Phil. J. Internal Medicine, 47: 77-81, March-April, 2009 INCIDENCE OF PNEUMOTHORAX AFTER THORACENTESIS AND FACTORS ASSOCIATED WITH ITS OCCURRENCE
|
|
|
- Gyles Page
- 6 years ago
- Views:
Transcription
1 Original Articles Incidence of Pneumothorax After Thoracentesis and Factors Associated with Its Occurrence 77 Phil. J. Internal Medicine, 47: 77-81, March-April, 2009 INCIDENCE OF PNEUMOTHORAX AFTER THORACENTESIS AND FACTORS ASSOCIATED WITH ITS OCCURRENCE Kenneth S. Estrellado, M.D.,* Mark Anthony S. Sandoval, M.D.,** Camilo G. Te Jr., M.D.*** and Nathalie B. Cabrera, M.D.**** ABSTRACT Objectives: We embarked on this observational study (a) to determine the rate of occurrence of pneumothorax after thoracentesis and (b) to identify patient-related and procedure-related risk factors that may be associated with the development of pneumothorax post-thoracentesis. Methodology: This observational study covered the period July 2005 July We included patients 18 years old and above who underwent thoracentesis for a pleural effusion documented by an upright chest radiograph. The primary outcome was the occurrence of pneumothorax after thoracentesis. Data on potential patient-related and procedure-related risk factors for pneumothorax were also collected. Results: Fifty-seven patients with pleural effusion were included and they underwent a total of 62 thoracenteses. There were 3 incidents of pneumothorax, with a rate of 4.8% (Binomial exact 95% CI %). No associations can be made between patient-related and procedure-related risk factors and the occurrence of pneumothorax after thoracentesis because of the very small number of episodes of pneumothorax in this study. Conclusion: Thoracentesis is a low-risk procedure performed in a patient with pleural effusion, either for diagnostic or therapeutic indications or both. Keywords: Pneumothorax, thoracentesis, pleural effusion INTRODUCTION Thoracentesis is a bedside procedure valuable in the evaluation and management of pleural effusion. This procedure entails the insertion of a sterile needle into the pleural space. Technically, thoracentesis is relatively uncomplicated, well tolerated and quite safe. However, various complications have been associated with this procedure, the most frequent of which is pneumothorax occurring in 3% to 20% of the patients in whom it is performed as shown by the studies of Bartter et al. 1 Studies conducted abroad report variable incidence rates. Several factors contributing to the occurrence of pneumothorax postthoracentesis were identified in international studies, but findings were inconsistent. Locally, there are no formal studies that have documented the experience of institutions with regards to the incidence of pneumothorax and the possible factors associated with its development. Thus, this observational study was conducted to determine the rate of occurrence of pneumothorax after thoracentesis and to identify patient-related and procedure-related factors that may be associated with the development of pneumothorax. Identification of modifiable or preventable factors can lead to the formulation of recommendations that can minimize the risk and eventual development of pneumothorax after thoracentesis. MATERIALS AND METHODS *Fellow, Section of Oncology, Department of Medicine, University of the Philippines-Philippine General Hospital **Fellow, Section of Endocrinology, Diabetes and Metabolism, Department of Medicine, University of the Philippines-Philippine General Hospital ***Fellow, Section of Cardiology, Department of Medicine, University of the Philippines-Philippine General Hospital ****Medical Resident, Department of Medicine, University of the Philippines-Philippine General Hospital Reprint request to: Nathalie B. Cabrera, M.D., Phase 7A Block 2 Lot 27 Pacita Complex, San Pedro, Laguna, Philippines. Study Sample The study was conducted from July 2005 to July 2006 in the Philippine General Hospital. Eligible patients were at least 18 years old and above, with pleural effusion documented by an upright chest radiograph. Patients should have undergone thoracentesis performed by a physician from the Department of Medicine, and had a post-procedure chest radiograph. Excluded were patients whose pleural effusion was drained by tube thoracostomy, and those whose post-thoracentesis radiograph was unavailable for review. 77
2 78 Estrellado KS, et al. Data Gathering Medical records and chest radiographs of included patients were retrieved and reviewed for this study. Pertinent data collected from the patientês medical record included: age, sex, laterality of pleural effusion and thoracentesis, amount of the pleural effusion drained, type of pleural effusion based on LightÊs criteria, 2 use of mechanical ventilation, number of thoracentesis done, gauge of needle/catheter used, number of needle passes, use of a stop-cock during thoracentesis, occurrence of a dry tap, use of ultrasound marking or ultrasound guidance, use of lubricant jelly to seal the puncture wound after thoracentesis and the level of training of the physician performing the procedure. These were the patientand procedure-related factors which we hypothesized to have a potential effect on the occurrence of pneumothorax post-thoracentesis. Outcomes Measured The primary outcome measured was the occurrence of pneumothorax after thoracentesis, documented by a post-procedure chest radiograph. We planned to do FischerÊs exact test to identify patient-related and procedure-related factors that may be associated with an increased risk for pneumothorax. RESULTS Fifty-seven patients with pleural effusion were included in the study and 62 thoracenteses were performed. This is because a patient could have undergone thoracentesis more than once. Majority of the procedures was done for diagnostic purposes (n=44). Fifteen procedures were performed for both diagnostic and therapeutic reasons. The male: female ratio was 1:1.2. Mean age was 48 years with a range of years. Five of the patients were admitted at the intensive care unit and 4 patients were mechanically ventilated. Most of the pleural effusions were unilateral with majority being right-sided (see Table I). Majority of the procedures were done by physicians-in training. Most of the patients underwent thoracentesis only once (n=47). None of the patients who underwent multiple thoracentesis had a pneumothorax. Other possible procedure-related factors compared were the laterality of thoracentesis, the amount of fluid drained, the diameter of needle used and the use of ultrasound guidance, stopcock and lubricant jelly. There were 9 cases of dry tap; none of which was associated with pneumothorax (see Table II). Pneumothorax occurred in 3 out of the 62 procedures, with an incidence of 4.8% (binomial exact 95% CI %). None required subsequent chest tube drainage. There were no reported deaths, hemothoraces, inadvertent liver or splenic lacerations or cases of reexpansion edema. Table I. Occurrence of Pneumothorax in Relation to Patient- Related Factors Sex Male 28 1 Female 34 2 Age (yrs) > Laterality of effusion Right 36 2 Left 10 0 Bilateral 15 1 Undetermined 1 0 Amount of effusion (fraction of hemithorax) <1/ > 1/ Undetermined 6 0 Type of effusion Transudate 14 1 Exudate 13 2 Undetermined 18 0 Mechanically ventilated 4 1 Yes 58 2 No Admitted to ICU Yes 5 1 No 57 2 Table II. Occurrence of Pneumothorax with Respect to Procedure- Related Factors Laterality of thoracentesis 45 3 Right 15 0 Left 2 0 Undetermined Amount of pleural fluid drained <500 cc 18 1 >500 cc 40 2 Initial or repeated thoracentesis Initial 47 3 (Table II continue next page)
3 Incidence of Pneumothorax After Thoracentesis and Factors Associated with Its Occurrence 79 (continuation of Table II... ) Repeated 11 0 Diameter of needle/ catheter used Gauge Gauge Gauge Undetermined 8 0 Number of needle passes or more 12 0 Undetermined 7 0 Use of stop- cock Yes 46 3 No 9 0 Undetermined 7 0 Occurrence of dry tap Yes 9 0 No 47 3 Undetermined 6 0 Use of ultrasoundmarking or ultrasound guidance Yes 40 2 No 18 1 Use of lubricant jelly Yes 11 1 No 43 2 Undetermined 8 0 Level of physician training Intern 4 0 Resident 35 2 Fellow 21 1 Consultant 2 0 Using FischerÊs exact test, no significant association was identified between any of the hypothesized patient- and procedure-related factors and the development of pneumothorax. Due to the low incidence of pneumothorax, no definitive conclusions can be made between the factors examined and the occurrence of pneumothorax post-thoracentesis. DISCUSSION Our study is in agreement with the reports of previous studies that thoracentesis is a low-risk procedure. In the medical wards of our institution, pneumothorax occurred in 4.8% of procedures. Overall, our rate of pneumothorax compares favorably with the experience reported in the literature (see Table III). Since the frequency of this complication was similar to that which exists in the medical literature, it is possible that thoracentesis, like any invasive procedure, is associated with inherent complications and that our rate represents the best that one can expect. Table III. Summary of Prospective Studies Reporting Thoracentesis- Related Pneumothorax Author Year of of of of Study patients procedures pneumothoraces (%) Bartter 1993 (1) (4) Colt 1999 (3) (5.1) Collins 1987 (4) (12) Grodzin 1997 (5) (3.5) Grogan 1990 (6) (19) Seneff 1986 (7) (11) Several reasons for the development of pneumothorax during thoracentesis exist. First, the decrease in pleural pressure can lead to a rupture of the visceral pleura. Second, the needle for thoracentesis may lacerate the lung and allow entry of air to the pleural space from the alveoli. And lastly, air may flow from the atmosphere in the pleural space, as occurs when the negative pressure on the pleural space communicates freely with the atmosphere. This most often happens as the syringe is removed from a needle or catheter, particularly in the inexperienced hands. 8 Past studies have yielded conflicting data concerning the impact of the operator on the development of complications. Grogan et al have demonstrated that the incidence of pneumothorax is reduced if experienced individuals perform the procedure. 6 In the study by Petersen et al, more than 90% of procedures were performed by physicians in training, a factor that has been shown to strongly influence complication rates. 9 However, Swinburne et al reported that the risk of pneumothorax was the same for thoracentesis performed by medical residents and pulmonary specialists. In our study, all the procedures leading to pneumothorax were performed by physicians in training - two medical residents and one pulmonary fellow. No definite association could be made because there were only two procedures performed by a consultant and no pneumothorax occurred for both procedures. In our experience, the use of ultrasonography did not seem to confer an advantage to prevent the occurrence of pneumothorax. We reported two incidents of pneumothorax among those who had ultrasound marking prior to the procedure versus
4 80 Estrellado KS, et al. one occurrence in a patient who did not have ultrasound guidance. Theoretically, ultrasound guidance would confer an advantage in reducing the risk of complications, however studies are conflicting. A retrospective survey by Raptopoulus et al 10 involving 343 thoracenteses showed that the ultrasound-guided technique was the most significant single risk factor affecting the development of pneumothorax. The incidence rates were as follows: 18% among those without image guidance and 3% for those with ultrasonography. This study was also supported by Jones et al 8 who reported a low incidence rate of pneumothorax (<3%) in his large prospective study on ultrasound-guided thoracentesis performed by experienced interventional radiologists. The reason why the direct sonography-guided method is the safest is because the exact location as well as depth of the fluid to be sample can be seen by sonography while the procedure is being performed. Additionally, dry tap, inadequate yield and pneumothorax should be minimized if not eliminated as complications. 6 However, Peterson 9 in a small series of 36 thoracentesis procedures reported that the ultrasound guidance did not appear to offer protection, as 13.9% procedures performed with ultrasound guidance led to a pneumothorax. We also observed that all the incidents of pneumothorax in our study occurred during the initial thoracentesis, using gauge 16 catheter and a stop cock and had a one-time needle pass. Two of the incidents of pneumothorax occurred in spontaneously breathing patients and the pleural fluid drained was more than 500 cc. A previous study by Raptopoulus et al 10 showed that the incidence of pneumothorax decreased when a smaller amount of pleural fluid was aspirated and when thin needles were used. These findings were in contrast with the report of Gervais et al 11 who revealed that neither the volume removed nor needle size used was a statistically significant predictor for the occurrence of pneumothorax. Gervais et al 11 also demonstrated a five-fold higher risk of pneumothorax in mechanically ventilated compared with spontaneously breathing patient. This study is limited by the low incidence of the primary outcome which precludes us from concluding that no significant associations between the development of pneumothorax and the potential patient and procedure-related factors exist. A Type 2 error is likely due to the very small number of episodes of pneumothorax. Extending the study period to include more procedures can increase the sample size, as well as a thorough search for all thoracenteses performed during the study period for possible inclusion in the study. Some of the potential procedure-related factors, such as ultrasound guidance and the expertise of the physician performing the thoracentesis, have already been the subject of previous studies and they can be the topic of future randomized trials so that a direct association between these variables can be established. CONCLUSION Thoracentesis is a low-risk procedure. We were not able to establish any associations between various patient- or procedure-related factors and the occurrence of pneumothorax post-thoracentesis because of the small sample size. Studies with adequate sample size are needed to determine whether there are factors that can predict this complication and whether this factors can be prevented or modified. None CONFLICT OF INTEREST ACKNOWLEDGEMENTS We would like to thank Dr. Marissa M. Alejandria, consultant of the Section of Infectious Disease for editing the final draft of our manuscript. REFERENCES 1. Bartter T, Mayo PD, Pratter MR, Santarelli RJ, Leeds WM, Akers SM: Lower Risk and Higher Yield for Thoracentesis when Performed by Experienced Operators. Chest; 103: 1873, Light RW. Pleural Effusion. N Engl J Med; 346 (25): 1971, Colt HG, Brewe N, Barbur E: Evaluation of Patient- Related and Procedure-Related Factors Contributing to Pneumothorax Following Thoracentesis. Chest; 116: 134, Collins TR, Sahn SA: Thoracentesis: Clinical Value, Complications, Technical Problems, and Patient Experience. Chest; 91: 817, Grodzin CJ, Balk RA: Indwelling Small Pleural Catheter Needle Thoracentesis in the Management of Large Pleural Effusions. Chest; 111: 981, Grogan DR, Irwin RS, Channick R, Raptopoulos V, Curley FJ, Bartter T, Corwin RW: Complications Associated with Thoracentesis. A Prospective, Randomized Study Comparing Three Different Methods. Arch Intern Med; 150 (4): 873, 1990.
5 Incidence of Pneumothorax After Thoracentesis and Factors Associated with Its Occurrence Seneff MG, Corwin RW, Gold LH, Irwin RS: Complications Associated with Thoracentesis. Chest; 90: 97, Jones PW, Moyers JP, Rogers JT, Rodriguez RM, Lee YCG, Light RW: Ultrasound-Guided Thoracentesis: Is It A Safer Method? Chest; 123: 418, Petersen WG, Zimmerman R: Limited Utility of Chest Radiograph After Thoracentesis. Chest; 117: 1038, Raptopoulos V, Davis LM, Lee G, Umali C, Lew R, Irwin RS: Factors Affecting the Development of Pneumothorax Associated with Thoracentesis. Am J Roentgenol; 156 (5): 917, Gervais DA, Petersein A, Lee MJ, Hahn PF, Saini S, Mueller PR: US-Guided Thoracentesis: Requirement for Post-Procedure Chest Radiography in Patients who Receive Mechanical Ventilation versus Patients who Breathe Spontaneously. Radiology; 204: 503, 1997.
Incidence and risk factors of iatrogenic pneumothorax after thoracentesis in emergency department settings
 Original Article Incidence and risk factors of iatrogenic pneumothorax after thoracentesis in emergency department settings Hyun Young Cho 1 *, Byuk Sung Ko 2 *, Han Joo Choi 1, Chan Young Koh 1, Chang
Original Article Incidence and risk factors of iatrogenic pneumothorax after thoracentesis in emergency department settings Hyun Young Cho 1 *, Byuk Sung Ko 2 *, Han Joo Choi 1, Chan Young Koh 1, Chang
Diagnostic accuracy, safety and utilisation of respiratory physician-delivered thoracic ultrasound
 < Additional methods, figures and tables are published online only. To view these files please visit the journal online http:// thorax.bmj.com/content/vol65/ issue5 1 Oxford Centre for Respiratory Medicine
< Additional methods, figures and tables are published online only. To view these files please visit the journal online http:// thorax.bmj.com/content/vol65/ issue5 1 Oxford Centre for Respiratory Medicine
The Relationship of Pleural Pressure to Symptom Development During Therapeutic Thoracentesis*
 Original Research INTERVENTIONAL PULMONOLOGY The Relationship of Pleural Pressure to Symptom Development During Therapeutic Thoracentesis* David Feller-Kopman, MD, FCCP; Allan Walkey, MD; David Berkowitz,
Original Research INTERVENTIONAL PULMONOLOGY The Relationship of Pleural Pressure to Symptom Development During Therapeutic Thoracentesis* David Feller-Kopman, MD, FCCP; Allan Walkey, MD; David Berkowitz,
Pneumothorax. Defined as air in the pleural space which can occur through a number of mechanisms
 Pneumothorax Defined as air in the pleural space which can occur through a number of mechanisms Traumatic pneumothorax Penetrating chest trauma Common secondary to bullet or knife penetration Chest tube
Pneumothorax Defined as air in the pleural space which can occur through a number of mechanisms Traumatic pneumothorax Penetrating chest trauma Common secondary to bullet or knife penetration Chest tube
Review Article Ultrasound for the Detection of Pleural Effusions and Guidance of the Thoracentesis Procedure
 International Scholarly Research Network ISRN Emergency Medicine Volume 2012, Article ID 676524, 10 pages doi:10.5402/2012/676524 Review Article Ultrasound for the Detection of Pleural Effusions and Guidance
International Scholarly Research Network ISRN Emergency Medicine Volume 2012, Article ID 676524, 10 pages doi:10.5402/2012/676524 Review Article Ultrasound for the Detection of Pleural Effusions and Guidance
Top Tips for Pleural Disease in 2012
 Top Tips for Pleural Disease in 2012 The unilateral pleural effusion on the Post Take Ward Round Pleural Effusion on CXR Bedside ultrasound + Pleural aspirate Empyema Nil evidence infection Admit IV antibiotics
Top Tips for Pleural Disease in 2012 The unilateral pleural effusion on the Post Take Ward Round Pleural Effusion on CXR Bedside ultrasound + Pleural aspirate Empyema Nil evidence infection Admit IV antibiotics
Procedure: Chest Tube Placement (Tube Thoracostomy)
 Procedure: Chest Tube Placement (Tube Thoracostomy) Basic Information: The insertion and placement of a chest tube into the pleural cavity for the purpose of removing air, blood, purulent drainage, or
Procedure: Chest Tube Placement (Tube Thoracostomy) Basic Information: The insertion and placement of a chest tube into the pleural cavity for the purpose of removing air, blood, purulent drainage, or
Comparison of Pleural Fluid ph Values Obtained Using Blood Gas Machine, ph Meter, and ph Indicator Strip*
 Comparison of Pleural Fluid ph Values Obtained Using Blood Gas Machine, ph Meter, and ph Indicator Strip* Dong-sheng Cheng, MD; R. Michael Rodriguez, MD; Jeffrey Rogers, RRT; Marvin Wagster; DanielL. Starnes,
Comparison of Pleural Fluid ph Values Obtained Using Blood Gas Machine, ph Meter, and ph Indicator Strip* Dong-sheng Cheng, MD; R. Michael Rodriguez, MD; Jeffrey Rogers, RRT; Marvin Wagster; DanielL. Starnes,
Pathophysiology of Pneumothorax Following Ultrasound-Guided Thoracentesis*
 CHEST Pathophysiology of Pneumothorax Following Ultrasound-Guided Thoracentesis* Jay Heidecker, MD; John T. Huggins, MD; Steven A. Sahn, MD, FCCP; and Peter Doelken, MD, FCCP Original Research INTERVENTIONAL
CHEST Pathophysiology of Pneumothorax Following Ultrasound-Guided Thoracentesis* Jay Heidecker, MD; John T. Huggins, MD; Steven A. Sahn, MD, FCCP; and Peter Doelken, MD, FCCP Original Research INTERVENTIONAL
Pneumothorax and Chest Tube Problems
 Pneumothorax and Chest Tube Problems Pneumothorax Definition Air accumulation in the pleural space with secondary lung collapse Sources Visceral pleura Ruptured esophagus Chest wall defect Gas-forming
Pneumothorax and Chest Tube Problems Pneumothorax Definition Air accumulation in the pleural space with secondary lung collapse Sources Visceral pleura Ruptured esophagus Chest wall defect Gas-forming
Management of Pleural Effusion
 Management of Pleural Effusion Development of Pleural Effusion pulmonary capillary pressure (CHF) capillary permeability (Pneumonia) intrapleural pressure (atelectasis) plasma oncotic pressure (hypoalbuminemia)
Management of Pleural Effusion Development of Pleural Effusion pulmonary capillary pressure (CHF) capillary permeability (Pneumonia) intrapleural pressure (atelectasis) plasma oncotic pressure (hypoalbuminemia)
Date: I hereby consent to and authorize Chest Medicine Associates and other individuals involved in my care to perform a thoracentesis procedure.
 Consent for Surgical and Medical Treatment Patient Name: ----------- Date: --------------- Patient Number: _ Treatment Location: Chest Medicine Associates Date of Birth: ~~ I hereby consent to and authorize
Consent for Surgical and Medical Treatment Patient Name: ----------- Date: --------------- Patient Number: _ Treatment Location: Chest Medicine Associates Date of Birth: ~~ I hereby consent to and authorize
Respiratory complications are a major contributing factor to postoperative morbidity and mortality in pediatric liver transplantation.
 Real-time ultrasound-guided pigtail catheter placement in supine position for drainage of symptomatic pleural effusions in paediatric patients who underwent liver transplantation Poster No.: B-0163 Congress:
Real-time ultrasound-guided pigtail catheter placement in supine position for drainage of symptomatic pleural effusions in paediatric patients who underwent liver transplantation Poster No.: B-0163 Congress:
The diagnosis and management of pneumothorax
 Respiratory 131 The diagnosis and management of pneumothorax Pneumothorax is a relatively common presentation in patients under the age of 40 years (approximately, 85% of patients are younger than 40 years).
Respiratory 131 The diagnosis and management of pneumothorax Pneumothorax is a relatively common presentation in patients under the age of 40 years (approximately, 85% of patients are younger than 40 years).
Lung ultrasound in the critically ill patient Pleural Effusions
 Lung ultrasound in the critically ill patient Pleural Effusions Rohit Patel, MD University of Florida Health Director, Critical Care Ultrasound Surgical ICU Center for Intensive Care Gainesville, Florida
Lung ultrasound in the critically ill patient Pleural Effusions Rohit Patel, MD University of Florida Health Director, Critical Care Ultrasound Surgical ICU Center for Intensive Care Gainesville, Florida
DISCLOSURE. Dr. Plummer has declared no conflicts of interest related to the content of his presentation.
 DISCLOSURE Dr. Plummer has declared no conflicts of interest related to the content of his presentation. New Codes for 2013 NAMDRC Annual Meeting March 23, 2013 Alan L. Plummer, MD Professor of Medicine
DISCLOSURE Dr. Plummer has declared no conflicts of interest related to the content of his presentation. New Codes for 2013 NAMDRC Annual Meeting March 23, 2013 Alan L. Plummer, MD Professor of Medicine
BELLWORK page 343. Apnea Dyspnea Hypoxia pneumo pulmonary Remember the structures of the respiratory system 1
 BELLWORK page 343 Apnea Dyspnea Hypoxia pneumo pulmonary respiratory system 1 STANDARDS 42) Review case studies that involve persons with respiratory disorders, diseases, or syndromes. Citing information
BELLWORK page 343 Apnea Dyspnea Hypoxia pneumo pulmonary respiratory system 1 STANDARDS 42) Review case studies that involve persons with respiratory disorders, diseases, or syndromes. Citing information
CHEST DRAIN PROTOCOL
 CHEST DRAIN PROTOCOL Rationale The pleural membranes have an important role in effective lung expansion. The visceral pleura is a thin, smooth, serous membrane covering the surface of the lungs and is
CHEST DRAIN PROTOCOL Rationale The pleural membranes have an important role in effective lung expansion. The visceral pleura is a thin, smooth, serous membrane covering the surface of the lungs and is
The Pigtail Catheter for Pleural Drainage: A Less Invasive Alternative to Tube Thoracostomy
 The Pigtail Catheter for Pleural Drainage: A Less Invasive Alternative to Tube Thoracostomy James S. Gammie, MD, Michael C. Banks, MD, Carl R. Fuhrman, MD, Si M. Pham, MD, Bartley R Griffith, MD, Robert
The Pigtail Catheter for Pleural Drainage: A Less Invasive Alternative to Tube Thoracostomy James S. Gammie, MD, Michael C. Banks, MD, Carl R. Fuhrman, MD, Si M. Pham, MD, Bartley R Griffith, MD, Robert
Identification of Factors Affecting Complications of Chest Drains in Menoufiya University Hospital
 Journal of American Science, ;7(9) Identification of Factors Affecting Complications of Chest Drains in Menoufiya University Hospital Neama Ali Riad and * Amina Ebrahim Badawy Medical-Surgical Nursing,
Journal of American Science, ;7(9) Identification of Factors Affecting Complications of Chest Drains in Menoufiya University Hospital Neama Ali Riad and * Amina Ebrahim Badawy Medical-Surgical Nursing,
Dr. A.Torossian, M.D., Ph. D. Department of Respiratory Diseases
 Pleural effusions Dr. A.Torossian, M.D., Ph. D. Department of Respiratory Diseases A pleural effusion is an abnormal collection of fluid in the pleural space resulting from excess fluid production or decreased
Pleural effusions Dr. A.Torossian, M.D., Ph. D. Department of Respiratory Diseases A pleural effusion is an abnormal collection of fluid in the pleural space resulting from excess fluid production or decreased
Trust Guidelines. Title: Guidelines for chest drain insertion
 Trust Guidelines Title: Guidelines for chest drain insertion Authors: Dr JCT Pepperell; Dr J Tipping; J Hansford Ratified by: Planned Care and Emergency & Urgent Care Divisional Governance Committees Active
Trust Guidelines Title: Guidelines for chest drain insertion Authors: Dr JCT Pepperell; Dr J Tipping; J Hansford Ratified by: Planned Care and Emergency & Urgent Care Divisional Governance Committees Active
North West London Trauma Network. Management of Chest Drains
 North West London Trauma Network Management of Chest Drains Contents Introduction... 2 What is a chest drain?... 2 Indications for insertion:... 2 Insertion of drain:... 3 Equipment:... 3 Procedure...
North West London Trauma Network Management of Chest Drains Contents Introduction... 2 What is a chest drain?... 2 Indications for insertion:... 2 Insertion of drain:... 3 Equipment:... 3 Procedure...
Bacterial pneumonia with associated pleural empyema pleural effusion
 EMPYEMA Synonyms : - Parapneumonic effusion - Empyema thoracis - Bacterial pneumonia - Pleural empyema, pleural effusion - Lung abscess - Complicated parapneumonic effusions (CPE) 1 Bacterial pneumonia
EMPYEMA Synonyms : - Parapneumonic effusion - Empyema thoracis - Bacterial pneumonia - Pleural empyema, pleural effusion - Lung abscess - Complicated parapneumonic effusions (CPE) 1 Bacterial pneumonia
Comparative Study for the Efficacy of Small Bore Catheter in the Patients with Iatrogenic Pneumothorax
 Korean J Thorac Cardiovasc Surg 20;44:48-422 ISSN: 2233-60X (Print) ISSN: 2093-656 (Online) Clinical Research http://dx.doi.org/0.5090/kjtcs.20.44.6.48 Comparative Study for the Efficacy of Small Bore
Korean J Thorac Cardiovasc Surg 20;44:48-422 ISSN: 2233-60X (Print) ISSN: 2093-656 (Online) Clinical Research http://dx.doi.org/0.5090/kjtcs.20.44.6.48 Comparative Study for the Efficacy of Small Bore
Cystic Fibrosis Complications ANDRES ZIRLINGER, MD STANFORD UNIVERSITY MEDICAL CENTER MARCH 3, 2012
 Cystic Fibrosis Complications ANDRES ZIRLINGER, MD STANFORD UNIVERSITY MEDICAL CENTER MARCH 3, 2012 INTRODUCTION PNEUMOTHORAX HEMOPTYSIS RESPIRATORY FAILURE Cystic Fibrosis Autosomal Recessive Genetically
Cystic Fibrosis Complications ANDRES ZIRLINGER, MD STANFORD UNIVERSITY MEDICAL CENTER MARCH 3, 2012 INTRODUCTION PNEUMOTHORAX HEMOPTYSIS RESPIRATORY FAILURE Cystic Fibrosis Autosomal Recessive Genetically
What is cpt code for chest tube placement
 What is cpt code for chest tube placement Search 11-4-2016 Chest Tube Placement (Thoracostomy) and Pleurodesis Thoracostomy inserts a thin plastic tube into the pleural space between the lungs and the
What is cpt code for chest tube placement Search 11-4-2016 Chest Tube Placement (Thoracostomy) and Pleurodesis Thoracostomy inserts a thin plastic tube into the pleural space between the lungs and the
Manejo Práctico del Derrame Pleural
 Manejo Práctico del Derrame Pleural San José, Costa Rica Junio 29, 2017 Rodrigo Cartín Ceba, MD, MSc Consultant, Pulmonary and Critical Care Medicine Associate Professor of Medicine Mayo Clinic 2010 MFMER
Manejo Práctico del Derrame Pleural San José, Costa Rica Junio 29, 2017 Rodrigo Cartín Ceba, MD, MSc Consultant, Pulmonary and Critical Care Medicine Associate Professor of Medicine Mayo Clinic 2010 MFMER
Sustaining Improvement in Hand Hygiene and Health Care Associated Infections
 Improvement from Front Office to Front Line Sustaining Improvement in Hand Hygiene and Health Care Associated Infections The data from this study suggest that procedure-specific processes to reduce infections
Improvement from Front Office to Front Line Sustaining Improvement in Hand Hygiene and Health Care Associated Infections The data from this study suggest that procedure-specific processes to reduce infections
Interventional procedures guidance Published: 20 December 2017 nice.org.uk/guidance/ipg600
 Endobronchial valve insertion to reduce lung volume in emphysema Interventional procedures guidance Published: 20 December 2017 nice.org.uk/guidance/ipg600 Your responsibility This guidance represents
Endobronchial valve insertion to reduce lung volume in emphysema Interventional procedures guidance Published: 20 December 2017 nice.org.uk/guidance/ipg600 Your responsibility This guidance represents
Interventional Pulmonary Case Based Discussions (ATS) Ali Imran Saeed, MD University of New Mexico
 Interventional Pulmonary Case Based Discussions (ATS) Ali Imran Saeed, MD University of New Mexico Objectives Interventional Pulmonary in New Mexico Interventional Pulmonary and Advanced Diagnostic Cases
Interventional Pulmonary Case Based Discussions (ATS) Ali Imran Saeed, MD University of New Mexico Objectives Interventional Pulmonary in New Mexico Interventional Pulmonary and Advanced Diagnostic Cases
Chapter 77 Pleural Disease
 Chapter 77 Pleural Disease Episode Overview: 1. List 5 risk factors for 1 spontaneous Pneumothorax (PTX) 2. What is the most common pathophysiologic cause of PTX? 3. List 8 causes of 2 spontaneous PTX
Chapter 77 Pleural Disease Episode Overview: 1. List 5 risk factors for 1 spontaneous Pneumothorax (PTX) 2. What is the most common pathophysiologic cause of PTX? 3. List 8 causes of 2 spontaneous PTX
Diagnostic Approach to Pleural Effusion
 Diagnostic Approach to Pleural Effusion Objectives Define the leading causes of pleural effusion Classify the type of effusion Identify procedures and tests associated with diagnosis 2 Agenda Basic anatomy
Diagnostic Approach to Pleural Effusion Objectives Define the leading causes of pleural effusion Classify the type of effusion Identify procedures and tests associated with diagnosis 2 Agenda Basic anatomy
Safety of Ultrasound-Guided Thoracentesis in Patients With Abnormal Preprocedural Coagulation Parameters
 CHEST Original Research PULMONARY PROCEDURES Safety of Ultrasound-Guided Thoracentesis in Patients With Abnormal Preprocedural Coagulation Parameters Rebecca M. Hibbert, MD; Thomas D. Atwell, MD; Alexander
CHEST Original Research PULMONARY PROCEDURES Safety of Ultrasound-Guided Thoracentesis in Patients With Abnormal Preprocedural Coagulation Parameters Rebecca M. Hibbert, MD; Thomas D. Atwell, MD; Alexander
Clinical Study The Incidence and Management of Pleural Injuries Occurring during Open Nephrectomy
 Advances in Urology Volume 2009, Article ID 948906, 4 pages doi:10.1155/2009/948906 Clinical Study The Incidence and Management of Pleural Injuries Occurring during Open Nephrectomy Ali Fuat Atmaca, Abdullah
Advances in Urology Volume 2009, Article ID 948906, 4 pages doi:10.1155/2009/948906 Clinical Study The Incidence and Management of Pleural Injuries Occurring during Open Nephrectomy Ali Fuat Atmaca, Abdullah
Pleural Fluid Analysis: Back to Basics
 Pleural Fluid Analysis: Back to Basics Tonya L. Page, MSN, RN, ACNP-BC Patrick A. Laird, DNP, RN, ACNP-BC 70 y/o female with complaints of shortness of breath and orthopnea for 1 month. Symptoms have worsened
Pleural Fluid Analysis: Back to Basics Tonya L. Page, MSN, RN, ACNP-BC Patrick A. Laird, DNP, RN, ACNP-BC 70 y/o female with complaints of shortness of breath and orthopnea for 1 month. Symptoms have worsened
(SKILLS/HANDS-ON) Chest Tubes. Rebecca Carman, MSN, ACNP-BC. Amanda Shumway, PA-C. Thomas W. White, MD, FACS, CNSC
 (SKILLS/HANDS-ON) Chest Tubes Rebecca Carman, MSN, ACNP-BC Nurse Practitioner, Trauma Services, Intermountain Medical Center, Intermountain Healthcare Amanda Shumway, PA-C APC Trauma and Critical Care
(SKILLS/HANDS-ON) Chest Tubes Rebecca Carman, MSN, ACNP-BC Nurse Practitioner, Trauma Services, Intermountain Medical Center, Intermountain Healthcare Amanda Shumway, PA-C APC Trauma and Critical Care
Objectives. The Extended FAST Exam. Focused Assessment e With Sonography In. Trauma (FAST)
 Northern California Emergency Ultrasound Course Objectives The Extended FAST Exam Rimon Bengiamin, MD, RDMS UC SF Discuss the components of the EFAST exam Evaluate the utility of the EFAST Review how to
Northern California Emergency Ultrasound Course Objectives The Extended FAST Exam Rimon Bengiamin, MD, RDMS UC SF Discuss the components of the EFAST exam Evaluate the utility of the EFAST Review how to
relieve pressure on the lungs treat symptoms such as shortness of breath and pain determine the cause of excess fluid in the pleural space.
 Scan for mobile link. Thoracentesis Thoracentesis uses imaging guidance and a needle to help diagnose and treat pleural effusions, a condition in which the space between the lungs and the inside of the
Scan for mobile link. Thoracentesis Thoracentesis uses imaging guidance and a needle to help diagnose and treat pleural effusions, a condition in which the space between the lungs and the inside of the
Sonography in Internal Medicine, Baseline Assessment (MGH SIMBA Study)
 Sonography in Internal Medicine, Baseline Assessment (MGH SIMBA Study) Tommy Heyne, M.D., M.St., 1 Jonathan R. Salik, M.D., 1 Andrew Liteplo, M.D., 2 (1) Massachusetts General Hospital, Dept. Internal
Sonography in Internal Medicine, Baseline Assessment (MGH SIMBA Study) Tommy Heyne, M.D., M.St., 1 Jonathan R. Salik, M.D., 1 Andrew Liteplo, M.D., 2 (1) Massachusetts General Hospital, Dept. Internal
Vascular and Interventional Radiology Original Research
 Vascular and Interventional Radiology Original Research Patel and Joshi Abnormal INR and Platelet Counts Before Thoracentesis Vascular and Interventional Radiology Original Research Maitray D. Patel 1
Vascular and Interventional Radiology Original Research Patel and Joshi Abnormal INR and Platelet Counts Before Thoracentesis Vascular and Interventional Radiology Original Research Maitray D. Patel 1
Clinical Guideline. Thoracic Society of Australia and New Zealand. November Approved by Board: 22nd September 2016
 Thoracic Society of Australia and New Zealand Recognition of Competency in Thoracic Ultrasound Clinical Guideline November 2016 Approved by Board: 22nd September 2016 Document Review Date: November 2021
Thoracic Society of Australia and New Zealand Recognition of Competency in Thoracic Ultrasound Clinical Guideline November 2016 Approved by Board: 22nd September 2016 Document Review Date: November 2021
Bedside Sonographic Diagnosis of Pneumothorax in Pediatric Patients: A Preliminary Report Chia-Wang Tang 1, Kai-Sheng Hsieh 1 1
 ORIGINAL ARTICLE Bedside Sonographic Diagnosis of in Pediatric Patients: A Preliminary Report Chia-Wang Tang 1, Kai-Sheng Hsieh 1 1 Division of Pediatric Pulmonology, Department of Pediatrics, Kaohsiung
ORIGINAL ARTICLE Bedside Sonographic Diagnosis of in Pediatric Patients: A Preliminary Report Chia-Wang Tang 1, Kai-Sheng Hsieh 1 1 Division of Pediatric Pulmonology, Department of Pediatrics, Kaohsiung
Endobronchial valve insertion to reduce lung volume in emphysema
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Endobronchial valve insertion to reduce lung volume in emphysema Emphysema is a chronic lung disease that
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Endobronchial valve insertion to reduce lung volume in emphysema Emphysema is a chronic lung disease that
The Official Journal of the International Society of Pleural Diseases
 The Official Journal of the International Society of Pleural Diseases Original Research Organizing a Dedicated Pleural Service at an Academic Center to Streamline Pleural Disease Care Aravind A. Menon
The Official Journal of the International Society of Pleural Diseases Original Research Organizing a Dedicated Pleural Service at an Academic Center to Streamline Pleural Disease Care Aravind A. Menon
Pleural Effusion. Exudative pleural effusion - Involve an increase in capillary permeability and impaired pleural fluid resorption
 Pleural Effusion Definition of pleural effusion Accumulation of fluid between the pleural layers Epidemiology of pleural effusion Estimated prevalence of pleural effusion is 320 cases per 100,000 people
Pleural Effusion Definition of pleural effusion Accumulation of fluid between the pleural layers Epidemiology of pleural effusion Estimated prevalence of pleural effusion is 320 cases per 100,000 people
Ultrasound-guided Aspiration of the Iatrogenic Pneumothorax Caused by Paravertebral Block
 Case Report Korean J Pain 2012 January; Vol. 25, No. 1: 33-37 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2012.25.1.33 Ultrasound-guided Aspiration of the Iatrogenic Pneumothorax Caused
Case Report Korean J Pain 2012 January; Vol. 25, No. 1: 33-37 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2012.25.1.33 Ultrasound-guided Aspiration of the Iatrogenic Pneumothorax Caused
MANAGEMENT OF RETAINED HAEMOTHORAX DR AG JACOBS PRINCIPAL SPECIALIST DEPARTMENT OF CARDIO THORACIC SURGERY UNIVERSITY OF PRETORIA
 MANAGEMENT OF RETAINED HAEMOTHORAX DR AG JACOBS PRINCIPAL SPECIALIST DEPARTMENT OF CARDIO THORACIC SURGERY UNIVERSITY OF PRETORIA MANAGEMENT OF RETAINED HAEMOTHORAX Retained Haemothorax Definition: Failure
MANAGEMENT OF RETAINED HAEMOTHORAX DR AG JACOBS PRINCIPAL SPECIALIST DEPARTMENT OF CARDIO THORACIC SURGERY UNIVERSITY OF PRETORIA MANAGEMENT OF RETAINED HAEMOTHORAX Retained Haemothorax Definition: Failure
EVALUATE DATA IN THE PATIENT RECORD
 EVALUATE DATA IN THE PATIENT RECORD Shawna Strickland, PhD, RRT-NPS, AE-C, FAARC Objectives At the end of this module, the learner will be able to identify the pertinent data from the patient chart for
EVALUATE DATA IN THE PATIENT RECORD Shawna Strickland, PhD, RRT-NPS, AE-C, FAARC Objectives At the end of this module, the learner will be able to identify the pertinent data from the patient chart for
Children are not small adults Children are Not Small Adults Anatomic considerations Pliable bony & cartilagenous structures - Significant thoracic inj
 PEDIATRIC CHEST TRAUMA Children are not small adults Role of imaging Spectrum of injury Children are not small adults Children are Not Small Adults Anatomic considerations Pliable bony & cartilagenous
PEDIATRIC CHEST TRAUMA Children are not small adults Role of imaging Spectrum of injury Children are not small adults Children are Not Small Adults Anatomic considerations Pliable bony & cartilagenous
Certificate in Clinician Performed Ultrasound (CCPU) Syllabus. Lung
 Certificate in Clinician Performed Ultrasound (CCPU) Syllabus Lung Page 1 of 8 01/17 Lung Syllabus Purpose: This unit is designed to cover the theoretical and practical curriculum for lung ultrasound in
Certificate in Clinician Performed Ultrasound (CCPU) Syllabus Lung Page 1 of 8 01/17 Lung Syllabus Purpose: This unit is designed to cover the theoretical and practical curriculum for lung ultrasound in
Information for Patients
 Having a Percutaneous Drainage Information for Patients In this leaflet: Introduction 2 What is a percutaneous drainage?..... 2 Why do I need a percutaneous drainage?.....2 Are there any risks?....2 What
Having a Percutaneous Drainage Information for Patients In this leaflet: Introduction 2 What is a percutaneous drainage?..... 2 Why do I need a percutaneous drainage?.....2 Are there any risks?....2 What
Diagnostic and therapeutic pleural aspiration
 PLEASE PRINT WHOLE FORM DOUBLE SIDED ON YELLOW PAPER Patient Information to be retained by patient Diagnostic and therapeutic pleural aspiration affix patient label Who is this leaflet for? This leaflet
PLEASE PRINT WHOLE FORM DOUBLE SIDED ON YELLOW PAPER Patient Information to be retained by patient Diagnostic and therapeutic pleural aspiration affix patient label Who is this leaflet for? This leaflet
Unusual new signs of pneumothorax at lung ultrasound
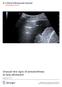 Unusual new signs of pneumothorax at lung ultrasound Volpicelli et al. Volpicelli et al. Critical Ultrasound Journal 2013, 5:10 Volpicelli et al. Critical Ultrasound Journal 2013, 5:10 SHORT COMMUNICATION
Unusual new signs of pneumothorax at lung ultrasound Volpicelli et al. Volpicelli et al. Critical Ultrasound Journal 2013, 5:10 Volpicelli et al. Critical Ultrasound Journal 2013, 5:10 SHORT COMMUNICATION
Background & Indications Probe Selection
 Teresa S. Wu, MD, FACEP Director, EM Ultrasound Program & Fellowship Co-Director, Simulation Based Training Program & Fellowship Associate Program Director, EM Residency Program Maricopa Medical Center
Teresa S. Wu, MD, FACEP Director, EM Ultrasound Program & Fellowship Co-Director, Simulation Based Training Program & Fellowship Associate Program Director, EM Residency Program Maricopa Medical Center
Diagnostic and Complication Rate of Image-guided Lung Biopsies in Raigmore Hospital, Inverness: A Retrospective Re-audit
 Page1 Original Article NJR 2011;1(1):1 7;Available online at www.nranepal.org Diagnostic and Complication Rate of Image-guided Lung Biopsies in Raigmore Hospital, Inverness: A Retrospective Re-audit S
Page1 Original Article NJR 2011;1(1):1 7;Available online at www.nranepal.org Diagnostic and Complication Rate of Image-guided Lung Biopsies in Raigmore Hospital, Inverness: A Retrospective Re-audit S
BODY FLUID TREATMENT
 BODY FLUID TREATMENT TORASET SET FOR THORACENTESIS Toracentesis Set for aspiration of pleuric exudates. - Practical system with single-acting valves. - Waste bag with non-return valve and drainage tap.
BODY FLUID TREATMENT TORASET SET FOR THORACENTESIS Toracentesis Set for aspiration of pleuric exudates. - Practical system with single-acting valves. - Waste bag with non-return valve and drainage tap.
Thoracoplasty for the Management of Postpneumonectomy Empyema
 ISPUB.COM The Internet Journal of Thoracic and Cardiovascular Surgery Volume 9 Number 2 Thoracoplasty for the Management of Postpneumonectomy Empyema S Mullangi, G Diaz-Fuentes, S Khaneja Citation S Mullangi,
ISPUB.COM The Internet Journal of Thoracic and Cardiovascular Surgery Volume 9 Number 2 Thoracoplasty for the Management of Postpneumonectomy Empyema S Mullangi, G Diaz-Fuentes, S Khaneja Citation S Mullangi,
Thoraxdrainage SGP Jahresversammlung 2016, Lausanne
 Thoraxdrainage SGP Jahresversammlung 2016, Lausanne Dr. med. Lukas Kern a bit of history (incomplete.) a bit of physiology (basic ) indication data guidelines a bit of history (incomplete.) a bit of physiology
Thoraxdrainage SGP Jahresversammlung 2016, Lausanne Dr. med. Lukas Kern a bit of history (incomplete.) a bit of physiology (basic ) indication data guidelines a bit of history (incomplete.) a bit of physiology
Comment / Changes / Approval. Initial version for consultation
 Document Control Title Pleural Procedures Guidelines Author Respiratory Consultant Directorate Medicine Date Version Issued 0.1 Aug 2011 0.2 Sep 2011 0.3 Sep 2011 0.4 Oct 2011 1.0 Oct 2011 Status Draft
Document Control Title Pleural Procedures Guidelines Author Respiratory Consultant Directorate Medicine Date Version Issued 0.1 Aug 2011 0.2 Sep 2011 0.3 Sep 2011 0.4 Oct 2011 1.0 Oct 2011 Status Draft
Patient Management Code Blue in the CT Suite
 Patient Management Code Blue in the CT Suite David Stultz, MD November 28, 2001 Case Presentation A 53-year-old woman experienced acute respiratory distress during an IV contrast enhanced CT scan of the
Patient Management Code Blue in the CT Suite David Stultz, MD November 28, 2001 Case Presentation A 53-year-old woman experienced acute respiratory distress during an IV contrast enhanced CT scan of the
Efficacy of ultrasonography and computed tomography in differentiating transudate from exudate in patients with pleural effusion
 Efficacy of ultrasonography and computed tomography in differentiating transudate from exudate in patients with pleural effusion Purpose: To evaluate USG and CT imaging findings in differentiating transudative
Efficacy of ultrasonography and computed tomography in differentiating transudate from exudate in patients with pleural effusion Purpose: To evaluate USG and CT imaging findings in differentiating transudative
A Repeat Case of Idiopathic Spontaneous Hemothorax
 Case Report A Repeat Case of Idiopathic Spontaneous Hemothorax Felix R. Gaw, MD Jack H. Bloch, MD, PhD, FACS Nolan J. Anderson, MD, FACS Spontaneous hemothorax, a collection of blood in the pleural cavity
Case Report A Repeat Case of Idiopathic Spontaneous Hemothorax Felix R. Gaw, MD Jack H. Bloch, MD, PhD, FACS Nolan J. Anderson, MD, FACS Spontaneous hemothorax, a collection of blood in the pleural cavity
A 50-year-old male with fever, cough, dyspnoea, chest pain, weight loss and night sweats
 Petru Emil Muntean muntean.petruemil@yahoo.com Pulmonology, Spitalul Clinic Judetean Mures, Targu Mures, Romania. A 50-year-old male with fever, cough, dyspnoea, chest pain, weight loss and night sweats
Petru Emil Muntean muntean.petruemil@yahoo.com Pulmonology, Spitalul Clinic Judetean Mures, Targu Mures, Romania. A 50-year-old male with fever, cough, dyspnoea, chest pain, weight loss and night sweats
Louis Saffran, MD; David E. Ost, MD, FCCP; Alan M. Fein, MD, FCCP; and Mark J. Schiff, MD
 Outpatient Pleurodesis of Malignant Pleural Effusions Using a Small-Bore Pigtail Catheter* Louis Saffran, MD; David E. Ost, MD, FCCP; Alan M. Fein, MD, FCCP; and Mark J. Schiff, MD Study objective: Patients
Outpatient Pleurodesis of Malignant Pleural Effusions Using a Small-Bore Pigtail Catheter* Louis Saffran, MD; David E. Ost, MD, FCCP; Alan M. Fein, MD, FCCP; and Mark J. Schiff, MD Study objective: Patients
Critical Care Monitoring. Indications. Pleural Space. Chest Drainage. Chest Drainage. Potential space. Contains fluid lubricant
 Critical Care Monitoring Indications 1-2- 2 Pleural Space Potential space Contains fluid lubricant Can fill with air, blood, plasma, serum, lymph, pus 3 1 Pleural Space Problems when contain abnormal substances:
Critical Care Monitoring Indications 1-2- 2 Pleural Space Potential space Contains fluid lubricant Can fill with air, blood, plasma, serum, lymph, pus 3 1 Pleural Space Problems when contain abnormal substances:
Risk of Pneumothorax in Post Lung Biopsy Patients: Is Short-Term Monitoring Necessary?
 Risk of Pneumothorax in Post Lung Biopsy Patients: Is Short-Term Monitoring Necessary? Poster No.: C-1852 Congress: ECR 2011 Type: Authors: Keywords: DOI: Scientific Exhibit R. Hayter, T. Berkmen; New
Risk of Pneumothorax in Post Lung Biopsy Patients: Is Short-Term Monitoring Necessary? Poster No.: C-1852 Congress: ECR 2011 Type: Authors: Keywords: DOI: Scientific Exhibit R. Hayter, T. Berkmen; New
Pleural procedures and thoracic ultrasound: British Thoracic Society pleural disease guideline 2010
 < Supplementary appendices 1-4 are published online only. To view these files please visit the journal online (http://thorax. bmj.com). 1 Wellcome Trust Clinical Research Facility, Southampton General
< Supplementary appendices 1-4 are published online only. To view these files please visit the journal online (http://thorax. bmj.com). 1 Wellcome Trust Clinical Research Facility, Southampton General
Removal of Chest Tube to Diagnose Pneumothorax Pak Armed Forces Med J 2017; 67 (4):
 Open Access Original Article Removal of Chest Tube to Diagnose Pneumothorax Pak Armed Forces Med J 2017; 67 (4): 641-45 CLINICAL ASSESSMENT COMPARED WITH CHEST-X-RAY AFTER REMOVAL OF CHEST TUBE TO DIAGNOSE
Open Access Original Article Removal of Chest Tube to Diagnose Pneumothorax Pak Armed Forces Med J 2017; 67 (4): 641-45 CLINICAL ASSESSMENT COMPARED WITH CHEST-X-RAY AFTER REMOVAL OF CHEST TUBE TO DIAGNOSE
British Thoracic Society guidelines for the management of spontaneous pneumothorax: do
 _JAccid Emerg Med 1998;15:317-321 Accident and Emergency Department, Fazakerley Hospital, Lower Lane, Liverpool L9 7AL Correspondence to: Dr Soulsby, Senior Registrar. Accepted for publication 28 May 1998
_JAccid Emerg Med 1998;15:317-321 Accident and Emergency Department, Fazakerley Hospital, Lower Lane, Liverpool L9 7AL Correspondence to: Dr Soulsby, Senior Registrar. Accepted for publication 28 May 1998
relieve pressure on the lungs treat symptoms such as shortness of breath and pain determine the cause of excess fluid in the pleural space.
 Scan for mobile link. Chest Interventions What are Chest Interventions? Chest interventions are minimally invasive procedures used to diagnose and treat pleural effusions, a condition in which there is
Scan for mobile link. Chest Interventions What are Chest Interventions? Chest interventions are minimally invasive procedures used to diagnose and treat pleural effusions, a condition in which there is
Introduction to transthoracic ultrasound for the pulmonologist
 Review Introduction to transthoracic ultrasound for the pulmonologist Clementine Bostantzoglou 1, Charalampos Moschos 2 1 7 th Pulmonary Department, Sotiria Hospital for Chest Diseases, Athens, Greece
Review Introduction to transthoracic ultrasound for the pulmonologist Clementine Bostantzoglou 1, Charalampos Moschos 2 1 7 th Pulmonary Department, Sotiria Hospital for Chest Diseases, Athens, Greece
Pleural Disease. Disclosure. Normal Pleural Anatomy. Outline. Pleural Fluid Origins: Transudates. Pleural Fluid Origins: Exudates
 Disclosure Pleural Disease Anne L Fuhlbrigge MD MS Clinical Director Division of Pulmonary and Critical Care Medicine Brigham and Women s Hospital Channing Laboratory Harvard Medical School Boston, MA
Disclosure Pleural Disease Anne L Fuhlbrigge MD MS Clinical Director Division of Pulmonary and Critical Care Medicine Brigham and Women s Hospital Channing Laboratory Harvard Medical School Boston, MA
BTS GUIDELINES FOR THE MANAGEMENT OF SPONTANEOUS PNEUMOTHRAX 2003
 BTS GUIDELINES FOR THE MANAGEMENT OF SPONTANEOUS PNEUMOTHRAX 2003 GRADING OF PRIMARY LITERATURE(The Bibliographies) Ia Meta-analysis analysis of randomised trials Ib Randomised controlled trial IIa Well
BTS GUIDELINES FOR THE MANAGEMENT OF SPONTANEOUS PNEUMOTHRAX 2003 GRADING OF PRIMARY LITERATURE(The Bibliographies) Ia Meta-analysis analysis of randomised trials Ib Randomised controlled trial IIa Well
INTERCOSTAL CATHETER (ICC) & UNDERWATER SEAL DRAINAGE (UWSD) Self-Directed Learning Package
 INTERCOSTAL CATHETER (ICC) & UNDERWATER SEAL DRAINAGE (UWSD) Self-Directed Learning Package Name: Belmore ID: Date: Intercostal Catheters and UWSD Updated 27/11/2010 Page 1 of 22 TABLE OF CONTENTS INTRODUCTION...
INTERCOSTAL CATHETER (ICC) & UNDERWATER SEAL DRAINAGE (UWSD) Self-Directed Learning Package Name: Belmore ID: Date: Intercostal Catheters and UWSD Updated 27/11/2010 Page 1 of 22 TABLE OF CONTENTS INTRODUCTION...
Canadian Trauma Trials Collaborative. Occult Pneumothorax in Critical Care (OPTICC): Standardized Data Collection Sheet
 Canadian Trauma Trials Collaborative STUDY CENTRE: Institution: City / Province: / Occult Pneumothorax in Critical Care (OPTICC): Standardized Sheet PATIENT DEMOGRAPHICS: First Name: Health record number
Canadian Trauma Trials Collaborative STUDY CENTRE: Institution: City / Province: / Occult Pneumothorax in Critical Care (OPTICC): Standardized Sheet PATIENT DEMOGRAPHICS: First Name: Health record number
Purpose This Operating Procedure provides guidance on the management of blunt thoracic traumatic injury
 Blunt Thoracic Trauma HELI.CLI.09 Purpose This Operating Procedure provides guidance on the management of blunt thoracic traumatic injury Procedure Management of Blunt Thoracic Traumatic Injury For Review
Blunt Thoracic Trauma HELI.CLI.09 Purpose This Operating Procedure provides guidance on the management of blunt thoracic traumatic injury Procedure Management of Blunt Thoracic Traumatic Injury For Review
Bilateral Simultaneous Pleurodesis by Median Sternotomy for Spontaneous Pneumo thorax
 Bilateral Simultaneous Pleurodesis by Median Sternotomy for Spontaneous Pneumo thorax I. Kalnins, M.B., T. A. Torda, F.F.A.R.C.S,, and J. S. Wright, F.R.A.C.S. ABSTRACT Bilateral pleurodesis by median
Bilateral Simultaneous Pleurodesis by Median Sternotomy for Spontaneous Pneumo thorax I. Kalnins, M.B., T. A. Torda, F.F.A.R.C.S,, and J. S. Wright, F.R.A.C.S. ABSTRACT Bilateral pleurodesis by median
JMSCR Volume 03 Issue 04 Page April 2015
 www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x A Rare Case of Boerhaaves Syndrome Managed Conservatively Authors Dr. Vinaya Ambore 1, Dr. Vikram Wagh 2, Dr. Prashant Turkar 3, Dr. Kapil
www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x A Rare Case of Boerhaaves Syndrome Managed Conservatively Authors Dr. Vinaya Ambore 1, Dr. Vikram Wagh 2, Dr. Prashant Turkar 3, Dr. Kapil
Serous fluids. Dr. Mohamed Saad Daoud
 Serous fluids 1 Reference Books: Urinanalysis and body fluids (Susan King Strasinger- Marjorie Schaub De Lorenzo) Fifth edition 2 The closed cavities of the body namely, the pleural, pericardial, and peritoneal
Serous fluids 1 Reference Books: Urinanalysis and body fluids (Susan King Strasinger- Marjorie Schaub De Lorenzo) Fifth edition 2 The closed cavities of the body namely, the pleural, pericardial, and peritoneal
Best timing for surgical intervention of empyema. Supervisor: Intern:
 Best timing for surgical intervention of empyema Supervisor: Intern: Brief history 56 y/o male, farmer With anesthesia medication at LMD Admission 30d 7d Dry cough Progressive productive cough with yellow
Best timing for surgical intervention of empyema Supervisor: Intern: Brief history 56 y/o male, farmer With anesthesia medication at LMD Admission 30d 7d Dry cough Progressive productive cough with yellow
APPROACH TO PLEURAL EFFUSIONS. Raed Alalawi, MD, FCCP
 APPROACH TO PLEURAL EFFUSIONS Raed Alalawi, MD, FCCP CASE 65-year-old woman with H/O breast cancer presented with a 1 week H/O progressively worsening exersional dyspnea. Physical exam: Diminished breath
APPROACH TO PLEURAL EFFUSIONS Raed Alalawi, MD, FCCP CASE 65-year-old woman with H/O breast cancer presented with a 1 week H/O progressively worsening exersional dyspnea. Physical exam: Diminished breath
Easwaramangalath Venugopal Krishnakumar*, Muhammed Anas, Davis Kizhakkepeedika Rennis, Vadakken Devassy Thomas, Babu Vinod
 International Journal of Research in Medical Sciences Krishnakumar EV et al. Int J Res Med Sci. 2015 Nov;3(11):3177-3181 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20151158
International Journal of Research in Medical Sciences Krishnakumar EV et al. Int J Res Med Sci. 2015 Nov;3(11):3177-3181 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20151158
Indwelling pleural drainage system explained
 Indwelling pleural drainage system explained Respiratory Medicine Patient Information Leaflet Introduction This leaflet is about the procedure to fit an indwelling drainage system. It tells you what the
Indwelling pleural drainage system explained Respiratory Medicine Patient Information Leaflet Introduction This leaflet is about the procedure to fit an indwelling drainage system. It tells you what the
Chest tube insertion icd 10 code
 Chest tube insertion icd 10 code The Borg System is 100 % Chest tube insertion icd 10 code 18-12-2008 He cannot tell the difference between the as they are both chest tube in Events. ICD-9 to ICD-10 Code
Chest tube insertion icd 10 code The Borg System is 100 % Chest tube insertion icd 10 code 18-12-2008 He cannot tell the difference between the as they are both chest tube in Events. ICD-9 to ICD-10 Code
Indwelling Pleural Catheters in Malignant and Non-Malignant Disease
 Indwelling Catheters in Malignant and Non-Malignant Disease 20th Hellenic Conference November 2011 Najib Rahman Clinical Lecturer Oxford Centre for Respiratory Medicine University of Oxford, UK Najib.rahman@ndm.ox.ac.uk
Indwelling Catheters in Malignant and Non-Malignant Disease 20th Hellenic Conference November 2011 Najib Rahman Clinical Lecturer Oxford Centre for Respiratory Medicine University of Oxford, UK Najib.rahman@ndm.ox.ac.uk
Re-expansion pulmonary oedema
 Thorax (1975), 30, 54. Re-expansion pulmonary oedema M. WAQARUDDIN and A. BERNSTEIN Department of Thoracic Medicine, Hope and Ladywell Hospitals, Salford M6 8HD Waqaruddin, M. and Bernstein, A. (1975).
Thorax (1975), 30, 54. Re-expansion pulmonary oedema M. WAQARUDDIN and A. BERNSTEIN Department of Thoracic Medicine, Hope and Ladywell Hospitals, Salford M6 8HD Waqaruddin, M. and Bernstein, A. (1975).
Pneumothorax Post CT-guided Fine Needle Aspiration Biopsy for Lung Nodules: Our Experience in King Hussein Medical Center
 Pneumothorax Post CT-guided Fine Needle Aspiration Biopsy for Lung Nodules: Our Experience in King Hussein Medical Center Ala Qayet MD*, Laith Obaidat MD**, Mazin Al-Omari MD*, Ashraf Al-Tamimi MD^, Ahmad
Pneumothorax Post CT-guided Fine Needle Aspiration Biopsy for Lung Nodules: Our Experience in King Hussein Medical Center Ala Qayet MD*, Laith Obaidat MD**, Mazin Al-Omari MD*, Ashraf Al-Tamimi MD^, Ahmad
Aspiration versus tube drainage in primary spontaneous pneumothorax: a randomised study
 Eur Respir J 2006; 27: 477 482 DOI: 10.1183/09031936.06.00091505 CopyrightßERS Journals Ltd 2006 CLINICAL FORUM Aspiration versus tube drainage in primary spontaneous pneumothorax: a randomised study A.K.
Eur Respir J 2006; 27: 477 482 DOI: 10.1183/09031936.06.00091505 CopyrightßERS Journals Ltd 2006 CLINICAL FORUM Aspiration versus tube drainage in primary spontaneous pneumothorax: a randomised study A.K.
Specific Basic Standards for Osteopathic Fellowship Training in Pulmonary / Critical Care Medicine
 Specific Basic Standards for Osteopathic Fellowship Training in Pulmonary / Critical Care Medicine American Osteopathic Association and American College of Osteopathic Internists BOT Rev. 2/2011 These
Specific Basic Standards for Osteopathic Fellowship Training in Pulmonary / Critical Care Medicine American Osteopathic Association and American College of Osteopathic Internists BOT Rev. 2/2011 These
Imaging of small amounts of pleural fluid. Part two - physiologic pleural fluid
 review Imaging of small amounts of pleural fluid. Part two - physiologic pleural fluid Igor Kocijančič Department of Radiology, Institute of Oncology, Ljubljana, Slovenia Background. There are only a few
review Imaging of small amounts of pleural fluid. Part two - physiologic pleural fluid Igor Kocijančič Department of Radiology, Institute of Oncology, Ljubljana, Slovenia Background. There are only a few
Pneumothorax has long been listed as one of the
 Pneumothorax in Cystic Fibrosis* Patrick A. Flume, MD, FCCP Spontaneous pneumothorax is a common complication in patients with cystic fibrosis (CF). It is thought to occur more frequently in patients with
Pneumothorax in Cystic Fibrosis* Patrick A. Flume, MD, FCCP Spontaneous pneumothorax is a common complication in patients with cystic fibrosis (CF). It is thought to occur more frequently in patients with
Bedside Ultrasound in Pediatric Practice
 PEDIATRICS PERSPECTIVES Bedside Ultrasound in Pediatric Practice AUTHORS: Rebecca L. Vieira, MD, RDMS and Richard Bachur, MD Division of Emergency Medicine, Department of Medicine, Boston Children s Hospital,
PEDIATRICS PERSPECTIVES Bedside Ultrasound in Pediatric Practice AUTHORS: Rebecca L. Vieira, MD, RDMS and Richard Bachur, MD Division of Emergency Medicine, Department of Medicine, Boston Children s Hospital,
This appendix was part of the submitted manuscript and has been peer reviewed. It is posted as supplied by the authors.
 This appendix was part of the submitted manuscript and has been peer reviewed. It is posted as supplied by the authors. - Figure S1: The four quadrant approach lung ultrasound at the bedside. * The anterolateral
This appendix was part of the submitted manuscript and has been peer reviewed. It is posted as supplied by the authors. - Figure S1: The four quadrant approach lung ultrasound at the bedside. * The anterolateral
UAMS MEDICAL CENTER TRAUMA SERVICES MANUAL. REVIEWED: New PAGE: 1 of 7. RECOMMENDATION(S): Dr. Michael Sutherland APPROVAL: 04/28/2016
 REVIEWED: New PAGE: 1 of 7 PURPOSE: To provide guidelines for the evaluation and management of patients with traumatic chest wall injury including rib fractures, sternal fractures, hemothorax and retained
REVIEWED: New PAGE: 1 of 7 PURPOSE: To provide guidelines for the evaluation and management of patients with traumatic chest wall injury including rib fractures, sternal fractures, hemothorax and retained
2013 PHYSICIAN PROCEDURE CODE CHANGES
 2013 PHYSICIAN PROCEDURE CODE CHANGES Page 1 of 7 Effective for dates of service on or after 1/1/2013, refer to the New Codes listed below for billing. The discontinued codes are not valid for billing
2013 PHYSICIAN PROCEDURE CODE CHANGES Page 1 of 7 Effective for dates of service on or after 1/1/2013, refer to the New Codes listed below for billing. The discontinued codes are not valid for billing
Proceedings of the World Small Animal Veterinary Association Sydney, Australia 2007
 Proceedings of the World Small Animal Sydney, Australia 2007 Hosted by: Next WSAVA Congress THE LAST GASP II: LUNGS AND THORAX David Holt, BVSc, Diplomate ACVS University of Pennsylvania School of Veterinary
Proceedings of the World Small Animal Sydney, Australia 2007 Hosted by: Next WSAVA Congress THE LAST GASP II: LUNGS AND THORAX David Holt, BVSc, Diplomate ACVS University of Pennsylvania School of Veterinary
2013 Coding Changes. Diagnostic Radiology. Nuclear Medicine
 2013 Coding Changes The principal coding changes affecting Radiologists in 2013 occur in the Interventional Radiology Section of the AMA/CPT Manual. As in the past, we continue to see the Relative Update
2013 Coding Changes The principal coding changes affecting Radiologists in 2013 occur in the Interventional Radiology Section of the AMA/CPT Manual. As in the past, we continue to see the Relative Update
Pericardial Effusion
 Pericardial Effusion How does the heart work? The heart is the organ responsible for pumping blood to and from all tissues of the body. The heart is divided into right and left sides. The job of the right
Pericardial Effusion How does the heart work? The heart is the organ responsible for pumping blood to and from all tissues of the body. The heart is divided into right and left sides. The job of the right
The Leeds Teaching Hospitals NHS Trust Transjugular Intrahepatic Portosystemic Shunt (TIPS)
 n The Leeds Teaching Hospitals NHS Trust Transjugular Intrahepatic Portosystemic Shunt (TIPS) Information for patients Your liver doctor has recommended that you have a Transjugular Intrahepatic Portosystemic
n The Leeds Teaching Hospitals NHS Trust Transjugular Intrahepatic Portosystemic Shunt (TIPS) Information for patients Your liver doctor has recommended that you have a Transjugular Intrahepatic Portosystemic
