EXPOSURE OF the distal esophagus
|
|
|
- Cleopatra Short
- 5 years ago
- Views:
Transcription
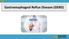
1 PAPER Elevated Body Mass Disrupts the Barrier to Gastroesophageal Reflux Shahjehan A. Wajed, FRCS; Christopher G. Streets, MRCS; Cedric G. Bremner, MD; Tom R. DeMeester, MD Hypothesis: Obesity impairs the antireflux function of a structurally intact barrier. Design: Retrospective analysis of body mass index in patients with normal esophageal manometric findings but with symptomatic and objectively confirmed gastroesophageal reflux. Setting: Specialist esophageal center. Patients: Patients symptomatic and diagnostic for gastroesophageal reflux, referred between October 1, 1998, and June 30, Exclusion criteria were a defective barrier, motility disorders, or previous surgery. Main Outcome Measures: Reflux was defined and quantified using the DeMeester score, and body mass index was calculated. Results: There was a strong correlation between body mass index and severity of gastroesophageal reflux. Patients who were overweight had significantly higher distal esophageal acid exposure. No significant difference in manometric findings was demonstrated between patients with normal weight and those who were overweight. Conclusion: The barrier to gastroesophageal reflux is rendered insufficient in patients who are overweight. Arch Surg. 2001;136: From the Department of Surgery, University of Southern California, Los Angeles. EXPOSURE OF the distal esophagus to pathologic levels of refluxed gastric juices causes the clinical phenomenon of gastroesophageal reflux disease (GERD) and its sequelae. Reflux is prevented by a mechanically competent lower esophageal sphincter (LES), which provides a barrier between the gastric and esophageal compartments, and a proper clearance activity of the esophageal body by appropriate LES relaxation and peristaltic contractions on swallowing. 1,2 Despite the presence of a structurally normal LES and effective esophageal clearance, excessive gastroesophageal reflux and consequent esophageal damage may still occur. In these patients, other factors must therefore exist that override the standard barrier to reflux. A possible simple explanation for the existence of GERD in this subgroup of patients might be a local impairment of the normal barrier mechanism. This may be caused by an external alteration in the anatomical and physiological characteristics of the LES or esophageal body. Excessive fat deposition could interfere directly with the LES esophageal body complex, preventing it from functioning effectively, or it could change the intra-abdominal pressure dynamics and render the barrier incompetent. We investigated the effect of body mass index (BMI), a standard marker for obesity and body fat content, as a possible factor in the generation of GERD in these individuals. RESULTS Patient demographics, esophageal characteristics, and disease variables are summarized in the Table. The mean age of the entire cohort was 48.6 years (range, years), with 41 men and 29 women. The primary presenting complaint was heartburn in 37 patients, with dysphagia and regurgitation representing another 15, totaling 52 with typical symptoms. The remainder presented with atypical symptoms still attributable to GERD. Body mass index was abnormally high in 55 patients, and no patient within this cohort qualified as being underweight. Of the 55 patients who were overweight, 37 were 1014
2 PATIENTS AND METHODS PATIENTS A retrospective analysis of data obtained between October 1, 1998, and June 30, 2000, was made of patients referred to the esophageal laboratory, Department of Surgery, University of Southern California, Los Angeles, for assessment of clinically suspected GERD. Patients with symptoms or a history strongly suggestive of GERD and with objective evidence of increased distal esophageal acid exposure on 24-hour ambulatory ph monitoring were identified. Those with any structural abnormality of the LES, incomplete LES relaxation, or any abnormality of esophageal body function were excluded. Patients with a history of esophagogastric surgery were also excluded. Patients were requested to discontinue any antacid medication 2 weeks before esophageal investigations. The remaining patients formed the study cohort and consisted of those with an apparently structurally normal LES and functional esophageal body, but with objective evidence of increased acid exposure to the esophagus. ESOPHAGEAL STUDIES Esophageal Manometry Manometry was performed using a single-catheter assembly consisting of 8 fluid-filled, perfused polyvinyl tubes bonded together with five 0.8-mm lateral openings placed 5 cm apart and radially oriented 120 from each other. The recording catheter was continuously perfused with distilled water using a low-compliance, pneumohydraulic capillary infusion pump (Arndorfer Medical Specialties, Greendale, Wis) at a rate of 0.5 ml/min. Each tube was connected to an external pressure transducer positioned at the midaxillary level. Before each test, the pressure transducers were calibrated using a mercury-filled manometer, so that a change in pressure of 1 mm Hg corresponded to 0.5 mm on the recording paper. A belt pneumograph was positioned around the chest to record respiratory excursions. A piezoelectric transducer was taped on the neck at the level of the cricoid cartilage to record pharyngeal swallows. Manometry was performed in the fasted state, and all medications were discontinued 24 hours before the test. The subject was placed in the supine position and encouraged to relax. The recording catheter was passed through an anesthetized nostril into the stomach and withdrawn at 1-cm increments every 20 seconds back into the esophagus. The 3 manometric characteristics of the distal esophageal sphincter measured were sphincter pressure, abdominal length, and overall length. The end respiratory gastric baseline pressure was used as a zero reference for pressure measurement. A persistent rise in pressure exceeding 2 mm Hg above the gastric baseline marked the distal border of the sphincter. The proximal border was marked by the point at which sphincter pressure dropped to end inspiratory esophageal baseline pressure. Five measurements of the distance between these 2 points were averaged and represented the overall length of the sphincter. The point at which the end inspiratory pressure changed from a positive to a negative deflection represented the respiratory inversion point. Five measurements of the distance between the respiratory inversion point and the distal border of the sphincter, that is, the length of the pressure wave that reflected positive excursions with respiration, were averaged and represented the abdominal length of the sphincter. The amplitude of the sphincter was measured as the difference (in millimeters of mercury) between the gastric baseline and the pressure at the respiratory inversion point during the middle of the respiratory Continued on next page classified as grade 1 overweight, 16 were grade 2 overweight, and 2 were grade 3 overweight. Manometric evidence of a hiatal hernia was present in 35 patients. No significant differences in patient characteristics, however, were noted between those with and without evidence of a hiatal hernia, including BMI and the esophageal and reflux severity variables presented in the Table. Similarly, subgrouping patients on the basis of sex or presenting symptoms (typical vs atypical) did not reveal any significant differences among any variables. A strong and significant correlation between BMI and DeMeester score was observed. Using Spearman analysis, a coefficient of 0.38, with P.001, was derived (Figure 1). A similar relationship was also noted between BMI and the total percentage duration the ph was less than 4 (coefficient 0.26, P=.03). Dichotomizing the cohort into normal and overweight subgroups based on BMI confirmed the major difference in the objective severity of esophageal acid exposure. For patients with a normal BMI, the mean DeMeester score was 21.5, and the total percentage duration the ph was less than 4 was 6.2%. This compared with a mean score of 34.7 and a percentage duration of 9.2% for the patients who were overweight. Using a Mann-Whitney analysis, this difference was significant, with P.001 for the DeMeester score (Figure 2) and P.01 for the total percentage duration the ph was less than 4. Nearly half the patients with a normal BMI had abnormal acid exposure during the postprandial period, while only a small number of the overweight group had the same problem, with 22 (40%) of these having upright reflux disease. Further subdivision of the overweight patients into their respective WHO classification groups reflected the trend of increasing distal esophageal acid exposure with increasing BMI, although these did not distinguish themselves from each other statistically. Of note, it appeared that weight alone, as opposed to weight and height, was the major discriminating factor between the 2 groups. Both groups had a similar mean height but contrasted markedly in weight. No significant differences with regard to patient details or manometric features were noted between the normal and overweight groups. Lower esophageal sphincter lengths and pressures were almost identical. However, the difference in manometric esophageal lengths, with a mean shorter value of 1.2 cm in patients who were overweight, approached significance in this study (P=.06). 1015
3 cycle. Five measurements of resting sphincter pressure were obtained and averaged to obviate the variation of pressures at each orifice due to the radial asymmetry of the sphincter. Normal values for the overall length of the sphincter, abdominal length of the sphincter, and resting sphincter pressure were defined as greater than 2 cm, greater than 1 cm, and 6 to 26 mm Hg, respectively, with values outside these limits representing the 2.5th percentile of a normal population distribution. 1 The presence of a double hump profile of the lower esophageal high pressure zone signified manometric evidence of a hiatal hernia, and measurements of the LES were made at the start of the most proximal hump, in these cases. Relaxation of the LES was determined by positioning 4 radially placed channels at the level of the respiratory inversion point, and the activity at this level and the channel 5 cm proximal to it (within the distal esophagus) was recorded in response to 5 separate swallows of 5-mL water boluses. Normal relaxation was recorded if the pressure in the LES fell to gastric baseline during the swallows. Esophageal body motility was investigated by placing the 5 recording channels along the length of the esophagus. The most proximal channel was located at a point 1 cm distal to the lower border of the upper esophageal sphincter, and pressure activity was assessed in response to 10 separate swallows each of a 5-mL water bolus. Normal esophageal motility was recorded only if normal peristalsis in the total absence of simultaneous or interrupted waves occurred, and if the pressure at each level was within normal 95th percentile limits for that level. Distal Esophageal Acid Exposure This was determined by 24-hour ambulatory ph monitoring. A 1-channel bipolar ph probe (Ingold; MUI Scientific, Mississauga, Ontario) was positioned to lie 5 cm proximal to the manometric upper border of the LES. Using a digital data recording device (MK III; Medtronic, Shoreview, Minn), ph in the distal esophagus was monitored for 24 hours, during which a test refluxogenic meal was given to induce postprandial reflux. To assess positional reflux, the patients were asked to maintain a diary to record activity. Calculation of a composite (DeMeester) score was used to assess severity of the reflux disease, 3,4 and the total duration that the esophageal ph was less than 4 was recorded and expressed as a percentage of total ambulatory duration. EVALUATION OF OBESITY Body mass index was calculated as weight in kilograms divided by the square of height in meters. Using the World Health Organization (WHO) classification, 5 a normal BMI was defined as a value between 18.5 and Values of 25.0 to 29.9 were defined as grade 1 overweight, 30.0 to 39.9 as grade 2 overweight (obese), and 40.0 or higher as grade 3 overweight (morbidly obese). STATISTICAL ANALYSIS Data were reported as mean±sem. Correlation between variables was assessed using Spearman analysis. Nonparametric testing between 2 groups of variables was carried out using a Mann-Whitney analysis, and a Fisher exact test was used for comparison between 2 sets of distinct subgroups. All tests were 2-tailed, with significance defined as P.05. Analysis was performed using standard commercially available biomedical software (SPSS, version 10.0; SPSS Inc, Chicago, Ill). COMMENT The key question in understanding the pathophysiology of GERD is what causes an overriding of the normal valve mechanism. Structural defects in the LES or esophageal body dysfunction predispose to disease evolution in most cases. 6,7 In this study, we identified a cohort of patients who shared the same manometric LES and esophageal body characteristics as 97.5% of the normal, asymptomatic general population, but whose distal esophagus was not protected from excessive gastric juice exposure. Fifty-five (79%) of these patients had an elevated BMI, and the increasing level of their obesity strongly correlated with the severity of the gastroesophageal reflux. This overweight subgroup of patients had a greater degree of reflux, as measured by ph probe, than the small number with a normal BMI. Patients with a normal BMI in this study had a mild level of increased distal esophageal acid exposure, predominantly during the postprandial period. Obesity is now regarded as a worldwide disease of epidemic proportions, which may induce ill health through several means. It is strongly associated with a wide spectrum of medical diseases, including diabetes mellitus, cardiovascular and respiratory disorders, cholelithiasis, and malignancy. 8,9 The etiology of its role in each of these conditions is complex and varied, but results in altered local and general anatomy or in changes in physiological and metabolic body function. In essence, the body is forced to deal with the storage of increased quantities of fat, resulting in the visceral deposition of adipose tissue within the upper body. The intraabdominal compartment and regions around the thoracic cage are favored locations, and this gives rise to the phenomenon of upper body obesity, which in itself comprises a risk factor for disease. 10 Barrier function could be modulated in several ways, resulting from the consequences of obesity. Widespread deposition of adipose tissue within the mesenteries, omentum, and preperitoneal regions and viscera, as well as around the gastroesophageal junction itself, may interfere with the complex local anatomical and physiological factors that contribute to valve competency, or it may cause a global change in the intra-abdominal environment. The presence of excess fat in and around the gastroesophageal junction could alter the anatomical structure and, hence, the geometry of the cardia, placing the sphincter at a mechanical disadvantage to counter gas distension forces attempting to pull it open. The acute angle 1016
4 Patient, Esophageal, and Reflux Variables* All Patients (N = 70) Normal Weight (n = 15) Overweight (n = 55) Patient Details Age, y 48.6 ± ± ± 1.8 Sex Male 41 (59) 9 (60) 32 (58) Female 29 (41) 6 (40) 23 (42) Weight, kg 85.0 ± ± ± 2.2 Height, m 1.72 ± ± ± 0.01 Body mass index, kg/m ± ± ± 0.7 Symptoms Typical 52 (75) 10 (67) 42 (76) Atypical 18 (25) 5 (33) 13 (24) Esophageal Characteristics LES overall length, cm 3.2 ± ± ± 0.01 LES abdominal length, cm 1.9 ± ± ± 0.01 LES resting pressure, mm Hg 15.4 ± ± ± 0.8 Esophageal length, cm 20.9 ± ± ± 0.3 Hiatal hernia Absent 35 (50) 5 (33) 30 (55) Present 35 (50) 10 (67) 25 (45) Reflux Disease DeMeester score 31.9 ± ± ± 2.2 Percentage duration ph ± ± ± 0.6 Position Upright 24 (34) 2 (13) 22 (40) Supine 18 (26) 3 (20) 15 (27) Bipositional 15 (21) 3 (20) 12 (22) Postprandial 12 (17) 7 (47) 5 (9) None 1 (1) 0 1 (1) *Values are mean ± SEM. Figures in parentheses denote percentage for column. LES indicates lower esophageal sphincter. Some percentages do not sum to 100 because of rounding. Significant difference between normal and overweight subgroups, P.01, Mann-Whitney test. DeMeester Score Normal Overweight Body Mass Index, kg/m 2 Figure 1. Scatterplot of body mass index against DeMeester score. Correlation coefficient, 0.38; significance, P.001. DeMeester Score n=15 n=55 Normal Overweight Body Mass Index, kg/m 2 Figure 2. Mean±SEM DeMeester scores for patients with normal weight and overweight. Significance, P.001. of His, an important anatomical structure preventing gastric wall tension from pulling the LES apart, 11,12 may become blunted, thus enabling moderate levels of gastric distension to more readily induce transient sphincter opening. Similarly, the potentiation effect on sphincter competency derived from the diaphragmatic crural sling 13 may be attenuated if this region is surrounded by cushions of fatty tissue. Obese individuals have a higher intra-abdominal resting pressure, and this relates to the sagittal abdominal diameter. 14 Excess fat deposition in and around abdominal viscera, in addition to elevating intra-abdominal pressure, may interfere with and delay gastric emptying. 15 This promotes fundic distension, with corresponding sphincter unfolding and length shortening, reducing its ability to function as an effective barrier. 16 The restriction of free space within the peritoneal cavity is likely to result in reduced pressure compliance within the abdominal compartment. Fluctuations in the intra-abdominal pressure, such as occurs with positional or postural change, coughing, or straining, are therefore exaggerated, with sudden sharp rises in gastric pressure overcoming LES resistance. The finding of similar values for the LES characteristics in both groups suggests that the barrier intrinsically is not at fault in causing reflux in the patients who were overweight. It has been argued that a neural phenomenon is primarily responsible for generating gastroesophageal reflux, through so-called transient LES relaxations. 17 Therefore, by some unexplained mechanism, obesity invokes an increased frequency or duration of these events. There is no obvious evidence for this and no clear reason why progressive increases in BMI should potentiate this effect. A direct, multifactorial mechanical process, interfering with the ability of the LES to prevent shortening or to offer adequate resistance to gastric pressure, is a more obvious explanation for the observations in this study. Observation of the association between obesity and reflux disease, in general, has yielded conflicting conclusions among different studies; hence, the benefit of weight loss is also controversial. In a recent large, Swedish population interview-based study, Lagergren et al 18 concluded that the presence of gastroesophageal reflux symptoms occurred independently of BMI. However, this group (with the addition of Lindgren) 19 have previously linked the presence of gastroesophageal reflux as a risk factor for esophageal adenocarcinoma, and Lagergren et al 20 have shown that this complication of GERD is, in fact, strongly associated with BMI. In a similar populationbased study, using a questionnaire among the residents of Olmstead County, Minnesota, BMI was indepen- 1017
5 dently associated with GERD. 21 Studies of the massively obese 22,23 and investigations of the effect of weight loss therapy in symptomatic improvement 24,25 have been contradictory in their conclusions. This study investigated patients with definitive symptoms and proven disease and then specifically examined those in whom reflux would not normally be expected to occur. This population will thus differ from more generalized studies. Among these patients, those who have a normal BMI have a mild form of disease and might benefit therapeutically from simple conservative measures, including lifestyle changes. Patients who are overweight, however, have a more severe form of disease. There may be some benefit achieved from simple weight reduction, although compliance with this form of treatment is likely to vary considerably, depending on the individual patient. There is also a potential role of surgical intervention. Because the barrier to reflux in these patients is rendered ineffective, augmentation of LES resting pressure and length could provide sufficient reserve to prevent the mechanistic overriding from taking place. Simple endoscopic procedures or laparoscopic Nissen fundoplication will prevent loss of length with gastric distension 26 and thus restore barrier competency. Presented at the 72nd Annual Meeting of the Pacific Coast Surgical Association, Banff, Canada, February 18, Corresponding author and reprints: Cedric G. Bremner, MD, Department of Surgery, University of Southern California, 1510 San Pablo St, Suite 514, Los Angeles, CA ( bremner@hsc.usc.edu). REFERENCES 1. Zaninotto G, DeMeester TR, Schwizer W, Johansson KE, Cheng SC. The lower esophageal sphincter in health and disease. Am J Surg. 1988;155: Kahrilas PJ, Dodds WJ, Hogan WJ. Effect of peristaltic dysfunction on esophageal volume clearance. Gastroenterology. 1988;94: Johnson LF, DeMeester TR. Twenty-four-hour ph monitoring of the distal esophagus: a quantitative measure of gastroesophageal reflux. Am J Gastroenterol. 1974; 62: Jamieson JR, Stein HJ, DeMeester TR, et al. Ambulatory 24-h esophageal ph monitoring: normal values, optimal thresholds, specificity, sensitivity, and reproducibility. Am J Gastroenterol. 1992;87: World Health Organization Expert Committee. Physical Status: The Use and Interpretation of Anthropometry. Geneva, Switzerland: World Health Organization; WHO Technical Report Series Stein HJ, Barlow AP, DeMeester TR, Hinder RA. Complications of gastroesophageal reflux disease: role of the lower esophageal sphincter, esophageal acid and acid/alkaline exposure, and duodenogastric reflux. Ann Surg. 1992;216: Stein HJ, Eypasch EP, DeMeester TR, Smyrk TC. Circadian esophageal motor function in patients with gastroesophageal reflux disease. Surgery. 1990;108: Kopelman PG. Obesity as a medical problem. Nature. 2000;404: Willett WC, Dietz WH, Colditz GA. Guidelines for healthy weight. N Engl J Med. 1999;341: Folsom AR, Kaye SA, Sellers TA, et al. Body fat distribution and 5-year risk of death in older women. JAMA. 1993;269: Pettersson GB, Bombeck CT, Nyhus LM. The lower esophageal sphincter: mechanism of opening and closure. Surgery. 1980;88: Marchand P. The gastro-oesophageal sphincter and mechanism of regurgitation. Br J Surg. 1955;42: Mittal RK, Rochester DF, McCallum RW. Electrical and mechanical activity in the human lower esophageal sphincter during diaphragmatic contraction. J Clin Invest. 1988;81: Sugarman H, Windsor A, Bessos M, Wolfe L. Intra-abdominal pressure, sagittal abdominal diameter and obesity comorbidity. J Intern Med. 1997;241: Maddox A, Horowitz M, Wishart J, Collins P. Gastric and oesophageal emptying in obesity. Scand J Gastroenterol. 1989;24: DeMeester TR, Ireland AP. Gastric pathology as an initiator and potentiator of gastroesophageal reflux disease. Dis Esophagus. 1997;10: Dodds WJ, Dent J, Hogan WJ, et al. Mechanisms of gastroesophageal reflux in patients with reflux esophagitis. N Engl J Med. 1982;307: Lagergren J, Bergstrom R, Nyren O. No relation between body mass and gastrooesophageal reflux symptoms in a Swedish population based study. Gut. 2000; 47: Lagergren J, Bergstrom R, Lindgren A, Nyren O. Symptomatic gastroesophageal reflux as a risk factor for esophageal adenocarcinoma. N Engl J Med. 1999; 340: Lagergren J, Bergstrom R, Nyren O. Association between body mass and adenocarcinoma of the esophagus and gastric cardia. Ann Intern Med. 1999;130: Locke, GR, Talley NJ, Fett SL. Risk factors associated with symptoms of gastroesophageal reflux. Am J Med. 1999;106: Lundell L, Ruth M, Sandberg N, Bove-Nielsen M. Does massive obesity promote abnormal gastroesophageal reflux? Dig Dis Sci. 1995;40: Fisher BL, Pennathur A, Mutnick JL, Little AG. Obesity correlates with gastroesophageal reflux. Dig Dis Sci. 1999;44: Kjellin A, Ramel S, Rossner S, Thor K. Gastroesophageal reflux in obese patients is not reduced by weight reduction. Scand J Gastroenterol. 1996;31: Fraser-Moodie CA, Norton B, Gornall C, Magnago S, Weale AR, Holmes GK. Weight loss has an independent beneficial effect on symptoms of gastro-oesophageal reflux in patients who are overweight. Scand J Gastroenterol. 1999;34: Mason RJ, DeMeester TR, Lund RJ, et al. Nissen fundoplication prevents shortening of the sphincter during gastric distention. Arch Surg. 1997;132: DISCUSSION Carlos Pellegrini, MD, Seattle, Wash: As you know, primarily because of the work done by the World Health Organization, body mass index has emerged as the best proxy to measure the effects of overweight on health. It has been clearly shown that several diseases, like hypertension, degenerative joint diseases, diabetes, and even small increases in BMI, significantly change health. The authors of this study examined the relationship between the BMI and esophageal acid exposure in a group of 70 patients who had 24-hour ph monitoring demonstration of pathologic reflux and symptoms of abnormal gastroesophageal reflux. They found that in 55 of the 70 patients who had BMIs greater than 25, and would therefore be considered obese under the WHO classification, acid exposure was greater than in the 15 patients who had a BMI in the normal range. They also found a direct correlation between BMI and specific DeMeester score. Previous studies looking at obesity and the presence of abnormal gastroesophageal reflux have yielded conflicting information. Some studies have shown that, indeed, there is a positive correlation, and some large studies have failed to show that. What, then, is unique about the study you have heard today? There are 2 aspects of this study that make it unique. First, the authors have an objective demonstration of gastroesophageal reflux. Many of the previous studies have been based simply on questionnaires. Secondly, the authors limited the study to a group of patients who have a structurally competent LES, that is, people who would normally not be expected to be refluxing. That is what I want to focus on. Limiting the study to a group of patients with the structurally competent LES eliminates a number of potential confounding factors and allows one to look at the effects of BMI on acid exposure. On the other hand, what concerns me is that if one is trying to determine the effects of obesity on reflux, limiting the study to just patients with a structurally normal sphincter eliminates essentially all patients with very severe reflux and eliminates, in fact, most patients with abnormal gastroesophageal reflux. Thus, the overall impact of obesity on acid exposure may be missed altogether. Is it possible, for example, that obesity, by increases in intragastric pressure as they suggested, leads to the devel- 1018
6 opment of hiatal hernia or shortening of the sphincter? None of these patients would have been included in the study. Therefore, it would be important for the authors to tell us what the overall relationship is in their database between BMI and acid exposure in all patients, not just those with structurally incompetent sphincter. The second question would be, since they postulated that increases in intra-abdominal pressure may be the result of an increase in BMI, was the intragastric pressure in these patients increased? Intragastric pressure is a good way to measure intra-abdominal pressure. Did they look at the transient LES relaxation in these patients?...increases in frequency or duration? Lastly, from the point of view of a practical surgeon, is decreasing BMI and decreasing body weight really a cure for gastroesophageal reflux? Have they had any experience measuring acid exposure before and after losing significant amounts of weight? We have looked at symptoms and weight loss in a very small group of 6 patients who took the challenge of losing a significant amount of weight and were surprised to see that we did not see any decrease in symptoms or any decrease in acid exposure, despite the loss of weight, suggesting that, once a certain threshold is crossed in weight gain, in a certain individual, a certain damage occurs to the antireflux mechanism that cannot be repaired simply by losing weight. Richard J. Finley, MD, Vancouver, British Columbia: There is a difference in distribution of fat between men and women. Males tend to have a greater percentage of fat in their peritoneal cavity than females, which may increase intraabdominal pressure. Did the authors notice a difference in reflux between the sexes? My other experience is that it is very difficult to get patients to lose weight when there is poor control of their reflux. What are your strategies for weight loss in patients with significant GERD? Ronald W. Busuttil, MD, Los Angeles, Calif: Although the sphincter was hindered with obesity, was there a higher incidence of esophagitis, ulcers, or Barrett s disease in these patients vs the nonobese? Secondly, did the proton-pump blockers have any kind of effect, or was it blunted in these obese patients compared with the normal patients? Dr Bremner: Dr Pellegrini, your first question was what is the relationship of BMI to acid exposure overall, and there was, in fact, no relationship in our study. You asked about relaxation of the LES, and relaxation was normal in both groups of patients. From a practical point of view, you asked is decreasing the BMI effective in improving the LES? Studies previously suggest not, and we haven t, in fact, had the opportunity to do that ourselves. This would make an excellent study to assess whether obesity reduction restores barrier competency. Dr Finley, there was no difference in the relation of sex to reflux in our series. You asked a practical question: how could we get these people to lose weight? Well, this is, as you know, a tremendous problem today, and perhaps there will one day be an alternative to bariatric surgery, which is the way we are all pushing at the moment. There was a question about esophagitis: was esophagitis greater in the morbidly obese patients or the obese patients in our series? Our study was confined to manometric and ph studies alone, and we do not have the endoscopic details. All of these patients were off PPIs [proton-pump inhibitors] for the study. IN OTHER AMA JOURNALS ARCHIVES OF INTERNAL MEDICINE Risk Factors for the Rising Rates of Primary Liver Cancer in the United States Hashem B. El-Serag, MD, MPH; Andrew C. Mason, MD Background: A recent increase in the incidence of hepatocellular carcinoma was reported in the United States. The cause of this witnessed rise remains unknown. Methods: We examined the temporal changes in both age-specific and age-standardized hospitalization rates of primary liver cancer associated with hepatitis C, hepatitis B, and alcoholic cirrhosis in the Department of Veterans Affairs Medical Center s Patient Treatment File. Results: A total of 1605 patients were diagnosed with primary liver cancer between 1993 and The overall age-adjusted proportional hospitalization rate for primary liver cancer increased from 36.4 per (95% confidence interval [CI], ) between 1993 and 1995 to 47.5 per (95% CI, ) between 1996 and There was a 3-fold increase in the age-adjusted rates for primary liver cancer associated with hepatitis C virus, from 2.3 per (95% CI, ) between 1993 and 1995 to 7.0 per (95% CI, ) between 1996 and Concomitant with this rise, the age-specific rates for primary liver cancer associated with hepatitis C also shifted toward younger patients. During the same periods, the age-adjusted rates for primary liver cancer associated with either hepatitis B virus (2.2 vs 3.1 per ) or alcoholic cirrhosis (8.4 vs 9.1 per ) remained stable. The rates for primary liver cancer without risk factors also remained without a statistically significant change, from 17.5 (95% CI, ) between 1993 and 1995 to 19.0 per (95% CI, ) between 1996 and Conclusions: Hepatitis C virus infection accounts for most of the increase in the number of cases of primary liver cancer among US veterans. The rates of primary liver cancer associated with alcoholic cirrhosis and hepatitis B virus infection have remained stable. (2000;160: ) Reprints: Hashem B. El-Serag, MD, MPH, Houston VA Medical Center (152), 2002 Holcombe Blvd, Houston, TX ( hasheme@bcm.tmc.edu). 1019
Obesity Is Associated With Increased Transient Lower Esophageal Sphincter Relaxation. Introduction. Predisposing factor. Introduction.
 Obesity Is Associated With Increased Transient Lower Esophageal Sphincter Relaxation Gastro Esophageal Reflux Disease (GERD) JUSTIN CHE-YUEN WU, et. al. The Chinese University of Hong Kong Gastroenterology,
Obesity Is Associated With Increased Transient Lower Esophageal Sphincter Relaxation Gastro Esophageal Reflux Disease (GERD) JUSTIN CHE-YUEN WU, et. al. The Chinese University of Hong Kong Gastroenterology,
The Frequency of Gastroesophageal Reflux Disease in Nutcracker Esophagus and the Effect of Acid-Reduction Therapy on the Motor Abnormality
 Bahrain Medical Bulletin, Vol.22, No.4, December 2000 The Frequency of Gastroesophageal Reflux Disease in Nutcracker Esophagus and the Effect of Acid-Reduction Therapy on the Motor Abnormality Saleh Mohsen
Bahrain Medical Bulletin, Vol.22, No.4, December 2000 The Frequency of Gastroesophageal Reflux Disease in Nutcracker Esophagus and the Effect of Acid-Reduction Therapy on the Motor Abnormality Saleh Mohsen
RECENT STUDIES have shown
 PAPER The Pattern of Esophageal Acid Exposure in Gastroesophageal Reflux Disease Influences the Severity of the Disease Guilherme M. R. Campos, MD; Jeffrey H. Peters, MD; Tom R. DeMeester, MD; Stefan Öberg,
PAPER The Pattern of Esophageal Acid Exposure in Gastroesophageal Reflux Disease Influences the Severity of the Disease Guilherme M. R. Campos, MD; Jeffrey H. Peters, MD; Tom R. DeMeester, MD; Stefan Öberg,
Falk Symposium, , , Portorož. Physiology of Swallowing and Anti-Gastroesophageal. Reflux-Mechanisms. Mechanisms: C.
 Falk Symposium, 15.-16.6.07, 16.6.07, Portorož Physiology of Swallowing and Anti-Gastroesophageal Reflux-Mechanisms Mechanisms: Anything new from a radiologist s view? C.Kulinna-Cosentini Cosentini Medical
Falk Symposium, 15.-16.6.07, 16.6.07, Portorož Physiology of Swallowing and Anti-Gastroesophageal Reflux-Mechanisms Mechanisms: Anything new from a radiologist s view? C.Kulinna-Cosentini Cosentini Medical
Putting Chronic Heartburn On Ice
 Putting Chronic Heartburn On Ice Over the years, gastroesophageal reflux disease has proven to be one of the most common complaints facing family physicians. With quicker diagnosis, this pesky ailment
Putting Chronic Heartburn On Ice Over the years, gastroesophageal reflux disease has proven to be one of the most common complaints facing family physicians. With quicker diagnosis, this pesky ailment
ORIGINAL ARTICLES ALIMENTARY TRACT. Bravo Catheter-Free ph Monitoring: Normal Values, Concordance, Optimal Diagnostic Thresholds, and Accuracy
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:60 67 ORIGINAL ARTICLES ALIMENTARY TRACT Bravo Catheter-Free ph Monitoring: Normal Values, Concordance, Optimal Diagnostic Thresholds, and Accuracy SHAHIN
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:60 67 ORIGINAL ARTICLES ALIMENTARY TRACT Bravo Catheter-Free ph Monitoring: Normal Values, Concordance, Optimal Diagnostic Thresholds, and Accuracy SHAHIN
The Lower Esophageal Sphincter in Health and Disease. Steven R. DeMeester Professor and Clinical Scholar Department of Surgery
 The Lower Esophageal Sphincter in Health and Disease Steven R. DeMeester Professor and Clinical Scholar Department of Surgery The Lower Esophageal Sphincter Dual function: allow bolus from esophagus into
The Lower Esophageal Sphincter in Health and Disease Steven R. DeMeester Professor and Clinical Scholar Department of Surgery The Lower Esophageal Sphincter Dual function: allow bolus from esophagus into
Primary and secondary esophageal contractions in patients with gastroesophageal reflux disease
 Brazilian Journal of Medical and Biological Research (6) 39: 27-31 ISSN -879X 27 Primary and secondary esophageal contractions in patients with gastroesophageal reflux disease C.G. Aben-Athar and R.O.
Brazilian Journal of Medical and Biological Research (6) 39: 27-31 ISSN -879X 27 Primary and secondary esophageal contractions in patients with gastroesophageal reflux disease C.G. Aben-Athar and R.O.
Gastroesophageal Reflux Disease, Paraesophageal Hernias &
 530.81 553.3 & 530.00 43289, 43659 1043432842, MD Assistant Clinical Professor of Surgery, UH JABSOM Associate General Surgery Program Director Director of Minimally Invasive & Bariatric Surgery Programs
530.81 553.3 & 530.00 43289, 43659 1043432842, MD Assistant Clinical Professor of Surgery, UH JABSOM Associate General Surgery Program Director Director of Minimally Invasive & Bariatric Surgery Programs
Abstract. Abnormal peristaltic waves like aperistalsis of the esophageal body, high amplitude and broader waves,
 Original Article Esophageal Motility Disorders in Diabetics Waquaruddin Ahmed, Ejaz Ahmed Vohra Department of Medicine, Dr. Ziauddin Medical University, Karachi. Abstract Objective: To see the presence
Original Article Esophageal Motility Disorders in Diabetics Waquaruddin Ahmed, Ejaz Ahmed Vohra Department of Medicine, Dr. Ziauddin Medical University, Karachi. Abstract Objective: To see the presence
NIH Public Access Author Manuscript Arch Surg. Author manuscript; available in PMC 2013 April 01.
 NIH Public Access Author Manuscript Published in final edited form as: Arch Surg. 2012 April ; 147(4): 352 357. doi:10.1001/archsurg.2012.17. Do large hiatal hernias affect esophageal peristalsis? Sabine
NIH Public Access Author Manuscript Published in final edited form as: Arch Surg. 2012 April ; 147(4): 352 357. doi:10.1001/archsurg.2012.17. Do large hiatal hernias affect esophageal peristalsis? Sabine
ORIGINAL ARTICLE. in which elements of the abdominal cavity herniate. Anatomic disruption of the esophagogastric junction (EGJ), phrenoesophageal
 ORIGINAL ARTICLE Effects of on Esophageal Peristalsis Sabine Roman, MD, PhD; Peter J. Kahrilas, MD; Leila Kia, MD; Daniel Luger, BA; Nathaniel Soper, MD; John E. Pandolfino, MD Hypothesis: Anatomic changes
ORIGINAL ARTICLE Effects of on Esophageal Peristalsis Sabine Roman, MD, PhD; Peter J. Kahrilas, MD; Leila Kia, MD; Daniel Luger, BA; Nathaniel Soper, MD; John E. Pandolfino, MD Hypothesis: Anatomic changes
ORIGINAL ARTICLE. Factors Affecting Esophageal Motility in Gastroesophageal Reflux Disease
 ORIGINAL ARTICLE Factors Affecting Esophageal Motility in Gastroesophageal Reflux Disease Emmanuel Chrysos, MD; George Prokopakis, MD; Elias Athanasakis, MD; George Pechlivanides, MD; John Tsiaoussis,
ORIGINAL ARTICLE Factors Affecting Esophageal Motility in Gastroesophageal Reflux Disease Emmanuel Chrysos, MD; George Prokopakis, MD; Elias Athanasakis, MD; George Pechlivanides, MD; John Tsiaoussis,
Metoclopramide in gastrooesophageal reflux
 Metoclopramide in gastrooesophageal reflux C. STANCIU AND JOHN R. BENNETT From the Gastrointestinal Unit, Hull Royal Infirmary Gut, 1973, 14, 275-279 SUMMARY In 3 patients with gastrooesophageal reflux,
Metoclopramide in gastrooesophageal reflux C. STANCIU AND JOHN R. BENNETT From the Gastrointestinal Unit, Hull Royal Infirmary Gut, 1973, 14, 275-279 SUMMARY In 3 patients with gastrooesophageal reflux,
Obesity Is Associated With Increased Transient Lower Esophageal Sphincter Relaxation
 GASTROENTEROLOGY 2007;132:883 889 Obesity Is Associated With Increased Transient Lower Esophageal Sphincter Relaxation JUSTIN CHE YUEN WU, LIK MAN MUI, CARRIAN MAN YUEN CHEUNG, YAWEN CHAN, and JOSEPH JAO
GASTROENTEROLOGY 2007;132:883 889 Obesity Is Associated With Increased Transient Lower Esophageal Sphincter Relaxation JUSTIN CHE YUEN WU, LIK MAN MUI, CARRIAN MAN YUEN CHEUNG, YAWEN CHAN, and JOSEPH JAO
Esophageal Manometry. John M. Wo, M.D. October 1, 2009
 Esophageal Manometry John M. Wo, M.D. October 1, 2009 Esophageal Manometry Anatomy and physiology of the esophagus Conventional esophageal manometry High resolution esophageal manometry (Pressure Topography)
Esophageal Manometry John M. Wo, M.D. October 1, 2009 Esophageal Manometry Anatomy and physiology of the esophagus Conventional esophageal manometry High resolution esophageal manometry (Pressure Topography)
ESOPHAGEAL CANCER AND GERD. Prof Salman Guraya FRCS, Masters MedEd
 ESOPHAGEAL CANCER AND GERD Prof Salman Guraya FRCS, Masters MedEd Learning objectives Esophagus anatomy and physiology Esophageal cancer Causes, presentations of esophageal cancer Diagnosis and management
ESOPHAGEAL CANCER AND GERD Prof Salman Guraya FRCS, Masters MedEd Learning objectives Esophagus anatomy and physiology Esophageal cancer Causes, presentations of esophageal cancer Diagnosis and management
Color Atlas of High Resolution Manometry
 Color Atlas of High Resolution Manometry Color Atlas of High Resolution Manometry Edited by Jeffrey Conklin, MD GI Motility Program Mark Pimentel, MD, FRCP(C) Cedars-Sinai Medical Center Edy Soffer, MD
Color Atlas of High Resolution Manometry Color Atlas of High Resolution Manometry Edited by Jeffrey Conklin, MD GI Motility Program Mark Pimentel, MD, FRCP(C) Cedars-Sinai Medical Center Edy Soffer, MD
Achalasia is a rare disease with an annual incidence estimated REVIEWS. Erroneous Diagnosis of Gastroesophageal Reflux Disease in Achalasia
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2011;9:1020 1024 REVIEWS Erroneous Diagnosis of Gastroesophageal Reflux Disease in Achalasia BOUDEWIJN F. KESSING, ALBERT J. BREDENOORD, and ANDRÉ J. P. M. SMOUT
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2011;9:1020 1024 REVIEWS Erroneous Diagnosis of Gastroesophageal Reflux Disease in Achalasia BOUDEWIJN F. KESSING, ALBERT J. BREDENOORD, and ANDRÉ J. P. M. SMOUT
127 Chapter 1 Chapter 2 Chapter 3
 CHAPTER 8 Summary Summary 127 In Chapter 1, a general introduction on the principles and applications of intraluminal impedance monitoring in esophageal disorders is provided. Intra-esophageal impedance
CHAPTER 8 Summary Summary 127 In Chapter 1, a general introduction on the principles and applications of intraluminal impedance monitoring in esophageal disorders is provided. Intra-esophageal impedance
oesophageal sphincter pressure in man
 Gut, 1987, 28, 1564-1568 Effect of the diaphragmatic contraction on lower oesophageal sphincter pressure in man R K MITTAL, D F ROCHESTER, AND R W McCALLUM From the Department of Internal Medicine, University
Gut, 1987, 28, 1564-1568 Effect of the diaphragmatic contraction on lower oesophageal sphincter pressure in man R K MITTAL, D F ROCHESTER, AND R W McCALLUM From the Department of Internal Medicine, University
Interventional procedures guidance Published: 16 December 2015 nice.org.uk/guidance/ipg540
 Electrical stimulation of the lower oesophageal sphincter for treating gastro-oesophageal reflux disease Interventional procedures guidance Published: 16 December 2015 nice.org.uk/guidance/ipg540 Your
Electrical stimulation of the lower oesophageal sphincter for treating gastro-oesophageal reflux disease Interventional procedures guidance Published: 16 December 2015 nice.org.uk/guidance/ipg540 Your
Clearance mechanisms of the aperistaltic esophagus. The pump-gun hypothesis.
 Gut Online First, published on December 14, 2005 as 10.1136/gut.2005.085423 Clearance mechanisms of the aperistaltic esophagus. The pump-gun hypothesis. Radu Tutuian 1, Daniel Pohl 1, Donald O Castell
Gut Online First, published on December 14, 2005 as 10.1136/gut.2005.085423 Clearance mechanisms of the aperistaltic esophagus. The pump-gun hypothesis. Radu Tutuian 1, Daniel Pohl 1, Donald O Castell
A.J. Bredenoord B.L.A.M. Weusten S. Carmagnola A.J.P.M. Smout
 5 Double-peaked high-pressure zone at the esophagogastric junction in controls and in patients with a hiatal hernia: A study using high-resolution manometry A.J. Bredenoord B.L.A.M. Weusten S. Carmagnola
5 Double-peaked high-pressure zone at the esophagogastric junction in controls and in patients with a hiatal hernia: A study using high-resolution manometry A.J. Bredenoord B.L.A.M. Weusten S. Carmagnola
Oesophageal Disorders
 Oesophageal Disorders Anatomy Upper sphincter Oesophageal body Diaphragm Lower sphincter Gastric Cardia Symptoms Of Oesophageal Disorders Dysphagia Odynophagia Heartburn Atypical Chest Pain Regurgitation
Oesophageal Disorders Anatomy Upper sphincter Oesophageal body Diaphragm Lower sphincter Gastric Cardia Symptoms Of Oesophageal Disorders Dysphagia Odynophagia Heartburn Atypical Chest Pain Regurgitation
On the relationship between gastric ph and pressure
 Gut, 1979, 20, 59-63 On the relationship between gastric ph and pressure in the normal human lower oesophageal sphincter M. D. KAYE1 From the Gastroenterology Unit, Department of Medicine, University of
Gut, 1979, 20, 59-63 On the relationship between gastric ph and pressure in the normal human lower oesophageal sphincter M. D. KAYE1 From the Gastroenterology Unit, Department of Medicine, University of
GERD. Gastroesophageal reflux disease, or GERD, occurs when acid from the. stomach backs up into the esophagus. Normally, food travels from the
 GERD What is GERD? Gastroesophageal reflux disease, or GERD, occurs when acid from the stomach backs up into the esophagus. Normally, food travels from the mouth, down through the esophagus and into the
GERD What is GERD? Gastroesophageal reflux disease, or GERD, occurs when acid from the stomach backs up into the esophagus. Normally, food travels from the mouth, down through the esophagus and into the
GASTROESOPHAGEAL REFLUX DISEASE. William M. Brady
 Drugs of Today 1998, 34(1): 25-30 Copyright PROUS SCIENCE GASTROESOPHAGEAL REFLUX DISEASE William M. Brady Section of General Internal Medicine, Temple University School of Medicine, Philadelphia, Pennsylvania,
Drugs of Today 1998, 34(1): 25-30 Copyright PROUS SCIENCE GASTROESOPHAGEAL REFLUX DISEASE William M. Brady Section of General Internal Medicine, Temple University School of Medicine, Philadelphia, Pennsylvania,
Precipitating causes of acid reflux episodes in ambulant patients with gastro-oesophageal reflux
 Gut 1995; 36: 505-510 University Department of Surgery, Bristol Royal Infirmary, Bristol C P Barham D C Gotley A Mills D Alderson Correspondence to: Mr C P Barham, University Department of Surgery, Bristol
Gut 1995; 36: 505-510 University Department of Surgery, Bristol Royal Infirmary, Bristol C P Barham D C Gotley A Mills D Alderson Correspondence to: Mr C P Barham, University Department of Surgery, Bristol
The effects of a weakly acidic meal on gastric buffering and postprandial gastro-oesophageal reflux
 Alimentary Pharmacology and Therapeutics The effects of a weakly acidic meal on gastric buffering and postprandial gastro-oesophageal reflux K. Ravi*, D. L. Francis*, J. A. See, D. M. Geno* & D. A. Katzka*
Alimentary Pharmacology and Therapeutics The effects of a weakly acidic meal on gastric buffering and postprandial gastro-oesophageal reflux K. Ravi*, D. L. Francis*, J. A. See, D. M. Geno* & D. A. Katzka*
GERD: A linical Clinical Clinical Update Objectives
 GERD: A Clinical Update Jeff Gilbert, M.D. University i of Kentucky Gastroenterology 11/6/08 Objectives To review the basic pathophysiology underlying gastroesophageal reflux disease To highlight current
GERD: A Clinical Update Jeff Gilbert, M.D. University i of Kentucky Gastroenterology 11/6/08 Objectives To review the basic pathophysiology underlying gastroesophageal reflux disease To highlight current
It is estimated that up to 11% of the US population experience. Ambulatory 24-hour Esophageal ph Monitoring
 J Clin Gastroenterol 2003;37(1):14 22. 2003 Lippincott Williams & Wilkins, Inc. Clinical Review Esophageal and Gastric Diseases Ambulatory 24-hour Esophageal ph Monitoring Why, When, and What to Do Christopher
J Clin Gastroenterol 2003;37(1):14 22. 2003 Lippincott Williams & Wilkins, Inc. Clinical Review Esophageal and Gastric Diseases Ambulatory 24-hour Esophageal ph Monitoring Why, When, and What to Do Christopher
Surgical Evaluation for Benign Esophageal Disease. Kimberly Howard, PA-C, MHS Duke University Medical Center April 7, 2018
 Surgical Evaluation for Benign Esophageal Disease Kimberly Howard, PA-C, MHS Duke University Medical Center April 7, 2018 Disclosures No disclosures relevant to this presentation. Objectives (for CME purposes)
Surgical Evaluation for Benign Esophageal Disease Kimberly Howard, PA-C, MHS Duke University Medical Center April 7, 2018 Disclosures No disclosures relevant to this presentation. Objectives (for CME purposes)
Gastro esophageal reflux disease DR. AMMAR I. ABDUL-LATIF
 Gastro esophageal reflux disease )GERD( DR. AMMAR I. ABDUL-LATIF GERD DEFINITION EPIDEMIOLOGY CAUSES PATHOGENESIS SIGNS &SYMPTOMS COMPLICATIONS DIAGNOSIS TREATMENT Definition Montreal consensus defined
Gastro esophageal reflux disease )GERD( DR. AMMAR I. ABDUL-LATIF GERD DEFINITION EPIDEMIOLOGY CAUSES PATHOGENESIS SIGNS &SYMPTOMS COMPLICATIONS DIAGNOSIS TREATMENT Definition Montreal consensus defined
Endoscopic Appearance of the Gastroesophageal Valve
 Diagnostic and Therapeutic Endoscopy, 1996, Vol. 2, pp. 147-150 Reprints available directly from the publisher Photocopying permitted by license only (C) 1996 OPA (Overseas Publishers Association) Amsterdam
Diagnostic and Therapeutic Endoscopy, 1996, Vol. 2, pp. 147-150 Reprints available directly from the publisher Photocopying permitted by license only (C) 1996 OPA (Overseas Publishers Association) Amsterdam
4/24/2015. History of Reflux Surgery. Recent Innovations in the Surgical Treatment of Reflux
 Recent Innovations in the Surgical Treatment of Reflux Scott Carpenter, DO, FACOS, FACS Mercy Hospital Ardmore Ardmore, OK History of Reflux Surgery - 18 th century- first use of term heartburn - 1934-
Recent Innovations in the Surgical Treatment of Reflux Scott Carpenter, DO, FACOS, FACS Mercy Hospital Ardmore Ardmore, OK History of Reflux Surgery - 18 th century- first use of term heartburn - 1934-
Clinical Study Management of Gastroesophageal Reflux Disease: A Review of Medical and Surgical Management
 Hindawi Publishing Corporation Minimally Invasive Surgery Volume 2014, Article ID 654607, 5 pages http://dx.doi.org/10.1155/2014/654607 Clinical Study Management of Gastroesophageal Reflux Disease: A Review
Hindawi Publishing Corporation Minimally Invasive Surgery Volume 2014, Article ID 654607, 5 pages http://dx.doi.org/10.1155/2014/654607 Clinical Study Management of Gastroesophageal Reflux Disease: A Review
Lower oesophageal sphincter tone in patients with peptic stricture
 Thorax, 1978, 33, 574578 Lower oesophageal sphincter tone in patients with peptic stricture R LOBELLO,1 M STEKELMAN, AND D A W EDWARDS2 From the Surgical Unit, University College Hospital Medical School,
Thorax, 1978, 33, 574578 Lower oesophageal sphincter tone in patients with peptic stricture R LOBELLO,1 M STEKELMAN, AND D A W EDWARDS2 From the Surgical Unit, University College Hospital Medical School,
David Markowitz, MD. Physicians and Surgeons
 Esophageal Motility David Markowitz, MD Columbia University, College of Columbia University, College of Physicians and Surgeons Alimentary Tract Motility Propulsion Movement of food and endogenous secretions
Esophageal Motility David Markowitz, MD Columbia University, College of Columbia University, College of Physicians and Surgeons Alimentary Tract Motility Propulsion Movement of food and endogenous secretions
Combined Manometric-pH Recording Catheter for Esophageal Function Tests
 HOW TO DO T Combined Manometric-pH Recording Catheter for Esophageal Function Tests Mark B. Orringer, M.D., Robert Lee, M.S., and Herbert Sloan, M.D. ABSTRACT A combined manometric-ph recording catheter
HOW TO DO T Combined Manometric-pH Recording Catheter for Esophageal Function Tests Mark B. Orringer, M.D., Robert Lee, M.S., and Herbert Sloan, M.D. ABSTRACT A combined manometric-ph recording catheter
Duke Masters of Minimally Invasive Thoracic Surgery Orlando, FL. September 17, Session VI: Minimally Invasive Thoracic Surgery: Miscellaneous
 Duke Masters of Minimally Invasive Thoracic Surgery Orlando, FL September 17, 2016 Session VI: Minimally Invasive Thoracic Surgery: Miscellaneous NOTES and POEM James D. Luketich MD, FACS Henry T. Bahnson
Duke Masters of Minimally Invasive Thoracic Surgery Orlando, FL September 17, 2016 Session VI: Minimally Invasive Thoracic Surgery: Miscellaneous NOTES and POEM James D. Luketich MD, FACS Henry T. Bahnson
Symptoms of gastroesophageal reflux disease (GERD) are. Effects of Age on the Gastroesophageal Junction, Esophageal Motility, and Reflux Disease
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2007;5:1392 1398 Effects of Age on the Gastroesophageal Junction, Esophageal Motility, and Reflux Disease JACQUELINE LEE,* ANGELA ANGGIANSAH, ROY ANGGIANSAH, ALASDAIR
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2007;5:1392 1398 Effects of Age on the Gastroesophageal Junction, Esophageal Motility, and Reflux Disease JACQUELINE LEE,* ANGELA ANGGIANSAH, ROY ANGGIANSAH, ALASDAIR
Manometry Conundrums
 Manometry Conundrums Gastroenterology and Hepatology Symposium February 10, 2018 Reena V. Chokshi, MD Assistant Professor of Medicine Division of Gastroenterology, Hepatology, & Nutrition Department of
Manometry Conundrums Gastroenterology and Hepatology Symposium February 10, 2018 Reena V. Chokshi, MD Assistant Professor of Medicine Division of Gastroenterology, Hepatology, & Nutrition Department of
Long-term effects of anti-reflux surgery on the physiology of the esophagogastric junction
 Surg Endosc (2015) 29:3726 3732 DOI 10.1007/s00464-015-4144-7 and Other Interventional Techniques Long-term effects of anti-reflux surgery on the physiology of the esophagogastric junction Boudewijn F.
Surg Endosc (2015) 29:3726 3732 DOI 10.1007/s00464-015-4144-7 and Other Interventional Techniques Long-term effects of anti-reflux surgery on the physiology of the esophagogastric junction Boudewijn F.
Maximizing Outcome of Extraesophageal Reflux Disease. (GERD) is often accompanied
 ...PRESENTATIONS... Maximizing Outcome of Extraesophageal Reflux Disease Based on a presentation by Peter J. Kahrilas, MD Presentation Summary Gastroesophageal reflux disease (GERD) accompanied by regurgitation
...PRESENTATIONS... Maximizing Outcome of Extraesophageal Reflux Disease Based on a presentation by Peter J. Kahrilas, MD Presentation Summary Gastroesophageal reflux disease (GERD) accompanied by regurgitation
34th Annual Toronto Thoracic Surgery Refresher Course
 34th Annual Toronto Thoracic Surgery Refresher Course TREATMENT OPTIONS FOR ACHALASIA Dr. Carmine Simone Director, Intensive Care Unit Head, Division of Critical Care Departments of Medicine and Surgery
34th Annual Toronto Thoracic Surgery Refresher Course TREATMENT OPTIONS FOR ACHALASIA Dr. Carmine Simone Director, Intensive Care Unit Head, Division of Critical Care Departments of Medicine and Surgery
Myogenic Control. Esophageal Motility. Enteric Nervous System. Alimentary Tract Motility. Determinants of GI Tract Motility.
 Myogenic Control Esophageal Motility David Markowitz, MD Columbia University, College of Physicians and Surgeons Basic Electrical Rythym: intrinsic rhythmic fluctuation of smooth muscle membrane potential
Myogenic Control Esophageal Motility David Markowitz, MD Columbia University, College of Physicians and Surgeons Basic Electrical Rythym: intrinsic rhythmic fluctuation of smooth muscle membrane potential
Esophageal Motility. Alimentary Tract Motility
 Esophageal Motility David Markowitz, MD Columbia University, College of Physicians and Surgeons Alimentary Tract Motility Propulsion Movement of food and endogenous secretions Mixing Allows for greater
Esophageal Motility David Markowitz, MD Columbia University, College of Physicians and Surgeons Alimentary Tract Motility Propulsion Movement of food and endogenous secretions Mixing Allows for greater
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: esophageal_ph_monitoring 4/2011 5/2017 5/2018 5/2017 Description of Procedure or Service Acid reflux is the
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: esophageal_ph_monitoring 4/2011 5/2017 5/2018 5/2017 Description of Procedure or Service Acid reflux is the
WHAT IS GASTROESOPHAGEAL REFLUX DISEASE (GERD)?
 WHAT IS GASTROESOPHAGEAL REFLUX DISEASE (GERD)? The term gastroesophageal reflux describes the movement (or reflux) of stomach contents back up into the esophagus, the muscular tube that extends from the
WHAT IS GASTROESOPHAGEAL REFLUX DISEASE (GERD)? The term gastroesophageal reflux describes the movement (or reflux) of stomach contents back up into the esophagus, the muscular tube that extends from the
Aerophagia, gastric, and supragastric belching: a study using intraluminal electrical impedance monitoring
 14 Aerophagia, gastric, and supragastric belching: a study using intraluminal electrical impedance monitoring A.J. Bredenoord B.L.A.M. Weusten D. Sifrim R. Timmer A.J.P.M. Smout Dept. of Gastroenterology,
14 Aerophagia, gastric, and supragastric belching: a study using intraluminal electrical impedance monitoring A.J. Bredenoord B.L.A.M. Weusten D. Sifrim R. Timmer A.J.P.M. Smout Dept. of Gastroenterology,
Medical Policy Manual. Topic: Gastric Reflux Surgery Date of Origin: November Section: Surgery Last Reviewed Date: March 2014
 Medical Policy Manual Topic: Gastric Reflux Surgery Date of Origin: November 2012 Section: Surgery Last Reviewed Date: March 2014 Policy No: 186 Effective Date: May 1, 2014 IMPORTANT REMINDER Medical Policies
Medical Policy Manual Topic: Gastric Reflux Surgery Date of Origin: November 2012 Section: Surgery Last Reviewed Date: March 2014 Policy No: 186 Effective Date: May 1, 2014 IMPORTANT REMINDER Medical Policies
Response of the gullet to gastric reflux in patients with hiatus hernia and oesophagitis
 Thorax (1970), 5, 459. Response of the gullet to gastric reflux in patients with hiatus hernia and oesophagitis D. A. K. WOODWARD1 Oesophageal Laboratory, Queen Elizabeth Hospital, Birmingham 15 The variability
Thorax (1970), 5, 459. Response of the gullet to gastric reflux in patients with hiatus hernia and oesophagitis D. A. K. WOODWARD1 Oesophageal Laboratory, Queen Elizabeth Hospital, Birmingham 15 The variability
MEDICAL POLICY SUBJECT: MAGNETIC ESOPHAGEAL RING/ MAGNETIC SPHINCTER AUGMENTATION FOR THE TREATMENT OF GASTROESOPHAGEAL REFLUX DISEASE (GERD)
 MEDICAL POLICY SUBJECT: MAGNETIC ESOPHAGEAL RING/ MAGNETIC SPHINCTER PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial
MEDICAL POLICY SUBJECT: MAGNETIC ESOPHAGEAL RING/ MAGNETIC SPHINCTER PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial
L ANELLO MAGNETICO NELLA TERAPIA DEL REFLUSSO
 L ANELLO MAGNETICO NELLA TERAPIA DEL REFLUSSO GASTROESOFAGEO Greta Saino University of Milan Department of Biomedical Sciences for Health Division of General Surgery IRCCS Policlinico San Donato TOP TEN
L ANELLO MAGNETICO NELLA TERAPIA DEL REFLUSSO GASTROESOFAGEO Greta Saino University of Milan Department of Biomedical Sciences for Health Division of General Surgery IRCCS Policlinico San Donato TOP TEN
Physiologic Mechanism and Preoperative Prediction of New-Onset Dysphagia After Laparoscopic Nissen Fundoplication
 Physiologic Mechanism and Preoperative Prediction of New-Onset Dysphagia After Laparoscopic Nissen Fundoplication Dennis Blom, M.D., Jeffrey H. Peters, M.D., Tom R. DeMeester, M.D., Peter F. Crookes, M.D.,
Physiologic Mechanism and Preoperative Prediction of New-Onset Dysphagia After Laparoscopic Nissen Fundoplication Dennis Blom, M.D., Jeffrey H. Peters, M.D., Tom R. DeMeester, M.D., Peter F. Crookes, M.D.,
Esophageal Manometry: Assessment of Interpreter Consistency
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:218 224 ORIGINAL ARTICLES Esophageal Manometry: Assessment of Interpreter Consistency DEVJIT S. NAYAR, FARAH KHANDWALA, EDGAR ACHKAR, STEVEN S. SHAY, JOEL
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:218 224 ORIGINAL ARTICLES Esophageal Manometry: Assessment of Interpreter Consistency DEVJIT S. NAYAR, FARAH KHANDWALA, EDGAR ACHKAR, STEVEN S. SHAY, JOEL
ACG Clinical Guideline: Diagnosis and Management of Gastroesophageal Reflux Disease
 ACG Clinical Guideline: Diagnosis and Management of Gastroesophageal Reflux Disease Philip O. Katz MD 1, Lauren B. Gerson MD, MSc 2 and Marcelo F. Vela MD, MSCR 3 1 Division of Gastroenterology, Einstein
ACG Clinical Guideline: Diagnosis and Management of Gastroesophageal Reflux Disease Philip O. Katz MD 1, Lauren B. Gerson MD, MSc 2 and Marcelo F. Vela MD, MSCR 3 1 Division of Gastroenterology, Einstein
Symptomatic outcome following laparoscopic anterior 180 partial fundoplication: Our initial experience
 International Journal of Medicine and Medical Sciences Vol. 2(4), pp. 128-132, April 2010 Available online http://www.academicjournals.org/ijmms ISSN 2006-9723 2010 Academic Journals Full Length Research
International Journal of Medicine and Medical Sciences Vol. 2(4), pp. 128-132, April 2010 Available online http://www.academicjournals.org/ijmms ISSN 2006-9723 2010 Academic Journals Full Length Research
THE NORMAL HUMAN ESOPHAGEAL MUCOSA: A HISTOLOGICAL REAPPRAISAL
 GASTROENTEROLOGY 68:40-44, 1975 Copyright 1975 by The Williams & Wilkins Co. Vol. 68, No.1 Printed in U.S.A. THE NORMAL HUMAN ESOPHAGEAL MUCOSA: A HISTOLOGICAL REAPPRAISAL WILFRED M. WEINSTEIN, M.D., EARL
GASTROENTEROLOGY 68:40-44, 1975 Copyright 1975 by The Williams & Wilkins Co. Vol. 68, No.1 Printed in U.S.A. THE NORMAL HUMAN ESOPHAGEAL MUCOSA: A HISTOLOGICAL REAPPRAISAL WILFRED M. WEINSTEIN, M.D., EARL
A CURIOUS CASE OF HYPERTENSIVE LES. Erez Hasnis Department of Gastroenterology Rambam Health Care Campus
 A CURIOUS CASE OF HYPERTENSIVE LES Erez Hasnis Department of Gastroenterology Rambam Health Care Campus CASE DESCRIPTION 63yo, F, single, attending nurse. PMH includes T2DM (Sitagliptin/Metformin), Hyperlipidemia
A CURIOUS CASE OF HYPERTENSIVE LES Erez Hasnis Department of Gastroenterology Rambam Health Care Campus CASE DESCRIPTION 63yo, F, single, attending nurse. PMH includes T2DM (Sitagliptin/Metformin), Hyperlipidemia
COMPARATIVE EFFECTS OF METOCLOPRAMIDE AND BETHANECHOL ON LOWER ESOPHAGEAL SPHINCTER PRESSURE IN REFLUX PATIENTS
 GASTROENTEROLOGY 68: 111-1118, 1975 Copyright 1975 by The Williams & Wilkins Co. Vol. 68, No. 5, Part 1 Printed in U.S.A. COMPARATIVE EFFECTS OF METOCLOPRAMIDE AND BETHANECHOL ON LOWER ESOPHAGEAL SPHINCTER
GASTROENTEROLOGY 68: 111-1118, 1975 Copyright 1975 by The Williams & Wilkins Co. Vol. 68, No. 5, Part 1 Printed in U.S.A. COMPARATIVE EFFECTS OF METOCLOPRAMIDE AND BETHANECHOL ON LOWER ESOPHAGEAL SPHINCTER
Four-Day Bravo ph Capsule Monitoring With and Without Proton Pump Inhibitor Therapy
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:1083 1088 Four-Day Bravo ph Capsule Monitoring With and Without Proton Pump Inhibitor Therapy IKUO HIRANO, QING ZHANG, JOHN E. PANDOLFINO, and PETER J. KAHRILAS
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:1083 1088 Four-Day Bravo ph Capsule Monitoring With and Without Proton Pump Inhibitor Therapy IKUO HIRANO, QING ZHANG, JOHN E. PANDOLFINO, and PETER J. KAHRILAS
Hiatal Hernias and Barrett s esophagus. Dr Sajida Ahad Mercy General Surgery
 Hiatal Hernias and Barrett s esophagus Dr Sajida Ahad Mercy General Surgery Objectives Identify the use of different diagnostic modalities for hiatal hernias List the different types of hiatal hernias
Hiatal Hernias and Barrett s esophagus Dr Sajida Ahad Mercy General Surgery Objectives Identify the use of different diagnostic modalities for hiatal hernias List the different types of hiatal hernias
ENDOLUMINAL THERAPIES FOR GERD. University of Colorado Department of Surgery Grand Rounds March 31st, 2008
 ENDOLUMINAL THERAPIES FOR GERD University of Colorado Department of Surgery Grand Rounds March 31st, 2008 Overview GERD Healthcare significance Definitions Treatment objectives Endoscopic options Plication
ENDOLUMINAL THERAPIES FOR GERD University of Colorado Department of Surgery Grand Rounds March 31st, 2008 Overview GERD Healthcare significance Definitions Treatment objectives Endoscopic options Plication
TBURN TBURN BURN ARTBURN EARTBURN EART HEARTBURN: HOW TO GET IT OFF YOUR CHEST
 TBURN BURN TBURN ARTBURN. EARTBURN EART N EARTBURN HEARTBURN: HOW TO GET IT OFF YOUR CHEST Do you sometimes wake up at night with a sharp, burning sensation in your chest? Does this sometimes happen during
TBURN BURN TBURN ARTBURN. EARTBURN EART N EARTBURN HEARTBURN: HOW TO GET IT OFF YOUR CHEST Do you sometimes wake up at night with a sharp, burning sensation in your chest? Does this sometimes happen during
What can you expect from the lab?
 Role of the GI Motility Lab in the Diagnosis and Treatment of Esophageal Disorders Kenneth R. DeVault MD, FACG, FACP Professor and Chair Department of Medicine Mayo Clinic Florida What can you expect from
Role of the GI Motility Lab in the Diagnosis and Treatment of Esophageal Disorders Kenneth R. DeVault MD, FACG, FACP Professor and Chair Department of Medicine Mayo Clinic Florida What can you expect from
Gastroesophageal Reflux Disease (GERD)
 Gastroesophageal Reflux Disease (GERD) Acid Reflux Acid reflux occurs when acid from the stomach moves backwards into the esophagus. Heartburn Heartburn is a symptom of acid reflux and GERD. It may feel
Gastroesophageal Reflux Disease (GERD) Acid Reflux Acid reflux occurs when acid from the stomach moves backwards into the esophagus. Heartburn Heartburn is a symptom of acid reflux and GERD. It may feel
La tasca acida nella MRGE: aspetti patogenetici e terapeutici
 La tasca acida nella MRGE: aspetti patogenetici e terapeutici Prof. VINCENZO SAVARINO Professore Ordinario di Gastroenterologia, Università degli Studi di Genova Direttore della Clinica Gastroenterologica
La tasca acida nella MRGE: aspetti patogenetici e terapeutici Prof. VINCENZO SAVARINO Professore Ordinario di Gastroenterologia, Università degli Studi di Genova Direttore della Clinica Gastroenterologica
/2014/106/1/22-29 Revista Española de Enfermedades Digestivas Vol. 106, N.º 1, pp , 2014 ORIGINAL PAPERS
 1130-0108/2014/106/1/22-29 Revista Española de Enfermedades Digestivas Copyright 2014 Arán Ediciones, S. L. Rev Esp Enferm Dig (Madrid Vol. 106, N.º 1, pp. 22-29, 2014 ORIGINAL PAPERS How useful is esophageal
1130-0108/2014/106/1/22-29 Revista Española de Enfermedades Digestivas Copyright 2014 Arán Ediciones, S. L. Rev Esp Enferm Dig (Madrid Vol. 106, N.º 1, pp. 22-29, 2014 ORIGINAL PAPERS How useful is esophageal
DON T LET OBESITY SPOIL YOUR HEALTH AND YOUR LIFE
 July 2015 Issue No.17 DON T LET OBESITY SPOIL YOUR HEALTH AND YOUR LIFE www.sghgroup.com JEDDAH RIYADH MEDINA ASEER HAIL SANAA DUBAI CAIRO Definitions Over View and General Facts General Key facts! Worldwide
July 2015 Issue No.17 DON T LET OBESITY SPOIL YOUR HEALTH AND YOUR LIFE www.sghgroup.com JEDDAH RIYADH MEDINA ASEER HAIL SANAA DUBAI CAIRO Definitions Over View and General Facts General Key facts! Worldwide
Refractory GERD : case presentation and discussion
 Refractory GERD : case presentation and discussion Ping-Huei Tseng National Taiwan University Hospital May 19, 2018 How effective is PPI based on EGD? With GERD symptom 75% erosive 25% NERD Endoscopy 81%
Refractory GERD : case presentation and discussion Ping-Huei Tseng National Taiwan University Hospital May 19, 2018 How effective is PPI based on EGD? With GERD symptom 75% erosive 25% NERD Endoscopy 81%
Systematic comparison of conventional oesophageal manometry with oesophageal motility while eating. bread ALIMENTARY TRACT
 1264 Gut, 1991,32, 1264-1269 ALIMENTARY TRACT Department of Medicine, Royal Infirmary of Edinburgh, Edinburgh EH3 9YW P J Howard L Maher A Pryde R C Heading Correspondence to: Dr P J Howard. Accepted for
1264 Gut, 1991,32, 1264-1269 ALIMENTARY TRACT Department of Medicine, Royal Infirmary of Edinburgh, Edinburgh EH3 9YW P J Howard L Maher A Pryde R C Heading Correspondence to: Dr P J Howard. Accepted for
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Achalasia, barium esophagography for, 57 58 Acid pocket, 18 19 Acid-sensing ion, 20 Acupuncture, 128 Adiponectin, in obesity, 166 ADX10059 metabotropic
Note: Page numbers of article titles are in boldface type. A Achalasia, barium esophagography for, 57 58 Acid pocket, 18 19 Acid-sensing ion, 20 Acupuncture, 128 Adiponectin, in obesity, 166 ADX10059 metabotropic
Citation for the published paper: Epidemiology May;24(3): Abdominal fat and male excess of esophageal adenocarcinoma
 This is an author produced version of a paper published in Epidemiology. This paper has been peer-reviewed but does not include the final publisher proof-corrections or journal pagination. Citation for
This is an author produced version of a paper published in Epidemiology. This paper has been peer-reviewed but does not include the final publisher proof-corrections or journal pagination. Citation for
Gastroesophageal Reflux Disease:
 Gastroesophageal Reflux Disease: Introduction Gastroesophageal reflux is the involuntary movement of gastric contents to the esophagus. It is a common disease, occurring in one third of the population
Gastroesophageal Reflux Disease: Introduction Gastroesophageal reflux is the involuntary movement of gastric contents to the esophagus. It is a common disease, occurring in one third of the population
Esophageal Disorders. Learning Objectives. Introduction. Gastroesophageal Reflux Disease. Reza Shaker, MD, and Benson T.
 Esophageal Disorders Reza Shaker, MD, and Benson T. Massey, MD, FACP Learning Objectives AFTER COMPLETING THIS CHAPTER, THE LEARNER SHOULD BE ABLE TO: 1. Recognize the typical and atypical presentations
Esophageal Disorders Reza Shaker, MD, and Benson T. Massey, MD, FACP Learning Objectives AFTER COMPLETING THIS CHAPTER, THE LEARNER SHOULD BE ABLE TO: 1. Recognize the typical and atypical presentations
Restoration of Normal Distensive Characteristics of the Esophagogastric Junction After Fundoplication
 ORIGINAL ARTICLES Restoration of Normal Distensive Characteristics of the Esophagogastric Junction After Fundoplication John E. Pandolfino, MD, Jennifer Curry, MD, Guoxiang Shi, MD, Raymond J. Joehl, MD,
ORIGINAL ARTICLES Restoration of Normal Distensive Characteristics of the Esophagogastric Junction After Fundoplication John E. Pandolfino, MD, Jennifer Curry, MD, Guoxiang Shi, MD, Raymond J. Joehl, MD,
Oesophageal motor responses to gastro-oesophageal reflux in healthy controls and reflux patients
 6 Department of Surgery, Guy s Hospital, St Thomas Street, London SE1 9RT, UK A Anggiansah R E K Marshall N F Bright WAOwen WJOwen Department of Radiological Sciences, Guy s Hospital, London, UK G Taylor
6 Department of Surgery, Guy s Hospital, St Thomas Street, London SE1 9RT, UK A Anggiansah R E K Marshall N F Bright WAOwen WJOwen Department of Radiological Sciences, Guy s Hospital, London, UK G Taylor
Does oesophageal motor function improve with time after successful antireflux surgery? Results of
 82 Department of Surgery L Rydberg L Lundell Department of Otorhinolaryngeology, Sahlgrenska University Hospital, University of Goteborg, Goteborg, Sweden M Ruth Correspondence to: Dr Lars Lundell, Department
82 Department of Surgery L Rydberg L Lundell Department of Otorhinolaryngeology, Sahlgrenska University Hospital, University of Goteborg, Goteborg, Sweden M Ruth Correspondence to: Dr Lars Lundell, Department
Health-related quality of life and physiological measurements in achalasia
 Diseases of the Esophagus (2017) 30, 1 5 DOI: 10.1111/dote.12494 Original Article Health-related quality of life and physiological measurements in achalasia Daniel Ross, 1 Joel Richter, 2 Vic Velanovich
Diseases of the Esophagus (2017) 30, 1 5 DOI: 10.1111/dote.12494 Original Article Health-related quality of life and physiological measurements in achalasia Daniel Ross, 1 Joel Richter, 2 Vic Velanovich
JNM Journal of Neurogastroenterology and Motility
 JNM Journal of Neurogastroenterology and Motility J Neurogastroenterol Motil, Vol. 19 No. 1 January, 2013 pissn: 2093-0879 eissn: 2093-0887 http://dx.doi.org/10.5056/jnm.2013.19.1.42 Original Article Observations
JNM Journal of Neurogastroenterology and Motility J Neurogastroenterol Motil, Vol. 19 No. 1 January, 2013 pissn: 2093-0879 eissn: 2093-0887 http://dx.doi.org/10.5056/jnm.2013.19.1.42 Original Article Observations
High Resolution Esophageal Manometry
 High Resolution Esophageal Manometry Dr. Geoffrey Turnbull MD, FRCPC Dalhousie University Dr. Yvonne Tse MD, FRCPC University of Toronto Name: Dr. Geoffrey Turnbull Conflict of Interest Disclosure (over
High Resolution Esophageal Manometry Dr. Geoffrey Turnbull MD, FRCPC Dalhousie University Dr. Yvonne Tse MD, FRCPC University of Toronto Name: Dr. Geoffrey Turnbull Conflict of Interest Disclosure (over
JNM Journal of Neurogastroenterology and Motility
 JNM Journal of Neurogastroenterology and Motility J Neurogastroenterol Motil, Vol. 20 No. 1 January, 2014 pissn: 2093-0879 eissn: 2093-0887 http://dx.doi.org/10.5056/jnm.2014.20.1.74 Original Article Utilizing
JNM Journal of Neurogastroenterology and Motility J Neurogastroenterol Motil, Vol. 20 No. 1 January, 2014 pissn: 2093-0879 eissn: 2093-0887 http://dx.doi.org/10.5056/jnm.2014.20.1.74 Original Article Utilizing
History. Prevalence at Endoscopy. Prevalence and Reflux Sx. Prevalence at Endoscopy. Barrett s Esophagus: Controversy and Management
 Barrett s Esophagus: Controversy and Management History Norman Barrett (1950) Chronic Peptic Ulcer of the Oesophagus and Oesophagitis Allison and Johnstone (1953) The Oesophagus Lined with Gastric Mucous
Barrett s Esophagus: Controversy and Management History Norman Barrett (1950) Chronic Peptic Ulcer of the Oesophagus and Oesophagitis Allison and Johnstone (1953) The Oesophagus Lined with Gastric Mucous
The Combined Collis-Nissen Operation: Early Assessment of Reflwx Control
 ORIGINAL ARTICLES The Combined Collis-Nissen Operation: Early Assessment of Reflwx Control Mark B. Orringer, M.D., and Jay S. Orringer, M.D. ABSTRACT This report summarizes the clinical experience with
ORIGINAL ARTICLES The Combined Collis-Nissen Operation: Early Assessment of Reflwx Control Mark B. Orringer, M.D., and Jay S. Orringer, M.D. ABSTRACT This report summarizes the clinical experience with
Acidic and Non-Acidic Reflux During Sleep Under Conditions of Powerful Acid Suppression*
 Original Research SLEEP MEDICINE Acidic and Non-Acidic Reflux During Sleep Under Conditions of Powerful Acid Suppression* William C. Orr, PhD; Andrea Craddock, PhD; and Suanne Goodrich, PhD Background:
Original Research SLEEP MEDICINE Acidic and Non-Acidic Reflux During Sleep Under Conditions of Powerful Acid Suppression* William C. Orr, PhD; Andrea Craddock, PhD; and Suanne Goodrich, PhD Background:
High-resolution Manometry in Patients with Gastroesophageal Reflux Disease Before and After Fundoplication
 JNM J Neurogastroenterol Motil, Vol. 23 No. 1 January, 2017 pissn: 2093-0879 eissn: 2093-0887 https://doi.org/.5056/jnm16062 Original Article High-resolution Manometry in Patients with Gastroesophageal
JNM J Neurogastroenterol Motil, Vol. 23 No. 1 January, 2017 pissn: 2093-0879 eissn: 2093-0887 https://doi.org/.5056/jnm16062 Original Article High-resolution Manometry in Patients with Gastroesophageal
Mechanisms of Gastroesophageal Reflux in Ambulant Healthy Human Subjects
 GASTROENTEROLOGY 1995;108:83-91 Mechanisms of Gastroesophageal Reflux in Ambulant Healthy Human Subjects MARK N. SCHOEMAN,* MARCUS DEM. TIPPETT,* LOUIS M. A. AKKERMANS,* JOHN DENT,* and RICHARD H. HOLLOWAY*
GASTROENTEROLOGY 1995;108:83-91 Mechanisms of Gastroesophageal Reflux in Ambulant Healthy Human Subjects MARK N. SCHOEMAN,* MARCUS DEM. TIPPETT,* LOUIS M. A. AKKERMANS,* JOHN DENT,* and RICHARD H. HOLLOWAY*
Achalasia is diagnosed by showing dysfunction of lower
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2013;11:131 137 ALIMENTARY TRACT A Comparison of Symptom Severity and Bolus Retention With Chicago Classification Esophageal Pressure Topography Metrics in Patients
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2013;11:131 137 ALIMENTARY TRACT A Comparison of Symptom Severity and Bolus Retention With Chicago Classification Esophageal Pressure Topography Metrics in Patients
Gastroesophageal reflux (GER) Gastroesophageal reflux (GER), the passage of gastric contents into the esophagus, is a normal physiologic process that
 Gastroesophageal reflux (GER) Gastroesophageal reflux (GER), the passage of gastric contents into the esophagus, is a normal physiologic process that may occur daily in healthy infants, children and adults.
Gastroesophageal reflux (GER) Gastroesophageal reflux (GER), the passage of gastric contents into the esophagus, is a normal physiologic process that may occur daily in healthy infants, children and adults.
Barrett s Esophagus. Abdul Sami Khan, M.D. Gastroenterologist Aurora Healthcare Burlington, Elkhorn, Lake Geneva, WI
 Barrett s Esophagus Abdul Sami Khan, M.D. Gastroenterologist Aurora Healthcare Burlington, Elkhorn, Lake Geneva, WI A 58 year-old, obese white man has had heartburn for more than 20 years. He read a magazine
Barrett s Esophagus Abdul Sami Khan, M.D. Gastroenterologist Aurora Healthcare Burlington, Elkhorn, Lake Geneva, WI A 58 year-old, obese white man has had heartburn for more than 20 years. He read a magazine
Effects of anti-reflux surgery on chronic cough and asthma in patients with gastro-oesophageal reflux disease
 RESPIRATORY MEDICINE (2000) 94, 1166 1170 doi:10.1053/rmed.2000.0944, available online at http://www.idealibrary.com on Effects of anti-reflux surgery on chronic cough and asthma in patients with gastro-oesophageal
RESPIRATORY MEDICINE (2000) 94, 1166 1170 doi:10.1053/rmed.2000.0944, available online at http://www.idealibrary.com on Effects of anti-reflux surgery on chronic cough and asthma in patients with gastro-oesophageal
Am J Gastroenterol Feb;109(2):171-7
 This is an author produced version of a paper accepted by The American Journal of Gastroenterology. This paper has been peer-reviewed but does not include the final publisher proof-corrections or journal
This is an author produced version of a paper accepted by The American Journal of Gastroenterology. This paper has been peer-reviewed but does not include the final publisher proof-corrections or journal
The Risk Factors and Quality of Life in Patients with Overlapping Functional Dyspepsia or Peptic Ulcer Disease with Gastroesophageal Reflux Disease
 Gut and Liver, Vol. 8, No. 2, March 2014, pp. 160-164 ORiginal Article The Risk Factors and Quality of Life in Patients with Overlapping Functional Dyspepsia or Peptic Ulcer Disease with Gastroesophageal
Gut and Liver, Vol. 8, No. 2, March 2014, pp. 160-164 ORiginal Article The Risk Factors and Quality of Life in Patients with Overlapping Functional Dyspepsia or Peptic Ulcer Disease with Gastroesophageal
The impact of continuous positive airway pressure on the lower esophageal sphincter
 Am J Physiol Gastrointest Liver Physiol 292: G1200 G1205, 2007. First published January 18, 2007; doi:10.1152/ajpgi.00476.2006. The impact of continuous positive airway pressure on the lower esophageal
Am J Physiol Gastrointest Liver Physiol 292: G1200 G1205, 2007. First published January 18, 2007; doi:10.1152/ajpgi.00476.2006. The impact of continuous positive airway pressure on the lower esophageal
Relations among autonomic nerve dysfunction, oesophageal motility, and gastric emptying in gastro-oesophageal reflux disease
 1436 Gut, 1991,32,1436-1440 ALIMENTARY TRACT Departments of Medicine K M Cunningham M Horowitz J M Wishart and Surgery, University of Adelaide P S Riddell G J Maddern J C Myers G G Jamieson Gastroenterology
1436 Gut, 1991,32,1436-1440 ALIMENTARY TRACT Departments of Medicine K M Cunningham M Horowitz J M Wishart and Surgery, University of Adelaide P S Riddell G J Maddern J C Myers G G Jamieson Gastroenterology
Manometric and symptomatic spectrum of motor dysphagia in a tertiary referral center in northern India
 Indian J Gastroenterol 2010(January February):29(1):18 22 ORIGINAL ARTICLE Manometric and symptomatic spectrum of motor dysphagia in a tertiary referral center in northern India Asha Misra Dipti Chourasia
Indian J Gastroenterol 2010(January February):29(1):18 22 ORIGINAL ARTICLE Manometric and symptomatic spectrum of motor dysphagia in a tertiary referral center in northern India Asha Misra Dipti Chourasia
Esophageal Motility Disorders. Disclosures
 Esophageal Motility Disorders V. Raman Muthusamy, MD FACG Director of Endoscopy Clinical i l Professor of Medicine i David Geffen School of Medicine at UCLA UCLA Health System Disclosures I am an interventional
Esophageal Motility Disorders V. Raman Muthusamy, MD FACG Director of Endoscopy Clinical i l Professor of Medicine i David Geffen School of Medicine at UCLA UCLA Health System Disclosures I am an interventional
Paraesophageal Hernia
 Paraesophageal Hernia Inderpal (Netu) S. Sarkaria, M.D. Vice Chairman, Clinical Affairs Director, Robotic Thoracic Surgery Co-Director, Esophageal and Lung Surgery Institute Speaker/Education: Intuitive
Paraesophageal Hernia Inderpal (Netu) S. Sarkaria, M.D. Vice Chairman, Clinical Affairs Director, Robotic Thoracic Surgery Co-Director, Esophageal and Lung Surgery Institute Speaker/Education: Intuitive
