Device closure of congenital ventricular septal defects with Amplatzer devices: first experiences in Turkey
|
|
|
- Amber Turner
- 5 years ago
- Views:
Transcription
1 The Turkish Journal of Pediatrics 2008; 50: Original Device closure of congenital ventricular septal defects with Amplatzer devices: first experiences in Turkey Alpay Çeliker, Süheyla Özkutlu, Tevfik Karagöz, İlkay Erdoğan Sema Özer, Ebru Aypar Pediatric Cardiology Unit, Department of Pediatrics, Hacettepe University Faculty of Medicine, Ankara, Turkey SUMMARY: Çeliker A, Özkutlu S, Karagöz T, Erdoğan İ, Özer S, Aypar E. Device closure of congenital ventricular septal defects with Amplatzer devices: first experiences in Turkey. Turk J Pediatr 2008; 50: Ventricular septal defects (VSD), which cause volume overload, may be closed by interventional method. The success depends on the precise anatomic definition of the defect and its relation to other cardiac structures. We report our first experiences of transcatheter closure of perimembranous and muscular VSD. Between May 2005 and September 2006, transcatheter closure of VSD was attempted in 38 patients. Implantation was successful in 37 patients. In one patient, the procedure failed because of the long sheath kinking. We observed important complications in three patients: severe tricuspid valve regurgitation, residual VSD and tricuspid valve regurgitation and right bundle branch block in the short-term follow-up. Transcatheter device closure with Amplatzer device seems to be effective and safe in the treatment of perimembranous and muscular VSDs. Tricuspid valve incompetence may cause problems. Long-term results are required to determine the efficacy and safety. Key words: ventricular septal defect, Amplatzer, perimembranous, membranous, perventricular. Ventricular septal defects (VSDs) must be repaired to prevent pulmonary hypertension, ventricular dilatation, aortic regurgitation, and endocarditis. Various occlusion systems allow percutaneous closure of muscular and membranous congenital and acquired VSD 1-4. Technically, VSD closure by a device is more difficult than with the other defects 1. The success depends on the precise anatomic definition of the defect and its relation to other cardiac structures. Defects that are close to the semilunar or atrioventricular valves are not suitable for closure with device. With the development of new self-centering Amplatzer devices, an increasing number of defects could be closed in muscular and membranous septae 5-7,8-10. We report our preliminary experience of transcatheter closure of VSD in different locations. Material and Methods Between May 2005 and September 2006, transcatheter closure of VSD was attempted in 38 patients (39 procedures). Ages of patients ranged between 4 months and 27 years (mean: 9 years, median: 8 years). We closed echocardiographically (enlargement of left ventricle [LV] on echocardiography) and angiographically significant VSDs. Mean body weight was 32.5 kg (range: 4-80 kg, median 21 kg) (Table I). Perimembranous VSD (PMVSD) was seen in 25 patients and muscular VSD in 13 patients (multiple muscular VSD in 1). Associated lesion was present in four patients: 1 operated tetralogy of Fallot, 2 patent ductus arteriosus (PDA) which were closed via transcatheter route, and 1 coarctation of aorta (Table I). On echocardiography, the diameter of VSD ranged from 2 to 10 mm (median: 5 mm). Before transcatheter closure, the ventricular septal anatomy was examined by a detailed transthoracic echocardiography. The ratio of pulmonary to systemic blood flow (Qp/Qs) ranged from 1 to 2.9 (median: 1.8). Pulmonary artery systolic pressure ranged between mmhg (median: 26.5 mmhg).
2 Volume 50 Number 2 VSD Closure with Amplatzer Devices 107 Table I. Demographic and Diagnostic Data Total patients 38 Male 17 Female 21 Age at implantation 9 years (2 months-27 years) Muscular VSD 13 patients, 14 interventions (multiple in 1) Perimembranous VSD 24 Multiple VSD 1 Associated defects: PDA Aortic coarctation Operated tetralogy of Fallot VSD size 2-10 mm (median 5 mm) Qp/Qs (median 1.8) Pulmonary artery systolic pressure mmhg (median 26.5 mmhg) Device size 4-11 (median 6) Failed case 1 PDA: Patent ductus arteriosus. VSD: Ventricular septal defect. Procedure Written informed consent for device placement and follow-up evaluation was obtained from the patient or parent/legal guardian. The catheterization procedure was performed under deep sedation and transthoracic echocardiography in 11 patients and general anesthesia and transesophageal echocardiography (TEE) in 27 patients. Heparin was administered during the procedure with 100 IU/kg and repeated if the procedure exceeded 90 minutes with a 50 IU/kg dose. Each patient underwent right and left heart catheterization through the percutaneous transfemoral route. The left anterior oblique (LAO) view with cranial angulation that best profiled the VSD was determined (Fig. 1). The size of the VSD and its distance from the atrioventricular valve was reconfirmed on cineangiography. Perimembranous VSD Closure To cross the VSD from the LV, we used 5 Fr cut pigtail and glide wire or Roadrunner and advanced it to the pulmonary artery. The catheter was advanced over the wire and exchanged with the noodle wire. This noodle wire was snared in the pulmonary artery or vena cava superior and pulled out through the femoral vein (Fig. 2). Delivery sheath was advanced over the noodle wire and the dilator slowly drawn back, and the sheath was pushed toward the apex of the LV. The device, which was 1-2 mm larger than the size of the VSD, was screwed into the Fig. 1. Aneurysmal VSD: Left ventricular angiogram reveals large aneurysmal VSD (arrow). Fig. 2. Creation of arteriovenous loop: A: Cut pig-tail catheter was advanced to the left pulmonary artery via VSD, B: Noodle wire was caught at right pulmonary artery with a snare catheter, C and D: Snare catheter was pulled from the femoral vein and arteriovenous loop was created.
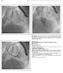
3 108 Çeliker A, et al The Turkish Journal of Pediatrics March- April 2008 cable. Pin vise was tightened to the cable at the end of the hub of the pusher catheter to prevent premature dislodgement of the device. The device was then advanced through the sheath and the LV disc was delivered midway between the anterior mitral valve leaflet and the left ventricular outflow tract. The entire system is pulled back to the septum. After angiographic and echocardiographic control, the waist was delivered followed by the right ventricular (RV) disc (Fig. 3). Once a good position was confirmed, the pin vise was loosened and the pusher catheter was retracted over the cable. The device was then released by counter-clockwise rotation of the pin vise. A repeat angiogram in the LV was done to assess position of the device and any residual shunt (Fig. 4). If the catheter could be passed easily from the VSD via the RV, there was no need to cross the defect from the LV. Muscular VSD Femoral artery and vein were accessed routinely, but internal jugular vein was preferred in the case of VSD located in posterior or apical septum. Angiography was done to define the location and size of the defect. The appropriate device size was chosen 1-2 mm larger than the size of the defect. A long sheath was then placed across the VSD. Once the VSD was crossed, a J exchange length wire was positioned in the pulmonary artery. This wire was snared and pulled out to form an arteriovenous loop. An appropriate-sized delivery sheath was then advanced from the femoral or right internal jugular vein over the wire to the apex of the LV and the exchange wire was removed. The left-sided retention disc was delivered in the mid-lv cavity and the entire assembly (sheath-device, cable) was pulled back to the septum. The waist was then delivered by retracting the sheath over the cable. Further retraction of the sheath over the cable will deploy the RV disc (Fig. 5). If the VSD was single, angiography in the LV was sufficient to delineate the position of the device and monitor the steps. However, if multiple VSDs were present, both angiography and TEE were used to verify the device position. Once the correct device position was confirmed, the device was released from the delivery cable using the pin vise. Fig. 3. Release of both discs: A: Both discs were opened, B: Angiography revealed closure of VSD. Fig. 5. Closure of midmuscular VSD: A: Both discs were opened, B: There was no shunt after the detachment. Fig. 4. After detachment: A: Disappearance of shunt on left ventriculogram, B: No aortic regurgitation on aortography. Perventricular Closure Protocol The perventricular approach was preferred in one four-month-old child with intractable heart failure. The procedure was done in the operating room under TEE guidance. The child was intubated via transnasal approach and a median sternotomy was done. The diameter of the defect was measured as 5 mm by TEE. For RV puncture, a 5-0 polypropylene purse-string
4 Volume 50 Number 2 VSD Closure with Amplatzer Devices 109 was placed at the carefully chosen location on the beating heart. An 18-gauge needle was introduced into the RV cavity and a guide wire was passed through the needle and advanced into the LV cavity. A 8 Fr short introducer sheath with a dilator was fed over the wire into the LV cavity. The dilator was removed and the sheath tip positioned in the LV cavity. The 6 mm device was then screwed to the cable and pulled inside a 7 Fr loader. The device was released by the same method described in the previous method of muscular VSD closure. After the release of the device, TEE was repeated to control the residual shunt. Cefazolin was administered during the procedure and subacute bacterial endocarditis (SBE) prophylaxis was recommended for six months following complete closure of the defect. All the patients except two - the hybrid procedure and patient with right bundle branch block - were hospitalized one day. Aspirin at a dose of 2-4 mg/kg/day and SBE prophylaxis for six months were advised. Patients were scheduled for follow-up at 1, 3, 6 and 12 months, with physical examination, telecardiogram, ECG, transthoracic echocardiography (Fig. 6) and 24-hour Holter monitoring. crossed from the LV and arteriovenous loop created in 23. In one, the VSD was crossed from the RV and procedure was uneventful (Table II). The mean diameters of VSD base and tip were 7.1±3.2 mm and 4.4±1.7 mm, respectively. The median device diameter was 6 mm. In this group, scopy and procedure time were 25±12 minutes and 109±26 minutes, respectively. All cases were closed successfully in those with muscular VSD (Table III). In seven patients (54%) with anterior or midmuscular VSD, we used femoral vein to load the device. In the other five patients, four with midmuscular and one with multiple apical muscular VSD, internal jugular vein was used for closure protocol. In the patient with multiple muscular VSD and pulmonary vascular disease, who had a previous operation for perimembranous large VSD, two Amplatzer muscular VSD devices were implanted to apical muscular VSDs in separate procedures. During the third attempt, we found multiple tiny muscular VSDs and suprasystemic pulmonary artery pressure and we abandoned the procedure. In this group, the mean VSD diameter was 6.2±1.8 mm. The scopy time and procedure time were 30±16 minutes and 104 ±50 minutes, respectively. An infant with large midmuscular VSD was closed by hybrid procedure uneventfully. At follow-up with a mean of 12.5±5.2 months, no patient had developed intravascular hemolysis or infective endocarditis. The device position remained stable and there was no evidence of problem in the device. Fig. 6. Echocardiographic appearance of midmuscular VSD after closure with Amplatzer muscular VSD closure device: Both discs were visible (arrow). Results Transcatheter deployment of the device was successful in 37 of 38 patients (97.4%). VSD closure resulted in complete disappearance of flow immediately across the defect in 34 procedures (91%). Two procedures were performed in only one patient. Perimembranous VSD was closed in 24 out of 25 patients (96%). In one patient, the procedure failed because of kinking of the long sheath in spite of repeated procedures. VSD was Complications There were two major (1 in muscular and 1 in perimembranous group) and one minor complication in our patients. One patient with high muscular VSD had moderate tricuspid valve regurgitation and residual shunt on the VSD on echocardiography. This patient underwent open heart surgery for the closure of the VSD and device removal. During the surgery, we observed that the chordae tendineae of the septal leaflet of the tricuspid valve had been attached to the rim of the device. In another patient, with perimembranous VSD and aneurysm formation, the device caused moderate to severe tricuspid valve regurgitation six months after the implantation. Repair of
5 110 Çeliker A, et al The Turkish Journal of Pediatrics March- April 2008 Table II. Clinical, Hemodynamic and Procedure Data in Patients with Perimembranous Ventricular Septal Defects Age Weight (kg) LVEDD VSD Type Qp/Qs PAP (mmhg) VSD Type VSD Base Device ST (min) PT (min) Follow-up (mos) Complication PM PM-AP PM-AP PM-AP PM PM PM-AP PM-AP PM PM RBBB PM-AP PM PM PM PM PM PM PM PM PM-AP PM PM PM-AP TR PM AP: Aneurysmal perimembranous. LVEDD: Left ventricle end diastolic dimension. PAP: Pulmonary artery systolic pressure. PM: Perimembranous. PT: Procedure time. RBBB: Right bundle branch block. ST: Scopy time. TR: Tricuspid regurgitation.
6 Volume 50 Number 2 VSD Closure with Amplatzer Devices 111 Table III. Clinical, Hemodynamic and Procedure Data in Patients with Muscular Ventricular Septal Defects Follow-up (mos) Complication PT (min) ST (min) Device VSD Type VSD Diameter PAP (mmhg) LVEDD Qp/Qs Weight (kg) Age (years) MM AM TR MM VPB AM * A AM AM ** MM MM MM MM MM MM *: Multiple apical VSD. **: Hybrid procedure. AM: Anterior muscular. A: Apical. LVEDD: Left ventricle end diastolic dimension. PAP: Pulmonary artery systolic pressure. MM: Midmuscular. ST: Scopy time. PT: Procedure time. TR: Tricuspid regurgitation. VPB: Ventricular premature beats. VSD: Ventricular septal defect. RV disc-associated tricuspid septal leaflet motion abnormality was attempted by valve plasty procedure. In one patient, we observed right bundle branch block on the ECG on the day of the procedure. There was no sign of secondor third-degree atrioventricular block in Holter recordings during a follow-up of 10 months. We observed two temporary problems. There was moderate tricuspid regurgitation in one patient with high muscular VSD following device closure, which disappeared after one day. Frequent ventricular ectopic beats following closure of midmuscular VSD disappeared at eight months of follow-up. Discussion This report describes the experience of a single center in transcatheter closure of congenital perimembranous and muscular VSDs with Amplatzer perimembranous and muscular VSD devices. Amplatzer muscular VSD closure device has gained worldwide acceptance since it was first used and there have been several reports describing the effectiveness and safety of this device 8, However, this device is not suitable for closure of perimembranous VSD due to close proximity of this type of defect to aortic valves 11. After the development and use of Amplatzer perimembranous VSD closure device, the closure rate of perimembranous VSDs has increased. This device has a special design that prevents aortic valve damage. Since its first use, this device has emerged as having a very high implantation rate and a very low acute complication rate 15. In our patient group, we successfully used this device in 97% of patients. One patient was abandoned because of sheath kinking. In one patient, VSD was crossed from the RV, which was very useful regarding procedure time, and arteriovenous loop creation was not needed. Amplatzer PMVSD device has a unique design for closure of these defects, but due to the close proximity of the conduction system and perimembranous VSD, atrioventricular conduction problem may occur in a significant number of patients 16,17. Atrioventricular conduction problems may occur during the procedure, in the immediate period after closure, or late during follow-up ). The block may occur after a very straightforward procedure. Occurrence of intraprocedural rhythm
7 112 Çeliker A, et al The Turkish Journal of Pediatrics March- April 2008 disturbance or difficulty in crossing the VSD with long sheath may forewarn the increased possibility of heart block. The mechanism of conduction problem is not known exactly, but edema or mechanical rubbing of device retention discs are among the suggested theories 18,20. The resolution of atrioventricular block after treatment with high-dose corticosteroids suggests edema as the main mechanism 18. The most dreadful complication regarding the conduction system is late atrioventricular block 19. In one large study, left anterior hemiblock and incomplete right bundle branch block were observed in 4% and 3.7%, respectively. There was early complete atrioventricular block in 1.1% of patients. In these two patients, complete AV block was resolved after one and two months with residual left anterior hemiblock 16. In a multicenter study, complete AV block, which was treated by pacemaker implantation, was observed in one patient (2.5%) 13. In our study group, we observed complete right bundle branch block in one patient (4%) during the procedure that persisted after six months of follow-up without sign of second or complete atrioventricular block. We did not see advanced atrioventricular block in the study group, which was evaluated by serial 24-hour ambulatory ECG monitoring at every follow-up exam. The morphology of perimembranous VSD has major importance on closure rates. The closure rate was found as 100% in patients with single VSD and as 98% in patients with single hole with aneurysmatic VSD at follow-up. However, closure rate was approximately 89% in patients with aneurysmal VSD with multiple holes. In our study group, one patient with aneurysmal VSD with multiple holes had mild residual shunt at eight months of follow-up. The presence of aneurysm with single VSD is a very good anatomy for device closure, since the left disc and aortic valve apparatus are not in close proximity to each other. We observed moderate to severe tricuspid regurgitation in one patient with perimembranous aneurysmal VSD after six months. The development of tricuspid regurgitation is an important concern for device closure of PMVSD. This might be related to entrapment of the tricuspid valve by the device. This complication may be prevented by careful entry to the RV using a balloon catheter 15. Before the device release, a thorough echocardiographic assessment of the tricuspid valve is mandatory 15,21,22. In patients with superiorly located muscular VSD, one should be very attentive regarding tricuspid valve apparatus and device interaction. In our study group, we observed one temporary tricuspid valve incompetence, which disappeared in 24 hours. This finding may be explained by tricuspid valve septal leaflet chorda trapping by the right retention disc. Surgery was performed in one patient with superiorly located muscular VSD in our study group. There was a large residual shunt and moderate tricuspid regurgitation in this patient. This may be related to malposition of the right retention disc of the device due to tricuspid valve chorda entrapment. We were unable to overcome this malposition during the procedure. After that patient, we used balloon catheters to pass the tricuspid valve to reach the RV and pulmonary artery for snaring the noodle wire. Small infants with large VSD should be treated by hybrid procedures in the operating room We treated one infant with large midmuscular VSD by this method, and the child recovered uneventfully. REFERENCES 1. Lock JE, Block PC, McKay RG, Baim DS, Keane JF. Transcatheter closure of ventricular septal defects. Circulation 1988; 78: Bridges ND, Perry SB, Keane JF, et al. Preoperative transcatheter closure of congenital muscular ventricular septal defects. N Engl J Med 1991; 324: Sideris EB, Walsh KP, Haddad JL, Chen CR, Ren SG, Kulkarni H. Occlusion of congenital ventricular septal defects by the buttoned device. Buttoned device Clinical Trials International Register. Heart 1997; 77: Thanopoulos BD, Tsaousis GS, Konstadopoulou GN, Zarayelyan AG. Transcatheter closure of muscular ventricular septal defect occluder: initial clinical application in children. J Am Coll Cardiol 1999; 33: Hijazi ZM, Hakim F, Al-Fadley F, et al. Transcatheter closure of single muscular ventricular septal defects using the Amplatzer Muscular VSD Occluder: initial results and technical considerations. Catheter Cardiovasc Interv 2000; 49: Gu X, Han YM, Titus JL, et al. Transcatheter closure of membranous ventricular septal defects with a new nitinol prosthesis in a natural swine model. Catheter Cardiovasc Interv 2000; 50: Le TP, Vaessen P, Freudenthal F, Grabitz RG, Sievert H. Transcatheter closure of subaortic ventricular septal defect (VSD) using a nickel-titanium spiral coil (NitOcclud): animal study and initial clinical result. Prog Pediatr Cardiol 2001; 14:
8 Volume 50 Number 2 VSD Closure with Amplatzer Devices Hijazi ZM, Hakim F, Hawaleh AA, et al. Catheter closure of perimembranous ventricular septal defects using the new Amplatzer membranous VSD occluder: initial clinical experience. Catheter Cardiovasc Interv 2002; 56: Thanapoulos BD, Tsaousis GS, Karanasios E, Eleftherakis NG, Paphitis C. Transcatheter closure of perimembranous ventricular septal defects with the Amplatzer asymmetric ventricular septal defect occluder: preliminary experience in children. Heart 2003; 89: Bilgiç A, Çeliker A, Özkutlu S, et al. Transcatheter closure of secundum atrial septal defects, a ventricular septal defect, and a patent arterial duct. Turk J Pediatr 2001; 43: Arora R, Trehan V, Thakur AK, Mehta V, Sengupta PP, Nigam M. Transcatheter closure of congenital muscular ventricular septal defect. J Interven Cardiol 2004; 17: Holzer R, Balzer D, Cao QL, et al. Device closure of muscular ventricular septal defects using the Amplatzer muscular ventricular septal defect occluder: immediate and mid-term results of a U.S. registry. J Am Coll Cardiol 2004; 43: Carminati M, Butera G, Chessa M, Drago M, Negura D, Piazza L. Transcatheter closure of congenital ventricular septal defect with Amplatzer septal occluders. Am J Cardiol 2005; 96 (Suppl): 52L-58L. 14. Vogel M, Rigby ML, Shore D. Perforation of the right aortic valve cusp: complication of ventricular septal defect closure with a modified Rashkind umbrella. Pediatr Cardiol 1996; 17: Pedra CA, Pedra SR, Esteves CA, et al. Percutaneous closure of perimembranous ventricular septal defects with the Amplatzer device: technical and morphological considerations. Catheter Cardiovasc Interv 2004; 61: Masura J, Gao W, Gavora P, et al. Percutaneous closure of perimembranous ventricular septal defects with the eccentric Amplatzer device: multicenter follow-up. Pediatr Cardiol 2005; 26: Fu YC, Bass J, Amin Z, et al. Transcatheter closure of perimembranous ventricular septal defects using the new Amplatzer membranous VSD occluder: results of the US phase I trial. J Am Coll Cardiol 2006; 47: Yip WC, Zimmerman F, Hijazi ZM. Heart block and empirical therapy after transcatheter closure of perimembranous ventricular septal defect. Catheter Cardiovasc Interv 2005; 66: Butera G, Massimo C, Mario C. Late complete atriovenous block after percutaneous closure of a perimembranous ventricular septal defect. Catheter Cardiovasc Interv 2006; 67: Walsh MA, Bialkowski J, Szkutnik M, Pawelec-Wojtalik M, Bobkowski W, Walsh KP. Atrioventricular block after transcatheter closure of perimembranous ventricular septal defects. Heart 2006; 92: Yen Ho S, Mccarthy KP, Rigby ML. Morphology of perimembranous ventricular septal defects: implications for transcatheter device closure. J Interven Cardiol 2004; 17: Mullins CE. Transcatheter closure of ventricular septal defects. In: Mullins CE (ed). Cardiac Catheterization in Congenital Heart Disease: Pediatric and Adult (1 st ed). Massachusetts: Blackwell Futura; 2006: Amin Z, Berry JM, Foker JE, et al. Intraoperative closure of muscular ventricular septal defect in a canine model and applicability of the technique in a baby. J Thorac Cardiovasc Surg 1998; 115: Amin Z, Gu X, Berry JM, et al. Perventricular [correction of Periventricular] closure of ventricular septal defects without cardiopulmonary bypass. Ann Thorac Surg 1999; 68: Rodes J, Piechaud JF, Ouaknine R, et al. Transcatheter closure of apical ventricular muscular septal defect combined with arterial switch operation in a newborn infant. Catheter Cardiovasc Interv 2000; 49: Akintuerk H, Michel-Behnke I, Bartram U, Müller M, Bauer J, Schranz D. Arterial switch operation for transposition of great arteries combined with closure of paramembranous ventricular septal defect using the Amplatzer membranous ventricular septal occluder. Am J Cardiol 2005; 96: Bacha EA, Cao QL, Galantowicz ME, et al. Multicenter experience with perventricular device closure of muscular ventricular septal defects. Pediatr Cardiol 2005; 26:
Hybrid Muscular VSD Closure in Small Weight Children
 Hybrid Muscular VSD Closure in Small Weight Children Shakeel A Qureshi, on behalf of: John P. Cheatham, MD George H. Dunlap Endowed Chair in Interventional Cardiology Director Cardiac Catheterization &
Hybrid Muscular VSD Closure in Small Weight Children Shakeel A Qureshi, on behalf of: John P. Cheatham, MD George H. Dunlap Endowed Chair in Interventional Cardiology Director Cardiac Catheterization &
For Personal Use. Copyright HMP 2013
 Case Report J INVASIVE CARDIOL 2013;25(2):E42-E44 Percutaneous Closure of Iatrogenic Ventricular Septal Defect Following Surgical Aortic Valve Replacement Using Two Different Approaches Takashi Matsumoto,
Case Report J INVASIVE CARDIOL 2013;25(2):E42-E44 Percutaneous Closure of Iatrogenic Ventricular Septal Defect Following Surgical Aortic Valve Replacement Using Two Different Approaches Takashi Matsumoto,
Percutaneous Device Closure of Congenital VSDs Current techniques and results for treating ventricular septal defects.
 Percutaneous Device Closure of Congenital VSDs Current techniques and results for treating ventricular septal defects. BY KARIM A. DIAB, MD; QI-LING CAO, MD; AND ZIYAD M. HIJAZI, MD, MPH During the past
Percutaneous Device Closure of Congenital VSDs Current techniques and results for treating ventricular septal defects. BY KARIM A. DIAB, MD; QI-LING CAO, MD; AND ZIYAD M. HIJAZI, MD, MPH During the past
Percutaneous VSD closure
 Percutaneous VSD closure Gianfranco Butera San Donato Milanese - Italy Patients selection Pts having hemodynamically significant VSD Left ventricular enlargement (left ventricular overload),defined as
Percutaneous VSD closure Gianfranco Butera San Donato Milanese - Italy Patients selection Pts having hemodynamically significant VSD Left ventricular enlargement (left ventricular overload),defined as
Journal of the American College of Cardiology Vol. 33, No. 5, by the American College of Cardiology ISSN /99/$20.
 Journal of the American College of Cardiology Vol. 33, No. 5, 1999 1999 by the American College of Cardiology ISSN 0735-1097/99/$20.00 Published by Elsevier Science Inc. PII S0735-1097(99)00011-X Transcatheter
Journal of the American College of Cardiology Vol. 33, No. 5, 1999 1999 by the American College of Cardiology ISSN 0735-1097/99/$20.00 Published by Elsevier Science Inc. PII S0735-1097(99)00011-X Transcatheter
Risk Factors and Outcomes of Post-Procedure Heart Blocks After Transcatheter Device Closure of Perimembranous Ventricular Septal Defect
 JACC: CARDIOVASCULAR INTERVENTIONS VOL. 5, NO. 4, 2012 2012 BY THE AMERICAN COLLEGE OF CARDIOLOGY FOUNDATION ISSN 1936-8798/$36.00 PUBLISHED BY ELSEVIER INC. DOI: 10.1016/j.jcin.2012.01.015 Risk Factors
JACC: CARDIOVASCULAR INTERVENTIONS VOL. 5, NO. 4, 2012 2012 BY THE AMERICAN COLLEGE OF CARDIOLOGY FOUNDATION ISSN 1936-8798/$36.00 PUBLISHED BY ELSEVIER INC. DOI: 10.1016/j.jcin.2012.01.015 Risk Factors
Imaging Evaluation of the Ventricular Septum
 Imaging Evaluation of the Ventricular Septum Craig E Fleishman, MD FACC FASE The Heart Center at Arnold Palmer Hospital for Children, Orlando SCAI Fall Fellows Course 2013 Las Vegas Disclosure Information
Imaging Evaluation of the Ventricular Septum Craig E Fleishman, MD FACC FASE The Heart Center at Arnold Palmer Hospital for Children, Orlando SCAI Fall Fellows Course 2013 Las Vegas Disclosure Information
Perimembranous ventricular septal defects (pmvsds) are
 Transcatheter Closure of Congenital Perimembranous Ventricular Septal Defect in Children Using Symmetric Occluders: An 8-Year Multiinstitutional Experience Lei Wang, MD, PhD,* Sancheng Cao, MD, Jun Li,
Transcatheter Closure of Congenital Perimembranous Ventricular Septal Defect in Children Using Symmetric Occluders: An 8-Year Multiinstitutional Experience Lei Wang, MD, PhD,* Sancheng Cao, MD, Jun Li,
Case Report. Martin L. Bocks, MD and Aimee K. Armstrong, MD
 Catheterization and Cardiovascular Interventions 74:488 493 (2009) Case Report Novel Method for Delivering the Amplatzer 1 Muscular VSD Occluder in a Patient With Double Outlet Right Ventricle After Bidirectional
Catheterization and Cardiovascular Interventions 74:488 493 (2009) Case Report Novel Method for Delivering the Amplatzer 1 Muscular VSD Occluder in a Patient With Double Outlet Right Ventricle After Bidirectional
Efficacy and Safety of Using Amplatzer Ductal Occluder for Transcatheter Closure of Perimembranous Ventricular Septal Defect in Pediatrics
 Iran J Pediatr. 2015 April; 25(2):e386. Published online 2015 April 18. DOI: 10.5812/ijp.386 Research Article Efficacy and Safety of Using Amplatzer Ductal Occluder for Transcatheter Closure of Perimembranous
Iran J Pediatr. 2015 April; 25(2):e386. Published online 2015 April 18. DOI: 10.5812/ijp.386 Research Article Efficacy and Safety of Using Amplatzer Ductal Occluder for Transcatheter Closure of Perimembranous
Jian Fang 1, Shaobo Xie 2, Lunchao Ma 2, Chao Yang 2. Original Article
 Original Article Anatomic and surgical factors affecting the switch from minimally invasive transthoracic occlusion to open surgery during ventricular septal defect repair Jian Fang 1, Shaobo Xie 2, Lunchao
Original Article Anatomic and surgical factors affecting the switch from minimally invasive transthoracic occlusion to open surgery during ventricular septal defect repair Jian Fang 1, Shaobo Xie 2, Lunchao
Type Size AP/PS RP/RS Qp/Qs. Ia Resistive <0.3 < Ib Resistive <0.3 < IIa Resistive <0.5 >2
 Transcatheter closure of VSD using Duct Occluder device Nguyen Lan Hieu, MD, PhD Hanoi Medical University Vietnam Heart Institute Anatomy of VSD 1. Perimembranous VSD: Aneurysm septal membranous(tv or
Transcatheter closure of VSD using Duct Occluder device Nguyen Lan Hieu, MD, PhD Hanoi Medical University Vietnam Heart Institute Anatomy of VSD 1. Perimembranous VSD: Aneurysm septal membranous(tv or
Transcatheter closure of the patent ductus arteriosus using the new Amplatzer duct occluder: Initial clinical applications in children
 Transcatheter closure of the patent ductus arteriosus using the new Amplatzer duct occluder: Initial clinical applications in children Basil Thanopoulos, MD, PhD, a Nikolaos Eleftherakis, MD, a Konstantinos
Transcatheter closure of the patent ductus arteriosus using the new Amplatzer duct occluder: Initial clinical applications in children Basil Thanopoulos, MD, PhD, a Nikolaos Eleftherakis, MD, a Konstantinos
CARDIAC INTERVENTIONS IN PEDIATRIC CARDIOLOGY: THE FUTURE
 CARDIAC INTERVENTIONS IN PEDIATRIC CARDIOLOGY: THE FUTURE Vikas Kohli From the: Senior Consultant Pediatric Cardiology, Apollo Centre of Advance Pediatrics, Indraprastha Apollo Hospitals, New Delhi-110044.
CARDIAC INTERVENTIONS IN PEDIATRIC CARDIOLOGY: THE FUTURE Vikas Kohli From the: Senior Consultant Pediatric Cardiology, Apollo Centre of Advance Pediatrics, Indraprastha Apollo Hospitals, New Delhi-110044.
Percutaneous VSD closure: Problems in the mid- and long-term
 Percutaneous VSD closure: Problems in the mid- and long-term Lee Benson MD Professor Pediatrics (Cardiology) Director, Cardiac Diagnostic & Interventional Unit The Hospital for Sick Children Toronto, Canada
Percutaneous VSD closure: Problems in the mid- and long-term Lee Benson MD Professor Pediatrics (Cardiology) Director, Cardiac Diagnostic & Interventional Unit The Hospital for Sick Children Toronto, Canada
Follow-up after VSD closure- what to look for?
 The 3rd Congress of Congenital heart disease Ventricular Septal Defect from A-Z January 9-11. 2013, Ho Chi Minh City, Vietnam Follow-up after VSD closure- what to look for? Nina Wunderlich University Hospital
The 3rd Congress of Congenital heart disease Ventricular Septal Defect from A-Z January 9-11. 2013, Ho Chi Minh City, Vietnam Follow-up after VSD closure- what to look for? Nina Wunderlich University Hospital
INTEGRATING ECHOCARDIOGRAPHY WITH CATHETER INTERVENTIONS FOR CONGENITAL HEART DISEASE. Krishna Kumar SevenHills Hospital, Mumbai, India
 INTEGRATING ECHOCARDIOGRAPHY WITH CATHETER INTERVENTIONS FOR CONGENITAL HEART DISEASE Krishna Kumar SevenHills Hospital, Mumbai, India Why talk about it? What is the big deal? Are we not stating the obvious?
INTEGRATING ECHOCARDIOGRAPHY WITH CATHETER INTERVENTIONS FOR CONGENITAL HEART DISEASE Krishna Kumar SevenHills Hospital, Mumbai, India Why talk about it? What is the big deal? Are we not stating the obvious?
Perventricular Closure of Muscular VSD
 Perventricular Closure of Muscular VSD John P. Cheatham, MD, MSCAI George H. Dunlap Endowed Chair in Interventional Cardiology Co-Director, The Heart Center, Nationwide Children s Hospital Professor, Pediatrics
Perventricular Closure of Muscular VSD John P. Cheatham, MD, MSCAI George H. Dunlap Endowed Chair in Interventional Cardiology Co-Director, The Heart Center, Nationwide Children s Hospital Professor, Pediatrics
Percutaneous closure of large VSD using a home-made fenestrated atrial septal occluder in 18-year-old with pulmonary hypertension
 Kamali et al. BMC Cardiovascular Disorders 2014, 14:74 CASE REPORT Percutaneous closure of large VSD using a home-made fenestrated atrial septal occluder in 18-year-old with pulmonary hypertension Hacer
Kamali et al. BMC Cardiovascular Disorders 2014, 14:74 CASE REPORT Percutaneous closure of large VSD using a home-made fenestrated atrial septal occluder in 18-year-old with pulmonary hypertension Hacer
Percutaneous atrial septal defect closure with the Occlutech Figulla Flex ASD Occluder.
 Percutaneous atrial septal defect closure with the Occlutech Figulla Flex ASD Occluder. First case with a novel delivery system. Werner Budts, Md, PhD, FESC Congenital and Structural Cardiology University
Percutaneous atrial septal defect closure with the Occlutech Figulla Flex ASD Occluder. First case with a novel delivery system. Werner Budts, Md, PhD, FESC Congenital and Structural Cardiology University
Ventricular septal defects (VSD) are one of the most
 Treatment of Isolated Ventricular Septal Defects in Children: Amplatzer Versus Surgical Closure Pierre Oses, MD, Nicolas Hugues, MD, Nagib Dahdah, MD, Suzanne J. Vobecky, MD, Joaquim Miro, MD, Michel Pellerin,
Treatment of Isolated Ventricular Septal Defects in Children: Amplatzer Versus Surgical Closure Pierre Oses, MD, Nicolas Hugues, MD, Nagib Dahdah, MD, Suzanne J. Vobecky, MD, Joaquim Miro, MD, Michel Pellerin,
Perimembranous VSD: When Do We Ask For A Surgical Closure? LI Xin. Department of Cardiothoracic Surgery Queen Mary Hospital Hong Kong
 Perimembranous VSD: When Do We Ask For A Surgical Closure? LI Xin Department of Cardiothoracic Surgery Queen Mary Hospital Hong Kong Classification (by Kirklin) I. Subarterial (10%) Outlet, conal, supracristal,
Perimembranous VSD: When Do We Ask For A Surgical Closure? LI Xin Department of Cardiothoracic Surgery Queen Mary Hospital Hong Kong Classification (by Kirklin) I. Subarterial (10%) Outlet, conal, supracristal,
5.8 Congenital Heart Disease
 5.8 Congenital Heart Disease Congenital heart diseases (CHD) refer to structural or functional heart diseases, which are present at birth. Some of these lesions may be discovered later. prevalence of Chd
5.8 Congenital Heart Disease Congenital heart diseases (CHD) refer to structural or functional heart diseases, which are present at birth. Some of these lesions may be discovered later. prevalence of Chd
Nit-Occlud. Coil System for PDA Closure IMPLANTATION POCKET GUIDE. Rx only CV / B. Braun Interventional Systems Inc.
 Refer to the Nit-Occlud PDA Instructions for Use for relevant warnings, precautions, complications and contraindications. This device has been designed for single use only. Nit-Occlud Coil System for PDA
Refer to the Nit-Occlud PDA Instructions for Use for relevant warnings, precautions, complications and contraindications. This device has been designed for single use only. Nit-Occlud Coil System for PDA
Transcatheter closure of atrial septal defects with transthoracic echocardiography
 Cardiology in the Young (2011), 21, 204 208 doi:10.1017/s1047951110001782 r Cambridge University Press, 2010 Original Article Transcatheter closure of atrial septal defects with transthoracic echocardiography
Cardiology in the Young (2011), 21, 204 208 doi:10.1017/s1047951110001782 r Cambridge University Press, 2010 Original Article Transcatheter closure of atrial septal defects with transthoracic echocardiography
CONGENITAL HEART DEFECTS IN ADULTS
 CONGENITAL HEART DEFECTS IN ADULTS THE ROLE OF CATHETER INTERVENTIONS Mario Carminati CONGENITAL HEART DEFECTS IN ADULTS CHD in natural history CHD with post-surgical sequelae PULMONARY VALVE STENOSIS
CONGENITAL HEART DEFECTS IN ADULTS THE ROLE OF CATHETER INTERVENTIONS Mario Carminati CONGENITAL HEART DEFECTS IN ADULTS CHD in natural history CHD with post-surgical sequelae PULMONARY VALVE STENOSIS
Atrial Septal Defect Closure. Stephen Brecker Director, Cardiac Catheterisation Labs
 Stephen Brecker Director, Cardiac Catheterisation Labs ADVANCED ANGIOPLASTY Incorporating The Left Main 5 Plus Course Conflicts of Interest The following companies have supported educational courses held
Stephen Brecker Director, Cardiac Catheterisation Labs ADVANCED ANGIOPLASTY Incorporating The Left Main 5 Plus Course Conflicts of Interest The following companies have supported educational courses held
Giovanni Di Salvo MD, PhD, FESC Second University of Naples Monaldi Hospital
 Giovanni Di Salvo MD, PhD, FESC Second University of Naples Monaldi Hospital VSD is one of the most common congenital cardiac abnormalities in the newborn. It can occur as an isolated finding or in combination
Giovanni Di Salvo MD, PhD, FESC Second University of Naples Monaldi Hospital VSD is one of the most common congenital cardiac abnormalities in the newborn. It can occur as an isolated finding or in combination
TRANSCATHETER CLOSURE OF PERSISTENT DUCTUS ARTERIOSUS USING THE AMPLATZER DUCT OCCLUDER IN INFANTS
 TRANSCATHETER CLOSURE OF PERSISTENT DUCTUS ARTERIOSUS USING THE AMPLATZER DUCT OCCLUDER IN INFANTS Al-Hakim FA 1, Harahsheh AS 2 & Hijazi IS 3 ABSTRACT Background: Despite technical improvements over the
TRANSCATHETER CLOSURE OF PERSISTENT DUCTUS ARTERIOSUS USING THE AMPLATZER DUCT OCCLUDER IN INFANTS Al-Hakim FA 1, Harahsheh AS 2 & Hijazi IS 3 ABSTRACT Background: Despite technical improvements over the
Echocardiographic Guidance During Placement of the Buttoned Double-Disk Device for Atrial Septa1 Defect Closure
 Echocardiographic Guidance During Placement of the Buttoned Double-Disk Device for Atrial Septa1 Defect Closure L. LUANN MINICH, M.D., and A. REBECCA SNIDER, M.D. Department of Pediatrics, C.S. Mott Children
Echocardiographic Guidance During Placement of the Buttoned Double-Disk Device for Atrial Septa1 Defect Closure L. LUANN MINICH, M.D., and A. REBECCA SNIDER, M.D. Department of Pediatrics, C.S. Mott Children
Case submission for CSI Asia-Pacific Case 2
 Case submission for CSI Asia-Pacific 2018- Case 2 Title Page Case category: Coarctation and ducts, valves Title: Simultaneous balloon aortic valvuloplasty with transcatheter closure of large hypertensive
Case submission for CSI Asia-Pacific 2018- Case 2 Title Page Case category: Coarctation and ducts, valves Title: Simultaneous balloon aortic valvuloplasty with transcatheter closure of large hypertensive
Atrial Septal Defects
 Supplementary ACHD Echo Acquisition Protocol for Atrial Septal Defects The following protocol for echo in adult patients with atrial septal defects (ASDs) is a guide for performing a comprehensive assessment
Supplementary ACHD Echo Acquisition Protocol for Atrial Septal Defects The following protocol for echo in adult patients with atrial septal defects (ASDs) is a guide for performing a comprehensive assessment
Percutaneous occluder device closure through femoral vein guidance by transthoracic echocardiography in adult atrial septal defect patients
 Original Article Percutaneous occluder device closure through femoral vein guidance by transthoracic echocardiography in adult atrial septal defect patients Yixin Jia, Xu Meng, Yan Li, Chunlei Xu, Wen
Original Article Percutaneous occluder device closure through femoral vein guidance by transthoracic echocardiography in adult atrial septal defect patients Yixin Jia, Xu Meng, Yan Li, Chunlei Xu, Wen
Transcatheter Closure of Atrial Septal Defects with Superior-anterior Rim Deficiency Using Amplatzer Septal Occluder
 ORIGINAL ARTICLE Transcatheter Closure of Atrial Septal Defects with Superior-anterior Rim Deficiency Using Amplatzer Septal Occluder Chien-Fu Huang, 1 Chih-Yuan Fang, 2 Sheung-Fat Ko, 3 Shao-Ju Chien,
ORIGINAL ARTICLE Transcatheter Closure of Atrial Septal Defects with Superior-anterior Rim Deficiency Using Amplatzer Septal Occluder Chien-Fu Huang, 1 Chih-Yuan Fang, 2 Sheung-Fat Ko, 3 Shao-Ju Chien,
ECHOCARDIOGRAPHIC APPROACH TO CONGENITAL HEART DISEASE: THE UNOPERATED ADULT
 ECHOCARDIOGRAPHIC APPROACH TO CONGENITAL HEART DISEASE: THE UNOPERATED ADULT Karen Stout, MD, FACC Divisions of Cardiology University of Washington Medical Center Seattle Children s Hospital NO DISCLOSURES
ECHOCARDIOGRAPHIC APPROACH TO CONGENITAL HEART DISEASE: THE UNOPERATED ADULT Karen Stout, MD, FACC Divisions of Cardiology University of Washington Medical Center Seattle Children s Hospital NO DISCLOSURES
IMAGES. in PAEDIATRIC CARDIOLOGY
 IMAGES in PAEDIATRIC CARDIOLOGY Images Paediatr Cardiol. 2005 Jan-Mar; 7(1): 12 17. PMCID: PMC3232568 Stent implantation for coarctation facilitated by the anterograde trans-septal approach N Sreeram and
IMAGES in PAEDIATRIC CARDIOLOGY Images Paediatr Cardiol. 2005 Jan-Mar; 7(1): 12 17. PMCID: PMC3232568 Stent implantation for coarctation facilitated by the anterograde trans-septal approach N Sreeram and
Transthoracic closure of atrial septal defect and ventricular septal defect without cardiopulmonary bypass
 Transthoracic closure of atrial septal defect and ventricular septal defect without cardiopulmonary bypass L. Wan, B.-T. Yu, Q.-C. Wu, L. Zeng, Q. Wang, J. Tang, Q.-R. Xu, H. Xu, W.-J. Wang, Y.-P. Cao
Transthoracic closure of atrial septal defect and ventricular septal defect without cardiopulmonary bypass L. Wan, B.-T. Yu, Q.-C. Wu, L. Zeng, Q. Wang, J. Tang, Q.-R. Xu, H. Xu, W.-J. Wang, Y.-P. Cao
Absent Pulmonary Valve Syndrome
 Absent Pulmonary Valve Syndrome Fact sheet on Absent Pulmonary Valve Syndrome In this condition, which has some similarities to Fallot's Tetralogy, there is a VSD with narrowing at the pulmonary valve.
Absent Pulmonary Valve Syndrome Fact sheet on Absent Pulmonary Valve Syndrome In this condition, which has some similarities to Fallot's Tetralogy, there is a VSD with narrowing at the pulmonary valve.
Transcatheter Closure of Ventricular Septal Defect
 Home SVCC Area: English - Español - Português Transcatheter Closure of Ventricular Septal Defect Zhong-Dong Du, MD; Ziyad M Hijazi, MD Section of Pediatric Cardiology, Department of Pediatrics, University
Home SVCC Area: English - Español - Português Transcatheter Closure of Ventricular Septal Defect Zhong-Dong Du, MD; Ziyad M Hijazi, MD Section of Pediatric Cardiology, Department of Pediatrics, University
HISTORY. Question: What category of heart disease is suggested by this history? CHIEF COMPLAINT: Heart murmur present since early infancy.
 HISTORY 18-year-old man. CHIEF COMPLAINT: Heart murmur present since early infancy. PRESENT ILLNESS: Although normal at birth, a heart murmur was heard at the six week check-up and has persisted since
HISTORY 18-year-old man. CHIEF COMPLAINT: Heart murmur present since early infancy. PRESENT ILLNESS: Although normal at birth, a heart murmur was heard at the six week check-up and has persisted since
Index. cardiology.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A ACHD. See Adult congenital heart disease (ACHD) Adult congenital heart disease (ACHD), 503 512 across life span prevalence of, 504 506
Index Note: Page numbers of article titles are in boldface type. A ACHD. See Adult congenital heart disease (ACHD) Adult congenital heart disease (ACHD), 503 512 across life span prevalence of, 504 506
Foetal Cardiology: How to predict perinatal problems. Prof. I.Witters Prof.M.Gewillig UZ Leuven
 Foetal Cardiology: How to predict perinatal problems Prof. I.Witters Prof.M.Gewillig UZ Leuven Cardiopathies Incidence : 8-12 / 1000 births ( 1% ) Most frequent - Ventricle Septum Defect 20% - Atrium Septum
Foetal Cardiology: How to predict perinatal problems Prof. I.Witters Prof.M.Gewillig UZ Leuven Cardiopathies Incidence : 8-12 / 1000 births ( 1% ) Most frequent - Ventricle Septum Defect 20% - Atrium Septum
Percutaneous closure of ventricular septal defects in children aged <12: early and mid-term results
 European Heart Journal (2006) 27, 2889 2895 doi:10.1093/eurheartj/ehl340 Clinical research Congenital heart disease Percutaneous closure of ventricular septal defects in children aged
European Heart Journal (2006) 27, 2889 2895 doi:10.1093/eurheartj/ehl340 Clinical research Congenital heart disease Percutaneous closure of ventricular septal defects in children aged
Notes by Sandra Dankwa 2009 HF- Heart Failure DS- Down Syndrome IE- Infective Endocarditis ET- Exercise Tolerance. Small VSD Symptoms -asymptomatic
 Congenital Heart Disease: Notes. Condition Pathology PC Ix Rx Ventricular septal defect (VSD) L R shuntsdefect anywhere in the ventricle, usually perimembranous (next to the tricuspid valve) 30% 1)small
Congenital Heart Disease: Notes. Condition Pathology PC Ix Rx Ventricular septal defect (VSD) L R shuntsdefect anywhere in the ventricle, usually perimembranous (next to the tricuspid valve) 30% 1)small
The earliest application of intracardiac imaging
 Intracardiac Echocardiography for Structural Heart Defects A review of ICE innovations, devices, and techniques. BY ZAHID AMIN, MD; QI-LING CAO, MD; AND ZIYAD M. HIJAZI, MD The earliest application of
Intracardiac Echocardiography for Structural Heart Defects A review of ICE innovations, devices, and techniques. BY ZAHID AMIN, MD; QI-LING CAO, MD; AND ZIYAD M. HIJAZI, MD The earliest application of
Congenital heart disease. By Dr Saima Ali Professor of pediatrics
 Congenital heart disease By Dr Saima Ali Professor of pediatrics What is the most striking clinical finding in this child? Learning objectives By the end of this lecture, final year student should be able
Congenital heart disease By Dr Saima Ali Professor of pediatrics What is the most striking clinical finding in this child? Learning objectives By the end of this lecture, final year student should be able
Transcatheter closure of interatrial
 372 Br HeartJf 1994;72:372-377 PRACTICE REVIEWED Department of Paediatric Cardiology, Royal Brompton Hospital, London A N Redington M L Rigby Correspondence to: Dr A N Redington, Department of Paediatric
372 Br HeartJf 1994;72:372-377 PRACTICE REVIEWED Department of Paediatric Cardiology, Royal Brompton Hospital, London A N Redington M L Rigby Correspondence to: Dr A N Redington, Department of Paediatric
Secundum atrial septal defect (ASD) is a common congenital heart disease and
 Device closure of atrial septal defects with the Amplatzer septal occluder: Safety and outcome in infants Karim A. Diab, MD, a Qi-Ling Cao, MD, a Emile A. Bacha, MD, b and Ziyad M. Hijazi, MD, MPH a Objective:
Device closure of atrial septal defects with the Amplatzer septal occluder: Safety and outcome in infants Karim A. Diab, MD, a Qi-Ling Cao, MD, a Emile A. Bacha, MD, b and Ziyad M. Hijazi, MD, MPH a Objective:
Adult Echocardiography Examination Content Outline
 Adult Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 4 5 Anatomy and Physiology Pathology Clinical Care and Safety Measurement Techniques, Maneuvers,
Adult Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 4 5 Anatomy and Physiology Pathology Clinical Care and Safety Measurement Techniques, Maneuvers,
Muscular VSD Occluder
 Muscular VSD Occluder Instructions for Use Device Description The AMPLATZER Muscular VSD Occluder is a self-expanding, double-disc device made from a nitinol wire mesh. The 2 discs are linked together
Muscular VSD Occluder Instructions for Use Device Description The AMPLATZER Muscular VSD Occluder is a self-expanding, double-disc device made from a nitinol wire mesh. The 2 discs are linked together
Research Article A New Coated Nitinol Occluder for Transcatheter Closure of Ventricular Septal Defects in a Canine Model
 BioMed Research International Volume 2013, Article ID 507919, 7 pages http://dx.doi.org/10.1155/2013/507919 Research Article A New Coated Nitinol Occluder for Transcatheter Closure of Ventricular Septal
BioMed Research International Volume 2013, Article ID 507919, 7 pages http://dx.doi.org/10.1155/2013/507919 Research Article A New Coated Nitinol Occluder for Transcatheter Closure of Ventricular Septal
Congenital heart disease: When to act and what to do?
 Leading Article Congenital heart disease: When to act and what to do? Duminda Samarasinghe 1 Sri Lanka Journal of Child Health, 2010; 39: 39-43 (Key words: Congenital heart disease) Congenital heart disease
Leading Article Congenital heart disease: When to act and what to do? Duminda Samarasinghe 1 Sri Lanka Journal of Child Health, 2010; 39: 39-43 (Key words: Congenital heart disease) Congenital heart disease
Patient guide: pfm Nit-Occlud PDA coil occlusion system. Catheter occlusion of. Patent Ductus Arteriosus. with the
 Patient guide: Catheter occlusion of Patent Ductus Arteriosus with the pfm Nit-Occlud PDA coil occlusion system pfm Produkte für die Medizin - AG Wankelstr. 60 D - 50996 Cologne Phone: +49 (0) 2236 96
Patient guide: Catheter occlusion of Patent Ductus Arteriosus with the pfm Nit-Occlud PDA coil occlusion system pfm Produkte für die Medizin - AG Wankelstr. 60 D - 50996 Cologne Phone: +49 (0) 2236 96
ΔΙΑΧΕΙΡΙΣΗ ΑΣΘΕΝΩΝ ΜΕ ΜΕΣΟΚΟΛΠΙΚΗ ΕΠΙΚΟΙΝΩΝΙΑ ΖΑΧΑΡΑΚΗ ΑΓΓΕΛΙΚΗ ΚΑΡΔΙΟΛΟΓΟΣ ΗΡΑΚΛΕΙΟ - ΚΡΗΤΗ
 ΔΙΑΧΕΙΡΙΣΗ ΑΣΘΕΝΩΝ ΜΕ ΜΕΣΟΚΟΛΠΙΚΗ ΕΠΙΚΟΙΝΩΝΙΑ ΖΑΧΑΡΑΚΗ ΑΓΓΕΛΙΚΗ ΚΑΡΔΙΟΛΟΓΟΣ ΗΡΑΚΛΕΙΟ - ΚΡΗΤΗ European Accreditation in TTE, TEE and CHD Echocardiography NOTHING TO DECLARE ATRIAL SEPTAL DEFECT TYPES SECUNDUM
ΔΙΑΧΕΙΡΙΣΗ ΑΣΘΕΝΩΝ ΜΕ ΜΕΣΟΚΟΛΠΙΚΗ ΕΠΙΚΟΙΝΩΝΙΑ ΖΑΧΑΡΑΚΗ ΑΓΓΕΛΙΚΗ ΚΑΡΔΙΟΛΟΓΟΣ ΗΡΑΚΛΕΙΟ - ΚΡΗΤΗ European Accreditation in TTE, TEE and CHD Echocardiography NOTHING TO DECLARE ATRIAL SEPTAL DEFECT TYPES SECUNDUM
IMAGES. in PAEDIATRIC CARDIOLOGY. Abstract
 IMAGES in PAEDIATRIC CARDIOLOGY Images Paediatr Cardiol. 2008 Apr-Jun; 10(2): 11 17. PMCID: PMC3232589 Transcatheter closure of symptomatic aortopulmonary window in an infant F Pillekamp, 1 T Hannes, 1
IMAGES in PAEDIATRIC CARDIOLOGY Images Paediatr Cardiol. 2008 Apr-Jun; 10(2): 11 17. PMCID: PMC3232589 Transcatheter closure of symptomatic aortopulmonary window in an infant F Pillekamp, 1 T Hannes, 1
Transcatheter Closure of Patent Ductus Arteriosus Using ADO Device: Retrospective Study of 149 Patients
 Original Article Transcatheter Closure of Patent Ductus Arteriosus Using ADO Device: Retrospective Study of 149 Patients ABSTRACT Sadiq M. Al-Hamash, Hussein Abdul Wahab 1, Zayir H. Khalid 1, Isam V. Nasser
Original Article Transcatheter Closure of Patent Ductus Arteriosus Using ADO Device: Retrospective Study of 149 Patients ABSTRACT Sadiq M. Al-Hamash, Hussein Abdul Wahab 1, Zayir H. Khalid 1, Isam V. Nasser
Case 47 Clinical Presentation
 93 Case 47 C Clinical Presentation 45-year-old man presents with chest pain and new onset of a murmur. Echocardiography shows severe aortic insufficiency. 94 RadCases Cardiac Imaging Imaging Findings C
93 Case 47 C Clinical Presentation 45-year-old man presents with chest pain and new onset of a murmur. Echocardiography shows severe aortic insufficiency. 94 RadCases Cardiac Imaging Imaging Findings C
Initial Human Experience. Objectives: To evaluate the feasibility, safety, and efficacy of the Occlutech VR
 Catheterization and Cardiovascular Interventions 00:00 00 (2015) Original Studies The New Occlutech V R PDA Occluder: Initial Human Experience M. A. Elbashier Abdelbasit, 1 * MBBS, MD, Mazeni Alwi, 1 MBBS,
Catheterization and Cardiovascular Interventions 00:00 00 (2015) Original Studies The New Occlutech V R PDA Occluder: Initial Human Experience M. A. Elbashier Abdelbasit, 1 * MBBS, MD, Mazeni Alwi, 1 MBBS,
Transcatheter device occlusion of patent ductus arteriosus
 CONGENITAL HEART DISEASE The New Occlutech Duct Occluder: Immediate Results, Procedural Challenges, and Short-Term Follow-Up Vikram Kudumula, MRCPCH; Demetris Taliotis, MRCPCH; Christopher Duke, FRCP ABSTRACT:
CONGENITAL HEART DISEASE The New Occlutech Duct Occluder: Immediate Results, Procedural Challenges, and Short-Term Follow-Up Vikram Kudumula, MRCPCH; Demetris Taliotis, MRCPCH; Christopher Duke, FRCP ABSTRACT:
Anatomy & Physiology
 1 Anatomy & Physiology Heart is divided into four chambers, two atrias & two ventricles. Atrioventricular valves (tricuspid & mitral) separate the atria from ventricles. they open & close to control flow
1 Anatomy & Physiology Heart is divided into four chambers, two atrias & two ventricles. Atrioventricular valves (tricuspid & mitral) separate the atria from ventricles. they open & close to control flow
Index. interventional.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Alagille syndrome, pulmonary artery stenosis in, 143 145, 148 149 Amplatz devices for atrial septal defect closure, 42 46 for coronary
Index Note: Page numbers of article titles are in boldface type. A Alagille syndrome, pulmonary artery stenosis in, 143 145, 148 149 Amplatz devices for atrial septal defect closure, 42 46 for coronary
Transcatheter Closure Versus Repeat Surgery for the Treatment of Postoperative Left-to-Right Shunts: A Single Center 15-Year Experience
 Original Article Cardiol Res. 2017;8(6):286-292 Transcatheter Closure Versus Repeat Surgery for the Treatment of Postoperative Left-to-Right Shunts: A Single Center 15-Year Experience Xinghua Gu a, Qiuwang
Original Article Cardiol Res. 2017;8(6):286-292 Transcatheter Closure Versus Repeat Surgery for the Treatment of Postoperative Left-to-Right Shunts: A Single Center 15-Year Experience Xinghua Gu a, Qiuwang
How to assess an adult with a Ventricular Septal Defect. When it should be closed and how?
 TTE AND TEE VDS ASSESSMENT. WHAT S S THE SIZE, WHERE ARE THE MARGINS? How to assess an adult with a Ventricular Septal Defect. When it should be closed and how? Dr Gianfranco Butera, MD, PhD Dr Gianfranco
TTE AND TEE VDS ASSESSMENT. WHAT S S THE SIZE, WHERE ARE THE MARGINS? How to assess an adult with a Ventricular Septal Defect. When it should be closed and how? Dr Gianfranco Butera, MD, PhD Dr Gianfranco
A case report: Percutaneous transcatheter treatment of Lutembacher syndrome
 A case report: Percutaneous transcatheter treatment of Lutembacher syndrome Dr. Sainath Hegde* Dr. Tukaram Aute** *Registrar, Dept of Cardiology, M.G.M Hospital, Aurangabad. **Asst. Prof, Dept of Cardiology,
A case report: Percutaneous transcatheter treatment of Lutembacher syndrome Dr. Sainath Hegde* Dr. Tukaram Aute** *Registrar, Dept of Cardiology, M.G.M Hospital, Aurangabad. **Asst. Prof, Dept of Cardiology,
Congenital Heart Defects
 Normal Heart Congenital Heart Defects 1. Patent Ductus Arteriosus The ductus arteriosus connects the main pulmonary artery to the aorta. In utero, it allows the blood leaving the right ventricle to bypass
Normal Heart Congenital Heart Defects 1. Patent Ductus Arteriosus The ductus arteriosus connects the main pulmonary artery to the aorta. In utero, it allows the blood leaving the right ventricle to bypass
Device Closure of ASD in Children Using the Amplatzer Devices: Indications and catheter preparations, technique, and outcome [15]
![Device Closure of ASD in Children Using the Amplatzer Devices: Indications and catheter preparations, technique, and outcome [15] Device Closure of ASD in Children Using the Amplatzer Devices: Indications and catheter preparations, technique, and outcome [15]](/thumbs/73/69533656.jpg) Device Closure of ASD in Children Using the Amplatzer Devices: Indications and catheter preparations, technique, and outcome [15] SCAI Fellow Course Fall 2014 Ralf J Holzer MD MSc FSCAI Medical Director
Device Closure of ASD in Children Using the Amplatzer Devices: Indications and catheter preparations, technique, and outcome [15] SCAI Fellow Course Fall 2014 Ralf J Holzer MD MSc FSCAI Medical Director
Transcatheter Atrial Septa1 Defect Closure: Preliminary Experience with the Rashkind Occluder Device
 Transcatheter Atrial Septa1 Defect Closure: Preliminary Experience with the Rashkind Occluder Device ROBERT H. BEEKMAN, M.D., ALBERT P. ROCCHINI, M.D., A. REBECCA SNIDER, M.D., and AMNON ROSENTHAL, M.D.
Transcatheter Atrial Septa1 Defect Closure: Preliminary Experience with the Rashkind Occluder Device ROBERT H. BEEKMAN, M.D., ALBERT P. ROCCHINI, M.D., A. REBECCA SNIDER, M.D., and AMNON ROSENTHAL, M.D.
Echocardiography in Adult Congenital Heart Disease
 Echocardiography in Adult Congenital Heart Disease Michael Vogel Kinderherz-Praxis München CHD missed in childhood Subsequent lesions after repaired CHD Follow-up of cyanotic heart disease CHD missed in
Echocardiography in Adult Congenital Heart Disease Michael Vogel Kinderherz-Praxis München CHD missed in childhood Subsequent lesions after repaired CHD Follow-up of cyanotic heart disease CHD missed in
TRANSCATHETER REPLACEMENT OF THE PULMONARY VALVE (PPVI)
 TRANSCATHETER REPLACEMENT OF THE PULMONARY VALVE (PPVI) BASIL D. THANOPOULOS MD, PhD Director Interventional Cardiology of CHD Euroclinic ATHENS - GREECE TRANSCATHETER REPLACEMENT OF THE PULMONARY VALVE
TRANSCATHETER REPLACEMENT OF THE PULMONARY VALVE (PPVI) BASIL D. THANOPOULOS MD, PhD Director Interventional Cardiology of CHD Euroclinic ATHENS - GREECE TRANSCATHETER REPLACEMENT OF THE PULMONARY VALVE
Uptofate Study Summary
 CONGENITAL HEART DISEASE Uptofate Study Summary Acyanotic Atrial septal defect Ventricular septal defect Patent foramen ovale Patent ductus arteriosus Aortic coartation Pulmonary stenosis Cyanotic Tetralogy
CONGENITAL HEART DISEASE Uptofate Study Summary Acyanotic Atrial septal defect Ventricular septal defect Patent foramen ovale Patent ductus arteriosus Aortic coartation Pulmonary stenosis Cyanotic Tetralogy
JOINT MEETING 2 Tricuspid club Chairpersons: G. Athanassopoulos, A. Avgeropoulou, M. Khoury, G. Stavridis
 JOINT MEETING 2 Tricuspid club Chairpersons: G. Athanassopoulos, A. Avgeropoulou, M. Khoury, G. Stavridis Similarities and differences in Tricuspid vs. Mitral Valve Anatomy and Imaging. Echo evaluation
JOINT MEETING 2 Tricuspid club Chairpersons: G. Athanassopoulos, A. Avgeropoulou, M. Khoury, G. Stavridis Similarities and differences in Tricuspid vs. Mitral Valve Anatomy and Imaging. Echo evaluation
Multifenestrated Septal Occluder Cribriform
 Multifenestrated Septal Occluder Cribriform Instructions for Use Device Description The AMPLATZER Multifenestrated Septal Occluder Cribriform (Cribriform Occluder) is a self-expanding double-disc nitinol
Multifenestrated Septal Occluder Cribriform Instructions for Use Device Description The AMPLATZER Multifenestrated Septal Occluder Cribriform (Cribriform Occluder) is a self-expanding double-disc nitinol
Index. interventional.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Ablation, of mitral leaflets, 80 Accucinch Annuloplasty system, for mitral regurgitation, 79, 94 95 Accutrak delivery system, for CoreValve
Index Note: Page numbers of article titles are in boldface type. A Ablation, of mitral leaflets, 80 Accucinch Annuloplasty system, for mitral regurgitation, 79, 94 95 Accutrak delivery system, for CoreValve
Pediatric Echocardiography Examination Content Outline
 Pediatric Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 Anatomy and Physiology Normal Anatomy and Physiology 10% 2 Abnormal Pathology and Pathophysiology
Pediatric Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 Anatomy and Physiology Normal Anatomy and Physiology 10% 2 Abnormal Pathology and Pathophysiology
Edwards Sapien. Medtronic CoreValve. Inoperable FDA approved High risk: in trials. FDA approved
 Transcatheter Aortic Valve Replacement Symptomatic Aortic Stenosis Asymptomatic Juan Crestanello, MD Interim Director, Division of Cardiac Surgery Associate Professor Division of Cardiac Surgery The Ohio
Transcatheter Aortic Valve Replacement Symptomatic Aortic Stenosis Asymptomatic Juan Crestanello, MD Interim Director, Division of Cardiac Surgery Associate Professor Division of Cardiac Surgery The Ohio
Mitral Valve Disease, When to Intervene
 Mitral Valve Disease, When to Intervene Swedish Heart and Vascular Institute Ming Zhang MD PhD Interventional Cardiology Structure Heart Disease Conflict of Interest None Current ACC/AHA guideline Stages
Mitral Valve Disease, When to Intervene Swedish Heart and Vascular Institute Ming Zhang MD PhD Interventional Cardiology Structure Heart Disease Conflict of Interest None Current ACC/AHA guideline Stages
Intracardiac echocardiography: an ideal guiding tool for device closure of interatrial communications
 Eur J Echocardiography (2005) 6, 92e96 Intracardiac echocardiography: an ideal guiding tool for device closure of interatrial communications Thomas Bartel a, *, Thomas Konorza a, Ulrich Neudorf b, Tiko
Eur J Echocardiography (2005) 6, 92e96 Intracardiac echocardiography: an ideal guiding tool for device closure of interatrial communications Thomas Bartel a, *, Thomas Konorza a, Ulrich Neudorf b, Tiko
Glenmark Cardiac Centre Mumbai, India
 ASD device closure: Long term follow up Bharat Dalvi, MD Glenmark Cardiac Centre Mumbai, India Our experience 1998 to 2011 1566 patients 912 patients > 4 years FU Exclusive with ASO Clinical, electrocardiographic
ASD device closure: Long term follow up Bharat Dalvi, MD Glenmark Cardiac Centre Mumbai, India Our experience 1998 to 2011 1566 patients 912 patients > 4 years FU Exclusive with ASO Clinical, electrocardiographic
The role of intraoperative TOE in congenital cardiac surgery
 The role of intraoperative TOE in congenital cardiac surgery Justiaan Swanevelder Dept of Anaesthesia Groote Schuur and Red Cross War Memorial Children s Hospitals University of Cape Town, South Africa
The role of intraoperative TOE in congenital cardiac surgery Justiaan Swanevelder Dept of Anaesthesia Groote Schuur and Red Cross War Memorial Children s Hospitals University of Cape Town, South Africa
Cardiac MRI in ACHD What We. ACHD Patients
 Cardiac MRI in ACHD What We Have Learned to Apply to ACHD Patients Faris Al Mousily, MBChB, FAAC, FACC Consultant, Pediatric Cardiology, KFSH&RC/Jeddah Adjunct Faculty, Division of Pediatric Cardiology
Cardiac MRI in ACHD What We Have Learned to Apply to ACHD Patients Faris Al Mousily, MBChB, FAAC, FACC Consultant, Pediatric Cardiology, KFSH&RC/Jeddah Adjunct Faculty, Division of Pediatric Cardiology
TCTAP C-217 Bilateral Pulmonary Arterio Venus Fistula Managed by Vascular Plugs and Coil Manotosh Panja 1 1 BelleVue Clinic, India
 S450 JOURNAL OF THE AMERICAN COLLEGE OF CARDIOLOGY, VOL. 65, NO. 17, SUPPL S, 2015 Case Summary. Aneurysm at LVOT is a rare complication after Bentall operation and the aneurysm may increase in size. In
S450 JOURNAL OF THE AMERICAN COLLEGE OF CARDIOLOGY, VOL. 65, NO. 17, SUPPL S, 2015 Case Summary. Aneurysm at LVOT is a rare complication after Bentall operation and the aneurysm may increase in size. In
Case Report Hemostasis of Left Atrial Appendage Bleed With Lariat Device
 273 Case Report Hemostasis of Left Atrial Appendage Bleed With Lariat Device Amena Hussain MD, Muhamed Saric MD, Scott Bernstein MD, Douglas Holmes MD, Larry Chinitz MD NYU Langone Medical Center, United
273 Case Report Hemostasis of Left Atrial Appendage Bleed With Lariat Device Amena Hussain MD, Muhamed Saric MD, Scott Bernstein MD, Douglas Holmes MD, Larry Chinitz MD NYU Langone Medical Center, United
Perventricular Closure of Muscular VSD s
 Perventricular Closure of Muscular VSD s Dr Damien Kenny, MB, MD Assistant Professor of Pediatrics Director of the Cardiac Catheterization Hybrid Suite Co-Director of the Rush Adult Congenital Heart Disease
Perventricular Closure of Muscular VSD s Dr Damien Kenny, MB, MD Assistant Professor of Pediatrics Director of the Cardiac Catheterization Hybrid Suite Co-Director of the Rush Adult Congenital Heart Disease
Successful Percutaneous Closure of Mitral Bioprosthetic Paravalvular Leak Using Figulla ASD Occluder
 Hans R. Figulla, M.D., PhD ; Ali Hamadanchi, M.D. Medicine, Pneumology Universitity Hospital, Jena, Germany Successful Percutaneous Closure of Mitral Bioprosthetic Paravalvular Leak Using Figulla ASD Occluder
Hans R. Figulla, M.D., PhD ; Ali Hamadanchi, M.D. Medicine, Pneumology Universitity Hospital, Jena, Germany Successful Percutaneous Closure of Mitral Bioprosthetic Paravalvular Leak Using Figulla ASD Occluder
Transcatheter closure of ventricular septal defects with nitinol wire occluders of type patent ductus arteriosus
 Pediatric cardiology Transcatheter closure of ventricular septal defects with nitinol wire occluders of type patent ductus arteriosus Arkadiusz Wierzyk 1, Małgorzata Szkutnik 1, Roland Fiszer 1, Paweł
Pediatric cardiology Transcatheter closure of ventricular septal defects with nitinol wire occluders of type patent ductus arteriosus Arkadiusz Wierzyk 1, Małgorzata Szkutnik 1, Roland Fiszer 1, Paweł
NEONATAL HYBRID PROCEDURES STRATEGIES TO REDUCE MORBIDITY AND MORTALITY
 NEONATAL HYBRID PROCEDURES STRATEGIES TO REDUCE MORBIDITY AND MORTALITY FOTIOS A. MITROPOULOS, MD, PHD DEPARTMENT OF PEDIATRIC AND ADULT CONGENITAL HEART SURGERY MITERA HYGEIA HOSPITALS, ATHENS, GREECE
NEONATAL HYBRID PROCEDURES STRATEGIES TO REDUCE MORBIDITY AND MORTALITY FOTIOS A. MITROPOULOS, MD, PHD DEPARTMENT OF PEDIATRIC AND ADULT CONGENITAL HEART SURGERY MITERA HYGEIA HOSPITALS, ATHENS, GREECE
Assessing Cardiac Anatomy With Digital Subtraction Angiography
 485 JACC Vol. 5, No. I Assessing Cardiac Anatomy With Digital Subtraction Angiography DOUGLAS S., MD, FACC Cleveland, Ohio The use of intravenous digital subtraction angiography in the assessment of patients
485 JACC Vol. 5, No. I Assessing Cardiac Anatomy With Digital Subtraction Angiography DOUGLAS S., MD, FACC Cleveland, Ohio The use of intravenous digital subtraction angiography in the assessment of patients
Paediatrics Revision Session Cardiology. Emma Walker 7 th May 2016
 Paediatrics Revision Session Cardiology Emma Walker 7 th May 2016 Cardiovascular Examination! General:! Make it fun!! Change how you act depending on their age! Introduction! Introduce yourself & check
Paediatrics Revision Session Cardiology Emma Walker 7 th May 2016 Cardiovascular Examination! General:! Make it fun!! Change how you act depending on their age! Introduction! Introduce yourself & check
ADULT CONGENITAL HEART DISEASE. Stuart Lilley
 ADULT CONGENITAL HEART DISEASE Stuart Lilley More adults than children have congenital heart disease Huge variety of congenital lesions from minor to major Heart failure, re-operation and arrhythmia are
ADULT CONGENITAL HEART DISEASE Stuart Lilley More adults than children have congenital heart disease Huge variety of congenital lesions from minor to major Heart failure, re-operation and arrhythmia are
Transcatheter Closure of Acute Myocardial Infarction VSD
 The 10 th Anniversary, Interventional Vascular Therapeutics ANGIOPLASTY SUMMIT 2005 TCT ASIA PACIFIC Transcatheter Closure of Acute Myocardial Infarction VSD Dr. Mullasari S Ajit Senior Consultant Cardiologist
The 10 th Anniversary, Interventional Vascular Therapeutics ANGIOPLASTY SUMMIT 2005 TCT ASIA PACIFIC Transcatheter Closure of Acute Myocardial Infarction VSD Dr. Mullasari S Ajit Senior Consultant Cardiologist
Διαδερμική θεραπεία των παραβαλβιδικών διαφυγών Σ.Ράμμος
 ΔΜΙΝΑΡΙΟ ΔΠΙΣΗΜΟΝΙΚΩΝ ΔΝΩΔΩΝ ΔΛΛΗΝΙΚΟΤ ΚΟΛΛΔΓΙΟΤ ΚΑΡ ΙΟΛΟΓΙΑ 2-4.10.2015 Δπιζηημονική Ένωζη Δπεμβαηικής Καρδιολογίας Βαλβιδοπάθειες, Γιαδερμικές παρεμβάζεις Διαδερμική θεραπεία των παραβαλβιδικών διαφυγών
ΔΜΙΝΑΡΙΟ ΔΠΙΣΗΜΟΝΙΚΩΝ ΔΝΩΔΩΝ ΔΛΛΗΝΙΚΟΤ ΚΟΛΛΔΓΙΟΤ ΚΑΡ ΙΟΛΟΓΙΑ 2-4.10.2015 Δπιζηημονική Ένωζη Δπεμβαηικής Καρδιολογίας Βαλβιδοπάθειες, Γιαδερμικές παρεμβάζεις Διαδερμική θεραπεία των παραβαλβιδικών διαφυγών
Treatment of Inter-MitraClip Regurgitation Due to Posterior Leaflet Cleft by Use of The Amplatzer Vascular Plug II device
 Volume 1, Issue 3 Case Report ISSN: 2572-9292 Treatment of Inter-MitraClip Regurgitation Due to Posterior Leaflet Cleft by Use of The Amplatzer Vascular Plug II device Neha M. Mantri, Gagan D. Singh, Thomas
Volume 1, Issue 3 Case Report ISSN: 2572-9292 Treatment of Inter-MitraClip Regurgitation Due to Posterior Leaflet Cleft by Use of The Amplatzer Vascular Plug II device Neha M. Mantri, Gagan D. Singh, Thomas
COMPLEMENTARY TECHNIQUES OF PERCUTANEOUS CLOSURE OF DUCTUS ARTERIOSUS USING DETACHABLE COOK COILS AND AMPLATZER DEVICES
 214 East African Medical Journal July 2013 East African Medical Journal Vol. 90 No. 7 July 2013 COMPLEMENTARY TECHNIQUES OF PERCUTANEOUS CLOSURE OF DUCTUS ARTERIOSUS USING DETACHABLE COOK COILS AND AMPLATZER
214 East African Medical Journal July 2013 East African Medical Journal Vol. 90 No. 7 July 2013 COMPLEMENTARY TECHNIQUES OF PERCUTANEOUS CLOSURE OF DUCTUS ARTERIOSUS USING DETACHABLE COOK COILS AND AMPLATZER
Diversion of the inferior vena cava following repair of atrial septal defect causing hypoxemia
 Marshall University Marshall Digital Scholar Internal Medicine Faculty Research Spring 5-2004 Diversion of the inferior vena cava following repair of atrial septal defect causing hypoxemia Ellen A. Thompson
Marshall University Marshall Digital Scholar Internal Medicine Faculty Research Spring 5-2004 Diversion of the inferior vena cava following repair of atrial septal defect causing hypoxemia Ellen A. Thompson
T his article provides a review of the interventional
 1168 REVIEW Interventional cardiac catheterisation in congenital heart disease R E Andrews, R M R Tulloh... As a result of recent technological advances, more types of congenital heart disease are amenable
1168 REVIEW Interventional cardiac catheterisation in congenital heart disease R E Andrews, R M R Tulloh... As a result of recent technological advances, more types of congenital heart disease are amenable
Recent technical advances and increasing experience
 Pediatric Open Heart Operations Without Diagnostic Cardiac Catheterization Jean-Pierre Pfammatter, MD, Pascal A. Berdat, MD, Thierry P. Carrel, MD, and Franco P. Stocker, MD Division of Pediatric Cardiology,
Pediatric Open Heart Operations Without Diagnostic Cardiac Catheterization Jean-Pierre Pfammatter, MD, Pascal A. Berdat, MD, Thierry P. Carrel, MD, and Franco P. Stocker, MD Division of Pediatric Cardiology,
Early and Late Complications Associated With Transcatheter Occlusion of Secundum Atrial Septal Defect
 Journal of the American College of Cardiology Vol. 39, No. 6, 2002 2002 by the American College of Cardiology Foundation ISSN 0735-1097/02/$22.00 Published by Elsevier Science Inc. PII S0735-1097(02)01711-4
Journal of the American College of Cardiology Vol. 39, No. 6, 2002 2002 by the American College of Cardiology Foundation ISSN 0735-1097/02/$22.00 Published by Elsevier Science Inc. PII S0735-1097(02)01711-4
Adult Congenital Heart Disease: What All Echocardiographers Should Know Sharon L. Roble, MD, FACC Echo Hawaii 2016
 1 Adult Congenital Heart Disease: What All Echocardiographers Should Know Sharon L. Roble, MD, FACC Echo Hawaii 2016 DISCLOSURES I have no disclosures relevant to today s talk 2 Why should all echocardiographers
1 Adult Congenital Heart Disease: What All Echocardiographers Should Know Sharon L. Roble, MD, FACC Echo Hawaii 2016 DISCLOSURES I have no disclosures relevant to today s talk 2 Why should all echocardiographers
CIPG Transcatheter Aortic Valve Replacement- When Is Less, More?
 CIPG 2013 Transcatheter Aortic Valve Replacement- When Is Less, More? James D. Rossen, M.D. Professor of Medicine and Neurosurgery Director, Cardiac Catheterization Laboratory and Interventional Cardiology
CIPG 2013 Transcatheter Aortic Valve Replacement- When Is Less, More? James D. Rossen, M.D. Professor of Medicine and Neurosurgery Director, Cardiac Catheterization Laboratory and Interventional Cardiology
