MDS 3.0 Quality Measures USER S MANUAL
|
|
|
- Lucas Anthony
- 5 years ago
- Views:
Transcription
1 MDS 3.0 Quality Measures USER S MANUAL Effective April 1, 2017 Prepared for: The Centers for Medicare & Medicaid Services under Contract No. HHSM I (HHSM-500-T0001). (RTI Project Number )
2 [This page intentionally left blank.]
3 QUALITY MEASURES (QM) USER S MANUAL CONTENTS Chapter 1 QM Sample and Record Selection Methodology...1 Section 1: Definitions...1 Section 2: Selecting the QM Samples...3 Section 3: Short Stay Record Definitions...4 Section 4: Long Stay Record Definitions...6 Chapter 2 MDS 3.0 Quality Measures Logical Specifications...9 Section 1: Short Stay Quality Measures...10 MDS 3.0 Measure: Percent of Residents Who Self-Report Moderate to Severe Pain (Short Stay)...10 MDS 3.0 Measure: Percent of Residents With Pressure Ulcers That Are New or Worsened (Short Stay)...11 MDS 3.0 Measure: Percent of Residents Who Were Assessed and Appropriately Given the Seasonal Influenza Vaccine (Short Stay)...13 MDS 3.0 Measure: Percent of Residents Who Received the Seasonal Influenza Vaccine (Short Stay)...14 MDS 3.0 Measure: Percent of Residents Who Were Offered and Declined the Seasonal Influenza Vaccine (Short Stay)...15 MDS 3.0 Measure: Percent of Residents Who Did Not Receive, Due to Medical Contraindication, the Seasonal Influenza Vaccine (Short Stay)...16 MDS 3.0 Measure: Percent of Residents Who Newly Received an Antipsychotic Medication (Short Stay)...17 MDS 3.0 Measure: Percent of Residents Who Made Improvements in Function (Short Stay)...18 Section 2: Long Stay Quality Measures...21 MDS 3.0 Measure: Percent of Residents Experiencing One or More Falls with Major Injury (Long Stay)...21 RTI International April 2017 (v11.0) i
4 MDS 3.0 Measure: Percent of Residents Who Self-Report Moderate to Severe Pain (Long Stay)...22 MDS 3.0 Measure: Percent of High-Risk Residents With Pressure Ulcers (Long Stay)...23 MDS 3.0 Measure: Percent of Residents Assessed and Appropriately Given the Seasonal Influenza Vaccine (Long Stay)...24 MDS 3.0 Measure: Percent of Residents Who Received the Seasonal Influenza Vaccine (Long Stay)...25 MDS 3.0 Measure: Percent of Residents Who Were Offered and Declined the Seasonal Influenza Vaccine (Long Stay)...26 MDS 3.0 Measure: Percent of Residents Who Did Not Receive, Due to Medical Contraindication, the Seasonal Influenza Vaccine (Long Stay)...27 MDS 3.0 Measure: Percent of Residents with a Urinary Tract Infection (Long Stay)...28 MDS 3.0 Measure: Percent of Residents Who Have/Had a Catheter Inserted and Left in Their Bladder (Long Stay)...29 MDS 3.0 Measure: Percent of Residents Who Were Physically Restrained (Long Stay)...30 MDS 3.0 Measure: Percent of Residents Whose Need for Help with Activities of Daily Living Has Increased (Long Stay)...31 MDS 3.0 Measure: Percent of Residents Who Lose Too Much Weight (Long Stay)...33 MDS 3.0 Measure: Percent of Residents Who Received an Antipsychotic Medication (Long-Stay)...34 MDS 3.0 Measure: Percent of Residents Who Used Antianxiety or Hypnotic Medication (Long Stay)...35 MDS 3.0 Measure: Percent of Residents Whose Ability to Move Independently Worsened (Long Stay)...36 Appendix A: Technical Details... A-1 Appendix B: Parameters Used for Each Quarter...B-1 Appendix C: Episode and Stay Determination Logic...C-1 Appendix D: Measures Withdrawn from NQF Submission... D-1 Appendix E: Surveyor Quality Measures... E-1 Appendix F: Specifications for the Facility Characteristics Report... F-1 RTI International April 2017 (v11.0) ii
5 Chapter 1 QM Sample and Record Selection Methodology The purpose of this chapter is to describe the methodology that is used to select the short and long stay samples as well as the key records that are used to compute the QMs for each of those samples. The first section below will present definitions that are used to describe the selection methodology. The second section describes the selection of the two samples. The third and fourth sections describe the selection of the key records within each of the two samples. The logic presented below depends upon the concepts of stays and episodes. Detailed specifications for the identification of stays and episodes are presented in Appendix C of this document. Section 1: Definitions Target period. The span of time that defines the QM reporting period (e.g., a calendar quarter). Stay. The period of time between a resident s entry into a facility and either (a) a discharge, or (b) the end of the target period, whichever comes first. A stay is also defined as a set of contiguous days in a facility. The start of a stay is either: An admission entry (A0310F = [01] and A1700 = [1]), or A reentry (A0310F = [01] and A1700 = [2]). The end of a stay is the earliest of the following: Any discharge assessment (A0310F = [10, 11]), or A death in facility tracking record (A0310F = [12]), or The end of the target period. Episode. A period of time spanning one or more stays. An episode begins with an admission (defined below) and ends with either (a) a discharge, or (b) the end of the target period, whichever comes first. An episode starts with: An admission entry (A0310F = [01] and A1700 = [1]). The end of an episode is the earliest of the following: A discharge assessment with return not anticipated (A0310F = [10]), or A discharge assessment with return anticipated (A0310F = [11]) but the resident did not return within 30 days of discharge, or A death in facility tracking record (A0310F = [12]), or The end of the target period. RTI International April 2017 (v11.0) 1
6 Admission. An admission entry record (A0310F = [01] and A1700 = [1]) is required when any one of the following occurs: Resident has never been admitted to this facility before; or Resident has been in this facility previously and was discharged return not anticipated; or Resident has been in this facility previously and was discharged return anticipated and did not return within 30 days of discharge. Reentry. A reentry record (A0310F = [01] and A1700 = [2]) is required when all of the following occurred prior to this entry, the resident was: Discharged return anticipated, and Returned to facility within 30 days of discharge. Cumulative days in facility (CDIF). The total number of days within an episode during which the resident was in the facility. It is the sum of the number of days within each stay included in an episode. If an episode consists of more than one stay separated by periods of time outside the facility (e.g., hospitalizations), only those days within the facility would count towards CDIF. Any days outside of the facility (e.g., hospital, home, etc.) would not count towards the CDIF total. The following rules are used when computing CDIF: When counting the number of days until the end of the episode, counting stops with (a) the last record in the target period if that record is a discharge assessment (A0310F = [10, 11]), (b) the last record in the target period if that record is a death in facility (A0310F = [12]), or (c) the end of the target period is reached, whichever is earlier. When counting the duration of each stay within an episode, include the day of entry (A1600) but not the day of discharge (A2000) unless the entry and discharge occurred on the same day in which case the number of days in the stay is equal to 1. While death in facility records (A0310F = [12]) end CDIF counting, these records are not used as target records because they contain only tracking information and do not include clinical information necessary for QM calculation. Special rules for influenza vaccination measures. Influenza vaccination measures are calculated only once per 12-month influenza season, which begins July 1 of a given year and ends on June 30 of the subsequent year. For these measures, the target period begins on October 1 and ends on March 31. This means that the end-of-episode date will be March 31 for an episode that is ongoing at the end of the influenza season and that March 31 should be used as the end date when computing CDIF and for classifying stays as long or short for the influenza vaccination measures. o Short stay. An episode with CDIF less than or equal to 100 days as of the end of the target period. Long stay. An episode with CDIF greater than or equal to 101 days as of the end of the target period. RTI International April 2017 (v11.0) 2
7 Target date. The event date for an MDS record, defined as follows: For an entry record (A0310F = [01]), the target date is equal to the entry date (A1600). For a discharge record (A0310F = [10, 11]) or death-in-facility record (A0310F = [12]), the target date is equal to the discharge date (A2000). For all other records, the target date is equal to the assessment reference date (A2300). Section 2: Selecting the QM Samples Two resident samples are selected for computing the QMs: a short-stay sample and a long-stay sample. These samples are selected using the following steps: 1. Select all residents whose latest episode either ends during the target period or is ongoing at the end of the target period. This latest episode is selected for QM calculation. 2. For each episode that is selected, compute the cumulative days in the facility (CDIF). 3. If the CDIF is less than or equal to 100 days, the resident is included in the short-stay sample. 4. If the CDIF is greater than or equal to 101 days, the resident is included in the long-stay sample. Note that all residents who are selected in Step 1 above will be placed in either the short- or long-stay sample and that the two samples are mutually exclusive. If a resident has multiple episodes within the target period, only the latest episode is used. Within each sample, certain key records are identified which are used for calculating individual measures. These records are defined in the following sections. RTI International April 2017 (v11.0) 3
8 Section 3: Short Stay Record Definitions ASSESSMENT SELECTED PROPERTY SELECTION SPECIFICATIONS Target assessment Initial assessment Selection period Qualifying RFAs 1 Selection logic Rationale Selection period Qualifying RFAs Selection logic Rationale Most recent 6 months (the short stay target period). A0310A = [01, 02, 03, 04, 05, 06] or A0310B = [01, 02, 03, 04, 05, 06] or A0310F = [10, 11] Latest assessment that meets the following criteria: (a) it is contained within the resident s selected episode, (b) it has a qualifying RFA, and (c) its target date is no more than 120 days 2 before the end of the episode. Records with a qualifying RFA contain all of the items needed to define the QMs. The target assessment need not have a target date within the target period, but it must occur within 120 days before the end of the resident s selected episode (either the target date of a discharge assessment or death in facility record that is the last record in the target period or the end of the target period if the episode is ongoing). 120 days allows 93 days between quarterly assessments plus an additional 27 days to allow for late assessments. The target assessment represents the resident s status at the end of the episode. First assessment following the admission entry record at the beginning of the resident s selected episode. A0310A = [01] or A0310B = [01, 06] or A0310F = [10, 11] Earliest assessment that meets the following criteria: (a) it is contained within the resident s selected episode, (b) it has a qualifying RFA, (c) it has the earliest target date that is greater than or equal to the admission entry date starting the episode, and (d) its target date is no more than 130 days prior to the target date of the target record. The initial assessment cannot be the same as the target assessment. If the same assessment qualifies as both the initial and target assessments, it is used as the target assessment and the initial assessment is considered to be missing. Records with a qualifying RFA contain all of the items needed to define the QMs. The initial assessment need not have a target date within the target period. The initial assessment represents the resident s status as soon as possible after the admission that marks the beginning of the episode. If the initial assessment is more than 130 days prior to the target assessment, it is not used and the initial record is considered to be missing. This prevents the use of an initial assessment for a short stay in which a large portion of the resident s episode was spent outside the facility. 130 days allows for as many as 30 days of a 100-day stay to occur outside of the facility. (continued) RTI International April 2017 (v11.0) 4
9 Short Stay Record Definitions (continued) ASSESSMENT SELECTED PROPERTY SELECTION SPECIFICATIONS Look-back Scan Selection period Scan all assessments within the current episode. Qualifying RFAs A0310A = [01, 02, 03, 04, 05, 06] or A0310B = [01, 02, 03, 04, 05, 06] or A0310F = [10, 11] Selection logic Include the target assessment and qualifying earlier assessments in the scan. Include an earlier assessment in the scan if it meets all of the following conditions: (a) it is contained within the resident s episode, (b) it has a qualifying RFA, and (c) its target date is on or before the target date for the target assessment. The target assessment and qualifying earlier assessments are scanned to determine whether certain events or conditions occurred during the look-back period. These events and conditions are specified in the definitions of measures that utilize the look-back scan. Rationale Some measures utilize MDS items that record events or conditions that occurred since the prior assessment was performed. The purpose of the look-back scan is to determine whether such events or conditions occurred during the lookback period. All assessments with target dates within the episode are examined to determine whether the event or condition of interest occurred at any time during the episode. Influenza vaccination Selection period Scan all assessments with target dates on or after October 1 of the most recently completed influenza season. assessment Qualifying RFAs A0310A = [01, 02, 03, 04, 05, 06] or A0310B = [01, 02, 03, 04, 05, 06] or A0310F = [10, 11] Selection logic Select the record with the latest target date that meets all of the following conditions: a) It has a qualifying RFA, and b) Target date is on or after October 1st of the most recently completed influenza season, and c) A1600 (entry date) is on or before March 31st of the most recently completed influenza season. Rationale The selection logic defined above is intended to identify the latest assessment that reports the influenza vaccine status for a resident who was in the facility for at least one day from October 1 through March 31. NOTES: 1 RFA: reason for assessment. 2 A short stay episode can span more than 100 calendar days because days outside of the facility are not counted in defining a 100-day or less short stay episode. RTI International April 2017 (v11.0) 5
10 Section 4: Long Stay Record Definitions ASSESSMENT SELECTED PROPERTY SELECTION SPECIFICATIONS Target assessment Selection period Most recent 3 months (the long stay target period). Qualifying RFAs A0310A = [01, 02, 03, 04, 05, 06] or A0310B = [01, 02, 03, 04, 05, 06] or A0310F = [10, 11] Selection logic Latest assessment that meets the following criteria: (a) it is contained within the resident s selected episode, (b) it has a qualifying RFA, and (c) its target date is no more than 120 before the end of the episode. Rationale Records with a qualifying RFA contain all of the items needed to define the QMs. The target assessment need not have a target date within the target period, but it must occur within 120 days of the end of the resident s episode (either the last discharge in the target period or the end of the target period if the episode is ongoing). 120 days allows 93 days between quarterly assessments plus an additional 27 days to allow for late assessments. The target assessment represents the resident s status at the end of the episode. Prior assessment Selection period Latest assessment that is 46 to 165 days before the target assessment. Qualifying RFAs A0310A = [01, 02, 03, 04, 05, 06] or A0310B = [01, 02, 03, 04, 05, 06] or A0310F = [10, 11] Selection logic Latest assessment that meets the following criteria: (a) it is contained within the resident s episode, (b) it has a qualifying RFA, and (c) its target date is contained in the window that is 46 days to 165 days preceding the target date of the target assessment. If no qualifying assessment exists, the prior assessment is considered missing. Rationale Records with a qualifying RFA contain all of the items needed to define the QMs. The prior assessment need not have a target date within the target period, but it must occur within the defined window. The window covers 120 days, which allows 93 days between quarterly assessments plus an additional 27 days to allow for late assessments. Requiring a 45 day gap between the prior assessment and the target assessment insures that the gap between the prior and target assessment will not be small (gaps of 45 days or less are excluded). (continued) RTI International April 2017 (v11.0) 6
11 Long Stay Record Definitions (continued) ASSESSMENT SELECTED PROPERTY SELECTION SPECIFICATIONS Look-back Scan Selection period Scan all assessments within the current episode that have target dates no more than 275 days prior to the target assessment. Qualifying RFAs A0310A = [01, 02, 03, 04, 05, 06] or A0310B = [01, 02, 03, 04, 05, 06] or A0310F = [10, 11] Selection logic Include the target assessment and all qualifying earlier assessments in the scan. Include an earlier assessment in the scan if it meets all of the following conditions: (a) it is contained within the resident s episode, (b) it has a qualifying RFA, (c) its target date is on or before the target date for the target assessment, and (d) its target date is no more than 275 days prior to the target date of the target assessment. The target assessment and qualifying earlier assessments are scanned to determine whether certain events or conditions occurred during the look-back period. These events and conditions are specified in the definitions of measures that utilize the lookback scan. Rationale Some measures utilize MDS items that record events or conditions that occurred since the prior assessment was performed. The purpose of the look-back scan is to determine whether such events or conditions occurred during the lookback period. These measures trigger if the event or condition of interest occurred any time during a one year period. A 275 day time period is used to include up to three quarterly OBRA assessments. The earliest of these assessments would have a look-back period of up to 93 days which would cover a total of about one year. All assessments with target dates in this time period are examined to determine whether the event or condition of interest occurred at any time during the time interval. (continued) RTI International April 2017 (v11.0) 7
12 Long Stay Record Definitions (continued) ASSESSMENT SELECTED PROPERTY SELECTION SPECIFICATIONS Influenza vaccination assessment Selection period Qualifying RFAs Selection logic Rationale Scan all assessments with target dates on or after October 1 of the most recently completed influenza season. A0310A = [01, 02, 03, 04, 05, 06] or A0310B = [01, 02, 03, 04, 05, 06] or A0310F = [10, 11] Select the record with the latest target date that meets all of the following conditions: a) It has a qualifying RFA, and b) Target date is on or after October 1st of the most recently completed influenza season, and c) A1600 (entry date) is on or before March 31st of the most recently completed influenza season. The selection logic defined above is intended to identify the latest assessment that reports the influenza vaccine status for a resident who was in the facility for at least one day from October 1 through March 31. RTI International April 2017 (v11.0) 8
13 Chapter 2 MDS 3.0 Quality Measures Logical Specifications RTI International April 2017 (v11.0) 9
14 Section 1: Short Stay Quality Measures MDS 3.0 Measure: Percent of Residents Who Self-Report Moderate to Severe Pain (Short Stay) 1 MEASURE DESCRIPTION MEASURE SPECIFICATIONS COVARIATES CMS: N NQF: 0676 This measure captures the percent of short stay residents, with at least one episode of moderate/severe pain or horrible/excruciating pain of any frequency, in the last 5 days. Numerator Short-stay residents with a selected target assessment where the target assessment meets either or both of the following two conditions: 1. Condition #1: resident reports daily pain with at least one episode of moderate/severe pain. Both of the following conditions must be met: 1.1. Almost constant or frequent pain (J0400=[1,2]) and 1.2. At least one episode of moderate to severe pain (J0600A = [05, 06, 07, 08, 09] or J0600B = [2, 3]). 2. Condition #2: resident reports very severe/horrible pain of any frequency (J0600A = [10] or J0600B = [4]). Denominator All short-stay residents with a selected target assessment, except those with exclusions. Exclusions If the resident is not included in the numerator (the resident did not meet the pain symptom conditions for the numerator) and any of the following conditions are true: 1. The pain assessment interview was not completed (J0200= [0, -, ^]). 2. The pain presence item was not completed (J0300 = [9, -, ^]). 3. For residents with pain or hurting at any time in the last 5 days (J0300 = [1]), any of the following are true: 3.1. The pain frequency item was not completed (J0400 = [9, -, ^]) Neither of the pain intensity items was completed (J0600A = [99, -, ^] and J0600B= [9, -,, ^]) The numeric pain intensity item indicates no pain (J0600A = [00]). Not applicable. NOTE: 1 This measure is used in the Five-Star Quality Rating System. RTI International April 2017 (v11.0) 10
15 MDS 3.0 Measure: Percent of Residents With Pressure Ulcers That Are New or Worsened (Short Stay) 1 MEASURE DESCRIPTION MEASURE SPECIFICATIONS COVARIATES CMS: N NQF: 0678 This measure captures the percentage of shortstay residents with new or worsening Stage II-IV pressure ulcers. Numerator Short-stay residents for which a look-back scan indicates one or more new or worsening Stage II-IV pressure ulcers Where on any assessment in the look-back scan: 1. Stage II (M0800A) >[0] or 2. Stage III (M0800B >[0] or 3. Stage IV (M0800C >[0]. Denominator All residents with one or more assessments that are eligible for a lookback scan, except those with exclusions. Exclusions 1. Residents are excluded if none of the assessments that are included in the look-back scan has a usable response for M0800A, M0800B, or M0800C. This situation is identified as follows: 1.1 If none of M0800A, M0800B, or M0800C > [0] and any one of these items is missing [-], then the assessment is not usable and is discarded. 1.2 If all of the assessments that are eligible for the look-back scan are discarded and no usable assessments remain, then the resident is excluded from the numerator and the denominator. 2. Resident is excluded if there is no initial assessment available to derive data for risk adjustment (covariates). 1. Indicator of requiring limited or more assistance in bed mobility selfperformance on the initial assessment: Covariate = [1] if (G0110A1 = [2, 3, 4, 7, 8]) Covariate = [0] if (G0110A1 = [0, 1, -]) 2. Indicator of bowel incontinence at least occasionally on the initial assessment: Covariate = [1] if (H0400 = [1, 2, 3]) Covariate = [0] if (H0400 = [0, 9, -, ^]) 3. Have diabetes or peripheral vascular disease on initial assessment: Covariate = [1] if any of the following are true: 3.1. (I0900 = [1]) (checked) 3.2. (I2900 = [1]) (checked) 3.3. I8000A through I8000J contains any of the following peripheral vascular disease diagnosis codes: [250.7, , , , , , , , , , 443.9]. Covariate = [0] if (I0900 = [0, - 2 ]) and (I2900 = [0, -]) and I8000A through I8000J do not contain any of the peripheral vascular disease diagnosis codes listed above. (continued) RTI International April 2017 (v11.0) 11
16 MDS 3.0 Measure: Percent of Residents With Pressure Ulcers That Are New or Worsened (Short Stay) 1 (continued) MEASURE DESCRIPTION MEASURE SPECIFICATIONS COVARIATES 4. Indicator of Low Body Mass Index, based on Height (K0200A) and Weight (K0200B) on the initial assessment: Covariate = [1] if BMI [12.0] and [19.0] Covariate = [0] if BMI has a value which is less than 12.0 or greater than 19.0 or if BMI cannot be computed because (K0200A = [0, -]) or (K0200B = [0, -]) Where: BMI = (weight * 703 / height 2 ) = ((K0200B) * 703) / (K0200A 2 ) and the resulting value is rounded to one decimal. 5. All covariates are missing if no initial assessment is available. NOTES: 1 This measure is used in the Five-Star Quality Rating System. 2 Item I0900 can be missing on assessments with target dates prior to 4/1/2012 where the item subset code is equal to NP or NQ. The item was not active on those assessments. RTI International April 2017 (v11.0) 12
17 MDS 3.0 Measure: Percent of Residents Who Were Assessed and Appropriately Given the Seasonal Influenza Vaccine (Short Stay) MEASURE DESCRIPTION MEASURE SPECIFICATIONS COVARIATES CMS: N NQF: 0680 The measure reports the percent of shortstay residents who are given, appropriately, the influenza vaccination during the most recent influenza season. Numerator Residents meeting any of the following criteria on the selected influenza vaccination assessment: 1. Resident received the influenza vaccine during the most recent influenza season, either in the facility (O0250A = [1]) or outside the facility (O0250C = [2]); or 2. Resident was offered and declined the influenza vaccine (O0250C = [4]); or 3. Resident was ineligible due to contraindication(s) (O0250C = [3]) (e.g., anaphylactic hypersensitivity to eggs or other components of the vaccine, history of Guillain-Barre Syndrome within 6 weeks after a previous influenza vaccination, bone marrow transplant within the past 6 months). Denominator All short-stay residents with a selected influenza vaccination assessment, except those with exclusions. Exclusions Resident s age on target date of selected target assessment is 179 days or less. Notes This measure is only calculated once per 12-month influenza season which begins on July 1 of a given year and ends on June 30 of the subsequent year, and reports data for residents who were in the facility for at least one day during the target period of October 1 through March 31 Not applicable. RTI International April 2017 (v11.0) 13
18 MDS 3.0 Measure: Percent of Residents Who Received the Seasonal Influenza Vaccine (Short Stay) MEASURE DESCRIPTION MEASURE SPECIFICATIONS COVARIATES CMS: N NQF: 0680A The measure reports the percent of shortstay residents who received the influenza vaccination during the most recent influenza season. Numerator Residents meeting the following criteria on the selected influenza vaccination assessment: 1. Resident received the influenza vaccine during the most recent influenza season, either in the facility (O0250A = [1]) or outside the facility (O0250C = [2]). Denominator All short-stay residents with a selected influenza vaccination assessment, except those with exclusions. Exclusions 1. Resident s age on target date of selected influenza vaccination assessment is 179 days or less. Notes This measure is only calculated once per 12-month influenza season which begins on July 1 of a given year and ends on June 30 of the subsequent year and reports data for residents who were in the facility for at least one day during the target period of October 1 through March 31. Not applicable. RTI International April 2017 (v11.0) 14
19 MDS 3.0 Measure: Percent of Residents Who Were Offered and Declined the Seasonal Influenza Vaccine (Short Stay) MEASURE DESCRIPTION MEASURE SPECIFICATIONS COVARIATES CMS: N NQF: 0680B The measure reports the percent of shortstay residents who are offered and declined the influenza vaccination during the most recent influenza season. Numerator Residents meeting the following criteria on the selected influenza vaccination assessment: 1. Resident was offered and declined the influenza vaccine during the most recent influenza season (O0250C = [4]). Denominator All short-stay residents with a selected influenza vaccination assessment, except those with exclusions. Exclusions 1. Resident s age on target date of selected influenza vaccination assessment is 179 days or less. Notes This measure is only calculated once per 12-month influenza season which begins on July 1 of a given year and ends on June 30 of the subsequent year and reports data for residents who were in the facility for at least one day during the target period of October 1 through March 31. Not applicable. RTI International April 2017 (v11.0) 15
20 MDS 3.0 Measure: Percent of Residents Who Did Not Receive, Due to Medical Contraindication, the Seasonal Influenza Vaccine (Short Stay) MEASURE DESCRIPTION MEASURE SPECIFICATIONS COVARIATES CMS: N NQF: 0680C The measure reports the percent of shortstay residents who did not receive, due to medical contraindication, the influenza vaccination during the most recent influenza season. Numerator Residents meeting the following criteria on the selected influenza vaccination assessment: 1. Resident was ineligible for the influenza vaccine during the most recent influenza season due to contraindication(s) (O0250C = [3]) (e.g., anaphylactic hypersensitivity to eggs or other components of the vaccine, history of Guillian-Barré Syndrome within 6 weeks after a previous influenza vaccination, bone marrow transplant within the past 6 months). Denominator All short-stay residents with a selected influenza vaccination assessment, except those with exclusions. Exclusions 1. Resident s age on target date of selected influenza vaccination assessment is 179 days or less. Notes This measure is only calculated once per 12-month influenza season which begins on July 1 of a given year and ends on June 30 of the subsequent year and reports data for residents who were in the facility for at least one day during the target period of October 1 through March 31 Not applicable. RTI International April 2017 (v11.0) 16
21 MDS 3.0 Measure: Percent of Residents Who Newly Received an Antipsychotic Medication (Short Stay) 1,2 MEASURE DESCRIPTION MEASURE SPECIFICATIONS COVARIATES CMS: N NQF: none This measure reports the percentage of short-stay residents who are receiving an antipsychotic medication during the target period but not on their initial assessment. Numerator Short-stay residents for whom one or more assessments in a look-back scan (not including the initial assessment) indicates that antipsychotic medication was received: 1. For assessments with target dates on or before 03/31/2012: (N0400A = [1]). 2. For assessments with target dates on or after 04/01/2012: (N0410A = [1, 2, 3, 4, 5, 6, 7]). Note that residents are excluded from this measure if their initial assessment indicates antipsychotic medication use or if antipsychotic medication use is unknown on the initial assessment (see exclusion #3, below). Denominator All short-stay residents who do not have exclusions and who meet all of the following conditions: 1. The resident has a target assessment, and 2. The resident has an initial assessment, and 3. The target assessment is not the same as the initial assessment. Exclusions 1. The following is true for all assessments in the look-back scan (excluding the initial assessment): 1.1. For assessments with target dates on or before 03/31/2012: (N0400A = [-]) For assessments with target dates on or after 04/01/2012: (N0410A = [-]). 2. Any of the following related conditions are present on any assessment in a look-back scan: 2.1. Schizophrenia (I6000 = [1]) Tourette s syndrome (I5350 = [1]) Huntington s disease (I5250 = [1]). 3. The resident s initial assessment indicates antipsychotic medication use or antipsychotic medication use is unknown: 3.1. For initial assessments with target dates on or before 03/31/2012: (N0400A = [1, -]) For initial assessments with target dates on or after 04/01/2012: (N0410A = [1, 2, 3, 4, 5, 6, 7, -]). Not applicable. NOTES: 1 This measure has not been submitted to NQF for endorsement. 2 This measure is used in the Five-Star Quality Rating System. RTI International April 2017 (v11.0) 17
22 MDS 3.0 Measure: Percent of Residents Who Made Improvements in Function (Short Stay) 1,2 MEASURE DESCRIPTION MEASURE SPECIFICATIONS COVARIATES CMS: N NQF: none This measure reports the percentage of short-stay residents who were discharged from the nursing home that gained more independence in transfer, locomotion, and walking during their episodes of care. NOTE: 1. A valid preceding 5-day assessment or admission assessment refers to the date of the earliest assessment if a resident has both 5-day (A0310B = [01]) and admission assessments (A0310A = [01]). 2. A valid discharge assessment refers to a discharge assessment with a date closest to the valid preceding 5-day or admission assessment where a return is not anticipated (A0310F = [10]). 3. The 5-day or admission assessment should be used to calculate the tercile cutoffs. If resident has both a 5-day and an admission assessment, calculate covariate using the assessment with the earlier date. Terciles are recalculated in each quarter. Numerator Short-stay residents who: 1. Have a valid discharge assessment (A0310F = [10]) and a valid preceding 5-day assessment or admission assessment; and 2. Have a change in performance score that is negative ([valid discharge assessment] - [valid preceding 5-day or admission assessment] < [0]). Performance is calculated as the sum of G0110B1 (transfer: selfperformance), G0110E1 (locomotion on unit: self-performance), and G0110D1 (walk in corridor: self-performance), with 7 s (activity occurred only once or twice) and 8's (activity did not occur) recoded to 4's (total dependence). Denominator Short-stay residents who meet all of the following conditions, except those with exclusions: 1. Have a valid discharge assessment (A0310F = [10]), and 2. Have a valid preceding 5-day assessment (A0310B = [01]) or admission assessment (A0310A = [01]). All covariates used throughout this measure are calculated using the valid preceding 5-day assessment or admission assessment described in the NOTE at the top of the measure specifications. 1. Age on the 5-day or admission assessment as calculated by subtracting date of birth (A0900) from the date of assessment (A2300) If (MONTH(A2300) > MONTH(A0900)) or (MONTH(A2300) = MONTH(A0900) and DAY(A2300) >= DAY(A0900)) then Age = YEAR(A2300)-YEAR(A0900) else Age = YEAR(A2300)-YEAR(A0900) Covariate Age Category<54 = 1 if Age =<54 and Covariate Age Category<54 = 0 if Age >54) 1.2 Covariate Age Category 54 to 84 = 1 if Age >54 and <=84 and Covariate Age Category 54 to 84 = 0 if Age <=54 or Age > 84) (reference) 1.3 Covariate Age Category >84 = 1 if Age >84 and Covariate Age Category >84 = 0 if Age <=84) (continued) RTI International April 2017 (v11.0) 18
23 MDS 3.0 Measure: Percent of Residents Who Made Improvements in Function (Short Stay) 1,2 (continued) MEASURE DESCRIPTION MEASURE SPECIFICATIONS COVARIATES Exclusions 1. Residents satisfying any of the following conditions: 1.1. Comatose (B0100 = [1]) on the 5-day or admission assessment, whichever was used in the QM Life expectancy of less than 6 months (J1400 = [1]) on the 5- day or admission assessment, whichever was used in the QM Hospice (O0100K2 = [1]) on the 5-day or admission assessment, whichever was used in the QM Residents with G0110B1, G0110D1, or G0110E1 missing on any of the assessments used to calculate the QM (i.e., discharge assessment, and 5-day or admission assessment, whichever was used in the QM) Residents with no impairment (sum of G0110B1, G0110D1 and G0110E1 = [0]) on the 5-day or admission assessment, whichever was used in the QM Residents with an unplanned discharge on any assessment during the care episode (A0310G = [2]) 2. Gender 2.1 Covariate = 1 if (A0800 = [2]) (Female) 2.2 Covariate = 0 if (A0800 = [1]) (Male) 3. Severe cognitive impairment 3.1 Covariate = 1 if (C1000 = [3] and C0700 = [1]) or BIMS summary score (C0500) < [7] 3.2 Covariate = 0 if either of the following criteria are met: (C1000 = [0, 1, 2] or C0700 = [0]) and (C0500 = [>7, ^, -, 99]) (C0500 > [7]) and (C1000 = [0, 1, 2, ^, -] or C0700 = [0, ^, - ]) 3.3 If Covariate has not been set to 1 or 0 based on logic in 3.1 and 3.2, then Covariate = [0]. 4. Long Form ADL (LFADL) Scale (G0110A1 + G0110B1 + G0110E1 + G0110G1 + G0110H1 + G0110I1 + G0110JI) 4.1 Covariate = 0 if LFADL = (middle tercile 3 or highest tercile) or if any (G0110A1, G0110B1, G0110E1, G0110G1, G0110H1, G0110I1, G0110J1) = [-] Covariate = 1 if LFADL = lowest tercile (continued) RTI International April 2017 (v11.0) 19
24 MDS 3.0 Measure: Percent of Residents Who Made Improvements in Function (Short Stay) 1,2 (continued) MEASURE DESCRIPTION MEASURE SPECIFICATIONS COVARIATES NOTES: 1 This measure has not been submitted to NQF for endorsement. 2 This measure is used in the Five-Star Quality Rating System. 3 Long Form ADL Scale terciles are recalculated in each quarter using the 5-day or admission assessment. 4.2 Covariate =0 if (lowest tercile or highest tercile) Covariate = 1 if LFADL = middle tercile (reference) 4.3 Covariate =0 if (lowest tercile or middle tercile) 5. Covariate = 1 if LFADL = highest tercile 6. Heart failure 6.1 Covariate = 1 if (I0600 = [1]) 6.2 Covariate = 0 if (I0600 = [0, -]) 7. CVA, TIA, or Stroke 7.1 Covariate = 1 if (I4500 = [1]) 8. Covariate = 0 if (I4500 = [0, -]) 9. Hip Fracture 9.1 Covariate = 1 if (I3900 = [1]) 9.2 Covariate = 0 if (I3900 = [0, -]) 10. Other Fracture 10.1 Covariate = 1 if (I4000 = [1]) 10.2 Covariate = 0 if (I4000 = [0, -]) RTI International April 2017 (v11.0) 20
25 Section 2: Long Stay Quality Measures MDS 3.0 Measure: Percent of Residents Experiencing One or More Falls with Major Injury (Long Stay) 1 MEASURE DESCRIPTION MEASURE SPECIFICATIONS COVARIATES CMS: N NQF: 0674 This measure reports the percent of longstay residents who have experienced one or more falls with major injury reported in the target period or look-back period. Numerator Long-stay residents with one or more look-back scan assessments that indicate one or more falls that resulted in major injury (J1900C = [1, 2]). Denominator All long-stay nursing home residents with a one or more look-back scan assessments except those with exclusions. Exclusions Resident is excluded if one of the following is true for all of the look-back scan assessments: 1. The occurrence of falls was not assessed (J1800 = [-]), or 2. The assessment indicates that a fall occurred (J1800 = [1]) and the number of falls with major injury was not assessed (J1900C = [-]). Not applicable. NOTE: 1 This measure is used in the Five-Star Quality Rating System. RTI International April 2017 (v11.0) 21
26 MDS 3.0 Measure: Percent of Residents Who Self-Report Moderate to Severe Pain (Long Stay) 1 MEASURE DESCRIPTION MEASURE SPECIFICATIONS COVARIATES CMS: N NQF: 0677 This measure captures the percent of long-stay residents who report either (1) almost constant or frequent moderate to severe pain in the last 5 days or (2) any very severe/horrible in the last 5 days. Numerator Long-stay residents with a selected target assessment where the target assessment meets either or both of the following two conditions: 1. Condition #1: resident report almost constant or frequent moderate to severe pain in the last 5 days. Both of the following conditions must be met: 1.1. Almost constant or frequent pain (J0400 = [1, 2]), and 1.2. At least one episode of moderate to severe pain: (J0600A = [05, 06, 07, 08, 09] or J600B = [2, 3]). 2. Condition #2: resident reports very severe/horrible pain of any frequency (J0600A = [10] or J0600B = [4]). Denominator All long-stay residents with a selected target assessment, except those with exclusions. Exclusions 1. The target assessment is an admission assessment, a PPS 5-day assessment, or a PPS readmission/return assessment (A0310A = [01] or A0310B = [01, 06]). 2. The resident is not included in the numerator (the resident did not meet the pain symptom conditions for the numerator) and any of the following conditions are true: 2.1. The pain assessment interview was not completed (J0200 = [0, -, ^]) The pain presence item was not completed (J0300 = [9, -, ^]) For residents with pain or hurting at any time in the last 5 days (J0300 = [1]), any of the following are true: The pain frequency item was not completed (J0400 = [9, -, ^]) Neither of the pain intensity items was completed (J0600A = [99, -, ^] and J0600B = [9, -. ^]) The numeric pain intensity item indicates no pain (J0600A = [00]). Independence or modified independence in daily decision making on the prior assessment Covariate = 1 if (C1000 = [0, 1] or if C0500 [13] and C0500 [15]). Covariate = 0 if any of the following is true: 1. (C1000 = [2, 3]) or 2. (C0500 [00] and C0500 [12]) or 3. (C0500 = [99, -, ^] and C1000 = [-, ^]). All covariates are missing if no prior assessment is available. NOTE: 1 This measure is used in the Five-Star Quality Rating System. RTI International April 2017 (v11.0) 22
27 MDS 3.0 Measure: Percent of High-Risk Residents With Pressure Ulcers (Long Stay) 1 MEASURE DESCRIPTION MEASURE SPECIFICATIONS COVARIATES CMS: N NQF: 0679 This measure captures the percentage of longstay, high-risk residents with Stage II-IV pressure ulcers. Numerator All long-stay residents with a selected target assessment that meets both of the following conditions: 1. Condition #1: There is a high risk for pressure ulcers, where high-risk is defined in the denominator definition below. 2. Condition #2: Stage II-IV or unstageable pressure ulcers are present, as indicated by any of the following six conditions: 2.1 (M0300B1 = [1, 2, 3, 4, 5, 6, 7, 8, 9]) or 2.2 (M0300C1 = [1, 2, 3, 4, 5, 6, 7, 8, 9]) or 2.3 (M0300D1 = [1, 2, 3, 4, 5, 6, 7, 8, 9]). Denominator All long-stay residents with a selected target assessment who meet the definition of high risk, except those with exclusions. Residents are defined as high-risk if they meet one or more of the following three criteria on the target assessment: 1. Impaired bed mobility or transfer indicated, by either or both of the following: 1.1 Bed mobility, self-performance (G0110A1 = [3, 4, 7, 8]). 1.2 Transfer, self-performance (G0110B1 = [3, 4, 7, 8]). 2. Comatose (B0100 = [1]). 3. Malnutrition or at risk of malnutrition (I5600 = [1]) (checked). Not applicable. Exclusions 1. Target assessment is an admission assessment (A0310A = [01]) or a PPS 5-day or readmission/return assessment (A0310B = [01, 06]). 2. If the resident is not included in the numerator (the resident did not meet the pressure ulcer conditions for the numerator) and any of the following conditions are true: 2.1 (M0300B1 = [-]). 2.2 (M0300C1 = [-]). 2.3 (M0300D1 = [-]). NOTE: 1 This measure is used in the Five-Star Quality Rating System. RTI International April 2017 (v11.0) 23
28 MDS 3.0 Measure: Percent of Residents Assessed and Appropriately Given the Seasonal Influenza Vaccine (Long Stay) MEASURE DESCRIPTION MEASURE SPECIFICATIONS COVARIATES CMS: N NQF: 0681 The measure reports the percent of longstay residents who are given, appropriately, the influenza vaccination during the most recent influenza season. Numerator Residents meeting any of the following criteria on the selected influenza vaccination assessment: 1. Resident received the influenza vaccine during the most recent influenza season, either in the facility (O0250A= [1]) or outside the facility (O0250C = [2]); or 2. Resident was offered and declined the influenza vaccine (O0250C = [4]); or 3. Resident was ineligible due to contraindication(s) (O0250C = [3]) (e.g., anaphylactic hypersensitivity to eggs or other components of the vaccine, history of Guillain-Barre Syndrome within 6 weeks after a previous influenza vaccination, bone marrow transplant within the past 6 months). Denominator All long-stay residents with a selected influenza vaccination assessment, except those with exclusions. Exclusions Resident s age on target date of selected influenza vaccination assessment is 179 days or less. Notes This measure is only calculated once per 12-month influenza season which begins on July 1 of a given year and ends on June 30 of the subsequent year and reports data for residents who were in the facility for at least one day during the target period of October 1 through March 31. Not applicable. RTI International April 2017 (v11.0) 24
29 MDS 3.0 Measure: Percent of Residents Who Received the Seasonal Influenza Vaccine (Long Stay) MEASURE DESCRIPTION MEASURE SPECIFICATIONS COVARIATES CMS: N NQF: 0681A The measure reports the percent of longstay residents who received the influenza vaccination during the most recent influenza season. Numerator Residents meeting the following criteria on the selected influenza vaccination assessment: 1. Resident received the influenza vaccine during the most recent influenza season, either in the facility (O0250A = [1]) or outside the facility (O0250C = [2]). Denominator All long-stay residents with a selected influenza vaccination assessment, except those with exclusions. Exclusions Resident s age on target date of selected influenza vaccination assessment is 179 days or less. Notes This measure is only calculated once per 12-month influenza season which begins on July 1 of a given year and ends on June 30 of the subsequent year and reports data for residents who were in the facility for at least one day during the target period of October 1 through March 31. Not applicable. RTI International April 2017 (v11.0) 25
30 MDS 3.0 Measure: Percent of Residents Who Were Offered and Declined the Seasonal Influenza Vaccine (Long Stay) MEASURE DESCRIPTION MEASURE SPECIFICATIONS COVARIATES CMS: N NQF: 0681B The measure reports the percent of longstay residents who are offered and declined the influenza vaccination during the most recent influenza season. Numerator Residents meeting the following criteria on the selected influenza vaccination assessment: 1. Resident was offered and declined the influenza vaccine during the most recent influenza season (O0250C = [4]). Denominator All long-stay residents with a selected influenza vaccination assessment, except those with exclusions. Exclusions Resident s age on target date of selected influenza vaccination assessment is 179 days or less. Notes This measure is only calculated once per 12-month influenza season which begins on July 1 of a given year and ends on June 30 of the subsequent year and reports data for residents who were in the facility for at least one day during the target period of October 1 through March 31. Not applicable. RTI International April 2017 (v11.0) 26
31 MDS 3.0 Measure: Percent of Residents Who Did Not Receive, Due to Medical Contraindication, the Seasonal Influenza Vaccine (Long Stay) MEASURE DESCRIPTION MEASURE SPECIFICATIONS COVARIATES CMS: N NQF: 0681C The measure reports the percent of longstay residents who did not receive, due to medical contraindication, the influenza vaccination during the most recent influenza season. Numerator Residents meeting the following criteria on the selected influenza vaccination assessment: 1. Resident was ineligible for the influenza vaccine during the most recent influenza season due to contraindication(s) (O0250C = [3]) (e.g., anaphylactic hypersensitivity to eggs or other components of the vaccine, history of Guillian-Barré Syndrome within 6 weeks after a previous influenza vaccination, bone marrow transplant within the past 6 months). Denominator All long-stay residents with a selected influenza vaccination assessment, except those with exclusions. Exclusions Resident s age on target date of selected influenza vaccination assessment is 179 days or less. Notes This measure is only calculated once per 12-month influenza season which begins on July 1 of a given year and ends on June 30 of the subsequent year and reports data for residents who were in the facility for at least one day during the target period of October 1 through March 31. Not applicable. RTI International April 2017 (v11.0) 27
32 MDS 3.0 Measure: Percent of Residents with a Urinary Tract Infection (Long Stay) 1 MEASURE DESCRIPTION MEASURE SPECIFICATIONS COVARIATES CMS: N NQF: 0684 The measure reports the percentage of long stay residents who have a urinary tract infection Numerator Long-stay residents with a selected target assessment that indicates urinary tract infection within the last 30 days (I2300 = [1]). Denominator All long-stay residents with a selected target assessment, except those with exclusions. Exclusions 1. Target assessment is an admission assessment (A0310A = [01]) or a PPS 5-day or readmission/return assessment (A0310B = [01, 06]). 2. Urinary tract infection value is missing (I2300 = [-]). Not applicable. NOTE: 1 This measure is used in the Five-Star Quality Rating System. RTI International April 2017 (v11.0) 28
33 MDS 3.0 Measure: Percent of Residents Who Have/Had a Catheter Inserted and Left in Their Bladder (Long Stay) 1 MEASURE DESCRIPTION MEASURE SPECIFICATIONS COVARIATES CMS: N NQF: 0686 This measure reports the percentage of residents who have had an indwelling catheter in the last 7 days. Numerator Long-stay residents with a selected target assessment that indicates the use of indwelling catheters (H0100A = [1]). Denominator All long-stay residents with a selected target assessment, except those with exclusions. Exclusions 1. Target assessment is an admission assessment (A0310A = [01]) or a PPS 5-day or readmission/return assessment (A0310B = [01, 06]). 2. Target assessment indicates that indwelling catheter status is missing (H0100A = [-]). 3. Target assessment indicates neurogenic bladder (I1550 = [1]) or neurogenic bladder status is missing (I1550 = [-]). 4. Target assessment indicates obstructive uropathy (I1650 = [1]) or obstructive uropathy status is missing (I1650 = [-]). 1. Frequent bowel incontinence on prior assessment (H0400 = [2, 3]). 1.1 Covariate = [1] if (H0400 = [2, 3]). 1.2 Covariate = [0] if (H0400 = [0, 1, 9, -]). 2. Pressure ulcers at stages II, III, or IV on prior assessment: 2.1 Covariate = [1] if any of the following are true: (M0300B1 = [1, 2, 3, 4, 5, 6, 7, 8, 9]), or (M0300C1 = [1, 2, 3, 4, 5, 6, 7, 8, 9]), or (M0300D1 = [1, 2, 3, 4, 5, 6, 7, 8, 9]). 2.2 Covariate = [0] if the following is true: (M0300B1 = [0, -, ^]) and (M0300C1 = [0, -, ^]) and (M0300D1 = [0, -, ^]). 3. All covariates are missing if no prior assessment is available. NOTE: 1 This measure is used in the Five-Star Quality Rating System. RTI International April 2017 (v11.0) 29
QM Reports Technical Specifications: Version 1.0
 Exhibit 271 Introduction The measures contained on the Quality Measure (QM) Reports are calculated in two major steps. In the first step, two samples of assessments are selected: a long-stay sample and
Exhibit 271 Introduction The measures contained on the Quality Measure (QM) Reports are calculated in two major steps. In the first step, two samples of assessments are selected: a long-stay sample and
QUALITY MEASURES NELIA ADACI RNC, BSN, CDONA, C-NE, RAC-CT VICE PRESIDENT, THE CHARTS GROUP
 HCANJ QUALITY MEASURES NELIA ADACI RNC, BSN, CDONA, C-NE, RAC-CT VICE PRESIDENT, THE CHARTS GROUP 1 OUTLINE What are Quality Measures? 4 Purposes of QM s Key Definitions Review the QM s Managing the QM
HCANJ QUALITY MEASURES NELIA ADACI RNC, BSN, CDONA, C-NE, RAC-CT VICE PRESIDENT, THE CHARTS GROUP 1 OUTLINE What are Quality Measures? 4 Purposes of QM s Key Definitions Review the QM s Managing the QM
Welcome and thank you for viewing What s your number? Understanding the Long- Stay Catheter Inserted/Left in Bladder Quality Measure.
 Welcome and thank you for viewing What s your number? Understanding the Long- Stay Catheter Inserted/Left in Bladder Quality Measure. This presentation is one in a series of videos explaining the 13 quality
Welcome and thank you for viewing What s your number? Understanding the Long- Stay Catheter Inserted/Left in Bladder Quality Measure. This presentation is one in a series of videos explaining the 13 quality
QI Version #: 6.3 MDS 2.0 Form Type: QUARTERLY ASSESSMENT FORM-TWO PAGE DOMAIN: ACCIDENTS
 DOMAIN: ACCIDENTS 1. Incidence of new fractures 1 1.1A0001 Residents with new fractures on most recent Residents who did not have fractures on the previous new hip fracture (J4c is checked on most recent
DOMAIN: ACCIDENTS 1. Incidence of new fractures 1 1.1A0001 Residents with new fractures on most recent Residents who did not have fractures on the previous new hip fracture (J4c is checked on most recent
Improving the Vaccination Long Stay Quality Measures
 Improving the Vaccination Long Stay Quality Measures 1 Objectives Become familiar with the QM specifications Understand how MDS coding triggers the QM Tips for Improvement 2 Critical Resources: Methodology
Improving the Vaccination Long Stay Quality Measures 1 Objectives Become familiar with the QM specifications Understand how MDS coding triggers the QM Tips for Improvement 2 Critical Resources: Methodology
Lori Hintz, RN Quality Improvement Advisor Great Plains Quality Innovation Network SD Foundation for Medical Care
 Lori Hintz, RN Quality Improvement Advisor Great Plains Quality Innovation Network SD Foundation for Medical Care What s Your Number? Understanding the Quality Measure Composite Score and Composite Score
Lori Hintz, RN Quality Improvement Advisor Great Plains Quality Innovation Network SD Foundation for Medical Care What s Your Number? Understanding the Quality Measure Composite Score and Composite Score
Hospice Quality Reporting Program: Specifications for the Hospice Item Set- Based Quality Measures
 April 2016 Hospice Quality Reporting Program: Specifications for the Hospice Item Set- Based Quality Measures Prepared for Center for Clinical Standards and Quality Centers for Medicare & Medicaid Services
April 2016 Hospice Quality Reporting Program: Specifications for the Hospice Item Set- Based Quality Measures Prepared for Center for Clinical Standards and Quality Centers for Medicare & Medicaid Services
QAPI Relay Residents Who Self-Report Moderate to Severe Pain Long-Stay Quality Measure Coding Improvements
 QAPI Relay Residents Who Self-Report Moderate to Severe Pain Long-Stay Quality Measure Coding Improvements Stacy Gordon, RN, MS, RAC-CT Senior Quality Improvement Facilitator May 2018 1 Today s Call is
QAPI Relay Residents Who Self-Report Moderate to Severe Pain Long-Stay Quality Measure Coding Improvements Stacy Gordon, RN, MS, RAC-CT Senior Quality Improvement Facilitator May 2018 1 Today s Call is
Global Immunization Measures. Developed by: Kathy Wonderly RN, MSEd, CPHQ Consultant Created: September, 2011 Most recent update: December, 2018
 Global Immunization Measures Developed by: Kathy Wonderly RN, MSEd, CPHQ Consultant Created: September, 2011 Most recent update: December, 2018 Global Immunization Measure Set Since these measures are
Global Immunization Measures Developed by: Kathy Wonderly RN, MSEd, CPHQ Consultant Created: September, 2011 Most recent update: December, 2018 Global Immunization Measure Set Since these measures are
QUALITY INDICATORS FOR RESIDENTIAL CARE FACILITIES Maine Bureau of Medical Services
 1.) Prevalence of Bladder Incontinence (High Degree of Incontinence) Previous QI103 2.) Prevalence of Bladder Incontinence (Low Degree of Incontinence) Previous QI104 3.) Prevalence of Bowel Incontinence
1.) Prevalence of Bladder Incontinence (High Degree of Incontinence) Previous QI103 2.) Prevalence of Bladder Incontinence (Low Degree of Incontinence) Previous QI104 3.) Prevalence of Bowel Incontinence
Hospice. Hospice Item Set (HIS) Submission Requirements. Quality Reporting Program Provider Training
 Hospice Quality Reporting Program Provider Training Hospice Item Set (HIS) Submission Requirements Presenter: Brenda Karkos, M.S.N./M.B.A., R.N., CHPN Date: January 18, 2017 Objectives Discuss the Hospice
Hospice Quality Reporting Program Provider Training Hospice Item Set (HIS) Submission Requirements Presenter: Brenda Karkos, M.S.N./M.B.A., R.N., CHPN Date: January 18, 2017 Objectives Discuss the Hospice
Getting to the core of customer satisfaction in skilled nursing and assisted living. Satisfaction Questionnaire & User s Manual
 Getting to the core of customer satisfaction in skilled nursing and assisted living. Satisfaction Questionnaire & User s Manual Questionnaire Development Nick Castle, Ph.D., from the University of Pittsburgh
Getting to the core of customer satisfaction in skilled nursing and assisted living. Satisfaction Questionnaire & User s Manual Questionnaire Development Nick Castle, Ph.D., from the University of Pittsburgh
MDS ACCURACY REVIEW TOOL
 MDS ACCURACY REVIEW TOOL RESIDENT INFORMATION Name: Medical Record #: Admission Date: MDS Assessment Reference Date: _ Reason for Audit: Complete-all sections Partial-specific section(s) Other: Codes for
MDS ACCURACY REVIEW TOOL RESIDENT INFORMATION Name: Medical Record #: Admission Date: MDS Assessment Reference Date: _ Reason for Audit: Complete-all sections Partial-specific section(s) Other: Codes for
The DHS MN Risk-Adjusted Quality Indicators: A Brief Guide
 The DHS MN Risk-Adjusted Quality Indicators: A Brief Guide DHS measures 26 quality indicators (QIs) from your facility s MDS assessments. These MN QIs allow for a better picture of the true quality of
The DHS MN Risk-Adjusted Quality Indicators: A Brief Guide DHS measures 26 quality indicators (QIs) from your facility s MDS assessments. These MN QIs allow for a better picture of the true quality of
Identification Information.
 Section A. Identification Information. A1200. Marital Status. 1. Never married. 2. Married. 3. Widowed. 4. Separated. 5. Divorced. A1300. Optional Resident Items. A. Medical record number: B. Room number:
Section A. Identification Information. A1200. Marital Status. 1. Never married. 2. Married. 3. Widowed. 4. Separated. 5. Divorced. A1300. Optional Resident Items. A. Medical record number: B. Room number:
Measure Information Form
 Measure Information Form Project Title: Vascular Access Project Overview: Date: The Centers for Medicare & Medicaid Services (CMS) has contracted with the University of Michigan Kidney Epidemiology and
Measure Information Form Project Title: Vascular Access Project Overview: Date: The Centers for Medicare & Medicaid Services (CMS) has contracted with the University of Michigan Kidney Epidemiology and
Influenza Immunization (IMM) National Quality/MBQIP Measure. July 9, 2015
 Influenza Immunization (IMM) National Quality/MBQIP Measure July 9, 2015 Objective Understanding the components of IMM, MBQIP measure including Patient Population (who), Description(what), Start Date(when),
Influenza Immunization (IMM) National Quality/MBQIP Measure July 9, 2015 Objective Understanding the components of IMM, MBQIP measure including Patient Population (who), Description(what), Start Date(when),
MEASURE TYPE. Percentage of female patients aged 65 years and older who were assessed for the presence or absence of urinary incontinence
 Clinicians in the MIPS track will be required to comply the QPP by reporting on six quality measures, including an outcome measure, for a minimum of 90 days. To help providers figure out what MIPS measures
Clinicians in the MIPS track will be required to comply the QPP by reporting on six quality measures, including an outcome measure, for a minimum of 90 days. To help providers figure out what MIPS measures
Table 3. Assessment Indicator Second Digit Table
 6 6.4 6-8 Table 2. Assessment Indicator First Digit Table 1st Digit Values Assessment Type (abbreviation) Standard* Scheduled Payment Period 0 Unscheduled PPS assessment (unsched) Not applicable 1 PPS
6 6.4 6-8 Table 2. Assessment Indicator First Digit Table 1st Digit Values Assessment Type (abbreviation) Standard* Scheduled Payment Period 0 Unscheduled PPS assessment (unsched) Not applicable 1 PPS
MARCH 5, 2018 DSRIP MEASURE SPECIFICATIONS FOR PALLIATIVE CARE PROVIDER SELECTED BY CCC. Page 1
 MARCH 5, 2018 DSRIP MEASURE SPECIFICATIONS FOR PALLIATIVE CARE PROVIDER SELECTED BY CCC Page 1 Table of Contents Bundle G1 Palliative Care Introduction... 3 G1-276: Hospice and Palliative Care Pain Assessment...
MARCH 5, 2018 DSRIP MEASURE SPECIFICATIONS FOR PALLIATIVE CARE PROVIDER SELECTED BY CCC Page 1 Table of Contents Bundle G1 Palliative Care Introduction... 3 G1-276: Hospice and Palliative Care Pain Assessment...
N ATIONAL Q UALITY F ORUM. National Voluntary Consensus Standards for Influenza and Pneumococcal Immunizations A CONSENSUS REPORT
 N ATIONAL Q UALITY F ORUM National Voluntary Consensus Standards for Influenza and Pneumococcal Immunizations A CONSENSUS REPORT NATIONAL QUALITY FORUM Foreword The millions of physicians, nurses, technologists,
N ATIONAL Q UALITY F ORUM National Voluntary Consensus Standards for Influenza and Pneumococcal Immunizations A CONSENSUS REPORT NATIONAL QUALITY FORUM Foreword The millions of physicians, nurses, technologists,
Fri Nov 02 09:11:33 EDT 2012 QIES Workbench. Record Layout Report
 file:///c:/users/hpmresdacsw1/appdata/local/temp/qwu_j78975_p1_mds_3 NH_... Page 1 of 24 11/27/212 Fri Nov 2 9:11:33 EDT 212 QIES Workbench Record Layout Report For Job: MDS 3. NH All Elements 4/1/212
file:///c:/users/hpmresdacsw1/appdata/local/temp/qwu_j78975_p1_mds_3 NH_... Page 1 of 24 11/27/212 Fri Nov 2 9:11:33 EDT 212 QIES Workbench Record Layout Report For Job: MDS 3. NH All Elements 4/1/212
2018 CMS Web Interface
 CMS Web Interface PREV-7 (NQF 0041): Preventive Care and Screening: Influenza Immunization Measure Steward: PCPI CMS Web Interface V2.1 Page 1 of 19 06/25/ Contents INTRODUCTION... 3 CMS WEB INTERFACE
CMS Web Interface PREV-7 (NQF 0041): Preventive Care and Screening: Influenza Immunization Measure Steward: PCPI CMS Web Interface V2.1 Page 1 of 19 06/25/ Contents INTRODUCTION... 3 CMS WEB INTERFACE
MDS 3.0 Updates Cassie Crafton R.N., CDP, RAC-CT
 MDS 3.0 Updates 2018 Cassie Crafton R.N., CDP, RAC-CT Objectives Understand new MDS 3.0 items in Sections GG, I, J, M, N and O that will be effective October 1 st, 2018 Know which MDS 3.0 items that will
MDS 3.0 Updates 2018 Cassie Crafton R.N., CDP, RAC-CT Objectives Understand new MDS 3.0 items in Sections GG, I, J, M, N and O that will be effective October 1 st, 2018 Know which MDS 3.0 items that will
2018 CMS Web Interface
 CMS Web Interface PREV-7 (NQF 0041): Preventive Care and Screening: Influenza Immunization Measure Steward: PCPI CMS Web Interface V2.0 Page 1 of 19 11/13/2017 Contents INTRODUCTION... 3 CMS WEB INTERFACE
CMS Web Interface PREV-7 (NQF 0041): Preventive Care and Screening: Influenza Immunization Measure Steward: PCPI CMS Web Interface V2.0 Page 1 of 19 11/13/2017 Contents INTRODUCTION... 3 CMS WEB INTERFACE
Healthcare Personnel Safety Component. Healthcare Personnel Vaccination Module Influenza Vaccination Summary. Outpatient Dialysis Facilities
 Healthcare Personnel Safety Component Healthcare Personnel Vaccination Module Influenza Vaccination Summary Outpatient Dialysis Facilities National Center for Emerging and Zoonotic Infectious Diseases
Healthcare Personnel Safety Component Healthcare Personnel Vaccination Module Influenza Vaccination Summary Outpatient Dialysis Facilities National Center for Emerging and Zoonotic Infectious Diseases
Measure #110 (NQF 0041): Preventive Care and Screening: Influenza Immunization National Quality Strategy Domain: Community/Population Health
 Measure #110 (NQF 0041): Preventive Care and Screening: Influenza Immunization National Quality Strategy Domain: Community/Population Health 2017 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE
Measure #110 (NQF 0041): Preventive Care and Screening: Influenza Immunization National Quality Strategy Domain: Community/Population Health 2017 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE
ICD-10-CM Coding and Documentation for Long Term Care
 ICD-10-CM Coding and Documentation for Long Term Care June 3, 2014 Chris Hoskins, MA, RHIA, CTR, CHC Karen Fabrizio, RHIA CHTS-CP AHIMA Approved ICD-10-CM/PCS Trainers Objectives Review 2014 Coding Guidelines
ICD-10-CM Coding and Documentation for Long Term Care June 3, 2014 Chris Hoskins, MA, RHIA, CTR, CHC Karen Fabrizio, RHIA CHTS-CP AHIMA Approved ICD-10-CM/PCS Trainers Objectives Review 2014 Coding Guidelines
NEW JERSEY 2011 HOSPITAL PERFORMANCE REPORT TECHNICAL REPORT: METHODOLOGY RECOMMENDED CARE (PROCESS OF CARE) MEASURES
 NEW JERSEY 2011 HOSPITAL PERFORMANCE REPORT TECHNICAL REPORT: METHODOLOGY RECOMMENDED CARE (PROCESS OF CARE) MEASURES New Jersey Department of Health and Senior Services Health Care Quality Assessment
NEW JERSEY 2011 HOSPITAL PERFORMANCE REPORT TECHNICAL REPORT: METHODOLOGY RECOMMENDED CARE (PROCESS OF CARE) MEASURES New Jersey Department of Health and Senior Services Health Care Quality Assessment
Measure Information Form
 Last Updated: Version 3.2 NQF-ENDORSED VOLUNTARY CONSENSUS STANDARDS FOR HOSPITAL CARE Measure Information Form Measure Set: Surgical Care Improvement Project (SCIP) Set Measure ID#: SCIP- Performance
Last Updated: Version 3.2 NQF-ENDORSED VOLUNTARY CONSENSUS STANDARDS FOR HOSPITAL CARE Measure Information Form Measure Set: Surgical Care Improvement Project (SCIP) Set Measure ID#: SCIP- Performance
Healthcare Personnel Influenza Vaccination Report
 Healthcare Personnel Influenza Vaccination Report Introduction As of Friday, November 1, 2013, the Healthcare Personnel Influenza Vaccination Report is available for facilities to complete through the
Healthcare Personnel Influenza Vaccination Report Introduction As of Friday, November 1, 2013, the Healthcare Personnel Influenza Vaccination Report is available for facilities to complete through the
Behavioral Health Evaluation
 This document is intended to serve as a template for a behavioral health committee meeting in an extended care facility. The State Operations Manual (SOM), Appendix PP - "Guidance to Surveyors for Long
This document is intended to serve as a template for a behavioral health committee meeting in an extended care facility. The State Operations Manual (SOM), Appendix PP - "Guidance to Surveyors for Long
MDS 3.0. Acronyms. Terminology & Definitions 8/22/2016 CAA CAT ADL BMI BIMS PT/OT/ST QI QM MDS RAI OMRA (SOT) OBRA RUG CMS COT OMRA ARD
 MDS 3.0 Acronyms MDS RAI OMRA (SOT) OBRA RUG CMS COT OMRA ARD CAA CAT ADL BMI BIMS PT/OT/ST QI QM Terminology & Definitions Active Disease Diagnosis Acute Change in Mental Status Period Reference Date
MDS 3.0 Acronyms MDS RAI OMRA (SOT) OBRA RUG CMS COT OMRA ARD CAA CAT ADL BMI BIMS PT/OT/ST QI QM Terminology & Definitions Active Disease Diagnosis Acute Change in Mental Status Period Reference Date
2018 CMS Web Interface
 CMS Web Interface PREV-5 (NQF 2372): Breast Cancer Screening Measure Steward: NCQA CMS Web Interface V2.1 Page 1 of 18 06/25/ Contents INTRODUCTION... 3 CMS WEB INTERFACE SAMPLING INFORMATION... 4 BENEFICIARY
CMS Web Interface PREV-5 (NQF 2372): Breast Cancer Screening Measure Steward: NCQA CMS Web Interface V2.1 Page 1 of 18 06/25/ Contents INTRODUCTION... 3 CMS WEB INTERFACE SAMPLING INFORMATION... 4 BENEFICIARY
Measure Applications Partnership. Hospital Workgroup In-Person Meeting Follow- Up Call
 Measure Applications Partnership Hospital Workgroup In-Person Meeting Follow- Up Call December 21, 2016 Feedback on Current Measure Sets for IQR, HACs, Readmissions, and VBP 2 Previously Identified Crosscutting
Measure Applications Partnership Hospital Workgroup In-Person Meeting Follow- Up Call December 21, 2016 Feedback on Current Measure Sets for IQR, HACs, Readmissions, and VBP 2 Previously Identified Crosscutting
Section H Bladder and Bowel
 Instructor Guide Section H Bladder and Bowel Objectives State the intent of Section H Bladder and Bowel. Describe how to conduct the assessment for urinary incontinence. Describe how to conduct the assessment
Instructor Guide Section H Bladder and Bowel Objectives State the intent of Section H Bladder and Bowel. Describe how to conduct the assessment for urinary incontinence. Describe how to conduct the assessment
2019 CMS Web Interface
 CMS Web Interface PREV-5 (NQF 2372): Breast Cancer Screening Measure Steward: NCQA CMS Web Interface V3.0 Page 1 of 18 xx/xx/2018 Contents INTRODUCTION... 3 CMS WEB INTERFACE SAMPLING INFORMATION... 4
CMS Web Interface PREV-5 (NQF 2372): Breast Cancer Screening Measure Steward: NCQA CMS Web Interface V3.0 Page 1 of 18 xx/xx/2018 Contents INTRODUCTION... 3 CMS WEB INTERFACE SAMPLING INFORMATION... 4
NEW JERSEY 2012 HOSPITAL PERFORMANCE REPORT TECHNICAL REPORT: METHODOLOGY RECOMMENDED CARE (PROCESS OF CARE) MEASURES
 NEW JERSEY 2012 HOSPITAL PERFORMANCE REPORT TECHNICAL REPORT: METHODOLOGY RECOMMENDED CARE (PROCESS OF CARE) MEASURES New Jersey Department of Health Health Care Quality Assessment June 2013 NEW JERSEY
NEW JERSEY 2012 HOSPITAL PERFORMANCE REPORT TECHNICAL REPORT: METHODOLOGY RECOMMENDED CARE (PROCESS OF CARE) MEASURES New Jersey Department of Health Health Care Quality Assessment June 2013 NEW JERSEY
Modular Program Report
 Modular Program Report Disclaimer The following report(s) provides findings from an FDA initiated query using Sentinel. While Sentinel queries may be undertaken to assess potential medical product safety
Modular Program Report Disclaimer The following report(s) provides findings from an FDA initiated query using Sentinel. While Sentinel queries may be undertaken to assess potential medical product safety
Urinary Catheter or Urinary Tract Infection Critical Element Pathway
 Use this pathway for a resident who has a symptomatic urinary tract infection (UTI) and/or an indwelling urinary catheter. Review the Following in Advance to Guide Observations and Interviews: Review the
Use this pathway for a resident who has a symptomatic urinary tract infection (UTI) and/or an indwelling urinary catheter. Review the Following in Advance to Guide Observations and Interviews: Review the
Quality ID #342: Pain Brought Under Control Within 48 Hours National Quality Strategy Domain: Person and Caregiver-Centered Experience and Outcomes
 Quality ID #342: Pain Brought Under Control Within 48 Hours National Quality Strategy Domain: Person and Caregiver-Centered Experience and Outcomes 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE
Quality ID #342: Pain Brought Under Control Within 48 Hours National Quality Strategy Domain: Person and Caregiver-Centered Experience and Outcomes 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE
Troy Hillman Manager, Analytical Services Uniform Data System for Medical Rehabilitation
 Avoiding Confusion between Payment and Quality Items on the New IRF-PAI, Part II: Other Implications Troy Hillman Manager, Analytical Services Uniform Data System for Medical Rehabilitation 2016 Uniform
Avoiding Confusion between Payment and Quality Items on the New IRF-PAI, Part II: Other Implications Troy Hillman Manager, Analytical Services Uniform Data System for Medical Rehabilitation 2016 Uniform
Emergency Department Stroke Registry Process of Care Indicator Specifications (July 1, 2011 June 30, 2012 Dates of Service)
 Specifications Description Methodology NIH Stroke Scale (NIHSS) Performed in Initial Evaluation used to assess the percentage of adult stroke patients who had the NIHSS performed during their initial evaluation
Specifications Description Methodology NIH Stroke Scale (NIHSS) Performed in Initial Evaluation used to assess the percentage of adult stroke patients who had the NIHSS performed during their initial evaluation
Section K Swallowing/ Nutritional Status
 Instructor Guide Section K Swallowing/ Nutritional Status Objectives State the intent of Section K Swallowing and Nutritional Status. Describe how to conduct an assessment of a resident s nutritional status.
Instructor Guide Section K Swallowing/ Nutritional Status Objectives State the intent of Section K Swallowing and Nutritional Status. Describe how to conduct an assessment of a resident s nutritional status.
PQS Summary of Pharmacy/ Medication-Related Updates in the CY 2020 Final Call Letter
 Managing Performance Information in a Quality Driven World PQS Summary of Pharmacy/ Medication-Related Updates in the CY 2020 Final Call Letter REGULATORY UPDATE PQS Summary of Pharmacy/ Medication-Related
Managing Performance Information in a Quality Driven World PQS Summary of Pharmacy/ Medication-Related Updates in the CY 2020 Final Call Letter REGULATORY UPDATE PQS Summary of Pharmacy/ Medication-Related
Measure #154 (NQF: 0101): Falls: Risk Assessment National Quality Strategy Domain: Patient Safety
 Measure #154 (NQF: 0101): Falls: Risk Assessment National Quality Strategy Domain: Patient Safety 2017 OPTIONS FOR INDIVIDUAL MEASURES: CLAIMS ONLY MEASURE TYPE: Process This is a two-part measure which
Measure #154 (NQF: 0101): Falls: Risk Assessment National Quality Strategy Domain: Patient Safety 2017 OPTIONS FOR INDIVIDUAL MEASURES: CLAIMS ONLY MEASURE TYPE: Process This is a two-part measure which
NORTHEAST HOSPITAL CORPORATION
 NORTHEAST HOSPITAL CORPORATION Title: Influenza and Pneumococcal Immunization Date Effective: 11/04 Date Revised: 7/08, 2/6/12, 3/15/13; 9/13/13 Date Reviewed: Joint Commission Chapter: Provision of Care,
NORTHEAST HOSPITAL CORPORATION Title: Influenza and Pneumococcal Immunization Date Effective: 11/04 Date Revised: 7/08, 2/6/12, 3/15/13; 9/13/13 Date Reviewed: Joint Commission Chapter: Provision of Care,
2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY. MEASURE TYPE: Outcome
 Quality ID #345 (NQF 1543): Rate of Asymptomatic Patients Undergoing Carotid Artery Stenting (CAS) Who Are Stroke Free or Discharged Alive National Quality Strategy Domain: Effective Clinical Care 2018
Quality ID #345 (NQF 1543): Rate of Asymptomatic Patients Undergoing Carotid Artery Stenting (CAS) Who Are Stroke Free or Discharged Alive National Quality Strategy Domain: Effective Clinical Care 2018
Modular Program Report
 Disclaimer The following report(s) provides findings from an FDA initiated query using Sentinel. While Sentinel queries may be undertaken to assess potential medical product safety risks, they may also
Disclaimer The following report(s) provides findings from an FDA initiated query using Sentinel. While Sentinel queries may be undertaken to assess potential medical product safety risks, they may also
MEASURE INFORMATION FORM
 MEASURE INFORMATION FORM Project Title: Dialysis Facility Compare Mineral Metabolism Project Overview: The Centers for Medicare & Medicaid Services (CMS) has contracted with the University of Michigan
MEASURE INFORMATION FORM Project Title: Dialysis Facility Compare Mineral Metabolism Project Overview: The Centers for Medicare & Medicaid Services (CMS) has contracted with the University of Michigan
Hospital Outpatient Quality Reporting. Benchmarks and Trends. Fourth Quarter 2013 through Fourth Quarter 2014
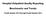 Hospital Outpatient Quality Reporting s and Trends Fourth Quarter through Fourth Quarter Hospital Outpatient Quality Reporting (Hospital OQR) Acute Myocardial Infarction (AMI), Surgery, and Stroke Data
Hospital Outpatient Quality Reporting s and Trends Fourth Quarter through Fourth Quarter Hospital Outpatient Quality Reporting (Hospital OQR) Acute Myocardial Infarction (AMI), Surgery, and Stroke Data
CMS Hospice Quality Reporting Program: Challenges & Opportunities
 1 CMS Hospice Quality Reporting Program: Challenges & Opportunities Carol Spence, PhD, RN National Hospice and Palliative Care Organization TODAY WE WILL COVER: Changes to HIS data collection CMS quality
1 CMS Hospice Quality Reporting Program: Challenges & Opportunities Carol Spence, PhD, RN National Hospice and Palliative Care Organization TODAY WE WILL COVER: Changes to HIS data collection CMS quality
Quality ID #110 (NQF 0041): Preventive Care and Screening: Influenza Immunization National Quality Strategy Domain: Community/Population Health
 Quality ID #110 (NQF 0041): Preventive Care and Screening: Influenza Immunization National Quality Strategy Domain: Community/Population Health 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE
Quality ID #110 (NQF 0041): Preventive Care and Screening: Influenza Immunization National Quality Strategy Domain: Community/Population Health 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE
Hospice Quality Reporting Program Provider Training
 Hospice Quality Reporting Program Provider Training Hospice Quality Reporting Program (HQRP) Data Submission and Requirements Presenters: Brenda Karkos, M.S.N./M.B.A., R.N., CHPN, Nurse Researcher/Associate,
Hospice Quality Reporting Program Provider Training Hospice Quality Reporting Program (HQRP) Data Submission and Requirements Presenters: Brenda Karkos, M.S.N./M.B.A., R.N., CHPN, Nurse Researcher/Associate,
Partial Hospitalization Program Program for Evaluating Payment Patterns Electronic Report. User s Guide Sixth Edition. Prepared by
 Partial Hospitalization Program Program for Evaluating Payment Patterns Electronic Report User s Guide Sixth Edition Prepared by Partial Hospitalization Program Program for Evaluating Payment Patterns
Partial Hospitalization Program Program for Evaluating Payment Patterns Electronic Report User s Guide Sixth Edition Prepared by Partial Hospitalization Program Program for Evaluating Payment Patterns
Performance Measures for Adult Immunization
 Performance Measures for Adult Immunization Reva Winkler, MD, MPH Senior Director, Performance Measures May 15, 2012 1 NQF-endorsed consensus standards for adult immunizations Influenza immunization 0431
Performance Measures for Adult Immunization Reva Winkler, MD, MPH Senior Director, Performance Measures May 15, 2012 1 NQF-endorsed consensus standards for adult immunizations Influenza immunization 0431
Appendix Identification of Study Cohorts
 Appendix Identification of Study Cohorts Because the models were run with the 2010 SAS Packs from Centers for Medicare and Medicaid Services (CMS)/Yale, the eligibility criteria described in "2010 Measures
Appendix Identification of Study Cohorts Because the models were run with the 2010 SAS Packs from Centers for Medicare and Medicaid Services (CMS)/Yale, the eligibility criteria described in "2010 Measures
Get With the Guidelines Stroke PMT. Quality Measure Descriptions
 Get With the Guidelines Stroke PMT Quality Measure s Last Updated July 2016 Print Measure s Dysphagia Screen Stroke Education Rehabilitation Considered Time to Intravenous Thrombolytic Therapy 60 min LDL
Get With the Guidelines Stroke PMT Quality Measure s Last Updated July 2016 Print Measure s Dysphagia Screen Stroke Education Rehabilitation Considered Time to Intravenous Thrombolytic Therapy 60 min LDL
2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY. MEASURE TYPE: Process
 Quality ID #44 (NQF 0236): Coronary Artery Bypass Graft (CABG): Preoperative Beta-Blocker in Patients with Isolated CABG Surgery National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR
Quality ID #44 (NQF 0236): Coronary Artery Bypass Graft (CABG): Preoperative Beta-Blocker in Patients with Isolated CABG Surgery National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR
Data Sources, Methods and Limitations
 Data Sources, Methods and Limitations The main data sources, methods and limitations of the data used in this report are described below: Local Surveys Rapid Risk Factor Surveillance System Survey The
Data Sources, Methods and Limitations The main data sources, methods and limitations of the data used in this report are described below: Local Surveys Rapid Risk Factor Surveillance System Survey The
Measure Information Form
 Measure Information Form Project Title: Mineral and Bone Disorder Project Overview: Date: The Centers for Medicare & Medicaid Services (CMS) has contracted with the University of Michigan Kidney Epidemiology
Measure Information Form Project Title: Mineral and Bone Disorder Project Overview: Date: The Centers for Medicare & Medicaid Services (CMS) has contracted with the University of Michigan Kidney Epidemiology
Program Objectives Hospice Compare
 Program Objectives Hospice Compare March 27, 2018 Jennifer Kennedy, EdD, MA, BSN, RN, CHC, NHPCO Kristi Dudash, MS, NHPCO National Hospice and Palliative Care Organization Describe the CASPER reports available
Program Objectives Hospice Compare March 27, 2018 Jennifer Kennedy, EdD, MA, BSN, RN, CHC, NHPCO Kristi Dudash, MS, NHPCO National Hospice and Palliative Care Organization Describe the CASPER reports available
DESCRIPTION: Percentage of women years of age who had a mammogram to screen for breast cancer
 Quality ID #112 (NQF 2372): Breast Cancer Screening National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES: CLAIMS ONLY MEASURE TYPE: Process DESCRIPTION: Percentage
Quality ID #112 (NQF 2372): Breast Cancer Screening National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES: CLAIMS ONLY MEASURE TYPE: Process DESCRIPTION: Percentage
Quality ID #112 (NQF 2372): Breast Cancer Screening National Quality Strategy Domain: Effective Clinical Care
 Quality ID #112 (NQF 2372): Breast Cancer Screening National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Process DESCRIPTION: Percentage
Quality ID #112 (NQF 2372): Breast Cancer Screening National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Process DESCRIPTION: Percentage
Improving Influenza Vaccination Rates in Critical Access Hospitals 10/26/2016
 Improving Influenza Vaccination Rates in Critical Access Hospitals 10/26/2016 Objectives Provide an overview of OP 27 Influenza Vaccination Among Healthcare Personnel (HCP) and IMM 2 Immunization for influenza
Improving Influenza Vaccination Rates in Critical Access Hospitals 10/26/2016 Objectives Provide an overview of OP 27 Influenza Vaccination Among Healthcare Personnel (HCP) and IMM 2 Immunization for influenza
Quality ID #113 (NQF 0034): Colorectal Cancer Screening National Quality Strategy Domain: Effective Clinical Care
 Quality ID #113 (NQF 0034): Colorectal Cancer Screening National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES: CLAIMS ONLY MEASURE TYPE: Process DESCRIPTION: Percentage
Quality ID #113 (NQF 0034): Colorectal Cancer Screening National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES: CLAIMS ONLY MEASURE TYPE: Process DESCRIPTION: Percentage
Unnecessary Medications Sampling Algorithm for QIS
 Overview ASE-Q selects five Census Sample residents for the Unnecessary Medications sample. The sampling algorithm is based on surveyor responses to selected questions in the Census Sample resident observation,
Overview ASE-Q selects five Census Sample residents for the Unnecessary Medications sample. The sampling algorithm is based on surveyor responses to selected questions in the Census Sample resident observation,
Preventive Care and Screening: Influenza Immunization
 e Title e Identifier ( Authoring Tool) Preventive Care and Screening: Influenza Immunization 147 e Version number 6.1.000 NQF Number 0041 GUID a244aa29-7d11-4616-888a-86e376bfcc6f ment Period Steward Developer
e Title e Identifier ( Authoring Tool) Preventive Care and Screening: Influenza Immunization 147 e Version number 6.1.000 NQF Number 0041 GUID a244aa29-7d11-4616-888a-86e376bfcc6f ment Period Steward Developer
NQF-ENDORSED VOLUNTARY CONSENSUS STANDARD FOR HOSPITAL CARE. Measure Information Form Collected For: CMS Outcome Measures (Claims Based)
 Last Updated: Version 4.3 NQF-ENDORSED VOLUNTARY CONSENSUS STANDARD FOR HOSPITAL CARE Measure Information Form Collected For: CMS Outcome Measures (Claims Based) Measure Set: CMS Readmission Measures Set
Last Updated: Version 4.3 NQF-ENDORSED VOLUNTARY CONSENSUS STANDARD FOR HOSPITAL CARE Measure Information Form Collected For: CMS Outcome Measures (Claims Based) Measure Set: CMS Readmission Measures Set
INPATIENT CONSULT SERVICE
 INPATIENT CONSULT SERVICE Patient Care OBJECTIVES BEGINNER Obtain essential and accurate information and present it in a concise but thorough format Perform a rehabilitation medicine focused consultation
INPATIENT CONSULT SERVICE Patient Care OBJECTIVES BEGINNER Obtain essential and accurate information and present it in a concise but thorough format Perform a rehabilitation medicine focused consultation
Objectives 1/10/2013. Hospital Outpatient Quality Reporting Specifications Manual Updates January 1, 2013
 Hospital Outpatient Quality Reporting Specifications Manual Updates January 1, 2013 Wanda Johnson, OFMQ Casey Thompson, OFMQ Kari Johnston, OFMQ Hospital Outpatient Quality Reporting Program Announcements
Hospital Outpatient Quality Reporting Specifications Manual Updates January 1, 2013 Wanda Johnson, OFMQ Casey Thompson, OFMQ Kari Johnston, OFMQ Hospital Outpatient Quality Reporting Program Announcements
REHABILITATION UNIT ANNUAL OUTCOMES REPORT Prepared by
 REHABILITATION UNIT ANNUAL OUTCOMES Prepared by REPORT - 2014 Keir Ringquist, PT, PhD, GCS Rehabilitation Program Manager Director of Occupational and Physical Therapy DEMOGRAPHICS OF THE REHABILITATION
REHABILITATION UNIT ANNUAL OUTCOMES Prepared by REPORT - 2014 Keir Ringquist, PT, PhD, GCS Rehabilitation Program Manager Director of Occupational and Physical Therapy DEMOGRAPHICS OF THE REHABILITATION
a guide to Reimbursement of Intermittent Catheters Know your options M2116N 04.08
 a guide to Reimbursement of Intermittent Catheters 1 Know your options Coloplast Corp. Minneapolis, MN 55411 1.800.533.0464 usmedweb@coloplast.com www.us.coloplast.com is a registered trademark of Coloplast
a guide to Reimbursement of Intermittent Catheters 1 Know your options Coloplast Corp. Minneapolis, MN 55411 1.800.533.0464 usmedweb@coloplast.com www.us.coloplast.com is a registered trademark of Coloplast
(i) This FAQ does not deal with clinical issues (eg What is the definition of a stroke unit? or
 STROKE INTEGRATED PERFORMANCE MEASURE RETURN (IPMR) FREQUENTLY ASKED QUESTIONS (FAQ) Prepared by NHS North West, Lancashire & Cumbria Cardiac & Stroke Network, Cheshire and Merseyside Clinical Networks
STROKE INTEGRATED PERFORMANCE MEASURE RETURN (IPMR) FREQUENTLY ASKED QUESTIONS (FAQ) Prepared by NHS North West, Lancashire & Cumbria Cardiac & Stroke Network, Cheshire and Merseyside Clinical Networks
MINIMUM DATA SET (MDS) - Version 3.0 RESIDENT ASSESSMENT AND CARE SCREENING Swing Bed Discharge (SD) Item Set
 MINIMUM DATA SET (MDS) - Version 3.0 RESIDENT ASSESSMENT AND CARE SCREENING Swing Bed Discharge (SD) Item Set Section A. Identification Information. A0100. Facility Provider Numbers. A. National Provider
MINIMUM DATA SET (MDS) - Version 3.0 RESIDENT ASSESSMENT AND CARE SCREENING Swing Bed Discharge (SD) Item Set Section A. Identification Information. A0100. Facility Provider Numbers. A. National Provider
Quality ID #113 (NQF 0034): Colorectal Cancer Screening National Quality Strategy Domain: Effective Clinical Care
 Quality ID #113 (NQF 0034): Colorectal Cancer Screening National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Process DESCRIPTION:
Quality ID #113 (NQF 0034): Colorectal Cancer Screening National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Process DESCRIPTION:
NQF-ENDORSED VOLUNTARY CONSENSUS STANDARDS FOR HOSPITAL CARE. Measure Information Form Collected For: CMS Outcome Measures (Claims Based)
 Last Updated: Version 4.3 NQF-ENDORSED VOLUNTARY CONSENSUS STANDARDS FOR HOSPITAL CARE Measure Information Form Collected For: CMS Outcome Measures (Claims Based) Measure Set: CMS Mortality Measures Set
Last Updated: Version 4.3 NQF-ENDORSED VOLUNTARY CONSENSUS STANDARDS FOR HOSPITAL CARE Measure Information Form Collected For: CMS Outcome Measures (Claims Based) Measure Set: CMS Mortality Measures Set
SECTION H: BLADDER AND BOWEL. H0100: Appliances. Item Rationale Health-related Quality of Life. Planning for Care
 SECTION H: BLADDER AND BOWEL Intent: The intent of the items in this section is to gather information on the use of bowel and bladder appliances, the use of and response to urinary toileting programs,
SECTION H: BLADDER AND BOWEL Intent: The intent of the items in this section is to gather information on the use of bowel and bladder appliances, the use of and response to urinary toileting programs,
Management of Heart Failure: Review of the Performance Measures by the Performance Measurement Committee of the American College of Physicians
 Performance Measurement Management of Heart Failure: Review of the Performance Measures by the Performance Measurement Committee of the American College of Physicians Writing Committee Amir Qaseem, MD,
Performance Measurement Management of Heart Failure: Review of the Performance Measures by the Performance Measurement Committee of the American College of Physicians Writing Committee Amir Qaseem, MD,
PQRS in TRAKnet 2015 GUIDE TO SUBMIT TING AND REPORTING PQRS IN 2015 THROUGH TRAKNET
 PQRS in TRAKnet 2015 GUIDE TO SUBMITTING AND REPORTING PQRS IN 2015 THROUGH TRAKNET What is PQRS? PQRS is a quality reporting program that uses negative payment adjustments to promote reporting of quality
PQRS in TRAKnet 2015 GUIDE TO SUBMITTING AND REPORTING PQRS IN 2015 THROUGH TRAKNET What is PQRS? PQRS is a quality reporting program that uses negative payment adjustments to promote reporting of quality
WHI Extension Appendix A, Form 33D Medical History Update (Detail) (Ver. 9) Page 1
 WHI Extension Appendix A, Form 33D Medical History Update (Detail) (Ver. 9) Page 1 FORM: 33D - MEDICAL HISTORY UPDATE (Detail) Version: 9 March 30, 2007 Description: When used: Self-administered or interviewer-administered;
WHI Extension Appendix A, Form 33D Medical History Update (Detail) (Ver. 9) Page 1 FORM: 33D - MEDICAL HISTORY UPDATE (Detail) Version: 9 March 30, 2007 Description: When used: Self-administered or interviewer-administered;
DESCRIPTION: Percent of asymptomatic patients undergoing CEA who are discharged to home no later than post-operative day #2
 Measure #260: Rate of Carotid Endarterectomy (CEA) for Asymptomatic Patients, without Major Complications (Discharged to Home by Post-Operative Day #2) National Quality Strategy Domain: Patient Safety
Measure #260: Rate of Carotid Endarterectomy (CEA) for Asymptomatic Patients, without Major Complications (Discharged to Home by Post-Operative Day #2) National Quality Strategy Domain: Patient Safety
PIN BENCHMARKING DATA DEFINITIONS DICTIONARY
 CORE MEASURES PIN BENCHMARKING DATA DEFINITIONS DICTIONARY 1 Total number of CAH acute care patient admissions. Report all CAH acute care only patient admissions for the quarter. Exclude CAH swing bed,
CORE MEASURES PIN BENCHMARKING DATA DEFINITIONS DICTIONARY 1 Total number of CAH acute care patient admissions. Report all CAH acute care only patient admissions for the quarter. Exclude CAH swing bed,
TECHNICAL NOTES APPENDIX SUMMER
 TECHNICAL NOTES APPENDIX SUMMER Hospital Performance Report Summer Update INCLUDES PENNSYLVANIA INPATIENT HOSPITAL DISCHARGES FROM July 1, 2005 through June 30, 2006 The Pennsylvania Health Care Cost Containment
TECHNICAL NOTES APPENDIX SUMMER Hospital Performance Report Summer Update INCLUDES PENNSYLVANIA INPATIENT HOSPITAL DISCHARGES FROM July 1, 2005 through June 30, 2006 The Pennsylvania Health Care Cost Containment
Hospice Quality Reporting Program. CAHPS and HIS. HQRP HIS Submission Requirements
 Hospice Quality Reporting CAHPS and HIS Katie Wehri, CHPC Healthcare Provider Solutions, Inc. KWehri@healthcareprovidersolutions.com Hospice Quality Reporting Program Hospice Item Set (HIS) Admission Discharge
Hospice Quality Reporting CAHPS and HIS Katie Wehri, CHPC Healthcare Provider Solutions, Inc. KWehri@healthcareprovidersolutions.com Hospice Quality Reporting Program Hospice Item Set (HIS) Admission Discharge
Fall Risk Assessment and Prevention in the Post-Acute Setting A Road Map
 Fall Risk Assessment and Prevention in the Post-Acute Setting A Road Map Cora M. Butler, JD, RN, CHC HealthCore Value Advisors, Inc. Juli A. James, RN Primaris Holdings, Inc. Objectives Explore the burden
Fall Risk Assessment and Prevention in the Post-Acute Setting A Road Map Cora M. Butler, JD, RN, CHC HealthCore Value Advisors, Inc. Juli A. James, RN Primaris Holdings, Inc. Objectives Explore the burden
Quality ID #236 (NQF 0018): Controlling High Blood Pressure National Quality Strategy Domain: Effective Clinical Care
 Quality ID #236 (NQF 0018): Controlling High Blood Pressure National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS F INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Intermediate Outcome
Quality ID #236 (NQF 0018): Controlling High Blood Pressure National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS F INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Intermediate Outcome
Appendix G Explanation/Clarification Summary
 Appendix G Explanation/Clarification Summary Summary of Changes for Recommendations Alignment of measures with VBP by fiscal year Measures and service dates were adjusted to be consistent with the FY2016
Appendix G Explanation/Clarification Summary Summary of Changes for Recommendations Alignment of measures with VBP by fiscal year Measures and service dates were adjusted to be consistent with the FY2016
Colorado State Innovation Model (SIM) Clinical Quality Measures (CQMs) Reporting Schedules
 Colorado State Innovation Model (SIM) Clinical Quality Measures (CQMs) Reporting Schedules 1 SIM Clinical Quality Measure (CQM) Reporting Schedules: Cohort 3 Table of Contents Reporting Schedules... 3
Colorado State Innovation Model (SIM) Clinical Quality Measures (CQMs) Reporting Schedules 1 SIM Clinical Quality Measure (CQM) Reporting Schedules: Cohort 3 Table of Contents Reporting Schedules... 3
IQSS 2019 QCDR and MIPS Measure Specifications
 IQSS1 Hypogonadism: Serum T, CBC, PSA, IPSS within 6 months of Rx Percentage of patients with a Effective Clinical Patients with documented new diagnosis of hypogonadism receiving androgen replacement
IQSS1 Hypogonadism: Serum T, CBC, PSA, IPSS within 6 months of Rx Percentage of patients with a Effective Clinical Patients with documented new diagnosis of hypogonadism receiving androgen replacement
TECHNICAL NOTES APPENDIX SUMMER
 TECHNICAL NOTES APPENDIX SUMMER Hospital Performance Report Summer Update INCLUDES PENNSYLVANIA INPATIENT HOSPITAL DISCHARGES FROM JULY 1, 2006 THROUGH JUNE 30, 2007 The Pennsylvania Health Care Cost Containment
TECHNICAL NOTES APPENDIX SUMMER Hospital Performance Report Summer Update INCLUDES PENNSYLVANIA INPATIENT HOSPITAL DISCHARGES FROM JULY 1, 2006 THROUGH JUNE 30, 2007 The Pennsylvania Health Care Cost Containment
DENOMINATOR: All female patients aged 65 years and older with a visit during the measurement period
 Measure #48: Urinary Incontinence: Assessment of Presence or Absence of Urinary Incontinence in Women Aged 65 Years and Older National Quality Strategy Domain: Effective Clinical Care 2017 OPTIONS FOR
Measure #48: Urinary Incontinence: Assessment of Presence or Absence of Urinary Incontinence in Women Aged 65 Years and Older National Quality Strategy Domain: Effective Clinical Care 2017 OPTIONS FOR
Working together, pressure ulcer prevention IS possible!
 How can we prevent Edna s skin from breaking down? Consider following these steps to help prevent skin damage from pressure ulcers: Understand why Edna is at risk. Develop a care plan to prevent pressure
How can we prevent Edna s skin from breaking down? Consider following these steps to help prevent skin damage from pressure ulcers: Understand why Edna is at risk. Develop a care plan to prevent pressure
Talking the same language for effective care of older people
 Introducing the interrai Home Care Talking the same language for effective care of older people interrai has developed an entire range of instruments and screeners to support assessment in a wide array
Introducing the interrai Home Care Talking the same language for effective care of older people interrai has developed an entire range of instruments and screeners to support assessment in a wide array
Nancy Hailpern, Director, Regulatory Affairs K Street, NW, Suite 1000 Washington, DC 20005
 Summary of Infection Prevention Issues in the Centers for Medicare & Medicaid Services (CMS) FY 2014 Inpatient Prospective Payment System (IPPS) Final Rule Hospital Readmissions Reduction Program-Fiscal
Summary of Infection Prevention Issues in the Centers for Medicare & Medicaid Services (CMS) FY 2014 Inpatient Prospective Payment System (IPPS) Final Rule Hospital Readmissions Reduction Program-Fiscal
UPDATE ON IMMUNIZATION GUIDELINES AND PRACTICES
 DISCLOSURES UPDATE ON IMMUNIZATION GUIDELINES AND PRACTICES Nothing to disclose Kylie Mueller, Pharm.D., BCPS Clinical Specialist, Infectious Diseases Spartanburg Regional Medical Center LEARNING OBJECTIVES
DISCLOSURES UPDATE ON IMMUNIZATION GUIDELINES AND PRACTICES Nothing to disclose Kylie Mueller, Pharm.D., BCPS Clinical Specialist, Infectious Diseases Spartanburg Regional Medical Center LEARNING OBJECTIVES
The table below includes the quality measures an ACO is required to submit to CMS as a participant in an MSSP Track 3 ACO
 The table below includes the quality measures an ACO is required to submit to CMS as a participant in an MSSP Track 3 ACO ACO-1 ACO-2 Getting Timely Care, Appointments, and Information How Well Your Providers
The table below includes the quality measures an ACO is required to submit to CMS as a participant in an MSSP Track 3 ACO ACO-1 ACO-2 Getting Timely Care, Appointments, and Information How Well Your Providers
Psychotropic Medication. Including Role of Gradual Dose Reductions
 Psychotropic Medication Including Role of Gradual Dose Reductions What are they? The phrase psychotropic drugs is a technical term for psychiatric medicines that alter chemical levels in the brain which
Psychotropic Medication Including Role of Gradual Dose Reductions What are they? The phrase psychotropic drugs is a technical term for psychiatric medicines that alter chemical levels in the brain which
Troubleshooting Audio
 Welcome Audio for this event is available via ReadyTalk Internet streaming. No telephone line is required. Computer speakers or headphones are necessary to listen to streaming audio. Limited dial-in lines
Welcome Audio for this event is available via ReadyTalk Internet streaming. No telephone line is required. Computer speakers or headphones are necessary to listen to streaming audio. Limited dial-in lines
Patient sample criteria for the Preventive Care Measure Group are patients aged 50 years and older with a specific patient encounter:
 2016 Physician Quality Reporting System Data Collection Form: Preventive Care (for patients aged 50 and older) NOTE: Individual measures may have more restrictive age and gender requirements. IMPORTANT:
2016 Physician Quality Reporting System Data Collection Form: Preventive Care (for patients aged 50 and older) NOTE: Individual measures may have more restrictive age and gender requirements. IMPORTANT:
