Composite of pneumonia, re-intubation, or death within 30 days of randomisation.
|
|
|
- Marian Hoover
- 5 years ago
- Views:
Transcription
1 Appendix: definitions Clinical outcome measures Primary outcome measure Composite of pneumonia, re-intubation, or death within 30 days of randomisation. Pneumonia Care will be taken to distinguish between tracheal colonisation, upper respiratory tract infections and early onset pneumonia. Pneumonia must meet the following criteria: Two or more serial chest radiographs with at least one of the following features (one radiograph is sufficient for patients with no underlying pulmonary or cardiac disease): a) new or progressive and persistent infiltrate b) consolidation c) cavitation AND at least one of the following: a) fever (>38 C) with no other recognised cause b) leucopaenia (< 4 x 10 9 /L) or leucocytosis (>12 x 10 9 /L) c) for adults >70 years old altered mental status with no other cause AND at least two of the following: a) new onset of purulent sputum or change in character of sputum or increased respiratory secretions or increased suctioning requirements b) new onset or worsening cough or dyspnoea, or tachypnoea c) rales or bronchial breath sounds d) worsening gas exchange (hypoxia, increased oxygen requirement, increased ventilator demand) PRISM Protocol version th April 2017 Page 1 of 14
2 Endotracheal re-intubation Re-insertion of an endotracheal tube after the patient has been extubated following the completion of the index surgical procedure. Endotracheal extubation is defined as an intentional clinical decision to remove an endotracheal tube. Extubation does not include accidental or inadvertent removal of an endotracheal tube. Re-intubation does not include intubation and anaesthesia for subsequent surgical procedures within the follow-up period, unless the patient in not extubated at the end of the later surgical procedure. Secondary outcome measures (listed alphabetically) Acute Kidney Injury According to the KIDGO consensus definition of moderate or severe acute kidney injury (2012): a) a two-fold increase in serum creatinine compared the preoperative baseline measurement b) or an increase in serum creatinine 354 μmol/l ( 4.0 mg/dl) with an acute rise of > 44 μmol/l (0.5mg/dL) c) or oliguria of < 0.5 ml/kg/hour for twelve consecutive hours d) or the initiation of new renal replacement therapy Note: Cannot be diagnosed in patients with existing end stage renal failure. Acute psychosis or delirium An acute episode of severe confusion or personality change, which may result in hallucinations or delusional beliefs in the absence of a pre-existing diagnosis, which may account for the clinical symptoms and signs. PRISM Protocol version th April 2017 Page 2 of 14
3 Acute respiratory distress syndrome According to the Berlin consensus criteria (2012): a) Within one week of a known clinical insult or new worsening respiratory symptoms b) AND bilateral opacities on chest imaging, not fully explained by effusions, lobar/lung collapse, or nodules c) AND respiratory failure not explained by cardiac failure or fluid overload (requires objective assessment e.g. echocardiogram to exclude hydrostatic oedema if no risk factors are present) d) AND supplemental oxygenation (requires correcting if altitude >1000m): - Mild: PaO 2 :FiO kpa with PEEP or CPAP 5cmH 2 O - Moderate: PaO 2 :FiO kpa with PEEP 5cmH 2 O - Severe: PaO 2 :FiO kpa with PEEP 5cmH 2 O Anastamotic leak Demonstrated at laparotomy or by contrast enhanced radiograph or CT scan. Aspiration pneumonitis Acute lung injury after the inhalation of gastric contents. Bowel infarction Demonstrated at laparotomy. PRISM Protocol version th April 2017 Page 3 of 14
4 Bronchospasm Newly detected expiratory wheeze treated with bronchodilators. Cardiac events Myocardial infarction Increase in serum cardiac biomarker values (preferably cardiac troponin) with at least one value above the 99 th percentile upper reference limit and at least one of the following criteria: a) symptoms of new ischaemia b) new or presumed new significant ST segment or T wave ECG changes or new left bundle branch block c) development or pathological Q waves on ECG d) radiological or echocardiographic evidence of new loss of viable myocardium or new regional wall motion abnormality e) identification of intracoronary thrombus at angiography or autopsy Arrhythmia ECG evidence of cardiac rhythm disturbance. Cardiac arrest with successful resuscitation Cardiac arrest according to UK Resuscitation Council definition. Successful resuscitation is defined as return of spontaneous circulation for at least one hour. Cardiogenic pulmonary oedema Appropriate clinical history and examination with consistent chest radiograph. PRISM Protocol version th April 2017 Page 4 of 14
5 Infective complications Infection, source uncertain Strong clinical suspicion of infection but the course has not been confirmed. Requires two or more of the following criteria: a) core temperature <36 o C or >38 o C b) white cell count >12 x 10 9 /L or <4 x 10 9 /L c) respiratory rate >20 breaths per minute or PaCO 2 < 4.5 kpa d) pulse rate >90 beats per minute Urinary tract infection This is a simplified version of the CDC criteria taken from the ESA-ESICM consensus on perioperative outcome measures (Jammer et al. 2014). Urinary tract infection is defined as a positive urine culture of 10 5 colony forming units per ml with no more than two species of micro-organisms AND with at least one of the following signs or symptoms: a) fever (>38 o C) b) urgency c) frequency d) dysuria e) suprapubic tenderness PRISM Protocol version th April 2017 Page 5 of 14
6 f) costo-vertebral angle pain or tenderness with no other recognised cause Surgical site infection (superficial) A superficial surgical site infection must meet the following criteria: Infection occurs within 30 days after the operative procedure AND involves only skin and subcutaneous tissue of the incision AND patient has at least one of the following: a) purulent drainage from the superficial incision; b) organisms isolated from an aseptically obtained culture of fluid or tissue from the superficial incision; c) at least one of the following signs or symptoms of infection: pain or tenderness, localised swelling, redness, or heat, and superficial incision is deliberately opened by surgeon, unless incision is culture-negative; d) diagnosis of superficial incisional surgical site infection by the surgeon or attending physician. Surgical site infection (deep) A deep incisional surgical site infection must meet the following criteria: Infection occurs within 30 days after the operative procedure AND involves deep soft tissues (e.g., fascial and muscle layers) of the incision AND patient has at least one of the following: a) purulent drainage from the deep incision but not from the organ/space component of the surgical site b) a deep incision spontaneously dehisces or is deliberately opened by a surgeon when the patient has at least one of the following signs or symptoms: fever (>38 o C) or localised pain or tenderness, unless incision is culture-negative PRISM Protocol version th April 2017 Page 6 of 14
7 c) an abscess or other evidence of infection involving the deep incision is found on direct examination, during reoperation, or by histopathological or radiologic examination d) diagnosis of a deep incisional surgical site infection by a surgeon or attending physician An infection that involves both superficial and deep incision sites should be classified as a deep incisional surgical site infection. Surgical site infection (organ/space) An organ/space surgical site infection involves any part of the body, excluding the skin incision, fascia, or muscle layers that is opened or manipulated during the operative procedure. An organ/space surgical site infection must meet the following criteria: Infection occurs within 30 days after the operative procedure AND appears related to the previous surgery AND the infection involves any part of the body, excluding the skin incision, fascia, or muscle layers opened or manipulated during the operative procedure AND patient has at least one of the following: a) purulent drainage from a drain that is placed through a stab wound into the organ/space; b) organisms isolated from an aseptically obtained culture of fluid or tissue in the organ/ space; c) an abscess or other evidence of infection involving the organ/space that is found on direct examination, during reoperation, or by histopathologic or radiologic examination; d) diagnosis of an organ/space surgical site infection by a surgeon or attending physician. PRISM Protocol version th April 2017 Page 7 of 14
8 Laboratory-confirmed bloodstream infection Requires at least one of the following criteria: a) Patient has a recognised pathogen cultured from one or more blood cultures and the organism cultured from blood is not related to an infection at another site. b) Patient has a fever (>38 o C), chills, or hypotension and at least one of the following: a. Common skin contaminant is cultured from two or more blood cultures drawn on separate occasions; b. Common skin contaminant is cultured from at least one blood culture from a patient with an intravascular line, and the physician institutes appropriate antimicrobial therapy; c. Positive antigen blood test. Perforated viscus Demonstrated at laparotomy or by contrast enhanced radiograph or CT scan. For example perforated bowel, gall bladder etc. Pleural effusion Radiological evidence of significant fluid accumulation in the pleural cavity. Most commonly this will be detected using a chest radiograph or an ultrasound scan. PRISM Protocol version th April 2017 Page 8 of 14
9 Pneumothorax Air in the pleural cavity with no visceral bed surrounding the visceral pleura. Usually results from damage to the pleural membranes or lung tissue. Postoperative haemorrhage Gastro-intestinal bleed Unambiguous clinical evidence or endoscopy showing blood in gastro-intestinal tract. Other postoperative haemorrhage Overt blood loss, not from the gastro-intestinal tract, requiring transfusion of two or more units of blood in two hours. Pulmonary embolism A new blood clot or thrombus within the pulmonary arterial system identified by computed tomography pulmonary angiogram (CTPA) with an appropriate clinical history. Stroke Clinical diagnosis with confirmation by computed tomography (CT) scan. PRISM Protocol version th April 2017 Page 9 of 14
10 Definitions of pre-defined adverse events related to CPAP Interface intolerance due to excessive air leak Air leaks associated with delivery device sufficient to prevent effective CPAP. Subjective assessment by clinician. Pain Pain associated with contact of delivery device against the skin, sufficient to prevent effective CPAP. Subjective assessment of severity by the investigator. Cutaneous pressure sore or pressure area Pressure sore or pressure area associated with contact of the delivery device against the skin. Assessment of severity to be completed by investigator and reported on page two of the supplementary adverse event form according to Waterlow grading 16 : a) Grade 1: discolouration of intact skin, not affected by light pressure b) Grade 2: partial thickness skin loss/damage involving the dermis or epidermis c) Grade 3: Full thickness skin loss/damage involving the subcutaneous tissue but not the underlying fascia. d) Grade 4: Full thickness skin loss/damage with extensive destruction and necrosis of the underlying tissue. Claustrophobia Claustrophobia associated with the delivery device sufficient to prevent effective CPAP. Subjective assessment of severity by investigator. Oronasal dryness Oronasal dryness associated with delivery device sufficient to prevent effective CPAP. Subjective assessment of severity by the investigator. PRISM Protocol version th April 2017 Page 10 of 14
11 Hypercapnia Hypercapnia directly resulting from CPAP and sufficient to prevent effective CPAP. This should not include hypercapnia not directly caused by CPAP. Subjective assessment by investigator and to record peak PaCO 2 on page two of the supplementary adverse event form. Haemodynamic instability Systolic blood pressure of less than 70 mmhg or need for inotropic drugs to maintain systolic blood pressure higher than 85 mmhg for two hours or more, or electrocardiogram evidence of ischemia or significant ventricular arrhythmias. Vomiting Vomiting, which is sufficient to prevent effective CPAP. Subjective assessment of severity by investigator. Aspiration of gastric contents Inhalation of regurgitated gastric contents directly related to CPAP. PRISM Protocol version th April 2017 Page 11 of 14
12 Other definitions Active cancer A current diagnosis of cancer excluding non-melanoma skin cancers. A previous diagnosis of cancer where the patient underwent curative treatment with remission is not considered active cancer. A surgical procedure where the indication is a presumed diagnosis of cancer, but which has not yet been confirmed with histology, should be considered active cancer. Cancer surgery Intended to be a curative treatment The surgical procedure is intended to cure the cancer. Intended to be palliative treatment The surgical procedure is not intended to cure the cancer. For example surgical debulking in metastatic disease, partial removal of a tumour or for the purpose of pain or other symptom control. End of surgery Completion of surgery. Usually marked by suturing of the wound and application of dressing(s). Intraoperative recruitment manoeuvre A technique used by the anaesthetist to transiently increase the transpulmonary pressure. This is usually by increasing tidal volume or inspiratory pressure for at least one breath. Levels of care after surgery Level 3 care: Critical care unit A clinical area capable of providing invasive mechanical ventilation or support to at least two organ systems. PRISM Protocol version th April 2017 Page 12 of 14
13 Level 2 care: Critical care unit or step-down unit A clinical area capable of providing support to a single organ system, but not including invasive mechanical ventilation, which is considered level 3 care. Post-anaesthesia care unit (PACU) Short-stay clinical area dedicated to caring for patients that are recovering from anaesthesia. If the PACU is providing level 2 care then level 2 care should be recorded on the CRF. Surgical ward Hospital ward environment not offering single-organ support or dedicated to patients recovering from anaesthesia. Critical care unit admission Either level two or level three care, as defined above. Open surgical technique Open abdominal surgery is usually distinguished from laparoscopic by the fact that for laparoscopic surgery the incision is only large enough to remove the resected specimen. Some procedures may involve the use of a laparoscope as well as an open incision, where the incision is larger than required to remove the specimen this is considered open surgery. Preoperative oxygen saturation (SpO 2 ) Pulse-oximetry on room air before surgery. Primary hospital admission The hospital admission for elective surgery during which the participant was randomised as part of the PRISM trial. The duration of the primary hospital stay PRISM Protocol version th April 2017 Page 13 of 14
14 should be calculated from the date of randomisation. Respiratory support Invasive mechanical ventilation Positive pressure ventilation via an endotracheal tube or supraglottic airway device. Non-invasive mechanical ventilation Positive pressure mechanical ventilation via a face-mask, hood or helmet, or nasal device. However, Continuous Positive Airway Pressure (CPAP) is not considered non-invasive mechanical ventilation. High flow nasal oxygen Humidified oxygen therapy delivered via large-bore nasal prongs at flow rates greater than 50 litres per minute. Maximum positive end expiratory pressure (PEEP) during surgery The maximum pressure, above atmospheric pressure, that exists at the end of expiration and provided by mechanical ventilation. Maximum set tidal volume (Vt) during surgery The maximum volume of air displaced between inspiration and expiration during mechanical ventilation as set on the ventilator. Start of surgery Time of the induction of anaesthesia before the surgical procedure. PRISM Protocol version th April 2017 Page 14 of 14
Table of Contents. Definitions document
 Definitions document Table of Contents Definitions of preoperative risk factors... 3 What is the definition of neurosurgery?... 3 What should I do if some important medical co-morbidities are not included
Definitions document Table of Contents Definitions of preoperative risk factors... 3 What is the definition of neurosurgery?... 3 What should I do if some important medical co-morbidities are not included
SECTION 1: INCLUSION, EXCLUSION & RANDOMISATION INFORMATION
 SECTION 1: INCLUSION, EXCLUSION & RANDOMISATION INFORMATION DEMOGRAPHIC INFORMATION Given name Family name Date of birth Consent date Gender Female Male Date of surgery INCLUSION & EXCLUSION CRITERIA YES
SECTION 1: INCLUSION, EXCLUSION & RANDOMISATION INFORMATION DEMOGRAPHIC INFORMATION Given name Family name Date of birth Consent date Gender Female Male Date of surgery INCLUSION & EXCLUSION CRITERIA YES
SECTION 1: INCLUSION, EXCLUSION & RANDOMISATION INFORMATION
 SECTION 1: INCLUSION, EXCLUSION & RANDOMISATION INFORMATION DEMOGRAPHIC INFORMATION Given name Family name Date of birth Consent date (DD/MMM/YYYY) (DD/MMM/YYYY) Gender Female Male Date of surgery (DD/MMM/YYYY)
SECTION 1: INCLUSION, EXCLUSION & RANDOMISATION INFORMATION DEMOGRAPHIC INFORMATION Given name Family name Date of birth Consent date (DD/MMM/YYYY) (DD/MMM/YYYY) Gender Female Male Date of surgery (DD/MMM/YYYY)
Schematic of diagnosing surgical site infections
 Schematic of diagnosing surgical site infections Infection occurred within 30 days after an operation if no implant is in place within one year if an implant is in place eg. hip replacement Do NOT report
Schematic of diagnosing surgical site infections Infection occurred within 30 days after an operation if no implant is in place within one year if an implant is in place eg. hip replacement Do NOT report
PATIENT CHARACTERISTICS AND PREOPERATIVE DATA (ecrf 1).
 PATIENT CHARACTERISTICS AND PREOPERATIVE DATA (ecrf 1). 1 Inform Consent Date: / / dd / Mmm / yyyy 2 Patient identifier: Please enter the 6 digit Patient identification number from your site patient log
PATIENT CHARACTERISTICS AND PREOPERATIVE DATA (ecrf 1). 1 Inform Consent Date: / / dd / Mmm / yyyy 2 Patient identifier: Please enter the 6 digit Patient identification number from your site patient log
LAS VEGAS Case Report Form 1 Intra-Operative
 LAS VEGAS Case Report Form 1 Intra-Operative Patient Informed Consent 1. Informed consent applicable: yes no (choose no if waived by local EC) 1.1 If applicable; was consent obtained? yes no 1.2 If yes,
LAS VEGAS Case Report Form 1 Intra-Operative Patient Informed Consent 1. Informed consent applicable: yes no (choose no if waived by local EC) 1.1 If applicable; was consent obtained? yes no 1.2 If yes,
NON-INVASIVE VENTILATION. Lijun Ding 23 Jan 2018
 NON-INVASIVE VENTILATION Lijun Ding 23 Jan 2018 Learning objectives What is NIV The difference between CPAP and BiPAP The indication of the use of NIV Complication of NIV application Patient monitoring
NON-INVASIVE VENTILATION Lijun Ding 23 Jan 2018 Learning objectives What is NIV The difference between CPAP and BiPAP The indication of the use of NIV Complication of NIV application Patient monitoring
Annex 4. Case definitions of infections
 Protocol for validation of PPS of HAIs and antimicrobial use in European LTCF TECHNICAL DOCUMENT Annex 4. Case definitions of infections Healthcare-associated infections and antimicrobial use in European
Protocol for validation of PPS of HAIs and antimicrobial use in European LTCF TECHNICAL DOCUMENT Annex 4. Case definitions of infections Healthcare-associated infections and antimicrobial use in European
Scottish Surveillance of Healthcare Associated Infection Programme (SSHAIP) Health Protection Scotland (HPS) SSI Surveillance Protocol 7th Edition
 1 Contents Female reproductive system operations (Abdominal hysterectomy and Caesarean section)... 3 Intra-abdominal infections... 3 Endometritis... 4 Other infections of the female reproductive tract...
1 Contents Female reproductive system operations (Abdominal hysterectomy and Caesarean section)... 3 Intra-abdominal infections... 3 Endometritis... 4 Other infections of the female reproductive tract...
SURGICAL SITE INFECTIONS: SURVEILLANCE & PREVENTION
 SURGICAL SITE INFECTIONS: SURVEILLANCE & PREVENTION Facts There were an estimated 157,500 surgical site infections associated with inpatient surgeries in 2011. SSIs were the most common healthcare-associated
SURGICAL SITE INFECTIONS: SURVEILLANCE & PREVENTION Facts There were an estimated 157,500 surgical site infections associated with inpatient surgeries in 2011. SSIs were the most common healthcare-associated
Data Collection Tool. Standard Study Questions: Admission Date: Admission Time: Age: Gender:
 Data Collection Tool Standard Study Questions: Admission Date: Admission Time: Age: Gender: Specifics of Injury: Time of Injury: Mechanism of Injury Blunt vs Penetrating? Injury Severity Score? Injuries:
Data Collection Tool Standard Study Questions: Admission Date: Admission Time: Age: Gender: Specifics of Injury: Time of Injury: Mechanism of Injury Blunt vs Penetrating? Injury Severity Score? Injuries:
Trial protocol - NIVAS Study
 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 Trial protocol - NIVAS Study METHODS Study oversight The Non-Invasive Ventilation after Abdominal Surgery
1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 Trial protocol - NIVAS Study METHODS Study oversight The Non-Invasive Ventilation after Abdominal Surgery
INFECTION PREVENTION AND CONTROL
 INFECTION PREVENTION AND CONTROL Health Care-Associated Infection (HAI) Definitions May 28, 2012 The Capital Health Infection Prevention Control (IPAC) department conducts ongoing surveillance reports
INFECTION PREVENTION AND CONTROL Health Care-Associated Infection (HAI) Definitions May 28, 2012 The Capital Health Infection Prevention Control (IPAC) department conducts ongoing surveillance reports
Landmark articles on ventilation
 Landmark articles on ventilation Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity ARDS AECC DEFINITION-1994 ALI Acute onset Bilateral chest infiltrates PCWP
Landmark articles on ventilation Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity ARDS AECC DEFINITION-1994 ALI Acute onset Bilateral chest infiltrates PCWP
NIV - BI-LEVEL POSITIVE AIRWAY PRESSURE (BIPAP)
 Introduction NIV - BI-LEVEL POSITIVE AIRWAY PRESSURE (BIPAP) Noninvasive ventilation (NIV) is a method of delivering oxygen by positive pressure mask that allows for the prevention or postponement of invasive
Introduction NIV - BI-LEVEL POSITIVE AIRWAY PRESSURE (BIPAP) Noninvasive ventilation (NIV) is a method of delivering oxygen by positive pressure mask that allows for the prevention or postponement of invasive
ISF criteria (International sepsis forum consensus conference of infection in the ICU) Secondary peritonitis
 Appendix with supplementary material. This appendix was part of the submitted manuscript and has been peer reviewed. It is posted as supplied by the authors. Supplementary Tables Table S1. Definitions
Appendix with supplementary material. This appendix was part of the submitted manuscript and has been peer reviewed. It is posted as supplied by the authors. Supplementary Tables Table S1. Definitions
Acute Kidney Injury: Acute kidney injury, AKI (stage 3), is an abrupt (within 48 hours) reduction of kidney function defined as:
 COMPLICATIONS Acute Kidney Injury: Acute kidney injury, AKI (stage 3), is an abrupt (within 48 hours) reduction of kidney function defined as: Increase in serum creatinine (SCr) of more than or equal to
COMPLICATIONS Acute Kidney Injury: Acute kidney injury, AKI (stage 3), is an abrupt (within 48 hours) reduction of kidney function defined as: Increase in serum creatinine (SCr) of more than or equal to
Handling Common Problems & Pitfalls During. Oxygen desaturation in patients receiving mechanical ventilation ACUTE SEVERE RESPIRATORY FAILURE
 Handling Common Problems & Pitfalls During ACUTE SEVERE RESPIRATORY FAILURE Pravit Jetanachai, MD QSNICH Oxygen desaturation in patients receiving mechanical ventilation Causes of oxygen desaturation 1.
Handling Common Problems & Pitfalls During ACUTE SEVERE RESPIRATORY FAILURE Pravit Jetanachai, MD QSNICH Oxygen desaturation in patients receiving mechanical ventilation Causes of oxygen desaturation 1.
Supplementary Online Content 2
 Supplementary Online Content 2 van Meenen DMP, van der Hoeven SM, Binnekade JM, et al. Effect of on demand vs routine nebulization of acetylcysteine with salbutamol on ventilator-free days in intensive
Supplementary Online Content 2 van Meenen DMP, van der Hoeven SM, Binnekade JM, et al. Effect of on demand vs routine nebulization of acetylcysteine with salbutamol on ventilator-free days in intensive
Discussion of Complex Clinical Scenarios and Variable Review ACS NSQIP Clinical Support Team
 Discussion of Complex Clinical Scenarios and Variable Review CS NSQIP Clinical Support Team SCR Open Q& Calls The CS NSQIP Clinical Team is trialing Open format Q& calls for NSQIP SCRs Participation in
Discussion of Complex Clinical Scenarios and Variable Review CS NSQIP Clinical Support Team SCR Open Q& Calls The CS NSQIP Clinical Team is trialing Open format Q& calls for NSQIP SCRs Participation in
Quality ID #357: Surgical Site Infection (SSI) National Quality Strategy Domain: Effective Clinical Care
 Quality ID #357: Surgical Site Infection (SSI) National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Outcome DESCRIPTION: Percentage
Quality ID #357: Surgical Site Infection (SSI) National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Outcome DESCRIPTION: Percentage
Competency Title: Continuous Positive Airway Pressure
 Competency Title: Continuous Positive Airway Pressure Trainee Name: ------------------------------------------------------------- Title: ---------------------------------------------------------------
Competency Title: Continuous Positive Airway Pressure Trainee Name: ------------------------------------------------------------- Title: ---------------------------------------------------------------
Care of the Deteriorating Patient in Recovery NADIA TICEHURST : CLINICAL NURSE EDUCATOR PERI ANAESTHETICS BENDIGO HEALTH
 Care of the Deteriorating Patient in Recovery NADIA TICEHURST : CLINICAL NURSE EDUCATOR PERI ANAESTHETICS BENDIGO HEALTH Intended learning outcomes Describe the components of a comprehensive clinician
Care of the Deteriorating Patient in Recovery NADIA TICEHURST : CLINICAL NURSE EDUCATOR PERI ANAESTHETICS BENDIGO HEALTH Intended learning outcomes Describe the components of a comprehensive clinician
1.1.2 CPAP therapy is used for patients who are suffering from an acute type 1 respiratory failure (Pa02 <8kPa with a normal or low Pac02).
 Guidelines for initiating and managing CPAP (Continuous Positive Airway Pressure) on a general ward. B25/2006 1.Introduction and Who Guideline applies to 1.1.1 This document provides guidance for Healthcare
Guidelines for initiating and managing CPAP (Continuous Positive Airway Pressure) on a general ward. B25/2006 1.Introduction and Who Guideline applies to 1.1.1 This document provides guidance for Healthcare
Weaning from Mechanical Ventilation. Dr Azmin Huda Abdul Rahim
 Weaning from Mechanical Ventilation Dr Azmin Huda Abdul Rahim Content Definition Classification Weaning criteria Weaning methods Criteria for extubation Introduction Weaning comprises 40% of the duration
Weaning from Mechanical Ventilation Dr Azmin Huda Abdul Rahim Content Definition Classification Weaning criteria Weaning methods Criteria for extubation Introduction Weaning comprises 40% of the duration
NON INVASIVE LIFE SAVERS. Non Invasive Ventilation (NIV)
 Table 1. NIV: Mechanisms Of Action Decreases work of breathing Increases functional residual capacity Recruits collapsed alveoli Improves respiratory gas exchange Reverses hypoventilation Maintains upper
Table 1. NIV: Mechanisms Of Action Decreases work of breathing Increases functional residual capacity Recruits collapsed alveoli Improves respiratory gas exchange Reverses hypoventilation Maintains upper
DAILY SCREENING FORM
 DAILY SCREENING FORM Patient s initials: Date of admission: Time of admission: Gender: M F Year of Birth: Type of admission: Medical/Surgical/Postoperative (elective) Days Date Mechanical ventilation Lung
DAILY SCREENING FORM Patient s initials: Date of admission: Time of admission: Gender: M F Year of Birth: Type of admission: Medical/Surgical/Postoperative (elective) Days Date Mechanical ventilation Lung
Information Often Given to the Nurse at the Time of Admission to the Postanesthesia Care Unit
 Information Often Given to the Nurse at the Time of Admission to the Postanesthesia Care Unit * Patient s name and age * Surgical procedure and type of anesthetic including drugs used * Other intraoperative
Information Often Given to the Nurse at the Time of Admission to the Postanesthesia Care Unit * Patient s name and age * Surgical procedure and type of anesthetic including drugs used * Other intraoperative
POSTGRADUATE INSTITUTE OF MEDICINE UNIVERSITY OF COLOMBO
 POSTGRADUATE INSTITUTE OF MEDICINE UNIVERSITY OF COLOMBO MD (ANAESTHESIOLOGY) FINAL EXAMINATION AUGUST 2013 Date : 2 nd August 2013 Time : 1.00 p.m. 4.00 p.m. Answer any three questions. Answer each question
POSTGRADUATE INSTITUTE OF MEDICINE UNIVERSITY OF COLOMBO MD (ANAESTHESIOLOGY) FINAL EXAMINATION AUGUST 2013 Date : 2 nd August 2013 Time : 1.00 p.m. 4.00 p.m. Answer any three questions. Answer each question
Acute Respiratory Distress Syndrome (ARDS) An Update
 Acute Respiratory Distress Syndrome (ARDS) An Update Prof. A.S.M. Areef Ahsan FCPS(Medicine) MD(Critical Care Medicine) MD ( Chest) Head, Dept. of Critical Care Medicine BIRDEM General Hospital INTRODUCTION
Acute Respiratory Distress Syndrome (ARDS) An Update Prof. A.S.M. Areef Ahsan FCPS(Medicine) MD(Critical Care Medicine) MD ( Chest) Head, Dept. of Critical Care Medicine BIRDEM General Hospital INTRODUCTION
ARDS Management Protocol
 ARDS Management Protocol February 2018 ARDS Criteria Onset Within 1 week of a known clinical insult or new or worsening respiratory symptoms Bilateral opacities not fully explained by effusions, lobar/lung
ARDS Management Protocol February 2018 ARDS Criteria Onset Within 1 week of a known clinical insult or new or worsening respiratory symptoms Bilateral opacities not fully explained by effusions, lobar/lung
Interventional procedures guidance Published: 20 December 2017 nice.org.uk/guidance/ipg600
 Endobronchial valve insertion to reduce lung volume in emphysema Interventional procedures guidance Published: 20 December 2017 nice.org.uk/guidance/ipg600 Your responsibility This guidance represents
Endobronchial valve insertion to reduce lung volume in emphysema Interventional procedures guidance Published: 20 December 2017 nice.org.uk/guidance/ipg600 Your responsibility This guidance represents
Supplementary material 1. Definitions of study endpoints (extracted from the Endpoint Validation Committee Charter) 1.
 Rationale, design, and baseline characteristics of the SIGNIFY trial: a randomized, double-blind, placebo-controlled trial of ivabradine in patients with stable coronary artery disease without clinical
Rationale, design, and baseline characteristics of the SIGNIFY trial: a randomized, double-blind, placebo-controlled trial of ivabradine in patients with stable coronary artery disease without clinical
Moving from VAP to VAC
 Moving from VAP to VAC Cindy Munro, PhD, RN, ANP-BC, FAANP, FAAN Associate Dean of Research and Innovation Professor College of Nursing Conflict of interest: No relationships with pharmaceutical companies,
Moving from VAP to VAC Cindy Munro, PhD, RN, ANP-BC, FAANP, FAAN Associate Dean of Research and Innovation Professor College of Nursing Conflict of interest: No relationships with pharmaceutical companies,
Analgesia for chest trauma - RVI
 Analgesia for chest trauma - RVI Northern Network Initial Management Patients with blunt chest trauma will be managed in a standard fashion within the context of the well established trauma systems at
Analgesia for chest trauma - RVI Northern Network Initial Management Patients with blunt chest trauma will be managed in a standard fashion within the context of the well established trauma systems at
Critical Care of the Post-Surgical Patient
 Critical Care of the Post-Surgical Patient, Dr med vet, DEA, DECVIM-CA Many critically ill patients require surgical treatments. These patients often have multisystem abnormalities during the immediate
Critical Care of the Post-Surgical Patient, Dr med vet, DEA, DECVIM-CA Many critically ill patients require surgical treatments. These patients often have multisystem abnormalities during the immediate
COBIS Management of airway burns and inhalation injury PAEDIATRIC
 COBIS Management of airway burns and inhalation injury PAEDIATRIC 1 A multidisciplinary team should provide the management of the child with inhalation injury. Childhood inhalation injury mandates transfer
COBIS Management of airway burns and inhalation injury PAEDIATRIC 1 A multidisciplinary team should provide the management of the child with inhalation injury. Childhood inhalation injury mandates transfer
Oxygenation. Chapter 45. Re'eda Almashagba 1
 Oxygenation Chapter 45 Re'eda Almashagba 1 Respiratory Physiology Structure and function Breathing: inspiration, expiration Lung volumes and capacities Pulmonary circulation Respiratory gas exchange: oxygen,
Oxygenation Chapter 45 Re'eda Almashagba 1 Respiratory Physiology Structure and function Breathing: inspiration, expiration Lung volumes and capacities Pulmonary circulation Respiratory gas exchange: oxygen,
LAPAROSCOPIC APPENDICECTOMY
 LAPAROSCOPIC APPENDICECTOMY WHAT IS THE APPENDIX? The appendix is a small, fingerlike pouch of the intestinal tract located where the small and large join. It has no known use. It is postulated that the
LAPAROSCOPIC APPENDICECTOMY WHAT IS THE APPENDIX? The appendix is a small, fingerlike pouch of the intestinal tract located where the small and large join. It has no known use. It is postulated that the
What is the next best step?
 Noninvasive Ventilation William Janssen, M.D. Assistant Professor of Medicine National Jewish Health University of Colorado Denver Health Sciences Center What is the next best step? 65 year old female
Noninvasive Ventilation William Janssen, M.D. Assistant Professor of Medicine National Jewish Health University of Colorado Denver Health Sciences Center What is the next best step? 65 year old female
RECOGNISINGSURGICAL SITE INFECTIONS(SSIs) NOVEMBER 2017
 RECOGNISINGSURGICAL SITE INFECTIONS(SSIs) NOVEMBER 2017 Welcome to this training resource. It has been designed for all healthcare workers involved in coordinating SSI surveillance, SSI surveillance data
RECOGNISINGSURGICAL SITE INFECTIONS(SSIs) NOVEMBER 2017 Welcome to this training resource. It has been designed for all healthcare workers involved in coordinating SSI surveillance, SSI surveillance data
Does proning patients with refractory hypoxaemia improve mortality?
 Does proning patients with refractory hypoxaemia improve mortality? Clinical problem and domain I selected this case because although this was the second patient we had proned in our unit within a week,
Does proning patients with refractory hypoxaemia improve mortality? Clinical problem and domain I selected this case because although this was the second patient we had proned in our unit within a week,
Pulmonary Pathophysiology
 Pulmonary Pathophysiology 1 Reduction of Pulmonary Function 1. Inadequate blood flow to the lungs hypoperfusion 2. Inadequate air flow to the alveoli - hypoventilation 2 Signs and Symptoms of Pulmonary
Pulmonary Pathophysiology 1 Reduction of Pulmonary Function 1. Inadequate blood flow to the lungs hypoperfusion 2. Inadequate air flow to the alveoli - hypoventilation 2 Signs and Symptoms of Pulmonary
Pediatric SCR Discussion of Complex Clinical Scenarios NSQIP Annual Meeting July 26, 2015
 Pediatric SCR Discussion of Complex Clinical Scenarios NSQIP Annual Meeting July 26, 2015 Scenario 1: Postoperative SSI A 16 year-old patient Principal Operative Procedure: Incision and Drainage for monoarticular
Pediatric SCR Discussion of Complex Clinical Scenarios NSQIP Annual Meeting July 26, 2015 Scenario 1: Postoperative SSI A 16 year-old patient Principal Operative Procedure: Incision and Drainage for monoarticular
Heart failure for syndicate
 Heart failure for syndicate By M.Wafaie Aboleineen,MD,FACC ESC Guidelines for the diagnosis and treatment of heart failure Part I 1 4 2 Common ECG abnormalities in HF 3 Common CXR abnormalities in HF Common
Heart failure for syndicate By M.Wafaie Aboleineen,MD,FACC ESC Guidelines for the diagnosis and treatment of heart failure Part I 1 4 2 Common ECG abnormalities in HF 3 Common CXR abnormalities in HF Common
Q3 Sex Male Female. Q9b Pre-operative PPOSSUM Morbidity: Mortality:
 Case Report Form Q1 Study ID Q2 Age at admission to study (years) Q3 Sex Male Female Q4 Comorbidities CCF Y/N COPD Y/N CVA Y/N Dementia Y/N Hemiplegia Y/N CKD Y/N Leukaemia Y/N DM(complicated) Y/N Lymphoma
Case Report Form Q1 Study ID Q2 Age at admission to study (years) Q3 Sex Male Female Q4 Comorbidities CCF Y/N COPD Y/N CVA Y/N Dementia Y/N Hemiplegia Y/N CKD Y/N Leukaemia Y/N DM(complicated) Y/N Lymphoma
INternational observational study To Understand the impact and BEst practices of airway management in critically ill patients CASE REPORT FORM
 INternational observational study To Understand the impact and BEst practices of airway management in critically ill patients Study acronym identifier: INTUBE CASE REPORT FORM Centre ID number: Patient
INternational observational study To Understand the impact and BEst practices of airway management in critically ill patients Study acronym identifier: INTUBE CASE REPORT FORM Centre ID number: Patient
COMMISSION ON ACCREDITATION FOR RESPIRATORY CARE TMC DETAILED CONTENT OUTLINE COMPARISON
 A. Evaluate Data in the Patient Record I. PATIENT DATA EVALUATION AND RECOMMENDATIONS 1. Patient history e.g., admission data orders medications progress notes DNR status / advance directives social history
A. Evaluate Data in the Patient Record I. PATIENT DATA EVALUATION AND RECOMMENDATIONS 1. Patient history e.g., admission data orders medications progress notes DNR status / advance directives social history
SESSION 3 OXYGEN THERAPY
 SESSION 3 OXYGEN THERAPY Harith Eranga Yapa Department of Nursing Faculty of Health Sciences The Open University of Sri Lanka 1 Outline Methods of delivery Complications of oxygen therapy Artificial airways
SESSION 3 OXYGEN THERAPY Harith Eranga Yapa Department of Nursing Faculty of Health Sciences The Open University of Sri Lanka 1 Outline Methods of delivery Complications of oxygen therapy Artificial airways
Index. Note: Page numbers of article titles are in boldface type
 Index Note: Page numbers of article titles are in boldface type A Acute coronary syndrome, perioperative oxygen in, 599 600 Acute lung injury (ALI). See Lung injury and Acute respiratory distress syndrome.
Index Note: Page numbers of article titles are in boldface type A Acute coronary syndrome, perioperative oxygen in, 599 600 Acute lung injury (ALI). See Lung injury and Acute respiratory distress syndrome.
Prepared by : Bayan Kaddourah RN,MHM. GICU Clinical Instructor
 Mechanical Ventilation Prepared by : Bayan Kaddourah RN,MHM. GICU Clinical Instructor 1 Definition Is a supportive therapy to facilitate gas exchange. Most ventilatory support requires an artificial airway.
Mechanical Ventilation Prepared by : Bayan Kaddourah RN,MHM. GICU Clinical Instructor 1 Definition Is a supportive therapy to facilitate gas exchange. Most ventilatory support requires an artificial airway.
The use of proning in the management of Acute Respiratory Distress Syndrome
 Case 3 The use of proning in the management of Acute Respiratory Distress Syndrome Clinical Problem This expanded case summary has been chosen to explore the rationale and evidence behind the use of proning
Case 3 The use of proning in the management of Acute Respiratory Distress Syndrome Clinical Problem This expanded case summary has been chosen to explore the rationale and evidence behind the use of proning
Information on Laparoscopic Extended Right Hemicolectomy. Colon surgery. The Colon. Laparoscopic Extended Right Hemicolectomy
 Colon surgery Patients undergo colon surgery for a number of conditions including: colorectal cancer, polyps, inflammatory bowel disease (Crohn s disease and ulcerative colitis), colonic inertia, stricture
Colon surgery Patients undergo colon surgery for a number of conditions including: colorectal cancer, polyps, inflammatory bowel disease (Crohn s disease and ulcerative colitis), colonic inertia, stricture
SUPPLEMENTAL MATERIAL. Supplemental digital content 1, Appendix 1. Ischemic symptoms and electrocardiography
 SUPPLEMENTAL MATERIAL Supplemental digital content 1, Appendix 1. Ischemic symptoms and electrocardiography findings 1. Ischemic symptoms included any of the following: chest discomfort, arm discomfort,
SUPPLEMENTAL MATERIAL Supplemental digital content 1, Appendix 1. Ischemic symptoms and electrocardiography findings 1. Ischemic symptoms included any of the following: chest discomfort, arm discomfort,
FRCA Final SOE 2 Example Question: Clinical Anaesthesia FINAL SOE
 FINAL SOE Category Clinical Long Information given to candidate You are asked to assess a 70-yr-old man on the ICU who underwent elective liver resection two days ago. Anaesthesia and surgery straightforward.
FINAL SOE Category Clinical Long Information given to candidate You are asked to assess a 70-yr-old man on the ICU who underwent elective liver resection two days ago. Anaesthesia and surgery straightforward.
Acute Kidney Injury: Acute kidney injury, AKI (stage 3), is an abrupt reduction of kidney function defined as:
 HOSPITAL COMPLICATIONS Acute Kidney Injury: Acute kidney injury, AKI (stage 3), is an abrupt reduction of kidney function defined as: Increase in serum creatinine (SCr) of more than or equal to 3x baseline
HOSPITAL COMPLICATIONS Acute Kidney Injury: Acute kidney injury, AKI (stage 3), is an abrupt reduction of kidney function defined as: Increase in serum creatinine (SCr) of more than or equal to 3x baseline
CHEST INJURIES. Jacek Piątkowski M.D., Ph. D.
 CHEST INJURIES Jacek Piątkowski M.D., Ph. D. CHEST INJURIES 3-4% of all injuries 8% of patients hospitalized due to injuries 65% of patients who died at the accident place CLASSIFICATION OF THE CHEST INJURIES
CHEST INJURIES Jacek Piątkowski M.D., Ph. D. CHEST INJURIES 3-4% of all injuries 8% of patients hospitalized due to injuries 65% of patients who died at the accident place CLASSIFICATION OF THE CHEST INJURIES
Accurate Diagnosis Of Postoperative Pneumonia Requires Objective Data
 Accurate Diagnosis Of Postoperative Pneumonia Requires Objective Data David Ebler, MD David Skarupa, MD Andrew J. Kerwin, MD, FACS Jhun de Villa, MD Michael S. Nussbaum, MD, FACS J.J. Tepas III, MD, FACS
Accurate Diagnosis Of Postoperative Pneumonia Requires Objective Data David Ebler, MD David Skarupa, MD Andrew J. Kerwin, MD, FACS Jhun de Villa, MD Michael S. Nussbaum, MD, FACS J.J. Tepas III, MD, FACS
AORTIC GRAFT INFECTION
 NURSING CARE Theresa O Keefe NUM Vascular Unit PAH Vascular infections are serious They are associated with high morbidity and mortality The primary cause of surgical wound infections is contamination
NURSING CARE Theresa O Keefe NUM Vascular Unit PAH Vascular infections are serious They are associated with high morbidity and mortality The primary cause of surgical wound infections is contamination
Head injuries. Severity of head injuries
 Head injuries ED Teaching day 23 rd October Severity of head injuries Minor GCS 14-15 Must not have any of the following: Amnesia 10min Neurological sign or symptom Skull fracture (clinically or radiologically)
Head injuries ED Teaching day 23 rd October Severity of head injuries Minor GCS 14-15 Must not have any of the following: Amnesia 10min Neurological sign or symptom Skull fracture (clinically or radiologically)
Healthcare-associated infections and antimicrobial use in European long-term care facilities (HALT-3) RESIDENT QUESTIONNAIRE
 Healthcare-associated infections and antimicrobial use in European long-term care facilities (HALT-3) RESIDENT QUESTIONNAIRE RESIDENT DATA GENDER Male Female BIRTH YEAR (YYYY) LENGTH OF STAY IN THE FACILITY
Healthcare-associated infections and antimicrobial use in European long-term care facilities (HALT-3) RESIDENT QUESTIONNAIRE RESIDENT DATA GENDER Male Female BIRTH YEAR (YYYY) LENGTH OF STAY IN THE FACILITY
Paramedic Rounds. Pre-Hospital Continuous Positive Airway Pressure (CPAP)
 Paramedic Rounds Pre-Hospital Continuous Positive Airway Pressure (CPAP) Morgan Hillier MD Class of 2011 Dr. Mike Peddle Assistant Medical Director SWORBHP Objectives Outline evidence for pre-hospital
Paramedic Rounds Pre-Hospital Continuous Positive Airway Pressure (CPAP) Morgan Hillier MD Class of 2011 Dr. Mike Peddle Assistant Medical Director SWORBHP Objectives Outline evidence for pre-hospital
LOKUN! I got stomach ache!
 LOKUN! I got stomach ache! Mr L is a 67year old Chinese gentleman who is a non smoker, social drinker. He has a medical history significant for Hypertension, Hyperlipidemia, Type 2 Diabetes Mellitus, Chronic
LOKUN! I got stomach ache! Mr L is a 67year old Chinese gentleman who is a non smoker, social drinker. He has a medical history significant for Hypertension, Hyperlipidemia, Type 2 Diabetes Mellitus, Chronic
Endobronchial valve insertion to reduce lung volume in emphysema
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Endobronchial valve insertion to reduce lung volume in emphysema Emphysema is a chronic lung disease that
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Endobronchial valve insertion to reduce lung volume in emphysema Emphysema is a chronic lung disease that
University of Wisconsin - Madison Cardiovascular Medicine Fellowship Program UW CICU Rotation Goals and Objectives
 Background: The field of critical care cardiology has evolved considerably over the past 2 decades. Contemporary critical care cardiology is increasingly focused on the management of patients with advanced
Background: The field of critical care cardiology has evolved considerably over the past 2 decades. Contemporary critical care cardiology is increasingly focused on the management of patients with advanced
The diagnosis and management of pneumothorax
 Respiratory 131 The diagnosis and management of pneumothorax Pneumothorax is a relatively common presentation in patients under the age of 40 years (approximately, 85% of patients are younger than 40 years).
Respiratory 131 The diagnosis and management of pneumothorax Pneumothorax is a relatively common presentation in patients under the age of 40 years (approximately, 85% of patients are younger than 40 years).
NIV in Acute Respiratory Failure: Where we fail? Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity
 NIV in Acute Respiratory Failure: Where we fail? Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity Use of NIV 1998-2010 50 45 40 35 30 25 20 15 10 5 0 1998
NIV in Acute Respiratory Failure: Where we fail? Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity Use of NIV 1998-2010 50 45 40 35 30 25 20 15 10 5 0 1998
Web Appendix 1: Literature search strategy. BTS Acute Hypercapnic Respiratory Failure (AHRF) write-up. Sources to be searched for the guidelines;
 Web Appendix 1: Literature search strategy BTS Acute Hypercapnic Respiratory Failure (AHRF) write-up Sources to be searched for the guidelines; Cochrane Database of Systematic Reviews (CDSR) Database of
Web Appendix 1: Literature search strategy BTS Acute Hypercapnic Respiratory Failure (AHRF) write-up Sources to be searched for the guidelines; Cochrane Database of Systematic Reviews (CDSR) Database of
University of Bristol - Explore Bristol Research
 Rogers, C., Capoun, R., Scott, L., Taylor, J., Angelini, G., Narayan, P.,... Ascione, R. (2017). Shortening cardioplegic arrest time in patients undergoing combined coronary and valve surgery: results
Rogers, C., Capoun, R., Scott, L., Taylor, J., Angelini, G., Narayan, P.,... Ascione, R. (2017). Shortening cardioplegic arrest time in patients undergoing combined coronary and valve surgery: results
Dr. Rami M. Adil Al-Hayali Assistant Professor in Medicine
 Dr. Rami M. Adil Al-Hayali Assistant Professor in Medicine Venous thromboembolism: pulmonary embolism (PE) deep vein thrombosis (DVT) 1% of all patients admitted to hospital 5% of in-hospital mortality
Dr. Rami M. Adil Al-Hayali Assistant Professor in Medicine Venous thromboembolism: pulmonary embolism (PE) deep vein thrombosis (DVT) 1% of all patients admitted to hospital 5% of in-hospital mortality
Dr Yuen Wai-Cheung HA Convention 2011
 Dr Yuen Wai-Cheung HA Convention 2011 Outlines Why HA benchmarks hospitals? How to do a successful benchmarking? Using SOMIP as an example How to read and understand SOMIP report? Benchmarking Benchmarking
Dr Yuen Wai-Cheung HA Convention 2011 Outlines Why HA benchmarks hospitals? How to do a successful benchmarking? Using SOMIP as an example How to read and understand SOMIP report? Benchmarking Benchmarking
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv
 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv.8.18.18 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) SUDDEN PROGRESSIVE FORM OF ACUTE RESPIRATORY FAILURE ALVEOLAR CAPILLARY MEMBRANE BECOMES DAMAGED AND MORE
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv.8.18.18 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) SUDDEN PROGRESSIVE FORM OF ACUTE RESPIRATORY FAILURE ALVEOLAR CAPILLARY MEMBRANE BECOMES DAMAGED AND MORE
Bronchoalveolar lavage (BAL) with surfactant in pediatric ARDS
 Bronchoalveolar lavage (BAL) with surfactant in pediatric ARDS M. Luchetti, E. M. Galassini, A. Galbiati, C. Pagani,, F. Silla and G. A. Marraro gmarraro@picu.it www.picu.it Anesthesia and Intensive Care
Bronchoalveolar lavage (BAL) with surfactant in pediatric ARDS M. Luchetti, E. M. Galassini, A. Galbiati, C. Pagani,, F. Silla and G. A. Marraro gmarraro@picu.it www.picu.it Anesthesia and Intensive Care
Our Commitment to Quality and Patient Safety Core Measures
 Calvert Memorial Hospital is committed to our community, with a focus on patient-centered care. High quality and safe patient care is not our goal, it is our priority. That means delivering the best possible
Calvert Memorial Hospital is committed to our community, with a focus on patient-centered care. High quality and safe patient care is not our goal, it is our priority. That means delivering the best possible
1.40 Prevention of Nosocomial Pneumonia
 1.40 Prevention of Nosocomial Pneumonia Purpose Audience Policy Statement: The guideline is designed to reduce the incidence of pneumonia and other acute lower respiratory tract infections. All UTMB healthcare
1.40 Prevention of Nosocomial Pneumonia Purpose Audience Policy Statement: The guideline is designed to reduce the incidence of pneumonia and other acute lower respiratory tract infections. All UTMB healthcare
Bronchoconstriction is also treated with medications that inhibit bronchiolar constriction such as: Ipratropium (Atrovent)
 Patients with difficulty breathing (dyspnea) may have problems with: Oxygenation due to alveolar problems Ventilation due to bronchiolar problems Oxygenation due to lung perfusion problems Combinations
Patients with difficulty breathing (dyspnea) may have problems with: Oxygenation due to alveolar problems Ventilation due to bronchiolar problems Oxygenation due to lung perfusion problems Combinations
OBJECTIVES OF TRAINING FOR THE ANAESTHESIA TERM
 College of Intensive Care Medicine of Australia and New Zealand ABN: 16 134 292 103 Document type: Training Date established: 2007 Date last reviewed: 2014 OBJECTIVES OF TRAINING FOR THE ANAESTHESIA TERM
College of Intensive Care Medicine of Australia and New Zealand ABN: 16 134 292 103 Document type: Training Date established: 2007 Date last reviewed: 2014 OBJECTIVES OF TRAINING FOR THE ANAESTHESIA TERM
I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device
 I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device II. Policy: Continuous Positive Airway Pressure CPAP by the Down's system will be instituted by Respiratory Therapy personnel
I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device II. Policy: Continuous Positive Airway Pressure CPAP by the Down's system will be instituted by Respiratory Therapy personnel
Thrombolysis Delivery, Care, and Monitoring. 5 Acute Trusts - 6 Primary Care Trusts Ambulance Trust 4 Local Authorities
 Thrombolysis Delivery, Care, and Monitoring Documentation & Pathways Need to follow locally agreed policies and procedures Follow thrombolysis pathway? Need to complete Sits database Weight Dose matters!
Thrombolysis Delivery, Care, and Monitoring Documentation & Pathways Need to follow locally agreed policies and procedures Follow thrombolysis pathway? Need to complete Sits database Weight Dose matters!
Infection Control: Surgical Site Infections
 Infection Control: Surgical Site Infections Infectious Disease Epidemiology Section Office of Public Health Louisiana Dept of Health & Hospitals 800-256-2748 www.oph.dhh.louisiana.gov Your taxes at work
Infection Control: Surgical Site Infections Infectious Disease Epidemiology Section Office of Public Health Louisiana Dept of Health & Hospitals 800-256-2748 www.oph.dhh.louisiana.gov Your taxes at work
Noninvasive ventilation: Selection of patient, interfaces, initiation and weaning
 CME article Johnson S, et al: Noninvasive ventilation Noninvasive ventilation: Selection of patient, interfaces, initiation and weaning Saumy Johnson, Ramesh Unnikrishnan * Email: ramesh.unnikrishnan@manipal.edu
CME article Johnson S, et al: Noninvasive ventilation Noninvasive ventilation: Selection of patient, interfaces, initiation and weaning Saumy Johnson, Ramesh Unnikrishnan * Email: ramesh.unnikrishnan@manipal.edu
Subarachnoid haemorrhage: the management of neurogenic pulmonary oedema
 Subarachnoid haemorrhage: the management of neurogenic pulmonary oedema Clinical problem and domain I chose this case because I had not encountered neurogenic pulmonary oedema previously and was unfamiliar
Subarachnoid haemorrhage: the management of neurogenic pulmonary oedema Clinical problem and domain I chose this case because I had not encountered neurogenic pulmonary oedema previously and was unfamiliar
Case 1. What does the CXR show? How would you manage this patient? Discussion overleaf.
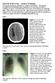 Tutorial of the week cerebral challenge. This has previously been published in Update in anaesthesia. Examples of investigations demonstrating typical appearances of commonly encountered conditions are
Tutorial of the week cerebral challenge. This has previously been published in Update in anaesthesia. Examples of investigations demonstrating typical appearances of commonly encountered conditions are
PATIENT INFORMATION FROM YOUR SURGEON & SAGES. Laparoscopic Colon Resection
 Patient Information published on: 03/2004 by the Society of American Gastrointestinal and Endoscopic Surgeons (SAGES) PATIENT INFORMATION FROM YOUR SURGEON & SAGES Laparoscopic Colon Resection About Conventional
Patient Information published on: 03/2004 by the Society of American Gastrointestinal and Endoscopic Surgeons (SAGES) PATIENT INFORMATION FROM YOUR SURGEON & SAGES Laparoscopic Colon Resection About Conventional
Respiratory Diseases and Disorders
 Chapter 9 Respiratory Diseases and Disorders Anatomy and Physiology Chest, lungs, and conducting airways Two parts: Upper respiratory system consists of nose, mouth, sinuses, pharynx, and larynx Lower
Chapter 9 Respiratory Diseases and Disorders Anatomy and Physiology Chest, lungs, and conducting airways Two parts: Upper respiratory system consists of nose, mouth, sinuses, pharynx, and larynx Lower
Approach to type 2 Respiratory Failure
 Approach to type 2 Respiratory Failure Changing Nature of NIV Not longer just the traditional COPD patients Increasingly Obesity Neuromuscular Pneumonias 3 fold increase in patients with Ph 7.25 and below
Approach to type 2 Respiratory Failure Changing Nature of NIV Not longer just the traditional COPD patients Increasingly Obesity Neuromuscular Pneumonias 3 fold increase in patients with Ph 7.25 and below
Keeping Patients Off the Vent: Bilevel, HFNC, Neither?
 Keeping Patients Off the Vent: Bilevel, HFNC, Neither? Robert Kempainen, MD Pulmonary and Critical Care Medicine Hennepin County Medical Center University of Minnesota School of Medicine Objectives Summarize
Keeping Patients Off the Vent: Bilevel, HFNC, Neither? Robert Kempainen, MD Pulmonary and Critical Care Medicine Hennepin County Medical Center University of Minnesota School of Medicine Objectives Summarize
Anaesthetic considerations for laparoscopic surgery in canines
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk Anaesthetic considerations for laparoscopic surgery in canines Author : Chris Miller Categories : Canine, Companion animal,
Vet Times The website for the veterinary profession https://www.vettimes.co.uk Anaesthetic considerations for laparoscopic surgery in canines Author : Chris Miller Categories : Canine, Companion animal,
Pet owners are often very anxious about veterinary procedures that involve anesthesia. This handout attempts to alleviate some of these concerns.
 Printable Version Anesthesia for Cats Pet owners are often very anxious about veterinary procedures that involve anesthesia. This handout attempts to alleviate some of these concerns. The word anesthesia
Printable Version Anesthesia for Cats Pet owners are often very anxious about veterinary procedures that involve anesthesia. This handout attempts to alleviate some of these concerns. The word anesthesia
CARDIAC PROBLEMS IN PREGNANCY
 CARDIAC PROBLEMS IN PREGNANCY LAS VEGAS, NEVADA, USA 27 February 1 March 2016 SUCCESSFUL TREATMENT WITH RECOMBINANT TISSUE PLASMINOGEN ACTIVATOR OF MASSIVE PULMONARY EMBOLISM IN THE 16 TH WEEK OF PREGNANCY
CARDIAC PROBLEMS IN PREGNANCY LAS VEGAS, NEVADA, USA 27 February 1 March 2016 SUCCESSFUL TREATMENT WITH RECOMBINANT TISSUE PLASMINOGEN ACTIVATOR OF MASSIVE PULMONARY EMBOLISM IN THE 16 TH WEEK OF PREGNANCY
Yes No Unknown. Major Infection Information
 Rehospitalization Intervention Check any that occurred during this hospitalization. Pacemaker without ICD ICD Atrial arrhythmia ablation Ventricular arrhythmia ablation Cardioversion CABG (coronary artery
Rehospitalization Intervention Check any that occurred during this hospitalization. Pacemaker without ICD ICD Atrial arrhythmia ablation Ventricular arrhythmia ablation Cardioversion CABG (coronary artery
Canadian Trauma Trials Collaborative. Occult Pneumothorax in Critical Care (OPTICC): Standardized Data Collection Sheet
 Canadian Trauma Trials Collaborative STUDY CENTRE: Institution: City / Province: / Occult Pneumothorax in Critical Care (OPTICC): Standardized Sheet PATIENT DEMOGRAPHICS: First Name: Health record number
Canadian Trauma Trials Collaborative STUDY CENTRE: Institution: City / Province: / Occult Pneumothorax in Critical Care (OPTICC): Standardized Sheet PATIENT DEMOGRAPHICS: First Name: Health record number
ARDS: an update 6 th March A. Hakeem Al Hashim, MD, FRCP SQUH
 ARDS: an update 6 th March 2017 A. Hakeem Al Hashim, MD, FRCP SQUH 30M, previously healthy Hx: 1 week dry cough Gradually worsening SOB No travel Hx Case BP 130/70, HR 100/min ph 7.29 pco2 35 po2 50 HCO3
ARDS: an update 6 th March 2017 A. Hakeem Al Hashim, MD, FRCP SQUH 30M, previously healthy Hx: 1 week dry cough Gradually worsening SOB No travel Hx Case BP 130/70, HR 100/min ph 7.29 pco2 35 po2 50 HCO3
Respiratory Failure. Causes of Acute Respiratory Failure (ARF): a- Intrapulmonary:
 Respiratory failure exists whenever the exchange of O 2 for CO 2 in the lungs cannot keep up with the rate of O 2 consumption & CO 2 production in the cells of the body. This results in a fall in arterial
Respiratory failure exists whenever the exchange of O 2 for CO 2 in the lungs cannot keep up with the rate of O 2 consumption & CO 2 production in the cells of the body. This results in a fall in arterial
ANAESTHESIA FOR BLEEDING TONSIL
 ANAESTHESIA FOR BLEEDING TONSIL BY Dr.S.C.Ganeshprabu, MD., D.A., Professor of Anaesthesiology, Madurai Medical College & Govt. Rajaji Hospital, Madurai -652 020. A 5-year-old child who had tonsillectomy
ANAESTHESIA FOR BLEEDING TONSIL BY Dr.S.C.Ganeshprabu, MD., D.A., Professor of Anaesthesiology, Madurai Medical College & Govt. Rajaji Hospital, Madurai -652 020. A 5-year-old child who had tonsillectomy
The Role of the Anaesthesiologist in the Perioperative Management of Preeclampsia. RA Dyer Interlaken 2017
 The Role of the Anaesthesiologist in the Perioperative Management of Preeclampsia RA Dyer Interlaken 2017 6 In preeclampsia - Understanding of pathophysiology Assessment of disease severity Prediction
The Role of the Anaesthesiologist in the Perioperative Management of Preeclampsia RA Dyer Interlaken 2017 6 In preeclampsia - Understanding of pathophysiology Assessment of disease severity Prediction
ICU management and referral guidelines for severe hypoxic respiratory failure
 Aim: ICU management and referral guidelines for severe hypoxic respiratory failure 1) To provide a concise management plan Non ventilatory Ventilatory 2) Timeline for referring patient with refractory
Aim: ICU management and referral guidelines for severe hypoxic respiratory failure 1) To provide a concise management plan Non ventilatory Ventilatory 2) Timeline for referring patient with refractory
Test Bank Pilbeam's Mechanical Ventilation Physiological and Clinical Applications 6th Edition Cairo
 Instant dowload and all chapters Test Bank Pilbeam's Mechanical Ventilation Physiological and Clinical Applications 6th Edition Cairo https://testbanklab.com/download/test-bank-pilbeams-mechanical-ventilation-physiologicalclinical-applications-6th-edition-cairo/
Instant dowload and all chapters Test Bank Pilbeam's Mechanical Ventilation Physiological and Clinical Applications 6th Edition Cairo https://testbanklab.com/download/test-bank-pilbeams-mechanical-ventilation-physiologicalclinical-applications-6th-edition-cairo/
Categorizing Wound Infections: A Comparison between ACS-NSQIP and an Institutional Surgical Secondary Events Database
 : A Comparison between ACS-NSQIP and an Institutional Surgical Secondary Events Database Luke V. Selby MD, Daniel D. Sjoberg MS, Danielle Cassella MA, Mindy Sovel MPH MS, David R. Jones MD, Vivian E. Strong
: A Comparison between ACS-NSQIP and an Institutional Surgical Secondary Events Database Luke V. Selby MD, Daniel D. Sjoberg MS, Danielle Cassella MA, Mindy Sovel MPH MS, David R. Jones MD, Vivian E. Strong
