Annals of Internal Medicine. 1993;118:45-58.
|
|
|
- Kory Chapman
- 6 years ago
- Views:
Transcription
1 NIH CONFERENCE Epstein-Barr Virus Infections: Biology, Pathogenesis, and Management Moderator: Stephen E. Straus, MD; Discussants: Jeffrey I. Cohen, MD; Giovanna Tosato, MD; and Jeffery Meier, MD Epstein-Barr virus (EBV) encodes genes that ensure its persistence in human B lymphocytes. Some of the genes encourage B-cell proliferation; others are poised to evade or defeat immune recognition. Immune restraints on the virus, however, are typically so effective that most infections are never symptomatic. In contrast, acute infectious mononucleosis, a self-limited lymphoproliferative illness, is common in adolescents and young adults. Unbridled proliferative illnesses arise when cellular immunity is grossly defective. Treatment of EBV-associated syndromes is largely supportive. Antiviral drugs have no proven role except in patients with oral hairy leukoplakia. Vaccine development is technically feasible but is not considered a high priority for developed nations. Annals of Internal Medicine. 1993;118: An edited summary of a Clinical Staff Conference held 25 March 1992 at the Amphitheater, Building 10, Bethesda, Maryland. The conference was sponsored by the National Institute of Allergy and Infectious Diseases, National Institutes of Health, and the Center for Biologies Evaluation and Research, Food and Drug Administration, U.S. Department of Health and Human Services. Authors who wish to cite a section of the conference and specifically indicate its author may use this example for the form of reference: Cohen JI. Molecular biology of Epstein-Barr virus and its mechanism of B-cell transformation, pp In: Straus SE, moderator. Epstein-Barr virus infections: biology, pathogenesis, and management. Ann Intern Med. 1992;118: Dr. Stephen E. Straus (Medical Virology Section, Laboratory of Clinical Investigation, National Institute of Allergy and Infectious Diseases [NIAID], National Institutes of Health [NIH], Bethesda, Maryland): Epstein-Barr virus (EBV) is a ubiquitous pathogen that has evolved an effective strategy for infection, persistence, and spread; EBV infection occurs in more than 90% of the population, most often without evident consequences (1, 2). The clinical outcome of infection rests on the compromise struck between the virus and the host a fragile interplay of competing forces. Epstein- Barr virus, for its part, unswervingly pursues a genetic mission to infect B lymphocytes, to endow them with an endless potential to pass the virus on to their progeny, and to do so while evading immune clearance. The host response is less predictable and determines whether an EBV infection becomes symptomatic. An ineffectual response, which occurs in persons with congenital or acquired immunodeficiency, permits the unbridled proliferation of virus-infected B cells. In contrast, the curious predilection of adolescents and adults to experience symptomatic infection and the features of the mononucleosis syndrome that ensues suggests that an excessive host response to EBV can also lead to illness. The biology of EBV, the diseases it provokes, the nature of the virus-host interaction and how it is controlled or subverted, and the limited means available to manage EBV infections are the subjects of this conference. Epidemiology The paradigmatic disease associated with EBV is infectious mononucleosis. The description and epidemiology of infectious mononucleosis predated by decades the recognition of EBV as its dominant cause; cytomegalovirus, human immunodeficiency virus (HIV), and Toxoplasma gondii are infrequent causes of mononucleosis-like illness (3, 4). Infectious mononucleosis occurs at all ages, but most cases occur during adolescence and early adulthood (5). It is now understood that the restricted age distribution of infectious mononucleosis is delimited at the lower end by the greater capacity of children to resolve a primary EBV infection with few or no symptoms. Although adults do not handle EBV as well as children, by the age of 25 years most are already seropositive and not susceptible to reinfection. In developing countries, EBV infection occurs early in life. Nearly the entire population of a developing country becomes infected before adolescence. Thus, symptomatic infectious mononucleosis is uncommon in Abbreviations and Glossary EA early antigen: a complex of viral nonstructural proteins expressed during active infection EBV Epstein-Barr virus EBER Epstein-Barr virus-encoded RNA: a viral RNA that is expressed in the cell nucleus during latent infection EBNA Epstein-Barr virus nuclear antigen: a complex of viral proteins in the cell nucleus expressed during latent infection IL interleukin: an immunomodulatory protein encoded by the cellular genome LMP Epstein-Barr virus latent membrane protein: a viral protein expressed on the surface of the cell during latent infection VCA viral capsid antigen: a complex of viral structural proteins expressed during active infection 1 January 1993 Annals of Internal Medicine Volume 118 Number 1 45
2 Table 1. The Most Common Symptoms and Signs of Infectious Mononucleosis* Variable Percent Symptom Sore throat 82 Malaise 57 Headache 51 Anorexia 21 Myalgias Chills Nausea 12 Abdominal discomfort 9 Cough 5 Vomiting 5 Arthralgias 2 Sign Lymphadenopathy Pharyngitis Fever Splenomegaly Hepatomegaly Palatal enanthem Rash 10 Jaundice 9 * Adapted from Schooley and Dolin (14), with permission. such countries. In areas with high standards of hygiene, such as the United States and western Europe, where EBV infection may be delayed until adulthood, infectious mononucleosis is more prevalent. The increase in the incidence of infectious mononucleosis with improved sanitary conditions may explain why this disease was not described until the latter half of the nineteenth century (3). Mononucleosis-like infections may occur more than once, but such episodes are generally not caused by a resurgence of viral activity. Reactivation disease appears exclusively in transplant recipients and similarly impaired persons (6); there has never been a confirmed case of symptomatic reactivation EBV disease in a healthy person. Most serial mononucleosis-like episodes are caused by sequential infections with different pathogens. Thus, EBV infection stands in stark contrast to other herpesvirus infections, which have a definite proclivity toward recurrences. Salivary tissues are the recognized repositories of EBV, and periodic shedding from such tissue is a necessary feature of this virus's biology. Shedding is sustained for months after infection and then falls gradually; in 15% to 20% of all attempts, the virus can be recovered from saliva (7). Immune compromise in transplant recipients and patients with the acquired immunodeficiency syndrome (AIDS) leads to higher rates of shedding (average, 50% to 80%) (8). Evidence of the virus's presence in cervical epithelium and semen has emerged, but sexual transmission has not been proved (9). Exchange of saliva would appear sufficient to explain EBV transfer to partners and the corresponding difficulty of transmitting this virus in the home, in the hospital, or in other confined quarters where the issue has been carefully examined (5, 10). The virus can be transmitted to susceptible recipients by blood transfusion or bone marrow transplantation (11, 12), but such transmission is rare. Studies of natural or experimental transmission of infectious mononucleosis documented an incubation period of 3 to 7 weeks (13). Clinical Spectrum Infectious Mononucleosis The classic syndrome of mononucleosis is defined as a clinical triad of fever, pharyngitis, and adenopathy (14), although many other symptoms and signs also occur (Table 1). The diagnosis of acute EBV infectious mononucleosis is based on clinical presentation and supportive laboratory findings, including an absolute lymphocytosis in which more than 10% of cells are atypical, as well as heterophil antibody titers of at least 1:56 by the traditional Paul-Bunnell-Davidsohn test or positive rapid slide assays such as the Mono-Latex test (Wampole Laboratories, Cranbury, New Jersey) (15). About 93% of patients who fulfill the above criteria have primary EBV infection; if the criteria are relaxed, the proportion decreases (16). The fortuitous discovery in 1967 that EBV causes infectious mononucleosis led quickly to the development of virus-specific antibody tests that, despite broad Table 2. Serologic Responses of Patients with Epstein-Barr Virus-associated Diseases* Condition Anti-VCA Anti-EA Anti-EBNA Heterophile IgM IgG IgA Diffuse Restricted (IgM) EA EA Uninfected - Infectious mononucleosis ± Convalescent ± + ± Past infection Chronic active infection ± ± Post-transplant _ + + ± + + ± - lymphoproliferative disease Burkitt lymphoma ± Nasopharyngeal carcinoma ± + ~ * Adapted from Okano and colleagues (17), with permission. The symbols denote the absence (-), variable presence (±), or usual presence in relatively low ( + ), moderate (++), or high (+ + + ) titers of the indicated antibodies. Anti-VCA = antibody to the Epstein-Barr viral capsid antigen; Anti-EA = antibody to the Epstein-Barr virus early antigen; Anti-EBNA = antibody to Epstein-Barr virus nuclear antigen January 1993 Annals of Internal Medicine Volume 118 Number 1
3 Table 3. Complications of Infectious Mononucleosis* Hematologic Neurologic Cardiac Respiratory Dermatologic Renal Hepatic Splenic Immunologic Hemolytic anemia, thrombocytopenia, granulocytopenia, aplastic anemia, hemophagocytic syndrome Encephalitis, transverse myelitis, the Reye syndrome, the Guillain-Barre syndrome, Bell palsy, psychosis, optic neuritis Myocarditis, pericarditis Streptococcal pharyngitis, laryngotonsillar obstruction, pneumonia, pleuritis, hilar lymphadenopathy, lymphocytic interstitial pneumonitis, nasopharyngeal carcinoma Ampicillin-associated rash, leukocytoclastic vasculitis, acrocyanosis, cold-mediated urticaria, oral hairy leukoplakia Interstitial nephritis, glomerulonephritis Hepatitis, massive hepatic necrosis, Reye syndrome Rupture Anergy, hypogammaglobulinemia, hypergammaglobulinemia, X-linked and non-x-linked lymphoproliferative syndromes, Burkitt and non-hodgkin B- and T-cell lymphomas * Reproduced from Straus (19), with permission. misunderstanding and overinterpretation, remain useful serologic tools, primarily for the diagnosis of primary illness but also as adjuncts in the evaluation of chronic or malignant sequelae of EBV infection (Table 2) (4, 17). Immunoglobulin M antibodies to the EBV viral capsid antigen (anti-vca) evolve quickly with infection, persist for weeks to months, and do not reappear. Thus, their detection is presumptive evidence of recent primary infection. Analysis of paired acute and convalescent sera shows a rise, a subsequent fall, and a lifelong persistence of IgG anti-vca, usually in titers ranging from 1:40 to 1:2560. Measurement of IgA anti-vca is not useful except in the diagnosis and management of nasopharyngeal carcinoma. Antibodies to viral early (pre-dna synthesis) antigens (anti-ea) of the diffuse or restricted types develop in most primary infections, peak in titers of less than 1:640, and wane with time. They persist frequently enough, though, that their presence in low titers is of no diagnostic significance (18). Antibodies to EBV nuclear antigen (anti-ebna) are detected in traditional assays relatively late after the onset of symptoms in infectious mononucleosis, so that their absence in a previously well person who develops acute illness suggests an ongoing EBV infection. The EBV-specific serologic tests were all originally done by immunofluorescence microscopy. The titers discussed above apply only to those assays. Newer tests involving enzyme-linked techniques, Western blots, or other immunoassays yield results that are not directly comparable to these standard methods. Moreover, even for a given assay, performance standards differ considerably from laboratory to laboratory, making the scrutiny of results acquired at different times in different places a fruitless exercise. Infectious mononucleosis is, with rare exceptions, a self-limited disease. Adenopathy or splenomegaly can persist for weeks and provoke some anxiety about their cause, but unless symptoms or signs progress well beyond the period of the acute illness, further workup is not warranted. Primary EBV infections, with or without the features of infectious mononucleosis, have many recognized complications (Table 3) that fall into various categories mostly dependent on immunopathologic responses to the virus. Ominous complications such as severe autoimmune hemolysis, airway obstruction from grossly enlarged tonsils, splenic rupture, and encephalitis, among others, are seen in otherwise healthy patients. Agranulocytosis, aplastic anemia, and other rare but grave features of acute, progressive EBV infection can arise in healthy patients but may indicate a demonstrable deficiency of cellular immunity (19). Lymphoproliferative Disorders Many EBV-associated lymphoproliferative lesions are recognized in persons with congenital or acquired cellular immune deficiency (20). X-linked lymphoproliferative disease is a rare disorder of young boys who develop fulminant mononucleosis after EBV infection. The disease is characterized by B- and T-cell infiltration of organs with displacement of bone marrow elements (21). Over two thirds of affected patients die of hemorrhage or infection within weeks, and 100% die by 40 years of age. Survivors of the acute infection experience aplastic anemia, hypo- or hypergammaglobulinemia, opportunistic infections, or lymphomas. Epstein- Barr virus-associated lymphoproliferative disease also occurs in 1% to 3% of bone marrow, kidney, or liver transplant recipients. About 5% to 10% of heart or heart-lung transplants have developed EBV-associated B-cell tumors (20). The marked degree of immunosuppression in these patients may allow outgrowth of EBVinfected B cells, resulting in lymphoproliferative lesions. The reversal of some of these lesions after a reduction in immunosuppressive therapy emphasizes the role of the immune system in controlling EBV infection in the normal host. In transplant recipients, as well as in patients with AIDS, EBV-associated B-cell tumors may have either polyclonal, monoclonal, or mixed phenotypes. Death from progressive expansion of tumors, immunodeficiency, and opportunistic infections is frequent. Chronic infectious mononucleosis is a rare, heterogeneous, and poorly understood syndrome that arises in previously well men and women (22, 23). During the past 13 years, we have studied six patients, including one girl, who developed chronic mononucleosis between the ages of 7 and 23 years. Their illnesses lasted 2 to 14 years and, thus far, three of the patients have died. Prominent features include reactive adenopathy and hepatosplenomegaly, uveitis, pneumonitis, and polyneuropathy. Progressive cellular and humoral im- 1 January 1993 Annals of Internal Medicine Volume 118 Number 1 47
4 mune deficiencies evolve in the course of follow-up, making it impossible to discern whether active infection causes the immune impairment or persists because of it. The features of chronic infectious mononucleosis establish it as distinct from the far more common chronic fatigue syndrome (23). Other Syndromes Nasopharyngeal carcinoma, Burkitt lymphoma, non- Hodgkin B-cell and central nervous system (CNS) lymphomas, rare T-cell lymphomas (24), and some thymomas have been associated with EBV infection. One particularly instructive disorder caused by EBV is oral hairy leukoplakia, which is characterized by an exophytic growth of epithelial cells of the tongue and buccal mucosa (25). None of these chronic or lymphoproliferative sequelae can be diagnosed by serologic methods alone. The persistence of anti-ea and of higher-than-usual levels of IgG anti-vca and the absence of anti-ebnas are common in patients with disorders described above, but these features can also be seen in any patient with cellular immune impairment. Very high titers of anti-ea (> 1:640) and IgG anti-vca (> 1:5120), which can sometimes be seen in immunodeficient patients, are compatible with chronic mononucleosis. As indicated earlier, isolation of the virus in seropositive persons is too common for it to be of diagnostic value (7, 8). Diagnoses are established histologically, and evidence of increased EBV levels in the tissues must be confirmed by immunohistochemical or nucleic acid hybridization techniques (23). Molecular Biology of Epstein-Barr Virus and Its Mechanism of B-Cell Transformation Structure and Replication Dr. Jeffrey I. Cohen (Medical Virology Section, Laboratory of Clinical Investigation, NIAID, NIH, Bethesda, Maryland): The EBV genome is a doublestranded DNA molecular of approximately base pairs; as in other herpesviruses, the molecule is divided into unique, internal repeat, and terminal repeat domains (26) (Figure 1). The genome encodes approximately 80 proteins. The function of many of the genes involved in viral replication has been inferred from their homology to herpes simplex virus genes; however, genes expressed during latent infection of B cells do not have recognized counterparts in other human herpesviruses. Two strains, or types, of EBV infect humans. These strains differ in the sequences of the viral genes expressed during latent infection and in their ability to transform B lymphocytes. Although earlier studies suggested that type A (or EBV-1) virus infection was more prevalent in North America and Europe and that type B (or EBV-2) virus infection was more prevalent in Africa, more recent studies suggest that both strains are prevalent in the United States (27) and that persons can be coinfected with both strains. Epstein-Barr virus infects epithelial cells of the oropharynx (28) and of the cervix (9) and resting B lymphocytes. The receptor for the virus on epithelial cells and B lymphocytes is the CD21 molecule, formerly called CR2, which is also the receptor for the C3d component of complement (29). Infection of epithelial Figure 1. The structure of the Epstein-Barr virus genome and the location of some of its important genes. The genome consists of about base pairs of double-stranded DNA (top line) that are organized in a series of unique (Ul to U5), internal repeat (IR1 to IR4), and terminal repeat (TR) domains (second line). Shorter repeated regions occur but are not shown. Several of the Epstein-Barr virus genes expressed during the viral replication cycle (third line) and during viral latency in B lymphocytes (fourth line) are depicted. The coding regions of EBNA (Epstein-Barr virus nuclear antigen)-!.?, LMP (latent membrane protein)-1, and LMP-2A and LMP-2B are spliced (A) from discontinuous portions of the genome; LMP-2A and LMP-2B begin at the right end of the circularized genome and extend across the terminal repeats to the left end of the genome. EBERs = Epstein-Barr virus encoded RNAs; ZEBRA = Z Epstein-Barr virus replication activator January 1993 Annals of Internal Medicine Volume 118 Number 1
5 Table 4. Diseases Associated with Persistent Epstein-Barr Virus Gene Expression* Disease Latency Proteins Replication Proteins EBERs EBNA-1 EBNA-2 LMP-1 ZEBRA gp350 Burkitt lymphoma + + _ Not studied _ Nasopharyngeal + + ± Not studied Not studied carcinoma Lymphoproliferative Not studied - disease Hodgkin disease + Not studied - + Not studied - Oral hairy - Not studied Not studied leukoplakia * EBERs = Epstein-Barr-virus-encoded RNAs; EBNA-1 = Epstein-Barr virus nuclear antigen 1; EBNA-2 = Epstein-Barr virus nuclear antigen 2; LMP = latent membrane protein 1. ZEBRA = Z Epstein-Barr virus replication activator. The symbols denote the usual expression ( + ), occasional expression (±), or lack of expression (-) of the proteins indicated. cells results in replication of the virus, with release of progeny virions from the cells. In contrast, infection of B lymphocytes usually results in latent infection without replication or release of virus. Recently, the CD21 molecule was inserted into epithelial cell lines that normally are not infectable by EBV. Thus, these cells can be infected with EBV, with the resulting expression of certain latent gene products and production of infectious virus (30). The virus can be reactivated from latently infected B lymphocytes by certain chemicals or by antibody to immunoglobulin. These stimuli lead to expression of the EBV BZLF1 gene product, or ZEBRA (Z EBV replication activator) protein, an immediate early gene product. The ZEBRA protein acts as the switch that triggers viral replication in latently infected B cells (31). This protein also transactivates (or up-regulates) expression of other immediate early genes as well as expression of ZEBRA itself. These genes, in turn, up-regulate the expression of early gene products, which include the viral DNA polymerase and thymidine kinase, important for viral DNA replication. Thymidine kinase phosphorylates acyclovir, thus permitting the drug to inhibit viral replication (32). Finally, the late gene products are made, including structural components of the virion such as the VCA and gp350, which is the major envelope glycoprotein of the virus. Another late viral protein, termed BCRF1, shares 70% amino acid identity with human interleukin-10 (33); this aspect is discussed more fully in the section on lymphocyte responses to EBV. Latency and Transformation When EBV infects B lymphocytes, its linear genome circularizes to form an episome, or extrachromosomal element, in the nucleus of the cell (34). The result is a transformation of the infected B cells, which acquire the capacity to proliferate indefinitely. In vitro, these latently infected B cells express only 10 of the approximately 80 genes encoded by the virus (see Figure 1). The state of latent infection is maintained by the EBNA-1 protein; it binds to a nucleotide sequence, termed orip, which is part of the viral origin of DNA replication. The binding of EBNA-1 to orip allows the viral genome to be maintained in the nucleus of the B cell. Two of the EBV latent genes encode proteins that transactivate other viral genes. Epstein-Barr virus nuclear antigen 1 leads to transactivation of the EBNA proteins, whereas EBNA-2 transactivates the expression of two EBV latent membrane proteins, LMP-1 and LMP-2. Epstein-Barr virus latent gene products also transactivate the expression of B-cell genes. Epstein- Barr virus nuclear antigen 2 transactivates CD21, CD23, and c-fgr; EBNA-3C also transactivates CD21, whereas LMP-1 transactivates CD23 and the intercellular adhesion molecules ICAM-1, LFA-1, and LFA-3. The secreted (truncated) form of CD23 may be a B-cell growth factor, but the full-length molecule may be a receptor, thus providing autocrine stimulation of EBV-infected B cells (35); CD23, also a low-affinity receptor for IgE, may be important for antigen presentation in association with major histocompatibility complex (MHC) II antigens and was recently shown to interact with CD21 (36). A member of the src oncogene family, c-fgr encodes a protein kinase that may be important for the regulation of B-cell growth. Two latent gene products, the EBV-encoded RNAs (EBERs), are the most abundant RNAs expressed in vitro; they do not code for proteins and are dispensable for transformation in vitro (37). One EBV latent gene product, LMP-1, acts as a direct oncogene in transformation assays (34). Expression of LMP-1 in epithelial cells transforms them morphologically (38), and in B-lymphoma cells, LMP-1 prevents programmed cell death, or apoptosis (39). Latent membrane protein 2 associates with a cellular tyrosine kinase and colocalizes in the cell with LMP-1 (42). Genetic analyses using viral mutants indicate that EBNA-2 and LMP-1 are essential for transformation (41). Thus, transformation of B cells is a complex process requiring the function of several EBV gene products that serve together to maintain the viral genome in the cell, transactivate viral and cellular gene products important for B-cell growth, interact with B-cell proteins, and prevent apoptosis. Lymphoproliferation and Neoplasia Studies have begun to clarify the molecular properties of several EBV-associated lymphoproliferative and neoplastic diseases, as well as the role of the virus in their development (Table 4). Burkitt lymphoma is a mono- 1 January 1993 Annals of Internal Medicine Volume 118 Number 1 49
6 Figure 2. Lymph node specimens from patients with Epstein- Barr virus lymphoproliferative disease. Specimens were stained with monoclonal antibody to Epstein-Barr virus nuclear antigen 2 (EBNA-2) (top panel) or latent membrane protein 1 (LMP-1) [bottom panel). Note the nuclear staining with nucleolar exclusion with EBNA-2 antibody and cytoplasmic membrane staining with LMP-1 antibody. Reproduced with permission from Gilligan and colleagues (51) (top panel) and Cohen (20) (bottom panel). clonal cell tumor typically containing an 8/14 or 8/22 chromosomal translocation that leads to dysregulation of the endogenous c-myc oncogene. In Africa, more than 90% of Burkitt lymphomas contain EBV genomes, whereas only 205 of such lymphomas in the United States contain EBV DNA. Cells in Burkitt lymphoma tissues express EBNA-1 and the EBERs but not EBNA-2, EBNA-3, or LMP (40). As indicated, EBNA-1 is essential for maintaining the viral genome in latently infected B cells, and its expression would be expected in Burkitt lymphoma. The chromosomal translocations associated with Burkitt lymphoma, however, may supplant the need for expression of additional EBV latent, growth-transforming genes. Further, EBNA-2, EBNA-3 A, EBNA-3C, and LMP-1 are targets for the destruction of EBV-infected B cells by cytotoxic T cells (43, 44). Thus, the expression of these genes would enhance the immune clearance of cells; their downregulation would facilitate tumor survival. Nasopharyngeal carcinoma is endemic in persons from southern China and in certain native North Americans. Viral genomes are present in tissues from all patients with nonkeratinizing nasopharyngeal carcinoma. Tissues from patients with the disease show expression of EBNA-1, the EBERs, and occasionally LMP-1 (in 40% to 70% of cases) (45). Although expression of LMP-1 provides a target for immune destruction, the growth-transforming advantage afforded by LMP-1 (34, 38) may result in a selective advantage for some of these tumors. The B-cell lymphoproliferative disorders arise in congenially immunosuppressed infants and children, as well as in immunosuppressed organ or bone marrow transplant recipients (20). These disorders can evolve during acute EBV infection, but most often they result from previous infection with the virus. The lesions may exhibit B-cell hyperplasia or lymphoma; regardless of the pathologic findings, the chromosomal translocations characteristic of Burkitt lymphoma are usually not present. Tissues from immunocompromised patients with B-cell lymphoproliferation contain EBV genomes and usually express the full complement of latent gene products (46, 47) (Figure 2). The marked degree of immunosuppression may allow EBV-infected B cells to express all the latency proteins and still expand without selective pressure from cytotoxic T cells. About one third of B-cell lymphomas in patients with AIDS contain EBV genomes (20). Unlike the tumors seen in congenitally or iatrogenically immunosuppressed patients, these tumors show a Burkitt or Burkitt-like histology and contain chromosomal translocations similar to those seen in Burkitt lymphoma in patients without AIDS. Most of these tumors in patients with AIDS also express the full repertoire of latent genes. Patients with Hodgkin disease often have elevated levels of antibody to EBV antigens before or at the time of presentation of lymphoma; this condition was long presumed to reflect evolving impairment in cellular immunity. Recently, however, tissues from 20% to 40% of patients with Hodgkin disease were found to contain EBV genomes, usually within the Reed-Sternberg cells (48). Most cases associated with EBV are of the more aggressive, nodular sclerosing or mixed cellularity subtypes of Hodgkin disease (49). Tumors that contain EBV DNA show expression of LMP-1 but not of EBNA-2. Unlike the EBV-associated tumors discussed above, oral hairy leukoplakia represents a nonmalignant infection of epithelial cells, with extensive replication of EBV. Lesions contain EBV DNA in the upper epithelial layers, and herpesvirus-like particles have been seen on electron microscopy (25); EBV DNA is not present in the lower layers. Thus, EBV may not be latent in the lower layers of the epithelium, and infection may be sustained by continuous infection of maturing cells in the upper layers. EBV replicative genes (such as ZEBRA, VCA, gp350) and LMP-1 are expressed, but the EBERs are not (50, 51). Lymphocyte Responses to Epstein-Barr Virus Infection Dr. Giovanna Tosato (Laboratory of Immunology, Center for Biologies Evaluation and Research, Food and Drug Administration, U.S. Department of Health and Human Services, Bethesda, Maryland): Most normal adults harbor EBV-infected B lymphocytes that have the potential for unlimited growth; however, lym January 1993 Annals of Internal Medicine Volume 118 Number 1
7 phoproliferative disorders involving EBV-infected cells only rarely occur. The successful restraint of EBVinfected B cells is primarily attributable to T-cell immunity (52, 53). Several observations form the basis for this assertion. First, if T cells are removed or functionally inactivated from the blood mononuclear cells of most normal EBV-seropositive persons, EBV-immortalized cell lines spontaneously arise in vitro (52). Second, after injection of EBV-seropositive blood intraperitoneally into mice with severe combined immunodeficiency, tumors that are composed of EBV-infected human B cells often arise (54) because of both the immunodeficiency of the host and the limited survival of the human T cells in the murine host. Finally, severe T-cell immunodeficiency in humans, such as occurs in solid organ transplant recipients and in patients with AIDS, is associated with lymphoproliferative syndromes involving B lymphocytes naturally infected with EBV (20). B Cells Infected with Epstein-Barr Virus Most of the studies of immunity to EBV infection used EBV-immortalized B cells as targets for monitoring immune functions. During the past several years, it has become apparent that EBV-immortalized B cells undergo several phenotypic changes that facilitate immortalization. One important change is the establishment of an autocrine loop whereby the EBV-immortalized B cells produce growth factors that stimulate their proliferation (55, 56). The existence of this process was suggested by the observation that EBV-immortalized cell lines die if cultured at critically low cell densities; supplementation of the culture medium with cell-free "conditioned" supernatants of EBV-immortalized cell lines cultured at optimal cell densities prevents this outcome, however. Recently, the growth stimulatory factors in the conditioned media of EBV-immortalized cells were shown to include lactic acid and interleukin-6. Lactic acid alone accounts for most of the stimulatory activity in serum-free supernatants of EBV-immortalized cell lines (57). Under culture conditions that include serum, stimulatory compounds other than lactic acid and interleukin-6 may also be involved (36, 58). Little is known about the requirements for growth and survival of EBV-infected B cells in vivo. During acute EBV-induced infectious mononucleosis, at least 1 in 10 4 circulating B cells is infected with EBV (52). These cells probably become infected with the virus as they travel through lymphoid tissues in the oral cavity. In normal EBV-seropositive persons, however, the proportion of circulating B cells that are chronically EBVinfected is less than 1 in 10 5 (Figure 3) (52). There has been controversy over the derivation of this pool of residual B cells infected with the virus. Moss and colleagues (59) noted that EBV can be detected frequently in the saliva years after the primary infection, and they proposed that virus in the oropharynx serves as a reservoir to repeatedly infect B cells, which then migrate to the periphery where they are susceptible to killing by cytotoxic T cells (59). In this view, the pool of virally infected B cells would be turning over constantly. An alternative model, now more widely accepted, is that the EBV-infected cells are long-lived; they are perhaps the very cells that were originally infected or their progeny (60). In support of this latter model, acyclovir therapy was shown to eliminate, or at least reduce, EBV shedding in the saliva, but it had no effect on the number of circulating B cells infected with EBV (52, 61). Moreover, repeated analyses of circulating EBVinfected cells during a 3-year period in a patient who had undergone ablative therapy and subsequent bone marrow transplantation showed them to be donor derived (62). During these 3 years, no B cells that carried the recipient's precise viral genotype could be found. Thus, EBV-infected cells can be long-lived, and de novo infection with virus intermittently released in the oropharynx or elsewhere may be uncommon after primary infection. T-Cell Regulation of Epstein-Barr Virus Infection Persons who are EBV seropositive and patients with acute EBV-induced infectious mononucleosis harbor EBV-infected B cells with the potential for unlimited growth. That all infected persons do not succumb to lymphoproliferative disorders points to the existence of potent, durable restraints on the EBV-transformed cells. Figure 3. Frequency and geometric mean of spontaneous B-cell outgrowth in the peripheral blood of patients with acute Epstein- Barr-virus-induced infectious mononucleosis and of normal persons seropositive for Epstein-Barr virus. The geometric mean is indicated by the horizontal bar. 1 January 1993 Annals of Internal Medicine Volume 118 Number 1 51
8 Figure 4. Inhibition of the proliferation of normal phytohemagglutinin-stimulated T cells by human and viral interleukin-10. The T cells were cultured for 3 days in phytohemagglutinin (PHA), 0.5 Mg/mL, either alone or with interleukin-10, 0.1 to 10 U/mL. Proliferation was measured as counts per minute (cpm) of 3 H-thymidine incorporation during the final 18 hours of culture. IL = interleukin. Early in the course of acute infectious mononucleosis, activated cytotoxic T cells are found in the peripheral blood, but they disappear during convalescence (52, 53). These cytotoxic cells are neither EBV-specific nor HLA-restricted, because they kill EBV-negative and MHC-incompatible targets. Thus, they resemble activated killer cells induced in vitro by T-cell exposure to mitogens, interleukin-2, or EBV-immortalized cells. In addition to this predominantly virus-nonspecific response, cytotoxic T-cell clones that are both specific for virus-infected cells and HLA-restricted can be derived from the blood of patients with infectious mononucleosis (53). Other T-cell clones that inhibit the growth of EBV-infected cells without killing them can also be derived from the blood of patients with infectious mononucleosis (63). Recent studies have shown extensive homology in the predicted amino acid sequences of murine interleukin- 10, human interleukin-10, and the protein product of BCRF-1 (viral interleukin-10); BCRF-1 is an open-reading frame in the EBV genome known to be expressed during replication (see Figure 1) (32). Functionally, human and viral interleukin-10 share several properties, including inhibition of gamma-interferon secretion and suppression of T-cell proliferation in response to antigen and mitogen (64) (Figure 4). Although it is not yet known whether viral interleukin-10 is produced during acute infectious mononucleosis, the generally poor response of T cells from patients with infectious mononucleosis to in-vitro stimulation with mitogens and antigens could be an effect of viral interleukin-10. It is intriguing to note that during evolution, EBV may have captured a cellular gene that aids its survival. By inhibiting T-cell growth and gamma-interferon production, viral interleukin-10 may limit host responses directed at eliminating the virus. Although present during acute EBV-induced infectious mononucleosis, activated cytotoxic and suppressor cells are not detected among T cells from persons who have recovered from the infection; however, by culturing T cells from EBV-seropositive persons under conditions that involve restimulation with autologous EBV-infected B cells, both cytotoxic and suppressor T-cell activities directed against EBV-positive B cells can be elicited (52, 53). Early studies showed that cytotoxic T cells derived in this manner have strong reactivity against autologous EBV-infected targets but fail to kill EBV-negative targets, even those that have been activated by mitogens and that are restricted by HLA class I determinants. Recently, the virus specificity of cytotoxic T-cell clones derived from EBV-seropositive persons was mapped. These clones recognized EBNA-2, EBNA-3A, EBNA-3C, and LMP (65-67). Interestingly, no cytotoxic T-cell clones that recognize EBNA-1 have yet been isolated. The lack of detectable EBNA-1-specific T-cell clones may have important implications regarding the cellular immune containment of EBV-infected cells. Epstein-Barr virus nuclear antigen is required to maintain the EBV episomal genome in B cells, so its expression is obligatory; however, the expression of other latency genes if not required (68). The failure of EBV to express certain genes, such as LMP and EBNA-2, in vivo may allow B cells to avoid cytotoxic T-cell recognition and clearance. Epstein-Barr Virus-related Lymphoproliferative Disorders Cellular immune restraints on EBV-infected B cells sometimes fail, and lymphoproliferative disorders involving EBV-infected B cells occur. Recent attention has focused on the potential role of growth factors as contributors to the various processes of transformation (69). Because EBV-immortalized cells respond to interleukin-6 with increased proliferation in vitro, the effects of interleukin-6 on B-cell tumorigenesis have been assessed (70, 71). Expression of the human interleukin-6 gene in EBV-transformed human B cells rendered them tumorigenic in athymic mice (70, 71). The parental cells and those clones transduced with a control plasmid (interleukin-6-nonexpressing) were generally nontumorigenic. The studies showed that the mechanism of interleukin-6 tumorigenicity was unrelated to a direct oncogenic effect of this cytokine on the EBV-immortalized cells. Rather, interleukin-6 appeared to inhibit markedly cytotoxic functions in the mouse, and it was the further reduction in immune effector activity that permitted tumor outgrowth (71). What relevance might these observations have to the development of tumors in humans? One study found that serum interleukin-6 levels are abnormally elevated in HIV-seropositive persons, a group predisposed to EBV-positive lymphomas (72). Six of seven patients who developed EBV-associated post-transplant lymphoproliferative disorders had markedly abnormal serum interleukin-6 levels (85 to 1040 U/mL) at various times after they received the transplant; in contrast, none of six patients with normal interleukin-6 levels (5 to 15 U/mL) developed post-transplant lymphoproliferative disorders (range, 45 to 215 days) (73). Thus, interleukin-6, an autocrine and paracrine growth factor of 52 1 January 1993 Annals of Internal Medicine Volume 118 Number 1
9 EBV-immortalized B cells in vitro, appears to be associated with increased tumorigenicity of EBV-immortalized cells in athymic mice and an increased rate of post-transplant lymphoproliferative disorders. Interleukin-6 may play an important role in the pathogenesis of EBV-related lymphoproliferative disorders, either by further limiting host immune responses or by directly promoting the growth of the EBV-infected B cells. A better understanding of the role of interleukin-6 in the multistep process of lymphomagenesis by EBV-infected B cells may provide a rational basis for novel approaches to therapy. Management and Prevention of Epstein-Barr Virus Infections Dr. Jeffery I. Meier (Medical Virology Section, Laboratory of Clinical Investigation, NIAID, NIH, Bethesda, Maryland): Epstein-Barr virus infections pose few problems for which more than supportive care is warranted. When required, the adjunctive therapeutic options often reflect strategies that either directly target the replication of EBV or, more often, the immunopathologic responses to viral infection. Uncomplicated Acute Infectious Mononucleosis General Considerations Patients with uncomplicated acute infectious mononucleosis usually require only symptomatic therapy. Contact sports should be avoided for at least 1 month or until resolution of splenomegaly has been verified. Splenic enlargement is not always clinically appreciable and generally resolves within the first month of illness. The enlarged spleen is susceptible to rupture (74, 75); an ultrasonographic examination can exclude subclinical splenomegaly. The exudative tonsillopharyngitis that accompanies infectious mononucleosis often leads to a search for bacterial infection. The percent of random-surveillance throat cultures in patients with infectious mononucleosis that grow group A beta-hemolytic streptococci ranges widely, from 3% to 30%, and as many as 30% of these show serologic evidence of recent streptococcal infection (76). Accordingly, treatment of beta-hemolytic streptococci with penicillin or erythromycin for 10 days is warranted to prevent poststreptococcal sequelae. Ampicillin- or amoxicillin-containing regimens should not be used in persons with infectious mononucleosis, because they frequently cause a rash. Corticosteroid Therapy The use of glucocorticoids for the routine management of acute infectious mononucleosis is controversial. The cumulative results of several small controlled clinical studies (Table 5) suggest that corticosteroids hasten the resolution of fever and tonsillopharyngeal symptoms of uncomplicated acute infectious mononucleosis, but they do not provide significant or reproducible benefit for lymphadenopathy or hepatosplenic involvement (77-82). Despite these studies, corticosteroids are still used by some physicians with the goal of quickly returning students to school. In part because of rare reports of an association between encephalitis or myocarditis and corticosteroid use in patients with acute infectious mononucleosis (83-85), other investigators have cautioned against the use of corticosteroids. Further, corticosteroids might adversely influence the biology of the infection the longterm immunity to EBV or the number of lymphocytes latently infected by the virus. On balance, we support recent guidelines that advise against the routine use of corticosteroids in patients with uncomplicated acute infectious mononucleosis (86). Table 5. Results of Controlled Studies of Corticosteroid or Corticotropin Therapy for Uncomplicated Acute Infectious Mononucleosis Study Study Patients, n Corticosteroid, Initial Time of P Value for Effects of (Reference) Design Dose, and Taper Assessment Fever Symptoms Signst Corticosteroids,* Placebo Cortico Duration steroid Therapy Bennike (76) Unblinded Corticotropin, 60 IU intramuscularly, Dailyt P < Not studied None 5 days Antila et al. Double-blind 5 8 Prednisone, 60 mg/d 2 d None Not studied Not studied (77) orally, 5 days without 2 d None None None taper Schumacher Double-blind Paramethasone, 16 mg/d Daily P = 0.01 None None et al. (78) orally, variable Prout and Case-control Prednisolone, 80 mg/d Variable P < Not studied Not studied Dalrymple orally, 6 days (79) Bender (80) Double-blind Paramethasone, 10 mg/d 12 h Not studied P = 0.01 Not studied orally, 9 days 36 h 60 h Not studied P = 0.05 Not studied None Not studied Not studied Klein et al. (81) Double-blind Prednisone, 60 mg/d 1 wk Not studied Trend Trend orally, 6 days 4 wk Not studied None None * P value reflects shortening of the duration of symptoms or signs by corticosteroids. t The laboratory and physical examination indices that were monitored varied; tonsillopharyngitis, lymphadenopathy, and hepatosplenic abnormalities were often evaluated. X Daily assessments until substantial overall improvement was observed. Trend = beneficial trend, not statistically significant. 1 January 1993 Annals of Internal Medicine Volume 118 Number 1 53
10 Table 6. Results of Double-Blind, Placebo-controlled Trials of Acyclovir Therapy for Acute Infectious Mononucleosis Study (Reference) Patients, n Dosage Day of Viral Shedding Overall Clinical Culture Improvement Placebo Acyclovir fr m Placebo Acyclovir Group Group Start of Group Group Therapy Pagano et al. (88) mg/m 2 body surface 0 1/5* 4/6 None significant area per day intrave- 5 2/4 0/6 (weight loss)t nously for 5 days 10 2/5 1/5 Andersson et al. (89) mg/kg, per day intrave- 0 15/16 14/15 None significant nously for 7 days /16 0/14$ (weight loss, fever, 7 16/16 1/15$ tonsillopharyngitis in 28 13/15 12/14 combined analysis) Andersson et al. (90) mg 5x/d, p.o., 7 d 0 19/20 16/ /18 10/ /20 8/16 None significant 14 9/9 6/ /20 16/16 van der Horst et al. (91) mg 5 times a day 0 50% 52% None significant orally for 10 days 10 38% 17% * The proportion (expressed as n/n or as a percent) of saliva specimens from which Epstein-Barr virus could be isolated. t Difference was statistically significant. %P < P < 0.01; differences in individual indices were not significant. Significant decrease in geometric mean virus titer, P < Antiviral Therapy Several antiviral agents, such as acyclovir, ganciclovir, bromovinyldeoxyuridine, zidovudine, and foscarnet, as well as human alpha-, beta-, and gamma-interferon, effectively inhibit the replication of EBV or initial B-cell transformation by the virus in vitro (87). Only EBV DNA synthesis dependent on the viral polymerase (the linear form of the genome) is susceptible to inhibition. The latent circular form of the genome, which replicates in concert with the cell cycle using the cellular DNA polymerase, is not selectively inhibited. Because both forms of replication transpire in the course of infectious mononucleosis, it was initially uncertain whether antiviral therapy would prove to be beneficial. The efficacy of acyclovir has been assessed in controlled studies of uncomplicated acute infectious mononucleosis (Table 6) (88-91). Oropharyngeal shedding of EBV is inhibited by intravenous or high-dose oral acyclovir therapy that yields peak serum levels exceeding 1 jug/ml, the concentration needed to suppress EBV genome replication by 50% in in-vitro studies. This effect is temporary, however; viral shedding resumes shortly after therapy is discontinued. Despite this virologic response, the trials documented little or no clinical benefit in treating uncomplicated acute infectious mononucleosis with acyclovir. Complications of Acute Infectious Mononucleosis Complications of acute infectious mononucleosis usually necessitate additional supportive measures such as tracheostomy for airway obstruction or transfusions for critical hemolytic anemia or thrombocytopenia. Corticosteroids may be useful for some of these complications. Small case series indicate that corticosteroids quickly reduce obstructive tonsillar enlargement so as to obviate tracheostomy in some instances (78, 92). Such therapy may also ameliorate autoimmune hemolytic anemia and thrombocytopenia (93, 94). Reports that aplastic anemia responds to corticosteroids or antithymocyte globulin suggest that these therapies can be contemplated as an initial alternative to bone marrow transplantation (95-97). In addition to these uses, corticosteroids may be cautiously considered in cases of encephalitis, myocarditis, and pericarditis (86). Acyclovir might be given with corticosteroids to restrict the potentially enhanced opportunity of the virus to replicate in the setting of steroid-induced immunosuppression. Andersson and Ernberg (85) conducted an open clinical trial in which the combination of prednisolone and acyclovir was assessed for treating immunocompetent patients with complicated acute infectious mononucleosis. They showed that acyclovir could suppress oropharyngeal shedding of EBV even when corticosteroids were given. Although the combined regimen appeared to be clinically beneficial, the individual contribution of acyclovir to this effect was not delineated. Acute Progressive Infection Treatment of fulminant infections that develop in the setting of immunologic deficiency has been disappointing (19). This result is typified by the general experience in patients with X-linked lymphoproliferative disease, in whom neither acyclovir nor corticosteroids seem to alter the explosive progression of primary EBV infection or its sequelae (98, 99). Gamma-interferon and the combination of alpha-interferon and immunoglobulin may provide transient benefit to such patients (100, 101). Chronic Infectious Mononucleosis Anecdotal reports have linked intravenous acyclovir therapy with improvement of fever, interstitial pneumonitis, and lymphocyte CD4/CD8 ratio in patients with 54 1 January 1993 Annals of Internal Medicine Volume 118 Number 1
11 chronic infectious mononucleosis (22). During the past 13 years, we have found that only one of six such patients responded to acyclovir and that three of five responded well to long-term treatment with prednisone plus a cytotoxic agent. In the isolated instances where alpha- or gamma-interferon or intravenous immunoglobulin was used, no evidence of benefit was seen. Other EBV-associated Disorders Oral Hairy Leukoplakia A benign lesion commonly found in HIV-infected persons, oral hairy leukoplakia is associated with minimal symptoms (or none) and may resolve spontaneously (26, 102). Interestingly, this is the only lesion that appears to arise as a direct consequence of replication of the linear genome of EBV and, therefore, is amenable to antiviral therapy. Several small series suggest that intravenous or oral acyclovir is effective in resolving hairy leukoplakia, but lesions frequently recur after therapy is discontinued (103). It has also been reported that hairy leukoplakia responds to ganciclovir. Lymphoproliferative Disorders The EBV-associated lymphoproliferative disorders that arise in solid organ and bone marrow transplant recipients pose another problem for which the treatment options are often unsatisfactory and untested by controlled trials. Measures should be taken to improve immune function by withdrawing or reducing immunosuppressive therapy, if possible. Otherwise, several regimens can be considered. Remissions of both polyclonal and monoclonal tumors have been associated with the combination of alpha-interferon and intravenous gammaglobulin (104). An initial report indicates that infusions of anti-b-cell antibodies hold promise for oligoclonal lymphoproliferative disorders not involving the central nervous system (105). Although earlier studies suggested that acyclovir was effective in cases of polyclonal lymphoproliferative disorders, subsequent research has cast doubt on this conclusion (20). Surgical resection of localized tumors appears to be beneficial in certain cases; debulking of extensive tumors may also be useful. Aggressive tumors may require cytotoxic or radiation therapy, or both. Lymphomas associated with EBV that arise in persons with AIDS or congenital immunodeficiency syndromes are typically aggressive, high-grade B-cell tumors that may respond to cytotoxic agents or radiation therapy. Prevention Restricting intimate contact during acute mononucleosis can reduce the transmission of EBV but will needlessly hamper contact with many persons who are already seropositive and, in cases of susceptible children, may even delay virus acquisition to an age when symptomatic mononucleosis is more likely. In addition, the transmissibility of EBV during asymptomatic viral shedding remains problematic long after the acute illness. Nevertheless, avoidance of intimate contact is reasonable in the few instances when the complications of 1 January 1993 infection could be devastating. Nosocomial transmission of EBV is largely preventable by attention to universal precautions and hand-washing. Isolation of persons with acute infectious mononucleosis is generally unnecessary (106). Because recipients of EBV-containing blood products or tissue allografts may become infected, the use of irradiated blood products or EBV-negative tissues in seronegative persons is justified in special circumstances (for children with severe combined immunodeficiency and selected transplant recipients, for example). Vaccine Development The major impetus for vaccine development arises from the desire to prevent infection in regions of the world where EBV-associated malignancies are highly endemic and to prevent infection in persons with immunodeficiency disorders. In addition, vaccination of all children in developed countries could be considered for the prevention of infectious mononucleosis. Because a live EBV vaccine, however attenuated, could retain its oncogenic potential, research is being concentrated on a subunit vaccine or an inactivated virus vaccine. Subunit vaccine development has focused on use of the EBV gp350 envelope glycoprotein, which binds to the virus receptor on B cells. Serum from humans infected with EBV contains antibodies to gp350 antigens. These antibodies are active in in-vitro assays such as virus neutralization, complement fixation, and antibody-dependent cellular cytotoxicity. In addition, most persons also have salivary IgA antibodies to gp350. Moreover, gp350 elicits a cellular immune response, and CD4-positive T-cell clones from infected humans recognize epitopes on gp350. Experimental preparations of gp350 appear to be promising. Cotton-top tamarins (Old World primates) invariably develop EBV-associated lymphoproliferation within 3 weeks after infection. After vaccination with gp350, the animals develop substantial levels of EBVneutralizing antibody and are protected from B-cell tumors after subsequent challenge with EBV (107). Despite the progress made in technical aspects of EBV vaccine development, several obstacles remain. There is concern that vaccine-induced immunity would wane and merely delay the age of primary infection or alter immune responses to the infection and make the disease worse. Also, it is not known whether the existing candidate vaccines would protect against virus acquired by a natural route of infection. It will be some time before a vaccine is considered suitable for routine prevention of EBV infection in the United States. Acknowledgments: The authors thank S. E. Pike, K. Jones, K. Taga, P. Frugoni, J. Tanner, M. K. Breinig, J. McKnight, and A. Rosenberg for helping with this work; B. R. Marshall, E. Caruso, and M. Stoughton for providing editorial assistance; and S. Rosen for organizing this conference and providing invaluable advice on the manuscript. Requests for Reprints: Stephen E. Straus, MD, Medical Virology Section, Laboratory of Clinical Investigation, NIAID, NIH, Building 10, Room 11N228, Bethesda, MD Current Author Addresses: Drs. Straus, Cohen, and Meier: Medical Virology Section, Laboratory of Clinical Investigation, NIAID, NIH, Building 10, Room 11N228, Bethesda, MD Annals of Internal Medicine Volume 118 Number 1 55
12 Dr. Tosato: Laboratory of Immunology, Center for Biologies, Evaluation, and Research, Food and Drug Administration, Building 29, Room 501, Bethesda, MD References 1. Miller G. Epstein-Barr virus: biology, pathogenesis, and medical aspects. In: Fields BN, Knipe DM, eds. Virology. Second edition. New York: Raven Press; 1990: Schlossberg D, ed. Infectious Mononucleosis. Second edition. New York: Springer-Verlag; Filatow NJ. Lektush ob ostriku infektsion Nikh Lolieznyak [Lectures on acute infectious diseases of children]. Moscow: U Deitel; Henle G, Henle W, Diehl V. Relation of Burkitfs tumor-associated herpes-type virus to infectious mononucleosis. Proc Natl Acad Sci USA. 1968;59: Straus SE, Fleisher GR. Infectious mononucleosis epidemiology and pathogenesis. In: Schlossberg D, ed. Infectious Mononucleosis. Second edition. New York: Springer-Verlag; 1989: Ho M, Jaffe R, Miller G, Breinig MK, Dummer JS, Makowa L, et al. The frequency of Epstein-Barr virus infection and associated lymphoproliferative syndrome after transplantation and its manifestations in children. Transplantation. 1988;45: Golden HD, Chang RS, Prescott W, Simpson E, Cooper TY. Leukocyte-transforming agents: prolonged excretion by patients with mononucleosis and excretion by normal individuals. J Infect Dis. 1973;127: Sumaya CV, Boswell RN, Ench Y, Kisner DL, Hersh EM, Reuben JM, et al. Enhanced serological and virological findings of Epstein- Barr virus in patients with AIDS and AIDS-related complex. J Infect Dis. 1986;154: Sixbey JW, Lemon SM, Pagano JS. A second site of Epstein-Barr virus shedding: the uterine cervix. Lancet. 1986;2: Nye FJ, Lambert HP. Epstein-Barr virus antibody in cases and contacts of infectious mononucleosis: a family study. J Hyg (Lond). 1973;71: Gerber P, Walsh JH, Rosenblum EN, Purcell RH. Association of EB-virus infection with the post-perfusion syndrome. Lancet. 1969;1: Shearer WT, Ritz J, Finegold MJ, Guerra IC, Rosenblatt HM, Lewis DE, et al. Epstein-Barr virus-associated B-cell proliferations of diverse clonal origins after bone marrow transplantation in a 12-year-old patient with severe combined immunodeficiency. N Engl J Med. 1985;312: Svedmyr E, Ernberg I, Seeley J, Weiland O, Masucci G, Blomogren H, et al. Virologic, immunologic, and clinical observations on a patient during the incubation, acute, and convalescent phases of infectious mononucleosis. Clin Immunol Immunopathol. 1984;30: Schooley RT, Dolin R. Epstein-Barr virus (infectious mononucleosis). In: Mandell GL, Douglas RG Jr, Bennett JE, eds. Principles and Practice of Infectious Diseases. Third edition. New York: Churchill Livingstone; 1990: Kano K, Milgram F. Heterophile antigens and antibodies in medicine. Curr Top Microbiol Immunol. 1977;77: Evans AS, Niederman JC, Cenabre LC, West B, Richards VA. A prospective evaluation of heterophile and Epstein-Barr virus-specific IgM antibody tests in clinical and subclinical infectious mononucleosis: specificity and sensitivity of the tests and persistence of antibody. J Infect Dis. 1975;12: Okano M, Thiele GM, Davis JR, Grierson HL, Purtillo DT. Epstein-Barr virus and human diseases: recent advances in diagnosis. Clin Microbiol. Rev. 1988;1: Horwitz CA, Henle W, Henle G, Rudnick H, Latts E. Long-term serological follow-up of patients for Epstein-Barr virus after recovery from infectious mononucleosis. J Infect Dis. 1985;151: Straus SE. Acute progressive Epstein-Barr virus infections. Annu Rev Med. 1992;43: Cohen JI. Epstein-Barr virus lymphoproliferative disease associated with acquired immunodeficiency. Medicine (Baltimore). 1991; 70: Purtilo DT, DeFlorio D Jr, Huff LM, Bhawan J, Yang JP, Otto R, et al. Variable phenotypic expression of an X-linked lymphoproliferative syndrome. N Engl J Med. 1977;297: Schooley RT, Carey RW, Miller G, Henle W, Eastman R, Mark EJ, et al. Chronic Epstein-Barr virus infections associated with fever and interstitial pneumonitis. Ann Intern Med. 1986;104: Straus SE. The chronic mononucleosis syndrome. J Infect Dis. 1988;157: Jones JF, Shurin S, Abramowsky C, Tubbs RR, Sciotto CG, Wahl R, et al. T-cell lymphomas containing Epstein-Barr viral DNA in patients with chronic Epstein-Barr virus infections. N Engl J Med. 1988;318: Greenspan JS, Greenspan D, Lennett ET, Abrams DI, Conant MA, Petersen V, et al. Replication of Epstein-Barr virus within the epithelial cells of oral "hairy" leukoplakia, an AIDS-associated lesion. N Engl J Med. 1985;313: Baer R, Bankier AT, Biggin MD, Deininger PL, Farrell PJ, Gibson TJ, et al. DNA sequence and expression of the B95-8 Epstein-Barr virus genome. Nature. 1984;310: Sixbey J, Shirley P, Chesney P, Buntin DM, Resnick L. Detection of a second widespread strain of Epstein-Barr virus. Lancet. 1989; 2: Sixbey JW, Nedrud JG, Raab-Traub N, Hanes RA, Pagano JS. Epstein-Barr virus replication in oropharyngeal epithelial cells. N Engl J Med. 1984;310: Fingeroth JD, Weis J J, Tedder TF, Strominger JL, Biro PA, Fearon DT. Epstein-Barr virus receptor of human B lymphocytes is the C3d receptor CR2. Proc Natl Acad Sci USA. 1984;81: Li QX, Young LS, Niedobitek G, Dawson CW, Birkenbach M, Wang F, Rickinson AB. Epstein-Barr virus infection and replication in a human epithelial cell system. Nature. 1992;356: Miller G. The switch between latency and replication of Epstein- Barr virus. J Infect Dis. 1990;161: Colby BM, Shaw JE, Elion GB, Pagano JS. Effect of acyclovir [9-(2-hydroxyethoxymethyl)guanine] on Epstein-Barr virus DNA replication. J Virol. 1980;34: Hsu DH, de Waal Malefyt R, Fiorentino DF, Dang MN, Vieira P, de Vries J, et al. Expression of interleukin-10 activity by Epstein-Barr virus protein BCRF1. Science. 1990;250: Kieff E, Liebowitz D. Epstein-Barr virus and its replication. In: Fields BN, Knipe DM, eds. Virology. New York: Raven Press; 1990: Swendeman S, Thorley-Lawson DA. The activation antigen BLAST-2, when shed, is an autocrine BCGF for normal and transformed B cells. EMBO J. 1987;6: Aubry JP, Pochon S, Graber P, Jansen KU, Bonnefoy JY. CD21 is a ligand for CD23 and regulates IgE production. Nature. 1992;358: Swaminathan S, Tomkinson B, Kieff E. Recombinant Epstein-Barr virus with small RNA (EBER) genes deleted transforms lymphocytes and replicates in vitro. Proc Natl Acad Sci USA ;88: Fahraeus R, Rymo R, Rhim JS, Klein G. Morphological transformation of human keratinocytes expressing the LMP gene of Epstein-Barr virus. Nature. 1990;345: Henderson S, Rowe M, Gregory C, Croom-Carter D, Wang F, Longnecker R, et al. Induction of bcl-2 expression by Epstein-Barr virus latent membrane protein 1 protects infected B cells from programmed cell death. Cell. 1991;65: Longnecker R, Druker B, Roberts TM, Kieff E. An Epstein-Barr virus protein associated with cell growth transformation interacts with a tyrosine kinase. J Virol. 1991;65: Cohen JI, Wang F, Mannick J, Kieff E. Epstein-Barr virus nuclear protein 2 is a key determinant of lymphocyte transformation. Proc Natl Acad Sci USA. 1989;86: Rowe M, Gregory C. Epstein-Barr virus and Burkitt's lymphoma. Adv Viral Oncol. 1989;8: Murray RJ, Kurilla MG, Griffin HM, Brooks JM, Mackett M, Arrand JR, et al. Human cytotoxic T cell responses against Epstein-Barr virus nuclear antigens demonstrated using recombinant vaccinia viruses. Proc Natl Acad Sci USA. 1990;87: Murray RJ, Wang D, Young LS, Wang F, Rowe M, Kieff E, et al. Epstein-Barr virus-specific cytotoxic T-cell recognition of transfectants expressing the virus-coded latent membrane protein LMP. J Virol. 1988;62: Young LS, Dawson CW, Clark D, Rupani H, Busson P, Tursz T, et al. Epstein-Barr virus gene expression in nasopharyngeal carcinoma. J Gen Virol. 1988;69: Young L, Alfieri C, Hennessy K, Evans H, O'Hara C, Anderson KC, et al. Expression of Epstein-Barr virus transformation-associated genes in tissues of patients with EBV lymphoproliferative disease. N Engl J Med. 1989;321: Thomas JA, Hotchin NA, Allday MJ, Amlot P, Rose M, Yacoub M, et al. Immunohistology of Epstein-Barr virus-associated antigens in B cell disorders from immunocompromised individuals. Transplantation. 1990;49: Weiss LM, Movahed LA, Warnke RA, Sklar J. Detection of Epstein-Barr viral genomes in Reed-Sternberg cells of Hodgkin's disease. N Engl J Med. 1989;320: Pallesen G, Hamilton-Dutoit SJ, Rowe M, Young LS. Expression of Epstein-Barr virus latent gene products in tumour cells of Hodgkin's disease. Lancet. 1991;337: Young LS, Lau R, Rowe M, Niedobitek G, Packham G, Shanahan F, et al. Differentiation-associated expression of the Epstein-Barr virus BZLF1 transactivator protein in oral hairy leukoplakia. J Virol. 1991;65: Gilligan K, Rajadurai P, Resnick L, Raab-Traub N. Epstein-Barr virus small nuclear RNAs are not expressed in permissively infected cells in AIDS-associated leukoplakia. Proc Natl Acad Sci USA. 1990;87: January 1993 Annals of Internal Medicine Volume 118 Number 1
13 52. Tosato G. The Epstein-Barr virus and the immune system. In: Klein G, Weinhouse S, eds. Advances in Cancer Research. London: Academic Press; 1987: Rickinson AB. Cellular immunological responses to the virus infection. In: Epstein MA, Achong BG, eds. The Epstein-Barr Virus: Recent Advances. New York: Wiley Medical Publications; 1990: Rowe M, Young LS, Crocker J, Stockes H, Henderson S, Rickinson AB. Epstein-Barr virus (EBV)-associated lymphoproliferative disease in the SCID mouse model: implications for the pathogenesis of EBV-positive lymphomas in man. J Exp Med. 1991;173: Gordon J, Ley SC, Melamed MD, Aman P, Hughes-Jones NC. Soluble factor requirements for the autostimulatory growth of B lymphocytes immortalized by Epstein-Barr virus. J Exp Med. 1984;159: Tosato G, Tanner G, Jones KD, Revel M, Pike SE. Identification of interleukin-6 as an autocrine growth factor for Epstein-Barr virusimmortalized B cells. J Virol. 1990;64: Pike SE, Markey SP, Ijames C, Jones KD, Tosato G. The role of lactic acid in autocrine B-cell growth stimulation. Proc Natl Acad Sci USA. 1991;88: Wakasugi H, Rimsky L, Mahe Y, Kamel AM, Fradelizi D, Tursz T, et al. Epstein-Barr virus-containing B-cell line produces interleukin-1 that it uses as a growth factor. Proc Natl Acad Sci USA. 1987;84: Moss DJ, Rickinson AB, Wallace LE, Epstein MA. Sequential appearance of Epstein-Barr virus nuclear and lymphocyte-detected membrane antigens in B cell transformation. Nature ;291: Klein G. Viral latency and transformation: the strategy of Epstein- Barr virus. Cell. 1989;58: Yao Qy, Ogan P, Rowe M, Wood M, Rickinson AB. Epstein-Barr virus-infected B cells persist in the circulation of acyclovir-treated virus carriers. Int J Cancer. 1989;43: Gratama JW, Oosterveer MAP, Zwaan FE, Lepoutre J, Klein G, Ernberg I. Eradication of Epstein-Barr virus by allogeneic marrow transplantation: implications for sites of viral latency. Proc Natl Acad Sci USA. 1988;85: Wang F, Blaese RM, Zoon KC, Tosato G. Suppressor T cell clones from patients with acute Epstein-Barr virus-induced infectious mononucleosis. J Clin Invest. 1987;79: Vieira P, DeWaal-Malefyt R, Dang MN, Johnson KC, Kastelein R, Fiorentino DF, et al. Isolation and expression of human cytokine inhibitory factor cdna clones: homology to Epstein-Barr open reading frame BCRF-1. Proc Natl Acad Sci USA. 1991;88: Thorley-Lawson DA, Israelsohn ES. Generation of specific cytotoxic T cells with a fragment of the Epstein-Barr virus-encoded p63/latent membrane protein. Proc Natl Acad Sci USA. 1987;84: Burrows SR, Sculley TB, Misko IS, Schmidt C, Moss DJ. An Epstein-Barr virus-specific cytotoxic T cell epitope in EBV nuclear antigen 3 (EBNA 3). J Exp Med. 1990;171: Burrows SR, Misco IS, Sculley TB, Schmidt C, Moss DJ. An Epstein-Barr virus-specific cytotoxic T-cell epitope present on A- and B-type transformants. J Virol. 1990;64: Yates JL, Warren N, Sugden B. Stable replication of plasmid derived from Epstein-Barr virus in various mammalian cells. Nature. 1985;313: Cross M, Dexter TM. Growth factors in development, transformation, and tumorigenesis. Cell. 1991;64: Scala G, Quinto I, Ruocco MR, Arcucci A, Mallardo M, Caretto P, et al. Expression of exogenous interleukin-6 gene in human Epstein-Barr virus B cells confers growth advantage and in vivo tumorigenicity. J Exp Med. 1990;172: Tanner J, Tosato G. Impairment of natural killer functions by interleukin-6 increases lymphoblastoid cell tumorigenicity in athymic mice. J Clin Invest. 1991;88: Birx D, Redfield RR, Tencer K, Fowler A, Burke DS, Tosato G. Induction of interleukin-6 during human immunodeficiency virus infection. Blood. 1990;76: Jones K, McKnight JLC, Breinig MC, Ho M, Tosato G. Abnormally elevated circulating IL-6 levels in patients with post-transplant lymphoproliferative disorders. Clin Res. 1992;[In press]. 74. Maki DG, Reich RM. Infectious mononucleosis in the athlete. Diagnosis, complications, and management. Am J Sports Med. 1982;10: Dommerby H, Stangerup SE, Stangerup M, Hancke S. Hepatosplenomegaly in infectious mononucleosis, assessed by ultrasonic scanning. J Laryngol Otol. 1986;100: Bennike T. Penicillin treatment of infectious mononucleosis: comparison of effects in ninety-nine patients with and in sixty-seven patients without penicillin therapy. Arch Intern Med. 1951;87: Antila V, Makela TE, Klemola E. Corticotropin in the treatment of infectious mononucleosis. Acta Med Scand. 1962;171: Schumacher HR, Jacobson WA, Bemiller CR. Treatment of infectious mononucleosis. Ann Intern Med. 1963;58: Prout C, Dalrymple W. A double-blind study of eighty-two cases of infectious mononucleosis treated with corticosteroids. J Am Coll Health Assoc. 1966;15: Bender CE. The value of corticosteroids in the treatment of infectious mononucleosis. JAMA. 1967;15: Klein EM, Cochran JF, Buck RL. The effects of short-term corticosteroid therapy on the symptoms of infectious mononucleosis pharyngotonsillitis: a double-blind study. J Am Coll Health Assoc. 1969;17: Collins M, Fleisher G, Kreisberg J, Fager S. Role of steroids in the treatment of infectious mononucleosis in the ambulatory college student. J Am Coll Health. 1984;33: Frenkel EP, Shiver CB, Berg P, et al. Meningoencephalitis in infectious mononucleosis: report of a case treated with cortisone. JAMA. 1956;162: Waldo RT. Neurologic complications of infectious mononucleosis after steroid therapy. South Med J. 1981;74: Andersson J, Ernberg I. Management of Epstein-Barr virus infections. Am J Med. 1988;85: McGowan JE Jr, Chesney PJ, Crossley KB, LaForce FM. Guidelines for the use of systemic glucocorticosteroids in the management of selected infections. Working Group on Steroid Use, Antimicrobial Agents Committee, Infectious Diseases Society of America. J Infect Dis. 1992;165: Straus SE. Epstein-Barr virus and human herpesvirus type 6. In: Galasso GJ, Whitely RJ, Merigan TC, eds. Antiviral Agents and Viral Diseases of Man. Third edition. New York: Raven Press; 1990: Pagano JS, Sixbey JW, Lin JC. Acyclovir and Epstein-Barr virus infection. J Antimicrob Chemother. 1983;12(Suppl B): Andersson J, Britton S, Ernberg I, Andersson U, Henle W, Skoldenberg B, et al. Effect of acyclovir on infectious mononucleosis: a double-blind, placebo-controlled study. J Infect Dis. 1986;153: Andersson J, Skoldenberg B, Henle W, Giesecke G, Ortqvist A, Julander I, et al. Acyclovir treatment in infectious mononucleosis: a clinical and virological study. Infection. 1987;15: van der Horst C, Joncas J, Ahronheim G, Gustafson N, Stein G, Gurwith M, et al. Lack of effect of peroral acyclovir for the treatment of infectious mononucleosis. J Infect Dis. 1991; 164: Brandfonbrener A, Epstein A, Wu S, Phair J. Corticosteroid therapy in Epstein-Barr virus infection. Effect on lymphocyte class, subset, and response to early antigen. Arch Intern Med. 1986; 146: Copeman HA. Infectious mononucleosis with severe thrombocytopenic purpura. Med J Aust. 1956;43: Smith JN. Complications of infectious mononucleosis. Ann Intern Med. 1956;44: Lazarus KH, Baehner RL. Aplastic anemia complicating infectious mononucleosis: a case report and review of the literature. Pediatrics. 1981;67: Grishaber JE, McClain KL, Mahoney DH Jr, Fernback DJ. Successful outcome of severe aplastic anemia folowing Epstein-Barr virus infection. Am J Hematol. 1988;28: Baranski B, Armstrong G, Truman JT, Quinnan GV Jr, Straus SE, Young NS. Epstein-Barr virus in the bone marrow of patients with aplastic anemia. Ann Intern Med. 1988;109: Grierson H, Purtilo DT. Epstein-Barr virus infections in males with the X-linked lymphoproliferative syndrome. Ann Intern Med. 1987; 106: Sullivan JL, Byron KS, Brewster FE, Sakamoto K, Show JE, Pagano JS. Treatment of life-threatening Epstein-Barr virus infection with acyclovir. Am J Med. 1982;73: Okana M, Pirruccelo SJ, Grierson HL, Johnson DR, Thiele GM, Purtilo DT. Immunovirological studies of fatal infectious mononucleosis in a patient with X-linked lymphoproliferative syndrome treated with intravenous immunoglobulin and interferon-alpha. Clin Immun Immunopathol. 1990;54: Okano M, Thiele GM, Kobayashi RH, Davis JR, Synovec MS, Grierson HL, et al. Interferon-gamma in a family with X-linked lymphoproliferative syndrome with acute Epstein-Barr virus infection. J Clin Immunol. 1989;9: Katz MH, Greenspan D, Heinic GS, Chan AK, Hollander H, Chernoff D, et al. Resolution of hairy leukoplakia: an observational trial of zidovudine versus no treatment [Letter]. J Infect Dis. 1991; 164: Resnick L, Herbst JS, Ablashi DV, Atherton S, Frank B, Rosen L, et al. Regression of oral hairy leukoplakia after orally administered acyclovir therapy. JAMA. 1988;259: Shapiro RS, Chauvenet A, McGuire W, Pearson A, Craft AW, 1 January 1993 Annals of Internal Medicine Volume 118 Number 1 57
Infectious Mononucleosis The Virus Pathophysiology: Age: History: Fever. Lymphadenopathy
 Infectious Mononucleosis The Virus A member of the Herpesvirus family Infects human B lymphocytes Herpes viruses contain double-stranded DNA, and they have an icosahedral capsid and a glycoprotein-containing
Infectious Mononucleosis The Virus A member of the Herpesvirus family Infects human B lymphocytes Herpes viruses contain double-stranded DNA, and they have an icosahedral capsid and a glycoprotein-containing
Epstein-Barr Virus 1
 Epstein-Barr Virus 1 Herpesviruses dsdna, linear, enveloped, 180-200 nm Large genome, codes for 75 viral proteins 50-70% similarity Cross reactivity between HSV and VZV HSV-2 virus particle. Note that
Epstein-Barr Virus 1 Herpesviruses dsdna, linear, enveloped, 180-200 nm Large genome, codes for 75 viral proteins 50-70% similarity Cross reactivity between HSV and VZV HSV-2 virus particle. Note that
EBV and Infectious Mononucleosis. Infectious Disease Definitions. Infectious Diseases
 Infectious Disease Definitions Infection when a microorganism invades a host and multiplies enough to disrupt normal function by causing signs and symptoms Pathogencity ability of an organism to cause
Infectious Disease Definitions Infection when a microorganism invades a host and multiplies enough to disrupt normal function by causing signs and symptoms Pathogencity ability of an organism to cause
Clinical Aspect and Application of Laboratory Test in Herpes Virus Infection. Masoud Mardani M.D,FIDSA
 Clinical Aspect and Application of Laboratory Test in Herpes Virus Infection Masoud Mardani M.D,FIDSA Shahidhid Bh BeheshtiMdi Medical lui Universityit Cytomegalovirus (CMV), Epstein Barr Virus(EBV), Herpes
Clinical Aspect and Application of Laboratory Test in Herpes Virus Infection Masoud Mardani M.D,FIDSA Shahidhid Bh BeheshtiMdi Medical lui Universityit Cytomegalovirus (CMV), Epstein Barr Virus(EBV), Herpes
EBV infection B cells and lymphomagenesis. Sridhar Chaganti
 EBV infection B cells and lymphomagenesis Sridhar Chaganti How EBV infects B-cells How viral genes influence the infected B cell Differences and similarities between in vitro and in vivo infection How
EBV infection B cells and lymphomagenesis Sridhar Chaganti How EBV infects B-cells How viral genes influence the infected B cell Differences and similarities between in vitro and in vivo infection How
Herpesviruses. Virion. Genome. Genes and proteins. Viruses and hosts. Diseases. Distinctive characteristics
 Herpesviruses Virion Genome Genes and proteins Viruses and hosts Diseases Distinctive characteristics Virion Enveloped icosahedral capsid (T=16), diameter 125 nm Diameter of enveloped virion 200 nm Capsid
Herpesviruses Virion Genome Genes and proteins Viruses and hosts Diseases Distinctive characteristics Virion Enveloped icosahedral capsid (T=16), diameter 125 nm Diameter of enveloped virion 200 nm Capsid
VZV, EBV, and HHV-6-8
 VZV, EBV, and HHV-6-8 Anne Gershon Common Features of Herpesviruses Morphology Basic mode of replication Primary infection followed by latency Ubiquitous Ability to cause recurrent infections (reactivation
VZV, EBV, and HHV-6-8 Anne Gershon Common Features of Herpesviruses Morphology Basic mode of replication Primary infection followed by latency Ubiquitous Ability to cause recurrent infections (reactivation
Epstein-Barr Virus in a Toddler. Elaine Bullock, MD Pediatrics LSU Health Shreveport Louisiana Chapter AAP Pediatric Potpourri on the Bayou
 Epstein-Barr Virus in a Toddler Elaine Bullock, MD Pediatrics LSU Health Shreveport Louisiana Chapter AAP Pediatric Potpourri on the Bayou Disclosure Presenter: Elaine Bullock, MD I have nothing to disclose
Epstein-Barr Virus in a Toddler Elaine Bullock, MD Pediatrics LSU Health Shreveport Louisiana Chapter AAP Pediatric Potpourri on the Bayou Disclosure Presenter: Elaine Bullock, MD I have nothing to disclose
Human Herpesviruses. VZV, EBV, and HHV-6-8. The rash of VZV is vesicular. MID 34
 VZV, EBV, and HHV-6-8 Anne Gershon Human Herpesviruses Replication (lytic infection) occurs in a cascade Latency occurs when the cascade is interrupted Transcription of viral genome and protein synthesis
VZV, EBV, and HHV-6-8 Anne Gershon Human Herpesviruses Replication (lytic infection) occurs in a cascade Latency occurs when the cascade is interrupted Transcription of viral genome and protein synthesis
Class 10. DNA viruses. I. Seminar: General properties, pathogenesis and clinial features of DNA viruses from Herpesviridae family
 English Division, 6-year programme Class 10 DNA viruses I. Seminar: General properties, pathogenesis and clinial features of DNA viruses from Herpesviridae family II. Assays to be performed: 1. Paul-Bunnel-Davidsohn
English Division, 6-year programme Class 10 DNA viruses I. Seminar: General properties, pathogenesis and clinial features of DNA viruses from Herpesviridae family II. Assays to be performed: 1. Paul-Bunnel-Davidsohn
Persistent Infections
 Persistent Infections Lecture 17 Biology 3310/4310 Virology Spring 2017 Paralyze resistance with persistence WOODY HAYES Acute vs persistent infections Acute infection - rapid and self-limiting Persistent
Persistent Infections Lecture 17 Biology 3310/4310 Virology Spring 2017 Paralyze resistance with persistence WOODY HAYES Acute vs persistent infections Acute infection - rapid and self-limiting Persistent
Properties of Herpesviruses
 Herpesviruses Properties of Herpesviruses Structure and Composition Spherical icosahedron, 150-200 nm Double-stranded DNA, linear More than 35 proteins Enveloped Replication from nucleus (budding) Features
Herpesviruses Properties of Herpesviruses Structure and Composition Spherical icosahedron, 150-200 nm Double-stranded DNA, linear More than 35 proteins Enveloped Replication from nucleus (budding) Features
Human Herpes Viruses (HHV) Mazin Barry, MD, FRCPC, FACP, DTM&H Assistant Professor and Consultant Infectious Diseases KSU
 Human Herpes Viruses (HHV) Mazin Barry, MD, FRCPC, FACP, DTM&H Assistant Professor and Consultant Infectious Diseases KSU HERPES VIRUS INFECTIONS objectives: ØTo know the clinically important HHVs. ØTo
Human Herpes Viruses (HHV) Mazin Barry, MD, FRCPC, FACP, DTM&H Assistant Professor and Consultant Infectious Diseases KSU HERPES VIRUS INFECTIONS objectives: ØTo know the clinically important HHVs. ØTo
Medical Virology Immunology. Dr. Sameer Naji, MB, BCh, PhD (UK) Head of Basic Medical Sciences Dept. Faculty of Medicine The Hashemite University
 Medical Virology Immunology Dr. Sameer Naji, MB, BCh, PhD (UK) Head of Basic Medical Sciences Dept. Faculty of Medicine The Hashemite University Human blood cells Phases of immune responses Microbe Naïve
Medical Virology Immunology Dr. Sameer Naji, MB, BCh, PhD (UK) Head of Basic Medical Sciences Dept. Faculty of Medicine The Hashemite University Human blood cells Phases of immune responses Microbe Naïve
BIT 120. Copy of Cancer/HIV Lecture
 BIT 120 Copy of Cancer/HIV Lecture Cancer DEFINITION Any abnormal growth of cells that has malignant potential i.e.. Leukemia Uncontrolled mitosis in WBC Genetic disease caused by an accumulation of mutations
BIT 120 Copy of Cancer/HIV Lecture Cancer DEFINITION Any abnormal growth of cells that has malignant potential i.e.. Leukemia Uncontrolled mitosis in WBC Genetic disease caused by an accumulation of mutations
Viral Diseases in the Hematolymphatics. By:Ass. Prof. Nader Alaridah
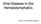 Viral Diseases in the Hematolymphatics By:Ass. Prof. Nader Alaridah Parvoviruses Members of the family Parvoviridae, are small (diameter, ~22 nm), nonenveloped, icosahedral viruses with a linear single-strand
Viral Diseases in the Hematolymphatics By:Ass. Prof. Nader Alaridah Parvoviruses Members of the family Parvoviridae, are small (diameter, ~22 nm), nonenveloped, icosahedral viruses with a linear single-strand
EBV Infection and Immunity. Andrew Hislop Institute for Cancer Studies University of Birmingham
 EBV Infection and Immunity Andrew Hislop Institute for Cancer Studies University of Birmingham EBV Introduction Large ds DNA virus Spread by saliva contact Lifelong infection Predominantly B-lymphotropic
EBV Infection and Immunity Andrew Hislop Institute for Cancer Studies University of Birmingham EBV Introduction Large ds DNA virus Spread by saliva contact Lifelong infection Predominantly B-lymphotropic
Viruses. Poxviridae. DNA viruses: 6 families. Herpesviridae Adenoviridae. Hepadnaviridae Papovaviridae Parvoviridae
 Viruses DNA viruses: 6 families Poxviridae Herpesviridae Adenoviridae Hepadnaviridae Papovaviridae Parvoviridae Human herpesviruses Three subfamilies (genome structure, tissue tropism, cytopathologic effect,
Viruses DNA viruses: 6 families Poxviridae Herpesviridae Adenoviridae Hepadnaviridae Papovaviridae Parvoviridae Human herpesviruses Three subfamilies (genome structure, tissue tropism, cytopathologic effect,
Human Herpesviruses. Medical Virology, 27 Nov 2015.
 Human Herpesviruses Assoc.Prof. Murat Sayan Kocaeli Üniversitesi, Rutin PCR Lab. Sorumlu Öğt.Üyesi Yakın Doğu Üniversitesi, DESAM Kurucu Öğrt. Üyesi sayanmurat@hotmail.com 0533 6479020 Medical Virology,
Human Herpesviruses Assoc.Prof. Murat Sayan Kocaeli Üniversitesi, Rutin PCR Lab. Sorumlu Öğt.Üyesi Yakın Doğu Üniversitesi, DESAM Kurucu Öğrt. Üyesi sayanmurat@hotmail.com 0533 6479020 Medical Virology,
2017 CST-Astellas Canadian Transplant Fellows Symposium. EBV Post Transplantation Implications and Approach to Management
 2017 CST-Astellas Canadian Transplant Fellows Symposium EBV Post Transplantation Implications and Approach to Management Atul Humar, MD Atul Humar is a Professor in the Department of Medicine, University
2017 CST-Astellas Canadian Transplant Fellows Symposium EBV Post Transplantation Implications and Approach to Management Atul Humar, MD Atul Humar is a Professor in the Department of Medicine, University
COURSE: Medical Microbiology, PAMB 650/720 - Fall 2008 Lecture 16
 COURSE: Medical Microbiology, PAMB 650/720 - Fall 2008 Lecture 16 Tumor Immunology M. Nagarkatti Teaching Objectives: Introduction to Cancer Immunology Know the antigens expressed by cancer cells Understand
COURSE: Medical Microbiology, PAMB 650/720 - Fall 2008 Lecture 16 Tumor Immunology M. Nagarkatti Teaching Objectives: Introduction to Cancer Immunology Know the antigens expressed by cancer cells Understand
Dr. Yi-chi M. Kong August 8, 2001 Benjamini. Ch. 19, Pgs Page 1 of 10 TRANSPLANTATION
 Benjamini. Ch. 19, Pgs 379-399 Page 1 of 10 TRANSPLANTATION I. KINDS OF GRAFTS II. RELATIONSHIPS BETWEEN DONOR AND RECIPIENT Benjamini. Ch. 19, Pgs 379-399 Page 2 of 10 II.GRAFT REJECTION IS IMMUNOLOGIC
Benjamini. Ch. 19, Pgs 379-399 Page 1 of 10 TRANSPLANTATION I. KINDS OF GRAFTS II. RELATIONSHIPS BETWEEN DONOR AND RECIPIENT Benjamini. Ch. 19, Pgs 379-399 Page 2 of 10 II.GRAFT REJECTION IS IMMUNOLOGIC
Medical Virology. Herpesviruses, Orthomyxoviruses, and Retro virus. - Herpesviruses Structure & Composition: Herpesviruses
 Medical Virology Lecture 2 Asst. Prof. Dr. Dalya Basil Herpesviruses, Orthomyxoviruses, and Retro virus - Herpesviruses Structure & Composition: Herpesviruses Enveloped DNA viruses. All herpesviruses have
Medical Virology Lecture 2 Asst. Prof. Dr. Dalya Basil Herpesviruses, Orthomyxoviruses, and Retro virus - Herpesviruses Structure & Composition: Herpesviruses Enveloped DNA viruses. All herpesviruses have
Immunodeficiencies HIV/AIDS
 Immunodeficiencies HIV/AIDS Immunodeficiencies Due to impaired function of one or more components of the immune or inflammatory responses. Problem may be with: B cells T cells phagocytes or complement
Immunodeficiencies HIV/AIDS Immunodeficiencies Due to impaired function of one or more components of the immune or inflammatory responses. Problem may be with: B cells T cells phagocytes or complement
Epstein-Barr virus and immunity
 Epstein-Barr virus and immunity Elena Kashuba, PhD Associate Professor Department of Microbiology, Tumor and Cell Biology (MTC) Karolinska Institutet 1 Epstein-Barr virus EBV Everybody s virus 200 nm Enveloped
Epstein-Barr virus and immunity Elena Kashuba, PhD Associate Professor Department of Microbiology, Tumor and Cell Biology (MTC) Karolinska Institutet 1 Epstein-Barr virus EBV Everybody s virus 200 nm Enveloped
Human Immunodeficiency Virus. Acquired Immune Deficiency Syndrome AIDS
 Human Immunodeficiency Virus Acquired Immune Deficiency Syndrome AIDS Sudden outbreak in USA of opportunistic infections and cancers in young men in 1981 Pneumocystis carinii pneumonia (PCP), Kaposi s
Human Immunodeficiency Virus Acquired Immune Deficiency Syndrome AIDS Sudden outbreak in USA of opportunistic infections and cancers in young men in 1981 Pneumocystis carinii pneumonia (PCP), Kaposi s
EBV in HSCT 2015 update of ECIL guidelines
 ECIL-6 EBV in HSCT 2015 update of ECIL guidelines Jan Styczynski (Poland, chair), Walter van der Velden (Netherlands), Christopher Fox (United Kingdom), Dan Engelhard (Israel), Rafael de la Camara (Spain),
ECIL-6 EBV in HSCT 2015 update of ECIL guidelines Jan Styczynski (Poland, chair), Walter van der Velden (Netherlands), Christopher Fox (United Kingdom), Dan Engelhard (Israel), Rafael de la Camara (Spain),
Hepatitis B (Part 1 - intro)
 Hepatitis B (Part 1 - intro) The Hepatitis B virus (HBV) l Virology Discovered in 1966 double-stranded DNA virus l family of hepadnaviruses l HBV unique to Humans (Primates too in laboratory studies) no
Hepatitis B (Part 1 - intro) The Hepatitis B virus (HBV) l Virology Discovered in 1966 double-stranded DNA virus l family of hepadnaviruses l HBV unique to Humans (Primates too in laboratory studies) no
Primary Immunodeficiency
 Primary Immunodeficiency DiGeorge Syndrome Severe Combined Immunodeficiency SCID X-Linked Agammaglobulinemia Common variable immunodeficiency (CVID) IgA deficiency Hyper- IgM Syndrome Wiskott-Aldrich syndrome
Primary Immunodeficiency DiGeorge Syndrome Severe Combined Immunodeficiency SCID X-Linked Agammaglobulinemia Common variable immunodeficiency (CVID) IgA deficiency Hyper- IgM Syndrome Wiskott-Aldrich syndrome
5.15 INFECTIOUS MONONUCLEOSIS
 5.15 INFECTIOUS MONONUCLEOSIS Narendra Rathi INTRODUCTION Infectious mononucleosis (IM) is an acute infection caused by Epstein-Barr virus (EBV), characterized by fever, lymphadenopathy, sore throat and
5.15 INFECTIOUS MONONUCLEOSIS Narendra Rathi INTRODUCTION Infectious mononucleosis (IM) is an acute infection caused by Epstein-Barr virus (EBV), characterized by fever, lymphadenopathy, sore throat and
Human Immunodeficiency Virus
 Human Immunodeficiency Virus Virion Genome Genes and proteins Viruses and hosts Diseases Distinctive characteristics Viruses and hosts Lentivirus from Latin lentis (slow), for slow progression of disease
Human Immunodeficiency Virus Virion Genome Genes and proteins Viruses and hosts Diseases Distinctive characteristics Viruses and hosts Lentivirus from Latin lentis (slow), for slow progression of disease
Gastroenteritis and viral infections
 Gastroenteritis and viral infections A Large number of viruses are found in the human gut; these include some that are associated with gastroenteritis Rotaviruses Adenoviruses 40/41 Caliciviruses Norwalk-like
Gastroenteritis and viral infections A Large number of viruses are found in the human gut; these include some that are associated with gastroenteritis Rotaviruses Adenoviruses 40/41 Caliciviruses Norwalk-like
Immunosuppressants. Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia
 Immunosuppressants Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Immunosuppressive Agents Very useful in minimizing the occurrence of exaggerated or inappropriate
Immunosuppressants Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Immunosuppressive Agents Very useful in minimizing the occurrence of exaggerated or inappropriate
Immune system. Aims. Immune system. Lymphatic organs. Inflammation. Natural immune system. Adaptive immune system
 Aims Immune system Lymphatic organs Inflammation Natural immune system Adaptive immune system Major histocompatibility complex (MHC) Disorders of the immune system 1 2 Immune system Lymphoid organs Immune
Aims Immune system Lymphatic organs Inflammation Natural immune system Adaptive immune system Major histocompatibility complex (MHC) Disorders of the immune system 1 2 Immune system Lymphoid organs Immune
Results. Clinical reports of transplant recipients
 Cloning of EBV genes as fusion proteins with Renilla luciferase for Luciferase Immunoprecipitation System (LIPS) analysis A panel of 13 different EBV proteins was generated as Renilla luciferase (Ruc)
Cloning of EBV genes as fusion proteins with Renilla luciferase for Luciferase Immunoprecipitation System (LIPS) analysis A panel of 13 different EBV proteins was generated as Renilla luciferase (Ruc)
Third line of Defense
 Chapter 15 Specific Immunity and Immunization Topics -3 rd of Defense - B cells - T cells - Specific Immunities Third line of Defense Specific immunity is a complex interaction of immune cells (leukocytes)
Chapter 15 Specific Immunity and Immunization Topics -3 rd of Defense - B cells - T cells - Specific Immunities Third line of Defense Specific immunity is a complex interaction of immune cells (leukocytes)
Test Bank for Basic Immunology Functions and Disorders of the Immune System 4th Edition by Abbas
 Test Bank for Basic Immunology Functions and Disorders of the Immune System 4th Edition by Abbas Chapter 04: Antigen Recognition in the Adaptive Immune System Test Bank MULTIPLE CHOICE 1. Most T lymphocytes
Test Bank for Basic Immunology Functions and Disorders of the Immune System 4th Edition by Abbas Chapter 04: Antigen Recognition in the Adaptive Immune System Test Bank MULTIPLE CHOICE 1. Most T lymphocytes
Confirmed (Laboratory Tests) Serum positive for IgM anti-hbc or, hepatitis B surface antigen (HbsAg).
 Hepatitis B Hepatitis B is a liver disease that results from infection with the Hepatitis B virus. It can range in severity from a mild illness lasting a few weeks to a serious, lifelong illness. Hepatitis
Hepatitis B Hepatitis B is a liver disease that results from infection with the Hepatitis B virus. It can range in severity from a mild illness lasting a few weeks to a serious, lifelong illness. Hepatitis
Immunity to Viruses. Patricia Fitzgerald-Bocarsly September 25, 2008
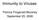 Immunity to Viruses Patricia Fitzgerald-Bocarsly September 25, 2008 The Immune System Deals with a Huge Range of Pathogens Roitt, 2003 Immune Responses to Viruses Viruses are dependent on the host cell
Immunity to Viruses Patricia Fitzgerald-Bocarsly September 25, 2008 The Immune System Deals with a Huge Range of Pathogens Roitt, 2003 Immune Responses to Viruses Viruses are dependent on the host cell
Coronaviruses cause acute, mild upper respiratory infection (common cold).
 Coronaviruses David A. J. Tyrrell Steven H. Myint GENERAL CONCEPTS Clinical Presentation Coronaviruses cause acute, mild upper respiratory infection (common cold). Structure Spherical or pleomorphic enveloped
Coronaviruses David A. J. Tyrrell Steven H. Myint GENERAL CONCEPTS Clinical Presentation Coronaviruses cause acute, mild upper respiratory infection (common cold). Structure Spherical or pleomorphic enveloped
Human Papillomavirus
 Human Papillomavirus Dawn Palaszewski, MD Assistant Professor of Obstetrics and Gynecology University of February 18, 2018 9:40 am Dawn Palaszewski, MD Assistant Professor Department of Obstetrics and
Human Papillomavirus Dawn Palaszewski, MD Assistant Professor of Obstetrics and Gynecology University of February 18, 2018 9:40 am Dawn Palaszewski, MD Assistant Professor Department of Obstetrics and
Immunology. Anas Abu-Humaidan M.D. Ph.D. Transplant immunology+ Secondary immune deficiency
 Immunology Anas Abu-Humaidan M.D. Ph.D. Transplant immunology+ Secondary immune deficiency Transplant Immunology Transplantation is the process of moving cells, tissues or organs from one site to another
Immunology Anas Abu-Humaidan M.D. Ph.D. Transplant immunology+ Secondary immune deficiency Transplant Immunology Transplantation is the process of moving cells, tissues or organs from one site to another
Immunology Lecture 4. Clinical Relevance of the Immune System
 Immunology Lecture 4 The Well Patient: How innate and adaptive immune responses maintain health - 13, pg 169-181, 191-195. Immune Deficiency - 15 Autoimmunity - 16 Transplantation - 17, pg 260-270 Tumor
Immunology Lecture 4 The Well Patient: How innate and adaptive immune responses maintain health - 13, pg 169-181, 191-195. Immune Deficiency - 15 Autoimmunity - 16 Transplantation - 17, pg 260-270 Tumor
Non-Hodgkin lymphomas (NHLs) Hodgkin lymphoma )HL)
 Non-Hodgkin lymphomas (NHLs) Hodgkin lymphoma )HL) Lymphoid Neoplasms: 1- non-hodgkin lymphomas (NHLs) 2- Hodgkin lymphoma 3- plasma cell neoplasms Non-Hodgkin lymphomas (NHLs) Acute Lymphoblastic Leukemia/Lymphoma
Non-Hodgkin lymphomas (NHLs) Hodgkin lymphoma )HL) Lymphoid Neoplasms: 1- non-hodgkin lymphomas (NHLs) 2- Hodgkin lymphoma 3- plasma cell neoplasms Non-Hodgkin lymphomas (NHLs) Acute Lymphoblastic Leukemia/Lymphoma
7 Omar Abu Reesh. Dr. Ahmad Mansour Dr. Ahmad Mansour
 7 Omar Abu Reesh Dr. Ahmad Mansour Dr. Ahmad Mansour -Leukemia: neoplastic leukocytes circulating in the peripheral bloodstream. -Lymphoma: a neoplastic process in the lymph nodes, spleen or other lymphatic
7 Omar Abu Reesh Dr. Ahmad Mansour Dr. Ahmad Mansour -Leukemia: neoplastic leukocytes circulating in the peripheral bloodstream. -Lymphoma: a neoplastic process in the lymph nodes, spleen or other lymphatic
MedChem401 Herpesviridae. Herpesviridae
 MedChem401 Herpesviridae Members of the herpesvirus family have been identified in more than 80 different animal species Eight have been identified as human pathogens Herpes viruses are a leading cause
MedChem401 Herpesviridae Members of the herpesvirus family have been identified in more than 80 different animal species Eight have been identified as human pathogens Herpes viruses are a leading cause
Viral Hepatitis Diagnosis and Management
 Viral Hepatitis Diagnosis and Management CLINICAL BACKGROUND Viral hepatitis is a relatively common disease (25 per 100,000 individuals in the United States) caused by a diverse group of hepatotropic agents
Viral Hepatitis Diagnosis and Management CLINICAL BACKGROUND Viral hepatitis is a relatively common disease (25 per 100,000 individuals in the United States) caused by a diverse group of hepatotropic agents
Chapter 24 The Immune System
 Chapter 24 The Immune System The Immune System Layered defense system The skin and chemical barriers The innate and adaptive immune systems Immunity The body s ability to recognize and destroy specific
Chapter 24 The Immune System The Immune System Layered defense system The skin and chemical barriers The innate and adaptive immune systems Immunity The body s ability to recognize and destroy specific
Case Report Traumatic Haemorrhagic Cervical Lymphadenopathy with Underlying Infectious Mononucleosis
 Hindawi Case Reports in Radiology Volume 2017, Article ID 3097414, 4 pages https://doi.org/10.1155/2017/3097414 Case Report Traumatic Haemorrhagic Cervical Lymphadenopathy with Underlying Infectious Mononucleosis
Hindawi Case Reports in Radiology Volume 2017, Article ID 3097414, 4 pages https://doi.org/10.1155/2017/3097414 Case Report Traumatic Haemorrhagic Cervical Lymphadenopathy with Underlying Infectious Mononucleosis
Dr. Ahmed K. Ali. Outcomes of the virus infection for the host
 Lec. 9 Dr. Ahmed K. Ali Outcomes of the virus infection for the host In the previous few chapters we have looked at aspects of the virus replication cycle that culminate in the exit of infective progeny
Lec. 9 Dr. Ahmed K. Ali Outcomes of the virus infection for the host In the previous few chapters we have looked at aspects of the virus replication cycle that culminate in the exit of infective progeny
Central tolerance. Mechanisms of Immune Tolerance. Regulation of the T cell response
 Immunoregulation: A balance between activation and suppression that achieves an efficient immune response without damaging the host. Mechanisms of Immune Tolerance ACTIVATION (immunity) SUPPRESSION (tolerance)
Immunoregulation: A balance between activation and suppression that achieves an efficient immune response without damaging the host. Mechanisms of Immune Tolerance ACTIVATION (immunity) SUPPRESSION (tolerance)
Mechanisms of Immune Tolerance
 Immunoregulation: A balance between activation and suppression that achieves an efficient immune response without damaging the host. ACTIVATION (immunity) SUPPRESSION (tolerance) Autoimmunity Immunodeficiency
Immunoregulation: A balance between activation and suppression that achieves an efficient immune response without damaging the host. ACTIVATION (immunity) SUPPRESSION (tolerance) Autoimmunity Immunodeficiency
Fayth K. Yoshimura, Ph.D. September 7, of 7 HIV - BASIC PROPERTIES
 1 of 7 I. Viral Origin. A. Retrovirus - animal lentiviruses. HIV - BASIC PROPERTIES 1. HIV is a member of the Retrovirus family and more specifically it is a member of the Lentivirus genus of this family.
1 of 7 I. Viral Origin. A. Retrovirus - animal lentiviruses. HIV - BASIC PROPERTIES 1. HIV is a member of the Retrovirus family and more specifically it is a member of the Lentivirus genus of this family.
Viral Hepatitis. Background
 Viral Hepatitis Background Hepatitis or inflammation of the liver can be caused by infectious and noninfectious problems. Infectious etiologies include viruses, bacteria, fungi and parasites. Noninfectious
Viral Hepatitis Background Hepatitis or inflammation of the liver can be caused by infectious and noninfectious problems. Infectious etiologies include viruses, bacteria, fungi and parasites. Noninfectious
Human Herpesviruses. Varicella-zoster virus. Human Herpesvirus (VZV) phospholipid envelope, tegument, icosahedral capsid, DNA core
 Common Features of Herpesviruses Morphology Basic mode of replication Primary infection followed by latency Ubiquitous Ability to cause recurrent infections (reactivation of latent virus), reinfections
Common Features of Herpesviruses Morphology Basic mode of replication Primary infection followed by latency Ubiquitous Ability to cause recurrent infections (reactivation of latent virus), reinfections
T-cell activation T cells migrate to secondary lymphoid tissues where they interact with antigen, antigen-presenting cells, and other lymphocytes:
 Interactions between innate immunity & adaptive immunity What happens to T cells after they leave the thymus? Naïve T cells exit the thymus and enter the bloodstream. If they remain in the bloodstream,
Interactions between innate immunity & adaptive immunity What happens to T cells after they leave the thymus? Naïve T cells exit the thymus and enter the bloodstream. If they remain in the bloodstream,
T-cell activation T cells migrate to secondary lymphoid tissues where they interact with antigen, antigen-presenting cells, and other lymphocytes:
 Interactions between innate immunity & adaptive immunity What happens to T cells after they leave the thymus? Naïve T cells exit the thymus and enter the bloodstream. If they remain in the bloodstream,
Interactions between innate immunity & adaptive immunity What happens to T cells after they leave the thymus? Naïve T cells exit the thymus and enter the bloodstream. If they remain in the bloodstream,
VIRAL AND AUTOIMMUNE HEPATITIS WHAT IS HEPATITIS?
 VIRAL AND AUTOIMMUNE HEPATITIS Arthur M. Magun, M.D. Clinical Professor of Medicine WHAT IS HEPATITIS? Inflammation of the liver Almost always, inflammation implies elevation in liver enzymes AST and ALT
VIRAL AND AUTOIMMUNE HEPATITIS Arthur M. Magun, M.D. Clinical Professor of Medicine WHAT IS HEPATITIS? Inflammation of the liver Almost always, inflammation implies elevation in liver enzymes AST and ALT
Commonly Asked Questions About Chronic Hepatitis C
 Commonly Asked Questions About Chronic Hepatitis C From the American College of Gastroenterology 1. How common is the hepatitis C virus? The hepatitis C virus is the most common cause of chronic viral
Commonly Asked Questions About Chronic Hepatitis C From the American College of Gastroenterology 1. How common is the hepatitis C virus? The hepatitis C virus is the most common cause of chronic viral
cure research HIV & AIDS
 Glossary of terms HIV & AIDS cure research Antiretroviral Therapy (ART) ART involves the use of several (usually a cocktail of three or more) antiretroviral drugs to halt HIV replication. ART drugs may
Glossary of terms HIV & AIDS cure research Antiretroviral Therapy (ART) ART involves the use of several (usually a cocktail of three or more) antiretroviral drugs to halt HIV replication. ART drugs may
Chapters 21-26: Selected Viral Pathogens
 Chapters 21-26: Selected Viral Pathogens 1. DNA Viral Pathogens 2. RNA Viral Pathogens 1. DNA Viral Pathogens Smallpox (pp. 623-4) Caused by variola virus (dsdna, enveloped): portal of entry is the respiratory
Chapters 21-26: Selected Viral Pathogens 1. DNA Viral Pathogens 2. RNA Viral Pathogens 1. DNA Viral Pathogens Smallpox (pp. 623-4) Caused by variola virus (dsdna, enveloped): portal of entry is the respiratory
Tumor Immunology. Wirsma Arif Harahap Surgical Oncology Consultant
 Tumor Immunology Wirsma Arif Harahap Surgical Oncology Consultant 1) Immune responses that develop to cancer cells 2) Escape of cancer cells 3) Therapies: clinical and experimental Cancer cells can be
Tumor Immunology Wirsma Arif Harahap Surgical Oncology Consultant 1) Immune responses that develop to cancer cells 2) Escape of cancer cells 3) Therapies: clinical and experimental Cancer cells can be
3. Lymphocyte proliferation (fig. 15.4): Clones of responder cells and memory cells are derived from B cells and T cells.
 Chapter 15 Adaptive, Specific Immunity and Immunization* *Lecture notes are to be used as a study guide only and do not represent the comprehensive information you will need to know for the exams. Specific
Chapter 15 Adaptive, Specific Immunity and Immunization* *Lecture notes are to be used as a study guide only and do not represent the comprehensive information you will need to know for the exams. Specific
Introduction to Viruses That Infect Humans: The DNA Viruses
 Chapter 24 Introduction to Viruses That Infect Humans: The DNA Viruses Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. 24.1 Viruses in Human Infections and Diseases
Chapter 24 Introduction to Viruses That Infect Humans: The DNA Viruses Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. 24.1 Viruses in Human Infections and Diseases
Form 2033 R3.0: Wiskott-Aldrich Syndrome Pre-HSCT Data
 Key Fields Sequence Number: Date Received: - - CIBMTR Center Number: CIBMTR Recipient ID: Has this patient's data been previously reported to USIDNET? USIDNET ID: Today's Date: - - Date of HSCT for which
Key Fields Sequence Number: Date Received: - - CIBMTR Center Number: CIBMTR Recipient ID: Has this patient's data been previously reported to USIDNET? USIDNET ID: Today's Date: - - Date of HSCT for which
Third line of Defense. Topic 8 Specific Immunity (adaptive) (18) 3 rd Line = Prophylaxis via Immunization!
 Topic 8 Specific Immunity (adaptive) (18) Topics - 3 rd Line of Defense - B cells - T cells - Specific Immunities 1 3 rd Line = Prophylaxis via Immunization! (a) A painting of Edward Jenner depicts a cow
Topic 8 Specific Immunity (adaptive) (18) Topics - 3 rd Line of Defense - B cells - T cells - Specific Immunities 1 3 rd Line = Prophylaxis via Immunization! (a) A painting of Edward Jenner depicts a cow
Return tissue fluid to the bloodstream (fluid balance) Immunity. Transport fats from the digestive tract to the bloodstream
 Lymphatic System L Y M P H A T I C C O M P O N E N T S What is a Lymphatic System? The lymphatic system is a complex system of fluid drainage and transport, immune response, and disease resistance. Fluid
Lymphatic System L Y M P H A T I C C O M P O N E N T S What is a Lymphatic System? The lymphatic system is a complex system of fluid drainage and transport, immune response, and disease resistance. Fluid
Virology Introduction. Definitions. Introduction. Structure of virus. Virus transmission. Classification of virus. DNA Virus. RNA Virus. Treatment.
 DEVH Virology Introduction Definitions. Introduction. Structure of virus. Virus transmission. Classification of virus. DNA Virus. RNA Virus. Treatment. Definitions Virology: The science which study the
DEVH Virology Introduction Definitions. Introduction. Structure of virus. Virus transmission. Classification of virus. DNA Virus. RNA Virus. Treatment. Definitions Virology: The science which study the
The Lymphatic System and Body Defenses
 PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Lymphatic System and Body Defenses 12PART B Adaptive Defense System: Third Line of Defense Immune
PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Lymphatic System and Body Defenses 12PART B Adaptive Defense System: Third Line of Defense Immune
Common Features of Herpesviruses
 Common Features of Herpesviruses Morphology Basic mode of replication Primary infection followed by latency Ubiquitous Ability to cause recurrent infections (reactivation of latent virus), reinfections
Common Features of Herpesviruses Morphology Basic mode of replication Primary infection followed by latency Ubiquitous Ability to cause recurrent infections (reactivation of latent virus), reinfections
Alphaherpesvirinae. Simplexvirus (HHV1&2/ HSV1&2) Varicellovirus (HHV3/VZV)
 Alphaherpesvirinae Simplexvirus (HHV1&2/ HSV1&2) Varicellovirus (HHV3/VZV) HERPES SIMPLEX VIRUS First human herpesvirus discovered (1922) Two serotypes recognised HSV-1 & HSV-2 (1962) HSV polymorphism
Alphaherpesvirinae Simplexvirus (HHV1&2/ HSV1&2) Varicellovirus (HHV3/VZV) HERPES SIMPLEX VIRUS First human herpesvirus discovered (1922) Two serotypes recognised HSV-1 & HSV-2 (1962) HSV polymorphism
Human Herpesviruses. Varicella-zoster virus. Human Herpesvirus (VZV) phospholipid envelope, tegument, icosahedral capsid, DNA core
 Common Features of Herpesviruses Morphology Basic mode of replication Primary infection followed by latency Ubiquitous Human Herpesvirus (VZV) phospholipid envelope, tegument, icosahedral capsid, DNA core
Common Features of Herpesviruses Morphology Basic mode of replication Primary infection followed by latency Ubiquitous Human Herpesvirus (VZV) phospholipid envelope, tegument, icosahedral capsid, DNA core
Transplantation. Immunology Unit College of Medicine King Saud University
 Transplantation Immunology Unit College of Medicine King Saud University Objectives To understand the diversity among human leukocyte antigens (HLA) or major histocompatibility complex (MHC) To know the
Transplantation Immunology Unit College of Medicine King Saud University Objectives To understand the diversity among human leukocyte antigens (HLA) or major histocompatibility complex (MHC) To know the
VIRUSES AND CANCER Michael Lea
 VIRUSES AND CANCER 2010 Michael Lea VIRAL ONCOLOGY - LECTURE OUTLINE 1. Historical Review 2. Viruses Associated with Cancer 3. RNA Tumor Viruses 4. DNA Tumor Viruses HISTORICAL REVIEW Historical Review
VIRUSES AND CANCER 2010 Michael Lea VIRAL ONCOLOGY - LECTURE OUTLINE 1. Historical Review 2. Viruses Associated with Cancer 3. RNA Tumor Viruses 4. DNA Tumor Viruses HISTORICAL REVIEW Historical Review
Chronic Hepatitis C. Risk Factors
 Chronic Hepatitis C The hepatitis C virus is one of the most important causes of chronic liver disease in the United States. Almost 4 million Americans or 1.8 percent of the U.S. population have an antibody
Chronic Hepatitis C The hepatitis C virus is one of the most important causes of chronic liver disease in the United States. Almost 4 million Americans or 1.8 percent of the U.S. population have an antibody
Hepatitis and Herpes Viruses. These two virus groups are very diverse, but cause much human morbidity and mortality
 Hepatitis and Herpes Viruses These two virus groups are very diverse, but cause much human morbidity and mortality Liver Functions Performs 3 major functions: Regulation: of blood composition glucose levels,
Hepatitis and Herpes Viruses These two virus groups are very diverse, but cause much human morbidity and mortality Liver Functions Performs 3 major functions: Regulation: of blood composition glucose levels,
virology MCQs 2- A virus commonly transmitted by use of contaminated surgical tools & needles produces a disease called serum hepatitis.
 virology MCQs 1- A virus which causes AIDS is: a- Small pox virus. b- Coxsackie B virus. c- Mumps virus. d- Rubella virus. e- HIV-III virus. 2- A virus commonly transmitted by use of contaminated surgical
virology MCQs 1- A virus which causes AIDS is: a- Small pox virus. b- Coxsackie B virus. c- Mumps virus. d- Rubella virus. e- HIV-III virus. 2- A virus commonly transmitted by use of contaminated surgical
Lymphoma: What You Need to Know. Richard van der Jagt MD, FRCPC
 Lymphoma: What You Need to Know Richard van der Jagt MD, FRCPC Overview Concepts, classification, biology Epidemiology Clinical presentation Diagnosis Staging Three important types of lymphoma Conceptualizing
Lymphoma: What You Need to Know Richard van der Jagt MD, FRCPC Overview Concepts, classification, biology Epidemiology Clinical presentation Diagnosis Staging Three important types of lymphoma Conceptualizing
10/31/2017. Immunodeficiencies. Outline. Discuss EBV. Non-destructive Polymorphic Monomorphic Therapies Challenges
 I have no financial disclosures Joo Y. Song, MD Assistant Professor of Clinical Pathology City of Hope National Medical Center Immunodeficiencies Outline Transplant Congenital Autoimmunity T-cell/immune
I have no financial disclosures Joo Y. Song, MD Assistant Professor of Clinical Pathology City of Hope National Medical Center Immunodeficiencies Outline Transplant Congenital Autoimmunity T-cell/immune
11/2/2017. Immunodeficiencies. Joo Y. Song, MD Assistant Professor of Clinical Pathology. I have no financial disclosures.
 I have no financial disclosures Joo Y. Song, MD Assistant Professor of Clinical Pathology City of Hope National Medical Center Immunodeficiencies Transplant Autoimmunity Drugs T-cell dysfunction (Age,
I have no financial disclosures Joo Y. Song, MD Assistant Professor of Clinical Pathology City of Hope National Medical Center Immunodeficiencies Transplant Autoimmunity Drugs T-cell dysfunction (Age,
Viruses. CLS 212: Medical Microbiology Miss Zeina Alkudmani
 Viruses CLS 212: Medical Microbiology Miss Zeina Alkudmani History Through the 1800s, many scientists discovered that something smaller than bacteria could cause disease and they called it virion (Latin
Viruses CLS 212: Medical Microbiology Miss Zeina Alkudmani History Through the 1800s, many scientists discovered that something smaller than bacteria could cause disease and they called it virion (Latin
Immunological Aspects of Parasitic Diseases in Immunocompromised Individuals. Taniawati Supali. Department of Parasitology
 Immunological Aspects of Parasitic Diseases in Immunocompromised Individuals Taniawati Supali Department of Parasitology 1 Defense mechanism in human Th17 (? ) Acute Chronic Th1 Th 2 Intracellular Treg
Immunological Aspects of Parasitic Diseases in Immunocompromised Individuals Taniawati Supali Department of Parasitology 1 Defense mechanism in human Th17 (? ) Acute Chronic Th1 Th 2 Intracellular Treg
See external label 2 C-8 C Σ=96 tests Cat # EBV-VCA IgA. Cat # EBV -VCA IgA ELISA. ELISA: Enzyme Linked Immunosorbent Assay
 DIAGNOSTIC AUTOMATION, INC. 23961 Craftsman Road, Suite D/E/F, Calabasas, CA 91302 Tel: (818) 591-3030 Fax: (818) 591-8383 onestep@rapidtest.com technicalsupport@rapidtest.com www.rapidtest.com See external
DIAGNOSTIC AUTOMATION, INC. 23961 Craftsman Road, Suite D/E/F, Calabasas, CA 91302 Tel: (818) 591-3030 Fax: (818) 591-8383 onestep@rapidtest.com technicalsupport@rapidtest.com www.rapidtest.com See external
Physiology Unit 3. ADAPTIVE IMMUNITY The Specific Immune Response
 Physiology Unit 3 ADAPTIVE IMMUNITY The Specific Immune Response In Physiology Today The Adaptive Arm of the Immune System Specific Immune Response Internal defense against a specific pathogen Acquired
Physiology Unit 3 ADAPTIVE IMMUNITY The Specific Immune Response In Physiology Today The Adaptive Arm of the Immune System Specific Immune Response Internal defense against a specific pathogen Acquired
Viral hepatitis. Supervised by: Dr.Gaith. presented by: Shaima a & Anas & Ala a
 Viral hepatitis Supervised by: Dr.Gaith presented by: Shaima a & Anas & Ala a Etiology Common: Hepatitis A Hepatitis B Hepatitis C Hepatitis D Hepatitis E Less common: Cytomegalovirus EBV Rare: Herpes
Viral hepatitis Supervised by: Dr.Gaith presented by: Shaima a & Anas & Ala a Etiology Common: Hepatitis A Hepatitis B Hepatitis C Hepatitis D Hepatitis E Less common: Cytomegalovirus EBV Rare: Herpes
PUO in the Immunocompromised Host: CMV and beyond
 PUO in the Immunocompromised Host: CMV and beyond PUO in the immunocompromised host: role of viral infections Nature of host defect T cell defects Underlying disease Treatment Nature of clinical presentation
PUO in the Immunocompromised Host: CMV and beyond PUO in the immunocompromised host: role of viral infections Nature of host defect T cell defects Underlying disease Treatment Nature of clinical presentation
Principles of Adaptive Immunity
 Principles of Adaptive Immunity Chapter 3 Parham Hans de Haard 17 th of May 2010 Agenda Recognition molecules of adaptive immune system Features adaptive immune system Immunoglobulins and T-cell receptors
Principles of Adaptive Immunity Chapter 3 Parham Hans de Haard 17 th of May 2010 Agenda Recognition molecules of adaptive immune system Features adaptive immune system Immunoglobulins and T-cell receptors
HBV : Structure. HBx protein Transcription activator
 Hepatitis B Virus 1 Hepatitis B Virus 2 Properties of HBV a member of the hepadnavirus group Enveloped, partially double-stranded DNA viruses, smallest DNA virus Replication involves a reverse transcriptase
Hepatitis B Virus 1 Hepatitis B Virus 2 Properties of HBV a member of the hepadnavirus group Enveloped, partially double-stranded DNA viruses, smallest DNA virus Replication involves a reverse transcriptase
Nephrology Grand Rounds
 Nephrology Grand Rounds PTLD in Kidney Transplantation Charles Le University of Colorado 6/15/12 Objectives Background Pathogenesis Epidemiology and Clinical Manifestation Incidence Risk Factors CNS Lymphoma
Nephrology Grand Rounds PTLD in Kidney Transplantation Charles Le University of Colorado 6/15/12 Objectives Background Pathogenesis Epidemiology and Clinical Manifestation Incidence Risk Factors CNS Lymphoma
4100: Cellular Therapy Essential Data Follow-Up Form
 4100: Cellular Therapy Essential Data Follow-Up Form Registry Use Only Sequence Number: Date Received: Key Fields CIBMTR Center Number: Event date: Visit: 100 day 6 months 1 year 2 years >2 years, Specify:
4100: Cellular Therapy Essential Data Follow-Up Form Registry Use Only Sequence Number: Date Received: Key Fields CIBMTR Center Number: Event date: Visit: 100 day 6 months 1 year 2 years >2 years, Specify:
Barry Slobedman. University of Sydney. Viruses in May 11 th May, 2013
 Barry Slobedman University of Sydney Viruses in May 11 th May, 2013 Outline Human cytomegalovirus (CMV) impact on the community Three phases of infection Focus on the dormant (latent) phase of infection
Barry Slobedman University of Sydney Viruses in May 11 th May, 2013 Outline Human cytomegalovirus (CMV) impact on the community Three phases of infection Focus on the dormant (latent) phase of infection
+ Intermittent shedding in urine, + Urinary tract
 Table 16.3 Examples of s in humans Microorganism Site of persistence Infectiousness of microorganism Viruses Consequence Herpes simplex Dorsal root ganglia Activation, cold sore + Salivary glands + Not
Table 16.3 Examples of s in humans Microorganism Site of persistence Infectiousness of microorganism Viruses Consequence Herpes simplex Dorsal root ganglia Activation, cold sore + Salivary glands + Not
Is it CVID? Not Necessarily HAIG TCHEUREKDJIAN, MD
 Is it CVID? Not Necessarily HAIG TCHEUREKDJIAN, MD Current Paradigm of Pathogenesis Genetic defect(s) Molecular defect(s) Cellular defect(s) Clinical disease Current Paradigm of Pathogenesis Genetic defect(s)
Is it CVID? Not Necessarily HAIG TCHEUREKDJIAN, MD Current Paradigm of Pathogenesis Genetic defect(s) Molecular defect(s) Cellular defect(s) Clinical disease Current Paradigm of Pathogenesis Genetic defect(s)
Concern for recurrence Stable virus especially in freeze dried form High infectivity in humans Vaccine supplies are limited No specific antiviral
 poxviruses Poxviruses Infect humans, birds, mammals, and insects. DsDNA brick shaped, enveloped multiply in the cytoplasm, 100x200x300 nm. lack normal capsid instead, layers of lipoprotiens and fibrils
poxviruses Poxviruses Infect humans, birds, mammals, and insects. DsDNA brick shaped, enveloped multiply in the cytoplasm, 100x200x300 nm. lack normal capsid instead, layers of lipoprotiens and fibrils
HIV 101: Overview of the Physiologic Impact of HIV and Its Diagnosis Part 2: Immunologic Impact of HIV and its Effects on the Body
 HIV 101: Overview of the Physiologic Impact of HIV and Its Diagnosis Part 2: Immunologic Impact of HIV and its Effects on the Body Melissa Badowski, PharmD, BCPS, AAHIVP Clinical Assistant Professor University
HIV 101: Overview of the Physiologic Impact of HIV and Its Diagnosis Part 2: Immunologic Impact of HIV and its Effects on the Body Melissa Badowski, PharmD, BCPS, AAHIVP Clinical Assistant Professor University
Bihong Zhao, M.D, Ph.D Department of Pathology
 Bihong Zhao, M.D, Ph.D Department of Pathology 04-28-2009 Is tumor self or non-self? How are tumor antigens generated? What are they? How does immune system respond? Introduction Tumor Antigens/Categories
Bihong Zhao, M.D, Ph.D Department of Pathology 04-28-2009 Is tumor self or non-self? How are tumor antigens generated? What are they? How does immune system respond? Introduction Tumor Antigens/Categories
The pathogenesis of nervous distemper
 Veterinary Sciences Tomorrow - 2004 The pathogenesis of nervous distemper Marc Vandevelde Canine distemper is a highly contagious viral disease of dogs and of all animals in the Canidae, Mustellidae and
Veterinary Sciences Tomorrow - 2004 The pathogenesis of nervous distemper Marc Vandevelde Canine distemper is a highly contagious viral disease of dogs and of all animals in the Canidae, Mustellidae and
