Percutaneous closure of ventricular septal defects in children aged <12: early and mid-term results
|
|
|
- Myron Webster
- 5 years ago
- Views:
Transcription
1 European Heart Journal (2006) 27, doi: /eurheartj/ehl340 Clinical research Congenital heart disease Percutaneous closure of ventricular septal defects in children aged <12: early and mid-term results Gianfranco Butera*, Mario Carminati, Massimo Chessa, Luciane Piazza, Raul Abella, Diana Gabriella Negura, Alessandro Giamberti, Bussadori Claudio, Angelo Micheletti, Youssef Tammam, and Alessandro Frigiola Department of Pediatric Cardiology and Cardiac Surgery, Istituto Policlinico San Donato, Via Morandi, 30, San Donato Milanese, Italy Received 30 January 2006; revised 19 September 2006; accepted 5 October 2006; online publish-ahead-of-print 19 October 2006 KEYWORDS Septal defect; Children; Treatment; Percutaneous Introduction Surgical closure of a ventricular septal defect (VSD) is now a routine procedure. The morbidity and mortality related to surgical procedures have been reported in the literature. 1 8 In the last decade, percutaneous techniques to close cardiac defects have been developed. Closure of atrial septal defects and patent ductus arteriosus using transcatheter devices has been widely reported, 9 12 and these techniques can now be used even in very young children. 13,14 More recently percutaneous techniques and devices have been developed specifically for closure of muscular VSD (mvsd) and perimembranous VSD (pmvsd). The initial experience in humans appears encouraging, but there are no datafromlargeseriesofchildrenwithanadequatefollow-up. Here, we report our early and mid-term follow-up results of percutaneous closure of mvsd and pmvsd in 88 subjects aged,12. Methods Between January 2000 and June 2005, we prospectively collected data on 140 patients who underwent transcatheter closure of a VSD at our institution. Eighty-eight of these 140 subjects were * Corresponding author. Tel: þ ; fax: þ address: gianfra.but@lycos.com Aims The aim of the article is to study the safety, efficacy, and follow-up of percutaneous closure of muscular ventricular septal defect (mvsd) and perimembranous ventricular septal defect (pmvsd) in children. Methods and results Between January 2000 and June 2005, among 140 patients who underwent percutaneous closure of an mvsd or a pmvsd, 88 were aged lt;12. Two different Amplatzer devices were used: the mvsd occluder and the pmvsd occluder. Mean age and weight at procedure were years and kg, respectively. Percutaneous closure was successfully achieved in 83 subjects (94%). No deaths occurred. Thirteen patients (14.7%) had early complications: device embolization (n ¼ 4), vascular complications (n ¼ 3), and rhythm abnormalities (n ¼ 6). These were transient complications in all but one case [1.1% complete atrioventricular block (cavb) needing pacemaker implantation]. During a median follow-up of 24 months, three subjects treated for a pmvsd needed pacemaker implantation due to the occurrence of cavb. Multivariable analysis using Cox s proportional hazard regression showed that age was the only risk factor associated with the occurrence of cavb (P ¼ 0.028; relative risk: 0.25). Conclusion Percutaneous closure of mvsd and pmvsd in children can be performed safely and successfully. The occurrence of cavb is a major concern in young children with pmvsd. children aged,12 (range years). Patients were assessed by a standard echocardiographic protocol: all patients underwent transthoracic echocardiography (TTE) that was performed with a Vingmed 800 (Vingmed Sound, Horten, Norway) and a System Five performance ultrasound system (Vingmed Sound) using a transducer appropriate to each patient s size and body weight. Inclusion and exclusion criteria The criteria for inclusion in this study were clinical and/or echocardiographic evidence of a significant left-to-right shunt through an mvsd or a pmvsd in patients under 12 years of age. A left-to-right shunt was considered significant when the following were found: (i) cardiomegaly on chest X-ray; (ii) left atrial enlargement, defined as a left atrial-to-aortic ratio.1.5; (iii) left ventricular enlargement (left ventricular volume overload), defined as a left ventricular end-diastolic diameter.þ2 standard deviations (SD) above the mean for the patient s age; (iv) symptoms: frequent respiratory infections and/or failure to thrive. Frequent respiratory infections were defined as more than six events per year. 19 Failure to thrive was defined according to Hamil et al. 20 We intended that patients should weigh at least 5 kg to be eligible for percutaneous closure of a VSD, although we did treat some subjects weighing,5 kg, who had significant post-operative residual VSD. We undertook a percutaneous procedure when we could use long sheaths of the following sizes according to weight: 6 8 Fr in subjects weighing from kg, 7 9 Fr in subjects weighing from 6 8 kg, and 8 10 Fr in subjects weighing. 8 kg. This enabled us to close & The European Society of Cardiology All rights reserved. For Permissions, please journals.permissions@oxfordjournals.org
2 2890 G. Butera et al. mvsd of up to 8 12 mm in subjects weighing kg, mm in subjects weighing 6 8 kg, and. 14 mm in subjects weighing. 8 kg, whereas we could close pmvsd of up to 6 8 mm in subjects weighing kg, 8 10 mm in subjects weighing 6 8 kg, and. 12 mm in subjects weighing. 8 kg. A defect was defined too large to be closed percutaneously when a device and a long sheath larger than the one possible for body weight would have been needed. Only subjects with a rim of at least 1 mm separating the aortic valve from the pmvsd were included. We excluded patients with an infundibular defect, patients with pmvsd and prolapse of an aortic cusp, and patients with mal-aligned VSD. Parents gave their informed written consent to the procedure. The general characteristics of the patients are reported in Table 1. Devices and delivery systems used Two different Amplatzer devices (AGA Medical Corp) were used: the mvsd occluder (MVSD-O) and the pmvsd occluder (pmvsd-o) These devices have a woven mesh of 72 nitinol wires with shape memory. They are made of a in. nitinol wire with a polyester mesh inside. These devices and their delivery systems have been previously described. 16 Procedures Percutaneous closure of a VSD is performed under general anaesthesia with oro-tracheal intubation. Patients are given heparin 100 IU/kg and antibiotics intravenously. The procedure is performed under fluoroscopic and transoesophageal echocardiographic (TEE) control. Access is through the right internal jugular vein and right femoral artery for mid-muscular and apical VSD, whereas right femoral vein and left femoral artery accesses are used for high mvsd and pmvsd. Standard right and left cardiac catheterization, standard left ventriculography to study mvsd and pmvsd and angiography of the ascending aorta are performed in all cases. The size of the VSD and its relation to the aorta are confirmed. The diameter of the VSD is calculated by integrating data from TEE and angiographic measurements. A device 1 2 mm larger than the measured VSD diameter is chosen. The VSD is crossed from the left ventricle using a right coronary artery catheter (Cordis Corp., USA) or an Amplatzer right coronary catheter (Cordis Corp., USA), and an exchange floppy Terumo guidewire (Terumo Corp., Japan) advanced into the pulmonary artery or the superior or inferior vena cava. The wire is then snared (EV3, MN, USA) to establish an arteriovenous circuit. Procedures for mid-muscular (Figure 1), apical VSD, and high mvsd and pmvsd (Figures 2 and 3) have been previously reported in detail. 16 Early in our experience, we closed some cases of high mvsd with a.5 mm rim towards the aortic valve using a retrograde aortic approach and an mvsd-o. In these cases, the VSD is crossed from the left ventricle and the wire is placed in the apex of the right ventricle. The long sheath is advanced from the aorta through the VSD into the right ventricular apex. The device is advanced in the long sheath, and then the distal disc is opened in the right ventricle and withdrawn to the septum. The proximal disc is then opened, taking care to avoid any entrapment of the aortic valve with the disc of the device. Finally, the correct position is confirmed and the device is released. VSD analysis The diameter of the VSD was measured by TTE and TEE, using twodimensional imaging and colour flow Doppler on long- and short-axis views. The vertical diameter was measured during left ventricular angiography using the views described earlier. Table 1 The locations of the VSD are reported in Table 1. A ventricular septal aneurysm was present in 25 patients (28%). All subjects with an aneurysm had a pmvsd. Associated lesions were encountered in five subjects. Multiple defects were found in three patients. Residual shunt and valve regurgitation A residual shunt was considered to be present when colour Doppler flow mapping showed a left-to-right shunt across the interventricular septum. A shunt was defined trivial (,1 mm colour jet width), small (1 2 mm colour jet width), moderate (2 4 mm colour jet width), or large (.4 mm colour jet width). Valve regurgitation was evaluated by colour Doppler flow imaging in a standard way. Ten subjects had trivial aortic regurgitation. Seven out of 10 patients had a pmvsd. Twenty patients had trivial to mild tricuspid regurgitation. Finally, eight subjects had trivial to mild mitral regurgitation related to mitral annulus dilatation due to volume overload of the left ventricle. Follow-up General characteristics N 88 Sex (F/M) 48/40 Age (years) (range years) Weight (kg) ( kg) VSD location Perimembranous 56 patients High muscular 8 patients Mid-muscular 16 patients Apical 5 patients Multiple 3 patients (two mvsd and one pmvsd) All subjects underwent clinical examination, electrocardiography, chest X-rays, 24 h EKG-Holter monitoring, and TTE before discharge and at 1, 6, and 12 months after the procedure and yearly thereafter. Before discharge, urinalysis was performed to exclude haemolysis. Platelet anti-aggregation therapy with aspirin 5 mg/kg per day p.o. and endocarditis prophylaxis were prescribed for 6 months. Statistical methods Data are expressed as a frequency or percentage for nominal variables, as the median (range) for categorical variables and as the mean + SD for continuous variables. The STATISTIX package version 8 was used for the statistical computations. The following dependent outcome variables were analyzed: total complications, complete atrioventricular block (cavb), device embolization, and vascular complications. The following independent variables were included in the analysis: age, weight, gender, defect type (congenital, residual post-surgery), defect position (perimembranous, muscular), device type (muscular Amplatzer device, eccentric Amplatzer device), device diameter, complex procedures (yes/no), multiple defects (yes/no), ventricular septal aneurysm (yes/no), device diameter/defect diameter measured on TTE, and device diameter/patient weight. Univariate analysis was performed using the x 2 test, Fisher s exact test, unpaired Student s t-test, Wilcoxon rank sum test, one-way ANOVA, the Kruskall Wallis test, log-rank test, and Cox regression analysis, as appropriate. Multivariable analysis to study risk factors for the occurrence of early complications was performed using multiple logistic regression analysis. The regression model diagnostic was performed by obtaining the standardized residuals and Cook s D-values and examining them using Wilk Shapiro and rankit plot tests. Independent
3 Percutaneous closure of VSDs 2891 Figure 1 Percutaneous closure of an mvsds. Top right: the angiogram demonstrates a single mid-mvsd; top left: a cine angiogram demonstrating snaring of the guide-wire passed from the left ventricle up to the superior vena cava; low right: the long sheath is in the ascending aorta coming from the right ventricle through the VSD; low left: left ventriculography showing almost complete VSD closure. variables with a P-value,0.2 in the univariate analysis were included in the multivariable model. Odds ratios (OR) and their 95% confidence intervals were calculated for independent variables included in the multivariable model. Multivariable analysis using Cox s proportional hazard regression analysis was performed to study the role of independent variables on the occurrence of cavb in the early period and during the follow-up. Evaluation of proportional hazards assumption was performed by using the goodness of fit testing approach. All tests were two sided. A probability value of P, 0.05 was considered statistically significant. Results Procedural data During the period of the study, all subjects with the inclusion criteria were sent to the catheterization laboratory with the intention to treat the defect percutaneously (Table 2). In 83 of 88 patients, the defect was successfully closed (94%). In four subjects, the procedure was aborted (see section on Complications for details) and one subject was sent for surgery after device embolization (see section on Complications for details). An internal jugular venous approach was used in 23 subjects, whereas a venous femoral access was used in 65. Complex procedures Complex procedures (combined procedures, hybrid procedures, closure of multiple VSD, post-surgical residual VSD) were performed in 17 children (19%). Five subjects underwent combined procedures: pulmonary valve dilatation in two subjects, atrial septal defect closure in one, patent ductus arteriosus in one, and atrial septal defect and small patent ductus arteriosus closure in one. Hybrid procedures were performed in three patients. Two subjects underwent VSD closure before surgical debanding of the pulmonary artery and one before repair of aortic coarctation. One of these subjects had multiple defects that were closed using two devices. Two more subjects were treated for multiple VSD. Finally, seven patients underwent percutaneous closure of a post-surgical residual VSD. Two of these were treated in an acute setting since they could not be weaned from mechanical support. Five more subjects were treated electively. These patients had undergone surgery, a median of 1.5 years (range: 7 months 4.5 years), before the percutaneous procedure. Complications Early post-procedural complications No deaths occurred. In five subjects, the procedure was aborted. In two patients (two 8-year-old girls with
4 2892 G. Butera et al. Figure 2 Percutaneous closure of a pmvsd. Left: the angiogram demonstrates a single pmvsd and left ventricular overload; middle: snaring of the guide-wire passed from the left ventricle in the left pulmonary artery; right: cine image showing the position of the delivery sheath in the apex of the left ventricle. Figure 3 Percutaneous closure of a pmvsd. Right: left ventricular angiogram after device release, showing good device position and no residual shunt. Note the platinum marker located in the left ventricular disk pointing towards the left ventricular apex; left: an ascending aortic angiogram demonstrating no aortic regurgitation. Table 2 Procedural data and devices used Fluoroscopic time (min) (range ) Procedure time (min) (range ) Qp/Qs (range 1.5 4) Systolic PA pressure (mmhg) Mean PA pressure (mmhg) VSD diameter on TTE (mm) (range ) Mean size of the device (range 4 16) used (mm) [(Device diameter)/(vsd % (range ) diameter on TTE)]*100 Types of devices used mvsd-o 30 patients pmvsd-o 53 patients Multiple devices 3 patients Qp/Qs, pulmonary-to-systemic flow ratio; PA, pulmonary artery. mal-aligned pmvsd), it was impossible to obtain a stable position of the device, which was retrieved before unscrewing it. One 6-month-old girl was sent for surgery after device embolization to the pulmonary artery; this baby had previously undergone an operation to correct aortic coarctation. These subjects were treated very early in our experience and it is possible that there was an error in their selection or a lack in operator s experience. In two patients with pmvsd (a 3.5-year-old female and a 6-year-old boy), cavb developed during manoeuvres of the catheter or Terumo guide-wire. The procedure was stopped in both subjects, and they both recovered sinus rhythm within 1 2h. A total of 13 significant complications occurred (14.7%). These were device embolization (n ¼ 4), vascular complications (n ¼ 3), and rhythm abnormalities (n ¼ 6). However, in all but one child (1.1%) who needed pacemaker implantation, these were transient complications and the patients had no sequelae. Univariate analysis showed that no variable predicted the occurrence of early complications. Only two variables showed a trend towards significance (device diameter/ patient weight: no complication vs. complication ; P ¼ 0.06; device measure: no complication mm vs. complication ; P ¼ 0.09). In the multivariable model, defect position (P ¼ 0.15) was also included. However, no risk factors were found. Device embolization This complication occurred in four patients (4.5%). In one already described case with a large mvsd, the patient was sent to surgery. In three other cases, the device was
5 Percutaneous closure of VSDs 2893 recaptured in the right pulmonary artery (two cases) or in the descending aorta (one case) using a goose-neck snare and a Mullins long sheath. In these cases, a larger device was chosen and successfully implanted. The occurrence of device embolization was not related to any of the independent variables studied. Vascular complications Femoral arterial thrombosis occurred in three patients (3.4%). In a 4-year-old girl (18 kg), vascular surgery of the femoral artery was needed for safe removal of a 10 Fr arterial sheath used to recapture an 8 mm PMVSD-O device that had embolized in the descending aorta. In two 1-year-old girls (7.5 and 7 kg), thrombolysis with r-tpa was successful. The occurrence of vascular complications was not related to any of the independent variables studied. Arrhythmic complications Significant arrhythmias occurred in six patients with a pmvsd (6.8%). cavb occurred during the procedure in two subjects in whom the procedure was aborted (described in the section on Early post-procedural complications). cavb occurred soon after device release in two subjects with a pmvsd. In one child (a 2-year-old boy, 10 mm PMVSD-O), it was a transient event, whereas in the second (a 3.4-year-old girl), it persisted for some hours after implantation of a 10 mm PMVSD-O. The girl was sent for surgery and recovered stable sinus rhythm after surgical closure and device removal. cavb developed 24 h after implantation of a 12 mm PMVSD-O in a 2-year-old boy. A permanent pacemaker was implanted into this child who has recovered stable sinus rhythm during follow-up. Finally, a 3.4-year-old boy treated with an 8 mm PMVSD-O developed cavb 5 days after the procedure. He had a heart rate of 50 b.p.m. and was asymptomatic. We decided to treat him with corticoid therapy (1 mg/kg) for 2 weeks. The cavb disappeared completely, and he is still in stable sinus rhythm 8 months after the procedure. Transient minor complications Transient atrial fibrillation occurred in one 5-year-old boy: no treatment was needed. A transient right bundle branch block occurred in three subjects, whereas a transient left bundle branch block occurred in two other patients. Three subjects developed moderate groin haematoma. Transient, mild haemolysis was recorded in two subjects, but resolved spontaneously within 48 h after the procedure. Valve regurgitation and residual shunts Pre-operative aortic, tricuspid or mitral valve regurgitation remained unchanged after the procedure. No significant new regurgitation of valves occurred. A trivial intraprosthetic residual shunt was present in 28 subjects (33%) at the end of the procedure. At discharge, 12 patients (14%) showed a tiny residual shunt and none had signs of haemolysis. TTE at 1, 6 and 12 months showed a trivial residual shunt in one patient (1.2%) due to a small fenestration within the aneurysm. Hospital stay All subjects in whom the percutaneous procedure was uneventful stayed in hospital for 2 days after the procedure. In cases with minor arrhythmic abnormalities, even transient bundle branch blocks, the hospital stay was prolonged to 72 h. The mean hospital stay was days. Follow-up Follow-up data were obtained from all patients. The median duration of follow-up was 24 months (range 3 66 months). No deaths or cases of endocarditis occurred. Patients with failure to thrive had complete recovery of growth (from the 10th percentile up to the 50th percentile during the follow-up). Subjects with frequent respiratory infections had no significant recurrences. Left ventricular dimensions returned to normal in all subjects but one. During the entire follow-up period, three subjects developed cavb. Two of these three experienced syncope (a 4-year-old boy and a 1.2-year-old girl both treated with an 8 mm PMVSD-O) due to paroxysmal cavb, 4 and 20 months after procedure, respectively. Another patient (a 2.7-year-old boy treated with a 12 mm PMVSD-O) developed asymptomatic cavb with a heart rate of 40 b.p.m. 12 months after defect closure. An endocardial ventricular pacemaker was implanted into all these subjects. Analysis of risk factors for the occurrence of cavb A total of nine patients experienced cavb during the period of the study. All of them had a pmvsd. This rhythm abnormality occurred early in six patients, whereas in three it was a late event. Pacemaker implantation was needed in 17% of the cases of early cavb (1/6) and in 100% of the cases of late cavb (3/3). Univariate analysis showed that the following variables were significantly associated with the occurrence of cavb: VSD location (pmvsd: 9/56 vs. mvsd: 0/32; P ¼ 0.02) and age (Cox regression analysis: P ¼ 0.033; relative risk: 0.62). In patients with pmvsd, the occurrence of cavb was not associated with either the ratio of the device measure to VSD diameter measured on TTE (Cox regression analysis: P ¼ 0.9) or the presence of aneurysm of the ventricular septum (Log-rank test: P ¼ 0.9). In multivariable analysis, other than age, patient s weight was included. However, only age was statistically correlated to the occurrence of cavb during follow-up (P ¼ 0.028; relative risk: 0.25). The site of the VSD was not entered into this model because cavb did not occur in any patients with an mvsd. Discussion VSDs account for 20% of all forms of congenital hearts defects. 21 The majority of VSD (60%) is perimembranous or membranous. mvsds account for 15% of VSD. Children with volume overload of the left chamber due to a VSD require closure of the defect in order to prevent ventricular dilatation and dysfunction, arrhythmias, aortic regurgitation, pulmonary arterial hypertension, endocarditis, or a double-chambered right ventricle. 22 Surgery is the gold standard for VSD closure, and there is a large body of data about surgical VSD closure in children. Although this is generally a safe procedure, it does have some potential risks, including cavb in 1 5%, 1,2,6,8 significant residual VSD in 1 10%, 1,3 5 the necessity for re-operation in 2%, 1 and even death in 0.6 5%. 1,4 7
6 2894 G. Butera et al. Furthermore, infections, tachy-arrhythmias, and neurological complications may occur. 1 In the last decade, percutaneous approaches to the closure of VSD have been developed However, only the recent introduction of Amplatzer mvsd-o and pmvsd-o has increased the number of subjects in whom percutaneous closure is feasible Although there are various reports about percutaneous closure of VSD, there is a lack of data on the safety, feasibility, and efficacy of percutaneous VSD closure in children. Literature data about percutaneous VSD closure are reported in Table In our series of 88 children, the percutaneous procedure was achieved successfully in 94%. Early complications occurred in 13 subjects (14.7%). However, in all but one case (1.1%), the complications were transient and the patients had no sequelae. Multivariable analysis showed that no variable predicted the occurrence of early complications. There were no serious complications related to the closure of mvsds either early or late after the procedure. The only serious concern of percutaneous VSD closure is the occurrence of cavb. This complication required pacemaker implantation in four subjects (4.5%) with pmvsd in our series. The cavb rates reported in the literature are very low, but it should be noted that only early post-procedural results have been published. In our series, the median follow-up was 24 months and cavb was a late event in three out of the four subjects requiring pacemaker implantation. In multivariable analysis, the only variable associated with the occurrence of cavb was age at procedure. In particular, the relative risk was 0.25, showing that younger subjects were at higher risk for the occurrence of cavb. Although, some authors have underlined that an oversized device is a risk factor for the occurrence of cavb, in particular, in subjects with pmvsd, this was not confirmed by our data. Finally, some authors 32 have suggested that a course of steroids should be used in an effort to avoid Table 3 Literature on percutaneous VSD closure Type of defect No. of patients Age at procedure (years) Success rate (%) pacemaker implantation. We used this approach successfully in one subject. However, although this therapy may be useful in an acute setting, we believe it is unlikely to be useful for late events occurring during the follow-up. It should be appreciated that cavb block can also occur after surgical closure of a VSD; indeed, this complication develops in about 1 5% of subjects so treated. 1,2,6,8 However, compared with surgery in which cavb usually appears early after the operation, in patients treated percutaneously, the occurrence of cavb is quite unpredictable and it is usually a late problem. This complication is related to the proximity of the conduction system to the margins of the pmvsd. Therefore, both surgery and device implantation may interfere with atrioventricular conduction. Various mechanisms may be considered as causative. It is possible that the presence of the device may disturb atrioventricular conduction by direct traumatic compression. Furthermore, the device may give rise to an inflammatory reaction or scar formation in the conduction tissue. However, there are no direct data about the mechanisms involved in the occurrence of cavb after percutaneous closure of a pmvsd. Large studies are needed to clarify the real impact of arrhythmic problems in these patients and the mechanism of the events. Clinical implications The percutaneous technique of VSD closure is widely appreciated by patients and their parents because it has less psychological impact (given the absence of a skin scar), the time spent in hospital is shorter, the procedure causes less pain and discomfort, and there is no need for admission to an intensive care unit. In the current era, percutaneous VSD closure provides a valuable alternative to surgery even in cases with complex morphology and in very young children. However, the decision to perform percutaneous closure of pmvsd in young subjects must be carefully weighed, given the challenging nature of this technique and the risk of Major complication (%) Description c-avb needing PM (%) Hijazi et al. 25 pmvsd / 0 / Bass et al. 15 pmvsd Acute aortic 0 / regurgitation: 1 patient Thanopoulos et al. 26 pmvsd / 0 3 Thanopoulos et al. 27 mvsd / Arora et al. 28 mvsd and cavb: 2 patients 1.9 / pmvsd Masura et al. 29 pmvsd Transient cavb: 0 / 2 patients Hijazi 16 mvsd Death: 2 patients 0 / Stroke: 1 patient Device embolization: 2 patients Cardiac perforation: 1 patient Hijazi et al. 30 mvsd / 0 / Pedra et al. 31 pmvsd / 0 3 Follow-up (months)
7 Percutaneous closure of VSDs 2895 cavb. Finally, due to the late occurrence of cavb, careful monitoring of rhythm and atrioventricular conduction is mandatory during the follow-up. Study limitations First of all, only in very experienced hands can these techniques be carried out safely and complications managed in the proper way. Furthermore, highly specialized surgical back-up must always be available. Secondly, although the techniques of percutaneous closure appear to be safe in the medium-term follow-up, it is not known whether they are safe in the very long-term, whereas the long-term safety and efficacy of surgery are well documented. Conclusions The percutaneous technique of closing VSD in children, even very young and symptomatic ones, is associated with excellent success and closure rates, no mortality, and low morbidity. In current day practice, percutaneous closure of muscular and perimembranous defects is a valuable alternative to surgery. Longer follow-up data and improvements in device characteristics are needed to reduce the risk of cavb. Conflict of interest: none declared. References 1. Mavroudis C, Backer CL, Jacobs JP. Ventricular septal defect. Pediatric Cardiac Surgery. 3rd ed. Mosby, Inc.; p Ross-Hesselink JW, Mejiboom FJ, Spitaels SEC, Van Domberg R, Van Rijen EH, Utens EM, Bogers AJ, Simons ML. Outcome of patients after surgical closure of ventricular septal defect at young age: longitudinal follow-up of years. Eur Heart J 2004;24: Kitagawa T, Durham LA, Mosca RS, Bove EL. Techniques and results in the management of multiple ventricular septal defects. J Thorac Cardiovasc Surg 1998;115: Wollenek G, Wyse R, Sullivan I, Elliot M, de Leval M, Stark J. Closure of muscular ventricular septal defects through a left ventriculotomy. Eur J Cardiothorac Surg 1996;10: Serraf A, Lacour-Gayet F, Bruniaux J, Ouaknine R, Losay J, Petit J, Binet JP, Planche C. Surgical management of isolated multiple ventricular septal defects: logical approach in 130 cases. J Thorac Cardiovasc Surg 1992;103: Hobbins SM, Izukawa T, Radford DJ, Williams WG, Trusler GA. Conduction disturbances after surgical correction of ventricular septal defect by the atrial approach. Br Heart J 1979;41: Backer CL, Winters RC, Zales VR, Takami H, Muster AJ, Benson DW, Mavroudis C. The restrictive muscular ventricular septal defect: how small is too small to close? Ann Thorac Surg 1993;56: Bol-Raap G, Weerheim J, Kappetein AP, Witsenburg M, Bogers AJ. Follow-up after surgical closure of congenital ventricular septal defects. Eur J Cardiothorac Surg 2003;24: Chessa M, Carminati M, Butera G, Bini RM, Drago M, Rosti L, Giamberti A, Pomè G, Bossone E, Carminati M. Early and late complications associated with transcatheter occlusion of secundum atrial septal defect. JACC 2002;39: Du Zhong-Dong, Hijazi Z, Kleinman CS, Silverman NH, Lamtz K, for the Amplatzer Investigators. Comparison between transcatheter and surgical closure of secundum atrial septal defect in children and adults. JACC 2002;39: Faella HJ, Hijazi Z. Closure of the patent ductus arteriosus with the Amplatzer PDA device: immediate results of the international clinical trial. Cathet Cardiovasc Intervent 2000;51: Pass RH, Hijazi Z, Hsu DT, Lewis V, Hellenbrand WE. Multicenter USA Amplatzer patent ductus arteriosus occlusion device trial. JACC 2004;44: Butera G, De Rosa G, Chessa M, Rosti L, Negura G, Piazza L, Giamberti A, Bossone E, Carminati M. Transcatheter closure of atrial septal defect in young children. Results follow-up JACC 2003;42: Butera G, De Rosa G, Chessa M, Piazza L, Delogu A, Frigiola A, Carminati M. Transcatheter closure of persistent ductus arteriosus with the Amplatzer duct occluder in very young symptomatic children. Heart 2004;90: Bass JL, Kalra GS, Arora R, Masura J, Gavora P, Thanoupoulos B, Torres W, Sievert H, Carminati M, Fisher G, Ewert P. Initial human experience with the Amplatzer perimembranous ventricular septal occluder device. Cathet Cardiovasc Intervent 2003;58: Hijazi Z. Device closure of ventricular septal defects. Cathet Cardiovasc Intervent 2003;60: Holzer R, Balzer D, Qi-Ling C, Lock K, Hijazi Z for the Amplatzer Muscular Ventricular Septal Defect Investigators. Device closure of muscular ventricular septal defects using the Amplatzer muscular ventricular septal defect occluder. JACC 2004;43: Chessa M, Carminati M, Cao QL, Butera G, Giusti S, Bini RM, Hijazi Z. Transcatheter closure of congenital and acquired ventricular septal defects using the Amplatzer occluder. J Invasive Cardiol 2002;14: Burgio GR. Il bambino con infezioni ricorrenti. In: Plebani A, ed., Immunologia Pediatrica. Mc Graw Hill Libri Italia Milano; p Hamil PV, Drizd TA, Johnson CL, Reed RB, Roche AF, Moore WM. Physical growth: National Center for Health Statistics percentiles. Am J Clin Nutr 1979;32: Rudolph AM. Ventricular septal defect. In: Rudolph AM, ed., Congenital Diseases of the Heart: Clinical-Physiological Considerations. 2nd ed. Armonk, NY: Futura Publishing Company; p Kidd L, Discroll DJ, Gersony WH, Hayes CJ, Keane JF, O Follon WM, Pieroni DR, Wolfe RR, Weidman WH. Second natural history study of congenital heart defects: results of treatment of patients with ventricular septal defects. Circulation 1993;87(Suppl. I): Lock JE, Block PC, McKay RG, Baim DS, Keane JF. Transcatheter closure of ventricular septal defects. Circulation 1988;78: Kalra GS, Verma PK, Dhall A, Singh S, Arora R. Transcatheter device closure of ventricular septal defects: immediate results and intermediate-term follow-up. Am Heart J 1999;138: Hijazi Z, Hakim F, Haweleh AA, Madani A, Tarawna H, Hiari A, Cao QL. Catheter closure of perimembranous ventricular septal defects using the new Amplatzer membranous VSD occluder: initial clinical experience. Cathet Cardiovasc Interv 2002;56: Thanopoulos BD, Tsaousis GS, Karanasios E, Eleftherakis NG, Paphitis C. Transcatheter closure of perimembranous ventricular septal defects with the Amplatzer asymmetric ventricular septal defect occluder: preliminary experience in children. Heart 2003;89: Thanopoulos BD, Tsaousis GS, Konstadopoulou GN, Zarayelyan AG. Transcatheter closure of muscular ventricular septal defects with the Amplatzer ventricular septal defect occluder: preliminary experience in children. J Am Coll Cardiol 1999;33: Arora R, Trehna V, Kumar A, Kalra GS, Nigam M. Transcatheter closure of congenital ventricular septal defects: experience with various devices. J Interv Cardiol 2003;16: Masura J, Gao W, Gavora P, Sun K, Zhan AO, Jiang S, Tiang-Liang C, Wang Y. Percutaneous closure of perimembranous ventricular septal defects with the eccentric Amplatzer device: multicenter follow-up study. Pediatr Cardiol 2005;26: Hijazi ZM, Hakim F, Al Fadley F, Abdelhamid J, Cao QL. Transcatheter closure of single muscular ventricular septal defects using the Amplatzer muscular VSD occluder: initial results and technical considerations. Cathet Cardiovasc Interv 2000;49: Pedra AC, Pedra SRF, Esteves CA, Pontes SC, Braga SL, Arrieta SR, Santana MV, Fontes VF, Masura J. Percutaneous closure of perimembranous ventricular septal defects with the Amplatzer device: technical and morphological considerations. Cathet Cardiovasc Interv 2004;61: Yip WC, Zimmermann F Hijazi ZM. Heart block and empirical therapy after transcatheter closure of perimembranous ventricular septal defect. Catheter Cardiovasc Interv 2005;66:
Percutaneous VSD closure
 Percutaneous VSD closure Gianfranco Butera San Donato Milanese - Italy Patients selection Pts having hemodynamically significant VSD Left ventricular enlargement (left ventricular overload),defined as
Percutaneous VSD closure Gianfranco Butera San Donato Milanese - Italy Patients selection Pts having hemodynamically significant VSD Left ventricular enlargement (left ventricular overload),defined as
Transcatheter Closure of Atrial Septal Defect in Young Children Results and Follow-Up
 Journal of the American College of Cardiology Vol. 42, No. 2, 2003 2003 by the American College of Cardiology Foundation ISSN 0735-1097/03/$30.00 Published by Elsevier Inc. doi:10.1016/s0735-1097(03)00589-8
Journal of the American College of Cardiology Vol. 42, No. 2, 2003 2003 by the American College of Cardiology Foundation ISSN 0735-1097/03/$30.00 Published by Elsevier Inc. doi:10.1016/s0735-1097(03)00589-8
Risk Factors and Outcomes of Post-Procedure Heart Blocks After Transcatheter Device Closure of Perimembranous Ventricular Septal Defect
 JACC: CARDIOVASCULAR INTERVENTIONS VOL. 5, NO. 4, 2012 2012 BY THE AMERICAN COLLEGE OF CARDIOLOGY FOUNDATION ISSN 1936-8798/$36.00 PUBLISHED BY ELSEVIER INC. DOI: 10.1016/j.jcin.2012.01.015 Risk Factors
JACC: CARDIOVASCULAR INTERVENTIONS VOL. 5, NO. 4, 2012 2012 BY THE AMERICAN COLLEGE OF CARDIOLOGY FOUNDATION ISSN 1936-8798/$36.00 PUBLISHED BY ELSEVIER INC. DOI: 10.1016/j.jcin.2012.01.015 Risk Factors
Perimembranous ventricular septal defects (pmvsds) are
 Transcatheter Closure of Congenital Perimembranous Ventricular Septal Defect in Children Using Symmetric Occluders: An 8-Year Multiinstitutional Experience Lei Wang, MD, PhD,* Sancheng Cao, MD, Jun Li,
Transcatheter Closure of Congenital Perimembranous Ventricular Septal Defect in Children Using Symmetric Occluders: An 8-Year Multiinstitutional Experience Lei Wang, MD, PhD,* Sancheng Cao, MD, Jun Li,
Percutaneous Device Closure of Congenital VSDs Current techniques and results for treating ventricular septal defects.
 Percutaneous Device Closure of Congenital VSDs Current techniques and results for treating ventricular septal defects. BY KARIM A. DIAB, MD; QI-LING CAO, MD; AND ZIYAD M. HIJAZI, MD, MPH During the past
Percutaneous Device Closure of Congenital VSDs Current techniques and results for treating ventricular septal defects. BY KARIM A. DIAB, MD; QI-LING CAO, MD; AND ZIYAD M. HIJAZI, MD, MPH During the past
Transcatheter closure of congenital ventricular septal defects: results of the European Registry
 European Heart Journal (2007) 28, 2361 2368 doi:10.1093/eurheartj/ehm314 Clinical research Congenital heart disease Transcatheter closure of congenital ventricular septal defects: results of the European
European Heart Journal (2007) 28, 2361 2368 doi:10.1093/eurheartj/ehm314 Clinical research Congenital heart disease Transcatheter closure of congenital ventricular septal defects: results of the European
Type Size AP/PS RP/RS Qp/Qs. Ia Resistive <0.3 < Ib Resistive <0.3 < IIa Resistive <0.5 >2
 Transcatheter closure of VSD using Duct Occluder device Nguyen Lan Hieu, MD, PhD Hanoi Medical University Vietnam Heart Institute Anatomy of VSD 1. Perimembranous VSD: Aneurysm septal membranous(tv or
Transcatheter closure of VSD using Duct Occluder device Nguyen Lan Hieu, MD, PhD Hanoi Medical University Vietnam Heart Institute Anatomy of VSD 1. Perimembranous VSD: Aneurysm septal membranous(tv or
Atrial Septal Defect Closure. Stephen Brecker Director, Cardiac Catheterisation Labs
 Stephen Brecker Director, Cardiac Catheterisation Labs ADVANCED ANGIOPLASTY Incorporating The Left Main 5 Plus Course Conflicts of Interest The following companies have supported educational courses held
Stephen Brecker Director, Cardiac Catheterisation Labs ADVANCED ANGIOPLASTY Incorporating The Left Main 5 Plus Course Conflicts of Interest The following companies have supported educational courses held
Device closure of congenital ventricular septal defects with Amplatzer devices: first experiences in Turkey
 The Turkish Journal of Pediatrics 2008; 50: 106-113 Original Device closure of congenital ventricular septal defects with Amplatzer devices: first experiences in Turkey Alpay Çeliker, Süheyla Özkutlu,
The Turkish Journal of Pediatrics 2008; 50: 106-113 Original Device closure of congenital ventricular septal defects with Amplatzer devices: first experiences in Turkey Alpay Çeliker, Süheyla Özkutlu,
CONGENITAL HEART DEFECTS IN ADULTS
 CONGENITAL HEART DEFECTS IN ADULTS THE ROLE OF CATHETER INTERVENTIONS Mario Carminati CONGENITAL HEART DEFECTS IN ADULTS CHD in natural history CHD with post-surgical sequelae PULMONARY VALVE STENOSIS
CONGENITAL HEART DEFECTS IN ADULTS THE ROLE OF CATHETER INTERVENTIONS Mario Carminati CONGENITAL HEART DEFECTS IN ADULTS CHD in natural history CHD with post-surgical sequelae PULMONARY VALVE STENOSIS
Efficacy and Safety of Using Amplatzer Ductal Occluder for Transcatheter Closure of Perimembranous Ventricular Septal Defect in Pediatrics
 Iran J Pediatr. 2015 April; 25(2):e386. Published online 2015 April 18. DOI: 10.5812/ijp.386 Research Article Efficacy and Safety of Using Amplatzer Ductal Occluder for Transcatheter Closure of Perimembranous
Iran J Pediatr. 2015 April; 25(2):e386. Published online 2015 April 18. DOI: 10.5812/ijp.386 Research Article Efficacy and Safety of Using Amplatzer Ductal Occluder for Transcatheter Closure of Perimembranous
Percutaneous VSD closure: Problems in the mid- and long-term
 Percutaneous VSD closure: Problems in the mid- and long-term Lee Benson MD Professor Pediatrics (Cardiology) Director, Cardiac Diagnostic & Interventional Unit The Hospital for Sick Children Toronto, Canada
Percutaneous VSD closure: Problems in the mid- and long-term Lee Benson MD Professor Pediatrics (Cardiology) Director, Cardiac Diagnostic & Interventional Unit The Hospital for Sick Children Toronto, Canada
Hybrid Muscular VSD Closure in Small Weight Children
 Hybrid Muscular VSD Closure in Small Weight Children Shakeel A Qureshi, on behalf of: John P. Cheatham, MD George H. Dunlap Endowed Chair in Interventional Cardiology Director Cardiac Catheterization &
Hybrid Muscular VSD Closure in Small Weight Children Shakeel A Qureshi, on behalf of: John P. Cheatham, MD George H. Dunlap Endowed Chair in Interventional Cardiology Director Cardiac Catheterization &
Ventricular septal defects (VSD) are one of the most
 Treatment of Isolated Ventricular Septal Defects in Children: Amplatzer Versus Surgical Closure Pierre Oses, MD, Nicolas Hugues, MD, Nagib Dahdah, MD, Suzanne J. Vobecky, MD, Joaquim Miro, MD, Michel Pellerin,
Treatment of Isolated Ventricular Septal Defects in Children: Amplatzer Versus Surgical Closure Pierre Oses, MD, Nicolas Hugues, MD, Nagib Dahdah, MD, Suzanne J. Vobecky, MD, Joaquim Miro, MD, Michel Pellerin,
Transcatheter closure of the patent ductus arteriosus using the new Amplatzer duct occluder: Initial clinical applications in children
 Transcatheter closure of the patent ductus arteriosus using the new Amplatzer duct occluder: Initial clinical applications in children Basil Thanopoulos, MD, PhD, a Nikolaos Eleftherakis, MD, a Konstantinos
Transcatheter closure of the patent ductus arteriosus using the new Amplatzer duct occluder: Initial clinical applications in children Basil Thanopoulos, MD, PhD, a Nikolaos Eleftherakis, MD, a Konstantinos
IMAGES. in PAEDIATRIC CARDIOLOGY. Abstract
 IMAGES in PAEDIATRIC CARDIOLOGY Images Paediatr Cardiol. 2008 Apr-Jun; 10(2): 11 17. PMCID: PMC3232589 Transcatheter closure of symptomatic aortopulmonary window in an infant F Pillekamp, 1 T Hannes, 1
IMAGES in PAEDIATRIC CARDIOLOGY Images Paediatr Cardiol. 2008 Apr-Jun; 10(2): 11 17. PMCID: PMC3232589 Transcatheter closure of symptomatic aortopulmonary window in an infant F Pillekamp, 1 T Hannes, 1
Journal of the American College of Cardiology Vol. 33, No. 5, by the American College of Cardiology ISSN /99/$20.
 Journal of the American College of Cardiology Vol. 33, No. 5, 1999 1999 by the American College of Cardiology ISSN 0735-1097/99/$20.00 Published by Elsevier Science Inc. PII S0735-1097(99)00011-X Transcatheter
Journal of the American College of Cardiology Vol. 33, No. 5, 1999 1999 by the American College of Cardiology ISSN 0735-1097/99/$20.00 Published by Elsevier Science Inc. PII S0735-1097(99)00011-X Transcatheter
Early and Late Complications Associated With Transcatheter Occlusion of Secundum Atrial Septal Defect
 Journal of the American College of Cardiology Vol. 39, No. 6, 2002 2002 by the American College of Cardiology Foundation ISSN 0735-1097/02/$22.00 Published by Elsevier Science Inc. PII S0735-1097(02)01711-4
Journal of the American College of Cardiology Vol. 39, No. 6, 2002 2002 by the American College of Cardiology Foundation ISSN 0735-1097/02/$22.00 Published by Elsevier Science Inc. PII S0735-1097(02)01711-4
Jian Fang 1, Shaobo Xie 2, Lunchao Ma 2, Chao Yang 2. Original Article
 Original Article Anatomic and surgical factors affecting the switch from minimally invasive transthoracic occlusion to open surgery during ventricular septal defect repair Jian Fang 1, Shaobo Xie 2, Lunchao
Original Article Anatomic and surgical factors affecting the switch from minimally invasive transthoracic occlusion to open surgery during ventricular septal defect repair Jian Fang 1, Shaobo Xie 2, Lunchao
How to assess an adult with a Ventricular Septal Defect. When it should be closed and how?
 TTE AND TEE VDS ASSESSMENT. WHAT S S THE SIZE, WHERE ARE THE MARGINS? How to assess an adult with a Ventricular Septal Defect. When it should be closed and how? Dr Gianfranco Butera, MD, PhD Dr Gianfranco
TTE AND TEE VDS ASSESSMENT. WHAT S S THE SIZE, WHERE ARE THE MARGINS? How to assess an adult with a Ventricular Septal Defect. When it should be closed and how? Dr Gianfranco Butera, MD, PhD Dr Gianfranco
Percutaneous atrial septal defect closure with the Occlutech Figulla Flex ASD Occluder.
 Percutaneous atrial septal defect closure with the Occlutech Figulla Flex ASD Occluder. First case with a novel delivery system. Werner Budts, Md, PhD, FESC Congenital and Structural Cardiology University
Percutaneous atrial septal defect closure with the Occlutech Figulla Flex ASD Occluder. First case with a novel delivery system. Werner Budts, Md, PhD, FESC Congenital and Structural Cardiology University
For Personal Use. Copyright HMP 2013
 Case Report J INVASIVE CARDIOL 2013;25(2):E42-E44 Percutaneous Closure of Iatrogenic Ventricular Septal Defect Following Surgical Aortic Valve Replacement Using Two Different Approaches Takashi Matsumoto,
Case Report J INVASIVE CARDIOL 2013;25(2):E42-E44 Percutaneous Closure of Iatrogenic Ventricular Septal Defect Following Surgical Aortic Valve Replacement Using Two Different Approaches Takashi Matsumoto,
CARDIAC INTERVENTIONS IN PEDIATRIC CARDIOLOGY: THE FUTURE
 CARDIAC INTERVENTIONS IN PEDIATRIC CARDIOLOGY: THE FUTURE Vikas Kohli From the: Senior Consultant Pediatric Cardiology, Apollo Centre of Advance Pediatrics, Indraprastha Apollo Hospitals, New Delhi-110044.
CARDIAC INTERVENTIONS IN PEDIATRIC CARDIOLOGY: THE FUTURE Vikas Kohli From the: Senior Consultant Pediatric Cardiology, Apollo Centre of Advance Pediatrics, Indraprastha Apollo Hospitals, New Delhi-110044.
Adult Echocardiography Examination Content Outline
 Adult Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 4 5 Anatomy and Physiology Pathology Clinical Care and Safety Measurement Techniques, Maneuvers,
Adult Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 4 5 Anatomy and Physiology Pathology Clinical Care and Safety Measurement Techniques, Maneuvers,
Case submission for CSI Asia-Pacific Case 2
 Case submission for CSI Asia-Pacific 2018- Case 2 Title Page Case category: Coarctation and ducts, valves Title: Simultaneous balloon aortic valvuloplasty with transcatheter closure of large hypertensive
Case submission for CSI Asia-Pacific 2018- Case 2 Title Page Case category: Coarctation and ducts, valves Title: Simultaneous balloon aortic valvuloplasty with transcatheter closure of large hypertensive
INTEGRATING ECHOCARDIOGRAPHY WITH CATHETER INTERVENTIONS FOR CONGENITAL HEART DISEASE. Krishna Kumar SevenHills Hospital, Mumbai, India
 INTEGRATING ECHOCARDIOGRAPHY WITH CATHETER INTERVENTIONS FOR CONGENITAL HEART DISEASE Krishna Kumar SevenHills Hospital, Mumbai, India Why talk about it? What is the big deal? Are we not stating the obvious?
INTEGRATING ECHOCARDIOGRAPHY WITH CATHETER INTERVENTIONS FOR CONGENITAL HEART DISEASE Krishna Kumar SevenHills Hospital, Mumbai, India Why talk about it? What is the big deal? Are we not stating the obvious?
ΔΙΑΧΕΙΡΙΣΗ ΑΣΘΕΝΩΝ ΜΕ ΜΕΣΟΚΟΛΠΙΚΗ ΕΠΙΚΟΙΝΩΝΙΑ ΖΑΧΑΡΑΚΗ ΑΓΓΕΛΙΚΗ ΚΑΡΔΙΟΛΟΓΟΣ ΗΡΑΚΛΕΙΟ - ΚΡΗΤΗ
 ΔΙΑΧΕΙΡΙΣΗ ΑΣΘΕΝΩΝ ΜΕ ΜΕΣΟΚΟΛΠΙΚΗ ΕΠΙΚΟΙΝΩΝΙΑ ΖΑΧΑΡΑΚΗ ΑΓΓΕΛΙΚΗ ΚΑΡΔΙΟΛΟΓΟΣ ΗΡΑΚΛΕΙΟ - ΚΡΗΤΗ European Accreditation in TTE, TEE and CHD Echocardiography NOTHING TO DECLARE ATRIAL SEPTAL DEFECT TYPES SECUNDUM
ΔΙΑΧΕΙΡΙΣΗ ΑΣΘΕΝΩΝ ΜΕ ΜΕΣΟΚΟΛΠΙΚΗ ΕΠΙΚΟΙΝΩΝΙΑ ΖΑΧΑΡΑΚΗ ΑΓΓΕΛΙΚΗ ΚΑΡΔΙΟΛΟΓΟΣ ΗΡΑΚΛΕΙΟ - ΚΡΗΤΗ European Accreditation in TTE, TEE and CHD Echocardiography NOTHING TO DECLARE ATRIAL SEPTAL DEFECT TYPES SECUNDUM
Case Report. Martin L. Bocks, MD and Aimee K. Armstrong, MD
 Catheterization and Cardiovascular Interventions 74:488 493 (2009) Case Report Novel Method for Delivering the Amplatzer 1 Muscular VSD Occluder in a Patient With Double Outlet Right Ventricle After Bidirectional
Catheterization and Cardiovascular Interventions 74:488 493 (2009) Case Report Novel Method for Delivering the Amplatzer 1 Muscular VSD Occluder in a Patient With Double Outlet Right Ventricle After Bidirectional
Perimembranous VSD: When Do We Ask For A Surgical Closure? LI Xin. Department of Cardiothoracic Surgery Queen Mary Hospital Hong Kong
 Perimembranous VSD: When Do We Ask For A Surgical Closure? LI Xin Department of Cardiothoracic Surgery Queen Mary Hospital Hong Kong Classification (by Kirklin) I. Subarterial (10%) Outlet, conal, supracristal,
Perimembranous VSD: When Do We Ask For A Surgical Closure? LI Xin Department of Cardiothoracic Surgery Queen Mary Hospital Hong Kong Classification (by Kirklin) I. Subarterial (10%) Outlet, conal, supracristal,
Congenital heart disease. By Dr Saima Ali Professor of pediatrics
 Congenital heart disease By Dr Saima Ali Professor of pediatrics What is the most striking clinical finding in this child? Learning objectives By the end of this lecture, final year student should be able
Congenital heart disease By Dr Saima Ali Professor of pediatrics What is the most striking clinical finding in this child? Learning objectives By the end of this lecture, final year student should be able
TRANSCATHETER CLOSURE OF PERSISTENT DUCTUS ARTERIOSUS USING THE AMPLATZER DUCT OCCLUDER IN INFANTS
 TRANSCATHETER CLOSURE OF PERSISTENT DUCTUS ARTERIOSUS USING THE AMPLATZER DUCT OCCLUDER IN INFANTS Al-Hakim FA 1, Harahsheh AS 2 & Hijazi IS 3 ABSTRACT Background: Despite technical improvements over the
TRANSCATHETER CLOSURE OF PERSISTENT DUCTUS ARTERIOSUS USING THE AMPLATZER DUCT OCCLUDER IN INFANTS Al-Hakim FA 1, Harahsheh AS 2 & Hijazi IS 3 ABSTRACT Background: Despite technical improvements over the
Echocardiographic Guidance During Placement of the Buttoned Double-Disk Device for Atrial Septa1 Defect Closure
 Echocardiographic Guidance During Placement of the Buttoned Double-Disk Device for Atrial Septa1 Defect Closure L. LUANN MINICH, M.D., and A. REBECCA SNIDER, M.D. Department of Pediatrics, C.S. Mott Children
Echocardiographic Guidance During Placement of the Buttoned Double-Disk Device for Atrial Septa1 Defect Closure L. LUANN MINICH, M.D., and A. REBECCA SNIDER, M.D. Department of Pediatrics, C.S. Mott Children
Secundum atrial septal defect (ASD) is a common congenital heart disease and
 Device closure of atrial septal defects with the Amplatzer septal occluder: Safety and outcome in infants Karim A. Diab, MD, a Qi-Ling Cao, MD, a Emile A. Bacha, MD, b and Ziyad M. Hijazi, MD, MPH a Objective:
Device closure of atrial septal defects with the Amplatzer septal occluder: Safety and outcome in infants Karim A. Diab, MD, a Qi-Ling Cao, MD, a Emile A. Bacha, MD, b and Ziyad M. Hijazi, MD, MPH a Objective:
Percutaneous closure of large VSD using a home-made fenestrated atrial septal occluder in 18-year-old with pulmonary hypertension
 Kamali et al. BMC Cardiovascular Disorders 2014, 14:74 CASE REPORT Percutaneous closure of large VSD using a home-made fenestrated atrial septal occluder in 18-year-old with pulmonary hypertension Hacer
Kamali et al. BMC Cardiovascular Disorders 2014, 14:74 CASE REPORT Percutaneous closure of large VSD using a home-made fenestrated atrial septal occluder in 18-year-old with pulmonary hypertension Hacer
Follow-up after VSD closure- what to look for?
 The 3rd Congress of Congenital heart disease Ventricular Septal Defect from A-Z January 9-11. 2013, Ho Chi Minh City, Vietnam Follow-up after VSD closure- what to look for? Nina Wunderlich University Hospital
The 3rd Congress of Congenital heart disease Ventricular Septal Defect from A-Z January 9-11. 2013, Ho Chi Minh City, Vietnam Follow-up after VSD closure- what to look for? Nina Wunderlich University Hospital
Paediatrica Indonesiana
 Paediatrica Indonesiana VOLUME 53 July NUMBER 4 Original Article Transcatheter vs. surgical closure of patent ductus arteriosus: outcomes and cost analysis Mulyadi M Djer, Mochammading, Mardjanis Said
Paediatrica Indonesiana VOLUME 53 July NUMBER 4 Original Article Transcatheter vs. surgical closure of patent ductus arteriosus: outcomes and cost analysis Mulyadi M Djer, Mochammading, Mardjanis Said
A case report: Percutaneous transcatheter treatment of Lutembacher syndrome
 A case report: Percutaneous transcatheter treatment of Lutembacher syndrome Dr. Sainath Hegde* Dr. Tukaram Aute** *Registrar, Dept of Cardiology, M.G.M Hospital, Aurangabad. **Asst. Prof, Dept of Cardiology,
A case report: Percutaneous transcatheter treatment of Lutembacher syndrome Dr. Sainath Hegde* Dr. Tukaram Aute** *Registrar, Dept of Cardiology, M.G.M Hospital, Aurangabad. **Asst. Prof, Dept of Cardiology,
Uptofate Study Summary
 CONGENITAL HEART DISEASE Uptofate Study Summary Acyanotic Atrial septal defect Ventricular septal defect Patent foramen ovale Patent ductus arteriosus Aortic coartation Pulmonary stenosis Cyanotic Tetralogy
CONGENITAL HEART DISEASE Uptofate Study Summary Acyanotic Atrial septal defect Ventricular septal defect Patent foramen ovale Patent ductus arteriosus Aortic coartation Pulmonary stenosis Cyanotic Tetralogy
Pathophysiology: Left To Right Shunts
 Pathophysiology: Left To Right Shunts Daphne T. Hsu, MD dh17@columbia.edu Learning Objectives Learn the relationships between pressure, blood flow, and resistance Review the transition from fetal to mature
Pathophysiology: Left To Right Shunts Daphne T. Hsu, MD dh17@columbia.edu Learning Objectives Learn the relationships between pressure, blood flow, and resistance Review the transition from fetal to mature
Diversion of the inferior vena cava following repair of atrial septal defect causing hypoxemia
 Marshall University Marshall Digital Scholar Internal Medicine Faculty Research Spring 5-2004 Diversion of the inferior vena cava following repair of atrial septal defect causing hypoxemia Ellen A. Thompson
Marshall University Marshall Digital Scholar Internal Medicine Faculty Research Spring 5-2004 Diversion of the inferior vena cava following repair of atrial septal defect causing hypoxemia Ellen A. Thompson
For Personal Use. Copyright HMP 2013
 Case Report With Brief Review J INVASIVE CARDIOL 2013;25(4):E78-E80 Percutaneous Transjugular Device Closure of Postoperative Residual Atrial Septal Defect Saktheeswaran Mahesh Kumar, MD, DM, Sasidharan
Case Report With Brief Review J INVASIVE CARDIOL 2013;25(4):E78-E80 Percutaneous Transjugular Device Closure of Postoperative Residual Atrial Septal Defect Saktheeswaran Mahesh Kumar, MD, DM, Sasidharan
Research Article A New Coated Nitinol Occluder for Transcatheter Closure of Ventricular Septal Defects in a Canine Model
 BioMed Research International Volume 2013, Article ID 507919, 7 pages http://dx.doi.org/10.1155/2013/507919 Research Article A New Coated Nitinol Occluder for Transcatheter Closure of Ventricular Septal
BioMed Research International Volume 2013, Article ID 507919, 7 pages http://dx.doi.org/10.1155/2013/507919 Research Article A New Coated Nitinol Occluder for Transcatheter Closure of Ventricular Septal
5.8 Congenital Heart Disease
 5.8 Congenital Heart Disease Congenital heart diseases (CHD) refer to structural or functional heart diseases, which are present at birth. Some of these lesions may be discovered later. prevalence of Chd
5.8 Congenital Heart Disease Congenital heart diseases (CHD) refer to structural or functional heart diseases, which are present at birth. Some of these lesions may be discovered later. prevalence of Chd
Transcatheter Closure of Atrial Septal Defects with Superior-anterior Rim Deficiency Using Amplatzer Septal Occluder
 ORIGINAL ARTICLE Transcatheter Closure of Atrial Septal Defects with Superior-anterior Rim Deficiency Using Amplatzer Septal Occluder Chien-Fu Huang, 1 Chih-Yuan Fang, 2 Sheung-Fat Ko, 3 Shao-Ju Chien,
ORIGINAL ARTICLE Transcatheter Closure of Atrial Septal Defects with Superior-anterior Rim Deficiency Using Amplatzer Septal Occluder Chien-Fu Huang, 1 Chih-Yuan Fang, 2 Sheung-Fat Ko, 3 Shao-Ju Chien,
HISTORY. Question: What category of heart disease is suggested by this history? CHIEF COMPLAINT: Heart murmur present since early infancy.
 HISTORY 18-year-old man. CHIEF COMPLAINT: Heart murmur present since early infancy. PRESENT ILLNESS: Although normal at birth, a heart murmur was heard at the six week check-up and has persisted since
HISTORY 18-year-old man. CHIEF COMPLAINT: Heart murmur present since early infancy. PRESENT ILLNESS: Although normal at birth, a heart murmur was heard at the six week check-up and has persisted since
Congenital heart disease: When to act and what to do?
 Leading Article Congenital heart disease: When to act and what to do? Duminda Samarasinghe 1 Sri Lanka Journal of Child Health, 2010; 39: 39-43 (Key words: Congenital heart disease) Congenital heart disease
Leading Article Congenital heart disease: When to act and what to do? Duminda Samarasinghe 1 Sri Lanka Journal of Child Health, 2010; 39: 39-43 (Key words: Congenital heart disease) Congenital heart disease
Transcatheter closure of atrial septal defects with transthoracic echocardiography
 Cardiology in the Young (2011), 21, 204 208 doi:10.1017/s1047951110001782 r Cambridge University Press, 2010 Original Article Transcatheter closure of atrial septal defects with transthoracic echocardiography
Cardiology in the Young (2011), 21, 204 208 doi:10.1017/s1047951110001782 r Cambridge University Press, 2010 Original Article Transcatheter closure of atrial septal defects with transthoracic echocardiography
IMAGES. in PAEDIATRIC CARDIOLOGY
 IMAGES in PAEDIATRIC CARDIOLOGY Images Paediatr Cardiol. 2005 Jan-Mar; 7(1): 12 17. PMCID: PMC3232568 Stent implantation for coarctation facilitated by the anterograde trans-septal approach N Sreeram and
IMAGES in PAEDIATRIC CARDIOLOGY Images Paediatr Cardiol. 2005 Jan-Mar; 7(1): 12 17. PMCID: PMC3232568 Stent implantation for coarctation facilitated by the anterograde trans-septal approach N Sreeram and
Transcatheter Closure Versus Repeat Surgery for the Treatment of Postoperative Left-to-Right Shunts: A Single Center 15-Year Experience
 Original Article Cardiol Res. 2017;8(6):286-292 Transcatheter Closure Versus Repeat Surgery for the Treatment of Postoperative Left-to-Right Shunts: A Single Center 15-Year Experience Xinghua Gu a, Qiuwang
Original Article Cardiol Res. 2017;8(6):286-292 Transcatheter Closure Versus Repeat Surgery for the Treatment of Postoperative Left-to-Right Shunts: A Single Center 15-Year Experience Xinghua Gu a, Qiuwang
Glenmark Cardiac Centre Mumbai, India
 ASD device closure: Long term follow up Bharat Dalvi, MD Glenmark Cardiac Centre Mumbai, India Our experience 1998 to 2011 1566 patients 912 patients > 4 years FU Exclusive with ASO Clinical, electrocardiographic
ASD device closure: Long term follow up Bharat Dalvi, MD Glenmark Cardiac Centre Mumbai, India Our experience 1998 to 2011 1566 patients 912 patients > 4 years FU Exclusive with ASO Clinical, electrocardiographic
Transcatheter closure of interatrial
 372 Br HeartJf 1994;72:372-377 PRACTICE REVIEWED Department of Paediatric Cardiology, Royal Brompton Hospital, London A N Redington M L Rigby Correspondence to: Dr A N Redington, Department of Paediatric
372 Br HeartJf 1994;72:372-377 PRACTICE REVIEWED Department of Paediatric Cardiology, Royal Brompton Hospital, London A N Redington M L Rigby Correspondence to: Dr A N Redington, Department of Paediatric
Implantation of Cardioverter Defibrillator After Percutaneous Closure of Atrial Septal Defect
 The Ochsner Journal 10:27 31, 2010 f Academic Division of Ochsner Clinic Foundation Implantation of Cardioverter Defibrillator After Percutaneous Closure of Atrial Septal Defect Anas Bitar, MD, Maria Malaya
The Ochsner Journal 10:27 31, 2010 f Academic Division of Ochsner Clinic Foundation Implantation of Cardioverter Defibrillator After Percutaneous Closure of Atrial Septal Defect Anas Bitar, MD, Maria Malaya
Pathophysiology: Left To Right Shunts
 Pathophysiology: Left To Right Shunts Daphne T. Hsu, MD dh17@columbia.edu Learning Objectives Learn the relationships between pressure, blood flow, and resistance Review the transition from fetal to mature
Pathophysiology: Left To Right Shunts Daphne T. Hsu, MD dh17@columbia.edu Learning Objectives Learn the relationships between pressure, blood flow, and resistance Review the transition from fetal to mature
Atrial Septal Defects
 Supplementary ACHD Echo Acquisition Protocol for Atrial Septal Defects The following protocol for echo in adult patients with atrial septal defects (ASDs) is a guide for performing a comprehensive assessment
Supplementary ACHD Echo Acquisition Protocol for Atrial Septal Defects The following protocol for echo in adult patients with atrial septal defects (ASDs) is a guide for performing a comprehensive assessment
Pediatric Echocardiography Examination Content Outline
 Pediatric Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 Anatomy and Physiology Normal Anatomy and Physiology 10% 2 Abnormal Pathology and Pathophysiology
Pediatric Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 Anatomy and Physiology Normal Anatomy and Physiology 10% 2 Abnormal Pathology and Pathophysiology
Transcatheter closure of patent foramen ovale using the internal jugular venous approach
 New methods in diagnosis and therapy Transcatheter closure of patent foramen ovale using the internal jugular venous approach Przemysław Węglarz 1,2, Ewa Konarska-Kuszewska 2, Tadeusz Zębik 2, Piotr Kuszewski
New methods in diagnosis and therapy Transcatheter closure of patent foramen ovale using the internal jugular venous approach Przemysław Węglarz 1,2, Ewa Konarska-Kuszewska 2, Tadeusz Zębik 2, Piotr Kuszewski
Intracardiac echocardiography: an ideal guiding tool for device closure of interatrial communications
 Eur J Echocardiography (2005) 6, 92e96 Intracardiac echocardiography: an ideal guiding tool for device closure of interatrial communications Thomas Bartel a, *, Thomas Konorza a, Ulrich Neudorf b, Tiko
Eur J Echocardiography (2005) 6, 92e96 Intracardiac echocardiography: an ideal guiding tool for device closure of interatrial communications Thomas Bartel a, *, Thomas Konorza a, Ulrich Neudorf b, Tiko
COMPLEMENTARY TECHNIQUES OF PERCUTANEOUS CLOSURE OF DUCTUS ARTERIOSUS USING DETACHABLE COOK COILS AND AMPLATZER DEVICES
 214 East African Medical Journal July 2013 East African Medical Journal Vol. 90 No. 7 July 2013 COMPLEMENTARY TECHNIQUES OF PERCUTANEOUS CLOSURE OF DUCTUS ARTERIOSUS USING DETACHABLE COOK COILS AND AMPLATZER
214 East African Medical Journal July 2013 East African Medical Journal Vol. 90 No. 7 July 2013 COMPLEMENTARY TECHNIQUES OF PERCUTANEOUS CLOSURE OF DUCTUS ARTERIOSUS USING DETACHABLE COOK COILS AND AMPLATZER
8 th International Workshop on Interventional Pediatric Cardiology Milan, March 31 st - April 2 nd 2011
 8 th International Workshop on Interventional Pediatric Cardiology Milan, March 31 st - April 2 nd 2011 MARCH 31 st 2011 7.15-7.50 REGISTRATION 7.50-8.00 WELCOME AND INTRODUCTION M. Carminati (Italy) 8.00-10.00
8 th International Workshop on Interventional Pediatric Cardiology Milan, March 31 st - April 2 nd 2011 MARCH 31 st 2011 7.15-7.50 REGISTRATION 7.50-8.00 WELCOME AND INTRODUCTION M. Carminati (Italy) 8.00-10.00
Original Policy Date
 MP 7.01.46 Transcatheter Closure of Patent Ductus Arteriosus Medical Policy Section Surgery Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature search/12:2013 Return
MP 7.01.46 Transcatheter Closure of Patent Ductus Arteriosus Medical Policy Section Surgery Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature search/12:2013 Return
AMPLATZER Septal Occluder
 AMPLATZER Septal Occluder A Patient s Guide to the Non-Surgical Closure of the Atrial Septal Defect Using the AMPLATZER Septal Occluder System leadership through innovation TM AGA Medical Corporation 5050
AMPLATZER Septal Occluder A Patient s Guide to the Non-Surgical Closure of the Atrial Septal Defect Using the AMPLATZER Septal Occluder System leadership through innovation TM AGA Medical Corporation 5050
Initial Human Experience. Objectives: To evaluate the feasibility, safety, and efficacy of the Occlutech VR
 Catheterization and Cardiovascular Interventions 00:00 00 (2015) Original Studies The New Occlutech V R PDA Occluder: Initial Human Experience M. A. Elbashier Abdelbasit, 1 * MBBS, MD, Mazeni Alwi, 1 MBBS,
Catheterization and Cardiovascular Interventions 00:00 00 (2015) Original Studies The New Occlutech V R PDA Occluder: Initial Human Experience M. A. Elbashier Abdelbasit, 1 * MBBS, MD, Mazeni Alwi, 1 MBBS,
Fabien Praz, Andreas Wahl, Sophie Beney, Stephan Windecker, Heinrich P. Mattle*, Bernhard Meier
 Procedural Outcome after Percutaneous Closure of Patent Foramen Ovale using the Amplatzer PFO Occluder Without Intra-Procedural Echocardiography in 1,000 Patients Fabien Praz, Andreas Wahl, Sophie Beney,
Procedural Outcome after Percutaneous Closure of Patent Foramen Ovale using the Amplatzer PFO Occluder Without Intra-Procedural Echocardiography in 1,000 Patients Fabien Praz, Andreas Wahl, Sophie Beney,
Notes by Sandra Dankwa 2009 HF- Heart Failure DS- Down Syndrome IE- Infective Endocarditis ET- Exercise Tolerance. Small VSD Symptoms -asymptomatic
 Congenital Heart Disease: Notes. Condition Pathology PC Ix Rx Ventricular septal defect (VSD) L R shuntsdefect anywhere in the ventricle, usually perimembranous (next to the tricuspid valve) 30% 1)small
Congenital Heart Disease: Notes. Condition Pathology PC Ix Rx Ventricular septal defect (VSD) L R shuntsdefect anywhere in the ventricle, usually perimembranous (next to the tricuspid valve) 30% 1)small
Clinical material and methods. Fukui Cardiovascular Center, Fukui, Japan
 Mitral Valve Regurgitation after Atrial Septal Defect Repair in Adults Shohei Yoshida, Satoshi Numata, Yasushi Tsutsumi, Osamu Monta, Sachiko Yamazaki, Hiroyuki Seo, Takaaki Samura, Hirokazu Ohashi Fukui
Mitral Valve Regurgitation after Atrial Septal Defect Repair in Adults Shohei Yoshida, Satoshi Numata, Yasushi Tsutsumi, Osamu Monta, Sachiko Yamazaki, Hiroyuki Seo, Takaaki Samura, Hirokazu Ohashi Fukui
Transcatheter closure of right coronary artery fistula to the right ventricle
 Case Report Transcatheter closure of right coronary artery fistula to the right ventricle Abstract Coronary artery fistula (CAF) is an uncommon anomaly usually congenital but can be acquired. Although,
Case Report Transcatheter closure of right coronary artery fistula to the right ventricle Abstract Coronary artery fistula (CAF) is an uncommon anomaly usually congenital but can be acquired. Although,
Concomitant procedures using minimally access
 Surgical Technique on Cardiac Surgery Concomitant procedures using minimally access Nelson Santos Paulo Cardiothoracic Surgery, Centro Hospitalar de Vila Nova de Gaia, Oporto, Portugal Correspondence to:
Surgical Technique on Cardiac Surgery Concomitant procedures using minimally access Nelson Santos Paulo Cardiothoracic Surgery, Centro Hospitalar de Vila Nova de Gaia, Oporto, Portugal Correspondence to:
Transcatheter device occlusion of patent ductus arteriosus
 CONGENITAL HEART DISEASE The New Occlutech Duct Occluder: Immediate Results, Procedural Challenges, and Short-Term Follow-Up Vikram Kudumula, MRCPCH; Demetris Taliotis, MRCPCH; Christopher Duke, FRCP ABSTRACT:
CONGENITAL HEART DISEASE The New Occlutech Duct Occluder: Immediate Results, Procedural Challenges, and Short-Term Follow-Up Vikram Kudumula, MRCPCH; Demetris Taliotis, MRCPCH; Christopher Duke, FRCP ABSTRACT:
Percutaneous occluder device closure through femoral vein guidance by transthoracic echocardiography in adult atrial septal defect patients
 Original Article Percutaneous occluder device closure through femoral vein guidance by transthoracic echocardiography in adult atrial septal defect patients Yixin Jia, Xu Meng, Yan Li, Chunlei Xu, Wen
Original Article Percutaneous occluder device closure through femoral vein guidance by transthoracic echocardiography in adult atrial septal defect patients Yixin Jia, Xu Meng, Yan Li, Chunlei Xu, Wen
Transcatheter Closure of Secundum Atrial Septal Defects in the Elderly
 REVIEW DOI 10.4070 / kcj.2009.39.2.47 Print ISSN 1738-5520 / On-line ISSN 1738-5555 Copyright c 2009 The Korean Society of Cardiology Transcatheter Closure of Secundum Atrial Septal Defects in the Elderly
REVIEW DOI 10.4070 / kcj.2009.39.2.47 Print ISSN 1738-5520 / On-line ISSN 1738-5555 Copyright c 2009 The Korean Society of Cardiology Transcatheter Closure of Secundum Atrial Septal Defects in the Elderly
Surgical Repair of Ventricular Septal Defect; Contemporary Results and Risk Factors for a Complicated Course
 Pediatr Cardiol (2017) 38:264 270 DOI 10.1007/s00246-016-1508-2 ORIGINAL ARTICLE Surgical Repair of Ventricular Septal Defect; Contemporary Results and Risk Factors for a Complicated Course Maartje Schipper
Pediatr Cardiol (2017) 38:264 270 DOI 10.1007/s00246-016-1508-2 ORIGINAL ARTICLE Surgical Repair of Ventricular Septal Defect; Contemporary Results and Risk Factors for a Complicated Course Maartje Schipper
AMPLATZER Septal Occluder Structural Heart Therapy. Over 15 years of. Demonstrated. Clinical Experience. We ll show you our data. Ask to see theirs.
 AMPLATZER Septal Occluder Structural Heart Therapy Over 15 years of Demonstrated Clinical Experience We ll show you our data. Ask to see theirs. Leading the Standard of Care 1,2 The AMPLATZER Septal Occluder
AMPLATZER Septal Occluder Structural Heart Therapy Over 15 years of Demonstrated Clinical Experience We ll show you our data. Ask to see theirs. Leading the Standard of Care 1,2 The AMPLATZER Septal Occluder
Perventricular Closure of Muscular VSD s
 Perventricular Closure of Muscular VSD s Dr Damien Kenny, MB, MD Assistant Professor of Pediatrics Director of the Cardiac Catheterization Hybrid Suite Co-Director of the Rush Adult Congenital Heart Disease
Perventricular Closure of Muscular VSD s Dr Damien Kenny, MB, MD Assistant Professor of Pediatrics Director of the Cardiac Catheterization Hybrid Suite Co-Director of the Rush Adult Congenital Heart Disease
Transcatheter Closure of Secundum Atrial Septal Defect in Patients Over 60 Years Old
 Original Article Print ISSN 1738-5520 On-line ISSN 1738-5555 Korean Circulation Journal Transcatheter Closure of Secundum Atrial Septal Defect in Patients Over 60 Years Old Saet Byul Woo, MD 1, So-Ick
Original Article Print ISSN 1738-5520 On-line ISSN 1738-5555 Korean Circulation Journal Transcatheter Closure of Secundum Atrial Septal Defect in Patients Over 60 Years Old Saet Byul Woo, MD 1, So-Ick
Giovanni Di Salvo MD, PhD, FESC Second University of Naples Monaldi Hospital
 Giovanni Di Salvo MD, PhD, FESC Second University of Naples Monaldi Hospital VSD is one of the most common congenital cardiac abnormalities in the newborn. It can occur as an isolated finding or in combination
Giovanni Di Salvo MD, PhD, FESC Second University of Naples Monaldi Hospital VSD is one of the most common congenital cardiac abnormalities in the newborn. It can occur as an isolated finding or in combination
2) VSD & PDA - Dr. Aso
 2) VSD & PDA - Dr. Aso Ventricular Septal Defect (VSD) Most common cardiac malformation 25-30 % Types of VSD: According to position perimembranous, inlet, muscular. According to size small, medium, large.
2) VSD & PDA - Dr. Aso Ventricular Septal Defect (VSD) Most common cardiac malformation 25-30 % Types of VSD: According to position perimembranous, inlet, muscular. According to size small, medium, large.
Transcatheter Closure of Patent Ductus Arteriosus Using ADO Device: Retrospective Study of 149 Patients
 Original Article Transcatheter Closure of Patent Ductus Arteriosus Using ADO Device: Retrospective Study of 149 Patients ABSTRACT Sadiq M. Al-Hamash, Hussein Abdul Wahab 1, Zayir H. Khalid 1, Isam V. Nasser
Original Article Transcatheter Closure of Patent Ductus Arteriosus Using ADO Device: Retrospective Study of 149 Patients ABSTRACT Sadiq M. Al-Hamash, Hussein Abdul Wahab 1, Zayir H. Khalid 1, Isam V. Nasser
Index. cardiology.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A ACHD. See Adult congenital heart disease (ACHD) Adult congenital heart disease (ACHD), 503 512 across life span prevalence of, 504 506
Index Note: Page numbers of article titles are in boldface type. A ACHD. See Adult congenital heart disease (ACHD) Adult congenital heart disease (ACHD), 503 512 across life span prevalence of, 504 506
Patient guide: pfm Nit-Occlud PDA coil occlusion system. Catheter occlusion of. Patent Ductus Arteriosus. with the
 Patient guide: Catheter occlusion of Patent Ductus Arteriosus with the pfm Nit-Occlud PDA coil occlusion system pfm Produkte für die Medizin - AG Wankelstr. 60 D - 50996 Cologne Phone: +49 (0) 2236 96
Patient guide: Catheter occlusion of Patent Ductus Arteriosus with the pfm Nit-Occlud PDA coil occlusion system pfm Produkte für die Medizin - AG Wankelstr. 60 D - 50996 Cologne Phone: +49 (0) 2236 96
First Transfemoral Aortic Valve Implantation In Bulgaria - Crossing The Valve With The Device Is Not Always
 ISPUB.COM The Internet Journal of Cardiology Volume 9 Number 2 First Transfemoral Aortic Valve Implantation In Bulgaria - Crossing The Valve With The Device Is Not T D, J P. Citation T D, J P.. First Transfemoral
ISPUB.COM The Internet Journal of Cardiology Volume 9 Number 2 First Transfemoral Aortic Valve Implantation In Bulgaria - Crossing The Valve With The Device Is Not T D, J P. Citation T D, J P.. First Transfemoral
J. Schwitter, MD, FESC Section of Cardiology
 J. Schwitter, MD, FESC Section of Cardiology CMR Center of the CHUV University Hospital Lausanne - CHUV Switzerland Centre de RM Cardiaque J. Schwitter, MD, FESC Section of Cardiology CMR Center of the
J. Schwitter, MD, FESC Section of Cardiology CMR Center of the CHUV University Hospital Lausanne - CHUV Switzerland Centre de RM Cardiaque J. Schwitter, MD, FESC Section of Cardiology CMR Center of the
Incidence And Predictors Of Left Bundle Branch Block After Transcatheter Aortic Valve Implantation
 Incidence And Predictors Of Left Bundle Branch Block After Transcatheter Aortic Valve Implantation Ömer Aktug 1, MD; Guido Dohmen 2, MD; Kathrin Brehmer 1, MD; Verena Deserno 1 ; Ralf Herpertz 1 ; Rüdiger
Incidence And Predictors Of Left Bundle Branch Block After Transcatheter Aortic Valve Implantation Ömer Aktug 1, MD; Guido Dohmen 2, MD; Kathrin Brehmer 1, MD; Verena Deserno 1 ; Ralf Herpertz 1 ; Rüdiger
Determinants of Cardiopulmonary Functional Improvement After Transcatheter Atrial Septal Defect Closure in Asymptomatic Adults
 Journal of the American College of Cardiology Vol. 43, No. 10, 2004 2004 by the American College of Cardiology Foundation ISSN 0735-1097/04/$30.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2003.10.067
Journal of the American College of Cardiology Vol. 43, No. 10, 2004 2004 by the American College of Cardiology Foundation ISSN 0735-1097/04/$30.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2003.10.067
TRANSCATHETER REPLACEMENT OF THE PULMONARY VALVE (PPVI)
 TRANSCATHETER REPLACEMENT OF THE PULMONARY VALVE (PPVI) BASIL D. THANOPOULOS MD, PhD Director Interventional Cardiology of CHD Euroclinic ATHENS - GREECE TRANSCATHETER REPLACEMENT OF THE PULMONARY VALVE
TRANSCATHETER REPLACEMENT OF THE PULMONARY VALVE (PPVI) BASIL D. THANOPOULOS MD, PhD Director Interventional Cardiology of CHD Euroclinic ATHENS - GREECE TRANSCATHETER REPLACEMENT OF THE PULMONARY VALVE
Index. interventional.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Alagille syndrome, pulmonary artery stenosis in, 143 145, 148 149 Amplatz devices for atrial septal defect closure, 42 46 for coronary
Index Note: Page numbers of article titles are in boldface type. A Alagille syndrome, pulmonary artery stenosis in, 143 145, 148 149 Amplatz devices for atrial septal defect closure, 42 46 for coronary
Nit-Occlud. Coil System for PDA Closure IMPLANTATION POCKET GUIDE. Rx only CV / B. Braun Interventional Systems Inc.
 Refer to the Nit-Occlud PDA Instructions for Use for relevant warnings, precautions, complications and contraindications. This device has been designed for single use only. Nit-Occlud Coil System for PDA
Refer to the Nit-Occlud PDA Instructions for Use for relevant warnings, precautions, complications and contraindications. This device has been designed for single use only. Nit-Occlud Coil System for PDA
Covered stents in patients with complex aortic coarctations
 Covered stents in patients with complex aortic coarctations Gianfranco Butera, MD, PhD, a Luciane Piazza, MD, a Massimo Chessa, MD, PhD, a Diana Gabriella Negura, MD, a Luca Rosti, MD, a Raul Abella, MD,
Covered stents in patients with complex aortic coarctations Gianfranco Butera, MD, PhD, a Luciane Piazza, MD, a Massimo Chessa, MD, PhD, a Diana Gabriella Negura, MD, a Luca Rosti, MD, a Raul Abella, MD,
Perventricular Closure of Muscular VSD
 Perventricular Closure of Muscular VSD John P. Cheatham, MD, MSCAI George H. Dunlap Endowed Chair in Interventional Cardiology Co-Director, The Heart Center, Nationwide Children s Hospital Professor, Pediatrics
Perventricular Closure of Muscular VSD John P. Cheatham, MD, MSCAI George H. Dunlap Endowed Chair in Interventional Cardiology Co-Director, The Heart Center, Nationwide Children s Hospital Professor, Pediatrics
Foetal Cardiology: How to predict perinatal problems. Prof. I.Witters Prof.M.Gewillig UZ Leuven
 Foetal Cardiology: How to predict perinatal problems Prof. I.Witters Prof.M.Gewillig UZ Leuven Cardiopathies Incidence : 8-12 / 1000 births ( 1% ) Most frequent - Ventricle Septum Defect 20% - Atrium Septum
Foetal Cardiology: How to predict perinatal problems Prof. I.Witters Prof.M.Gewillig UZ Leuven Cardiopathies Incidence : 8-12 / 1000 births ( 1% ) Most frequent - Ventricle Septum Defect 20% - Atrium Septum
Case # 1. Page: 8. DUKE: Adams
 Case # 1 Page: 8 1. The cardiac output in this patient is reduced because of: O a) tamponade physiology O b) restrictive physiology O c) coronary artery disease O d) left bundle branch block Page: 8 1.
Case # 1 Page: 8 1. The cardiac output in this patient is reduced because of: O a) tamponade physiology O b) restrictive physiology O c) coronary artery disease O d) left bundle branch block Page: 8 1.
Transcatheter Atrial Septal Defect Closure with Right Aortic Arch Is it really difficult? M Tokue, H Hara, K Sugi, M Nakamura
 5th Asia Pacific Congenital & Structural Heart Intervention Symposium 2014 10 12 October 2014, Hong Kong Convention and Exhibition Centre Organizer: Hong Kong Society of Congenital & Structural Heart Disease
5th Asia Pacific Congenital & Structural Heart Intervention Symposium 2014 10 12 October 2014, Hong Kong Convention and Exhibition Centre Organizer: Hong Kong Society of Congenital & Structural Heart Disease
List of Videos. Video 1.1
 Video 1.1 Video 1.2 Video 1.3 Video 1.4 Video 1.5 Video 1.6 Video 1.7 Video 1.8 The parasternal long-axis view of the left ventricle shows the left ventricular inflow and outflow tract. The left atrium
Video 1.1 Video 1.2 Video 1.3 Video 1.4 Video 1.5 Video 1.6 Video 1.7 Video 1.8 The parasternal long-axis view of the left ventricle shows the left ventricular inflow and outflow tract. The left atrium
Long-Term Results of Transcatheter Closure of Patent Ductus Arteriosus in Infants Using Amplatzer Duct Occluder
 Original Article Iran J Pediatr Aug 2013; Vol 23 (No 4), Pp: 411-416 Long-Term Results of Transcatheter Closure of Patent Ductus Arteriosus in Infants Using Amplatzer Duct Occluder Mostafa Behjati-Ardakani*
Original Article Iran J Pediatr Aug 2013; Vol 23 (No 4), Pp: 411-416 Long-Term Results of Transcatheter Closure of Patent Ductus Arteriosus in Infants Using Amplatzer Duct Occluder Mostafa Behjati-Ardakani*
Edwards Sapien. Medtronic CoreValve. Inoperable FDA approved High risk: in trials. FDA approved
 Transcatheter Aortic Valve Replacement Symptomatic Aortic Stenosis Asymptomatic Juan Crestanello, MD Interim Director, Division of Cardiac Surgery Associate Professor Division of Cardiac Surgery The Ohio
Transcatheter Aortic Valve Replacement Symptomatic Aortic Stenosis Asymptomatic Juan Crestanello, MD Interim Director, Division of Cardiac Surgery Associate Professor Division of Cardiac Surgery The Ohio
Transcatheter Closure of Atrial Septal Defects in a Center With Limited Resources: Outcomes and Short Term Follow-Up
 Iran J Pediatr. 2015 December; 25(6): e3906. Published online 2015 December 23. doi: 10.5812/ijp.3906 Research Article Transcatheter Closure of Atrial Septal Defects in a Center With Limited Resources:
Iran J Pediatr. 2015 December; 25(6): e3906. Published online 2015 December 23. doi: 10.5812/ijp.3906 Research Article Transcatheter Closure of Atrial Septal Defects in a Center With Limited Resources:
TCTAP C-217 Bilateral Pulmonary Arterio Venus Fistula Managed by Vascular Plugs and Coil Manotosh Panja 1 1 BelleVue Clinic, India
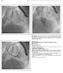 S450 JOURNAL OF THE AMERICAN COLLEGE OF CARDIOLOGY, VOL. 65, NO. 17, SUPPL S, 2015 Case Summary. Aneurysm at LVOT is a rare complication after Bentall operation and the aneurysm may increase in size. In
S450 JOURNAL OF THE AMERICAN COLLEGE OF CARDIOLOGY, VOL. 65, NO. 17, SUPPL S, 2015 Case Summary. Aneurysm at LVOT is a rare complication after Bentall operation and the aneurysm may increase in size. In
Transcatheter closure of ventricular septal defects with nitinol wire occluders of type patent ductus arteriosus
 Pediatric cardiology Transcatheter closure of ventricular septal defects with nitinol wire occluders of type patent ductus arteriosus Arkadiusz Wierzyk 1, Małgorzata Szkutnik 1, Roland Fiszer 1, Paweł
Pediatric cardiology Transcatheter closure of ventricular septal defects with nitinol wire occluders of type patent ductus arteriosus Arkadiusz Wierzyk 1, Małgorzata Szkutnik 1, Roland Fiszer 1, Paweł
가천의대길병원소아심장과최덕영 PA C IVS THE EVALUATION AND PRINCIPLES OF TREATMENT STRATEGY
 가천의대길병원소아심장과최덕영 PA C IVS THE EVALUATION AND PRINCIPLES OF TREATMENT STRATEGY PA c IVS (not only pulmonary valve disease) Edwards JE. Pathologic Alteration of the right heart. In: Konstam MA, Isner M, eds.
가천의대길병원소아심장과최덕영 PA C IVS THE EVALUATION AND PRINCIPLES OF TREATMENT STRATEGY PA c IVS (not only pulmonary valve disease) Edwards JE. Pathologic Alteration of the right heart. In: Konstam MA, Isner M, eds.
LONG TERM COMPLICATIONS FOLLOWING PERCUTANEOUS ASD CLOSURE
 LONG TERM COMPLICATIONS FOLLOWING PERCUTANEOUS ASD CLOSURE Zakaria Jalal Cardiopathies congénitales de l enfant et de l adulte Hôpital cardiologique Haut Lévêque Pessac CHU Bordeaux INTRODUCTION Percutaneous
LONG TERM COMPLICATIONS FOLLOWING PERCUTANEOUS ASD CLOSURE Zakaria Jalal Cardiopathies congénitales de l enfant et de l adulte Hôpital cardiologique Haut Lévêque Pessac CHU Bordeaux INTRODUCTION Percutaneous
The earliest application of intracardiac imaging
 Intracardiac Echocardiography for Structural Heart Defects A review of ICE innovations, devices, and techniques. BY ZAHID AMIN, MD; QI-LING CAO, MD; AND ZIYAD M. HIJAZI, MD The earliest application of
Intracardiac Echocardiography for Structural Heart Defects A review of ICE innovations, devices, and techniques. BY ZAHID AMIN, MD; QI-LING CAO, MD; AND ZIYAD M. HIJAZI, MD The earliest application of
