Clinical Efficacy and Safety of Methotrexate versus Hydroxychloroquine in Preventing Lichen Planopilaris Progress: A Randomized Clinical Trial
|
|
|
- Sabrina Baldwin
- 5 years ago
- Views:
Transcription
1 Original Article Clinical Efficacy and Safety of Methotrexate versus Hydroxychloroquine in Preventing Lichen Planopilaris Progress: A Randomized Clinical Trial Abstract Background: Lichen planopilaris is an inflammatory cicatricial alopecia, and its management is a challenge for dermatologists. We aimed to compare the efficacy of methotrexate and hydroxychloroquine on refractory lichen planopilaris. Methods: In a randomized clinical trial, 29 patients were randomly allocated to receive either 15 mg methotrexate/week or 200 mg hydroxychloroquine twice a day for 6 months. Side effects, symptoms/signs, and laboratory tests were assessed periodically. Lichen Planopilaris Activity Index (LPPAI) was measured before intervention and at 2, 4, and 6 months after. The changes from baseline to the end of the study were analyzed within each group and between the two groups by per protocol and intention to treat analysis. Results: After 2 months, mean (standard deviation [SD]) decrease in LPPAI in methotrexate group was significantly more than that in hydroxychloroquine group (1.68 [1.24] vs. 0.8 [0.71], respectively, P = 0.047). Furthermore, after 6 months, mean (SD) decrease in LPPAI in methotrexate group was significantly higher than that in hydroxychloroquine group (3.3 [2.09] vs [0.91], respectively, P = 0.01). The following symptoms/signs showed significant improvements in frequency and/or severity in methotrexate group after intervention: pruritus (P = 0.007), erythema (P = 0.01), perifollicular erythema (P = 0.01), perifollicular scaling (P = 0.08), spreading (P = 0.001), and follicular keratosis (P = 0.04). In hydroxychloroquine group, only erythema (P = 0.004) showed significant improvement. Conclusions: Methotrexate was more effective than hydroxychloroquine in treating refractory lichen planopilaris. Farahnaz Fatemi Naeini, Mina Saber, Ali Asilian, Sayed Mohsen Hosseini 1 Department of Dermatology, Skin Diseases and Leishmaniasis Research Center, School of Medicine, Isfahan University of Medical Sciences, Isfahan, Iran, 1 Department of Biostatics and Epidemiology, School of Public Health, Isfahan University of Medical Sciences, Isfahan, Iran Keywords: Hydroxychloroquine, lichen planopilaris, methotrexate Introduction Lichen planopilaris, a common form of primary cicatricial alopecia, is mediated by chronic lymphocytic inflammation around the isthmus of the hair follicle leading to the destruction of follicle germ cells. [1 3] The main clinical finding is progressive patchy scarring alopecia usually seen in middle aged women. The clinical symptoms include itching, burning, and pain of the scalp that may impair the quality of life. [3 5] Different medications have been applied to treat lichen planopilaris, both topically such as intralesional corticosteroids, and systematically such as hydroxychloroquine. [6 8] Hydroxychloroquine may reduce the symptoms and signs in prolonged treatment. [8] Immunosuppressive agents such as mycophenolate mofetil and azathioprine have been administered for more severe cases. [9 11] Adalimumab, oral retinoids, thalidomide, and cyclosporine have been used to treat resistant and This is an open access article distributed under the terms of the Creative Commons Attribution-NonCommercial-ShareAlike 3.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms. For reprints contact: reprints@medknow.com refractory lichen planopilaris. [12 15] Methotrexate, with or without topical corticosteroids, has been employed to treat oral, [16] vulvovaginal, [17,18] anogenital, and generalized lichen planus [18 20] with acceptable clinical efficacy. Given the persistence inflammation and lymphocytic infiltrations in pathophysiology of lichen planopilaris, [6] strong anti inflammatory effects of methotrexate may cease the inflammation in this chronic inflammatory diseases. [5] The aim of this study was to evaluate the safety and efficacy of 6 month methotrexate versus hydroxychloroquine in patients with refractory lichen planopilaris. Methods Study design and participants The current study was a randomized clinical trial conducted from February 2015 to December This study was done in dermatologic clinic affiliated with Isfahan University of Medical Sciences, approved by the Institutional Review Board and Ethics How to cite this article: Naeini FF, Saber M, Asilian A, Hosseini SM. Clinical efficacy and safety of methotrexate versus hydroxychloroquine in preventing lichen planopilaris progress: A randomized clinical trial. Int J Prev Med 2017;8:37. Address for correspondence: Dr. Mina Saber, Department of Dermatology, Skin Diseases and Leishmaniasis Research Center, School of Medicine, Isfahan University of Medical Sciences, Isfahan, Iran. E mail: mina.saber33@yahoo. com Access this article online Website: DOI: /ijpvm.IJPVM_156_17 Quick Response Code: 2017 International Journal of Preventive Medicine Published by Wolters Kluwer Medknow 1
2 Committee of the university and was registered in Iranian Registry of Clinical Trials (IRCT N1). Forty two patients, 18 years, diagnosed with active refractory lichen planopilaris were assessed for eligibility to participate in the study [Figure 1]. The diagnosis was made based on clinical evaluation and was established by histopathological confirmation. Refractory lichen planopilaris defined as no response to treatment with topical agents/systematic medications in the past 6 months. Written informed consent was obtained from all the participants. Four patients refused to participate [Figure 1]. Complete physical examination including ophthalmologic examination and the following laboratory evaluations were carried out for all consented patients: complete blood count, renal function tests, liver function tests, viral markers, and baseline activity of glucose 6 phosphate dehydrogenase measurement. Exclusion criteria were pregnancy, breastfeeding, gastrointestinal disorders, vision problems/retinopathy, porphyria, psoriasis, anemia (Hb <9 mg/dl), leukopenia (white blood cells <4000/dl), thrombocytopenia (platelets <100,000/dl), increased liver enzymes more than three times of the upper normal limit, significant liver disease, positive viral hepatic markers, history of convulsion, and excessive alcohol intake. Nine patients were excluded after application of exclusion criteria [Figure 1]. The following withdrawal criteria were applied: not showing up for follow up visits, not taking the medication according to the study protocol, receiving other topical or immunosuppressive agents during the study, and nontolerable side effects. Four patients withdrew from the study [Figure 1]. Treatment protocol All medications were discontinued at least 1 month before the start of the study. Twenty nine patients were randomly allocated to receive either 15 mg methotrexate per week or 200 mg hydroxychloroquine twice a day for 6 months. History taking including medication side effects, physical examination, and the following laboratory evaluations were carried out periodically: complete blood count, renal function tests, and liver function tests. The patients were instructed to record/report any side effect experienced. Figure 1: Consort flow chart of the study 2 International Journal of Preventive Medicine 2017, 8: 37
3 Outcome measures The activity of lichen planopilaris in each patient was measured using Lichen Planopilaris Activity Index (LPPAI) scoring system and photographic examination. LPPAI was measured before the intervention and at 2, 4, and 6 months after intervention. LPPAI was calculated as (itch + pain + burn)/3 + (scalp erythema + perifollicular erythema + perifollicular scale)/ (pull test) (spreading/2). Follicular keratosis was also evaluated at baseline and 2, 4, and 6 months after intervention. Photography was assessed at baseline and at the end of the study by two dermatologists who were blind to group allocation. The most active point was tattooed and surrounded by ink mark in a circle of 0.5 inch radius. A standardized seven point scale was used to interpret photography. The scale included greatly decreased = 3, moderately decreased = 2, slightly decreased = 1, no change = 0, slightly increased = +1, moderately increased = +2, and greatly increased = +3. There was a don t know option which denoted the photographs were not suitable for proper clinical evaluation. [21] Medication side effects were carefully monitored to evaluate the safety of administered medications. Statistical analysis Disease characteristics at baseline and after 2, 4, and 6 months were compared between the two groups using Chi square and Fisher exact tests for categorical variables, Mann Whitney U test for nonparametric variables and Student s t test for parametric variables. The changes from the baseline to the end of study period within each group were tested using Wilcoxon signed rank test for nonparametric variables and paired t test for parametric variables. Spearmen correlation was conducted to evaluate the correlation between the two subspecialty assessments of photography. Per protocol analysis was carried out on all patients remained in the study. To avoid the bias associated with the nonrandom loss of patients, intention to treat (ITT) analysis was conducted on all enrolled patients at the baseline. The worst case scenario was considered for patients who were lost to follow up. P <0.05 was considered statistically significant. SPSS version 17 (Chicago, IL, USA) was used for data analysis. Results Baseline characteristics Forty two patients were assessed, four refused to participate, and nine were excluded [Figure 1]. Fifteen and 14 patients were enrolled in methotrexate and hydroxychloroquine groups, respectively. Thirteen (86.7%) and 8 (57.1%) ones were females in methotrexate and hydroxychloroquine groups, respectively. The difference was not significant (P = 0.1). The mean (standard deviation [SD]) age of participants was 44.9 (11.1) years in methotrexate group and 40.8 (11.7) years in hydroxychloroquine group (P = 0.4). The mean age of disease diagnosis was 42.3 (12.8) and 37.6 (11) years in methotrexate and hydroxychloroquine groups, receptively (P = 0.3). Moreover, disease duration was 3 (2) and 3.14 (4.22) years, respectively (P = 0.9). Furthermore, there was no significant baseline difference between the two groups in terms of family history, organ involvements, clinical findings, and past therapeutic measurements [Table 1]. Similarly, there was no significant difference in frequency of symptoms/signs between the two groups at baseline. The only exception was pull test [Table 2]. The mean LPPAI at baseline in methotrexate group was significantly higher than that in hydroxychloroquine group [Table 3]. Between groups per protocol analysis after intervention Mean (SD) LPPAI in methotrexate group at baseline, 4.63 (1.83), was significantly higher than that in hydroxychloroquine group, 3.46 (0.94), (P = 0.04). Table 3 reveals LPPAI difference between the two groups at baseline and during the study. Mean (SD) decrease in LPPAI in methotrexate group after 2 months was significantly higher than that in hydroxychloroquine group [Table 3]. Similarly, at the end of the study, LPPAI in methotrexate group decreased more significantly than that in hydroxychloroquine group [Table 3]. Figure 2 demonstrates the trend of LPPAI change in both groups during the study. The sharper declines of LPPAI in methotrexate group versus the milder declines in hydroxychloroquine group during the first and the last 2 months of study are noticeable. The decline in LPPAI in methotrexate group is steady and continuous during all study period whereas the decline in LPPAI in hydroxychloroquine group is unremarkable in the last 2 months [Figure 2]. Photographic assessment conducted by two different subspecialists showed also no significant difference between the two groups [Table 4]. Spearmen correlation was conducted to understand the correlation between the two assessments. The results Figure 2: The pattern of decease in Lichen Planopilaris Activity Index in both groups International Journal of Preventive Medicine 2017, 8: 37 3
4 Table 1: Family history, organ involvements, and past therapeutic experiences compared between the two groups Disease characteristics Methotrexate, n (%) Hydroxychloroquine, n (%) P Positive family history 2 (13.3) 1 (7.1) 0.6 Skin involvement 3 (20.0) 4 (28.6) 0.7 Pigmentary changes 1 (6.7) 3 (21.4) 0.2 Telangiectasia 2 (13.3) 3 (21.4) 0.7 Crusting 3 (20) 3 (21.4) 0.2 Pustules 1 (6.7) Atrophy 1 (6.7) 2 (14.3) 0.6 Nail involvement 0 0 NA Mucosal involvement 2 (13.3) 2 (14.3) 0.7 Follicular lichen planus 3 (20.0) 1 (7.1) 0.6 Frontal fibrosing alopecia 1 (6.70) 1 (7.1) 0.8 Recent treatments before the current study Topical corticosteroids 15 (100) 14 (100) NA Systemic corticosteroids 8 (53.3) 6 (42.8) 0.7 Chloroquine 2 (13.3) Mycophenolate mofetil 4 (26.7) 3 (21.4) 0.6 Cyclosporine 4 (26.7) 1 (7.1) 0.3 Acitretin 2 (13.3) Isotretinoin 2 (13.3) Pioglitazone 1 (6.70) NA=Not available showed substantial (r = 0.50) and significant (P = 0.013) correlation. Within group per protocol analysis after intervention Table 2 demonstrates the frequency and severity of nine symptoms/signs at baseline and during the study. Five symptoms/signs showed significant improvement in frequency and/or severity in methotrexate group after 6 months intervention compared to the baseline. The corresponding P values for all nine symptoms/ signs were as follow pain (P = 0.06), burning (P = 0.1), pruritus (P = 0.007), erythema (P = 0.01), perifollicular erythema (P = 0.01), perifollicular scaling (P = 0.08), pull test (P = 0.06), spreading (P = 0.001), and follicular keratosis (P = 0.04). On the contrary, only erythema showed a significant improvement in frequency and/or severity in hydroxychloroquine group after 6 months intervention compared to the baseline. The corresponding P values for all symptoms and signs were as follow pain (P = 0.75), burning (P = 0.25), pruritus (P = 0.08), erythema (P = 0.004), perifollicular erythema (P = 0.2), perifollicular scaling (P = 0.8), pull test (P = 0.9), spreading (P = 0.06), and follicular keratosis (P = 0.2). Table 3 reveals LPPAI difference within both groups at baseline and during the study. Consistent decrease in LPPAI was observed within methotrexate group at month 2 compared to the baseline (P = 0.006), at month 4 compared to the month 2 (P = 0.005), and at month 6 compared to the month 4 (P = 0.03). On the other hand, LPPAI decreased significantly within hydroxychloroquine group at month 2 compared to the baseline (P = 0.002) and at month 4 compared to the month 2 (P = 0.01). No significant decrease in LPPAI at month 6 compared to the month 4 was observed within hydroxychloroquine group (P = 0.8). Intention to treat analysis The worst case scenario was considered for lost to follow up patients. After 4 months, mean (SD) decrease in LPPAI in methotrexate group was significantly higher than that in hydroxychloroquine group [Table 3]. Similarly, at the end of the study, mean (SD) decrease in LPPAI in methotrexate group was significantly more than that in hydroxychloroquine group [Table 3]. Consistent decrease in LPPAI was observed within methotrexate group; at month 2 compared to the baseline (P = 0.01), at month 4 compared to the month 2 (P = 0.001), and at month 6 compared to the month 4 (P = 0.03). On the other hand, LPPAI decreased significantly within hydroxychloroquine group, at month 2 compared to the baseline (P = 0.005) and at month 4 compared to the month 2 (P = 0.02). The significance of the difference in photographic assessment was not changed when analyzed by either assessor [Table 4]. Medication side effects Two patients experienced medication side effects. One (6.7%) in methotrexate group who showed elevated liver enzymes and the other (7.1%) in hydroxychloroquine group who demonstrated drug eruption. Discussion The current study demonstrated higher therapeutic effects of methotrexate than hydroxychloroquine on lichen planopilaris 4 International Journal of Preventive Medicine 2017, 8: 37
5 Table 2: Frequency of symptoms and signs compared between the two groups Baseline Month 2 Month 4 Month 6 Methotrexate Hydroxychloroquine P Methotrexate Hydroxychloroquine P Methotrexate Hydroxychloroquine P M H P Pain, n (%) No 11 (73.3) 11 (78.6) (60) 12 (85.7) (80) 12 (85.7) (93.3) 9 (64.3) 0.5 Mild 3 (20) 1 (7.1) 0 1 (7.1) (14.2) Moderate 0 2 (14.2) 1 (6.7) 0 1 (6.7) Severe 1 (6.7) Burning, n (%) No 12 (80) 10 (71.4) (46.7) 10 (71.4) (67) 10 (71.4) (86.7) 10 (71.4) 0.7 Mild 1 (6.7) 2 (14.2) 1 (6.7) 0 2 (13.3) 2 (16.7) 0 1 (7.1) Moderate 1 (6.7) 0 2 (13.3) 1 (7.1) 1 (6.7) 0 1 (6.7) 0 Severe 1 (6.7) 2 (14.3) 0 2 (15.4) Pruritus, n (%) No 2 (13.3) 3 (21.4) (13.3) 5 (38.5) (53.3) 7 (58.3) (67) 6 (42.7) 0.4 Mild 4 (26.7) 3 (21.4) 4 (26.7) 3 (23.1) 1 (6.7) 2 (16.7) 1 (6.7) 1 (7.1) Moderate 2 (13.3) 2 (14.2) 3 (20) 3 (23.1) 3 (20) 1 (8.3) 2 (13.3) 2 (14.2) Severe 7 (46.7) 6 (43) 1 (6.7) 2 (15.4) 1 (6.7) 2 (16.7) 1 (6.7) 2 (14.2) Erythema, n (%) No 5 (33.3) 4 (28.6) (53.3) 6 (43) (67) 10 (71.4) (80) 10 (71.4) 0.8 Mild 5 (33.3) 4 (28.6) 2 (13.3) 3 (21.4) 1 (6.7) 1 (7.1) 0 0 Moderate 4 (26.7) 2 (14.2) 0 4 (28.5) 2 (13.3) 1 (7.1) 2 (13.3) 1 (7.1) Severe 1 (6.7) 4 (28.6) Perifollicular erythema, n (%) No 0 1 (7.1) (26.7) 3 (21.4) (26.7) 5 (35.7) (40) 3 (21.4) 0.1 Mild 7 (46.7) 5 (35.7) 4 (26.7) 6 (43) 7 (46.7) 4 6 (40) 5 (35.7) Moderate 5 (33.3) 3 (21.4) 1 (6.7) 2 (14.2) 1 (6.7) 3 2 (13.3) 0 Severe 3 (20) 5 (35.7) 1 (6.7) 2 (14.2) 1 (6.7) (21.4) Perifollicular scaling, n (%) No 4 (26.7) 7 (58.3) (33.3) 8 (57) (40) (46.7) 4 (28.5) 0.4 Mild 4 (26.7) 2 (14.2) 2 (13.3) 1 (7.1) 5 (33.3) 3 3 (20) 2 (14.2) Moderate 1 (6.7) 3 (21.4) 0 2 (14.2) 1 (6.7) 1 (7.1) 4 (26.7) 4 (28.5) Severe 6 (40) 2 (14.2) 3 (20) 2 (14.2) 1 (6.7) 1 (7.1) 0 1 (7.1) Pull test, n (%) No 10 (67) 14 (100) (53.3) 13 (93) (73.3) 12 (85.7) (93.3) 11 (78.6) NA Presence 5 (33.3) 0 2 (13.3) 0 2 (13.3) Spreading, n (%) No 0 1 (7.1) (6.7) 1 (7.1) (20) 2 (14.2) (46.7) 5 (35.7) 0.5 Intermediate 1 (6.7) 3 (21.4) 3 (20) 4 (28.5) 5 (33.3) 3 5 (33.3) 2 (14.2) Presence 14 (93.3) 10 (71.4) 6 (40) 8 (57) 5 (33.3) 7 2 (13.3) 4 (28.5) Follicular keratosis, n (%) Contd.. International Journal of Preventive Medicine 2017, 8: 37 5
6 Table 2: Contd... Baseline Month 2 Month 4 Month 6 Methotrexate Hydroxychloroquine P Methotrexate Hydroxychloroquine P Methotrexate Hydroxychloroquine P M H P No 1 (6.7) (6.7) 3 (21.4) (13.3) 2 (14.2) (20) 1 (7.1) 0.8 Mild 4 (26.7) 5 (35.7) 4 (26.7) 5 (35.7) 6 (40) 6 6 (40) 6 (43) Moderate 3 (20) 5 (35.7) 5 (33.3) 4 (28.5) 1 (6.7) 2 (14.2) 4 (46.7) 4 (28.5) Severe 7 (46.7) 4 (28.6) 0 1 (7.1) 4 (26.7) 2 (14.2) 1 (6.7) 0 in a 6 month randomized clinical trial. Considerable improvements were recorded in frequency and severity of follicular keratosis, pruritus, perifollicular erythema, spreading, and erythema in patients received methotrexate whereas only erythema improved significantly in patients who received hydroxychloroquine. When disease remission occurred, probably, follicular keratosis was the last sign which was improved significantly only in methotrexate group. The significant improvements in symptoms and signs plus more than 70% drop in LPPAI in methotrexate group at the end of study versus <45% drop in final LPPAI in hydroxychloroquine group were the most remarkable findings of the study. In other words, the mean LPPAI at the end of the study was less than one third of the baseline in patients received methotrexate and more than half of the baseline in patients received hydroxychloroquine. The trend of change was sharp and significant in methotrexate group at all time points during the study whereas it was not significant after month four in hydroxychloroquine group. These findings were observed in both per protocol and ITT analyses. When ITT analysis was applied, the mean LPPAI difference was increased in both groups at all time points after baseline. However, the increments did not change the significance of findings. Photographic examination might be able to detect improvements in severe cases. Subtle but significant improvements could be easily overlooked in photographic assessment. Both medications were tolerated very well with minimum side effects. Diverse results have been achieved when different anti inflammatory medications such as hydroxychloroquine, pioglitazone, tetracycline, mycophenolate mofetil, and cyclosporine were employed to treat lichen planopilaris. [6 14] Some reports showed the promising effect of hydroxychloroquine whereas some others showed the reverse. [8,22] Similarly, although cyclosporine demonstrated considerable effects on LPP, its discontinuation might be associated with high relapse rate. [23] Similar therapeutic effects of mycophenolate mofetil and topical clobetasol have been also shown. [9] It seems the current research is the first clinical randomized trial applied to evaluate the therapeutic effects of methotrexate on lichen planopilaris. This is a cell mediated autoimmune disorder with activated T lymphocytes target follicular antigens. [6] Possible pharmacological mechanisms of methotrexate that might modify the path of disease include inhibition of purine and pyrimidine synthesis, suppression of transmethylation reactions with an accumulation of polyamines and reduction of antigen dependent T cell proliferation. [24,25] Given the favorable efficacy, reasonable cost, safety profile, and the ease of administration, methotrexate might be a new effective medication in treating lichen planopilaris. The strengths of our randomized clinical trial were the novel medication applied and the combined assessments of LPPAI, 6 International Journal of Preventive Medicine 2017, 8: 37
7 Table 3: Lichen Planopilaris Activity Index changes compared between the two groups LPPAI difference Per protocol analysis Intention to treat analysis Methotrexate (n=14) Hydroxychloroquine (n=11) P Methotrexate (n=15) Hydroxychloroquine (n=14) P Mean SD Mean SD Mean SD Mean SD Baseline month Baseline month Baseline month LPPAI=Lichen Planopilaris Activity Index, SD=Standard deviation Table 4: Photographic assessment conducted by two different subspecialists at baseline and at the end of the study. They were compared between the two groups by both per protocol and intention to treat analyses Per protocol analysis Intention to treat analysis Methotrexate Hydroxychloroquine P Methotrexate Hydroxychloroquine P Global photographic assessment 1, n (%) Slightly decreased 2 (14.3) 1 (9.1) (13.3) 1 (7.1) 0.6 No change 4 (28.6) 3 (27.3) 4 (26.7) 3 (21.4) Slightly increased 4 (28.6) 4 (36.4) 4 (26.7) 4 (28.6) Moderately increased 2 (14.3) 3 (27.3) 2 (13.3) 3 (21.4) Greatly increased 2 (14.3) 0 3 (20.0) 3 (21.4) Global photographic assessment 2, n (%) Slightly decreased 1 (7.1) (6.7) No change 4 (28.6) 4 (36.4) 4 (26.7) 4 (28.6) Slightly increased 3 (21.4) 4 (36.4) 3 (20.0) 4 (28.6) Moderately increased 6 (42.9) 3 (27.3) 6 (40.0) 3 (21.4) Greatly increased (6.7) 3 (21.4) follicular keratosis, and photographic examination. The limitations of the current study were low sample size, relatively short follow up, and lack of histopathologic evaluations. Conclusions Methotrexate was more effective than hydroxychloroquine in treating refractory lichen planopilaris. Further multi center studies with larger sample sizes and longer follow ups are warranted. Financial support and sponsorship This study was supported by Isfahan University of Medical Sciences. Conflicts of interest There are no conflicts of interest. Received: 30 Jan 17 Accepted: 22 Mar 17 Published: 25 May 17 References 1. Olsen EA. Female pattern hair loss and its relationship to permanent/cicatricial alopecia: A new perspective. J Investig Dermatol Symp Proc 2005;10: Ochoa BE, King LE Jr., Price VH. Lichen planopilaris: Annual incidence in four hair referral centers in the United States. J Am Acad Dermatol 2008;58: Assouly P, Reygagne P. Lichen planopilaris: Update on diagnosis and treatment. Semin Cutan Med Surg 2009;28: Kang H, Alzolibani AA, Otberg N, Shapiro J. Lichen planopilaris. Dermatol Ther 2008;21: Chiang YZ, Bundy C, Griffiths CE, Paus R, Harries MJ. The role of beliefs: Lessons from a pilot study on illness perception, psychological distress and quality of life in patients with primary cicatricial alopecia. Br J Dermatol 2015;172: Manousaridis I, Manousaridis K, Peitsch WK, Schneider SW. Individualizing treatment and choice of medication in lichen planus: A step by step approach. J Dtsch Dermatol Ges 2013;11: Baibergenova A, Donovan J. Lichen planopilaris: Update on pathogenesis and treatment. Skinmed 2013;11: Chiang C, Sah D, Cho BK, Ochoa BE, Price VH. Hydroxychloroquine and lichen planopilaris: Efficacy and introduction of lichen planopilaris activity index scoring system. J Am Acad Dermatol 2010;62: Lajevardi V, Ghodsi SZ, Goodarzi A, Hejazi P, Azizpour A, Beygi S. Comparison of systemic mycophenolate mofetil with topical clobetasol in lichen planopilaris: A parallel group, assessor and analyst blinded, randomized controlled trial. Am J Clin Dermatol 2015;16: Tursen U, Api H, Kaya T, Ikizoglu G. Treatment of lichen planopilaris with mycophenolate mofetil. Dermatol Online J 2004;10: Mirmirani P, Willey A, Price VH. Short course of oral cyclosporine in lichen planopilaris. J Am Acad Dermatol 2003;49: Kreutzer K, Effendy I. Therapy resistant folliculitis decalvans and lichen planopilaris successfully treated with adalimumab. J Dtsch Dermatol Ges 2014;12: Spano F, Donovan JC. Efficacy of oral retinoids in treatment resistant lichen planopilaris. J Am Acad Dermatol 2014;71: George SJ, Hsu S. Lichen planopilaris treated with thalidomide. J Am Acad Dermatol 2001;45: International Journal of Preventive Medicine 2017, 8: 37 7
8 15. Harries MJ, Messenger A. Treatment of frontal fibrosing alopecia and lichen planopilaris. J Eur Acad Dermatol Venereol 2014;28: Lajevardi V, Ghodsi SZ, Hallaji Z, Shafiei Z, Aghazadeh N, Akbari Z. Treatment of erosive oral lichen planus with methotrexate. J Dtsch Dermatol Ges 2016;14: Jang N, Fischer G. Treatment of erosive vulvovaginal lichen planus with methotrexate. Australas J Dermatol 2008;49: Nylander Lundqvist E, Wahlin YB, Hofer PA. Methotrexate supplemented with steroid ointments for the treatment of severe erosive lichen ruber. Acta Derm Venereol 2002;82: Hazra SC, Choudhury AM, Khondker L, Khan SI. Comparative efficacy of methotrexate and mini pulse betamethasone in the treatment of lichen planus. Mymensingh Med J 2013;22: Kanwar AJ, De D. Methotrexate for treatment of lichen planus: Old drug, new indication. J Eur Acad Dermatol Venereol 2013;27:e Olsen EA, Whiting DA, Savin R, Rodgers A, Johnson Levonas AO, Round E, et al. Global photographic assessment of men aged 18 to 60 years with male pattern hair loss receiving finasteride 1 mg or placebo. J Am Acad Dermatol 2012;67: Donati A, Assouly P, Matard B, Jouanique C, Reygagne P. Clinical and photographic assessment of lichen planopilaris treatment efficacy. J Am Acad Dermatol 2011;64: Rácz E, Gho C, Moorman PW, Noordhoek Hegt V, Neumann HA. Treatment of frontal fibrosing alopecia and lichen planopilaris: A systematic review. J Eur Acad Dermatol Venereol 2013;27: Tian H, Cronstein BN. Understanding the mechanisms of action of methotrexate: Implications for the treatment of rheumatoid arthritis. Bull NYU Hosp Jt Dis 2007;65: Brown PM, Pratt AG, Isaacs JD. Mechanism of action of methotrexate in rheumatoid arthritis, and the search for biomarkers. Nat Rev Rheumatol 2016;12: International Journal of Preventive Medicine 2017, 8: 37
Lichen planopilaris in a Latin American (Chilean) population: demographics, clinical profile and treatment experience
 Original article CED Clinical and Experimental Dermatology Lichen planopilaris in a Latin American (Chilean) population: demographics, clinical profile and treatment experience F. Mardones 1 and J. Shapiro
Original article CED Clinical and Experimental Dermatology Lichen planopilaris in a Latin American (Chilean) population: demographics, clinical profile and treatment experience F. Mardones 1 and J. Shapiro
Frontal fibrosing alopecia severity index (FFASI): a validated scoring system for assessing frontal fibrosing alopecia
 Received Date : 22-Jul-2015 Accepted Article Revised Date : 10-Jan-2016 Accepted Date : 11-Jan-2016 Article type : Research Letter Frontal fibrosing alopecia severity index (FFASI): a validated scoring
Received Date : 22-Jul-2015 Accepted Article Revised Date : 10-Jan-2016 Accepted Date : 11-Jan-2016 Article type : Research Letter Frontal fibrosing alopecia severity index (FFASI): a validated scoring
Strathprints Institutional Repository
 Strathprints Institutional Repository Holmes, S. and Ryan, T. and Young, D. and Harries, M. (2016) Frontal fibrosing alopecia severity index (FFASI) : a validated scoring system for assessing frontal fibrosing
Strathprints Institutional Repository Holmes, S. and Ryan, T. and Young, D. and Harries, M. (2016) Frontal fibrosing alopecia severity index (FFASI) : a validated scoring system for assessing frontal fibrosing
Comparison of the narrow band UVB versus systemic corticosteroids in the treatment of lichen planus: A randomized clinical trial
 Received: 10.7.2011 Accepted: 5.12.2011 Original Article Comparison of the narrow band UVB versus systemic corticosteroids in the treatment of lichen planus: A randomized clinical trial Fariba Iraji, 1
Received: 10.7.2011 Accepted: 5.12.2011 Original Article Comparison of the narrow band UVB versus systemic corticosteroids in the treatment of lichen planus: A randomized clinical trial Fariba Iraji, 1
What Are the Different Forms?
 SCARRING/CICATRICIAL ALOPECIA Scarring alopecia also known as cicatricial alopecia, refers to a collection of hair loss disorders that may be diagnosed in up to 3% of hair loss patients. It occurs worldwide
SCARRING/CICATRICIAL ALOPECIA Scarring alopecia also known as cicatricial alopecia, refers to a collection of hair loss disorders that may be diagnosed in up to 3% of hair loss patients. It occurs worldwide
Therapeutic updates for Lichen planopilaris and Frontal fibrosing alopecia: a systematic
 Therapeutic updates for Lichen planopilaris and Frontal fibrosing alopecia: a systematic review Abstract Background: Lichen planopilaris (LPP) and frontal fibrosing alopecia (FFA) are skin diseases. A
Therapeutic updates for Lichen planopilaris and Frontal fibrosing alopecia: a systematic review Abstract Background: Lichen planopilaris (LPP) and frontal fibrosing alopecia (FFA) are skin diseases. A
Diagnosis and Management of the Hair Loss Patient: Pearls and Pitfalls
 Diagnosis and Management of the Hair Loss Patient: Pearls and Pitfalls U033 July 30 th 2017 7:30-8:30AM Paradi Mirmirani, MD The Permanente Medical Group, Vallejo, CA Regional Director, Hair Disorders
Diagnosis and Management of the Hair Loss Patient: Pearls and Pitfalls U033 July 30 th 2017 7:30-8:30AM Paradi Mirmirani, MD The Permanente Medical Group, Vallejo, CA Regional Director, Hair Disorders
SHORT REPORT FRONTAL FIBROSING ALOPECIA IN A PREMENOPAUSAL WOMAN: IMMUNOHISTOCHEMICAL AND IMMUNOFLUORESCENCE ANALYSIS
 EUROPEAN JOURNAL OF INFLAMMATION Vol. 5, no. 1, 23-27 (2007) SHORT REPORT FRONTAL FIBROSING ALOPECIA IN A PREMENOPAUSAL WOMAN: IMMUNOHISTOCHEMICAL AND IMMUNOFLUORESCENCE ANALYSIS G.I. ATHANASIADIS, E.
EUROPEAN JOURNAL OF INFLAMMATION Vol. 5, no. 1, 23-27 (2007) SHORT REPORT FRONTAL FIBROSING ALOPECIA IN A PREMENOPAUSAL WOMAN: IMMUNOHISTOCHEMICAL AND IMMUNOFLUORESCENCE ANALYSIS G.I. ATHANASIADIS, E.
It is not invisible! A case report of 2 patients with scalp Lichen Planopilaris mimicking Androgenic Alopecia
 Open Access Annals of Dermatological Research Case Report It is not invisible! A case report of 2 patients with scalp Lichen Planopilaris mimicking Androgenic Alopecia Sorbellini Elisabetta 1, Pinto Daniela
Open Access Annals of Dermatological Research Case Report It is not invisible! A case report of 2 patients with scalp Lichen Planopilaris mimicking Androgenic Alopecia Sorbellini Elisabetta 1, Pinto Daniela
Clearance in vulvar lichen sclerosus: a realistic treatment endpoint or a chimera?
 DOI: 10.1111/jdv.14516 JEADV SHORT REPORT Clearance in vulvar lichen sclerosus: a realistic treatment endpoint or a chimera? A. Borghi,* A. Virgili, S. Minghetti, G. Toni, M. Corazza Dipartimento di Scienze
DOI: 10.1111/jdv.14516 JEADV SHORT REPORT Clearance in vulvar lichen sclerosus: a realistic treatment endpoint or a chimera? A. Borghi,* A. Virgili, S. Minghetti, G. Toni, M. Corazza Dipartimento di Scienze
An Epidemiological Study of 198 Cases of Primary Cicatricial Alopecia in Iran
 British Journal of Medicine & Medical Research 20(4): 1-6, 2017; Article no.bjmmr.27476 ISSN: 2231-0614, NLM ID: 101570965 SCIENCEDOMAIN international www.sciencedomain.org An Epidemiological Study of
British Journal of Medicine & Medical Research 20(4): 1-6, 2017; Article no.bjmmr.27476 ISSN: 2231-0614, NLM ID: 101570965 SCIENCEDOMAIN international www.sciencedomain.org An Epidemiological Study of
Antonella Tosti Fredric Brandt Endowed Professor of Dermatology & Cutaneous Surgery
 Dermoscopy in the evaluation and treatment of hair loss Antonella Tosti Fredric Brandt Endowed Professor of Dermatology & Cutaneous Surgery DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY Antonella Tosti, MD
Dermoscopy in the evaluation and treatment of hair loss Antonella Tosti Fredric Brandt Endowed Professor of Dermatology & Cutaneous Surgery DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY Antonella Tosti, MD
Tips on Evaluation and Diagnosis of Scarring Alopecias. Melissa Peck Piliang, MD Dermatology and Anatomic Pathology Cleveland Clinic
 Tips on Evaluation and Diagnosis of Scarring Alopecias Melissa Peck Piliang, MD Dermatology and Anatomic Pathology Cleveland Clinic Disclosures I do not have any relevant relationships with industry Investigator:
Tips on Evaluation and Diagnosis of Scarring Alopecias Melissa Peck Piliang, MD Dermatology and Anatomic Pathology Cleveland Clinic Disclosures I do not have any relevant relationships with industry Investigator:
Lichen planopilaris and its variants. Antonella Tosti. Fredric Brandt Endowed Professor of Dermatology & Cutaneous Surgery
 Lichen planopilaris and its variants Antonella Tosti Fredric Brandt Endowed Professor of Dermatology & Cutaneous Surgery DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY Antonella Tosti, MD S023 Lichen planopilaris
Lichen planopilaris and its variants Antonella Tosti Fredric Brandt Endowed Professor of Dermatology & Cutaneous Surgery DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY Antonella Tosti, MD S023 Lichen planopilaris
FAST FACTS FOR BOARD REVIEW
 FAST FACTS FOR BOARD REVIEW Series Editor: William W. Huang, MD, MPH Common Hair Disorders Rita Pichardo-Geisinger, MD Dr. Pichardo-Geisinger is Associate Professor of Dermatology, Wake Forest Baptist
FAST FACTS FOR BOARD REVIEW Series Editor: William W. Huang, MD, MPH Common Hair Disorders Rita Pichardo-Geisinger, MD Dr. Pichardo-Geisinger is Associate Professor of Dermatology, Wake Forest Baptist
Efficacy of Topical Diphencyprone in the Treatment of Alopecia Areata
 Original Article Efficacy of Topical Diphencyprone in the Treatment of Alopecia Areata Maryam Akhiani, MD Hasan Seyrafi, MD Farshad Farnaghi, MD Parastoo Banan, MD Vahideh Lajvardi, MD Department of Dermatology,
Original Article Efficacy of Topical Diphencyprone in the Treatment of Alopecia Areata Maryam Akhiani, MD Hasan Seyrafi, MD Farshad Farnaghi, MD Parastoo Banan, MD Vahideh Lajvardi, MD Department of Dermatology,
Dutasteride female pattern hair loss management 49, 50 male baldness management 41, 42 Dyeing, see Hair care
 Subject Index Acne keloidalis nuchae, ethnic patients 146, 147 Actinic keratosis, ultraviolet radiation exposure 108 Aging hair effects 4, 5 melanocyte aging 130 132 molecular mechanisms 5 7 pigment loss,
Subject Index Acne keloidalis nuchae, ethnic patients 146, 147 Actinic keratosis, ultraviolet radiation exposure 108 Aging hair effects 4, 5 melanocyte aging 130 132 molecular mechanisms 5 7 pigment loss,
Ann Dermatol Vol. 27, No. 6,
 IK Yeo, et al Ann Dermatol Vol. 27, No. 6, 2015 http://dx.doi.org/10.5021/ad.2015.27.6.676 ORIGINAL ARTICLE Comparison of High-Dose Corticosteroid Pulse Therapy and Combination Therapy Using Oral Cyclosporine
IK Yeo, et al Ann Dermatol Vol. 27, No. 6, 2015 http://dx.doi.org/10.5021/ad.2015.27.6.676 ORIGINAL ARTICLE Comparison of High-Dose Corticosteroid Pulse Therapy and Combination Therapy Using Oral Cyclosporine
Frontal fibrosing alopecia: A review of 60 cases. Alison MacDonald, MRCP, Colin Clark, FRCP, and Susan Holmes, FRCP, MD Glasgow, United Kingdom
 Frontal fibrosing alopecia: A review of 60 cases Alison MacDonald, MRCP, Colin Clark, FRCP, and Susan Holmes, FRCP, MD Glasgow, United Kingdom Background: Frontal fibrosing alopecia (FFA) is a variant
Frontal fibrosing alopecia: A review of 60 cases Alison MacDonald, MRCP, Colin Clark, FRCP, and Susan Holmes, FRCP, MD Glasgow, United Kingdom Background: Frontal fibrosing alopecia (FFA) is a variant
Discoid Lupus Erythematosus
 S023 Hair and Scalp Dermoscopy Discoid Lupus Erythematosus Bruna Duque Estrada, M.D. Instituto de Dermatologia Prof. Rubem David Azulay Rio de Janeiro, Brazil. Disclosure of Relationship with Industry
S023 Hair and Scalp Dermoscopy Discoid Lupus Erythematosus Bruna Duque Estrada, M.D. Instituto de Dermatologia Prof. Rubem David Azulay Rio de Janeiro, Brazil. Disclosure of Relationship with Industry
Tips on getting the most from your alopecia pathology reports. D irector, H a ir C linic, Boston Medical C e n ter
 Tips on getting the most from your alopecia pathology reports Lynne J. Goldberg, MD J a g Bhawan Professor o f Dermatology a n d Pathology & Laboratory Medicine Boston U n iversity School of Medicine D
Tips on getting the most from your alopecia pathology reports Lynne J. Goldberg, MD J a g Bhawan Professor o f Dermatology a n d Pathology & Laboratory Medicine Boston U n iversity School of Medicine D
Snapshot Dx Quiz: September 2018 Detailed Answers
 Snapshot Dx Quiz: September 2018 Detailed Answers Cynthia X. Wang, BA 1 Milan J. Anadkat, MD 1,2 1 Washington University School of Medicine, St. Louis, Missouri 2 Division of Dermatology, St. Louis, Missouri
Snapshot Dx Quiz: September 2018 Detailed Answers Cynthia X. Wang, BA 1 Milan J. Anadkat, MD 1,2 1 Washington University School of Medicine, St. Louis, Missouri 2 Division of Dermatology, St. Louis, Missouri
Treatment of alopecia universalis with topical Janus kinase inhibitors a double blind, placebo, and active controlled pilot study
 Report Treatment of alopecia universalis with topical Janus kinase inhibitors a double blind, placebo, and active controlled pilot study Laita Bokhari, MPhil Med, and Rodney Sinclair, MBBS, MD, FACD Sinclair
Report Treatment of alopecia universalis with topical Janus kinase inhibitors a double blind, placebo, and active controlled pilot study Laita Bokhari, MPhil Med, and Rodney Sinclair, MBBS, MD, FACD Sinclair
Elements for a Public Summary
 VI.2 VI.2.1 Elements for a Public Summary Overview of disease epidemiology Psoriasis (excluding widespread plaque psoriasis) Psoriasis is a common chronic skin disorder. Estimates of the prevalence (proportion
VI.2 VI.2.1 Elements for a Public Summary Overview of disease epidemiology Psoriasis (excluding widespread plaque psoriasis) Psoriasis is a common chronic skin disorder. Estimates of the prevalence (proportion
FIBROSING ALOPECIA IN A PATTERN DISTRIBUTION IN TWO BROTHERS WITH PILI MULTIGEMINI
 FIBROSING ALOPECIA IN A PATTERN DISTRIBUTION IN TWO BROTHERS WITH PILI MULTIGEMINI B D S B S M Department of Dermatology and Venereology, ed al a lty, ed al n er ty o a Summary. presence of several hairs
FIBROSING ALOPECIA IN A PATTERN DISTRIBUTION IN TWO BROTHERS WITH PILI MULTIGEMINI B D S B S M Department of Dermatology and Venereology, ed al a lty, ed al n er ty o a Summary. presence of several hairs
COMPLEX CUTANEOUS LUPUS CASES PEARLS AND PITFALLS
 COMPLEX CUTANEOUS LUPUS CASES PEARLS AND PITFALLS Benjamin F. Chong, MD, MSCS February 17, 2018 CONFLICTS OF INTEREST D I S CLOSURE OF R E LATI ONSHIPS W I T H I NDUSTRY Benjamin Chong, MD, MSCS F059 Complex
COMPLEX CUTANEOUS LUPUS CASES PEARLS AND PITFALLS Benjamin F. Chong, MD, MSCS February 17, 2018 CONFLICTS OF INTEREST D I S CLOSURE OF R E LATI ONSHIPS W I T H I NDUSTRY Benjamin Chong, MD, MSCS F059 Complex
Poonkiat Suchonwanit, MD Hair and Scalp Disorders Unit Division of Dermatology Department of Medicine Ramathibodi Hospital
 Poonkiat Suchonwanit, MD Hair and Scalp Disorders Unit Division of Dermatology Department of Medicine Ramathibodi Hospital Hair loss Excessive hair growth Hair haft abnormalities Hair color Anagen Catagen
Poonkiat Suchonwanit, MD Hair and Scalp Disorders Unit Division of Dermatology Department of Medicine Ramathibodi Hospital Hair loss Excessive hair growth Hair haft abnormalities Hair color Anagen Catagen
Ann Dermatol Vol. 25, No. 1,
 Ann Dermatol Vol. 25, No. 1, 2013 http://dx.doi.org/10.5021/ad.2013.25.1.12 ORIGINAL ARTICLE Combination Therapy with Cyclosporine and Psoralen Plus Ultraviolet A in the Patients with Severe Alopecia Areata:
Ann Dermatol Vol. 25, No. 1, 2013 http://dx.doi.org/10.5021/ad.2013.25.1.12 ORIGINAL ARTICLE Combination Therapy with Cyclosporine and Psoralen Plus Ultraviolet A in the Patients with Severe Alopecia Areata:
INTRALESIONAL PLATELET RICH PLASMA vs INTRALESIONAL TRIAMCINOLONE IN THE TREATMENT OF ALOPECIA AREATA: A COMPARATIVE STUDY
 International Journal of Medical Research & Health Sciences www.ijmrhs.com Volume 4 Issue 1 Coden: IJMRHS Copyright @214 ISSN: 2319-5886 Received: 3 rd Oct 214 Revised: 7 th Dec 214 Accepted: 17 th Dec
International Journal of Medical Research & Health Sciences www.ijmrhs.com Volume 4 Issue 1 Coden: IJMRHS Copyright @214 ISSN: 2319-5886 Received: 3 rd Oct 214 Revised: 7 th Dec 214 Accepted: 17 th Dec
Combination Nonbiologic Therapy in Psoriasis. Sushil Tahiliani, MBBS, MD
 Combination Nonbiologic Therapy in Psoriasis Sushil Tahiliani, MBBS, MD Agenda Rationale Preferred and less preferred combination Morphology-specific preferred combinations Doses used in combinations Potential
Combination Nonbiologic Therapy in Psoriasis Sushil Tahiliani, MBBS, MD Agenda Rationale Preferred and less preferred combination Morphology-specific preferred combinations Doses used in combinations Potential
CHAPTER 22 Brocq s alopecia (pseudopelade of Brocq) and burnt out scarring alopecia
 CHAPTER 22 Brocq s alopecia (pseudopelade of Brocq) and burnt out scarring alopecia BROCQ S ALOPECIA The term pseudopelade of Brocq is a source of much confusion and fruitless debate, and should be abandoned.
CHAPTER 22 Brocq s alopecia (pseudopelade of Brocq) and burnt out scarring alopecia BROCQ S ALOPECIA The term pseudopelade of Brocq is a source of much confusion and fruitless debate, and should be abandoned.
Treatment with steroids and immunosuppressants
 Treatment with steroids and immunosuppressants Donna Culton, MD, PhD University of North Carolina IPPF 2017 Annual Patient Conference Newport Beach, CA September 16, 2017 Factors that will influence therapy
Treatment with steroids and immunosuppressants Donna Culton, MD, PhD University of North Carolina IPPF 2017 Annual Patient Conference Newport Beach, CA September 16, 2017 Factors that will influence therapy
Sarcoidosis Case. Robert P. Baughman Interstitial Lung Disease and Sarcoidosis Clinic University of Cincinnati, USA. WASOG: educational material
 Sarcoidosis Case Robert P. Baughman Interstitial Lung Disease and Sarcoidosis Clinic University of Cincinnati, USA WASOG: educational material Sarcoidosis Case patient is a Caucasian male age 46 was diagnosed
Sarcoidosis Case Robert P. Baughman Interstitial Lung Disease and Sarcoidosis Clinic University of Cincinnati, USA WASOG: educational material Sarcoidosis Case patient is a Caucasian male age 46 was diagnosed
CLASSIFICATION OF AGA IN MALES: THE HAMILTON-NORWOOD SYSTEM DISCLOSURE OF CONFLICTS OF INTEREST
 DISCLOSURE OF CONFLICTS OF INTEREST Investigator: Allergan, Intendis, Procter & Gamble, Abbott, Samumed, Cassiopea, Bayer, Galderma Amy McMichael, MD Professor and Chair Department of Dermatology Wake
DISCLOSURE OF CONFLICTS OF INTEREST Investigator: Allergan, Intendis, Procter & Gamble, Abbott, Samumed, Cassiopea, Bayer, Galderma Amy McMichael, MD Professor and Chair Department of Dermatology Wake
This PDF is available for free download from a site hosted by Medknow Publications
 Net Study Comparison of clinical efficacy of topical tazarotene.1% cream with topical clobetasol propionate.5% cream in chronic plaque psoriasis: A double-blind, randomized, right-left comparison study
Net Study Comparison of clinical efficacy of topical tazarotene.1% cream with topical clobetasol propionate.5% cream in chronic plaque psoriasis: A double-blind, randomized, right-left comparison study
Brazilian Experience of the Treatment of Alopecia Universalis with the Novel Antirheumatic Therapy Tofacitinib: A Case Series
 Rheumatol Ther (2017) 4:503 508 DOI 10.1007/s40744-017-0069-z CASE SERIES Brazilian Experience of the Treatment of Alopecia Universalis with the Novel Antirheumatic Therapy Tofacitinib: A Case Series Morton
Rheumatol Ther (2017) 4:503 508 DOI 10.1007/s40744-017-0069-z CASE SERIES Brazilian Experience of the Treatment of Alopecia Universalis with the Novel Antirheumatic Therapy Tofacitinib: A Case Series Morton
The Benefits of Leflunomide
 Page 1 of 5 Angell Navigation Site Navigation Emergency The Benefits of Leflunomide By Doug Brum, DVM www.angell.org/internalmedicine internalmedicine@angell.org 617-541-5186 Leflunomide is a newer immunosuppressant
Page 1 of 5 Angell Navigation Site Navigation Emergency The Benefits of Leflunomide By Doug Brum, DVM www.angell.org/internalmedicine internalmedicine@angell.org 617-541-5186 Leflunomide is a newer immunosuppressant
Comparison of Bier's Block and Systemic Analgesia for Upper Extremity Procedures: A Randomized Clinical Trial
 J Arch Mil Med. 1 August; (3): e1977. Published online 1 August 3. DOI: 1.81/jamm.1977 Research Article Comparison of Bier's Block and Systemic Analgesia for Upper Extremity Procedures: A Randomized Clinical
J Arch Mil Med. 1 August; (3): e1977. Published online 1 August 3. DOI: 1.81/jamm.1977 Research Article Comparison of Bier's Block and Systemic Analgesia for Upper Extremity Procedures: A Randomized Clinical
Immunosuppressants. Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia
 Immunosuppressants Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Immunosuppressive Agents Very useful in minimizing the occurrence of exaggerated or inappropriate
Immunosuppressants Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Immunosuppressive Agents Very useful in minimizing the occurrence of exaggerated or inappropriate
A case of rosacea fulminans in a pregnant woman
 Hong Kong J. Dermatol. Venereol. (2018) 26, 122-126 Views and Practice A case of rosacea fulminans in a pregnant woman JE Seol, SH Park, JU Kim, GJ Cho, SH Moon, H Kim Introduction Rosacea fulminans (RF)
Hong Kong J. Dermatol. Venereol. (2018) 26, 122-126 Views and Practice A case of rosacea fulminans in a pregnant woman JE Seol, SH Park, JU Kim, GJ Cho, SH Moon, H Kim Introduction Rosacea fulminans (RF)
EFFICACY AND SAFETY OF CLOBETASOL PROPIONATE SHAMPOO IN THERAPY OF PSORIASIS OF THE SCALP
 WORLD JOURNAL OF PHARMACY AND PHARMACEUTICAL SCIENCES Platonova et al. SJIF Impact Factor 2.786 Volume 4, Issue 04, 238-246. Research Article ISSN 2278 4357 EFFICACY AND SAFETY OF CLOBETASOL PROPIONATE
WORLD JOURNAL OF PHARMACY AND PHARMACEUTICAL SCIENCES Platonova et al. SJIF Impact Factor 2.786 Volume 4, Issue 04, 238-246. Research Article ISSN 2278 4357 EFFICACY AND SAFETY OF CLOBETASOL PROPIONATE
Acute generalized lichen planus with diffuse palmoplantar involvement in a 4-year old child: A case report and review
 CASE REPORT Acute generalized lichen planus with diffuse palmoplantar involvement in a 4-year old child: A case report and review Arun Joshi, MD, Manish Rijhwani, MD, Mohammed Alajmi, MD Department of
CASE REPORT Acute generalized lichen planus with diffuse palmoplantar involvement in a 4-year old child: A case report and review Arun Joshi, MD, Manish Rijhwani, MD, Mohammed Alajmi, MD Department of
Effects of Acupuncture on Chinese Adult Patients with Psoriatic Arthritis: A Prospective Cohort Study
 Effects of Acupuncture on Chinese Adult Patients with Psoriatic Arthritis: A Prospective Cohort Study Peiyi Chen 1, Tiantian Xin 2* and Yingchun Zeng 3,4 1 School of Nursing, Guangzhou University of Chinese
Effects of Acupuncture on Chinese Adult Patients with Psoriatic Arthritis: A Prospective Cohort Study Peiyi Chen 1, Tiantian Xin 2* and Yingchun Zeng 3,4 1 School of Nursing, Guangzhou University of Chinese
What caused this refractory pruritic eruption? Patient Presentation
 What caused this refractory pruritic eruption? Patient Presentation A 67 year-old female presented with greater than 3 years of refractory and debilitating intermittent bouts of recurrent pruritus on the
What caused this refractory pruritic eruption? Patient Presentation A 67 year-old female presented with greater than 3 years of refractory and debilitating intermittent bouts of recurrent pruritus on the
REGISTRY OF SEVERE CUTANEOUS ADVERSE REACTIONS TO DRUGS AND COLLECTION OF BIOLOGICAL SAMPLES. R e g i S C A R PATIENT'S DATA. Age country of birth
 REGISTRY OF SEVERE CUTANEOUS ADVERSE REACTIONS TO DRUGS AND COLLECTION OF BIOLOGICAL SAMPLES R e g i S C A R PATIENT'S DATA Initials of the patient date of birth Age country of birth Gender male female
REGISTRY OF SEVERE CUTANEOUS ADVERSE REACTIONS TO DRUGS AND COLLECTION OF BIOLOGICAL SAMPLES R e g i S C A R PATIENT'S DATA Initials of the patient date of birth Age country of birth Gender male female
New Patient Hair Loss: Now What? Melissa Piliang, MD Cleveland Clinic Dermatology and Pathology
 New Patient Hair Loss: Now What? Melissa Piliang, MD Cleveland Clinic Dermatology and Pathology Conflict of Interest No relevant conflicts Investigator for Samumed, Kythera, Incyte, Concert, Allergan Advisory
New Patient Hair Loss: Now What? Melissa Piliang, MD Cleveland Clinic Dermatology and Pathology Conflict of Interest No relevant conflicts Investigator for Samumed, Kythera, Incyte, Concert, Allergan Advisory
JERRY SHAPIRO, MD, FAAD PROFESSOR
 The Ronald O. Perelman Department of Dermatology Novel treatments for hair regrowth Where are we? JERRY SHAPIRO, MD, FAAD PROFESSOR AAD Chicago 2018 Disclosures Consultant/Investigator for: Aclaris Samumed
The Ronald O. Perelman Department of Dermatology Novel treatments for hair regrowth Where are we? JERRY SHAPIRO, MD, FAAD PROFESSOR AAD Chicago 2018 Disclosures Consultant/Investigator for: Aclaris Samumed
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,350 108,000 1.7 M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,350 108,000 1.7 M Open access books available International authors and editors Downloads Our
The reliability of three psoriasis assessment tools: Psoriasis area and severity index, body surface area and physician global assessment
 Original papers The reliability of three psoriasis assessment tools: Psoriasis area and severity index, body surface area and physician global assessment Agnieszka Bożek A F, Adam Reich A F Department
Original papers The reliability of three psoriasis assessment tools: Psoriasis area and severity index, body surface area and physician global assessment Agnieszka Bożek A F, Adam Reich A F Department
Dermoscopic Approach to a Small Round to Oval Hairless Patch on the Scalp
 Ann Dermatol Vol. 26, No. 2, 2014 http://dx.doi.org/10.5021/ad.2014.26.2.214 ORIGINAL ARTICLE Dermoscopic Approach to a Small Round to Oval Hairless Patch on the Scalp Woo-Haing Shim 1, Seung-Wook Jwa
Ann Dermatol Vol. 26, No. 2, 2014 http://dx.doi.org/10.5021/ad.2014.26.2.214 ORIGINAL ARTICLE Dermoscopic Approach to a Small Round to Oval Hairless Patch on the Scalp Woo-Haing Shim 1, Seung-Wook Jwa
Cutanous Manifestation of Lupus Erythematosus. Presented By: Dr. Naif S. Al Shahrani Salman Bin Abdaziz university
 Cutanous Manifestation of Lupus Erythematosus Presented By: Dr. Naif S. Al Shahrani Salman Bin Abdaziz university A 50-year old lady, who is otherwise healthy, presented to the dermatology clinic with
Cutanous Manifestation of Lupus Erythematosus Presented By: Dr. Naif S. Al Shahrani Salman Bin Abdaziz university A 50-year old lady, who is otherwise healthy, presented to the dermatology clinic with
News in erosive lichen planus of the vulva
 News in erosive lichen planus of the vulva Anne Lise Helgesen Dermatologist, Postdoc, National Centre of Womens Health, Oslo University Hospital, Oslo, Norway - a great challenge WHY? No evidence based
News in erosive lichen planus of the vulva Anne Lise Helgesen Dermatologist, Postdoc, National Centre of Womens Health, Oslo University Hospital, Oslo, Norway - a great challenge WHY? No evidence based
PSORIASIS PSORIASIS. Anatomic sites FACTS ABOUT PROSIASIS PSORIASIS 11/16/2017 STIGMATA OF PSORIASIS
 PSORIASIS Dr. Sami Alsuwaidan President, Saudi Society of Dermatology & Dermatologic Surgery Associate Professor and Consultant Department of Dermatology, College of Medicine King Saud University PSORIASIS
PSORIASIS Dr. Sami Alsuwaidan President, Saudi Society of Dermatology & Dermatologic Surgery Associate Professor and Consultant Department of Dermatology, College of Medicine King Saud University PSORIASIS
Quality of life in patients with alopecia areata attending dermatology department in a tertiary care centre - A cross-sectional study
 Original Article Quality of life in patients with alopecia areata attending dermatology department in a tertiary care centre - A cross-sectional study Fasalul Abideen, Anoop Thy Valappil, Pretty Mathew,
Original Article Quality of life in patients with alopecia areata attending dermatology department in a tertiary care centre - A cross-sectional study Fasalul Abideen, Anoop Thy Valappil, Pretty Mathew,
INFORMATION ON HYDROXYCHLOROQUINE (PLAQUENIL)
 750 West Broadway Suite 905 - Vancouver BC V5Z 1H8 Phone: 604.283.9299 Fax: 604.648.9003 Email: vancouveroffice@donovanmedical.com Web: www.donovanmedical.com INFORMATION ON HYDROXYCHLOROQUINE (PLAQUENIL)
750 West Broadway Suite 905 - Vancouver BC V5Z 1H8 Phone: 604.283.9299 Fax: 604.648.9003 Email: vancouveroffice@donovanmedical.com Web: www.donovanmedical.com INFORMATION ON HYDROXYCHLOROQUINE (PLAQUENIL)
Clinical Trial Report Synopsis
 Clinical Trial Report Synopsis A phase 2a, proof of concept trial, testing twice daily application of LEO 124249 ointment 30 mg/g in the treatment of mild to moderate inverse psoriasis Design of trial:
Clinical Trial Report Synopsis A phase 2a, proof of concept trial, testing twice daily application of LEO 124249 ointment 30 mg/g in the treatment of mild to moderate inverse psoriasis Design of trial:
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,500 108,000 1.7 M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,500 108,000 1.7 M Open access books available International authors and editors Downloads Our
S003 CPC Self-Assessment
 S003 CPC Self-Assessment Alina G. Bridges, D.O. Associate Professor Program Director, Dermatopathology Fellowship Department of Dermatology, Division of Dermatopathology and Cutaneous Immunopathology Mayo
S003 CPC Self-Assessment Alina G. Bridges, D.O. Associate Professor Program Director, Dermatopathology Fellowship Department of Dermatology, Division of Dermatopathology and Cutaneous Immunopathology Mayo
Etanercept for Treatment of Hidradenitis
 Home Search Browse Resources Help What's New About Purpose Etanercept for Treatment of Hidradenitis This study is currently recruiting patients. Sponsors and Collaborators: University of Pennsylvania Amgen
Home Search Browse Resources Help What's New About Purpose Etanercept for Treatment of Hidradenitis This study is currently recruiting patients. Sponsors and Collaborators: University of Pennsylvania Amgen
Evaluation of efficacy and safety of finasteride 1 mg in 3177 Japanese men with androgenetic alopecia
 doi:./j.46-88.2.78.x Journal of Dermatology 22; 9: 27 2 ORIGINAL ARTICLE Evaluation of efficacy and safety of finasteride mg in 77 Japanese men with androgenetic alopecia Akio SATO, Akira TAKEDA 2 Tokyo
doi:./j.46-88.2.78.x Journal of Dermatology 22; 9: 27 2 ORIGINAL ARTICLE Evaluation of efficacy and safety of finasteride mg in 77 Japanese men with androgenetic alopecia Akio SATO, Akira TAKEDA 2 Tokyo
Modified Atkins diet in adult with refractory epilepsy: A controlled randomized clinical trial
 Iranian Journal of Neurology Original Paper Iran J Neurol 2017; 16(2): 72-7 Modified Atkins diet in adult with refractory epilepsy: A controlled randomized clinical trial Received: 17 Dec. 2016 Accepted:
Iranian Journal of Neurology Original Paper Iran J Neurol 2017; 16(2): 72-7 Modified Atkins diet in adult with refractory epilepsy: A controlled randomized clinical trial Received: 17 Dec. 2016 Accepted:
ALOPECIA AREATA (AA) IS A
 STUDY Alefacept for Severe Alopecia Areata A Randomized, Double-blind, Placebo-Controlled Study Bruce E. Strober, MD, PhD; Kavita Menon, MD; Amy McMichael, MD; Maria Hordinsky, MD; Gerald Krueger, MD;
STUDY Alefacept for Severe Alopecia Areata A Randomized, Double-blind, Placebo-Controlled Study Bruce E. Strober, MD, PhD; Kavita Menon, MD; Amy McMichael, MD; Maria Hordinsky, MD; Gerald Krueger, MD;
Quality of life in patients with primary axillary hyperhidrosis before and after treatment with fractionated microneedle radiofrequency
 Original Article Quality of life in patients with primary axillary hyperhidrosis before and after treatment with fractionated microneedle radiofrequency Bahareh Abtahi-Naeini, Farahnaz Fatemi Naeini, Neda
Original Article Quality of life in patients with primary axillary hyperhidrosis before and after treatment with fractionated microneedle radiofrequency Bahareh Abtahi-Naeini, Farahnaz Fatemi Naeini, Neda
Pharmacy Prior Authorization
 Pharmacy Prior Authorization AETA BETTER HEALTH PESLVAIA & AETA BETTER HEALTH KIDS Humira (Medicaid) This fax machine is located in a secure location as required by HIPAA regulations. Complete/review information,
Pharmacy Prior Authorization AETA BETTER HEALTH PESLVAIA & AETA BETTER HEALTH KIDS Humira (Medicaid) This fax machine is located in a secure location as required by HIPAA regulations. Complete/review information,
Conflicts of interest
 Vulvar Cases 2 nd PANHELLANIC CONGRESS on Lower Genital Tract Disorders December 14-16 Grand Hyatt Athens Lynette J. Margesson MD FRCPC Assistant Professor of Obstetrics & Gynecology and Surgery(Dermatology)
Vulvar Cases 2 nd PANHELLANIC CONGRESS on Lower Genital Tract Disorders December 14-16 Grand Hyatt Athens Lynette J. Margesson MD FRCPC Assistant Professor of Obstetrics & Gynecology and Surgery(Dermatology)
KEY MESSAGES. Psoriasis patients are more prone to cardiovascular diseases, stroke, lymphoma and non-melanoma skin cancers, and increased mortality.
 KEY MESSAGES Psoriasis is a genetically determined, systemic immune-mediated chronic inflammatory disease that affects primarily the skin and joints. Psoriasis Vulgaris is characterised by well-demarcated
KEY MESSAGES Psoriasis is a genetically determined, systemic immune-mediated chronic inflammatory disease that affects primarily the skin and joints. Psoriasis Vulgaris is characterised by well-demarcated
World Journal of Pharmaceutical Research
 Shraddhamayananda SJIF Impact Factor 5.045 Volume 3, Issue 6, 618-625. Research Article ISSN 2277 7105 EFFICACY OF HOMEOPATHIC MEDICINES IN THE TREATMENT OF ACNE *Swami Shraddhamayananda Ramakrishna Mission
Shraddhamayananda SJIF Impact Factor 5.045 Volume 3, Issue 6, 618-625. Research Article ISSN 2277 7105 EFFICACY OF HOMEOPATHIC MEDICINES IN THE TREATMENT OF ACNE *Swami Shraddhamayananda Ramakrishna Mission
Dermatopathology Workshop Summary, Berlin 2004
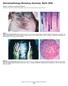 Dermatopathology Workshop Summary, Berlin 2004 David A. Whiting and Rolf Hoffmannw Baylor Hair Research and Treatment Center, Dallas, Texas, USA; wdermatology Practice, Freiburg, Germany Figure 1 Case
Dermatopathology Workshop Summary, Berlin 2004 David A. Whiting and Rolf Hoffmannw Baylor Hair Research and Treatment Center, Dallas, Texas, USA; wdermatology Practice, Freiburg, Germany Figure 1 Case
Prescribing Information
 Prescribing Information Pr DERMOVATE Cream (clobetasol propionate cream, USP) Pr DERMOVATE Ointment (clobetasol propionate ointment, USP) Topical corticosteroid TaroPharma Preparation Date: A Division
Prescribing Information Pr DERMOVATE Cream (clobetasol propionate cream, USP) Pr DERMOVATE Ointment (clobetasol propionate ointment, USP) Topical corticosteroid TaroPharma Preparation Date: A Division
Adrenocorticotropic hormone gel in patients with refractory rheumatoid arthritis: a case series
 International Journal of Clinical Rheumatology For reprint orders, please contact: reprints@futuremedicine.com Adrenocorticotropic hormone gel in patients with refractory rheumatoid arthritis: a case series
International Journal of Clinical Rheumatology For reprint orders, please contact: reprints@futuremedicine.com Adrenocorticotropic hormone gel in patients with refractory rheumatoid arthritis: a case series
Psoriatic Scarring Alopecia
 Psoriatic Scarring Alopecia Ming-Hsiung Yeh 1 Tsen-Fang Tsai 2 Cheng-Hsiang Hsiao 3 Psoriasis affects approximately 0.123% of the population in China. Scalp is the first site of involvement in nearly 50%
Psoriatic Scarring Alopecia Ming-Hsiung Yeh 1 Tsen-Fang Tsai 2 Cheng-Hsiang Hsiao 3 Psoriasis affects approximately 0.123% of the population in China. Scalp is the first site of involvement in nearly 50%
The Egyptian Journal of Hospital Medicine (January 2019) Vol. 74 (6), Page
 The Egyptian Journal of Hospital Medicine (January 2019) Vol. 74 (6), Page 1416-1422 Trichoscopic Clues for Diagnosis of Patchy Scalp Alopecia in the Egyptian Patients Abd Elrauof Mohamed AL Mohsen, Mohamed
The Egyptian Journal of Hospital Medicine (January 2019) Vol. 74 (6), Page 1416-1422 Trichoscopic Clues for Diagnosis of Patchy Scalp Alopecia in the Egyptian Patients Abd Elrauof Mohamed AL Mohsen, Mohamed
A Comparative Study of Oral Cyclosporine and Betamethasone Minipulse Therapy in the Treatment of Alopecia Areata
 Cyclosporine and Steroid Minipulse Therapy in AA pissn 1013-9087ㆍeISSN 2005-3894 Ann Dermatol Vol. 28, No. 5, 2016 http://dx.doi.org/10.5021/ad.2016.28.5.569 ORIGINAL ARTICLE A Comparative Study of Oral
Cyclosporine and Steroid Minipulse Therapy in AA pissn 1013-9087ㆍeISSN 2005-3894 Ann Dermatol Vol. 28, No. 5, 2016 http://dx.doi.org/10.5021/ad.2016.28.5.569 ORIGINAL ARTICLE A Comparative Study of Oral
What s New in Alopecia Areata
 AN UPDATE ON THE LAST 12 MONTHS What s New in Alopecia Areata PhD FRCPC Dermatologist Assistant Professor, University of Toronto Getting information out to Physicians Five new studies to discuss Can cholesterol
AN UPDATE ON THE LAST 12 MONTHS What s New in Alopecia Areata PhD FRCPC Dermatologist Assistant Professor, University of Toronto Getting information out to Physicians Five new studies to discuss Can cholesterol
Alopecia. Antonella Tosti. Fredric Brandt Endowed Professor of Dermatology&Cutaneous Surgery Miller School of Medicine, University of Miami
 Alopecia Antonella Tosti Fredric Brandt Endowed Professor of Dermatology&Cutaneous Surgery Miller School of Medicine, University of Miami DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY Antonella Tosti, MD S049
Alopecia Antonella Tosti Fredric Brandt Endowed Professor of Dermatology&Cutaneous Surgery Miller School of Medicine, University of Miami DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY Antonella Tosti, MD S049
74 B4 C 36 #%&' $ ./ 14U 1 / : )'"/%& '" #$. %* #& 1#/V W&, X-/2 1,*E! #G! 1%/V C YV 1 :7? #:Z2 #? :! +!" #$ %&' ( )' * -2 + :
 1392915: 13921119: 1392,(&' () #*#$%)! 269 #$"!: 2 2 1! 2 3 ()& * "# $%& #%&' $! " #$%& '( ) (Pseudocatalasesuperoxide dismutase PSD) :. #7. * 8 4 #*! *9:&! $;
1392915: 13921119: 1392,(&' () #*#$%)! 269 #$"!: 2 2 1! 2 3 ()& * "# $%& #%&' $! " #$%& '( ) (Pseudocatalasesuperoxide dismutase PSD) :. #7. * 8 4 #*! *9:&! $;
Comparison the effectiveness of pyruvic acid 50% and salicylic acid 30% in the treatment of acne
 Original Article Comparison the effectiveness of pyruvic acid 50% and salicylic acid 30% in the treatment of acne Fariba Jaffary, Gita Faghihi 1, Sara Saraeian 2, Sayed Mohsen Hosseini 3 Skin Diseases
Original Article Comparison the effectiveness of pyruvic acid 50% and salicylic acid 30% in the treatment of acne Fariba Jaffary, Gita Faghihi 1, Sara Saraeian 2, Sayed Mohsen Hosseini 3 Skin Diseases
Psoriasis is a lifelong condition, with onset
 THERAPEUTICS FOR THE CLINICIAN Clobetasol Propionate Lotion in the Treatment of Moderate to Severe Plaque-Type Psoriasis Jacques Decroix, MD; Henrik Pres, MD; Nicolaï Tsankov, MD; Michel Poncet, PhD; Stéphanie
THERAPEUTICS FOR THE CLINICIAN Clobetasol Propionate Lotion in the Treatment of Moderate to Severe Plaque-Type Psoriasis Jacques Decroix, MD; Henrik Pres, MD; Nicolaï Tsankov, MD; Michel Poncet, PhD; Stéphanie
Index. derm.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Abatacept for DLE, 493 for SLE, 497 Ablative therapies, localized, for cutaneous T-cell lymphoma, 502 506. See also Cutaneous T-cell lymphoma,
Note: Page numbers of article titles are in boldface type. A Abatacept for DLE, 493 for SLE, 497 Ablative therapies, localized, for cutaneous T-cell lymphoma, 502 506. See also Cutaneous T-cell lymphoma,
Update on systemic therapies and emerging treatments How do I choose a systemic agent?
 Update on systemic therapies and emerging treatments How do I choose a systemic agent? Amy S. Paller, M.D. Walter J. Hamlin Professor and Chair of Dermatology Professor of Pediatrics Northwestern University
Update on systemic therapies and emerging treatments How do I choose a systemic agent? Amy S. Paller, M.D. Walter J. Hamlin Professor and Chair of Dermatology Professor of Pediatrics Northwestern University
A study of treatment modalities in psoriasis in dermatology outpatient department of a tertiary care teaching hospital
 Original article A study of treatment modalities in psoriasis in dermatology outpatient department of a tertiary care teaching hospital 1Y Roja Ramani, 2 Benu Panigrahy, 3 Sailenkumar Mishra, 4 BTPS Singh
Original article A study of treatment modalities in psoriasis in dermatology outpatient department of a tertiary care teaching hospital 1Y Roja Ramani, 2 Benu Panigrahy, 3 Sailenkumar Mishra, 4 BTPS Singh
Alopecia areata: Workup and treatment
 Alopecia areata: Workup and treatment Carolyn Goh Assistant Clinical Professor David Geffen School of Medicine at UCLA Department of Medicine-Dermatology February 2018 DISCLOSURE OF RELATIONSHIPS WITH
Alopecia areata: Workup and treatment Carolyn Goh Assistant Clinical Professor David Geffen School of Medicine at UCLA Department of Medicine-Dermatology February 2018 DISCLOSURE OF RELATIONSHIPS WITH
Analysis of causation of Stevens Johnson Syndrome in a patient of rheumatoid arthritis with increased dose of methotrexate
 Original Research Article Analysis of causation of Stevens Johnson Syndrome in a patient of rheumatoid arthritis with increased dose of methotrexate Manab Nandy 1, Sangeeta De 2*, Mustafa Asad 2, Nirmal
Original Research Article Analysis of causation of Stevens Johnson Syndrome in a patient of rheumatoid arthritis with increased dose of methotrexate Manab Nandy 1, Sangeeta De 2*, Mustafa Asad 2, Nirmal
GENERAL OVERVIEW OF TYPES OF HAIR LOSS AND ALOPECIA TELOGEN EFFLUVIUM
 GENERAL OVERVIEW OF TYPES OF HAIR LOSS AND ALOPECIA TELOGEN EFFLUVIUM Telogen effluvium is a form of diffuse hair loss that occurs during the telogen or resting phase of the hair growth cycle. Telogen
GENERAL OVERVIEW OF TYPES OF HAIR LOSS AND ALOPECIA TELOGEN EFFLUVIUM Telogen effluvium is a form of diffuse hair loss that occurs during the telogen or resting phase of the hair growth cycle. Telogen
The value of dermoscopy in diagnosing eyebrow loss in patients with alopecia areata and frontal fibrosing alopecia
 DOI: 10.1111/jdv.15279 JEADV ORIGINAL ARTICLE The value of dermoscopy in diagnosing eyebrow loss in patients with alopecia areata and frontal fibrosing alopecia A. Waskiel-Burnat, 1 A. Rakowska, 1, * M.
DOI: 10.1111/jdv.15279 JEADV ORIGINAL ARTICLE The value of dermoscopy in diagnosing eyebrow loss in patients with alopecia areata and frontal fibrosing alopecia A. Waskiel-Burnat, 1 A. Rakowska, 1, * M.
Case 1 History. William Tremaine, M.D. CP
 Extraintestinal Manifestations of IBD Case Studies William Tremaine, M.D. Case 1 History 18 year-old woman with Crohn s disease Onset at age 5: colonic & perianal Sulfasalazine, prednisone, mercaptopurine
Extraintestinal Manifestations of IBD Case Studies William Tremaine, M.D. Case 1 History 18 year-old woman with Crohn s disease Onset at age 5: colonic & perianal Sulfasalazine, prednisone, mercaptopurine
Clinical Study Narrow-Band Ultraviolet B versus Oral Minocycline in Treatment of Unstable Vitiligo: A Prospective Comparative Trial
 Dermatology Research and Practice, Article ID 240856, 4 pages http://dx.doi.org/10.1155/2014/240856 Clinical Study Narrow-Band Ultraviolet B versus Oral Minocycline in Treatment of Unstable Vitiligo: A
Dermatology Research and Practice, Article ID 240856, 4 pages http://dx.doi.org/10.1155/2014/240856 Clinical Study Narrow-Band Ultraviolet B versus Oral Minocycline in Treatment of Unstable Vitiligo: A
LUPUS CAN DO EVERYTHING, BUT NOT EVERYTHING IS LUPUS LUPUS 101 SLE SUBSETS AUTOIMMUNE DISEASE 11/4/2013 HOWARD HAUPTMAN, MD IDIOPATHIC DISCOID LUPUS
 LUPUS 101 LUPUS CAN DO EVERYTHING, BUT NOT EVERYTHING IS LUPUS HOWARD HAUPTMAN, MD IDIOPATHIC DISCOID LUPUS SLE SUBSETS SUBACUTE CUTANEOUS LUPUS DRUG INDUCED LUPUS NEONATAL LUPUS LATE ONSET LUPUS ANTI-PHOSPHOLIPID
LUPUS 101 LUPUS CAN DO EVERYTHING, BUT NOT EVERYTHING IS LUPUS HOWARD HAUPTMAN, MD IDIOPATHIC DISCOID LUPUS SLE SUBSETS SUBACUTE CUTANEOUS LUPUS DRUG INDUCED LUPUS NEONATAL LUPUS LATE ONSET LUPUS ANTI-PHOSPHOLIPID
DATA SHEET. Betamethasone dipropionate equivalent to betamethasone 0.5mg/g (0.05% w/w).
 DATA SHEET 1. DIPROSONE DIPROSONE (0.05% w/w) cream DIPROSONE (0.05% w/w) ointment 2. QUALITATIVE AND QUANTITATIVE COMPOSITION Betamethasone dipropionate equivalent to betamethasone 0.5mg/g (0.05% w/w).
DATA SHEET 1. DIPROSONE DIPROSONE (0.05% w/w) cream DIPROSONE (0.05% w/w) ointment 2. QUALITATIVE AND QUANTITATIVE COMPOSITION Betamethasone dipropionate equivalent to betamethasone 0.5mg/g (0.05% w/w).
LOCALLY AVAILABLE BIOLOGIC AGENTS IN THE TREATMENT OF PSORIATIC ARTHRITIS
 Locally Available Biologic Agents in the Treatment of Psoriatic Arthritis 253 Phil. J. Internal Medicine, 47: 253-259, Nov.-Dec., 2009 LOCALLY AVAILABLE BIOLOGIC AGENTS IN THE TREATMENT OF PSORIATIC ARTHRITIS
Locally Available Biologic Agents in the Treatment of Psoriatic Arthritis 253 Phil. J. Internal Medicine, 47: 253-259, Nov.-Dec., 2009 LOCALLY AVAILABLE BIOLOGIC AGENTS IN THE TREATMENT OF PSORIATIC ARTHRITIS
Androgenetic alopecia (AGA) or common baldness
 Original Article Access this article online Website: www.ijtrichology.com DOI: 10.4103/ijt.ijt_75_16 Quick Response Code: A Comparative Study of Microneedling with Platelet rich Plasma Plus Topical Minoxidil
Original Article Access this article online Website: www.ijtrichology.com DOI: 10.4103/ijt.ijt_75_16 Quick Response Code: A Comparative Study of Microneedling with Platelet rich Plasma Plus Topical Minoxidil
How to decipher a pathology report for alopecia
 How to decipher a pathology report for alopecia DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY Lynne J. Goldberg, MD S063-Hair Disorders Made Easier DISCLOSURES I do not have any relationships with industry
How to decipher a pathology report for alopecia DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY Lynne J. Goldberg, MD S063-Hair Disorders Made Easier DISCLOSURES I do not have any relationships with industry
Coverage Criteria: Express Scripts, Inc. monograph dated 12/15/ months or as otherwise noted by indication
 BENEFIT DESCRIPTION AND LIMITATIONS OF COVERAGE ITEM: PRODUCT LINES: COVERED UNDER: DESCRIPTION: CPT/HCPCS Code: Company Supplying: Setting: Kineret (anakinra subcutaneous injection) Commercial HMO/PPO/CDHP
BENEFIT DESCRIPTION AND LIMITATIONS OF COVERAGE ITEM: PRODUCT LINES: COVERED UNDER: DESCRIPTION: CPT/HCPCS Code: Company Supplying: Setting: Kineret (anakinra subcutaneous injection) Commercial HMO/PPO/CDHP
Letter to the Editor: Nail Lichen Planus: A True Nail Emergency. Journal of the American Academy of Dermatology
 Accepted Manuscript Letter to the Editor: Nail Lichen Planus: A True Nail Emergency Shari R. Lipner, MD, PhD PII: S0190-9622(19)30128-8 DOI: https://doi.org/10.1016/j.jaad.2018.11.065 Reference: YMJD 13102
Accepted Manuscript Letter to the Editor: Nail Lichen Planus: A True Nail Emergency Shari R. Lipner, MD, PhD PII: S0190-9622(19)30128-8 DOI: https://doi.org/10.1016/j.jaad.2018.11.065 Reference: YMJD 13102
Vaginal involvement in genital erosive lichen planus
 Acta Obstetricia et Gynecologica. 2010; 89: 966 970 SHORT REPORT Vaginal involvement in genital erosive lichen planus ANNE LISE ORDING HELGESEN 1,2,3, PETTER GJERSVIK 3,4, PETER JEBSEN 5, ROLF KIRSCHNER
Acta Obstetricia et Gynecologica. 2010; 89: 966 970 SHORT REPORT Vaginal involvement in genital erosive lichen planus ANNE LISE ORDING HELGESEN 1,2,3, PETTER GJERSVIK 3,4, PETER JEBSEN 5, ROLF KIRSCHNER
Update on African American Hair and Scalp Disorders
 Update on African American Hair and Scalp Disorders Heather Woolery-Lloyd, M.D. Director of Ethnic Skin Care Voluntary Assistant Professor Miller/University of Miami School of Medicine Department of Dermatology
Update on African American Hair and Scalp Disorders Heather Woolery-Lloyd, M.D. Director of Ethnic Skin Care Voluntary Assistant Professor Miller/University of Miami School of Medicine Department of Dermatology
Patients who achieved the primary criterion for response i.e.: complete clearance or a reduction
 MC 9101 F Study Page3 ABSTRACT Background: Cyclosporin A has been shown to be an effective systemic treatment in severe psoriasis but with the disadvantage of dose-dependent toxic effects particularly
MC 9101 F Study Page3 ABSTRACT Background: Cyclosporin A has been shown to be an effective systemic treatment in severe psoriasis but with the disadvantage of dose-dependent toxic effects particularly
CONTROVERSIES IN MANAGEMENT AND TREATMENT OF CUTANEOUS LUPUS PATIENTS
 CONTROVERSIES IN MANAGEMENT AND TREATMENT OF CUTANEOUS LUPUS PATIENTS Benjamin F. Chong, MD, MSCS February 19, 2018 CONFLICTS OF INTEREST D I S CLOSURE OF R E LATI ONSHIPS W I T H I NDUSTRY Benjamin Chong,
CONTROVERSIES IN MANAGEMENT AND TREATMENT OF CUTANEOUS LUPUS PATIENTS Benjamin F. Chong, MD, MSCS February 19, 2018 CONFLICTS OF INTEREST D I S CLOSURE OF R E LATI ONSHIPS W I T H I NDUSTRY Benjamin Chong,
Trichoscopic findings in cicatricial alopecias and hair shaft disorders and its application in histopathology
 International Journal of Research in Medical Sciences Khadatkar AS et al. Int J Res Med Sci. 2017 Dec;5(12):5254-5259 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Original Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20175435
International Journal of Research in Medical Sciences Khadatkar AS et al. Int J Res Med Sci. 2017 Dec;5(12):5254-5259 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Original Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20175435
Quality of life evaluation in patients with pemphigus vulgaris
 Original Article Quality of life evaluation in patients with pemphigus vulgaris Pouran Layegh, MD 1 Yalda Nahidi, MD 1 Iman Malekzadeh, MD 1 Mohammad Taghi Shakeri, MD 2 1. Research Center for Cutaneous
Original Article Quality of life evaluation in patients with pemphigus vulgaris Pouran Layegh, MD 1 Yalda Nahidi, MD 1 Iman Malekzadeh, MD 1 Mohammad Taghi Shakeri, MD 2 1. Research Center for Cutaneous
