Clinical Policy Title: Bone graft substitutes
|
|
|
- Jonah Pierce
- 6 years ago
- Views:
Transcription
1 Clinical Policy Title: Bone graft substitutes Clinical Policy Number: Effective Date: July 1, 2016 Initial Review Date: May 18, 2016 Most Recent Review Date: May 19, 2017 Next Review Date: May 2018 Policy contains: Bone graft substitutes. Related policies: CP# CP# Bone marrow transplant Spinal surgeries ABOUT THIS POLICY: AmeriHealth Caritas Pennsylvania has developed clinical policies to assist with making coverage determinations. AmeriHealth Caritas Pennsylvania s clinical policies are based on guidelines from established industry sources, such as the Centers for Medicare & Medicaid Services (CMS), state regulatory agencies, the American Medical Association (AMA), medical specialty professional societies, and peer-reviewed professional literature. These clinical policies along with other sources, such as plan benefits and state and federal laws and regulatory requirements, including any state- or plan-specific definition of medically necessary, and the specific facts of the particular situation are considered by AmeriHealth Caritas Pennsylvania when making coverage determinations. In the event of conflict between this clinical policy and plan benefits and/or state or federal laws and/or regulatory requirements, the plan benefits and/or state and federal laws and/or regulatory requirements shall control. AmeriHealth Caritas Pennsylvania s clinical policies are for informational purposes only and not intended as medical advice or to direct treatment. Physicians and other health care providers are solely responsible for the treatment decisions for their patients. AmeriHealth Caritas Pennsylvania s clinical policies are reflective of evidence-based medicine at the time of review. As medical science evolves, AmeriHealth Caritas Pennsylvania will update its clinical policies as necessary. AmeriHealth Caritas Pennsylvania s clinical policies are not guarantees of payment. Coverage policy AmeriHealth Caritas Pennsylvania considers the use of the following bone graft substitutes, alone or in combination, to be clinically proven and, therefore, medically necessary for enhancement of bone healing. Bone graft and graft substitutes: Autograft based, used alone. Allograft-based, allograft bone used alone or in combination with other materials, including demineralized bone matrix (DBM). Ceramic or polymer-based synthetic bone graft substitutes. Bone graft substitutes containing an organic bone material (e.g., bovine or coral) when used alone or combined with another covered bone graft substitute. Note: Refer to the chart on page three in this policy for the list of bone graft substitutes. 0
2 Limitations: AmeriHealth Caritas Pennsylvania considers all other uses of bone graft substitutes to be investigational and, therefore, not medically necessary: Mesenchymal stem cell therapy is considered investigational for all orthopedic applications, including, but not limited to, use in repair or regeneration of musculoskeletal tissue. Allograft bone products containing viable stem cells is considered investigational for all orthopedic applications, including, but not limited to, DBM with stem cells. Cms.gov: Local Coverage Determination (LCD) L33382 Lumbar Spinal Fusion for Instability and Degenerative Disc Conditions does not address lumbar spinal fusion techniques, devices, and instrumentation or bone graft substitutes. Some of the emerging techniques and associated tools (e.g., devices, spinal instrumentation, and bone graft substitutes) are investigational, and this LCD does not endorse such procedures. The scope of this LCD is the indications and medical need of lumbar spinal fusion for instability and degenerative disc conditions. Alternative covered services: None. Background Bone grafting is a surgical procedure that replaces missing bone with material from patient s own body, or an artificial, synthetic, or natural substitute. Bone grafting is possible because bone tissue has the ability to regenerate completely if provided the space into which it has to grow. As natural bone grows, it generally replaces the graft material completely, resulting in a fully integrated region of new bone. The Centers for Disease Control and Prevention (CDC) gave an update: allograft-associated bacterial infections United States, Tissue allografts are commonly used in orthopedic surgical procedures; in 1999, approximately 650,000 musculoskeletal allografts were distributed by tissue processors. A rare complication of musculoskeletal allografts is bacterial infection. After the reported death of a recipient of an allograft contaminated with Clostridium spp. (an anaerobic spore and toxin-forming organism), CDC investigated this case and solicited additional reports of allograft-associated infections; 26 cases have been identified. This report summarizes the investigation of these cases and describes additional steps given to a tissue processor to enhance tissue transplant safety. Classification of bone grafts based on material groups: 1
3 Allograft-based bone graft involves allograft bone, used alone or in combination with other materials (e.g., Grafton or OrthoBlast). Factor-based bone graft are natural and recombinant growth factors, used alone or in combination with other materials such as transforming growth factor-beta (TGF-beta), platelet-derived growth factor (PDGF), fibroblast growth factors (FGF), and bone morphogeneic protein (BMP). Cell-based bone grafts use cells to generate new tissue alone or are added onto a support matrix, such as mesenchymal stem cells. Ceramic-based bone graft substitutes include calcium phosphate, calcium sulphate, and bioglass used alone or in combination, such as OsteoGraf, ProOsteon, or OsteoSet. Polymer-based bone graft uses degradable and nondegradable polymers alone or in combination with other materials, such as open-porosity polylactic acid polymer. The past and existing bone grafts, graft substitutes, and the clinical evidence to support their use in the management of orthopedic cases are reviewed as also future direction of research (Table 1). Table 1: Bone graft and graft substitutes Class Description Examples Properties of action Autograft based Used alone Osteoconductive Osteoinductive Osteogenic Allograft based Factor based Cell based Ceramic based Polymer based Allograft bone used alone or in combination with other materials Natural and recombinant growth factors used alone or in combination with other materials Cells used to generate new tissue alone or seeded onto a support matrix Includes calcium phosphate, calcium sulfate, and bioactive glass used alone or in combination Includes degradable and nondegradable polymers used alone and in combination with other materials Allegro, Orthoblast, Grafton TGF-β, PDGF, FGF, BMP Mesenchymal stem cells Osteograf,, Osteoset, NovaBone Cortoss, OPLA, Immix Osteoconductive Osteoinductive Osteoinductive Both osteoconductive and osteoinductive with carrier materials Osteogenic Both osteogenic and osteoconductive with carrier materials Osteoconductive Limited osteoinductive when mixed with bone marrow Osteoconductive Bioresorbable in degradable polymer Miscellaneous (Laurencin C, 2006) Coral hydrogel-hydroxyapatite (HA) granules, blocks and composite ProOsteon Osteoconductive Bioresorbable Types and tissue sources of bone graft substitute: When a block graft will be performed, autogenous bone is the most preferred material because there is 2
4 less risk of graft rejection as the graft is originated from the patient s body. It would be osteoinductive and osteogenic, as well as osteoconductive. A disadvantage of autologous grafts is that an additional surgical site is required, which is another location for potential postoperative pain and complications. Synthetic variants: Flexible HA composite is a variant that has a mineral-to-organic matrix ratio approximating that of human bone. Artificial bone can be created from ceramics, such as calcium phosphates (e.g., HA and tricalcium phosphate), bioglass, and calcium sulphate that are biologically active depending on solubility in physiological environment. These materials combine with growth factors, ions such as strontium, or are mixed with bone marrow aspirate to increase biological activity. The presence of elements such as strontium can result in higher bone mineral density (BMD) and enhanced osteoblast proliferation. Xenografts are bone grafts from a species other than human, such as a bovine species, and are used as a calcified matrix. Alloplastic grafts: Alloplastic grafts may be made from hydroxyapatite, a naturally occurring mineral (main mineral component of bone), made from bioactive glass. Hydroxyapatite is a synthetic bone graft, which is the most used now due to its osteoconduction, hardness, and acceptability by bone. Some synthetic bone grafts are made of calcium carbonate, which starts to decrease in usage because it is completely resorbable in a short time and makes breaking of the bone easier. Finally used is the tricalcium phosphate in combination with hydroxyapatite and thus giving effect of both osteoconduction and resorbability. Ceramic-based bone graft substitutes: The majority of bone grafts available involve ceramics, either alone or in combination with another material (e.g., calcium sulfate, bioactive glass, or calcium phosphate). Ceramics like calcium phosphates use calcium hydroxyapatite, which is osteoconductive and osteointegrative and, in some cases, osteoinductive. Ceramics require high temperatures for scaffold formation and have brittle properties. Growth factors: Growth factors-enhanced grafts are produced using recombinant DNA technology. They consist of either human growth factors or morphogens (BMPs in conjunction with a carrier medium, such as collagen). Polymer-based bone graft substitutes: 3
5 These can be divided into natural polymers and synthetic polymers, and subclassified into degradable and nondegradable types. Polymer-based bone graft substitutes include: Healos, a natural polymer-based product and polymer-ceramic composite consisting of collagen fibers coated with hydroxyapatite and indicated for spinal fusions. Cortoss, an injectable resin-based product with applications for load-bearing sites. The most common use of bone grafting is in application of dental implants to restore the edentulous area of a missing tooth. In general, bone grafts are either used in block (such as from chin or ascending ramus area of lower jaw) or particulated to be able to adapt better to a defect. The grafted, vascularized fibulas have been used to restore skeletal integrity to long bones of limbs in which congenital bone defects exist and to replace segments of bone after trauma or malignant tumor invasion. The periosteum and nutrient artery are generally removed with a piece of bone so the graft will remain alive and grow when transplanted into a new host site. Once the transplanted bone is secured into its new location, it generally restores blood supply to the bone on which it has been attached. Besides the main use of bone grafting in dental implants, this procedure is used to fuse joints to prevent movement, repair broken bones that have bone loss, and repair broken bones that have not yet healed. Searches AmeriHealth Caritas Pennsylvania searched PubMed and the databases of: UK National Health Services Centre for Reviews and Dissemination. Agency for Healthcare Research and Quality s National Guideline Clearinghouse and other evidence-based practice centers. The Centers for Medicare & Medicaid Services (CMS). We conducted searches on April 12, Search terms were: allograft, autograft, bone reconstruction, bone repair, calcium sulphate, ceramic, hydroxyapatite, implant, polymer. We included: Systematic reviews, which pool results from multiple studies to achieve larger sample sizes and greater precision of effect estimation than in smaller primary studies. Systematic reviews use predetermined transparent methods to minimize bias, effectively treating the review as a scientific endeavor, and are thus rated highest in evidence-grading hierarchies. Guidelines based on systematic reviews. Economic analyses, such as cost-effectiveness, and benefit or utility studies (but not simple cost studies), reporting both costs and outcomes sometimes referred to as efficiency studies which also rank near the top of evidence hierarchies. Findings 4
6 The ideal bone-graft substitute is biocompatible, bioresorbable, osteoconductive, osteoinductive, structurally similar to bone, easy to use, and cost-effective. Currently marketed products are variable in their composition and claimed mechanisms of action. It is reasonable that not all bone-graft substitute products will perform the same. Future biosynthetic bone implants may obviate the need for autologous bone grafts. There is increasing interest in combining an osteoconductive protein in an osteoconductive carrier medium to facilitate timed-release delivery and/or to provide a material scaffold for bone formation. Further, advances in tissue engineering, with the integration of the biological, physical, and engineering sciences, will generate new carrier constructs that repair, regenerate, and restore tissue to its functional state. These constructs are likely to encompass additional families of growth factors, evolving biological scaffolds, and incorporation of mesenchymal stem cells. Ultimately, the development of ex vivo bioreactors capable of bone manufacture with the appropriate biomechanical cues will provide tissue-engineered constructs for direct use in the skeletal system. Finally, as researchers continue to find new materials and biologic approaches to bone repair, the future of bone graft substitutes continues to be an expanding topic of interest. The U.S. Food and Drug Administration (FDA) requires that the manufacturers of human allograft products be registered. The Musculoskeletal Transplant Foundation is listed in the FDA s Human Cell and Tissue Establishment Registration database. Please enter Musculoskeletal Transplant Foundation in the Establishment Name window in the FDA Human Cell and Tissue Establishment Registration database: playsearch&cfid= &cftoken=985566c088c8989f-1f22e2a5-cd46-2d0d-fe6c7a28b417f791. Accessed April 12, Policy updates: A narrative review (Zhang, 2017) assessed the need for natural bone substitutes with specific mention of nacre, or mother-of-pearl, as an organic matrix-calcium carbonate coupled shell structure. Nacre is produced by molluscs. In vivo and in vitro studies have revealed that nacre is osteoinductive, osteoconductive, biocompatible, and biodegradable. The authors concluded that there is great potential clinically for nacre as a bone graft substitute. Summary of clinical evidence: Citation Zhang (2017) Nacre, a natural, multi-use, and timely biomaterial for bone graft Content, Methods, Recommendations Key points: There is a huge and rapidly increasing clinical need for bone regeneration and repair. Bone substitutes are more and more often seen as a potential solution. Major innovation efforts are underway to develop such substitutes, some having advanced even to clinical practice (i.e., natural biomaterials). Nacre, or mother-of-pearl, is an organic matrix-calcium carbonate coupled shell structure produced by molluscs. 5
7 Citation Content, Methods, Recommendations substitution In vivo and in vitro studies have revealed that nacre is osteoinductive, osteoconductive, biocompatible, and biodegradable. The review sums up the current needs in orthopedic clinics and the challenges for the development of bone substitutes, and the potential use of nacre as a bone graft substitute. Grabowski Key points: (2013) Bone graft and bone graft substitutes in spine surgery Bone grafting is frequently used to augment bone healing with the numerous approaches to reconstructing or replacing skeletal defects. Autologous cancellous bone graft remains the most effective grafting material because it provides the three elements required for bone regeneration: osteoconduction, osteoinduction, and osteogenic cells. Autologous cortical bone graft provides these three components to a limited extent as well and also provides the structural integrity important in reconstruction of larger defects. However, because autogenous grafting is associated with several shortcomings and complications, including limited quantities of bone for harvest and donor-site morbidity, alternatives have been used in a wide range of orthopedic pathologic conditions. Grafting substitutes currently available include cancellous and cortical allograft bone, ceramics, demineralized bone matrix, bone marrow, and composite grafts. No single alternative graft material provides all three components for bone regeneration. The clinical applications for each type of material are dictated by its particular structural and biochemical properties. Composite grafts consisting of several materials are often used to maximize bone healing, especially where the grafting site is compromised. Kirkpatrick (2010) Bone void fillers Bucholz (1989) Interporous hydroxyapatit e as a bone graft substitute in tibial plateau fractures Damien (1991) Bone graft and bone graft =Fulltext# Key points: For this technology overview, the tools of evidence based medicine were used to summarize information on the effectiveness and clinical outcomes related to the usage of bone void fillers specifically, synthetic graft materials. Comprehensive literature searches were conducted to address five key questions, which the task force that prepared the report posed as follows: - Question 1 addressed the use of synthetic bone void fillers alone. - Question 2 was designed to determine whether synthetic bone void fillers could successfully serve as graft extenders and eliminate the need for iliac crest bone graft. - Questions 3, 4, and 5 addressed the use of allografts as a comparison with synthetic fillers because clinical results with allografts are perceived as being much closer to autografts in these areas of the spine. Key points: The metaphyseal defects in 40 patients with displaced tibial plateau fractures necessitating surgical repair were filled with either cancellous autograft or interporous hydroxyapatite. Roentgenographic and clinical assessments at follow-up periods averaging 15.4 months (autograft) and 34.5 months (hydroxyapatite) demonstrated no significant differences in the two groups. Interporous hydroxyapatite is a safe, effective alternative to autogenous cancellous bone for the filling of metaphyseal defects associated with tibial plateau fractures. Key points: The morbidity associated with autogenous bone graft harvest and the recent concern regarding the transmission of live virus through the use of allografts have been the impetus for research into a variety of materials that could take the place of these standard materials for bone grafting. The positive results reported with various ceramics and/or bone derivatives suggest the possibility of a 6
8 Citation substitutes: a review of current technology and applications Content, Methods, Recommendations material with osteoconductive and/or osteoinductive properties for use with or in place of bone graft. This review discusses a variety of bone graft and bone graft substitute materials. Among the osteoconductive materials outlined are the hydroxyapatite and tricalcium phosphate ceramics as well as some reportedly osteoactive polymers. While osteoconduction is a favorable quality, much interest has focused on the use of osteoinductive or osteogenic materials, such as demineralized bone matrix or bone derivatives, that is, BMP osteogenin and others. It is increasingly apparent that these materials require a carrier vehicle for optimal expression of osteoactivity. Therefore, the review finishes with a comparison of the various materials suggested for use as carriers. References Professional society guidelines/other: Bone-graft substitutes in orthopaedic surgery. American Academy of OrthopaedicSurgeons (AAOS). AAOS Website: Accessed April 12, Centers for Disease Control and Prevention. Septic arthritis following anterior cruciate ligament reconstruction using tendon allografts: Florida and Louisiana, MMWR Morb Mortal Wkly Rep. 2001; 50: Centers for Disease Control and Prevention (CDC) Update: Allograft-associated bacterial infections: United States, MMWR Morb Mortal Wkly Rep. 2002; 51: Peer-reviewed references: Alex Jahangir, MD; Ryan M. Nunley, MD; Samir Mehta, MD. Bone-graft substitutes in orthopaedic surgery. Journal of the American Academy of Orthopaedic Surgeons: January Volume 21 - Issue Bansal S, Chauhan V, Sharma S, Maheshwari R, Juyal A, Raghuvanshi S. Evaluation of hydroxyapatite and beta-tricalcium phosphate mixed with bone marrow aspirate as a bone graft substitute for posterolateral spinal fusion. Indian J Orthop. 2009;43: Bisla RS, Singh K, Singh J, Chawla SK. Clinical and 16. radiographic studies on evaluation of entire segment cortical bone grafts in goats. Indian J Anim Sci 1991; 61 : Bucholz RW, Carlton A, Holmes R: Interporous hydroxyapatite as a bone graft substitute in tibial plateau fractures. Clin Orthop Relat Res 1989; 240: Conrad EU, Gretch DR, Obermeyer KR, Moogk MS, Sayers M, Wilson JJ, et al. Transmission of the 7
9 hepatitis-c virus by tissue transplantation. J Bone Joint Surg Am. 1995;77: Damien CJ, Parsons JR. Bone graft and bone graft substitutes: a review of current technology and applications. (1991)J Appl Biomater Fall;2(3): Giannoudis PV, Dinopoulos H, Tsiridis E. Bone substitutes: An update. Injury. 2005;36(Suppl 3):S20 7. Grabowski M, Gregory D; Cornett A. Bone Graft and Bone Graft Substitutes in Spine Surgery: Current Concepts and Controversies. Journal of the American Academy of Orthopaedic Surgeons.2013;21 (1): Kirkpatrick, John S. MD; Cornell, Charles N. MD; Hoang, Bone Void Fillers. Journal of the American Academy of Orthopaedic Surgeons. 2010;18(9): Laurencin C, Khan Y, El-Amin SF. Bone graft substitutes. Expert Rev Med Devices. Indian j med res. 2010;3: Parikh SN. Bone graft substitutes: past, present, future. J Postgrad Med. 2002;48(2): Prasanna K, Belliappa V, Ghousia F. Bone grafts in dentistry. J Pharm Bioallied Sci. 2013; 5(Suppl 1): S125 S127. Sengupta DK, Truumees E, Patel CK, et al. Outcome of local bone versus autogenous iliac crest bone graft in the instrumented posterolateral fusion of the lumbar spine. Spine (Phila Pa 1976) 2006;31(9): Zhang G, Brion A, Willemin AS, et al. Nacre, a natural, multi-use, and timely biomaterial for bone graft substitution. J Biomed Mater Res A. 2017;105(2): CMS National Coverage Determinations (NCDs): No NCDs identified as of the writing of this policy. Local Coverage Determinations (LCDs) No LCDs identified as of the writing of this policy. Commonly submitted codes Below are the most commonly submitted codes for the service(s)/item(s) subject to this policy. This is not an exhaustive list of codes. Providers are expected to consult the appropriate coding manuals and bill accordingly. 8
10 CPT Code Description Comments N/A ICD-10 Code Description Comments Diagnoses too numerous HCPCS Level II Code C9359 C9362 Description Porous purified collagen matrix bone void filler (Integra Mozaik Osteoconductive Scaffold Putty, Integra OS Osteoconductive Scaffold Putty) per 0.5 cc Porous purified collagen matrix bone void filler (Integra Mozaik Osteoconductive Scaffold Strip) per 0.5cc Comments 9
Clinical Policy Title: Bone graft substitutes
 Clinical Policy Title: Bone graft substitutes Clinical Policy Number: 14.02.09 Effective Date: July 1, 2016 Initial Review Date: May 18, 2016 Most Recent Review Date: May 1, 2018 Next Review Date: May
Clinical Policy Title: Bone graft substitutes Clinical Policy Number: 14.02.09 Effective Date: July 1, 2016 Initial Review Date: May 18, 2016 Most Recent Review Date: May 1, 2018 Next Review Date: May
BIOACTIVE SYNTHETIC GRAFT
 B U I L D S T R O N G B O N E F A S T Putty Particulate Morsels A BIOACTIVE SYNTHETIC BONE FOR FASTER HEALING NovaBone is a 100% bioactive synthetic material composed from elements that occur naturally
B U I L D S T R O N G B O N E F A S T Putty Particulate Morsels A BIOACTIVE SYNTHETIC BONE FOR FASTER HEALING NovaBone is a 100% bioactive synthetic material composed from elements that occur naturally
Inion BioRestore. Bone Graft Substitute. Product Overview
 Inion BioRestore Bone Graft Substitute Product Overview Inion BioRestore Introduction Inion BioRestore is a synthetic bone graft substitute, which remodels into bone and is easy to use. Inion BioRestore
Inion BioRestore Bone Graft Substitute Product Overview Inion BioRestore Introduction Inion BioRestore is a synthetic bone graft substitute, which remodels into bone and is easy to use. Inion BioRestore
B U I L D S T R O N G B O N E F A S T
 B U I L D S T R O N G B O N E F A S T Putty MIS Particulate Morsels A BIOACTIVE SYNTHETIC BONE FOR FASTER HEALING NovaBone is a 100% bioactive synthetic material composed from elements that occur naturally
B U I L D S T R O N G B O N E F A S T Putty MIS Particulate Morsels A BIOACTIVE SYNTHETIC BONE FOR FASTER HEALING NovaBone is a 100% bioactive synthetic material composed from elements that occur naturally
Clinical Policy Title: Zoster (shingles) vaccine
 Clinical Policy Title: Zoster (shingles) vaccine Clinical Policy Number: 18.02.10 Effective Date: June 1, 2018 Initial Review Date: April 10, 2018 Most Recent Review Date: May 1, 2018 Next Review Date:
Clinical Policy Title: Zoster (shingles) vaccine Clinical Policy Number: 18.02.10 Effective Date: June 1, 2018 Initial Review Date: April 10, 2018 Most Recent Review Date: May 1, 2018 Next Review Date:
chronos Bone Void Filler. Beta-Tricalcium Phosphate ( β-tcp) bone graft substitute.
 chronos Bone Void Filler. Beta-Tricalcium Phosphate ( β-tcp) bone graft substitute. Osteoconductive Resorbable Synthetic chronos Bone Void Filler chronos granules and preforms are synthetic, porous, osteoconductive,
chronos Bone Void Filler. Beta-Tricalcium Phosphate ( β-tcp) bone graft substitute. Osteoconductive Resorbable Synthetic chronos Bone Void Filler chronos granules and preforms are synthetic, porous, osteoconductive,
Clinical Policy Title: Cardiac rehabilitation
 Clinical Policy Title: Cardiac rehabilitation Clinical Policy Number: 04.02.02 Effective Date: September 1, 2013 Initial Review Date: February 19, 2013 Most Recent Review Date: February 6, 2018 Next Review
Clinical Policy Title: Cardiac rehabilitation Clinical Policy Number: 04.02.02 Effective Date: September 1, 2013 Initial Review Date: February 19, 2013 Most Recent Review Date: February 6, 2018 Next Review
Clinical Policy Title: Dental bone grafting
 Clinical Policy Title: Dental bone grafting Clinical Policy Number: 14.03.06 Effective Date: April 1, 2017 Initial Review Date: March 15, 2017 Most Recent Review Date: March 15, 2017 Next Review Date:
Clinical Policy Title: Dental bone grafting Clinical Policy Number: 14.03.06 Effective Date: April 1, 2017 Initial Review Date: March 15, 2017 Most Recent Review Date: March 15, 2017 Next Review Date:
Bone Grafting and Bone Graft Substitutes. Original Author: James Krieg, MD Revision Author: David Hak, MD Last Revision May 2010
 Bone Grafting and Bone Graft Substitutes Original Author: James Krieg, MD Revision Author: David Hak, MD Last Revision May 2010 Bone Graft Function Structural support of articular fracture Tibial plateau
Bone Grafting and Bone Graft Substitutes Original Author: James Krieg, MD Revision Author: David Hak, MD Last Revision May 2010 Bone Graft Function Structural support of articular fracture Tibial plateau
ADVANCED BONE GRAFT SYSTEM OVERVIEW
 ADVANCED BONE GRAFT SYSTEM OVERVIEW NANOSS BIOACTIVE ADVANCED BONE GRAFT Table Of Contents INTRODUCTION System Overview... 1 NANOSS BIOACTIVE COMPONENTS Comparison of nanoss Bioactive and Human Bone...
ADVANCED BONE GRAFT SYSTEM OVERVIEW NANOSS BIOACTIVE ADVANCED BONE GRAFT Table Of Contents INTRODUCTION System Overview... 1 NANOSS BIOACTIVE COMPONENTS Comparison of nanoss Bioactive and Human Bone...
Ankle and subtalar arthrodesis
 OSTEOAMP Allogeneic Morphogenetic Proteins Ankle Nonunions OSTEOAMP Case Report ANKLE NONUNIONS Dr. Jason George DeVries Orthopedic & Sports Medicine, Bay Care Clinic, 501 N. 10th Street, Manitowoc, WI
OSTEOAMP Allogeneic Morphogenetic Proteins Ankle Nonunions OSTEOAMP Case Report ANKLE NONUNIONS Dr. Jason George DeVries Orthopedic & Sports Medicine, Bay Care Clinic, 501 N. 10th Street, Manitowoc, WI
Biomaterials Line. MIS Corporation. All Rights Reserved.
 7. Biomaterials Line MIS Corporation. All Rights Reserved. 6. MIS s Quality System complies with international quality standards: ISO 13485: 2003 - Quality Management System for Medical Devices, ISO 9001:
7. Biomaterials Line MIS Corporation. All Rights Reserved. 6. MIS s Quality System complies with international quality standards: ISO 13485: 2003 - Quality Management System for Medical Devices, ISO 9001:
Versatile grafting Solutions
 Versatile grafting Solutions A Canadian company serving Canadian dentists since 1997 Here s why your colleagues are calling us for their bone regeneration needs Founded in 1997 Citagenix has been providing
Versatile grafting Solutions A Canadian company serving Canadian dentists since 1997 Here s why your colleagues are calling us for their bone regeneration needs Founded in 1997 Citagenix has been providing
CONFORM FlEX. Demineralized cancellous bone
 CONFORM FlEX Demineralized cancellous bone TABlE OF CONTENTS introduction 2 FEATURES AND BENEFiTS 4 PROCESSiNg AND PACKAgiNg information 5 MUSCUlOSKElETAl TRANSPlANT FOUNDATiON (MTF) 6 ORDERiNg information
CONFORM FlEX Demineralized cancellous bone TABlE OF CONTENTS introduction 2 FEATURES AND BENEFiTS 4 PROCESSiNg AND PACKAgiNg information 5 MUSCUlOSKElETAl TRANSPlANT FOUNDATiON (MTF) 6 ORDERiNg information
SPINE BIOMATERIALS Crop Bleed
 A comprehensive guide to biomaterials offered by Posterolateral DBX PUTTY DBX STRIP DBX MIX DBX INJECT chronos Strip chronos Granules chronos Preforms PROCURE CHOICE Marrow Aspiration Kit Bone Marrow Aspiration
A comprehensive guide to biomaterials offered by Posterolateral DBX PUTTY DBX STRIP DBX MIX DBX INJECT chronos Strip chronos Granules chronos Preforms PROCURE CHOICE Marrow Aspiration Kit Bone Marrow Aspiration
Clinical Policy Title: Abdominal aortic aneurysm screening
 Clinical Policy Title: Abdominal aortic aneurysm screening Clinical Policy Number: 08.01.10 Effective Date: August 1, 2017 Initial Review Date: June 22, 2017 Most Recent Review Date: July 20, 2017 Next
Clinical Policy Title: Abdominal aortic aneurysm screening Clinical Policy Number: 08.01.10 Effective Date: August 1, 2017 Initial Review Date: June 22, 2017 Most Recent Review Date: July 20, 2017 Next
More than bone regeneration. A total solution.
 More than bone regeneration. A total solution. More than a dental implant company. A total solution. When it comes to treatment options, your patients want positive results both functionally and esthetically.
More than bone regeneration. A total solution. More than a dental implant company. A total solution. When it comes to treatment options, your patients want positive results both functionally and esthetically.
Clinical Policy Title: Strep testing
 Clinical Policy Title: Strep testing Clinical Policy Number: 07.01.09 Effective Date: December 1, 2017 Initial Review Date: October 19, 2017 Most Recent Review Date: November 16, 2017 Next Review Date:
Clinical Policy Title: Strep testing Clinical Policy Number: 07.01.09 Effective Date: December 1, 2017 Initial Review Date: October 19, 2017 Most Recent Review Date: November 16, 2017 Next Review Date:
A WIDE RANGE OF REGENERATIVE SOLUTIONS
 A WIDE RANGE OF REGENERATIVE SOLUTIONS INDICATIONS: 1/ SOCKET AND RIDGE PRESERVATION 2/ FILLING OF EXTRACTION SOCKETS Biomaterials offers portfolio of regenerative materials for implantology, aimed at
A WIDE RANGE OF REGENERATIVE SOLUTIONS INDICATIONS: 1/ SOCKET AND RIDGE PRESERVATION 2/ FILLING OF EXTRACTION SOCKETS Biomaterials offers portfolio of regenerative materials for implantology, aimed at
Orthopedic & Sports Medicine, Bay Care Clinic, 501 N. 10th Street, Manitowoc, WI Procedure. Subtalar arthrodesis
 OSTEOAMP Allogeneic Morphogenetic Proteins Subtalar Nonunions OSTEOAMP Case Report SUBTALAR NONUNIONS Dr. Jason George DeVries and Dr. Brandon M. Scharer Orthopedic & Sports Medicine, Bay Care Clinic,
OSTEOAMP Allogeneic Morphogenetic Proteins Subtalar Nonunions OSTEOAMP Case Report SUBTALAR NONUNIONS Dr. Jason George DeVries and Dr. Brandon M. Scharer Orthopedic & Sports Medicine, Bay Care Clinic,
Clinical Policy Title: Genetic testing for G1691A polymorphism factor V Leiden
 Clinical Policy Title: Genetic testing for G1691A polymorphism factor V Leiden Clinical Policy Number: 05.01.03 Effective Date: January 1, 2016 Initial Review Date: July 15, 2015 Most Recent Review Date:
Clinical Policy Title: Genetic testing for G1691A polymorphism factor V Leiden Clinical Policy Number: 05.01.03 Effective Date: January 1, 2016 Initial Review Date: July 15, 2015 Most Recent Review Date:
Bone Tissue Biology & The Application of Synthetic Compounds for the Facilitation of Bone Tissue Healing
 Bone Tissue Biology & The Application of Synthetic Compounds for the Facilitation of Bone Tissue Healing Ryan T. Jones Western Michigan University May 2011 Introduction Bone has unique properties: Tensile
Bone Tissue Biology & The Application of Synthetic Compounds for the Facilitation of Bone Tissue Healing Ryan T. Jones Western Michigan University May 2011 Introduction Bone has unique properties: Tensile
P105 Predictable Bone Grafting for Site Preparation for Implants and Prosthetics Workshop JAMES GRISDALE, DDS THURSDAY, FEBRUARY 26
 P105 Predictable Bone Grafting for Site Preparation for Implants and Prosthetics Workshop JAMES GRISDALE, DDS THURSDAY, FEBRUARY 26 Please complete the speaker evaluation form in the Midwinter Meeting
P105 Predictable Bone Grafting for Site Preparation for Implants and Prosthetics Workshop JAMES GRISDALE, DDS THURSDAY, FEBRUARY 26 Please complete the speaker evaluation form in the Midwinter Meeting
Bone Grafting for Socket Preservation
 Bone Grafting for Socket Preservation Dr. Karl R. Koerner Normal extraction facial bone loss. Excessive force. Commonly the thickness of facial bone. Hussain, A. et al. Ridge preservation comparing a nonresorbable
Bone Grafting for Socket Preservation Dr. Karl R. Koerner Normal extraction facial bone loss. Excessive force. Commonly the thickness of facial bone. Hussain, A. et al. Ridge preservation comparing a nonresorbable
Comparative Animal Study of OssiMend and Healos 13,14
 Comparative Animal Study of OssiMend and Healos 13,14 Objective This study was conducted to evaluate the use of OssiMend as compared with Healos in combination with autologous bone marrow as a bone grafting
Comparative Animal Study of OssiMend and Healos 13,14 Objective This study was conducted to evaluate the use of OssiMend as compared with Healos in combination with autologous bone marrow as a bone grafting
BONE AUGMENTATION AND GRAFTING
 1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
Calcium Phosphate Cement
 Calcium Phosphate Cement Fast-Setting Bone Graft and AutoGraft Extender. * Ossilix is a high performance next generation calcium phosphate cement indicated for filling bony defects in cancellous bone.
Calcium Phosphate Cement Fast-Setting Bone Graft and AutoGraft Extender. * Ossilix is a high performance next generation calcium phosphate cement indicated for filling bony defects in cancellous bone.
Spine A Preliminary Study of the Efficacy of Beta-Tricalcium Phosphate as a Bone Graft Expander for Instrumented Posterolateral Fusions
 Bibliography Spine Epstein, N.E., A Preliminary Study of the Efficacy of Beta-Tricalcium Phosphate as a Bone Graft Expander for Instrumented Posterolateral Fusions. Journal of Spinal Disorders and Techniques,
Bibliography Spine Epstein, N.E., A Preliminary Study of the Efficacy of Beta-Tricalcium Phosphate as a Bone Graft Expander for Instrumented Posterolateral Fusions. Journal of Spinal Disorders and Techniques,
Developments in bone grafting in veterinary orthopaedics part one
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk Developments in bone grafting in veterinary orthopaedics part one Author : John Innes, Peter Myint Categories : Vets Date
Vet Times The website for the veterinary profession https://www.vettimes.co.uk Developments in bone grafting in veterinary orthopaedics part one Author : John Innes, Peter Myint Categories : Vets Date
ORTHOPEDICS BONE Recalcitrant nonunions In total hip replacement total knee surgery increased callus volume
 ORTHOPEDICS Orthopedics has to do with a variety of tissue: bone, cartilage, tendon, ligament, muscle. In this regard orthopedic and sports medicine share the same tissue targets. Orthopedics is mostly
ORTHOPEDICS Orthopedics has to do with a variety of tissue: bone, cartilage, tendon, ligament, muscle. In this regard orthopedic and sports medicine share the same tissue targets. Orthopedics is mostly
CONFORM SHEET. Demineralized cancellous bone
 CONFORM SHEET Demineralized cancellous bone TABLE OF CONTENTS INTRODUCTION 2 FEATURES AND BENEFITS 4 HYDRATION INFORMATION 5 PROCESSING AND PACKAGING INFORMATION 6 MUSCULOSKELETAL TRANSPLANT FOUNDATION
CONFORM SHEET Demineralized cancellous bone TABLE OF CONTENTS INTRODUCTION 2 FEATURES AND BENEFITS 4 HYDRATION INFORMATION 5 PROCESSING AND PACKAGING INFORMATION 6 MUSCULOSKELETAL TRANSPLANT FOUNDATION
Clinical Policy Title: Subtalar arthroereisis (implant)
 Clinical Policy Title: Subtalar arthroereisis (implant) Clinical Policy Number: 14.03.05 Effective Date: April 1, 2017 Initial Review Date: August 17, 2016 Most Recent Review Date: September 21, 2017 Next
Clinical Policy Title: Subtalar arthroereisis (implant) Clinical Policy Number: 14.03.05 Effective Date: April 1, 2017 Initial Review Date: August 17, 2016 Most Recent Review Date: September 21, 2017 Next
BONE OR SOFT TISSUE HEALING AND FUSION ENHANCEMENT PRODUCTS
 BONE OR SOFT TISSUE HEALING AND FUSION ENHANCEMENT PRODUCTS UnitedHealthcare Commercial Medical Policy Policy Number: 2017T0410S Effective Date: March 1, 2017 Table of Contents Page INSTRUCTIONS FOR USE...
BONE OR SOFT TISSUE HEALING AND FUSION ENHANCEMENT PRODUCTS UnitedHealthcare Commercial Medical Policy Policy Number: 2017T0410S Effective Date: March 1, 2017 Table of Contents Page INSTRUCTIONS FOR USE...
DEMINERALIZED BONE MATRIX
 DEMINERALIZED BONE MATRIX DEMINERALIZED BONE MATRIX GRAFT OVERVIEW BioAdapt is a pre-formed demineralized bone matrix (DBM) comprised of 00 percent donated human musculoskeletal tissue. BioAdapt DBM provides
DEMINERALIZED BONE MATRIX DEMINERALIZED BONE MATRIX GRAFT OVERVIEW BioAdapt is a pre-formed demineralized bone matrix (DBM) comprised of 00 percent donated human musculoskeletal tissue. BioAdapt DBM provides
THE BUILDING BLOCKS OF BONE FUSION. Medline Demineralized Bone Allografts Safe and Effective Grafting Options
 THE BUILDING BLOCKS OF BONE FUSION. Medline Demineralized Bone Allografts Safe and Effective Grafting Options 2 MEDLINE BUILD ON QUALITY. Successful bone fusion and osteogenesis depend on a number of factors
THE BUILDING BLOCKS OF BONE FUSION. Medline Demineralized Bone Allografts Safe and Effective Grafting Options 2 MEDLINE BUILD ON QUALITY. Successful bone fusion and osteogenesis depend on a number of factors
Clinical Policy Title: Bone growth stimulators for non-healing fractures
 Clinical Policy Title: Bone growth stimulators for non-healing fractures Clinical Policy Number: 14.02.03 Effective Date: January 1, 2015 Initial Review Date: July 16, 2014 Most Recent Review Date: March
Clinical Policy Title: Bone growth stimulators for non-healing fractures Clinical Policy Number: 14.02.03 Effective Date: January 1, 2015 Initial Review Date: July 16, 2014 Most Recent Review Date: March
Clinical Policy Title: Ketamine for treatment-resistant depression
 Clinical Policy Title: Ketamine for treatment-resistant depression Clinical Policy Number: 00.02.13 Effective Date: January 1, 2016 Initial Review Date: August 19, 2015 Most Recent Review Date: January
Clinical Policy Title: Ketamine for treatment-resistant depression Clinical Policy Number: 00.02.13 Effective Date: January 1, 2016 Initial Review Date: August 19, 2015 Most Recent Review Date: January
Bioactive Glass Biphasic β-tcp & HA Granules Alkylene Oxide Polymer Carrier. MEDLINEUNITE Bioactive Bone Graft
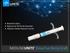 Bioactive Glass Biphasic β-tcp & HA Granules Alkylene Oxide Polymer Carrier Principles of Bone Healing Reparative Phase Healing Cascade 1. Cellular infiltration and migration to site (fibroblasts, macrophages,
Bioactive Glass Biphasic β-tcp & HA Granules Alkylene Oxide Polymer Carrier Principles of Bone Healing Reparative Phase Healing Cascade 1. Cellular infiltration and migration to site (fibroblasts, macrophages,
Basic science symposium I: bone graft substitutes.
 Basic science symposium I: bone graft substitutes. Todd Boyce, Osteotech, Inc. Joseph M. Lane, Hospital for Special Surgery New York Scott D Boden, Emory University Jeffrey C. Wang, UCLA Comprehensive
Basic science symposium I: bone graft substitutes. Todd Boyce, Osteotech, Inc. Joseph M. Lane, Hospital for Special Surgery New York Scott D Boden, Emory University Jeffrey C. Wang, UCLA Comprehensive
Subject: Non-Invasive Electrical Bone Growth Stimulators (EBGS)
 09-E0000-22 Original Effective Date: 06/15/00 Reviewed: 04/28/16 Revised: 05/15/16 Subject: Non-Invasive Electrical Bone Growth Stimulators (EBGS) THIS MEDICAL COVERAGE GUIDELINE IS NOT AN AUTHORIZATION,
09-E0000-22 Original Effective Date: 06/15/00 Reviewed: 04/28/16 Revised: 05/15/16 Subject: Non-Invasive Electrical Bone Growth Stimulators (EBGS) THIS MEDICAL COVERAGE GUIDELINE IS NOT AN AUTHORIZATION,
OssiMend Bone Graft Matrix
 OssiMend All-Natural Mineral-Collagen Bone Grafting Matrix Anorganic bone mineral and type I collagen Highly purified, biocompatible matrix Osteoconductive Osteoinductive and Osteogenic in conjunction
OssiMend All-Natural Mineral-Collagen Bone Grafting Matrix Anorganic bone mineral and type I collagen Highly purified, biocompatible matrix Osteoconductive Osteoinductive and Osteogenic in conjunction
Most cells in the human body have an assigned purpose. They are liver cells, fat cells, bone cells,
 What is a Stem Cell? Most cells in the human body have an assigned purpose. They are liver cells, fat cells, bone cells, and so on. These cells can replicate more of their own kind of cell, but they cannot
What is a Stem Cell? Most cells in the human body have an assigned purpose. They are liver cells, fat cells, bone cells, and so on. These cells can replicate more of their own kind of cell, but they cannot
In the last decade of the 20 th century, special emphasis was put on an emerging field of science: Tissue engineering,which combines the state of the
 In the last decade of the 20 th century, special emphasis was put on an emerging field of science: Tissue engineering,which combines the state of the art materials science with concepts from the life sciences.
In the last decade of the 20 th century, special emphasis was put on an emerging field of science: Tissue engineering,which combines the state of the art materials science with concepts from the life sciences.
Clinical Policy Title: Genicular nerve block
 Clinical Policy Title: Genicular nerve block Clinical Policy Number: 14.01.10 Effective Date: October 1, 2017 Initial Review Date: September 21, 2017 Most Recent Review Date: October 19, 2017 Next Review
Clinical Policy Title: Genicular nerve block Clinical Policy Number: 14.01.10 Effective Date: October 1, 2017 Initial Review Date: September 21, 2017 Most Recent Review Date: October 19, 2017 Next Review
Innovative Range of Regenerative Solutions
 TM Innovative Range of Regenerative Solutions MIS Implant Technologies Ltd. All rights reserved. Optimal volumes and quality of hard and soft tissue are required to satisfy the goals of oral rehabilitation
TM Innovative Range of Regenerative Solutions MIS Implant Technologies Ltd. All rights reserved. Optimal volumes and quality of hard and soft tissue are required to satisfy the goals of oral rehabilitation
Radiology Case Reports. Bone Graft Extruded From an Intramedullary Nail Tract in the Tibia. Penelope J. Galbraith, M.D., and Felix S. Chew, M.D.
 Radiology Case Reports Volume 2, Issue 4, 2007 Bone Graft Extruded From an Intramedullary Nail Tract in the Tibia Penelope J. Galbraith, M.D., and Felix S. Chew, M.D. A 33-year-old man presented for follow
Radiology Case Reports Volume 2, Issue 4, 2007 Bone Graft Extruded From an Intramedullary Nail Tract in the Tibia Penelope J. Galbraith, M.D., and Felix S. Chew, M.D. A 33-year-old man presented for follow
Clinical Policy Title: Genetic testing for G1691A polymorphism factor V Leiden
 Clinical Policy Title: Genetic testing for G1691A polymorphism factor V Leiden Clinical Policy Number: 05.01.03 Effective Date: January 1, 2016 Initial Review Date: July 15, 2015 Most Recent Review Date:
Clinical Policy Title: Genetic testing for G1691A polymorphism factor V Leiden Clinical Policy Number: 05.01.03 Effective Date: January 1, 2016 Initial Review Date: July 15, 2015 Most Recent Review Date:
NEW FIXATION STRATEGIES FOR OSTEOPOROTIC BONE
 NEW FIXATION STRATEGIES FOR OSTEOPOROTIC BONE THE PROBLEMS Fixation failure Malunion F 83 yrs 2 Months 6 Months F 81 yrs 3 Months FIXATION AUGMENTATION TECHNIQUES (FATs) Surgical procedures aimed at increasing
NEW FIXATION STRATEGIES FOR OSTEOPOROTIC BONE THE PROBLEMS Fixation failure Malunion F 83 yrs 2 Months 6 Months F 81 yrs 3 Months FIXATION AUGMENTATION TECHNIQUES (FATs) Surgical procedures aimed at increasing
AttraX. Portfolio. Surface Drives Performance
 Portfolio Surface Drives Performance Advanced Biomaterial Microarchitecture Drives Bone Formation Traditional calcium phosphate materials generally do not give rise to bone formation when implanted in
Portfolio Surface Drives Performance Advanced Biomaterial Microarchitecture Drives Bone Formation Traditional calcium phosphate materials generally do not give rise to bone formation when implanted in
GRAFTON DEMINERALIZED BONE: FIBER TECHNOLOGY AND PERFORMANCE IMPLICATIONS
 GRAFTON DEMINERALIZED BONE: FIBER TECHNOLOGY AND PERFORMANCE IMPLICATIONS Based Upon the Published Source: Martin GJ, Jr., Boden SD, Titus L, Scarborough NL. New formulations of demineralized bone matrix
GRAFTON DEMINERALIZED BONE: FIBER TECHNOLOGY AND PERFORMANCE IMPLICATIONS Based Upon the Published Source: Martin GJ, Jr., Boden SD, Titus L, Scarborough NL. New formulations of demineralized bone matrix
Clinical UM Guideline
 Clinical UM Guideline Subject: Biological Materials to Aid in Soft and Hard Tissue Grafting Guideline #: 03-401 Current Effective Date: 03/24/2017 Status: New Last Review Date: 02/08/2017 Description This
Clinical UM Guideline Subject: Biological Materials to Aid in Soft and Hard Tissue Grafting Guideline #: 03-401 Current Effective Date: 03/24/2017 Status: New Last Review Date: 02/08/2017 Description This
Clinical Policy Title: Platelet rich plasma
 Clinical Policy Title: Platelet rich plasma Clinical Policy Number: 05.02.10 Effective Date: February 1, 2017 Initial Review Date: November 16, 2016 Most Recent Review Date: November 16, 2016 Next Review
Clinical Policy Title: Platelet rich plasma Clinical Policy Number: 05.02.10 Effective Date: February 1, 2017 Initial Review Date: November 16, 2016 Most Recent Review Date: November 16, 2016 Next Review
Clinical Policy Title: Abdominal aortic aneurysm screening
 Clinical Policy Title: Abdominal aortic aneurysm screening Clinical Policy Number: 08.01.10 Effective Date: August 1, 2017 Initial Review Date: June 22, 2017 Most Recent Review Date: June 5, 2018 Next
Clinical Policy Title: Abdominal aortic aneurysm screening Clinical Policy Number: 08.01.10 Effective Date: August 1, 2017 Initial Review Date: June 22, 2017 Most Recent Review Date: June 5, 2018 Next
THE NEXT FRONTIER OF BONE REGENERATION. where Technology meets Nature
 THE NEXT FRONTIER OF BONE REGENERATION where Technology meets Nature SmartBone is a new hybrid bioactive bone substitute specifically developed for bone regeneration in reconstructive surgery. SmartBone
THE NEXT FRONTIER OF BONE REGENERATION where Technology meets Nature SmartBone is a new hybrid bioactive bone substitute specifically developed for bone regeneration in reconstructive surgery. SmartBone
REASONS TO USE R.T.R.
 3 REASONS TO USE R.T.R. AFTER EACH EXTRACTION Fully resorbable ß-TCP material RTR 3raisons 120x280.indd 1 16/06/15 10:52 1AVOID SPONTANEOUS RIDGE RESORPTION After tooth extraction, spontaneous healing
3 REASONS TO USE R.T.R. AFTER EACH EXTRACTION Fully resorbable ß-TCP material RTR 3raisons 120x280.indd 1 16/06/15 10:52 1AVOID SPONTANEOUS RIDGE RESORPTION After tooth extraction, spontaneous healing
THE NEXT FRONTIER OF BONE REGENERATION. where Technology meets Nature
 THE NEXT FRONTIER OF BONE REGENERATION where Technology meets Nature SmartBone is a new hybrid bioactive bone substitute specifically developed for bone regeneration in reconstructive surgery. SmartBone
THE NEXT FRONTIER OF BONE REGENERATION where Technology meets Nature SmartBone is a new hybrid bioactive bone substitute specifically developed for bone regeneration in reconstructive surgery. SmartBone
ctive Bone Bonding Bone Regeneration Osteostimulation*
 www.bonalive.com ctive Bone Bonding Bone Regeneration Osteostimulation* A revolution in bone grafting Osteoconductive bone graft substitute with osteostimulative* properties *non-osteoinductive Before
www.bonalive.com ctive Bone Bonding Bone Regeneration Osteostimulation* A revolution in bone grafting Osteoconductive bone graft substitute with osteostimulative* properties *non-osteoinductive Before
Clinical Policy Title: Abdominal aortic aneurysm screening
 Clinical Policy Title: Abdominal aortic aneurysm screening Clinical Policy Number: 08.01.10 Effective Date: August 1, 2017 Initial Review Date: June 22, 2017 Most Recent Review Date: June 5, 2018 Next
Clinical Policy Title: Abdominal aortic aneurysm screening Clinical Policy Number: 08.01.10 Effective Date: August 1, 2017 Initial Review Date: June 22, 2017 Most Recent Review Date: June 5, 2018 Next
Osteocel. An introduction to
 An introduction to Osteocel This booklet provides general information on Osteocel cellular allografts as a bone graft substitute in your spinal fusion surgery. It is not meant to replace any personal conversations
An introduction to Osteocel This booklet provides general information on Osteocel cellular allografts as a bone graft substitute in your spinal fusion surgery. It is not meant to replace any personal conversations
rhpdgf-bb/β-tcp TECHNOLOGY OVERVIEW AUGMENT Bone Graft THE FIRST AND ONLY PROVEN ALTERNATIVE TO AUTOGRAFT IN ANKLE AND HINDFOOT ARTHRODESIS
 rhpdgf-bb/β-tcp TECHNOLOGY OVERVIEW AUGMENT Bone Graft THE FIRST AND ONLY PROVEN ALTERNATIVE TO AUTOGRAFT IN ANKLE AND HINDFOOT ARTHRODESIS AUGMENT Bone Graft T HE F I R S T A ND O N LY PROV EN A LT ERN
rhpdgf-bb/β-tcp TECHNOLOGY OVERVIEW AUGMENT Bone Graft THE FIRST AND ONLY PROVEN ALTERNATIVE TO AUTOGRAFT IN ANKLE AND HINDFOOT ARTHRODESIS AUGMENT Bone Graft T HE F I R S T A ND O N LY PROV EN A LT ERN
BIOACTIVE BASICS. Bioactive materials elicit a controlled action and reaction in the physiological environment.
 BIOACTIVE BASICS Bioactive materials elicit a controlled action and reaction in the physiological environment. Bioglass is a glass ceramic composed of silicon dioxide (SiO 2 ), sodium oxide (Na 2 O), calcium
BIOACTIVE BASICS Bioactive materials elicit a controlled action and reaction in the physiological environment. Bioglass is a glass ceramic composed of silicon dioxide (SiO 2 ), sodium oxide (Na 2 O), calcium
Clinical Policy Title: Dental bone grafting
 Clinical Policy Title: Dental bone grafting Clinical Policy Number: 14.03.06 Effective Date: April 1, 2017 Initial Review Date: March 15, 2017 Most Recent Review Date: March 6, 2018 Next Review Date: March
Clinical Policy Title: Dental bone grafting Clinical Policy Number: 14.03.06 Effective Date: April 1, 2017 Initial Review Date: March 15, 2017 Most Recent Review Date: March 6, 2018 Next Review Date: March
Cigna Medical Coverage Policy
 Cigna Medical Coverage Policy Subject Bone Graft Substitutes for Use in Bone Repair Table of Contents Coverage Policy... 1 General Background... 2 Coding/Billing Information... 14 References... 16 Effective
Cigna Medical Coverage Policy Subject Bone Graft Substitutes for Use in Bone Repair Table of Contents Coverage Policy... 1 General Background... 2 Coding/Billing Information... 14 References... 16 Effective
CLINICAL EXPERIENCES OF SINGLE AND MULTI-LEVEL LUMBAR SPINE FUSIONS USING A DBM/CALCIUM SULFATE/BMA COMPOSITE GRAFT TO EXTEND LOCAL BONE
 CLINICAL EXPERIENCES OF SINGLE AND MULTI-LEVEL LUMBAR SPINE FUSIONS USING A DBM/CALCIUM SULFATE/BMA COMPOSITE GRAFT TO EXTEND LOCAL BONE Bruce M. Frankel, MD and Susan G. Capps, PhD CLINICAL EXPERIENCES
CLINICAL EXPERIENCES OF SINGLE AND MULTI-LEVEL LUMBAR SPINE FUSIONS USING A DBM/CALCIUM SULFATE/BMA COMPOSITE GRAFT TO EXTEND LOCAL BONE Bruce M. Frankel, MD and Susan G. Capps, PhD CLINICAL EXPERIENCES
TREATMENT OF CARTILAGE LESIONS
 TREATMENT OF CARTILAGE LESIONS Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati Medical Center -Associate Professor
TREATMENT OF CARTILAGE LESIONS Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati Medical Center -Associate Professor
Technique Guide. chronos Strip. Osteoconductive betatricalcium phosphate ( -TCP) composite.
 Technique Guide chronos Strip. Osteoconductive betatricalcium phosphate ( -TCP) composite. Table of Contents Introduction chronos Strip 2 Indications and Contraindications 3 Surgical Technique Preparation
Technique Guide chronos Strip. Osteoconductive betatricalcium phosphate ( -TCP) composite. Table of Contents Introduction chronos Strip 2 Indications and Contraindications 3 Surgical Technique Preparation
Clinical Policy Title: Fluorescence in situ hybridization for cervical cancer screening
 Clinical Policy Title: Fluorescence in situ hybridization for cervical cancer screening Clinical Policy Number: 01.01.02 Effective Date: April 1, 2015 Initial Review Date: January 21, 2015 Most Recent
Clinical Policy Title: Fluorescence in situ hybridization for cervical cancer screening Clinical Policy Number: 01.01.02 Effective Date: April 1, 2015 Initial Review Date: January 21, 2015 Most Recent
BONE-GRAFT SUBSTITUTES: FACTS, FICTIONS & APPLICATIONS
 BONE-GRAFT SUBSTITUTES: FACTS, FICTIONS & APPLICATIONS AMERICAN ACADEMY OF ORTHOPAEDIC SURGEONS 76TH ANNUAL MEETING FEBRUARY 25-28, 2009 LAS VEGAS, NEVADA ORTHOPAEDIC DEVICE FORUM PREPARED BY: A. SETH
BONE-GRAFT SUBSTITUTES: FACTS, FICTIONS & APPLICATIONS AMERICAN ACADEMY OF ORTHOPAEDIC SURGEONS 76TH ANNUAL MEETING FEBRUARY 25-28, 2009 LAS VEGAS, NEVADA ORTHOPAEDIC DEVICE FORUM PREPARED BY: A. SETH
synthetic CANCELLOUS BONE technical monograph Presented by Barbara Blum, Ph.D.
 C E L L P L E X TCP synthetic CANCELLOUS BONE technical monograph Presented by Barbara Blum, Ph.D. TECHNICAL MONOGRAPH CELLPLEX TCP SYNTHETIC CANCELLOUS BONE CELLPLEX TCP synthetic CANCELLOUS BONE introduction
C E L L P L E X TCP synthetic CANCELLOUS BONE technical monograph Presented by Barbara Blum, Ph.D. TECHNICAL MONOGRAPH CELLPLEX TCP SYNTHETIC CANCELLOUS BONE CELLPLEX TCP synthetic CANCELLOUS BONE introduction
Kade Huntsman, MD a, Steven Scott, MD ab, Mauricio Berdugo, MD a, Stephen Roper, PA a Gregory Juda, PhD c
 EuroSpine 2011 Milan, Italy Kade Huntsman, MD a, Steven Scott, MD ab, Mauricio Berdugo, MD a, Stephen Roper, PA a Gregory Juda, PhD c a Salt Lake Orthopaedic Clinic, 1160 East 3900 South, Suite 5000, Salt
EuroSpine 2011 Milan, Italy Kade Huntsman, MD a, Steven Scott, MD ab, Mauricio Berdugo, MD a, Stephen Roper, PA a Gregory Juda, PhD c a Salt Lake Orthopaedic Clinic, 1160 East 3900 South, Suite 5000, Salt
Clinical Policy Title: Discography
 Clinical Policy Title: Discography Clinical Policy Number: 03.01.01 Effective Date: January 1, 2017 Initial Review Date: October 19, 2016 Most Recent Review Date: October 19, 2017 Next Review Date: October
Clinical Policy Title: Discography Clinical Policy Number: 03.01.01 Effective Date: January 1, 2017 Initial Review Date: October 19, 2016 Most Recent Review Date: October 19, 2017 Next Review Date: October
CELLPLEX TCP SYNTHETIC CANCELLOUS BONE
 CELLPLEX TCP SYNTHETIC CANCELLOUS BONE 129257-9 The following languages are included in this packet: English (en) Deutsch (de) Nederlands (nl) Français (fr) Español (es) Italiano (it) Português (pt) -
CELLPLEX TCP SYNTHETIC CANCELLOUS BONE 129257-9 The following languages are included in this packet: English (en) Deutsch (de) Nederlands (nl) Français (fr) Español (es) Italiano (it) Português (pt) -
Bone, Cartilage and Ligament Graft Substitutes
 Medical Coverage Policy Effective Date... 2/15/2018 Next Review Date... 2/15/2019 Coverage Policy Number... 0118 Bone, Cartilage and Ligament Graft Substitutes Table of Contents Coverage Policy... 1 Overview...
Medical Coverage Policy Effective Date... 2/15/2018 Next Review Date... 2/15/2019 Coverage Policy Number... 0118 Bone, Cartilage and Ligament Graft Substitutes Table of Contents Coverage Policy... 1 Overview...
POSTERIOR LUMBAR FUSION SURGICAL TECHNIQUE USING A BONE VOID FILLER. Magnifuse. Bone Graft
 POSTERIOR LUMBAR FUSION SURGICAL TECHNIQUE USING A BONE VOID FILLER Magnifuse Bone Graft PREPARATION INSTRUCTIONS Soft tissue should be completely removed from the posterior elements of the spinal segments
POSTERIOR LUMBAR FUSION SURGICAL TECHNIQUE USING A BONE VOID FILLER Magnifuse Bone Graft PREPARATION INSTRUCTIONS Soft tissue should be completely removed from the posterior elements of the spinal segments
BioVin Collagen Membrane
 BioVin Collagen Membrane Resorbable cross-linked collagen membrane BioVin Bovine Bone Bovine Bone Substitute OToss Synthetic Bone Synthetic Resorbable Biphasic Calcium Phosphate OToss Synthetic Bone Inject
BioVin Collagen Membrane Resorbable cross-linked collagen membrane BioVin Bovine Bone Bovine Bone Substitute OToss Synthetic Bone Synthetic Resorbable Biphasic Calcium Phosphate OToss Synthetic Bone Inject
Bone augmentation with biomaterials
 Patient information dental bone & tissue regeneration botiss biomaterials Bone augmentation with biomaterials established safe natural X100 Implantation stability is crucial for success Atrophy of the
Patient information dental bone & tissue regeneration botiss biomaterials Bone augmentation with biomaterials established safe natural X100 Implantation stability is crucial for success Atrophy of the
MASTERGRAFT Putty. Technical Guide
 MASTERGRAFT Putty Technical Guide MASTERGRAFT Putty is a malleable-cohesive, osteoconductive scaffold composed of collagen that is physically mixed with resorbable ceramic granules. Mixing Process Collagen
MASTERGRAFT Putty Technical Guide MASTERGRAFT Putty is a malleable-cohesive, osteoconductive scaffold composed of collagen that is physically mixed with resorbable ceramic granules. Mixing Process Collagen
Void Fillers: White Paste or Bone
 J. TRACY WATSON M.D. PROFESSOR OF ORTHOPAEDIC SURGERY CHIEF ORTHOPAEDIC TRAUMA SERVICE ST. LOUIS UNIVERSITY SCHOOL OF MEDICINE Void Fillers: White Paste or Bone Void Fillers: White Paste or Bone INJECTABLE
J. TRACY WATSON M.D. PROFESSOR OF ORTHOPAEDIC SURGERY CHIEF ORTHOPAEDIC TRAUMA SERVICE ST. LOUIS UNIVERSITY SCHOOL OF MEDICINE Void Fillers: White Paste or Bone Void Fillers: White Paste or Bone INJECTABLE
BONE void FILLER. Beta-tricalcium phosphate ( b-tcp) bone graft substitute. OvERvIEW BROCHURE
 chronos BONE void FILLER Beta-tricalcium phosphate ( b-tcp) bone graft substitute OvERvIEW BROCHURE chronos STRIP chronos Strip is a synthetic bone void filler manufactured from chronos Beta-Tricalcium
chronos BONE void FILLER Beta-tricalcium phosphate ( b-tcp) bone graft substitute OvERvIEW BROCHURE chronos STRIP chronos Strip is a synthetic bone void filler manufactured from chronos Beta-Tricalcium
OSTEOCHONDRAL ALLOGRAFT RECONSTRUCTION FOR MASSIVE BONE DEFECT
 OSTEOCHONDRAL ALLOGRAFT RECONSTRUCTION FOR MASSIVE BONE DEFECT Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati
OSTEOCHONDRAL ALLOGRAFT RECONSTRUCTION FOR MASSIVE BONE DEFECT Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati
Clinical Policy Title: Computerized gait analysis
 Clinical Policy Title: Computerized gait analysis Clinical Policy Number: 15.01.01 Effective Date: October 1, 2014 Initial Review Date: May 21, 2014 Most Recent Review Date: June 22, 2017 Next Review Date:
Clinical Policy Title: Computerized gait analysis Clinical Policy Number: 15.01.01 Effective Date: October 1, 2014 Initial Review Date: May 21, 2014 Most Recent Review Date: June 22, 2017 Next Review Date:
Re-growing the Skeleton: Approaches in Tissue Engineering and Regenerative Medicine
 Re-growing the Skeleton: Approaches in Tissue Engineering and Regenerative Medicine How we fix things now Total Knee Replacements Fracture Plates Fusing Joints Defining Regenerative Medicine restore form
Re-growing the Skeleton: Approaches in Tissue Engineering and Regenerative Medicine How we fix things now Total Knee Replacements Fracture Plates Fusing Joints Defining Regenerative Medicine restore form
Clinical Policy Title: Platelet rich plasma
 Clinical Policy Title: Platelet rich plasma Clinical Policy Number: 05.02.10 Effective Date: February 1, 2017 Initial Review Date: November 16, 2016 Most Recent Review Date: November 16, 2017 Next Review
Clinical Policy Title: Platelet rich plasma Clinical Policy Number: 05.02.10 Effective Date: February 1, 2017 Initial Review Date: November 16, 2016 Most Recent Review Date: November 16, 2017 Next Review
Symbios Xenograft Granules Porcine Bone Graft Material
 Symbios Xenograft Granules Porcine Bone Graft Material 32671122-USX-1607_Symbios Highlight Brochure.indd 1 2016-09-27 12:12 Symbios Xenograft Granules Porcine bone graft material Symbios Xenograft Granules
Symbios Xenograft Granules Porcine Bone Graft Material 32671122-USX-1607_Symbios Highlight Brochure.indd 1 2016-09-27 12:12 Symbios Xenograft Granules Porcine bone graft material Symbios Xenograft Granules
Clinical Policy Title: Altered auditory feedback devices for speech dysfluency (stuttering)
 Clinical Policy Title: Altered auditory feedback devices for speech dysfluency (stuttering) Clinical Policy Number: 17.02.02 Effective Date: January 1, 2016 Initial Review Date: August 19, 2015 Most Recent
Clinical Policy Title: Altered auditory feedback devices for speech dysfluency (stuttering) Clinical Policy Number: 17.02.02 Effective Date: January 1, 2016 Initial Review Date: August 19, 2015 Most Recent
PRO-STIM Injectable Inductive Graft TECHNICAL MONOGRAPH
 PRO-STIM Injectable Inductive Graft TECHNICAL MONOGRAPH PRO-STIM Injectable Inductive Graft TECHNICAL MONOGRAPH Headline Contents Headline Appendix 4 5 7 8 13 14 Clinical Benefits Self-Forming Porous Scaffold
PRO-STIM Injectable Inductive Graft TECHNICAL MONOGRAPH PRO-STIM Injectable Inductive Graft TECHNICAL MONOGRAPH Headline Contents Headline Appendix 4 5 7 8 13 14 Clinical Benefits Self-Forming Porous Scaffold
Treatment of Distal Radius Bone Defects with Injectable Calcium Sulphate Cement
 Treatment of Distal Radius Bone Defects with Injectable Calcium Sulphate Cement Deng Lei, Ma Zhanzhong, Yang Huaikuo, Xue Lei and Yang Gongbo Orthopaedic Department, Beijing XiYuan Hospital, China Academy
Treatment of Distal Radius Bone Defects with Injectable Calcium Sulphate Cement Deng Lei, Ma Zhanzhong, Yang Huaikuo, Xue Lei and Yang Gongbo Orthopaedic Department, Beijing XiYuan Hospital, China Academy
Synthetic and absorbable autograft substitute with osteoinduction
 putty Synthetic and absorbable autograft substitute with osteoinduction Quality made in Germany Synthetic and absorbable autograft substitute with osteoinduction Information on the synthetic bone grafting
putty Synthetic and absorbable autograft substitute with osteoinduction Quality made in Germany Synthetic and absorbable autograft substitute with osteoinduction Information on the synthetic bone grafting
Stem cells, growth factors and scaffolds in craniofacial regenerative medicine
 Stem cells, growth factors and scaffolds in craniofacial regenerative medicine Viktor Tollemar, Zach J. Collier, Maryam K. Mohammed, Michael J. Lee, Guillermo A. Ameer, and Russell R. Reid Genes Dis. 2016
Stem cells, growth factors and scaffolds in craniofacial regenerative medicine Viktor Tollemar, Zach J. Collier, Maryam K. Mohammed, Michael J. Lee, Guillermo A. Ameer, and Russell R. Reid Genes Dis. 2016
POWER TO RESTORE WITHOUT LEAVING A TRACE. The only remaining evidence of the trauma
 POWER TO RESTORE WITHOUT LEAVING A TRACE The only remaining evidence of the trauma Perfect partner for your trauma and non-unions Your choice of synthetic bone graft not only influences the efficiency
POWER TO RESTORE WITHOUT LEAVING A TRACE The only remaining evidence of the trauma Perfect partner for your trauma and non-unions Your choice of synthetic bone graft not only influences the efficiency
Clinical Policy Title: Vacuum assisted closure in surgical wounds
 Clinical Policy Title: Vacuum assisted closure in surgical wounds Clinical Policy Number: 17.03.00 Effective Date: September 1, 2015 Initial Review Date: June 16, 2013 Most Recent Review Date: August 17,
Clinical Policy Title: Vacuum assisted closure in surgical wounds Clinical Policy Number: 17.03.00 Effective Date: September 1, 2015 Initial Review Date: June 16, 2013 Most Recent Review Date: August 17,
Bone augmentation with maxgraft
 Patient information bone & tissue regeneration botiss biomaterials Bone augmentation with maxgraft established safe X100 natural Implantation stability is crucial for success Atrophy of the jaw bone loss
Patient information bone & tissue regeneration botiss biomaterials Bone augmentation with maxgraft established safe X100 natural Implantation stability is crucial for success Atrophy of the jaw bone loss
OSTEOCHONDRAL ALLOGRAFTS AND AUTOGRAFTS IN THE TREATMENT OF FOCAL ARTICULAR CARTILAGE LESIONS
 Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-115 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-115 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Horizontal bone augmentation by means of guided bone regeneration
 Periodontology 2000, Vol. 66, 2014, 13 40 2014 John Wiley & Sons A/S. Published by John Wiley & Sons Ltd Printed in Singapore. All rights reserved PERIODONTOLOGY 2000 Horizontal bone augmentation by means
Periodontology 2000, Vol. 66, 2014, 13 40 2014 John Wiley & Sons A/S. Published by John Wiley & Sons Ltd Printed in Singapore. All rights reserved PERIODONTOLOGY 2000 Horizontal bone augmentation by means
Mesenchymal Stem Cell Therapy for Orthopedic Indications. Original Policy Date
 MP 2.01.59 Mesenchymal Stem Cell Therapy for Orthopedic Indications Medical Policy Section Medicine Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Local policy created/12:2013 Return
MP 2.01.59 Mesenchymal Stem Cell Therapy for Orthopedic Indications Medical Policy Section Medicine Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Local policy created/12:2013 Return
Resorbable bilayer synthetic membrane Biomimetic tissue-engineered matrix for GBR and GTR
 Resorbable bilayer synthetic membrane Biomimetic tissue-engineered matrix for GBR and GTR Patented Jet-Spraying technology: Full barrier effect during 4 weeks, and complete resorption in 6 months PATENTED
Resorbable bilayer synthetic membrane Biomimetic tissue-engineered matrix for GBR and GTR Patented Jet-Spraying technology: Full barrier effect during 4 weeks, and complete resorption in 6 months PATENTED
