Journal of Breast Cancer
|
|
|
- Cassandra Lyons
- 6 years ago
- Views:
Transcription
1 Journal of Breast Cancer ORIGINAL ARTICLE J Breast Cancer 2017 March; 20(1): Patient Satisfaction with Implant Based Breast Reconstruction Associated with Implant Volume and Mastectomy Specimen Weight Ratio Woo Yeol Baek, Il Hwan Byun, Young Seok Kim, Dae Hyun Lew, Joon Jeong 1, Tai Suk Roh Institute of Human Tissue Restoration, Department of Plastic & Reconstructive Surgery, and 1 Department of Surgery, Yonsei University College of Medicine, Seoul, Korea Purpose: Breast volume assessment is one of the most important steps during implant-based breast reconstruction because it is critical in selecting implant size. According to previous studies, there is a close relationship between the mastectomy specimen weight and resected breast volume. The aim of this study was to evaluate long-term patient satisfaction with implantbased breast reconstruction guided by the ratio of implant volume to mastectomy specimen weight. In doing so, we describe the ideal ratio for patient satisfaction. Methods: A total of 84 patients who underwent implant-based breast reconstruction for breast cancer were included in this study. The patients were grouped by the ratio of implant size to mastectomy specimen weight (group 1, <65%; group 2, 65% 75%; and group 3, > 75%). Outcome analysis was performed using a questionnaire of patient satisfaction and the desired implant size. Results: Patient satisfaction scores concerning the postoperative body image, size, and position of the reconstructed breast were significantly higher in group 2. The average ratio of the ideal implant volume to mastectomy specimen weight for each group was 71.9% (range, 54.5% 96.7%), with the differences across the three groups being not significant (p= 0.244). Conclusion: Since there is an increase in breast reconstruction, selecting the appropriate breast implant is undoubtedly important. Our novel technique using the ratio of implant volume to mastectomy specimen weight provides physicians a firm guide to intraoperative selection of the proper implant in reconstructive breast surgery. Key Words: Breast implants, Mammaplasty, Patient satisfaction INTRODUCTION The demand for postmastectomy reconstruction of breast tissue following cancer is increasing worldwide [1]. Approximately 18% to 25% of patients who receive a mastectomy undergo breast reconstruction [2,3]. The breast reconstruction methods vary, including the use of autologous tissue, prosthetic material, or a combination of the two [4]. Deciding which method to use involves multiple factors, such as patient preference, risk factors, and physical characteristics [2]. While autologous tissue reconstruction using a transverse rectus abdominis musculocutaneous flap is one of the gold standards for breast reconstruction, the increasing use of a tissue expander or implant-based reconstruction represent additional reasonable methods [5]. A two-stage procedure that involves Correspondence to: Tai Suk Roh Department of Plastic and Reconstructive Surgery, Yonsei University College of Medicine, 50 Yonsei-ro, Seodaemun-gu, Seoul 03722, Korea Tel: , Fax: ROHTS@yuhs.ac Received: September 6, 2016 Accepted: December 7, 2016 tissue expansion with a temporary expander, followed by replacement with a permanent implant, is a safe and popular method of reconstruction [6]. Today, immediate implant reconstruction is also a well-accepted reconstruction method. Approximately 15% to 20% of breast reconstructions are performed with this technique [7]. The ideal candidate for implant-based reconstruction is a slim patient who requires bilateral reconstruction or a slim patient with small, minimally ptotic breasts and sufficient soft tissue who requires unilateral reconstruction [5,8]. The physician must consider sufficiency and quality of soft tissue coverage, symmetry of inframammary folds, and implant position and size to achieve suitable aesthetic result of implant-based breast reconstruction. Among these factors, proper implant size selection is undoubtedly crucial in achieving satisfactory aesthetic result of reconstruction [9]. Preoperative breast volume measurement is a determining factor for selecting implant size that closely matches the contralateral breast [10,11]. Furthermore, mastectomy specimen weight is proportionate to the volume required to fill the residual defect [11]. This weight measurement enables the reconstructive surgeon to select the appro Korean Breast Cancer Society. All rights reserved. pissn This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License ( eissn licenses/by-nc/4.0) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
2 Patient Satisfaction with Implant Based Breast Reconstruction 99 priate implant. Spear and Spittler [5] have reported that mastectomy specimen weight in grams correlates with the volume of the selected implant in cubic centimeters and should serve as important information. We assumed that the selected implant volume is closely associated with mastectomy specimen weight and hypothesized that there is an ideal ratio of implant volume to mastectomy specimen weight. The aim of this study was to evaluate long-term patient satisfaction with implant breast reconstruction associated with the ratio of implant volume to mastectomy specimen weight. METHODS Between 2004 and 2012, 84 patients who were treated with postmastectomy breast reconstruction using an implant at a single institution were surveyed retrospectively. The reconstructions included a two-stage procedure that involved the insertion of a tissue expander followed by an implant after a few months (n = 69) and a one-stage method of immediate insertion of the implant at the time of mastectomy (n = 15). The two-stage reconstructions were performed on patients who underwent total mastectomy, while the immediate implant reconstructions were performed on those who underwent nipple or skin sparing mastectomy. In tissue expander cases, the permanent implants were inserted about three months after the initial operation. Tissue expanders or permanent silicone implants were placed with the assistance of an acellular dermal matrix (ADM). The ADM was fixed on the lower margin of the origin of the dissected pectoralis major muscle on the superior side and connected to the serratus anterior muscle on the lateral side, as well as to the chest wall on the medial and inferior side. This created a supportive pocket for expander or implant placement against the chest wall. The ADMs used in this study were AlloDerm (LifeCell Corp., Branchburg, USA) and CGDerm (CGBio Corp., Seoul, Korea). Patients who underwent immediate and unilateral reconstructions were included in this study, while those who underwent delayed or bilateral reconstructions were not. We also excluded patients who underwent simultaneous contralateral breast reduction, mastopexy, and augmentation because we planned to analyze patient satisfaction with the reconstructed breast compared to the contralateral (intact) breast. The independent clinical variables obtained by review of medical records included patient age, weight, height, stage of breast cancer, and history of radiation or chemotherapy (Table 1). Patients were either contacted by telephone or interviewed in person at our outpatient clinic. We developed a new questionnaire for this study. The questionnaire contained 11 rating scale questions (0 10 scale) and one subjective question, and required approximately 10 minutes to complete. The rating scale contained three categories to determine patient satisfaction with (1) postoperative body image, (2) size and position of the reconstructed breast compared to the intact one, and (3) the breast reconstruction procedure itself (Supplementary Table 1, available online). All procedures were performed by three other plastic surgeons who did not participate in the reconstruction (response rate, 75.0% [84/112]). The patients were grouped based on their ratio of implant volume to mastectomy specimen weight (group 1, < 65%; Table 1. Patient characteristics Characteristic Total (n= 84) Expander+implant (n=69) Immediate implant (n=15) p-value Age (yr) 43.0± ± ± Height (cm) 160.0± ± ± Weight (kg) 54.1± ± ± BMI (kg/m 2 ) 21.1± ± ± Follow-up (yr) 3.1± ± ± Stage (33.3) 23 (33.3) 5 (33.3) I 28 (33.3) 20 (29.0) 8 (53.3) II 26 (40.0) 24 (34.8) 2 (13.3) III/IV 2 (2.4) 2 (2.9) 0 Specimen weight (g) 386.6± ± ± Implant volume (ml) 275.3± ± ± Ratio (%)* 75.5± ± ± Radiation 18 (21.4) 15 (21.7) 3 (20.0) Chemotherapy 54 (64.3) 46 (66.7) 8 (53.3) Data are presented as mean± SD or number (%). BMI= body mass index. *Ratio (%), implant volume/specimen weight 100.
3 100 Woo Yeol Baek, et al. group 2, 65% 75%; and group 3, > 75%) and type of reconstruction (expander+implant vs. immediate implant). Data analysis was performed using SAS version 9.2 (SAS Institute Inc., Cary, USA). Patient satisfaction in each group was compared using a one-way analysis of variance. Values were expressed as the mean± standard deviation, and the significance level was set at p< We considered scores of 8 or greater for rating scale questions as excellent satisfaction. The comparison and trend of excellent satisfaction rates for different ratios of implant volume to specimen weight were analyzed using Youden s index. This study was approved by the Institutional Review Board of Yonsei University (IRB number: ) and was conducted in accordance with the Declaration of Helsinki. RESULTS Of 84 patients, the mean age was 43.0 ± 9.3 years and the average body mass index was 21.1 ± 2.2. The mean implant size was 275.3± 55.2 ml, and the mean mastectomy specimen weight was 386.6± g. The mean ratio of implant size to mastectomy specimen weight was 75.5 ± The mean follow-up period was 3.1 ± 2.6. Sixty-nine patients (82.1%) underwent expander+implant breast reconstruction, and the remaining 15 (17.9%) underwent immediate implant reconstruction (Table 1). The patients were divided, based on their ratio of implant volume to mastectomy specimen weight, into group 1 (n=25), group 2 (n=28), or group 3 (n=31), for which the average specimen weights were 479.2±114.2 g, 390.5±81.7 g, and 308.5± 86.4 g, respectively. The specimen weights of group 1 were generally heavier than those of the other groups (p< 0.001). The average implant volume of each group was ± 54.8 ml, ± 56.9 ml, and ± 54.7 ml, respectively (p= 0.613). The mean ratios were 56.2% ± 6.2%, 70.0% ± 3.1%, and 96.1%± 23.4%, respectively. Demographic data were similar between the three groups, except for weight (Table 2). Among the groups, the patient satisfaction scores were generally higher in group 2 than in the other groups. The mean satisfaction score regarding postoperative body image (category 1, questions Q1 Q5) was 8.9± 0.9 in group 2, which was significantly higher than that in the other groups (p< 0001). The mean score of Q1 was the highest in the first category. The scores involving standing position (Q2 and Q3) were higher than those involving supine position (Q4 and Q5), regardless of whether the patient was wearing a brassiere. We assumed that these results were due to the character of a reconstructed breast, which is less ptotic and more prominent when lying down. The patients in group 2 were more satisfied with the size or position of the reconstructed breast than were patients in the other groups (category 2, p< 0.001) and reconstruction itself (category 3, p= 0.005). In addition, we asked a subjective question about the ideal reconstructed breast size compared to their existing one (Q12). The patients in group 1 wanted larger implants by a mean 23.2%± 13.5%, but those in group 3 wanted smaller implants by mean 21.1% ± 11.2%. Meanwhile, the ideal implant size requested by group 2 was similar to the existing breast (1.4%± 5.9%). Based on these results, we calculated that the ratio of ideal implant volume to mastectomy specimen weight for each group was 71.9%± 11.8%, with Table 2. Patient classification based on the ratio of implant volume to mastectomy specimen weight Characteristic Group 1 (n= 25) Group 2 (n=28) Group 3 (n=31) p-value Age (yr) 44.5± ± ± Height (cm) 160.9± ± ± Weight (kg) 56.8± ± ± BMI (kg/m 2 ) 22.0± ± ± Follow-up (yr) 3.2± ± ± Stage (36.0) 9 (32.1) 10 (32.3) I 6 (24.0) 10 (35.7) 12 (38.7) II 9 (36.0) 9 (32.1) 8 (25.8) III/IV 1 (4.0) 0 1 (3.2) Specimen weight (g) 479.2± ± ±86.4 < Implant volume (ml) 267.1± ± ± Ratio (%)* 56.2± ± ± Radiation 7 (28.0) 6 (21.4) 5 (16.1) Chemotherapy 18 (72.0) 20 (71.4) 16 (51.6) Data are presented as mean± SD or number (%). The patients were grouped based on their ratio of implant volume to mastectomy specimen weight (group 1, < 65%, group 2, 65% 75%, and group 3, > 75%). *Ratio (%), implant size/specimen weight 100.
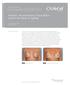
4 Patient Satisfaction with Implant Based Breast Reconstruction 101 Table 3. Scores of the questionnaire for each group Category Group 1 (n= 27) Group 2 (n= 28) Group 3 (n= 31) p-value Category 1 Q1 7.4± ± ± 1.2 < Q2 7.1± ± ± 1.1 < Q3 6.7± ± ± 1.1 < Q4 6.8± ± ± 1.1 < Q5 6.1± ± ± 0.9 < Total 6.8± ± ± 1.2 < Category 2 Q6 6.7± ± ± 1.2 < Q7 7.6± ± ± Total 7.1± ± ± 1.6 < Category 3 Q8 9.0± ± ± Q9 9.0± ± ± Q10 7.6± ± ± 1.1 < Total 8.5± ± ± Q11 7.2± ± ± 1.5 < Ideal size (%)* 123.2± ± ± New ratio (%) 68.7± ± ± Data are presented as mean± SD. *Ideal size: ideal reconstructed breast size which patient wants, compared to existing one; New ratio: the ratio of ideal implant size to mastectomy specimen weight. New ratio (%) Table 4. Rate of excellent satisfaction* Category Group 1 (n=27) No. (%) Ratio (%) Figure 1. The ideal new ratio in relation to the original ratio of implant volume to specimen weight. X-axis, the ratio of implant volume to mastectomy specimen weight (%); Y-axis, the new ratio recalculated with the ideal implant volume which patients desired (%). Sixty-one patients (61/84, 72.6%) resulted new ratios located within 65.0% to 75.0%. Group 2 (n=28) No. (%) the differences across the three groups being insignificant (p= 0.244) (Table 3, Figure 1). We considered scores of 8 or greater as indicating excellent satisfaction. In group 2, the proportion with an average score of 8 or greater was 96.4%. In contrast, the percentages of patients indicating excellent satisfaction were 29.6% in group 1 and 25.8% in group 3 (p < 0.001) (Table 4). We also used Youden s index (J) to determine the upper and lower margins of the ratio that result in a predictable excellent satisfaction for a patient. J is formally defined as J = sensitivity+specificity 1. The cutoff value that achieved maximum J was used to find the ratio (implant volume to specimen weight) of the predictable greatest satisfaction. In category 1, the maximum J was (sensitivity, 1.0; specificity, ) when the ratio was 76.9%. The odd ratio (OR) at this ratio was (95% confidence interval, ). This implies that when the ratio is more than 76.9%, the possibility of excellent satisfaction decreases by a factor of When the ratio is less than 76.9%, the possibility of excellent satisfaction is increased. The cutoff values of category 2 and Q11 were 76.9% and 80.0%, respectively. A ratio of less than 76.9% in category 2 and 80.0% in Q11 increased the possibility of excellent satisfaction among patients. However, in category 3, the cutoff value was 61.1%, and the OR at this ratio was This implies that when the ratio was greater than 61.1%, the possibility of excellent satisfaction among patients increased. Based on these results, we predicted that a ratio of implant volume to mastectomy specimen weight of 61.1% to 76.9% increases the possibility of excellent satisfaction. This range matched the range of group 2 (65.0% 75.0%), which showed the greatest patient satisfaction. DISCUSSION Group 3 (n=31) No. (%) p-value Category (18.5) 26 (92.9) 1 (2.7) < Category (25.9) 25 (89.3) 7 (22.6) < Category (77.8) 28 (100) 27 (87.1) < Q (37.0) 28 (100) 11 (35.5) < Total 8 (29.6) 27 (96.4) 8 (25.8) < *Excellent satisfaction, average scores of 8 or greater in scale question. Breast reconstruction is now widely considered to be an important component of the treatment of breast cancer [1]. During this process, the principle aesthetic objective is the restoration of volumetric symmetry [12]. Accurate volume assessment is a prerequisite in breast reconstruction and provides a guideline for implant size selection. Although breast volume assessment is undoubtedly important, it is not conducted routinely in some institutions because of the absence of a commonly accepted standard method [10,12-19]. There are numerous techniques for preoperative and intraoperative estimation of implant size, but most are inaccurate and inconsistent [9]. Moreover, this estimation depends on the surgeon s experience, skill, and surgical ability in many
5 102 Woo Yeol Baek, et al. cases. According to previous studies, preoperative estimation techniques include anthropometric volume estimation and volumetric analysis using ultrasonography, mammography, computed tomography, magnetic resonance imaging, and three-dimensional scanners [13,18-22]. Although these exams may occur during the cancer staging workup, they require other specialized staff, including radiographers and radiologists [9]. Furthermore, the thickness of the remnant skin envelop after mastectomy cannot be estimated preoperatively using these tests. Intraoperative estimation techniques include implant sizers method and gauze swab implant-estimation method [9]. While using an implant sizer is a commonly available method, it is expensive [9]. Moreover, it has different characteristics compared to a permanent implant, which can result in intraoperative trial and error [9]. Caulfield and Niranjan [9] used surgical gauze swabs and reported that the gauze swab implant-estimation method is an easily reproducible and inexpensive method that produces reliable results. However, the sizes and characteristics of gauzes differ across manufacturers, thereby complicating the process of estimating the volume of a saline-soaked gauze swab, which is used as an intraoperative trial sizer. It is also possible to mistakenly leave gauze inside the breast when using this method. Thus, we introduced a novel technique of using mastectomy specimen weight to select implant size. Although selecting breast implant size according to removed breast volume (mastectomy specimen volume) may be the most accurate method, it is more difficult and time-consuming to assess the specimen volume instead of weight, intraoperatively. Several studies have clarified the close relationship between mastectomy specimen weight and resected breast volume, and thus we decided to use specimen weight in this study [23,24]. We surveyed patient satisfaction with an original questionnaire and analyzed the ideal reconstructed breast size that patients desired. By analyzing the ideal volume, we calculated the new ratio (the ratio of ideal implant volume to mastectomy specimen weight), and found that 72.6% (61/84) of new ratios in patients were 65% to 75% (Figure 1). We hypothesized that a 65% to 75% ratio of implant size to mastectomy specimen weight will lead to symmetric and aesthetically pleasing results, which is supported by questionnaire scores (Table 3). A ratio of 65.0% to 75.0% is preferable over 100% because of density differences between the implant and the specimen. Furthermore, since general surgeons remove the tail portion of the breast as well as the body of the breast, the implant that does not cover the tail should be smaller than the total specimen weight. Thus, we thought that the implant volume should be smaller than the specimen weight, yet large enough to fulfill the symmetry of bilateral breasts, and such implants resulted in the greatest level of satisfaction among participants of group 2. We also think that such a ratio, which was not too large, produced a satisfactory shape and natural form while allowing for movement. Interestingly, in operations with greater specimen weights, the operator chose an implant of lesser ratio. We believe that in cases of large specimen weights, other variables, such as the breast width and height, restricted the choices of implants and, thus, smaller ratios. In addition, one can see that the specimen weight range was quite wide for each group, and so, it is difficult to definitively state that patients with large specimen weights used small implants. Nevertheless, the patient survey showed the greatest level of satisfaction in group 2, and we carefully concluded that a ratio between 65.0% and 75.0% produced the greatest level of patient satisfaction. Therefore, choosing an implant volume using specimen weight and size as guides is a powerful method. We do acknowledge that such a ratio is quite specific to our institute with a consistent style of general surgeons, yet this will provide a helpful guide to the general rules of reconstruction and other institutes, where surgeons can establish specific ratios unique to their environment. For breast surgeons, the most difficult, but most important, goal is achieving symmetry during breast reconstruction. Every person has a unique shape and volume, with even the breasts of a single person differing. Although implants have variations in styles and sizes, they cannot meet the unique circumstances and needs of each patient. While base width and projection are important, choosing implants based on natural projection sometimes results in an insufficient volume. There are many variables to consider and, in this study, we mainly focused on specimen weight and ratio. Although shape and other factors are important, we believe that volume is a more critical factor to patient satisfaction. This is because fixed implant styles are limited in matching the exact shape of the contralateral side; however, when wearing a brassier, a similar volume confers a stable feeling of symmetry and great satisfaction on the patient. This study has several limitations. First, the follow-up period was shorter in group 2 (2.2 ± 2.3 years) than in the other groups (group 1, 3.2± 2.7 years; group 3, 3.7± 2.6 years). This difference can affect patient satisfaction and aesthetic outcome. Hu et al. [25] reported that satisfaction with a reconstructed breast including appearance, shape, softness, size, and projection, diminished by the time of long-term followup ( > 8 years). Because the mean follow-up period of all groups was shorter than 8 years, patient satisfaction may decrease in the future. Second, we created a survey focusing on the size and position of the reconstructed breast; however,
6 Patient Satisfaction with Implant Based Breast Reconstruction 103 other factors, such as rippling and capsular contracture, may affect satisfaction as well. Moreover, ancillary procedures, such as autologous fat injection, inframammary fold repositioning, and scar revision, which are performed along with nipple-areolar complex reconstruction, may have affected patient satisfaction. In addition, the density differences between implant and specimen as well as between the specimens among patients may have affected the results. In the future, a large-scale study with more subdivided groups and a longterm follow-up period is necessary. Despite the few limitations, to our knowledge, this is the first report of patient satisfaction analysis involving the ratio of implant volume to mastectomy specimen weight in breast reconstruction. In this time of increasing breast reconstruction, selecting the appropriate breast implant is undoubtedly of crucial importance. Our novel technique that makes use of the ratio of implant volume to mastectomy specimen weight provides physicians with a useful guide for intraoperative selection of the proper implant for reconstructive breast surgery. CONFLICT OF INTEREST The authors declare that they have no competing interests. REFERENCES 1. Tzafetta K, Ahmed O, Bahia H, Jerwood D, Ramakrishnan V. Evaluation of the factors related to postmastectomy breast reconstruction. Plast Reconstr Surg 2001;107: Vega S, Smartt JM Jr, Jiang S, Selber JC, Brooks CJ, Herrera HR, et al. 500 Consecutive patients with free TRAM flap breast reconstruction: a single surgeon s experience. Plast Reconstr Surg 2008;122: Duggal CS, Grudziak J, Metcalfe DB, Carlson GW, Losken A. The effects of breast size in unilateral postmastectomy breast reconstruction. Ann Plast Surg 2013;70: Noone RB. Thirty-five years of breast reconstruction: eleven lessons to share. Plast Reconstr Surg 2009;124: Spear SL, Spittler CJ. Breast reconstruction with implants and expanders. Plast Reconstr Surg 2001;107: Radovan C. Breast reconstruction after mastectomy using the temporary expander. Plast Reconstr Surg 1982;69: Salzberg CA, Ashikari AY, Koch RM, Chabner-Thompson E. An 8-year experience of direct-to-implant immediate breast reconstruction using human acellular dermal matrix (AlloDerm). Plast Reconstr Surg 2011; 127: Roostaeian J, Pavone L, Da Lio A, Lipa J, Festekjian J, Crisera C. Immediate placement of implants in breast reconstruction: patient selection and outcomes. Plast Reconstr Surg 2011;127: Caulfield RH, Niranjan NS. Innovative techniques: a novel technique for intraoperative estimation of breast implant size in aesthetic and reconstructive breast surgery. Aesthetic Plast Surg 2008;32: Kayar R, Civelek S, Cobanoglu M, Gungor O, Catal H, Emiroglu M. Five methods of breast volume measurement: a comparative study of measurements of specimen volume in 30 mastectomy cases. Breast Cancer (Auckl) 2011;5: Shamoun JM, Hartrampf CR. Mastectomy specimen weight and skin dimensions as an adjunct in breast reconstruction. Ann Plast Surg 1996; 36: Yoo A, Minn KW, Jin US. Magnetic resonance imaging-based volumetric analysis and its relationship to actual breast weight. Arch Plast Surg 2013;40: Katariya RN, Forrest AP, Gravelle IH. Breast volumes in cancer of the breast. Br J Cancer 1974;29: Malini S, Smith EO, Goldzieher JW. Measurement of breast volume by ultrasound during normal menstrual cycles and with oral contraceptive use. Obstet Gynecol 1985;66: Fowler PA, Casey CE, Cameron GG, Foster MA, Knight CH. Cyclic changes in composition and volume of the breast during the menstrual cycle, measured by magnetic resonance imaging. Br J Obstet Gynaecol 1990;97: Daly SE, Kent JC, Huynh DQ, Owens RA, Alexander BF, Ng KC, et al. The determination of short-term breast volume changes and the rate of synthesis of human milk using computerized breast measurement. Exp Physiol 1992;77: Ward C, Harrison B. The search for volumetric symmetry in reconstruction of the breast after mastectomy. Br J Plast Surg 1986;39: Bulstrode N, Bellamy E, Shrotria S. Breast volume assessment: comparing five different techniques. Breast 2001;10: Yip JM, Mouratova N, Jeffery RM, Veitch DE, Woodman RJ, Dean NR. Accurate assessment of breast volume: a study comparing the volumetric gold standard (direct water displacement measurement of mastectomy specimen) with a 3D laser scanning technique. Ann Plast Surg 2012;68: Caruso MK, Guillot TS, Nguyen T, Greenway FL. The cost effectiveness of three different measures of breast volume. Aesthetic Plast Surg 2006; 30: Palin WE Jr, von Fraunhofer JA, Smith DJ Jr. Measurement of breast volume: comparison of techniques. Plast Reconstr Surg 1986;77: Longo B, Farcomeni A, Ferri G, Campanale A, Sorotos M, Santanelli F. The BREAST-V: a unifying predictive formula for volume assessment in small, medium, and large breasts. Plast Reconstr Surg 2013;132:1e-7e. 23. Parmar C, West M, Pathak S, Nelson J, Martin L. Weight versus volume in breast surgery: an observational study. JRSM Short Rep 2011;2: Aslan G, Terzioğlu A, Tuncali D, Bingul F. Breast reduction: weight versus volume. Plast Reconstr Surg 2003;112: Hu ES, Pusic AL, Waljee JF, Kuhn L, Hawley ST, Wilkins E, et al. Patientreported aesthetic satisfaction with breast reconstruction during the long-term survivorship period. Plast Reconstr Surg 2009;124:1-8.
Is Unilateral Implant or Autologous Breast Reconstruction Better in Obtaining Breast Symmetry?
 ORIGINAL ARTICLE Is Unilateral Implant or Autologous Breast Reconstruction Better in Obtaining Breast Symmetry? Oriana Cohen, MD, Kevin Small, MD, Christina Lee, BA, Oriana Petruolo, MD, Nolan Karp, MD,
ORIGINAL ARTICLE Is Unilateral Implant or Autologous Breast Reconstruction Better in Obtaining Breast Symmetry? Oriana Cohen, MD, Kevin Small, MD, Christina Lee, BA, Oriana Petruolo, MD, Nolan Karp, MD,
Assessment of Breast Volume Change after Transverse Rectus Abdominis Myocutaneous Flap
 Assessment of Breast Volume Change after Transverse Rectus Abdominis Myocutaneous Flap Sang Uk Park, Jeong Su Shim Department of Plastic and Reconstructive Surgery, Catholic University of Daegu School
Assessment of Breast Volume Change after Transverse Rectus Abdominis Myocutaneous Flap Sang Uk Park, Jeong Su Shim Department of Plastic and Reconstructive Surgery, Catholic University of Daegu School
Breast cancer reconstruction surgery (immediate and delayed) across Ontario: Patient indications and appropriate surgical options
 A Quality Initiative of the Program in Evidence-Based Care (PEBC), Cancer Care Ontario (CCO) Breast cancer reconstruction surgery (immediate and delayed) across Ontario: Patient indications and appropriate
A Quality Initiative of the Program in Evidence-Based Care (PEBC), Cancer Care Ontario (CCO) Breast cancer reconstruction surgery (immediate and delayed) across Ontario: Patient indications and appropriate
Selective salvage of zones 2 and 4 in the pedicled TRAM flap: a focus on reducing fat necrosis and improving aesthetic outcomes
 DOI 10.1186/s40064-016-1714-7 RESEARCH Open Access Selective salvage of zones 2 and 4 in the pedicled TRAM flap: a focus on reducing fat necrosis and improving aesthetic outcomes Chi Sun Yoon and Kyu Nam
DOI 10.1186/s40064-016-1714-7 RESEARCH Open Access Selective salvage of zones 2 and 4 in the pedicled TRAM flap: a focus on reducing fat necrosis and improving aesthetic outcomes Chi Sun Yoon and Kyu Nam
Allograft Based Breast Reconstruction: Opportunity for a Second Look
 Allograft Based Breast Reconstruction: Opportunity for a Second Look Martin I. Newman, MD, FACS Director of Resident Education and Associate Program Director Department of Plastic and Reconstructive Surgery
Allograft Based Breast Reconstruction: Opportunity for a Second Look Martin I. Newman, MD, FACS Director of Resident Education and Associate Program Director Department of Plastic and Reconstructive Surgery
Treatment of Pseudoangiomatous Stromal Hyperplasia of the Breast: Implant-Based Reconstruction with a Vascularized Dermal Sling
 Treatment of Pseudoangiomatous Stromal Hyperplasia of the Breast: Implant-Based Reconstruction with a Vascularized Dermal Sling Idea and Innovation Bok Ki Jung 1, Ji Hae Nahm 2, Dae Hyun Lew 1, Dong Won
Treatment of Pseudoangiomatous Stromal Hyperplasia of the Breast: Implant-Based Reconstruction with a Vascularized Dermal Sling Idea and Innovation Bok Ki Jung 1, Ji Hae Nahm 2, Dae Hyun Lew 1, Dong Won
Breast Reconstruction Postmastectomy. Using DermaMatrix Acellular Dermis in breast reconstruction with tissue expander.
 Breast Reconstruction Postmastectomy. Using DermaMatrix Acellular Dermis in breast reconstruction with tissue expander. Strong and flexible Bacterially inactivated Provides implant support Breast Reconstruction
Breast Reconstruction Postmastectomy. Using DermaMatrix Acellular Dermis in breast reconstruction with tissue expander. Strong and flexible Bacterially inactivated Provides implant support Breast Reconstruction
NIPPLE SPARING PRE-PECTORAL BREAST RECONSTRUCTION
 NIPPLE SPARING PRE-PECTORAL BREAST RECONSTRUCTION 42 yo female healthy athlete Right breast mass. Past medical history: none Family history: aunt with Breast cancer Candidates for nipple-sparing mastectomy
NIPPLE SPARING PRE-PECTORAL BREAST RECONSTRUCTION 42 yo female healthy athlete Right breast mass. Past medical history: none Family history: aunt with Breast cancer Candidates for nipple-sparing mastectomy
How To Make a Good Mastectomy for Reconstruction Based on the Anatomy. Zhang Jin, Ph.D MD
 How To Make a Good Mastectomy for Reconstruction Based on the Anatomy Zhang Jin, Ph.D MD Deputy Director and Professor Tianjin Medical University Cancer Institute and Hospital People s Republic of China
How To Make a Good Mastectomy for Reconstruction Based on the Anatomy Zhang Jin, Ph.D MD Deputy Director and Professor Tianjin Medical University Cancer Institute and Hospital People s Republic of China
Clinical Accuracy of Portrait 3D Surgical Simulation Platform in Breast Augmentation. Ryan K. Wong MD, David T Pointer BS, Kamran Khoobehi MD FACS
 Clinical Accuracy of Portrait 3D Surgical Simulation Platform in Breast Augmentation Ryan K. Wong MD, David T Pointer BS, Kamran Khoobehi MD FACS Division of Plastic, Reconstructive & Reconstructive Surgery,
Clinical Accuracy of Portrait 3D Surgical Simulation Platform in Breast Augmentation Ryan K. Wong MD, David T Pointer BS, Kamran Khoobehi MD FACS Division of Plastic, Reconstructive & Reconstructive Surgery,
A new classification system of nasal contractures
 Original Article J Cosmet Med 2017;1(2):106-111 https://doi.org/10.25056/jcm.2017.1.2.106 pissn 2508-8831, eissn 2586-0585 A new classification system of nasal contractures Geunuck Chang 1, Donghak Jung
Original Article J Cosmet Med 2017;1(2):106-111 https://doi.org/10.25056/jcm.2017.1.2.106 pissn 2508-8831, eissn 2586-0585 A new classification system of nasal contractures Geunuck Chang 1, Donghak Jung
The Effect of Acellular Dermal Matrix in Implant-Based Immediate Breast Reconstruction with Latissimus Dorsi Flap
 ORIGINAL ARTICLE https://doi.org/10.14730/.2017.23.1.17 Arch Aesthetic Plast Surg 2017;23(1):17-23 pissn: 2234-0831 eissn: 2288-9337 The Effect Acellular Dermal Matrix in Implant-Based Immediate Breast
ORIGINAL ARTICLE https://doi.org/10.14730/.2017.23.1.17 Arch Aesthetic Plast Surg 2017;23(1):17-23 pissn: 2234-0831 eissn: 2288-9337 The Effect Acellular Dermal Matrix in Implant-Based Immediate Breast
Breast Reconstruction: Current Strategies and Future Opportunities
 Breast Reconstruction: Current Strategies and Future Opportunities Hani Sbitany, MD Assistant Professor of Surgery University of California, San Francisco Division of Plastic and Reconstructive Surgery
Breast Reconstruction: Current Strategies and Future Opportunities Hani Sbitany, MD Assistant Professor of Surgery University of California, San Francisco Division of Plastic and Reconstructive Surgery
More women are surviving breast cancer BREAST
 BREAST Patient-Reported Aesthetic Satisfaction with Breast Reconstruction during the Long-Term Survivorship Period Emily S. Hu, M.D. Andrea L. Pusic, M.D. Jennifer F. Waljee, M.D., M.P.H. Latoya Kuhn,
BREAST Patient-Reported Aesthetic Satisfaction with Breast Reconstruction during the Long-Term Survivorship Period Emily S. Hu, M.D. Andrea L. Pusic, M.D. Jennifer F. Waljee, M.D., M.P.H. Latoya Kuhn,
JMSCR Vol 06 Issue 01 Page January 2018
 www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v6i1.35 Breast Volume estimation by Anthropometry
www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v6i1.35 Breast Volume estimation by Anthropometry
Pocket Conversion Made Easy: A Simple Technique Using Alloderm to Convert Subglandular Breast Implants to the Dual-Plane Position
 Breast Surgery Pocket Conversion Made Easy: A Simple Technique Using Alloderm to Convert Subglandular Breast Implants to the Dual-Plane Position M. Mark Mofid, MD; and Navin K. Singh, MD Background: The
Breast Surgery Pocket Conversion Made Easy: A Simple Technique Using Alloderm to Convert Subglandular Breast Implants to the Dual-Plane Position M. Mark Mofid, MD; and Navin K. Singh, MD Background: The
Infectious Complications Leading to Explantation in Implant-Based Breast Reconstruction With AlloDerm
 Infectious Complications Leading to Explantation in Implant-Based Breast Reconstruction With AlloDerm Minh-Doan Nguyen, MD, PhD, a Chen Chen, MS, b Salih Colakoğlu, MD, b Donald J. Morris, MD, b Adam M.
Infectious Complications Leading to Explantation in Implant-Based Breast Reconstruction With AlloDerm Minh-Doan Nguyen, MD, PhD, a Chen Chen, MS, b Salih Colakoğlu, MD, b Donald J. Morris, MD, b Adam M.
Current Strategies in Breast Reconstruction
 Current Strategies in Breast Reconstruction Hani Sbitany, MD Assistant Professor of Surgery University of California, San Francisco Division of Plastic and Reconstructive Surgery 12 th Annual School of
Current Strategies in Breast Reconstruction Hani Sbitany, MD Assistant Professor of Surgery University of California, San Francisco Division of Plastic and Reconstructive Surgery 12 th Annual School of
The biplanar oncoplastic technique case series: a 2-year review
 Original Article The biplanar oncoplastic technique case series: a 2-year review Alexander J. Kaminsky 1, Ketan M. Patel 2, Costanza Cocilovo 1, Maurice Y. Nahabedian 2, Reza Miraliakbari 3 1 INOVA Fairfax
Original Article The biplanar oncoplastic technique case series: a 2-year review Alexander J. Kaminsky 1, Ketan M. Patel 2, Costanza Cocilovo 1, Maurice Y. Nahabedian 2, Reza Miraliakbari 3 1 INOVA Fairfax
Advances in Localized Breast Cancer
 Advances in Localized Breast Cancer Melissa Camp, MD, MPH and Fariba Asrari, MD June 18, 2018 Moderated by Elissa Bantug 1 Advances in Surgery for Breast Cancer Melissa Camp, MD June 18, 2018 2 Historical
Advances in Localized Breast Cancer Melissa Camp, MD, MPH and Fariba Asrari, MD June 18, 2018 Moderated by Elissa Bantug 1 Advances in Surgery for Breast Cancer Melissa Camp, MD June 18, 2018 2 Historical
Diagnosis and Treatment of Patients with Primary and Metastatic Breast Cancer. Oncoplastic and Reconstructive Surgery
 Diagnosis and Treatment of Patients with Primary and Metastatic Breast Cancer Oncoplastic and Reconstructive Surgery Plastic-reconstructive aspects after mastectomy Versions 2002 2017: Audretsch / Bauerfeind
Diagnosis and Treatment of Patients with Primary and Metastatic Breast Cancer Oncoplastic and Reconstructive Surgery Plastic-reconstructive aspects after mastectomy Versions 2002 2017: Audretsch / Bauerfeind
Breast Reconstruction Options
 Breast Reconstruction Options Natural reconstruction using your ABDOMINAL tissue: TRAM Flap (Transverse Rectus Abdominis Myocutaneous) There are various forms of TRAM flap reconstruction that are commonly
Breast Reconstruction Options Natural reconstruction using your ABDOMINAL tissue: TRAM Flap (Transverse Rectus Abdominis Myocutaneous) There are various forms of TRAM flap reconstruction that are commonly
Frederick J. Duffy, Jr., MD, FACS and Brice W. McKane, MD, FACS BREAST RECONSTRUCTION
 Frederick J. Duffy, Jr., MD, FACS and Brice W. McKane, MD, FACS BREAST RECONSTRUCTION BREAST RECONSTRUCTION: A WOMAN S DECISION Options and Information Our approach to breast reconstruction entails a very
Frederick J. Duffy, Jr., MD, FACS and Brice W. McKane, MD, FACS BREAST RECONSTRUCTION BREAST RECONSTRUCTION: A WOMAN S DECISION Options and Information Our approach to breast reconstruction entails a very
Contralateral Prophylactic Mastectomy with Immediate Reconstruction: Added Benefits, Added Risks
 Contralateral Prophylactic Mastectomy with Immediate Reconstruction: Added Benefits, Added Risks Grant W. Carlson Wadley R. Glenn Professor of Surgery Divisions of Plastic Surgery & Surgical Oncology Emory
Contralateral Prophylactic Mastectomy with Immediate Reconstruction: Added Benefits, Added Risks Grant W. Carlson Wadley R. Glenn Professor of Surgery Divisions of Plastic Surgery & Surgical Oncology Emory
Prevention of Implant Malposition in Inframammary Augmentation Mammaplasty
 Prevention of Implant Malposition in Inframammary Augmentation Mammaplasty Yoon Ji Kim, Yang Woo Kim, Young Woo Cheon Department of Plastic and Reconstructive Surgery, Gachon University Gil Medical Center,
Prevention of Implant Malposition in Inframammary Augmentation Mammaplasty Yoon Ji Kim, Yang Woo Kim, Young Woo Cheon Department of Plastic and Reconstructive Surgery, Gachon University Gil Medical Center,
PROS AND CONS OF IMMEDIATE PROSTHETIC IMPLANTS VS USE OF EXPANDER FOR POST MASTECTOMY BREAST RECONSTRUCTIONS
 PROS AND CONS OF IMMEDIATE PROSTHETIC IMPLANTS VS USE OF EXPANDER FOR POST MASTECTOMY BREAST Dr Tienie van Rooyen Mediclinic Kloof Hospital Pretoria IMMEDIATE Since 1990 s Skin sparing mastectomies proven
PROS AND CONS OF IMMEDIATE PROSTHETIC IMPLANTS VS USE OF EXPANDER FOR POST MASTECTOMY BREAST Dr Tienie van Rooyen Mediclinic Kloof Hospital Pretoria IMMEDIATE Since 1990 s Skin sparing mastectomies proven
Advances and Innovations in Breast Reconstruction and Brest Surgery Presented by PCMC plastic surgeons
 Advances and Innovations in Breast Reconstruction and Brest Surgery Presented by PCMC plastic surgeons Options for reconstruction after mastectomy Implants Autologous tissue = from your own body: skin
Advances and Innovations in Breast Reconstruction and Brest Surgery Presented by PCMC plastic surgeons Options for reconstruction after mastectomy Implants Autologous tissue = from your own body: skin
Reconstruction of the Breast after Cancer An Overview of Procedures and Options by Karen M. Horton, MD, MSc, FRCSC
 Downloaded from Reconstruction of the Breast after Cancer An Overview of Procedures and Options by Karen M. Horton, MD, MSc, FRCSC What is Breast Reconstruction? Reconstruction of the breast involves recreating
Downloaded from Reconstruction of the Breast after Cancer An Overview of Procedures and Options by Karen M. Horton, MD, MSc, FRCSC What is Breast Reconstruction? Reconstruction of the breast involves recreating
Breast Augmentation and Mastopexy Using a Pectoral Muscle Loop
 Aesth Plast Surg (2011) 35:333 340 DOI 10.1007/s00266-010-9612-9 ORIGINAL ARTICLE Breast Augmentation and Mastopexy Using a Pectoral Muscle Loop André Auersvald Luiz Augusto Auersvald Received: 28 April
Aesth Plast Surg (2011) 35:333 340 DOI 10.1007/s00266-010-9612-9 ORIGINAL ARTICLE Breast Augmentation and Mastopexy Using a Pectoral Muscle Loop André Auersvald Luiz Augusto Auersvald Received: 28 April
Breast Reconstruction. Westmead Breast Cancer Institute
 Breast Reconstruction Westmead Breast Cancer Institute What is breast reconstruction? Breast reconstruction is a surgical procedure that creates a shape on the chest wall following a mastectomy. Occasionally,
Breast Reconstruction Westmead Breast Cancer Institute What is breast reconstruction? Breast reconstruction is a surgical procedure that creates a shape on the chest wall following a mastectomy. Occasionally,
Prepectoral breast reconstruction and radiotherapy a closer look
 Original Article Prepectoral breast reconstruction and radiotherapy a closer look Steven Sigalove Scottsdale Center for Plastic Surgery, Scottsdale, AZ, USA Correspondence to: Steven Sigalove, MD, FACS.
Original Article Prepectoral breast reconstruction and radiotherapy a closer look Steven Sigalove Scottsdale Center for Plastic Surgery, Scottsdale, AZ, USA Correspondence to: Steven Sigalove, MD, FACS.
A Comparative Study of CG CryoDerm and AlloDerm in Direct-to-Implant Immediate Breast Reconstruction
 A Comparative Study of CG CryoDerm and AlloDerm in Direct-to-Implant Immediate Breast Reconstruction Original Article Jun Ho Lee 1, Ki Rin Park 1, Tae Gon Kim 1, Ju-Ho Ha 1, Kyu-Jin Chung 1, Yong-Ha Kim
A Comparative Study of CG CryoDerm and AlloDerm in Direct-to-Implant Immediate Breast Reconstruction Original Article Jun Ho Lee 1, Ki Rin Park 1, Tae Gon Kim 1, Ju-Ho Ha 1, Kyu-Jin Chung 1, Yong-Ha Kim
Breast Reconstruction Surgery
 Breast Reconstruction Surgery I. Policy University Health Alliance (UHA) will reimburse for Breast Reconstruction Surgery when it is determined to be medically necessary and when it meets the medical criteria
Breast Reconstruction Surgery I. Policy University Health Alliance (UHA) will reimburse for Breast Reconstruction Surgery when it is determined to be medically necessary and when it meets the medical criteria
Medical Review Criteria Breast Surgeries
 Medical Review Criteria Breast Surgeries Subject: Breast Surgeries Authorization: Prior authorization is required for the following procedures requested for members enrolled in HPHC commercial (HMO, POS,
Medical Review Criteria Breast Surgeries Subject: Breast Surgeries Authorization: Prior authorization is required for the following procedures requested for members enrolled in HPHC commercial (HMO, POS,
Nipple-Areolar Complex Reconstruction: A Review of the Literature and Introduction of the Rectangle-to-Cube Nipple Flap
 Nipple-Areolar Complex Reconstruction: A Review of the Literature and Introduction of the Rectangle-to-Cube Nipple Flap Joshua T. Henderson, BA, a ThomasJ.Lee,MD, b Andrew M. Swiergosz, BS, a Andrea R.
Nipple-Areolar Complex Reconstruction: A Review of the Literature and Introduction of the Rectangle-to-Cube Nipple Flap Joshua T. Henderson, BA, a ThomasJ.Lee,MD, b Andrew M. Swiergosz, BS, a Andrea R.
A Prospective Analysis of Dynamic Loss of Breast Projection in Tissue Expander-Implant Reconstruction
 A Prospective Analysis of Dynamic Loss of Breast Projection in Tissue Expander-Implant Reconstruction Lauren M Mioton 1 *, Sumanas W Jordan 2 *, John YS Kim 2 1 Department of Plastic Surgery, Vanderbilt
A Prospective Analysis of Dynamic Loss of Breast Projection in Tissue Expander-Implant Reconstruction Lauren M Mioton 1 *, Sumanas W Jordan 2 *, John YS Kim 2 1 Department of Plastic Surgery, Vanderbilt
BREAST AUGMENTATION TECHNIQUES
 BREAST AUGMENTATION TECHNIQUES Breast Augmentation Top Surgical Procedure in 2015 (Worldwide) Surgical Procedure : Breast Augmentation Rank : 1 Total : 1,488,992 Percent of Total Surgical Procedures :
BREAST AUGMENTATION TECHNIQUES Breast Augmentation Top Surgical Procedure in 2015 (Worldwide) Surgical Procedure : Breast Augmentation Rank : 1 Total : 1,488,992 Percent of Total Surgical Procedures :
Reconstructive Breast Surgery and Management of Breast Implants
 Reconstructive Breast Surgery and Management of Breast Implants Policy Number: 7.01.22 Last Review: 1/2018 Origination: 3/1993 Next Review: 1/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue
Reconstructive Breast Surgery and Management of Breast Implants Policy Number: 7.01.22 Last Review: 1/2018 Origination: 3/1993 Next Review: 1/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue
SIMPOSIO Ricostruzione mammaria ed implicazioni radioterapiche Indicazioni
 SIMPOSIO Ricostruzione mammaria ed implicazioni radioterapiche Indicazioni Icro Meattini, MD Radiation Oncology Department - University of Florence Azienda Ospedaliero Universitaria Careggi Firenze Breast
SIMPOSIO Ricostruzione mammaria ed implicazioni radioterapiche Indicazioni Icro Meattini, MD Radiation Oncology Department - University of Florence Azienda Ospedaliero Universitaria Careggi Firenze Breast
The decision to repair a partial mastectomy CME. State of the Art and Science in Postmastectomy Breast Reconstruction.
 CME State of the Art and Science in Postmastectomy Breast Reconstruction Steven J. Kronowitz, M.D. Houston, Texas Learning Objectives: After reading this article, the participant should be able to: 1.
CME State of the Art and Science in Postmastectomy Breast Reconstruction Steven J. Kronowitz, M.D. Houston, Texas Learning Objectives: After reading this article, the participant should be able to: 1.
Radiation Therapy And Expander-Implant Breast Reconstruction: Analysis Of Timing And Complications
 Yale University EliScholar A Digital Platform for Scholarly Publishing at Yale Yale Medicine Thesis Digital Library School of Medicine January 2013 Radiation Therapy And Expander-Implant Breast Reconstruction:
Yale University EliScholar A Digital Platform for Scholarly Publishing at Yale Yale Medicine Thesis Digital Library School of Medicine January 2013 Radiation Therapy And Expander-Implant Breast Reconstruction:
Outcome of Management of Local Recurrence after Immediate Transverse Rectus Abdominis Myocutaneous Flap Breast Reconstruction
 Outcome of Management of Local Recurrence after Immediate Transverse Rectus bdominis Myocutaneous Flap reast Reconstruction Taik Jong Lee 1, Wu Jin Hur 1, Eun Key Kim 1, Sei Hyun hn 2 1 Department of Plastic
Outcome of Management of Local Recurrence after Immediate Transverse Rectus bdominis Myocutaneous Flap reast Reconstruction Taik Jong Lee 1, Wu Jin Hur 1, Eun Key Kim 1, Sei Hyun hn 2 1 Department of Plastic
The use of postmastectomy radiation therapy (PMRT) to prevent
 NORTHEASTERN SOCIETY OF PLASTIC SURGEONS Postmastectomy Radiation Therapy and Breast An Analysis of Complications and Patient Satisfaction Bernard T. Lee, MD,* Tolulope A. Adesiyun, BS,* Salih Colakoglu,
NORTHEASTERN SOCIETY OF PLASTIC SURGEONS Postmastectomy Radiation Therapy and Breast An Analysis of Complications and Patient Satisfaction Bernard T. Lee, MD,* Tolulope A. Adesiyun, BS,* Salih Colakoglu,
Plastic surgery of the breast includes; augmentation, reduction, Plastic Surgery of the Breast. Abstract. Continuing Education Column
 Plastic Surgery of the Breast Keuk Shun Shin, M.D. Keuk SHUN SHIN s Asthetic Plastic Surgery E mail: drsks@drsks.co.kr Abstract Plastic surgery of the breast includes; augmentation, reduction, reconstruction
Plastic Surgery of the Breast Keuk Shun Shin, M.D. Keuk SHUN SHIN s Asthetic Plastic Surgery E mail: drsks@drsks.co.kr Abstract Plastic surgery of the breast includes; augmentation, reduction, reconstruction
Medical Review Criteria Breast Surgeries
 Medical Review Criteria Breast Surgeries Effective Date: November 8, 2016 Subject: Breast Surgeries Policy: HPHC covers medically necessary breast surgeries including mastectomy, breast reconstruction,
Medical Review Criteria Breast Surgeries Effective Date: November 8, 2016 Subject: Breast Surgeries Policy: HPHC covers medically necessary breast surgeries including mastectomy, breast reconstruction,
A long term review of augmentation mastopexy in muscle splitting biplane
 Topic: Aesthetic Surgery of the Breast A long term review of augmentation mastopexy in muscle splitting biplane Umar Daraz Khan Aesthetic Plastic Surgeon, Reshape House, West Malling, Kent ME19 6QR, UK.
Topic: Aesthetic Surgery of the Breast A long term review of augmentation mastopexy in muscle splitting biplane Umar Daraz Khan Aesthetic Plastic Surgeon, Reshape House, West Malling, Kent ME19 6QR, UK.
Strattice Reconstructive Tissue Matrix used in the repair of rippling
 Clinical case study Strattice Tissue Matrix Strattice Reconstructive Tissue Matrix used in the repair of rippling Steven Teitelbaum, MD* Santa Monica, CA Case summary A 48-year-old woman with a history
Clinical case study Strattice Tissue Matrix Strattice Reconstructive Tissue Matrix used in the repair of rippling Steven Teitelbaum, MD* Santa Monica, CA Case summary A 48-year-old woman with a history
Tackling challenging revision breast augmentation cases
 the BREAST Careful preoperative consultations can reduce the need for revision breast surgery. Second Time Around Tackling challenging revision breast augmentation cases By Adam D. Schaffner, MD, FACS
the BREAST Careful preoperative consultations can reduce the need for revision breast surgery. Second Time Around Tackling challenging revision breast augmentation cases By Adam D. Schaffner, MD, FACS
ARTICLE COVERSHEET SERVER-BASED
 ARTICLE COVERSHEET LWW_CONDENSED-FLA(7.75X10.75) SERVER-BASED Template version : 8.1 Revised: 08/23/2012 Article :SAP22670 Creator : jteves Date : Saturday September 8th 2012 Time : 05:19:34 Number of
ARTICLE COVERSHEET LWW_CONDENSED-FLA(7.75X10.75) SERVER-BASED Template version : 8.1 Revised: 08/23/2012 Article :SAP22670 Creator : jteves Date : Saturday September 8th 2012 Time : 05:19:34 Number of
Predictability of anthropomorphic measurements in implant selection for breast reconstruction: a retrospective cohort study
 Eur J Plast Surg (2017) 40:203 212 DOI 10.1007/s00238-016-1261-z ORIGINAL PAPER Predictability of anthropomorphic measurements in implant selection for breast reconstruction: a retrospective cohort study
Eur J Plast Surg (2017) 40:203 212 DOI 10.1007/s00238-016-1261-z ORIGINAL PAPER Predictability of anthropomorphic measurements in implant selection for breast reconstruction: a retrospective cohort study
Breast Reconstruction
 Steven E. Copit, M.D. Chief- Division of Plastic Surgery Thomas Jefferson University Hospital Philadelphia, PA analysis of The Defect Skin Breast Volume Nipple Areola Complex analysis of The Defect the
Steven E. Copit, M.D. Chief- Division of Plastic Surgery Thomas Jefferson University Hospital Philadelphia, PA analysis of The Defect Skin Breast Volume Nipple Areola Complex analysis of The Defect the
Pre-pectoral Breast Reconstruction in Nipple Sparing Mastectomy
 September 2017 Issue 9 Pre-pectoral Breast Reconstruction in Nipple Sparing Mastectomy Aldona J. Spiegel, MD Director and Founder of the Center for Breast Restoration at the Institute for Reconstructive
September 2017 Issue 9 Pre-pectoral Breast Reconstruction in Nipple Sparing Mastectomy Aldona J. Spiegel, MD Director and Founder of the Center for Breast Restoration at the Institute for Reconstructive
Prophylactic Mastectomy & Reconstructive Implications
 Prophylactic Mastectomy & Reconstructive Implications Minas T Chrysopoulo, MD PRMA Center For Advanced Breast Reconstruction Prophylactic Mastectomy Surgical removal of one or both breasts to reduce the
Prophylactic Mastectomy & Reconstructive Implications Minas T Chrysopoulo, MD PRMA Center For Advanced Breast Reconstruction Prophylactic Mastectomy Surgical removal of one or both breasts to reduce the
JPRAS Open 3 (2015) 1e5. Contents lists available at ScienceDirect. JPRAS Open. journal homepage:
 JPRAS Open 3 (2015) 1e5 Contents lists available at ScienceDirect JPRAS Open journal homepage: http://www.journals.elsevier.com/ jpras-open Case report The pedicled transverse partial latissimus dorsi
JPRAS Open 3 (2015) 1e5 Contents lists available at ScienceDirect JPRAS Open journal homepage: http://www.journals.elsevier.com/ jpras-open Case report The pedicled transverse partial latissimus dorsi
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Breast Reconstructive Surgery After Mastectomy Page 1 of 8 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Breast Reconstructive Surgery After Mastectomy PRE-DETERMINATION
Breast Reconstructive Surgery After Mastectomy Page 1 of 8 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Breast Reconstructive Surgery After Mastectomy PRE-DETERMINATION
Goals of Care. Restore shape and function after cancer
 Goals of Care Restore shape and function after cancer Aid in physiological and psychological benefit Relationship with significant other Self esteem and positive body image Feeling of a whole body Avoid
Goals of Care Restore shape and function after cancer Aid in physiological and psychological benefit Relationship with significant other Self esteem and positive body image Feeling of a whole body Avoid
The success of breast conservation protocols BREAST. Implant Reconstruction in Breast Cancer Patients Treated with Radiation Therapy
 BREAST Implant Reconstruction in Breast Cancer Patients Treated with Radiation Therapy Jeffrey A. Ascherman, M.D. Matthew M. Hanasono, M.D. Martin I. Newman, M.D. Duncan B. Hughes, M.D. New York, N.Y.
BREAST Implant Reconstruction in Breast Cancer Patients Treated with Radiation Therapy Jeffrey A. Ascherman, M.D. Matthew M. Hanasono, M.D. Martin I. Newman, M.D. Duncan B. Hughes, M.D. New York, N.Y.
Skin sparing mastectomy: Technique and suggested methods of reconstruction
 Journal of the Egyptian National Cancer Institute (2014) 26, 153 159 Cairo University Journal of the Egyptian National Cancer Institute www.nci.cu.adu.eg www.sciencedirect.com Full Length Article Skin
Journal of the Egyptian National Cancer Institute (2014) 26, 153 159 Cairo University Journal of the Egyptian National Cancer Institute www.nci.cu.adu.eg www.sciencedirect.com Full Length Article Skin
Advances in Breast Surgery. Catherine Campo, D.O. Breast Surgeon Meridian Health System April 17, 2015
 Advances in Breast Surgery Catherine Campo, D.O. Breast Surgeon Meridian Health System April 17, 2015 Objectives Understand the surgical treatment of breast cancer Be able to determine when a lumpectomy
Advances in Breast Surgery Catherine Campo, D.O. Breast Surgeon Meridian Health System April 17, 2015 Objectives Understand the surgical treatment of breast cancer Be able to determine when a lumpectomy
Outcomes Evaluation Following Bilateral Breast Reconstruction Using Latissimus Dorsi Myocutaneous Flaps
 BREAST SURGERY Outcomes Evaluation Following Bilateral Breast Reconstruction Using Latissimus Dorsi Myocutaneous Flaps Albert Losken, MD, FACS, Claire S. Nicholas, MD, Ximena A. inell, MD, and Grant W.
BREAST SURGERY Outcomes Evaluation Following Bilateral Breast Reconstruction Using Latissimus Dorsi Myocutaneous Flaps Albert Losken, MD, FACS, Claire S. Nicholas, MD, Ximena A. inell, MD, and Grant W.
The Case FOR Oncoplastic Surgery in Small Breasts. Barbara L. Smith, MD, PhD Massachusetts General Hospital Harvard Medical School Boston, MA USA
 The Case FOR Oncoplastic Surgery in Small Breasts Barbara L. Smith, MD, PhD Massachusetts General Hospital Harvard Medical School Boston, MA USA Changing issues in breast cancer management Early detection
The Case FOR Oncoplastic Surgery in Small Breasts Barbara L. Smith, MD, PhD Massachusetts General Hospital Harvard Medical School Boston, MA USA Changing issues in breast cancer management Early detection
Preoperative planning and breast implant selection for volume difference management in asymmetrical breasts
 . Plast Aesthet Res 2017;4:108-15 DOI: 10.20517/2347-9264.2017.36 Original Article Plastic and Aesthetic Research www.parjournal.net Open Access Preoperative planning and breast implant selection for volume
. Plast Aesthet Res 2017;4:108-15 DOI: 10.20517/2347-9264.2017.36 Original Article Plastic and Aesthetic Research www.parjournal.net Open Access Preoperative planning and breast implant selection for volume
Vertical mammaplasty has been developed
 BREAST Y-Scar Vertical Mammaplasty David A. Hidalgo, M.D. New York, N.Y. Background: Vertical mammaplasty is an effective alternative to inverted-t methods. Among other benefits, it results in a significantly
BREAST Y-Scar Vertical Mammaplasty David A. Hidalgo, M.D. New York, N.Y. Background: Vertical mammaplasty is an effective alternative to inverted-t methods. Among other benefits, it results in a significantly
BREAST RECONSTRUCTION FOLLOWING PROPHYLACTIC OR THERAPEUTIC MASTECTOMY FOR BREAST CANCER
 BREAST RECONSTRUCTION FOLLOWING PROPHYLACTIC OR THERAPEUTIC MASTECTOMY FOR BREAST CANCER Effective Date: September 2013 The recommendations contained in this guideline are a consensus of the Alberta Provincial
BREAST RECONSTRUCTION FOLLOWING PROPHYLACTIC OR THERAPEUTIC MASTECTOMY FOR BREAST CANCER Effective Date: September 2013 The recommendations contained in this guideline are a consensus of the Alberta Provincial
BREAST RECONSTRUCTION POST MASTECTOMY
 UnitedHealthcare Commercial Coverage Determination Guideline BREAST RECONSTRUCTION POST MASTECTOMY Guideline Number: SUR057 Effective Date: January 1, 2019 Table of Contents Page INSTRUCTIONS FOR USE...
UnitedHealthcare Commercial Coverage Determination Guideline BREAST RECONSTRUCTION POST MASTECTOMY Guideline Number: SUR057 Effective Date: January 1, 2019 Table of Contents Page INSTRUCTIONS FOR USE...
MASTECTOMY AND IMMEDIATE BREAST RECONSTRUCTION IN INVASIVE CARCINOMA
 MASTECTOMY AND IMMEDIATE BREAST RECONSTRUCTION IN INVASIVE CARCINOMA Node-postive breast cancer Delayed-immediate reconstruction versus delayed reconstruction DBCG RT Recon-Protocol Tine Engberg Damsgaard
MASTECTOMY AND IMMEDIATE BREAST RECONSTRUCTION IN INVASIVE CARCINOMA Node-postive breast cancer Delayed-immediate reconstruction versus delayed reconstruction DBCG RT Recon-Protocol Tine Engberg Damsgaard
F ORUM. Is One-Stage Breast Augmentation With Mastopexy Safe and Effective? A Review of 186 Primary Cases
 Is One-Stage Breast Augmentation With Mastopexy Safe and Effective? A Review of 186 Primary Cases W. Grant Stevens, MD; David A. Stoker, MD; Mark E. Freeman, MD; Suzanne M. Quardt, MD; Elliot M. Hirsch,
Is One-Stage Breast Augmentation With Mastopexy Safe and Effective? A Review of 186 Primary Cases W. Grant Stevens, MD; David A. Stoker, MD; Mark E. Freeman, MD; Suzanne M. Quardt, MD; Elliot M. Hirsch,
Columella Lengthening with a Full-Thickness Skin Graft for Secondary Bilateral Cleft Lip and Nose Repair
 Original Article Columella Lengthening with a Full-Thickness Skin Graft for Secondary Bilateral Cleft Lip and Nose Repair Yoon Seok Lee 1, Dong Hyeok Shin 1, Hyun Gon Choi 1, Jee Nam Kim 1, Myung Chul
Original Article Columella Lengthening with a Full-Thickness Skin Graft for Secondary Bilateral Cleft Lip and Nose Repair Yoon Seok Lee 1, Dong Hyeok Shin 1, Hyun Gon Choi 1, Jee Nam Kim 1, Myung Chul
A New Breast Shape Classification
 A New Breast Shape Classification plasticsurgerypractice.com/2011/10/a-new-breast-shape-classification Class 1: Appears natural with no superior pole fullness. Class 2: Appears natural with mild superior
A New Breast Shape Classification plasticsurgerypractice.com/2011/10/a-new-breast-shape-classification Class 1: Appears natural with no superior pole fullness. Class 2: Appears natural with mild superior
Mitchell Buller, MEng, a Adee Heiman, BA, a Jared Davis, MD, b ThomasJ.Lee,MD, b Nicolás Ajkay, MD, FACS, c and Bradon J. Wilhelmi, MD, FACS b
 Immediate Breast Reconstruction of a Nipple Areolar Lumpectomy Defect With the L-Flap Skin Paddle Breast Reduction Design and Contralateral Reduction Mammoplasty Symmetry Procedure: Optimizing the Oncoplastic
Immediate Breast Reconstruction of a Nipple Areolar Lumpectomy Defect With the L-Flap Skin Paddle Breast Reduction Design and Contralateral Reduction Mammoplasty Symmetry Procedure: Optimizing the Oncoplastic
INNOVATIVE RECONSTRUCTIVE STRATEGIES IN BREAST CANCER SURGERY
 INNOVATIVE RECONSTRUCTIVE STRATEGIES IN BREAST CANCER SURGERY Jane L. Kakkis, MD, MPH Breast Surgeon, Director Orange Coast Memorial Medical Center, Fountain Valley, CA USA WHEN RADIATION IS NECESSARY
INNOVATIVE RECONSTRUCTIVE STRATEGIES IN BREAST CANCER SURGERY Jane L. Kakkis, MD, MPH Breast Surgeon, Director Orange Coast Memorial Medical Center, Fountain Valley, CA USA WHEN RADIATION IS NECESSARY
BREAST RECONSTRUCTION POST MASTECTOMY
 UnitedHealthcare Commercial Coverage Determination Guideline BREAST RECONSTRUCTION POST MASTECTOMY Guideline Number: SUR057 Effective Date: February 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE...
UnitedHealthcare Commercial Coverage Determination Guideline BREAST RECONSTRUCTION POST MASTECTOMY Guideline Number: SUR057 Effective Date: February 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE...
Breast Cancer after Augmentation: Oncologic and Reconstructive Considerations among Women Undergoing Mastectomy.
 BREAST Breast Cancer after Augmentation: Oncologic and Reconstructive Considerations among Women Undergoing Mastectomy Eugenia H. Cho, B.S. Ronnie L. Shammas, B.S. Brett T. Phillips, M.D., M.B.A. Rachel
BREAST Breast Cancer after Augmentation: Oncologic and Reconstructive Considerations among Women Undergoing Mastectomy Eugenia H. Cho, B.S. Ronnie L. Shammas, B.S. Brett T. Phillips, M.D., M.B.A. Rachel
A Clinical Anatomic Study of Internal Mammary Perforators as Recipient Vessels for Breast Reconstruction
 A Clinical Anatomic Study of Internal Mammary Perforators as Recipient Vessels for Breast Reconstruction In-Soo Baek 1, Jae-Pil You 1, Sung-Mi Rhee 1, Gil-Su Son 2, Deok-Woo Kim 1, Eun-Sang Dhong 1, Seung-Ha
A Clinical Anatomic Study of Internal Mammary Perforators as Recipient Vessels for Breast Reconstruction In-Soo Baek 1, Jae-Pil You 1, Sung-Mi Rhee 1, Gil-Su Son 2, Deok-Woo Kim 1, Eun-Sang Dhong 1, Seung-Ha
AESTHETIC SURGERY OF THE BREAST: MASTOPEXY, AUGMENTATION & REDUCTION
 CHAPTER 18 AESTHETIC SURGERY OF THE BREAST: MASTOPEXY, AUGMENTATION & REDUCTION Ali A. Qureshi, MD and Smita R. Ramanadham, MD Aesthetic surgery of the breast aims to either correct ptosis with a mastopexy,
CHAPTER 18 AESTHETIC SURGERY OF THE BREAST: MASTOPEXY, AUGMENTATION & REDUCTION Ali A. Qureshi, MD and Smita R. Ramanadham, MD Aesthetic surgery of the breast aims to either correct ptosis with a mastopexy,
INFORMED CONSENT-BREAST RECONSTRUCTION WITH TRAM ABDOMINAL MUSCLE FLAP
 INFORMED CONSENT-BREAST RECONSTRUCTION WITH TRAM ABDOMINAL MUSCLE FLAP 2000 American Society of Plastic Surgeons. Purchasers of the Patient Consultation Resource Book are given a limited license to modify
INFORMED CONSENT-BREAST RECONSTRUCTION WITH TRAM ABDOMINAL MUSCLE FLAP 2000 American Society of Plastic Surgeons. Purchasers of the Patient Consultation Resource Book are given a limited license to modify
Two-stage prepectoral breast reconstruction
 Original Article Two-stage prepectoral breast reconstruction Maurice Y. Nahabedian 1, Steven R. Jacobson 2 1 National Center for Plastic Surgery, McLean, VA, USA; 2 Jacobson Plastic Surgery, Rochester,
Original Article Two-stage prepectoral breast reconstruction Maurice Y. Nahabedian 1, Steven R. Jacobson 2 1 National Center for Plastic Surgery, McLean, VA, USA; 2 Jacobson Plastic Surgery, Rochester,
Information about breast augmentation (enlargement) surgery Part 1 of 3
 Information about breast augmentation (enlargement) surgery Part 1 of 3 This leaflet explains breast augmentation surgery. It is important that you read this information carefully and completely. Please
Information about breast augmentation (enlargement) surgery Part 1 of 3 This leaflet explains breast augmentation surgery. It is important that you read this information carefully and completely. Please
Breast Restoration Surgery After a mastectomy
 UW MEDICINE PATIENT EDUCATION Breast Restoration Surgery After a mastectomy This handout explains the most common procedures that are used at University of Washington Medical Center (UWMC) to restore a
UW MEDICINE PATIENT EDUCATION Breast Restoration Surgery After a mastectomy This handout explains the most common procedures that are used at University of Washington Medical Center (UWMC) to restore a
 This article was published in an Elsevier journal. The attached copy is furnished to the author for non-commercial research and education use, including for instruction at the author s institution, sharing
This article was published in an Elsevier journal. The attached copy is furnished to the author for non-commercial research and education use, including for instruction at the author s institution, sharing
Current perspectives on radiation therapy in autologous and prosthetic breast reconstruction
 Review Article Current perspectives on radiation therapy in autologous and prosthetic breast reconstruction Mark W. Clemens, Steven J. Kronowitz Department of Plastic Surgery, The University of Texas M.D.
Review Article Current perspectives on radiation therapy in autologous and prosthetic breast reconstruction Mark W. Clemens, Steven J. Kronowitz Department of Plastic Surgery, The University of Texas M.D.
Anatomical Landmarks for Safe Elevation of the Deep Inferior Epigastric Perforator Flap: A Cadaveric Study
 Anatomical Landmarks for Safe Elevation of the Deep Inferior Epigastric Perforator Flap: A Cadaveric Study Saeed Chowdhry, MD, Ron Hazani, MD, Philip Collis, BS, and Bradon J. Wilhelmi, MD University of
Anatomical Landmarks for Safe Elevation of the Deep Inferior Epigastric Perforator Flap: A Cadaveric Study Saeed Chowdhry, MD, Ron Hazani, MD, Philip Collis, BS, and Bradon J. Wilhelmi, MD University of
Acellular Dermal Matrix in Primary Breast Reconstruction
 Supplemental Article Acellular Dermal Matrix in Primary Breast Reconstruction Hani Sbitany, MD; and Howard N. Langstein, MD Traditional implant-based breast reconstruction is relatively simple to perform
Supplemental Article Acellular Dermal Matrix in Primary Breast Reconstruction Hani Sbitany, MD; and Howard N. Langstein, MD Traditional implant-based breast reconstruction is relatively simple to perform
COPE Library Sample
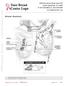 Breast Anatomy LOBULE LOBE ACINI (MILK PRODUCING UNITS) NIPPLE AREOLA COMPLEX ENLARGEMENT OF DUCT AND LOBE LOBULE SUPRACLAVICULAR NODES INFRACLAVICULAR NODES DUCT DUCT ACINI (MILK PRODUCING UNITS) 8420
Breast Anatomy LOBULE LOBE ACINI (MILK PRODUCING UNITS) NIPPLE AREOLA COMPLEX ENLARGEMENT OF DUCT AND LOBE LOBULE SUPRACLAVICULAR NODES INFRACLAVICULAR NODES DUCT DUCT ACINI (MILK PRODUCING UNITS) 8420
Aesthetic Subunits of the Breast
 Aesthetic Subunits of the Breast Scott L. Spear, M.D., and Steven P. Davison, D.D.S., M.D. Washington, D.C. Surgery for breast cancer has traditionally addressed the breast as if it were a geometric circle
Aesthetic Subunits of the Breast Scott L. Spear, M.D., and Steven P. Davison, D.D.S., M.D. Washington, D.C. Surgery for breast cancer has traditionally addressed the breast as if it were a geometric circle
Aesthetic reconstruction of the nasal tip using a folded composite graft from the ear
 The British Association of Plastic Surgeons (2004) 57, 238 244 Aesthetic reconstruction of the nasal tip using a folded composite graft from the ear Yong Oock Kim*, Beyoung Yun Park, Won Jae Lee Institute
The British Association of Plastic Surgeons (2004) 57, 238 244 Aesthetic reconstruction of the nasal tip using a folded composite graft from the ear Yong Oock Kim*, Beyoung Yun Park, Won Jae Lee Institute
Breast reconstruction has an important role BREAST. A Two-Year Prospective Analysis of Trunk Function in TRAM Breast Reconstructions
 BREAST A Two-Year Prospective Analysis of Trunk Function in TRAM Breast Reconstructions Amy K. Alderman, M.D. William M. Kuzon, Jr., M.D., Ph.D. Edwin G. Wilkins, M.D. Ann Arbor, Mich. Background: Functional
BREAST A Two-Year Prospective Analysis of Trunk Function in TRAM Breast Reconstructions Amy K. Alderman, M.D. William M. Kuzon, Jr., M.D., Ph.D. Edwin G. Wilkins, M.D. Ann Arbor, Mich. Background: Functional
Neil J. Zemmel, MD, FACS Steven J. Montante, MD Megan J. Russell, PA-C. Your Guide To BREAST RECONSTRUCTION
 Neil J. Zemmel, MD, FACS Steven J. Montante, MD Megan J. Russell, PA-C Your Guide To BREAST RECONSTRUCTION Introduction The diagnosis of breast cancer begins a journey of making many informed decisions
Neil J. Zemmel, MD, FACS Steven J. Montante, MD Megan J. Russell, PA-C Your Guide To BREAST RECONSTRUCTION Introduction The diagnosis of breast cancer begins a journey of making many informed decisions
Reconstructive Breast Surgery following Mastectomy for Breast Cancer: A Review
 Research Article http://www.alliedacademies.org/advanced-surgical-research/ Reconstructive Breast Surgery following Mastectomy for Breast Cancer: A Review Gurnam Virdi* Department of surgery, Queen Elizabeth
Research Article http://www.alliedacademies.org/advanced-surgical-research/ Reconstructive Breast Surgery following Mastectomy for Breast Cancer: A Review Gurnam Virdi* Department of surgery, Queen Elizabeth
Predictors of Contralateral Prophylactic Mastectomy and the Impact on Breast Reconstruction
 CLINICAL PAPER Predictors of Contralateral Prophylactic Mastectomy and the Impact on Breast Reconstruction Ximena A. Pinell-White, MD, Keli Kolegraff, MD, and Grant W. Carlson, MD Background: Contralateral
CLINICAL PAPER Predictors of Contralateral Prophylactic Mastectomy and the Impact on Breast Reconstruction Ximena A. Pinell-White, MD, Keli Kolegraff, MD, and Grant W. Carlson, MD Background: Contralateral
Outcomes of Acellular Dermal Matrix for Immediate Tissue Expander Reconstruction with Radiotherapy: A Retrospective Cohort Study
 Breast Surgery 5 Outcomes of Acellular Dermal Matrix for Immediate Tissue Expander Reconstruction with Radiotherapy: A Retrospective Cohort Study Aesthetic Surgery Journal 2018, 1 11 2018 The American
Breast Surgery 5 Outcomes of Acellular Dermal Matrix for Immediate Tissue Expander Reconstruction with Radiotherapy: A Retrospective Cohort Study Aesthetic Surgery Journal 2018, 1 11 2018 The American
MICHAEL R. ZENN, M.D. INFORMATION ABOUT BREAST RECONSTRUCTION
 MICHAEL R. ZENN, M.D. INFORMATION ABOUT BREAST RECONSTRUCTION The purpose of breast reconstruction is to restore body image and to enable you to wear all types of clothes without restriction. Most women
MICHAEL R. ZENN, M.D. INFORMATION ABOUT BREAST RECONSTRUCTION The purpose of breast reconstruction is to restore body image and to enable you to wear all types of clothes without restriction. Most women
Augmentation of the Ptotic Breast: Simultaneous Periareolar Mastopexy/Breast Augmentation By: Laurence Kirwan, M.D., F.R.C.S
 Augmentation of the Ptotic Breast: Simultaneous Periareolar Mastopexy/Breast Augmentation By: Laurence Kirwan, M.D., F.R.C.S Background: Submusculofascial augmentation of the ptotic breast can result in
Augmentation of the Ptotic Breast: Simultaneous Periareolar Mastopexy/Breast Augmentation By: Laurence Kirwan, M.D., F.R.C.S Background: Submusculofascial augmentation of the ptotic breast can result in
A multiple logistic regression analysis of complications following microsurgical breast reconstruction
 Original Article A multiple logistic regression analysis of complications following microsurgical breast reconstruction Samir Rao 1, Ellen C. Stolle 1, Sarah Sher 1, Chun-Wang Lin 1, Bahram Momen 2, Maurice
Original Article A multiple logistic regression analysis of complications following microsurgical breast reconstruction Samir Rao 1, Ellen C. Stolle 1, Sarah Sher 1, Chun-Wang Lin 1, Bahram Momen 2, Maurice
National Medical Policy
 National Medical Policy Subject: Policy Number: Breast Reconstructive Surgery NMP492 Effective Date*: February 2013 Updated: April 2016 This National Medical Policy is subject to the terms in the IMPORTANT
National Medical Policy Subject: Policy Number: Breast Reconstructive Surgery NMP492 Effective Date*: February 2013 Updated: April 2016 This National Medical Policy is subject to the terms in the IMPORTANT
Implant selection in the setting of prepectoral breast reconstruction
 Review Article Implant selection in the setting of prepectoral breast reconstruction Allen Gabriel, G. Patrick Maxwell Department of Plastic Surgery, Loma Linda University Medical Center, Loma Linda, CA,
Review Article Implant selection in the setting of prepectoral breast reconstruction Allen Gabriel, G. Patrick Maxwell Department of Plastic Surgery, Loma Linda University Medical Center, Loma Linda, CA,
Correction of Long Standing Proximal Interphalangeal Flexion Contractures with Cross Finger Flaps and Vigorous Postoperative Exercises
 Original Article DOI 10.3349/ymj.2010.51.4.574 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 51(4):574-578, 2010 Correction of Long Standing Proximal Interphalangeal Flexion Contractures with Cross Finger
Original Article DOI 10.3349/ymj.2010.51.4.574 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 51(4):574-578, 2010 Correction of Long Standing Proximal Interphalangeal Flexion Contractures with Cross Finger
Medical Policy Original Effective Date: Revised Date: Page 1 of 8
 Page 1 of 8 Disclaimer Description Coverage Determination Refer to the member s specific benefit plan and Schedule of Benefits to determine coverage. This may not be a benefit on all plans, or the plan
Page 1 of 8 Disclaimer Description Coverage Determination Refer to the member s specific benefit plan and Schedule of Benefits to determine coverage. This may not be a benefit on all plans, or the plan
Breast Reconstruction with Superficial Inferior Epigastric Artery Flaps: A Prospective Comparison with TRAM and DIEP Flaps
 Breast Reconstruction with Superficial Inferior Epigastric Artery Flaps: A Prospective Comparison with TRAM and DIEP Flaps Pierre M. Chevray, M.D., Ph.D. Houston, Texas Breast reconstruction using the
Breast Reconstruction with Superficial Inferior Epigastric Artery Flaps: A Prospective Comparison with TRAM and DIEP Flaps Pierre M. Chevray, M.D., Ph.D. Houston, Texas Breast reconstruction using the
