Endoscopic Ultrasound Guided Fine Needle Aspiration in the Diagnosis of Mediastinal Masses of Unknown Origin
|
|
|
- Eleanore Briggs
- 6 years ago
- Views:
Transcription
1 THE AMERICAN JOURNAL OF GASTROENTEROLOGY Vol. 97, No. 10, by Am. Coll. of Gastroenterology ISSN /02/$22.00 Published by Elsevier Science Inc. PII S (02) Endoscopic Ultrasound Guided Fine Needle Aspiration in the Diagnosis of Mediastinal Masses of Unknown Origin Marc F. Catalano, M.D., Mark L. Rosenblatt, M.D., Amitabh Chak, M.D., Michael V. Sivak, Jr., M.D., James Scheiman, M.D., and Frank Gress, M.D. St. Luke s Medical Center, Pancreatic Biliary Center, Milwaukee, Wisconsin; University Hospitals of Cleveland, Cleveland, Ohio; University of Michigan, Ann Arbor, Michigan; Winthrop Hospital, Long Island, New York OBJECTIVES: The ability of endosonography to diagnose a variety of gastrointestinal pathology has been significantly advanced with the introduction of endoscopic ultrasound guided fine needle aspiration (EUS-FNA) biopsy. EUS- FNA technology can also be applied to the evaluation of non-gi disorders. The role of EUS-FNA to establish the diagnosis of unexplained mediastinal masses has not been previously described. The aim of this study was to determine the diagnostic accuracy, impact on subsequent workup, and role of EUS-FNA in treating mediastinal masses of unknown cause. METHODS: A total of 26 patients (15 men and 11 women, mean age 61 yr, range yr) underwent EUS-FNA in patients presenting with unexplained mediastinal masses at four tertiary referral centers. Presenting symptoms included: chest pain (10 patients), dysphagia (eight), cough (seven), fever (six), night sweats (three), and no symptoms/abnormal x-ray (five patients). Five of 26 patients had prior history of cancer (three lung, one tracheal, and one esophageal). RESULTS: Final diagnosis using EUS-FNA, surgery, autopsy, other diagnostic study, or long-term follow-up was available in all patients. EUS-FNA results were classified under three disease categories: 1) infectious, 2) benign/ inflammatory, and 3) malignant. Final diagnosis included infectious in five patents, benign/inflammatory in nine, and malignant in 12. EUS-FNA was successful in 21 of 26 patients (81%) for all disease categories (infectious 60%, benign/inflammatory 78%, and malignant 92%). EUS-FNA was successful in directing subsequent workup in 77% (20 of 26) and therapy in 73% (19 of 26). Mean EUS-FNA passes for adequate tissue sampling was lower of nonmalignant disease categories (3.0 and 3.4) versus malignant disease (4.4). No complications were seen during the course of this study. CONCLUSIONS: EUS-FNA in patients presenting with idiopathic mediastinal masses establishes the diagnosis in the vast majority of cases, particularly for those with malignant disease. The emergence of transesophageal EUS-FNA of the mediastinum provides the ability to alter subsequent workup and therapy, obviating the need for more invasive diagnostic studies such as thoracotomy. (Am J Gastroenterol 2002;97: by Am. Coll. of Gastroenterology) INTRODUCTION Thoracic imaging of mediastinal masses is challenging. CT of the chest is the current standard by which the mediastinum is visualized. Problems then arise as to various tissue sampling modalities. In well-selected patients, CT-guided fine needle aspiration (FNA), mediastinoscopy, thoracoscopic mediastinal biopsy, or transbronchial biopsy has been used. Morbidity, time, and costs have limited their applicability. The advent of endoscopic ultrasonography (EUS) has made it possible to image the GI tract and surrounding extraluminal tissues. EUS-FNA has become the preferred method for staging of upper GI tract cancers. The esophagus affords an excellent acoustic window through which to scan the mediastinum, a fact that extends the usefulness of this examination. Recently, EUS-FNA has been shown to have a valuable role in identifying posterior mediastinal involvement when staging nongastrointestinal malignancies (1, 2). The purpose of this study was to assess the diagnostic accuracy of EUS-FNA on a heterogenous group of patients presenting with idiopathic mediastinal mass lesions, and to assess the impact of EUS-FNA on subsequent workup and therapy. MATERIALS AND METHODS A total of 26 patients underwent EUS-FNA in patients presenting with idiopathic and mediastinal masses at four tertiary referral centers. This group included 15 men and 11 women, with a mean age of 61 yr (range yr). Inclusion criteria included age 18 yr with informed consent, absence of tissue diagnosis at the time of EUS, and final diagnosis established. Exclusion criteria included previ-
2 2560 Catalano et al. AJG Vol. 97, No. 10, 2002 ously established diagnosis, inaccessible masses for EUS- FNA, coagulopathy, or final diagnosis not available at follow-up. CT was obtained in all patients before referral for EUS, and was abnormal (demonstrating a mediastinal mass in the absence of lymphadenopathy) in 23 of 26 patients (89%). The remaining three patients had incidental mass found within the mediastinum on EUS Presenting symptoms included chest pain in 10 patients, dysphagia in eight, cough in seven, fever in six, night sweats in three, and no symptoms/abnormal x-ray in five. Five of 26 patients had a prior history of cancer, including three patients with lung cancer, one with laryngeal cancer, and one with esophageal cancer, but were believed to be free of disease after surgical therapy (16 months to 3.5 yr before EUS). Final diagnosis using EUS-FNA, surgery, autopsy, and other diagnostic study or long-term follow-up was available in all patients. EUS FNA results were classified under three disease categories: 1) infectious, 2) benign/ inflammatory, and 3) malignant mediastinal. All patients underwent radial endosonography (Olympus EUM-20, Olympus America, Lake Success, NY) followed by linear array endosonography (Pentax FG32-UA, Pentax, Orangeburg, NY, or Olympus GFUC-30P). Fine needle aspiration was accomplished using two different needle types: a 22-gauge, 8-cm, adjustable length needle (Wilson- Cook, Winston-Salem, NC) and a 22-gauge, 12-cm, adjustable length needle (GIP, Medi-Globe, Tempe, AZ). A cytopathologist was present in all cases to evaluate adequacy of each EUS-FNA sample. The impact of EUS-FNA results in terms of changing clinical management (theoretic vs actual plan), including eventual workup and treatment, was determined by each endoscopist for each individual case. The change in clinical management definition was the difference between the theoretical plan (pre-eus) and the actual plan (post-eus). As this was a retrospective study, ability of EUS to alter subsequent therapy and workup was based on a theoretical plan in the absence of EUS (i.e., CT-FNA, mediastinoscopy, or thoracotomy with biopsy to establish the diagnosis) and actual plan (after EUS-FNA). The latter included the diagnosis of malignancy with avoidance of surgery. Patients with nondiagnostic FNA had, by definition, failure of the study to alter subsequent therapy and workup. RESULTS Figure 1. Mediastinal masses of unknown cause: final diagnosis. All 26 patients underwent successful EUS-FNA tissue sampling (two to seven passes/patient). Histopathology was determined to be adequate by a bedside cytopathologist in all cases. Final patient diagnosis by disease category included five patients with benign/infectious masses, nine with inflammatory masses, and 12 with malignant mediastinal masses (Fig. 1). EUS-FNA was successful in establishing the diagnosis in 21 of 26 patients (81%) for all disease categories, including infectious in three of five patients (60%), benign/inflammatory in seven of nine patients (78%), and malignant mediastinal in 11 of 12 patients (92%). Final diagnosis by histopathology and special stains (Table 1) included the following: 1) infectious in five patients, including two abscess, two histoplasmosis, and one tuberculosis (by acid-fast staining); 2) benign/inflammatory in nine patients, including five cysts (bronchogenic and duplication), three fibrosis, and two nonspecific inflammatory masses; 3) malignant mediastinal (12 patients), including two adenocarcinoma of unknown primary (Fig. 2 4), four metastatic lung cancer (non small cell and small cell), three lymphoma (Fig. 5 7), two metastatic (tracheal and esophageal), and one papillary carcinoma of thyroid. Patients with lymphoma were established by presence of characteristic, small, morphologically identical lymphocytes with high nuclear to cytoplasmic ratio. Because this was suspicious for lymphoma, the bedside cytopathologist requested samples for flow cytometry. The five patients with duplication and bronchogenic cysts had classic appearance by endosonography (anechoic, thin walled structures adjacent to the esophageal lumen). FNA of the lesion, specifically the wall, and aspiration of fluid was performed for cytologic analysis given the presenting symptoms (including weight loss, chest pain, or fever). The ability of EUS-FNA to alter subsequent workup included three of five patients with infectious mediastinal masses (60%), six of nine patients with benign/inflammatory mediastinal masses (67%), and 11 of 12 patients with malignant mediastinal masses (92%). The ability of EUS-FNA to alter subsequent therapy included three of five patients with infectious mediastinal masses (60%), seven of nine patients with benign/inflammatory mediastinal masses (78%), and Table 1. Ability of EUS-FNA to Alter Subsequent Workup and Therapy Disease Classification Patients (n) EUS Final Diagnosis (%) Alters Workup Alters Therapy Infectious 5 3 (60%) 3 (60%) Benign/inflammatory 9 6 (67%) 7 (78%) Malignant mediastinal (92%) 9 (75%) Total (77%) 19 (73%)
3 AJG October, 2002 EUS-FNA in Diagnosis of Mediastinal Masses 2561 Figure 2. EUS demonstrating 4.2-cm mediastinal mass adjacent to the esophagus at 25-cm. LCA left carotid artery; LSV left subclavian vein; RCA right carotid artery. nine of 12 patients with malignant mediastinal masses (75%) (Table 1). EUS-FNA passes (mean) for adequate tissue sampling was lower in nonmalignant disease categories (3.0 and 3.4) versus malignant disease (4.4) but did not reach statistical significance. No complications were seen during the course of the study. DISCUSSION Mediastinal mass lesions represent a heterogenous group of tumors that can involve various components of the mediastinal space. They are most frequently located in the anterosuperior mediastinum (54%), with the posterior (26%) and middle mediastinum (20%) being less frequently involved. Figure 3. EUS-FNA of patient in Figure 1.
4 2562 Catalano et al. AJG Vol. 97, No. 10, 2002 Figure 4. Histology of patient in Figures 1 and 2 demonstrating adenocarcinoma. The masses that occur most commonly in each of the three anatomic subdivisions and the relative incidence with which they occur are shown in Table 2 (3). In the anterosuperior mediastinum, the most frequent neoplasms are thymoma (31%), lymphoma (23%), and germ cell tumor (17%). Posterior mediastinal lesions are usually neurogenic tumors (52%), bronchogenic cysts (22%), and enteric cysts (7%). Middle mediastinal masses are usually pericardial cysts (35%), lymphomas (21%), and bronchogenic cysts (15%). Overall, malignant neoplasms represent 25 42% of mediastinal masses (4). Because of the characteristic location of many mediastinal masses, the site of the mass establishes a useful differential diagnosis that aids in planning the diagnostic evaluation. Imaging-guided percutaneous transthoracic biopsy has become widely accepted. CT, an effective minimally invasive technique for the diagnosis of a variety of intrathoracic lesions that are otherwise not readily accessible, has been the preferred guidance modality for difficult parenchymal, hilar, and mediastinal lesions. The major drawback of CT guided biopsy is the lack of real-time guidance, the need to perform multiple section acquisitions, the longer procedure time, the inaccessibility of smaller lesions obstructed by overlying bone, and a higher frequency of pneumothorax. Alternatives to CT are more invasive. These include thoracoscopy, limited thoracotomy, cervical mediastinoscopy, anterior mediastinoscopy, bronchoscopy with transbronchial needle biopsy, and, more recently, EUS-FNA. Cervical mediastinoscopy has traditionally been considered as the gold standard complement to CT in the preoperative staging of the mediastinum in non small cell lung carcinoma. It provides access to paratracheal lymph nodes and, to a lesser extent, subcarinal lymph nodes. The major limitations are the poorly accessed aortopulmonary region, subcarinal lymph nodes, and the inferior mediastinum. Significant morbidity limits this high risk procedure. General anesthesia is preferred by the thoracic surgeon to provide better control and flexibility in terms of surgical manipulation. Anterior mediastinal masses may cause airway obstruction and cardiovascular collapse after induction of anesthesia. Contraindications include superior vena cava obstruction, tracheal deviation, and aneurysm of the thoracic aorta. Complications occur in up to 3.0%. Hemorrhage and pneumothorax are the most common. Not uncommon are recurrent laryngeal nerve injury, mediastinitis, hemothorax, and chylothorax (5). Inpatient recovery and cost further limit this modality. Recently, it has been shown that EUS may be used to Figure 5. EUS depicting a 4-cm mediastinal mass in a patient presenting with dysphagia and chest pain.
5 AJG October, 2002 EUS-FNA in Diagnosis of Mediastinal Masses 2563 Figure 6. EUS-FNA of patient represented in Figure 4. image the posterior mediastinum to evaluate periesophageal masses or to detect lymphadenopathy in patients with esophageal or non small cell lung cancer (6). EUS has been demonstrated to be superior to CT scanning in diagnosing local metastatic lymph nodes in patients with esophageal cancer (7, 8). EUS-FNA has also been shown to detect mediastinal sarcoidosis, silicoanthracosis, histoplasmosis, and retrosternal goiters (9). Unlike previously published articles on EUS-FNA of mediastinal masses and lymph nodes (2, 4, 10 12), our report details the evaluation and tissue sampling of nongastrointestinal lesions. Although some diagnoses demonstrated lymphatic origin, all cases had pre-eus CT describing the mass lesions in the absence of lymphadenopathy. The above-mentioned articles (2, 4, 10 12) collectively Figure 7. Histology of patient in Figures 4 and 5, demonstrating large cell lymphoma. reported on only 29 patients with mediastinal masses, a number similar to that in our current report. In a comprehensive report on EUS-FNA, Giovannini et al. (4) described the results of 141 consecutive patients, which included 18 with mediastinal masses. The accuracy for this indication was reportedly 89%. In their report, Hunerbein et al. (2) presented 25 patients with mediastinal lesions, including six patients with nonlymph node masses, all correctly diagnosed by EUS-FNA. Unlike our study, no attempt was made to describe the impact of accurate EUS Table 2. Anatomic Location of Primary Tumors and Cysts of the Mediastinum Type of Tumor/Cyst Percentage Anterosuperior mediastinum Thymic neoplasms 31 Lymphomas 23 Germ cell tumors (benign and malignant) 17 Carcinoma 13 Cysts 6 Mesenchymal 4 Endocrine 5 Other 1 Middle mediastinum Cysts 61 Lymphomas 20 Mesenchymal 8 Carcinoma 6 Other 5 Posterior mediastinum Neurogenic 52 Cysts 32 Mesenchymal 10 Other 6
6 2564 Catalano et al. AJG Vol. 97, No. 10, 2002 Table 3. Density and Topographical Approach for Classifying Mediastinal Masses Location Lipidic Liquid Vascular Soft Tissue Misc AM Thymolipoma Thymic/Pleural/pericardic cysts Goiter adenoma Thymoma MM Bronchogenic cyst Aortic arch aneurysm Lymph node PM Neurinoma, neurofibroma Meningocele Descending aortic Thrombotic aneurysm aneurysm Any Lipomatosis, teratoma Hydatic cyst Ganglioma Melanoma Lymph node mediastinitis AM Anterior mediastinum; Misc miscellaneous; MM middle mediastinum; PM posterior mediastinum. tissue sampling. Several unique features of endosonography make it favorable when specifically compared with CT imaging. Real-time visualization during the procedure permits continuous imaging assessment. EUS uses a multiplanar capability, which allows use of an oblique, angled approach if necessary. CT is limited somewhat by volume effects that occur because of discrete scan thickness. This is exemplified when attempting to visualize the region of the left atrium and the aortopulmonary window. In addition, problems with inadequate contrast or streak artifact generated from soft tissue-air interfaces with the main bronchi and trachea are not present with endosonography. Additionally, the principal complication of CT-guided biopsy is pneumothorax occurring in 25 43% of patients, which is somewhat higher than the average rate of approximately 25 30% after fluoroscopically guided thoracic biopsy (13). In a recent report by Panelli et al. (14), EUS was described to assist in the evaluation of mediastinal masses in 33 patients. Of these, only 25 had EUS-FNA. Three of these had a diagnosis of malignancy established by standard endoscopic biopsy, whereas eight others had FNA of malignant mediastinal lymph nodes. The remaining 14 patients had mediastinal masses diagnosed by EUS-FNA. The authors postulated that EUS-FNA provided a less invasive modality in establishing the diagnosis of mediastinal masses. We successfully used EUS-FNA to obtain diagnostic biopsies in 26 consecutive patients with idiopathic mediastinal masses. Our results show that EUS-FNA is a safe and effective guidance modality for transesophageal biopsy of mediastinal lesions. In fact, we were able to perform EUS- FNA with an overall accuracy of 81% for defining the cause of the mediastinal mass. A recent study to evaluate nodal spread in non small cell lung cancer used EUS-FNA to accurately differentiate benign from malignant nodal involvement in 84% of patients (6). These recent descriptions of real-time evaluation of mediastinal lesions further strengthen the clinical utility of this imaging technique. Performance of EUS-FNA relies heavily upon skilled endosonographers. A fundamental knowledge of the mediastinal anatomy and pathology that are unique to each compartment may help in determining the etiology (Table 3). With the exclusion of sampling error, it is unclear why the yield for malignant mediastinal lesions was higher than that for the benign/inflammatory or the infectious groups. This may have been the result of more FNA needle passes in malignant (mean 4.4) compared with benign (mean 3 and 3.4) disease categories. It is our experience that in patients with high index of suspicion for malignancy, either on the basis of clinical presentation or atypical cells obtained on initial FNA passes, more aggressive tissue sampling is performed. In our experience, FNA of any organ or tissue should be performed with an attendant cytopathologist or cytotechnologist who can readily examine specimens as they are aspirated. It is generally agreed that immediate feedback regarding the adequacy of aspirated materials for pathological diagnosis decreases the chance of a false negative diagnosis. We determined that the ability of EUS-FNA affected subsequent workup and therapy in 73% and 71% of patients, respectively. No complications occurred as a result of EUS- FNA. Specifically, there were no cases of mediastinitis as a result of transesophageal bacterial migration, contrary to what one might expect. Furthermore, no patients received prophylactic antibiotics, including the two patients with mediastinal abscesses. Although we cannot recommend the routine use of antibiotics, it seems prudent to use prophylactic antibiotics if the preprocedural index of suspicion for bacterial contamination is high (i.e., cystic lesions). Perhaps the only limitation of EUS are the regions of the anterior mediastinum and the contralateral trachea, both of which are of primary concern in patients with suspected lung cancer. This may have an impact on the role of EUS- FNA in preoperative staging of the mediastinum. Therefore, EUS-FNA should be considered in all patients with suspicious posterior mediastinal lesions and in those patients with an indeterminate result on CT (13). Anterior mediastinal lesions can be visualized in contrast to lymph nodes in this area because of marked size differences, and these masses are invariably paraesophageal (no air artifact between lesion and esophageal wall). Mediastinoscopy should be reserved for patients with enlarged anterior masses or for patients with suspicious lesions that are not successfully sampled by EUS. The current role of EUS-FNA to assess the mediastinum is limited by the availability of this application, combined with a lack of awareness of the technique on the part of thoracic surgeons and pulmonologists. As clinical algorithms regarding specific indications validate this approach,
7 AJG October, 2002 EUS-FNA in Diagnosis of Mediastinal Masses 2565 it is likely that EUS-FNA of idiopathic mediastinal lesions will play an increasing role. Reprint requests and correspondence: Marc F. Catalano, M.D., 2801 W. KK River Parkway, Suite 1030, Milwaukee, WI Received Feb. 7, 2001; accepted Apr. 26, REFERENCES 1. Hawes RH, Gress F, Kesler KA, et al. Endoscopic ultrasound versus computed tomography in the evaluation of the mediastinum in inpatients with non-small cell lung CA. Endoscopy 1994;26: Hunerbein M, Chadimi BM, Haensch W, Schlag PM. Transesophageal biopsy of mediastinal and pulmonary tumors by means of endoscopic ultrasound guidance. J Thorac Cardiovasc Surg 1998;116: Davis RD, Sabistan DC. Primary tumors and cysts of the mediosturum. In: Sabistan DC, Lyerly HK, eds. Textbook of surgery. WB Saunders, 1997: Giovannini M, Seitz JF, Monges G, et al. Fine needle aspiration cytology guided by endoscopic ultrasonography: Results in 141 patients. Endoscopy 1995;27: Eisenkraft JB, Coe NE, Caplin SA, et al. Cervical mediostinoscopy. In: Barash PG, Collen BF, Stoelting RK, eds. Clinical anesthesia. Lippincott: 1999: Gress F, Sividas TJ, Sandler A, et al. EUS/FNA biopsy guided by ultrasound and CT in the preop staging of non-small cell lung CA. A comparative study. Ann Intern Med 1997;127: Tio TL, Cohen P, Coene PP, et al. Endoscopic ultrasound and computed tomography in staging of esophageal carcinoma. Gastroenterology 1989;96: Botet JF, Lightdale CJ, Gellar A. Preoperative staging of esophageal carcinoma: Comparison of endoscopy ultrasound and dynamic CT. Radiology 1991;181: Wiersema MJ, Chak A, Lehman GA. Mediastinal histoplasmosis: Evaluation by EUS and EUS/FNA biopsy. Gastrointest Endosc 1994;40: Williams DB, Sahai AV, Aabakken L, et al. Endoscopic ultrasound guided fine needle aspiration biopsy: A large single centre experience. Gut 1999;44: Wiersema MJ, Harada N, Daiehagh P, et al. Evaluation of mediastinal lymphadenopathy with transesophageal endosonography guided fine needle aspiration biopsy. Acta Endoscopica 1998;28: Silvestri GA, Hoffman BJ, Bhutani MS, et al. Endoscopic ultrasound with fine needle aspiration in the diagnosis and staging of lung cancer. Ann Thorac Surg 1996;61: Gobien RD, Stanley JH, Vujic I, et al. Thoracic biopsy. CT guidance of thin-needle aspiration. Am J Radiology 1984;142: Panelli F, Erickson RA, Prasad VM. Evaluation of mediastinal masses by endoscopic ultrasound and ultrasound-guided fine needle aspiration. Am J Gastroenterology 2001;96:401 8.
Sectional Anatomy Quiz II
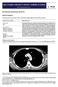 Sectional Anatomy II Rashid Hashmi Rural Clinical School, University of New South Wales, Wagga Wagga, New South Wales, Australia A R T I C L E I N F O Article type: Article history: Received: 3 Aug 2017
Sectional Anatomy II Rashid Hashmi Rural Clinical School, University of New South Wales, Wagga Wagga, New South Wales, Australia A R T I C L E I N F O Article type: Article history: Received: 3 Aug 2017
Mediastinal Tumors: Imaging
 Mediastinal Tumors: Imaging References Imaging in Oncology, Husband and Reznek Computed Tomography and Magnetic Resonance of the thorax, Naidich, Zerhouni, Siegelman, Mediastinal compartments Anterior:
Mediastinal Tumors: Imaging References Imaging in Oncology, Husband and Reznek Computed Tomography and Magnetic Resonance of the thorax, Naidich, Zerhouni, Siegelman, Mediastinal compartments Anterior:
Endoscopic Ultrasound-Guided Fine Needle Aspiration for Staging Patients With Carcinoma of the Lung
 Endoscopic Ultrasound-Guided Fine Needle Aspiration for Staging Patients With Carcinoma of the Lung Michael B. Wallace, MD, MPH, Gerard A. Silvestri, MD, MS, Anand V. Sahai, MD, MS (Epid), Robert H. Hawes,
Endoscopic Ultrasound-Guided Fine Needle Aspiration for Staging Patients With Carcinoma of the Lung Michael B. Wallace, MD, MPH, Gerard A. Silvestri, MD, MS, Anand V. Sahai, MD, MS (Epid), Robert H. Hawes,
Preoperative Evaluation of Lymph Node Metastasis in Esophageal Cancer
 Review Preoperative Evaluation of Lymph Node Metastasis in Esophageal Cancer Yoko Murata, Masaho Ohta, Kazuhiko Hayashi, Hiroko Ide, and Ken Takasaki Lymph node metastasis (LMN) in esophageal cancer occurs
Review Preoperative Evaluation of Lymph Node Metastasis in Esophageal Cancer Yoko Murata, Masaho Ohta, Kazuhiko Hayashi, Hiroko Ide, and Ken Takasaki Lymph node metastasis (LMN) in esophageal cancer occurs
Mediastinal Staging. Samer Kanaan, M.D.
 Mediastinal Staging Samer Kanaan, M.D. Overview Importance of accurate nodal staging Accuracy of radiographic staging Mediastinoscopy EUS EBUS Staging TNM Definitions T Stage Size of the Primary Tumor
Mediastinal Staging Samer Kanaan, M.D. Overview Importance of accurate nodal staging Accuracy of radiographic staging Mediastinoscopy EUS EBUS Staging TNM Definitions T Stage Size of the Primary Tumor
Karoline Nowillo, MD. February 1, 2008
 Case Presentation Karoline Nowillo, MD SUNY Downstate t February 1, 2008 Case Presentation Chief complaint enlarging goiter x 8 months History of present illness shortness of breath, heaviness in chest
Case Presentation Karoline Nowillo, MD SUNY Downstate t February 1, 2008 Case Presentation Chief complaint enlarging goiter x 8 months History of present illness shortness of breath, heaviness in chest
Diagnostic Value of EBUS-TBNA in Various Lung Diseases (Lymphoma, Tuberculosis, Sarcoidosis)
 Diagnostic Value of EBUS-TBNA in Various Lung Diseases (Lymphoma, Tuberculosis, Sarcoidosis) Sevda Sener Cömert, MD, FCCP. SBU, Kartal Dr.Lütfi Kırdar Training and Research Hospital Department of Pulmonary
Diagnostic Value of EBUS-TBNA in Various Lung Diseases (Lymphoma, Tuberculosis, Sarcoidosis) Sevda Sener Cömert, MD, FCCP. SBU, Kartal Dr.Lütfi Kırdar Training and Research Hospital Department of Pulmonary
MEDIASTINAL STAGING surgical pro
 MEDIASTINAL STAGING surgical pro Paul E. Van Schil, MD, PhD Department of Thoracic and Vascular Surgery University of Antwerp, Belgium Mediastinal staging Invasive techniques lymph node mapping cervical
MEDIASTINAL STAGING surgical pro Paul E. Van Schil, MD, PhD Department of Thoracic and Vascular Surgery University of Antwerp, Belgium Mediastinal staging Invasive techniques lymph node mapping cervical
Mediastinoscopy, Mediastinotomy And Thoracoscopy For Mediastinal Lesions. Alper Toker, MD
 Mediastinoscopy, Mediastinotomy And Thoracoscopy For Mediastinal Lesions Alper Toker, MD Istanbul University, Istanbul Medical School Department of Thoracic Surgery The mediastinum is a complex anatomic
Mediastinoscopy, Mediastinotomy And Thoracoscopy For Mediastinal Lesions Alper Toker, MD Istanbul University, Istanbul Medical School Department of Thoracic Surgery The mediastinum is a complex anatomic
Bronchogenic Carcinoma
 A 55-year-old construction worker has smoked 2 packs of ciggarettes daily for the past 25 years. He notes swelling in his upper extremity & face, along with dilated veins in this region. What is the most
A 55-year-old construction worker has smoked 2 packs of ciggarettes daily for the past 25 years. He notes swelling in his upper extremity & face, along with dilated veins in this region. What is the most
Endoscopic Ultrasound-Guided Fine- Needle Aspiration for Non-small Cell Lung Cancer Staging* A Systematic Review and Metaanalysis
 CHEST Endoscopic Ultrasound-Guided Fine- Needle Aspiration for Non-small Cell Lung Cancer Staging* A Systematic Review and Metaanalysis Carlos G. Micames, MD; Douglas C. McCrory, MD; Darren A. Pavey, MD;
CHEST Endoscopic Ultrasound-Guided Fine- Needle Aspiration for Non-small Cell Lung Cancer Staging* A Systematic Review and Metaanalysis Carlos G. Micames, MD; Douglas C. McCrory, MD; Darren A. Pavey, MD;
Basic Data. Sex:Male 31 years old Occupation: 搬家工人
 Basic Data Sex:Male 31 years old Occupation: 搬家工人 Chief Complaint Intermittent chest pain with shortness of breath for 2-3 months. Present Illness 4 months ago, he started having occasional chest pain
Basic Data Sex:Male 31 years old Occupation: 搬家工人 Chief Complaint Intermittent chest pain with shortness of breath for 2-3 months. Present Illness 4 months ago, he started having occasional chest pain
Hong Kong Society of Upper Gastrointestinal Surgeons CLINICAL MEETING 29 NOV 2012
 Hong Kong Society of Upper Gastrointestinal Surgeons CLINICAL MEETING 29 NOV 2012 Esophageal Leiomyoma Introduction Case presentation Operative video Discussion Esophageal Leiomyoma Benign tumors of the
Hong Kong Society of Upper Gastrointestinal Surgeons CLINICAL MEETING 29 NOV 2012 Esophageal Leiomyoma Introduction Case presentation Operative video Discussion Esophageal Leiomyoma Benign tumors of the
MEDIASTINAL LYMPH NODE METASTASIS IN PATIENTS WITH CLINICAL STAGE I PERIPHERAL NON-SMALL-CELL LUNG CANCER
 MEDIASTINAL LYMPH NODE METASTASIS IN PATIENTS WITH CLINICAL STAGE I PERIPHERAL NON-SMALL-CELL LUNG CANCER Tsuneyo Takizawa, MD a Masanori Terashima, MD a Teruaki Koike, MD a Hideki Akamatsu, MD a Yuzo
MEDIASTINAL LYMPH NODE METASTASIS IN PATIENTS WITH CLINICAL STAGE I PERIPHERAL NON-SMALL-CELL LUNG CANCER Tsuneyo Takizawa, MD a Masanori Terashima, MD a Teruaki Koike, MD a Hideki Akamatsu, MD a Yuzo
Esophageal seeding after endoscopic ultrasound-guided fine-needle aspiration of a mediastinal tumor
 Esophageal seeding after endoscopic ultrasound-guided fine-needle aspiration of a mediastinal tumor Authors Kensuke Yokoyama 1,JunUshio 1,NorikatsuNumao 1, Kiichi Tamada 1, Noriyoshi Fukushima 2, Alan
Esophageal seeding after endoscopic ultrasound-guided fine-needle aspiration of a mediastinal tumor Authors Kensuke Yokoyama 1,JunUshio 1,NorikatsuNumao 1, Kiichi Tamada 1, Noriyoshi Fukushima 2, Alan
Repeat Thyroid Nodule Fine-Needle Aspiration in Patients With Initial Benign Cytologic Results
 Anatomic Pathology / REPEAT THYROID FINE-NEEDLE ASPIRATION Repeat Thyroid Nodule Fine-Needle Aspiration in Patients With Initial Benign Cytologic Results Melina B. Flanagan, MD, MSPH, 1 N. Paul Ohori,
Anatomic Pathology / REPEAT THYROID FINE-NEEDLE ASPIRATION Repeat Thyroid Nodule Fine-Needle Aspiration in Patients With Initial Benign Cytologic Results Melina B. Flanagan, MD, MSPH, 1 N. Paul Ohori,
Evaluation of Neck Mass. Disclosure. Learning Objectives 3/24/2014. Karen T. Pitman MD, FACS Banner MDACC, Gilbert AZ. Nothing to disclose
 Evaluation of Neck Mass Karen T. Pitman MD, FACS Banner MDACC, Gilbert AZ Nothing to disclose Disclosure Learning Objectives 1. Describe a systematic method to evaluate a patient with a neck mass 2. Select
Evaluation of Neck Mass Karen T. Pitman MD, FACS Banner MDACC, Gilbert AZ Nothing to disclose Disclosure Learning Objectives 1. Describe a systematic method to evaluate a patient with a neck mass 2. Select
The Various Methods to Biopsy the Lung PROF SHITRIT DAVID HEAD, PULMONARY DEPARTMENT MEIR MEDICAL CENTER, ISRAEL
 The Various Methods to Biopsy the Lung PROF SHITRIT DAVID HEAD, PULMONARY DEPARTMENT MEIR MEDICAL CENTER, ISRAEL Conflict of Interest This presentation is supported by AstraZeneca Two main steps before
The Various Methods to Biopsy the Lung PROF SHITRIT DAVID HEAD, PULMONARY DEPARTMENT MEIR MEDICAL CENTER, ISRAEL Conflict of Interest This presentation is supported by AstraZeneca Two main steps before
Case of the Day Chest
 Case of the Day Chest Darin White MDCM FRCPC Department of Radiology, Mayo Clinic 76 th Annual Scientific Meeting Canadian Association of Radiologists Montreal, QC April 26, 2013 2013 MFMER slide-1 Disclosures
Case of the Day Chest Darin White MDCM FRCPC Department of Radiology, Mayo Clinic 76 th Annual Scientific Meeting Canadian Association of Radiologists Montreal, QC April 26, 2013 2013 MFMER slide-1 Disclosures
Transbronchial fine needle aspiration
 Thorax 1982;37 :270-274 Transbronchial fine needle aspiration J LEMER, E MALBERGER, R KONIG-NATIV From the Departments of Cardio-thoracic Surgery and Cytology, Rambam Medical Center, Haifa, Israel ABSTRACT
Thorax 1982;37 :270-274 Transbronchial fine needle aspiration J LEMER, E MALBERGER, R KONIG-NATIV From the Departments of Cardio-thoracic Surgery and Cytology, Rambam Medical Center, Haifa, Israel ABSTRACT
UCLA General Surgery Residency Program Rotation Educational Policy Goals and Objectives
 UPDATED: July 2009 ROTATION: THORACIC SURGERY UCLA General Surgery Residency Program ROTATION DIRECTOR: Mary Maish, M.D. CHIEF OF CARDIAC SURGERY: Robert Cameron, M.D. SITES: UCLA Medical Center - Westwood
UPDATED: July 2009 ROTATION: THORACIC SURGERY UCLA General Surgery Residency Program ROTATION DIRECTOR: Mary Maish, M.D. CHIEF OF CARDIAC SURGERY: Robert Cameron, M.D. SITES: UCLA Medical Center - Westwood
Video-Mediastinoscopy Thoracoscopy (VATS)
 Surgical techniques Video-Mediastinoscopy Thoracoscopy (VATS) Gunda Leschber Department of Thoracic Surgery ELK Berlin Chest Hospital, Berlin, Germany Teaching Hospital of Charité Universitätsmedizin Berlin
Surgical techniques Video-Mediastinoscopy Thoracoscopy (VATS) Gunda Leschber Department of Thoracic Surgery ELK Berlin Chest Hospital, Berlin, Germany Teaching Hospital of Charité Universitätsmedizin Berlin
A Study of Thyroid Swellings and Correlation between FNAC and Histopathology Results
 International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 6 Number 4 (2017) pp. 265-269 Journal homepage: http://www.ijcmas.com Original Research Article https://doi.org/10.20546/ijcmas.2017.604.030
International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 6 Number 4 (2017) pp. 265-269 Journal homepage: http://www.ijcmas.com Original Research Article https://doi.org/10.20546/ijcmas.2017.604.030
Assessing the lung and mediastinum in cancer-is tissue the issue? George Santis
 1 Assessing the lung and mediastinum in cancer-is tissue the issue? George Santis Optimal management of Cancer Histological diagnosis & accurate staging at presentation Molecular analysis of primary tumour
1 Assessing the lung and mediastinum in cancer-is tissue the issue? George Santis Optimal management of Cancer Histological diagnosis & accurate staging at presentation Molecular analysis of primary tumour
Endoscopic UltraSound (EUS) Endoscopic Mucosal Resection (EMR) Moishe Liberman Director C.E.T.O.C.
 Endoscopic UltraSound (EUS) Endoscopic Mucosal Resection (EMR) Moishe Liberman Director C.E.T.O.C. Division of Thoracic Surgery Centre Hospitalier de l Université de Montréal Research Grants: Disclosures
Endoscopic UltraSound (EUS) Endoscopic Mucosal Resection (EMR) Moishe Liberman Director C.E.T.O.C. Division of Thoracic Surgery Centre Hospitalier de l Université de Montréal Research Grants: Disclosures
Standardized transbronchial needle aspiration procedure for intrathoracic lymph node staging of non-small cell lung cancer
 Original Article on Transbronchial Needle Aspiration (TBNA) Standardized transbronchial needle aspiration procedure for intrathoracic lymph node staging of non-small cell lung cancer Xu-Ru Jin 1 *, Min
Original Article on Transbronchial Needle Aspiration (TBNA) Standardized transbronchial needle aspiration procedure for intrathoracic lymph node staging of non-small cell lung cancer Xu-Ru Jin 1 *, Min
Endobronchial Ultrasound in the Diagnosis & Staging of Lung Cancer
 Endobronchial Ultrasound in the Diagnosis & Staging of Lung Cancer Dr Richard Booton PhD FRCP Lead Lung Cancer Clinician, Consultant Respiratory Physician & Speciality Director Manchester University NHS
Endobronchial Ultrasound in the Diagnosis & Staging of Lung Cancer Dr Richard Booton PhD FRCP Lead Lung Cancer Clinician, Consultant Respiratory Physician & Speciality Director Manchester University NHS
Endoscopic Ultrasound With Fine-Needle Aspiration in the Diagnosis and Staging of Lung Cancer
 Endoscopic Ultrasound With Fine-Needle Aspiration in the Diagnosis and Staging of Lung Cancer Gerard A. Silvestri, MD, Brenda J. Hoffman, MD, Manoop S. Bhutani, MD, Robert H. Hawes, MD, Lynn Coppage, MD,
Endoscopic Ultrasound With Fine-Needle Aspiration in the Diagnosis and Staging of Lung Cancer Gerard A. Silvestri, MD, Brenda J. Hoffman, MD, Manoop S. Bhutani, MD, Robert H. Hawes, MD, Lynn Coppage, MD,
ROSE in EUS guided FNA of Pancreatic Lesions
 ROSE in EUS guided FNA of Pancreatic Lesions Guy s Hospital, London, 16 April 2018 Laxmi Batav Imperial College NHS Trust Imperial College NHS Trust Cytology Workload Cervical Cytology 57,500 (decreases
ROSE in EUS guided FNA of Pancreatic Lesions Guy s Hospital, London, 16 April 2018 Laxmi Batav Imperial College NHS Trust Imperial College NHS Trust Cytology Workload Cervical Cytology 57,500 (decreases
4/22/2010. Hakan Korkmaz, MD Assoc. Prof. of Otolaryngology Ankara Dıșkapı Training Hospital-Turkey.
 Management of Differentiated Thyroid Cancer: Head Neck Surgeon Perspective Hakan Korkmaz, MD Assoc. Prof. of Otolaryngology Ankara Dıșkapı Training Hospital-Turkey Thyroid gland Small endocrine gland:
Management of Differentiated Thyroid Cancer: Head Neck Surgeon Perspective Hakan Korkmaz, MD Assoc. Prof. of Otolaryngology Ankara Dıșkapı Training Hospital-Turkey Thyroid gland Small endocrine gland:
EBUS-TBNA in PET-positive lymphadenopathies in treated cancer patients
 ORIGINAL ARTICLE LUNG IMAGING EBUS-TBNA in PET-positive lymphadenopathies in treated cancer patients Juliana Guarize 1, Monica Casiraghi 1, Stefano Donghi 1, Chiara Casadio 2, Cristina Diotti 1, Niccolò
ORIGINAL ARTICLE LUNG IMAGING EBUS-TBNA in PET-positive lymphadenopathies in treated cancer patients Juliana Guarize 1, Monica Casiraghi 1, Stefano Donghi 1, Chiara Casadio 2, Cristina Diotti 1, Niccolò
Diagnostic and Complication Rate of Image-guided Lung Biopsies in Raigmore Hospital, Inverness: A Retrospective Re-audit
 Page1 Original Article NJR 2011;1(1):1 7;Available online at www.nranepal.org Diagnostic and Complication Rate of Image-guided Lung Biopsies in Raigmore Hospital, Inverness: A Retrospective Re-audit S
Page1 Original Article NJR 2011;1(1):1 7;Available online at www.nranepal.org Diagnostic and Complication Rate of Image-guided Lung Biopsies in Raigmore Hospital, Inverness: A Retrospective Re-audit S
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of endobronchial ultrasound-guided transbronchial needle aspiration for mediastinal
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of endobronchial ultrasound-guided transbronchial needle aspiration for mediastinal
VOLUME 19 NUMBER 2 * FEBRUARY 1975
 THE ANNALS OF THORACIC SURGERY Journal of The Society of Thoracic Surgeons and the Southern Thoracic Surgical Association VOLUME 9 NUMBER 2 * FEBRUARY 975 Medias tinoscopy Its Application in Central Versus
THE ANNALS OF THORACIC SURGERY Journal of The Society of Thoracic Surgeons and the Southern Thoracic Surgical Association VOLUME 9 NUMBER 2 * FEBRUARY 975 Medias tinoscopy Its Application in Central Versus
In 1982 Pearson and colleagues [1] from Toronto published
![In 1982 Pearson and colleagues [1] from Toronto published In 1982 Pearson and colleagues [1] from Toronto published](/thumbs/95/124110746.jpg) Transition From Mediastinoscopy to Endoscopic Ultrasound for Lung Cancer Staging Mark I. Block, MD Division of Thoracic Surgery, Memorial Healthcare System, Hollywood, Florida Background. Esophageal endoscopic
Transition From Mediastinoscopy to Endoscopic Ultrasound for Lung Cancer Staging Mark I. Block, MD Division of Thoracic Surgery, Memorial Healthcare System, Hollywood, Florida Background. Esophageal endoscopic
5/18/2013. Most thyroid nodules are benign. Thyroid nodules: new techniques in evaluation
 Most thyroid nodules are benign Thyroid nodules: new techniques in evaluation Incidence Etiology Risk factors Diagnosis Gene classification system Treatment Postgraduate Course in General Surgery Jessica
Most thyroid nodules are benign Thyroid nodules: new techniques in evaluation Incidence Etiology Risk factors Diagnosis Gene classification system Treatment Postgraduate Course in General Surgery Jessica
Lecture 2: Clinical anatomy of thoracic cage and cavity II
 Lecture 2: Clinical anatomy of thoracic cage and cavity II Dr. Rehan Asad At the end of this session, the student should be able to: Identify and discuss clinical anatomy of mediastinum such as its deflection,
Lecture 2: Clinical anatomy of thoracic cage and cavity II Dr. Rehan Asad At the end of this session, the student should be able to: Identify and discuss clinical anatomy of mediastinum such as its deflection,
Use and Abuse of Onsite Adequacy for EUS-FNA of the Pancreas
 Use and Abuse of Onsite Adequacy for EUS-FNA of the Pancreas Nirag Jhala MD Director of Cytopathology Perelman Center for Advanced Medicine Surgical Pathologist- GI Subspecialty Dept of Path and Lab Medicine
Use and Abuse of Onsite Adequacy for EUS-FNA of the Pancreas Nirag Jhala MD Director of Cytopathology Perelman Center for Advanced Medicine Surgical Pathologist- GI Subspecialty Dept of Path and Lab Medicine
Case Scenario 1. The patient has now completed his neoadjuvant chemoradiation and has been cleared for surgery.
 Case Scenario 1 July 10, 2010 A 67-year-old male with squamous cell carcinoma of the mid thoracic esophagus presents for surgical resection. The patient has completed preoperative chemoradiation. This
Case Scenario 1 July 10, 2010 A 67-year-old male with squamous cell carcinoma of the mid thoracic esophagus presents for surgical resection. The patient has completed preoperative chemoradiation. This
Thyroid nodules 3/22/2011. Most thyroid nodules are benign. Thyroid nodules: differential diagnosis
 Most thyroid nodules are benign Thyroid nodules Postgraduate Course in General Surgery thyroid nodules occur in 77% of the world s population palpable thyroid nodules occur in about 5% of women and 1%
Most thyroid nodules are benign Thyroid nodules Postgraduate Course in General Surgery thyroid nodules occur in 77% of the world s population palpable thyroid nodules occur in about 5% of women and 1%
Thyroid Ultrasound for the Endocrine Surgeon: A Valuable Clinical Tool that Enhances Diagnostic and Therapeutic Outcomes
 Thyroid Ultrasound for the Endocrine Surgeon: A Valuable Clinical Tool that Enhances Diagnostic and Therapeutic Outcomes Allan Siperstein MD The Cleveland Clinic Audience Quiz Taken ultrasound course Perform
Thyroid Ultrasound for the Endocrine Surgeon: A Valuable Clinical Tool that Enhances Diagnostic and Therapeutic Outcomes Allan Siperstein MD The Cleveland Clinic Audience Quiz Taken ultrasound course Perform
CT Chest. Verification of an opacity seen on the straight chest X ray
 CT Chest Indications: To assess equivocal plain x-ray findings Staging of lung neoplasm Merastatic workup of extra thoraces malignancies Diagnosis of diffuse lung diseases with HRCT Assessment of bronchietasis
CT Chest Indications: To assess equivocal plain x-ray findings Staging of lung neoplasm Merastatic workup of extra thoraces malignancies Diagnosis of diffuse lung diseases with HRCT Assessment of bronchietasis
Primary mediastinal tumours
 Primary mediastinal tumours Thorax (1974), 29, 475. YOUSF D. AL-NAAMAN, MOHAMAD S. AL-AN, and MUAYYAD M. AL-OMER Department of Thoracic and Cardiovascular Surgery, College of Medicine, University of Baghdad,
Primary mediastinal tumours Thorax (1974), 29, 475. YOUSF D. AL-NAAMAN, MOHAMAD S. AL-AN, and MUAYYAD M. AL-OMER Department of Thoracic and Cardiovascular Surgery, College of Medicine, University of Baghdad,
Joseph B. Zwischenberger, MD, FCCP; Clare Savage, MD; Scott K. Alpard, BA; Carryn M. Anderson, BA; Santiago Marroquin, MD; and Brian W.
 Mediastinal Transthoracic Needle and Core Lymph Node Biopsy* Should It Replace Mediastinoscopy? Joseph B. Zwischenberger, MD, FCCP; Clare Savage, MD; Scott K. Alpard, BA; Carryn M. Anderson, BA; Santiago
Mediastinal Transthoracic Needle and Core Lymph Node Biopsy* Should It Replace Mediastinoscopy? Joseph B. Zwischenberger, MD, FCCP; Clare Savage, MD; Scott K. Alpard, BA; Carryn M. Anderson, BA; Santiago
Endoscopic ultrasonography in suspected pancreatic malignancy and indecisive CT
 O r i g i n a l a r t i c l e Endoscopic ultrasonography in suspected pancreatic malignancy and indecisive CT O.L.M. Meijer 1, R.K. Weersma 1, E.J. van der Jagt 2, H.M. van Dullemen 1 * Departments of
O r i g i n a l a r t i c l e Endoscopic ultrasonography in suspected pancreatic malignancy and indecisive CT O.L.M. Meijer 1, R.K. Weersma 1, E.J. van der Jagt 2, H.M. van Dullemen 1 * Departments of
May 2017 Imaging Case of the Month. Prasad M. Panse, MD and Michael B. Gotway, MD. Department of Radiology Mayo Clinic Arizona Scottsdale, Arizona USA
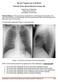 May 2017 Imaging Case of the Month Prasad M. Panse, MD and Michael B. Gotway, MD Department of Radiology Mayo Clinic Arizona Scottsdale, Arizona USA Clinical History: A 32-year-old man presented for routine
May 2017 Imaging Case of the Month Prasad M. Panse, MD and Michael B. Gotway, MD Department of Radiology Mayo Clinic Arizona Scottsdale, Arizona USA Clinical History: A 32-year-old man presented for routine
Case Scenario 1. The patient agreed to a CT guided biopsy of the left upper lobe mass. This was performed and confirmed non-small cell carcinoma.
 Case Scenario 1 An 89 year old male patient presented with a progressive cough for approximately six weeks for which he received approximately three rounds of antibiotic therapy without response. A chest
Case Scenario 1 An 89 year old male patient presented with a progressive cough for approximately six weeks for which he received approximately three rounds of antibiotic therapy without response. A chest
Radiology Pathology Conference
 Radiology Pathology Conference Sharlin Johnykutty,, MD, Cytopathology Fellow Sara Majewski, MD, Radiology Resident Friday, August 28, 2009 Presentation material is for education purposes only. All rights
Radiology Pathology Conference Sharlin Johnykutty,, MD, Cytopathology Fellow Sara Majewski, MD, Radiology Resident Friday, August 28, 2009 Presentation material is for education purposes only. All rights
Thyroid nodules. Most thyroid nodules are benign
 Thyroid nodules Postgraduate Course in General Surgery Jessica E. Gosnell MD Assistant Professor March 22, 2011 Most thyroid nodules are benign thyroid nodules occur in 77% of the world s population palpable
Thyroid nodules Postgraduate Course in General Surgery Jessica E. Gosnell MD Assistant Professor March 22, 2011 Most thyroid nodules are benign thyroid nodules occur in 77% of the world s population palpable
Volume 2 Issue ISSN
 Volume 2 Issue 3 2012 ISSN 2250-0359 Correlation of fine needle aspiration and final histopathology in thyroid disease: a series of 702 patients managed in an endocrine surgical unit *Chandrasekaran Maharajan
Volume 2 Issue 3 2012 ISSN 2250-0359 Correlation of fine needle aspiration and final histopathology in thyroid disease: a series of 702 patients managed in an endocrine surgical unit *Chandrasekaran Maharajan
Preoperative Evaluation
 Preoperative Evaluation Lateral compartment lymph nodes are easier to detect and are amenable to FNA Central compartment lymph nodes are much more difficult to detect and FNA (Tg washout testing is compromised)
Preoperative Evaluation Lateral compartment lymph nodes are easier to detect and are amenable to FNA Central compartment lymph nodes are much more difficult to detect and FNA (Tg washout testing is compromised)
Pathology of Mediastinal Tumors
 SAMO Meeting Lucerne 2009 Pathology of Mediastinal Tumors Alex Soltermann Most common lesions (adults) Clinical presentation 50% of the patients are asymptomatic, lesion discovered incidentally Symptoms
SAMO Meeting Lucerne 2009 Pathology of Mediastinal Tumors Alex Soltermann Most common lesions (adults) Clinical presentation 50% of the patients are asymptomatic, lesion discovered incidentally Symptoms
Reoperative central neck surgery
 Reoperative central neck surgery R. Pandev, I. Tersiev, M. Belitova, A. Kouizi, D. Damyanov University Clinic of Surgery, Section Endocrine Surgery University Hospital Queen Johanna ISUL Medical University
Reoperative central neck surgery R. Pandev, I. Tersiev, M. Belitova, A. Kouizi, D. Damyanov University Clinic of Surgery, Section Endocrine Surgery University Hospital Queen Johanna ISUL Medical University
Thyroid Neoplasm. ORL-Head and neck Surgery 2014
 In The Name of God Thyroid Neoplasm ORL-Head and neck Surgery 2014 Malignant Neoplasm By age 90, virtually everyone has nodules Estimates of cancer prevalence at autopsy 4% to 36% Why these lesions are
In The Name of God Thyroid Neoplasm ORL-Head and neck Surgery 2014 Malignant Neoplasm By age 90, virtually everyone has nodules Estimates of cancer prevalence at autopsy 4% to 36% Why these lesions are
Update on Thyroid FNA The Bethesda System. Shikha Bose M.D. Associate Professor Cedars Sinai Medical Center
 Update on Thyroid FNA The Bethesda System Shikha Bose M.D. Associate Professor Cedars Sinai Medical Center Thyroid Nodules Frequent occurrence Palpable: 4-7% of adults Ultrasound: 10-31% Majority benign
Update on Thyroid FNA The Bethesda System Shikha Bose M.D. Associate Professor Cedars Sinai Medical Center Thyroid Nodules Frequent occurrence Palpable: 4-7% of adults Ultrasound: 10-31% Majority benign
Respiratory Interactive Session. Elaine Borg
 Respiratory Interactive Session Elaine Borg Case 1 Respiratory Cytology 55 year old gentleman Anterior mediastinal mass EBUS FNA Case 1 Respiratory Cytology 55 year old gentleman with anterior mediastinal
Respiratory Interactive Session Elaine Borg Case 1 Respiratory Cytology 55 year old gentleman Anterior mediastinal mass EBUS FNA Case 1 Respiratory Cytology 55 year old gentleman with anterior mediastinal
Endoscopic Ultrasonography Clinical Impact. Giancarlo Caletti. Gastroenterologia Università di Bologna. Caletti
 Clinical Impact Giancarlo Gastroenterologia Università di Bologna AUSL di Imola,, Castel S. Pietro Terme (BO) 1982 Indications Diagnosis of Submucosal Tumors (SMT) Staging of Neoplasms Evaluation of Pancreato-Biliary
Clinical Impact Giancarlo Gastroenterologia Università di Bologna AUSL di Imola,, Castel S. Pietro Terme (BO) 1982 Indications Diagnosis of Submucosal Tumors (SMT) Staging of Neoplasms Evaluation of Pancreato-Biliary
Improving the Inaccuracies of Clinical Staging of Patients with NSCLC: A Prospective Trial
 Improving the Inaccuracies of Clinical Staging of Patients with NSCLC: A Prospective Trial Robert James Cerfolio, MD, FACS, Ayesha S. Bryant, MD, MSPH, Buddhiwardhan Ojha, MD, MPH, and Mohammad Eloubeidi,
Improving the Inaccuracies of Clinical Staging of Patients with NSCLC: A Prospective Trial Robert James Cerfolio, MD, FACS, Ayesha S. Bryant, MD, MSPH, Buddhiwardhan Ojha, MD, MPH, and Mohammad Eloubeidi,
Vishnu Sharma M 1*, Janso Kollanur 1, Manjunath. M 1, Alka C Bhat 1, V.Viswambhar 2
 e - ISSN - 2349-8005 INTERNATIONAL JOURNAL OF ADVANCES IN CASE REPORTS Journal homepage: www.mcmed.us/journal/ijacr ELDERLY SMOKER WITH LEFT SIDED CHEST PAIN Vishnu Sharma M 1*, Janso Kollanur 1, Manjunath.
e - ISSN - 2349-8005 INTERNATIONAL JOURNAL OF ADVANCES IN CASE REPORTS Journal homepage: www.mcmed.us/journal/ijacr ELDERLY SMOKER WITH LEFT SIDED CHEST PAIN Vishnu Sharma M 1*, Janso Kollanur 1, Manjunath.
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 4/30/2011 Radiology Quiz of the Week # 18 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 4/30/2011 Radiology Quiz of the Week # 18 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Ultrasound for Pre-operative Evaluation of Well Differentiated Thyroid Cancer
 Ultrasound for Pre-operative Evaluation of Well Differentiated Thyroid Cancer Its Not Just About the Nodes AACE Advances in Medical and Surgical Management of Thyroid Cancer - 2017 Robert A. Levine, MD,
Ultrasound for Pre-operative Evaluation of Well Differentiated Thyroid Cancer Its Not Just About the Nodes AACE Advances in Medical and Surgical Management of Thyroid Cancer - 2017 Robert A. Levine, MD,
Mediastinal lymphadenopathy is a common finding in
 ORIGINAL ARTICLE Endobronchial Ultrasound-Guided Transbronchial Needle Aspiration for the Diagnosis of Intrathoracic Lymphadenopathy in Patients with Extrathoracic Malignancy A Multicenter Study Neal Navani,
ORIGINAL ARTICLE Endobronchial Ultrasound-Guided Transbronchial Needle Aspiration for the Diagnosis of Intrathoracic Lymphadenopathy in Patients with Extrathoracic Malignancy A Multicenter Study Neal Navani,
Research Article The Utility of Repeat Endoscopic Ultrasound-Guided Fine Needle Aspiration for Suspected Pancreatic Cancer
 Gastroenterology Research and Practice Volume 2010, Article ID 268290, 4 pages doi:10.1155/2010/268290 Research Article The Utility of Repeat Endoscopic Ultrasound-Guided Fine Needle Aspiration for Suspected
Gastroenterology Research and Practice Volume 2010, Article ID 268290, 4 pages doi:10.1155/2010/268290 Research Article The Utility of Repeat Endoscopic Ultrasound-Guided Fine Needle Aspiration for Suspected
Sectional Anatomy Quiz - III
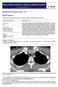 Sectional Anatomy - III Rashid Hashmi * Rural Clinical School, University of New South Wales (UNSW), Wagga Wagga, NSW, Australia A R T I C L E I N F O Article type: Article history: Received: 30 Jun 2018
Sectional Anatomy - III Rashid Hashmi * Rural Clinical School, University of New South Wales (UNSW), Wagga Wagga, NSW, Australia A R T I C L E I N F O Article type: Article history: Received: 30 Jun 2018
Utilizing EBUS (Endobronchial Ultrasound) for Diagnosis of Lung Cancer and other Pulmonary Diseases
 Utilizing EBUS (Endobronchial Ultrasound) for Diagnosis of Lung Cancer and other Pulmonary Diseases Akintayo Sokunbi, M.D MidMichigan Hospital Midland, Michigan Objectives Discuss EBUS guided biopsy principles
Utilizing EBUS (Endobronchial Ultrasound) for Diagnosis of Lung Cancer and other Pulmonary Diseases Akintayo Sokunbi, M.D MidMichigan Hospital Midland, Michigan Objectives Discuss EBUS guided biopsy principles
ACG Clinical Guideline: Diagnosis and Management of Pancreatic Cysts
 ACG Clinical Guideline: Diagnosis and Management of Pancreatic Cysts Grace H. Elta, MD, FACG 1, Brintha K. Enestvedt, MD, MBA 2, Bryan G. Sauer, MD, MSc, FACG (GRADE Methodologist) 3 and Anne Marie Lennon,
ACG Clinical Guideline: Diagnosis and Management of Pancreatic Cysts Grace H. Elta, MD, FACG 1, Brintha K. Enestvedt, MD, MBA 2, Bryan G. Sauer, MD, MSc, FACG (GRADE Methodologist) 3 and Anne Marie Lennon,
Thoracic Surgery; An Overview
 Thoracic Surgery What we see Thoracic Surgery; An Overview James P. Locher, Jr, MD Methodist Cardiovascular and Thoracic Surgery Lung cancer Mets Fungus and TB Lung abcess and empyema Pleural based disease
Thoracic Surgery What we see Thoracic Surgery; An Overview James P. Locher, Jr, MD Methodist Cardiovascular and Thoracic Surgery Lung cancer Mets Fungus and TB Lung abcess and empyema Pleural based disease
Appendix 9: Endoscopic Ultrasound in Gastroenterology
 Appendix 9: Endoscopic Ultrasound in Gastroenterology This curriculum is intended for clinicians who perform endoscopic ultrasonography (EUS) in gastroenterology. It includes standards for theoretical
Appendix 9: Endoscopic Ultrasound in Gastroenterology This curriculum is intended for clinicians who perform endoscopic ultrasonography (EUS) in gastroenterology. It includes standards for theoretical
Endoscopic Ultrasound and Positron Emission Tomography for Lung Cancer Staging
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2006;4:846 851 Endoscopic Ultrasound and Positron Emission Tomography for Lung Cancer Staging MANDEEP S. SAWHNEY,*, ROBERT A. KRATZKE, FRANK A. LEDERLE, AMY M.
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2006;4:846 851 Endoscopic Ultrasound and Positron Emission Tomography for Lung Cancer Staging MANDEEP S. SAWHNEY,*, ROBERT A. KRATZKE, FRANK A. LEDERLE, AMY M.
Thyroid Nodule. Disclosure. Learning Objectives P A P A P A 3/18/2014. Nothing to disclose.
 Thyroid Nodule Evaluating the patient with a thyroid nodule and some management options. Miguel V. Valdez PA C Disclosure Nothing to disclose. Learning Objectives Examination of thyroid gland Options for
Thyroid Nodule Evaluating the patient with a thyroid nodule and some management options. Miguel V. Valdez PA C Disclosure Nothing to disclose. Learning Objectives Examination of thyroid gland Options for
Undergraduate Teaching
 Prof. James F Meaney Undergraduate Teaching Chest X-Ray Understanding the normal anatomical by reference to cross sectional imaging Radiology? It s FUN! Cryptic puzzle Sudoku (Minecraft?) It s completely
Prof. James F Meaney Undergraduate Teaching Chest X-Ray Understanding the normal anatomical by reference to cross sectional imaging Radiology? It s FUN! Cryptic puzzle Sudoku (Minecraft?) It s completely
SETTING Fudan University Shanghai Cancer Center. RESPONSIBLE PARTY Haiquan Chen MD.
 OFFICIAL TITLE A Phase Ⅲ Study of Left Side Thoracotomy Approach (SweetProcedure) Versus Right Side Thoracotomy Plus Midline Laparotomy Approach (Ivor-Lewis Procedure) Esophagectomy in Middle or Lower
OFFICIAL TITLE A Phase Ⅲ Study of Left Side Thoracotomy Approach (SweetProcedure) Versus Right Side Thoracotomy Plus Midline Laparotomy Approach (Ivor-Lewis Procedure) Esophagectomy in Middle or Lower
Large veins of the thorax Brachiocephalic veins
 Large veins of the thorax Brachiocephalic veins Right brachiocephalic vein: formed at the root of the neck by the union of the right subclavian & the right internal jugular veins. Left brachiocephalic
Large veins of the thorax Brachiocephalic veins Right brachiocephalic vein: formed at the root of the neck by the union of the right subclavian & the right internal jugular veins. Left brachiocephalic
Endoscopic Ultrasound-Guided Fine-Needle Aspiration in Patients With Non-Small Cell Lung Cancer and Prior Negative Mediastinoscopy
 Endoscopic Ultrasound-Guided Fine-Needle Aspiration in Patients With Non-Small Cell Lung Cancer and Prior Negative Mediastinoscopy Mohamad A. Eloubeidi, MD, MHS, Ashutosh Tamhane, MD, MSPH, Victor K. Chen,
Endoscopic Ultrasound-Guided Fine-Needle Aspiration in Patients With Non-Small Cell Lung Cancer and Prior Negative Mediastinoscopy Mohamad A. Eloubeidi, MD, MHS, Ashutosh Tamhane, MD, MSPH, Victor K. Chen,
performed to help sway the clinician in what the appropriate diagnosis is, which can substantially alter the treatment of management.
 Hello, I am Maura Polansky at the University of Texas MD Anderson Cancer Center. I am a Physician Assistant in the Department of Gastrointestinal Medical Oncology and the Program Director for Physician
Hello, I am Maura Polansky at the University of Texas MD Anderson Cancer Center. I am a Physician Assistant in the Department of Gastrointestinal Medical Oncology and the Program Director for Physician
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/44702 holds various files of this Leiden University dissertation. Author: Von Bartheld, M.B. Title: Advancements in pulmonary endosonography : the new standard
Cover Page The handle http://hdl.handle.net/1887/44702 holds various files of this Leiden University dissertation. Author: Von Bartheld, M.B. Title: Advancements in pulmonary endosonography : the new standard
VIDEO-ASSISTED MEDIASTINOSCOPY FOR MEDIASTINAL STAGING OF LUNG CANCER
 VIDEO-ASSISTED MEDIASTINOSCOPY FOR MEDIASTINAL STAGING OF LUNG CANCER Christophoros N. Foroulis Associate Professor of Thoracic Surgery Aristotle University of Thessaloniki 1 st International Course on
VIDEO-ASSISTED MEDIASTINOSCOPY FOR MEDIASTINAL STAGING OF LUNG CANCER Christophoros N. Foroulis Associate Professor of Thoracic Surgery Aristotle University of Thessaloniki 1 st International Course on
Thyroid nodules - medical and surgical management. Endocrinology and Endocrine Surgery Manchester Royal Infirmary
 Thyroid nodules - medical and surgical management JRE Davis NR Parrott Endocrinology and Endocrine Surgery Manchester Royal Infirmary Thyroid nodules - prevalence Thyroid nodules common, increase with
Thyroid nodules - medical and surgical management JRE Davis NR Parrott Endocrinology and Endocrine Surgery Manchester Royal Infirmary Thyroid nodules - prevalence Thyroid nodules common, increase with
Role of EBUS in mediastinal staging of lung cancer. -Dr. Nandakishore Baikunje
 Role of EBUS in mediastinal staging of lung cancer -Dr. Nandakishore Baikunje Overview of the seminar Introduction Endosonography to stage the mediastinum Technical aspects of EBUS-TBNA for mediastinal
Role of EBUS in mediastinal staging of lung cancer -Dr. Nandakishore Baikunje Overview of the seminar Introduction Endosonography to stage the mediastinum Technical aspects of EBUS-TBNA for mediastinal
Pulmonary Sarcoidosis - Radiological Evaluation
 Original Research Article Pulmonary Sarcoidosis - Radiological Evaluation Jayesh Shah 1, Darshan Shah 2*, C. Raychaudhuri 3 1 Associate Professor, 2 1 st Year Resident, 3 Professor and HOD Radiology Department,
Original Research Article Pulmonary Sarcoidosis - Radiological Evaluation Jayesh Shah 1, Darshan Shah 2*, C. Raychaudhuri 3 1 Associate Professor, 2 1 st Year Resident, 3 Professor and HOD Radiology Department,
Bronchoscopy and endobronchial ultrasound for diagnosis and staging of lung cancer
 FRANCISCO AÉCIO ALMEIDA, MD, MS, FCCP Associate Staff Member, Director, Interventional Pulmonary Medicine Fellowship Program, Respiratory Institute, Cleveland Clinic, Cleveland, OH Bronchoscopy and endobronchial
FRANCISCO AÉCIO ALMEIDA, MD, MS, FCCP Associate Staff Member, Director, Interventional Pulmonary Medicine Fellowship Program, Respiratory Institute, Cleveland Clinic, Cleveland, OH Bronchoscopy and endobronchial
Radiology Pathology Conference
 Radiology Pathology Conference Nadia F. Yusaf, M.D. PGY-3 1/29/2010 Presentation material is for education purposes only. All rights reserved. 2010 URMC Radiology Page 1 of 90 Case 1 60 year- old man presents
Radiology Pathology Conference Nadia F. Yusaf, M.D. PGY-3 1/29/2010 Presentation material is for education purposes only. All rights reserved. 2010 URMC Radiology Page 1 of 90 Case 1 60 year- old man presents
Endoscopic ultrasound-guided needle aspiration in lung cancer
 ORIGINAL ARTICLE Artur Szlubowski 1, Marcin Zieliński 1, Joanna Figura 1, Jolanta Hauer 1, Witold Sośnicki 1, Juliusz Pankowski 2, Anna Obrochta 2, Magdalena Jakubiak 2 1 Department of Thoracic Surgery
ORIGINAL ARTICLE Artur Szlubowski 1, Marcin Zieliński 1, Joanna Figura 1, Jolanta Hauer 1, Witold Sośnicki 1, Juliusz Pankowski 2, Anna Obrochta 2, Magdalena Jakubiak 2 1 Department of Thoracic Surgery
The diagnostic efficacy and safety of endobronchial ultrasound-guided transbronchial needle aspiration as an initial diagnostic tool
 ORIGINAL ARTICLE Korean J Intern Med 2013;28.660-667 The diagnostic efficacy and safety of endobronchial ultrasound-guided transbronchial needle aspiration as an initial diagnostic tool Young Rak Choi
ORIGINAL ARTICLE Korean J Intern Med 2013;28.660-667 The diagnostic efficacy and safety of endobronchial ultrasound-guided transbronchial needle aspiration as an initial diagnostic tool Young Rak Choi
Lung Cancer - Suspected
 Lung Cancer - Suspected Shared Decision Making Lung Cancer: http://www.enhertsccg.nhs.uk/ Patient presents with abnormal CXR Lung cancer - clinical presentation History and Examination Incidental finding
Lung Cancer - Suspected Shared Decision Making Lung Cancer: http://www.enhertsccg.nhs.uk/ Patient presents with abnormal CXR Lung cancer - clinical presentation History and Examination Incidental finding
UNDERSTANDING SERIES LUNG CANCER BIOPSIES LungCancerAlliance.org
 UNDERSTANDING SERIES LUNG CANCER BIOPSIES 1-800-298-2436 LungCancerAlliance.org CONTENTS What is a Biopsy?...2 Non-Surgical Biopsies...3 Surgical Biopsies...5 Biopsy Risks...6 Biopsy Results...6 Questions
UNDERSTANDING SERIES LUNG CANCER BIOPSIES 1-800-298-2436 LungCancerAlliance.org CONTENTS What is a Biopsy?...2 Non-Surgical Biopsies...3 Surgical Biopsies...5 Biopsy Risks...6 Biopsy Results...6 Questions
Ultrasonography of the Neck as an Adjunct to FNA. Nicole Massoll M.D.
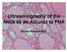 Ultrasonography of the Neck as an Adjunct to FNA Nicole Massoll M.D. Basic Features of Head and Neck Ultrasound and Anatomy Nicole Massoll M.D. University of Arkansas for Medical Sciences, Little Rock
Ultrasonography of the Neck as an Adjunct to FNA Nicole Massoll M.D. Basic Features of Head and Neck Ultrasound and Anatomy Nicole Massoll M.D. University of Arkansas for Medical Sciences, Little Rock
Minimally Invasive Mediastinal Staging of Non Small-Cell Lung Cancer: Emphasis on Ultrasonography-Guided Fine-Needle Aspiration
 Endobronchial ultrasound and endoscopic ultrasound-guided lymph node biopsy may represent an alternative to cervical mediastinoscopy. Dorothy Fox, Rough Seas. Acrylic on canvas, 36ʺ 36ʺ. Minimally Invasive
Endobronchial ultrasound and endoscopic ultrasound-guided lymph node biopsy may represent an alternative to cervical mediastinoscopy. Dorothy Fox, Rough Seas. Acrylic on canvas, 36ʺ 36ʺ. Minimally Invasive
Accurate mediastinal staging is a critical component
 Endobronchial Ultrasound for Lung Cancer Staging: How Many Stations Should Be Sampled? Mark I. Block, MD Thoracic Surgery, Memorial Healthcare System, Hollywood, Florida Background. No guidelines exist
Endobronchial Ultrasound for Lung Cancer Staging: How Many Stations Should Be Sampled? Mark I. Block, MD Thoracic Surgery, Memorial Healthcare System, Hollywood, Florida Background. No guidelines exist
GUIDELINE RECOMMENDATIONS
 European Journal of Cardio-Thoracic Surgery 48 (2015) 1 15 doi:10.1093/ejcts/ezv194 Cite this article as: Vilmann P, Frost Clementsen P, Colella S, Siemsen M, De Leyn P, Dumonceau J-M et al. Combined endobronchial
European Journal of Cardio-Thoracic Surgery 48 (2015) 1 15 doi:10.1093/ejcts/ezv194 Cite this article as: Vilmann P, Frost Clementsen P, Colella S, Siemsen M, De Leyn P, Dumonceau J-M et al. Combined endobronchial
Recommendations 1 For mediastinal nodal staging in patients with suspected or proven non-small-cell lung cancer
 Guideline 545 Combined endobronchial and esophageal endosonography for the diagnosis and staging of lung cancer: European Society of Gastrointestinal Endoscopy (ESGE) Guideline, in cooperation with the
Guideline 545 Combined endobronchial and esophageal endosonography for the diagnosis and staging of lung cancer: European Society of Gastrointestinal Endoscopy (ESGE) Guideline, in cooperation with the
The right middle lobe is the smallest lobe in the lung, and
 ORIGINAL ARTICLE The Impact of Superior Mediastinal Lymph Node Metastases on Prognosis in Non-small Cell Lung Cancer Located in the Right Middle Lobe Yukinori Sakao, MD, PhD,* Sakae Okumura, MD,* Mun Mingyon,
ORIGINAL ARTICLE The Impact of Superior Mediastinal Lymph Node Metastases on Prognosis in Non-small Cell Lung Cancer Located in the Right Middle Lobe Yukinori Sakao, MD, PhD,* Sakae Okumura, MD,* Mun Mingyon,
Owing to the recent attention given to lung cancer
 Electromagnetic : A Surgeon s Perspective Todd S. Weiser, MD, Kevin Hyman, MD, Jaime Yun, MD, Virginia Litle, MD, Cythinia Chin, MD, and Scott J. Swanson, MD Department of Cardiothoracic Surgery, Mount
Electromagnetic : A Surgeon s Perspective Todd S. Weiser, MD, Kevin Hyman, MD, Jaime Yun, MD, Virginia Litle, MD, Cythinia Chin, MD, and Scott J. Swanson, MD Department of Cardiothoracic Surgery, Mount
Endoscopic Ultrasound in Patients Over 80 Years Old
 DOI 10.1007/s10620-011-1718-7 ORIGINAL ARTICLE Endoscopic Ultrasound in Patients Over 80 Years Old Tan Attila Douglas O. Faigel Received: 11 January 2011 / Accepted: 8 April 2011 Ó Springer Science+Business
DOI 10.1007/s10620-011-1718-7 ORIGINAL ARTICLE Endoscopic Ultrasound in Patients Over 80 Years Old Tan Attila Douglas O. Faigel Received: 11 January 2011 / Accepted: 8 April 2011 Ó Springer Science+Business
endoscopic ultrasound-guided fine-needle aspiration
 Original article 213 Endoscopic ultrasound-guided fine-needle aspiration for the diagnosis of sarcoidosis Authors M. B. von Bartheld 1, M. Veseliç-Charvat 2, K. F. Rabe 1, J. T. Annema 1 Institutions 1
Original article 213 Endoscopic ultrasound-guided fine-needle aspiration for the diagnosis of sarcoidosis Authors M. B. von Bartheld 1, M. Veseliç-Charvat 2, K. F. Rabe 1, J. T. Annema 1 Institutions 1
A Case of Pediatric Plasma Cell Granuloma
 August 2001 A Case of Pediatric Plasma Cell Granuloma Nii Tetteh, Harvard Medical School Year IV Our Patient 8 year old male with history of recurrent left lower lobe and lingular pneumonias since 1994.
August 2001 A Case of Pediatric Plasma Cell Granuloma Nii Tetteh, Harvard Medical School Year IV Our Patient 8 year old male with history of recurrent left lower lobe and lingular pneumonias since 1994.
Abstracting Upper GI Cancer Incidence and Treatment Data Quiz 1 Multiple Primary and Histologies Case 1 Final Pathology:
 Abstracting Upper GI Cancer Incidence and Treatment Data Quiz 1 Multiple Primary and Histologies Case 1 A 74 year old male with a history of GERD presents complaining of dysphagia. An esophagogastroduodenoscopy
Abstracting Upper GI Cancer Incidence and Treatment Data Quiz 1 Multiple Primary and Histologies Case 1 A 74 year old male with a history of GERD presents complaining of dysphagia. An esophagogastroduodenoscopy
Suspicious Cytologic Diagnostic Category in Endoscopic Ultrasound-Guided FNA of the Pancreas: Follow-Up and Outcomes
 Suspicious Cytologic Diagnostic Category in Endoscopic Ultrasound-Guided FNA of the Pancreas: Follow-Up and Outcomes Evan A. Alston, MD 1 ; Sejong Bae, PhD 2 ; and Isam A. Eltoum, MD, MBA 1 BACKGROUND:
Suspicious Cytologic Diagnostic Category in Endoscopic Ultrasound-Guided FNA of the Pancreas: Follow-Up and Outcomes Evan A. Alston, MD 1 ; Sejong Bae, PhD 2 ; and Isam A. Eltoum, MD, MBA 1 BACKGROUND:
Non-neoplastic Conditions in the Mediastinum
 2017 WCTI Non-neoplastic Conditions in the Mediastinum Mi Young Kim, MD, PhD Hyun Jung Koo, MD Jae Woo Song, MD, PhD Department of Radiology and Research Institute of Radiology Asan Medical Center, University
2017 WCTI Non-neoplastic Conditions in the Mediastinum Mi Young Kim, MD, PhD Hyun Jung Koo, MD Jae Woo Song, MD, PhD Department of Radiology and Research Institute of Radiology Asan Medical Center, University
The Itracacies of Staging Patients with Suspected Lung Cancer
 The Itracacies of Staging Patients with Suspected Lung Cancer Gerard A. Silvestri, MD,MS, FCCP Professor of Medicine Medical University of South Carolina Charleston, SC silvestri@musc.edu Staging Lung
The Itracacies of Staging Patients with Suspected Lung Cancer Gerard A. Silvestri, MD,MS, FCCP Professor of Medicine Medical University of South Carolina Charleston, SC silvestri@musc.edu Staging Lung
