Protocol for the Examination of Specimens From Patients With Carcinoma of the Penis
|
|
|
- Joella O’Brien’
- 5 years ago
- Views:
Transcription
1 Protocol for the Examination of Specimens From Patients With Carcinoma of the Penis Version: Protocol Posting Date: June 2017 Includes ptnm requirements from the 8 th Edition, AJCC Staging Manual For accreditation purposes, this protocol should be used for the following procedures AND tumor types: Procedure Description Penectomy Includes specimens designated partial penectomy and total penectomy. Circumcision Required if margins can be assessed. Tumor Type Description Carcinoma Includes carcinomas arising from foreskin glands or penile shaft. This protocol is NOT required for accreditation purposes for the following: Procedure Biopsy (incisional or excisional) Primary resection specimen with no residual cancer (eg, following neoadjuvant therapy) Cytologic specimens The following tumor types should NOT be reported using this protocol: Tumor Type Urothelial carcinoma (consider Urethra protocol) Lymphoma (consider the Hodgkin or non-hodgkin Lymphoma protocols) Sarcoma (consider the Soft Tissue protocol) Authors Antonio L. Cubilla, MD*; Ming Zhou, MD, PhD*; Robert Allan, MD; Mahul B. Amin, MD; Jonathan I. Epstein, MD; David J. Grignon, MD; Peter A. Humphrey, MD, PhD; Curtis A. Pettaway, MD; Jason Pettus, MD; Victor E. Reuter, MD; John R. Srigley, MD; Elsa F. Velazquez, MD With guidance from the CAP Cancer Committee and CAP Pathology Electronic Reporting Committee. * Denotes primary author. All other contributing authors are listed alphabetically College of American Pathologists (CAP). All rights reserved. For Terms of Use please visit
2 Accreditation Requirements This protocol can be utilized for a variety of procedures and tumor types for clinical care purposes. For accreditation purposes, only the definitive primary cancer resection specimen is required to have the core and conditional data elements reported in a synoptic format. Core data elements are required in reports to adequately describe appropriate malignancies. For accreditation purposes, essential data elements must be reported in all instances, even if the response is not applicable or cannot be determined. Conditional data elements are only required to be reported if applicable as delineated in the protocol. For instance, the total number of lymph nodes examined must be reported, but only if nodes are present in the specimen. Optional data elements are identified with + and although not required for CAP accreditation purposes, may be considered for reporting as determined by local practice standards. The use of this protocol is not required for recurrent tumors or for metastatic tumors that are resected at a different time than the primary tumor. Use of this protocol is also not required for pathology reviews performed at a second institution (ie, secondary consultation, second opinion, or review of outside case at second institution). Circumcision is NOT considered to be the definitive resection specimen, even though the entire cancer may be removed. A protocol is recommended for reporting such specimens for clinical care purposes, but this is not required for accreditation purposes. Synoptic Reporting All core and conditionally required data elements outlined on the surgical case summary from this cancer protocol must be displayed in synoptic report format. Synoptic format is defined as: Data element: followed by its answer (response), outline format without the paired "Data element: Response" format is NOT considered synoptic. The data element must be represented in the report as it is listed in the case summary. The response for any data element may be modified from those listed in the case summary, including Cannot be determined if appropriate. Each diagnostic parameter pair (Data element: Response) is listed on a separate line or in a tabular format to achieve visual separation. The following exceptions are allowed to be listed on one line: o Anatomic site or specimen, laterality, and procedure o Pathologic Stage Classification (ptnm) elements o Negative margins, as long as all negative margins are specifically enumerated where applicable The synoptic portion of the report can appear in the diagnosis section of the pathology report, at the end of the report or in a separate section, but all Data element: Responses must be listed together in one location Organizations and pathologists may choose to list the required elements in any order, use additional methods in order to enhance or achieve visual separation, or add optional items within the synoptic report. The report may have required elements in a summary format elsewhere in the report IN ADDITION TO but not as replacement for the synoptic report i.e. all required elements must be in the synoptic portion of the report in the format defined above. CAP Laboratory Accreditation Program Protocol Required Use Date: March 2018* * Beginning January 1, 2018, the 8th edition AJCC Staging Manual should be used for reporting ptnm. CAP Penis Protocol Summary of Changes Version errata: Size of Largest Metastatic Deposit MODIFIED Unit of measure from millimeters to centimeters Version : The following data elements were modified: Pathologic Stage Classification (ptnm, AJCC 8 th Edition) 2
3 CAP Approved Surgical Pathology Cancer Case Summary Protocol posting date: June 2017 PENIS: Note: This case summary is recommended for reporting biopsy specimens, but is not required for accreditation purposes. Select a single response unless otherwise indicated. Procedure Incisional biopsy Excisional biopsy Partial penectomy Total penectomy Circumcision Other (specify): Not specified Foreskin (presence and type) (select all that apply) (Note A) Present (uncircumcised) + Short + Medium + Long + Phimotic Not identified (circumcised) Cannot be determined Tumor Site (select all that apply) Glans Foreskin mucosal surface Foreskin skin surface Coronal sulcus (balanopreputial sulcus) Skin of the shaft Shaft Penile urethra Penis, NOS Tumor Size Greatest dimension (centimeters): cm + Additional dimensions (centimeters): x cm Cannot be determined (explain): + Tumor Focality + Unifocal + Multifocal + Tumor Macroscopic Features (select all that apply) + Flat + Ulcerated + Polypoid + Verruciform + Necrosis + Hemorrhage + Data elements preceded by this symbol are not required for accreditation purposes. These optional elements may be clinically important but are not yet validated or regularly used in patient management. 3
4 CAP Approved + Other (specify): + Tumor Deep Borders (select all that apply) (Note C) + Pushing (broad base) + Infiltrative (jagged) + Other (specify): Histologic Type (Note D) Non-HPV-related squamous cell carcinoma Squamous cell carcinoma, usual type Pseudohyperplastic carcinoma Pseudoglandular carcinoma Verrucous carcinoma Carcinoma cuniculatum Papillary squamous cell carcinoma, NOS Adenosquamous carcinoma Sarcomatoid squamous cell carcinoma HPV-related squamous cell carcinoma Basaloid squamous cell carcinoma Papillary-basaloid squamous cell carcinoma Warty carcinoma Warty-basaloid squamous cell carcinoma Clear cell squamous cell carcinoma Lymphoepithelioma-like carcinoma Paget disease Adnexal carcinoma (specify type): Carcinoma, type cannot be determined Other histologic type not listed (specify): Histologic Grade (Note E) G1: Well differentiated G2: Moderately differentiated G3: Poorly differentiated GX: Cannot be assessed Not applicable Tumor Extension (select all that apply) No evidence of primary tumor Carcinoma in situ Noninvasive localized squamous cell carcinoma Tumor invades lamina propria Tumor invades dermis Tumor invades dartos fascia Tumor invades corpus spongiosum Tumor invades corpus cavernosum Tumor invades tunica albuginea Tumor invades Buck s fascia Tumor invades penile (distal) urethra Tumor invades regional skin (pubis, inguinal) Tumor invades into adjacent structures (ie, scrotum, prostate, pubic bone) (specify): Tumor invades other structures (specify): Cannot be assessed (explain): + Data elements preceded by this symbol are not required for accreditation purposes. These optional elements may be clinically important but are not yet validated or regularly used in patient management. 4
5 CAP Approved + Tumor Thickness or Depth of Invasion (Note F) + Specify (millimeters): mm Margins (select all that apply) (Note G) Cannot be assessed Uninvolved Involved (specify for penectomy or circumcision specimens below) Invasive carcinoma Noninvasive carcinoma/ carcinoma in situ For penectomy specimens: Urethral Periurethral tissues (subepithelial connective tissue [lamina propria], corpus spongiosum, Buck s fascia) Corpus cavernosum Buck s fascia at penile shaft Skin Other (specify): For circumcision specimens: Coronal sulcus mucosal margin Cutaneous margin Lymphovascular Invasion (Note H) Not identified Present Cannot be determined Perineural Invasion (Note I) Not identified Present Cannot be determined Regional Lymph Nodes (Note B) No lymph nodes submitted or found Lymph Node Examination (required only if lymph nodes are present in the specimen) Number of Lymph Nodes Involved: Number cannot be determined (explain): Specify Site(s) (if applicable): # # Note: Sites may include sentinel, inguinal, pelvic, or other lymph nodes. If inguinal lymph nodes involved, specify: Number of Inguinal Lymph Nodes Involved: Number cannot be determined (explain): Laterality of Inguinal Lymph Nodes Involved (required only if applicable) Unilateral Bilateral Cannot be determined (explain): Number of Lymph Nodes Examined: Number cannot be determined (explain): + Size of Largest Metastatic Deposit (centimeters): cm + Specify Site: + Data elements preceded by this symbol are not required for accreditation purposes. These optional elements may be clinically important but are not yet validated or regularly used in patient management. 5
6 CAP Approved + Size of Largest Lymph Node Involved (centimeters): cm + Specify Site: Extranodal Extension (required only if lymph nodes involved) Not identified Present Cannot be determined Pathologic Stage Classification (ptnm, AJCC 8 th Edition) (Note J) Note: Reporting of pt, pn, and (when applicable) pm categories is based on information available to the pathologist at the time the report is issued. Only the applicable T, N, or M category is required for reporting; their definitions need not be included in the report. The categories (with modifiers when applicable) can be listed on 1 line or more than 1 line. TNM Descriptors (required only if applicable) (select all that apply) m (multiple primary tumors) r (recurrent) y (posttreatment) Primary Tumor (pt) ptx: Primary tumor cannot be assessed pt0: No evidence of primary tumor ptis: Carcinoma in situ (penile intraepithelial neoplasia [PeIN]) pta: Noninvasive localized squamous cell carcinoma pt1: Glans: Tumor invades lamina propria Foreskin: Tumor invades dermis, lamina propria, or dartos fascia Shaft: Tumor invades connective tissue between epidermis and corpora regardless of location All sites with or without lymphovascular invasion or perineural invasion and is or is not high grade pt1a: Tumor is without lymphovascular invasion or perineural invasion and is not high grade (ie, grade 3 or sarcomatoid) pt1b: Tumor exhibits lymphovascular invasion and/or perineural invasion or is high grade (ie, grade 3 or sarcomatoid) pt2: Tumor invades into corpus spongiosum (either glans or ventral shaft) with or without urethral invasion pt3: Tumor invades into corpora cavernosum (including tunica albuginea) with or without urethral invasion pt4: Tumor invades into adjacent structures (ie, scrotum, prostate, pubic bone) Regional Lymph Nodes (pn) pnx: Lymph node metastasis cannot be established pn0: No lymph node metastasis pn1: 2 unilateral inguinal metastases, no ENE pn2: 3 unilateral inguinal metastases or bilateral metastases, no ENE pn3: ENE of lymph node metastases or pelvic lymph node metastases Distant Metastasis (pm) (required only if confirmed pathologically in this case) pm1: Distant metastasis present # Specify site(s), if known: # Including lymph node metastasis outside the true pelvis, lung, liver, cutaneous nodules distant from the primary site, and bone. + Data elements preceded by this symbol are not required for accreditation purposes. These optional elements may be clinically important but are not yet validated or regularly used in patient management. 6
7 CAP Approved + Additional Pathologic Findings (select all that apply) (Note K) + None identified + HPV-related penile intraepithelial neoplasia (PeIN), warty type + HPV-related penile intraepithelial neoplasia (PeIN), basaloid type + HPV-related penile intraepithelial neoplasia (PeIN), warty-basaloid type + Non-HPV-related PeIN (differentiated [simplex] penile intraepithelial neoplasia) + Pleomorphic PeIN + Spindle PeIN + Clear cell PEIN + Pagetoid PEIN + Lichen sclerosus + Squamous hyperplasia + Condyloma acuminatum + Other (specify): + Ancillary Studies + Specify: + Not performed + Comment(s) + Data elements preceded by this symbol are not required for accreditation purposes. These optional elements may be clinically important but are not yet validated or regularly used in patient management. 7
8 Explanatory Notes A. Types of Foreskin There are three foreskin types: in the short foreskin, the preputial orifice is located behind the glans corona; in the medium foreskin, the orifice is between the corona and the meatal orifice; in the long foreskin, the entire glans is covered and the meatus is not identified without retracting the foreskin. Phimotic foreskins are unretractable and long. 1 Phimosis is present in up to one-half of patients with penile carcinoma, 1 and its presence is considered a risk factor for the development of this tumor. 2-4 B. Number of Involved Lymph Nodes and Extension of the Lymphadenectomy The presence of more than two positive lymph nodes in one inguinal basin increases the likelihood of contralateral inguinal and ipsilateral pelvic nodal involvement. 5 In such cases, prophylactic contralateral inguinal and ipsilateral pelvic lymphadenectomy is advised. The number and percentage of positive nodes involved also has an impact on survival. 6,7 C. Tumor Base of Infiltration Two patterns are recognized: infiltrating (invasion in blocks of small solid strands of cell tumors broadly infiltrating the stroma) and pushing infiltration (tumor cells invading in large cell blocks with well-defined tumor-stroma interface). The infiltrating pattern of invasion is associated with a higher risk for nodal involvement. 8 D. Histologic Subtype of Squamous Cell Carcinoma The World Health Organization (WHO) classification of tumors of the penis was recently published. 9 Most penile cancers are squamous cell carcinomas (SCC), and most arise from the epithelium of the distal portion of the penis (including glans, coronal sulcus, and mucosal surface of the prepuce). Squamous cell carcinoma of the usual type (keratinizing SCC) comprises about 50% to 60% of all cases There are other SCC variants showing distinctive morphological and outcome features The different histological subtypes correlate with different rates of regional/nodal and systemic dissemination. Penile cancer subtypes can be prognostically stratified in three groups. The low-risk group includes verruciform tumors such as verrucous, papillary, and warty/condylomatous carcinomas. 13,14 More recently described subtypes, such as pseudohyperplastic and carcinoma cuniculatum of the penis, also belong to this category of excellent prognosis. 15,16 The high-risk category is comprised by basaloid, sarcomatoid, adenosquamous, and poorly differentiated SCC of the usual type There is an intermediate category of metastatic risk that includes most SCCs of the usual type, some mixed neoplasms (such as hybrid verrucous carcinomas), and high-grade variants of warty/condylomatous carcinomas. 14 E. Histologic Grade Histological grade has been consistently reported as an influential predictive factor of groin metastasis and dissemination of penile cancer We recommend a method to grade penile SCCs as follows: Grade 1 is an extremely well-differentiated carcinoma, with a minimal deviation from the morphology of normal/hyperplastic squamous epithelium. Grade 2 tumors show a more disorganized growth as compared to grade 1 lesions, higher nuclear-tocytoplasmic ratio, evident mitoses, and, although present, less prominent keratinization. Grade 3 are tumors showing any proportion of anaplastic cells, identified as solid sheets or irregular small aggregates, cords or nests of cells with little or no keratinization, high nuclear-to-cytoplasmic ratio, thick nuclear membranes, nuclear pleomorphism, clumped chromatin, prominent nucleoli, and numerous mitosis A tumor should be graded according to the least differentiated component. Any proportion of grade 3 should be noted in the report. 23 F. Depth of Invasion The tumor depth in small lesions is best obtained by perpendicularly sectioning along the tumor central axis. For 8
9 large glans tumors, it is preferred to section the specimen longitudinally in half, with additional parallel sections of each half, using as an axis the central and ventral penile urethra. The depth of invasion of SCC is defined as a measurement in millimeters from the epithelial-stromal junction of the adjacent nonneoplastic epithelium to the deepest point of invasion. In larger tumors, especially verruciform ones, the previously mentioned system is not applicable, and we measure the thickness from the surface (excluding the keratin layer) to the deepest point of invasion. Depth of invasion and tumor thickness are of equivalent significance. There is a correlation between depth of invasion and outcome in penile cancers. Minimal risk for metastasis was reported for tumors measuring less than 5 mm in thickness. 22,24 Tumors invading deeper into penile anatomical levels are usually associated with a higher risk for nodal involvement. There is also a correlation between deeper infiltration and higher histological grade, although some exceptions do occur. 26 Tumors invading corpus cavernosum are at higher risk for presenting nodal metastases than those invading only corpus spongiosum, 26,27 and the deepest erectile tissue invaded should be clearly stated in the final pathology report. Per AJCC 8 th edition, tumor invading into subepithelial connective tissue (lamina propria), Dartos muscle, and Buck s fascia is staged as T1; tumor invading into corpus spongiosum (either glans or ventral shaft) with or without urethral invasion is staged as T2; tumor invading into corpora cavernosum (including tunica albuginea) with or without urethral invasion is staged as T3; and tumor invading into adjacent structures (ie, scrotum, prostate, pubic bone) is staged as T4. G. Resection Margins Positive margins adversely affect prognosis in patients with penile squamous cell carcinomas. 10,12,28 Important margins to be examined in partial penectomy specimens include: (1) proximal urethra and surrounding periurethral cylinder consisting of epithelium, subepithelial connective tissue (lamina propria), corpus spongiosum, and penile fascia; (2) proximal shaft with corresponding corpora cavernosa separated and surrounded by the tunica albuginea and Buck s fascia; and (3) skin of shaft with underlying corporal dartos 27 (Figure 1). The coronal sulcus mucosal margin and cutaneous margin should be entirely examined when evaluating circumcision specimens. Figure 1. Partial penectomy specimen; anatomical structures of proximal resection margin. The ventral urethra (U) is surrounded by the corpus spongiosum (CS) and a delicate white tunica albuginea (A). The latter is also surrounding the corpora cavernosa (CC). The penile fascia (Buck s fascia) (BF) is located underneath skin (S) and dartos (D). The proximal margin of resection should be cut en face and all the structures including the entire circumference of the urethra with periurethral cylinder should be examined. The 3 important margins to be examined include (1) skin of the shaft with underlying dartos and penile fascia, (2) the corpora cavernosa with surrounding tunica albuginea, and (3) the urethra and periurethral cylinder that includes the lamina propria, corpus spongiosum, albuginea, and penile fascia. Abbreviations: CCA, cavernous artery; DDV, deep dorsal vein; SDV, superficial dorsal vein. 9
10 H. Lymphovascular Invasion Vascular invasion, lymphatic or venous, adversely affects prognosis of penile cancer The TNM staging classification in the 8th edition of the AJCC Cancer Staging Manual subdivides T1 tumors into T1a and T1b based on the absence or presence of lymphovascular invasion or poorly differentiated tumors. 34 Embolic involvement of lymphatic vascular spaces occurs usually near the invasive tumor front, but it may also be found at a certain distance from the primary tumor in anatomical areas such as the lamina propria, penile fascia, and especially in the subepithelial connective tissues surrounding penile urethra. Venous invasion indicates a more advanced stage of the disease and is related to the compromise of the specialized erectile venous structures of corpora spongiosa and cavernosa. I. Nomograms, Risk Groups, and Perineural Invasion An evaluation of clinical and pathological variables using a nomogram was recently developed. 31 The selected factors were clinical stage of lymph nodes, microscopic growth pattern, grade, vascular invasion, and invasion of corpora spongiosa and cavernosa and urethra. The probability of nodal metastasis as predicted by the nomogram was close to the real incidence of metastasis observed at follow up. A second nomogram to estimate predictions of survival at 5 years with the same clinical and pathological factors gave similar results. 32 More recently, perineural invasion and histological grade were found to be the strongest independent predictors of mortality in penile tumors 5 to 10 mm thick. A nomogram considering the predictive value of perineural invasion and histological grade was accordingly constructed. 21 Risk groups stratification systems are available to predict the likelihood of inguinal nodal involvement and for therapeutic planning and are based on a combination of histological grade and pt stage Strongest predictive power results from the combination of histological grade, deepest anatomical level of infiltration, and presence of perineural invasion. These factors are used for constructing the prognostic index. 27 J. TNM Staging Classification The protocol recommends the use of the TNM staging system of the American Joint Committee on Cancer (AJCC) for carcinoma of the penis. 34 By AJCC convention, the designation T refers to a primary tumor that has not been previously treated. The symbol p refers to the pathologic classification of the TNM, as opposed to the clinical classification, and is based on gross and microscopic examination. pt entails a resection of the primary tumor or a biopsy adequate to evaluate the highest pt category, pn entails removal of nodes adequate to validate lymph node metastasis, and pm implies microscopic examination of distant lesion. Pathologic staging is usually performed after surgical resection of the primary tumor. The summary of changes in the TNM staging classification in the 8th edition of the AJCC Cancer Staging Manual is as follows: Change Histologic Grade (G) Details of Change The 3-tiered World Health Organization (WHO)/International Society of Urological Pathology (ISUP) grading system has been adopted. Any proportion of anaplastic cells is sufficient to categorize a tumor as grade 3. Definition of Primary Tumor (T) Definition of Primary Tumor (T) Definition of Primary Tumor (T) Definition of Primary Tumor (T) Definition of Primary Tumor (T) Definition of Regional Lymph Nodes (N) Definition of Regional Lymph Nodes (N) Ta definition is now broadened to include noninvasive localized squamous carcinoma. T1a and T1b have been separated by an additional prognostic indicator the presence or absence or perineural invasion. T1a or T1b are described by the site where they occur on the penis and are designated glans, foreskin, or shaft. Anatomic layers invaded are described for the three locations. T2 definition includes corpus spongiosum invasion. T3 definition now involves corpora cavernosum invasion. pn1 is defined as 2 unilateral inguinal metastases, no extranodal extension. pn2 is defined as 3 unilateral inguinal metastases or bilateral metastases 10
11 Additional Descriptor The m suffix indicates the presence of multiple primary tumors and is recorded in parentheses, eg, pta(m)n0m0. Anatomic Stage/Prognostic Groups Group T N M Stage 0is Tis N0 M0 Stage 0a Ta N0 M0 Stage I T1a N0 M0 Stage IIA T1b N0 M0 Stage IIA T2 N0 M0 Stage IIB T3 N0 M0 Stage IIIA T1-3 N1 M0 Stage IIIB T1-3 N2 M0 Stage IV T4 Any N M0 Stage IV Any T N3 M0 Stage IV Any T Any N M1 Prognostic Factors (Site-Specific Factors) Factors required for staging: None. Clinically significant factors: Involvement of corpus spongiosum Involvement of corpus cavernosum Percentage of tumor that is poorly differentiated Verrucous carcinoma depth of invasion Size of largest lymph node metastasis Extranodal/extracapsular extension Human papillomavirus (HPV) status K. Penile Intraepithelial Neoplasia Penile Intraepithelial Neoplasia (PeIN) may be subclassified as differentiated (simplex), warty, basaloid, and warty/basaloid (mixed). 39,40 Differentiated PeIN shows parakeratosis, epithelial thickening, elongation of rete ridges, prominent bridges, basal cell atypia, enlarged nuclei, and prominent nucleoli. Differentiated PeIN is frequently associated with lichen sclerosus. It is considered HPV-unrelated, there is no koilocytosis, and p16 immunohistochemical staining results (surrogate of high-risk types of HPV) are usually negative. Basaloid PeIN is characterized by a replacement of the normal epithelium by small, uniform cells with round nuclei and scant cytoplasm. Numerous mitosis and apoptotic cells are usually present. Warty PeIN shows a spiky surface with parakeratosis. The normal epithelium is replaced by markedly pleomorphic cells showing prominent koilocytosis. Mixed warty-basaloid lesions are not infrequent. Warty and basaloid PeIN are HPV-related lesions and usually overexpress p16. L. Handling of the Specimen Circumcision Specimen Take measurements, describe specimen, and identify and describe tumor. Identify and ink the mucosal and cutaneous margins with different colors. Most SCCs arise from the mucosal surface of the foreskin, therefore the coronal sulcus (mucosal) margin is especially important. Lightly stretch and pin the specimen to a cardboard. Fix for several hours in formalin. Cut vertically the whole specimen labeling from 1 to 12, clockwise. Penectomy Specimen Take measurements, describe specimen, and identify and describe tumor. Most SCCs of the penis arise from the epithelium of the distal portion of the organ (glans, coronal sulcus, and mucosal surface of the prepuce; the tumor may involve one or more of these anatomical compartments). 41 If present, classify the foreskin as short, medium, long, and/or phimotic. 2 Cut the proximal margin of resection en face making sure to include the entire circumference of the urethra (Figure 1). If the urethra has been retracted, it is important to identify its resection 11
12 margin and submit it entirely. The resection margin can be divided in three important areas that need to be analyzed: the skin of the shaft with underlying dartos and penile fascia; corpora cavernosa with albuginea; and urethra with periurethral cylinder that includes subepithelial connective tissue (lamina propria), corpus spongiosum, albuginea, and penile fascia (Figure 1). The urethra and periurethral cylinder can be placed in one cassette. The skin of the shaft with dartos and fascia can be included together with the corpora cavernosa. Because this is a large specimen, it may need to be included in several cassettes to include the entire resection margin. Fix the rest of the specimen overnight. Then, in the fixed state and if the tumor is large and involves most of the glans, cut longitudinally and centrally by using the meatus and the proximal urethra as reference points. Do not probe the urethra. Separate the specimen into halves, left and right (Figures 2 and 3). Then cut two to six serial sections of each half. If tumor is small and asymmetrically located in the dorsal or ventral area, the central portion of the tumor may be used as the axis of sectioning. If the tumor is large involving multiples sites (glans, sulcus and foreskin), it is important not to remove the foreskin leaving the entire specimen intact for sectioning. In cases of small carcinomas exclusively located in the glans with no foreskin involvement, one may choose to remove the foreskin leaving a 3-mm redundant edge around the sulcus. Proceed cutting the foreskin as indicated for circumcision specimens. If the primary tumor is located in the glans, one should still submit the foreskin serially and in orderly fashion labeled from 1 to 12 clockwise. The rest of the penectomy specimen should be handled as described above. Figure 2. Partial penectomy specimen. After submitting the proximal resection margin, the specimen is cut in half longitudinally. Parallel serial sections will follow. Abbreviations: CA, carcinoma; CC, corpus cavernosum; F, foreskin; G, glans; TA, tunica albuginea; U, urethra. 12
13 Figure 3. Longitudinal and central section showing the ventral urethra (U) and the penile main anatomic compartments: glans (GL), coronal sulcus (COS), and foreskin (F). The Buck s (penile) fascia (PF) encases the shaft and inserts into the coronal sulcus. Abbreviations: ALB, albuginea; CC, corpus cavernosum; CS, corpus spongiosum; DT, dartos; E, epithelium; LP, lamina propria; MU, urethral meatus. M. Pathology Report for Penile Squamous Cell Carcinoma The report should contain the following information: primary tumor: tumor site or sites, size in centimeters, histologic subtype, histologic grade, anatomical level of invasion, tumor thickness in millimeters, and vascular and perineural invasion. In penectomy specimens, the margins of resection to be reported are urethral/periurethral, corporal, and skin of the shaft. 28 In circumcision specimens, margins include coronal sulcus mucosal margin and cutaneous margin. Common associated lesions to be reported are penile intraepithelial neoplasia (differentiated or undifferentiated), lichen sclerosus, and other inflammatory dermatologic conditions. If the specimen is accompanied by inguinal nodes, the number and size of nodes should be described. All nodes should be included for microscopic examination. The number of positive nodes and total number of nodes examined should be reported as well as the presence of extracapsular extension and the number and site (eg, inguinal versus pelvic) of metastatic nodes. The distinction between superficial and deep inguinal lymph nodes has been eliminated in the seventh edition TNM classification. 34 References 1. Velazquez EF, Bock A, Soskin A, Codas R, Arbo M, Cubilla AL. Preputial variability and preferential association of long phimotic foreskins with penile cancer: an anatomic comparative study of types of foreskin in a general population and cancer patients. Am J Surg Pathol. 2003;27(7): Daling J, Madeleine MM, Johnson LG, et al. Penile cancer: importance of circumcision, human papillomavirus and smoking in in situ and invasive disease. Int J Cancer. 2005;116(4): Tsen HF, Morgenstern H, Mack T, Peters RK. Risk factors for penile cancer: results of a population-based case-control study in Los Angeles County (United States). Cancer Causes Control. 2002;12(3): Madsen BS, van den Brule AJ, Jensen HL, Wholfahrt J, Frisch M. Risk factors for squamous cell carcinoma of the penis: population-based case-control study in Denmark. Cancer Epidemiol Biomarkers Prev. 2008;17(10): Lont AP, Kroon BK, Gallee MP, van Tinteren H, Moonen LM, Horenblas S. Pelvic lymph node dissection for penile carcinoma: extent of inguinal lymph node involvement as an indicator for pelvic lymph node involvement and survival. J Urol. 2007;177(3): Svatek RS, Munsell M, Kincaid JM, et al. Association between lymph node density and disease specific survival in patients with penile cancer. J Urol. In press. 7. Pandey D, Mahajan V, Kannan RR. Prognostic factors in node-positive carcinoma of the penis. J Surg Oncol. 2006;93(2):
14 8. Guimarães G, Lopes A, Campos RS, et al. Front pattern of invasion in squamous cell carcinoma of the penis: new prognostic factor for predicting risk of lymph node metastases. Urology. 2006;68(1): Moch H, Humphrey PA, Ulbright TM, Reuter VE. WHO Classification of Tumours of the Urinary System and Male Genital Organs. Geneva, Switzerland: WHO Press; Epstein JH, Humphrey PA, Cubilla AL. Tumors of the Prostate Gland, Seminal Vesicles, Male Urethra, Penis and Scrotum. Washington, DC: Armed Forces Institute of Pathology; 2011 Atlas of Tumor Pathology. 11. Cubilla AL, Dillner J, Schellhammer PF, Horenblas S. Malignant epithelial tumors. In: Eble JN, Sauter G, Epstein J, Sesterhenn I, eds. Pathology and Genetics of Tumors of the Urinary System and Male Genital Organs. Lyon, France: IARC Press; World Health Organization Classification of Tumours. 12. Velazquez EF, Barreto JE, Ayala G, Cubilla AL. Penis. In: Mills SE, Carter D, Greenson JK, et al, eds. Sternberg s Diagnostic Surgical Pathology. 5 th ed. Philadelphia, PA: Lippincot Williams & Wilkins; Cubilla AL, Reuter V, Velazquez E, Piris A, Saito S, Young RH. Histologic classification of penile carcinoma and its relation to outcome in 61 patients with primary resection. Int J Surg Pathol. 2001;9(2): Cubilla AL, Velazques EF, Reuter VE, Oliva E, Mihm MC Jr, Young RH. Warty (condylomatous) squamous cell carcinoma of the penis: a report of 11 cases and proposed classification of verruciform tumors penile tumors. Am J Surg Pathol. 2000;24(4): Cubilla AL, Velazquez EF, Young RH. Pseudohyperplastic squamous cell carcinoma of the penis associated with lichen sclerosus an extremely well-differentiated nonverruciform neoplasm that preferentially affects the foreskin and is frequently misdiagnosed: a report of 10 cases of a distinctive clinicopathologic entity. Am J Surg Pathol. 2004;28(7): Barreto JE, Velazquez EF, Ayala E, Torres J, Cubilla AL. Carcinoma cuniculatum of the penis a distinctive variant of penile squamous cell carcinoma: report of 7 cases. Am J Surg Pathol. 2007;31(1): Cubilla AL, Reuter VE, Gregoire L, et al. Basaloid squamous cell carcinoma: a distinctive HPV related penile neoplasm: a report of 20 cases. Am J Surg Pathol. 1998;22(6): Velazquez EF, Melamed J, Barreto JE, Aguero F, Cubilla AL. Sarcomatoid carcinoma of the penis: a clinicopathological study of 14 cases. Am J Surg Pathol. 2005;29(9): Cubilla AL, Ayala MT, Barreto JE, Bellasai JG, Nöel JC. Surface adenosquamous carcinoma of the penis: a report of three cases. Am J Surg Pathol. 1996;20(2): Slaton JW, Morgenstern N, Levy DA, et al. Tumor stage, vascular invasion and the percentage of poorly differentiated cancer: independent prognosticators for inguinal node metastasis in penile squamous cancer. J Urol. 2001;165(4): Cubilla AL, Velazquez EF, Ayala GE, Chaux A, Torres J, Reuter V. Identification of prognostic pathologic parameters in squamous cell carcinoma of the penis: significance and difficulties. Pathol Case Rev. 2005;10: Velazquez EF, Ayala G, Liu H, et al. Histologic grade and perineural invasion are more important than tumor thickness as predictor of nodal metastasis in penile squamous cell carcinoma invading 5 to 10 mm. Am J Surg Pathol. 2008;32(7): Chaux A, Torres J, Pfannl R, et al. Histologic grade in penile squamous cell carcinoma: visual estimation versus digital measurement of proportions of grades, adverse prognosis with any proportion of grade 3 and correlation of a Gleason-like system with nodal metastasis. Am J Surg Pathol. 2009;33: Emerson RE, Ulbright TM, Eble JN, Geary WA, Eckert GJ, Cheng L. Predicting cancer progression in patients with penile squamous cell carcinoma: the importance of depth of invasion and vascular invasion. Mod Pathol. 2001;14(10): Guimaraes GC, Cunha IW, et al. Penile squamous cell carcinoma clinicopathological features, nodal metastasis and outcome in 333 cases. J Urol. 2009;182(2): Leijte J, Gallee M, Antonini N, Horenblas S. Evaluation of current TNM classification of penile carcinoma. J Urol. 2008;180(3): Chaux A, Caballero C, Soares F, et al. The prognostic index: a useful pathologic guide for prediction of nodal metastases and survival in penile squamous cell carcinoma. Am J Surg Pathol. 2009;33(7): Velazquez EF, Soskin A, Bock A, Codas R, Barreto JE, Cubilla AL. Positive resection margins in partial penectomies: sites of involvement and proposal of local routes of spread of penile squamous cell carcinoma. Am J Surg Pathol. 2004;28(3): Lopes A, Hidalgo GS, Kowalski LP, Torloni H, Rossi BM, Fonseca FP. Prognostic factors in carcinoma of the penis: multivariate analysis of 145 patients treated with amputation and lymphadenectomy. J Urol. 1996;156(5):
15 30. Ficarra V, Zattoni F, Cunisco SC, et al. Lymphatic and vascular embolizations are independent predictive variables of inguinal node involvement in patients with squamous cell carcinoma of the penis: Gruppo Uro- Oncologico del Nord Est (Northeast Uro-Oncological Group) Penile Cancer data base data. Cancer. 2005;103(12): Ficarra V, Zattoni F, Artibani W, et al; GUONE Penile Cancer Project Members. Nomogram predictive of pathological inguinal lymph node involvement in patients with squamous cell carcinoma of the penis. J Urol. 2006;175(6): Kattan MW, Ficarra V, Artibani W, et al; GUONE Penile Cancer Project Members. Nomogram predictive of cancer specific survival in patients undergoing partial or total amputation for squamous cell carcinoma of the penis. J Urol. 2006;175(6): Novara G, Galfano A, De Marco V, Artibani W, Ficarra V. Prognostic factors in squamous cell carcinoma of the penis. Nat Clin Pract Urol. 2007;4(3): Amin MB, Edge SB, Greene FL, et al, eds. AJCC Cancer Staging Manual. 8th ed. New York, NY: Springer; Solsona E, Algaba F, Horenblas S, Pizzocaro G, Windahl T; European Association of Urology. EAU guidelines on penile cancer. Eur Urol. 2004;46(1): Solsona E, Iborra I, Rubio J, Casanova JL, Ricos JV, Calabuig C. Prospective validation of the association of local tumor stage and grade as a predictive factor for occult lymph node micrometastasis in patients with penile carcinoma and clinically negative inguinal lymph nodes. J Urol. 2001;165(5): Hungerhuber E, Schlenker B, et al. Risk stratification in penile carcinoma: 25-year experience with surgical inguinal lymph node staging. Urology. 2006;68(3): Ornellas AA, Nóbrega BL, Wei Kin Chin E, et al. Prognostic factors in invasive squamous cell carcinoma of the penis: analysis of 196 patients treated at the Brazilian National Cancer Institute. J Urol. 2008;180(4): Cubilla AL, Pfannl R, Rodriguez I, et al. Morphological characterization and distribution of penile precancerous lesions using a simplified nomenclature: a study of 198 lesions in 115 patients. Lab Invest. 2008;88:696(A). 40. Pfannl R, Hernandez M, Velazquez EF, et al. Expression of p53 and p16 in differentiated and warty/basaloid penile intraepithelial neoplasia (PeIN). Lab Invest. 2008;88:807(A). 41. Cubilla AL, Piris A, Pfanni R, Rodriguez I, Agüero F, Young RH. Anatomic levels: important landmarks in penectomy specimens; a detailed anatomic and histologic study based on the examination of 44 specimens. Am J Surg Pathol. 2001;25:
Protocol for the Examination of Specimens from Patients with Carcinoma of the Penis
 Protocol for the Examination of Specimens from Patients with Carcinoma of the Penis Protocol applies to primary carcinoma of the penis. Primary urethral carcinomas and melanomas are not included. Version:
Protocol for the Examination of Specimens from Patients with Carcinoma of the Penis Protocol applies to primary carcinoma of the penis. Primary urethral carcinomas and melanomas are not included. Version:
Penile cancer teams in UK. Common variants. Penile cancer teams. Basaloid squamous carcinoma. The Pathology of Penile Tumours
 The Pathology of Penile Tumours Dr Jonathan H Shanks The Christie NHS Foundation Trust, Manchester, UK Penile cancer teams in UK 12 centres for penile cancer work (10 in England and Wales, 2 in Scotland)
The Pathology of Penile Tumours Dr Jonathan H Shanks The Christie NHS Foundation Trust, Manchester, UK Penile cancer teams in UK 12 centres for penile cancer work (10 in England and Wales, 2 in Scotland)
ACCME/Disclosures. 52 year old man who consulted for a long-standing mass on the distal penis 4/13/2016
 ACCME/Disclosures United States and Canadian Academy of Pathology Seattle, WA 2016 Elsa F Velazquez, MD Director of Dermatopathology, V.P. Clinical Assistant Professor of Dermatology Tufts University,
ACCME/Disclosures United States and Canadian Academy of Pathology Seattle, WA 2016 Elsa F Velazquez, MD Director of Dermatopathology, V.P. Clinical Assistant Professor of Dermatology Tufts University,
INTERNATIONAL SOCIETY OF UROLOGICAL PATHOLOGISTS USCAP COMPANION MEETING PROGRAM WASHINGTON D.C. New Concepts and Entities in Penile Cancer Pathology
 INTERNATIONAL SOCIETY OF UROLOGICAL PATHOLOGISTS USCAP COMPANION MEETING PROGRAM WASHINGTON D.C. New Concepts and Entities in Penile Cancer Pathology Elsa F. Velazquez, MD Brigham and Women s Hospital
INTERNATIONAL SOCIETY OF UROLOGICAL PATHOLOGISTS USCAP COMPANION MEETING PROGRAM WASHINGTON D.C. New Concepts and Entities in Penile Cancer Pathology Elsa F. Velazquez, MD Brigham and Women s Hospital
Pathological risk-group stratifcatioo systems for peoile caocer maoagemeot: A study of 198 patieots with iovasive squamous cell carciooma
 Alcides Chaux Office of Scientific Research Norte University Rev UN Med 2013 2(1): 69-92 Pathological risk-group stratifcatioo systems for peoile caocer maoagemeot: A study of 198 patieots with iovasive
Alcides Chaux Office of Scientific Research Norte University Rev UN Med 2013 2(1): 69-92 Pathological risk-group stratifcatioo systems for peoile caocer maoagemeot: A study of 198 patieots with iovasive
Case Report Warty Carcinoma Penis: An Uncommon Variant
 Hindawi Case Reports in Pathology Volume 2017, Article ID 2937592, 4 pages https://doi.org/10.1155/2017/2937592 Case Report Warty Carcinoma Penis: An Uncommon Variant Sushma Thapa, 1 Arnab Ghosh, 1 Santosh
Hindawi Case Reports in Pathology Volume 2017, Article ID 2937592, 4 pages https://doi.org/10.1155/2017/2937592 Case Report Warty Carcinoma Penis: An Uncommon Variant Sushma Thapa, 1 Arnab Ghosh, 1 Santosh
GUIDELINES ON PENILE CANCER
 GUIDELINES ON PENILE CANCER (Text update April 2010) G. Pizzocaro, F. Algaba, S. Horenblas, E. Solsona, S. Tana, H. Van Der Poel, N. Watkin 78 Penile Cancer Eur Urol 2010 Jun;57(6):1002-12 Introduction
GUIDELINES ON PENILE CANCER (Text update April 2010) G. Pizzocaro, F. Algaba, S. Horenblas, E. Solsona, S. Tana, H. Van Der Poel, N. Watkin 78 Penile Cancer Eur Urol 2010 Jun;57(6):1002-12 Introduction
Protocol for the Examination of Specimens From Patients With Carcinoma of the Urethra and Periurethral Glands
 Protocol for the Examination of Specimens From Patients With Carcinoma of the Urethra and Periurethral Glands Version: Protocol Posting Date: June 2017 Includes ptnm requirements from the 8 th Edition,
Protocol for the Examination of Specimens From Patients With Carcinoma of the Urethra and Periurethral Glands Version: Protocol Posting Date: June 2017 Includes ptnm requirements from the 8 th Edition,
GUIDELINEs ON PENILE CANCER
 GUIDELINEs ON PENILE CANCER (update April 2010) G. Pizzocaro, F. Algaba, S. Horenblas, E. Solsona, S. Tana, H. Van Der Poel, N. Watkin Eur Urol 2010, doi:10.1016/j.eururo.2010.01.039 Introduction Over
GUIDELINEs ON PENILE CANCER (update April 2010) G. Pizzocaro, F. Algaba, S. Horenblas, E. Solsona, S. Tana, H. Van Der Poel, N. Watkin Eur Urol 2010, doi:10.1016/j.eururo.2010.01.039 Introduction Over
VULVAR CARCINOMA. Page 1 of 5
 VULVAR CARCINOMA EXAMPLE OF A VULVAR CARCINOMA USING PROPOSED TEMPLATE Case: Invasive squamous cell carcinoma arising in D-VIN Tumor in left labia major Left partial vaginectomy and sentinel lymph node
VULVAR CARCINOMA EXAMPLE OF A VULVAR CARCINOMA USING PROPOSED TEMPLATE Case: Invasive squamous cell carcinoma arising in D-VIN Tumor in left labia major Left partial vaginectomy and sentinel lymph node
UICC TNM 8 th Edition Errata
 UICC TNM 8 th Edition Errata ions are in italics Page 28 Oropharynx p16 positive Pathological Stage II,T2 N2 M0 T3 N0,N1 M0 Stage II,T2 N2 M0 T3,T4 N0,N1 M0 Page 61 Oesophagus Adenocarcinoma Pathological
UICC TNM 8 th Edition Errata ions are in italics Page 28 Oropharynx p16 positive Pathological Stage II,T2 N2 M0 T3 N0,N1 M0 Stage II,T2 N2 M0 T3,T4 N0,N1 M0 Page 61 Oesophagus Adenocarcinoma Pathological
Definition of Synoptic Reporting
 Definition of Synoptic Reporting The CAP has developed this list of specific features that define synoptic reporting formatting: 1. All required cancer data from an applicable cancer protocol that are
Definition of Synoptic Reporting The CAP has developed this list of specific features that define synoptic reporting formatting: 1. All required cancer data from an applicable cancer protocol that are
GUIDELINES ON PENILE CANCER
 GUIDELINES ON PENILE CANCER (Text updated March 2005) G. Pizzocaro (chairman), F. Algaba, S. Horenblas, H. van der Poel, E. Solsona, S. Tana, N. Watkin 58 Penile Cancer Eur Urol 2004;46(1);1-8 Introduction
GUIDELINES ON PENILE CANCER (Text updated March 2005) G. Pizzocaro (chairman), F. Algaba, S. Horenblas, H. van der Poel, E. Solsona, S. Tana, N. Watkin 58 Penile Cancer Eur Urol 2004;46(1);1-8 Introduction
UICC TNM 8 th Edition Errata
 UICC TNM 8 th Edition Errata ions are in italics Head and Neck Tumours Pages 20, p27, p34, p38, p41, and p49 ly pn2a Metastasis in a single ipsilateral lymph node, less than 3cm in greatest dimension with
UICC TNM 8 th Edition Errata ions are in italics Head and Neck Tumours Pages 20, p27, p34, p38, p41, and p49 ly pn2a Metastasis in a single ipsilateral lymph node, less than 3cm in greatest dimension with
EAU GUIDELINES ON PENILE CANCER
 EAU GUIDELINES ON PENILE CANCER (Text update April 2014) O.W. Hakenberg (Chair), N. Watkin, E. Compérat, S. Minhas, A. Necchi, C. Protzel Introduction and epidemiology The incidence of penile cancer increases
EAU GUIDELINES ON PENILE CANCER (Text update April 2014) O.W. Hakenberg (Chair), N. Watkin, E. Compérat, S. Minhas, A. Necchi, C. Protzel Introduction and epidemiology The incidence of penile cancer increases
EAU GUIDELINES ON PENILE CANCER
 EAU GUIDELINES ON PENILE CANCER (Text update April 2014) O.W. Hakenberg (Chair), E. Compérat, S. Minhas, A. Necchi, C. Protzel, N. Watkin Guidelines Associate: R. Robinson Introduction and epidemiology
EAU GUIDELINES ON PENILE CANCER (Text update April 2014) O.W. Hakenberg (Chair), E. Compérat, S. Minhas, A. Necchi, C. Protzel, N. Watkin Guidelines Associate: R. Robinson Introduction and epidemiology
Carcinoma of the Urinary Bladder Histopathology
 Carcinoma of the Urinary Bladder Histopathology Reporting Proforma (Radical & Partial Cystectomy, Cystoprostatectomy) Includes the International Collaboration on Cancer reporting dataset denoted by * Family
Carcinoma of the Urinary Bladder Histopathology Reporting Proforma (Radical & Partial Cystectomy, Cystoprostatectomy) Includes the International Collaboration on Cancer reporting dataset denoted by * Family
GUIDELINES ON PENILE CANCER
 46 E. Solsona (chairman), F. Algaba, S. Horenblas, G. Pizzocaro, T. Windahl Eur Urol 2002;42(3):199-203 Introduction Penile carcinoma is an uncommon malignant disease with an incidence ranging from 0.1
46 E. Solsona (chairman), F. Algaba, S. Horenblas, G. Pizzocaro, T. Windahl Eur Urol 2002;42(3):199-203 Introduction Penile carcinoma is an uncommon malignant disease with an incidence ranging from 0.1
Urinary Bladder, Ureter, and Renal Pelvis
 Urinary Bladder, Ureter, and Renal Pelvis Protocol applies to all carcinomas of the urinary bladder, ureter, and renal pelvis. Protocol revision date: January 2005 Based on AJCC/UICC TNM, 6th edition Procedures
Urinary Bladder, Ureter, and Renal Pelvis Protocol applies to all carcinomas of the urinary bladder, ureter, and renal pelvis. Protocol revision date: January 2005 Based on AJCC/UICC TNM, 6th edition Procedures
Warty carcinoma of the penis: A clinicopathological study from South India
 Original Article Warty carcinoma of the penis: A clinicopathological study from South India Marie Therese Manipadam, Suresh Kumar Bhagat 1, Ganesh Gopalakrishnan 1, Nitin S. Kekre 1, Ninan K. Chacko 1,
Original Article Warty carcinoma of the penis: A clinicopathological study from South India Marie Therese Manipadam, Suresh Kumar Bhagat 1, Ganesh Gopalakrishnan 1, Nitin S. Kekre 1, Ninan K. Chacko 1,
Prognostic factors of genitourinary tumors: Do we have to care?
 Prognostic factors of genitourinary tumors: Do we have to care? Jae Y. Ro, MD, PhD Professor and Director of Surgical Pathology The Methodist Hospital, Weill Medical College of Cornell University, Houston,
Prognostic factors of genitourinary tumors: Do we have to care? Jae Y. Ro, MD, PhD Professor and Director of Surgical Pathology The Methodist Hospital, Weill Medical College of Cornell University, Houston,
EUROPEAN UROLOGY 58 (2010)
 EUROPEAN UROLOGY 58 (2010) 742 747 available at www.sciencedirect.com journal homepage: www.europeanurology.com Penile Cancer Prognostic Factors for Occult Inguinal Lymph Node Involvement in Penile Carcinoma
EUROPEAN UROLOGY 58 (2010) 742 747 available at www.sciencedirect.com journal homepage: www.europeanurology.com Penile Cancer Prognostic Factors for Occult Inguinal Lymph Node Involvement in Penile Carcinoma
Although SCCP is a rare disease in the Brazilian male
 Prognostic Factors in Invasive Squamous Cell Carcinoma of the Penis: Analysis of 196 Patients Treated at the Brazilian National Cancer Institute Antonio Augusto Ornellas,* Bernardo Lindenberg Braga Nóbrega,
Prognostic Factors in Invasive Squamous Cell Carcinoma of the Penis: Analysis of 196 Patients Treated at the Brazilian National Cancer Institute Antonio Augusto Ornellas,* Bernardo Lindenberg Braga Nóbrega,
Carcinoma of the Renal Pelvis and Ureter Histopathology
 Carcinoma of the Renal Pelvis and Ureter Histopathology Reporting Proforma (NEPHROURETERECTOMY AND URETERECTOMY) Includes the International Collaboration on Cancer reporting dataset denoted by * Family
Carcinoma of the Renal Pelvis and Ureter Histopathology Reporting Proforma (NEPHROURETERECTOMY AND URETERECTOMY) Includes the International Collaboration on Cancer reporting dataset denoted by * Family
S1.04 Principal clinician. G1.01 Comments. G2.01 *Specimen dimensions (prostate) S2.02 *Seminal vesicles
 Prostate Cancer Histopathology Reporting Proforma (Radical Prostatectomy) Includes the International Collaboration on Cancer reporting dataset denoted by * Family name Given name(s) Date of birth Sex Male
Prostate Cancer Histopathology Reporting Proforma (Radical Prostatectomy) Includes the International Collaboration on Cancer reporting dataset denoted by * Family name Given name(s) Date of birth Sex Male
PATIENTS AND METHODS. We reviewed patients with SCC of the penis from five different urological centres. The
 2008 The Authors; Journal compilation 2008 BJU International Original Article LYMPH-NODE METASTASES IN INTERMEDIATE-RISK SQUAMOUS CELL CARCINOMA OF THE PENIS NAUMANN et al. BJUI BJU INTERNATIONAL Lymph-node
2008 The Authors; Journal compilation 2008 BJU International Original Article LYMPH-NODE METASTASES IN INTERMEDIATE-RISK SQUAMOUS CELL CARCINOMA OF THE PENIS NAUMANN et al. BJUI BJU INTERNATIONAL Lymph-node
Protocol for the Examination of Specimens From Patients With Carcinoma of the Prostate Gland
 Protocol for the Examination of Specimens From Patients With Carcinoma of the Prostate Gland Version: Protocol Posting Date: June 2017 Includes ptnm requirements from the 8 th Edition, AJCC Staging Manual
Protocol for the Examination of Specimens From Patients With Carcinoma of the Prostate Gland Version: Protocol Posting Date: June 2017 Includes ptnm requirements from the 8 th Edition, AJCC Staging Manual
The pathology of bladder cancer
 1 The pathology of bladder cancer Charles Jameson Introduction Carcinoma of the bladder is the seventh most common cancer worldwide [1]. It comprises 3.2% of all cancers, with an estimated 260 000 new
1 The pathology of bladder cancer Charles Jameson Introduction Carcinoma of the bladder is the seventh most common cancer worldwide [1]. It comprises 3.2% of all cancers, with an estimated 260 000 new
TOPICS FOR DISCUSSION
 INTERNATIONAL SOCIETY OF UROLOGIC PATHOLOGY PATHOLOGIC STAGING OF SELECT UROLOGIC MALIGNANCIES Mahul B. Amin, MD Professor and Chairman Pathology and Laboratory Medicine Cedars-Sinai Medical Center Los
INTERNATIONAL SOCIETY OF UROLOGIC PATHOLOGY PATHOLOGIC STAGING OF SELECT UROLOGIC MALIGNANCIES Mahul B. Amin, MD Professor and Chairman Pathology and Laboratory Medicine Cedars-Sinai Medical Center Los
Protocol for the Examination of Specimens From Patients With Merkel Cell Carcinoma of the Skin
 Protocol for the Examination of Specimens From Patients With Merkel Cell Carcinoma of the Skin Version: Protocol Posting Date: June 2017 Includes ptnm requirements from the 8 th Edition, AJCC Staging Manual
Protocol for the Examination of Specimens From Patients With Merkel Cell Carcinoma of the Skin Version: Protocol Posting Date: June 2017 Includes ptnm requirements from the 8 th Edition, AJCC Staging Manual
Uterine Cervix. Protocol applies to all invasive carcinomas of the cervix.
 Uterine Cervix Protocol applies to all invasive carcinomas of the cervix. Protocol revision date: January 2005 Based on AJCC/UICC TNM, 6 th edition and FIGO 2001 Annual Report Procedures Cytology (No Accompanying
Uterine Cervix Protocol applies to all invasive carcinomas of the cervix. Protocol revision date: January 2005 Based on AJCC/UICC TNM, 6 th edition and FIGO 2001 Annual Report Procedures Cytology (No Accompanying
CARCINOMA OF THE PENIS STRUCTURED REPORTING PROTOCOL. (1st Edition 2018)
 CARCINOMA OF THE PENIS STRUCTURED REPORTING PROTOCOL (1st Edition 2018) Incorporating the: International Collaboration on Cancer Reporting (ICCR) Dataset for the reporting of Carcinoma of the Penis and
CARCINOMA OF THE PENIS STRUCTURED REPORTING PROTOCOL (1st Edition 2018) Incorporating the: International Collaboration on Cancer Reporting (ICCR) Dataset for the reporting of Carcinoma of the Penis and
Handling and Pathology Reporting of Circumcision and Penectomy Specimens $
 European Urology European Urology 46 (2004) 434 439 Review Handling and Pathology Reporting of Circumcision and Penectomy Specimens $ Gregor Mikuz a,*, Alison M. Winstanley b, Claude C. Schulman c, Frans
European Urology European Urology 46 (2004) 434 439 Review Handling and Pathology Reporting of Circumcision and Penectomy Specimens $ Gregor Mikuz a,*, Alison M. Winstanley b, Claude C. Schulman c, Frans
Squamous carcinoma of the penis: a case report
 Squamous carcinoma of the penis: a case report De Fiores A., Diosi D., Bella G., De Marco V. Introdution Penile cancer is a relatively rare neoplasm in the developed world and 95% of the cases histologically
Squamous carcinoma of the penis: a case report De Fiores A., Diosi D., Bella G., De Marco V. Introdution Penile cancer is a relatively rare neoplasm in the developed world and 95% of the cases histologically
Descriptor Definition Author s notes TNM descriptors Required only if applicable; select all that apply multiple foci of invasive carcinoma
 S5.01 The tumour stage and stage grouping must be recorded to the extent possible, based on the AJCC Cancer Staging Manual (7 th Edition). 11 (See Tables S5.01a and S5.01b below.) Table S5.01a AJCC breast
S5.01 The tumour stage and stage grouping must be recorded to the extent possible, based on the AJCC Cancer Staging Manual (7 th Edition). 11 (See Tables S5.01a and S5.01b below.) Table S5.01a AJCC breast
Procedures Needle Biopsy Transurethral Prostatic Resection Suprapubic or Retropubic Enucleation (Subtotal Prostatectomy) Radical Prostatectomy
 Prostate Gland Protocol applies to invasive carcinomas of the prostate gland. Protocol web posting date: July 2006 Protocol effective date: April 2007 Based on AJCC/UICC TNM, 6 th edition Procedures Needle
Prostate Gland Protocol applies to invasive carcinomas of the prostate gland. Protocol web posting date: July 2006 Protocol effective date: April 2007 Based on AJCC/UICC TNM, 6 th edition Procedures Needle
Epithelial abnormalities and precancerous lesions of anterior urethra in patients with penile carcinoma: a report of 89 cases
 & 2005 USCAP, Inc All rights reserved 0893-3952/05 $30.00 www.modernpathology.org Epithelial abnormalities and precancerous lesions of anterior urethra in patients with penile carcinoma: a report of 89
& 2005 USCAP, Inc All rights reserved 0893-3952/05 $30.00 www.modernpathology.org Epithelial abnormalities and precancerous lesions of anterior urethra in patients with penile carcinoma: a report of 89
Update on staging colorectal carcinoma, the 8 th edition AJCC. General overview of staging. When is staging required? 11/1/2017
 Update on staging colorectal carcinoma, the 8 th edition AJCC Dale C. Snover, MD November 3, 2017 General overview of staging Reason for uniform staging Requirements to use AJCC manual and/or CAP protocols
Update on staging colorectal carcinoma, the 8 th edition AJCC Dale C. Snover, MD November 3, 2017 General overview of staging Reason for uniform staging Requirements to use AJCC manual and/or CAP protocols
Small Intestine. Protocol revision date: January 2005 Based on AJCC/UICC TNM, 6 th edition
 Small Intestine Protocol applies to all invasive carcinomas of the small intestine, including those with focal endocrine differentiation. Excludes carcinoid tumors, lymphomas, and stromal tumors (sarcomas).
Small Intestine Protocol applies to all invasive carcinomas of the small intestine, including those with focal endocrine differentiation. Excludes carcinoid tumors, lymphomas, and stromal tumors (sarcomas).
Staging and Grading Last Updated Friday, 14 November 2008
 Staging and Grading Last Updated Friday, 14 November 2008 There is a staging graph below Blood in the urine is the most common indication that something is wrong. Often one will experience pain or difficulty
Staging and Grading Last Updated Friday, 14 November 2008 There is a staging graph below Blood in the urine is the most common indication that something is wrong. Often one will experience pain or difficulty
CAP Cancer Protocol and ecc Summary of Changes for August 2014 Thyroid Agile Release
 CAP Cancer Protocol and ecc Summary of Changes for August 2014 Thyroid Agile Release 2 REVISION HISTORY Date Author / Editor Comments 5/19/2014 Jaleh Mirza Created the document 8/12/2014 Samantha Spencer/Jaleh
CAP Cancer Protocol and ecc Summary of Changes for August 2014 Thyroid Agile Release 2 REVISION HISTORY Date Author / Editor Comments 5/19/2014 Jaleh Mirza Created the document 8/12/2014 Samantha Spencer/Jaleh
UICC 8 th Edition Errata 25 th of May 2018
 UICC 8 th Edition Errata 25 th of May 2018 ions are in italics Head and Neck Tumours Page 19 Oral Cavity T2 T3 T4a Tumour 2 cm or less in greatest dimension and more than 5 mm but no more than 10 mm depth
UICC 8 th Edition Errata 25 th of May 2018 ions are in italics Head and Neck Tumours Page 19 Oral Cavity T2 T3 T4a Tumour 2 cm or less in greatest dimension and more than 5 mm but no more than 10 mm depth
CUT-UP PROTOCOL Foreskin SCC, Glansectomy, and Penectomy BASIC ANATOMY
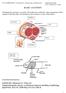 BASIC ANATOMY Orientating the specimen is essential. The urethra runs within the corpus spongiosum which expands to form the glans. The frenulum of the foreskin is on the ventral aspect. DORSAL Proximal
BASIC ANATOMY Orientating the specimen is essential. The urethra runs within the corpus spongiosum which expands to form the glans. The frenulum of the foreskin is on the ventral aspect. DORSAL Proximal
Thyroid Gland. Protocol applies to all malignant tumors of the thyroid gland, except lymphomas.
 Thyroid Gland Protocol applies to all malignant tumors of the thyroid gland, except lymphomas. Procedures Cytology (No Accompanying Checklist) Partial Thyroidectomy Total Thyroidectomy With/Without Lymph
Thyroid Gland Protocol applies to all malignant tumors of the thyroid gland, except lymphomas. Procedures Cytology (No Accompanying Checklist) Partial Thyroidectomy Total Thyroidectomy With/Without Lymph
Colon and Rectum. Protocol revision date: January 2005 Based on AJCC/UICC TNM, 6th edition
 Colon and Rectum Protocol applies to all invasive carcinomas of the colon and rectum. Carcinoid tumors, lymphomas, sarcomas, and tumors of the vermiform appendix are excluded. Protocol revision date: January
Colon and Rectum Protocol applies to all invasive carcinomas of the colon and rectum. Carcinoid tumors, lymphomas, sarcomas, and tumors of the vermiform appendix are excluded. Protocol revision date: January
Kidney Case 1 SURGICAL PATHOLOGY REPORT
 Kidney Case 1 Surgical Pathology Report February 9, 2007 Clinical History: This 45 year old woman was found to have a left renal mass. CT urography with reconstruction revealed a 2 cm medial mass which
Kidney Case 1 Surgical Pathology Report February 9, 2007 Clinical History: This 45 year old woman was found to have a left renal mass. CT urography with reconstruction revealed a 2 cm medial mass which
S1.04 PRINCIPAL CLINICIAN G1.01 COMMENTS S2.01 SPECIMEN LABELLED AS G2.01 *SPECIMEN DIMENSIONS (PROSTATE) S2.03 *SEMINAL VESICLES
 Prostate Cancer Histopathology Reporting Proforma (Radical Prostatectomy) Includes the International Collaboration on Cancer reporting dataset denoted by * Family name Given name(s) Date of birth Indigenous
Prostate Cancer Histopathology Reporting Proforma (Radical Prostatectomy) Includes the International Collaboration on Cancer reporting dataset denoted by * Family name Given name(s) Date of birth Indigenous
Tumours of the Oesophagus & Gastro-Oesophageal Junction Histopathology Reporting Proforma
 Tumours of the Oesophagus & Gastro-Oesophageal Junction Histopathology Reporting Proforma Mandatory questions (i.e. protocol standards) are in bold (e.g. S1.01). S1.01 Identification Family name Given
Tumours of the Oesophagus & Gastro-Oesophageal Junction Histopathology Reporting Proforma Mandatory questions (i.e. protocol standards) are in bold (e.g. S1.01). S1.01 Identification Family name Given
6/5/2010. Renal vein invasion & Capsule Penetration (T3a) Adrenal Gland involvement (T4 vs. M1) Beyond Gerota s Fascia? (?T4).
 GU Cancer Staging: Updates and Challenging Areas 13 th Current Issues in Surgical Pathology San Francisco, CA June 5, 2010 Jeffry P. Simko, PhD, MD Associate Professor Departments of Urology and Anatomic
GU Cancer Staging: Updates and Challenging Areas 13 th Current Issues in Surgical Pathology San Francisco, CA June 5, 2010 Jeffry P. Simko, PhD, MD Associate Professor Departments of Urology and Anatomic
Protocol applies to melanoma of cutaneous surfaces only.
 Melanoma of the Skin Protocol applies to melanoma of cutaneous surfaces only. Procedures Biopsy (No Accompanying Checklist) Excision Re-excision Protocol revision date: January 2005 Based on AJCC/UICC
Melanoma of the Skin Protocol applies to melanoma of cutaneous surfaces only. Procedures Biopsy (No Accompanying Checklist) Excision Re-excision Protocol revision date: January 2005 Based on AJCC/UICC
Protocol for the Examination of Cystectomy Specimens From Patients With Carcinoma of the Urinary Bladder
 Protocol for the Examination of Cystectomy Specimens From Patients With Carcinoma of the Urinary Bladder Version: UrinaryBladder 4.0.1.1 Protocol Posting Date: February 2019 CAP Laboratory Accreditation
Protocol for the Examination of Cystectomy Specimens From Patients With Carcinoma of the Urinary Bladder Version: UrinaryBladder 4.0.1.1 Protocol Posting Date: February 2019 CAP Laboratory Accreditation
MUSCLE - INVASIVE AND METASTATIC BLADDER CANCER
 10 MUSCLE - INVASIVE AND METASTATIC BLADDER CANCER Recommendations from the EAU Working Party on Muscle Invasive and Metastatic Bladder Cancer G. Jakse (chairman), F. Algaba, S. Fossa, A. Stenzl, C. Sternberg
10 MUSCLE - INVASIVE AND METASTATIC BLADDER CANCER Recommendations from the EAU Working Party on Muscle Invasive and Metastatic Bladder Cancer G. Jakse (chairman), F. Algaba, S. Fossa, A. Stenzl, C. Sternberg
A215- Urinary bladder cancer tissues
 A215- Urinary bladder cancer tissues (formalin fixed) For research use only Specifications: No. of cases: 45 Tissue type: Urinary bladder cancer tissues No. of spots: 2 spots from each cancer case (90
A215- Urinary bladder cancer tissues (formalin fixed) For research use only Specifications: No. of cases: 45 Tissue type: Urinary bladder cancer tissues No. of spots: 2 spots from each cancer case (90
Bladder Case 1 SURGICAL PATHOLOGY REPORT. Procedure: Cystoscopy, transurethral resection of bladder tumor (TURBT)
 Bladder Case 1 February 17, 2007 Specimen (s) received: Bladder Tumor Pre-operative Diagnosis: Bladder Cancer Post operative Diagnosis: Bladder Cancer Procedure: Cystoscopy, transurethral resection of
Bladder Case 1 February 17, 2007 Specimen (s) received: Bladder Tumor Pre-operative Diagnosis: Bladder Cancer Post operative Diagnosis: Bladder Cancer Procedure: Cystoscopy, transurethral resection of
STAGE CATEGORY DEFINITIONS
 CLINICAL Extent of disease before any treatment y clinical staging completed after neoadjuvant therapy but before subsequent surgery TX Tis Tis (DCIS) Tis (LCIS) Tis (Paget s) T1 T1mi T1a T1b T1c a b c
CLINICAL Extent of disease before any treatment y clinical staging completed after neoadjuvant therapy but before subsequent surgery TX Tis Tis (DCIS) Tis (LCIS) Tis (Paget s) T1 T1mi T1a T1b T1c a b c
Penis/Scrotum. 5.1 Extramammary Paget disease vs. High-grade penile intraepithelial
 5 Penis/Scrotum 5.1 Extramammary Paget disease vs. High-grade penile intraepithelial neoplasia 5.2 Pseudoepitheliomatous squamous cell carcinoma vs. Pseudoepitheliomatous hyperplasia 5.3 Verrucous squamous
5 Penis/Scrotum 5.1 Extramammary Paget disease vs. High-grade penile intraepithelial neoplasia 5.2 Pseudoepitheliomatous squamous cell carcinoma vs. Pseudoepitheliomatous hyperplasia 5.3 Verrucous squamous
Urinary Bladder, Ureter, and Renal Pelvis
 Urinary Bladder, Ureter, and Renal Pelvis Protocol applies to all carcinomas of the urinary bladder, ureter, and renal pelvis. Protocol revision date: January 2005 Based on AJCC/UICC TNM, 6th edition Procedures
Urinary Bladder, Ureter, and Renal Pelvis Protocol applies to all carcinomas of the urinary bladder, ureter, and renal pelvis. Protocol revision date: January 2005 Based on AJCC/UICC TNM, 6th edition Procedures
Protocol for the Examination of Specimens From Patients With Squamous Cell Carcinoma of the Skin
 Protocol for the Examination of Specimens From Patients With Squamous Cell Carcinoma of the Skin Protocol applies to invasive squamous cell carcinomas of the skin. Squamous cell carcinomas of the eyelid,
Protocol for the Examination of Specimens From Patients With Squamous Cell Carcinoma of the Skin Protocol applies to invasive squamous cell carcinomas of the skin. Squamous cell carcinomas of the eyelid,
Protocol for the Examination of Lymphadenectomy Specimens From Patients With Malignant Germ Cell and Sex Cord-Stromal Tumors of the Testis
 Protocol for the Examination of Specimens From Patients With Malignant Germ Cell and Sex Cord-Stromal Tumors of the Testis Version: Testis 4.0.1.1 Protocol Posting Date: February 2019 Accreditation Requirements
Protocol for the Examination of Specimens From Patients With Malignant Germ Cell and Sex Cord-Stromal Tumors of the Testis Version: Testis 4.0.1.1 Protocol Posting Date: February 2019 Accreditation Requirements
A five year study on differential diagnosis of verruciform penile lesions
 Original Research Article A five year study on differential diagnosis of verruciform penile lesions S. Sujatha 1, V. Srinivas Kumar 2*, K. Durga 3 1 Associate Professor, 2 Assistant Professor, 3 Professor
Original Research Article A five year study on differential diagnosis of verruciform penile lesions S. Sujatha 1, V. Srinivas Kumar 2*, K. Durga 3 1 Associate Professor, 2 Assistant Professor, 3 Professor
This form may provide more data elements than required for collection by standard setters such as NCI SEER, CDC NPCR, and CoC NCDB.
 1 Terms of Use The cancer staging form is a specific document in the patient record; it is not a substitute for documentation of history, physical examination, and staging evaluation, or for documenting
1 Terms of Use The cancer staging form is a specific document in the patient record; it is not a substitute for documentation of history, physical examination, and staging evaluation, or for documenting
Penis Cancer. What is penis cancer? Symptoms. Patient Information. Pagina 1 / 9. Patient Information - Penis Cancer
 Patient Information English 31 Penis Cancer The underlined terms are listed in the glossary. What is penis cancer? Cancer is abnormal cell growth in the skin or organ tissue. When this cell growth starts
Patient Information English 31 Penis Cancer The underlined terms are listed in the glossary. What is penis cancer? Cancer is abnormal cell growth in the skin or organ tissue. When this cell growth starts
INTRADUCTAL LESIONS OF THE PROSTATE. Jonathan I. Epstein
 INTRADUCTAL LESIONS OF THE PROSTATE Jonathan I. Epstein Topics Prostatic intraepithelial neoplasia (PIN) Intraductal adenocarcinoma (IDC-P) Intraductal urothelial carcinoma Ductal adenocarcinoma High Prostatic
INTRADUCTAL LESIONS OF THE PROSTATE Jonathan I. Epstein Topics Prostatic intraepithelial neoplasia (PIN) Intraductal adenocarcinoma (IDC-P) Intraductal urothelial carcinoma Ductal adenocarcinoma High Prostatic
This form may provide more data elements than required for collection by standard setters such as NCI SEER, CDC NPCR, and CoC NCDB.
 1 Terms of Use The cancer staging form is a specific document in the patient record; it is not a substitute for documentation of history, physical examination, and staging evaluation, or for documenting
1 Terms of Use The cancer staging form is a specific document in the patient record; it is not a substitute for documentation of history, physical examination, and staging evaluation, or for documenting
Penis Cancer. What is penis cancer? Symptoms. Patient Information. Pagina 1 / 9. Patient Information - Penis Cancer
 Patient Information English 31 Penis Cancer The underlined terms are listed in the glossary. What is penis cancer? Cancer is abnormal cell growth in the skin or organ tissue. When this cell growth starts
Patient Information English 31 Penis Cancer The underlined terms are listed in the glossary. What is penis cancer? Cancer is abnormal cell growth in the skin or organ tissue. When this cell growth starts
Gastric Cancer Histopathology Reporting Proforma
 Gastric Cancer Histopathology Reporting Proforma Mandatory questions (i.e. protocol standards) are in bold (e.g. S1.01). S1.01 Identification Family name Given name(s) Date of birth Sex Male Female Intersex/indeterminate
Gastric Cancer Histopathology Reporting Proforma Mandatory questions (i.e. protocol standards) are in bold (e.g. S1.01). S1.01 Identification Family name Given name(s) Date of birth Sex Male Female Intersex/indeterminate
ACCME/Disclosures. Cribriform Lesions of the Prostate. Case
 Cribriform Lesions of the Prostate Ming Zhou, MD, PhD Departments of Pathology and Urology New York University Langone Medical Center New York, NY Ming.Zhou@NYUMC.ORG ACCME/Disclosures The USCAP requires
Cribriform Lesions of the Prostate Ming Zhou, MD, PhD Departments of Pathology and Urology New York University Langone Medical Center New York, NY Ming.Zhou@NYUMC.ORG ACCME/Disclosures The USCAP requires
Recommendations for the Reporting of Prostate Carcinoma
 Recommendations for the Reporting of Prostate Carcinoma Association of Directors of Anatomic and Surgical Pathology * ADASP Reporting Guidelines It has been evident for decades that pathology reports are
Recommendations for the Reporting of Prostate Carcinoma Association of Directors of Anatomic and Surgical Pathology * ADASP Reporting Guidelines It has been evident for decades that pathology reports are
Primary Cutaneous Melanoma Pathology Reporting Proforma DD MM YYYY. *Tumour site. *Specimen laterality. *Specimen type
 Primary Cutaneous Melanoma Pathology Reporting Proforma Includes the International Collaboration on Cancer reporting dataset denoted by * Family name Given name(s) Date of birth DD MM YYYY Sex Male Female
Primary Cutaneous Melanoma Pathology Reporting Proforma Includes the International Collaboration on Cancer reporting dataset denoted by * Family name Given name(s) Date of birth DD MM YYYY Sex Male Female
Protocol for the Examination of Specimens From Patients With Thymic Tumors
 Protocol for the Examination of Specimens From Patients With Thymic Tumors Version: Protocol Posting Date: June 2017 Includes ptnm requirements from the 8 th Edition, AJCC Staging Manual For accreditation
Protocol for the Examination of Specimens From Patients With Thymic Tumors Version: Protocol Posting Date: June 2017 Includes ptnm requirements from the 8 th Edition, AJCC Staging Manual For accreditation
Malignant tumors of melanocytes : Part 3. Deba P Sarma, MD., Omaha
 Malignant tumors of melanocytes : Part 3 Deba P Sarma, MD., Omaha Let s go over one case of melanoma using the following worksheet. Of the various essential information that needs to be included in the
Malignant tumors of melanocytes : Part 3 Deba P Sarma, MD., Omaha Let s go over one case of melanoma using the following worksheet. Of the various essential information that needs to be included in the
Protocol for the Examination of Specimens From Patients With Carcinoma of the Urinary Bladder
 Protocol for the Examination of Specimens From Patients With Carcinoma of the Urinary Bladder Version: Protocol Posting Date: June 2017 Includes ptnm requirements from the 8 th Edition, AJCC Staging Manual
Protocol for the Examination of Specimens From Patients With Carcinoma of the Urinary Bladder Version: Protocol Posting Date: June 2017 Includes ptnm requirements from the 8 th Edition, AJCC Staging Manual
Vulvar Carcinoma. Definition: Cases should be classified as carsinoma of the vulva when the primary site growth is in the vulva Malignant melanoma sho
 Carcinoma Vulva & Vagina Subdivisi Onkologi Ginekologi Bagian Obgin FK USU Vulvar Carcinoma. Definition: Cases should be classified as carsinoma of the vulva when the primary site growth is in the vulva
Carcinoma Vulva & Vagina Subdivisi Onkologi Ginekologi Bagian Obgin FK USU Vulvar Carcinoma. Definition: Cases should be classified as carsinoma of the vulva when the primary site growth is in the vulva
Colorectal Cancer Structured Pathology Reporting Proforma DD MM YYYY
 Colorectal Cancer Structured Pathology Reporting Proforma Mandatory questions (i.e. protocol standards) are in bold (e.g. S1.03). Family name Given name(s) Date of birth DD MM YYYY S1.02 Clinical details
Colorectal Cancer Structured Pathology Reporting Proforma Mandatory questions (i.e. protocol standards) are in bold (e.g. S1.03). Family name Given name(s) Date of birth DD MM YYYY S1.02 Clinical details
The International Association for the Study of Lung Cancer (IASLC) Lung Cancer Staging Project, Data Elements
 Page 1 Contents 1.1. Registration... 2 1.2. Patient Characteristics... 3 1.3. Laboratory Values at Diagnosis... 5 1.4. Lung Cancers with Multiple Lesions... 6 1.5. Primary Tumour Description... 10 1.6.
Page 1 Contents 1.1. Registration... 2 1.2. Patient Characteristics... 3 1.3. Laboratory Values at Diagnosis... 5 1.4. Lung Cancers with Multiple Lesions... 6 1.5. Primary Tumour Description... 10 1.6.
Protocol for the Examination of Specimens From Patients With Carcinoma of the Anus
 Protocol for the Examination of Specimens From Patients With Carcinoma of the Anus Version: Protocol Posting Date: June 2017 Includes ptnm requirements from the 8 th Edition, AJCC Staging Manual For accreditation
Protocol for the Examination of Specimens From Patients With Carcinoma of the Anus Version: Protocol Posting Date: June 2017 Includes ptnm requirements from the 8 th Edition, AJCC Staging Manual For accreditation
Prostate cancer ~ diagnosis and impact of pathology on prognosis ESMO 2017
 Prostate cancer ~ diagnosis and impact of pathology on prognosis ESMO 2017 Dr Puay Hoon Tan Division of Pathology Singapore General Hospital Prostate cancer (acinar adenocarcinoma) Invasive carcinoma composed
Prostate cancer ~ diagnosis and impact of pathology on prognosis ESMO 2017 Dr Puay Hoon Tan Division of Pathology Singapore General Hospital Prostate cancer (acinar adenocarcinoma) Invasive carcinoma composed
Benign and malignant epithelial lesions: Seborrheic keratosis: A common benign pigmented epidermal tumor occur in middle-aged or older persons more
 Benign and malignant epithelial lesions: Seborrheic keratosis: A common benign pigmented epidermal tumor occur in middle-aged or older persons more common on the trunk; but extremities, head and neck are
Benign and malignant epithelial lesions: Seborrheic keratosis: A common benign pigmented epidermal tumor occur in middle-aged or older persons more common on the trunk; but extremities, head and neck are
*OPERATIVE PROCEDURE. Serum tumour markers within normal limits S1.04 PRINCIPAL CLINICIAN
 Neoplasia of the Testis - Orchidectomy Histopathology Reporting Proforma Includes the International Collaboration on Cancer reporting dataset denoted by * Family name Given name(s) Date of birth Indigenous
Neoplasia of the Testis - Orchidectomy Histopathology Reporting Proforma Includes the International Collaboration on Cancer reporting dataset denoted by * Family name Given name(s) Date of birth Indigenous
Protocol for the Examination of Specimens From Patients With Merkel Cell Carcinoma of the Skin
 Protocol for the Examination of Specimens From Patients With Merkel Cell Carcinoma of the Skin Protocol applies to Merkel cell carcinoma of cutaneous surfaces only. Based on AJCC/UICC TNM, 7th edition
Protocol for the Examination of Specimens From Patients With Merkel Cell Carcinoma of the Skin Protocol applies to Merkel cell carcinoma of cutaneous surfaces only. Based on AJCC/UICC TNM, 7th edition
46. Merkel Cell Carcinoma
 1 Terms of Use The cancer staging form is a specific document in the patient record; it is not a substitute for documentation of history, physical examination, and staging evaluation, or for documenting
1 Terms of Use The cancer staging form is a specific document in the patient record; it is not a substitute for documentation of history, physical examination, and staging evaluation, or for documenting
Pathology of the skin. 2nd Department of Pathology, Semmelweis University
 Pathology of the skin 2nd Department of Pathology, Semmelweis University Histology of the skin Epidermis: Stratum corneum Stratum granulosum Stratum spinosum Stratum basale Dermis: papillary and reticular
Pathology of the skin 2nd Department of Pathology, Semmelweis University Histology of the skin Epidermis: Stratum corneum Stratum granulosum Stratum spinosum Stratum basale Dermis: papillary and reticular
Objective. Results. Patients and Methods. Conclusions. Keywords <squamous cell carcinoma of the penis, prognostics, cancerspecific mortality, nomogram
 Development and external validation of a prognostic tool for prediction of cancer-specific mortality after complete loco-regional pathological staging for squamous cell carcinoma of the penis Maxine Sun,
Development and external validation of a prognostic tool for prediction of cancer-specific mortality after complete loco-regional pathological staging for squamous cell carcinoma of the penis Maxine Sun,
Pathologic Assessment of Invasion in TUR Specimens. A. Lopez-Beltran. T1 (ct1)
 Pathologic Assessment of Invasion in TUR Specimens A. Lopez-Beltran T1 (ct1) 1 Prognostic factors for progression/invasive disease Ta,T1,CIS- NMIBC :TNM 2017 ESSENTIAL: Grade T stage CIS Number of lesions
Pathologic Assessment of Invasion in TUR Specimens A. Lopez-Beltran T1 (ct1) 1 Prognostic factors for progression/invasive disease Ta,T1,CIS- NMIBC :TNM 2017 ESSENTIAL: Grade T stage CIS Number of lesions
Update on 8 th Edition Cutaneous AJCC Staging of Primary Cutaneous Melanoma. Michael T. Tetzlaff MD, PhD
 Update on 8 th Edition Cutaneous AJCC Staging of Primary Cutaneous Melanoma Michael T. Tetzlaff MD, PhD Associate Professor Departments of Pathology (Dermatopathology) and Translational and Molecular Pathology
Update on 8 th Edition Cutaneous AJCC Staging of Primary Cutaneous Melanoma Michael T. Tetzlaff MD, PhD Associate Professor Departments of Pathology (Dermatopathology) and Translational and Molecular Pathology
A RARE CASE OF VERRUCOUS CARCINOMA IN MIDDLE AGED MALE
 A RARE CASE OF VERRUCOUS CARCINOMA IN MIDDLE AGED MALE *Alagar Samy R. and Elankumar S. ESIC Medical College and Hospital, Coimbatore, Tamilnadu, India *Author for Correspondence ABSTRACT Penile verrucous
A RARE CASE OF VERRUCOUS CARCINOMA IN MIDDLE AGED MALE *Alagar Samy R. and Elankumar S. ESIC Medical College and Hospital, Coimbatore, Tamilnadu, India *Author for Correspondence ABSTRACT Penile verrucous
Large blocks in prostate and bladder pathology
 Large blocks in prostate and bladder pathology Farkas Sükösd Department of Pathology, University of Szeged The history of the large block technique in radical prostatectomy and cystectomy The first large
Large blocks in prostate and bladder pathology Farkas Sükösd Department of Pathology, University of Szeged The history of the large block technique in radical prostatectomy and cystectomy The first large
25 TH ICRO DEHRADUN STAGING OF GENITOURINARY MALIGNANCIES
 25 TH ICRO DEHRADUN STAGING OF GENITOURINARY MALIGNANCIES SPEAKER DR DEEPAK ABROL CLINICAL ONCOLOGIST JAND K HEALTH SERVICES CONSULTANT ONCOLOGIST MAHARISHI DAYANAND HOSPITAL AND MEDICAL RESEARCH CENTER
25 TH ICRO DEHRADUN STAGING OF GENITOURINARY MALIGNANCIES SPEAKER DR DEEPAK ABROL CLINICAL ONCOLOGIST JAND K HEALTH SERVICES CONSULTANT ONCOLOGIST MAHARISHI DAYANAND HOSPITAL AND MEDICAL RESEARCH CENTER
Pancreas (Exocrine) Protocol applies to all carcinomas of the exocrine pancreas.
 Pancreas (Exocrine) Protocol applies to all carcinomas of the exocrine pancreas. Protocol revision date: January 2005 Based on AJCC/UICC TNM, 6 th edition Procedures Cytology (No Accompanying Checklist)
Pancreas (Exocrine) Protocol applies to all carcinomas of the exocrine pancreas. Protocol revision date: January 2005 Based on AJCC/UICC TNM, 6 th edition Procedures Cytology (No Accompanying Checklist)
Protocol for the Examination of Specimens From Patients With Invasive Carcinoma of the Breast
 Protocol for the Examination of Specimens From Patients With Invasive Carcinoma of the Breast Version: Protocol Posting Date: June 2017 Includes ptnm requirements from the 8 th Edition, AJCC Staging Manual
Protocol for the Examination of Specimens From Patients With Invasive Carcinoma of the Breast Version: Protocol Posting Date: June 2017 Includes ptnm requirements from the 8 th Edition, AJCC Staging Manual
ARTHUR PURDY STOUT SOCIETY COMPANION MEETING: DIFFICULT NEW DIFFERENTIAL DIAGNOSES IN PROSTATE PATHOLOGY. Jonathan I. Epstein.
 1 ARTHUR PURDY STOUT SOCIETY COMPANION MEETING: DIFFICULT NEW DIFFERENTIAL DIAGNOSES IN PROSTATE PATHOLOGY Jonathan I. Epstein Professor Pathology, Urology, Oncology The Reinhard Professor of Urological
1 ARTHUR PURDY STOUT SOCIETY COMPANION MEETING: DIFFICULT NEW DIFFERENTIAL DIAGNOSES IN PROSTATE PATHOLOGY Jonathan I. Epstein Professor Pathology, Urology, Oncology The Reinhard Professor of Urological
Staging Challenges in Lower GI Cancers. Disclosure of Relevant Financial Relationships. AJCC 8 th edition and CAP protocol updates
 Staging Challenges in Lower GI Cancers Sanjay Kakar, MD University of California, San Francisco March 05, 2017 Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education
Staging Challenges in Lower GI Cancers Sanjay Kakar, MD University of California, San Francisco March 05, 2017 Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education
GUIDELINES ON NON-MUSCLE- INVASIVE BLADDER CANCER
 GUIDELINES ON NON-MUSCLE- INVASIVE BLADDER CANCER (Limited text update December 21) M. Babjuk, W. Oosterlinck, R. Sylvester, E. Kaasinen, A. Böhle, J. Palou, M. Rouprêt Eur Urol 211 Apr;59(4):584-94 Introduction
GUIDELINES ON NON-MUSCLE- INVASIVE BLADDER CANCER (Limited text update December 21) M. Babjuk, W. Oosterlinck, R. Sylvester, E. Kaasinen, A. Böhle, J. Palou, M. Rouprêt Eur Urol 211 Apr;59(4):584-94 Introduction
Vulva Cancer Histopathology Reporting Proforma
 Vulva Cancer Histopathology Reporting Proforma Mandatory questions (i.e. protocol standards) are in bold (e.g. S1.01). S1.01 Identification Family name Given name(s) Ethnicity Unknown AboriginalTorres
Vulva Cancer Histopathology Reporting Proforma Mandatory questions (i.e. protocol standards) are in bold (e.g. S1.01). S1.01 Identification Family name Given name(s) Ethnicity Unknown AboriginalTorres
MUSCLE-INVASIVE AND METASTATIC BLADDER CANCER
 MUSCLE-INVASIVE AND METASTATIC BLADDER CANCER (Text update March 2008) A. Stenzl (chairman), N.C. Cowan, M. De Santis, G. Jakse, M. Kuczyk, A.S. Merseburger, M.J. Ribal, A. Sherif, J.A. Witjes Introduction
MUSCLE-INVASIVE AND METASTATIC BLADDER CANCER (Text update March 2008) A. Stenzl (chairman), N.C. Cowan, M. De Santis, G. Jakse, M. Kuczyk, A.S. Merseburger, M.J. Ribal, A. Sherif, J.A. Witjes Introduction
Diseases of the vulva
 Diseases of the vulva 1. Bartholin Cyst - Infection of the Bartholin gland produces an acute inflammation within the gland (adenitis) and may result in an abscess. Bartholin duct cysts - Are relatively
Diseases of the vulva 1. Bartholin Cyst - Infection of the Bartholin gland produces an acute inflammation within the gland (adenitis) and may result in an abscess. Bartholin duct cysts - Are relatively
