A cardiac prevention and rehabilitation programme for all patients at first presentation with coronary artery disease
|
|
|
- Giles Johns
- 5 years ago
- Views:
Transcription
1 Heart 2001;85: Cardiovascular Medicine, Imperial College School of Medicine, National Heart and Lung Institute, Charing Cross Campus, Fulham Palace Road, London W6 8RF, UK KFFox DAWood M Wright S J SutcliVe Bromley Hospitals NHS Trust, Farnborough Hospital, Farnborough Common, Orpington, Kent BR6 8ND, UK M Nuttall B Arora E Dawson P Devane K Stock K Brown Correspondence to: Professor Wood d.wood@ic.ac.uk Accepted 5 December 2000 A cardiac prevention and rehabilitation programme for all patients at first presentation with coronary artery disease K F Fox, M Nuttall, D A Wood, M Wright, B Arora, E Dawson, P Devane, K Stock, S J SutcliVe, K Brown Abstract Objective To develop and test a cardiac prevention and rehabilitation programme for achieving sustained lifestyle, risk factor, and therapeutic targets in patients presenting for the first time with exertional angina, acute coronary syndromes, or coronary revascularisation. Design A descriptive study. Setting A hospital based 12 week outpatient programme. Interventions A multiprofessional family based programme of lifestyle and risk factor modification. Main outcome measures Non-smoking status, body mass index, blood pressure, plasma cholesterol, use of prophylactic drugs. Results 158 patients (82% of 194 possible cases) were recruited over 15 months, with 72% completing the programme. Targets for achieving non-smoking status, blood pressure < 140/90 mm Hg, and total cholesterol < 4.8 mmol/l were achieved in 92%, 73%, and 62%, respectively, and the proportion on aspirin, β blockers, and lipid lowering treatment was 95%, 58%, and 64% on referral back to general practice for continuing care. Conclusions A comprehensive cardiac prevention and rehabilitation programme can be overed to all patients presenting for the first time with coronary heart disease, including those with exertional angina who are normally managed in primary care. Lifestyle, risk factor, and therapeutic targets can be successfully achieved in most patients with such a hospital based programme. (Heart 2001;85: ) Keywords: preventive policy; rehabilitation; coronary artery disease Prevention of coronary heart disease is one of the central targets of the National service framework for coronary heart disease. 1 This can be achieved by primary prevention, improved treatment of acute disease episodes, revascularisation, and secondary prevention. A community register of coronary heart disease in Bromley in south east London has recently shown that exertional angina is the most common presentation of coronary heart disease. 2 Sudden cardiac death accounts for less than one in five, and acute myocardial infarction for about one third of all first presentations of coronary heart disease in the community. Thus the opportunities for secondary prevention before loss of myocardium from infarction (the most important determinant of mortality in patients with coronary heart disease) 3 are considerably greater if patients with angina are targeted. The risk of a major coronary event is increased in the first year after presentation with exertional angina, 4 and therefore prevention should start soon after diagnosis. There is strong scientific evidence for coronary prevention through lifestyle measures, 5 aspirin, 6 post-myocardial infarction treatment with β blockers, 7 statins, 8 10 and angiotensin converting enzyme (ACE) inhibitors, and surgical revascularisation. 3 This evidence applies to patients with angina (lipid lowering treatment 8 and aspirin 6 ) as well as to those who have had an infarct or a revascularisation procedure. However, the full potential of these secondary prevention measures has not been realised in clinical practice: in the ASPIRE (action on secondary prevention through intervention to reduce events) survey of secondary prevention practice in 2583 patients from 24 specialist cardiac centres and district general hospitals in the UK, 13 19% were still smoking cigarettes, 18% had a blood pressure of > 160/ 90 mm Hg, and 72% had a total cholesterol of > 5.0 mmol/l. Traditional cardiac rehabilitation programmes have focused on patients after myocardial infarction or revascularisation, thus excluding the majority of patients with incident (new) coronary heart disease. Among those patients currently targeted for rehabilitation uptake is low. 14 The recent Joint British Societies recommendations on coronary prevention 15 advocate that the care of coronary patients should embrace all aspects of cardiac prevention and rehabilitation, and such an integrated service should be available to all patients with coronary heart disease, including exertional angina and acute coronary syndromes. We established a cardiac prevention and rehabilitation programme at Bromley Hospitals NHS Trust, south east London, for all incident (new) cases of coronary heart disease. The objective was to achieve defined lifestyle, risk factor, and therapeutic targets.
2 534 Fox, Nuttall, Wood, et al Time 0 weeks Figure 1 12 weeks Incident case of coronary artery disease (Rapid Access Chest Pain Clinic/inpatients) Recruitment < 2 working days < 2 working days Home visit Explore attitudes and knowledge 1 week Initial cardiovascular screening Health Promotion Sessions (8 weeks) Lectures and workshops/group discussions Exercise sessions Monitoring and treatment of BP/lipids/glucose Re-screening and report letter to GP and practice nurse The Changes for Life programme and the flow of patients. n = 194 n = 158 n = 148 n = 133 n = 113 n = 102 Methods Bromley Health Authority (population ) is served by 151 general practitioners in 59 practices. All patients registered with 80 general practitioners, selected at random from all practices, were eligible for the programme. Bromley Hospital (with the cardiac care unit and accident and emergency department) and Farnborough Hospital provide secondary cardiac care, while the specialist cardiac centres at King s College Hospital, the Royal Brompton, and St Thomas Hospital provide tertiary care. All new cases of coronary heart disease could be identified because of a contemporaneous epidemiological study of the incidence of coronary heart disease within the same population. 2 All records of admissions through the accident and emergency department were screened by a research nurse and presentations consistent with coronary heart disease identified. Patients were followed up on the wards, and incident (new) cases of exertional angina, unstable angina, or myocardial infarction identified. All identified patients presenting in primary care with suspected cardiac chest pain but not requiring acute hospital admission were referred to a dedicated rapid access chest pain clinic (RACPC) for evaluation. The RACPC opened in 1996 and the majority of incident (new) exertional angina cases were identified through this service. Completeness of case identification for new exertional angina has been confirmed by an audit of nitrate prescriptions in a random sample of general practices. 2 A small traditional cardiac rehabilitation programme already existed for patients after myocardial infarction or coronary revascularisation. The new programme, Changes for Life, (fig 1) was established in October 1997 for all cases of incident coronary heart disease, and replaced the traditional service. Two full time nurses, a physiotherapist (one fifth time), and a dietician (one fifth time) ran the programme with the support of other health care professionals. RECRUITMENT Inpatients with a first diagnosis of coronary heart disease and registered with a general practitioner allocated to the new programme were visited on the ward by one of the cardiac prevention nurses and overed a place. This nurse would remain as the patient s primary nurse throughout the duration of the programme. If the patient agreed to participate, a home visit followed, usually within two working days of hospital discharge. Patients identified through the RACPC as a first diagnosis of coronary heart disease, and also registered with a general practitioner allocated to the programme, were contacted to arrange a home visit, usually within two working days of being assessed in the RACPC. At the home visit the patient was given a copy of the Cardiofax (a filofax format) containing information about the Changes for Life programme, the causes of coronary disease, lifestyle, other risk factors, and other documentation. The patient s partner was encouraged to be present at this home visit and at all subsequent meetings, and cardiovascular screening was overed to partners and ovspring (> 16 years old). Patients who did not wish to participate in the programme received usual care. THE CHANGES FOR LIFE PROGRAMME The Changes for Life cardiac prevention and rehabilitation programme ran for about 12 weeks and consisted of the following: x a home visit and questionnaire to explore patient and family knowledge and attitudes to coronary heart disease prevention; x cardiovascular screening of patients and partners at the hospital and the over to screen first degree blood relatives; x an eight week rolling health promotion programme of lectures and group discussions, together with weekly exercise sessions; x a nurse protocol for repeat assessment and management of blood pressure and cholesterol; x a final rescreening at the hospital of patients and family members for coronary heart disease risk factors; x a comprehensive electronic report to the patient s general practitioner specifying lifestyle, risk factor, and therapeutic targets. Behavioural change in the programme was based on the Procheska and DeClimente cycle of change, 16 promoted by the Health Education Authority, encouraging thinking about change, preparing to change, making changes, maintaining changes, and addressing relapse. The cardiac prevention nurses and other members of the Changes for Life team were all trained in this approach by a clinical psychologist. The initial cardiovascular screening of patients and family members included an assessment of lifestyle (smoking, diet, and physical activity), height and weight (to calculate body mass index (BMI: weight (kg)/height (m 2 )), blood pressure (two readings at rest), random
3 Cardiac prevention and rehabilitation programme 535 Table 1 Process of recruitment cholesterol and fasting lipids, blood glucose, and pharmacological treatment. A dietician was responsible for individual or family dietary assessment and advice. Lifestyle changes were negotiated and targets discussed: complete cessation of tobacco smoking by the patient and family members; BMI < 25 kg/m 2 (desirable body weight); blood pressure < 140/ 90 mm Hg; total cholesterol < 4.8 mmol/l; and compliance with prophylactic drug treatment: aspirin (or other platelet modifying drugs), β blockers after myocardial infarction, and cholesterol modification. A policy of evidence based prescribing was followed, using the doses of drugs employed in clinical trials which have reported both eycacy, in terms of clinical events, and safety. After the cardiovascular screening the multidisciplinary health promotion programme took place over eight weekly sessions, usually starting within a week or so of hospital discharge or RACPC assessment. The following subjects were covered: coronary heart disease risk factors; family support and change; stopping smoking; diet and weight; physical activity; stress management; drug treatment; and the role of support groups. A group discussion was held one week after each lecture to allow participants time to assimilate the facts and formulate questions. At each weekly session supervised exercise for one hour was led by a physiotherapist and included a warm up period, three groups of exercises, and a cool down period. At the end of the eight weekly sessions each patient was given an individual exercise plan by the physiotherapist. The nurses had protocols for assessment and management of blood pressure, blood lipids, and glucose. Blood pressure was monitored twice a week and the target for blood pressure was < 140/90 mm Hg. A physician was responsible for optimising antihypertensive treatment. Patients who had an acute coronary syndrome were started immediately on a statin in hospital if the initial random cholesterol concentration was > 6.0 mmol/l. If the cholesterol was < 6.0 mmol/l this was repeated eight weeks later on three separate occasions (including one fasting lipid profile). If the average total cholesterol was > 4.8 mmol/l a statin was prescribed by a physician. For all other coronary patients, Total (n=194) Recruited (n=158) (% recruited) Source RACPC (80) 74 Inpatients (84) 36 Other 4 3 (75) 3 Diagnosis Exertional angina (78) 66 Unstable angina 14 9 (65) 7 Acute MI (93) 31 Other diagnoses (eg, recent MI) (86) 9 Sex Male (83) 78 Female (79) 35 Age (years) < (82) 74 > (81) 39 MI, myocardial infarction; RACPC, rapid access chest pain clinic. Completed programme (n=113) regardless of their initial cholesterol concentration, the same protocol was followed with three separate measurements (including one fasting) during the programme and treatment initiated by a physician if the average concentration was > 4.8 mmol/l. Patients with a random glucose concentration of > 6.7 mmol/l had a measurement of haemoglobin A1c. If this was abnormal they were referred to a diabetes specialist (KB) for evaluation and management. The patients symptoms and medical status were monitored throughout the programme and referral back to the consultant physician(s) responsible for their care done as required. RESCREENING On completion of the health promotion sessions patients and screened family members were rescreened for lifestyle, blood pressure, cholesterol, glucose, and use of drug treatment. An electronic report was prepared and sent to the patients general practitioner and the practice nurse, giving the results in relation to the defined lifestyle, risk factor, and therapeutic targets and what further action, if any, was required. ONE YEAR FOLLOW UP Patients were sent a letter inviting them for interview one year after completing the programme, which included questions on lifestyle and drug treatment and measurements of BMI, blood pressure (two readings at rest), and non-fasting total cholesterol. STATISTICS All patient data were entered directly by the nurses onto a dedicated Microsoft Access database. Data were analysed using SPSS for Windows and Stata software. Continuous variables were analysed using t tests and discrete factors by χ 2 tests. Results In all, 417 incident cases of coronary heart disease were identified from the population of over 15 months, between October 1997 and December Of these, 194 were registered with general practitioners allocated to the Changes for Life programme, and 158 (response rate 82%) were recruited to the programme (table 1). Mean age was 65 years (range years), men 64 years; women 66 years. Eighty seven patients (55%) presented with exertional angina and the rest had an acute coronary syndrome or some other coronary heart disease diagnosis. The flow of patients through the programme is shown in fig 1; 72% completed the programme and 65% attended for rescreening. Completion of the programme did not diver significantly by diagnosis, place of recruitment, age, or sex. Ninety six (72%) patients who participated in the programme attended for the one year follow up, which was completed in December Table 2 shows initial screening results for all 133 patients, and separately for those 102 patients who subsequently attended for rescreening at 12 weeks, together with the one
4 536 Fox, Nuttall, Wood, et al Table 2 Cardiovascular risk factors at initial screening examination, rescreening at the end of the programme, and one year follow up Characteristic All patients screened Initial screening (n=133) Patients attending for rescreening at end of programme Screening (n=102) Rescreening (n=102) Participating patients One year follow up (n=96) Non-smoking status (%) Weight (kg) (mean (SD)) 77.8 (12.7) 77.4 (11.8) 76.6 (12.1) 77.7 (12.5) Body mass index (kg/m 2 ) (mean (SD)) 27.6 (4.6) 27.4 (4.6) 27.1 (4.6) 27.4 (4.5) %BMI<25kg/m Systolic BP (mm Hg) (mean (SD)) 135 (21) 132 (20) 134 (18) 134 (20) Diastolic BP (mm Hg) (mean (SD)) 80 (14) 78 (12) 77 (10) 78 (12) % < 140/90 mm Hg * 58** Total cholesterol (mmol/l) (mean (SD)) 5.3 (1.1) 5.3 (1.1) 4.7 (0.84)* 4.9 (1.1) % < 4.8 mmol/l Plasma glucose (mmol/l) Aspirin treatment (%) ** β Blocker treatment (%) Lipid lowering treatment (%) * 56 Initial screening results for those attending for re-screening; *p < rescreening v screening; **p < 0.05 one year follow up v rescreening. BMI, body mass index; BP, blood pressure. year follow up data on those patients who participated in the programme. Eighty seven per cent of patients were not smoking at the start of the programme and this increased by a further 5% (four patients quit smoking) to 92% at rescreening. There was a small fall in weight and BMI, but the proportion achieving the target BMI of < 25 kg/m 2 did not change during the programme. Although there were no significant reductions in mean systolic or diastolic blood pressure, the proportion achieving a blood pressure of < 140/90 mm Hg increased by 6%, from 67% to 73% (p < 0.001). There was a reduction in mean total blood cholesterol, and the proportion achieving a cholesterol of < 4.8 mmol/l increased by 30%, from 32% to 62% (p < 0.001). Ninety five per cent of patients reported taking aspirin (all > 75 mg a day and six were also taking ticlopidine in addition). Fifty eight per cent of patients were taking a β blocker (typically atenolol 50 mg) at rescreening, and among those with acute myocardial infarction 22 of 31 patients (71%) were on this drug. The proportion taking lipid modifying treatment (most often simvastatin 20 mg) increased by 29% from 35% to 64% (p < 0.001). The improvements in lifestyle, risk factors, and drug treatment were not all maintained at one year, with a fall in the proportion of patients taking aspirin, β blockers, and lipid lowering treatment, and a decrease in the proportion of patients maintaining the blood pressure and cholesterol targets. Discussion The prevention of coronary heart disease is a government priority, and cardiac rehabilitation is one of the key elements of the National service framework for coronary heart disease.wehave shown how a comprehensive cardiac prevention and rehabilitation programme can be organised for all patients presenting for the first time with any symptomatic manifestation of coronary heart disease, including angina pectoris. A high recruitment rate (average 81%) was achieved across all diagnoses. Our hospital based programme met targets for lifestyle (92% non-smoking status), blood pressure control (73% < 140/90 mm Hg), total cholesterol (62%< 4.8 mmol/l), and drug treatment (95% aspirin, 71% β blocker post-myocardial infarction, 64% lipid treatment). The Joint British Societies recommendations on coronary prevention in clinical practice 15 define patients with established coronary heart disease or other atherosclerotic disease as the top priority; the report recommended that in hospitals the care of such patients should embrace all aspects of cardiac prevention and rehabilitation, and be overed to all coronary patients, not only those who had had a myocardial infarct or a revascularisation procedure. Providing such a service is recognised as a hospiral trust responsibility in the National service framework for coronary heart disease. Historically, cardiac rehabilitation focused on supervised exercise sessions but is now evolving into comprehensive lifestyle programmes providing risk factor management and psychosocial and vocational support. This evolution in cardiac rehabilitation is reflected in the World Health Organization s changed definition, with the addition of the following words...the sum of activities required to influence favourably the underlying cause of the disease,.... Our Changes for Life programme meets this definition and also fulfils the joint British Societies recommendation of inclusivity by recruiting all patients with coronary disease, most commonly exertional angina. Our cardiac prevention and rehabilitation programme was one part of an integrated strategy for the care of all patients presenting with coronary heart disease in Bromley, south east London. Most patients with acute coronary syndromes in this district were admitted to the coronary care unit or cardiology ward and were seen on a daily basis by the consultant cardiologist on call. The three cardiologists followed a common policy for secondary prevention and this combined with the special interest in prevention of one of them, and two cardiac prevention nurses meant that secondary prevention measures were commonly in place before patients entered the programme. The rapid access chest pain clinic provided a same day assessment service for new cases of chest pain in general practice or in the accident and emergency department, and this meant that all new cases of exertional angina were evaluated by the cardiology service, and the same policy of secondary prevention measures was followed throughout. This integrated approach to the care of all coronary patients presenting from the community resulted in the high use of aspirin, β blockers, and statins recorded at the start of the programme. The additional improvements achieved through the programme must be seen in this context, as not all coronary patients are as evectively managed before entering a cardiac rehabilitation service. Our programme focused on those presenting for the first time with coronary disease. We believe that patients at the symptomatic onset of their disease are more open to making lifestyle changes, managing risk factors, and
5 Cardiac prevention and rehabilitation programme 537 complying with drug treatment. This is not an argument for excluding those with existing disease, as risk factor management is very successful in reducing risk in those with prevalent disease. However, the structure and content of a programme for recurrent disease may have diverent emphases, particularly if patients have already been exposed to prevention and rehabilitation services in the same health care setting. Patients were actively recruited shortly after diagnosis (not simply referred) to the Changes for Life programme. This explains the very high recruitment rate 82% of all eligible patients, compared with 41% in other rehabilitation programmes. 14 There were no diverences in recruitment rates by age, sex, or diagnosis. Patients with angina (either exertional or unstable) were as likely to participate in the programme as those who had had a myocardial infarct. A home visit by the nurses provided a valuable professional bridge for patients during a vulnerable period between hospital diagnosis and the start of the outpatient phase of the programme. They were also able to assess the potential for lifestyle change by the household, and the whole family was encouraged to participate. For married couples there is concordance for lifestyle and risk factors such as obesity, blood pressure, lipids, and glucose, 17 and also concordance for changes in these risk factors. 18 Patients and families were asked to take personal responsibility for lifestyle change, and this is integral to the Procheska and DeClimente cycle of change model. 16 Clear lifestyle, risk factor, and therapeutic targets were defined in the protocol. Most patients stopped smoking following the diagnosis of coronary heart disease, and just 8% of all patients were still using tobacco to some extent at the end of the programme. Weight loss averaged 1 2 kg and the proportion of patients with BMI of > 25 kg/m 2 remained the same. Although there is a confounding evect of weight gain in patients who stop smoking cigarettes, 19 this observation shows the diyculties in achieving substantial weight loss, despite professional dietary advice. However, despite the small weight reduction the majority of patients achieved the blood pressure target of less than 140/90 mm Hg. This represents a substantial improvement on ASPIRE, where one in two patients had not achieved this target. 13 While the cardiac prevention nurses monitored blood pressure at each visit, and followed a blood pressure reduction protocol, they could not prescribe drugs. A physician had to modify drug treatment, and changes were not made as often as the protocol required. Extending the cardiac prevention nurse s responsibility to drug titration in a defined therapeutic protocol may further improve blood pressure control. The proportion of patients achieving the target cholesterol concentration (< 4.8 mmol/l) improved significantly between the start of the programme and rescreening, and those achieving the current Joint British Societies target of < 5.0 mmol/l, 15 (70%) represent a substantial improvement on ASPIRE, where four of five patients had a cholesterol concentration above this value at follow up. 13 In the same way as for blood pressure control, nurse uptitration of statin treatment with appropriate safeguards may further increase the proportion achieving the cholesterol target. Sixty four per cent of patients were on lipid modifying treatment on completing this programme, compared with 16% in ASPIRE. Aspirin use was almost universal, reflecting the prescribing policy in the coronary care units, the wards, and the RACPC, and there was just a small (2%) further improvement during the programme. Similarly, the use of β blockers was high for the same reasons, particularly following a myocardial infarction where 68% were on a β blocker at rescreening, compared with 38% in the ASPIRE survey. Other approaches to raising the standard of secondary prevention have been rather disappointing. In the SHIP (Southampton heart integrated care project) trial specialist liaison nurses sought to improve communication between hospital and general practice by encouraging general practice nurses to provide structured follow up of coronary patients, including those with angina. Although BMI was slightly lower in the intervention group at one year, there were no diverences in smoking, fitness, blood pressure, or lipid concentrations compared with control patients. In this trial, 20 5% of patients had a blood pressure of > 160 mm Hg systolic or > 100 mm Hg diastolic which was untreated; 38% had a cholesterol concentration of > 5.5 mmol/l but were not taking lipid lowering drugs; and 42% of the index patients had attended at least one cardiac rehabilitation session (18% more than control) but with no significant impact on risk factor control. In primary care, the POST (postal prompts after a coronary event) study used postal prompts to patients (myocardial infarction or unstable angina) and general practitioners at two weeks and three months after discharge from hospital. There was no diverence in the use of β blockers or cholesterol lowering drugs in the intervention group compared with the controls (although a significantly higher proportion of patients had their cholesterol measured in the intervention group). 21 Ninety per cent of the intervention group in POST were taking aspirin, but only 38% were using a β blocker and 28% a cholesterol lowering drug. A health promotion trial in general practice for patients with angina reported no significant diverences at two years in smoking habit, systolic or diastolic blood pressure, cholesterol concentration, or BMI. 22 Specific drug treatments were not reported. In a randomised controlled trial of nurse run clinics in general practice in north east Scotland, coronary patients experienced significant improvements in chest pain and physical activity at one year. There was no evect on blood pressure, lipid management, or smoking status. 23 Our Changes for Life programme has several advantages over these other approaches to secondary prevention (table 3). First, the patient s
6 538 Fox, Nuttall, Wood, et al Table 3 Key features of the Changes for Life cardiac prevention and rehabilitation programme + All incident (new) cases of coronary heart disease were eligible + Recruitment was immediately after the diagnosis of disease + The programme was an integral part of the cardiology department s care + Patients were visited at home + Partner and relative involvement + Targets for lifestyle, risk factors, and drug treatments were defined and assessed + Rescreening at the end of the programme enabled evaluation cardiological management is completely integrated with all aspects of secondary prevention and rehabilitation, from CCU to the wards and the RACPC. Second, all professional stav required for this multidisciplinary programme, and the necessary resources, are available in hospital. Third, the organisation of group sessions for education, health promotion, physical activity, and so on is much easier for both patients and stav alike when centred on a single facility. At the end of the hospital phase of Changes for Life, the patient s lifestyle, risk factors, and drug treatment were re-evaluated and reports sent both to general practitioners and practice nurses. Integration of this type of hospital programme with primary care is essential for continuity of care by physicians and other health professionals over the long term. The challenge in the community is to sustain and improve on patients lifestyle, risk factor, and therapeutic targets. CONCLUSIONS A comprehensive cardiac prevention and rehabilitation programme can be overed to all patients presenting for the first time with coronary artery disease. A high recruitment rate can be achieved in all diagnostic groups, including patients presenting with exertional angina through a rapid access chest pain clinic. Lifestyle, risk factor, and therapeutic targets can be successfully achieved in most patients with such a hospital based programme and therefore they can expect a corresponding reduction in coronary morbidity and mortality as long as these results are sustained in general practice. The Changes for Life programme was supported by the British Heart Foundation and by unrestricted educational grants from Merck Sharp and Dohme and Novartis. Bromley Hospitals NHS Trust consultant cardiologists: Dr Ed Langford, Dr Fawas Akhras (locum), and Professor David Wood. We are grateful for the professional advice and training provided by Sheila Doherty (psychologist). We thank Clive Beech (pharmacist), C Perry (health promotion advisor), Janet Webb (occupational therapist), Margaret Tipson (diabetes nurse specialist), Vanessa Douglas (practice nurse coordinator) and Michael Oliver. We thank the general practitioners of Bromley Health Authority for their support. 1 Department of Health. The National Service framework for coronary heart disease. London: DOH, SutcliVe SJ, SutcliVe AK, Wood DA. The clinical incidence of fatal and non-fatal coronary heart disease in the population [abstract]. Heart 1999;81(suppl 1):28. 3 Yusuf S, Zucker D, Peduzzi P, et al.evect of coronary artery bypass graft surgery on survival: overview of 10 year results from randomized trials by the coronary artery bypass graft surgery trialists collaboration. Lancet 1994;344: Ghandi MM, Lampe F, Wood DA. Incidence, clinical characteristics and short-term prognosis of angina pectoris. Heart 1995;73: Law M, Tang JL. An analysis of the evectiveness of interventions intended to help people stop smoking. Arch Intern Med 1995;155: Antiplatelet Trialists Collaboration. Collaborative overview of randomised trials of antiplatelet therapy. 1. Prevention of death, myocardial infarction and stroke by prolonged antiplatelet therapy in various categories of patients. BMJ 1994;308: Freemantle N, Cleland J, Young P, et al. Beta blockade after myocardial infarction: systematic review and meta regression analysis. BMJ 1999;318: Scandinavian Simvastatin Survival Study. A randomised trial of cholesterol lowering in 4444 patients with coronary heart disease: the Scandinavian simvastatin survival study (4S). Lancet 1994;344: Sacks FM, PfeVer MA, Moye LA, et al. The evect of pravastatin on coronary events after myocardial infarction in patients with average lipid levels. N Engl J Med 1996;335: The Long-Term Intervention with Pravastatin in Ischaemic Disease (LIPID) Study Group. Prevention of cardiovascular events and death with pravastatin in patients with coronary heart disease and a broad range of initial cholesterol levels. N Engl J Med 1998;339: Acute Infarction Ramipril EYcacy (AIRE) Investigators. EVects of ramipril on morbidity and mortality of survivors of acute myocardial infarction with clinical evidence of heart failure. Lancet 1993;342: Yusuf S, Sleight P, Pogue J, et al. EVects of an angiotensinconverting enzyme inhibitor, ramipril, on cardiovascular events in high risk patients. N Engl J Med 2000;342: Aspire Steering Group. A British Cardiac Society survey of the potential for the secondary prevention of coronary disease: ASPIRE (action on secondary prevention through intervention to reduce events). Principal results. Heart 1996;75: Cooper R, Lloyd G, Weinmaman J, et al. Why patients do not attend cardiac rehabilitation: role of intentions and illness beliefs. Heart 1999;82: Wood DA, Durrington P, Poulter N, et al. Joint British recommendations on prevention of coronary heart disease in clinical practice. Heart 1999;80(suppl 2):S Prochaska JO, DiClemente CC. Toward a comprehensive model of change. In: Treating addictive behaviour: processes of change. New York: Plenum Press, 1986: Sackett DL, Anderson GD, Milner R, et al. Concordance for coronary risk factors among spouses. Circulation 1975;52: Pyke SDM, Wood DA, Kinmouth AL, et al, on behalf of the BHFS group. Changes in coronary risk and risk factor levels in couples following lifestyle intervention: the British family heart study. Arch Fam Med 1997;6: Thomson R, Pyke SDM, Scott EA, et al. Dietary change after smoking cessation: a prospective study. Br J Nutr 1995;74: Jolly K, Bradley F, Sharp S, et al. Randomised controlled trial of follow up care in general practice of patients with myocardial infarction and angina: final results of the Southampton heart integrated care project (SHIP). BMJ 1999;318: Feder G, GriYths C, Eldridge S, et al. EVect of postal prompts to patients and general practitioners on the quality of primary care after a coronary event (POST): randomised control trial. BMJ 1999;318: Cupples ME, McKnight A. Randomised controlled trial of health promotion in general practice for patients at high cardiovascular risk. BMJ 1994;309: Campbell NC, Ritchie LD, Thain J, et al. Secondary prevention in coronary heart disease: a randomised trial of nurse led clinics in primary care. Heart 1998;80:
Repeat ischaemic heart disease audit of primary care patients ( ): Comparisons by age, sex and ethnic group
 Repeat ischaemic heart disease audit of primary care patients (2002-2003): Comparisons by age, sex and ethnic group Baseline-repeat ischaemic heart disease audit of primary care patients: a comparison
Repeat ischaemic heart disease audit of primary care patients (2002-2003): Comparisons by age, sex and ethnic group Baseline-repeat ischaemic heart disease audit of primary care patients: a comparison
Management of ischaemic heart disease in primary care: towards better practice
 Journal of Public Health Medicine Vol. 21, No. 2, pp. 179 184 Printed in Great Britain Management of ischaemic heart disease in primary care: towards better practice Krish Thiru, Jeremy Gray and Azeem
Journal of Public Health Medicine Vol. 21, No. 2, pp. 179 184 Printed in Great Britain Management of ischaemic heart disease in primary care: towards better practice Krish Thiru, Jeremy Gray and Azeem
Guidelines on cardiovascular risk assessment and management
 European Heart Journal Supplements (2005) 7 (Supplement L), L5 L10 doi:10.1093/eurheartj/sui079 Guidelines on cardiovascular risk assessment and management David A. Wood 1,2 * 1 Cardiovascular Medicine
European Heart Journal Supplements (2005) 7 (Supplement L), L5 L10 doi:10.1093/eurheartj/sui079 Guidelines on cardiovascular risk assessment and management David A. Wood 1,2 * 1 Cardiovascular Medicine
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE QUALITY AND OUTCOMES FRAMEWORK (QOF) INDICATOR DEVELOPMENT PROGRAMME Briefing paper QOF indicator area: Peripheral arterial disease Potential output:
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE QUALITY AND OUTCOMES FRAMEWORK (QOF) INDICATOR DEVELOPMENT PROGRAMME Briefing paper QOF indicator area: Peripheral arterial disease Potential output:
Secondary Prevention of Coronary Heart Disease in Primary Health Care
 & Secondary Prevention of Coronary Heart Disease in Primary Health Care Olivera Batić-Mujanović¹*, Muharem Zildžić², Azijada Beganlić¹ 1. House of Health Tuzla, Family Medicine Teaching Center, Albina
& Secondary Prevention of Coronary Heart Disease in Primary Health Care Olivera Batić-Mujanović¹*, Muharem Zildžić², Azijada Beganlić¹ 1. House of Health Tuzla, Family Medicine Teaching Center, Albina
Cardiac Rehabilitation after Primary Coronary Intervention CONTRA
 DEBATE SESSION Is there a role for cardiac rehabilitation in the modern era of Percutaneous coronary intervention and coronary artery bypass grafting? Cardiac Rehabilitation after Primary Coronary Intervention
DEBATE SESSION Is there a role for cardiac rehabilitation in the modern era of Percutaneous coronary intervention and coronary artery bypass grafting? Cardiac Rehabilitation after Primary Coronary Intervention
National Medicines Information Centre
 National Medicines Information Centre VOLUME 8 NUMBER 6 2002 ST. JAMES S HOSPITAL DUBLIN 8 TEL 01-4730589 or 1850-727-727 FAX 01-4730596 E-Mail: nmic@stjames.ie If you would like to receive NMIC publications
National Medicines Information Centre VOLUME 8 NUMBER 6 2002 ST. JAMES S HOSPITAL DUBLIN 8 TEL 01-4730589 or 1850-727-727 FAX 01-4730596 E-Mail: nmic@stjames.ie If you would like to receive NMIC publications
LIST OF ABBREVIATIONS
 Diabetes & Endocrinology 2005 Royal College of Physicians of Edinburgh Diabetes and lipids 1 G Marshall, 2 M Fisher 1 Research Fellow, Department of Cardiology, Glasgow Royal Infirmary, Glasgow, Scotland,
Diabetes & Endocrinology 2005 Royal College of Physicians of Edinburgh Diabetes and lipids 1 G Marshall, 2 M Fisher 1 Research Fellow, Department of Cardiology, Glasgow Royal Infirmary, Glasgow, Scotland,
Preventive Cardiology Scientific evidence
 Preventive Cardiology Scientific evidence Professor David A Wood Garfield Weston Professor of Cardiovascular Medicine International Centre for Circulatory Health Imperial College London Primary prevention
Preventive Cardiology Scientific evidence Professor David A Wood Garfield Weston Professor of Cardiovascular Medicine International Centre for Circulatory Health Imperial College London Primary prevention
Coronary heart disease prevention and age inequalities:
 Coronary heart disease prevention and age inequalities: the first year of the National Service Framework for CHD Julia Hippisley-Cox, Michael Pringle, Ruth Cater, Carol Coupland and Andy Meal ABSTRACT
Coronary heart disease prevention and age inequalities: the first year of the National Service Framework for CHD Julia Hippisley-Cox, Michael Pringle, Ruth Cater, Carol Coupland and Andy Meal ABSTRACT
Coronary heart disease and stroke
 4 Coronary heart disease and stroke Overview of cardiovascular disease Cardiovascular disease (CVD), also called circulatory disease, describes a group of diseases which are caused by blockage or rupture
4 Coronary heart disease and stroke Overview of cardiovascular disease Cardiovascular disease (CVD), also called circulatory disease, describes a group of diseases which are caused by blockage or rupture
Unstable angina and NSTEMI
 Issue date: March 2010 Unstable angina and NSTEMI The early management of unstable angina and non-st-segment-elevation myocardial infarction This guideline updates and replaces recommendations for the
Issue date: March 2010 Unstable angina and NSTEMI The early management of unstable angina and non-st-segment-elevation myocardial infarction This guideline updates and replaces recommendations for the
Cwm Taf NHS Trust Cardiac Rehabilitation ROYAL GLAMORGAN HOSPITAL LLANTRISANT
 Cwm Taf NHS Trust Cardiac Rehabilitation ROYAL GLAMORGAN HOSPITAL LLANTRISANT Meet the Team Clinical Specialist Nurse Manager Band 8a x1 WTE Cardiac Rehabilitation Specialist Nurse Band 7 x 1 WTE Cardiac
Cwm Taf NHS Trust Cardiac Rehabilitation ROYAL GLAMORGAN HOSPITAL LLANTRISANT Meet the Team Clinical Specialist Nurse Manager Band 8a x1 WTE Cardiac Rehabilitation Specialist Nurse Band 7 x 1 WTE Cardiac
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE QUALITY AND OUTCOMES FRAMEWORK (QOF) INDICATOR DEVELOPMENT PROGRAMME Briefing paper QOF indicator area: Primary prevention of CVD Potential output:
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE QUALITY AND OUTCOMES FRAMEWORK (QOF) INDICATOR DEVELOPMENT PROGRAMME Briefing paper QOF indicator area: Primary prevention of CVD Potential output:
Cardiac rehabilitation: The psychological changes that predict health outcome and healthy behaviour
 Psychology, Health & Medicine, February 2005; 10(1): 88 95 Cardiac rehabilitation: The psychological changes that predict health outcome and healthy behaviour SUSAN MICHIE 1, DARYL O CONNOR 2, JULIAN BATH
Psychology, Health & Medicine, February 2005; 10(1): 88 95 Cardiac rehabilitation: The psychological changes that predict health outcome and healthy behaviour SUSAN MICHIE 1, DARYL O CONNOR 2, JULIAN BATH
South Tyneside Exercise Referral and Weight Management Programme
 South Tyneside Exercise Referral and Weight Management Programme Referral Guidance Document 2011/2012 1 2 South Tyneside Exercise Referral and Community Weight Management Programme Introduction An Exercise
South Tyneside Exercise Referral and Weight Management Programme Referral Guidance Document 2011/2012 1 2 South Tyneside Exercise Referral and Community Weight Management Programme Introduction An Exercise
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Myocardial infarction: secondary prevention in primary and secondary care for patients following a myocardial infarction 1.1
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Myocardial infarction: secondary prevention in primary and secondary care for patients following a myocardial infarction 1.1
General practice. Introduction. Abstract. Participants and methods
 Editorial by Hobbs and Murray Primary Medical Care, University of Southampton, Aldermoor Health Centre, Southampton SO16 5ST Kate Jolly, senior registrar Fiona Bradley, research fellow Helen Smith, senior
Editorial by Hobbs and Murray Primary Medical Care, University of Southampton, Aldermoor Health Centre, Southampton SO16 5ST Kate Jolly, senior registrar Fiona Bradley, research fellow Helen Smith, senior
Secondary prevention in coronary heart disease: a randomised trial of nurse led clinics in primary care
 Heart 1998;80:447 452 447 Department of General Practice and Primary Care, Foresterhill Health Centre, Aberdeen, UK N C Campbell L D Ritchie H G Deans Denburn Health Centre, Rosemount Viaduct, Aberdeen,
Heart 1998;80:447 452 447 Department of General Practice and Primary Care, Foresterhill Health Centre, Aberdeen, UK N C Campbell L D Ritchie H G Deans Denburn Health Centre, Rosemount Viaduct, Aberdeen,
the high CVD risk smoker
 Smoking Cessation: population and patients A comprehensive approach to the smoker the high CVD risk smoker Catriona Jennings Cardiovascular Specialist Research Nurse Imperial College London European Society
Smoking Cessation: population and patients A comprehensive approach to the smoker the high CVD risk smoker Catriona Jennings Cardiovascular Specialist Research Nurse Imperial College London European Society
Program Metrics. New Unique ID. Old Unique ID. Metric Set Metric Name Description. Old Metric Name
 Program Metrics The list below includes the metrics that will be calculated by the PINNACLE Registry for the outpatient office setting. These include metrics for, Atrial Fibrillation, Hypertension and.
Program Metrics The list below includes the metrics that will be calculated by the PINNACLE Registry for the outpatient office setting. These include metrics for, Atrial Fibrillation, Hypertension and.
Development of a Primary Care Model for Cardiac Rehabilitation and Secondary Prevention
 Development of a Primary Care Model for Cardiac Rehabilitation and Secondary Prevention Kristine Battye, Colleen Bichel, Kerry Kelly 5th National Rural Health Conference Adelaide, South Australia, 14-17th
Development of a Primary Care Model for Cardiac Rehabilitation and Secondary Prevention Kristine Battye, Colleen Bichel, Kerry Kelly 5th National Rural Health Conference Adelaide, South Australia, 14-17th
CONCISE GUIDE National Clinical Guidelines for Stroke 2nd Edition
 CONCISE GUIDE 2004 National for Stroke 2nd Edition This concise guide summarises the recommendations, graded according to the evidence, from the National 2nd edition. As critical aspects of care are not
CONCISE GUIDE 2004 National for Stroke 2nd Edition This concise guide summarises the recommendations, graded according to the evidence, from the National 2nd edition. As critical aspects of care are not
The Role of Cardiac Rehabilitation in Recovery & Secondary Prevention. Loren M Stabile, MS Cardiac & Pulmonary Rehab Program Manager
 The Role of Cardiac Rehabilitation in Recovery & Secondary Prevention Loren M Stabile, MS Cardiac & Pulmonary Rehab Program Manager Objectives Core Components of Cardiac Rehab Program CR Indications &
The Role of Cardiac Rehabilitation in Recovery & Secondary Prevention Loren M Stabile, MS Cardiac & Pulmonary Rehab Program Manager Objectives Core Components of Cardiac Rehab Program CR Indications &
Cardiac Rehabilitation. Questions and Answers Information for Patients
 Cardiac Rehabilitation Questions and Answers Information for Patients Cardiac Rehabilitation Dept 01625 663083 Leaflet Ref: 10985 Published: 01/17 Review: 12/19 Page 1 Contacts Cardiac Rehabilitation Service
Cardiac Rehabilitation Questions and Answers Information for Patients Cardiac Rehabilitation Dept 01625 663083 Leaflet Ref: 10985 Published: 01/17 Review: 12/19 Page 1 Contacts Cardiac Rehabilitation Service
New PINNACLE Measures The below measures for PINNACLE will be added as new measures to the outcomes reporting starting with Version 2.0.
 New PINNACLE Measures The below measures for PINNACLE will be added as new measures to the outcomes reporting starting with Version 2.0. Measure Steward Measure Name Measure Description Rationale for Adding
New PINNACLE Measures The below measures for PINNACLE will be added as new measures to the outcomes reporting starting with Version 2.0. Measure Steward Measure Name Measure Description Rationale for Adding
Practice-Level Executive Summary Report
 PINNACLE Registry Metrics 0003, Test Practice_NextGen [Rolling: 1st April 2015 to 31st March 2016 ] Generated on 5/11/2016 11:37:35 AM American College of Cardiology Foundation National Cardiovascular
PINNACLE Registry Metrics 0003, Test Practice_NextGen [Rolling: 1st April 2015 to 31st March 2016 ] Generated on 5/11/2016 11:37:35 AM American College of Cardiology Foundation National Cardiovascular
The EUROASPIRE surveys: lessons learned in cardiovascular disease prevention
 Brief Report The EUROASPIRE surveys: lessons learned in cardiovascular disease prevention Kornelia Kotseva 1,2 ; on behalf of the EUROASPIRE Investigators 1 National Heart & Lung Institute, Imperial College
Brief Report The EUROASPIRE surveys: lessons learned in cardiovascular disease prevention Kornelia Kotseva 1,2 ; on behalf of the EUROASPIRE Investigators 1 National Heart & Lung Institute, Imperial College
Secondary prevention and systems approaches: Lessons from EUROASPIRE and EUROACTION
 Secondary prevention and systems approaches: Lessons from EUROASPIRE and EUROACTION Dr Kornelia Kotseva National Heart & Lung Insitute Imperial College London, UK on behalf of all investigators participating
Secondary prevention and systems approaches: Lessons from EUROASPIRE and EUROACTION Dr Kornelia Kotseva National Heart & Lung Insitute Imperial College London, UK on behalf of all investigators participating
Nursing in Scotland. Glasgow & Clyde Weight Management Service
 Nursing in Scotland Glasgow & Clyde Weight Management Service Contact: Dr Marie L Prince Chartered Clinical Psychologist marie.prince@ggc.scot.nhs.uk GCWMS Ward 23 Surgical Block Glasgow Royal Infirmary
Nursing in Scotland Glasgow & Clyde Weight Management Service Contact: Dr Marie L Prince Chartered Clinical Psychologist marie.prince@ggc.scot.nhs.uk GCWMS Ward 23 Surgical Block Glasgow Royal Infirmary
Quality Payment Program: Cardiology Specialty Measure Set
 Measure Title * Reportable via PINNACLE α Reportable via Diabetes Collaborative CQMC v1.0 Measure High Priority Measure Cross Cutting Measure Heart Failure (HF): Angiotensin- Converting Enzyme (ACE) Inhibitor
Measure Title * Reportable via PINNACLE α Reportable via Diabetes Collaborative CQMC v1.0 Measure High Priority Measure Cross Cutting Measure Heart Failure (HF): Angiotensin- Converting Enzyme (ACE) Inhibitor
GOVERNING BODY REPORT
 GOVERNING BODY REPORT DATE OF MEETING: 20th September 2012 TITLE OF REPORT: KEY MESSAGES: NHS West Cheshire Clinical Commissioning Group has identified heart disease as one of its six strategic clinical
GOVERNING BODY REPORT DATE OF MEETING: 20th September 2012 TITLE OF REPORT: KEY MESSAGES: NHS West Cheshire Clinical Commissioning Group has identified heart disease as one of its six strategic clinical
How many patients with coronary heart disease are not achieving their risk-factor targets? Experience in Victoria versus
 How many patients with coronary heart disease are not achieving their risk-factor targets? Experience in Victoria 1996 1998 versus Margarite J Vale, Michael V Jelinek, James D Best, on behalf of the COACH
How many patients with coronary heart disease are not achieving their risk-factor targets? Experience in Victoria 1996 1998 versus Margarite J Vale, Michael V Jelinek, James D Best, on behalf of the COACH
CORONARY ARTERY DISEASE (CAD) MEASURES GROUP OVERVIEW
 CONARY ARTERY DISEASE (CAD) MEASURES GROUP OVERVIEW 2014 PQRS OPTIONS F MEASURES GROUPS: 2014 PQRS MEASURES IN CONARY ARTERY DISEASE (CAD) MEASURES GROUP: #6. Coronary Artery Disease (CAD): Antiplatelet
CONARY ARTERY DISEASE (CAD) MEASURES GROUP OVERVIEW 2014 PQRS OPTIONS F MEASURES GROUPS: 2014 PQRS MEASURES IN CONARY ARTERY DISEASE (CAD) MEASURES GROUP: #6. Coronary Artery Disease (CAD): Antiplatelet
Smoking Counselling and Cessation Service in Hospital Authority 7 May HA Convention 2014
 Smoking Counselling and Cessation Service in Hospital Authority 7 May 2014 - HA Convention 2014 On behalf of COC (Family Medicine) Dr Maria Leung Consultant, Department of Family Medicine New Territories
Smoking Counselling and Cessation Service in Hospital Authority 7 May 2014 - HA Convention 2014 On behalf of COC (Family Medicine) Dr Maria Leung Consultant, Department of Family Medicine New Territories
PREVENTIVE AND REHABILITATIVE MANAGEMENT OF ACUTE CORONARY SYNDROMES (NSTEMI, STEMI, PCI)
 PREVENTIVE AND REHABILITATIVE MANAGEMENT OF ACUTE CORONARY SYNDROMES (NSTEMI, STEMI, PCI) Dato Dr. Balachandran Kandasamy Institut Jantung Negara 12 th November 2016 KEY MESSAGES 1. Initiate a long-term
PREVENTIVE AND REHABILITATIVE MANAGEMENT OF ACUTE CORONARY SYNDROMES (NSTEMI, STEMI, PCI) Dato Dr. Balachandran Kandasamy Institut Jantung Negara 12 th November 2016 KEY MESSAGES 1. Initiate a long-term
2010 National Audit of Dementia (Care in General Hospitals) Guy's and St Thomas' NHS Foundation Trust
 Royal College of Psychiatrists 2010 National Audit of Dementia (Care in General Hospitals) Organisational checklist results and commentary for: Guy's and St Thomas' NHS Foundation Trust The 2010 national
Royal College of Psychiatrists 2010 National Audit of Dementia (Care in General Hospitals) Organisational checklist results and commentary for: Guy's and St Thomas' NHS Foundation Trust The 2010 national
Medicines Management Optimisation Achieving your 5 a day post-mi Medication WORKSHOP
 Medicines Management Optimisation Achieving your 5 a day post-mi Medication WORKSHOP What is Medicines Optimisation? the safe and effective use of medicines to enable the best possible outcomes NICE ng
Medicines Management Optimisation Achieving your 5 a day post-mi Medication WORKSHOP What is Medicines Optimisation? the safe and effective use of medicines to enable the best possible outcomes NICE ng
Cardiovascular Disease
 NEW ZEALAND HEALTH STRATEGY DHB TOOLKIT Cardiovascular Disease To reduce the incidence of cardiovascular disease 2003 Edition 2: February 2003 Contents Contents...2 Executive summary...4 Introduction...5
NEW ZEALAND HEALTH STRATEGY DHB TOOLKIT Cardiovascular Disease To reduce the incidence of cardiovascular disease 2003 Edition 2: February 2003 Contents Contents...2 Executive summary...4 Introduction...5
EUROACTION. A European Society of Cardiology Demonstration Project in Preventive Cardiology FINAL RESULTS
 EUROACTION A European Society of Cardiology Demonstration Project in Preventive Cardiology FINAL RESULTS Professor David Wood on behalf of the EUROACTION Group EUROACTION 8 countries 24 centres 962 subjects
EUROACTION A European Society of Cardiology Demonstration Project in Preventive Cardiology FINAL RESULTS Professor David Wood on behalf of the EUROACTION Group EUROACTION 8 countries 24 centres 962 subjects
How would you manage Ms. Gold
 How would you manage Ms. Gold 32 yo Asian woman with dyslipidemia Current medications: Simvastatin 20mg QD Most recent lipid profile: TC = 246, TG = 100, LDL = 176, HDL = 50 What about Mr. Williams? 56
How would you manage Ms. Gold 32 yo Asian woman with dyslipidemia Current medications: Simvastatin 20mg QD Most recent lipid profile: TC = 246, TG = 100, LDL = 176, HDL = 50 What about Mr. Williams? 56
Evidence Briefing for NHS Bradford and Airedale. Physical health monitoring for people with schizophrenia or other serious mental illness
 Evidence Briefing for NHS Bradford and Airedale Physical health monitoring for people with schizophrenia or other serious mental illness The NICE clinical guideline on schizophrenia 1 recommends that GPs
Evidence Briefing for NHS Bradford and Airedale Physical health monitoring for people with schizophrenia or other serious mental illness The NICE clinical guideline on schizophrenia 1 recommends that GPs
Quality Payment Program: Cardiology Specialty Measure Set
 Quality Payment Program: Cardiology Specialty Set Title Number CMS Reporting Method(s) Heart Failure (HF): Angiotensin- Converting Enzyme (ACE) Inhibitor or Angiotensin Receptor Blocker (ARB) Therapy for
Quality Payment Program: Cardiology Specialty Set Title Number CMS Reporting Method(s) Heart Failure (HF): Angiotensin- Converting Enzyme (ACE) Inhibitor or Angiotensin Receptor Blocker (ARB) Therapy for
Coronary Heart Disease
 Coronary Heart Disease This document is a final specification of the PRIMIS Comparative Analysis Service (CAS) MIQUEST query set to enable analyses in support of the NSF for CHD. The specification has
Coronary Heart Disease This document is a final specification of the PRIMIS Comparative Analysis Service (CAS) MIQUEST query set to enable analyses in support of the NSF for CHD. The specification has
Models of preventive care in clinical practice to achieve 25 by 25
 Models of preventive care in clinical practice to achieve 25 by 25 Professor David A Wood Garfield Weston Professor of Cardiovascular Medicine International Centre for Circulatory Health Imperial College
Models of preventive care in clinical practice to achieve 25 by 25 Professor David A Wood Garfield Weston Professor of Cardiovascular Medicine International Centre for Circulatory Health Imperial College
Clinical Considerations of High Intensity Interval Training (HIIT)
 Clinical Considerations of High Intensity Interval Training (HIIT) Jenna Taylor Exercise Physiologist & Dietitian The Wesley Hospital PhD Candidate The University of Queensland What is High Intensity Interval
Clinical Considerations of High Intensity Interval Training (HIIT) Jenna Taylor Exercise Physiologist & Dietitian The Wesley Hospital PhD Candidate The University of Queensland What is High Intensity Interval
This booklet has been published by CREST (the Clinical Resource Efficiency Support Team).
 This booklet has been published by CREST (the Clinical Resource Efficiency Support Team). CREST is a small committee of health care professionals established under the auspices of the Central Medical Advisory
This booklet has been published by CREST (the Clinical Resource Efficiency Support Team). CREST is a small committee of health care professionals established under the auspices of the Central Medical Advisory
Commissioning for Better Outcomes in COPD
 Commissioning for Better Outcomes in COPD Dr Matt Kearney Primary Care & Public Health Advisor Respiratory Programme, Department of Health General Practitioner, Runcorn November 2011 What are the Commissioning
Commissioning for Better Outcomes in COPD Dr Matt Kearney Primary Care & Public Health Advisor Respiratory Programme, Department of Health General Practitioner, Runcorn November 2011 What are the Commissioning
The importance of follow-up after a cardiac event: CARDIAC REHABILITATION. Dr. Guy Letcher
 The importance of follow-up after a cardiac event: CARDIAC REHABILITATION Dr. Guy Letcher The National Medicare Experience Mortality After Angioplasty 225,915 patients Mortality After Bypass Surgery 357,885
The importance of follow-up after a cardiac event: CARDIAC REHABILITATION Dr. Guy Letcher The National Medicare Experience Mortality After Angioplasty 225,915 patients Mortality After Bypass Surgery 357,885
Performance and Quality Measures 1. NQF Measure Number. Coronary Artery Disease Measure Set
 Unless indicated, the PINNACLE Registry measures are endorsed by the American College of Cardiology Foundation and the American Heart Association and may be used for purposes of health care insurance payer
Unless indicated, the PINNACLE Registry measures are endorsed by the American College of Cardiology Foundation and the American Heart Association and may be used for purposes of health care insurance payer
Primary care. Abstract. Introduction. Tom Marshall, Andrew Rouse
 Resource implications and health benefits of primary prevention strategies for cardiovascular disease in people aged 30 to 74: mathematical modelling study Tom Marshall, Andrew Rouse Abstract Objective
Resource implications and health benefits of primary prevention strategies for cardiovascular disease in people aged 30 to 74: mathematical modelling study Tom Marshall, Andrew Rouse Abstract Objective
Measurement Name Beta-Blocker Therapy Prior Myocardial Infarction (MI)
 Program Metrics The list below includes the metrics that will be calculated by the PINNACLE Registry for the outpatient office setting. These include metrics for Artery, Atrial Fibrillation, Hypertension
Program Metrics The list below includes the metrics that will be calculated by the PINNACLE Registry for the outpatient office setting. These include metrics for Artery, Atrial Fibrillation, Hypertension
Coronary Heart Disease and Stroke, Primary and Secondary Prevention Guidelines (Cholesterol)
 CLINICAL GUIDELINE Coronary Heart Disease and Stroke, Primary and Secondary Prevention Guidelines (Cholesterol) A guideline is intended to assist healthcare professionals in the choice of disease-specific
CLINICAL GUIDELINE Coronary Heart Disease and Stroke, Primary and Secondary Prevention Guidelines (Cholesterol) A guideline is intended to assist healthcare professionals in the choice of disease-specific
PRESENTED BY BECKY BLAAUW OCT 2011
 PRESENTED BY BECKY BLAAUW OCT 2011 Introduction In 1990 top 5 causes of death and disease around the world: Lower Respiratory Tract Infections Diarrhea Conditions arising during pregnancy Major Depression
PRESENTED BY BECKY BLAAUW OCT 2011 Introduction In 1990 top 5 causes of death and disease around the world: Lower Respiratory Tract Infections Diarrhea Conditions arising during pregnancy Major Depression
APPENDIX B: LIST OF THE SELECTED SECONDARY STUDIES
 APPENDIX B: LIST OF THE SELECTED SECONDARY STUDIES Main systematic reviews secondary studies on the general effectiveness of statins in secondary cardiovascular prevention (search date: 2003-2006) NICE.
APPENDIX B: LIST OF THE SELECTED SECONDARY STUDIES Main systematic reviews secondary studies on the general effectiveness of statins in secondary cardiovascular prevention (search date: 2003-2006) NICE.
I t is established that regular light to moderate drinking is
 32 CARDIOVASCULAR MEDICINE Taking up regular drinking in middle age: effect on major coronary heart disease events and mortality S G Wannamethee, A G Shaper... See end of article for authors affiliations...
32 CARDIOVASCULAR MEDICINE Taking up regular drinking in middle age: effect on major coronary heart disease events and mortality S G Wannamethee, A G Shaper... See end of article for authors affiliations...
Proof of Concept: NHS Wales Atlas of Variation for Cardiovascular Disease. Produced on behalf of NHS Wales and Welsh Government
 Proof of Concept: NHS Wales Atlas of Variation for Cardiovascular Disease Produced on behalf of NHS Wales and Welsh Government April 2018 Table of Contents Introduction... 3 Variation in health services...
Proof of Concept: NHS Wales Atlas of Variation for Cardiovascular Disease Produced on behalf of NHS Wales and Welsh Government April 2018 Table of Contents Introduction... 3 Variation in health services...
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE. Proposed Health Technology Appraisal
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Proposed Health Technology Appraisal Vorapaxar for the secondary prevention of atherothrombotic events after myocardial infarction Draft scope (pre-referral)
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Proposed Health Technology Appraisal Vorapaxar for the secondary prevention of atherothrombotic events after myocardial infarction Draft scope (pre-referral)
Article by Anette Marina Rodrigues Nursing, Texila American University, India Abstract
 Perception of Patients about Cardiovascular Disease (CVD) and Effect of Communication by Physician and the Assisting Registered Nurse to Enhance Assessment of Risk and Bridge a Gap of Accurate Perception
Perception of Patients about Cardiovascular Disease (CVD) and Effect of Communication by Physician and the Assisting Registered Nurse to Enhance Assessment of Risk and Bridge a Gap of Accurate Perception
EUROACTION A model for secondary and primary preventive care to achieve 25 by 25
 EUROACTION A model for secondary and primary preventive care to achieve 25 by 25 Professor David A Wood Garfield Weston Professor of Cardiovascular Medicine International Centre for Circulatory Health
EUROACTION A model for secondary and primary preventive care to achieve 25 by 25 Professor David A Wood Garfield Weston Professor of Cardiovascular Medicine International Centre for Circulatory Health
2. Quality and Outcomes Framework: new NICE recommendations
 Proposed Changes to the GMS Contract 2013/14 1. GP pay and expenses uplift It is proposed GP pay and expenses is uplifted by 1.5%. This increased investment will allow for an average pay increase of up
Proposed Changes to the GMS Contract 2013/14 1. GP pay and expenses uplift It is proposed GP pay and expenses is uplifted by 1.5%. This increased investment will allow for an average pay increase of up
Stroke secondary prevention. Gill Cluckie Stroke Nurse Consultant St. George s Hospital
 Stroke secondary prevention Gill Cluckie Stroke Nurse Consultant St. George s Hospital Stroke recurrence The risk of recurrent stroke is greatest after first stroke 2 3% of survivors of a first stroke
Stroke secondary prevention Gill Cluckie Stroke Nurse Consultant St. George s Hospital Stroke recurrence The risk of recurrent stroke is greatest after first stroke 2 3% of survivors of a first stroke
Survivorship Guidelines. September 2013 (updated August 2015)
 Survivorship Guidelines September 2013 (updated August 2015) CONTENTS Contents 1 Introduction... 3 2 Background... 3 3 Recommendations and Rationale... 4 Appendix 1: Holistic Needs Assessment... 9 Appendix
Survivorship Guidelines September 2013 (updated August 2015) CONTENTS Contents 1 Introduction... 3 2 Background... 3 3 Recommendations and Rationale... 4 Appendix 1: Holistic Needs Assessment... 9 Appendix
PRESCRIBING SUPPORT TEAM AUDIT: ACE Inhibitors in the treatment of stable angina (October 2007) PRESCRIBING SUPPORT TECHNICIAN:
 PRESCRIBING SUPPORT TEAM AUDIT: ACE Inhibitors in the treatment of stable angina (October 2007) DATE OF AUTHORISATION: AUTHORISING GP: PRESCRIBING SUPPORT TECHNICIAN: SUMMARY SIGN Guideline No. 96 Management
PRESCRIBING SUPPORT TEAM AUDIT: ACE Inhibitors in the treatment of stable angina (October 2007) DATE OF AUTHORISATION: AUTHORISING GP: PRESCRIBING SUPPORT TECHNICIAN: SUMMARY SIGN Guideline No. 96 Management
Country report Serbia April 2017
 Country report Serbia April 2017 Report by Vojislav Giga, MD, PhD, Cardiologist et al. National CVD Prevention Coordinator for Serbia Cardiology Clinic, Clinical Center of Serbia, Belgrade, Serbia Prepared
Country report Serbia April 2017 Report by Vojislav Giga, MD, PhD, Cardiologist et al. National CVD Prevention Coordinator for Serbia Cardiology Clinic, Clinical Center of Serbia, Belgrade, Serbia Prepared
2010 National Audit of Dementia (Care in General Hospitals)
 Royal College of Psychiatrists 2010 National Audit of Dementia (Care in General Hospitals) Organisational checklist results and commentary for: Barking, Havering and Redbridge Hospitals NHS Trust The 2010
Royal College of Psychiatrists 2010 National Audit of Dementia (Care in General Hospitals) Organisational checklist results and commentary for: Barking, Havering and Redbridge Hospitals NHS Trust The 2010
NRT Voucher redemption scheme service specification
 NRT Voucher redemption scheme service specification Updated March 2016 Review date March 2018 Page 1 of 7 1. Introduction The NRT voucher scheme is for NHS Fife stop smoking advisors who have been deemed
NRT Voucher redemption scheme service specification Updated March 2016 Review date March 2018 Page 1 of 7 1. Introduction The NRT voucher scheme is for NHS Fife stop smoking advisors who have been deemed
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE General practice Indicators for the NICE menu
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE General practice Indicators for the NICE menu Indicator area: Pulse rhythm assessment for AF Indicator: NM146 Date: June 2017 Introduction There is evidence
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE General practice Indicators for the NICE menu Indicator area: Pulse rhythm assessment for AF Indicator: NM146 Date: June 2017 Introduction There is evidence
Reliability of the incremental shuttle walk test and the Chester step test in cardiac rehabilitation
 Reliability of the incremental shuttle walk test and the Chester step test in cardiac rehabilitation Item Type Thesis or dissertation Authors Reardon, Melanie Publisher University of Chester Download date
Reliability of the incremental shuttle walk test and the Chester step test in cardiac rehabilitation Item Type Thesis or dissertation Authors Reardon, Melanie Publisher University of Chester Download date
SCHEDULE 2 THE SERVICES
 1 SCHEDULE 2 THE SERVICES A. Service Specifications Mandatory headings 1 4: mandatory but detail for local determination and agreement Optional headings 5-7: optional to use, detail for local determination
1 SCHEDULE 2 THE SERVICES A. Service Specifications Mandatory headings 1 4: mandatory but detail for local determination and agreement Optional headings 5-7: optional to use, detail for local determination
ST-elevation myocardial infarctions (STEMIs)
 Guidelines for Treating STEMI: Case-Based Questions As many as 25% of eligible patients presenting with STEMI do not receive any form of reperfusion therapy. The ACC/AHA guidelines highlight steps to improve
Guidelines for Treating STEMI: Case-Based Questions As many as 25% of eligible patients presenting with STEMI do not receive any form of reperfusion therapy. The ACC/AHA guidelines highlight steps to improve
C-Reactive Protein and Your Heart
 C-Reactive Protein and Your Heart By: James L. Holly, MD Inflammation is the process by which the body responds to injury. Laboratory evidence and findings at autopsy studies suggest that the inflammatory
C-Reactive Protein and Your Heart By: James L. Holly, MD Inflammation is the process by which the body responds to injury. Laboratory evidence and findings at autopsy studies suggest that the inflammatory
2010 National Audit of Dementia (Care in General Hospitals) North West London Hospitals NHS Trust
 Royal College of Psychiatrists 2010 National Audit of Dementia (Care in General Hospitals) Organisational checklist results and commentary for: rth West London Hospitals NHS Trust The 2010 national audit
Royal College of Psychiatrists 2010 National Audit of Dementia (Care in General Hospitals) Organisational checklist results and commentary for: rth West London Hospitals NHS Trust The 2010 national audit
D epression occurs concurrently with
 RESEARCH Depression after cardiac hospitalisation The Identifying Depression as a Comorbid Condition (IDACC) study Victoria Wade, FRACGP, MPsych, is former Director, Primary Mental Health Care Australian
RESEARCH Depression after cardiac hospitalisation The Identifying Depression as a Comorbid Condition (IDACC) study Victoria Wade, FRACGP, MPsych, is former Director, Primary Mental Health Care Australian
Randomized comparison of single versus double mammary coronary artery bypass grafting: 5 year outcomes of the Arterial Revascularization Trial
 Randomized comparison of single versus double mammary coronary artery bypass grafting: 5 year outcomes of the Arterial Revascularization Trial Embargoed until 10:45 a.m. CT, Monday, Nov. 14, 2016 David
Randomized comparison of single versus double mammary coronary artery bypass grafting: 5 year outcomes of the Arterial Revascularization Trial Embargoed until 10:45 a.m. CT, Monday, Nov. 14, 2016 David
Clinical Practice Guideline
 Clinical Practice Guideline Secondary Prevention for Patients with Coronary and Other Vascular Disease Since the 2001 update of the American Heart Association (AHA)/American College of Cardiology (ACC)
Clinical Practice Guideline Secondary Prevention for Patients with Coronary and Other Vascular Disease Since the 2001 update of the American Heart Association (AHA)/American College of Cardiology (ACC)
Role of Clopidogrel in Acute Coronary Syndromes. Hossam Kandil,, MD. Professor of Cardiology Cairo University
 Role of Clopidogrel in Acute Coronary Syndromes Hossam Kandil,, MD Professor of Cardiology Cairo University ACS Treatment Strategies Reperfusion/Revascularization Therapy Thrombolysis PCI (with/ without
Role of Clopidogrel in Acute Coronary Syndromes Hossam Kandil,, MD Professor of Cardiology Cairo University ACS Treatment Strategies Reperfusion/Revascularization Therapy Thrombolysis PCI (with/ without
HEALTH TARGETS IN PRIMARY CARE
 HEALTH TARGETS IN PRIMARY CARE MORE HEART AND DIABETES CHECKS BETTER HELP FOR SMOKERS TO QUIT Better Help for Smokers to Quit 90% of enrolled patients who smoke and are seen by General Practice, will be
HEALTH TARGETS IN PRIMARY CARE MORE HEART AND DIABETES CHECKS BETTER HELP FOR SMOKERS TO QUIT Better Help for Smokers to Quit 90% of enrolled patients who smoke and are seen by General Practice, will be
Myocardial Ischaemia National Audit Project (MINAP): Improving data capture and use across South Wales
 Myocardial Ischaemia National Audit Project (MINAP): Improving data capture and use across South Wales Author Owner Document Reference Alison Turner Cardiovascular Audit and Primary Care Nurse South Wales
Myocardial Ischaemia National Audit Project (MINAP): Improving data capture and use across South Wales Author Owner Document Reference Alison Turner Cardiovascular Audit and Primary Care Nurse South Wales
Prescribing for substance misuse: alcohol detoxification. Clinical background
 Prescribing for substance misuse: alcohol detoxification POMH-UK Quality Improvement Programme. Topic 14a: baseline Clinical background 1 2014 The Royal College of Psychiatrists. For further information
Prescribing for substance misuse: alcohol detoxification POMH-UK Quality Improvement Programme. Topic 14a: baseline Clinical background 1 2014 The Royal College of Psychiatrists. For further information
NHS QIS National Measurement of Audit Acute Coronary Syndrome
 NHS QIS National Measurement of Audit Acute Coronary Syndrome Things have changed based on the experience and feedback from the first cycle of measurement and, for the better we think! The Acute Coronary
NHS QIS National Measurement of Audit Acute Coronary Syndrome Things have changed based on the experience and feedback from the first cycle of measurement and, for the better we think! The Acute Coronary
2017 MSSP Clinical Quality Measures
 *The information contained in this document relies heavily on information supplied by CMS. GPRO CARE-1 (NQF 0097): Medication Reconciliation Post-Discharge DESCRIPTION: Percentage of discharges from any
*The information contained in this document relies heavily on information supplied by CMS. GPRO CARE-1 (NQF 0097): Medication Reconciliation Post-Discharge DESCRIPTION: Percentage of discharges from any
HA Corporate Scholarship Program:
 HA Corporate Scholarship Program: Substance Abuse Service in Psychiatry Ronnie Pao 02-10-10 The Maudsley Hospital Marina House Community Drug & Alcohol Team London Borough of Southwark Provides a Tier
HA Corporate Scholarship Program: Substance Abuse Service in Psychiatry Ronnie Pao 02-10-10 The Maudsley Hospital Marina House Community Drug & Alcohol Team London Borough of Southwark Provides a Tier
Guidelines for Integrated Management of. Cardiovascular Diseases and Diabetes. in Clinics and Ri-hospitals
 Guidelines for Integrated Management of Cardiovascular Diseases and Diabetes in Clinics and Ri-hospitals Ministry of Public Health DPR Korea January 2013 Rationale ncommunicable diseases such as cardiovascular
Guidelines for Integrated Management of Cardiovascular Diseases and Diabetes in Clinics and Ri-hospitals Ministry of Public Health DPR Korea January 2013 Rationale ncommunicable diseases such as cardiovascular
Service organisation for the secondary prevention of ischaemic heart disease in primary care.
 Royal College of Surgeons in Ireland e-publications@rcsi General Practice Articles Department of General Practice 1-1-2010 Service organisation for the secondary prevention of ischaemic heart disease in
Royal College of Surgeons in Ireland e-publications@rcsi General Practice Articles Department of General Practice 1-1-2010 Service organisation for the secondary prevention of ischaemic heart disease in
2016 Physician Quality Reporting System Data Collection Form: Coronary Artery Disease (CAD) (for patients aged 18 and older)
 2016 Physician Quality Reporting System Data Collection Form: Coronary Artery Disease (CAD) (for patients aged 18 and older) IMPORTANT: Any measure with a 0% performance rate (100% for inverse measures)
2016 Physician Quality Reporting System Data Collection Form: Coronary Artery Disease (CAD) (for patients aged 18 and older) IMPORTANT: Any measure with a 0% performance rate (100% for inverse measures)
Heart Failure (HF) - Primary Care Flow Charts. Pre diagnosis Symptoms or signs suggestive of HF
 Heart Failure (HF) - Primary Care Flow Charts Pre diagnosis Symptoms or signs suggestive of HF 12 lead ECG Normal examination and 12 lead ECG HF highly unlikely Abnormal 12 lead ECG HF Possible Arrange
Heart Failure (HF) - Primary Care Flow Charts Pre diagnosis Symptoms or signs suggestive of HF 12 lead ECG Normal examination and 12 lead ECG HF highly unlikely Abnormal 12 lead ECG HF Possible Arrange
Heart Failure (HF) - Primary Care Flow Charts. Symptoms or signs suggestive of HF. Pre diagnosis. Refer to the Heart Failure Clinic at VHK for
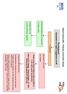 Heart Failure (HF) - Primary Care Flow Charts Pre diagnosis Symptoms or signs suggestive of HF 12 lead ECG Normal examination and 12 lead ECG HF highly unlikely Abnormal 12 lead ECG HF Possible Arrange
Heart Failure (HF) - Primary Care Flow Charts Pre diagnosis Symptoms or signs suggestive of HF 12 lead ECG Normal examination and 12 lead ECG HF highly unlikely Abnormal 12 lead ECG HF Possible Arrange
BEST PRACTICE FRAMEWORK QUESTIONNAIRE
 CAPTURE the FRACTURE BEST PRACTICE FRAMEWORK QUESTIONNAIRE INTRODUCTION Capture the Fracture invites Fracture Liaison Services (FLS) to apply for Capture the Fracture Best Practice Recognition programme.
CAPTURE the FRACTURE BEST PRACTICE FRAMEWORK QUESTIONNAIRE INTRODUCTION Capture the Fracture invites Fracture Liaison Services (FLS) to apply for Capture the Fracture Best Practice Recognition programme.
SIGN 149 Risk estimation and the prevention of cardiovascular disease. Quick Reference Guide July Evidence
 SIGN 149 Risk estimation and the prevention of cardiovascular disease Quick Reference Guide July 2017 Evidence ESTIMATING CARDIOVASCULAR RISK R Individuals with the following risk factors should be considered
SIGN 149 Risk estimation and the prevention of cardiovascular disease Quick Reference Guide July 2017 Evidence ESTIMATING CARDIOVASCULAR RISK R Individuals with the following risk factors should be considered
2010 National Audit of Dementia (Care in General Hospitals) Chelsea and Westminster Hospital NHS Foundation Trust
 Royal College of Psychiatrists 2010 National Audit of Dementia (Care in General Hospitals) Organisational checklist results and commentary for: NHS Foundation Trust The 2010 national audit of dementia
Royal College of Psychiatrists 2010 National Audit of Dementia (Care in General Hospitals) Organisational checklist results and commentary for: NHS Foundation Trust The 2010 national audit of dementia
Cardiovascular Risk Assessment and Management Making a Difference
 Cardiovascular Risk Assessment and Management Making a Difference Norman Sharpe March 2014 Numbers and age-standardised mortality rates from all causes, by sex, 1950 2010 Death rates halved Life expectancy
Cardiovascular Risk Assessment and Management Making a Difference Norman Sharpe March 2014 Numbers and age-standardised mortality rates from all causes, by sex, 1950 2010 Death rates halved Life expectancy
Date of Meeting: Ratified Date: 03/06/2009
 Document Type: PROTOCOL Title: Management And Transfer Of Patients With Acute Scope: Cardiac Network-wide Author/Originator and Title: Dr Ranjit More & members of the Cardiac Network Clinical Advisory
Document Type: PROTOCOL Title: Management And Transfer Of Patients With Acute Scope: Cardiac Network-wide Author/Originator and Title: Dr Ranjit More & members of the Cardiac Network Clinical Advisory
 Five chapters 1. What is CVD prevention 2. Why is CVD prevention needed 3. Who needs CVD prevention 4. How is CVD prevention applied 5. Where should CVD prevention be offered Shorter, more adapted to clinical
Five chapters 1. What is CVD prevention 2. Why is CVD prevention needed 3. Who needs CVD prevention 4. How is CVD prevention applied 5. Where should CVD prevention be offered Shorter, more adapted to clinical
Smoking and CVD. .what role for the Cardiologist? Dr Sandeep Gupta, MD, FRCP
 Smoking and CVD.what role for the Cardiologist? Dr Sandeep Gupta, MD, FRCP Consultant Cardiologist Whipps Cross/BartsHealth NHS Trusts Hospitals, London, UK Therapeutic Advances in the Treatment of Cardiovascular
Smoking and CVD.what role for the Cardiologist? Dr Sandeep Gupta, MD, FRCP Consultant Cardiologist Whipps Cross/BartsHealth NHS Trusts Hospitals, London, UK Therapeutic Advances in the Treatment of Cardiovascular
Update on Lipid Management in Cardiovascular Disease: How to Understand and Implement the New ACC/AHA Guidelines
 Update on Lipid Management in Cardiovascular Disease: How to Understand and Implement the New ACC/AHA Guidelines Paul Mahoney, MD Sentara Cardiology Specialists Lipid Management in Cardiovascular Disease
Update on Lipid Management in Cardiovascular Disease: How to Understand and Implement the New ACC/AHA Guidelines Paul Mahoney, MD Sentara Cardiology Specialists Lipid Management in Cardiovascular Disease
The CARI Guidelines Caring for Australians with Renal Impairment. Cardiovascular Risk Factors
 Cardiovascular Risk Factors ROB WALKER (Dunedin, New Zealand) Lipid-lowering therapy in patients with chronic kidney disease Date written: January 2005 Final submission: August 2005 Author: Rob Walker
Cardiovascular Risk Factors ROB WALKER (Dunedin, New Zealand) Lipid-lowering therapy in patients with chronic kidney disease Date written: January 2005 Final submission: August 2005 Author: Rob Walker
Cardiac Rehabilitation Should be Paid in Korea?
 Cardiac Rehabilitation Should be Paid in Korea? Cardiac prevention & Rehabilitation Center, Heart Institute, Asan Medical Center, Seoul, Korea Jong-Young Lee, MD. NO CONFLICT OF INTEREST TO DECLARE Before
Cardiac Rehabilitation Should be Paid in Korea? Cardiac prevention & Rehabilitation Center, Heart Institute, Asan Medical Center, Seoul, Korea Jong-Young Lee, MD. NO CONFLICT OF INTEREST TO DECLARE Before
Professor Norman Sharpe. Heart Foundation West Coast
 Professor Norman Sharpe Heart Foundation West Coast Primary Care the Keystone to Heart Health Improvement Norman Sharpe June 2013 The heart health continuum and the keystone position The culprit disease
Professor Norman Sharpe Heart Foundation West Coast Primary Care the Keystone to Heart Health Improvement Norman Sharpe June 2013 The heart health continuum and the keystone position The culprit disease
