. Chapter 18 ENDOCRINE GLANDS
 BIOLOGY 2402 Anatomy and Physiology Lecture Chapter 18 ENDOCRINE GLANDS 1 ENDOCRINE GLANDS Homeostasis depends on the precise regulation of the organs and organ systems of the body. Together the nervous
BIOLOGY 2402 Anatomy and Physiology Lecture Chapter 18 ENDOCRINE GLANDS 1 ENDOCRINE GLANDS Homeostasis depends on the precise regulation of the organs and organ systems of the body. Together the nervous
Thyroid gland. Thyroid hormones
 Thyroid gland Thyroid hormones 2/8 thyroid gland consists of two lobes weighing 20 g thyroid cells surround follicles filled with a colloid (thyroglobulin glycoprotein): storage thyroid gland produces
Thyroid gland Thyroid hormones 2/8 thyroid gland consists of two lobes weighing 20 g thyroid cells surround follicles filled with a colloid (thyroglobulin glycoprotein): storage thyroid gland produces
Chapter 11. Endocrine System
 Chapter 11 Endocrine System 1 Introduction A. The endocrine system is made up of the cells, tissues, and organs that secrete hormones into body fluids. B. Hormones diffuse into the bloodstream to act target
Chapter 11 Endocrine System 1 Introduction A. The endocrine system is made up of the cells, tissues, and organs that secrete hormones into body fluids. B. Hormones diffuse into the bloodstream to act target
Ch 8: Endocrine Physiology
 Ch 8: Endocrine Physiology Objectives 1. Review endocrine glands of body. 2. Understand how hypothalamus controls endocrine system & sympathetic epinephrine response. 3. Learn anterior pituitary hormones
Ch 8: Endocrine Physiology Objectives 1. Review endocrine glands of body. 2. Understand how hypothalamus controls endocrine system & sympathetic epinephrine response. 3. Learn anterior pituitary hormones
03-Dec-17. Thyroid Disorders GOITRE. Grossly enlarged thyroid - in hypothyroidism in hyperthyroidism - production of anatomical symptoms
 Thyroid Disorders GOITRE Grossly enlarged thyroid - in hypothyroidism in hyperthyroidism - production of anatomical symptoms 1 Physiological Goiter load on thyroid supply of I - limited stress due to:
Thyroid Disorders GOITRE Grossly enlarged thyroid - in hypothyroidism in hyperthyroidism - production of anatomical symptoms 1 Physiological Goiter load on thyroid supply of I - limited stress due to:
Human Anatomy and Physiology - Problem Drill 16: The Endocrine System
 Human Anatomy and Physiology - Problem Drill 16: The Endocrine System Question No. 1 of 10 The endocrine system is made up of a number of organs and glands. Which one of the following is not an organ or
Human Anatomy and Physiology - Problem Drill 16: The Endocrine System Question No. 1 of 10 The endocrine system is made up of a number of organs and glands. Which one of the following is not an organ or
Thyroid Disorders Towards a Healthy Endocrine System
 Thyroid Disorders Towards a Healthy Endocrine System What are Thyroid Disorders? The thyroid is a butterfly-shaped gland in the middle of the lower neck. Through the release of hormones, the thyroid regulates
Thyroid Disorders Towards a Healthy Endocrine System What are Thyroid Disorders? The thyroid is a butterfly-shaped gland in the middle of the lower neck. Through the release of hormones, the thyroid regulates
Mastering Thyroid Disorders. Douglas C. Bauer, MD UCSF Division of General Internal Medicine
 Mastering Thyroid Disorders Douglas C. Bauer, MD UCSF Division of General Internal Medicine Cases 68 yr old female with new atrial fibrillation and no other findings except TSH=0.04, normal free T4 79
Mastering Thyroid Disorders Douglas C. Bauer, MD UCSF Division of General Internal Medicine Cases 68 yr old female with new atrial fibrillation and no other findings except TSH=0.04, normal free T4 79
Should every pregnant woman be screened for thyroid disease?
 Should every pregnant woman be screened for thyroid disease? Tal Biron-Shental Rinat Gabbay-Benziv Is there a debate? Thyroid screening Guidelines Targeted case finding criteria Age > 30 years Personal
Should every pregnant woman be screened for thyroid disease? Tal Biron-Shental Rinat Gabbay-Benziv Is there a debate? Thyroid screening Guidelines Targeted case finding criteria Age > 30 years Personal
Program Outline / page 1. I. Get Acquainted With Your Hormone System. III. Learn Why The Thyroid Gland is Important for Your Health
 Program Outline / page 1 Module 1 I. Get Acquainted With Your Hormone System What is the endocrine system? What are hormonal rhythms? What are the main hormonal networks and axis? II. Know Your Thyroid
Program Outline / page 1 Module 1 I. Get Acquainted With Your Hormone System What is the endocrine system? What are hormonal rhythms? What are the main hormonal networks and axis? II. Know Your Thyroid
Critical illness and endocrinology. ICU Fellowship Training Radboudumc
 Critical illness and endocrinology ICU Fellowship Training Radboudumc Critical illness Ultimate form of severe physical stress Generates an orchestrated endocrine response to provide the energy for fight
Critical illness and endocrinology ICU Fellowship Training Radboudumc Critical illness Ultimate form of severe physical stress Generates an orchestrated endocrine response to provide the energy for fight
DRUGS. 4- Two molecules of DIT combine within the thyroglobulinto form L-thyroxine (T4)' One molecule of MIT & one molecule of DIT combine to form T3
 THYROID HORMONEs & ANTITHYROID The thyroid secretes 2 types of hormones: DRUGS 1- Iodine containing amino acids (are important for growth, development and metabolism) and these are: triodothyronine, tetraiodothyronine,(
THYROID HORMONEs & ANTITHYROID The thyroid secretes 2 types of hormones: DRUGS 1- Iodine containing amino acids (are important for growth, development and metabolism) and these are: triodothyronine, tetraiodothyronine,(
Endocrine and Reproductive Systems. Chapter 39: Biology II
 Endocrine and Reproductive Systems Chapter 39: Biology II The Endocrine System Made up of glands that release their products into the bloodstream These products broadcast messages throughout the body Chemicals
Endocrine and Reproductive Systems Chapter 39: Biology II The Endocrine System Made up of glands that release their products into the bloodstream These products broadcast messages throughout the body Chemicals
THYROID AWARENESS. By: Karen Carbone. January is thyroid awareness month. At least 30 million Americans
 THYROID AWARENESS By: Karen Carbone January is thyroid awareness month. At least 30 million Americans have a thyroid disorder and half-15 million-are silent sufferers who are undiagnosed, according to
THYROID AWARENESS By: Karen Carbone January is thyroid awareness month. At least 30 million Americans have a thyroid disorder and half-15 million-are silent sufferers who are undiagnosed, according to
Endocrine System Notes
 Endocrine System Notes is the tendency to maintain a stable internal environment. - parts of the body that secrete hormones directly into the body. - parts of the body that make secretions which travel
Endocrine System Notes is the tendency to maintain a stable internal environment. - parts of the body that secrete hormones directly into the body. - parts of the body that make secretions which travel
Thyrotoxicosis in Pregnancy: Diagnose and Management
 Thyrotoxicosis in Pregnancy: Diagnose and Management Yuanita Asri Langi email: meralday@yahoo.co.id Endocrinology & Metabolic Division, Internal Medicine Department, Prof.dr.R.D. Kandou Hospital/ Sam Ratulangi
Thyrotoxicosis in Pregnancy: Diagnose and Management Yuanita Asri Langi email: meralday@yahoo.co.id Endocrinology & Metabolic Division, Internal Medicine Department, Prof.dr.R.D. Kandou Hospital/ Sam Ratulangi
Chapter 12 Endocrine System (export).notebook. February 27, Mar 17 2:59 PM. Mar 17 3:09 PM. Mar 17 3:05 PM. Mar 17 3:03 PM.
 Endocrine System Hormones Chemical messengers released directly into the bloodstream Regulate: *May have wide spread effect or only affect certain tissues ** : cells with receptors that respond to specific
Endocrine System Hormones Chemical messengers released directly into the bloodstream Regulate: *May have wide spread effect or only affect certain tissues ** : cells with receptors that respond to specific
Back to the Basics: Thyroid Gland Structure, Function and Pathology
 Back to the Basics: Thyroid Gland Structure, Function and Pathology JANELLE M. CHIASERA LEARNING OBJECTIVES 1. Explain the HPT feedback system involving the thyroid gland. Include the hormone produced
Back to the Basics: Thyroid Gland Structure, Function and Pathology JANELLE M. CHIASERA LEARNING OBJECTIVES 1. Explain the HPT feedback system involving the thyroid gland. Include the hormone produced
Thyroid Gland 甲状腺. Huiping Wang ( 王会平 ), PhD Department of Physiology Rm C541, Block C, Research Building, School of Medicine Tel:
 Thyroid Gland 甲状腺 Huiping Wang ( 王会平 ), PhD Department of Physiology Rm C541, Block C, Research Building, School of Medicine Tel: 88208292 Outline Thyroid Hormones Types Biosynthesis Storage and Release
Thyroid Gland 甲状腺 Huiping Wang ( 王会平 ), PhD Department of Physiology Rm C541, Block C, Research Building, School of Medicine Tel: 88208292 Outline Thyroid Hormones Types Biosynthesis Storage and Release
Your Thyroid By Lawrence C. F Wood M.D., Chester Ridgway READ ONLINE
 Your Thyroid By Lawrence C. F Wood M.D., Chester Ridgway READ ONLINE The thyroid is a gland located below the larynx (voice box), and its function is to regulate metabolism. Metabolism is the chemical
Your Thyroid By Lawrence C. F Wood M.D., Chester Ridgway READ ONLINE The thyroid is a gland located below the larynx (voice box), and its function is to regulate metabolism. Metabolism is the chemical
2004 Where Do We Go from Here? Summary of Working Group Discussions on Thyroid Function and Gestational Outcomes
 THYROID Volume 15, Number 1, 2005 Mary Ann Liebert, Inc. 2004 Where Do We Go from Here? Summary of Working Group Discussions on Thyroid Function and Gestational Outcomes Joseph G. Hollowell, 1 Stephen
THYROID Volume 15, Number 1, 2005 Mary Ann Liebert, Inc. 2004 Where Do We Go from Here? Summary of Working Group Discussions on Thyroid Function and Gestational Outcomes Joseph G. Hollowell, 1 Stephen
The Investigations of the Thyroid gland
 The Investigations of the Thyroid gland Essential for understanding this presentation: 1) Anatomy: The Thyroid Gland and it s surroundings 2) Biochemistry: Hormones produced by the Thyroid Gland 3) Physiology:
The Investigations of the Thyroid gland Essential for understanding this presentation: 1) Anatomy: The Thyroid Gland and it s surroundings 2) Biochemistry: Hormones produced by the Thyroid Gland 3) Physiology:
The Presence of Thyroid Autoantibodies in Pregnancy
 The Presence of Thyroid Autoantibodies in Pregnancy Dr. O Sullivan does not have any financial relationships with any commercial interests. KATIE O SULLIVAN, MD FELLOW, ADULT/PEDIATRIC ENDOCRINOLOGY ENDORAMA
The Presence of Thyroid Autoantibodies in Pregnancy Dr. O Sullivan does not have any financial relationships with any commercial interests. KATIE O SULLIVAN, MD FELLOW, ADULT/PEDIATRIC ENDOCRINOLOGY ENDORAMA
Hypothalamic Control of Posterior Pituitary
 Hypothalamic Control of Posterior Pituitary Hypothalamus neuron cell bodies produce ADH: supraoptic nuclei Oxytocin: paraventricular nuclei Transported along the hypothalamohypophyseal tract Stored in
Hypothalamic Control of Posterior Pituitary Hypothalamus neuron cell bodies produce ADH: supraoptic nuclei Oxytocin: paraventricular nuclei Transported along the hypothalamohypophyseal tract Stored in
Grave s Disease. of the endocrine system known as Grave s disease. This disease condition which affects the
 Grave s Disease The proper functioning of the human body is dependant upon the normal working of the systems of the human body. The coordination of these systems is essential for maintaining all the normal
Grave s Disease The proper functioning of the human body is dependant upon the normal working of the systems of the human body. The coordination of these systems is essential for maintaining all the normal
Endocrine System. Chemical Control
 Endocrine System Chemical Control Endocrine System - the system that secretes hormones in the body - hormones can last for minutes or for hours - a major gland, once called the master gland, is the pituitary
Endocrine System Chemical Control Endocrine System - the system that secretes hormones in the body - hormones can last for minutes or for hours - a major gland, once called the master gland, is the pituitary
DISORDERS OF THE THYROID GLAND SIGNS, SYMPTOMS, & TREATMENT ENDOCRINE SYSTEM AT A GLANCE OBJECTIVES ANATOMY OF THE THYROID
 OBJECTIVES DISORDERS OF THE THYROID GLAND SIGNS, SYMPTOMS, & TREATMENT Stephanie Blackburn, MHS, MLS(ASCP) CM LSU Health Shreveport Clinical Laboratory Science Program Discuss the synthesis and action
OBJECTIVES DISORDERS OF THE THYROID GLAND SIGNS, SYMPTOMS, & TREATMENT Stephanie Blackburn, MHS, MLS(ASCP) CM LSU Health Shreveport Clinical Laboratory Science Program Discuss the synthesis and action
9.2 Hormonal Regulation of Growth
 9.2 Hormonal Regulation of Growth Hormonal Regulation of Growth Pituitary gland regulates growth and development Thyroid gland regulates metabolic rate (exception: some hormones for growth and development)
9.2 Hormonal Regulation of Growth Hormonal Regulation of Growth Pituitary gland regulates growth and development Thyroid gland regulates metabolic rate (exception: some hormones for growth and development)
Review Article Think Thyroid - Think Life: Pregnancy with Thyroid Disorders
 Chettinad Health City Medical Journal Muthukumaran Jayapaul* Consultant Endocrinologist, Arka Center for Hormonal Health, Chennai, India Dr. Muthu Kumaran Jayapaul is a Consultant Endocrinologist and also
Chettinad Health City Medical Journal Muthukumaran Jayapaul* Consultant Endocrinologist, Arka Center for Hormonal Health, Chennai, India Dr. Muthu Kumaran Jayapaul is a Consultant Endocrinologist and also
Graves Disease in Pediatrics
 Graves Disease in Pediatrics Graves disease is a common cause of an overactive thyroid. It occurs in about 1 in 5000 children and teens. It occurs more often in females than males. This booklet is designed
Graves Disease in Pediatrics Graves disease is a common cause of an overactive thyroid. It occurs in about 1 in 5000 children and teens. It occurs more often in females than males. This booklet is designed
Part I Initial Office Visit. Questions NATIONAL CENTER FOR CASE STUDY TEACHING IN SCIENCE
 Thyroid Troubles: A Case Study in Negative Feedback Regulation by Breanna N. Harris Department of Biological Sciences Texas Tech University, Lubbock, TX Part I Initial Office Visit You are six months into
Thyroid Troubles: A Case Study in Negative Feedback Regulation by Breanna N. Harris Department of Biological Sciences Texas Tech University, Lubbock, TX Part I Initial Office Visit You are six months into
THE TREATMENT OF HYPOTHYROIDISM IN PREGNANCY
 2017 ILEX PUBLISHING HOUSE, Bucharest, Roumania http://www.jrdiabet.ro Rom J Diabetes Nutr Metab Dis. 24(2):155-160 doi: 10.1515/rjdnmd-2017-0020 THE TREATMENT OF HYPOTHYROIDISM IN PREGNANCY Rucsandra
2017 ILEX PUBLISHING HOUSE, Bucharest, Roumania http://www.jrdiabet.ro Rom J Diabetes Nutr Metab Dis. 24(2):155-160 doi: 10.1515/rjdnmd-2017-0020 THE TREATMENT OF HYPOTHYROIDISM IN PREGNANCY Rucsandra
Subclinical Hypothyroidism and Isolated Hypothyroxinemia during Pregnancy and Their Association with Pregnancy Outcome: A 2-Year Study
 Open Journal of Obstetrics and Gynecology, 2017, 7, 693-701 http://www.scirp.org/journal/ojog ISSN Online: 2160-8806 ISSN Print: 2160-8792 Subclinical Hypothyroidism and Isolated Hypothyroxinemia during
Open Journal of Obstetrics and Gynecology, 2017, 7, 693-701 http://www.scirp.org/journal/ojog ISSN Online: 2160-8806 ISSN Print: 2160-8792 Subclinical Hypothyroidism and Isolated Hypothyroxinemia during
Alvin C. Powers, M.D. 1/27/06
 Thyroid Histology Follicular Cells ECF side Apical lumen Thyroid Follicles -200-400 um Parafollicular or C-cells Colloid Photos from University of Manchester and tutorial created by Dr. James Crimando,
Thyroid Histology Follicular Cells ECF side Apical lumen Thyroid Follicles -200-400 um Parafollicular or C-cells Colloid Photos from University of Manchester and tutorial created by Dr. James Crimando,
Hyperthyroidism Diagnosis and Treatment. April Janet A. Schlechte, M.D.
 Hyperthyroidism Diagnosis and Treatment Family Practice Refresher Course April 2015 Janet A. Schlechte, M.D. Disclosure of Financial Relationships Janet A. Schlechte, M.D. has no relationships with any
Hyperthyroidism Diagnosis and Treatment Family Practice Refresher Course April 2015 Janet A. Schlechte, M.D. Disclosure of Financial Relationships Janet A. Schlechte, M.D. has no relationships with any
Hypothyroidism in Women
 Illustration istock Collection / thinkstockphotos.com T Hypothyroidism in Women Donna Dunn Thyroid disease is a major health issue in the United States. Approximately 20 million Americans have been diagnosed
Illustration istock Collection / thinkstockphotos.com T Hypothyroidism in Women Donna Dunn Thyroid disease is a major health issue in the United States. Approximately 20 million Americans have been diagnosed
Pancreas. Endocrine pancreas - Islets of Langerhans A or alpha cells glucagon B or beta cells insulin Delta cells somatostatin
 Endocrine System Pancreas Endocrine pancreas - Islets of Langerhans A or alpha cells glucagon B or beta cells insulin Delta cells somatostatin Glucagon & Metabolism Produced by beta cells of Islets Primary
Endocrine System Pancreas Endocrine pancreas - Islets of Langerhans A or alpha cells glucagon B or beta cells insulin Delta cells somatostatin Glucagon & Metabolism Produced by beta cells of Islets Primary
Chapter 45-Hormones and the Endocrine System. Simple Hormone Pathways
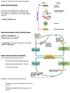 Chapter 45-Hormones and the Endocrine System Simple Hormone s Low ph in duodenum Hormones are released from an endocrine, travel through the bloodstream, and interact with the receptor or a target to cause
Chapter 45-Hormones and the Endocrine System Simple Hormone s Low ph in duodenum Hormones are released from an endocrine, travel through the bloodstream, and interact with the receptor or a target to cause
Thyroid hormone. Functional anatomy of thyroid gland
 Thyroid hormone ส ว ฒณ ค ปต ว ฒ ต กจ ฑาธ ช ห อง 101 Aims Functional anatomy of thyroid gland Synthesis, secretion and metabolism of the thyroid hormones The mechanism of thyroid hormone action Role of
Thyroid hormone ส ว ฒณ ค ปต ว ฒ ต กจ ฑาธ ช ห อง 101 Aims Functional anatomy of thyroid gland Synthesis, secretion and metabolism of the thyroid hormones The mechanism of thyroid hormone action Role of
