Case Report. Martin L. Bocks, MD and Aimee K. Armstrong, MD
|
|
|
- Linette Black
- 5 years ago
- Views:
Transcription
1 Catheterization and Cardiovascular Interventions 74: (2009) Case Report Novel Method for Delivering the Amplatzer 1 Muscular VSD Occluder in a Patient With Double Outlet Right Ventricle After Bidirectional Glenn Procedure and Pulmonary Artery Band Martin L. Bocks, MD and Aimee K. Armstrong, MD We report the first use of bilateral femoral venovenous rail creation for the delivery of an Amplatzer 1 Muscular Ventricular Septal Defect Occluder in a patient with a large mid-to-apical muscular ventricular septal defect before Rastelli operation. The presence of a right-sided bidirectional Glenn shunt, a banded main pulmonary artery, and double outlet right ventricle anatomy precluded the use of standard delivery techniques. The patient underwent successful transcatheter device placement followed by Rastelli operation on the following day. ' 2009 Wiley-Liss, Inc. Key words: congenital heart defects; heart catheterization; heart septal defects; ventricular; infants; echocardiography; transesophageal INTRODUCTION The standard percutaneous technique for closing mid-to-apical muscular ventricular septal defects (mvsds) with the Amplatzer 1 Muscular Ventricular Septal Defect Occluder (AMVSDO) has been well described [1 3]. This procedure involves either the formation of an arteriovenous loop from a femoral artery to the right internal jugular (RIJ) vein (Fig. 1a) or a venovenous loop from a femoral vein to the RIJ vein, using an existing interatrial communication or via transseptal atrial puncture. The device is typically delivered antegrade into the left ventricle (LV) from a right ventricular (RV) approach via the RIJ venous sheath. Retrograde delivery of the AMVSDO from the aorta can also be used, if kinking of the sheath is encountered when approaching from the RIJ vein [1], but this technique can lead to femoral arterial injury and aortic insufficiency in smaller children [1,4,5]. There are, however, particular congenital and post-surgical cardiac configurations that preclude the use of these standard delivery techniques. First, the presence of a cavopulmonary anastomosis, such as a bidirectional Glenn shunt (BDG), or of superior vena cava occlusion prohibits standard rail or loop formation, due to the lack of accessibility to the RIJ vein. Second, patients with unrepaired double outlet right ventricle (DORV) with D-malposed great arteries are not candidates for standard arteriovenous rail creation, because of the presence of the aorta on the RV side of the defect. Any rail involving the aorta requires crossing through both VSDs (RV?LV?RV) and could increase the risk of kinking the delivery sheath and of developing heart block. Lastly, creating the throughand-through loop is difficult in the presence of a main pulmonary artery band (PAB), which makes the standard location for snaring the wire inaccessible. We report a novel technique using a bifemoral venovenous loop, to deliver an AMVSDO in a patient with DORV, D-malposed great arteries, large subpulmonary VSD, and multiple apical and mid mvsds, who had previously undergone right BDG and PAB in preparation for single ventricle palliation at an outside institution. Division of Pediatric Cardiology, University of Michigan Health System, Ann Arbor, Michigan Conflict of interest: Nothing to report. *Correspondence to: Martin L. Bocks, MD, Division of Pediatric Cardiology, University of Michigan Health System, L1242 Women s, SPC 5204, 1500 E. Medical Center Drive, Ann Arbor, MI mbocks@umich.edu Received 24 September 2008; Revision accepted 23 December 2008 DOI /ccd Published online 24 August 2009 in Wiley InterScience (www. interscience.wiley.com). ' 2009 Wiley-Liss, Inc.
2 Novel Delivery Technique for AMVSDO Fig. 1. (a) Diagram of standard arteriovenous loop formation for closure of apical and midmuscular VSDs using the AMVSDO. (b) Diagram of bifemoral venovenous loop used in delivering the AMVSDO in this patient with DORV status-post PAB and BDG. [Color figure can be viewed in the online issue, which is available at CASE REPORT A 23 month-old, 7.5 kg female was referred for transcatheter closure of a large mid-to-apical mvsd before undergoing Rastelli procedure. The patient was born prematurely at 30 weeks of gestation, weighing approximately 900 grams. Her cardiac diagnoses included DORV, D-malposed great arteries, a large sub-pulmonary VSD, multiple mvsds, a large secundum atrial septal defect, an aberrant right subclavian artery, a bicuspid pulmonary valve, and mild subpulmonary stenosis. Her small size and the presence of abnormal tricuspid valve attachments to the crest of the outlet septum initially precluded her from a complex biventricular repair. She underwent PAB and atrial septectomy at 2 months of age at an outside institution. At 6 months of age, as part of a single ventricle palliation pathway, a right BDG was performed, and her banded pulmonary artery was left intact. The patient was subsequently referred to our institution for consideration of a biventricular repair. Upon evaluation of the patient s echocardiogram, it was determined that a Rastelli operation was possible, despite the presence of abnormal septal attachments of the tricuspid valve. The largest of the multiple mvsds, a large mid-to-apical mvsd, was in a location that would make it difficult to close surgically. Because of the extensive nature of the proposed surgery, perventricular device placement was not considered, as not to prolong the length of the already complex operation. Therefore, she was referred for transcatheter closure of the largest of the mvsds on the day before surgical intervention. Preoperative 2D echocardiography confirmed the above described anatomy, with the largest mvsd measuring approximately 10 mm on the LV side (Fig. 2). Three dimensional transthoracic echocardiography further demonstrated that this defect was divided on the RV side by a prominent muscle bundle/moderator band. The muscle bundle divided the defect on the RV side into a 5 7-mm defect superiorly and a smaller 2 3-mm defect inferiorly. The patient s aspirin was discontinued 2 days before the cardiac catheterization, as the surgery was planned for the following day. The cardiac catheterization was performed under general anesthesia with transesophageal echocardiographic (TEE) guidance. Access was obtained in the right femoral artery, bilateral femoral veins, and right subclavian vein. Heparin (100 units/ kg) was administered, and activated clotting times (ACT) were maintained above 200 sec. A right and left heart catheterization was performed. Pulmonary artery systolic pressure was 12 mm Hg with a right ventricular pressure of 77/7 mm Hg, suggesting a tight PAB. A retrograde left ventriculogram was performed
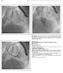
3 490 Bocks and Armstrong Fig. 2. Apical four-chamber view demonstrating muscular VSD in 2D and with color flow mapping. [Color figure can be viewed in the online issue, which is available at www. interscience.wiley.com.] detailing the location and size of the mvsds (Fig. 3). A 6-Fr balloon wedge catheter was placed into the left femoral venous (LFV) sheath and was advanced up through the atrial septal defect and into the apex of the left ventricle. A inch stiff-angled Glidewire 1 (Terumo Medical, Somerset, NJ) was used to access the largest mvsd. Following over the wire the catheter was advanced into the RV and out the aortic valve to the ascending aorta. A second balloon wedge catheter was placed in the right femoral venous (RFV) sheath and advanced through the right atrium, into the RV, and out the ascending aorta. Care was taken to ensure that both balloons were inflated at all times while passing through the right ventricle and into the ascending aorta. A 10-mm Amplatz Goose Neck 1 Snare retrieval device (EV3, Plymouth, MN) placed in the RFV balloon catheter was then used to snare a inch J-exchange guidewire from the LFV catheter. The guidewire was pulled across the aortic and tricuspid valves and exteriorized out of the RFV sheath, creating a bifemoral venovenous rail across the large mvsd (Fig. 1b). An 8-mm AMVSDO was selected for transcatheter closure based on angiographic and TEE measurements and taking into consideration the prominent right ventricular muscle bundle. A 7-French, 45 degree Amplatzer delivery sheath (AGA Medical, Golden Valley, MN) was prepared, and an inch Amplatz Super Fig. 3. Left ventriculogram in the long axial oblique projection revealing location of muscular VSD (thick arrow) and outlet VSD (thin arrow). Stiff TM exchange wire (Boston Scientific, Natick, MA) was advanced through the rail catheter antegrade across the tricuspid valve for a right-sided approach. Passage of the Super Stiff TM wire resulted in severe, reversible
4 Novel Delivery Technique for AMVSDO Fig. 4. Transesophageal echocardiogram with color flow mapping demonstrating severe TVR during use of Super-stiff exchange wire through the loop. [Color figure can be viewed in the online issue, which is available at wiley.com.] tricuspid valve regurgitation (TVR) and subsequent systemic hypotension (Fig. 4). This wire was replaced with a less stiff inch J-exchange guidewire (Argon Medical, Athens, TX), which was used to advance the delivery sheath across the mvsd into the LV with minimal TVR. Advancement of the AMVSDO toward the LV resulted in significant kinking of the sheath at the septum, despite keeping the LFV catheter and guidewire within the delivery sheath, using the kissing technique. The device and delivery cable were removed. A inch Platinum Plus TM stiff wire (Boston Scientific, Natick, MA) was then loaded alongside the device and delivery cable and was advanced out the end of the delivery sheath and into the LFV catheter. This provided the needed stiffness with which to advance the AMVSDO across the ventricular septum without kinking of the delivery sheath. The device was then delivered in the mvsd under fluoroscopic and TEE guidance using techniques previously described [1 3]. Before releasing the device, the arterial angiographic catheter was advanced retrograde into the left ventricle, and an angiocardiogram was performed. The presence of the Fig. 5. Repeat left ventriculogram after AMVSDO delivery showing proper placement of the device across the large muscular VSD. large subpulmonary VSD made it difficult to discern the degree of residual shunt through the mid-to-apical mvsd, but the TEE suggested that there was significantly less mvsd shunt with the AMVSDO in place. The device was subsequently released from the delivery cable. After waiting a period of 10 min, a left ventriculogram revealed good placement of the device and less residual shunting across the apical portion of the ventricular septum (Fig. 5). On the following day, the patient underwent Rastelli procedure with surgical enlargement of the outlet VSD, atrial septal defect closure, and placement of a 14-mm Contegra 1 heterograft (Medtronic, Minneapolis, MN) from the right ventricle to the distal end of the divided main pulmonary artery. Direct pressure measurements at the end of the surgical repair revealed a RV systolic pressure of 35 mm Hg and a LV systolic pressure of 90 mm Hg. Intraoperative TEE revealed multiple small residual leaks at the VSD patch margin, with estimated cumulative shunt being small-to-moderate. The remainder of the hospital course was unremarkable, and the patient was discharged from the hospital on the eighth postoperative day. DISCUSSION Surgical closure of multiple mvsds, especially in patients with other associated complex congenital heart defects, is often associated with significant morbidity and mortality. Because of the difficulty in accessing and completely closing these defects, multiple mvsds continue
5 492 Bocks and Armstrong to pose a major challenge to the surgeon and cardiologist despite improvements in surgical technique and pre- and intraoperative echocardiographic imaging [6 9]. The development of devices specifically designed to close mvsds via the transcatheter route has provided an alternative approach to surgical closure and a means for patients potentially to avoid surgery altogether. With the transcatheter approach, it has been well established that mid and apical mvsds are best closed from a rail system that includes RIJ venous access. This provides the smoothest sheath course with the fewest number of bends and usually results in less delivery sheath kinking [1,10,11]. As the hybrid approach for repairing both simple and complex congenital heart defects becomes more common, novel methods of intervention and device delivery need to evolve. Although the use of the bifemoral venovenous approach has been reported in a patient with a membranous VSD and prosthetic aortic valve to deliver the AMVSDO, we report the first use of the bifemoral venovenous rail to deliver this device into a mid-to-apical mvsd [12]. Although technical success was achieved in this case, several observations are worth noting. First, atrioventricular valve regurgitation, specifically TVR, is a known complication of AMVSDO delivery [13 15]. It is usually secondary to the wire loop or sheath crossing through the chordae tendineae of the tricuspid valve and is rarely permanent or severe. Irreversible TVR, however, has been reported when device delivery results in entrapment of the chordal apparatus or when the device directly impinges on the tricuspid valve leaflets [3,14 16]. Despite making efforts to establish a wire loop that did not involve the chordae of the tricuspid valve in this case, the bifemoral venovenous loop still impinged on the tricuspid valve and caused reversible, severe TVR. The acute wire angle from the inferior vena cava across the tricuspid valve and down into the mid-to-apical portion of the RV put significant stress on the posterior and lateral leaflets of the tricuspid valve. This stress was increased with the use of the very stiff Amplatz Super Stiff guidewire, and in our patient with unrepaired DORV, severe and acute TVR resulted in considerable systemic hypotension. A less stiff wire, such as a standard J-exchange wire or the Amplatz Noodle TM wire, results in less stenting-open of the tricuspid valve leaflets. Second, delivery sheath kinking, which is a well known problem with AMVSDO delivery, was encountered due to the acute angle formed when crossing the VSD [1,3,10,14,17]. Although it was not available at the time of this case, the more recently developed Amplatzer TorqVue Delivery and Exchange System (AGA Medical, Golden Valley, MN) offers greater flexibility and resistance to kinking and is now the recommended sheath for delivering the AMVSDO. In addition, the use of a 180 degree sheath may have caused less kinking than the 45 degree sheath. As has been previously reported, using a inch stiff wire alongside the delivery cable provided the necessary stiffness to successfully position the device in the left ventricle [1,10]. Lastly, perventricular delivery of the AMVSDO should be considered for patients with complex anatomy when the ideal route of device delivery is not an option. The safety and efficacy of perventricular delivery of the AMVSDO when additional cardiac surgeries are required has been well established [15,17,18]. Bacha, et al. reported the largest series of patients (n 5 10) in whom simultaneous perventricular AMVSDO delivery and cardiac surgical interventions were performed [15]. Most of the additional procedures performed included takedown of PAB, pulmonary artery augmentation, and coarctation repair. One patient in the series had congenital heart defects similar to the patient in this case, including previous surgical intervention with BDG and PAB. This patient underwent perventricular AMVSDO placement after initial VSD enlargement and interventricular baffling of the left ventricle to the aorta. Preoperatively, the defect was thought to be insignificant but, in the operating room, was found to be causing a large residual left-to-right shunt that prevented weaning from cardiopulmonary bypass. The device was placed in the operating room, using the perventricular approach. To our knowledge, there has been no patient described in the literature in whom the preoperative plan included perventricular device placement simultaneously with such a complex surgery. Although a perventricular approach may have made device delivery technically easier, preoperative closure of this remote mvsd allowed the surgeons to spend valuable time focusing on the more complex part of the operation. CONCLUSIONS A transcatheter bifemoral venovenous rail can be used for successful delivery of the AMVSDO into midto-apical mvsds in patients with complex congenital heart lesions, including DORV and particularly when the RIJ vein is not accessible. Severe TVR caused during delivery sheath placement can be overcome by using a less stiff guidewire, and sheath kinking can be prevented with the use of a kink resistant delivery sheath. Perventricular device delivery should be considered in patients with complex congenital heart disease, along with novel methods of transcatheter delivery. REFERENCES 1. Hijazi ZM, Hakim F, Al Fadley F, Abdelhamid J, Cao QL. Transcatheter closure of single muscular ventricular septal defects using the Amplatzer muscular VSD occluder: initial
6 Novel Delivery Technique for AMVSDO results and technical considerations. Catheter Cardiovasc Interv 2000;49: Thanopoulos BD, Tsaousis GS, Konstadopoulou GN, Zarayelyan AG. Transcatheter closure of muscular ventricular septal defects with the Amplatzer ventricular septal defect occluder: Initial clinical applications in children. J Am Coll Cardiol 1999;33: Hijazi Z. Device closure of ventricular septal defects. Catheter Cardiovasc Interv 2003;60: Arora R, Trehan V, Kumar A, Kalra GS, Nigam M. Transcatheter closure of congenital ventricular septal defects: Experience with various devices. J Interv Cardiol 2003;16: Behnke-Michel I, Le TP, Waldecker B, Akintuerk H, Valeske K, Schranz D. Percutaneous closure of congenital and acquired ventricular septal defects-considerations on the selection of the occlusion device. J Interven Cardiol 2005;18: Kitagawa T, Durham LA, Mosca RS, Bove EL. Techniques and results in the management of multiple ventricular septal defects. J Thorac Cardiovasc Surg 1998;115: Kleinert S, Sano T, Weintraub RG, Mee RB, Karl TR, Wilkinson JL. Anatomic features and surgical strategies in double-outlet right ventricle. Circulation 1997;96: Seddio F, Reddy VM, McElhinney DB, Tworetzky W, Silverman NH, Hanley FL. Multiple ventricular septal defects: How and when should they be repaired?. J Thorac Cardiovasc Surg 1999;117: Aoki M, Forbess JM, Jonas RA, Mayer JE Jr, Castaneda AR. Results of biventricular repair for double-outlet right ventricle. J Thorac Cardiovasc Surg. 1994;107: Carminati M, Butera G, Chessa M, Drago M, Negra D, Piazza L. Transcatheter closure of congenital ventricular septal defects with Amplatzer occluders. Am J Cardiol 2005;96 (suppl.):52l-58l. 11. Lock JE, Block PC, McKay RG, Baim DS, Keane JF. Transcatheter closure of ventricular septal defects. Circulation 1988;78: Klein AJ, Garcia JA, Carroll JD. Percutaneous closure of an iatrogenic ventricular septal defect following mechanical aortic valve replacement using the transseptal technique. Catheter Cardiovasc Interv 2007;70: Carminati M, Butera G, Chessa M, De Giovanni J, Fisher G, Gewillig M, Peuster M, Piechaud JF, Santoro G, Sievert H, Spadoni I, Walsh K. Investigators of the European VSD Registry. Transcatheter closure of congenital ventricular septal defects: Results of the European Registry. Eur Heart J 2007;28: Waight DJ, Bacha EA, Kahana M, Cao QL, Heitschmidt M, Hijazi ZM. Catheter therapy of swiss cheese ventricular septal defects using the Amplatzer muscular VSD occluder. Catheter Cardiovasc Interv 2002;55: Bacha EA, Cao QL, Galantowicz ME, Cheatham JP, Fleishman CE, Weinstein SW, Becker PA, Hill SL, Koenig P, Alboliras E, Abdulla R, Starr JP, Hijazi ZM. Multicenter experience with perventricular device closure of muscular ventricular septal defects. Pediatr Cardiol 2005;26: Diab KA, Cao QL, Hijazi ZM. Device closure of congenital ventricular septal defects. Congenit Heart Dis 2007;2: Diab KA, Cao QL, Mora BN, Hijazi ZM. Device closure of muscular ventricular septal defects in infants less than one year of age using the Amplatzer devices: Feasibility and outcome. Catheter Cardiovasc Interv 2007;70: Holzer R, Balzer D, Qi-Ling C, Lock K, Hijazi ZM. Amplatzer muscular ventricular septal defect investigators. Device closure of muscular ventricular septal defects using the Amplatzer muscular ventricular septal defect occluder. J Am Coll Cardiol 2004;43:
Hybrid Muscular VSD Closure in Small Weight Children
 Hybrid Muscular VSD Closure in Small Weight Children Shakeel A Qureshi, on behalf of: John P. Cheatham, MD George H. Dunlap Endowed Chair in Interventional Cardiology Director Cardiac Catheterization &
Hybrid Muscular VSD Closure in Small Weight Children Shakeel A Qureshi, on behalf of: John P. Cheatham, MD George H. Dunlap Endowed Chair in Interventional Cardiology Director Cardiac Catheterization &
For Personal Use. Copyright HMP 2013
 Case Report J INVASIVE CARDIOL 2013;25(2):E42-E44 Percutaneous Closure of Iatrogenic Ventricular Septal Defect Following Surgical Aortic Valve Replacement Using Two Different Approaches Takashi Matsumoto,
Case Report J INVASIVE CARDIOL 2013;25(2):E42-E44 Percutaneous Closure of Iatrogenic Ventricular Septal Defect Following Surgical Aortic Valve Replacement Using Two Different Approaches Takashi Matsumoto,
Percutaneous Device Closure of Congenital VSDs Current techniques and results for treating ventricular septal defects.
 Percutaneous Device Closure of Congenital VSDs Current techniques and results for treating ventricular septal defects. BY KARIM A. DIAB, MD; QI-LING CAO, MD; AND ZIYAD M. HIJAZI, MD, MPH During the past
Percutaneous Device Closure of Congenital VSDs Current techniques and results for treating ventricular septal defects. BY KARIM A. DIAB, MD; QI-LING CAO, MD; AND ZIYAD M. HIJAZI, MD, MPH During the past
Device closure of congenital ventricular septal defects with Amplatzer devices: first experiences in Turkey
 The Turkish Journal of Pediatrics 2008; 50: 106-113 Original Device closure of congenital ventricular septal defects with Amplatzer devices: first experiences in Turkey Alpay Çeliker, Süheyla Özkutlu,
The Turkish Journal of Pediatrics 2008; 50: 106-113 Original Device closure of congenital ventricular septal defects with Amplatzer devices: first experiences in Turkey Alpay Çeliker, Süheyla Özkutlu,
Percutaneous VSD closure
 Percutaneous VSD closure Gianfranco Butera San Donato Milanese - Italy Patients selection Pts having hemodynamically significant VSD Left ventricular enlargement (left ventricular overload),defined as
Percutaneous VSD closure Gianfranco Butera San Donato Milanese - Italy Patients selection Pts having hemodynamically significant VSD Left ventricular enlargement (left ventricular overload),defined as
Journal of the American College of Cardiology Vol. 33, No. 5, by the American College of Cardiology ISSN /99/$20.
 Journal of the American College of Cardiology Vol. 33, No. 5, 1999 1999 by the American College of Cardiology ISSN 0735-1097/99/$20.00 Published by Elsevier Science Inc. PII S0735-1097(99)00011-X Transcatheter
Journal of the American College of Cardiology Vol. 33, No. 5, 1999 1999 by the American College of Cardiology ISSN 0735-1097/99/$20.00 Published by Elsevier Science Inc. PII S0735-1097(99)00011-X Transcatheter
IMAGES. in PAEDIATRIC CARDIOLOGY. Abstract
 IMAGES in PAEDIATRIC CARDIOLOGY Images Paediatr Cardiol. 2008 Apr-Jun; 10(2): 11 17. PMCID: PMC3232589 Transcatheter closure of symptomatic aortopulmonary window in an infant F Pillekamp, 1 T Hannes, 1
IMAGES in PAEDIATRIC CARDIOLOGY Images Paediatr Cardiol. 2008 Apr-Jun; 10(2): 11 17. PMCID: PMC3232589 Transcatheter closure of symptomatic aortopulmonary window in an infant F Pillekamp, 1 T Hannes, 1
Jian Fang 1, Shaobo Xie 2, Lunchao Ma 2, Chao Yang 2. Original Article
 Original Article Anatomic and surgical factors affecting the switch from minimally invasive transthoracic occlusion to open surgery during ventricular septal defect repair Jian Fang 1, Shaobo Xie 2, Lunchao
Original Article Anatomic and surgical factors affecting the switch from minimally invasive transthoracic occlusion to open surgery during ventricular septal defect repair Jian Fang 1, Shaobo Xie 2, Lunchao
Transcatheter closure of the patent ductus arteriosus using the new Amplatzer duct occluder: Initial clinical applications in children
 Transcatheter closure of the patent ductus arteriosus using the new Amplatzer duct occluder: Initial clinical applications in children Basil Thanopoulos, MD, PhD, a Nikolaos Eleftherakis, MD, a Konstantinos
Transcatheter closure of the patent ductus arteriosus using the new Amplatzer duct occluder: Initial clinical applications in children Basil Thanopoulos, MD, PhD, a Nikolaos Eleftherakis, MD, a Konstantinos
Perventricular Closure of Muscular VSD
 Perventricular Closure of Muscular VSD John P. Cheatham, MD, MSCAI George H. Dunlap Endowed Chair in Interventional Cardiology Co-Director, The Heart Center, Nationwide Children s Hospital Professor, Pediatrics
Perventricular Closure of Muscular VSD John P. Cheatham, MD, MSCAI George H. Dunlap Endowed Chair in Interventional Cardiology Co-Director, The Heart Center, Nationwide Children s Hospital Professor, Pediatrics
IMAGES. in PAEDIATRIC CARDIOLOGY
 IMAGES in PAEDIATRIC CARDIOLOGY Images Paediatr Cardiol. 2005 Jan-Mar; 7(1): 12 17. PMCID: PMC3232568 Stent implantation for coarctation facilitated by the anterograde trans-septal approach N Sreeram and
IMAGES in PAEDIATRIC CARDIOLOGY Images Paediatr Cardiol. 2005 Jan-Mar; 7(1): 12 17. PMCID: PMC3232568 Stent implantation for coarctation facilitated by the anterograde trans-septal approach N Sreeram and
Type Size AP/PS RP/RS Qp/Qs. Ia Resistive <0.3 < Ib Resistive <0.3 < IIa Resistive <0.5 >2
 Transcatheter closure of VSD using Duct Occluder device Nguyen Lan Hieu, MD, PhD Hanoi Medical University Vietnam Heart Institute Anatomy of VSD 1. Perimembranous VSD: Aneurysm septal membranous(tv or
Transcatheter closure of VSD using Duct Occluder device Nguyen Lan Hieu, MD, PhD Hanoi Medical University Vietnam Heart Institute Anatomy of VSD 1. Perimembranous VSD: Aneurysm septal membranous(tv or
Giovanni Di Salvo MD, PhD, FESC Second University of Naples Monaldi Hospital
 Giovanni Di Salvo MD, PhD, FESC Second University of Naples Monaldi Hospital VSD is one of the most common congenital cardiac abnormalities in the newborn. It can occur as an isolated finding or in combination
Giovanni Di Salvo MD, PhD, FESC Second University of Naples Monaldi Hospital VSD is one of the most common congenital cardiac abnormalities in the newborn. It can occur as an isolated finding or in combination
Transcatheter Closure of Acute Myocardial Infarction VSD
 The 10 th Anniversary, Interventional Vascular Therapeutics ANGIOPLASTY SUMMIT 2005 TCT ASIA PACIFIC Transcatheter Closure of Acute Myocardial Infarction VSD Dr. Mullasari S Ajit Senior Consultant Cardiologist
The 10 th Anniversary, Interventional Vascular Therapeutics ANGIOPLASTY SUMMIT 2005 TCT ASIA PACIFIC Transcatheter Closure of Acute Myocardial Infarction VSD Dr. Mullasari S Ajit Senior Consultant Cardiologist
Percutaneous atrial septal defect closure with the Occlutech Figulla Flex ASD Occluder.
 Percutaneous atrial septal defect closure with the Occlutech Figulla Flex ASD Occluder. First case with a novel delivery system. Werner Budts, Md, PhD, FESC Congenital and Structural Cardiology University
Percutaneous atrial septal defect closure with the Occlutech Figulla Flex ASD Occluder. First case with a novel delivery system. Werner Budts, Md, PhD, FESC Congenital and Structural Cardiology University
INTEGRATING ECHOCARDIOGRAPHY WITH CATHETER INTERVENTIONS FOR CONGENITAL HEART DISEASE. Krishna Kumar SevenHills Hospital, Mumbai, India
 INTEGRATING ECHOCARDIOGRAPHY WITH CATHETER INTERVENTIONS FOR CONGENITAL HEART DISEASE Krishna Kumar SevenHills Hospital, Mumbai, India Why talk about it? What is the big deal? Are we not stating the obvious?
INTEGRATING ECHOCARDIOGRAPHY WITH CATHETER INTERVENTIONS FOR CONGENITAL HEART DISEASE Krishna Kumar SevenHills Hospital, Mumbai, India Why talk about it? What is the big deal? Are we not stating the obvious?
Transcatheter closure of patent foramen ovale using the internal jugular venous approach
 New methods in diagnosis and therapy Transcatheter closure of patent foramen ovale using the internal jugular venous approach Przemysław Węglarz 1,2, Ewa Konarska-Kuszewska 2, Tadeusz Zębik 2, Piotr Kuszewski
New methods in diagnosis and therapy Transcatheter closure of patent foramen ovale using the internal jugular venous approach Przemysław Węglarz 1,2, Ewa Konarska-Kuszewska 2, Tadeusz Zębik 2, Piotr Kuszewski
Transcatheter closure of interatrial
 372 Br HeartJf 1994;72:372-377 PRACTICE REVIEWED Department of Paediatric Cardiology, Royal Brompton Hospital, London A N Redington M L Rigby Correspondence to: Dr A N Redington, Department of Paediatric
372 Br HeartJf 1994;72:372-377 PRACTICE REVIEWED Department of Paediatric Cardiology, Royal Brompton Hospital, London A N Redington M L Rigby Correspondence to: Dr A N Redington, Department of Paediatric
In 1980, Bex and associates 1 first introduced the initial
 Technique of Aortic Translocation for the Management of Transposition of the Great Arteries with a Ventricular Septal Defect and Pulmonary Stenosis Victor O. Morell, MD, and Peter D. Wearden, MD, PhD In
Technique of Aortic Translocation for the Management of Transposition of the Great Arteries with a Ventricular Septal Defect and Pulmonary Stenosis Victor O. Morell, MD, and Peter D. Wearden, MD, PhD In
NEONATAL HYBRID PROCEDURES STRATEGIES TO REDUCE MORBIDITY AND MORTALITY
 NEONATAL HYBRID PROCEDURES STRATEGIES TO REDUCE MORBIDITY AND MORTALITY FOTIOS A. MITROPOULOS, MD, PHD DEPARTMENT OF PEDIATRIC AND ADULT CONGENITAL HEART SURGERY MITERA HYGEIA HOSPITALS, ATHENS, GREECE
NEONATAL HYBRID PROCEDURES STRATEGIES TO REDUCE MORBIDITY AND MORTALITY FOTIOS A. MITROPOULOS, MD, PHD DEPARTMENT OF PEDIATRIC AND ADULT CONGENITAL HEART SURGERY MITERA HYGEIA HOSPITALS, ATHENS, GREECE
Intracardiac echocardiography: an ideal guiding tool for device closure of interatrial communications
 Eur J Echocardiography (2005) 6, 92e96 Intracardiac echocardiography: an ideal guiding tool for device closure of interatrial communications Thomas Bartel a, *, Thomas Konorza a, Ulrich Neudorf b, Tiko
Eur J Echocardiography (2005) 6, 92e96 Intracardiac echocardiography: an ideal guiding tool for device closure of interatrial communications Thomas Bartel a, *, Thomas Konorza a, Ulrich Neudorf b, Tiko
Pediatric Echocardiography Examination Content Outline
 Pediatric Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 Anatomy and Physiology Normal Anatomy and Physiology 10% 2 Abnormal Pathology and Pathophysiology
Pediatric Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 Anatomy and Physiology Normal Anatomy and Physiology 10% 2 Abnormal Pathology and Pathophysiology
Perimembranous ventricular septal defects (pmvsds) are
 Transcatheter Closure of Congenital Perimembranous Ventricular Septal Defect in Children Using Symmetric Occluders: An 8-Year Multiinstitutional Experience Lei Wang, MD, PhD,* Sancheng Cao, MD, Jun Li,
Transcatheter Closure of Congenital Perimembranous Ventricular Septal Defect in Children Using Symmetric Occluders: An 8-Year Multiinstitutional Experience Lei Wang, MD, PhD,* Sancheng Cao, MD, Jun Li,
Echocardiographic Guidance During Placement of the Buttoned Double-Disk Device for Atrial Septa1 Defect Closure
 Echocardiographic Guidance During Placement of the Buttoned Double-Disk Device for Atrial Septa1 Defect Closure L. LUANN MINICH, M.D., and A. REBECCA SNIDER, M.D. Department of Pediatrics, C.S. Mott Children
Echocardiographic Guidance During Placement of the Buttoned Double-Disk Device for Atrial Septa1 Defect Closure L. LUANN MINICH, M.D., and A. REBECCA SNIDER, M.D. Department of Pediatrics, C.S. Mott Children
The earliest application of intracardiac imaging
 Intracardiac Echocardiography for Structural Heart Defects A review of ICE innovations, devices, and techniques. BY ZAHID AMIN, MD; QI-LING CAO, MD; AND ZIYAD M. HIJAZI, MD The earliest application of
Intracardiac Echocardiography for Structural Heart Defects A review of ICE innovations, devices, and techniques. BY ZAHID AMIN, MD; QI-LING CAO, MD; AND ZIYAD M. HIJAZI, MD The earliest application of
CARDIAC INTERVENTIONS IN PEDIATRIC CARDIOLOGY: THE FUTURE
 CARDIAC INTERVENTIONS IN PEDIATRIC CARDIOLOGY: THE FUTURE Vikas Kohli From the: Senior Consultant Pediatric Cardiology, Apollo Centre of Advance Pediatrics, Indraprastha Apollo Hospitals, New Delhi-110044.
CARDIAC INTERVENTIONS IN PEDIATRIC CARDIOLOGY: THE FUTURE Vikas Kohli From the: Senior Consultant Pediatric Cardiology, Apollo Centre of Advance Pediatrics, Indraprastha Apollo Hospitals, New Delhi-110044.
Imaging Evaluation of the Ventricular Septum
 Imaging Evaluation of the Ventricular Septum Craig E Fleishman, MD FACC FASE The Heart Center at Arnold Palmer Hospital for Children, Orlando SCAI Fall Fellows Course 2013 Las Vegas Disclosure Information
Imaging Evaluation of the Ventricular Septum Craig E Fleishman, MD FACC FASE The Heart Center at Arnold Palmer Hospital for Children, Orlando SCAI Fall Fellows Course 2013 Las Vegas Disclosure Information
The Double Switch Using Bidirectional Glenn and Hemi-Mustard. Frank Hanley
 The Double Switch Using Bidirectional Glenn and Hemi-Mustard Frank Hanley No relationships to disclose CCTGA Interesting Points for Discussion What to do when. associated defects must be addressed surgically:
The Double Switch Using Bidirectional Glenn and Hemi-Mustard Frank Hanley No relationships to disclose CCTGA Interesting Points for Discussion What to do when. associated defects must be addressed surgically:
Case Report Hemostasis of Left Atrial Appendage Bleed With Lariat Device
 273 Case Report Hemostasis of Left Atrial Appendage Bleed With Lariat Device Amena Hussain MD, Muhamed Saric MD, Scott Bernstein MD, Douglas Holmes MD, Larry Chinitz MD NYU Langone Medical Center, United
273 Case Report Hemostasis of Left Atrial Appendage Bleed With Lariat Device Amena Hussain MD, Muhamed Saric MD, Scott Bernstein MD, Douglas Holmes MD, Larry Chinitz MD NYU Langone Medical Center, United
JOINT MEETING 2 Tricuspid club Chairpersons: G. Athanassopoulos, A. Avgeropoulou, M. Khoury, G. Stavridis
 JOINT MEETING 2 Tricuspid club Chairpersons: G. Athanassopoulos, A. Avgeropoulou, M. Khoury, G. Stavridis Similarities and differences in Tricuspid vs. Mitral Valve Anatomy and Imaging. Echo evaluation
JOINT MEETING 2 Tricuspid club Chairpersons: G. Athanassopoulos, A. Avgeropoulou, M. Khoury, G. Stavridis Similarities and differences in Tricuspid vs. Mitral Valve Anatomy and Imaging. Echo evaluation
Percutaneous closure of large VSD using a home-made fenestrated atrial septal occluder in 18-year-old with pulmonary hypertension
 Kamali et al. BMC Cardiovascular Disorders 2014, 14:74 CASE REPORT Percutaneous closure of large VSD using a home-made fenestrated atrial septal occluder in 18-year-old with pulmonary hypertension Hacer
Kamali et al. BMC Cardiovascular Disorders 2014, 14:74 CASE REPORT Percutaneous closure of large VSD using a home-made fenestrated atrial septal occluder in 18-year-old with pulmonary hypertension Hacer
Since first successfully performed by Jatene et al, the
 Long-Term Predictors of Aortic Root Dilation and Aortic Regurgitation After Arterial Switch Operation Marcy L. Schwartz, MD; Kimberlee Gauvreau, ScD; Pedro del Nido, MD; John E. Mayer, MD; Steven D. Colan,
Long-Term Predictors of Aortic Root Dilation and Aortic Regurgitation After Arterial Switch Operation Marcy L. Schwartz, MD; Kimberlee Gauvreau, ScD; Pedro del Nido, MD; John E. Mayer, MD; Steven D. Colan,
Adult Congenital Heart Disease: What All Echocardiographers Should Know Sharon L. Roble, MD, FACC Echo Hawaii 2016
 1 Adult Congenital Heart Disease: What All Echocardiographers Should Know Sharon L. Roble, MD, FACC Echo Hawaii 2016 DISCLOSURES I have no disclosures relevant to today s talk 2 Why should all echocardiographers
1 Adult Congenital Heart Disease: What All Echocardiographers Should Know Sharon L. Roble, MD, FACC Echo Hawaii 2016 DISCLOSURES I have no disclosures relevant to today s talk 2 Why should all echocardiographers
Secundum atrial septal defect (ASD) is a common congenital heart disease and
 Device closure of atrial septal defects with the Amplatzer septal occluder: Safety and outcome in infants Karim A. Diab, MD, a Qi-Ling Cao, MD, a Emile A. Bacha, MD, b and Ziyad M. Hijazi, MD, MPH a Objective:
Device closure of atrial septal defects with the Amplatzer septal occluder: Safety and outcome in infants Karim A. Diab, MD, a Qi-Ling Cao, MD, a Emile A. Bacha, MD, b and Ziyad M. Hijazi, MD, MPH a Objective:
Techniques for repair of complete atrioventricular septal
 No Ventricular Septal Defect Patch Atrioventricular Septal Defect Repair Carl L. Backer, MD *, Osama Eltayeb, MD *, Michael C. Mongé, MD *, and John M. Costello, MD For the past 10 years, our center has
No Ventricular Septal Defect Patch Atrioventricular Septal Defect Repair Carl L. Backer, MD *, Osama Eltayeb, MD *, Michael C. Mongé, MD *, and John M. Costello, MD For the past 10 years, our center has
CONGENITAL HEART DEFECTS IN ADULTS
 CONGENITAL HEART DEFECTS IN ADULTS THE ROLE OF CATHETER INTERVENTIONS Mario Carminati CONGENITAL HEART DEFECTS IN ADULTS CHD in natural history CHD with post-surgical sequelae PULMONARY VALVE STENOSIS
CONGENITAL HEART DEFECTS IN ADULTS THE ROLE OF CATHETER INTERVENTIONS Mario Carminati CONGENITAL HEART DEFECTS IN ADULTS CHD in natural history CHD with post-surgical sequelae PULMONARY VALVE STENOSIS
T who has survived first-stage palliative surgical management
 Intermediate Procedures After First-Stage Norwood Operation Facilitate Subsequent Repair Richard A. Jonas, MD Department of Cardiac Surgery, Children s Hospital, Boston, Massachusetts Actuarial analysis
Intermediate Procedures After First-Stage Norwood Operation Facilitate Subsequent Repair Richard A. Jonas, MD Department of Cardiac Surgery, Children s Hospital, Boston, Massachusetts Actuarial analysis
HISTORY. Question: What category of heart disease is suggested by this history? CHIEF COMPLAINT: Heart murmur present since early infancy.
 HISTORY 18-year-old man. CHIEF COMPLAINT: Heart murmur present since early infancy. PRESENT ILLNESS: Although normal at birth, a heart murmur was heard at the six week check-up and has persisted since
HISTORY 18-year-old man. CHIEF COMPLAINT: Heart murmur present since early infancy. PRESENT ILLNESS: Although normal at birth, a heart murmur was heard at the six week check-up and has persisted since
For Personal Use. Copyright HMP 2013
 Case Report With Brief Review J INVASIVE CARDIOL 2013;25(4):E78-E80 Percutaneous Transjugular Device Closure of Postoperative Residual Atrial Septal Defect Saktheeswaran Mahesh Kumar, MD, DM, Sasidharan
Case Report With Brief Review J INVASIVE CARDIOL 2013;25(4):E78-E80 Percutaneous Transjugular Device Closure of Postoperative Residual Atrial Septal Defect Saktheeswaran Mahesh Kumar, MD, DM, Sasidharan
Mid-term Result of One and One Half Ventricular Repair in a Patient with Pulmonary Atresia and Intact Ventricular Septum
 Mid-term Result of One and One Half Ventricular Repair in a Patient with Pulmonary Atresia and Intact Ventricular Septum Kagami MIYAJI, MD, Akira FURUSE, MD, Toshiya OHTSUKA, MD, and Motoaki KAWAUCHI,
Mid-term Result of One and One Half Ventricular Repair in a Patient with Pulmonary Atresia and Intact Ventricular Septum Kagami MIYAJI, MD, Akira FURUSE, MD, Toshiya OHTSUKA, MD, and Motoaki KAWAUCHI,
Diversion of the inferior vena cava following repair of atrial septal defect causing hypoxemia
 Marshall University Marshall Digital Scholar Internal Medicine Faculty Research Spring 5-2004 Diversion of the inferior vena cava following repair of atrial septal defect causing hypoxemia Ellen A. Thompson
Marshall University Marshall Digital Scholar Internal Medicine Faculty Research Spring 5-2004 Diversion of the inferior vena cava following repair of atrial septal defect causing hypoxemia Ellen A. Thompson
Percutaneous occluder device closure through femoral vein guidance by transthoracic echocardiography in adult atrial septal defect patients
 Original Article Percutaneous occluder device closure through femoral vein guidance by transthoracic echocardiography in adult atrial septal defect patients Yixin Jia, Xu Meng, Yan Li, Chunlei Xu, Wen
Original Article Percutaneous occluder device closure through femoral vein guidance by transthoracic echocardiography in adult atrial septal defect patients Yixin Jia, Xu Meng, Yan Li, Chunlei Xu, Wen
Transcatheter closure of atrial septal defects with transthoracic echocardiography
 Cardiology in the Young (2011), 21, 204 208 doi:10.1017/s1047951110001782 r Cambridge University Press, 2010 Original Article Transcatheter closure of atrial septal defects with transthoracic echocardiography
Cardiology in the Young (2011), 21, 204 208 doi:10.1017/s1047951110001782 r Cambridge University Press, 2010 Original Article Transcatheter closure of atrial septal defects with transthoracic echocardiography
A case report: Percutaneous transcatheter treatment of Lutembacher syndrome
 A case report: Percutaneous transcatheter treatment of Lutembacher syndrome Dr. Sainath Hegde* Dr. Tukaram Aute** *Registrar, Dept of Cardiology, M.G.M Hospital, Aurangabad. **Asst. Prof, Dept of Cardiology,
A case report: Percutaneous transcatheter treatment of Lutembacher syndrome Dr. Sainath Hegde* Dr. Tukaram Aute** *Registrar, Dept of Cardiology, M.G.M Hospital, Aurangabad. **Asst. Prof, Dept of Cardiology,
Atrial Septal Defects
 Supplementary ACHD Echo Acquisition Protocol for Atrial Septal Defects The following protocol for echo in adult patients with atrial septal defects (ASDs) is a guide for performing a comprehensive assessment
Supplementary ACHD Echo Acquisition Protocol for Atrial Septal Defects The following protocol for echo in adult patients with atrial septal defects (ASDs) is a guide for performing a comprehensive assessment
Repair of Complete Atrioventricular Septal Defects Single Patch Technique
 Repair of Complete Atrioventricular Septal Defects Single Patch Technique Fred A. Crawford, Jr., MD The first repair of a complete atrioventricular septal defect was performed in 1954 by Lillehei using
Repair of Complete Atrioventricular Septal Defects Single Patch Technique Fred A. Crawford, Jr., MD The first repair of a complete atrioventricular septal defect was performed in 1954 by Lillehei using
Ebstein s anomaly is defined by a downward displacement
 Repair of Ebstein s Anomaly Sylvain Chauvaud, MD Ebstein s anomaly is a tricuspid valve anomaly associated with poor right ventricular contractility in severe cases. Surgery is indicated in all symptomatic
Repair of Ebstein s Anomaly Sylvain Chauvaud, MD Ebstein s anomaly is a tricuspid valve anomaly associated with poor right ventricular contractility in severe cases. Surgery is indicated in all symptomatic
TRANSCATHETER REPLACEMENT OF THE PULMONARY VALVE (PPVI)
 TRANSCATHETER REPLACEMENT OF THE PULMONARY VALVE (PPVI) BASIL D. THANOPOULOS MD, PhD Director Interventional Cardiology of CHD Euroclinic ATHENS - GREECE TRANSCATHETER REPLACEMENT OF THE PULMONARY VALVE
TRANSCATHETER REPLACEMENT OF THE PULMONARY VALVE (PPVI) BASIL D. THANOPOULOS MD, PhD Director Interventional Cardiology of CHD Euroclinic ATHENS - GREECE TRANSCATHETER REPLACEMENT OF THE PULMONARY VALVE
Perimembranous VSD: When Do We Ask For A Surgical Closure? LI Xin. Department of Cardiothoracic Surgery Queen Mary Hospital Hong Kong
 Perimembranous VSD: When Do We Ask For A Surgical Closure? LI Xin Department of Cardiothoracic Surgery Queen Mary Hospital Hong Kong Classification (by Kirklin) I. Subarterial (10%) Outlet, conal, supracristal,
Perimembranous VSD: When Do We Ask For A Surgical Closure? LI Xin Department of Cardiothoracic Surgery Queen Mary Hospital Hong Kong Classification (by Kirklin) I. Subarterial (10%) Outlet, conal, supracristal,
Appendix A.1: Tier 1 Surgical Procedure Terms and Definitions
 Appendix A.1: Tier 1 Surgical Procedure Terms and Definitions Tier 1 surgeries AV Canal Atrioventricular Septal Repair, Complete Repair of complete AV canal (AVSD) using one- or two-patch or other technique,
Appendix A.1: Tier 1 Surgical Procedure Terms and Definitions Tier 1 surgeries AV Canal Atrioventricular Septal Repair, Complete Repair of complete AV canal (AVSD) using one- or two-patch or other technique,
5.8 Congenital Heart Disease
 5.8 Congenital Heart Disease Congenital heart diseases (CHD) refer to structural or functional heart diseases, which are present at birth. Some of these lesions may be discovered later. prevalence of Chd
5.8 Congenital Heart Disease Congenital heart diseases (CHD) refer to structural or functional heart diseases, which are present at birth. Some of these lesions may be discovered later. prevalence of Chd
Mitral Valve Disease, When to Intervene
 Mitral Valve Disease, When to Intervene Swedish Heart and Vascular Institute Ming Zhang MD PhD Interventional Cardiology Structure Heart Disease Conflict of Interest None Current ACC/AHA guideline Stages
Mitral Valve Disease, When to Intervene Swedish Heart and Vascular Institute Ming Zhang MD PhD Interventional Cardiology Structure Heart Disease Conflict of Interest None Current ACC/AHA guideline Stages
Treatment of Inter-MitraClip Regurgitation Due to Posterior Leaflet Cleft by Use of The Amplatzer Vascular Plug II device
 Volume 1, Issue 3 Case Report ISSN: 2572-9292 Treatment of Inter-MitraClip Regurgitation Due to Posterior Leaflet Cleft by Use of The Amplatzer Vascular Plug II device Neha M. Mantri, Gagan D. Singh, Thomas
Volume 1, Issue 3 Case Report ISSN: 2572-9292 Treatment of Inter-MitraClip Regurgitation Due to Posterior Leaflet Cleft by Use of The Amplatzer Vascular Plug II device Neha M. Mantri, Gagan D. Singh, Thomas
Hypoplastic Left Heart Syndrome: Echocardiographic Assessment
 Hypoplastic Left Heart Syndrome: Echocardiographic Assessment Craig E Fleishman, MD, FACC, FASE Director, Non-invasive Cardiac Imaging The Hear Center at Arnold Palmer Hospital for Children, Orlando SCAI
Hypoplastic Left Heart Syndrome: Echocardiographic Assessment Craig E Fleishman, MD, FACC, FASE Director, Non-invasive Cardiac Imaging The Hear Center at Arnold Palmer Hospital for Children, Orlando SCAI
Case Report. Stent Placement in a Neonate with Sano Modification of the Norwood using Semi-Elective Extracorporeal Membrane Oxygenation.
 Stent Placement in a Neonate with Sano Modification of the Norwood using Semi-Elective Extracorporeal Membrane Oxygenation Mustafa Gulgun and Michael Slack Associated Profesor Children National Medical
Stent Placement in a Neonate with Sano Modification of the Norwood using Semi-Elective Extracorporeal Membrane Oxygenation Mustafa Gulgun and Michael Slack Associated Profesor Children National Medical
Case submission for CSI Asia-Pacific Case 2
 Case submission for CSI Asia-Pacific 2018- Case 2 Title Page Case category: Coarctation and ducts, valves Title: Simultaneous balloon aortic valvuloplasty with transcatheter closure of large hypertensive
Case submission for CSI Asia-Pacific 2018- Case 2 Title Page Case category: Coarctation and ducts, valves Title: Simultaneous balloon aortic valvuloplasty with transcatheter closure of large hypertensive
8/31/2016. Mitraclip in Matthew Johnson, MD
 Mitraclip in 2016 Matthew Johnson, MD 1 Abnormal Valve Function Valve Stenosis Obstruction to valve flow during that phase of the cardiac cycle when the valve is normally open. Hemodynamic hallmark - pressure
Mitraclip in 2016 Matthew Johnson, MD 1 Abnormal Valve Function Valve Stenosis Obstruction to valve flow during that phase of the cardiac cycle when the valve is normally open. Hemodynamic hallmark - pressure
A New Amplatzer Device to Maintain Patency of Fontan Fenestrations and Atrial Septal Defects
 Catheterization and Cardiovascular Interventions 57:246 251 (2002) Pediatric Interventions A New Amplatzer Device to Maintain Patency of Fontan Fenestrations and Atrial Septal Defects Zahid Amin, 1,2 *
Catheterization and Cardiovascular Interventions 57:246 251 (2002) Pediatric Interventions A New Amplatzer Device to Maintain Patency of Fontan Fenestrations and Atrial Septal Defects Zahid Amin, 1,2 *
Repair or Replacement
 Surgical intervention post MitraClip Device: Repair or Replacement Saudi Heart Association, February 21-24 Rüdiger Lange, MD, PhD Nicolo Piazza, MD, FRCPC, FESC German Heart Center, Munich, Germany Division
Surgical intervention post MitraClip Device: Repair or Replacement Saudi Heart Association, February 21-24 Rüdiger Lange, MD, PhD Nicolo Piazza, MD, FRCPC, FESC German Heart Center, Munich, Germany Division
ATRIAL SEPTAL CLOSURE AND LEFT ATRIAL APPENDAGE OCCLUSION: INDICATIONS AND GUIDANCE ECHOCARDIOGRAPHY IN INTERVENTIONAL CARDIOLOGY
 ATRIAL SEPTAL CLOSURE AND LEFT ATRIAL APPENDAGE OCCLUSION: INDICATIONS AND GUIDANCE Aristides G. Panlilio, MD, FPCP, FPCC,FPSE, FASE Philippine Heart Center Chinese General Hospital and Medical Center
ATRIAL SEPTAL CLOSURE AND LEFT ATRIAL APPENDAGE OCCLUSION: INDICATIONS AND GUIDANCE Aristides G. Panlilio, MD, FPCP, FPCC,FPSE, FASE Philippine Heart Center Chinese General Hospital and Medical Center
Recent technical advances and increasing experience
 Pediatric Open Heart Operations Without Diagnostic Cardiac Catheterization Jean-Pierre Pfammatter, MD, Pascal A. Berdat, MD, Thierry P. Carrel, MD, and Franco P. Stocker, MD Division of Pediatric Cardiology,
Pediatric Open Heart Operations Without Diagnostic Cardiac Catheterization Jean-Pierre Pfammatter, MD, Pascal A. Berdat, MD, Thierry P. Carrel, MD, and Franco P. Stocker, MD Division of Pediatric Cardiology,
Ping-Pong Guide Catheter Technique for Retrograde Intervention of a Chronic Total Occlusion Through an Ipsilateral Collateral
 Catheterization and Cardiovascular Interventions 78:395 399 (2011) Case Reports Ping-Pong Guide Catheter Technique for Retrograde Intervention of a Chronic Total Occlusion Through an Ipsilateral Collateral
Catheterization and Cardiovascular Interventions 78:395 399 (2011) Case Reports Ping-Pong Guide Catheter Technique for Retrograde Intervention of a Chronic Total Occlusion Through an Ipsilateral Collateral
Dual Arterial Access for Stenting of Aortic Coarctation in Patients with Near-Total Descending Aortic Interruption
 DOI 10.1007/s40119-015-0048-9 CASE SERIES Dual Arterial Access for Stenting of Aortic Coarctation in Patients with Near-Total Descending Aortic Interruption Tahir Hamid. Syed Ibrahim Jamallulail. Bernard
DOI 10.1007/s40119-015-0048-9 CASE SERIES Dual Arterial Access for Stenting of Aortic Coarctation in Patients with Near-Total Descending Aortic Interruption Tahir Hamid. Syed Ibrahim Jamallulail. Bernard
Tetralogy of Fallot (TOF) with atrioventricular (AV)
 Tetralogy of Fallot with Atrioventricular Canal Defect: Two Patch Repair Sitaram M. Emani, MD, and Pedro J. del Nido, MD Tetralogy of Fallot (TOF) with atrioventricular (AV) canal defect is classified
Tetralogy of Fallot with Atrioventricular Canal Defect: Two Patch Repair Sitaram M. Emani, MD, and Pedro J. del Nido, MD Tetralogy of Fallot (TOF) with atrioventricular (AV) canal defect is classified
Anatomy & Physiology
 1 Anatomy & Physiology Heart is divided into four chambers, two atrias & two ventricles. Atrioventricular valves (tricuspid & mitral) separate the atria from ventricles. they open & close to control flow
1 Anatomy & Physiology Heart is divided into four chambers, two atrias & two ventricles. Atrioventricular valves (tricuspid & mitral) separate the atria from ventricles. they open & close to control flow
Introduction. Study Design. Background. Operative Procedure-I
 Risk Factors for Mortality After the Norwood Procedure Using Right Ventricle to Pulmonary Artery Shunt Ann Thorac Surg 2009;87:178 86 86 Addressor: R1 胡祐寧 2009/3/4 AM7:30 SICU 討論室 Introduction Hypoplastic
Risk Factors for Mortality After the Norwood Procedure Using Right Ventricle to Pulmonary Artery Shunt Ann Thorac Surg 2009;87:178 86 86 Addressor: R1 胡祐寧 2009/3/4 AM7:30 SICU 討論室 Introduction Hypoplastic
"Giancarlo Rastelli Lecture"
 "Giancarlo Rastelli Lecture" Surgical treatment of Malpositions of the Great Arteries Pascal Vouhé Giancarlo Rastelli (1933 1970) Cliquez pour modifier les styles du texte du masque Deuxième niveau Troisième
"Giancarlo Rastelli Lecture" Surgical treatment of Malpositions of the Great Arteries Pascal Vouhé Giancarlo Rastelli (1933 1970) Cliquez pour modifier les styles du texte du masque Deuxième niveau Troisième
Implantation of Cardioverter Defibrillator After Percutaneous Closure of Atrial Septal Defect
 The Ochsner Journal 10:27 31, 2010 f Academic Division of Ochsner Clinic Foundation Implantation of Cardioverter Defibrillator After Percutaneous Closure of Atrial Septal Defect Anas Bitar, MD, Maria Malaya
The Ochsner Journal 10:27 31, 2010 f Academic Division of Ochsner Clinic Foundation Implantation of Cardioverter Defibrillator After Percutaneous Closure of Atrial Septal Defect Anas Bitar, MD, Maria Malaya
Coarctation of the aorta
 T H E P E D I A T R I C C A R D I A C S U R G E R Y I N Q U E S T R E P O R T Coarctation of the aorta In the normal heart, blood flows to the body through the aorta, which connects to the left ventricle
T H E P E D I A T R I C C A R D I A C S U R G E R Y I N Q U E S T R E P O R T Coarctation of the aorta In the normal heart, blood flows to the body through the aorta, which connects to the left ventricle
TCTAP C-217 Bilateral Pulmonary Arterio Venus Fistula Managed by Vascular Plugs and Coil Manotosh Panja 1 1 BelleVue Clinic, India
 S450 JOURNAL OF THE AMERICAN COLLEGE OF CARDIOLOGY, VOL. 65, NO. 17, SUPPL S, 2015 Case Summary. Aneurysm at LVOT is a rare complication after Bentall operation and the aneurysm may increase in size. In
S450 JOURNAL OF THE AMERICAN COLLEGE OF CARDIOLOGY, VOL. 65, NO. 17, SUPPL S, 2015 Case Summary. Aneurysm at LVOT is a rare complication after Bentall operation and the aneurysm may increase in size. In
Percutaneous Intervention for totally Occluded Coarctation Of Aorta. John Jose, Vipin Kumar, Ommen K George Dept Of Cardiology
 Percutaneous Intervention for totally Occluded Coarctation Of Aorta John Jose, Vipin Kumar, Ommen K George Dept Of Cardiology Background Coarctation of aorta (CoA) forms 5-7% of congenital heart diseases
Percutaneous Intervention for totally Occluded Coarctation Of Aorta John Jose, Vipin Kumar, Ommen K George Dept Of Cardiology Background Coarctation of aorta (CoA) forms 5-7% of congenital heart diseases
Transthoracic closure of atrial septal defect and ventricular septal defect without cardiopulmonary bypass
 Transthoracic closure of atrial septal defect and ventricular septal defect without cardiopulmonary bypass L. Wan, B.-T. Yu, Q.-C. Wu, L. Zeng, Q. Wang, J. Tang, Q.-R. Xu, H. Xu, W.-J. Wang, Y.-P. Cao
Transthoracic closure of atrial septal defect and ventricular septal defect without cardiopulmonary bypass L. Wan, B.-T. Yu, Q.-C. Wu, L. Zeng, Q. Wang, J. Tang, Q.-R. Xu, H. Xu, W.-J. Wang, Y.-P. Cao
Double Outlet Right Ventricle with Anterior and Left-Sided Aorta and Subpulmonary Ventricular Septal Defect
 Case Report Double Outlet Right Ventricle with Anterior and Left-Sided rta and Subpulmonary Ventricular Septal Defect Luciana Braz Peixoto, Samira Morhy Borges Leal, Carlos Eduardo Suaide Silva, Sandra
Case Report Double Outlet Right Ventricle with Anterior and Left-Sided rta and Subpulmonary Ventricular Septal Defect Luciana Braz Peixoto, Samira Morhy Borges Leal, Carlos Eduardo Suaide Silva, Sandra
An understanding of the many factors involved in the
 Atrioventricular Valve Dysfunction: Evaluation by Doppler and Cross-Sectional Ultrasound Norman H. Silverman, MD, and Doff B. McElhinney, MD Division of Pediatric Cardiology, Department of Pediatrics,
Atrioventricular Valve Dysfunction: Evaluation by Doppler and Cross-Sectional Ultrasound Norman H. Silverman, MD, and Doff B. McElhinney, MD Division of Pediatric Cardiology, Department of Pediatrics,
Repair of very severe tricuspid regurgitation following detachment of the tricuspid valve
 OPEN ACCESS Images in cardiology Repair of very severe tricuspid regurgitation following detachment of the tricuspid valve Ahmed Mahgoub 1, Hassan Kamel 2, Walid Simry 1, Hatem Hosny 1, * 1 Aswan Heart
OPEN ACCESS Images in cardiology Repair of very severe tricuspid regurgitation following detachment of the tricuspid valve Ahmed Mahgoub 1, Hassan Kamel 2, Walid Simry 1, Hatem Hosny 1, * 1 Aswan Heart
The goal of the hybrid approach for hypoplastic left heart
 The Hybrid Approach to Hypoplastic Left Heart Syndrome Mark Galantowicz, MD The goal of the hybrid approach for hypoplastic left heart syndrome (HLHS) is to lessen the cumulative impact of staged interventions,
The Hybrid Approach to Hypoplastic Left Heart Syndrome Mark Galantowicz, MD The goal of the hybrid approach for hypoplastic left heart syndrome (HLHS) is to lessen the cumulative impact of staged interventions,
An anterior aortoventriculoplasty, known as the Konno-
 The Konno-Rastan Procedure for Anterior Aortic Annular Enlargement Mark E. Roeser, MD An anterior aortoventriculoplasty, known as the Konno-Rastan procedure, is a useful tool for the cardiac surgeon. Originally,
The Konno-Rastan Procedure for Anterior Aortic Annular Enlargement Mark E. Roeser, MD An anterior aortoventriculoplasty, known as the Konno-Rastan procedure, is a useful tool for the cardiac surgeon. Originally,
CATHETERIZATION PROTOCOL Prepared by Matthew Crystal ( )
 CATHETERIZATION PROTOCOL Prepared by Matthew Crystal (2006-06-21) Cath Procedure Diagnosis: Hospitalization Requirement Blood on hold Cath Lab Fontan Yes (CCU after completion) Yes (as per OR protocols)
CATHETERIZATION PROTOCOL Prepared by Matthew Crystal (2006-06-21) Cath Procedure Diagnosis: Hospitalization Requirement Blood on hold Cath Lab Fontan Yes (CCU after completion) Yes (as per OR protocols)
The modified Konno procedure, or subaortic ventriculoplasty,
 Modified Konno Procedure for Left Ventricular Outflow Tract Obstruction David P. Bichell, MD The modified Konno procedure, or subaortic ventriculoplasty, first described by Cooley and Garrett in1986, 1
Modified Konno Procedure for Left Ventricular Outflow Tract Obstruction David P. Bichell, MD The modified Konno procedure, or subaortic ventriculoplasty, first described by Cooley and Garrett in1986, 1
The Heart. Happy Friday! #takeoutyournotes #testnotgradedyet
 The Heart Happy Friday! #takeoutyournotes #testnotgradedyet Introduction Cardiovascular system distributes blood Pump (heart) Distribution areas (capillaries) Heart has 4 compartments 2 receive blood (atria)
The Heart Happy Friday! #takeoutyournotes #testnotgradedyet Introduction Cardiovascular system distributes blood Pump (heart) Distribution areas (capillaries) Heart has 4 compartments 2 receive blood (atria)
Balloon valvuloplasty and angioplasty in congenital
 Br Heart J 1985; 54: 285-9 Balloon valvuloplasty and angioplasty in congenital heart disease GRAHAM A H MILLER From the Brompton Hospital, London SUMMARY Balloon dilatation valvuloplasty was performed
Br Heart J 1985; 54: 285-9 Balloon valvuloplasty and angioplasty in congenital heart disease GRAHAM A H MILLER From the Brompton Hospital, London SUMMARY Balloon dilatation valvuloplasty was performed
Ventricular septal defects (VSD) are one of the most
 Treatment of Isolated Ventricular Septal Defects in Children: Amplatzer Versus Surgical Closure Pierre Oses, MD, Nicolas Hugues, MD, Nagib Dahdah, MD, Suzanne J. Vobecky, MD, Joaquim Miro, MD, Michel Pellerin,
Treatment of Isolated Ventricular Septal Defects in Children: Amplatzer Versus Surgical Closure Pierre Oses, MD, Nicolas Hugues, MD, Nagib Dahdah, MD, Suzanne J. Vobecky, MD, Joaquim Miro, MD, Michel Pellerin,
Surgery For Ebstein Anomaly
 Surgery For Ebstein Anomaly Christian Pizarro, MD Chief, Pediatric Cardiothoracic Surgery Director, Nemours Cardiac Center Alfred I. dupont Hospital for Children Professor of Surgery and Pediatrics Sidney
Surgery For Ebstein Anomaly Christian Pizarro, MD Chief, Pediatric Cardiothoracic Surgery Director, Nemours Cardiac Center Alfred I. dupont Hospital for Children Professor of Surgery and Pediatrics Sidney
Delayed Infective Endocarditis with Mycotic Aneurysm Rupture below the Mechanical Valved Conduit after the Bentall Procedure
 Case Report Acta Cardiol Sin 2014;30:341 345 Delayed Infective Endocarditis with Mycotic Aneurysm Rupture below the Mechanical Valved Conduit after the Bentall Procedure Mei-Ling Chen, 1,3 Michael Y. Chen,
Case Report Acta Cardiol Sin 2014;30:341 345 Delayed Infective Endocarditis with Mycotic Aneurysm Rupture below the Mechanical Valved Conduit after the Bentall Procedure Mei-Ling Chen, 1,3 Michael Y. Chen,
the Cardiovascular System I
 the Cardiovascular System I By: Dr. Nabil A Khouri MD, MsC, Ph.D MEDIASTINUM 1. Superior Mediastinum 2. inferior Mediastinum Anterior mediastinum. Middle mediastinum. Posterior mediastinum Anatomy of
the Cardiovascular System I By: Dr. Nabil A Khouri MD, MsC, Ph.D MEDIASTINUM 1. Superior Mediastinum 2. inferior Mediastinum Anterior mediastinum. Middle mediastinum. Posterior mediastinum Anatomy of
A Novel Balloon Assisted Two-Stents Telescoping Technique for Repositioning an Embolized Stent in the Pulmonary Conduit
 Catheterization and Cardiovascular Interventions 84:219 223 (2014) A Novel Balloon Assisted Two-Stents Telescoping Technique for Repositioning an Embolized Stent in the Pulmonary Conduit Daisuke Kobayashi,*
Catheterization and Cardiovascular Interventions 84:219 223 (2014) A Novel Balloon Assisted Two-Stents Telescoping Technique for Repositioning an Embolized Stent in the Pulmonary Conduit Daisuke Kobayashi,*
Transcatheter Closures for Fistula Tract and Paravalvular Leak after Mitral Valve Replacement and Tricuspid Annuloplasty
 Case Report Print ISSN 1738-5520 On-line ISSN 1738-5555 Korean Circulation Journal Transcatheter Closures for Fistula Tract and Paravalvular Leak after Mitral Valve Replacement and Tricuspid nnuloplasty
Case Report Print ISSN 1738-5520 On-line ISSN 1738-5555 Korean Circulation Journal Transcatheter Closures for Fistula Tract and Paravalvular Leak after Mitral Valve Replacement and Tricuspid nnuloplasty
Congenital Heart Defects
 Normal Heart Congenital Heart Defects 1. Patent Ductus Arteriosus The ductus arteriosus connects the main pulmonary artery to the aorta. In utero, it allows the blood leaving the right ventricle to bypass
Normal Heart Congenital Heart Defects 1. Patent Ductus Arteriosus The ductus arteriosus connects the main pulmonary artery to the aorta. In utero, it allows the blood leaving the right ventricle to bypass
Although most patients with Ebstein s anomaly live
 Management of Neonatal Ebstein s Anomaly Christopher J. Knott-Craig, MD, FACS Although most patients with Ebstein s anomaly live through infancy, those who present clinically as neonates are a distinct
Management of Neonatal Ebstein s Anomaly Christopher J. Knott-Craig, MD, FACS Although most patients with Ebstein s anomaly live through infancy, those who present clinically as neonates are a distinct
Percutaneous mitral valve repair/replacement. Jan Van der Heyden MD, PhD St.Antonius Hospital Nieuwegein
 Percutaneous mitral valve repair/replacement Jan Van der Heyden MD, PhD St.Antonius Hospital Nieuwegein Mitral Valve anatomy Difference between AoV and MV Aortic Valve Mitral Valve Transcatheter Mitral
Percutaneous mitral valve repair/replacement Jan Van der Heyden MD, PhD St.Antonius Hospital Nieuwegein Mitral Valve anatomy Difference between AoV and MV Aortic Valve Mitral Valve Transcatheter Mitral
Surgical Treatment for Double Outlet Right Ventricle. Masakazu Nakao Consultant, Paediatric Cardiothoracic Surgery
 for Double Outlet Right Ventricle Masakazu Nakao Consultant, Paediatric Cardiothoracic Surgery 1 History Intraventricular tunnel (Kawashima) First repair of Taussig-Bing anomaly (Kirklin) Taussig-Bing
for Double Outlet Right Ventricle Masakazu Nakao Consultant, Paediatric Cardiothoracic Surgery 1 History Intraventricular tunnel (Kawashima) First repair of Taussig-Bing anomaly (Kirklin) Taussig-Bing
The Adolescent and Adult Congenital Heart Disease Program
 The Adolescent and Adult Congenital Heart Disease Program The Heart Center at Nationwide Children s Hospital & The Ohio State University D- Transposition of the Great Vessels D- transposition of the great
The Adolescent and Adult Congenital Heart Disease Program The Heart Center at Nationwide Children s Hospital & The Ohio State University D- Transposition of the Great Vessels D- transposition of the great
Atrial Septal Defect Closure. Stephen Brecker Director, Cardiac Catheterisation Labs
 Stephen Brecker Director, Cardiac Catheterisation Labs ADVANCED ANGIOPLASTY Incorporating The Left Main 5 Plus Course Conflicts of Interest The following companies have supported educational courses held
Stephen Brecker Director, Cardiac Catheterisation Labs ADVANCED ANGIOPLASTY Incorporating The Left Main 5 Plus Course Conflicts of Interest The following companies have supported educational courses held
For Personal Use. Copyright HMP 2013
 12-00415 Case Report J INVASIVE CARDIOL 2013;25(4):E69-E71 A Concert in the Heart. Bilateral Melody Valve Implantation in the Branch Pulmonary Arteries Nicola Maschietto, MD, PhD and Ornella Milanesi,
12-00415 Case Report J INVASIVE CARDIOL 2013;25(4):E69-E71 A Concert in the Heart. Bilateral Melody Valve Implantation in the Branch Pulmonary Arteries Nicola Maschietto, MD, PhD and Ornella Milanesi,
Bioprosthetic Mitral Valve Dysfunction: Innovation and Evolution of a New Therapeutic Technique
 Bioprosthetic Mitral Valve Dysfunction: Innovation and Evolution of a New Therapeutic Technique Charanjit S. Rihal MD MBA Professor and Chair Division of Cardiovascular Diseases Mayo Clinic DISCLOSURES
Bioprosthetic Mitral Valve Dysfunction: Innovation and Evolution of a New Therapeutic Technique Charanjit S. Rihal MD MBA Professor and Chair Division of Cardiovascular Diseases Mayo Clinic DISCLOSURES
Transcatheter Closure of Atrial Septal Defects with Superior-anterior Rim Deficiency Using Amplatzer Septal Occluder
 ORIGINAL ARTICLE Transcatheter Closure of Atrial Septal Defects with Superior-anterior Rim Deficiency Using Amplatzer Septal Occluder Chien-Fu Huang, 1 Chih-Yuan Fang, 2 Sheung-Fat Ko, 3 Shao-Ju Chien,
ORIGINAL ARTICLE Transcatheter Closure of Atrial Septal Defects with Superior-anterior Rim Deficiency Using Amplatzer Septal Occluder Chien-Fu Huang, 1 Chih-Yuan Fang, 2 Sheung-Fat Ko, 3 Shao-Ju Chien,
Patent Foramen Ovale Closure Without Echocardiographic Control: Use of Standby Intracardiac Ultrasound
 JACC: CARDIOVASCULAR INTERVENTIONS VOL. 1, NO. 4, 2008 2008 BY THE AMERICAN COLLEGE OF CARDIOLOGY FOUNDATION ISSN 1936-8798/08/$34.00 PUBLISHED BY ELSEVIER INC. DOI: 10.1016/j.jcin.2008.05.006 Patent Foramen
JACC: CARDIOVASCULAR INTERVENTIONS VOL. 1, NO. 4, 2008 2008 BY THE AMERICAN COLLEGE OF CARDIOLOGY FOUNDATION ISSN 1936-8798/08/$34.00 PUBLISHED BY ELSEVIER INC. DOI: 10.1016/j.jcin.2008.05.006 Patent Foramen
THE HEART OBJECTIVES: LOCATION OF THE HEART IN THE THORACIC CAVITY CARDIOVASCULAR SYSTEM
 BIOLOGY II CARDIOVASCULAR SYSTEM ACTIVITY #3 NAME DATE HOUR THE HEART OBJECTIVES: Describe the anatomy of the heart and identify and give the functions of all parts. (pp. 356 363) Trace the flow of blood
BIOLOGY II CARDIOVASCULAR SYSTEM ACTIVITY #3 NAME DATE HOUR THE HEART OBJECTIVES: Describe the anatomy of the heart and identify and give the functions of all parts. (pp. 356 363) Trace the flow of blood
The CardioMEMS HF system (Abbott Vascular,
 How to Implant the CardioMEMS Heart Failure Sensor A step-by-step review of the sensor implantation procedure, including pre- and postprocedural assessment. BY DAVID M. SHAVELLE, MD, FACC, FSCAI The CardioMEMS
How to Implant the CardioMEMS Heart Failure Sensor A step-by-step review of the sensor implantation procedure, including pre- and postprocedural assessment. BY DAVID M. SHAVELLE, MD, FACC, FSCAI The CardioMEMS
Cardiac ultrasound protocols
 Cardiac ultrasound protocols IDEXX Telemedicine Consultants Two-dimensional and M-mode imaging planes Right parasternal long axis four chamber Obtained from the right side Displays the relative proportions
Cardiac ultrasound protocols IDEXX Telemedicine Consultants Two-dimensional and M-mode imaging planes Right parasternal long axis four chamber Obtained from the right side Displays the relative proportions
