Cases. A Case of Primary Syphilis: Emergency Department Evaluation and Management
|
|
|
- Ronald Watkins
- 6 years ago
- Views:
Transcription
1 Cases O F N O T E Advanced Emergency Nursing Journal Vol. 30, No. 4, pp Copyright c 2008 Wolters Kluwer Health Lippincott Williams & Wilkins Column Editor: Elda G. Ramirez, PhD, RN, FNP-BC, FAANP A Case of Primary Syphilis: Emergency Department Evaluation and Management Courtney Elizabeth Reinisch, DNP; Janice L. Smolowitz, EdD, DNP, APN Abstract Syphilis is a systemic disease caused by Treponema pallidum spirochete. The majority of young, sexually active patients who have genital ulcers also have genital herpes, syphilis, or chanroid. Syphilis is therefore known as the great imitator because many of the characteristics of syphilis are indistinguishable from those of other sexually transmitted infections. Patients who contract syphilis may seek treatment of related complaints on the basis of varying stages of infection. It is important for the advance practice nurse to screen, diagnose, and appropriately treat all patients at risk for syphilis and other sexually transmitted infections. This article presents an interesting case of a 21-year-old man with a genital lesion who presented to the emergency department. The role of the emergency department advance practice nurse in the treatment and management of patients with syphilis is outlined herein. Key words: chancre, genital ulcer, primary syphilis, sexual transmitted infection (STI), sexually transmitted disease (STD) EPIDEMIOLOGY In the United States, the majority of young, sexually active patients who have genital ulcers have genital herpes, syphilis, or chanroid. The frequency of each condition differs by geographic area and patient population; however, genital herpes is the most prevalent of these diseases. More than one of these diseases can be present in a patient who has genital ulcers. All three of these diseases have From the School of Nursing, Columbia University, New York. Corresponding author: Courtney Elizabeth Reinisch, DNP, School of Nursing, Columbia University, New York, NY ( cer2117@columbia.edu). been associated with an increased risk for HIV infection. The overall increase in rates of syphilis among adults and adolescents from 2004 to 2005 was driven primarily by increases among men having sex with men (MSM), with the rate increasing 8.5% (from 4.7 in 2004 to 5.1 per 100,000 populations in 2005). Trends were also seen among women, as the rate of reported cases increased for the first time in more than 10 years. Primary and secondary syphilis rates increased among African Americans for the second year in 2005 after a decade of decline (Centers for Disease Control and Prevention [CDC], Workowski, & Berman, 2006). Among 18- to 49-year-olds in the United States, the prevalence of syphilis 310
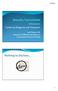
2 October December 2008 Vol. 30, No. 4 Primary Syphilis in the Emergency Department 311 seroreactivity was 0.71% with Blacks having the highest rate of seroprevalence at 4.3%, followed by Mexican Americans 0.98% and Whites 0.07%. Syphilis seroprevalence was higher among those who had first sex before the age of 15 years and among those persons who reported greater than five lifetime sex partners (Gottlieb et al., 2008). PATHOPHYSIOLOGY Syphilis is a systemic disease caused by Treponema pallidum spirochete. Treponema pallidum readily crosses intact mucosa (Fig 1). The route of transmission of syphilis is by sexual contact, although there are cases of congenital syphilis via transmission in utero (CDC, Workowski, & Berman, 2006). The incubation period from contact to infection for syphilis ranges from 9 to 90 days, usually about 21 days. The infection devel- ops at site of contact. Typically the initial presentation is a single, painless, clean-based, indurated ulcer with firm raised borders. See Table 1 for a description of the different stages of syphilis. THE CASE A 21-year-old African American man with a chief complaint of recheck of a rash presented to a suburban community hospital emergency department (ED). The patient stated that he was diagnosed and treated for scabies 5 days earlier at a health center. He reported that he applied permethrin lotion and left it on overnight before washing it off. According to the patient, my rash and itching improved. Three days ago he noticed a painless pimple on his penis. He was sexually active with only women and used protection (e.g., condoms) all the time. The patient denied having a serious girlfriend or being in a committed relationship. The patient also stated that it had been a long time since he had intercourse without wearing a condom although he was unable to specify how long it had been. Review of Systems The patient denied fever, fatigue, recent weight loss, weakness, headache, seizures, gait abnormities, paralysis, heat or cold intolerance, excessive sweating, or excessive thirst or hunger. He stated that he had noticed swollen lymph nodes in the groin. The patient denied any urinary frequency, urgency, hesitancy, hematuria, or penile discharge. Figure 1. Chancre of primary syphilis. From Greenberg s Text-Atlas of Emergency Medicine, by M. I. Greenberg, R. G. Hendrickson, M. Silverberg, C. J. Capbell, A. P. Morocco, C. A. Salvaggio, et al., 2005, Philadelphia, PA: Lippincott Williams & Wilkins, p Reprinted with permission of Sweet and Gibbs. Medical History The patient s medical history was significant for scabies and varicella as a child. Pasthospitalizations and surgeries. None Allergies. No known allergies to food or medications Immunizations. Tetanus immunization was 7yearsago Current medications. None
3 312 Advanced Emergency Nursing Journal Table 1. Signs and symptoms of syphilis infection Syphilis infection Primary infection Secondary infection Tertiary infection Signs and symptoms Ulcer or chancre at the infection site Single ulcerated lesion with a surrounding red areola. The edge and base have a cartilaginous consistency on palpation. 70% of men present with lesion on penis or scrotum 50% of women present with lesion on the vulva, cervix, or perineum Extra genital chancres occur most commonly above the neck, usually involving the lips or oral cavity Regional lymph nodes are firm, discrete, and nontender Abrading the chancre releases highly infectious clear exudate containing numerous Treponema pallidum organisms Manifestations that include, but are not limited to, skin rash, mucocutaneous lesions, and lymphadenopathy Patchy alopecia Cardiac or ophthalmic manifestations, auditory abnormalities, or gummatous lesions Note. Adapted from Sexually Transmitted Diseases Treatment Guidelines, by K. A. Workowski and S. M. Berman, 2006, Morbidity and Mortality Weekly Report. Social History The patient was a full-time college student. He lived in an apartment with three male roommates. The patient denied alcohol abuse; he stated, I drink alcohol socially on weekends at college, approximately six to twelve beers per week. He denied any recreational drug use. The patient stated he was a smoker approximately one half pack of cigarettes daily for the last 4 years (two pack years). Family History The family history was significant for hypertension, diabetes, cardiovascular disease, renal disease, and stroke. There was no history of seizure disorder or cancer. Physical Examination The physical examination revealed that a 21- year-old African American man appeared to be his stated age. He was in no acute distress. His affect and mood were anxious. Vital signs were blood pressure 138/72 mmhg, pulse rate 92/min, respirations 20/min, temperature 97.9 F by mouth, pain 0, and oxygen saturation 99% on room air. Pertinent positive physical findings were a painless 1-cm reddened, raised lesion to the glans of the penis without bleeding or drainage, testicles without masses, and no penile discharge noted (see Fig 1). Lymphatic examination revealed three enlarged, nontender inguinal nodes bilaterally ranging in size from 0.5 to 1.5 cm. Neurologic examination revealed the patient to be alert and oriented to person, place, and time. Cranial nerves II XII were without abnormality. Motor function for upper and lower extremities was equal bilaterally, strength was 5/5 bilaterally, and deep tendon reflexes were +2 bilaterally. DIFFERENTIAL DIAGNOSIS The history, physical examination, and risk factors made primary syphilis the most likely diagnosis for this patient. Consideration was given to chancroid and herpes simplex virus; however, in the absence of pain, herpes simplex virus was less likely. Table 2 lists the differential diagnoses considered for patients who present with genital lesions.
4 October December 2008 Vol. 30, No. 4 Primary Syphilis in the Emergency Department 313 Table 2. Differential diagnosis for syphilis Amyloidosis Lichen Chancroid Condyloma acuminata Herpes simplex Leprosy Lymphogranuloma venereum Genital warts Rubella Acute febrile exanthem Infectious mononucleosis Drug eruptions Erythema multiforme Pityriasis rosea Pityriasis rubra pilaris Psoriasis Sarcoidosis Scabies Stevens-Johnson syndrome Tinea corporis Lichen planus Oral thrush Note. Adapted from Sexually Transmitted Diseases Treatment Guidelines, by K. A. Workowski and S. M. Berman, 2006, Morbidity and Mortality Weekly Report. LABS A diagnosis based only on the patient s medical history and physical examination frequently is inaccurate. Therefore, all patients who have genital ulcers should be examined with a serologic test for syphilis and a diagnostic evaluation for genital herpes. In settings where chancroid is prevalent, a test for Haemophilus ducreyi should also be performed. Dark field examinations and direct fluorescent antibody tests of lesion exudates or tissue are the definitive methods for diagnosing early syphilis. A presumptive diagnosis is possible with the use of two types of serologic tests: (1) nontreponemal tests (e.g., Venereal Disease Research Laboratory and rapid plasma reagin) and (2) treponemal tests (e.g., fluorescent treponemal antibody absorption and T. pallidum particle agglutination). The use of only one type of serologic test is insufficient for diagnosis because false-positive nontreponemal test results are sometimes associated with various medical conditions Table 3. Diagnostic tests recommended for evaluation of genital ulcers Syphilis Herpes Chancroid Specific tests for evaluation of genital ulcers Serology and either darkfield examination or direct immunofluorescence test for Treponema pallidum Culture or antigen test for herpes simplex virus Culture for Haemophilus ducreyi Note. Adapted from Sexually Transmitted Diseases Treatment Guidelines, 2006, by Centers for Disease Control and Prevention, K. A. Workowski, and S. M. Berman, 2006, Morbidity and Mortality Weekly Report Recommendations and Reports, 55(RR-11), pp unrelated to syphilis (CDC, Workowski, & Berman, 2006). Table 3 identifies needed evaluation for genital ulcers and Table 4 discusses diagnostics specific to syphilis. A rapid plasma reagin was drawn for serologic evaluation for syphilis. Although the patient lacked dysuria and signs of urethritis, screening for chlamydia, gonorrhea, and human immunodeficiency virus (HIV) infection were indicated. Gonorrhea and chlamydia cultures were obtained. HIV testing was not performed in the ED because the patient was uninsured, posttest counseling was not available in this setting, and referral to the sexual transmitted infection (STI) clinic provided a comprehensive follow-up. Treatment Patients who have syphilis may seek treatment of signs or symptoms of related complaints on the basis of varying stages of infection. This patient presented 3 days after symptoms began. The patient was treated empirically, with penicillin G benzathine (Bicillin L-A) (2.4 units im), the treatment of choice for syphilis.
5 314 Advanced Emergency Nursing Journal Table 4. Diagnostic evaluation for syphilis Primary and secondary infection In suspected acquired syphilis, perform nontreponemal serology screening using VDRL, RPR, or the recently developed ICE syphilis recombinant antigen test Dark-field microscopy is essential in evaluating moist cutaneous lesions Direct immunofluorescence staining of fixed smears (direct fluorescent antibody Treponema pallidum) is an option Both procedures detect the causative organism at a rate of approximately 85% 92% Test sera yielding a positive or equivocal reaction by the fluorescent treponemal antibody-absorption, quantitative VDRL/RPR, and microhemagglutination assay Treponema pallidum tests Primary syphilis: Skin lesions reveal perivascular infiltration, chiefly by lymphocytes, plasma cells, and macrophages, with capillary endothelial proliferation and subsequent obliteration of small blood vessels Tertiary infection Biopsy may be necessary to differentiate gummas from coincidental granulomatous conditions Lumbar puncture for cerebrospinal fluid examination is indicated with neurologic signs or symptoms, treatment failure or plans to administer treatment other than penicillin, a serum reagin titer of greater than or equal to 1:32, seropositive HIV, and other changes indicative of active syphilis (e.g., gumma, aortitis) The only means by which the occurrence of asymptomatic neurosyphilis in latent syphilis can be excluded is via cerebrospinal fluid examination Note: VDRL = Venereal Disease Research Laboratory; RPR = rapid plasma reagin. Adapted from Sexually Transmitted Diseases Treatment Guidelines, 2006, by Centers for Disease Control and Prevention, K. A. Workowski, and S. M. Berman, 2006, Morbidity and Mortality Weekly Report Recommendations and Reports, 55(RR-11), pp Penicillin G, administered parenterally, is the preferred drug for treatment of all stages of syphilis. The preparation(s) used (i.e., benzathine, aqueous procaine, or aqueous crystalline), the dosage, and the length of treatment depend on the stage and clinical manifestations of the disease. However, neither combinations of benzathine penicillin and procaine penicillin nor oral penicillin preparations are considered appropriate for the treatment of syphilis (CDC, Workowski, & Berman, 2006). No proven alternatives to penicillin are available for treating neurosyphilis, congenital syphilis, or syphilis in pregnant women. Penicillin is also recommended for use, whenever possible, in HIV-infected patients (CDC, Workowski, & Berman, 2006). Of the adult U.S. population, 3% 10% have experienced urticaria, angioedema, or anaphylaxis (i.e., upper airway obstruction, bronchospasm, or hypotension) after penicillin therapy. Readministration of penicillin to these patients can cause severe, immediate reactions. Because anaphylactic reactions to penicillin can be fatal, every effort should be made to avoid administering penicillin to penicillin-allergic patients, unless they undergo acute desensitization to eliminate anaphylactic sensitivity (CDC, Workowski, & Berman, 2006). An estimated 10% of persons who report a history of severe allergic reactions to penicillin remain allergic. There are limited research data to support the use of alternatives to penicillin in early syphilis. Nonpregnant individuals with definite penicillin allergy and primary or secondary syphilis can be effectively treated with an alternative regimen of doxycycline, in a dosage of 100 mg
6 October December 2008 Vol. 30, No. 4 Primary Syphilis in the Emergency Department 315 orally twice daily for 14 days or tetracycline HCl 500 mg orally 6 hourly for 14 days. Doxycycline is generally better tolerated than an equivalent tetracycline regimen, which may enhance treatment compliance. Erythromycin, in a dosage of 500 mg orally four times daily for 2 weeks, is a second alternative, although it is not as effective as doxycycline. Evidence for the effectiveness of ceftriaxone (Rocephin) is limited but a regimen of 1 g daily, given intramuscularly or intravenously for 8 10 days, may maintain adequate treponemacidal levels. Azithromycin 2 g as a single oral dose may be effective. Careful monitoring of the serologic response is necessary to ensure eradication of the organism whenever an alternative regimen is used (Workowski & Berman, 2006). COUNSELING The patient was counseled regarding the diagnosis of syphilis, risks for STI, prevention, and need for HIV testing. The patient was also advised that he is at highest risk for this condition on the basis of his age, race, sexual practices, college student status, and high-risk behavior that included heavy alcohol use on weekends. The patient was referred to the local sexually transmitted disease (STD) clinic for follow-up within 72 hr where he would receive results of ED diagnostics, further treatment if needed, HIV counseling and testing, and partner management using a sliding fee scale. PREVENTION OF STIs Primary prevention of STIs begins with changing the sexual behaviors that place persons at risk for infection. Healthcare providers have a unique opportunity to provide education and counseling to their patients. As part of the clinical interview, healthcare providers should routinely obtain sexual histories from their patients and address risk reduction (CDC, Workowski, & Berman, 2006). Counseling skills, characterized by respect, Table 5. Key techniques to facilitate rapport with patients Open-ended questions Key techniques to facilitate rapport with patients Understandable language Normalizing language Tell me about any new sex partners you ve had since your last visit. What s your experience with using condoms been like? Have you ever had a sore or scab on your penis? Some of my patients have difficulty using a condom with every sex act. How is it for you? Note. Adapted from Sexually Transmitted Diseases Treatment Guidelines, 2006, by Centers for Disease Control and Prevention, K. A. Workowski, and S. M. Berman, 2006, Morbidity and Mortality Weekly Report Recommendations and Reports, 55(RR-11), pp compassion, and a nonjudgmental attitude toward all patients, are essential to obtaining a thorough sexual history and to delivering prevention messages effectively, outlined in Table 5. The Five Ps Open communication with patients is necessary when gathering information and educating to prevent the spread of STIs. The CDC, Workowski, and Berman (2006) identify the five key areas of interest as the Five Ps partners, prevention of pregnancy, protection from STDs, practices, and past history of STD. Eliciting information concerning five key areas of interest is outlined in Table 6. Abstinence The most reliable way to avoid transmission of STDs is to abstain from sex (i.e., oral, vaginal, or anal sex) or to be in a long-term, mutually monogamous relationship with an
7 316 Advanced Emergency Nursing Journal Table 6. The five Ps: Patient interview questions The five Ps: Partners, prevention of pregnancy, protection from STDs, practices, past history of STDs Partners Prevention of pregnancy Protection from STDs Practices Past history of STDs Do you have sex with men, women, or both? In the past 2 months, how many partners have you had sex with? In the past 12 months, how many partners have you had sex with? Are you or your partner trying to get pregnant? If no, What are you doing to prevent pregnancy? What do you do to protect yourself from STDs and HIV? To understand your risks for STDs, I need to understand the kind of sex you have had recently. Have you had vaginal sex, meaning penis in vagina sex? If yes, Do you use condoms: never, sometimes, or always? Have you had anal sex, meaning penis in rectum/anus sex? If yes, Do you use condoms: never, sometimes, or always? Have you had oral sex, meaning mouth on penis/vagina? For condom answers If never : Why don t you use condoms? If sometimes : In what situations or with whom, do you not use condoms? Have you ever had an STD? Note. STD = sexually transmitted disease. Adapted from Sexually Transmitted Diseases Treatment Guidelines, 2006, by Centers for Disease Control and Prevention, K. A. Workowski, and S. M. Berman, 2006, Morbidity and Mortality Weekly Report Recommendations and Reports, 55(RR-11), pp uninfected partner. Counseling that encourages abstinence from sexual intercourse is crucial for persons who are being treated for an STD (or whose partners are undergoing treatment) and for persons who want to avoid the possible consequences of sex completely (e.g., STD/HIV and unintended pregnancy; CDC, Workowski, & Berman, 2006). Because the incidence of syphilis has increased in HIV-infected persons, the use of client-centered STD counseling for HIVinfected persons has received strong emphasis from public health agencies. All patients who have syphilis should be tested for HIV infection, and in geographic areas where the prevalence of HIV is high, patients who have primary syphilis should be retested for HIV after 3 months if the first HIV test result was negative (CDC, Workowski, & Berman, 2006). More than 60% of new syphilis infections are estimated to occur in MSM (Gottlieb et al., 2008). Condom Education Patients should be advised that condoms must be used consistently and correctly to be effective in preventing STIs. The recommendations in Table 7 ensure the proper use of male condoms. Patient Follow-up Treatment failure can occur with any regimen. Assessing response to treatment frequently is difficult, and definitive criteria for cure or failure have not been established. Nontreponemal test titers might decline more slowly for persons who previously had syphilis. Patients should be reexamined clinically and serologically 6 and 12 months after treatment; more frequent evaluation might be prudent if follow-up is uncertain (CDC, Workowski, & Berman, 2006). Patients who have persistent signs or recurrent symptoms or who have a sustained
8 October December 2008 Vol. 30, No. 4 Primary Syphilis in the Emergency Department 317 Table 7. Patient education: Condom use Use a new condom with each sex act (e.g., oral, vaginal, and anal) Carefully handle the condom to avoid damaging it with fingernails, teeth, or other sharp objects Put the condom on after the penis is erect and before any genital, oral, or anal contact with the partner Use only water-based lubricants (e.g., K-Y Jelly, Astroglide, AquaLube, and glycerin) with latex condoms. Oil-based lubricants (e.g., petroleum jelly, shortening, mineral oil, massage oils, body lotions, and cooking oil) can weaken latex Ensure adequate lubrication during vaginal and anal sex, which might require the use of exogenous water-based lubricants To prevent the condom from slipping off, hold the condom firmly against the base of the penis during withdrawal and withdraw while the penis is still erect Note. Adapted from Sexually Transmitted Diseases Treatment Guidelines, 2006, by Centers for Disease Control and Prevention, K. A. Workowski, and S. M. Berman, 2006, Morbidity and Mortality Weekly Report Recommendations and Reports, 55(RR-11), pp fourfold increase in nontreponemal test titer have probably failed treatment or were reinfected. These patients should be retreated and reevaluated for HIV infection. Treatment failure usually cannot be reliably distinguished from reinfection with T. pallidum; therefore, a cerebrospinal fluid analysis should also be performed (CDC, Workowski, & Berman, 2006). Partner Management Partner notification is the process by which healthcare providers or public health authorities can seek information and help arrange for evaluation and treatment of sex partners, either directly or with assistance from state and local health departments. The intensity of partner services and the specific STIs for which they are offered vary among providers, agencies, and geographic areas. These services should be accompanied by health counseling and might include referral of patients and their partners for other services (CDC, Workowski, & Berman, 2006). Public Health Implications Sexual contact without barrier protection is the second highest cause of the global burden of disease. Twelve million people per year acquire syphilis, primarily in Africa, where congenital syphilis is a major cause of still birth (Peterman & Furness, 2007). Because syphilis is on the rise in particular groups, public health efforts need to continue. Prevention efforts include information campaigns aimed at MSM of the risk of syphilis (Peterman & Furness, 2007). An urgent need exists to amplify effective use of evidence-based measures to diminish this burden of disease, including barrier methods that protect against both STI and pregnancy (male and female condoms). The limited effect of public health campaigns to promote effective use of these barrier methods might be attributable to scare tactics that emphasize adverse consequences of sexual acts without protection. Promotion of pleasure in use of male and female condoms can facilitate consistent use of condoms and boost their effectiveness to protect against STI and pregnancy (Philpott, Knerr, & Maher, 2006). Therefore, the effect of public-health initiatives that emphasize positive outcomes of use of male and female condoms as barrier methods, and positive results of practicing other forms of safer sex, need to be investigated (Philpott, Knerr, & Maher, 2006). Such work includes the potential for safer sex to contribute to good health and hygiene in general, to reduce anxiety about risk of STI and pregnancy, and make sex more pleasurable (Philpott, Knerr, & Maher, 2006). FUTURE RECOMMENDATIONS AND CONCLUSION This patient was treated and discharged from the ED uneventfully. He was counseled and
9 318 Advanced Emergency Nursing Journal educated appropriately and verbalized understanding of the importance for STI evaluation at the local clinic. He planned to discuss his diagnosis with his sexual partner so that she could undergo evaluation and treatment. Patients who contract syphilis may seek treatment in the ED setting. Advance practice nurses need to be aware that syphilis is once again rising in prevalence and to be vigilant for individuals at increased risk for this infection, such as Blacks and MSM. Partners may also present in the ED and require screening, treatment, and counseling. Advance practice nurses need to be aware that treatment failure can occur and to be certain to retreat or refer patients appropriately. The advance practice nurse in the ED is in a position to identify, appropriately treat, educate, counsel, and refer these patients for continued care to avoid a further spread and rise in infection rates. REFERENCES Centers for Disease Control and Prevention, Workowski, K. A., & Berman, S. M. (2006). Sexually transmitted diseases treatment guidelines, [erratum appears in MMWR Recommendations and Reports, 15;55(36):997.] Morbidity and Mortality Weekly Report Recommendations and Reports, 55(RR-11), Gottlieb, S. L., Pope, V., Sternberg, M. R., McQuillan, G. M., Beltrami, J. F., Berman, S. M., et al. (2008). Prevalence of syphilis seroreactivity in the United States: Data from the National Health and Nutrition Examination Surveys (NHANES) Sexually Transmitted Diseases, 35(5), Greenberg, M. I., Hendrickson, R. G., Silverberg, M., Capbell, C. J., Morocco, A. P., Salvaggio, C. A., et al. (2005). Greenberg s text-atlas of emergency medicine. Philadelphia, PA: Lippincott Williams & Wilkins. Peterman, T. A., & Furness, B. W. (2007). The resurgence of syphilis among men who have sex with men. Current Opinion in Infectious Diseases, 20(1), Philpott, A., Knerr, W., & Maher, D. (2006). Promoting protection and pleasure: Amplifying the effectiveness of barriers against sexually transmitted infections and pregnancy. Lancet, 368(9551), Workowski, K. A., & Berman, S. M. (2006). Sexually transmitted diseases treatment guidelines. Morbidity and Mortality Weekly Report. Centers for Disease Control and Prevention. (Recommendations and reports ISSN No )
Syphilis Treatment Protocol
 STD, HIV, AND TB SECTION Syphilis Treatment Protocol CLINICAL GUIDANCE FOR PRIMARY AND SECONDARY SYPHILIS AND LATENT SYPHILIS www.lekarzol.com (4/2016) Page 1 of 8 Table of Contents Description... 3 Stages
STD, HIV, AND TB SECTION Syphilis Treatment Protocol CLINICAL GUIDANCE FOR PRIMARY AND SECONDARY SYPHILIS AND LATENT SYPHILIS www.lekarzol.com (4/2016) Page 1 of 8 Table of Contents Description... 3 Stages
Timby/Smith: Introductory Medical-Surgical Nursing, 9/e
 Timby/Smith: Introductory Medical-Surgical Nursing, 9/e Chapter 62: Caring for Clients With Sexually Transmitted Diseases Slide 1 Epidemiology Introduction Study of the occurrence, distribution, and causes
Timby/Smith: Introductory Medical-Surgical Nursing, 9/e Chapter 62: Caring for Clients With Sexually Transmitted Diseases Slide 1 Epidemiology Introduction Study of the occurrence, distribution, and causes
Management of Syphilis in Patients with HIV
 Management of Syphilis in Patients with HIV Adult Clinical Guideline from the New York State Department of Health AIDS Institute www.hivguidelines.org Purpose of the Guideline Increase the numbers of NYS
Management of Syphilis in Patients with HIV Adult Clinical Guideline from the New York State Department of Health AIDS Institute www.hivguidelines.org Purpose of the Guideline Increase the numbers of NYS
Sexually Transmitted Diseases Treatment Guidelines, 2015
 Morbidity and Mortality Weekly Report Recommendations and Reports / Vol. 64 / No. 3 June 5, 2015 Sexually Transmitted Diseases Treatment Guidelines, 2015 U.S. Department of Health and Human Services Centers
Morbidity and Mortality Weekly Report Recommendations and Reports / Vol. 64 / No. 3 June 5, 2015 Sexually Transmitted Diseases Treatment Guidelines, 2015 U.S. Department of Health and Human Services Centers
The Great Imitator Revealed: Syphilis
 The Great Imitator Revealed: Syphilis Jeffrey D. Klausner, MD, MPH Professor of Medicine and Public Health University of California Los Angeles David Geffen School of Medicine Los Angeles, California Learning
The Great Imitator Revealed: Syphilis Jeffrey D. Klausner, MD, MPH Professor of Medicine and Public Health University of California Los Angeles David Geffen School of Medicine Los Angeles, California Learning
9/9/2015. Began to see a shift in 2012 Early syphilis cases more than doubled from year before
 George Walton, MPH, CPH, MLS(ASCP) CM STD Program Manager Bureau of HIV, STD, and Hepatitis September 15, 2015 1 1) Discuss the changing epidemiology of syphilis in Iowa; 2) Explore key populations affected
George Walton, MPH, CPH, MLS(ASCP) CM STD Program Manager Bureau of HIV, STD, and Hepatitis September 15, 2015 1 1) Discuss the changing epidemiology of syphilis in Iowa; 2) Explore key populations affected
Syphilis Technical Instructions for Civil Surgeons
 National Center for Emerging and Zoonotic Infectious Diseases Syphilis Technical Instructions for Civil Surgeons Joanna J. Regan, MD, MPH, FAAP Medical Officer Medical Assessment and Policy Team Immigrant,
National Center for Emerging and Zoonotic Infectious Diseases Syphilis Technical Instructions for Civil Surgeons Joanna J. Regan, MD, MPH, FAAP Medical Officer Medical Assessment and Policy Team Immigrant,
WHAT DO U KNOW ABOUT STIS?
 WHAT DO U KNOW ABOUT STIS? Rattiya Techakajornkeart MD. Bangrak STIs Cluster, Bureau of AIDS, TB and STIs, Department of Disease Control, MOPH, Thailand SEXUALLY TRANSMITTED INFECTIONS? STIs Infections
WHAT DO U KNOW ABOUT STIS? Rattiya Techakajornkeart MD. Bangrak STIs Cluster, Bureau of AIDS, TB and STIs, Department of Disease Control, MOPH, Thailand SEXUALLY TRANSMITTED INFECTIONS? STIs Infections
Chapter 11. Sexually Transmitted Diseases
 Chapter 11. Sexually Transmitted Diseases General Guidelines Persons identified as having one sexually transmitted disease (STD) are at risk for others and should be screened as appropriate. Partners of
Chapter 11. Sexually Transmitted Diseases General Guidelines Persons identified as having one sexually transmitted disease (STD) are at risk for others and should be screened as appropriate. Partners of
Learning Objectives. Syphilis. Lessons. Epidemiology: Disease in the U.S. Syphilis Definition. Transmission. Treponema pallidum
 Learning Objectives Syphilis Treponema pallidum 1 Upon completion of this content, the learner will be able to 1. Describe the epidemiology of syphilis in the U.S. 2. Describe the pathogenesis of T. pallidum.
Learning Objectives Syphilis Treponema pallidum 1 Upon completion of this content, the learner will be able to 1. Describe the epidemiology of syphilis in the U.S. 2. Describe the pathogenesis of T. pallidum.
SYPHILIS (REPORTABLE)
 SYPHILIS (REPORTABLE) PREAMBLE In BC, the diagnosis of syphilis is determined by the BCCDC Provincial STI/HIV Clinic physician directly or in coordination with the*physician or nurse practitioner (NP)
SYPHILIS (REPORTABLE) PREAMBLE In BC, the diagnosis of syphilis is determined by the BCCDC Provincial STI/HIV Clinic physician directly or in coordination with the*physician or nurse practitioner (NP)
Chancroid Table of Contents
 Subsection: Chancroid Page 1 of 8 Chancroid Table of Contents Chancroid Fact Sheet Subsection: Chancroid Page 2 of 8 Chancroid (Haemophilus ducreyi) Overview (1,2) For a more complete description of chancroid,
Subsection: Chancroid Page 1 of 8 Chancroid Table of Contents Chancroid Fact Sheet Subsection: Chancroid Page 2 of 8 Chancroid (Haemophilus ducreyi) Overview (1,2) For a more complete description of chancroid,
Replaces: 04/13/17. / Formulated: 7/05 SYPHLIS
 Effective Date: 81017 Replaces: 041317 Page 1 of 7 POLICY: The Texas Department of Criminal Justice (TDCJ) will identify, test, and manage all offenders with suspected or confirmed syphilis with a uniform
Effective Date: 81017 Replaces: 041317 Page 1 of 7 POLICY: The Texas Department of Criminal Justice (TDCJ) will identify, test, and manage all offenders with suspected or confirmed syphilis with a uniform
SYPHILIS. The Great Pretender K. Amen Eguakun, MSN, APRN, AAHIVS
 SYPHILIS The Great Pretender K. Amen Eguakun, MSN, APRN, AAHIVS Learning Objectives At the end of this presentation, the participants will be able to 1. Describe the epidemiology of syphilis in the United
SYPHILIS The Great Pretender K. Amen Eguakun, MSN, APRN, AAHIVS Learning Objectives At the end of this presentation, the participants will be able to 1. Describe the epidemiology of syphilis in the United
Nothing to disclose.
 Update on Diagnosis and Treatment Lisa Winston, MD University of California, San Francisco/ Zuckerberg San Francisco General Nothing to disclose. 1 This talk will be a little depressing Rising incidence
Update on Diagnosis and Treatment Lisa Winston, MD University of California, San Francisco/ Zuckerberg San Francisco General Nothing to disclose. 1 This talk will be a little depressing Rising incidence
5/1/2017. Sexually Transmitted Diseases Burning Questions
 Sexually Transmitted Diseases Burning Questions Jeffrey D. Klausner, MD, MPH Professor of Medicine and Public Health University of California Los Angeles Los Angeles, California FORMATTED: 04-03-17 Financial
Sexually Transmitted Diseases Burning Questions Jeffrey D. Klausner, MD, MPH Professor of Medicine and Public Health University of California Los Angeles Los Angeles, California FORMATTED: 04-03-17 Financial
STDs and Hepatitis C
 STDs and Hepatitis C Catherine S. O Neal, MD Assistant Professor of Clinical Medicine, Infectious Diseases Louisiana State University Health Sciences Center March 3, 2018 Objectives Review patient risk
STDs and Hepatitis C Catherine S. O Neal, MD Assistant Professor of Clinical Medicine, Infectious Diseases Louisiana State University Health Sciences Center March 3, 2018 Objectives Review patient risk
SEXUALLY TRANSMITED DISEASES SYPHILIS ( LUES ) Dr D. Tenea Department of Dermatology University of Pretoria
 SEXUALLY TRANSMITED DISEASES SYPHILIS ( LUES ) Dr D. Tenea Department of Dermatology University of Pretoria INTRODUCTION Venereal disease = old term STD infections transmitted by sexual contact Sexually
SEXUALLY TRANSMITED DISEASES SYPHILIS ( LUES ) Dr D. Tenea Department of Dermatology University of Pretoria INTRODUCTION Venereal disease = old term STD infections transmitted by sexual contact Sexually
Sexually Transmitted Disease Treatment Tables
 Sexually Transmitted Disease Treatment Tables Federal Bureau of Prisons Clinical Practice Guidelines June 2011 Clinical guidelines are made available to the public for informational purposes only. The
Sexually Transmitted Disease Treatment Tables Federal Bureau of Prisons Clinical Practice Guidelines June 2011 Clinical guidelines are made available to the public for informational purposes only. The
STI s. (Sexually Transmitted Infections)
 STI s (Sexually Transmitted Infections) Build Awareness In Canada and around the world, the trend is clear: sexually transmitted infections (STIs) are on the rise. One of the primary defenses in the fight
STI s (Sexually Transmitted Infections) Build Awareness In Canada and around the world, the trend is clear: sexually transmitted infections (STIs) are on the rise. One of the primary defenses in the fight
Sexually Transmi/ed Diseases
 Sexually Transmi/ed Diseases Chapter Fourteen 2013 McGraw-Hill Higher Education. All rights reserved. Also known as sexually transmitted infections The Major STDs (STIs) HIV/AIDS Chlamydia Gonorrhea Human
Sexually Transmi/ed Diseases Chapter Fourteen 2013 McGraw-Hill Higher Education. All rights reserved. Also known as sexually transmitted infections The Major STDs (STIs) HIV/AIDS Chlamydia Gonorrhea Human
Quick Study: Sexually Transmitted Infections
 Quick Study: Sexually Transmitted Infections Gonorrhea What is it: A bacterial infection of the genitals, anus, or throat. How common: The CDC estimates 820,000 people in the United States get Gonorrhea
Quick Study: Sexually Transmitted Infections Gonorrhea What is it: A bacterial infection of the genitals, anus, or throat. How common: The CDC estimates 820,000 people in the United States get Gonorrhea
How to Prevent Sexually Transmitted Diseases
 ACOG publications are protected by copyright and all rights are reserved. ACOG publications may not be reproduced in any form or by any means without written permission from the copyright owner. This includes
ACOG publications are protected by copyright and all rights are reserved. ACOG publications may not be reproduced in any form or by any means without written permission from the copyright owner. This includes
Practice Steps for Implementation of Guidelines Recommendations The guideline recommendations are shown schematically -
 ASK SCREEN Test for HIV and STI Practice Steps for Implementation of Guidelines Recommendations The guideline recommendations are shown schematically - Routinely obtain a thorough sexual history from all
ASK SCREEN Test for HIV and STI Practice Steps for Implementation of Guidelines Recommendations The guideline recommendations are shown schematically - Routinely obtain a thorough sexual history from all
ALASKA NATIVE MEDICAL CENTER SEXUALLY TRANSMITTED DISEASE SCREENING AND TREATMENT GUIDELINES
 ALASKA NATIVE MEDICAL CENTER SEXUALLY TRANSMITTED DISEASE SCREENING AND TREATMENT GUIDELINES A. Screening Page Chlamydia and Gonorrhea 1 HIV 1 Syphilis 1 Genital Herpes 2 Hepatitis A 2 Hepatitis B 2 Hepatitis
ALASKA NATIVE MEDICAL CENTER SEXUALLY TRANSMITTED DISEASE SCREENING AND TREATMENT GUIDELINES A. Screening Page Chlamydia and Gonorrhea 1 HIV 1 Syphilis 1 Genital Herpes 2 Hepatitis A 2 Hepatitis B 2 Hepatitis
SYPHILIS (Treponema pallidum) IMMEDIATE NOTIFICATION STD PROGRAM
 SYPHILIS (Treponema pallidum) IMMEDIATE NOTIFICATION STD PROGRAM Event Name: Event Time Period: Clinical Description (CDC 2014) Syphilis 180 days Syphilis is a complex sexually transmitted disease that
SYPHILIS (Treponema pallidum) IMMEDIATE NOTIFICATION STD PROGRAM Event Name: Event Time Period: Clinical Description (CDC 2014) Syphilis 180 days Syphilis is a complex sexually transmitted disease that
Clinical Education Initiative CHANCROID: CLINICAL UPDATE. Speaker: Patricia Coury-Doniger, FNP-C, ANC
 Clinical Education Initiative Support@ceitraining.org CHANCROID: CLINICAL UPDATE Speaker: Patricia Coury-Doniger, FNP-C, ANC 2/8/2017 Chancroid: Clinical Update [video transcript] 00:00:11 I have no disclosures.
Clinical Education Initiative Support@ceitraining.org CHANCROID: CLINICAL UPDATE Speaker: Patricia Coury-Doniger, FNP-C, ANC 2/8/2017 Chancroid: Clinical Update [video transcript] 00:00:11 I have no disclosures.
Sexually Transmitted Infections in the Adolescent Population. Abraham Lichtmacher MD FACOG Chief of Women s Services Lovelace Health System
 Sexually Transmitted Infections in the Adolescent Population Abraham Lichtmacher MD FACOG Chief of Women s Services Lovelace Health System STI in the Adolescent High school students nationwide, 34.2% were
Sexually Transmitted Infections in the Adolescent Population Abraham Lichtmacher MD FACOG Chief of Women s Services Lovelace Health System STI in the Adolescent High school students nationwide, 34.2% were
Sexually transmitted infections (in women)
 Sexually transmitted infections (in women) Timothy Kremer, MD Assistant Professor, Department of Obstetrics and Gynecology University of North Texas Health Science Center Last official CDC guidelines:
Sexually transmitted infections (in women) Timothy Kremer, MD Assistant Professor, Department of Obstetrics and Gynecology University of North Texas Health Science Center Last official CDC guidelines:
What You Need to Know. Sexually Transmitted Infections (STIs)
 What You Need to Know Sexually Transmitted Infections (STIs) What You Need to Know About STIs What are STIs? Sexually transmitted infections (STIs) are diseases that spread through sexual contact. If you
What You Need to Know Sexually Transmitted Infections (STIs) What You Need to Know About STIs What are STIs? Sexually transmitted infections (STIs) are diseases that spread through sexual contact. If you
Sexually transmitted infections (in women)
 Sexually transmitted infections (in women) Timothy Kremer, MD Assistant Professor, Department of Obstetrics and Gynecology University of North Texas Health Science Center Last official CDC guidelines:
Sexually transmitted infections (in women) Timothy Kremer, MD Assistant Professor, Department of Obstetrics and Gynecology University of North Texas Health Science Center Last official CDC guidelines:
The Resurgence of Syphilis in British Columbia: Who is affected? What are the challenges? How can we improve our response?
 The Resurgence of Syphilis in British Columbia: Who is affected? What are the challenges? How can we improve our response? Gillian Hill-Carroll Travis Salway Hottes Pacific AIDS Network Webinar Series
The Resurgence of Syphilis in British Columbia: Who is affected? What are the challenges? How can we improve our response? Gillian Hill-Carroll Travis Salway Hottes Pacific AIDS Network Webinar Series
Sexually Transmitted Diseases. Summary of CDC Treatment Guidelines
 DC 2015 Sexually Transmitted Diseases Summary of CDC Treatment Guidelines These summary guidelines reflect the June 2015 update to the 2010 CDC Guidelines for Treatment of Sexually Transmitted Diseases.
DC 2015 Sexually Transmitted Diseases Summary of CDC Treatment Guidelines These summary guidelines reflect the June 2015 update to the 2010 CDC Guidelines for Treatment of Sexually Transmitted Diseases.
Sexually Transmitted Infections (STIs)
 Sexually Transmitted Infections (STIs) Overview Definition of STIs: What are they? Transmission: How are they spread? Types of infection: Bacterial (Chlamydia, Gonorrhea, Syphilis) Viral (Hepatitis B,
Sexually Transmitted Infections (STIs) Overview Definition of STIs: What are they? Transmission: How are they spread? Types of infection: Bacterial (Chlamydia, Gonorrhea, Syphilis) Viral (Hepatitis B,
WOMENCARE. Herpes. Source: PDR.net Page 1 of 8. A Healthy Woman is a Powerful Woman (407)
 WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 Herpes Basics: Herpes is a common viral disease characterized by painful blisters of the mouth or genitals. The herpes simplex virus (HSV) causes
WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 Herpes Basics: Herpes is a common viral disease characterized by painful blisters of the mouth or genitals. The herpes simplex virus (HSV) causes
Sexually Transmitted Infections
 Sexually Transmitted Infections STI Director/ Centers for Disease Control Overview Definition of STIs: What are they? Transmission: How are they spread? Types of infection: -Bacterial (Chlamydia, LGV,
Sexually Transmitted Infections STI Director/ Centers for Disease Control Overview Definition of STIs: What are they? Transmission: How are they spread? Types of infection: -Bacterial (Chlamydia, LGV,
January Dear Physician:
 Richard F. Daines, M.D. Commissioner Wendy E. Saunders Executive Deputy Commissioner January 2009 Dear Physician: The purpose of this letter is to bring your attention to the significant increase in reported
Richard F. Daines, M.D. Commissioner Wendy E. Saunders Executive Deputy Commissioner January 2009 Dear Physician: The purpose of this letter is to bring your attention to the significant increase in reported
Syphilis Update: New Presentations of an Old Disease
 Syphilis Update: New Presentations of an Old Disease Bradley Stoner, MD, PhD Washington University in St. Louis Disclosure: Bradley Stoner, MD, PhD STDs in the United States Where do we stand right now?
Syphilis Update: New Presentations of an Old Disease Bradley Stoner, MD, PhD Washington University in St. Louis Disclosure: Bradley Stoner, MD, PhD STDs in the United States Where do we stand right now?
Syphilis in the 21 st Century: Sex, Sores, Science, and Surveillance. Syphilis in Men
 Syphilis in the 21 st Century: Sex, Sores, Science, and Surveillance Syphilis in Men Kenneth A. Katz, MD, MSc, MSCE Kaiser Permanente, San Francisco, CA AAD Annual Meeting Washington, D.C. March 2, 2019
Syphilis in the 21 st Century: Sex, Sores, Science, and Surveillance Syphilis in Men Kenneth A. Katz, MD, MSc, MSCE Kaiser Permanente, San Francisco, CA AAD Annual Meeting Washington, D.C. March 2, 2019
S403- Update on STIs for the Generalists
 S403- Update on STIs for the Generalists Mobeen H. Rathore, MD Professor and Director University of Florida Center for HIV/AIDS Research Education and Service (UF CARES) Chief, Pediatric Infectious Diseases
S403- Update on STIs for the Generalists Mobeen H. Rathore, MD Professor and Director University of Florida Center for HIV/AIDS Research Education and Service (UF CARES) Chief, Pediatric Infectious Diseases
Sexually Transmitted Infections
 Sexually Transmitted Infections Introduction Sexually transmitted diseases, or STDs, are some of the most common infectious diseases. Sexually transmitted diseases are also called sexually transmitted
Sexually Transmitted Infections Introduction Sexually transmitted diseases, or STDs, are some of the most common infectious diseases. Sexually transmitted diseases are also called sexually transmitted
CLINICAL MANAGEMENT OF STDS
 CLINICAL MANAGEMENT OF STDS Diana Torres-Burgos MD, MPH NYC STD/HIV Prevention Training Center STD/HIV Update Conference Grand Rapids, MI 3/11/2014 Outline Essential components of STD care management Sexual
CLINICAL MANAGEMENT OF STDS Diana Torres-Burgos MD, MPH NYC STD/HIV Prevention Training Center STD/HIV Update Conference Grand Rapids, MI 3/11/2014 Outline Essential components of STD care management Sexual
Public/Private Partnerships: Intervening in the Spread of Syphilis
 Public/Private Partnerships: Intervening in the Spread of Diana Torres-Burgos MD, MPH Gerard Castaneda, BSN Alana Thomas, BS STD/HIV Update Conference Grand Rapids, MI 3/11/2014 Outline overview Stages
Public/Private Partnerships: Intervening in the Spread of Diana Torres-Burgos MD, MPH Gerard Castaneda, BSN Alana Thomas, BS STD/HIV Update Conference Grand Rapids, MI 3/11/2014 Outline overview Stages
Syphilis among MSM: Clinical Care and Public Health Reporting
 Massachusetts Department of Public Health Bureau of Infectious Disease and Laboratory Sciences Syphilis among MSM: Clinical Care and Public Health Reporting Kevin Ard, MD, MPH, Medical Director, National
Massachusetts Department of Public Health Bureau of Infectious Disease and Laboratory Sciences Syphilis among MSM: Clinical Care and Public Health Reporting Kevin Ard, MD, MPH, Medical Director, National
To view an archived recording of this presentation please click the following link:
 To view an archived recording of this presentation please click the following link: http://pho.adobeconnect.com/p16lj8z0qm3/ Please scroll down this file to view a copy of the slides from the session.
To view an archived recording of this presentation please click the following link: http://pho.adobeconnect.com/p16lj8z0qm3/ Please scroll down this file to view a copy of the slides from the session.
Sexually Transmitted. Diseases
 Sexually Transmitted Diseases How can I get an STD? Many STDs are carried and transmitted through semen and vaginal fluids. Some STDs can be spread through skin to skin contact Mother to child STDs: Signs
Sexually Transmitted Diseases How can I get an STD? Many STDs are carried and transmitted through semen and vaginal fluids. Some STDs can be spread through skin to skin contact Mother to child STDs: Signs
MYTHS OF STIs True or False
 MYTHS OF STIs True or False 1. Most people with an STD experience painful symptoms. 2. Birth control pills prevent the spread of STDs. 3. Douching will cure and STD. 4. Abstinence is the best way to prevent
MYTHS OF STIs True or False 1. Most people with an STD experience painful symptoms. 2. Birth control pills prevent the spread of STDs. 3. Douching will cure and STD. 4. Abstinence is the best way to prevent
STD. Are sexually transmitted infections (STIs) different from sexually transmitted diseases (STDs)?
 What are sexually transmitted diseases (STDs)? STD Sexually transmitted diseases are diseases that can be passed from person to person through sexual contact. Depending on the STD, sexual contact that
What are sexually transmitted diseases (STDs)? STD Sexually transmitted diseases are diseases that can be passed from person to person through sexual contact. Depending on the STD, sexual contact that
In Canada and around the world, the trend is clear: sexually transmitted infections (STIs) are on the rise.
 Adapted From: Sexually Transmitted Infections Pamphlet. Public Health Agency of Canada, 2007 In Canada and around the world, the trend is clear: sexually transmitted infections (STIs) are on the rise.
Adapted From: Sexually Transmitted Infections Pamphlet. Public Health Agency of Canada, 2007 In Canada and around the world, the trend is clear: sexually transmitted infections (STIs) are on the rise.
Sexually Transmitted Infections. Kim Dawson October 2010
 Sexually Transmitted Infections Kim Dawson October 2010 Objectives: You will learn about: Sexually Transmitted Infections (STI s). How they are transferred. High risk behavior. The most common STI s. How
Sexually Transmitted Infections Kim Dawson October 2010 Objectives: You will learn about: Sexually Transmitted Infections (STI s). How they are transferred. High risk behavior. The most common STI s. How
Disclosures. STD Screening for Women. Chlamydia & Gonorrhea. I have no disclosures or conflicts of interest to report.
 Disclosures Management of STIs: Challenges in Practice I have no disclosures or conflicts of interest to report. Alison O. Marshall, MSN, FNP-C Associate Professor of Practice & Director of the Family
Disclosures Management of STIs: Challenges in Practice I have no disclosures or conflicts of interest to report. Alison O. Marshall, MSN, FNP-C Associate Professor of Practice & Director of the Family
STDs. Lesson 5.1. By Carone Fitness. Sexually Transmitted Diseases
 Lesson 5.1 STDs By Carone Fitness The Silent Epidemic An epidemic is an outbreak of an infectious disease that affects a large population. Epidemics have afflicted people since the beginning of time, not
Lesson 5.1 STDs By Carone Fitness The Silent Epidemic An epidemic is an outbreak of an infectious disease that affects a large population. Epidemics have afflicted people since the beginning of time, not
How is it transferred?
 STI s What is a STI? It is a contagious infection that is transferred from one person to another through sexual intercourse or other sexually- related behaviors. How is it transferred? The organisms live
STI s What is a STI? It is a contagious infection that is transferred from one person to another through sexual intercourse or other sexually- related behaviors. How is it transferred? The organisms live
Use of Treponemal Immunoassays for Screening and Diagnosis of Syphilis
 Use of Treponemal Immunoassays for Screening and Diagnosis of Syphilis Guidance for Medical Providers and Laboratories in California These guidelines were developed by the California Department of Public
Use of Treponemal Immunoassays for Screening and Diagnosis of Syphilis Guidance for Medical Providers and Laboratories in California These guidelines were developed by the California Department of Public
2/13/ Graphic photographs or cartoons used during this presentation might be offensive to some; for this I apologize in advance.
 Leon Bullard, MD, MA Medical Consultant, DHEC, DADE The 23 rd Annual APRN Conference Charleston, SC February 24, 2017 1. Provide a brief (very) review of the syphilis story. 2. Define and discuss the stages
Leon Bullard, MD, MA Medical Consultant, DHEC, DADE The 23 rd Annual APRN Conference Charleston, SC February 24, 2017 1. Provide a brief (very) review of the syphilis story. 2. Define and discuss the stages
Clinical Practice Guideline with Delegation of Function
 1 of 8 1.0 Purpose 1.1 To improve and focus efforts to treat those at risk for undiagnosed/untreated incubating, primary, secondary, or early latent infectious syphilis. 2.0 Scope and Goal 2.1 Antibiotic
1 of 8 1.0 Purpose 1.1 To improve and focus efforts to treat those at risk for undiagnosed/untreated incubating, primary, secondary, or early latent infectious syphilis. 2.0 Scope and Goal 2.1 Antibiotic
SEXUALLY TRANSMITTED INFECTIONS (STIS)
 SEXUALLY TRANSMITTED INFECTIONS (STIS) CONTENTS Causes Prevention Methods of Transmission Decisions to Have Sexual Intercourse Signs and symptoms Screening Pop Quiz Diagnosis Management: Public Health
SEXUALLY TRANSMITTED INFECTIONS (STIS) CONTENTS Causes Prevention Methods of Transmission Decisions to Have Sexual Intercourse Signs and symptoms Screening Pop Quiz Diagnosis Management: Public Health
Learning Objectives. Epidemiology 5/3/2013. Treponema pallidum Diagnosis, Treatment and Prevention. Anne Rompalo, MD, ScM Professor of Medicine
 Treponema pallidum Diagnosis, Treatment and Prevention Anne Rompalo, MD, ScM Professor of Medicine Learning Objectives Describe the epidemiology of syphilis in the U.S.Describe the pathogenesis of Treponema
Treponema pallidum Diagnosis, Treatment and Prevention Anne Rompalo, MD, ScM Professor of Medicine Learning Objectives Describe the epidemiology of syphilis in the U.S.Describe the pathogenesis of Treponema
Lisa Villarroel, MD MPH Medical Director, Division of Public Health Preparedness Arizona Department of Health Services.
 Lisa Villarroel, MD MPH Medical Director, Division of Public Health Preparedness Arizona Department of Health Services Disclosures: None 1 PRIMARY Fitzgerald TJ, Cleveland P, Johnson RC et al: Scanning
Lisa Villarroel, MD MPH Medical Director, Division of Public Health Preparedness Arizona Department of Health Services Disclosures: None 1 PRIMARY Fitzgerald TJ, Cleveland P, Johnson RC et al: Scanning
SEXUALLY TRANSMITTED DISEASES
 SEXUALLY TRANSMITTED DISEASES Kaya Süer MD, Near East University Faculty of Medicine Infectious Diseases and Clinical Microbiology True or false 1. Most people with an STD experience painful symptoms.
SEXUALLY TRANSMITTED DISEASES Kaya Süer MD, Near East University Faculty of Medicine Infectious Diseases and Clinical Microbiology True or false 1. Most people with an STD experience painful symptoms.
OVERVIEW SEXUALLY TRANSMITTED INFECTIONS REPORTS STI BASICS WATCH OUT! HOW TO PREVENT STIs. Sexually Transmitted Infections Reports
 UNIT NINE: UNDERSTANDING & PREVENTING SEXUALLY TRANSMITTED INFECTIONS OVERVIEW SEXUALLY TRANSMITTED INFECTIONS REPORTS STI BASICS WATCH OUT! HOW TO PREVENT STIs Overview When compared to the other industrialized
UNIT NINE: UNDERSTANDING & PREVENTING SEXUALLY TRANSMITTED INFECTIONS OVERVIEW SEXUALLY TRANSMITTED INFECTIONS REPORTS STI BASICS WATCH OUT! HOW TO PREVENT STIs Overview When compared to the other industrialized
Sexuality/Reproduction CALM Summer 2015
 Female Reproduction Sexuality/Reproduction CALM Summer 2015 Male Reproduction Reproduction https://www.youtube.com/watch?v=_7rsh2loiy8 1 About Sex How to use a condom Set Limits Think about how far you
Female Reproduction Sexuality/Reproduction CALM Summer 2015 Male Reproduction Reproduction https://www.youtube.com/watch?v=_7rsh2loiy8 1 About Sex How to use a condom Set Limits Think about how far you
A Man with a Rash and Pink Eye. STD Case Studies from the Denver Metro Health Clinic
 A Man with a Rash and Pink Eye STD Case Studies from the Denver Metro Health Clinic Case 45 year-old HIV+ gay male, presented to the STD clinic as a contact to gonorrhea Generalized rash since 6 weeks
A Man with a Rash and Pink Eye STD Case Studies from the Denver Metro Health Clinic Case 45 year-old HIV+ gay male, presented to the STD clinic as a contact to gonorrhea Generalized rash since 6 weeks
Sexually Transmitted Infections
 Sexually Transmitted Infections What is a Sexually Transmitted Infection or STI? STI s are infections that are spread from person to person through intimate sexual contact. STI s are dangerous because
Sexually Transmitted Infections What is a Sexually Transmitted Infection or STI? STI s are infections that are spread from person to person through intimate sexual contact. STI s are dangerous because
Bacteriology. Spirochetes. Three important genera: 1. Treponema 2. Borrelia 3. Leptospira. Treponema pallidum. Causes syphilis.
 Bacteriology Spirochetes Three important genera: 1. Treponema 2. Borrelia 3. Leptospira Treponema pallidum Causes syphilis Organism: - Spirochetes with 6-14 regularly spaced spirals - Its length is the
Bacteriology Spirochetes Three important genera: 1. Treponema 2. Borrelia 3. Leptospira Treponema pallidum Causes syphilis Organism: - Spirochetes with 6-14 regularly spaced spirals - Its length is the
6/11/15. BACTERIAL STDs IN A POST- HIV WORLD. Learning Objectives. How big a problem are STIs in the U.S.?
 BACTERIAL STDs IN A POST- HIV WORLD Tracey Graney, PhD, MT(ASCP) Monroe Community College Learning Objectives Describe the epidemiology and incidence of bacterial STDs in the U.S. Describe current detection
BACTERIAL STDs IN A POST- HIV WORLD Tracey Graney, PhD, MT(ASCP) Monroe Community College Learning Objectives Describe the epidemiology and incidence of bacterial STDs in the U.S. Describe current detection
Michigan Guidelines: HIV, Syphilis, HBV in Pregnancy
 Michigan Guidelines: HIV, Syphilis, HBV in Pregnancy Presenter: Theodore B. Jones, MD Maternal Fetal Medicine Wayne State University School of Medicine Beaumont Dearborn Hospital HIV, Syphilis, HBV in
Michigan Guidelines: HIV, Syphilis, HBV in Pregnancy Presenter: Theodore B. Jones, MD Maternal Fetal Medicine Wayne State University School of Medicine Beaumont Dearborn Hospital HIV, Syphilis, HBV in
Preventing Sexual Transmitted Diseases
 Preventing Sexual Transmitted Diseases Chapter 12 Card game Lie Sexually Transmitted Diseases Sexuality is an intrinsic part of human nature and affects many things People are not always honest about their
Preventing Sexual Transmitted Diseases Chapter 12 Card game Lie Sexually Transmitted Diseases Sexuality is an intrinsic part of human nature and affects many things People are not always honest about their
CHAPTER-X SYPHILIS R.KAVITHA, M.PHARM, LECTURER, DEPARTMENT OF PHARMACEUTICS, SRM COLLEGE OF PHARMACY, SRM UNIVERSITY, KATTANKULATHUR.
 CHAPTER-X SYPHILIS R.KAVITHA, M.PHARM, LECTURER, DEPARTMENT OF PHARMACEUTICS, SRM COLLEGE OF PHARMACY, SRM UNIVERSITY, KATTANKULATHUR. Trepanoma pallidum D. Clinical Infection: Syphilis Transmission Usually
CHAPTER-X SYPHILIS R.KAVITHA, M.PHARM, LECTURER, DEPARTMENT OF PHARMACEUTICS, SRM COLLEGE OF PHARMACY, SRM UNIVERSITY, KATTANKULATHUR. Trepanoma pallidum D. Clinical Infection: Syphilis Transmission Usually
Sexually transmitted infections
 Sexually transmitted infections Dr Caroline CHARLIER-WOERTHER Université Paris Descartes Paris, France Learning objectives Counsel patients about the risk of STD Know how to diagnose and treat a sexuallytransmitted
Sexually transmitted infections Dr Caroline CHARLIER-WOERTHER Université Paris Descartes Paris, France Learning objectives Counsel patients about the risk of STD Know how to diagnose and treat a sexuallytransmitted
Trends in Reportable Sexually Transmitted Diseases in the United States, 2007
 Trends in Reportable Sexually Transmitted Diseases in the United States, 2007 National Surveillance Data for Chlamydia, Gonorrhea, and Syphilis Sexually transmitted diseases (STDs) remain a major public
Trends in Reportable Sexually Transmitted Diseases in the United States, 2007 National Surveillance Data for Chlamydia, Gonorrhea, and Syphilis Sexually transmitted diseases (STDs) remain a major public
STDs in HIV Clinical Care: New Guidelines on Treatment and Prevention
 STDs in HIV Clinical Care: New Guidelines on Treatment and Prevention Palliative Care Conference Faculty Development Conference August 13, 2015 Steven C. Johnson M.D. Director, University of Colorado HIV/AIDS
STDs in HIV Clinical Care: New Guidelines on Treatment and Prevention Palliative Care Conference Faculty Development Conference August 13, 2015 Steven C. Johnson M.D. Director, University of Colorado HIV/AIDS
STI Treatment Guidelines. Teodora Wi. Training Course in Sexual and Reproductive Health Research
 Teodora Wi Geneva, 28 August 2017 STI Treatment Guidelines Teodora Wi Training Course in Sexual and Reproductive Health Research 2017 Twitter @HRPresearch 1 STI treatment guidelines Neisseria gonorrhoeae
Teodora Wi Geneva, 28 August 2017 STI Treatment Guidelines Teodora Wi Training Course in Sexual and Reproductive Health Research 2017 Twitter @HRPresearch 1 STI treatment guidelines Neisseria gonorrhoeae
STI & HIV PRE-TEST ANSWER KEY
 Name: STI & HIV PRE-TEST ANSWER KEY 1. You can catch a STI or HIV from door knobs, toilet seats, or FALSE drinking fountains. STIs are transmitted sexually, requiring sexual contact. Some STIs can be transmitted
Name: STI & HIV PRE-TEST ANSWER KEY 1. You can catch a STI or HIV from door knobs, toilet seats, or FALSE drinking fountains. STIs are transmitted sexually, requiring sexual contact. Some STIs can be transmitted
PROTECT YOURSELF + PROTECT YOUR PARTNER. syphilis THE FACTS
 PROTECT YOURSELF + PROTECT YOUR PARTNER syphilis THE FACTS PROTECT YOURSELF + PROTECT YOUR PARTNER THE FACTS Syphilis (SI fi lis) is a sexually transmitted disease (STD). Anyone can get syphilis. Many
PROTECT YOURSELF + PROTECT YOUR PARTNER syphilis THE FACTS PROTECT YOURSELF + PROTECT YOUR PARTNER THE FACTS Syphilis (SI fi lis) is a sexually transmitted disease (STD). Anyone can get syphilis. Many
Chapter 25 Notes Lesson 1
 Chapter 25 Notes Lesson 1 The Risk of STIs 1) What is a sexually transmitted disease (STD)? Referred to as a sexually transmitted infection (STI) infectious diseases spread from person to person through
Chapter 25 Notes Lesson 1 The Risk of STIs 1) What is a sexually transmitted disease (STD)? Referred to as a sexually transmitted infection (STI) infectious diseases spread from person to person through
What you need to know to: Keep Yourself SAFE!
 What you need to know to: Keep Yourself SAFE! What are sexually transmitted diseases (STDs)? How are they spread? What are the different types of STDs? How do I protect myself? STDs are infections or diseases
What you need to know to: Keep Yourself SAFE! What are sexually transmitted diseases (STDs)? How are they spread? What are the different types of STDs? How do I protect myself? STDs are infections or diseases
STI Indicators by STI
 STI Indicators by STI Table of Contents pg. 2 Sexual History pg. 3-4 Syphilis pg. 5-6 Gonorrhea pg. 7-9 Chlamydia pg. 10 HIV/PrEP 1 Sexual History Comprehensive Sexual History Elements Percentage of patients
STI Indicators by STI Table of Contents pg. 2 Sexual History pg. 3-4 Syphilis pg. 5-6 Gonorrhea pg. 7-9 Chlamydia pg. 10 HIV/PrEP 1 Sexual History Comprehensive Sexual History Elements Percentage of patients
Summary Guidelines for the Use of Herpes Simplex Virus (HSV) Type 2 Serologies
 Summary Guidelines for the Use of Herpes Simplex Virus (HSV) Type 2 Serologies Genital herpes is one of the most prevalent sexually transmitted diseases, affecting more than one in five sexually active
Summary Guidelines for the Use of Herpes Simplex Virus (HSV) Type 2 Serologies Genital herpes is one of the most prevalent sexually transmitted diseases, affecting more than one in five sexually active
Selassie AW (DBBE) 1. Overview 12 million incident cases per year $10 billion economic impact More than 25 organisms.
 Infectious Disease Epidemiology BMTRY 713 (A. Selassie, DrPH) Lecture 12 Sexually Transmitted Diseases Learning Objectives 1. Review the epidemiology of sexually Transmitted Diseases 2. Assess the personal
Infectious Disease Epidemiology BMTRY 713 (A. Selassie, DrPH) Lecture 12 Sexually Transmitted Diseases Learning Objectives 1. Review the epidemiology of sexually Transmitted Diseases 2. Assess the personal
SEX AND SEXUALLY TRANSMITTED INFECTIONS
 SEX AND SEXUALLY TRANSMITTED INFECTIONS Sex and STIs Be fully informed, Be safe! Prevent Pregnancy Practice abstinence Use effective birth control Use Emergency Contraception Prevent STI s Practice Abstinence
SEX AND SEXUALLY TRANSMITTED INFECTIONS Sex and STIs Be fully informed, Be safe! Prevent Pregnancy Practice abstinence Use effective birth control Use Emergency Contraception Prevent STI s Practice Abstinence
SEXUALLY TRANSMITTED DISEASES (INFECTIONS)
 SEXUALLY TRANSMITTED DISEASES (INFECTIONS) HIV/AIDS - TRANSMISSION Sexual intercourse Anal, oral, & vaginal Multiple partners Sharing needles Mother to infant Born or breast milk Blood transfusions Open
SEXUALLY TRANSMITTED DISEASES (INFECTIONS) HIV/AIDS - TRANSMISSION Sexual intercourse Anal, oral, & vaginal Multiple partners Sharing needles Mother to infant Born or breast milk Blood transfusions Open
Urogenital Tract / 3 rd year Syphilis, HPV. Dr Hamed Al-Zoubi MD, PhD Associate Prof. of Medical Microbiology
 Urogenital Tract / 3 rd year Syphilis, HPV Dr Hamed Al-Zoubi MD, PhD Associate Prof. of Medical Microbiology What you need to know about syphilis? Etiology of syphilis Transmission & Epidemiology Pathogenesis
Urogenital Tract / 3 rd year Syphilis, HPV Dr Hamed Al-Zoubi MD, PhD Associate Prof. of Medical Microbiology What you need to know about syphilis? Etiology of syphilis Transmission & Epidemiology Pathogenesis
Several of the most common STDs are often asymptomatic. Asymptomatic
 What Are STDs? Several of the most common STDs are often asymptomatic. Asymptomatic Individuals show no symptoms, or the symptoms are mild and disappear after the onset of the infection Common STDs There
What Are STDs? Several of the most common STDs are often asymptomatic. Asymptomatic Individuals show no symptoms, or the symptoms are mild and disappear after the onset of the infection Common STDs There
- (Have NO cure yet, but are controllable) - (Can be cured if caught early enough)
 Myths or Facts of STD s 1. Most people with an STD experience painful symptoms. 2. Abstinence is the best way to prevent STD s. 3. If you get an STD once, and are treated, you can t get it again. 4. A
Myths or Facts of STD s 1. Most people with an STD experience painful symptoms. 2. Abstinence is the best way to prevent STD s. 3. If you get an STD once, and are treated, you can t get it again. 4. A
Emerging Issues in STDs and Resistance
 Emerging Issues in STDs and Resistance Toye H. Brewer, MD Asst. Professor of Clinical Medicine University of Miami School of Medicine Co-Director- Fogarty International Training Program Outline Syphilis-
Emerging Issues in STDs and Resistance Toye H. Brewer, MD Asst. Professor of Clinical Medicine University of Miami School of Medicine Co-Director- Fogarty International Training Program Outline Syphilis-
Learning Objectives. STI Update. Case 1 6/1/2016
 Learning Objectives STI Update June 16 th, 2016 Madhu Choudhary, MD. FIDSA Assoc. Prof of Medicine Albany Medical College Review screening recommendations for STI in different patient populations Describe
Learning Objectives STI Update June 16 th, 2016 Madhu Choudhary, MD. FIDSA Assoc. Prof of Medicine Albany Medical College Review screening recommendations for STI in different patient populations Describe
STI S SEXUALLY TRANSMITTED INFECTIONS
 STI S SEXUALLY TRANSMITTED INFECTIONS Mandatory teaching in the State of Utah We teach Abstinence prior to marriage Regarding STI/HIV, most teens think that Talking about STI/HIV prevention is.. What issues,
STI S SEXUALLY TRANSMITTED INFECTIONS Mandatory teaching in the State of Utah We teach Abstinence prior to marriage Regarding STI/HIV, most teens think that Talking about STI/HIV prevention is.. What issues,
Dermatologist Venereologist MD, PhD
 Vassiliki Mousatou Dermatologist Venereologist MD, PhD Genital warts Genital herpes Syphilis Gonococcal and no gonococcal urethritis HIV Hepatitis B and C Also: Lymphogranuloma venereum and Granuloma
Vassiliki Mousatou Dermatologist Venereologist MD, PhD Genital warts Genital herpes Syphilis Gonococcal and no gonococcal urethritis HIV Hepatitis B and C Also: Lymphogranuloma venereum and Granuloma
How Do You Catch An Infection?
 How Do You Catch An Infection? Animals Insects Water People Food Infectious Diseases Considerations for the 21 st Century Viruses, bacteria, fungi, protozoa, helminths Infectious diseases are the second
How Do You Catch An Infection? Animals Insects Water People Food Infectious Diseases Considerations for the 21 st Century Viruses, bacteria, fungi, protozoa, helminths Infectious diseases are the second
September 2006 HepTalk Listserv
 Mon, Oct 29, 2007 12:47 PM Subject: September 2006 HepTalk Listserv Date: Monday, October 2, 2006 9:22 PM From: Kathryn Anderson To: Conversation:
Mon, Oct 29, 2007 12:47 PM Subject: September 2006 HepTalk Listserv Date: Monday, October 2, 2006 9:22 PM From: Kathryn Anderson To: Conversation:
Case 1. Case 1. Physical exam
 11/13/2012 Case 28 year-old woman Complains of very painful lesions in vulvar area Increasing severity since 4 days Pain aggravated by urination She has a slight fever and also complains of headache and
11/13/2012 Case 28 year-old woman Complains of very painful lesions in vulvar area Increasing severity since 4 days Pain aggravated by urination She has a slight fever and also complains of headache and
Lymphogranuloma Venereum (LGV) Surveillance Project
 Lymphogranuloma Venereum (LGV) Surveillance Project Lymphogranuloma venereum (LGV) is a systemic, sexually transmitted disease (STD) caused by a type of Chlamydia trachomatis (serovars L1, L2, L3) that
Lymphogranuloma Venereum (LGV) Surveillance Project Lymphogranuloma venereum (LGV) is a systemic, sexually transmitted disease (STD) caused by a type of Chlamydia trachomatis (serovars L1, L2, L3) that
Professor Adrian Mindel
 Causes of genital ulceration viruses and others Professor Adrian Mindel University of Sydney VIM 16 th August 2012 Outline Definition Causes Epidemiology Diagnosis Definition of genital ulcer A defect
Causes of genital ulceration viruses and others Professor Adrian Mindel University of Sydney VIM 16 th August 2012 Outline Definition Causes Epidemiology Diagnosis Definition of genital ulcer A defect
Dr. R. Someshwaran, MBBS, MD., Assistant professor, Dept. of Microbiology, KFMS&R
 Dr. R. Someshwaran, MBBS, MD., Assistant professor, Dept. of Microbiology, KFMS&R 1 What is Syphilis? Syphilis is a systemic, sexually transmitted disease (STD) caused by the Treponema pallidum bacterium.
Dr. R. Someshwaran, MBBS, MD., Assistant professor, Dept. of Microbiology, KFMS&R 1 What is Syphilis? Syphilis is a systemic, sexually transmitted disease (STD) caused by the Treponema pallidum bacterium.
Biology 3201 Unit 2 Reproduction: Sexually Transmitted Infections (STD s/sti s)
 Biology 3201 Unit 2 Reproduction: Sexually Transmitted Infections (STD s/sti s) STI s once called venereal diseases More than 20 STIs have now been identified most prevalent among teenagers and young adults.
Biology 3201 Unit 2 Reproduction: Sexually Transmitted Infections (STD s/sti s) STI s once called venereal diseases More than 20 STIs have now been identified most prevalent among teenagers and young adults.
CASE-BASED SMALL GROUP DISCUSSION
 MHD I, Session IV, STUDENT Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION MHD I SESSION IV Wednesday, September 18, 2013 MHD I, Session IV, STUDENT Copy Page 2 Resource for cases: Robbins Basic Pathology,
MHD I, Session IV, STUDENT Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION MHD I SESSION IV Wednesday, September 18, 2013 MHD I, Session IV, STUDENT Copy Page 2 Resource for cases: Robbins Basic Pathology,
University Health Services at CMU STI Awareness Month specials for students:
 University Health Services at CMU STI Awareness Month specials for students: -Free condoms during April (10 per student) -Free walk-in rapid HIV testing April 22-27 (no appointment needed) -STI Screening
University Health Services at CMU STI Awareness Month specials for students: -Free condoms during April (10 per student) -Free walk-in rapid HIV testing April 22-27 (no appointment needed) -STI Screening
