Guidelines for Recognition of Private Hospital-Based Rehabilitation Services March 2016
|
|
|
- Emmeline Barker
- 5 years ago
- Views:
Transcription
1 Guidelines for Recognition of Private Hospital-Based Rehabilitation Services March 2016 Developed by the Consultative Committee on Private Rehabilitation
2 Guidelines for Recognition of Private Hospital-Based Rehabilitation Services (The Guidelines) Contents Page Introduction 1 Guidelines Criterion 1 Rehabilitation care provided by a specialist rehabilitation team on an admitted or non-admitted basis in a specialist rehabilitation unit (a separate physical space). and Criterion 2 Rehabilitation care provided by a multidisciplinary team which is under the clinical management of a Consultant Physician in Rehabilitation medicine or equivalent. The service is multidisciplinary and will ensure specialist rehabilitation is available 7 days per week. and Criterion 3 Rehabilitation care provided for a person with impairment or disability and for whom there is reasonable expectation of functional gain. and Criterion 4 Rehabilitation care for which the primary treatment goal is improvement in functional status. and Criterion 5 Rehabilitation care which is evidenced in the medical record by: an individualized and documented initial and discharge assessment of functional ability by use of a recognised functional assessment measure; an individualized multidisciplinary rehabilitation plan which includes negotiated rehabilitation goals and indicative time frames; and hospital-specific documented programmes or treatment plan Appendix 1 Standardised Nomenclature and Admission Guidelines 11 Guidelines for Recognition of Private Hospital based Rehabilitation Services November 2015
3 Introduction The purpose of specialist rehabilitation units in the private sector is to treat patients requiring specialist rehabilitation. This particular group of patients, as defined in these Guidelines, requires multidisciplinary rehabilitation treatment in a specialist rehabilitation unit for the clinical intent or treatment goal of improving the functional status of a patient with an impairment, disability or handicap within a clinically appropriate timeframe. There may be multiple entry paths (e.g. from place of residence, another hospital or hospital ward) to a specialist multidisciplinary rehabilitation service. Referral source is not an indicator of appropriateness for admission to a specialist rehabilitation service, but patients must be admitted to the services under the direction of a Consultant Physician in Rehabilitation Medicine or equivalent and be assessed as appropriate in accordance with the admission criteria in these Guidelines. Private facilities providing multidisciplinary rehabilitation care which meet all the criteria in these Guidelines may be eligible for private health insurance payments. The Guidelines have been developed in consultation with the Australasian Faculty of Rehabilitation Medicine (AFRM) a Faculty of the Royal Australasian College of Physicians. They have also been endorsed by the Consultative Committee on Private Rehabilitation (CCPR), which has independent industry Representation 1. The industry recognizes the Functional Independence Measure (FIM) as the functional measure of choice for inpatient rehabilitation, thus ensuring industry data requirements are met as defined by the Australasian Rehabilitation Outcomes Centre (AROC). It is intended that the Guidelines will guide hospitals and health insurers in their contract negotiations. The definition of a rehabilitation patient is also relevant and can be found in Schedule 1, Part 2, 8 of the Private Health Insurance (Benefit Requirements) Rules made under the Private Health Insurance Act In addition, these Guidelines are a component of the quality criteria for private hospital and day hospital facilities with rehabilitation services seeking eligibility for Second Tier default benefits. These Guidelines have been developed for the delivery of private rehabilitation services. They may also be of assistance to State and Territory health authorities in the treatment of private and public patients in public hospitals. It is anticipated that the elements in these requirements will be reviewed biennially by the CCPR. 1 The Consultative Committee on Private Rehabilitation is a national industry committee comprising representatives of the Australasian Faculty of Rehabilitation Medicine, Private Healthcare Australia, the Australian Private Hospitals Association, the Department of Veterans Affairs and the Private Health Insurance Ombudsman. Guidelines for Recognition of Private Hospital based Rehabilitation Services March 2016 Page 3
4 Criterion 1 Rehabilitation care provided by a specialist rehabilitation team on an admitted or nonadmitted patient basis in a specialist rehabilitation unit (a separate physical space) Specialist Rehabilitation Team Rehabilitation care must be provided by a multidisciplinary team which is defined as: - a medical practitioner who is a Consultant Physician in Rehabilitation Medicine and who is a Fellow of the Australasian Faculty of Rehabilitation Medicine (Royal Australasian College of Physicians) or equivalent 2 ; - nursing staff skilled and experienced in rehabilitation nursing, appropriate to the rehabilitation casemix of the hospital; - allied health professionals with relevant experience, including FIM credentialing and registered or recognised by the appropriate professional bodies, appropriate to the rehabilitation casemix of the hospital; and - delivery of defined and documented rehabilitation programmes, reviewed as appropriate. The Consultant Physician in Rehabilitation Medicine is responsible for the co-ordination of treatment for each patient Specialist Multidisciplinary Rehabilitation Service Rehabilitation care should be provided in a dedicated facility/unit/ward. It is generally not recommended that overnight inpatient rehabilitation patients will be accommodated outside the dedicated rehabilitation unit/ward other than in situations of short term unavoidable operational requirements. The design of the facility/unit will be dependent on the casemix of the facility/unit. However, the following features will be included: - disability access to all areas including bed units, wards, dedicated rooms for individual therapy, dining rooms, toilets and accessible outside areas; - a physiotherapy area with appropriate equipment and which has dedicated rooms for individual therapy and assessment as well as large open space for gait training and general exercise; - an occupational therapy area that has space for group activities, rooms for individual therapy and assessment, a therapy workshop and dedicated areas for community assessment of Activities of Daily Living (ADL); 2 There may be circumstances in which an alternative qualification to AFRM or equivalent is appropriate, such as where: - patients are receiving sub-specialty rehabilitation and the qualifications and experience of the medical specialist are applicable to the casemix of the programme; or patients are receiving sub specialty specialty rehabilitation and the qualifications and experience of the medical specialist are applicable to the casemix of the programme; or - the specialist has extensive experience in rehabilitation.is an experienced physician or surgeon experienced in multidisciplinary rehabilitation medicine. Guidelines for Recognition of Private Hospital based Rehabilitation Services March 2016 Page 4
5 - individual therapy or consultation areas suitable for quiet clinical consultation or mental state examination or speech therapy, assessment and treatment or psychological assessment, counselling and treatment where appropriate; - a meeting room suitable for case conferences and family meetings; - hydrotherapy pool conforming to the relevant Australian Design Standards (if hydrotherapy is appropriate for casemix). In circumstances where hydrotherapy is recommended for individual patients as per their treatment plans and the hospital does not have hydrotherapy pool on site, it must be able to demonstrate that safe and appropriate access to a hydrotherapy pool is available Equipment The facility/unit s equipment will be dependent on the casemix of the facility/unit: - parallel bars; - ergometer, and treadmill calibrated to measure distance/units; - gym equipment, including weights, pressures and pulleys, suitable for muscle strengthening; - an area and equipment for provision of personal and domestic ADL training; - range of wheelchairs and mobility aids; - appropriate mental state and cognitive screening and assessment tools; - appropriate speech and language assessment and treating tools; - appropriate tools for patient and family education; and - stairs with handrails and turning area at top of stairs. 1.4 Rehabilitation Settings Rehabilitation services may be provided on an admitted or non-admitted basis including the continuum of services between inpatient and ambulatory settings according to the medical and functional requirements of the patient. This ensures the efficient running of the service and assists with early discharge home whilst maximising functional outcomes. Where overnight inpatient multidisciplinary rehabilitation is not clinically indicated, multidisciplinary rehabilitation may be offered through a full Day Rehabilitation Programme, a Half-Day Rehabilitation Programme or a Sessional Therapy Programme. It should be noted that, within an episode of care, a patient s rehabilitation needs may vary, and that, for example, patients who are receiving a day programme may move progressively between full-day, half-day and sessional programmes. Clinical assessment will direct the appropriate selection of programmes for a patient. For the purposes of these Guidelines, a session is defined as functional task management by an appropriately qualified health professional over a period which approximates 30 minutes. Guidelines for Recognition of Private Hospital based Rehabilitation Services March 2016 Page 5
6 1.4.1 Full-Day Rehabilitation Programme Day Rehabilitation Programmes 3 are suitable for those patients who have established rehabilitation needs, do not require overnight inpatient care, and whose rehabilitation programmes and goals require the involvement of a multidisciplinary team, under the direction of a Consultant Physician in Rehabilitation Medicine or equivalent. Day Rehabilitation Programmes provide a coordinated programme of care on an admitted same day basis which is documented in an individualised multidisciplinary rehabilitation plan which includes negotiated rehabilitation goals and indicative time frames. The number of sessions associated with a full-day rehabilitation programme will be more than 5 sessions Half-Day Rehabilitation Programme Half-day Rehabilitation Programmes are suitable for those patients who have established rehabilitation needs, do not require overnight inpatient care, and whose rehabilitation programmes and goals require the involvement of a multidisciplinary team, under the direction of a Consultant Physician in Rehabilitation Medicine or equivalent. Half-Day Rehabilitation Programmes provide a coordinated programme of care on a an admitted same day basis which is documented in an individualised multidisciplinary rehabilitation plan which includes negotiated rehabilitation goals and indicative time frames. The number of sessions associated with a half-day rehabilitation programme will be 3 to 5 sessions Sessional Therapy Programme When a patient has established rehabilitation needs and goals as determined by a Consultant in Rehabilitation Medicine or equivalent, does not require overnight inpatient care and requires a single mode of therapy not involving the coordination of multidisciplinary care, such needs may be met through a Sessional Therapy Programme. A Sessional Therapy Programme provides a single modality of therapy of up to 2 sessions in a given day which is documented in an individualised rehabilitation plan which includes negotiated rehabilitation goals and indicative time frames Inpatient Rehabilitation Programme Inpatient Rehabilitation Programmes are suitable for those patients who have established rehabilitation needs, but who are also assessed as requiring 24 hour nursing care. Their rehabilitation programs and goals require the involvement of a multidisciplinary team, under the direction of a Consultant in Rehabilitation Medicine or equivalent and should be confirmed with the patient on admission. The multi-disciplinary service will be available 7 days per week ensuring specialist rehabilitation care is available regardless of day of admission. Inpatient Rehabilitation Programmes provide a daily coordinated programme of care that is documented in an individualised multidisciplinary rehabilitation plan and which includes negotiated rehabilitation goals and indicative time frames. 3 Due to differing definitions of admitted and non-admitted care in different states of Australia for their respective data collections, Day Rehabilitation Programmes may be named variously as same day day only half day or non-admitted episodes of care according to the location of the facility. Guidelines for Recognition of Private Hospital based Rehabilitation Services March 2016 Page 6
7 Criterion 2 Rehabilitation care provided by a multidisciplinary team which is under the clinical management of a Consultant Physician in Rehabilitation Medicine or equivalent Clinical Staffing Rehabilitation care must be provided by a multidisciplinary team The multidisciplinary rehabilitation team will be under the clinical direction of a Consultant Physician in Rehabilitation Medicine or equivalent 4. Each programme shall be supervised by a Consultant Physician in Rehabilitation Medicine or equivalent and staffed by an appropriately qualified multidisciplinary team relevant to the therapeutic needs of the patients being treated and have access to consultative services which are appropriate to the programmes offered Other clinical staff, both professional and support staff, will be appropriately skilled, experienced and provided in sufficient numbers to provide individual and group therapy programmes for the casemix of patients being serviced Policy and Programme Review A facility/unit must have: - a comprehensive manual of policy and procedures applying to and within the facility, and there should be evidence that this is reviewed on an annual basis and updated as per accreditation requirements or legislative changes; - a demonstrated process for reviewing programmes and patient outcomes. 4 There may be circumstances in which an alternative qualification to AFRM or equivalent is appropriate, such as where: - patients are receiving sub-specialty rehabilitation and the qualifications and experience of the medical specialist are applicable to the casemix of the programme, or - the specialist is an experienced physician or surgeon experienced in multidisciplinary rehabilitation. Guidelines for Recognition of Private Hospital based Rehabilitation Services March 2016 Page 7
8 2.3. Data Collection and Outcome Measures A facility/unit must: - submit rehabilitation data in AN-SNAP3 5 format (or update versions) to the Australasian Rehabilitation Outcomes Centre (AROC) targeting 100% of all inpatient rehabilitation episodes for assessment and national benchmarking; - ensure all rehabilitation episodes will be scored for Functional Independence Measure (FIM) by a FIM-credentialed staff member. 5 Australian National Sub-Acute and Non-Acute Patient classification system. Guidelines for Recognition of Private Hospital based Rehabilitation Services March 2016 Page 8
9 Criterion 3 Rehabilitation care provided for a person with impairment or disability and for whom there is reasonable expectation of functional gain Impairment Codes Each patient is assigned an impairment code using the current version of the AROC Impairment Coding Guidelines. These guidelines were originally based on the UDSmr Guidelines. The 2013 AROC Guidelines is available on line: Classifications include: - stroke - brain dysfunction - neurological conditions - spinal cord dysfunction - amputation of limb - arthritis - chronic pain - orthopaedic disorders - cardiac - pulmonary disorders - burns - congenital deformities - major multiple trauma - developmental disabilities - reconditioning/restorative - other disabling impairments The episode should be classified according to the primary clinical reason for the current episode of rehabilitation care. The AROC impairment code identifies the major focus of rehabilitation and the primary subject of the rehabilitation plan. Guidelines for Recognition of Private Hospital based Rehabilitation Services March 2016 Page 9
10 Criterion 4 Rehabilitation care for which the primary treatment goal is improvement in functional status Assessment and Admission Rehabilitation care must be provided for a person who has all of the following: - an impairment with associated functional loss; - a reasonable expectation of functional gain; and - the primary treatment goal is improvement in functional status Acceptable rehabilitation impairments are the current version of the AROC Impairment Codes as described in the AROC Impairment Coding Guidelines w pdf Prior to commencement of the rehabilitation programme, a comprehensive and documented rehabilitation assessment should be undertaken Appropriate outcome measures must be used to document initial assessment of functional ability for all patients The pre-admission assessment should also indicate that the patient has an understanding of and commitment to the rehabilitation process The pre-programme assessment will take into account the most appropriate hospitalbased setting for rehabilitation care Admission Guidelines Programmes offered by private rehabilitation facilities that meet these Guidelines would be expected to include the features described in Appendix 1: Standardised Nomenclature and Admission Guidelines for Rehabilitation Patients in Private Facilities Admissions to a rehabilitation programme should conform to the admission criteria of that programme as set out in Appendix I Guidelines for Recognition of Private Hospital based Rehabilitation Services March 2016 Page 10
11 Criterion 5 Rehabilitation care which is evidenced in the medical record by: an individualised and documented initial and discharge assessment of functional ability by use of a recognised functional assessment measure; an individualised multidisciplinary rehabilitation plan which includes negotiated rehabilitation goals and indicative time frames; and hospital-specific documented programmes or treatment plan 5.1. Assessing Functional Ability Appropriate outcome measures must be used to document admission and discharge assessment of functional ability Utilisation of other standardised outcome instruments dependent on casemix Development and implementation of a Multidisciplinary Rehabilitation Programme for each individual patient A written patient specific rehabilitation plan must be developed by the multidisciplinary team and include: - clearly stated multidisciplinary goals and outcomes of the planned rehabilitation; - predicted period of rehabilitation (length of stay); - functional gain; - discharge destination; - reflect the needs of the patient, family and carers as well as all members of the multidisciplinary team; and - meeting industry-accepted reporting requirements (for example the relevant Clinical Indicators developed by the Australian Council on Healthcare Standards) For patient review and multidisciplinary care conferences: - there must be regular meetings whilst the patient is in a rehabilitation programme; - there must be a documented policy for regular review of patients; - this policy must include regular interdisciplinary case conferences which evaluate and document the progress of the patient against the established plan.in the medical record. The patient, family members and carers should be kept informed and contribute to the decisions of the rehabilitation team Discharge Planning All patients will have a comprehensive documented discharge plan. This discharge plan must Guidelines for Recognition of Private Hospital based Rehabilitation Services March 2016 Page 11
12 be commenced and documented on admission and activated on discharge. The discharge plan will take into account: - the needs of the patient and family; - home assessment where appropriate; - relevant discharge destination end point; - liaison with community services and communication with the referring doctor and Local Medical Officer; and - ongoing treatment requirements and care setting. A copy of the discharge plan will be sent to the patient s General Practitioner and will include details of medications currently prescribed for the patient. Guidelines for Recognition of Private Hospital based Rehabilitation Services March 2016 Page 12
13 Guidelines for Recognition of Private Hospital-Based Rehabilitation Services APPENDIX 1 STARDISED NOMENCLATURE and ADMISSION GUIDELINES for REHABILITATION PATIENTS IN PRIVATE FACILITIES Note: These Guidelines apply to rehabilitation facilities and services that meet the Guidelines for Recognition of Private Hospital-Based Rehabilitation Services March 2016 Guidelines for Recognition of Private Hospital based Rehabilitation Services March 2016 Page 13
14 Orthopaedic Programme Upper Limb Lower Limb Complex Joint Replacement Spinal post surgical 1. UPPER LIMB THOPAEDIC PROGRAMME Clinical Criteria for Admission: 1. Following upper limb orthopaedic procedures, trauma, injuries or fractures which directly result in disability which requires a rehabilitation programme targeted at developing skills in personal activities of daily living. 2. Patient fitted with an upper limb orthosis this may require a short term rehabilitation programme directed at developing skills in personal activities of daily living. 3. The patient has co-morbidities which result in the need for rehabilitation Including, but not limited to: a. Significant balance problems where walking aid is ordinarily held by the affected arm. b. Widespread generalised arthritis. c. Neurological or cognitive dysfunction. 4. Access Indications Because of upper limb orthopaedic procedures there are mobility and balance changes resulting in safety problems which would benefit from multidisciplinary rehabilitation treatment. 5. The presence of post-operative complications which restrict function. 6. The patient is able to actively participate in a rehabilitation programme with or without the aid of a carer. Guidelines for Recognition of Private Hospital based Rehabilitation Services November 2015 Page 14
15 2. LOWER LIMB THOPAEDIC Clinical Criteria for Admission 1. Following lower limb orthopaedic procedures, trauma, injuries or pelvic fractures which result in disability which requires a rehabilitation programme directed at developing skills in personal activities of daily living. 2. Fractures requiring acquisition of specific balance or mobility skills for safety. 3. Bilateral weight bearing limb fractures. 4. Multiple fractures with major trauma. 5. Lower limb fractures with co-morbidities which result in the need for rehabilitation; Including, but not limited to: a. Widespread generalised rheumatoid or osteoarthritis. b. Significant balance problems which includes Parkinson s disease, early Alzheimer s disease and other neurological and cognitive dysfunctions, vestibular problems, previous stroke. c. Factors which effect ability to weight bear with appropriate aid such as other joint, replacements, status of upper limb joints, significant respiratory or cardiac disease. d. Post-operative complications. 6. Access Indications Because of lower limb orthopaedic procedures there are mobility and balance changes resulting in safety problems which would benefit from multidisciplinary rehabilitation. 7. The patient is able to actively participate in a rehabilitation programme with or without the aid of a carer. Guidelines for Recognition of Private Hospital based Rehabilitation Services November 2015 Page 15
16 3. JOINT REPLACEMENT Clinical criteria for Admission: 1. Lower limb joint replacement with or without local complications of the procedure which result in disability which requires a rehabilitation programme directed at developing skills in personal activities of daily living. 2 Lower limb joint replacement with co-morbidities which result in the need for rehabilitation, Including but not limited to: a. Widespread generalised rheumatoid or osteoarthritis. b. Significant balance problems which includes Parkinson s disease, early Alzheimer s disease, vestibular problems, previous stroke. c. Factors which effect ability to weight bear with appropriate aid such as other joint replacements, status of upper limb joints, significant respiratory or cardiac disease. d. Patients that have difficulty in complying with safety instructions to ensure the protection of the new joint. e. Neurological or cognitive dysfunctions. 3 Access indications such that the lower limb joint replacement causes mobility changes which result in balance and safety issues. 4 The patient is able to actively participate in a rehabilitation programme with or without the aid of a carer. Guidelines for Recognition of Private Hospital based Rehabilitation Services November 2015 Page 16
17 4. SPINAL POST SURGICAL Clinical Criteria for Admission 1. Following spinal surgery or spinal intervention such as laminectomy 2. The patient has persisting disability and dependency due to: 2.1 Post-operative complications which restrict function. 2.2 Co-morbidities which result in the need for rehabilitation because of balance and safety issues. 2.3 Impairment in muscle strength, joint instability (e.g. Halo brace), limited and painful range of movement, disturbance of peripheral joint sensation, postural and gait dysfunction A condition which results in disability which requires a rehabilitation programme directed at developing skills in personal activities of daily living. 2.5 Access Indications Because of spinal intervention there are mobility and balance changes resulting in safety problems which would benefit from multidisciplinary rehabilitation. 3 The patient is able to actively participate in a rehabilitation programme with or without the aid of a carer. Guidelines for Recognition of Private Hospital based Rehabilitation Services November 2015 Page 17
18 Neurological Programme Non Stroke e.g.: Parkinson s & Extra Pyramidal Disorders Non Stroke - Peripheral Non Stroke Neurological Traumatic brain Non traumatic brain Stroke 1. NON STROKE PARKINSON S & EXTRA PYRAMIDAL DISDERS Clinical Criteria for Admission Indications are: 1. Recent onset or deterioration in mobility and function requiring medication manipulation as an adjunct to the rehabilitation received. 2. Parkinson s disease / Extra pyramidal disorders with: 2.1 Recurrent falls + sequelae. 2.2 Swallowing disorders with subsequent problems, e.g. Dietary, chest Infection. 2.3 Communication disorder. 4 The patient is able to actively participate in a rehabilitation programme with or without the aid of a carer. Guidelines for Recognition of Private Hospital based Rehabilitation Services November 2015 Page 18
19 2. NON STROKE PERIPHERAL Clinical Criteria for Admission 1. The patient has suffered a recent onset of neurological condition. 2. The patient has suffered deterioration of functional ability in association with an established neurological condition. / Including but not limited to: a. Guillain-Barre Syndrome. b. Other Neuropathies. c. Myopathies. d. Peripheral Nerve injuries. 3. The disability is assessed as being likely to respond to rehabilitation. 4 The patient is able to actively participate in a rehabilitation programme with or without the aid of a carer. Guidelines for Recognition of Private Hospital based Rehabilitation Services November 2015 Page 19
20 3. NON STROKE NEUROLOGICAL Clinical Criteria for Admission 1. The patient has suffered deterioration of functional ability in association with an established neurological condition Including but not limited to: a. Multiple sclerosis. b. Other Multi focal conditions. This would exclude conditions that primarily manifest as dementia e.g. Alzheimer s disease 2. The patient has persisting disability and dependency due to: 2.1. Nerve root damage. / 2.2 Spinal Cord damage including Cauda Equina syndrome involving bladder or bowel. 3. The disability is assessed as being likely to respond to rehabilitation. 4. The patient is able to actively participate in a rehabilitation programme with or without the aid of a carer. Guidelines for Recognition of Private Hospital based Rehabilitation Services November 2015 Page 20
21 4 STROKE Clinical Criteria for Admission: 1. The patient has suffered a recent onset of stroke with functional loss 2. The patient has suffered deterioration of functional ability following a previous stroke. / 3. The disability is assessed as being likely to respond to rehabilitation. 4. The patient is able to actively participate in a rehabilitation programme with or without the aid of a carer. Guidelines for Recognition of Private Hospital based Rehabilitation Services November 2015 Page 21
22 5. TRAUMATIC BRAIN INJURY Clinical Criteria for Admission 1. The patient has suffered a recent traumatic brain injury. / 2. The patient s impairment (cognitive, behavioural and/or communicative impairment) is such that the functional deficit requires specific care which cannot be safely provided at home or in an outpatient setting. / 3. The patient and/or carer requires intensive daily therapy in a multidisciplinary setting. / 4. The disability is assessed as being likely to respond to rehabilitation. 5. The patient is able to actively participate in a rehabilitation programme with or without the aid of a carer. Guidelines for Recognition of Private Hospital based Rehabilitation Services November 2015 Page 22
23 6. NON TRAUMATIC BRAIN INJURY Conditions causing brain injury including but not limited to hypoxia, post-surgical infection, post subarachnoid haemorrhage, and following neurosurgery for brain tumour. Clinical Criteria for Admission 1. The patient has suffered a recent brain injury or brain surgery or emerges from coma or vegetative state. 2. The patient has experienced a recent or progressive deterioration in functional capability following previous non traumatic brain injury. 3. The patient s impairment (cognitive, behavioural and/or communicative impairment) is such that the functional deficit requires specific care which cannot be safely provided at home or in an outpatient setting. / 4. The patient requires intensive daily therapy in a multidisciplinary setting. 5. The disability is assessed as being likely to respond to rehabilitation. 6. The patient is able to actively participate in a rehabilitation programme with or without the aid of a carer. Guidelines for Recognition of Private Hospital based Rehabilitation Services November 2015 Page 23
24 Pain Programme Clinical Criteria for Admission: 1. Diagnosis of chronic/intractable pain condition or patient pain levels and medication use resulting in a deficit in balance, mobility and functioning which requires multidisciplinary intervention. 2. Assessment indicates the patient is in an appropriate psychological state to participate, with potential for positive response to intervention. / 3. Aiming to avoid surgical intervention and minimise/rationalise medication use. / 4. The disability is assessed as being likely to respond to rehabilitation. 5. The patient is able to actively participate in a rehabilitation programme with or without the aid of a carer. Guidelines for Recognition of Private Hospital based Rehabilitation Services November 2015 Page 24
25 Re-conditioning Programme Clinical Criteria for Admission: Where a rehabilitation programme aims to maximise or restore functional independence, exercise tolerance and endurance in a patient who is deconditioned: 1. Following an acute surgical intervention. 2. Following an acute medical condition or exacerbation Including, but not limited to: a. Septicaemia. b. Renal failure. c. Liver failure. d. Cardiac or respiratory illness. 3. Patient is experiencing an acute exacerbation of inflammatory arthritis (e.g. As evidenced by multiple joints, ESR elevation, mobility of upper and lower limbs diminished) with concurrent disability. 4. Following exacerbation of chronic illness. 5. Patient is deconditioned as a result of cancer or following treatment from cancer. 6. The acute episode has resulted in a functional deterioration to a level that the patient requires support and guidance with basic ADL tasks and/or increased inability to transfer and ambulate. 7. The patient s disability is assessed as being likely to respond to multidisciplinary rehabilitation therapy within appropriate time frames and the rehabilitation therapy is not part of respite care. 8. The patient is able to actively participate in a rehabilitation programme with or without the aid of a carer. Guidelines for Recognition of Private Hospital based Rehabilitation Services November 2015 Page 25
26 Amputee Programme Clinical Criteria for Admission: 1. Below Knee Amputation (transtibial), Symes, Through Knee Amputation, Above Knee Amputation (transfemoral), Above Elbow Amputation and Below Elbow Amputation or higher complication. 2. Bilateral amputations. 3. Functional education and training for prosthesis. 4. Any of the above amputation or fracture with other significant co-morbidities, including, but not limited to stroke, rheumatoid arthritis, cardiac diseases. 5. Following amputation: Failed stump healing or wound breakdown. Debilitating amputation-related pain. Contractures restricting mobility. Phantom pain. 6. The patient is able to actively participate in a rehabilitation programme with or without the aid of a carer. Guidelines for Recognition of Private Hospital based Rehabilitation Services November 2015 Page 26
27 Cardiac Programme Clinical Criteria for Admission: Where a rehabilitation programme aims to maximise or restore functional independence, exercise tolerance and endurance: 1. Following a recent cardiac event. 2. The patient is medically stable: Post-operative cases afebrile for 48 hours No arrhythmia changes for 48 hours Wounds are sound Cardiac Failure controlled and stabilised Angina controlled and stabilised / 3. There is associated persisting disability and dependency following the cardiac event e.g.: Recent Stroke, Respiratory Compromise, Significant Comorbidities e.g. Generalised Arthritis, previous Stroke. 4. The Patient s disability is assessed as being likely to respond to multidisciplinary rehabilitation, with rehabilitation goals being identified, within appropriate timeframes. 5. The patient is able to actively participate in a rehabilitation programme with or without the aid of a carer. Guidelines for Recognition of Private Hospital based Rehabilitation Services November 2015 Page 27
AROC Intensity of Therapy Project. AFRM Conference 18 September 2013
 AROC Intensity of Therapy Project AFRM Conference 18 September 2013 What is AROC? AROC began as a joint initiative of the whole Australian rehabilitation sector (providers, payers, regulators and consumers)
AROC Intensity of Therapy Project AFRM Conference 18 September 2013 What is AROC? AROC began as a joint initiative of the whole Australian rehabilitation sector (providers, payers, regulators and consumers)
AROC Outcome Targets Report Inpatient Pathway 3
 AROC Outcome Targets Report Inpatient Pathway 3 Anywhere Hospital January 2013 December 2013 Australasian Faculty of Rehabilitation Medicine AROC impairment specific benchmarking process...3 Introducing
AROC Outcome Targets Report Inpatient Pathway 3 Anywhere Hospital January 2013 December 2013 Australasian Faculty of Rehabilitation Medicine AROC impairment specific benchmarking process...3 Introducing
Subacute inpatient rehabilitation across a range of impairments: intensity of therapy received and outcomes
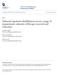 University of Wollongong Research Online Australian Health Services Research Institute Faculty of Business 2013 Subacute inpatient rehabilitation across a range of impairments: intensity of therapy received
University of Wollongong Research Online Australian Health Services Research Institute Faculty of Business 2013 Subacute inpatient rehabilitation across a range of impairments: intensity of therapy received
AROC Reports for Any Health Fund (AHF) January December 2004
 University of Wollongong Research Online Australasian Rehabilitation Outcomes Centre - AROC Centre for Health Service Development - CHSD 2005 AROC Reports for Any Health Fund (AHF) January 2004 - December
University of Wollongong Research Online Australasian Rehabilitation Outcomes Centre - AROC Centre for Health Service Development - CHSD 2005 AROC Reports for Any Health Fund (AHF) January 2004 - December
NATIONAL REHABILITATION HOSPITAL (NRH) THE SPINAL CORD SYSTEM OF CARE (SCSC) PROGRAMME INPATIENT SCOPE OF SERVICE
 NATIONAL REHABILITATION HOSPITAL (NRH) THE SPINAL CORD SYSTEM OF CARE (SCSC) PROGRAMME INPATIENT SCOPE OF SERVICE NATIONAL REHABILITATION HOSPITAL SCOPE OF SERVICE FOR THE SPINAL CORD SYSTEM OF CARE PROGRAMME
NATIONAL REHABILITATION HOSPITAL (NRH) THE SPINAL CORD SYSTEM OF CARE (SCSC) PROGRAMME INPATIENT SCOPE OF SERVICE NATIONAL REHABILITATION HOSPITAL SCOPE OF SERVICE FOR THE SPINAL CORD SYSTEM OF CARE PROGRAMME
19 Date clinically ready for DD/MM/YYYY Record date patient was clinically ready for discharge after delay 2
 Australian Rehabilitation Outcomes Centre (AROC) Amputation Impairment specific adjunct module to the AROC dataset Please use this excel workbook to record additional data on your amputatee patients. Collection
Australian Rehabilitation Outcomes Centre (AROC) Amputation Impairment specific adjunct module to the AROC dataset Please use this excel workbook to record additional data on your amputatee patients. Collection
Frequently Asked Questions: Riverview Rehabilitation Center
 Frequently Asked Questions: Riverview Rehabilitation Center WHAT SERVICES ARE PROVIDED? Riverview Rehabilitation Center provides a comprehensive, interdisciplinary and functionally based treatment program
Frequently Asked Questions: Riverview Rehabilitation Center WHAT SERVICES ARE PROVIDED? Riverview Rehabilitation Center provides a comprehensive, interdisciplinary and functionally based treatment program
Initial analysis of newly added data items. Do they provide insights of value?
 University of Wollongong Research Online Australian Health Services Research Institute Faculty of Business 2013 Initial analysis of newly added data items. Do they provide insights of value? Frances Simmonds
University of Wollongong Research Online Australian Health Services Research Institute Faculty of Business 2013 Initial analysis of newly added data items. Do they provide insights of value? Frances Simmonds
Inpatient Acute Rehabilitation
 Inpatient Acute Rehabilitation A massive stroke. A major illness. A debilitating injury. At first, you can t imagine how life will ever be the same. Affiliated with the renowned Dignity Health Neurological
Inpatient Acute Rehabilitation A massive stroke. A major illness. A debilitating injury. At first, you can t imagine how life will ever be the same. Affiliated with the renowned Dignity Health Neurological
Part B - Health Facility Briefing and Planning. PLANNING Functional Areas Functional Relationships
 650 INDEX SUB-ACUTE CARE UNIT 650.1.00 Description INTRODUCTION Description PLANNING Functional Areas Functional Relationships DESIGN General COMPONENTS OF THE UNIT Introduction s Non- s APPENDICES Schedule
650 INDEX SUB-ACUTE CARE UNIT 650.1.00 Description INTRODUCTION Description PLANNING Functional Areas Functional Relationships DESIGN General COMPONENTS OF THE UNIT Introduction s Non- s APPENDICES Schedule
NATIONAL REHABILITATION HOSPITAL SPINAL CORD SYSTEM OF CARE (SCSC) OUTPATIENT SCOPE OF SERVICE
 NATIONAL REHABILITATION HOSPITAL SPINAL CORD SYSTEM OF CARE (SCSC) OUTPATIENT SCOPE OF SERVICE Introduction: The Spinal Cord System of Care (SCSC) at the National Rehabilitation Hospital (NRH) provides
NATIONAL REHABILITATION HOSPITAL SPINAL CORD SYSTEM OF CARE (SCSC) OUTPATIENT SCOPE OF SERVICE Introduction: The Spinal Cord System of Care (SCSC) at the National Rehabilitation Hospital (NRH) provides
Surgery saved my life. Rehab is restoring my future.
 The Best Way Back Baylor Institute for Rehabilitation offers care for the most challenging and medically complex patients, including those with traumatic brain injury, traumatic spinal cord injury and
The Best Way Back Baylor Institute for Rehabilitation offers care for the most challenging and medically complex patients, including those with traumatic brain injury, traumatic spinal cord injury and
Rehabilitation/Geriatrics ADMISSION CRITERIA. Coordinated Entry System
 Rehabilitation/Geriatrics ADMISSION CRITERIA Coordinated Entry System Table of Contents Rehabilitation and Geriatric Service Sites 3 Overview of Coordinated Entry System...4 Geriatric Rehabilitation Service
Rehabilitation/Geriatrics ADMISSION CRITERIA Coordinated Entry System Table of Contents Rehabilitation and Geriatric Service Sites 3 Overview of Coordinated Entry System...4 Geriatric Rehabilitation Service
POSITION DESCRIPTION Grade 4 Physiotherapist Physiotherapy Department
 POSITION DESCRIPTION Grade 4 Physiotherapist Physiotherapy Department Date revised: June 2015 POSITION: AWARD/AGREEMENT: Grade 4 Physiotherapists Health Professionals (Public Sector Victoria) CLASSIFICATION
POSITION DESCRIPTION Grade 4 Physiotherapist Physiotherapy Department Date revised: June 2015 POSITION: AWARD/AGREEMENT: Grade 4 Physiotherapists Health Professionals (Public Sector Victoria) CLASSIFICATION
restoring hope rebuilding lives
 Spinal Cord Injury Brain Injury Stroke Neurologic Diseases Orthopedic Conditions Amputation Cancer Cardiac Recovery The patient experience: 2015 in review restoring hope rebuilding lives Advancing care
Spinal Cord Injury Brain Injury Stroke Neurologic Diseases Orthopedic Conditions Amputation Cancer Cardiac Recovery The patient experience: 2015 in review restoring hope rebuilding lives Advancing care
2014 Report Card. 62 acute inpatient rehabilitation beds days
 Lovelace Rehabilitation Hospital is dedicated helping each patient overcome the effects of illness and injury through our comprehensive inpatient and outpatient programs. Our highly specialized physicians
Lovelace Rehabilitation Hospital is dedicated helping each patient overcome the effects of illness and injury through our comprehensive inpatient and outpatient programs. Our highly specialized physicians
Diabetes (DIA) Measures Document
 Diabetes (DIA) Measures Document DIA Version: 2.1 - covering patients discharged between 01/07/2016 and present. Programme Lead: Liz Kanwar Clinical Lead: Dr Aftab Ahmad Number of Measures In Clinical
Diabetes (DIA) Measures Document DIA Version: 2.1 - covering patients discharged between 01/07/2016 and present. Programme Lead: Liz Kanwar Clinical Lead: Dr Aftab Ahmad Number of Measures In Clinical
HEAL Protocol for GPs and Practice Nurses
 HEAL Protocol for GPs and Practice Nurses Exercise Pathway Co-ordinator Sport & Active Leisure West Offices Station Rise York YO1 6GA Telephone: 01904 555755 Email: angela.shephard@york.gov.uk 1 P a g
HEAL Protocol for GPs and Practice Nurses Exercise Pathway Co-ordinator Sport & Active Leisure West Offices Station Rise York YO1 6GA Telephone: 01904 555755 Email: angela.shephard@york.gov.uk 1 P a g
Selective Dorsal Rhizotomy (SDR) Scotland Service Pathway
 Selective Dorsal Rhizotomy (SDR) Scotland Service Pathway This pathway should to be read in conjunction with the attached notes. The number in each text box refers to the note that relates to the specific
Selective Dorsal Rhizotomy (SDR) Scotland Service Pathway This pathway should to be read in conjunction with the attached notes. The number in each text box refers to the note that relates to the specific
Spinal Cord Injury Fact Sheet
 TIRR Memorial Hermann is a nationally recognized rehabilitation hospital that returns lives interrupted by neurological illness, trauma or other debilitating conditions back to independence. Some of the
TIRR Memorial Hermann is a nationally recognized rehabilitation hospital that returns lives interrupted by neurological illness, trauma or other debilitating conditions back to independence. Some of the
Casa Colina Centers for Rehabilitation: A unique physician-directed model of care that works
 Casa Colina Centers for Rehabilitation: A unique physician-directed model of care that works Emily R. Rosario, PhD Why is Casa Colina unique? Continuum of care offering medical and rehabilitation services
Casa Colina Centers for Rehabilitation: A unique physician-directed model of care that works Emily R. Rosario, PhD Why is Casa Colina unique? Continuum of care offering medical and rehabilitation services
Your Orthotics service is changing
 Your Orthotics service is changing Important for referrers on changes effective from January 2015 Why is the service changing? As demand for the orthotics service increases and budgets remain relatively
Your Orthotics service is changing Important for referrers on changes effective from January 2015 Why is the service changing? As demand for the orthotics service increases and budgets remain relatively
2017 Report Card. 62 acute inpatient rehabilitation beds 13 DAYS
 Lovelace UNM Rehabilitation Hospital is dedicated helping each patient overcome the effects of illness and injury through our comprehensive inpatient and outpatient programs. Our highly specialized physicians
Lovelace UNM Rehabilitation Hospital is dedicated helping each patient overcome the effects of illness and injury through our comprehensive inpatient and outpatient programs. Our highly specialized physicians
SPINAL CORD INJURY Rehab Definitions Framework Self-Assessment Tool inpatient rehab Survey for Spinal Cord Injury (SCI)
 SPINAL CORD INJURY Rehab s Framework Self-Assessment Tool inpatient rehab Survey for Spinal Cord Injury (SCI) INTRODUCTION: In response to a changing rehab landscape in which rehabilitation is offered
SPINAL CORD INJURY Rehab s Framework Self-Assessment Tool inpatient rehab Survey for Spinal Cord Injury (SCI) INTRODUCTION: In response to a changing rehab landscape in which rehabilitation is offered
SPINAL CORD INJURY Rehab Definitions Framework Self-Assessment Tool Outpatient/ambulatory rehab Survey for Spinal Cord Injury (SCI)
 SPINAL CORD INJURY Rehab s Framework Self-Assessment Tool Outpatient/ambulatory rehab Survey for Spinal Cord Injury (SCI) INTRODUCTION: In response to a changing rehab landscape in which rehabilitation
SPINAL CORD INJURY Rehab s Framework Self-Assessment Tool Outpatient/ambulatory rehab Survey for Spinal Cord Injury (SCI) INTRODUCTION: In response to a changing rehab landscape in which rehabilitation
Acute Rehabilitation. Giving Courage l Creating Hope l Building Strength
 Acute Rehabilitation Giving Courage l Creating Hope l Building Strength What is Acute Rehabilitation? Rehabilitation is a team of healthcare professionals working together to help people regain function
Acute Rehabilitation Giving Courage l Creating Hope l Building Strength What is Acute Rehabilitation? Rehabilitation is a team of healthcare professionals working together to help people regain function
Department of Physical Medicine and Rehabilitation
 For enquiries and appointments, please contact us at: 物理醫學及復康科部 Department of Physical Medicine and Rehabilitation Department of Physical Medicine and Rehabilitation 5/F, Li Shu Pui Block, Hong Kong Sanatorium
For enquiries and appointments, please contact us at: 物理醫學及復康科部 Department of Physical Medicine and Rehabilitation Department of Physical Medicine and Rehabilitation 5/F, Li Shu Pui Block, Hong Kong Sanatorium
InterQual Level of Care 2018 Index
 InterQual Level of Care 2018 Index Rehabilitation Criteria Index Words by Subset The Index is an alphabetical listing of conditions and/or diagnoses designed to guide the user to the criteria subset where
InterQual Level of Care 2018 Index Rehabilitation Criteria Index Words by Subset The Index is an alphabetical listing of conditions and/or diagnoses designed to guide the user to the criteria subset where
PREVIOUS EMPLOYMENT. Associate OT : CJ Occupational Therapy * Assessment and treatment for adults with neurological conditions
 CURRICULUM VITAE Katie Hanagarth Green Owl Therapy Office 3, 36 Greenhill Street Stratford-upon-Avon CV37 6LE Tel: 01789 413960 / 07966 573317 Email: katie@greenowltherapy.co.uk - Web: www.greenowltherapy.co.uk
CURRICULUM VITAE Katie Hanagarth Green Owl Therapy Office 3, 36 Greenhill Street Stratford-upon-Avon CV37 6LE Tel: 01789 413960 / 07966 573317 Email: katie@greenowltherapy.co.uk - Web: www.greenowltherapy.co.uk
Functional Outcomes among the Medically Complex Population
 Functional Outcomes among the Medically Complex Population Paulette Niewczyk, PhD, MPH Director of Research Uniform Data System for Medical Rehabilitation 2015 Uniform Data System for Medical Rehabilitation,
Functional Outcomes among the Medically Complex Population Paulette Niewczyk, PhD, MPH Director of Research Uniform Data System for Medical Rehabilitation 2015 Uniform Data System for Medical Rehabilitation,
Young onset dementia service Doncaster
 Young onset dementia service Doncaster RDaSH Older People s Mental Health Services Introduction The following procedures and protocols will govern the operational working and function of the Doncaster
Young onset dementia service Doncaster RDaSH Older People s Mental Health Services Introduction The following procedures and protocols will govern the operational working and function of the Doncaster
Neurodegenerative diseases Includes multiple sclerosis, Parkinson s disease, postpolio syndrome, rheumatoid arthritis, lupus
 TIRR Memorial Hermann is a nationally recognized rehabilitation hospital that returns lives interrupted by neurological illness, trauma or other debilitating conditions back to independence. Some of the
TIRR Memorial Hermann is a nationally recognized rehabilitation hospital that returns lives interrupted by neurological illness, trauma or other debilitating conditions back to independence. Some of the
Introduction. Peripheral arterial disease. Hospital inpatient data - 5,498 FCE (2009/10), & 530 deaths in England alone
 1 Introduction 2 Introduction Peripheral arterial disease Affects 20% adults in Europe and North America In the UK 500-1000/million PAD, 1-2% require amputation LLA 8-15% in people with diabetes with up
1 Introduction 2 Introduction Peripheral arterial disease Affects 20% adults in Europe and North America In the UK 500-1000/million PAD, 1-2% require amputation LLA 8-15% in people with diabetes with up
Specialty Rehabilitation Fact Sheet
 TIRR Memorial Hermann is a nationally recognized rehabilitation hospital that returns lives interrupted by neurological illness, trauma or other debilitating conditions back to independence. Some of the
TIRR Memorial Hermann is a nationally recognized rehabilitation hospital that returns lives interrupted by neurological illness, trauma or other debilitating conditions back to independence. Some of the
INPATIENT CONSULT SERVICE
 INPATIENT CONSULT SERVICE Patient Care OBJECTIVES BEGINNER Obtain essential and accurate information and present it in a concise but thorough format Perform a rehabilitation medicine focused consultation
INPATIENT CONSULT SERVICE Patient Care OBJECTIVES BEGINNER Obtain essential and accurate information and present it in a concise but thorough format Perform a rehabilitation medicine focused consultation
We Have a Great Story to Tell
 We Have a Great Story to Tell Inpatient Outpatient Day Neuro Baylor Scott & White Institute for Rehabilitation Frisco is dedicated to helping patients find their way back from all types of injuries, illnesses,
We Have a Great Story to Tell Inpatient Outpatient Day Neuro Baylor Scott & White Institute for Rehabilitation Frisco is dedicated to helping patients find their way back from all types of injuries, illnesses,
Physiotherapy Department. Grade 2 Physiotherapist Aged and Transitional Care Stream. Health Professionals (Public Sector Victoria)
 POSITION DESCRIPTION Grade 2 Physiotherapist Physiotherapy Department DATE REVISED: April 2016 POSITION: AWARD/AGREEMENT: Grade 2 Physiotherapist Aged and Transitional Care Stream Health Professionals
POSITION DESCRIPTION Grade 2 Physiotherapist Physiotherapy Department DATE REVISED: April 2016 POSITION: AWARD/AGREEMENT: Grade 2 Physiotherapist Aged and Transitional Care Stream Health Professionals
BURKE S ACUTE REHAB: PERSONALIZED FOR MAXIMUM RECOVERY
 WELCOME TO BURKE No one plans to experience a life-changing illness or traumatic injury. So it is comforting to know that for the past 100 years, Burke Rehabilitation Hospital has been a leader in rehabilitation
WELCOME TO BURKE No one plans to experience a life-changing illness or traumatic injury. So it is comforting to know that for the past 100 years, Burke Rehabilitation Hospital has been a leader in rehabilitation
A Best Practice Clinical Care Pathway for Major Amputation Surgery
 A Best Practice Clinical Care Pathway for Major Amputation Surgery April 2016 Introduction The perioperative mortality rate after major lower limb amputation in the UK is unacceptably high in modern medical
A Best Practice Clinical Care Pathway for Major Amputation Surgery April 2016 Introduction The perioperative mortality rate after major lower limb amputation in the UK is unacceptably high in modern medical
They are updated regularly as new NICE guidance is published. To view the latest version of this NICE Pathway see:
 Chronic fatigue syndrome myalgic encephalomyelitis elitis overview bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated
Chronic fatigue syndrome myalgic encephalomyelitis elitis overview bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated
2010 National Audit of Dementia (Care in General Hospitals)
 Royal College of Psychiatrists 2010 National Audit of Dementia (Care in General Hospitals) Organisational checklist results and commentary for: Barking, Havering and Redbridge Hospitals NHS Trust The 2010
Royal College of Psychiatrists 2010 National Audit of Dementia (Care in General Hospitals) Organisational checklist results and commentary for: Barking, Havering and Redbridge Hospitals NHS Trust The 2010
2010 National Audit of Dementia (Care in General Hospitals) Guy's and St Thomas' NHS Foundation Trust
 Royal College of Psychiatrists 2010 National Audit of Dementia (Care in General Hospitals) Organisational checklist results and commentary for: Guy's and St Thomas' NHS Foundation Trust The 2010 national
Royal College of Psychiatrists 2010 National Audit of Dementia (Care in General Hospitals) Organisational checklist results and commentary for: Guy's and St Thomas' NHS Foundation Trust The 2010 national
Geriatric Medicine I) OBJECTIVES
 Geriatric Medicine I) OBJECTIVES 1 To provide a broad training and in-depth experience at a level sufficient for trainees to acquire competence and professionalism required of a specialist in Geriatric
Geriatric Medicine I) OBJECTIVES 1 To provide a broad training and in-depth experience at a level sufficient for trainees to acquire competence and professionalism required of a specialist in Geriatric
General Medical Rehabilitation
 General Medical Rehabilitation Outcomes Report 20 Rehabilitation Hospital is part of the Rehabilitation system of care, a post-acute provider of neuro-rehabilitation for over 45 years. Our 160-bed acute,
General Medical Rehabilitation Outcomes Report 20 Rehabilitation Hospital is part of the Rehabilitation system of care, a post-acute provider of neuro-rehabilitation for over 45 years. Our 160-bed acute,
Audit and Implementation Guide: Clinical guidelines for the pre and post operative physiotherapy management of adults with lower limb amputations
 2nd Edition- 2016 Audit and Implementation Guide: Clinical guidelines for the pre and post operative physiotherapy British Association of Chartered Physiotherapists in Amputee Rehabilitation NICE has accredited
2nd Edition- 2016 Audit and Implementation Guide: Clinical guidelines for the pre and post operative physiotherapy British Association of Chartered Physiotherapists in Amputee Rehabilitation NICE has accredited
Appendix E : Evidence table 9 Rehabilitation: Other Key Documents
 Appendix E : Evidence table 9 Rehabilitation: Other Key Documents 1. Cameron et al. Geriatric rehabilitation following following fractures in older people: a systematic review. Health Technology Assessment
Appendix E : Evidence table 9 Rehabilitation: Other Key Documents 1. Cameron et al. Geriatric rehabilitation following following fractures in older people: a systematic review. Health Technology Assessment
2010 National Audit of Dementia (Care in General Hospitals) Chelsea and Westminster Hospital NHS Foundation Trust
 Royal College of Psychiatrists 2010 National Audit of Dementia (Care in General Hospitals) Organisational checklist results and commentary for: NHS Foundation Trust The 2010 national audit of dementia
Royal College of Psychiatrists 2010 National Audit of Dementia (Care in General Hospitals) Organisational checklist results and commentary for: NHS Foundation Trust The 2010 national audit of dementia
Recognition of Skills and Training Q. Does the Greens support direct referrals to selected medical specialist services?
 22 September 2014 Colleen Hartland, MLC 75 Victoria Street SEDDON VIC 3011 Dear Ms Hartland, The Australian Physiotherapy Association represents more than 4,100 Victorian physiotherapists and over 16,500
22 September 2014 Colleen Hartland, MLC 75 Victoria Street SEDDON VIC 3011 Dear Ms Hartland, The Australian Physiotherapy Association represents more than 4,100 Victorian physiotherapists and over 16,500
Aiming for Excellence in Stroke Care
 Training Centre in Sub-acute Care (TRACS WA) Aiming for Excellence in Stroke Care A tool for quality improvement in stroke care Developed by TRAining Centre in Subacute Care (TRACS WA) February 2016 For
Training Centre in Sub-acute Care (TRACS WA) Aiming for Excellence in Stroke Care A tool for quality improvement in stroke care Developed by TRAining Centre in Subacute Care (TRACS WA) February 2016 For
Neurodegenerative diseases Includes multiple sclerosis, Parkinson s disease, postpolio syndrome, rheumatoid arthritis, lupus
 TIRR Memorial Hermann is a nationally recognized rehabilitation hospital that returns lives interrupted by neurological illness, trauma or other debilitating conditions back to independence. Some of the
TIRR Memorial Hermann is a nationally recognized rehabilitation hospital that returns lives interrupted by neurological illness, trauma or other debilitating conditions back to independence. Some of the
More capacity for healing. More focus on you.
 REHABILITATION PROGRAM small means more. More capacity for healing. More focus on you. The Rehabilitation Center at Mt. Ascutney Hospital offering patient-centered rehabilitative care for your best possible
REHABILITATION PROGRAM small means more. More capacity for healing. More focus on you. The Rehabilitation Center at Mt. Ascutney Hospital offering patient-centered rehabilitative care for your best possible
Freedom of Information Act Request Physiotherapy Services for Neurological Conditions
 Freedom of Information Act Request Physiotherapy Services for Neurological Conditions 1. In total how many physiotherapists does C&V UHB employ? s services 33 qualified paediatric physiotherapy staff in
Freedom of Information Act Request Physiotherapy Services for Neurological Conditions 1. In total how many physiotherapists does C&V UHB employ? s services 33 qualified paediatric physiotherapy staff in
2010 National Audit of Dementia (Care in General Hospitals) North West London Hospitals NHS Trust
 Royal College of Psychiatrists 2010 National Audit of Dementia (Care in General Hospitals) Organisational checklist results and commentary for: rth West London Hospitals NHS Trust The 2010 national audit
Royal College of Psychiatrists 2010 National Audit of Dementia (Care in General Hospitals) Organisational checklist results and commentary for: rth West London Hospitals NHS Trust The 2010 national audit
DELINEATION OF PRIVILEGES - REHABILITATION MEDICINE
 KALEIDA HEALTH Name ABMS Board DELINEATION OF PRIVILEGES - REHABILITATION MEDICINE Certification: Please circle all that apply: Board Qualified: Inpatient Rehab Care: Admitting Privileges** (**e: Admitting
KALEIDA HEALTH Name ABMS Board DELINEATION OF PRIVILEGES - REHABILITATION MEDICINE Certification: Please circle all that apply: Board Qualified: Inpatient Rehab Care: Admitting Privileges** (**e: Admitting
South East Coast Operational Delivery Network. Critical Care Rehabilitation
 South East Coast Operational Delivery Networks Hosted by Medway Foundation Trust South East Coast Operational Delivery Network Background Critical Care Rehabilitation The optimisation of recovery from
South East Coast Operational Delivery Networks Hosted by Medway Foundation Trust South East Coast Operational Delivery Network Background Critical Care Rehabilitation The optimisation of recovery from
Ratified by: Care and Clinical Policies Date: 17 th February 2016
 Clinical Guideline Reference Number: 0803 Version 5 Title: Physiotherapy guidelines for the Management of People with Multiple Sclerosis Document Author: Henrieke Dimmendaal / Laura Shenton Date February
Clinical Guideline Reference Number: 0803 Version 5 Title: Physiotherapy guidelines for the Management of People with Multiple Sclerosis Document Author: Henrieke Dimmendaal / Laura Shenton Date February
The Role of Physiatry in the Care of Adults and Children with Hydrocephalus
 The Role of Physiatry in the Care of Adults and Children with Hydrocephalus Scott E. Brown, MD Chairman Department of Physical Medicine and Rehabilitation Sinai Hospital of Baltimore Who Are We? PHYSICAL
The Role of Physiatry in the Care of Adults and Children with Hydrocephalus Scott E. Brown, MD Chairman Department of Physical Medicine and Rehabilitation Sinai Hospital of Baltimore Who Are We? PHYSICAL
General Rehabilitation Sub-Acute Model of Care
 Central Adelaide Local Health Network Central Adelaide Rehabilitation Service General Rehabilitation Sub-Acute Model of Care November 2016 Page 1 Contents ABBREVIATION LIST... 4 1. Purpose of Document...
Central Adelaide Local Health Network Central Adelaide Rehabilitation Service General Rehabilitation Sub-Acute Model of Care November 2016 Page 1 Contents ABBREVIATION LIST... 4 1. Purpose of Document...
What to expect following spinal cord injury. Information for patients Therapy Services
 What to expect following spinal cord injury Information for patients Therapy Services Introduction This leaflet aims to explain what spinal cord injury is and what to expect over the next few months. What
What to expect following spinal cord injury Information for patients Therapy Services Introduction This leaflet aims to explain what spinal cord injury is and what to expect over the next few months. What
NZ Organised Stroke Rehabilitation Service Specifications (in-patient and community)
 NZ Organised Stroke Rehabilitation Service Specifications (in-patient and community) Prepared by the National Stroke Network to outline minimum and strongly recommended standards for DHBs. Date: December
NZ Organised Stroke Rehabilitation Service Specifications (in-patient and community) Prepared by the National Stroke Network to outline minimum and strongly recommended standards for DHBs. Date: December
Chapter. CPT only copyright 2008 American Medical Association. All rights reserved. 28Physical Medicine and Rehabilitation
 Chapter 28Physical Medicine and Rehabilitation 28 28.1 Enrollment...................................................... 28-2 28.2 Benefits, Limitations, and Authorization Requirements......................
Chapter 28Physical Medicine and Rehabilitation 28 28.1 Enrollment...................................................... 28-2 28.2 Benefits, Limitations, and Authorization Requirements......................
LLANDUDNO HOSPITAL PROJECT CYCLE ONE REPORT FOR REHABILITATION PROJECT TEAM: ASSESSMENT OF POTENTIAL SOLUTIONS FOR DEVELOPING SERVICES MARCH 2010
 LLANDUDNO HOSPITAL PROJECT CYCLE ONE REPORT FOR REHABILITATION PROJECT TEAM: ASSESSMENT OF POTENTIAL SOLUTIONS FOR DEVELOPING SERVICES MARCH 2010 SITUATION The Rehabilitation Project Team has been established
LLANDUDNO HOSPITAL PROJECT CYCLE ONE REPORT FOR REHABILITATION PROJECT TEAM: ASSESSMENT OF POTENTIAL SOLUTIONS FOR DEVELOPING SERVICES MARCH 2010 SITUATION The Rehabilitation Project Team has been established
American Board of Physical Medicine & Rehabilitation. Part I Curriculum & Weights
 American Board of Physical Medicine & Rehabilitation Part I Curriculum & Weights Neurologic Disorders 30% Stroke Spinal Cord Injury Traumatic Brain Injury Neuropathies a) Mononeuropathies b) Polyneuropathies
American Board of Physical Medicine & Rehabilitation Part I Curriculum & Weights Neurologic Disorders 30% Stroke Spinal Cord Injury Traumatic Brain Injury Neuropathies a) Mononeuropathies b) Polyneuropathies
Australian, Finland and South Africa - Delving into Data to Investigate Differences in Stroke Rehabilitation
 University of Wollongong Research Online Australasian Rehabilitation Outcomes Centre - AROC Centre for Health Service Development - CHSD 2005 Australian, Finland and South Africa - Delving into Data to
University of Wollongong Research Online Australasian Rehabilitation Outcomes Centre - AROC Centre for Health Service Development - CHSD 2005 Australian, Finland and South Africa - Delving into Data to
NATIONAL REHABILITATION HOSPITAL PROSTHETIC, ORTHOTIC & LIMB ABSENCE REHABILITATION PROGRAMME
 NATIONAL REHABILITATION HOSPITAL PROSTHETIC, ORTHOTIC & LIMB ABSENCE REHABILITATION PROGRAMME SCOPE OF SERVICE 1 Introduction: The Prosthetic, Orthotic & Limb Absence Rehabilitation Programme (POLAR) at
NATIONAL REHABILITATION HOSPITAL PROSTHETIC, ORTHOTIC & LIMB ABSENCE REHABILITATION PROGRAMME SCOPE OF SERVICE 1 Introduction: The Prosthetic, Orthotic & Limb Absence Rehabilitation Programme (POLAR) at
Neurodegenerative Diseases, Debilitating Conditions and Multiple Trauma Program (Neuromuscular Rehab)
 Neurodegenerative Diseases, Debilitating Conditions and Multiple Trauma Program (Neuromuscular Rehab) TIRR Memorial Hermann is a nationally recognized rehabilitation hospital that returns lives interrupted
Neurodegenerative Diseases, Debilitating Conditions and Multiple Trauma Program (Neuromuscular Rehab) TIRR Memorial Hermann is a nationally recognized rehabilitation hospital that returns lives interrupted
National Osteoarthritis Strategy DRAFT for Consultation Online survey responses submitted by DAA, October 2018
 National Osteoarthritis Strategy DRAFT for Consultation Online survey responses submitted by DAA, October 2018 1. Which state or territory are you in? National a member association that represents Accredited
National Osteoarthritis Strategy DRAFT for Consultation Online survey responses submitted by DAA, October 2018 1. Which state or territory are you in? National a member association that represents Accredited
Your Orthotics service is changing
 Your Orthotics service is changing Important information for service users on changes effective from July 2015 Why is the service changing? As demand for the Orthotics service increases, Livewell Southwest
Your Orthotics service is changing Important information for service users on changes effective from July 2015 Why is the service changing? As demand for the Orthotics service increases, Livewell Southwest
Nathan Schomburg PT, NCS 2535 Shellburne Dr. Wexford, PA (412)
 Nathan Schomburg PT, NCS 2535 Shellburne Dr. Wexford, PA 15090 (412) 310-6837 schomburgn@upmc.edu EDUCATION Duquesne University, Pittsburgh, PA Masters of Physical Therapy 1997-2002 2001 Recipient of John
Nathan Schomburg PT, NCS 2535 Shellburne Dr. Wexford, PA 15090 (412) 310-6837 schomburgn@upmc.edu EDUCATION Duquesne University, Pittsburgh, PA Masters of Physical Therapy 1997-2002 2001 Recipient of John
物理治療中心. Physiotherapy Centre. Multi-disciplinary Chronic Pain Rehabilitation Programme. Physiotherapy Centre. Physiotherapy Centre
 物理治療中心 Physiotherapy Centre Multi-disciplinary Chronic Pain Rehabilitation Programme For enquiries and appointments, please contact us at: Physiotherapy Centre 5/F, Li Shu Pui Block Hong Kong Sanatorium
物理治療中心 Physiotherapy Centre Multi-disciplinary Chronic Pain Rehabilitation Programme For enquiries and appointments, please contact us at: Physiotherapy Centre 5/F, Li Shu Pui Block Hong Kong Sanatorium
Criteria for Registering as a Developmental Paediatrician
 Criteria for Registering as a Developmental Paediatrician A doctor can apply to be registered as a Developmental Paediatrician if he/she fulfils ALL the following requirements: 1 A recognised basic medical
Criteria for Registering as a Developmental Paediatrician A doctor can apply to be registered as a Developmental Paediatrician if he/she fulfils ALL the following requirements: 1 A recognised basic medical
MUSCULOSKELETAL AND NEUROLOGICAL DISORDERS
 MUSCULOSKELETAL AND NEUROLOGICAL DISORDERS There are a wide variety of Neurologic and Musculoskeletal disorders which can impact driving safety. Impairment may be the result of altered muscular, skeletal,
MUSCULOSKELETAL AND NEUROLOGICAL DISORDERS There are a wide variety of Neurologic and Musculoskeletal disorders which can impact driving safety. Impairment may be the result of altered muscular, skeletal,
Rehabilitation Programs
 Rehabilitation Programs Inpatient and Half-Day Rehabilitation Program Information and Referral Form WELCOME TO ST LUKE S CARE Thank you for choosing St Luke s Care for your rehabilitation. With an unwavering
Rehabilitation Programs Inpatient and Half-Day Rehabilitation Program Information and Referral Form WELCOME TO ST LUKE S CARE Thank you for choosing St Luke s Care for your rehabilitation. With an unwavering
What is Occupational Therapy? Introduction to Occupational Therapy. World Federation of Occupational Therapists 2012
 World Federation of Occupational Therapists 2012 Introduction to Occupational Therapy Suki HUI Occupational Therapist I Statement on Occupational Therapy Occupational therapy is a client-centred health
World Federation of Occupational Therapists 2012 Introduction to Occupational Therapy Suki HUI Occupational Therapist I Statement on Occupational Therapy Occupational therapy is a client-centred health
Expert Transfers in Rehabilitation: A Safety and Utilisation Review
 Expert Transfers in Rehabilitation: A Safety and Utilisation Review Robert Mehan Meaghan Mackenzie Kim Brock Rehabilitation Care Centre NAHC 2007 - Hobart An important focus in stroke rehabilitation is
Expert Transfers in Rehabilitation: A Safety and Utilisation Review Robert Mehan Meaghan Mackenzie Kim Brock Rehabilitation Care Centre NAHC 2007 - Hobart An important focus in stroke rehabilitation is
1. Can self-propel, or use their foot to push (punt), a standard manual wheelchair 1 and be safe and able to do essential daily tasks.
 Disability Support Services Equipment and Modifications Competency Framework Wheeled Mobility and Postural Management Introduction The Wheeled Mobility and Postural Management Credential recognises that
Disability Support Services Equipment and Modifications Competency Framework Wheeled Mobility and Postural Management Introduction The Wheeled Mobility and Postural Management Credential recognises that
Primary Health Networks
 Primary Health Networks Drug and Alcohol Treatment Activity Work Plan 2016-17 to 2018-19 Hunter New England & Central Coast Please note: This Activity Work Plan was developed in response to the HNECC PHN
Primary Health Networks Drug and Alcohol Treatment Activity Work Plan 2016-17 to 2018-19 Hunter New England & Central Coast Please note: This Activity Work Plan was developed in response to the HNECC PHN
Orthopaedic Therapy Service inpatient guide. Information for patients MSK Orthopaedic Inpatients (Therapy)
 Orthopaedic Therapy Service inpatient guide Information for patients MSK Orthopaedic Inpatients (Therapy) This leaflet is designed to answer any queries you may have about the Orthopaedic Therapy Service.
Orthopaedic Therapy Service inpatient guide Information for patients MSK Orthopaedic Inpatients (Therapy) This leaflet is designed to answer any queries you may have about the Orthopaedic Therapy Service.
Joint replacement reviews conducted by physiotherapists Bernarda Cavka Advanced Practice Physiotherapist The Royal Melbourne Hospital
 Joint replacement reviews conducted by physiotherapists Bernarda Cavka Advanced Practice Physiotherapist The Royal Melbourne Hospital 2014 The Quantum Leap The Royal Melbourne Hospital (RMH) One of two
Joint replacement reviews conducted by physiotherapists Bernarda Cavka Advanced Practice Physiotherapist The Royal Melbourne Hospital 2014 The Quantum Leap The Royal Melbourne Hospital (RMH) One of two
9 Diabetes care. Back to contents
 Back to contents Diabetes is a major risk factor for the development of peripheral vascular disease and 349/628 (55.6%) of the patients in this study had diabetes. Hospital inpatients with diabetes are
Back to contents Diabetes is a major risk factor for the development of peripheral vascular disease and 349/628 (55.6%) of the patients in this study had diabetes. Hospital inpatients with diabetes are
Albury Wodonga Health Albury Campus Physiotherapy placements
 Albury Wodonga Health Albury Campus Physiotherapy placements Welcome to the Albury campus of Albury Wodonga Health, it is also referred to as the Albury Hospital and occasionally Albury Base Hospital.
Albury Wodonga Health Albury Campus Physiotherapy placements Welcome to the Albury campus of Albury Wodonga Health, it is also referred to as the Albury Hospital and occasionally Albury Base Hospital.
Center for Optimal Aging
 Center for Optimal Aging Center for Optimal Aging Program Summary The Center for Optimal Aging is an outpatient program offered exclusively at Providence Little Company of Mary Medical Center San Pedro.
Center for Optimal Aging Center for Optimal Aging Program Summary The Center for Optimal Aging is an outpatient program offered exclusively at Providence Little Company of Mary Medical Center San Pedro.
MSK Rehab Definitions Framework - hip fractures Self assessment Survey Outpatient Rehab
 MSK Rehab Definitions Framework - hip fractures Self assessment Survey Outpatient Rehab In response to a changing rehab landscape in which rehabilitation is offered in many different settings with variations
MSK Rehab Definitions Framework - hip fractures Self assessment Survey Outpatient Rehab In response to a changing rehab landscape in which rehabilitation is offered in many different settings with variations
Implementing Best Practice Rehabilitative Care for Patients with Hip Fracture & Total Joint Replacement
 Implementing Best Practice Rehabilitative Care for Patients with Hip Fracture & Total Joint Replacement A Toolkit for Implementing the RCA s TJR and Hip Fracture Best Practice Frameworks January 2018 Purpose
Implementing Best Practice Rehabilitative Care for Patients with Hip Fracture & Total Joint Replacement A Toolkit for Implementing the RCA s TJR and Hip Fracture Best Practice Frameworks January 2018 Purpose
Comprehensive Acute. Rehabilitation Unit
 Comprehensive Acute Rehabilitation Unit The Comprehensive Acute Rehabilitation Unit at Thomas Jefferson University Hospital has provided excellence in patient-focused acute rehabilitative care since 1963.
Comprehensive Acute Rehabilitation Unit The Comprehensive Acute Rehabilitation Unit at Thomas Jefferson University Hospital has provided excellence in patient-focused acute rehabilitative care since 1963.
Shaping Diabetes Services in Southern Derbyshire. A vision for Diabetes Services For Southern Derbyshire CCG
 Shaping Diabetes Services in Southern Derbyshire A vision for Diabetes Services For Southern Derbyshire CCG Vanessa Vale Commissioning Manager September 2013 Contents 1. Introduction 3 2. National Guidance
Shaping Diabetes Services in Southern Derbyshire A vision for Diabetes Services For Southern Derbyshire CCG Vanessa Vale Commissioning Manager September 2013 Contents 1. Introduction 3 2. National Guidance
LIFE-CHANGING CARE INPATIENT CARE
 LIFE-CHANGING CARE INPATIENT CARE Helping Patients Get the Most out of Rehab When a stroke, accident or other traumatic incident turns a person s world upside down, there s a place in Indiana where he
LIFE-CHANGING CARE INPATIENT CARE Helping Patients Get the Most out of Rehab When a stroke, accident or other traumatic incident turns a person s world upside down, there s a place in Indiana where he
Draft Falls Prevention Strategy
 Cheshire West & Chester Council Draft Falls Prevention Strategy 2017-2020 Visit: cheshirewestandchester.gov.uk Visit: cheshirewestandchester.gov.uk 02 Cheshire West and Chester Council Draft Falls Prevention
Cheshire West & Chester Council Draft Falls Prevention Strategy 2017-2020 Visit: cheshirewestandchester.gov.uk Visit: cheshirewestandchester.gov.uk 02 Cheshire West and Chester Council Draft Falls Prevention
A. Service Specification
 A. Service Specification Service Specification No: 1767 Service Adult Highly Specialist Pain Management Services Commissioner Lead For local completion Lead For local completion 1. Scope 1.1 Prescribed
A. Service Specification Service Specification No: 1767 Service Adult Highly Specialist Pain Management Services Commissioner Lead For local completion Lead For local completion 1. Scope 1.1 Prescribed
Service Specific Documentation Guidelines. Service Area: Inpatient MSK / Amputee Rehab October 2007
 1. Standards of Practice Service Specific Documentation Guidelines Service Area: Inpatient MSK / Amputee Rehab October 2007 Informed Consent for Assessment and Treatment Check box on assessment form. 2.
1. Standards of Practice Service Specific Documentation Guidelines Service Area: Inpatient MSK / Amputee Rehab October 2007 Informed Consent for Assessment and Treatment Check box on assessment form. 2.
Centre for Research on Ageing [influencing policy improving practice enhancing quality of life]
![Centre for Research on Ageing [influencing policy improving practice enhancing quality of life] Centre for Research on Ageing [influencing policy improving practice enhancing quality of life]](/thumbs/73/69177132.jpg) Centre for Research on Ageing [influencing policy improving practice enhancing quality of life] Associate Professor Barbara Horner (PhD) Director, Centre for Research on Ageing, Faculty of Health Sciences.
Centre for Research on Ageing [influencing policy improving practice enhancing quality of life] Associate Professor Barbara Horner (PhD) Director, Centre for Research on Ageing, Faculty of Health Sciences.
OUTCOMES AND DATA 2016
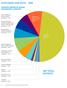 AND DATA 2016 SERVED BY REHAB IMPAIRMENT CATEGORY 20 patients 5.1% MAJOR MULTIPLE TRAUMA W/BRAIN OR SPINAL CORD INJURY 24 patients 6.2% TRAUMATIC 39 patients 10.0% AMPUTATION LOWER EXTREMITY 26 patients
AND DATA 2016 SERVED BY REHAB IMPAIRMENT CATEGORY 20 patients 5.1% MAJOR MULTIPLE TRAUMA W/BRAIN OR SPINAL CORD INJURY 24 patients 6.2% TRAUMATIC 39 patients 10.0% AMPUTATION LOWER EXTREMITY 26 patients
Rehabilitation - Reducing costs and hospital stay. Dr Elizabeth Aitken Consultant Physician
 Rehabilitation - Reducing costs and hospital stay Dr Elizabeth Aitken Consultant Physician What factors affect outcome? Comorbidities Cardiac Respiratory Neurological Nutritional issues Diabetes Anaemia
Rehabilitation - Reducing costs and hospital stay Dr Elizabeth Aitken Consultant Physician What factors affect outcome? Comorbidities Cardiac Respiratory Neurological Nutritional issues Diabetes Anaemia
Guidelines for exercise and orthoses in children with neuromuscular disorders
 Guidelines for exercise and orthoses in children with neuromuscular disorders These guidelines were drawn following a workshop held in Newcastle 2002. Several experts from different disciplines including
Guidelines for exercise and orthoses in children with neuromuscular disorders These guidelines were drawn following a workshop held in Newcastle 2002. Several experts from different disciplines including
This page is for information. Do not submit.
 This page is for information. Do not submit. AISH Application - Part B Medical Report Information for Physicians Your patient (the applicant) is applying for the Assured Income for the Severely Handicapped
This page is for information. Do not submit. AISH Application - Part B Medical Report Information for Physicians Your patient (the applicant) is applying for the Assured Income for the Severely Handicapped
National Stroke Association s Guide to Choosing Stroke. Rehabilitation Services
 National Stroke Association s Guide to Choosing Stroke Rehabilitation Services Rehabilitation, often referred to as rehab, is an important part of stroke recovery. Through rehab, you: Re-learn basic skills
National Stroke Association s Guide to Choosing Stroke Rehabilitation Services Rehabilitation, often referred to as rehab, is an important part of stroke recovery. Through rehab, you: Re-learn basic skills
Foreword. The 2014 survey monitors the effect of the ACFI and members experiences and perceptions of its implementation.
 ACFI Survey 2014 Australian Physiotherapy Association ACFI Survey 2014 2 Foreword The Australian Physiotherapy Association (APA) advocates for equitable access to quality physiotherapy and optimal health
ACFI Survey 2014 Australian Physiotherapy Association ACFI Survey 2014 2 Foreword The Australian Physiotherapy Association (APA) advocates for equitable access to quality physiotherapy and optimal health
Fall Risk Assessment and Prevention in the Post-Acute Setting A Road Map
 Fall Risk Assessment and Prevention in the Post-Acute Setting A Road Map Cora M. Butler, JD, RN, CHC HealthCore Value Advisors, Inc. Juli A. James, RN Primaris Holdings, Inc. Objectives Explore the burden
Fall Risk Assessment and Prevention in the Post-Acute Setting A Road Map Cora M. Butler, JD, RN, CHC HealthCore Value Advisors, Inc. Juli A. James, RN Primaris Holdings, Inc. Objectives Explore the burden
Knowsley Community. Stroke Team.
 Knowsley Community Stroke Team julia.owens@lhch.nhs.uk marie.florian@lhch.nhs.uk 0151 244 3369 Knowsley Cardiovascular Disease Service Community Cardiovascular Service Rehabilitation services One stop
Knowsley Community Stroke Team julia.owens@lhch.nhs.uk marie.florian@lhch.nhs.uk 0151 244 3369 Knowsley Cardiovascular Disease Service Community Cardiovascular Service Rehabilitation services One stop
