Tanya A. Halse, Justine Edwards, Phyllis L. Cunningham, William J. Wolfgang, Nellie B. Dumas, Vincent E. Escuyer, and Kimberlee A.
|
|
|
- Polly Dixon
- 5 years ago
- Views:
Transcription
1 JOURNAL OF CLINICAL MICROBIOLOGY, Apr. 2010, p Vol. 48, No /10/$12.00 doi: /jcm Copyright 2010, American Society for Microbiology. All Rights Reserved. Combined Real-Time PCR and rpob Gene Pyrosequencing for Rapid Identification of Mycobacterium tuberculosis and Determination of Rifampin Resistance Directly in Clinical Specimens Tanya A. Halse, Justine Edwards, Phyllis L. Cunningham, William J. Wolfgang, Nellie B. Dumas, Vincent E. Escuyer, and Kimberlee A. Musser* Wadsworth Center, New York State Department of Health, Albany, New York Received 3 November 2009/Returned for modification 30 December 2009/Accepted 19 January 2010 Our laboratory has developed a rapid, sensitive, and specific molecular approach for detection in clinical, within 48 h of receipt, of both Mycobacterium tuberculosis complex (MTBC) DNA and mutations within the 81-bp core region of the rpob gene that are associated with rifampin (RIF) resistance. This approach, which combines an initial real-time PCR with internal inhibition assessment and a pyrosequencing assay, was validated for direct use with clinical. To assess the suitability of real-time PCR for use with respiratory, nonrespiratory, acid-fast bacillus (AFB)-positive and AFB-negative, we evaluated received in our laboratory between 11 October 2007 and 30 June With culture used as the gold standard, the sensitivity, specificity, and positive and negative predictive values were determined for 1,316 to be as follows: for respiratory, 94.7%, 99.9%, 99.6%, and 98.6%, respectively; for nonrespiratory, 88.5%, 100.0%, 100.0%, and 96.9%, respectively; for AFB-positive, 99.6%, 100.0%, 100.0%, and 97.7%, respectively; and for AFB-negative, 75.4%, 99.9%, 98.0%, and 98.4%, respectively. PCR inhibition was determined to be minimal in this assay, occurring in 0.2% of tests. The rpob gene pyrosequencing assay was evaluated in a similar prospective study, in which 148 clinical positive for MTBC DNA by real-time PCR were tested. The final results revealed that the results of direct testing of clinical by the pyrosequencing assay were 98.6% concordant with the results of conventional testing for susceptibility to RIF in liquid culture and that our assay displayed adequate sensitivity for 96.6% of the clinical tested. Used together, these assays provide reliable results that aid with the initial management of patients with suspected tuberculosis prior to the availability of the results for cultured material, and they also provide the ability to predict RIF resistance in Mycobacterium tuberculosis-positive in as little as 48 h from the time of clinical specimen receipt. One-third of the world s population is infected with Mycobacterium tuberculosis. In 2007 alone, 9.27 million new cases were identified and 1.6 million deaths occurred. Only 44% (4.1 million cases) of these were acid-fast bacillus (AFB) smear positive (24). The resurgence of tuberculosis (TB) in developed as well as developing countries since 1980 has been associated with the HIV epidemic, the emergence of drug-resistant strains, and increases in emigration from regions with high rates of disease endemicity (6, 9, 11). The rapid detection of M. tuberculosis is essential for disease management, because of the high risk of transmission from person to person. The CDC recommends that clinical received be analyzed simultaneously by culture, AFB staining, and nucleic acid amplification (NAA) protocols (2). Culture is the gold standard for final determination, but it is slow and may take up to 2 to 8 weeks. Staining for AFB is rapid but has a low sensitivity and a low specificity, since it does not distinguish nontuberculous mycobacteria (NTM) from members of the M. tuberculosis complex (MTBC). Thus, rapid identification, which is essential for effective control, relies on NAA. * Corresponding author. Mailing address: Wadsworth Center, New York State Department of Health, 120 New Scotland Avenue, Albany, NY Phone: (518) Fax: (518) Published ahead of print on 27 January A number of studies involving the detection of MTBC by PCR have been reported; these have targeted cfp10 (12), the senx3-regx3 intergenic region (4), the16s rrna gene (10), and the internal transcribed spacer (ITS) (21). However, the most commonly used target for the identification of MTBC is the multiple-copy-number insertion sequence IS6110 (also known as IS986) (4, 5, 8, 9, 14, 16, 20, 22), which is thought to provide the highest sensitivity. The assessment of rifampin (RIF) resistance in M. tuberculosis-infected patients is critically important to patient management and can affect both the treatment of individual patients and the spread of disease. The standard methods for drug susceptibility testing (DST) of M. tuberculosis can take weeks to months to provide results. Due to the emergence of multidrug-resistant tuberculosis (MDR-TB) and extensively drugresistant tuberculosis (XDR-TB), there is a critical need for new, rapid, and accurate DST methods. NAA assays for determination of mutations in an 81-bp region of the rpob gene have been published, and an excellent correlation between the presence of these mutations and RIF resistance has been demonstrated. Mutations in this region are believed to correlate with RIF resistance in 96% of all RIF-resistant M. tuberculosis strains (18). Several tests have been published that perform nucleic acid sequence analysis of mycobacterial isolates by methods that include single-nucleotide polymorphism analysis (3) and pyrosequencing (13, 17, 25) of isolates, but no meth- 1182
2 VOL. 48, 2010 REAL-TIME PCR AND PYROSEQUENCING OF M. TUBERCULOSIS 1183 odology yet reported has utilized rpob gene pyrosequencing analysis of the 81-bp core region directly with clinical positive for MTBC by real-time PCR. Here we describe a two-step molecular approach that will detect MTBC DNA and yield rpob gene mutation analysis results within 48 h from the time of receipt of the clinical specimen. MATERIALS AND METHODS Clinical. A total of 1,316 clinical received for routine mycobacterial cultivation in the Mycobacteriology Laboratory at the Wadsworth Center, New York State Department of Health (NYSDOH), between 11 October 2007 and 30 June 2009 were included in this study. Our laboratory also performs testing for treatment follow-up for diagnosed cases of TB. We have excluded these from the data analysis to best reflect the utility of the testing in a clinical microbiology laboratory that will utilize the test only for diagnostic purposes. Of these 1,316, 1,201 were respiratory, including sputum, bronchoalveolar lavage, and bronchial wash, and 115 were nonrespiratory, including abscess, aspirate, cerebrospinal fluid, gastric fluid, tissue, pleural fluid, wound, liver tissue, and lymph node. Each respiratory specimen was treated with an equal volume of 3.5% NaOH in a 50-ml conical centrifuge tube and vortexed for 30 s, to break up the mucin. The tubes were incubated at room temperature for 15 min to decontaminate the. Sterile phosphate buffer was added to stop the digestiondecontamination process (adjusting the volume to 50 ml), the contents of the tube were mixed by inversion, and the tubes were centrifuged at 3,000 g for 15 min. The supernatant was discarded, and the remaining pellet was resuspended in 3.0 ml of sterile phosphate-buffered saline (ph 6.8); smears were then prepared by the Ziehl-Neelsen acid-fast staining method. An aliquot was treated at 80 C for 1 h, cooled, and stored frozen at 20 C until it was tested by real-time PCR. The lung biopsy and tissue were minced with a scalpel, ground in disposable tissue grinders until they were homogeneous, and then processed as described above. Prior to the real-time PCR assay, a 100- l aliquot of the heat-treated specimen was processed by use of a GeneOhm lysis kit (BD Diagnostics, San Diego, CA), according to the manufacturer s instructions. MGIT inoculation and incubation and routine testing. Before inoculation, Bactec MGIT 960 tubes were supplemented as described by the manufacturer (MGIT [7-ml] package insert; Becton Dickinson). A 0.5-ml portion of the processed specimen was inoculated into the MGIT tube, and the tubes were introduced into the Bactec MGIT 960 instrument, as recommended by the manufacturer; the tubes were then incubated either until they were found to be positive by the instrument or for 8 weeks. Routine media, including a Lowenstein-Jensen slant and a Middlebrook 7H10/ 7H11 selective biplate, were also inoculated with 100 l of the processed specimen, incubated at 37 C, and held for 8 weeks. These plates were observed and the results were recorded during this period of time. Real-time PCR assay. An M. tuberculosis complex-specific primer and mgb probe set was adapted from those described in a previous report that targeted the multicopy IS6110 insertion element (22). The 5 end of the probe was labeled with the fluorescent reporter dye 6-carboxyfluorescein (FAM). An additional probe was used to target an inhibition control plasmid (IC). The 5 end of this probe was labeled with the fluorescent dye VIC, and the 3 end was labeled with the quencher dye 6-carboxytetramethylrhodamine (TAMRA). An additional set of primers that amplifies a portion of the rpob gene was also added to the real-time PCR mixture, and this was considered the first round of a nested PCR. Any real-time PCR-positive amplicon would then be added to the conventional pyrosequencing PCR assay mixture, as described below. The probes were obtained from Applied Biosystems (Foster City, CA), and the oligonucleotides were from Integrated DNA Technologies (Coralville, IA). Each patient sample was tested in duplicate, with one reaction including the IC. The real-time PCR assay was carried out in a 25- l volume with a LightCycler-FastStart DNA master hybridization probes kit (Roche Diagnostics Corporation, Indianapolis, IN). Each reaction mixture consisted of 1 LightCycler-FastStart DNA master hybridization probe mixture, 3.5 mm MgCl 2, 450 nm forward oligonucleotide primer TBC-F (5 -GGG-TAG-CAG- ACC-TCA-CCT-ATG-3 ), 1,350 nm reverse oligonucleotide primer TBC-R (5 -AGC-GTA-GGC-GTC-GGT-GA-3 ), 250 nm TBC probe (FAM-TCG- CCT-ACG-TGG-CCT-TT-MGBNFQ), 1 M forward primer rpob nest-f (5 -ATC-GAA-TAT-CTG-GTC-CGC-TTG-CAC-3 ), 1 M reverse primer rpob nest-r (5 -TCG-TGC-TCC-AGG-AAG-GGA-ATC-AT-3 ), sterile water, and 5 l of DNA template. The thermal cycling conditions were as follows: 1 cycle at 95 C for 10 min, followed by 45 cycles at 95 C for 15 s and 60 C for 1 min. Thermal cycling, fluorescent data collection, and data analysis were performed with an ABI 7000 sequence detection system or an ABI 7500 real-time PCR instrument, according to the manufacturer s instructions, with the passive reference dye carboxy-x-rhodamine turned off. Threshold cycle (C T ) values less than 37 were reported as positive, and samples with values greater than 37 were retested; if the results were the same, the result was reported as positive, and if they were not, they were reported as inconclusive. Internal inhibition control. The DNA isolated from each patient sample was also tested for the presence of PCR inhibitors. An internal control plasmid was constructed from a PCR product that contained fruit fly DNA and identical primer binding sites used for the MTBC IS6110 real-time PCR assay, thereby allowing coamplification to occur in the presence of M. tuberculosis complex DNA. This PCR product was cloned into a plasmid vector (pcr2.1-topo) with a TOPO TA cloning kit (Invitrogen Life Technologies, Carlsbad, CA), according to the manufacturer s instructions. For establishment of the optimal dilution, the plasmid was serially diluted to a level 2 log units higher than the level of detection. This control plasmid, along with 250 nm Inhib-probe (VIC-TCG- CTC-TGT-TTC-ATA-CCC-GGC-GA-TAMRA), was spiked into one of the duplicate PCR mixtures containing 5 l of the patient sample DNA, and the C T value obtained from this reaction was compared with that from a second reaction performed with a mixture containing only the control plasmid. The reaction was considered to be inhibited if the C T values differed by 3 or if a negative result was obtained for the reaction mixture containing the spiked control plasmid. Additionally, 1:5 dilutions of these were prepared if inhibition was detected in the initial test. If the specimen was positive despite some inhibition, the result was reported as positive; if the specimen was negative, it was reported as indeterminate. Real-time PCR assay sensitivity and specificity. The analytical sensitivity of the assay was determined through the use of a standard curve of 10-fold dilutions of DNA isolated from a strain of M. tuberculosis (containing one copy of IS6110) and is reported in units of CFU. Each dilution of template DNA was run in duplicate. The efficiency of the PCR was calculated from the r 2 value generated by the standard curve. The specificity of the assay was determined by testing approximately 10 6 genome copies of DNA purified from MTBC organisms, containing NTM, and other respiratory pathogens that can cause similar clinical symptoms. This testing included the following bacterial strains: Bordetella parapertussis, Bordetella pertussis, Chlamydophila pneumoniae, group A Streptococcus, Haemophilus influenzae type C, Legionella pneumophila, Mycobacterium abscessus (n 3 strains), M. africanum (n 3), M. avium complex, M. bovis (n 3), M. bovis BCG (n 3), M. canetti, M. celatum, M. chelonae (n 3), M. fortuitum (n 2), M. goodii (n 3), M. gordonae (n 2), M. haemophilum, M. interjectum, M. intracellulare, M. kansasii (n 2), M. kubicae, M. lentiflavum (n 2), M. malmoense, M. microti, M. mucogenicum, M. nebraskense, M. neoaurum, M. parascrofulaceum, M. peregrinum (n 2), M. porcinum (n 3), M. scrofulaceum, M. simiae, M. smegmatis, M. szulgai, M. terrae, M. tuberculosis (n 25, including strains with known number of copies of IS6110, ranging from partial to 21 copies), M. ulcerans, and M. xenopi (n 2). The strains were from either ATCC or the culture collection of the Wadsworth Center, NYSDOH. All bacterial strains from the Wadsworth Center used in the specificity panel underwent 16S rrna, hsp65, and rpob DNA sequence analysis for confirmation of their identities. rpob gene analysis by pyrosequencing. Amplification and sequencing primers were designed with PSQ assay design software (Biotage, Inc., Charlottesville, VA). A 289-bp product of the rpob gene was amplified by conventional PCR with the reverse primer biotin labeled for immobilization onto streptavidin-coated Sepharose beads. Two separate sequencing primers were used to assess the full 81-bp region of the rpob gene in two reactions with one PCR product. Real-time PCR-positive were subjected to conventional PCR. Each 100- l reaction mixture included 1 PCR buffer, 0.2 mm deoxynucleoside triphosphate mixture, 0.1 M each PCR primer-for (5 -AGA TCC GGG TCG GCA TGT-3 ) and PCR primer-rev (5-5Biosg/CAC ATC CGG CCG TAG TGC-3 ), 0.25 U/ l Taq DNA polymerase, mm MgCl 2,1 Q-solution (Taq PCR core kit; manufactured by Qiagen), and 1 l of the PCR product from the real-time PCR assay described above. The conditions were 95 C for 5 min; 50 cycles of 94 C for 30 s, 60 C for 30 s, and 72 C for 30 s; and 72 C for 7 min. The amplified products were visualized on a 2% agarose E-gel (Invitrogen Inc., Grand Island, NY) to confirm the presence of 289-bp products. When cultured material was to be tested during the validation, 5 l of a heat-treated suspension was used as the DNA template. Pyrosequencing analysis was performed, according to the manufacturer s instructions, on a PSQ 96ID system (Biotage, Inc., Qiagen). The protocol consisted
3 1184 HALSE ET AL. J. CLIN. MICROBIOL. of preparation of the single-stranded DNA with a vacuum preparation tool, annealing of the sequencing primers (primer rpobpyro-seq [5 -CCG CGA TCA AGG AGT-3 ] and primer rpobpyro-seq2 [5 -CGC TGT CGG GGT TGA-3 ]) at room temperature, and real-time sequencing with a pyrosequencer by use of a PSQ SQA reagent kit. The resultant sequences, reflected in the form of pyrograms, were compared against a library containing sequences of known mutations by means of the Identifire software. The specific nucleotide dispensation order strategy used for each sequencing reaction was as follows: for sequencing reaction 1, TCTCGACACAGCAGTCTGACGCATATCGATAGT ACGCAGACACACGCATGTCGTGAC3(CTAG)AGCGCGACTGTCAGTG CGCTGC, and for sequencing reaction 2, C3(TGAC)AGCGCGACTG3(TGA C)GCGC2(CTG). The specificity of the assay was determined by testing approximately 10 6 genome copies of DNA purified from potential respiratory pathogens and bacterial flora and included DNA from Bordetella pertussis, Chlamydophila pneumoniae, Escherichia coli, Haemophilus influenzae, Klebsiella pneumoniae, Legionella pneumophila, Mycobacterium kansasii, Mycoplasma pneumoniae, Neisseria meningitidis, Pseudomonas aeruginosa, Staphylococcus aureus, and Streptococcus pneumoniae. The strains were from either ATCC or the culture collection of the Wadsworth Center, NYSDOH. All bacterial strains from the Wadsworth Center used in the specificity panel underwent 16S rrna sequence analysis for confirmation of their identities. Validation of pyrosequencing analysis results for rpob gene mutation assessment. The pyrosequencing assay was validated with a panel of 60 M. tuberculosis isolates that included a total of 10 different previously identified rpob gene mutations, as well as wild-type rpob gene sequences. All strains had previously been analyzed by Sanger sequence analysis. Additionally, 148 MTBC real-time PCR-positive clinical received by our laboratory between 30 October 2007 and 9 July 2009 were analyzed by pyrosequencing of the rpob gene, and the results were compared to those of DST for RIF performed with the resulting MGIT liquid culture from the same specimen. The same set of clinical was also used to assess the sensitivity of the assay compared to the results of culture and microscopy to determine the utility of this assay for use as a direct test as part of a testing algorithm. Sanger DNA sequence analysis was carried out by the Applied Genomic Technologies Core Facility at the Wadsworth Center. RESULTS Sensitivity and specificity of MTBC real-time PCR assay. The analytical sensitivity of the MTBC real-time PCR assay was determined to be 0.05 CFU, the sensitivity with sputum was determined to be 0.5 CFU, and the efficiency of the assay was found to be 100%. The specificity of the assay was initially validated with MTBC and NTM reference cultures maintained at the Wadsworth Center. Thirty-seven samples of MTBC tested positive, and 50 strains of NTM and other bacteria found in respiratory tested negative, resulting in 100% specificity for the cohort (data not shown). Validation of MTBC real-time PCR for direct use with clinical. The results of our MTBC real-time PCR assay were compared to those of the amplified M. tuberculosis direct test (MTD; Gen-Probe, San Diego, CA), and before implementation, the sensitivity and specificity of the assay were found to be equivalent to those of MTD. However, our assay gave fewer inconclusive results; similar results have been found by others, when they compared the results of their assays to those of MTD (16, 20). We further evaluated the MTBC realtime PCR assay for use with routine clinical received between 11 October 2007 and 30 June After decontamination and concentration, the were tested in parallel by culture, microscopy, Ziehl-Neelsen staining for AFB, and the MTBC real-time PCR (Table 1). A total of 1,316 clinical were included in the evaluation, namely, 1,201 respiratory and 115 nonrespiratory. The MTBC real-time PCR assay result was in agreement with the culture result for 253 TABLE 1. Real-time PCR results for detection of MTBC in clinical a Specimen and direct microscopy and culture result (no. of ) No. of with the following real-time PCR result: Pos Neg Inconcl. Indet. Respiratory b AFB /C (229) 210 c AFB /C (38) AFB /C (40) AFB /C (912) Total (1,201) Nonrespiratory c AFB /C (14) AFB /C (5) AFB /C (9) AFB /C (87) Total (115) a Specimens were received between 11 October 2007 and 30 June Abbreviations: AFB, AFB positive; AFB, AFB negative; C, culture positive for MTBC; C, culture negative for MTBC; Pos, positive result; Neg, negative result; Inconcl., inconclusive result (result with a C T value that was high and not repeatable); Indet., indeterminate result (PCR inhibition). b Includes sputum, bronchoalveolar lavage, and bronchial wash. c Includes abscess, aspirate, cerebrospinal fluid, gastric, tissue, pleural fluid, wound, liver tissue, and lymph node. positive for MTBC and 1,038 negative for MTBC, or 98.1% agreement. A positive MTBC real-time PCR result was determined for one specimen that was culture negative and AFB negative. A negative real-time PCR result for MTBC was found for 17 that were culture positive (1 of these was AFB positive). To be sure that these 17 were not negative as a result of the IS6110 PCR target itself, we performed the MTBC real-time PCR assay with the liquid culture from these 17 to verify that the target was present and detectable. All 17 tested positive when the liquid culture was assessed. Additionally, the final culture plating results for these revealed that 6 had less than 10 colonies present on the plates and that the other 11 were negative on the plates but were positive by MGIT liquid culture, also indicating that the organism was present at a low level. The results for a total of three (0.2%) were reported to be indeterminate by MTBC real-time PCR, due to PCR inhibition, as determined by the internal inhibition control utilized in the MTBC real-time PCR assay. A total of seven (0.5%) were found to have an inconclusive result, with the C T value indicating that the concentration of DNA was at or near the analytical sensitivity of the assay. Detection of MTBC in respiratory and nonrespiratory. With culture applied as the gold standard and by the exclusion of samples with inconclusive and indeterminate molecular results, we calculated the sensitivity, specificity, and positive predictive value (PPV), and negative predictive value (NPV) for the MTBC real-time PCR assay (Table 2). The sensitivities for respiratory and nonrespiratory were 94.7% and 88.5%, respectively, and the specificities were 99.9% and 100.0%, respectively. PPV and NPV were 99.6% and 98.6%, respectively, for respiratory, and 100.0% and 96.9%, respectively, for nonrespiratory.
4 VOL. 48, 2010 REAL-TIME PCR AND PYROSEQUENCING OF M. TUBERCULOSIS 1185 TABLE 2. Performance characteristics of MTBC real-time PCR test compared to those of culture for respiratory, nonrespiratory, AFB-positive, and AFB-negative Parameter Respiratory Detection of MTBC between AFB-positive and AFB-negative. The sensitivities, specificities, PPVs, and NPVs for the real-time PCR assay were then calculated separately for AFB-positive (for which the results ranged from doubtful to numerous by microscopic observation) and AFBnegative (no AFB were seen by microscopic observation) (Table 2). The sensitivities, specificities, PPVs, and NPVs were 99.6%, 100.0%, 100.0%, and 97.7%, respectively, for AFB-positive and 75.4%, 99.9%, 98.0%, and 98.4%, respectively, for AFB-negative. Of 254 culture positive for NTM and not included in the data set described above, 241 were respiratory and 13 were nonrespiratory. A total of 247 of these were real-time PCR negative for MTBC, the results for 6 were inconclusive, and the result for 1 specimen was initially positive but the organism in the specimen was later identified as M. kansasii. In a second test of the latter specimen from the MGIT liquid culture, the MTBC real-time PCR was found to be negative. Validation of rpob gene analysis by pyrosequencing. Initial specificity testing indicated that the test was 100% specific for the detection of MTBC. To validate the rpob pyrosequencing assay, we tested 60 M. tuberculosis isolates retrospectively. This TABLE 3. Retrospective analysis of 60 M. tuberculosis isolates with known rpob gene sequence by rpob gene pyrosequencing rpob gene sequence (core 81-bp region) Nonrespiratory AFBpositive AFBnegative No. of isolates tested by Sanger and pyrosequencing Deletion... 2 Leu511Pro... 8 Gln513Glu... 2 Asp516Val... 5 His526Asp... 7 His526Tyr...14 His526Leu and Arg528Arg... 2 Arg528Arg (silent)... 4 Ser531Leu... 5 Leu533Pro... 4 Wild type... 7 All Sensitivity a (%) Specificity b (%) PPV c (%) NPV d (%) a Sensitivity was calculated as the number of true-positive with culture as the gold standard divided by the number of true-positive plus the number of false-negative (culture positive, PCR negative). b Specificity was calculated as the number of true-negative with culture as the gold standard divided by the number of true-negative plus the number of false-positive (culture negative, PCR positive). c PPV was calculated as the number of true-positive with culture as the gold standard divided by the number of true-positive plus the number of false-positive (culture negative, PCR positive). d NPV was calculated as the number of true-negative with culture as the gold standard divided by the number of true-negative plus the number of false-negative (culture positive, PCR negative). TABLE 4. rpob gene pyrosequencing results for detection of RIF resistance in 148 MTBC real-time PCR-positive clinical Direct microscopy and culture (no. of ) a No. of with the following pyrosequencing result: Wild type Mutation Inconclusive AFB /C (136) AFB /C (12) a AFB, AFB positive; AFB, AFB negative; C, culture positive for MTBC. set included isolates containing rpob gene point mutations, deletions, and the wild-type rpob gene sequence. Table 3 lists the rpob genotyping result obtained for these isolates by pyrosequencing analysis and Sanger sequence analysis. The results for all 60 isolates (100%) showed concordance between the two methods. A set of 148 MTBC real-time PCR-positive clinical received by our laboratory between 30 October 2007 and 9 July 2009 were tested by rpob gene pyrosequencing in parallel with culture, DST, and microscopy. To demonstrate the method s utility for the direct testing of clinical, a comparison of the results of rpob gene pyrosequencing to those of microscopy and culture is shown in Table 4. A total of 136 AFB-positive and MTBC culture-positive and 12 AFB-negative and MTBC culture-positive were examined. The wild-type rpob sequence was found in 140 of the (131 AFBpositive and 9 AFB-negative ), and an rpob gene point mutation was found in 3 (2 AFB-positive and 1 AFB-negative specimen). Overall, the results for five (three AFB-positive and two AFB-negative ) were found to be inconclusive; thus, this assay provided adequate sensitivity for 97.8% of the AFB-positive and 83.3% of the AFB-negative tested. In an additional comparison of this specimen group (Table 5), the results obtained by the gold standard assay, conventional DST for RIF in liquid culture, were compared to those of rpob gene pyrosequencing analysis directly with the clinical specimen. In this comparison, the isolates in 139 were found to be RIF susceptible and to have a wild-type rpob gene sequence. The isolates in two of the were RIF resistant, and an rpob gene point mutation was identified in the 81-bp region. The isolate in one specimen that was determined to be RIF susceptible had the rpob gene point mutation Asp516Tyr. No mutation was identified in the 81-bp region of TABLE 5. Comparison of conventional RIF DST to rpob gene pyrosequencing for 143 clinical a No. of Conventional RIF DST result Result of pyrosequencing of rpob 139 S Wild type (S) 2 R Mutation (R) 1 S Mutation (R) b 1 R Wild type (S) c a The data are for the same set of used to obtain the data presented in Table 4, but the five with inconclusive pyrosequencing results were excluded from this analysis. S, susceptible; R, resistant. b Asp516Tyr mutation with known poor predictive value. c Mutation determined to be within the rpob gene outside of the 81-bp region, Val176Phe.
5 1186 HALSE ET AL. J. CLIN. MICROBIOL. FIG. 1. Algorithm for integration of the molecular methods used for the direct testing for M. tuberculosis into an existing testing scheme. the rpob gene in the isolate in another specimen that was found to be RIF resistant. However, the isolate in this specimen was later determined to have an upstream rpob mutation (Val176Phe) outside of the 81-bp region of the rpob gene. Excluded from the analysis were five for which inconclusive pyrosequencing results had been obtained; the isolates in these were later determined to be RIF susceptible by DST. Overall, this testing revealed that 141 of 143 (98.6%) had concordant results. Algorithm for incorporation of direct testing of M. tuberculosis by molecular methods. As a result of the validation testing performed by our laboratory, we propose an algorithm for the integration of these tests into the work flow of testing for M. tuberculosis. Figure 1 illustrates a strategy that incorporates the MTBC real-time PCR on day 1 of testing, followed by rpob pyrosequencing on day 2. Culture plating, MGIT liquid culture, and microscopy are performed in parallel. For many, the use of this algorithm allows initial reports for the presence of MTBC and the results of rpob analysis directly with clinical to be released on day 1 or day 2 of testing, followed by additional culture and molecular testing for confirmation. DISCUSSION This report describes the development of a highly sensitive and specific real-time PCR assay for the rapid identification of MTBC, combined with an rpob gene pyrosequencing assay for the rapid assessment of RIF resistance, for utilization directly with clinical. As shown in Fig. 1, the assay pair allows the preliminary reporting of MTBC by direct detection in 24 h and the preliminary reporting of the results of rpob gene mutation analysis, which shows a strong correlation to RIF resistance, within 48 h of receipt of the clinical specimen. This approach provides a significant improvement in efficiency and accuracy over those of previous testing methods and offers patient and public health benefits that include facilitation of the detection of new cases of tuberculosis and cases of MDR TB and facilitation of strategies for treatment and infection control. The first assay of the pair, the MTBC real-time PCR assay, was evaluated with 1,316 routine clinical received for which the microscopy, culture, and MTBC real-time PCR results were compared. With culture considered the gold standard, the sensitivities, specificities, PPVs, and NPVs of the MTBC real-time PCR assay were calculated for respiratory, nonrespiratory, AFB-positive, and AFB-negative. This type of analysis, which entails the use of a real-time PCR assay directly with decontaminated clinical, is rare in the literature, and our study was performed with the largest cohort of samples analyzed by such methods to date. We found the sensitivity of the assay to be the highest for respiratory (94.7%) and AFB-positive (99.6%), as would be expected. However, we achieved good sensitivity with both nonrespiratory (88.5%) and AFB-negative (75.4%). Of importance, during this analysis we did not find any culture-positive MTBC for which IS6110 was absent, although this rare occurrence has been documented (1, 7). Overall, the assay yielded 18 discrepancies among the 1,316
6 VOL. 48, 2010 REAL-TIME PCR AND PYROSEQUENCING OF M. TUBERCULOSIS 1187 tested; 1 of these was MTBC real-time PCR positive and MTBC culture negative. This specimen had a reproducible C T above 37. The fact that the MTBC real-time PCR assay can detect DNA from nonviable as well as viable organisms may have been a factor, the patient could have been latently infected, or a technical error may have been the cause. No additional were received from this patient. The assessment of this MTBC real-time PCR assay also yielded 17 false-negative results (MTBC real time PCR negative, MTBC culture positive), which represented 1.3% of the tested; 16 of these were AFB negative and 1 was AFB positive. As described in the Results, these had the IS6110 target when the liquid culture was assessed, so this appeared to be due to the sensitivity of the assay. The culture plates either were negative or contained less than 10 colonies when they were observed. According to our protocol, 100 l of the processed specimen is plated and only 5 l of the same specimen is added to the MTBC real-time PCR assay mixture, once the heat treatment has been completed. If 10 colonies were present in 100 l, 0.5 colonies would be added to the PCR mixture, which would be just below the limit of detection of this assay. Additionally, seven (0.5%) were found to have inconclusive real-time PCR results: a C T value of 37 was detected, but the result was not reproducible when the specimen was retested. Finally, three (0.2%) were found to have indeterminate results (i.e., PCR inhibition was present). As a result of this analysis, we assess the data from our MTBC realtime PCR assay to be similar to or better than published data for other assays that have targeted the IS6110 insertion sequence (5, 8, 9, 14, 16, 19, 20). Importantly, we demonstrate that our in-house MTBC realtime PCR assay can effectively detect mycobacteria in challenging extrarespiratory and AFB-negative samples: relative to the findings obtained by a previously published assay (16), our assay shows superior sensitivity and comparable specificity. Utilization of microscopy for 46 that were AFB negative but positive by MTBC real-time PCR and/or culture led us to believe that the AFB smear, which is not specific to MTBC (14, 15), may not provide any added diagnostic benefit to the patient, once direct molecular testing has been incorporated into the testing scheme. Further work on the relationship between the results of diagnostic testing methods and the infectiousness of patients needs to be accomplished. We also found the MTBC real-time PCR to be an effective tool for the differentiation of containing MTBC from containing NTM. Among the 254 in which NTM was confirmed to have been identified, all but 1 specimen was found to be negative by the MTBC real-time PCR assay. The remaining specimen, reported to contain M. kansasii, was positive for MTBC DNA when the initial specimen was tested, but it was negative when a sample from liquid culture was later tested. This specimen could have been contaminated, it could initially have contained MTBC DNA, or it could have contained a mixed culture in which M. kansasii outgrew MTBC. One point of note is that 15 M. kansasiipositive tested MTBC real-time PCR negative during the time period spanned by the testing. For the specimen in question, the sample from the MGIT liquid culture was found to be MTBC real-time PCR negative, and culture and molecular methods were positive for M. kansasii; that combination of results indicates that the particular strain of M. kansasii does not represent a specificity issue for the MTBC real-time PCR assay. However, the example demonstrates the value of the utilization of an overall approach that entails both molecular and culture-based methods. Validation of the second assay of our pair, the rpob pyrosequencing assay, directly with clinical identified by real-time PCR to contain MTBC was also successful. In total, the isolates in 143 of the 148 (96.6%) were correctly identified by direct pyrosequencing analysis. The results for five were inconclusive by rpob pyrosequencing; the MTBC real-time PCR results for these showed C T values of between 31 and 36, and AFB smear testing gave a result of none or rare. The inconclusive results, indicating that rpob pyrosequencing could not be performed, may be explained on the basis of the fact that the latter assay has a slightly lower sensitivity than the preceding MTBC real-time PCR assay. Our specimen testing also compared the results of rpob gene pyrosequencing analysis obtained by direct use of the clinical specimen and the results of DST with the resulting liquid culture. The testing determined that the results of rpob gene pyrosequencing analysis obtained by direct use of the clinical specimen had 98.6% (141/143 ) concordance with the results of DST for this cohort. The two for which the results of DST and rpob pyrosequencing did not agree included one specimen containing an isolate that was RIF susceptible, and the mutation was confirmed to be Asp516Tyr. This mutation has been observed previously and is believed to have a low predictive value for RIF resistance, but its presence should nevertheless be noted (23). The isolate in the other specimen was found to be RIF resistant, but no mutation in the 81-bp region of rpob gene was identified. Further testing detected a rare mutation lying outside of the 81-bp region, Val176Phe. Again, this caveat should be borne in mind; the 81-bp region that is utilized in our assay is believed to predict 96% of cases of RIF resistance, but the remaining cases will be missed. It is for this reason that only results for which mutations are determined are reported immediately and results indicating the presence of the wild-type sequence require conventional DST before a report may be released. Of note, the two rpob mutations that were initially detected by pyrosequencing were reported in 48 h, thus providing critical treatment information before the confirmatory RIF-resistant DST result was reported 3 weeks later. As a result of the present evaluation and a previous comparison to the MTD assay, our laboratory has now adopted the MTBC real-time PCR and rpob gene pyrosequencing assays for the rapid detection of MTBC and drug resistance for use in routine testing. Furthermore, the real-time PCR assay proved effective for nonrespiratory and AFB-negative samples. From an institutional point of view, the lower cost ( $11.00 for real-time PCR with inhibition assessment and $1.00 for pyrosequencing analysis of the rpob gene), the short turnaround time ( 24 h and 48 h for the two assays, respectively), and the minimal hands-on time required for the assays will help to ensure that an adequate testing capacity is available as the demand for the rapid identification of MTBC-infected individuals continues to increase.
7 1188 HALSE ET AL. J. CLIN. MICROBIOL. ACKNOWLEDGMENTS We acknowledge the Wadsworth Center Applied Genomic Technologies Core Facility for Sanger DNA sequencing and Adriana Verschoor, Keith Derbyshire, and Ronald Limberger for critical reading of the manuscript. Jeff Driscoll, Michael McGarry, Jeremy Rivenburg, Elizabeth Nazarian, and Danielle Wroblewski are thanked for their technical contributions. REFERENCES 1. Agasino, C. B., A. Ponce de Leon, R. M. Jasmer, and P. M. Small Epidemiology of Mycobacterium tuberculosis strains in San Francisco that do not contain IS6110. Int. J. Tuber. Lung Dis. 2: Anonymous Updated guidelines for the use of nucleic acid amplification tests in the diagnosis of tuberculosis. MMWR Morb. Mortal. Wkly. Rep. 58: Arnold, C., L. Westland, G. Mowat, A. Underwood, J. Magee, and S. Gharbia Single-nucleotide polymorphism-based differentiation and drug resistance detection in Mycobacterium tuberculosis from isolates or directly from sputum. Clin. Microbiol. Infect. 11: Broccolo, F., P. Scarpellini, G. Locatelli, A. Zingale, A. M. Brambilla, P. Cichero, L. A. Sechi, A. Lazzarin, P. Lusso, and M. S. Malnati Rapid diagnosis of mycobacterial infections and quantitation of Mycobacterium tuberculosis load by two real-time calibrated PCR assays. J. Clin. Microbiol. 41: Cleary, T. J., G. Roudel, O. Casillas, and N. Miller Rapid and specific detection of Mycobacterium tuberculosis by using the Smart Cycler instrument and a specific fluorogenic probe. J. Clin. Microbiol. 41: Corbett, E. L., C. J. Watt, N. Walker, D. Maher, B. G. Williams, M. C. Raviglione, and C. Dye The growing burden of tuberculosis: global trends and interactions with the HIV epidemic. Arch. Intern. Med. 163: Das, S., C. N. Paramasivan, D. B. Lowrie, R. Prabhakar, and P. R. Narayanan IS6110 restriction fragment length polymorphism typing of clinical isolates of Mycobacterium tuberculosis from patients with pulmonary tuberculosis in Madras, south India. Tuber. Lung Dis. 76: Desjardin, L. E., Y. Chen, M. D. Perkins, L. Teixeira, M. D. Cave, and K. D. Eisenach Comparison of the ABI 7700 system (TaqMan) and competitive PCR for quantification of IS6110 DNA in sputum during treatment of tuberculosis. J. Clin. Microbiol. 36: Drouillon, V., P. H. Lagrange, and J. L. Herrmann Molecular diagnosis of pulmonary tuberculosis by automated extraction and real-time PCR on non-decontaminated pulmonary. Eur. J. Clin. Microbiol. Infect. Dis. 26: Foongladda, S., S. Pholwat, B. Eampokalap, P. Kiratisin, and R. Sutthent Multi-probe real-time PCR identification of common Mycobacterium species in blood culture broth. J. Mol. Diagn. 11: Frieden, T. R., and C. R. Driver Tuberculosis control: past 10 years and future progress. Tuberculosis (Edinb.) 83: Gopinath, K., and S. Singh Multiplex PCR assay for simultaneous detection and differentiation of Mycobacterium tuberculosis, Mycobacterium avium complexes and other mycobacterial species directly from clinical. J. Appl. Microbiol. 107: Jureen, P., L. Engstrand, S. Eriksson, A. Alderborn, M. Krabbe, and S. E. Hoffner Rapid detection of rifampin resistance in Mycobacterium tuberculosis by pyrosequencing technology. J. Clin. Microbiol. 44: Kibiki, G. S., B. Mulder, A. J. van der Ven, N. Sam, M. J. Boeree, A. van der Zanden, and W. M. Dolmans Laboratory diagnosis of pulmonary tuberculosis in TB and HIV endemic settings and the contribution of real time PCR for M. tuberculosis in bronchoalveolar lavage fluid. Trop. Med. Int. Health 12: Kim, T. C., R. S. Blackman, K. M. Heatwole, T. Kim, and D. F. Rochester Acid-fast bacilli in sputum smears of patients with pulmonary tuberculosis. Prevalence and significance of negative smears pretreatment and positive smears post-treatment. Am. Rev. Respir. Dis. 129: Lemaitre, N., S. Armand, A. Vachee, O. Capilliez, C. Dumoulin, and R. J. Courcol Comparison of the real-time PCR method and the Gen-Probe amplified Mycobacterium tuberculosis direct test for detection of Mycobacterium tuberculosis in pulmonary and nonpulmonary. J. Clin. Microbiol. 42: Marttila, H. J., J. Makinen, M. Marjamaki, and H. Soini Prospective evaluation of pyrosequencing for the rapid detection of isoniazid and rifampin resistance in clinical Mycobacterium tuberculosis isolates. Eur. J. Clin. Microbiol. Infect. Dis. 28: Musser, J. M Antimicrobial agent resistance in mycobacteria: molecular genetic insights. Clin. Microbiol. Rev. 8: Palomino, J. C Newer diagnostics for tuberculosis and multi-drug resistant tuberculosis. Curr. Opin. Pulm. Med. 12: Pounder, J. I., W. K. Aldous, and G. L. Woods Comparison of realtime polymerase chain reaction using the Smart Cycler and the Gen-Probe amplified Mycobacterium tuberculosis direct test for detection of M. tuberculosis complex in clinical. Diagn. Microbiol. Infect. Dis. 54: Richardson, E. T., D. Samson, and N. Banaei Rapid identification of Mycobacterium tuberculosis and nontuberculous mycobacteria by multiplex, real-time PCR. J. Clin. Microbiol. 47: Savelkoul, P. H., A. Catsburg, S. Mulder, L. Oostendorp, J. Schirm, H. Wilke, A. G. van der Zanden, and G. T. Noordhoek Detection of Mycobacterium tuberculosis complex with real time PCR: comparison of different primer-probe sets based on the IS6110 element. J. Microbiol. Methods 66: Van Deun, A., L. Barrera, I. Bastian, L. Fattorini, H. Hoffmann, K. M. Kam, L. Rigouts, S. Rusch-Gerdes, and A. Wright Mycobacterium tuberculosis strains with highly discordant rifampin susceptibility test results. J. Clin. Microbiol. 47: World Health Organization and Global Tuberculosis Programme. Global tuberculosis control: WHO report, p. v. Global Tuberculosis Programme, World Health Organization, Geneva, Switzerland. 25. Zhao, J. R., Y. J. Bai, Q. H. Zhang, Y. Wang, M. Luo, and X. J. Yan Pyrosequencing-based approach for rapid detection of rifampin-resistant Mycobacterium tuberculosis. Diagn. Microbiol. Infect. Dis. 51:
TB Updates for the Physician Rochester, Minnesota June 19, 2009
 TB Updates for the Physician Rochester, Minnesota June 19, 2009 Mycobacterial Laboratory Science Update Nancy L. Wengenack, Ph.D. Associate Professor of Laboratory Medicine and Pathology Division of Clinical
TB Updates for the Physician Rochester, Minnesota June 19, 2009 Mycobacterial Laboratory Science Update Nancy L. Wengenack, Ph.D. Associate Professor of Laboratory Medicine and Pathology Division of Clinical
TB 101 Disease, Clinical Assessment and Lab Testing
 TB 101 Disease, Clinical Assessment and Lab Testing Pacific Islands Tuberculosis Controllers Association Conference (PITCA) Clinical Laboratory Breakout None Disclosure Objectives Be able to list and explain
TB 101 Disease, Clinical Assessment and Lab Testing Pacific Islands Tuberculosis Controllers Association Conference (PITCA) Clinical Laboratory Breakout None Disclosure Objectives Be able to list and explain
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Sherman SI, Wirth LJ, Droz J-P, et al. Motesanib diphosphate
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Sherman SI, Wirth LJ, Droz J-P, et al. Motesanib diphosphate
TB Laboratory for Nurses
 TB Laboratory for Nurses Shea Rabley, RN, MN Consultant Mayo Clinic Center for Tuberculosis 2014 MFMER slide-1 Disclosures None 2014 MFMER slide-2 Objectives Participants will be able to: 1. Name 2 safety
TB Laboratory for Nurses Shea Rabley, RN, MN Consultant Mayo Clinic Center for Tuberculosis 2014 MFMER slide-1 Disclosures None 2014 MFMER slide-2 Objectives Participants will be able to: 1. Name 2 safety
CDPH - CTCA Joint Guidelines Guideline for Micobacteriology Services In California
 CDPH - CTCA Joint Guidelines Guideline for Micobacteriology Services In California These guidelines are intended to be used as an educational aid to help clinicians make informed decisions about patient
CDPH - CTCA Joint Guidelines Guideline for Micobacteriology Services In California These guidelines are intended to be used as an educational aid to help clinicians make informed decisions about patient
TB NAAT testing at the Los Angeles County Public Health Laboratory
 TB NAAT testing at the Los Angeles County Public Health Laboratory Hector Rivas Public Health Microbiology Supervisor II Los Angeles County Public Health Laboratory hrivas@ph.lacounty.gov April 2012 1
TB NAAT testing at the Los Angeles County Public Health Laboratory Hector Rivas Public Health Microbiology Supervisor II Los Angeles County Public Health Laboratory hrivas@ph.lacounty.gov April 2012 1
Ken Jost, BA, has the following disclosures to make:
 Diagnosis of TB Disease: Laboratory Ken Jost, BA May 10, 2017 TB Intensive May 9-12, 2017 San Antonio, TX EXCELLENCE EXPERTISE INNOVATION Ken Jost, BA, has the following disclosures to make: No conflict
Diagnosis of TB Disease: Laboratory Ken Jost, BA May 10, 2017 TB Intensive May 9-12, 2017 San Antonio, TX EXCELLENCE EXPERTISE INNOVATION Ken Jost, BA, has the following disclosures to make: No conflict
Microbiological Pathology, Sefako Makgatho Health Science University, Pretoria, South Africa 2
 The Incidence of discordant Rifampicin susceptibility results between genotypic and phenotypic methods in Mycobacterium tuberculosis complex isolates at Dr George Mukhari Hospital Tertiary Laboratory,
The Incidence of discordant Rifampicin susceptibility results between genotypic and phenotypic methods in Mycobacterium tuberculosis complex isolates at Dr George Mukhari Hospital Tertiary Laboratory,
Overview of Mycobacterial Culture, Identification, and Drug Susceptibility Testing
 Overview of Mycobacterial Culture, Identification, and Drug Susceptibility Testing 1. Essentials for the Mycobacteriology Laboratory: Promoting Quality Practices 1.1 Overview: Mycobacterial Culture, Identification,
Overview of Mycobacterial Culture, Identification, and Drug Susceptibility Testing 1. Essentials for the Mycobacteriology Laboratory: Promoting Quality Practices 1.1 Overview: Mycobacterial Culture, Identification,
Diagnosis of TB: Laboratory Ken Jost Tuesday April 1, 2014
 TB Nurse Case Management San Antonio, Texas April 1 3, 2014 Diagnosis of TB: Laboratory Ken Jost Tuesday April 1, 2014 Ken Jost, BA has the following disclosures to make: No conflict of interests No relevant
TB Nurse Case Management San Antonio, Texas April 1 3, 2014 Diagnosis of TB: Laboratory Ken Jost Tuesday April 1, 2014 Ken Jost, BA has the following disclosures to make: No conflict of interests No relevant
Nucleic Acid Amplification Testing for the Diagnosis of TB
 Roche Nucleic Acid Amplification Testing for the Diagnosis of TB David Warshauer, PhD Deputy Director, Communicable Diseases Wisconsin State Laboratory of Hygiene 19 th /20 th Century Traditional Algorithm
Roche Nucleic Acid Amplification Testing for the Diagnosis of TB David Warshauer, PhD Deputy Director, Communicable Diseases Wisconsin State Laboratory of Hygiene 19 th /20 th Century Traditional Algorithm
TB Intensive San Antonio, Texas November 11 14, 2014
 TB Intensive San Antonio, Texas November 11 14, 2014 Diagnosis of TB: Laboratory Ken Jost, BA November 12, 2014 Ken Jost, BA has the following disclosures to make: No conflict of interests No relevant
TB Intensive San Antonio, Texas November 11 14, 2014 Diagnosis of TB: Laboratory Ken Jost, BA November 12, 2014 Ken Jost, BA has the following disclosures to make: No conflict of interests No relevant
Harmonizing the Use of Molecular & Culture-based DST of Mycobacterium tuberculosis
 Harmonizing the Use of Molecular & Culture-based DST of Mycobacterium tuberculosis Grace Lin, MS. Research Scientist grace.lin@cdph.ca.gov APHL 8 th TB Lab Conference San Diego 8-19-13 Harmonizing? There
Harmonizing the Use of Molecular & Culture-based DST of Mycobacterium tuberculosis Grace Lin, MS. Research Scientist grace.lin@cdph.ca.gov APHL 8 th TB Lab Conference San Diego 8-19-13 Harmonizing? There
Diagnosis of TB: Laboratory Ken Jost Tuesday April 9, 2013
 TB Nurse Case Management San Antonio, Texas April 9-11, 2013 Diagnosis of TB: Laboratory Ken Jost Tuesday April 9, 2013 Ken Jost has the following disclosures to make: No conflict of interests No relevant
TB Nurse Case Management San Antonio, Texas April 9-11, 2013 Diagnosis of TB: Laboratory Ken Jost Tuesday April 9, 2013 Ken Jost has the following disclosures to make: No conflict of interests No relevant
Evaluation of a Single-Tube Multiplex Real-Time PCR for Differentiation of Members of the Mycobacterium tuberculosis Complex in Clinical Specimens
 JOUNAL O CLINICAL MICOBIOLOGY, July 2011, p. 2562 2567 Vol. 49, No. 7 0095-1137/11/$12.00 doi:10.1128/jcm.00467-11 Copyright 2011, American Society for Microbiology. All ights eserved. Evaluation of a
JOUNAL O CLINICAL MICOBIOLOGY, July 2011, p. 2562 2567 Vol. 49, No. 7 0095-1137/11/$12.00 doi:10.1128/jcm.00467-11 Copyright 2011, American Society for Microbiology. All ights eserved. Evaluation of a
AFB Identification Texas Approach
 AFB Identification Texas Approach Ken Jost Texas Department of State Health Services 6th National Conference on Laboratory Aspects of TB June 21, 2010 DSHS-Austin TB Lab Customers & Samples Year 2009 175
AFB Identification Texas Approach Ken Jost Texas Department of State Health Services 6th National Conference on Laboratory Aspects of TB June 21, 2010 DSHS-Austin TB Lab Customers & Samples Year 2009 175
NAAT in the Clinical Laboratory and Impact on Infection Control 9 th National Conference on Laboratory Aspects of Tuberculosis APHL
 NAAT in the Clinical Laboratory and Impact on Infection Control 9 th National Conference on Laboratory Aspects of Tuberculosis APHL Susan Novak-Weekley, S(M), ASCP, Ph.D., D(ABMM) Director of Microbiology,
NAAT in the Clinical Laboratory and Impact on Infection Control 9 th National Conference on Laboratory Aspects of Tuberculosis APHL Susan Novak-Weekley, S(M), ASCP, Ph.D., D(ABMM) Director of Microbiology,
MYCOBACTERIOLOGY SERVICE MANUAL
 MYCOBACTERIOLOGY SERVICE MANUAL The Office of Laboratory Services (OLS) provides primary isolation and identification of Mycobacterium species in human diagnostic specimens. Reference specimens of AFB
MYCOBACTERIOLOGY SERVICE MANUAL The Office of Laboratory Services (OLS) provides primary isolation and identification of Mycobacterium species in human diagnostic specimens. Reference specimens of AFB
Supplementary Table 3. 3 UTR primer sequences. Primer sequences used to amplify and clone the 3 UTR of each indicated gene are listed.
 Supplemental Figure 1. DLKI-DIO3 mirna/mrna complementarity. Complementarity between the indicated DLK1-DIO3 cluster mirnas and the UTR of SOX2, SOX9, HIF1A, ZEB1, ZEB2, STAT3 and CDH1with mirsvr and PhastCons
Supplemental Figure 1. DLKI-DIO3 mirna/mrna complementarity. Complementarity between the indicated DLK1-DIO3 cluster mirnas and the UTR of SOX2, SOX9, HIF1A, ZEB1, ZEB2, STAT3 and CDH1with mirsvr and PhastCons
c Tuj1(-) apoptotic live 1 DIV 2 DIV 1 DIV 2 DIV Tuj1(+) Tuj1/GFP/DAPI Tuj1 DAPI GFP
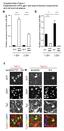 Supplementary Figure 1 Establishment of the gain- and loss-of-function experiments and cell survival assays. a Relative expression of mature mir-484 30 20 10 0 **** **** NCP mir- 484P NCP mir- 484P b Relative
Supplementary Figure 1 Establishment of the gain- and loss-of-function experiments and cell survival assays. a Relative expression of mature mir-484 30 20 10 0 **** **** NCP mir- 484P NCP mir- 484P b Relative
Microscopic Morphology in Smears Prepared from MGIT Broth Medium for Rapid Presumptive Identification of Mycobacterium tuberculosis
 Annals of Clinical & Laboratory Science, vol. 33, no. 2, 2003 179 Microscopic Morphology in Smears Prepared from MGIT Broth Medium for Rapid Presumptive Identification of Mycobacterium tuberculosis complex,
Annals of Clinical & Laboratory Science, vol. 33, no. 2, 2003 179 Microscopic Morphology in Smears Prepared from MGIT Broth Medium for Rapid Presumptive Identification of Mycobacterium tuberculosis complex,
Rapid differentiation of mycobacterium tuberculosis and mycobacterium leprae from sputum by polymerase chain reaction
 Original Article Nepal Medical College Journal 27; 9(1): Rapid differentiation of mycobacterium tuberculosis and mycobacterium leprae from sputum by polymerase chain reaction Bishwa Raj Sapkota, Chaman
Original Article Nepal Medical College Journal 27; 9(1): Rapid differentiation of mycobacterium tuberculosis and mycobacterium leprae from sputum by polymerase chain reaction Bishwa Raj Sapkota, Chaman
Table S1. Oligonucleotides used for the in-house RT-PCR assays targeting the M, H7 or N9. Assay (s) Target Name Sequence (5 3 ) Comments
 SUPPLEMENTAL INFORMATION 2 3 Table S. Oligonucleotides used for the in-house RT-PCR assays targeting the M, H7 or N9 genes. Assay (s) Target Name Sequence (5 3 ) Comments CDC M InfA Forward (NS), CDC M
SUPPLEMENTAL INFORMATION 2 3 Table S. Oligonucleotides used for the in-house RT-PCR assays targeting the M, H7 or N9 genes. Assay (s) Target Name Sequence (5 3 ) Comments CDC M InfA Forward (NS), CDC M
Evaluation of the Rapid MGIT TBc Identification Test for Culture Confirmation of Mycobacterium tuberculosis Complex Strain Detection
 JOURNAL OF CLINICAL MICROBIOLOGY, Mar. 2011, p. 802 807 Vol. 49, No. 3 0095-1137/11/$12.00 doi:10.1128/jcm.02243-10 Copyright 2011, American Society for Microbiology. All Rights Reserved. Evaluation of
JOURNAL OF CLINICAL MICROBIOLOGY, Mar. 2011, p. 802 807 Vol. 49, No. 3 0095-1137/11/$12.00 doi:10.1128/jcm.02243-10 Copyright 2011, American Society for Microbiology. All Rights Reserved. Evaluation of
MIC = Many Inherent Challenges Sensititre MIC for Antimicrobial Susceptibility Testing of Mycobacterium tuberculosis complex
 MIC = Many Inherent Challenges Sensititre MIC for Antimicrobial Susceptibility Testing of Mycobacterium tuberculosis complex Marie Claire Rowlinson, PhD D(ABMM) Florida Bureau of Public Health Laboratories
MIC = Many Inherent Challenges Sensititre MIC for Antimicrobial Susceptibility Testing of Mycobacterium tuberculosis complex Marie Claire Rowlinson, PhD D(ABMM) Florida Bureau of Public Health Laboratories
TB/HIV 2 sides of the same coin. Dr. Shamma Shetye, MD Microbiology Metropolis Healthcare, Mumbai
 TB/HIV 2 sides of the same coin Dr. Shamma Shetye, MD Microbiology Metropolis Healthcare, Mumbai Global- Tb new cases Diagnosis-Microscopy ZN,Flourescent microscopy(fm) Rapid, inexpensive test Specificity>95%
TB/HIV 2 sides of the same coin Dr. Shamma Shetye, MD Microbiology Metropolis Healthcare, Mumbai Global- Tb new cases Diagnosis-Microscopy ZN,Flourescent microscopy(fm) Rapid, inexpensive test Specificity>95%
Mycobacterial cell wall. Cell Cycle Lengths. Outline of Laboratory Methods. Laboratory Methods
 Laboratory Methods Cell Cycle Lengths Generation time (hrs) Days needed for 26 generations (colony) E. coli 0.33 0.36 Nancy Connell, PhD Professor, nfectious Disease Department of Medicine Center for Emerging
Laboratory Methods Cell Cycle Lengths Generation time (hrs) Days needed for 26 generations (colony) E. coli 0.33 0.36 Nancy Connell, PhD Professor, nfectious Disease Department of Medicine Center for Emerging
Supplemental Data. Shin et al. Plant Cell. (2012) /tpc YFP N
 MYC YFP N PIF5 YFP C N-TIC TIC Supplemental Data. Shin et al. Plant Cell. ()..5/tpc..95 Supplemental Figure. TIC interacts with MYC in the nucleus. Bimolecular fluorescence complementation assay using
MYC YFP N PIF5 YFP C N-TIC TIC Supplemental Data. Shin et al. Plant Cell. ()..5/tpc..95 Supplemental Figure. TIC interacts with MYC in the nucleus. Bimolecular fluorescence complementation assay using
Stacy White, PhD May 12, TB for Community Providers. Phoenix, Arizona
 Role of the Laboratory in TB Diagnosis Stacy White, PhD May 12, 2015 TB for Community Providers May 12, 2015 Phoenix, Arizona EXCELLENCE EXPERTISE INNOVATION Stacy White, PhD has the following disclosures
Role of the Laboratory in TB Diagnosis Stacy White, PhD May 12, 2015 TB for Community Providers May 12, 2015 Phoenix, Arizona EXCELLENCE EXPERTISE INNOVATION Stacy White, PhD has the following disclosures
Abbreviations: P- paraffin-embedded section; C, cryosection; Bio-SA, biotin-streptavidin-conjugated fluorescein amplification.
 Supplementary Table 1. Sequence of primers for real time PCR. Gene Forward primer Reverse primer S25 5 -GTG GTC CAC ACT ACT CTC TGA GTT TC-3 5 - GAC TTT CCG GCA TCC TTC TTC-3 Mafa cds 5 -CTT CAG CAA GGA
Supplementary Table 1. Sequence of primers for real time PCR. Gene Forward primer Reverse primer S25 5 -GTG GTC CAC ACT ACT CTC TGA GTT TC-3 5 - GAC TTT CCG GCA TCC TTC TTC-3 Mafa cds 5 -CTT CAG CAA GGA
Supplementary Document
 Supplementary Document 1. Supplementary Table legends 2. Supplementary Figure legends 3. Supplementary Tables 4. Supplementary Figures 5. Supplementary References 1. Supplementary Table legends Suppl.
Supplementary Document 1. Supplementary Table legends 2. Supplementary Figure legends 3. Supplementary Tables 4. Supplementary Figures 5. Supplementary References 1. Supplementary Table legends Suppl.
WSLH Testing and Surveillance Updates
 WSLH Testing and Surveillance Updates Wisconsin Mycobacteriology Laboratory Network annual conference November 4, 2015, Madison, WI Updates Outline Collection and Transport Smear and Culture Nucleic Acid
WSLH Testing and Surveillance Updates Wisconsin Mycobacteriology Laboratory Network annual conference November 4, 2015, Madison, WI Updates Outline Collection and Transport Smear and Culture Nucleic Acid
Culture Density (OD600) 0.1. Culture Density (OD600) Culture Density (OD600) Culture Density (OD600) Culture Density (OD600)
 A. B. C. D. E. PA JSRI JSRI 2 PA DSAM DSAM 2 DSAM 3 PA LNAP LNAP 2 LNAP 3 PAO Fcor Fcor 2 Fcor 3 PAO Wtho Wtho 2 Wtho 3 Wtho 4 DTSB Low Iron 2 4 6 8 2 4 6 8 2 22 DTSB Low Iron 2 4 6 8 2 4 6 8 2 22 DTSB
A. B. C. D. E. PA JSRI JSRI 2 PA DSAM DSAM 2 DSAM 3 PA LNAP LNAP 2 LNAP 3 PAO Fcor Fcor 2 Fcor 3 PAO Wtho Wtho 2 Wtho 3 Wtho 4 DTSB Low Iron 2 4 6 8 2 4 6 8 2 22 DTSB Low Iron 2 4 6 8 2 4 6 8 2 22 DTSB
Receipt within 1 day of specimen collection. Report AFB b smear result within 1 day from receipt of specimen
 Recommendation Promote rapid delivery of specimens to the laboratory Use fluorescent acid-fast staining and promptly transmit results by phone, FAX, or electronically Identify growth as acid-fast and use
Recommendation Promote rapid delivery of specimens to the laboratory Use fluorescent acid-fast staining and promptly transmit results by phone, FAX, or electronically Identify growth as acid-fast and use
Diagnosis of Tuberculosis by GeneXpert MTB/RIF Assay Technology: A Short Review
 International Journal of Advanced Microbiology and Health Research www.ijamhr.com Volume 1; Issue 1; September 2017; Page No. 20-24 Review Article Diagnosis of Tuberculosis by GeneXpert MTB/RIF Assay Technology:
International Journal of Advanced Microbiology and Health Research www.ijamhr.com Volume 1; Issue 1; September 2017; Page No. 20-24 Review Article Diagnosis of Tuberculosis by GeneXpert MTB/RIF Assay Technology:
A retrospective evaluation study of diagnostic accuracy of Xpert MTB/RIF assay, used for detection of Mycobacterium tuberculosis in Greece
 Örebro University School of Health and Medical Science Biomedical Laboratory Science Programme 180 credits Degree project in biomedical laboratory science, advanced course, 15 credits May 21, 2015 A retrospective
Örebro University School of Health and Medical Science Biomedical Laboratory Science Programme 180 credits Degree project in biomedical laboratory science, advanced course, 15 credits May 21, 2015 A retrospective
WELCOME. Lab Talk: What a Nurse Hears. April 18, NTNC Annual Meeting Lab Talk: What a Nurse Hears
 Lab Talk: What a Lab Talk: What a Max Salfinger, MD, FIDSA, FAAM Executive Director, Advanced Diagnostic Laboratories Laboratory Director, Mycobacteriology & Pharmacokinetics National Jewish Health Lisa
Lab Talk: What a Lab Talk: What a Max Salfinger, MD, FIDSA, FAAM Executive Director, Advanced Diagnostic Laboratories Laboratory Director, Mycobacteriology & Pharmacokinetics National Jewish Health Lisa
Frances Morgan, PhD October 21, Comprehensive Care of Patients with Tuberculosis and Their Contacts October 19 22, 2015 Wichita, KS
 The Laboratory s Role in Caring for Patients Diagnosed with TB Frances Morgan, PhD October 21, 2015 Comprehensive Care of Patients with Tuberculosis and Their Contacts October 19 22, 2015 Wichita, KS EXCELLENCE
The Laboratory s Role in Caring for Patients Diagnosed with TB Frances Morgan, PhD October 21, 2015 Comprehensive Care of Patients with Tuberculosis and Their Contacts October 19 22, 2015 Wichita, KS EXCELLENCE
A smart acid nanosystem for ultrasensitive. live cell mrna imaging by the target-triggered intracellular self-assembly
 Electronic Supplementary Material (ESI) for Chemical Science. This journal is The Royal Society of Chemistry 2017 A smart ZnO@polydopamine-nucleic acid nanosystem for ultrasensitive live cell mrna imaging
Electronic Supplementary Material (ESI) for Chemical Science. This journal is The Royal Society of Chemistry 2017 A smart ZnO@polydopamine-nucleic acid nanosystem for ultrasensitive live cell mrna imaging
Respiratory Pathogen Panel TEM-PCR Test Code:
 Respiratory Pathogen Panel TEM-PCR Test Code: 220000 Tests in this Panel Enterovirus group Human bocavirus Human coronavirus (4 types) Human metapneumovirus Influenza A - Human influenza Influenza A -
Respiratory Pathogen Panel TEM-PCR Test Code: 220000 Tests in this Panel Enterovirus group Human bocavirus Human coronavirus (4 types) Human metapneumovirus Influenza A - Human influenza Influenza A -
Supplementary Figure 1. ROS induces rapid Sod1 nuclear localization in a dosagedependent manner. WT yeast cells (SZy1051) were treated with 4NQO at
 Supplementary Figure 1. ROS induces rapid Sod1 nuclear localization in a dosagedependent manner. WT yeast cells (SZy1051) were treated with 4NQO at different concentrations for 30 min and analyzed for
Supplementary Figure 1. ROS induces rapid Sod1 nuclear localization in a dosagedependent manner. WT yeast cells (SZy1051) were treated with 4NQO at different concentrations for 30 min and analyzed for
A Rapid and Sensitive Chip-based Assay for Detection of rpob Gene Mutations Conferring Rifampicin Resistance in Mycobacterium tuberculosis (TB).
 A Rapid and Sensitive Chip-based Assay for Detection of rpob Gene Mutations Conferring Rifampicin Resistance in Mycobacterium tuberculosis (TB). Wanyuan Ao, Steve Aldous, Evelyn Woodruff, Brian Hicke,
A Rapid and Sensitive Chip-based Assay for Detection of rpob Gene Mutations Conferring Rifampicin Resistance in Mycobacterium tuberculosis (TB). Wanyuan Ao, Steve Aldous, Evelyn Woodruff, Brian Hicke,
Rapid Diagnosis of Extensively Drug-Resistant Tuberculosis by Use of a Reverse Line Blot Hybridization Assay
 JOURNAL OF CLINICAL MICROBIOLOGY, July 2011, p. 2546 2551 Vol. 49, No. 7 0095-1137/11/$12.00 doi:10.1128/jcm.02511-10 Copyright 2011, American Society for Microbiology. All Rights Reserved. Rapid Diagnosis
JOURNAL OF CLINICAL MICROBIOLOGY, July 2011, p. 2546 2551 Vol. 49, No. 7 0095-1137/11/$12.00 doi:10.1128/jcm.02511-10 Copyright 2011, American Society for Microbiology. All Rights Reserved. Rapid Diagnosis
The diagnostic value of gyrb RFLP PCR. Mycobacteria in patients with clinical. in Mazandaran
 Mazandaran University of Medical Sciences The diagnostic value of gyrb RFLP PCR test t in differentiation between pathogenic Mycobacteria in patients with clinical suspicions spicions of tuberculosis in
Mazandaran University of Medical Sciences The diagnostic value of gyrb RFLP PCR test t in differentiation between pathogenic Mycobacteria in patients with clinical suspicions spicions of tuberculosis in
Update on MALDI-TOF Validation
 Update on MALDI-TOF Validation Donald Busalacchi B.S. Microbiologist- WSLH WMLN 2015 Review Matrix-Assisted Laser Desorption Ionization Time-of- Flight A form of Mass Spectroscopy utilizing a soft ionization
Update on MALDI-TOF Validation Donald Busalacchi B.S. Microbiologist- WSLH WMLN 2015 Review Matrix-Assisted Laser Desorption Ionization Time-of- Flight A form of Mass Spectroscopy utilizing a soft ionization
Comparison of mechanical disruption techniques for the rapid inactivation of
 JCM Accepted Manuscript Posted Online 10 August 2016 J. Clin. Microbiol. doi:10.1128/jcm.01096-16 Copyright 2016, American Society for Microbiology. All Rights Reserved. 1 2 3 4 5 6 7 8 9 10 Comparison
JCM Accepted Manuscript Posted Online 10 August 2016 J. Clin. Microbiol. doi:10.1128/jcm.01096-16 Copyright 2016, American Society for Microbiology. All Rights Reserved. 1 2 3 4 5 6 7 8 9 10 Comparison
Research Article Use of Genotype MTBDRplus Assay for Diagnosis of Multidrug-Resistant Tuberculosis in Nepal
 Hindawi International Scholarly Research Notices Volume 2017, Article ID 1635780, 5 pages https://doi.org/10.1155/2017/1635780 Research Article Use of Genotype MTBDRplus Assay for Diagnosis of Multidrug-Resistant
Hindawi International Scholarly Research Notices Volume 2017, Article ID 1635780, 5 pages https://doi.org/10.1155/2017/1635780 Research Article Use of Genotype MTBDRplus Assay for Diagnosis of Multidrug-Resistant
Nature Structural & Molecular Biology: doi: /nsmb Supplementary Figure 1
 Supplementary Figure 1 U1 inhibition causes a shift of RNA-seq reads from exons to introns. (a) Evidence for the high purity of 4-shU-labeled RNAs used for RNA-seq. HeLa cells transfected with control
Supplementary Figure 1 U1 inhibition causes a shift of RNA-seq reads from exons to introns. (a) Evidence for the high purity of 4-shU-labeled RNAs used for RNA-seq. HeLa cells transfected with control
M. Khanna and S. Visuri
 The ProPneumo1 Assay: Detection of Chlamydophila pneumoniae, Mycoplasma pneumoniae, and an Internal Control Using Multiplex PCR on Multiple Real Time PCR Systems S. Dollhopf,, W. Majewski,, P. Douglass,
The ProPneumo1 Assay: Detection of Chlamydophila pneumoniae, Mycoplasma pneumoniae, and an Internal Control Using Multiplex PCR on Multiple Real Time PCR Systems S. Dollhopf,, W. Majewski,, P. Douglass,
Retrospective and Prospective Verification of the Cepheid Xpert Flu Assay
 JCM Accepts, published online ahead of print on 20 July 2011 J. Clin. Microbiol. doi:10.1128/jcm.01162-11 Copyright 2011, American Society for Microbiology and/or the Listed Authors/Institutions. All Rights
JCM Accepts, published online ahead of print on 20 July 2011 J. Clin. Microbiol. doi:10.1128/jcm.01162-11 Copyright 2011, American Society for Microbiology and/or the Listed Authors/Institutions. All Rights
Rapid detection of Mycobacterium tuberculosis complex from sputum samples using novel Loop-Mediated Isothermal Amplification
 Rapid detection of Mycobacterium tuberculosis complex from sputum samples using novel Loop-Mediated Isothermal Amplification Tetsu Hase, Ph.D. EIKEN CHEMICAL Co.,LTD. 1 Basic principle of LAMP method 2
Rapid detection of Mycobacterium tuberculosis complex from sputum samples using novel Loop-Mediated Isothermal Amplification Tetsu Hase, Ph.D. EIKEN CHEMICAL Co.,LTD. 1 Basic principle of LAMP method 2
Received 11 May 2010/Returned for modification 1 July 2010/Accepted 8 July 2010
 JOURNAL OF CLINICAL MICROBIOLOGY, Sept. 2010, p. 3073 3080 Vol. 48, No. 9 0095-1137/10/$12.00 doi:10.1128/jcm.00939-10 Copyright 2010, American Society for Microbiology. All Rights Reserved. Development
JOURNAL OF CLINICAL MICROBIOLOGY, Sept. 2010, p. 3073 3080 Vol. 48, No. 9 0095-1137/10/$12.00 doi:10.1128/jcm.00939-10 Copyright 2010, American Society for Microbiology. All Rights Reserved. Development
Clinical and Public Health Impact of Nucleic Acid Amplification Tests (NAATs) for Tuberculosis
 Clinical and Public Health Impact of Nucleic Acid Amplification Tests (NAATs) for Tuberculosis Amit S. Chitnis, MD, MPH; Pennan M. Barry, MD, MPH; Jennifer M. Flood, MD, MPH. California Tuberculosis Controllers
Clinical and Public Health Impact of Nucleic Acid Amplification Tests (NAATs) for Tuberculosis Amit S. Chitnis, MD, MPH; Pennan M. Barry, MD, MPH; Jennifer M. Flood, MD, MPH. California Tuberculosis Controllers
Public Health Mycobacteriology (TB) Laboratory Testing Services
 Public Health Mycobacteriology (TB) Laboratory Testing Services Gary Budnick Supervising Microbiologist Connecticut Department of Public Health Laboratory Branch Hartford, Connecticut Specimen Collection
Public Health Mycobacteriology (TB) Laboratory Testing Services Gary Budnick Supervising Microbiologist Connecticut Department of Public Health Laboratory Branch Hartford, Connecticut Specimen Collection
Latent Tuberculosis Infections Controversies in Diagnosis and Management Update 2016
 Latent Tuberculosis Infections Controversies in Diagnosis and Management Update 2016 Randy Culpepper, MD, MPH Deputy Heath Officer/Medical Director Frederick County Health Department March 16, 2016 2 No
Latent Tuberculosis Infections Controversies in Diagnosis and Management Update 2016 Randy Culpepper, MD, MPH Deputy Heath Officer/Medical Director Frederick County Health Department March 16, 2016 2 No
The MODS Assay for Detection of TB and TB Drug Resistance: A Multi-center Study
 The MODS Assay for Detection of TB and TB Drug Resistance: A Multi-center Study microscopic observation drug susceptibility Susan E. Dorman, MD Johns Hopkins University Afranio L. Kritski, MD, PhD Federal
The MODS Assay for Detection of TB and TB Drug Resistance: A Multi-center Study microscopic observation drug susceptibility Susan E. Dorman, MD Johns Hopkins University Afranio L. Kritski, MD, PhD Federal
Principles of laboratory diagnosis of M. tuberculosis. Anne-Marie Demers, MD, FRCPC 11 September 2017
 Principles of laboratory diagnosis of M. tuberculosis Anne-Marie Demers, MD, FRCPC 11 September 2017 QUESTION Which statement is false? 1) A smear can only be on a concentrated specimen 2) It is normal
Principles of laboratory diagnosis of M. tuberculosis Anne-Marie Demers, MD, FRCPC 11 September 2017 QUESTION Which statement is false? 1) A smear can only be on a concentrated specimen 2) It is normal
Research Methods for TB Diagnostics. Kathy DeRiemer, PhD, MPH University of California, Davis Shanghai, China: May 8, 2012
 Research Methods for TB Diagnostics Kathy DeRiemer, PhD, MPH University of California, Davis Shanghai, China: May 8, 2012 Overview Why do we need good TB diagnostics? What works? What doesn t work? How
Research Methods for TB Diagnostics Kathy DeRiemer, PhD, MPH University of California, Davis Shanghai, China: May 8, 2012 Overview Why do we need good TB diagnostics? What works? What doesn t work? How
DNA sequencing for the confirmation of rifampin resistance detected by Cepheid Xpert
 JCM Accepted Manuscript Posted Online 4 March 2015 J. Clin. Microbiol. doi:10.1128/jcm.03433-14 Copyright 2015, American Society for Microbiology. All Rights Reserved. 1 2 DNA sequencing for the confirmation
JCM Accepted Manuscript Posted Online 4 March 2015 J. Clin. Microbiol. doi:10.1128/jcm.03433-14 Copyright 2015, American Society for Microbiology. All Rights Reserved. 1 2 DNA sequencing for the confirmation
Nucleic Acid Amplification Test for Tuberculosis. Heidi Behm, RN, MPH Acting TB Controller HIV/STD/TB Program Oregon, Department of Health Services
 Nucleic Acid Amplification Test for Tuberculosis Heidi Behm, RN, MPH Acting TB Controller HIV/STD/TB Program Oregon, Department of Health Services What is this test? Nucleic Acid Amplification Test (NAAT)
Nucleic Acid Amplification Test for Tuberculosis Heidi Behm, RN, MPH Acting TB Controller HIV/STD/TB Program Oregon, Department of Health Services What is this test? Nucleic Acid Amplification Test (NAAT)
Supplementary Figure 1
 Supplementary Figure 1 Supplementary Figure 1: Cryopreservation alters CD62L expression by CD4 T cells. Freshly isolated (left) or cryopreserved PBMCs (right) were stained with the mix of antibodies described
Supplementary Figure 1 Supplementary Figure 1: Cryopreservation alters CD62L expression by CD4 T cells. Freshly isolated (left) or cryopreserved PBMCs (right) were stained with the mix of antibodies described
Molecular tests for rapid detection of rifampicin and isoniazid resistance in Mycobacterium tuberculosis.
 Title Molecular tests for rapid detection of rifampicin and isoniazid resistance in Mycobacterium. Author(s) Ho, PL; Yam, WC; Leung, CC; Yew, WW; Mok, TYW; Chan, KS; Tam, CM Citation Hong Kong Medical
Title Molecular tests for rapid detection of rifampicin and isoniazid resistance in Mycobacterium. Author(s) Ho, PL; Yam, WC; Leung, CC; Yew, WW; Mok, TYW; Chan, KS; Tam, CM Citation Hong Kong Medical
Xpert MTB/RIF Training. Indira Soundiram 2012
 Xpert MTB/RIF Training Indira Soundiram 2012 A Better Way to Platform Design GeneXpert Infinity-48 GeneXpert Module GX-I GX-II GX-IV GX-XVI 2 Defining Molecular Diagnostics Any Test Any Time Any Sample
Xpert MTB/RIF Training Indira Soundiram 2012 A Better Way to Platform Design GeneXpert Infinity-48 GeneXpert Module GX-I GX-II GX-IV GX-XVI 2 Defining Molecular Diagnostics Any Test Any Time Any Sample
The ABC s of AFB s Laboratory Testing for Tuberculosis. Gary Budnick Connecticut Department of Public Health Mycobacteriology Laboratory
 The ABC s of AFB s Laboratory Testing for Tuberculosis Gary Budnick Connecticut Department of Public Health Mycobacteriology Laboratory Laboratory TAT Goals Case Study Specimen Collection Testing Contact
The ABC s of AFB s Laboratory Testing for Tuberculosis Gary Budnick Connecticut Department of Public Health Mycobacteriology Laboratory Laboratory TAT Goals Case Study Specimen Collection Testing Contact
Role of the Laboratory in TB Diagnosis and Management
 Role of the Laboratory in TB Diagnosis and Management Michael Pentella, Ph.D., D(ABMM), CIC Associate Director University Hygienic Lab Clinical Associate Professor, College of Public Health, University
Role of the Laboratory in TB Diagnosis and Management Michael Pentella, Ph.D., D(ABMM), CIC Associate Director University Hygienic Lab Clinical Associate Professor, College of Public Health, University
Diagnosis of Extra Pulmonary Tuberculosis By Using Xpert MTB/RIF Assay (CBNAAT) And MGIT Liquid Culture.
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 9 Ver. 10 (September. 2018), PP 65-70 www.iosrjournals.org Diagnosis of Extra Pulmonary Tuberculosis
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 9 Ver. 10 (September. 2018), PP 65-70 www.iosrjournals.org Diagnosis of Extra Pulmonary Tuberculosis
Xpert MTB/RIF Ultra: Understanding this new diagnostic and who will have access to it
 Xpert MTB/RIF Ultra: Understanding this new diagnostic and who will have access to it Angela Starks, PhD Chief, Laboratory Branch Division of TB Elimination Matt Bankowski, PhD, MS, D(ABMM), HCLD/CC(ABB)
Xpert MTB/RIF Ultra: Understanding this new diagnostic and who will have access to it Angela Starks, PhD Chief, Laboratory Branch Division of TB Elimination Matt Bankowski, PhD, MS, D(ABMM), HCLD/CC(ABB)
Drug susceptibility testing for tuberculosis KRISTEN DICKS, MD, MPH DUKE UNIVERSITY MEDICAL CENTER
 Drug susceptibility testing for tuberculosis KRISTEN DICKS, MD, MPH DUKE UNIVERSITY MEDICAL CENTER Outline Drug resistant TB: definitions and epidemiology How does TB become resistant? Current drug susceptibility
Drug susceptibility testing for tuberculosis KRISTEN DICKS, MD, MPH DUKE UNIVERSITY MEDICAL CENTER Outline Drug resistant TB: definitions and epidemiology How does TB become resistant? Current drug susceptibility
Biology and Medicine
 eissn: 09748369 Diagnosis of pulmonary tuberculosis by smear microscopy and culture in a tertiary health care facility Biology and Medicine SI Khatib, MT Williamson, R Singh, JM Joshi Accepted: 28 th Feb
eissn: 09748369 Diagnosis of pulmonary tuberculosis by smear microscopy and culture in a tertiary health care facility Biology and Medicine SI Khatib, MT Williamson, R Singh, JM Joshi Accepted: 28 th Feb
Recommended laboratory tests to identify influenza A/H5 virus in specimens from patients with an influenza-like illness
 World Health Organization Recommended laboratory tests to identify influenza A/H5 virus in specimens from patients with an influenza-like illness General information Highly pathogenic avian influenza (HPAI)
World Health Organization Recommended laboratory tests to identify influenza A/H5 virus in specimens from patients with an influenza-like illness General information Highly pathogenic avian influenza (HPAI)
Diagnosis of drug resistant TB
 Diagnosis of drug resistant TB Megan Murray, MD, ScD Harvard School of Public Health Brigham and Women s Hospital Harvard Medical School Broad Institute Global burden of TB 9 million new cases year 2 million
Diagnosis of drug resistant TB Megan Murray, MD, ScD Harvard School of Public Health Brigham and Women s Hospital Harvard Medical School Broad Institute Global burden of TB 9 million new cases year 2 million
of clinical laboratory diagnosis in Extra-pulmonary Tuberculosis
 New approaches and the importance of clinical laboratory diagnosis in Extra-pulmonary Tuberculosis Bahrmand.AR, Hadizadeh Tasbiti.AR, Saifi.M, Yari.SH, Karimi.A, Fateh.A, Tuberculosis Dept. Pasteur Institute
New approaches and the importance of clinical laboratory diagnosis in Extra-pulmonary Tuberculosis Bahrmand.AR, Hadizadeh Tasbiti.AR, Saifi.M, Yari.SH, Karimi.A, Fateh.A, Tuberculosis Dept. Pasteur Institute
Towards Harmonization of Mycobacteriology in TB Trials. Study 31/ACTG 5349 Key Elements of Mycobacteriology Laboratory Procedures
 Study 31/ACTG 5349 Key Elements of Mycobacteriology Laboratory Procedures: Towards Harmonization of Mycobacteriology in TB Trials Title Author(s) Study 31/ACTG 5349 Key Elements of Mycobacteriology Laboratory
Study 31/ACTG 5349 Key Elements of Mycobacteriology Laboratory Procedures: Towards Harmonization of Mycobacteriology in TB Trials Title Author(s) Study 31/ACTG 5349 Key Elements of Mycobacteriology Laboratory
MYCOBACTERIA. Pulmonary T.B. (infect bird)
 MYCOBACTERIA SPP. Reservoir Clinical Manifestation Mycobacterium tuberculosis Human Pulmonary and dissem. T.B. M. lepra Human Leprosy M. bovis Human & cattle T.B. like infection M. avium Soil, water, birds,
MYCOBACTERIA SPP. Reservoir Clinical Manifestation Mycobacterium tuberculosis Human Pulmonary and dissem. T.B. M. lepra Human Leprosy M. bovis Human & cattle T.B. like infection M. avium Soil, water, birds,
Use of the BacT/ALERT MB Mycobacteria Blood Culture System for Detecting ACCEPTED
 JCM Accepts, published online ahead of print on December 00 J. Clin. Microbiol. doi:.11/jcm.011-0 Copyright 00, American Society for Microbiology and/or the Listed Authors/Institutions. All Rights Reserved.
JCM Accepts, published online ahead of print on December 00 J. Clin. Microbiol. doi:.11/jcm.011-0 Copyright 00, American Society for Microbiology and/or the Listed Authors/Institutions. All Rights Reserved.
When good genes go bad
 When good genes go bad Dr Kessendri Reddy NHLS Tygerberg Hospital Division of Clinical Microbiology Fakulteit Geneeskunde en Gesondheidswetenskappe Faculty of Medicine and Health Sciences Overview Cases
When good genes go bad Dr Kessendri Reddy NHLS Tygerberg Hospital Division of Clinical Microbiology Fakulteit Geneeskunde en Gesondheidswetenskappe Faculty of Medicine and Health Sciences Overview Cases
Molecular diagnosis of MDR-TB using GenoType MTBDRplus 96 assay in Ibadan, Nigeria
 Niger. J. Physiol. Sci. 28(December 2013) 187 191 www.njps.com.ng Molecular diagnosis of MDR-TB using GenoType MTBDRplus 96 assay in Ibadan, Nigeria * 1 Kehinde A.O. and 2 Adebiyi, E.O. Department of Medical
Niger. J. Physiol. Sci. 28(December 2013) 187 191 www.njps.com.ng Molecular diagnosis of MDR-TB using GenoType MTBDRplus 96 assay in Ibadan, Nigeria * 1 Kehinde A.O. and 2 Adebiyi, E.O. Department of Medical
Comparison of the Xpert MTB/RIF Assay and Real-time PCR for the Detection of Mycobacterium tuberculosis
 Available online at www.annclinlabsci.org Annals of Clinical & Laboratory Science, vol. 45, no. 3, 2015 327 Comparison of the Xpert MTB/RIF Assay and Real-time PCR for the Detection of Mycobacterium tuberculosis
Available online at www.annclinlabsci.org Annals of Clinical & Laboratory Science, vol. 45, no. 3, 2015 327 Comparison of the Xpert MTB/RIF Assay and Real-time PCR for the Detection of Mycobacterium tuberculosis
Research Article Factors Associated with Missed Detection of Mycobacterium tuberculosis by Automated BACTEC MGIT 960 System
 BioMed Research International Volume 2016, Article ID 5972021, 4 pages http://dx.doi.org/10.1155/2016/5972021 Research Article Factors Associated with Missed Detection of Mycobacterium tuberculosis by
BioMed Research International Volume 2016, Article ID 5972021, 4 pages http://dx.doi.org/10.1155/2016/5972021 Research Article Factors Associated with Missed Detection of Mycobacterium tuberculosis by
Evaluation of the Microscopic-Observation. Drug-Susceptibility Assay Drugs Concentration for Detection Of Multidrug-Resistant Tuberculosis
 Evaluation of the Microscopic-Observation Drug-Susceptibility Assay Drugs Concentration for Detection Of Multidrug-Resistant Tuberculosis ABSTRACT New diagnostic tools are urgently needed to interrupt
Evaluation of the Microscopic-Observation Drug-Susceptibility Assay Drugs Concentration for Detection Of Multidrug-Resistant Tuberculosis ABSTRACT New diagnostic tools are urgently needed to interrupt
TB Nurse Case Management. March 7-9, Diagnosis of TB: Ken Jost Wednesday March 7, 2012
 TB Nurse Case Management San Antonio, Texas March 7-9, 2012 Diagnosis of TB: Laboratory Ken Jost Wednesday March 7, 2012 Ken Jost has the following disclosures to make: No conflict of interests No relevant
TB Nurse Case Management San Antonio, Texas March 7-9, 2012 Diagnosis of TB: Laboratory Ken Jost Wednesday March 7, 2012 Ken Jost has the following disclosures to make: No conflict of interests No relevant
For in vitro Veterinary Diagnostics only. Kylt Rotavirus A. Real-Time RT-PCR Detection.
 For in vitro Veterinary Diagnostics only. Kylt Rotavirus A Real-Time RT-PCR Detection www.kylt.eu DIRECTION FOR USE Kylt Rotavirus A Real-Time RT-PCR Detection A. General Kylt Rotavirus A products are
For in vitro Veterinary Diagnostics only. Kylt Rotavirus A Real-Time RT-PCR Detection www.kylt.eu DIRECTION FOR USE Kylt Rotavirus A Real-Time RT-PCR Detection A. General Kylt Rotavirus A products are
Simultaneous and Rapid Detection of Causative Pathogens in Community-acquired Pneumonia by Real-time PCR (1167)
 From the Japanese Association of Medical Sciences The Japanese Association for Infectious Diseases Simultaneous and Rapid Detection of Causative Pathogens in Community-acquired Pneumonia by Real-time PCR
From the Japanese Association of Medical Sciences The Japanese Association for Infectious Diseases Simultaneous and Rapid Detection of Causative Pathogens in Community-acquired Pneumonia by Real-time PCR
PCR-Based Method To Differentiate the Subspecies of the Mycobacterium tuberculosis Complex on the Basis of Genomic Deletions
 JOURNAL OF CLINICAL MICROBIOLOGY, Apr. 2003, p. 1637 1650 Vol. 41, No. 4 0095-1137/03/$08.00 0 DOI: 10.1128/JCM.41.4.1637 1650.2003 Copyright 2003, American Society for Microbiology. All Rights Reserved.
JOURNAL OF CLINICAL MICROBIOLOGY, Apr. 2003, p. 1637 1650 Vol. 41, No. 4 0095-1137/03/$08.00 0 DOI: 10.1128/JCM.41.4.1637 1650.2003 Copyright 2003, American Society for Microbiology. All Rights Reserved.
CD31 5'-AGA GAC GGT CTT GTC GCA GT-3' 5 ' -TAC TGG GCT TCG AGA GCA GT-3'
 Table S1. The primer sets used for real-time RT-PCR analysis. Gene Forward Reverse VEGF PDGFB TGF-β MCP-1 5'-GTT GCA GCA TGA ATC TGA GG-3' 5'-GGA GAC TCT TCG AGG AGC ACT T-3' 5'-GAA TCA GGC ATC GAG AGA
Table S1. The primer sets used for real-time RT-PCR analysis. Gene Forward Reverse VEGF PDGFB TGF-β MCP-1 5'-GTT GCA GCA TGA ATC TGA GG-3' 5'-GGA GAC TCT TCG AGG AGC ACT T-3' 5'-GAA TCA GGC ATC GAG AGA
Multi-clonal origin of macrolide-resistant Mycoplasma pneumoniae isolates. determined by multiple-locus variable-number tandem-repeat analysis
 JCM Accepts, published online ahead of print on 30 May 2012 J. Clin. Microbiol. doi:10.1128/jcm.00678-12 Copyright 2012, American Society for Microbiology. All Rights Reserved. 1 2 Multi-clonal origin
JCM Accepts, published online ahead of print on 30 May 2012 J. Clin. Microbiol. doi:10.1128/jcm.00678-12 Copyright 2012, American Society for Microbiology. All Rights Reserved. 1 2 Multi-clonal origin
Diagnosis and Management of Active Tuberculosis
 Diagnosis and Management of Active Tuberculosis Zelalem Temesgen, MD FIDSA AAHIVS 2013 MFMER slide-1 Disclosures None 2013 MFMER slide-2 Objectives By the end of this session, participants should be able
Diagnosis and Management of Active Tuberculosis Zelalem Temesgen, MD FIDSA AAHIVS 2013 MFMER slide-1 Disclosures None 2013 MFMER slide-2 Objectives By the end of this session, participants should be able
Toluidin-Staining of mast cells Ear tissue was fixed with Carnoy (60% ethanol, 30% chloroform, 10% acetic acid) overnight at 4 C, afterwards
 Toluidin-Staining of mast cells Ear tissue was fixed with Carnoy (60% ethanol, 30% chloroform, 10% acetic acid) overnight at 4 C, afterwards incubated in 100 % ethanol overnight at 4 C and embedded in
Toluidin-Staining of mast cells Ear tissue was fixed with Carnoy (60% ethanol, 30% chloroform, 10% acetic acid) overnight at 4 C, afterwards incubated in 100 % ethanol overnight at 4 C and embedded in
Laboratory diagnosis of spinal tuberculosis: Past and Present. SA Patwardhan, S Joshi Abstract : Spinal tuberculosis often has an indolent course and
 Laboratory diagnosis of spinal tuberculosis: Past and Present. SA Patwardhan, S Joshi Abstract : Spinal tuberculosis often has an indolent course and can be a diagnostic challenge. Timely laboratory diagnosis
Laboratory diagnosis of spinal tuberculosis: Past and Present. SA Patwardhan, S Joshi Abstract : Spinal tuberculosis often has an indolent course and can be a diagnostic challenge. Timely laboratory diagnosis
Protocols for Laboratory Verification of Performance of the BioFire FilmArray Pneumonia Panel
 Protocols for Laboratory Verification of Performance of the BioFire FilmArray Pneumonia Panel Laboratory Protocols for Use with a ZeptoMetrix NATtrol Verification Panel Purpose The Clinical Laboratory
Protocols for Laboratory Verification of Performance of the BioFire FilmArray Pneumonia Panel Laboratory Protocols for Use with a ZeptoMetrix NATtrol Verification Panel Purpose The Clinical Laboratory
Laboratory Diagnostic Techniques. Hugo Donaldson Consultant Microbiologist Imperial College Healthcare NHS Trust
 Laboratory Diagnostic Techniques Hugo Donaldson Consultant Microbiologist Imperial College Healthcare NHS Trust Learning Objectives 1) When to consider a diagnosis of TB 2) When to consider a referral
Laboratory Diagnostic Techniques Hugo Donaldson Consultant Microbiologist Imperial College Healthcare NHS Trust Learning Objectives 1) When to consider a diagnosis of TB 2) When to consider a referral
a) Primary cultures derived from the pancreas of an 11-week-old Pdx1-Cre; K-MADM-p53
 1 2 3 4 5 6 7 8 9 10 Supplementary Figure 1. Induction of p53 LOH by MADM. a) Primary cultures derived from the pancreas of an 11-week-old Pdx1-Cre; K-MADM-p53 mouse revealed increased p53 KO/KO (green,
1 2 3 4 5 6 7 8 9 10 Supplementary Figure 1. Induction of p53 LOH by MADM. a) Primary cultures derived from the pancreas of an 11-week-old Pdx1-Cre; K-MADM-p53 mouse revealed increased p53 KO/KO (green,
*To whom correspondence should be addressed. This PDF file includes:
 www.sciencemag.org/cgi/content/full/science.1212182/dc1 Supporting Online Material for Partial Retraction to Detection of an Infectious Retrovirus, XMRV, in Blood Cells of Patients with Chronic Fatigue
www.sciencemag.org/cgi/content/full/science.1212182/dc1 Supporting Online Material for Partial Retraction to Detection of an Infectious Retrovirus, XMRV, in Blood Cells of Patients with Chronic Fatigue
MGIT 960) for Recovery of Mycobacteria from 9558 Extrapulmonary ACCEPTED. Specimens including Urine Samples
 JCM Accepts, published online ahead of print on September 00 J. Clin. Microbiol. doi:./jcm.00-0 Copyright 00, American Society for Microbiology and/or the Listed Authors/Institutions. All Rights Reserved.
JCM Accepts, published online ahead of print on September 00 J. Clin. Microbiol. doi:./jcm.00-0 Copyright 00, American Society for Microbiology and/or the Listed Authors/Institutions. All Rights Reserved.
Mycobacteriology William H. Benjamin, Jr.
 Mycobacteriology William H. Benjamin, Jr. William H. Benjamin, PhD Department of Pathology UAB 1 Mycobacteria sp. Acid Fast Bacilli (AFB) Mycolic acids (C78-91) Waxes Obligate aerobes Slow growing days
Mycobacteriology William H. Benjamin, Jr. William H. Benjamin, PhD Department of Pathology UAB 1 Mycobacteria sp. Acid Fast Bacilli (AFB) Mycolic acids (C78-91) Waxes Obligate aerobes Slow growing days
INTENSIFIED TB CASE FINDING
 INTENSIFIED TB CASE FINDING My friends call me Intensified Case Finding (ICF) I undertake regularly screening all people with, or at high risk of HIV, for symptoms of TB in health care facilities, communities
INTENSIFIED TB CASE FINDING My friends call me Intensified Case Finding (ICF) I undertake regularly screening all people with, or at high risk of HIV, for symptoms of TB in health care facilities, communities
Mycobacteria Diagnostic Testing in Manitoba. Dr. Michelle Alfa Medical Director, DSM Clin Micro Discipline
 Mycobacteria Diagnostic Testing in Manitoba Dr. Michelle Alfa Medical Director, DSM Clin Micro Discipline Acknowlegements: Assunta Rendina: Charge Tech HSC Lab Joyce Wolf & Dr. Meenu Sharma: NML Dr. Kanchana
Mycobacteria Diagnostic Testing in Manitoba Dr. Michelle Alfa Medical Director, DSM Clin Micro Discipline Acknowlegements: Assunta Rendina: Charge Tech HSC Lab Joyce Wolf & Dr. Meenu Sharma: NML Dr. Kanchana
CHAPTER 3: DEFINITION OF TERMS
 CHAPTER 3: DEFINITION OF TERMS NOTE: TB bacteria is used in place of Mycobacterium tuberculosis and Mycobacterium tuberculosis complex in most of the definitions presented here. 3.1 Acid-fast bacteria
CHAPTER 3: DEFINITION OF TERMS NOTE: TB bacteria is used in place of Mycobacterium tuberculosis and Mycobacterium tuberculosis complex in most of the definitions presented here. 3.1 Acid-fast bacteria
Figure S1. Analysis of genomic and cdna sequences of the targeted regions in WT-KI and
 Figure S1. Analysis of genomic and sequences of the targeted regions in and indicated mutant KI cells, with WT and corresponding mutant sequences underlined. (A) cells; (B) K21E-KI cells; (C) D33A-KI cells;
Figure S1. Analysis of genomic and sequences of the targeted regions in and indicated mutant KI cells, with WT and corresponding mutant sequences underlined. (A) cells; (B) K21E-KI cells; (C) D33A-KI cells;
The Clinical Impact of Rapid Nucleic Acid Amplification Tests for Detection of M. tuberculosis
 The Clinical Impact of Rapid Nucleic Acid Amplification Tests for Detection of M. tuberculosis DR. PHYLLIS DELLA-LATTA, D(ABMM), FAAM DIRECTOR, CLINICAL MICROBIOLOGY SERVICE PROFESSOR, CLINICAL PATHOLOGY
The Clinical Impact of Rapid Nucleic Acid Amplification Tests for Detection of M. tuberculosis DR. PHYLLIS DELLA-LATTA, D(ABMM), FAAM DIRECTOR, CLINICAL MICROBIOLOGY SERVICE PROFESSOR, CLINICAL PATHOLOGY
